Advances in research on the treatment. Removal Torque Analysis of Implants in Rabbit Tibia After Topical Application of Simvastatin Gel RESEARCH
|
|
|
- Sharleen White
- 6 years ago
- Views:
Transcription
1 RESEARCH Removal Torque Analysis of Implants in Rabbit Tibia After Topical Application of Simvastatin Gel Fatima Neves Faraco-Schwed, DDS, MD, PhD 1 * Luiz Macedo Mangueira, DDS, MS 2 Joao Vitor Albuquerque Ribeiro, DDS 1 Alexsandro Da Silva Antao, DDS 1 Jamil Awad Shibli, DDS, MD, PhD 3 The aim of this study was to evaluate the effects of topical application of simvastatin gel (7.5 mg) on the removal torque of titanium implants in the rabbit tibia. A total of 32 surgeries were performed on 16 New Zealand rabbits for the placement of 2 implants in 1 tibia of each rabbit. Only 1 of the surgical defects was injected with 30 mg/ml of simvastatin gel before implant placement. The initial torque was set at 20 N.cm, and removal torque testing was performed 28 and 56 days postoperatively with a Tonishi torque wrench. Surgical defects were divided into 4 groups: group IG-28 (test, 28 days), group IG-56 (test, 56 days), group I-28 (control, 28 days), and group I-56 (control, 56 days). Removal torque values were higher in group IG-56 than in groups IG- 28, I-28, and I-56 (P,.05). Groups IG-28, I-28, and I-56 showed similar values (P..05). Removal torque force increased under the influence of simvastatin, indicating that topical administration of a 7.5-mg dose of simvastatin gel is effective in improving the torque force required to remove implants inserted in the rabbit tibia. Key Words: statin, removal torque, dental implants INTRODUCTION Advances in research on the treatment of hyperlipidemia in the mid-1980s culminated in the development of a revolutionary class of drugs: the statins or vastatins. These lipid-lowering drugs can reduce low-density lipoprotein levels by 29%, reaching a 60% reduction in cholesterol levels in some cases. 1 3 All statins share the ability to inhibit endogenous cholesterol synthesis by competitively inhibiting 3-hydroxyl-3-methylglutaryl coenzyme A (HMG-CoA) reductase, thus preventing the conversion of HMG-CoA reductase to mevalonate. On the other hand, statins can increase bone mineral density, reducing the risk of osteoporosis and fracture Paulista University (UNIP), São Paulo, SP, Brazil. 2 Santo Amaro University (UNISA), São Paulo, SP, Brazil. 3 Guarulhos University, São Paulo, SP, Brazil. * Corresponding author, fatimafaraco@terra.com.br DOI: /AAID-JOI-D Topical statins alone and/or associated with a vehicle that slows their intestinal absorption and hepatic metabolism, such as gel, stimulate bone formation by acting on the mrna synthesis of bone morphogenetic protein-2 (BMP-2), which promotes osteoblast proliferation and differentiation. Since this mechanism precedes the increase in BMP-2 mrna expression, statins may also promote angiogenesis. 4 6 Bone morphogenetic protein-2, a member of the transforming growth factor beta family, may have direct effects on adjacent cells (paracrine effect) and/or act on osteoblasts (autocrine effect), thus aiding bone regeneration over a long period of time. This protein may progress into a component of bone remodeling over a long time, thus enhancing the pattern of bone mineral density. 7 Statins have also been demonstrated to induce osteoclast apoptosis and to inhibit bone resorption in vitro; after in vivo treatment, they promote a decrease in osteoclast numbers. 8,9 It is therefore Journal of Oral Implantology 53
2 Use of Simvastatin Gel in Implants Placed in Rabbit Tibia crucial to understand the effects of topical statin gel on surfaces and surgical defects in order to increase the success rate of implant osseointegration in patients with osteoporosis or other hypocalcemic disorders. 10,11 Complementary simvastatin partially prevented the ovariectomized-induced bone loss in 8-monthold rats. 3 Using a healing femur fracture model, simvastatin given orally in the diet resulted in a marked increase in callus amount, fracture-breaking strength, and energy absorption at day. 12 In addition, local application seems reasonable as currently available statins were developed to target liver metabolism. These statins are poorly distributed to bone, and very few of an oral dose reach the systemic circulation. Furthermore, local application avoids systemic side effects. 13 The aim of this study was to evaluate the effects of topical application of 30 mg/ml of simvastatin gel (7.5 mg) on the removal torque force of implants installed in the rabbit tibia. METHODS Sixteen male New Zealand rabbits, weighing between 3.0 and 3.4 kg and aged 11 to 15 months, were used in this study. The study was approved by the Research Ethics Committee of Santo Amaro University (UNISA), Brazil (protocol No. 133/05). All animals were bred in the animal facilities of Universidade Paulista and, during the experimental period, were individually housed in iron cages, under the same environmental conditions, and fed standard chow and water ad libitum. Rabbits were weighed before surgery to establish the optimal postoperative drug dose (0.6 ml of ketamine hydrochloride, 0.3 ml of midazolam, and 0.5 ml of meperidine intramuscularly) and anesthetic induction (1.0 ml of intramuscular ketamine, injected 10 minutes after preanesthetic medication; anesthetic maintenance consisted of 0.4 ml of ketamine every 15 minutes until the end of surgery). After sedation, trichotomy and preoperative skin antisepsis were performed. Prolacaine hydrochloride and felypressin (0.03 IU/mL) were used for infiltration anesthesia in the tibial region. Surgical technique A skin incision approximately 5 cm long was made in the anterior tibia. After incision of the muscle fascia, the periosteum was stripped using a Molt curette, leading to exposure of the underlying bone. A 16:1 contra-angle handpiece coupled to a surgical micromotor was previously set for 1700 rpm, and the peristaltic pump was set for maximum flow. Two drill holes were made at least 150 mm apart in the right tibia of rabbits to receive 2 implants. The first hole was initially drilled with a gun drill (2 mm) on the medial aspect of the tibia near the knee joint, avoiding distal cortical perforation. The second hole was made using the same drill, the farthest possible from the first hole, toward the paw joint. Distal cortical perforation was avoided to reduce fracture risk. A helicoidal drill (2.8 mm) was used subsequently. A threaded male fastener, with the same diameter of the implant, was then used to facilitate implant insertion and to uniformly control placement torque force, standardized at 20 N.cm. Implant placement Implants were inserted using a Torque-Lock torque wrench. Each animal received 2 titanium implants (LTX, 3i Innovation; mm, with surface treatment: blasting with aluminum oxide and acid attack) in the right tibia. Before implant placement, 0.25 ml simvastatin gel (30 mg/ml), at a dose of 7.5 mg, was injected in only 1 of the surgical defects (group test: IG). Before statin injections, a sterile gauze was applied to the surgical defect to absorb and stop bleeding, ensuring that the drug could spread along the wall of surgical defects. Only blood was left within the second defect before implant placement (group control: I). After implant placement, running sutures were performed for the inner layer and simple skin suture for the outer layer. Occlusive dressings were then applied to the wounds. Animals were killed after 28 and 56 days, when a new intervention was performed for exposure and removal of implants. A calibrated Tonishi torque wrench was used to record the torque force required to remove implants. Surgical defects were divided into 4 experimental groups, according to time of reopening and application of simvastatin gel to the surgical site, as follows: Group IG-28 (test, 28 days): Eight implants were installed following simvastatin gel injection (30 mg/ml); the sites were reopened 28 days after implant placement for removal torque testing. 54 Vol. XL/No. One/2014
3 Faraco-Schwed et al TABLE 1 Results from removal torque analysis* of implants in the rabbit tibia in groups IG-28 (test, 28 days, topical simvastatin gel), I-28 (control, 28 days, without topical simvastatin gel), IG-56 (test, 56 days, topical simvastatin gel), I-56 (control, 56 days without simvastatin gel) Animal No. IG-28 I-28 IG-56 I Mean 6 SD Mean 6 SD *Values are expressed as N.cm. Group IG-56 (test, 56 days): Eight implants were installed following simvastatin gel injection (30 mg/ml); the sites were reopened 56 days after implant placement for removal torque testing. Group I-28 (control, 28 days): Eight implants were installed without topical simvastatin gel; the sites were reopened 28 days after implant placement for removal torque testing. Group I-56 (control, 56 days): Eight implants were installed without topical simvastatin gel; the sites were reopened 56 days after implant placement for removal torque testing. After the animals were killed, their tibiae were immediately positioned and fixed in a splint to prevent any movement. Removal torque testing was then performed on all implants. An engaging device was used to maintain the torque wrench aligned along the axis of the implant. Statistical analysis of removal torque values was performed using a Student t test for 2 paired samples, with a significance level of.05. RESULTS Results from removal torque analysis of implants in the rabbit tibia performed 28 and 56 days after surgery are described in Table 1. Table 2 shows the analysis of differences found between groups IG-28 (test, 28 days) and I-28 (control, 28 days), between groups IG-56 (test, 56 days) and I-56 (control, 56 days), and between groups IG-56 (test, 56 days) and IG-28 (test, 28 days), using a Student t test (2 paired samples for mean values). Table 3 describes the differences found between IG-56 and I-28, I-56 and IG-28, and I-56 and I-28B using a Student t test (2 paired samples for mean values). Table 4 shows the results of analysis of variance, 2 criteria. Significant differences were observed in mean values between group IG-56 (test, 56 days) and group I-56 (control, 56 days; P ¼.04; Table 2). Removal torque values were higher in group IG-56 (test, 56 days) than in group I-56 (control, 56 days; Tables 1 and 2). Mean values for group IG-56 were not higher because of a discrepancy observed in the results for animal 16 (Table 1). There were no statistically significant differences in mean values between group IG-28 (test, 28 days) and group I-28 (control, 28 days; P ¼.448; Table 2). Removal torque force was evidently higher in group IG-28 (test, 28 days) than in group I-28 (control, 28 days); however, the statistical analysis revealed no significant differences because of a discrepancy observed in the results for animal 1 (Table 1). Significant differences were observed in mean values between group IG-28 (test, 28 days) and Journal of Oral Implantology 55
4 Use of Simvastatin Gel in Implants Placed in Rabbit Tibia TABLE 2 Removal torque analysis* 28 and 56 days after surgery between groups IG-28 (topical simvastatin, 28 days) and I-28 (without topical simvastatin, 28 days), groups IG-56 (topical simvastatin, 56 days) and I-56 (without simvastatin, 56 days) and groups IG-28 (topical simvastatin, 28 days) and IG-56 (topical simvastatin, 56 days) 28-Day Comparison 56-Day Comparison Test Group Comparison Groups IG-28 I-28 IG-56 I-56 IG-28 IG-56 Days of surgery Mean Variance Standard deviation Observations Start t P value Two-tailed critical t *Student t test (2 samples assuming equivalent variance). group IG-56 (test, 56 days; P ¼.003; Table 2). Our analysis revealed statistically significant differences in mean values between group IG-56 (test, 56 days) and group I-28 (control, 28 days; P ¼.002; Table 3). However, there were no significant differences in mean values between group IG-28 (test, 28 days) and group I-56 (control, 56 days; P ¼.21; Table 3). DISCUSSION The present study evaluated the effects of topical simvastatin gel on the removal torque force of implants inserted in the rabbit tibia. Several studies have associated statins with increased BMP-2 gene expression in bone cells. 3,6,10 14 This motivated us to study the role of statins in implant osseointegration in the rabbit tibia. Studies show that statins act by stimulating the formation of BMP-2, 3 14 by promoting osteoblast differentiation and bone formation, 4,15 and by encouraging angiogenesis. 3,12,15 Statins have also been associated with increased expression of BMP-2 gene in bone cells. 16,17 The time of sacrifice adopted in this study was based on studies by Marx and Garg, 17 who showed that the remodeling process of the bone-implant interface in rabbits lasts 6 weeks. Those authors also observed that the maturation of compact bone occurs in 18 months. Authors assessing the effect of statins when administered systemically or orally have not reported satisfactory results. 15,18 Therefore, the present study used topical simvastatin gel, injected into the surgical defect before implant placement. Topical statins alone and/or associated with a TABLE 3 Removal torque analysis* 28 and 56 days after surgery between groups IG-28 (topical simvastatin, 28 days) and I-56 (without simvastatin, 56 days), groups IG-56 (topical simvastatin, 56 days) and I-28 (without simvastatin, 28 days), and groups I-56 (without simvastatin, 56 days) and I-28 (without simvastatin, 28 days) Test 28 Days and Control 56-Day Comparison Test 56 Days and Control 28-Day Comparison Control Group Comparison Groups IG-28 I-56 IG-56 I-28 I-28 I-56 Days of surgery Mean Variance Standard deviation Observations Stat t P value Two-tailed critical t *Student t test (2 samples assuming equivalent variance). 56 Vol. XL/No. One/2014
5 Faraco-Schwed et al TABLE 4 Analysis of variance results GL SQ QM F P Treatments Blocks Error vehicle that slows their intestinal absorption and hepatic metabolism can promote bone formation. 4 6,19 In the present study, statin gel (7.5 mg simvastatin) had a positive effect on the removal torque force of implants inserted in the rabbit tibia. Group IG-56 (test, 56 days), when compared with the other groups, showed the highest mean removal torque force, suggesting that the action of statins is enhanced over time (Table 3). Although a comparison between mean values from groups IG-28 (test, 28 days) and I-28 (control, 28 days) showed no statistically significant differences (Table 2), there was a discrepancy in the results for animal 1, in which removal torque force in group I-28 (control, 28 days) was significantly greater than in group IG-28 (test, 28 days; Table 1). This fact could lead us to assume that in group IG-28, statin had no positive effect on removal torque force. However, overall results showed that statin increased removal torque force in all other animals at 28 days. The increase observed in removal torque force in group IG-28 (test, 28 days) may be interpreted as an improvement in the bone-implant interface (ie, we may assume that there was an improvement in bone mineral density). This suspicion may be confirmed by histological analysis of the areas of interest. The absence of such analysis may be considered a limitation of this study; therefore, studies using this approach are warranted to clarify the effects of statin. On the other hand, our results can and should be elucidated by understanding the mechanism by which statins perform their effects on bone and endothelial cells, a mechanism of action that has been demonstrated by several authors assessing statins as modulators of bone formation. 4 6,19 The simvastatin dose (7.5 mg) used in this study was based on previous studies reporting that a high dose of simvastatin formulated in a gel can stimulate cranial bone apposition and the bone formed remained for up to 22 days after dosing. 5 These findings pose the possibility that statins can be used for local bone repair to enhance new bone formation in orthopedic indications, in surgical repair of bone defects, and in conditions such as periodontal bone disease. There are numerous advantages for the local use of statins to stimulate bone formation: first, it is an inexpensive drug to manufacture compared with recombinant proteins, such as BMPs or fibroblast growth factors; second, it has a long history of clinical systemic usage with very acceptable good toxicity profiles; and finally, it is relatively easy to incorporate into biodegradable matrices that regulate its release to enhance its effectiveness. 17,18 When a surgical procedure is performed for placement of dental implants, the trauma necessary for the creation of surgical defects and the presence of implants may trigger a complex process involving several cellular and extracellular events. The relationship of these events with the use of topical statins has been discussed in the literature. Titanium implants installed after topical application of simvastatin have shown abundant formation of trabecular bone, thicker in the medullary canal, and an improvement in the bone-implant interface and bone mineral density when analyzed histologically. 3,8,20 Lee et al 13 showed that a 0.5-mg dose of simvastatin gel can induce a cumulative effect in new bone formation with minimal edema and without attenuation of mechanical properties, compared with the control group, suggesting that simvastatin injection is a comfortable and flexible method to initiate bone formation in areas of thin, vulnerable alveolar bone. Mundy et al 6 showed that lovastatin and simvastatin can specifically activate the BMP-2 promoter. Those authors used cultured bone cells from the calvaria of mice and observed that statins significantly increased the number of osteoblasts and the amount of new bone formation. A similar effect was observed in vivo when simvastatin was Journal of Oral Implantology 57
6 Use of Simvastatin Gel in Implants Placed in Rabbit Tibia FIGURE 1. Maximum, minimum, and median values of removal torque in groups IG-28, IG-56, I-28, and I-56 injected subcutaneously over the calvaria of mice at concentrations of 1 to 10 lm. In our study, group IG-56 (test, 56 days) had greater removal torque values than group I-56 (control, 56 days), suggesting that simvastatin may hasten the process of implant osseointegration (Tables 1 and 2) and that the increase in the removal torque force of implants is likely to be a result of the increase in the surface area of osseointegration. However, histomorphometric studies of the bone-implant interface are required to elucidate this issue. Ayukawa et al 20 and Thylin et al 5 investigated whether local simvastatin delivery affected cellular events and new bone formation in surgically created bone defects in rats. Histological and histomorphometric analyses demonstrated that local administration of simvastatin stimulates bone formation in the early stages of artificially created bone defects. 5,20 Our results revealed no statistically significant differences between groups IG-28 (test, 28 days) and I-28 (control, 28 days; Tables 1 and 2). However, mean removal torque force was greater, although not statistically significant, in group IG-28 than in group I-28 (Table 2). A discrepancy observed in the results for animal 1 is likely to be the reason for this statistical difference. Skoglund and Aspenberg 24 conducted a study in which simvastatin was either administered subcutaneously or directly applied to the fracture area in mice, with the goal of stimulating fracture repair. Simvastatin applied directly to the fracture area had a positive effect on fracture healing when biomechanical parameters were analyzed. 24 In the present study, topical simvastatin injected in surgical defects before implant placement promoted an increase in the removal torque force of implants in group IG-56 (test, 56 days) when compared with groups IG-28 (test, 28 days), I-28 (control, 28 days), and I-56 (control, 56 days). Our findings indicate that removal torque force increased under the influence of simvastatin, hastening the process of osseointegration among test animals, which is in agreement with studies reporting that topical delivery of simvastatin is associated with an improvement in bone regeneration. 4,6,14,19 22 CONCLUSION Our results indicate that topical administration of a 7.5-mg dose of simvastatin gel was effective in improving the torque force required to remove implants inserted in the rabbit tibia. ABBREVIATIONS BMP-2: bone morphogenic protein-2 HMG-CoA: 3-hydroxyl-3-methylglutaryl coenzyme A ACKNOWLEDGMENTS The authors thank the following individuals for their contributions to the present article: Prof Dr Wilson Roberto Sendyk (In Memoriam) and Prof Dr Alfredo Gromatzky of the Department of Graduate Studies of UNISA for their support of our research. REFERENCES 1. Anbinder AL, Junqueira JC, Mancini MNG, Balducci I, Rocha RF, Carvalho, YR. Influence of simvastatin on bone regeneration of tibial defects and blood cholesterol level in rats. Braz Dent J. 2006; 17: Park JW, Kim HK, Kim YJ, Jang JH, Son H, Hanawa T. Osteoblast response and osseointegration of a Ti-6AI-4V alloy implant incorporating strontium. Acta Biomaterial. 2010;6: Sugiyama M, Kodama T, Konishi K, Abe K, Asami S, Oikawa S. Compactin and simvastatin, but not pravastatin, induce bone morphogenetic protein-2 in human osteosarcoma cells. Biochem Biophys Res Commun. 2000;271: Garret IR, Gutierres G, Mundy G. The role of statins as potential targets for bone formation. Arthritis Res Ther. 2002;4: Thylin MR, McConnell JC, Schmid MJ, et al. Effects of simvastatin gels on murine calvarial bone. J Periodontol. 2002;73: Mundy G, Garret R, Harris S, et al. Stimulation of bone formation in vitro and in rodents by statins. Science. 1999;286: Marx RE, Garg AK. Bone structure, metabolism, and 58 Vol. XL/No. One/2014
7 Faraco-Schwed et al physiology: its impact on dental implantology. Implant Dent. 1998; 7: Ayukawa Y, Yasukawa E, Moriyama Y, et al. Local application of statin promotes bone repair through the suppression of osteoclasts and the enhancement of osteoclasts at bonehealing sites in rats. Oral Surg Oral Med Oral Pathol Oral Radiol and Endod. 2009;107: Rogers MJ. Statins: lower lipids and better bone? Nature Med. 2000;6: Pagkalos J, Cha JM, Kang Y, Heliotis M, Tsiridis E, Mantalaris A. Simvastatin induces osteogenic differentiation of murine embryonic stem cells. J Bone Miner Res. 2010;25: Song C, Guo Z, Ma Q, et al. Simvastatin induces osteoblastic differentiation and inhibits adipocytic differentiation in mouse bone marrow stromal cells. Biochem Biophy Res. 2003;308: Moriyama Y, Ayukawa Y, Ogino Y, et al. Local application of fluvastatin improves peri-implant bone quantity and mechanical properties: a rodent study. Acta Biomater. 2010;6: Lee Y, Schmid MJ, Marx DB, et al. The effect of local simvastatin delivery strategies on mandibular bone formation in vivo. Biomaterials. 2008;29: Alsaadi G, Quirynen M, Komárek A, van Steenberghe D. Impact of local and systemic factors on the incidence of oral implant failures, up to abutment connection. J Clin Periodontol. 2007;34: Inoue TM. Influence of simvastatin administered subcutaneously in the bone healing in rat tibia. Rev Pos Grad SP. 2003;10: Koka S, Babul NM, Norell AJ. Survival of dental implants in post-menopausal bisphosphonate users. J Prosthodont Res. 2010; 54: Garrett IR. Anabolic agents and the bone morphogenetic protein pathway. Curr Top Dev Biol. 2010;78: Von-Stechow D, Fish S, Yahalom D, et al. Does simvastatin stimulate bone formation in vivo? BMC Musculoskeltal Disord. 2003; 4: Wong RW, Rabie ABM. Early healing pattern of statininduced osteogenesis. Br J Oral Maxillofac Surg. 2005;43: Ayukawa Y, Okamura A, Koyamo K. Simvastatin promotes osteogenesis around titanium implants. Clin Oral Implants Res. 2004;15: Skoglund B, Aspenberg P. Locally applied simvastatin improves fracture healing in mice. BMC Musculoskeletal Disord. 2004;8: Edwards CJ, Spector TD. Statins as modulators of bone formation. Arthritis Res. 2002;4: Journal of Oral Implantology 59
Review The influence of statins on osseointegration: a systematic review of animal model studies
 J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2016 43; 873 882 Review The influence of statins on osseointegration: a systematic review of animal model studies D.I.SENDYK*,M.C.Z.DEBONI*,C.M.PANNUTI,
J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2016 43; 873 882 Review The influence of statins on osseointegration: a systematic review of animal model studies D.I.SENDYK*,M.C.Z.DEBONI*,C.M.PANNUTI,
DOCUMENTED CLINICAL SUCCESS
 DOCUMENTED CLINICAL SUCCESS Implants with enjoy outstanding clinical outcomes that further demonstrate the quality and performance of the coating. CUMULATIVE IMPLANT SURVIVAL RATE 100% 100% 100% 100% 97.9%
DOCUMENTED CLINICAL SUCCESS Implants with enjoy outstanding clinical outcomes that further demonstrate the quality and performance of the coating. CUMULATIVE IMPLANT SURVIVAL RATE 100% 100% 100% 100% 97.9%
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis
 Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Statins and osteoporosis: Can these lipid-lowering drugs also bolster bones?
 CURRENT DRUG THERAPY ABELARDO C. CRUZ, MD Division of Rheumatology, Department of Medicine, State University of New York at Stony Brook BARRY L. GRUBER, MD Head, Division of Rheumatology, Professor of
CURRENT DRUG THERAPY ABELARDO C. CRUZ, MD Division of Rheumatology, Department of Medicine, State University of New York at Stony Brook BARRY L. GRUBER, MD Head, Division of Rheumatology, Professor of
Microstructural changes in the bone tissue and in the bone callus of diabetic rats with and without insulin treatment
 Microstructural changes in the bone tissue and in the bone callus of diabetic rats with and without insulin treatment A. Zamarioli 1, M.S. Campos 1, A. Guimarães 1, M. Butezloff 1, G.B. Leoni 2, M.D. Sousa-Neto
Microstructural changes in the bone tissue and in the bone callus of diabetic rats with and without insulin treatment A. Zamarioli 1, M.S. Campos 1, A. Guimarães 1, M. Butezloff 1, G.B. Leoni 2, M.D. Sousa-Neto
Patient Guide. Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening
 Patient Guide Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening Introduction You have decided to have a limb lengthening operation. The surgery you have chosen uses a device
Patient Guide Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening Introduction You have decided to have a limb lengthening operation. The surgery you have chosen uses a device
Maryland AGD AE and Socket Grafting 2015
 The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
4766 Research Dr. San Antonio, TX insightdentalsystems.com
 OVERVIEW OF THE INSIGHT DENTAL IMPLANT DELIVERY SYSTEM The IDS system comes in a unit dose implant system where its advantage provides sterile instrumentation in one single-use kit. It is organized to
OVERVIEW OF THE INSIGHT DENTAL IMPLANT DELIVERY SYSTEM The IDS system comes in a unit dose implant system where its advantage provides sterile instrumentation in one single-use kit. It is organized to
PROXIMAL TIBIAL PLATE
 SURGICAL NÁSTROJE TECHNIQUE PRO ARTROSKOPII PROXIMAL INSTRUMENTS TIBIAL FOR PLATE ARTHROSCOPY Proximal Tibial Plate Description of medical device The Proximal Tibial Plate is used in epyphyseal and metaphyseal
SURGICAL NÁSTROJE TECHNIQUE PRO ARTROSKOPII PROXIMAL INSTRUMENTS TIBIAL FOR PLATE ARTHROSCOPY Proximal Tibial Plate Description of medical device The Proximal Tibial Plate is used in epyphyseal and metaphyseal
Enhancing implant stability with osseodensification a case report with 2-year follow-up
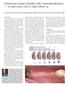 Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
in compact bone, large vertical canals carrying blood vessels and nerves. in compact bone, large horizontal canals carrying blood vessels and nerves.
 Carl Christensen, PhD Skeletal System (Bones`) Bio. 2304 Human Anatomy 1. Identify a term for each of the following: shaft of a long bone ends of a long bone ossified remnant of the "growth plate" connective
Carl Christensen, PhD Skeletal System (Bones`) Bio. 2304 Human Anatomy 1. Identify a term for each of the following: shaft of a long bone ends of a long bone ossified remnant of the "growth plate" connective
Musculoskeletal Clinical Correlates: Osseous Conditions in Dental Patients
 Musculoskeletal Clinical Correlates: Osseous Conditions in Dental Patients Learning Objectives Define osteoporosis and explain how it is diagnosed. Describe the main risk factors for developing osteoporosis.
Musculoskeletal Clinical Correlates: Osseous Conditions in Dental Patients Learning Objectives Define osteoporosis and explain how it is diagnosed. Describe the main risk factors for developing osteoporosis.
Effect of Locally Applied Fluvastat. Journal Journal of Hard Tissue Biology, 24(
 Effect of Locally Applied Fluvastat Titleturnover Osteoporosis Model Defect Mouse w Author(s) Ohira, T; Tanabe, K; Sasaki, H; Yos Alternative Yajima, Y Journal Journal of Hard Tissue Biology, 24( URL http://hdl.handle.net/10130/3929
Effect of Locally Applied Fluvastat Titleturnover Osteoporosis Model Defect Mouse w Author(s) Ohira, T; Tanabe, K; Sasaki, H; Yos Alternative Yajima, Y Journal Journal of Hard Tissue Biology, 24( URL http://hdl.handle.net/10130/3929
Cochlear Baha Attract Surgery. Aurélie Dewael Education Manager Cochlear Academy EMEA
 Cochlear Baha Attract Surgery Aurélie Dewael Education Manager Cochlear Academy EMEA Straightforward surgical procedure Mean surgery time: 40 min. 85% of the surgeries with the recommended C-shaped incision.
Cochlear Baha Attract Surgery Aurélie Dewael Education Manager Cochlear Academy EMEA Straightforward surgical procedure Mean surgery time: 40 min. 85% of the surgeries with the recommended C-shaped incision.
Effect of Locally Applied Fluvastat.
 Effect of Locally Applied Fluvastat Titleturnover Osteoporosis Model Defect Author(s) 大平, 貴士 Journal, (): - Mouse w URL http://hdl.handle.net/10130/3622 Right Posted at the Institutional Resources for
Effect of Locally Applied Fluvastat Titleturnover Osteoporosis Model Defect Author(s) 大平, 貴士 Journal, (): - Mouse w URL http://hdl.handle.net/10130/3622 Right Posted at the Institutional Resources for
Evaluation of Osseo Integrated Implants in Regenerated Jaw Bones after Cyst Enucleation
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 7, Issue 4 (May.- Jun. 2013), PP 01-06 Evaluation of Osseo Integrated Implants in Regenerated Jaw Bones
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 7, Issue 4 (May.- Jun. 2013), PP 01-06 Evaluation of Osseo Integrated Implants in Regenerated Jaw Bones
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
External Skeletal Fixation (ESF)
 External Skeletal Fixation (ESF) Technique for fracture repair in animals Introduction External Skeletal Fixation is a versatile and effective technique for fracture repair in animals, rigidly stabilizing
External Skeletal Fixation (ESF) Technique for fracture repair in animals Introduction External Skeletal Fixation is a versatile and effective technique for fracture repair in animals, rigidly stabilizing
INTRODUCTION. long-term results in the restoration of both totally and partially
 CLINICAL RESTORATION OF THE SOFT-TISSUE MARGIN IN SINGLE-TOOTH IMPLANT IN THE ANTERIOR MAXILLA Jamil Awad Shibli, DDS, MS, PhD Susana d Avila, DDS, MS KEY WORDS Dental implants Subepithelial connective
CLINICAL RESTORATION OF THE SOFT-TISSUE MARGIN IN SINGLE-TOOTH IMPLANT IN THE ANTERIOR MAXILLA Jamil Awad Shibli, DDS, MS, PhD Susana d Avila, DDS, MS KEY WORDS Dental implants Subepithelial connective
SKELETAL TISSUES CHAPTER 7 INTRODUCTION TO THE SKELETAL SYSTEM TYPES OF BONES
 SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
3.5 mm Locking Attachment Plate
 For Treatment of Periprosthetic Fractures 3.5 mm Locking Attachment Plate Surgical Technique Table of Contents Introduction 3.5 mm Locking Attachment Plate 2 Indications 4 Surgical Technique Preparation
For Treatment of Periprosthetic Fractures 3.5 mm Locking Attachment Plate Surgical Technique Table of Contents Introduction 3.5 mm Locking Attachment Plate 2 Indications 4 Surgical Technique Preparation
QUICK REFERENCE GUIDE. The PreFix Fixator (92000 Series) ALWAYS INNOVATING
 21 The PreFix Fixator (92000 Series) ALWAYS INNOVATING INTRODUCTION The PreFix fixator is designed to provide temporary external fixation. This may be needed when local facilities or the condition of the
21 The PreFix Fixator (92000 Series) ALWAYS INNOVATING INTRODUCTION The PreFix fixator is designed to provide temporary external fixation. This may be needed when local facilities or the condition of the
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
SURGICAL TECHNIQUE THE TENDON ANCHOR SYSTEM
 SURGICAL TECHNIQUE THE TENDON ANCHOR SYSTEM TABLE OF CONTENTS Introduction PAGE 1 Features and Benefits PAGE 1-2 Applications PAGE 3 Ordering Information PAGE 4 Indications & Contra-indications PAGE 5
SURGICAL TECHNIQUE THE TENDON ANCHOR SYSTEM TABLE OF CONTENTS Introduction PAGE 1 Features and Benefits PAGE 1-2 Applications PAGE 3 Ordering Information PAGE 4 Indications & Contra-indications PAGE 5
03 Best combination for thin ridge
 MILAkit TM BonEx kit TM 03 Best combination for thin ridge Joel A. Gonzales RDA Product Specialist Email: Cell: joelg@megagenus.com (480) 440-3927 Thor MEGAGEN Implant 28 29 Why Thor? 1. Simple & Strong
MILAkit TM BonEx kit TM 03 Best combination for thin ridge Joel A. Gonzales RDA Product Specialist Email: Cell: joelg@megagenus.com (480) 440-3927 Thor MEGAGEN Implant 28 29 Why Thor? 1. Simple & Strong
The development of modern Oral
 RESEARCH In Vitro Evaluation of the Removal Force of Abutments in Frictional Dental Implants João César Zielak, DDS, MSc, PhD* Murilo Rorbacker, DDS Rodrigo Gomes, DDS Celso Yamashita, DDS, MSc, PhD Carla
RESEARCH In Vitro Evaluation of the Removal Force of Abutments in Frictional Dental Implants João César Zielak, DDS, MSc, PhD* Murilo Rorbacker, DDS Rodrigo Gomes, DDS Celso Yamashita, DDS, MSc, PhD Carla
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Surgical Technique. Intramedullary locked Nailing With Screws for Humerus Fractures Solid/Cannulated. Humeral Interlocking Nail.
 Screws for Humerus Fractures Surgical Technique Humeral Interlocking Nail Approved by Humerus Nail Kit Code 08050001 Contents Introduction Implant design Indications Pre-operative planning Patient positioning
Screws for Humerus Fractures Surgical Technique Humeral Interlocking Nail Approved by Humerus Nail Kit Code 08050001 Contents Introduction Implant design Indications Pre-operative planning Patient positioning
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
A locking plate system that expands a surgeon s options in trauma surgery. Zimmer NCB Plating System
 A locking plate system that expands a surgeon s options in trauma surgery Zimmer NCB Plating System The Power of Choice The power of having true intraoperative options is at your fingertips. Using standard
A locking plate system that expands a surgeon s options in trauma surgery Zimmer NCB Plating System The Power of Choice The power of having true intraoperative options is at your fingertips. Using standard
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CASE REPORT. Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur
 PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
Surgical Technique. CONQUEST FN Femoral Neck Fracture System
 Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
BONE GRAFTING. Product Catalog
 BONE GRAFTING Product Catalog PRODUCT LINE Titanium Mesh Surgitime Titanium Titanium Foil Surgitime Titanium Seal Polytetraflouroethylene Membrane Surgitime PTFE Bone Screws Fixation Set We innovate to
BONE GRAFTING Product Catalog PRODUCT LINE Titanium Mesh Surgitime Titanium Titanium Foil Surgitime Titanium Seal Polytetraflouroethylene Membrane Surgitime PTFE Bone Screws Fixation Set We innovate to
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
A STUDY ON THE CORRELATION BETWEEN IMPLANT STABILITY VALUES AND INITIAL INSERTION TORQUE
 J Korean Acad Prosthodont : Volume 44, Number 3, 2006 A STUDY ON THE CORRELATION BETWEEN IMPLANT STABILITY VALUES AND INITIAL INSERTION TORQUE Jong-Hyuk Lee 1,2, D.D.S., M.S.D., Jae-Ho Yang 1, D.D.S.,
J Korean Acad Prosthodont : Volume 44, Number 3, 2006 A STUDY ON THE CORRELATION BETWEEN IMPLANT STABILITY VALUES AND INITIAL INSERTION TORQUE Jong-Hyuk Lee 1,2, D.D.S., M.S.D., Jae-Ho Yang 1, D.D.S.,
Module 2:! Functional Musculoskeletal Anatomy A! Semester 1! !!! !!!! Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb!
 Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Maxillary sinus augmentation without any graft material- A case Report
 A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
TSLP Thoracolumbar Spine Locking Plate
 Anterior thoracolumbar spine locking plate TSLP Thoracolumbar Spine Locking Plate Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use
Anterior thoracolumbar spine locking plate TSLP Thoracolumbar Spine Locking Plate Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use
Double Engine Orthopedic Bone Nail System Universal Humeral Nail
 Double Engine Orthopedic Bone Nail System ----------- Universal Humeral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic
Double Engine Orthopedic Bone Nail System ----------- Universal Humeral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic
Introduction of Dentium Implant. Help kit
 Introduction of Dentium Implant Help kit Fixture Remover [Application] For removal of fixture when it is broken, or there is no normal hex left, or critical damage was made in the internal thread so there
Introduction of Dentium Implant Help kit Fixture Remover [Application] For removal of fixture when it is broken, or there is no normal hex left, or critical damage was made in the internal thread so there
HISTORY. PERFORMANCE. SUCCESS.
 HISTORY. PERFORMANCE. SUCCESS. Zimmer MP-1 HA Technology Hydroxyapatite Surface Technology Celebrating Over Three Decades of Clinical Success DOCUMENTED CLINICAL SUCCESS Implants with enjoy outstanding
HISTORY. PERFORMANCE. SUCCESS. Zimmer MP-1 HA Technology Hydroxyapatite Surface Technology Celebrating Over Three Decades of Clinical Success DOCUMENTED CLINICAL SUCCESS Implants with enjoy outstanding
Surgical Technique. Distal Radius and Foot
 Surgical Technique Distal Radius and Foot JET-X BAR Unilateral Fixator Distal Radius and Foot Surgical Technique Contents Design Features...2 Distal Radius Surgical Technique Indications...10 Surgical
Surgical Technique Distal Radius and Foot JET-X BAR Unilateral Fixator Distal Radius and Foot Surgical Technique Contents Design Features...2 Distal Radius Surgical Technique Indications...10 Surgical
Does Hyperbaric Oxygen Therapy Improve Bone Regeneration With Mesenchymal Stem Cells
 Does Hyperbaric Oxygen Therapy Improve Bone Regeneration With Mesenchymal Stem Cells Johannes Schneppendahl, MD 1, Jan Grassmann, MD 1, Marcel Betsch, M.D. 2, Michael Wild, MD, PhD 3, Mohssen Hakimi, MD,
Does Hyperbaric Oxygen Therapy Improve Bone Regeneration With Mesenchymal Stem Cells Johannes Schneppendahl, MD 1, Jan Grassmann, MD 1, Marcel Betsch, M.D. 2, Michael Wild, MD, PhD 3, Mohssen Hakimi, MD,
» Guided Surgery. by MEDENTiKA « MEDENTIGUIDE SURGERY MANUAL MICROCONE. IPS Implant systems
 » Guided Surgery by MEDENTiKA «IPS Implant systems MEDENTIGUIDE MICROCONE SURGERY MANUAL » MedentiGuide «MedentiGuide drill sleeves support the surgeon in preparing the implant bed for MEDENTiKA implants.
» Guided Surgery by MEDENTiKA «IPS Implant systems MEDENTIGUIDE MICROCONE SURGERY MANUAL » MedentiGuide «MedentiGuide drill sleeves support the surgeon in preparing the implant bed for MEDENTiKA implants.
Instructions for Use DENTAL IMPLANTS
 HAHN TAPERED IMPLANT GUIDED SURGERY SYSTEM Instructions for Use English General Information IMPORTANT INFORMATION PLEASE READ Caution: U.S. federal law restricts this device to sale by, or on the order
HAHN TAPERED IMPLANT GUIDED SURGERY SYSTEM Instructions for Use English General Information IMPORTANT INFORMATION PLEASE READ Caution: U.S. federal law restricts this device to sale by, or on the order
BONE HEALING AT A FAILED IMPLANT SITE. HISTOLOGIC EVALUATIONS: ACASE REPORT Jun-Beom Park, DDS, MSD IN A TYPE II DIABETIC PATIENT: CLINICAL AND
 CLINICAL BONE HEALING AT A FAILED IMPLANT SITE IN A TYPE II DIABETIC PATIENT: CLINICAL AND HISTOLOGIC EVALUATIONS: ACASE REPORT Jun-Beom Park, DDS, MSD Placement of endosseous dental implants in diabetic
CLINICAL BONE HEALING AT A FAILED IMPLANT SITE IN A TYPE II DIABETIC PATIENT: CLINICAL AND HISTOLOGIC EVALUATIONS: ACASE REPORT Jun-Beom Park, DDS, MSD Placement of endosseous dental implants in diabetic
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues
 An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Owner's Guide to Natural Healing. Autologous Conditioned Plasma (ACP)
 An Owner's Guide to Natural Healing Autologous Conditioned Plasma (ACP) Healing after an injury involves a well-orchestrated and complex series of events where proteins in the blood have primary roles,
An Owner's Guide to Natural Healing Autologous Conditioned Plasma (ACP) Healing after an injury involves a well-orchestrated and complex series of events where proteins in the blood have primary roles,
POIEX/HACEX system - The key to success. - Clinical results and points to consider -
 POIEX/HACEX system - The key to success - Clinical results and points to consider - POIEX/HACEX system - The key to success - Clinical results and points to consider - POIEX/HACEX system - The key to success
POIEX/HACEX system - The key to success - Clinical results and points to consider - POIEX/HACEX system - The key to success - Clinical results and points to consider - POIEX/HACEX system - The key to success
Surgical Technique. 3.5mm and 4.5mm Lateral Proximal Tibia Locking Plates
 Surgical Technique 3.5mm and 4.5mm Lateral Proximal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System 3.5mm and 4.5mm Lateral Proximal Tibia Locking Plate Surgical Technique Contents Product
Surgical Technique 3.5mm and 4.5mm Lateral Proximal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System 3.5mm and 4.5mm Lateral Proximal Tibia Locking Plate Surgical Technique Contents Product
NCB Distal Femur System. Surgical Technique
 NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
» Guided Surgery. by MEDENTiKA « MEDENTIGUIDE SURGERY MANUAL QUATTROCONE QUATTROCONE30. IPS Implant systems
 » Guided Surgery by MEDENTiKA «IPS Implant systems MEDENTIGUIDE QUATTROCONE QUATTROCONE30 SURGERY MANUAL » MedentiGuide «MedentiGuide drill sleeves support the surgeon in preparing the implant bed for
» Guided Surgery by MEDENTiKA «IPS Implant systems MEDENTIGUIDE QUATTROCONE QUATTROCONE30 SURGERY MANUAL » MedentiGuide «MedentiGuide drill sleeves support the surgeon in preparing the implant bed for
BIOL 2457 CHAPTER 6 SI 1. irregular ectopic: sutural (Wormian) The is between the shaft and end. It contains cartilage that is
 BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
Conventus CAGE PH Surgical Techniques
 Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
In 1981, Dr. Albrektsson, a member of
 Osseodensification facilitates ridge expansion with enhanced implant stability in the maxilla: part II case report with 2-year follow-up Drs. Ann Marie Hofbauer and Salah Huwais offer another case study
Osseodensification facilitates ridge expansion with enhanced implant stability in the maxilla: part II case report with 2-year follow-up Drs. Ann Marie Hofbauer and Salah Huwais offer another case study
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS
 OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
Tobacco and Bone Health
 Tobacco and Bone Health Prof. Dr. Alok Chandra Agrawal MS Orthopaedics, DNB Orthopaedics, PhD Orthopaedics MAMS All India Institute of Medical Sciences Raipur CG Cigarette smoking is commonly identified
Tobacco and Bone Health Prof. Dr. Alok Chandra Agrawal MS Orthopaedics, DNB Orthopaedics, PhD Orthopaedics MAMS All India Institute of Medical Sciences Raipur CG Cigarette smoking is commonly identified
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
Technique Guide Hammertoe Correction System
 Technique Guide Hammertoe Correction System TM The ToeMATE Hammertoe Correction System is an easy to implant bone screw system intended for the correction of hammertoe deformity. It is provided in a complete
Technique Guide Hammertoe Correction System TM The ToeMATE Hammertoe Correction System is an easy to implant bone screw system intended for the correction of hammertoe deformity. It is provided in a complete
THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S.
 THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S. Skeletal anchorage, the concept of using the facial skeleton to control tooth
THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S. Skeletal anchorage, the concept of using the facial skeleton to control tooth
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system.
 LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Technique Guide This publication is not intended for distribution in the USA. Instruments
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Technique Guide This publication is not intended for distribution in the USA. Instruments
Posterior mandible and vertical augmentation
 CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
PRP Usage in Today's Implantology
 Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Skeletal System. The skeletal System... Components
 Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
In the process of tissue repair ENHANCEMENT OF OSSEOINTEGRATION BY GENERATING A DYNAMIC IMPLANT SURFACE RESEARCH. Eduardo A.
 RESEARCH ENHANCEMENT OF OSSEOINTEGRATION BY GENERATING A DYNAMIC IMPLANT SURFACE Eduardo A. Anitua, DDS, MD KEY WORDS Growth factors Titanium implants Osseointegration Preparations of autologous plasma
RESEARCH ENHANCEMENT OF OSSEOINTEGRATION BY GENERATING A DYNAMIC IMPLANT SURFACE Eduardo A. Anitua, DDS, MD KEY WORDS Growth factors Titanium implants Osseointegration Preparations of autologous plasma
Osseous Tissue and Bone Structure
 C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
Technique Guide. Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones.
 Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Supplementary Data. Supplementary Methods:
 Supplementary Data Supplementary Methods: Release kinetics of from collagen sponges in vivo. 2μg of human recombinant 165 was labeled with lexafluor 555 (Microscale Protein Labeling Kit; Invitrogen) as
Supplementary Data Supplementary Methods: Release kinetics of from collagen sponges in vivo. 2μg of human recombinant 165 was labeled with lexafluor 555 (Microscale Protein Labeling Kit; Invitrogen) as
Technique Guide. TomoFix Osteotomy System. A comprehensive plating system for stable fixation of osteotomies around the knee.
 Technique Guide TomoFix Osteotomy System. A comprehensive plating system for stable fixation of osteotomies around the knee. Table of Contents Introduction TomoFix Osteotomy System 2 AO Principles 4 Indications
Technique Guide TomoFix Osteotomy System. A comprehensive plating system for stable fixation of osteotomies around the knee. Table of Contents Introduction TomoFix Osteotomy System 2 AO Principles 4 Indications
REFERENCES for PLATELET RICH PLASMA (PRP)
 REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
Immediate post-extraction BIOMIMETIC CORAL IC implant placement in the anterior esthetic zone
 Immediate post-extraction BIOMIMETIC CORAL IC implant placement in the anterior esthetic zone AUTHORS Dr. Antonio Mallebrera Clinica Mallebrera Centro Dental (Petrer, Alicante) Sr. Juan José Sempere Matarredona
Immediate post-extraction BIOMIMETIC CORAL IC implant placement in the anterior esthetic zone AUTHORS Dr. Antonio Mallebrera Clinica Mallebrera Centro Dental (Petrer, Alicante) Sr. Juan José Sempere Matarredona
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics.
 In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
Surgical Technique. Anterolateral and Medial Distal Tibia Locking Plates
 Surgical Technique Anterolateral and Medial Distal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System Anterolateral and Medial Distal Tibia Locking Plates Surgical Technique Contents Product
Surgical Technique Anterolateral and Medial Distal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System Anterolateral and Medial Distal Tibia Locking Plates Surgical Technique Contents Product
S i m p l i c I t y, c o m f o r t, a e s t h e t i c s. axiom. The new dimension
 S i m p l i c I t y, c o m f o r t, a e s t h e t i c s axiom The new dimension 2 Implants by anthogyr axiom, t h e n e w g e n e r a t i o n i m p l a n t axiom characteristics represent the perfect synthesis
S i m p l i c I t y, c o m f o r t, a e s t h e t i c s axiom The new dimension 2 Implants by anthogyr axiom, t h e n e w g e n e r a t i o n i m p l a n t axiom characteristics represent the perfect synthesis
Dental Implants. From the beginning up to now. By: Dr Arash Khojasteh
 Dental Implants From the beginning up to now By: Dr Arash Khojasteh WHAT IS A DENTAL IMPLANT? Dental implant is an artificial fixture which is placed surgically into the jaw bone to substitute for a missing
Dental Implants From the beginning up to now By: Dr Arash Khojasteh WHAT IS A DENTAL IMPLANT? Dental implant is an artificial fixture which is placed surgically into the jaw bone to substitute for a missing
TITANIUM TIBIAL NAIL SySTEM
 TITANIUM TIBIAL NAIL SySTEM Solid and Cannulated Nails SURGICAL TEChNIqUE Table of contents Introduction Indications 2 Preoperative Implant Selection 6 Surgical Technique Instruments for Opening the Tibia
TITANIUM TIBIAL NAIL SySTEM Solid and Cannulated Nails SURGICAL TEChNIqUE Table of contents Introduction Indications 2 Preoperative Implant Selection 6 Surgical Technique Instruments for Opening the Tibia
Pathophysiology of fracture healing
 Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
Platelet-rich fibrin membrane in immediate dental implant loading
 original article Platelet-rich fibrin membrane in immediate dental implant loading Carlos Fernando de Almeida Barros MOURÃO 1, Natália Belmock Mascarenhas Freitas MOURÃO 2 104 Abstract / Introduction:
original article Platelet-rich fibrin membrane in immediate dental implant loading Carlos Fernando de Almeida Barros MOURÃO 1, Natália Belmock Mascarenhas Freitas MOURÃO 2 104 Abstract / Introduction:
scientific compendium
 scientific compendium Zimmer Tapered Screw-Vent Implant Success Stories in Stability and Survival Rates Zimmer Tapered Screw-Vent Implant Scientific Compendium table of contents CLINICAL & PRE-CLINICAL
scientific compendium Zimmer Tapered Screw-Vent Implant Success Stories in Stability and Survival Rates Zimmer Tapered Screw-Vent Implant Scientific Compendium table of contents CLINICAL & PRE-CLINICAL
TRAUMATOLOGY. Vortex. Distal Tibia plate
 TRAUMATOLOGY Vortex Distal Tibia plate 1 References Dr. László Vámhidy PhD. Head of Department, Clinical Director MSI Department of Traumatology and Hand Surgery Pécs, Hungary Prof. Dr. Endre Varga Professor
TRAUMATOLOGY Vortex Distal Tibia plate 1 References Dr. László Vámhidy PhD. Head of Department, Clinical Director MSI Department of Traumatology and Hand Surgery Pécs, Hungary Prof. Dr. Endre Varga Professor
Inion BioRestore. Bone Graft Substitute. Product Overview
 Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
Technique Guide. 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia Plates
Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia Plates
Cost-effective immediate restoration in the anterior region of the mandible (isy by CAMLOG)
 Cost-effective immediate restoration in the anterior region of the mandible (isy by CAMLOG) Many patients wish to have permanent dentures, and often this wish can be fulfilled by one of the greatest developments
Cost-effective immediate restoration in the anterior region of the mandible (isy by CAMLOG) Many patients wish to have permanent dentures, and often this wish can be fulfilled by one of the greatest developments
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture.
 Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine.
 Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine. Technique Guide Instruments and implants approved by the AO Foundation
Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine. Technique Guide Instruments and implants approved by the AO Foundation
Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft
 The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Abstract. Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University
 Bone marrow injection in patients with delayed union and non-union of long Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University Abstract In the process of bone formation and healing
Bone marrow injection in patients with delayed union and non-union of long Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University Abstract In the process of bone formation and healing
