Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate Loading Protocol: An In-Vivo Study
|
|
|
- Elwin Stone
- 5 years ago
- Views:
Transcription
1 J Indian Prosthodont Soc (Apr-June 2013) 13(2): DOI /s ORIGINAL ARTICLE Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate Loading Protocol: An In-Vivo Study Manesh Lahori A. S. Kaul Sidhartha Chandra Rahul Nagrath Himanshu Gupta Received: 19 October 2012 / Accepted: 14 December 2012 / Published online: 27 December 2012 Ó Indian Prosthodontic Society 2012 Abstract The aim of the present study was to evaluate the changes in periimplant bone quality, crestal bone level and the implant stability (periotest) for mandibular implant retained overdentures with ball attachments using delayed and immediate loading protocols. Ten completely edentulous patients had two alpha bio dental implants placed in the anterior part of the mandible. The loading protocols for the patients was chosen randomly by drawing lots. Five patients were loaded under immediate loading protocols and other five following delayed. Crestal bone loss and bone quality were assessed around each implant. Periotest values were recorded for each implant at 3, 6 and 12 months after loading. Two implants were lost and were excluded from the study. However mean crestal bone loss around implants was 0.81 mm from the time of prosthetic loading to 12 months after prosthetic loading was seen and no significant result was found between the two groups for the crestal bone loss and the periotest values. Though the periotest value decreased (indicates increased stability) over the time period. The bone density changes were significant for both the groups at coronal level at all time intervals but at middle level significant only after 12 months of prosthetic loading, although individual variation was high. This study concluded that the changes in crestal bone level and periotest values were insignificant for the two groups. But the implant stability increased over the time and the crestal bone loss was evident with decreased rate over the period of time. There was wide individual variation for the bone density changes but overall increase in the density was seen. M. Lahori (&) A. S. Kaul S. Chandra R. Nagrath H. Gupta Department of Prosthodontics, K. D. Dental College, Mathura, India maneshlahori@gmail.com Keywords Periotest Introduction Overdenture Crestal bone Implant stability Rehabilitation of the completely edentulous mandible using implants to retain a fixed prosthesis is a predictable long-term treatment modality. High implant success rates have also been achieved using 2 or more implants to anchor an overdenture. Two implant-retained overdentures with separated implants have been reported with similar implant success rates ( %) and functional improvement [1]. In case of completely edentulous arches, the residual ridge provides support to the complete denture and implant retained overdenture. Success of implant retained overdenture depends upon osseointegration and stability of implants. Bone quantity and quality are the two main prerequisite that influence successful osseointegration [2]. Bone quality and quantity both are determining factor not only in diagnosis, treatment planning, surgical approach, healing time but also in initial progressive loading during prosthetic construction. Implant stability which can occur at two different stages: primary and secondary. Primary stability of an implant comes from mechanical engagement with cortical bone. Secondary stability, on the other hand offers biological stability through bone regeneration and remodelling. Degree of implant stability may also depend on the condition of the surrounding tissues. Primary stability and absence of micromovement are considered fundamental prerequisites for the osseointegration of endosseous implants [3], for this reason three to six months of healing period before loading was usually recommended. However,
2 114 J Indian Prosthodont Soc (Apr-June 2013) 13(2): this healing period was empirically based and not experimentally ascertained. It is therefore justifiable to question whether this healing period is an absolute prerequisite to obtain osseointegration, or if under certain circumstances this period can be shortened without jeopardizing osseointegration and long term results. This study was conducted to evaluate amount of crestal bone loss and changes in bone density around the implants in time intervals of 3, 6 and 12 months in implant retained overdentures through dentascan and implant stability through periotest and the results were compared between the immediately loaded and delayed loaded groups. Materials and Methods Ten edentulous patients of age group years were selected to participate in within subject crossover clinical trial in Department of Prosthodontics, KD Dental College, Mathura. In this study 20 implants were placed to retain mandibular implant overdenture. The basic inclusion criteria was the edentulous patients with edentulism not less than 4 months and were not satisfied with the retention of mandibular prosthesis. At the inception, all the patients underwent an initial examination, including recording of their medical and dental histories and evaluation of their existing dentures. A presurgical dentascan was taken with the radiographic stent [4] in the patients mouth and the information from the dentascan was assessed for the placement of two implants in the interforaminal region according to standard technique. Out of 20 implants, 10 were loaded following delayed loading protocol and other 10 implants were placed following immediate loading protocol. The second dentascans were taken after the prosthetic loading and the data were assessed for bone quantity and quality. And the third, fourth and fifth dentascans were taken after a period of 3, 6 and 12 months of prosthetic loading to evaluate the changes in the crestal bone height and bone density in the patients. The patients were evaluated for implant stability by the use of periotest device after the initial healing period and 3, 6 and 12 months after the prosthetic loading (Figs. 1, 2, 3, 4, 5, 6, 7). Data Collection For Bone Quality For each of the sites, an image representing a 1 mm buccolingual slice immediately mesial to the implant and an image representing a 1-mm buccolingual slice immediately distal to the implant were selected for analysis. Using the dentascan HOUNSEFIELD UNIT for each point was calculated of 1 mm all along the implant length. The bone density was also be quantitatively evaluated for slices at an equal interval along the entire length of the implant. A rectangular area mapped relative to the onethird size of the implant was placed over the image. Bone density readings were then obtained from three separate subdivisions of the rectangular area: a coronal third, a middle third, and an apical third. Within the 20 implant sites, between mesial and distal images, the various subdivisions of the rectangular implant areas were compared with respect to the bone density values [3] (Fig. 8). For Crestal Bone Height The distance between the observed crestal bone level and the implant shoulder was measured at 1-mm buccolingual slice immediately mesial to the implant and an image representing a 1-mm buccolingual slice immediately distal to the implant (Fig. 9). Implant Stability The implant stability was checked using periotest. The periotest value for each implant was recorded and assessed for the implant stability. Results The peri-implant bone was studied for the changes in crestal bone height, bone density and implant stability (using periotest) at the various time intervals i.e., at the time of prosthetic loading, 3, 6 and 12 months after prosthetic loading. The patients were then divided into two groups the control group (delayed loading) and the test group (immediate loading).in the test group, 10 one-piece implants were placed, compared with 10 two-piece implants in the control group. One group II (immediate loading) participant was not available for follow-up because of implant failure and was therefore excluded. Crestal Bone Height Mean of Crestal Bone Loss The mean of mesial bone loss from the time of prosthetic loading to 3 months after prosthetic loading was 0.44 mm, to 6 months after prosthetic loading was 0.64 mm and 12 months after prosthetic loading was 0.82 mm. The crestal bone changes after 6 and 12 months of prosthetic loading from the time of prosthetic loading were found to be statistically significant. The crestal bone level change from 3 months after prosthetic loading to 6 and 12 months
3 J Indian Prosthodont Soc (Apr-June 2013) 13(2): Fig. 1 Preoperative dentascan with radiographic stent in patient s mouth after prosthetic loading was 0.20 and 0.38 mm, respectively and were statistically not significant. The mean change from 6 months after prosthetic loading to 12 months after prosthetic loading was 0.17 mm and found to be statistically not significant (Table 1). The mean of distal bone loss from the time of prosthetic loading to 3, 6 and 12 months after prosthetic loading was 0.51, 0.65 and 0.80 mm, respectively. The results were found to be statistically significant. The mean crestal bone level change from 3 months after prosthetic loading to 6 months after prosthetic loading was 0.14 mm and 12 months after prosthetic loading was 0.29 mm and were statistically not significant. The mean change from 6 months after prosthetic loading to 12 months after prosthetic loading was 0.15 mm and found to be statistically not significant (Table 1). The mean crestal bone loss was calculated from the baseline (at the time of prosthetic loading), from 3, 6 and 12 months after prosthetic loading. The mean loss of crestal bone height after 3 months of prosthetic loading from the baseline was 0.48 mm and at 6 months after prosthetic loading was 0.65 mm and 12 months after prosthetic loading was 0.81 mm. The changes were found to be statistically significant. The mean crestal bone loss from the 3 months after prosthetic loading to 6 months after prosthetic loading was 0.17 mm and not statistically significant and 12 months after prosthetic loading was 0.33 mm and was statistically significant. From 6 months of prosthetic loading to 12 months of prosthetic loading was 0.16 mm the changes were statistically not significant (Table 1).
4 116 J Indian Prosthodont Soc (Apr-June 2013) 13(2): Fig. 2 3D view of the presurgical dentascan Fig. 3 Radiographic stent Mean Crestal Bone Loss Compared Between the Two Groups (i.e., Delayed Loading Group and Immediate Loading Group) The mean crestal bone loss was computed for the control group and the test group at 3 months after prosthetic loading, 6 months after prosthetic loading and 12 months after prosthetic loading. No statistically significant differences were found between the two groups. The results obtained were 0.52 ± 0.63 mm (control group) and 0.43 ± 0.65 mm (test group) after 3 months of prosthetic loading, 0.69 ± 0.05 mm (control group) and 0.6 ± 0.06 mm (test group) after 6 months of prosthetic loading Fig. 4 Osteotomy site prepared and 0.85 ± 0.05 mm (control group) and 0.76 ± 0.10 mm (test group) after 12 months of prosthetic loading (Graph 1). Bone Density Changes in Bone Density Over the Time Period The mean bone density changes at the coronal level when compared from the time of prosthetic loading to the 3 months after prosthetic loading was ± 23.48, ± HU at 6 months after prosthetic loading
5 J Indian Prosthodont Soc (Apr-June 2013) 13(2): Fig. 5 Implants placed Fig. 6 Denture relieved over the corresponding site Fig. 7 Data collection for bone quality and ± HU at 12 months after prosthetic loading and was statistically significant. The bone density changes between the 3 months after prosthetic loading to 6 months after prosthetic loading was ± HU and 12 months after prosthetic loading was ± HU and found to be statistically significant. When the mean bone density was compared from 6 months after prosthetic loading to 12 months after prosthetic loading the change found was ± HU and was statistically significant. The mean bone density changes at the middle level when compared from the time of prosthetic loading to the 3 months after prosthetic loading was ± 42.28, ± HU at 6 months after prosthetic loading and ± HU at 12 months after prosthetic loading and was statistically significant. The changes between the 3 months after prosthetic loading to 6 months after prosthetic loading was ± HU and 12 months after prosthetic loading were ± HU and found to be statistically significant. When the mean bone density was compared from 6 months after prosthetic loading to 12 months after prosthetic loading the change found was ± HU and was statistically significant. The mean bone density changes at the apical level when compared from the time of prosthetic loading to the 3 months after prosthetic loading was 7.19 ± 45.07, ± HU at 6 months after prosthetic loading and ± HU at 12 months after prosthetic loading. The values were statistically significant when compared to 6 and 12 months after prosthetic loading. The changes between the 3 months after prosthetic loading to 6 months after prosthetic loading was ± HU and 12 months after prosthetic loading was ± HU and was statistically significant. When the mean bone density was compared from 6 months after prosthetic loading to 12 months after prosthetic loading the change found was 0.87 ± HU and was statistically insignificant (Graph 2). Mean Bone Density Changes Compared Between Control Group (Delayed Loading Group) and Test Group (Immediate Loading Group) The mean bone density change at the coronal level after 3 months of prosthetic loading for control group was HU and test group was HU. And statistically the results found to be significant. After 6 months of prosthetic loading the mean bone density for control group recorded was HU and for test group was HU. After 12 months of prosthetic loading the mean bone density for the control group was HU and for test group was HU. The results were statistically significant for both the time intervals. The bone density changes found to be statistically significant in delayed loading group than immediate loading group at the coronal level. The mean bone density after 3 months of prosthetic loading for control group was HU and test group was 4.10 HU. And statistically the results found to be non significant. After 6 months of prosthetic loading the mean bone density for control group recorded was and for test group was HU. The results were statistically not significant. After 12 months of prosthetic loading the mean bone density for the control group was HU and for
6 118 J Indian Prosthodont Soc (Apr-June 2013) 13(2): Fig. 8 Data collection for crestal bone height Fig. 9 Implant stability checked using periotest test group was HU. The results were statistically significant. The bone density changes were significant only after 12 months of prosthetic loading when compared between the two groups. The mean bone density change after 3 months of prosthetic loading for control group was 2.52 HU and test group was HU. After 6 months of prosthetic loading the mean bone density for control group recorded was HU and for test group was HU. After 12 months of prosthetic loading the mean bone density for the control group was HU and for test group was HU. All the results were statistically not Table 1 Mesial, distal and mean crestal bone loss after 3, 6 and 12 months of prosthetic loading and there intergroup comparison (post hoc Tukey test) I - time J - time Sites Mean difference (I - J) Std. error Sig. At the time of prosthetic loading 3 Months after prosthetic loading Mesial Distal Mean Months after prosthetic loading Mesial Distal Mean Months after prosthetic loading Mesial Distal Mean Months after prosthetic loading 6 Months after prosthetic loading Mesial Distal Mean Months after prosthetic loading Mesial Distal Mean Months after prosthetic loading 12 Months after prosthetic loading Mesial Distal Mean
7 J Indian Prosthodont Soc (Apr-June 2013) 13(2): Graph 1 The graph shows the mean crestal bone loss in mm (y-axis) at time intervals (x-axis) of 3, 6 and 12 months after prosthetic loading between control and test groups Graph 2 The graph shows the mean bone density changes in HU (yaxis) at coronal (blue), middle (red) and apical (green) at time intervals (x-axis) of 3, 6 and 12 months after prosthetic loading. (Color figure online) significant. Though increase in bone density was seen but not to significant level. Implant Stability Changes in Mean Periotest Value From the Time of Prosthetic Loading to 3, 6 and 12 Months After Prosthetic Loading The mean periotest value for the implants at the time of prosthetic loading was -2.06, after 3 months of prosthetic loading was -2.50, 6 months after prosthetic loading was and 12 months after prosthetic loading was The results were statistically not significant when compared from the time of prosthetic loading to 3 months after prosthetic loading. The results were statistically significant from the time of prosthetic loading to 6 and 12 months after prosthetic loading (Graph 3). Changes in Periotest Value Compared Between Control Group and Test Group The periotest value was compared between the delayed and immediate loading groups. The mean periotest value at the time of prosthetic loading was -2.6 ± 1.84 and ± 1.77 for the control and test Graph 3 The graph shows the mean periotest values (y-axis) for the the patients at time intervals (x-axis) group, respectively and after 12 months of prosthetic loading was -3.6 ± 1.78 and ± 1.64 for the control and test group, respectively. And the results found were not statistically significant (Table 2). Discussion The loss of teeth and eventual edentulism may constitute a severe handicap. Zarb and Schmitt [5] have presented a historical resume of the development of complete dentures from poorly fitting constructions of the last century to today s more optimized ones. However, inspite of an undisputable improvement in denture quality with modern prosthodontic techniques, poor retention, especially of the lower denture, is still a great problem for many patients. Branemarks seminal osseointegration research introduced a new era of prosthodontic therapy. Adequate stability of an implant in the surrounding bone is essential to allow undisturbed healing and bone formation to occur following placement and also to permit optimal stress
8 120 J Indian Prosthodont Soc (Apr-June 2013) 13(2): Table 2 Mean periotest values compared for the control group and test group at the time of prosthetic loading, 3, 6 and 12 months after prosthetic loading Time interval Groups Mean Std. deviation Std. error mean T test P value At the time of prosthetic loading Delayed loading Immediate loading Months after prosthetic loading Delayed loading Immediate loading Months after prosthetic loading Delayed loading Immediate loading Months after prosthetic loading Delayed loading Immediate loading distribution from masticatory and occlusal functional loads through the implant-tissue interface. The stability requirements for healing and function are rather different; primary stability is necessary at the time of implant placement, and secondary stability is needed following osseointegration, which occurs in function. Primary stability and absence of micromovement are considered fundamental prerequisites for the osseointegration of endosseous implants [3]. Therefore, to avoid high stress/strain in the surrounding bone in the adaptation period, it has been advocated to apply progressive loading on oral implants. A slight load on healing bone shortens healing rather than prolong it. Strains in healing bone not exceeding mild overload might improve healing. Clinical studies [6] have shown that immediately loaded oral implants acting as support for a prosthesis can osseointegrate providing that the forces and implant micro-motion can be controlled [7]. Changes in Mean Crestal Height The stiffness of oral implants of titanium or its alloys is several times greater than that of cortical bone. When an oral implant is occasionally loaded, the stress will be transferred to the bone, with the highest stress in the most coronal portion of the supporting bone. Therefore, an increased strain in the bone resulting in an overload would also be most likely to happen first in this area [7]. Some marginal bone loss around oral implants during the first year of function has been a common observation. Roe et al. [8] found the similar significant results in accordance to author when they compared eight completely edentulous patients (five men, three women) with a mean age of 69.1 years. Studies involving the bone loss in mandibular implant overdenture cases have reported periimplant crestal bone level changes ranging from 0.19 to 2.38 mm at time interval of 12 months [9 12] Periotest Value The values obtained by the author is in accordance with the recordings of Payne et al. [13] which states that the periotest value became more negative with time period and similar results were found by Chiapasco et al. [14], Rungcharassaeng et al. [15], Payne et al. [13], and Naert et al. [10]. The periotest values were compared between the control (conventional loading group) and test group (immediate loading group). Payne et al. [13] found the periotest values at baseline were (control group) versus (test group). Mean PTV after 1 year was -4.9 (control) versus (test). There was a trend of increasingly negative mean PTVs for all implants in both groups, without any significant differences between baseline and year 1. Chiapasco et al. [14] recorded the medians of periotest values in the test group were -4, -4, -4, -4.3 and control group -3, -4, -5 and -4.5 at the time of prosthetic loading and 6, 12 and 24 months after prosthetic loading, respectively. The results were statistically insignificant. Bone Density The changes in bone density as seen by the author is supported by the statement that it has been shown that more dense bone surrounds mechanically loaded oral implants than non-loaded implants in monkeys. The strength of the bone increases from the beginning of loading after surgical exposure and up to 1 year after loading, both because the bone becomes more dense and because of an increase in mineral content [7]. This increase in the mean bone density is also evident at the middle and apical level but when compared between the coronal, middle and apical level the mean bone density change is much more evident at the coronal level. When it is compared between the two groups: conventional loading and immediate loading groups the bone
9 J Indian Prosthodont Soc (Apr-June 2013) 13(2): density changes are significant when compared at the coronal level at all the time. At middle there were no significant changes after 3 and 6 months of prosthetic loading but the result was significant after 12 months of prosthetic loading. At apical level changes between the two groups were insignificant for all the time intervals. Thus, the changes at the coronal level were more pronounced than at the middle and the apical level. Conclusions The results obtained were compared statistically using SPSS software and following conclusions were made: (1) The mean crestal bone loss shows significant changes after 3, 6 and 12 months of prosthetic loading. Though the changes between 6 months after prosthetic loading and 12 months after prosthetic loading are not significant but crestal bone loss is still evident. (2) The periotest values become more negative with the time interval suggesting the increase in the implant stability with the time as the secondary stability is achieved with the bone modeling and remodeling. (3) There is increase in the bone density with the time period. And the changes are more pronounced at the coronal level than at middle level and very minimal increase in density is seen at apical level. (4) When compared between the delayed loading and immediate loading groups there was no significant difference between the crestal bone loss of the two groups. (5) The periotest values were compared between the two groups (delayed loading and immediate loading groups). The results were insignificant. (6) When compared between the two groups the results were significant for the mean bone density changes at the coronal level at 3, 6 and 12 months after prosthetic loading. At middle level the results were significant only after 12 months of prosthetic loading and at the apical level the changes were insignificant but increase in bone density was seen. References 1. Liddelow GJ, Henry PJ (2007) A prospective study of immediately loaded single implant-retained mandibular overdentures: preliminary one-year results. J Prosthet Dent 97(6 Suppl): S126 S Atsumi M, Park SH, Wang HL (2007) Methods used to assess implant stability : current status. Int J Oral Maxillofac Implants 22: Meredith N (1998) Assessment of implant stability as a prognostic determinant. Int J Prosthodont 11: Lima V, Morgano SM (1993) A dual purpose stent for the implant supported prosthesis. J Prosthet Dent 69: Zarb GA, Schmitt A (1995) Implant prosthodontic treatment options for the edentulous patient. J Oral Rehabil 22: Attard NJ, David LA, Zarb GA (2005) Immediate loading of implants with mandibular overdentures: one-year clinical results of a prospective study. Int J Prosthodont 18: Au-Yeung KM, Ahuja AT, Ching AS, Metreweli C (2001) Dentascan in oral imaging. Clin Radiol 56: Roe P et al (2010) Immediate loading of unsplinted implants in the anterior mandible for overdentures: a case series. Int J Oral Maxillofac Implants 25: Batenburg R, Meijer H, Raghoebar G, Vissink A (1998) Treatment concept for mandibular overdentures supported by endosseous implants: a literature review. Int J Oral Maxillofac Implants 13: Naert IE, Gizani S, Vuylsteke M, van Steenberghe D (1997) A randomized clinical trial on the influence of splinted and unsplinted oral implants in mandibular overdenture therapy. A 3-year report. Clin Oral Investig 1: Tawse-Smith A, Perio C, Payne AG, Kumara R, Thomson WM (2001) Onestage operative procedure using two different implant systems: a prospective study on implant overdentures in the edentulous mandible. Clin Implant Dent Relat Res 3: Heijdenrijk K, Raghoebar GM, Meijer HJA, van der Reijden WA, van Winkelhoff AJ, Stegenga B (2002) Two stage IMZ implants and ITI implants inserted in a single-stage procedure. Clin Oral Implants Res 13: Payne AGT, Tawse-Smith A, Duncan WD, Kumara R (2002) Conventional and early loading of unsplinted ITI implants supporting mandibular overdentures. Clin Oral Implants Res 13: Chiapasco M, Abati S, Romeo E, Vogel G (2001) Implant retained mandibular overdentures with Branemark system MKII implants: a prospective comparative study between delayed and immediate loading. Int J Oral Maxillofac Implants 16: Rungcharassaeng K, Lozada JL, Kan JYK, Kim JS, Campagni WV, Munoz CA (2002) Peri-implant tissue response of immediately loaded, threaded, HA-coated implants: 1-year results. J Prosthet Dent 87:
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
CHAPTER 1. General Introduction
 CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
While the protocol for direct bone-to-implant
 Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report
 Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen
![Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen](/thumbs/87/96311633.jpg) University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
The use of two interforaminal implants to retain/
 Immediate Loading of Unsplinted Implants in the Anterior Mandible for Overdentures: 3-Year Results Phillip Roe, DDS, MS 1 /Joseph Y. K. Kan, DDS, MS 2 / Kitichai Rungcharassaeng, DDS, MS 3 /Jaime L. Lozada,
Immediate Loading of Unsplinted Implants in the Anterior Mandible for Overdentures: 3-Year Results Phillip Roe, DDS, MS 1 /Joseph Y. K. Kan, DDS, MS 2 / Kitichai Rungcharassaeng, DDS, MS 3 /Jaime L. Lozada,
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Rehabilitation of an Edentulous Patient with Implant Supported Overdenture
 10.5005/jp-journals-10031-1036 CASE REPORT Rehabilitation of an Edentulous Patient with Implant Supported Overdenture Swapnali Mhatre, Sabita M Ram, Janani Mahadevan, Malika Karthik ABSTRACT The conventional
10.5005/jp-journals-10031-1036 CASE REPORT Rehabilitation of an Edentulous Patient with Implant Supported Overdenture Swapnali Mhatre, Sabita M Ram, Janani Mahadevan, Malika Karthik ABSTRACT The conventional
Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized Balanced Occlusion
 Med. J. Cairo Univ., Vol. 83, No. 2, June: 93-97, 2015 www.medicaljournalofcairouniversity.net Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized
Med. J. Cairo Univ., Vol. 83, No. 2, June: 93-97, 2015 www.medicaljournalofcairouniversity.net Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized
CHAPTER 7. General Discussion
 CHAPTER 7 General Discussion Chapter 7 A common complaint of edentulous patients wearing conventional dentures is the lack of stability and retention of their mandibular prosthesis. These problems can
CHAPTER 7 General Discussion Chapter 7 A common complaint of edentulous patients wearing conventional dentures is the lack of stability and retention of their mandibular prosthesis. These problems can
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Simplified Method for fabrication of O- Ring Implant Supported Overdenture- Case Report
 CASE REPORT Simplified Method for fabrication of O- Ring Implant Supported Overdenture- Case Report Dr. Vikas Punia 1, Dr. Mohit Handa 2, Dr.Nikhil Verma 3, Dr.Virender Singh 4, Dr. Vivek Lath 5. M.D.S.,
CASE REPORT Simplified Method for fabrication of O- Ring Implant Supported Overdenture- Case Report Dr. Vikas Punia 1, Dr. Mohit Handa 2, Dr.Nikhil Verma 3, Dr.Virender Singh 4, Dr. Vivek Lath 5. M.D.S.,
Effect of diameter and length on stress distribution of the alveolar crest around immediate loading implants.
 Effect of diameter and length on stress distribution of the alveolar crest around immediate loading implants. Ding X, Liao SH, Zhu XH, Zhang XH, Zhang L. Clin Implant Dent Relat Res. 2009 Dec;11(4):279-87.
Effect of diameter and length on stress distribution of the alveolar crest around immediate loading implants. Ding X, Liao SH, Zhu XH, Zhang XH, Zhang L. Clin Implant Dent Relat Res. 2009 Dec;11(4):279-87.
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Harsukh Educational Charitable Society International Journal of Community Health and Medical Research
 Harsukh Educational Charitable Society International Journal of Community Health and Medical Research Journal home page:www.ijchmr.com doi: 10.21276/ijchmr ISSN E: 2457-0117 ISSN P:2581-5040 Index Copernicus
Harsukh Educational Charitable Society International Journal of Community Health and Medical Research Journal home page:www.ijchmr.com doi: 10.21276/ijchmr ISSN E: 2457-0117 ISSN P:2581-5040 Index Copernicus
University of Groningen
 University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
CHAPTER 2. Zygogiannis K Wismeijer D Aartman IHA Osman RB. Int J Oral Maxillofac Implants 2016 Jan-Feb;31(1):63-72
 CHAPTER 2 A systematic review on immediate loading of implants used to support overdentures opposed by conventional prostheses: factors that might influence clinical outcomes Zygogiannis K Wismeijer D
CHAPTER 2 A systematic review on immediate loading of implants used to support overdentures opposed by conventional prostheses: factors that might influence clinical outcomes Zygogiannis K Wismeijer D
Consequences of insufficient treatment planning for flapless implant surgery for a mandibular overdenture: A clinical report
 Consequences of insufficient treatment planning for flapless implant surgery for a mandibular overdenture: A clinical report Avinash S., BDS, MS a University of Connecticut Health Center, Farmington, Conn.
Consequences of insufficient treatment planning for flapless implant surgery for a mandibular overdenture: A clinical report Avinash S., BDS, MS a University of Connecticut Health Center, Farmington, Conn.
Evaluation of Stress Distribution in Bone of Different Densities Using Different Implant Designs: A Three-Dimensional Finite Element Analysis
 J Indian Prosthodont Soc (Oct-Dec 2013) 13(4):555 559 DOI 10.1007/s13191-012-0189-7 ORIGINAL ARTICLE Evaluation of Stress Distribution in Bone of Different Densities Using Different Implant Designs: A
J Indian Prosthodont Soc (Oct-Dec 2013) 13(4):555 559 DOI 10.1007/s13191-012-0189-7 ORIGINAL ARTICLE Evaluation of Stress Distribution in Bone of Different Densities Using Different Implant Designs: A
Implant supported mandibular overdenture - a literature review of costs, maintenance and patient satisfaction
 Implant supported mandibular overdenture - a literature review of costs, maintenance and patient satisfaction Corina-Marinela Cristache 1, Ionela-Ruxandra Sfeatcu 2, Mihai Burlibaºa 3, Gheorghe Cristache
Implant supported mandibular overdenture - a literature review of costs, maintenance and patient satisfaction Corina-Marinela Cristache 1, Ionela-Ruxandra Sfeatcu 2, Mihai Burlibaºa 3, Gheorghe Cristache
Fixed Bicortical Screw and Blade Implants as a Non-Standard Solution to an Edentulous (Toothless) Mandible
 http://www.ijos.org.cn Strecha et al. Non-Standard Solution to an Edentulous Mandible doi: 10.4248/IJOS10030 Fixed Bicortical Screw and Blade Implants as a Non-Standard Solution to an Edentulous (Toothless)
http://www.ijos.org.cn Strecha et al. Non-Standard Solution to an Edentulous Mandible doi: 10.4248/IJOS10030 Fixed Bicortical Screw and Blade Implants as a Non-Standard Solution to an Edentulous (Toothless)
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Evaluation of Patient Satisfaction in Implant-supported Dentures retained with Ball and Bar Attachment /jp-journals
 Evaluation of Patient Satisfaction in Implant-supported Dentures retained with Ball and Bar Attachment 10.5005/jp-journals-10029-1144 through Verbal Rating System ORIGINAL ARTICLE Evaluation of Patient
Evaluation of Patient Satisfaction in Implant-supported Dentures retained with Ball and Bar Attachment 10.5005/jp-journals-10029-1144 through Verbal Rating System ORIGINAL ARTICLE Evaluation of Patient
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Mandibular Implant-Retained Overdentures with two Different Implant Designs. Ibrahim R. Eltorky
 Mandibular Implant-Retained Overdentures with two Different Implant Designs Ibrahim R. Eltorky Associate professor of Prosthodontics, Faculty of Dentistry, Tanta University, Egypt. ibrahim_eltorky@yahoo.com
Mandibular Implant-Retained Overdentures with two Different Implant Designs Ibrahim R. Eltorky Associate professor of Prosthodontics, Faculty of Dentistry, Tanta University, Egypt. ibrahim_eltorky@yahoo.com
Social changes, evolution in dentistry, and changes
 695-702 Naert 9/21/04 2:37 PM Page 695 A 10-year Randomized Clinical Trial on the Influence of Splinted and Unsplinted Oral Implants Retaining Mandibular Overdentures: Peri-implant Outcome Ignace Naert,
695-702 Naert 9/21/04 2:37 PM Page 695 A 10-year Randomized Clinical Trial on the Influence of Splinted and Unsplinted Oral Implants Retaining Mandibular Overdentures: Peri-implant Outcome Ignace Naert,
Since their introduction, mandibular overdentures
 A Systematic Review on Immediate Loading of Implants Used to Support Overdentures Opposed by Conventional Prostheses: Factors That Might Influence Clinical Outcomes Kostas Zygogiannis, DDS, RCSed 1 /Daniel
A Systematic Review on Immediate Loading of Implants Used to Support Overdentures Opposed by Conventional Prostheses: Factors That Might Influence Clinical Outcomes Kostas Zygogiannis, DDS, RCSed 1 /Daniel
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Specialty Dentistry. Dentistry has nine specialty fields recognized by the American Dental Association
 Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Radiographic Stent for Simplified Placement of Implants in the Mandible
 10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
Implant-retained Mandibular Overdentures: A Comparative Study of Immediate Loading vs Delayed Loading after One Year
 IJOICR 10.5005/JP-Journals-10012-1076 Implant-retained Mandibular Overdentures: A Comparative Study of Immediate Loading vs Delayed Loading after One Year ORIGINAL RESEARCH Implant-retained Mandibular
IJOICR 10.5005/JP-Journals-10012-1076 Implant-retained Mandibular Overdentures: A Comparative Study of Immediate Loading vs Delayed Loading after One Year ORIGINAL RESEARCH Implant-retained Mandibular
 A New Procedure Reduces Laboratory Time to 6 Hours for the Elaboration of Immediate Loading Prostheses with a Titanium Frame Following Implant Placement Huard C, Bessadet M, Nicolas E, Veyrune JL * International
A New Procedure Reduces Laboratory Time to 6 Hours for the Elaboration of Immediate Loading Prostheses with a Titanium Frame Following Implant Placement Huard C, Bessadet M, Nicolas E, Veyrune JL * International
SCD Case Study. Implant-supported overdentures
 SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT
 ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
Implant Overdentures: Guidelines for Immediate Loading
 Implant Overdentures: Guidelines for Immediate Loading Effective Date: 8/01/16 Expiration Date: 8/01/19 About the Author Dr. Scherer is an assistant clinical professor at Loma Linda University, a clinical
Implant Overdentures: Guidelines for Immediate Loading Effective Date: 8/01/16 Expiration Date: 8/01/19 About the Author Dr. Scherer is an assistant clinical professor at Loma Linda University, a clinical
Three dimensional finite element analysis of immediate loading mini over denture implants with and without acrylonitrile O ring
 Original Research Three dimensional finite element analysis of immediate loading mini over denture implants with and without acrylonitrile O ring Srinivasan Jayaraman, Sreekanth Mallan 1, Babu Rajan, Murugan
Original Research Three dimensional finite element analysis of immediate loading mini over denture implants with and without acrylonitrile O ring Srinivasan Jayaraman, Sreekanth Mallan 1, Babu Rajan, Murugan
(Assist. Prof), Dept. Of Prosthodontics, Govt. Dental College Thiruvananthapuram(Kerala).India
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 2 Ver. IV (February. 2017), PP 95-99 www.iosrjournals.org A Simple Technique to Rehabilitate
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 2 Ver. IV (February. 2017), PP 95-99 www.iosrjournals.org A Simple Technique to Rehabilitate
م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION
 Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness
 TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness DATE: 13 January 2015 CONTEXT AND POLICY ISSUES According to the World health Organization, the
TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness DATE: 13 January 2015 CONTEXT AND POLICY ISSUES According to the World health Organization, the
G03: Complications 12/7/2013 8:00AM 4:30PM
 American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
The effect of attachment type and implant number on satisfaction and quality of life of mandibular implant-retained overdenture wearers
 Original Article The effect of attachment type and implant number on satisfaction and quality of life of mandibular implant-retained overdenture wearers Emre Mumcu, Hakan Bilhan and Onur Geckili Department
Original Article The effect of attachment type and implant number on satisfaction and quality of life of mandibular implant-retained overdenture wearers Emre Mumcu, Hakan Bilhan and Onur Geckili Department
Fixed full-arch implant-supported acrylic resin prostheses
 Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
Evaluation of subjective satisfaction of dental implant patients
 ORIGINAL ARTICLE http://dx.doi.org/0.525/jkaoms.204.40.3.30 pissn 2234-7550 eissn 2234-5930 Evaluation of subjective satisfaction of dental implant patients Young-Kyun Kim, Hyun-Suk Kim, Yang-Jin Yi 2,
ORIGINAL ARTICLE http://dx.doi.org/0.525/jkaoms.204.40.3.30 pissn 2234-7550 eissn 2234-5930 Evaluation of subjective satisfaction of dental implant patients Young-Kyun Kim, Hyun-Suk Kim, Yang-Jin Yi 2,
Design and Manufacturing of Titanium Attachment for Single Implant Retained Mandibular Overdenture: A Review
 Original article: Design and Manufacturing of Titanium Attachment for Single Implant Retained Mandibular Overdenture: A Review *RupaliRaut 1, Dr. S. B. Jaju 2, Dr. N. H. Rathi 3 1Student, M. Tech CAD/CAM,
Original article: Design and Manufacturing of Titanium Attachment for Single Implant Retained Mandibular Overdenture: A Review *RupaliRaut 1, Dr. S. B. Jaju 2, Dr. N. H. Rathi 3 1Student, M. Tech CAD/CAM,
In 1977, Lew1 developed a passive
 CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study
 Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
REVIEWS. 10 Stomatologija, Baltic Dental and Maxillofacial Journal, 2008, Vol. 10, No. 1 SUMMARY
 Maxillary complete denture outcome with two-implant supported mandibular overdentures. A systematic review Vygandas Rutkunas, Hiroshi Mizutani, Vytaute Peciuliene, Ruta Bendinskaite, Tomas Linkevicius
Maxillary complete denture outcome with two-implant supported mandibular overdentures. A systematic review Vygandas Rutkunas, Hiroshi Mizutani, Vytaute Peciuliene, Ruta Bendinskaite, Tomas Linkevicius
Mandibular implant-supported hybrid prostheses
 Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. To systematically appraise the impact of mechanical/technical risk factors on
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. To systematically appraise the impact of mechanical/technical risk factors on
Prosthetic RehabilitationofaPatientwithAlzheimersDiseaseusingaCombinedBallBarandClipRetainedImplantSupportedOverdentureA Case Report
 Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
The earliest methods used
 RESEARCH EVALUATION OF THE PERIOTEST AS A DIAGNOSTIC TOOL FOR DENTAL IMPLANTS A. Norman Cranin, DDS, D.Eng Jack DeGrado, DDS Marc Kaufman, DDS Mylene Baraoidan, DDS Robert DiGregorio, PharmD George Batgitis,
RESEARCH EVALUATION OF THE PERIOTEST AS A DIAGNOSTIC TOOL FOR DENTAL IMPLANTS A. Norman Cranin, DDS, D.Eng Jack DeGrado, DDS Marc Kaufman, DDS Mylene Baraoidan, DDS Robert DiGregorio, PharmD George Batgitis,
University of Groningen. Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees
 University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
The treatment of the completely edentulous mandible
 A prosthetic solution to restoring the edentulous mandible with limited interarch space using an implant-tissue-supported overdenture: A clinical report Marianna Pasciuta, DDS, MS, a Yoav Grossmann, DMD,
A prosthetic solution to restoring the edentulous mandible with limited interarch space using an implant-tissue-supported overdenture: A clinical report Marianna Pasciuta, DDS, MS, a Yoav Grossmann, DMD,
Case Presentation Template for AO Master Certificate
 Case Presentation Template for AO Master Certificate You must have signed informed consent from patients (or relatives/guardians) before submitting an AO Case Presentation and ask them to sign the statement
Case Presentation Template for AO Master Certificate You must have signed informed consent from patients (or relatives/guardians) before submitting an AO Case Presentation and ask them to sign the statement
Since the introduction of osseointegrated dental implants
 CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Immediate Loading of a Multi-Threaded Implant
 Immediate Loading of a Multi-Threaded Implant Dr. Jonathan Yahav, DDS (Northwestern University, Chicago, IL) Aye Myat, BS in Biological Sciences (University of Illinois at Chicago, Chicago IL) Khasim Ali
Immediate Loading of a Multi-Threaded Implant Dr. Jonathan Yahav, DDS (Northwestern University, Chicago, IL) Aye Myat, BS in Biological Sciences (University of Illinois at Chicago, Chicago IL) Khasim Ali
Stress in the Mandible with Splinted Dental Implants caused by Limited Flexure on Mouth Opening: An in vitro Study
 10.5005/jp-journals-10029-1002 Marta Radnai et al RESEARCH ARTICLE Stress in the Mandible with Splinted Dental Implants caused by Limited Flexure on Mouth Opening: An in vitro Study Marta Radnai, Balázs
10.5005/jp-journals-10029-1002 Marta Radnai et al RESEARCH ARTICLE Stress in the Mandible with Splinted Dental Implants caused by Limited Flexure on Mouth Opening: An in vitro Study Marta Radnai, Balázs
Researcher 2017;9(7) Bone Changes in Dental Implant Combined with Laser Therapy: A Split Mouth Study
 Bone Changes in Dental Implant Combined with Laser Therapy: A Split Mouth Study Ali Fahd 1, Yousef Abd-El Ghaffar 2, Hanaa El-Shenawy 3, Mohamed Khalifa 4, and Mushira Dahaba 4 1. Oral and maxillofacial
Bone Changes in Dental Implant Combined with Laser Therapy: A Split Mouth Study Ali Fahd 1, Yousef Abd-El Ghaffar 2, Hanaa El-Shenawy 3, Mohamed Khalifa 4, and Mushira Dahaba 4 1. Oral and maxillofacial
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report
 Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
University of Groningen
 University of Groningen Mandibular Overdentures Supported by 6-mm Dental Implants Gulje, Felix; Raghoebar, Gerry; Ter Meulen, Jan-Willem P.; Vissink, Arjan; Meijer, Hendrikus; GuljÃ, Felix Published in:
University of Groningen Mandibular Overdentures Supported by 6-mm Dental Implants Gulje, Felix; Raghoebar, Gerry; Ter Meulen, Jan-Willem P.; Vissink, Arjan; Meijer, Hendrikus; GuljÃ, Felix Published in:
Immediate Loading of Brånemark System Implants Following Placement in Edentulous Patients: A Clinical Report
 Immediate Loading of Brånemark System Implants Following Placement in Edentulous Patients: A Clinical Report Katsuhiro Horiuchi, DDS, PhD 1 /Hiroya Uchida, DDS 2 / Kazuhiko Yamamoto, DDS, PhD 3 /Masahito
Immediate Loading of Brånemark System Implants Following Placement in Edentulous Patients: A Clinical Report Katsuhiro Horiuchi, DDS, PhD 1 /Hiroya Uchida, DDS 2 / Kazuhiko Yamamoto, DDS, PhD 3 /Masahito
Retreatment: Fractured Implants Due To Biomechanical Overload
 Glenn J. Wolfinger, DMD, FACP Retreatment: Fractured Implants Due To Biomechanical Overload Thomas J. Balshi, DDS, FACP he strength of osseointegration, T the biologic and biomechanical union of bone to
Glenn J. Wolfinger, DMD, FACP Retreatment: Fractured Implants Due To Biomechanical Overload Thomas J. Balshi, DDS, FACP he strength of osseointegration, T the biologic and biomechanical union of bone to
Ilser Turkyilmaz Lars Sennerby Celal Tumer Muhittin Yenigul Mehmet Avci
 Ilser Turkyilmaz Lars Sennerby Celal Tumer Muhittin Yenigul Mehmet Avci Stability and marginal bone level measurements of unsplinted implants used for mandibular overdentures: a 1-year randomized prospective
Ilser Turkyilmaz Lars Sennerby Celal Tumer Muhittin Yenigul Mehmet Avci Stability and marginal bone level measurements of unsplinted implants used for mandibular overdentures: a 1-year randomized prospective
GuidedService. The ultimate guide for precise implantations
 GuidedService The ultimate guide for precise implantations ABGuidedService The ultimate guide for precise implantations At A.B. Dental we've brought implantology into the future with a 3D digitally planned
GuidedService The ultimate guide for precise implantations ABGuidedService The ultimate guide for precise implantations At A.B. Dental we've brought implantology into the future with a 3D digitally planned
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
CASE REPORT. Prosthetic rehabilitation of edentulous mandible with two-implant retained fixed hybrid prosthesis: A case report.
 1828 CASE REPORT Prosthetic rehabilitation of edentulous mandible with two-implant retained fixed hybrid prosthesis: A case report Meisha Gul, Muhammad Rizwan Nazeer, Robia Ghafoor Abstract Removable complete
1828 CASE REPORT Prosthetic rehabilitation of edentulous mandible with two-implant retained fixed hybrid prosthesis: A case report Meisha Gul, Muhammad Rizwan Nazeer, Robia Ghafoor Abstract Removable complete
The restoration of partially and completely
 CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
The biologic predictability of dental implants has
 Prosthetic Complications with Dental Implants: From an Up-to-8-year Experience in Private Practice Rabah Nedir, DMD 1 /Mark Bischof, DMD 2 /Serge Szmukler-Moncler, DMD, PhD 3 / Urs C. Belser, DMD 4 /Jacky
Prosthetic Complications with Dental Implants: From an Up-to-8-year Experience in Private Practice Rabah Nedir, DMD 1 /Mark Bischof, DMD 2 /Serge Szmukler-Moncler, DMD, PhD 3 / Urs C. Belser, DMD 4 /Jacky
STABILITY OF IMPLANTS AND NATURAL TEETH MONTHS OF FUNCTION AS DETERMINED BY THE PERIOTEST OVER 60 CLINICAL
 CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
A SURVEY TO ASSESS PATIENT SATISFACTION AFTER RECEIVING COMPLETE DENTURE PROSTHESES IN A.B. SHETTY MEMORIAL INSTITUTE OF DENTAL SCIENCES
 Short Communication A SURVEY TO ASSESS PATIENT SATISFACTION AFTER RECEIVING COMPLETE DENTURE PROSTHESES IN A.B. SHETTY MEMORIAL INSTITUTE OF DENTAL SCIENCES 2 Vinaya S. Bhat, Krishna Prasad D. & Prakyath
Short Communication A SURVEY TO ASSESS PATIENT SATISFACTION AFTER RECEIVING COMPLETE DENTURE PROSTHESES IN A.B. SHETTY MEMORIAL INSTITUTE OF DENTAL SCIENCES 2 Vinaya S. Bhat, Krishna Prasad D. & Prakyath
The simplicity of the low-profile attachments
 The simplicity of the low-profile attachments Dds Roberto Scrascia Born in Taranto on October 6, 1982. He graduated from the University of Bari in Dentistry and Prosthodontics in 2009, with an experimental
The simplicity of the low-profile attachments Dds Roberto Scrascia Born in Taranto on October 6, 1982. He graduated from the University of Bari in Dentistry and Prosthodontics in 2009, with an experimental
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
An osseointegrated oral implant is characterized
 Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Dent Mater J 2011; 30(6): MATERIALS AND METHODS Attachment systems The attachment systems examined in this study were as follows (Fig. 1).
 2011; 30(6): 928 934 Stress analysis of mandibular two-implant overdenture with different attachment systems Shin TAKESHITA, Manabu KANAZAWA and Shunsuke MINAKUCHI Complete Denture Prosthodontics, Department
2011; 30(6): 928 934 Stress analysis of mandibular two-implant overdenture with different attachment systems Shin TAKESHITA, Manabu KANAZAWA and Shunsuke MINAKUCHI Complete Denture Prosthodontics, Department
Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry
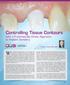 Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry Go online for in-depth content by Timothy F. Kosinski, DDS, MAGD With continual improvements in the design and production
Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry Go online for in-depth content by Timothy F. Kosinski, DDS, MAGD With continual improvements in the design and production
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function
 Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
The overall outcome of dental implant procedures
 Bone Density Assessments of Dental Implant Sites: 1. Quantitative Computed Tomography Masih Shahlaie, BDS 1 /Bernard Gantes, DDS 2 /Eloy Schulz, MD 3 /Matt Riggs, PhD 4 /Max Crigger, DDS 5 Purpose: This
Bone Density Assessments of Dental Implant Sites: 1. Quantitative Computed Tomography Masih Shahlaie, BDS 1 /Bernard Gantes, DDS 2 /Eloy Schulz, MD 3 /Matt Riggs, PhD 4 /Max Crigger, DDS 5 Purpose: This
Influence of Different Angulations of Force in Stress Distribution in Implant Retained Finger Prosthesis: A Finite Element Study
 World Journal of Medical Sciences 10 (2): 217-221, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.2.82275 Influence of Different Angulations of Force in Stress Distribution
World Journal of Medical Sciences 10 (2): 217-221, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.2.82275 Influence of Different Angulations of Force in Stress Distribution
Australian Dental Journal
 Australian Dental Journal The official journal of the Australian Dental Association SCIENTIFIC ARTICLE Australian Dental Journal 2012; 57: 440 445 doi: 10.1111/adj.12002 Load transfer in tilted implants
Australian Dental Journal The official journal of the Australian Dental Association SCIENTIFIC ARTICLE Australian Dental Journal 2012; 57: 440 445 doi: 10.1111/adj.12002 Load transfer in tilted implants
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics.
 In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
