New-onset diabetes after transplantation: focus on strategies to reduce risk
|
|
|
- Gerard Jenkins
- 5 years ago
- Views:
Transcription
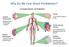
1 New-onset diabetes after transplantation: focus on strategies to reduce risk Adnan Sharif Practice Points New-onset diabetes after transplantation (NODAT) is one of the major medical complications associated with solid-organ transplantation. Risk factors for NODAT are both transplant specific and nonspecific. There are important similarities and differences between NODAT and diabetes mellitus that prevent simple translation of research findings between the two. Appreciation of non-modifiable NODAT risk factors will help devise individualized immunosuppressant regimens that balance the risks of graft rejection and cardio metabolic complications. An understanding of modifiable NODAT risk factors should guide clinical decision-making processes to help reverse, attenuate or delay the onset or progression of NODAT. Summary New-onset diabetes after transplantation (NODAT) is a major and frequent complication post-solid-organ transplantation with significant adverse outcomes associated with its development. Focus amongst transplant clinicians has shifted towards strategies to both predict and prevent the onset of NODAT. Our approach to this problem must incorporate both transplant-specific and nonspecific strategies and appreciate the differences between NODAT and diabetes mellitus with regards to pathophysiology, risk factors, clinical course and management. The complexity of these patients warrants cooperation between clinicians involved within both fields of transplantation and diabetes. This article aims to discuss current strategies to reduce the risk of NODAT and proposes future directions for clinical research. New-onset diabetes after transplantation (NODAT) is a major medical complication associated with solid-organ transplantation, with many adverse clinical outcomes attributed to its development [1 4]. Owing to its considerable prevalence amongst transplant recipients, with up to half of all nondiabetic transplant recipients (range: 2 53%) likely to be diagnosed with NODAT [5], the associated risk of morbidity, mortality, cost and adverse impact on patient quality of life (see Figure 1), attenuating the future risk of developing NODAT has become a clinical priority amongst transplant clinicians. Although there are parallels between such strategies in the transplant recipient and those in the general population, we should hesitate to Department of Nephrology & Transplantation, Renal Institute of Birmingham, Queen Elizabeth Hospital Birmingham, Edgbaston, Birmingham, UK; Tel.: ; Fax: ; sharif_adnan@hotmail.com /DMT Future Medicine Ltd Diabetes Manage. (2011) 1(3), ISSN
2 Sharif Cardiovascular disease Prevalence Death censored Graft failure Overall NODAT Patient inconvenience Increased cost Patient mortality Infectious complications Graft function Figure 1. Why reduce the risk of new-onset diabetes after transplantation? NODAT: New-onset diabetes after transplantation. simply translate strategies from one population to another. NODAT and diabetes mellitus have many similarities but there are also important clinical and pathophysiological differences [2] that make transplant recipients a unique highrisk population (see Table 1). Although some of these individuals would have developed diabetes mellitus regardless of solid-organ transplantation, the transplant event itself provides a trigger and exacerbates underlying risk (e.g., similar to gestational diabetes) that justifies the term new-onset diabetes after transplantation (superseding the previously used term post-transplant diabetes mellitus). Publication of NODAT consensus guidelines in 2003 provided transplant clinicians with clarification regarding screening, diagnosis and management options [6]. Prior to 2003 the diagnosis of NODAT lacked consistency owing to variable diagnostic criteria, center demographics and evolving immunosuppression regimens. The 2003 guidelines provided a consensus amongst transplant clinicians to adopt current American Diabetes Association (ADA) guidelines for the diagnosis of NODAT in line with the diagnosis of diabetes mellitus, and outlined treatment pathways with regards to management. However, in the current climate of new pharmacotherapy and clinical evidence, these guidelines are in need of urgent update with regards to preventative strategies. The purpose of this article is to review the transplantation literature, with the aim of discussing the evidence base behind strategies to reduce the risk of NODAT, and to suggest future directions. The aim is to assist clinicians in their attempts to devise focused and targeted risk-attenuation strategies for the development of NODAT in these high-risk patients. In the first half, the discussion will focus on how to predict the risk of developing NODAT. In the latter half of the article, the discussion will discuss strategies to attenuate or delay the development of NODAT and the evidence base for such therapeutic measures (see Figure 2). Prediction of NODAT Risk factors Risk factors for the development of NODAT, both modifiable and non-modifiable, that are either transplant specific or nonspecific have been the subject of a recent comprehensive review [7] and are shown in Box 1. The importance of documenting these risk factors cannot be overstated. Knowledge of non-modifiable risk factors is important as it will allow individualization of immunosuppression to balance both graft and cardio metabolic outcomes. Modifiable risk factors aid both prediction and prevention of NODAT and will be discussed in the second half of the article under preventative measures. In the context of predicting the risk of NODAT, it would be logical to assume a greater number of risk factors represents a higher likelihood of developing NODAT. In the general population, there are a variety of predictive risk factor models available that have epidemiologically demonstrated the ability to predict for the future risk of Type 2 diabetes mellitus [8]. No similar predictive models exist for a transplantspecific setting and it would be clinically advantageous to devise a specific NODAT predictive model for transplant recipients. Abnormal glucose metabolism Close surveillance of abnormal glycemia, regardless of timing or duration in the context of transplantation, identifies an individual with a heightened risk for the subsequent development of NODAT. Cosio et al. demonstrated an almost linear relationship between increasing levels of pre-transplantation fasting glycemia and subsequent post-transplantation risk of either impaired fasting glucose or NODAT [1]. From a postoperative perspective, Chakkera et al. recently demonstrated a relationship between inpatient hyperglycemia immediately post-transplantation and subsequent risk of developing NODAT [9]. Patients who 272 Diabetes Manage. (2011) 1(3) future science group
3 New-onset diabetes after transplantation: focus on strategies to reduce risk maintained normoglycemia whilst in hospital only had a 4% risk of NODAT at 1-year posttransplantation, in contrast with a 30% risk of NODAT for individuals with inpatient hyperglycemia requiring insulin therapy (patients with noninsulin-requiring hyperglycemia had an intermediate risk of developing NODAT of 18%). The considerable risk associated with insulin-requiring hyperglycemia is important as the authors have previously published work demonstrating that 66% of nondiabetic renal transplant recipients required insulin therapy upon discharge post-transplantation [10], although such percentages of insulin-on-discharge have not been observed from my own personal experience. Therefore the occurrence of hyperglycemia in any recipient post-transplantation, even if short term and self-limiting, should alert the clinician to the high-risk status of that individual for the subsequent development of NODAT. It should be highlighted that even self-limiting hyperglycemia that satisfies a diagnosis of diabetes but resolves should be classed as an episode of NODAT in accordance with the 2003 consensus guidelines, to allow appropriate risk stratification to be implemented to attenuate future NODAT risk. Oral glucose tolerance tests The oral glucose tolerance test (OGTT) should be considered the gold-standard diagnostic test post-transplantation on current evidence and diagnostic criteria are similar to the general population as suggested by the ADA (see Table 2). Its advantage lies in the ability to identify both fasting and postprandial hyperglycemia. Both are associated with disparate risks for development of diabetes and cardiovascular disease in the general population [11 13] due to their distinct pathophysiologies [14], with postprandial hyperglycemia having greater predictive power [11,15,16]. Similar epidemiological data for the predictive power of postprandial glucose is not available in transplant recipients and it remains to be seen whether postprandial hyperglycemia is a stronger risk factor than fasting hyperglycemia for clinical outcomes such as NODAT and cardiovascular disease post-transplantation. The clinical benefit of identifying postprandial hyperglycemia with an OGTT pre-transplantation has been demonstrated by Bergrem and colleagues [17], where a diagnosis of impaired glucose tolerance pretransplantation was associated with a 26% increased risk of developing post-transplantation hyperglycemia. The advantage of an OGTT post-transplantation has been confirmed in a number of publications [18,19], as it can provide greater predictive power than fasting glucose alone by unmasking NODAT with postprandial glucose assessment. Glycated hemoglobin The role of the A1c assay from a screening and risk stratification perspective remains controversial in the general population, with an additional layer of complexity in the context of transplantation. Hoban et al. have previously demonstrated glycated hemoglobin to be superior to fasting glucose as a screening test for NODAT in renal transplant recipients [20]. Sharif and Baboolal have commented on the benefits and caveats of utilizing the A1c assay in the context of transplantation [21]. Notably, the accuracy of the assay will be mitigated in the setting of myelotoxic immuosuppression and post-transplantation anemia. However, Table 1. Comparison of Type 2 diabetes mellitus with new-onset diabetes after transplantation. Comparator Type 2 diabetes mellitus NODAT Diagnosis ADA criteria 2003 Consensus guidelines (incorporating ADA criteria) Pathophysiology Combination of b cell dysfunction in context of insulin resistance Combination of b cell dysfunction in context of insulin resistance (exacerbated by immunosuppression) Risk factors Management Complications General (e.g., age, obesity, family history and ethnicity) Clinical evidence from randomized controlled trials Micro- and macro-vascular complications well documented ADA: American Diabetes Association; NODAT: New-onset diabetes after transplantation. General (but lack of evidence for some traditional risk like family history) Transplant specific No randomized controlled trials available to guide management Unclear if similar degree or severity of complications future science group 273
4 Sharif Awareness of risk factors Modify risk factors Individualize immunosuppression CMV prophylaxis Predictive tools Pleiotropic management Disposition index Surrogate markers Prediction Glycemic status NODAT risk reduction strategy Metabolic syndrome Insulin Dysglycemia resistance OGTT HbA1c Electrolyte correction Prevention Pharmacological prophylaxis Lifestyle modification Figure 2. Strategies to reduce risk of new-onset diabetes after transplantation. CMV: Cytomegalovirus; NODAT: New-onset diabetes after transplantation; OGTT: Oral glucose tolerance test. the benefits are likely to outweigh the limitations and further work is required to validate the use of the assay for screening and diagnosis in a post transplantation setting. Metabolic syndrome The metabolic syndrome is proposed as a cluster of known cardiovascular risk factors, inter-related by a common but speculative pathophysiological defect that symbolizes a heightened metabolic burden. The syndrome is not a disease itself but a marker of metabolic disturbance and a potential risk assessment tool for the development of diabetes and cardiovascular disease. The role of the metabolic syndrome is controversial with regards to NODAT risk stratification. Diagnosing metabolic syndrome in the context of solid-organ transplantation is associated with numerous adverse clinical outcomes and has been the subject of a comprehensive review article [22]. Notably, it is unclear whether there are pathophysiological differences between the metabolic syndrome in the general versus transplant population. There is emerging evidence of the utility of the metabolic syndrome in risk stratifying transplant recipients for future risk of NODAT, whether it is diagnosed pretransplantation [23] or post-transplantation [24]. Whether labeling transplant recipients with the metabolic syndrome has any clinical benefit over and above the presence of its individual components is unclear, but from an epidemiological viewpoint it certainly identifies high-risk patients who may merit further investigation or closer monitoring. Insulin resistance indexes New-onset diabetes after transplantation is characterized by the development of insufficient insulin secretion by the pancreatic b cell to compensate for the concomitant degree of insulin resistance [25 27]. Therefore, the development of insulin resistance is one of the early pathophysiological defects on the spectrum of dysglycemia and easy identification of deteriorating insulin resistance may be clinically advantageous. Gold standard techniques for assessing insulin sensitivity, such as euglycemic clamps or frequently sampled, intravenous glucose tolerance tests, are laborious and expensive academic tools. However, there are numerous surrogates available for estimation of insulin resistance in the context of transplantation, of which McAuley s index (calculated as: exp [ ln (insulin [in microunits per milliliter]) 0.31 ln (triglycerides [in millimoles per liter])) has been validated as one of the strongest 274 Diabetes Manage. (2011) 1(3) future science group
5 New-onset diabetes after transplantation: focus on strategies to reduce risk correlates (correlation r values ranging from ; p < 0.05) [28,29]. Clinical application of these surrogates are lacking and there is no evidence to suggest continuous monitoring of these surrogates predicts for the development of NODAT. Disposition index Although surrogate insulin resistance indexes could be useful as screening tools, screening of this pathophysiological phenomenon may be difficult to interpret in isolation. As previously highlighted, NODAT develops due to b cell dysfunction in the context of insulin resistance. This relationship is quantitatively represented as a mathematical constant (rectangular hyperbola) and qualitatively called the disposition index. In the context of falling insulin sensitivity (increasing insulin resistance), the pancreatic b cell secretes more insulin to compenstate in a reciprocal relationship. Despite these metabolic upheavals, the disposition index will remain constant and the patient remains normoglycemic. Only if the pancreatic b cells fails to adequately compensate for the degree of insulin resistance will the metabolic inter-relationship between insulin secretion and sensitivity fail and the disposition index falls, heralding the onset of hyperglycemia [26,30]. Therefore, as a more integrated representation of glycemic metabolism, surrogate markers for the disposition index itself may be better suited to track the evolution of glycemic abnormalities. In the general population, Utzschneider and colleagues demonstrated a surrogate for the disposition index that predicted for the development of future diabetes mellitus over and above that predicted by postprandial glucose [31]. In the transplant population, Sharif et al. have produced a surrogate formula for the disposition index (DI = Insulin 0 [3.33/(glucose 0 3.5)] exp [2.63 (0.28 ln {insulin 0 /6.945}) (0.31 ln trigycerides 0 )]), calculated in standard international units, which correlates well with the intravenous glucose tole rance test-derived disposition index, is statistically consistent with a mathematical hyperbola and is valid in subgroups of transplant recipients [32]. The advantage of the Sharif index compared with the Utzschneider index is the ability to utilize fasting rather than postprandial blood sampling. There is evidence that a high carbohydrate low glycemic index diet in the general population can modify the disposition index in patients with impaired glucose tolerance [33]. However, clinical application of this experimental surrogate post-transplantation is awaited and it remains to be seen whether serial monitoring of the disposition index is clinically advantageous. Prevention of NODAT Tailored immunosuppression As previously discussed, an awareness of risk factors for NODAT is important for predicting the likelihood of its development [7]. An understanding of non-modifiable risk factors allows individualization of immunosuppressive regimens prior to transplantation, balancing the efficacy of graft survival with minimization of complications. In the current era of Box 1. Risk factors for new-onset diabetes after transplantation. Non-modifiable Age Ethnicity Family history of diabetes mellitus? Cause of end-stage renal failure Gender? HLA mismatch? Genetics Innate immunity Donor characteristics? Education Modifiable Previous stress diabetes Obesity Metabolic syndrome Pre-transplant triglycerides Cytomegalovirus Hepatitis C Immunosuppression Tacrolimus Cyclosporin Sirolimus Corticosteroids Rejection episodes? Antihypertensives b-blockers Thiazide diuretics Biochemical abnormalities Magnesium Uric acid? Glomerular filtration rate? Italics represent transplant-specific risk factors. future science group 275
6 Sharif Table 2. Diagnosis of prediabetes based upon fasting glucose and oral glucose tolerance test (WHO). Glycemic state 0 h glucose (mmol/l) 2 h glucose (mmol/l) Normal <6.1 <7.8 IFG IGT NODAT >6.9 > mmol/l with American Diabetes Association. IFG: Impaired fasting glycemia; IGT: Impaired glucose tolerance; NODAT: New-onset diabetes after transplantation. immunosuppression there exists a variety of regimens providing comparable graft survival that could be appropriate for such patients at high risk of developing NODAT [34]. Examples of strategies with less diabetogenicity currently available include the use of cyclosporin rather than tacrolimus as the calcineurin inhibitor of choice [35], corticosteroid avoidance [36] or corticosteroid-sparing regimens [37]. The task for transplant clinicians is to balance the benefits of less diabetogenic immunosuppression with the potential increased risk of rejection with these strategies. Calcineurin inhibitor-free immunosuppression is one option but has its limitations. Transplant recipients poorly tolerate mtor inhibitors and incidentally these agents are themselves associated with a risk of NODAT [38]. Newer immunosuppressant agents such as belatacept and tasocitinib are on the horizon, and awaiting regulatory approval, and have been shown to be less diabetogenic with equivalent graft survival, albeit at risk of increased allograft rejection [39,40]. Obesity/metabolic syndrome Obesity, either alone or as a constituent of the metabolic syndrome, is one of the most important risk factors for the development of NODAT [23]. Putative evidence links pathophysiological mechanisms such as obesity, inflammation and adipocyte dysfunction as risk factors for NODAT [41]. A focus on obesity is important as it is common post-transplantation and associated with detrimental patient and graft outcomes [42]. However, there is currently no evidence to suggest pharmacologically or surgically targeting obesity post-transplantation has any favorable metabolic effects from a glycemic point of view. With regards to the metabolic syndrome, although it has shown to be a useful risk stratification tool, it remains debateable whether the diagnosis provides any additional therapeutic advantage over its individual components. Controversy remains as to the merit of the metabolic syndrome [43,44] and what value it has as a therapeutic target. Until a definitive underlying pathophysiological mechanism is elucidated, the metabolic syndrome is likely to remain an epidemiological rather than a clinical or therapeutic tool. Virus infection Cytomegalovirus infection Hjelmesaeth and colleagues have demonstrated an independent link between cytomegalovirus (CMV) infection and the development of NODAT, with putative mechanisms including direct virus-induced pancreatic b cell damage [45]. This raises the possibility of prophylactic agents to prevent CMV infection also indirectly attenuating the risk of developing NODAT. Current transplantation practice is to administer 100 days of antiviral prophylaxis (e.g., oral valganciclovir) to patients at high risk for CMV (usually donor CMV positive and recipient CMV negative). The recent Improved Protection Against Cytomegalovirus in Transplant (IMPACT) study explored the benefits of utilizing a 200 day approach compared with 100 days in renal transplant recipients at high risk for NODAT [46]. Although there were advantages with regards to a reduced incidence of CMV with the prolonged 200 day prophylaxis, there was no significant difference in the secondary end point of incidence of NODAT (although the study was not adequately powered for this ana lysis). It should, however, be noted that not all groups have shown a link between CMV and NODAT and any putative link between the two remains pathophysiologically speculative [47]. Hepatitis C Studies have shown that recipients with hepatitis C have a greater incidence of NODAT [48 50], although others have shown no statistically significant association and merely a trend [51]. Bloom et al. retrospectively performed multivariate logistic regression on 427 renal transplant recipients and identified hepatitis C as an independent risk factor, although a significant interaction existed between hepatitis C status and tacrolimus use [52]. The mechanism by which hepatitis C may cause NODAT is speculative but possible mechanisms suggested include impaired insulin action, defects in glucose 276 Diabetes Manage. (2011) 1(3) future science group
7 New-onset diabetes after transplantation: focus on strategies to reduce risk homeostasis secondary to liver disease or insulin resistance [52], with the latter emerging as the strongest causative factor [53]. This raises the possibility of antiviral treatment of hepatitis C attenuating the risk or progression of NODAT, although such evidence is lacking. Correction of biochemical abnormalities Biochemical abnormalities are common posttransplantation and likely secondary to both immunosuppression and tubular dysfunction (in the context of kidney transplantation). Van Laecke et al. demonstrated the detrimental effect of post-transplant hypomagnesemia on glucose metabolism in a retrospective singlecenter ana lysis of 254 renal transplant recipients [54]. Although this would suggest magnesium replacement may attenuate abnormal glucose metabolism, the authors paradoxically found the use of magnesium supplements to be associated with a risk of NODAT on a univariate ana lysis. Apart from hypomagnesemia, other common post-transplant biochemical abnormalities that may be associated with transplant-associated hyperglycemia include hyperuricemia and vitamin D deficiency [55]. Whether correction of any of these factors will attenuate abnormal glucose metabolism post transplantation is unknown. Antihypertensive therapy The differing diabetogenicity of hypertensive agents is well documented in the general population, with b blockers in particular noted for significant diabetogenic effects [56]. In the transplant population, Hjelmesaeth et al. observed detrimental effects of b blockers and thiazide diuretics on glucose metabolism, although this proved nonsignificant in a multivariate ana lysis [57]. The pathophysiological effect of b blockers on glucose metabolism post-transplantation may result from adipocyte dysfunction [58]. The choice of antihypertensive agents post-transplantation should be based on benefit on an individual basis but should acknowledge the possible diabetogenic risk attached to each agent in the context of pre-existing diabetic risk. Lifestyle modification Lifestyle modification has been shown to delay the onset of diabetes in nontransplant populations with abnormal glucose metabolism [59 62]. In a transplantation setting, Sharif et al. have demonstrated the successful use of aggressive lifestyle modifications [63]. Renal transplant recipients with abnormal postprandial glucose metabolism on an OGTT (impaired glucose tolerance and NODAT, n = 36) were selected to have aggressive lifestyle modifications (dietician referral, graded exercise program and weight loss advice), whilst renal transplant recipients with normal postprandial glucose metabolism (normal and impaired fasting glucose, n = 79) received leaflets advocating healthy lifestyle modifications alone. The dietary meal framework was derived from Diabetes UK advice [101] and consisted of 50% carbohydrate, 25% protein (meat, fish and beans) and 25% fiber (fruit and vegetables). A graded exercise program was commenced with the aim of maintaining 2 h of endurance exercise (e.g., walking, jogging or swimming) per week. Dieticians monitored all dietary and exercise diaries with reinforcement of lifestyle modification advice. The intensive regimen resulted in a statistically significant reduction in postprandial glucose levels (10.2 mmol/l to 8.7 mmol/l, D = -15%, p = 0.012) and improved reclassification of glycemic status on re-evaluation by OGTT 6 months later. By contrast, simple lifestyle modification advice by leaflets alone in the group with normal glucose tolerance (n = 79) resulted in a significant deterioration of postprandial glucose levels (5.9 mmol/l to 6.6 mmol/l, D = +12%, p = 0.001) and worse glycemic status reclassification on follow-up OGTT. Pharmacological prophylaxis for high risk patients Unlike in the general population [64 66], there is no evidence in the transplant population that the use of glucose-lowering agents as prophylaxis in patients deemed to be high risk for the development of NODAT or cardiovascular disease is beneficial. Randomized controlled trials targeting nondiabetic transplant recipients should be actively encouraged. In the context of overlapping metabolic disorders with shared pathophysiological mechanisms, it could be hypothesized that antiobesity or lipid-lowering agents may be beneficial owing to putative indirect effects on glucose metabolism, so-called pleiotropic effects. Statins for pleiotropic benefits Prasad et al. putatively suggested the link between the use of 3 hydroxy-3 methylglutarylcoenzyme A reductase inhibitors (statins) and a future science group 277
8 Sharif reduced incidence of NODAT in a retrospective ana lysis of 314 renal transplant recipients [67]. Based on this hypothesis, Sharif et al. conducted a randomized controlled, double-blind, placebocontrolled crossover study comparing the effects of rosuvastatin 10 mg once daily and placebo in 20 nondiabetic renal transplant recipients with an indication for statin treatment [68]. Physiological parameters of glucose metabolism were assessed with the use of a frequently sampled, intravenous, glucose tolerance test and a meal tolerance test at the end of a 12 week crossover in each arm. Despite being an effective lipid-lowering agent and with clinically but not statistically significant anti-inflammatory action, the study demonstrated no significant influence of shortterm rosuvastatin treatment on any physiological parameters of pancreatic b cell function and insulin sensitivity. It could be argued that the pleiotropic effects of statin treatment only manifest after long-term administration, but in the absence of any clear evidence this hypothesis remains pure speculation. Conclusion This article highlights our current understanding on the strategies available for predicting and preventing the development of NODAT. In view of the significant advances made in both our knowledge base and available pharmacological armamentarium, it provides a clinical update to outdated NODAT guidelines. Although there remains a lack of randomized controlled trials, clinicians are in a better position today to make informed decisions regarding the prevention, attenuation and management of transplantassociated hyperglycemia in a clinical setting. We hope the summary provided here not only guides risk reduction of NODAT, but inspires further research and clinical trials into preventative strategies focussing specifically on solid-organ transplant recipients. New-onset diabetes after transplantation is a major complication of solid-organ transplantation with associated morbidity, mortality and financial cost. Appropriate risk stratification should lead to adequate strategies to attenuate the risk of the development of NODAT this requires close attention to risk factors for NODAT on an individual basis. Attention must be given to targeted research on the pathophysiology, progression and management of NODAT as simple translation of clinical data from the general population may not be appropriate. With patient expectations of a successful allograft heightened in the current era, focusing on attenuating the adverse complications of solid-organ transplantation, such as NODAT, will dominate the direction of transplantation medicine in the years to come. Future perspective Interest in this area is likely to direct attention to strategies attenuating the development of NODAT and focusing on how to predict and prevent NODAT. With regards to attenuating abnormal glycemic metabolism, it is clear that NODAT has many similarities but also important differences with diabetes mellitus and that simple translation of research from the general to transplant population should be avoided. Focused and targeted clinical trials are specifically required in this high-risk population to help guide strategies to both predict and prevent development of NODAT, including prophylaxis for high-risk recipients and targeting of obesity and the metabolic syndrome. Collaborations between transplant clinicans and diabetologists should therefore be encouraged to ensure transplant recipients receive optimum care for transplant-associated hyperglycemia. Evolving research domains such as utilizing genomics and genetic polymorphisms to identify high-risk population groups are likely to add to the knowledge base of NODAT risk stratification and will help shed light on some of the pathophysiological mysteries associated with the disease. Transplant-specific randomized controlled trials are required to assess the potential for pharmacological prophylaxis to prevent the onset of NODAT in high-risk groups. Some agents such as metformin may be suitably attractive for their weight neutral properties, but close attention would need to be given to potential side effects. With the number of transplant recipients on the increase, future projects should be planned for by clinicians today. Financial & competing interests disclosure The author has no relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript. This includes employment, consultancies, honoraria, stock ownership or options, expert t estimony, grants or patents received or pending, or royalties. No writing assistance was utilized in the production of this manuscript. 278 Diabetes Manage. (2011) 1(3) future science group
9 New-onset diabetes after transplantation: focus on strategies to reduce risk Bibliography 1 Cosio FG, Kudva Y, Velde MVD et al.: New onset hyperglycemia and diabetes are associated with increased cardiovascular risk after kidney transplantation. Kidney Int. 67, (2005). 2 Crutchlow MF, Bloom RD: Transplantassociated hyperglycemia: a new look at an old problem. Clin. J. Am. Soc. Nephrol. 2, (2007). 3 Moore R, Ravindran V, Baboolal K: The burden of new-onset diabetes mellitus after transplantation. Clin. Transplant. 20(6), (2006). 4 Bodziak KA, Hricik DE: New-onset diabetes mellitus after solid organ transplantation. Transpl. Int. 22(5), (2009). 5 Davidson JA, Wilkinson A: New-Onset Diabetes after Transplantation 2003 International Consensus Guidelines: an endocrinologist s view. Diabetes Care 27(3), (2004). 6 Davidson J, Wilkinson A, Dantal J et al.: New-onset diabetes after transplantation: 2003 International consensus guidelines. Proceedings of an international expert panel meeting. Barcelona, Spain, 19 February Transplantation 75(Suppl. 10), SS3 S24 (2003). 7 Sharif A, Baboolal K: Risk factors for new-onset diabetes after kidney transplantation. Nat. Rev. Nephrol. 6(7), (2010). 8 Schwarz PE, Li J, Lindstrom J, Tuomilehto J: Tools for predicting the risk of Type 2 diabetes in daily practice. Horm. Metab. Res. 41(2), (2009). 9 Chakkera HA, Knowler WC, Devarapalli Y et al.: Relationship between inpatient hyperglycemia and insulin treatment after kidney transplantation and future new onset diabetes mellitus. Clin. J. Am. Soc. Nephrol. 5(9), (2010). 10 Chakkera HA, Weil EJ, Castro J et al.: Hyperglycemia during the immediate period after kidney transplantation. Clin. J. Am. Soc. Nephrol. 4(4), (2009). 11 Davies MJ, Raymond NT, Day JL, Hales CN, Burden AC: Impaired glucose tolerance and fasting hyperglycaemia have different characteristics. Diabet. Med. 17(6), (2000). 12 Unwin N, Shaw J, Zimmet P, Alberti KG: Impaired glucose tolerance and impaired fasting glycaemia: the current status on definition and intervention. Diabet. Med. 19(9), (2002). 13 Tominaga M, Eguchi H, Manaka H, Igarashi K, Kato T, Sekikawa A: Impaired glucose tolerance is a risk factor for cardiovascular disease, but not impaired fasting glucose. The Funagata Diabetes Study. Diabetes Care 22(6), (1999). 14 Meyer C, Pimenta W, Woerle HJ et al.: Different mechanisms for impaired fasting glucose and impaired postprandial glucose tolerance in humans. Diabetes Care 29(8), (2006). 15 Santaguida PL, Balion C, Hunt D et al.: Diagnosis, prognosis, and treatment of impaired glucose tolerance and impaired fasting glucose. Evid. Rep. Technol. Assess. (Summ.) 128, 1 11 (2005). 16 Zhang YF, Hong J, Zhan WW et al.: Hyperglycaemia after glucose loading is a major predictor of preclinical atherosclerosis in nondiabetic subjects. Clin. Endocrinol. (Oxf.) 64(2), (2006). 17 Bergrem HA, Valderhaug TG, Hartmann A, Bergrem H, Hjelmesaeth J, Jenssen T: Glucose tolerance before and after renal transplantation. Nephrol. Dial. Transplant. 25(3), (2010). 18 Sharif A, Moore RH, Baboolal K: The use of oral glucose tolerance tests to risk stratify for new-onset diabetes after transplantation: an underdiagnosed phenomenon. Transplantation 82(12), (2006). 19 Armstrong KA, Prins JB, Beller EM et al.: Should an oral glucose tolerance test be performed routinely in all renal transplant recipients? Clin. J. Am. Soc. Nephrol. 1, (2006). 20 Hoban R, Gielda B, Temkit M et al.: Utility of HbA1c in the detection of subclinical post renal transplant diabetes. Transplantation 81(3), (2006). 21 Sharif A, Baboolal K: Diagnostic application of the A(1c) assay in renal disease. J. Am. Soc. Nephrol. 21(3), (2010). 22 Sharif A: Metabolic syndrome and solid-organ transplantation. Am. J. Transplant. 10(1), (2010). 23 Bayer ND, Cochetti PT, Anil Kumar MS et al.: Association of metabolic syndrome with development of new-onset diabetes after transplantation. Transplantation 90(8), (2010). 24 Porrini E, Delgado P, Bigo C et al.: Impact of metabolic syndrome on graft function and survival after cadaveric renal transplantation. Am. J. Kidney Dis. 48(1), (2006). 25 Nam JH, Mun JI, Kim SI et al.: b-cell dysfunction rather than insulin resistance is the main contributing factor for the development of postrenal transplantation diabetes mellitus. Transplantation 71(10), (2001). 26 Pacini G: The hyperbolic equilibrium between insulin sensitivity and secretion. Nutr. Metab. Cardiovasc. Dis. 16(Suppl. 1), S22 S27 (2006). 27 Hjelmesaeth J, Hagen M, Hartmann A, Midtvedt K, Egeland T, Jenssen T: The impact of impaired insulin release and insulin resistance on glucose intolerance after renal transplantation. Clin. Transplant. 16(6), (2002). 28 Sharif A, Ravindran V, Moore RH et al.: Insulin resistance indexes in renal transplant recipients maintained on tacrolimus immunosuppression. Transplantation 89(3), (2010). 29 Oterdoom LH, de Vries AP, van Son WJ et al.: Validation of insulin resistance indexes in a stable renal transplant population. Diabetes Care 28(10), (2005). 30 Ekstrand AV, Eriksson JG, Gronhagen-Riska C, Ahonen PJ, Groop LC: Insulin resistance and insulin deficiency in the pathogenesis of posttransplantation diabetes in man. Transplantation 53(3), (1992). 31 Utzschneider KM, Prigeon RL, Faulenbach MV et al.: Oral disposition index predicts the development of future diabetes above and beyond fasting and 2 h glucose levels. Diabetes Care 32(2), (2009). 32 Sharif A, Ravindran VK, Dunseath G, Luzio SD, Owens DR, Baboolal K: Impending hyperglycemia in normoglycemic renal transplant recipients an experimental predictive surrogate. Transplantation 89(11), (2010). 33 Wolever TM, Mehling C: Highcarbohydrate-low-glycaemic index dietary advice improves glucose disposition index in subjects with impaired glucose tolerance. Br. J. Nutr. 87(5), (2002). 34 Chadban S: New-onset diabetes after transplantation should it be a factor in choosing an immunosuppressant regimen for kidney transplant recipients. Nephrol. Dial. Transplant. 23(6), (2008). 35 Vincenti F, Friman S, Scheuermann E et al.: Results of an international, randomized trial comparing glucose metabolism disorders and outcome with cyclosporine versus tacrolimus. Am. J. Transplant. 7(6), (2007). future science group 279
10 Sharif 36 Woodle ES, First MR, Pirsch J, Shihab F, Gaber AO, Van Veldhuisen P: A prospective, randomized, double-blind, placebocontrolled multicenter trial comparing early (7 day) corticosteroid cessation versus long-term, low-dose corticosteroid therapy. Ann. Surg. 248(4), (2008). 37 Knight SR, Morris PJ: Steroid avoidance or withdrawal after renal transplantation increases the risk of acute rejection but decreases cardiovascular risk. A meta-analysis. Transplantation 89(1), 1 14 (2010). 38 Johnston O, Rose CL, Webster AC, Gill JS: Sirolimus is associated with new-onset diabetes in kidney transplant recipients. J. Am. Soc. Nephrol. 19(7), (2008). 39 Vincenti F, Charpentier B, Vanrenterghem Y et al.: A Phase III study of Belatacept-based Immunosuppression Regimens versus Cyclosporine in Renal Transplant Recipients (BENEFIT study). Am. J. Transplant. 10(3), (2010). 40 Busque S, Leventhal J, Brennan DC et al.: Calcineurin-inhibitor-free immunosuppression based on the JAK inhibitor CP 690,550: a pilot study in de novo kidney allograft recipients. Am. J. Transplant. 9(8), (2009). 41 Bayes B, Granada ML, Pastor MC et al.: Obesity, adiponectin and inflammation as predictors of new-onset diabetes mellitus after kidney transplantation. Am. J. Transplant. 7(2), (2007). 42 Potluri K, Hou S: Obesity in kidney transplant recipients and candidates. Am. J. Kidney Dis. 56(1), (2010). 43 Alberti KG, Zimmet PZ: Should we dump the metabolic syndrome? No. BMJ 336(7645), 641 (2008). 44 Gale EA: Should we dump the metabolic syndrome? Yes. BMJ 336(7645), 640 (2008). 45 Hjelmesaeth J, Sagedal S, Hartmann A et al.: Asymptomatic cytomegalovirus infection is associated with increased risk of new-onset diabetes mellitus and impaired insulin release after renal transplantation. Diabetologia 47(9), (2004). 46 Humar A, Lebranchu Y, Vincenti F et al.: The efficacy and safety of 200 days valganciclovir cytomegalovirus prophylaxis in high-risk kidney transplant recipients. Am. J. Transplant. 10(5), (2010). 47 Gourishankar S, Jhangri GS, Tonelli M, Wales LH, Cockfield SM: Development of diabetes mellitus following kidney transplantation: a Canadian experience. Am. J. Transplant. 4(11), (2004). 48 Soule JL, Olyaei AJ, Boslaugh TA et al.: Hepatitis C infection increases the risk of new-onset diabetes after transplantation in liver allograft recipients. Am. J. Surg. 189(5), ; discussion 557 (2005). 49 Finni PE, Souza ER, Rioja S et al.: Is hepatitis C a risk factor to posttransplant diabetes mellitus after renal transplantation in patients using tacrolimus? Transplant. Proc. 36(4), (2004). 50 Fabrizi F, Messa P, Martin P, Takkouche B: Hepatitis C virus infection and post-transplant diabetes mellitus among renal transplant patients: a meta-ana lysis. Int. J. Artif. Organs 31(8), (2008). 51 Sens YA, Silva VD, Malafronte P, Souza JF, Miorin LA, Jabur P: Posttransplant diabetes mellitus in renal transplant patients with hepatitis C virus. Transplant. Proc. 36(4), (2004). 52 Bloom RD, Rao V, Weng F, Grossman RA, Cohen D, Mange KC: Association of hepatitis C with posttransplant diabetes in renal transplant patients on tacrolimus. J. Am. Soc. Nephrol. 13(5), (2002). 53 Baid-Agrawal S, Frei U, Reinke P et al.: Impaired insulin sensitivity as an underlying mechanism linking hepatitis C and posttransplant diabetes mellitus in kidney recipients. Am. J. Transplant. 9(12), (2009). 54 Van Laecke S, Van Biesen W, Verbeke F, De Bacquer D, Peeters P, Vanholder R: Posttransplantation hypomagnesemia and its relation with immunosuppression as predictors of new-onset diabetes after transplantation. Am. J. Transplant. 9(9), (2009). 55 Sharif A: Predictors of new-onset diabetes after transplantation: the overlooked confounders. Am. J. Transplant. 9, 2858 (2009). 56 Gress TW, Nieto FJ, Shahar E, Wofford MR, Brancati FL: Hypertension and antihypertensive therapy as risk factors for Type 2 diabetes mellitus. Atherosclerosis Risk in Communities Study. N. Engl. J. Med. 342(13), (2000). 57 Hjelmesaeth J, Midtvedt K, Jenssen T, Hartmann A: Insulin resistance after renal transplantation: impact of immunosuppressive and antihypertensive therapy. Diabetes Care 24(12), (2001). 58 Hjelmesaeth J, Flyvbjerg A, Jenssen T et al.: Hypoadiponectinemia is associated with insulin resistance and glucose intolerance after renal transplantation: impact of immunosuppressive and antihypertensive drug therapy. Clin. J. Am. Soc. Nephrol. 1(3), (2006). 59 Uusitupa M: Lifestyles matter in the prevention of Type 2 diabetes. Diabetes Care 25(9), (2002). 60 Lindstrom J, Eriksson JG, Valle TT et al.: Prevention of diabetes mellitus in subjects with impaired glucose tolerance in the Finnish Diabetes Prevention Study: results from a randomized clinical trial. J. Am. Soc. Nephrol. 14(7 Suppl. 2), S108 S113 (2003). 61 Tuomilehto J, Lindstrom J, Eriksson JG et al.: Prevention of Type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N. Engl. J. Med. 344(18), (2001). 62 Pan XR, Li GW, Hu YH et al.: Effects of diet and exercise in preventing NIDDM in people with impaired glucose tolerance. The Da Qing IGT and Diabetes Study. Diabetes Care 20(4), (1997). 63 Sharif A, Moore R, Baboolal K: Influence of lifestyle modification in renal transplant recipients with postprandial hyperglycemia. Transplantation 85(3), (2008). 64 Chiasson JL, Josse RG, Gomis R, Hanefeld M, Karasik A, Laakso M: Acarbose treatment and the risk of cardiovascular disease and hypertension in patients with impaired glucose tolerance: the STOP-NIDDM trial. JAMA 290(4), (2003). 65 Knowler WC, Barrett-Connor E, Fowler SE et al.: Reduction in the incidence of Type 2 diabetes with lifestyle intervention or metformin. N. Engl. J. Med. 346(6), (2002). 66 Gerstein HC, Yusuf S, Bosch J et al.: Effect of rosiglitazone on the frequency of diabetes in patients with impaired glucose tolerance or impaired fasting glucose: a randomised controlled trial. Lancet 368(9541), (2006). 67 Prasad GV, Kim SJ, Huang M et al.: Reduced incidence of new-onset diabetes mellitus after renal transplantation with 3 hydroxy-3 methylglutaryl-coenzyme a reductase inhibitors (statins). Am. J. Transplant. 4(11), (2004). 68 Sharif A, Ravindran V, Moore R et al.: The effect of rosuvastatin on insulin sensitivity and pancreatic b cell function in nondiabetic renal transplant recipients. Am. J. Transplant. 9(6), (2009). Website 101 Diabetes UK: Eating well Food and diabetes (2006) Food_and_recipes 280 Diabetes Manage. (2011) 1(3) future science group
New-onset diabetes after transplantation. Christophe Legendre Université Paris Descartes & Hôpital Necker, Paris.
 New-onset diabetes after transplantation Christophe Legendre Université Paris Descartes & Hôpital Necker, Paris. Actualités Jean Hamburger Paris, 23-24 avril 2012 NODAT IFG IGT CJ Yates et al, Am J Transplant
New-onset diabetes after transplantation Christophe Legendre Université Paris Descartes & Hôpital Necker, Paris. Actualités Jean Hamburger Paris, 23-24 avril 2012 NODAT IFG IGT CJ Yates et al, Am J Transplant
Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study
 Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study Laura F. DeFina, MD,* Gloria Lena Vega, PhD,Þ David Leonard, PhD,Þ and Scott M. Grundy,
Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study Laura F. DeFina, MD,* Gloria Lena Vega, PhD,Þ David Leonard, PhD,Þ and Scott M. Grundy,
Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis
 CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance
 CLINICAL PRACTICE Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance John MF. Adam*, Daniel Josten** ABSTRACT The American Diabetes Association has strongly recommended that fasting
CLINICAL PRACTICE Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance John MF. Adam*, Daniel Josten** ABSTRACT The American Diabetes Association has strongly recommended that fasting
Waist Circumference as an Independent Risk Factor for NODAT
 ORIGINAL PAPER ISSN 1425-9524 DOI: 10.12659/AOT.892067 Received: 2014.07.23 Accepted: 2014.10.21 Published: 2015.03.20 Waist Circumference as an Independent Risk Factor for Authors Contribution: Study
ORIGINAL PAPER ISSN 1425-9524 DOI: 10.12659/AOT.892067 Received: 2014.07.23 Accepted: 2014.10.21 Published: 2015.03.20 Waist Circumference as an Independent Risk Factor for Authors Contribution: Study
Diabetes: Staying Two Steps Ahead. The prevalence of diabetes is increasing. What causes Type 2 diabetes?
 Focus on CME at the University of University Manitoba of Manitoba : Staying Two Steps Ahead By Shagufta Khan, MD; and Liam J. Murphy, MD The prevalence of diabetes is increasing worldwide and will double
Focus on CME at the University of University Manitoba of Manitoba : Staying Two Steps Ahead By Shagufta Khan, MD; and Liam J. Murphy, MD The prevalence of diabetes is increasing worldwide and will double
Pretransplant Risk Score for New-Onset Diabetes After Kidney Transplantation
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Pretransplant Risk Score for New-Onset Diabetes After Kidney Transplantation HARINI A. CHAKKERA, MD, MPH 1 E. JENNIFER
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Pretransplant Risk Score for New-Onset Diabetes After Kidney Transplantation HARINI A. CHAKKERA, MD, MPH 1 E. JENNIFER
Validation of diagnostic utility of fasting plasma glucose and HbA1c in stable renal transplant recipients one year after transplantation
 Ussif et al. BMC Nephrology (2019) 20:12 https://doi.org/10.1186/s12882-018-1171-3 RESEARCH ARTICLE Open Access Validation of diagnostic utility of fasting plasma glucose and HbA1c in stable renal transplant
Ussif et al. BMC Nephrology (2019) 20:12 https://doi.org/10.1186/s12882-018-1171-3 RESEARCH ARTICLE Open Access Validation of diagnostic utility of fasting plasma glucose and HbA1c in stable renal transplant
Post-challenge hyperglycaemia is associated with premature death and macrovascular complications
 Diabetologia (2003) 46[Suppl1]:M17 M21 DOI 10.1007/s00125-002-0932-4 Post-challenge hyperglycaemia is associated with premature death and macrovascular complications Q. Qiao 1, 2, J. Tuomilehto 2, 3, K.
Diabetologia (2003) 46[Suppl1]:M17 M21 DOI 10.1007/s00125-002-0932-4 Post-challenge hyperglycaemia is associated with premature death and macrovascular complications Q. Qiao 1, 2, J. Tuomilehto 2, 3, K.
Impaired Glucose Tolerance
 Page 1 of 6 Impaired Glucose Tolerance If you have impaired glucose tolerance, your blood glucose is raised beyond the normal range but it is not so high that you have diabetes. However, if you have impaired
Page 1 of 6 Impaired Glucose Tolerance If you have impaired glucose tolerance, your blood glucose is raised beyond the normal range but it is not so high that you have diabetes. However, if you have impaired
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
OUT OF DATE. Choice of calcineurin inhibitors in adult renal transplantation: Effects on transplant outcomes
 nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
Early diagnosis, early treatment and the new diagnostic criteria of diabetes mellitus
 British Journal of Nutrition (2000), 84, Suppl. 2, S177±S181 S177 Early diagnosis, early treatment and the new diagnostic criteria of diabetes mellitus Takeshi Kuzuya* JA Shioya General Hospital, Tomita
British Journal of Nutrition (2000), 84, Suppl. 2, S177±S181 S177 Early diagnosis, early treatment and the new diagnostic criteria of diabetes mellitus Takeshi Kuzuya* JA Shioya General Hospital, Tomita
Laboratory analysis of the obese child recommendations and discussion. MacKenzi Hillard May 4, 2011
 Laboratory analysis of the obese child recommendations and discussion MacKenzi Hillard May 4, 2011 aka: What to do with Fasting Labs The Obesity Epidemic The prevalence of obesity in adolescents has tripled
Laboratory analysis of the obese child recommendations and discussion MacKenzi Hillard May 4, 2011 aka: What to do with Fasting Labs The Obesity Epidemic The prevalence of obesity in adolescents has tripled
Solid organ transplantation is currently an important
 REVIEW Post-Transplant Diabetes Mellitus: Causes, Treatment, and Impact on Outcomes Vijay Shivaswamy, Brian Boerner, and Jennifer Larsen Division of Diabetes, Endocrinology, and Metabolism (V.S., B.B.,
REVIEW Post-Transplant Diabetes Mellitus: Causes, Treatment, and Impact on Outcomes Vijay Shivaswamy, Brian Boerner, and Jennifer Larsen Division of Diabetes, Endocrinology, and Metabolism (V.S., B.B.,
Copyright 2017 by Sea Courses Inc.
 Pre-Diabetes: Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic, or mechanical,
Pre-Diabetes: Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic, or mechanical,
Discussion points. The cardiometabolic connection. Cardiometabolic Risk Management in the Primary Care Setting
 Session #5 Cardiometabolic Risk Management in the Primary Care Setting Sonja Reichert, MD MSc FCFP FACPM Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE S Discussion points Whom should we be
Session #5 Cardiometabolic Risk Management in the Primary Care Setting Sonja Reichert, MD MSc FCFP FACPM Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE S Discussion points Whom should we be
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care
 Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
WILL YOU USE HBA1C TO SCREEN & MONITOR DIABETES? Dr. Amany Mousa
 WILL YOU USE HBA1C TO SCREEN & MONITOR DIABETES? Dr. Amany Mousa Diabetes is clinically well defined by glycation of proteins 1. True 2. false So far, diabetes has been defined as a clinical condition
WILL YOU USE HBA1C TO SCREEN & MONITOR DIABETES? Dr. Amany Mousa Diabetes is clinically well defined by glycation of proteins 1. True 2. false So far, diabetes has been defined as a clinical condition
What is the Best Induction Immunosuppression Regimen in Kidney Transplantation? Richard Borrows: Queen Elizabeth Hospital Birmingham
 What is the Best Induction Immunosuppression Regimen in Kidney Transplantation? Richard Borrows: Queen Elizabeth Hospital Birmingham SYMPHONY Study Ekberg et al. NEJM 2008 Excluded: DCD kidneys; CIT>30hours;
What is the Best Induction Immunosuppression Regimen in Kidney Transplantation? Richard Borrows: Queen Elizabeth Hospital Birmingham SYMPHONY Study Ekberg et al. NEJM 2008 Excluded: DCD kidneys; CIT>30hours;
Reducing cardiovascular risk factors in patients with prediabetes
 REVIEW Reducing cardiovascular risk factors in patients with prediabetes Jean-Louis Chiasson 1 & Sophie Bernard 1 Practice Points The prevalence of prediabetes is high and on the rise. Subjects with impaired
REVIEW Reducing cardiovascular risk factors in patients with prediabetes Jean-Louis Chiasson 1 & Sophie Bernard 1 Practice Points The prevalence of prediabetes is high and on the rise. Subjects with impaired
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION Diagnostic and Therapeutic Implications of Relationships Between Fasting, 2-Hour Postchallenge Plasma Glucose and Hemoglobin A 1c Values Hans J. Woerle, MD; Walkyria P. Pimenta,
ORIGINAL INVESTIGATION Diagnostic and Therapeutic Implications of Relationships Between Fasting, 2-Hour Postchallenge Plasma Glucose and Hemoglobin A 1c Values Hans J. Woerle, MD; Walkyria P. Pimenta,
Reduced graft function (with or without dialysis) vs immediate graft function a comparison of long-term renal allograft survival
 Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting glucose: The Rancho Bernardo Study
 Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
T he prevalence of type 2 diabetes
 Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Two-Step Approach for the Prediction of Future Type 2 Diabetes Risk MUHAMMAD A. ABDUL-GHANI, MD, PHD 1 TAMAM ABDUL-GHANI, MSC 1 MICHAEL P.
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Two-Step Approach for the Prediction of Future Type 2 Diabetes Risk MUHAMMAD A. ABDUL-GHANI, MD, PHD 1 TAMAM ABDUL-GHANI, MSC 1 MICHAEL P.
New-onset diabetes after transplantation: focus on treatment strategies
 New-onset diabetes after transplantation: focus on treatment strategies Practice Points Anna Marino1, Aysha Inankur1 & Lisa Tannock 1,2 Screening for diabetes, cardiovascular risk factors and metabolic
New-onset diabetes after transplantation: focus on treatment strategies Practice Points Anna Marino1, Aysha Inankur1 & Lisa Tannock 1,2 Screening for diabetes, cardiovascular risk factors and metabolic
Metabolic Syndrome. Shon Meek MD, PhD Mayo Clinic Florida Endocrinology
 Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
The role of glycated hemoglobin in the screening and diagnosis of renal posttransplantation diabetes
 Federal University of Rio Grande do Sul Graduate Program in Endocrinology Brazil The role of glycated hemoglobin in the screening and diagnosis of renal posttransplantation diabetes Ana Laura Pimentel
Federal University of Rio Grande do Sul Graduate Program in Endocrinology Brazil The role of glycated hemoglobin in the screening and diagnosis of renal posttransplantation diabetes Ana Laura Pimentel
Optimizing Postpartum Maternal Health to Prevent Chronic Diseases
 Optimizing Postpartum Maternal Health to Prevent Chronic Diseases Amy Loden, MD, FACP, NCMP Disclosures Research: None Financial: none applicable to this presentation PRIUM QEssentials Market Research
Optimizing Postpartum Maternal Health to Prevent Chronic Diseases Amy Loden, MD, FACP, NCMP Disclosures Research: None Financial: none applicable to this presentation PRIUM QEssentials Market Research
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy
 Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
Emerging Drug List EVEROLIMUS
 Generic (Trade Name): Manufacturer: Everolimus (Certican ) Novartis Pharmaceuticals NO. 57 MAY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence: For use with cyclosporine
Generic (Trade Name): Manufacturer: Everolimus (Certican ) Novartis Pharmaceuticals NO. 57 MAY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence: For use with cyclosporine
Management of Diabetes After Solid Organ Transplantation
 Management of Diabetes After Solid Organ Transplantation Aidar R. Gosmanov, MD, PhD, FACE Chief, Endocrinology Section Stratton VAMC, Albany, NY Associate Professor of Medicine Division of Endocrinology,
Management of Diabetes After Solid Organ Transplantation Aidar R. Gosmanov, MD, PhD, FACE Chief, Endocrinology Section Stratton VAMC, Albany, NY Associate Professor of Medicine Division of Endocrinology,
Obesity Management in Patients with Diabetes Jamy D. Ard, MD Sunday, February 11, :15 a.m. 11:00 a.m.
 Obesity Management in Patients with Diabetes Jamy D. Ard, MD Sunday, February 11, 2018 10:15 a.m. 11:00 a.m. Type 2 diabetes mellitus (T2DM) is closely associated with obesity, primarily through the link
Obesity Management in Patients with Diabetes Jamy D. Ard, MD Sunday, February 11, 2018 10:15 a.m. 11:00 a.m. Type 2 diabetes mellitus (T2DM) is closely associated with obesity, primarily through the link
Andrew Cohen, MD and Neil S. Skolnik, MD INTRODUCTION
 2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
De novo posttransplant diabetes mellitus (PTDM) occurs
 CLINICAL TRAPLANTATION Home Glucometer Monitoring Markedly Improves Diagnosis of Post Renal Transplant Diabetes Mellitus in Renal Transplant Recipients Amish Shah, 1 Gwen Kendall, 1 Richard A. Demme, 1
CLINICAL TRAPLANTATION Home Glucometer Monitoring Markedly Improves Diagnosis of Post Renal Transplant Diabetes Mellitus in Renal Transplant Recipients Amish Shah, 1 Gwen Kendall, 1 Richard A. Demme, 1
Literature Review Transplantation
 Literature Review 2010- Transplantation Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney and Pancreas Transplant Programs University of
Literature Review 2010- Transplantation Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney and Pancreas Transplant Programs University of
Presenter Disclosure Information
 Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Why Do We Care About Prediabetes?
 Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS
 FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS Objective: We have recently shown the feasibility of a community-based,
FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS Objective: We have recently shown the feasibility of a community-based,
Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE
 Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE ORIGINAL ARTICLE Mohammed Arifulla 1, Lisha Jenny John 1, Jayadevan Sreedharan 2, Jayakumary Muttappallymyalil 3, Jenny
Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE ORIGINAL ARTICLE Mohammed Arifulla 1, Lisha Jenny John 1, Jayadevan Sreedharan 2, Jayakumary Muttappallymyalil 3, Jenny
The American Diabetes Association estimates
 DYSLIPIDEMIA, PREDIABETES, AND TYPE 2 DIABETES: CLINICAL IMPLICATIONS OF THE VA-HIT SUBANALYSIS Frank M. Sacks, MD* ABSTRACT The most serious and common complication in adults with diabetes is cardiovascular
DYSLIPIDEMIA, PREDIABETES, AND TYPE 2 DIABETES: CLINICAL IMPLICATIONS OF THE VA-HIT SUBANALYSIS Frank M. Sacks, MD* ABSTRACT The most serious and common complication in adults with diabetes is cardiovascular
associated with serious complications, but reduce occurrences with preventive measures
 Wk 9. Management of Clients with Diabetes Mellitus 1. Diabetes Mellitus body s inability to metabolize carbohydrates, fats, proteins hyperglycemia associated with serious complications, but reduce occurrences
Wk 9. Management of Clients with Diabetes Mellitus 1. Diabetes Mellitus body s inability to metabolize carbohydrates, fats, proteins hyperglycemia associated with serious complications, but reduce occurrences
Prevention of diabetes in the modern era of affluent society and economic constraints
 Prevention of diabetes in the modern era of affluent society and economic constraints KONSTANTINOS MAKRILAKIS, MD, MPH, PhD ASSOCIATE PROFESSOR IN INTERNAL MEDICINE NATIONAL AND KAPODISTRIAN UNIVERSITY
Prevention of diabetes in the modern era of affluent society and economic constraints KONSTANTINOS MAKRILAKIS, MD, MPH, PhD ASSOCIATE PROFESSOR IN INTERNAL MEDICINE NATIONAL AND KAPODISTRIAN UNIVERSITY
Objectives. Kidney Complications With Diabetes. Case 10/21/2015
 Objectives Kidney Complications With Diabetes Brian Boerner, MD Diabetes, Endocrinology, and Metabolism University of Nebraska Medical Center Review screening for, and management of, albuminuria Review
Objectives Kidney Complications With Diabetes Brian Boerner, MD Diabetes, Endocrinology, and Metabolism University of Nebraska Medical Center Review screening for, and management of, albuminuria Review
Eugene Barrett M.D., Ph.D. University of Virginia 6/18/2007. Diagnosis and what is it Glucose Tolerance Categories FPG
 Diabetes Mellitus: Update 7 What is the unifying basis of this vascular disease? Eugene J. Barrett, MD, PhD Professor of Internal Medicine and Pediatrics Director, Diabetes Center and GCRC Health System
Diabetes Mellitus: Update 7 What is the unifying basis of this vascular disease? Eugene J. Barrett, MD, PhD Professor of Internal Medicine and Pediatrics Director, Diabetes Center and GCRC Health System
Metabolic Syndrome Update The Metabolic Syndrome: Overview. Global Cardiometabolic Risk
 Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
NOTICE. Release of final Health Canada document: Standards for Clinical Trials in Type 2 Diabetes in Canada
 September 24, 2007 NOTICE Our file number: 07-122151-509 Release of final Health Canada document: Standards for Clinical Trials in Type 2 Diabetes in Canada The final version of the Health Canada guidance
September 24, 2007 NOTICE Our file number: 07-122151-509 Release of final Health Canada document: Standards for Clinical Trials in Type 2 Diabetes in Canada The final version of the Health Canada guidance
A 6-year prospective study on new onset diabetes mellitus, insulin release and insulin sensitivity in renal transplant recipients
 Nephrol Dial Transplant (2003) 18: 2154 2159 DOI: 10.1093/ndt/gfg338 Original Article A 6-year prospective study on new onset diabetes mellitus, insulin release and insulin sensitivity in renal transplant
Nephrol Dial Transplant (2003) 18: 2154 2159 DOI: 10.1093/ndt/gfg338 Original Article A 6-year prospective study on new onset diabetes mellitus, insulin release and insulin sensitivity in renal transplant
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable?
 Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
What s New. in Clinical Research
 What s New in Clinical Research This new department features articles discussing recent developments in drug therapy, as well as review articles on specific drug therapies or disease states. Articles will
What s New in Clinical Research This new department features articles discussing recent developments in drug therapy, as well as review articles on specific drug therapies or disease states. Articles will
Echocardiography analysis in renal transplant recipients
 Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Metabolic Syndrome: What s in a name?
 Commentary Metabolic Syndrome: What s in a name? Deborah P. Wubben, MD, MPH; Alexandra K. Adams, MD, PhD Abstract The term metabolic syndrome has recently become en vogue. But is the definition realistic,
Commentary Metabolic Syndrome: What s in a name? Deborah P. Wubben, MD, MPH; Alexandra K. Adams, MD, PhD Abstract The term metabolic syndrome has recently become en vogue. But is the definition realistic,
Prof. Armando Torres Nephrology Section Hospital Universitario de Canarias University of La Laguna Tenerife, Canary Islands, Spain.
 Does RAS blockade improve outcomes after kidney transplantation? Armando Torres, La Laguna, Spain Chairs: Hans De Fijter, Leiden, The Netherlands Armando Torres, La Laguna, Spain Prof. Armando Torres Nephrology
Does RAS blockade improve outcomes after kidney transplantation? Armando Torres, La Laguna, Spain Chairs: Hans De Fijter, Leiden, The Netherlands Armando Torres, La Laguna, Spain Prof. Armando Torres Nephrology
Glycemic control in type 2 diabetes. Exercise prescription in type 2 diabetes treatment. Target for diabetes intervention.
 Exercise prescription in type 2 diabetes treatment Glycemic control in type 2 diabetes Prof. L.J.C. van Loon The level of glycemia is associated with the development of cardiovascular complications Glycemic
Exercise prescription in type 2 diabetes treatment Glycemic control in type 2 diabetes Prof. L.J.C. van Loon The level of glycemia is associated with the development of cardiovascular complications Glycemic
Impaired Glucose Tolerance, Impaired Fasting Glycaemia and Cardiovascular Risk
 R E V I E W A R T I C L E Impaired Glucose Tolerance, Impaired Fasting Glycaemia and Cardiovascular Risk Harsinen Sanusi ABSTRACT Type 2 Diabetes Mellitus tends to increase year by year and it has high
R E V I E W A R T I C L E Impaired Glucose Tolerance, Impaired Fasting Glycaemia and Cardiovascular Risk Harsinen Sanusi ABSTRACT Type 2 Diabetes Mellitus tends to increase year by year and it has high
Victims of success: Do we still need clinical trials? Robert S. Gaston, MD CTI Clinical Trials and Consulting University of Alabama at Birmingham
 Victims of success: Do we still need clinical trials? Robert S. Gaston, MD CTI Clinical Trials and Consulting University of Alabama at Birmingham Disclosure Employee: CTI Clinical Trials and Consulting
Victims of success: Do we still need clinical trials? Robert S. Gaston, MD CTI Clinical Trials and Consulting University of Alabama at Birmingham Disclosure Employee: CTI Clinical Trials and Consulting
Implementing Type 2 Diabetes Prevention Programmes
 Implementing Type 2 Diabetes Prevention Programmes Jaakko Tuomilehto Department of Public Health University of Helsinki Helsinki, Finland FIN-D2D Survey 2004 Prevalence of previously diagnosed and screen-detected
Implementing Type 2 Diabetes Prevention Programmes Jaakko Tuomilehto Department of Public Health University of Helsinki Helsinki, Finland FIN-D2D Survey 2004 Prevalence of previously diagnosed and screen-detected
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS
 IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
Pharmacology notes Interleukin-2 receptor-blocking monoclonal antibodies: evaluation of 2 new agents
 BUMC Proceedings 1999;12:110-112 Pharmacology notes Interleukin-2 receptor-blocking monoclonal antibodies: evaluation of 2 new agents CHERYLE GURK-TURNER, RPH Department of Pharmacy Services, BUMC wo mouse/human
BUMC Proceedings 1999;12:110-112 Pharmacology notes Interleukin-2 receptor-blocking monoclonal antibodies: evaluation of 2 new agents CHERYLE GURK-TURNER, RPH Department of Pharmacy Services, BUMC wo mouse/human
Pasta: A High-Quality Carbohydrate Food
 Pasta: A High-Quality Carbohydrate Food Cyril W.C. Kendall Department of Nutritional Sciences, Faculty of Medicine, University of Toronto; Clinical Nutrition & Risk Factor Modification Center, St. Michael
Pasta: A High-Quality Carbohydrate Food Cyril W.C. Kendall Department of Nutritional Sciences, Faculty of Medicine, University of Toronto; Clinical Nutrition & Risk Factor Modification Center, St. Michael
and Training Standards for Diabetes Prevention [IMAGE] project) to provide
![and Training Standards for Diabetes Prevention [IMAGE] project) to provide and Training Standards for Diabetes Prevention [IMAGE] project) to provide](/thumbs/94/120124786.jpg) Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Insulin Sensitivity, b-cell Function, and Incretin Effect in Individuals With Elevated 1-h Postload Plasma Glucose Levels MARIA A. MARINI,
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Insulin Sensitivity, b-cell Function, and Incretin Effect in Individuals With Elevated 1-h Postload Plasma Glucose Levels MARIA A. MARINI,
Other Ways to Achieve Metabolic Control
 Other Ways to Achieve Metabolic Control Nestor de la Cruz- Muñoz, MD, FACS Associate Professor of Clinical Surgery Chief, Division of Laparoendoscopic and Bariatric Surgery DeWitt Daughtry Family Department
Other Ways to Achieve Metabolic Control Nestor de la Cruz- Muñoz, MD, FACS Associate Professor of Clinical Surgery Chief, Division of Laparoendoscopic and Bariatric Surgery DeWitt Daughtry Family Department
Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone
 Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Supplementary Online Content
 Supplementary Online Content Larsen JR, Vedtofte L, Jakobsen MSL, et al. Effect of liraglutide treatment on prediabetes and overweight or obesity in clozapine- or olanzapine-treated patients with schizophrenia
Supplementary Online Content Larsen JR, Vedtofte L, Jakobsen MSL, et al. Effect of liraglutide treatment on prediabetes and overweight or obesity in clozapine- or olanzapine-treated patients with schizophrenia
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Non-type 1 diabetes mellitus in Canadian children
 Non-type 1 diabetes mellitus in Canadian children Principal investigators Shazhan Amed, MD, FRCPC, FAAP, Division of Endocrinology, The Hospital for Sick Children, 555 University Ave, Toronto ON M5G 1X8;
Non-type 1 diabetes mellitus in Canadian children Principal investigators Shazhan Amed, MD, FRCPC, FAAP, Division of Endocrinology, The Hospital for Sick Children, 555 University Ave, Toronto ON M5G 1X8;
Effect of long-term steroid withdrawal in renal transplant recipients: a retrospective cohort study
 NDT Plus (2010) 3 [Suppl 2]: ii32 ii36 doi: 10.1093/ndtplus/sfq064 Effect of long-term steroid withdrawal in renal transplant recipients: a retrospective cohort study Miguel Gonzalez-Molina 1, Miguel Angel
NDT Plus (2010) 3 [Suppl 2]: ii32 ii36 doi: 10.1093/ndtplus/sfq064 Effect of long-term steroid withdrawal in renal transplant recipients: a retrospective cohort study Miguel Gonzalez-Molina 1, Miguel Angel
K For patients who have never been tested for HCV, it is. K It is suggested that HCV-infected patients not previously
 http://www.kidney-international.org & 2008 DIGO Guideline 4: Management of HCV-infected patients before and after kidney transplantation idney International (2008) 73 (Suppl 109), S53 S68; doi:10.1038/ki.2008.87
http://www.kidney-international.org & 2008 DIGO Guideline 4: Management of HCV-infected patients before and after kidney transplantation idney International (2008) 73 (Suppl 109), S53 S68; doi:10.1038/ki.2008.87
Community Based Diabetes Prevention
 Community Based Diabetes Prevention Melanie Davies Professor of Diabetes Medicine Outline NIHR Programme Grant proposal and update to progress The Vascular Check programme HbA1c debate Algorithm to detect
Community Based Diabetes Prevention Melanie Davies Professor of Diabetes Medicine Outline NIHR Programme Grant proposal and update to progress The Vascular Check programme HbA1c debate Algorithm to detect
CMV INFECTION IN KIDNEY TRANSPLANTATION
 CMV INFECTION IN KIDNEY TRANSPLANTATION PIERRE MERVILLE CHU BORDEAUX - UNIVERSITÉ BORDEAUX SEGALEN UMR-CNRS 5164 SUMMARY: 1.Epidemiology in kidney transplantation 2.T T cell response: αβ and γδ lymphocytes
CMV INFECTION IN KIDNEY TRANSPLANTATION PIERRE MERVILLE CHU BORDEAUX - UNIVERSITÉ BORDEAUX SEGALEN UMR-CNRS 5164 SUMMARY: 1.Epidemiology in kidney transplantation 2.T T cell response: αβ and γδ lymphocytes
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29755 holds various files of this Leiden University dissertation. Author: Moes, Dirk Jan Alie Roelof Title: Optimizing immunosuppression with mtor inhibitors
Cover Page The handle http://hdl.handle.net/1887/29755 holds various files of this Leiden University dissertation. Author: Moes, Dirk Jan Alie Roelof Title: Optimizing immunosuppression with mtor inhibitors
1472 Diabetes Care Volume 39, August 2016
 1472 Diabetes Care Volume 39, August 2016 Prediabetes : Are There Problems With This Label? No, We Need Heightened Awareness of This Condition! Diabetes Care 2016;39:1472 1477 DOI: 10.2337/dc16-1143 William
1472 Diabetes Care Volume 39, August 2016 Prediabetes : Are There Problems With This Label? No, We Need Heightened Awareness of This Condition! Diabetes Care 2016;39:1472 1477 DOI: 10.2337/dc16-1143 William
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Mayo Clinic Proceedings September 2018 Issue Summary
 Greetings, I am Dr Karl Nath, the Editor-in-Chief of Mayo Clinic Proceedings, and I am pleased to welcome you to the multimedia summary for the journal s September 2018 issue. There are 4 articles this
Greetings, I am Dr Karl Nath, the Editor-in-Chief of Mayo Clinic Proceedings, and I am pleased to welcome you to the multimedia summary for the journal s September 2018 issue. There are 4 articles this
Hemoglobin A1C and diabetes diagnosis: The Rancho Bernardo Study
 Diabetes Care Publish Ahead of Print, published online October 16, 2009 Hemoglobin A1c and diabetes Hemoglobin A1C and diabetes diagnosis: The Rancho Bernardo Study Running Title: Hemoglobin A1c and diabetes
Diabetes Care Publish Ahead of Print, published online October 16, 2009 Hemoglobin A1c and diabetes Hemoglobin A1C and diabetes diagnosis: The Rancho Bernardo Study Running Title: Hemoglobin A1c and diabetes
TIGAR Personalized Medicine in Diabetes
 TIGAR Personalized Medicine in Diabetes Frequently asked questions by Physicians This information is solely for use by an appropriately qualified health care professional. This manual is meant to be used
TIGAR Personalized Medicine in Diabetes Frequently asked questions by Physicians This information is solely for use by an appropriately qualified health care professional. This manual is meant to be used
Cancer in kidney transplant recipients: epidemiology and prevention
 BTS 2018, Brighton Cancer in kidney transplant recipients: epidemiology and prevention Adnan Sharif Queen Elizabeth Hospital Birmingham Outline 1. The burden of cancer after kidney transplantation 2. Epidemiology
BTS 2018, Brighton Cancer in kidney transplant recipients: epidemiology and prevention Adnan Sharif Queen Elizabeth Hospital Birmingham Outline 1. The burden of cancer after kidney transplantation 2. Epidemiology
Acute rejection and late renal transplant failure: Risk factors and prognosis
 Nephrol Dial Transplant (2004) 19 [Suppl 3]: iii38 iii42 DOI: 10.1093/ndt/gfh1013 Acute rejection and late renal transplant failure: Risk factors and prognosis Luis M. Pallardo Mateu 1, Asuncio n Sancho
Nephrol Dial Transplant (2004) 19 [Suppl 3]: iii38 iii42 DOI: 10.1093/ndt/gfh1013 Acute rejection and late renal transplant failure: Risk factors and prognosis Luis M. Pallardo Mateu 1, Asuncio n Sancho
Metformin should be considered in all patients with type 2 diabetes unless contra-indicated
 November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
Diagnostic criteria for diabetes Routine cases and Non-diabetic hyperglycaemia adapted with permission from Royal Devon and Exeter
 Diagnostic criteria for diabetes Routine cases and Non-diabetic hyperglycaemia adapted with permission from Royal Devon and Exeter Diabetes may be diagnosed on any of the following criteria (WHO 2006,
Diagnostic criteria for diabetes Routine cases and Non-diabetic hyperglycaemia adapted with permission from Royal Devon and Exeter Diabetes may be diagnosed on any of the following criteria (WHO 2006,
Prevention and management of new-onset diabetes mellitus in kidney transplantation
 REVIEW Prevention and management of new-onset diabetes mellitus in kidney transplantation M. Juan Khong, Ch. Ping Chong* Discipline of Clinical Pharmacy, School of Pharmaceutical Sciences, Universiti Sains
REVIEW Prevention and management of new-onset diabetes mellitus in kidney transplantation M. Juan Khong, Ch. Ping Chong* Discipline of Clinical Pharmacy, School of Pharmaceutical Sciences, Universiti Sains
Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab
 TRANSPLANTATION Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab Khadijeh Makhdoomi, 1,2 Saeed Abkhiz, 1,2 Farahnaz Noroozinia, 1,3
TRANSPLANTATION Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab Khadijeh Makhdoomi, 1,2 Saeed Abkhiz, 1,2 Farahnaz Noroozinia, 1,3
Management of Post-transplant hyperlipidemia
 Management of Post-transplant hyperlipidemia B. Gisella Carranza Leon, MD Assistant Professor of Medicine Lipid Clinic - Vanderbilt Heart and Vascular Institute Division of Diabetes, Endocrinology and
Management of Post-transplant hyperlipidemia B. Gisella Carranza Leon, MD Assistant Professor of Medicine Lipid Clinic - Vanderbilt Heart and Vascular Institute Division of Diabetes, Endocrinology and
Reviewing Diabetes Guidelines. Newsletter compiled by Danny Jaek, Pharm.D. Candidate
 Reviewing Diabetes Guidelines Newsletter compiled by Danny Jaek, Pharm.D. Candidate AL AS KA N AT IV E DI AB ET ES TE A M Volume 6, Issue 1 Spring 2011 Dia bet es Dis pat ch There are nearly 24 million
Reviewing Diabetes Guidelines Newsletter compiled by Danny Jaek, Pharm.D. Candidate AL AS KA N AT IV E DI AB ET ES TE A M Volume 6, Issue 1 Spring 2011 Dia bet es Dis pat ch There are nearly 24 million
Horizon Scanning Technology Summary. Liraglutide for type 2 diabetes. National Horizon Scanning Centre. April 2007
 Horizon Scanning Technology Summary National Horizon Scanning Centre Liraglutide for type 2 diabetes April 2007 This technology summary is based on information available at the time of research and a limited
Horizon Scanning Technology Summary National Horizon Scanning Centre Liraglutide for type 2 diabetes April 2007 This technology summary is based on information available at the time of research and a limited
Diabetes and the Heart
 Diabetes and the Heart Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 6, 2012 Outline Screening for diabetes in patients with CAD Screening for CAD in patients with
Diabetes and the Heart Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 6, 2012 Outline Screening for diabetes in patients with CAD Screening for CAD in patients with
Journal of the American College of Cardiology Vol. 48, No. 2, by the American College of Cardiology Foundation ISSN /06/$32.
 Journal of the American College of Cardiology Vol. 48, No. 2, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.03.043
Journal of the American College of Cardiology Vol. 48, No. 2, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.03.043
National Horizon Scanning Centre. Saxagliptin (BMS ) for type 2 diabetes. April 2008
 Saxagliptin (BMS 477118) for type 2 diabetes This technology summary is based on information available at the time of research and a limited literature search. It is not intended to be a definitive statement
Saxagliptin (BMS 477118) for type 2 diabetes This technology summary is based on information available at the time of research and a limited literature search. It is not intended to be a definitive statement
Risks and benefits of weight loss: challenges to obesity research
 European Heart Journal Supplements (2005) 7 (Supplement L), L27 L31 doi:10.1093/eurheartj/sui083 Risks and benefits of weight loss: challenges to obesity research Donna Ryan* Pennington Biomedical Research
European Heart Journal Supplements (2005) 7 (Supplement L), L27 L31 doi:10.1093/eurheartj/sui083 Risks and benefits of weight loss: challenges to obesity research Donna Ryan* Pennington Biomedical Research
Certified Clinical Transplant Nurse (CCTN) * Detailed Content Outline
 I. PRETRANSPLANTATION CARE 9 11 3 23 A. Evaluate End-Stage Organ Failure 1 1 1 3 1. History and physical assessment 2. Vital signs and / or hemodynamic parameters 3. Lab values 4. Diagnostic tests B. Monitor
I. PRETRANSPLANTATION CARE 9 11 3 23 A. Evaluate End-Stage Organ Failure 1 1 1 3 1. History and physical assessment 2. Vital signs and / or hemodynamic parameters 3. Lab values 4. Diagnostic tests B. Monitor
HHS Public Access Author manuscript Kidney Int. Author manuscript; available in PMC 2013 September 01.
 Choices in kidney transplantation in type 1 diabetes: Are there skeletal benefits of the endocrine pancreas? Julia J. Scialla, MD, MHS Division of Nephrology and Hypertension, Department of Medicine, University
Choices in kidney transplantation in type 1 diabetes: Are there skeletal benefits of the endocrine pancreas? Julia J. Scialla, MD, MHS Division of Nephrology and Hypertension, Department of Medicine, University
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29755 holds various files of this Leiden University dissertation. Author: Moes, Dirk Jan Alie Roelof Title: Optimizing immunosuppression with mtor inhibitors
Cover Page The handle http://hdl.handle.net/1887/29755 holds various files of this Leiden University dissertation. Author: Moes, Dirk Jan Alie Roelof Title: Optimizing immunosuppression with mtor inhibitors
Long-term prognosis of BK virus-associated nephropathy in kidney transplant recipients
 Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
European Risk Management Plan. Measures impairment. Retreatment after Discontinuation
 European Risk Management Plan Table 6.1.4-1: Safety Concern 55024.1 Summary of Risk Minimization Measures Routine Risk Minimization Measures Additional Risk Minimization Measures impairment. Retreatment
European Risk Management Plan Table 6.1.4-1: Safety Concern 55024.1 Summary of Risk Minimization Measures Routine Risk Minimization Measures Additional Risk Minimization Measures impairment. Retreatment
Review of Rituximab and renal transplantation. Dr.E Nemati. Professor of Nephrology
 Review of Rituximab and renal transplantation Dr.E Nemati Professor of Nephrology Introductio n Rituximab is a chimeric anti-cd20 monoclonal antibody. The CD20 antigen is a transmembrane nonglycosylated
Review of Rituximab and renal transplantation Dr.E Nemati Professor of Nephrology Introductio n Rituximab is a chimeric anti-cd20 monoclonal antibody. The CD20 antigen is a transmembrane nonglycosylated
Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
 Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
Dipeptidyl-Peptidase 4 (DPP-4) Inhibitors Drug Class Prior Authorization Protocol
 Dipeptidyl-Peptidase 4 (DPP-4) Inhibitors Drug Class Prior Authorization Protocol Line of Business: Medicaid P&T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has been developed
Dipeptidyl-Peptidase 4 (DPP-4) Inhibitors Drug Class Prior Authorization Protocol Line of Business: Medicaid P&T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has been developed
OBJECTIVES. Phases of Transplantation and Immunosuppression
 Transplant and Immunosuppression: Texas Transplant Center April 29, 2017 Regina L. Ramirez, Pharm.D., BCPS PGY1 Pharmacy Residency Program Director Clinical Practice Specialist Solid Organ Transplant and
Transplant and Immunosuppression: Texas Transplant Center April 29, 2017 Regina L. Ramirez, Pharm.D., BCPS PGY1 Pharmacy Residency Program Director Clinical Practice Specialist Solid Organ Transplant and
Welcome and Introduction
 Welcome and Introduction This presentation will: Define obesity, prediabetes, and diabetes Discuss the diagnoses and management of obesity, prediabetes, and diabetes Explain the early risk factors for
Welcome and Introduction This presentation will: Define obesity, prediabetes, and diabetes Discuss the diagnoses and management of obesity, prediabetes, and diabetes Explain the early risk factors for
EARLY VERSUS LATE STEROID WITHDRAWAL Julio Pascual, Barcelona, Spain Chairs: Ryszard Grenda, Warsaw, Poland
 EARLY VERSUS LATE STEROID WITHDRAWAL Julio Pascual, Barcelona, Spain Chairs: Ryszard Grenda, Warsaw, Poland Julio Pascual, Barcelona, Spain Prof. Julio Pascal Hospital del Mar Nephrology Department Barcelona,
EARLY VERSUS LATE STEROID WITHDRAWAL Julio Pascual, Barcelona, Spain Chairs: Ryszard Grenda, Warsaw, Poland Julio Pascual, Barcelona, Spain Prof. Julio Pascal Hospital del Mar Nephrology Department Barcelona,
