Evaluation of an Absorbable Collagen Membrane in Treating Class II. Furcation Defects
|
|
|
- Jesse Glenn
- 5 years ago
- Views:
Transcription
1 Evaluation of an Absorbable Collagen Membrane in Treating Class II Furcation Defects Horn-Lay Wang,* Robert. O'Neal,* Clifford L. Thomas/ Yu Shyr/ and R. Lamont MacNeil* 1029 Recent research has focused upon the utilization of an absorbable collagen membrane in guided tissue regeneration (GTR). Concern exists as to whether this type of membrane is beneficial in the treatment of periodontal defects. The purpose of this study was to evaluate the effect of a type I bovine collagen membrane on treatment of Class II furcation defects. Twelve systemically healthy patients (six male and six female, ages 32 to 68) were treated. Each had bilateral mandibular furcation defects with attachment loss >6 mm. Prior to surgery all patients completed initial therapy including scaling and root planing. At the time of the surgery, teeth were randomly assigned to either a control (flap debridement alone) or test (flap debridement plus collagen membrane) group. Data were collected on the day of surgery, and 2, 4, and 6 months post-surgery and at the 12 month re-entry surgery. Clinical measurements included probing depth (PD), clinical attachment level (CAL), gingival recession (GR), Stent to base of defect (SB), crestal bone to base of defect (CB), width of defect, and mobility. Statistical analysis was performed utilizing the paired t test. Both control and test groups demonstrated significant (P< 0.05) improvement at 12 months re-entry in PD, CAL, SB, and CB when compared to the presurgery status. While there is no significant difference in PD, CAL, GR, width of defect, and mobility between control and test groups, sites treated with the collagen membrane had significantly higher bone fill (SB and CB) at re-entry. A significant improvement of furcation horizontal bone repair and defect improvement was noted in the collagen membranes-treated sites as compared to the presurgery status. No foreign body reaction was observed in either group during this study. This study suggests that the use of absorbable collagen membrane may have beneficial effects in the treatment of Class II furcal defects. J Periodontol 1994; 65: Key Words: Collagen therapeutic use; furcation therapy; guided tissue regeneration; membranes, barrier; randomized clinical trial. Guided tissue regeneration (i.e., epithelial exclusion and selective repopulation of the root surface by multipotential cells) utilizing non-resorbable occlusive membranes has become an accepted mode of therapy in periodontics.12 Although proven efficacious in promoting new connective tissue attachment, non-resorbable membranes are not without their shortcomings. For example, recession with bacterial contamination is a common clinical finding.3 In addition, the need for a second surgical procedure to retrieve the membrane may also disrupt healing. We have been conducting research on an absorbable barrier composed of type * Department of Periodontics/Prevention/Geriatrics, School of Dentistry, University of Michigan, Ann Arbor, MI. 'Private practice, Cleveland, OH. 'Department of Biostatistics, School of Public Health, University of Michigan, Ann Arbor, MI. I collagen. Collagen has a number of properties which make 7 it practical for use as a barrier.4 Collagen is the most abundant protein in the body and the main constituent of periodontal connective tissue. It comprises approximately 30% of the human body and functions as the extracellular framework for all multi-cellular barrier is animals. The rationale for using collagen as a based on the following: First, collagen possesses hemostatic properties.8 Wikesjö et al. have indicated that in order for regeneration to occur, the developing clot must form and adhere to the root surface thereby facilitating proper wound maturation.9 Because collagen is a hemostatic agent by virtue of its ability to aggregate platelets, it may further facilitate wound maturation by enhancing the initial blood clot and fibrin linkage formation. This concept is supported by Haney et al. who indicated that clot stabilization, wound
2 1030 COLLAGEN MEMBRANES IN THE TREATMENT OF CLASS II FURCATIONS J Periodontol November 1994 stability, space provision, epithelial cell exclusion, and complete gingival coverage are critical factors for the success of the GTR procedure.10 Second, a collagen membrane, once infiltrated by vascular channels, may serve as a lattice for migrating periodontal ligament fibroblasts.11 Third, collagen has been found to be chemotactic for fibroblasts in vitro,12 a property that may enhance cell migration into the space formed between the root surface and the collagen membrane. Clinical trials and animal studies have shown most collagen membranes to be effective in inhibiting epithelial migration and promoting new connective tissue attachment.1314 Fourth, collagen can be formed into many shapes and can easily be manipulated and adapted to the root surface. Fifth, collagen is a weak immunogen.15 Sixth, collagen is a cross-linked material which, is bioabsorbable, eliminating the need for re-entry surgery to remove it.16 In total, these properties suggest that collagen may have applications as a barrier material for use in regeneration therapy. Thus, the following study was designed to evaluate the effect of a type I bovine collagen membrane in treatment of Class II furcation defects. MATERIALS AND METHODS Patients The research protocol herein described was approved by the Human Subjects Review Committee at the School of Dentistry, The University of Michigan. Twelve systemically healthy patients (ages 32 to 68), six males and six females, were included in the study. The following criteria were used to select the patients for this clinical study: 1) evidence of advanced Periodontitis; 2) bilateral Class II mandibular furcation defects exhibiting attachment loss >6 mm; 3) radiographie evidence of a Class II mandibular mo- no antibiotic lar defect; 4) excellent systemic health; 5) therapy in the past 6 months; and 7) no periodontal surgery in the past 12 months. Informed consent from all subjects who met the criteria and agreed to participate in the study were obtained. Patients entered the study either directly after a standard preparation stage (i.e., oral hygiene instruction, scaling and root planing, and other initial disease control procedures) or upon the decision that surgical intervention was needed during maintenance therapy. Measurements Clinical data including probing depths (PD) of the periodontal defects, gingival recession (GR), mobility and plaque (PI) and gingival (Gl) indices were collected at baseline (one week prior to the surgery) and 2, 4 and 6 months post surgery. PD were obtained using a North Carolina 15 mm probe: the deepest point at six sites of selected teeth was recorded. GR was measured from the cementoenamel junction (CEJ) to the free gingival margin. Tooth mobility was detected utilizing Miller's classification (0 = no mobility; 1 the first distinguishable sign of = movement greater than normal; 2 = movement of 1 mm from normal position in any direction; and 3 = movement of more than 1 mm in any direction).17 PI was recorded according to the criteria de- Silness and Löe.18 Gl was measured using scribed by Löe and Silness.19 Additional clinical measurements were performed at the time of periodontal surgery and at one year re-entry surgery. Clinical attachment levels (CAL) were measured using a pre-fabricated acrylic Stent and a North Carolina 15 mm probe; the Stent was grooved at the time of surgery to record the orientation of the probe. When placed in the osseous defect, an occlusal ledge served as an occlusal landmark. The following measurements were made: SB, stent to the base of defect, stent to the free gingival margin; CB, crest of bone to base of defect; and buccolingual/mesiodistal morphology of the furcation defects (Fig- 1). Surgical Protocol All surgical procedures were performed by the same periodontist. Bilateral mandibular furcation defects were randomly assigned by coin toss to receive either flap debridement plus collagen membrane (test) or flap debridement alone (control) before the defects were debrided. The surgical procedure involved the elevation of a full thickness mucoperiosteal flap with intracrevicular incisions, preserving as much keratinized tissue as possible. The furcation defects were debrided and all root surfaces were completely scaled and root planed by hand, ultrasonic, and rotating instrumentation. The test material was a collagen mem- Stent groove Figure 1. Method used to analyze the furcation defect. (I) occlusal surface of stent to a line drawn from the mesial to distal at the base of the defect (BD); (2) crest of bone (AC) to base of the defect (BD); (3) horizontal probing depth (horizontal PD) from a line tangential to the root surface to the horizontal extent of the defect; (4) vertical probing depth (vertical PD) measures the line from the mesial to the distal at the bottom of the furcation defect (modified from Paul, et al.23).
3 Volume 65 Number 11 WANG, O'NEAL, THOMAS, SHYR, MACNEIL 1031 Table 1. Clinical Parameters Comparison Between Collagen Treated and Flap Sites (mean ± standard error) at Different Time Periods (n 12 = per group) Debridement Control Clinical Parameters Groups Baseline 2 Months 4 Months 6 Months 12 Months Gingival index Plaque index Probing depths Collagen Control Collagen Control Collagen Control 0.92 ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ±0.47 Table 2. Clinical Measurements (mm) for Collagen and Flap Debridement Control Sites at Baseline (n = 12 per group) Measurement Probing depths Attachment level Stent to free gingival margin Stent to base of defect Crest bone to base of defect Furcation measurements Buccolingual width Mesiodistal width Area of defects Collagen Sites Control Sites 6.92 ± ± ± ± ± ± ± ± ± ±6.82 No statistically-significant difference = < ± ± ± ± ± ±7.22 brane8 prepared from purified chemically cross-linked form and supplied Difference 0.00 ± ± ± ± ± ± ± ±0.91 bovine Achilles tendon in a in individual 18 mm X 38 mm X mm sterile pieces. The material was individually cut to proper dimension and then placed over the defect extending 2 mm beyond the edge of the furcation defect. The membrane was not sutured unless the size of the defect necessitated such procedures. Any suturing of the membrane was accomplished with 5-0 chromic gut sutures. The flap was subsequently sutured securely to its original position with 4-0 black silk sutures, with care to ensure that no portion of the membrane was left exposed on the day of surgery. On the control side all surgical procedures were identical, except that no membrane was placed. All patients received routine written and oral postoperative instructions and were prescribed doxycycline 100 mg/day for 2 weeks. Each patient was instructed to rinse with 0.12% Chlorhexidine gluconate11 for a period of 6 weeks. Sutures were removed 7 to 10 days after the surgery of the membrane noted. Patients and any change in position returned weekly for 4 weeks for observation of any adverse tissue reactions. Patients were then seen at 2, 4, and 6 months post-surgery for Gl, PI, PD, and GR recording; tissue evaluation; plaque debridement; and oral hygiene review. One Year Re-Entry Surgery At the end of 12 months, the patients were scheduled for re-entry surgery. Clinical measurements (GI, PI, PD, CAL, BioMend (formerly Periobarrier), Calcitek Inc., Carlsbad, CA. "Peridex, Procter & Gamble, Cincinnati, OH. Stent to the free gingival margin, SB, CB, and mobility) of the involved tooth were recorded prior to the surgery. Surgical re-entry consisted of sulcular incisions to preserve attached gingiva and interdental papillae. Full-thickness mucoperiosteal flaps were designed to expose the previously treated furcation areas for clinical photographs and measurements as previously described. Flaps were then replaced and sutured. Patients were seen at one week post-surgery for suture removal, and then placed on a closely supervised 3-month schedule for supportive periodontal treatment. Statistical Analysis The data were organized, presented as means ± standard error and analyzed using the SAS system. Repeated measures analysis of variance (ANOVA) was used to evaluate changes in clinical parameters within groups at different times. The paired r-test was utilized to compare the clinical measurements between control and test groups at each time period. Significance was reported at the 0.05 level. = RESULTS Twelve patients (mean age ±9.15) with bilateral similar furcation defects were studied. During the course of this study, no adverse tissue reaction, infections, or delayed healing were reported. As shown in Table 1, GI and PI decreased dramatically in both test and control sites at two months post-surgery. This noticeable downward shift was maintained throughout the experimental (12 month) period. The mean PD was reduced significantly at 2, 4, 6, and 12 months post-surgery when compared to baseline in both groups. No significant differences of GI, PI, and mean PD were noted between the test and control sites at any time point. Only mid-buccal or -lingual furca measurements from stent to free gingival margin, SB, and CB were used for statistical analysis. No differences were noted at baseline between collagen treated sites and flap debridement control sites for any clinical parameters (Table 2). Table 3 presents a comparison of clinical measurements for test and control sites at one year re-entry. A statistically significant variance was observed in CB (crestal bone to base of defect) for test (collagen) site when compared to control site at one year re-entry. Other parameters, while showing positive trends and differences, did not demonstrate statistically significant changes.
4 - (1/ COLLAGEN MEMBRANES IN THE TREATMENT OF CLASS II FURCATIONS J Periodontol November 1994 Table 3. Clinical Measurements (mm) for Collagen and Flap Debridement Control Sites at One Year Re-Entry (n = 12 per group) Measurements Probing depths Attachment level Stent to free gingival margin Stent to base of defect Crest bone to base of defect Furcation measurements Buccolingual width Mesiodistal width Area of defects Collagen Sites ± ± ± ± ± ± ±6.21 'Statistically significant difference = <0.05. Control Sites 5.00 ± ± ± ± ± ± ± ±8.10 Difference ± ± ± ± ±0.43* ± ± ±1.37 Table 4. Clinical Changes in Class II Furcation Invasions (mm) One Year After Treatment With and Without Collagen Barrier Placement (n = 12 per group) Measurements Probing depths Attachment level Stent to free gingival margin Stent to base of defect Crest bone to base of defect Furcation measurements Buccolingual width Mesiodistal width Area of defects Collagen Sites 2.84 ±0.41* 1.67 ±0.22* ±0.29* 2.50 ±0.38* 2.83 ±0.41* Control Sites 1.92±0.67* 0.67 ± ±0.36* 1.50 ±0.26* 1.50±0.26* 2.04±0.43* 1.08± ± ± ±0.88* 2.07 ±1.48 *Statistically significant between baseline and one year reentry at <0.05. Statistically significant difference = <0.05. Difference 0.92 ± ± ± ± ±0.47* 0.96 ± ± ±1.28 When the one year re-entry values were compared to the baseline measurements, both treatment modalities showed significant reduction (P <0.05) in all clinical parameters from baseline (Table 4). The mean probing depth improvement for the collagen barrier-treated defects was 2.84 mm as compared to 1.92 mm for the controls. Collagen-treated sites showed statistically significant gain of attachment (1.67 mm), whereas there was no significant gain for the controls (0.67 mm). No difference was noted between test and control sites with regard to gingival recession. The collagen barrier sites showed an improvement in defect fill (stent to base of defect) (2.50 mm vs mm) and vertical bone fill (crest of bone to base of defect) (2.83 mm vs mm) which was statistically significant in comparison to the control sites. When considering the furcation measurements, the sites treated with collagen membrane showed a significant improvement in horizontal probing depths and defect improvement as compared to the baseline. Defect area improvement was calculated from this formula: defect area improvement = (1/2 X Horizontal "3' X Verticalinitial) X Horizontal"1-0"^ X Verticalrccntr"). No significant Table 5. Percentage Furcation Measurement After One Year (n 12) = Reduction in Vertical Bone Fill and Horizontal Clinical parameters Groups None 0-25% 26-50% >50% Vertical bone fill Horizontal bone fill Collagen 0 (0%) 0 (0%) 2 (16.7%) 10 (83.3%) Control 0 (0%) 4 (33.3%) 3 (25%) 5 (41.7%) Collagen 0 (0%) 2 (16.7%) 6 (50%) 4 (33.3%) Control 1 (8.3%) 6 (50%) 2 (16.7%) 3 (25%) improvement was noted on the control treated sites when compared to the pre-surgery measurements. At re-entry, the percent of improvement in vertical bone fill and furcation horizontal (bucco-lingual width) probing depth was calculated for each treatment site. The data were grouped in 25% increments (Table 5). The collagen sites had 10 of the 12 sites with vertical bone fill greater than 50% as compared to 5 out of 12 in the control groups. Ten furcations treated with collagen membrane showed a reduction in the horizontal probing depth greater than 25%, while less than half (5) of the controls demonstrated the same. No adverse gingival tissue reactions were observed. In addition, at no time was displacement of the collagen membrane noted. None of the treated teeth had a change in mobility at one year and no significant differences were noted between groups. Surgical procedures and treatment results are illustrated in Figures 2 and 3. DISCUSSION The use of collagen as a barrier to enhance cell/tissue regeneration to a previously diseased root has gained considerable attention recently.4-7 Here we describe the use of a bioabsorbable type I collagen membrane derived from bovine tendon. This membrane is biodegradable and its absorption rate is controlled by its degree of crosslinking, with an average retention time of 6 to 7 weeks.20 The membrane is semipermeable with a pore size of µ and can prevent epithelial cell penetration while permitting passage of nutrients. This study was designed to evaluate the barrier in treating Class II mandibular molar furcation defects in humans. The results of this one year re-entry clinical trial indicate that the placement of type I bovine collagen in Class II furcations results in significantly greater defect fill (2.50 mm vs mm) and vertical bone fill (2.83 mm vs mm) when compared to control sites. Similar results were reported by Blumenthal,21 who showed that sites treated with a different collagen membrane gained vertical open probing new attachment at 12 months re-entry when compared to baseline. Our results are also in agreement with the 3 months re-entry study by Van Swol et al.,6 who reported that collagen treated sites had significantly higher vertical bone fill (from CEJ to base of the bony defect) when compared to the control groups. Similar findings were also reported by Chung et al.7 in their one year study. When both treatment modalities (with and without col-
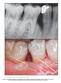
5 Volume 65 Number 11 WANG, O'NEAL, THOMAS, SHYR, MACNEIL Demonstration of clinical placement of collagen membrane in a molar tooth (#30) with Class II furcation involvement. A. pre-surgery; B. buccal initial incision designed to preserve papillary tissue with a vertical releasing incision on the mesial; C. surgical exposure of a class II furcation defect with evidence of cervical enamel projection; D. low speed diamond bur to remove the cervical enamel projection; E. membrane trimmed; F. membrane placed without suture. Figure both showed significant imclinical from baseline (Table in measurements provement The mean 4). probing depth improvement and attachment for the collagen barrier treated defects was 2.84 mm gain and 1.67 mm, respectively, as compared to 1.92 mm and 0.67 mm for the control sites. Although collagen-treated sites tended to respond more favorably, surgical intervention either with or without membrane placement resulted in lagen barrier) were compared, reducing probing depth at furcal sites. Similar results have been reported by Paul et al.22 The positive effect of collagen membrane treatment on furcation sites was most evident in improvement in horizontal probing depth and defect fill. The sites treated with collagen membrane showed a significant improvement in horizontal bone repair (2.04 ±0.43 mm) and defect improvement (3.90 ±0.88 mm) compared to baseline. How-
6 1034 COLLAGEN MEMBRANES IN THE TREATMENT OF CLASS II FURCATIONS J Periodontol November 1994 Figure 2. (Continued) G. tissues sutured; H. one-week post-surgery healing; I. one-year post surgery healing; J. one-year re-entry showed newly formed tissue; K. surgical exposure of the flap debridement treated control site; L. one year re-entry of the flap debridement treated control site indicated no gain of the newly formed tissue. significant improvement was noted on the control (1.08 ±0.61 mm and 2.07 ±1.48 mm respectively) compared to the baseline. This finding is in agreement with Anderson,23 who reported that collagen barrier treated sites had 87% of "approximate defect area" resolution in furcation areas compared to 49% restoration in the flap debridement control sites. In addition, several studies have reported on these criteria with use of expanded polytetrafluoroethylene (eptfe). Lekovic et al.24 showed only ever, no treated sites 0.12 mm horizontal fill at 6 month re-entry and Caffesse et al.25 reported 1.4 mm gain. This comparison indirectly suggests that collagen membrane may have better potential to regenerate horizontal bone fill than the eptfe non-absorbable membrane. The major benefit of using a bioabsorbable collagen membrane instead of eptfe barriers is that collagen is a natural protein of the human body which is degraded by host enzymes, hence eliminating the need for a second re-
7 Volume 65 Number 11 WANG, O'NEAL, THOMAS, SHYR, MACNEIL Figure 3. Results of collagen membrane treatment. A. surgical exposure of class II furcation defect with 5 mm vertical probing depth from the alveolar crest and 5 mm of horizontal probing component; B. one-year re-entry showing furcation filled with attached, dense, non-probeable tissue as seen in e-ptfe treated trieval surgery. cases. Thus, the possibility of losing attachment GTR procedure by secondary surgery is reduced.26 Also, animal studies by Pitaru et al.5 and Pfieffer et al.4 demonstrated that collagen membranes can prevent apical migration of epithelium and enhance new connective tissue attachment during periodontal wound healing to the same extent as eptfe membranes.1 Although, statistically significant gains in clinical attachment levels were not observed in this present study, positive clinical trends were observed for collagen membrane-treated sites. This observation agrees with a recent study by Blumenthal21 which reported that both collagen membrane and eptfe are effective in gaining vertical open probing new attachment and horizontal open and closed probing new attachment. In addition, it was also reported that sites treated with collagen membrane had less membrane exposure when compared to eptfe treated sites;21 we report similar findings in this study. Lack of membrane exposure may be explained by the fact that collagen is chemotactic for fibroblasts12 which may enhance initial flap stabilization and the potential for regeneration. This property may reduce the detrimental effects which we believed to accompany exposure of mem- gained through a 1035 brane during GTR procedure and microbial colonization of barrier materials following GTR therapy.3-27 Adverse tissue reaction, infections, or delayed healing were not observed following surgical placement of a bioabsorbable collagen barrier in this study. The presence of the collagen membrane did not increase plaque accumulation or gingival inflammation (Table 1), even though a mild host inflammatory response accompanied absorption of the membrane. A previous study has demonstrated that the presence of collagen membrane was not associated with increased bacterial colonization and did not alter the local microflora when compared to the flap debridement and untreated control sites.28 These findings are in agreement with Blumenthal21 and are further supported by Choi et al.,29 who reported that collagen matrix placed in a canine fenestration wound neither enhances nor inhibits periodontal healing. Also, Stein et al. showed that there were no adverse effects on the adjacent healthy sites when a collagen membrane was placed during GTR procedures.30 Kamer and Churukian reported that 2% of patients receiving injectable collagen experienced localized hypersensitivity reactions at the site of injection.31 No such reaction was noted in patients in this study. Johns et al. indicated that collagen membrane placed during GTR procedures does not elicit an antibody reaction.32 The low antigenicity of this product is likely related to the fact that the collagen membrane is treated with pepsin to remove its tyrosine (the most highly antigenic portion) content. Therefore, the product appears to be a biocompatible and safe material. The collagen barrier used in this study is easy to trim, adapt, and secure to the defect. When compared to eptfe membrane, the collagentreated sites tend to show better tissue response during early wound healing.21 Since collagen is a hemostatic agent by virtue of its ability to aggregate platelets, it may further facilitate wound maturation by enhancing the initial blood clot and fibrin linkage formation.8 This concept is supported by Haney et al. who indicated that clot stabilization, wound stability, space provision, epithelial cell exclusion, and complete gingival coverage are critical factors for the success of GTR procedures.10 A limitation of this study is the small sample size used; this shortcoming may have some affect or influence the power and significance of statistical tests used in this study. Future studies should include a larger sample size and longer follow-up time to determine the long-term effect of collagen membrane treatment. Within the scope of this initial study, the following conclusions can be drawn: 1) the placement of type I bovine collagen membrane during surgery on Class II furcations results in significantly higher defect fill and vertical bone fill when compared to the control sites; 2) sites treated with collagen membranes show a significant improvement in horizontal bone repair and defect improvement when compared to the presurgical status; 3) the collagen membrane-treated sites are twice as likely to have greater than 50% vertical bone fill than the control sites; 4) no significant differences were observed in attachment gain
8 1036 COLLAGEN MEMBRANES IN THE TREATMENT OF CLASS II FURCATIONS J Periodontol November 1994 probing depth reduction, or mobility; 5) the collagen membrane is well tolerated by the tissues with test and control sites exhibiting comparable recession pattern, in general tissue healing was similar to that observed following conventional flap therapy; and 6) surgical treatment with or without a collagen membrane showed significant improvement in clinical parameters from baseline. Acknowledgments The authors thank Dr. Frederic Smith for his assistance in the preparation of this manuscript. This study was supported, in part, by Colla-Tec (now Integra Life Sciences) Corporation, Princeton, NJ. REFERENCES 1. Gottlow J, Nyman S, Karring T, et al. New attachment formation as the result of controlled tissue regeneration. J Clin Periodontol 1984; 11: Pontoriero R, Lindhe J, Nyman S, et al. Guided tissue regeneration in degree II furcation-involved mandibular molars. A clinical study. J Clin Periodontol 1988; 15: Selvig KA, Kersten BG, Chamberlain ADH, Wikesjö UME, Nilveus RE. Regenerative surgery of intrabony periodontal defects using eptfe barrier membranes: Scanning electron microscopic evaluation of retrieved membranes versus clinical healing. J Periodontol 1992; 63: Pfeifer J, Van Swol RL, Ellinger R. Epithelial exclusion and tissue regeneration using a collagen membrane barrier in chronic periodontal defects: A histologie study. Ini J Periodontics Restorative Dent 1989; 9: Pitaru S, Tal H, Soldinger M, Noff M. Collagen membranes prevent apical migration of epithelium and support new connective tissue attachment during periodontal wound healing in dogs. J Periodont Res 1989; 24: Van Swol RL, Ellinger R, Pfeifer J, Barton NE, Blumenthal. Collagen membrane barrier therapy to guide regeneration in class II furcation in humans. J Periodontol 1993; 64: Chung KM, Salkin LM, Stein MD, Freedman AL. Clinical evaluation of a biodegradable collagen membrane in guided tissue regeneration. J Periodontol 1990; 61: Sableman E. Biology, Biotechnology and Biocompatibility of Collagen. Biocompatibility of Tissue Analogs, Vol 1. Boca Raton, Florida: CRC Press, Inc.; 1985; Wikesjö UME, Nilveus RE, Selvig KA. Significance of early healing events on periodontal repair. A review. J Periodontol 1992; 63: Haney JM, Nilveus RE, McMillan PJ, Wikesjö UME. Periodontal repair in dogs: Expanded polytetrafluoroethylene barrier membranes support wound stabilization and enhance bone regeneration. J Periodontol 1993; 64: Quteisch D, Singrao S, Dolby AE. Light and electron microscopic evaluation of biocompatibility, résorption and penetration characteristics of human collagen graft material. J Clin Periodontol 1991; 18: Posthlewaite AE, Seyer JM, Kang AH. Chemostasis attraction of human fibroblast to type I, II and III collagene and collagen derived Peptides. Proc Nat Acad Sci (USA) 1978; 75: Quteisch D, Dolby AE. The use of irradiated-crosslinked human collagen membrane in guided tissue regeneration. J Clin Periodontol 1992; 19: Eilender G, Hammond R, Papli R, et al. Osteogenic capacity of collagen in repair of established periodontal defects. Clin Mat 1992; 9: Cooperman L, Machaeli D. The immuno-genicity of injectable collagen I. A 1-year prospective study. J Am Acad Dermatol 1984; 10: Greenstein G, Caton JG. Biodegradable barriers and guided tissue regeneration. Periodontology ; 1: Miller SC. Textbook of Periodontia. Philadelphia: The Blakiston Company; 1938: Silness J, Löe H. Periodontal disease in pregnancy. II. Correlation condition. Acta Odontol Scand between oral hygiene and periodontal 1964; 22: Löe H, Silness J. Periodontal disease in pregnancy. I. Prevalence and severity. Acta Odontol Scand 1963; 21: North American Science Associates, Inc. Laboratory report No. 89T Eight week evaluation of a periodontal collagen barrier sponge following subcutaneous implant in the rat. 21. Blumenthal NM. A clinical comparison of collagen membranes with eptfe membranes in the treatment of human mandibular buccal class II furcation defects. J Periodontol 1993; 64: Paul BF, Mellonig JT, Towle HJ, Gray JL. Use of a collagen barrier to enhance healing in human periodontal furcation defects. Int J Periodontics Restorative Dent 1992; 12: Anderson HH. The effectiveness of a collagen membrane barrier in achieving new attachment in grade II furcation involvements. [Thesis] Kansas City, Missouri: University of Missouri-Kansas City, Lekovic V, Kenney EB, Kovacevic, Carranza FA. Evaluation of guided tissue regeneration in class II furcation defects. A clinical reentry study. J Periodontol 1989; 60: Caffesse RG, Smith BA, Duff B, et al. Class II furcation treated by guided tissue regeneration in humans: Case reports. J Periodontol 1990; 61: Hill RW, Ramfjord SP, Morrison EC, et al. Four types of periodontal treatment compared over two years. J Periodontol 1981; 52: Tempro PJ, Nalbandian J. Colonization of retrieved polytetrafluoroethylene membranes: Morphological and microbiological observation. J Periodontol 1993; 64: Thomas C, Wang H-L, Syed S. Effect of a resorbable membrane upon subgingival microflora. J Dent Res 1993; 72(Spec. Issue):207(Abstr. 829). 29. Choi SY, Nilveus RE, Minutello RD, Zimmerman GJ, Wikesjö UME. Effect of a collagen matrix on healing in periodontal fenestration defects in dogs. J Periodontol 1993; 64: Stein MD, Salkin LM, Freedman AL. The effects of guided tissue regeneration membrane placement on healthy periodontal sites. J Periodontol 1993; 64: Kamer FM, Churukian MM. The clinical use of injectable collagen: A three-year retrospective study. Arch Otolaryngol 1984; 110: Johns LP, Merritt K, Agarwal S, Ceravolo FJ. Immunogenicity of a bovine collagen membrane in guided tissue regeneration. J Dent Res 1992; 71(Spec. Issue):298(Abstr. 1538). Send reprint requests to: Dr. Horn-Lay Wang, University of Michigan, School of Dentistry, 1011 N. University Avenue, Ann Arbor, MI Accepted for publication June 4, 1994.
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth. Jose A. Moreno Rodríguez and Raúl G.
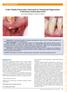 A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth Jose A. Moreno Rodríguez and Raúl G. Caffesse Introduction: Periodontal regeneration of hopeless teeth represents
A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth Jose A. Moreno Rodríguez and Raúl G. Caffesse Introduction: Periodontal regeneration of hopeless teeth represents
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Management of miller class II gingival recession by laterally positioned pedicle flap revised technique
 Management of miller class II gingival by laterally positioned pedicle flap revised technique Received: 2/4/206 Accepted: 3/0/206 Dildar Abdullah Othman* Abstract Background and objective: Gingival is
Management of miller class II gingival by laterally positioned pedicle flap revised technique Received: 2/4/206 Accepted: 3/0/206 Dildar Abdullah Othman* Abstract Background and objective: Gingival is
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
The ultimate goal in periodontal
 Volume 71 Number 4 Interleukin-1 Gene Polymorphisms and Long-Term Stability Following Guided Tissue Regeneration Therapy* Massimo De Sanctis and Giovanni Zucchelli Background: Specific interleukin (IL)-1
Volume 71 Number 4 Interleukin-1 Gene Polymorphisms and Long-Term Stability Following Guided Tissue Regeneration Therapy* Massimo De Sanctis and Giovanni Zucchelli Background: Specific interleukin (IL)-1
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Bone Levels - From Hypothesis To Facts
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 6, Issue 5 (May.- Jun. 2013), PP 19-23 Bone Levels - From Hypothesis To Facts Savitha B 1, Priyanka
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 6, Issue 5 (May.- Jun. 2013), PP 19-23 Bone Levels - From Hypothesis To Facts Savitha B 1, Priyanka
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
COPYRIGHT 2002 BY QUINTESSENCE PUBLISHING CO, INC.PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY.NO PART OF THIS ARTICLE MAY BERE-
 The International Journal of Periodontics & Restorative Dentistry Use of Bone Grafts for the Enhancement of a GTR-Based Root Coverage Procedure: A Pilot Case Study Hom-Lay Wang, DDS, MSD*/Kenneth Kimble,
The International Journal of Periodontics & Restorative Dentistry Use of Bone Grafts for the Enhancement of a GTR-Based Root Coverage Procedure: A Pilot Case Study Hom-Lay Wang, DDS, MSD*/Kenneth Kimble,
Evaluation of Guided Tissue Regeneration Following Third Molar Extraction by Bone Scintigraphy Using Tc99m-MDP
 CASE REPORT Evaluation of Guided Tissue Regeneration Following Third Molar Extraction by Bone Scintigraphy Using Tc99m-MDP Orit Oettinger-Barak, Eli E. Machtei, Zohar Keidar, Dan Mahler, Imad Abu EL-Naaj,
CASE REPORT Evaluation of Guided Tissue Regeneration Following Third Molar Extraction by Bone Scintigraphy Using Tc99m-MDP Orit Oettinger-Barak, Eli E. Machtei, Zohar Keidar, Dan Mahler, Imad Abu EL-Naaj,
ELIMINATE POCKETS. Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease
 ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
Dental Research Journal
 Dental Research Journal Case Report Treatment strategy for guided tissue regeneration in various class II furcation defect: Case series Pushpendra Kumar Verma 1, Ruchi Srivastava 1, K. K. Gupta 2, T. P.
Dental Research Journal Case Report Treatment strategy for guided tissue regeneration in various class II furcation defect: Case series Pushpendra Kumar Verma 1, Ruchi Srivastava 1, K. K. Gupta 2, T. P.
Many techniques have been proposed for root coverage:
 Case Series Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients Jaime A. Vergara* and Raul G. Caffesse Background: The surgical techniques used
Case Series Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients Jaime A. Vergara* and Raul G. Caffesse Background: The surgical techniques used
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Platelet Rich Fibrin- A New Hope for Regeneration of Osseous Defects in Aggressive Periodontitis Patients: A Case Report
 American Journal of Advanced Drug Delivery www.ajadd.co.uk Original Article Platelet Rich Fibrin- A New Hope for Regeneration of Osseous Defects in Aggressive Periodontitis Patients: A Case Report Jayant
American Journal of Advanced Drug Delivery www.ajadd.co.uk Original Article Platelet Rich Fibrin- A New Hope for Regeneration of Osseous Defects in Aggressive Periodontitis Patients: A Case Report Jayant
Minimally invasive techniques for periodontal regeneration
 2016; 2(12): 230-234 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2016; 2(12): 230-234 www.allresearchjournal.com Received: 04-10-2016 Accepted: 05-11-2016 Dr. Rizwan M Sanadi Professor,
2016; 2(12): 230-234 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2016; 2(12): 230-234 www.allresearchjournal.com Received: 04-10-2016 Accepted: 05-11-2016 Dr. Rizwan M Sanadi Professor,
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
HeliMEND Advanced. Absorbable Collagen Membrane. Instructions for Use
 HeliMEND Advanced Absorbable Collagen Membrane Instructions for Use 2 Indications HeliMEND Advanced absorbable collagen membrane is an absorbable, implantable material that is indicated for guided tissue
HeliMEND Advanced Absorbable Collagen Membrane Instructions for Use 2 Indications HeliMEND Advanced absorbable collagen membrane is an absorbable, implantable material that is indicated for guided tissue
Gingival recession causes periodontal
 J Periodontol October 2005 Factors Affecting the Outcomes of Coronally Advanced Flap Root Coverage Procedure Lien-Hui Huang,* Rodrigo E.F. Neiva, and Hom-Lay Wang Background: The coronally advanced flap
J Periodontol October 2005 Factors Affecting the Outcomes of Coronally Advanced Flap Root Coverage Procedure Lien-Hui Huang,* Rodrigo E.F. Neiva, and Hom-Lay Wang Background: The coronally advanced flap
The dentogingival junction to the
 Volume 79 Number 10 RedefiningtheBiologicWidthinSevere, Generalized, Chronic Periodontitis: Implications for Therapy M. John Novak,* Huda M. Albather, and John M. Close Background: Previous studies demonstrated
Volume 79 Number 10 RedefiningtheBiologicWidthinSevere, Generalized, Chronic Periodontitis: Implications for Therapy M. John Novak,* Huda M. Albather, and John M. Close Background: Previous studies demonstrated
Contemporary Periodontal Surgery
 Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Fundamental & Preventive Curvatures of Teeth and Tooth Development. Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L.
 Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Osseous surgery in periodontal treatment
 SCIENTIFIC SESSION Osseous surgery in periodontal treatment Essayist: Roberto Pontoriero Introduction In periodontally involved patients, periodontal therapy usually results in various degrees of soft-tissue
SCIENTIFIC SESSION Osseous surgery in periodontal treatment Essayist: Roberto Pontoriero Introduction In periodontally involved patients, periodontal therapy usually results in various degrees of soft-tissue
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
A clinical evaluation of bioactive glass particulate in the treatment of mandibular class II furcation defects
 Braz J Oral Sci. October-December 2007 - Vol. 6 - Number 23 Manoj Humagain 1 Dilip G Nayak 2 Ashita S Uppoor 3 1 Specialist Resident 2 Professor and Head 3 Professor Department of Periodontics, Manipal
Braz J Oral Sci. October-December 2007 - Vol. 6 - Number 23 Manoj Humagain 1 Dilip G Nayak 2 Ashita S Uppoor 3 1 Specialist Resident 2 Professor and Head 3 Professor Department of Periodontics, Manipal
Alarge number of sound clinical
 Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Efficacy of Palatal Connective Tissue Graft as a Membrane in the Treatment of Intrabony Defects
 Journal of Periodontology & Implant Dentistry Research Article Efficacy of Palatal Connective Tissue Graft as a Membrane in the Treatment of Intrabony Defects Hamid Moghaddas 1 Leila Soltani 2 Omid Moghaddas
Journal of Periodontology & Implant Dentistry Research Article Efficacy of Palatal Connective Tissue Graft as a Membrane in the Treatment of Intrabony Defects Hamid Moghaddas 1 Leila Soltani 2 Omid Moghaddas
GMJ, ASM 2013;2(S1):S120-S125 GULF MEDICAL JOURNAL
 Evaluate clinical effectiveness of autologous platelet rich plasma (PRP) using curasan technique in treating intrabony defects using regenerative material Bone graft / GTR membrane M Sesha Reddy College
Evaluate clinical effectiveness of autologous platelet rich plasma (PRP) using curasan technique in treating intrabony defects using regenerative material Bone graft / GTR membrane M Sesha Reddy College
When performing conventional crown
 Case of the Month Biologic Shaping Kurtzman Daniel Melker, DDS 1 Abstract When performing conventional crown lengthening, the existing margins of an old restoration or the cementoenamel junction (CEJ)
Case of the Month Biologic Shaping Kurtzman Daniel Melker, DDS 1 Abstract When performing conventional crown lengthening, the existing margins of an old restoration or the cementoenamel junction (CEJ)
Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery
 CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT
 TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT Dr Prashant Bhusari*, Dr Apoorva Saxena**, Dr Jaya Jain***,Dr Rashmi Rathore***, Dr Aditi
TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT Dr Prashant Bhusari*, Dr Apoorva Saxena**, Dr Jaya Jain***,Dr Rashmi Rathore***, Dr Aditi
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Double Papillary Flap - A Treatment for Gingival Recession
 World Journal of Medical Sciences 10 (2): 117-121, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.2.82175 Double Papillary Flap - A Treatment for Gingival Recession 1 1 1
World Journal of Medical Sciences 10 (2): 117-121, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.2.82175 Double Papillary Flap - A Treatment for Gingival Recession 1 1 1
Periodontal Regeneration
 Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Alveolar ridge preservation techniques
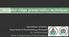 Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic case report.
 European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
Pradeep AR, Karthikeyan BV. Peri-implant papilla reconstruction: Realities and limitations. J Periodontol 2006:77:
 Machtei EE, Dunford R, Grossi SG, Genco RJ. Gingival recession and exposure of barrier membrane: Effect on guided tissue regeneration of Class II furcation defects. Int J Periodont Rest Dent 1995; 15:
Machtei EE, Dunford R, Grossi SG, Genco RJ. Gingival recession and exposure of barrier membrane: Effect on guided tissue regeneration of Class II furcation defects. Int J Periodont Rest Dent 1995; 15:
Efficacy of Lateral Pedicle Graft in the Treatment of Isolated Gingival Recession Defects
 International Journal of Pharmaceutical Science Invention ISSN (Online): 2319 6718, ISSN (Print): 2319 670X Volume 3 Issue 1 January 2014 PP.46-50 Efficacy of Lateral Pedicle Graft in the Treatment of
International Journal of Pharmaceutical Science Invention ISSN (Online): 2319 6718, ISSN (Print): 2319 670X Volume 3 Issue 1 January 2014 PP.46-50 Efficacy of Lateral Pedicle Graft in the Treatment of
The International Journal of Periodontics & Restorative Dentistry
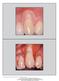 The International Journal of Periodontics & Restorative Dentistry 127 Comparison of Recombinant Human Platelet-Derived Growth Factor-BB Plus Beta Tricalcium Phosphate and a Collagen Membrane to Subepithelial
The International Journal of Periodontics & Restorative Dentistry 127 Comparison of Recombinant Human Platelet-Derived Growth Factor-BB Plus Beta Tricalcium Phosphate and a Collagen Membrane to Subepithelial
Esthetic Crown Lengthening
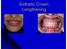 Esthetic Crown Lengthening Esthetic Crown Lengthening ACCELERATED OSTEOGENIC ORTHODOTNICS (WILKODONTICS) It is a technique developed by Wilko brothers. has roots in orthopedics, back to the early 1900s
Esthetic Crown Lengthening Esthetic Crown Lengthening ACCELERATED OSTEOGENIC ORTHODOTNICS (WILKODONTICS) It is a technique developed by Wilko brothers. has roots in orthopedics, back to the early 1900s
Socket Graft Plus. Case Presentation. Ideal Bone Graft for All Socket Grafting Situations. Case #1
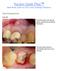 Socket Graft Plus Ideal Bone Graft for All Socket Grafting Situations Case Presentation Case #1 Tooth #3 presents with a buccal parulis, ensuring a buccal alveolar fenestration. The tooth will be remove
Socket Graft Plus Ideal Bone Graft for All Socket Grafting Situations Case Presentation Case #1 Tooth #3 presents with a buccal parulis, ensuring a buccal alveolar fenestration. The tooth will be remove
Townie Guest Editorial. Gingival Attachment Loss: Evaluation and Surgical Options. Daniel J. Melker, DDS. fig. 1
 Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts
 J Periodontol August 2005 A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts A. Hirsch,* M. Goldstein,* J. Goultschin,*
J Periodontol August 2005 A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts A. Hirsch,* M. Goldstein,* J. Goultschin,*
Delta Dental of Virginia Clinical Policy # 402
 Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12 Accepted on:22/05/12
 SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
REGENERATIONTIME. A Case Report by. Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option
 A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
A wide variety of membrane options
 A wide variety of membrane options BOVINE Bovine collagen membrane Neomem is a resorbable collagen membrane derived from highly purified type I collagen fibres from bovine Achilles tendon. The macromolecular
A wide variety of membrane options BOVINE Bovine collagen membrane Neomem is a resorbable collagen membrane derived from highly purified type I collagen fibres from bovine Achilles tendon. The macromolecular
AL-AZHAR. Dental Journal. Print ISSN Online ISSN ADJ-for Girls, Vol. 5, No. 1, January (2018) PP. 29:35
 AL-AZHAR Dental Journal F o r G i r l s The Official Publication of The Faculty of Dental Medicine For Girls, Al-Azhar University Cairo, Egypt. Print ISSN 2537-0308 Online ISSN 2537-0316 ADJ-for Girls,
AL-AZHAR Dental Journal F o r G i r l s The Official Publication of The Faculty of Dental Medicine For Girls, Al-Azhar University Cairo, Egypt. Print ISSN 2537-0308 Online ISSN 2537-0316 ADJ-for Girls,
The regeneration of the tooth supporting structures
 Position Paper Periodontal Regeneration* Untreated periodontal disease leads to tooth loss through destruction of the attachment apparatus and toothsupporting structures. The goals of periodontal therapy
Position Paper Periodontal Regeneration* Untreated periodontal disease leads to tooth loss through destruction of the attachment apparatus and toothsupporting structures. The goals of periodontal therapy
Everything You Wanted to Know About Extractions but Were Afraid to Ask
 Everything You Wanted to Know About Extractions but Were Afraid to Ask Tooth extraction is a surgical procedure with serious potential complications and should only be performed by a trained veterinarian.
Everything You Wanted to Know About Extractions but Were Afraid to Ask Tooth extraction is a surgical procedure with serious potential complications and should only be performed by a trained veterinarian.
The treatment of destructive periodontal disease, due to specific periodontopathic
 1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
Periosteal fenestration: A single stage surgical procedure for root coverage along with vestibular deepening
 2017; 3(2): 14-18 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2017; 3(2): 14-18 2017 IJADS www.oraljournal.com Received: 05-02-2017 Accepted: 06-03-2017 Dr. Hoti Lal Gupta MDS, Professor and Head
2017; 3(2): 14-18 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2017; 3(2): 14-18 2017 IJADS www.oraljournal.com Received: 05-02-2017 Accepted: 06-03-2017 Dr. Hoti Lal Gupta MDS, Professor and Head
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 257 Minimally Invasive Surgical Technique and Enamel Matrix Derivative in Intrabony Defects: 2. Factors Associated with Healing Outcomes
The International Journal of Periodontics & Restorative Dentistry 257 Minimally Invasive Surgical Technique and Enamel Matrix Derivative in Intrabony Defects: 2. Factors Associated with Healing Outcomes
The Sandwich Bone Augmentation Technique. Jia-Hui Fu* and Hom-Lay Wang*
 CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
Journal of Periodontology & Implant Dentistry. Research Article
 Journal of Periodontology & Implant Dentistry Research Article Clinical and Radiographic Evaluation of the Effect of Bovinederived Hydroxyapatite (Bio-Oss ) and A Synthetic HA/β-TCP (Osteon ) in the Treatment
Journal of Periodontology & Implant Dentistry Research Article Clinical and Radiographic Evaluation of the Effect of Bovinederived Hydroxyapatite (Bio-Oss ) and A Synthetic HA/β-TCP (Osteon ) in the Treatment
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Case Report Esthetic Root Coverage with Double Papillary Subepithelial Connective Tissue Graft: A Case Report
 Case Reports in Dentistry, Article ID 509319, 5 pages http://dx.doi.org/10.1155/2014/509319 Case Report Esthetic Root Coverage with Double Papillary Subepithelial Connective Tissue Graft: A Case Report
Case Reports in Dentistry, Article ID 509319, 5 pages http://dx.doi.org/10.1155/2014/509319 Case Report Esthetic Root Coverage with Double Papillary Subepithelial Connective Tissue Graft: A Case Report
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Triple Combination Therapy A 12 Month Case Series
 Triple Combination Therapy A 12 Month Case Series Kanakamedala Anilkumar 1, Theyagarajan Ramakrishnan 2, Geetha Ari 3, Monica Sharon A 4 1, 2, 3 M.D.S, Department of Periodontics, Meenakshi Ammal Dental
Triple Combination Therapy A 12 Month Case Series Kanakamedala Anilkumar 1, Theyagarajan Ramakrishnan 2, Geetha Ari 3, Monica Sharon A 4 1, 2, 3 M.D.S, Department of Periodontics, Meenakshi Ammal Dental
Surgical reconstruction of lost papilla around implant with a modified technique: A case report
 Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
CITRIC ACID ROOT BIOMODIFICATION IN RECESSION COVERAGE WITH LATERAL PEDICLE FLAP TECHNIQUE- A CASE REPORT
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 05 CITRIC ACID ROOT BIOMODIFICATION IN RECESSION COVERAGE WITH LATERAL PEDICLE FLAP TECHNIQUE- A CASE REPORT Mamta Singh
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 05 CITRIC ACID ROOT BIOMODIFICATION IN RECESSION COVERAGE WITH LATERAL PEDICLE FLAP TECHNIQUE- A CASE REPORT Mamta Singh
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
The effect of antifibrinolytic agents on the healing of modified Widman flaps in monkeys
 Journal of Periodontal Research 1984: 19: 210-213 Short Communication The effect of antifibrinolytic agents on the healing of modified Widman flaps in monkeys A. BERGENHOLTZ, R. G. CAFFESSE, C. E. NASJLETI,
Journal of Periodontal Research 1984: 19: 210-213 Short Communication The effect of antifibrinolytic agents on the healing of modified Widman flaps in monkeys A. BERGENHOLTZ, R. G. CAFFESSE, C. E. NASJLETI,
MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY
 MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY DR.H.Gharati Periodontist & Dental Implant Specialist Assistant Professor, School Of Dentistry Friedman(1957): DEFINITION Mucogingival surgery, Surgical
MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY DR.H.Gharati Periodontist & Dental Implant Specialist Assistant Professor, School Of Dentistry Friedman(1957): DEFINITION Mucogingival surgery, Surgical
Tooth Retained Implant: No More an Oxymoron
 بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
Inion GTR Biodegradable Membrane System
 Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS
 OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS DESCRIPTION OSSIX PLUS is a biodegradable and biocompatible collagen membrane intended for use during the process of guided
OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS DESCRIPTION OSSIX PLUS is a biodegradable and biocompatible collagen membrane intended for use during the process of guided
Pre op Failed endodontic treatment with sinus involvement.
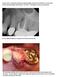 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
COMBINED PERIODONTAL-ENDODONTIC LESION. By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur
 COMBINED PERIODONTAL-ENDODONTIC LESION By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur Differential diagnosis For differential diagnostic purposed the endo-perio
COMBINED PERIODONTAL-ENDODONTIC LESION By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur Differential diagnosis For differential diagnostic purposed the endo-perio
A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran
 Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Subject: Osseous Surgery Guideline #: Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017
 Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Connective Tissue Graft for Gingival Recession in Mandibular Incisor Area: A Case Report
 Bull Tokyo Dent Coll (2017) 58(3): 155 162 Case Report doi:10.2209/tdcpublication.2016-0038 Connective Tissue Graft for Gingival Recession in Mandibular Incisor Area: A Case Report Masahiro Egawa 1), Satoru
Bull Tokyo Dent Coll (2017) 58(3): 155 162 Case Report doi:10.2209/tdcpublication.2016-0038 Connective Tissue Graft for Gingival Recession in Mandibular Incisor Area: A Case Report Masahiro Egawa 1), Satoru
Michael K. McGuire* and Martha Nunn
 Volume 74 Number 8 Evaluation of Human Recession Defects Treated with Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue. Part 1: Comparison of Clinical Parameters Michael
Volume 74 Number 8 Evaluation of Human Recession Defects Treated with Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue. Part 1: Comparison of Clinical Parameters Michael
Guided Tissue and Bone Regeneration
 Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
The use of platelet-rich plasma in combination with connective tissue grafts following treatment of gingival recessions
 RESEARCH REPORT 63 Sasha M Jankovic, Aleksic M Zoran, Lekovic M Vojislav, Dimitrijevic S Bozidar, Barry E Kenney The use of platelet-rich plasma in combination with connective tissue grafts following treatment
RESEARCH REPORT 63 Sasha M Jankovic, Aleksic M Zoran, Lekovic M Vojislav, Dimitrijevic S Bozidar, Barry E Kenney The use of platelet-rich plasma in combination with connective tissue grafts following treatment
Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in
 Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in a dog m Author(s) Fujita, T; Yamamoto, S; Ota, M; Shi Alternative Yamada, S International journal
Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in a dog m Author(s) Fujita, T; Yamamoto, S; Ota, M; Shi Alternative Yamada, S International journal
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Initial Therapy. Alessan"o Geminiani, DDS, MS. Oral sulcular epithelium. Oral. epithelium. Junctional. epithelium. Connective tissue.
 Oral sulcular epithelium Junctional epithelium E Oral epithelium Initial Therapy Connective tissue Bone Alessan"o Geminiani, DDS, MS Non-surgical Therapy Scaling: Instrumentation of the crown and root
Oral sulcular epithelium Junctional epithelium E Oral epithelium Initial Therapy Connective tissue Bone Alessan"o Geminiani, DDS, MS Non-surgical Therapy Scaling: Instrumentation of the crown and root
Extraction socket preservation using β tricalcium phosphate bone graft plug and platelet rich fibrin membrane A case series
 2014; 1(1): 39-43 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2014; 1(1): 39-43 2014 IJADS www.oraljournal.com Received: 02-01-2015 Accepted: 07-02-2015 Shantipriya Reddy Prof and Head, department
2014; 1(1): 39-43 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2014; 1(1): 39-43 2014 IJADS www.oraljournal.com Received: 02-01-2015 Accepted: 07-02-2015 Shantipriya Reddy Prof and Head, department
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT
 ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
Introduction to Periodontal and Implant Surgery
 Introduction to Periodontal and Implant Surgery Professor Jon B. Suzuki, DDS, PhD, MBA Temple University Professor of Microbiology and Immunology (Med) Professor of Periodontology and Oral Implantology
Introduction to Periodontal and Implant Surgery Professor Jon B. Suzuki, DDS, PhD, MBA Temple University Professor of Microbiology and Immunology (Med) Professor of Periodontology and Oral Implantology
Indications The selection of amalgam as a restorative material for class V cavity should involve the following considerations:
 1 Lec.7 د.عبد املنعم اخلفاجي CLASS V CAVITY PREPARATION FOR AMAGLAM Indications The selection of amalgam as a restorative material for class V cavity should involve the following considerations: 1- Caries:
1 Lec.7 د.عبد املنعم اخلفاجي CLASS V CAVITY PREPARATION FOR AMAGLAM Indications The selection of amalgam as a restorative material for class V cavity should involve the following considerations: 1- Caries:
