A Study of Patient Experience Using a Blood Glucose Meter With an In-Built Insulin Dose Calculator
|
|
|
- Tyrone Weaver
- 5 years ago
- Views:
Transcription
1 532489DSTXXX / Journal of Diabetes Science and TechnologyRamtoola et al research-article2014 Original Article A Study of Patient Experience Using a Blood Glucose Meter With an In-Built Insulin Dose Calculator Journal of Diabetes Science and Technology 2014, Vol. 8(4) Diabetes Technology Society Reprints and permissions: sagepub.com/journalspermissions.nav DOI: / dst.sagepub.com Shenaz Ramtoola, MD 1, Edward Jude, MD 2, Anthony Robinson, DM 3, Iqbal Malik, MD 4, Gerrard Rayman, MD 5, Cuong Dang, MD 6, Graham David RossMartin, MB ChB 7, and Amar Ali, MB ChB 1 Abstract Background: Accurate calculation and adjustment of insulin doses is integral to maintaining glycemic control in insulin treated patients. Difficulties with insulin dose calculations may lead to poor adherence to blood glucose monitoring and insulin treatment regimes, resulting in poor metabolic control. The main objective of this study was to evaluate ease of use and user preference of a high specification touch screen blood glucose meter, which has an in-built insulin calculator, compared to patients usual method of testing blood glucose and deciding insulin doses. Methods: Patients with diabetes on a multiple daily injection insulin regime used the Test Meter without the insulin calculator and 1 of 3 comparator meters, each for a 7-day period. They then used the Test Meter with the in-built calculator for 10 days. Patients completed an ease of use questionnaire after each 7-day period, a preference questionnaire after the second 7-day period, and a questionnaire comparing the Test Meter with their usual method after the final 10-day period. Results: Of 164 patients who completed the study, 76% stated a preference for the Test Meter as a diabetes management tool compared to their usual method. A small number of patients preferred familiar methods and/or calculating insulin doses themselves. The log book function of meters was important to most patients. Conclusions: The Test Meter system with in-built insulin calculator supports people to better manage their diabetes and increases their confidence. Patients have different needs and preferences which should be acknowledged and supported in a patient centered health service. Keywords blood glucose meter, bolus calculator, diabetes, insulin Patient self-management through blood glucose monitoring and accurate calculation and adjustment of insulin doses is integral to glycemic control in patients with insulin treated diabetes. This is a challenge for many patients as multiple variables need to be considered. There is evidence in adolescents suggesting that poor compliance with insulin regimes due to a lack of understanding of and/or frustration with the complexity of insulin dose calculations may contribute to poor metabolic control. 1 A recent study of patients with type 2 diabetes (T2D) showed that many lack the understanding and skills to apply selfmonitoring data to aid therapy adjustments. 2 High avoidance (avoiding thinking about blood glucose values and diabetes) and a sense of pointlessness of self-monitoring were associated with infrequent self-monitoring and use of self-monitoring data for insulin dose adjustments, and lack of sharing data with health care professionals. The authors suggested that if patients were guided in seeing the value of self-monitoring blood glucose it could improve adherence to self-monitoring. A blood glucose meter (BGM) which is easy to use with features to assist patients with dose calculations may promote increased frequency of glucose testing and improved diabetes self-management. The FreeStyle InsuLinx BGM 1 Royal Blackburn Hospital, Blackburn, UK 2 Tameside Hospital NHS Foundation Trust, Ashton-under-Lyne, UK 3 Royal United Hospital, Bath, UK 4 Ayr Hospital, Ayr, UK 5 Ipswich Hospital, Ipswich, UK 6 University of Salford Diabetes Centre, North Manchester General Hospital, Manchester, UK 7 Greenwood Medical Centre, Nottingham, UK Corresponding Author: Shenaz Ramtoola, MD, Consultant Physician, Royal Blackburn Hospital, Haslingden Road, Blackburn, BB2 3HH, UK. Shenaz.Ramtoola@elht.nhs.uk
2 Ramtoola et al 777 Group 1 Comparator BGM InsuLinx BG Mode only InsuLinx with Insulin Calculator (10 days) Group 2 InsuLinx BG Mode only Comparator BGM Day User Questionnaire #1 User Questionnaire #2 & Preference Questionnaire Preference Questionnaire InsuLinx v Usual Method Figure 1. Study design. contains an in-built bolus insulin dose calculator. Insulin, medication doses, food intake, physical activity, and health information can be logged. In easy mode the meter suggests the insulin dose based on a usual prescribed meal dose, current and target glucose levels. In advanced mode carbohydrate intake and insulin-to-carbohydrate ratios are also taken into account. The main objective of this study was to evaluate ease of use and user preference of this meter compared to patients usual method of testing blood glucose and deciding insulin doses. A secondary objective was to compare the ease of use of the meter with other leading BGMs. Patients and Methods This was a randomized, 2-arm, cross-over study conducted at 7 sites in the United Kingdom from September 2011 to April The clinical protocol Ease of Use of New BGM with In-Built Insulin Calculator at Home Study (ADC-PMS- INX-11011) was approved by the National Research Ethics Committee. The study was registered on ClinicalTrials.gov (NCT ). Study Participants Eligible patients were adults with type 1 diabetes (T1D) or T2D on a multiple daily injection (MDI) insulin regime (insulin adjusting) for at least 6 months, regularly doing 3 or more blood glucose tests per day, and willing to do at least 4 tests daily, who had no previous experience of the FreeStyle InsuLinx meter (Abbott Diabetes Care, Alameda, CA; Test Meter) or the assigned comparator meter. All patients gave written informed consent. Study Design and Plan Patients used the Test Meter without the insulin calculator (BG mode) and 1 of 3 assigned comparator BGMs (Accu- Chek Aviva Nano [Roche Diagnostics, Mannheim, Germany; Comparator 1], Bayer Contour USB [Bayer Consumer Care, Basel, Switzerland; Comparator 2], LifeScan Verio Pro [LifeScan Europe, Zug, Switzerland: Comparator 3]) each for a 7-day period (Figure 1). They completed an ease of use questionnaire after each 7-day period for the BGM used, and after the second 7-day period a preference questionnaire comparing the 2 BGMs used. They then used the Test Meter with the in-built insulin dose calculator (IC mode) for 10 days, after which they completed a 2-part questionnaire, part A comparing the Test Meter with their usual method of testing blood glucose and calculating insulin dose, and part B evaluating specific features of the Test Meter. Patients were randomized into 1 of 2 groups, to use either the Test Meter or comparator BGM first. A 1-hour training session was given to patients on use of the Test Meter in BG Mode and the comparator BGM, supported by use of a structured training checklist for each meter. A half-hour training session on use of the Test Meter in IC mode was given after completing the first 14 days of the study. Easy mode setup was used in patients using a pattern-based insulin regime. Advanced mode setup was used for patients
3 778 Journal of Diabetes Science and Technology 8(4) Table 1. Baseline Characteristics of Patients (n = 164). Characteristic 7 (4.3) Male sex 83 (50.6) Caucasian 161 (98.2) Completed college education 74 (45.1) BMI (31.1) T1D 128 (78.0) Experienced severe hypoglycemia 8 (4.9) episodes in last 6 months Experienced severe hyperglycemia episodes in last 6 months a Carbohydrate counting 82 (50) who used a carbohydrate-counting based insulin regime. No changes were made to patients usual insulin regimes. Statistical Analysis The exact binomial test for proportion was performed to determine the statistical significance of the inequality in preference, or inequality in agreement and disagreement with ease of use statements, in those patients stating a preference or an opinion. All analyses were conducted using SAS version Results Mean ± SD (range) 4.3 ± 1.9 (2-20) Age (years) 48.8 ± 13.0 (19-82) BMI (kg/m 2 ) 28.1 ± 5.5 ( ) Years since diagnosis 21 ± 13 (1-58) Number of blood glucose tests daily b HbA1c (%) b 8.8 ± 1.4 ( ) a Severe hyperglycemia was defined as a hyperglycemic event requiring attention from medical personnel and/or hospitalization. b n = 162 and 158, respectively. A total of 178 eligible adult patients were enrolled, of whom 164 completed the study. Baseline characteristics of these patients are shown in Table 1. Ease of use questionnaires showed that most patients found all 4 study meters with their test strips easy to use and gave them information on how they were doing with their blood glucose. A significant majority of patients also considered that the Test Meter and Comparators 2 and 3 gave them information on how they were doing with managing their diabetes as well as how they needed to manage their blood glucose (Table 2). The results of the preference questionnaire between the 2 meters used by each patient are shown in Table 3. The Test Meter was significantly favored over Comparator 1. There was no significant difference in patient preference between the Test Meter and Comparators 2 and 3. The meters were rated as about the same in questions on individual aspects of use by 23-73% of patients. Among patients who expressed a preference in these questions, the Test Meter was significantly favored over Comparator 1 for all responses except for the number of error messages, and over Comparator 3 for easier set up of date, time and language, and for wasting fewer strips. Altogether 133 patients (81%) said they would definitely or probably change their meter for a study meter; 98 patients (60%) would definitely or probably change for the Test Meter. Table 4 shows the meter features other than testing blood glucose levels indicated by patients to be important to them. The log book was by far the most valued feature. Table 5 shows patients evaluation of specific features of the Test Meter. Most patients considered that the touch screen was easy to use; the system helped them decide their insulin dose and feel more confident about it and about managing their diabetes. Table 6 shows the results of the questionnaire comparing the Test Meter as a diabetes management tool compared to the patients usual method of testing blood glucose and calculating insulin dose. There was a significant preference for the Test Meter over patients usual method (76% vs 17%, P <.0001). Over 70% of patients considered the Test Meter was a better system to manage their diabetes, gave them the information they need to help manage their diabetes, made them feel more confident when adjusting their mealtime insulin and about managing their diabetes, and was more helpful and easier to decide and log an insulin dose. Among the 125 patients expressing a preference for the Test Meter, the commonest reason cited in the free text section of the questionnaire related to the insulin calculator function (n = 55, 44%), followed by overall and specific aspects of ease of use (n = 40, 32%), and log book and other information functions (n = 26, 21%). Conversely, among the 27 patients who preferred their usual method, the most common cited reason (n = 9, 33%) also related to the insulin calculator, such as ability or preference to calculate own insulin doses or use prescribed doses, lack of trust in or inability to adapt to the insulin calculator, and self-reported hypoglycemia after taking the insulin dose recommended by the Test Meter. Four (15%) patients expressed not liking change, preferring or feeling more comfortable with usual routine. Two patients had an episode of severe hypoglycemia during the study; 1 of these was assessed as not related to study device met serious adverse event (SAE) criteria; the other was assessed as possibly related to the study device. Both patients were using the Test Meter. Another patient reported an increased frequency of hypoglycemia throughout the study, during use of both Comparator Meter and Test Meter, in BG or IC mode.
4 Ramtoola et al 779 Table 2. Responses From Ease of Use Questionnaires About Study Meters. Statement Meter a Yes No P value yes vs no The meter is easy to use Comparator 1 54 (91.5) 5 (8.5) <.0001 Comparator 2 50 (96.2) 2 (3.8) <.0001 Comparator 3 51 (98.1) 1 (1.9) <.0001 Test Meter 153 (93.9) 10 (6.1) <.0001 The strips are easy to use with this meter Comparator 1 49 (83.1) 9 (15.3) <.0001 Comparator 2 48 (92.3) 4 (7.7) <.0001 Comparator 3 45 (86.5) 7 (13.5) <.0001 Test Meter 148 (90.8) 15 (9.2) <.0001 The meter gives me information on how I am doing with my blood glucose The meter gives me information on how I am doing with managing my diabetes The meter gives me information on how I need to manage my blood glucose Comparator 1 47 (79.7) 12 (20.3) <.0001 Comparator 2 48 (92.3) 4 (7.7) <.0001 Comparator 3 44 (84.6) 8 (15.4) <.0001 Test Meter 149 (91.4) 14 (8.6) <.0001 Comparator 1 36 (61.0) 22 (37.3) ns Comparator 2 43 (82.7) 9 (17.3) <.0001 Comparator 3 36 (69.2) 15 (28.8) <.01 Test Meter 125 (76.7) 38 (23.3) <.0001 Comparator 1 35 (59.3) 24 (40.7) ns Comparator 2 34 (65.4) 18 (34.6) <.05 Comparator 3 33 (63.5) 17 (32.7) <.05 Test Meter 120 (73.6) 41 (25.2) <.0001 a Comparator 1 n = 59; Comparator 2 n = 52; Comparator 3 n = 52; Test Meter n = 163. Comparison meter ease of use questionnaire for 1 patient was lost, this patient excluded from above analysis. Where results do not add to 100% it is due to missing answers for that response. Discussion The main objective of the study was to evaluate the user preference and ease of use of a meter with an in-built insulin dose calculator, compared to patients usual method of testing blood glucose and deciding insulin doses, when used by patients on a MDI insulin regime. Of patients, 76% stated a preference for using the Test Meter system as a diabetes management tool over their usual method. Over 70% of patients felt more confident adjusting their insulin and managing their diabetes, and over 90% considered the system easy to use, and gave them information on how they were doing with their blood glucose. The fact that patients found the system helped in the interpretation of blood glucose test results and in using these to decide an insulin dose could help overcome the feelings of avoidance and pointlessness identified as obstacles to blood glucose self-monitoring. 2 A previous study showed that using the bolus calculator built into the Test Meter minimized errors in insulin dose determination. 4 Glaser et al observed a higher frequency of errors with conventional bolus calculation methods compared with an insulin dose calculation device. 1 They suggested that consistent use of the insulin dose calculation device may help to improve metabolic control. Maurizi et al demonstrated that using an insulin dose calculator did improve HbA1c levels in T1D patients compared to manual calculation. 5 A recent review on the use of BGMs with builtin bolus calculators concluded that these are effective motivational tools which empower the patient through an increased capability to translate self-monitored blood glucose values into appropriate therapeutic decisions. 6 A small proportion of patients, however, prefer familiar routines, calculating their own or using prescribed insulin doses; this must be acknowledged and supported. Potential risks of hypoglycemia in any automated system must also be borne in mind, and appropriate patient education in this respect is important. In recent years much progress has been made in BGM technology, which now provides an array of features additional to blood glucose testing. This study gave further insight into patients views on such additional features. The log book feature was overwhelmingly the additional feature most valued by patients. Among patients who stated a preference for the Test Meter over their current method, the calculator function, ease of use and log book and other information functions were the most frequent cited reasons for their preference. Budget constraints in many health care systems have resulted in restrictions on meter and test strip availability and choice, cost considerations being paramount irrespective of additional features. This study demonstrates patients
5 780 Journal of Diabetes Science and Technology 8(4) Table 3. Responses to the Preference Questionnaire Test Meter vs Comparator Meter. Question Response Which meter... Assigned comparator meter a Test Meter About the same Comparator meter P value Test Meter vs comparator meter Is easiest to setup date, time and Comparator 1 22 (37.3) 30 (50.8) 2 (3.4) <.0001 language? Comparator 2 9 (17.0) 33 (62.3) 9 (17.0) ns Comparator 3 10 (19.2) 38 (73.1) 2 (3.8) <.05 Is easier to test blood glucose with? Comparator 1 28 (47.5) 26 (44.1) 3 (5.1) <.0001 Comparator 2 14 (26.4) 22 (41.5) 16 (30.2) ns Comparator 3 13 (25.0) 25 (48.1) 14 (26.9) ns Is easier to use for blood glucose Comparator 1 34 (57.6) 19 (32.2) 4 (6.8) <.0001 monitoring? Comparator 2 18 (34.0) 17 (32.1) 18 (34.0) ns Comparator 3 17 (32.7) 23 (44.2) 12 (23.1) ns Gave fewer error messages? Comparator 1 14 (23.7) 32 (54.2) 9 (15.3) ns Comparator 2 9 (17.0) 30 (56.6) 5 (9.4) ns Comparator 3 15 (28.8) 25 (48.1) 7 (13.5) ns Did you waste fewer test strips Comparator 1 24 (40.7) 25 (42.4) 6 (10.2) <.01 with? Comparator 2 17 (32.1) 20 (37.7) 9 (17.0) ns Comparator 3 20 (38.5) 18 (34.6) 8 (15.4) <.05 Is easiest to use? Comparator 1 29 (49.2) 24 (40.7) 6 (10.2) Comparator 2 17 (32.1) 18 (34.0) 17 (32.1) ns Comparator 3 21 (40.4) 15 (28.8) 16 (30.8) ns Is the most user friendly? Comparator 1 37 (62.7) 16 (27.1) 5 (8.5) <.0001 Comparator 2 22 (41.5) 12 (22.6) 19 (35.8) ns Comparator 3 20 (38.5) 16 (30.8) 16 (30.8) ns Makes your life simpler? Comparator 1 32 (54.2) 21 (35.6) 5 (8.5) <.0001 Comparator 2 20 (37.7) 19 (35.8) 14 (26.4) ns Comparator 3 16 (30.8) 26 (50.0) 10 (19.2) ns Gives you the information you Comparator 1 36 (61.0) 20 (33.9) 3 (5.1) <.0001 need to help manage your Comparator 2 17 (32.1) 28 (52.8) 8 (15.1) ns diabetes? Comparator 3 15 (28.8) 29 (55.8) 8 (15.4) ns Is a better blood glucose Comparator 1 40 (67.8) 16 (27.1) 3 (5.1) <.0001 monitoring system to help you Comparator 2 20 (37.7) 20 (37.7) 13 (24.5) ns manage your diabetes? Comparator 3 18 (34.6) 24 (46.2) 10 (19.2) ns Do you prefer? Comparator 1 45 (76.3) 8 (13.6) 6 (10.2) <.0001 Comparator 2 26 (49.1) 5 (9.4) 22 (41.5) ns Comparator 3 25 (48.1) 6 (11.5) 19 (36.5) ns a Comparator 1 n = 59; Comparator 2 n = 53; Comparator 3 n = 52. Where results do not add to 100% it is due to missing answers for that response. different needs and preferences in respect of blood glucose monitoring, which should be acknowledged in any patient centered health care service. Clinicians should be supported to meet these individual needs and preferences, and thus promote patient collaboration, involvement and empowerment in managing their diabetes.
6 Ramtoola et al 781 Table 4. Blood Glucose Meter Features Important to Patients. What meter features are important to you? Log book 140 (85.4) Reports 75 (45.7) Alarms 42 (25.6) Upload software 42 (25.6) Weekly messages 34 (20.7) Personalization 25 (15.2) Other 17 (10.4) No answer 7 (4.3) Total number of patients = 164. Table 5. Patients Evaluation of Specific Features of the Test Meter. Statement Conclusion Response The Test Meter... Yes No N/A Gives me helpful information if an error occurs Auto-assist information was useful Active insulin feature was helpful Has a touch screen that is easy to use Helps you decide how much insulin to take Helps you feel confident about how much mealtime insulin to take Gives information that makes you feel more confident in managing your diabetes P value yes vs no 60 (36.6) 7 (4.3) 97 (59.1) < (47.0) 8 (4.9) 78 (47.6) < (54.9) 13 (7.9) 61 (37.2) < (90.9) 14 (8.5) N/A < (92.1) 13 (7.9) N/A < (91.5) 14 (8.5) N/A < (91.5) 14 (8.5) N/A <.0001 Total number of patients = 164. Where results do not add to 100% it is due to missing answers for that response. Over 70% of patients on a MDI insulin regime preferred the Test Meter, a BGM system with in-built insulin calculator, over their usual method of testing blood glucose and deciding insulin doses. They found it easy to use and felt more confident adjusting their mealtime insulin dose and managing their diabetes. This study has highlighted that patients have different preferences. Greater flexibility should be allowed by health care systems in supporting patients choices. Abbreviations BGM, blood glucose meter; MDI, multiple daily injection; SAE, serious adverse event; T1D, type 1 diabetes; T2D, type 2 diabetes. Table 6. Comparison of Test Meter to Patients Usual Method. Question Response Usual method P value test meter vs usual method Which method... Test Meter About the same Is a better system to 131 (79.9) 19 (11.6) 14 (8.5) <.0001 manage your diabetes? Gives you the information 137 (83.5) 20 (12.2) 7 (4.3) <.0001 you need to help manage your diabetes? Makes you feel more 122 (74.4) 29 (17.7) 13 (7.9) <.0001 confident about managing your diabetes? Is easier to use when 107 (65.2) 35 (21.3) 22 (13.4) <.0001 managing your diabetes? Is more helpful when 135 (82.3) 16 (9.8) 13 (7.9) <.0001 deciding your insulin dose? Is easier to decide an 132 (80.5) 21 (12.8) 11 (6.7) <.0001 insulin dose? Makes you feel more 119 (72.6) 27 (16.5) 18 (11.0) <.0001 confident when adjusting your mealtime insulin? Gave you fewer errors in 98 (59.8) 46 (28.0) 13 (7.9) <.0001 your insulin dose? Is easier to log an insulin 148 (90.2) 6 (3.7) 10 (6.1) <.0001 dose? Makes your life more 103 (62.8) 38 (23.2) 23 (14.0) <.0001 simple? Did you prefer? 125 (76.2) 12 (7.3) 27 (16.5) <.0001 Total number of patients = 164. Where results do not add to 100% it is due to missing answers for that response. Acknowledgments We thank the following for assistance: Study personnel at the 7 clinical sites for execution of this study; Walter Amor and Zoe Welsh (Abbott Diabetes Care) for assistance with statistical analysis. Declaration of Conflicting Interests The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The trial was designed by Abbott Diabetes Care with input from the chief investigator. FreeStyle and related brand marks are trademarks of Abbott Diabetes Care Inc in various jurisdictions. Funding The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was sponsored by Abbott Diabetes Care Ltd. References 1. Glaser NS, Iden SB, Green-Burgeson D, et al. Benefits of an insulin dosage calculation device for adolescents with type 1 diabetes mellitus. J Pediatr Endocrinol Metab. 2004;17(12):
7 782 Journal of Diabetes Science and Technology 8(4) 2. Polonsky WH, Fisher L, Hessler D, Edelman SV. What is so tough about self-monitoring of blood glucose? Perceived obstacles among patients with type 2 diabetes. Diabetes Med. 2014;31(1): SAS Institute Inc. SAS/STAT 9.2 User s Guide. Cary, NC: SAS Institute Inc; Sussman A, Taylor EJ, Patel M, Ward J, Alva S, Lawrence A, Ng R. Performance of a glucose meter with a built-in automated bolus calculator versus manual bolus calculation in insulin-using subjects. J Diabetes Sci Technol. 2012;6(2): Maurizi AR, Lauria A, Maggi D, et al. A novel insulin unit calculator for the management of type 1 diabetes. Diabetes Technol Ther. 2011;13(4): Colin IM, Paris I. Glucose meters with built-in automated bolus calculator: gadget or real value for insulin-treated diabetic patients? Diabetes Ther. 2013;4(1):1-11.
Designed with your patients lives in mind
 The Accu-Chek Insight diabetes therapy system Designed with your patients lives in mind With pre-filled insulin cartridge Designed for easy patient training The Accu-Chek Insight diabetes therapy system
The Accu-Chek Insight diabetes therapy system Designed with your patients lives in mind With pre-filled insulin cartridge Designed for easy patient training The Accu-Chek Insight diabetes therapy system
Better connected for better decisions
 Introducing the Accu-Chek Connect diabetes management system Better connected for better decisions Help your patients use the power of their mobile devices and the web to manage their diabetes How many
Introducing the Accu-Chek Connect diabetes management system Better connected for better decisions Help your patients use the power of their mobile devices and the web to manage their diabetes How many
DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS)
 Type 2 Diabetes DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Clinical Guideline Self-monitoring of blood glucose (SMBG) should be considered but not be routinely offered for adults with type 2 diabetes
Type 2 Diabetes DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Clinical Guideline Self-monitoring of blood glucose (SMBG) should be considered but not be routinely offered for adults with type 2 diabetes
DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS)
 DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Type 2 Diabetes Clinical Guideline Self-monitoring of blood glucose (SMBG) should be considered but not routinely offered for adults with type 2 diabetes
DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Type 2 Diabetes Clinical Guideline Self-monitoring of blood glucose (SMBG) should be considered but not routinely offered for adults with type 2 diabetes
Walsall CCG Supported Blood Glucose Meters April 2018
 Meter Name Picture Type Strips Lancets Information Company PRIMARY CARE INITIATION TEE2+ Uncomplicated Type 2 diabetes patient on TEE2 test CareSens Lancets Easy to use. Large clear display Bluetooth functionality
Meter Name Picture Type Strips Lancets Information Company PRIMARY CARE INITIATION TEE2+ Uncomplicated Type 2 diabetes patient on TEE2 test CareSens Lancets Easy to use. Large clear display Bluetooth functionality
Software Version 2.0. User s Guide
 Software Version 2.0 User s Guide Table of Contents Contents Contents Important Information About Your FreeStyle Auto-Assist Software...1 Intended Use...1 System Requirements...1 Connecting to your Abbott
Software Version 2.0 User s Guide Table of Contents Contents Contents Important Information About Your FreeStyle Auto-Assist Software...1 Intended Use...1 System Requirements...1 Connecting to your Abbott
Advances in Diabetes Care Technologies
 1979 Advances in Diabetes Care Technologies 2015 Introduction Insulin pump use: ~ 20% - 30% of patients with T1DM < 1% of insulin-treated patients with T2DM 2007 FDA estimates ~375,000 insulin pumps for
1979 Advances in Diabetes Care Technologies 2015 Introduction Insulin pump use: ~ 20% - 30% of patients with T1DM < 1% of insulin-treated patients with T2DM 2007 FDA estimates ~375,000 insulin pumps for
Report Reference Guide
 Report Reference Guide How to use this guide Each type of CareLink report and its components are described in the following sections. Report data used to generate the sample reports was from sample patient
Report Reference Guide How to use this guide Each type of CareLink report and its components are described in the following sections. Report data used to generate the sample reports was from sample patient
DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS)
 Type 2 Diabetes DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Clinical Guideline Self-monitoring of blood glucose should be offered to all newly diagnosed type 2 diabetic patients as an integral part
Type 2 Diabetes DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Clinical Guideline Self-monitoring of blood glucose should be offered to all newly diagnosed type 2 diabetic patients as an integral part
Advances in Diabetes Care Technologies
 1979 Advances in Diabetes Care Technologies 2015 Introduction Roughly 20% - 30% of patients with T1DM and fewer than 1% of insulin-treated patients with T2DM use an insulin pump In 2007, the US FDA estimated
1979 Advances in Diabetes Care Technologies 2015 Introduction Roughly 20% - 30% of patients with T1DM and fewer than 1% of insulin-treated patients with T2DM use an insulin pump In 2007, the US FDA estimated
When Will CGM Replace SMBG? Roy W. Beck, MD, PhD. JAEB Center for Health Research Tampa, Florida
 When Will CGM Replace SMBG? Roy W. Beck, MD, PhD JAEB Center for Health Research Tampa, Florida Financial Disclosures Dr. Beck does not have any personal conflicts of interest His employer, the JAEB Center
When Will CGM Replace SMBG? Roy W. Beck, MD, PhD JAEB Center for Health Research Tampa, Florida Financial Disclosures Dr. Beck does not have any personal conflicts of interest His employer, the JAEB Center
Diabetes Devices Workshop Angela Aldrich, PharmD, PhC April Mott, PharmD, PhC, BCPS Presbyterian Medical Group 28 January 2018
 Diabetes Devices Workshop Angela Aldrich, PharmD, PhC April Mott, PharmD, PhC, BCPS Presbyterian Medical Group 28 January 2018 Pumps & Sensors & Meters, Oh My! A Tale of Two Meters Technology for glucometers
Diabetes Devices Workshop Angela Aldrich, PharmD, PhC April Mott, PharmD, PhC, BCPS Presbyterian Medical Group 28 January 2018 Pumps & Sensors & Meters, Oh My! A Tale of Two Meters Technology for glucometers
Keywords diabetes software, insulin, self-management, self-monitoring of blood glucose, SMBG
 557188DSTXXX10.1177/1932296814557188Journal of Diabetes Science and TechnologyHinnen et al research-article2014 Original Article Use of Diabetes Data Management Software Reports by Health Care Providers,
557188DSTXXX10.1177/1932296814557188Journal of Diabetes Science and TechnologyHinnen et al research-article2014 Original Article Use of Diabetes Data Management Software Reports by Health Care Providers,
For more comprehensive information, please refer to the t:connect Application User Guide available online at: Getting Started Guide.
 Congratulations on the purchase of your new insulin pump from Tandem Diabetes Care. Your decision to use insulin pump therapy is a sign of your commitment to actively manage your diabetes. This guide provides
Congratulations on the purchase of your new insulin pump from Tandem Diabetes Care. Your decision to use insulin pump therapy is a sign of your commitment to actively manage your diabetes. This guide provides
The Current Status of Bolus Calculator Decision-Support Software. Introduction. David C. Klonoff, M.D., FACP EDITORIAL
 Journal of Diabetes Science and Technology Volume 6, Issue 5, September 2012 Diabetes Technology Society EDITORIAL The Current Status of Bolus Calculator Decision-Support Software David C., M.D., FACP
Journal of Diabetes Science and Technology Volume 6, Issue 5, September 2012 Diabetes Technology Society EDITORIAL The Current Status of Bolus Calculator Decision-Support Software David C., M.D., FACP
Diabetes Management App. Instruction Manual
 Diabetes Management App Instruction Manual Accu-Chek Connect Diabetes Management App Overview The Accu-Chek Connect diabetes management app (hereafter referred to as the app) is designed to help you: Transfer
Diabetes Management App Instruction Manual Accu-Chek Connect Diabetes Management App Overview The Accu-Chek Connect diabetes management app (hereafter referred to as the app) is designed to help you: Transfer
As the number of new glucose monitoring devices
 DIABETES TECHNOLOGY & THERAPEUTICS Volume 17, Number 9, 2015 ª Mary Ann Liebert, Inc. DOI: 10.1089/dia.2014.0417 ORIGINAL ARTICLE Development of a New Measure for Assessing Glucose Monitoring Device-Related
DIABETES TECHNOLOGY & THERAPEUTICS Volume 17, Number 9, 2015 ª Mary Ann Liebert, Inc. DOI: 10.1089/dia.2014.0417 ORIGINAL ARTICLE Development of a New Measure for Assessing Glucose Monitoring Device-Related
Welcome to CareLink Pro
 Reference Guide Welcome to CareLink Pro This guide was developed to serve as a reference for obtaining patient data and reviewing CareLink Pro reports. Getting Started with CareLink Pro Adding New Patients
Reference Guide Welcome to CareLink Pro This guide was developed to serve as a reference for obtaining patient data and reviewing CareLink Pro reports. Getting Started with CareLink Pro Adding New Patients
James J. Chamberlain, MD 1, Dana Dopita, RN, MSN, CDE 1, Emily Gilgen, RD, CD, CDE 1, and Annie Neuman, MPA, PA-C 1.
 604633DSTXXX10.1177/1932296815604633Journal of Diabetes Science and TechnologyChamberlain et al research-article2015 Original Article Impact of Frequent and Persistent Use of Continuous Glucose Monitoring
604633DSTXXX10.1177/1932296815604633Journal of Diabetes Science and TechnologyChamberlain et al research-article2015 Original Article Impact of Frequent and Persistent Use of Continuous Glucose Monitoring
Plug-and-play goes online
 The next-generation Accu-Chek T Smart Pix software Plug-and-play goes online Proven tools for efficient and effective diabetes management 1 even for patients who are not in your office How many of these
The next-generation Accu-Chek T Smart Pix software Plug-and-play goes online Proven tools for efficient and effective diabetes management 1 even for patients who are not in your office How many of these
Guidance for the choice of blood glucose testing meters, strips and lancets
 Guidance for the choice of blood glucose testing meters, strips and lancets This guidance is intended to assist healthcare professionals in their selection of appropriate blood glucose meters and testing
Guidance for the choice of blood glucose testing meters, strips and lancets This guidance is intended to assist healthcare professionals in their selection of appropriate blood glucose meters and testing
WOULD YOU LIKE TO REDUCE THE FEAR OF HYPOGLYCAEMIA FOR YOUR PATIENTS?
 WOULD YOU LIKE TO REDUCE THE FEAR OF HYPOGLYCAEMIA FOR YOUR PATIENTS? THE ONLY SYSTEM CLINICALLY PROVEN TO REDUCE HYPOGLYCAEMIA MINIMED 640G SYSTEM WITH SMARTGUARD TECHNOLOGY 1 HYPOGLYCAEMIA IS CHALLENGING
WOULD YOU LIKE TO REDUCE THE FEAR OF HYPOGLYCAEMIA FOR YOUR PATIENTS? THE ONLY SYSTEM CLINICALLY PROVEN TO REDUCE HYPOGLYCAEMIA MINIMED 640G SYSTEM WITH SMARTGUARD TECHNOLOGY 1 HYPOGLYCAEMIA IS CHALLENGING
WOULD YOU LIKE MORE CONFIDENCE IN YOUR HYPOGLYCAEMIC CONTROL? SMARTGUARD. PROVIDES PREDICTIVE PROTECTION
 WOULD YOU LIKE MORE CONFIDENCE IN YOUR HYPOGLYCAEMIC CONTROL? SMARTGUARD. PROVIDES PREDICTIVE PROTECTION 1,2 MINIMED 640G WITH SMARTGUARD HAVE YOU CONSIDERED THE REAL IMPACT HYPOGLYCAEMIA HAS ON YOUR LIFE?
WOULD YOU LIKE MORE CONFIDENCE IN YOUR HYPOGLYCAEMIC CONTROL? SMARTGUARD. PROVIDES PREDICTIVE PROTECTION 1,2 MINIMED 640G WITH SMARTGUARD HAVE YOU CONSIDERED THE REAL IMPACT HYPOGLYCAEMIA HAS ON YOUR LIFE?
UNCOVERING THE BENEFITS OF THE ACCU- CHEK BOLUS ADVISOR MICHAEL PORTER CDE
 UNCOVERING THE BENEFITS OF THE ACCU- CHEK BOLUS ADVISOR MICHAEL PORTER CDE 1 LEARNING OBJECTIVES By the end of this session participants should be able to understand: The benefits of bolus advisors The
UNCOVERING THE BENEFITS OF THE ACCU- CHEK BOLUS ADVISOR MICHAEL PORTER CDE 1 LEARNING OBJECTIVES By the end of this session participants should be able to understand: The benefits of bolus advisors The
THE ONLY SYSTEM^ CLINICALLY PROVEN TO REDUCE HYPOGLYCAEMIA
 THE ONLY SYSTEM^ CLINICALLY PROVEN TO REDUCE HYPOGLYCAEMIA MINIMED 640G system^ with SmartGuard technology HYPOGLYCAEMIA IS CHALLENGING FOR GLYCAEMIC CONTROL 1 AND quality of life 2 Achieving good glucose
THE ONLY SYSTEM^ CLINICALLY PROVEN TO REDUCE HYPOGLYCAEMIA MINIMED 640G system^ with SmartGuard technology HYPOGLYCAEMIA IS CHALLENGING FOR GLYCAEMIC CONTROL 1 AND quality of life 2 Achieving good glucose
Abstract. Mike Grady, Ph.D., 1 Denise Campbell, B.Sc., 1 Kirsty MacLeod, B.Sc., 1 and Aparna Srinivasan, Ph.D. 2 ORIGINAL ARTICLE.
 Journal of Diabetes Science and Technology Volume 7, Issue 4, July 2013 Diabetes Technology Society ORIGINAL ARTICLE Evaluation of a Blood Glucose Monitoring System with Automatic High- and Low-Pattern
Journal of Diabetes Science and Technology Volume 7, Issue 4, July 2013 Diabetes Technology Society ORIGINAL ARTICLE Evaluation of a Blood Glucose Monitoring System with Automatic High- and Low-Pattern
MINIMED 640G WITH SMARTGUARD GIVES YOU CONFIDENCE TO TAKE CONTROL OF YOUR DIABETES
 MINIMED 640G WITH SMARTGUARD GIVES YOU CONFIDENCE OF YOUR DIABETES HAVE YOU CONSIDERED THE REAL IMPACT HYPOS HAVE ON YOUR LIFE? AN ESTIMATED 1 HOUR EVERY DAY IS LOST TO THE MANAGEMENT OF 43% OF PEOPLE
MINIMED 640G WITH SMARTGUARD GIVES YOU CONFIDENCE OF YOUR DIABETES HAVE YOU CONSIDERED THE REAL IMPACT HYPOS HAVE ON YOUR LIFE? AN ESTIMATED 1 HOUR EVERY DAY IS LOST TO THE MANAGEMENT OF 43% OF PEOPLE
NEW TECHNOLOGIES FOR MANAGING DIABETES ANGELA THOMPSON DNP, FNP-C, BC-ADM, CDE, FAANP
 NEW TECHNOLOGIES FOR MANAGING DIABETES ANGELA THOMPSON DNP, FNP-C, BC-ADM, CDE, FAANP No commercial support or sponsorship was received for this project I have nothing to disclose OBJECTIVES Identify at
NEW TECHNOLOGIES FOR MANAGING DIABETES ANGELA THOMPSON DNP, FNP-C, BC-ADM, CDE, FAANP No commercial support or sponsorship was received for this project I have nothing to disclose OBJECTIVES Identify at
Performance-powered. The OneTouch. Ping insulin pump and meter-remote.
 Performance-powered. The OneTouch Ping insulin pump and meter-remote. I We don t just deliver insulin. We deliver outstanding clinical performance. P36337_OTP_DetAid_OmniPodUpdate_r12.indd 1 OneTouch Ping.
Performance-powered. The OneTouch Ping insulin pump and meter-remote. I We don t just deliver insulin. We deliver outstanding clinical performance. P36337_OTP_DetAid_OmniPodUpdate_r12.indd 1 OneTouch Ping.
CareLink. software REPORT REFERENCE GUIDE. Management Software for Diabetes
 CareLink Management Software for Diabetes software REPORT REFERENCE GUIDE How to use this guide Each type of CareLink report and its components are described in the following sections. Report data used
CareLink Management Software for Diabetes software REPORT REFERENCE GUIDE How to use this guide Each type of CareLink report and its components are described in the following sections. Report data used
The Diamond Study: Continuous Glucose Monitoring In Patients on Mulitple Daily Insulin Injections
 8/5/217 The Diamond Study: Continuous Glucose Monitoring In Patients on Mulitple Daily Insulin Injections Richard M. Bergenstal, MD Executive Director International Diabetes Center at Park Nicollet Minneapolis,
8/5/217 The Diamond Study: Continuous Glucose Monitoring In Patients on Mulitple Daily Insulin Injections Richard M. Bergenstal, MD Executive Director International Diabetes Center at Park Nicollet Minneapolis,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE GUIDANCE EXECUTIVE (GE)
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE GUIDANCE EXECUTIVE (GE) Review of TA151 Continuous subcutaneous insulin infusion for the treatment of diabetes mellitus This guidance was issued in
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE GUIDANCE EXECUTIVE (GE) Review of TA151 Continuous subcutaneous insulin infusion for the treatment of diabetes mellitus This guidance was issued in
Sponsor / Company: Sanofi Drug substance(s): Insulin Glargine. Study Identifiers: NCT
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Live life, less complicated. InPen MOBILE APP. Healthcare Provider INSTRUCTIONS FOR USE. CompanionMedical.com
 InPen MOBILE APP Healthcare Provider INSTRUCTIONS FOR USE TABLE OF CONTENTS Introduction...3 InPen Mobile App...3 Intended Use...3 Indications for Use...3 Contraindications...3 Start Orders...4 General
InPen MOBILE APP Healthcare Provider INSTRUCTIONS FOR USE TABLE OF CONTENTS Introduction...3 InPen Mobile App...3 Intended Use...3 Indications for Use...3 Contraindications...3 Start Orders...4 General
OneTouch Reveal web app Report Reference Guide
 OneTouch Reveal web app Report Reference Guide Your step-by-step guide to setting up and using the OneTouch Reveal web app OneTouch Verio meter OneTouch Verio Flex meter OneTouch Verio IQ meter OneTouch
OneTouch Reveal web app Report Reference Guide Your step-by-step guide to setting up and using the OneTouch Reveal web app OneTouch Verio meter OneTouch Verio Flex meter OneTouch Verio IQ meter OneTouch
Home Glucose Monitoring
 Home Glucose Monitoring Blood Glucose Monitors Name (Manufacturer/Distributor) Size (inches) Weight (ounces) Active (Roche) 4.6 X 1.07 X 0.9 2.01 without Advantage (Roche) 3.3 X 2.8 X 0.8 1.8 without Test
Home Glucose Monitoring Blood Glucose Monitors Name (Manufacturer/Distributor) Size (inches) Weight (ounces) Active (Roche) 4.6 X 1.07 X 0.9 2.01 without Advantage (Roche) 3.3 X 2.8 X 0.8 1.8 without Test
1. Continuous Glucose Monitoring
 1. Continuous Glucose Monitoring 1. Physiology of interstitial fluid glucose 2. Comparison of CGM and self-monitored blood glucose (SMBG) data 3. Insulin dosing indication in BGM vs. CGM & the FDA 4. Protection
1. Continuous Glucose Monitoring 1. Physiology of interstitial fluid glucose 2. Comparison of CGM and self-monitored blood glucose (SMBG) data 3. Insulin dosing indication in BGM vs. CGM & the FDA 4. Protection
Commissioning Statement. Flash Glucose Monitoring system (FreeStyle Libre ) March 2018
 Technology Commissioning Statement Flash Glucose Monitoring system (FreeStyle Libre ) March 2018 FreeStyle Libre (Abbott) Flash Glucose Monitoring System for use in adults, young people and children. Recommendation
Technology Commissioning Statement Flash Glucose Monitoring system (FreeStyle Libre ) March 2018 FreeStyle Libre (Abbott) Flash Glucose Monitoring System for use in adults, young people and children. Recommendation
Diabetes Management: Current High Tech Innovations
 Diabetes Management: Current High Tech Innovations How Far We ve Come in the Last 40 Years William V. Tamborlane, MD Department of Pediatrics Yale School of Medicine Disclosures I am a consultant for:
Diabetes Management: Current High Tech Innovations How Far We ve Come in the Last 40 Years William V. Tamborlane, MD Department of Pediatrics Yale School of Medicine Disclosures I am a consultant for:
Insulin Pump An information session to help you decide if you are ready to use an insulin pump.
 Insulin Pump An information session to help you decide if you are ready to use an insulin pump. Welcome Welcome to the insulin pump information session. We hope this session helps you to decide whether
Insulin Pump An information session to help you decide if you are ready to use an insulin pump. Welcome Welcome to the insulin pump information session. We hope this session helps you to decide whether
Software Version 1.0. User s Manual
 Software Version 1.0 User s Manual Table of Contents Contents 0 Important Information about Your FreeStyle Libre software...1 Intended Use...1 System Requirements...1 Customer Service...1 Getting to Know
Software Version 1.0 User s Manual Table of Contents Contents 0 Important Information about Your FreeStyle Libre software...1 Intended Use...1 System Requirements...1 Customer Service...1 Getting to Know
Corporate Medical Policy
 Corporate Medical Policy Continuous Monitoring of Glucose in the Interstitial Fluid File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_monitoring_of_glucose_in_the_interstitial_fluid
Corporate Medical Policy Continuous Monitoring of Glucose in the Interstitial Fluid File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_monitoring_of_glucose_in_the_interstitial_fluid
Blood glucose Meter Roche USA V6/ PMS 287 Proof Print Number 209 Advanced Owner s Booklet
 This file may not print or view at 100%. Die lines and color breaks do not print. Roche USA 50841 V6/1 06434258002 Black Proof Print Number 209 06434258002-0512 Roche USA 50841 V6/2 06434258002 Cyan Proof
This file may not print or view at 100%. Die lines and color breaks do not print. Roche USA 50841 V6/1 06434258002 Black Proof Print Number 209 06434258002-0512 Roche USA 50841 V6/2 06434258002 Cyan Proof
Report Reference Guide. THERAPY MANAGEMENT SOFTWARE FOR DIABETES CareLink Report Reference Guide 1
 Report Reference Guide THERAPY MANAGEMENT SOFTWARE FOR DIABETES CareLink Report Reference Guide 1 How to use this guide Each type of CareLink report and its components are described in the following sections.
Report Reference Guide THERAPY MANAGEMENT SOFTWARE FOR DIABETES CareLink Report Reference Guide 1 How to use this guide Each type of CareLink report and its components are described in the following sections.
Design of Insulin Watch
 Tentative design Our system is composed of two components: a portable insulin watch and a notepad sized device. Insulin Watch: The portable insulin watch provides the following functionalities: 1) Blood
Tentative design Our system is composed of two components: a portable insulin watch and a notepad sized device. Insulin Watch: The portable insulin watch provides the following functionalities: 1) Blood
USING THE MINIMED 670G SYSTEM
 USING THE MINIMED 670G SYSTEM Instructions for the Experienced MiniMed 630G System User USING THE MINIMED 670G SYSTEM: INSTRUCTIONS FOR THE EXPERIENCED USER Checklist for starting on your MiniMed 670G
USING THE MINIMED 670G SYSTEM Instructions for the Experienced MiniMed 630G System User USING THE MINIMED 670G SYSTEM: INSTRUCTIONS FOR THE EXPERIENCED USER Checklist for starting on your MiniMed 670G
ADAG Study Group Data Links A1C Levels with Empirically Measured Blood Glucose Values - New Treatment Guidelines Will Now be Needed
 529638DSTXXX10.1177/1932296814529638Journal of Diabetes Science and TechnologyKlonoff research-article2014 Editorial ADAG Study Group Data Links A1C Levels with Empirically Measured Blood Glucose Values
529638DSTXXX10.1177/1932296814529638Journal of Diabetes Science and TechnologyKlonoff research-article2014 Editorial ADAG Study Group Data Links A1C Levels with Empirically Measured Blood Glucose Values
Abbott FreeStyle Libre Pro System
 , the Professional CGM Abbott FreeStyle Libre Pro Reader Kit includes: Reader, USB cable, interactive tutorial on USB, and power adapter, user s manual, Quick Start Guide, Quick Reference Guide Kit includes:
, the Professional CGM Abbott FreeStyle Libre Pro Reader Kit includes: Reader, USB cable, interactive tutorial on USB, and power adapter, user s manual, Quick Start Guide, Quick Reference Guide Kit includes:
Diabetes and Technology. Saturday, September 9, 2017 Aimee G sell, APRN, ANP-C, CDE
 Diabetes and Technology Saturday, September 9, 2017 Aimee G sell, APRN, ANP-C, CDE Disclosure Speaker s Bureau: Janssan Pharmaceuticals Current Technology V-Go by Valeritas Continuous Sensors (personal
Diabetes and Technology Saturday, September 9, 2017 Aimee G sell, APRN, ANP-C, CDE Disclosure Speaker s Bureau: Janssan Pharmaceuticals Current Technology V-Go by Valeritas Continuous Sensors (personal
Quick Reference Guide
 FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the Interactive Tutorial. The Quick Reference Guide
FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the Interactive Tutorial. The Quick Reference Guide
Role of Mobile Technology to Improve Diabetes Care in Adults with Type 1 Diabetes: The Remote-T1D Study ibgstar Ò in Type 1 Diabetes Management
 Diabetes Ther (2017) 8:811 819 DOI 10.1007/s13300-017-0272-5 ORIGINAL RESEARCH Role of Mobile Technology to Improve Diabetes Care in Adults with Type 1 Diabetes: The Remote-T1D Study ibgstar Ò in Type
Diabetes Ther (2017) 8:811 819 DOI 10.1007/s13300-017-0272-5 ORIGINAL RESEARCH Role of Mobile Technology to Improve Diabetes Care in Adults with Type 1 Diabetes: The Remote-T1D Study ibgstar Ò in Type
Insulin Pumps and Continuous Glucose Sensors- Embracing Technology. Susan Cavalier, BS, RN, CDE Manager, Diabetes Educator Sanford Diabetes Education
 Insulin Pumps and Continuous Glucose Sensors- Embracing Technology Susan Cavalier, BS, RN, CDE Manager, Diabetes Educator Sanford Diabetes Education Diabetes Management Tools in 1974 Insulin pump history
Insulin Pumps and Continuous Glucose Sensors- Embracing Technology Susan Cavalier, BS, RN, CDE Manager, Diabetes Educator Sanford Diabetes Education Diabetes Management Tools in 1974 Insulin pump history
15 th Annual DAFNE collaborative meeting Tuesday 28 th June 2016
 15 th Annual DAFNE collaborative meeting Tuesday 28 th June 2016 Sponsored by: Abbott Diabetes Care and Lilly Diabetes The REPOSE Trial (Relative Effectiveness of Pumps over Structured Education) Background
15 th Annual DAFNE collaborative meeting Tuesday 28 th June 2016 Sponsored by: Abbott Diabetes Care and Lilly Diabetes The REPOSE Trial (Relative Effectiveness of Pumps over Structured Education) Background
Reader and Sensor Demo Kit. Quick Start Guide
 Reader and Sensor Demo Kit Quick Start Guide Contents Intended Use... 1 System Overview... 1 Reader................................................... 3 Sensor...................................................
Reader and Sensor Demo Kit Quick Start Guide Contents Intended Use... 1 System Overview... 1 Reader................................................... 3 Sensor...................................................
Quick Reference Guide
 FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the Interactive Tutorial. The Quick Reference Guide
FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the Interactive Tutorial. The Quick Reference Guide
Incorporating CGM Into Clinical Decision Making. Etie Moghissi, MD, FACE Clinical Associate Professor, David Geffen School of Medicine UCLA
 Incorporating CGM Into Clinical Decision Making Etie Moghissi, MD, FACE Clinical Associate Professor, David Geffen School of Medicine UCLA 1 Limitations of Current Glucose Monitoring Methods A1c Standard
Incorporating CGM Into Clinical Decision Making Etie Moghissi, MD, FACE Clinical Associate Professor, David Geffen School of Medicine UCLA 1 Limitations of Current Glucose Monitoring Methods A1c Standard
Advances in Technology in the Treatment of Diabetes Mellitus 2017 How far have we come-how far are we going? Is there a final frontier?
 Advances in Technology in the Treatment of Diabetes Mellitus 2017 How far have we come-how far are we going? Is there a final frontier? Alan B Schorr DO FAAIM FACE www.sugardoc.com abs@sugardoc.com Disclosures
Advances in Technology in the Treatment of Diabetes Mellitus 2017 How far have we come-how far are we going? Is there a final frontier? Alan B Schorr DO FAAIM FACE www.sugardoc.com abs@sugardoc.com Disclosures
Participants in the Program
 Type 2 Diabetes Performance Improvement Initiative: Chart Reviews Participants in the Program 318 clinicians have registered 192 have started the program 126 have started their initial chart review 26
Type 2 Diabetes Performance Improvement Initiative: Chart Reviews Participants in the Program 318 clinicians have registered 192 have started the program 126 have started their initial chart review 26
Comparison of Lancing Devices for Self-Monitoring of Blood Glucose Regarding Lancing Pain
 Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society ORIGINAL ARTICLES Comparison of Lancing Devices for Self-Monitoring of Blood Glucose Regarding Lancing
Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society ORIGINAL ARTICLES Comparison of Lancing Devices for Self-Monitoring of Blood Glucose Regarding Lancing
BLOOD GLUCOSE METER TEST STRIP STEP THERAPY CRITERIA
 BLOOD GLUCOSE METER TEST STRIP STEP THERAPY CRITERIA Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan.
BLOOD GLUCOSE METER TEST STRIP STEP THERAPY CRITERIA Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan.
medicines_management/correspondence/pathway-for-the-managed- Access-of-FreeStyle-Libre.
 Pathway for the Managed Access of FreeStyle Libre (Flash Glucose monitoring) for Adults and Children in the care of Trust Specialist Diabetes Clinics in Northern Ireland www.hscboard.hscni.net/download/publications/pharmacy_and_
Pathway for the Managed Access of FreeStyle Libre (Flash Glucose monitoring) for Adults and Children in the care of Trust Specialist Diabetes Clinics in Northern Ireland www.hscboard.hscni.net/download/publications/pharmacy_and_
USING THE MINIMED 670G SYSTEM. Instructions for the Experienced MiniMed 630G System User
 USING THE MINIMED 670G SYSTEM Instructions for the Experienced MiniMed 630G System User This is a supplemental guide. For complete instructions and safety information, please see your MiniMed 670G System
USING THE MINIMED 670G SYSTEM Instructions for the Experienced MiniMed 630G System User This is a supplemental guide. For complete instructions and safety information, please see your MiniMed 670G System
Control of Glycemic Variability for Reducing Hypoglycemia Jae Hyeon Kim
 Control of Glycemic Variability for Reducing Hypoglycemia Jae Hyeon Kim Division of Endocrinology and Metabolism, Samsung Medical Center, Sungkyunkwan University School of Medicine Conflict of interest
Control of Glycemic Variability for Reducing Hypoglycemia Jae Hyeon Kim Division of Endocrinology and Metabolism, Samsung Medical Center, Sungkyunkwan University School of Medicine Conflict of interest
Target Audience. approach this patient case scenario, including identifying an
 Activity Overview In this case-based webcast, meet LaWanda, a 57-year-old woman with type 2 diabetes. Her glycated hemoglobin (HbA1C) is 8.4%, she is currently taking basal insulin and fast-acting insulin,
Activity Overview In this case-based webcast, meet LaWanda, a 57-year-old woman with type 2 diabetes. Her glycated hemoglobin (HbA1C) is 8.4%, she is currently taking basal insulin and fast-acting insulin,
Quick Reference Guide
 FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide FreeStyle LibreLink app A FreeStyle Libre product IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the
FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide FreeStyle LibreLink app A FreeStyle Libre product IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the
FLIPS FreeStyle Libre in Pregnancy Study
 FLIPS FreeStyle Libre in Pregnancy Study Evaluation of the Accuracy of the FreeStyle Libre Flash Glucose Monitoring System Use in Pregnancy Label Extension Study (CE) Section 1: PARTICIPANT INFORMATION
FLIPS FreeStyle Libre in Pregnancy Study Evaluation of the Accuracy of the FreeStyle Libre Flash Glucose Monitoring System Use in Pregnancy Label Extension Study (CE) Section 1: PARTICIPANT INFORMATION
Insulin Pump Therapy. WakeMed Children s Endocrinology & Diabetes WakeMed Health & Hospitals Version 1.3, rev 5/21/13 MP
 Insulin Pump Therapy WakeMed Children s Endocrinology & Diabetes Overview What is an insulin pump? What are the advantages and disadvantages of an insulin pump? Lifestyle Changes Food Management Exercise
Insulin Pump Therapy WakeMed Children s Endocrinology & Diabetes Overview What is an insulin pump? What are the advantages and disadvantages of an insulin pump? Lifestyle Changes Food Management Exercise
The Realities of Technology in Type 1 Diabetes
 The Realities of Technology in Type 1 Diabetes May 6, 2017 Rosanna Fiallo-scharer, MD Margaret Frederick, RN Disclosures I have no conflicts of interest to disclose I will discuss some unapproved treatments
The Realities of Technology in Type 1 Diabetes May 6, 2017 Rosanna Fiallo-scharer, MD Margaret Frederick, RN Disclosures I have no conflicts of interest to disclose I will discuss some unapproved treatments
Getting Started. Learning Guide. with Insulin Pump Therapy. PUMP Foundations. for the MiniMed 530G with Enlite
 Getting Started with Insulin Pump Therapy for the MiniMed 530G with Enlite Learning Guide PUMP Foundations MiniMed 530G Insulin Pump Settings Form: We recommend that you record all settings on this form
Getting Started with Insulin Pump Therapy for the MiniMed 530G with Enlite Learning Guide PUMP Foundations MiniMed 530G Insulin Pump Settings Form: We recommend that you record all settings on this form
Introducing DIA-TEC CLOUDTM. Technology. Education. Community. Your NEW Strategy for Diabetes Cost Management from the Experts at DECM
 Introducing DIA-TEC CLOUDTM Technology. Education. Community. Your NEW Strategy for Diabetes Cost Management from the Experts at DECM Technology. Education. Community. Diabetes happens in real time. Now,
Introducing DIA-TEC CLOUDTM Technology. Education. Community. Your NEW Strategy for Diabetes Cost Management from the Experts at DECM Technology. Education. Community. Diabetes happens in real time. Now,
Basal Bolus Insulin Therapy Frequently Asked Questions
 1. What is Basal Bolus Insulin Therapy (BBIT)? 2. What evidence supports the use of subcutaneous Basal Bolus Insulin Therapy? 3. Does Basal Bolus Insulin Therapy apply to all patients? 4. What s wrong
1. What is Basal Bolus Insulin Therapy (BBIT)? 2. What evidence supports the use of subcutaneous Basal Bolus Insulin Therapy? 3. Does Basal Bolus Insulin Therapy apply to all patients? 4. What s wrong
Now you know. InPen MOBILE APP. Healthcare Provider INSTRUCTIONS FOR USE. CompanionMedical.com Companion Medical, Inc.
 InPen MOBILE APP Healthcare Provider INSTRUCTIONS FOR USE 2017 Companion Medical, Inc. LBL-00235-AC TABLE OF CONTENTS Introduction...3 InPen Mobile App...3 Intended Use...3 Indications for Use...3 Contraindications...3
InPen MOBILE APP Healthcare Provider INSTRUCTIONS FOR USE 2017 Companion Medical, Inc. LBL-00235-AC TABLE OF CONTENTS Introduction...3 InPen Mobile App...3 Intended Use...3 Indications for Use...3 Contraindications...3
This Diabetes Policy should be read in conjunction with the Dealing with Medical Conditions Policy of Goulburn Region Preschool Association Inc.
 DIABETES POLICY Mandatory Quality Area 2 The content of this policy was developed for KPV by advocacy and diabetes educators at Diabetes Australia Vic and the Royal Children s Hospital Melbourne s manager
DIABETES POLICY Mandatory Quality Area 2 The content of this policy was developed for KPV by advocacy and diabetes educators at Diabetes Australia Vic and the Royal Children s Hospital Melbourne s manager
THE SHEFFIELD AREA PRESCRIBING GROUP. Position Statement for Prescribing of Freestyle Libre In Type 1 Diabetes. Date: March 2018.
 THE SHEFFIELD AREA PRESCRIBING GROUP Position Statement for Prescribing of Freestyle Libre In Type 1 Diabetes Date: March 2018 Overview Freestyle Libre is a flash glucose sensor device that measures *interstitial
THE SHEFFIELD AREA PRESCRIBING GROUP Position Statement for Prescribing of Freestyle Libre In Type 1 Diabetes Date: March 2018 Overview Freestyle Libre is a flash glucose sensor device that measures *interstitial
Type 2 Diabetes Recommended SMBG
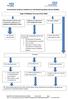 Herefordshire Diabetes Guideline for Self-Monitoring Blood Glucose (SMBG) Type 2 Diabetes Recommended SMBG Diet controlled/ metformin only/ combination of metformin and pioglitazone/dpp4/sglt2 or GLP1
Herefordshire Diabetes Guideline for Self-Monitoring Blood Glucose (SMBG) Type 2 Diabetes Recommended SMBG Diet controlled/ metformin only/ combination of metformin and pioglitazone/dpp4/sglt2 or GLP1
Case Study. Patient Profile. Baseline Report - Daily Patterns. Insights
 Case Study Patient Profile Sex/Age: Female, 48 years old Disease diagnosis: Type 2 for past 13 years, coronary artery disease for 3 years, complains of severe tiredness HbA1c: 9.0% Diabetes medication
Case Study Patient Profile Sex/Age: Female, 48 years old Disease diagnosis: Type 2 for past 13 years, coronary artery disease for 3 years, complains of severe tiredness HbA1c: 9.0% Diabetes medication
Placename CCG. Policies for the Commissioning of Healthcare
 Placename CCG Policies for the Commissioning of Healthcare Policy for the funding of insulin pumps and continuous glucose monitoring devices for patients with diabetes 1 Introduction 1.1 This document
Placename CCG Policies for the Commissioning of Healthcare Policy for the funding of insulin pumps and continuous glucose monitoring devices for patients with diabetes 1 Introduction 1.1 This document
mysugr Logbook User Manual
 mysugr Logbook User Manual Version: 3.49_Android - 2018-05-03 1 Indications for Use 1.1 Intended Use The mysugr Logbook is used to support the treatment of diabetes through daily diabetes-related data
mysugr Logbook User Manual Version: 3.49_Android - 2018-05-03 1 Indications for Use 1.1 Intended Use The mysugr Logbook is used to support the treatment of diabetes through daily diabetes-related data
Diabetes II Insulin pumps; Continuous glucose monitoring system (CGMS) Ernest Asamoah, MD FACE FACP FRCP (Lond)
 Diabetes II Insulin pumps; Continuous glucose monitoring system (CGMS) Ernest Asamoah, MD FACE FACP FRCP (Lond) 9501366-011 20110401 Objectives Understand the need for insulin pumps and CGMS in managing
Diabetes II Insulin pumps; Continuous glucose monitoring system (CGMS) Ernest Asamoah, MD FACE FACP FRCP (Lond) 9501366-011 20110401 Objectives Understand the need for insulin pumps and CGMS in managing
Inpatient Glycemic Management:
 Disclosure to Participants Conflict of Interest (COI) and Financial Relationship Disclosures: Dr. Seley attended Advisory Board Meeting: Alliance (Boehringer-Ingelheim/Lilly) Bayer Diabetes Care Sanofi
Disclosure to Participants Conflict of Interest (COI) and Financial Relationship Disclosures: Dr. Seley attended Advisory Board Meeting: Alliance (Boehringer-Ingelheim/Lilly) Bayer Diabetes Care Sanofi
INSPIRED BY GIVE HIM MORE. The MiniMed 670G system is the world s first insulin delivery system that automatically adapts to your child s needs.
 INSPIRED BY GIVE HIM MORE. The MiniMed 670G system is the world s first insulin delivery system that automatically adapts to your child s needs. * NOW APPROVED FOR AGES 7 AND UP. Waterproof to a depth
INSPIRED BY GIVE HIM MORE. The MiniMed 670G system is the world s first insulin delivery system that automatically adapts to your child s needs. * NOW APPROVED FOR AGES 7 AND UP. Waterproof to a depth
For patients uncontrolled on multiple daily injections of insulin. A quick-start guide for your practice ALL-DAY CONTROL WITH
 For patients uncontrolled on multiple daily injections of insulin A quick-start guide for your practice Dosing guidance 1,* V-Go: 3 options 1 For initiating V-Go in patients switching from MDI The majority
For patients uncontrolled on multiple daily injections of insulin A quick-start guide for your practice Dosing guidance 1,* V-Go: 3 options 1 For initiating V-Go in patients switching from MDI The majority
Research Article Measures of Adherence and Challenges in Using Glucometer Data in Youth with Type 1 Diabetes: Rethinking the Value of Self-Report
 Hindawi Diabetes Research Volume 2017, Article ID 1075428, 4 pages https://doi.org/10.1155/2017/1075428 Research Article Measures of Adherence and Challenges in Using Glucometer Data in Youth with Type
Hindawi Diabetes Research Volume 2017, Article ID 1075428, 4 pages https://doi.org/10.1155/2017/1075428 Research Article Measures of Adherence and Challenges in Using Glucometer Data in Youth with Type
Description of the technology
 Advice Note 2017/ 001 What is the clinical effectiveness, safety and budget impact of the Freestyle Libre System compared with current glucose monitoring methods for people aged 4 years and over with diabetes
Advice Note 2017/ 001 What is the clinical effectiveness, safety and budget impact of the Freestyle Libre System compared with current glucose monitoring methods for people aged 4 years and over with diabetes
Your pet s diabetes is manageable
 BLOOD GLUCOSE MONITORING SYSTEM Your pet s diabetes is manageable Treatment and Monitoring Plan for: Pet s Name: Clinic Name: Primary Vet: Clinic Phone No.: Clinic Email: Emergency Phone No: Today s Date:
BLOOD GLUCOSE MONITORING SYSTEM Your pet s diabetes is manageable Treatment and Monitoring Plan for: Pet s Name: Clinic Name: Primary Vet: Clinic Phone No.: Clinic Email: Emergency Phone No: Today s Date:
Advances in Diabetes Care Technologies
 Advances in Diabetes Care Technologies 1979 2015 Introduction Roughly 20% to 30% of patients with T1DM and fewer than 1% of insulin-treated patients with T2DM use an insulin pump In 2007, the U.S. FDA
Advances in Diabetes Care Technologies 1979 2015 Introduction Roughly 20% to 30% of patients with T1DM and fewer than 1% of insulin-treated patients with T2DM use an insulin pump In 2007, the U.S. FDA
Today s Goals 10/6/2017. New Frontiers in Diabetes Technology. Disclosures
 New Frontiers in Diabetes Technology Marie E. McDonnell, MD Director, Brigham and Women's Diabetes Program Division of Endocrinology, Diabetes and Hypertension Brigham and Women s Hospital Today s Goals
New Frontiers in Diabetes Technology Marie E. McDonnell, MD Director, Brigham and Women's Diabetes Program Division of Endocrinology, Diabetes and Hypertension Brigham and Women s Hospital Today s Goals
Self-assessment checklist
 Self-assessment checklist 1 1 All hospitals should have a fully staffed diabetes inpatient team, made up of the following 1 : consultant. Sufficient diabetes inpatient specialist nurses to run a daily
Self-assessment checklist 1 1 All hospitals should have a fully staffed diabetes inpatient team, made up of the following 1 : consultant. Sufficient diabetes inpatient specialist nurses to run a daily
C o n n e c t e d I n s u l i n D e l i v e r y S y s t e m
 Technology Innovation Alert C o n n e c t e d I n s u l i n D e l i v e r y S y s t e m 6 July 12 July, 2018 1 4 0 0 Start ups Companies Universities Individuals Interesting Innovation Compliance with
Technology Innovation Alert C o n n e c t e d I n s u l i n D e l i v e r y S y s t e m 6 July 12 July, 2018 1 4 0 0 Start ups Companies Universities Individuals Interesting Innovation Compliance with
CONTINUOUS GLUCOSE MONITORING SOLUTIONS Provided by Roche Diabetes Care
 CONTINUOUS GLUCOSE MONITORING SOLUTIONS Provided by Roche Diabetes Care More confidence for your patients 03 GIVING YOU THE CHOICE CGM solutions provided by Roche Diabetes Care Welcome to a world of new
CONTINUOUS GLUCOSE MONITORING SOLUTIONS Provided by Roche Diabetes Care More confidence for your patients 03 GIVING YOU THE CHOICE CGM solutions provided by Roche Diabetes Care Welcome to a world of new
What is diabetes? What happens in diabetes? The most common types of diabetes are type 1 and type 2. Type 2. Type 1. In people without diabetes:
 If you or someone you know has diabetes, you re not alone. Millions of people have diabetes. Diabetes cannot yet be cured. But it can be managed. The most common types of diabetes are type 1 and type 2
If you or someone you know has diabetes, you re not alone. Millions of people have diabetes. Diabetes cannot yet be cured. But it can be managed. The most common types of diabetes are type 1 and type 2
CONTINUOUS OR INTERMITTENT GLUCOSE MONITORING IN INTERSTITIAL FLUID
 FLUID Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
FLUID Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
Lessons From The Type 1 Diabetes Exchange
 Lessons From The Type 1 Diabetes Exchange Andrew Ahmann, MD Harold Schnitzer Diabetes Health Center at OHSU Presenter Disclosure Information In compliance with the accrediting board policies, the American
Lessons From The Type 1 Diabetes Exchange Andrew Ahmann, MD Harold Schnitzer Diabetes Health Center at OHSU Presenter Disclosure Information In compliance with the accrediting board policies, the American
Meeting the Challenge of Inpatient Glycemic Management in the Non-Critical Care Setting
 Meeting the Challenge of Inpatient Glycemic Management in the Non-Critical Care Setting Jane Jeffrie Seley, DNP, MPH, GNP, BC-ADM, CDE, CDTC, FAAN, FAADE Diabetes Nurse Practitioner, Inpatient Diabetes
Meeting the Challenge of Inpatient Glycemic Management in the Non-Critical Care Setting Jane Jeffrie Seley, DNP, MPH, GNP, BC-ADM, CDE, CDTC, FAAN, FAADE Diabetes Nurse Practitioner, Inpatient Diabetes
Commissioning Statement
 Commissioning Statement Treatment/ device For the treatment of Commissioning position Flash Glucose Monitoring Systems (including Freestyle Libre ) Monitoring glucose levels in adults and children over
Commissioning Statement Treatment/ device For the treatment of Commissioning position Flash Glucose Monitoring Systems (including Freestyle Libre ) Monitoring glucose levels in adults and children over
Pumping Insulin is it for your patients?
 Pumping Insulin is it for your patients? YOU CAN make managing diabetes easier. Fred Porcase D.O. Disclosures to Participants Conflicts Of Interest and Financial Relationships Disclosures: No professional
Pumping Insulin is it for your patients? YOU CAN make managing diabetes easier. Fred Porcase D.O. Disclosures to Participants Conflicts Of Interest and Financial Relationships Disclosures: No professional
Calgary Diabetes Centre Insulin Pump Therapy: Preparation and Expectations
 Calgary Diabetes Centre Insulin Pump Therapy: Preparation and Expectations This is a long and important document. It lists the steps for starting insulin pump therapy at the Calgary Diabetes Centre. It
Calgary Diabetes Centre Insulin Pump Therapy: Preparation and Expectations This is a long and important document. It lists the steps for starting insulin pump therapy at the Calgary Diabetes Centre. It
I. Promoting Student Independence
 The Nursing Support Services (NSS) Coordinator provides support according to the Provincial Standards: Supporting Students with Type 1 Diabetes in the School Setting. The NSS Coordinator delegates specific
The Nursing Support Services (NSS) Coordinator provides support according to the Provincial Standards: Supporting Students with Type 1 Diabetes in the School Setting. The NSS Coordinator delegates specific
More Than 1 Year of Hybrid Closed Loop in Pediatrics. Gregory P. Forlenza, MD Assistant Professor Barbara Davis Center
 More Than 1 Year of Hybrid Closed Loop in Pediatrics Gregory P. Forlenza, MD Assistant Professor Barbara Davis Center Disclosure Dr. Forlenza has served as a consultant for Abbott Diabetes Care and conducts
More Than 1 Year of Hybrid Closed Loop in Pediatrics Gregory P. Forlenza, MD Assistant Professor Barbara Davis Center Disclosure Dr. Forlenza has served as a consultant for Abbott Diabetes Care and conducts
