Diabetes is the most common
|
|
|
- Wilfrid Thompson
- 5 years ago
- Views:
Transcription
1 Cutaneous Manifestations of Diabetes Mellitus Michelle Duff, 1 Olga Demidova, 2 Stephanie Blackburn, 1 and Jay Shubrook 2 1 OhioHealth O Bleness Hospital, Athens, OH 2 Ohio University Heritage College of Osteopathic Medicine, Athens, OH Corresponding author: Jay Shubrook, shubrook@ohio.edu DOI: /diaclin by the American Diabetes Association. Readers may use this article as long as the work is properly cited, the use is educational and not for profit, and the work is not altered. See creativecommons.org/licenses/by-nc-nd/3.0 for details. Diabetes is the most common endocrine disorder, affecting 8.3% of the population (1). Skin disorders will be present in 79.2% of people with diabetes (2). A study of 750 patients with diabetes found that the most common skin manifestations were cutaneous infections (47.5%), xerosis (26.4%), and inflammatory skin diseases (20.7%) (2). Individuals with type 2 diabetes are more likely than those with type 1 diabetes to develop cutaneous manifestations. Cutaneous disease can appear as the first sign of diabetes or may develop at any time in the course of the disease. This review provides a brief overview of skin conditions that primary care providers (PCPs) may encounter when treating patients with diabetes. Conditions Associated With Insulin Resistance Acanthosis Nigricans Acanthosis nigricans (AN) is likely the most readily recognized skin manifestation of diabetes (3). It is present in up to 74% of obese adult patients and can be predictive of the existence of hyperinsulinemia (4). The presence of AN is a prognostic indicator for developing type 2 diabetes. There is also a possible genetic predisposition or increased sensitivity of the skin to hyperinsulinemia in different ethnic groups. At the same obesity rates, prevalence of AN is lowest in whites (0.5%), higher in Hispanics (5%), and even higher in African Americans (13%) (5). FIGURE 1. Acanthosis nigricans and acrochordans. AN is a hyperpigmented velvety thickening of skin folds, presenting predominantly in the neck, axilla, and groin areas (Fig. 1). Possible additional presentations could include skin tags and hyperkeratosis. Heredity, obesity, endocrine disorders, certain drugs, and malignancy are associated with AN. Benign AN type 2 is related to type 2 diabetes, and pseudo-an type 3 is associated with the metabolic syndrome. Type 2 diabetes related AN has an insidious onset and initially presents as hyperpigmentation. Both underlying conditions present with insulin resistance (3). Children aged 8 14 years who had AN were found to have insulin resistance, and 25% had disturbed glucose metabolism at the time of the study (6). Microscopically, AN presents as papillomatosis and hyperkeratosis (epidermis in irregular folds, exhibiting various degrees of acanthosis). Treatment consists of treating the underlying cause. Significant weight loss resolves AN type 2 and type CLINICAL.DIABETESJOURNALS.ORG
2 d u f f et al. Topical or systemic retinoids and topical retinolytics may be used to manage symptoms (7). Acrochordrons Acrochordons, or fibroepithelial polyps, skin tags, and soft fibromas, are pedunculated outgrowths of normal skin on a narrow stalk, most commonly located on the eyelids, neck, axillae, and groin (Fig. 1). They are found in ~25% of adults, and their number and prevalence increases with age (6). Familial history, obesity and AN have been related to acrochordons; the relationship between hyperinsulinemia and skin tags has been well established (8). Acrochordons are benign lesions, but may become symptomatic with abrasion or necrosis. Red or black skin tags are the result of twisting of the base, which cuts off the blood supply. The diagnosis of acrochordons is made by clinical appearance. Rarely, they may look suspicious for malignancy and should be sent for histological testing. Treatment is usually cosmetic or for cases involving irritation. Excision may be performed with forceps, finegrade scissors, cryosurgery with liquid nitrogen, or electrodesiccation (9). Diabetic Dermopathy Population studies from Sweden demonstrate that diabetic dermopathy (DD) affects 33% of patients with type 1 diabetes, 39% of patients with type 2 diabetes, and 2% of control subjects (9). However, a more recent study found that DD is present in only 0.2% of people with well-controlled type 2 diabetes (10). This condition presents as small (<1 cm), well-demarcated, atrophic depressions, macules, or papules on the pretibia and is considered to be a sign of insulin resistance (Fig. 2). Lesions heal and disappear within 1 2 years on their own, leaving atrophic hypopigmentation at the site of origin (3). Little is known about the relationship of DD to diabetes. On cadaveric skin biopsy, 4 of 14 samples demonstrated moderate to severe FIGURE 2. Diabetic dermopathy. arterial wall thickening, and 11 of 14 samples demonstrated mild basement membrane thickening. Stain findings suggested the presence of hemosiderin and melanin depositions in the epidermis of affected patients (11). No current treatment exists or is necessary for DD, which is asymptomatic and does not lead to morbidity (3). Eruptive Xanthoma Eruptive xanthoma (EX) presents on the buttocks, elbows, and knees as sudden onset crops of yellow papules with an erythematous base (Fig. 3) (12). EX is rare and occurs more often in patients with poorly controlled type 2 diabetes. The sudden appearance of EX can be worrisome to patients and may prompt a visit to the physician. These lesions can be the first sign of diabetes. The decrease in lipoprotein lipase activity seen in insulin-dependent diabetes results in an accumulation of serum triglycerides. Occasionally, when the serum triglyceride level reaches 2,000 mg/dl, lipids will deposit in the skin (13). Cutaneous presentation is associated with hypertriglyceridemia types I, III, IV, and V or secondary FIGURE 3. Eruptive xanthomas. hyperlipidemias. Types I, III, IV, and V show high concentrations of very-low-density lipoprotein and chylomicrons. EX lesions tend to resolve spontaneously within weeks (14). Diagnosis can be made clinically and confirmed with a biopsy of the lesions. It is important to obtain fasting lipid levels at presentation. People with EX are at higher risk from hypertriglyceridemia of early coronary artery disease and pancreatitis (13). Treatment should aim to lower the triglyceride concentration with diet modification and systemic medications to reverse this condition and decrease complications (15,16). Rubeosis Facei Rubeosis facei (RF), a relatively common skin manifestation associated with diabetes, is a microangiopathic complication. It may go unnoticed by patients and physicians. However, if recognized, it should alert physicians to look for other microangiopathic complications such as retinopathy (17). RF presents as a flushing to the face. This condition is seen in 3 5% of people with diabetes. In a study of 150 participants comparing facial redness association with diabetes, Gitelson et al. (18) showed that 59% of patients with diabetes had markedly red faces compared to slightly red or not red (21 and 20%, respectively). The appearance of RF correlates with poor glucose control. No treatment is needed. Strict glycemic control can improve the appearance and prevent complications of microangiopathy in other organ systems (12,19). Epidermal Necrolysis/Stevens- Johnson Syndrome Stevens-Johnson syndrome is a rare mucocutaneous necrotizing condition diagnosed in 1 6 cases per million people annually worldwide (20). A more severe form called toxic epidermal necrolysis is diagnosed at a rate of cases per million people per year (21). Because of their similar etiology, pathogenesis, and clinical and histological presentation, it has been VOLUME 33, NUMBER 1, WINTER
3 proposed to refer to both conditions as epidermal necrolysis (EN) (22). In most cases, EN begins on first exposure to an inciting drug, within 8 weeks of the first dose. The dipeptidyl peptidase-4 inhibitor sitagliptin has been associated with cases of Stevens-Johnson Syndrome (23). It could present with fever, headache, rhinitis, cough, malaise, burning eyes, and dysphagia (24). In 1 3 days, EN progresses to mucocutaneous ulcerations, necrosis and detachment of epidermis, severe stomatitis, and ocular involvement (25). Initial dusky red, pruritic macules are distributed symmetrically over the face, upper trunk, and proximal limbs, with distal limbs relatively spared (26). These lesions progressively coalesce and develop dark necrotic centers as they spread down the trunk. Nickolsky s sign displacement of epidermis with lateral pressure is positive over the blistering epidermis. The pathophysiology of EN is under-investigated. Presence of a strong cell-mediated immunological response involving natural killer cells and CD8 + T lymphocytes specific for the causative agent has been noted. This reaction also involves monocytes and granulocytes (27). Other factors that amplify the reaction are still being investigated. The end result of hypersensitivity is a full-thickness keratinocyte apoptosis of the epidermis and mucous membranes (28). Although drugs and their components are the most common etiologies, viruses, Mycoplasma pneumoniae, and immunizations are also suspected. More than 100 medications have been identified as causes of EN (29). If a person develops EN while on sitagliptin, the drug s manufacturer recommends discontinuing therapy as soon as a hypersensitivity reaction is noted (30). EN is a life-threatening emergency. Current treatments include withdrawal of all medications that would not be life-threatening. Discontinuation of medications started in the past 8 weeks is particularly important. EN is treated supportively as a massive burn, with emphasis on preservation of intact skin and supportive symptomatic measures. Patients presenting with EN should be transferred to a qualified intensive care unit as soon as possible (31). Immunosuppressive drugs have not proven to be helpful (24). Conditions Associated With Type 1 Diabetes Necrobiosis Lipoidica Necrobiosis lipoidica (NL) is rare, appearing in % of people with type 1 diabetes, more often in women than men (12,32). Typical lesions of NL occur in young and middle-aged patients and present most commonly on the pretibial skin as irregular, painless ovoid plaques with a yellow atrophic center and a red to purple periphery. The lesions are usually multiple and bilateral. Lesions may ulcerate spontaneously or from trauma (33,34). Of the patients with NL, 11 65% have type 1 diabetes at the time of cutaneous diagnosis (34). Ninety percent of people with NL who do not have diabetes eventually develop diabetes (mostly type 1 diabetes) (12). Glycemic control has no effect on the course of NL (16). NL is a benign condition, and dermatology referral is not usually necessary. The cause of NL is currently unknown. Proposed causes are localized trauma, microangiopathy, immunoglobulins and fibrin deposition, and metabolic changes (32,35). Although NL is benign, its appearance is cosmetically distressing to patients (Fig. 4). The mainstay of treatment is currently steroids, either topical, intralesional, or, rarely, systemic. Steroids are cost-effective and have low side-effect profiles. Steroid use is beneficial to control the initial erythema in early lesions but fails to help with the atrophic component of the lesions and can worsen atrophy. Stockings are advised to help with stasis changes and protect from FIGURE 4. Necrobiosis lipoidica. trauma (35). Other treatments that have been used include pentoxifyllin, cyclosporine, ticlopidine infliximab, and thalidomide. Some case reports have shown benefit from nicotinamide, clofazimine, cloroquine, and topical tretanoin. These later treatments do require dermatology referral to manage medications and potential side effects (32,36). Vitiligo Vitiligo affects % of world population, making it the most common depigmenting disorder. Patients present with patches of depigmentation of skin and hair (Fig. 5). Possible etiologies are both environmental and polygenetic. This condition affects males and females equally (37). Out of several subtypes, generalized vitiligo is most common. It is associated with autoimmune diseases in 20 30% of cases. The most common associations are with Hashimoto s thyroiditis, Grave s disease, rheumatoid arthritis, psoriasis, type 1 diabetes (usually adult-onset), pernicious anemia, systemic lupus erythematosus, and Addison s disease (38). A 2009 study of 50 patients with type 1 diabetes reported that 4% of subjects had vitiligo (39). Genetic vitiligo (GV) is most often a gradually progressive disorder and is unresponsive to treatment. However, some cases do stop progressing. GV complications are long duration, 42 CLINICAL.DIABETESJOURNALS.ORG
4 d u f f et al. FIGURE 5. Vitiligo. Koebner phenomenon, leukotrichia, and mucosal involvement (37). Dermatological therapy attempts to reduce T-cell response and induce melanocyte migration and regeneration. Corticosteroids with ultraviolet B or calcineurin inhibitors or systemic psoralen and ultraviolet A (PUVA) light are first-line treatments. Calcipotriol, topical PUVA, excimer laser, corticosteroid pulse therapy, and surgical melanocyte grafting are some of the treatment options. These treatments are long and complicated by numerous side effects. Use of sunscreen is recommended but also controversial because of ultraviolet B stimulation of melanocytes and the possibility of repopulation, as well as photo-adaptation of vitiligo-affected skin. Moderate exposure to sun is recommended. The psychosocial impact of vitiligo can be substantial, and patient support groups are available. Numerous nontraditional treatments are attempted by patients but should be investigated for safety before administration (40). Bullosis Diabeticorum Bullosis diabeticorum, or diabetic bullae, are seen in 0.5% of individuals with type 1 diabetes. This condition is seen more often in men and in those with longstanding peripheral neuropathy. The lesions arise spontaneously and are primarily on the dorsa and the sides of the lower legs and feet. Occasionally, they are seen on the forearms and hands. The lesions present as clear bulla on non-inflamed bases. They are painless and contain sterile fluid. Lesion size can range from a few millimeters to a few centimeters (16). Blister pathology is currently unknown. Diabetic bullae typically appear in individuals who have had type 1 diabetes for many years. However, this condition may be the first sign of diabetes (41). Lesions resolve on their own in 2 5 weeks. Differential diagnosis includes bullous pemphigoid, which can be ruled out by submitting a biopsy of the lesion for direct and indirect immunofluorescence. The lesions resemble those in acquired epidermolytic bullosa, porphyria cutanea tarda, autoimmune or impetiginous bullae, erythema multiforme, or drug eruption (42). Dermatologists often make the diagnosis of diabetic bulla; after diagnosis, this condition can be managed by PCPs. The treatment is focused on infection prevention (19). If the bullae become large and symptomatic, they can be aspirated, leaving the roof intact to protect the skin barrier (16). Individuals may use saline compresses for symptomatic relief. Topical antibiotics or steroids are generally not necessary (41). Other Diabetes-Related Conditions Psoriasis Psoriasis is a chronic, inflammatory, polygenic skin disorder with environmental triggers such as trauma, medications, and infection. Psoriasis is characterized by erythematous scaly papules and plaques with pustular and erythrodermic eruptions occurring most commonly in areas of friction such as scalp, elbows, knees, hands, feet, trunk, and nails. Koebner phenomenon is a well-documented factor, in which a plaque develops on the site of the injury. Histologically, Koebner phenomenon presents with alterations in epidermal growth (elongated rete ridges with dilated blood vessels, thinned suprapapillary plate, and differentiation), intermittent parakeratosis, and multiple biochemical, immunological, and vascular abnormalities (e.g., lymphocyte and neutrophil infiltration). This condition can develop at any age, with the most common onset between 15 and 30 years of age; it is uncommon in people <10 years of age. It affects 2 3% of the U.S. population. Approximately 9% of people with diabetes (type 1 or type 2) has psoriasis (42). Recent research shows that psoriasis may raise predisposition for developing diabetes mellitus, just as it does for heart attack and stroke. A 13-year study with 52,000 participants concluded that people with psoriasis have a 49 56% greater risk of developing type 2 diabetes later in life (43). Most people with psoriasis will be treated by a dermatologist. Treatment consists of topical and systemic immunomodulators, as well as ultraviolet light and laser application. Topical treatments are effective in most cases; however, they carry a 40% adherence rate because of time-consuming application and cosmetic inappropriateness (44). Both cream and ointment should be prescribed. Phototherapy with ultraviolet A, ultraviolet B, and psoralein has been used for several decades and has shown good response in mild cases (45). Lichen Planus Lichen planus is an uncommon disorder affecting <1% of the general population. Onset is common in middle age (30 60 years of age). However, the prevalence of lichen planus in people with type 1 or type 2 diabetes has been noted to be 2 4% (39,46). Lichen planus may affect the skin (termed cutaneous, with several variants), the oral cavity ( oral ), the genitalia ( vulvar or penile ), the scalp ( lichen planopilaris ), the nails, or the esophagus (47,48). Lichen planus presents as grouped, symmetric, erythematous to viola- VOLUME 33, NUMBER 1, WINTER
5 ceous, flat-topped, polygonal papules distributed mainly in flexural aspects of arms and legs and rarely can appear on the trunk ( Blaschkoid or zosteriform ) and inverse ( intertriginous ) (48). Variants may include ulcerative and perforating types. Koebner phenomenon is common, and pruritus associated with lichen planus is intense and heals with postinflammatory hyperpigmentation. Clinically, cutaneous lichen planus presents as flat-topped, violaceous papulosqamous eruptions on the skin. It is classically described as the four Ps : pruritic, purple (violaceous), polygonal, and papules or plaques. Papules may be isolated and a few millimeters in diameter or may coalesce to form larger plaques (48). Fine white lines may be visible on the surface of papules or plaques and are known as Wickham s striae. Diagnosis can be made based on clinical findings. If clinical recognition is questionable, a biopsy is indicated. Etiology of the condition is unknown. It is suspected that CD8+ T cells and a Th1 immune response (cell-mediated mechanism against keratinocytes) is involved (49). Most cases of lichen planus will be managed by a dermatologist. Treatment of cutaneous lichen planus is focused on pruritus control (47). The potency of topical steroids used depends on the site involved. On the trunk and extremities, high-potency corticosteroids are indicated, whereas on the face and intertriginous areas, medium- to low-potency ointments are used. This is because of steroid-induced atrophy. Treatment efficacy should to be checked in 3 weeks. With generalized involvement, light therapy may be added to the treatment plan. Intralesional corticosteroids are applied to thicker lesions (49). Systemic glucocorticoids, phototherapy with PUVA and ultraviolet B, and oral acitretin can be beneficial in people who are not candidates for topical steroid therapy. Few studies have been conducted on treatments because of the typical spontaneous remission of lichen planus (47,48). Xerosis Xerosis is another name for dry skin. It is the second most common skin manifestation in people with diabetes. In a study of 100 patients with diabetes and skin lesions, xerosis was present in 44% of the patients (50). Patients with renal disease also frequently suffer from xerosis. No referral to a dermatologist is necessary for xerosis. PCPs should educate patients about the importance of skin hygiene, including applying fragrance-free creams or lotions within 3 minutes of bathing to trap moisture within the skin. Sclerederma Diabeticorum Sclerederma diabeticorum is a condition of thick, indurated, erythematous plaques occurring on the upper back and neck. Lesions may have erythema. This condition is seen in ~2.5 14% of individuals with diabetes (51). The condition is more common in obese middle-aged men with type 2 diabetes. Patients with scleroderma diabeticorum are often asymptomatic; however, neck and back pain may occur. The diagnosis is often made clinically, although a definitive diagnosis is confirmed by skin biopsy. The pathogenesis of scleroderma diabeticorum is thought to be linked to increased stimulation of insulin and nonenzymatic glycosylation of collagen. This causes increased collagen cross-linking, rendering the collagen fibers resistant to degradation by collagenase and leading to increased amounts of collagen. Treatments have showed limited benefits. Some treatment options include steroids, methotrexate, and ultraviolet light phototherapy (15,52). Differential diagnosis includes Sclerederma Buschke, also associated with type 1 diabetes. Sclerederma Buschke presents as thickening mainly on the neck, shoulders, and upper limbs, often after an upper-respiratory infection. This condition clears spontaneously in a period of months or years. Women are affected more often than men. Sclerederma diabeticorum involves the fingers, hands, and trunk. It is in the family of diabetic thick skin called morphea and is the most severe, systemic sclerederma (53). Granuloma Annulare Granuloma annulare (GA) presents as erythematous to flesh-colored papules coalescing to form an oval or ring lesion. GA often presents asymptomatically but can cause pruritus or a burning sensation (54). The association between granuloma annulare and diabetes is controversial. One retrospective study showed a 12% association between GA and diabetes (55). Another study reported diabetes in 21% of 100 cases of generalized granuloma annulare (GGA) and in 9.7% of 1,350 cases of localized GA (56). Skin lesions may often precede diabetes. Struder et al. (55) suggest that patients with recurrent localized granuloma annulare or the disseminated form be given a glucose tolerance test. The pathogenesis of GA is currently unknown. Treatment options are topical steroids, intralesional steroids, isotretinoin, dapsone, antimalarials, and phototherapy. Untreated lesions may spontaneously regress; this is more common in the localized form of GA than in the disseminated form (57). Localized forms can be treated easily and followed by PCPs. Recurrent GA or disseminated GA can be worked up by PCPs and referred to a dermatologist. GGA tends to be idiopathic. However, it has been associated with diabetes and with diseases such as autoimmune thyroiditis, HIV, hepatitis C, Epstein-Barr virus infection, sarcoidosis, and internal malignancies (58). Acquired Perforating Dermatosis Acquired perforating dermatosis presents as dome-shaped papules and nodules with hyperkeratotic plugs. This condition is characterized by 44 CLINICAL.DIABETESJOURNALS.ORG
6 d u f f et al. the transepidermal elimination of some component of the dermis. The cutaneous perforating disorders have classically been divided into four types: elastosis perforans serpiginosa, reactive perforating collagenosis, perforating folliculitis, and Kyrle s disease. Perforating disorders have been associated with chronic renal failure, dialysis, and diabetes. Acquired perforating dermatitis is seen in both type 1 and type 2 diabetes (15,16,59). In most cases, the renal disease is a complication of diabetic nephropathy (60). The lesions of acquired perforating dermatosis are most commonly seen on the trunk and extremities and tend to be pruritic. It has been thought that the mechanism of action may be derived from epidermal trauma, a foreign-body reaction to the collagen in the dermis, or metabolic products from uremia (59,61). Dialysis has not shown therapeutic value, but renal transplant has been shown to be effective in clearing the lesions (60). Treatment options include avoidance of scratching, topical or systemic steroids, phototherapy, retinoid, and antihistamines. Onychodystrophy Onychodystrophy presents as excessive nail thickening and deformity, which may cause accumulation of debris and subsequent infection of the toe that should be treated as a diabetic ulcer. Poorly fitting shoes may cause repeated trauma and worsening of the injured site (61). In patients with diabetes, onychodystrophy is the result of poor peripheral circulation and diabetic neuropathy. The condition itself may cause diabetic foot ulcers (62). Proper nail care, well-fitting shoes, and immediate attention to nail infections are important. Periungual Telangectasias Periungual telangectasias present as nail fold erythema, dilated blood vessels visible to the naked eye, fingertip tenderness, and thick cuticles. Telangectasias arise in the nail beds of people with diabetes after loss of capillary loops and dilation of remaining capillaries. The condition is present in up to 49% of people with diabetes (63). Some patients also experience fingertip tenderness. No treatment is necessary for this condition. Infections Associated With Diabetes Cutaneous Infections Infections form the largest group of cutaneous conditions affecting people with diabetes. In a 2009 study of 50 patients, 55% of those with diabetes had infectious skin manifestations at some time (39). Another study reported a 61% prevalence rate in skin infections in people with diabetes (64). Cutaneous infections include candidiasis, dermatophytosis, and bacterial infections. These are described in more detail below. Candidiasis Mucocutaneous candidiasis is caused most commonly by Candida albicans and presents as red plaques with characteristic white adherent exudate and satellite pustules. The risk of infection is increased with hyperglycemia, which favors Candida proliferation. Candidal vulvovaginitis is the most common of all cases, and perianal candidiasis is also common in both males and females. Other presentations include thrush (infection of oral mucosa and perleche), angular cheilitis, intertrigo (infection of skinfolds and erosio interdigitalis blastomysetica chronica), finger web space infection, paronychia (infection of soft tissue around the nailplate), and onichomycosis (infection of the nail) (3). Common cutaneous fungal infections are summarized in Table 1. Rarely, critically ill patients with diabetic ketoacidosis (DKA) may be diagnosed with mucormycosis, an acute, severe, soft-tissue infection caused by Mucor, Rhizopus, and Absidia species. Saprophytic fungi prefer the low ph environments seen during DKA and thrive in hyperglycemia. Some fungi also utilize ketones as nutritional substance (3). An estimated 50 75% of cases of rhinocerebral mucormycosis occur in patients with diabetes (65). Mucormycosis is progressive and poorly responds to systemic antifungals. Treatment options include itraconazole, fluconazole, amphotericine B, and voriconazole. This condition is often fatal. Dermatophytosis Tinea or dermatophytoses are superficial infections of the skin, hair, and nails by fungus. Tinea corporis, tinea pedis (Fig. 6), and onychomycosis (Fig. 7) are common dermatophyte TABLE 1. Common Cutaneous Fungal Infections Infection Definition Candidal vulvovaginitis Infection of vaginal mucosa Perianal candidiasis Infection of perineum and perianal area Thrush Infection of the oral mucosa Perleche Infection of labial commissures of mouth angles Intertrigo Infection of skinfolds Erosion interdigitalis blastomysetica chronica Infection of finger web space Paronychia Infection of the soft tissue around the nail plate Onichomycosis Infection of the nail VOLUME 33, NUMBER 1, WINTER
7 FIGURE 6. Tinea pedis. FIGURE 7. Onchiomycosis. infections encountered in people with diabetes. In a 2013 study of 76 patients with tinea corporis, the main predisposing factor was xerosis (66). In a 2001 study of 171 people with diabetes compared with 276 control subjects, the most common infection in people with diabetes was tinea pedis, followed by distal subungual onychomycosis (65). This study did not show a correlation between dermatophytosis and duration or type of diabetes or its complications. Trichophyton rubrum, Trichophyton mentagrophytes, and Trichophyton tonsurans are the most common dermatophytes. Because dermatophyte infections are so common in the general population, no dermatology referral is necessary. Treatment consists of topical antifungals or systemic antifungal medication. Table 2 summarizes common fungal infections and the topical and oral antifungal therapies used to treat them. Bacterial Infections Cutaneous bacterial infections are more common, as well as more severe, TABLE 2. Treatment Options for Common Fungal Infections Cutaneous Fungal Treatment Options Infections Candidal vulvovaginitis Butoconazole vaginal 2% cream Clotrimazole vaginal 1% cream, 100 mg vaginal tablet Miconazole 2% cream, 100 mg vaginal suppository, 200 mg vaginal suppository, 1,200 mg vaginal suppository Ticonazole vaginal 6.5% ointment Fluconazole 150 mg 1 dose Nystatin vaginal 100,000-unit vaginal tablet Perianal candidiasis Miconazole topical 2% cream, 4% cream Miconazole insert 100 mg, 200 mg, 1,200 mg Diflucan 150 mg by mouth 1 Thrush Nystatin 100,000 U/mL Clotrimazole 10 mg Miconazole 50 mg Gentian violet topical 1% Perleche Nystatin/triamcinolone topical 100,000 U/0.1% Clotrimazole topical 1% Miconazole topical 2% Ketoconazole topical 2% Intertrigo Fluconazole 200 mg daily 2 4 weeks Itraconazole 200 mg daily 2 4 weeks Ketoconazole 200 mg daily 2 4 weeks Terbinafine 500 mg by mouth twice daily 6 8 weeks Nystatin topical 100,000 units/g ointment, powder, cream Erosion interdigitalis Clotrimazole 1% cream or solution blastomysetica chronica Paronychia Fluconazole 200 mg daily 2 4 weeks Itraconazole 200 mg daily 2 4 weeks Ketoconazole 200 mg daily 2 4 weeks Terbinafine 500 mg by mouth twice daily 6 8 weeks Onichomycosis Terbinafine 250 mg in people with diabetes. Diabetic foot ulcers are the leading type of morbidity in diabetes. They develop because of decreased sensation from diabetic neuropathy and unrecognized injury, with subsequent infection. White blood cell dysfunction resulting from increased glucose levels allows bacteria to proliferate. Staphylococcal folliculitis or skin abscesses are among the most common bacterial infections in uncontrolled diabetes. They respond well to antibiotics and surgical drainage. Pseudomonas aeruginosa is another common diabetic foot ulcer organism. External ear canal infection caused by Pseudomonas aeruginosa is also frequent in people with diabetes. Pseudomonads thrive in moist 46 CLINICAL.DIABETESJOURNALS.ORG
8 d u f f et al. environments full of oxygen. Lesions can be recognized by characteristic green-blue pigment, as well as fluorescence with Wood s lamp application. Microscopically, pseudomonads are identified as gram-negative rods. Patients may present with otalgia, otorrhea, hearing loss, and edema and erythema of the external ear canal. Treatment consists of drying the area and applying topical antibiotics to uncomplicated infections. Malignant external otitis media requires immediate recognition and systemic antibiotics such as fluoroquinolones, plus an antipseudomonal antibiotic (e.g., antipseudomonal penicillin, antipseudomonal cephalosporin, monobactam, aminoglycoside, or carbapenem). Higher doses and surgical debridement are required to prevent spreading of the infection to bone and the nervous system (67). Urgent treatment of otitis externa is important because of its potential to rapidly spread to bone and cranial nerves, which could lead to mortality (68). Summary Diabetes is the most common endocrine disorder, and many cutaneous disorders are associated with diabetes. Knowledge of these skin conditions can aid PCPs in the diagnosis of diabetes and the treatment of its associated skin conditions. Most conditions can be managed by PCPs, but referral to a dermatologist may be warranted in some cases. As the incidence and prevalence of diabetes increases, skin manifestations associated with diabetes will become more common. Thus, PCPs should familiarize themselves with their presentation and treatment. Duality of Interest Jay. Shubrook has received research grant support from Sanofi Aventis and serves on the Global Primary Care Diabetes Board of Eli Lilly. No other potential conflicts of interest relevant to this article were reported. References 1. Centers for Disease Control and Prevention National Diabetes Fact Sheet. Available from gov/diabetes//pubs/factsheet11.htm. Accessed 25 August Demirseren DD, Emre S, Akoglu G, et al. Relationship between skin diseases and extracutaneous complications of diabetes mellitus: clinical analysis of 750 patients. Am J Clin Dermatol 2014;15: Kalus AA, Chien AJ, Olerud JE. Chapter 151: Diabetes mellitus and other endocrine diseases. In Fitzpatrick s Dermatology in General Medicine. 8th ed. Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, Wolff K, Eds. New York, McGraw- Hill, Available online from accessmedicine.mhmedical.com/content. aspx?bookid=392§ionid= Accessed 11 November Hud JA Jr, Cohen JB, Wagner JM, Cruz PD Jr. Prevalence and significance of acanthosis nigricans in an adult obese population. Arch Dermatol 1992;128: Stuart CA, Pate CJ, Peters EJ. Prevalence of acanthosis nigricans in an unselected population. Am J Med 1989;87: Banik R, Lubach D. Skin tags: localization and frequencies according to sex and age. Dermatologica 1987;174: Brickman WJ, Huang J, Silverman BL, Metzger BE. Acanthosis nigricans identifies youth at high risk for metabolic abnormalities. J Pediatr 2010;156: Kahana M, Grossman E, Feinstein A, Ronnen M, Cohen M, Millet M. Skin tags: a cutaneous marker for diabetes mellitus. Acta Dermato-Venereologica 1987;67: Ko CJ. Dermal hypertrophies and benign fibroblastic/myofibroblastic tumors. In Fitzpatrick s Dermatology in General Medicine. 8th ed. Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Lefferr DJ, Wolf K, Eds. New York, McGraw-Hill, Available from mhmedical.com/content.aspx?bookid=392§ionid= Accessed 11 November Ragunatha S, Anitha B, Inamadar AC, Palit A, Devarmani SS. Cutaneous disorders in 500 diabetic patients attending diabetic clinic. Indian J Dermatol 2011;56: McCash S, Emanuel PO. Defining diabetic dermopathy. J Dermatol 2011;38: Paron NG, Lambert PW. Cutaneous manifestations of diabetes mellitus. Prim Care 2000;27: Martínez DP, Díaz JÓF, Bobes CM. Eruptive xanthomas and acute pancreatitis in a patient with hypertriglyceridemia. Int Arch Med 2008;1:6 14. Binić I, Janković A. Eruptive xanthomas associated with diabetes mellitus. Chin Med J 2009;122: Levy L, Zeichner JA. Dermatologic manifestation of diabetes. J Diabetes 2012;4: Ferringer T, Miller F 3rd. Cutaneous manifestations of diabetes mellitus. Dermatol Clin 2002;20: Namazi MR, Jorizzo JL, Fallahzadeh MK. Rubeosis faciei diabeticorum: a common, but often unnoticed, clinical manifestation of diabetes mellitus. ScientificWorldJournal 2010;10: Gitelson S, Wertheimer-Kaplinski N. Color of the face in diabetes mellitus: observations on a group of patients in Jerusalem. Diabetes 1965;14: Tabor CA, Parlette EC. Cutaneous manifestations of diabetes. Postgrad Med 2006;119: Chan HL, Stern RS, Arndt KA, et al. The incidence of erythema multiforme, Stevens-Johnson syndrome, and toxic epidermal necrolysis: a population based study with particular reference to reactions caused by drugs among outpatients. Arch Dermatol 1990;126: Rzany B, Mockenhaupt M, Baur S, et al. Epidemiology of erythema exsudativum multiforme majus, Stevens-Johnson syndrome, and toxic epidermal necrolysis in Germany ( ): structure and results of a population-based registry. J Clin Epidemiol 1996;49: Ruiz-Maldonado R. Acute disseminated epidermal necrosis types 1, 2, and 3: study of sixty cases. J Am Acad Dermatol 1985;13: Pathak R, Bridgeman MB. Dipeptidyl peptidase-4 (DPP-4) inhibitors in the management of diabetes. P T 2010;35: Valeyrie-Allanore L, Roujeau J. Epidermal necrolysis (Stevens Johnson syndrome and toxic epidermal necrolysis). In Fitzpatrick s Dermatology in General Medicine. 8th ed. Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, Wolff K, Eds. New York, McGraw-Hill, Available from mhmedical.com/content.aspx?bookid=392§ionid= Accessed 11 November Stevens AM, Johnson FC. A new eruptive fever associated with stomatitis and ophthalmia: report of two cases in children. Am J Dis Child 1922;24: Mockenhaupt M. Severe drug-induced skin reactions: clinical pattern, diagnostics and therapy. J Dtsch Dermatol Ges 2009;7: Paquet P, Nikkels A, Arrese JE, Vanderkelen A, Piérard GE. Macrophages and tumor necrosis factor alpha in toxic epidermal necrolysis. Arch Dermatol 1994;130: Sassolas B, Haddad C, Mockenhaupt M, et al. ALDEN, an algorithm for assessment of drug causality in Stevens-Johnson syndrome and toxic epidermal necrolysis: comparison with case-control analysis. Clin Pharmacol Ther 2010;88:60 68 VOLUME 33, NUMBER 1, WINTER
9 29. Roujeau JC, Stern RS. Severe adverse cutaneous reactions to drugs. N Engl J Med 1994;331: Januvia [package insert]. Whitehouse Station, NJ, Merck & Co., Ellis MW, Oster CN, Turiansky GW, Blanchard JR. A case report and a proposed algorithm for the transfer of patients with Stevens-Johnson syndrome and toxic epidermal necrolysis to a burn center. Mil Med 2002;167: Kota SK, Jammula S, Kota SK, Meher LK, Modi KD. Necrobiosis lipoidica diabeticorum: a case-based review of literature. Indian J Endocrinol Metab 2012;16: Lowitt MH, Dover JS. Necrobiosis lipoidica. J Am Acad Dermatol 1991;25: O Toole EA, Kennedy U, Nolan JJ, Young MM, Roger S, Barnes L. Necrobiosis lipoidica: only a minority of patients have diabetes mellitus. Br J Dermatol 1999;140: Roy S, Shayaan M. Unsightly rash on shin. necrobiosis lipoidica diabeticorum. J Fam Pract 2012;61: Cohen O, Yaniv R, Karasik A, Trau H. Necrobiosis lipoidica and diabetic control revisited. Med Hypotheses 1996;46: Hann SK, Park YK, Chun WH. Clinical features of vitiligo. Clin Dermatol 1997;15: Spritz R. The genetics of generalized vitiligo. Curr Dir Autoimmun 2008;10: Mahajan S, Koranne R, Sharma S. Cutaneous manifestation of diabetes melitus. Indian J Dermatol Venereol Leprol 2003;69: Birlea SA, Spritz RA, Norris DA. Chapter 74: Vitiligo. In Fitzpatrick s Dermatology in General Medicine. 8th ed. Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, Wolff K, Eds. New York, McGraw-Hill, Available from Accessed 11 Nomveber Lipsky BA, Baker PD, Ahroni JH. Diabetic bullae: 12 cases of a purportedly rare cutaneous disorder. Int J Dermatol 2000;39: Romano G, Moretti G, Di Benedetto A, et al. Skin lesions in diabetes mellitus: prevalence and clinical correlations. Diabetes Res Clin Pract 1998;39: Khalid U, Hansen PR, Gislason G, et al. Psoriasis is associated with increased risk of incident diabetes mellitus: a Danish nationwide cohort study. Eur Heart J 2012;33: Richards H, Fortune D, O Sullivan T, Main C, Griffiths C. Patients with psoriasis and their compliance with medication. J Am Acad Dermatol 1999;41: Hönigsmann H. Phototherapy for psoriasis. Clin Exp Dermatol 2001;26: Puri N. A study on cutaneous manifestations of diabetes mellitus. Our Dermatology Online 2012;3: Le Cleach L, Chosidow O. Lichen planus. N Engl J Med 2012;366: Wagner G, Rose C, Sachse MM. Clinical variants of lichen planus. J Dtsch Dermatol Ges 2013;11: Lehman JS, Tollefson MM, Gibson LE. Lichen planus. Int J Dermatol 2009;48: Goyal A, Raina S, Kaushal SS, Mahajan V, Sharma NL. Pattern of cutaneous manifestation in diabetes mellitus. Indian J Dermatol 2010;55: Cole GW, Headley J, Skowsky R. Scleredema diabeticorum: a common and distinct cutaneous manifestation of diabetes mellitus. Diabetes Care 1983;6: Thumpimukvatana N, Wongpraparut C, Lim HW. Scleredema diabeticorum successfully treated with ultraviolet A1 phototherapy. J Dermatol 2010;37: Van Hattem S, Bootsma AH, Thio HB. Skin manifestations of diabetes. Cleve Clin J Med 2008;75: Sahin MT, Türel-Ermertcan A, Oztürkcan S, Türkdogan P. Generalized granuloma annulare in a patient with type II diabetes mellitus: successful treatment with isotretinoin. J Eur Acad Dermatol Venereol 2006;20: Struder E, Calza A, Saurat J. Precipitating factors and associated disorders in 84 patients with granuloma annulare: a retrospective study. Dermatology 1996;193: Dabski K, Winkelmann R. Generalized granuloma annulare: clinical and laboratory findings in 100 patients. J Am Acad Dermatol 1989;20: Cyr PR. Diagnosis and management of granuloma annulare. Am Fam Phys 2006;74: Arroyo MP. Generalized granuloma annulare. Dermatol Online J 2003;9: Farrell A. Commentary: acquired perforating dermatosis in renal and diabetic patients. Lancet 1997;349: Maurice P, Neild GH. Acquired perforating dermatosis and diabetic nephropathy: a case report and review of the literature. Clin Exp Dermatol 1997;22: Mutluoglu M, Uzun G, Karabacak E. Toenail onychodystrophy of the diabetic foot. BMJ Case Rep 2012 Oct. 19; Millikan LE, Powell DW, Drake LA. Quality of life for patients with onychomycosis. Int J Dermatol 1999;38(Suppl. 2): Landau J, Davis E. The small blood vessels of the conjunctiva and nail bed in diabetes mellitus. Lancet 1960;2: Romano C, Massai L, Asta F, et al. Prevalence of dermatophytic skin and nail infections in diabetic patients. Mycoses 2001;44: Higa M. Clinical epidemiology of fungal infection in diabetes. Nihon Rinsho 2008;66: Qadim HH, Golforoushan F, Azimi H, Goldust M. Factor leading to dermatophytosis. Ann Parisitol 2013;59: Yeung C, Lee K. Community acquired fulminant pseudomonas infection of the gastrointestinal tract in previously healthy infants. J Paediatr Child Health 1998;34: Soheilipour S, Meidani M, Derakhshandi H, et al. Necrotizing external otitis: a case series. B-ENT 2013;9: CLINICAL.DIABETESJOURNALS.ORG
Diabetes and Skin. Benjamin Barankin, MD, FRCPC. Dermatologist & Director, Toronto Dermatology Centre
 Diabetes and Skin Benjamin Barankin, MD, FRCPC Dermatologist & Director, Toronto Dermatology Centre Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Diabetes and Skin Benjamin Barankin, MD, FRCPC Dermatologist & Director, Toronto Dermatology Centre Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
COMMON SKIN CONDITIONS IN PRIMARY CARE. Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio
 COMMON SKIN CONDITIONS IN PRIMARY CARE Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio DISCLOSURE The Speaker and members of the planning committee do not have a conflict of interest
COMMON SKIN CONDITIONS IN PRIMARY CARE Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio DISCLOSURE The Speaker and members of the planning committee do not have a conflict of interest
Saturday, 09 October :14 - Last Updated Sunday, 13 February :43
 1/9 2/9 Diabetic finding had 50.Diabetic pretibial asymmetrical superficial extravasated hyperpigmentation. behind diabetic inareas dermopathy diabetes. blood dermopathy dermopathy, erythrocytes distribution.
1/9 2/9 Diabetic finding had 50.Diabetic pretibial asymmetrical superficial extravasated hyperpigmentation. behind diabetic inareas dermopathy diabetes. blood dermopathy dermopathy, erythrocytes distribution.
Egyptian Dermatology Online Journal Vol. 5 No 2:5, December 2009
 Cutaneous Manifestations of Diabetes mellitus: A Hospital Based Study in Kashmir, India Mashkoor Ahmed Wani, MD 1 *; Iffat Hassan, MD 2 *; Mohd Hayat Bhat, DM 3 and Qazi Masood Ahmed, MD 4 * Egyptian Dermatology
Cutaneous Manifestations of Diabetes mellitus: A Hospital Based Study in Kashmir, India Mashkoor Ahmed Wani, MD 1 *; Iffat Hassan, MD 2 *; Mohd Hayat Bhat, DM 3 and Qazi Masood Ahmed, MD 4 * Egyptian Dermatology
Rashes Not To Be Missed In Children
 May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
Cutanous Manifestation of Lupus Erythematosus. Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university
 Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level
 Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level Dr Ng Su Yuen Paediatrician and Paediatric Dermatologist Hospital Pulau Pinang Outline Common inflammatory
Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level Dr Ng Su Yuen Paediatrician and Paediatric Dermatologist Hospital Pulau Pinang Outline Common inflammatory
=ﻰﻤاﻤﺤﻠا ﺔﻴﻘﻠﺤﻠا ﺔذﺒاﻨﻠا
 1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
My ear won t stop hurting!
 This month: 1. My ear won t stop hurting! 5. Cortisone Cream Didn t Help! 2. What are these red bumps? 6. Can my girlfriend get it? 3. Why won t this rash leave? 7. My wife noticed it! 4. What s the cause
This month: 1. My ear won t stop hurting! 5. Cortisone Cream Didn t Help! 2. What are these red bumps? 6. Can my girlfriend get it? 3. Why won t this rash leave? 7. My wife noticed it! 4. What s the cause
Swapna Kameti, Senthil Kumar, Vijaya Mohan Rao*, Penchala Reddy*, C Aruna
 Original Article Spectrum of cutaneous manifestations in diabetes mellitus and their association with duration of diabetes mellitus: An observational study in a tertiary care hospital of South India Swapna
Original Article Spectrum of cutaneous manifestations in diabetes mellitus and their association with duration of diabetes mellitus: An observational study in a tertiary care hospital of South India Swapna
Difference Between Seborrheic Dermatitis and Psoriasis
 Difference Between Seborrheic Dermatitis and Psoriasis www.differencebetween.com Key Difference Seborrheic Dermatitis vs Psoriasis Dermatological conditions are perhaps the most worrisome diseases in the
Difference Between Seborrheic Dermatitis and Psoriasis www.differencebetween.com Key Difference Seborrheic Dermatitis vs Psoriasis Dermatological conditions are perhaps the most worrisome diseases in the
Cutaneous Conditions Associated with Systemic Disease
 Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
السكري للداء مرافقة فقاعات diabeticorum= Bullosis
 1 / 6 Bullosis diabeticorum Bullous disease of diabetes (bullosis diabeticorum) is a distinct, spontaneous, noninflammatory, blistering condition of acral skin unique to patients with diabetes mellitus.
1 / 6 Bullosis diabeticorum Bullous disease of diabetes (bullosis diabeticorum) is a distinct, spontaneous, noninflammatory, blistering condition of acral skin unique to patients with diabetes mellitus.
الاكزيماتيد= Eczematid
 1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
Common Superficial Fungal Infections
 How to recognise and treat Common Superficial Fungal Infections Dr Lilianne Scholtz (MBBCh) Types of superficial fungal infections Ringworm (Tinea) Candida (Thrush) Body Groin Feet Skin Nappy rash Vagina
How to recognise and treat Common Superficial Fungal Infections Dr Lilianne Scholtz (MBBCh) Types of superficial fungal infections Ringworm (Tinea) Candida (Thrush) Body Groin Feet Skin Nappy rash Vagina
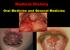
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
Psoriasis. What is Psoriasis? What causes psoriasis? Medical Topics Psoriasis
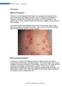 1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
Classification. Distal & Lateral Subungual OM. White Superficial OM. Proximal Subungual OM. Candidal OM. Total dystrophic OM
 Onychomycosis Commonest dermatological condition Definition: Infection of the nail caused by fungi that include dermatophytes, non-dermatophyte moulds and yeasts (mainly Candida). 80% of all OM affects
Onychomycosis Commonest dermatological condition Definition: Infection of the nail caused by fungi that include dermatophytes, non-dermatophyte moulds and yeasts (mainly Candida). 80% of all OM affects
Management of fungal infection
 Management of fungal infection HKDU symposium 17 th May 2015 Speaker: Dr. Thomas Chan MBBS (Hons), MRCP, FHKCP, FHKAM Synopsis Infection caused by fungus mycoses Skin infection by fungus is common in general
Management of fungal infection HKDU symposium 17 th May 2015 Speaker: Dr. Thomas Chan MBBS (Hons), MRCP, FHKCP, FHKAM Synopsis Infection caused by fungus mycoses Skin infection by fungus is common in general
Common Cutaneous Signs of Medical Illnesses
 Common Cutaneous Signs of Medical Illnesses DR COLIN THENG MBBS, MMED (FAM. MED), MRCP(UK), FAMS SENIOR CONSULTANT DERMATOLOGIST THE SKIN SPECIALISTS & LASER CLINIC MOUNT ALVERNIA MEDICAL CENTRE D, #07-61
Common Cutaneous Signs of Medical Illnesses DR COLIN THENG MBBS, MMED (FAM. MED), MRCP(UK), FAMS SENIOR CONSULTANT DERMATOLOGIST THE SKIN SPECIALISTS & LASER CLINIC MOUNT ALVERNIA MEDICAL CENTRE D, #07-61
Lichen planus along with Blaschko lines "Blaschkoian lichen planus"
 Original Article Lichen planus along with Blaschko lines "Blaschkoian lichen planus" Hossein Kavoussi, Mazaher Ramazani, Elias Salimi Dermatology Department, Kermanshah University of Medical Sciences,
Original Article Lichen planus along with Blaschko lines "Blaschkoian lichen planus" Hossein Kavoussi, Mazaher Ramazani, Elias Salimi Dermatology Department, Kermanshah University of Medical Sciences,
Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada
 Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses Inc. All rights reserved.
Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses Inc. All rights reserved.
Opportunistic Mycoses
 CANDIDIASIS SOFYAN LUBIS DEPARTEMEN MIKROBIOLOGI FAK.KEDOKTERAN USU MEDAN 2009 Opportunistic Mycoses Opportunistic mycoses are fungal infections that do not normally cause disease in healthy people, but
CANDIDIASIS SOFYAN LUBIS DEPARTEMEN MIKROBIOLOGI FAK.KEDOKTERAN USU MEDAN 2009 Opportunistic Mycoses Opportunistic mycoses are fungal infections that do not normally cause disease in healthy people, but
Skin & Endocrine Disorders: Beyond the Usual Diabetes and Dermatology
 Skin & Endocrine Disorders: Beyond the Usual Diabetes and Dermatology Michelle Tarbox, MD Assistant Professor of Dermatology and Dermatopathology Texas Tech University Health Sciences Center I have no
Skin & Endocrine Disorders: Beyond the Usual Diabetes and Dermatology Michelle Tarbox, MD Assistant Professor of Dermatology and Dermatopathology Texas Tech University Health Sciences Center I have no
Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])
![Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV]) Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])](/thumbs/89/99382632.jpg) Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Actinic keratosis (AK): Dr Sarma s simple guide
 Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
My Algorithm. Questions to ask. Do you or your family have a history of?... Allergic rhinitis, Sensitive skin, Asthma Skin Cancer
 Tracey C. Vlahovic, DPM Associate Professor, Temple University School of Podiatric Medicine My Algorithm Inflammatory Skin Disorder on Feet Family hx, clinical exam, look at hands! Defined plaques: Psoriasis
Tracey C. Vlahovic, DPM Associate Professor, Temple University School of Podiatric Medicine My Algorithm Inflammatory Skin Disorder on Feet Family hx, clinical exam, look at hands! Defined plaques: Psoriasis
Psoriasis: Causes, Symptoms, And Treatment
 Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
Facial Rash. Facial Rash 10/14/2013. Ten Look Alike Rashes Michelle DiBaise, MPAS, PA-C, DFAAPA Associate Clinical Professor NAU PA Program
 Ten Look Alike Rashes Michelle DiBaise, MPAS, PA-C, DFAAPA Associate Clinical Professor NAU PA Program Facial Rash Facial Rash Case 1 28 year female Progressive development of erythematous facial lesions
Ten Look Alike Rashes Michelle DiBaise, MPAS, PA-C, DFAAPA Associate Clinical Professor NAU PA Program Facial Rash Facial Rash Case 1 28 year female Progressive development of erythematous facial lesions
Thursday, 21 October :53 - Last Updated Thursday, 11 November :27
 1 / 15 2 / 15 3 / 15 4 / 15 Pityriasis Alba Background Pityriasis alba is a nonspecific dermatitis of unknown etiology that causes erythematous scaly patches. These resolve and leave areas of hypopigmentation
1 / 15 2 / 15 3 / 15 4 / 15 Pityriasis Alba Background Pityriasis alba is a nonspecific dermatitis of unknown etiology that causes erythematous scaly patches. These resolve and leave areas of hypopigmentation
Skin Problems. Issues for a Child. Skin Problems. Paediatric Palliative Care For Home Based Carers. Common in children with HIV
 Skin Problems Paediatric Palliative Care For Home Based Carers Funded by British High Commission, Pretoria Small Grant Scheme Skin Problems Common in children with HIV Often conditions common in all children
Skin Problems Paediatric Palliative Care For Home Based Carers Funded by British High Commission, Pretoria Small Grant Scheme Skin Problems Common in children with HIV Often conditions common in all children
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA)
 Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
DERMCASE. Doc, my baby s all spotty! Case 1
 Test Your Knowledge With Multiple-Choice Cases This month 5 cases: Case 1 1. Doc, my baby s all spotty! 2. A Mediterranean Matter 3. Mommy, what s wrong with my head? 4. Armed with Lesions 5. It s spreading!
Test Your Knowledge With Multiple-Choice Cases This month 5 cases: Case 1 1. Doc, my baby s all spotty! 2. A Mediterranean Matter 3. Mommy, what s wrong with my head? 4. Armed with Lesions 5. It s spreading!
It is estimated that about 26,000 new cases of
 Focus on CME at Dalhousie University Set On Soothing Psoriasis A. H. Murray, MD, FRCP(C) Presented at the 76th Annual Dalhousie Refresher Course It is estimated that about 26,000 new cases of psoriasis
Focus on CME at Dalhousie University Set On Soothing Psoriasis A. H. Murray, MD, FRCP(C) Presented at the 76th Annual Dalhousie Refresher Course It is estimated that about 26,000 new cases of psoriasis
A giant skin Tag over labium majus: An unusual location of skin tag
 A giant skin Tag over labium majus: An unusual location of skin tag Garima Gupta 1, Ruchi Sinha 2, Sulekha Pandey 3, L. K. Pandey 3 Department of Obstetrics and Gynecology, Institute of Medical Sciences,
A giant skin Tag over labium majus: An unusual location of skin tag Garima Gupta 1, Ruchi Sinha 2, Sulekha Pandey 3, L. K. Pandey 3 Department of Obstetrics and Gynecology, Institute of Medical Sciences,
Pathogens with Intermediate Virulence Dermatophytes opportunistic Pathogens
 Pathogens with Intermediate Virulence Dermatophytes opportunistic Pathogens Cryptococcus neoformans Candida albicans Aspergillus species Pneumocystis carinii 1 Dermatophytes Named for derma skin Cause
Pathogens with Intermediate Virulence Dermatophytes opportunistic Pathogens Cryptococcus neoformans Candida albicans Aspergillus species Pneumocystis carinii 1 Dermatophytes Named for derma skin Cause
Rameshwar Gutte and Uday Khopkar
 Extragenital unilateral lichen sclerosus et atrophicus in a child: a case report Rameshwar Gutte and Uday Khopkar Department of Dermatolgy, Seth GSMC and KEM Hospital, Parel, Mumbai-400012, India Egyptian
Extragenital unilateral lichen sclerosus et atrophicus in a child: a case report Rameshwar Gutte and Uday Khopkar Department of Dermatolgy, Seth GSMC and KEM Hospital, Parel, Mumbai-400012, India Egyptian
A. Erythema multiforme and related diseases
 Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Citation The Journal of Dermatology, 37(8), available at
 NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
Topical Calcipotriol Algorithm
 Topical Calcipotriol Algorithm Is this patient an adult previously diagnosed with psoriasis by a doctor? Do the skin patches look the same as those diagnosed as psoriasis? Is this psoriasis covering an
Topical Calcipotriol Algorithm Is this patient an adult previously diagnosed with psoriasis by a doctor? Do the skin patches look the same as those diagnosed as psoriasis? Is this psoriasis covering an
Dermclinic
 Dermclinic /Dermclinic A Photo Quiz to Hone Dermatologic Skills DAVID L. KAPLAN, MD Series Editor University of Missouri Kansas City, University of Kansas Case 1: Upon his return from a summer visit to
Dermclinic /Dermclinic A Photo Quiz to Hone Dermatologic Skills DAVID L. KAPLAN, MD Series Editor University of Missouri Kansas City, University of Kansas Case 1: Upon his return from a summer visit to
Time to Learn. 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service
 Time to Learn 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service The Red Face Rosacea Acne Seborrhoeic eczema eczema Psoriasis Slapped cheek syndrome Fungal infection Erysipelas...
Time to Learn 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service The Red Face Rosacea Acne Seborrhoeic eczema eczema Psoriasis Slapped cheek syndrome Fungal infection Erysipelas...
TINEA (FUNGAL) INFECTION
 1 Medical Topics - Tinea TINEA (FUNGAL) INFECTION Tinea infection There are 3 main groups of fungal organisms that can cause skin infections. They include dermatophytes, yeast and moulds. Dermatophytes
1 Medical Topics - Tinea TINEA (FUNGAL) INFECTION Tinea infection There are 3 main groups of fungal organisms that can cause skin infections. They include dermatophytes, yeast and moulds. Dermatophytes
Skin Deep: Cutaneous Lupus. Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016
 Skin Deep: Cutaneous Lupus Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016 Introduction: Cutaneous lupus erythematosus LE is an autoimmune disease with a range of clinical manifestations
Skin Deep: Cutaneous Lupus Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016 Introduction: Cutaneous lupus erythematosus LE is an autoimmune disease with a range of clinical manifestations
ISPUB.COM. A Case of Actinic Lichen Planus. K Choi, H Kim, H Kim, Y Park INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Dermatology Volume 8 Number K Choi, H Kim, H Kim, Y Park Citation K Choi, H Kim, H Kim, Y Park.. The Internet Journal of Dermatology. 2009 Volume 8 Number. Abstract The
ISPUB.COM The Internet Journal of Dermatology Volume 8 Number K Choi, H Kim, H Kim, Y Park Citation K Choi, H Kim, H Kim, Y Park.. The Internet Journal of Dermatology. 2009 Volume 8 Number. Abstract The
Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India.
 Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
CASE REPORT ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX
 ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa
 More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa Conflicts of Interest/Disclosure None Classification/Overview 1) Necrobiotic/Palisading
More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa Conflicts of Interest/Disclosure None Classification/Overview 1) Necrobiotic/Palisading
Test your knowledge with multiple-choice cases. What are these speckled spots?
 Test your knowledge with multiple-choice cases Case 1 What are these speckled spots? A speckled, pigmented lesion is noticed on the upper arm of a 10-year-old girl. Her mother says the lesion has been
Test your knowledge with multiple-choice cases Case 1 What are these speckled spots? A speckled, pigmented lesion is noticed on the upper arm of a 10-year-old girl. Her mother says the lesion has been
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
GROUP 15 TOPICAL PREPARATIONS
 - 105 - GROUP 15 15.1 DERMATOLOGICAL PREPARATIONS 15.1.1 TOPICAL ANTIFUNGALS CLOTRIMAZOLE Indication: Treatment of susceptible fungal infections, dermatophytoses, superficial mycoses, and cutaneous candidiasis
- 105 - GROUP 15 15.1 DERMATOLOGICAL PREPARATIONS 15.1.1 TOPICAL ANTIFUNGALS CLOTRIMAZOLE Indication: Treatment of susceptible fungal infections, dermatophytoses, superficial mycoses, and cutaneous candidiasis
Introduction. Study of fungi called mycology.
 Fungi Introduction Study of fungi called mycology. Some fungi are beneficial: ex a) Important in production of some foods, ex: cheeses, bread. b) Important in production of some antibiotics, ex: penicillin
Fungi Introduction Study of fungi called mycology. Some fungi are beneficial: ex a) Important in production of some foods, ex: cheeses, bread. b) Important in production of some antibiotics, ex: penicillin
Subspecialty Rotation: Dermatology
 Subspecialty Rotation: Dermatology Faculty: Wesley Galen, M.D. GOAL: Prevention, Counseling and Screening (Dermatology). Understand the pediatrician's role in preventing illness and dysfunction related
Subspecialty Rotation: Dermatology Faculty: Wesley Galen, M.D. GOAL: Prevention, Counseling and Screening (Dermatology). Understand the pediatrician's role in preventing illness and dysfunction related
Types of Skin Infections
 Anatomy of Skin Types of Skin Infections Bacterial Impetigo Folliculitis Acne Fungal /Parasitic Tinea Pedis Tinea Cruris Tinea Versicolor Tinea Corporis Toenail fungus Allergic/Irritation conditions Dermatitis
Anatomy of Skin Types of Skin Infections Bacterial Impetigo Folliculitis Acne Fungal /Parasitic Tinea Pedis Tinea Cruris Tinea Versicolor Tinea Corporis Toenail fungus Allergic/Irritation conditions Dermatitis
Medical History. Oral Medicine and General Medicine
 Medical History Oral Medicine and General Medicine Gingivitis herpetica acuta NECROTIZÁLÓ SIALOMETAPLASIA SOOR Medical History The life expectancy has recently increased and increasing By dental prevention
Medical History Oral Medicine and General Medicine Gingivitis herpetica acuta NECROTIZÁLÓ SIALOMETAPLASIA SOOR Medical History The life expectancy has recently increased and increasing By dental prevention
Emergency Dermatology. Emergency Dermatology
 Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Conflicts. Objectives. University of Texas Health Science Center at San Antonio. Pediatrics Grand Rounds 24 August Pediatric Dermatology 101
 Pediatric Dermatology 101 John C. Browning, MD, FAAD, FAAP Conflicts Investigator: ViroXis Advisor: ViroXis Advisory Board: TopMD Speaker: Galderma Objectives Understand the meaning and importance of cutaneous
Pediatric Dermatology 101 John C. Browning, MD, FAAD, FAAP Conflicts Investigator: ViroXis Advisor: ViroXis Advisory Board: TopMD Speaker: Galderma Objectives Understand the meaning and importance of cutaneous
Dr Janakan Natkunarajah (Dr Jana)
 Dr Janakan Natkunarajah (Dr Jana) Diagnosis Furuncle (Boil) Deep follicular abscess Anti-staph antibiotics Systemic & topical Carbuncle Deep abscess formed in a group of follicles Incise and Drain Recurrent
Dr Janakan Natkunarajah (Dr Jana) Diagnosis Furuncle (Boil) Deep follicular abscess Anti-staph antibiotics Systemic & topical Carbuncle Deep abscess formed in a group of follicles Incise and Drain Recurrent
A Vitiligo Update for Pharmacists: Current Practices and Future Advances
 A Vitiligo Update for Pharmacists: Current Practices and Future Advances Dalal Hammoudi Halat, RPh, MSc, PhD Assistant Professor School of Pharmacy, Lebanese International University Disclosure Dalal Hammoudi
A Vitiligo Update for Pharmacists: Current Practices and Future Advances Dalal Hammoudi Halat, RPh, MSc, PhD Assistant Professor School of Pharmacy, Lebanese International University Disclosure Dalal Hammoudi
Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady
 Hong Kong J. Dermatol. Venereol. (2009) 17, 151-155 Case Report Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady SKF Loo, LY
Hong Kong J. Dermatol. Venereol. (2009) 17, 151-155 Case Report Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady SKF Loo, LY
Tinea: Head to Toe A dermatophyte tour of human skin. Tour de Tinea Head to Toe. Tips for Tinea Head to Toe. Psoriasis. Non-inflammatory Tinea Capitis
 Tinea: Head to Toe A dermatophyte tour of human skin Renee Howard, MD Assistant Clinical Professor of Dermatology, UCSF Tour de Tinea Head to Toe Tips for Tinea Head to Toe Capitis Faciei Corporis Pedis
Tinea: Head to Toe A dermatophyte tour of human skin Renee Howard, MD Assistant Clinical Professor of Dermatology, UCSF Tour de Tinea Head to Toe Tips for Tinea Head to Toe Capitis Faciei Corporis Pedis
KEY MESSAGES. Psoriasis patients are more prone to cardiovascular diseases, stroke, lymphoma and non-melanoma skin cancers, and increased mortality.
 KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
LESIONS OF THE ORAL CAVITY ORAL CAVITY. Oral Cavity Subsites 4/10/2013 LIPS TEETH GINGIVA ORAL MUCOUS MEMBRANES PALATE TONGUE ORAL LYMPHOID TISSUES
 LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
What is Psoriasis? Common Areas Affected. Type Who Does it Affect Characteristics
 What is? is a term derived from the Greek word psōra which means itch and is a common, long lasting, inflammatory skin condition which affects 1-3% of the UK population and about 80 million people worldwide.
What is? is a term derived from the Greek word psōra which means itch and is a common, long lasting, inflammatory skin condition which affects 1-3% of the UK population and about 80 million people worldwide.
BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123
 BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123 M55. 4/7 tender lesions on knee, legs and arms. Also iritis/ weight loss/headache, synovitis.?vasculitis. Sarcoidosis. Biopsy from left elbow
BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123 M55. 4/7 tender lesions on knee, legs and arms. Also iritis/ weight loss/headache, synovitis.?vasculitis. Sarcoidosis. Biopsy from left elbow
Disorders of the vulva
 Vulval lesions Disorders of the vulva Terminology standardised by the International Society for the Study of Vulvovaginal Disease(ISSVD) Classification 1.Nonneoplastic epithelial disorders of vulva Lichen
Vulval lesions Disorders of the vulva Terminology standardised by the International Society for the Study of Vulvovaginal Disease(ISSVD) Classification 1.Nonneoplastic epithelial disorders of vulva Lichen
Questions. Answers. Share your photos and diagnoses with us!
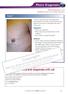 Illustrated quizzes on problems seen in everyday practice CASE 1 A 66-year-old male presents with ruddy-brown, pruritic papules on his chest and back that have been present for several years. The patient
Illustrated quizzes on problems seen in everyday practice CASE 1 A 66-year-old male presents with ruddy-brown, pruritic papules on his chest and back that have been present for several years. The patient
Skin lesions & Abrasions
 Skin lesions & Abrasions What Are Skin Lesions? A skin lesion is a part of the skin that has an abnormal growth or appearance compared to the skin around it Types of Skin Lesions Two types of skin lesions
Skin lesions & Abrasions What Are Skin Lesions? A skin lesion is a part of the skin that has an abnormal growth or appearance compared to the skin around it Types of Skin Lesions Two types of skin lesions
Cutaneous reactions to targeted therapies. Stavonnie Patterson, MD, FAAD Northwestern University Feinberg School of Medicine March 6, 2017
 Cutaneous reactions to targeted therapies Stavonnie Patterson, MD, FAAD Northwestern University Feinberg School of Medicine March 6, 2017 Disclosures I have no relevant disclosures Papulopustular Eruption
Cutaneous reactions to targeted therapies Stavonnie Patterson, MD, FAAD Northwestern University Feinberg School of Medicine March 6, 2017 Disclosures I have no relevant disclosures Papulopustular Eruption
Emergency Dermatology Dr Melissa Barkham
 Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
This PDF is available for free download from a site hosted by Medknow Publications
 Net Study Comparison of clinical efficacy of topical tazarotene.1% cream with topical clobetasol propionate.5% cream in chronic plaque psoriasis: A double-blind, randomized, right-left comparison study
Net Study Comparison of clinical efficacy of topical tazarotene.1% cream with topical clobetasol propionate.5% cream in chronic plaque psoriasis: A double-blind, randomized, right-left comparison study
COPYRIGHTED MATERIAL. Introduction CHAPTER 1. Introduction
 CHAPTER 1 Introduction OVERVIEW The clinical features of skin lesions are related to the underlying pathological processes. Broadly skin conditions fall into three clinical groups: (a) those with a well-defined
CHAPTER 1 Introduction OVERVIEW The clinical features of skin lesions are related to the underlying pathological processes. Broadly skin conditions fall into three clinical groups: (a) those with a well-defined
MERCY RETREAT Dermatology
 MERCY RETREAT 2016 Dermatology INFECTIONS IN DERMATOLOGY Why we do talk about infections today? These are some of the most commonly seen dermatologic diseases that present to primary care physician office
MERCY RETREAT 2016 Dermatology INFECTIONS IN DERMATOLOGY Why we do talk about infections today? These are some of the most commonly seen dermatologic diseases that present to primary care physician office
Dermatology GP Referral Guidelines
 Austin Health Dermatology Department holds 5 Clinic sessions to discuss and plan the treatment of with Dermatology conditions. Department of Health clinical urgency categories for specialist clinics Urgent:
Austin Health Dermatology Department holds 5 Clinic sessions to discuss and plan the treatment of with Dermatology conditions. Department of Health clinical urgency categories for specialist clinics Urgent:
Eczema. By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University
 Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
BMT CTN 0801 Protocol. Chronic GVHD Provider Survey. FOLLOW-UP v3.0
 BMT CTN 0801 Protocol Chronic GVHD Provider Survey FOLLOW-UP v3.0 Instructions: Please score a symptom only if you know or suspect it be related to chronic GVHD. Subjective are acceptable. For example,
BMT CTN 0801 Protocol Chronic GVHD Provider Survey FOLLOW-UP v3.0 Instructions: Please score a symptom only if you know or suspect it be related to chronic GVHD. Subjective are acceptable. For example,
Table of Contents: Part 1 Medical Dermatology. Chapter 1 Acneiform Disorders. Acne. Acne Vulgaris. Pomade Acne. Steroid Acne
 Table of Contents: Part 1 Medical Dermatology Chapter 1 Acneiform Disorders Acne Acne Vulgaris Pomade Acne Steroid Acne Infantile Acne Pediatric Perspectives Neonatal Acne (Acne Neonatorum) Pediatric Perspectives
Table of Contents: Part 1 Medical Dermatology Chapter 1 Acneiform Disorders Acne Acne Vulgaris Pomade Acne Steroid Acne Infantile Acne Pediatric Perspectives Neonatal Acne (Acne Neonatorum) Pediatric Perspectives
Skin Side Effects U N I V E R S I T Y OF V I E N N A, D E P A R T M E N T OF O N C O L O G Y, G E N E R A L H O S P I T A L V I E N N A
 Skin Side Effects Christiane Thallinger, M D U N I V E R S I T Y OF V I E N N A, D E P A R T M E N T OF O N C O L O G Y, G E N E R A L H O S P I T A L V I E N N A Targets Substances 1 Multi Kinase Inhibitors
Skin Side Effects Christiane Thallinger, M D U N I V E R S I T Y OF V I E N N A, D E P A R T M E N T OF O N C O L O G Y, G E N E R A L H O S P I T A L V I E N N A Targets Substances 1 Multi Kinase Inhibitors
BMT CTN 0801 Protocol. Chronic GVHD Provider Survey ENROLLMENT
 BMT CTN 0801 Protocol Chronic GVHD Provider Survey ENROLLMENT Instructions: Please score a symptom only if you know or suspect it be related to chronic GVHD. Subjective are acceptable. For example, joint
BMT CTN 0801 Protocol Chronic GVHD Provider Survey ENROLLMENT Instructions: Please score a symptom only if you know or suspect it be related to chronic GVHD. Subjective are acceptable. For example, joint
Name the condition: Canine sterile neutrophilic dermatosis (Sweet s syndrome)
 5-year-old male miniature Schnauzer dog with acute onset of severe macular erythema and multiple tender violaceus plaques all over the body. Which of the following is the most likely diagnosis? 1. Canine
5-year-old male miniature Schnauzer dog with acute onset of severe macular erythema and multiple tender violaceus plaques all over the body. Which of the following is the most likely diagnosis? 1. Canine
Questions. Answers. Share your photos and diagnoses with us!
 Illustrated quizzes on problems seen in everyday practice Case 1 A 56-year-old woman presented with a two-week history of pruritic urticarial plaques and tense bullae on both erythematous and normal skin.
Illustrated quizzes on problems seen in everyday practice Case 1 A 56-year-old woman presented with a two-week history of pruritic urticarial plaques and tense bullae on both erythematous and normal skin.
Misdiagnosed Case of Lepromatous Leprosy
 Bahrain Medical Bulletin, Vol. 36, No. 3, September 2014 Misdiagnosed Case of Lepromatous Leprosy Ahmed Anwer Aljowder, BSc, MD* Azad Kareem Kassim FRCPI, FRCP (Glasg), FAAD** Mazen Raees MB, BCh, BAO,
Bahrain Medical Bulletin, Vol. 36, No. 3, September 2014 Misdiagnosed Case of Lepromatous Leprosy Ahmed Anwer Aljowder, BSc, MD* Azad Kareem Kassim FRCPI, FRCP (Glasg), FAAD** Mazen Raees MB, BCh, BAO,
TREATMENT OPTIONS FOR PSORIASIS. Sandra Hanlon Dermatology Senior Charge Nurse NHS Ayrshire and Arran 07/03/17
 TREATMENT OPTIONS FOR PSORIASIS Sandra Hanlon Dermatology Senior Charge Nurse NHS Ayrshire and Arran 07/03/17 PSORIASIS A chronic, non-infectious inflammatory skin condition that has no cure Characterised
TREATMENT OPTIONS FOR PSORIASIS Sandra Hanlon Dermatology Senior Charge Nurse NHS Ayrshire and Arran 07/03/17 PSORIASIS A chronic, non-infectious inflammatory skin condition that has no cure Characterised
Cutaneous manifestations of diabetes mellitus
 Original Article Cutaneous manifestations of diabetes mellitus Tariq Mahmood*, Arfan ul Bari**, Humayun Agha * Department of Medicine, ** Department of Dermatology, PAF, Hospital, Sargodha. Department
Original Article Cutaneous manifestations of diabetes mellitus Tariq Mahmood*, Arfan ul Bari**, Humayun Agha * Department of Medicine, ** Department of Dermatology, PAF, Hospital, Sargodha. Department
Dermatology for the Internist DREW M ANDERSON, MD VOLUNTEER CLINICAL ASSISTANT PROFESSOR OF MEDICINE, INDIANA UNIVERSITY SCHOOL OF MEDICINE
 Dermatology for the Internist DREW M ANDERSON, MD VOLUNTEER CLINICAL ASSISTANT PROFESSOR OF MEDICINE, INDIANA UNIVERSITY SCHOOL OF MEDICINE Why Should I Care? 53% of all skin related visits are to non
Dermatology for the Internist DREW M ANDERSON, MD VOLUNTEER CLINICAL ASSISTANT PROFESSOR OF MEDICINE, INDIANA UNIVERSITY SCHOOL OF MEDICINE Why Should I Care? 53% of all skin related visits are to non
Psoriasis Penis - A Two Case Report
 Article ID: WMC003176 ISSN 2046-1690 Psoriasis Penis - A Two Case Report Corresponding Author: Dr. Ilko Bakardzhiev, MD, PhD, Medical College, Medical University of Varna, 9000 - Bulgaria Submitting Author:
Article ID: WMC003176 ISSN 2046-1690 Psoriasis Penis - A Two Case Report Corresponding Author: Dr. Ilko Bakardzhiev, MD, PhD, Medical College, Medical University of Varna, 9000 - Bulgaria Submitting Author:
Outline Dermatomycoses Definition: diseases or fungal infections of the skin Transmission of Dermatomycoses Case Report 1 Presentation of Disease
 Outline Dermatomycoses Tinea corporis,tinea capitis,tinea pedis, Tinea cruris, Definition: diseases or fungal infections of the skin Dermatophyte infections are caused by Trichophyton, Microsporum, and
Outline Dermatomycoses Tinea corporis,tinea capitis,tinea pedis, Tinea cruris, Definition: diseases or fungal infections of the skin Dermatophyte infections are caused by Trichophyton, Microsporum, and
A case of rosacea fulminans in a pregnant woman
 Hong Kong J. Dermatol. Venereol. (2018) 26, 122-126 Views and Practice A case of rosacea fulminans in a pregnant woman JE Seol, SH Park, JU Kim, GJ Cho, SH Moon, H Kim Introduction Rosacea fulminans (RF)
Hong Kong J. Dermatol. Venereol. (2018) 26, 122-126 Views and Practice A case of rosacea fulminans in a pregnant woman JE Seol, SH Park, JU Kim, GJ Cho, SH Moon, H Kim Introduction Rosacea fulminans (RF)
Three clinical cases. fungal infections
 Three clinical cases Diagnostic and treatment challenges in skin and mucosal fungal infections Else Svejgaard, MD, Merete Hædersdal, MD Dept. of Dermatology, Bispebjerg University Hospital, Copenhagen,
Three clinical cases Diagnostic and treatment challenges in skin and mucosal fungal infections Else Svejgaard, MD, Merete Hædersdal, MD Dept. of Dermatology, Bispebjerg University Hospital, Copenhagen,
CORNEAL CONDITIONS CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
HEADS UP. IT S OUR BIRTHDAY. Photo Diagnosis
 An illustrated quiz on problems seen in everyday practice Case 1 A 57-year-old male presented with a history of recurrent abdominal pain and weight loss over the last three months. A computed tomography
An illustrated quiz on problems seen in everyday practice Case 1 A 57-year-old male presented with a history of recurrent abdominal pain and weight loss over the last three months. A computed tomography
Diagnosis and Treatment of Infectious, Inflammatory and Neoplastic Nail Conditions
 OFFICE DERMATOLOGY, PART I 0025-7125/98 $8.00 +.OO NAIL DISORDERS Diagnosis and Treatment of Infectious, Inflammatory and Neoplastic Nail Conditions Phoebe Rich, MD Nail problems (Table 1) are common complaints
OFFICE DERMATOLOGY, PART I 0025-7125/98 $8.00 +.OO NAIL DISORDERS Diagnosis and Treatment of Infectious, Inflammatory and Neoplastic Nail Conditions Phoebe Rich, MD Nail problems (Table 1) are common complaints
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi Medical Microbiology
 1 Nursing college, Second stage Microbiology Medical Microbiology Lecture-1- Fungi (Mycosis) They are a diverse group of saprophytic and parasitic eukaryotic organisms. Human fungal diseases (mycoses)
1 Nursing college, Second stage Microbiology Medical Microbiology Lecture-1- Fungi (Mycosis) They are a diverse group of saprophytic and parasitic eukaryotic organisms. Human fungal diseases (mycoses)
Vulval dermatoses. Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough
 Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Objectives. 1. Recognizing benign skin lesions. 2.Know which patients will likely need surgical intervention.
 The Joy of Pediatric Skin Dr. Claire Sanger University of Kentucky Plastic & Reconstructive Surgery Objectives 1. Recognizing benign skin lesions 2.Know which patients will likely need surgical intervention.
The Joy of Pediatric Skin Dr. Claire Sanger University of Kentucky Plastic & Reconstructive Surgery Objectives 1. Recognizing benign skin lesions 2.Know which patients will likely need surgical intervention.
Granuloma annulare is a benign self-limited disease, first described by Colcott-Fox 1 in 1895 and Radcliffe-Crocker in 1902.
 Granuloma Annulare Granuloma annulare is a benign self-limited disease, first described by Colcott-Fox 1 in 1895 and Radcliffe-Crocker in 1902. EPIDEMIOLOGY Granuloma annulare is a relatively common disorder.
Granuloma Annulare Granuloma annulare is a benign self-limited disease, first described by Colcott-Fox 1 in 1895 and Radcliffe-Crocker in 1902. EPIDEMIOLOGY Granuloma annulare is a relatively common disorder.
Antifungal drugs Dr. Raz Muhammed
 Antifungal drugs 13. 12. 2018 Dr. Raz Muhammed 2. Flucytosine (5-FC) Is fungistatic Is a synthetic pyrimidine antimetabolite Is often used in combination with amphotericin B in the treatment of systemic
Antifungal drugs 13. 12. 2018 Dr. Raz Muhammed 2. Flucytosine (5-FC) Is fungistatic Is a synthetic pyrimidine antimetabolite Is often used in combination with amphotericin B in the treatment of systemic
Deep Dermatophytosis
 Deep Dermatophytosis 2016-11-06 MMTN/Bangkok Department of Dermatology Chang Gung Memorial Hospital, Linkou Branch Taoyuan, Taiwan Superficial dermatophytosis Wikimedia Stratum corneum Tinea faciei Tinea
Deep Dermatophytosis 2016-11-06 MMTN/Bangkok Department of Dermatology Chang Gung Memorial Hospital, Linkou Branch Taoyuan, Taiwan Superficial dermatophytosis Wikimedia Stratum corneum Tinea faciei Tinea
CASE REPORT GRANULOMA ANNULARE MIMICKING SARCOIDOSIS AND TREATED WITH ACITRETIN: A CASE REPORT
 GRANULOMA ANNULARE MIMICKING SARCOIDOSIS AND TREATED WITH ACITRETIN: A CASE REPORT M.G. Gopal 1, Divya Gupta 2, Sharath Kumar B.C 3, Ramesh M 4, Nandini 5 HOW TO CITE THIS ARTICLE: MG Gopal, Divya Gupta,
GRANULOMA ANNULARE MIMICKING SARCOIDOSIS AND TREATED WITH ACITRETIN: A CASE REPORT M.G. Gopal 1, Divya Gupta 2, Sharath Kumar B.C 3, Ramesh M 4, Nandini 5 HOW TO CITE THIS ARTICLE: MG Gopal, Divya Gupta,
