Comparison of clinical and radiographic status around dental implants placed in patients with and without prediabetes: 1-year follow-up outcomes
|
|
|
- Branden Anthony
- 6 years ago
- Views:
Transcription
1 Mohammad D. Al Amri Tariq S. Abduljabbar Abdulaziz A. Al-Kheraif Georgios E. Romanos Fawad Javed Comparison of clinical and radiographic status around dental implants placed in patients with and without prediabetes: 1-year follow-up outcomes Authors affiliations: Mohammad D. Al Amri, Tariq S. Abduljabbar, Department of Prosthetic Dental Sciences, College of Dentistry, King Saud University, Riyadh, Saudi Arabia Abdulaziz A. Al-Kheraif, Dental Health Department, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia Georgios E. Romanos, Department of Periodontology, School of Dental Medicine, Stony Brook University, Stony Brook, NY, USA and; Department of Oral Surgery and Implant Dentistry, Johann Wolfgang University, Frankfurt, Germany Fawad Javed, Department of General Dentistry, Eastman Institute for Oral Health, University of Rochester, Rochester, NY, USA Corresponding author: Dr Mohammad D. Al Amri Department of Prosthetic Dental Sciences College of Dentistry King Saud University P.O. Box 60169, Riyadh 11545, Saudi Arabia Tel.: Fax: Key words: clinical parameters, dental implant, marginal bone loss, prediabetes, success rate Abstract Objective: We hypothesized that peri-implant soft tissue inflammation is worse and peri-implant marginal bone loss (MBL) is higher around dental implants placed in patients with prediabetes compared to healthy subjects. The aim of the present 12-month follow-up study was to compare the clinical and radiographic status around dental implants placed in patients with and without prediabetes. Material and methods: Twelve patients with medically diagnosed prediabetes (Group-1) and 12 controls (Group-2) were included. All patients were indicated for single tooth maxillary or mandibular premolar replacement with the adjacent teeth intact. Success of the restored implants was assessed by comparing clinical (peri-implant bleeding on probing [BOP], and probing pocket depth [PPD]) and radiographic (peri-implant MBL) parameters at baseline and at 12-months followup. Statistical analysis was performed using one-way analysis of variance, and P-values <0.05 were considered statistically significant. Results: At 12 months of follow-up, there was no clinical evidence for the presence of plaque, BOP and peri-implant pockets with PPD 4 mm in both groups. At 12-month follow-up, the mean MBL among implants placed in groups 1 and 2 were mm and mm, respectively. Overall, the periodontal status (PI, BOP and PPD 4 mm) at 12-month follow-up was comparable among patients in both groups. Conclusion: Within the limitations of this study, it is concluded that dental implants inserted in prediabetic and healthy patients have similar success rates and remain clinically and radiographically stable after 1-year follow-up. Date: Accepted 30 December 2015 To cite this article: Al Amri MD, Abduljabbar TS, Al-Kheraif AA, Romanos GE, Javed F. Comparison of clinical and radiographic status around dental implants placed in patients with and without prediabetes: 1-year follow-up outcomes. Clin. Oral Impl. Res. 00, 2016, 1 5 doi: /clr It is known that chronic hyperglycemia negatively influences osseointegration of dental implants, and implant failure is a common manifestation in such patients (Alsaadi et al. 2008; Daubert et al. 2015). Chronic hyperglycemia has also been associated with the delayed cell proliferation and osteoblast differentiation (Colombo et al. 2011). In addition, chronic hyperglycemia has been associated with the dysregulation of bone factors such as transforming growth factor-beta, fibroblast growth factor, osteopontin, osteocalcin and osteoprotegerin in the peri-implant crevicular fluid (Ghiraldini et al. 2015). Although optimal glycemic control in patients with diabetes has been reported to enhance osseointegration (Javed & Romanos 2009), results from a recent clinical trial showed that elevated hemoglobin A1c (HbA1c) levels in patients with type 2 diabetes mellitus (T2DM) were not associated with altered implant success after 1 year of loading (Oates et al. 2014). However, alterations in early bone healing and implant stability were associated with chronic hyperglycemia (Oates et al. 2014). Similar results were reported in another clinical study (Ghiraldini et al. 2015). Prediabetes, a state of abnormal glucose homeostasis, is characterized by the presence of impaired fasting glucose, impaired glucose tolerance, or both (American Diabetes Association 2015a). Prediabetes designations have been defined by fasting glucose levels of milligrams per deciliter (mg/dl), hemoglobin A1c (HbA1c) levels between 5.7% and 6.4% and postglucose challenge levels of mg/dl (Olson et al. 2010; American Diabetes Association 2015b). Studies (Javed et al. 2012a,b, 2013, 2014a,b, 2015; Alshehri 2016 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd 1
2 & Javed 2015) have shown that scores of periodontal inflammatory parameters (such as bleeding on probing [BOP] and probing pocket depth [PPD]) are higher among patients with prediabetes compared with systemically healthy individuals (controls). Although marginal bone loss (MBL) as measured on radiograph is also higher in prediabetic patients compared with controls (Javed et al. 2014a,b); controversial results have also been reported (Kowall et al. 2015). As patients with prediabetes exhibit a poorer periodontal (clinical and radiographic) status compared with controls (Javed et al. 2014a,b), it is hypothesized that peri-implant soft tissue inflammation is worse and MBL is higher around dental implants placed in patients with prediabetes compared to healthy subjects. The aim of the present 1- year follow-up case-control study was to assess the clinical and radiographic status around dental implants placed in patients with prediabetes. Material and methods Ethical approvals The study was approved by the Research Ethics Review committee of the College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia. Volunteering individuals were requested to read and sign a consent form. Inclusion and exclusion criteria The inclusion criteria were (a) patients with medically diagnosed prediabetes and (b) selfreported systemically healthy controls. The exclusion criteria were as follows: (a) patients with systemic disorders other than prediabetes (such as type 1 diabetes mellitus, T2DM, renal disorders, acquired immune deficiency syndrome and cardiovascular disorders); (b) individuals using tobacco products (smokers and tobacco chewers); (c) pregnant and/or lactating females; (d) patients with a history of antibiotic and/or steroid intake within the past 3 months of implant placement; and (e) use of bone augmentation protocols. Participants In total, 24 male patients (12 patients with prediabetes [Group-1] and 12 controls [Group- 2]) were included. Patients in Group-1 were requested to present their medical records to determine the date of the most recent assessment of hemoglobin A1C, fasting plasma glucose or oral glucose tolerance test that confirmed the diagnosis of prediabetes in the study population. These individuals were recruited from the Department of Prosthetic Dental Sciences, College of Dentistry, King Saud University, Riyadh, Saudi Arabia. In both groups, patients had implants placed for the replacement of a single premolar tooth in the maxilla or mandible with adjacent teeth intact. All patients underwent full-mouth scaling using an ultrasonic scaler (VV DENTA, Guangxi, China) prior to implant placement. Measurement of hemoglobin A1c levels In both groups, HbA1c levels were measured at the time of surgery, after 6 months and 1 year of follow-up. Venous blood samples were drawn in the morning, and HbA1c levels were determined using the high-performance liquid chromatography method (Bio- Rad Laboratories, Inc., D-10TM; Hemoglobin Systems, Hercules, CA, USA) (Ozcelik et al. 2010). Individuals with HbA1c levels ranging between % and 4 5.5% were categorized as prediabetic individuals and controls, respectively (American Diabetes Association 2015a,b). Surgical protocol A 7-day course of wide-spectrum antibiotic (Amoxicillin 500 mg 8 h) was started 3 days before the participants were scheduled for implant surgery. Clindamycin (150 mg 6 h for 7 days) was prescribed as an alternate antibiotic for individuals with a self-reported history of penicillin allergy. Following local anesthesia, a crestal incision was made using a #15 blade and full-thickness mucoperiosteal flaps were raised to expose the bone. A total of 24 bone level implants (12 implants in Group-1 and 12 in Group-2) were placed in the center of the healed alveolar ridge (day 0) using an insertion torque of Ncm. The implants used had a diameter of 3.5 mm and ranging in length from 10 to 16 mm (Straumann â Dental Implant System, Institut Straumann, AG Peter Merian-Weg 12 CH-4002 Basel, Switzerland). Healing abutments were connected to the implants using hand torque (day 0). The flaps were sutured around the healing abutment using resorbable sutures (4/0 Vicryl), and digital intraoral postoperative radiographs were taken. After a mean duration of 3.5 months, final impressions were made for the fabrication of a definitive porcelain-fused-to-metal (PFM) implant-supported prosthesis (day 112). All implants were loaded with screw-retained PFM crowns. Postoperative management Participants were advised to complete the 7- day antibiotic course, which had started 3 days before surgery. Analgesics (Ibuprofen 600 mg 6 h for 5 days) were also prescribed for pain control. Acetaminophen (325 mg 6 h for 5 days) was prescribed as an alternate analgesic for individuals who reported to be allergic to ibuprofen. Participants in both groups were instructed to rinse with a 0.12% chlorhexidine gluconate solution (Corsodyl, Boots, Nottingham, UK) twice daily for 2 weeks. Oral hygiene instructions were given to all patients, and they were also enrolled in a 6-month follow-up dental prophylaxis program (ultrasonic cleaning) for 1 year. Patients were advised to maintain their serum glycemic levels and were also suggested to contact their primary care physicians in this regard. Clinical and radiographic parameters Peri-implant and full-mouth plaque index (PI), BOP and PPD 4 mm were assessed among individuals in both groups. These parameters were assessed at six sites per tooth/implant (mesiobuccal, midbuccal, distobuccal, mesiolingual, midlingual and distolingual). For the assessment of PPD, a metal periodontal probe with a tip diameter of 0.42 mm (Zeffiro, Lascod spa, Sesto Fiorentino, Italy) was inserted into the peri-implant sulcus and the most apically probable distance was recorded in millimeters (Abreu et al. 2007; Zitzmann & Berglundh 2008). In both groups, evidence of any radiolucency and mesial and/or distal marginal bone loss (MBL) around the implants was determined at 6 and 12 months of follow-up. Digital intraoral radiographs were taken and visualized on a computer screen. Radiographs were analyzed at 209 magnification using a software (CorelDraw 11.0, Corel Corp and Coral Ltd, Ottawa, Canada). MBL was defined as the distance from the widest supracrestal part of the implant to the crestal bone level (Mumcu et al. 2011). Criteria for implant success The criteria for implant success were (a) stable implants and superstructures, (b) no symptoms of pain, (c) no signs of BOP and/or purulent discharge, (d) MBL of 1 mm around the implant in the first year, and (e) absence of radiolucency around implants. Statistical analysis Statistical analysis was performed using a software program (SPSS Version 18, Chicago, IL, USA). BOP, PPD and MBL among patients 2 Clin. Oral Impl. Res. 0, 2016 / John Wiley & Sons A/S. Published by John Wiley & Sons Ltd
3 at 6 months and 12 months of follow-up in both groups were compared using the nonparametric Mann Whitney U-test. P-values less than 0.05 were considered statistically significant. Results General characteristics of the study population The mean age of participants in groups 1 and 2 were 44.5 years (41 49 years) and 43.3 years (39 47 years), respectively. At baseline, the mean HbA1c levels were significantly higher among patients in Group-1 compared to patients in Group-2 (P = 0.002). There was no statistically significant difference in mean HbA1c levels among patients in groups 1 and 2 at 6 and 12 months of follow-up (Table 1). In both groups, all implants were clinically stable with no signs of mobility and/or inflammation. None of the participants were allergic to amoxicillin or ibuprofen. Full-mouth plaque index, bleeding on probing and probing depth among individuals in groups 1 and 2 At baseline, there was no statistically significant difference of plaque, BOP and PPD 4 mm among patients in groups 1 and 2. In both groups, there was a statistically significant difference in PI, BOP and PPD 4 mm at 6 months (P = 0.00) and 12 months (P = 0.00) of follow-up. There was no significant difference in PI, BOP and PPD 4 mm at 6- and 12-month follow-ups among patients in groups 1 and 2 (Table 2). Peri-implant plaque index, bleeding on probing and probing depth among individuals in groups 1 and 2 after 6 and 12 months of follow-up In both groups, there was no clinical evidence of peri-implant pockets with PPD 4 mm at 6 and 12 months of followup. At 6 and 12 months of follow-up, there was no clinical evidence for the presence of plaque, BOP and peri-implant pockets with PPD 4 mm in both groups. Marginal bone loss among individuals in groups 1 and 2 after 6 and 12 months of follow-up There was no radiographic evidence of MBL around implants placed in groups 1 and 2 at 6-month follow-up. At 12-month follow-up, the mean MBL among implants placed in groups 1 and 2 were mm and mm, respectively (P = 0.12). Discussion To our knowledge from indexed literature, this is the first study, which assessed the clinical and radiographic parameters status of implants placed in patients with and without prediabetes. We reviewed the patients records to determine the date of the most recent assessment of HbA1C, fasting plasma glucose or oral glucose tolerance test which was performed. This was used mainly to confirm the prediabetic state of the participants. However, for the present study, we elected to measure HbA1c levels to have the most updated glycemic levels in the present study. In this study, it was hypothesized that the peri-implant soft tissue inflammation is worse and MBL is higher around dental implants placed in patients with prediabetes compared to controls. This hypothesis was based on the fact that chronic hyperglycemia is associated with an increased formation and accumulation of advanced glycation endproducts in periodontal tissues, which augment inflammation, and if hyperglycemia is left uncontrolled, it may lead to MBL around teeth (Lalla et al. 2000; Chang et al. 2013, 2014). Interestingly, the present results showed that all implants remained clinically stable up to 12 months of follow-up with no signs of soft tissue inflammation. An explanation in this regard could be derived from the fact that all participants were given strict oral hygiene maintenance instructions and were also enrolled in a 6-month dental prophylaxis program. In the dental prophylaxis program, ultrasonic scalers were used to eradicate any stagnated plaque from teeth Table 1. Mean HbA1c levels among patients in groups 1 and 2 at baseline and after 6 and 12 months of follow-up Study groups (n) Hemoglobin A1c (%) Baseline 6 months follow-up Group-1 (n = 12) * Group-2 (n = 12) *Compared to Group-2 at baseline (P = 0.002). SD, standard deviation. 12 months follow-up and implant surfaces, and at every visit, it was clinically ensured that the patients are maintaining good oral hygiene status. It is interesting to note that the overall periodontal status of individuals with and without prediabetes was comparable at 6 and 12 months of follow-up (Table 2). In a 10- year follow-up clinical study, Degidi et al. (2012) found that the long-term bone levels around dental implants can be maintained when levels of oral hygiene are kept adequate. Likewise, clinical results by Lin et al. (2011) demonstrated that a 100% success rate of implants can be achieved provided that oral hygiene maintenance and periimplant gingival health are ensured. Authors of the present study support the studies by Degidi et al. (2012) and Lin et al. (2011). However, from the present results, it is evident that optimal oral hygiene maintenance not only prevents MBL around implants in systemically healthy individuals, but also in hyperglycemic patients, such as those with prediabetes. It is therefore imperative for clinicians to educate patients about the importance of regular oral hygiene maintenance and its beneficial influences on teeth and implants. Studies have shown that non-surgical periodontal therapy (NSPT) plays a role in reducing periodontal inflammation and serum glycemic levels among patients with chronic hyperglycemia (Stewart et al. 2001; Simpson et al. 2010; Corbella et al. 2013; Javed et al. 2014a,b). However, it has also been reported that NSPT reduces periodontal inflammation but does not significantly affect metabolic control in hyperglycemic patients (Serrano et al. 2012; Alshehri & Javed 2015). In the present study, a trend toward decrease in HbA1c level was observed among patients with prediabetes (Group-1); however, compared to baseline glycemic levels, HbA1c levels measured at 12-months of follow-up failed to show any statistically significant difference. The present 1-year follow-up results support the study by Oates et al. (2014), which showed that elevated HbA1c levels in patients with type 2 diabetes were not associated with altered implant success 1 year after loading. Moreover, clinical evidence from several investigations has suggested that although glycemic control is an important consideration that may require modifications in the treatment protocols, hyperglycemia may not be as a contraindication to implant therapy in diabetic patients (Oates & Huynh-Ba 2012; Oates et al. 2013, 2014) John Wiley & Sons A/S. Published by John Wiley & Sons Ltd 3 Clin. Oral Impl. Res. 0, 2016 / 1 5
4 Table 2. Median standard deviation full-mouth plaque index, bleeding on probing and probing depth among individuals in groups 1 and 2 after 6 and 12 months of follow-up Parameters Baseline 6-month follow-up 12-month follow-up Baseline 6-month follow-up 12-month follow-up Plaque index (%) * Bleeding on probing (%) * Probing depth 4 mm (%) * *Compared to 6-month follow-up in Group-1 (P = 0.000). Compared to 12-month follow-up in Group-1 (P = 0.00). Compared to 6-month follow-up in Group-2 (P = 0.00). Compared to 12-month follow-up in Group-2 (P = 0.00). Group-1 (n = 12) Group-2 (n = 12) It is well-known that a history of periodontal disease is a significant risk factor for periimplant diseases (peri-implant mucositis and peri-implantitis) (Serino & Str om 2009; Renvert & Quirynen 2015). From the baseline assessment of periodontal inflammatory parameters (PI, BOP and PPD), it is noteworthy that all participants had a relatively good oral hygiene status, with plaque accumulation and periodontal pockets of 4 mm in less than 30% and 5% sites, respectively (Table 2). This suggests that participants in both groups had an acceptable oral hygiene status and were most likely maintaining good oral hygiene. However, it is speculated that a history of periodontal disease would have most likely influenced the success of dental implants placed in both groups. Further long-term prospective studies are needed in this regard. There are a few limitations of the present study. As the present results were based on 1-year follow-up results, it is hypothesized that optimal long-term oral hygiene maintenance among patients with prediabetes would positively influence the success of implants in these patients. Moreover, it is well-established that the outcomes of oral surgical interventions and marginal bone levels are compromised in smokers as compared to non-smokers (Javed et al. 2007, 2012a,b; Kotsakis et al. 2015). It is speculated that regardless of daily oral hygiene maintenance, habitual tobacco smoking jeopardizes the outcomes of implant treatment among patients with and without prediabetes by increasing MBL around implants. In the present study, strict eligibility criteria (such as absence of other systemic diseases, no use of antibiotics/steroids within the past 3 months and absence of tobacco habits) were established for the inclusion of prediabetic patients. It is therefore possible that such factors may have influenced the outcomes of the present study. Furthermore, in the present study, implants were placed in both arches. As the bone density varies between the maxilla and mandible (Fuster-Torres et al. 2011), it is hypothesized that in the long term, jaw location may influence MBL around implants. Further long-term clinical trials are needed to test the aforementioned hypothesis. Conclusion Within the limitations of this study, it is concluded that dental implants inserted in prediabetic and healthy patients have similar success rates and remain clinically and radiographically stable after 1-year follow-up. Regular oral hygiene maintenance plays a potentially vital role for implant therapy in patients with and without prediabetes. Acknowledgements: The project was financially supported by Vice Deanship of Research Chairs, King Saud University, Riyadh, Saudi Arabia. Conflict of interest and financial disclosure The authors declare no conflict of interest. There was no external source of funding for this study. References Abreu, M.H., Bianchini, M.A., Magini, R.S. & R osing, C.K. (2007) Clinical and radiographic evaluation of periodontal and peri-implant conditions in patients with implant-supported prosthesis. Acta Odontologica Latinoamericana 20: Alsaadi, G., Quirynen, M., Michiles, K., Teughels, W., Komarek, A. & van Steenberghe, D. (2008) Impact of local and systemic factors on the incidence of failures up to abutment connection with modified surface oral implants. Journal of Clinical Periodontology 35: Alshehri, F.A. & Javed, F. (2015) Impact of scaling and root planing on clinical periodontal status and glycemic levels in prediabetic patients. Interventional Medicine and Applied Science 7: American Diabetes Association. (2015a) Standards of medical care in diabetes-2015 abridged for primary care providers. Clinical Diabetes 33: American Diabetes Association. (2015b) Standards of medical care in diabetes 2015: summary of revisions. Diabetes Care 38(Suppl.): S4. Chang, P.C., Chien, L.Y., Yeo, J.F., Wang, Y.P., Chung, M.C., Chong, L.Y., Kuo, M.Y., Chen, C.H., Chiang, H.C., Ng, B.N., Lee, Q.Q., Phay, Y.K., Ng, J.R. & Erk, K.Y. (2013) Progression of periodontal destruction and the roles of advanced glycation end products in experimental diabetes. Journal of Periodontology 84: Chang, P.C., Tsai, S.C., Chong, L.Y. & Kao, M.J. (2014) N-phenacylthiazolium bromide inhibits the advanced glycation end product (age)-age receptor axis to modulate experimental periodontitis in rats. Journal of Periodontology 85: e268 e276. Colombo, J.S., Balani, D., Sloan, A.J., Crean, S.J., Okazaki, J. & Waddington, R.J. (2011) Delayed osteoblast differentiation and altered inflammatory response around implants placed in incisor sockets of type 2 diabetic rats. Clinical Oral Implants Research 22: Corbella, S., Francetti, L., Taschieri, S., De Siena, F. & Fabbro, M.D. (2013) Effect of periodontal treatment on glycemic control of patients with diabetes: a systematic review and meta-analysis. Journal of Diabetes Investigation 4: Daubert, D.M., Weinstein, B.F., Bordin, S., Leroux, B.G. & Flemming, T.F. (2015) Prevalence and predictive factors for peri-implant disease and implant failure: a cross-sectional analysis. Journal of Periodontology 86: Degidi, M., Nardi, D. & Piattelli, A. (2012) 10-year follow-up of immediately loaded implants with tiunite porous anodized surface. Clinical Implant Dentistry and Related Research 14: Fuster-Torres, M.A., Penarrocha-Diago, M. & Penarrocha-Oltra, D. (2011) Relationships between bone density values from cone beam computed tomography, maximum insertion torque, and resonance frequency analysis at implant placement: a pilot study. International Journal of Oral & Maxillofacial Implants 26: Ghiraldini, B., Conte, A., Casarin, R.C., Casati, M.Z., Pimentel, S.P., Cirano, F.R. & Ribeiro, F.V. (2015) Influence of glycemic control on peri- 4 Clin. Oral Impl. Res. 0, 2016 / John Wiley & Sons A/S. Published by John Wiley & Sons Ltd
5 implant bone healing: 12-month outcomes of local release of bone-related factors and implant stabilization in type 2 diabetics. Clinical Implant Dentistry and Related Research. doi: / cid Javed, F., Ahmed, H.B., Mehmood, A., Bain, C. & Romanos, G.E. (2014a) Effect of nonsurgical periodontal therapy (with or without oral doxycycline delivery) on glycemic status and clinical periodontal parameters in patients with prediabetes: a short-term longitudinal randomized case-control study. Clinical Oral Investigations 18: Javed, F., Al-Askar, M., Al-Rasheed, A., Babay, N., Galindo-Moreno, P. & Al-Hezaimi, K. (2012a) Comparison of self-perceived oral health, periodontal inflammatory conditions and socioeconomic status in individuals with and without prediabetes. The American Journal of the Medical Sciences 344: Javed, F., Al-Askar, M., Samaranayake, L.P. & Al- Hezaimi, K. (2013) Periodontal disease in habitual cigarette smokers and nonsmokers with and without prediabetes. The American Journal of the Medical Sciences 345: Javed, F., Al-Kheraif, A.A., Al Amri, M.D., Alshehri, M., Vohra, F., Al-Askar, M., Malmstrom, H. & Romanos, G.E. (2015) Periodontal status and whole salivary cytokine profile among smokers and never-smokers with and without prediabetes. Journal of Periodontology 86: Javed, F., Al-Rasheed, A., Almas, K., Romanos, G.E. & Al-Hezaimi, K. (2012b) Effect of cigarette smoking on the clinical outcomes of periodontal surgical procedures. The American Journal of the Medical Sciences 343: Javed, F., Nasstrom, K., Benchimol, D., Altamash, M., Klinge, B. & Engstrom, P.E. (2007) Comparison of periodontal and socioeconomic status between subjects with type 2 diabetes mellitus and non-diabetic controls. Journal of Periodontology 78: Javed, F. & Romanos, G.E. (2009) Impact of diabetes mellitus and glycemic control on the osseointegration of dental implants: a systematic literature review. Journal of Periodontology 80: Javed, F., Thafeed Alghamdi, A.S., Mikami, T., Mehmood, A., Ahmed, H.B., Samaranayake, L.P. & Tenenbaum, H.C. (2014b) Effect of glycemic control on self-perceived oral health, periodontal parameters, and alveolar bone loss among patients with prediabetes. Journal of Periodontology 85: Kotsakis, G.A., Javed, F., Hinrichs, J.E., Karoussis, I.K. & Romanos, G.E. (2015) Impact of cigarette smoking on clinical outcomes of periodontal flap surgical procedures: a systematic review and meta-analysis. Journal of Periodontology 86: Kowall, B., Holtfreter, B., Volzke, H., Schipf, S., Mundt, T., Rathmann, W. & Kocher, T. (2015) Prediabetes and well controlled diabetes are not associated with periodontal disease: the ship trend study. Journal of Clinical Periodontology 42: Lalla, E., Lamster, I.B., Feit, M., Huang, L., Spessot, A., Qu, W., Kislinger, T., Lu, Y., Stern, D.M. & Schmidt, A.M. (2000) Blockade of rage suppresses periodontitis-associated bone loss in diabetic mice. Journal of Clinical Investigation 105: Lin, I.C., Gonzalez, A.M., Chang, H.J., Kao, S.Y. & Chen, T.W. (2011) A 5-year follow-up of 80 implants in 44 patients placed immediately after the lateral trap-door window procedure to accomplish maxillary sinus elevation without bone grafting. The International Journal of Oral & Maxillofacial Implants 26: Mumcu, E., Bilhan, H. & Cekici, A. (2011) Marginal bone loss around implants supporting fixed restorations. Journal of Oral Implantology 37: Oates, T.W., Jr, Galloway, P., Alexander, P., Vargas Green, A., Huynh-Ba, G., Feine, J. & McMahan, C.A. (2014) The effects of elevated hemoglobin a (1c) in patients with type 2 diabetes mellitus on dental implants: survival and stability at one year. The Journal of the American Dental Association 145: Oates, T.W. & Huynh-Ba, G. (2012) Diabetes effects on dental implant survival. Forum Implantology 8: Oates, T.W., Huynh-Ba, G., Vargas, A., Alexander, P. & Feine, J. (2013) A critical review of diabetes, glycemic control, and dental implant therapy. Clinical Oral Implants Research 24: Olson, D.E., Rhee, M.K., Herrick, K., Ziemer, D.C., Twombly, J.G. & Phillips, L.S. (2010) Screening for diabetes and pre-diabetes with proposed a1cbased diagnostic criteria. Diabetes Care 33: Ozcelik, F., Yiginer, O., Arslan, E., Serdar, M.A., Uz, O., Kardesoglu, E. & Kurt, I. (2010) Association between glycemic control and the level of knowledge and disease awareness in type 2 diabetic patients. Polskie Archiwum Medycyny Wewneztrznej 120: Renvert, S. & Quirynen, M. (2015) Risk indicators for peri-implantitis. A narrative review. Clinical Oral Implants Research 26(Suppl. 11): Serino, G. & Str om, C. (2009) Peri-implantitis in partially edentulous patients: association with inadequate plaque control. Clinical Oral Implants Research 20: Serrano, C., Perez, C. & Sabogal, D. (2012) Effect of periodontal therapy on metabolic control and an inflammatory mediator in type 2 diabetic subjects: a report on 17 consecutive cases. Journal of the International Academy of Periodontology 14: Simpson, T.C., Needleman, I., Wild, S.H., Moles, D.R. & Mills, E.J. (2010) Treatment of periodontal disease for glycaemic control in people with diabetes. Cochrane Database Systematic Reviews: CD Stewart, J.E., Wager, K.A., Friedlander, A.H. & Zadeh, H.H. (2001) The effect of periodontal treatment on glycemic control in patients with type 2 diabetes mellitus. Journal of Clinical Periodontology 28: Zitzmann, N.U. & Berglundh, T. (2008) Definition and prevalence of peri-implant diseases. Journal of Clinical Periodontology 35: John Wiley & Sons A/S. Published by John Wiley & Sons Ltd 5 Clin. Oral Impl. Res. 0, 2016 / 1 5
Tariq Abduljabbar DMSc 1 Nawwaf Al-Hamoudi MSc 2 Zeyad H. Al-Sowygh MSc 1 Mohammed Alajmi BDS 1 Fawad Javed PhD 3 Fahim Vohra MRD 1.
 Received: 31 October 2017 Revised: 5 November 2017 Accepted: 6 November 2017 DOI: 10.1111/cid.12564 ORIGINAL ARTICLE Comparison of peri-implant clinical and radiographic status around short (6 mm in length)
Received: 31 October 2017 Revised: 5 November 2017 Accepted: 6 November 2017 DOI: 10.1111/cid.12564 ORIGINAL ARTICLE Comparison of peri-implant clinical and radiographic status around short (6 mm in length)
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Periodontal Disease in Habitual Cigarette Smokers and Nonsmokers With and Without Prediabetes
 CLINICAL INVESTIGATION Periodontal Disease in Habitual Cigarette Smokers and Nonsmokers With and Without Prediabetes Fawad Javed, PhD, Mansour Al-Askar, MSc, Lakshman P. Samaranayake, FRCPath and Khalid
CLINICAL INVESTIGATION Periodontal Disease in Habitual Cigarette Smokers and Nonsmokers With and Without Prediabetes Fawad Javed, PhD, Mansour Al-Askar, MSc, Lakshman P. Samaranayake, FRCPath and Khalid
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space
 Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Periodontal parameters in prediabetes, type 2 diabetes mellitus, and non-diabetic patients
 Original Research Periodontics Periodontal parameters in prediabetes, type 2 diabetes mellitus, and non-diabetic patients Mohammed ALASQAH (a) Sameer MOKEEM (b) Ali ALRAHLAH (c) Nawwaf AL-HAMOUDI (b) Tariq
Original Research Periodontics Periodontal parameters in prediabetes, type 2 diabetes mellitus, and non-diabetic patients Mohammed ALASQAH (a) Sameer MOKEEM (b) Ali ALRAHLAH (c) Nawwaf AL-HAMOUDI (b) Tariq
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Clinical Perspectives
 Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Fawad Javed,* Tariq Abduljabbar, Fahim Vohra, Hans Malmstrom,* Irfan Rahman, and Georgios E. Romanos i
 Comparison of Periodontal Parameters and Self-Perceived Oral Symptoms Among Cigarette Smokers, Individuals Vaping Electronic Cigarettes, and Never-Smokers Fawad Javed,* Tariq Abduljabbar, Fahim Vohra,
Comparison of Periodontal Parameters and Self-Perceived Oral Symptoms Among Cigarette Smokers, Individuals Vaping Electronic Cigarettes, and Never-Smokers Fawad Javed,* Tariq Abduljabbar, Fahim Vohra,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy
 Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Peri-implant health and peri-implant bone stability after immediate implant placement
 2 First report of a two-year retrospective study with a newly developed bone-level implant system Peri-implant health and peri-implant bone stability after immediate implant placement DR-MEDIC STOM. HENRIETTE
2 First report of a two-year retrospective study with a newly developed bone-level implant system Peri-implant health and peri-implant bone stability after immediate implant placement DR-MEDIC STOM. HENRIETTE
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
implants placed at crestal and subcrestal levels.
 Mohammad D. Al Amri Sulieman S. Al-Johany Abdulaziz M. Al Baker Mohammad Q. Al Rifaiy Tariq S. Abduljabbar Abdulaziz A. Al-Kheraif Soft tissue changes and crestal bone loss around platform-switched implants
Mohammad D. Al Amri Sulieman S. Al-Johany Abdulaziz M. Al Baker Mohammad Q. Al Rifaiy Tariq S. Abduljabbar Abdulaziz A. Al-Kheraif Soft tissue changes and crestal bone loss around platform-switched implants
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Comparison of clinical and radiographic status around immediately-loaded versus
 Received Date : 24-May-2016 Revised Date : 25-Nov-2016 Accepted Date : 04-Dec-2016 Article type : Original Article Comparison of clinical and radiographic status around immediately-loaded versus conventional
Received Date : 24-May-2016 Revised Date : 25-Nov-2016 Accepted Date : 04-Dec-2016 Article type : Original Article Comparison of clinical and radiographic status around immediately-loaded versus conventional
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
The use of the LiteTouch Er:YAG laser in peri-implantitis treatment
 The use of the LiteTouch Er:YAG laser in peri-implantitis treatment Authors_Prof. Tzi Kang Peng, Taiwan & Prof. Georgi Tomov, Bulgaria _Introduction With oral implantology experience its Renaissance, the
The use of the LiteTouch Er:YAG laser in peri-implantitis treatment Authors_Prof. Tzi Kang Peng, Taiwan & Prof. Georgi Tomov, Bulgaria _Introduction With oral implantology experience its Renaissance, the
3. Guarantee conditions
 Straumann Guarantee Straumann Guarantee (Valid as of April 1, 2012) 1. Guarantee beneficiary and scope This guarantee (the Straumann Guarantee as defined below) from the Institut Straumann AG, Basel, Switzerland
Straumann Guarantee Straumann Guarantee (Valid as of April 1, 2012) 1. Guarantee beneficiary and scope This guarantee (the Straumann Guarantee as defined below) from the Institut Straumann AG, Basel, Switzerland
Amount of bone loss after maxillary dental implant loading in smoker and non-smoker patients
 Amount of bone loss after maxillary dental implant loading in smoker and non-smoker patients Taha Y. Hamad, B.D.S., H.D.D., M.Sc. (1) Background: Excessive crestal bone loss after dental implant occurs
Amount of bone loss after maxillary dental implant loading in smoker and non-smoker patients Taha Y. Hamad, B.D.S., H.D.D., M.Sc. (1) Background: Excessive crestal bone loss after dental implant occurs
INDIAN DENTAL JOURNAL
 ACHIEVING OPTIMAL AESTHETICS WITH IMMEDIATE IMPLANT PLACEMENT Dr. Mayank Singh 1 Dr. Lakshya Kumar 2 Dr. Shahid Ahmad Shah 3 Dr. Ronak Bhatt 4 1, 2 Assistant Professor, Department of Prosthodontics, King
ACHIEVING OPTIMAL AESTHETICS WITH IMMEDIATE IMPLANT PLACEMENT Dr. Mayank Singh 1 Dr. Lakshya Kumar 2 Dr. Shahid Ahmad Shah 3 Dr. Ronak Bhatt 4 1, 2 Assistant Professor, Department of Prosthodontics, King
Volume 2 Issue
 Volume 2 Issue 2 2017 Page 333 to 340 Research Article Oral Health and Dentistry ISSN: 2573-4989 The Anti-Inflammatory Actions of an Intra-Oral Adhesive Patch Containing Botanical Extracts Exert Inhibitory
Volume 2 Issue 2 2017 Page 333 to 340 Research Article Oral Health and Dentistry ISSN: 2573-4989 The Anti-Inflammatory Actions of an Intra-Oral Adhesive Patch Containing Botanical Extracts Exert Inhibitory
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
GuidedService. The ultimate guide for precise implantations
 GuidedService The ultimate guide for precise implantations ABGuidedService The ultimate guide for precise implantations At A.B. Dental we've brought implantology into the future with a 3D digitally planned
GuidedService The ultimate guide for precise implantations ABGuidedService The ultimate guide for precise implantations At A.B. Dental we've brought implantology into the future with a 3D digitally planned
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Peri-implant marginal bone loss: What is the current concensus? an academic controversy or a clinical challenge?
 Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
From planning to surgery: a totally digital working flow for Leone implants placement
 Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review
 The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
Submission to Clinical Oral Implants Research (adjusted version)
 Submission to Clinical Oral Implants Research (adjusted version) Title A prospective cohort study on the impact of smoking on soft tissue alterations around single implants Running title Soft tissue alterations
Submission to Clinical Oral Implants Research (adjusted version) Title A prospective cohort study on the impact of smoking on soft tissue alterations around single implants Running title Soft tissue alterations
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
SCD Case Study. The ability of the integrated implant to bear a load must be greater than the anticipated load during function.
 SCD Case Study Dental implants offer an effective and predictable way to replace teeth. Function, aesthetics and phonetics are regained. The long-term success clinically and aesthetically depends upon
SCD Case Study Dental implants offer an effective and predictable way to replace teeth. Function, aesthetics and phonetics are regained. The long-term success clinically and aesthetically depends upon
Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study
 R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Application of the Straumann BLT Ø 2.9mm implant in a narrow interdental space
 C A S E R E P O R T Application of the Straumann BLT Ø 2.9mm implant in a narrow interdental space Michael Kristensen 1 This case report describes the application of the Straumann BLT Ø 2.9 mm implant
C A S E R E P O R T Application of the Straumann BLT Ø 2.9mm implant in a narrow interdental space Michael Kristensen 1 This case report describes the application of the Straumann BLT Ø 2.9 mm implant
Volume 27 No. 11 August New Information and Reminders for Dental Services
 State of New Jersey Department of Human Services Division of Medical Assistance & Health Services Volume 27 No. 11 August 2017 To: Subject: Dental Providers - For Action Managed Care Organizations For
State of New Jersey Department of Human Services Division of Medical Assistance & Health Services Volume 27 No. 11 August 2017 To: Subject: Dental Providers - For Action Managed Care Organizations For
JMSCR Vol 06 Issue 07 Page July 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i7.101 Immediate Implant Following
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i7.101 Immediate Implant Following
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Self-perceived oral health and periodontal parameters in chronic periodontitis patients with and without rheumatoid arthritis
 Journal of Investigative and Clinical Dentistry (2014), 5, 1 6 ORIGINAL ARTICLE Periodontics Self-perceived oral health and periodontal parameters in chronic periodontitis patients with and without rheumatoid
Journal of Investigative and Clinical Dentistry (2014), 5, 1 6 ORIGINAL ARTICLE Periodontics Self-perceived oral health and periodontal parameters in chronic periodontitis patients with and without rheumatoid
Featured Patient Case #1: Complete Mouth Reconstruction with Hybrid Restorations
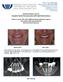 Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Effect of thread size on the implant neck area: preliminary results at 1 year of function
 Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Screw retained implant crown restoration with digital workflow using scan body and surgical guide
 Dr. Anthony Mak W Dental Screw retained implant crown restoration with digital workflow using scan body and surgical guide Solutions featured: 3Shape TRIOS 3Shape Implant Studio 3Shape scan bodies 3Shape
Dr. Anthony Mak W Dental Screw retained implant crown restoration with digital workflow using scan body and surgical guide Solutions featured: 3Shape TRIOS 3Shape Implant Studio 3Shape scan bodies 3Shape
Linking Research to Clinical Practice
 Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Comparison of Self-Perceived Oral Health, Periodontal Inflammatory Conditions and Socioeconomic Status in Individuals With and Without Prediabetes
 CLINICAL INVESTIGATION Comparison of Self-Perceived Oral Health, Periodontal Inflammatory Conditions and Socioeconomic Status in Individuals With and Without Prediabetes Fawad Javed, PhD, Mansour Al-Askar,
CLINICAL INVESTIGATION Comparison of Self-Perceived Oral Health, Periodontal Inflammatory Conditions and Socioeconomic Status in Individuals With and Without Prediabetes Fawad Javed, PhD, Mansour Al-Askar,
PREVENTIVE DENTISTRY. Straumann Next Generation Dentistry Prevent. Restore. Enhance.
 PREVENTIVE DENTISTRY Prevent. Restore. Enhance. 2 Next Generation Dentistry: Take a holistic approach with innovative solutions that enable preventive dentistry. If given the option, we all prefer prevention
PREVENTIVE DENTISTRY Prevent. Restore. Enhance. 2 Next Generation Dentistry: Take a holistic approach with innovative solutions that enable preventive dentistry. If given the option, we all prefer prevention
AMERICAN ACADEMY OF IMPLANT DENTISTRY
 AMERICAN ACADEMY OF IMPLANT DENTISTRY 211 East Chicago Ave., Suite 750, Chicago IL 60611-2616 312/335-1550 GUIDELINES FOR CASE REPORTS FOR FELLOW MEMBERSHIP* General Information Each Fellow candidate must
AMERICAN ACADEMY OF IMPLANT DENTISTRY 211 East Chicago Ave., Suite 750, Chicago IL 60611-2616 312/335-1550 GUIDELINES FOR CASE REPORTS FOR FELLOW MEMBERSHIP* General Information Each Fellow candidate must
Immediate loading in heavy smokers
 case report Immediate loading in heavy smokers Dr Dr Branislav Fatori & Dr Inge Schmitz, Germany Today, numerous implant systems and many modifications thereof are available on the market, and it may be
case report Immediate loading in heavy smokers Dr Dr Branislav Fatori & Dr Inge Schmitz, Germany Today, numerous implant systems and many modifications thereof are available on the market, and it may be
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
Stability and bone loss around submerged and non-submerged implants in diabetic and non-diabetic patients: a 7-year follow-up
 Original Research Implantodontology Stability and bone loss around submerged and non-submerged implants in diabetic and non-diabetic patients: a 7-year follow-up Saeed AL ZAHRANI (a) Abdullah Abdulaziz
Original Research Implantodontology Stability and bone loss around submerged and non-submerged implants in diabetic and non-diabetic patients: a 7-year follow-up Saeed AL ZAHRANI (a) Abdullah Abdulaziz
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Devoted to the Advancement of Implant Dentistry
 Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Background. crestal bone loss, immediate loading, conventional loading, type 2 diabetes mellitus. Accepted for publication 4 December 2016
 J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2017 44; 220 228 Comparison of clinical and radiographic status around immediately loaded versus conventional loaded implants placed
J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2017 44; 220 228 Comparison of clinical and radiographic status around immediately loaded versus conventional loaded implants placed
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
The Endodontic / Implant Controversy
 The Endodontic / Implant Controversy Innovations in Endodontics Series Robert Handysides DDS Associate Professor and Chair Department of Endodontics Loma Linda University School of Dentistry Endodontic
The Endodontic / Implant Controversy Innovations in Endodontics Series Robert Handysides DDS Associate Professor and Chair Department of Endodontics Loma Linda University School of Dentistry Endodontic
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Short implants in the posterior maxilla to avoid sinus augmentation procedure: 5-year results from a retrospective cohort study
 Lorenz et al. International Journal of Implant Dentistry (2019) 5:3 https://doi.org/10.1186/s40729-018-0155-1 International Journal of Implant Dentistry RESEARCH Open Access Short implants in the posterior
Lorenz et al. International Journal of Implant Dentistry (2019) 5:3 https://doi.org/10.1186/s40729-018-0155-1 International Journal of Implant Dentistry RESEARCH Open Access Short implants in the posterior
Xive. Scientific Summary
 Xive Scientific Summary Comprehensive solutions for all phases of implant dentistry Welcome Are you looking for information about the excellent results on primary stability and immediate loading when using
Xive Scientific Summary Comprehensive solutions for all phases of implant dentistry Welcome Are you looking for information about the excellent results on primary stability and immediate loading when using
ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12 Accepted on:22/05/12
 SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
A CRITICAL REVIEW INTO PROSTHODONTIC FACTORS FOR BONE LOSS ASSOCIATED WITH DENTAL IMPLANTS
 A CRITICAL REVIEW INTO PROSTHODONTIC FACTORS FOR BONE LOSS ASSOCIATED WITH DENTAL IMPLANTS DR CHRISTOPHER C.K. HO ORAL RESTORATIVE SCIENCES PROSTHODONTICS REGISTRAR SUPERVISOR: PROF IVEN KLINEBERG INTRODUCTION
A CRITICAL REVIEW INTO PROSTHODONTIC FACTORS FOR BONE LOSS ASSOCIATED WITH DENTAL IMPLANTS DR CHRISTOPHER C.K. HO ORAL RESTORATIVE SCIENCES PROSTHODONTICS REGISTRAR SUPERVISOR: PROF IVEN KLINEBERG INTRODUCTION
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
Effect of Glycemic Control on Self- Perceived Oral Health, Periodontal Parameters, and Alveolar Bone Loss Among Patients With Prediabetes
 Volume 85 Number 2 Effect of Glycemic Control on Self- Perceived Oral Health, Periodontal Parameters, and Alveolar Bone Loss Among Patients With Prediabetes Fawad Javed,* Ali Saad Thafeed AlGhamdi, Toshinari
Volume 85 Number 2 Effect of Glycemic Control on Self- Perceived Oral Health, Periodontal Parameters, and Alveolar Bone Loss Among Patients With Prediabetes Fawad Javed,* Ali Saad Thafeed AlGhamdi, Toshinari
More than a beautiful smile. A new quality of life with dental implants.
 More than a beautiful smile. A new quality of life with dental implants. Why tooth loss matters Think of tooth loss and the first thing that comes to mind may be an unattractive appearance. It s true that
More than a beautiful smile. A new quality of life with dental implants. Why tooth loss matters Think of tooth loss and the first thing that comes to mind may be an unattractive appearance. It s true that
MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT
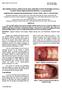 ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
High Crown to Implant Ratio as Stress Factor in Short Implants Therapy
 10.1515/bjdm-2016-0015 BALKAN JOURNAL OF DENTAL MEDICINE ISSN 2335-0245 STOMATOLOGICAL SOCIETY High Crown to Implant Ratio as Stress Factor in Short Implants Therapy SUMMARY Background/Aim: The purpose
10.1515/bjdm-2016-0015 BALKAN JOURNAL OF DENTAL MEDICINE ISSN 2335-0245 STOMATOLOGICAL SOCIETY High Crown to Implant Ratio as Stress Factor in Short Implants Therapy SUMMARY Background/Aim: The purpose
Case Presentation. Overall Health. Oral Hygiene. Chief Complaint. I hate my upper denture. I can t taste food. I want an implant solution
 Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
CASE REPORT MEGAGEN IMPLANT. AnyRidge. CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP
 AnyRidge CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP AnyRidge Clinical Case Ⅰ. Dr. Davide Farronato Baseline - fractured tooth Baseline - fractured tooth #25 Rx view Atraumatic avulsion technique
AnyRidge CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP AnyRidge Clinical Case Ⅰ. Dr. Davide Farronato Baseline - fractured tooth Baseline - fractured tooth #25 Rx view Atraumatic avulsion technique
Cronicon DENTAL SCIENCE. Review Article Dental Implant Survival: A Literature Review
 Cronicon OPEN ACCESS DENTAL SCIENCE Review Article Dental Implant Survival: A Literature Review Janice Diaz-Rodriguez 1, Robin Weltman 1, Duong T Tran 2, Lawrence Friedman 1 and Isabel C Gay 3 * 1 Department
Cronicon OPEN ACCESS DENTAL SCIENCE Review Article Dental Implant Survival: A Literature Review Janice Diaz-Rodriguez 1, Robin Weltman 1, Duong T Tran 2, Lawrence Friedman 1 and Isabel C Gay 3 * 1 Department
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Implant Restorations: A Step-By-Step Guide
 Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
DIGITAL DIAGNOSIS AND TREATMENT PLANNING FOR PLACEMENT AND RESTORATION OF SINGLE IMPLANTS IN THE POSTERIOR MAXILLA By Timothy Kosinski, DDS
 DIGITAL DIAGNOSIS AND TREATMENT PLANNING FOR PLACEMENT AND RESTORATION OF SINGLE IMPLANTS IN THE POSTERIOR MAXILLA By Timothy Kosinski, DDS Dental implants have undergone many positive advances in recent
DIGITAL DIAGNOSIS AND TREATMENT PLANNING FOR PLACEMENT AND RESTORATION OF SINGLE IMPLANTS IN THE POSTERIOR MAXILLA By Timothy Kosinski, DDS Dental implants have undergone many positive advances in recent
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
4. What about age? There is no age limit. After puberty, anyone can get dental implants.
 Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
