A new implant for glaucoma
|
|
|
- Priscilla Holland
- 5 years ago
- Views:
Transcription
1 Brit. 1. Ophthal. (I97 I) 55, 28 A new implant for glaucoma Effect of removing implants A. C. B. MOLTENO Department of Ophthalmology, University of the Witwatersrand, and Baragwanath Hospital, Johannesburg, South Africa A new type of draining implant and the results of 47 operations have been discussed by Molteno (I969a). This implant consists of a translimbal tube rigidly attached to, and opening onto the external surface of a thin circular acrylic plate 8 mm. in diameter. This plate is curved to fit and is sutured firmly to sclera. When covered by a flap of conjunctiva and Tenon's capsule the plate forms the floor of a uniocular bleb in free communication with the anterior chamber, which cannot shrink to an area less than that of the plate. These implants controlled the intraocular pressure in 83 per cent. of patients with medically uncontrollable glaucoma and in all nine patients who received systemic steroids to reduce bleb fibrosis. Several of the earlier cases developed excessively fibrosed blebs, and 32 per cent. of them needed long-term local steroid medication to prevent attacks of iridocyclitis. The removal of implants was considered because, both in the rabbit and in man, a firm fibrous bleb formed around the implant so that it could be removed after a suitable lapse of time leaving both fistula and bleb intact. This removal would avoid corneal complications from the presence of the plastic and inflammatory reaction at points of relative movement between eye and implant (Molteno, I969b) which might be causing continuous deposition of fibrous tissue in the bleb wall. The blebs and fistulae left on removal could be expected to persist indefinitely since they would be lined by mature fibrous tissue which had already passed the stages of early contraction and late cicatrization (Walter and Israel, I965), during which shrinkage had been forcibly prevented by the implants. Furthermore, the large diameter and unilocular nature of the blebs would result in a given intraocular pressure exerting a far larger force stretching the bleb wall than would be the case with a smaller bleb, since the force stretching the wall of a vesicle is equal to the pressure within multiplied by its radius of curvature (Young, i805; Laplace, I807). The implants were accordingly removed from nineteen eyes. In three eyes (Cases 7 and 8) implants of Perspex were removed because they caused intractable uveitis; in one case a Stellon implant was removed because the bleb became overfibrosed and the glaucoma remained uncontrollable. In the remaining fifteen eyes, Stellon implants were removed in an attempt to improve adequate drainage and obviate the need for long-term local steroid medication. The surgical techniques used for removal and the results obtained are the subject of this communication. Received for publication July 3, I970 Address for reprints: Department of Ophthalmology, University of the Witwatersrand, Johannesburg, South Africa
2 New implant for glaucoma Design of clinical trial Patients with advanced glaucoma, in whom the visual acuity had fallen to 6/6o or less, were admitted to hospital for full evaluation and a trial of medical therapy. Those in whom the intraocular pressure could not be reduced to 20 mm. Hg had implants inserted. In most cases they remained in hospital until the removal of the implants between 5 weeks and 7 months later. Those discharged from hospital were readmitted for evaluation of their condition before the implant was removed. After the removal they remained in hospital for between 6 weeks and one year, after which they were followed as outpatients. Diagnosis and evaluation All cases were examined by the author and underwent a full ophthalmic examination, including applanation tonometry, tonography, and gonioscopy. The trial of medical therapy lasted at least 7 days. The following dosages were used: (i) Diamox 250 mg. four times a day with potassium supplement (2) Glycerol I50 ml. four times a day for up to 2 weeks (3) Gutt. Epitrate 2 per cent. four times a day (4) Gutt. Phospholine iodide o-o6-o- 125 per cent. or, if tolerated, Gutt. Tosmelin o 2s 5 per cent. Foliow-up During hospitalization, the patients were seen daily and had at least weekly slit-lamp examinations with applanation tonometry. At outpatient visits applanation tonometry and slit-lamp examination were routine and tonography was performed at longer intervals to confirm that the changes observed in the intraocular pressure were actually due to changes in outflow. Methods used The intraocular pressure was measured with a Goldmann applanation tonometer fitted to a Haag- Streit goo slit lamp. Tonography was carried out for 4 minutes using a Schwartzer electronic tonometer with continuous strip recorder (both instruments were regularly checked using the calibration standards provided by the makers). Surgical techniques TIME OF OPERATION It was soon discovered that at least 3 months' delay after the insertion of an implant was needed for a firm bleb to form. Removal before 3 months (Cases 5, 6, 7, I2, and 13) gave relatively poor results, while accurate watertight closure of the incision into the bleb was very difficult. Therefore most implants were removed between 3 and 7 months after insertion, but there was no technical advantage in waiting more than 4 months as they attained their greatest thickness by the end of the third month. ANAESTHESIA AND HYPOTONY General anaesthesia was preferred but when it was not available, local anaesthesia and akinesia were used as for a cataract extraction. Hypotony was produced either by intravenous infusion of IO per cent. Mannitol solution or by the administration of 500 mg. Diamox and 150 ml. glycerol by mouth. 2g
3 30 STEPS IN SURGICAL TECHNIQUE 3A. C. B. Molteno (i) Exposure of the bleb was provided by a speculum and a superior rectus stitch carefully inserted to avoid the bleb. (2) A circumferential conjunctival incision was made 3 mm. behind the bleb and its limbal edge was retracted to expose the posterior edge of the bleb. (3) After all bleeding points had been lightly cauterized a Bard-Parker knife was used to make a single clean incision into the bleb cavity. This incision was placed I mm. anterior to the posterior edge of the inner fibrous bleb and carried across the full width of the episcleral plate. (4) The posterior stitch holding the implant to the sclera was cut and an iris repositor was used to ease the posterior edge of the episcleral plate away from the bleb cavity. (5) The two anterior sutures holding the implant to the sclera were cut by sliding a Tooke's knife forward between the episcleral plate of the implant and the sclera. The implant was then grasped with a pair of toothed forceps and gently removed (Fig. i). F IG. I Removing implantfirom bleb FIG. 2 Bleb cavlty lined by,fibrous tissue. (6) A sliver of tissue comprising the full thickness of the bleb wall together with overlying conj'unctiva was removed from the anterior lip of the incision, using curved scissors, a watertight closure of the inner fibrous layer of the bleb was then effected by five or six interrupted edge-to-edge sutures of 7-0 silk and the anterior chamber was re-formed by injecting a medium-sized air bubble into the bleb (Fig. 2). (7) The conj'unctiva was closed by a continuous suture Of 7 0 silk and the operation was completed by the inj'ection of Lincomycin with Depo-Medrol beneath the conj'unctiva in the quadrant opposite the bleb. During the removal of the implant the utmost care was taken to avoid stretching or otherwise inj'uring the inner fibrous layer of the bleb. In two cases, part-of the bleb was lifted from the sclera, so demonstrating that the attachment of bleb to sclera formed a plane of weakness. POSTOPERATIVE CARE All eyes were single-padded for 24 hours, after which the patients were allowed up, wearing dark glasses. Gutt. Sofradex and gutt. Phenylephrine io per cent, wer-e given until the eyes became quiet after 2 to 4 weeks. One patient (two eyes), a 15-year-old girl (Case I4), received systemic steroids for 4 months after the implants were removed in order to suppress fibrous tissue activity in the blebs. Two patients (three eyes) in whom Perspex implants excited a severe uveitis (Cases 7 and 8) received systemic steroids for 6 weeks and 7 months respectively after the removal of' the implants.
4 New implant for glaucoma OPERATIVE AND POSTOPERATIVE COMPLICATIONS In this small series of nineteen operations for removal of implants no operative complications were encountered. The only postoperative complications occurred in Case 2 (two eyes) in whom malignant glaucoma developed 4 days and 7 months respectively after removal of the implants. The attacks occurred 3 days apart a week after the patient had finished a 7-day course of Orenzyme which had been given to determine whether it would improve drainage. In both eyes the glaucoma was successfully treated by withdrawing fluid posterior vitreous through a pars plana incision, combined with re-formation of the anterior chambers by means of air inserted through a singlethrust cyclodialysis. Both anterior chambers remained deep and drainage was re-established and has persisted in both eyes for a year since these episodes. Results BLEB BEHAVIOUR AFTER REMOVAL OF IMPLANT In the immediate postoperative period, except for the three eyes in which Perspex implants had been used (Cases 7 and 8) the eyes remained quiet with a mild inflammatory reaction along the suture line. The blebs were all distended while the intraocular pressures rose within I o days to the levels present immediately before removal of the particular implants. At this stage aqueous could easily be displaced from eye to bleb and vice versa (Fig. 5, below). After I to 4 months, the blebs showed definite changes, either increasing in area with an associated fall in intraocular pressure or starting to shrink with an associated rise in intraocular pressure. (Bleb spread occurred in the eight patients aged 50 years or more when 3 or more months had passed between insertion and removal of implants (Table I)). Table I Case Age Sex No. (yrs) I 53 2 R 79 L Results in eight patients over 50 years old (eleven eyes) M M M M Diagnosis 4 6i M 5 R 65 M L 65 M Glaucoma secondary to trauma 6 67 M 7 R 53 L Range Mean 64 M F + or - 3 mths before removal (months) + Malignant + glaucoma - Perspex F Uveitis Total follow-up Intraocular Pressure (mm. Hg) Before removal I9 23.I 8 Final 20 I8-5 I I6 I7 i6.5 I9 I6 I8 I I 22 I I I I5.6 Bleb shrinkage occurred in six out of the eight eyes belonging to the six patients less than thirty years old, and in all cases in which the implants were removed before 3 months had elapsed (Table II). 31
5 32 Table H Case Age Sex No. (yrs) Results in six patients under 30 years old (eight eyes) Diagnosis 9 25 F 10 i6 F Glaucoma associated with Sturge Weber syndrome i i R 4 F Buphthalmos L 4 F Buphthalmos F I3 29 M Glaucoma secondary to old perforating injury I4R L Range Mean '4 ' I6 F F + or - 3 mths before removal Steroids + fsteroids A. C. B. Molteno Intraocular pressure Total (mm. Hg) follow-up (mths) Before Final removal 3I I9 I I I I I3 13 I 2-3 I i '5 ' The only exceptions to the above rules were a so-year-old woman (Case 8) with Perspex uveitis in whom bleb shrinkage occurred and two eyes in a Is-year-old girl (Case I4) who was given large doses of systemic steroids for 4 months and in whom both blebs extended in area. BLEB SPREAD (Fig. 3) Where this occurred, the sharply demarcated fibrosed and elevated bleb, which remained after removal of its contained implant, gradually flattened and spread posteriorly and circumferentially while becoming less fibrosed. FIG 3 Bleb spread: Appearance of bleb 3 months after removal of implant
6 _ty ''.a.r2f. 9.- R.S ~~~~~~~~~~removal JNew implantfor glaucoma 33 Ultimately (after ij to 3 months) a large area, sometimes a whole quadrant, became covered by the bleb which consisted of well-vascularized but oedematous conjunctival and episcleral tissue. On massage of the globe this heaped up slightly and extended peripherally. Gonioscopy of these eyes showed at first an open fistula where the translimbal tube had been but, by the end of the third month after removal, all those fistulae which could be clearly seen had become filled by a delicate network of fibrous tissue. During this period of spread, the intraocular pressure gradually fell to a stable level of between 7 5 and 20 mm. Hg approximately 3 months after the removal of the implant. Drainage Routes Observed In most cases in which the bleb had spread, the obvious oedema of the episcleral tissues suggested that most aqueous escaped from the bleb via the subconjunctival lymphatics. However, several blebs showed signs of transconjunctival drainage: both localized thin areas with a positive Seidel sign and diffuse areas where oedema of the episcleral tissues involved the conjunctiva so that numerous tiny microcysts formed in the epithelium on massage of the eyes. In two cases prominent aqueous veins formed in addition to the routes described above. Although one of the blebs was found to be grossly overfibrosed on of the implant, all blebs which spread gradually lost their fibrosed walls and ultimately (after more than a year in one case) all signs of fibrous tissues having been laid down had vanished. BLEB SHRINKAGE (Figs 4 to 7) This occurred in all six patients less than 30 years old who did not receive systemic steroids. The sharply-defined, well-vascularized, fibrosed and heaped bleb which remained after removal of the implant remained unchanged for several weeks, and then slowly shrank over a period of up to I8 months to leave a small nubbin of heavily-fibrosed conjunctiva over the fistula. Gonioscopy showed that the fistula became filled with a tenuous network of fibrous tissue, which gradually became denser and ultimately consolidated to leave merely a dimple in the sclera to mark the site of the fistula. FIG. 4 Bleb shrinkage: Appearance of bleb 4 months after insertion of implant and shortly before
7 34 as in Fig. 4, I week after removal of iml t; ~~~~~~~~~~~~~...P.. ~~~~fibrosed A. C. B. Molteno FIG. 5 Same bleb ~~~FIG. 6 Same bleh, as in Fig. 4, heavily and shrinking- 4 months later Br J Ophthalmol: first published as /bjo on 1 January Downloaded from During the period of shrinkage, the intraocular pressure rose steadily until as the bleb, disappeared the preoperative level was regained. Once all drainage had ceased the fibrosed nubbin became thinner and less fibrosed until it had reverted to the appearance. of normal conjunctiva between 6 and 12 months later. Drainage Routes Observed Virtually no drainage of aqueous was observed from shrinking blebs, apart from a minimal amount of transconjunctival drainage over the fistulae when the blebs were almost obliter-, ated and the intraocular pressure markedly raised. on 2 April 2019 by guest. Protected by copyright.
8 NVew implant for glaucoma FIG. Same eye as in Figs 4 to 6, 27 4eekmont/s after removal of implant, showing reversion of bleb to normal conjunc-tiva. A second implant has been inserted in the nasal quadrant. In all cases except those with Perspex uveitis, the eyes remained quiet and by the fourth week after removal topical steroids and mydriatics were discontinued. One patient (Case i) developed a mild iritis io months after removal of the implant; this was treated with steroid and cycloplegic drops, responded rapidly, and has remained quiet without medication during a further year of follow up. EFFECT OF EARLY REMOVAL ON TENDENCY TO IRITIS When implants were removed before the end of the third month, the behaviour of the eye varied according to the age of the patient. In those over 50 years old the blebs persisted but were smaller and less adequate than those which remained after the implants had been left in situ for 3 months or more. In the group under 30 years old there were only two cases of early removal. In one the bleb became obliterated within 8 weeks of removal, and in the other rapid shrinkage occurred but the bleb "roof" became ischaemic and transconjunctival drainage was established and has persisted. Discussion In the elderly the effect of removing the implant was to maintain or reduce the preremoval intraocular pressure and to elimninate the need for long-term steroid medication. Renmoval after 5 months uniformly resulted in a large, flat, thick-walled, moderatelyvascular bleb, which extended in all directions on massage of the eye. This type of bleb is safe and permanent and always drains well (intraocular pressure mm. Hg; C values ). In young patients removal, even when delayed for several months, resulted in a higher intraocular pressure in every case, except where systemic steroids were given to the limit of tolerance for 4 months after removal. Good drainage was obtained in this particular case, with flat extensible "permanent" type blebs, but it is not safe to give steroids in this manner as a routine. 35
9 36 A. C. B. Molteno Although the results are based on small numbers of cases, the effect of age on bleb behaviour was so marked that the removal of implants in patients less than 50 years old seems to be contraindicated. Young patients fortunately tolerate implants very well. In the elderly, removal gives an ideal result, but the reason why there should be this marked difference between the age groups is not immediately obvious. The overall results of insertion followed by removal were: (I) Control of intraocular pressure without medication: twelve cases (9 over 50 years) (2) Control of intraocular pressure with medication: one case (over 50 years) (3) Failure: six cases (5 under 30 years). POSSIBLE CAUSE OF BLEB SHRINKAGE IN THE YOUNG The persistent vascularity and increasing fibrosis of shrinking blebs in young patients was associated with markedly raised intraocular pressures, but was followed by complete disappearance of the heavily-fibrosed bleb wall once all drainage of aqueous had ceased. This behaviour suggested that in these cases the aqueous exerted an irritant effect on the bleb wall. Epstein (1959) demonstrated histologically that the aqueous from an eye with absolute glaucoma had a fibrosing effect on the episcleral tissues, which caused failure of a seton operation in approximately 4 weeks. There is no direct evidence of the nature of the irritating factor, but ischaemia of any tissue results in the release of vasodilating factors while necrosis and autolysis of tissue releases factors which excite an acute inflammatory response followed later by fibrosis (Walter and Israel, i965). In these cases with nearly absolute glaucoma the pressure had been reduced by the initial insertion of the implant and in three cases in young patients the pressure had been below 30 mm. Hg for between 4 and 6 months, making it seem unlikely that tissue breakdown products from the intraocular structures would persist so long. However, in cases of rubeosis iridis, there is generally a lapse of several months between central vein occlusion and the onset of neovascularization. In this condition, a vasoformative factor produced by destruction of intraocular structures was postulated by Smith (1955, I961), Ashton (i 96I), and Sanders (i 96I) as the cause of the neovascularization. The persistence of this factor months after the occlusion suggests that the "Epstein factor" could likewise persist for several months after normalization of the pressure and could be responsible for the fibrosis which obliterates the blebs, and that both factors have a common origin in destruction of intraocular tissue. In older patients the glaucoma was equally advanced, but because aged tissues respond less actively to all stimuli the fibrosing response of the bleb walls was insufficient to raise the intraocular pressure or contract the blebs, and the blebs therefore remained until all tissue breakdown products had been eliminated, after which gradual loss of fibrous tissue occurred. The loss of fibrous tissue in these cases could be a manifestation of the degenerative action of normal aqueous on the episcleral tissues described by Teng, Chi, and Katzin (I959), but that it is not the only process leading to loss of collagen is shown by the defibrosis which occurred in shrunken blebs after all drainage of aqueous had ceased. INDICATIONS FOR REMOVAL OF IMPLANTS Since the initial publication of the results obtained by inserting implants (Molteno I 969a,b) the number of such operations has risen to eighty. The more recent cases have confirmed
10 New implantfor glaucoma the value of systemic steroids in avoiding overfibrosis of the blebs and eliminating late postoperative iridocyclitis. Thus, at present, the author routinely inserts implants under steroid cover and leaves them in. Removal is helpful in elderly patients to whom systemic steroids cannot be given for medical reasons, in elderly patients who live so far away that supervision is impossible, and to forestall perforation of a bleb if the implant has been incorrectly inserted. If guided by these indications removal will increase the usefulness of implants and further improve the overall results. Summary (I) The theoretical advantages of removing the author's glaucoma implants after a suitable period are stated. (2) The surgical techniques for removal are described and the results obtained in a series of nineteen removal operations are reported. (3) The effect of the patient's age on the results is stressed and a possible causative mechanism discussed. (4) The present indications for removing an implant are given. I wish to thank Prof. M. H. Luntz for his help and encouragement. My thanks are due to the Superintendents of Baragwanath Hospital and St. John's Eye Hospital for their co-operation and assistance. This work was assisted bylgrants from the University of the Witwatersrand and the Council for Scientific and Industrial Research. References ASHTON, N. (x96i) Trans. ophthal. Soc. U.K., 8i, 145 EPSTEIN, E. (I959) Brit. J. Ophthal., 43, 64I LAPLACE, P. S. (I807) "Traite de mecanique celeste (Supplement au Xe livre), i.e. Supplement a la theorie de l'action capillaire." Courcier, Paris MOLTENO, A. C. B. (I969a) Brit. J. Ophthal., 53, 6o6 - (i969b) Ibid., 53, i6i SMITH, R. (955) "XVII Conc. Ophthal., Canada, U.S.A. Acta", vol. 2, p. I I64 SMITH, R. (i96i) Trans. ophthal. Soc. U.K., 8I, 125 SANDERS, A. G. (196i) Ibid., 8i, 125 TENG, C. C., CHI, H. H., and KATZIN, H. M. (I959) Amer. J. Ophthal., 47, I6 WALTER, j. B., and ISRAEL, M. S. (x965) "General Pathology," 2nd ed., pp. 1I 2, 15I, 755. Churchhill, London YOUNG, T. (i8o5) Phil. Trans. roy. Soc. Lond., 95, 65 37
New implant for drainage in glaucoma
 Brit. J. Ophthal. (I969) 53, 6o6 New implant for drainage in glaucoma Clinical trial A. C. B. MOLTENO Department of Ophthalmology, University of the Wnitwatersrand and Baragwanath Hospital, 7ohannesburg,
Brit. J. Ophthal. (I969) 53, 6o6 New implant for drainage in glaucoma Clinical trial A. C. B. MOLTENO Department of Ophthalmology, University of the Wnitwatersrand and Baragwanath Hospital, 7ohannesburg,
Implants for draining neovascular glaucoma
 British Journal of Ophthalmology, 1977, 61, 120-125 Implants for draining neovascular glaucoma A. C. B. MOLTENO, M. M. B. VAN ROOYEN, AND R. S. BARTHOLOMEW From the Departments of Ophthalmology of the
British Journal of Ophthalmology, 1977, 61, 120-125 Implants for draining neovascular glaucoma A. C. B. MOLTENO, M. M. B. VAN ROOYEN, AND R. S. BARTHOLOMEW From the Departments of Ophthalmology of the
Third Generation. Glaucoma Drainage Device
 MOLTENO 3 Third Generation Glaucoma Drainage Device A Step by Step Guide to Inserting the Molteno3 Glaucoma Drainage Device for Delayed or Immediate Drainage and either translimal or pars plana insertion
MOLTENO 3 Third Generation Glaucoma Drainage Device A Step by Step Guide to Inserting the Molteno3 Glaucoma Drainage Device for Delayed or Immediate Drainage and either translimal or pars plana insertion
Third Generation. Glaucoma Drainage Device
 MOLTENO 3 Third Generation Glaucoma Drainage Device A Step by Step Guide to Inserting the Molteno3 Glaucoma Drainage Device for Delayed or Immediate Drainage and either Translimbal or Pars Plana Insertion
MOLTENO 3 Third Generation Glaucoma Drainage Device A Step by Step Guide to Inserting the Molteno3 Glaucoma Drainage Device for Delayed or Immediate Drainage and either Translimbal or Pars Plana Insertion
Sinus trabeculectomy. Preliminary results of IOO operations
 Brit. J. Ophthal. (I 972) 56, 833 Sinus trabeculectomy Preliminary results of IOO operations A. P. NESTEROV, N. V. FEDEROVA, AND Y. E. BATMANOV Department of Ophthalmology, Kazan Medical Institute, Kazan,
Brit. J. Ophthal. (I 972) 56, 833 Sinus trabeculectomy Preliminary results of IOO operations A. P. NESTEROV, N. V. FEDEROVA, AND Y. E. BATMANOV Department of Ophthalmology, Kazan Medical Institute, Kazan,
Angle recession and secondary glaucoma
 Brit. j. Ophthal. (I973) 57, 6o8 Angle recession and secondary glaucoma D. MOONEY Kent County Ophthalmic and Aural Hospital, Maidstone In a previous article (Mooney, I972), the incidence and extent of
Brit. j. Ophthal. (I973) 57, 6o8 Angle recession and secondary glaucoma D. MOONEY Kent County Ophthalmic and Aural Hospital, Maidstone In a previous article (Mooney, I972), the incidence and extent of
Lymphangiectasia haemorrhagica
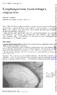 Brit. 7. Ophthal. (i 969) 53, 274 Lymphangiectasia haemorrhagica conjunctivae PHILIP AWDRY Moorfields Eye Hospital, City Road, London, E.C. I Leber (i 88o) described a condition in which a connexion between
Brit. 7. Ophthal. (i 969) 53, 274 Lymphangiectasia haemorrhagica conjunctivae PHILIP AWDRY Moorfields Eye Hospital, City Road, London, E.C. I Leber (i 88o) described a condition in which a connexion between
AQUEOUS VEINS IN RABBITS*
 Brit. J. Ophthal., 35, 119. AQUEOUS VEINS IN RABBITS* BY D. P. GREAVES AND E. S. PERKINS Institute of Ophthalmology, London Director of Research, Sir Stewart Duke-Elder IN the course of investigations
Brit. J. Ophthal., 35, 119. AQUEOUS VEINS IN RABBITS* BY D. P. GREAVES AND E. S. PERKINS Institute of Ophthalmology, London Director of Research, Sir Stewart Duke-Elder IN the course of investigations
Diffuse infiltrating retinoblastoma
 Brit. 1. Ophthal. (I 971) 55, 6oo Diffuse infiltrating retinoblastoma GWYN MORGAN Department of Pathology, Institute of Ophthalmology, University of London The term "diffuse infiltrating retinoblastoma"
Brit. 1. Ophthal. (I 971) 55, 6oo Diffuse infiltrating retinoblastoma GWYN MORGAN Department of Pathology, Institute of Ophthalmology, University of London The term "diffuse infiltrating retinoblastoma"
non-perforating injury
 Brit. J. Ophthal. (I 972) 56, 418 Anterior chamber angle tears after non-perforating injury DAVID MOONEY Croydon Eye Unit, Croydon, Surrey Recession of the anterior chamber angle is a common finding after
Brit. J. Ophthal. (I 972) 56, 418 Anterior chamber angle tears after non-perforating injury DAVID MOONEY Croydon Eye Unit, Croydon, Surrey Recession of the anterior chamber angle is a common finding after
Trabeculectomy - A Short Term Follow-up
 Trabeculectomy - A Short Term Follow-up Pages with reference to book, From 193 To 196 K.S. Hasan, G. Rabbani, S. Hashmani, M.M. Hasan ( Department of Ophthalmology Civil Hospital and Dow Medical College.
Trabeculectomy - A Short Term Follow-up Pages with reference to book, From 193 To 196 K.S. Hasan, G. Rabbani, S. Hashmani, M.M. Hasan ( Department of Ophthalmology Civil Hospital and Dow Medical College.
Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique
 Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique Kirti Nath Jha Professor of Ophthalmology Mahatma Gandhi Medical College & Research Institute,Pondy-Cuddalore
Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique Kirti Nath Jha Professor of Ophthalmology Mahatma Gandhi Medical College & Research Institute,Pondy-Cuddalore
Iridocyclo-retraction in narrow-angle
 Brit. 3. Ophthal. (I 97 I) 55, 389 Iridocyclo-retraction in narrow-angle glaucoma M. XI. KRASNOV Second Medical Institute, Moscow, USSR No specific way has so far been found to treat the organic (synechial)
Brit. 3. Ophthal. (I 97 I) 55, 389 Iridocyclo-retraction in narrow-angle glaucoma M. XI. KRASNOV Second Medical Institute, Moscow, USSR No specific way has so far been found to treat the organic (synechial)
STAB INCISION GLAUCOMA SURGERY (SIGS) AMAR AGARWAL
 STAB INCISION GLAUCOMA SURGERY (SIGS) AMAR AGARWAL SIGS or Stab Incision Glaucoma Surgery is a guarded filtration procedure that was introduced by me and is slowly but surely becoming popular amongst many
STAB INCISION GLAUCOMA SURGERY (SIGS) AMAR AGARWAL SIGS or Stab Incision Glaucoma Surgery is a guarded filtration procedure that was introduced by me and is slowly but surely becoming popular amongst many
Trabeculectomy combined with cataract extraction: a follow-up study
 British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
Encircling silicone rod without drainage
 Brit. J. Ophthal. (I 973) 57, 53 7 Encircling silicone rod without drainage for retinal detachment with giant breaks ABDEL-LATIF SIAM Ophthalmology Department, Ain Shams University, Cairo, Egypt Giant
Brit. J. Ophthal. (I 973) 57, 53 7 Encircling silicone rod without drainage for retinal detachment with giant breaks ABDEL-LATIF SIAM Ophthalmology Department, Ain Shams University, Cairo, Egypt Giant
STAB INCISION GLAUCOMA SURGERY (SIGS)
 STAB INCISION GLAUCOMA SURGERY (SIGS) DR. SOOSAN JACOB Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Youtube channel*: Dr. Soosan Jacob SIGS or Stab Incision Glaucoma Surgery is a guarded
STAB INCISION GLAUCOMA SURGERY (SIGS) DR. SOOSAN JACOB Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Youtube channel*: Dr. Soosan Jacob SIGS or Stab Incision Glaucoma Surgery is a guarded
chamber pigment in the anterior L beration of iris phenylephrine hydrochloride solution. After instillation of io per cent.
 Brit.. Ophthal. (I 97 I) 55, 544 L beration of iris chamber After instillation of io per cent. hydrochloride solution J. L. AGGARWAL AND B. BEVERIDGE Wolverhampton and Midland Counties Eye Infirmary pigment
Brit.. Ophthal. (I 97 I) 55, 544 L beration of iris chamber After instillation of io per cent. hydrochloride solution J. L. AGGARWAL AND B. BEVERIDGE Wolverhampton and Midland Counties Eye Infirmary pigment
Haemorrhagic glaucoma
 Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
A METHOD OF TRABECULOTOMY WITH SOME PRELIMINARY RESULTS*t
 Brit. J. Ophthal. (1967) 51, 539 A METHOD OF TRABECULOTOMY WITH SOME PRELIMINARY RESULTS*t BY I. M. STRACHAN Ophthalmic Department, Royal Infirmary, Dundee IT HAS long been suspected that the cause of
Brit. J. Ophthal. (1967) 51, 539 A METHOD OF TRABECULOTOMY WITH SOME PRELIMINARY RESULTS*t BY I. M. STRACHAN Ophthalmic Department, Royal Infirmary, Dundee IT HAS long been suspected that the cause of
Family studies in glaucoma
 Brit. j. Ophthal. (I 974) 58, 529 Family studies in glaucoma E. S. PERKINS Institute of Ophthalmology, University of London There is now strong evidence for a genetic basis to glaucoma. Numerous family
Brit. j. Ophthal. (I 974) 58, 529 Family studies in glaucoma E. S. PERKINS Institute of Ophthalmology, University of London There is now strong evidence for a genetic basis to glaucoma. Numerous family
Prednisolone-2 I -stearoylglycolate in scleritis
 Brit. j. Ophthal. (1970) 54, 394 Prednisolone- -stearoylglycolate in scleritis S. S. HAYREH* AND P. G. WATSON Scleritis Clinic, Moorfields Eye Hospital, City Road, London, E.C. i Scleritis is one of the
Brit. j. Ophthal. (1970) 54, 394 Prednisolone- -stearoylglycolate in scleritis S. S. HAYREH* AND P. G. WATSON Scleritis Clinic, Moorfields Eye Hospital, City Road, London, E.C. i Scleritis is one of the
LEUKAEMIA*t INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC. pattemn * Received for pubiication November io, i967.
 Brit. J. Ophthal. (1968) 52, 781 INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC LEUKAEMIA*t BY BRIAN MARTIN The General Infirmary, Leeds OCULAR involvement is common in the leukaemias though the anterior
Brit. J. Ophthal. (1968) 52, 781 INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC LEUKAEMIA*t BY BRIAN MARTIN The General Infirmary, Leeds OCULAR involvement is common in the leukaemias though the anterior
COMMUNICATIONS PHOTOCOAGULATION OF THE RETINA* OPHTHALMOSCOPIC AND HISTOLOGICAL FINDINGS. photocoagulation of the rabbit's retina.
 Brit. J. Ophthal. (1963) 47, 577. COMMUNICATIONS PHOTOCOAGULATION OF THE RETINA* OPHTHALMOSCOPIC AND HISTOLOGICAL FINDINGS BY A. LAVYEL Haifa, Israel SINCE the introduction of the photocoagulator by Meyer-Schwickerath
Brit. J. Ophthal. (1963) 47, 577. COMMUNICATIONS PHOTOCOAGULATION OF THE RETINA* OPHTHALMOSCOPIC AND HISTOLOGICAL FINDINGS BY A. LAVYEL Haifa, Israel SINCE the introduction of the photocoagulator by Meyer-Schwickerath
(PSEUDOPHAKOI)*t PERSONAL TECHNIQUES OF PSEUDOPHAKIA
 Brit. J. Ophthal. (1967) 51, 767 IRIS-CLIP AND IRIIDO-CAPSULAR LENS IMPLANTS (PSEUDOPHAKOI)*t PERSONAL TECHNIQUES OF PSEUDOPHAKIA BY C. D. BINKHORST Terneuzen, Netherlands THE iris-clip lens implant or
Brit. J. Ophthal. (1967) 51, 767 IRIS-CLIP AND IRIIDO-CAPSULAR LENS IMPLANTS (PSEUDOPHAKOI)*t PERSONAL TECHNIQUES OF PSEUDOPHAKIA BY C. D. BINKHORST Terneuzen, Netherlands THE iris-clip lens implant or
arthritis "Contact lens" cornea in rheumatoid (opposite). Brit. J. Ophthal. (I970) 54, 410 Peterborough District Hospital
 Brit. J. Ophthal. (I970) 54, 410 "Contact lens" cornea in rheumatoid arthritis A. J. LYNE Peterborough District Hospital It has been noted that patients suffering from long-standing rheumatoid arthritis
Brit. J. Ophthal. (I970) 54, 410 "Contact lens" cornea in rheumatoid arthritis A. J. LYNE Peterborough District Hospital It has been noted that patients suffering from long-standing rheumatoid arthritis
Corneal blood staining after hyphaema
 Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Therapeutic keratoplasty in
 Brit. J. Ophthal. (I 97 I) 55, 326 Therapeutic keratoplasty in Pseudomonas pyocyaneus corneal ulcers S. R. K. MALIK AND GURBAX SINGH Maulana Azad Medical College and Associated Irwin and G.B. Pant Hospital,
Brit. J. Ophthal. (I 97 I) 55, 326 Therapeutic keratoplasty in Pseudomonas pyocyaneus corneal ulcers S. R. K. MALIK AND GURBAX SINGH Maulana Azad Medical College and Associated Irwin and G.B. Pant Hospital,
Plate/Valve Specifications: Thickness: 0.9mm Width: 13.00mm Length: 16.00mm Surface Area: mm 2
 Distribué en France par FCI S.A.S. France Chirurgie Instrumentation SAS 20/22 rue Louis Armand 75015 PARIS Tél. 01.53.98.98.98 / Fax. 01.53.98.98.99 fci@fci.fr / www.fci.fr CATALOGUE DE VENTE Features:
Distribué en France par FCI S.A.S. France Chirurgie Instrumentation SAS 20/22 rue Louis Armand 75015 PARIS Tél. 01.53.98.98.98 / Fax. 01.53.98.98.99 fci@fci.fr / www.fci.fr CATALOGUE DE VENTE Features:
RETINITIS PIGMENTOSA* A NEW THERAPEUTIC APPROACH
 Brit. J. Ophthal. (1963) 47, 144. RETINITIS PIGMENTOSA* A NEW THERAPEUTIC APPROACH BY LALIT P. AGARWAL, S. R. K. MALIK, MADAN MOHAN, AND P. R. KARWAL From the Department of Ophthalmology, All-India Institute
Brit. J. Ophthal. (1963) 47, 144. RETINITIS PIGMENTOSA* A NEW THERAPEUTIC APPROACH BY LALIT P. AGARWAL, S. R. K. MALIK, MADAN MOHAN, AND P. R. KARWAL From the Department of Ophthalmology, All-India Institute
STAB INCISION GLAUCOMA SURGERY (SIGS)
 STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
Provocative tests in closed-angle glaucoma
 Brit. 7. Ophthal. (I976) 6o, I 5 Provocative tests in closed-angle glaucoma R. MAPSTONE From St Paul's Eye Hospital, Liverpool The absence of a provocative test with proved predictive value, in s at risk
Brit. 7. Ophthal. (I976) 6o, I 5 Provocative tests in closed-angle glaucoma R. MAPSTONE From St Paul's Eye Hospital, Liverpool The absence of a provocative test with proved predictive value, in s at risk
Retinal dialysis. procedures. The purpose of the present paper is to report the results of treatment of 62
 Brit. J. Ophthal. (I973) 57, 572 Retinal dialysis A. H. CHIGNELL Moorfields Eye Hospital, City Road, London, E.C. i Retinal dialysis is an important cause of retinal detachment and subsequent reduction
Brit. J. Ophthal. (I973) 57, 572 Retinal dialysis A. H. CHIGNELL Moorfields Eye Hospital, City Road, London, E.C. i Retinal dialysis is an important cause of retinal detachment and subsequent reduction
Comparative trial of Dexon (polyglycolic acid), collagen,
 Brit. Y. Ophthal. (1975) 59, 736 Comparative trial of Dexon (polyglycolic acid), collagen, and silk sutures in ophthalmic surgery S. CHATTERJEE From the Department of Ophthalmology, Birmingham and Midland
Brit. Y. Ophthal. (1975) 59, 736 Comparative trial of Dexon (polyglycolic acid), collagen, and silk sutures in ophthalmic surgery S. CHATTERJEE From the Department of Ophthalmology, Birmingham and Midland
WGA. The Global Glaucoma Network
 The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
EXP11677SK. Financial Disclosure. None to be Declared EXP11677SK
 Financial Disclosure None to be Declared Presentation overview Glaucoma Surgical History Complications of trabeculectomy Express Device Specifications Surgical Steps Clinical advantages, indications and
Financial Disclosure None to be Declared Presentation overview Glaucoma Surgical History Complications of trabeculectomy Express Device Specifications Surgical Steps Clinical advantages, indications and
Surgical management of Duane's
 Brit. J. Ophthal. (I974) 58, 30 I Surgical management of Duane's syndrome M. H. GOBIN ljniversity Eye Clinic, Leyden, IHolland Ten years ago I introduced a surgical technique for the correction of Duane's
Brit. J. Ophthal. (I974) 58, 30 I Surgical management of Duane's syndrome M. H. GOBIN ljniversity Eye Clinic, Leyden, IHolland Ten years ago I introduced a surgical technique for the correction of Duane's
Primary Angle Closure Glaucoma
 www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
PARTIAL CYCLECTOMY* BY H. B. STALLARD
 Brit. J. Ophthal. (1961) 45, 797. PARTIAL CYCLECTOMY* BY H. B. STALLARD London SURGICAL exploration of part of the ciliary body is justifiable when gonioscopic examination shows an extension of a malignant
Brit. J. Ophthal. (1961) 45, 797. PARTIAL CYCLECTOMY* BY H. B. STALLARD London SURGICAL exploration of part of the ciliary body is justifiable when gonioscopic examination shows an extension of a malignant
Mechanics of the Ahmed Glaucoma Valve
 Dr. A. Mateen Ahmed President & CEO - New World Medical, Inc. New World Medical, Inc. (NWMI) is a high tech medical device company whose goal is to help humanity lead a better life through improved technology
Dr. A. Mateen Ahmed President & CEO - New World Medical, Inc. New World Medical, Inc. (NWMI) is a high tech medical device company whose goal is to help humanity lead a better life through improved technology
INTRAVENOUS UREA IN GLAUCOMA*
 Brit. J. Ophthal. (1961) 45, 307. NTRAVENOUS UREA N GLAUCOMA* BY C. G. KETH London HYPERTONC solutions have been used to reduce the intra-ocular pressure in glaucoma since Cantonnet (1904) first used hypertonic
Brit. J. Ophthal. (1961) 45, 307. NTRAVENOUS UREA N GLAUCOMA* BY C. G. KETH London HYPERTONC solutions have been used to reduce the intra-ocular pressure in glaucoma since Cantonnet (1904) first used hypertonic
EX-PRESS Glaucoma Filtration Device Surgical Procedure
 EX-PRESS Glaucoma Filtration Device Surgical Procedure Surgical Recommendations EX-PRESS Glaucoma Filtration Device preloaded device (plus 1 back-up) Sterile caliper Lid speculum Corneal forceps 0.12 forceps
EX-PRESS Glaucoma Filtration Device Surgical Procedure Surgical Recommendations EX-PRESS Glaucoma Filtration Device preloaded device (plus 1 back-up) Sterile caliper Lid speculum Corneal forceps 0.12 forceps
TECHNIQUE OF GONIOTOMY*
 Brit. J. Ophthal. (1965) 49, 594 TECHNIQUE OF GONIOTOMY* BY A. LISTER Moorfields Hospital, London EXPERIENCE in treating over one hundred cases of congenital glaucoma during the past sixteen years has
Brit. J. Ophthal. (1965) 49, 594 TECHNIQUE OF GONIOTOMY* BY A. LISTER Moorfields Hospital, London EXPERIENCE in treating over one hundred cases of congenital glaucoma during the past sixteen years has
Cataract in childhood: photographic methods in assessment
 British Journal of Ophthalmology, 1977, 61, 135-140 Cataract in childhood: photographic methods in assessment NICHOLAS BROWN The slit-lamp examination of the child's lens with cataract can yield useful
British Journal of Ophthalmology, 1977, 61, 135-140 Cataract in childhood: photographic methods in assessment NICHOLAS BROWN The slit-lamp examination of the child's lens with cataract can yield useful
Humanity s Vision Is Our Focus. The Ahmed Glaucoma Valve
 Humanity s Vision Is Our Focus The Ahmed Glaucoma Valve Dr. A. Mateen Ahmed President - New World Medical New World Medical is a high tech medical device company whose goal is to help humanity lead a better
Humanity s Vision Is Our Focus The Ahmed Glaucoma Valve Dr. A. Mateen Ahmed President - New World Medical New World Medical is a high tech medical device company whose goal is to help humanity lead a better
Pseudophakic pupillary-block glaucoma
 British Journal of Ophthalmology, 1977, 61, 329-333 DAVID WERNER AND MARTIN KABACK From the Department of Ophthalmology, Jewish General Hospital, Montreal, Canada SUMMARY Four cases of iris-supported pseudophakic
British Journal of Ophthalmology, 1977, 61, 329-333 DAVID WERNER AND MARTIN KABACK From the Department of Ophthalmology, Jewish General Hospital, Montreal, Canada SUMMARY Four cases of iris-supported pseudophakic
The O'Connor cinch revisited
 The O'Connor cinch revisited British Journal of Ophthalmology, 1978, 62, 765-769 A. THOMAS WILLIAMS, HENRY S. METZ, AND ARTHUR JAMPOLSKY From the Smith-Kettlewell Institute of Visual Sciences, San Francisco,
The O'Connor cinch revisited British Journal of Ophthalmology, 1978, 62, 765-769 A. THOMAS WILLIAMS, HENRY S. METZ, AND ARTHUR JAMPOLSKY From the Smith-Kettlewell Institute of Visual Sciences, San Francisco,
GLAUCOMA TREATED WITH DIAMOX*t PRELIMINARY REPORT OF 20 CASES
 Brit. J. Ophthal. (1955) 39, 659. GLAUCOA TREATED WITH DIAOX*t PRELIINARY REPORT O 20 CASES BY S.. DRANCE Oxford THE use of Diamox in logically follows riedenwald's concept that the bicarbonate ion is
Brit. J. Ophthal. (1955) 39, 659. GLAUCOA TREATED WITH DIAOX*t PRELIINARY REPORT O 20 CASES BY S.. DRANCE Oxford THE use of Diamox in logically follows riedenwald's concept that the bicarbonate ion is
CORNEO-SCLERAL TONOGRAPHY* t BY T. H. HODGSON AND R. K. MACDONALD From the Department of Ophthalmology, University of Toronto, Canada
 Brit. J. Ophthal. (1957) 41, 301. CORNEO-SCLERAL TONOGRAPHY* t BY T. H. HODGSON AND R. K. MACDONALD From the Department of Ophthalmology, University of Toronto, Canada THAT pressure exerted on the eyeball
Brit. J. Ophthal. (1957) 41, 301. CORNEO-SCLERAL TONOGRAPHY* t BY T. H. HODGSON AND R. K. MACDONALD From the Department of Ophthalmology, University of Toronto, Canada THAT pressure exerted on the eyeball
CORNEAL VASCULARIZATION AFTER CATARACT EXTRACTION BY ZONULYSIS*
 Brit. J. Ophthal (1959) 43, 325. CORNEAL VASCULARIZATION AFTER CATARACT EXTRACTION BY ZONULYSIS* BY D. W. HILL St. Bartholomew's Hospital, London CATARACT extraction, after the zonule has been dissolved
Brit. J. Ophthal (1959) 43, 325. CORNEAL VASCULARIZATION AFTER CATARACT EXTRACTION BY ZONULYSIS* BY D. W. HILL St. Bartholomew's Hospital, London CATARACT extraction, after the zonule has been dissolved
Anterior segment imaging
 Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
Relationship between limbal incisions. angle. and the structures of the anterior chamber
 Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
T O Normal male 0 Normal female II U* Affected male % t7 8 t
 Brit. J. Ophthal. (I974) 58, 536 Familial glaucoma In nine generations of a South Hampshire family J. P. MARTIN AND E. C. ZORAB Southampton Eye Hospital A. Zorab (1932) reported a family suffering from
Brit. J. Ophthal. (I974) 58, 536 Familial glaucoma In nine generations of a South Hampshire family J. P. MARTIN AND E. C. ZORAB Southampton Eye Hospital A. Zorab (1932) reported a family suffering from
HYPERTENSION IN MARFAN'S SYNDROME*
 Brit. J. Ophthal. (1960) 44, 123. BILATERAL SECONDARY GLAUCOMA AND SYSTEMIC HYPERTENSION IN MARFAN'S SYNDROME* BY The Benn Hospital, Belfast SINCE Marfan (1896) first described the condition of "dolichostenomalie",
Brit. J. Ophthal. (1960) 44, 123. BILATERAL SECONDARY GLAUCOMA AND SYSTEMIC HYPERTENSION IN MARFAN'S SYNDROME* BY The Benn Hospital, Belfast SINCE Marfan (1896) first described the condition of "dolichostenomalie",
INTRA-CORNEAL LAMELLAR KERATOPLASTY*
 Brit. J. Ophthal. (1960) 44, 629. INTRA-CORNEAL LAMELLAR KERATOPLASTY* BY TADEUSZ KRWAWICZ Ophthalmological Clinic, Medical Academy, Lublin, Poland THE operative technique of lamellar keratoplasty is still
Brit. J. Ophthal. (1960) 44, 629. INTRA-CORNEAL LAMELLAR KERATOPLASTY* BY TADEUSZ KRWAWICZ Ophthalmological Clinic, Medical Academy, Lublin, Poland THE operative technique of lamellar keratoplasty is still
A ptosis repair of aponeurotic defects by the posterior approach
 British Journal of Ophthalmology, 1979, 63, 586-590 A ptosis repair of aponeurotic defects by the posterior approach J. R. 0. COLLIN From the Department of Clinical Ophthalmology, Moorfields Eye Hospital,
British Journal of Ophthalmology, 1979, 63, 586-590 A ptosis repair of aponeurotic defects by the posterior approach J. R. 0. COLLIN From the Department of Clinical Ophthalmology, Moorfields Eye Hospital,
SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP*
 Brit. J. Ophthal. (1959) 43, 361. SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP* BY V. CAVKA Belgrade, Yugoslavia AMONG the various operative procedures carried out for detachment of the retina,
Brit. J. Ophthal. (1959) 43, 361. SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP* BY V. CAVKA Belgrade, Yugoslavia AMONG the various operative procedures carried out for detachment of the retina,
Written by Administrator Wednesday, 13 January :27 - Last Updated Thursday, 21 January :34
 angle closure glaucoma A type of glaucoma caused by a sudden and severe rise in eye pressure. Occurs when the pupil enlarges too much or too quickly, and the outer edge of the iris blocks the eye s drainage
angle closure glaucoma A type of glaucoma caused by a sudden and severe rise in eye pressure. Occurs when the pupil enlarges too much or too quickly, and the outer edge of the iris blocks the eye s drainage
PERIPHERAL IRI]DECTOMY IN CLOSED-ANGLE GLAUCOMA*
![PERIPHERAL IRI]DECTOMY IN CLOSED-ANGLE GLAUCOMA* PERIPHERAL IRI]DECTOMY IN CLOSED-ANGLE GLAUCOMA*](/thumbs/92/109283083.jpg) Brit. J. Ophthal. (1959) 43, 114. PERIPHERAL IRI]DECTOMY IN CLOSED-ANGLE GLAUCOMA* BY Manchester Royal Eye Hospital PERIPHERAL iridectomy has become an accepted method of treating closedangle glaucoma.
Brit. J. Ophthal. (1959) 43, 114. PERIPHERAL IRI]DECTOMY IN CLOSED-ANGLE GLAUCOMA* BY Manchester Royal Eye Hospital PERIPHERAL iridectomy has become an accepted method of treating closedangle glaucoma.
EFFECTS OF PREDNISOLONE EYE DROPS*t
 Brit. J. Ophthal. (1967) 51, 398 EFFECTS OF PREDNISOLONE EYE DROPS*t A TRIAL OF THE EFFECTS OF PREDNISOLONE PHOSPHATE EYE DROPS ON THE INTRA-OCULAR PRESSURE OF NORMAL VOLUNTEERS BY T. G. RAMSELL, W. TRILLWOOD,
Brit. J. Ophthal. (1967) 51, 398 EFFECTS OF PREDNISOLONE EYE DROPS*t A TRIAL OF THE EFFECTS OF PREDNISOLONE PHOSPHATE EYE DROPS ON THE INTRA-OCULAR PRESSURE OF NORMAL VOLUNTEERS BY T. G. RAMSELL, W. TRILLWOOD,
cryotherapy Pigment fallout and uveitis after (Lincoff, Baras, and McLean, I965). Moorfields Eye Hospital, City Road, London, E.C.
 Brit. J. Ophthal. (I 97) 57, 156 Pigment fallout and uveitis after cryotherapy A. H. CHIGNELL, R. S. CLEMETT, AND I. H. S. REVIE Moorfields Eye Hospital, City Road, London, E.C. i Cryotherapy, first advocated
Brit. J. Ophthal. (I 97) 57, 156 Pigment fallout and uveitis after cryotherapy A. H. CHIGNELL, R. S. CLEMETT, AND I. H. S. REVIE Moorfields Eye Hospital, City Road, London, E.C. i Cryotherapy, first advocated
M-Sphere Orbital Implant Surgical Guide
 MOLTENO Orbital Implant Surgical Guide A Step by Step Guide to inserting the Natural Hydroxyapatite Orbital Implant 0316-SG/MS Anthony C. B. Molteno, FRCS, FRACO Copyright Anthony C. B. Molteno Molteno,
MOLTENO Orbital Implant Surgical Guide A Step by Step Guide to inserting the Natural Hydroxyapatite Orbital Implant 0316-SG/MS Anthony C. B. Molteno, FRCS, FRACO Copyright Anthony C. B. Molteno Molteno,
Cronicon EC OPHTHALMOLOGY. Research Article Trephine Assisted Trabeculectomy Technique. Idrees* Introduction
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Article Idrees* Al Dara Hospital and Medical Center at Riyadh, Saudi Arabia *Corresponding Author: Dr Idrees, Al Dara Hospital and Medical Center at Riyadh,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Article Idrees* Al Dara Hospital and Medical Center at Riyadh, Saudi Arabia *Corresponding Author: Dr Idrees, Al Dara Hospital and Medical Center at Riyadh,
implants Marks V, VII, and VIII
 Brit. J. Ophthal. (1975) 59, 99 Long-term results of the Choyce anterior chamber lens implants Marks V, VII, and VIII JOHN L. PEARCE Redditch, Worcs This paper continues the assessment of the long-term
Brit. J. Ophthal. (1975) 59, 99 Long-term results of the Choyce anterior chamber lens implants Marks V, VII, and VIII JOHN L. PEARCE Redditch, Worcs This paper continues the assessment of the long-term
Basic microsurgical suturing techniques for beginners
 ESCRS 2014 Basic microsurgical suturing techniques for beginners Trauma, sclera, trabeculectomy B.O. Bachmann Dept. of Ophthalmology, University of Cologne, Germany Financial interests: none Investigating
ESCRS 2014 Basic microsurgical suturing techniques for beginners Trauma, sclera, trabeculectomy B.O. Bachmann Dept. of Ophthalmology, University of Cologne, Germany Financial interests: none Investigating
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
frontalis muscle while the patient makes an attempt to open the eye. With the first and third classes I am not now concerned, except
 OPERATION FOR THE RELIEF OF CONGENITAL PTOSIs 741 AN OPERATION FOR THE RELIEF OF CONGENITAL PTOSIS* BY R. AFFLECK GREEVES LONDON CASES of congenital ptosis may be conveniently divided, clinically, into
OPERATION FOR THE RELIEF OF CONGENITAL PTOSIs 741 AN OPERATION FOR THE RELIEF OF CONGENITAL PTOSIS* BY R. AFFLECK GREEVES LONDON CASES of congenital ptosis may be conveniently divided, clinically, into
Auditors Desk Reference
 Auditors Desk Reference 2016 Contents Chapter 1. Auditing Processes and Protocols... 1 Claims Reimbursement... 1 Role of Audits... 6 Medical Record Documentation... 9 Chapter 2. Focusing and Performing
Auditors Desk Reference 2016 Contents Chapter 1. Auditing Processes and Protocols... 1 Claims Reimbursement... 1 Role of Audits... 6 Medical Record Documentation... 9 Chapter 2. Focusing and Performing
ROLE OF ORAL GLYCEROL IN GLAUCOMA*
 Brit. J. Ophthal. (1965) 49, 660 ROLE OF ORAL GLYCEROL IN GLAUCOMA* BY P. AWASTHI AND S. N. SRIVASTAVA Department of Ophthalmology,_Sarojni Naidu Medical College, Agra, India IN cases of acute glaucoma
Brit. J. Ophthal. (1965) 49, 660 ROLE OF ORAL GLYCEROL IN GLAUCOMA* BY P. AWASTHI AND S. N. SRIVASTAVA Department of Ophthalmology,_Sarojni Naidu Medical College, Agra, India IN cases of acute glaucoma
Trabeculectomy A Review and 2 Year Follow Up
 ORIGINAL ARTICLE Trabeculectomy A Review and 2 Year Follow Up F Jaais, (MRCOphth) Department of Ophthalmology, University Malaya Medical Center, Faculty of Medicine, 50603 Kuala Lumpur Summary This study
ORIGINAL ARTICLE Trabeculectomy A Review and 2 Year Follow Up F Jaais, (MRCOphth) Department of Ophthalmology, University Malaya Medical Center, Faculty of Medicine, 50603 Kuala Lumpur Summary This study
Malawi. Ocular leprosy in. Clinical and therapeutic survey of 8,325 leprosy. patients
 Brit. 5. Ophthal. (I 970) 54, I 07 Ocular leprosy in Malawi Clinical and therapeutic survey of 8,325 leprosy patients U. TICHO AND I. BEN SIRA Eye Department, Hadassah Medical Centre, Jerusalem, Israel
Brit. 5. Ophthal. (I 970) 54, I 07 Ocular leprosy in Malawi Clinical and therapeutic survey of 8,325 leprosy patients U. TICHO AND I. BEN SIRA Eye Department, Hadassah Medical Centre, Jerusalem, Israel
Federov iris-supported intraocular acrylic lens
 Brit. j. Ophthal. (I974) 58, 718 Federov iris-supported intraocular acrylic lens P. JARDINE AND J. H. SANDFORD-SMITH Bristol Eye Hospital, Bristol The use of intraocular lenses in the correction of aphakia
Brit. j. Ophthal. (I974) 58, 718 Federov iris-supported intraocular acrylic lens P. JARDINE AND J. H. SANDFORD-SMITH Bristol Eye Hospital, Bristol The use of intraocular lenses in the correction of aphakia
RETINAL DETACHMENT AT THE POSTERIOR POLE*
 Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
TRABECULECTOMY. Dr. Sandra M. Johnson, MD
 TRABECULECTOMY Dr. Sandra M. Johnson, MD FILTRATION OPTIONS Trabeculotomy, Schlemn s canal, internal Deep Non-penetrating Sclerectomy filtering to a scleral lake, or viscocanulostomy Trabeculectomy shunting
TRABECULECTOMY Dr. Sandra M. Johnson, MD FILTRATION OPTIONS Trabeculotomy, Schlemn s canal, internal Deep Non-penetrating Sclerectomy filtering to a scleral lake, or viscocanulostomy Trabeculectomy shunting
VASCULAR CHANGES THAT OCCUR DURING THE CHRONIC GLAUCOMA* PHASIC VARIATIONS OF TENSION IN
 Brit. J. Ophthal. (1953) 37, 293. VASCULAR CHANGES THAT OCCUR DURING THE PHASIC VARIATIONS OF TENSION IN CHRONIC GLAUCOMA* BY J. H. DOBREE From the Glaucoma Clinic, Institute of Ophthalmology, University
Brit. J. Ophthal. (1953) 37, 293. VASCULAR CHANGES THAT OCCUR DURING THE PHASIC VARIATIONS OF TENSION IN CHRONIC GLAUCOMA* BY J. H. DOBREE From the Glaucoma Clinic, Institute of Ophthalmology, University
Beginner (score = 3) Can hold goniolens but hesitates to move to visualize a different angle.
 Instructions: Use one form per trainee For each competency, allocate a score to the trainee s level of execution of said skill: Novice (Score = 2), Beginner (Score = 3), Advanced (Score 4), and Competent
Instructions: Use one form per trainee For each competency, allocate a score to the trainee s level of execution of said skill: Novice (Score = 2), Beginner (Score = 3), Advanced (Score 4), and Competent
Injection Techniques Principles and Practice. Introduction. Learning Objectives 5/18/2015. Richard E. Castillo, OD, DO
 Injection Techniques Principles and Practice Richard E. Castillo, OD, DO Administering injections is considered a routine clinic activity Safety demands knowledge of: Anatomy & Physiology Pharmacology
Injection Techniques Principles and Practice Richard E. Castillo, OD, DO Administering injections is considered a routine clinic activity Safety demands knowledge of: Anatomy & Physiology Pharmacology
Surgical outcome of phacoemulsification combined with the Pearce trabeculect~m~ in patients with glaucoma
 Surgical outcome of phacoemulsification combined with the Pearce trabeculect~m~ in patients with glaucoma Louis R. Pasquale, M.D., S. Gregory Smith, M.D. ABSTRACT The safety and efficacy of phacoemulsification
Surgical outcome of phacoemulsification combined with the Pearce trabeculect~m~ in patients with glaucoma Louis R. Pasquale, M.D., S. Gregory Smith, M.D. ABSTRACT The safety and efficacy of phacoemulsification
Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk cases
 European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
SECOND SEASON PREDNISONE TREATMENT IN VERNAL CONJUNCTIVITIS WITH SPECIAL REFERENCE TO CORNEAL COMPLICATIONS*
 Brit. J. Ophthal. (1958) 42, 674. SECOND SEASON PREDNISONE TREATMENT IN VERNAL CONJUNCTIVITIS WITH SPECIAL REFERENCE TO CORNEAL COMPLICATIONS* BY ELI NEUMANN From the Department of Ophthalmology, Hadassah
Brit. J. Ophthal. (1958) 42, 674. SECOND SEASON PREDNISONE TREATMENT IN VERNAL CONJUNCTIVITIS WITH SPECIAL REFERENCE TO CORNEAL COMPLICATIONS* BY ELI NEUMANN From the Department of Ophthalmology, Hadassah
UNIQUE CHANGES IN THE RETINAL VEINS OF A DIABETIC PATIENT*
 Brit. J. Ophthal. (1962) 46, 737. UNIQUE CHANGES IN THE RETINAL VEINS OF A DIABETIC PATIENT* BY Nuffield Laboratory of Ophthalmology, Oxford, and Cape Town, Union of South Africa THis paper illustrates
Brit. J. Ophthal. (1962) 46, 737. UNIQUE CHANGES IN THE RETINAL VEINS OF A DIABETIC PATIENT* BY Nuffield Laboratory of Ophthalmology, Oxford, and Cape Town, Union of South Africa THis paper illustrates
PLATE 34. (Received for publication, June 6, 1921.)
 Published Online: 1 November, 1921 Supp Info: http://doi.org/10.1084/jem.34.5.435 Downloaded from jem.rupress.org on October 18, 2018 REMOTE RESULTS OF COMPLETE HOMOTRANSPLAN- TATION OF THE CORNEA, BY
Published Online: 1 November, 1921 Supp Info: http://doi.org/10.1084/jem.34.5.435 Downloaded from jem.rupress.org on October 18, 2018 REMOTE RESULTS OF COMPLETE HOMOTRANSPLAN- TATION OF THE CORNEA, BY
STRUCTURE OF THE VITREOUS BODY*
 Brit. J. Ophthal. (1953) 37, 343. STRUCTURE OF THE VITREOUS BODY* OBSERVATIONS BY MEANS OF THE PHASE-CONTRAST MICROSCOPE BY ANTONIO A. ROSSI From the Institute of Ophthalmology, London (Director of Research,
Brit. J. Ophthal. (1953) 37, 343. STRUCTURE OF THE VITREOUS BODY* OBSERVATIONS BY MEANS OF THE PHASE-CONTRAST MICROSCOPE BY ANTONIO A. ROSSI From the Institute of Ophthalmology, London (Director of Research,
Glaucoma. How is Glaucoma Diagnosed? Glaucoma Testing
 Glaucoma How is Glaucoma Diagnosed? Glaucoma Testing There is no single test for glaucoma. The diagnosis is made by evaluating the patient from a number of perspectives, using specialized instruments.
Glaucoma How is Glaucoma Diagnosed? Glaucoma Testing There is no single test for glaucoma. The diagnosis is made by evaluating the patient from a number of perspectives, using specialized instruments.
EPISCLERAL VESSELS* EFFECT OF RAISED OCULAR TENSION ON THE. general concensus of opinion as to how, or why, the vascular changes develop.
 Brit. J. Ophthal. (1954) 38, 500. EFFECT OF RAISED OCULAR TENSION ON THE EPISCLERAL VESSELS* DEVELOPMENT OF THE CAPUT MEDUSAE IN PRIMARY GLAUCOMA BY J. H. DOBREE From the Glaucoma Clinic, Institute of
Brit. J. Ophthal. (1954) 38, 500. EFFECT OF RAISED OCULAR TENSION ON THE EPISCLERAL VESSELS* DEVELOPMENT OF THE CAPUT MEDUSAE IN PRIMARY GLAUCOMA BY J. H. DOBREE From the Glaucoma Clinic, Institute of
Objectives. Tubes, Ties and Videotape: Financial Disclosure. Five Year TVT Results IOP Similar
 Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
JMSCR Volume 03 Issue 01 Page January 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Pterygium Excision and Conjunctival Autograft A Study Authors Dr. M. Premanandam 1, Dr. A. Geetha 2, Dr. Himabindu 3 1 MS, Associate Professor,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Pterygium Excision and Conjunctival Autograft A Study Authors Dr. M. Premanandam 1, Dr. A. Geetha 2, Dr. Himabindu 3 1 MS, Associate Professor,
VISUAL PROGNOSIS OF PROLIFERATING DIABETIC
 Brit. J. Ophthal. (1963) 47, 611. VISUAL PROGNOSIS OF PROLIFERATING DIABETIC RETINOPATHY* BY WILLIAM PARKES BEETHAM From the Harvard Medical School, the Massachusetts Eye and Ear Infirmary, and the New
Brit. J. Ophthal. (1963) 47, 611. VISUAL PROGNOSIS OF PROLIFERATING DIABETIC RETINOPATHY* BY WILLIAM PARKES BEETHAM From the Harvard Medical School, the Massachusetts Eye and Ear Infirmary, and the New
PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL
 PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL Endothelial keratoplasty (EK) has evolved at a brisk pace and the volume of data accumulated over the past 10 years has demonstrated that
PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL Endothelial keratoplasty (EK) has evolved at a brisk pace and the volume of data accumulated over the past 10 years has demonstrated that
EVALUATION OF SUSTAINED-RELEASE ACETAZOLAMIDE*t
 Brit. J. Ophthal. (1963) 47, 31. From the EVALUATION OF SUSTAINED-RELEASE ACETAZOLAMIDE*t BY CARLOS MESTRE, MILES A. GALIN, AND JOHN M. McLEANt Department of Surgery (Ophthalmology) of The New York Hospital-Cornell
Brit. J. Ophthal. (1963) 47, 31. From the EVALUATION OF SUSTAINED-RELEASE ACETAZOLAMIDE*t BY CARLOS MESTRE, MILES A. GALIN, AND JOHN M. McLEANt Department of Surgery (Ophthalmology) of The New York Hospital-Cornell
Information for Patients. Deep sclerectomy for the treatment of Glaucoma
 Manchester Royal Eye Hospital Glaucoma Services Information for Patients Deep sclerectomy for the treatment of Glaucoma Introduction This leaflet provides information for patients being offered deep sclerectomy
Manchester Royal Eye Hospital Glaucoma Services Information for Patients Deep sclerectomy for the treatment of Glaucoma Introduction This leaflet provides information for patients being offered deep sclerectomy
Vascular changes in the iris in chronic
 Vascular changes in the iris in chronic anterior uveitis LEILA LAATIKAINEN From the Department of Ophthalmology, University of Helsinki, Finland British Journal of Ophthalmology, 1979, 63, 145-149 SUMMARY
Vascular changes in the iris in chronic anterior uveitis LEILA LAATIKAINEN From the Department of Ophthalmology, University of Helsinki, Finland British Journal of Ophthalmology, 1979, 63, 145-149 SUMMARY
Subject Index. Canaloplasty aqueous outflow system evaluation 110, 111 complications 118, 119 historical perspective 109, 110
 Subject Index Ab externo Schlemm canal surgery, see Canaloplasty, Viscocanalostomy Ab interno Schlemm canal surgery, see istent, Trabectome Adjustable sutures 14, 15 AGV glaucoma drainage implants 43,
Subject Index Ab externo Schlemm canal surgery, see Canaloplasty, Viscocanalostomy Ab interno Schlemm canal surgery, see istent, Trabectome Adjustable sutures 14, 15 AGV glaucoma drainage implants 43,
Glaucoma. What is glaucoma? Eye Words to Know. What causes glaucoma?
 2014 2015 Glaucoma What is glaucoma? Glaucoma is a disease that damages your eye s optic nerve. It usually happens when fluid builds up in the front part of your eye. That extra fluid increases the pressure
2014 2015 Glaucoma What is glaucoma? Glaucoma is a disease that damages your eye s optic nerve. It usually happens when fluid builds up in the front part of your eye. That extra fluid increases the pressure
Surgery of the glaucomas
 Surgery of the glaucomas P. G. WATSON Cambridge Once the decision to operate has been made, one question remains: which surgical procedure is best for that patient? As time has passed the choice of procedure
Surgery of the glaucomas P. G. WATSON Cambridge Once the decision to operate has been made, one question remains: which surgical procedure is best for that patient? As time has passed the choice of procedure
INSERTION* SURGICAL ANATOMY OF THE LEVATOR PALPEBRAE. impossible to dissect and separate these layers. That the levator aponeurosis
 Brit. J. Ophthal. (1962) 46, 503. SURGICAL ANATOMY OF THE LEVATOR PALPEBRAE INSERTION* BY EDWARD EPSTEIN Johannesburg, Union of South Africa THE text-book description of the anatomy of the upper eyelid
Brit. J. Ophthal. (1962) 46, 503. SURGICAL ANATOMY OF THE LEVATOR PALPEBRAE INSERTION* BY EDWARD EPSTEIN Johannesburg, Union of South Africa THE text-book description of the anatomy of the upper eyelid
_ Assessment of the anterior chamber. Review of anatomy of the angle
 Assessment of the anterior chamber Dr Simon Barnard PhD BSc FCOptom FAAO DCLP Department of Optometry & Visual Science City University London, UK Review of anatomy of the angle Figure 1. Anatomical section
Assessment of the anterior chamber Dr Simon Barnard PhD BSc FCOptom FAAO DCLP Department of Optometry & Visual Science City University London, UK Review of anatomy of the angle Figure 1. Anatomical section
Trabeculectomy with ologen implant versus trabeculectomy with mitomycin-c in primary open angle glaucoma: A 2-year study
 World Journal of Pharmaceutical Sciences ISSN (Print): 2321-3310; ISSN (Online): 2321-3086 Available online at: http://www.wjpsonline.org/ Original Article Trabeculectomy with ologen implant versus trabeculectomy
World Journal of Pharmaceutical Sciences ISSN (Print): 2321-3310; ISSN (Online): 2321-3086 Available online at: http://www.wjpsonline.org/ Original Article Trabeculectomy with ologen implant versus trabeculectomy
