Article. HLA-DQ Mismatches and Rejection in Kidney Transplant Recipients
|
|
|
- Mark Harrell
- 6 years ago
- Views:
Transcription
1 Article HLA-DQ Mismatches and Rejection in Kidney Transplant Recipients Wai H. Lim,* Jeremy R. Chapman, Patrick T. Coates, Joshua R. Lewis, Graeme R. Russ, Narelle Watson, Rhonda Holdsworth,** and Germaine Wong Abstract Background and objectives The current allocation algorithm for deceased donor kidney transplantation takes into consideration HLA mismatches at the ABDR loci but not HLA mismatches at other loci, including HLA-DQ. However, the independent effects of incompatibilities for the closely linked HLA-DQ antigens in the context of HLA-DR antigen matched and mismatched allografts are uncertain. We aimed to determine the effect of on renal allograft outcomes. Design, setting, participants, & measurements Using data from the Australia and New Zealand Dialysis and Transplant Registry, we examined the association between and acute rejections in primary live and deceased donor kidney transplant recipients between 2004 and 2012 using adjusted Cox regression models. Results Of the 788 recipients followed for a median of 2.8 years (resulting in 2891 person-years), 321 (40.7%) and 467 (59.3%) received zero and one or two HLA-DQ mismatched kidneys, respectively. Compared with recipients who have received zero HLA-DQ mismatched kidneys, those who have received one or two HLA-DQ mismatched kidneys experienced greater numbers of any rejection (50 of 321 versus 117 of 467; P,0.01), late rejections (occurring.6 months post-transplant; 8 of 321 versus 27 of 467; P=0.03), and antibody-mediated rejections (AMRs; 12 of 321 versus 38 of 467; P=0.01). Compared with recipients of zero HLA-DQ mismatched kidneys, the adjusted hazard ratios for any and late rejections in recipients who had received one or two HLA-DQ mismatched kidneys were 1.54 (95% confidence interval [95% CI], 1.08 to 2.19) and 2.85 (95% CI, 1.05 to 7.75), respectively. HLA-DR was an effect modifier between and AMR (P value for interaction =0.02), such that the association between and AMR was statistically significant in those who have received one or two HLA-DR mismatched kidneys, with adjusted hazard ratio of 2.50 (95% CI, 1.05 to 5.94). Conclusions are associated with acute rejection, independent of HLA-ABDR mismatches and initial immunosuppression. Clinicians should be aware of the potential importance of HLA-DQ matching in the assessment of immunologic risk in kidney transplant recipients. Clin J Am Soc Nephrol 11: , doi: /CJN Introduction Matching at the HLA-ABDR loci remains the cornerstone of deceased donor kidney allocation in Australia and worldwide because of the association between incremental HLA-ABDR mismatches and increased risk of rejection and/or graft loss after kidney transplantation (1 3). Although differences in HLA-DQ matching between donors and recipients have been shown to be associated with adverse graft outcomes, matching at the HLA-DQ locus is not explicitly considered in the allocation algorithm for deceased donor kidney transplantation (4,5). There is a general consensus suggesting that are unlikely to have a major effect on graft survival, because serologic compatibility for HLA-DR usually ensures a corresponding compatibility for HLA-DQ (6 8). However, different HLA-DR alleles within an antigen group may be associated with different DQ antigens, resulting in HLA-DR antigen matched but HLA-DQ antigen mismatched grafts, which may result in a differential effect in graft outcomes. In acute graft versus host disease after hematopoietic stem cell transplantation, donor-recipient incompatibility at the HLA-DQ locus is associated with almost a twofold greater risk of acute graft versus host disease, independent of compatibility at the HLA-DR locus (9,10). Recent studies have also shown that increasing numbers of HLA-DQ epitope mismatches and/or the development of donor specific anti HLA-DQ antibody after kidney transplantation may contribute to poorer graft outcomes, including the risk of developing transplant glomerulopathy and late graft loss (4,11,12). Despite these findings, the clinical importance of broad antigen in predicting acute rejection after kidney transplantation independent of the effects of HLA *Department of Renal Medicine, Sir Charles Gairdner Hospital, Perth, Western Australia, Australia; Australia and New Zealand Dialysis and Transplant Registry, Adelaide, South Australia, Australia; Centre for Transplant and Renal Research, Westmead Hospital, Sydney, New South Wales, Australia; Central and Northern Adelaide Renal and Transplantation Services, Royal Adelaide Hospital, Adelaide, South Australia, Australia; Centre for Kidney Research, The Children s Hospital at Westmead, Sydney School of Public Health, University of Sydney, Sydney, New South Wales, Australia; New South Wales Transplantation and Immunogenetic Services, Australian Red Cross Service, Sydney, New South Wales, Australia; and **Transplantation Services, Australian Red Cross Services, Melbourne, Victoria, Australia Correspondence: Dr. Wai H. Lim, Department of Renal Medicine, Sir Charles Gairdner Hospital, Perth, WA 6009, Australia. wai. lim@health.wa.gov.au Vol 11 May, 2016 Copyright 2016 by the American Society of Nephrology 875
2 876 Clinical Journal of the American Society of Nephrology matching at the ABDR loci has not been examined (7). The aims of this study are to examine the association between and acute rejection and graft loss after kidney transplantation and assess whether in the presence of compatibility for HLA-DR have any significant effect on graft outcomes. Materials and Methods Study Population All primary live donor and deceased donor kidney transplant recipients in Australia and New Zealand between 2004 and 2012 were included in the analyses. We excluded recipients of multiple organ grafts, those with prior grafts, and those whose data on HLA-DQ matching were not available. Molecular HLA typing was introduced into clinical practice in 1997, with all HLA typing laboratories using this method (and therefore, reporting molecular HLA typing) from The number of HLA mismatches is provided to the Australia and New Zealand Dialysis and Transplant (ANZDATA) Registry from the National Organ Matching, a computerized system designed to allocate donor kidneys to potential kidney transplant recipients according to blood group and tissue compatibility. The clinical and research activities being reported are consistent with the Principles of the Declaration of Istanbul as outlined in the Declaration of Istanbul on Organ Trafficking and Transplant Tourism. Data Collection The baseline data included donor characteristics of age and type; recipient characteristics of age, sex, race, cause of ESRD, preemptive transplantation, waiting time pretransplant, diabetes, coronary artery disease, and smoking history; and transplant-related characteristics, including use of induction antibody therapy, peak panel reactive antibody (PRA) expressed as a percentage, total ischemic time, type of initial immunosuppressive agents (categorized as calcineurin inhibitor, antimetabolite, and prednisolone), transplant era (categorized as , , and ), and transplant state/country (New South Wales, Victoria, South Australia, Queensland, Western Australia, and New Zealand). Clinical Outcomes The primary clinical outcomes of this study were acute rejection (including early rejection occurring at #6 months, late rejection occurring at.6 months, any rejection, and humoral rejection [i.e., antibody-mediated rejection (AMR)]), overall graft loss (defined as death or returned to dialysis), death censored graft loss (DCGL), and graft function (egfr) at 1 and 5 years after transplantation. The various types of rejection are coded as the absence or presence of cellular, vascular, and humoral rejections. The diagnosis of AMR required at least two of the following three criteria: (1) positive C4d staining on immunofluorescence, (2) presence of donor specific anti HLA antibody, and (3) characteristic histologic changes of AMR. The dates of the first episode of acute rejection that occurred within the first 6 months after transplantation were available starting in 1997, whereas the dates of subsequent episodes were only consistently reported starting in As such, we have restricted the inclusion period from 2004 to Statistical Analyses Comparisons of the baseline characteristics between recipients stratified by HLA-DQ matched and mismatched kidney transplants were made by chi-squared test, ANOVA, and Mann Whitney U test for categorical, parametric, and nonparametric continuous variables, respectively. Acute rejection, overall graft loss, and DCGL were examined using the adjusted and random effects Cox proportional hazard regression models, accounting for the potential intracluster correlation within transplant states and country. Linear regression was used to examine the association between and egfr at 1 and 5 years. The covariates included in the Cox and linear regression models were donor-, recipient-, and transplant-related characteristics outlined above. Results were expressed as hazard ratios (HRs) or mean differences with 95% confidence intervals (95% CIs). Effect modification was tested between the study factor and other covariates using two way interaction terms in the adjusted models. Only covariates that were associated with rejection (overall and DCGL) and egfr at 1 and 5 years with P values of,0.10 in the unadjusted analyses were included in the multivariable-adjusted analyses. All analyses were undertaken using the SPSS V10 statistical software program (SPSS Inc., Chicago, IL) and SAS statistical software 9.4 (SAS Institute Inc., Cary, NC). Results Study Population Of 6107 recipients who were transplanted between 2004 and 2012, 5319 (87%) were excluded from the analyses because of missing HLA-DQ molecular typing. Apart from age and donor type, there were no significant differences in the sensitization status (peak PRA.50%; 5.4% versus 7.1%; P=0.06), the incidence of acute rejection (23.3% versus 21.2%; P=0.12), and other demographic characteristics, such as sex (men: 63.7% versus 61.9%; P=0.30), pretransplant diabetes (14.1% versus 11.7%; P=0.06), and race (white recipients: 79.6% versus 79.2%; P=0.45), among those who were excluded compared with those who were included in the analyses. Recipients excluded from the analyses were older (mean age 6SD: versus years old; P=0.001), had received kidneys from older donors (mean age 6SD: versus years old; P,0.001), and were more likely to have received live donor kidney transplants (44.6% versus 31.1%; P,0.001) compared with those included in the analyses. Initial types of immunosuppressive agents, era, and transplanting state/country were similar in both groups. Table 1 shows the baseline characteristics of the study population stratified by recipients with HLA-DQ matched and mismatched kidneys. There were 788 kidney transplant recipients between 2004 and 2012 followed for a median of 2.8 years (interquartile range, years), resulting in 2891 person-years. Of these, 321 (40.7%) received zero HLA-DQ mismatched kidneys, and 467 (59.3%) received one or two HLA-DQ mismatched kidneys (393 [49.9%] and 74 [9.4%] received one and two HLA-DQ mismatched kidneys, respectively). Compared with kidney transplant recipients who have received kidneys with one or two, those who have
3 Clin J Am Soc Nephrol 11: , May, 2016 HLA-DQ Mismatches and Kidney Transplant Outcomes, Lim et al. 877 Table 1. Baseline characteristics of kidney transplant recipients stratified by (n=788) Characteristics and Outcomes Zero HLA-DQ Mismatch, n=321 One or Two HLA-DQ Mismatches, n=467 P Value Demographics Median age (25% 75%), yr 45 (32 56) 47 (34 57) 0.51 Men, n (%) 189 (38.7) 299 (61.3) 0.14 White, n (%) 257 (80.1) 367 (78.6) Preemptive, n (%) 45 (14.0) 36 (7.7) Median BMI (25% 75%), kg/m ( ) 25.7 ( ) 0.13 Diabetes, n (%) 30 (9.3) 61 (13.1) 0.11 Coronary artery disease, n (%) 18 (5.6) 36 (7.7) 0.25 Former/current smoker, n (%) 121 (38.0) 201 (42.3) 0.33 Cause of ESRD, n (%) 0.22 GN 126 (39.3) 184 (39.4) Diabetes 22 (6.9) 47 (10.1) Cystic 48 (15.0) 78 (16.7) Median waiting time (25% 75%), yr 1.7 ( ) 1.9 ( ) 0.02 Donor characteristics Median age (25% 75%), yr 47 (32 57) 46 (33 55) 0.57 Live donor, n (%) 104 (32.4) 141 (30.2) 0.51 Immunology/transplant HLA-A mismatches, n (%), (26.8) 58 (12.4) 1or2 235 (73.2) 409 (87.6) HLA-B mismatches, n (%), (21.5) 30 (6.4) 1or2 252 (78.5) 437 (93.6) HLA-DR mismatches, n (%), (45.5) 26 (5.6) 1or2 175 (54.5) 441 (94.4) Peak PRA.50%, n (%) 19 (5.9) 24 (5.1) 0.64 Median ischemic time (25% 75%), h 9 (4 13) 9 (4 13) 0.94 Induction, n (%) 233 (72.6) 319 (68.3) 0.20 Initial prednisolone, n (%) 306 (95.3) 437 (93.6) 0.30 Initial CNI, n (%) 310 (96.6) 440 (94.2) 0.84 Initial antimetabolite, n (%) 0.88 None 22 (6.9) 35 (7.5) Azathioprine 2 (0.6) 2 (0.4) MMF 297 (92.5) 430 (92.1) Outcomes Mean6SD egfr, ml/min per 1.73 m 2 1-yr egfr, n= yr egfr, n= Acute rejection, n (%) First 6 mo 42 (13.1) 90 (19.3) 0.02 Late rejection 8 (2.5) 27 (5.8) 0.03 Any 50 (15.6) 117 (25.1) AMR 12 (3.7) 38 (8.1) 0.01 Mean6SD total rejection episodes Graft loss, n (%) 42 (13.1) 62 (13.3) 0.94 DCGL, n (%) 20 (6.2) 44 (9.4) 0.11 Data are expressed as numbers (proportions), medians (25th 75th percentiles), or means6sds. BMI, body mass index; PRA, panel reactive antibody; CNI, calcineurin inhibitor; MMF, mycophenolate; AMR, antibody-mediated rejection; DCGL, death censored graft loss. received kidneys with zero were more likely to be white and have received preemptive kidney transplants. The proportion of recipients with with zero to six HLA-ABDR mismatches is shown in Supplemental Figure 1. Only 26 (3%) recipients had no mismatches at the HLA-A, HLA-B, HLA-DR, and HLA-DQ loci. Of the recipients who received zero HLA-DQ mismatched kidneys (n=321), 235 (73%), 252 (78%), and 175 (54%) had mismatches at the HLA-A, HLA-B, and HLA-DR loci, respectively. Of those who had received one or two HLA-DQ mismatched kidneys (n=467), 58 (12%), 30 (6%), and 26 (6%) had zero mismatches at the HLA-A, HLA-B, and HLA-DR loci, respectively. Of those with zero HLA-DR
4 878 Clinical Journal of the American Society of Nephrology mismatched kidneys, 15% were mismatched at the HLA-DQ locus. A greater proportion of kidney transplant recipients whohavereceivedhla-dqmismatchedkidneysexperienced early acute rejection episodes (19.3% and 13.1%, respectively; P=0.02), late rejection (5.8% and 2.5%, respectively; P=0.03), any rejection episodes (25.1% and 15.6%, respectively; P=0.001), and AMR (8.1% and 3.7%, respectively; P=0.01) compared with recipients with zero HLA-DQ mismatched kidneys. The incidences of overall graft loss and DCGL were similar in the two groups. HLA-DQ Mismatches, Overall Graft Loss, and DCGL There were no statistically significant associations between, overall graft loss, and DCGL in the unadjusted and adjusted Cox regression models (Table 2). In the random effects models, the adjusted HRs of one or two HLA-DQ mismatched grafts for overall graft loss and DCGL were 0.95 (95% CI, 0.64 to 1.40) and 1.26 (95% CI, 0.84 to 2.44), respectively, compared with zero HLA-DQ mismatched grafts. Of those who have experienced graft loss, the proportions of recipients who had received HLA-DQ matched and mismatched kidneys and had graft loss that was attributed to acute rejection were 4.8% and 16.1%, respectively (P=0.07). HLA-DQ Mismatches and the Timing of Acute Rejection In the unadjusted models, one or two HLA-DQ mismatched kidneys were associated with a significantly greater risk of any rejection, early rejection, and late rejection, with unadjusted HRs of 1.71 (95% CI, 1.23 to 2.38; P=0.002), 1.53 (95% CI, 1.06 to 2.21; P=0.02), and 2.41 (95% CI, 1.09 to 5.31; P=0.03), respectively, compared with zero HLA-DQ mismatched kidneys. Compared with recipients who have received zero HLA-DQ mismatched kidneys, the adjusted HRs of recipients who have received one or two HLA-DQ mismatched kidneys for any rejection, early rejection, and late rejection were 1.54 (95% CI, 1.08 to 2.19; P=0.02), 1.38 (95% CI, 0.95 to 2.01; P=0.09), and 2.85 (95% CI, 1.05 to 7.75; P=0.04), respectively, independent of age, HLA mismatches at the ABDR loci, and era (Figure 1); similar adjusted HRs were observed in the random effects models (any rejection: HR, 1.51; 95% CI, 1.06 to 2.14; P=0.02; early rejection: HR, 1.42; 95% CI, 0.98 to 2.07; P=0.06; and late rejection: HR, 2.50; 95% CI, 1.06 to 5.86; P=0.03). Other covariates associated with any, early, and late rejections are shown in Table 2. The median (interquartile range) time to the occurrence of late rejection was 18 (10 44) months after transplant, with 40% of late rejections being AMR. HLA-A, HLA-B, and HLA-DR mismatches were not effect modifiers between and any rejection, early rejection, and late rejection. The adjusted cumulative incidence curve for any rejection is shown in Figure 2. The incidences of any rejection of recipients who have received zero and one or two HLA-DQ mismatched kidneys were 12% and 19%, respectively, at 3 months, 13% and 22%, respectively, at 12 months, 14% and 23%, respectively, at 2 years, and 15% and 23%, respectively, at 3 years after transplantation (log rank P=0.001). HLA-DQ Mismatches and AMR Compared with recipients who have received zero HLA- DQ mismatched kidneys, recipients of one or two HLA-DQ mismatched kidneys were associated with unadjusted and adjusted HRs of 2.22 (95% CI, 1.16 to 4.25; P=0.02) and 2.33 (95% CI, 1.19 to 4.58; P=0.01), respectively, independent of age, HLA mismatches at the other loci, and era (Figure 1). In the random effects model, the adjusted HR for AMR was 2.18 (95% CI, 1.14 to 4.16; P=0.02) for recipients of one or two HLA-DQ mismatched kidneys. Other covariates associated with AMR are shown in Table 2. HLA-DR was an effect modifier between and risk of AMR (P value for interaction =0.02). In the analyses stratified by HLA-DR mismatches, the association between and AMR was only observed in recipients who have received one or two HLA-DR mismatched kidneys (n=616), with adjusted HR of 2.50 (95% CI, 1.05 to 5.94; P=0.04), but not observed in those who have received zero HLA-DR mismatched kidneys (n=172; adjusted HR, 1.50; 95% CI, 0.20 to 9.99; P=0.46). The adjusted cumulative incidence curves for AMR are shown in Figure 3. The incidences of AMR of recipients who have received HLA-DQ matched and mismatched kidneys were 3% and 5%, respectively, at 3 months, 3% and 7%, respectively, at 12 months, 3% and 7%, respectively, at 2 years, and 4% and 8%, respectively, at 3 years after transplantation (log rank P=0.01). HLA-DQ Mismatches and Graft Function The mean (SD) egfrs at 1 and 5 years for recipients who have received HLA-DQ matched and mismatched kidneys are shown in Table 1. There were no associations between and mean egfr at 1 and 5 years in unadjusted and adjusted linear regression models. Compared with recipients of HLA-DQ matched kidneys, the mean egfr was 4.20 ml/min per 1.73 m 2 (95% CI, to 2.76; P=0.24) lower at 1 year and 5.43 ml/min per 1.73 m 2 (95% CI, to 1.14; P=0.10) lower at 5 years in recipients of HLA-DQ mismatched kidneys when adjusted for sex, donor and recipient ages, and body mass index. Discussion In our study involving 788 kidney transplant recipients with a median follow-up time of 2.8 years, we have shown that the inclusion of to conventional HLA-ABDR mismatches improved the risk stratification of acute rejection, particularly in those at risk of late rejection and AMR, independent of initial immunosuppression and sensitization status. We have also shown that HLA-DR was an effect modifier between and risk of AMR, such that the association between HLA-DQ mismatches and risk of AMR may be more important in recipients who have received HLA-DR mismatched kidneys. An association between HLA-ABDR mismatches and acute rejection risk in live and deceased donor kidney transplantation has been shown in multiple studies, with this association persisting even in the era of modern immunosuppression (3). In a retrospective study of 82 pediatric kidney transplant recipients with prior failed grafts, #30% of recipients developed de novo anti HLA antibody predominantly against HLA-DQ (13). Similarly, it has been
5 Clin J Am Soc Nephrol 11: , May, 2016 HLA-DQ Mismatches and Kidney Transplant Outcomes, Lim et al. 879 Table 2. Association between and rejection, overall graft loss, and death censored graft loss in adjusted Cox regression models Clinical Outcomes Adjusted Hazard Ratio (95% CI) P Value Timing of acute rejection Any rejection 1 or (1.08 to 2.19) 0.02 Waiting time per 1 yr longer 1.07 (1.02 to 1.13) 0.01 Early rejection 1 or (0.90 to 2.01) 0.09 Waiting time per yr longer 1.08 (1.02 to 1.14) 0.01 HLA-B mismatches 1 or (1.07 to 5.02) 0.03 Late rejection 1 or (1.05 to 7.75) 0.04 Age per yr 0.96 (0.94 to 0.98) Types of acute rejection Antibody-mediated rejection 1or2 a 2.33 (1.19 to 4.58) or 2 with 0 HLA-DR mismatches 2.50 (1.05 to 5.94) or 2 with 1 or 2 HLA-DR mismatches 1.50 (0.20 to 9.99) 0.46 Peak PRA every 10% higher 1.01 (1.00 to 1.02) 0.07 Graft loss Overall graft loss 1 or (0.55 to 1.35) 0.51 Ischemic time per h 1.06 (1.01 to 1.12) 0.02 BMI per kg/m 2 higher 1.05 (1.01 to 1.09) 0.02 Race White 1.00 Nonwhite 1.73 (0.80 to 3.76) 0.16 Indigenous 3.45 (1.94 to 6.14),0.001 Death censored graft loss 1 or (0.62 to 2.16) 0.64 Recipient age per yr 0.97 (0.95 to 0.99),0.01 Ischemic time per h 1.09 (1.01 to 1.17) 0.02 BMI per kg/m 2 higher 1.07 (1.02 to 1.13) 0.01 Race White 1.00 Nonwhite 2.09 (0.78 to 5.57) 0.14 Indigenous 4.72 (2.40 to 9.28),0.001 Data presented are adjusted hazard ratios with 95% CIs for acute rejection and overall and death censored graft loss. In the models adjusted for recipient age, donor age, donor type, BMI, HLA-ABDR mismatches, peak PRA, era, race, ischemic time, waiting time, induction therapy, and initial immunosuppression, only covariates (except ) remaining in the most parsimonious models are shown. 95% CI, 95% confidence interval; PRA, panel reactive antibody; BMI, body mass index. a Interaction between and HLA-DR mismatches (P value for interaction =0.02), with adjusted hazard ratios (95% CIs) of one or two HLA-DQ mismatched kidneys shown for zero and one or two HLA-DR mismatched kidneys compared with zero HLA-DQ mismatched kidneys.
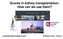
6 880 Clinical Journal of the American Society of Nephrology Figure 1. Incidence and forest plots of the adjusted hazard ratios of timing and types of acute rejection after kidney transplantation stratified by HLA-DQ matched and mismatched kidney transplants adjusted for donor and recipient age, race, donor type, body mass index, era, number of HLA-ABDR mismatches, panel reactive antibody, waiting time, ischemic time, induction therapy, and initial immunosuppression. *Interaction between HLA-DQ and HLA-DR mismatches with adjusted hazard ratio of one or two compared to zero HLA-DQ mismatch for zero and one or two HLA-DR mismatched kidneys; # incidence of antibody mediated rejection in recipients of zero HLA-DR and one or two HLA-DQ mismatched kidneys, and one or two HLA-DR and one or two HLA-DQ mismatched kidneys. 95% CI, 95% confidence interval. shown that increasing epitope mismatches at both HLA- DR and HLA-DQ loci was strongly predictive of developing de novo class 2 donor specific antibody, suggesting that matching at the HLA-DQ locus is likely to improve the stratification of immunologic risk (and therefore, risk of developing rejection, de novo antibody, and/or long term graft outcomes), particularly for recipients who may require retransplantation (4). Studies involving pediatric and adult kidney transplant only and kidney-pancreas transplant recipients have also shown that the development of de novo donor specific anti HLA-DQ antibody was associated with a #10-fold greater risk of developing early and late AMR, which was often associated with development of transplant glomerulopathy and early graft loss (14 16). In our study, we have highlighted the importance of class 2 mismatches and the risk of acute rejection. We have shown an independent association between and acute rejection, including AMR. It is important to point out that the majority of acute rejection (approximately 80%) occurred within the first 6 months after transplantation, suggesting the potential contribution of pretransplant donor specific anti HLA-DQ antibody to the risk of early rejection. However, information pertaining to the development of antibodies before and after transplantation and histologic data on transplant glomerulopathy are not available within the registry. The lack of direct association between and longer term graft outcomes is interesting and may imply that the causes of allograft failure are multifactorial. A large retrospective study of.12,000 primary deceased donor kidney transplant recipients showed that the addition of does not improve the prediction of graft survival, independent of HLA-ABDR matching. However, these studies were using data from before 2000, when the utility of molecular HLA typing and the use of modern induction and maintenance immunosuppressive agents were not available (7,8). Similarly, our study did not report an association between HLA-DQ mismatches and graft loss and may reflect the shorter median follow-up time compared with that in previous studies. Long term follow-up of this cohort will be important to establish the clinical significance of HLA-DQ mismatches. There is also considerable variability in the immunogenicity of individual HLA, and matching at the epitope level may improve our understanding of otherwise unexplained sensitization status induced by a given HLA mismatch (17). Although HLA-DQ and -DR may be closely related at an antigen level, it has been shown that small differences in one or more epitopes between donors and recipients at either locus are sufficient to generate a humoral and/or T cell mediated immune response (18,19). In a nested casecontrol study of a cohort of 52 kidney transplant recipients with established transplant glomerulopathy, an increasing number of HLA-DQ and HLA-DR eplet mismatches was associated with an increased risk of developing transplant glomerulopathy, suggesting that epitope mismatches at either HLA-DQ or HLA-DR locus are equally important in predicting graft outcomes (5). Future studies evaluating both broad antigen and epitope are
7 Clin J Am Soc Nephrol 11: , May, 2016 HLA-DQ Mismatches and Kidney Transplant Outcomes, Lim et al. 881 Figure 2. Adjusted cumulative incidence curves for any rejection after kidney transplantation according to HLA-DQ matched and mismatched kidney transplants (log rank P value <0.01). MM, mismatched. crucial in establishing a better understanding of the association between and clinical outcomes. Our study has several strengths and limitations. Using data from the ANZDATA Registry, we have established an association between and rejection risk in kidney transplant recipients in the era of molecular HLA typing and modern immunosuppression. Selection bias may exist, because there may be systematic differences in the management of kidney transplant recipients between transplanting centers and clinicians. There were numerous recipients without donor-recipient HLA-DQ typing, likely reflecting variations in practices of HLA typing across the country and era. Although multiple confounding factors were adjusted for, there may be unmeasured residual Figure 3. Adjusted cumulative incidence curves for antibody-mediated rejection after kidney transplantation according to HLA-DQ matched and mismatched kidney transplants (log rank P value <0.01). MM, mismatched.
8 882 Clinical Journal of the American Society of Nephrology confounders, such as the intensity of immunosuppression (i.e., therapeutic drug levels), the number of epitope mismatches, and the presence of pre and post transplant donor specific anti HLA antibodies, which are not collected by the ANZDATA Registry. In view of the lack of detailed descriptor within the ANZDATA Registry, misclassification bias of the outcomes could potentially occur, but the bias is likely to be random and nondifferential between the exposed and unexposed groups. We were unable to examine the effect of the incremental number of HLA- DQ mismatches and outcomes because of the small number of recipients who had received two HLA-DQ mismatched kidneys, and therefore, we would have had insufficient power to detect a significant difference between HLA-DQ matched and mismatched kidney transplants. The ANZDATA Registry does not collect data on HLA-DP mismatches, which has also been shown to be associated with rejection in case series and observational studies (20). In the current deceased donor allocation algorithm used in Australia, additional points are assigned for patients who are highly sensitized (with peak PRA.80%) and those with zero to two HLA-ABDR mismatches, particularly zero HLA-DR mismatches, because lower numbers of HLA-ABDR mismatches are associated with improved graft outcomes. Currently, matching at the HLA-DQ locus is not considered in the allocation pathway for deceased donor kidneys. Our data have shown that improved HLA- DQ matching may reduce the overall risk of acute rejection but has no effect on the overall long term graft survival. Although there is insufficient evidence to suggest that the current point allocation should be changed, we believe that our data add to the current debate as to whether adding bonus points to HLA-DQ and HLA-DR matching may improve access for highly sensitized and minority kidney transplant candidates, in whom the disparity in HLA matching occurs largely as a result of incompatibility to common class 1 HLA antigens found in the white donor population. An economic evaluation examining the addition of HLA-DQ matching to the current allocation model is prudent before considering potential changes to the current allocation pathway. are associated with an increased risk of any rejection, late rejection, and AMR, independent of HLA-ABDR mismatches, sensitization status, and initial immunosuppression. Our study findings highlight the importance of establishing before transplantation to better define the immunologic risk of each potential kidney transplant candidate and potentially minimize sensitization against HLA-DQ antigen and subsequent development of de novo antibody, which may be particularly important in pediatric or younger patients who are likely to require future retransplantation. Future studies further defining the association between HLA-DQ mismatches, pretransplant and de novo HLA-DQ antibodies, and long term graft outcomes could improve the understanding of the importance of HLA-DQ matching in kidney transplantation in addition to the conventional matching at HLA-ABDR loci. Acknowledgments The authors acknowledge the substantial contributions of the entire Australian and New Zealand nephrology community (physicians, surgeons, database managers, nurses, renal operators, and patients), which provides information to and maintains the ANZDATA Database. The data reported here have been supplied by the ANZDATA. The interpretation and reporting of these data are the responsibility of the authors and in no way should be seen as official policy or interpretation of the ANZDATA. Disclosures W.H.L., P.T.C., and G.R.R. have participated in industry sponsored clinical trials and symposia and received educational grants, travel support, or honoraria from companies producing immunosuppressant drugs, including Novartis (Basel, Switzerland), Alexion (New Haven, CT), Genzyme (Sanofi US, Bridgewater, NJ), and Pfizer (New York, New York). References 1. Wissing KM, Fomegné G, Broeders N, Ghisdal L, Hoang AD, Mikhalski D, Donckier V, Vereerstraeten P, Abramowicz D: HLA mismatches remain risk factors for acute kidney allograft rejection in patients receiving quadruple immunosuppression with antiinterleukin-2 receptorantibodies. Transplantation 85: , Beckingham IJ, Dennis MJ, Bishop MC, Blamey RW, Smith SJ, Nicholson ML: Effect of human leucocyte antigen matching on the incidence of acute rejection in renal transplantation. Br J Surg 81: , Lim WH, Chadban SJ, Clayton P, Budgeon CA, Murray K, Campbell SB, Cohney S, Russ GR, McDonald SP: Human leukocyte antigen mismatches associated with increased risk of rejection, graft failure, and death independent of initial immunosuppression in renal transplant recipients. Clin Transplant 26: E428 E437, Wiebe C, Pochinco D, Blydt-Hansen TD, Ho J, Birk PE, Karpinski M, Goldberg A, Storsley LJ, Gibson IW, Rush DN, Nickerson PW: Class II HLA epitope matching-a strategy to minimize de novo donor-specific antibody development and improve outcomes. Am J Transplant 13: , Sapir-Pichhadze R, Tinckam K, Quach K, Logan AG, Laupacis A, John R, Beyene J, Kim SJ: HLA-DR and -DQ eplet mismatches and transplant glomerulopathy: A nested case-control study. Am J Transplant 15: , Bushell A, Higgins RM, Wood KJ, Morris PJ: between donor and recipient in the presence of HLA-DR compatibility do not influence the function or outcome of renal transplants. Hum Immunol 26: , Sasaki N, Idica A: The HLA-matching effect in different cohorts of kidney transplant recipients: 10 years later. Clin Transpl 2010: , Freedman BI, Thacker LR, Heise ER, Adams PL: HLA-DQ matching in cadaveric renal transplantation. Clin Transplant 11: , Petersdorf EW, Longton GM, Anasetti C, Mickelson EM, Smith AG, Martin PJ, Hansen JA: Definition of HLA-DQ as a transplantation antigen. Proc Natl Acad Sci U S A 93: , Fernández-Vi~na MA, Klein JP, Haagenson M, Spellman SR, Anasetti C, Noreen H, Baxter-Lowe LA, Cano P, Flomenberg N, Confer DL, Horowitz MM, Oudshoorn M, Petersdorf EW, Setterholm M, Champlin R, Lee SJ, de Lima M: Multiple mismatches at the low expression HLA loci DP, DQ, and DRB3/4/5 associate with adverse outcomes in hematopoietic stem cell transplantation. Blood 121: , Kosmoliaptsis V, Gjorgjimajkoska O, Sharples LD, Chaudhry AN, Chatzizacharias N, Peacock S, Torpey N, Bolton EM, Taylor CJ, Bradley JA: Impact of donor mismatches at individual HLA-A, -B, -C, -DR, and -DQ loci on the development of HLA-specific antibodies in patients listed for repeat renal transplantation. Kidney Int 86: , DeVos JM, Gaber AO, Knight RJ, Land GA, Suki WN, Gaber LW, Patel SJ: Donor-specific HLA-DQ antibodies may contribute to poor graft outcome after renal transplantation. Kidney Int 82: , 2012
9 Clin J Am Soc Nephrol 11: , May, 2016 HLA-DQ Mismatches and Kidney Transplant Outcomes, Lim et al Tagliamacco A, Cioni M, Comoli P, Ramondetta M, Brambilla C, Trivelli A, Magnasco A, Biticchi R, Fontana I, Dulbecco P, Palombo D, Klersy C, Ghiggeri GM, Ginevri F, Cardillo M, Nocera A: DQ molecules are the principal stimulators of de novo donor-specific antibodies in nonsensitized pediatric recipients receiving a first kidney transplant. Transplant Int 27: , Willicombe M, Brookes P, Sergeant R, Santos-Nunez E, Steggar C, Galliford J, McLean A, Cook TH, Cairns T, Roufosse C, Taube D: De novo DQ donor-specific antibodies are associated with a significant risk of antibody-mediated rejection and transplant glomerulopathy. Transplantation 94: , Ginevri F, Nocera A, Comoli P, Innocente A, Cioni M, Parodi A, Fontana I, Magnasco A, Nocco A, Tagliamacco A, Sementa A, Ceriolo P, Ghio L, Zecca M, Cardillo M, Garibotto G, Ghiggeri GM, Poli F: Posttransplant de novo donor-specific hla antibodies identify pediatric kidney recipients at risk for late antibody-mediated rejection. Am J Transplant 12: , Devos JM, Gaber AO, Teeter LD, Graviss EA, Patel SJ, Land GA, Moore LW, Knight RJ: Intermediate-term graft loss after renal transplantation is associated with both donor-specific antibody and acute rejection. Transplantation 97: , Lucas DP, Leffell MS, Zachary AA: Differences in immunogenicity of HLA antigens and the impact of cross-reactivity on the humoral response. Transplantation 99: 77 85, Duquesnoy RJ: A structurally based approach to determine HLA compatibility at the humoral immune level. Hum Immunol 67: , Dankers MK, Witvliet MD, Roelen DL, de Lange P, Korfage N, Persijn GG, Duquesnoy R, Doxiadis II, Claas FH: The number of amino acid triplet differences between patient and donor is predictive for the antibody reactivity against mismatched human leukocyte antigens. Transplantation 77: , Jolly EC, Key T, Rasheed H, Morgan H, Butler A, Pritchard N, Taylor CJ, Clatworthy MR: Preformed donor HLA-DP-specific antibodies mediate acute and chronic antibody-mediated rejection following renal transplantation. Am J Transplant 12: , 2012 Received: November 3, 2015 Accepted: February 4, 2016 Published online ahead of print. Publication date available at www. cjasn.org. See related editorial, HLA-DQ Mismatching: Mounting Evidence for a Role in Kidney Transplant Rejection, on pages This article contains supplemental material online at asnjournals.org/lookup/suppl/doi: /cjn /-/ DCSupplemental.
Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
 Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Should red cells be matched for transfusions to patients listed for renal transplantation?
 Should red cells be matched for transfusions to patients listed for renal transplantation? Dr M.Willicombe Imperial College Renal and Transplant Centre, Hammersmith Hospital Should red cells be matched
Should red cells be matched for transfusions to patients listed for renal transplantation? Dr M.Willicombe Imperial College Renal and Transplant Centre, Hammersmith Hospital Should red cells be matched
Acceptable mismatching at the class II epitope level: the Canadian experience
 REVIEW C URRENT OPINION Acceptable mismatching at the class II epitope level: the Canadian experience Chris Wiebe a and Peter Nickerson a,b Purpose of review To summarize the evidence concerning human
REVIEW C URRENT OPINION Acceptable mismatching at the class II epitope level: the Canadian experience Chris Wiebe a and Peter Nickerson a,b Purpose of review To summarize the evidence concerning human
Chapter 7. Australian Waiting List. ANZDATA Registry 39th Annual Report. Data to 31-Dec-2015
 Chapter 7 Australian Waiting List 216 ANZDATA Registry 39th Annual Report Data to 31-Dec-215 Stock and Flow The waiting list data reported here are derived from the Australian National Organ Matching System
Chapter 7 Australian Waiting List 216 ANZDATA Registry 39th Annual Report Data to 31-Dec-215 Stock and Flow The waiting list data reported here are derived from the Australian National Organ Matching System
The new Banff vision of the role of HLA antibodies in organ transplantation: Improving diagnostic system and design of clinical trials
 The new Banff vision of the role of HLA antibodies in organ transplantation: Improving diagnostic system and design of clinical trials Carmen Lefaucheur 1 2 Banff 2015: Integration of HLA-Ab for improving
The new Banff vision of the role of HLA antibodies in organ transplantation: Improving diagnostic system and design of clinical trials Carmen Lefaucheur 1 2 Banff 2015: Integration of HLA-Ab for improving
Predicting HLA Class II Alloantigen Immunogenicity From the Number and Physiochemical Properties of Amino Acid Polymorphisms
 CLINICAL AND TRANSLATIONAL RESEARCH Predicting HLA Class II Alloantigen Immunogenicity From the Number and Physiochemical Properties of Amino Acid Polymorphisms Vasilis Kosmoliaptsis, 1,2,6 Linda D. Sharples,
CLINICAL AND TRANSLATIONAL RESEARCH Predicting HLA Class II Alloantigen Immunogenicity From the Number and Physiochemical Properties of Amino Acid Polymorphisms Vasilis Kosmoliaptsis, 1,2,6 Linda D. Sharples,
Table S1. Clinical outcomes of the acceptable mismatch allocation model.
 Table S1. Clinical outcomes of the acceptable mismatch allocation model. Recipient Age PRA Waiting Time (months) HLA mismatch (A/B/DR) HLAMatchmaker acceptable mismatch (years) (%) Actual Simulation Change
Table S1. Clinical outcomes of the acceptable mismatch allocation model. Recipient Age PRA Waiting Time (months) HLA mismatch (A/B/DR) HLAMatchmaker acceptable mismatch (years) (%) Actual Simulation Change
Human leukocyte antigen (HLA) matching has a beneficial
 IMMUNOBIOLOGY AND GENOMICS Predicting the Immunogenicity of Human Leukocyte Antigen Class I Alloantigens Using Structural Epitope Analysis Determined by HLAMatchmaker Vasilis Kosmoliaptsis, 1,2 J. Andrew
IMMUNOBIOLOGY AND GENOMICS Predicting the Immunogenicity of Human Leukocyte Antigen Class I Alloantigens Using Structural Epitope Analysis Determined by HLAMatchmaker Vasilis Kosmoliaptsis, 1,2 J. Andrew
Allocation of deceased donor kidneys. Phil Clayton NSW Renal Group 14 June 2012
 Allocation of deceased donor kidneys Phil Clayton NSW Renal Group 14 June 2012 Outline Why study kidney allocation? Equity vs utility Current Australian model Previous work in Australia US allocation research
Allocation of deceased donor kidneys Phil Clayton NSW Renal Group 14 June 2012 Outline Why study kidney allocation? Equity vs utility Current Australian model Previous work in Australia US allocation research
Mortality among Younger and Older Recipients of Kidney Transplants from Expanded Criteria Donors Compared with Standard Criteria Donors
 Article Mortality among Younger and Older Recipients of Kidney Transplants from Expanded Criteria Donors Compared with Standard Criteria Donors Maggie K.M. Ma,* Wai H. Lim, Jonathan C. Craig, Graeme R.
Article Mortality among Younger and Older Recipients of Kidney Transplants from Expanded Criteria Donors Compared with Standard Criteria Donors Maggie K.M. Ma,* Wai H. Lim, Jonathan C. Craig, Graeme R.
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
Kidney Transplant Outcomes for Prolonged Cold Ischemic Times in the Context of Kidney Paired Donation
 Kidney Transplant Outcomes for Prolonged Cold Ischemic Times in the Context of Kidney Paired Donation by Yayuk Joffres Thesis Submitted in Partial Fulfillment of the Requirements for the Degree of Master
Kidney Transplant Outcomes for Prolonged Cold Ischemic Times in the Context of Kidney Paired Donation by Yayuk Joffres Thesis Submitted in Partial Fulfillment of the Requirements for the Degree of Master
Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
 Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
BK virus infection in renal transplant recipients: single centre experience. Dr Wong Lok Yan Ivy
 BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
Organ transplantation in Bulgaria
 Cell Tissue Banking (28) 9:337 342 DOI 1.17/s1561-7-935-2 Organ transplantation in Bulgaria Elissaveta Naumova Æ Petar Panchev Æ Pencho J. Simeonov Æ Anastassia Mihaylova Æ Kalina Penkova Æ Petia Boneva
Cell Tissue Banking (28) 9:337 342 DOI 1.17/s1561-7-935-2 Organ transplantation in Bulgaria Elissaveta Naumova Æ Petar Panchev Æ Pencho J. Simeonov Æ Anastassia Mihaylova Æ Kalina Penkova Æ Petia Boneva
Should Pediatric Patients Wait for HLA-DR-Matched Renal Transplants?
 American Journal of Transplantation 2008; 8: 2056 2061 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2008; 8: 2056 2061 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
Peter Chang,* Jagbir Gill,* James Dong,* Caren Rose,* Howard Yan,* David Landsberg,* Edward H. Cole, and John S. Gill*
 Article Living Donor Age and Kidney Allograft Half-Life: Implications for Living Donor Paired Exchange Programs Peter Chang,* Jagbir Gill,* James Dong,* Caren Rose,* Howard Yan,* David Landsberg,* Edward
Article Living Donor Age and Kidney Allograft Half-Life: Implications for Living Donor Paired Exchange Programs Peter Chang,* Jagbir Gill,* James Dong,* Caren Rose,* Howard Yan,* David Landsberg,* Edward
Debate: HLA matching matters in children
 Annual Congress 2018 14 th to 16 th March, the Brighton Centre, Brighton Debate: HLA matching matters in children Presenting the case for - Dr Jon Jin (JJ) Kim, Nottingham Richard & Ronald Herrick 23 Dec
Annual Congress 2018 14 th to 16 th March, the Brighton Centre, Brighton Debate: HLA matching matters in children Presenting the case for - Dr Jon Jin (JJ) Kim, Nottingham Richard & Ronald Herrick 23 Dec
Australia & New Zealand Pancreas. Transplant Registry Report
 Australia & New Zealand Pancreas Transplant Registry Report 1984-2007 This report is a compilation of data provided by the five current Pancreas transplant units in Australia and New Zealand: Auckland
Australia & New Zealand Pancreas Transplant Registry Report 1984-2007 This report is a compilation of data provided by the five current Pancreas transplant units in Australia and New Zealand: Auckland
Chronic renal histological changes at implantation and subsequent deceased donor kidney transplant outcomes: a single-centre analysis
 Chronic renal histological changes at implantation and subsequent deceased donor kidney transplant outcomes: a single-centre analysis Benedict Phillips 1, Kerem Atalar 1, Hannah Wilkinson 1, Nicos Kessaris
Chronic renal histological changes at implantation and subsequent deceased donor kidney transplant outcomes: a single-centre analysis Benedict Phillips 1, Kerem Atalar 1, Hannah Wilkinson 1, Nicos Kessaris
Effect of previously failed kidney transplantation on peritoneal dialysis outcomes in the Australian and New Zealand patient populations
 NDT Advance Access published November 9, 2005 Nephrol Dial Transplant (2005) 1 of 8 doi:10.1093/ndt/gfi248 Original Article Effect of previously failed kidney transplantation on peritoneal dialysis outcomes
NDT Advance Access published November 9, 2005 Nephrol Dial Transplant (2005) 1 of 8 doi:10.1093/ndt/gfi248 Original Article Effect of previously failed kidney transplantation on peritoneal dialysis outcomes
Effects of HLA-Matched Blood Transfusion for Patients Awaiting Renal Transplantation
 CLINICAL AND TRANSLATIONAL RESEARCH Effects of HLA-Matched Blood Transfusion for Patients Awaiting Renal Transplantation Bernadette A. Magee, 1,4 Jeanie Martin, 1 Miceal P. Cole, 1 Kieran G. Morris, 2
CLINICAL AND TRANSLATIONAL RESEARCH Effects of HLA-Matched Blood Transfusion for Patients Awaiting Renal Transplantation Bernadette A. Magee, 1,4 Jeanie Martin, 1 Miceal P. Cole, 1 Kieran G. Morris, 2
Article. Simultaneous Pancreas Kidney Transplant versus Other Kidney Transplant Options in Patients with Type 2 Diabetes
 Article Simultaneous Pancreas Kidney Transplant versus Other Kidney Transplant Options in Patients with Type 2 Diabetes Alexander C. Wiseman* and Jane Gralla Summary Background and objectives Current organ
Article Simultaneous Pancreas Kidney Transplant versus Other Kidney Transplant Options in Patients with Type 2 Diabetes Alexander C. Wiseman* and Jane Gralla Summary Background and objectives Current organ
Association between causes of peritoneal dialysis technique failure and all-cause mortality
 www.nature.com/scientificreports Received: 27 September 2017 Accepted: 21 February 2018 Published: xx xx xxxx OPEN Association between causes of peritoneal dialysis technique failure and all-cause mortality
www.nature.com/scientificreports Received: 27 September 2017 Accepted: 21 February 2018 Published: xx xx xxxx OPEN Association between causes of peritoneal dialysis technique failure and all-cause mortality
Australia & New Zealand Pancreas. Transplant Registry Report
 Australia & New Zealand Pancreas Transplant Registry Report 1984-2009 This report is a compilation of data provided by the three current Pancreas transplant units in Australia and New Zealand: Auckland
Australia & New Zealand Pancreas Transplant Registry Report 1984-2009 This report is a compilation of data provided by the three current Pancreas transplant units in Australia and New Zealand: Auckland
Chapter 6: Transplantation
 Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS
 COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS A COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS KEVIN C. MANGE, M.D.,
COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS A COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS KEVIN C. MANGE, M.D.,
The New Kidney Allocation Policy: Implications for Your Patients and Your Practice
 The New Kidney Allocation Policy: Implications for Your Patients and Your Practice Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Explain
The New Kidney Allocation Policy: Implications for Your Patients and Your Practice Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Explain
Progress in Pediatric Kidney Transplantation
 Send Orders for Reprints to reprints@benthamscience.net The Open Urology & Nephrology Journal, 214, 7, (Suppl 2: M2) 115-122 115 Progress in Pediatric Kidney Transplantation Jodi M. Smith *,1 and Vikas
Send Orders for Reprints to reprints@benthamscience.net The Open Urology & Nephrology Journal, 214, 7, (Suppl 2: M2) 115-122 115 Progress in Pediatric Kidney Transplantation Jodi M. Smith *,1 and Vikas
APHERESIS FOR DESENSITIZATION OF NON-RENAL TRANSPLANTS
 APHERESIS FOR DESENSITIZATION OF NON-RENAL TRANSPLANTS GOW AREPALLY, MD MEDICAL DIRECTOR DUKE THERAPEUTIC APHERESIS SERVICE ASSOCIATE PROFESSOR, MEDICINE AMERICAN SOCIETY FOR APHERESIS MAY 25 TH 2013 OVERVIEW
APHERESIS FOR DESENSITIZATION OF NON-RENAL TRANSPLANTS GOW AREPALLY, MD MEDICAL DIRECTOR DUKE THERAPEUTIC APHERESIS SERVICE ASSOCIATE PROFESSOR, MEDICINE AMERICAN SOCIETY FOR APHERESIS MAY 25 TH 2013 OVERVIEW
Basel - 6 September J.-M. Tiercy National Reference Laboratory for Histocompatibility (LNRH) University Hospital Geneva
 Basel - 6 eptember 2012 J.-M. Tiercy National Reference Laboratory for Histocompatibility (LNRH) University Hospital Geneva Outline the HLA system is (a) complex anti-hla immunisation and alloreactivity
Basel - 6 eptember 2012 J.-M. Tiercy National Reference Laboratory for Histocompatibility (LNRH) University Hospital Geneva Outline the HLA system is (a) complex anti-hla immunisation and alloreactivity
Long-Term Renal Allograft Survival in the United States: A Critical Reappraisal
 American Journal of Transplantation 2011; 11: 450 462 Wiley Periodicals Inc. C 2010 The Authors Journal compilation C 2010 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2011; 11: 450 462 Wiley Periodicals Inc. C 2010 The Authors Journal compilation C 2010 The American Society of Transplantation and the American Society of Transplant
Chapter 10. Cancer. ANZDATA gratefully acknowledges the contributions of the Cancer Working Group convened by Germaine Wong.
 Chapter Cancer ANZDATA gratefully acknowledges the contributions of the Cancer Working Group convened by Germaine Wong Contents: Cancer -1 Incidence of Cancer on Renal Replacement Therapy -2 Kidney Cancer
Chapter Cancer ANZDATA gratefully acknowledges the contributions of the Cancer Working Group convened by Germaine Wong Contents: Cancer -1 Incidence of Cancer on Renal Replacement Therapy -2 Kidney Cancer
Even in this era of efficient immunosuppression, a positive
 OVERVIEW Enhanced Kidney Allocation to Highly Sensitized Patients by the Acceptable Mismatch Program Frans H. J. Claas, 1 Axel Rahmel, 2 and IIias I. N. Doxiadis 1 Even in this era of efficient immunosuppression,
OVERVIEW Enhanced Kidney Allocation to Highly Sensitized Patients by the Acceptable Mismatch Program Frans H. J. Claas, 1 Axel Rahmel, 2 and IIias I. N. Doxiadis 1 Even in this era of efficient immunosuppression,
Hong Kong Journal Nephrol of 2000;(2): Nephrology 2000;2(2): BR HAWKINS ORIGINAL A R T I C L E A point score system for allocating cadaver
 Hong Kong Journal Nephrol of 2000;(2):79-83. Nephrology 2000;2(2):79-83. ORIGINAL A R T I C L E A point score system for allocating cadaveric kidneys for transplantation based on patient age, waiting time
Hong Kong Journal Nephrol of 2000;(2):79-83. Nephrology 2000;2(2):79-83. ORIGINAL A R T I C L E A point score system for allocating cadaveric kidneys for transplantation based on patient age, waiting time
Transplantation in Australia and New Zealand
 Transplantation in Australia and New Zealand Matthew D. Jose MBBS (Adel), FRACP, FASN, PhD (Monash), AFRACMA Professor of Medicine, UTAS Renal Physician, Royal Hobart Hospital Overview CKD in Australia
Transplantation in Australia and New Zealand Matthew D. Jose MBBS (Adel), FRACP, FASN, PhD (Monash), AFRACMA Professor of Medicine, UTAS Renal Physician, Royal Hobart Hospital Overview CKD in Australia
Chapter 12. End Stage Kidney Disease in Indigenous Peoples of Australia and Aotearoa/New Zealand. ANZDATA Registry 39th Annual Report
 Chapter 12 End Stage Kidney Disease in Indigenous Peoples of and Aotearoa/ 216 ANZDATA Registry 39th Annual Report Data to 31-Dec-215 Introduction In this chapter, the rates and practice patterns for end-stage
Chapter 12 End Stage Kidney Disease in Indigenous Peoples of and Aotearoa/ 216 ANZDATA Registry 39th Annual Report Data to 31-Dec-215 Introduction In this chapter, the rates and practice patterns for end-stage
Older Living Kidney Donors and Recipients. Charles Le University of Colorado 6/24/11
 Older Living Kidney Donors and Recipients Charles Le University of Colorado 6/24/11 Clinical Scenario HPI: 60 y/o healthy AAM with h/o CKD5 on HD x 2 yrs 2/2 HTN, was evaluated in transplant clinic for
Older Living Kidney Donors and Recipients Charles Le University of Colorado 6/24/11 Clinical Scenario HPI: 60 y/o healthy AAM with h/o CKD5 on HD x 2 yrs 2/2 HTN, was evaluated in transplant clinic for
The New Kidney Allocation System: What You Need to Know. Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health
 The New Kidney Allocation System: What You Need to Know Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health ~6% of patients die each year on the deceased donor waiting
The New Kidney Allocation System: What You Need to Know Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health ~6% of patients die each year on the deceased donor waiting
Corneal transplantation: HLA and age
 L Aquila, 24 novembre 2012 Corneal transplantation: HLA and age Federico Genzano Besso*, Paola Magistroni, Piera Santoro*, Silvano Battaglio*, Raffaella Giacometti, Morteza Mansouri and Antonio Amoroso
L Aquila, 24 novembre 2012 Corneal transplantation: HLA and age Federico Genzano Besso*, Paola Magistroni, Piera Santoro*, Silvano Battaglio*, Raffaella Giacometti, Morteza Mansouri and Antonio Amoroso
Reduced graft function (with or without dialysis) vs immediate graft function a comparison of long-term renal allograft survival
 Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Princess Alexandra Hospital, Brisbane
 Princess Alexandra Hospital Coagulase Negative Staphylococcal Peritonitis in Australian Peritoneal Dialysis Patients Predictors, Treatment and Outcomes in 936 cases Dr Magid Fahim Princess Alexandra Hospital,
Princess Alexandra Hospital Coagulase Negative Staphylococcal Peritonitis in Australian Peritoneal Dialysis Patients Predictors, Treatment and Outcomes in 936 cases Dr Magid Fahim Princess Alexandra Hospital,
Clinical Study Over Ten-Year Kidney Graft Survival Determinants
 International Nephrology Volume 2012, Article ID 302974, 5 pages doi:10.1155/2012/302974 Clinical Study Over Ten-Year Kidney Graft Survival Determinants Anabela Malho Guedes, 1, 2 Jorge Malheiro, 1 Isabel
International Nephrology Volume 2012, Article ID 302974, 5 pages doi:10.1155/2012/302974 Clinical Study Over Ten-Year Kidney Graft Survival Determinants Anabela Malho Guedes, 1, 2 Jorge Malheiro, 1 Isabel
The Kidney Allocation System Changed in a Substantive Way on December 5, Your Patients Have Been, and Will Be, Affected by These Changes
 The Kidney Allocation System Changed in a Substantive Way on December 5, 2014 Your Patients Have Been, and Will Be, Affected by These Changes 1 The New Kidney Allocation System Terms of Importance Pediatric
The Kidney Allocation System Changed in a Substantive Way on December 5, 2014 Your Patients Have Been, and Will Be, Affected by These Changes 1 The New Kidney Allocation System Terms of Importance Pediatric
Access and Outcomes Among Minority Transplant Patients, , with a Focus on Determinants of Kidney Graft Survival
 American Journal of Transplantation 2010; 10 (Part 2): 1090 1107 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
American Journal of Transplantation 2010; 10 (Part 2): 1090 1107 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
Survival of recipients of cadaveric kidney transplants compared with those receiving dialysis treatment in Australia and New Zealand,
 Nephrol Dial Transplant (2002) 17: 2212 2219 Original Article Survival of recipients of cadaveric kidney transplants compared with those receiving dialysis treatment in Australia and New Zealand, 1991
Nephrol Dial Transplant (2002) 17: 2212 2219 Original Article Survival of recipients of cadaveric kidney transplants compared with those receiving dialysis treatment in Australia and New Zealand, 1991
End Stage Kidney Disease Among Indigenous Peoples of Australia and New Zealand
 Chapter 12 End Stage Kidney Disease Among Indigenous Peoples of and New Zealand 216 ANZDATA Registry 39th Annual Report Data to 31-Dec-215 Introduction In this chapter, rates of end-stage kidney disease
Chapter 12 End Stage Kidney Disease Among Indigenous Peoples of and New Zealand 216 ANZDATA Registry 39th Annual Report Data to 31-Dec-215 Introduction In this chapter, rates of end-stage kidney disease
Transplant Update New Kidney Allocation System Transplant Referral Strategies. Antonia Harford, MD University of New Mexico
 Transplant Update New Kidney Allocation System Transplant Referral Strategies Antonia Harford, MD University of New Mexico Financial Disclosures Doctor Harford has received financial support for dialysis
Transplant Update New Kidney Allocation System Transplant Referral Strategies Antonia Harford, MD University of New Mexico Financial Disclosures Doctor Harford has received financial support for dialysis
Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation
 Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation Titte R Srinivas, MD, FAST Medical Director, Kidney and Pancreas Transplant Programs Objectives: Describe trends
Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation Titte R Srinivas, MD, FAST Medical Director, Kidney and Pancreas Transplant Programs Objectives: Describe trends
IMPACT OF PREFORMED AND DE NOVO ANTI-HLA DP ANTIBODIES
 IMPACT OF PREFORMED AND DE NOVO ANTI-HLA DP ANTIBODIES IN RENAL ALLOGRAFT SURVIVAL Dolores Redondo-Pachón 1, Julio Pascual 1*, María J. Pérez-Sáez 1, Carmen García 2, Juan José Hernández 2, Javier Gimeno
IMPACT OF PREFORMED AND DE NOVO ANTI-HLA DP ANTIBODIES IN RENAL ALLOGRAFT SURVIVAL Dolores Redondo-Pachón 1, Julio Pascual 1*, María J. Pérez-Sáez 1, Carmen García 2, Juan José Hernández 2, Javier Gimeno
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20898 holds various files of this Leiden University dissertation. Author: Jöris, Monique Maria Title: Challenges in unrelated hematopoietic stem cell transplantation.
Cover Page The handle http://hdl.handle.net/1887/20898 holds various files of this Leiden University dissertation. Author: Jöris, Monique Maria Title: Challenges in unrelated hematopoietic stem cell transplantation.
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,700 108,500 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,700 108,500 1.7 M Open access books available International authors and editors Downloads Our
6/19/2012. Who is in the room today? What is your level of understanding of Donor Antigens and Candidate Unacceptables in KPD?
 6/19/212 KPD Webinar Series: Part 3 Demystifying the OPTN Kidney Paired Donation Pilot Program Unacceptable HLA antigens: The key to finding a compatible donor for your patient M. Sue Leffell, Ph.D. J.
6/19/212 KPD Webinar Series: Part 3 Demystifying the OPTN Kidney Paired Donation Pilot Program Unacceptable HLA antigens: The key to finding a compatible donor for your patient M. Sue Leffell, Ph.D. J.
CHAPTER 10 CANCER REPORT. Jeremy Chapman. and. Angela Webster
 CHAPTER 10 CANCER REPORT Jeremy Chapman and Angela Webster CANCER REPORT ANZDATA Registry 2004 Report This report summarises the cancer (excluding nonmelanocytic skin cancer) experience of patients treated
CHAPTER 10 CANCER REPORT Jeremy Chapman and Angela Webster CANCER REPORT ANZDATA Registry 2004 Report This report summarises the cancer (excluding nonmelanocytic skin cancer) experience of patients treated
Epitope matching in solid organ transplantation: T-cell epitopes
 Epitope matching in solid organ transplantation: T-cell epitopes Eric Spierings (e.spierings@umcutrecht.nl) Laboratory for Translational Immunology, UMC Utrecht conflict of interest: the UMCU has filed
Epitope matching in solid organ transplantation: T-cell epitopes Eric Spierings (e.spierings@umcutrecht.nl) Laboratory for Translational Immunology, UMC Utrecht conflict of interest: the UMCU has filed
J Am Soc Nephrol 14: , 2003
 J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
NAPRTCS Annual Transplant Report
 North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2014 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE II TRANSPLANTATION Section
North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2014 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE II TRANSPLANTATION Section
Pediatric Transplantation DOI: /j x
 Pediatr Transplantation 2007: 11: 77 81 Copyright Ó 2007 Blackwell Munksgaard Pediatric Transplantation DOI: 10.1111/j.1399-3046.2006.00617.x Intravenous immunoglobulin, HLA allele typing and HLAMatchmaker
Pediatr Transplantation 2007: 11: 77 81 Copyright Ó 2007 Blackwell Munksgaard Pediatric Transplantation DOI: 10.1111/j.1399-3046.2006.00617.x Intravenous immunoglobulin, HLA allele typing and HLAMatchmaker
ORIGINAL ARTICLE. Received April 30, 2007; accepted June
 LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009
 Western University Scholarship@Western Electronic Thesis and Dissertation Repository June 2015 Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009 Ngan Lam The University
Western University Scholarship@Western Electronic Thesis and Dissertation Repository June 2015 Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009 Ngan Lam The University
Steroid Minimization: Great Idea or Silly Move?
 Steroid Minimization: Great Idea or Silly Move? Disclosures I have financial relationship(s) within the last 12 months relevant to my presentation with: Astellas Grants ** Bristol Myers Squibb Grants,
Steroid Minimization: Great Idea or Silly Move? Disclosures I have financial relationship(s) within the last 12 months relevant to my presentation with: Astellas Grants ** Bristol Myers Squibb Grants,
Impact of HLA Mismatch at First Kidney Transplant on Lifetime With Graft Function in Young Recipients
 American Journal of Transplantation 2014; 14: 876 885 Wiley Periodicals Inc. C Copyright 2014 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12643
American Journal of Transplantation 2014; 14: 876 885 Wiley Periodicals Inc. C Copyright 2014 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12643
Management of Rejection
 Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
The Use of HLA /HPA Selected Platelets
 The Use of HLA /HPA Selected Platelets Dr Colin Brown PhD FRCPath. Consultant Clinical Scientist Histocompatibility and Immunogenetics HLA and Transfusion Human Leucocyte Antigens HLA Human Platelet Antigens
The Use of HLA /HPA Selected Platelets Dr Colin Brown PhD FRCPath. Consultant Clinical Scientist Histocompatibility and Immunogenetics HLA and Transfusion Human Leucocyte Antigens HLA Human Platelet Antigens
NAPRTCS Annual Transplant Report
 North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2010 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE I INTRODUCTION 1 II
North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2010 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE I INTRODUCTION 1 II
DSA Positive and then To biopsy or not?
 DSA Positive and then To biopsy or not? Banff SCT 2017 29 March 2017 Peter Nickerson, MD, FRCPC, FCAHS Flynn Family Chair in Renal Transplantation Professor of Internal Medicine and Immunology Relevant
DSA Positive and then To biopsy or not? Banff SCT 2017 29 March 2017 Peter Nickerson, MD, FRCPC, FCAHS Flynn Family Chair in Renal Transplantation Professor of Internal Medicine and Immunology Relevant
Sylwia Mizia, 1 Dorota Dera-Joachimiak, 1 Malgorzata Polak, 1 Katarzyna Koscinska, 1 Mariola Sedzimirska, 1 and Andrzej Lange 1, 2. 1.
 Bone Marrow Research Volume 2012, Article ID 873695, 5 pages doi:10.1155/2012/873695 Clinical Study Both Optimal Matching and Procedure Duration Influence Survival of Patients after Unrelated Donor Hematopoietic
Bone Marrow Research Volume 2012, Article ID 873695, 5 pages doi:10.1155/2012/873695 Clinical Study Both Optimal Matching and Procedure Duration Influence Survival of Patients after Unrelated Donor Hematopoietic
The Acceptable Mismatch program of Eurotransplant.
 The Acceptable Mismatch program of Eurotransplant. Frans Claas Leiden University Medical Center Eurotransplant Reference Laboratory Leiden, the Netherlands. Hinterzarten, December 7, 2013 Main problem
The Acceptable Mismatch program of Eurotransplant. Frans Claas Leiden University Medical Center Eurotransplant Reference Laboratory Leiden, the Netherlands. Hinterzarten, December 7, 2013 Main problem
Hasan Fattah 3/19/2013
 Hasan Fattah 3/19/2013 AASK trial Rational: HTN is a leading cause of (ESRD) in the US, with no known treatment to prevent progressive declines leading to ESRD. Objective: To compare the effects of 2 levels
Hasan Fattah 3/19/2013 AASK trial Rational: HTN is a leading cause of (ESRD) in the US, with no known treatment to prevent progressive declines leading to ESRD. Objective: To compare the effects of 2 levels
Transplantation in highly sensitised patients treated with intravenous immunoglobulin and Rituximab
 ORIGINAL ARTICLE Advance Access publication 1 February 2010 Transplantation in highly sensitised patients treated with intravenous immunoglobulin and Rituximab Ana Carina Ferreira 1, Sandra Brum 1, Vasco
ORIGINAL ARTICLE Advance Access publication 1 February 2010 Transplantation in highly sensitised patients treated with intravenous immunoglobulin and Rituximab Ana Carina Ferreira 1, Sandra Brum 1, Vasco
Utility of protocol kidney biopsies for de novo donor- specific antibodies
 Received: 6 June 2017 Revised: 24 July 2017 Accepted: 29 July 2017 DOI: 10.1111/ajt.14466 BRIEF COMMUNICATION Utility of protocol kidney biopsies for de novo donor- specific antibodies Sandesh Parajuli
Received: 6 June 2017 Revised: 24 July 2017 Accepted: 29 July 2017 DOI: 10.1111/ajt.14466 BRIEF COMMUNICATION Utility of protocol kidney biopsies for de novo donor- specific antibodies Sandesh Parajuli
Simultaneous Pancreas Kidney Transplantation:
 Simultaneous Pancreas Kidney Transplantation: What is the added advantage, and for whom? Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney
Simultaneous Pancreas Kidney Transplantation: What is the added advantage, and for whom? Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney
PEER REVIEW HISTORY ARTICLE DETAILS TITLE (PROVISIONAL)
 PEER REVIEW HISTORY BMJ Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form (http://bmjopen.bmj.com/site/about/resources/checklist.pdf)
PEER REVIEW HISTORY BMJ Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form (http://bmjopen.bmj.com/site/about/resources/checklist.pdf)
Long-term prognosis of BK virus-associated nephropathy in kidney transplant recipients
 Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
For broad-split groups where the broad antigen was very rare, we excluded the broad antigen and analyzed each child antigen as their own category.
 Description of categorization of broad and split antigens HLA antigen classifications have evolved over time as assay development has allowed the detection of differences in antigens ( split categories)
Description of categorization of broad and split antigens HLA antigen classifications have evolved over time as assay development has allowed the detection of differences in antigens ( split categories)
Renal Transplantation: Allocation challenges and changes. Renal Transplantation. The Numbers 1/13/2014
 Renal Transplantation: Allocation challenges and changes Mark R. Wakefield, M.D., F.A.C.S. Associate Professor of Surgery/Urology Director Renal Transplantation Renal Transplantation Objectives: Understand
Renal Transplantation: Allocation challenges and changes Mark R. Wakefield, M.D., F.A.C.S. Associate Professor of Surgery/Urology Director Renal Transplantation Renal Transplantation Objectives: Understand
Induction Immunosuppressive Therapy in the Elderly Kidney Transplant Recipient in the United States
 Article Induction Immunosuppressive Therapy in the Elderly Kidney Transplant Recipient in the United States Jagbir Gill,* Marcelo Sampaio, John S. Gill,* James Dong,* Hung-Tien Kuo, Gabriel M. Danovitch,
Article Induction Immunosuppressive Therapy in the Elderly Kidney Transplant Recipient in the United States Jagbir Gill,* Marcelo Sampaio, John S. Gill,* James Dong,* Hung-Tien Kuo, Gabriel M. Danovitch,
ORIGINAL ARTICLE. Eric F. Martin, 1 Jonathan Huang, 3 Qun Xiang, 2 John P. Klein, 2 Jasmohan Bajaj, 4 and Kia Saeian 1
 LIVER TRANSPLANTATION 18:914 929, 2012 ORIGINAL ARTICLE Recipient Survival and Graft Survival are Not Diminished by Simultaneous Liver-Kidney Transplantation: An Analysis of the United Network for Organ
LIVER TRANSPLANTATION 18:914 929, 2012 ORIGINAL ARTICLE Recipient Survival and Graft Survival are Not Diminished by Simultaneous Liver-Kidney Transplantation: An Analysis of the United Network for Organ
Virtual Crossmatch in Kidney Transplantation
 Virtual Crossmatch in Kidney Transplantation Shiva Samavat Associate Professor of Nephrology Labbafinejad Hospital SBMU 2018.11.21 All transplant candidates are screened to determine the degree of humoral
Virtual Crossmatch in Kidney Transplantation Shiva Samavat Associate Professor of Nephrology Labbafinejad Hospital SBMU 2018.11.21 All transplant candidates are screened to determine the degree of humoral
Kidney Transplant Outcomes In Elderly Patients. Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania
 Kidney Transplant Outcomes In Elderly Patients Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Case Discussion 70 year old Asian male, neuropsychiatrist, works full
Kidney Transplant Outcomes In Elderly Patients Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Case Discussion 70 year old Asian male, neuropsychiatrist, works full
OUT OF DATE. Choice of calcineurin inhibitors in adult renal transplantation: Effects on transplant outcomes
 nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
Scores in kidney transplantation: How can we use them?
 Scores in kidney transplantation: How can we use them? Actualités Néphrologiques 2017 M Hazzan (Lille France ) Contents Scores to estimate the quality of the graft Scores to estimate old candidates to
Scores in kidney transplantation: How can we use them? Actualités Néphrologiques 2017 M Hazzan (Lille France ) Contents Scores to estimate the quality of the graft Scores to estimate old candidates to
Prevalence and Outcomes of Multiple-Listing for Cadaveric Kidney and Liver Transplantation
 American Journal of Transplantation 24; 4: 94 1 Blackwell Munksgaard Copyright C Blackwell Munksgaard 23 doi: 1.146/j.16-6135.23.282.x Prevalence and Outcomes of Multiple-Listing for Cadaveric Kidney and
American Journal of Transplantation 24; 4: 94 1 Blackwell Munksgaard Copyright C Blackwell Munksgaard 23 doi: 1.146/j.16-6135.23.282.x Prevalence and Outcomes of Multiple-Listing for Cadaveric Kidney and
The privilege of induction avoidance and calcineurin inhibitors withdrawal in 2 haplotype HLA matched white kidney transplantation
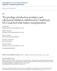 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 The privilege of induction avoidance and calcineurin inhibitors withdrawal in 2 haplotype HLA matched white
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 The privilege of induction avoidance and calcineurin inhibitors withdrawal in 2 haplotype HLA matched white
Pancreas After Islet Transplantation: A First Report of the International Pancreas Transplant Registry
 American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
HLA Amino Acid Polymorphisms and Kidney Allograft Survival. Supplemental Digital Content
 HLA Amino Acid Polymorphisms and Kidney Allograft Survival Supplemental Digital Content Malek Kamoun, MD, PhD a, Keith P. McCullough, MS b, Martin Maiers, MS c, Marcelo A. Fernandez Vina, MD, PhD d, Hongzhe
HLA Amino Acid Polymorphisms and Kidney Allograft Survival Supplemental Digital Content Malek Kamoun, MD, PhD a, Keith P. McCullough, MS b, Martin Maiers, MS c, Marcelo A. Fernandez Vina, MD, PhD d, Hongzhe
Current strategies to kidney allocation
 Current strategies to kidney allocation Dr Marie Alice Macher Dr Christian Jacquelinet Emilie Savoye Dr Corinne Antoine Direction Prélèvement Greffe organes - tissus From organ sharing to organ allocation
Current strategies to kidney allocation Dr Marie Alice Macher Dr Christian Jacquelinet Emilie Savoye Dr Corinne Antoine Direction Prélèvement Greffe organes - tissus From organ sharing to organ allocation
Literature Review Transplantation
 Literature Review 2010- Transplantation Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney and Pancreas Transplant Programs University of
Literature Review 2010- Transplantation Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney and Pancreas Transplant Programs University of
Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function
 ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
Association of Kidney Transplantation with Survival in Patients with Long Dialysis Exposure
 Article Association of Kidney Transplantation with Survival in Patients with Long Dialysis Exposure Caren Rose,* Jagbir Gill,* and John S. Gill* Abstract Background and objectives Evidence that kidney
Article Association of Kidney Transplantation with Survival in Patients with Long Dialysis Exposure Caren Rose,* Jagbir Gill,* and John S. Gill* Abstract Background and objectives Evidence that kidney
Clinical correlates, outcomes and healthcare costs associated with early mechanical ventilation after kidney transplantation
 The American Journal of Surgery (2013) 206, 686-692 Association of Women Surgeons: Clinical Science Clinical correlates, outcomes and healthcare costs associated with early mechanical ventilation after
The American Journal of Surgery (2013) 206, 686-692 Association of Women Surgeons: Clinical Science Clinical correlates, outcomes and healthcare costs associated with early mechanical ventilation after
RECURRENT GLOMERULONEPHRITIS RISK OF RENAL ALLOGRAFT LOSS FROM RECURRENT GLOMERULONEPHRITIS. Data Collection
 RISK OF RENAL ALLOGRAFT LOSS FROM RECURRENT GLOMERULONEPHRITIS ESTHER M. BRIGANTI, M.B., B.S., M.CLIN.EPI., GRAEME R. RUSS, M.B., B.S., PH.D., JOHN J. MCNEIL, M.B., B.S., PH.D., ROBERT C. ATKINS, M.B.,
RISK OF RENAL ALLOGRAFT LOSS FROM RECURRENT GLOMERULONEPHRITIS ESTHER M. BRIGANTI, M.B., B.S., M.CLIN.EPI., GRAEME R. RUSS, M.B., B.S., PH.D., JOHN J. MCNEIL, M.B., B.S., PH.D., ROBERT C. ATKINS, M.B.,
Australia & New Zealand Pancreas. Transplant Registry Report Inquiries or comments should be directed to the secretariat at:
 Australia & New Zealand Pancreas Transplant Registry Report 1984-2013 This report is a compilation of data provided by the four current Pancreas transplant units in Australia and New Zealand: Auckland
Australia & New Zealand Pancreas Transplant Registry Report 1984-2013 This report is a compilation of data provided by the four current Pancreas transplant units in Australia and New Zealand: Auckland
SHORT COMMUNICATION. G. Joshy & P. Dunn & M. Fisher & R. Lawrenson
 Diabetologia (2009) 52:1474 1478 DOI 10.1007/s00125-009-1380-1 SHORT COMMUNICATION Ethnic differences in the natural progression of nephropathy among diabetes patients in New Zealand: hospital admission
Diabetologia (2009) 52:1474 1478 DOI 10.1007/s00125-009-1380-1 SHORT COMMUNICATION Ethnic differences in the natural progression of nephropathy among diabetes patients in New Zealand: hospital admission
Desensitization in Kidney Transplant. James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver
 Desensitization in Kidney Transplant James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Organ Shortage Currently there are >90,000 patients on the kidney
Desensitization in Kidney Transplant James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Organ Shortage Currently there are >90,000 patients on the kidney
Does Kidney Donor Risk Index implementation lead to the transplantation of more and higher-quality donor kidneys?
 Nephrol Dial Transplant (2017) 32: 1934 1938 doi: 10.1093/ndt/gfx257 Advance Access publication 21 August 2017 Does Kidney Donor Risk Index implementation lead to the transplantation of more and higher-quality
Nephrol Dial Transplant (2017) 32: 1934 1938 doi: 10.1093/ndt/gfx257 Advance Access publication 21 August 2017 Does Kidney Donor Risk Index implementation lead to the transplantation of more and higher-quality
DE-MYSTIFYING THE BLACK BOX OF TRANSPLANT IMMUNOLOGY
 2016 DE-MYSTIFYING THE BLACK BOX OF TRANSPLANT IMMUNOLOGY James H Lan, MD, FRCP(C), D(ABHI) Clinical Assistant Professor, University of British Columbia Nephrology & Kidney Transplantation, Vancouver General
2016 DE-MYSTIFYING THE BLACK BOX OF TRANSPLANT IMMUNOLOGY James H Lan, MD, FRCP(C), D(ABHI) Clinical Assistant Professor, University of British Columbia Nephrology & Kidney Transplantation, Vancouver General
The time interval between kidney and pancreas transplantation and the clinical outcomes of pancreas after kidney transplantation
 Clin Transplant 2012: 26: 403 410 DOI: 10.1111/j.1399-0012.2011.01519.x ª 2011 John Wiley & Sons A/S. The time interval between kidney and pancreas transplantation and the clinical outcomes of pancreas
Clin Transplant 2012: 26: 403 410 DOI: 10.1111/j.1399-0012.2011.01519.x ª 2011 John Wiley & Sons A/S. The time interval between kidney and pancreas transplantation and the clinical outcomes of pancreas
Echocardiography analysis in renal transplant recipients
 Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Diabetes Mellitus GUIDELINES UNGRADED SUGGESTIONS FOR CLINICAL CARE IMPLEMENTATION AND AUDIT BACKGROUND
 Diabetes Mellitus Date written: November 2011 Author: Scott Campbell GUIDELINES a. We recommend that diabetes should not on its own preclude a patient from being considered for kidney transplantation (1D).
Diabetes Mellitus Date written: November 2011 Author: Scott Campbell GUIDELINES a. We recommend that diabetes should not on its own preclude a patient from being considered for kidney transplantation (1D).
