Chronic oedema affects over 100,000
|
|
|
- Irma Kennedy
- 6 years ago
- Views:
Transcription
1 Diabetic foot ulceration: the impact of oedema KEY WORDS Compression therapy Diabetic foot ulceration Lower limb oedema Lower limb ulceration The impact of diabetic foot disease on people with diabetes is profound and is associated with disability, amputation and premature death (National Diabetes Foot Care Audit Report, 2016). Diabetic foot ulceration (DFU) is common in people with diabetes, with around 10% of this group having a foot ulceration at some point in their lifetime (National Institute of Health and Care Excellence [NICE], 2015). There are significant costs to the NHS in caring for patients with DFU; with annual costs estimated at 650 million; equating to 1 in every 150 spent by the NHS (Kerr, 2012). Delayed healing is a common factor with DFU; Guest, Fuller and Vowden (2017) report that only 35% of patients with DFU will heal within a 12-month period. This article looks at the importance of oedema management and encourages practitioners to actively undertake education and training in the science and art of compression therapy. DR LEANNE ATKIN Lecturer practitioner/vascular Nurse Consultant, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust JUSTINE TANSLEY Specialist Podiatrist in diabetes and wound management; Podiatrist for the Lower Limb Therapy Service (Specialist leg ulcer service), Torbay and South Devon NHS Foundation Trust JOHN STEPHENSON Senior Lecturer in Biomedical Statistics, School of Human and Health Sciences, University of Huddersfield Chronic oedema affects over 100,000 people in the UK (Lewis and Morgan, 2008), with the prevalence of lower leg chronic oedema increasing year-on-year as a result of an aging population and rising obesity rates. Oedema in isolation is frequently recognised but often not treated (Atkin, 2014). However, many practitioners are aware of the importance of addressing the oedema to facilitate leg ulcer healing in patients with leg ulceration (Lymphoedema Framework, 2006). A cornerstone to the management of oedema is compression therapy, which is known to reduce oedema in a number of ways; including the direct application of pressure to ensure that less fluid is allowed to leak out of the capillary vessels whilst simultaneously encouraging more fluid to be reabsorbed into the venous and lymphatic systems (Wounds International, 2013). The reduction and management of oedema in the lower limbs is known to improve healing rates in lower limb ulceration (Wounds International, 2013). Where patients have evidence of both DFU and lower limb oedema, compression therapy is not always considered. Oedema can affect all or part of the lower limb; the toes, the dorsum of foot, ankle or gaiter region can be affected in isolation but often is present throughout the whole of the lower limb. The presence of oedema in patients with DFU has been found to be linked with poorer outcomes: lower limb oedema is more common in patients who require amputation, or in those who subsequently die; compared to patients who heal (Apelqvist et al, 1990). This may be due to the complexities of these patients, who often have concomitant conditions, such as renal and/or heart failure and are generally in poor health. This article will deliver an overview of the important aspects of DFU management in combination with lower limb oedema and will provide details of results of a local audit investigating the incidence of lower limb oedema in patients with DFU. ASSESSMENT The NICE guidelines for the management of patients with DFU (NICE, 2015) advocates neurovascular screening of every patient every time a foot problem arises. For those who develop an active foot ulcer, a referral should be made immediately to the diabetes foot specialist team. If specialist teams are considering oedema reduction as part of management, the following underlying conditions need to be explored as they can influence types of oedema and treatment options: diabetes control; heart failure; kidney disease/failure; recent surgery; deep vein thrombosis; Charcot arthropathy; lifestyle factors, Wounds UK Vol 14 No
2 i.e. obesity, immobility, concordance (NICE, 2015; Wounds UK, 2016). Vascular assessment is imperative if compression therapy is to be considered for oedema reduction to ensure the patient has no evidence of Peripheral Arterial Disease (PAD) where compression therapy may be contradicted (NICE, 2012). Palpating pedal pulses and listening to arterial sounds with a handheld Doppler is a simple test which will provide information of an individual s vascular status. A biphasic or triphasic signal would suggest that there is no evidence of occlusive or stenotic arterial disease, whereas a monophasic signal suggests the presence of PAD. The calculation of the Ankle Brachial Pressure Index (ABPI) is a useful tool in establishing whether a patient has any evidence of PAD and therefore in assessing their suitability of compression therapy. However, in patients with diabetes, caution is required when interpreting the ABPI, as diabetes is known to increase the presence of medial arterial wall calcification, which can lead to incompressible arteries or a falsely elevated ABPI result (Al-Qaisi et al, 2009). However, it is important to remember that an elevated ABPI does not preclude patients from having compression therapy, in these cases the arterial supply needs to be assessed using other methods such as pulse palpation, an arterial duplex scan, magnetic resource angiograms or through onward referral to specialist services. Where there is evidence of severe oedema, Doppler and ABPI assessment can be challenging, simply due to the size of the lower leg. In these cases, larger size blood pressure cuffs and Doppler probes designed to look deeper into tissue (5 MhZ) may be required. In cases where arterial wall calcification is presence or where ABPI cannot be calculated, the use of Toe Brachial Pressure Index (TBPI) may be useful, and this is argued to be more reliable in diabetic patients, due to the distal arteries being less likely to be affected by arterial wall calcification (Aiello et al, 2014). COMPRESSION THERAPY Compression therapy should only be instigated by a professional with the appropriate underlying skills and competency in lower limb assessment/compression therapy. There are a number of compression systems available. These include: compression hosiery (treatment hosiery/ulcer kits, toe caps, preventative hosiery); compression wrap systems; or multicomponent compression bandaging. Compression hosiery kits Treatment hosiery kits are designed to apply a graduated compression value of 40 mmhg at the ankle. Hosiery kits have been proven to be as equally effective at healing venous leg ulcers compared to multi-component bandages (Ashby, 2014). Furthermore, hosiery kits have additional advantages over multi-component bandages: they are less expensive; are less bulky and therefore do not restrict patients choice of footwear or clothing; offer guaranteed levels of compression, which is not practitioner dependent; allow patients to self-care; and reduce nursing time as they are quicker to apply (Atkin, 2015). However, they are not suitable where the patient has irregular limb shapes, gross amount of oedema or if the patient has heavily exuding wounds where the exudate is not contained within the dressings (Wounds UK, 2016). Where toe oedema is present, toe caps, a type of glove for the foot, can offer an advantage at reducing oedema. They provide an alternative to toe bandaging and can be used on top of dressings (Elwell and Wig, 2015). Compression wraps Compression wraps are a valuable alternative to delivering sustained compression. Compression wrap systems are adjustable devices which consist of low elastic material sections that wrap across the limb and are secured with hook and loop fasteners. They are designed for self-application over the short- or long-term, enabling the patient or carer to apply or adjust the device as required, in their own setting. It is important to remember that where ulceration is present, clinicians should aim to treat their patients with full strength compression of 40 mmhg at the ankle wherever possible to optimise the healing. The advantage of the compression wrap system is that it may be adjusted to meet comfort levels, can be easily adjusted as limb volume is reduced, and allows selfcare. All of these factors can facilitate concordance with compression. The separate leg and foot pieces which can be adjusted independently of one another can hold advantages, as they allow modification to accommodate specific foot problems. The compression wrap systems are designed to apply a graduated compression of 40 mmhg 34 Wounds UK Vol 14 No
3 at the ankle, and some systems do have builtin pressure measurements. However, not all compression wrap systems are able to guarantee the level of compression applied, as the amount of compression delivered is dependent on the application technique. Compression wrap systems can hold advantages in patients where limb volume will reduce quickly, where there is limb deformity or where the patient wishes to self-care; they are not suitable for patients who have heavily exuding wounds where exudate is not controlled within the dressing (Wounds UK, 2016). Multicomponent bandaging Multicomponent bandaging is required where patients have gross oedema/congestion, irregular shaped limbs and/or foot deformities, or where the exudate is not contained within the dressings; due to the adaptability of bandages and the ability to reshape the limb and absorb a degree of exudate. Bandage systems have been proven to improve venous and lymphatic return (O'Meara et al, 2012). However, the application of compression bandaging requires a high level of skill and can only be applied by an appropriately trained and competent professional. In cases where interdigital ulceration or gross toe oedema is present, lymphoedema toe caps or specialist bandaging techniques, including toe bandaging, stump techniques or stirrup bandaging may be required (Atkin and Sykes, 2015). There are, however, some disadvantages for the patient in using compression bandages which can affect their concordance with the compression therapy, as they can be bulky and restrict choice of clothing and footwear (Miller et al, 2011). Additionally, compression bandaging has been shown to affect the ankle range of movement, and therefore may increase the risk of falling in elderly patients (Atkin et al, 2016). The complexity of foot ulcerations in patients with diabetes means that factors such as neuropathy, neuropathic pain, arterial disease or foot deformity need to be considered prior to the application of compression. The choice of which compression system should be used is based on a number of factors, and should not be solely influenced by clinical effectiveness but important factors such as: patient lifestyle; clinical presentation of the wound and the limb; patient choice; practitioners own knowledge and skills; and treatment costs. These factors should all have a role in decision making (Moffatt et al, 2009). WOUND CARE Wound bed preparation is an important aspect to promote healing in patients with diabetic foot ulceration. Dressings should be selected according to the type of tissue present, presence of infection/ biofilm, the levels of exudate and the overall treatment aims. Where lymphorrhea is present (lymph fluid exudating onto the surface of the skin), appropriate compression therapy is key to effectively reducing and managing the levels of exudate. The amount of exudate can significantly impact on patient quality of life resulting in wet clothing, footwear and bedding. If left unmanaged, lymphoedema can cause moisture damage and maceration to the skin, leading to increased areas of ulceration. In cases where exudate levels are often high, super absorbent dressing can aid exudate management, and the use of skin protectors can help protect the peri-wound area from further excoriation or moisture. Effective management of high exudate levels, especially lymphorrhea presents significant challenges to practitioners. It is vital that appropriate treatment is commenced immediately to prevent further skin breakdown and to reduce the risk of infection (Todd et al, 2017). SKIN CARE Skin care is an essential part to both the management of patients with lower limb oedema and diabetic foot ulceration. Healthy, hydrated and intact skin provides the most effective barrier to reduce the risk of infection in an already immunocompromised patient. Skin care should be embedded in patients everyday practice, with patients being encouraged to build a daily routine including inspection of the skin, careful washing and use of emollients (McIntosh and Green, 2009). LIFESTYLE ADVICE Patients should be encouraged to elevate their legs for short periods during the day and to sleep in bed at night. Sleeping in a chair should be discouraged- even in reclining chairs. Periods of elevation of the lower limbs aids venous and lymphatic return. The benefits of a healthy balanced diet should be discussed, and if the patient is obese, interventions to aid weight loss 36 Wounds UK Vol 14 No
4 Table 1. Checklist used and definitions used to describe co-factors which are present in each individual identified with lower limb oedema Venous insufficiency Peripheral neuropathy Visual signs/skin changes associated with venous insufficiency: ankle flare, varicose eczema, haemosiderin staining, atrophie blanche, varicose veins etc Patient scored 4/5 or less in 10g monofilament test on one or both feet Obesity BMI of greater than 30 kg/m 2 Heart Lung Liver Kidney Mobility Has the patient been diagnosed with heart failure? Has the patient been diagnosed with asthma or chronic obstructive pulmonary disease? Has the patient been diagnosed with liver disease? (Check liver function test) Has the patient been diagnosed with chronic kidney disease? (Review patient s egfr) Ask patient about activity levels should be encouraged. Reduction in weight will aid both the control of diabetes and oedema reduction as obesity impedes lymphatic flow (McIntosh and Green, 2009; Wing et al, 2011). CLINICAL AUDIT An audit was carried out aiming to document the prevalence of lower limb oedema in patients with either type 1 or type 2 diabetes in an area of South Devon. The patients had either an active foot ulcer or recent history of ulceration, and therefore classed as ulcerated or high risk respectively. The audit took place within a Community NHS Trust and ran over a period of 12 weeks. Data from 7 podiatry clinics was collecwted and a total of 80 patients, selected at random, were included in the audit. Each clinic was booked by other members of the Podiatry team and included a mix of both diabetic and non-diabetic foot ulcers and diabetic patients classed as high risk. The auditing podiatrist then screened patients to see whether they were suitable for the audit. Although individuals often returned to the clinics on a weekly basis for treatment, each individual was only counted once. The total number of patients attending the podiatry clinics over the audited time frame was 120. If the patient had an active foot ulcer, the audit was also used to document the prevalence of evidence of lower limb oedema or lymphorrhea. For each patient, a series of observations were undertaken. These included: Assessment of oedema visual observation of whether oedema was present, palpation of the skin for signs of pitting oedema and assessment using the Stemmer s sign'. Stemmer's sign is a clinical sign, indicating the presence of lymphedema. It is positive if the skin of the forefoot cannot be pinched and lifted. Testing for Stemmer's sign consists of trying to lift the skin over the second toe, using the thumb and index finger in a pinching movement The location of any ulceration and whether the wound occurred on or below the level of the malleoli Where active foot ulcer was present, the evidence of lymphorrhea was recorded, using the definition of water-like fluid accumulating on the base of the wound/running or dripping from the wound after drying/blotting wound with sterile gauze swab If oedema was present, individual factors known to influence oedema and cross referencing with the patients medical history, were recorded using a check list (Table 1) Whether each patient was using any kind of compression therapy or diuretics to help manage their oedema. RESULTS A total of 80 diabetic patients were included in the audit. Their ages ranged from 44 to 98 years (median age = 76 years). Table 2 shows the total number of patients observed to have a diabetic foot ulcer and/ or lower limb oedema in the total sample. The table further reports the number of patients who presented with both conditions (to potentially explore whether this could be an additional risk factor in the diabetic foot); the total number of patients from the sample group observed to have a diabetic foot ulcer and lymphorrhea; and the number of patients presenting with oedema who were prescribed an intervention to help manage the oedema. Table 2 indicates that a substantial minority (19 out of 44; 43.2%) of diabetic patients presenting with oedema are prescribed an intervention to help manage the oedema; with diuretic Wounds UK Vol 14 No
5 Table 2. Audit data indicating numbers of patients with diabetic foot ulceration (with associated lymphorrhea) and/or lower limb oedema (with use of compression therapy or medication) Condition Frequency (valid %) Diabetes 80 (100%) Diabetic foot ulceration Yes Presenting with lymphorrhea Not presenting with lymphorrhea No Lower limb oedema Yes Using compression therapy* Using diuretic medication Not using compression therapy or diuretic medication No Multiple conditons Both diabetic foot ulceration and lower limb oedema Diabetic foot ulceration only Lower limb oedema only Neither condition * including bandaging, hosiery or wrap systems 38 (47.5%) 7 (8.75%) 31 (38.75%) 42 (52.5%) 44 (55.0%) 3 (3.75%) 16 (20.0%) 25 (31.25%) 36 (45.0%) 21 (26.25%) 17 (21.25%) 23 (28.75%) 19 (23.75%) medication amounting to the majority of such interventions. Hence interventions are being considered in this group of patients; however, compression therapy is not being widely used (only 3 out of 44 (6.8%) oedema patients are given compression therapy). This raises the issue of why this treatment is not widely given in those patients with diabetes, especially in those with an adequate vascular supply. Table 2 also indicates that lymphorrhea is a fairly uncommon, but not unknown, comorbidity amongst patients with lower limb oedema. The seven patients in this cohort who also presented with lymphorrhea represented 18.4% of the 38 patients with lower limb oedema; suggesting that the concomitant presence of lymphorrhea in patients with lower limb oedema is something that those treating diabetic foot ulcers need to be aware of, and have a plan for its management. Table 2 further reports the number of patients who presented with both conditions; demonstrating that lower limb oedema may co-exist in those with diabetes and diabetic foot ulcers. The prevalence of the common factors influencing lower limb oedema in the sample group was assessed, to explore whether the disease process of diabetes, which can be responsible for complications such as peripheral neuropathy and renal impairment, directly influences lower limb oedema in this group of patients; or whether other factors co-exist which potentially could also be taken into account when managing this group of patients. Venous insufficiency was the most commonly occurring comorbidity; being present in over half of the assessed patients, with significant numbers of patients also found to have obesity and/or peripheral neuropathy. All co-factors associated with presence of lower limb oedema are summarised graphically in Figure 1. SUMMARY Diabetic foot ulcers are complex, and a multidisciplinary approach to management is essential. It is widely accepted that there any many factors which impact healing of diabetic foot ulceration: peripheral arterial disease, peripheral neuropathy, renal disease and foot deformity; but this audit highlights that oedema also needs to be considered and appropriately managed. The rising prevalence of the elderly- and lifestylerelated chronic illness means that chronic lower limb oedema is encountered by many practitioners 38 Wounds UK Vol 14 No
6 Liver disease = 1 Heart failure = 1 Lung disease = 10 Kidney disease = 16 Immobility = 25 Peripheral neuropathy = 28 Obesity = 30 Venous insufficiency = Figure 1. Co-factors associated with presence of lower limb oedema (Todd et al, 2017). Obesity and sedentary lifestyle, which are common factors in patient with diabetes, seriously impact on the development and progression of chronic oedema. Chronic oedema can have devastating physical and psychological effects on the patient. The extra weight of the swollen limb can affect gait and mobility, and cause pain in the surrounding joints and muscles (Todd et al, 2017) This extra weight of the limb will impact the healing of the diabetic foot ulceration and the ability to reduce the pressure load. Compression therapy is the mainstay in oedema management, and with correct specialist team involvement, regular monitoring and a treatment plan tailored to each individual patient, this practice is safe in patients with diabetes and adequate peripheral arterial circulation (Scottish Intercollegiate Guidelines Network, 2010; Wounds UK, 2016). Treatment of lower limb oedema in patients with DFU can improve outcomes for patients with DFU (Ho et al, 2013). Therefore, it is important that all practitioners managing patients with DFU are aware of the importance of oedema management and wherever possible undertake education and training in the art of compression therapy. Wuk REFERENCES Aiello A, Anichini R, Brocco E et al (2014) Treatment of peripheral arterial disease in diabetes: A consensus of the Italian Societies of Diabetes (SID, AMD), Radiology (SIRM) and Vascular Endovascular Surgery (SICVE). Nutr Metab Cardiovasc Dis 24(4): Al-Qaisi M, Nott DM, King DH et al (2009) Ankle brachial pressure index (ABPI): An update for practitioners. Vasc Health Risk Manag 5: Apelqvist J, Larsson J, Agardh C (1990) The importance of peripheral pulses, peripheral oedema and local pain for the outcome of diabetic foot ulcers. Diabet Med 7(7): Ashby RL, Gabe R, Ali S et al (2014) Clinical and cost-effectiveness of compression hosiery versus compression bandages in treatment of venous leg ulcers (Venous leg Ulcer Study IV, VenUS IV): A randomised controlled trial. Lancet 383(9920): Atkin L (2014) Lower-limb oedema: assessment, treatment and challenges. Br J Community Nurs 19 (Suppl 10): S22 8 Atkin L (2015) Modern Management of Venous Leg Ulceration. Journal of General Practice Nursing: Skills for practice 1(4): 26 7 Atkin L, Stephenson J, Parfitt G et al (2016) An investigation to assess ankle mobility in healthy individuals from the application of multi-component compression bandages and compression hosiery. J Foot Ankle Res 9(1):18 Atkin L, Sykes R (2015) Inovations in compression for chronic odema: Using specialist bandage techniques to improve outcomes. Br J Community Nursing 20(5 Suppl): S8 11 Elwell R, Wig J (2015) Microfine toe caps: an innovative and cost-saving solution. Br J Community Nurs 20(4) Suppl: S30, S32, S34 6 Guest JF, Fuller GW, Vowden P (2017) Diabetic foot ulcer management in clinical practice in the UK: costs and outcomes. International Wound Journal 15(1): Ho TK, Leigh RD, Tsui J (2013) Diabetic foot disease and oedema. The British Journal of Diabetes & Vascular Disease. The British Journal of Diabetes and Vascular Diease 13(1): Kerr M (2012) Foot Care for People with Diabetes: the Economic Case for Change. Available at: dia-foot-care-mtg-kerr pdf (accessed ) Lewis M, Morgan K (2008) Managing chronic oedema: a collaborative community approach. B J Community Nurs 13(2): S25 6, S Lymphoedema Framework (2006) Best Practice for the Management of Lymphoedema. Available at: issues/210/files/content_175.pdf (accessed ) McIntosh C, Green T (2009) An overview of lower limb lymphoedema and diabetes: clinical review. Journal of Lymphoedema 4(1): Miller C, Kapp, Newall N et al (2011) Predicting concordance with multilayer compression bandaging. J Wound Care 20(3): Moffatt C, Kommala D, Dourdin N et al (2009) Venous leg ulcers: patient concordance with compression therapy and its impact on healing and prevention of recurrence. Int Wound J 6(5): National Diabetes Foot Care Audit Report (2016) National Diabetes Foot Care Audit for England and Wales Clinical Audit and Registries Management Service. Available at: (accessed ) National Institute for Health and Care Excellence (2012) Lower Limb Peripheral Arterial Disease: Diagnosis and Management. Available at: org.uk/guidance/cg147/evidence/cg147-lower-limb-peripheral-arterialdisease-full-guideline3 (accessed ) National Institute for Health and Care Excellence (2015) Diabetic Foot Problems: Prevention and Management. Available at: uk/guidance/ng19/resources/diabetic-foot-problems-prevention-andmanagement (accessed ) O'Meara SO, Cullum N, Nelson AE et al (2012) Compression for venous leg ulcers. Cochrane Database Syst Rev 11:CD Scottish Intercollegiate Guidelines Network (2010) Management of Chronic Venous Leg Ulcers: A National Clinical Guideline 120. Available at: (accessed ) Todd M, Lay-Flurrie K, Drake J (2017) Managing ulceration and lymphorrhea in chronic oedema. British Journal of Community Nursing 22(Sup 5): S34 S41 Wing RR, Lang W, Wadden TA et al (2011) Benefits of modest weight loss in improving cardiovascular risk factors in overweight and obese individuals with type 2 diabetes. Diabetes Care 34(7): Wounds International (2013) Principles of Compression in Venous Disease: a Practitioner s Guide to Treatment and Prevention of Venous Leg Ulcers. Available at: content_10802.pdf (accessed ) Wounds UK (2016) Best Practice Statement: Holistic management of venous leg ulceration. Available at: pdf (accessed ) Wounds UK Vol 14 No
JoyTickle, Tissue Viability Nurse Specialist, Shropshire Community Health NHS Trust
 Lower limb Ulceration Pathway: Leanne Atkin, Lecturer practitioner/vascular Nurse Specialist, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust, E mail: l.atkin@hud.ac.uk
Lower limb Ulceration Pathway: Leanne Atkin, Lecturer practitioner/vascular Nurse Specialist, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust, E mail: l.atkin@hud.ac.uk
Managing venous leg ulcers and oedema using compression hosiery
 Managing venous leg ulcers and oedema using compression hosiery Tickle J (2015) Managing venous leg ulcers and oedema using compression hosiery. Nursing Standard. 30, 8, 57-63. Date of submission: July
Managing venous leg ulcers and oedema using compression hosiery Tickle J (2015) Managing venous leg ulcers and oedema using compression hosiery. Nursing Standard. 30, 8, 57-63. Date of submission: July
It is estimated that 730,000 patients suffer with
 The leg ulceration pathway: impact of implementation Leg ulceration continues to be a common cause of suffering for patients and the treatment of these patients continues to place a significant burden
The leg ulceration pathway: impact of implementation Leg ulceration continues to be a common cause of suffering for patients and the treatment of these patients continues to place a significant burden
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES
 ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Between 1% and 2% of the. Juxta CURES : when is it appropriate?
 Juxta CURES : when is it appropriate? Compression therapy is the optimum treatment for venous leg ulcers (Nelson, 2011). Through case study evidence, this article challenges the view that the current gold
Juxta CURES : when is it appropriate? Compression therapy is the optimum treatment for venous leg ulcers (Nelson, 2011). Through case study evidence, this article challenges the view that the current gold
Promoting best practice in leg ulcer management
 Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS
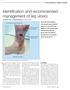 Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Prevention and Management of Leg Ulcers
 EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND
 GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING
 HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
Venous and lymphatic disease
 Welcome to JCN s learning zone. By reading the article in each issue, you can learn all about the key principles of subjects that are vital to your role as a community nurse. Once you have read the article,
Welcome to JCN s learning zone. By reading the article in each issue, you can learn all about the key principles of subjects that are vital to your role as a community nurse. Once you have read the article,
Leg ulcer assessment and management
 Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
All WALES LYMPHOEDEMA GUIDANCE:
 All WALES LYMPHOEDEMA GUIDANCE: Lymphoedema Vascular Assessment Policy (Toe Brachial Pressure Index / TBPI) April 2013 Created by the All Wales Lymphoedema Service Leads 1 Background The presence of peripheral
All WALES LYMPHOEDEMA GUIDANCE: Lymphoedema Vascular Assessment Policy (Toe Brachial Pressure Index / TBPI) April 2013 Created by the All Wales Lymphoedema Service Leads 1 Background The presence of peripheral
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
Obesity and Lymphoedema : a clinical dilemma
 Obesity and Lymphoedema : a clinical dilemma Professor Christine Moffatt CBE Professor of Clinical Nursing Research & Nurse consultant Royal Derby Hospital Foundation Trust Lymphoedema Service Chair ILF
Obesity and Lymphoedema : a clinical dilemma Professor Christine Moffatt CBE Professor of Clinical Nursing Research & Nurse consultant Royal Derby Hospital Foundation Trust Lymphoedema Service Chair ILF
Leg ulcers are non-healing
 Clinical Chronic REVIEW WOUNDS Doppler assessment: getting it right Full leg ulcer assessments are important in order to identify the aetiology of patients leg ulcer and Doppler ultrasounds form a part
Clinical Chronic REVIEW WOUNDS Doppler assessment: getting it right Full leg ulcer assessments are important in order to identify the aetiology of patients leg ulcer and Doppler ultrasounds form a part
The key to successful. Impact of compression therapy on chronic. venous disease
 Acute WOUNDS Impact of compression therapy on chronic venous disease Chronic venous disease is known to affect up to 50% of the adult population and it is estimated that 1% of individuals will suffer from
Acute WOUNDS Impact of compression therapy on chronic venous disease Chronic venous disease is known to affect up to 50% of the adult population and it is estimated that 1% of individuals will suffer from
Compression therapy can
 What are the benefits of using cohesive inelastic compression bandages in the community? Compression therapy can play a vital role in improving the quality of life for those with chronic venous insufficiency,
What are the benefits of using cohesive inelastic compression bandages in the community? Compression therapy can play a vital role in improving the quality of life for those with chronic venous insufficiency,
compression should be applied at the strongest class that the patient can tolerate.
 Sponsored feature A simple and effective solution to preventing recurrent venous leg ulcers When trying to prevent the recurrence of leg ulcers, many Leg ulcers It is widely accepted that good compression
Sponsored feature A simple and effective solution to preventing recurrent venous leg ulcers When trying to prevent the recurrence of leg ulcers, many Leg ulcers It is widely accepted that good compression
Treating your leg ulcer
 Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
West Gloucestershire Primary Care Trust Community Nursing Service. Leg Ulcer Audit. Gloucestershire Primary & Community Care Audit Group
 West Gloucestershire Primary Care Trust Community Nursing Service Leg Ulcer Audit 2006 Gloucestershire Primary & Community Care Audit Group Contents Page number Background 3 Audit Aims 4 Methodology 4
West Gloucestershire Primary Care Trust Community Nursing Service Leg Ulcer Audit 2006 Gloucestershire Primary & Community Care Audit Group Contents Page number Background 3 Audit Aims 4 Methodology 4
Wound Healing Community Outreach Service
 Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
Leg ulcers. Causes and management. OBJECTIVE This article outlines the assessment and management of patients with leg ulceration.
 THEME Wounds Leg ulcers Causes and management BACKGROUND A leg ulcer is not a disease but the manifestation of an underlying problem that requires a clear diagnosis. Sandra Dean RN, is nurse consultant
THEME Wounds Leg ulcers Causes and management BACKGROUND A leg ulcer is not a disease but the manifestation of an underlying problem that requires a clear diagnosis. Sandra Dean RN, is nurse consultant
In line with the professional requirements of the Nursing and Midwifery Council
 STANDARDS OF PRACTICE FOR LEG CLUB STAFF October 2010 Foreword In line with the professional requirements of the Nursing and Midwifery Council Code: Standards of conduct, performance and ethics for nurses
STANDARDS OF PRACTICE FOR LEG CLUB STAFF October 2010 Foreword In line with the professional requirements of the Nursing and Midwifery Council Code: Standards of conduct, performance and ethics for nurses
Leg Ulcer Case Study
 Leg Ulcer Case Study Wound Healing Community Outreach Service Mrs Ivy Hurtzalot, a 71-year-old lady, presents to her general practitioner with an ulcer on her right medial malleolus. Ivy reveals that the
Leg Ulcer Case Study Wound Healing Community Outreach Service Mrs Ivy Hurtzalot, a 71-year-old lady, presents to her general practitioner with an ulcer on her right medial malleolus. Ivy reveals that the
Wound debridement: guidelines and practice to remove barriers to healing
 Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Practical Point in Holistic Diabetic Foot Care 3 March 2016
 Diabetic Foot Ulcer : Vascular Management Practical Point in Holistic Diabetic Foot Care 3 March 2016 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai
Diabetic Foot Ulcer : Vascular Management Practical Point in Holistic Diabetic Foot Care 3 March 2016 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai
PROCEDURE FOR VASCULAR ASSESSMENT BY DOPPLER ULTRASOUND
 PROCEDURE FOR VASCULAR ASSESSMENT BY DOPPLER ULTRASOUND (to achieve Ankle Brachial Pressure Index) First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One To enable nurses
PROCEDURE FOR VASCULAR ASSESSMENT BY DOPPLER ULTRASOUND (to achieve Ankle Brachial Pressure Index) First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One To enable nurses
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Wounds UK. Development and evaluation of a hosiery selection algorithm in an acute and community healthcare NHS Trust
 Reprint Volume 9 Issue 4 Wounds UK Development and evaluation of a hosiery selection algorithm in an acute and community healthcare NHS Trust Authors Jackie Stephen-Haynes, Rachael Sykes RESEARCH AND
Reprint Volume 9 Issue 4 Wounds UK Development and evaluation of a hosiery selection algorithm in an acute and community healthcare NHS Trust Authors Jackie Stephen-Haynes, Rachael Sykes RESEARCH AND
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
AWMA MODULE ACCREDITATION. Module Three: Assessment and Management of Lower Leg Ulceration
 AWMA MODULE ACCREDITATION Module Three: Assessment and Management of Lower Leg Ulceration Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Three: Assessment and Management of Lower Leg Ulceration Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
Compression Bandaging Formulary 2017
 Area Drugs Therapeutics Committee Compression Bandaging Formulary 2017 Compression Bandaging Formulary 2017 Developed by the NHS Fife Wound and Skin Care Forum (WSCF) Group Approved: October 2017 Review:
Area Drugs Therapeutics Committee Compression Bandaging Formulary 2017 Compression Bandaging Formulary 2017 Developed by the NHS Fife Wound and Skin Care Forum (WSCF) Group Approved: October 2017 Review:
AN INTRODUCTION TO DOPPLER. Sarah Gardner, Clinical lead, Tissue viability service. Oxford Health NHS Foundation Trust.
 AN INTRODUCTION TO DOPPLER Sarah Gardner, Clinical lead, Tissue viability service. Oxford Health NHS Foundation Trust. THE DOPPLER EFFECT The Doppler Principle was described by Physicist and mathematician
AN INTRODUCTION TO DOPPLER Sarah Gardner, Clinical lead, Tissue viability service. Oxford Health NHS Foundation Trust. THE DOPPLER EFFECT The Doppler Principle was described by Physicist and mathematician
ORTHOTICS COMPETENCY FRAMEWORK FOR THE PREVENTION, TREATMENT AND MANAGEMENT OF DIABETIC FOOT DISEASE - 1 -
 ORTHOTICS COMPETENCY FRAMEWORK FOR THE PREVENTION, TREATMENT AND MANAGEMENT OF DIABETIC FOOT DISEASE - 1 - THE ORTHOTICS COMPETENCY FRAMEWORK FOR THE PREVENTION, TREATMENT AND MANAGEMENT OF DIABETIC FOOT
ORTHOTICS COMPETENCY FRAMEWORK FOR THE PREVENTION, TREATMENT AND MANAGEMENT OF DIABETIC FOOT DISEASE - 1 - THE ORTHOTICS COMPETENCY FRAMEWORK FOR THE PREVENTION, TREATMENT AND MANAGEMENT OF DIABETIC FOOT
Wound Care People Ltd. Holistic assessment and
 Understanding compression: part 2 holistic assessment and clinical decision-making in leg ulcer management Georgina Ritchie, Helen Taylor The second in this four-part series exploring leg ulcer management
Understanding compression: part 2 holistic assessment and clinical decision-making in leg ulcer management Georgina Ritchie, Helen Taylor The second in this four-part series exploring leg ulcer management
Wound Assessment Report
 Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Address: Left Leg. other: Nails: thick yellow brittle fungus abnormal thick yellow brittle fungus abnormal
 South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Model of Care for the Diabetic Foot
 Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
Wound management accounts for
 An audit to determine the clinical effectiveness of a pathway for managing wound infection KEY WORDS Wound management Infection risk Clinical pathway Audit Prevention of wound infection is a key objective
An audit to determine the clinical effectiveness of a pathway for managing wound infection KEY WORDS Wound management Infection risk Clinical pathway Audit Prevention of wound infection is a key objective
Wound management accounts for
 An audit to determine the clinical effectiveness of a pathway for managing wound infection. KEY WORDS Wound management Infection risk Clinical pathway Audit Prevention of wound infection is a key objective
An audit to determine the clinical effectiveness of a pathway for managing wound infection. KEY WORDS Wound management Infection risk Clinical pathway Audit Prevention of wound infection is a key objective
Jackie Stephen-Haynes. Compression therapies- Does. Jackie Stephen-Haynes 2011
 Jackie Stephen-Haynes Compression therapies- Does compression meet the patients needs? 2011 Aims For practitioner to be able to consider compression options and the impact for the patient Leg Ulcer Definition
Jackie Stephen-Haynes Compression therapies- Does compression meet the patients needs? 2011 Aims For practitioner to be able to consider compression options and the impact for the patient Leg Ulcer Definition
Venous leg ulcers: importance of early assessment and intervention for long-term success
 Venous leg ulcers: importance of early assessment and intervention for long-term success Introduction A venous leg ulcer (VLU) can be defined as: an open lesion between the knee and ankle joint that occurs
Venous leg ulcers: importance of early assessment and intervention for long-term success Introduction A venous leg ulcer (VLU) can be defined as: an open lesion between the knee and ankle joint that occurs
POSITION PAPER FOR ANKLE BRACHIAL PRESSURE INDEX (ABPI)
 Best Practice, Leadership, Support POSITION PAPER FOR ANKLE BRACHIAL PRESSURE INDEX (ABPI) Informing decision making prior to the application of compression therapy @BritishLymph The British Lymphology
Best Practice, Leadership, Support POSITION PAPER FOR ANKLE BRACHIAL PRESSURE INDEX (ABPI) Informing decision making prior to the application of compression therapy @BritishLymph The British Lymphology
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Level 2 Leg Ulcer Management Service. Service Level Agreement Background. Contents:
 Level 2 Leg Ulcer Management Service Service Level Agreement 2016-2019 Contents: 1. Background to Leg Ulcer Management Service 2. Service Details 3. Accreditation 4. Service Standards 5. Finance Details
Level 2 Leg Ulcer Management Service Service Level Agreement 2016-2019 Contents: 1. Background to Leg Ulcer Management Service 2. Service Details 3. Accreditation 4. Service Standards 5. Finance Details
Foot protection for people with diabetes a focus on prevention
 Foot protection for people with diabetes a focus on prevention Presentation by Mike Townson Independent Podiatry Consultant. Facilitated by Angela Farrell Neubourg Pharma UK Ltd. Foot Assessment training
Foot protection for people with diabetes a focus on prevention Presentation by Mike Townson Independent Podiatry Consultant. Facilitated by Angela Farrell Neubourg Pharma UK Ltd. Foot Assessment training
PDP SELF-TEST QUESTIONNAIRE LEG ULCERS. Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring.
 Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS UPDATED PDP SELF-TEST QUESTIONNAIRE SEPTEMBER 2013 Ulcer Full thickness loss of
Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS UPDATED PDP SELF-TEST QUESTIONNAIRE SEPTEMBER 2013 Ulcer Full thickness loss of
TREATING LOWER LIMB LYMPHOEDEMA WITH COMPRESSION BANDAGING
 TREATING LOWER LIMB LYMPHOEDEMA WITH COMPRESSION BANDAGING Debra Doherty is Senior Lecturer, Centre for Research and implementation of Clinical Practice, Thames Valley University Multilayer continues to
TREATING LOWER LIMB LYMPHOEDEMA WITH COMPRESSION BANDAGING Debra Doherty is Senior Lecturer, Centre for Research and implementation of Clinical Practice, Thames Valley University Multilayer continues to
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Lower Leg Ulceration. Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network;
 Lower Leg Ulceration Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network; wendy.mcinnes@sa.gov.au 0447 051 036 1 Lower Leg Ulceration A manifestation of underlying pathology/disease
Lower Leg Ulceration Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network; wendy.mcinnes@sa.gov.au 0447 051 036 1 Lower Leg Ulceration A manifestation of underlying pathology/disease
Root Cause Analysis The Tools. Angie Abbott Head of Podiatry and Orthotics Torbay and Southern Devon
 Root Cause Analysis The Tools Angie Abbott Head of Podiatry and Orthotics Torbay and Southern Devon Why do RCA s? To understand if the amputation was avoidable or unavoidable Learn and improve Identify
Root Cause Analysis The Tools Angie Abbott Head of Podiatry and Orthotics Torbay and Southern Devon Why do RCA s? To understand if the amputation was avoidable or unavoidable Learn and improve Identify
Six step guide to improving diabetes footcare. Putting feet. first
 Six step guide to improving diabetes footcare Putting feet first In England there are over 140 leg, foot or toe amputations a week. Diabetes related amputations and foot ulcers cost the NHS in England
Six step guide to improving diabetes footcare Putting feet first In England there are over 140 leg, foot or toe amputations a week. Diabetes related amputations and foot ulcers cost the NHS in England
Practical advice when treating feet
 Practical advice when treating feet Helen Mandic Clinical Lead Podiatrist in Health Promotion and Student Mentor Department of Podiatry and Foot Health Dawlish Hospital Falls Prevention The Role of the
Practical advice when treating feet Helen Mandic Clinical Lead Podiatrist in Health Promotion and Student Mentor Department of Podiatry and Foot Health Dawlish Hospital Falls Prevention The Role of the
PDP SELF-TEST QUESTIONNAIRE
 Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring
Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline
 Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Vascular Assessment of the Lower Limb. Anita Roberts RGN MBA
 Vascular Assessment of the Lower Limb Anita Roberts RGN MBA Peripheral Arterial Disease A marker for future vascular disease (CHD and stroke) In Europe and North America an estimated 27 million people
Vascular Assessment of the Lower Limb Anita Roberts RGN MBA Peripheral Arterial Disease A marker for future vascular disease (CHD and stroke) In Europe and North America an estimated 27 million people
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
4-layer compression bandaging system (includes microbe binding wound contact layer) Latex-free, 4-layer compression bandaging system
 JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT. SCOPE: Western Australia. Clinical Protocol for Venous Leg Ulcer Management
 CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT SCOPE: Western Australia Clinical Protocol for Venous Leg Ulcer The following protocol outlines the sequence of events in the assessment and management of
CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT SCOPE: Western Australia Clinical Protocol for Venous Leg Ulcer The following protocol outlines the sequence of events in the assessment and management of
Improving customer care in compression hosiery
 Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
Sores That Will Not Heal
 Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY Do not include made to measure on the prescription; the community pharmacy/dispensing practice will endorse
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY Do not include made to measure on the prescription; the community pharmacy/dispensing practice will endorse
How to manage leg ulcers in the elderly
 How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Diabetes Foot Screening and Risk Stratification Tool
 Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Graduated compression and moist wound
 PRODUCT EVALUATION Managing venous leg ulcers using compression therapy and dressings Gail Powell, Gill Wicks and Katrin Will Graduated compression and moist wound healing are the foundation of venous
PRODUCT EVALUATION Managing venous leg ulcers using compression therapy and dressings Gail Powell, Gill Wicks and Katrin Will Graduated compression and moist wound healing are the foundation of venous
Independent evaluation of BEMER physical vascular regulation therapy
 of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
Leg ulceration is a chronic condition affecting
 Effect of super-absorbent dressings on compression sub-bandage pressure Leanne Cook Leanne Cook, Vascular Nurse Specialist, Mid Yorkshire NHS Trust Email: Leanne.cook@midyorks.nhs.uk Leg ulceration is
Effect of super-absorbent dressings on compression sub-bandage pressure Leanne Cook Leanne Cook, Vascular Nurse Specialist, Mid Yorkshire NHS Trust Email: Leanne.cook@midyorks.nhs.uk Leg ulceration is
NHS RightCare scenario: The variation between standard and optimal pathways
 January 2017 NHS RightCare scenario: The variation between standard and optimal pathways Betty s story: Wound care Appendix 1: Summary slide pack January 2017 Betty s story This is the story of Betty s
January 2017 NHS RightCare scenario: The variation between standard and optimal pathways Betty s story: Wound care Appendix 1: Summary slide pack January 2017 Betty s story This is the story of Betty s
2008 American Medical Association and National Committee for Quality Assurance. All Rights Reserved. CPT Copyright 2007 American Medical Association
 Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
HDiag 37 - Vascular Assist 03 27/4/07 17:11 Page 1. Vascular Assessment Systems and Electronic Patient Record Software. DIAGNOSTIC Products Division
 HDiag 37 - Vascular Assist 03 27/4/07 17:11 Page 1 Vascular Assessment Systems and Electronic Patient Record Software DIAGNOSTIC Products Division HDiag 37 - Vascular Assist 03 27/4/07 17:12 Page 2 The
HDiag 37 - Vascular Assist 03 27/4/07 17:11 Page 1 Vascular Assessment Systems and Electronic Patient Record Software DIAGNOSTIC Products Division HDiag 37 - Vascular Assist 03 27/4/07 17:12 Page 2 The
Keeping the diabetic foot healed How effective is the Newcastle Foot Protection Team?
 Keeping the diabetic foot healed How effective is the Newcastle Foot Protection Team? Linda Robertshaw Advanced Podiatrist Nicola Coates Principal Podiatrist (Diabetes) Background Risk factors for diabetic
Keeping the diabetic foot healed How effective is the Newcastle Foot Protection Team? Linda Robertshaw Advanced Podiatrist Nicola Coates Principal Podiatrist (Diabetes) Background Risk factors for diabetic
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC
 High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
Arterial Studies And The Diabetic Foot Patient
 Arterial Studies And The Patient George L. Berdejo, BA, RVT, FSVU gberdejo@wphospital.org Disclosures I have nothing to disclose! Diabetes mellitus continues to grow in global prevalence and to consume
Arterial Studies And The Patient George L. Berdejo, BA, RVT, FSVU gberdejo@wphospital.org Disclosures I have nothing to disclose! Diabetes mellitus continues to grow in global prevalence and to consume
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
Simplifying ankle brachial pressure index for leg ulcer management
 Product focus feature Simplifying ankle brachial pressure index for leg ulcer management Sylvie Hampton Compression therapy is a key component of venous leg ulcer management. Best practice guidelines recommend
Product focus feature Simplifying ankle brachial pressure index for leg ulcer management Sylvie Hampton Compression therapy is a key component of venous leg ulcer management. Best practice guidelines recommend
Implementing the updated NICE Guidance on the Diabetic Foot
 Implementing the updated NICE Guidance on the Diabetic Foot Rachel Berrington Senior Diabetes Specialist Nurse Foot Lead University Hospitals of Leicester NHS Trust Key Priorities for Implementation NG19
Implementing the updated NICE Guidance on the Diabetic Foot Rachel Berrington Senior Diabetes Specialist Nurse Foot Lead University Hospitals of Leicester NHS Trust Key Priorities for Implementation NG19
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
HOW TO USE A DOPPLER IN YOUR PRACTICE
 GPCME Conference June 2014 Bridget Rood USL Medical Presents.. HOW TO USE A DOPPLER IN YOUR PRACTICE Disclosure I am a NZRN and currently work at USL Medical as a Product Manager USL Medical are the exclusive
GPCME Conference June 2014 Bridget Rood USL Medical Presents.. HOW TO USE A DOPPLER IN YOUR PRACTICE Disclosure I am a NZRN and currently work at USL Medical as a Product Manager USL Medical are the exclusive
Best Practice Statement
 WUK BPS Best Practice Statement Holistic Management of Venous Leg Ulceration 2016 Assessment and diagnosis Classification of venous leg ulcers Wound and skin management Compression Holistic management
WUK BPS Best Practice Statement Holistic Management of Venous Leg Ulceration 2016 Assessment and diagnosis Classification of venous leg ulcers Wound and skin management Compression Holistic management
A retrospective chart review will be done at the start and end of the study (anticipated 1 year duration) measuring rates of the following:
 Project name: Renal Foot Care Program Supervisor: Shaoyee Yao Background: Hemodialysis patients have significant co-morbidities including diabetes, peripheral vascular disease, neuropathy and lower limb
Project name: Renal Foot Care Program Supervisor: Shaoyee Yao Background: Hemodialysis patients have significant co-morbidities including diabetes, peripheral vascular disease, neuropathy and lower limb
Primary hypertension in adults
 Primary hypertension in adults NICE provided the content for this booklet which is independent of any company or product advertised Hypertension Welcome NICE published an updated guideline on the diagnosis
Primary hypertension in adults NICE provided the content for this booklet which is independent of any company or product advertised Hypertension Welcome NICE published an updated guideline on the diagnosis
Prevalence of leg ulceration in a London population
 Q J Med 2004; 97:431 437 doi:10.1093/qjmed/hch075 Prevalence of leg ulceration in a London population C.J. MOFFATT 1, P.J. FRANKS 1, D.C. DOHERTY 1, R. MARTIN 2, R. BLEWETT 2 and F. ROSS 3 From the 1 Centre
Q J Med 2004; 97:431 437 doi:10.1093/qjmed/hch075 Prevalence of leg ulceration in a London population C.J. MOFFATT 1, P.J. FRANKS 1, D.C. DOHERTY 1, R. MARTIN 2, R. BLEWETT 2 and F. ROSS 3 From the 1 Centre
Welcome to Allied Health Telehealth
 Welcome to Allied Health Telehealth Paediatric lymphoedema A challenge for clinicians and families To receive an attendance certificate please complete your online evaluation at: https://www.surveymonkey.com/s/paedlymphoedema
Welcome to Allied Health Telehealth Paediatric lymphoedema A challenge for clinicians and families To receive an attendance certificate please complete your online evaluation at: https://www.surveymonkey.com/s/paedlymphoedema
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
How to prevent blood clots whilst in hospital and after your return home
 How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
Use of a velcro wrap system in the management of lower limb lymphoedema/chronic oedema. Sue Lawrance
 Use of a velcro wrap system in the management of lower limb lymphoedema/chronic oedema Sue Lawrance Abstract Lymphoedema and chronic lower limb oedema are conventionally treated with multi-layer bandaging,
Use of a velcro wrap system in the management of lower limb lymphoedema/chronic oedema Sue Lawrance Abstract Lymphoedema and chronic lower limb oedema are conventionally treated with multi-layer bandaging,
Leg ulceration is a chronic condition which,
 Preventing unnecessary suffering: an audit of a leg ulcer clinic Jenny Bentley Jenny Bentley is Lecturer, Florence Nightingale School of Nursing and Midwifery, King s College, London Leg ulceration is
Preventing unnecessary suffering: an audit of a leg ulcer clinic Jenny Bentley Jenny Bentley is Lecturer, Florence Nightingale School of Nursing and Midwifery, King s College, London Leg ulceration is
University of Huddersfield Repository
 University of Huddersfield Repository Newton, Veronica and Roberts, Peter Foot Inspection or Foot Assessment? Original Citation Newton, Veronica and Roberts, Peter (2011) Foot Inspection or Foot Assessment?
University of Huddersfield Repository Newton, Veronica and Roberts, Peter Foot Inspection or Foot Assessment? Original Citation Newton, Veronica and Roberts, Peter (2011) Foot Inspection or Foot Assessment?
The management of patients with lymphoedema
 Juxta-Fit compression garments in lymphoedema management Julie Mullings Julie Mullings, Tissue Viabilty Specialist Nurse, University Hospital of South Manchester - Community Services Email: Julie.mullings@uhsm.nhs.uk
Juxta-Fit compression garments in lymphoedema management Julie Mullings Julie Mullings, Tissue Viabilty Specialist Nurse, University Hospital of South Manchester - Community Services Email: Julie.mullings@uhsm.nhs.uk
Total Contact Cast System
 Total Contact Cast System Instructions for Use Products Included in Cutimed Off-Loader Select kit Qty Cutimed Cavity Sterile 1 ea. Cutisorb Cotton Gauze 2" x 2" 4 ea. Delta-Lite Conformable Fiberglass
Total Contact Cast System Instructions for Use Products Included in Cutimed Off-Loader Select kit Qty Cutimed Cavity Sterile 1 ea. Cutisorb Cotton Gauze 2" x 2" 4 ea. Delta-Lite Conformable Fiberglass
