A model of GLP-1 action on insulin secretion in nondiabetic subjects
|
|
|
- Gilbert Butler
- 6 years ago
- Views:
Transcription
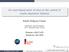
1 Am J Physiol Endocrinol Metab 298: E1115 E1121, 21. First published February 23, 21; doi:1.1152/ajpendo A model of GLP-1 action on insulin secretion in nondiabetic subjects Chiara Dalla Man, 1 Francesco Micheletto, 1 Airani Sathananthan, 2 Robert A. Rizza, 2 Adrian Vella, 2 and Claudio Cobelli 1 1 Department of Information Engineering, University of Padova, Padua, Italy; and 2 Division of Endocrinology, Diabetes, Metabolism, and Nutrition, Mayo Clinic College of Medicine, Rochester, Minnesota Submitted 3 November 29; accepted in final form 19 February 21 Dalla Man C, Micheletto F, Sathananthan A, Rizza RA, Vella A, Cobelli C. A model of GLP-1 action on insulin secretion in nondiabetic subjects. Am J Physiol Endocrinol Metab 298: E1115 E1121, 21. First published February 23, 21; doi:1.1152/ajpendo Glucagon-like peptide-1 (GLP-1)-based therapies for diabetes have aroused interest because of their effects on insulin secretion and glycemic control. However, a mechanistic model enabling quantitation of pancreatic response to GLP-1 has never been developed. To develop such a model we studied 88 healthy individuals (age yr, BMI kg/m 2 ) by use of a hyperglycemic clamp. A variable infusion maintained glucose concentrations at 15 mg/dl for 24 min. At 12 min, an intravenous infusion of GLP-1 was started (.75 pmol kg 1 min1 from min, 1.5 pmol kg 1 min1 from min). Consequently, plasma C-peptide concentration rose from 1, pmol/l at 12 min to 4, pmol/l at 18 min and to 6, pmol/l at 24 min. Four models of GLP-1 action on insulin secretion were considered. All models share the common assumption that insulin secretion is made up of two components, one proportional to glucose rate of change through dynamic responsivity, d, and one proportional to glucose through static responsivity, s, but differing by modality of GLP-1 control. The model that best fit C-peptide data assumes that above-basal insulin secretion depends linearly on GLP-1 concentration and its rate of change. An index () measuring the percentage increase of secretion due to GLP-1 is derived. Before GLP-1 infusion, d and s min 1. Under GLP-1 stimulus, % per pmol/l, meaning that an increase of 5 pmol/l in peripheral GLP-1 concentrations induces an 6% increase in over-basal insulin secretion. glucagon-like peptide-1; incretins; C-peptide; hyperglycemic clamp; -cell responsivity; parameter estimation Address for reprint requests and other correspondence: C. Cobelli, Dept. of Information Engineering, Univ. of Padova, Via Gradenigo 6/B, I Padua, Italy ( cobelli@dei.unipd.it). GLUCAGON-LIKE PEPTIDE-1 (GLP-1) is produced by the enteroendocrine L cells of the intestinal mucosa and is released into the portal circulation in response to meal ingestion (2). It arises from the posttranslational processing of proglucagon by prohormone convertase-1 (PC-1) in the enteroendocrine L cells of the intestinal mucosa (16). GLP-1 enhances insulin secretion and inhibits glucagon release in a glucose-dependent manner (17), prompting the development of GLP-1-based therapies for the treatment of diabetes (11). However, infused GLP-1 is rapidly inactivated by the widely distributed enzyme dipeptidyl peptidase-4 (DPP-4), which removes the two NH 2 -terminal amino acids, consequently requiring constant infusion to maintain its effects on insulin secretion. GLP-1-based therapy for type 2 diabetes has required the development of GLP-1 receptor agonists that resist the action of DPP-4 (21) or compounds that inhibit DPP-4, thereby raising endogenous concentrations of active GLP-1 (1). It has previously been suggested that genetic differences may explain some of the variation to GLP-1 response in prior studies (25). Several studies are available on GLP-1 action on insulin secretion both at the cellular (13, 14, 18) and at the whole body levels (1, 2, 1, 15, 17, 19); however, none of them has ever aimed to mechanistically model GLP-1 action on insulin secretion. In fact, quantitating the effect of GLP-1 on insulin secretion is not straightforward, given that GLP-1 delays gastric emptying (26) and is a glucose-dependent secretagogue. Consequently, measuring the response to an oral meal challenge has required the use of modeling techniques to account for changes in insulin secretion in response to changing glucose concentrations. Changes in gastric emptying alter the rate of portal appearance of meal-derived glucose and consequently need to be accounted for in such situations. These considerations have often led to the use of a hyperglycemic clamp to quantitate response to GLP-1 infusion. However, peripheral insulin concentrations do not represent insulin secretion but rather the sum of pancreatic insulin secretion, hepatic insulin extraction, and distribution into the circulating compartment. Thus, more accurate measurements of insulin secretion are based on deconvolution (12, 24 27) from C-peptide concentrations, given that both are secreted in an equimolar fashion and C-peptide is not extracted by the liver. However, to mechanistically describe pancreatic insulin secretion and derive indexes of -cell function, one can use the C-peptide minimal model (4), which allows exploration of the influence of glucose concentrations on insulin secretion, after a glucose perturbation. Furthermore, infusion of GLP-1 adds a second secretagogue that influences insulin secretion in concert with hyperglycemia. Developing a modification of the C-peptide minimal model that allows quantitation of the effect of hyperglycemia and GLP-1 on -cell secretion would therefore be an important tool with which to explore the basis for interindividual differences in insulin secretion in response to GLP-1. We therefore studied a group of healthy subjects by use of a hyperglycemic clamp and two infusion rates of GLP-1 (halfmaximal and maximal). We subsequently used glucose, GLP-1, and C-peptide data to develop a model to describe these data and quantitate the percentage increase of secretion due to GLP-1. RESEARCH DESIGN AND METHODS Subjects After approval from the Mayo Institutional Review Board, 88 subjects with an overnight fasting glucose 5.3 mmol/l gave written informed consent to participate in the study. All subjects were in good health, were at a stable weight, and did not engage in regular vigorous exercise. Subjects (52 females and 36 males) were 4 yr of age (average yr) at the time of participation and had no history /1 Copyright 21 the American Physiological Society E1115
2 E1116 of impaired fasting glucose or diabetes or of prior therapy with antidiabetic medication. Subjects had a BMI between 19 and 4 kg/m 2 (average kg/m 2 ) and no history of chronic disease or prior abdominal surgery. All subjects were instructed to follow a weight maintenance diet containing 55% carbohydrate, 3% fat, and 15% protein for the period of study. Body composition was measured using dual-energy X-ray absorptiometry (DPX scanner; Lunar, Madison, WI). Experimental Design Subjects were admitted to the CRU at 17 on the evening prior to the study. Subsequently, they consumed a standard 1 cal/kg meal (55% carbohydrate, 3% fat, and 15% protein), after which they fasted overnight. At 6 (6 min) a forearm vein was cannulated with an 18-gauge needle to allow infusions to be performed. An 18-gauge cannula was inserted retrogradely into a vein of the dorsum of the contralateral hand. This was placed in a heated Plexiglas box maintained at 55 C to allow sampling of arterialized venous blood. At time min a primed (.1 g/kg over 4 min), continuous infusion of 5% dextrose was initiated. The dextrose infusion rate was varied to maintain peripheral glucose concentrations at 15 mg/dl (Fig. 1). At 12 min, GLP-1(7 36) amide (Bachem, San Diego, CA) was infused (15 pmol/kg lean body mass over 1 min and then at a rate of.75 pmol kg 1 min1 ). At 18 min, the infusion rate was increased to 1.5 pmol kg 1 min1. Prior experience with infusion of GLP-1 at a fixed rate (1.2 pmol kg 1 min1 ) has suggested that such an infusion requires 2 3 min to reach adequate concentrations of GLP-1 (32). Given the short duration of infusion, we used a higher infusion rate for the first 1 min to rapidly achieve elevated GLP-1 concentrations. We did not use a GLP-1 bolus over 2 3 min, in order to avoid potential nausea and vomiting associated with a rapid, sudden rise of GLP-1 concentrations. Blood was collected at frequent intervals over the duration of the study (24 min). Analytic Techniques Plasma samples were placed on ice, centrifuged at 4 C, separated, and stored at 2 C until assayed. Glucose concentrations were Fig. 1. Average glucose infusion rate used to maintain glucose level at 15 mg/dl, despite change in GLP-1 induced C-peptide concentrations. Error bars represent standard error. measured using a glucose oxidase method (Yellow Springs Instruments, Yellow Springs, OH). Plasma GLP-1, glucagon, and C-peptide were measured by RIA using reagents supplied by Linco Research (St. Louis, MO). Sample tubes utilized for measurement of active GLP-1 had 1 M of DPP-4 inhibitor (Linco Research, St. Louis, MO) added. C-peptide Minimal Model The model used to describe C-peptide secretion before GLP-1 infusion is the C-peptide minimal model originally proposed in Ref. 28 for graded up-and-down glucose infusion and then employed also during an oral test (4). Briefly, the pancreatic secretion (SR) is linked to plasma C-peptide concentration by the two-compartment model of C-peptide kinetics originally proposed by Eaton et al. (12): ĊP1(t) k1 k21] CP1(t) k12 CP2(t) SR(t) CP1() CP1b k 21 (1) ĊP 2 (t) k 21 CP 1 (t) k 12 CP 2 (t) CP 2 () CP 2b CP 1b k 12 where CP 1 and CP 2 (pmol/l) are C-peptide concentrations in the accessible and peripheral compartments, respectively, and k 1, k 12, and k 21 (min 1 ) are C-peptide kinetic parameters fixed to standard values (3) to ensure numerical identification of the overall model. The model also assumes that SR is made up of a basal (SR b), a static (SR s), and a dynamic (SR d) component: SR(t) SR b (t) SR s (t) SR d (t) (2) SR s is assumed equal to the provision of releasable insulin to -cells, controlled by glucose concentration above a threshold level h: ṠR s (t) [SR s (t) s (G(t) h)] (3) Basically, the static secretion component is proportional, through parameter s, to delayed glucose concentration above a threshold h, with a time delay equal to 1/. s is the static -cell responsivity to glucose and measures the ability of glucose to stimulate SR s. SRd represents the secretion of insulin from the promptly releasable pool and is proportional to the rate of increase of glucose: SR d (t) d dg(t) if dg(t) otherwise and G(t) G b (4) where d is the dynamic -cell responsivity to glucose and measures the ability of glucose rate of change to stimulate SR d. The over-basal insulin secretion (SR) is thus SR(t) SR s (t) SR d (t) (5) GLP-1 Minimal Models Since several reports in the literature indicate that GLP-1 acts only on above-basal insulin secretion while it has no effect on basal secretion, (2, 13, 17), we assumed that GLP-1 potentiates only above-basal insulin secretion. Four models of increasing complexity of GLP-1 action have been tested. Model 1. Model 1 assumes a proportional action of GLP-1 on over-basal insulin secretion: SR glp1 (t) SR(t) [a GLP1(t) 1] (6) with SR(t) the glucose-dependent secretion rate before GLP-1 infusion, SR glp1 (t) the glucose-dependent secretion rate after GLP-1 infusion, GLP1(t) the over-basal hormone concentration, and a model parameter. Model 2. Model 2 assumes a proportional plus derivative action of GLP-1 on SR : AJP-Endocrinol Metab VOL 298 JUNE 21
3 SR glp1 SR(t) dglp1t a GLP1(t) b SR(t) [a GLP1(t) 1] 1 if dglp1(t) otherwise (7) with a and b model parameters representing the percentage increase of SR due to the GLP-1 and GLP-1 rate of change, respectively. Model 3. Our data show that the relationship between GLP-1 and C-peptide concentrations is likely to be nonlinear (see RESULTS, Plasma C-peptide and GLP-1 concentration). Thus, model 3 is proposed, which assumes a nonlinear (Michaelis-Menten) action of GLP-1 on SR: c SR glp1 (t) SR(t) 1 (8) d GLP1(t) with c and d model parameters representing, respectively, the maximum percentage increase of SR due to GLP-1 and the value of the above-basal GLP-1 concentration at which the half-maximum percentage increase is obtained. Model 4. Finally, model 4 assumes a nonlinear and derivative action of GLP-1 on SR: SR SR(t) glp1 1 c GLP1(t) dglp1(t) b dglp1t d GLP1(t) if (9) c SR(t) 1 otherwise d GLP1(t) with b, c, and d defined as above. The GLP-1 Potentiation Index It is useful to quantify the ability of GLP-1 to control insulin secretion through a potentiation index (). The index is defined as the ratio between the average percent increase in over-basal insulin secretion and average GLP-1 plasma concentration. With this definition, (% per pmol/l) can be derived for all the above models. However, since model 2 was selected as the most parsimonious (see RESULTS), we report the derivation of only for model 2: SR glp1 (t) SR(t) SR(t) 1 GLP1(t) a GLP1(t) b dglp1(t) GLP1(t) 1 dglp1(t) a b 1 GLP1(t) max a b 1 (1) AUCGLP1t) with AUC denoting the area under the curve and GLP1 max the peak value of over-basal GLP-1 concentration. Parameter Estimation and Model Comparison The GLP-1 models have been incorporated into the C-peptide model to describe SR as function of glucose and GLP-1 concentrations. All models were numerically identified on C-peptide data by nonlinear least squares (6, 7), as implemented in SAAM II [Simulation Analysis and modelling software (3)]. Error of C-peptide data was assumed to be independent, Gaussian, and with zero mean and known variance (29). Glucose and GLP-1 concentrations and, for models 2 and 4, GLP-1 rate of change are the model-forcing functions, assumed to be known without error. Since cost and blood volume considerations limited the number of GLP-1 data points available, we calculated the derivative on a virtually continuous signal reconstructed by stochastic deconvolution (9). Models were compared on the basis of the following criteria (see Ref. 7 for details): ability to describe the data (weighted residual square sum, WRSS), precision of parameter estimates (expressed as CV), model parsimony (Akaike information criterion, AIC), and residual independence (Anderson run test). Moreover, since more complex models collapsed into simpler models when one or more parameters were estimated to be, we also considered as a criterion the percentage of identifications for which all parameters were nonzero. Statistical Analysis Data are presented as means SE, if not differently indicated. Two-sample comparisons were done by Wilcoxon signed rank test (significance level set to 5%). Pearson s correlation was used to evaluate univariate correlation. RESULTS E1117 Plasma C-Peptide and GLP-1 Concentration Basal plasma C-peptide concentration was pmol/l; at 12 min, before the intravenous infusion of GLP-1 was started, C-peptide concentration was 1, pmol/l, due to the rise in glucose concentration, and plasma GLP-1 was pmol/l. After the GLP-1 infusion, plasma GLP-1 concentration increased to pmol/l at 18 min and to pmol/l at 24 min (all differences were statistically significant, P.1), and consequently C- peptide concentration rose to 4, and 6, at 18 and 24 min, respectively (all differences were statistically significant, P.1) (Fig. 2). The ratios between above-basal C-peptide and above-basal GLP-1 concentrations were and at 18 and 24 min, respectively, and the difference was statistically significant (P.1). As already mentioned, this result supports the hypothesis that GLP-1 acts nonlinearly on C-peptide secretion. Model Comparison Table 1 shows the criteria used for model selection. All the tested models fit the data well as confirmed by the Run Test, which supported randomness of residuals in 7% of the subjects. Time courses of weighted residuals obtained with the four models are shown in Fig. 3. Model 4 provided, on average, the best fit. As expected, increasing the complexity of the model (and the number of parameters), worsens the precision of parameter estimates (increased CV), but the parsimony criterion indicates model 4 as the most parsimonious (lowest AIC). On the other hand, model 4 collapsed into simpler models in most cases: e.g., to model 3 in 11 subjects, since parameter b was zero, to model 2 in 43 subjects, since parameter d was very high, and even to model 1 in 17 subjects, since both changes in parameters b and d occurred. Even if in the remaining 21 subjects model 4 was superior to the other models, we are inclined to select model 2 as the best model, AJP-Endocrinol Metab VOL 298 JUNE 21
4 E1118 Fig. 2. Average plasma glucose (top left), insulin (top right) C-peptide (bottom left), and GLP-1 concentrations (bottom right). Error bars represent standard error. since it is the most parsimonious to adequately fit the data in most cases. In addition (see below), it provides estimates of the potentiation index only modestly different from that of model 4, which is the most complex among the proposed models. Model Indexes model parameters are reported in Table 2 together with their precision. Before GLP-1 infusion, -cell responsivity indexes were: s min 1 and d Under GLP-1 stimulus, the potentiation index estimated with model 2 was % per pmol/l. This means that, if peripheral active GLP-1 concentration increases of 5 pmol/l, as occurs after a meal, over-basal insulin secretion is increased by 6%. Note that if potentiation index were estimated with more complex models, similar results would have been obtained; e.g., with model 4, % per pmol/l (correlation with model 2 index: R.95 P.1). This confirms that model 2, despite being less accurate than model 4 in some cases, still provides good estimates of the efficiency of the GLP-1 control on over-basal insulin secretion. DISCUSSION GLP-1 is a potent insulin secretagogue that stimulates insulin secretion in a glucose-dependent manner. When infused in supraphysiological concentrations, it delays gastric emptying and promotes satiety (8), leading to weight loss (33). Since these actions are useful in the treatment of type 2 diabetes, GLP-1-based therapy for type 2 diabetes has been developed for clinical use in humans. The role of such therapies in the treatment algorithm for type 2 diabetes is as yet uncertain; consequently, neither DPP-4 inhibitors nor GLP-1 receptor agonists are used as first-line therapy. However, there has been some suggestion that there is interindividual heterogeneity in response to GLP-1, raising the possibility that some individuals may benefit more from such therapy than others earlier in the disease (25, 31). Given the potential expense and side effects from such intervention, it would be reasonable to develop a quantitative measure of GLP-1-induced insulin secretion that can be used to examine differences in individual response to this hormone. Several studies are available on GLP-1 action on insulin secretion (1, 2, 1, 13 15, 17 19), however, to the best of our knowledge, none of them has ever aimed to mechanistically model GLP-1 Table 1. Comparison of GLP-1 action models Residual Independence (Run Test) Data Fit (WRSS) Precision (CV) Parsimony Criterion (AIC) No. Parameters %Nonzero Parameters Model 1 68% 192 7% % Model 2 75% % % Model 3 7% % % Model 4 71% 19 28% % AJP-Endocrinol Metab VOL 298 JUNE 21
5 E1119 Fig. 3. Average weighted residuals obtained with models 1, 2, 3, and 4. Error bars represent standard deviation. action on -cells. For instance, other investigators have previously utilized a hyperglycemic clamp to measure insulin secretion from deconvoluted C-peptide data. However, such a methodology does not take into account potential changes in glucose concentration during the hyperglycemic clamp or the changing GLP-1 concentrations prevailing during the experiment. The only model that indirectly accounts for a potentiation due to incretin is the one proposed by Mari et al. (2). It introduced a potentiating factor, which modulates the doseresponse relation between insulin secretion and plasma glucose to better fit the C-peptide data, but it did not explicitly describe the incretin effect. Other studies (e.g., Ref. 1) also found a correlation between GLP-1 and the potentiating factor or utilized the model to assess different hormone responses in the morning vs. the afternoon (19). Another method used to assess incretin potentiation was that employed in Ref. 5. There the -cell responsivities to glucose, s, and d were calculated for both oral and intravenous matched glucose infusions, using the C-peptide minimal model originally proposed by Toffolo et al. for graded up-and-down glucose infusion (28) and then em- Table 2. Estimates of model parameters Model 1 Model 2 Model 3 Model 4 [min 1 ] (1) (1) (1) (1) h [mg/dl] (4) (4) (4) (4) d [1 9 ] (5) (5) (5) (5) s [1 9 min1 ] (8) (8) (8) (8) a [l/pmol] (7) (6) b [l min/pmol] (21) (25) c [dimensionless] (16) (11) d [pmol/l] (36) (33) Values are means SE. Numbers in parentheses represent CV%. AJP-Endocrinol Metab VOL 298 JUNE 21
6 E112 ployed during an oral test (4). The difference between oral and intravenous indexes provided an indirect measure of the incretin effect; there was an 6% difference between the two indexes, implying that the incretin effect is responsible for such potentiation. However, in none of the above studies was there an attempt to mechanistically describe GLP-1 action on insulin secretion. The novelty of the present study is thus the development and validation against experimental data of a model of GLP-1 action on insulin secretion that, in contrast to other methods, allows simultaneous estimation of both -cell responsivity to glucose and of the ability of GLP-1 to enhance secretion. This model is a potential tool to quantitate between-subject variation in response to GLP-1. To this end, 88 healthy individuals were studied. They underwent a hyperglycemic clamp with an exogenous infusion of GLP-1 (Fig. 1), which brought hormone concentration first to physiological and then to supraphysiological concentrations (Fig. 2). Four models have been tested. All of them are based on the common assumption that insulin secretion is made up of a basal component; a dynamic component, proportional to glucose rate of change through the dynamic responsivity index d (1 9 ); and a static index, proportional to glucose through the static responsivity s (1 9 min 1 ) (4). Moreover, since it is known that GLP-1 enhances insulin secretion in a glucosedependent manner (2, 13, 17), all of the tested models assume that GLP-1 concentration modulates the above-basal insulin secretion. Models differ in the modalities with which GLP-1 controls insulin secretion, e.g., linear or nonlinear, static or derivative control. We found that model 2 was the most parsimonious (Table 1). In fact, it better fit the C-peptide data and provided precise parameter estimates in the largest number of subjects. It provides a potentiation index, % per pmol/l, measuring the ability of GLP-1 to promote above-basal insulin secretion. To appreciate the meaning of this index, consider that, during hyperglycemic conditions (15 mg/dl), an increase of 5 pmol/l in peripheral GLP-1 concentrations, similar to that occurring after a meal, is predicted to induce a 63% increase in glucose-stimulated insulin secretion. This finding is comparable with the results reported in Ref. 5 for an OGTT, although the levels of GLP-1 were not reported. Furthermore, we also identified the original C-peptide model separately in the intervals 12 min (no incretin stimulation) and min (incretin stimulation) and estimated two different s, i.e., s 12 and s s was 326% higher on average than s 12, due to an average increase in GLP-1 of 29 pmol/l. This is in agreement with Ref. 5 if one assumes that an average 5 pmol/l increase of GLP-1 is likely to occur during an oral test. As observed in RESULTS, model selection criteria would have indicated model 4 as the most parsimonious. However, model 4 reduces to model 3 in 11 subjects, since parameter b was zero, to model 2 in 43 subjects, since parameter d was very high, and to model 1 in 17 subjects, since both changes in parameters b and d occurred. One can thus speculate that model 4 is the most general model that is able to predict the C-peptide concentration in very challenging conditions, such as during a hyperglycemic clamp with GLP-1 at physiological and supraphysiological concentration, whereas in most subjects or different experimental conditions, e.g., during a meal, a simpler model (but derived from model 4) may be sufficient; e.g., model 2 is a better candidate when plasma GLP-1 excursions are smaller; thus, the use of a nonlinear model may be not necessary. Of note, the potentiation index provided by model 2 is virtually identical to that obtained with model 4 ( % vs % per pmol/l, R.95, P.1). This supports that, even though simpler, model 2 is robust enough to adequately quantify the action of GLP-1 on glucose-dependent insulin secretion. Finally, it is interesting to note that the model describing the glucose-dependent insulin secretion (4, 28) is linear in both d and s ; i.e., doubling d or s results in doubling SR d or SR s, respectively. Therefore, all the models described in the section GLP-1 Minimal Models can be rewritten in terms of GLP-1 action of -cell responsivity indexes; i.e., can be defined as the percentage increase of s and d due to GLP-1. This means that GLP-1 produces the same potentiation on both the dynamic and the static phases. The assumption that both d and s are similarly modulated by GLP-1 relies on the evidence provided in Ref. 5, where the percentage increases of d and s due to incretins were similar (58 and 63%, respectively). The adopted protocol design does not allow us to verify this assumption. In fact, when GLP-1 is infused, i.e., from t 12 to 24 min, glucose is approximately constant and the dynamic phase of insulin secretion is virtually absent. This makes it impossible to separately assess GLP-1 potentiation on the dynamic phase ( d ). As a matter of fact, four additional models, similar in structure to models 1, 2 3 and 4, respectively, but assuming GLP-1 action on static phase ( s ) only, performed similarly to their counterparts. However, we believe that, in light of the applicability of the model to different protocols, the GLP-1 action on dynamic insulin secretion has to be included in the model. In conclusion, a model of GLP-1 action of insulin secretion in nondiabetic subjects has been proposed. The model has been tested on data obtained from a hyperglycemic clamp with exogenous infusion of GLP-1. Further studies are needed to assess its validity during different protocols, e.g., meal or OGTT, and its applicability in type 2 diabetic patients. GRANTS We acknowledge the support of the Mayo Clinic CTSA Grant RR-2415 and Minnesota Obesity Center Grant DK A. Vella and C. Cobelli are supported by DK and R. A. Rizza by DK DISCLOSURES One or more authors is employed by and/or has a total financial interest worth more than $1, (from consultancy honoraria/expert testimony/corporate grants/patents pending/royalties/other) and/or has a 5% equity in an entity related to the subject matter discussed in the paper. A. Vella has received research grants from Merck and has consulted for Sanofi Aventis and CPEX Pharmaceuticals. REFERENCES 1. Ahrén B, Holst JJ, Mari A. Characterization of GLP-1 effects on beta-cell function after meal ingestion in humans. Diabetes Care 26: , Baggio LL, Drucker DJ. Biology of incretins: GLP-1 and GIP (Review). Gastroenterology 132: , Barrett PH, Bell BM, Cobelli C, Golde H, Schumitzky A, Vicini P, Foster D. SAAM II: Simulation, Analysis, and modeling software for tracer and pharmacokinetic studies. Metabolism 47: , AJP-Endocrinol Metab VOL 298 JUNE 21
7 E Breda E, Cavaghan MK, Toffolo G, Polonsky KS, Cobelli C. Oral glucose tolerance test minimal model indexes of beta-cell function and insulin sensitivity. Diabetes 5: , Campioni M, Toffolo G, Shuster LT, Service FJ, Rizza RA, Cobelli C. Incretin effect potentiates -cell responsivity to glucose as well as to its rate of change: OGTT and matched intravenous study. Am J Physiol Endocrinol Metab 292: E54 E6, Carson ER, Cobelli C, Finkelstein L. The Mathematical modeling of Endocrine-Metabolic Systems. Model Formulation, Identification and Validation. New York: Wiley, Cobelli C, Foster D, Toffolo G. Tracer Kinetics in Biomedical Research: from Data to Model. Kluwer Academic/Plenum, New York, Delgado-Aros S, Kim DY, Burton DD, Thomforde GM, Stephens D, Brinkmann BH, Vella A, Camilleri M. Effect of GLP-1 on gastric volume, emptying, maximum volume ingested, and postprandial symptoms in humans. Am J Physiol Gastrointest Liver Physiol 282: G424 G431, De Nicolao G, Sparacino G, Cobelli C. Nonparametric input estimation in physiological systems: problems, methods, and case studies. Automatica 33: , Drucker DJ. Therapeutic potential of dipeptidyl peptidase IV inhibitors for the treatment of type 2 diabetes. Expert Opin Investig Drugs 12: 87 1, Drucker DJ, Nauck MA. The incretin system: glucagon-like peptide-1 receptor agonists and dipeptidyl peptidase-4 inhibitors in type 2 diabetes. Lancet 368: , Eaton RP, Allen RC, Schade DS, Erickson KM, Standefer J. Prehepatic insulin production in man: kinetic analysis using peripheral connecting peptide behavior. J Clin Endocrinol Metab 51: , Farilla L, Bulotta A, Hirshberg B, Li Calzi S, Khoury N, Noushmehr H, Bertolotto C, Di Mario U, Harlan DM, Perfetti R. Glucagon-like peptide 1 inhibits cell apoptosis and improves glucose responsiveness of freshly isolated human islets. Endocrinology 144: , Fujimoto W, Miki T, Ogura T, Zhang M, Seino Y, Satin LS, Nakaya H, Seino S. Niflumic acid-sensitive ion channels play an important role in the induction of glucose-stimulated insulin secretion by cyclic AMP in mice. Diabetologia 52: , Højberg PV, Zander M, Vilsbøll T, Knop FK, Krarup T, Vølund A, Holst JJ, Madsbad S. Near normalisation of blood glucose improves the potentiating effect of GLP-1 on glucose-induced insulin secretion in patients with type 2 diabetes. Diabetologia 51: , Holst JJ, Bersani M, Johnsen AH, Kofod H, Hartmann B, Orskov C. Proglucagon processing in porcine and human pancreas. J Biol Chem 269: , Holst JJ, Toft-Nielsen MB, Orskov C, Nauck M, Willms B. On the effects of glucagon-like peptide-1 on blood glucose regulation in normal and diabetic subjects. Ann NY Acad Sci 85: , Kwan EP, Gao X, Leung YM, Gaisano HY. Activation of exchange protein directly activated by cyclic adenosine monophosphate and protein kinase A regulate common and distinct steps in promoting plasma membrane exocytic and granule-to-granule fusions in rat islet beta cells. Pancreas 35: e45 e54, Lindgren O, Mari A, Deacon CF, Carr RD, Winzell MS, Vikman J, Ahrén B. Differential islet and incretin hormone responses in morning versus afternoon after standardized meal in healthy men. J Clin Endocrinol Metab 94: , Mari A, Schmitz O, Gastaldelli A, Oestergaard T, Nyholm B, Ferrannini E. Meal and oral glucose tests for assessment of -cell function: modeling analysis in normal subjects. Am J Physiol Endocrinol Metab 283: E1159 E1166, Nauck MA, Meier JJ. Glucagon-like peptide 1 and its derivatives in the treatment of diabetes. Regul Pept 128: , Pillonetto G, Sparacino G, Cobelli C. Reconstructing insulin secretion rate after a glucose stimulus by an improved stochastic deconvolution method. IEEE Trans Biomed Eng 48: , Polonsky KS, Rubenstein AH. C-peptide as a measure of the secretion and hepatic extraction of insulin: Pitfalls and limitations. Diabetes 33: , Polonsky KS, Licinio-Paixao J, Given BD, Pugh W, Rue P, Galloway J, Karrison T, Frank B. Use of biosynthetic human C-peptide in the measurement of insulin secretion rates in normal volunteers and type I diabetic patients. J Clin Invest 51: 98 15, Schafer SA, Tschritter O, Machicao F, Thamer C, Stefan N, Gallwitz B, Holst JJ, Dekker JM, t Hart LM, Nijpels G, van Haeften TW, Haring HU, Fritsche A. Impaired glucagon-like peptide-1-induced insulin secretion in carriers of transcription factor 7-like 2 (TCF7L2) gene polymorphisms. Diabetologia 5: , Schirra J, Wank U, Arnold R, Goke B, Katschinski M. Effects of glucagon-like peptide-1(7 36)amide on motility and sensation of the proximal stomach in humans. Gut 5: , Sparacino G, Cobelli C. A stochastic deconvolution method to reconstruct insulin secretion rate after a glucose stimulus. IEEE Trans Biomed Eng 43: , Toffolo G, Breda Cavaghan MK E, Ehrmann DA, Polonsky KS, Cobelli C. Quantitative indexes of -cell function during graded up-anddown glucose infusion from C-peptide minimal models. Am J Physiol Endocrinol Metab 28: E2 E1, Toffolo G, Campioni M, Basu R, Rizza RA, Cobelli C. A minimal model of insulin secretion and kinetics to assess hepatic insulin extraction. Am J Physiol Endocrinol Metab 29: E169 E176, Van Cauter E, Mestrez F, Sturis J, Polonsky KS. Estimation of insulin secretion rates from C-peptide levels. Comparison of individual and standard kinetic parameters for C-peptide clearance. Diabetes 41: , Vella A, Camilleri M. Pharmacogenetics: potential role in the treatment of diabetes and obesity. Expert Opin Pharmacother 9: , Vella A, Shah P, Basu R, Basu A, Holst JJ, Rizza RA. Effect of glucagon-like peptide 1(7 36) amide on glucose effectiveness and insulin action in people with type 2 diabetes. Diabetes 49: , Zander M, Madsbad S, Madsen JL, Holst JJ. Effect of 6-week course of glucagon-like peptide 1 on glycaemic control, insulin sensitivity, and beta-cell function in type 2 diabetes: a parallel-group study. Lancet 359: , 22. AJP-Endocrinol Metab VOL 298 JUNE 21
The oral meal or oral glucose tolerance test. Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol
 Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol Minimal Model Assessment of -Cell Responsivity and Insulin Sensitivity in Nondiabetic Individuals Chiara Dalla Man,
Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol Minimal Model Assessment of -Cell Responsivity and Insulin Sensitivity in Nondiabetic Individuals Chiara Dalla Man,
Electronic Supplementary Material to the article entitled Altered pattern of the
 Electronic Supplementary Material to the article entitled Altered pattern of the incretin effect as assessed by modelling in individuals with glucose tolerance ranging from normal to diabetic Integrated
Electronic Supplementary Material to the article entitled Altered pattern of the incretin effect as assessed by modelling in individuals with glucose tolerance ranging from normal to diabetic Integrated
Quantitative indexes of -cell function during graded up&down glucose infusion from C-peptide minimal models
 Am J Physiol Endocrinol Metab 280: E2 E10, 2001. Quantitative indexes of -cell function during graded up&down glucose infusion from C-peptide minimal models GIANNA TOFFOLO, 1 ELENA BREDA, 1 MELISSA K.
Am J Physiol Endocrinol Metab 280: E2 E10, 2001. Quantitative indexes of -cell function during graded up&down glucose infusion from C-peptide minimal models GIANNA TOFFOLO, 1 ELENA BREDA, 1 MELISSA K.
Dipeptidyl Peptidase-4 Inhibition by Vildagliptin and the Effect on Insulin Secretion and Action in Response to Meal Ingestion in Type 2 Diabetes
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Dipeptidyl Peptidase-4 Inhibition by Vildagliptin and the Effect on Insulin Secretion and Action in Response to Meal
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Dipeptidyl Peptidase-4 Inhibition by Vildagliptin and the Effect on Insulin Secretion and Action in Response to Meal
The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans
 The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Seoul National University College of Medicine Plasma glucose
The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Seoul National University College of Medicine Plasma glucose
Characterization of GLP-1 Effects on -Cell Function After Meal Ingestion in Humans
 Emerging Treatments and Technologies O R I G I N A L A R T I C L E Characterization of GLP-1 Effects on -Cell Function After Meal Ingestion in Humans BO AHRÉN, MD, PHD 1 JENS J. HOLST, MD, PHD 2 ANDREA
Emerging Treatments and Technologies O R I G I N A L A R T I C L E Characterization of GLP-1 Effects on -Cell Function After Meal Ingestion in Humans BO AHRÉN, MD, PHD 1 JENS J. HOLST, MD, PHD 2 ANDREA
Management of Type 2 Diabetes
 Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
la prise en charge du diabète de
 N21 XIII Congrès National de Diabétologie, 29 mai 2011, Alger Intérêt et place des Anti DPP4 dans la prise en charge du diabète de type 2 Nicolas PAQUOT, MD, PhD CHU Sart-Tilman, Université de Liège Belgique
N21 XIII Congrès National de Diabétologie, 29 mai 2011, Alger Intérêt et place des Anti DPP4 dans la prise en charge du diabète de type 2 Nicolas PAQUOT, MD, PhD CHU Sart-Tilman, Université de Liège Belgique
GLP-1 agonists. Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK
 GLP-1 agonists Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What do GLP-1 agonists do? Physiology of postprandial glucose regulation Meal ❶ ❷ Insulin Rising plasma
GLP-1 agonists Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What do GLP-1 agonists do? Physiology of postprandial glucose regulation Meal ❶ ❷ Insulin Rising plasma
28 Regulation of Fasting and Post-
 28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE. CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010
 Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Scope. History. History. Incretins. Incretin-based Therapy and DPP-4 Inhibitors
 Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
New and Emerging Therapies for Type 2 DM
 Dale Clayton MHSc, MD, FRCPC Dalhousie University/Capital Health April 28, 2011 New and Emerging Therapies for Type 2 DM The science of today, is the technology of tomorrow. Edward Teller American Physicist
Dale Clayton MHSc, MD, FRCPC Dalhousie University/Capital Health April 28, 2011 New and Emerging Therapies for Type 2 DM The science of today, is the technology of tomorrow. Edward Teller American Physicist
Chief of Endocrinology East Orange General Hospital
 Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Alternative insulin delivery systems: how demanding should the patient be?
 Diabetologia (1997) 4: S97 S11 Springer-Verlag 1997 Alternative insulin delivery systems: how demanding should the patient be? K.S. Polonsky, M. M. Byrne, J. Sturis Department of Medicine, The University
Diabetologia (1997) 4: S97 S11 Springer-Verlag 1997 Alternative insulin delivery systems: how demanding should the patient be? K.S. Polonsky, M. M. Byrne, J. Sturis Department of Medicine, The University
Agus Kartono, Egha Sabila Putri, Ardian Arif Setiawan, Heriyanto Syafutra and Tony Sumaryada
 American Journal of Applied Sciences Original Research Paper Study of Modified Oral Minimal Model using n-order Decay Rate of Plasma Insulin for the Oral Glucose Tolerance Test in Subjects with Normal,
American Journal of Applied Sciences Original Research Paper Study of Modified Oral Minimal Model using n-order Decay Rate of Plasma Insulin for the Oral Glucose Tolerance Test in Subjects with Normal,
The Oral Minimal Model Method
 Diabetes Volume 63, April 2014 1203 Claudio Cobelli, 1 Chiara Dalla Man, 1 Gianna Toffolo, 1 Rita Basu, 2 Adrian Vella, 2 and Robert Rizza 2 The Oral Minimal Model Method The simultaneous assessment of
Diabetes Volume 63, April 2014 1203 Claudio Cobelli, 1 Chiara Dalla Man, 1 Gianna Toffolo, 1 Rita Basu, 2 Adrian Vella, 2 and Robert Rizza 2 The Oral Minimal Model Method The simultaneous assessment of
Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP
 Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP KEY POINTS sitagliptin (Januvia) is a DPP-4 inhibitor that blocks the breakdown of the
Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP KEY POINTS sitagliptin (Januvia) is a DPP-4 inhibitor that blocks the breakdown of the
Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function
 Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function Background. Following meal ingestion, several hormones are released from the gastrointestinal tract. Some
Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function Background. Following meal ingestion, several hormones are released from the gastrointestinal tract. Some
GLP 1 agonists Winning the Losing Battle. Dr Bernard SAMIA. KCS Congress: Impact through collaboration
 GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
The Mediterranean Diet: HOW and WHY It Works So Well for T2DM
 The Mediterranean Diet: HOW and WHY It Works So Well for T2DM Susan L. Barlow, RD, CDE. Objectives 1. Discuss the effects of meal size on GLP-1 concentrations. 2. Compare and contrast the specific effects
The Mediterranean Diet: HOW and WHY It Works So Well for T2DM Susan L. Barlow, RD, CDE. Objectives 1. Discuss the effects of meal size on GLP-1 concentrations. 2. Compare and contrast the specific effects
INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES
 INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES ARSHNA SANGHRAJKA DIABETES SPECIALIST PRESCRIBING PHARMACIST OBJECTIVES EXPLORE THE TYPES OF INSULIN AND INJECTABLE DIABETES TREATMENTS AND DEVICES AVAILABLE
INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES ARSHNA SANGHRAJKA DIABETES SPECIALIST PRESCRIBING PHARMACIST OBJECTIVES EXPLORE THE TYPES OF INSULIN AND INJECTABLE DIABETES TREATMENTS AND DEVICES AVAILABLE
Glucagon-like peptide 1(GLP-1)
 Emerging Treatments and Technologies O R I G I N A L A R T I C L E Differential Effects of Acute and Extended Infusions of Glucagon-Like Peptide-1 on First- and Second-Phase Insulin Secretion in Diabetic
Emerging Treatments and Technologies O R I G I N A L A R T I C L E Differential Effects of Acute and Extended Infusions of Glucagon-Like Peptide-1 on First- and Second-Phase Insulin Secretion in Diabetic
Abnormalities in the secretion and insulinotropic
 ORIGINAL ARTICLE GIP Does Not Potentiate the Antidiabetic Effects of GLP-1 in Hyperglycemic Patients With Type 2 Diabetes Nikolaos Mentis, 1 Irfan Vardarli, 1 Lars D. Köthe, 1 Jens J. Holst, 2 Carolyn
ORIGINAL ARTICLE GIP Does Not Potentiate the Antidiabetic Effects of GLP-1 in Hyperglycemic Patients With Type 2 Diabetes Nikolaos Mentis, 1 Irfan Vardarli, 1 Lars D. Köthe, 1 Jens J. Holst, 2 Carolyn
Diabetes 2013: Achieving Goals Through Comprehensive Treatment. Session 2: Individualizing Therapy
 Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Near normalisation of blood glucose improves the potentiating effect of GLP-1 on glucose-induced insulin secretion in patients with type 2 diabetes
 Diabetologia (28) 1:632 64 DOI 1.17/s1-8-943-x ARTICLE Near normalisation of blood glucose improves the potentiating effect of GLP-1 on glucose-induced insulin secretion in patients with type 2 diabetes
Diabetologia (28) 1:632 64 DOI 1.17/s1-8-943-x ARTICLE Near normalisation of blood glucose improves the potentiating effect of GLP-1 on glucose-induced insulin secretion in patients with type 2 diabetes
Intact Glucagon-like Peptide-1 Levels are not Decreased in Japanese Patients with Type 2 Diabetes
 Or i g i n a l Advance Publication Intact Glucagon-like Peptide-1 Levels are not Decreased in Japanese Patients with Type 2 Diabetes Soushou Lee*, Daisuke Yabe**, Kyoko Nohtomi*, Michiya Takada*, Ryou
Or i g i n a l Advance Publication Intact Glucagon-like Peptide-1 Levels are not Decreased in Japanese Patients with Type 2 Diabetes Soushou Lee*, Daisuke Yabe**, Kyoko Nohtomi*, Michiya Takada*, Ryou
Discussion & Conclusion
 Discussion & Conclusion 7. Discussion DPP-4 inhibitors augment the effects of incretin hormones by prolonging their half-life and represent a new therapeutic approach for the treatment of type 2 diabetes
Discussion & Conclusion 7. Discussion DPP-4 inhibitors augment the effects of incretin hormones by prolonging their half-life and represent a new therapeutic approach for the treatment of type 2 diabetes
NIH Public Access Author Manuscript Diabetologia. Author manuscript; available in PMC 2014 February 01.
 NIH Public Access Author Manuscript Published in final edited form as: Diabetologia. 2013 February ; 56(2): 231 233. doi:10.1007/s00125-012-2788-6. Lipotoxicity impairs incretin signalling V. Poitout 1,2
NIH Public Access Author Manuscript Published in final edited form as: Diabetologia. 2013 February ; 56(2): 231 233. doi:10.1007/s00125-012-2788-6. Lipotoxicity impairs incretin signalling V. Poitout 1,2
Pathogenesis of Type 2 Diabetes
 9/23/215 Multiple, Complex Pathophysiological Abnmalities in T2DM incretin effect gut carbohydrate delivery & absption pancreatic insulin secretion pancreatic glucagon secretion HYPERGLYCEMIA? Pathogenesis
9/23/215 Multiple, Complex Pathophysiological Abnmalities in T2DM incretin effect gut carbohydrate delivery & absption pancreatic insulin secretion pancreatic glucagon secretion HYPERGLYCEMIA? Pathogenesis
Contribution of Endogenous Glucagon-Like Peptide 1 to Glucose Metabolism After Roux-en-Y Gastric Bypass
 Diabetes Volume 63, February 2014 483 Meera Shah, 1 Jennie H. Law, 1 Francesco Micheletto, 2 Matheni Sathananthan, 1 Chiara Dalla Man, 2 Claudio Cobelli, 2 Robert A. Rizza, 1 Michael Camilleri, 3 Alan
Diabetes Volume 63, February 2014 483 Meera Shah, 1 Jennie H. Law, 1 Francesco Micheletto, 2 Matheni Sathananthan, 1 Chiara Dalla Man, 2 Claudio Cobelli, 2 Robert A. Rizza, 1 Michael Camilleri, 3 Alan
ORIGINAL ARTICLE. Effect of Linagliptin on Incretin-axis and Glycaemic Variability in T1DM
 28 ORIGINAL ARTICLE Effect of Linagliptin on Incretin-axis and Glycaemic Variability in T1DM S Mukherjee 1, SK Bhadada 1*, N Sachdeva 1, D Badal 1, S Bhansali 1, P Dutta 1, A Bhansali 1 Abstract Backgrounds
28 ORIGINAL ARTICLE Effect of Linagliptin on Incretin-axis and Glycaemic Variability in T1DM S Mukherjee 1, SK Bhadada 1*, N Sachdeva 1, D Badal 1, S Bhansali 1, P Dutta 1, A Bhansali 1 Abstract Backgrounds
An integrated glucose homeostasis model of glucose, insulin, C-peptide, GLP-1, GIP and glucagon in healthy subjects and patients with type 2 diabetes
 An integrated glucose homeostasis model of glucose, insulin, C-peptide, GLP-1, GIP and glucagon in healthy subjects and patients with type 2 diabetes Oskar Alskär, Jonatan Bagger, Rikke Røge, Kanji Komatsu,
An integrated glucose homeostasis model of glucose, insulin, C-peptide, GLP-1, GIP and glucagon in healthy subjects and patients with type 2 diabetes Oskar Alskär, Jonatan Bagger, Rikke Røge, Kanji Komatsu,
A Minimal C-Peptide Sampling Method to Capture Peak and Total Prehepatic Insulin Secretion in Model-Based Experimental Insulin Sensitivity Studies
 Journal of Diabetes Science and Technology Volume 3, Issue 4, July 29 Diabetes Technology Society ORIGINAL ARTICLES A Minimal C-Peptide Sampling Method to Capture Peak and Total Prehepatic Insulin Secretion
Journal of Diabetes Science and Technology Volume 3, Issue 4, July 29 Diabetes Technology Society ORIGINAL ARTICLES A Minimal C-Peptide Sampling Method to Capture Peak and Total Prehepatic Insulin Secretion
Abstract. Effect of sitagliptin on glycemic control in patients with type 2 diabetes. Introduction. Abbas Mahdi Rahmah
 Effect of sitagliptin on glycemic control in patients with type 2 diabetes Abbas Mahdi Rahmah Correspondence: Dr. Abbas Mahdi Rahmah Consultant Endocrinologist, FRCP (Edin) Director of Iraqi National Diabetes
Effect of sitagliptin on glycemic control in patients with type 2 diabetes Abbas Mahdi Rahmah Correspondence: Dr. Abbas Mahdi Rahmah Consultant Endocrinologist, FRCP (Edin) Director of Iraqi National Diabetes
T2DM is a global epidemic with
 : a new option for the management of type 2 diabetes Marc Evans MRCP, MD, Consultant Diabetologist, Llandough Hospital, Cardiff Incretin-based therapies for the treatment of diabetes mellitus (T2DM) present
: a new option for the management of type 2 diabetes Marc Evans MRCP, MD, Consultant Diabetologist, Llandough Hospital, Cardiff Incretin-based therapies for the treatment of diabetes mellitus (T2DM) present
Defective amplification of the late phase insulin response to glucose by GIP in obese Type II diabetic patients
 Diabetologia (2002) 45:1111 1119 DOI 10.1007/s00125-002-0878-6 Defective amplification of the late phase insulin response to glucose by GIP in obese Type II diabetic patients T. Vilsbøll 1, 2, T. Krarup
Diabetologia (2002) 45:1111 1119 DOI 10.1007/s00125-002-0878-6 Defective amplification of the late phase insulin response to glucose by GIP in obese Type II diabetic patients T. Vilsbøll 1, 2, T. Krarup
Treating Type 2 Diabetes with Bariatric Surgery. Goal of Treating T2DM. Remission of T2DM with Bariatric
 Treating Type 2 Diabetes with Bariatric Surgery Number (in Millions) of Persons with Diagnosed Diabetes, United States, 198 25 The number of Americans with diabetes increased from 5.6 to 15.8 million Guilherme
Treating Type 2 Diabetes with Bariatric Surgery Number (in Millions) of Persons with Diagnosed Diabetes, United States, 198 25 The number of Americans with diabetes increased from 5.6 to 15.8 million Guilherme
Blood glucose concentrations in healthy humans
 ORIGINAL ARTICLE Effect of Glycemia on Plasma Incretins and the Incretin Effect During Oral Glucose Tolerance Test Marzieh Salehi, 1 Benedict Aulinger, 1 and David A. D Alessio 1,2 The incretin effect,
ORIGINAL ARTICLE Effect of Glycemia on Plasma Incretins and the Incretin Effect During Oral Glucose Tolerance Test Marzieh Salehi, 1 Benedict Aulinger, 1 and David A. D Alessio 1,2 The incretin effect,
Role of incretins in the treatment of type 2 diabetes
 Role of incretins in the treatment of type 2 diabetes Jens Juul Holst Department of Medical Physiology Panum Institute University of Copenhagen Denmark Diabetes & Obesity Spanish Society of Internal Medicine
Role of incretins in the treatment of type 2 diabetes Jens Juul Holst Department of Medical Physiology Panum Institute University of Copenhagen Denmark Diabetes & Obesity Spanish Society of Internal Medicine
Ulrike Pielmeier*. Mark L. Rousing* Steen Andreassen*
 Preprints of the 19th World Congress The International Federation of Automatic Control Pancreatic secretion, hepatic extraction, and plasma clearance of insulin from steady-state insulin and C-peptide
Preprints of the 19th World Congress The International Federation of Automatic Control Pancreatic secretion, hepatic extraction, and plasma clearance of insulin from steady-state insulin and C-peptide
An event-based point of view on the control of insulin-dependent diabetes
 An event-based point of view on the control of insulin-dependent diabetes Brigitte Bidégaray-Fesquet Laboratoire Jean Kuntzmann Univ. Grenoble Alpes, France Réunion e-baccuss September 4th 20 Réunion e-baccuss,
An event-based point of view on the control of insulin-dependent diabetes Brigitte Bidégaray-Fesquet Laboratoire Jean Kuntzmann Univ. Grenoble Alpes, France Réunion e-baccuss September 4th 20 Réunion e-baccuss,
Type 2 DM in Adolescents: Use of GLP-1 RA. Objectives. Scope of Problem: Obesity. Background. Pathophysiology of T2DM
 Type 2 DM in Adolescents: Use of GLP-1 RA Objectives Identify patients in the pediatric population with T2DM that would potentially benefit from the use of GLP-1 RA Discuss changes in glycemic outcomes
Type 2 DM in Adolescents: Use of GLP-1 RA Objectives Identify patients in the pediatric population with T2DM that would potentially benefit from the use of GLP-1 RA Discuss changes in glycemic outcomes
LUP. Lund University Publications Institutional Repository of Lund University
 LUP Lund University Publications Institutional Repository of Lund University This is an author produced version of a paper published in The Journal of clinical endocrinology and metabolism. This paper
LUP Lund University Publications Institutional Repository of Lund University This is an author produced version of a paper published in The Journal of clinical endocrinology and metabolism. This paper
ARTICLE. P. V. Højberg & T. Vilsbøll & R. Rabøl & F. K. Knop & M. Bache & T. Krarup & J. J. Holst & S. Madsbad
 Diabetologia (29) 52:199 27 DOI 1.17/s125-8-1195-5 ARTICLE Four weeks of near-normalisation of blood glucose improves the insulin response to glucagon-like peptide-1 and glucose-dependent insulinotropic
Diabetologia (29) 52:199 27 DOI 1.17/s125-8-1195-5 ARTICLE Four weeks of near-normalisation of blood glucose improves the insulin response to glucagon-like peptide-1 and glucose-dependent insulinotropic
Current Status of Incretin Based Therapies in Type 2 Diabetes
 Current Status of Incretin Based Therapies in Type 2 Diabetes DR.M.Mukhyaprana Prabhu Professor of Internal Medicine Kasturba Medical College, Manipal, Manipal University, India 2 nd International Endocrine
Current Status of Incretin Based Therapies in Type 2 Diabetes DR.M.Mukhyaprana Prabhu Professor of Internal Medicine Kasturba Medical College, Manipal, Manipal University, India 2 nd International Endocrine
METABOLISM CLINICAL AND EXPERIMENTAL XX (2011) XXX XXX. available at Metabolism.
 METABOLISM CLINICAL AND EXPERIMENTAL XX (211) XXX XXX available at www.sciencedirect.com Metabolism www.metabolismjournal.com Estimation of prehepatic insulin secretion: comparison between standardized
METABOLISM CLINICAL AND EXPERIMENTAL XX (211) XXX XXX available at www.sciencedirect.com Metabolism www.metabolismjournal.com Estimation of prehepatic insulin secretion: comparison between standardized
Diabetes: What is the scope of the problem?
 Diabetes: What is the scope of the problem? Elizabeth R. Seaquist MD Division of Endocrinology and Diabetes Department of Medicine Director, General Clinical Research Center Pennock Family Chair in Diabetes
Diabetes: What is the scope of the problem? Elizabeth R. Seaquist MD Division of Endocrinology and Diabetes Department of Medicine Director, General Clinical Research Center Pennock Family Chair in Diabetes
Incretinas e inhibidores de la DPP-4. Dr. Ramon Gomis Hospital Clínic Barcelona
 Incretinas e inhibidores de la DPP-4 Dr. Ramon Gomis Hospital Clínic Barcelona El páncreas normal y el islote de Langerhans lóbulos conducto intralobulillar islote vaso Islote de Langerhans Adaptado de
Incretinas e inhibidores de la DPP-4 Dr. Ramon Gomis Hospital Clínic Barcelona El páncreas normal y el islote de Langerhans lóbulos conducto intralobulillar islote vaso Islote de Langerhans Adaptado de
Appetite, Glycemia and Entero-Insular Hormone Responses Differ Between Oral, Gastric-Remnant and Duodenal Administration of a Mixed Meal Test After
 Appetite, Glycemia and Entero-Insular Hormone Responses Differ Between Oral, Gastric-Remnant and Duodenal Administration of a Mixed Meal Test After Roux-en-Y Gastric Bypass June 2018 How a surgical complication
Appetite, Glycemia and Entero-Insular Hormone Responses Differ Between Oral, Gastric-Remnant and Duodenal Administration of a Mixed Meal Test After Roux-en-Y Gastric Bypass June 2018 How a surgical complication
GLP-1 receptor agonists for type 2 diabetes A rationale drug. development. Bo Ahrén
 PROF. BO AHREN (Orcid ID : 0000-0002-9804-5340) Article type : Mini Review GLP-1 receptor agonists for type 2 diabetes A rationale drug development Bo Ahrén Department of Clinical Sciences Lund, Lund University,
PROF. BO AHREN (Orcid ID : 0000-0002-9804-5340) Article type : Mini Review GLP-1 receptor agonists for type 2 diabetes A rationale drug development Bo Ahrén Department of Clinical Sciences Lund, Lund University,
TCF7L2 Variant rs Affects the Risk of Type 2 Diabetes by Modulating Incretin Action
 ORIGINAL ARTICLE TCF7L2 Variant rs793146 Affects the Risk of Type 2 Diabetes by Modulating Incretin Action Dennis T. Villareal, 1 Heather Robertson, 1 Graeme I. Bell, 2 Bruce W. Patterson, 1 Hung Tran,
ORIGINAL ARTICLE TCF7L2 Variant rs793146 Affects the Risk of Type 2 Diabetes by Modulating Incretin Action Dennis T. Villareal, 1 Heather Robertson, 1 Graeme I. Bell, 2 Bruce W. Patterson, 1 Hung Tran,
(Incretin) ( glucagon-like peptide-1 GLP-1 ) GLP-1. GLP-1 ( dipeptidyl peptidase IV DPP IV ) GLP-1 DPP IV GLP-1 exenatide liraglutide FDA 2 2 2
 007 18 189-194 (Incretin) Incretin ( ) -1 ( glucagon-like peptide-1 ) ( dipeptidyl peptidase IV ) liraglutide FDA ( Type diabetes mellitus ) -1 ( Glucagon-like peptide-1, ) ( Incretin ) ( Dipeptidyl peptidase
007 18 189-194 (Incretin) Incretin ( ) -1 ( glucagon-like peptide-1 ) ( dipeptidyl peptidase IV ) liraglutide FDA ( Type diabetes mellitus ) -1 ( Glucagon-like peptide-1, ) ( Incretin ) ( Dipeptidyl peptidase
INJECTABLE THERAPIES IN DIABETES. Barbara Ann McKee Diabetes Specialist Nurse
 INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
Insulin Secretion and Hepatic Extraction during Euglycemic Clamp Study: Modelling of Insulin and C-peptide data
 Insulin Secretion and Hepatic Extraction during Euglycemic Clamp Study: Modelling of Insulin and C-peptide data Chantaratsamon Dansirikul Mats O Karlsson Division of Pharmacokinetics and Drug Therapy Department
Insulin Secretion and Hepatic Extraction during Euglycemic Clamp Study: Modelling of Insulin and C-peptide data Chantaratsamon Dansirikul Mats O Karlsson Division of Pharmacokinetics and Drug Therapy Department
Initially more rapid small intestinal glucose delivery increases plasma. insulin, GIP and GLP-1, but does not improve overall glycemia in
 Articles in PresS. Am J Physiol Endocrinol Metab (May 10, 2005). doi:10.1152/ajpendo.00099.2005 E-00099-2005.R1 Final accepted version 1 Initially more rapid small intestinal glucose delivery increases
Articles in PresS. Am J Physiol Endocrinol Metab (May 10, 2005). doi:10.1152/ajpendo.00099.2005 E-00099-2005.R1 Final accepted version 1 Initially more rapid small intestinal glucose delivery increases
Non-insulin treatment in Type 1 DM Sang Yong Kim
 Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Glucagon secretion in relation to insulin sensitivity in healthy subjects
 Diabetologia (2006) 49: 117 122 DOI 10.1007/s00125-005-0056-8 ARTICLE B. Ahrén Glucagon secretion in relation to insulin sensitivity in healthy subjects Received: 4 July 2005 / Accepted: 12 September 2005
Diabetologia (2006) 49: 117 122 DOI 10.1007/s00125-005-0056-8 ARTICLE B. Ahrén Glucagon secretion in relation to insulin sensitivity in healthy subjects Received: 4 July 2005 / Accepted: 12 September 2005
Reduction of insulinotropic properties of GLP-1 and GIP after glucocorticoid-induced insulin resistance
 Diabetologia (5) 5:9 9 DOI.7/s5-5-5-y ARTICLE Reduction of insulinotropic properties of GLP- and GIP after glucocorticoid-induced insulin resistance Marie Eriksen & David H. Jensen & Siri Tribler & Jens
Diabetologia (5) 5:9 9 DOI.7/s5-5-5-y ARTICLE Reduction of insulinotropic properties of GLP- and GIP after glucocorticoid-induced insulin resistance Marie Eriksen & David H. Jensen & Siri Tribler & Jens
GLP-1. GLP-1 is produced by the L-cells of the gut after food intake in two biologically active forms It is rapidly degraded by DPP-4.
 GLP-1 GLP-1 is produced by the L-cells of the gut after food intake in two biologically active forms It is rapidly degraded by DPP-4 Food intake éinsulin Gut églucose uptake Pancreas Beta cells Alpha cells
GLP-1 GLP-1 is produced by the L-cells of the gut after food intake in two biologically active forms It is rapidly degraded by DPP-4 Food intake éinsulin Gut églucose uptake Pancreas Beta cells Alpha cells
Data from an epidemiologic analysis of
 CLINICAL TRIAL RESULTS OF GLP-1 RELATED AGENTS: THE EARLY EVIDENCE Lawrence Blonde, MD, FACP, FACE ABSTRACT Although it is well known that lowering A 1c (also known as glycated hemoglobin) is associated
CLINICAL TRIAL RESULTS OF GLP-1 RELATED AGENTS: THE EARLY EVIDENCE Lawrence Blonde, MD, FACP, FACE ABSTRACT Although it is well known that lowering A 1c (also known as glycated hemoglobin) is associated
Personalized therapeutics in diabetes
 Personalized therapeutics in diabetes Leen M. t Hart Molecular Cell Biology & Molecular Epidemiology Leiden University Medical Center Epidemiology & Biostatistics VU University Medical Center Diabetes
Personalized therapeutics in diabetes Leen M. t Hart Molecular Cell Biology & Molecular Epidemiology Leiden University Medical Center Epidemiology & Biostatistics VU University Medical Center Diabetes
The Many Faces of T2DM in Long-term Care Facilities
 The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
My Journey in Endocrinology. Samuel Cataland M.D
 My Journey in Endocrinology Samuel Cataland M.D. 1968-2015 Drs Berson M.D. Yalow phd Insulin Radioimmunoassay Nobel Prize Physiology or Medicine 1977 Rosalyn Yalow: Radioimmunoassay Technology Andrew Schally
My Journey in Endocrinology Samuel Cataland M.D. 1968-2015 Drs Berson M.D. Yalow phd Insulin Radioimmunoassay Nobel Prize Physiology or Medicine 1977 Rosalyn Yalow: Radioimmunoassay Technology Andrew Schally
SOCIETA ITALIANA DI NUTRIZIONE UMANA Milano novembre Geltrude Mingrone. Istituto di Clinica Medica Università Cattolica S.
 SOCIETA ITALIANA DI NUTRIZIONE UMANA Milano 29-30 novembre 2007 Geltrude Mingrone Istituto di Clinica Medica Università Cattolica S. Cuore Roma Treatment Goals for Type II Achieve normal or near-normal
SOCIETA ITALIANA DI NUTRIZIONE UMANA Milano 29-30 novembre 2007 Geltrude Mingrone Istituto di Clinica Medica Università Cattolica S. Cuore Roma Treatment Goals for Type II Achieve normal or near-normal
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Zibar K., Knežević Ćuća J., Blaslov K., Bulum T., Smirčić-Duvnjak L. (2015) Difference in glucagon-like peptide-1 concentrations between C-peptide negative type 1 diabetes
Središnja medicinska knjižnica Zibar K., Knežević Ćuća J., Blaslov K., Bulum T., Smirčić-Duvnjak L. (2015) Difference in glucagon-like peptide-1 concentrations between C-peptide negative type 1 diabetes
Difference in glucagon-like peptide-1 concentrations between C-peptide negative type 1 diabetes mellitus patients and healthy controls
 Original Article Annals of Clinical Biochemistry 2015, Vol. 52(2) 220 225! The Author(s) 2014 Reprints and permissions: sagepub.co.uk/journalspermissions.nav DOI: 10.1177/0004563214544709 acb.sagepub.com
Original Article Annals of Clinical Biochemistry 2015, Vol. 52(2) 220 225! The Author(s) 2014 Reprints and permissions: sagepub.co.uk/journalspermissions.nav DOI: 10.1177/0004563214544709 acb.sagepub.com
22 Emerging Therapies for
 22 Emerging Therapies for Treatment of Type 2 Diabetes Siddharth N Shah Abstract: The prevalence of Diabetes is progressively increasing world-wide and the growth of the disease in our country is phenomenal.
22 Emerging Therapies for Treatment of Type 2 Diabetes Siddharth N Shah Abstract: The prevalence of Diabetes is progressively increasing world-wide and the growth of the disease in our country is phenomenal.
EXENDIN-4 IS A 39-amino acid reptilian peptide that
 0021-972X/04/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 89(7):3469 3473 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/jc.2003-032001 Exendin-4 Normalized Postcibal
0021-972X/04/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 89(7):3469 3473 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/jc.2003-032001 Exendin-4 Normalized Postcibal
Cordoba 01/02/2008. Slides Professor Pierre LEFEBVRE
 Cordoba 01/02/2008 Slides Professor Pierre LEFEBVRE Clinical Research in Type 2 Diabetes : Current Status and Future Approaches Pierre Lefèbvre* University of Liège Belgium Granada, Spain, February 2008
Cordoba 01/02/2008 Slides Professor Pierre LEFEBVRE Clinical Research in Type 2 Diabetes : Current Status and Future Approaches Pierre Lefèbvre* University of Liège Belgium Granada, Spain, February 2008
DPP-4 inhibitor. The new class drug for Diabetes
 DPP-4 inhibitor The new class drug for Diabetes 1 Cause of Death in Korea 1 st ; Neoplasm 2 nd ; Cardiovascular Disease 3 rd ; Cerebrovascular Disease Diabetes 2 Incidence of Fatal or Nonfatal MI During
DPP-4 inhibitor The new class drug for Diabetes 1 Cause of Death in Korea 1 st ; Neoplasm 2 nd ; Cardiovascular Disease 3 rd ; Cerebrovascular Disease Diabetes 2 Incidence of Fatal or Nonfatal MI During
SELECTED ABSTRACTS AND POSTER PRESENTATIONS
 SELECTED ABSTRACTS AND POSTER PRESENTATIONS The following summaries are based on abstracts and posters presented at the American Diabetes Association s 65th Annual Scientific Sessions held in San Diego,
SELECTED ABSTRACTS AND POSTER PRESENTATIONS The following summaries are based on abstracts and posters presented at the American Diabetes Association s 65th Annual Scientific Sessions held in San Diego,
ARTICLE. D. H. Jensen & K. Aaboe & J. E. Henriksen & A. Vølund & J. J. Holst & S. Madsbad & T. Krarup
 Diabetologia () :1 11 DOI.7/s--9-7 ARTICLE Steroid-induced insulin resistance and impaired glucose tolerance are both associated with a progressive decline of incretin effect in first-degree relatives
Diabetologia () :1 11 DOI.7/s--9-7 ARTICLE Steroid-induced insulin resistance and impaired glucose tolerance are both associated with a progressive decline of incretin effect in first-degree relatives
Oral glutamine increases circulating glucagon-like peptide 1, glucagon, and insulin concentrations in lean, obese, and type 2 diabetic subjects 1 4
 Oral glutamine increases circulating glucagon-like peptide 1, glucagon, and insulin concentrations in lean, obese, and type 2 diabetic subjects 1 4 Jerry R Greenfield, I Sadaf Farooqi, Julia M Keogh, Elana
Oral glutamine increases circulating glucagon-like peptide 1, glucagon, and insulin concentrations in lean, obese, and type 2 diabetic subjects 1 4 Jerry R Greenfield, I Sadaf Farooqi, Julia M Keogh, Elana
Targeting simultaneously GLP-1, GIP and glucagon receptors : a new paradigm for treating obesity and diabetes
 SHORT COMMENT FOR NATURE REVIEWS ENDOCRINOLOGY Targeting simultaneously GLP-1, GIP and glucagon receptors : a new paradigm for treating obesity and diabetes André J. SCHEEN (1), Nicolas PAQUOT (2) (1)
SHORT COMMENT FOR NATURE REVIEWS ENDOCRINOLOGY Targeting simultaneously GLP-1, GIP and glucagon receptors : a new paradigm for treating obesity and diabetes André J. SCHEEN (1), Nicolas PAQUOT (2) (1)
VIRTUAL PATIENTS DERIVED FROM THE
 VIRTUAL PATIENTS DERIVED FROM THE CARELINK DATABASE Benyamin Grosman PhD Senior Principle Scientist Medtronic Diabetes WHY VIRTUAL PATIENT MODELING? Reduce the cost of clinical trials Use models in conjunction
VIRTUAL PATIENTS DERIVED FROM THE CARELINK DATABASE Benyamin Grosman PhD Senior Principle Scientist Medtronic Diabetes WHY VIRTUAL PATIENT MODELING? Reduce the cost of clinical trials Use models in conjunction
adenosine triphosphate-sensitive K[ Citation Journal of Diabetes Investigation ( modifications or adaptations are ma
 Fructose induces glucose-dependent Titleglucagon-like peptide-1 and insulin adenosine triphosphate-sensitive K[ Seino, Yusuke; Ogata, Hidetada; Mae Author(s) Takako; Iida, Atsushi; Harada, Nori Susumu;
Fructose induces glucose-dependent Titleglucagon-like peptide-1 and insulin adenosine triphosphate-sensitive K[ Seino, Yusuke; Ogata, Hidetada; Mae Author(s) Takako; Iida, Atsushi; Harada, Nori Susumu;
Expanding Treatment Options for Diabetes: GLP-1 Receptor Agonists. Copyright
 CLINICAL Viewpoint Expanding Treatment Options for Diabetes: GLP-1 Receptor Agonists Advancements in Diabetes Management: A Canadian Diabetes Steering Committee Report Copyright Not for Sale or Commercial
CLINICAL Viewpoint Expanding Treatment Options for Diabetes: GLP-1 Receptor Agonists Advancements in Diabetes Management: A Canadian Diabetes Steering Committee Report Copyright Not for Sale or Commercial
Pramlintide & Weight. Diane M Karl MD. The Endocrine Clinic & Oregon Health & Science University Portland, Oregon
 Pramlintide & Weight Diane M Karl MD The Endocrine Clinic & Oregon Health & Science University Portland, Oregon Conflict of Interest Speakers Bureau: Amylin Pharmaceuticals Consultant: sanofi-aventis Grant
Pramlintide & Weight Diane M Karl MD The Endocrine Clinic & Oregon Health & Science University Portland, Oregon Conflict of Interest Speakers Bureau: Amylin Pharmaceuticals Consultant: sanofi-aventis Grant
In conjunction with the rising prevalence of diabetes,
 65S Incretin-Based Therapies A Clinical Need Filled by Unique Metabolic Effects Learning Objectives List the 2 major pathophysiologic defects associated with type 2 diabetes. Discuss the barriers to achieving
65S Incretin-Based Therapies A Clinical Need Filled by Unique Metabolic Effects Learning Objectives List the 2 major pathophysiologic defects associated with type 2 diabetes. Discuss the barriers to achieving
David C. Polidori, 1 Richard N. Bergman, 2 Stephanie T. Chung, 3 and Anne E. Sumner 3
 1556 Diabetes Volume 65, June 2016 David C. Polidori, 1 Richard N. Bergman, 2 Stephanie T. Chung, 3 and Anne E. Sumner 3 Hepatic and Extrahepatic Insulin Clearance Are Differentially Regulated: Results
1556 Diabetes Volume 65, June 2016 David C. Polidori, 1 Richard N. Bergman, 2 Stephanie T. Chung, 3 and Anne E. Sumner 3 Hepatic and Extrahepatic Insulin Clearance Are Differentially Regulated: Results
Hyperglycaemia increases dipeptidyl peptidase IV activity in diabetes mellitus
 Diabetologia (2005) 48: 1168 1172 DOI 10.1007/s00125-005-1749-8 ARTICLE E. Mannucci. L. Pala. S. Ciani. G. Bardini. A. Pezzatini. I. Sposato. F. Cremasco. A. Ognibene. C. M. Rotella Hyperglycaemia increases
Diabetologia (2005) 48: 1168 1172 DOI 10.1007/s00125-005-1749-8 ARTICLE E. Mannucci. L. Pala. S. Ciani. G. Bardini. A. Pezzatini. I. Sposato. F. Cremasco. A. Ognibene. C. M. Rotella Hyperglycaemia increases
Accurate Measurement of Postprandial Glucose Turnover: Why Is It Difficult and How Can It Be Done (Relatively) Simply?
 Diabetes Volume 65, May 2016 1133 Robert A. Rizza, 1 Gianna Toffolo, 2 and Claudio Cobelli 2 Accurate Measurement of Postprandial Glucose Turnover: Why Is It Difficult and How Can It Be Done (Relatively)
Diabetes Volume 65, May 2016 1133 Robert A. Rizza, 1 Gianna Toffolo, 2 and Claudio Cobelli 2 Accurate Measurement of Postprandial Glucose Turnover: Why Is It Difficult and How Can It Be Done (Relatively)
Type 2 diabetes results from the interaction of
 ORIGINAL ARTICLE Separate Impact of Obesity and Glucose Tolerance on the Incretin Effect in Normal Subjects and Type 2 Diabetic Patients Elza Muscelli, 1 Andrea Mari, 2 Arturo Casolaro, 1 Stefania Camastra,
ORIGINAL ARTICLE Separate Impact of Obesity and Glucose Tolerance on the Incretin Effect in Normal Subjects and Type 2 Diabetic Patients Elza Muscelli, 1 Andrea Mari, 2 Arturo Casolaro, 1 Stefania Camastra,
Diabetes: Three Core Deficits
 Diabetes: Three Core Deficits Fat Cell Dysfunction Impaired Incretin Function Impaired Appetite Suppression Obesity and Insulin Resistance in Muscle and Liver Hyperglycemia Impaired Insulin Secretion Islet
Diabetes: Three Core Deficits Fat Cell Dysfunction Impaired Incretin Function Impaired Appetite Suppression Obesity and Insulin Resistance in Muscle and Liver Hyperglycemia Impaired Insulin Secretion Islet
Effect of Glucagon-Like Peptide-1 on - and -Cell Function in C-Peptide-Negative Type 1 Diabetic Patients
 ORIGINAL ARTICLE Endocrine Research Brief Report Effect of Glucagon-Like Peptide-1 on - and -Cell Function in C-Peptide-Negative Type 1 Diabetic Patients Urd Kielgast, Meena Asmar, Sten Madsbad, and Jens
ORIGINAL ARTICLE Endocrine Research Brief Report Effect of Glucagon-Like Peptide-1 on - and -Cell Function in C-Peptide-Negative Type 1 Diabetic Patients Urd Kielgast, Meena Asmar, Sten Madsbad, and Jens
Mathematical model of standard oral glucose tolerance test for characterization of insulin potentiation in health
 Università Politecnica delle Marche Scuola di Dottorato di Ricerca in Scienze dell Ingegneria Curriculum in Elettromagnetismo e Bioingegneria ----------------------------------------------------------------------------------------
Università Politecnica delle Marche Scuola di Dottorato di Ricerca in Scienze dell Ingegneria Curriculum in Elettromagnetismo e Bioingegneria ----------------------------------------------------------------------------------------
Professor Rudy Bilous James Cook University Hospital
 Professor Rudy Bilous James Cook University Hospital Rate per 100 patient years Rate per 100 patient years 16 Risk of retinopathy progression 16 Risk of developing microalbuminuria 12 12 8 8 4 0 0 5 6
Professor Rudy Bilous James Cook University Hospital Rate per 100 patient years Rate per 100 patient years 16 Risk of retinopathy progression 16 Risk of developing microalbuminuria 12 12 8 8 4 0 0 5 6
The Contribution of Endogenous Glucagon-Like Peptide-1 to Glucose Metabolism after Roux-en-Y Gastric Bypass
 Page 1 of 39 Diabetes 1 The Contribution of Endogenous Glucagon-Like Peptide-1 to Glucose Metabolism after Roux-en-Y Gastric Bypass *Meera Shah MD 1, *Jennie H. Law MD 1, Francesco Micheletto PhD 2, Matheni
Page 1 of 39 Diabetes 1 The Contribution of Endogenous Glucagon-Like Peptide-1 to Glucose Metabolism after Roux-en-Y Gastric Bypass *Meera Shah MD 1, *Jennie H. Law MD 1, Francesco Micheletto PhD 2, Matheni
Adapting to insulin resistance in obesity: role of insulin secretion and clearance
 Diabetologia (218) 61:681 687 https://doi.org/1.17/s125-17-4511- ARTICLE Adapting to insulin resistance in obesity: role of insulin secretion and clearance Sang-Hee Jung 1 & Chan-Hee Jung 2 & Gerald M.
Diabetologia (218) 61:681 687 https://doi.org/1.17/s125-17-4511- ARTICLE Adapting to insulin resistance in obesity: role of insulin secretion and clearance Sang-Hee Jung 1 & Chan-Hee Jung 2 & Gerald M.
Adeterioration in -cell function is an independent
 Relationships Among Age, Proinsulin Conversion, and -Cell Function in Nondiabetic Humans Andreas Fritsche, Alexander Madaus, Norbert Stefan, Otto Tschritter, Elke Maerker, Anna Teigeler, Hans Häring, and
Relationships Among Age, Proinsulin Conversion, and -Cell Function in Nondiabetic Humans Andreas Fritsche, Alexander Madaus, Norbert Stefan, Otto Tschritter, Elke Maerker, Anna Teigeler, Hans Häring, and
GLP-1 Receptor Agonists and SGLT-2 Inhibitors. Debbie Hicks
 GLP-1 Receptor Agonists and SGLT-2 Inhibitors Debbie Hicks Prescribing and Adverse Event reporting information is available at this meeting from the AstraZeneca representative The views expressed by the
GLP-1 Receptor Agonists and SGLT-2 Inhibitors Debbie Hicks Prescribing and Adverse Event reporting information is available at this meeting from the AstraZeneca representative The views expressed by the
Insulin Administration for People with Type 1 diabetes
 Downloaded from orbit.dtu.dk on: Nov 17, 1 Insulin Administration for People with Type 1 diabetes Boiroux, Dimitri; Finan, Daniel Aaron; Poulsen, Niels Kjølstad; Madsen, Henrik; Jørgensen, John Bagterp
Downloaded from orbit.dtu.dk on: Nov 17, 1 Insulin Administration for People with Type 1 diabetes Boiroux, Dimitri; Finan, Daniel Aaron; Poulsen, Niels Kjølstad; Madsen, Henrik; Jørgensen, John Bagterp
Vildagliptin is a potent and selective
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Effects of the Dipeptidyl Peptidase-IV Inhibitor Vildagliptin on Incretin Hormones, Islet Function, and Postprandial
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Effects of the Dipeptidyl Peptidase-IV Inhibitor Vildagliptin on Incretin Hormones, Islet Function, and Postprandial
Preserved insulin secretory capacity and weight loss are the predominant predictors
 Page 1 of 23 Preserved insulin secretory capacity and weight loss are the predominant predictors of glycemic control in patients with type 2 diabetes randomized to Roux-en-Y gastric bypass Kim T. Nguyen,
Page 1 of 23 Preserved insulin secretory capacity and weight loss are the predominant predictors of glycemic control in patients with type 2 diabetes randomized to Roux-en-Y gastric bypass Kim T. Nguyen,
An integrated glucose-insulin model to describe oral glucose tolerance test data in healthy volunteers
 Title: An integrated glucose-insulin model to describe oral glucose tolerance test data in healthy volunteers Authors: Hanna E. Silber 1, Nicolas Frey 2 and Mats O. Karlsson 1 Address: 1 Department of
Title: An integrated glucose-insulin model to describe oral glucose tolerance test data in healthy volunteers Authors: Hanna E. Silber 1, Nicolas Frey 2 and Mats O. Karlsson 1 Address: 1 Department of
GLP-1-based therapies in the management of type 2 diabetes
 GLP-1-based therapies in the management of type 2 diabetes Makbul Aman Mansyur Division Endocrine & Metabolism Department of Internal Medicine Faculty of Medicine Hasanuddin University/ RSUP Dr. Wahidin
GLP-1-based therapies in the management of type 2 diabetes Makbul Aman Mansyur Division Endocrine & Metabolism Department of Internal Medicine Faculty of Medicine Hasanuddin University/ RSUP Dr. Wahidin
Glucagon Response to Oral Glucose Challenge in Type 1 Diabetes: Lack of Impact of Euglycemia
 1076 Diabetes Care Volume 37, April 2014 Glucagon Response to Oral Glucose Challenge in Type 1 Diabetes: Lack of Impact of Euglycemia Caroline K. Kramer, 1,2 Carla A. Borgo~no, 3 Paula Van Nostrand, 1
1076 Diabetes Care Volume 37, April 2014 Glucagon Response to Oral Glucose Challenge in Type 1 Diabetes: Lack of Impact of Euglycemia Caroline K. Kramer, 1,2 Carla A. Borgo~no, 3 Paula Van Nostrand, 1
Clinical Overview of Combination Therapy with Sitagliptin and Metformin
 Clinical Overview of Combination Therapy with Sitagliptin and Metformin 1 Contents Pathophysiology of type 2 diabetes and mechanism of action of sitagliptin Clinical data overview of sitagliptin: Monotherapy
Clinical Overview of Combination Therapy with Sitagliptin and Metformin 1 Contents Pathophysiology of type 2 diabetes and mechanism of action of sitagliptin Clinical data overview of sitagliptin: Monotherapy
