Glucagon, Catecholamine and Pancreatic Polypeptide Secretion
|
|
|
- Brianne Alexander
- 6 years ago
- Views:
Transcription
1 Glucagon, Catecholamine and Pancreatic Polypeptide Secretion in Type I Diabetic Recipients of Pancreas Allografts Peter Diem,* J. Bruce Redmon,* Munir Abid,* Antoinette Moran,* David E. R. Sutherland,* Jeffrey B. Halter,' and R. Paul Robertson* *Diabetes Center and Division ofendocrinology, Department ofmedicine, tdepartment ofpediatrics, Department ofsurgery, University ofminnesota, Minneapolis, Minnesota; and 'Department ofmedicine, University ofmichigan and the Veterans Administration Medical Center, Ann Arbor, Michigan Abstract Successful pancreas transplantation in type I diabetic patients restores normal fasting glucose levels and biphasic insulin responses to glucose. However, virtually no data from pancreas recipients are available relative to other islet hormonal responses or hormonal counterregulation of hypoglycemia. Consequently, glucose, glucagon, catecholamine, and pancreatic polypeptide responses to insulin-induced hypoglycemia and to stimulation with arginine and secretin were examined in 38 diabetic pancreas recipients, 54 type I diabetic nonrecipients, and 26 nondiabetic normal control subjects. Glucose recovery after insulin-induced hypoglycemia in pancreas recipients was significantly improved. Basal glucagon levels were significantly higher in recipients compared with nonrecipients and normal subjects. Glucagon responses to insulin-induced hypoglycemia were significantly greater in the pancreas recipients compared with nonrecipients and similar to that observed in control subjects. Glucagon responses to intravenous arginine were significantly greater in pancreas recipients than that observed in both the nonrecipients and normal subjects. No differences were observed in epinephrine responses during insulin-induced hypoglycemia. No differences in pancreatic polypeptide responses to hypoglycemia were observed when comparing the recipient and nonrecipient groups, both of which were less than that observed in the control subjects. Our data demonstrate significant improvement in glucose recovery after hypoglycemia which was associated with improved glucagon secretion in type I diabetic recipients of pancreas transplantation. (J. Clin. Invest : ) Key words: pancreas transplantation * glucagon - catecholamines - pancreatic polypeptide Presented in part at the 11st Annual Meeting of the Association of American Physicians, Washington, May 1988, the 48th Annual Meeting of the American Diabetes Association, New Orleans, June 1988, and at the 13th International Diabetes Federation Congress, Sydney, Australia, November Address correspondence and reprint requests to Dr. R. Paul Robertson, The Diabetes Center, Box 11 UMHC, University of Minnesota, Minneapolis, MN Receivedfor publication 26 February 199 and in revisedform 13 July 199. J. Clin. Invest. The American Society for Clinical Investigation, Inc /9/12/28/6 $2. Volume 86, December 199, Introduction After successful pancreas transplantation, recipients with type I diabetes mellitus achieve a return to normal fasting plasma glucose levels, normal oral glucose tolerance tests, and normal levels of HbA,C (1-7). However, whether recipients undergo alterations in counterregulatory hormonal responses to glycopenia, or improvement in counterregulation of hypoglycemia, has not been determined. These are important considerations because type I diabetic patients commonly have defective glucagon and epinephrine responses to hypoglycemia and, consequently, deranged counterregulation of hypoglycemia with its attendant risks (8-13). Therefore, presence or absence of improvement in these responses are highly relevant factors in the evaluation of the overall benefits of pancreas transplantation. Moreover, since the transplanted pancreas is denervated and since islet alpha cell and pancreatic polypeptide cell function is neurally modulated, investigation of pancreas recipients offers a unique opportunity to assess regulation of glucagon and pancreatic polypeptide secretion from the pancreas in humans in the setting of absent central nervous system input into the islet. To evaluate hormonal counterregulation of hypoglycemia in patients with type I diabetes mellitus who have received successful pancreas allografts, we have examined glucose, glucagon, pancreatic polypeptide, and catecholamine responses during insulin-induced hypoglycemia. We have also assessed glucagon and pancreatic polypeptide responsivity to direct stimulators of alpha and pancreatic polypeptide cells (arginine and secretin, respectively) to ascertain whether possible alterations in secretory responses in pancreas recipients are specific for hypoglycemic signaling or more general in nature. In this study, the responses of pancreas recipients were compared with responses of patients with similar durations of type I diabetes mellitus, who had not received pancreas transplantation, and to nondiabetic control subjects. Methods Subjects. 38 type I diabetic recipients of pancreas allografts with iliac vessel anastomoses and with intact native pancreases who had been transplanted between 3 and 6 mo previously were studied (Table I). All recipients were normoglycemic, had normal hemoglobin A,C levels and mildly elevated serum creatinine levels, and none were receiving exogenous insulin or other medication for diabetes. Immunosuppression was achieved with the triple-drug regimen of aathioprine, cyclosporine, and prednisone (14). 54 patients with type I diabetes and with similar age, sex distribution, body-mass index, serum creatinine levels, and duration ofdiabetes, as well as 26 normal volunteers of similar age, sex distribution, and body-mass index, were studied to obtain control data. All subjects were admitted to the University 28 P. Diem, J. Redmon, M. Abid, A. Moran, D. Sutherland, J. Halter, and R. Robertson
2 Table L Characteristics of Type I Diabetic Recipients ofpancreas Allografts, Type I Diabetic Nonrecipients, and Normal Control Subjects Recipients Nonrecipients Controls n Age (y) 34±6 33±8 34±14 Duration of diabetes mellitus (y) 22±6 22±7 BMI (kg/m2) 23.4± ±3. 23.±3.1 HbA1C (%) 5.2±.7 9.± ±.5 Serum creatinine (,umol/liter) 136±7 162±27 77±3 Duration after pancreas 22±6 transplantation (mo) (range: 3-6) Twelve of the diabetic subjects were studied before and after pancreas transplantation. All data are expressed as mean± 1 SD. of Minnesota Clinical Research Center and tests were begun at 8: a.m. with the subjects at bedrest after fasting overnight. Informed written consent was obtained from all subjects and the test procedures had been approved by the University of Minnesota Human Subjects Committee. All tests were not performed on all subjects. Insulin-induced hypoglycemia. 24 type I diabetic recipients, 48 type I diabetic nonrecipients, and 16 normal control subjects underwent insulin tolerance tests. An intravenous line was placed in an antecubital vein to draw samples for glucose, glucagon, pancreatic polypeptide, and catecholamines. In type I diabetic nonrecipients normoglycemia was first established with an intravenous insulin infusion for 6-12 h overnight. Two baseline samples were withdrawn during normoglycemia 5 and min before insulin was injected intravenously to induce hypoglycemia. Pancreas recipients and nonrecipients were given U/kg, whereas controls were given.5 U/kg of insulin as an intravenous pulse to achieve similar glucose nadirs in all groups. Additional blood samples were withdrawn at 5, 1, 15, 2, 25, 3, 35, 4, 45, 5, and 6 min after the insulin pulse. Patients who experienced extreme drowsiness and/or who complained of severe discomfort received 25 g of intravenous glucose to terminate hypoglycemia. Arginine and secretin stimulation. To compare glucagon responses induced by hypoglycemia with responses induced by a more directly acting secretagogue, 25 type I diabetic recipients, 47 type I diabetic nonrecipients, and 18 normal control subjects were given a maximally effective pulse of arginine (5 g in 25 ml of water IV). To compare pancreatic polypeptide responses to hypoglycemia with a more directly acting agonist, 25 recipients, 17 type I diabetic nonrecipients, and 17 normal control subjects responses received a maximally effective pulse of secretin (2 U/kg body weight in.9% NaCl IV). Three baseline samples and additional samples 2, 3, 4, 5, 7, and 1 min after the respective injections were withdrawn for determination of glucagon or hpp levels, respectively. Analytical methods. Serum glucose was immediately measured with a Beckman Glucose Analyer II (Beckman Instruments Inc., Fullerton, CA). Samples for glucagon determinations were collected into prechilled tubes containing 2.5 mg EDTA and 5 U Trasylol per milliliter blood, put on ice, and centrifuged immediately. Glucagon was measured by radioimmunoassay (15) with antibody 4A obtained from Dr. R. H. Unger (University of Texas, Dallas). Pancreatic polypeptide was measured by radioimmunoassay (16) according to Chance et al. using antibody kindly provided by Dr. R. E. Chance (Ely Lilly and Co., Indianapolis, IN). Catecholamines were measured using a radioenymatic method described previously (17). Data analysis. Data are expressed as mean±sem unless otherwise stated. Statistics for intergroup compansons were performed by analysis of variance followed by Fisher's least significant difference. When applicable, Student's paired or unpaired t test were used. Discrete variables were compared by chi-squares analysis. Least-squares linear regression was used to assess bivariate interdependency. All P values were for two-tailed distributions and P <.5 was considered statistically significant. Results Glucose suppression and recovery during insulin tolerance testing. Similar blood glucose nadirs were obtained in all three groups (1.8±.1 mm in recipients, 2.±.1 mm in nonrecipients, and 2.±.1 mm in controls; P = NS). However, the fall in glucose tended to be somewhat slower in the nonrecipients than in the two other groups (Fig. 1). Blood glucose recovery after insulin-induced hypoglycemia in diabetic nonrecipients was severely impaired, the maximal blood glucose recovery being only 8±2% of decrement. Blood glucose recovery was significantly better in recipients (34±4% of decrement; P <.1) but significantly lower than that observed in controls (58±3% of decrement; P <.1). All normal subjects and diabetic patients reached glucose levels below 2.6 mm and all completed at least 35 min of this test from the time of insulin injection. Only 2 of 24 recipients could not complete the test because of symptoms ofhypoglycemia. In contrast, the test was prematurely terminated by giving intravenous glucose because of marked symptoms of hypoglycemia in 19 out of 48 nonrecipients (P <.1). Consequently, the mean data illustrated in Figs. 1, 5, and 6 most likely result in an overestimation of blood glucose recovery and of hormonal responses during the last third of the test in the nonrecipient group because only those nonrecipients with comparatively less impaired hormonal responses were able to complete the test. In a subset of 12 type I diabetic patients who were studied before and after pancreas transplantation, blood glucose recovery after insulin-induced hypoglycemia improved in each individual and the difference in blood glucose recovery was highly significant (13±6% vs. 42±6% of decrement; P <.1; Fig. 2). Glucagon responses to insulin-induced hypoglycemia and to stimulation with arginine. Basal glucagon levels at normoglycemia were higher in recipients (192±23 ng/liter) than in nonrecipients (115±9 ng/liter; P <.1) and controls (1 13±12 ng/liter; P <.1; Fig. 1). During insulin-induced hypoglycemia very little increase in glucagon levels was observed in the nonrecipients. In contrast, glucagon levels increased significantly during hypoglycemia in recipients and in normal control subjects. Maximal incremental glucagon responses to hypoglycemia (Amax) in recipients (17±31 ng/ liter) were significantly greater (P <.1) than nonrecipients (37±7 ng/liter, P <.1), and similar to that observed in controls (125±15 ng/liter). In the subset of 12 type I diabetics studied before and after pancreas transplantation, maximal incremental glucagon responses were significantly improved (52±15 vs. 225±57 ng/liter; P <.2). Blood glucose recovery correlated significantly with incremental glucagon responses when all recipient data were used (r =.49, n = 24, P <.1), but in the subset of 12 recipients this correlation was not significant (r =.38, n = 12). The effect of beta adrenergic blockade on glucagon secretion during hypoglycemia in three pancreas recipients was examined to ascertain whether improved glucagon responses were related to beta adrenergic input. Glucagon responses were unaffected by an Glucagon, Catecholamine, and Pancreatic Polypeptide in Pancreas Recipients 29
3 6- INSULINI 8 8 a E E U' 4-1 6/16 22/ /4 8 Us U cc a u' n i 1 c O O I I I T INSULIN * I PRE-TX POST-TX PRE-TX POST-TX Figure 2. Glucose and glucagon data obtained at 6 min after the injection of insulin in 12 type I diabetic recipients who were tested before and after pancreas transplantation. Glucose data are expressed as a percentage of the absolute fall in glucose levels (pretest levels minus nadir levels), and glucagon levels are expressed as peak increments over pretest glucagon values. These 12 type I diabetic recipients were tested before and after pancreas transplantation. Differences in plasma glucose recovery at 6 min are significant at P <.1, and differences in maximal glucagon increments are significant at P < i Figure 1. Circulating glucose and glucagon levels before and during insulin-induced hypoglycemia in 24 type I diabetic recipients of pancreas allografts (closed squares), 48 type I diabetic nonrecipients (open squares), and 16 nondiabetic normal control subjects (open circles). The test was completed in 22/24 type I diabetic recipients, 27/48 type I diabetic nonrecipients, and 16/16 normal controls. The dashed line represents an estimation of the theoretical 6-min glucose level that would have been achieved had the 21/48 nonrecipients completed their test. This estimation was made based upon the last three plasma glucose levels before premature discontinuation of this test by injecting intravenous glucose because of severe discomfort. Plasma glucose recovery in recipients of pancreas allografts was significantly improved compared with type I diabetic nonrecipients (P <.1), but still significantly lower than that observed in normal control subjects (P <.1). Basal levels of glucagon were significantly elevated in pancreas recipients compared with nonrecipients (P <.1) and controls (P <.1). The maximal incremental glucagon responses in recipients were significantly greater (P <.1) than nonrecipients and not significantly different than controls. intravenous infusion of propranolol (8,ug/min) given before and during hypoglycemia (Fig. 3). Glucagon responses to arginine were also determined in recipients, nonrecipients, and normal control subjects to compare alpha cell responsiveness with direct stimulation. Basal glucagon values were approximately two-fold elevated in recipients compared with nonrecipients and controls (Fig. 4), and integrated incremental glucagon responses under the curve were significantly greater in recipients (191±27) compared with nonrecipients (71±7; P <.1) and with controls (1 19±162 ng/liter X min, P <.1). Catecholamine responses to insulin-induced hypoglycemia. Epinephrine responses to insulin-induced hypoglycemia were highly variable in all three groups (Fig. 5), with a trend towards impaired responses in nonrecipients. However, no significant differences in basal levels or in peak incremental epinephrine responses were observed among nonrecipients (2.2±.3), recipients (2.3±.4), and controls (2.6±.4 nmol/liter). The results obtained from 6 type I diabetics studied before and after pancreas transplantation also showed no improvement in peak 1.-% 8 -..O 6 4 A61w%p 2 PROPRANOLOL (8 INSULIN jig/min) Figure 3. Lack of effect of f,-adenergic blockade (propranolol, 8 jg/ min i.v. infusion) on plasma glucagon levels during insulin-induced hypoglycemia in three type I diabetic recipients of pancreas allografts (after pancreas transplantation and without propranolol, closed squares; after pancreas transplantation and with propranolol, closed circles; and before pancreas transplantation, open squares). I 21 P. Diem, J. Redmon, M. Abid, A. Moran, D. Sutherland, J. Halter, and R. Robertson
4 ARGININE Figure 4. Plasma gluca- 6 gon levels before and after arginine (5 g i.v.) S 4 in 25 type I diabetic re cipients of pancreas allografts (closed squares), Q 2-46 type I diabetic (2 nonrecipients (open squares), and 18 normal control subjects (open circles). Glucagon secretion expressed as area under the curve from -1 min was significantly greater in type I diabetic pancreas recipients compared with nonrecipients (P <.1), and compared with normal control subjects (P <.1). 1asma epinephrine levels before and during insulin toler- recipients. It is interesting how this increased glucagon re- Figure 5. F ance testinig in 14 type I diabetic recipients of pancreas allografts sponsivity in recipients is not peculiar to glycopenic signaling, (closed squtares), 19 type I diabetic nonrecipients (open squares), and because increased secretion in recipients was also observed 1 normal control subjects (open circles). There were no significant during stimulation with arginine. Our data also suggest that differences among the three groups. islet alpha cells in humans do not require central nervous SECRETIN IN ISULIN t 2- E I~~~~~ XL 1-1 I Figure 6. Circulating hpp levels before and during insulin tolerance testing in 24 type I diabetic recipients of pancreas allografts (closed squares), 46 type I diabetic nonrecipients (open squares), and 16 normal controls (open -'--' circles). Peak pancreatic 5 6 polypeptide responses to hypoglycemia were significantly diminished in pancreas recipients (P <.1) and in nonrecipients (P <.1) compared with normal control subjects. No differences were observed among the three groups after a 1 stimulation with intravenous secretin (2 U/kg). incremental epinephrine responses to hypoglycemia (2.3±.6 1 nmol/liter vs. 2.3±.6). Similarly, norepinephrine responses Z sn showed no differences between the three groups (peak incremental norepinephrine responses: 1.2±.2 in nonrecipients, n = 14; in recipients, n = 19; and 1.3±.2 nmol/liter in controls, n = 1) Pancreatic polypeptide responses to hypoglycemia and to secretin stimulation. Basal pancreatic polypeptide levels at normoglycemia did not differ among the three groups (41±7 I111llIII in nnnrfnrinientc in re inientc qnd 74+6 nmvl/litir in _ tide, and catecholamines. Our data demonstrate significant controls; IFig. 6). Peak incremental pancreatic polypeptide re- improvement in, although not normaliation of, the magni- hypoglycemia were significantly diminished in tude of recovery of circulating glucose levels after insulin-in- sponses to nonrecipioents (79±15; P <.1) and in recipients (7±15; P duced hypoglycemia. The improvement in glucose recovery is <.1) ( compared iomulatio withcontrol iontraveou subjects subjecrtin, (195±37 peak9±7pa pmol/liter). eret evident when cross-sectionally comparing the glucose reimulation During sti.tinrvnusr sponses of pancreas recipients with those of normal controls polypepti( de responses (average of three highest values minus basal valu.ie for eahsuecircpins6±4n=and nonrecipients, and when comparing prospectively the efor each suject) inrecipients(67±24; n ' glucose responses in the subset of recipients we studied before nonrecipiients n = ( ), and normal control subjects and after pancreas transplantation. A marked increase in basal (37±11 pimol/liter; n = 17) did not differ. and stimulated glucagon secretion was associated with the improved glucose recovery after hypoglycemia in the pancreas Discuss oion recipients. In this subset, 4 of the 12 recipients had no im- The studies described herein were designed to determine the provement in glucagon responses but two had improved episuccessful, pancreas transplantation in type I diabetic nephnne responses (in the other two epinephnne data were effects of not patients obtained), which may explain the improvement in glucose u recovery. The reason for the elevated basal glucagon levels is uncertain. Systemic venous drainage of the allograft may be an 3 important factor since glucagon secreted by the allograft would INSULIN reach the systemic circulation before and not after metabolism Z-. by the liver. The liver is known to be an important site of Ea glucagon metabolism with normal hepatic glucagon extraction - 2 estimated at 2-25% (18, 19). The other possible explanations include diminished renal function and steroid therapy. Ul However, Ostman et al. reported that basal glucagon levels in = pancreas transplant recipients with systemic venous drainage w 1 of their graft were elevated compared with kidney transplant I 6 recipients with similar renal function and the same immunosuppressive regimen (2). Regardless of the explanation for w elevated basal glucagon levels in our patients, it seems reason- _,,,,,, able to contend that the marked increase in glucagon secretion during insulin-induced hypoglycemia is related to the im- proved glucose recovery after hypoglycemia in our pancreas Glucagon, Catecholamine, and Pancreatic Polypeptide in Pancreas Recipients 211
5 system inputs to respond to glycopenia, although it is generally accepted that central nervous system inputs into the endocrine pancreas participate in islet alpha cell responses to hypoglycemia. The contention that our patients' allografts remained denervated at the time of study seems reasonable since many of our patients were studied by 3 mo after pancreas transplantation. Moreover, even if reinnervation was to occur, it is extremely unlikely that this would establish the normal neural mechanisms inherent in the native pancreas because our patients allografts were positioned in an heterotopic position in the pelvis rather than in the area surrounding the normal pancreatic bed. An alternative interpretation of our data is that return to normoglycemia for an extended period of time may have improved alpha cell function so that hypoglycemia could stimulate secretion from the native pancreas. There are not a great deal of reported data to argue against this possibility, although it has been reported that patients treated with insulin pumps and achieving normoglycemia for a period of up to 12 mo still had defective glucagon responses to hypoglycemia (21, 22). Although there are very few studies of this nature and glucose control with intensive insulin treatment is not as fine as one can obtain through pancreas transplantation, we think it is worth considering that the marked improvement in glucagon secretion in pancreas recipients could be due to the allograft exclusively, since it is well appreciated that alpha cells respond to hypoglycemia in the absence of sympathetic or parasympathetic innervation. In our study, no significant differences were observed in pancreatic polypeptide responses or catecholamine responses during insulin-induced hypoglycemia when comparing recipients and nonrecipients of pancreas allografts. Interestingly, glucagon responses to arginine, which are not neurally mediated, were greater in the recipients compared with nonrecipients, whereas no significant differences between these two groups were observed in pancreatic polypeptide responses to secretin, which require vagal innervation of the islet (23, 24). This further suggests that the transplanted allografts in our patients remained denervated up to the time of our studies. That pancreatic polypeptide secretion is quantitatively similar in recipients and nonrecipients suggests that secretion of this hormone in both groups occurs from native pancreas only. If this reasoning is correct, serial monitoring of pancreatic polypeptide responses may provide a valuable metabolic marker for possible future allograft reinnervation should it occur. Although there appeared to be a trend towards improvement in the epinephrine responses in pancreas recipients, there were no significant differences in the epinephrine responses among the three groups. Regardless, because of this trend and because of the possibility of denervation hypersensitivity to adrenergic stimulation, we wished to establish whether the improved glucagon responses in the recipients might be related to increased adenergic input into pancreatic islet alpha cells through betaadenergic stimulation (25). That propranolol failed to diminish the glucagon responses to hypoglycemia reinforces the possibility that these responses may have been due to direct sensing by the alpha cells of glycopenia rather than concurrent beta-adenergic stimulation from circulating catecholamines. The effects of pancreas transplantation in humans with type I diabetes mellitus on glucose and hormonal counterregulatory responses to hypoglycemia, and on secretion of glucagon, catecholamines, and pancreatic polypeptide in general, have not been previously reported. The only other report addressing glucagon responsivity after hypoglycemia or other stimulation in pancreas recipients is that of Bosi et al. (26) who reported intact glucagon responses to hypoglycemia in five of six patients who received segmental pancreas allografts. However, this study did not include control data from diabetics or normal subjects for comparison, nor did it provide pretransplantation data from their recipients. Hence, one cannot be certain from their report alone whether segmental transplantation improved glucagon responses or counterregulation of hypoglycemia. The only other relevant report is from Ostman et al. (2) who reported only basal but not stimulated glucagon levels. The importance of these studies at a pragmatic level lies in the widely recognied observation that absence of glucagon responses to hypoglycemia in patients with type I diabetes mellitus is an important consequence which generally begins to become evident several years after diagnosis of the disease. This leads to deranged counterregulation of hypoglycemia and significant clinical risks. In view of the augmented glucagon responses and improved counterregulation of hypoglycemia demonstrated in our study, it may be reasonable to consider pancreas transplantation in type I diabetic patients who are at proven risk for serious episodes of insulin-induced hypoglycemia and who demonstrate refractoriness to conventional medical management with diet, alteration of insulin dosage, and exogenous glucagon injections. Acknowledgments We are indebted to the nursing and laboratory staffofthe University of Minnesota General Clinical Research Center for skilled patient care and excellent technical assistance. In addition we thank Ms. Paula Rossin for help with the preparation of this manuscript. This work was supported by grants (RO 1-DK and MO 1-RR- 4) from the National Institutes of Health and the Medical Research Service of the Department of Veterans Affairs. Dr. Diem was in part supported by a grant from the Swiss National Science Foundation. References 212 P. Diem, J. Redmon, M. Abid, A. Moran, D. Sutherland, J. Halter, and R. Robertson 1. Sutherland, D. E. R., J. S. Najarian, B. Z. Greenberg, B. J. Senske, G. E. Anderson, R. S. Francis, and F. C. Goet Hormonal and metabolic effects of a pancreatic endocrine graft. Ann. Int. Med. 95: Poa, G., J. Traeger, J. M. Dubernard, A. Secchi, A. E. Pontiroli, E. Bosi, M. C. Malik, A. Ruitton, and N. Blanc Endocrine responses oftype 1 (insulin-dependent) diabetic patients following successful pancreas transplantation. Diabetologia. 24: Traeger, J., J. M. Dubernard, G. Poa, E. Bosi, A. Secchi, A. E. Pontiroli, J. L. Touraine, H. Betuel, S. El Yafi, F. Da Ponte, D. Cantarovich, N. Diab, C. Cardoo, X. Martin, G. Kamel, and A. Gelet Influence of immunosuppressive therapy on the endocrine function of segmental pancreatic allografts. Transplant. Proc. 15: Poa, G., E. Bosi, A. Secchi, P. M. Piatti, J. L. Touraine, A. Gelet, A. E. Pontiroli, J. M. Dubernard, and J. Traeger Metabolic control of type I (insulin-dependent) diabetes after pancreas transplantation. Brit. Med. J. 291: Dafoe, D. C., D. A. Campbell, R. M. Merion, L. Rosenberg, L. L. Rocher, A. I. Vinik, A. K. Vine, and J. G. Turcotte Pancreatic transplantation-university of Michigan. Transplant. Proc. 19(Suppl): Land, W., R. Landgraf, W.-D. Illner, D. Abendroth, A. Kampik, U. Jensen, F. P. Lenhart, D. Burg, G. Hillebrand, L. A. Castro, M. M. C. Landgraf-Leurs, L. Frey, M. Gokel, St. Schleibner, J. Nusser,
6 and M. Ulbig Clinical pancreatic transplantation using the prolamine duct occlusion technique-the Munich experience. Transplant. Proc. 19(Suppl): Diem, P., M. Abid, J. B. Redmon, D. E. R. Sutherland, and R. P. Robertson Systemic venous drainage of pancreas allografts as independent cause of hyperinsulinemia in type I diabetic recipients. Diabetes. 39: Gerich, J. E Glucose counterregulation and its impact on diabetes mellitus. Diabetes. 37: Gerich, J. E., M. Langlois,. Noacco, J. H. Karam, and P. H. Forsham Lack of glucagon response to hypoglycemia in diabetes: evidence for an intrinsic pancreatic alpha cell defect. Science (Wash. DC). 182: Campbell, L. V., E. W. Kraegen, H. Meler, and L. Laarus Hormonal responses to insulin infusion in diabetes mellitus. Diabetologia. 16: Boden, G., G. A. Reichard, R. D. Hoeldtke, I. Revani, and. E. Owen Severe insulin induced hypoglycemia associated with deficiencies in the release of counterregulatory hormones. N. Engl. J. Med. 35: Benson, J. W. Jr., D. G. Johnson, J. P. Palmer, P. L. Werner, and J. W. Ensinck Glucagon and catecholamine secretion during hypoglycemia in normal diabetic man. J. Clin. Endocrinol. Metab. 44: Maher, T. D., R. J. Taneberg, B. Z. Greenberg, J. E. Hoffman, R. P. Doe, and F. C. Goet Lack of glucagon secretion during hypoglycemia in diabetic autonomic neuropathy. Diabetes. 26: Sutherland, D. E. R., D. L. Dunn, F. C. Goet, W. Kennedy, R. C. Ramsay, M. W. Steffes, S. M. Mauer, R. Gruessner, K. C. Moudry-Munns, P. Morel, A. Viste, R. P. Robertson, and J. S. Najarian A 1-year experience with 29 pancreas transplants at a single institution. Ann. Surg. 21: Harris, V., G. R. Faloona, and R. H. Unger Glucagon. In Methods of Hormone Radioimmunoassay. B. M. Jaffe and H. R. Behrman, editors. Academic Press, New York Chance, R. E., N. E. Moon, and M. G. Johnson Human pancreatic polypeptide (HPP) and bovine pancreatic polypeptide (BPP). In Methods of Hormone Radioimmunoassay. B. M. Jaffe and H. R. Behrman, editors. Academic Press, New York Evans, M. I., J. B. Halter, and D. Porte, Jr Comparison of double and single isotope enymatic derivative methods for measurement of catecholamines in human plasma. Clin. Chem. 24: Marco, J., J. Diego, M. Villanueva, M. Dray-Fierros, I. Valverde, and J. Segovia Elevated plasma glucagon levels in cirrhosis of the liver. N. Engi. J. Med. 289: Jaspan, J. B., K. S. Polonsky, M. Lewis, J. Pensler, W. Pugh, A. R. Moossa, and A. H. Rubenstein Hepatic metabolism of glucagon in the dog. Am. J. Physiol. 24:E Ostman, J., J. Bolinder, R. Gunnarson, C. Brattstrom, G. Tyden, J. Wahren, and C.-G. Groth Effects of pancreas transplantation on metabolic and hormonal profiles in IDDM patients. Diabetes. 38(Suppl. 1): Bergenstal, R. M., K. S. Polonsky, G. Pons, J. B. Jaspan, and A. H. Rubenstein Lack ofglucagon response to hypoglycemia in type I diabetics after long-term optimal therapy with a continuous subcutaneous insulin infusion pump. Diabetes. 32: Bolli, G., G. Calabrese, P. De Feo, P. Compagnucci, G. Zegra, G. Angeletti, M. G. Cartechini, F. Santeusanio, and P. Brunetti Lack of glucagon response in glucose counterregulation in type I (insulin-dependent) diabetics: absence of recovery after prolonged optimal insulin therapy. Diabetologia. 22: Schwart, T. W Pancreatic polypeptide: a hormone under vagal control. Gastroenterology. 84: Glaser, B., A. I. Vinik, A. A. Sive, and J. C. Floyd, Jr Plasma human pancreatic polypeptide responses to administered secretin: effects of surgical vagotomy, cholinergic blockade, and chronic pancreatitis. J. Clin. Endocrinol. & Metab. 5: Gerich, J. E., M. Loreni, E. Tsalikian, and J. H. Karam Studies on the mechanism of epinephrine-induced hyperglycemia in man. Diabetes. 25: Bosi, E., P. M. Piatti, A. Secchi, L. D. Monti, J. Traeger, J. M. Dubernard, and G. Poa Response of glucagon and insulin secretion to insulin-induced hypoglycemia in type I diabetic recipients after pancreatic transplantation. Diab. Nutr. Metab. 1: Glucagon, Catecholamine, and Pancreatic Polypeptide in Pancreas Recipients 213
Glucagon response to hypoglycemia in sympathectomized man.
 Glucagon response to hypoglycemia in sympathectomized man. J P Palmer,, D G Johnson, J W Ensinck J Clin Invest. 1976;57(2):522-525. https://doi.org/10.1172/jci108305. Research Article Hypoglycemia stimulates
Glucagon response to hypoglycemia in sympathectomized man. J P Palmer,, D G Johnson, J W Ensinck J Clin Invest. 1976;57(2):522-525. https://doi.org/10.1172/jci108305. Research Article Hypoglycemia stimulates
Insulin Secretion in Diabetes Mellitus
 A Role for AlphaAdrenergic Receptors in Abnormal nsulin Secretion in Diabetes Mellitus R. PAUL ROBERTSON, JEFFREY B. HALTER, and DANiEL PORTE, JR. From the University of Washington School of Medicine and
A Role for AlphaAdrenergic Receptors in Abnormal nsulin Secretion in Diabetes Mellitus R. PAUL ROBERTSON, JEFFREY B. HALTER, and DANiEL PORTE, JR. From the University of Washington School of Medicine and
Diabetologia 9 Springer-Verlag 1991
 Diabetologia (1991) 34 [Suppl 1]: $61-$67 0012186X91001t4A Diabetologia 9 Springer-Verlag 1991 Metabolic and hormonal studies of Type 1 (insulin-dependent) diabetic patients after successful pancreas and
Diabetologia (1991) 34 [Suppl 1]: $61-$67 0012186X91001t4A Diabetologia 9 Springer-Verlag 1991 Metabolic and hormonal studies of Type 1 (insulin-dependent) diabetic patients after successful pancreas and
Intrahepatic islet transplantation has been demonstrated
 Intrahepatic Islet Transplantation in Type 1 Diabetic Patients Does Not Restore Hypoglycemic Hormonal Counterregulation or Symptom Recognition After Insulin Independence Breay W. Paty, 1,2 Edmond A. Ryan,
Intrahepatic Islet Transplantation in Type 1 Diabetic Patients Does Not Restore Hypoglycemic Hormonal Counterregulation or Symptom Recognition After Insulin Independence Breay W. Paty, 1,2 Edmond A. Ryan,
Diabetologia. Key words: Catecholamines, cortisol, glucagon, glucose counter-regulation, growth hormone, hypoglycaemia. Subjects and Protocols
 Diabetologia (1982) 22:100-105 Diabetologia 9 Springer-Verlag 1982 Lack of Glucagon Response in Glucose Counter-Regulation in Type 1 (Insulin-Dependent) Diabetics: Absence of Recovery After Prolonged Optimal
Diabetologia (1982) 22:100-105 Diabetologia 9 Springer-Verlag 1982 Lack of Glucagon Response in Glucose Counter-Regulation in Type 1 (Insulin-Dependent) Diabetics: Absence of Recovery After Prolonged Optimal
This document reviews the safety,
 T E C H N I C A L R E V I E W Pancreas Transplantation for Patients With Diabetes Mellitus AMERICAN DIABETES ASSOCIATION This document reviews the safety, efficacy, and indications for pancreas and islet
T E C H N I C A L R E V I E W Pancreas Transplantation for Patients With Diabetes Mellitus AMERICAN DIABETES ASSOCIATION This document reviews the safety, efficacy, and indications for pancreas and islet
Diabetologia 9 Springer-Verlag t991
 Diabetologia (1991) 34 [Suppl 1]: S 113-S 117 0012186X9100126B Diabetologia 9 Springer-Verlag t991 Follow-up study of sensory-motor polyneuropathy in Type 1 (insulin-dependent) diabetic subjects after
Diabetologia (1991) 34 [Suppl 1]: S 113-S 117 0012186X9100126B Diabetologia 9 Springer-Verlag t991 Follow-up study of sensory-motor polyneuropathy in Type 1 (insulin-dependent) diabetic subjects after
Abs tract. To characterize glucose counterregulatory
 Defective Glucose Counterregulation After Subcutaneous Insulin in Noninsulin-dependent Diabetes Mellitus Paradoxical Suppression of Glucose Utilization and Lack of Compensatory Increase in Glucose Production,
Defective Glucose Counterregulation After Subcutaneous Insulin in Noninsulin-dependent Diabetes Mellitus Paradoxical Suppression of Glucose Utilization and Lack of Compensatory Increase in Glucose Production,
Circulating insulin inhibits glucagon secretion induced by arginine in type 1 diabetes
 European Journal of Endocrinology (2000) 142 30 34 ISSN 0804-4643 CLINICAL STUDY Circulating insulin inhibits glucagon secretion induced by arginine in type 1 diabetes Per R Oskarsson 1, Per-Eric Lins
European Journal of Endocrinology (2000) 142 30 34 ISSN 0804-4643 CLINICAL STUDY Circulating insulin inhibits glucagon secretion induced by arginine in type 1 diabetes Per R Oskarsson 1, Per-Eric Lins
Eilandjes transplantatie. Eelco de Koning, LUMC 14 februari 2008
 Eilandjes transplantatie Eelco de Koning, LUMC 14 februari 2008 Pancreas or islets? What tissue do we wish to transplant? Is there competition for donor pancreas? How does the islet isolation and transplantation
Eilandjes transplantatie Eelco de Koning, LUMC 14 februari 2008 Pancreas or islets? What tissue do we wish to transplant? Is there competition for donor pancreas? How does the islet isolation and transplantation
Diabetologia 9 Springer-Verlag 1989
 Diabetologia (1989) 32:61-66 Diabetologia 9 Springer-Verlag 1989 Effects of chronic feeding on the impaired glucagon and epinephrine responses to insulin-induced hypoglycaemia in streptozotocin diabetic
Diabetologia (1989) 32:61-66 Diabetologia 9 Springer-Verlag 1989 Effects of chronic feeding on the impaired glucagon and epinephrine responses to insulin-induced hypoglycaemia in streptozotocin diabetic
Diabetologia 9 Springer-Verlag 1984
 Diabetologia (1984) 26:203 207 Diabetologia 9 Springer-Verlag 1984 How does glucose regulate the human pancreatic A cell in vivo? C. M. Asplin*, P. M. Hollander** and J. P. Palmer Diabetes Research Center
Diabetologia (1984) 26:203 207 Diabetologia 9 Springer-Verlag 1984 How does glucose regulate the human pancreatic A cell in vivo? C. M. Asplin*, P. M. Hollander** and J. P. Palmer Diabetes Research Center
Clinical Policy: Pancreas Transplantation Reference Number: PA.CP.MP.102
 Clinical Policy: Reference Number: PA.CP.MP.102 Effective Date: 01/18 Last Review Date: 03/17 Revision Log Coding Implications Description This policy describes the medical necessity requirements for pancreas
Clinical Policy: Reference Number: PA.CP.MP.102 Effective Date: 01/18 Last Review Date: 03/17 Revision Log Coding Implications Description This policy describes the medical necessity requirements for pancreas
Pancreas After Islet Transplantation: A First Report of the International Pancreas Transplant Registry
 American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
Counterregulation in Man
 Mechanisms of Postprandial Glucose Counterregulation in Man PHYSIOLOGIC ROLS OF GLUCAGON AND PINPHRIN VIS-A-VIS INSULIN IN TH PRVNTION OF HYPOGLYCMIA LAT AFTR GLUCOS INGSTION THOMAS F. TS, WILLIAM. CLUTTR,
Mechanisms of Postprandial Glucose Counterregulation in Man PHYSIOLOGIC ROLS OF GLUCAGON AND PINPHRIN VIS-A-VIS INSULIN IN TH PRVNTION OF HYPOGLYCMIA LAT AFTR GLUCOS INGSTION THOMAS F. TS, WILLIAM. CLUTTR,
Somatostatin is an endogenous peptide and neurotransmitter
 Rapid Publication Somatostatin Impairs Clearance of Exogenous Insulin in Humans ELI IPP, YSEF SINAI, BENJAMIN BAR-Z, RAFAEL NESHER, AND ERL CERASI SUMMARY Somatostatin has been widely used to suppress
Rapid Publication Somatostatin Impairs Clearance of Exogenous Insulin in Humans ELI IPP, YSEF SINAI, BENJAMIN BAR-Z, RAFAEL NESHER, AND ERL CERASI SUMMARY Somatostatin has been widely used to suppress
Glucagon secretion in relation to insulin sensitivity in healthy subjects
 Diabetologia (2006) 49: 117 122 DOI 10.1007/s00125-005-0056-8 ARTICLE B. Ahrén Glucagon secretion in relation to insulin sensitivity in healthy subjects Received: 4 July 2005 / Accepted: 12 September 2005
Diabetologia (2006) 49: 117 122 DOI 10.1007/s00125-005-0056-8 ARTICLE B. Ahrén Glucagon secretion in relation to insulin sensitivity in healthy subjects Received: 4 July 2005 / Accepted: 12 September 2005
Glucagon Regulation of Plasma Ketone Body Concentration
 Glucagon Regulation of Plasma Ketone Body Concentration in Human Diabetes DAVID S. ScHADE and R. PHiIp EATON From the Department of Medicine, University of New Mexico School of Medicine, Albuquerque, New
Glucagon Regulation of Plasma Ketone Body Concentration in Human Diabetes DAVID S. ScHADE and R. PHiIp EATON From the Department of Medicine, University of New Mexico School of Medicine, Albuquerque, New
the natural history and underlying pathophysiology
 Pathophysiology/Complications O R I G I N A L A R T I C L E Early Loss of the Glucagon Response to Hypoglycemia in Adolescents With Type 1 Diabetes ARIS SIAFARIKAS, FRACP, MD 1,2,3 ROBERT J. JOHNSTON,
Pathophysiology/Complications O R I G I N A L A R T I C L E Early Loss of the Glucagon Response to Hypoglycemia in Adolescents With Type 1 Diabetes ARIS SIAFARIKAS, FRACP, MD 1,2,3 ROBERT J. JOHNSTON,
associated with serious complications, but reduce occurrences with preventive measures
 Wk 9. Management of Clients with Diabetes Mellitus 1. Diabetes Mellitus body s inability to metabolize carbohydrates, fats, proteins hyperglycemia associated with serious complications, but reduce occurrences
Wk 9. Management of Clients with Diabetes Mellitus 1. Diabetes Mellitus body s inability to metabolize carbohydrates, fats, proteins hyperglycemia associated with serious complications, but reduce occurrences
Islet and Pancreas Transplantation
 Islet and Pancreas Transplantation Julie Wardle Specialist Nurse Coordinator Indication for Transplant Treatment option for a select groups of patients with type 1 diabetes Aged 18 years or over Recurrent
Islet and Pancreas Transplantation Julie Wardle Specialist Nurse Coordinator Indication for Transplant Treatment option for a select groups of patients with type 1 diabetes Aged 18 years or over Recurrent
Arginine-Stimulated Acute Phase of Insulin and Glucagon
 Arginine-Stimulated Acute Phase of Insulin and Glucagon Secretion in Diabetic Subjects JERRY P. PALMER, JAMES W. BENSON, ROBERT M. WALTER, and JoHN W. ENSINCK From the Department of Medicine and Diabetes
Arginine-Stimulated Acute Phase of Insulin and Glucagon Secretion in Diabetic Subjects JERRY P. PALMER, JAMES W. BENSON, ROBERT M. WALTER, and JoHN W. ENSINCK From the Department of Medicine and Diabetes
therapy, is increased two- to threefold in patients practicing intensive insulin therapy ( 1, 2). This phenomenon has become
 Impaired Hormonal Responses to Hypoglycemia in Spontaneously Diabetic and Recurrently Hypoglycemic Rats Reversibility and Stimulus Specificity of the Deficits Anthony M. Powell, Robert S. Sherwin, and
Impaired Hormonal Responses to Hypoglycemia in Spontaneously Diabetic and Recurrently Hypoglycemic Rats Reversibility and Stimulus Specificity of the Deficits Anthony M. Powell, Robert S. Sherwin, and
In established (i.e., C-peptide negative) type 1 diabetes,
 Hypoglycemia-Associated Autonomic Failure in Advanced Type 2 Diabetes Scott A. Segel, Deanna S. Paramore, and Philip E. Cryer We tested the hypotheses that the glucagon response to hypoglycemia is reduced
Hypoglycemia-Associated Autonomic Failure in Advanced Type 2 Diabetes Scott A. Segel, Deanna S. Paramore, and Philip E. Cryer We tested the hypotheses that the glucagon response to hypoglycemia is reduced
Counterregulatory responses to hypoglycemia in patients with maturity-onset diabetes of the young caused by HNF-1a gene mutations (MODY3)
 European Journal of Endocrinology (2001) 144 45±49 ISSN 0804-4643 CLINICAL STUDY Counterregulatory responses to hypoglycemia in patients with maturity-onset diabetes of the young caused by HNF-1a gene
European Journal of Endocrinology (2001) 144 45±49 ISSN 0804-4643 CLINICAL STUDY Counterregulatory responses to hypoglycemia in patients with maturity-onset diabetes of the young caused by HNF-1a gene
Management of Type 2 Diabetes
 Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Alternative insulin delivery systems: how demanding should the patient be?
 Diabetologia (1997) 4: S97 S11 Springer-Verlag 1997 Alternative insulin delivery systems: how demanding should the patient be? K.S. Polonsky, M. M. Byrne, J. Sturis Department of Medicine, The University
Diabetologia (1997) 4: S97 S11 Springer-Verlag 1997 Alternative insulin delivery systems: how demanding should the patient be? K.S. Polonsky, M. M. Byrne, J. Sturis Department of Medicine, The University
The Contribution of Endogenous Insulin Secretion to the Ketogenic Response to Glucagon in Man* D. S. Schade and R. P. Eaton
 Diabetologia 11,555-559 (1975) 9 by Springer-Verlag 1975 The Contribution of Endogenous Insulin Secretion to the Ketogenic Response to Glucagon in Man* D. S. Schade and R. P. Eaton Dept. of Medicine, Univ.
Diabetologia 11,555-559 (1975) 9 by Springer-Verlag 1975 The Contribution of Endogenous Insulin Secretion to the Ketogenic Response to Glucagon in Man* D. S. Schade and R. P. Eaton Dept. of Medicine, Univ.
EFFECT OF VAGOTOMY AND PYLOROPLASTY: THE ORAL GLUCOSE TOLERANCE TEST
 GASTROENTEROLOGY 64: 217-222, 1973 Copyright 1973 by The Williams & Wilkins Co. Vol. 64, No.2 Printed in U.S.A. EFFECT OF VAGOTOMY AND PYLOROPLASTY: THE ORAL GLUCOSE TOLERANCE TEST W, H, HALL, M,D" L.
GASTROENTEROLOGY 64: 217-222, 1973 Copyright 1973 by The Williams & Wilkins Co. Vol. 64, No.2 Printed in U.S.A. EFFECT OF VAGOTOMY AND PYLOROPLASTY: THE ORAL GLUCOSE TOLERANCE TEST W, H, HALL, M,D" L.
Kidney Transplantation
 Kidney Tran nsplantation Historical per rspective and current practice Piyanut Poo otracool, M.D. Departmen nt of Surgery, Ramathibo odi Hospital, Mahidol University Kidney Transplantation DDKT Adult deceased
Kidney Tran nsplantation Historical per rspective and current practice Piyanut Poo otracool, M.D. Departmen nt of Surgery, Ramathibo odi Hospital, Mahidol University Kidney Transplantation DDKT Adult deceased
Uniphasic Insulin Responses to Secretin Stimulation in Man
 Uniphasic Insulin Responses to Stimulation in Man ROGER L. LERNER and DANIEL PORTE, JR. From the University of Washington School of Medicine and Veterans Administration Hospital, Seattle, Washington 98108
Uniphasic Insulin Responses to Stimulation in Man ROGER L. LERNER and DANIEL PORTE, JR. From the University of Washington School of Medicine and Veterans Administration Hospital, Seattle, Washington 98108
The oral meal or oral glucose tolerance test. Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol
 Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol Minimal Model Assessment of -Cell Responsivity and Insulin Sensitivity in Nondiabetic Individuals Chiara Dalla Man,
Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol Minimal Model Assessment of -Cell Responsivity and Insulin Sensitivity in Nondiabetic Individuals Chiara Dalla Man,
9.3 Stress Response and Blood Sugar
 9.3 Stress Response and Blood Sugar Regulate Stress Response Regulate Blood Sugar Stress Response Involves hormone pathways that regulate metabolism, heart, rate and breathing The Adrenal Glands a pair
9.3 Stress Response and Blood Sugar Regulate Stress Response Regulate Blood Sugar Stress Response Involves hormone pathways that regulate metabolism, heart, rate and breathing The Adrenal Glands a pair
Stabilisation of diabetic retinopathy following simultaneous pancreas and kidney transplant
 736 St Paul s Eye Unit, Royal Liverpool University Hospital, Liverpool L7 8XP I A Pearce B Ilango D Wong Transplant Unit R A Sells Correspondence to: Mr D Wong, St Paul s Eye Unit, Royal Liverpool University
736 St Paul s Eye Unit, Royal Liverpool University Hospital, Liverpool L7 8XP I A Pearce B Ilango D Wong Transplant Unit R A Sells Correspondence to: Mr D Wong, St Paul s Eye Unit, Royal Liverpool University
Simple Measures to Monitor b -Cell Mass and Assess Islet Graft Dysfunction
 American Journal of Transplantation 2007; 7: 303 308 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant Surgeons
American Journal of Transplantation 2007; 7: 303 308 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant Surgeons
Increasing the Decrement in Insulin Secretion Improves Glucagon Responses to Hypoglycemia in Advanced Type 2 Diabetes
 Emerging Treatments and Technologies O R I G I N A L A R T I C L E Increasing the Decrement in Insulin Secretion Improves Glucagon Responses to Hypoglycemia in Advanced Type 2 Diabetes ZARMEN ISRAELIAN,
Emerging Treatments and Technologies O R I G I N A L A R T I C L E Increasing the Decrement in Insulin Secretion Improves Glucagon Responses to Hypoglycemia in Advanced Type 2 Diabetes ZARMEN ISRAELIAN,
Orthostatic Hypotension in Kidney Pancreas Transplant Patients and its Relation to Preexisting Autonomic Neuropathy
 Orthostatic Hypotension in Kidney Pancreas Transplant Patients and its Relation to Preexisting Autonomic Neuropathy Anand Khurana, 1 Charles F McCuskey, 2 Elena G Slavcheva 1 Abstract Objectives: Orthostatic
Orthostatic Hypotension in Kidney Pancreas Transplant Patients and its Relation to Preexisting Autonomic Neuropathy Anand Khurana, 1 Charles F McCuskey, 2 Elena G Slavcheva 1 Abstract Objectives: Orthostatic
Metabolic follow-up after long-term pancreas graft survival
 European Journal of Endocrinology (2007) 156 603 610 ISSN 0804-4643 CLINICAL STUDY Metabolic follow-up after long-term pancreas graft survival Christoph D Dieterle, Helmut Arbogast 1, Wolf-Dieter Illner
European Journal of Endocrinology (2007) 156 603 610 ISSN 0804-4643 CLINICAL STUDY Metabolic follow-up after long-term pancreas graft survival Christoph D Dieterle, Helmut Arbogast 1, Wolf-Dieter Illner
(7). Not all patients with these clinical syndromes respond to leucine, and the phrase "leucine-sensitive"
 Journal of Clinical Investigation Vol. 41, No. 3, 1962 THE USE OF INSULIN IN THE PRODUCTION OF L-LEUCINE- INDUCED HYPOGLYCEMIA IN NORMAL DOGS * By G. REAVEN AND C. LUCAS f (From the Department of Internal
Journal of Clinical Investigation Vol. 41, No. 3, 1962 THE USE OF INSULIN IN THE PRODUCTION OF L-LEUCINE- INDUCED HYPOGLYCEMIA IN NORMAL DOGS * By G. REAVEN AND C. LUCAS f (From the Department of Internal
Control of Blood Glucose in the ICU: Reconciling the Conflicting Data
 Control of Blood Glucose in the ICU: Reconciling the Conflicting Data Steven E. Nissen MD Disclosure Consulting: Many pharmaceutical companies Clinical Trials: AbbVie, Amgen, Astra Zeneca, Esperion, Eli
Control of Blood Glucose in the ICU: Reconciling the Conflicting Data Steven E. Nissen MD Disclosure Consulting: Many pharmaceutical companies Clinical Trials: AbbVie, Amgen, Astra Zeneca, Esperion, Eli
Diabetes mellitus is a complex of syndromes characterized metabolically by hyperglycemia and altered glucose metabolism, and associated
 Diabetes mellitus is a complex of syndromes characterized metabolically by hyperglycemia and altered glucose metabolism, and associated pathologically with specific microvascular and macrovascular complications.
Diabetes mellitus is a complex of syndromes characterized metabolically by hyperglycemia and altered glucose metabolism, and associated pathologically with specific microvascular and macrovascular complications.
Iatrogenic hypoglycemia is the limiting factor in the
 Sleep-Related Hypoglycemia-Associated Autonomic Failure in Type 1 Diabetes Reduced Awakening From Sleep During Hypoglycemia Salomon Banarer and Philip E. Cryer Given that iatrogenic hypoglycemia often
Sleep-Related Hypoglycemia-Associated Autonomic Failure in Type 1 Diabetes Reduced Awakening From Sleep During Hypoglycemia Salomon Banarer and Philip E. Cryer Given that iatrogenic hypoglycemia often
David Bruyette, DVM, DACVIM Medical Director
 VCAWLAspecialty.com David Bruyette, DVM, DACVIM Medical Director The pancreas is made up of endocrine and exocrine tissue. The endocrine pancreas is composed of islets of Langerhans, which make up approximately
VCAWLAspecialty.com David Bruyette, DVM, DACVIM Medical Director The pancreas is made up of endocrine and exocrine tissue. The endocrine pancreas is composed of islets of Langerhans, which make up approximately
Effect of sex on counterregulatory responses to exercise after antecedent hypoglycemia in type 1 diabetes
 Am J Physiol Endocrinol Metab 287: E16 E24, 2004. First published March 2, 2004; 10.1152/ajpendo.00480.2002. Effect of sex on counterregulatory responses to exercise after antecedent hypoglycemia in type
Am J Physiol Endocrinol Metab 287: E16 E24, 2004. First published March 2, 2004; 10.1152/ajpendo.00480.2002. Effect of sex on counterregulatory responses to exercise after antecedent hypoglycemia in type
Iatrogenic hypoglycemia is the limiting factor, both
 Limited Impact of Vigorous Exercise on Defenses Against Hypoglycemia Relevance to Hypoglycemia-Associated Autonomic Failure Veronica P. McGregor, 1 Jeffrey S. Greiwe, 2 Salomon Banarer, 1 and Philip E.
Limited Impact of Vigorous Exercise on Defenses Against Hypoglycemia Relevance to Hypoglycemia-Associated Autonomic Failure Veronica P. McGregor, 1 Jeffrey S. Greiwe, 2 Salomon Banarer, 1 and Philip E.
The second meal phenomenon in type 2 diabetes
 Diabetes Care Publish Ahead of Print, published online April 14, 2009 Second meal phenomenon and diabetes The second meal phenomenon in type 2 diabetes Ana Jovanovic MD, Jean Gerrard SRN, Roy Taylor MD
Diabetes Care Publish Ahead of Print, published online April 14, 2009 Second meal phenomenon and diabetes The second meal phenomenon in type 2 diabetes Ana Jovanovic MD, Jean Gerrard SRN, Roy Taylor MD
Corporate Medical Policy
 Corporate Medical Policy Pancreas Transplant File Name: Origination: Last CAP Review: Next CAP Review: Last Review: pancreas_transplant 1/2000 5/2017 5/2018 8/2017 Description of Procedure or Service Transplantation
Corporate Medical Policy Pancreas Transplant File Name: Origination: Last CAP Review: Next CAP Review: Last Review: pancreas_transplant 1/2000 5/2017 5/2018 8/2017 Description of Procedure or Service Transplantation
Adrenal gland And Pancreas
 Adrenal gland And Pancreas Structure Cortex Glucocorticoids Effects Control of secretion Mineralocorticoids Effects Control of secretion Sex steroids Medulla Catecholamines Adrenal cortex 80% of an adrenal
Adrenal gland And Pancreas Structure Cortex Glucocorticoids Effects Control of secretion Mineralocorticoids Effects Control of secretion Sex steroids Medulla Catecholamines Adrenal cortex 80% of an adrenal
Timely!Insulinization In!Type!2! Diabetes,!When!and!How
 Timely!Insulinization In!Type!2! Diabetes,!When!and!How, FACP, FACE, CDE Professor of Internal Medicine UT Southwestern Medical Center Dallas, Texas Current Control and Targets 1 Treatment Guidelines for
Timely!Insulinization In!Type!2! Diabetes,!When!and!How, FACP, FACE, CDE Professor of Internal Medicine UT Southwestern Medical Center Dallas, Texas Current Control and Targets 1 Treatment Guidelines for
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation
 Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Week 3, Lecture 5a. Pathophysiology of Diabetes. Simin Liu, MD, ScD
 Week 3, Lecture 5a Pathophysiology of Diabetes Simin Liu, MD, ScD General Model of Peptide Hormone Action Hormone Plasma Membrane Activated Nucleus Cellular Trafficking Enzymes Inhibited Receptor Effector
Week 3, Lecture 5a Pathophysiology of Diabetes Simin Liu, MD, ScD General Model of Peptide Hormone Action Hormone Plasma Membrane Activated Nucleus Cellular Trafficking Enzymes Inhibited Receptor Effector
Diabetes: What is the scope of the problem?
 Diabetes: What is the scope of the problem? Elizabeth R. Seaquist MD Division of Endocrinology and Diabetes Department of Medicine Director, General Clinical Research Center Pennock Family Chair in Diabetes
Diabetes: What is the scope of the problem? Elizabeth R. Seaquist MD Division of Endocrinology and Diabetes Department of Medicine Director, General Clinical Research Center Pennock Family Chair in Diabetes
Autonomic regulation of islet hormone secretion
 Autonomic regulation of islet hormone secretion Implications for health and disease Billy & Bree Paper 1: Autonomic regulation of islet hormone secretion : Implications for health and disease By Team BBB
Autonomic regulation of islet hormone secretion Implications for health and disease Billy & Bree Paper 1: Autonomic regulation of islet hormone secretion : Implications for health and disease By Team BBB
feeding reflects the number of functional PP cells present in the pancreas. Impaired PP release after feeding might, therefore, be a manifestation of
 Postgraduate Medical Journal (October 1981) 57, 617-621 Basal and postprandial serum concentrations of pancreatic polypeptide in pancreatitis and after pancreaticoduodenectomy C. B. H. W. LAMRS M.D. Division
Postgraduate Medical Journal (October 1981) 57, 617-621 Basal and postprandial serum concentrations of pancreatic polypeptide in pancreatitis and after pancreaticoduodenectomy C. B. H. W. LAMRS M.D. Division
VICTOSA and Renal impairment DR.R.S.SAJAD
 VICTOSA and Renal impairment DR.R.S.SAJAD February 2019 Main effect of GLP-1 is : Stimulating glucose dependent insulin release from the pancreatic islets. Slow gastric emptying Inhibit inappropriate
VICTOSA and Renal impairment DR.R.S.SAJAD February 2019 Main effect of GLP-1 is : Stimulating glucose dependent insulin release from the pancreatic islets. Slow gastric emptying Inhibit inappropriate
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Allogeneic Pancreas Transplant
 Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14 The following
Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14 The following
Role of Academia In Achieving Targets in Diabetes Care
 Role of Academia In Achieving Targets in Diabetes Care Disclosures Member of NovoNordisk, Lilly, Metavention, Sanofi, and Janssen Diabetes Advisory Boards Role of Academia in Discovering New Treatments
Role of Academia In Achieving Targets in Diabetes Care Disclosures Member of NovoNordisk, Lilly, Metavention, Sanofi, and Janssen Diabetes Advisory Boards Role of Academia in Discovering New Treatments
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Dysglycaemia In Acute Patients With Nutritional Therapy Mechanisms And Consequences Of Dysglycaemia In Patients Receiving Nutritional Therapy M. León- Sanz (ES) Mechanisms and
ESPEN Congress Madrid 2018 Dysglycaemia In Acute Patients With Nutritional Therapy Mechanisms And Consequences Of Dysglycaemia In Patients Receiving Nutritional Therapy M. León- Sanz (ES) Mechanisms and
CANINE PANCREATIC ALLOTRANSPLANTATION WITH DUODENUM (PANCREATICODUODENAL TRANSPLANTATION) USING CYCLOSPORIN A
 Nagoya J. Med. Sci. 47. 57-66, 1984 CANINE PANCREATIC ALLOTRANSPLANTATION WITH DUODENUM (PANCREATICODUODENAL TRANSPLANTATION) USING CYCLOSPORIN A TAKESHI MORIMOTO, M.D.*, HIROSHI TAKAGI, M.D.* and TATSUHEI
Nagoya J. Med. Sci. 47. 57-66, 1984 CANINE PANCREATIC ALLOTRANSPLANTATION WITH DUODENUM (PANCREATICODUODENAL TRANSPLANTATION) USING CYCLOSPORIN A TAKESHI MORIMOTO, M.D.*, HIROSHI TAKAGI, M.D.* and TATSUHEI
The endocrine system is complex and sometimes poorly understood.
 1 CE Credit Testing the Endocrine System for Adrenal Disorders and Diabetes Mellitus: It Is All About Signaling Hormones! David Liss, BA, RVT, VTS (ECC) Platt College Alhambra, California For more information,
1 CE Credit Testing the Endocrine System for Adrenal Disorders and Diabetes Mellitus: It Is All About Signaling Hormones! David Liss, BA, RVT, VTS (ECC) Platt College Alhambra, California For more information,
Human Type 1 Diabetes Is Characterized by an Early, Marked, Sustained, and Islet-Selective Loss of Sympathetic Nerves
 2322 Diabetes Volume 65, August 2016 Thomas O. Mundinger, 1 Qi Mei, 1 Alan K. Foulis, 2 Corinne L. Fligner, 3 Rebecca L. Hull, 1,4 and Gerald J. Taborsky Jr. 1,4 Human Type 1 Diabetes Is Characterized
2322 Diabetes Volume 65, August 2016 Thomas O. Mundinger, 1 Qi Mei, 1 Alan K. Foulis, 2 Corinne L. Fligner, 3 Rebecca L. Hull, 1,4 and Gerald J. Taborsky Jr. 1,4 Human Type 1 Diabetes Is Characterized
NIH Public Access Author Manuscript Transplant Proc. Author manuscript; available in PMC 2010 September 22.
 NIH Public Access Author Manuscript Published in final edited form as: Transplant Proc. 1990 February ; 22(1): 57 59. Effect of Hepatic Dysfunction and T Tube Clamping on FK 506 Pharmacokinetics and Trough
NIH Public Access Author Manuscript Published in final edited form as: Transplant Proc. 1990 February ; 22(1): 57 59. Effect of Hepatic Dysfunction and T Tube Clamping on FK 506 Pharmacokinetics and Trough
Chapter 13 worksheet
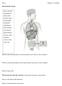 Name: Chapter 13 worksheet The Endocrine System Please label the: hypothalamus pineal gland pituitary gland thyroid gland parathyroid gland thymus heart stomach liver adrenal glands kidneys pancreas small
Name: Chapter 13 worksheet The Endocrine System Please label the: hypothalamus pineal gland pituitary gland thyroid gland parathyroid gland thymus heart stomach liver adrenal glands kidneys pancreas small
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
Future Therapies in the Treatment of Diabetes: Islet Transplantation
 Future Therapies in the Treatment of Diabetes: Islet Transplantation Michael R. Rickels, MD, MS Associate Professor of Medicine University of Pennsylvania Perelman School of Medicine Medical Director,
Future Therapies in the Treatment of Diabetes: Islet Transplantation Michael R. Rickels, MD, MS Associate Professor of Medicine University of Pennsylvania Perelman School of Medicine Medical Director,
Endocrine System. Regulating Blood Sugar. Thursday, December 14, 17
 Endocrine System Regulating Blood Sugar Stress results in nervous and hormonal responses. The adrenal glands are located above each kidney. Involved in stress response. Stress Upsets Homeostasis Stress
Endocrine System Regulating Blood Sugar Stress results in nervous and hormonal responses. The adrenal glands are located above each kidney. Involved in stress response. Stress Upsets Homeostasis Stress
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Fundamentals of Exercise Physiology and T1D
 COMPLIMENTARY CE Fundamentals of Exercise Physiology and T1D Jointly Provided by Developed in collaboration with 1 INTRODUCTION TO PHYSICAL ACTIVITY AND T1D 2 Many People with T1D Have Lower Levels of
COMPLIMENTARY CE Fundamentals of Exercise Physiology and T1D Jointly Provided by Developed in collaboration with 1 INTRODUCTION TO PHYSICAL ACTIVITY AND T1D 2 Many People with T1D Have Lower Levels of
Reversal by Methysergide of Inhibition of Insulin
 Reversal by Methysergide of Inhibition of Insulin Secretion by Prostaglandin E in the Dog R. PAUL ROBERTSON and ROBERT J. GUEST, Division of Clinical Pharmacology, Department of Medicine, University of
Reversal by Methysergide of Inhibition of Insulin Secretion by Prostaglandin E in the Dog R. PAUL ROBERTSON and ROBERT J. GUEST, Division of Clinical Pharmacology, Department of Medicine, University of
Moving to an A1C-Based Screening & Diagnosis of Diabetes. By Prof.M.Assy Diabetes&Endocrinology unit
 Moving to an A1C-Based Screening & Diagnosis of Diabetes By Prof.M.Assy Diabetes&Endocrinology unit is the nonenzymatic glycated product of the hemoglobin beta-chain at the valine terminal residue. Clin
Moving to an A1C-Based Screening & Diagnosis of Diabetes By Prof.M.Assy Diabetes&Endocrinology unit is the nonenzymatic glycated product of the hemoglobin beta-chain at the valine terminal residue. Clin
My Journey in Endocrinology. Samuel Cataland M.D
 My Journey in Endocrinology Samuel Cataland M.D. 1968-2015 Drs Berson M.D. Yalow phd Insulin Radioimmunoassay Nobel Prize Physiology or Medicine 1977 Rosalyn Yalow: Radioimmunoassay Technology Andrew Schally
My Journey in Endocrinology Samuel Cataland M.D. 1968-2015 Drs Berson M.D. Yalow phd Insulin Radioimmunoassay Nobel Prize Physiology or Medicine 1977 Rosalyn Yalow: Radioimmunoassay Technology Andrew Schally
Article. Reference. Effect of insulin on glucose- and arginine-stimulated somatostatin secretion from the isolated perfused rat pancreas
 Article Effect of insulin on glucose- and arginine-stimulated somatostatin secretion from the isolated perfused rat pancreas GERBER, Pietro, et al. Abstract The effects of exogenous insulin on somatostatin
Article Effect of insulin on glucose- and arginine-stimulated somatostatin secretion from the isolated perfused rat pancreas GERBER, Pietro, et al. Abstract The effects of exogenous insulin on somatostatin
Acute and Steady-State Insulin Responses
 Acute and Steady-State nsulin Responses to Glucose in Nonobese Diabetic Subjects ROGER L. LERNER and DANEL PORTE, JR. From the University of Washington School of Medicine and Veterans Administration Hospital,
Acute and Steady-State nsulin Responses to Glucose in Nonobese Diabetic Subjects ROGER L. LERNER and DANEL PORTE, JR. From the University of Washington School of Medicine and Veterans Administration Hospital,
Pancreatic Insulinoma Presenting. with Episodes of Hypoinsulinemic. Hypoglycemia in Elderly ---- A Case Report
 2008 19 432-436 Pancreatic Insulinoma Presenting with Episodes of Hypoinsulinemic Hypoglycemia in Elderly ---- A Case Report Chieh-Hsiang Lu 1, Shih-Che Hua 1, and Chung-Jung Wu 2,3 1 Division of Endocrinology
2008 19 432-436 Pancreatic Insulinoma Presenting with Episodes of Hypoinsulinemic Hypoglycemia in Elderly ---- A Case Report Chieh-Hsiang Lu 1, Shih-Che Hua 1, and Chung-Jung Wu 2,3 1 Division of Endocrinology
Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus. Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre
 Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre Outline How big is the problem? Natural progression of type 2 diabetes What
Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre Outline How big is the problem? Natural progression of type 2 diabetes What
Role of Counterregulatory Hormones for Glucose Metabolism in Children and Adolescents with Type 1 Diabetes
 Clin Pediatr Endocrinol 2011; 20(4), 73-80 Copyright 2011 by The Japanese Society for Pediatric Endocrinology Original Article Role of Counterregulatory Hormones for Glucose Metabolism in Children and
Clin Pediatr Endocrinol 2011; 20(4), 73-80 Copyright 2011 by The Japanese Society for Pediatric Endocrinology Original Article Role of Counterregulatory Hormones for Glucose Metabolism in Children and
Medical Endocrinology / Introduction 4 Medical Endocrinology
 Medical Endocrinology / Introduction 4 Medical Endocrinology 1 2 : Positive feedback control of labor contractions during birth of a baby. The solid return arrow symbolizes positive feedback. If the response
Medical Endocrinology / Introduction 4 Medical Endocrinology 1 2 : Positive feedback control of labor contractions during birth of a baby. The solid return arrow symbolizes positive feedback. If the response
What systems are involved in homeostatic regulation (give an example)?
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
A Comparison of Leucine- and Acetoacetate-induced Hypoglycemia in Man *
 Journal of Clinical Investigation Vol. 43, No. 1, 1964 A Comparison of Leucine- and Acetoacetate-induced Hypoglycemia in Man * STEFAN S. FAJANS, JOHN C. FLOYD, JR., RALPH F. KNOPF, AND JEROME W. CONN (From
Journal of Clinical Investigation Vol. 43, No. 1, 1964 A Comparison of Leucine- and Acetoacetate-induced Hypoglycemia in Man * STEFAN S. FAJANS, JOHN C. FLOYD, JR., RALPH F. KNOPF, AND JEROME W. CONN (From
Pancreas Transplantation From Living Donors: A Single Center Experience of 20 Cases
 American Journal of Transplantation 2016; 16: 2413 2420 Wiley Periodicals Inc. Copyright 2016 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.13738
American Journal of Transplantation 2016; 16: 2413 2420 Wiley Periodicals Inc. Copyright 2016 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.13738
28 Regulation of Fasting and Post-
 28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
PREVENTION OF NOCTURNAL HYPOGLYCEMIA USING PREDICTIVE LOW GLUCOSE SUSPEND (PLGS)
 PREVENTION OF NOCTURNAL HYPOGLYCEMIA USING PREDICTIVE LOW GLUCOSE SUSPEND (PLGS) Pathways for Future Treatment and Management of Diabetes H. Peter Chase, MD Carousel of Hope Symposium Beverly Hilton, Beverly
PREVENTION OF NOCTURNAL HYPOGLYCEMIA USING PREDICTIVE LOW GLUCOSE SUSPEND (PLGS) Pathways for Future Treatment and Management of Diabetes H. Peter Chase, MD Carousel of Hope Symposium Beverly Hilton, Beverly
EXENDIN-4 IS A 39-amino acid reptilian peptide that
 0021-972X/04/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 89(7):3469 3473 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/jc.2003-032001 Exendin-4 Normalized Postcibal
0021-972X/04/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 89(7):3469 3473 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/jc.2003-032001 Exendin-4 Normalized Postcibal
Latest Achievements of Diabetes Research Reviewed Contents of 1984's Major Diabetes Congresses
 Latest Achievements of Diabetes Research Reviewed Contents of 1984's Major Diabetes Congresses Frontiers in Diabetes Vol. 7 Series Editor F. Belfiore, Catania karger s. Karger Basel Munchen Paris London
Latest Achievements of Diabetes Research Reviewed Contents of 1984's Major Diabetes Congresses Frontiers in Diabetes Vol. 7 Series Editor F. Belfiore, Catania karger s. Karger Basel Munchen Paris London
Beta-Cell Replacement by Transplantation in Diabetes Mellitus: When Pancreas, When Islets, and How To Allocate the Pancreas?
 Trends David E.R. in Transplant. Sutherland 2010;4:99-107 and Dixon B. Kaufmann: Beta-Cell Replacement by Transplantation in Diabetes Mellitus Beta-Cell Replacement by Transplantation in Diabetes Mellitus:
Trends David E.R. in Transplant. Sutherland 2010;4:99-107 and Dixon B. Kaufmann: Beta-Cell Replacement by Transplantation in Diabetes Mellitus Beta-Cell Replacement by Transplantation in Diabetes Mellitus:
ENERGY FROM INGESTED NUTREINTS MAY BE USED IMMEDIATELY OR STORED
 QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
Allogeneic Pancreas Transplant
 Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14, 05/15, 05/16,
Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14, 05/15, 05/16,
Diabetes Mellitus Type 2 Evidence-Based Drivers
 This module is supported by an unrestricted educational grant by Aventis Pharmaceuticals Education Center. Copyright 2003 1 Diabetes Mellitus Type 2 Evidence-Based Drivers Driver One: Reducing blood glucose
This module is supported by an unrestricted educational grant by Aventis Pharmaceuticals Education Center. Copyright 2003 1 Diabetes Mellitus Type 2 Evidence-Based Drivers Driver One: Reducing blood glucose
PANCREAS TRANSPLANTATION WAS first described
 0163-769X/04/$20.00/0 Endocrine Reviews 25(6):919 946 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/er.2002-0036 Pancreas Transplantation: Indications and Consequences JENNIFER
0163-769X/04/$20.00/0 Endocrine Reviews 25(6):919 946 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/er.2002-0036 Pancreas Transplantation: Indications and Consequences JENNIFER
J Am Soc Nephrol 14: , 2003
 J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
One of the primary physiologic functions of insulin is
 M I N I R E V I E W Minireview: The Role of the Autonomic Nervous System in Mediating the Glucagon Response to Hypoglycemia Gerald J. Taborsky, Jr. and Thomas O. Mundinger Veterans Affairs Puget Sound
M I N I R E V I E W Minireview: The Role of the Autonomic Nervous System in Mediating the Glucagon Response to Hypoglycemia Gerald J. Taborsky, Jr. and Thomas O. Mundinger Veterans Affairs Puget Sound
Simultaneous pancreas-kidney transplant versus kidney transplant alone in diabetic patients
 Kidney International, Vol. 41(1992), pp. 924 929 Simultaneous pancreas-kidney transplant versus kidney transplant alone in diabetic patients ALAN H. S. CHEUNG, DAVID E. R. SUTHERLAND, KRISTEN J. GILLINGHAM,
Kidney International, Vol. 41(1992), pp. 924 929 Simultaneous pancreas-kidney transplant versus kidney transplant alone in diabetic patients ALAN H. S. CHEUNG, DAVID E. R. SUTHERLAND, KRISTEN J. GILLINGHAM,
Ch. 39 Endocrine System
 Ch. 39 Endocrine System The Endocrine System The endocrine system is made up of glands that release their products into the bloodstream These products deliver messages throughout the body Hormones Hormones
Ch. 39 Endocrine System The Endocrine System The endocrine system is made up of glands that release their products into the bloodstream These products deliver messages throughout the body Hormones Hormones
THE MEDICAL BENEFITS OF PANCREATIC TRANSPLANTATION
 THE MEDICAL BENEFITS OF PANCREATIC TRANSPLANTATION Carlos E. Marroquin, M.D., F.A.C.S. Chief, Transplant and Hepatobiliary Surgery Department of Surgery Learning Objectives Describe historic events in
THE MEDICAL BENEFITS OF PANCREATIC TRANSPLANTATION Carlos E. Marroquin, M.D., F.A.C.S. Chief, Transplant and Hepatobiliary Surgery Department of Surgery Learning Objectives Describe historic events in
Sponsor / Company: Sanofi Drug substance(s): insulin glargine (HOE901) According to template: QSD VERSION N 4.0 (07-JUN-2012) Page 1
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Combining Complex Pathophysiologic Concepts: Diabetes Mellitus
 Chapter 18 Combining Complex Pathophysiologic Concepts: Diabetes Mellitus KEY TERMS dawn phenomenon diabetes mellitus endocrine pancreas exocrine pancreas hyperglycemia hyperketonemia hypoglycemia insulin
Chapter 18 Combining Complex Pathophysiologic Concepts: Diabetes Mellitus KEY TERMS dawn phenomenon diabetes mellitus endocrine pancreas exocrine pancreas hyperglycemia hyperketonemia hypoglycemia insulin
The In-Clinic Close Loop Experience in the US
 The In-Clinic Close Loop Experience in the US Keystone Symposium, Practical Ways to Achieve Targets in Diabetes Care July 14, 2012 Francine Ratner Kaufman, MD Chief Medical Officer, VP Global Medical,
The In-Clinic Close Loop Experience in the US Keystone Symposium, Practical Ways to Achieve Targets in Diabetes Care July 14, 2012 Francine Ratner Kaufman, MD Chief Medical Officer, VP Global Medical,
History of Investigation
 Acini - Pancreatic juice (1º) (2º) Secretions- neuronal and hormonal mechanisms 1) Secretin - bicarbonate rich 2) Cholecystokinin - enzyme rich Islets of Langerhans (contain 4 cell types) Alpha cells (α)-
Acini - Pancreatic juice (1º) (2º) Secretions- neuronal and hormonal mechanisms 1) Secretin - bicarbonate rich 2) Cholecystokinin - enzyme rich Islets of Langerhans (contain 4 cell types) Alpha cells (α)-
ARTICLE. F. Porcellati & S. Pampanelli & P. Rossetti & N. Busciantella Ricci & S. Marzotti & P. Lucidi & F. Santeusanio & G. B. Bolli & C. G.
 DO00519; No of Pages 8 Diabetologia (2007) 50:422 430 DOI 10.1007/s00125-006-0519-6 ARTICLE Effect of the amino acid alanine on glucagon secretion in non-diabetic and type 1 diabetic subjects during hyperinsulinaemic
DO00519; No of Pages 8 Diabetologia (2007) 50:422 430 DOI 10.1007/s00125-006-0519-6 ARTICLE Effect of the amino acid alanine on glucagon secretion in non-diabetic and type 1 diabetic subjects during hyperinsulinaemic
