Osseous Surgery for Crown Lengthening: A 6-Month Clinical Study
|
|
|
- Gerald Johns
- 5 years ago
- Views:
Transcription
1 Volume 75 Number 9 Case Series Osseous Surgery for Crown Lengthening: A 6-Month Clinical Study David E. Deas,* Alan J. Moritz,* Howard T. McDonnell,* Charles A. Powell,* and Brian L. Mealey* Background: Despite the fact that surgical crown lengthening is a commonly performed treatment, little is known about the specific surgical endpoints of the procedure or the stability of the newly attained crown height over time. Recent clinical reports have ranged across a spectrum from significant tissue rebound to remarkable stability using similar surgical techniques. The purpose of this study was to assess the stability of surgical crown lengthening procedures performed by various surgeons using specific guidelines to determine surgical endpoints. Specifically, we sought to determine the following: 1) What is the immediate increase in clinical crown height following surgery? 2) How stable is the established crown length over a 6-month period? 3) How much supporting bone is removed to establish the new crown length? 4) How does the position of the flap margin relative to the alveolar bone at surgical closure relate to the stability of crown height? Methods: Twenty-five patients requiring crown lengthening of 43 teeth were included in this study. Clinical indices recorded at eight sites on each molar and six sites on each premolar included plaque, bleeding on probing, probing depth, and relative attachment level from a customized probing stent. Surgical measurements at the same sites included the distance from stent to alveolar bone both before and after osseous surgery and the distance from flap margin to alveolar bone after suturing. Clinical measurements were repeated at 1, 3, and 6 months after surgery. Sites were divided into three groups. All sites on teeth targeted for crown lengthening were labeled treated sites (TT). Interproximal sites on neighboring teeth were labeled adjacent (AA) if they shared a proximal surface with a treated tooth and nonadjacent (AN) if they were on the opposite side, away from the treated tooth. * U.S. Air Force Periodontics Residency, Wilford Hall Medical Center, Lackland Air Force Base, TX. The views expressed in this article are those of the authors and are not to be construed as official nor as reflecting the views of the United States Air Force or Department of Defense. Results: Throughout the entire 6-month healing period, descriptive statistics revealed no significant time or group differences in plaque and bleeding scores. At treated sites, the mean gain of crown height at surgery was 2.27 ± 1.1 mm. This was reduced to 1.91 ± 1.08 mm at 1 month, 1.69 ± 1.02 mm at 3 months, and 1.57 ± 1.01 mm at 6 months. At adjacent sites, the gain of crown length was 2.18 ± 0.98 mm, 1.61 ± 0.98 mm, 1.43 ± 0.96 mm, and 1.30 ± 0.96 mm at surgery, 1, 3, and 6 months, respectively. At non-adjacent sites the crown height increased 1.06 ± 1.07 mm, 1.00 ± 0.93 mm, 0.84 ± 1.00 mm, and 0.76 ± 0.85 mm, respectively. These mean measurements were significantly different for each treatment group at each time interval and appeared not to have stabilized between 3 and 6 months. The mean osseous reduction at treated, adjacent, and non-adjacent sites was 1.13 ± 0.90 mm, 0.78 ± 0.75 mm, and ± 0.69 mm, respectively. Frequency distribution of osseous reduction demonstrated that 23.6% of treated sites had 0 mm, 44.3% had 1 mm, 25.4% had 2 mm, 6.2% had 3 mm, and less than 1% had 4 mm of bone removed to establish crown height. More bone removal was noted at premolar than at molar sites; however, this was not statistically significant. When tissue rebound following surgery was plotted against post-surgical flap position, it was noted that the closer the flap margin was sutured to the alveolar crest, the greater the tissue rebound during the post-surgical period. This rebound ranged from 1.33 ± 1.02 mm when the flap was sutured 1 mm from the alveolar crest, to 0.16 ± 1.15 mm when the flap was sutured 4 mm from the alveolar crest. Conclusions: These data suggest that there is a significant tissue rebound following crown-lengthening surgery that has not fully stabilized by 6 months. The amount of tissue rebound seems related to the position of the flap relative to the alveolar crest at suturing. These findings support the premise that clinicians should establish proper crown height during surgery without overreliance on flap placement at the osseous crest. J Periodontol 2004;75: KEY WORDS Alveolar bone; follow-up studies; surgical flaps; tooth/anatomy and histology; tooth crown/surgery. 1288
2 J Periodontol September 2004 Deas, Moritz, McDonnell, Powell, Mealey According to the 2003 American Academy of Periodontology Practice Profile Survey, one of the most common reasons for periodontal surgery is for purposes of crown lengthening. 1 The crown lengthening procedure is often necessary both to provide adequate retention and resistance form by gaining supracrestal tooth length, 2-5 as well as to prevent impingement of restoration margins on the attachment apparatus by reestablishing the biologic width. 6,7 While many restorative dentists are very specific in their requests for crown lengthening, others simply trust the surgeon to return the patient to them with longer crowns that will allow for adequate restoration. Without specific guidance, the surgical goal may become nothing more than to make the tooth a little longer. In addition, there is scant information in the literature relating post-surgical flap position at the alveolar crest to the stability of crown lengthening over time. Knowing that an optimal flap placement will enhance the outcome of these procedures may be of significant benefit to the surgeon and restorative dentist alike. Consistent with studies of the dimensions of the periodontal attachment apparatus described as the biologic width, 8,9 several authors have proposed that crown lengthening procedures optimally create at least 3 mm of tooth structure between the alveolar crest and future restorative margin to allow for proper restoration Ingber et al., 10 for example, proposed 3 mm to allow 1 mm for the connective tissue attachment, 1 mm for the epithelial attachment, and 1 mm for placement of a margin. Although some clinicians have favored an amount >3 mm, 4,13 the 3 mm distance from crest to crown margin has over the years become fairly ingrained in the dental literature. Attempting to attribute a fixed measurement to the biologic width may indeed disregard surface-to-surface, tooth-to-tooth, and patient-topatient variability; however, it is our observation that many practitioners delivering surgical crown lengthening therapies commonly rely on the 3 mm figure. While numerous technique and case report articles are available, few controlled examinations of the postsurgical changes following crown lengthening surgery have been published. Of the controlled studies we reviewed, two had as a surgical goal a 3 mm distance between the alveolar crest and restorative margin 14,15 and a third did not mention a surgical endpoint. 16 Interestingly, each of these studies reported that the desired amount of crown lengthening was either not predictably attained or was subject to change over time. More recently, Lanning et al. described a technique of measuring the biologic width by presurgical bone sounding. 17 That measurement was added to the amount of supracrestal tooth structure needed for margin placement and used as a guideline to determine the surgical reduction of the alveolar crest. This resulted in 3 mm of bone removal at 90% of treated sites, which is far in excess of that reported in the prior studies. However, the authors reported no significant change in the position of the free gingival margin between 3 and 6 months post-surgery. The purpose of the present investigation was to further assess the short-term stability of surgical crown lengthening procedures using an osseous resective technique and specific guidelines to determine the surgical endpoint. This study sought to answer the following questions: 1) What is the immediate increase in crown height following surgery? 2) What happens to this newly established crown height over time? 3) How much supporting bone is removed during crown lengthening surgery? 4) How does the position of the flap margin relative to the alveolar crest at surgical closure relate to the stability of surgically created crown height? MATERIALS AND METHODS The experimental protocol was approved by the Institutional Review Board for human studies, Wilford Hall Medical Center (WHMC), Lackland Air Force Base, San Antonio, Texas. This study evaluated 25 consecutively treated periodontally healthy patients (18 males, seven females) referred to the Department of Periodontics at WHMC for crown lengthening surgery on 43 posterior teeth between December 2001 and August Medical and dental histories were reviewed and no contraindications to surgical therapy were noted. All but one patient required crown lengthening prior to complete coverage crown or fixed partial denture fabrication; the other patient required surgical access for placement of an amalgam restoration. All patients were restored by the end of the study and prosthetic treatment was begun no sooner than 6 weeks after surgery. Each patient received an initial examination and treatment planning session. Oral hygiene procedures were reviewed, and scaling and/or prophylaxis were scheduled if deemed necessary by the examining periodontist. After treatment plan presentation, patients were provided information about the study and indicated willingness to participate by providing written informed consent. An alginate impression was then made of each arch to be surgically treated in order to fabricate customized probing stents. Full-arch probing stents were made from a 2 mm clear copolyester plastic using a pressure form matrix machine. To insure proper fit after restorative procedures, the teeth to be restored were overwaxed by 1 mm. The stent was then made from a duplicate of the waxed cast and seated firmly on the remaining teeth on which no additional wax was applied. Stents were trimmed to the height of contour of all teeth, and grooves were placed at the sites to be measured with an 1169 fissure bur. To improve visualization, the apical margin of the probing stent was Splint Biocryl, Great Lakes Orthodontics, Ltd., Tonawanda, NY. BioStar, Great Lakes Orthodontics, Ltd. 1289
3 Crown Lengthening: A 6-Month Clinical Study Volume 75 Number 9 traced with a black permanent marker. All measurements were taken by one of two calibrated examiners (DD, AM) using a UNC-15 manual probe. Surgical procedures were accomplished under local anesthesia with intravenous or oral sedation at patient request. Clinicians included both faculty and residents of the Department of Periodontics at Wilford Hall Medical Center. Three guidelines were given to each surgeon to determine the surgical endpoint for crown lengthening. The first guideline was to place the alveolar crest at a level at least 3 mm from the anticipated crown margin. To allow sufficient room for tooth preparation, the second guideline required surgeons, where possible, to leave at least 9 mm of clinical crown height coronal 1290 Figure 1. Measurement sites for treatment groups. Eight sites were measured on each molar and six sites on each premolar. Sequence of Clinical Measurements Baseline Pre- Post- (presurgery) Osseous Suturing 1 Month 3 Months 6 Months Pl S-AB(P) S-GM(X) Pl Pl Pl PD S-AB(X) PD PD PD BOP GM-AB(X) BOP BOP BOP SGM SGM SGM SGM RAL RAL RAL RAL to the osseous crest. This calculation was derived from anticipating that a tooth in occlusion and awaiting a crown restoration would Table 1. require 2 mm of occlusal reduction for restorative space, 4 mm axial wall length, and 3 mm distance from restorative margin to the bone. The third surgical guideline was to place flap margins either at or apical to the anticipated restorative margin following suturing. Each case included intrasulcular and/or internally beveled incisions and elevation of full thickness flaps on the buccal and lingual aspects of the alveolar process. Where required, flap thinning was performed in order to minimize tissue thickness. After flap reflection and supracrestal soft tissue removal, osteoplasty and ostectomy were performed using rotating carbide steel burs and hand chisels. Subsequently, all root surfaces were scaled and root planed with sharp curets and/or ultrasonic instrumentation to remove any possible remnants of connective tissue attachment supracrestally. Both treated and adjacent teeth were monitored for this study and measured sites were divided into three groups. All sites on teeth to be restored and the specific targets of the crown lengthening procedures were identified as treated tooth (TT) sites. Interproximal sites on adjacent teeth were labeled adjacent tooth/adjacent surface (AA) sites if they shared a proximal surface with a treated tooth and adjacent tooth/non-adjacent surface (AN) sites if they were on the side away from a treated tooth (Fig. 1). Measurements were recorded at eight predetermined sites (mesio-facial, MF; mesiofacial furcation, MFF; disto-facial furcation, DFF; distofacial, DF; disto-lingual, DL; disto-lingual furcation, DLF; mesio-lingual furcation, MLF; mesio-lingual, ML) on each treated molar and six sites (MF, F, DF, DL, L, ML) on each treated premolar in the surgical field. On adjacent teeth, four sites (MF, DF, DL, ML) were recorded for both molars and premolars. The sequence of clinical measurements is described in Table 1. Using the probing stent, the following baseline measurements were taken for each site at the surgical appointment prior to administering local anesthetic: 1) the presence or absence of plaque (PL); 2) probing depth (PD); 3) the presence or absence of bleeding on probing (BOP); 4) the distance from stent to gingival margin (S-GM); and 5) relative attachment level from base of sulcus to stent (RAL). Following administration of anesthetic, flap reflection, and debridement, a measurement was made from the stent to the alveolar crest [S-AB(P)]. After osseous resection, a measurement was made at each site from the stent to the post-resection osseous crest [S-AB(X)]. Flaps were then sutured and pressure was applied for 3 minutes, after which a measurement was made from the stent to the sutured marginal tissue position [S-GM(X)]. The probe was then placed under the tissue at each site, and the distance from the sutured flap margin to the bony crest was measured [GM-AB(X)]. The use of periodontal dressing was at the discretion of the surgeon, but dressing use was the exception rather than the rule following surgery. All patients were prescribed analgesics and twice daily 0.12% chlorhexidine gluconate rinses for the first Hu-Friedy, Chicago, IL. Peridex, Procter & Gamble, Cincinnati, OH.
4 J Periodontol September 2004 Deas, Moritz, McDonnell, Powell, Mealey 2 weeks following surgery. Patients were seen for suture removal and prophylaxis between 7 and 10 days and a plaque control regimen was instituted. Additional postoperative visits (including prophylaxis) were performed at 2 and 4 weeks to assess healing and reinforce early oral hygiene measures. Baseline measurements of PL, PD, BOP, S-GM, and RAL were repeated at 1, 3, and 6 months following surgery. Statistical Analysis Data obtained for each type of site per patient were averaged and assessed for differences between baseline to post-surgery and to 1, 3, and 6 months. Data were analyzed by repeated measures analysis of variance (ANOVA) to determine presence of an overall effect and Tukey s honestly significant differences (HSD) post-hoc test for multiple comparisons was used to determine which site pairs differed significantly and the extent of those differences. Differences in probing depths and attachment levels at each time point were examined using paired and one sample t tests. RESULTS Twenty-four of the original 25 patients completed the study and no post-surgical complications were observed. One treated tooth was extracted after 1 month due to non-restorable caries. One patient moved from the area after the 3-month post-surgical appointment and was lost to further follow up. Thus, 1- and 3-month data are reported for 25 patients, while 3- and 6-month data are reported for 24 patients. Attachment loss was noted for each of the three treatment groups, as expected, and was noted to be significant for each group compared to presurgical baseline (P <0.05). By 6 months, attachment loss at TT, AA, and AN sites was 1.24 ± 1.09 mm, 0.99 ± 1.14 mm, and 0.49 ± 0.83 mm, respectively. Change in Crown Length The mean change in the distance from the probing stent to the free gingival margin from surgery to months 1, 3, and 6 is presented in Table 3. At TT sites, the mean increase in crown length following surgery was 2.27 ± 1.1 mm. This newly established crown height was reduced to 1.91 ± 1.08 mm by 1 month, 1.69 ± 1.02 mm by 3 months, and 1.57 ± 1.01 mm by 6 months. At each time point there was a significant increase in crown height compared to baseline, but the trend toward reduced crown height over time was confirmed by the fact that the mean measurements at 1, 3, and 6 months were all significantly less than the immediate post-surgical values (P <0.005). The amount of crown lengthening post-surgically at TT molar sites was not significantly different from that at TT premolar sites (2.28 ± 1.14 mm versus 2.19 ± 0.80 mm). For AA sites, an initial mean crown height increase of 2.18 ± 0.98 mm was reduced to 1.61 ± 0.98 mm by 1 month, 1.43 ± 0.96 mm by 3 months, and 1.30 ± Table 2. Probing Depth Clinical Indices The mean percentage of TT sites with BOP was 26.6% at baseline. This decreased slightly to 18.6% at 1 month, then rebounded to 23.5% and 22.0% at 3 and 6 months. These differences were not significant at any time point. Similarly, the percentage of TT sites with plaque was 26.3% at baseline, increased slightly to 32.5% and 34.4% at 1 and 3 months, then reduced to 25.7% at 6 months. There was no significant difference between the percentage of TT sites with plaque at any time point. Similarly, no significant changes in PL or BOP Table 3. were noted at AA or AN sites. Mean PD measurements for all three treatment groups are reported in Table 2. TT, AA, and AN sites experienced an initial decrease in PD followed by a gradual return toward baseline by 6 months. The decrease in probing depth was statistically significant from baseline to 1, 3, and 6 months for all three groups (P <0.05). Time Treated (TT) Adjacent (AA) Non-Adjacent (AN) Baseline 2.29 ± ± ± month 1.71 ± ± ± months 1.86 ± ± ± months 1.95 ± ± ± 0.69 Within each group, PD decreased significantly from baseline to 1, 3, and 6 months (P <0.05). Crown Lengthening: Treated and Adjacent Teeth Treated (TT) Adjacent (AA) Non-Adjacent (AN) Time N Change ± SD N Change ± SD N Change ± SD Baseline/post-surgery ± ± ± 1.07 Baseline/1 month ± ± ± 0.93 Baseline/3 months ± ± ± 1.00 Baseline/6 months ± ± ± 0.85 Changes in crown length were significant (P <0.005) for each treatment group at each time interval. 1291
5 Crown Lengthening: A 6-Month Clinical Study Volume 75 Number mm by 6 months. At AN sites the crown length was increased by 1.06 ± 1.07 mm at surgery, which decreased to 0.76 ± 0.85 mm by 6 months. For both groups, the mean crown heights at all time points were also significantly different (P <0.005). The amount of osseous reduction needed to achieve this additional crown length is reported in Table 4. At TT sites, a mean of 1.13 ± 0.90 mm of bone was removed, compared to 0.78 ± 0.75 mm at AA sites and ± 0.69 mm at AN sites. This reduction was statistically significant from baseline for both TT and AA sites (P <0.001) but not at AN sites. The frequency with which different amounts of bone removal at TT sites was achieved is shown in Table 5. At 67.9% of all treated sites, 1 mm of osseous reduction was performed during the crown lengthening procedure. Two mm of Table 4. Osseous Reduction 1292 Treated (TT) Adjacent (AA) Non-Adjacent (AN) N Sites Change ± SD N Sites Change ± SD N Sites Change ± SD ± ± ± 0.69 A significant reduction in bone height was achieved at treated and adjacent sites (P <0.001) but not at non-adjacent sites. Table 5. Osseous Reduction at Treated Sites Reduction N Percentage 0 mm mm mm mm mm Table 6. Tissue Rebound at 6 Months Related to Post-Suturing Flap Position All Sites GM/AB(X) N Change ± SD 1 mm ± mm ± mm ± mm ± 1.15 osseous reduction was achieved at 25.4% of TT sites and 3 mm reduction was noted for 6.5% of sites. For treated teeth, osseous reduction at premolar sites was greater than at molar sites (1.37 ± 0.99 mm versus 1.08 ± 0.88 mm), but the differences were not statistically significant. Tissue Rebound Following Surgery In order to investigate the phenomenon of tissue rebound following crown lengthening surgery, the change in crown length from post-surgery to 6 months was plotted against the flap position relative to the alveolar crest immediately after suturing [GM-AB(X)]. After reviewing the number and distribution of data points, it was decided to group the [GM-AB(X)] measurements into four levels: 1 mm, 2 mm, 3 mm, and 4 mm. As noted in Table 6, the mean amount of tissue rebound by 6 months was greatest when the flaps were positioned within 1 mm of the alveolar crest and was least when the flap position was initially more coronal. This relationship held true regardless of treatment group, or whether the sites were interproximal or facial/lingual (Tables 7 and 8). No significant difference in tissue rebound was found between premolars and molars in any of the groups. The overall Pearson correlation coefficient between post-suturing flap to bony crest position and post-surgical tissue rebound was (P <0.01). DISCUSSION The results of this clinical investigation demonstrated that 6 months following surgical crown lengthening procedures, teeth may exhibit a progressive marginal soft tissue rebound which reduces the surgically established crown height. This coronal shift of the soft tissues appears to be related to the positioning of the sutured flap post-surgery relative to the newly created alveolar crestal position both interproximally as well as facial/lingually. Overall, 14.5% of sites were sutured within 1 mm of the post-surgical alveolar crest and rebounded coronally a mean 1.33 ± 1.02 mm by 6 months. Similarly, 43.7% of sites were sutured at 2 mm from the bone margin, 28.7% at 3 mm, and 13.1% at 4 mm; these sites were found at 6 months to have rebounded 0.90 ± 0.89 mm, 0.47 ± 0.79 mm, and 0.16 ± 1.15 mm, respectively. There was a significant inverse correlation between the distance from flap to bony crest at the time of suturing and the amount of tissue rebound, indicating a greater rebound when the flap margin was positioned closer to the bony crest. These findings reflect the tendency of the healing periodontium to reform a new supracrestal gingival unit in order to regain that dimension referred to as the biologic width. Most recently, Lanning et al. 17 confirmed the suggestion from prior studies 4,10-13 that the biologic width will reestablish itself after crown length-
6 J Periodontol September 2004 Deas, Moritz, McDonnell, Powell, Mealey Table 7. Tissue Rebound at 6 Months Related to Post-Suturing Flap Position (treated versus adjacent sites) Treated (TT) Adjacent (AA) Non-Adjacent (AN) GM/AB(X) N Change ± SD N Change ± SD N Change ± SD 1 mm ± ± ± mm ± ± ± mm ± ± ± mm ± ± ± 0.85 Table 8. Tissue Rebound at 6 Months Related to Post-Suturing Flap Position (interproximal versus facial/lingual sites) Interproximal Facial/Lingual GM/AB(X) N Change ± SD N Change ± SD 0 mm 0 N/A ± mm ± ± mm ± ± mm ± ± mm ± ± 1.17 ening procedures to its original vertical dimension by 6 months. The current study suggests that in anticipation of the reconstitution of the supracrestal attachment and sulcus, suturing the post-surgical flap less than 3 mm from the bone may of necessity result in significant marginal soft tissue rebound. One may thus clinically question the practice of apically positioning the flap margins to the level of the bony crest during crown lengthening procedures. It would appear that positioning the flap somewhat coronal to the alveolar crest might result in a more predictable and stable amount of surgically created crown length. This may require more aggressive osseous resection if the restorative goal is to provide supragingival crown margins. Few studies in the literature on surgical crown lengthening report results on the movement of the healing gingival margin based on the initial sutured flap position relative to the alveolar crest. Bragger et al. examined changes in marginal soft tissue levels after 6 weeks and 6 months of healing. 14 This study also sought to create a distance of 3 mm from alveolar crest level to the future restorative margin, and surgical flaps were positioned at the osseous crest. Looking at 43 test teeth in 25 patients, they found that at 96% of sites, 2 mm of bone was removed on test teeth and bone removal of 3 mm was done in only 4% of sites. This compares favorably to the present study where 93% of sites had 2 mm of bone resection and 7% had 3 mm. Additionally, they found that when the means of all sites were examined, the 1.3 mm apical displacement of the gingival margin after surgery was maintained at the 6-month examination (1.4 mm). This differs from the current study in which the initial 2.27 mm average apical displacement of the gingival margin at the time of surgery was reduced to 1.57 mm at 6 months. In a study by Pontoriero et al., 84 teeth in 30 patients receiving surgical crown lengthening were evaluated over a 12-month period. 16 There was no mention of a surgical endpoint given in this study and adjacent teeth were included with the data for crown-lengthened teeth. Mean bone removal was 0.9 mm at interproximal and 1.0 mm at buccal/lingual sites and bone removal 2 mm was reported in only 8% of sites. Based on reported data, surgical flaps were placed subcrestally at interproximal sites, leaving the interdental areas denuded, whereas buccal/lingual sites had flaps placed at the bony crest. Such positioning seemed to promote a significant coronal displacement of marginal tissues of 3.2 mm at interproximal and 2.9 mm at buccal/lingual sites, with a resultant mean crown length difference between baseline and 12-month examination of only 0.5 mm interproximally and 1.2 mm at buccal/lingual sites. These results have cast a doubt on the stability of crown lengthening procedures over longer time periods and, similar to our study, seem to indicate that gingival margin regrowth may still be occurring beyond 6 months. Additionally, based on their findings, the authors 16 propose that greater bone removal during crown lengthening procedures should be considered in order to maximize final crown length. Postoperative marginal flap positioning is not discussed in their conclusions as potentially contributing to the amount of rebound witnessed. In an effort to determine whether a target goal of 3 mm from osseous crest to planned restorative margin was routinely achieved, Herrero et al. evaluated crown lengthening outcomes on 21 teeth in 16 patients treated by surgeons of various skill levels. 15 They noted that the target objective of 3 mm was not routinely achieved. The mean distance from prosthetic margin to alveolar crest was 2.4 mm with the greatest removal at the facial aspects of teeth (2.6 mm) and the least at the distal-lingual aspect (2.2 mm). More recently, in a 6-month study Lanning et al. followed 72 treated sites in 18 patients receiving crownlengthening surgery. 17 Individual presurgical biologic 1293
7 Crown Lengthening: A 6-Month Clinical Study Volume 75 Number 9 width measurements were used to customize the amount of bone removal indicated from anticipated prosthetic margins. Flaps were subsequently sutured at the alveolar crest; however, post-surgical flap position relative to the bony crest was not measured. A greater amount of osseous resection was done in this study than what has previously been reported in the literature, with 90% of treated sites having had 3 mm of bone removed. Additionally, 21% of non-adjacent sites and 39% of adjacent sites on adjacent teeth had 3 mm of bone removed. This resulted in a stable gingival margin between the 3- and 6-month examinations, with total mean displacement at 6 months for treated sites being 3.33 mm. The authors 17 concluded that the amount of bone removal in their study may have been a significant factor contributing to the stability of the gingival margin over time. In the current study, it was noted that the request for crown lengthening came most often for only one or two tooth surfaces rather than the entire tooth. At surgery, this request translated to an amount of osseous resection that was not uniform at all sites around the treated teeth. In fact, it was common for two or three sites on a given tooth to have 2 mm osseous reduction, while the remaining sites had minimal or even no reduction. This tended to make the mean osseous reduction (and subsequent increased crown height) at TT sites smaller than actually provided at required sites. Many factors seem to contribute to the maintenance of tooth structure gained through surgical crown lengthening procedures. Individual patient healing characteristics, reformation of the biologic width, adequacy of positive osseous architecture created during surgery, timing of restorative procedures, and post-operative plaque control may be among these factors. Another factor may be the position of the flap margin after surgery, which was examined in the present study. Some degree of marginal tissue rebound can be anticipated following crown lengthening surgery. It is possible that earlier marginal tissue stability can be achieved if the gingival margin is placed at the time of suturing in a position that accounts for the reformation of the biologic width. In conclusion, the data presented in this study suggest that there is a significant marginal soft tissue rebound following crown-lengthening surgery that has not fully stabilized by 6 months. The amount of coronal rebound appears to be related to the position of the flap relative to the alveolar crest at suturing. These findings support the premise that clinicians should establish proper crown height during surgery without overreliance on flap placement at the osseous crest to gain necessary crown length. ACKNOWLEDGMENTS The authors gratefully acknowledge the contribution of Dr. Anneke Bush, Clinical Research Squadron, 59th Medical Wing, Lackland AFB, Texas, for statistical support and Col. John Boyle, Dental Laboratory Flight Commander, 1st Dental Squadron, Langley AFB, Virginia, for his laboratory expertise. We would also like to thank SSgt. Amy Swindells and SSgt. LaTonya Jefferson, 59th Dental Squadron, Lackland AFB, for their technical assistance. REFERENCES 1. American Academy of Periodontology Practice Profile Survey: Characteristics and Trends in Private Periodontal Practice. Chicago: American Academy of Periodontology; Palomo F, Kopczyk RA. Rationale and methods for crown lengthening. J Am Dent Assoc 1978;96: Lundergan W, Hughes WR. Crown lengthening: A surgical flap approach. Compend Contin Educ Dent 1996; 17: Rosenberg ES, Garber DA, Evian C. Tooth lengthening procedures. Compend Contin Educ Dent 1980;1: Rosenberg ES, Cho SC, Garber DA. Crown lengthening revisited. Compend Contin Educ Dent 1999;20: Carnevale G, Sterrantino SF, Di Febo G. Soft and hard tissue wound healing following tooth preparation to the alveolar crest. Int J Periodontics Restorative Dent 1983; 3(6) Oakley E, Rhyu IC, Karatzas S, Gandini-Santiago L, Nevins M, Caton J. Formation of the biologic width following crown lengthening in nonhuman primates. Int J Periodontics Restorative Dent 1999;19: Gargiulo A, Wentz F, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol 1961;32: Vacek JS, Gher ME, Assad DA, Richardson AC, Giambarres LI. The dimensions of the human dentogingival junction. Int J Periodontics Restorative Dent 1994;14: Ingber FJS, Rose LF, Coslet JG. The biologic width. A concept in periodontics and restorative dentistry. Alpha Omegan 1977;70: Nevins M, Skurow HM. The intracrevicular restorative margin, the biological width, and maintenance of the gingival margin. Int J Periodontics Restorative Dent 1984; 4(3): Fugazzotto P. Periodontal restorative interrelationships: The isolated restoration. J Am Dent Assoc 1985;110: Wagenberg BD, Eskow RN, Langer B. Exposing adequate tooth structure for restorative dentistry. Int J Periodontics Restorative Dent 1989;9: Bragger U, Lauchenauer D, Lang NP. Surgical lengthening of the clinical crown. J Clin Periodontol 1992;19: Herrero F, Scott JP, Maropis PS, Yukna RA. Clinical comparison of desired versus actual amount of surgical crown lengthening. J Periodontol 1995;66: Pontoriero R, Carnevale G. Surgical crown lengthening: A 12-month clinical wound healing study. J Periodontol 2001;72: Lanning SK, Waldrop TC, Gunsolley JC, Maynard JG. Surgical crown lengthening: Evaluation of the biologic width. J Periodontol 2003;74: Correspondence: Col. David E. Deas, 59th Medical Wing/MRDT, 2450 Pepperrell Street, Lackland Air Force Base, TX Accepted for publication January 23,
Radiographic evaluation of the alveolar bone level change before and after crown-lengthening procedures in a dental school setting
 RESEARCH REPORT 197 Publication Jackie Chi, Srinivas M Susarla, David M Kim, Nadeem Y Karimbux Radiographic evaluation of the alveolar bone level change bee and after crown-lengthening procedures in a
RESEARCH REPORT 197 Publication Jackie Chi, Srinivas M Susarla, David M Kim, Nadeem Y Karimbux Radiographic evaluation of the alveolar bone level change bee and after crown-lengthening procedures in a
The preservation of a healthy periodontium
 Volume 74 Number 4 Surgical Crown Lengthening: Evaluation of the Biological Width Sharon K. Lanning,* homas C. Waldrop, John C. Gunsolley, and J. Gary Maynard Background: Previous surgical crown lengthening
Volume 74 Number 4 Surgical Crown Lengthening: Evaluation of the Biological Width Sharon K. Lanning,* homas C. Waldrop, John C. Gunsolley, and J. Gary Maynard Background: Previous surgical crown lengthening
Clinical Study A Comparative Evaluation for Biologic Width following Surgical Crown Lengthening Using Gingivectomy and Ostectomy Procedure
 International Dentistry Volume, Article ID 4794, 9 pages doi:.//4794 Clinical Study A Comparative Evaluation for Biologic Width following Surgical Crown Lengthening Using Gingivectomy and Ostectomy Procedure
International Dentistry Volume, Article ID 4794, 9 pages doi:.//4794 Clinical Study A Comparative Evaluation for Biologic Width following Surgical Crown Lengthening Using Gingivectomy and Ostectomy Procedure
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 55 Supracrestal Gingival Tissue Measurements in Healthy Human Periodontium Eliane Porto Barboza, CD, MScD, DScD* Raul Feres MonteAlto,
The International Journal of Periodontics & Restorative Dentistry 55 Supracrestal Gingival Tissue Measurements in Healthy Human Periodontium Eliane Porto Barboza, CD, MScD, DScD* Raul Feres MonteAlto,
Treatment of Altered Passive Eruption: Periodontal Plastic Surgery of the Dentogingival Junction
 CASE REPORT Publication Treatment of Altered Passive Eruption: Periodontal Plastic Surgery of the Dentogingival Junction Roberto Rossi, DDS, MScD Private Practice Genoa, Italy Remo Benedetti, MD, DDS Private
CASE REPORT Publication Treatment of Altered Passive Eruption: Periodontal Plastic Surgery of the Dentogingival Junction Roberto Rossi, DDS, MScD Private Practice Genoa, Italy Remo Benedetti, MD, DDS Private
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
Is Biologic Width of Anterior and Posterior Teeth Similar?
 ORIGINAL ARTICLE Is Biologic Width of Anterior and Posterior Teeth Similar? Amir Alireza Rasouli Ghahroudi 1, Afshin Khorsand 1, Siamak Yaghobee 1,2, and Farideh Haghighati 1 1 Department of Periodontology,
ORIGINAL ARTICLE Is Biologic Width of Anterior and Posterior Teeth Similar? Amir Alireza Rasouli Ghahroudi 1, Afshin Khorsand 1, Siamak Yaghobee 1,2, and Farideh Haghighati 1 1 Department of Periodontology,
Root Reshaping: An Integral Component of Periodontal Surgery
 1 Root Reshaping: An Integral Component of Periodontal Surgery Daniel J. Melker, DDS* Christopher R. Richardson, DMD, MS** It is the aim of this article to present a surgical option to the traditional
1 Root Reshaping: An Integral Component of Periodontal Surgery Daniel J. Melker, DDS* Christopher R. Richardson, DMD, MS** It is the aim of this article to present a surgical option to the traditional
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
The following resources related to this article are available online at jada.ada.org ( this information is current as of June 20, 2010 ):
 Contemporary Crown-Lengthening Therapy: A Review Timothy J. Hempton and John T. Dominici J Am Dent Assoc 2010;141;647-655 The following resources related to this article are available online at jada.ada.org
Contemporary Crown-Lengthening Therapy: A Review Timothy J. Hempton and John T. Dominici J Am Dent Assoc 2010;141;647-655 The following resources related to this article are available online at jada.ada.org
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques Mohammad Assaf Assistant Professor, Faculty of Dentistry, Al-Quds University, Jerusalem, Palestine. ABSTRACT Correspondence
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques Mohammad Assaf Assistant Professor, Faculty of Dentistry, Al-Quds University, Jerusalem, Palestine. ABSTRACT Correspondence
Biologic width: Understanding and its preservation Malathi K 1, Singh A 2
 Biologic width: Understanding and its preservation Malathi K 1, Singh A 2 Review Article 1 Dr K Malathi Professor & Head, Periodontics Government Dental college and Hospital Tamil Nadu, India 2 Dr Arjun
Biologic width: Understanding and its preservation Malathi K 1, Singh A 2 Review Article 1 Dr K Malathi Professor & Head, Periodontics Government Dental college and Hospital Tamil Nadu, India 2 Dr Arjun
Restorative Dentistry and Papilla Reconstruction in Reduced Periodontium
 CLINICAL AND RESEARCH REPORT Restorative Dentistry and Papilla Reconstruction in Reduced Periodontium Robert Azzi, Daniel Etienne, Bernard Schweitz Restoring the loss of periodontal soft and hard tissues
CLINICAL AND RESEARCH REPORT Restorative Dentistry and Papilla Reconstruction in Reduced Periodontium Robert Azzi, Daniel Etienne, Bernard Schweitz Restoring the loss of periodontal soft and hard tissues
Crown Lengthening Procedure: Various Techniques A Case Series
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. VIII (June. 2017), PP 40-46 www.iosrjournals.org Crown Lengthening Procedure: Various
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. VIII (June. 2017), PP 40-46 www.iosrjournals.org Crown Lengthening Procedure: Various
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
Crown Lengthening Procedures after Orthodontic Treatment and before Placement of Prosthetic Crowns
 British Journal of Medicine & Medical Research 17(8): 1-6, 2016, Article no.bjmmr.27398 ISSN: 2231-0614, NLM ID: 101570965 SCIENCEDOMAIN international www.sciencedomain.org Crown Lengthening Procedures
British Journal of Medicine & Medical Research 17(8): 1-6, 2016, Article no.bjmmr.27398 ISSN: 2231-0614, NLM ID: 101570965 SCIENCEDOMAIN international www.sciencedomain.org Crown Lengthening Procedures
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association
 All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association Patients have traditionally sought treatment when concerned with the way their teeth look, function or feel. Over the past
All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association Patients have traditionally sought treatment when concerned with the way their teeth look, function or feel. Over the past
Osseous surgery in periodontal treatment
 SCIENTIFIC SESSION Osseous surgery in periodontal treatment Essayist: Roberto Pontoriero Introduction In periodontally involved patients, periodontal therapy usually results in various degrees of soft-tissue
SCIENTIFIC SESSION Osseous surgery in periodontal treatment Essayist: Roberto Pontoriero Introduction In periodontally involved patients, periodontal therapy usually results in various degrees of soft-tissue
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic case report.
 European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
Hemisection as an Alternative Treatment for Decayed Multirooted Abutment: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 7, Issue 4 (May.- Jun. 2013), PP 32-36 Hemisection as an Alternative Treatment for Decayed Multirooted
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 7, Issue 4 (May.- Jun. 2013), PP 32-36 Hemisection as an Alternative Treatment for Decayed Multirooted
The dentogingival junction to the
 Volume 79 Number 10 RedefiningtheBiologicWidthinSevere, Generalized, Chronic Periodontitis: Implications for Therapy M. John Novak,* Huda M. Albather, and John M. Close Background: Previous studies demonstrated
Volume 79 Number 10 RedefiningtheBiologicWidthinSevere, Generalized, Chronic Periodontitis: Implications for Therapy M. John Novak,* Huda M. Albather, and John M. Close Background: Previous studies demonstrated
Over the years, restorative
 Periodontics Combining perio-restorative protocols to maximize function Lloyd M. Tucker, DMD, MSD n Daniel J. Melker, DDS n Howard M. Chasolen, DMD CDE 2 HOURS CREDIT This article describes a team approach
Periodontics Combining perio-restorative protocols to maximize function Lloyd M. Tucker, DMD, MSD n Daniel J. Melker, DDS n Howard M. Chasolen, DMD CDE 2 HOURS CREDIT This article describes a team approach
ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12 Accepted on:22/05/12
 SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
Minimally invasive techniques for periodontal regeneration
 2016; 2(12): 230-234 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2016; 2(12): 230-234 www.allresearchjournal.com Received: 04-10-2016 Accepted: 05-11-2016 Dr. Rizwan M Sanadi Professor,
2016; 2(12): 230-234 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2016; 2(12): 230-234 www.allresearchjournal.com Received: 04-10-2016 Accepted: 05-11-2016 Dr. Rizwan M Sanadi Professor,
Alarge number of sound clinical
 Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
For many years, patients with
 Dr. Robert Lowe is one of the great teachers in dentistry. Recently, he received the Gordon J. Christensen Award from the Chicago Dental Society in recognition of his excellence in teaching. Some of my
Dr. Robert Lowe is one of the great teachers in dentistry. Recently, he received the Gordon J. Christensen Award from the Chicago Dental Society in recognition of his excellence in teaching. Some of my
Biologic Width: An Important Link between. Periodontics and Restorative Dentistry REVIEW ARTICLE BIOLOGIC WIDTH
 JDSOR REVIEW ARTICLE Biologic Width: An Important Link between 10.5005/jp-journals-10039-1125 Periodontics and Restorative Dentistry Biologic Width: An Important Link between Periodontics and Restorative
JDSOR REVIEW ARTICLE Biologic Width: An Important Link between 10.5005/jp-journals-10039-1125 Periodontics and Restorative Dentistry Biologic Width: An Important Link between Periodontics and Restorative
Many techniques have been proposed for root coverage:
 Case Series Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients Jaime A. Vergara* and Raul G. Caffesse Background: The surgical techniques used
Case Series Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients Jaime A. Vergara* and Raul G. Caffesse Background: The surgical techniques used
ELIMINATE POCKETS. Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease
 ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
Educational Training Document
 Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Topographie Classification of Deformities of the Alveolar
 Topographie Classification of Deformities of the Alveolar Process* Kenneth W. Karn.f Howard P. Shockett^ William C. Moffitt and Jonathan L. Gray Accepted for publication 1 August 1983 A system of nomenclature
Topographie Classification of Deformities of the Alveolar Process* Kenneth W. Karn.f Howard P. Shockett^ William C. Moffitt and Jonathan L. Gray Accepted for publication 1 August 1983 A system of nomenclature
Volume 27 No. 11 August New Information and Reminders for Dental Services
 State of New Jersey Department of Human Services Division of Medical Assistance & Health Services Volume 27 No. 11 August 2017 To: Subject: Dental Providers - For Action Managed Care Organizations For
State of New Jersey Department of Human Services Division of Medical Assistance & Health Services Volume 27 No. 11 August 2017 To: Subject: Dental Providers - For Action Managed Care Organizations For
GINGIVAL SURGICAL TECHNIQUES
 Gingival Surgical Procedures GINGIVAL SURGICAL TECHNIQUES! limited to the gingival and not involving underlying osseous structures! Gingival Curettage! Gingivectomy! Gingivoplasty! Gingival Flap Gingival
Gingival Surgical Procedures GINGIVAL SURGICAL TECHNIQUES! limited to the gingival and not involving underlying osseous structures! Gingival Curettage! Gingivectomy! Gingivoplasty! Gingival Flap Gingival
ESTEHETIC SMILE A CONCERN DUE TO ALTERED PASSIVE ERUPTION - CASE REPORTS
 ESTEHETIC SMILE A CONCERN DUE TO ALTERED PASSIVE ERUPTION - CASE REPORTS Savitha A.N 1 * Sahar Razack 2 Rosh R.M 3 1. Professor, Department of Periodontics, The Oxford Dental College, 10 th Milestone,
ESTEHETIC SMILE A CONCERN DUE TO ALTERED PASSIVE ERUPTION - CASE REPORTS Savitha A.N 1 * Sahar Razack 2 Rosh R.M 3 1. Professor, Department of Periodontics, The Oxford Dental College, 10 th Milestone,
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Clinical UM Guideline
 Clinical UM Guideline Subject: Clinical Crown Lengthening Guideline #: 04-206 Current Effective Date: 03/24/2017 Status: New Last Review Date: 02/08/2017 Description This document addresses the procedure
Clinical UM Guideline Subject: Clinical Crown Lengthening Guideline #: 04-206 Current Effective Date: 03/24/2017 Status: New Last Review Date: 02/08/2017 Description This document addresses the procedure
Fundamental & Preventive Curvatures of Teeth and Tooth Development. Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L.
 Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Subject: Clinical Crown Lengthening Guideline #: Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018
 Dental Policy Subject: Clinical Crown Lengthening Guideline #: 04-206 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses the procedure of clinical
Dental Policy Subject: Clinical Crown Lengthening Guideline #: 04-206 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses the procedure of clinical
When performing conventional crown
 Case of the Month Biologic Shaping Kurtzman Daniel Melker, DDS 1 Abstract When performing conventional crown lengthening, the existing margins of an old restoration or the cementoenamel junction (CEJ)
Case of the Month Biologic Shaping Kurtzman Daniel Melker, DDS 1 Abstract When performing conventional crown lengthening, the existing margins of an old restoration or the cementoenamel junction (CEJ)
(Images are at the end of article)
 Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Bone Levels - From Hypothesis To Facts
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 6, Issue 5 (May.- Jun. 2013), PP 19-23 Bone Levels - From Hypothesis To Facts Savitha B 1, Priyanka
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 6, Issue 5 (May.- Jun. 2013), PP 19-23 Bone Levels - From Hypothesis To Facts Savitha B 1, Priyanka
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 2011 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY.. 357 Laser-Assisted Flapless Crown
The International Journal of Periodontics & Restorative Dentistry 2011 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY.. 357 Laser-Assisted Flapless Crown
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
PERIODONTAL STABILITY IN SURGICAL CROWN LENGTHENING PREPROSTHETIC INTERVENTIONS -A SYSTEMATIC REVIEW
 PERIODONTAL STABILITY IN SURGICAL CROWN LENGTHENING PREPROSTHETIC INTERVENTIONS -A SYSTEMATIC REVIEW LUMINIŢA OANCEA 1, ROXANA GEORGIANA MOISE 2, MARINA GIURGIU 3 1,3 Carol Davila University of Medicine
PERIODONTAL STABILITY IN SURGICAL CROWN LENGTHENING PREPROSTHETIC INTERVENTIONS -A SYSTEMATIC REVIEW LUMINIŢA OANCEA 1, ROXANA GEORGIANA MOISE 2, MARINA GIURGIU 3 1,3 Carol Davila University of Medicine
Townie Guest Editorial. Gingival Attachment Loss: Evaluation and Surgical Options. Daniel J. Melker, DDS. fig. 1
 Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Smile Design. Daniel H Ward DDS 1080 Polaris Pkwy Ste 130 Columbus OH
 Smile Design Daniel H Ward DDS 1080 Polaris Pkwy Ste 130 Columbus OH 43240 614-430-8990 dward@columbus.rr.com Incisal Placement Incisal plane parallel to the interpupillary line Vertical midline in the
Smile Design Daniel H Ward DDS 1080 Polaris Pkwy Ste 130 Columbus OH 43240 614-430-8990 dward@columbus.rr.com Incisal Placement Incisal plane parallel to the interpupillary line Vertical midline in the
Active Clinical Treatment Case 48
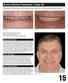 Active Clinical Treatment Case 48 Treating Clinicians: Drs. Jung Nam, Scott G. Cohen and Soojin Kim Initial smile Final smile Initial Presentation: January 2004 Age at Initial Presentation: 59 Active Treatment
Active Clinical Treatment Case 48 Treating Clinicians: Drs. Jung Nam, Scott G. Cohen and Soojin Kim Initial smile Final smile Initial Presentation: January 2004 Age at Initial Presentation: 59 Active Treatment
"Designing a fixed partial denture without a pontic"- Case report
 Article ID: ISSN 2046-1690 "Designing a fixed partial denture without a pontic"- Peer review status: No Corresponding Author: Dr. Khurshid Mattoo, Assistant Professor, Prosthodontics, College of Dental
Article ID: ISSN 2046-1690 "Designing a fixed partial denture without a pontic"- Peer review status: No Corresponding Author: Dr. Khurshid Mattoo, Assistant Professor, Prosthodontics, College of Dental
REGENERATIONTIME. A Case Report by. Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option
 A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
Efficacy of Lateral Pedicle Graft in the Treatment of Isolated Gingival Recession Defects
 International Journal of Pharmaceutical Science Invention ISSN (Online): 2319 6718, ISSN (Print): 2319 670X Volume 3 Issue 1 January 2014 PP.46-50 Efficacy of Lateral Pedicle Graft in the Treatment of
International Journal of Pharmaceutical Science Invention ISSN (Online): 2319 6718, ISSN (Print): 2319 670X Volume 3 Issue 1 January 2014 PP.46-50 Efficacy of Lateral Pedicle Graft in the Treatment of
The patient gave a history of hypertension and gastritis for which was taking Lacidipine 4mg, Omeprazole 20mg and Simvastatin 40mg.
 A.S. was referred by her general dental practitioner for assessment for possible implant placement to restore the space where her bridge replacing her maxillary central incisors had recently failed. Fig
A.S. was referred by her general dental practitioner for assessment for possible implant placement to restore the space where her bridge replacing her maxillary central incisors had recently failed. Fig
Case Report Alveolar Ridge Augmentation using Subepithelial Connective Tissue Grafts: A Case report
 Alveolar Ridge Augmentation using Subepithelial Connective Tissue Grafts: A Case report Po-Yu Lai, DDS, MS School of Dentistry, National Yang-Ming University Shing-Wai Yip, DDS, MS, DScD Prosthodontics
Alveolar Ridge Augmentation using Subepithelial Connective Tissue Grafts: A Case report Po-Yu Lai, DDS, MS School of Dentistry, National Yang-Ming University Shing-Wai Yip, DDS, MS, DScD Prosthodontics
Free Gingival Autograft: A Case Report
 CASE REPORT Free Gingival Autograft: A Case Report Veena Ashok. P. MDS, Bhargav Neetha BDS Abstract: Gingival recession is defined as Displacement of soft tissue margin apical to the cemento-enamel junction
CASE REPORT Free Gingival Autograft: A Case Report Veena Ashok. P. MDS, Bhargav Neetha BDS Abstract: Gingival recession is defined as Displacement of soft tissue margin apical to the cemento-enamel junction
Introduction to Periodontal and Implant Surgery
 Introduction to Periodontal and Implant Surgery Professor Jon B. Suzuki, DDS, PhD, MBA Temple University Professor of Microbiology and Immunology (Med) Professor of Periodontology and Oral Implantology
Introduction to Periodontal and Implant Surgery Professor Jon B. Suzuki, DDS, PhD, MBA Temple University Professor of Microbiology and Immunology (Med) Professor of Periodontology and Oral Implantology
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clinical Study Altered Passive Eruption and Familial Trait: A Preliminary Investigation
 International Dentistry, Article ID 874092, 5 pages http://dx.doi.org/10.1155/2014/874092 Clinical Study Altered Passive Eruption and Familial Trait: A Preliminary Investigation Roberto Rossi, 1 Giorgio
International Dentistry, Article ID 874092, 5 pages http://dx.doi.org/10.1155/2014/874092 Clinical Study Altered Passive Eruption and Familial Trait: A Preliminary Investigation Roberto Rossi, 1 Giorgio
Senior Dental Insurance Scheduled Allowance
 Senior Dental Insurance Scheduled Allowance LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental services which will be considered for payment by The American Progressive Life
Senior Dental Insurance Scheduled Allowance LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental services which will be considered for payment by The American Progressive Life
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Clinical Perspectives
 Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
HDS PROCEDURE CODE GUIDELINES
 D4000 - D4999 Local anesthesia is usually considered to be part of Periodontal procedures. General Guidelines 1. Periodontal services are only benefited when performed on natural teeth for treatment of
D4000 - D4999 Local anesthesia is usually considered to be part of Periodontal procedures. General Guidelines 1. Periodontal services are only benefited when performed on natural teeth for treatment of
Core build-up using post systems
 Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Note: The short arm of the BLPG tip is of the same length and measurement as the long arm of the T-bar and the Inline tip.
 Crown Lengthening CROWN LENGTHENING (CL) GAUGE: The Crown Lengthening Gauge has the Biologic Periogauge (BLPG) tip on one end and the Papilla tip on the opposite end. The BLPG tip is used to achieve the
Crown Lengthening CROWN LENGTHENING (CL) GAUGE: The Crown Lengthening Gauge has the Biologic Periogauge (BLPG) tip on one end and the Papilla tip on the opposite end. The BLPG tip is used to achieve the
LIST OF COVERED DENTAL SERVICES
 LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental Services which will be considered for payment by Constitution Life Insurance Company after the expiration of any applicable
LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental Services which will be considered for payment by Constitution Life Insurance Company after the expiration of any applicable
Subject: Osseous Surgery Guideline #: Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017
 Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Amalgam restoration of posterior proximal cavities with deep and concave gingival outlines
 Amalgam restoration of posterior proximal cavities with deep and concave gingival outlines M. Darveniza, MDSc, FRACDS* Abstract A technique for making a matrix and wedges for amalgam restoration of deep
Amalgam restoration of posterior proximal cavities with deep and concave gingival outlines M. Darveniza, MDSc, FRACDS* Abstract A technique for making a matrix and wedges for amalgam restoration of deep
Evaluation of fixed partial denture in relation to gingival recession and other factors
 Evaluation of fixed partial denture in relation to gingival recession and other factors Faiza M. Abdul Ameer,B.D.S., M. Sc. (1) Zainab M. Abdul Ameer,B.D.S., M. Sc (2) ABSTRACT Background: Gingival recession
Evaluation of fixed partial denture in relation to gingival recession and other factors Faiza M. Abdul Ameer,B.D.S., M. Sc. (1) Zainab M. Abdul Ameer,B.D.S., M. Sc (2) ABSTRACT Background: Gingival recession
Periodontal Maintenance
 Periodontal Maintenance Friday, February 20, 2015 1:06 PM Periodontal disease control always begins with patient education - Plaque control, diet, smoking cessation, impact that systemic health has on
Periodontal Maintenance Friday, February 20, 2015 1:06 PM Periodontal disease control always begins with patient education - Plaque control, diet, smoking cessation, impact that systemic health has on
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Gum Graft? Patient Need a. Does My. 66 JANUARY 2017 // dentaltown.com. by Dr. Brian S. Gurinsky
 by Dr. Brian S. Gurinsky Dr. Brian S. Gurinsky was born in Dallas and attended college at the University of Texas at Austin. He continued his education at Baylor College of Dentistry in Dallas, where he
by Dr. Brian S. Gurinsky Dr. Brian S. Gurinsky was born in Dallas and attended college at the University of Texas at Austin. He continued his education at Baylor College of Dentistry in Dallas, where he
Esthetic crown restorations require precise control of
 CLINICAL Technique REVIEW Crown Restorations A Review of the Positive Influence of Crown Contours on Soft-Tissue Esthetics Richard P. Kinsel, DDS; Bryan I. Pope, DMD, MSD; and Daniele Capoferri Abstract:
CLINICAL Technique REVIEW Crown Restorations A Review of the Positive Influence of Crown Contours on Soft-Tissue Esthetics Richard P. Kinsel, DDS; Bryan I. Pope, DMD, MSD; and Daniele Capoferri Abstract:
Alveolar bone development before the placement
 CLINICIAN S CORNER A novel approach for implant site development through root tipping Flavio Uribe, a Thomas Taylor, b David Shafer, c and Ravindra Nanda d Farmington, Conn Implant site development through
CLINICIAN S CORNER A novel approach for implant site development through root tipping Flavio Uribe, a Thomas Taylor, b David Shafer, c and Ravindra Nanda d Farmington, Conn Implant site development through
Clinical UM Guideline
 Clinical UM Guideline Subject: Teeth With A Poor or Guarded Prognosis Guideline #: Admin -01 Current Effective Date: 01/01/2016 Status: New Last Review Date: 02/08/2017 Description This document addresses
Clinical UM Guideline Subject: Teeth With A Poor or Guarded Prognosis Guideline #: Admin -01 Current Effective Date: 01/01/2016 Status: New Last Review Date: 02/08/2017 Description This document addresses
Dr.Adel F.Ibraheem Partial Veneer Crown(Three quarter crown) Three quarter (¾ )crown: Uses: Indications ---- For posterior teeth ;
 Lecture.9 Dr.Adel F.Ibraheem Partial Veneer Crown(Three quarter crown) *It is a cast metal crown restoration that cover only a part of the clinical crown, most commonly used type of partial veneer crown
Lecture.9 Dr.Adel F.Ibraheem Partial Veneer Crown(Three quarter crown) *It is a cast metal crown restoration that cover only a part of the clinical crown, most commonly used type of partial veneer crown
Dental Policy Subject: Teeth with a Poor or Guarded Prognosis Guideline #: Clinical Policy - 01 Publish Date: 03/15/2018 Status:
 Dental Policy Subject: Teeth with a Poor or Guarded Prognosis Guideline #: Clinical Policy - 01 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses
Dental Policy Subject: Teeth with a Poor or Guarded Prognosis Guideline #: Clinical Policy - 01 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses
Periodontal evaluation of crown-root fractured teeth following modified crown lengthening surgery
 cia.apractice Periodontal evaluation of crown-root fractured teeth following modified crown lengthening surgery VERIFIABLE CPD 2017BrtishDentalAsM. Zhen, 1 C. Wang, 1 W-J. Hu,* 1 H. Zhang, 2 L-S. Li, 2
cia.apractice Periodontal evaluation of crown-root fractured teeth following modified crown lengthening surgery VERIFIABLE CPD 2017BrtishDentalAsM. Zhen, 1 C. Wang, 1 W-J. Hu,* 1 H. Zhang, 2 L-S. Li, 2
Lec. 3-4 Dr. Saif Alarab Clinical Technique for Class I Amalgam Restorations The outline form
 Lec. 3-4 Dr. Saif Alarab Clinical Technique for Class I Amalgam Restorations Class I refers to -Restorations on the occlusal surfaces of posterior teeth, - The occlusal two thirds of facial and lingual
Lec. 3-4 Dr. Saif Alarab Clinical Technique for Class I Amalgam Restorations Class I refers to -Restorations on the occlusal surfaces of posterior teeth, - The occlusal two thirds of facial and lingual
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MDG Dental Plan Comparison
 D0999 Office visit during regular hours, general dentist only Evaluations D0120 Periodic oral examination - established patient D0140 Limited oral evaluation - problem focused D0145 Oral evaluation for
D0999 Office visit during regular hours, general dentist only Evaluations D0120 Periodic oral examination - established patient D0140 Limited oral evaluation - problem focused D0145 Oral evaluation for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Summary of Benefits Dental Coverage - New Dental Option
 Summary of Benefits Dental Coverage - New Dental Option Managed Dental Plan MET225 - Texas Code Description Co-Payment Diagnostic Treatment D0120 Periodic Oral Evaluation established patient $0 D0150 Comprehensive
Summary of Benefits Dental Coverage - New Dental Option Managed Dental Plan MET225 - Texas Code Description Co-Payment Diagnostic Treatment D0120 Periodic Oral Evaluation established patient $0 D0150 Comprehensive
Aetna Dental Inc. One Prudential Circle Sugar Land, TX SUMMARY OF COVERAGE
 Aetna Dental Inc. One Prudential Circle Sugar Land, TX 77478 1-877-238-6200 SUMMARY OF COVERAGE CONTRACT HOLDER: Clear Creek ISD GROUP AGREEMENT: 620318 PLAN EFFECTIVE: September 1, 2014 The benefits shown
Aetna Dental Inc. One Prudential Circle Sugar Land, TX 77478 1-877-238-6200 SUMMARY OF COVERAGE CONTRACT HOLDER: Clear Creek ISD GROUP AGREEMENT: 620318 PLAN EFFECTIVE: September 1, 2014 The benefits shown
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
SECURE CHOICE INDIVIDUAL COPAYMENT SCHEDULE
 DentiCare of Alabama, Inc. 3595 Grandview Parkway, Suite 650 Birmingham, AL 35243 SECURE CHOICE INDIVIDUAL COPAYMENT SCHEDULE SECTION I: PLAN DENTIST SERVICES (Subject to Exclusions and Limitations Listed
DentiCare of Alabama, Inc. 3595 Grandview Parkway, Suite 650 Birmingham, AL 35243 SECURE CHOICE INDIVIDUAL COPAYMENT SCHEDULE SECTION I: PLAN DENTIST SERVICES (Subject to Exclusions and Limitations Listed
Aetna Dental Inc. One Prudential Circle Sugar Land, TX SUMMARY OF COVERAGE
 Aetna Dental Inc. One Prudential Circle Sugar Land, TX 77478 1-877-238-6200 SUMMARY OF COVERAGE CONTRACT HOLDER: BNSF Railway Company GROUP AGREEMENT: 727796 PLAN EFFECTIVE: January 1, 2016 The benefits
Aetna Dental Inc. One Prudential Circle Sugar Land, TX 77478 1-877-238-6200 SUMMARY OF COVERAGE CONTRACT HOLDER: BNSF Railway Company GROUP AGREEMENT: 727796 PLAN EFFECTIVE: January 1, 2016 The benefits
Schedule of Benefits (GR-9N S )
 Schedule of Benefits (GR-9N S-01-001-01) Employer: Group Policy Number: BNSF Railway Company GP-727796 Issue Date: January 1, 2016 Effective Date: January 1, 2016 Schedule: 1A Cert Base: 1 For: DMO - All
Schedule of Benefits (GR-9N S-01-001-01) Employer: Group Policy Number: BNSF Railway Company GP-727796 Issue Date: January 1, 2016 Effective Date: January 1, 2016 Schedule: 1A Cert Base: 1 For: DMO - All
Linking Research to Clinical Practice
 Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Schedule of Benefits (GR-9N S )
 Schedule of Benefits (GR-9N S-01-001-01) Employer: Group Policy Number: Roman Catholic Diocese Of Dallas GP-870560-WI Issue Date: February 9, 2015 Effective Date: January 1, 2015 Schedule: 7A Cert Base:
Schedule of Benefits (GR-9N S-01-001-01) Employer: Group Policy Number: Roman Catholic Diocese Of Dallas GP-870560-WI Issue Date: February 9, 2015 Effective Date: January 1, 2015 Schedule: 7A Cert Base:
Maintenance in the Periodontally Compromised Patient. Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club
 Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS
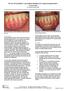 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
