PENETRATING KERATOPLASTY
|
|
|
- Emma Barnett
- 5 years ago
- Views:
Transcription
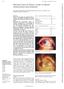
1 CLINICAL SCIENCES Risk Factors for Various Causes of Failure in Initial Corneal Grafts Marianne O. Price, PhD; Robert W. Thompson, Jr, MD; Francis W. Price, Jr, MD Objective: To determine the risk factors for specific causes of initial corneal graft failure. Methods: This study analyzed corneal graft survival rates in a longitudinal noncomparative case series of 3992 consecutive penetrating keratoplasties performed at a single large referral center. Regrafts (n=352) were excluded from the analysis of risk factors for initial graft failure. Data were collected retrospectively from August 1, 1982, through December 31, 1986, and prospectively from January 1, 1987, through August 31, Patients were examined preoperatively, at 1, 3, 6, 9, 12, 18, and 24 months posttransplantation, and annually thereafter. Potential risk factors were evaluated individually by Kaplan-Meier survival analysis. Cox proportional hazards regression modeling was then used to investigate the impact of each independent variable, adjusted for the confounding influence of the other independent variables. Results: The use of topical glaucoma medications was a significant risk factor for corneal graft failure by 3 major causes: rejection, endothelial decompensation without a documented immunologic reaction, and ocular surface disease. Deep stromal vascularization was an independent risk factor for rejection failure. Diabetes mellitus, peripheral anterior synechiae, recipient race, and small trephination size were significant risk factors for endothelial failure. Conclusion: Independent risk factors differentially impact specific causes of corneal graft failure. Arch Ophthalmol. 2003;121: From the Cornea Research Foundation of America, Indianapolis, Ind (Dr M. O. Price); the Kansas City Eye Clinic, Overland Park, Kan (Dr Thompson); and Corneal Consultants of Indiana, Indianapolis (Dr F. W. Price). The authors have no relevant financial interest in this article. PENETRATING KERATOPLASTY (PKP) is one of the most successful and frequently performed transplantation procedures. Recent long-term studies 1-3 report 10-year corneal graft survival rates of 59% to 80%. Because more than corneal transplantations are performed each year, 4 the cumulative number of graft failures is significant despite the relatively high survival rates. It is particularly important to prevent initial grafts from failing, because survival rates for regrafts are greatly reduced. 2,3,5-8 The identification of risk factors for initial graft failure can help surgeons determine which eyes are at increased risk, so that those eyes can be more aggressively treated. Graft failure can be broadly defined as any irreversible change in the graft preventing recovery of useful vision. Risk factors for graft failure in general include prior graft failure in that eye, glaucoma, 1,3,5 peripheral anterior synechiae, 3,5,6 and corneal vascularization. 2,3,5-8 However, graft failure represents a common end point that can be reached by distinctly different pathways. Among the most frequent causes of graft failure are immunologic allograft rejection, endothelial decompensation in the absence of any documented immunologic reaction episodes, ocular surface disease, glaucoma, and astigmatism. 3,9,10 This study determines how different risk factors impact various failure causes in initial corneal grafts, because a better understanding of causes and effects could ultimately lead to improved treatment methods. METHODS This study reports findings from a longitudinal noncomparative case series of 3992 consecutive PKPs performed by surgeons at a tertiary care referral center, Corneal Consultants of Indiana, between August 1, 1982, and August 31, Regrafts (n=352) were excluded from the analysis. Data were collected retrospectively through December 31, 1986, and prospectively thereafter. Each patient provided written informed consent. Surgical technique and postoperative care were as previously described. 11 All patients underwent a complete ophthalmic examination before PKP, and medical history was documented. Defined postoperative examinations 1087
2 were performed at 1, 3, 6, 9, 12, 18, and 24 months and annually thereafter. DETERMINATION OF OUTCOMES Grafts that did not clear within 2 weeks of transplantation were considered primary donor failures. These events were rare, occurring in only 21 eyes (0.5%). Because primary donor failures were caused by difficulties with donor tissue survivability unrelated to recipient characteristics, when these grafts were repeated, the repeat grafts were entered into the database as initial grafts for outcome analysis. Any graft that initially cleared but later irreversibly changed, preventing recovery of useful vision, was counted as a graft failure. The time of failure was defined as the first postoperative examination that the patient was seen with a failed graft. An eye was dropped from further analysis when graft failure was recorded. An eye was considered lost to follow-up when a patient had not been examined for more than 1 year from the first missed postoperative examination period. There were 2667 initial grafts with 2 or more years of follow-up and 1250 with 5 or more years of follow-up. Grafts that failed because of endothelial decompensation were classified as failures by rejection if there was any postoperative history of possible allograft rejection, such as ciliary flush with keratic precipitates on the donor endothelium, definite rejection episodes such as an endothelial rejection line, or signs of stromal or epithelial rejection. A graft failure was classified as a rejection failure even if the endothelial failure occurred months or years after any immunologic reactions. Grafts that failed because of endothelial decompensation in the absence of any documented immunologic reactions were classified as endothelial failure. Grafts that failed as a result of ocular surface-related problems, such as melts, ulcers, or exposure keratitis, were classified as surface disease failures. Less prevalent failure modes, such as astigmatism, did not result in a sufficient number of failures to perform separate risk factor analyses. A history of preoperative glaucoma was determined by the patient s use of medications to reduce intraocular pressure. Stromal vascularization was defined as vascularization of the middle or deep stroma, extending into the area of trephination at surgery. Eyes first seen with a diagnosis of interstitial keratitis were only classified as positive for stromal vascularization if clinically significant blood flow was present. STATISTICAL ANALYSIS To adjust for varying lengths of follow-up, survival analysis was used to individually evaluate possible prognostic risk factors for graftfailure. SurvivalcurvesweregeneratedusingtheKaplan-Meier product limit method, and differences between subgroups were assessed using the log-rank test. Relative risks and adjusted survival probabilities were estimated using the Cox proportional hazards regression model with forward and backward selection algorithms. Multivariate models were separately determined for any cause of graft failure and for specific causes of graft failure. Whenever many characteristics are analyzed, there is an increased risk of reporting a type I error (a false-positive error). P.05 was consideredsignificant. However, thegreatestconfidencecanbeplaced inthoseriskfactorshavingthelowestpvalues. Thestatisticalpower to detect risk factors increases with sample size, and was higher for the analysis of all graft failures (n=272) compared with the separate analyses of the endothelial failures (n=82), rejection failures (n=76), and surface complication failures (n=49). RESULTS The patient cohort was 63.8% female, and the mean patient age was 67 years (range, 1-98 years). The mean±sd follow-up was 43±34 months (range, 1 month to 15 years). The primary preoperative diagnoses for the 3640 eyes undergoing an initial PKP were as follows: Diagnosis No. (%) of Eyes Pseudophakic bullous keratopathy 1288 (35.4) Fuchs dystrophy 908 (24.9) Keratoconus 449 (12.3) Aphakic bullous keratopathy 311 (8.5) Corneal scars or ulcers 337 (9.3) Interstitial keratitis 97 (2.7) Herpetic keratitis 77 (2.1) Other 173 (4.8) As described elsewhere, 12 overall graft survival rates for this patient cohort varied depending on the preoperative diagnosis, with patients with keratoconus and Fuchs dystrophy having the highest graft survival rates, 97.4% and 96.9%, respectively, at 5 years. Graft survival rates were also favorable, although somewhat lower, for patients with other preoperative diagnoses (88.1% for those with pseudophakic bullous keratopathy, 83.2% for those with aphakic bullous keratopathy, and 80.2% for those with corneal scars or ulcers) at 5 years. When the initial diagnoses were grouped into 2 categories, lower risk (keratoconus and Fuchs dystrophy) and higher risk (all others), the relative risk of graft failure was 3.5 (95% confidence interval, ) times greater for the higher-risk group (P.001). Graft failures occurred in 272 (7.5%) of 3640 initial grafts. Rejection, endothelial decompensation without an immunologic reaction, and ocular surface disease were the primary causes of graft failure, accounting for 27.9%, 30.1%, and 18.0% of the failed grafts, respectively. The remaining graft failures resulted from astigmatism (4.8%), glaucoma (2.9%), and other less frequent causes (together, 16.2%). Characteristics considered potential risk factors for graft failure were first individually evaluated using Kaplan- Meier survival analysis. Survival analysis adjusts for different lengths of follow-up by evaluating all time points to determine if there is a significant difference between groups. Recipient characteristics having a significant effect on initial graft failure rates are shown in Table 1, along with comparative failure rates at the 5-year point. Separate survival analyses were performed to identify risk factors for the major failure causes The risk factors most strongly associated with overall graft failure were a history of preoperative glaucoma medication use, deep stromal vascularization, peripheral anterior synechiae, recipient race, and unusually small or large recipient bed sizes (Table 1). A small recipient horizontal corneal diameter and diabetes mellitus were also significant risk factors for graft failure by any cause. Most of the identified risk factors were associated with only 1 or 2 of the major categories of graft failure, with the exception that use of a glaucoma medication was a risk factor for all 3. The presence of peripheral anterior synechiae or being African American increased the risk of failure by rejection or endothelial decompensation, but not by ocular surface disease. Deep stromal vascularization specifically increased the risk of failure due to rejection. Diabetes mellitus specifically increased the risk of endothelial decompensation, as did a recipient horizontal corneal diameter of mm or less. 1088
3 Table 1. Recipient Risk Factors That Impacted Initial Graft Outcomes, as Determined by Kaplan-Meier Survival Analysis 5-y Graft Failure Rate, % Risk Factor No. of Grafts All Failures Rejection Failures Endothelial Failures Surface Failures Preoperative glaucoma medication No Yes P value* NA Peripheral anterior synechiae No Yes P value* NA Deep stromal vascularization No Yes P value* NA Diabetes mellitus No Yes P value* NA Race White African American P value* NA Horizontal corneal diameter, mm P value* NA Recipient bed size, mm P value* NA Abbreviation: NA, data not applicable. *Based on the log-rank statistic. The choice of recipient and donor tissue trephine sizes was influenced by recipient corneal diameter size, vascularization, and scarring. Overall, variation in recipient horizontal corneal diameter size accounted for 49% of the variance in recipient trephine size. Small recipient beds ( 7 mm) were associated with an increased risk of endothelial failure and rejection failure (Table 1). Results were similar for unusually small donor button sizes ( 7.25 mm) (data not shown). The sizes of the recipient bed and donor button were highly correlated (R 2 =0.89), because it was routine practice to use a donor trephine size of approximately 0.25 mm larger than the recipient trephine size for all initial diagnoses other than keratoconus. For keratoconus, the donor button was often sized the same as, or slightly smaller than, the recipient bed. An unusually large recipient bed size ( 8.5 mm) was associated with an increased risk of failure by rejection or ocular surface disease (Table 1). However, only 23 grafts had a recipient bed exceeding 8.5 mm. Thirteen were placed to treat large cones in eyes with keratoconus, and none of those 13 grafts failed during the study. In contrast, the remaining 10 grafts were primarily placed to treat large corneal scars and ulcers, and 5 of those 10 failed. This was well in excess of the 13.1% graft failure rate for any eyes first seen with corneal scars or ulcers (P.001). These results indicate that the outcomes for grafts exceeding 8.5 mm primarily depended on the underlying corneal condition requiring the use of an unusually large graft. The surgeon s choice of suture method was influenced by the characteristics of the recipient eye, and interrupted sutures were often selected for high-risk recipients. For example, interrupted sutures were used in 83.1% of the eyes with deep stromal vascularization, compared with only 27.1% of the eyes without such vascularization, a significant difference (P.001). Interrupted sutures were also preferentially selected for small ( mm) recipient corneal diameters (P.001). Grafts secured with interrupted sutures were more likely to fail by all 3 major causes compared with grafts secured with running or combination sutures (P.002). However, this was likely because of underlying recipient risk factors, rather than a direct effect of suture method, because grafts secured with interrupted sutures were no more likely to fail than those secured with running sutures in eyes with keratoconus, which are generally low-risk eyes (P=.22). 3,9 Recipient characteristics that did not significantly influence graft failure rates included sex, age, and hy- 1089
4 Table 2. Recipient Characteristics That Did Not Affect Initial Graft Outcomes* Characteristic No. of Grafts 5-y Graft Failure Rate, % Sex Male Female Age, y Hypertension No Yes Secondary IOL with PKP No Yes Corneal diameter recipient bed, mm P Value Abbreviations: IOL, intraocular lens; PKP, penetrating keratoplasty. *Characteristics were evaluated by Kaplan-Meier survival analysis, and P values were determined by the log-rank statistic. pertension (Table 2). The placement of an intraocular lens secondary to PKP had no impact on graft survival rate, nor did the size difference between the recipient horizontal corneal diameter and the recipient bed (Table 2). No donor corneal characteristics had a significant effect on graft outcome. Characteristics that were analyzed included donor age (mean, 39 years; SD, 16 years) (P=.16), sex (70.2% male) (P=.65), death to enucleation time (mean, 5.7 hours; SD, 3.7 hours) (P=.60), time to cornea preservation (mean, 6.4 hours; SD, 4.3 hours) (P=.28), time to use (mean, 85 hours; SD, 33 hours) (P=.69), corneal storage solution (McCarey-Kaufman, K- Sol, DexSol, Optisol, or corneal storage medium) (P=.94), and cause of death (58.2% medical, 20.1% violence, and 21.7% other trauma or unintentional injuries) (P=.59). (Kaplan-Meier survival analysis and the log-rank statistic were used for continuous variables, and a Cox proportional hazards regression analysis was used for categorical variables.) Donor age was not randomized in this study, because it was routine practice to use donor tissue younger than the recipient whenever possible. The potential risk factors identified by survival analysis (Table 1) were correlated to some extent. For example, eyes with peripheral anterior synechiae were more likely than other eyes to also have glaucoma (P.001). To investigate the impact of each independent variable, adjusted for the confounding influence of the other independent variables, multivariate Cox proportional hazards regression models were analyzed. Five significant risk factors were included in the final regression model for failure by any cause (Table 3). Patients classified as having glaucoma before PKP, based on their use of glaucoma medications, were twice as likely to experience graft failure as patients who did not have preoperative glaucoma. The presence of peripheral anterior synechiae or deep stromal vascularization each independently increased the relative risk of overall graft failure by 2-fold. African Americans were twice as likely to experience graft failure compared with white persons or persons of other races. In addition, recipient bed sizes of 7 mm or less were at almost a 3-fold higher risk of graft failure compared with larger bed sizes. The final regression model for failure by immunologic rejection contained 3 independent risk factors (Table 3). Eyes with preoperative glaucoma were at a 2-fold increased risk of failure due to rejection compared with eyes without preoperative glaucoma (Table 3). Eyes with deep stromal vascularization were almost 3 times more likely to experience rejection failure compared with eyes without such vascularization. In addition, the risk of rejection failure was 3-fold higher in eyes with unusually small recipient beds ( 7 mm) compared with those with larger recipient beds ( 7 mm). Five independent risk factors were identified in the final model of failure by endothelial decompensation without an immunologic reaction (Table 3). The use of glaucoma medications increased the risk of endothelial failure by almost 2-fold. Peripheral anterior synechiae conferred a 3-fold increased risk of endothelial failure. The risk of endothelial failure was twice as high in patients with diabetes mellitus as in patients without diabetes mellitus. African Americans had a 3.6-fold increased relative risk of endothelial decompensation compared with white persons and others. Unusually small recipient beds ( 7 mm) were associated with an almost 5-fold increased relative risk of endothelial decompensation compared with recipient beds exceeding 7 mm. The only significant risk factor for ocular surfacerelated failures was use of glaucoma medications, which conferred a 3-fold increased risk (Table 3). COMMENT The purpose of this study was to identify the risk factors associated with distinct causes of graft failure in initial corneal transplantations. We individually examined risk factors for rejection, endothelial decompensation without evidence of rejection, and ocular surface disease, because these were the most prevalent causes in the patient cohort and together accounted for 76.1% of the initial graft failures. We believe it is particularly important to anticipate and prevent failure of initial grafts, because regrafts have a much poorer prognosis. Although prior studies 5,10,13 have identified risk factors for rejection failures, to our knowledge, this is the first study to determine risk factors not only for rejection but also for endothelial decompensation and ocular surface-related failure causes. Patients using glaucoma medications were at an increased risk of graft failure by all 3 major causes, even after adjusting for other confounding risk factors (Table 3). The incidence of preoperative glaucoma was 15%, comparable to published rates of 9% to 28%. 1,14,15 Overall, grafts in eyes with preoperative glaucoma were twice as likely to fail as those in eyes that were not being treated for glaucoma, supporting findings in other studies. 1,
5 Table 3. Adjusted RRs for Factors Impacting Various Causes of Initial Graft Failure* Failure Type Risk Factor Any Type Rejection Endothelial Surface Preoperative glaucoma medication RR (95% CI) 2.1 ( ) 2.2 ( ) 1.8 ( ) 2.8 ( ) P value Peripheral anterior synechiae RR (95% CI) 2.0 ( ) 1.7 ( ) 2.9 ( ) 1.1 ( ) P value Deep stromal vascularization RR (95% CI) 1.9 ( ) 2.7 ( ) 1.1 ( ) 1.6 ( ) P value Diabetes mellitus RR (95% CI) 1.3 ( ) 1.3 ( ) 2.3 ( ) 1.2 ( ) P value Recipient race RR (95% CI) 2.4 ( ) 2.2 ( ) 3.6 ( ) 0.6 ( ) P value Recipient bed 7mm RR (95% CI) 2.6 ( ) 3.2 ( ) 4.8 ( ) 2.0 ( ) P value Abbreviations: CI, confidence interval; RR, relative risk. *The RRs and P values were determined by Cox proportional hazards regression modeling. P.05 was considered significant. Preoperative glaucoma was an independent predictor of endothelial failure, consistent with clinical observations by one of us (F.W.P.) that a high intraocular pressure can lead to rapid endothelial decompensation, perhaps through direct damage to endothelial cells. 16 Interestingly, patients being treated with glaucoma medications were also at a significantly increased risk for rejection and ocular surface-related failures. Increased leukocyte and fibrocyte accumulation in conjunctival and limbal tissue has been reported secondary to the use of topical glaucoma medications. 17,18 This inflammatory cell response may increase the likelihood of recipient immunologic recognition of donor tissue, leading to immunologic graft rejection. The inflammatory reaction seems to be primarily related to the preservatives, such as benzalkonium chloride, rather than the medications themselves. 18,19 Benzalkonium chloride has cumulative toxic effects on the corneal-conjunctival surface, and its detergent properties can also adversely alter tear film fluidity and breakup time. 20 This may be particularly problematic following PKP, because the donor corneas are neurotrophic and, therefore, more susceptible to exposure and toxicity. Therefore, in patients with glaucoma, transplantation surgeons should consider the use of glaucoma medications with noninflammatory preservatives (such as sodium chlorite [Purite]), the use of noncorticosteroid immunosuppressants after PKP to minimize corticosteroid-responsive increases in intraocular pressure, or earlier intervention with surgical alternatives for intraocular pressure control. In the United States, there is only 1 approved topical glaucoma medication using sodium chlorite, brimonidine tartrate (Alphagan-P; Allergan, Inc, Irvine, Calif). The most potent topical antiglaucoma medications are the prostamides, 21 but they have inflammatory preservatives, and this group of drugs seems to have an inherent propensity to cause increased inflammation in some eyes. None of the eyes in our patient cohort received topical prostamides, and further studies will need to be performed to evaluate their effect on graft survival. Further studies comparing the effect of earlier surgical intervention with long-term use of glaucoma medications on corneal graft survival are also needed. Increased graft failure rates have been reported following certain types of glaucoma surgery, particularly with the use of glaucoma setons. 22,23 Flat anterior chambers, which can directly damage the endothelium of the graft, often develop following standard filtration surgery with trabeculectomy; this procedure is also prone to complications from hypotony, such as suprachoroidal hemorrhages and cataract progression. Newer nonpenetrating glaucoma filtration techniques have a lower complication rate compared with trabeculectomy. 24,25 Because of the reduced incidence of complications, such as flat anterior chambers and suprachoroidal hemorrhages, nonpenetrating filtration surgical procedures may provide a valuable alternative to multiple long-term topical medications for intraocular pressure control after PKP. Peripheral anterior synechiae were associated with an increased risk of rejection failures and endothelial failures without rejection episodes. Anterior synechiae place the donor endothelium in closer proximity to blood vessels that may increase the risk of rejection. 16 Furthermore, anterior synechiae may accelerate loss of endothelial cells through either direct traction or indirect increased anterior segment inflammation. 16 Our findings support studies showing that peripheral anterior synechiae can increase the overall graft failure rate 6,13,26 and the rejection failure rate. 13,27 Deep stromal vascularization increased the risk of failure due to rejection by 2.7-fold (P.001), but had no impact on rates of ocular surface-related failures or endothelial failures without an immunologic reaction. Corneal vascularization has been defined in different ways in various studies. Our results support the concept that 1091
6 vascularization can facilitate an immunologic response against the corneal graft. 14,27-29 Diabetes mellitus was specifically a risk factor for endothelial failure. Although diabetes mellitus is not typically investigated as a risk factor for corneal graft failure, it is associated with excess glycosylation of blood proteins, impaired circulation, breakdown of the blood/aqueous barrier, and deterioration of various organ systems. African Americans comprised a relatively small minority of the patient cohort, reflecting the racial distribution in Indiana during the study period. 30 African Americans experienced a 3- to 4-fold higher risk of endothelial failure, compared with white persons and others, despite similar rates of follow-up. Another study 13 did not find recipient race to be a risk factor for graft failure, perhaps reflecting differences in patient demographics. Recipient beds of 7 mm or smaller were used infrequently and only as necessary to accommodate a small recipient corneal diameter, scarring, or vascularization. Grafts with small recipient beds ( 7 mm) were at almost a 5-fold higher risk of endothelial failure compared with those with larger beds (Table 3). Smaller grafts may be more prone to endothelial failure because they have a smaller pool of intact endothelial cells to maintain corneal clarity. An unusually small recipient bed size was also associated with an increased risk of rejection failure, consistent with findings in high-risk eyes in the Collaborative Corneal Transplantation Studies. 13 Recipient bed sizes of less than 7 mm were likewise associated with an increased risk of overall graft failure in the large Australian Corneal Graft Registry. 3 Neither recipient age nor sex affected graft outcomes in this large cohort of initial grafts. There are conflicting reports 1,3,6-8,13,28,29,31-33 in the literature regarding these characteristics. None of the donor corneal characteristics analyzed in this study had an impact on graft outcome. This is generally consistent with the consensus of other studies. 3,13,14,34 Donor age was not randomized in our patient cohort, because it was routine practice to use donor tissue younger than the recipient whenever possible. The effect of donor age is under further investigation in the prospective randomized Cornea Donor Study. 35 In conclusion, independent risk factors were differentially associated with specific causes of initial corneal graft failure. The use of topical glaucoma medications was a significant risk factor for corneal graft failure by 3 major causes: rejection, endothelial decompensation without a documented immunologic reaction, and ocular surface disease. Deep stromal vascularization was an independent risk factor for rejection failures. Diabetes mellitus, peripheral anterior synechiae, recipient race, and small trephination size were significant risk factors for endothelial failure in the absence of an immunologic reaction. Submitted for publication September 5, 2002; final revision received March 7, 2003; accepted March 25, This study was supported by a grant from the Indiana Lion s Eye Bank, Indianapolis. We thank Barry Katz, PhD, Indiana University, Indianapolis, for his assistance in performing the analyses for this study. Corresponding author and reprints: Francis W. Price, Jr, MD, Corneal Consultants of Indiana, 9002 N Meridian St, Suite 207, Indianapolis, IN ( REFERENCES 1. Ing JJ, Ing HH, Nelson LR, et al. Ten-year postoperative results of penetrating keratoplasty. Ophthalmology. 1998;105: Inoue K, Amano S, Oshika T, et al. A 10-year review of penetrating keratoplasty. Jpn J Ophthalmol. 2000;44: Williams KA, Muehlberg SM, Bartlett CM, et al. The Australian Corneal Graft Registry: 1999 Report. Adelaide, Australia: Snap Printing; Frequently asked questions. Eye Bank Association of America Web site. Available at: Accessibility verified March Price FW Jr, Whitson WE, Johns S, et al. Risk factors for corneal graft failure. J Refract Surg. 1996;12: Sit M, Weisbrod DJ, Naor J, et al. Corneal graft outcome study. Cornea. 2001; 20: Vail A, Gore SM, Bradley BA, Easty DL, Rogers CA, for the Corneal Transplant Follow-up Study Collaborators. Corneal graft survival and visual outcome: a multicenter study. Ophthalmology. 1994;101: Dandona L, Naduvilath TJ, Janarthanan M, et al. Survival analysis and visual outcome in a large series of corneal transplants in India. Br J Ophthalmol. 1997; 81: Price FW Jr, Whitson WE, Collins KS, et al. Five-year corneal graft survival: a large, single-center patient cohort. Arch Ophthalmol. 1993;111: Dandona L, Naduvilath TJ, Janarthanan M, et al. Causes of corneal graft failure in India. Indian J Ophthalmol. 1998;46: Price FW Jr, Whitson WE, Marks RG. Graft survival in four common groups of patients undergoing penetrating keratoplasty. Ophthalmology. 1991;98: Thompson RW Jr, Price MO, Bowers PJ, et al. Long-term graft survival following penetrating keratoplasty. Ophthalmology. In press. 13. Maguire MG, Stark WJ, Gottsch JD, et al, for the Collaborative Corneal Transplantation Studies Research Group. Risk factors for corneal graft failure and rejection in the collaborative corneal transplantation studies. Ophthalmology. 1994; 101: Boisjoly HM, Tourigny R, Bazin R, et al. Risk factors of corneal graft failure. Ophthalmology. 1993;100: Chipman ML, Slomovic AS, Rootman D, et al. Changing risk for early transplant failure. Can J Ophthalmol. 1993;28: Wilson SE, Kaufman HE. Graft failure after penetrating keratoplasty. Surv Ophthalmol. 1990;34: Sherwood MB, Grierson I, Millar L, et al. Long-term morphologic effects of antiglaucoma drugs on the conjunctiva and Tenon s capsule in glaucomatous patients. Ophthalmology. 1989;96: Baudouin C, Pisella PJ, Fillacier K, et al. Ocular surface inflammatory changes induced by topical antiglaucoma drugs. Ophthalmology. 1999;106: Burstein NL. Corneal cytotoxicity of topically applied drugs, vehicles and preservatives. Surv Ophthalmol. 1980;25: Baudouin C. Side effects of antiglaucomatous drugs on the ocular surface. Curr Opin Ophthalmol. 1996;7: Cantor LB. Bimatoprost. Expert Opin Investig Drugs. 2001;10: Beebe WE, Starita RJ, Fellman RL, et al. The use of Molteno implant and anterior chamber tube shunt to encircling band for the treatment of glaucoma in keratoplasty patients. Ophthalmology. 1990;97: McDonnell PJ, Robin JB, Schanzlin DJ, et al. Molteno implant for control of glaucoma in eyes after penetrating keratoplasty. Ophthalmology. 1988;95: Lachkar Y, Hamard P. Nonpenetrating filtering surgery. Curr Opin Ophthalmol. 2002;13: Hamard P, Lachkar Y. Non penetrating filtering surgery: evolution and results [in French]. J Fr Ophtalmol. 2002;25: Tragakis MP, Brown SI. The significance of anterior synechiae after corneal transplantation. Am J Ophthalmol. 1972;74: Arentsen JJ. Corneal transplant allograft reaction: possible predisposing factors. Trans Am Ophthalmol Soc. 1983;81: Volker-Dieben HJ, D Amaro J, Kok van Alphen CC. Hierarchy of prognostic factors for corneal allograft survival. Aust N Z J Ophthalmol. 1987;15: Hill JC. The relative importance of risk factors used to define high-risk keratoplasty. Ger J Ophthalmol. 1996;5: The World Almanac and Book of Facts Manwah, NJ: World Almanac Education Group; Musch DC, Meyer RF. Risk of endothelial rejection after bilateral penetrating keratoplasty. Ophthalmology. 1989;96: Boisjoly HM, Bernard PM, Dube I, et al. Effect of factors unrelated to tissue matching on corneal transplant endothelial rejection. Am J Ophthalmol. 1989;107: Barraquer RI, Kargacin M. Prognostic factors in penetrating keratoplasty. Dev Ophthalmol. 1989;18: Vail A, Gore SM, Bradley BA, et al. Influence of donor and histocompatibility factors on corneal graft outcome. Transplantation. 1994;58: Beck RW, Gal RL, Mannis MJ, et al. Is donor age an important determinant of graft survival? Cornea. 1999;18:
Corneal graft rejection in African Americans at Howard University Hospital
 Saudi Journal of Ophthalmology (2011) 25, 285 289 King Saud University Saudi Journal of Ophthalmology www.saudiophthaljournal.com www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE Corneal graft rejection
Saudi Journal of Ophthalmology (2011) 25, 285 289 King Saud University Saudi Journal of Ophthalmology www.saudiophthaljournal.com www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE Corneal graft rejection
PATIENT INFORMATION ON CORNEAL GRAFT
 PATIENT INFORMATION ON CORNEAL GRAFT (TRANSPLANT) SURGERY M ANANDAN What is the cornea? The clear window of the eye approximately 0.5mm thick and 12mm across. It lies in front of the fluid filled anterior
PATIENT INFORMATION ON CORNEAL GRAFT (TRANSPLANT) SURGERY M ANANDAN What is the cornea? The clear window of the eye approximately 0.5mm thick and 12mm across. It lies in front of the fluid filled anterior
Clinical Indications for Penetrating Keratoplasty in Maharaj Nakorn Chiang Mai Hospital,
 Thai J Ophthalmol Clinical Indications for Penetrating Keratoplasty in Maharaj Nakorn Chiang Mai Hospital, 1990-1 995 Somsanguan Ausayakhun, M.D.* Jinda Juntaramanee** ABSTRACT The preoperative clinical
Thai J Ophthalmol Clinical Indications for Penetrating Keratoplasty in Maharaj Nakorn Chiang Mai Hospital, 1990-1 995 Somsanguan Ausayakhun, M.D.* Jinda Juntaramanee** ABSTRACT The preoperative clinical
Donor Risk Factors for Graft Failure in the Cornea Donor Study
 CLINICAL SCIENCE Donor Risk Factors for Graft Failure in the Cornea Donor Study Joel Sugar, MD,* Monty Montoya, MBA, Mariya Dontchev, MPH, Jean Paul Tanner, MPH, Roy Beck, MD, PhD, Robin Gal, MSPH, Shawn
CLINICAL SCIENCE Donor Risk Factors for Graft Failure in the Cornea Donor Study Joel Sugar, MD,* Monty Montoya, MBA, Mariya Dontchev, MPH, Jean Paul Tanner, MPH, Roy Beck, MD, PhD, Robin Gal, MSPH, Shawn
Visual outcome in patients undergoing penetrating keratoplasty
 International Journal of Research in Medical Sciences Singh G et al. Int J Res Med Sci. 2015 Jan;3(1):244-249 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: 10.5455/2320-6012.ijrms20150144
International Journal of Research in Medical Sciences Singh G et al. Int J Res Med Sci. 2015 Jan;3(1):244-249 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: 10.5455/2320-6012.ijrms20150144
CHAPTER 2 CORNEAL TRANSPLANTATION. Editors: Dr. Shamala Retnasabapathy Dr. Choong Yean Yaw Dr. Michael Law Sie Haur
 CHAPTER 2 Editors: Dr. Shamala Retnasabapathy Dr. Choong Yean Yaw Dr. Michael Law Sie Haur Expert Panel: Dr. Shamala Retnasabapathy (Chair) Dr. Choong Yean Yaw (Co-chair) Dr. Jonathan Choon Siew Cheong
CHAPTER 2 Editors: Dr. Shamala Retnasabapathy Dr. Choong Yean Yaw Dr. Michael Law Sie Haur Expert Panel: Dr. Shamala Retnasabapathy (Chair) Dr. Choong Yean Yaw (Co-chair) Dr. Jonathan Choon Siew Cheong
Influence of advanced recipient and donor age on the outcome of corneal transplantation
 British Journal of Ophthalmology 1997;81:835 839 835 Department of Ophthalmology, Flinders University of South Australia, Australia K A Williams S M Muehlberg R F Lewis D J Coster Correspondence to: Dr
British Journal of Ophthalmology 1997;81:835 839 835 Department of Ophthalmology, Flinders University of South Australia, Australia K A Williams S M Muehlberg R F Lewis D J Coster Correspondence to: Dr
FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM
 FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM ΙΟΑΝΝΙS Α. MALLIAS, MD, PHD Director of the Dept. of Ophthalmology, Mediterraneo Hospital, Glyfada, Athens, Greece Clinical Fellow in Cornea and
FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM ΙΟΑΝΝΙS Α. MALLIAS, MD, PHD Director of the Dept. of Ophthalmology, Mediterraneo Hospital, Glyfada, Athens, Greece Clinical Fellow in Cornea and
Subject Index. Atopic keratoconjunctivitis (AKC) management 16 overview 15
 Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
Outcome of Penetrating Keratoplasty from a Corneal Unit in Pakistan
 Original Article Outcome of Penetrating Keratoplasty from a Corneal Unit in Pakistan Muhammad Nasir Bhatti, Yawar Zaman, P.S. Mahar, Azizur Rahman, Muhammad Fazal Kamal, Mazhar-ul-Hassan, Partab Rai Pak
Original Article Outcome of Penetrating Keratoplasty from a Corneal Unit in Pakistan Muhammad Nasir Bhatti, Yawar Zaman, P.S. Mahar, Azizur Rahman, Muhammad Fazal Kamal, Mazhar-ul-Hassan, Partab Rai Pak
Repeat penetrating keratoplasty: indications and prognosis,
 European Journal of Ophthalmology / Vol. 19 no. 3, 2009 / pp. 362-368 Repeat penetrating keratoplasty: indications and prognosis, 1995-2005 ZULEYHA YALNIZ-AKKAYA, AYSE BURCU NUROZLER, ELVIN HATICE YILDIZ,
European Journal of Ophthalmology / Vol. 19 no. 3, 2009 / pp. 362-368 Repeat penetrating keratoplasty: indications and prognosis, 1995-2005 ZULEYHA YALNIZ-AKKAYA, AYSE BURCU NUROZLER, ELVIN HATICE YILDIZ,
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endothelial_keratoplasty 9/2009 6/2018 6/2019 6/2018 Description of Procedure or Service Endothelial keratoplasty
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endothelial_keratoplasty 9/2009 6/2018 6/2019 6/2018 Description of Procedure or Service Endothelial keratoplasty
PENETRATING KERATOPLASTY IS
 LABORATORY SCIENCES Mechanical Stability of Microkeratome-Assisted Intracorneal Keratoprosthesis Implantation Melanie H. Erb, MD; Mehran Taban, MD; Charles A. Barsam, MD; Paula M. Sweet, MT; Roy S. Chuck,
LABORATORY SCIENCES Mechanical Stability of Microkeratome-Assisted Intracorneal Keratoprosthesis Implantation Melanie H. Erb, MD; Mehran Taban, MD; Charles A. Barsam, MD; Paula M. Sweet, MT; Roy S. Chuck,
Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes The cornea
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes The cornea
Deep Anterior Lamellar Keratoplasty - Techniques
 Deep Anterior Lamellar Keratoplasty - Techniques SHERAZ DAYA MD FACP FACS FRCS(Ed) FRCOphth Financial Disclosure Company Code 1. Abbott Medical Optics Inc. S 2. Bausch + Lomb C,L 3. Carl Zeiss Meditec
Deep Anterior Lamellar Keratoplasty - Techniques SHERAZ DAYA MD FACP FACS FRCS(Ed) FRCOphth Financial Disclosure Company Code 1. Abbott Medical Optics Inc. S 2. Bausch + Lomb C,L 3. Carl Zeiss Meditec
Endothelial Keratoplasty
 Endothelial Keratoplasty Policy Number: 9.03.22 Last Review: 11/2017 Origination: 11/2015 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Endothelial
Endothelial Keratoplasty Policy Number: 9.03.22 Last Review: 11/2017 Origination: 11/2015 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Endothelial
Cataract and cornea. Miltos O. Balidis PhD, FEBOphth,ICOphth ATHENS
 Cataract and cornea Miltos O. Balidis PhD, FEBOphth,ICOphth CATARACT and Stromal opacities Keratoplasty Keratoconus Endothelial pathology Scars PTK Trypan blue 0.01%. Work at the transparent side of cornea
Cataract and cornea Miltos O. Balidis PhD, FEBOphth,ICOphth CATARACT and Stromal opacities Keratoplasty Keratoconus Endothelial pathology Scars PTK Trypan blue 0.01%. Work at the transparent side of cornea
Protocol. Endothelial Keratoplasty
 Protocol Endothelial Keratoplasty (90322) Medical Benefit Effective Date: 04/01/14 Next Review Date: 11/18 Preauthorization No Review Dates: 01/14, 11/14, 11/15, 11/16, 11/17 Preauthorization is not required.
Protocol Endothelial Keratoplasty (90322) Medical Benefit Effective Date: 04/01/14 Next Review Date: 11/18 Preauthorization No Review Dates: 01/14, 11/14, 11/15, 11/16, 11/17 Preauthorization is not required.
Windows2016 Update What s New in My Specialty? cornea. May 20, 2016 OGDEN SURGICAL-MEDICAL SOCIETY CONFERENCE
 Windows2016 Update What s New in My Specialty? cornea May 20, 2016 OGDEN SURGICAL-MEDICAL SOCIETY CONFERENCE This presentation has no commercial content, promotes no commercial vendor and is not supported
Windows2016 Update What s New in My Specialty? cornea May 20, 2016 OGDEN SURGICAL-MEDICAL SOCIETY CONFERENCE This presentation has no commercial content, promotes no commercial vendor and is not supported
Five-year Treatment Outcomes in the Ahmed Baerveldt Comparison (ABC)Study
 Five-year Treatment Outcomes in the Ahmed Baerveldt Comparison (ABC)Study Donald L Budenz, MD, MPH; Keith Barton, MD; Steven J Gedde, MD; William J Feuer, MS; Joyce Schiffman, MS; Vital P Costa, MD; David
Five-year Treatment Outcomes in the Ahmed Baerveldt Comparison (ABC)Study Donald L Budenz, MD, MPH; Keith Barton, MD; Steven J Gedde, MD; William J Feuer, MS; Joyce Schiffman, MS; Vital P Costa, MD; David
Long-term Evaluation of Endothelial Cell Changes in Fuchs Corneal Dystrophy: The Influence of Phacoemulsification and Penetrating Keratoplasty
 pissn: 111-8942 eissn: 292-9382 Korean J Ophthalmol 213;27(6):49-415 http://dx.doi.org/1.3341/kjo.213.27.6.49 Original Article Long-term Evaluation of Endothelial Cell Changes in Corneal Dystrophy: The
pissn: 111-8942 eissn: 292-9382 Korean J Ophthalmol 213;27(6):49-415 http://dx.doi.org/1.3341/kjo.213.27.6.49 Original Article Long-term Evaluation of Endothelial Cell Changes in Corneal Dystrophy: The
GENERAL INFORMATION CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL TRANSPLANTATION WHAT IS CORNEAL TRANSPLANTATION? A corneal transplant is an operation where a damaged or diseased cornea is replaced with donated, healthy tissue. Also called
GENERAL INFORMATION CORNEAL TRANSPLANTATION WHAT IS CORNEAL TRANSPLANTATION? A corneal transplant is an operation where a damaged or diseased cornea is replaced with donated, healthy tissue. Also called
Objectives. Tubes, Ties and Videotape: Financial Disclosure. Five Year TVT Results IOP Similar
 Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Indications for Corneal Transplantation at a Tertiary Referral Center in Tehran
 Original Article Indications for Corneal Transplantation at a Tertiary Referral Center in Tehran Mohammad Zare, MD; Mohammad-Ali Javadi, MD; Bahram Einollahi, MD Alireza Baradaran-Rafii, MD; Siamak Zarei
Original Article Indications for Corneal Transplantation at a Tertiary Referral Center in Tehran Mohammad Zare, MD; Mohammad-Ali Javadi, MD; Bahram Einollahi, MD Alireza Baradaran-Rafii, MD; Siamak Zarei
UPDATE ON CORNEAL TRANSPLANTATION. Frank S. Hwang M.D. Assistant Professor Cornea, External Disease and Refractive Surgery
 UPDATE ON CORNEAL TRANSPLANTATION Frank S. Hwang M.D. Assistant Professor Cornea, External Disease and Refractive Surgery OBJECTIVES Types of corneal transplantation Donor Selection of corneal tissue Penetrating
UPDATE ON CORNEAL TRANSPLANTATION Frank S. Hwang M.D. Assistant Professor Cornea, External Disease and Refractive Surgery OBJECTIVES Types of corneal transplantation Donor Selection of corneal tissue Penetrating
Various Landmark. Clinical Clinical Trials: Trials: Cornea. Cornea is the first refractive media and also is the major. Sandeep Gupta MS,DNB
 Clinical Clinical Trials: Trials: Cornea Various Landmark Corneal Clinical Trials Sandeep Gupta MS,DNB Sandeep Gupta MS,DNB, Parth Patel MBBS, B.V. Rao MS,DNB, Gagandeep Kaur MBBS, V.S. Gurunadh MS, M.A.
Clinical Clinical Trials: Trials: Cornea Various Landmark Corneal Clinical Trials Sandeep Gupta MS,DNB Sandeep Gupta MS,DNB, Parth Patel MBBS, B.V. Rao MS,DNB, Gagandeep Kaur MBBS, V.S. Gurunadh MS, M.A.
Corneal Transplantation (PK) Penetrating Keratoplasty
 Corneal Transplantation (PK) Penetrating Keratoplasty Why do you need a corneal transplant? The cornea is a window of transparent tissue at the front of the eyeball. It allows light to pass into the eye
Corneal Transplantation (PK) Penetrating Keratoplasty Why do you need a corneal transplant? The cornea is a window of transparent tissue at the front of the eyeball. It allows light to pass into the eye
Sclerokeratoplasty David S. Chu, M.D. Cases
 Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Indications for keratoplasty in Nepal:
 Original article Indications for keratoplasty in Nepal: 2005-2010 Bajracharya L 1, Gurung R 1, DeMarchis EH 2, Oliva M 3, Ruit S 1, Tabin G 4 1 Tilganga Institute of Ophthalmology, Gaushala, Kathmandu,
Original article Indications for keratoplasty in Nepal: 2005-2010 Bajracharya L 1, Gurung R 1, DeMarchis EH 2, Oliva M 3, Ruit S 1, Tabin G 4 1 Tilganga Institute of Ophthalmology, Gaushala, Kathmandu,
Assistant Professor, Department of Ophthalmology, Rajindra Hospital, Patiala, Punjab, India 3
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 79-85, p-issn: 79-86.Volume 6, Issue 7 Ver. X (July. 7), PP 5-5 www.iosrjournals.org A Randomized Controlled Prospective Study To Assess
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 79-85, p-issn: 79-86.Volume 6, Issue 7 Ver. X (July. 7), PP 5-5 www.iosrjournals.org A Randomized Controlled Prospective Study To Assess
OCULAR HERPES simplex virus
 CLINICAL SCIENCES Oral Acyclovir After Penetrating Keratoplasty for Herpes Simplex Keratitis Fabiana P. Tambasco, MD; Elisabeth J. Cohen, MD; Lien H. Nguyen, MD; Christopher J. Rapuano, MD; Peter R. Laibson,
CLINICAL SCIENCES Oral Acyclovir After Penetrating Keratoplasty for Herpes Simplex Keratitis Fabiana P. Tambasco, MD; Elisabeth J. Cohen, MD; Lien H. Nguyen, MD; Christopher J. Rapuano, MD; Peter R. Laibson,
2009 Eye Banking Statistical Report Eye Bank Association of America th Street, N.W. Suite 1010 Washington, DC Phone (202) Fax
 2009 Eye Banking Statistical Report Eye Bank Association of America 1015 18th Street, N.W. Suite 1010 Washington, DC 20036 Phone (202) 775-4999 Fax (202) 429-6036 www.restoresight.org Introduction 2009
2009 Eye Banking Statistical Report Eye Bank Association of America 1015 18th Street, N.W. Suite 1010 Washington, DC 20036 Phone (202) 775-4999 Fax (202) 429-6036 www.restoresight.org Introduction 2009
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk cases
 European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
Outcomes of Penetrating Keratoplasty for Macular Corneal Dystrophy
 Outcomes of Penetrating Keratoplasty for Macular Corneal Dystrophy Farid Karimian, MD; Ali-Reza Baradaran-Rafii, MD; Sepehr Feizi, MD Mohammad Zare, MD; Mohammad-Reza Jafarinasab, MD; Mohammad-Ali Javadi,
Outcomes of Penetrating Keratoplasty for Macular Corneal Dystrophy Farid Karimian, MD; Ali-Reza Baradaran-Rafii, MD; Sepehr Feizi, MD Mohammad Zare, MD; Mohammad-Reza Jafarinasab, MD; Mohammad-Ali Javadi,
Original Article Retrospective analysis of corneal transplantation: a tertiary hospital database study over ten years
 Int J Clin Exp Med 2018;11(7):6824-6831 www.ijcem.com /ISSN:1940-5901/IJCEM0069798 Original Article : a tertiary hospital database study over ten years Yaping Jiang 1,2, Minjie Sheng 1, Yue Zhang 3, Xiaoyan
Int J Clin Exp Med 2018;11(7):6824-6831 www.ijcem.com /ISSN:1940-5901/IJCEM0069798 Original Article : a tertiary hospital database study over ten years Yaping Jiang 1,2, Minjie Sheng 1, Yue Zhang 3, Xiaoyan
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Pachymetry Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Pachymetry Professional Institutional Original Effective Date: March 11, 2004 Original Effective
Pachymetry Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Pachymetry Professional Institutional Original Effective Date: March 11, 2004 Original Effective
Review of the Ahmed versus Baerveldt study 5-year treatment outcomes
 Perspective Page 1 of 5 Review of the Ahmed versus Baerveldt study 5-year treatment outcomes Victor Koh 1,2, Cecilia Maria Aquino 1, Paul Chew 1,2 1 Department of Ophthalmology, National University Hospital,
Perspective Page 1 of 5 Review of the Ahmed versus Baerveldt study 5-year treatment outcomes Victor Koh 1,2, Cecilia Maria Aquino 1, Paul Chew 1,2 1 Department of Ophthalmology, National University Hospital,
Subject Index. Canaloplasty aqueous outflow system evaluation 110, 111 complications 118, 119 historical perspective 109, 110
 Subject Index Ab externo Schlemm canal surgery, see Canaloplasty, Viscocanalostomy Ab interno Schlemm canal surgery, see istent, Trabectome Adjustable sutures 14, 15 AGV glaucoma drainage implants 43,
Subject Index Ab externo Schlemm canal surgery, see Canaloplasty, Viscocanalostomy Ab interno Schlemm canal surgery, see istent, Trabectome Adjustable sutures 14, 15 AGV glaucoma drainage implants 43,
Landmark Tube Trials
 SECTION EDITOR: BARBARA SMIT, MD, PhD Landmark Tube Trials A review of key findings from recent multicenter randomized clinical trials involving tube shunts. BY AMBIKA HOGUET, MD, AND STEVEN J. GEDDE,
SECTION EDITOR: BARBARA SMIT, MD, PhD Landmark Tube Trials A review of key findings from recent multicenter randomized clinical trials involving tube shunts. BY AMBIKA HOGUET, MD, AND STEVEN J. GEDDE,
Ruba Alobaidy Jia Y Ng Sathish Srinivasan
 Ruba Alobaidy Jia Y Ng Sathish Srinivasan Department of Ophthalmology, University Hospital Ayr, Ayr, Scotland The authors have no financial interests to declare. Continuous curvilinear capsulorhexis (CCC)
Ruba Alobaidy Jia Y Ng Sathish Srinivasan Department of Ophthalmology, University Hospital Ayr, Ayr, Scotland The authors have no financial interests to declare. Continuous curvilinear capsulorhexis (CCC)
Lamellar Keratoplasty for the Treatment of Fungal Keratitis
 Cornea 21(1): 33 37, 2002. 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Lamellar Keratoplasty for the Treatment of Fungal Keratitis Lixin Xie, M.D., Weiyun Shi, M.D., Zhaosheng Liu, M.D., and
Cornea 21(1): 33 37, 2002. 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Lamellar Keratoplasty for the Treatment of Fungal Keratitis Lixin Xie, M.D., Weiyun Shi, M.D., Zhaosheng Liu, M.D., and
Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
PRESENTED By DR. FAISAL ALMOBARAK, MD
 PRESENTED By DR. FAISAL ALMOBARAK, MD Early FAC associated with hypotony is an important complication after glaucoma filtering procedures, especially trabeculectomy. The reported incidence after trabeculectomy
PRESENTED By DR. FAISAL ALMOBARAK, MD Early FAC associated with hypotony is an important complication after glaucoma filtering procedures, especially trabeculectomy. The reported incidence after trabeculectomy
ASCRS 2016 Instructional Course Mastering Femtosecond Laser Assisted Phacoemulsification. An Evidence-Based Review
 ASCRS 2016 Instructional Course 07-410 Mastering Femtosecond Laser Assisted Phacoemulsification An Evidence-Based Review TIMOTHY V ROBERTS MBBS (NSW), MMed (Syd), FRANZCO, FRACS, GAICD Vision Eye Institute,
ASCRS 2016 Instructional Course 07-410 Mastering Femtosecond Laser Assisted Phacoemulsification An Evidence-Based Review TIMOTHY V ROBERTS MBBS (NSW), MMed (Syd), FRANZCO, FRACS, GAICD Vision Eye Institute,
Trabeculectomy combined with cataract extraction: a follow-up study
 British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
Managing & Avoiding Post-Op Complications in Tube Surgeries
 Managing & Avoiding Post-Op Complications in Tube Surgeries K. Sheng Lim St. Thomas Hospital, London shenglim@gmail.com Current GDD Molteno 1969 Baerveldt 1990 Ahmed 1993 Current GDD GDD Plate Material
Managing & Avoiding Post-Op Complications in Tube Surgeries K. Sheng Lim St. Thomas Hospital, London shenglim@gmail.com Current GDD Molteno 1969 Baerveldt 1990 Ahmed 1993 Current GDD GDD Plate Material
Endothelial Keratoplasty
 Endothelial Keratoplasty Policy Number: 9.03.22 Last Review: 11/2018 Origination: 11/2015 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Endothelial
Endothelial Keratoplasty Policy Number: 9.03.22 Last Review: 11/2018 Origination: 11/2015 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Endothelial
Degenerations. Conditions with cloudy cornea at birth or in infancy
 Dermoids The lesions are choristomas, which are congenital masses of tissue that have been dislocated from their normal position Limbal dermoids--overlapping the cornea and sclera, often inferotemporally
Dermoids The lesions are choristomas, which are congenital masses of tissue that have been dislocated from their normal position Limbal dermoids--overlapping the cornea and sclera, often inferotemporally
Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification
 Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification Mohammad Pakravan, MD; Homayoun Nikkhah, MD; Shahin Yazdani, MD Camelia Shahabi, MD; Massih Sedigh-Rahimabadi, MD Labbafinejad
Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification Mohammad Pakravan, MD; Homayoun Nikkhah, MD; Shahin Yazdani, MD Camelia Shahabi, MD; Massih Sedigh-Rahimabadi, MD Labbafinejad
Influence of HLA-A, HLA-B, and HLA-DR matching on rejection of random corneal grafts using corneal tissue for retrospective DNA HLA typing
 Br J Ophthalmol 1;85:1341 1346 1341 Ophthalmology, University Hospital Rotterdam, M C Bartels Medical Immunology, University Medical Centre Utrecht, H G Otten Ophthalmo-Immunology, The Ophthalmic Research
Br J Ophthalmol 1;85:1341 1346 1341 Ophthalmology, University Hospital Rotterdam, M C Bartels Medical Immunology, University Medical Centre Utrecht, H G Otten Ophthalmo-Immunology, The Ophthalmic Research
Research Article Corneal Endothelial Changes in Patients of Type 2 Diabetes Mellitus Using Specular Microscopy
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Article Corneal Endothelial Changes in Patients of Type 2 Diabetes Mellitus Using Specular Microscopy Sumit 1, Shashi Ahuja 2 *, Chanaveerappa Bammigatti
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Article Corneal Endothelial Changes in Patients of Type 2 Diabetes Mellitus Using Specular Microscopy Sumit 1, Shashi Ahuja 2 *, Chanaveerappa Bammigatti
Long-Term Follow-up of Corneal and Sclero- Corneal Grafting in Severe Eye Perforations
 Original Article Long-Term Follow-up of Corneal and Sclero- Corneal Grafting in Severe Eye Perforations Qasim Mansoor, Roa Rashad Qamar, S. Biswas, H.P. Adhikary Pak J Ophthalmol 2006, Vol. 22 No.2.................................................................................................
Original Article Long-Term Follow-up of Corneal and Sclero- Corneal Grafting in Severe Eye Perforations Qasim Mansoor, Roa Rashad Qamar, S. Biswas, H.P. Adhikary Pak J Ophthalmol 2006, Vol. 22 No.2.................................................................................................
Meet Libby. Corneal Dysgenesis, Degeneration, and Dystrophies Definitions. Dr. Victor Malinovsky
 Meet Libby Corneal Dysgenesis, Degeneration, and Dystrophies 2006 Dr. Victor Malinovsky Definitions Dysgenesis: (congenital anomalies) A development disorder that results in a congenital malformation of
Meet Libby Corneal Dysgenesis, Degeneration, and Dystrophies 2006 Dr. Victor Malinovsky Definitions Dysgenesis: (congenital anomalies) A development disorder that results in a congenital malformation of
Medical Policy. MP Endothelial Keratoplasty. BCBSA Ref. Policy: Last Review: 03/29/2018 Effective Date: 03/29/2018 Section: Other
 Medical Policy BCBSA Ref. Policy: 9.03.22 Last Review: 03/29/2018 Effective Date: 03/29/2018 Section: Other Related Policies 9.03.01 Keratoprosthesis 9.03.18 Optical Coherence Tomography of the Anterior
Medical Policy BCBSA Ref. Policy: 9.03.22 Last Review: 03/29/2018 Effective Date: 03/29/2018 Section: Other Related Policies 9.03.01 Keratoprosthesis 9.03.18 Optical Coherence Tomography of the Anterior
Preoperative risk factors and incidence of glaucoma after penetrating keratoplasty
 International Journal of Clinical Trials Hemanth Raj MN et al. Int J Clin Trials. 2014 Aug;1(2):55-61 http://www.ijclinicaltrials.com pissn 2349-3240 eissn 2349-3259 Research Article DOI: 10.5455/2349-3259.ijct20140804
International Journal of Clinical Trials Hemanth Raj MN et al. Int J Clin Trials. 2014 Aug;1(2):55-61 http://www.ijclinicaltrials.com pissn 2349-3240 eissn 2349-3259 Research Article DOI: 10.5455/2349-3259.ijct20140804
Laser Assisted Keratoplasty
 Laser Assisted Keratoplasty Elizabeth H. Gauger and Kenneth M. Goins, M.D. October 15, 2009 Chief Complaint: Worsening vision in right eye History of Present Illness: 63 yo female with known history of
Laser Assisted Keratoplasty Elizabeth H. Gauger and Kenneth M. Goins, M.D. October 15, 2009 Chief Complaint: Worsening vision in right eye History of Present Illness: 63 yo female with known history of
Non-Descemet Stripping Automated Endothelial Keratoplasty for Bullous Keratopathy in Buphthalmic Eye
 DOI: 10.1159/000446103 Published online: June 2, 2016 2016 The Author(s) Published by S. Karger AG, Basel This article is licensed under the Creative Commons Attribution-NonCommercial 4.0 International
DOI: 10.1159/000446103 Published online: June 2, 2016 2016 The Author(s) Published by S. Karger AG, Basel This article is licensed under the Creative Commons Attribution-NonCommercial 4.0 International
WGA. The Global Glaucoma Network
 The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
Secondary Intraocular Lens Implantation in University Hospital l, Kuala Lumpur
 Secondary Intraocular Lens Implantation in University Hospital l, Kuala Lumpur Fathilah Jaais, MRCOphth, Department of Ophthalmology, Faculty of Medicine, University of Malaya, Lembah Pantai, 50603 Kuala
Secondary Intraocular Lens Implantation in University Hospital l, Kuala Lumpur Fathilah Jaais, MRCOphth, Department of Ophthalmology, Faculty of Medicine, University of Malaya, Lembah Pantai, 50603 Kuala
Messages From the Advanced Glaucoma Intervention Study
 Landmark Studies Section editor: Ronald L. Fellman, MD Take-Home Messages From the Advanced Glaucoma Intervention Study By Leon W. Herndon, MD, and Daniel B. Moore, MD I tasked Leon W. Herndon, MD, and
Landmark Studies Section editor: Ronald L. Fellman, MD Take-Home Messages From the Advanced Glaucoma Intervention Study By Leon W. Herndon, MD, and Daniel B. Moore, MD I tasked Leon W. Herndon, MD, and
No-Touch Technique and a New Donor Adjuster for Descemet s Stripping Automated Endothelial Keratoplasty
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
INTRODUCTION. Trans Am Ophthalmol Soc 2007;105:
 ENDOTHELIAL KERATOPLASTY: CLINICAL OUTCOMES IN THE TWO YEARS FOLLOWING DEEP LAMELLAR ENDOTHELIAL KERATOPLASTY (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) BY Mark A. Terry MD ABSTRACT Purpose: To evaluate
ENDOTHELIAL KERATOPLASTY: CLINICAL OUTCOMES IN THE TWO YEARS FOLLOWING DEEP LAMELLAR ENDOTHELIAL KERATOPLASTY (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) BY Mark A. Terry MD ABSTRACT Purpose: To evaluate
Table 1. Characteristics of patients. Postoperative Comorbidity acuity band keratopathy. Visual Cause of. Case Age (Yr) Sex F/U (Month)
 착색양막을이용한띠각막병증의미용적치료 1459 Table 1. Characteristics of patients Case Age (Yr) Sex F/U (Month) Visual Cause of Postoperative Comorbidity acuity band keratopathy complications 1 19 M 13 NLP * PHPV Injection,
착색양막을이용한띠각막병증의미용적치료 1459 Table 1. Characteristics of patients Case Age (Yr) Sex F/U (Month) Visual Cause of Postoperative Comorbidity acuity band keratopathy complications 1 19 M 13 NLP * PHPV Injection,
FACTORS AFFECTING THE OUTCOME OF CORNEAL REGRAFT SRINIVAS K. H & H. HARIPRASAD
 TJPRC: International Journal of Ophthalmic Surgery and Ocular Pharmacology (TJPRC: IJOSOP) Vol. 1, Issue 1, Jun 2017, 33-48 TJPRC Pvt. Ltd. FACTORS AFFECTING THE OUTCOME OF CORNEAL REGRAFT ABSTRACT SRINIVAS
TJPRC: International Journal of Ophthalmic Surgery and Ocular Pharmacology (TJPRC: IJOSOP) Vol. 1, Issue 1, Jun 2017, 33-48 TJPRC Pvt. Ltd. FACTORS AFFECTING THE OUTCOME OF CORNEAL REGRAFT ABSTRACT SRINIVAS
Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma
 Original Article Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma Irfan Qayyum Malik, M. Moin, A. Rehman, Mumtaz Hussain
Original Article Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma Irfan Qayyum Malik, M. Moin, A. Rehman, Mumtaz Hussain
Corneal transplantation: HLA and age
 L Aquila, 24 novembre 2012 Corneal transplantation: HLA and age Federico Genzano Besso*, Paola Magistroni, Piera Santoro*, Silvano Battaglio*, Raffaella Giacometti, Morteza Mansouri and Antonio Amoroso
L Aquila, 24 novembre 2012 Corneal transplantation: HLA and age Federico Genzano Besso*, Paola Magistroni, Piera Santoro*, Silvano Battaglio*, Raffaella Giacometti, Morteza Mansouri and Antonio Amoroso
Corneal blood staining after hyphaema
 Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Why DMEK? EK: Complications and Controversies
 Why DMEK? EK: Complications and Controversies Quicker visual recovery Lower rejection rate Michael J. Taravella, MD Director: Cornea and Refractive Surgery University of Colorado 1 Less stroma? Potential
Why DMEK? EK: Complications and Controversies Quicker visual recovery Lower rejection rate Michael J. Taravella, MD Director: Cornea and Refractive Surgery University of Colorado 1 Less stroma? Potential
The Evolution of Corneal Transplantation
 e-issn 2329-0358 DOI: 10.12659/AOT.905498 Received: 2017.05.25 Accepted: 2017.07.19 Published: 2017.12.15 The Evolution of Corneal Transplantation Authors Contribution: Study Design A Data Collection B
e-issn 2329-0358 DOI: 10.12659/AOT.905498 Received: 2017.05.25 Accepted: 2017.07.19 Published: 2017.12.15 The Evolution of Corneal Transplantation Authors Contribution: Study Design A Data Collection B
Introduction. Donor tissue preparation for Descemet Membrane Endothelial ASCRS Aim of dissection. DMEK graft preparation
 Introduction Donor tissue preparation for Descemet Membrane Endothelial keratoplasty (DMEK) ASCRS - 2015 Endothelial Keratoplasty DSAEK / DSEK DMEK Donor lamellae stroma + DM + endothelium DM + endothelium
Introduction Donor tissue preparation for Descemet Membrane Endothelial keratoplasty (DMEK) ASCRS - 2015 Endothelial Keratoplasty DSAEK / DSEK DMEK Donor lamellae stroma + DM + endothelium DM + endothelium
Journal of Ophthalmic Medical Technology. Fuchs Dystrophy Amy Hischier
 Journal of Ophthalmic Medical Technology Volume 8, Number 1 October 2013 www.jomtonline.com Fuchs Dystrophy Amy Hischier Patient History: A 55 year old female complained that both of her eyes were red,
Journal of Ophthalmic Medical Technology Volume 8, Number 1 October 2013 www.jomtonline.com Fuchs Dystrophy Amy Hischier Patient History: A 55 year old female complained that both of her eyes were red,
NEW OPPORTUNITIES OF USING THERAPEUTICAL CONTACT LENSES IN OCULAR SURGERY
 NEW OPPORTUNITIES OF USING THERAPEUTICAL CONTACT LENSES IN OCULAR SURGERY Authors: Prof univ. dr. Adriana Stănilă, Dr. Elena Mihai, Dr. Adrian Teodoru, Dr. IonuŃ Costache The Clinical Department of Op
NEW OPPORTUNITIES OF USING THERAPEUTICAL CONTACT LENSES IN OCULAR SURGERY Authors: Prof univ. dr. Adriana Stănilă, Dr. Elena Mihai, Dr. Adrian Teodoru, Dr. IonuŃ Costache The Clinical Department of Op
Are You a Candidate for Corneal Transplantation?
 Are You a Candidate for Corneal Transplantation? www.fleyedocs.com Se Habla Español Are You a Candidate for Corneal Transplantation? Close to 50,000 cornea transplants are now performed in the United States
Are You a Candidate for Corneal Transplantation? www.fleyedocs.com Se Habla Español Are You a Candidate for Corneal Transplantation? Close to 50,000 cornea transplants are now performed in the United States
Mooren s ulcer in China: a study of clinical characteristics and treatment
 1244 Zhongshan Ophthalmic Center, Sun Yat-sen University of Medical Sciences, Guangzhou, PR China J Chen H Xie Z Wang B Yang Z Liu L Chen X Gong Y Lin Correspondence to: Dr Jiaqi Chen, Zhongshan Ophthalmic
1244 Zhongshan Ophthalmic Center, Sun Yat-sen University of Medical Sciences, Guangzhou, PR China J Chen H Xie Z Wang B Yang Z Liu L Chen X Gong Y Lin Correspondence to: Dr Jiaqi Chen, Zhongshan Ophthalmic
rhngf for neurotrophic keratitis first line
 September 2015 Horizon Scanning Research & Intelligence Centre rhngf for neurotrophic keratitis first line LAY SUMMARY This briefing is based on information available at the time of research and a limited
September 2015 Horizon Scanning Research & Intelligence Centre rhngf for neurotrophic keratitis first line LAY SUMMARY This briefing is based on information available at the time of research and a limited
DALK IN DANGEROUS INFECTIONS
 32 INTERNATIONAL CONGRESS of the HELLENIC SOCIETY OF INTRAOCULAR IMPLANT AND REFRACTIVE SURGERY CORNEA ROUND TABLE: STROMAL REPAIR DALK IN DANGEROUS INFECTIONS, MD Clinica Degli Occhi Sarnicola, Grosseto
32 INTERNATIONAL CONGRESS of the HELLENIC SOCIETY OF INTRAOCULAR IMPLANT AND REFRACTIVE SURGERY CORNEA ROUND TABLE: STROMAL REPAIR DALK IN DANGEROUS INFECTIONS, MD Clinica Degli Occhi Sarnicola, Grosseto
Medical Affairs Policy
 Medical Affairs Policy Service: Corneal Treatments and Specialized Contact Lenses (Corneal remodeling, Corneal transplant, Corneal collagen crosslinking, Intrastromal Rings- INTACS, Keratoconus treatments,
Medical Affairs Policy Service: Corneal Treatments and Specialized Contact Lenses (Corneal remodeling, Corneal transplant, Corneal collagen crosslinking, Intrastromal Rings- INTACS, Keratoconus treatments,
Cornea/Anterior Segment OCT. User Experience
 Cornea/Anterior Segment OCT User Experience User Experience Case#1 Post Penetrating Keratoplasty Tokyo Medical University / Kohsei Chuo General Hospital Hideki Mori MD, PhD Almost eight years have passed
Cornea/Anterior Segment OCT User Experience User Experience Case#1 Post Penetrating Keratoplasty Tokyo Medical University / Kohsei Chuo General Hospital Hideki Mori MD, PhD Almost eight years have passed
Corneal densitometry using Pentacam based scheimpflug imaging system: Indian rural population
 Original article: Corneal densitometry using Pentacam based scheimpflug imaging system: Indian rural population Dr Nikhil Mahajan*, Prof. Swati Tomar** **Professor,*Resident Department of Ophthalmology,
Original article: Corneal densitometry using Pentacam based scheimpflug imaging system: Indian rural population Dr Nikhil Mahajan*, Prof. Swati Tomar** **Professor,*Resident Department of Ophthalmology,
Corneal Graft or Transplant Patient information leaflet
 Corneal Graft or Transplant Patient information leaflet Corneal Graft or Transplant/MQ/ST/08.2012/v1.2 review 08.2015 Page 1 Corneal Graft or Transplant The Cornea is the clear window at the front of the
Corneal Graft or Transplant Patient information leaflet Corneal Graft or Transplant/MQ/ST/08.2012/v1.2 review 08.2015 Page 1 Corneal Graft or Transplant The Cornea is the clear window at the front of the
Introduction. Fuchs Endothelial Corneal Dystrophy (FECD) represents a non-inflammatory dystrophy of the corneal endothelial layer which
 Romanian Journal of Ophthalmology, Volume 59, Issue 3, July-September 2015. pp:159-163 GENERAL ARTICLE FUCHS ENDOTHELIAL CORNEAL DYSTROPHY: IS FEMTOSECOND LASER ASSISTED CATARACT SURGERY THE RIGHT APPROACH?
Romanian Journal of Ophthalmology, Volume 59, Issue 3, July-September 2015. pp:159-163 GENERAL ARTICLE FUCHS ENDOTHELIAL CORNEAL DYSTROPHY: IS FEMTOSECOND LASER ASSISTED CATARACT SURGERY THE RIGHT APPROACH?
Trabeculectomy A Review and 2 Year Follow Up
 ORIGINAL ARTICLE Trabeculectomy A Review and 2 Year Follow Up F Jaais, (MRCOphth) Department of Ophthalmology, University Malaya Medical Center, Faculty of Medicine, 50603 Kuala Lumpur Summary This study
ORIGINAL ARTICLE Trabeculectomy A Review and 2 Year Follow Up F Jaais, (MRCOphth) Department of Ophthalmology, University Malaya Medical Center, Faculty of Medicine, 50603 Kuala Lumpur Summary This study
Human lamellar tendon graft in corneal surgery
 Human lamellar tendon graft in corneal surgery Armando Signorelli, Jr, MD, Carlos Roberto Signorelli, MD, Ernest Rifgatovich Muldashev, MD Refractive and Corneal surgery - 1993 - V.9(2) - P. 135-139 ABSTRACT
Human lamellar tendon graft in corneal surgery Armando Signorelli, Jr, MD, Carlos Roberto Signorelli, MD, Ernest Rifgatovich Muldashev, MD Refractive and Corneal surgery - 1993 - V.9(2) - P. 135-139 ABSTRACT
TO DETERMINE THE LONG-TERM SAFETY AND EFFIcacy
 Five-year Follow-up of the Fluorouracil Filtering Surgery Study THE FLUOROURACIL FILTERING SURGERY STUDY GROUP* PURPOSE: To determine the efficacy and safety of subconjunctival 5-fluorouracil injections
Five-year Follow-up of the Fluorouracil Filtering Surgery Study THE FLUOROURACIL FILTERING SURGERY STUDY GROUP* PURPOSE: To determine the efficacy and safety of subconjunctival 5-fluorouracil injections
JMSCR Vol 06 Issue 11 Page November 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i11.77 Short-Term Outcome of Penetrating
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i11.77 Short-Term Outcome of Penetrating
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
What are some common conditions that affect the cornea?
 What are some common conditions that affect the cornea? Injuries After minor injuries or scratches, the cornea usually heals on its own. Deeper injuries can cause corneal scarring, resulting in a haze
What are some common conditions that affect the cornea? Injuries After minor injuries or scratches, the cornea usually heals on its own. Deeper injuries can cause corneal scarring, resulting in a haze
Ferrara Technique of Deep Anterior Lamellar Keratoplasty for Keratoconus Treatment
 10.5005/jp-journals-10025-1050 Original Article IJKECD Ferrara Technique of Deep Anterior Lamellar Keratoplasty for Keratoconus Treatment Paulo Ferrara, Guilherme Ferrara, Leonardo Torquetti Abstract Purpose:
10.5005/jp-journals-10025-1050 Original Article IJKECD Ferrara Technique of Deep Anterior Lamellar Keratoplasty for Keratoconus Treatment Paulo Ferrara, Guilherme Ferrara, Leonardo Torquetti Abstract Purpose:
Post-LASIK infections
 Post-LASIK infections By Mohamed El-moddather Assiss. Prof. and head of department of ophthalmology AL-Azhar unizersity Assuit LASIK has become a common refractive procedure and is generally considered
Post-LASIK infections By Mohamed El-moddather Assiss. Prof. and head of department of ophthalmology AL-Azhar unizersity Assuit LASIK has become a common refractive procedure and is generally considered
Slide 1. Slide 2. Slide 3. An EK For All Reasons: When and How to Perform DSAEK and DMEK. Financial Disclosure
 Slide 1 An EK For All Reasons: When and How to Perform DSAEK and DMEK M I C H A E L T A R A V E L L A, M D R I C H A R D D A V I D S O N, M D V I P U L S H A H, M D A A R O N W A I T E, M D Slide 2 Financial
Slide 1 An EK For All Reasons: When and How to Perform DSAEK and DMEK M I C H A E L T A R A V E L L A, M D R I C H A R D D A V I D S O N, M D V I P U L S H A H, M D A A R O N W A I T E, M D Slide 2 Financial
Preliminary Programme
 In conjunction with the Serbian Society of Cataract and Refractive Surgeons 9 11 February 2018 Preliminary Programme General Information Venue Sava Centar, Milentija Popovića 9, Beograd 11070, Serbia Local
In conjunction with the Serbian Society of Cataract and Refractive Surgeons 9 11 February 2018 Preliminary Programme General Information Venue Sava Centar, Milentija Popovića 9, Beograd 11070, Serbia Local
REAL-WORLD UTILIZATION PATTERNS OF CYCLOSPORINE OPHTHALMIC EMULSION 0.05% WITHIN MANAGED CARE
 REAL-WORLD UTILIZATION PATTERNS OF CYCLOSPORINE OPHTHALMIC EMULSION 0.05% WITHIN MANAGED CARE Tina H Chiang 1, John G Walt 1, John P McMahon, Jr. 2, James E Mansfield, Jr. 2, Susan Simonyi 3 1 Allergan
REAL-WORLD UTILIZATION PATTERNS OF CYCLOSPORINE OPHTHALMIC EMULSION 0.05% WITHIN MANAGED CARE Tina H Chiang 1, John G Walt 1, John P McMahon, Jr. 2, James E Mansfield, Jr. 2, Susan Simonyi 3 1 Allergan
Corneal astigmatism in leprosy and its importance for cataract surgery
 Lepr Rev (2017) 88, 154 158 Corneal astigmatism in leprosy and its importance for cataract surgery BENJAMIN NONGRUM*, SHIRLEY CHACKO**, PRIYA THOMAS MATHEW** & PAULSON** *North Eastern Indira Gandhi Regional
Lepr Rev (2017) 88, 154 158 Corneal astigmatism in leprosy and its importance for cataract surgery BENJAMIN NONGRUM*, SHIRLEY CHACKO**, PRIYA THOMAS MATHEW** & PAULSON** *North Eastern Indira Gandhi Regional
Fleck. Pre-Descemet Dystrophies (generally good vision and comfort) Primary Pre-Descemet Dystrophy
 Fleck Etiology: bilateral, sometimes asymmetric, autosomal dominant opacities located in all levels of stroma as early as 1 st decade Slit lamp: well demarcated, small round gray-white doughnut-like, wreath-like
Fleck Etiology: bilateral, sometimes asymmetric, autosomal dominant opacities located in all levels of stroma as early as 1 st decade Slit lamp: well demarcated, small round gray-white doughnut-like, wreath-like
Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995
 Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995 Steven H. Belle, Kimberly C. Beringer, and Katherine M. Detre T he Scientific Liver Transplant Registry (LTR) was established
Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995 Steven H. Belle, Kimberly C. Beringer, and Katherine M. Detre T he Scientific Liver Transplant Registry (LTR) was established
Surgeon Preference Form
 Surgeon Preference Form Please complete this form and fax it to 608.338.0044. If you have any questions, please contact our Tissue Distribution Coordinator at 877.233.2354 option 2. LEBW looks forward
Surgeon Preference Form Please complete this form and fax it to 608.338.0044. If you have any questions, please contact our Tissue Distribution Coordinator at 877.233.2354 option 2. LEBW looks forward
MEDICAL POLICY. SUBJECT: AQUEOUS DRAINAGE DEVICES (STENTS AND SHUNTS) POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community.
MEDICAL POLICY Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community.
ULTRATHIN DSAEK: THE PRESENT STATUS. Massimo Busin, MD FORLI - ITALY
 ULTRATHIN DSAEK: THE PRESENT STATUS Massimo Busin, MD FORLI - ITALY DSAEK TODAY GOLD STANDARD FOR THE SURGICAL TREATMENT OF ENDOTHELIAL DECOMPENSATION DSAEK VISUAL OUTCOME 20/40 BSCVA 38% to 100% at 3-6
ULTRATHIN DSAEK: THE PRESENT STATUS Massimo Busin, MD FORLI - ITALY DSAEK TODAY GOLD STANDARD FOR THE SURGICAL TREATMENT OF ENDOTHELIAL DECOMPENSATION DSAEK VISUAL OUTCOME 20/40 BSCVA 38% to 100% at 3-6
Outcomes of Pars Plana Vitrectomy in Combination With Penetrating Keratoplasty
 Original Manuscript Outcomes of Pars Plana Vitrectomy in Combination With Penetrating Keratoplasty Journal of VitreoRetinal Diseases 2017, Vol. 1(2) 116-121 ª The Author(s) 2017 Reprints and permission:
Original Manuscript Outcomes of Pars Plana Vitrectomy in Combination With Penetrating Keratoplasty Journal of VitreoRetinal Diseases 2017, Vol. 1(2) 116-121 ª The Author(s) 2017 Reprints and permission:
