What s New. in Clinical Research
|
|
|
- Candace Pitts
- 5 years ago
- Views:
Transcription
1 What s New in Clinical Research This new department features articles discussing recent developments in drug therapy, as well as review articles on specific drug therapies or disease states. Articles will discuss new drugs, new indications for existing drugs, and large, multicentre Phase III and IV trials. All articles have been reviewed by our board of editorial consultants. 96 The Canadian Journal of Diagnosis / June 2007
2 Current Research on the Prevention and Treatment of Type 2 Diabetes 1. University of British Columbia, Vancouver, British Columbia. 2. Institut universitaire de cardiologie et de pneumologie de Québec, Hôpital Laval, Ste-Foy, Quebec. By Keith Dawson 1 MD, FRCPC and Claude Garceau 2 MD, FRCPC The incidence of diabetes mellitus, which affects approximately 5% of adults worldwide, 1 has increased greatly during the past 20 years. 2 In particular, there has been an alarming rise in the incidence of type 2 diabetes, which is attributable to the rapid increase in obesity rates and the aging of the population. 3 In light of these demographic factors, it is imperative that healthcare professionals provide optimal treatment to their patients not only to manage diabetes and prevent its complications, but also to prevent its development in the first place. A number of lifestyle and pharmacological interventions are known to be effective in helping patients optimally manage their glycemic levels. There are also emerging data to suggest that pharmacotherapy can be effective in preventing the progression of disease from pre-diabetic states (e.g., impaired fasting glucose [IFG] and impaired glucose tolerance [IGT]) to overt type 2 diabetes. This review will briefly review the impact of type 2 diabetes and provide a brief discussion of the disease s pathophysiology. The focus will then shift to treatment modalities, focusing on the results of recent landmark clinical trials in the prevention and management of type 2 diabetes. Copyright Not for Sale or Commercial Distribution Unauthorised use prohibited. Authorised users can download, display, viewand print a single copy for personal use THE IMPACT OF TYPE 2 DIABETES The impact of type 2 diabetes a chronic, progressively worsening disease is well documented. There are associations with cardiovascular disease the primary cause of death in type 2 diabetes significant reductions in life expectancy, 4 and a high morbidity load. Hypertension, dyslipidemia, and macrovascular and microvascular events (e.g., retinopathy, neuropathy) are all common complications that seriously compromise patients quality of life and place enormous burdens on the healthcare system. PATHOPHYSIOLOGY OF TYPE 2 DIABETES Type 2 diabetes is a metabolic disorder that is characterized by a progression of hyperglycemia caused by defective insulin secretion, insulin action or both. 5 The disease s dynamic quality makes it especially challenging to identify initially and, subsequently, demands both careful monitoring and timely therapeutic responses to its progression. While the precise pathophysiology of type 2 diabetes is not understood, it typically results from a prolonged period during which the individual undergoes IFG and/or IGT. Recent research has shown that glucose deterioration occurs in a stepwise fashion. 6 In a three-step process, glucose levels first begin to progressively increase in the daytime postprandial period, followed by the morning period, and lastly in the The Canadian Journal of Diagnosis / June
3 Current Research on the Prevention and Treatment of Type 2 Diabetes overnight fasting period. These key stages in the progression from postprandial to fasting hyperglycemia, and finally to overt diabetes, can be seen as part of a continuum that begins long before the disease becomes clinically evident. Insulin resistance (inability of insulin to adequately facilitate the uptake or use of glucose) is thought to be a major factor in the disease s development. Impairment of insulin secretion also plays a key role. Initially, if a patient experiences insulin resistance, the pancreas compensates by producing more insulin. This may be initially sufficient to control glycemia. Over time, however, the pancreas becomes unable to produce enough insulin to continue to overcome the resistance, leading to the development and subsequent progression of type 2 diabetes. The vicious cycle then continues, as elevated glucose further impairs pancreatic beta-cell function, which, in turn, reduces insulin production. Evidence from the United Kingdom Prospective Diabetes Study (UKPDS) has shown that decline in β-cell function is directly correlated with the duration of disease and suggests that the decline actually typically begins long before the diagnosis of diabetes is made. 7 These insights serve to emphasize the potential importance of long-term glucose control to help preserve β-cell function. Indeed, Harris et al observed that glycemic control, for type 2 diabetes patients, eroded significantly with increasing duration of diabetes in spite of increasing therapeutic intervention. 8 TYPE 2 DIABETES: THE CHALLENGES OF MANAGEMENT Clearly, type 2 diabetes confronts clinicians with complex and enduring management challenges, including identifying patients at risk of developing the disease, despite the likelihood of their condition (e.g., IFG and/or IGT) being asymptomatic. Once the disease develops, implementing and maintaining a successful and optimal treatment strategy involving both nonpharmacologic and pharmacologic interventions is also challenging. In fact, in spite of increasing therapeutic intervention, glycemic control has been found to progressively diminish with the increasing duration of the disease, 8 a result that is consistent with the UKPDS clinical findings about the progressive nature of type 2 diabetes. 7 The goals of management in type 2 diabetes are therefore threefold: to improve A1C levels, to slow progression of diabetes, and to reduce complications. However, before arriving at these goals, one should consider ways by which the risk of type 2 diabetes can be reduced. PREVENTION OF TYPE 2 DIABETES The importance of lifestyle intervention, with an emphasis on diet and fitness goals, has become widely accepted as an important component in preventing the development of type 2 diabetes. In the Diabetes Prevention Program (DPP), researchers set goals of 7% weight loss and 150 minutes of physical activity per week for patients in the lifestyle intervention arm of the study. Following this protocol resulted in a 58% reduction in the incidence of type 2 diabetes. 9 However, the success of the lifestyle interventions in the DPP reflected, to a certain degree, the intensity with which participants were monitored and received professional assistance and guidance in adhering to program goals. The extent to which primary-care physicians, who are predominantly charged with the management of type 2 diabetes, can hope to achieve such effective adherence as was found in the DPP study and achieve the concomitant benefits of lifestyle intervention is seriously in doubt. There exists, then, a pressing need for additional means of early and effective intervention to supplement lifestyle modification as a means of preventing the development of type 2 diabetes. Three types of antihyperglycemic agents have also demonstrated an ability to prevent the development of type 2 diabetes. The alpha-glucosidase inhibitor acarbose was investigated in the Study to Prevent Non-Insulin-Dependent Diabetes Mellitus (STOP-NIDDM), 10 which randomized 1,429 patients with impaired glucose tolerance to acarbose 100 mg t.i.d. or placebo. For the primary endpoint of development of diabetes, acarbose reduced the relative risk by 25% versus placebo (p=0.0015). Furthermore, acarbose significantly increased reversion of impaired glucose tolerance to normal glucose tolerance (p < ). Similarly, the DPP also included a metformin arm. Compared to placebo, metformin was found to reduce the risk of type 2 diabetes by 31% among 3,234 men and women with a body mass index of 34 ± 6.7 kg/m 2 and IFG or IGT. 11 In the washout phase, which averaged 11 days, there was a partial loss of efficacy of metformin in preventing diabetes compared to placebo. 12 The rate of diabetes increased by 5.4% in the metformin group compared to a 3.3% increase in the placebo group, but 98 The Canadian Journal of Diagnosis / June 2007
4 the Prevention and Treatment of Type 2 Diabetes FIGURE 1 DREAM Study:Time to Occurrence of Type 2 Diabetes or Death Rosiglitazone Placebo Cumulative hazard Years Number at risk Placebo 2,634 2,470 2,150 1, Rosiglitazone 2,635 2,538 2,414 1, metformin continued to prevent diabetes in 25% of patients in the metfornin group. More recently, the Diabetes Reduction Assessment with ramipril and rosiglitazone Medication (DREAM) study evaluated the efficacy of rosiglitazone 8 mg daily versus placebo in preventing type 2 diabetes among 5,269 adults, aged 30 or more, with IFG or IGT or both. 13 Over the trial s three-year duration, rosiglitazone at 8 mg daily reduced the risk of diabetes or death (primary endpoint) by 60% compared to placebo (Figure 1). The number needed to treat (NNT) was approximately seven; for every seven people with IFG or IGT who are prescribed rosiglitazone for three years, one will be prevented from developing diabetes. 13 In addition to the primary endpoint result, rosiglitazone also increased the likelihood of regression to normoglycemia by about 70-80% compared to placebo. Figure 2 shows the distribution of patients in the two treatment arms with diabetes, IFG or IGT and normoglycemia (as defined as fasting plasma glucose [FPG] < 6.1 mmol/l). 13 In a washout phase where medications were stopped for three to six months, there was a similar rate of diabetes in the rosiglitazone and placebo groups. 14 When the trial and washout data are analyzed together, there is an overall benefit to treatment with rosiglitazone for a median of three years. PHARMACOLOGIC MANAGEMENT OF TYPE 2 DIABETES As is the case with prevention, the cornerstone of management of type 2 diabetes is lifestyle modification. However, primary-care physicians have identified noncompliance with diet (72%) and exercise (71%) as the most common barriers to achieving glycemic targets through lifestyle modification. 8 Further complicating treatment is the problem of clinical inertia : whereby physicians, while recognizing problems, fail to act or to alter therapy appropriately. 15 According to Phillips et al, physicians are able to identify patients failing to meet their glycemic targets, but tend to overestimate the effectiveness of the care that they are providing. 15 This misinterpretation can lead physicians to rationalize their continued emphasis on compliance with lifestyle modifications, even though they recognize that patients failure to comply is responsible for their inability to control their diabetes. Beyond continuation of that ineffective treatment course, many The Canadian Journal of Diagnosis / June
5 Current Research on the Prevention and Treatment of Type 2 Diabetes FIGURE 2 Proportion of Participants who Developed Diabetes, Regressed to Normal, or Continued to Have IFG, IGT or Both (DREAM Study) Rosiglitazone Placebo Proportional % p < Diabetes IGT, IFG or both Normal + FPG < 6.1 mmol/l physicians seem to be unaware of and, thus, at a loss to prescribe alternative treatments. 15 The Canadian Diabetes Association (CDA) s clinical practice guidelines recommend that the management of type 2 diabetes patients should aim to achieve glycemic levels as close to normal as possible, as early as possible. 5 Thus, if those with type 2 diabetes are not successful in achieving glycemic targets through lifestyle changes within two to three months, the CDA guidelines recommend the initiation of antihyperglycemic agents with concomitant lifestyle counselling. 5 There are a number of pharmacotherapeutic agents available to Canadian physicians and their patients. The choice of antihyperglycemic agent(s) should be based on the individual patient and an understanding of the individual profiles of the various agents. The agents recommended by the Canadian guidelines include metformin, sulfonylureas (e.g., gliclazide, glyburide, glimepiride), alpha-glucosidase inhibitors (e.g., acarbose), TZDs (e.g., pioglitazone, rosiglitazone) and insulin. 5 The following section details recent findings with the TZD class of agents. TZDs. The American Heart Association (AHA) and American Diabetes Association (ADA) 2003 consensus statement identified pioglitazone and rosiglitazone as effective agents in achieving glycemic goals and in reducing diabetes-related end-organ disease. 16 TZDs are indicated either as monotherapy or in combination with sulfonylurea or metformin when lifestyle interventions and single agents do not produce adequate glycemic control. In addition to lowering blood glucose, the AHA/ADA assert that both drugs may benefit cardiovascular parameters, such as lipid, blood pressure, inflammatory biomarkers, endothelial function, and fibrinolytic status. 17,18 TZDs are not associated with hypoglycemia. However, they are contraindicated in those with either hepatic dysfunction or pronounced cardiac failure. Leiter et al evaluated the efficacy of rosiglitazone in 705 patients with type 2 diabetes treated in primary care in Canada. 19 The study was comprised of two separate comparisons: lifestyle modifications alone (n=64) versus rosiglitazone plus lifestyle modifications (n=405) among drug-naïve patients; and metformin at augmented doses plus lifestyle modifications versus metformin plus addition of rosiglitazone plus lifestyle modifications among metformin-treated patients. In the first comparison, mean change in A1C from baseline at 32 weeks (primary efficacy variable), treatment with rosiglitazone resulted in a decrease from a baseline A1C of 0.62% (p < 0.001), while there was no significant reduction in the lifestyle alone group (Figure 3). In the second comparison, the combination of rosiglitazone with metformin resulted in a significant decrease 100 The Canadian Journal of Diagnosis / June 2007
6 the Prevention and Treatment of Type 2 Diabetes FIGURE 3 Changes in A1C Over Time 19 Cohort 1 = = lifestyle (n=50) = rosiglitazone + lifestyle (n=362) Cohort 2 = = metformin + lifestyle (n=70) = metformin + rosiglitazone + lifestyle (n=144) Mean A1C (%) Duration of treatment (weeks) in AlC compared with metformin. Adding rosiglitazone to metformin reduced A1C from 7.5 to 7.0%, while augmenting the dose of metformin alone resulted in a reduction from 7.5 to 7.4% (Figure 3). The results suggest then that combining rosiglitazone and metformin is a more effective approach than the usual strategy of maximizing the dose of metformin monotherapy. Rosenstock et al also evaluated the efficacy of rosiglitazone/metformin combination therapy in a multicentre, open-label trial involving 190 patients with an A1C greater than 11% or FPG greater than 15 mmol/l. 20 Patients in this study initially received the rosiglitazone/metformin therapy in a 4 mg/1000 mg fixed-dose combination therapy. The dose was subsequently uptitrated in increments of 2 mg/500 mg at four-week intervals, to a daily dose of 8 mg/2000 mg or the maximum tolerated dose. At 24 weeks, a clinically significant mean reduction in A1C from 11.8 to 7.8% (p <.0001) and a mean FPG reduction from 16.9 to 9.2 mmol/l (p <.0001) were observed. Nearly half of the patients reached an A1C level less than 7% and nearly one-third reached an A1C level of 6.5% or less. In addition, a clinically significant reduction in FPG (of 5.2 mmol/l) was observed after four weeks of fixed-dose combination therapy. In a subsequent multicentre trial, Rosenstock et al studied the efficacy of rosiglitazone/metformin combination therapy versus monotherapy with either rosiglitazone or metformin in a double-blind design. 21 Study subjects had an A1C between 7.5 and 11%, and FPG less than or equal to 15 mmol/l. Patients were randomized to receive an initial daily dose of rosiglitazone/metformin (fixed-dose combination) 2 mg/500 mg, metformin 500 mg, or rosiglitazone 4 mg; doses could be uptitrated to 8 mg/2000 mg, 2000 mg, and 8 mg, respectively. After 32 weeks, patients on the rosiglitazone/ metformin combination therapy achieved a 2.3% reduction in A1C. This result was significantly greater than reductions with metformin ( 1.8%) or rosiglitazone ( 1.6%) monotherapy. Target A1Cs of less than or equal to 6.5% or less than 7% were reached by more patients in the rosiglitazone/metformin group (60% and 77%) than the metformin (39% and 57%) or rosiglitazone (35% and 58%) groups. Furthermore, there was a significantly greater mean decrease in FPG with the fixed-dose combination therapy ( 4.1 mmol/l) compared with metformin ( 2.8 mmol/l; p < ) or rosiglitazone ( 2.6 mmol/l; p < ). Because it is desirable to slow or halt the progression of disease as soon as possible, it is desirable to consider the relative efficacy of possible first-line monotherapies in achieving this goal. A large (n=4,360) clinical trial, A Diabetes Outcome Progression Trial (ADOPT), recently evaluated rosiglitazone, metformin, and glyburide as initial treatment in recently diagnosed, drug-naïve patients with type 2 diabetes. 22 The Canadian Journal of Diagnosis / June
7 Current Research on the Prevention and Treatment of Type 2 Diabetes FIGURE 4 Kaplan-Meier Estimates of the Cumulative Incidence of Monotherapy Failure at 5 Years (ADOPT) 22 Cumulative incidence of monotherapy failure (%) Hazard ratio (95% CI) Rosiglitazone vs. metformin 0.68 ( ); p < Rosiglitazone vs. glyburide 0.37 ( ); p < Glyburide Metformin Rosiglitazone Years Number at risk Rosiglitazone 1,393 1,207 1, Metformin 1,397 1,205 1, Glyburide 1,337 1, The primary outcome of this study was time to monotherapy failure, defined as plasma glucose levels of more than 180 mg per deciliter (> 10.0 mmol/l) after an overnight fast. The mean duration of the study was 4.0 years. The primary results showed that there was a cumulative incidence of monotherapy failure at 5 years of 15% with rosiglitazone, 21% with metformin, and 34% with glyburide (Figure 4). This represents a risk reduction of 32% for rosiglitazone compared with metformin and 63% compared with glyburide. 22 This result indicates that rosiglitazone is superior to metformin and glyburide in delaying the progressive loss of glycemic control. Indeed, rosiglitazone maintained a mean level of A1C at less than 7% longer (57 months) than metformin (45 months) and glyburide (33 months) (Figure 5). In addition, rosiglitazone was more effective in improving insulin sensitivity than either metformin or glyburide (Figure 6). There was also an indication that rosiglitazone was more effective in slowing the annual rate of decline in β-cell function compared to metformin. Further analysis is required to extract the significance of this result. Although rosiglitazone was associated with weight gain, redistribution of body fat and varying patterns of adipokine release may account for the observed improvement in insulin sensitivity despite the weight gain. Subgroup analysis revealed that the rosiglitazone treatment effect was greater with older patients than metformin and amongst those with a larger waist circumference (> 110 cm). Rosiglitazone was more effective than glyburide in all subgroups. As with any agent, when considering the use of an antihyperglycemic agent, one must weigh the potential risks against the expected benefit. In the case of rosiglitazone, some concern has been raised about associated weight gain and the possibility of increased risk of congestive heart failure (CHF). As well, the ADOPT study showed a 4.2% increase in extremity fractures in women taking rosiglitazone compared with metformin. 22 These findings remain to be clarified, but this was not an identified primary outcome in the study. In the first Rosenstock study, the investigators wrote that the fixed-dose combination was well tolerated as a first-line therapy and no new tolerability issues were iden- 102 The Canadian Journal of Diagnosis / June 2007
8 the Prevention and Treatment of Type 2 Diabetes FIGURE 5 Changes in A1C Over Five Years by Treatment Group (ADOPT) Treatment difference (95% CI) Rosiglitazone vs. metformin, 0.13 ( 0.22 to 0.05); p = Rosiglitazone vs. glyburide, 0.42 ( 0.50 to 0.33); p < Annualized slope (95% CI) Rosiglitazone, 0.07 (0.06 to 0.09) Metformin, 0.14 (0.13 to 0.16)* Glyburide, 0.24 (0.23 to 0.26)* Glycated hemoglobin (%) Years Number of patients Rosiglitazone 4,012 3,308 2,991 2,583 2, FIGURE 6 Changes in Insulin Sensitivity Over Five Years by Treatment Group (ADOPT) Treatment difference (95% CI) Rosiglitazone vs. metformin, 12.6 (8.1 to 17.3); p < Rosiglitazone vs. glyburide, 41.2 (35.2 to 47.4); p < Annualized slope (95% CI) Rosiglitazone, 6.9 (6.0 to 7.7) Metformin, 5.8 (4.9 to 6.6) Glyburide, 4.9 (3.9 to 5.8)* Insulin sensitivity (%) Years Number of patients 3,634 3,193 2,776 2,367 2, The Canadian Journal of Diagnosis / June
9 Current Research on the Prevention and Treatment of Type 2 Diabetes tified. A mean increase of 2.6 kg in body weight was less than previously reported with rosiglitazone monotherapy and considerably less than what might have been expected given the large improvement in glycaemic control. 20 In the DREAM study, the investigators stated, for every 1,000 people treated with rosiglitazone for three years, about 144 cases of diabetes will be prevented, with an excess of four to five cases of CHF. 13 In the ADOPT study, the authors found that the rate of CHF associated with rosiglitazone was similar to that in studies involving low-risk populations and to that associated with metformin, but higher than that associated with glyburide. 22 CONCLUSION More than 8% of adults worldwide have either IGT or IFG, and every year 5-10% of that group will develop diabetes with the concomitant disease burden. As the increasing prevalence of diabetes in an aging Canadian population places an increasing burden on a healthcare system that is already stressed, there is an urgent need References 1. Secree R, Shaw J, Zimmer P. Diabetes and impaired glucose tolerance prevalence and projection. In Allgot B, King H, et al, (eds.) Diabetes atlas, 2nd ed. Brussels: International Diabetes Federation, 2003: WHO. Global Strategy on diet, physical activity and health: diabetes. Jan. 1, (Accessed April 28, 2006). 3. Trends in diabetes prevalence, incidence, and mortality in Ontario, Canada : a population-based study, p U.K. Prospective Diabetes Study (UKPDS) Group. U.K. Prospective Diabetes Study 16. Overview of 6 years therapy of type II diabetes: a progressive disease. Diabetes 1995; 44(11): Canadian Diabetes Association 2003 Clinical Practice Guideline Expert Committee. Canadian Diabetes Association 2003 clinical practice guidelines for the prevention and management of diabetes in Canada. Can J Diabetes 2003; 27(suppl 2):S1-S Monnier L, Colette C, Dunseath GJ, et al. The loss of postprandial glycemic control precedes stepwise deterioration of fasting with worsening diabetes. Diabetes Care 2007; 30(2): Matthews DR, Cull CA, Stratton IM, et al. UKPDS 26: sulphonylurea failure in non-insulin-dependent diabetic patients over six years. UK Prospective Diabetes (UKPDS) Group. Diabetes Med 1998; 15(4): Harris SB, Ekoe JM, Zdanowicz Y, et al. Glycemic control and morbidity in the Canadian primary care setting (results of the diabetes in Canada evaluation study). Diabetes Res Clin Pract 2005; 70(1): The Diabetes Prevention Program (DPP) Research Group. The Diabetes Prevention Program. Diabetes Care 2002; 25(12): Chiasson, JL, Josse RG, Gomis R, et al. Acarbose for prevention of type 2 diabetes mellitus: the STOP-NIDDM randomised trial. Lancet 2002; 359(9323): Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention of metformin. N Engl J Med 2002; 346(6): The Diabetes Prevention Program Research Group. Effects of withdrawal from metformin on the development of diabetes in the Diabetes Prevention Program. Diabetes Care 2003; 26(4): for more effective intervention in the prevention and treatment of the disease. Recognition of the importance of early and effective glycemic control has led the CDA to recommend pharmacologic intervention when lifestyle modification has not achieved glycemic targets within two to three months. The evidence is accumulating showing the effectiveness and safety of rosiglitazone throughout the spectrum of disease. The DREAM study has shown that rosiglitazone can help prevent the emergence of type 2 diabetes in those with IFG and/or IGT; the ADOPT study showed that rosiglitazone is superior to metformin or glyburide monotherapy in delaying the progression of type 2 diabetes. Even so, these results do show that all tested monotherapies fail relatively quickly. The use of effective combination therapies is therefore imperative. Previous studies have shown that rosiglitazone is also effective as part of a combination antihyperglycemic regimen. In optimizing the management of type 2 diabetes, evidence therefore indicates that rosiglitazone can play a major role at several stages of the disease. 13. DREAM (Diabetes REduction Assessment with ramipril and rosiglitazone Medication) Trial Investigators; Gerstein HC, Yusuf S, Bosch J, et al. Effect of rosiglitazone on the frequency of diabetes in patients with impaired glucose tolerance or impaired fasting glucose: a randomised controlled trial. Lancet 2006; 368(9541): Holman RR. Late-breaking trials: DREAM washout period results. Program and abstracts of the 19th World Diabetes Congress; December 3-7, 2006; Cape Town, South Africa. 15. Phillips LS, Branch WT, Cook CB, et al. Clinical inertia. Ann Intern Med 2001; 135(9): Nesto RW, Bell D, Bonow RO, et al; American Heart Association; American Diabetes Association. Thiazolidinedione use, fluid retention, and congestive heart failure: a consensus statement from the American Heart Association and American Diabetes Association. October 7, Circulation 2003; 108: Parulkar AA, Pendergrass ML, Granada-Ayala R, et al. Nonhypoglycemic effects of thiazolidinediones. Ann Intern Med 2001; 134(1): Haffner SM, Greenberg AS, Weston WM, et al. Effects of rosiglitazone treatment on nontraditional markers of cardiovascular disease in patients with type 2 diabetes mellitus. Circulation 2002; 106(6): Leiter LA, Harris SB, Chiasson J-L, et al. Efficacy and safety of rosiglitazone as monotherapy or in combination with metformin in primary care settings. Can J Diabetes 2005; 29(4): Rosenstock J, Rood J, Cobitz A, et al. Improvement in glycaemic control with rosiglitazone/metformin fixed-dose combination therapy in patients with type 2 diabetes with very poor glycaemic control. Diabetes Obes Metab 2006; 8(6): Rosenstock J, Rood J, Cobitz A, et al. Initial treatment with rosiglitazone/metformin fixed-dose combination therapy compared with either rosiglitazone or metformin patients with uncontrolled type 2 diabetes. Diabetes Obes Metab 2006; 8(6): Kahn SE, Haffner SM, Heise MA, et al. Glycemic durability of rosiglitazone, metformin, or glyburide monotherapy. N Engl J Med 2006; 355(23): The Canadian Journal of Diagnosis / June 2007
Choosing a Diabetes Strategy Where to Start and Where to Go
 Choosing a Diabetes Strategy Where to Start and Where to Go Erin Keely, MD, FRCPC; and Sharon Brez, RN, BScN, MA(Ed), CDE As presented at the University of Ottawa's 52nd Annual Refresher Course for Family
Choosing a Diabetes Strategy Where to Start and Where to Go Erin Keely, MD, FRCPC; and Sharon Brez, RN, BScN, MA(Ed), CDE As presented at the University of Ottawa's 52nd Annual Refresher Course for Family
Diabetes: Staying Two Steps Ahead. The prevalence of diabetes is increasing. What causes Type 2 diabetes?
 Focus on CME at the University of University Manitoba of Manitoba : Staying Two Steps Ahead By Shagufta Khan, MD; and Liam J. Murphy, MD The prevalence of diabetes is increasing worldwide and will double
Focus on CME at the University of University Manitoba of Manitoba : Staying Two Steps Ahead By Shagufta Khan, MD; and Liam J. Murphy, MD The prevalence of diabetes is increasing worldwide and will double
Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes
 Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes Genetics, environment, and lifestyle (obesity, inactivity, poor diet) Impaired fasting glucose Decreased β-cell
Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes Genetics, environment, and lifestyle (obesity, inactivity, poor diet) Impaired fasting glucose Decreased β-cell
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable?
 Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
NOTICE. Release of final Health Canada document: Standards for Clinical Trials in Type 2 Diabetes in Canada
 September 24, 2007 NOTICE Our file number: 07-122151-509 Release of final Health Canada document: Standards for Clinical Trials in Type 2 Diabetes in Canada The final version of the Health Canada guidance
September 24, 2007 NOTICE Our file number: 07-122151-509 Release of final Health Canada document: Standards for Clinical Trials in Type 2 Diabetes in Canada The final version of the Health Canada guidance
Copyright 2017 by Sea Courses Inc.
 Pre-Diabetes: Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic, or mechanical,
Pre-Diabetes: Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic, or mechanical,
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy
 Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
Canadian Diabetes Association 2013
 Spring 2014 Canadian Diabetes Association 2013 clinical practice guidelines - Do claims data align to the guidelines? Canadian Diabetes Association 2013 clinical practice guidelines - Do claims data align
Spring 2014 Canadian Diabetes Association 2013 clinical practice guidelines - Do claims data align to the guidelines? Canadian Diabetes Association 2013 clinical practice guidelines - Do claims data align
Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus. Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre
 Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre Outline How big is the problem? Natural progression of type 2 diabetes What
Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre Outline How big is the problem? Natural progression of type 2 diabetes What
Eugene Barrett M.D., Ph.D. University of Virginia 6/18/2007. Diagnosis and what is it Glucose Tolerance Categories FPG
 Diabetes Mellitus: Update 7 What is the unifying basis of this vascular disease? Eugene J. Barrett, MD, PhD Professor of Internal Medicine and Pediatrics Director, Diabetes Center and GCRC Health System
Diabetes Mellitus: Update 7 What is the unifying basis of this vascular disease? Eugene J. Barrett, MD, PhD Professor of Internal Medicine and Pediatrics Director, Diabetes Center and GCRC Health System
Diabetes Mellitus: Implications of New Clinical Trials and New Medications
 Diabetes Mellitus: Implications of New Clinical Trials and New Medications Estimates of Diagnosed Diabetes in Adults, 2005 Alka M. Kanaya, MD Asst. Professor of Medicine UCSF, Primary Care CME October
Diabetes Mellitus: Implications of New Clinical Trials and New Medications Estimates of Diagnosed Diabetes in Adults, 2005 Alka M. Kanaya, MD Asst. Professor of Medicine UCSF, Primary Care CME October
Metabolic Karma. - Essential Solution in Type2 DM - Eun Gyoung Hong, M.D., Ph.D
 2014 ICDM Breakfast Symposium. Oct 18, 2014 Grand Hilton, Seoul Metabolic Karma - Essential Solution in Type2 DM - Eun Gyoung Hong, M.D., Ph.D Department of Endocrinology and Metabolism, Hallym University
2014 ICDM Breakfast Symposium. Oct 18, 2014 Grand Hilton, Seoul Metabolic Karma - Essential Solution in Type2 DM - Eun Gyoung Hong, M.D., Ph.D Department of Endocrinology and Metabolism, Hallym University
Hanyang University Guri Hospital Chang Beom Lee
 Hanyang University Guri Hospital Chang Beom Lee Meal prayer, Van Brekelenkam 17 th C Introduction 2012 ADA/EASD Position Statement Proper Patients for Pioglitazone β-cell Preservation by Pioglitazone Benefit
Hanyang University Guri Hospital Chang Beom Lee Meal prayer, Van Brekelenkam 17 th C Introduction 2012 ADA/EASD Position Statement Proper Patients for Pioglitazone β-cell Preservation by Pioglitazone Benefit
Diabetes Mellitus Type 2 Evidence-Based Drivers
 This module is supported by an unrestricted educational grant by Aventis Pharmaceuticals Education Center. Copyright 2003 1 Diabetes Mellitus Type 2 Evidence-Based Drivers Driver One: Reducing blood glucose
This module is supported by an unrestricted educational grant by Aventis Pharmaceuticals Education Center. Copyright 2003 1 Diabetes Mellitus Type 2 Evidence-Based Drivers Driver One: Reducing blood glucose
Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone
 Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care
 Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
Early treatment for patients with Type 2 Diabetes
 Israel Society of Internal Medicine Kibutz Hagoshrim, June 22, 2012 Early treatment for patients with Type 2 Diabetes Eduard Montanya Hospital Universitari Bellvitge-IDIBELL CIBERDEM University of Barcelona
Israel Society of Internal Medicine Kibutz Hagoshrim, June 22, 2012 Early treatment for patients with Type 2 Diabetes Eduard Montanya Hospital Universitari Bellvitge-IDIBELL CIBERDEM University of Barcelona
Non-insulin treatment in Type 1 DM Sang Yong Kim
 Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
DIABETES IN 2007 What snew
 DIABETES IN 2007 What snew 1 Objectives 1. Review recently published clinical trials in diabetes What does this mean to us? 1. Discuss novel concepts in the treatment of diabetes What should we expect?
DIABETES IN 2007 What snew 1 Objectives 1. Review recently published clinical trials in diabetes What does this mean to us? 1. Discuss novel concepts in the treatment of diabetes What should we expect?
A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes
 A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Hypotheses: Among individuals with type 2 diabetes, the risks of major microvascular
A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Hypotheses: Among individuals with type 2 diabetes, the risks of major microvascular
The New Diabetes Standard of Care: More Than Just Glycemic Control. Copyright
 CLINICAL Viewpoint The New Diabetes Standard of Care: More Than Just Glycemic Control Advancement in Diabetes Management: A Canadian Diabetes Steering Committee Report Copyright Not for Sale or Commercial
CLINICAL Viewpoint The New Diabetes Standard of Care: More Than Just Glycemic Control Advancement in Diabetes Management: A Canadian Diabetes Steering Committee Report Copyright Not for Sale or Commercial
Rosiglitazone in Canada: experience in clinical practice
 Drug Evaluation Rosiglitazone in Canada: experience in clinical practice 1. Introduction 2. Materials and methods 3. Conclusion and discussion 4. Expert opinion Beata Patasi, Deborah MacNair, Ryan J Marble
Drug Evaluation Rosiglitazone in Canada: experience in clinical practice 1. Introduction 2. Materials and methods 3. Conclusion and discussion 4. Expert opinion Beata Patasi, Deborah MacNair, Ryan J Marble
CME/CE QUIZ CME/CE QUESTIONS
 CME/CE QUIZ CME/CE QUESTIONS Continuing Medical Education Accreditation The University of Cincinnati College of Medicine designates this educational activity for a maximum of two (2) AMA PRA Category 1
CME/CE QUIZ CME/CE QUESTIONS Continuing Medical Education Accreditation The University of Cincinnati College of Medicine designates this educational activity for a maximum of two (2) AMA PRA Category 1
National Horizon Scanning Centre. Saxagliptin (BMS ) for type 2 diabetes. April 2008
 Saxagliptin (BMS 477118) for type 2 diabetes This technology summary is based on information available at the time of research and a limited literature search. It is not intended to be a definitive statement
Saxagliptin (BMS 477118) for type 2 diabetes This technology summary is based on information available at the time of research and a limited literature search. It is not intended to be a definitive statement
Type 2 Diabetes Mellitus 2011
 2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
The Many Faces of T2DM in Long-term Care Facilities
 The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
Sulfoniluree e glinidi: pro e contro
 Sulfoniluree e glinidi: pro e contro Giorgio Sesti Università Magna Graecia di Catanzaro ITALY T2DM anti-hyperglycaemic therapy: general recommendations Diabetes Care 35:1364-1379, 2012; Diabetologia 55:1577-1596,
Sulfoniluree e glinidi: pro e contro Giorgio Sesti Università Magna Graecia di Catanzaro ITALY T2DM anti-hyperglycaemic therapy: general recommendations Diabetes Care 35:1364-1379, 2012; Diabetologia 55:1577-1596,
GLP 1 agonists Winning the Losing Battle. Dr Bernard SAMIA. KCS Congress: Impact through collaboration
 GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
Comparative Effectiveness and Safety of Diabetes Medications for Adults with Type 2 Diabetes
 Draft Comparative Effectiveness Review Comparative Effectiveness and Safety of Diabetes Medications for Adults with Type Diabetes Prepared for: Agency for Healthcare Research and Quality U.S. Department
Draft Comparative Effectiveness Review Comparative Effectiveness and Safety of Diabetes Medications for Adults with Type Diabetes Prepared for: Agency for Healthcare Research and Quality U.S. Department
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS
 IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
Current Diabetes Care for Internists:2011
 Current Diabetes Care for Internists:2011 Petch Rawdaree, DM, MSc, DLSHTM Faculty of Medicine Vajira Hospital University of Bangkok Metropolis 19 th January 2011 ก ก 1. ก ก ก ก 2. ก ก ก ก ก 3. ก ก ก ก
Current Diabetes Care for Internists:2011 Petch Rawdaree, DM, MSc, DLSHTM Faculty of Medicine Vajira Hospital University of Bangkok Metropolis 19 th January 2011 ก ก 1. ก ก ก ก 2. ก ก ก ก ก 3. ก ก ก ก
COMMISSIONING POLICY RECOMMENDATION TREATMENT ADVISORY GROUP Policy agreed by (Vale of York CCG/date)
 Drug, Treatment, Device name ( Vipidia; Takeda) COMMISSIONING POLICY RECOMMENDATION TREATMENT ADVISORY GROUP Policy agreed by (Vale of York CCG/date) Licensed indication To improve glycaemic control in
Drug, Treatment, Device name ( Vipidia; Takeda) COMMISSIONING POLICY RECOMMENDATION TREATMENT ADVISORY GROUP Policy agreed by (Vale of York CCG/date) Licensed indication To improve glycaemic control in
Long-Term Care Updates
 Long-Term Care Updates January 2019 By Kristina Nikl, PharmD Several recent studies evaluating the management of diabetes in older adults have concluded that 25-52% of elderly patients are currently being
Long-Term Care Updates January 2019 By Kristina Nikl, PharmD Several recent studies evaluating the management of diabetes in older adults have concluded that 25-52% of elderly patients are currently being
Insulin Intensification: A Patient-Centered Approach
 MARTIN J. ABRAHAMSON, MD Harvard Medical School, Boston, MA Insulin Intensification: A Patient-Centered Approach Dr Abrahamson is associate professor of medicine at Harvard Medical School and medical director
MARTIN J. ABRAHAMSON, MD Harvard Medical School, Boston, MA Insulin Intensification: A Patient-Centered Approach Dr Abrahamson is associate professor of medicine at Harvard Medical School and medical director
Why Do We Care About Prediabetes?
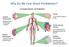 Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
DICE Study Backgrounder
 DICE Study Backgrounder Diabetes In Canada Evaluation (DICE), the largest diabetes study of its kind in Canada, examines the management and control of type 2 diabetes in the Canadian family practice setting.
DICE Study Backgrounder Diabetes In Canada Evaluation (DICE), the largest diabetes study of its kind in Canada, examines the management and control of type 2 diabetes in the Canadian family practice setting.
LATE BREAKING STUDIES IN DM AND CAD. Will this change the guidelines?
 LATE BREAKING STUDIES IN DM AND CAD Will this change the guidelines? Objectives 1. Discuss current guidelines for prevention of CHD in diabetes. 2. Discuss the FDA Guidance for Industry regarding evaluating
LATE BREAKING STUDIES IN DM AND CAD Will this change the guidelines? Objectives 1. Discuss current guidelines for prevention of CHD in diabetes. 2. Discuss the FDA Guidance for Industry regarding evaluating
Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes!
 Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Jaini Patel, PharmD, BCACP Assistant Professor of Pharmacy Practice Midwestern University Chicago College of Pharmacy Kathleen
Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Jaini Patel, PharmD, BCACP Assistant Professor of Pharmacy Practice Midwestern University Chicago College of Pharmacy Kathleen
Effective Health Care
 Number 8 Effective Health Care Comparative Effectiveness and Safety of Oral Diabetes Medications for Adults With Type 2 Diabetes Executive Summary Background Type 2 diabetes is characterized by insulin
Number 8 Effective Health Care Comparative Effectiveness and Safety of Oral Diabetes Medications for Adults With Type 2 Diabetes Executive Summary Background Type 2 diabetes is characterized by insulin
Metabolic Syndrome Update The Metabolic Syndrome: Overview. Global Cardiometabolic Risk
 Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
Old oral antidiabetic agents in the armamentarium of diabetes mellitus treatment: Safety and efficacy
 Old oral antidiabetic agents in the armamentarium of diabetes mellitus treatment: Safety and efficacy Melpomeni Peppa Assistant Professor of Endocrinology 2 nd Dept of Internal Medicine-Propaedeutic, Athens
Old oral antidiabetic agents in the armamentarium of diabetes mellitus treatment: Safety and efficacy Melpomeni Peppa Assistant Professor of Endocrinology 2 nd Dept of Internal Medicine-Propaedeutic, Athens
Age-adjusted Percentage of U.S. Adults Who Were Obese or Who Had Diagnosed Diabetes
 Age-adjusted Percentage of U.S. Adults Who Were Obese or Who Had Diagnosed Diabetes Obesity (BMI 30 kg/m 2 ) 1994 2000 2009 No Data 26.0% Diabetes 1994 2000 2009
Age-adjusted Percentage of U.S. Adults Who Were Obese or Who Had Diagnosed Diabetes Obesity (BMI 30 kg/m 2 ) 1994 2000 2009 No Data 26.0% Diabetes 1994 2000 2009
A Call to Action: Addressing Diabetes Medication Safety
 A Call to Action: Addressing Diabetes Medication Safety Evan M. Klass, M.D., F.A.C.P. Senior Associate Dean, Statewide Initiatives Reducing ED visits for insulin induced hypoglycemia is a Healthy People
A Call to Action: Addressing Diabetes Medication Safety Evan M. Klass, M.D., F.A.C.P. Senior Associate Dean, Statewide Initiatives Reducing ED visits for insulin induced hypoglycemia is a Healthy People
Comprehensive Diabetes Treatment
 Comprehensive Diabetes Treatment Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism The George Washington University School of Medicine Diabetes
Comprehensive Diabetes Treatment Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism The George Washington University School of Medicine Diabetes
Insulin Delivery and Glucose Monitoring Methods for Diabetes Mellitus: Comparative Effectiveness
 Insulin Delivery and Glucose Monitoring Methods for Diabetes Mellitus: Comparative Effectiveness Prepared for: Agency for Healthcare Research and Quality (AHRQ) www.ahrq.gov Outline of Material Introduction
Insulin Delivery and Glucose Monitoring Methods for Diabetes Mellitus: Comparative Effectiveness Prepared for: Agency for Healthcare Research and Quality (AHRQ) www.ahrq.gov Outline of Material Introduction
Prediabetes Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Disclosures/Conflict of Interest.
 Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Jaini Patel, PharmD, BCACP Assistant Professor of Pharmacy Practice Midwestern University Chicago College of Pharmacy Kathleen
Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Jaini Patel, PharmD, BCACP Assistant Professor of Pharmacy Practice Midwestern University Chicago College of Pharmacy Kathleen
The Burden of the Diabetic Heart
 The Burden of the Diabetic Heart Dr. Ghaida Kaddaha (MBBS, MRCP-UK, FRCP-london) Diabetes Unit Rashid Hospital Dubai U.A.E Risk of CVD in Diabetes Morbidity and mortality from CVD is 2-4 fold higher than
The Burden of the Diabetic Heart Dr. Ghaida Kaddaha (MBBS, MRCP-UK, FRCP-london) Diabetes Unit Rashid Hospital Dubai U.A.E Risk of CVD in Diabetes Morbidity and mortality from CVD is 2-4 fold higher than
DIABETES DEBATE - IS NEW BETTER?
 DIABETES DEBATE - IS NEW BETTER? WHAT MEDICATION CLASS AFTER METFORMIN TO CONTROL BLOOD SUGAR Dr. Lydia Hatcher, MD, CCFP, FCFP, CHE, D-CAPM Associate Clinical Professor of Family Medicine, McMaster Chief
DIABETES DEBATE - IS NEW BETTER? WHAT MEDICATION CLASS AFTER METFORMIN TO CONTROL BLOOD SUGAR Dr. Lydia Hatcher, MD, CCFP, FCFP, CHE, D-CAPM Associate Clinical Professor of Family Medicine, McMaster Chief
IDF Regions and global projections of the number of people with diabetes (20-79 years), 2013 and Diabetes Atlas -sixth Edition: IDF 2013
 IDF Regions and global projections of the number of people with diabetes (20-79 years), 2013 and 2035 Diabetes Atlas -sixth Edition: IDF 2013 Diabetes Atlas -sixth Edition: IDF 2013 Chronic complications
IDF Regions and global projections of the number of people with diabetes (20-79 years), 2013 and 2035 Diabetes Atlas -sixth Edition: IDF 2013 Diabetes Atlas -sixth Edition: IDF 2013 Chronic complications
Management of Type 2 Diabetes
 Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Glycemic control a matter of life and death
 Glycemic control a matter of life and death Linda Garcia Mellbin MD PhD Specialist in Cardiology & Internal medicine Dep of Cardiology Karolinska University Hospital /Karolinska Institutet Mortality (%)
Glycemic control a matter of life and death Linda Garcia Mellbin MD PhD Specialist in Cardiology & Internal medicine Dep of Cardiology Karolinska University Hospital /Karolinska Institutet Mortality (%)
CADTH Optimal use report
 Canadian Agency for Drugs and Technologies in Health Agence canadienne des médicaments et des technologies de la santé CADTH Optimal use report Volume 3, Issue 1D July 2013 Optimal Use Recommendations
Canadian Agency for Drugs and Technologies in Health Agence canadienne des médicaments et des technologies de la santé CADTH Optimal use report Volume 3, Issue 1D July 2013 Optimal Use Recommendations
Primary Prevention of T2DM. KW Chan Endocrine & Diabetes Team Department of M&G, PMH 22 March 2009
 Primary Prevention of T2DM KW Chan Endocrine & Diabetes Team Department of M&G, PMH 22 March 2009 Primary Prevention of T2DM Why to intervene? When to intervene? Lifestyle intervention Pharmacological
Primary Prevention of T2DM KW Chan Endocrine & Diabetes Team Department of M&G, PMH 22 March 2009 Primary Prevention of T2DM Why to intervene? When to intervene? Lifestyle intervention Pharmacological
Efficacy and Safety of Initial Combination Therapy in Treatment-Naïve Type 2 Diabetes Patients: A Systematic Review and Meta-analysis
 Diabetes Ther (2018) 9:1995 2014 https://doi.org/10.1007/s13300-018-0493-2 ORIGINAL RESEARCH Efficacy and Safety of Initial Combination Therapy in Treatment-Naïve Type 2 Diabetes Patients: A Systematic
Diabetes Ther (2018) 9:1995 2014 https://doi.org/10.1007/s13300-018-0493-2 ORIGINAL RESEARCH Efficacy and Safety of Initial Combination Therapy in Treatment-Naïve Type 2 Diabetes Patients: A Systematic
Diabetes 2013: Achieving Goals Through Comprehensive Treatment. Session 2: Individualizing Therapy
 Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Comparative Effectiveness, Safety, and Indications of Insulin Analogues in Premixed Formulations for Adults With Type 2 Diabetes Executive Summary
 Number 14 Effective Health Care Comparative Effectiveness, Safety, and Indications of Insulin Analogues in Premixed Formulations for Adults With Type 2 Diabetes Executive Summary Background and Key Questions
Number 14 Effective Health Care Comparative Effectiveness, Safety, and Indications of Insulin Analogues in Premixed Formulations for Adults With Type 2 Diabetes Executive Summary Background and Key Questions
Management of Type 2 Diabetes. Why Do We Bother to Achieve Good Control in DM2. Insulin Secretion. The Importance of BP and Glucose Control
 Insulin Secretion Management of Type 2 Diabetes DG van Zyl Why Do We Bother to Achieve Good Control in DM2 % reduction 0-5 -10-15 -20-25 -30-35 -40 The Importance of BP and Glucose Control Effects of tight
Insulin Secretion Management of Type 2 Diabetes DG van Zyl Why Do We Bother to Achieve Good Control in DM2 % reduction 0-5 -10-15 -20-25 -30-35 -40 The Importance of BP and Glucose Control Effects of tight
GUIDELINES FOR DYSLIPIDEMIA MANAGEMENT AND EDUCATION THROUGH NOVA SCOTIA DIABETES CENTRES
 GUIDELINES FOR DYSLIPIDEMIA MANAGEMENT AND EDUCATION THROUGH NOVA SCOTIA DIABETES CENTRES Prepared by DCPNS Action Committee Dr. Lynne Harrigan Brenda Cook Peggy Dunbar Bev Harpell with the assistance
GUIDELINES FOR DYSLIPIDEMIA MANAGEMENT AND EDUCATION THROUGH NOVA SCOTIA DIABETES CENTRES Prepared by DCPNS Action Committee Dr. Lynne Harrigan Brenda Cook Peggy Dunbar Bev Harpell with the assistance
1/28/2014. The Metabolic Syndrome: Early History. Insulin Resistance: Early Diagnosis and Treatment to Prevent Cardiovascular Disease
 : Early Diagnosis and Treatment to Prevent Cardiovascular Disease Henry N. Ginsberg, M.D. Irving Professor of Medicine Columbia University College of Physicans and Surgeons The Metabolic Syndrome: Early
: Early Diagnosis and Treatment to Prevent Cardiovascular Disease Henry N. Ginsberg, M.D. Irving Professor of Medicine Columbia University College of Physicans and Surgeons The Metabolic Syndrome: Early
How to Reduce CVD Complications in Diabetes?
 How to Reduce CVD Complications in Diabetes? Chaicharn Deerochanawong M.D. Diabetes and Endocrinology Unit Department of Medicine Rajavithi Hospital, Ministry of Public Health Framingham Heart Study 30-Year
How to Reduce CVD Complications in Diabetes? Chaicharn Deerochanawong M.D. Diabetes and Endocrinology Unit Department of Medicine Rajavithi Hospital, Ministry of Public Health Framingham Heart Study 30-Year
Metformin should be considered in all patients with type 2 diabetes unless contra-indicated
 November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Scottish Medicines Consortium
 Scottish Medicines Consortium liraglutide 6mg/mL prefilled pen for injection (3mL) (Victoza ) Novo Nordisk Ltd. No. (585/09) 06 November 2009 The Scottish Medicines Consortium (SMC) has completed its assessment
Scottish Medicines Consortium liraglutide 6mg/mL prefilled pen for injection (3mL) (Victoza ) Novo Nordisk Ltd. No. (585/09) 06 November 2009 The Scottish Medicines Consortium (SMC) has completed its assessment
Contents. I. CV disease and insulin resistance: Challenges and opportunities. II. Insulin sensitizers: Surrogate and clinical outcomes studies
 Contents I. CV disease and insulin resistance: Challenges and opportunities II. Insulin sensitizers: Surrogate and clinical outcomes studies IV. Identifying and treating patients with insulin resistance
Contents I. CV disease and insulin resistance: Challenges and opportunities II. Insulin sensitizers: Surrogate and clinical outcomes studies IV. Identifying and treating patients with insulin resistance
Mae Sheikh-Ali, M.D. Assistant Professor of Medicine Division of Endocrinology University of Florida College of Medicine- Jacksonville
 Mae Sheikh-Ali, M.D. Assistant Professor of Medicine Division of Endocrinology University of Florida College of Medicine- Jacksonville Pathogenesis of Diabetes Mellitus (DM) Criteria for the diagnosis
Mae Sheikh-Ali, M.D. Assistant Professor of Medicine Division of Endocrinology University of Florida College of Medicine- Jacksonville Pathogenesis of Diabetes Mellitus (DM) Criteria for the diagnosis
Multiple Small Feedings of the Mind: Diabetes. Sonja K Fredrickson, MD, BC-ADM March 7, 2014
 Multiple Small Feedings of the Mind: Diabetes Sonja K Fredrickson, MD, BC-ADM March 7, 2014 Question 1: Setting A1c Goals Describe the evidence based approach to determining the target HgbA1c in different
Multiple Small Feedings of the Mind: Diabetes Sonja K Fredrickson, MD, BC-ADM March 7, 2014 Question 1: Setting A1c Goals Describe the evidence based approach to determining the target HgbA1c in different
Diabetes Overview. How Food is Digested
 Diabetes Overview You are The Teacher, The Coach and the Fan Pathophysiology of Diabetes Complications Know the Numbers Treatment Can Good Control Make a Difference? Can Tight Control Be too Tight? How
Diabetes Overview You are The Teacher, The Coach and the Fan Pathophysiology of Diabetes Complications Know the Numbers Treatment Can Good Control Make a Difference? Can Tight Control Be too Tight? How
Type 1 diabetes, although the most common
 ADDRESSING THE 21ST CENTURY DIABETES EPIDEMIC * Based on a presentation by David M. Nathan, MD ABSTRACT Type 2 diabetes is an epidemic disorder. Although its complications can be treated, prevented, or
ADDRESSING THE 21ST CENTURY DIABETES EPIDEMIC * Based on a presentation by David M. Nathan, MD ABSTRACT Type 2 diabetes is an epidemic disorder. Although its complications can be treated, prevented, or
DIABETES AND METABOLIC SYNDROME
 TRIALS NUMBER OF PARTICIPANTS NUMBER OF WOMEN PERCENTAGE OF WOMEN MEAN AGE MEAN - (YEARS) TRIALS WITH ANALYSIS BY GENDER N, (%) 48,508 20,091 41.4% 61.1 4.3 4/7 (57.1%) HR PROactive (Dormandy et al 61
TRIALS NUMBER OF PARTICIPANTS NUMBER OF WOMEN PERCENTAGE OF WOMEN MEAN AGE MEAN - (YEARS) TRIALS WITH ANALYSIS BY GENDER N, (%) 48,508 20,091 41.4% 61.1 4.3 4/7 (57.1%) HR PROactive (Dormandy et al 61
Discussion points. The cardiometabolic connection. Cardiometabolic Risk Management in the Primary Care Setting
 Session #5 Cardiometabolic Risk Management in the Primary Care Setting Sonja Reichert, MD MSc FCFP FACPM Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE S Discussion points Whom should we be
Session #5 Cardiometabolic Risk Management in the Primary Care Setting Sonja Reichert, MD MSc FCFP FACPM Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE S Discussion points Whom should we be
Quick Reference Guide
 2013 Clinical Practice Guidelines Quick Reference Guide (Updated November 2016) 416569-16 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Copyright 2016 Canadian Diabetes Association SCREENING
2013 Clinical Practice Guidelines Quick Reference Guide (Updated November 2016) 416569-16 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Copyright 2016 Canadian Diabetes Association SCREENING
Sanofi Announces Results of ORIGIN, the World s Longest and Largest Randomised Clinical Trial in Insulin in Pre- and Early Diabetes
 PRESS RELEASE Sanofi Announces Results of ORIGIN, the World s Longest and Largest Randomised Clinical Trial in Insulin in Pre- and Early Diabetes Dublin, Ireland (15 June 2012) Sanofi presented results
PRESS RELEASE Sanofi Announces Results of ORIGIN, the World s Longest and Largest Randomised Clinical Trial in Insulin in Pre- and Early Diabetes Dublin, Ireland (15 June 2012) Sanofi presented results
The Diabetes Link to Heart Disease
 The Diabetes Link to Heart Disease Anthony Abe DeSantis, MD September 18, 2015 University of WA Division of Metabolism, Endocrinology and Nutrition Oswald Toosweet Case #1 68 yo M with T2DM Diagnosed DM
The Diabetes Link to Heart Disease Anthony Abe DeSantis, MD September 18, 2015 University of WA Division of Metabolism, Endocrinology and Nutrition Oswald Toosweet Case #1 68 yo M with T2DM Diagnosed DM
Evidence-Based Glucose Management in Type 2 Diabetes
 Evidence-Based Glucose Management in Type 2 Diabetes James R. Gavin III, MD, PhD CEO and Chief Medical Officer Healing Our Village, Inc. Clinical Professor of Medicine Emory University School of Medicine
Evidence-Based Glucose Management in Type 2 Diabetes James R. Gavin III, MD, PhD CEO and Chief Medical Officer Healing Our Village, Inc. Clinical Professor of Medicine Emory University School of Medicine
3. NEW DIAGNOSTIC CRITERIA, NEW CLASSIFICATION OF DM AND MODERN THERAPY APPROACH
 3. NEW DIAGNOSTIC CRITERIA, NEW CLASSIFICATION OF DM AND MODERN THERAPY APPROACH 1.1 Introduction Ivana Pavlić-Renar, Ph.D. Vuk Vrhovac University Clinic, Zagreb, Croatia The current classification of
3. NEW DIAGNOSTIC CRITERIA, NEW CLASSIFICATION OF DM AND MODERN THERAPY APPROACH 1.1 Introduction Ivana Pavlić-Renar, Ph.D. Vuk Vrhovac University Clinic, Zagreb, Croatia The current classification of
Pre-diabetes. Pharmacological Approaches to Delay Progression to Diabetes
 Pre-diabetes Pharmacological Approaches to Delay Progression to Diabetes Overview Definition of Pre-diabetes Risk Factors for Pre-diabetes Clinical practice guidelines for diabetes Management, including
Pre-diabetes Pharmacological Approaches to Delay Progression to Diabetes Overview Definition of Pre-diabetes Risk Factors for Pre-diabetes Clinical practice guidelines for diabetes Management, including
Cardiovascular Management of a Patient with Diabetes
 Cardiovascular Management of a Patient with Diabetes Dr Jeremy Krebs Clinical Leader Endocrinology and Diabetes Wellington Hospital Summary People with diabetes take a lot of medication Compliance and
Cardiovascular Management of a Patient with Diabetes Dr Jeremy Krebs Clinical Leader Endocrinology and Diabetes Wellington Hospital Summary People with diabetes take a lot of medication Compliance and
Why is Earlier and More Aggressive Treatment of T2 Diabetes Better?
 Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
MOA: Long acting glucagon-like peptide 1 receptor agonist
 Alexandria Rydz MOA: Long acting glucagon-like peptide 1 receptor agonist Increases glucose dependent insulin secretion Decreases inappropriate glucagon secretion Increases β- cell growth and replication
Alexandria Rydz MOA: Long acting glucagon-like peptide 1 receptor agonist Increases glucose dependent insulin secretion Decreases inappropriate glucagon secretion Increases β- cell growth and replication
Microvascular Complications in Diabetes:
 Microvascular Complications in Diabetes: Perspectives on Glycemic Control to Prevent Microvascular Complications Discussion Outline: Glycemia and Microvascular Compliations Clinical Trials - A Brief History
Microvascular Complications in Diabetes: Perspectives on Glycemic Control to Prevent Microvascular Complications Discussion Outline: Glycemia and Microvascular Compliations Clinical Trials - A Brief History
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE. CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010
 Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Keywords Cardiovascular diseases. Diabetes. Diabetic nephropathy. Dysglycaemia. Renal. Risk
 Diabetologia (005) 48: 749 755 DOI 0.007/s005-005-858-4 ARTICLE H. C. Gerstein. J. Pogue. J. F. E. Mann. E. Lonn. G. R. Dagenais. M. McQueen. S. Yusuf. HOPE investigators The relationship between dysglycaemia
Diabetologia (005) 48: 749 755 DOI 0.007/s005-005-858-4 ARTICLE H. C. Gerstein. J. Pogue. J. F. E. Mann. E. Lonn. G. R. Dagenais. M. McQueen. S. Yusuf. HOPE investigators The relationship between dysglycaemia
Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes
 Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes Geneva Clark Briggs, PharmD, BCPS Adjunct Professor at University of Appalachia College of Pharmacy Clinical Associate, Medical
Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes Geneva Clark Briggs, PharmD, BCPS Adjunct Professor at University of Appalachia College of Pharmacy Clinical Associate, Medical
T2DM is a global epidemic with
 : a new option for the management of type 2 diabetes Marc Evans MRCP, MD, Consultant Diabetologist, Llandough Hospital, Cardiff Incretin-based therapies for the treatment of diabetes mellitus (T2DM) present
: a new option for the management of type 2 diabetes Marc Evans MRCP, MD, Consultant Diabetologist, Llandough Hospital, Cardiff Incretin-based therapies for the treatment of diabetes mellitus (T2DM) present
Diabetes Treatment Update
 Diabetes Treatment Update Timothy C. Evans, MD PhD FACP University of Washington Department of Medicine Disclosure: Dr. Evans has no significant financial interest in any of the products or manufacturers
Diabetes Treatment Update Timothy C. Evans, MD PhD FACP University of Washington Department of Medicine Disclosure: Dr. Evans has no significant financial interest in any of the products or manufacturers
Choice of monotherapy in newly diagnosed Type 2 diabetic patients: clinical perspective of ADOPT
 CLINICAL TRIAL REPORT Choice of monotherapy in newly diagnosed Type 2 diabetic patients: clinical perspective of ADOPT Janaka Karalliedde & Robin E Buckingham Author for correspondence King s College &
CLINICAL TRIAL REPORT Choice of monotherapy in newly diagnosed Type 2 diabetic patients: clinical perspective of ADOPT Janaka Karalliedde & Robin E Buckingham Author for correspondence King s College &
Welcome and Introduction
 Welcome and Introduction This presentation will: Define obesity, prediabetes, and diabetes Discuss the diagnoses and management of obesity, prediabetes, and diabetes Explain the early risk factors for
Welcome and Introduction This presentation will: Define obesity, prediabetes, and diabetes Discuss the diagnoses and management of obesity, prediabetes, and diabetes Explain the early risk factors for
Moving to an A1C-Based Screening & Diagnosis of Diabetes. By Prof.M.Assy Diabetes&Endocrinology unit
 Moving to an A1C-Based Screening & Diagnosis of Diabetes By Prof.M.Assy Diabetes&Endocrinology unit is the nonenzymatic glycated product of the hemoglobin beta-chain at the valine terminal residue. Clin
Moving to an A1C-Based Screening & Diagnosis of Diabetes By Prof.M.Assy Diabetes&Endocrinology unit is the nonenzymatic glycated product of the hemoglobin beta-chain at the valine terminal residue. Clin
Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Diabetes sections of the Guidelines)
 Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Diabetes sections of the Guidelines) Authors: Dr. M. Love, Kathy Harrigan Reviewers:
Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Diabetes sections of the Guidelines) Authors: Dr. M. Love, Kathy Harrigan Reviewers:
Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study
 Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study Laura F. DeFina, MD,* Gloria Lena Vega, PhD,Þ David Leonard, PhD,Þ and Scott M. Grundy,
Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study Laura F. DeFina, MD,* Gloria Lena Vega, PhD,Þ David Leonard, PhD,Þ and Scott M. Grundy,
Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications
 Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications Nathan Woolever, Pharm.D., Resident Pharmacist Pharmacy Grand Rounds November 6 th, 2018 Franciscan Healthcare La Crosse, WI 2017
Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications Nathan Woolever, Pharm.D., Resident Pharmacist Pharmacy Grand Rounds November 6 th, 2018 Franciscan Healthcare La Crosse, WI 2017
Diabetes: Definition Pathophysiology Treatment Goals. By Scott Magee, MD, FACE
 Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
INSIGHT INTO MANAGING AND TREATING TYPE 2 DIABETES ISRAEL HARTMAN MD FACE
 INSIGHT INTO MANAGING AND TREATING TYPE 2 DIABETES ISRAEL HARTMAN MD FACE Type 2 Diabetes Mellitus (T2DM) Is an Epidemic The Centers for Disease Control and Prevention statistics from 2007 estimated that
INSIGHT INTO MANAGING AND TREATING TYPE 2 DIABETES ISRAEL HARTMAN MD FACE Type 2 Diabetes Mellitus (T2DM) Is an Epidemic The Centers for Disease Control and Prevention statistics from 2007 estimated that
Glycemic control A combination of life style interaction and the use of drugs
 Multifactorial management to reduce cardiovascular risk in patients with diabetes mellitus Glycemic control A combination of life style interaction and the use of drugs Eberhard Standl Munich Diabetes
Multifactorial management to reduce cardiovascular risk in patients with diabetes mellitus Glycemic control A combination of life style interaction and the use of drugs Eberhard Standl Munich Diabetes
Barriers to Achieving A1C Targets: Clinical Inertia and Hypoglycemia. KM Pantalone Endocrinology
 Barriers to Achieving A1C Targets: Clinical Inertia and Hypoglycemia KM Pantalone Endocrinology Disclosures Speaker Bureau AstraZeneca, Merck, Novo Nordisk, Sanofi Consultant Novo Nordisk, Eli Lilly, Merck
Barriers to Achieving A1C Targets: Clinical Inertia and Hypoglycemia KM Pantalone Endocrinology Disclosures Speaker Bureau AstraZeneca, Merck, Novo Nordisk, Sanofi Consultant Novo Nordisk, Eli Lilly, Merck
Practical Diabetes. Nic Crook. (and don t use so many charts) Kuirau Specialists 1239 Ranolf Street Rotorua. Rotorua Hospital Private Bag 3023 Rotorua
 Practical Diabetes (and don t use so many charts) Nic Crook Rotorua Hospital Private Bag 3023 Rotorua Kuirau Specialists 1239 Ranolf Street Rotorua Worldwide rates of diabetes mellitus: predictions 80
Practical Diabetes (and don t use so many charts) Nic Crook Rotorua Hospital Private Bag 3023 Rotorua Kuirau Specialists 1239 Ranolf Street Rotorua Worldwide rates of diabetes mellitus: predictions 80
Managing Diabetes for Improved Health and Economic Outcomes
 Managing Diabetes for Improved Health and Economic Outcomes Based on a presentation by David McCulloch, MD Presentation Summary The contribution of postprandial glucose to diabetes progression and diabetes-related
Managing Diabetes for Improved Health and Economic Outcomes Based on a presentation by David McCulloch, MD Presentation Summary The contribution of postprandial glucose to diabetes progression and diabetes-related
Obesity Management in Patients with Diabetes Jamy D. Ard, MD Sunday, February 11, :15 a.m. 11:00 a.m.
 Obesity Management in Patients with Diabetes Jamy D. Ard, MD Sunday, February 11, 2018 10:15 a.m. 11:00 a.m. Type 2 diabetes mellitus (T2DM) is closely associated with obesity, primarily through the link
Obesity Management in Patients with Diabetes Jamy D. Ard, MD Sunday, February 11, 2018 10:15 a.m. 11:00 a.m. Type 2 diabetes mellitus (T2DM) is closely associated with obesity, primarily through the link
Impaired Glucose Tolerance
 Page 1 of 6 Impaired Glucose Tolerance If you have impaired glucose tolerance, your blood glucose is raised beyond the normal range but it is not so high that you have diabetes. However, if you have impaired
Page 1 of 6 Impaired Glucose Tolerance If you have impaired glucose tolerance, your blood glucose is raised beyond the normal range but it is not so high that you have diabetes. However, if you have impaired
Diabete: terapia nei pazienti a rischio cardiovascolare
 Diabete: terapia nei pazienti a rischio cardiovascolare Giorgio Sesti Università Magna Graecia di Catanzaro Cardiovascular mortality in relation to diabetes mellitus and a prior MI: A Danish Population
Diabete: terapia nei pazienti a rischio cardiovascolare Giorgio Sesti Università Magna Graecia di Catanzaro Cardiovascular mortality in relation to diabetes mellitus and a prior MI: A Danish Population
