Practice-Based Evidence from 29-Year Outcome Analysis of Management of the Edentulous Jaw Using Osseointegrated Dental Implants
|
|
|
- Charlotte May
- 5 years ago
- Views:
Transcription
1 Practice-Based Evidence from 29-Year Outcome Analysis of Management of the Edentulous Jaw Using Osseointegrated Dental Implants Matilda Dhima, DMD, MS, 1 Vladimira Paulusova, MD, 2 Christine Lohse, MS, 3 Thomas J. Salinas, DDS, 4 & Alan B. Carr, DMD, MS 5 1 Assistant Professor, Mayo Clinic College of Medicine and Chief Resident, Prosthodontics and Maxillofacial Prosthetics, Department of Dental Specialties, Division of Prosthetic and Esthetic Dentistry, Mayo Clinic, Rochester, MN 2 Assistant Professor, Department of Dentistry, Faculty of Medicine and University Hospital in Hradec Králové, Charles University, Prague, Czech Republic 3 Statistician, Department of Biostatistics, Mayo Clinic, Rochester, MN 4 Professor, Mayo Clinic College of Medicine and Consultant, Department of Dental Specialties, Division of Prosthetic and Esthetic Dentistry, Mayo Clinic, Rochester, MN 5 Professor, Mayo Clinic College of Medicine and Consultant, Chair, Department of Dental Specialties, Division of Prosthetic and Esthetic Dentistry, Mayo Clinic, Rochester, MN Keywords Edentulous jaw; dental implants; outcome analysis; practice-based evidence; hybrid; implant-retained dental prosthesis; complications; follow-up; management. Correspondence Alan B. Carr, DMD, MS, Mayo Clinic 200 1st St. SW, Rochester, MN carr.alan@mayo.edu The findings of this manuscript were presented at the American College of Prosthodontists Annual Session, Baltimore, Maryland The authors deny any conflicts of interest. Accepted April 27, 2013 doi: /jopr Abstract Purpose: The aim of this retrospective study was to summarize practice-based evidence associated with long-term outcomes (>20 years) in the management of edentulous patients. The patient population was managed with implant-supported prostheses, following the original osseointegration protocol, provided over the period from 1983 to 1991 in the group prosthodontics practice at the Mayo Clinic. The data are an example of practice quality assurance monitoring and are used to refine care delivery when needed and to provide information regarding expected outcomes in a shared decision-making interaction with prospective patients. Materials and Methods: Two hundred and sixty four patients with at least one edentulous jaw were identified. Of these, 255 completed their care and follow-up at the Mayo Clinic (209 mandible only, 35 maxilla only, 11 mandible and maxilla). Prosthodontic outcomes categorized as anticipated or unanticipated prosthetic and biologic events and the respective interventions required for each were recorded to assess follow-up event dynamics for this care modality. Results: The mean duration of follow-up for 190 of the 255 patients (65 died at a mean follow-up of 12.6 years) was 13.0 years (median 13.6; range 0.3 to 28). At least one prosthetic event was experienced by 148 patients (58%), and 81 (32%) experienced at least one biologic event. Overall, patients experienced 3.8 times more prosthetic events than biologic events. Twenty-four (9%) patients experienced 35 implant failures. Overall survival rates at 20 years were 86% for prostheses, 15% survived free of any event, and 92% experienced survival free of implant failure (95% confidence interval). Conclusion: Anticipated and unanticipated prosthetic events occur throughout the life of the hybrid prosthesis. Prosthetic events significantly surpass (four times more) biologic events and occur significantly later in the follow-up. For this patient group, 8.6% (22/255) had implant-supported prostheses remade during follow-up in this patient population. These findings support the recommendation that prosthodontic care for missing teeth be thought of in a chronic condition context, recognizing that long-term outcome monitoring to provide realistic care expectations is important for demonstrating care value in oral health promotion. Journal of Prosthodontics 23 (2014) C 2013 by the American College of Prosthodontists 173
2 Edentulous Jaw and Implants, 29-Year Outcome Analysis Dhima et al Management of tooth loss over the past three decades has grown in scope due to the demonstrated predictability of dental implants. The original introduction of dental implants to North America demonstrated a predictable application for the edentulous jaw, 1 and similar clinical application began across the United States and Canada as a result. 2,3 Conscientious clinicians, using a shared decision-making 4 approach in consultation (i.e., informing patients as to the difference between and results of options available to them), have provided edentulous patients evidence as to benefit and harm based on published reports that now reach three decades. 5 Meaningful decision making with patients seeking prosthodontic care involves sharing clinical outcome evidence that reflects the patient perspective of the care provided and is associated with a period of time that has significance relative to the care expectations of patients. 6 For the permanent condition tooth loss, the expectation of replacements providing adequate performance for an extended period of time is understandable. In this long-term health-care context, tooth loss is similar to other chronic conditions in medicine and requires long-term management 7 of time-dependent events, which are often unique to the selected prosthetic management option. 8 This perspective suggests that outcome measures discussed with patients should reflect meaning from a patient perspective over a period of time that captures time-dependent differences of value to shared decision-making needs. 9 Much research has been reported from clinical trials related to implant outcomes The applicability of clinical trial-based evidence to practice has been the subject of many reports. 13,14 Expressed concerns over trials in general and those involving procedural specialties 15 include issues of generalizability, the use of surrogate outcomes, and short-term outcome applicability or meaningfulness. 16 Evidence obtained from practice settings that provide care outcomes of importance to patients can add valuable insight to providers interested in monitoring quality and patients interested in hearing about care expectations. Care outcomes from practice, termed practice-based evidence (PBE 16 ) is complementary to trial-based evidence (complementary in that trial evidence demonstrates which treatment is effective; practice evidence demonstrates what results are observed when an effective treatment is provided), as it addresses evidence needs when trials are not performed or when care outcomes are needed for long-term chronic conditions. This report provides practice evidence for the management of edentulism using cantilevered fixed implant prostheses for patients presenting to the Mayo Clinic from 1983 to The report provides outcome data for prosthesis survival and biological and technical outcomes for original osseointegrated surgical and prosthetic protocols, and represents PBE over a period of care of up to 29 years. Materials and methods A retrospective cohort was identified of all patients receiving edentulous implant care from 1983 to Appropriate institutional review board approval was obtained. The cohort comprised 308 patients with at least one edentulous jaw receiving an implant-supported prosthesis following the original Brånemark protocol. 17,18 Complete records review (electronic Table 1 Characteristics of data collected Patient characteristics Clinical characteristics Event(s) characteristics Age Gender Geographical identity Living status Smoking history Medical comorbidities Implant dates by stage Prosthesis type Prosthesis placement date Opposing dentition Event type/date Event interventions/number/date Visits to last appointment and paper) resulted in 28 patients being excluded due to incomplete or missing documentation, and 15 patients excluded due to written patient requests on file for their records not to be used for research. The remaining 265 patient records were reviewed, and data were sought from diagnostic, treatment, and follow-up phases. Data were abstracted by two clinicians familiar with the record environment and the data exposures sought. Initial abstraction efforts were formally reviewed by duplicating abstraction for 12 charts to assure completeness and accuracy. All data were collected on a secure Microsoft Excel 2010 file. Data abstracted included both patient and clinical characteristics and event-related data (Table 1), following event reporting designations used in clinical-trial monitoring for human protection. 19 Prosthetic and biological outcome events are categorized as anticipated (when prosthetically functional; biologically reversible) or unanticipated (when prosthetically harmful with continued function; biologically irreversible and requiring care) (Table 2). Overall survival, survival free of event, and survival free of implant failure were estimated using the Kaplan-Meier method. Overall survival was designated by prosthesis presence in the mouth with or without anticipated events. Survival free of event was defined as prosthesis present and with no record of any event(s). The duration of follow-up for overall survival was calculated from the date of implant placement to the date of patient death or last check-up. The duration of survival free of event was calculated from the date of implant to the date of the first event or last check-up. The duration of survival free of implant failure was calculated from the date of implant to the date of first implant failure or last follow-up. All statistical analyses were performed using the SAS software package (SAS Institute, Cary, NC). Results The mean duration of follow-up for 190 of the 255 patients (65 died at a mean follow-up of 12.6 years) was 13.0 years (median 13.6; range 0.3 to 28). The majority of the 255 patients (97%) underwent surgery and prosthesis placement at Mayo Clinic, while 9 (3%) had their prosthesis fabricated elsewhere. Relative to age, gender, and arch restored, there were no differences 174 Journal of Prosthodontics 23 (2014) C 2013 by the American College of Prosthodontists
3 Dhima et al Edentulous Jaw and Implants, 29-Year Outcome Analysis Table 2 Description of anticipated and unanticipated prosthetic and biologic events Prosthetic events Anticipated Lip biting Change of opposing dentition Loose opposing denture Lost composite filling Difficulty cleaning under prosthesis Loose opposing overdenture Loose O rings Tooth broken opposing partial denture Lost gold matrix Prosthesis tooth fracture Prosthesis tooth wear Tooth broken on opposing denture Loose gold screw Anticipated Plaque/calculus Hyperplasia Tingling when flossing Paresthesia Biologic events Unanticipated Fractured gold screw Loose abutment Fractured abutment screw Fractured multiple abutment screws Prosthesis fracture Broken opposing denture Fractured acrylic base Distorted implant platform Removal of failed implant Unanticipated Periapical radiolucency Infection Mobile implant Benign/malignant process All events types were collected and categorized. Anticipated/unanticipated designations were chosen to assist clarification of recall dynamics. An event associated with continued functional performance and reversible return to biological health is considered as less disruptive to follow-up, which is anticipated. An event that leads to harm with function and is irreversible biologically would be more demanding at follow-up, both an unanticipated and undesirable outcome. between patient groups. Regarding residence, 78% (7 of 9) of the patients restored elsewhere where National residents, compared to 44% National residents in the Mayo-treated cohort (Table 3). Single-arch prostheses were provided the majority of the time (209 mandibular, 35 maxillary), and 11 patients received both mandibular and maxillary prostheses. The 255 patients received 1325 implants, 1089 in the mandible and 236 in the maxilla. The average age of cohort patients was 56.4 years [68 (27%) less than 50 years of age, 83 (33%) between 50 and 60 years of age, 104 (41%) over 60 years of age] at the time of implant placement. In this group of implant patients, these patients were largely existing denture wearers with a history of maladaptation to removable prostheses. Patients were followed an average of 11.8 years from the time of implant placement to last check-up [140 (53%) followed over 10 years, 96 (36%) followed over 15 years, and 58 (23%) followed over 20 years]. Patients returned for an average of five visits per year after prosthesis placement. Overview of prosthesis survival Overall prosthesis survival rates at 5, 10, 15, and 20 years following the date of implant reveal a 20-year survival rate of 86% (Fig 1). Survival free of prosthetic or biologic events for the same time intervals reveals 51% at 5 years and 11% at Table 3 Summary of patient specific features Feature (n = 255 completed rehabilitations) Mean (range) Age at first implant in years 56.4 (9 82) Years from first implant to last check-up 11.8 ( ) Overall number of visits 23.8 (0 113) Number of visits per year 4.3 (0 69) Sex N (%) Female 190 (75) Male 65 (25) Residence National 111 (44) Local 84 (33) Regional 53 (21) International 7 (3) Arch restored Mandible 209 (82) Maxilla 35 (14) Both mandible and maxilla 11 (4) Prosthetic design Metal acrylic 229 (90) Spark erosion 8 (3) Bar with RPD 7 (3) Metal ceramic 3 (1) Bar milled/od 1 (<1) Metal acrylic switch to spark erosion 4 (2) Metal acrylic switch to bar with RPD 2 (1) Metal acrylic switch to metal ceramic 1 (<1) Smoker 82 (32) Cardiovascular disease 136 (53) Osteoporosis 59 (23) GERD 28 (11) Hypertension 185 (73) Hyperlipidemia 164 (64) Carcinoma 34 (13) Feature (n = 9 prostheses placed elsewhere) Mean (median; range) Age at first implant in years 60.6 (61; 43 81) Years from first implant to last check-up 0.5 (0.5; ) Sex N (%) Female 6 (67) Male 3 (33) Residence National 7 (78) Regional 2 (22) Arch restored Mandible 7 (78) Maxilla 1 (11) Both mandible and maxilla 1 (11) Prosthetic design Metal acrylic 2 (22) Spark erosion 1 (11) Unknown 6 (67) Local: State of Minnesota. Regional: North Dakota, South Dakota, Nebraska, Wisconsin, Iowa. National: United States of America excluding local and regional. International: Outside the United States of America. Journal of Prosthodontics 23 (2014) C 2013 by the American College of Prosthodontists 175
4 Edentulous Jaw and Implants, 29-Year Outcome Analysis Dhima et al 5 years 97% (94 99; 179) 10 years 94% (90 97; 131) 15 years 88% (83 94; 85) 20 years 86% (80 92; 47) (95% CI; # at risk) Figure 1 Overall prosthesis survival. 100 Survival free of any events (%) years 50% (45 58; 94) 10 years 35% (29 43; 49) 15 years 18% (13 26; 21) 20 years 11% (6 19; 6) (95% CI; # at risk) Years from placement Figure 2 Prosthesis survival free of any events. 20 years (Fig 2). Prosthesis survival free of any prosthetic events is shown in Figure 3. Survival free of implant failure rates for the same time intervals reveals that at 20 years, 12% of the prostheses had experienced implant failure (Fig 4). Of the prostheses, 15% survived free of any event, and 92% experienced survival free of implant failure (95% confidence interval). Twenty two of the cohort patients (8.6%) had a prosthesis remake. The timing of the remakes ranged from 1.2 to 25.6 years following the date of implant insertion (mean 9.6 years). The most common reason for a prosthesis remake was due to prosthetic events, and was often related to repeated events suggesting the need for improved prosthesis-implant fit. Overview of events A summary of prosthetic and biologic events, both those anticipated and unanticipated, is shown in Table 4. There were over three times as many prosthetic events as biologic events in this patient group. Regarding the prosthetic events, unanticipated events occurred more commonly, they required fewer than two visits on average to resolve, and were seen from year 1 through year 26 of follow-up (mean 7.6 years from implant placement). Regarding biologic events, anticipated events occurred more than twice as frequently as unanticipated events, both types were resolved in two or fewer visits, and each type was seen sooner, on average, than prosthetic events. The mean number of prosthetic events observed per patient was two times more than the mean number of biologic events observed per patient (4.3 and 2.1, respectively). The mean number of unanticipated prosthetic events observed per patient was 4, while the mean number of unanticipated biologic events observed per patient was 1.5. On average, the first anticipated prosthetic events occurred 10.5 years after implant placement and significantly later than the first anticipated biologic event, which occurred 4.1 years after implant placement (Table 4). The mean number of visits 176 Journal of Prosthodontics 23 (2014) C 2013 by the American College of Prosthodontists
5 Dhima et al Edentulous Jaw and Implants, 29-Year Outcome Analysis Survival free of any prosthetic events (%) years 65% (58 71; 115) 10 years 41% (34 49; 56) 15 years 27% (21 36; 30) 20 years 15% (10 24; 10) (95% CI; # at risk) Figure 3 Prosthesis survival free of any prosthetic events Years from Prosthesis Insertion 5 years 91% (88 95; 166) 10 years 91% (87 95; 126) 15 years 88% (83 93; 82) 20 years 88% (83 93; 47) (95% CI; # at risk) Figure 4 Prosthesis survival free of implant failure. to address anticipated prosthetic events were 2.8 (range 1 to 8) with 43% of them addressed in one visit. The mean number of visits to address anticipated biologic events was 1.4 (range 1 to 9) with 72% of them addressed in one visit (Table 4). Table 5 summarizes events at the patient level. Over one-third of the patients experienced no prosthetic or biologic events over the period of follow-up. Nearly one-fourth of the patients experienced both types of events, one-third experienced only prosthetic events, and less than one-tenth experienced only biologic events. Well over half (58%) experienced at least one prosthetic event, and for the patients with at least one event (i.e., at least one prosthetic or biologic event) the mean time to their first event was approximately 5 years. Most common prosthetic and biologic events Table 6 shows fractured screws and abutments were the top two prosthetic events observed; occurring at the 6- to 7-year mean time period and requiring a single visit to address more than 85% of the time. The third most common prosthetic event observed, wear, occurred at a much later mean time period (14 years) and, as would be expected, required more visits to address. The most frequent prosthetic event was fracture of a single gold screw, which on average occurred 7.4 years after prosthesis insertion. The most frequent biologic event was peri-implant soft tissue hyperplasia, which on average occurred 3.3 years after implant placement. Implant failures Fewer than 10% of the patients experienced 35 implant failures over the course of the observation period. Ten failures occurred less than 1 year after implant placement, with the remaining 25 implant failures occurring in patients a mean of 4.7 years (range 1 to 13.1) after implant placement. Nineteen of the implant failures occurred in the mandible and 16 in the maxilla. Journal of Prosthodontics 23 (2014) C 2013 by the American College of Prosthodontists 177
6 Edentulous Jaw and Implants, 29-Year Outcome Analysis Dhima et al Table 4 Summary of anticipated and unanticipated events and visits to address events Visits to resolve event N (%) Years from implant placement Visits to resolve event N Mean (Range) N 1 2 >2 Prosthetic 643 Anticipated ( ) 2.8 (1 8) 107 (43) 40 (16) 104 (41) Unanticipated ( ) 1.7 (1 12) 312 (80) 27 (7) 53 (14) Biologic 169 Anticipated ( ) 1.4 (1 9) 85 (72) 27 (23) 5 (4) Unanticipated ( ) 2.1 (1 8) 18 (35) 23 (44) 11 (21) All values are listed for sample sizes 3. Table 5 Summary of patient experiences with events Years from implant placement Patients N (%) to the first event Event type N total = 255 Mean (range) At least one prosthetic 148 (58) 4.9 (2.6; 17 days to 26.0 years) At least one biologic 81 (32) Only prosthetic 86 (34) Only biologic 19 (7) Prosthetic and biologic 62 (24) None 88 (35) This failure cohort also experienced mostly unanticipated prosthetic events. Of particular note for this edentulous population is the finding that opposing dentition type did not have a statistically significant impact on implant failure or time of failure. For the group, 60% had an opposing complete denture, and 31% had natural opposing dentition. Discussion The evidence-based history in prosthodontics is longstanding. It began with a formal scholarly exposure to the principles involved at McMaster University in the early 1990s, followed by educational workshops targeting dissemination of these principles to residency directors and educators, and included publication of prosthodontic-specific evidence-based learning and practice aids modeled after those originally published in medicine. 20 Since that time, progress has been made in the understanding of clinical evidence and its application to the clinical encounter of patient care. Yet clinical trial reports consistently fall short of providing outcomes that delineate long-term expectations that patients and providers use to understand complex care decisions in prosthodontics. 21 This does not mean that evidence-based efforts are not worthwhile, but does suggest the need to consider defining best practice using evidence complimentary to trialbased evidence and doing so with careful understanding as to how much confidence we can infer from evidence sources to our unique situations. 13 This article suggests that evidence from practice, systematically collected and studied by conscientious practitioners, should be considered. Long-term practice outcome data The data in this report represent outcomes from a time frame of care beginning 29 years ago; it serves as an example of a database maintenance report used as part of practice monitoring, and its specific use will be to (1) guide decisions regarding scheduling of maintenance visits, and (2) inform shared decision-making discussions with patients in a group prosthodontic practice. The practice scope requires database use to systematically monitor care quality, and for the chronic condition of missing teeth, doing so allows identification of time-dependent influences on the clinical course, categorized Table 6 The three most common prosthetic and biologic events and how they were addressed Years from implant placement to the first event Visits to address N Visits to address N (%) Event Top 3 N (%) Mean (range) 1 visit 2 visits >2 visits Prosthetic N = 643 Fractured screw 113 (18) 7.4 ( ) 1.4 (1 9) 100 (89) 4 (4) 9 (8) Fractured abutment 73 (11) 6.4 ( ) 1.3 (1 5) 64 (88) 3 (4) 6 (8) Wear 63 (8) 13.9 ( ) 4.6 (1 8) 5 (8) 4 (6) 56 (86) Biologic N = 169 Hyperplasia 97 (57) 3.3 ( ) 1.4 (1 9) 68 (70) 25 (26) 4 (4) Mobile implant 23 (14) 3.4 ( ) 1.7 (1 4) 11 (48) 10 (43) 2 (9) Infection 15 (9) 6.3 ( ) 2.2 (1 5) 3 (20) 8 (53) 4 (27) 178 Journal of Prosthodontics 23 (2014) C 2013 by the American College of Prosthodontists
7 Dhima et al Edentulous Jaw and Implants, 29-Year Outcome Analysis Table 7 Summary of patient-centered questions for informed health care decisions as suggested by the Patient-Centered Outcomes Research Institute. Available online at research-we-support/pcor/. Patient centered questions to ask 1 Given my personal characteristics, conditions and preferences, what should I expect will happen to me? 2 What are my options and what are the potential benefits and harms of those options? 3 What can I do to improve the outcomes that are most important to me? 4 How can clinicians and the care delivery systems they work in help me make the best decisions about my health and healthcare? Last accessed on February 9, as clinical outcomes. Such a systematic monitoring, analyzing, and responding to outcomes of care with a quality target in mind is a longstanding goal of outcomes research. 22 Outcomes research Outcomes research has meant various things to different groups over the past few decades. Lee et al share a historical perspective of this confusing field and summarize current understanding of outcomes research as being concerned with improving clinical practice as applied to patients treated outside clinical trials. 23 Specific to the field of prosthodontics, outcomes are the consequences of management decisions for missing and defective teeth, made at the individual patient level, involving multiple factors of importance to the patient and, based on the clinical findings, the clinician. A fundamental principle involved in the patient-provider interaction is that the patient elects to pursue care for self-defined reasons. 24 Therefore, in shared decision-making discussions, all factors important to a management decision must have value to the individual electing the intervention. 9 Consequently, pertinent outcomes should be identified as consistent with patient expectations, helpful to providers in quality assurance (QA) monitoring relative to meeting treatment targets, and providing data for summary and sharing with patients considering care. When outcomes directly address common patient concerns regarding expectations, options, benefit and risk, and self-care they directly inform best practices (Table 7). Outcome comparison It is important to view the evidence in this report against previous reports. Favorable long-term outcomes have been shown for edentulous patients treated using a two-stage surgical protocol, machined titanium implants, and implant-supported cantilevered prostheses at the abutment level. 11,12,18 Several articles have also reported implant and prosthetic component performance events such as loose and fractured screws, prosthesis superstructure wear and fracture, alteration of opposing dentition, and even the need for prosthesis replacement. 18,25-28 Reports of prosthesis maintenance needs and the impact of implant failures on long-term care are important, yet when reports are limited in patient sample size and length of follow-up, 12,18 and when concern exists as to how applicable the outcomes are to an individual practice, it is difficult to know with surety if practice change is required. This overall prosthesis survival of 86% at 20 years is similar to the lower limit of previous reports in the literature, which ranged from 84% to 34% 12 to 100%. 11 Material fatigue of superstructure and first-generation implant components contributed to the events observed. Unlike other studies that showed minimal prosthetic events, 10,11 this study reveals significantly more prosthetic events than biologic events. Furthermore, prosthetic events occurred significantly later than biologic events. The anticipated prosthetic events occurred on average more than 10 years after initial treatment, while unanticipated prosthetic events occurred on average almost 8 years after initial treatment. As suggested in the literature, 10-12,17 time-dependent outcomes are critical to understand from a prosthetic maintenance perspective. The comparative difference between event types (four times more prosthetic events than biologic events) is not in agreement with previous reports, which described minimal screw fractures, screw loosening, wear, and loss of access fillings. Prosthesis tooth wear was the third most common event with 65 (10%) patients, consistent with previous literature 12 when differences in the size of the patient population were taken into account (308 patients in this study vs. 45 to 58 patients). An early study 10 showed that, on average, a patient received 2.27 implant-retained prostheses (range 1 to 4), more than reported in this study. Population characteristics The population in this report represents approximately six times more patients than similar patient populations reviewed in the literature. Regarding the comparability of patients, the patients in this cohort included all patients from implant care inception through No selection bias is expected, and all data are part of the current clinical outcome database used prospectively. The inclusion of a large portion of patients who travel some distance for care (44% National patients) is unique, yet followup remains robust, as 140 (53%) patients have been followed for 10 years, 96 (36%) for more than 15 years, and 58 (23%) for more than 20 years. Events With 75% of this patient population still living after 30 years of initial treatment, the data reveal that time-dependent events become more frequent. Also, biologic events reflect a remarkable biological tolerance over time. 29 Although the majority of the prosthetic events could be addressed in one or two visits, visits ranged from 1 to 9. This information is valuable for describing potential long-term care needs, and financial and maintenance expectations associated with such treatment. One in three patients experienced no events during follow-up; one of four experienced both a biological and prosthetic event; 58% had at least one prosthetic event. Prosthetic events were felt to be related to cantilever constructions and are not unexpected, given previous reports. 30,31 Screw loosening related to the prosthetic screw is known to have a design safety feature of this original system, placing the most at-risk component in a retrievable location. The Journal of Prosthodontics 23 (2014) C 2013 by the American College of Prosthodontists 179
8 Edentulous Jaw and Implants, 29-Year Outcome Analysis Dhima et al data support the finding that prosthetic events were managed in timely manner on average. Biologic events can be characterized as low in severity, resolved in a timely manner, and when involving a failure of an implant, this did not always detract from prosthesis function. Regarding implant failure, approximately one out three (10/35) failed in the first year, and failure was not associated with opposing dentition type. This implant survival finding of 88% (83 to 93, 95% CI) at 20 years is consistent with other studies of a similar patient population Prosthesis-specific survival The findings of this report suggest that patients considering similar care have a very good chance (86%) that at 20 years they will have a functioning prosthesis. When we found the need to remake a prosthesis, it occurred infrequently (22 of 255 patients) and at varying times after the original prosthesis (from 1.2 to 25.6 years). This outcome compares very favorably with conventional fixed prostheses, where one systematic review describes an 89% 10-year survival estimate. 32 Practice application As this practice evolves, we are faced with considering what key findings from this time period can best inform current and future care. The patient population in this report is more homogenous than edentulous patients seen in the last 5 to 10 years. In 1983 when this treatment approach was implemented, presenting patients had been edentulous for several years and were considered for care based on presentation with significant residual alveolar ridge resorption and attendant maladaptation to conventional prostheses. This type of patient with such significant residual ridge resorption resulted in a significantly large restorative space to accommodate implant and prosthetic components for resin to metal prostheses. On the contrary, current populations being managed with implant-supported prostheses also include patients who received elective extractions, creating situations with potentially limited restorative space. This situation more often requires consideration of strategically prescribed terminal implants, which reduces or eliminates cantilever influences. Conclusion This report of practice-based outcome evidence from a 29- year follow-up period of implant prostheses provides long-term data useful for practice QA and shared decision-making patient discussions. The clinical events associated with patient follow-up visits revealed the following: 1. Overall prosthesis survival at 20 years was 86%. 2. Prosthetic events occur significantly later and more frequently than biologic events. 3. The most common prosthetic event was fractured gold screws, and the most common biologic event was hyperplasia. These findings support the suggestion that prosthodontic care for edentulism be managed within a chronic condition context for a more realistic understanding of maintenance expectations for patients and providers. Acknowledgments The authors acknowledge the contributions to the clinical work reviewed in this report from all consultants, residents, and allied staff providing patient care within the Department of Dental Specialties at Mayo Clinic since References 1. Branemark PI, Adell R, Albrektsson T, et al: Osseointegrated titanium fixtures in the treatment of edentulousness. Biomaterials 1983;4: Laney WR, Tolman DE, Keller EE, et al: Dental implants: tissue-integrated prosthesis utilizing the osseointegration concept. Mayo Clin Proc 1986;61: Cox JF, Zarb GA: The longitudinal clinical efficacy of osseointegrated dental implants: a 3-year report. Int J Oral Maxillofac Implants 1987;2: Legare F, Ratte S, Stacey D, et al: Interventions for improving the adoption of shared decision making by healthcare professionals. Cochrane Database Syst Rev 2010:CD Branemark PI, Albrektsson T: Titanium implants permanently penetrating human skin. Scand J Plast Reconstr Surg 1982;16: Cronin M, Meaney S, Jepson NJ, et al: A qualitative study of trends in patient preferences for the management of the partially dentate state. Gerodontology 2009;26: Griffin S, Kinmonth AL: Diabetes care: the effectiveness of systems for routine surveillance for people with diabetes. Cochrane Database Syst Rev 2000:CD Carr AB: Effect of prosthetic remedial treatments on the oral health status of individuals and populations. Int J Prosthodont 2003;16(Suppl): Carr AB: Successful long-term treatment outcomes in the field of osseointegrated implants: prosthodontic determinants. Int J Prosthodont 1998;11: Attard NJ, Zarb GA: Long-term treatment outcomes in edentulous patients with implant-fixed prostheses: the Toronto study. Int J Prosthodont 2004;17: Ekelund JA, Lindquist LW, Carlsson GE, et al: Implant treatment in the edentulous mandible: a prospective study on Branemark system implants over more than 20 years. Int J Prosthodont 2003;16: Astrand P, Ahlqvist J, Gunne J, et al: Implant treatment of patients with edentulous jaws: a 20-year follow-up. Clin Implant Dent Relat Res 2008;10: Feinstein AR, Horwitz RI: Problems in the evidence of evidence-based medicine. Am J Med 1997;103: Berwick DM: Broadening the view of evidence-based medicine. Qual Saf Health Care 2005;14: Cook JA: The challenges faced in the design, conduct and analysis of surgical randomised controlled trials. Trials 2009;10:9 16. Pincus T, Sokka T: Evidence-based practice and practice-based evidence. Nat Clin Pract Rheumatol 2006;2: Adell R, Lekholm U, Rockler B, et al: A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Maxillofac Surg 1981;10: Attard NJ, Zarb GA: Long-term treatment outcomes in edentulous patients with implant overdentures: the Toronto study. Int J Prosthodont 2004;17: Journal of Prosthodontics 23 (2014) C 2013 by the American College of Prosthodontists
9 Dhima et al Edentulous Jaw and Implants, 29-Year Outcome Analysis 19. Office for Human Research Protections (OHRP): Draft guidance on reporting and reviewing adverse events and unanticipated problems involving risks to subjects or others. Available online at htpp:// Last accessed on February 9, McGivney GP: Evidence-based dentistry article series. J Prosthet Dent 2000;83: Abt E, Carr AB, Worthington HV: Interventions for replacing missing teeth: partially absent dentition. Cochrane Database Syst Rev 2012;2:CD AHRQ Outcomes Research Fact Sheet: AHRQ Publication No. 00-P011, March Rockville, MD, Agency for Healthcare Research and Quality. Available on line at clinic/outfact.htm. Last accessed on February 9, Lee SJ, Earle CC, Weeks JC: Outcomes research in oncology: history, conceptual framework, and trends in the literature. J Natl Cancer Inst 2000;92: Davies AR: Patient defined outcomes. Qual Health Care 1994;3(Suppl): Henry PJ, Bower RC, Wall CD: Rehabilitation of the edentulous mandible with osseointegrated dental implants: 10 year follow-up. Aust Dent J 1995;40: Carlsson GE, Lindquist LW, Jemt T: Long-term marginal periimplant bone loss in edentulous patients. Int J Prosthodont 2000;13: Snauwaert K, Duyck J, van Steenberghe D, et al: Time dependent failure rate and marginal bone loss of implant supported prostheses: a 15-year follow-up study. Clin Oral Investig 2000;4: Ferrigno N, Laureti M, Fanali S, et al: A long-term follow-up study of non-submerged ITI implants in the treatment of totally edentulous jaws. Part I: ten-year life table analysis of a prospective multicenter study with 1286 implants. Clin Oral Implants Res 2002;13: Koka S, Zarb G: On osseointegration: the healing adaptation principle in the context of osseosufficiency, osseoseparation, and dental implant failure. Int J Prosthodont 2012;25: Zurdo J, Romao C, Wennstrom JL: Survival and complication rates of implant-supported fixed partial dentures with cantilevers: a systematic review. Clin Oral Implants Res 2009;20(Suppl 4): Aglietta M, Siciliano VI, Zwahlen M, et al: A systematic review of the survival and complication rates of implant supported fixed dental prostheses with cantilever extensions after an observation period of at least 5 years. Clin Oral Implants Res 2009;20: Jokstad A: After 10 years seven out of ten fixed dental prostheses (FDP) remain intact and nine out of ten FDPs remain in function following biological and technical complications that have been repaired. J Evid Based Dent Pract 2010;10:39-40 Journal of Prosthodontics 23 (2014) C 2013 by the American College of Prosthodontists 181
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible
 A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
The restoration of partially and completely
 CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Retrospective Cohort Study of the Clinical Performance of 1-Stage Dental Implants
 Retrospective Cohort Study of the Clinical Performance of 1-Stage Dental Implants Alan B. Carr, DMD, MS 1 /Yong-Geun Choi, DDS, MPH, MPH 2 / Steven E. Eckert, DDS, MS 1 /Ronald P. Desjardins, DMD, MS 3
Retrospective Cohort Study of the Clinical Performance of 1-Stage Dental Implants Alan B. Carr, DMD, MS 1 /Yong-Geun Choi, DDS, MPH, MPH 2 / Steven E. Eckert, DDS, MS 1 /Ronald P. Desjardins, DMD, MS 3
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
 C L I N I C A L P R A C T I C E Implant Prosthodontic Management of Anterior Partial Edentulism: Long-Term Follow-Up of a Prospective Study John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
C L I N I C A L P R A C T I C E Implant Prosthodontic Management of Anterior Partial Edentulism: Long-Term Follow-Up of a Prospective Study John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
Mandibular implant-supported hybrid prostheses
 Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
AO Certificate in Implant Dentistry Certificate
 AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Fixed full-arch implant-supported acrylic resin prostheses
 Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
Since the early 1980s, when the concept of
 Retention of Teeth Versus Extraction and Implant Placement: Treatment Preferences of Dental Faculty and Dental Students Peter M. Di Fiore, D.D.S., M.S.; Lawrence Tam, D.D.S.; Ha T. Thai, D.D.S.; Eugene
Retention of Teeth Versus Extraction and Implant Placement: Treatment Preferences of Dental Faculty and Dental Students Peter M. Di Fiore, D.D.S., M.S.; Lawrence Tam, D.D.S.; Ha T. Thai, D.D.S.; Eugene
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Frequency and Type of Prosthetic Complications Associated with Interim, Immediately Loaded Full-Arch Prostheses: A 2-Year Retrospective Chart Review
 Frequency and Type of Prosthetic Complications Associated with Interim, Immediately Loaded Full-Arch Prostheses: A 2-Year Retrospective Chart Review Carl Drago, DDS, MS, FACP 1,2,3 1 Department of Dental
Frequency and Type of Prosthetic Complications Associated with Interim, Immediately Loaded Full-Arch Prostheses: A 2-Year Retrospective Chart Review Carl Drago, DDS, MS, FACP 1,2,3 1 Department of Dental
G03: Complications 12/7/2013 8:00AM 4:30PM
 American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Implants are a part of IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY CLINICAL
 CLINICAL IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY Clifford B. Starr, DMD Mohamed A. Maksoud, DMD KEY WORDS Dental implants General dentistry Resident
CLINICAL IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY Clifford B. Starr, DMD Mohamed A. Maksoud, DMD KEY WORDS Dental implants General dentistry Resident
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Featured Patient Case #1: Complete Mouth Reconstruction with Hybrid Restorations
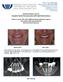 Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
KAREN O. From Failure to Fantastic
 KAREN O From Failure to Fantastic THE Pi TEAM THOMAS J. BALSHI, DDS, PhD, FACP GLENN J. WOLFINGER, DMD, FACP JAMES R. BOWERS, DDS IAN SMITH, DMD KAREN O Karen suffered from painful and swollen gum tissue
KAREN O From Failure to Fantastic THE Pi TEAM THOMAS J. BALSHI, DDS, PhD, FACP GLENN J. WOLFINGER, DMD, FACP JAMES R. BOWERS, DDS IAN SMITH, DMD KAREN O Karen suffered from painful and swollen gum tissue
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Implant Restorations: A Step-By-Step Guide
 Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Lect. 14 Prosthodontics Dr. Osama
 Lect. 14 Prosthodontics Dr. Osama Principles of Removable Partial Denture Design Difference in Prosthesis Support and Influence on Design: For a tooth-supported prosthesis, the movement potential is less
Lect. 14 Prosthodontics Dr. Osama Principles of Removable Partial Denture Design Difference in Prosthesis Support and Influence on Design: For a tooth-supported prosthesis, the movement potential is less
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
REMOVABLE PROSTHODONTICS
 REMOVABLE PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG020.03 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
REMOVABLE PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG020.03 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function
 Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options
 Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
 Case Report International Journal of Dental and Health Sciences Volume 02,Issue 01 RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
Case Report International Journal of Dental and Health Sciences Volume 02,Issue 01 RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report
 Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
In 1977, Lew1 developed a passive
 CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Removable partial dentures
 Removable partial dentures Feb, 4, 2015 McCracken's Removable Partial Prosthodontics, Twelfth Edition Carr, Alan B 1 Prosthesis that replaces the missing teeth and associated supporting structures in a
Removable partial dentures Feb, 4, 2015 McCracken's Removable Partial Prosthodontics, Twelfth Edition Carr, Alan B 1 Prosthesis that replaces the missing teeth and associated supporting structures in a
The removable implant supported prosthesis for the upper jaw
 Implant placement in the atrophied maxilla The removable implant supported Drs. Alan Rosenfeld and George Mandelaris Diplomates, American Board of Periodontology Initial Exam: Patient with ill fitting,
Implant placement in the atrophied maxilla The removable implant supported Drs. Alan Rosenfeld and George Mandelaris Diplomates, American Board of Periodontology Initial Exam: Patient with ill fitting,
Many of the problems reported by conventional
 Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION
 Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
4. What about age? There is no age limit. After puberty, anyone can get dental implants.
 Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Fixed Partial Dentures /FPDs/, Implant Supported. in implant prosthodontics
 Fixed Partial Dentures /FPDs/, Implant Supported Prosthesis/ISP/ in implant prosthodontics Prof.dr.Tamas Divinyi Semmelweis University, Faculty of Dentistry Department of Oral and Maxillofacial Surgery
Fixed Partial Dentures /FPDs/, Implant Supported Prosthesis/ISP/ in implant prosthodontics Prof.dr.Tamas Divinyi Semmelweis University, Faculty of Dentistry Department of Oral and Maxillofacial Surgery
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
The costs and benefits of prosthodontic interventions:
 PROSTHODONTICS 4th year - Fall 2008 The costs and benefits of prosthodontic interventions: Treatment outcomes in prosthodontics and importance of oral hygiene compliance and good control routines Asbjørn
PROSTHODONTICS 4th year - Fall 2008 The costs and benefits of prosthodontic interventions: Treatment outcomes in prosthodontics and importance of oral hygiene compliance and good control routines Asbjørn
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers
 Turk J Med Sci 31 (2001) 445-449 TÜB TAK Filiz KEYF Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers Received: November 30,
Turk J Med Sci 31 (2001) 445-449 TÜB TAK Filiz KEYF Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers Received: November 30,
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
From planning to surgery: a totally digital working flow for Leone implants placement
 Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Prosthetic RehabilitationofaPatientwithAlzheimersDiseaseusingaCombinedBallBarandClipRetainedImplantSupportedOverdentureA Case Report
 Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Specialty Dentistry. Dentistry has nine specialty fields recognized by the American Dental Association
 Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
JOMI on CD-ROM, 1990 Mar ( ): The Applicability of Osseointegrated Oral Imp
 The Applicability of Osseointegrated Oral Implants in the Rehabilitation of Partial Edentulism: A Prospective Multicenter Study on 558 Fixtures Daniel van Steenberghe, MD, PhD/Ulf Lekholm, DDS, PhD/Charles
The Applicability of Osseointegrated Oral Implants in the Rehabilitation of Partial Edentulism: A Prospective Multicenter Study on 558 Fixtures Daniel van Steenberghe, MD, PhD/Ulf Lekholm, DDS, PhD/Charles
Predictors of implant loss with rehabilitation of edentulous jaws with implant-assisted complete prostheses
 C L I N I C A L Predictors of implant loss with rehabilitation of edentulous jaws with implant-assisted complete prostheses Johan Hartshorne 1 A critical appraisal of a systematic review: Kern J-S, Kern
C L I N I C A L Predictors of implant loss with rehabilitation of edentulous jaws with implant-assisted complete prostheses Johan Hartshorne 1 A critical appraisal of a systematic review: Kern J-S, Kern
Saudi Journal of Oral and Dental Research. DOI: /sjodr. ISSN (Print) Dubai, United Arab Emirates Website:
 DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
The Importance of Implant Surface Characteristics in the Replacement of Failed Implants
 The Importance of Implant Surface Characteristics in the Replacement of Failed Implants Ghada Alsaadi, DDS, MSc 1 /Marc Quirynen, DDS, PhD 2 /Daniel van Steenberghe, MD, PhD, Dr hc 3 Purpose: The purpose
The Importance of Implant Surface Characteristics in the Replacement of Failed Implants Ghada Alsaadi, DDS, MSc 1 /Marc Quirynen, DDS, PhD 2 /Daniel van Steenberghe, MD, PhD, Dr hc 3 Purpose: The purpose
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
30/01/2012. Aim. Learning Objectives. Learning Objectives. We know that. Learning Objectives. Diagnosing. Treatment planning.
 Aim Advanced Partial Dentures A contradiction or a true advance? Looking to the Partial denture option Learning Objectives Diagnosing Treatment planning Learning Objectives Expectations have greatly overtaken
Aim Advanced Partial Dentures A contradiction or a true advance? Looking to the Partial denture option Learning Objectives Diagnosing Treatment planning Learning Objectives Expectations have greatly overtaken
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
oral implantology 52 Stoma.eduJ (2014) 1 (1) Abstract Introduction
 Cite this article: Kempler J. An implant supported maxillary fixed prosthesis with a substructure/suprastructure design: a clinical case. Stoma Edu J. 2014; 1(1);52-58. oral implantology An Implant Supported
Cite this article: Kempler J. An implant supported maxillary fixed prosthesis with a substructure/suprastructure design: a clinical case. Stoma Edu J. 2014; 1(1);52-58. oral implantology An Implant Supported
While the protocol for direct bone-to-implant
 Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Monday Morning Pearls of Practice by Bobby Baig
 Oct 17, 2016 Monday Morning Pearls of Practice by Bobby Baig baig@buildyoursmile.com Prosthodontic Associates 2300 Yonge St, suite 905 Toronto, M4P1E4 www.buildyoursmile.com Mechanical Integrity of Retrieved
Oct 17, 2016 Monday Morning Pearls of Practice by Bobby Baig baig@buildyoursmile.com Prosthodontic Associates 2300 Yonge St, suite 905 Toronto, M4P1E4 www.buildyoursmile.com Mechanical Integrity of Retrieved
Implants- immediate restoration of postextraction edentation both esthetically and functionally
 Implants- immediate restoration of postextraction edentation both esthetically and functionally Otilia Stana (Gag), LileIoana Elena, Freiman Paul, Mugur Popescu, Elisei Gabriela, Sebesan Voicu, Vincze
Implants- immediate restoration of postextraction edentation both esthetically and functionally Otilia Stana (Gag), LileIoana Elena, Freiman Paul, Mugur Popescu, Elisei Gabriela, Sebesan Voicu, Vincze
Fabrication of a Hybrid Screw-Retained and Cement-Retained Implant Prosthesis: A Case Report
 Journal Dental School 2012; 30(2):198-202 Case Report Fabrication of a Hybrid Screw-Retained and Cement-Retained Implant Prosthesis: A Case Report 1 Abolfazl Saboury * 2 Hamid Neshandar Asli 1 Associate
Journal Dental School 2012; 30(2):198-202 Case Report Fabrication of a Hybrid Screw-Retained and Cement-Retained Implant Prosthesis: A Case Report 1 Abolfazl Saboury * 2 Hamid Neshandar Asli 1 Associate
Solid Zirconia Full-Arch Implant Prosthesis (Protocol C All-CAD with Multi-Unit Abutments) BruxZir. FIRST Appointment. The BruxZir
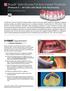 (Protocol C All-CAD with Multi-Unit Abutments) Step-by-Step Restorative Protocol C The BruxZir Full-Arch Implant Prosthesis offers a fixed, all-zirconia implant solution for edentulous patients desiring
(Protocol C All-CAD with Multi-Unit Abutments) Step-by-Step Restorative Protocol C The BruxZir Full-Arch Implant Prosthesis offers a fixed, all-zirconia implant solution for edentulous patients desiring
Implant treatment in patients with severely
 Rehabilitation of Patients with Severely Resorbed Maxillae by Means of Implants With or Without Bone Grafts: A 3- to 5-Year Follow-up Clinical Report Göran Widmark, LDS, Odont Dr 1 /Bernt Andersson, LDS,
Rehabilitation of Patients with Severely Resorbed Maxillae by Means of Implants With or Without Bone Grafts: A 3- to 5-Year Follow-up Clinical Report Göran Widmark, LDS, Odont Dr 1 /Bernt Andersson, LDS,
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Indian Journal of Medical Research and Pharmaceutical Sciences August 2016;3(8) ISSN: ISSN: DOI: /zenodo Impact Factor: 3.
 HYBRID VS CERAMOMETAL IMPLANT PROSTHESIS Dr.Rahul Patil* *Mds Prosthodontics, Senior Lecturer Sddc Dental College, Parbhani Keywords: Abstract A completely edentulous patient has few treatment options
HYBRID VS CERAMOMETAL IMPLANT PROSTHESIS Dr.Rahul Patil* *Mds Prosthodontics, Senior Lecturer Sddc Dental College, Parbhani Keywords: Abstract A completely edentulous patient has few treatment options
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident
 Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Research Article Interdental Papilla Length and the Perception of Aesthetics in Asymmetric Situations
 International Dentistry Volume 2015, Article ID 125146, 5 pages http://dx.doi.org/10.1155/2015/125146 Research Article Interdental Papilla Length and the Perception of Aesthetics in Asymmetric Situations
International Dentistry Volume 2015, Article ID 125146, 5 pages http://dx.doi.org/10.1155/2015/125146 Research Article Interdental Papilla Length and the Perception of Aesthetics in Asymmetric Situations
Locator retained mandibular complete prosthesis (isy Implant System)
 Locator retained mandibular complete prosthesis (isy Implant System) Mucosa-supported complete prostheses with poor fit greatly reduce people's quality of life. This is why the importance of implant-supported
Locator retained mandibular complete prosthesis (isy Implant System) Mucosa-supported complete prostheses with poor fit greatly reduce people's quality of life. This is why the importance of implant-supported
CHAPTER 1. General Introduction
 CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
Element-Z Screw-Retained Hybrid
 Element-Z Screw-Retained Hybrid Implant-Level Restoration Step-by-Step Restorative Protocol The Element-Z Screw-Retained Hybrid offers a fixed, all-ceramic implant solution for edentulous patients desiring
Element-Z Screw-Retained Hybrid Implant-Level Restoration Step-by-Step Restorative Protocol The Element-Z Screw-Retained Hybrid offers a fixed, all-ceramic implant solution for edentulous patients desiring
Simulation Training in Implant Restorative Care for Single- Tooth Sites and Implant Overdenture Prosthetic Rehabilitation
 Original Publication Simulation Training in Implant Restorative Care for Single- Tooth Sites and Implant Overdenture Prosthetic Rehabilitation Joseph A. Toljanic, DDS*, Preetha P. Kanjirath, Ryan R. Vahdani,
Original Publication Simulation Training in Implant Restorative Care for Single- Tooth Sites and Implant Overdenture Prosthetic Rehabilitation Joseph A. Toljanic, DDS*, Preetha P. Kanjirath, Ryan R. Vahdani,
Zygomaticus Implants: A New Treatment Modality for the Edentulous Maxilla
 Zygomaticus Implants: A New Treatment Modality for the Edentulous Maxilla Thomas Salinas, DDS*/Avishai Sadan, DMD **/Tom Peterson, CDT, MDT***/ Bundhit Jirajariyavej, DDS, MSc****/Michael Block, DMD*****
Zygomaticus Implants: A New Treatment Modality for the Edentulous Maxilla Thomas Salinas, DDS*/Avishai Sadan, DMD **/Tom Peterson, CDT, MDT***/ Bundhit Jirajariyavej, DDS, MSc****/Michael Block, DMD*****
 A New Procedure Reduces Laboratory Time to 6 Hours for the Elaboration of Immediate Loading Prostheses with a Titanium Frame Following Implant Placement Huard C, Bessadet M, Nicolas E, Veyrune JL * International
A New Procedure Reduces Laboratory Time to 6 Hours for the Elaboration of Immediate Loading Prostheses with a Titanium Frame Following Implant Placement Huard C, Bessadet M, Nicolas E, Veyrune JL * International
Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete Denture and Mandibular Teeth supported Overdenture
 Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Placement of osseointegrated implants is an increasingly
 Dental Implants in the Elderly Population: A Long-Term Follow-up Sharon M. Compton, PhD 1 /Danielle Clark, BSc 2 /Stephanie Chan, BSc 3 / Iris Kuc, DDS 4 /Berhanu A. Wubie, MSc 5 /Liran Levin, DMD 6 Purpose:
Dental Implants in the Elderly Population: A Long-Term Follow-up Sharon M. Compton, PhD 1 /Danielle Clark, BSc 2 /Stephanie Chan, BSc 3 / Iris Kuc, DDS 4 /Berhanu A. Wubie, MSc 5 /Liran Levin, DMD 6 Purpose:
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
For more than 20 years, the standard protocol for
 Immediate Loading of Splinted Locking-Taper Implants: 1-Year Survival Estimates and Risk Factors for Failure Mohammed S. Erakat, BS 1 /Sung-Kiang Chuang, DMD, MD 2 /Roy H. Yoo, DMD 3 / Meghan Weed, BS
Immediate Loading of Splinted Locking-Taper Implants: 1-Year Survival Estimates and Risk Factors for Failure Mohammed S. Erakat, BS 1 /Sung-Kiang Chuang, DMD, MD 2 /Roy H. Yoo, DMD 3 / Meghan Weed, BS
Low-Cost Implant Overdenture Option for Patients Treated in a Predoctoral Dental School Curriculum
 Milieu in Dental School and Practice Low-Cost Implant Overdenture Option for Patients Treated in a Predoctoral Dental School Curriculum Michael S. McCracken, D.D.S., Ph.D.; Ruth Aponte-Wesson, D.D.S.,
Milieu in Dental School and Practice Low-Cost Implant Overdenture Option for Patients Treated in a Predoctoral Dental School Curriculum Michael S. McCracken, D.D.S., Ph.D.; Ruth Aponte-Wesson, D.D.S.,
(Images are at the end of article)
 Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
CASE REPORT. Prosthetic rehabilitation of edentulous mandible with two-implant retained fixed hybrid prosthesis: A case report.
 1828 CASE REPORT Prosthetic rehabilitation of edentulous mandible with two-implant retained fixed hybrid prosthesis: A case report Meisha Gul, Muhammad Rizwan Nazeer, Robia Ghafoor Abstract Removable complete
1828 CASE REPORT Prosthetic rehabilitation of edentulous mandible with two-implant retained fixed hybrid prosthesis: A case report Meisha Gul, Muhammad Rizwan Nazeer, Robia Ghafoor Abstract Removable complete
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy
 Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
All authors abide by the Association for Medical Ethics (AME) ethical rules of disclosure.
 Fogli V, Michele C, Lauritano D, Carinci F. Intraoraly welded titanium bar for immediate restoration in maxilla: Case report and review of the literature. Annals of Oral & Maxillofacial Surgery 2014 Mar
Fogli V, Michele C, Lauritano D, Carinci F. Intraoraly welded titanium bar for immediate restoration in maxilla: Case report and review of the literature. Annals of Oral & Maxillofacial Surgery 2014 Mar
TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness
 TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness DATE: 13 January 2015 CONTEXT AND POLICY ISSUES According to the World health Organization, the
TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness DATE: 13 January 2015 CONTEXT AND POLICY ISSUES According to the World health Organization, the
Determination of the Rate of Need for Relining Complete Dentures in Patients Referring to a Department of Prosthodontics
 ISS: 2203-1413 Vol.04 o.02 Determination of the Rate of eed for Relining Complete Dentures in Patients Referring to a Department of Prosthodontics Ramin egahdari 1, Seyyed Mahdi Vahid Pakdel 2, Sepideh
ISS: 2203-1413 Vol.04 o.02 Determination of the Rate of eed for Relining Complete Dentures in Patients Referring to a Department of Prosthodontics Ramin egahdari 1, Seyyed Mahdi Vahid Pakdel 2, Sepideh
(Assist. Prof), Dept. Of Prosthodontics, Govt. Dental College Thiruvananthapuram(Kerala).India
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 2 Ver. IV (February. 2017), PP 95-99 www.iosrjournals.org A Simple Technique to Rehabilitate
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 2 Ver. IV (February. 2017), PP 95-99 www.iosrjournals.org A Simple Technique to Rehabilitate
Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report
 Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
