Nasolabial Soft Tissue Changes After Le Fort I Advancement
|
|
|
- Ralf Paul
- 5 years ago
- Views:
Transcription
1 J Oral Maxillofac Surg 70:e270-e277, 2012 Nasolabial Soft Tissue Changes After Le Fort I Advancement Sivabalan Vasudavan, BDSc, MDSc, MPH,* Yasas S. N. Jayaratne, BDS, and Bonnie L. Padwa, DMD, MD Purpose: To identify the nasolabial soft tissue changes that occur after Le Fort I advancement. Materials and Methods: A prospective study of patients who had Le Fort I advancement at the Children s Hospital Boston from 2005 to The pre- and postoperative anthropometeric nasolabial measurements were recorded by a single examiner. Results: A total of 37 patients with a mean age of 18.6 years at the time of operation and a mean follow-up of 12.6 months were recruited. Nearly one half of the study sample (16 of 37) had cleft lip/palate. Direct anthropometry showed a reduction of the nasal length by 1.3 mm while the nasal tip protrusion increased by 1.1 mm. The nasofrontal angle decreased by 9.8 and the upper lip moved forward by 4.15 mm, reflecting the advancement in the maxilla. The height of the cutaneous upper lip increased by 0.4 mm. No significant differences were found in the soft tissue response observed between the cleft and noncleft subjects. Conclusions: Le Fort I advancement produces elevation of the nasal tip, as seen by a reduction in the nasal length, an increase in the nasal tip protrusion, and a concomitant reduction in the nasofrontal angle. Additionally, the cutaneous lip height increased, most likely due to an unfurling of the upper lip American Association of Oral and Maxillofacial Surgeons J Oral Maxillofac Surg 70:e270-e277, 2012 A combined surgical orthodontic approach is routinely used to correct significant dentofacial deformities. Surgical movement of the maxilla influences the overlying soft tissue and nasal morphology. Therefore, quantitative data on alterations in the nasolabial region that occur with the skeletal movements need to be considered during treatment planning for patients undergoing Le Fort I advancement. *Private Specialist Orthodontic Practice, Perth, Australia, Adjunct Faculty, Department of Developmental Biology, Harvard School of Dental Medicine and Department of Dentistry, Children s Hospital Boston. Department of Plastic and Oral Surgery, Children s Hospital Boston, Harvard Medical School, and Discipline of Oral and Maxillofacial Surgery, University of Hong Kong Faculty of Dentistry, Hong Kong, People s Republic of China. Department of Plastic and Oral Surgery, Children s Hospital Boston, Harvard Medical School, and Harvard School of Dental Medicine, Boston, MA. Address correspondence and reprint requests to Dr Padwa: Department of Plastic and Oral Surgery, Children s Hospital Boston, 300 Longwood Avenue, Boston, MA 02115; bonnie.padwa@ childrens.harvard.edu 2012 American Association of Oral and Maxillofacial Surgeons /12/7004-0$36.00/0 doi: /j.joms The published data are replete with studies using lateral cephalometry to document the soft tissue changes that occur with orthognathic surgery. Although this technique permits evaluation of the profile alterations, it does not give information on what occurs in the transverse dimension, which is especially important in assessing the nasolabial changes. Moreover, patients are used to viewing themselves in the mirror as a three-dimensional (3D) object and could find it difficult to relate to information presented solely as profile analysis. Anthropometry is an objective technique for quantifying facial morphology using a series of linear and angular measurements derived from a set of welldefined landmarks. 1 It permits measurements in all three dimensions and calculation of proportions to evaluate facial harmony. 2 The sagittal and transverse soft tissues measurements obtained with anthropometry can be correlated with the osseous movements and can be incorporated into prediction algorithms. This type of information will potentially provide better predictions of the sagittal and transverse changes that occur with Le Fort I osteotomy. The objectives of the present study were to quantify the nasolabial soft tissue changes that occur with Le Fort I advancement, and to identify the role of gender, the magnitude of surgical movement, and the diagnosis of a cleft lip/palate (CLP) on the nasolabial soft tissue changes that occur with Le Fort I advancement. e270
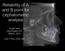
2 VASUDAVAN, JAYARATNE, AND PADWA e271 FIGURE 1. Anthropometric landmarks: en, endocanthion; n, nasion; sn, subnasale; al, alare; pr, pronasale; c, highest point of Columella; ls, labiale superius; sto, stomion; cph, crista philtri inferior. Materials and Methods SAMPLE SELECTION The study cohort consisted of a series of consecutively treated patients who had undergone Le Fort I osteotomy performed by a single surgeon (B.L.P.) at Children s Hospital Boston (Boston, MA) from 2005 to All subjects who met the following criteria were included in the present study: 1. Single piece Le Fort I osteotomy and advancement with rigid fixation 2. Preoperative and at least 6-month postoperative lateral cephalograms available 3. No concomitant mandibular osteotomy or adjunctive nasal procedures performed within the observation period The Children s Hospital, Boston, institutional review board approved the present study (protocol no. M ). SURGICAL TECHNIQUE All patients underwent standard Le Fort I osteotomy with rigid internal fixation. The right and left alar bases were sutured with 3.0 Prolene to a hole surgically created in the anterior nasal spine. The alar base width was narrowed by 2 to 3 mm. The wound was closed with running horizontal mattress suture without V Y advancement. ANTHROPOMETRIC EVALUATION Preoperative (T1) and postoperative (T2) standard anthropometeric nasolabial measurements (Fig 1 and Table 1) were recorded using a caliper and nasal angleometer, as described by Farkas. 3 All measurements were performed by a single examiner (B.L.P.) with more than 15 years experience in direct anthropometric techniques. Proportional indexes were calculated based on the linear measurements (Table 2). For transverse proportional indices, the intercanthal distance was used as a base measurement, because this region was unaffected by the operation. CEPHALOMETRIC ASSESSMENT Surgical changes to the craniofacial skeleton were objectively evaluated using routine lateral cephalometric analysis. The pre- and postoperative
3 e272 NASOLABIAL CHANGES AFTER LE FORT I ADVANCEMENT Table 1. LINEAR AND ANGULAR ANTHROPOMETRIC MEASUREMENTS Measurement Intercanthal distance Nasal height Nasal width Nasal length Nasal tip protrusion Columellar length Cutaneous upper labial height Overall upper labial height Vermilion height of upper lip Lower prolabial width Sagittal position of upper lip Maxillary incisor teeth display at rest Nasofrontal angle Nasal tip angle Nasolabial angle en-en n-sn al-al n-prn sn-prn sn-c sn-ls sn-sto ls-sto cphi-cphi t-ls incisal show Landmarks Angle between proximal nasal bridge contour and anterior surface of forehead below glabella Angle formed by lines following general direction of columella and nasal bridge Angle between surfaces of columella and upper lip skin Abbreviations: en, endocanthion; n, nasion; sn, subnasale; al, alare; pr, pronasale; c, highest point of columella; ls, labiale superius; st, stomion; cphi, crista philtri inferior. Vasudavan, Jayaratne, and Padwa. Nasolabial Changes After Le Fort I Advancement. J Oral Maxillofac Surg lateral cephalograms were scanned and digitized using the Dolphin Imaging Program, premium version 10.5 (Dolphin Imaging and Management Solutions, Chatsworth, CA) by a single examiner (S.V.). The mean enlargement factor was recorded for each radiograph. All linear measurements were transformed by the respective enlargement factors using the imaging software to enable direct comparison. A customized cephalometric analysis using an x and y coordinate system allowed measurement of the linear distances from the horizontal and vertical reference lines. The horizontal reference line was parallel to the Frankfort-Horizontal plane and passed through nasion. The vertical reference line, perpendicular to the horizontal reference line, originated at nasion and extended inferiorly (Fig 2). The horizontal and vertical change in the maxillary position between T1 and T2 was documented using the difference in N-A (HP) in millimeters and N-ANS (perp HP) in millimeters, respectively. Measurement error for the cephalometric analysis was assessed in 10 randomly selected patients, whose lateral cephalometric radiographs were redigitized and remeasured by the same examiner 1 month later. The coefficient of variation was calculated. STATISTICAL ANALYSIS Simple descriptive statistics (mean, standard deviation, and frequency distributions) were used to summarize the data. The initial tests for normality (assessment for skewness, kurtosis, and Shapiro-Wilk) were performed to determine, where appropriate, the parametric and nonparametric univariate analysis testing for the continuous variables (Table 2). Paired t tests and Wilcoxon rank sum tests were used to examine the differences in the anthropometric and cephalometric outcomes between T1 and T2. To examine the independent association of several factors with changes in the anthropometric measures, multivariate linear regression analyses were used to study the association between the independent and outcome variables. The outcome variables included changes in anthropometric measurements (T2 T1). 4 The predictor variables were selected on an a priori knowledge of influencing soft tissue change and included gender, the amount of horizontal and vertical maxillary skeletal change, and the presence of a CLP. All regression models were built using the ordinary least squares approach. R-square values were computed to examine the amount of variance explained by the predictor variables. Corrections were made for multiplicity using a modified Bonferonni method to reduce the likelihood of type I errors; an threshold for statistical significance for multiple comparisons was set at Univariate analyses were performed using SAS, version 9.2 (SAS Institute, Cary, NC), and multivariate linear regression analyses were performed using SPSS for Windows, version 16 (SPSS, Chicago, IL). Results A total of 37 patients (19 males and 18 females), who had a Le Fort I advancement at Children s Hospital Boston, from 2005 and 2007, with a mean age of 18.6 years (range 13.9 to 41.6), were included in the present study. This sample included 16 patients with CLP, equally distributed between unilateral (n 8) and bilateral (n 8). Of the 37 patients, 13 underwent maxillary sagittal advancement only, 10 simultaneous inferior repositioning, and 14 superior repositioning. Malar augmentation with Medpore implants was performed in 22 (59%) of all 37 patients and in 13 (80%) of the 16 patients with CLP. The postoperative (T2) lateral cephalograms and anthropometric measurements were taken more than 6 months after Le Fort I advancement (mean 12.6 months, range 7.6 to 20).
4 VASUDAVAN, JAYARATNE, AND PADWA e273 Table 2. CHANGES IN ANTHROPOMETRIC MEASURES FROM T1 TO T2 (n 37) Anthropometric Parameter T1 T2 T2-T1 95% CI P Value Linear measurements Intercanthal distance (en-en) , * Nasal height (n-sn) , Nasal width (al-al) , * Nasal length (n-prn) , Nasal tip protrusion (sn-prn) , Columellar length (sn-c) , Cutaneous height of upper lip (sn-ls) , Overall upper lip height (sn-sto) , Vermilion height of upper lip (ls-sto) , Lower prolabial width (cphi-cphi) , Maxillary incisor display , * Right tragion to labiale superious , distance (t-ls) Angular measurements Nasofrontal angle ( ) , Nasal tip angle ( ) , Nasolabial angle ( ) , Proportional indexes Nasal index (al-al/n-sn 100) , * Nasal bridge index (n-prn/n-sn 100) , Nasal tip protrusion-width index (snprn/al-al , ) al-al/en-en , * chpi-chpi/en-en , Abbreviations: CI, confidence interval; en, endocanthion; n, nasion; sn, subnasale; al, alare; pr, pronasale; c, highest point of columella; ls, labiale superius; st, stomion; cphi, crista philtri inferior. Data presented as mean standard deviation. *P.05. P.001. P.01. ANTHROPOMETRIC MEASUREMENTS After Le Fort I maxillary advancement, a number of statistically significant nasolabial anthropometric changes were observed (Table 2). The nasal length decreased by 1.3 mm (two-sided P.0001, 95% confidence interval 1.79 to 0.73), and the nasal tip protrusion increased by 1.1 mm (two-sided P.001, 95% confidence interval 0.5 to 1.79). No statistically significant differences were observed for the changes in nasal height, alar base width, nasal tip angle, nasolabial angle, or columellar length. Among the proportional indices, the nasal bridge index showed a statistically significant reduction of 2% (two-sided P.001, 95% confidence interval 3.42 to 0.98). The height of the cutaneous upper lip increased by 0.4 mm (two-sided P.01, 95% confidence interval 0.1 to 0.7 mm), and the upper lip had advanced forward by 4.15 mm (two-sided P.01, 95% confidence interval 2.89 to 5.42), as evident from the change in the linear distance from the right tragion to labiale superius (t-ls). No significant differences were observed for changes in vermillion height, philtrum width, or maxillary incisal tooth display at rest. Patients with CLP had a wider nose (P.01) at baseline (Table 3). No statistically significant differences were found in the anthropometric changes that occurred with Le Fort I advancement between the non-clp and CLP groups at an level of Subgroup analysis among the 3 types of maxillary movements (ie, pure advancement, advancement with superior repositioning, and advancement with inferior repositioning) did not result in statistically significant differences with respect to the soft tissue changes at an level of CEPHALOMETRIC MEASUREMENTS A number of statistically significant changes were found in the cephalometric measures that reflected the sagittal advancement of the maxilla [SNA, ANB, WITS, N-A (HP), midface length, and palatal length; Table 4]. Concomitant improvement was found in patient profile, with an increase in facial convexity of approximately 5. Measurement error was assessed by the coefficient of variation, which was less than 5% for all the cephalometric variables on repeated measures in a random subset of patients.
5 e274 NASOLABIAL CHANGES AFTER LE FORT I ADVANCEMENT FIGURE 2. Cephalometric planes used for assessing maxillary advancement. MULTIVARIATE LINEAR REGRESSION ANALYSES The multivariate linear regression analysis suggested that the horizontal change in maxillary position, gender, and the diagnosis of CLP were significant predictors of changes in a number of nasolabial anthropometric measurements (Table 5). Nasal Height (n-sn) A marginal association was found between male gender and the changes observed in nasal height. A 1-mm increase occurred in nasal height in the males compared with the females, at an level of The independent predictors accounted for 31.8% of the variance observed in the changes in nasal height resulting from Le Fort I maxillary osteotomy. Change in Maxillary Incisal Display at Rest (U1) The change observed in the maxillary incisal tooth display at rest (in millimeters) was significantly associated with the diagnosis of CLP. After controlling for surgical movements and baseline measurements, the patients with CLP had 1.3 mm less incisal display than the non-clp subjects. The independent predictors accounted for 68.3% of the variance observed in the changes in maxillary in-
6 VASUDAVAN, JAYARATNE, AND PADWA e275 Table 3. PREOPERATIVE ANTHROPOMETRIC PARAMETERS (T1) AND AMOUNT OF CHANGE ( T) STRATIFIED ACCORDING TO PRESENCE OR ABSENCE OF CLEFT LIP/PALATE Anthropometric Parameter T1 T T2 T1 Non-CLP CLP P Value Non-CLP CLP P Value Linear measurements Intercanthal distance (en-en) Nasal height (n-sn) Nasal width (al-al) Nasal length (n-prn) Nasal tip protrusion (sn-prn) * Columellar length (sn-c) Cutaneous upper labial height (sn-ls) Overall upper labial height (sn-sto) * Vermilion height of upper lip (ls-sto) Lower prolabial width (cphi-cphi) Maxillary incisor display Right tragus-ls Angular measurements Nasofrontal angle ( ) Nasal tip angle ( ) Nasolabial angle ( ) Proportional indexes Nasal index (al-al/n-sn 100) Nasal bridge index (n-prn/n-sn 100) Nasal tip protrusion-width index (snprn/al-al ) al-al/en-en chpi-chpi/en-en Abbreviations: T1, baseline; T2, postoperative; T; change from T1 to T2; CLP, cleft lip/palate; en, endocanthion; n, nasion; sn, subnasale; al, alare; pr, pronasale; c, highest point of columella; ls, labiale superius; st, stomion; cphi, crista philtri inferior. *P.05. cisal display at rest (in millimeters) resulting from Le Fort I maxillary advancement. Change in Nasolabial Angle The changes observed in the nasolabial angle were significantly associated with the baseline measurement and horizontal skeletal change. When all other factors (eg, cleft type, gender, vertical changes) were controlled, for every 1-mm advancement, a 1.35 increase was found in the nasolabial angle. The independent predictors accounted for 61.7% of variance observed in the changes in the nasolabial angle resulting from Le Fort I maxillary advancement. Table 4. CEPHALOMETRIC MEASURES AT T1, T2, AND T T2 T1 (N 37) Variable T1 T2 T T2 T1 95% CI P Value Horizontal skeletal SNA ( ) , * ANB ( ) , * Wits (FOP) (mm) , * N-A (HP) (mm) , * Vertical skeletal N-ANS (Perp HP) (mm) , U1-NF (Perp NF) (mm) , U6-NF (Perp NF) (mm) , Overjet (mm) , * Overbite (mm) , * Abbreviations: T1, baseline; T2, postoperative; T; change from T1 to T2; CI, confidence interval; NF, nasion Frankfort perpendicular. *P.001.
7 e276 NASOLABIAL CHANGES AFTER LE FORT I ADVANCEMENT Table 5. PREDICTORS OF NASOLABIAL SOFT TISSUE CHANGE Parameter Predictor R 2 Regression Equation Nasal height (mm) Maxillary incisor display at rest (mm) Nasolabial angle ( ) Baseline variable, gender Baseline variable, CLP Baseline variable, horizontal change Change in nasal height (n-sn) 6.67 [0.152 (n-sn at T1)] 1.01 (male) (CLP) (horizontal advancement) (vertical change) Change in maxillary incisal display at rest (U1) [0.461 (U1 at T1)] (male) (CLP) (horizontal advancement) (vertical change) Change in nasolabial angle [0.421 (nasolabial angle at T1)] (male) 6.17 (CLP) 1.35 (horizontal advancement) (vertical change) Abbreviations: n, nasion; sn, subnasale. Discussion The 3D nature of the skeletal alignment and the variation in the characteristics of the overlying soft tissues confound the esthetic outcomes after orthognathic surgery. Skeletal maneuvers can not only change the soft tissue morphology in the immediate vicinity, but also that in distant regions owing to the 3D composite anatomy of the craniofacial region. These changes affect the overall esthetic balance of the face. Thus, maxillofacial surgeons must pay due attention to alterations in the facial form before performing orthognathic surgery. Although plain radiography and computed tomography provide excellent hard tissue images, the information that can be extracted pertaining to the soft tissue counterparts and their surface anatomy is limited. The response of the facial soft tissues to Le Fort I advancement was assessed in the present study using direct anthropometric measurements. This permitted evaluation of the frontal, as well as the profile, changes. The linear distance from the right tragus to the labiale superius increased after maxillary advancement. This might have resulted from the forward movement of the upper lip, as well as from the increase in the transverse dimension of the facial middle third owing to the new soft tissue support being given by the maxillary advancement. The nasal length (n-prn) and nasofrontal angle decreased with a concomitant increase in the nasal tip protrusion (sn-prn), indicating an elevation of the nasal tip. Similar changes in the nasal tip have been reported in studies using lateral cephalograms. 5,6 The cutaneous lip height also increased, most likely from an unfurling of the upper lip. Apart from lateral cephalometry, two-dimensional photogrammetry and nasal casts have been used to assess nasolabial soft tissue changes after Le Fort I advancement. The poor definition and superimposition of the midline and lateral soft tissue outlines are some of the main drawbacks of lateral cephalometry. Although linear measurements can be performed on two-dimensional frontal photographs, they are not appropriate for assessing changes in facial depth. Betts et al 7 used 31 nasal casts constructed from impressions taken with custom-made trays to evaluate soft tissue response to Le Fort I osteotomy. They observed a widening of the nasal base (average 9%) in all patients, irrespective of the vector of maxillary movement. Nasal tip protrusion and the nasolabial angle decreased in 65% of the patients. However, it was not possible to draw conclusions on the significance of these changes, because the investigators did not perform a statistical analysis to compare the preand postoperative outcomes. In addition to the discomfort and potential for soft tissue compression during impression taking, nasal cast analysis can also be confounded by the errors induced from the dimensional changes of the impression and cast materials. Yamada et al 8 evaluated the soft tissue changes occurring after Le Fort I osteotomy using a 3D laser scanner. They reported a statistically significant increase in the nasal width (al-al) and nasal tip protrusion (n-prn). Recently, Rauso et al 9 also reported on the nasolabial changes using direct anthropometry, with a general trend toward widening of the alar base and a concomitant shortening of the columellar length even after performing the alar c-inch and a midline V Y extension. They did not observe such a trend in relation to the upper lip. In addition to the direct transverse measurements, we calculated proportion indices for a better understanding of the relative soft tissue changes that occur with maxillary advancement. The intercanthal distance was selected as the base measure, because no surgical intervention was performed in this region. Although an increase in the nasal width has been reported to occur after Le Fort I advancement, 10 we did not observe a statistically significant increase in the transverse nasal measurements or their proportional indices in our sample. This might be because
8 VASUDAVAN, JAYARATNE, AND PADWA e277 meticulous attention was given to narrowing the alar base width 2 to 3 mm by suturing the right and left alar bases to the anterior nasal spine in all patients at the time of maxillary advancement. Apart from the nasal bridge index (n-prn/n-sn 100), other proportional indices did not reach the P.01 level of statistical significance. The increase in the nasal bridge index is a result of the forward and upward movement of the nasal tip with maxillary advancement. Although a simple hard/soft tissue movement ratio that fits all patients would be desirable, such ratios do not exist. Considerable individual variation among patients would confound the predictions given by such simple ratios. The use of multiple regression equations could be a possible solution, because these consider some of the other factors that affect the esthetic outcomes. In the present study, we have generated some regression equations that could be used in the prediction of certain soft tissue parameters (Table 5). Patients with CLP had nasolabial repair as infants, and although scar tissue is present in the area, the established anthropometric landmarks are used in this patient population. 11 In addition, the paired t test was used to compare the CLP and non-clp groups. In respect to the baseline values (T1), only the nasal width was significantly larger in the CLP group. However, the net soft tissue change ( T) before (T1) and after (T2) surgery was not significantly different between the 2 groups at an level of 0.01 ( T T2 T1; Table 3). Many patients who require Le Fort I osteotomy have maxillary hypoplasia that extends to the infraorbital rims. A standard Le Fort I advancement does not change the deficiency in the superior aspect of the middle third of the face. 12 Therefore, malar augmentation with implants in the infraorbital region that extend to the zygomatic arch were placed in several patients at the time of Le Fort I to improve the projection of the upper midface. However, it was not possible to quantify the changes in the malar complex with conventional anthropometric techniques. With the availability of stereophotography, it will be possible to monitor the alterations in the malar region using 3D color maps. 13,14 In addition, stereophotography will facilitate the collection of anthropometric measurements. Le Fort I advancement produces elevation of the nasal tip, as evident by the reduction in the nasal length and nasofrontal angle, along with an increase in the nasal tip protrusion. Additionally, the cutaneous lip height is observed to be increased, most likely from an unfurling of the upper lip. A lack of understanding of the 3D nature of the soft tissue response to orthognathic surgery can result in undesirable esthetic outcomes. A thorough soft tissue examination must be a part of the preoperative evaluation. It is important to appreciate the nasolabial changes that occur with maxillary advancement and to include these in the treatment plan. Acknowledgment We would like to thank Drs Stephen Sullivan, Veerasathpurush Allareddy, and Heather Baer for their helpful comments. References 1. Kolar JC, Salter EM: Craniofacial Anthropometry: Practical Measurement of the Head and Face for Clinical, Surgical, and Research Use. Springfield, IL, Charles C Thomas, Farkas LG, Hreczko TA, Kolar JC, et al: Vertical and horizontal proportions of the face in young adult North American Caucasians: Revision of neoclassical canons. Plast Reconstr Surg 75: 328, Farkas LG: Anthropometry of the Head and Face (ed 2). New York, Raven, Bailey LJ, Dover AJ, Proffit WR: Long-term soft tissue changes after orthodontic and surgical corrections of skeletal Class III malocclusions. Angle Orthod 77:389, Mommaerts MY, Lippens F, Abeloos JV, et al: Nasal profile changes after maxillary impaction and advancement surgery. J Oral Maxillofac Surg 58:470, Rosen HM: Lip-nasal aesthetics following Le Fort I osteotomy. Plast Reconstr Surg 81:171, Betts NJ, Vig KW, Vig P, et al: Changes in the nasal and labial soft tissues after surgical repositioning of the maxilla. Int J Adult Orthodon Orthognath Surg 8:7, Yamada T, Mishima K, Moritani N, et al: Nasolabial morphologic changes after a Le Fort I osteotomy: A three-dimensional anthropometric study. J Craniofac Surg 21:1089, Rauso R, Tartaro G, Tozzi U, et al: Nasolabial changes after maxillary advancement. J Craniofac Surg 22:809, Betts NJ, Dowd KF: Soft tissue changes associated with orthognathic surgery. Atlas Oral Maxillofac Surg Clin North Am 8:13, Farkas LG, Forrest CR, Phillips JH: Comparison of the morphology of the cleft face and the normal face: Defining the anthropometric differences. J Craniofac Surg 11:76, Marsh JL, Galić M: Maxillofacial osteotomies for patients with cleft lip and palate. Clin Plast Surg 16:803, Jayaratne YS, Zwahlen RA, Lo J, et al: Facial soft tissue response to anterior segmental osteotomies: A systematic review. Int J Oral Maxillofac Surg 39:1050, Jayaratne YS, Zwahlen RA, Lo J, et al: Three-dimensional color maps: A novel tool for assessing craniofacial changes. Surg Innov 17:198, 2010
Maxillary Advancement Surgery and Nasolabial Soft Tissue Changes
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 3 Ver. VIII (March. 2017), PP 23-29 www.iosrjournals.org Maxillary Advancement Surgery and
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 3 Ver. VIII (March. 2017), PP 23-29 www.iosrjournals.org Maxillary Advancement Surgery and
Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients
 Original Article Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients Ming Tak Chew a Abstract: Cephalometric studies have shown that the Chinese race tends to have a greater
Original Article Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients Ming Tak Chew a Abstract: Cephalometric studies have shown that the Chinese race tends to have a greater
AESTHETIC ORTHOGNATHIC SURGERY
 c0435 ESTHETIC ORTHOGNTHIC SURGERY Stephen. aker, MD, DDS, and Harvey Rosen, MD, DMD CHPTER 87 s0010 p0010 s0020 p0015 s0025 p0020 s0030 p0025 s0035 p0030 s0040 p0035 s0045 p0040 1. What is orthognathic
c0435 ESTHETIC ORTHOGNTHIC SURGERY Stephen. aker, MD, DDS, and Harvey Rosen, MD, DMD CHPTER 87 s0010 p0010 s0020 p0015 s0025 p0020 s0030 p0025 s0035 p0030 s0040 p0035 s0045 p0040 1. What is orthognathic
How predictable is orthognathic surgery?
 European Journal of Orthodontics 26 (2004) 303 309 European Journal of Orthodontics vol. 26 no. 3 European Orthodontic Society 2004; all rights reserved. How predictable is orthognathic surgery? Charlotte
European Journal of Orthodontics 26 (2004) 303 309 European Journal of Orthodontics vol. 26 no. 3 European Orthodontic Society 2004; all rights reserved. How predictable is orthognathic surgery? Charlotte
Changes in soft tissue thickness after Le Fort I osteotomy in different cleft types
 Arja Heliövaara, DDS, PhD Orthodontist Jyri Hukki, MD, PhD Senior Consultant in Plastic Surgery Reijo Ranta, DDS, PhD Docent and Senior Orthodontist Aarne Rintala, MD, PhD Assistant Professor of Plastic
Arja Heliövaara, DDS, PhD Orthodontist Jyri Hukki, MD, PhD Senior Consultant in Plastic Surgery Reijo Ranta, DDS, PhD Docent and Senior Orthodontist Aarne Rintala, MD, PhD Assistant Professor of Plastic
Nasal Changes after Surgical Correction of Skeletal Class III Malocclusion in Koreans
 Original Article Nasal Changes after Surgical Correction of Skeletal Class III Malocclusion in Koreans Chooryung Chung a ; Yebert Lee b ; Kwang-Ho Park c ; Sun-Hyung Park d ; Young-Chel Park e ; Kyung-Ho
Original Article Nasal Changes after Surgical Correction of Skeletal Class III Malocclusion in Koreans Chooryung Chung a ; Yebert Lee b ; Kwang-Ho Park c ; Sun-Hyung Park d ; Young-Chel Park e ; Kyung-Ho
Patients with cleft lip and palate (CLP) usually
 Comparison of Treatment Outcome and Stability Between Distraction Osteogenesis and LeFort I Osteotomy in Cleft Patients With Maxillary Hypoplasia Seung-Hak Baek, DDS, MSD, PhD,* Jin-Kyung Lee, DDS, 1 Jong-Ho
Comparison of Treatment Outcome and Stability Between Distraction Osteogenesis and LeFort I Osteotomy in Cleft Patients With Maxillary Hypoplasia Seung-Hak Baek, DDS, MSD, PhD,* Jin-Kyung Lee, DDS, 1 Jong-Ho
LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS
 POLSKI PRZEGLĄD CHIRURGICZNY 2009, 81, 1, 23 27 10.2478/v10035-009-0004-2 LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS PRADEEP JAIN, ANAND AGARWAL, ARVIND SRIVASTAVA Department of Plastic
POLSKI PRZEGLĄD CHIRURGICZNY 2009, 81, 1, 23 27 10.2478/v10035-009-0004-2 LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS PRADEEP JAIN, ANAND AGARWAL, ARVIND SRIVASTAVA Department of Plastic
Effect of Preoperative Nasal Retainer on Nasal Growth in Patients with Bilateral Incomplete Cleft Lip: A 3-Year Follow-Up Study
 Effect of Preoperative Nasal Retainer on Nasal Growth in Patients with Bilateral Incomplete Cleft Lip: A 3-Year Follow-Up Study Original Article Young Chul Kim, Woo Shik Jeong, Tae Suk Oh, Jong Woo Choi,
Effect of Preoperative Nasal Retainer on Nasal Growth in Patients with Bilateral Incomplete Cleft Lip: A 3-Year Follow-Up Study Original Article Young Chul Kim, Woo Shik Jeong, Tae Suk Oh, Jong Woo Choi,
A CROSS-SECTIONAL STUDY OF SOFT TISSUE FACIAL MORPHOMETRY IN CHILDREN AND ADOLESCENTS
 Malaysian Journal of Medical Sciences, Vol. 13, No. 1, January 2006 (25-29) ORIGINAL ARTICLE A CROSS-SECTIONAL STUDY OF SOFT TISSUE FACIAL MORPHOMETRY IN CHILDREN AND ADOLESCENTS Nizam Abdullah*, Lin Naing**,
Malaysian Journal of Medical Sciences, Vol. 13, No. 1, January 2006 (25-29) ORIGINAL ARTICLE A CROSS-SECTIONAL STUDY OF SOFT TISSUE FACIAL MORPHOMETRY IN CHILDREN AND ADOLESCENTS Nizam Abdullah*, Lin Naing**,
PREDICTING LOWER LIP AND CHIN RESPONSE TO MANDIBULAR ADVANCEMENT WITH GENIOPLASTY A CEPHALOMETRIC STUDY
 PREDICTING LOWER LIP AND CHIN RESPONSE TO MANDIBULAR ADVANCEMENT WITH GENIOPLASTY A CEPHALOMETRIC STUDY Dr. Deepthi T. Amanna Authors : Dr. Deepthi T. Amanna Assistant Professor Dr. E.T. Roy Professor
PREDICTING LOWER LIP AND CHIN RESPONSE TO MANDIBULAR ADVANCEMENT WITH GENIOPLASTY A CEPHALOMETRIC STUDY Dr. Deepthi T. Amanna Authors : Dr. Deepthi T. Amanna Assistant Professor Dr. E.T. Roy Professor
The America Association of Oral and Maxillofacial Surgeons classify occlusion/malocclusion in to the following three categories:
 Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 02 SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT Amit Dahiya 1,Minakshi
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 02 SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT Amit Dahiya 1,Minakshi
Surgically assisted rapid palatal expansion (SARPE) prior to combined Le Fort I and sagittal osteotomies: A case report
 200 Carlos Alberto E. Tavares, DDS, MS, DOrth Professor Department of Orthodontics Associação Brasileira de Odontologia - RS Porto Alegre, Brazil Miguel Scheffer, DDS, MS Chairman Department of Oral and
200 Carlos Alberto E. Tavares, DDS, MS, DOrth Professor Department of Orthodontics Associação Brasileira de Odontologia - RS Porto Alegre, Brazil Miguel Scheffer, DDS, MS Chairman Department of Oral and
Incisal and Soft Tissue Effects of Maxillary Premolar Extraction in Class II Treatment
 Original Article Incisal and Soft Tissue Effects of Maxillary Premolar Extraction in Class II Treatment Nevenka Tadic a ; Michael G. Woods b ABSTRACT Objective: This retrospective study was designed to
Original Article Incisal and Soft Tissue Effects of Maxillary Premolar Extraction in Class II Treatment Nevenka Tadic a ; Michael G. Woods b ABSTRACT Objective: This retrospective study was designed to
Balanced Angular Profile Analysis
 Cosmetic Balanced Angular Profile Analysis Seung Chul Rhee, M.D., So Ra Kang, M.D., Ph.D., and Heung Sik Park, M.D., Ph.D. Seoul, Republic of Korea To evaluate current preferences and ethnic differences
Cosmetic Balanced Angular Profile Analysis Seung Chul Rhee, M.D., So Ra Kang, M.D., Ph.D., and Heung Sik Park, M.D., Ph.D. Seoul, Republic of Korea To evaluate current preferences and ethnic differences
ORIGINAL ARTICLES. Three-Dimensional Analysis of the Child Cleft Face
 ORIGINAL ARTICLES Three-Dimensional Analysis of the Child Cleft Face S. DUFFY, B.CH.D., F.D.S.R.C.S., M.SC., M.ORTH. J. H. NOAR, B.D.S., F.D.S.R.C.S., M.SC., M.ORTH. R. D. EVANS, B.D.S., F.D.S.R.C.S.,
ORIGINAL ARTICLES Three-Dimensional Analysis of the Child Cleft Face S. DUFFY, B.CH.D., F.D.S.R.C.S., M.SC., M.ORTH. J. H. NOAR, B.D.S., F.D.S.R.C.S., M.SC., M.ORTH. R. D. EVANS, B.D.S., F.D.S.R.C.S.,
Evaluation of maxillary protrusion malocclusion treatment effects with prosth-orthodontic method in old adults
 Evaluation of maxillary protrusion malocclusion treatment effects with prosth-orthodontic method in old adults Peicheng Xu, DDS, MSD, a and Honghu Liu, DDS, PhD b a Shanghai Xuhui Dental Hospital and b
Evaluation of maxillary protrusion malocclusion treatment effects with prosth-orthodontic method in old adults Peicheng Xu, DDS, MSD, a and Honghu Liu, DDS, PhD b a Shanghai Xuhui Dental Hospital and b
MAHP Orthognathic Surgery Guidelines. Medical Policy Statement. Criteria
 Introduction The word orthognathic comes from the Greek words for straighten and jaw. Orthognathic surgery is the surgical correction of abnormalities of the mandible and/or maxilla. 1 It involves the
Introduction The word orthognathic comes from the Greek words for straighten and jaw. Orthognathic surgery is the surgical correction of abnormalities of the mandible and/or maxilla. 1 It involves the
The changes of soft tissue profile. skeletal class II patients with mandibular retrognathy treated with extraction of maxillary first premolars
 The changes of soft tissue profile in skeletal class II patients with mandibular retrognathy (Hendri et al) The changes of soft tissue profile in skeletal class II patients with mandibular retrognathy
The changes of soft tissue profile in skeletal class II patients with mandibular retrognathy (Hendri et al) The changes of soft tissue profile in skeletal class II patients with mandibular retrognathy
CLINICAL NOTE. Long-Term Results in the Bilateral Cleft Lip Repair by Mulliken s Method
 CLINICAL NOTE Long-Term Results in the Bilateral Cleft Lip Repair by Mulliken s Method Seok-Kwun Kim, MD, PhD, Myung-Hoon Kim, MD, Yong-Seok Kwon, MD, and Keun-Cheol Lee, MD, PhD Purpose: To evaluate long-term
CLINICAL NOTE Long-Term Results in the Bilateral Cleft Lip Repair by Mulliken s Method Seok-Kwun Kim, MD, PhD, Myung-Hoon Kim, MD, Yong-Seok Kwon, MD, and Keun-Cheol Lee, MD, PhD Purpose: To evaluate long-term
Soft Tissue Changes after Upper Premolar Extraction in Class II Camouflage Therapy
 Original Article Soft Tissue Changes after Upper Premolar Extraction in Class II Camouflage Therapy R. Scott Conley a ; Christopher Jernigan b Abstract: The long-term effect on the facial profile has led
Original Article Soft Tissue Changes after Upper Premolar Extraction in Class II Camouflage Therapy R. Scott Conley a ; Christopher Jernigan b Abstract: The long-term effect on the facial profile has led
Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient
 Case Report Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient Masayoshi Kawakami, DDS, PhD a ; Takakazu Yagi, DDS, PhD b ; Kenji
Case Report Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient Masayoshi Kawakami, DDS, PhD a ; Takakazu Yagi, DDS, PhD b ; Kenji
Three-Dimensional Analysis of Nasal Symmetry Following Primary Correction of Unilateral Cleft Lip Nasal Deformity
 The Cleft Palate Craniofacial Journal 00(00) pp. 000 000 Month 0000 Ó Copyright 2016 American Cleft Palate Craniofacial Association ORIGINAL ARTICLE Three-Dimensional Analysis of Nasal Symmetry Following
The Cleft Palate Craniofacial Journal 00(00) pp. 000 000 Month 0000 Ó Copyright 2016 American Cleft Palate Craniofacial Association ORIGINAL ARTICLE Three-Dimensional Analysis of Nasal Symmetry Following
Morphologic Changes of Nose after LeFort I osteotomy of Skeletal Class III Patients
 Morphologic Changes of Nose after LeFort I osteotomy of Skeletal Class III Patients Yebert Lee, D.D.S. The Graduate School Yonsei University Department of Dentistry Morphologic Changes of Nose after LeFort
Morphologic Changes of Nose after LeFort I osteotomy of Skeletal Class III Patients Yebert Lee, D.D.S. The Graduate School Yonsei University Department of Dentistry Morphologic Changes of Nose after LeFort
Topic: Orthognathic Surgery Date of Origin: October 5, Section: Surgery Last Reviewed Date: December 2013
 Medical Policy Manual Topic: Orthognathic Surgery Date of Origin: October 5, 2004 Section: Surgery Last Reviewed Date: December 2013 Policy No: 137 Effective Date: March 1, 2014 IMPORTANT REMINDER Medical
Medical Policy Manual Topic: Orthognathic Surgery Date of Origin: October 5, 2004 Section: Surgery Last Reviewed Date: December 2013 Policy No: 137 Effective Date: March 1, 2014 IMPORTANT REMINDER Medical
Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair
 Original Article Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair Yoon Seok Lee 1, Dong Hyeok Shin 1, Hyun Gon Choi 1, Jee Nam Kim 1, Myung Chul
Original Article Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair Yoon Seok Lee 1, Dong Hyeok Shin 1, Hyun Gon Choi 1, Jee Nam Kim 1, Myung Chul
Orthognathic treatment of facial asymmetry due to temporomandibular joint ankylosis
 Orthognathic treatment of facial asymmetry due to temporomandibular joint ankylosis Ayse Gulsen 1, Serhat Sibar 2, Selahattin Ozmen 3 1 Department of Plastic, Reconstructive, and Aesthetic Surgery, Gazi
Orthognathic treatment of facial asymmetry due to temporomandibular joint ankylosis Ayse Gulsen 1, Serhat Sibar 2, Selahattin Ozmen 3 1 Department of Plastic, Reconstructive, and Aesthetic Surgery, Gazi
Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery
 European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
Virtual model surgery and wafer fabrication for orthognathic surgery
 Int. J. Oral Maxillofac. Surg. 2009; 38: 1306 1323 available online at http://www.sciencedirect.com Technical Note Orthognathic Surgery Virtual model surgery and wafer fabrication for orthognathic surgery
Int. J. Oral Maxillofac. Surg. 2009; 38: 1306 1323 available online at http://www.sciencedirect.com Technical Note Orthognathic Surgery Virtual model surgery and wafer fabrication for orthognathic surgery
Sensitivity of a Method for the Analysis of Facial Mobility. II. Interlandmark Separation
 Sensitivity of a Method for the Analysis of Facial Mobility. II. Interlandmark Separation CARROLL-ANN TROTMAN, B.D.S., M.A., M.S. JULIAN J. FARAWAY, PH.D. Objective: This study demonstrates a method of
Sensitivity of a Method for the Analysis of Facial Mobility. II. Interlandmark Separation CARROLL-ANN TROTMAN, B.D.S., M.A., M.S. JULIAN J. FARAWAY, PH.D. Objective: This study demonstrates a method of
Severe Malocclusion: Appropriately Timed Treatment. This article discusses challenging issues clinicians face when treating
 Severe Malocclusion: The Importance of Appropriately Timed Treatment A Synchronized and Simultaneous Interdisciplinary Plan Using Cosmetic Dentistry Principles David M. Sarver, DMD, MS Abstract This article
Severe Malocclusion: The Importance of Appropriately Timed Treatment A Synchronized and Simultaneous Interdisciplinary Plan Using Cosmetic Dentistry Principles David M. Sarver, DMD, MS Abstract This article
Comparison of craniofacial characteristics of typical Chinese and Caucasian young adults
 European Journal of Orthodontics 33 (2011) 205 211 doi:10.1093/ejo/cjq054 Advance Access Publication 13 August 2010 The Author 2010. Published by Oxford University Press on behalf of the European Orthodontic
European Journal of Orthodontics 33 (2011) 205 211 doi:10.1093/ejo/cjq054 Advance Access Publication 13 August 2010 The Author 2010. Published by Oxford University Press on behalf of the European Orthodontic
Orthognathic surgery. Dr. Mohamed Rahil. ((Maxillofacial surgeon))
 Orthognathic surgery Dr. Mohamed Rahil ((Maxillofacial surgeon)) Tikrit dentistry college 2015 2016 Orthognathic surgery is the art and science of diagnosis, and treatment of facial disproportion. These
Orthognathic surgery Dr. Mohamed Rahil ((Maxillofacial surgeon)) Tikrit dentistry college 2015 2016 Orthognathic surgery is the art and science of diagnosis, and treatment of facial disproportion. These
The three-dimensional effects of orthodontic treatment on the facial soft tissues a preliminary study.
 IN BRIEF l Orthodontic treatment can effect the appearance of the face in all three dimensions of space. The extent of these effects can be accurately assessed using an imaging technique such as three-dimensional
IN BRIEF l Orthodontic treatment can effect the appearance of the face in all three dimensions of space. The extent of these effects can be accurately assessed using an imaging technique such as three-dimensional
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS Dr. Masatoshi Sana Year: ESLO 01 RÉSUMÉ OF CASE 8 CASE CATEGORY: TRANS / VERTICAL DISCREPANCY NAME: Akiko T. BORN : 15/03/1973 SEX: F PRE-TREATMENT RECORDS: AGE:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS Dr. Masatoshi Sana Year: ESLO 01 RÉSUMÉ OF CASE 8 CASE CATEGORY: TRANS / VERTICAL DISCREPANCY NAME: Akiko T. BORN : 15/03/1973 SEX: F PRE-TREATMENT RECORDS: AGE:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER : 13 Dr. Masatoshi Sana CASE NUMBER : Year : ESLO 01 RÉSUMÉ OF CASE 2 CASE CATEGORY: CLASS I MALOCCLUSION NAME: BORN: SEX: Yukari K. 08/03/1979
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER : 13 Dr. Masatoshi Sana CASE NUMBER : Year : ESLO 01 RÉSUMÉ OF CASE 2 CASE CATEGORY: CLASS I MALOCCLUSION NAME: BORN: SEX: Yukari K. 08/03/1979
Facial planning for orthodontists and oral surgeons
 ADVANCES IN ORTHODONTICS & DENTOFACIAL SURGERY Facial planning for orthodontists and oral surgeons G. William Arnett, DDS, FACD, a and Michael J. Gunson, DDS, MD b Santa Barbara, Calif The bite indicates
ADVANCES IN ORTHODONTICS & DENTOFACIAL SURGERY Facial planning for orthodontists and oral surgeons G. William Arnett, DDS, FACD, a and Michael J. Gunson, DDS, MD b Santa Barbara, Calif The bite indicates
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER:44 CASE NUMBER: 2 Year: 2010 ESLO 01 RÉSUMÉ OF CASE 5 CASE CATEGORY: CLASS II DIVISION 1 MALOCCLUSION A MALOCCLUSION WITH SIGNIFICANT MANDIBULAR
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER:44 CASE NUMBER: 2 Year: 2010 ESLO 01 RÉSUMÉ OF CASE 5 CASE CATEGORY: CLASS II DIVISION 1 MALOCCLUSION A MALOCCLUSION WITH SIGNIFICANT MANDIBULAR
Morphologic outcome of bimaxillary surgery An anthropometric appraisal
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.19978 http://dx.doi.org/doi:10.4317/medoral.19978 An anthropometric appraisal Gregor F. Raschke 1, Ulrich M. Rieger 2, Andre
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.19978 http://dx.doi.org/doi:10.4317/medoral.19978 An anthropometric appraisal Gregor F. Raschke 1, Ulrich M. Rieger 2, Andre
ORTHOGNATHIC SURGERY
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Original Research. Figure 1: (a) Unilateral complete cleft of the lip and palate, (b) unilateral complete skeletal cleft with a Simonart s band.
 Received: 14 th August 2015 Accepted: 19 th November 2015 Conflicts of Interest: None Source of Support: Nil Original Research Simonart s Bands and Facial Growth in Unilateral Cleft Lip and Palate Patients:
Received: 14 th August 2015 Accepted: 19 th November 2015 Conflicts of Interest: None Source of Support: Nil Original Research Simonart s Bands and Facial Growth in Unilateral Cleft Lip and Palate Patients:
Long Term Stability and Prediction of Soft Tissue Changes Following LeFort I Surgery
 University of Connecticut DigitalCommons@UConn SoDM Masters Theses School of Dental Medicine June 1991 Long Term Stability and Prediction of Soft Tissue Changes Following LeFort I Surgery Gregory A. Hack
University of Connecticut DigitalCommons@UConn SoDM Masters Theses School of Dental Medicine June 1991 Long Term Stability and Prediction of Soft Tissue Changes Following LeFort I Surgery Gregory A. Hack
NIH Public Access Author Manuscript J Oral Maxillofac Surg. Author manuscript; available in PMC 2010 July 27.
 NIH Public Access Author Manuscript Published in final edited form as: J Oral Maxillofac Surg. 2009 October ; 67(10): 2123 2129. doi:10.1016/j.joms.2009.03.007. Orthopedic Traction of the Maxilla With
NIH Public Access Author Manuscript Published in final edited form as: J Oral Maxillofac Surg. 2009 October ; 67(10): 2123 2129. doi:10.1016/j.joms.2009.03.007. Orthopedic Traction of the Maxilla With
Contents. Section 1: Introduction and History. 1. Cephalometry in Orthodontics Section 2: Classification of Cephalometric Landmarks
 Contents Section 1: Introduction and History 1. Cephalometry in Orthodontics... 3 Technical Aspects 4 Cephalometric X-ray Tracing Techniques 4 Section 2: Classification of Cephalometric Landmarks 2. Classification
Contents Section 1: Introduction and History 1. Cephalometry in Orthodontics... 3 Technical Aspects 4 Cephalometric X-ray Tracing Techniques 4 Section 2: Classification of Cephalometric Landmarks 2. Classification
Evaluating Upper Lip and Nose Changes after Alveolar Bone Grafting in Unilateral Cleft Lip and Palate Patients Using 3D Stereophotogrammetry
 Evaluating Upper Lip and Nose Changes after Alveolar Bone Grafting in Unilateral Cleft Lip and Palate Patients Using 3D Stereophotogrammetry Atchariyaporn Ranchan DDS*, Poonsak Pisek DDS, MS, FRCDT*, Supaporn
Evaluating Upper Lip and Nose Changes after Alveolar Bone Grafting in Unilateral Cleft Lip and Palate Patients Using 3D Stereophotogrammetry Atchariyaporn Ranchan DDS*, Poonsak Pisek DDS, MS, FRCDT*, Supaporn
Patients with small lower jaws may derive aesthetic
 Operative Strategies Enlarging the Deficient Mandible Michael J. Yaremchuk, MD; Yi-Chieh Chen, MD Dr. Yaremchuk is Clinical Professor of Surgery, Harvard Medical School and Chief of Craniofacial Surgery,
Operative Strategies Enlarging the Deficient Mandible Michael J. Yaremchuk, MD; Yi-Chieh Chen, MD Dr. Yaremchuk is Clinical Professor of Surgery, Harvard Medical School and Chief of Craniofacial Surgery,
Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction
 Case Report Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction Roberto M. A. Lima, DDS a ; Anna Leticia Lima, DDS b Abstract:
Case Report Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction Roberto M. A. Lima, DDS a ; Anna Leticia Lima, DDS b Abstract:
Three-Dimensional Cephalometry Using Helical Computer Tomography: Measurement Error Caused by Head Inclination
 Original Article Three-Dimensional Cephalometry Using Helical Computer Tomography: Measurement Error Caused by Head Inclination Kumiko Togashi, DDS a ; Hideki Kitaura, DDS, PhD b ; Koichi Yonetsu, DDS,
Original Article Three-Dimensional Cephalometry Using Helical Computer Tomography: Measurement Error Caused by Head Inclination Kumiko Togashi, DDS a ; Hideki Kitaura, DDS, PhD b ; Koichi Yonetsu, DDS,
Longitudinal study of cephalometric soft tissue profile traits between the ages of 6 and 18 years
 Original Article Longitudinal study of cephalometric soft tissue profile traits between the ages of 6 and 18 years Robert T. Bergman a ; John Waschak b ; Ali Borzabadi-Farahani c ; Neal C. Murphy d ABSTRACT
Original Article Longitudinal study of cephalometric soft tissue profile traits between the ages of 6 and 18 years Robert T. Bergman a ; John Waschak b ; Ali Borzabadi-Farahani c ; Neal C. Murphy d ABSTRACT
Orthodontics-surgical combination therapy for Class III skeletal malocclusion
 [Downloaded free from http://www.contempclindent.org on Tuesday, July 16, 2013, IP: 164.100.31.82] Click here to download free Android application for this jou Orthodontics-surgical combination therapy
[Downloaded free from http://www.contempclindent.org on Tuesday, July 16, 2013, IP: 164.100.31.82] Click here to download free Android application for this jou Orthodontics-surgical combination therapy
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.]
![06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.] 06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.]](/thumbs/84/91182117.jpg) Reference #: MC/B002 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS)
Reference #: MC/B002 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS)
Mixed-reality simulation for orthognathic surgery
 Fushima and Kobayashi Maxillofacial Plastic and Reconstructive Surgery (2016) 38:13 DOI 10.1186/s40902-016-0059-z METHODOLOGY Mixed-reality simulation for orthognathic surgery Kenji Fushima 1* and Masaru
Fushima and Kobayashi Maxillofacial Plastic and Reconstructive Surgery (2016) 38:13 DOI 10.1186/s40902-016-0059-z METHODOLOGY Mixed-reality simulation for orthognathic surgery Kenji Fushima 1* and Masaru
Dental Research Journal
 Dental Research Journal Original Article Comparative assessment of soft-tissue changes in Class II Division 1 patients following extraction and non-extraction treatment Sneh Lata Verma 1, Vijay Prakash
Dental Research Journal Original Article Comparative assessment of soft-tissue changes in Class II Division 1 patients following extraction and non-extraction treatment Sneh Lata Verma 1, Vijay Prakash
An Anterior Tooth Size Comparison in Unilateral and Bilateral Congenitally Absent Maxillary Lateral Incisors
 An Anterior Tooth Size Comparison in Unilateral and Bilateral Congenitally Absent Maxillary Lateral Incisors Abstract The purpose of this study is to compare the anterior tooth size width in patients with
An Anterior Tooth Size Comparison in Unilateral and Bilateral Congenitally Absent Maxillary Lateral Incisors Abstract The purpose of this study is to compare the anterior tooth size width in patients with
Reliability of A and B point for cephalometric analysis
 Reliability of A and B point for cephalometric analysis Angle East Washington DC March, 2015 Carl P Roy, DDS, MS 1 History Orthodontic profession has always attempted to classify malocclusions. A-P relationship
Reliability of A and B point for cephalometric analysis Angle East Washington DC March, 2015 Carl P Roy, DDS, MS 1 History Orthodontic profession has always attempted to classify malocclusions. A-P relationship
Longitudinal dento-skeletal changes in UCLP patients following maxillary distraction osteogenesis using RED system
 J Med Dent Sci 2004; 51: 27 33 Original Article Longitudinal dento-skeletal changes in UCLP patients following maxillary distraction osteogenesis using RED system Eduardo Yugo Suzuki, Nobuyoshi Motohashi
J Med Dent Sci 2004; 51: 27 33 Original Article Longitudinal dento-skeletal changes in UCLP patients following maxillary distraction osteogenesis using RED system Eduardo Yugo Suzuki, Nobuyoshi Motohashi
Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report
 Case Report Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report 1 Vinni Arora, 2 Rekha Sharma, 3 Sachin Parashar 1 Senior Resident, 2 Professor and Head of Department, 3 Former Resident
Case Report Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report 1 Vinni Arora, 2 Rekha Sharma, 3 Sachin Parashar 1 Senior Resident, 2 Professor and Head of Department, 3 Former Resident
SURGICAL MODEL ACCURACY DEVICE. 25 years - manufacturing and distribution - around the globe research - design - manufacturing - distribution
 SURGICAL MODEL ACCURACY DEVICE 25 years - manufacturing and distribution - around the globe research - design - manufacturing - distribution 2 SMAD - SURGICAL MODEL ACCURACY DEVICE SMAD has be designed
SURGICAL MODEL ACCURACY DEVICE 25 years - manufacturing and distribution - around the globe research - design - manufacturing - distribution 2 SMAD - SURGICAL MODEL ACCURACY DEVICE SMAD has be designed
/jp-journals Effects of Bimax and Segmental Surgeries for Correction of Bimaxillary Dentoalveolar Protrusion Class I on Soft
 10.5005/jp-journals-10024-1456 ORIGINAL research Effects of Bimax and Segmental Surgeries for Correction of Bimaxillary Dentoalveolar Protrusion Class I on Soft Tissue Parameters: Upper lip Thickness and
10.5005/jp-journals-10024-1456 ORIGINAL research Effects of Bimax and Segmental Surgeries for Correction of Bimaxillary Dentoalveolar Protrusion Class I on Soft Tissue Parameters: Upper lip Thickness and
Does a correlation exist between nasal airway volume and craniofacial morphology: A cone beam computed tomography study
 Original Research Does a correlation exist between nasal airway volume and craniofacial morphology: A cone beam computed tomography study Jeenal V Gupta, Makhija PG, Gupta KC 1 Departments of Orthodontics
Original Research Does a correlation exist between nasal airway volume and craniofacial morphology: A cone beam computed tomography study Jeenal V Gupta, Makhija PG, Gupta KC 1 Departments of Orthodontics
OF LINGUAL ORTHODONTICS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: KDr. KP. kanarelis CASE NUMBER: 1 Year: 2010 WBLO 01 RESUME OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME : IOANNIS.G BORN: 03.01.1989 SEX:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: KDr. KP. kanarelis CASE NUMBER: 1 Year: 2010 WBLO 01 RESUME OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME : IOANNIS.G BORN: 03.01.1989 SEX:
UNILATERAL UPPER MOLAR DISTALIZATION IN A SEVERE CASE OF CLASS II MALOCCLUSION. CASE PRESENTATION. 1*
 UNILATERAL UPPER MOLAR DISTALIZATION IN A SEVERE CASE OF CLASS II MALOCCLUSION. CASE PRESENTATION. 1* Department of Orthodontics and Pedodontics 1 Faculty of Dental Medicine, University of Medicine and
UNILATERAL UPPER MOLAR DISTALIZATION IN A SEVERE CASE OF CLASS II MALOCCLUSION. CASE PRESENTATION. 1* Department of Orthodontics and Pedodontics 1 Faculty of Dental Medicine, University of Medicine and
The characteristics of profile facial types and its relation with mandibular rotation in a sample of Iraqi adults with different skeletal relations
 The characteristics of profile facial types and its relation with mandibular rotation in a sample of Iraqi adults with different skeletal relations Sara M. Al-Mashhadany, B.D.S., M.Sc. (1) Nagham M.J.
The characteristics of profile facial types and its relation with mandibular rotation in a sample of Iraqi adults with different skeletal relations Sara M. Al-Mashhadany, B.D.S., M.Sc. (1) Nagham M.J.
Original Research. This appraisal is based on a system of cephalometric analysis that was developed at Indiana University by Burstone and Legan.
 Received: 08 th June 2015 Accepted: 13 th September 2015 Conflicts of Interest: None Source of Support: Nil Original Research Hard Tissue Cephalometric Norms for Orthognathic Surgery in Karnataka Population
Received: 08 th June 2015 Accepted: 13 th September 2015 Conflicts of Interest: None Source of Support: Nil Original Research Hard Tissue Cephalometric Norms for Orthognathic Surgery in Karnataka Population
 Evaluation of the maxillary morphological changes following distraction in CLP patients decrease in the Ul to NF except for Case 6. me [35] instance,血e small maxillary advancement of 2.4 mm and maxillary
Evaluation of the maxillary morphological changes following distraction in CLP patients decrease in the Ul to NF except for Case 6. me [35] instance,血e small maxillary advancement of 2.4 mm and maxillary
Class II. Bilateral Cleft Lip and Palate. Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Cleft Lip and Palate.
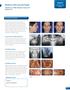 Bilateral Cleft Lip and Palate Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Class II Cleft Lip and Palate Pretreatment Diagnosis Class II dolichofacial female, age 22 years 11 months, presented
Bilateral Cleft Lip and Palate Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Class II Cleft Lip and Palate Pretreatment Diagnosis Class II dolichofacial female, age 22 years 11 months, presented
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
Comparison between the external gonial angle in panoramic radiographs and lateral cephalograms of adult patients with Class I malocclusion
 425 Journal of Oral Science, Vol. 51, No. 3, 425-429, 2009 Original Comparison between the external gonial angle in panoramic radiographs and lateral cephalograms of adult patients with Class I malocclusion
425 Journal of Oral Science, Vol. 51, No. 3, 425-429, 2009 Original Comparison between the external gonial angle in panoramic radiographs and lateral cephalograms of adult patients with Class I malocclusion
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS KANARELIS PANAGIOTIS (TAKIS) CASE NUMBER: 1 Year: 2012 WBLO 1 RÉSUMÉ OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS KANARELIS PANAGIOTIS (TAKIS) CASE NUMBER: 1 Year: 2012 WBLO 1 RÉSUMÉ OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME:
Scientific Treatment Goals for Oral and Facial Harmony
 Scientific Treatment Goals for Oral and Facial Harmony AAO Lecture May 7, 2013 Philadelphia, PA Will A. Andrews, D.D.S. Optimal oral and facial harmony implies a state of maximum health, function and appearance
Scientific Treatment Goals for Oral and Facial Harmony AAO Lecture May 7, 2013 Philadelphia, PA Will A. Andrews, D.D.S. Optimal oral and facial harmony implies a state of maximum health, function and appearance
Surgical correction of septal deviation after Le Fort I osteotomy
 Shin et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:21 DOI 10.1186/s40902-016-0067-z Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Surgical correction of septal
Shin et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:21 DOI 10.1186/s40902-016-0067-z Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Surgical correction of septal
Original Article Soft-tissue facial characteristics of attractive Chinese men compared to normal men
 Int J Clin Exp Med 2015;8(5):7977-7982 www.ijcem.com /ISSN:1940-5901/IJCEM0007360 Original Article Soft-tissue facial characteristics of attractive Chinese men compared to normal men Feng Wu 1, Junfang
Int J Clin Exp Med 2015;8(5):7977-7982 www.ijcem.com /ISSN:1940-5901/IJCEM0007360 Original Article Soft-tissue facial characteristics of attractive Chinese men compared to normal men Feng Wu 1, Junfang
Copyright by 2018 Gaziantep University School of Medicine - Available online at
 DOI: 10.5152/EurJTher.2018.743 Manuscript Type: Original Article Title: EFFECT OF VERTICAL GROWTH PATTERN ON MAXILLARY AND FRONTAL SINUS SIZE Authors: 1 Merve Göymen, 2 Güzin Bilgin, 1 Ayşegül Güleç Institutions:
DOI: 10.5152/EurJTher.2018.743 Manuscript Type: Original Article Title: EFFECT OF VERTICAL GROWTH PATTERN ON MAXILLARY AND FRONTAL SINUS SIZE Authors: 1 Merve Göymen, 2 Güzin Bilgin, 1 Ayşegül Güleç Institutions:
In clinical practice the quantitative evaluation of
 Scientific Foundations Relation Between Anthropometric and Cephalometric Measurements and Proportions of the Face of Healthy Young White Adult Men and Women Maria Budai, DDS, Dip ORTHO* Leslie G. Farkas,
Scientific Foundations Relation Between Anthropometric and Cephalometric Measurements and Proportions of the Face of Healthy Young White Adult Men and Women Maria Budai, DDS, Dip ORTHO* Leslie G. Farkas,
Arch dimensional changes following orthodontic treatment with extraction of four first premolars
 Received: 14 June. 2015 Accepted: 7 Dec. 2015 Arch dimensional changes following orthodontic treatment with extraction of four first premolars Abstract Asghar Ebadifar DDS, MSc 1, Mohammad Hossien Shafazand
Received: 14 June. 2015 Accepted: 7 Dec. 2015 Arch dimensional changes following orthodontic treatment with extraction of four first premolars Abstract Asghar Ebadifar DDS, MSc 1, Mohammad Hossien Shafazand
Orthodontic and Orthognathic Surgical Correction of a Skeletal Class III Malocclusion
 Dental Medicine Research 30 2) 161 166, 2010 161 Case Report Orthodontic and Orthognathic Surgical Correction of a Skeletal Class III Malocclusion Tetsutaro Yamaguchi, Yoko Tomoyasu, Tatsuo Shirota*, Masashi
Dental Medicine Research 30 2) 161 166, 2010 161 Case Report Orthodontic and Orthognathic Surgical Correction of a Skeletal Class III Malocclusion Tetsutaro Yamaguchi, Yoko Tomoyasu, Tatsuo Shirota*, Masashi
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER: 44 CASE NUMBER: 1 Year: ESLO 01 RÉSUMÉ OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME: K.N BORN: 03/03/1980 SEX: Male PRE-TREATMENT RECORDS:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER: 44 CASE NUMBER: 1 Year: ESLO 01 RÉSUMÉ OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME: K.N BORN: 03/03/1980 SEX: Male PRE-TREATMENT RECORDS:
Maxillary Growth Control with High Pull Headgear- A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 01 Ver. X January. (2018), PP 09-13 www.iosrjournals.org Maxillary Growth Control with High
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 01 Ver. X January. (2018), PP 09-13 www.iosrjournals.org Maxillary Growth Control with High
Quantitation of transverse maxillary dimensions using computed tomography: a methodological and reproducibility study
 European Journal of Orthodontics 26 (2004) 209 215 European Journal of Orthodontics vol. 26 no. 2 European Orthodontic Society 2004; all rights reserved. Quantitation of transverse maxillary dimensions
European Journal of Orthodontics 26 (2004) 209 215 European Journal of Orthodontics vol. 26 no. 2 European Orthodontic Society 2004; all rights reserved. Quantitation of transverse maxillary dimensions
Research & Reviews: Journal of Dental Sciences
 Research & Reviews: Journal of Dental Sciences Orthodontic Camouflage of Skeletal Class I, Class II and Class III Malocclusion in Borderline Cases Report of Three Cases Dr. Seema Kapil Lahoti 1 *, Dr.
Research & Reviews: Journal of Dental Sciences Orthodontic Camouflage of Skeletal Class I, Class II and Class III Malocclusion in Borderline Cases Report of Three Cases Dr. Seema Kapil Lahoti 1 *, Dr.
CASE: EXTRACTION Dr. TRAINING M (CA) Caucasian AGE: 8.6 VISUAL NORMS RMO X: 02/06/ R: 02/21/2003 MISSING PERMANENT TEETH RMO 2003
 O C RMO CASE: EXTRACTION Dr. TRAINING M (CA) Caucasian AGE:. X: // - R: // MISSING PERMANENT TEETH VISUAL NORMS RMO R L RMO Diagnostic Services RMO, Inc. ()- Post Office Box ()- Canoga Park, CA - EXTRACTION
O C RMO CASE: EXTRACTION Dr. TRAINING M (CA) Caucasian AGE:. X: // - R: // MISSING PERMANENT TEETH VISUAL NORMS RMO R L RMO Diagnostic Services RMO, Inc. ()- Post Office Box ()- Canoga Park, CA - EXTRACTION
Unilateral cleft nasal deformity is a clinical term referring to a nose
 ORIGINAL ARTICLE Assessment of Secondary Cleft Rhinoplasty Using Resorbable Plates at the Age of Primary School Arun K. Gosain, MD and Amir H. Fathi, MD Background: Secondary rhinoplasty after a cleft
ORIGINAL ARTICLE Assessment of Secondary Cleft Rhinoplasty Using Resorbable Plates at the Age of Primary School Arun K. Gosain, MD and Amir H. Fathi, MD Background: Secondary rhinoplasty after a cleft
Early Mixed Dentition Period
 REVIEW ARTIC CLE AODMR The Effects of a Prefabricated Functional Appliance in Early Mixed Dentition Period Toshio Iwata 1, Takashi Usui 2, Nobukazu Shirakawa 2, Toshitsugu Kawata 3 1 Doctor of Philosophy
REVIEW ARTIC CLE AODMR The Effects of a Prefabricated Functional Appliance in Early Mixed Dentition Period Toshio Iwata 1, Takashi Usui 2, Nobukazu Shirakawa 2, Toshitsugu Kawata 3 1 Doctor of Philosophy
Cephalometric Analysis
 Cephalometric Analysis of Maxillary and Mandibular Growth and Dento-Alveolar Change Part III In two previous articles in the PCSO Bulletin s Faculty Files, we discussed the benefits and limitations of
Cephalometric Analysis of Maxillary and Mandibular Growth and Dento-Alveolar Change Part III In two previous articles in the PCSO Bulletin s Faculty Files, we discussed the benefits and limitations of
Sample Case #1. Disclaimer
 ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
Implications for Nasal Recontouring: Nasion Position Preferences as Determined by a Survey of White North Americans
 Aesth. Plast. Surg. 27:438 445, 2004 DOI: 10.1007/s00266-004-3083-9 Implications for Nasal Recontouring: Nasion Position Preferences as Determined by a Survey of White North Americans Arian Mowlavi, M.D.,
Aesth. Plast. Surg. 27:438 445, 2004 DOI: 10.1007/s00266-004-3083-9 Implications for Nasal Recontouring: Nasion Position Preferences as Determined by a Survey of White North Americans Arian Mowlavi, M.D.,
Quantitative Determination of
 The Application of 3D Images for Quantitative Determination of Zygoma in an Asian Population Shih-Hsuan Mao, Yu-Hsuan Hsieh, Chih-Hao Chen, Chien-Tzung Chen Department of Plastic and Reconstructive Surgery,
The Application of 3D Images for Quantitative Determination of Zygoma in an Asian Population Shih-Hsuan Mao, Yu-Hsuan Hsieh, Chih-Hao Chen, Chien-Tzung Chen Department of Plastic and Reconstructive Surgery,
A Modified Three-piece Base Arch for en masse Retraction and Intrusion in a Class II Division 1 Subdivision Case
 Dhaval Ranjitbhai Lekhadia, Gautham Hegde RESEARCH ARTICLE 10.5005/jp-journals-10029-1149 A Modified Three-piece Base Arch for en masse Retraction and Intrusion in a Class II Division 1 Subdivision Case
Dhaval Ranjitbhai Lekhadia, Gautham Hegde RESEARCH ARTICLE 10.5005/jp-journals-10029-1149 A Modified Three-piece Base Arch for en masse Retraction and Intrusion in a Class II Division 1 Subdivision Case
OF LINGUAL ORTHODONTICS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: KDr. KP. kanarelis CASE NUMBER: 2 Year: 2010 WBLO 01 RESUME OF CASE 2 CASE CATEGORY: ADULT MALOCCLUSION NAME : MARIA A. BORN: 18.04.1983 SEX:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: KDr. KP. kanarelis CASE NUMBER: 2 Year: 2010 WBLO 01 RESUME OF CASE 2 CASE CATEGORY: ADULT MALOCCLUSION NAME : MARIA A. BORN: 18.04.1983 SEX:
RMO VISUAL NORMS. CASE: CHINESE SAMPLE Dr. TRAINING F (CH) Chinese AGE: 12.4 X: 09/30/ R: 02/21/2003 MISSING PERMANENT TEETH
 O C RMO CASE: CHINESE SAMPLE Dr. TRAINING F (CH) Chinese AGE:. X: // - R: // MISSING PERMANENT TEETH VISUAL NORMS RMO R L RMO Diagnostic Services RMO, Inc. ()- Post Office Box ()- Canoga Park, CA - CHINESE
O C RMO CASE: CHINESE SAMPLE Dr. TRAINING F (CH) Chinese AGE:. X: // - R: // MISSING PERMANENT TEETH VISUAL NORMS RMO R L RMO Diagnostic Services RMO, Inc. ()- Post Office Box ()- Canoga Park, CA - CHINESE
The Long Term Outcome of Mandibular Orthognathic Surgery
 The Long Term Outcome of Mandibular Orthognathic Surgery Mohammed Ibrahim Al-Ajmi B.D.S (Ireland), MFDS RCPS (Glasgow) Thesis submitted for the degree of Doctorate of Clinical Dentistry (Oral and Maxillofacial
The Long Term Outcome of Mandibular Orthognathic Surgery Mohammed Ibrahim Al-Ajmi B.D.S (Ireland), MFDS RCPS (Glasgow) Thesis submitted for the degree of Doctorate of Clinical Dentistry (Oral and Maxillofacial
ORTHOGNATHIC SURGERY
 ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital,
 Dr. Ellen Wen-Ching Ko, DDS, MS Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital, Taipei, Taiwan Professor, Graduate Institute of Craniofacial and Dental Science, Chang
Dr. Ellen Wen-Ching Ko, DDS, MS Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital, Taipei, Taiwan Professor, Graduate Institute of Craniofacial and Dental Science, Chang
TWO PHASE FOR A BETTER FACE!! TWIN BLOCK AND HEADGEAR FOLLOWED BY FIXED THERAPY FOR CLASS II CORRECTION
 Case Report NUJHS Vol. 5, No.2, June 2015, ISSN 2249-7110 TWO PHASE FOR A BETTER FACE!! TWIN BLOCK AND HEADGEAR FOLLOWED BY FIXED THERAPY FOR CLASS II CORRECTION 1 2 3 4 U S Krishna Nayak, Ashutosh Shetty,
Case Report NUJHS Vol. 5, No.2, June 2015, ISSN 2249-7110 TWO PHASE FOR A BETTER FACE!! TWIN BLOCK AND HEADGEAR FOLLOWED BY FIXED THERAPY FOR CLASS II CORRECTION 1 2 3 4 U S Krishna Nayak, Ashutosh Shetty,
Individual and ethnic aspects of preoperative planning for posttraumatic rhinoplasty
 Eur J Plast Surg (2011) 34:245 249 DOI 10.1007/s00238-010-0502-9 ORIGINAL PAPER Individual and ethnic aspects of preoperative planning for posttraumatic rhinoplasty Paweł Szychta & Jan Rykała & Julia Kruk-Jeromin
Eur J Plast Surg (2011) 34:245 249 DOI 10.1007/s00238-010-0502-9 ORIGINAL PAPER Individual and ethnic aspects of preoperative planning for posttraumatic rhinoplasty Paweł Szychta & Jan Rykała & Julia Kruk-Jeromin
IJCMR 553. ORIGINAL RESEARCH Different Population- Different Analysis A Cephalometric Study. Sachin Singh 1, Jayesh Rahalkar 2 ABSTRACT INTRODUCTION
 IJCMR 553 ORIGINAL RESEARCH Different Population- Different Analysis A Cephalometric Study Sachin Singh 1, Jayesh Rahalkar 2 ABSTRACT Introduction: Cephalometric norms derived for Caucasian population
IJCMR 553 ORIGINAL RESEARCH Different Population- Different Analysis A Cephalometric Study Sachin Singh 1, Jayesh Rahalkar 2 ABSTRACT Introduction: Cephalometric norms derived for Caucasian population
Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report
 Case Report Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/506 Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report Ahmed Alassiry Assistant
Case Report Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/506 Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report Ahmed Alassiry Assistant
