A novel case of compound heterozygous congenital hyperinsulinism without high insulin levels
|
|
|
- Justina McLaughlin
- 5 years ago
- Views:
Transcription
1 Brady et al. International Journal of Pediatric Endocrinology (2015) 2015:16 DOI /s CASE REPORT Open Access A novel case of compound heterozygous congenital hyperinsulinism without high insulin levels Cassandra Brady 1*, Andrew A. Palladino 2 and Iris Gutmark-Little 1 Abstract Background: Congenital hyperinsulinism leads to unregulated insulin secretion and hypoglycemia. Diagnosis can be difficult and genetic testing may be warranted. Case: This patient initially presented at 11 months with seizure activity secondary to severe hypoglycemia. Her diagnostic evaluation included genetic studies, which confirmed congenital hyperinsulinism. A novel combination of mutations in the ABCC8 gene leading to diffuse, diazoxide-unresponsive congenital hyperinsulinism was identified. Mutation analysis of ABCC8 showed three variants (R1215W paternal, pathogenic; W739C maternal, variant of unknown significance; R1393L maternal, variant of unknown significance). Her clinical course continues to be complicated by severe, refractory hypoglycemia at age 3 years. Conclusion: We describe a novel compound heterozygous mutation leading to diffuse, diazoxide-unresponsive congenital hyperinsulinism. This case illustrates challenges associated with diagnosing and managing congenital hyperinsulinism and the importance of genetic testing. Keywords: Congenital hyperinsulinism, ABCC8, Octreotide, Diazoxide-unresponsive Background Congenital hyperinsulinism (CHI) leads to hypoglycemia in infants and children due to inappropriately elevated insulin levels. Mutations leading to CHI have been described in nine genes [1]. The most common mutations occur in ABCC8 and KCNJ11, which encode for the ATP-sensitive potassium (K ATP ) channel present on the beta-cell plasma membrane. During normal glucose-stimulated insulin secretion, the K ATP channel closes in response to an increase in the energy potential of the beta-cell. Closure of this channel results in depolarization of the beta-cell plasma membrane leading to calcium influx into the beta-cell and insulin secretion. Certain mutations in ABCC8 and KCNJ11 lead to defective K ATP channels that are either unable to open or cannot localize to the plasma membrane [2]. Defective channels lead to continued depolarization of the plasma membrane and insulin secretion regardless of the plasma glucose level. Patients with these mutations * Correspondence: cassie.brady@vanderbilt.edu 1 Cincinnati Children s Hospital Medical Center, Division of Endocrinology, 3333 Burnet Ave, MLC 7012, Cincinnati, OH 45229, USA Full list of author information is available at the end of the article can be classified as diazoxide-responsive or unresponsive [1, 3]. Diazoxide is a K ATP channel agonist which keeps the channel in an open state resulting in the suppression of insulin secretion [4]. Severe forms of CHI can lead to complete destruction of channel activity and are therefore unresponsive to diazoxide [2]. Inheritance of ABCC8 and KCNJ11 mutations occurs in either a dominant or recessive fashion [1]. These mutations, dependent on inheritance pattern, may lead to focal or diffuse disease histologically (i.e. localized islet cell abnormalities versus effects throughout pancreas). Homozygous or compound heterozygous recessive mutations are associated with diffuse disease, and are typically managed medically or with near total pancreatectomy, as indicated. The diagnosis of CHI can be made during a fasting challenge. At the time of hypoglycemia (glucose <50 mg/dl (2.775 mmol/l)) [2, 3], a blood sample ( critical sample ) is obtained to assess the presence or absence of key metabolic indices and counter-regulatory hormones which serve as alternative fuels and stimulants to raise serum glucose. Often, the fasting challenge does not yield confirmatory or clear diagnostic evidence of CHI and a repeat 2015 Brady et al. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
2 Brady et al. International Journal of Pediatric Endocrinology (2015) 2015:16 Page 2 of 5 fasting evaluation may be necessary. Genetic testing is also recommended to assess for the common CHI-causing mutations in patients with a known or suspected diagnosis of hyperinsulinism. Once CHI is confirmed, defining the extent of disease is a critical next step to determine ideal intervention. Previously, imaging studies such as ultrasound, computed tomography, and magnetic resonance imaging have been implemented for the purpose of distinguishing focal from diffuse disease. However, these studies have not been shown to be effective for this purpose. The radiotracer 18 fluoro-l- dihydroxyphenylalanine ( 18 F-DOPA), which concentrates in insulin-secreting beta cells of the pancreas, has been used in specialized CHI care centers for the past decade to classify disease. In the largest series, the specificity of this imaging technique to detect focal disease was 96 % [5]. This case demonstrates a novel compound heterozygous mutation causing CHI, the natural history of this mutation, and the associated challenges in management. This case also outlines the pitfalls of interpreting insulin levels at the time of hypoglycemia and emphasizes the importance of genetic testing in this setting. Case presentation An 11-month-old African-American female presented to neurology due to seizure-like activity. She was a former term infant with a birthweight of kg. At presentation she weighed 9.6 kg (56th%) and was 77 cm (89th%) tall. During her evaluation, a glucose value of 38 mg/dl (1.998 mmol/l) and bicarbonate of 24 mmol/l were noted. During a subsequent fasting challenge, her serum glucose decreased to 32 mg/dl (1.776 mmol/l) within 5.5 h. The results of the critical sample are presented in Table 1. Specifically, her insulin level was appropriately low, while her beta-hydroxybutyrate (BOHB) was minimally elevated, and free fatty acids were inappropriately within the normal range. Additionally, her growth hormone was low. All other laboratory results including ammonia, *urine organic acids, *serum amino acids, and Table 1 Fasting challenge results Test name (Normal range) Laboratory result IGFBP-1 (ng/ml) (5 9 years: 15 95; no reference range 61 for patients <5 years) Insulin (<2-13 μiu/ml fasting) 0.2 Glucose (>70 mg/dl/3.885 mmol/l) 32/1.776 C-peptide ( ng/ml) 0.5 BOHB (0 3.0 mg/dl) 4.3 (0.41 mmol/l) Free Fatty Acids ( mmol/l) 0.46 Growth Hormone (>7 ng/ml) 3 *acylcarnitine profile were normal (*drawn in the fed state). A glucagon stimulation to assess glycemic response at the time of hypoglycemia was attempted but was unsuccessful. Based on the critical sample results, she was thought to have growth hormone deficiency and was started on growth hormone therapy. She was discharged after several inpatient days with improved glucose levels. In the interim, the insulin-like growth factor-1 (IGF-1) (prior to growth hormone therapy) resulted at ng/ml (approximately the 80th% for age and sex), and insulinlike growth factor binding protein-3 (IGFBP-3) was 2800 ng/ml (above the mean for age and sex). While at home, she was noted to have a glucose of 19 mg/dl ( mmol/l) despite growth hormone therapy. Given the severity of her hypoglycemia, she was readmitted for further assessment. An arginine/clonidine growth hormone stimulation test done after discontinuation of growth hormone revealed a peak growth hormone level of 7.9 ng/dl (radioimmunoassay). In the setting of continued hypoglycemia despite growth hormone therapy, her critical sample obtained at her initial admission was reviewed and determined to be concerning for CHI. Therefore genetic studies for CHI were sent (Athena Diagnostics, Worcester, Massachusetts). While genetic studies were pending, diazoxide treatment was initiated and titrated to 15 mg/kg/day divided three times daily. However, she continued to have hypoglycemia. After one week of diazoxide therapy, octreotide was added. Octreotide was increased to 15 mcg/kg/day, with subsequent improvement but not resolution of hypoglycemia. Frequent feeds and uncooked cornstarch were implemented to avert hypoglycemia. Her hyperinsulinism was deemed diazoxide-unresponsive and diazoxide was discontinued. Mutational analysis confirmed a diagnosis of CHI as three variants in ABCC8 were identified (Table 2). The R1215W variant was found to be paternally-inherited while the W739C and R1393L variants were maternally inherited. The paternal change was a known mutation described previously (at Children s Hospital of Philadelphia) in a patient with diffuse disease. In this previously described patient, the inheritance pattern was thought to be recessive, given a normal maternal ABCC8 gene copy. In our patient, the significance of the maternal variants was unclear as they had not been previously described in Table 2 Genetic results (ABCC8 Mutation) Mutation Inheritance Interpretation c. R1215W Paternal Pathogenic c. W739C Maternal VUS c. R1393L Maternal VUS VUS variant of unknown significance
3 Brady et al. International Journal of Pediatric Endocrinology (2015) 2015:16 Page 3 of 5 CHI cases. Therefore, for our patient, we were unable to predict focal versus diffuse disease pathology based on mutational analysis alone. Our patient was transferred to Children s Hospital of Philadelphia for an 18-fluoro L-3, 4-dihydroxyphenylalanine positron emission tomography ( 18 -F-DOPA-PET) scan. There was no focal uptake of isotope by the pancreas (Fig. 1), which suggested, but did not confirm diffuse disease. A pancreatic biopsy was subsequently recommended in order to further delineate her pathology, but was declined by the family. A gastrostomy tube was placed for enteral dextrose administration (overnight glucose infusion rate (GIR) of 7 mg/kg/min). Over several months, the child has continued to have intermittent, daily hypoglycemia despite adjustments of her treatment regimen. The GIR of her fluids has been gradually increased. Her current treatmentregimenatage3yearsconsistsofoctreotide20 mcg/kg/day divided three times daily and overnight dextrose (14 h, GIR of 9 mg/kg/min) through her gastrostomy tube. She continues to have daytime hypoglycemia [glucose <70 mg/dl (3.885 mmol/l)]. Speech delay that was noted shortly after diagnosis persists despite therapy. Considering her disease and failure of medical management, a near-total pancreatectomy may be necessary to achieve normal blood glucose levels. Other treatment options that are also being considered include continuous glucagon via an insulin pump [6, 7] and continuous octreotide via an insulin pump [8]. These treatments have not been pursued based on parental requests. Conclusions This case reveals a new compound heterozygous mutation in ABCC8 that leads to diffuse, diazoxide-unresponsive CHI. It highlights the severity of disease due to this combination of mutations and the difficulty of diagnosis and management. To diagnose CHI, laboratory tests known as the critical sample, are utilized and include: plasma glucose, plasma insulin, c-peptide, insulin-like growth factor binding protein-1 (IGFBP-1), BOHB, free fatty acids, ammonia, lactate, pyruvate, acylcarnitine profile, free and total carnitine, organic acids (urine), growth hormone, and cortisol [3]. The diagnosis of CHI can be made in the setting of hypoglycemia when elevated insulin levels are present with suppression of BOHB and free fatty acids. Often, the initial fasting challenge does not yield confirmatory or clear diagnostic evidence of CHI and repeat fasting evaluations may be necessary. In the critical sample, insulin and c-peptide levels help to establish the presence of inappropriate elevations in insulin and to distinguish between excess endogenous and exogenous insulin, respectively. Interpretation of insulin levels at the time of hypoglycemia can be difficult, as evidenced by this case. Insulin levels may be elevated, decreased, or normal [9]. This may be due to periodic release of insulin [3], insulin degrading enzymes in hemolyzed blood samples [9 11], insulin antibodies [12], and rapid hepatic clearance [9, 13]. At room temperature, research shows that >90 % of insulin can be degraded due to massive hemolysis which induces degrading enzymes [11]. Maintaining the Fig. 1 Results of F -Dopa PET Scan. This image demonstrates the results of our patient s F -Dopa PET scan. The pancreas is circled in black. There is no evidence of focal tracer uptake on this image, suggesting diffuse disease. However the finding of diffuse uptake on F -Dopa PET scan does not exclude a focal lesion
4 Brady et al. International Journal of Pediatric Endocrinology (2015) 2015:16 Page 4 of 5 sample at colder temperatures (4 C) may decrease degrading enzyme activity [11], however this can make critical sample collection more difficult. Interfering insulin antibodies may also lead to falsely low insulin levels as demonstrated in immunoradiometric assays and electrochemiluminescent assays in prior reports [12].Insulinisalsorapidlydegradedbythebodyata rate of 2 percent per minute with about 50 % removed by the liver [13, 9]. These issues may have played a role in our patient s decreased insulin level on her fasting challenge. Another important indicator of hyperinsulinism is the glycemic response to glucagon at the time of hypoglycemia [14]. A glucose rise after glucagon of greater than 30 mg/dl (1.665 mmol/l) may reflect hyperinsulinism with a sensitivity of 91 % and specificity of 93 % [14, 9]. This glycemic excursion after glucagon reflects the suppressive effects of insulin on the release of glycogen stores from the liver. In our patient s evaluation, the glucagon challenge was not completed in a way that it would have been interpretable. The fasting challenge is an important opportunity to obtain and interpret other counter-regulatory mechanisms that maintain euglycemia. Elevation in BOHB is a measure of appropriate ketogenesis during fasting. BOHB values less than 2.7 mmol/liter (28.1 mg/dl) during hypoglycemia have a reported sensitivity and specificity of 100 % in hyperinsulinemia induced by an insulinoma [9, 15]. The patient in this case had a relatively low BOHB value, which may have been an indicator of high insulin levels. Growth hormone and cortisol act as counter-regulatory hormones to increase lipolysis and gluconeogenesis, respectively. Growth hormone and cortisol are expected to be increased during hypoglycemia if these hormonal systems are intact [16]. The child in this case was started on growth hormone due to the low value at the time of hypoglycemia. However, decreased growth hormone and cortisol levels at the time of hypoglycemia are not diagnostic of deficiencies, and 65 % of children in a study by Kelly et al. were misdiagnosed with growth hormone deficiency during a fasting challenge [17]. Our patient subsequently had a normal growth hormone response during further evaluation. Shortly after diagnosis in our patient s clinical course, it became evident that the CHI was likely diazoxideunresponsive. Diazoxide-unresponsive CHI is typically due to defects in the K ATP channel [18]. However genetic analysis and determination of inheritance pattern is extremely helpful for both prediction of disease pathology and response to therapy. Inheritance of ABCC8 and KCNJ11 mutations occurs in either a dominant or recessive fashion [1]. Further, depending on inheritance pattern, these mutations may lead to focal or diffuse disease histologically. Autosomal recessive mutations from both parents typically cause diffuse disease. A paternally-inherited recessive mutation in the K ATP channel with maternal loss of heterozygosity leads to paternal uniparental disomy and the development of focal disease [3, 1]. The genetic results for this patient demonstrated a paternally-inherited known pathogenic recessive mutation, but the pathogenicity of the maternal mutations was unclear. We have recently learned (from a patient at Children s Hospital of Philadelphia) that the W739C maternal variant has been identified in a patient with diffuse disease indicating that it likely acts recessively. We suspect the R1393L variant is pathogenic and could act either recessively or dominantly. Of note, our patient s brother is a carrier of the paternal mutation, but did not inherit either of the maternal mutations. Both of her parents and her brother have no signs or symptoms of hypoglycemia. An 18 -F-Dopa-PET scan was obtained. This noninvasive imaging technique has been used to further delineate between focal and diffuse CHI [19]. However, diffuse uptake on this scan does not rule out focal disease [3]. In the largest series, the specificity of this imaging technique to detect focal disease was 96 %, with a positive predictive value of 96 %. In this series, 105 patients with confirmed CHI underwent pancreatectomy. Of these, 53 had a postoperative diagnosis of focal CHI. However, preoperative 18 -F-Dopa-PET imaging in 8 of these 53 was reported erroneously as diffuse [5]. Finally, there are reports of clinical improvement in individuals with heterozygous ABCC8 mutations [20] or those with severe disease [21] with time. Whether improvement will occur in this patient, remains to be determined, but is becoming less likely. We speculate that the late presentation of this patient is more likely due to late detection as opposed to the genetic mutations. We describe a novel compound heterozygous mutation leading to diffuse, diazoxide-unresponsive CHI. This case illustrates the pitfalls and challenges associated with diagnosing CHI and the importance of genetic testing and how it can guide management decisions, including whether or not imaging studies are warranted. Lastly, the case illustrates the difficulty of medically-managing a patient with diffuse CHI. Consent Written informed consent was obtained from the patient for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal. Abbreviations CHI: Congenital hyperinsulinism; K ATP : ATP-sensitive potassium; IGF-1: Insulin-like growth factor-1; IGFBP-3: Insulin-like growth factor binding protein-3; IGFBP-1: Insulin-like growth factor binding protein-1; BOHB: beta-hydroxybutyrate; GIR: Glucose infusion rate; 18 -F-DOPA-PET: 18-fluoro L-3,4-dihydroxyphenylalanine positron emission tomography; 18 -F-DOPA: 18-fluoro L-3,4-dihydroxyphenylalanine.
5 Brady et al. International Journal of Pediatric Endocrinology (2015) 2015:16 Page 5 of 5 Competing interests The authors declare that they have no competing interests. Authors contributions CB and IL provided initial care for patient at home institution and continue to provide care to patient. AP provided subsequent care of patient at Children s Hospital of Philadelphia and interpreted genetic results and imaging. CB drafted the manuscript. AP and IL provided edits to manuscript. All authors read and approved final version of manuscript. Acknowledgements We thank Lisa J. States for her input regarding the F-Dopa PET scan and Kara Boodhansingh for her guidance in genetic interpretation. Author details 1 Cincinnati Children s Hospital Medical Center, Division of Endocrinology, 3333 Burnet Ave, MLC 7012, Cincinnati, OH 45229, USA. 2 Children s Hospital of Philadelphia, Division of Endocrinology, 34th Street and Civic Center Boulevard, Philadelphia, PA 19104, USA. 17. Kelly A, Tang R, Becker S, Stanley CA. Poor specificity of low growth hormone and cortisol levels during fasting hypoglycemia for the diagnoses of growth hormone deficiency and adrenal insufficiency. Pediatrics. 2008;122:e Flanagan S, Damhuis A, Banerjee I, Rokicki D, Jefferies C, Kapoor R, et al. Partial ABCC8 gene deletion mutations causing diazoxide-unresponsive hyperinsulinaemic hypoglycaemia. Pediatr Diabetes. 2012;13: Ribeiro MJ, De Lonlay P, Delzescaux T, Boddaert N, Jaubert F, Bourgeois S, et al. Characterization of hyperinsulinism in infancy assessed with PET and 18 F-fluoro-L-DOPA. J Nucl Med. 2005;46: Kapoor RR, Flanagan SE, Arya VB, Shield JP, Ellard S, Hussain K. Clinical and molecular characterisation of 300 patients with congenital hyperinsulinism. Eur J Endocrinol. 2013;168: Aynsley-Green A, Hussain K, Hall J, Saudubray JM, Nihoul-Fekete C, De Lonlay-Debeney P, et al. Practical management of hyperinsulinism in infancy. Arch Dis Child Fetal Neonatal Ed. 2000;82:F Received: 6 April 2015 Accepted: 1 July 2015 References 1. Snider KE, Becker S, Boyajian L, Shyng SL, MacMullen C, Hughes N, et al. Genotype and phenotype correlations in 417 children with congenital hyperinsulinism. J Clin Endocrinol Metab. 2013;98:E Palladino AA, Stanley CA. A specialized team approach to diagnosis and medical versus surgical treatment of infants with congenital hyperinsulinism. Semin Pediatr Surg. 2011;20: Palladino AA, Bennett MJ, Stanley CA. Hyperinsulinism in infancy and childhood: when an insulin level is not always enough. Clin Chem. 2008;54: Sarafoglou K, Hoffman G. Pediatric endocrinology and inborn errors of metabolism. New York: McGraw-Hill Medical; Laje P, States LJ, Zhuang H, Becker SA, Palladino AA, Stanley CA, et al. Accuracy of PET/CT Scan in the diagnosis of the focal form of congenital hyperinsulinism. J Pediatr Surg. 2013;48: Neylon OM, Moran MM, Pellicano A, Nightingale M, O'Connell MA. Successful subcutaneous glucagon use for persistent hypoglycaemia in congenital hyperinsulinism. J Pediatr Endocrinol Metab. 2013;26: Mohnike K, Blankenstein O, Pfuetzner A, Potzsch S, Schober E, Steiner S, et al. Long-term non-surgical therapy of severe persistent congenital hyperinsulinism with glucagon. Horm Res. 2008;70: Yorifuji T, Kawakita R, Hosokawa Y, Fujimaru R, Matsubara K, Aizu K, et al. Efficacy and safety of long-term, continuous subcutaneous octreotide infusion for patients with different subtypes of KATP-channel hyperinsulinism. Clin Endocrinol (Oxf). 2013;78: De Leon DD, Stanley CA. Determination of insulin for the diagnosis of hyperinsulinemic hypoglycemia. Best Pract Res Clin Endocrinol Metab. 2013;27: Cantrell JW, Hochholzer JM, Frings CS. Effect of hemolysis on the apparent concentration of insulin in plasma. Clin Chem. 1972;18: Chevenne D, Letailleur A, Trivin F, Porquet D. Effect of hemolysis on the concentration of insulin in serum determined by RIA and IRMA. Clin Chem. 1998;44: Sapin R. The interference of insulin antibodies in insulin immunometric assays. Clin Chem Lab Med. 2002;40: Berson SA, Yalow RS, Bauman A, Rothschild MA, Newerly K. Insulin-I131 metabolism in human subjects: demonstration of insulin binding globulin in the circulation of insulin treated subjects. J Clin Invest. 1956;35: Finegold DN, Stanley CA, Baker L. Glycemic response to glucagon during fasting hypoglycemia: an aid in the diagnosis of hyperinsulinism. J Pediatr. 1980;96: Placzkowski KA, Vella A, Thompson GB, Grant CS, Reading CC, Charboneau JW, et al. Secular trends in the presentation and management of functioning insulinoma at the Mayo Clinic, J Clin Endocrinol Metab. 2009;94: Sperling M. Pediatric endocrinology. Fourthth ed. Philadelphia, PA: Elsevier Saunders; Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Patient Demographics 5/12/2016
 Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Pediatric Endocrine Nursing Society May 14, 2016 Enyo Dzata, MSN, CRNP Congenital Hyperinsulinism Center Division
Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Pediatric Endocrine Nursing Society May 14, 2016 Enyo Dzata, MSN, CRNP Congenital Hyperinsulinism Center Division
THE IMPORTANCE OF GENETICS WHEN TREATING HYPERINSULINISM
 THE IMPORTANCE OF GENETICS WHEN TREATING HYPERINSULINISM HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS HYPERINSULINISM? The leading cause of hypoglycemia in infants and
THE IMPORTANCE OF GENETICS WHEN TREATING HYPERINSULINISM HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS HYPERINSULINISM? The leading cause of hypoglycemia in infants and
Congenital hyperinsulinism
 SWISS SOCIETY OF NEONATOLOGY Winner of the Case of the Year Award 2012 Congenital hyperinsulinism FEBRUARY 2012 2 Morgillo D, Berger TM, Caduff JH, Barthlen W, Mohnike K, Mohnike W, Neonatal and Pediatric
SWISS SOCIETY OF NEONATOLOGY Winner of the Case of the Year Award 2012 Congenital hyperinsulinism FEBRUARY 2012 2 Morgillo D, Berger TM, Caduff JH, Barthlen W, Mohnike K, Mohnike W, Neonatal and Pediatric
Surgery in Congenital Hyperinsulinismless. Winfried Barthlen
 Surgery in Congenital Hyperinsulinismless may be more Winfried Barthlen congenital hyperinsulinism - very rare (1:40.000) - uncontrolled insulin secretion - life threatening hypoglycemia symptoms - unconsciousness,
Surgery in Congenital Hyperinsulinismless may be more Winfried Barthlen congenital hyperinsulinism - very rare (1:40.000) - uncontrolled insulin secretion - life threatening hypoglycemia symptoms - unconsciousness,
Challenging diagnosis of congenital hyperinsulinism in two infants of diabetic mothers with rare pathogenic KCNJ11 and HNF4A gene variants
 Huerta-Saenz et al. International Journal of Pediatric Endocrinology (2018) 2018:5 https://doi.org/10.1186/s13633-018-0060-7 CASE REPORT Open Access Challenging diagnosis of congenital hyperinsulinism
Huerta-Saenz et al. International Journal of Pediatric Endocrinology (2018) 2018:5 https://doi.org/10.1186/s13633-018-0060-7 CASE REPORT Open Access Challenging diagnosis of congenital hyperinsulinism
The Surgeon General s Call to Action and the
 Case of the Month Pamela Heaberlin, MS, RN, NNP-BC Section Editor 2.3 HOURS Continuing Education Congenital Hyperinsulinism Exclusive Human Milk and Breastfeeding Taryn M. Edwards, MSN, CRNP, NNP-BC ;
Case of the Month Pamela Heaberlin, MS, RN, NNP-BC Section Editor 2.3 HOURS Continuing Education Congenital Hyperinsulinism Exclusive Human Milk and Breastfeeding Taryn M. Edwards, MSN, CRNP, NNP-BC ;
Hypoglycemia in congenital hyperinsulinism
 How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
Remission in Non-Operated Patients with Diffuse Disease and Long-Term Conservative Treatment.
 5th Congenital Hyperinsulinism International Family Conference Milan, September 17-18 Remission in Non-Operated Patients with Diffuse Disease and Long-Term Conservative Treatment. PD Dr. Thomas Meissner
5th Congenital Hyperinsulinism International Family Conference Milan, September 17-18 Remission in Non-Operated Patients with Diffuse Disease and Long-Term Conservative Treatment. PD Dr. Thomas Meissner
Managing Congenital Hyperinsulinism in the Neonatal Period Vall d Hebron Hospital s Approach and Experience
 Managing Congenital Hyperinsulinism in the Alejandro Vargas Pieck Miquel Gussinyer Canadell María Clemente León Diego Yeste Fernández Universidad Autónoma de Barcelona Antonio Carrascosa Lezcano The first
Managing Congenital Hyperinsulinism in the Alejandro Vargas Pieck Miquel Gussinyer Canadell María Clemente León Diego Yeste Fernández Universidad Autónoma de Barcelona Antonio Carrascosa Lezcano The first
Overview. o Limitations o Normal regulation of blood glucose o Definition o Symptoms o Clinical forms o Pathophysiology o Treatment.
 Pål R. Njølstad MD PhD KG Jebsen Center for Diabetes Research University of Bergen, Norway Depertment of Pediatrics Haukeland University Hospital Broad Institute of Harvard & MIT Cambridge, MA, USA Hypoglycemia
Pål R. Njølstad MD PhD KG Jebsen Center for Diabetes Research University of Bergen, Norway Depertment of Pediatrics Haukeland University Hospital Broad Institute of Harvard & MIT Cambridge, MA, USA Hypoglycemia
Not Your Typical Case of Ketotic Hypoglycemia
 Not Your Typical Case of Ketotic Hypoglycemia Linda Steinkrauss, RN, MSN, CPNP Objectives By the end of this session, attendees should be able to: 1. Discuss the difference between idiopathic ketotic hypoglycemia
Not Your Typical Case of Ketotic Hypoglycemia Linda Steinkrauss, RN, MSN, CPNP Objectives By the end of this session, attendees should be able to: 1. Discuss the difference between idiopathic ketotic hypoglycemia
Case Reports. Diffuse Type Hyperinsulinaemic Hypoglycaemia of Infancy: Case Report of Management without Pancreatectomy
 HK J Paediatr (new series) 2014;19:252-256 Case Reports Diffuse Type Hyperinsulinaemic Hypoglycaemia of Infancy: Case Report of Management without Pancreatectomy THY TAN, KL NG Abstract Key words Congenital
HK J Paediatr (new series) 2014;19:252-256 Case Reports Diffuse Type Hyperinsulinaemic Hypoglycaemia of Infancy: Case Report of Management without Pancreatectomy THY TAN, KL NG Abstract Key words Congenital
Use of Lanreotide (long acting Somatostatin analogue) in Congenital Hyperinsulinism (CHI)
 Use of Lanreotide (long acting Somatostatin analogue) in Congenital Hyperinsulinism (CHI) Dr Pratik Shah Clinical Research fellow in Hyperinsulinism Clinical Molecular Genetics Unit Institute of Child
Use of Lanreotide (long acting Somatostatin analogue) in Congenital Hyperinsulinism (CHI) Dr Pratik Shah Clinical Research fellow in Hyperinsulinism Clinical Molecular Genetics Unit Institute of Child
4/23/2015. Linda Steinkrauss, MSN, PNP. No conflicts of interest
 Linda Steinkrauss, MSN, PNP No conflicts of interest 1 5 year old African-American female presented to our Endocrinology Clinic with hypoglycemia Abnormal chromosomes Duplication of 11q13.5-11p14.1 affecting
Linda Steinkrauss, MSN, PNP No conflicts of interest 1 5 year old African-American female presented to our Endocrinology Clinic with hypoglycemia Abnormal chromosomes Duplication of 11q13.5-11p14.1 affecting
Neonatal Hypoglycaemia
 Neonatal Hypoglycaemia Dr Shubha Srinivasan Paediatric Endocrinologist The Children s Hospital at Westmead Hypoglycaemia and the Brain CSF glucose is 2/3 that of plasma Intracerebral glucose 1/3 that of
Neonatal Hypoglycaemia Dr Shubha Srinivasan Paediatric Endocrinologist The Children s Hospital at Westmead Hypoglycaemia and the Brain CSF glucose is 2/3 that of plasma Intracerebral glucose 1/3 that of
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA
 NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
Management of Glucose in the Preterm Infant. Charles A. Stanley, MD Division of Endocrinology Children s Hospital of Philadelphia
 Management of Glucose in the Preterm Infant Charles A. Stanley, MD Division of Endocrinology Children s Hospital of Philadelphia Disclosures Charles Stanley, MD I have no relevant financial relationships
Management of Glucose in the Preterm Infant Charles A. Stanley, MD Division of Endocrinology Children s Hospital of Philadelphia Disclosures Charles Stanley, MD I have no relevant financial relationships
Cook Children s HI Center. Paul Thornton Medical Director Cook Children s Hyperinsulinism Center
 Cook Children s HI Center Paul Thornton Medical Director Cook Children s Hyperinsulinism Center Formed in Oct 2010 Cook Children s HI Center Mission: To provide excellence in medical care to patients with
Cook Children s HI Center Paul Thornton Medical Director Cook Children s Hyperinsulinism Center Formed in Oct 2010 Cook Children s HI Center Mission: To provide excellence in medical care to patients with
PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS. A17/S(HSS)/a Congenital hyperinsulinism service (Children)
 A17/S(HSS)/a 2013/14 NHS STANDARD CONTRACT FOR CONGENITAL HYPERINSULINISM SERVICE (CHILDREN) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner
A17/S(HSS)/a 2013/14 NHS STANDARD CONTRACT FOR CONGENITAL HYPERINSULINISM SERVICE (CHILDREN) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner
Pancreatic Insulinoma Presenting. with Episodes of Hypoinsulinemic. Hypoglycemia in Elderly ---- A Case Report
 2008 19 432-436 Pancreatic Insulinoma Presenting with Episodes of Hypoinsulinemic Hypoglycemia in Elderly ---- A Case Report Chieh-Hsiang Lu 1, Shih-Che Hua 1, and Chung-Jung Wu 2,3 1 Division of Endocrinology
2008 19 432-436 Pancreatic Insulinoma Presenting with Episodes of Hypoinsulinemic Hypoglycemia in Elderly ---- A Case Report Chieh-Hsiang Lu 1, Shih-Che Hua 1, and Chung-Jung Wu 2,3 1 Division of Endocrinology
Congenital hyperinsulinism: clinical and molecular characterisation of compound heterozygous ABCC8 mutation responsive to Diazoxide therapy
 Arya et al. International Journal of Pediatric Endocrinology 2014, 2014:24 CASE REPORT Open Access Congenital hyperinsulinism: clinical and molecular characterisation of compound heterozygous ABCC8 mutation
Arya et al. International Journal of Pediatric Endocrinology 2014, 2014:24 CASE REPORT Open Access Congenital hyperinsulinism: clinical and molecular characterisation of compound heterozygous ABCC8 mutation
Congenital hyperinsulinism (HI) is the leading cause of
 ORIGINAL ARTICLE High Risk of Diabetes and Neurobehavioral Deficits in Individuals With Surgically Treated Hyperinsulinism Katherine Lord, Jerilynn Radcliffe, Paul R. Gallagher, N. Scott Adzick, Charles
ORIGINAL ARTICLE High Risk of Diabetes and Neurobehavioral Deficits in Individuals With Surgically Treated Hyperinsulinism Katherine Lord, Jerilynn Radcliffe, Paul R. Gallagher, N. Scott Adzick, Charles
A novel mutation of ABCC8 gene in a patient with diazoxide-unresponsive congenital hyperinsulinism
 Case report Park Korean JS, J et Pediatr al. Congenital 2016;59(Suppl hyperinsulinism 1):S116-120with a novel mutation of ABCC8 pissn 1738-1061 eissn 2092-7258 Korean J Pediatr A novel mutation of ABCC8
Case report Park Korean JS, J et Pediatr al. Congenital 2016;59(Suppl hyperinsulinism 1):S116-120with a novel mutation of ABCC8 pissn 1738-1061 eissn 2092-7258 Korean J Pediatr A novel mutation of ABCC8
Neonatal Hypoglycemia
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
ORE Open Research Exeter
 ORE Open Research Exeter TITLE - A Case Report. AUTHORS Khawash, P; Hussain, K; Flanagan, SE; et al. JOURNAL Journal of Clinical Research in Pediatric Endocrinology DEPOSITED IN ORE 03 March 2016 This
ORE Open Research Exeter TITLE - A Case Report. AUTHORS Khawash, P; Hussain, K; Flanagan, SE; et al. JOURNAL Journal of Clinical Research in Pediatric Endocrinology DEPOSITED IN ORE 03 March 2016 This
History of Hyperinsulinism (HI) in Pediatrics and Overview of Diagnostic/Therapeutic Algorithm. Charles A. Stanley, MD CHOP HI Center
 History of Hyperinsulinism (HI) in Pediatrics and Overview of Diagnostic/Therapeutic Algorithm Charles A. Stanley, MD CHOP HI Center Discovery of Hypoglycemia January, 1922 (? by J.B. Collip) In the Beginning
History of Hyperinsulinism (HI) in Pediatrics and Overview of Diagnostic/Therapeutic Algorithm Charles A. Stanley, MD CHOP HI Center Discovery of Hypoglycemia January, 1922 (? by J.B. Collip) In the Beginning
بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری
 بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری Serum glucose< 35 mg/dl 1-3 hr of life < 40 mg/dl 3-24 hr < 45 mg/dl after 24 hr 10% NL newborns can t maintain BS>30 if delayed feeding >3-6 hrs
بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری Serum glucose< 35 mg/dl 1-3 hr of life < 40 mg/dl 3-24 hr < 45 mg/dl after 24 hr 10% NL newborns can t maintain BS>30 if delayed feeding >3-6 hrs
Advances in the diagnosis and management of hyperinsulinemic hypoglycemia
 Advances in the diagnosis and management of hyperinsulinemic hypoglycemia Ritika R Kapoor, Chela James and Khalid Hussain* SUMMARY Hyperinsulinemic hypoglycemia (HH) is a consequence of unregulated insulin
Advances in the diagnosis and management of hyperinsulinemic hypoglycemia Ritika R Kapoor, Chela James and Khalid Hussain* SUMMARY Hyperinsulinemic hypoglycemia (HH) is a consequence of unregulated insulin
Learning Objectives. At the conclusion of this module, participants should be better able to:
 Learning Objectives At the conclusion of this module, participants should be better able to: Treat asymptomatic neonatal hypoglycemia with buccal dextrose gel Develop patient-specific approaches to intravenous
Learning Objectives At the conclusion of this module, participants should be better able to: Treat asymptomatic neonatal hypoglycemia with buccal dextrose gel Develop patient-specific approaches to intravenous
Diazoxide-responsive Hyperinsulinism
 Diazoxide-responsive Hyperinsulinism Linda Boyajian, CRNP Diva D. De León-Crutchlow, MD, MSCE Congenital Hyperinsulinism Center The Children s Hospital of Philadelphia Picture courtesy of Dr. Colin Hawkes
Diazoxide-responsive Hyperinsulinism Linda Boyajian, CRNP Diva D. De León-Crutchlow, MD, MSCE Congenital Hyperinsulinism Center The Children s Hospital of Philadelphia Picture courtesy of Dr. Colin Hawkes
Cook Children s Hyperinsulinism Center
 Cook Children s Hyperinsulinism Center Dear friends and colleagues, It is my privilege to present Cook Children s Hyperinsulinism Center, one of only two of its kind in the country. At Cook Children s,
Cook Children s Hyperinsulinism Center Dear friends and colleagues, It is my privilege to present Cook Children s Hyperinsulinism Center, one of only two of its kind in the country. At Cook Children s,
Hyperinsulinemic hypoglycemia, a major cause of severe hypoglycemia
 brief report Sirolimus Therapy in Infants with Severe Hyperinsulinemic Hypoglycemia Senthil Senniappan, M.D., Sanda Alexandrescu, M.D., Nina Tatevian, M.D., Pratik Shah, M.D., Ved Arya, M.D., Sarah Flanagan,
brief report Sirolimus Therapy in Infants with Severe Hyperinsulinemic Hypoglycemia Senthil Senniappan, M.D., Sanda Alexandrescu, M.D., Nina Tatevian, M.D., Pratik Shah, M.D., Ved Arya, M.D., Sarah Flanagan,
A Multicenter Experience with Long-Acting Somatostatin Analogues in Patients with Congenital Hyperinsulinism
 Syddansk Universitet A Multicenter Experience with Long-Acting Somatostatin Analogues in Patients with van der Steen, Ivo; van Albada, Mirjam E; Mohnike, Klaus; Thybo Christesen, Henrik; Empting, Susann;
Syddansk Universitet A Multicenter Experience with Long-Acting Somatostatin Analogues in Patients with van der Steen, Ivo; van Albada, Mirjam E; Mohnike, Klaus; Thybo Christesen, Henrik; Empting, Susann;
THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals
 Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Long-term treatment with Lanreotide in CHI
 Long-term treatment with Lanreotide in CHI Oliver Blankenstein Institute for Experimental Paediatric Endocrinology Charité-Universitätsmedizin Berlin U N I V E R S I T Ä T S M E D I Z I N B E R L I N 5
Long-term treatment with Lanreotide in CHI Oliver Blankenstein Institute for Experimental Paediatric Endocrinology Charité-Universitätsmedizin Berlin U N I V E R S I T Ä T S M E D I Z I N B E R L I N 5
Permanent neonatal diabetes mellitus. Case Report
 Rawal Medical Journal An official publication of Pakistan Medical Association Rawalpindi Islamabad branch Established 1975 Volume 36 Number 4 October - December 2011 Case Report Permanent neonatal diabetes
Rawal Medical Journal An official publication of Pakistan Medical Association Rawalpindi Islamabad branch Established 1975 Volume 36 Number 4 October - December 2011 Case Report Permanent neonatal diabetes
PES Recommendations for Evaluation and Management of Hypoglycemia in Neonates, Infants, and Children Paul S. Thornton On behalf of the Team
 Cook Children s 1 PES Recommendations for Evaluation and Management of Hypoglycemia in Neonates, Infants, and Children Paul S. Thornton On behalf of the Team Cook Children s 2 Co-Chair: Charles Stanley
Cook Children s 1 PES Recommendations for Evaluation and Management of Hypoglycemia in Neonates, Infants, and Children Paul S. Thornton On behalf of the Team Cook Children s 2 Co-Chair: Charles Stanley
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
David Bruyette, DVM, DACVIM Medical Director
 VCAWLAspecialty.com David Bruyette, DVM, DACVIM Medical Director The pancreas is made up of endocrine and exocrine tissue. The endocrine pancreas is composed of islets of Langerhans, which make up approximately
VCAWLAspecialty.com David Bruyette, DVM, DACVIM Medical Director The pancreas is made up of endocrine and exocrine tissue. The endocrine pancreas is composed of islets of Langerhans, which make up approximately
Neonatal Diabetes. Objectives. Conflicts of Interest Disclosure. No conflicts of interest related to the content of this presentation
 Neonatal Diabetes Shannon Abernethy BSN, RN, CPN Pediatric Nurse Navigator Bon Secours Virginia Medical Group Pediatric Endocrinology and Diabetes Associates 1 Objectives Identify and define neonatal diabetes
Neonatal Diabetes Shannon Abernethy BSN, RN, CPN Pediatric Nurse Navigator Bon Secours Virginia Medical Group Pediatric Endocrinology and Diabetes Associates 1 Objectives Identify and define neonatal diabetes
Inactivating mutations of the b-cell ATP-sensitive
 ORIGINAL ARTICLE Diazoxide-Unresponsive Congenital Hyperinsulinism in Children With Dominant Mutations of the b-cell Sulfonylurea Receptor SUR1 Courtney M. MacMullen, 1 Qing Zhou, 2 Kara E. Snider, 1 Paul
ORIGINAL ARTICLE Diazoxide-Unresponsive Congenital Hyperinsulinism in Children With Dominant Mutations of the b-cell Sulfonylurea Receptor SUR1 Courtney M. MacMullen, 1 Qing Zhou, 2 Kara E. Snider, 1 Paul
Hyperinsulinaemic Hypoglycaemia
 Review 157 Hyperinsulinaemic Hypoglycaemia Authors V. B. Arya 1, Z. Mohammed 1, O. Blankenstein 2, P. De Lonlay 3, K. Hussain 1 Affiliations Key words congenital hyperinsulinism hyperinsulinaemic hypoglycaemia
Review 157 Hyperinsulinaemic Hypoglycaemia Authors V. B. Arya 1, Z. Mohammed 1, O. Blankenstein 2, P. De Lonlay 3, K. Hussain 1 Affiliations Key words congenital hyperinsulinism hyperinsulinaemic hypoglycaemia
Endocrine topic reviews. Artit Sangkakam, MD 19, september 2013
 Endocrine topic reviews Artit Sangkakam, MD 19, september 2013 Hypoglycemia in Non-DM Definition In diabetic mellitus : Plasma glucose 70 mg/dl In Non-diabetic mellitus : Plasma glucose 55 mg/dl Normal
Endocrine topic reviews Artit Sangkakam, MD 19, september 2013 Hypoglycemia in Non-DM Definition In diabetic mellitus : Plasma glucose 70 mg/dl In Non-diabetic mellitus : Plasma glucose 55 mg/dl Normal
CONGENITAL HYPERINSULINISM SURGICAL TREATMENT AND COMPLICATIONS
 Acta Chirurg 2011; 8: 21-25 CONGENITAL HYPERINSULINISM SURGICAL TREATMENT AND COMPLICATIONS Running head: Congenital Hyperinsulinism Authors: Marko Bogovic, M.D. Stipe Batinica, M.D., Prof. Tomislav Luetic,
Acta Chirurg 2011; 8: 21-25 CONGENITAL HYPERINSULINISM SURGICAL TREATMENT AND COMPLICATIONS Running head: Congenital Hyperinsulinism Authors: Marko Bogovic, M.D. Stipe Batinica, M.D., Prof. Tomislav Luetic,
PET Scan in Practice for CHI
 PET Scan in Practice for CHI - Basics, strength and weakness - Oliver Blankenstein Institute for Experimental Paediatric Endocrinology Charité-Universitätsmedizin Berlin U N I V E R S I T Ä T S M E D I
PET Scan in Practice for CHI - Basics, strength and weakness - Oliver Blankenstein Institute for Experimental Paediatric Endocrinology Charité-Universitätsmedizin Berlin U N I V E R S I T Ä T S M E D I
Conservatively treated Congenital Hyperinsulinism (CHI) due to K-ATP channel gene mutations: reducing severity over time
 Salomon-Estebanez et al. Orphanet Journal of Rare Diseases (2016) 11:163 DOI 10.1186/s13023-016-0547-3 RESEARCH Conservatively treated Congenital Hyperinsulinism (CHI) due to K-ATP channel gene mutations:
Salomon-Estebanez et al. Orphanet Journal of Rare Diseases (2016) 11:163 DOI 10.1186/s13023-016-0547-3 RESEARCH Conservatively treated Congenital Hyperinsulinism (CHI) due to K-ATP channel gene mutations:
Linda Boyajian, RN, MSN, CRNP Congenital Hyperinsulinism Center Children s Hospital of Philadelphia
 Linda Boyajian, RN, MSN, CRNP Congenital Hyperinsulinism Center Children s Hospital of Philadelphia Congenital Hyperinsulinism refers to a variety of congenital disorders in which hypoglycemia is caused
Linda Boyajian, RN, MSN, CRNP Congenital Hyperinsulinism Center Children s Hospital of Philadelphia Congenital Hyperinsulinism refers to a variety of congenital disorders in which hypoglycemia is caused
Case Report Metastatic Insulinoma Managed with Radiolabeled Somatostatin Analog
 Case Reports in Endocrinology Volume 2013, Article ID 252159, 4 pages http://dx.doi.org/10.1155/2013/252159 Case Report Metastatic Insulinoma Managed with Radiolabeled Somatostatin Analog Ricardo Costa,
Case Reports in Endocrinology Volume 2013, Article ID 252159, 4 pages http://dx.doi.org/10.1155/2013/252159 Case Report Metastatic Insulinoma Managed with Radiolabeled Somatostatin Analog Ricardo Costa,
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
Received 21 August 2011 accepted 12 February 2012
 Original article 49 Near-total pancreatectomy for persistent hyperinsulinemic hypoglycemia of infancy (nesidioblastosis): Mansoura experience Adham Elsaied a, Mohammed El-Ghazaly a, Basem Saied a and Ashraf
Original article 49 Near-total pancreatectomy for persistent hyperinsulinemic hypoglycemia of infancy (nesidioblastosis): Mansoura experience Adham Elsaied a, Mohammed El-Ghazaly a, Basem Saied a and Ashraf
What systems are involved in homeostatic regulation (give an example)?
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
Week 3, Lecture 5a. Pathophysiology of Diabetes. Simin Liu, MD, ScD
 Week 3, Lecture 5a Pathophysiology of Diabetes Simin Liu, MD, ScD General Model of Peptide Hormone Action Hormone Plasma Membrane Activated Nucleus Cellular Trafficking Enzymes Inhibited Receptor Effector
Week 3, Lecture 5a Pathophysiology of Diabetes Simin Liu, MD, ScD General Model of Peptide Hormone Action Hormone Plasma Membrane Activated Nucleus Cellular Trafficking Enzymes Inhibited Receptor Effector
Persistent Hyperinsulinemic Hypoglycemia of Infancy-Case Report
 Human Journals Case Report June 2018 Vol.:9, Issue:4 All rights are reserved by Suraiya Begum et al. Persistent Hyperinsulinemic Hypoglycemia of Infancy-Case Report Keywords: Persistent hyperinsulinemic
Human Journals Case Report June 2018 Vol.:9, Issue:4 All rights are reserved by Suraiya Begum et al. Persistent Hyperinsulinemic Hypoglycemia of Infancy-Case Report Keywords: Persistent hyperinsulinemic
Hyperglycaemia. Clinical presentation. Definition of hyperglycaemia. Approach to the problem
 Hyperglycaemia 1 Clinical presentation Hyperglycaemia is usually picked up incidentally on routine blood glucose assessment or in response to finding glycosuria. It may be noted as part of the workup of
Hyperglycaemia 1 Clinical presentation Hyperglycaemia is usually picked up incidentally on routine blood glucose assessment or in response to finding glycosuria. It may be noted as part of the workup of
Proceedings of the Southern European Veterinary Conference - SEVC -
 Close this window to return to IVIS www.ivis.org Proceedings of the Southern European Veterinary Conference - SEVC - Sep. 30-Oct. 3, 2010, Barcelona, Spain Next SEVC Conference: Sep. 30-Oct. 2, 2011 -
Close this window to return to IVIS www.ivis.org Proceedings of the Southern European Veterinary Conference - SEVC - Sep. 30-Oct. 3, 2010, Barcelona, Spain Next SEVC Conference: Sep. 30-Oct. 2, 2011 -
Insulinoma Masquerading as Idiopathic Partial Complex Epilepsy: A Case Report
 Scientific Times Journal of Open Access Paediatrics Scientific Times Journal of Paediatrics Scientific Times Case Report Case Report Insulinoma Masquerading as Idiopathic Partial Complex Epilepsy: A Case
Scientific Times Journal of Open Access Paediatrics Scientific Times Journal of Paediatrics Scientific Times Case Report Case Report Insulinoma Masquerading as Idiopathic Partial Complex Epilepsy: A Case
Persistent Hyperinsulinaemic Hypoglycaemia of Infancy in 43 Children: Long-term Clinical and Surgical Follow-up
 19 th Congress of AAPS Persistent Hyperinsulinaemic Hypoglycaemia of Infancy in 43 Children: Long-term Clinical and Surgical Follow-up Saleh Al-Nassar, Nadia Sakati, Abdullah Al-Ashwal and Bassam Bin-Abbas,
19 th Congress of AAPS Persistent Hyperinsulinaemic Hypoglycaemia of Infancy in 43 Children: Long-term Clinical and Surgical Follow-up Saleh Al-Nassar, Nadia Sakati, Abdullah Al-Ashwal and Bassam Bin-Abbas,
W1A- Cases I Learned From
 W1A- Cases I Learned From David H Adamkin, MD Professor of Pediatrics Director, Division of Neonatology Director of Nutritional Research Rounsavall Chair of Neonatal Medicine Co-Director of Neonatal Fellowship
W1A- Cases I Learned From David H Adamkin, MD Professor of Pediatrics Director, Division of Neonatology Director of Nutritional Research Rounsavall Chair of Neonatal Medicine Co-Director of Neonatal Fellowship
Insulinoma - 72 hour Fast Protocol - RNS Endocrinology
 Page 1 of 9 - RNS Endocrinology Test name 72 hour fast Alternate test names. Related Tests Mixed meal test Indication(s) Differential diagnosis of causes of hypoglycaemia. Hypoglycaemia is rare in persons
Page 1 of 9 - RNS Endocrinology Test name 72 hour fast Alternate test names. Related Tests Mixed meal test Indication(s) Differential diagnosis of causes of hypoglycaemia. Hypoglycaemia is rare in persons
Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing
 Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing Jean-Pierre Chanoine, MD Endocrinology and Diabetes Unit British Columbia s Children s Hospital Objectives 1. Interpret the
Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing Jean-Pierre Chanoine, MD Endocrinology and Diabetes Unit British Columbia s Children s Hospital Objectives 1. Interpret the
Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia
 Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Hormonal regulation of. Physiology Department Medical School, University of Sumatera Utara
 Hormonal regulation of nutrient metabolism Physiology Department Medical School, University of Sumatera Utara Homeostasis & Controls Successful compensation Homeostasis reestablished Failure to compensate
Hormonal regulation of nutrient metabolism Physiology Department Medical School, University of Sumatera Utara Homeostasis & Controls Successful compensation Homeostasis reestablished Failure to compensate
NEONATAL CLINICAL PRACTICE GUIDELINE
 NEONATAL CLINICAL PRACTICE GUIDELINE 1.0 PURPOSE AND INTENT Title: Approval Date: March 2016 Approved by: Neonatal Patient Care Teams, HSC & SBH Women s Health Maternal Newborn Committee Child Health Standards
NEONATAL CLINICAL PRACTICE GUIDELINE 1.0 PURPOSE AND INTENT Title: Approval Date: March 2016 Approved by: Neonatal Patient Care Teams, HSC & SBH Women s Health Maternal Newborn Committee Child Health Standards
An Unusual Case of Concurrent Insulinoma and Nesidioblastosis
 CASE REPORT An Unusual Case of Concurrent Insulinoma and Nesidioblastosis Elizabeth Bright 1, Giuseppe Garcea 1, Seok L Ong 1, Webster Madira 2, David P Berry 1, Ashley R Dennison 1 Departments of 1 Hepatobiliary
CASE REPORT An Unusual Case of Concurrent Insulinoma and Nesidioblastosis Elizabeth Bright 1, Giuseppe Garcea 1, Seok L Ong 1, Webster Madira 2, David P Berry 1, Ashley R Dennison 1 Departments of 1 Hepatobiliary
Guidelines for the Prevention and Management of Hypoglycaemia
 ASHFORD & ST PETER S HOSPITALS NHS TRUST CHILDREN S SERVICES Guidelines for the Prevention and Management of Hypoglycaemia 1. The Care Plan for Prevention of Hypoglycaemia on Labour Ward and the Postnatal
ASHFORD & ST PETER S HOSPITALS NHS TRUST CHILDREN S SERVICES Guidelines for the Prevention and Management of Hypoglycaemia 1. The Care Plan for Prevention of Hypoglycaemia on Labour Ward and the Postnatal
Introduction SHORT COMMUNICATION
 Diabetologia (2005) 48: 2236 2240 DOI 10.1007/s00125-005-1933-x SHORT COMMUNICATION M. E. Patti. G. McMahon. E. C. Mun. A. Bitton. J. J. Holst. J. Goldsmith. D. W. Hanto. M. Callery. R. Arky. V. Nose.
Diabetologia (2005) 48: 2236 2240 DOI 10.1007/s00125-005-1933-x SHORT COMMUNICATION M. E. Patti. G. McMahon. E. C. Mun. A. Bitton. J. J. Holst. J. Goldsmith. D. W. Hanto. M. Callery. R. Arky. V. Nose.
Glucose Metabolism in 105 Children and Adolescents After Pancreatectomy for Congenital Hyperinsulinism
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Glucose Metabolism in 105 Children and Adolescents After Pancreatectomy for Congenital Hyperinsulinism JACQUES BELTRAND,
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Glucose Metabolism in 105 Children and Adolescents After Pancreatectomy for Congenital Hyperinsulinism JACQUES BELTRAND,
An Unexpected Cause of Hypoglycemia
 An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
28 Regulation of Fasting and Post-
 28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
Congenital hyperinsulinism: current status and future perspectives
 Review article http://dx.doi.org/10.6065/apem.2014.19.2.57 Ann Pediatr Endocrinol Metab 2014;19:57-68 Congenital hyperinsulinism: current status and future perspectives Tohru Yorifuji, MD, PhD Department
Review article http://dx.doi.org/10.6065/apem.2014.19.2.57 Ann Pediatr Endocrinol Metab 2014;19:57-68 Congenital hyperinsulinism: current status and future perspectives Tohru Yorifuji, MD, PhD Department
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
72 hour Fast Protocol
 Page 1 of 5 Principle This procedure provides instruction on how to conduct a prolonged fast. During the fast, a careful record must be kept of exactly what was done, what blood samples were taken and
Page 1 of 5 Principle This procedure provides instruction on how to conduct a prolonged fast. During the fast, a careful record must be kept of exactly what was done, what blood samples were taken and
Vineland adaptive behavior scales to identify neurodevelopmental problems in children with Congenital Hyperinsulinism (CHI)
 Salomon-Estebanez et al. Orphanet Journal of Rare Diseases (2017) 12:96 DOI 10.1186/s13023-017-0648-7 RESEARCH Vineland adaptive behavior scales to identify neurodevelopmental problems in children with
Salomon-Estebanez et al. Orphanet Journal of Rare Diseases (2017) 12:96 DOI 10.1186/s13023-017-0648-7 RESEARCH Vineland adaptive behavior scales to identify neurodevelopmental problems in children with
Relationship between incident types and impact on patients in drug name errors: a correlational study
 Tsuji et al. Journal of Pharmaceutical Health Care and Sciences (2015) 1:11 DOI 10.1186/s40780-015-0011-x RESEARCH ARTICLE Open Access Relationship between incident types and impact on patients in drug
Tsuji et al. Journal of Pharmaceutical Health Care and Sciences (2015) 1:11 DOI 10.1186/s40780-015-0011-x RESEARCH ARTICLE Open Access Relationship between incident types and impact on patients in drug
Pediatric non-diabetic ketoacidosis: a caseseries
 Bai et al. BMC Pediatrics (2017) 17:209 DOI 10.1186/s12887-017-0960-3 RESEARCH ARTICLE Open Access Pediatric non-diabetic ketoacidosis: a caseseries report Ke Bai 1, Yueqiang Fu 1, Chengjun Liu 1*, Feng
Bai et al. BMC Pediatrics (2017) 17:209 DOI 10.1186/s12887-017-0960-3 RESEARCH ARTICLE Open Access Pediatric non-diabetic ketoacidosis: a caseseries report Ke Bai 1, Yueqiang Fu 1, Chengjun Liu 1*, Feng
Pediatric Toxic Hypoglycemia. Sara Kazim, MD, FRCP (EM) Clinical Pharmacology and Medical Toxicology Fellowship IEMC May Antalya
 Pediatric Toxic Hypoglycemia Sara Kazim, MD, FRCP (EM) Clinical Pharmacology and Medical Toxicology Fellowship IEMC May 2016 - Antalya Conflicts of Interests... None Learning Needs... By the end of this
Pediatric Toxic Hypoglycemia Sara Kazim, MD, FRCP (EM) Clinical Pharmacology and Medical Toxicology Fellowship IEMC May 2016 - Antalya Conflicts of Interests... None Learning Needs... By the end of this
Fundamentals of Exercise Physiology and T1D
 COMPLIMENTARY CE Fundamentals of Exercise Physiology and T1D Jointly Provided by Developed in collaboration with 1 INTRODUCTION TO PHYSICAL ACTIVITY AND T1D 2 Many People with T1D Have Lower Levels of
COMPLIMENTARY CE Fundamentals of Exercise Physiology and T1D Jointly Provided by Developed in collaboration with 1 INTRODUCTION TO PHYSICAL ACTIVITY AND T1D 2 Many People with T1D Have Lower Levels of
Hormonal Regulations Of Glucose Metabolism & DM
 Hormonal Regulations Of Glucose Metabolism & DM What Hormones Regulate Metabolism? What Hormones Regulate Metabolism? Insulin Glucagon Thyroid hormones Cortisol Epinephrine Most regulation occurs in order
Hormonal Regulations Of Glucose Metabolism & DM What Hormones Regulate Metabolism? What Hormones Regulate Metabolism? Insulin Glucagon Thyroid hormones Cortisol Epinephrine Most regulation occurs in order
Approach to hypoglycemia in infants and children
 Review Article Approach to hypoglycemia in infants and children Kajal Gandhi Section of Endocrinology, Nationwide Children s Hospital, Columbus, OH, USA Correspondence to: Kajal Gandhi, DO, MPH. Section
Review Article Approach to hypoglycemia in infants and children Kajal Gandhi Section of Endocrinology, Nationwide Children s Hospital, Columbus, OH, USA Correspondence to: Kajal Gandhi, DO, MPH. Section
RECENTLY, WE AND others described an unusual form
 0013-7227/01/$03.00/0 The Journal of Clinical Endocrinology & Metabolism 86(8):3724 3728 Printed in U.S.A. Copyright 2001 by The Endocrine Society Acute Insulin Responses to Leucine in Children with the
0013-7227/01/$03.00/0 The Journal of Clinical Endocrinology & Metabolism 86(8):3724 3728 Printed in U.S.A. Copyright 2001 by The Endocrine Society Acute Insulin Responses to Leucine in Children with the
CARE OF THE NEWBORN HYPOGLYCAEMIA
 CARE OF THE NEWBORN HYPOGLYCAEMIA Background Definition A true blood glucose of less than 2.6 mmol/l venous sample. Neonatal hypoglycaemia is commonly defined as a true blood glucose of less than 2.6 mmol/l
CARE OF THE NEWBORN HYPOGLYCAEMIA Background Definition A true blood glucose of less than 2.6 mmol/l venous sample. Neonatal hypoglycaemia is commonly defined as a true blood glucose of less than 2.6 mmol/l
Heartland Genetics and Newborn Screening Collaborative Conference
 Heartland Genetics and Newborn Screening Collaborative Conference Laurel K. Willig, MD Assistant Medical Director for the Center for Pediatric Genomic Medicine and Joshua E. Petrikin, MD Director of Neonatal
Heartland Genetics and Newborn Screening Collaborative Conference Laurel K. Willig, MD Assistant Medical Director for the Center for Pediatric Genomic Medicine and Joshua E. Petrikin, MD Director of Neonatal
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
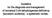 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Case Report Asymptomatic Congenital Hyperinsulinism due to a Glucokinase-Activating Mutation, Treated as Adrenal Insufficiency for Twelve Years
 Hindawi Case Reports in Endocrinology Volume 2017, Article ID 4709262, 6 pages https://doi.org/10.1155/2017/4709262 Case Report Asymptomatic Congenital Hyperinsulinism due to a Glucokinase-Activating Mutation,
Hindawi Case Reports in Endocrinology Volume 2017, Article ID 4709262, 6 pages https://doi.org/10.1155/2017/4709262 Case Report Asymptomatic Congenital Hyperinsulinism due to a Glucokinase-Activating Mutation,
Hyperinsulinemic hypoglycemia has
 R E V I E W A R T I C L E Hyperinsulinemic Hypoglycemia in Infancy: Current Concepts in Diagnosis and Management SHRENIK VORA, SURESH CHANDRAN, VICTOR SAMUEL RAJADURAI AND # KHALID HUSSAIN From Department
R E V I E W A R T I C L E Hyperinsulinemic Hypoglycemia in Infancy: Current Concepts in Diagnosis and Management SHRENIK VORA, SURESH CHANDRAN, VICTOR SAMUEL RAJADURAI AND # KHALID HUSSAIN From Department
Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption),
 Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption), in which blood glucose predominantly originates from
Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption), in which blood glucose predominantly originates from
OVERVIEW OF PEDIATRIC DIABETES Alan B. Cortez, M.D. Pediatric Endocrinology Chief, Department of Pediatrics Kaiser-Permanente, Orange County
 OVERVIEW OF PEDIATRIC DIABETES 2011 Alan B. Cortez, M.D. Pediatric Endocrinology Chief, Department of Pediatrics Kaiser-Permanente, Orange County Outline of Pediatric Diabetes Presentation Types of Pediatric
OVERVIEW OF PEDIATRIC DIABETES 2011 Alan B. Cortez, M.D. Pediatric Endocrinology Chief, Department of Pediatrics Kaiser-Permanente, Orange County Outline of Pediatric Diabetes Presentation Types of Pediatric
Heterozygous ABCC8 mutations are a cause of MODY
 Diabetologia (2012) 55:123 127 DOI 10.1007/s00125-011-2319-x SHORT COMMUNICATION Heterozygous ABCC8 mutations are a cause of MODY P. Bowman & S. E. Flanagan & E. L. Edghill & A. Damhuis & M. H. Shepherd
Diabetologia (2012) 55:123 127 DOI 10.1007/s00125-011-2319-x SHORT COMMUNICATION Heterozygous ABCC8 mutations are a cause of MODY P. Bowman & S. E. Flanagan & E. L. Edghill & A. Damhuis & M. H. Shepherd
Complications of diazoxide treatment in
 Archives of Disease in Childhood, 1989, 64, 1496-1500 Complications of diazoxide treatment in neonatal hyperinsulinism Y K ABU-OSBA,* K B MANASRA, AND P M MATHEWt persistent *NeonatologylPerinatology Section,
Archives of Disease in Childhood, 1989, 64, 1496-1500 Complications of diazoxide treatment in neonatal hyperinsulinism Y K ABU-OSBA,* K B MANASRA, AND P M MATHEWt persistent *NeonatologylPerinatology Section,
Neonatal hypoglycemia Sharon Straussman and Lynne L. Levitsky
 Neonatal hypoglycemia Sharon Straussman and Lynne L. Levitsky Pediatric Endocrine Unit, Massachusetts General Hospital, Boston, Massachusetts, USA Correspondence to Lynne L. Levitsky, MD, Chief, Pediatric
Neonatal hypoglycemia Sharon Straussman and Lynne L. Levitsky Pediatric Endocrine Unit, Massachusetts General Hospital, Boston, Massachusetts, USA Correspondence to Lynne L. Levitsky, MD, Chief, Pediatric
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
ENERGY FROM INGESTED NUTREINTS MAY BE USED IMMEDIATELY OR STORED
 QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
Diagnosis and treatment of hyperinsulinaemic hypoglycaemia and its implications for paediatric endocrinology
 Demirbilek et al. International Journal of Pediatric Endocrinology (2017) 2017:9 DOI 10.1186/s13633-017-0048-8 REVIEW Diagnosis and treatment of hyperinsulinaemic hypoglycaemia and its implications for
Demirbilek et al. International Journal of Pediatric Endocrinology (2017) 2017:9 DOI 10.1186/s13633-017-0048-8 REVIEW Diagnosis and treatment of hyperinsulinaemic hypoglycaemia and its implications for
Cordoba 01/02/2008. Slides Professor Pierre LEFEBVRE
 Cordoba 01/02/2008 Slides Professor Pierre LEFEBVRE Clinical Research in Type 2 Diabetes : Current Status and Future Approaches Pierre Lefèbvre* University of Liège Belgium Granada, Spain, February 2008
Cordoba 01/02/2008 Slides Professor Pierre LEFEBVRE Clinical Research in Type 2 Diabetes : Current Status and Future Approaches Pierre Lefèbvre* University of Liège Belgium Granada, Spain, February 2008
Controversies in Neonatal Hypoglycemia PAC / LAC CONFERENCE, JUNE 1 ST 2017
 Controversies in Neonatal Hypoglycemia PRIYA JEGATHEESAN, MD PAC / LAC CONFERENCE, JUNE 1 ST 2017 Disclosure I have no conflicts of interest to disclose Objectives Review Recommendations from different
Controversies in Neonatal Hypoglycemia PRIYA JEGATHEESAN, MD PAC / LAC CONFERENCE, JUNE 1 ST 2017 Disclosure I have no conflicts of interest to disclose Objectives Review Recommendations from different
By: Dr. Doaa Khater Yassin, MM and M.D Paed Sr. specialist of Pediatrics SQUH
 By: Dr. Doaa Khater Yassin, MM and M.D Paed Sr. specialist of Pediatrics SQUH Born SGA with birth weight of 2.4 kg, had IUGR Hospitalized at the age of 2 month with severe dehydration Diagnosed as DKA
By: Dr. Doaa Khater Yassin, MM and M.D Paed Sr. specialist of Pediatrics SQUH Born SGA with birth weight of 2.4 kg, had IUGR Hospitalized at the age of 2 month with severe dehydration Diagnosed as DKA
For more information about how to cite these materials visit
 Author(s): Arno Kumagai, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Arno Kumagai, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
EAT TO LIVE: THE ROLE OF THE PANCREAS. Felicia V. Nowak, M.D., Ph.D. Ohio University COM 22 January, 2008
 EAT TO LIVE: THE ROLE OF THE PANCREAS Felicia V. Nowak, M.D., Ph.D. Ohio University COM 22 January, 2008 THE ROLE OF THE PANCREAS Exocrine pancreas Endocrine pancreas THE ROLE OF THE PANCREAS EXOCRINE
EAT TO LIVE: THE ROLE OF THE PANCREAS Felicia V. Nowak, M.D., Ph.D. Ohio University COM 22 January, 2008 THE ROLE OF THE PANCREAS Exocrine pancreas Endocrine pancreas THE ROLE OF THE PANCREAS EXOCRINE
Inactivating mutations in the genes encoding the
 ORIGINAL ARTICLE GLP-1 Receptor Antagonist Exendin-(9-39) Elevates Fasting Blood Glucose Levels in Congenital Hyperinsulinism Owing to Inactivating Mutations in the ATP-Sensitive K + Channel Andrew C.
ORIGINAL ARTICLE GLP-1 Receptor Antagonist Exendin-(9-39) Elevates Fasting Blood Glucose Levels in Congenital Hyperinsulinism Owing to Inactivating Mutations in the ATP-Sensitive K + Channel Andrew C.
