Medical and Surgical Management of GI Disorders in Dogs and Cats March 14, 2010
|
|
|
- Richard Blake
- 5 years ago
- Views:
Transcription
1 METROPOLITAN NEW JERSEY VETERINARY MEDICAL ASSOCIATION Medical and Surgical Management of GI Disorders in Dogs and Cats March 14, 2010 Gary Oswald, DVM, Diplomate ACVIM (Internal Medicine) Tampa Bay Veterinary Specialists & Emergency Care Center 1501-A Belcher Rd S. Largo, Florida Use of GI Blood Panels in diagnosis and treatment of chronic GI disease. Why run more GI panels? What does serum cobalamin & folate really tell me? Gastrointestinal/Pancreatic-specific blood panels include serum cobalamin (vitamin B12), folate, TLI and PLI determination. These tests may help in the management of patients with chronic vomiting, weight loss, diarrhea, or in poor body condition. Submission of a fasted serum sample for this evaluation is recommended prior to advanced GI diagnostics such as endoscopic biopsy or significant longterm treatment trials (ie prednisone) as the results may provide alternative treatment suggestions. The entire panel should be evaluated as the pancreatic tests must be assessed before cobalamin and folate levels can be interpreted as they may be abnormal in animals with EPI. The GI Laboratory at Texas A&M or major national labs (ANTECH, Idexx) are the recommended providers of this test at this time. What does a low cobalamin level indicate? How do I treat? Cobalamin is absorbed in the distal small intestine (specifically in the ileum). Values below the control range are seen in patients with EPI, bacterial overgrowth in the upper small intestine, or disease affecting the distal small intestine. There is no known significance of values exceeding the control range. There is compelling evidence that significant tissue-level cobalamin deficiency is present in some companion animal patients with gastrointestinal disease. The significance of this finding for the clinical management of these patients is also becoming clearer as it is evident that many GI patients experience sub-optimal treatment response unless their concurrent cobalamin deficiency is corrected via parenteral supplementation. As cobalamin deficiency in companion animals is usually secondary to reduced cobalamin absorptive capacity, the use of dietary cobalamin supplementation is at best highly inefficient, and most likely ineffective, in the restoration of bodily cobalamin stores. The route of choice for cobalamin supplementation is by parenteral injection. Generic formulations of cobalamin are readily available and extremely cost effective. Most generic cobalamin preparations are 1mg/ml (1000µg/ml). Multi-vitamin and B-complex injectable formulations contain very much lower concentrations of cobalamin, and often cause pain at the injection site, their use is not recommended. Cobalamin is non-irritant and may be given subcutaneously or intramuscularly. The recommended treatment schedule is one dose weekly for six weeks, one dose every two weeks for six weeks, then dose monthly. You can remeasure serum cobalamin concentrations one month after last administration if GI signs are relapsing. Unless the intestinal disease is totally resolved, it is likely that the patient will continue to
2 require regular cobalamin supplementation, the frequency necessary is assessed control of GI signs and/or by regular measurement of serum cobalamin concentration. Animal Bodyweight Range Dose/injection Domestic cats, dogs up to 5kg (10 lb) 250 µg Dogs, 5-15kg (10-30 lb) 500 µg Dogs > 15kg (>30 lb) 1000 µg What does an elevated serum folate level suggest? How do I treat? Folate is absorbed in the proximal small intestine only. Values above the control range are suggestive of bacterial overgrowth in the upper small intestine. Values below the control range are suggestive of non-bacterial disease affecting the proximal small intestine. Antibiotic therapy is generally indicated in GI-symptomatic patients with elevated serum folate levels since this finding suggests bacterial-induced disease. Low serum folate levels do not require direct supplementation but further diagnostics and appropriate treatment of suspected proximal SI disease is recommended. What does the TLI test tell me? Pancreatic acinar cells synthesize and secrete trypsinogen. Almost all trypsinogen is released into the duct system and is released into the duodenum. However, a small portion is released into the vascular space and can be measured by use of speciesspecific immunoassays for measurement of trypsin-like immunoreactivity (TLI). Dogs and cats with exocrine pancreatic insufficiency (EPI) have a lack of pancreatic acinar cells and thus a decreased secretion of pancreatic enzymes into the duodenum. At the same time the amount of trypsinogen released into the vascular space is also decreased leading to a decreased serum TLI concentration. A canine TLI concentration of < 2.5 μg/l has been shown to be highly sensitive and specific for EPI in the dog. In cats a serum feline TLI concentration < 8 μg/l has been shown to be highly specific for EPI. Pancreatic inflammation can lead to an increased release of trypsinogen into the vascular space thus serum TLI concentration can be increased in dogs and cats with pancreatitis. A significantly increased serum TLI concentration (> 50 μg/l in dogs and > 100 μg/l in cats) is highly specific for pancreatitis but has a limited sensitivity of 30-60%. Therefore, elevated serum ctli concentration is of little clinical use for the diagnosis of canine or feline pancreatitis as superior diagnostic tests are now available (ie cpli, fpli). What does the PLI test tell me? Assays for measurement of pancreatic lipase immunoreactivity in dogs and cats (cpli and fpli) have been more recently developed and validated. In contrast to assays for the measurement of lipase activity which measure lipase from a variety of tissue origins, use of immunoassays allows for specific measurement of lipase originating only from the exocrine pancreas. Serum PLI concentration is highly sensitive and specific for the diagnosis of pancreatitis in dogs and cats. A commercial assay for measurement of cpli & fpli (Spec cpl & fpli ) has recently been released by a major diagnostic company (Idexx) and is also
3 available through the Gastrointestinal Laboratory at Texas A&M University ( In cats, values greater than 5.4 µg/l are consistent with pancreatic inflammatory disease (sensitivity of the fpli was 100% in moderate to severe cases of pancreatitis and 54% in mild cases, specificity of the fpli was 100% in healthy cats and 67% in symptomatic cats with histologically normal pancreas). In dogs, values greater than 200 µg/l are consistent with pancreatic inflammatory disease (sensitivity and specificity approach 95%). PLI is a pancreatic leakage enzyme so other causes of pancreatic disease; such as primary or metastatic pancreatic neoplasia, infectious or toxic diseases affecting the pancreas, will also result in an elevated value. Serum cpli was measured in a group of dogs with exocrine pancreatic insufficiency and the median serum cpli concentration was significantly decreased compared to clinically healthy dogs. When should I be concerned about elevated liver enzymes? The clinician is constantly presented with patients that have abnormal liver enzymes identified on the routine biochemical profile. The question often asked is does this patient have liver disease. The answer is often no; not primary hepatic disease but rather secondary hepatic involvement resulting from some extrahepatic event or drugs, referred to as secondary or reactive hepatopathy. Consequently it is important that the clinician must first evaluate the entire patient when encountering the animal with abnormal enzymes to exclude the possibility of a secondary reactive hepatopathy. Management of the reactive liver involves treating the primary disease condition and providing optimal hepatic support to maintain normal liver function. When a patient presents with abnormal liver enzymes (such as ALP, ALT) the clinician must evaluate the animal carefully to first rule out the possibility that the liver enzyme abnormalities are not secondary to a primary non-hepatic disorder. The most common cause for abnormal ALT and ALP values in dogs is not primary hepatic disease but rather secondary hepatic changes as a result of a non-hepatic disease process. These secondary changes are generally reversible once the primarily disease is treated. Asymptomatic patients having abnormal liver enzymes in which an underlying nonhepatic disease is not identified should be re-evaluated at a later date, perhaps in 4 to 6 weeks. An important principle that should be kept in mind when evaluating the patient with abnormal liver enzymes is that the liver has a great reserve capacity and clinical signs of liver disease often do not appear until the disease is quite advanced. Continued abnormal liver enzymes would be a strong indication for further investigation of the liver. Further investigation should include evaluating hepatic function (bile acids) and liver tissue biopsy. Liver function tests become abnormal only when significant liver dysfunction is present. Because the liver is involved in so many metabolic functions and there are variable hepatic responses to an insult there is no ideal liver function test to tell us the extent of liver damage. Of the test available, bile acids (urine or serum) are a reflection of the efficiency and integrity of the enterohepatic circulation of these bile acids. Abnormal bile acid concentrations support the presence of portal vascular anomalies or hepatic insufficiency. When serum bile acid concentrations are greater than 25 umol/l for the dog and cat there is a high probability that the histological findings will define a lesion.
4 One study found the optimal test combination of abnormal serum ALT activity and abnormal bile acid concentrations provided the best sensitivity and specificity for the diagnosis of chronic hepatitis in the dog. Bile Acid testing Blood or Urine?? Bile acids are formed and conjugated in the liver and secreted in the bile. After a meal cholecystokinin stimulates gall bladder contraction and release of bile into the duodenum. Conjugated bile acids play a crucial role in fat absorption as they help to emulsify fat. A small amount of bile acids are deconjugated by the small intestinal microflora. These unconjugated bile acids are absorbed in the small intestine and are no longer available for fat emulsification. In contrast, conjugated bile acids are absorbed in the large intestine, reach the vascular space, and are extracted from the portal blood by the liver. Pre- and postprandial bile acid concentrations are used for the diagnosis of hepatic impairment and portosystemic shunting. Food is withheld from the patient for 12 hours and a serum sample is collected. A small amount of food, rich in fat, is fed to stimulate gall bladder contraction and another serum sample is collected 2 hours later. When hepatic function is significantly impaired extraction of bile acids from the portal blood becomes less efficient and both pre- and postprandial serum bile acid concentrations increase. In patients with portosystemic vascular anomalies pre-prandial bile acid concentrations may be only slightly increased, while post-prandial serum bile acid concentrations are often severely increased. In some normal patients paradoxical results are observed in that pre-prandial bile acid concentrations are higher than post-prandial concentrations. It has been speculated that this finding is due to gall bladder contraction without food intake. Recently, increased pre-prandial bile acid concentrations have also been found in dogs with evidence of an altered small intestinal microflora. Recently, the use of sulfated and non-sulfated urinary bile acid concentrations in dogs and cats with suspected hepatic disease has been described and validated and may provide an advantage as patients do not require fasting, a single sample is required and the urine sample can be obtained at home. How do I proceed to work-up a patient with suspected liver disease? Unexplained persistent abnormal liver enzymes or animals with abnormal hepatic function determined by bile acids warrant further liver evaluation. Liver evaluation would include imaging studies and liver biopsy. Ultrasonography is very useful to evaluate the character of the liver parenchyma and the biliary system. Masses, nodules, choleliths, obstructed biliary system and vascular abnormalities are generally detected. Frequently fine needle aspiration (FNA) for cytological evaluation is performed in conjunction with ultrasound. Although FNA is safe and easy to perform interpretation of the cytological diagnosis of disease can be variable. One must be cautious in the interpretation of the results and use those FNA findings in conjunction with other diagnostics to make a diagnosis. Although there are a number of indications for performing a liver biopsy and one must carefully evaluate each case on its own merits. If presented with a patient with abnormal liver enzymes and clinical evidence of liver disease and when the liver biopsy will offer useful information about the case a liver biopsy would be indicated. Additional reasons to perform a liver biopsy would be to explain the cause of abnormal liver enzymes or function tests such as serum bile acids. The method of liver biopsy procurement involves surgery, ultrasound needle biopsy or laparoscopy. Each method has certain advantages and disadvantages.
5 Better than Prednisone?? Non-steroidal treatment options for chronic GI disease. What are the best treatments for IBD in dogs and cats? There are many causes of gastrointestinal (GI) inflammation. The term inflammatory bowel disease (IBD) is an idiopathic (unexplained) chronic inflammation of the GI tract in dogs and cats. It is based on histopathologic biopsy findings and a diagnosis of exclusion. An inflammatory GI condition is often suspected in patients with ongoing chronic GI signs, so initial symptomatic therapy is often directed at eliminating possible antigenic stimuli, e.g., diet, bacteria and parasites. Managing or decreasing the inflammatory response with immunosuppressive or immunomodulatory drugs should be reserved for patients with histologic IBD and exclusion of other known factors. DIET There are multiple diet selections that should be thoroughly investigated in patients with poorly responding IBD. Low fat/higher carbohydrate intestinal prescription diets may be useful especially in patients with chronic diarrhea and/or concurrent pancreatitis. Higher fiber/lower fat prescription diets may be useful especially in cases with colonic involvement. Novel protein/cho prescription or home-made diets are often used with success in reducing clinical signs in patients with food-antigen hypersensitivity. Hydrolyzed diets may also be helpful as their reduced molecular weight constituents may avoid GI immune detection. Treatment of PLE cases involves use of ultra-low fat diets for long term successful management. Corticosteroid treatment (and cyclosporine) may be useful in early treatment following diagnosis to reduce associated intestinal inflammation while the GI tract adjusts to the ultra-low fat diet. Royal Canin Digestive Low Fat, home-prepared ultra-low fat diet or enteral nutrition supplements (Vivonex TEN) can be used. COBALAMIN Animals with GI disease may not absorb and process cobalamin normally. All cells in the body require cobalamin for normal function including the GI enterocytes. Cobalamin deficiency may contribute to the ongoing clinical signs seen in animals with GI disease. Clinical studies and experience suggests that patients with serum cobalamin deficiency can benefit when supplemented with parenteral cobalamin. METRONIDAZOLE Metronidazole has antibacterial (especially anaerobic), antiprotozoal, anti-inflammatory and antifibrotic activities. It can be effective as a sole agent in some mild cases of inflammatory bowel disorders (primary or secondary). The recommended dose for IBD may be lower than that for antibacterial and antiprotozoal purposes. A starting dose of 15 mg/kg q 12 hours is often used and can be tapered to the lowest effective dose. Periodic bolus dosing or long-term continuous use is acceptable if this drug helps reduce or manage clinical signs. It may also be used in combination with other drugs, most commonly CCS and may allow the CCS dose to be reduced. Side effects include occasional nausea and vomiting. Significant neurologic (vestibular) side effects can be seen in some patients but this is an uncommon unpredictable idiosyncratic reaction and is not caused by higher dosages. It has a bitter taste and can cause salivation especially in cats but is easily formulated into palatable liquids. TYLOSIN
6 Tylosin is a macrolide antibiotic with activity against GI gram-positive bacteria. It may be used successfully in some dogs and cats with inflammatory bowel disorders. Tylosin may also have anti-inflammatory properties but the mechanism of action is unknown. It has a very bitter taste and is most easily administered to cats placed in a gelatin capsule. Side effects have not been reported in the dog or cat. A starting dose of 40 mg/kg q 12 hours is recommended and it can be tapered to the lowest effective dose. Periodic bolus dosing or long-term continuous use is acceptable if this drug helps reduce or manage clinical signs. (1/8 tsp = 325mg tylosin base). MESALAMINE PREPARATIONS Mesalamine or 5-aminosalicylic acid (5-ASA) can be used for colitis dogs, and cats. Sulfasalazine has been most commonly used and is composed of a molecule of 5-ASA linked to sulfapyridine via an azo bond. Side effects such as keratoconjunctivitis sicca (KCS), typical of sulfa drugs may be seen with sulfasalazine. Other preparations of 5- ASA that do not contain sulfapyridine are available. Olsalazine is composed of two 5- ASA molecules linked via an azo bond and sulfasalazine is composed of a single 5-ASA molecule. These preparations are delivered relatively intact to the distal small intestine and colon where bacteria in the GI tract break the azo bond and release the active molecules. The 5-ASA is poorly absorbed and has local anti-inflammatory effects by inhibiting lipoxygenase. It may also act as a oxygen derived free radical scavenger. Doses must be adjusted for cats due to their salicylate sensitivity, but can be used safely at lower doses and for shorter durations as compared to the dog. The dose for sulfasalazine in dogs is mg/kg q 8-12 hours for 2 weeks tapered to the lowest effective dose. Schirmer tear tests should be done periodically to monitor for KCS. The starting dose for cats is mg/kg q 24 hours tapered to the lowest effective dose. Olsalazine has been used at a dose of 5-10 mg/kg q 12 hours. A dose for cats has not been established, but 5-10 mg/kg q 24 hours has been reported. URSODEOXYCHOLIC ACID Ursodeoxycholic acid (ursodiol) is used classically as a hepatoprotective agent. It has been used anecdotally in the therapy of IBD. Ursodiol may decrease antibody production by B cells (IgG, IgA) and decrease IL2 production by T cells. No studied have been published on its use in IBD in dogs and cats. The reported dose for liver disease is mg/kg q 24 hours. OTHER THERAPIES Antioxidant therapy may play an important role in scavenging free oxygen radicals that are produced during the inflammatory process and thus reducing acute flare-ups and reducing chronic GI and pancreatic inflammation and fibrosis. S-adenosylmethionine (SAM-E), Vitamin E and omega-3-fatty acids are considerations. S-adenosylmethionine The naturally occurring molecule, S-adenosylmethionine (SAMe), is synthesized in all living cells and is essential in intermediary metabolism having both hepatoprotective and antioxidant properties. Some of the highest concentrations of SAMe occur in the liver. SAMe is derived from the amino acid methionine and ATP driven by the enzyme SAMe synthetase. The liver normally produces abundant SAMe but there is also evidence to suggest conversion from methionine to SAMe by SAMe synthetase mediated is hindered in liver disease. Once SAMe is formed it then is used in three major biochemical
7 pathways of metabolism: transmethylation, transsulfuration and aminopropylation. The products of SAMe have an influence on modulating inflammation, promotion of cell replication, and protein synthesis. SAMe also plays a major role in membrane function and is an essential precursor for the essential intracellular antioxidant GSH. SAMe pharmacology has been studied in both dogs and cats. Oral SAMe is bound to a stable salt and should be enteric coated. Without enteric coating the product can be oxidized readily and broken down. Tablets should be foil wrapped and should not be divided to prevent breakdown. When given on an empty stomach there is also better bioavailability. SAMe is rapidly absorbed and peak plasma levels can be detected for up to 6-8 hours. Studies in normal dogs and cats given SAMe for 12 and 16 weeks respectively found it was well tolerated without adverse side effects. Doses used were 20 mg/kg/day. Studies have also found that all SAMe products are not similar in bioavability and the concentration of SAMe in the product. SAMe is available as Denosyl (Nutramax). Clinical experience with SAMe is considerable both with experimental studies and through management of clinical cases in dogs and cats. A placebo-controlled feline model of oxidant injury from acetaminophen and found SAMe treated cats had reduced Heinz body formation and erythrocyte destruction and evidence of protection in hepatic GSH in the treated cats as well. Vitamin E (alpha tocopherol) is a membrane bound antioxidant that functions in preventing lipid membrane peroxidation. Vitamin E provides protection against copper, iron, bile acids and certain hepatic toxins. One study we found vitamin E improved the GSH:GSSG ratio (glutathione concentrations as a measure of oxidatitive damage) in dogs with chronic hepatitis. Doses of IU/kg/day are recommended. Omega 3 fatty acids may also be considered in the therapy of IBD in dogs and cats and are provided in an enhanced level in many GI friendly prescription diets. Is probiotic therapy useful in managing GI patients? Probiotics and prebiotics have the potential to alter the GI microflora and have proposed benefits for patients with GI disease. Both have been shown to reduce inflammation in mouse models of IBD The microbes used in probiotics are non-pathogenic organisms, such Bifidobacterium or Lactobacillus, or non-bacterial organisms such as Saccromyces spp. Criteria for probiotic organisms include resistance to low gastric ph, adherence to intestinal mucosa, ability to proliferate and colonise the colon, activity against pathogenic microorganisms, and modulation of the immune system. They must also have no pathogenic, toxic, mutagenic or carcinogenic effects. The proposed benefits of probiotics include increased competition against pathogenic species of bacteria, reduction of bacterial translocation, and production of antimicrobial products. Potential uses for probiotics are prevention of diarrhea associated with dietary amendments, antibiotic (penicillins, tetracyclines, clindamycin), immunosuppressive and chemotherapy treatments. Prevention of stress-induced diarrhea is also a possible place for the use of pre-emptive probiotic treatment. These supplements may also hasten GI recovery following toxic or infectious (parvovirus) GI insults. Their use has also been proposed in the management of stable IBD patients. A concern over probiotic use is the formulation of each brand as there is no regulation in the US. Purina has introduced Fortiflora in the veterinary market and their has been some early excitement regarding its use. Nutramax Proviable and Iams Prostora are also available as veterinary-licensed products.
8 Are pancreatic enzyme supplements helpful in IBD management? Why pancreatic enzyme supplements do not always work in EPI? There can be multiple problems with pancreatic enzyme supplements. The oral pill formulations just do not work well in some patients likely due to poor degradation and enzyme release. The powder forms seem to work best in my experience in most patients. You do not need to preincubate the food as some have suggested. The dosage has to be individualized for each patient. Some patients will require a large dose in order to obtain improved fecal consistency. Large powder volumes in the food can irritate the lips and palate of some patients necessitating either a dose reduction or use of fresh pancreas tissue obtained from a butcher shop. Other causes of poor response to pancreatic enzyme supplementation include uncorrected cobalamin deficiency and small intestinal bacterial overgrowth. The importance of checking serum cobalamin and folate levels in suspected EPI cases cannot be underestimated! Immunosuppressive Treatment Options for chronic IBD patients. CORTICOSTEROIDS Corticosteroids are the most frequently prescribed anti-inflammatory and immunosuppressive medications for chronic idiopathic IBD patients. You may use any corticosteroid preparation (prednisone, prednisolone, methylprednisolone, dexamethasone, triamcinolone) for initial management in dogs. Based on recent studies cats would likely respond best to prednisolone due to their unique hepatic metabolism. The most important thing to remember is that IBD is an immunologic disease so an immunsuppressive dose is required for initial management similar to any other immunemediated disorder. If improvement in clinical signs is observed then the CCS dosage can be sequentially reduced every 2-4 weeks to a maintenance dose (ideally qd or qod) that provided clinical control. Patients that experience adverse CCS side effects and require ongoing treatment can be switched to budesonide (corticosteroid with hepatoenteric recirculation and less systemic effects) or an alternate non-steroidal immunosuppressive agent can be added and the CCS can be gradually tapered or eliminated. BUDESONIDE An orally administered glucocorticoid with limited systemic effects that has shown efficacy in treating IBD in patients that are either refractory to or intolerant of systemic corticosteroids. It is a potent glucocorticoid (15X more potent than prednisolone) with high topical activity. The oral formulation allows delayed dissolution until reaching the duodenum with subsequent controlled release allowing topical anti-inflammatory activity within the intestine. The drug is absorbed from the intestines into the portal circulation, but has a high first-pass metabolism effect through the liver that reduces systemic blood levels. However, significant suppression of the HPA-axis can still occur in some patients. Some clinician prefer budesonide as the CCS of choice for IBD patients. Expense can be an issue as it is only available in a human-approved product (Entocort EC) as a 3mg capsule; it often requires compounding to smaller dosage strengths. Canine : 1 mg PO once daily for small dogs and 2 mg PO once daily for large dogs. Feline : 1 mg PO once daily.
9 AZATHIOPRINE Azathioprine is a synthetic purine analog that interferes with DNA and RNA coding and transcription inhibiting antigen induced lymphocyte transformation thus has greater effects on humoral as compared to cell mediated immunity. Azathioprine is metabolized to 6-mercaptopurine which acts as the active component. It has been used successfully as an adjunct therapy in dogs and cats with severe or refractory IBD. It does not take effect immediately, and a lag time of 2-6 weeks can be expected before improvement is seen. Side effects can include hepatic disease and bone marrow suppression. It can be quite toxic in cats causing severe bone marrow suppression. Due to the possibility of this severe side effect, I prefer to use other drugs such as chlorambucil in cats. Canine : 2 mg/kg q 24 hours for 2 weeks then the dose is tapered to every other day for 2-4 weeks then 1 mg/kg every other day indefinitely if possible. Complete blood counts should be done initially to monitor for bone marrow suppression. The drug should be discontinued and an alternate found if bone marrow suppression occurs. Acute pancreatitis is also a potential side effect. CHLORAMBUCIL Chlorambucil is an alkylating agent that interferes with DNA replication, RNA transcription ultimately disrupting nucleic acid formation. It can be used in cats for severe or refractory cases of IBD as an alternative to azathioprine. Chlorambucil is the my second choice after CCS for refractory or severe IBD in cats. Side effects include vomiting, anorexia, and bone marrow suppression. Feline : >5 kg are started at 2mg/cat q 48 hours for 2-4 weeks then tapered to the lowest effective dose (2 mg/cat q hours). Cats <5kg are started at 1mg/cat q 48 hours or 2mg/cat q 72 hours. Complete blood counts should be performed q 2 weeks initially and q 3 months thereafter. The drug should be discontinued and an alternative found if bone marrow suppression occurs. CYCLOSPORINE Cyclosporine inhibits T cell activation and cytokine and has been used for immunosuppression in a variety of immunologic disorders in dogs and cats. To date, no studies have been published in regard to the use of cyclosporine for treatment if IBD in dogs and cats, but it has been used anecdotally. It is not cytotoxic nor myelotoxic, nor nephrotoxic or hepatotoxic in dogs and cats unless very high levels are maintained. Several preparations are available and possess very different bioavailability. Modified cyclosporine (generic, Neoral ) is more bioavailable compared to Sandimmune and is generally recommended. Recently approved for use in dogs with atopy is the veterinary formulation of a modified cyclosporine Atopica which thought to have similar bioavailability to Neoral. Modified cyclosporine is started at a dose of 2-3mg/kg q hours for cats and 5 mg/kg q 12 hours in the dog. Blood levels can be very individual so it is recommended to evaluate trough blood levels of the drug if a satisfactory response is not seen with initial dosing; desired whole blood trough level for first month is 500 ng/ml. May be able to reduce trough levels to 250 ng/ml after one month if satisfactory response is maintained. It has a very unpleasant taste and should be administered via intact capsules. There may be an increased risk for opportunistic infections and possibly tumor formation with longterm use.
10 OTHER IMMUNOSUPPRESSANT Methotrexate inhibits folic acid reductase. It has been shown to reduce the requirements for CCS in some human patients with Crohn's disease. Gastrointestinal toxicity is the main side effect. Methotrexate is used in dogs and cats as an antineoplastic agent, AND has been reported for use in chronic-active hepatitis and IBD. In my experience significant GI side effects limits its use in most patients. A variety of dosage regimens area published. Tacrolimus (FK 506) has a similar mechanism of action as that of cyclosporine, but is reportedly times more potent. It also inhibits B cell proliferation and this antibody production via an unknown mechanism. It is replacing the use of cyclosporine in human transplant medicine. Tacrolimus has been used in people with refractory ulcerative colitis with some success. Use of tacrolimus for IBD in dogs and cats has not been published, but it is widely accepted for topical therapy of perianal fistulas in dogs. It is available in a human-approved oral capsule. Mycophenolate mofetil (Cellcept ) is hydrolyzed by liver esterases to mycophenolic acid which is cytostatic for lymphocytes. It is a relatively selective inhibitor of T and B cell proliferation. In one study, approximately 40% of human patients with refractory IBD achieved remission and complete steroid withdrawal on mycophenolate. An initial dose of 20mg/kg BID is proposed but should be tapered to 10mg/kg BID within a few weeks as side effects including GI hemorrhage, anorexia, and diarrhea are seen with prolonged use of the higher dose. Yellow Cat does not = Dead Cat. Feeding sick GI and/or Hepatic Lipidosis Cats. Are all yellow (icteric) cats dead cats? Hepatic lipidosis is a distinct clinical condition in common in cats but uncommon in dogs. Hepatic lipidosis occurs either as a primary idiopathic disease syndrome or secondary to a number of primary disease conditions. Lipid accumulation in the liver is simply the result of nutritional, metabolic or toxic insults to the liver and the degree of lipid accumulation can be quite variable. Feline idiopathic hepatic lipidosis however appears to be a distinct syndrome observed in obese older cats that have undergone a stressful episode associated with anorexia. Cats will present with an acute history of rapid weight loss, depression and icterus. A liver FNA cytology or biopsy confirms diffuse hepatic lipidosis. Treatment involves aggressive tube feeding and general liver support. What can I do to prevent or save the fatty liver cat? Hepatic lipidosis in cats is essentially a consequence of catabolism from anorexia due to any cause. Lipidosis can develop within a few days but may also take 2 weeks to occur. Some cats can withstand prolonged fasting without developing clinically significant lipidosis at all. The precise pathogenesis of lipidosis is not known in detail, but catabolism leads to decreased insulin-to-glucagon ratio in the circulation, which stimulates hormone-sensitive lipase to release fatty acids. The liver is the main place for their metabolism. One of the principle routes by which the liver can make fat stores suitable for use in other tissues is by the formation of very low-density lipoproteins (VLDL). One of the essences of this complex metabolic disorder is the unavailability of
11 essential amino acids. These are necessary for different liver functions, such as formation of apoproteins for composition of VLDL in which form accumulating triglycerides can be exported from the liver cells, and the urea cycle in which arginine is essential. For treatment of both HE and lipidosis it is therefore essential to restore the energy balance especially by giving proteins. High-energy diets containing predominantly fats or sugars do not help these cats. Feeding liquefied baby food or commercial high-energy and high-protein veterinary formulations are equally good. The goal is to restore the energy balance and supplement amino acid deficiencies, especially arginine and taurine. L-carnitine may be an important factor because it may help the hepatocytes to exploit fatty acids in beta oxidation. In cats that present with anorexia or weight loss, one of the first things to consider in treatment planning is the day rule. This rule is used as a guideline when considering nutritional support. If the cat hasn't eaten in 3 days, start planning to implement nutritional support; if the cat hasn't eaten in 5 days, implement nutritional support immediately; and finally, if the cat hasn't eaten in 7 days, the cat is developing protein/calorie malnutrition-begin immediate nutritional support. Once the determination is made that nutritional support is needed, the next step is to determine how to provide that nutrition. Again, the rule of thumb is: if the gut works use it, and use as much of the GI tract that is functional-in other words, provide nutrition as high up (close to the mouth) as is feasible. There are a wide variety of options available for providing enteral nutrition to cats, including oral/force feeding, pharmacologic appetite stimulation, nasoesophageal tube feeding, esophageal (E) tube feeding, gastrostomy (G) tube feeding, or jejunostomy (J) tube feeding. Each of these different feeding methods have pro's and con's that may influence the decision to use that method. However, one key is that the feeding method selected should be able to provide all of the cat's protein and energy needs, without significantly increasing morbidity or stress to the cat. For example, while force feeding a cat orally does not require placement of a feeding tube, in most cats it is difficult, if not impossible to attain their caloric needs by this method. Further, in some cats, this will result in significant stress to the cat (and caregivers), and may also result in development of food adversion-to the foods being force-fed. This is the only form of HE requiring higher instead of lower-protein feeding. A daily caloric intake around 60 kcal/kg is adequate for most ill cats. Supplementation of multivitamins may be beneficial in cats with long-term anorexia. Feeding is often required for several weeks until the cat starts eating spontaneously. Review of select feline, canine and human enteral diet considerations is provided. It may be dangerous to stimulate appetite by diazepam administration. The risk for HE is a contraindication for drugs activating the GABA/benzodiazepine receptor system, over stimulation of which is part of the pathogenesis of HE. Cats with hepatic lipidosis can easily develop insulin resistance with hyperglycemia, which may gradually increase to glucose levels as seen in diabetes mellitus. The insulin resistance implies that very large doses of insulin would be needed, with the inherent risk for sudden hypoglycemia. A benefit of treatment with insulin has never been demonstrated, and it is advised to restrict therapy to forced feeding. Glucocorticoids are also contraindicated because they stimulate lipolysis and fatty acid accumulation in the liver, induce catabolism, and increase the risk for hyperglycemia. Some authors advocate the use of antibiotics for cats with hepatic lipidosis, but a positive effect has never been proven. Antibiotics are not given as a routine.
Lymphoplasmacytic-Plasmacytic Gastroenteritis
 Lymphoplasmacytic-Plasmacytic Gastroenteritis (Inflammation of the Stomach and Intestines, Characterized by the Presence of Lymphocytes and Plasmacytes [Types of White Blood Cell]) Basics OVERVIEW An inflammatory
Lymphoplasmacytic-Plasmacytic Gastroenteritis (Inflammation of the Stomach and Intestines, Characterized by the Presence of Lymphocytes and Plasmacytes [Types of White Blood Cell]) Basics OVERVIEW An inflammatory
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
10/13 Tuesday 2:30-3:20 PM UPDATE ON FELINE LIVER DISEASE David C. Twedt, DVM, Diplomate ACVIM Colorado State University Fort Collins, CO
 10/13 Tuesday 2:30-3:20 PM UPDATE ON FELINE LIVER DISEASE David C. Twedt, DVM, Diplomate ACVIM Colorado State University Fort Collins, CO There are a number of specific liver diseases unique to the cat
10/13 Tuesday 2:30-3:20 PM UPDATE ON FELINE LIVER DISEASE David C. Twedt, DVM, Diplomate ACVIM Colorado State University Fort Collins, CO There are a number of specific liver diseases unique to the cat
HOW TO DEAL WITH THOSE ABNORMAL LIVER ENZYMES David C. Twedt DVM, DACVIM Colorado State University Fort Collins, CO
 HOW TO DEAL WITH THOSE ABNORMAL LIVER ENZYMES David C. Twedt DVM, DACVIM Colorado State University Fort Collins, CO The identification of abnormal liver enzymes usually indicates liver damage but rarely
HOW TO DEAL WITH THOSE ABNORMAL LIVER ENZYMES David C. Twedt DVM, DACVIM Colorado State University Fort Collins, CO The identification of abnormal liver enzymes usually indicates liver damage but rarely
The Case of the Limping Poodle
 The Case of the Limping Poodle David C. Twedt DVM, Diplomate ACVIM Case Summary Signalment: Beau 6 yr N/M standard poodle History: Mild intermittent right front leg lameness No current medications Plan:
The Case of the Limping Poodle David C. Twedt DVM, Diplomate ACVIM Case Summary Signalment: Beau 6 yr N/M standard poodle History: Mild intermittent right front leg lameness No current medications Plan:
Crohn's disease CAUSES COURSE OF CROHN'S DISEASE TREATMENT. Sulfasalazine
 Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Cholangitis/ Cholangiohepatitis Syndrome (Inflammation of the Bile Duct System and Liver) Basics
 Glendale Animal Hospital 623-934-7243 www.familyvet.com Cholangitis/ Cholangiohepatitis Syndrome (Inflammation of the Bile Duct System and Liver) Basics OVERVIEW The liver is the largest gland in the body;
Glendale Animal Hospital 623-934-7243 www.familyvet.com Cholangitis/ Cholangiohepatitis Syndrome (Inflammation of the Bile Duct System and Liver) Basics OVERVIEW The liver is the largest gland in the body;
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
Digestive System. Why do we need to eat? Growth Maintenance (repair tissue) Energy
 Digestive System Why do we need to eat? Growth Maintenance (repair tissue) Energy Nutrients Nutrient = chemical that must be obtained by an organism from it s environment in order to survive; nutrients
Digestive System Why do we need to eat? Growth Maintenance (repair tissue) Energy Nutrients Nutrient = chemical that must be obtained by an organism from it s environment in order to survive; nutrients
The Importance of Glutamine and Antioxidant Vitamin Supplementation in HIV
 The Importance of Glutamine and Antioxidant Vitamin Supplementation in HIV An Introduction to Glutamine Glutamine is the most abundant amino acid in the human body, and plays extremely important role in
The Importance of Glutamine and Antioxidant Vitamin Supplementation in HIV An Introduction to Glutamine Glutamine is the most abundant amino acid in the human body, and plays extremely important role in
Summary of Product Characteristics
 Brand Name: OXALO [Pre Probiotic] Capsules Therapeutic Category: Prevention of Stone Formation Urinary tract stone disease has been a part of the human condition for millennia; in fact, bladder and kidney
Brand Name: OXALO [Pre Probiotic] Capsules Therapeutic Category: Prevention of Stone Formation Urinary tract stone disease has been a part of the human condition for millennia; in fact, bladder and kidney
Doncaster & Bassetlaw Medicines Formulary
 Doncaster & Bassetlaw Medicines Formulary Section 1.5 Chronic Bowel Disorders (including IBD) Aminosalicylates: Mesalazine 400mg and 800mg MR Tablets (Octasa) Mesalazine 1.2g MR Tablets (Mezavant XL) Mesalazine
Doncaster & Bassetlaw Medicines Formulary Section 1.5 Chronic Bowel Disorders (including IBD) Aminosalicylates: Mesalazine 400mg and 800mg MR Tablets (Octasa) Mesalazine 1.2g MR Tablets (Mezavant XL) Mesalazine
Crohn's Disease. What causes Crohn s disease? What are the symptoms?
 Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
Week 3 The Pancreas: Pancreatic ph buffering:
 Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Fibrosis and Cirrhosis of the Liver
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Fibrosis and Cirrhosis of the Liver Basics OVERVIEW The liver is the largest gland
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Fibrosis and Cirrhosis of the Liver Basics OVERVIEW The liver is the largest gland
My dog or cat has problems with the stomach, intestines or liver... what do I do now?
 Dietary food for the targeted tackling of gastrointestinal and/or liver problems in dogs and cats My dog or cat has problems with the stomach, intestines or liver... what do I do now? reliable and and
Dietary food for the targeted tackling of gastrointestinal and/or liver problems in dogs and cats My dog or cat has problems with the stomach, intestines or liver... what do I do now? reliable and and
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
What is Crohn's disease?
 What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
Understanding probiotics and health
 Understanding probiotics and health Gemma Laws MSc Student Microbiology and Immunology Department The gut microbiota The name given to the total microbial population living in our intestine Bacteria, fungi,
Understanding probiotics and health Gemma Laws MSc Student Microbiology and Immunology Department The gut microbiota The name given to the total microbial population living in our intestine Bacteria, fungi,
The Small Intestine. The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine.
 The Small Intestine The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine. approximately six metres (the longest section of your digestive
The Small Intestine The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine. approximately six metres (the longest section of your digestive
Canine Chronic Idiopathic Hepatitis
 Canine Chronic Idiopathic Hepatitis David C. Twedt DVM, DACVIM Problem Acute Rt rear leg lameness History Probably stepped on by owner s horse Healthy otherwise No medications Physical exam Possible partial
Canine Chronic Idiopathic Hepatitis David C. Twedt DVM, DACVIM Problem Acute Rt rear leg lameness History Probably stepped on by owner s horse Healthy otherwise No medications Physical exam Possible partial
Exocrine Pancreatic Insufficiency Historical perspective, serum TLI, and cats. David A. Williams MA VetMB PhD
 Exocrine Pancreatic Insufficiency ----- Historical perspective, serum TLI, and cats David A. Williams MA VetMB PhD Exocrine pancreatic 1850s - Bernard 1950s - Anderson 1970s - Sateri 1980s - Batt
Exocrine Pancreatic Insufficiency ----- Historical perspective, serum TLI, and cats David A. Williams MA VetMB PhD Exocrine pancreatic 1850s - Bernard 1950s - Anderson 1970s - Sateri 1980s - Batt
e. Undigested material is compacted and stored until the colon is full. When the colon is full, a signal to empty it is sent by sensors in the walls
 Digestive System 1. General a. Animals obtain energy by breaking food molecules into smaller pieces. b. The basic fuel molecules are amino acids, lipids and sugars c. Digestion is the chemical breakdown
Digestive System 1. General a. Animals obtain energy by breaking food molecules into smaller pieces. b. The basic fuel molecules are amino acids, lipids and sugars c. Digestion is the chemical breakdown
The Benefits of Leflunomide
 Page 1 of 5 Angell Navigation Site Navigation Emergency The Benefits of Leflunomide By Doug Brum, DVM www.angell.org/internalmedicine internalmedicine@angell.org 617-541-5186 Leflunomide is a newer immunosuppressant
Page 1 of 5 Angell Navigation Site Navigation Emergency The Benefits of Leflunomide By Doug Brum, DVM www.angell.org/internalmedicine internalmedicine@angell.org 617-541-5186 Leflunomide is a newer immunosuppressant
ESPEN Congress The Hague 2017
 ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
INFLAMMATORY BOWEL DISEASE
 INFLAMMATORY BOWEL DISEASE What is inflammatory bowel disease? Inflammatory Bowel Disease (IBD) is a syndrome rather than a specific disease, with a number of possible causes. Occasionally, the stomach
INFLAMMATORY BOWEL DISEASE What is inflammatory bowel disease? Inflammatory Bowel Disease (IBD) is a syndrome rather than a specific disease, with a number of possible causes. Occasionally, the stomach
C International Veterinary Branding
 C International Veterinary Branding The pancreas is a gland that is located in the front part of the abdomen. It lies just below the stomach and directly beside the upper part of the small intestine. The
C International Veterinary Branding The pancreas is a gland that is located in the front part of the abdomen. It lies just below the stomach and directly beside the upper part of the small intestine. The
Glucosuria osmotic diuresis Compensatory polydipsia If can t drink enough to compensate dehydration
 How to deal with concurrent pancreatitis and diabetes in dogs and cats Linda Fleeman Animal Diabetes Australia Boronia Veterinary Clinic: 03 9762 3177 Rowville Veterinary Clinic: 03 9763 1799 Lort Smith
How to deal with concurrent pancreatitis and diabetes in dogs and cats Linda Fleeman Animal Diabetes Australia Boronia Veterinary Clinic: 03 9762 3177 Rowville Veterinary Clinic: 03 9763 1799 Lort Smith
Pancreatitis. Acute Pancreatitis
 Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Physiology Unit 4 DIGESTIVE PHYSIOLOGY
 Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
Digestion and Absorption
 Digestion and Absorption Digestion and Absorption Digestion is a process essential for the conversion of food into a small and simple form. Mechanical digestion by mastication and swallowing Chemical digestion
Digestion and Absorption Digestion and Absorption Digestion is a process essential for the conversion of food into a small and simple form. Mechanical digestion by mastication and swallowing Chemical digestion
Digestive Care Advisor Training #1. Digestion 101 & H.O.P.E.
 Digestive Care Advisor Training #1 & H.O.P.E. The Digestive System in Brief The Process of Digestion The human digestive system is a complex series of organs and glands that process food and excrete waste.
Digestive Care Advisor Training #1 & H.O.P.E. The Digestive System in Brief The Process of Digestion The human digestive system is a complex series of organs and glands that process food and excrete waste.
PHYSIOLOGY OF THE DIGESTIVE SYSTEM
 Student Name CHAPTER 26 PHYSIOLOGY OF THE DIGESTIVE SYSTEM D igestion is the process of breaking down complex nutrients into simpler units suitable for absorption. It involves two major processes: mechanical
Student Name CHAPTER 26 PHYSIOLOGY OF THE DIGESTIVE SYSTEM D igestion is the process of breaking down complex nutrients into simpler units suitable for absorption. It involves two major processes: mechanical
CHM333 LECTURE 34: 11/30 12/2/09 FALL 2009 Professor Christine Hrycyna
 Lipid Metabolism β-oxidation FA Acetyl-CoA Triacylglycerols (TAGs) and glycogen are the two major forms of stored energy in vertebrates Glycogen can supply ATP for muscle contraction for less than an hour
Lipid Metabolism β-oxidation FA Acetyl-CoA Triacylglycerols (TAGs) and glycogen are the two major forms of stored energy in vertebrates Glycogen can supply ATP for muscle contraction for less than an hour
Protein Content (grams) 25 g 5 g 30 g 0 g 28 g 2 g. 20 g 10 g 30 g 0 g 27 g 3 g. 20 g 10 g 20 g 10 g 26 g 4 g. 10 g 20 g 10 g 20 g 10 g 20 g
 Digestive Enzymes Introduction: A person is eating a food item. The food contains 30 grams of starch (a polysaccharide), 30 grams of protein and 30 grams of triglycerides (a lipid). Samples of digestive
Digestive Enzymes Introduction: A person is eating a food item. The food contains 30 grams of starch (a polysaccharide), 30 grams of protein and 30 grams of triglycerides (a lipid). Samples of digestive
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Welcome to the Solving Leaky Gut Tough Case Protocol
 Welcome to the Solving Leaky Gut Tough Case Protocol solvingleakygut.com A 3-Pronged Approach Is Needed for Solving Leaky Gut Before reading this you should have watched the training videos as they explain
Welcome to the Solving Leaky Gut Tough Case Protocol solvingleakygut.com A 3-Pronged Approach Is Needed for Solving Leaky Gut Before reading this you should have watched the training videos as they explain
a. parotid b. sublingual c. submandibular
 Bozeman Science/ Nature The Digestive System Watch the videos, and answer the questions below. Please write your answers in complete sentences, and explain all concepts thoroughly. 1. What are the four
Bozeman Science/ Nature The Digestive System Watch the videos, and answer the questions below. Please write your answers in complete sentences, and explain all concepts thoroughly. 1. What are the four
Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4)
 Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
PEDIATRIC INFLAMMATORY BOWEL DISEASE
 PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
Immunosuppressants. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
ph Dependent Drug Delivery System: Review
 ph Dependent Drug Delivery System: Review Korake.S.P. SVERI s College of Pharmacy (Poly.), Pandharpur The ph-dependent CTDDS exploit the generally accepted view that ph of the human GIT increases progressively
ph Dependent Drug Delivery System: Review Korake.S.P. SVERI s College of Pharmacy (Poly.), Pandharpur The ph-dependent CTDDS exploit the generally accepted view that ph of the human GIT increases progressively
Clinically proven to quickly relieve symptoms of common gastrointestinal disorders. TERRAGASTRO - Good health starts in the gut
 Clinically proven to quickly relieve symptoms of common gastrointestinal disorders GASTROINTESTINAL DISEASE Referred to as gastrointestinal diseases, they are common disorders which affect the esophagus,
Clinically proven to quickly relieve symptoms of common gastrointestinal disorders GASTROINTESTINAL DISEASE Referred to as gastrointestinal diseases, they are common disorders which affect the esophagus,
To help protect your privacy, PowerPoint prevented this external picture from being automatically downloaded. To download and display this picture,
 To help protect your privacy, PowerPoint prevented this external picture from being automatically downloaded. To download and display this picture, click Options in the Message Bar, and then click Enable
To help protect your privacy, PowerPoint prevented this external picture from being automatically downloaded. To download and display this picture, click Options in the Message Bar, and then click Enable
Pathology of the Liver and Biliary Tract 5 Diseases of the Biliary Tract. Shannon Martinson, April 2016
 Pathology of the Liver and Biliary Tract 5 Diseases of the Biliary Tract Shannon Martinson, April 2016 http://people.upei.ca/smartinson/ OUTLINE Normal anatomy & function Hepatobiliary Injury and responses
Pathology of the Liver and Biliary Tract 5 Diseases of the Biliary Tract Shannon Martinson, April 2016 http://people.upei.ca/smartinson/ OUTLINE Normal anatomy & function Hepatobiliary Injury and responses
UNDERSTANDING THE DIGESTIVE SYSTEM
 UNDERSTANDING THE DIGESTIVE SYSTEM Understanding Digestion The key to solving food and digestive issues starts with an understanding of how the digestive and intestinal system works If you know what is
UNDERSTANDING THE DIGESTIVE SYSTEM Understanding Digestion The key to solving food and digestive issues starts with an understanding of how the digestive and intestinal system works If you know what is
Summary of chemical breakdown of food by hydrolytic enzymes (Protein enzymes).
 Biology 12 Digestive System Digestion Overview: The digestive process can be divided into 4 phases: 1. ingestion - includes swallowing and peristalsis 2. digestion - the physical (by teeth) and chemical
Biology 12 Digestive System Digestion Overview: The digestive process can be divided into 4 phases: 1. ingestion - includes swallowing and peristalsis 2. digestion - the physical (by teeth) and chemical
Biology 12 - Digestion Notes
 Biology 12 - Digestion Notes Anatomy Physiology Functions of the Digestive System -------------------------------------------------------------------------------------- food (enzymes, bile, HCl) to assist
Biology 12 - Digestion Notes Anatomy Physiology Functions of the Digestive System -------------------------------------------------------------------------------------- food (enzymes, bile, HCl) to assist
UNDERSTANDING THE DIGESTIVE SYSTEM
 Slide 1 UNDERSTANDING THE DIGESTIVE SYSTEM Slide 2 Understanding Digestion The key to solving food and digestive issues starts with an understanding of how the digestive and intestinal system works If
Slide 1 UNDERSTANDING THE DIGESTIVE SYSTEM Slide 2 Understanding Digestion The key to solving food and digestive issues starts with an understanding of how the digestive and intestinal system works If
Digestive System. How your body obtains nutrients. Wednesday, March 2, 16
 Digestive System How your body obtains nutrients Vocabulary Ingestion: food enters the system Physical and enzymatic breakdown begins Digestion: Further breakdown Chemical/enzymatic Vocabulary Absorption:
Digestive System How your body obtains nutrients Vocabulary Ingestion: food enters the system Physical and enzymatic breakdown begins Digestion: Further breakdown Chemical/enzymatic Vocabulary Absorption:
Welcome to Week 2 of the Crohn s & Colitis Foundation of America (CCFA) Online Support Group.
 Welcome to Week 2 of the Crohn s & Colitis Foundation of America (CCFA) Online. Last week s material consisted of an overview of inflammatory bowel diseases (IBD), specifically Crohn s disease and ulcerative
Welcome to Week 2 of the Crohn s & Colitis Foundation of America (CCFA) Online. Last week s material consisted of an overview of inflammatory bowel diseases (IBD), specifically Crohn s disease and ulcerative
VITAMINS, MINERALS AND THE GUT
 VITAMINS, MINERALS AND THE GUT Nutrients Looking at individual nutrients that are involved with gut health can be misleading This is not about taking individual nutrients It supports more a whole food
VITAMINS, MINERALS AND THE GUT Nutrients Looking at individual nutrients that are involved with gut health can be misleading This is not about taking individual nutrients It supports more a whole food
Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE. Drug: TACROLIMUS Protocol number: CV 43
 Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE Drug: TACROLIMUS Protocol number: CV 43 Indications: RENAL, PANCREAS OR COMBINED RENAL PANCREAS TRANSPLANTATION IN ADULTS.
Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE Drug: TACROLIMUS Protocol number: CV 43 Indications: RENAL, PANCREAS OR COMBINED RENAL PANCREAS TRANSPLANTATION IN ADULTS.
Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, ,
 IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
Thornton Natural Healthcare s Better Health News
 September, 2010 Volume 5, Issue 9 Special Interest Articles: Bowel flora Vitamin A Supplementation and Diet and GAGs and Vitamin C Risks for Thornton Natural Healthcare s Better Health News www.thornton-health.com
September, 2010 Volume 5, Issue 9 Special Interest Articles: Bowel flora Vitamin A Supplementation and Diet and GAGs and Vitamin C Risks for Thornton Natural Healthcare s Better Health News www.thornton-health.com
Chronic GI PROBLEMS in Cats & dogs
 Chronic GI PROBLEMS in Cats & dogs Chronic vomiting, diarrhea or both are fairly common problems in dogs and cats. They may be related to relatively minor causes, such as chronic swallowing of hair, or
Chronic GI PROBLEMS in Cats & dogs Chronic vomiting, diarrhea or both are fairly common problems in dogs and cats. They may be related to relatively minor causes, such as chronic swallowing of hair, or
HOW THE MICROBIOME AFFECTS OUR HEALTH
 HOW THE MICROBIOME AFFECTS OUR HEALTH THE INTESTINAL BARRIER AND INTESTINAL PERMEABILITY Intestinal Barrier: a functional body Defense from translocation of dietary antigens, bacteria or bacterial endotoxins
HOW THE MICROBIOME AFFECTS OUR HEALTH THE INTESTINAL BARRIER AND INTESTINAL PERMEABILITY Intestinal Barrier: a functional body Defense from translocation of dietary antigens, bacteria or bacterial endotoxins
Biology 12 Unit 5 Pretest
 Biology Unit 5 Pretest Name: Date: Block:. Chewing aids digestion by A. stimulating release of bile B. increasing surface area of food C. breaking up polymers into monomers D. stimulating water absorption.
Biology Unit 5 Pretest Name: Date: Block:. Chewing aids digestion by A. stimulating release of bile B. increasing surface area of food C. breaking up polymers into monomers D. stimulating water absorption.
Diabetes Oral Agents Pharmacology. University of Hawai i Hilo Pre-Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 Diabetes Oral Agents Pharmacology University of Hawai i Hilo Pre-Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 Learning Objectives Understand the role of the utilization of free
Diabetes Oral Agents Pharmacology University of Hawai i Hilo Pre-Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 Learning Objectives Understand the role of the utilization of free
CHRONIC DIARRHEA DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE THAN 4 WEEKS
 DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
LAB 5 - Enzymes BACKGROUND INFORMATION
 LAB 5 - Enzymes BACKGROUND INFORMATION Chemical Reactions The cells of organisms, from bacteria to plants to animals, carry out hundreds to thousands of chemical reactions that must be properly coordinated
LAB 5 - Enzymes BACKGROUND INFORMATION Chemical Reactions The cells of organisms, from bacteria to plants to animals, carry out hundreds to thousands of chemical reactions that must be properly coordinated
Routes of drug administration
 Routes of drug administration Definition:- A route of administration in pharmacy is the path by which a drug is taken into the body. Classification:- The various routes of administrations are classified
Routes of drug administration Definition:- A route of administration in pharmacy is the path by which a drug is taken into the body. Classification:- The various routes of administrations are classified
CHRONIC HEPATIC DISEASE IN DOGS: EARLY DIAGNOSIS MAKES THE DIFFERENCE
 CHRONIC HEPATIC DISEASE IN DOGS: EARLY DIAGNOSIS MAKES THE DIFFERENCE Michael D Willard, DVM, MS, DACVIM CHRONIC INFLAMMATORY/NECROTIC DISEASES Adverse drug reactions may cause mild to fatal hepatic disease.
CHRONIC HEPATIC DISEASE IN DOGS: EARLY DIAGNOSIS MAKES THE DIFFERENCE Michael D Willard, DVM, MS, DACVIM CHRONIC INFLAMMATORY/NECROTIC DISEASES Adverse drug reactions may cause mild to fatal hepatic disease.
Gut Microbiota and IBD. Vahedi. H M.D Associate Professor of Medicine DDRI
 Gut Microbiota and IBD Vahedi. H M.D Associate Professor of Medicine DDRI 1393.3.1 2 GUT MICROBIOTA 100 Trillion Microbes - 10 times more than cells in our body Collective weight of about 1kg in human
Gut Microbiota and IBD Vahedi. H M.D Associate Professor of Medicine DDRI 1393.3.1 2 GUT MICROBIOTA 100 Trillion Microbes - 10 times more than cells in our body Collective weight of about 1kg in human
more intense treatments are needed to get rid of the infection.
 What Is Clostridium Difficile (C. Diff)? Clostridium difficile, or C. diff for short, is an infection from a bacterium that can grow in your intestines and cause bad GI symptoms. The main risk of getting
What Is Clostridium Difficile (C. Diff)? Clostridium difficile, or C. diff for short, is an infection from a bacterium that can grow in your intestines and cause bad GI symptoms. The main risk of getting
My dog or cat has pancreas problems what do I do now?
 TROVET Digestion Support, dietary supplement for the targeted tackling of pancreas problems in dogs and cats My dog or cat has pancreas problems what do I do now? reliable and affordable dietary pet food
TROVET Digestion Support, dietary supplement for the targeted tackling of pancreas problems in dogs and cats My dog or cat has pancreas problems what do I do now? reliable and affordable dietary pet food
Targeted Health Regimen Every Targeted Health Regimen builds upon the Foundations of Optimal Health Regimen. Blood Glucose Maintenance Regimen
 Targeted Health Regimen Every Targeted Health Regimen builds upon the Foundations of Optimal Health Regimen. Blood Glucose Maintenance Regimen Every year we are faced with weight gain and increasingly
Targeted Health Regimen Every Targeted Health Regimen builds upon the Foundations of Optimal Health Regimen. Blood Glucose Maintenance Regimen Every year we are faced with weight gain and increasingly
An overview of the digestive system. mouth pharynx esophagus stomach small intestine large intestine rectum anus
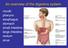 An overview of the digestive system mouth pharynx esophagus stomach small intestine large intestine rectum anus Why GIT? What are the main steps in the digestive process? Ingestion intake of food via the
An overview of the digestive system mouth pharynx esophagus stomach small intestine large intestine rectum anus Why GIT? What are the main steps in the digestive process? Ingestion intake of food via the
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
Gastroporesis or Leaky Gut
 Dr Wendy Wells 8595 E Bell Rd D101 Scottsdale, AZ 85260 (480) 607-0299 Gastroporesis or Leaky Gut From the mouth to anus is an enfolding of our skin. As you know, our skin contains a layer of cells and
Dr Wendy Wells 8595 E Bell Rd D101 Scottsdale, AZ 85260 (480) 607-0299 Gastroporesis or Leaky Gut From the mouth to anus is an enfolding of our skin. As you know, our skin contains a layer of cells and
Diabetes Management. Understanding and Organization
 Diabetes Management Understanding and Organization -What is Diabetes Me"itus? History The term diabetes is typically used to describe the condition Diabetes Mellitus. Diabetes mellitus is literally translated
Diabetes Management Understanding and Organization -What is Diabetes Me"itus? History The term diabetes is typically used to describe the condition Diabetes Mellitus. Diabetes mellitus is literally translated
Corporate Medical Policy Fecal Microbiota Transplantation
 Corporate Medical Policy Fecal Microbiota Transplantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: Fecal_microbiota_transplantation 7/2014 11/2017 11/2018 11/2017 Description
Corporate Medical Policy Fecal Microbiota Transplantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: Fecal_microbiota_transplantation 7/2014 11/2017 11/2018 11/2017 Description
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM
 ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM The digestive system also known as the alimentary canal or gastrointestinal tract consists of a series of hollow organs joined in a
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM The digestive system also known as the alimentary canal or gastrointestinal tract consists of a series of hollow organs joined in a
Bacteriology. Mycology. Patient: SAMPLE PATIENT DOB: Sex: MRN: Rare. Rare. Positive. Brown. Negative *NG. Negative
 Patient: SAMPLE PATIENT DOB: Sex: MRN: 3.2 0.9-26.8 U/g 1.2 0.2-3.3 mg/g 2.2 1.3-8.6 micromol/g 1.1 1.3-23.7 mg/g 1.1 0.2-3.5 mg/g Rare 1.0 0.2-8.8 mg/g Rare 4.4 2.6-32.4 mg/g 64.6 >= 13.6 micromol/g Bacteriology
Patient: SAMPLE PATIENT DOB: Sex: MRN: 3.2 0.9-26.8 U/g 1.2 0.2-3.3 mg/g 2.2 1.3-8.6 micromol/g 1.1 1.3-23.7 mg/g 1.1 0.2-3.5 mg/g Rare 1.0 0.2-8.8 mg/g Rare 4.4 2.6-32.4 mg/g 64.6 >= 13.6 micromol/g Bacteriology
Chapter 26 The Digestive System
 Chapter 26 The Digestive System Digestive System Gastroenterology is the study of the stomach and intestine. Digestion Catabolism Absorption Anabolism The actions of the digestive system are controlled
Chapter 26 The Digestive System Digestive System Gastroenterology is the study of the stomach and intestine. Digestion Catabolism Absorption Anabolism The actions of the digestive system are controlled
Lipid Digestion. An Introduction to Lipid Transport and Digestion with consideration of High Density and Low Density Lipoproteins.
 Digestion An Introduction to Transport and Digestion with consideration of High Density and Low Density Lipoproteins By Noel Ways Suspension and Nutralization of Chyme ph Boli containing lipids enters
Digestion An Introduction to Transport and Digestion with consideration of High Density and Low Density Lipoproteins By Noel Ways Suspension and Nutralization of Chyme ph Boli containing lipids enters
10/23/2013 ANIMAL NUTRITION ANIMAL NUTRITION ESSENTIAL NUTRIENTS AN ANIMAL S DIET MUST STUPPLY: AMINO ACIDS
 ANIMAL NUTRITION Food is taken in, taken apart, and taken up in the process of animal nutrition In general, animals fall into three categories: Herbivores Carnivores Omnivores ANIMAL NUTRITION Chapter
ANIMAL NUTRITION Food is taken in, taken apart, and taken up in the process of animal nutrition In general, animals fall into three categories: Herbivores Carnivores Omnivores ANIMAL NUTRITION Chapter
Chronic Vomiting in Cats. Jinelle Webb DVM, DVSc, Dipl ACVIM
 Chronic Vomiting in Cats Jinelle Webb DVM, DVSc, Dipl ACVIM Is a vomiting cat normal? l At my house maybe? Or maybe I should attend my own lecture. l Cats do tend to vomit more readily than dogs l Hairballs
Chronic Vomiting in Cats Jinelle Webb DVM, DVSc, Dipl ACVIM Is a vomiting cat normal? l At my house maybe? Or maybe I should attend my own lecture. l Cats do tend to vomit more readily than dogs l Hairballs
the only oral supplement so quick and effective:
 The Product the only oral supplement so quick and effective: 30 days to increase ferritinemia and syderemia to +50% [90-120 days with common oral supplementation with iron]. After 1 week the subject will
The Product the only oral supplement so quick and effective: 30 days to increase ferritinemia and syderemia to +50% [90-120 days with common oral supplementation with iron]. After 1 week the subject will
Bacteriology. Mycology. Genova Diagnostics SAMPLE REPORT. Rare. Rare. Negative. Brown. Negative *NG. Negative
 Completed: November 2010 Genova Diagnostics eceived: October 2010 Collected: October 2010 oute Number:7 4.2 0.9-26.8 U/g 0.9 0.2-3.3 mg/g 0.8 1.3-8.6 micromol/g 42.7 1.3-23.7 mg/g 1.7 0.2-3.5 mg/g are
Completed: November 2010 Genova Diagnostics eceived: October 2010 Collected: October 2010 oute Number:7 4.2 0.9-26.8 U/g 0.9 0.2-3.3 mg/g 0.8 1.3-8.6 micromol/g 42.7 1.3-23.7 mg/g 1.7 0.2-3.5 mg/g are
Recuperation. dog. Getting them back to optimal health has never been this easy. Developed by vets for vets
 To obtain optimal recuperation, Viyo Recuperation should be given for at least a period of 14 consecutive days. Developed by vets for vets Recuperation dog Getting them back to optimal health has never
To obtain optimal recuperation, Viyo Recuperation should be given for at least a period of 14 consecutive days. Developed by vets for vets Recuperation dog Getting them back to optimal health has never
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint
 GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
Corticosteroids. Veterinary Pharmacology Endocrine System. University of Tehran Faculty of Veterinary Medicine Academic Year
 Veterinary Pharmacology Endocrine System Corticosteroids University of Tehran Faculty of Veterinary Medicine Academic Year 2008-9 Goudarz Sadeghi, DVM, PhD, DSc Associate Professor of Pharmacology Introduction
Veterinary Pharmacology Endocrine System Corticosteroids University of Tehran Faculty of Veterinary Medicine Academic Year 2008-9 Goudarz Sadeghi, DVM, PhD, DSc Associate Professor of Pharmacology Introduction
Chapter 14: The Digestive System
 Chapter 14: The Digestive System Digestive system consists of Muscular tube (digestive tract) alimentary canal Accessory organs teeth, tongue, glandular organs 6 essential activities 1. 2. 3. 4. 5. 6.
Chapter 14: The Digestive System Digestive system consists of Muscular tube (digestive tract) alimentary canal Accessory organs teeth, tongue, glandular organs 6 essential activities 1. 2. 3. 4. 5. 6.
Amy-Jo Hooley Specialist Clinical Pharmacist
 Gut Decontamination Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the Safe Administration
Gut Decontamination Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the Safe Administration
Soft palate elevates, closing off the nasopharynx. Hard palate Tongue Bolus Epiglottis. Glottis Larynx moves up and forward.
 The Cephalic Phase Chemical and mechanical digestion begins in the mouth Saliva is an exocrine secretion Salivary secretion is under autonomic control Softens and lubricates food Chemical digestion: salivary
The Cephalic Phase Chemical and mechanical digestion begins in the mouth Saliva is an exocrine secretion Salivary secretion is under autonomic control Softens and lubricates food Chemical digestion: salivary
Subject Index. rationale for supplementation in cancer patients 260, 273 surgical cancer patient supplementation
 Acute-phase response, cytokine mediation in cachexia 157, 158 ß 2 -Adrenergic agonist, effects on rat tumor models 264 Alcohol breast cancer studies 107, 108, 111, 112, 116 ß-carotene interactions 53 lung
Acute-phase response, cytokine mediation in cachexia 157, 158 ß 2 -Adrenergic agonist, effects on rat tumor models 264 Alcohol breast cancer studies 107, 108, 111, 112, 116 ß-carotene interactions 53 lung
New Studies Continue to Reveal the Health Benefits of Colostrum
 New Studies Continue to Reveal the Health Benefits of Colostrum by Barbara L. Minton (see all articles by this author) (NaturalNews) Colostrum is the thin yellowish fluid produced during the first few
New Studies Continue to Reveal the Health Benefits of Colostrum by Barbara L. Minton (see all articles by this author) (NaturalNews) Colostrum is the thin yellowish fluid produced during the first few
Physiology 12. Overview. The Gastrointestinal Tract. Germann Ch 19
 Physiology 12 The Gastrointestinal Tract Germann Ch 19 Overview 1 Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Physiology 12 The Gastrointestinal Tract Germann Ch 19 Overview 1 Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Introduction to Human Anatomy & Physiology Chapter 35
 Biology Introduction to Human Anatomy & Physiology Chapter 35 Digestion The breakdown of complex biological molecules into their component parts. Lipids to fatty acids Proteins to individual amino acids
Biology Introduction to Human Anatomy & Physiology Chapter 35 Digestion The breakdown of complex biological molecules into their component parts. Lipids to fatty acids Proteins to individual amino acids
TASTE THE RAINBOW A HEALTHY GUT
 TASTE THE RAINBOW A HEALTHY GUT HAVE YOU.. Taken antibiotics in the past two years? Used anti-inflammatory drugs such as aspirin or ibuprofen? Eaten processed foods? Drink sodas? Eaten foods with chemical
TASTE THE RAINBOW A HEALTHY GUT HAVE YOU.. Taken antibiotics in the past two years? Used anti-inflammatory drugs such as aspirin or ibuprofen? Eaten processed foods? Drink sodas? Eaten foods with chemical
Digestive System. Part A Multiple Choice. 1. Which of the following is NOT a digestive enzyme? A. Pepsin. B. Ptyalin. C. Gastrin. D. Trypsin.
 Digestive System Part A Multiple Choice 1. Which of the following is NOT a digestive enzyme? A. Pepsin. B. Ptyalin. C. Gastrin. D. Trypsin. 2. The presence of large numbers of mitochondria in the cells
Digestive System Part A Multiple Choice 1. Which of the following is NOT a digestive enzyme? A. Pepsin. B. Ptyalin. C. Gastrin. D. Trypsin. 2. The presence of large numbers of mitochondria in the cells
Cardiac Nutrition Healthy eating for a strong heart beating
 Cardiac Nutrition Healthy eating for a strong heart beating Julia Shih VMD, DACVIM (Cardiology) Key Topics Role of Nutrition Optimal Weight Important Nutrients Restricted Nutrients Supplements The Individual
Cardiac Nutrition Healthy eating for a strong heart beating Julia Shih VMD, DACVIM (Cardiology) Key Topics Role of Nutrition Optimal Weight Important Nutrients Restricted Nutrients Supplements The Individual
KRISHNA TEJA PHARMACY COLLEGE HUMAN ANATOMY AND PHYSIOLOGY. DIGESTIVE SYSTEM Dr.B.Jyothi
 KRISHNA TEJA PHARMACY COLLEGE HUMAN ANATOMY AND PHYSIOLOGY DIGESTIVE SYSTEM Dr.B.Jyothi Prof, Dept. Of Pharmacology KTPC The Digestive System Food undergoes six major processes: 1. Ingestion : process
KRISHNA TEJA PHARMACY COLLEGE HUMAN ANATOMY AND PHYSIOLOGY DIGESTIVE SYSTEM Dr.B.Jyothi Prof, Dept. Of Pharmacology KTPC The Digestive System Food undergoes six major processes: 1. Ingestion : process
Ch 7 Nutrition in humans
 Ch 7 Nutrition in humans Think about (Ch 7, p.2) 1. The stomach churns food into smaller pieces physically. The stomach wall secretes proteases to chemically digest proteins. It also releases hydrochloric
Ch 7 Nutrition in humans Think about (Ch 7, p.2) 1. The stomach churns food into smaller pieces physically. The stomach wall secretes proteases to chemically digest proteins. It also releases hydrochloric
Chapter 6, Part Read Activity 6A - Choosing a Meal and orally attempt the procedure and discussion on page 99.
 Science 9 Unit 1 Worksheet Chapter 6, Part 1. 1. Read Activity 6A - Choosing a Meal and orally attempt the procedure and discussion on page 99. 2. Your body is made up of,,,, and many other materials.
Science 9 Unit 1 Worksheet Chapter 6, Part 1. 1. Read Activity 6A - Choosing a Meal and orally attempt the procedure and discussion on page 99. 2. Your body is made up of,,,, and many other materials.
Chapter 15 Gastrointestinal System
 Chapter 15 Gastrointestinal System Dr. LL Wang E-mail: wanglinlin@zju.edu.cn Rm 608, Block B, Research Building, School of Medicine, Zijingang Campus Pancreatic Secretion The exocrine cells in the pancreas
Chapter 15 Gastrointestinal System Dr. LL Wang E-mail: wanglinlin@zju.edu.cn Rm 608, Block B, Research Building, School of Medicine, Zijingang Campus Pancreatic Secretion The exocrine cells in the pancreas
The Digestive System. Prepares food for use by all body cells.
 The Digestive System Prepares food for use by all body cells. Digestion The chemical breakdown of complex biological molecules into their component parts. Lipids to fatty acids Proteins to individual amino
The Digestive System Prepares food for use by all body cells. Digestion The chemical breakdown of complex biological molecules into their component parts. Lipids to fatty acids Proteins to individual amino
Lipid Digestion. and Human Nutrition. An Introduction to Lipid Transport and Digestion with consideration of High Density and Low Density Lipoproteins
 Digestion and Human Nutrition An Introduction to Transport and Digestion with consideration of High Density and Low Density Lipoproteins By Noel Ways Emulsification of s and release of Pancreatic Lipase
Digestion and Human Nutrition An Introduction to Transport and Digestion with consideration of High Density and Low Density Lipoproteins By Noel Ways Emulsification of s and release of Pancreatic Lipase
Intestinal Rehabilitation and Transplantation
 Intestinal Rehabilitation and Transplantation Joel Lim, MD Associate Professor of Pediatrics Children s Mercy Hospital University of Missouri in Kansas City Objective: Intestinal Failure/Short Bowel Syndrome
Intestinal Rehabilitation and Transplantation Joel Lim, MD Associate Professor of Pediatrics Children s Mercy Hospital University of Missouri in Kansas City Objective: Intestinal Failure/Short Bowel Syndrome
