Occlusion periodontal health
|
|
|
- Bernadette Baldwin
- 5 years ago
- Views:
Transcription
1 9 Occlusion and periodontal health J. De Boever, A. De Boever Synopsis Periodontal structures depend on functional occlusal forces to activate the periodontal mechanoreceptors in the neuromuscular physiology of the masticatory system. Occlusal forces stimulate the receptors in the periodontal ligament to regulate jaw movements and the occlusal forces. Without antagonists the periodontal ligament shows some non-functional atrophy. Tooth mobility is the clinical expression of the viscoelastic properties of the ligament and the functional response. Tooth mobility can change due to general metabolic influences, a traumatic occlusion and inflammation. Premature contacts between the arches can result in trauma to the periodontal structures. A traumatic occlusion on a healthy periodontium leads to an increased mobility but not to attachment loss. In inflamed periodontal structures traumatic occlusion contributes to a further and faster spread of the inflammation apically and to more bone loss. A traumatic occlusion, as in a deep bite, may cause stripping of the gingival margins. It is not clear if prematurities or steep occlusal guidance contribute to the occurrence of gingival recession. On implants, prematurities may result in breakdown of osseointegration. In some cases occlusal corrections will be necessary to eliminate the traumatic influence of a nonphysiological occlusion. Key points Healthy periodontal structures and occlusal forces Physiology and clinical aspects of tooth mobility Tooth mobility Types of occlusal forces Trauma from occlusion: Primary trauma in healthy non-inflamed periodontium Primary trauma in healthy but reduced periodontal structures Secondary trauma in the progression of periodontitis Implants and occlusal trauma Gingival recession and occlusal trauma Clinical consequence and procedures HEALTHY PERIODONTAL STRUCTURES AND OCCLUSAL FORCES The healthy periodontal structures, including root cementum, periodontal ligament and alveolar bone, form a functional unit or organ. The periodontal ligament is a very specialised interface between tooth and the alveolar bone. It serves as a structural, sensory and nutritive unit supporting the normal oral functions of chewing, swallowing, speaking, etc. It has a very dense network of interconnecting fibres attached to the bone. The supracrestal fibres are especially important because they maintain the relative position of the teeth in the arch. The collagen fibres in the periodontal ligament are very dense and represent up to 75% of the volume. These so-called Sharpey fibres are apically oriented and embedded both in the alveolar bone and the root cement. The natural dentition has been compared, because of these interconnecting supracrestal fibres, to beads on a string. Teeth function together but have their individual mobility in the 83
2 SECTION 3 CLINICAL PRACTICE AND THE OCCLUSION alveolus. The entire periodontal ligament has viscoelastic characteristics. The ligament provides tooth fixation, and also force absorption. The thickness of the periodontal ligament is directly related to the forces exerted on it. The periodontal ligament has a rich and dense vascular and nervous network. The ligament contains proprioceptors for movement and positioning and mechanoreceptors for touch, pain and pressure. They regulate muscle function and occlusal forces to avoid overload and damage of the teeth and the alveolar bone. The periodontal ligament distributes and absorbs forces. Under physiological conditions the occlusal forces are transferred to alveolar bone and further to the mandible, the maxilla and the entire skull. The alveolar process has a pronounced capacity for modelling and remodelling under functional loading. The alveolar process remodels at a rate of 20% per year. The basal bone does not have this capacity. The periodontal ligament and alveolar bone need the functional stimulus of the occlusion to maintain their physiological, healthy condition. TOOTH MOBILITY Physiological tooth mobility is the result of the histological characteristics of the periodontal ligament. Physiological tooth mobility, in the horizontal as well as in the vertical direction, is different between single root and multirooted teeth and is determined by the width, height and quality of the periodontal ligament (Fig. 9.1). In the vertical direction, the displacement is 0.02 mm by small forces up to 1 N. Under larger vertical forces, the tooth is moved in an apical direction because venous fluid and blood of the periodontal structures is pushed towards the venous lacunae and the cancellous bone. It takes 1 2 minutes before the tooth returns to its normal position after releasing an applied occlusal force. This explains the fact that tooth mobility is decreased after chewing, and the tooth is then in a more apical position. In healthy conditions, the teeth move in a horizontal plane, under a force of 500 g, as follows (Mühlemann 1960): incisors: mm canines: mm premolars: mm molars: mm. Tooth mobility can also be estimated using the Periotest (Siemens AG, Germany), an electronic device that measures the reaction of the periodontium to a defined percussion force. Under higher occlusal loads, the forces are transmitted to the bone, with slight deformation of the alveolar process as a result. The force is also transmitted to neighbouring teeth through the interproximal contacts. Evaluation of tooth mobility The exact measurement of individual tooth mobility (periodontometry) is necessary for research purposes. Clinically, an estimation of tooth mobility is performed by loading the tooth in an anterolateral direction with two instruments. Four possible grades of tooth mobility are considered: grade 0: physiological mobility grade 1: increased mobility but less than 1 mm in total grade 2: pronounced increase; more than 1 mm in total grade 3: more than 1 mm displacement combined with a displacement in vertical direction (tooth can be intruded). Increased mobility can also be observed on radiographs: there is a widening of the periodontal space without vertical or angular bone resorption and without increased probing depth of the periodontal pocket (Figs 9.2 and 9.3). Aetiological factors of hyper- and hypomobility Fig. 9.1 Physiological tooth mobility in a healthy periodontium is determined by the bone height, the form of the root and the magnitude of the applied force, and the extent is limited. Excessive occlusal forces or premature contacts on teeth are the primary aetiologic factors for hypermobility. There is an increased mobility during pregnancy because of the increase in the fluid content of the periodontal structures, an increased vascularity and a proliferation of 84
3 OCCLUSION AND PERIODONTAL HEALTH 9 Fig. 9.2 Forces applied in one direction on the tooth give a widening of the periodontal ligament at the bone margin at the other side and in the apical area on the same side of the force. capillaries into the periodontal tissues. Systemic diseases such as non-hodgkin s lymphoma, scleroderma and Cushing s syndrome may lead to increased mobility. Hypermobility may be observed in cases of severe periodontal inflammation (periodontitis), teeth with a healthy but reduced periodontal support (that is, in patients after successful periodontal treatment), or in the first weeks after periodontal surgery. Normal physiological mobility is decreased in the elderly and in the absence of antagonist teeth. In cases of severe bruxism and clenching the mobility decreases ( ankylosing effect ). Without antagonists and therefore without functional stimulation, teeth will either overerupt or become ankylosed. The periodontal ligament becomes thinner and non-functional. Evaluation of the changes in occlusal mobility can be helpful in the diagnosis of occlusal dysfunction, parafunction and in the evaluation of occlusal treatment procedures. TYPES OF OCCLUSAL FORCES The reaction of the bone and ligament depends on the magnitude, duration and direction of the forces. Different types of occlusal forces can be recognised: Physiologically normal occlusal forces in chewing and swallowing: small and rarely exceeding 5 N. They provide the positive stimulus to maintaining the periodontium and the alveolar bone in a healthy and functional condition. Impact forces: mainly high but of short duration. The periodontium can sustain high forces during a short period; however, forces exceeding the viscoelastic buffer capacities of the periodontal ligament will result in fracture of tooth and bone. Continuous forces: very low forces (for example, orthodontic forces), but continuously applied in one direction are effective in displacing a tooth by remodelling the alveolus. Jiggling forces: intermittent forces in two different directions (premature contacts on, for example, crowns, fillings) result in widening of the alveolus and in increased mobility. TRAUMA FROM OCCLUSION Fig. 9.3 Widening of the periodontal space as observed on radiographs. Trauma from occlusion has been defined as structural and functional changes in the periodontal tissues caused by excessive occlusal forces. Some of these changes are adaptive, while others should be considered pathological. Occlusal trauma can be acute if caused by external impact 85
4 SECTION 3 CLINICAL PRACTICE AND THE OCCLUSION A B C Fig. 9.4 Clinical example of a primary occlusal trauma in a young girl with a deep bite and a persistent deciduous canine. A Frontal view showing the deep bite. B Palatal view, with the primary trauma on the palatal mucosa caused by the lower canine. When the patient closes, the lower canine is forced in between the upper canine and the central and lateral incisors. C This traumatic occlusion causes the widening of the periodontal space, as seen on the radiograph. forces or chronic if caused by internal occlusal factors (premature contacts, grinding). Chronic occlusal trauma can be understood as primary and secondary trauma. Occlusal trauma is the overall process by which traumatic occlusion (that is, an occlusion that produces forces that cause injury) produces injury to the attachment apparatus. Primary occlusal trauma Primary occlusal trauma is caused by excessive and nonphysiological forces exerted on teeth with a normal, healthy and non-inflamed periodontium. The forces may be exerted on the periodontal structures in one direction (orthodontic forces) or as jiggling forces. Forces in one direction: orthodontic forces Forces in one direction cause tipping of the tooth in the opposite direction or tooth displacement parallel to the force resulting in a bodily movement. In the periodontal ligament, zones of compression and zones of tension are found, inducing increased resorption. The clinical result is a (temporary) increased mobility. However, there are no changes in the supracrestal fibres, no loss of periodontal attachment, or an increased probing pocket depth. The increased tooth mobility is functional adaptation to the forces exerted on that tooth. If the forces are too high and above the adaptation level, an aseptic necrosis in the tension zone of the periodontal ligament occurs, characterised by hyalinisation. In the compression zone, pressure stimulates osteoclasts in the adjacent bone and the alveolar wall is resorbed until a new connection is formed with the hyalinised bone ( undermining resorption ). In the tension zone, bone apposition and rupture of the collagen fibres occur. After removal of the force the periodontal ligament is reorganised and after some time develops a normal histological appearance. If the applied forces are too high, root resorption occurs in the middle of the hyalinised tissues. This resorption continues for a variable time, resulting in shorter roots, frequently seen after orthodontic treatment. Jiggling forces Jiggling forces, coming from different and opposite directions, cause more complex histological changes in the ligament. Theoretically the same events (hyalinisation, resorption) occur, however, they are not clearly separated. There are no distinct zones of pressure and tension. Histologically, there is apposition and resorption on either side of the periodontal ligament, resulting in a widening of the periodontal space (Fig. 9.4). This may be observed on radiographs. This phenomenon explains the increased mobility without pocket formation, migration and tipping. The clinical phenomena are not only dependent on the magnitude of the forces, but also on the crown root relationship, the position in the arch, the direction of the long axis, and the pressure of tongue and cheek musculature (Fig. 9.5). The interarch relationship (for example, deep bite) influences the extent of the trauma caused by jiggling forces. The hypermobility is found as long as the forces are exerted on the tooth: there is no adaptation. Hypermobility is therefore not a sign of an ongoing process, but may be the result of a previous jiggling force. The long-term prognosis of teeth with increased mobility is poor, and is a complicating factor if they are used as abutment in prosthodontic reconstruction. Successful periodontal treatment leads to healthy but reduced periodontal structures. Jiggling forces exerted on the teeth in this condition result in a pronounced increase in tooth mobility because the point of rotation (fulcrum) is closer to the apex than normal. This is uncomfortable for 86
5 OCCLUSION AND PERIODONTAL HEALTH 9 Fig. 9.5 Under jiggling forces in a healthy periodontium, the periodontal ligament space is widened, resulting in more tooth mobility but not in marginal bone resorption or attachment loss. Fig. 9.6 In cases of a healthy but reduced periodontium the tooth mobility (measured at the crown level) is increased for the same force, as compared with a tooth with a complete periodontium, because of the more apical position of the fulcrum. the patient and might be an indication for splinting of teeth (Fig. 9.6). Secondary occlusal trauma Secondary trauma from occlusion is defined as the trauma caused by excessive and premature occlusal forces on teeth with an inflamed periodontium. A number of animal experiments and clinical epidemiological studies investigated the role of occlusion in the pathogenesis of periodontitis. In his original studies in the 1960s, Glickman (Glickman & Smulow 1967) formulated the hypothesis that premature contacts and excessive occlusal forces could be a co-factor in the progression of periodontal disease by changing the pathway and spread of inflammation into the deeper periodontal tissues. Glickman hypothesised that the gingival zone was a zone for irritation by the microbial plaque; the supracrestal fibres were then considered to be a zone of co-destruction under the influence of a faulty occlusion (Fig. 9.7). Clinically, vertical bone resorption and the formation of infrabony defects should be an indication for occlusal trauma. Animal experiments Animal experiments investigating the influence of a faulty occlusion on the progression of periodontal disease were published by Swedish investigators between 1970 A B Fig. 9.7 Role of traumatic occlusion in the progression of periodontitis according to Glickman & Smulow (1967). In the presence of microbial plaque and inflammation, A is the zone of irritation and B the zone of co-destruction where the prematurities are co-destructive by changing the inflammatory pathway. and 1980 using the beagle dog model, and by American investigators using the squirrel monkey model. In spite of the many remaining questions and controversies, few animal studies have been published since then. From these studies the following conclusions may be drawn: 87
6 SECTION 3 CLINICAL PRACTICE AND THE OCCLUSION In the absence of marginal inflammation, jiggling forces do not induce more bone resorption nor a shift of the epithelial attachment in an apical direction. In the case of marginal inflammation (gingivitis), occlusal overload has no influence. Jiggling forces on teeth with periodontal disease result in more bone loss and more loss of connective tissue attachment (Ericsson & Lindhe 1982). Jiggling forces induce a faster shift of microbial plaque in the apical direction in the pocket (Fig. 9.8). One single trauma does not influence the pathogenesis; the forces have to be chronic. Treatment of periodontal inflammation without elimination of the premature contacts results in decreased tooth mobility, an increase in bone density, but no change of bone level. After periodontal treatment with scaling and rootplaning, the presence or absence of prematurities have no influence on the microbial repopulation of the deepened pockets. It must be mentioned that some animal studies did not reach the same definitive conclusions, due to differences in experimental setup and different animal models. The results of experimental animal studies cannot therefore be directly extrapolated to the human situation. Fig. 9.8 In applying jiggling forces on an inflamed, untreated periodontium with existing infrabony pockets (A), the bone destruction is accelerated and the bacteria move more apically (B). Clinical epidemiological studies Given the complexity of the occlusal and periodontal interaction and the multifactorial aspect of the pathology, very few human studies have been published. Most studies have a limited number of subjects and the results are analysed on a subject basis rather than on a tooth basis. The studies have been recently summarised by Hallmon (Hallmon 1999). A number of cross-sectional epidemiological studies found either no relationship between the presence of premature contacts and increased probing depth or bone loss, while others reported that mobility and radiographic evidence of a widened periodontal ligament were associated with increased pocket depth, attachment loss and bone loss (Jin & Cao 1992). More recent longitudinal studies (Harrel & Nunn 2001) found that teeth with premature contacts at initial examination had a deeper probing pocket depth, an increased mobility and a worse prognosis. At the 1 year examination, teeth without premature contacts originally, or teeth where premature contacts had been removed, showed a 66% reduced chance of a worsening periodontal situation. After a few months, teeth with prematurities showed an increased probing depth compared with the teeth receiving occlusal adjustment. It was concluded that premature contacts are a catalyst in the progression of periodontal disease. It has also been shown that in the same patient more periodontopathogens are found in pockets around hypermobile teeth, than in teeth with normal mobility. This can lead to the hypothesis that the increased mobility changes the ecosystem in the pocket, favouring growth of these bacteria. TRAUMA FROM OCCLUSION AND IMPLANTS Endosseous implants have no periodontal ligament as an intimate implant alveolar bone contact exists ( functional ankylosis ). Implant failure can occur not only because of bacterial infection (peri-implantitis) but also because of occlusal overload (biomechanical failure) in combination with immunological host factors (Esposito et al 1998). Occlusal overload results in osseodisintegration over the complete implant surface without clinically detectable pocket formation or signs of inflammation. Often the implant has no increased mobility in spite of pronounced bone resorption along its entire surface. Clinical measurement of implant mobility is not an accurate tool for evaluating osseointegration or disintegration of an implant until late in the pathological process. If increased implant mobility occurs, osseointegration is by then usually destroyed. 88
7 OCCLUSION AND PERIODONTAL HEALTH 9 GINGIVAL TRAUMA FROM OCCLUSION Gingival recession may be provoked by direct contact of the teeth with the gingiva, as in severe overbite, where the upper incisors damage the buccal gingiva of the lower incisors. This problem is not easy to solve and may involve orthodontic treatment, orthognathic surgery or extensive prosthetic rehabilitation requiring an increase in vertical dimension. It has been stated that gingival recession occurs with functional overload and/or premature contacts, as in the buccal surface of upper canines where there is a steep lateral canine guidance. Those cervical surfaces also show enamel abfraction. There is still controversy regarding whether or not overload is an aetiological factor in the recession, and consequently whether or not the occlusion and the lateral guidance should be changed. PRACTICAL CLINICAL CONCLUSIONS AND GUIDELINES In a healthy non-inflamed dentition, traumatic occlusion leads to hypermobility of some teeth; if hypermobility, radiological widening of periodontal ligament space or pronounced cervical abfraction is found, the occlusion should be analysed and corrected. Simple uncomplicated, non-time-consuming procedures are in most cases adequate to restore a physiological situation and to reduce hypermobility. In cases of a healthy but reduced periodontium, increased mobility may also be reduced by occlusal adjustment; it should be recognised that tooth mobility in such cases, based on the mechanical situation, is nevertheless increased. It may be necessary to splint the teeth to increase the functional comfort and to avoid direct fracture. This may include very mobile teeth with a healthy but reduced periodontium, but complicates the clinical procedures. In cases of secondary occlusal trauma, treating the inflammation is of primary importance and should be the first step in treatment planning. From the literature it can be concluded that prematurities may play a role in the progression of the periodontitis. A simple correction of the occlusion, if necessary, should be included in the initial phase of periodontal treatment. This results in more gain in attachment level during periodontal treatment, and may contribute to better healing of periodontal tissues. There are some indications that removing premature tooth contacts improves the prognosis of periodontally involved tissues. If some teeth do not react to conventional periodontal treatment as expected, further investigation should not only include periodontal re-examination and microbiological testing, but also more extensive occlusal analysis. As implant overload leads to bone resorption without the warning signal of inflammation, deep peri-implantitis pockets or (in the early stage) increased mobility, evaluation of the occlusion and radiographs should be included in regular maintenance programmes. References Ericsson I, Lindhe J 1982 The effect of long standing jiggling on the experimental marginal periodontitis in the beagle dog. Journal of Clinical Periodontology 9:495 Esposito M, Hirsch J M, Lekholm U, Thomsen P 1998 Biological factors contributing to failures of osseointegrated implants. II. Etiopathogenesis. European Journal of Oral Sciences 106: Glickman I, Smulow I B 1967 Further observation on the effects of trauma from occlusion. Journal of Periodontology 38:280 Hallmon W 1999 Occlusal trauma: effect and impact on the periodontium. Annals of Periodontology 4:102 Harrel S K, Nunn M E 2001 The effect of occlusal discrepancies upon periodontitis. II. Relationships of occlusal treatment to the progression of periodontal disease. Journal of Periodontology 72: Jin L, Cao C 1992 Clinical diagnosis of trauma from occlusion and its relation with severity of periodontitis. Journal of Clinical Periodontology 19:92 97 Mühlemann H R 1960 Ten years of tooth mobility measurements. Journal of Periodontology 31: Further reading Beertsen W, McCulloch C A G, Sodek J 1997 The periodontal ligament: a unique, multifunctional connective tissue. Periodontology :20 40 Burgett F G, Ramfjord S P, Nissle R R et al 1992 A randomized trial of occlusal adjustment in the treatment of periodontitis. Journal of Clinical Periodontology 19: Gher M 1996 Non surgical pocket therapy: dental occlusion. Annals of Periodontology 1: Giargia M, Lindhe J 1997 Tooth mobility and periodontal disease. Journal of Clinical Periodontology 24: Grant D A, Flynn M J, Slots J 1995 Periodontal microbiota of mobile and non-mobile teeth. Journal of Periodontology 66: Kaufman H, Carranza F A, Enders B, Neuman M G, Murphy N 1984 Influence of trauma from occlusion on the bacterial re-population of periodontal pockets in dogs. Journal of Periodontology 55:86 92 McCulloch C A G, Kekic P, McKee M D 2000 Role of physical forces in regulating the form and function of the periodontal ligament. Periodontology 24:56 72 Polson A M II 1974 Co-destructive factors of periodontitis and mechanically produced injury. Journal of Periodontal Research 9: Schulte W, Hoedt B, Lukas D, Maune M, Steppeler M 1992 Periotest for measuring periodontal characteristics. Correlation with periodontal bone loss. Journal of Periodontal Research 27: Wang H, Burgett F G, Shyt Y, Ramfjord S 1994 The influence of molar furcation involvement and mobility on future clinical periodontal attachment loss. Journal of Periodontology 65:
8
The periodontium attempts to accommodate to the forces exerted to the crown. This adaptive capacity varies in different persons and in the same person
 The periodontium attempts to accommodate to the forces exerted to the crown. This adaptive capacity varies in different persons and in the same person at different times. The effect of occlusal forces
The periodontium attempts to accommodate to the forces exerted to the crown. This adaptive capacity varies in different persons and in the same person at different times. The effect of occlusal forces
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Periodontal ligament
 Periodontal ligament The periodontium The periodontium includes: The gingiva Cementum Periodontal ligament Alveolar bone Def: The periodontal ligament is the dense fibrous connective tissue that occupies
Periodontal ligament The periodontium The periodontium includes: The gingiva Cementum Periodontal ligament Alveolar bone Def: The periodontal ligament is the dense fibrous connective tissue that occupies
Fundamental & Preventive Curvatures of Teeth and Tooth Development. Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L.
 Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Plaque and Occlusion in Periodontal Disease Wednesday, February 25, :54 AM
 Plaque and Occlusion in Periodontal Disease Wednesday, February 25, 2015 9:54 AM 1. The definition of Trauma From Occlusion: Primary TFO, Secondary TFO, and Combined TFO 2. Clinical and Radiographic signs
Plaque and Occlusion in Periodontal Disease Wednesday, February 25, 2015 9:54 AM 1. The definition of Trauma From Occlusion: Primary TFO, Secondary TFO, and Combined TFO 2. Clinical and Radiographic signs
Tooth eruption and movement
 Tooth eruption and movement Dr. Krisztián Nagy Diphydont dentition Deciduous dentition primary dentition Diphydont dentition Permanent dentition secondary dentition Mixed Dentition: Presence of both dentitions
Tooth eruption and movement Dr. Krisztián Nagy Diphydont dentition Deciduous dentition primary dentition Diphydont dentition Permanent dentition secondary dentition Mixed Dentition: Presence of both dentitions
Esthetic Crown Lengthening
 Esthetic Crown Lengthening Esthetic Crown Lengthening ACCELERATED OSTEOGENIC ORTHODOTNICS (WILKODONTICS) It is a technique developed by Wilko brothers. has roots in orthopedics, back to the early 1900s
Esthetic Crown Lengthening Esthetic Crown Lengthening ACCELERATED OSTEOGENIC ORTHODOTNICS (WILKODONTICS) It is a technique developed by Wilko brothers. has roots in orthopedics, back to the early 1900s
Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report
 Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition. By: Kimberly Hawrylyshyn
 Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
FRACTURES AND LUXATIONS OF PERMANENT TEETH
 FRACTURES AND LUXATIONS OF PERMANENT TEETH 1. Treatment guidelines and alveolar bone Followup Procedures INFRACTION Clinical findings Radiographic findings Treatment Follow-Up Favorable Outcome Unfavorable
FRACTURES AND LUXATIONS OF PERMANENT TEETH 1. Treatment guidelines and alveolar bone Followup Procedures INFRACTION Clinical findings Radiographic findings Treatment Follow-Up Favorable Outcome Unfavorable
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Eruption and Shedding of Teeth
 Eruption and Shedding of Teeth Mixed Dentition: Presence of both dentitions Figure from Ten Cate s Oral Histology, Ed., Antonio Nanci, 6 th edition Tooth eruption is the process by which developing teeth
Eruption and Shedding of Teeth Mixed Dentition: Presence of both dentitions Figure from Ten Cate s Oral Histology, Ed., Antonio Nanci, 6 th edition Tooth eruption is the process by which developing teeth
Core build-up using post systems
 Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Root Proximity Characteristics and Type of Alveolar Bone Loss: A Case-control Study
 Journal of the International Academy of Periodontology 011 13/3: 73-79 Root Proximity Characteristics and Type of Alveolar Bone Loss: A Case-control Study 1 1 1 Maria-Anna Loukideli, Alexandra Tsami, Eudoxie
Journal of the International Academy of Periodontology 011 13/3: 73-79 Root Proximity Characteristics and Type of Alveolar Bone Loss: A Case-control Study 1 1 1 Maria-Anna Loukideli, Alexandra Tsami, Eudoxie
Infrabony Pockets and Reduced Alveolar Bone Height in Relation to Orthodontic Therapy
 > Home I TOC I Bndex Infrabony Pockets and Reduced Alveolar Bone Height in Relation to Orthodontic Therapy Birgit Thilander Experimental animal studies have shown that orthodontic movement
> Home I TOC I Bndex Infrabony Pockets and Reduced Alveolar Bone Height in Relation to Orthodontic Therapy Birgit Thilander Experimental animal studies have shown that orthodontic movement
ABSTRACT INTRODUCTION
 ABSTRACT Purpose: Evaluation of stress distribution maxilla under parafunctional loading on short dental implant using 3-dimensional (3D) finite element models. Material and method: 3D maxillary and mandibular
ABSTRACT Purpose: Evaluation of stress distribution maxilla under parafunctional loading on short dental implant using 3-dimensional (3D) finite element models. Material and method: 3D maxillary and mandibular
ORTHODONTICS Treatment of malocclusion Assist.Lec.Kasem A.Abeas University of Babylon Faculty of Dentistry 5 th stage
 Lec: Treatment of class I malocclusion Class I occlusion can be defined by Angles, classification as the mesiobuccal cusp of the upper 1 st permanent molar occlude with the developmental groove of the
Lec: Treatment of class I malocclusion Class I occlusion can be defined by Angles, classification as the mesiobuccal cusp of the upper 1 st permanent molar occlude with the developmental groove of the
ANATOMY OF THE PERIODONTIUM. Dr. Fatin Awartani
 ANATOMY OF THE PERIODONTIUM Part II Cementum and Alveolar bone Associate Professor Periodontal division King Saud university Cementum Calcified mesenchymal tissue that forms the outer covering of the anatomic
ANATOMY OF THE PERIODONTIUM Part II Cementum and Alveolar bone Associate Professor Periodontal division King Saud university Cementum Calcified mesenchymal tissue that forms the outer covering of the anatomic
Everything You Wanted to Know About Extractions but Were Afraid to Ask
 Everything You Wanted to Know About Extractions but Were Afraid to Ask Tooth extraction is a surgical procedure with serious potential complications and should only be performed by a trained veterinarian.
Everything You Wanted to Know About Extractions but Were Afraid to Ask Tooth extraction is a surgical procedure with serious potential complications and should only be performed by a trained veterinarian.
Principle of Occlusion
 Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
The treatment of destructive periodontal disease, due to specific periodontopathic
 1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
COMBINED PERIODONTAL-ENDODONTIC LESION. By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur
 COMBINED PERIODONTAL-ENDODONTIC LESION By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur Differential diagnosis For differential diagnostic purposed the endo-perio
COMBINED PERIODONTAL-ENDODONTIC LESION By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur Differential diagnosis For differential diagnostic purposed the endo-perio
WHAT IS THE PURPOSE OF WHAT WE DO? TEAM PERIODONTICS: WORKING TOGETHER TO IMPROVE PATIENT CARE YOU ARE THE PERIODONTISTS IN YOUR PRACTICE!
 Setter Periodontics 2075 SW 1 st Ave #2L Portland, OR 97201 503-222-9961 michael@setterperio.com WHAT IS THE PURPOSE OF WHAT WE DO? Gum Gardeners Study Club 2.27.17 TEAM PERIODONTICS: WORKING TOGETHER
Setter Periodontics 2075 SW 1 st Ave #2L Portland, OR 97201 503-222-9961 michael@setterperio.com WHAT IS THE PURPOSE OF WHAT WE DO? Gum Gardeners Study Club 2.27.17 TEAM PERIODONTICS: WORKING TOGETHER
IMPACTED CANINES. Unfortunately, this important tooth is the second most common tooth to be impacted after third molars
 IMPACTED CANINES After we talked about impacted third molars, today we ll discuss about maxillary impacted canines in upper dental arch, how to manage these cases as a dental surgeon. You will study about
IMPACTED CANINES After we talked about impacted third molars, today we ll discuss about maxillary impacted canines in upper dental arch, how to manage these cases as a dental surgeon. You will study about
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
Diagnosis. overt Examination. Definitive Examination. History. atient interview. Personal History. Clinical Examination.
 Diagnosis overt Examination History Definitive Examination atient interview Personal History Mental Attitude Medical History Dental History Clinical Examination Extra Oral Oral Radiographic Evaluation
Diagnosis overt Examination History Definitive Examination atient interview Personal History Mental Attitude Medical History Dental History Clinical Examination Extra Oral Oral Radiographic Evaluation
OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC
 Oral Anatomy and Occlusion Prosthodontic Component OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC By: Dr. Babak Shokati, DDS, MSc. MSc. Prosthodontics Definition of Masticatory System by The Academy of Prosthodontics
Oral Anatomy and Occlusion Prosthodontic Component OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC By: Dr. Babak Shokati, DDS, MSc. MSc. Prosthodontics Definition of Masticatory System by The Academy of Prosthodontics
14/09/15. Assessment of Periodontal Disease. Outline. Why is Periodontal assessment needed? The Basics of Periodontal assessment
 Assessment of Periodontal Disease Dr Wendy Turner Outline Why is Periodontal assessment needed? The Basics of Periodontal assessment Probing: Basic Periodontal Examination for adults and children. Detailed
Assessment of Periodontal Disease Dr Wendy Turner Outline Why is Periodontal assessment needed? The Basics of Periodontal assessment Probing: Basic Periodontal Examination for adults and children. Detailed
Multidisciplinary treatment in a case of loss of posterior vertical dimension
 J. Stomat. Occ. Med. (2014) 7:25 31 DOI 10.1007/s12548-013-0096-5 Multidisciplinary treatment in a case of loss of posterior vertical dimension Teresa Pinho Ana Norton Manuel Neves Received: 25 June 2013
J. Stomat. Occ. Med. (2014) 7:25 31 DOI 10.1007/s12548-013-0096-5 Multidisciplinary treatment in a case of loss of posterior vertical dimension Teresa Pinho Ana Norton Manuel Neves Received: 25 June 2013
Managing the failing dentition
 C L I N I C A L Managing the failing dentition Kamal Suri 1 Increasingly, the numbers of patients walking through the doors of our practices are those whose dentition is slowly in decline. I am presented
C L I N I C A L Managing the failing dentition Kamal Suri 1 Increasingly, the numbers of patients walking through the doors of our practices are those whose dentition is slowly in decline. I am presented
Teeth under High Occlusal Force may Reflect Occlusal Trauma-associated Periodontal Conditions in Subjects with Untreated Chronic Periodontitis
 under High Occlusal Force may Reflect Occlusal Trauma-associated Periodontal Conditions in Subjects with Untreated Chronic Periodontitis Shuang Ying ZHOU 1, Hina MAHMOOD 2, Cai Fang CAO 1, Li Jian JIN
under High Occlusal Force may Reflect Occlusal Trauma-associated Periodontal Conditions in Subjects with Untreated Chronic Periodontitis Shuang Ying ZHOU 1, Hina MAHMOOD 2, Cai Fang CAO 1, Li Jian JIN
Tooth Retained Implant: No More an Oxymoron
 بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
Implant Occlusion. Dora Kompotiati Boris Stein David Wilson
 Implant Occlusion Dora Kompotiati Boris Stein David Wilson Disclaimer Currently, there is no evidence-based, implant-specific concept of occlusion Future studies are needed to clarify the relationship
Implant Occlusion Dora Kompotiati Boris Stein David Wilson Disclaimer Currently, there is no evidence-based, implant-specific concept of occlusion Future studies are needed to clarify the relationship
You know you would like to stop swearing at the computer after each shot. Troubleshooting oral radiography
 You know you would like to stop swearing at the computer after each shot Troubleshooting oral radiography Goals of oral radiology Achieve diagnostic images of the teeth and surrounding bone. Images should
You know you would like to stop swearing at the computer after each shot Troubleshooting oral radiography Goals of oral radiology Achieve diagnostic images of the teeth and surrounding bone. Images should
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
NATIONAL EXAMINING BOARD FOR DENTAL NURSES
 NATIONAL EXAMINING BOARD FOR DENTAL NURSES NATIONAL DIPLOMA EXAMINATION DENTAL CHARTING NEBDN is a limited company registered in England & Wales No. 5580200 Registered with the Charity Commisioners No.
NATIONAL EXAMINING BOARD FOR DENTAL NURSES NATIONAL DIPLOMA EXAMINATION DENTAL CHARTING NEBDN is a limited company registered in England & Wales No. 5580200 Registered with the Charity Commisioners No.
ELIMINATE POCKETS. Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease
 ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery
 CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
THE SYNDROME OF THE DISTAL MOLAR TOOTH
 Prosthetic Dentistry THE SYNDROME OF THE DISTAL MOLAR TOOTH V. Burlui 1, Carmen Stadoleanu 1, Corina Cristescu 2 1 Prof. PhD, Dept. Prosthetic Dentistry, Fac. Med. Dent., U. Apollonia of Iasi 1 Prof. PhD,
Prosthetic Dentistry THE SYNDROME OF THE DISTAL MOLAR TOOTH V. Burlui 1, Carmen Stadoleanu 1, Corina Cristescu 2 1 Prof. PhD, Dept. Prosthetic Dentistry, Fac. Med. Dent., U. Apollonia of Iasi 1 Prof. PhD,
6610 NE 181st Street, Suite #1, Kenmore, WA
 660 NE 8st Street, Suite #, Kenmore, WA 9808 www.northshoredentalacademy.com.08.900 READ CHAPTER The Professional Dental Assistant (p.-9) No Key Terms Recall Questions:,,,, and 6 CLASS SYLLABUS DAY READ
660 NE 8st Street, Suite #, Kenmore, WA 9808 www.northshoredentalacademy.com.08.900 READ CHAPTER The Professional Dental Assistant (p.-9) No Key Terms Recall Questions:,,,, and 6 CLASS SYLLABUS DAY READ
Arrangement of the artificial teeth:
 Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
The fundamental biomechanics of oral implants. Dr. Szűcs Attila
 The fundamental biomechanics of oral implants Dr. Szűcs Attila Physical elements I. Mechanics solving of technical problems by physical laws»» investigation of prosthesis and the connection to abutments
The fundamental biomechanics of oral implants Dr. Szűcs Attila Physical elements I. Mechanics solving of technical problems by physical laws»» investigation of prosthesis and the connection to abutments
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
PERIODONTAL CASE PRESENTATION - 1
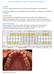 PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
Dental Morphology and Vocabulary
 Dental Morphology and Vocabulary Palate Palate Palate 1 2 Hard Palate Rugae Hard Palate Palate Palate Soft Palate Palate Palate Soft Palate 4 Palate Hard Palate Soft Palate Maxillary Arch (Maxilla) (Uppers)
Dental Morphology and Vocabulary Palate Palate Palate 1 2 Hard Palate Rugae Hard Palate Palate Palate Soft Palate Palate Palate Soft Palate 4 Palate Hard Palate Soft Palate Maxillary Arch (Maxilla) (Uppers)
Periapical Radiography
 Periapical Radiography BARBARA E. DIXON B.D.S., M.Sc., D.P.D.S. Main Indications Detection of Apical infection/inflammation Assessment of the periodontal status After trauma Assessment of Unerupted teeth
Periapical Radiography BARBARA E. DIXON B.D.S., M.Sc., D.P.D.S. Main Indications Detection of Apical infection/inflammation Assessment of the periodontal status After trauma Assessment of Unerupted teeth
Combined Periodontal and Prosthetic Treatment of Patients With Advanced Periodontal Disease
 A Longitudinal Study of Combined Periodontal and Prosthetic Treatment of Patients With Advanced Periodontal Disease by Sture Nyman Jan Lindhe Clinical and laboratory research endeavors have revealed unanimously
A Longitudinal Study of Combined Periodontal and Prosthetic Treatment of Patients With Advanced Periodontal Disease by Sture Nyman Jan Lindhe Clinical and laboratory research endeavors have revealed unanimously
It is well-known that osseointegrated implants do not
 Infraposition of Implant-Retained Maxillary Incisor Crown Placed in an Adult Patient: Case Report Roberto Cocchetto, MD, DDS 1 /Luigi Canullo, DDS 2 /Renato Celletti, MD, DDS 3 Several studies have clearly
Infraposition of Implant-Retained Maxillary Incisor Crown Placed in an Adult Patient: Case Report Roberto Cocchetto, MD, DDS 1 /Luigi Canullo, DDS 2 /Renato Celletti, MD, DDS 3 Several studies have clearly
Sample Case #1. Disclaimer
 ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
Dr Mohammed Alfarsi Page 1 9 December Principles of Occlusion
 Dr Mohammed Alfarsi Page 1 9 December 2013 Principles of Occlusion Overview: The occlusion is a very large, yet easy to manage once properly understood, topic. Thus, no one handout is enough to fully understand
Dr Mohammed Alfarsi Page 1 9 December 2013 Principles of Occlusion Overview: The occlusion is a very large, yet easy to manage once properly understood, topic. Thus, no one handout is enough to fully understand
Dental Anatomy and Occlusion
 CHAPTER 53 Dental Anatomy and Occlusion Ma Lou C. Sabino DDS, and Emily G. Smythe, DDS What numerical system is used most commonly in the United States for designating the adult dentition? Pediatric dentition?
CHAPTER 53 Dental Anatomy and Occlusion Ma Lou C. Sabino DDS, and Emily G. Smythe, DDS What numerical system is used most commonly in the United States for designating the adult dentition? Pediatric dentition?
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Mesial Step Class I or Class III Dependent upon extent of step seen clinically and patient s growth pattern Refer for early evaluation (by 8 years)
 Orthodontics and Dentofacial Development Overview Development of Dentition Treatment Retention and Relapse Growth of Naso-Maxillary Complex Develops postnatally entirely by intramenbranous ossification
Orthodontics and Dentofacial Development Overview Development of Dentition Treatment Retention and Relapse Growth of Naso-Maxillary Complex Develops postnatally entirely by intramenbranous ossification
6. Timing for orthodontic force
 6. Timing for orthodontic force Orthodontic force is generally less than 300gm, so early mechanical stability is enough for immediate orthodontic force. There is no actually difference in success rate
6. Timing for orthodontic force Orthodontic force is generally less than 300gm, so early mechanical stability is enough for immediate orthodontic force. There is no actually difference in success rate
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Adult performance horse dental care in, 505 519 bit seat reduction in, 514 515 canine teeth disorders, 515 diagnostic nerve blocks in,
Index Note: Page numbers of article titles are in boldface type. A Adult performance horse dental care in, 505 519 bit seat reduction in, 514 515 canine teeth disorders, 515 diagnostic nerve blocks in,
Interdisciplinary management of Impacted teeth in an adult with Orthodontics & Free Gingival graft : A Case Report
 Original article: Interdisciplinary management of Impacted teeth in an adult with Orthodontics & Free Gingival graft : A Case Report Dr Renuka Patel, Dr Falguni Mehta, Dr. Ashish Pandey Assistant Professor,
Original article: Interdisciplinary management of Impacted teeth in an adult with Orthodontics & Free Gingival graft : A Case Report Dr Renuka Patel, Dr Falguni Mehta, Dr. Ashish Pandey Assistant Professor,
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Root resorptions are not multifactorial, complex, controversial or polemical!
 O r t h o d o n t i c I n s i g h t The concept of root resorptions or Root resorptions are not multifactorial, complex, controversial or polemical! Alberto Consolaro* Abstract The mechanisms of root resorptions
O r t h o d o n t i c I n s i g h t The concept of root resorptions or Root resorptions are not multifactorial, complex, controversial or polemical! Alberto Consolaro* Abstract The mechanisms of root resorptions
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Alveolar Bone Remodeling and Development after Immediate Orthodontic Root Movement
 Journal of Dental Health, Oral Disorders & Therapy Alveolar Bone Remodeling and Development after Immediate Orthodontic Root Abstract Introduction: Adult orthodontics is rapidly expanding primarily due
Journal of Dental Health, Oral Disorders & Therapy Alveolar Bone Remodeling and Development after Immediate Orthodontic Root Abstract Introduction: Adult orthodontics is rapidly expanding primarily due
Concepts of occlusion Balanced occlusion. Monoplane occlusion. Lingualized occlusion. Figure (10-1)
 Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Examination of teeth and gingiva
 Examination of teeth and gingiva Siriporn Chattipakorn, DDS, PhD. SUBJECTIVE HISTORY Chief complaint In patient s own words My tooth hurts when I chew hard foods I can t drink cold drink I have bad breath
Examination of teeth and gingiva Siriporn Chattipakorn, DDS, PhD. SUBJECTIVE HISTORY Chief complaint In patient s own words My tooth hurts when I chew hard foods I can t drink cold drink I have bad breath
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
STABILITY OF IMPLANTS AND NATURAL TEETH MONTHS OF FUNCTION AS DETERMINED BY THE PERIOTEST OVER 60 CLINICAL
 CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
Finite Element Analysis of Dental Implant as Orthodontic Anchorage
 JCDP 10.5005/jp-journals-10024-1044 ORIGINAL RESEARCH Finite Element Analysis of Dental Implant as Orthodontic Anchorage Finite Element Analysis of Dental Implant as Orthodontic Anchorage Anirban Sarmah,
JCDP 10.5005/jp-journals-10024-1044 ORIGINAL RESEARCH Finite Element Analysis of Dental Implant as Orthodontic Anchorage Finite Element Analysis of Dental Implant as Orthodontic Anchorage Anirban Sarmah,
Primary Teeth Chapter 18. Dental Anatomy 2016
 Primary Teeth Chapter 18 Dental Anatomy 2016 Primary Teeth - Introduction Synonyms deciduous teeth, baby teeth, temporary teeth, milk teeth. There are 20 primary teeth, designated as A thru T in the Universal
Primary Teeth Chapter 18 Dental Anatomy 2016 Primary Teeth - Introduction Synonyms deciduous teeth, baby teeth, temporary teeth, milk teeth. There are 20 primary teeth, designated as A thru T in the Universal
Conventional immediate implant placement and immediate placement with socket-shield technique Which is better
 International Journal of Clinical Medicine Research 2014; 1(5): 176-180 Published online December 30, 2014 (http://www.aascit.org/journal/ijcmr) ISSN: 2375-3838 Conventional immediate implant placement
International Journal of Clinical Medicine Research 2014; 1(5): 176-180 Published online December 30, 2014 (http://www.aascit.org/journal/ijcmr) ISSN: 2375-3838 Conventional immediate implant placement
Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
 ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
ORTHODONTIC INITIAL ASSESSMENT FORM (OIAF) w/ INSTRUCTIONS
 Use the accompanying Tip Sheet and How to Score the Orthodontic Initial Assessment Form for guidance in completion of the assessment form. You will need this score sheet and a disposable ruler (or a Boley
Use the accompanying Tip Sheet and How to Score the Orthodontic Initial Assessment Form for guidance in completion of the assessment form. You will need this score sheet and a disposable ruler (or a Boley
Avoiding Restorative Failure
 Avoiding Restorative Failure Lee Ann Brady, DMD Dr. Brady has no relevant financial relationships to disclose. Presentation partially sponsored by DMG and GC America Friday, June 15, 2018 1:30pm 4:30pm
Avoiding Restorative Failure Lee Ann Brady, DMD Dr. Brady has no relevant financial relationships to disclose. Presentation partially sponsored by DMG and GC America Friday, June 15, 2018 1:30pm 4:30pm
AETIOLOGY AND SEVERITY OF GINGIVAL RECESSION AMONG YOUNG INDIVIDUALS IN BELGAUM DISTRICT IN INDIA
 AETIOLOGY AND SEVERITY OF GINGIVAL RECESSION AMONG YOUNG INDIVIDUALS IN BELGAUM DISTRICT IN INDIA V. Dodwad. Aetiology and severity of gingival recession among young individuals in Belgaum district in
AETIOLOGY AND SEVERITY OF GINGIVAL RECESSION AMONG YOUNG INDIVIDUALS IN BELGAUM DISTRICT IN INDIA V. Dodwad. Aetiology and severity of gingival recession among young individuals in Belgaum district in
Implant placement in the esthetic zone after completion of growth
 See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/281824061 Implant placement in the esthetic zone after completion of growth Article October
See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/281824061 Implant placement in the esthetic zone after completion of growth Article October
Small Animal Dentistry. Presented by: Rebecca Dodge, CVT
 Small Animal Dentistry Presented by: Rebecca Dodge, CVT Topics to be discussed Anatomy and oral examination Common dental problems for canines and felines Client knowledge and prevention tips Anatomy Dog
Small Animal Dentistry Presented by: Rebecca Dodge, CVT Topics to be discussed Anatomy and oral examination Common dental problems for canines and felines Client knowledge and prevention tips Anatomy Dog
Medical NBDE-II. Dental Board Exams Part I.
 Medical NBDE-II Dental Board Exams Part I http://killexams.com/exam-detail/nbde-ii Question: 149 Anatomically, the term "clinical root" can be defined as which of the following: A. The space in the tooth
Medical NBDE-II Dental Board Exams Part I http://killexams.com/exam-detail/nbde-ii Question: 149 Anatomically, the term "clinical root" can be defined as which of the following: A. The space in the tooth
Archived SECTION 14 - SPECIAL DOCUMENTATION REQUIREMENTS
 SECTION 14 - SPECIAL DOCUMENTATION REQUIREMENTS 14.1 CERTIFICATE OF MEDICAL NECESSITY...2 14.2 OPERATIVE REPORT...2 14.2.A PROCEDURES REQUIRING A REPORT...2 14.3 PRIOR AUTHORIZATION REQUEST...2 14.3.A
SECTION 14 - SPECIAL DOCUMENTATION REQUIREMENTS 14.1 CERTIFICATE OF MEDICAL NECESSITY...2 14.2 OPERATIVE REPORT...2 14.2.A PROCEDURES REQUIRING A REPORT...2 14.3 PRIOR AUTHORIZATION REQUEST...2 14.3.A
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics.
 In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
Longitudinal Measurements of Tooth Mobility during Orthodontic Treatment Using a Periotest
 Original Article Longitudinal Measurements of Tooth Mobility during Orthodontic Treatment Using a Periotest Eiji Tanaka, DDS, PhD a ; Kazuhiro Ueki, DDS, PhD b ; Mayu Kikuzaki, DDS c ; Eitaro Yamada, DDS
Original Article Longitudinal Measurements of Tooth Mobility during Orthodontic Treatment Using a Periotest Eiji Tanaka, DDS, PhD a ; Kazuhiro Ueki, DDS, PhD b ; Mayu Kikuzaki, DDS c ; Eitaro Yamada, DDS
Prof. Trimurni Abidin, drg.,m.kes.,sp.kg(k) Department of Conservative Dentistry Faculty of Dentistry University of Sumatera Utara 2013
 Biomechanics in Restorative Dentistry Prof. Trimurni Abidin, drg.,m.kes.,sp.kg(k) Department of Conservative Dentistry Faculty of Dentistry University of Sumatera Utara 2013 FORCES EXERTED DURING OCCLUSION
Biomechanics in Restorative Dentistry Prof. Trimurni Abidin, drg.,m.kes.,sp.kg(k) Department of Conservative Dentistry Faculty of Dentistry University of Sumatera Utara 2013 FORCES EXERTED DURING OCCLUSION
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Attachment G. Orthodontic Criteria Index Form Comprehensive D8080. ABBREVIATIONS CRITERIA for Permanent Dentition YES NO
 First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
Educational Training Document
 Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Immediate Implant Placement:
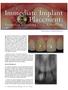 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
RAJ M. SAINI, DDS, MSD
 Restoring and Maintaining Periodontal Health with Orthodontic Treatment RAJ M. SAINI, DDS, MSD rajmsaini@yahoo.com Diplomate Of The American Board Of Orthodontics Clinical Professor Of Orthodontics New
Restoring and Maintaining Periodontal Health with Orthodontic Treatment RAJ M. SAINI, DDS, MSD rajmsaini@yahoo.com Diplomate Of The American Board Of Orthodontics Clinical Professor Of Orthodontics New
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Prosthetic V. Removable dentures I.
 Prosthetic V. Removable dentures I. Removable dentures Partial Complete (full) lenka.roubalikova@tiscali.cz 2 Prosthetic dentistry replacement of Damaged teeth reconstruction of the crown (inlays, crowns)
Prosthetic V. Removable dentures I. Removable dentures Partial Complete (full) lenka.roubalikova@tiscali.cz 2 Prosthetic dentistry replacement of Damaged teeth reconstruction of the crown (inlays, crowns)
APPENDIX A. MEDICAID ORTHODONTIC INITIAL ASSESSMENT FORM (IAF) You will need this scoresheet and a disposable ruler (or a Boley Gauge)
 APPENDIX A MEDICAID ORTHODONTIC INITIAL ASSESSMENT FORM (IAF) You will need this scoresheet and a disposable ruler (or a Boley Gauge) Name: _ I. D. Number: Conditions: 1. Cleft palate deformities 2. Deep
APPENDIX A MEDICAID ORTHODONTIC INITIAL ASSESSMENT FORM (IAF) You will need this scoresheet and a disposable ruler (or a Boley Gauge) Name: _ I. D. Number: Conditions: 1. Cleft palate deformities 2. Deep
Active Clinical Treatment Case 48
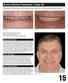 Active Clinical Treatment Case 48 Treating Clinicians: Drs. Jung Nam, Scott G. Cohen and Soojin Kim Initial smile Final smile Initial Presentation: January 2004 Age at Initial Presentation: 59 Active Treatment
Active Clinical Treatment Case 48 Treating Clinicians: Drs. Jung Nam, Scott G. Cohen and Soojin Kim Initial smile Final smile Initial Presentation: January 2004 Age at Initial Presentation: 59 Active Treatment
Periodontal Regeneration
 Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Evaluation of fixed partial denture in relation to gingival recession and other factors
 Evaluation of fixed partial denture in relation to gingival recession and other factors Faiza M. Abdul Ameer,B.D.S., M. Sc. (1) Zainab M. Abdul Ameer,B.D.S., M. Sc (2) ABSTRACT Background: Gingival recession
Evaluation of fixed partial denture in relation to gingival recession and other factors Faiza M. Abdul Ameer,B.D.S., M. Sc. (1) Zainab M. Abdul Ameer,B.D.S., M. Sc (2) ABSTRACT Background: Gingival recession
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
