Comparative Effectiveness of Liver Transplant Strategies for End-Stage Liver Disease Patients on Renal Replacement Therapy
|
|
|
- Annabella Miles
- 5 years ago
- Views:
Transcription
1 LIVER TRANSPLANTATION 20: , 2014 ORIGINAL ARTICLE Comparative Effectiveness of Liver Transplant Strategies for End-Stage Liver Disease Patients on Renal Replacement Therapy Yaojen Chang, 1 Lorenzo Gallon, 2 Colleen Jay, 2 Kirti Shetty, 3 Bing Ho, 2 Josh Levitsky, 2 Talia Baker, 2 Daniela Ladner, 2 John Friedewald, 2 Michael Abecassis, 2 Gordon Hazen, 4 and Anton I. Skaro 2 1 Lombardi Comprehensive Cancer Center, Department of Oncology, Cancer Prevention and Control Program, Georgetown University School of Medicine, Washington, DC; 2 Comprehensive Transplant Center, Northwestern University Feinberg School of Medicine, Chicago, IL; 3 Division of Gastroenterology and Hepatology, Sibley Memorial Hospital, Johns Hopkins Medicine, Washington, DC; and 4 Department of Industrial Engineering and Management Sciences, Northwestern University McCormick School of Engineering, Evanston, IL There are complex risk-benefit tradeoffs with different transplantation strategies for end-stage liver disease patients on renal support. Using a Markov discrete-time state transition model, we compared survival for this group with 3 strategies: simultaneous liver-kidney (SLK) transplantation, liver transplantation alone (LTA) followed by immediate kidney transplantation if renal function did not recover, and LTA followed by placement on the kidney transplant wait list. Patients were followed for 30 years from the age of 50 years. The probabilities of events were synthesized from population data and clinical trials according to Model for End-Stage Liver Disease (MELD) scores (21-30 and >30) to estimate input parameters. Sensitivity analyses tested the impact of uncertainty on survival. Overall, the highest survival rates were seen with SLK transplantation for both MELD score groups (82.8% for MELD scores of and 82.5% for MELD scores > 30 at 1 year), albeit at the cost of using kidneys that might not be needed. Liver transplantation followed by kidney transplantation led to higher survival rates (77.3% and 76.4%, respectively, at 1 year) than placement on the kidney transplant wait list (75.1% and 74.3%, respectively, at 1 year). When uncertainty was considered, the results indicated that the waiting time and renal recovery affected conclusions about survival after SLK transplantation and liver transplantation, respectively. The subgroups with the longest durations of pretransplant renal replacement therapy and highest MELD scores had the largest absolute increases in survival with SLK transplantation versus sequential transplantation. In conclusion, the findings demonstrate the inherent tension in choices about the use of available kidneys and suggest that performing liver transplantation and using renal transplantation only for those who fail to recover their native renal function could free up available donor kidneys. These results could inform discussions about transplantation policy. Liver Transpl 20: , VC 2014 AASLD. Received June 27, 2013; accepted April 9, See Editorial on Page 1017 Abbreviations: CI, confidence interval; ECD, extended criteria donor; ESLD, end-stage liver disease; KTA, kidney transplantation alone; LTA, liver transplantation alone; MELD, Model for End-Stage Liver Disease; NMH, Northwestern Memorial Hospital; OPTN, Organ Procurement and Transplantation Network; r, weekly rate; RRT, renal replacement therapy; SLK, simultaneous liver-kidney; SRTR, Scientific Registry of Transplant Recipients; t, 1 week. The authors have no conflicts of interest to declare. This research was supported in part by the Cancer Intervention and Surveillance Modeling Network (grant U01 CA from the National Cancer Institute) and the National Institute on Disability and Rehabilitation Research (grant H133P from the Department of Education). Address reprint requests to Yaojen Chang, Dr.P.H., M.S., M.P.H., Lombardi Comprehensive Cancer Center, Department of Oncology, Cancer Prevention and Control Program, Georgetown University School of Medicine, 3300 Whitehaven Street, Suite 4100, Washington, DC Telephone: ; FAX: ; yc377@georgetown.edu DOI /lt View this article online at wileyonlinelibrary.com. LIVER TRANSPLANTATION.DOI /lt. Published on behalf of the American Association for the Study of Liver Diseases VC 2014 American Association for the Study of Liver Diseases.
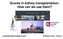
2 LIVER TRANSPLANTATION, Vol. 20, No. 9, 2014 CHANG ET AL Figure 1. Schematic diagram of the Markov simulation model used to compare survival rates for 50-year-old ESLD patients on pretransplant RRT by transplant strategy. Death could occur with any health state or SLK/LTA transplant surgery. There are approximately 15,000 individuals in the United States each year with end-stage liver disease (ESLD) who are on waiting lists for liver transplantation. 1 Many of these individuals also have associated renal impairment. Comorbid renal disease increases the risk of death while a person is on the liver transplant waiting list. 2-5 Moreover, those who undergo liver transplantation in the setting of cirrhosis with renal impairment have a particularly poor prognosis, especially when their renal function does not improve after liver transplantation. 6-8 Therefore, simultaneous liver-kidney (SLK) transplantation has been suggested as a strategy for improving posttransplant survival. 2,9,10 In fact, its use has increased 2-fold since criteria that consider both liver and kidney function [the Model for End-Stage Liver Disease (MELD) system] were implemented in 2002 for transplant waiting-list prioritization. 11 However, the increase in the number of SLK transplants could have other unintended consequences, such as increased wait-list times due to the need to have 2 matched organs and the use of kidneys that might not have been needed in patients destined to have improved renal function after liver transplantation. Sequential approaches have been proposed as alternatives: liver transplant is performed first, and renal transplant is then performed only for the subset of patients who do not experience renal recovery. For this group, however, the added time on the renal transplant waiting list after liver transplantation could increase mortality Because of the complexity of these alternative transplant strategies, they are difficult to compare directly in clinical trials. To our knowledge, no previous studies have compared the outcomes of these alternative transplant strategies or examined multiple approaches according to the severity of liver and kidney disease. Moreover, procedures and outcomes are not tracked in national registries with sufficient detail for outcomes to be directly estimated. 1,15 In such situations, in which there are different tradeoffs with the benefits and harms associated with various transplant scenarios, modeling can be a useful scientific method for comparing and quantifying the outcomes of alternative transplantation approaches. This study used simulation modeling to compare survival with 3 different transplant strategies for 2 groups of ESLD patients at the age of 50 years with renal disease who were already on pretransplant renal replacement therapy (RRT). The 2 groups were patients with MELD scores of 21 and 30 and patients with scores > 30 because, by definition, being on RRT means that individuals have a score of 21 or higher. Increasing scores indicate a higher risk of mortality. For each of these 2 groups, we examined (1) SLK transplantation, (2) liver transplantation alone (LTA) followed by placement on the wait list for renal transplantation according to the current allocation policy, and (3) LTA followed by kidney transplantation for recipients who did not recover native renal function. The results are intended to inform clinical decision making and policy discussions about US transplant strategies. PATIENTS AND METHODS Model Overview A Markov discrete-time state transition model was constructed with TreeAge Pro 2009 (version , TreeAge Software, Williamstown, MA) to evaluate the 3 strategies for 2 groups of 50-year-old patients (based on MELD scores) with ESLD (regardless of etiology); all patients were receiving pretransplant RRT (Fig. 1). We selected the age of 50 years to start the simulation because the largest proportion of ESLD patients are 50 to 64 years old. The model consisted of a finite number of mutually exclusive health states, which are called Markov states. 16,17 In each simulation, according to the strategy being evaluated, a patient moved through the model to experience events (eg, undergo liver-kidney transplant surgery) and transitioned between all the different health states that followed from that strategy (eg, graft rejection and recovery of renal function) until death or the end of a 30-year time horizon. Patients could move
3 1036 CHANG ET AL. LIVER TRANSPLANTATION, September 2014 TABLE 1. Values of Parameters Used in a Markov Simulation Model Comparing Transplant Strategies for 50-Year-Old ESLD Patients on Pretransplant RRT Parameter Base Case* Source Time to liver transplant by MELD score (days) OPTN/SRTR 15 (2008) ( ) ( ) > ( ) Time to kidney transplant for 50- to 64-year-old ( ) OPTN/SRTR 15 (2008) candidates under current allocation policy (days) Annual liver wait-list death rates per 1000 OPTN/SRTR 15 (2008) patient-years by MELD score > Annual kidney wait-list death rate per OPTN/SRTR 15 (2008) patient-years Annual dialysis death rate per 1000 patientyears 133 Wolfe et al. 19 (1999) LTA recipient survival without renal recovery at 64 Northup et al. 18 (2010) 90 days (%) LTA recipient survival without renal recovery at 15 Northup et al. 18 (2010) 1500 days (%) LTA recipient survival for group with MELD 78 Gonwa et al. 7 (2006) scores of after renal recovery at 5 years (%) LTA recipient survival for group with MELD 72 Gonwa et al. 7 (2006) scores > 30 after renal recovery at 5 years (%) SLK recipient survival for group with MELD 71.5 Gonwa et al. 7 (2006) scores of at 5 years (%) SLK recipient survival for group with MELD 68 Gonwa et al. 7 (2006) scores > 30 at 5 years (%) KTA recipient survival at 10 years with non OPTN/SRTR 15 (2008) ECD deceased donor kidneys (%) Probability of liver transplant operative mortality (%) 3 Llovet et al. 20 (1999), Jonas et al. 21 (2001), Mazzaferro et al. 22 (1996) Probability of kidney transplant operative 1.3 Hollingsworth et al. 23 (2007) mortality (%) Probability of SLK transplant operative mortality (%) 4.3 Llovet et al. 20 (1999), Jonas et al. 21 (2001), Mazzaferro et al. 22 (1996), Hollingsworth et al. 23 (2007) Probability of SLK acute graft failure (%) 1.3 NMH data Probability of post-lta renal recovery with pretransplant 70.8 Northup et al. 18 (2010) RRT for <30 days (%) Probability of post-lta renal recovery with pretransplant 56.3 Northup et al. 18 (2010) RRT for days (%) Probability of post-lta renal recovery with pretransplant 23.5 Northup et al. 18 (2010) RRT for days (%) Probability of post-lta renal recovery with pretransplant 11.5 Northup et al. 18 (2010) RRT for >90 days (%) Post-KTA renal graft survival at 3 months (%) 95.7 OPTN/SRTR 15 (2008) Post-LTA liver graft survival at 3 months (%) 88.1 OPTN/SRTR 15 (2008) Post-LTA liver graft survival at 5 years (%) 62.8 OPTN/SRTR 15 (2008) Post-LTA kidney graft survival at 10 years (%) 27 Ojo et al. 24 (2003) Post-SLK liver/renal graft survival at 97.3 NMH data 3 months (%) Post-SLK liver graft survival at 5 years (%) 62 Pham et al. 25 (2007) Post-SLK kidney graft survival at 5 years (%) 60 Pham et al. 25 (2007)
4 LIVER TRANSPLANTATION, Vol. 20, No. 9, 2014 CHANG ET AL TABLE 1. Continued Parameter Base Case* Source Post-KTA kidney graft survival at 10 years with 42.4 OPTN/SRTR 15 (2008) non-ecd deceased donor kidneys (%) *The data within parentheses are 95% CIs for the national median waiting times. Northwestern University Enterprise Data Warehouse. The declining exponential function was used to convert the parameter values in the literature into weekly values. To convert the rates into probabilities, the following equation was used: P e 2rt where r is the weekly rate and t is 1 week. The probability of post-lta renal recovery was terminated in the 12th posttransplant week in the model because the likelihood of recovering renal function more than 3 months after transplantation was very low. between states at 1-week intervals; this reflected how disease progression is tracked in the MELD score system. Thirty years was selected as the time horizon because few 50-year-old patients with ESLD will live beyond this span. This study was deemed exempt from IRB review due to only secondary, de-identified data used in the simulation model. At the start of the model, each patient followed 1 of the 3 transplant strategies. If the patient survived the transplant surgery, the new organ(s) could be accepted or rejected. Posttransplant renal recovery could occur or not occur. Because renal recovery or the development of renal graft function was unlikely to occur more than 3 months after transplantation, 18 patients who did not have recovery of renal function remained on RRT and were placed on the kidney transplant waiting list. They either died on the kidney waiting list or survived to undergo kidney transplantation alone (KTA). This kidney could either function or be rejected. Additionally, chronic liver and kidney failure could occur after transplantation and result in the patient being wait-listed for liver retransplantation, kidney retransplantation, or both, although this group would be expected to be small because of the high rates of chronic complications and wait-list mortality. Death could occur before any of the transplants while the patient was on the waiting list, during surgery, or at any time after transplantation; mortality was assumed to be due to liver-kidney disease and not unrelated causes. The primary outcome of the model was the survival rate for each transplant strategy. As noted previously, we grouped the patients into 2 groups on the basis of their MELD scores: 21 to 30 and >30. By definition, because our patient population had ESLD and was already on RRT, they all would have had MELD scores of 21 or more at the start of the simulation. Because RRT could be stopped and/or reinitiated while patients were on the waiting list, the model considered the probabilities of transitions between the initial MELD score and higher or lower scores over time. Transition probabilities occurred between states defined by MELD score quintiles. These new MELD scores, in turn, affected the wait-list position at any point in time. Data Sources The parameter values and ranges used in the model to estimate the probabilities of all transitions between states and the prevalence of events were estimated from multiple data sources. If available, data from clinical trials were used; otherwise, large populationbased observational data sets were used. Because all transplant candidates are represented in transplant registries, these data sources were considered as population estimates. Because all transition probabilities occurred in 1-week cycles, some data required a conversion from annual values to weekly values. The values and sources of all parameters are summarized on Table 1 and are highlighted in the following narrative. Waiting Time The number of days from listing to the date of liver transplantation was based on data from the 2008 Organ Procurement and Transplantation Network (OPTN)/Scientific Registry of Transplant Recipients (SRTR) annual report for each MELD score quintile. 15 The median was used as the point estimate, and the 95% confidence interval (CI) of the median was used to determine a range for testing the impact of the initial wait time on survival outcomes in sensitivity analyses. Waiting-list times for kidneys after liver transplantation without renal recovery were assumed to be 16 weeks because the recovery of native renal function was less likely to occur more than 3 months after transplantation. 18 Times on the waiting list for repeat liver or kidney transplantation after organ rejection were based on the national median waiting time for each MELD quintile. 15 We assumed an equal wait-list time within MELD score groups regardless of the type of liver transplant (ie, with or without a renal transplant) because the registries did not differentiate these procedures. We tested the impact of this assumption in a sensitivity analysis. For liver transplant candidates on the wait list, the probability of changing MELD score groups over time was estimated from data reported in the 2008 United Network for Organ Sharing/OPTN data set.
5 1038 CHANG ET AL. LIVER TRANSPLANTATION, September 2014 TABLE 2. Markov Model Estimates of Posttransplant Survival Rates for 50-Year-Old ESLD Patients on Pretransplant RRT by Transplant Strategy and MELD Scores Survival Rate by Transplant Strategy 1 Year 2 Years 3 Years 5 Years 10 Years MELD scores of SLK transplant with standard criteria donor kidneys Liver transplant and subsequent kidney transplant if needed with current allocation wait time Liver transplant and subsequent kidney transplant if needed with 16-week wait time MELD scores > 30 SLK transplant with standard criteria donor kidneys Liver transplant and subsequent kidney transplant if needed with current allocation wait time Liver transplant and subsequent kidney transplant if needed with 16-week wait time NOTE: The data are presented as percentages. Posttransplant Events Beyond operative mortality (discussed later), 2 posttransplant events affect survival: graft rejection and recovery of renal function. After transplantation, organ(s) can be acutely or chronically rejected. Because Markov model states do not have a memory of prior health, we made the simplifying assumption that the probability of acute and chronic liver and kidney graft failure was unaffected by previous MELD scores. We assumed that only standard criteria donor kidney grafts were used for KTA. Mortality Mortality can occur over time in several ways, including death due to organ failure or its complications while the patient is on the waiting list, operative mortality during transplantation, postoperative mortality due to complications, death due to acute or chronic organ rejection and failure, and death due to other causes related to the underlying ESLD. The mortality rate on the initial waiting list for each MELD score quintile was derived from the 2008 OPTN/SRTR annual report. 15 Operative mortality was based on the published literature The probabilities of posttransplant mortality were significantly affected by renal function. We assumed that the long-term survival of liver transplant recipients undergoing either simultaneous or single transplantation was based on a constant hazard of death. We also assumed that liver recipients who did not recover their native renal function had a much higher posttransplant mortality rate on the basis of observational data reported by Northup et al. 18 Analysis Simulations were replicated 500,000 times for each scenario, and the results were summarized with Stata 11 (StataCorp LP, College Station, TX). The primary outcome was the survival associated with each of the 3 transplant strategies by MELD score group. We examined the absolute 1-, 3-, 5-, and 10-year survival rates because these were felt to be the most relevant to clinical decision making for the respective transplant recipients. We did not examine survival beyond 10 years because of the shortage of long-term observed data for validating model outcomes. Results were also stratified by the time on pretransplant RRT. To fully reflect the impact of different waiting times (eg, subsequent kidney transplantation 52 weeks after liver transplantation) and dialysis durations (>90 days) on survival, we assessed the impact of these factors on 2-year survival. One-way sensitivity analyses were conducted to test the impact of uncertainty on parameter estimates for waiting times, renal recovery, and chronic renal graft survival after liver transplantation. Initial median waiting times for LTA varied over the 95% CI range because of variability at the regional, donor service area, and transplant center levels. Patients undergoing SLK transplantation could have different waitlist times than those undergoing LTA. Alternatively, because of the need to match 2 organs, the waitinglist time could be longer for SLK transplantation versus LTA. Therefore, we used wait-list times ranging from 50% to 200% of the national median wait-list time for SLK transplantation. We also varied the range of times for kidney transplants after LTA (16, 26, and 52 weeks). Renal recovery was varied and based on 50% to 200% of the values observed for each period of RRT duration (<30, 30-60, 60-90, and >90 days) 18 ; 50% to 200% of the baseline renal graft survival after liver transplantation was tested in the sensitivity analysis. 24 The results of these 1-way sensitivity analyses are summarized in tornado diagrams. In this format, the results are arranged from the largest impact to the least impact of varying a given parameter on survival rates. In this manner, the uncertainty of the parameter associated with the largest bar, the one at
6 LIVER TRANSPLANTATION, Vol. 20, No. 9, 2014 CHANG ET AL Figure 2. Survival rates for transplant recipients in the MELD score categories of 21 to 30 and >30 by transplant strategy. LTA indicates liver transplant recipients with the option of being placed on the kidney wait list when renal recovery failed; LTA_KTA16wk indicates liver transplant recipients with the option of subsequent kidney transplantation 16 weeks after transplantation when renal recovery failed; and SLK indicates SLK transplant recipients. TABLE 3. Markov Model Estimates of 1-Year Posttransplant Survival Rates for 50-Year-Old ESLD Patients on Pretransplant RRT by Transplant Strategy and MELD Scores Stratified by the Duration of Pretransplant RRT Pretransplant RRT Duration (Days) 1-Year Survival Rate < >90 MELD scores of SLK transplant with standard criteria donor kidneys Liver transplant and subsequent kidney transplant if needed with current allocation wait time Liver transplant and subsequent kidney transplant if needed with 16-week wait time MELD scores > 30 SLK transplant with standard criteria donor kidneys Liver transplant and subsequent kidney transplant if needed with current allocation wait time Liver transplant and subsequent kidney transplant if needed with 16-week wait time NOTE: The data are presented as percentages. the top of the chart, has the maximum impact on the survival result, with each successive parameter uncertainty (lower bars) having a lesser impact. RESULTS In this population of 50-year-old ESLD patients on pretransplant RRT, survival decreased over time with all 3 strategies, and it was lower for the patients in the more severe MELD score category (>30; Table 2). The scenario with the highest survival rate was SLK transplantation (Table 2 and Fig. 2), which was followed by LTA with the option of subsequent kidney transplantation at 16 weeks or placement on the kidney transplant wait list when renal recovery failed (77.3% and 75.1% at 1 year, respectively, for the lower MELD score group). This was true for both MELD score groups (82.8% and 82.5% with SLK transplantation for the lower and higher MELD score groups, respectively, at 1 year). However, when LTA was
7 1040 CHANG ET AL. LIVER TRANSPLANTATION, September 2014 Figure 3. Two-year survival rates for SLK transplant candidates and LTA candidates by the MELD score category with different assumptions about the waiting time. Figure 4. Two-year survival rates for LTA recipients in the MELD score categories of 21 to 30 and >30 when kidney transplantation for those who failed to recover renal function was subsequently performed at 16, 26, and 52 weeks or on the basis of the current kidney graft allocation policy. performed initially and renal recovery did not occur within the first 3 months, patients immediately undergoing renal transplantation had higher survival rates than those who were allocated kidneys according to routine policies. As shown in Table 2, the differ- ences in the survival rates of SLK transplant recipients and liver transplant recipients under the current kidney allocation policy were larger (8.2% and 7.7% at 1 year and 9.9% and 9.2% at 3 years for the MELD score categories of >30 and 21-30,
8 LIVER TRANSPLANTATION, Vol. 20, No. 9, 2014 CHANG ET AL Figure 5. One-year survival rates for liver transplant recipients in the MELD score categories of >30 and 21 to 30 when renal recovery during each period of RRT duration was varied in the range of 50% to 200% of the baseline values. respectively) than the differences between the other strategies. Also, we noted that the survival advantage of SLK transplantation versus liver transplantation with the option of subsequent kidney transplantation 16 weeks after liver transplantation was narrowed to 6.1% and 5.5% at 1 year, 5% and 4.4% at 3 years, and 3.9% and 3.2% at 5 years for the higher and lower MELD score groups, respectively. During the 30-year simulation period, the cumulative incidence of renal transplantation after LTA was 18.4% with the current kidney allocation policy/wait time (data not shown). When we considered the duration of pretransplant RRT (Table 3), the ranking of the strategies remained similar across all durations in terms of 1-year survival, with SLK transplantation leading to substantially higher survival than initial LTA. Additionally, there was little reduction in survival as the duration of pretransplant rental replacement therapy increased with the simultaneous transplant strategy. However, with LTA, survival decreased substantially with an increasing duration of prior renal support therapy. For instance, for the group with higher MELD scores, 1-year survival decreased from 74.3% to 52.8% as the duration of pretransplant RRT increased from <30 days to >90 days under the current kidney allocation policy. Sensitivity Analysis Survival after SLK transplantation was related to the uncertainty of the waiting time, with improved survival associated with waiting times 50% shorter than the national median and with reductions in survival associated with waiting times 200% greater than the national median (Fig. 3). The reduction in survival was less for those with MELD scores of 21 to 30 versus those with MELD scores > 30. However, survival rates varied by less than 63% when the waiting time was varied less dramatically over the 95% CI of the national median waiting time. Among those undergoing LTA and subsequent kidney transplantation, outcomes were also affected by the uncertainty of the waiting time (Fig. 4). Overall, across all strategies, patients had the best survival with the shortest transplant waiting times. When chronic renal graft survival after liver transplantation was varied from 50% to 200% of the baseline values, the changes in the 3- and 5-year survival rates were modest (20.64% to 10.41% and 21.24% to 10.81% for the group with MELD scores > 30 and 20.72% to 10.50% and 21.59% to 10.82% for the group with MELD scores of 21-30). A sensitivity analysis of the probability of renal recovery after liver
9 1042 CHANG ET AL. LIVER TRANSPLANTATION, September 2014 transplantation for each pretransplant RRT duration (<30, 30-60, 60-90, and >90 days) with MELD scores > 30 and MELD scores of 21 to 30 is displayed in Fig. 5. For instance, the 1-year survival rate for the liver transplant recipients with MELD scores > 30 receiving pretransplant RRT for <30 days changed in the range of 25.66% to 16.59% when the probability of renal recovery was varied from 50% to 200% of the baseline value. The various probabilities of renal recovery after liver transplantation had a significant impact on the survival of the liver transplant recipients. DISCUSSION This is the first study to use simulation modeling to directly compare and quantify the expected outcomes of current or proposed clinical transplantation strategies among middle-aged patients with ESLD who are on pretransplant renal support. Overall, the SLK transplant strategies led to higher survival rates than sequential transplantation approaches. There were no major differences between MELD score groups, but patients who had been on RRT for the longest period seemed to benefit the most with respect to survival from simultaneous transplantation versus sequential transplantation. Finally, performing liver transplantation first and then performing renal transplantation only for those who fail to recover their native renal function could free up available donor kidneys, and this could be a good alternative to simultaneous transplantation if waiting times are short. Our model results suggest that among the alternatives considered, SLK transplantation results in the greatest short- and long-term survival for liver transplant candidates receiving pretransplant RRT. This result is consistent with other analyses comparing LTA and SLK transplantation for dialysis-dependent patients. 7,8,26,27 The 1 study with a different conclusion included patients undergoing SLK transplantation or sequential liver-kidney transplantation when subsequent kidney transplants provided to liver transplant recipients and SLK transplants provided to ESLD patients on RRT were performed in the same period of time. 12 Thus, the 2 groups were getting very similar treatments that were essentially simultaneous transplants. Northup et al. 18 noted that ESLD patients on renal dialysis who undergo LTA have a very low survival rate (16% at 4 years) if they do not recover renal function. Because of the current wait time of multiple years for renal transplantation, many of these patients will not survive. However, our results suggest that SLK transplantation could prevent this wait-list mortality and dramatically increase survival (56%-64% at 5 years). The model results for SLK transplantation and liver transplantation among those receiving pretransplant renal support are very similar to those observed in clinical practice for this same group of patients. For instance, Gonwa et al. 7 reported survival rates for 632 SLK transplant recipients and 1103 liver transplant recipients at 1, 2, and 3 years after transplantation of 83.6%, 79%, and 74.8% and 75.2%, 71.2%, and 68.3%, respectively. These rates are within 65% of our model results. The consistency of our results with this large clinical series supports the validity of the model employed in our study. Additionally, our model results are consistent with clinical observational studies showing that the longer the duration of pretransplant RRT is, the greater the benefits will be from SLK transplantation. For example, Northup et al. 18 demonstrated an inverse doseresponse relationship between the pretransplant RRT duration and the probability of renal recovery after liver transplantation. However, 1 study did not observe better survival with simultaneous transplantation versus sequential transplantation for a subgroup on RRT for <3 months, 5 whereas our model results indicated survival benefits with SLK over LTA even when the pretransplant dialysis duration was <30 days. However, our model projected that the difference in the survival benefit observed between a pretransplant RRT duration < 30 days and a pretransplant RRT duration > 90 days would be substantial. In comparison with the current deceased donor kidney graft allocation policy, the strategy of subsequent kidney transplantation 16 weeks after liver transplantation improved the survival of liver transplant recipients who received pretransplant RRT. A more significant survival advantage with this strategy was found for the subgroup of liver transplant recipients with MELD scores of 21 to 30 who received pretransplant RRT for the longest duration (>90 days). On the other hand, the difference in survival between SLK transplant recipients and liver transplant recipients decreased when kidney transplantation was subsequently performed 16 weeks after transplantation for those who did not recover renal function. Because of the approximately 6% annual wait-list mortality rate among end-stage renal disease patients who are 50 to 64 years old and the likelihood of recovering native renal function after liver transplantation, liver transplantation with subsequent kidney transplantation at 16 weeks might be a very good alternative strategy for ESLD patients on pretransplant RRT. With this strategy, unnecessary SLK transplants can be avoided, and additional kidney grafts can be released to endstage renal disease patients on kidney transplant wait lists. Current MELD-based liver allocation has given priority to ESLD patients with renal impairment. Consequently, the number of SLK transplants has steadily increased since the implementation of the MELD system in As the number of kidney grafts allocated to SLK transplantation has increased, the kidney transplant waiting period has been lengthened, and more kidney wait-list deaths could occur. Thus, this comparison of liver-based transplant strategies underscores the dynamic tradeoffs between approaches and raises interesting allocation questions. The current model examined approaches for only a subset of ESLD patients, so we cannot fully
10 LIVER TRANSPLANTATION, Vol. 20, No. 9, 2014 CHANG ET AL address equity and allocation issues. Although it would be very complex, an examination of multiple conditions affected by organ allocation in future models would be interesting for placing liver disease strategies in a broader context. This work (and clinical decisions) could be facilitated by new data for accurately identifying ESLD patients who will not recover renal function after transplantation. There are many strengths of this modeling study, including the direct comparison of 3 alternative transplant strategies, the use of the best available data, the detailed assessment of the impact of parameter uncertainty on outcomes, and the robust conclusions that are consistent with clinical observations. Despite these strengths, there are also several limitations that should be considered in an evaluation of our results. First, the population targeted in this study was very narrowly defined, and the results will not apply to all ESLD patients, such as the 25% of those receiving SLK transplants who are not on pretransplant dialysis. Second, among the subset of patients who had been on RRT for <30 days, improvements in survival after SLK transplantation may not be related to the receipt of a new kidney. To the extent that this is true, we may have overestimated survival, although estimates for those on pretransplant RRT for longer durations are more likely to reflect true benefits from receiving a new kidney. Third, as noted previously, the model was restricted to outcomes among our target population and did not assess the effects of the different transplant strategies on organ allocation and availability for other groups of patients. Fourth, there were insufficient data to model intermediate outcomes that would be relevant to decision making and/or the assessment of costs, such as retransplantation rates. Finally, simulation modeling does not provide tests of statistical significance, nor does it determine levels of clinically meaningful improvements in survival rates. The United Network for Organ Sharing is developing SLK transplant guidelines in response to the dramatically increasing number of SLK transplants and the variations among transplant centers in indications for this procedure. 28 The proposed guidelines focus on offering SLK transplantation only to ESLD patients who are unlikely to regain renal function after liver transplantation (eg, on the basis of the length of time on dialysis and the baseline renal function). The results of our model support these guidelines because we have demonstrated that maximal gains in survival after SLK transplantation accrue to those who have high MELD scores (>30) and those who have been on RRT for >90 days. In conclusion, there are dynamic and complex tradeoffs in the risks and benefits of different transplantation strategies for middle-aged ESLD patients requiring renal support. This study used simulation modeling to compare and quantify the outcomes of 3 clinically prevalent transplant approaches for this population. Models allow direct comparisons of large numbers of individuals that might not be feasible in clinical trials. The results suggest that SLK transplantation yields higher survival rates than liver transplantation under the current kidney graft allocation policy. When kidney transplantation was subsequently available to those who failed to recover renal function 16 weeks after transplantation, differences in the survival rates associated with SLK transplantation and liver transplantation became limited. Liver transplantation with subsequent kidney transplantation might be an alternative strategy for decreasing the tradeoff between the mortality risk after liver transplantation and unnecessary SLK transplantation, but important equity allocation issues are raised. ACKNOWLEDGMENT The authors acknowledge Dr. Mandelblatt (Georgetown-Lombardi Cancer Center) for her assistance with manuscript editing. REFERENCES 1. Organ Procurement and Transplantation Network (OPTN) and Scientific Registry of Transplant Recipients (SRTR). OPTN/SRTR 2011 Annual Data Report. Rockville, MD: Department of Health and Human Services, Health Resources and Services Administration, Healthcare Systems Bureau, Division of Transplantation; Testino G, Ferro C. Hepatorenal syndrome: a review. Hepatogastroenterology 2010;57: Ruiz R, Kunitake H, Wilkinson AH, Danovitch GM, Farmer DG, Ghobrial RM, et al. Long-term analysis of combined liver and kidney transplantation at a single center. Arch Surg 2006;141: Myers RP, Shaheen AA, Aspinall AI, Quinn RR, Burak KW. Gender, renal function, and outcomes on the liver transplant waiting list: assessment of revised MELD including estimated glomerular filtration rate. J Hepatol 2011;54: Locke JE, Warren DS, Singer AL, Segev DL, Simpkins CE, Maley WR, et al. Declining outcomes in simultaneous liverkidney transplantation in the MELD era: ineffective usage of renal allografts. Transplantation 2008;85: Moreno JM, Cuervas-Mons V, Rubio E, Pons F, Herreros de TA, Turrion VS, Millan I. Chronic renal dysfunction after liver transplantation in adult patients: prevalence, risk factors, and impact on mortality. Transplant Proc 2003;35: Gonwa TA, McBride MA, Anderson K, Mai ML, Wadei H, Ahsan N. Continued influence of preoperative renal function on outcome of orthotopic liver transplant (OLTX) in the US: where will MELD lead us? Am J Transplant 2006;6: Nair S, Verma S, Thuluvath PJ. Pretransplant renal function predicts survival in patients undergoing orthotopic liver transplantation. Hepatology 2002;35: Moreno-Gonzalez E, Meneu-Diaz JC, Garcıa G, Jimenez Romero C, Loinaz Segurola C, Gomez Sanz R, et al. Simultaneous liver-kidney transplant for combined renal and hepatic end-stage disease. Transplant Proc 2003;35: Lang M, Neumann U, Kahl A, Steinm uller T, Settmacher U, Neuhaus P. Long-term outcome of 27 patients after combined liver-kidney transplantation. Transplant Proc 2001;33: Papafragkakis H, Martin P, Akalin E. Combined liver and kidney transplantation. Curr Opin Organ Transplant 2010;15:
11 1044 CHANG ET AL. LIVER TRANSPLANTATION, September Simpson N, Cho YW, Cicciarelli JC, Selby RR, Fong TL. Comparison of renal allograft outcomes in combined liver-kidney transplantation versus subsequent kidney transplantation in liver transplant recipients: analysis of UNOS database. Transplantation 2006;82: Thompson JA, Lake JR. The impact of MELD allocation on simultaneous liver-kidney transplantation. Curr Gastroenterol Rep 2009;11: Ruiz R, Barri YM, Jennings LW, Chinnakotla S, Goldstein RM, Levy MF, et al. Hepatorenal syndrome: a proposal for kidney after liver transplantation (KALT). Liver Transpl 2007;13: Annual Report of the U.S. Organ Procurement and Transplantation Network and the Scientific Registry of Transplant Recipients: Transplant Data Accessed January Sonnenberg FA, Beck JR. Markov models in medical decision making: a practical guide. Med Decis Making 1993;13: Siebert U, Alagoz O, Bayoumi AM, Jahn B, Owens DK, Cohen DJ, Kuntz KM; for ISPOR-SMDM Modeling Good Research Practices Task Force. State-transition modeling: a report of the ISPOR-SMDM Modeling Good Research Practices Task Force 3. Value Health 2012;15: Northup PG, Argo CK, Bakhru MR, Schmitt TM, Berg CL, Rosner MH. Pretransplant predictors of recovery of renal function after liver transplantation. Liver Transpl 2010; 16: Wolfe RA, Ashby VB, Milford EL, Ojo AO, Ettenger RE, Agodoa LY, et al. Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N Engl J Med 1999;341: Llovet JM, Fuster J, Bruix J. Intention-to-treat analysis of surgical treatment for early hepatocellular carcinoma: resection versus transplantation. Hepatology 1999;30: Jonas S, Bechstein WO, Steinm uller T, Herrmann M, Radke C, Berg T, et al. Vascular invasion and histopathologic grading determine outcome after liver transplantation for hepatocellular carcinoma in cirrhosis. Hepatology 2001;33: Mazzaferro V, Regalia E, Doci R, Andreola S, Pulvirenti A, Bozzetti F, et al. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med 1996;334: Hollingsworth JM, Hollenbeck BK, Englesbe MJ, DeMonner S, Krein SL. Operative mortality after renal transplantation does surgeon type matter? J Urol 2007; 177: Ojo AO, Held PJ, Port FK, Wolfe RA, Leichtman AB, Young EW, et al. Chronic renal failure after transplantation of a nonrenal organ. N Engl J Med 2003;349: Pham PT, Pham PC, Wilkinson AH. Renal function outcomes following liver transplantation and combined liver-kidney transplantation. Nat Clin Pract Nephrol 2007;3: Eason JD, Gonwa TA, Davis CL, Sung RS, Gerber D, Bloom RD. Proceedings of consensus conference on simultaneous liver kidney transplantation (SLK). Am J Transplant 2008;8: Schmitt TM, Kumer SC, Al-Osaimi A, Shah N, Argo CK, Berg C, et al. Combined liver-kidney and liver transplantation in patients with renal failure outcomes in the MELD era. Transpl Int 2009;22: Organ Procurement and Transplantation Network. III. Policy proposals. Accessed January 2014.
ORIGINAL ARTICLE. Eric F. Martin, 1 Jonathan Huang, 3 Qun Xiang, 2 John P. Klein, 2 Jasmohan Bajaj, 4 and Kia Saeian 1
 LIVER TRANSPLANTATION 18:914 929, 2012 ORIGINAL ARTICLE Recipient Survival and Graft Survival are Not Diminished by Simultaneous Liver-Kidney Transplantation: An Analysis of the United Network for Organ
LIVER TRANSPLANTATION 18:914 929, 2012 ORIGINAL ARTICLE Recipient Survival and Graft Survival are Not Diminished by Simultaneous Liver-Kidney Transplantation: An Analysis of the United Network for Organ
Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors?
 Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
2 Biostatistics and 3 Surgery, University of Michigan, Ann
 LIVER TRANSPLANTATION 22:71 79, 2016 ORIGINAL ARTICLE Propensity Score-Based Survival Benefit of Simultaneous Liver-Kidney Transplant Over Liver Transplant Alone for Recipients With Pretransplant Renal
LIVER TRANSPLANTATION 22:71 79, 2016 ORIGINAL ARTICLE Propensity Score-Based Survival Benefit of Simultaneous Liver-Kidney Transplant Over Liver Transplant Alone for Recipients With Pretransplant Renal
Outcome and natural course of renal dysfunction in liver transplant recipients with severely impaired kidney function prior to transplantation
 Original Article Outcome and natural course of renal dysfunction in liver transplant recipients with severely impaired kidney function prior to transplantation United European Gastroenterology Journal
Original Article Outcome and natural course of renal dysfunction in liver transplant recipients with severely impaired kidney function prior to transplantation United European Gastroenterology Journal
Trends in Organ Donation and Transplantation in the United States,
 American Journal of Transplantation 2010; 10 (Part 2): 961 972 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
American Journal of Transplantation 2010; 10 (Part 2): 961 972 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
MORTALITY IN PATIENTS ON DIALYSIS AND TRANSPLANT RECIPIENTS
 MORTALITY IN PATIENTS ON DIALYSIS AND TRANSPLANT RECIPIENTS COMPARISON OF MORTALITY IN ALL PATIENTS ON DIALYSIS, PATIENTS ON DIALYSIS AWAITING TRANSPLANTATION, AND RECIPIENTS OF A FIRST CADAVERIC TRANSPLANT
MORTALITY IN PATIENTS ON DIALYSIS AND TRANSPLANT RECIPIENTS COMPARISON OF MORTALITY IN ALL PATIENTS ON DIALYSIS, PATIENTS ON DIALYSIS AWAITING TRANSPLANTATION, AND RECIPIENTS OF A FIRST CADAVERIC TRANSPLANT
Simultaneous Liver Kidney Allocation Policy: A Proposal to Optimize Appropriate Utilization of Scarce Resources
 American Journal of Transplantation 2016; 16: 758 766 Wiley Periodicals Inc. Special Article Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
American Journal of Transplantation 2016; 16: 758 766 Wiley Periodicals Inc. Special Article Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
New Organ Allocation Policy in Liver Transplantation in the United States
 REVIEW New Organ Allocation Policy in Liver Transplantation in the United States David A. Goldberg, M.D., M.S.C.E.,*,, Richard Gilroy, and Michael Charlton, MD., F.R.C.P. The number of potential recipients
REVIEW New Organ Allocation Policy in Liver Transplantation in the United States David A. Goldberg, M.D., M.S.C.E.,*,, Richard Gilroy, and Michael Charlton, MD., F.R.C.P. The number of potential recipients
The pediatric end-stage liver disease (PELD) score
 Selection of Pediatric Candidates Under the PELD System Sue V. McDiarmid, 1 Robert M. Merion, 2 Dawn M. Dykstra, 2 and Ann M. Harper 3 Key Points 1. The PELD score accurately predicts the 3 month probability
Selection of Pediatric Candidates Under the PELD System Sue V. McDiarmid, 1 Robert M. Merion, 2 Dawn M. Dykstra, 2 and Ann M. Harper 3 Key Points 1. The PELD score accurately predicts the 3 month probability
Geographic Differences in Event Rates by Model for End-Stage Liver Disease Score
 American Journal of Transplantation 2006; 6: 2470 2475 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2006; 6: 2470 2475 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
Hepatorenal Syndrome: a Proposal for Kidney After Liver Transplantation (KALT)
 LIVER TRANSPLANTATION 13:838-843, 2007 ORIGINAL ARTICLE Hepatorenal Syndrome: a Proposal for Kidney After Liver Transplantation (KALT) Richard Ruiz, Yousri M. Barri, Linda W. Jennings, Srinath Chinnakotla,
LIVER TRANSPLANTATION 13:838-843, 2007 ORIGINAL ARTICLE Hepatorenal Syndrome: a Proposal for Kidney After Liver Transplantation (KALT) Richard Ruiz, Yousri M. Barri, Linda W. Jennings, Srinath Chinnakotla,
Removing Patients from the Liver Transplant Wait List: A Survey of US Liver Transplant Programs
 LIVER TRANSPLANTATION 14:303-307, 2008 ORIGINAL ARTICLE Removing Patients from the Liver Transplant Wait List: A Survey of US Liver Transplant Programs Kevin P. Charpentier 1 and Arun Mavanur 2 1 Rhode
LIVER TRANSPLANTATION 14:303-307, 2008 ORIGINAL ARTICLE Removing Patients from the Liver Transplant Wait List: A Survey of US Liver Transplant Programs Kevin P. Charpentier 1 and Arun Mavanur 2 1 Rhode
Differential Simultaneous Liver and Kidney Transplant Benefit Based on Severity of Liver Damage at the Time of Transplantation
 Differential Simultaneous Liver and Kidney Transplant Benefit Based on Severity of Liver Damage at the Time of Transplantation Item Type Article Authors Habib, Shahid; Khan, Khalid; Hsu, Chiu-Hsieh; Meister,
Differential Simultaneous Liver and Kidney Transplant Benefit Based on Severity of Liver Damage at the Time of Transplantation Item Type Article Authors Habib, Shahid; Khan, Khalid; Hsu, Chiu-Hsieh; Meister,
Clinical Questions of Combined Liver Kidney Transplantation
 Clinical Questions of Combined Liver Kidney Transplantation Miklos Z Molnar, MD, PhD, FEBTM, FERA, FASN Associate Professor of Medicine Methodist University Hospital, Transplant Institute Division of Transplantation,
Clinical Questions of Combined Liver Kidney Transplantation Miklos Z Molnar, MD, PhD, FEBTM, FERA, FASN Associate Professor of Medicine Methodist University Hospital, Transplant Institute Division of Transplantation,
Implications of the Statewide Sharing Variance on Kidney Transplantation Geographic Inequity and Allocation Efficiency
 Implications of the Statewide Sharing Variance on Kidney Transplantation Geographic Inequity and Allocation Efficiency Ashley E Davis 1, 2, Sanjay Mehrotra 1, 2, 3, Lisa McElroy 2,4, John J Friedewald
Implications of the Statewide Sharing Variance on Kidney Transplantation Geographic Inequity and Allocation Efficiency Ashley E Davis 1, 2, Sanjay Mehrotra 1, 2, 3, Lisa McElroy 2,4, John J Friedewald
Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
 Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
Effect of Body Mass Index on the Survival Benefit of Liver Transplantation
 LIVER TRANSPLANTATION 13:1678-1683, 2007 ORIGINAL ARTICLE Effect of Body Mass Index on the Survival Benefit of Liver Transplantation Shawn J. Pelletier, 1 Douglas E. Schaubel, 2,3 Guanghui Wei, 2 Michael
LIVER TRANSPLANTATION 13:1678-1683, 2007 ORIGINAL ARTICLE Effect of Body Mass Index on the Survival Benefit of Liver Transplantation Shawn J. Pelletier, 1 Douglas E. Schaubel, 2,3 Guanghui Wei, 2 Michael
Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation
 Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation July 26, 2006 Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation A paper prepared
Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation July 26, 2006 Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation A paper prepared
Historically, hepatocellular carcinoma (HCC)
 Delayed Hepatocellular Carcinoma Model for End-Stage Liver Disease Exception Score Improves Disparity in Access to Liver Transplant in the United States Julie K. Heimbach, 1 Ryutaro Hirose, 2 Peter G.
Delayed Hepatocellular Carcinoma Model for End-Stage Liver Disease Exception Score Improves Disparity in Access to Liver Transplant in the United States Julie K. Heimbach, 1 Ryutaro Hirose, 2 Peter G.
In the United States, the Model for End-Stage Liver. Re-weighting the Model for End-Stage Liver Disease Score Components
 GASTROENTEROLOGY 2008;135:1575 1581 Re-weighting the Model for End-Stage Liver Disease Score Components PRATIMA SHARMA,* DOUGLAS E. SCHAUBEL,, CAMELIA S. SIMA,, ROBERT M. MERION,, and ANNA S. F. LOK* *Division
GASTROENTEROLOGY 2008;135:1575 1581 Re-weighting the Model for End-Stage Liver Disease Score Components PRATIMA SHARMA,* DOUGLAS E. SCHAUBEL,, CAMELIA S. SIMA,, ROBERT M. MERION,, and ANNA S. F. LOK* *Division
Following the introduction of adult-to-adult living
 LIVER FAILURE/CIRRHOSIS/PORTAL HYPERTENSION Liver Transplant Recipient Survival Benefit with Living Donation in the Model for Endstage Liver Disease Allocation Era Carl L. Berg, 1 Robert M. Merion, 2 Tempie
LIVER FAILURE/CIRRHOSIS/PORTAL HYPERTENSION Liver Transplant Recipient Survival Benefit with Living Donation in the Model for Endstage Liver Disease Allocation Era Carl L. Berg, 1 Robert M. Merion, 2 Tempie
Access and Outcomes Among Minority Transplant Patients, , with a Focus on Determinants of Kidney Graft Survival
 American Journal of Transplantation 2010; 10 (Part 2): 1090 1107 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
American Journal of Transplantation 2010; 10 (Part 2): 1090 1107 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
What Is the Real Gain After Liver Transplantation?
 LIVER TRANSPLANTATION 15:S1-S5, 9 AASLD/ILTS SYLLABUS What Is the Real Gain After Liver Transplantation? James Neuberger Organ Donation and Transplantation, NHS Blood and Transplant, Bristol, United Kingdom;
LIVER TRANSPLANTATION 15:S1-S5, 9 AASLD/ILTS SYLLABUS What Is the Real Gain After Liver Transplantation? James Neuberger Organ Donation and Transplantation, NHS Blood and Transplant, Bristol, United Kingdom;
Serum Sodium and Survival Benefit of Liver Transplantation
 LIVER TRANSPLANTATION 21:308 313, 2015 ORIGINAL ARTICLE Serum Sodium and Survival Benefit of Liver Transplantation Pratima Sharma, 1 Douglas E. Schaubel, 2 Nathan P. Goodrich, 4 and Robert M. Merion 3,4
LIVER TRANSPLANTATION 21:308 313, 2015 ORIGINAL ARTICLE Serum Sodium and Survival Benefit of Liver Transplantation Pratima Sharma, 1 Douglas E. Schaubel, 2 Nathan P. Goodrich, 4 and Robert M. Merion 3,4
Prevalence and Outcomes of Multiple-Listing for Cadaveric Kidney and Liver Transplantation
 American Journal of Transplantation 24; 4: 94 1 Blackwell Munksgaard Copyright C Blackwell Munksgaard 23 doi: 1.146/j.16-6135.23.282.x Prevalence and Outcomes of Multiple-Listing for Cadaveric Kidney and
American Journal of Transplantation 24; 4: 94 1 Blackwell Munksgaard Copyright C Blackwell Munksgaard 23 doi: 1.146/j.16-6135.23.282.x Prevalence and Outcomes of Multiple-Listing for Cadaveric Kidney and
Improvements in immunosuppressive medication, organ
 JASN Express. Published on April 27, 2005 as doi: 10.1681/ASN.2004121092 Impact of Cadaveric Renal Transplantation on Survival in Patients Listed for Transplantation Gabriel C. Oniscu,* Helen Brown, John
JASN Express. Published on April 27, 2005 as doi: 10.1681/ASN.2004121092 Impact of Cadaveric Renal Transplantation on Survival in Patients Listed for Transplantation Gabriel C. Oniscu,* Helen Brown, John
Long-Term Renal Allograft Survival in the United States: A Critical Reappraisal
 American Journal of Transplantation 2011; 11: 450 462 Wiley Periodicals Inc. C 2010 The Authors Journal compilation C 2010 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2011; 11: 450 462 Wiley Periodicals Inc. C 2010 The Authors Journal compilation C 2010 The American Society of Transplantation and the American Society of Transplant
ORIGINAL ARTICLE. Simultaneous Liver-Kidney Transplantation for Adult Recipients With Irreversible End-Stage Renal Disease
 ORIGINAL ARTICLE Simultaneous Liver-Kidney Transplantation for Adult Recipients With Irreversible End-Stage Renal Disease E. Moreno-Gonzalez, MD, PhD, FACS(Hon); J. C. Meneu-Diaz, MD, PhD; I. Garcia, MD;
ORIGINAL ARTICLE Simultaneous Liver-Kidney Transplantation for Adult Recipients With Irreversible End-Stage Renal Disease E. Moreno-Gonzalez, MD, PhD, FACS(Hon); J. C. Meneu-Diaz, MD, PhD; I. Garcia, MD;
Liver Sharing and Organ Procurement Organization Performance
 LIVER TRANSPLANTATION 21:293 299, 2015 ORIGINAL ARTICLE Liver Sharing and Organ Procurement Organization Performance Sommer E. Gentry, 1,2 Eric K. H. Chow, 1 Allan Massie, 1,3 Xun Luo, 1 David Zaun, 4
LIVER TRANSPLANTATION 21:293 299, 2015 ORIGINAL ARTICLE Liver Sharing and Organ Procurement Organization Performance Sommer E. Gentry, 1,2 Eric K. H. Chow, 1 Allan Massie, 1,3 Xun Luo, 1 David Zaun, 4
Kidney vs. Liver: Where are We Really with Allocation in Kidney Transplantation?
 Kidney vs. Liver: Where are We Really with Allocation in Kidney Transplantation? Mark D. Stegall,, MD Chair, UNOS/OPTN Kidney Allocation Review Subcommittee Different Allocation Factors Liver Wait list
Kidney vs. Liver: Where are We Really with Allocation in Kidney Transplantation? Mark D. Stegall,, MD Chair, UNOS/OPTN Kidney Allocation Review Subcommittee Different Allocation Factors Liver Wait list
Wait List Management. John J. Friedewald, Darshika Chhabra, and Baris Ata. The US Transplant System. National Wait List
 Wait List Management John J. Friedewald, Darshika Chhabra, and Baris Ata 4 Abbreviations CDC Centers for Disease Control and Prevention CPRAs Calculated panel reactive antibodies DCD Donation after cardiac
Wait List Management John J. Friedewald, Darshika Chhabra, and Baris Ata 4 Abbreviations CDC Centers for Disease Control and Prevention CPRAs Calculated panel reactive antibodies DCD Donation after cardiac
Receiving a Kidney Transplant in the Ninth Decade of Life
 Trends Edmund in Transplant. Huang and 2011;5:121-7 Suphamai Bunnapradist: Receiving a Kidney Transplant in the Ninth Decade of Life Receiving a Kidney Transplant in the Ninth Decade of Life Edmund Huang
Trends Edmund in Transplant. Huang and 2011;5:121-7 Suphamai Bunnapradist: Receiving a Kidney Transplant in the Ninth Decade of Life Receiving a Kidney Transplant in the Ninth Decade of Life Edmund Huang
Kidney and Pancreas Transplantation in the United States,
 American Journal of Transplantation 2006; 6 (Part 2): 1153 1169 Blackwell Munksgaard No claim to original US government works Journal compilation C 2006 The American Society of Transplantation and the
American Journal of Transplantation 2006; 6 (Part 2): 1153 1169 Blackwell Munksgaard No claim to original US government works Journal compilation C 2006 The American Society of Transplantation and the
J Am Soc Nephrol 14: , 2003
 J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
ORIGINAL ARTICLE. Received December 4, 2013; accepted March 9, 2014.
 LIVER TRANSPLANTATION 20:728 735, 2014 ORIGINAL ARTICLE Inferior Long-Term Outcomes of Liver-Kidney Transplantation Using Donation After Cardiac Death Donors: Single-Center and Organ Procurement and Transplantation
LIVER TRANSPLANTATION 20:728 735, 2014 ORIGINAL ARTICLE Inferior Long-Term Outcomes of Liver-Kidney Transplantation Using Donation After Cardiac Death Donors: Single-Center and Organ Procurement and Transplantation
Should Liver Transplantation in Patients with Model for End-Stage Liver Disease Scores < 14 Be Avoided? A Decision Analysis Approach
 LIVER TRANSPLANTATION 15:242-254, 2009 ORIGINAL ARTICLE Should Liver Transplantation in Patients with Model for End-Stage Liver Disease Scores < 14 Be Avoided? A Decision Analysis Approach James D. Perkins,
LIVER TRANSPLANTATION 15:242-254, 2009 ORIGINAL ARTICLE Should Liver Transplantation in Patients with Model for End-Stage Liver Disease Scores < 14 Be Avoided? A Decision Analysis Approach James D. Perkins,
Repeat Organ Transplantation in the United States,
 American Journal of Transplantation 2007; 7 (Part 2): 1424 1433 Blackwell Munksgaard No claim to original US government works Journal compilation C 2007 The American Society of Transplantation and the
American Journal of Transplantation 2007; 7 (Part 2): 1424 1433 Blackwell Munksgaard No claim to original US government works Journal compilation C 2007 The American Society of Transplantation and the
Kidney and Pancreas Transplantation in the United States, : Access for Patients with Diabetes and End-Stage Renal Disease
 American Journal of Transplantation 29; 9 (Part 2): 894 96 Wiley Periodicals Inc. No claim to original US government works Journal compilation C 29 The American Society of Transplantation and the American
American Journal of Transplantation 29; 9 (Part 2): 894 96 Wiley Periodicals Inc. No claim to original US government works Journal compilation C 29 The American Society of Transplantation and the American
Scores in kidney transplantation: How can we use them?
 Scores in kidney transplantation: How can we use them? Actualités Néphrologiques 2017 M Hazzan (Lille France ) Contents Scores to estimate the quality of the graft Scores to estimate old candidates to
Scores in kidney transplantation: How can we use them? Actualités Néphrologiques 2017 M Hazzan (Lille France ) Contents Scores to estimate the quality of the graft Scores to estimate old candidates to
PATIENTS AND METHODS. Data Source
 LIVER TRANSPLANTATION 20:1045 1056, 2014 ORIGINAL ARTICLE Waiting Time Predicts Survival After Liver Transplantation for Hepatocellular Carcinoma: A Cohort Study Using the United Network for Organ Sharing
LIVER TRANSPLANTATION 20:1045 1056, 2014 ORIGINAL ARTICLE Waiting Time Predicts Survival After Liver Transplantation for Hepatocellular Carcinoma: A Cohort Study Using the United Network for Organ Sharing
Organ donation and transplantation trends in the United States, 2001
 American Journal of Transplantation 2003; 3 (Suppl. 4): 7 12 Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1601-2577 Organ donation and transplantation trends in the United States, 2001 Friedrich
American Journal of Transplantation 2003; 3 (Suppl. 4): 7 12 Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1601-2577 Organ donation and transplantation trends in the United States, 2001 Friedrich
Disparities in Liver Transplant Allocation: An Update on MELD Allocation System
 Disparities in Liver Transplant Allocation: An Update on MELD Allocation System Naudia L. Jonassaint, MD MHS Assistant Professor of Medicine and Surgery University of Pittsburgh School of Medicine Historical
Disparities in Liver Transplant Allocation: An Update on MELD Allocation System Naudia L. Jonassaint, MD MHS Assistant Professor of Medicine and Surgery University of Pittsburgh School of Medicine Historical
Kidney Allocation- Will it ever be fair? Peter G Stock MD, PhD UCSF Department of Surgery. Would you accept this offer?
 Kidney Allocation- Will it ever be fair? Peter G Stock MD, PhD UCSF Department of Surgery Question 1: A 19 y/o deceased donor kidney (O mismatch) from NYC is allocated to a 72 y/o highly sensitized caucasian
Kidney Allocation- Will it ever be fair? Peter G Stock MD, PhD UCSF Department of Surgery Question 1: A 19 y/o deceased donor kidney (O mismatch) from NYC is allocated to a 72 y/o highly sensitized caucasian
Association of Kidney Transplantation with Survival in Patients with Long Dialysis Exposure
 Article Association of Kidney Transplantation with Survival in Patients with Long Dialysis Exposure Caren Rose,* Jagbir Gill,* and John S. Gill* Abstract Background and objectives Evidence that kidney
Article Association of Kidney Transplantation with Survival in Patients with Long Dialysis Exposure Caren Rose,* Jagbir Gill,* and John S. Gill* Abstract Background and objectives Evidence that kidney
Impact of the Etiology of Acute Kidney Injury on Outcomes Following Liver Transplantation: Acute Tubular Necrosis Versus Hepatorenal Syndrome
 LIVER TRANSPLANTATION 18:539-548, 2012 ORIGINAL ARTICLE Impact of the Etiology of Acute Kidney Injury on Outcomes Following Liver Transplantation: Acute Tubular Necrosis Versus Hepatorenal Syndrome Mitra
LIVER TRANSPLANTATION 18:539-548, 2012 ORIGINAL ARTICLE Impact of the Etiology of Acute Kidney Injury on Outcomes Following Liver Transplantation: Acute Tubular Necrosis Versus Hepatorenal Syndrome Mitra
Concepts for Kidney Allocation
 ORGAN PROCUREMENT AND TRANSPLANTATION NETWORK Concepts for Kidney Allocation The Organ Procurement and Transplantation Network (OPTN) is seeking feedback regarding the use of two concepts in the allocation
ORGAN PROCUREMENT AND TRANSPLANTATION NETWORK Concepts for Kidney Allocation The Organ Procurement and Transplantation Network (OPTN) is seeking feedback regarding the use of two concepts in the allocation
Early Changes in Kidney Distribution under the New Allocation System
 Early Changes in Kidney Distribution under the New Allocation System Allan B. Massie,* Xun Luo,* Bonnie E. Lonze,* Niraj M. Desai,* Adam W. Bingaman, Matthew Cooper, and Dorry L. Segev* *Department of
Early Changes in Kidney Distribution under the New Allocation System Allan B. Massie,* Xun Luo,* Bonnie E. Lonze,* Niraj M. Desai,* Adam W. Bingaman, Matthew Cooper, and Dorry L. Segev* *Department of
Current status of kidney and pancreas transplantation in the United States,
 American Journal of Transplantation 25; 5 (Part 2): 94 915 Blackwell Munksgaard Blackwell Munksgaard 25 Current status of kidney and pancreas transplantation in the United States, 1994 23 Gabriel M. Danovitch
American Journal of Transplantation 25; 5 (Part 2): 94 915 Blackwell Munksgaard Blackwell Munksgaard 25 Current status of kidney and pancreas transplantation in the United States, 1994 23 Gabriel M. Danovitch
Table S1. Clinical outcomes of the acceptable mismatch allocation model.
 Table S1. Clinical outcomes of the acceptable mismatch allocation model. Recipient Age PRA Waiting Time (months) HLA mismatch (A/B/DR) HLAMatchmaker acceptable mismatch (years) (%) Actual Simulation Change
Table S1. Clinical outcomes of the acceptable mismatch allocation model. Recipient Age PRA Waiting Time (months) HLA mismatch (A/B/DR) HLAMatchmaker acceptable mismatch (years) (%) Actual Simulation Change
Predictors of renal recovery in patients with pre-orthotopic liver transplant (OLT) renal dysfunction
 Iglesias et al. BMC Nephrology 2013, 14:147 RESEARCH ARTICLE Open Access Predictors of renal recovery in patients with pre-orthotopic liver transplant (OLT) renal dysfunction Jose Iglesias 1,2,3*, Elliot
Iglesias et al. BMC Nephrology 2013, 14:147 RESEARCH ARTICLE Open Access Predictors of renal recovery in patients with pre-orthotopic liver transplant (OLT) renal dysfunction Jose Iglesias 1,2,3*, Elliot
Case 1 AND. Treatment of HCV: Pre- vs Post- Transplant. 58 yo male, ESRD/diabetic nephropathy, HD for 3 weeks
 Treatment of HCV: Pre- vs Post- Transplant Roy D. Bloom MD Professor of Medicine University of Pennsylvania Roy D. Bloom MD Professor of Medicine Medical Director, Kidney Transplant Program University
Treatment of HCV: Pre- vs Post- Transplant Roy D. Bloom MD Professor of Medicine University of Pennsylvania Roy D. Bloom MD Professor of Medicine Medical Director, Kidney Transplant Program University
Journal of the American College of Cardiology Vol. 60, No. 1, by the American College of Cardiology Foundation ISSN /$36.
 Journal of the American College of Cardiology Vol. 60, No. 1, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2012.02.031
Journal of the American College of Cardiology Vol. 60, No. 1, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2012.02.031
Organ allocation for liver transplantation: Is MELD the answer? North American experience
 Organ allocation for liver transplantation: Is MELD the answer? North American experience Douglas M. Heuman, MD Virginia Commonwealth University Richmond, VA, USA March 1998: US Department of Health and
Organ allocation for liver transplantation: Is MELD the answer? North American experience Douglas M. Heuman, MD Virginia Commonwealth University Richmond, VA, USA March 1998: US Department of Health and
Chapter 6: Transplantation
 Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Does Kidney Donor Risk Index implementation lead to the transplantation of more and higher-quality donor kidneys?
 Nephrol Dial Transplant (2017) 32: 1934 1938 doi: 10.1093/ndt/gfx257 Advance Access publication 21 August 2017 Does Kidney Donor Risk Index implementation lead to the transplantation of more and higher-quality
Nephrol Dial Transplant (2017) 32: 1934 1938 doi: 10.1093/ndt/gfx257 Advance Access publication 21 August 2017 Does Kidney Donor Risk Index implementation lead to the transplantation of more and higher-quality
journal of medicine The new england
 The new england journal of medicine established in 1812 february 5, 2004 vol. 350 no. 6 Effect of Changing the Priority for HLA Matching on the Rates and Outcomes of Kidney Transplantation in Minority
The new england journal of medicine established in 1812 february 5, 2004 vol. 350 no. 6 Effect of Changing the Priority for HLA Matching on the Rates and Outcomes of Kidney Transplantation in Minority
Increasing Trends in Transplantation of HCV-positive Livers into Uninfected Recipients
 Accepted Manuscript Increasing Trends in Transplantation of HCV-positive Livers into Uninfected Recipients George Cholankeril, MD, Andrew A. Li, MD, Brittany B. Dennis, PhD, Alice E. Toll, MS, Donghee
Accepted Manuscript Increasing Trends in Transplantation of HCV-positive Livers into Uninfected Recipients George Cholankeril, MD, Andrew A. Li, MD, Brittany B. Dennis, PhD, Alice E. Toll, MS, Donghee
CJASN epress. Published on September 2, 2010 as doi: /CJN
 CJASN epress. Published on September 2, 2010 as doi: 10.2215/CJN.02950410 An Emerging Population: Kidney Candidates Who Are Placed on the Waiting List after Liver, Heart, and Lung ation Titte R. Srinivas,*
CJASN epress. Published on September 2, 2010 as doi: 10.2215/CJN.02950410 An Emerging Population: Kidney Candidates Who Are Placed on the Waiting List after Liver, Heart, and Lung ation Titte R. Srinivas,*
An Economic Analysis of the Cost Effectiveness of Blood Gene Expression
 Research Article imedpub Journals http://www.imedpub.com Journal of Health & Medical Economics ISSN 2471-9927 DOI: 10.21767/2471-9927.100029 Abstract An Economic Analysis of the Cost Effectiveness of Blood
Research Article imedpub Journals http://www.imedpub.com Journal of Health & Medical Economics ISSN 2471-9927 DOI: 10.21767/2471-9927.100029 Abstract An Economic Analysis of the Cost Effectiveness of Blood
Nearly half of a million individuals in the United
 Access to Kidney Transplantation among the Elderly in the United States: A Glass Half Full, not Half Empty Elke S. Schaeffner,* Caren Rose, and John S. Gill *Division of Nephrology, Charité University
Access to Kidney Transplantation among the Elderly in the United States: A Glass Half Full, not Half Empty Elke S. Schaeffner,* Caren Rose, and John S. Gill *Division of Nephrology, Charité University
Kidney Transplant Outcomes In Elderly Patients. Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania
 Kidney Transplant Outcomes In Elderly Patients Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Case Discussion 70 year old Asian male, neuropsychiatrist, works full
Kidney Transplant Outcomes In Elderly Patients Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Case Discussion 70 year old Asian male, neuropsychiatrist, works full
ORIGINAL ARTICLE LIVER TRANSPLANTATION 17: , 2011
 LIVER TRANSPLANTATION 17:789-797, 2011 ORIGINAL ARTICLE Outcomes of Adult Living Donor Liver Transplantation: Comparison of the Adult-to-Adult Living Donor Liver Transplantation Cohort Study and the National
LIVER TRANSPLANTATION 17:789-797, 2011 ORIGINAL ARTICLE Outcomes of Adult Living Donor Liver Transplantation: Comparison of the Adult-to-Adult Living Donor Liver Transplantation Cohort Study and the National
Incidence of Rejection in Renal Transplant Surgery in the LVHN Population Leading to Graft Failure: 6 Year Review
 Incidence of Rejection in Renal Transplant Surgery in the LVHN Population Leading to Graft Failure: 6 Year Review Jessica Ludolph 1 Lynsey Biondi, MD 1,2 and Michael Moritz, MD 1,2 1 Department of Surgery,
Incidence of Rejection in Renal Transplant Surgery in the LVHN Population Leading to Graft Failure: 6 Year Review Jessica Ludolph 1 Lynsey Biondi, MD 1,2 and Michael Moritz, MD 1,2 1 Department of Surgery,
Influence of kidney offer acceptance behavior on metrics of allocation efficiency
 Accepted: 11 July 2017 DOI: 10.1111/ctr.13057 ORIGINAL ARTICLE Influence of kidney offer acceptance behavior on metrics of allocation efficiency Andrew Wey 1 Nicholas Salkowski 1 Bertram L. Kasiske 1,2
Accepted: 11 July 2017 DOI: 10.1111/ctr.13057 ORIGINAL ARTICLE Influence of kidney offer acceptance behavior on metrics of allocation efficiency Andrew Wey 1 Nicholas Salkowski 1 Bertram L. Kasiske 1,2
Clinical Study The Impact of the Introduction of MELD on the Dynamics of the Liver Transplantation Waiting List in São Paulo, Brazil
 Transplantation, Article ID 219789, 4 pages http://dx.doi.org/1.1155/214/219789 Clinical Study The Impact of the Introduction of MELD on the Dynamics of the Liver Transplantation Waiting List in São Paulo,
Transplantation, Article ID 219789, 4 pages http://dx.doi.org/1.1155/214/219789 Clinical Study The Impact of the Introduction of MELD on the Dynamics of the Liver Transplantation Waiting List in São Paulo,
Older Living Kidney Donors and Recipients. Charles Le University of Colorado 6/24/11
 Older Living Kidney Donors and Recipients Charles Le University of Colorado 6/24/11 Clinical Scenario HPI: 60 y/o healthy AAM with h/o CKD5 on HD x 2 yrs 2/2 HTN, was evaluated in transplant clinic for
Older Living Kidney Donors and Recipients Charles Le University of Colorado 6/24/11 Clinical Scenario HPI: 60 y/o healthy AAM with h/o CKD5 on HD x 2 yrs 2/2 HTN, was evaluated in transplant clinic for
Liver and intestine transplantation: summary analysis,
 American Journal of Transplantation 25; 5 (Part 2): 916 933 Blackwell Munksgaard Blackwell Munksgaard 25 Liver and intestine transplantation: summary analysis, 1994 23 Douglas W. Hanto a,, Thomas M. Fishbein
American Journal of Transplantation 25; 5 (Part 2): 916 933 Blackwell Munksgaard Blackwell Munksgaard 25 Liver and intestine transplantation: summary analysis, 1994 23 Douglas W. Hanto a,, Thomas M. Fishbein
Regulatory Realities Redefining Benefit of Lung Transplant in the Current Era
 Regulatory Realities Redefining Benefit of Lung Transplant in the Current Era Gundeep S Dhillon, MD, MPH Associate Professor of Medicine Medical Director, Lung & Heart-Lung Transplantation Program Stanford
Regulatory Realities Redefining Benefit of Lung Transplant in the Current Era Gundeep S Dhillon, MD, MPH Associate Professor of Medicine Medical Director, Lung & Heart-Lung Transplantation Program Stanford
Kidney transplantation is the treatment of choice
 SPECIAL ARTICLES Evidence-based Organ Allocation* Stefanos A. Zenios, PhD, Lawrence M. Wein, PhD, Glenn M. Chertow, MD, MPH BACKGROUND: There are not enough cadaveric kidneys to meet the demands of transplant
SPECIAL ARTICLES Evidence-based Organ Allocation* Stefanos A. Zenios, PhD, Lawrence M. Wein, PhD, Glenn M. Chertow, MD, MPH BACKGROUND: There are not enough cadaveric kidneys to meet the demands of transplant
KIDNEY TRANSPLANTATION IS THE
 ORIGINAL CONTRIBUTION Deceased-Donor Characteristics and the Survival Benefit of Kidney Transplantation Robert M. Merion, MD Valarie B. Ashby, MA Robert A. Wolfe, PhD Dale A. Distant, MD Tempie E. Hulbert-Shearon,
ORIGINAL CONTRIBUTION Deceased-Donor Characteristics and the Survival Benefit of Kidney Transplantation Robert M. Merion, MD Valarie B. Ashby, MA Robert A. Wolfe, PhD Dale A. Distant, MD Tempie E. Hulbert-Shearon,
Despite recent advances in the care of patients with
 Liver Transplantation for Hepatocellular Carcinoma: Lessons from the First Year Under the Model of End- Stage Liver Disease (MELD) Organ Allocation Policy Francis Y. Yao, 1,2 Nathan M. Bass, 1 Nancy L.
Liver Transplantation for Hepatocellular Carcinoma: Lessons from the First Year Under the Model of End- Stage Liver Disease (MELD) Organ Allocation Policy Francis Y. Yao, 1,2 Nathan M. Bass, 1 Nancy L.
Impact of the Center on Graft Failure After Liver Transplantation
 LIVER TRANSPLANTATION 19:957 964, 2013 ORIGINAL ARTICLE Impact of the Center on Graft Failure After Liver Transplantation Sumeet K. Asrani, 1,6 W. Ray Kim, 1,2 Erick B. Edwards, 7 Joseph J. Larson, 3 Gabriel
LIVER TRANSPLANTATION 19:957 964, 2013 ORIGINAL ARTICLE Impact of the Center on Graft Failure After Liver Transplantation Sumeet K. Asrani, 1,6 W. Ray Kim, 1,2 Erick B. Edwards, 7 Joseph J. Larson, 3 Gabriel
Waitlist Priority for Hepatocellular Carcinoma Beyond Milan Criteria: A Potentially Appropriate Decision Without a Structured Approach
 American Journal of Transplantation 2014; 14: 79 87 Wiley Periodicals Inc. C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12530
American Journal of Transplantation 2014; 14: 79 87 Wiley Periodicals Inc. C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12530
Should Pediatric Patients Wait for HLA-DR-Matched Renal Transplants?
 American Journal of Transplantation 2008; 8: 2056 2061 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2008; 8: 2056 2061 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
Reconsidering Liver Transplantation for HCC in a Era of Organ shortage
 Reconsidering Liver Transplantation for HCC in a Era of Organ shortage Professor Didier Samuel Centre Hépatobiliaire Inserm-Paris Sud Research Unit 1193 Departement Hospitalo Universitaire Hepatinov Hôpital
Reconsidering Liver Transplantation for HCC in a Era of Organ shortage Professor Didier Samuel Centre Hépatobiliaire Inserm-Paris Sud Research Unit 1193 Departement Hospitalo Universitaire Hepatinov Hôpital
Liver Transplantation: The End of the Road in Chronic Hepatitis C Infection
 University of Massachusetts Medical School escholarship@umms UMass Center for Clinical and Translational Science Research Retreat 2012 UMass Center for Clinical and Translational Science Research Retreat
University of Massachusetts Medical School escholarship@umms UMass Center for Clinical and Translational Science Research Retreat 2012 UMass Center for Clinical and Translational Science Research Retreat
Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
 Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Questions and Answers for Transplant Candidates about the Kidney Allocation System
 TA L K I N G A B O U T T R A N S P L A N TAT I O N Questions and Answers for Transplant Candidates about the Kidney Allocation System United Network for Organ Sharing (UNOS) is a non-profit charitable
TA L K I N G A B O U T T R A N S P L A N TAT I O N Questions and Answers for Transplant Candidates about the Kidney Allocation System United Network for Organ Sharing (UNOS) is a non-profit charitable
OPTN/SRTR 2016 Annual Data Report: Preface
 OPTN/SRTR 2016 Annual Data Report: Preface This Annual Data Report of the US Organ Procurement and Transplantation Network (OPTN) and the Scientific Registry of Transplant Recipients (SRTR) is the twenty-sixth
OPTN/SRTR 2016 Annual Data Report: Preface This Annual Data Report of the US Organ Procurement and Transplantation Network (OPTN) and the Scientific Registry of Transplant Recipients (SRTR) is the twenty-sixth
New National Allocation Policy for Deceased Donor Kidneys in the United States and Possible Effect on Patient Outcomes
 New National Allocation Policy for Deceased Donor Kidneys in the United States and Possible Effect on Patient Outcomes Ajay K. Israni,* Nicholas Salkowski,* Sally Gustafson,* Jon J. Snyder,* John J. Friedewald,
New National Allocation Policy for Deceased Donor Kidneys in the United States and Possible Effect on Patient Outcomes Ajay K. Israni,* Nicholas Salkowski,* Sally Gustafson,* Jon J. Snyder,* John J. Friedewald,
The New Kidney Allocation Policy: Implications for Your Patients and Your Practice
 The New Kidney Allocation Policy: Implications for Your Patients and Your Practice Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Explain
The New Kidney Allocation Policy: Implications for Your Patients and Your Practice Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Explain
Update on Kidney Allocation
 Update on Kidney Allocation 23rd Annual Conference Association for Multicultural Affairs in Transplantation Silas P. Norman, M.D., M.P.H. Associate Professor Division of Nephrology September 23, 2015 Disclosures
Update on Kidney Allocation 23rd Annual Conference Association for Multicultural Affairs in Transplantation Silas P. Norman, M.D., M.P.H. Associate Professor Division of Nephrology September 23, 2015 Disclosures
Simultaneous Pancreas Kidney Transplantation:
 Simultaneous Pancreas Kidney Transplantation: What is the added advantage, and for whom? Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney
Simultaneous Pancreas Kidney Transplantation: What is the added advantage, and for whom? Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney
The Kidney Allocation System Changed in a Substantive Way on December 5, Your Patients Have Been, and Will Be, Affected by These Changes
 The Kidney Allocation System Changed in a Substantive Way on December 5, 2014 Your Patients Have Been, and Will Be, Affected by These Changes 1 The New Kidney Allocation System Terms of Importance Pediatric
The Kidney Allocation System Changed in a Substantive Way on December 5, 2014 Your Patients Have Been, and Will Be, Affected by These Changes 1 The New Kidney Allocation System Terms of Importance Pediatric
Optimizing Patient Selection, Organ Allocation, and Outcomes in Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC)
 XXVI SETH Congress- 30 November 2017 Optimizing Patient Selection, Organ Allocation, and Outcomes in Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC) Neil Mehta, MD University of California,
XXVI SETH Congress- 30 November 2017 Optimizing Patient Selection, Organ Allocation, and Outcomes in Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC) Neil Mehta, MD University of California,
The principal goals of kidney transplantation are to improve
 Is Kidney Transplantation for Everyone? The Example of the Older Dialysis Patient Greg A. Knoll Division of Nephrology, Kidney Research Centre, and the Clinical Epidemiology Program, Ottawa Hospital Research
Is Kidney Transplantation for Everyone? The Example of the Older Dialysis Patient Greg A. Knoll Division of Nephrology, Kidney Research Centre, and the Clinical Epidemiology Program, Ottawa Hospital Research
Organ Allocation in Pennsylvania: Current concepts and future directions
 Organ Allocation in Pennsylvania: Current concepts and future directions David Goldberg, MD, MSCE Assistant Professor of Medicine and Epidemiology Medical Director of Living Donor Liver Transplantation
Organ Allocation in Pennsylvania: Current concepts and future directions David Goldberg, MD, MSCE Assistant Professor of Medicine and Epidemiology Medical Director of Living Donor Liver Transplantation
High mortality in orthotopic liver transplant recipients who require hemodialysis
 Clin Transplant 2011: 25: 213 221 DOI: 10.1111/j.1399-0012.2010.01238.x ª 2010 John Wiley & Sons A/S. High mortality in orthotopic liver transplant recipients who require hemodialysis Zand MS, Orloff MS,
Clin Transplant 2011: 25: 213 221 DOI: 10.1111/j.1399-0012.2010.01238.x ª 2010 John Wiley & Sons A/S. High mortality in orthotopic liver transplant recipients who require hemodialysis Zand MS, Orloff MS,
PRE-ASSESSMENT. Living Donor Liver Transplantation
 No. 24 Oct 2003 Before decides to undertake a health technology assessment, a pre-assessment of the literature is performed. Pre-assessments are based on a limited literature search; they are not extensive,
No. 24 Oct 2003 Before decides to undertake a health technology assessment, a pre-assessment of the literature is performed. Pre-assessments are based on a limited literature search; they are not extensive,
Survival Benefit-Based Deceased-Donor Liver Allocation
 American Journal of Transplantation 2009; 9 (Part 2): 970 981 Wiley Periodicals Inc. No claim to original US government works Journal compilation C 2009 The American Society of Transplantation and the
American Journal of Transplantation 2009; 9 (Part 2): 970 981 Wiley Periodicals Inc. No claim to original US government works Journal compilation C 2009 The American Society of Transplantation and the
Morbidity and Mortality After Living Kidney Donation, : Survey of United States Transplant Centers
 American Journal of Transplantation 2003; 3: 830 834 Copyright # Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1600-6135 Morbidity and Mortality After Living Kidney Donation, 1999 2001: Survey of
American Journal of Transplantation 2003; 3: 830 834 Copyright # Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1600-6135 Morbidity and Mortality After Living Kidney Donation, 1999 2001: Survey of
Effects of Allocating Livers for Transplantation Based on Model for End-stage Liver Disease-Sodium Scores on Patient Outcomes
 Accepted Manuscript Effects of Allocating Livers for Transplantation Based on Model for End-stage Liver Disease-Sodium Scores on Patient Outcomes Shunji Nagai, MD, PhD, Lucy C Chau, HBSc, MMI, Randolph
Accepted Manuscript Effects of Allocating Livers for Transplantation Based on Model for End-stage Liver Disease-Sodium Scores on Patient Outcomes Shunji Nagai, MD, PhD, Lucy C Chau, HBSc, MMI, Randolph
OHSU Digital Commons. Oregon Health & Science University. Barry Schlansky. Scholar Archive. July 2013
 Oregon Health & Science University OHSU Digital Commons Scholar Archive July 2013 Waitlist time predicts survival after liver transplantation for hepatocellular carcinoma : a cohort study in the United
Oregon Health & Science University OHSU Digital Commons Scholar Archive July 2013 Waitlist time predicts survival after liver transplantation for hepatocellular carcinoma : a cohort study in the United
Allogeneic Pancreas Transplant
 Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14, 05/15, 05/16,
Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14, 05/15, 05/16,
Glomerular Filtration Rate Equations for Liver-Kidney Transplantation in Patients With Cirrhosis: Validation of Current Recommendations
 Glomerular Filtration Rate Equations for Liver-Kidney Transplantation in Patients With Cirrhosis: Validation of Current Recommendations Claire Francoz, 1,2 Mitra K. Nadim, 3 Aurore Baron, 1,2 Dominique
Glomerular Filtration Rate Equations for Liver-Kidney Transplantation in Patients With Cirrhosis: Validation of Current Recommendations Claire Francoz, 1,2 Mitra K. Nadim, 3 Aurore Baron, 1,2 Dominique
Are two better than one?
 Are two better than one? Disclosures Ryutaro Hirose, MD Professor in Clinical Surgery University of California, San Francisco I have no relevant disclosures related to this presentation The PROBLEM There
Are two better than one? Disclosures Ryutaro Hirose, MD Professor in Clinical Surgery University of California, San Francisco I have no relevant disclosures related to this presentation The PROBLEM There
ORIGINAL ARTICLE. Sarah K. Alver, 1 Douglas J. Lorenz, 1 Michael R. Marvin, 2 and Guy N. Brock 1 SEE EDITORIAL ON PAGE 1321 ORIGINAL ARTICLE 1343
 ORIGINAL ARTICLE Projected Outcomes of 6-Month Delay in Exception Points Versus an Equivalent Model for End-Stage Liver Disease Score for Hepatocellular Carcinoma Liver Transplant Candidates Sarah K. Alver,
ORIGINAL ARTICLE Projected Outcomes of 6-Month Delay in Exception Points Versus an Equivalent Model for End-Stage Liver Disease Score for Hepatocellular Carcinoma Liver Transplant Candidates Sarah K. Alver,
Improving liver allocation: MELD and PELD
 American Journal of Transplantation 24; 4 (Suppl. 9): 114 131 Blackwell Munksgaard Blackwell Munksgaard 24 Improving liver allocation: MELD and PELD Richard B. Freeman Jr a,, Russell H. Wiesner b, John
American Journal of Transplantation 24; 4 (Suppl. 9): 114 131 Blackwell Munksgaard Blackwell Munksgaard 24 Improving liver allocation: MELD and PELD Richard B. Freeman Jr a,, Russell H. Wiesner b, John
Long-term Outcomes After Third Liver Transplant
 ArtıcLe Long-term Outcomes After Third Liver Transplant C. Burcin Taner, 1 Deniz Balci, 1 Darrin L. Willingham, 1 Andrew P. Keaveny, 1 Barry G. Rosser, 1 Juan M. Canabal, 1 Timothy S. J. Shine, 2 Denise
ArtıcLe Long-term Outcomes After Third Liver Transplant C. Burcin Taner, 1 Deniz Balci, 1 Darrin L. Willingham, 1 Andrew P. Keaveny, 1 Barry G. Rosser, 1 Juan M. Canabal, 1 Timothy S. J. Shine, 2 Denise
