University of Groningen. Maxillary overdentures on dental implants Boven, Geessien Catharina
|
|
|
- Aileen Parsons
- 5 years ago
- Views:
Transcription
1 University of Groningen Maxillary overdentures on dental implants Boven, Geessien Catharina IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version below. Document Version Publisher's PDF, also known as Version of record Publication date: 2018 Link to publication in University of Groningen/UMCG research database Citation for published version (APA): Boven, G. C. (2018). Maxillary overdentures on dental implants. [Groningen]: Rijksuniversiteit Groningen. Copyright Other than for strictly personal use, it is not permitted to download or to forward/distribute the text or part of it without the consent of the author(s) and/or copyright holder(s), unless the work is under an open content license (like Creative Commons). Take-down policy If you believe that this document breaches copyright please contact us providing details, and we will remove access to the work immediately and investigate your claim. Downloaded from the University of Groningen/UMCG research database (Pure): For technical reasons the number of authors shown on this cover page is limited to 10 maximum. Download date:
2 implant surface at placemen Does a large dehiscent implant surface at placement affect 5-years treatment outcome? An assessment of implants placed to support a maxillary overdenture This chapter is an edited version of the manuscript: Boven GC, Meijer HJA, Slot W, Vissink A, Raghoebar GM Does a large dehiscent implant surface at placement t affect the 5-year treatment years outcome? An assessment of implants placed to support a maxillary overdenture. J Craniomaxillofac Surg. 2015;4(9):
3 Abstract Objective The aim of this study was to assess the 5 years clinical and radiographic outcome of implants with a dehiscent surface at implant placement. Material and methods A total of 26 consecutive patients (61.6±8.0 years) with at least one implant with a dehiscent implant surface of ⅔ of the implant length at the labial side were included. All implants were placed to support a maxillary overdenture. The implants were placed with adequate primary stability and the dehiscent surface was covered with autologous bone, anorganic bovine bone and a resorbable membrane. Outcome measures were soft tissue conditions, change of radiographic marginal bone level and implant survival. Baseline data (at loading, T0) were compared with 1 (T1) and 5 (T5) years post loading data. Results Of the 116 implants, 40 implants had no dehiscences, 16 a buccal dehiscence <⅔ of the implant length and 60 implants a dehiscence ⅔. The peri-implant tissue was healthy and 5-years marginal bone loss was well within normal limits (0.4mm [ ]). One implant was lost during the osseointegration period. Conclusions Placing implants with a dehiscence ⅔ of the buccal implant surface with good initial stability combined with covering of the dehiscent surface with autologous bone, anorganic bone and a resorbable membrane is accompanied by a favourable 5-years peri-implant health. 50
4 Introduction Nowadays, a great variety of evaluations on performance of dental implants is done. Most evaluations employ inclusion criteria implying placement of implants in nearly ideal conditions, i.e., sufficient quantity and quality of bone and no infection at the implant site (1). With the dissemination of implant treatment and increasing patients demands, there is a growing pressure in implant dentistry to perform rehabilitations with implants placed in non-ideal conditions including placement of implants in fresh extraction sockets, periodontal compromised areas, and sites with low bone density and/or quantity. The latter condition is accompanied by an increase on presence of dehiscences or fenestrations at implant placement (2 4). Evidence on how implants can be reliably inserted with large dehiscences of the implant surface at time of placement particularly with regard to the long term outcome is sparse. A finite element analysis showed that presence of buccal or lingual dehiscences is accompanied with an increase in marginal bone strain at the mesial and distal sites of the implant. This increased strain increases the risk of bone tissue overload at such locations (5). Deeper peri-implant pockets and greater clinical attachment loss have been reported for implants inserted in sites with dehiscences and guided bone regeneration than in healed sites without dehiscences (6). To prevent attachment loss related to dehiscences at the time of implant placement, a variety of membranes, autologous bone and bone substitutes has been used (7). Even though placing implants without a complete coverage by bone at placement might be suboptimal, such approaches are commonly applied in routine clinical practice, also in the severely resorbed maxilla. As it is not well known how implants, used to retain a maxillary denture, that were placed with a dehiscence of the implant surface perform on the long run. The aim of the present study was to assess the clinical and radiographic outcome of such implants that have been in function for five years. Materials and methods Patient selection A total of 26 consecutive patients (61.6±8.0 years) in whom at least one implant with a dehiscent implant surface of ⅔ of the implant length at the 51
5 labial side was placed between January 2006 and December 2009 were included (8). All implants were placed to support a maxillary overdenture. In short, these fully edentulous patients suffered from lack of retention and stability of the upper denture and had been referred to the Department of Oral and Maxillofacial Surgery (University Medical Centre Groningen, the Netherlands). The patients were at least 18 years of age, non-smoking, were capable of understanding and giving informed consent, were at least 1 year edentulous in the maxilla and mandible, had a sufficient volume of bone to place implants in the anterior maxillary and mandibular region, and had bone dimensions allowing for implant placement with sufficient primary stability. The study was approved by the Medical Ethical Committee of the University Medical Centre Groningen (ABR NL ). As mentioned above, patients for the present study were included if the exposed implant surface (measured with a pair of calipers during surgery) of at least one implant was ⅔ of the implant length (either 4 or 6 implants were placed in the maxilla, thus a maximum of six implants was placed with an exposed implant surface of ⅔ of the implant length). The decision to set a dehiscence <⅔ of the labial implant surface as a cut-off point for this study is based on the following. Previously, it was proposed that a non-mobile implant demonstrating over 50% of vertical bone loss was a failure and has to be removed (9). However, treatment of peri-implantitis often converts a situation from unfavourable to favourable with respect to implant retention and arresting disease progression (10 12). Therefore, a criterion of >50% is too low to denote whether an implant is prone to failure. For this study we stated that a fixture should be characterized as prone to fail when ⅔ of the supporting peri-implant bone has been resorbed and there are signs of inflammation. This limit is arbitrary, but we presume that the potential to predictably place an implant with such a large dehiscence of the implant surface might be lower. The scoring was done by the surgeon (GMR). Implants of included patients were divided into three groups: ⅔ exposed surface at implant placement, <⅔ exposed surface at implant placement and no exposed surface at implant placement. The three groups of implants were compared to each other. After loading (T0), and one year (T1) and five years (T5) after overdenture placement, all patients were recalled. 52
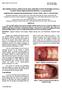
6 Treatment procedure All surgical procedures were performed by one experienced oral and maxillofacial surgeon (GMR). The prosthetic procedures were accomplished by three experienced prosthodontists. Manufacturing of the superstructure was done by a single experienced dental laboratory (8). In short, four or six dental implants with a length of at least 11 mm and a diameter of 4 mm were inserted in the maxillary anterior region (OsseoSpeed 4.0 S dental implants, Astra Tech AB, Mölndal, Sweden). The implants were placed at crestal bone level in predefined positions (positions 15, 1, 11, 21, 2, 25 in the six implants group; positions 1, 11, 21, 2 in the four implants group; Slot et al., 201) with help of a surgical template in a two-stage procedure. All implants were inserted with a minimum of 2 mm bone thickness on the palatal side. All implants were inserted with adequate primary stability (insertion torque of 45 Ncm) (Figure 1). Figure 1. The implants are placed with large dehiscences. The dehiscence or fenestration of the implants was augmented with bone grafts harvested from the maxillary tuberosity region. The bone graft was harvested using chisels and shaped with forceps. The bone grafts were placed buccally of the implant in order to cover the surface and were fixed to the alveolar bone with titanium screws (Martin Medizin Technik, Germany) (diameter 1.5 mm) (Figure 2). 5
7 Figure 2. The dehiscences of the implants are covered with bone grafts harvested from the maxillary tuberosity region and fixed to the alveolar bone with titanium screws. The remaining bone particles and the autogenous bone chips collected during implant bed preparation were used to fill the small gaps between the bone graft and the implant. After this, the reconstructed region was bucally covered with anorganic bovine bone (Bio-Oss, Geistlich Pharma AG, Wolhusen, Switzerland) and a resorbable membrane (Bio-Gide, Geistlich Pharma AG, Wolhusen, Switzerland). The mucoperiostal flap was replaced and wound closure was performed by using resorbable suture material Vicryl 4.0 (Ethicon, Norderstedt, Germany). Two weeks after implant placement, the patient was allowed to wear the removable dentures again after adjustment of the prostheses with a resilient lining material (Soft liner; GC Corporation, Tokyo, Japan). After a -months osseointegration period, second stage surgery was performed and the titanium screws were removed and healing abutments (Uni Healing Abutments, Astra Tech AB, Mölndal, Sweden) were placed (Figure ). The denture was adjusted in the area of the healing abutments and relined again with a resilient lining material. The design of the overdentures was full coverage of the alveolar process, but without palatal coverage in the maxilla. All implants were splinted with a bar. 54
8 Figure. Situation after a -months osseointegration period. Outcome measures Soft tissue conditions For presence of plaque, the index according to Mombelli et al. (1) was used (score 0: no detection of plaque, score 1: plaque can be detected by running a probe across the smooth marginal surface of the abutment and implant, score 2: plaque can be seen by the naked eye, score : abundance amount of plaque). The presence of calculus (score 1) or the absence of calculus (score 0) was scored. To qualify the degree of peri-implant inflammation, the modified Löe & Silness index (14) was used (score 0: normal peri-implant mucosa, score 1: mild inflammation; slight change in colour, slight oedema, score 2: moderate inflammation; redness, oedema and glazing, score : severe inflammation; marked redness and oedema, ulceration). For bleeding, the bleeding index according to Mombelli et al. (1) was used (score 0: no bleeding when using a periodontal probe, score 1: isolated bleeding spots visible, score 2: a confluent red line of blood along the mucosa margin, score : heavy or profuse bleeding). Probing depth was measured at four sites of each implant (mesial, labial, 55
9 distal, and lingual) by using a manual periodontal probe (Williams Color- Coded Probe; Hu-Friedy, Chicago, Il, USA) after removal of the bar; the distance between the marginal border of the mucosa and the tip of the periodontal probe was scored as the probing depth. For each implant the deepest probing depth was recorded. All parameters were scored at T0, T1 and T5. Implant survival Implant survival was defined as the percentage of implants initially placed that were still present and not mobile at follow-up. Lost implants were scored any time after placement. Mobile implants were scored by percussion after removal of the bar. Change of radiographic bone level Standardized intra-oral radiographs were taken at T0, T1 and T5. The intraoral radiographs were taken according to a long-cone paralleling technique with an individualized X-ray holder (15). The digital images were analysed using computer software (Biomedical Engineering, University Medical Centre Groningen, the Netherlands) to perform linear measurements on digital radiographs. Reference line for bone level evaluation was the outer border of the neck of the implant. Mesial and distal bone changes in this region were considered as radiographic bone height change and were defined as the difference in bone height between the radiograph taken at T0, T1 and T5. The selected imaging technique showed an acceptable accuracy for peri-implant bone level measurements with an overall error of about 0.5 mm (16). Measuring was done by one observer (HJAM). Statistics Data collection was done by JWAS and analysis of the radiographs was done by HJAM. The worst score per implant of the clinical and radiographic parameters was used in the data analysis. The homogeneity between the implants with and without dehiscence was verified using the Pearson Χ 2 test. A Χ 2 value <0.05 was considered to represent a statistically significant difference. Because no statistical difference was observed between the three groups, the implant was used as the statistical unit. In each group, all variables were expressed in millimetres. Variables were not normally distributed. Descriptive statistics (e.g., median (interquartile range 56
10 (IQR) described as first quartile (Q1) - third quartile (Q))) were used to characterize the subject population. The comparisons of the variables between the groups at T1 and T5 were performed using the Kruskal-Wallis test. A pairwise comparison was done if a significant difference was found. A P-value <0.05 was considered to represent a statistically significant difference. The data analysis was performed using Statistical Package for Social Sciences (version 22.0; SPSS Inc.: An IBM Company, IBM Corporation, Chicago, IL, USA). Results Patient characteristics are shown in Table 1. Forty implants were placed without dehiscence of the implant surface, 16 implants with a dehiscence <⅔ and 60 implants with a dehiscence ⅔. One patient died, not related to the implant therapy during the first year of evaluation (25 patients completed T1). Another patient died, again not related to the implant therapy, during the fourth year after implant. One patient was not able to visit for T5 because of severe dementia (2 patients completed T5). The mean age of the patients at implant placement was 61.6±8.0 years (range ). During the surgical procedure there was no extensive bleeding at the donor site. Two patients had an antral perforation through the maxillary sinuses after harvesting the tuberosity bone. The wound was primary closed. Healing was uneventful. No objective signs of sinusitis were encountered during the evaluation period. Wound healing after surgery was undisturbed with the exception of one patient with a slightly disturbed bone healing because of a small bone sequester. After removal of the bone sequester the wound healing was undisturbed. Soft tissue conditions No significant change in probing depth was seen between the three groups at T1 and T5 (Table 2). Mean scores of the indices for plaque, calculus, gingiva, and bleeding were very low too and did not change with time (Table 1). 57
11 Table 1. Characteristics of the subject population at the time of implant placement. Age (years ± SD) 61.6 ± 8.0 Gender (%) 14 female (54%) 12 male (46%) T0 T1 T5 Plaque-score (median [IQR]) 0.0 [0.0;0.0] 0.0 [0.0;0.0] 0.0 [0.0;1.0] Gingiva-score (median [IQR]) 0.0 [0.0;0.0] 0.0 [0.0;0.0] 0.0 [0.0;1.0] Bleeding-score (median [IQR]) 0.0 [0.0;1.0] 0.0 [0.0;1.0] 0.0 [0.0;1.0] Calculus-score (median [IQR]) 0.0 [0.0;0.0] 0.0 [0.0;0.0] 0.0 [0.0;0.0] Differences between different T0, T1 and T5 were tested with the related-samples McNemar test (p<0.05). No significant differences were found. IQR: interquartile range. Table 2. Median values and interquartile range (IQR) of radiographic bone loss in mm, probing depth in mm, and frequency distribution of bone loss 1 year and 5 years after placement of the overdenture of the implants placed with and without dehiscence. Loss of marginal bone between T0 and T1 in mm (median [IQR]) mm > mm > mm > mm >2.0 mm Missing data/implant loss Loss of marginal bone between T0 and T5 in mm (median [IQR]) mm > mm > mm > mm >2.0 mm Missing data Change in probing depth between T0 and T1 (median [IQR]) Change in probing depth between T0 and T5 (median [IQR]) Group 1. No dehiscence (n=40) -0.1 [-0.4;0.0] 82.5% 17.5% 0% -0.4 [-1.0; 0.0] 52.5% 20.0% 12.5% 5.0% 5.0% 5.0% Group 2. Dehiscence <⅔ (n=16) 0.0 [-0.2;0.0]* 100% 0% -0.2 [-0.9;0.0] 62.5% 6.% 12.5% 6.% 12.5% Group. Dehiscence ⅔ (n=60) -0.2 [-0.5;-0.1]* 76.7% 15.0% 5.0% 1.7% 1.7% -0.5 [-0.8;-0.1] 50.0% 0.0% 15.0% 5.0% 0.0 [ ] [ ] [ ] [ ] [-0. 1.] 0.0 [ ] *A Kruskal-Wallis H test showed that there was a statistically significant difference in change of bone height between the different groups. 1 A negative change in probing depth reflects a less deep pocket. IQR, interquartile range. 58
12 Implant survival One implant placed with a ⅔ dehiscence was lost during the osseointegration period of months. No other implants were lost during follow-up yielding a 1-year survival and 5-years survival of both 99.1%. Because a bar-supported overdenture could be made on the remaining five implants, there was no need to replace the implant. Change of radiographic bone level The amount of bone loss for all groups at T1 and T5 is shown in table 2 and figure 4. A Kruskal-Wallis H test showed that there was a statistically significant difference in change of bone height between the different groups (p = 0.044). Pairwise comparison revealed there was a significant difference between group 2 and (p = 0.048) and no difference between group 1 and group 2 (p = 0.504) or group (p = 0.554). Thus, at T1, bone loss was higher, though clinical not relevant, for implants with a dehiscence ⅔ (-0.2 mm [-0.5;-0.1]) compared to implants with a dehiscence < ⅔ (0.0 mm [-0.2; 0.0]). No significant differences in bone loss were seen at T5. 59
13 *Significant difference between groups 2 and at T1 (p = 0.01). Figure 4. Box and whisker plot of the difference in marginal bone height between T0 and T1 (1 year), and T0 and T5 (5 years) as measured on the intra-oral radiographs. Discussion Analysis of the data of this study revealed that placing implants with a dehiscence of the implant surface in the maxilla to support a maxillary overdenture does not result in worse per-implant health and implant survival under the condition that the implant is placed with primary stability and the dehiscence is covered with autologous bone, anorganic bovine bone and a resorbable membrane. This eliminates the need for a two surgical interventions (pre implant placement augmentation and abutment connection surgery) thus reducing morbidity and speeding up prosthodontic rehabilitation. 60
14 The incidence of complications, like sensory deficits in the lower lip and mental foramen area, among intraoral donor sites is more significant for the mandibular symphysis and the ramus area than the maxillary tuberosity (17,18). This observation is in line with the results of our study as the donor site (maxillary tuberosity) did not cause complications. Another advantage of choosing the tuberosity as the donor site is that harvesting of bone can be performed through the same incision as for the insertion of the implants. The mean peri-implant probing depths and indices for plaque, calculus, gingiva and bleeding were very low at T1 and T5, and comparable to the scores reported in the literature (19,20). Also the implant survival rate was comparable to survival rates for implants placed in the maxilla (21). Because the measurements were done on intra-oral radiographs, we have to deal with a measurement error of 0.5 mm (16). The minor difference observed between the groups at T1 has no clinical relevance and had resolved at T5. Moreover, the radiographic bone loss observed (at T5) was small and well within the accepted limits (22). Conclusion Placing implants with a dehiscence ⅔ of the buccal implant surface with good initial stability combined with covering of the dehiscent surface with autologous bone, anorganic bone and a resorbable membrane is accompanied by a favourable 5-years peri-implant health. 61
15 References 1. Malo P, Nobre MDA, Lopes A. Immediate rehabilitation of completely edentulous arches with a four-implant prosthesis concept in difficult conditions: an open cohort study with a mean follow-up of 2 years. Int J Oral Maxillofac Implants. 2012;27(5): Malo P, De Araujo Nobre M, Rangert B. Implants placed in immediate function in periodontally compromised sites: A five-year retrospective and one-year prospective study. J Prosthet Dent. 2007;97(6 Suppl):S Vanden Bogaerde L, Rangert B, Wendelhag I. Immediate/early function of Brånemark System TiUnite implants in fresh extraction sockets in maxillae and posterior mandibles: an 18-month prospective clinical study. C Clin Implant Dent Relat Res. 2005;7 Suppl 1:S Mattsson T, Gynther II, Fredholm U. Implant treatment without bone grafting in severely resorbed edentulous maxillae. J Oral Maxillofac Surg. 1999;57(): Van Oosterwyck H, Duyck J, Vander Sloten J, Van Der Perre G, Naert I. Periimplant bone tissue strains in cases of dehiscence: a finite element study. Clin Oral Implants Res. 2002;1(): Siciliano VI, Salvi GE, Matarasso S, Cafiero C, Blasi A, Lang NP. Soft tissues healing at immediate transmucosal implants placed into molar extraction sites with buccal self-contained dehiscences. A 12-month controlled clinical trial. Clin Oral Implants Res. 2009;20(5): Palmer RM, Floyd PD, Palmer PJ, Smith BJ, Johansson CB, Albrektsson T. Healing of implant dehiscence defects with and without expanded polytetrafluoroethylene membranes: a controlled clinical and histological study. Clin Oral Implants Res Jun;5(2): Slot W, Raghoebar GM, Vissink A, Meijer HJA. Maxillary overdentures supported by four or six implants in the anterior region; 1-year results from a randomized controlled trial. J Clin Periodontol. 201 Mar;40(): Misch CE, Perel ML, Wang H-L, Sammartino G, Galindo-Moreno P, Trisi P, et al. Implant success, survival, and failure: the International Congress of Oral Implantologists (ICOI) Pisa Consensus Conference. Implant Dent. 2008;17(1): Khoshkam V, Chan HL, Lin GH, MacEachern MP, Monje A, Suarez F, et al. Reconstructive procedures for treating periimplantitis: a systematic review. J Dent Res. 201;92(12 Suppl):11S 8S. 11. Materni A. Managing an extreme peri-implantitis. Minerva Stomatol. 201;62(9): Parma-Benfenati S, Roncati M, Tinti C. Treatment of peri-implantitis: surgical therapeutic approaches based on periimplantitis defects. Int J Periodontics Restorative Dent. 201;(5): Mombelli a, van Oosten M a, Schurch E, Land NP. The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiol Immunol. 1987;2(4): Loë H, Silness J. Periodontal disease in 62
16 pregnancy. I. Prevalence and severity. Acta Odontol Scand. 196 Dec;21: Meijndert L, Meijer HJA, Raghoebar GM, Vissink A. A technique for standardized evaluation of soft and hard peri-implant tissues in partially edentulous patients. J Periodontol. 2004;75(5): De Smet E, Jacobs R, Gijbels F, Naert I. The accuracy and reliability of radiographic methods for the assessment of marginal bone level around oral implants. Dentomaxillofacial Radiol. 2002;1(): Boronat A, Carrillo C, Penarrocha M, Pennarocha M. Dental implants placed simultaneously with bone grafts in horizontal defects: a clinical retrospective study with 7 patients. Int J Oral Maxillofac Implants. 2010;25(1): Silva FMS, Cortez ALV, Moreira RWF, Mazzonetto R. Complications of intraoral donor site for bone grafting prior to implant placement. Implant Dent. 2006;15(4): Meijer HJA, Raghoebar GM, Batenburg RH, Visser A, Vissink A. Mandibular overdentures supported by two or four endosseous implants: a 10 year clinical trial. Clin Oral Implants Res. 2009;20(7): Meijer HJA, Raghoebar GM, Batenburg R, Vissink A. Mandibular overdentures supported by two Branemark, IMZ or ITI implants: a 5-year prospective study. J Clin Periodontol. 2004;1(9): Raghoebar GM, Meijer HJA, Slot W, Slater JJR, Vissink A. A systematic review of implant-supported overdentures in the edentulous maxilla, compared to the mandible: how many implants? Eur J Oral Implantol. 2014;7 Suppl 2:S Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986;1(1):
17 64
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen
![Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen](/thumbs/87/96311633.jpg) University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
University of Groningen
 University of Groningen Mandibular Overdentures Supported by 6-mm Dental Implants Gulje, Felix; Raghoebar, Gerry; Ter Meulen, Jan-Willem P.; Vissink, Arjan; Meijer, Hendrikus; GuljÃ, Felix Published in:
University of Groningen Mandibular Overdentures Supported by 6-mm Dental Implants Gulje, Felix; Raghoebar, Gerry; Ter Meulen, Jan-Willem P.; Vissink, Arjan; Meijer, Hendrikus; GuljÃ, Felix Published in:
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Many of the problems reported by conventional
 Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident
 Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
University of Groningen. Immediate dental implant placement in the aesthetic zone Slagter, Kirsten
 University of Groningen Immediate dental implant placement in the aesthetic zone Slagter, Kirsten IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Immediate dental implant placement in the aesthetic zone Slagter, Kirsten IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
University of Groningen. Implant treatment for patients with severe hypodontia Filius, Marieke Adriana Pieternella
 University of Groningen Implant treatment for patients with severe hypodontia Filius, Marieke Adriana Pieternella IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Implant treatment for patients with severe hypodontia Filius, Marieke Adriana Pieternella IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study
 26 News No.26 January 2011 The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study Make it Simple 2 The Use Of 6mm Long Implants In Cases With Limited Bone
26 News No.26 January 2011 The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study Make it Simple 2 The Use Of 6mm Long Implants In Cases With Limited Bone
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
SCD Case Study. Implant-supported overdentures
 SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
Vertical and horizontal alveolar ridge augmentation
 CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
University of Groningen
 University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
Posterior mandible and vertical augmentation
 CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
Vertical Augmentation
 Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Citation for published version (APA): Schortinghuis, J. (2004). Ultrasound stimulation of mandibular bone defect healing s.n.
 University of Groningen Ultrasound stimulation of mandibular bone defect healing Schortinghuis, Jurjen IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Ultrasound stimulation of mandibular bone defect healing Schortinghuis, Jurjen IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate Loading Protocol: An In-Vivo Study
 J Indian Prosthodont Soc (Apr-June 2013) 13(2):113 121 DOI 10.1007/s13191-012-0240-8 ORIGINAL ARTICLE Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate
J Indian Prosthodont Soc (Apr-June 2013) 13(2):113 121 DOI 10.1007/s13191-012-0240-8 ORIGINAL ARTICLE Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
Clinical Paper Pre-Implant Surgery
 Int. J. Oral Maxillofac. Surg. 2009; 38: 736 743 doi:10.1016/j.ijom.2009.03.002, available online at http://www.sciencedirect.com Clinical Paper Pre-Implant Surgery Comparison of procedures for immediate
Int. J. Oral Maxillofac. Surg. 2009; 38: 736 743 doi:10.1016/j.ijom.2009.03.002, available online at http://www.sciencedirect.com Clinical Paper Pre-Implant Surgery Comparison of procedures for immediate
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region
 CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
JMSCR Vol 06 Issue 07 Page July 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i7.101 Immediate Implant Following
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i7.101 Immediate Implant Following
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
AO Certificate in Implant Dentistry Certificate
 AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps
 CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT
 ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
University of Groningen. Maxillary overdentures on dental implants Boven, Geessien Catharina
 University of Groningen Maxillary overdentures on dental implants Boven, Geessien Catharina IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Maxillary overdentures on dental implants Boven, Geessien Catharina IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen. Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees
 University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Samantha W. Chou, D.M.D N. Southport Ave. Chicago, Illinois Phone: Fax:
 Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
 227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
Clinical Perspectives
 Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
CASE REPORT MEGAGEN IMPLANT. AnyRidge. CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP
 AnyRidge CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP AnyRidge Clinical Case Ⅰ. Dr. Davide Farronato Baseline - fractured tooth Baseline - fractured tooth #25 Rx view Atraumatic avulsion technique
AnyRidge CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP AnyRidge Clinical Case Ⅰ. Dr. Davide Farronato Baseline - fractured tooth Baseline - fractured tooth #25 Rx view Atraumatic avulsion technique
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Short implants in the posterior maxilla to avoid sinus augmentation procedure: 5-year results from a retrospective cohort study
 Lorenz et al. International Journal of Implant Dentistry (2019) 5:3 https://doi.org/10.1186/s40729-018-0155-1 International Journal of Implant Dentistry RESEARCH Open Access Short implants in the posterior
Lorenz et al. International Journal of Implant Dentistry (2019) 5:3 https://doi.org/10.1186/s40729-018-0155-1 International Journal of Implant Dentistry RESEARCH Open Access Short implants in the posterior
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
University of Groningen
 University of Groningen Maxillary overdentures supported by four or six implants in the anterior region Slot, Wim; Raghoebar, Gerry; Cune, Marco; Vissink, Arjan; Meijer, Hendrikus Published in: Journal
University of Groningen Maxillary overdentures supported by four or six implants in the anterior region Slot, Wim; Raghoebar, Gerry; Cune, Marco; Vissink, Arjan; Meijer, Hendrikus Published in: Journal
Dental Research Journal
 Dental Research Journal Original Article Survival and success rate of one piece implant inserted in molar sites Francesco Carinci 1 1 Department of Medical-Surgical Sciences of Communication and Behavior,
Dental Research Journal Original Article Survival and success rate of one piece implant inserted in molar sites Francesco Carinci 1 1 Department of Medical-Surgical Sciences of Communication and Behavior,
Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure
 Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure Leonard Krekmanov, DDS, PhD 1 The purpose of this investigation was to modify
Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure Leonard Krekmanov, DDS, PhD 1 The purpose of this investigation was to modify
The effect of peri-implant bone exposure on soft tissue healing and bone loss in two adjacent implants
 Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options
 Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Radiographic Stent for Simplified Placement of Implants in the Mandible
 10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
University of Groningen. Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees
 University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique
 e116 Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique Sang-Hoon Park, DDS, MS* Hom-Lay Wang, DDS, MSD, PhD** This paper presents three cases of peri-implant
e116 Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique Sang-Hoon Park, DDS, MS* Hom-Lay Wang, DDS, MSD, PhD** This paper presents three cases of peri-implant
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Ridge Split Procedure
 Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
The alternative to connective tissue grafts. Geistlich Fibro-Gide
 The alternative to connective tissue grafts Geistlich Fibro-Gide CONTENTS From Then to Now 2 Geistlich Fibro-Gide in a Nutshell 4 Treatment Concepts Staged Approach After Implant Placement 8 Interview
The alternative to connective tissue grafts Geistlich Fibro-Gide CONTENTS From Then to Now 2 Geistlich Fibro-Gide in a Nutshell 4 Treatment Concepts Staged Approach After Implant Placement 8 Interview
Bringing you Geistlich biocompatibility with improved application and handling benefits. Your combination for success
 Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Retrospective success and survival rates of dental implants placed with simultaneous bone augmentation in partially edentulous patients
 Nima Bazrafshan Ivan Darby Retrospective success and survival rates of dental implants placed with simultaneous bone augmentation in partially edentulous patients Authors affiliations: Nima Bazrafshan,
Nima Bazrafshan Ivan Darby Retrospective success and survival rates of dental implants placed with simultaneous bone augmentation in partially edentulous patients Authors affiliations: Nima Bazrafshan,
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae
 Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae Jonas P. Becktor, DDS 1 /Sten Isaksson, MD, DDS, PhD 2 /Lars Sennerby, DDS, PhD 3 Purpose: The aim of this study was
Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae Jonas P. Becktor, DDS 1 /Sten Isaksson, MD, DDS, PhD 2 /Lars Sennerby, DDS, PhD 3 Purpose: The aim of this study was
International Journal of Dentistry and Oral Health
 ISSN 2471-657X Case Report Open Access Immediate Implantation and Alveolar Reconstruction of Compromised Socket Helme Altaee *1, Ana Luisa Santos 2 1 Consultant Maxillofacial surgeon and dental Implantologist
ISSN 2471-657X Case Report Open Access Immediate Implantation and Alveolar Reconstruction of Compromised Socket Helme Altaee *1, Ana Luisa Santos 2 1 Consultant Maxillofacial surgeon and dental Implantologist
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
Retrospective Clinical Study on Flapless Implant Placement
 ORIGINAL ARTICLE J Korean Dent Sci. 2012;5(2):54-59 http://dx.doi.org/10.5856/jkds.2012.5.2.54 ISSN 2005-4742 Retrospective Clinical Study on Flapless Implant Placement Jong-Hee Kim 1, Young-Kyun Kim 1,
ORIGINAL ARTICLE J Korean Dent Sci. 2012;5(2):54-59 http://dx.doi.org/10.5856/jkds.2012.5.2.54 ISSN 2005-4742 Retrospective Clinical Study on Flapless Implant Placement Jong-Hee Kim 1, Young-Kyun Kim 1,
Peri-Implant Augmentation
 Indication Sheet PIR - Special Edition Peri-Implant ugmentation Long-term stability KEY TO SUCCESS 3.5-year follow-up by Dr. Paul Stone, University of Edinburgh Dental Institute and lackhills Specialist
Indication Sheet PIR - Special Edition Peri-Implant ugmentation Long-term stability KEY TO SUCCESS 3.5-year follow-up by Dr. Paul Stone, University of Edinburgh Dental Institute and lackhills Specialist
Ridge Augmentation. Selection of Applicable Abstracts and Posters. Using Titanium-Reinforced PTFE Membranes
 Ridge Augmentation Selection of Applicable Abstracts and Posters Using Titanium-Reinforced PTFE Membranes Gultekin BA, Cansiz E, Borahan MO. Clinical and 3-Dimensional Radiographic Evaluation of Autogenous
Ridge Augmentation Selection of Applicable Abstracts and Posters Using Titanium-Reinforced PTFE Membranes Gultekin BA, Cansiz E, Borahan MO. Clinical and 3-Dimensional Radiographic Evaluation of Autogenous
Rehabilitation of a Patient with Completely Edentulous Maxillary Arch using All on 4 Concept of Implantation
 IJopRD K Harshakumar et al CASE REPORT 10.5005/jp-journals-10019-1179 Rehabilitation of a Patient with Completely Edentulous Maxillary Arch using All on 4 Concept of Implantation 1 K Harshakumar, 2 Nimisha
IJopRD K Harshakumar et al CASE REPORT 10.5005/jp-journals-10019-1179 Rehabilitation of a Patient with Completely Edentulous Maxillary Arch using All on 4 Concept of Implantation 1 K Harshakumar, 2 Nimisha
Evaluation of immediate loading of single dental implants in the maxillary esthetic zone: Clinical and radiographical comparative study
 Evaluation of immediate loading of single dental implants in the maxillary esthetic zone: Clinical and radiographical comparative study Received: 9/6/2013 Accepted: 30/7/2013 Serwan Saeb Al Naqshabandi
Evaluation of immediate loading of single dental implants in the maxillary esthetic zone: Clinical and radiographical comparative study Received: 9/6/2013 Accepted: 30/7/2013 Serwan Saeb Al Naqshabandi
