The time interval between kidney and pancreas transplantation and the clinical outcomes of pancreas after kidney transplantation
|
|
|
- Justina Sparks
- 5 years ago
- Views:
Transcription
1 Clin Transplant 2012: 26: DOI: /j x ª 2011 John Wiley & Sons A/S. The time interval between kidney and pancreas transplantation and the clinical outcomes of pancreas after kidney transplantation Luan FL, Kommareddi M, Cibrik DM, Samaniego M, Ojo AO. The time interval between kidney and pancreas transplantation and the clinical outcomes of pancreas after kidney transplantation. Abstract: Pancreas after kidney (PAK) transplantation is one of the accepted pancreas transplant modalities. We studied the impact of time interval between kidney and pancreas transplantation on the outcomes of PAK transplantation. Using OPTN/SRTR data, we included 1853 PAK transplants performed between 1996 and 2005 with follow-up until November 1, Kaplan Meier survival and multivariate Cox regression analyses were performed using the time interval between kidney and pancreas transplantation either as a categorical (less than one yr, between one and less than three yr, and greater than or equal to three yr) or as a continuous variable (months) to assess kidney graft and patient survival. Patients who received a pancreas transplant three yr or later after kidney transplantation had higher risk of death-censored kidney graft loss (HR 1.56, 95% CI 1.04, 2.32, p = 0.03). Each month beyond three yr between kidney and pancreas transplantation incurred 1% higher risk of subsequent death-censored kidney graft loss (HR 1.01, 95% CI 1.001, 1.02, p = 0.03). In conclusion, time interval between pancreas and kidney transplantation is an independent risk factor of kidney graft loss following pancreas transplantation. Shortening the time interval between pancreas and kidney transplantation to less than three yr may reduce the risk of kidney graft loss in qualified PAK transplant candidates. Fu L. Luan, Mallika Kommareddi, Diane M. Cibrik, Millie Samaniego and Akinlolu O. Ojo Internal Medicine, Division of Nephrology, University of Michigan, Ann Arbor, MI, USA Key words: death-censored kidney graft failure pancreas after kidney transplantation time interval Abbreviations: amdrd, abbreviated Modification of Diet in Renal Disease; ANOVA, analysis of variance; ATG, anti-thymocyte globulin; BMI, body mass index; CI, confidence interval; CNIs, calcineurin inhibitors; DCD, donor after cardiac death; ECD, expanded criteria donor; egfr, estimated glomerular filtration rate; ESRD, end-stage renal disease; HLA, human leukocyte antigens; HR, hazard ratio; HRSA, Health Resources and Services Administration; IL2, interleukin 2; IRB, institutional review board; OPTN/SRTR, Organ Procurement and Transplantation Network/ Scientific Registry of Transplant Recipients; PAK, pancreas after kidney; PRA, panel reactive antibodies; SCD, standard criteria donor. Corresponding author: Fu L. Luan, MD, Internal Medicine, Division of Nephrology, University of Michigan, 3914 Taubman Center, Box 0364, 1500 East Medical Center Drive, Ann Arbor, MI , USA. Tel.: ; fax: ; fluan@med.umich.edu Conflict of interest: The authors of this manuscript have no conflicts of interest to disclose. Accepted for publication 19 July 2011 Pancreas after kidney (PAK) transplantation is one of the accepted pancreas transplant modalities (1, 2). PAK transplantation allows uremic type 1 diabetic patients to receive a life-saving kidney transplant first and then a subsequent pancreas transplant to correct hyperglycemia (3). Historically, PAK transplants have a lower pancreas graft survival rate compared with simultaneous pancreas 403
2 Luan et al. and kidney transplants although lately some singlecenter studies have reported comparable results (3 5). Furthermore, one study has suggested that PAK transplant recipients had inferior patient survival compared with wait-listed PAK candidates treated with conventional insulin therapy (6). Several investigators over the years have examined the potential risk factors associated with poor PAK outcome, including the timing elapsed between pancreas and kidney transplantation (7, 8). The number of patients included in these studies was limited. One recent study, however, did show that timing of pancreas transplantation has an impact on the clinical outcome as the time interval between kidney and pancreas transplantation longer than one yr was associated with inferior uncensored kidney graft survival post-pancreas transplantation (8). We hypothesized that the longer time interval between kidney and pancreas transplantation could predispose kidney transplant to the development of chronic injuries, immunologic or not, and thus negatively impact kidney graft and/or patient survival after pancreas transplantation. We undertook a retrospective analysis of national registry data to determine the effect of time interval on pancreas and kidney graft survival and mortality risk among PAK transplant patients. Materials and methods We included all adult primary PAK transplants performed between January 1, 1996 and December 31, 2005 in the United States with follow-up until November 1, Data were collected and provided by the Organ Procurement and Transplantation Network (OPTN)/Scientific Registry of Transplant Recipients (SRTR). The SRTR data system includes data on all donors, wait-listed candidates, and transplant recipients in the United States, submitted by the members of the OPTN, and has been described elsewhere (9). The Health Resources and Services Administration (HRSA), US Department of Health and Human Services, provides oversight to the activities of the OPTN and SRTR contractors. The study was approved by the Institutional Review Board (IRB). We identified the date of kidney and pancreas transplantation and calculated the time interval elapsed between kidney and pancreas transplantation. This time interval was then utilized either as a categorical variable separating all PAK transplant recipients into three groups (less than one yr, one to less than three yr, and greater than or equal to three yr) or as a continuous variable (months) and incorporated into multivariate analyses separately. As Group 3 included a larger proportion of kidney transplant patients from 1995 or earlier, to account for the possible influence of era in transplant care, we created era 1995 or earlier and era after 1995 as an indicator variable. This era covariate was incorporated into all multivariate analyses. In addition, baseline recipient- and donor-related characteristics were examined and used in multivariate analyses as well. Other important variables considered in the multivariate analyses included the baseline renal allograft function post-kidney transplant and at the time of pancreas transplantation, expressed as estimated glomerular filtration rate (egfr) and calculated using the abbreviated Modification of Diet in Renal Disease (amdrd) prediction equation, surgical modality in exocrine pancreas drainage (bladder vs. enteric), the use of various immunosuppressive agents at the time of kidney and pancreas transplantation, induction and maintenance, and center volume of pancreas transplants performed at a given year. Demographic and baseline characteristics from the time of pancreas transplantation were compared using ANOVA and chi-square test among the three groups of PAK patients. The time at risk of the outcomes of interest, death and deathcensored kidney graft loss, started at the time of pancreas transplantation as both outcomes could not happen prior to pancreas transplantation by the nature of study design. Kaplan Meier survival analyses were carried out for composite event-free survival, for death-censored pancreas and kidney transplants survival, and patient survival. Several sets of multivariate Cox proportional hazards regression models using a backward selection approach were performed to assess the effects of time interval and to identify other independent risk factors on death-censored pancreas and kidney graft loss and death. Analyses were performed using SAS 9.1, (Cary, NC, USA) and statistical significance was set at p Results We identified a total of 1853 PAK transplant recipients during the study period with complete information on the date of both organ transplants and clinical follow-up. The mean and median time between kidney and pancreas transplant was 31.7 (±35.8) and 17.1 (0.1, 200.7) months, respectively. The mean age was 41.5 (±7.6) yr. African American patients accounted for 7.3% of PAK patients. The majority of kidney transplants were from a living donor (70.9%). The mean egfr at the time of pancreas transplant was 60.4 (±17.8) ml/min. 404
3 Time interval and PAK transplantation PAK transplant recipients were separated into three groups according to the time interval between kidney and pancreas transplantation: Group 1 with less than one yr, Group 2 from one to less than three yr, and Group 3 with three or more years between the two transplant events. PAK transplant recipients from the three groups differed in several demographic and baseline characteristics (Table 1). PAK transplant recipients from Group 3 were older (42.9 yr vs and 41.1 yr in Group 1 and 2, respectively, p < 0.001) and had shorter duration of diabetes at kidney transplant (24.8 yr vs and 25.0 yr in Group 1 and 2, respectively, p = 0.002). They received less often a preemptive kidney transplant (16.3% vs. 32.1% and 26.7% in Group 1 and 2, respectively, p < 0.001) and had fewer living donor kidney transplants (60.6% vs. 77.3% and 72.3% in Group 1 and 2, respectively, p < 0.001), although the kidney donor age was younger for Group 3 PAK transplant recipients (34.9 yr vs and 38.5 yr in Group 1 and 2, respectively, p < 0.001). Bladder drainage of pancreas transplant was more frequently utilized among patients from Group 3 (48.4% vs. 38.3% and 30.4% in Group 1 and 2, respectively, p < 0.001). There were also significant differences in immunosuppression regimens at the time of kidney transplantation as PAK transplant recipients from Group 3 often received no induction (71.8% vs. 44.5% and 49.7% in Group 1 and 2, respectively, p < 0.001), more frequently used cyclosporine (81.7% vs. 36.1% and 47.2% in Group 1 and 2, respectively, p < 0.001) and less frequently mycophenolates (32.2% vs. 73.7% and 73.3% in Group 1 and 2, respectively, p < 0.001). However, at the time of pancreas transplantation, the difference in immunosuppression regimens was much less striking (Table 1). While baseline renal function post-kidney transplant was comparable, the renal function at the time of pancreas transplantation was significantly lower for PAK transplant recipients in Group 3 (57.2 vs and 61.6 ml/min in Group 1 and 2, respectively, p < 0.001). Following pancreas transplantation, PAK transplant recipients from Group 3 displayed overall inferior clinical outcome (Fig. 1A, log-rank p = 0.01). This was mainly related to reduced death-censored kidney graft survival as well as patient survival (Fig. 1B and C, log-rank p < and p < 0.001, respectively). Pancreas allograft survival, early (within 90 d) and during subsequent years, was not different between the three groups (data not shown). Multivariate Cox proportional hazards regression analyses demonstrated that the time interval equal to or greater than three yr between kidney and pancreas transplantation was independently and significantly associated with increased risk of deathcensored kidney graft loss (HR 1.56, 95% CI 1.04, 2.32, p = 0.03 with era as a covariate) (Table 2). This was further confirmed in an alternate analysis using the time interval between kidney and pancreas transplantation as a continuous variable. Each month beyond three yr between kidney and pancreas transplantation incurred 1% increase in the risk of kidney graft loss (HR 1.01, 95% CI 1.001, 1.02, p = 0.03). As an alternative analytic approach, we performed a different set of multivariate Cox proportional hazards regression analyses using pancreas transplantation as a timedependent covariate and with starting point at the time of kidney transplantation, and we found an even greater increase in the risk associated with longer time interval (HR 1.66, 95% CI 1.18, 2.35, p = for time interval between one and less than three yr and HR 2.27, 95% CI 1.54, 3.33, p < for time interval greater than or equal to three yr, respectively) although we felt that a greater bias was created because of inclusion of all patients prior to pancreas transplantation in the reference group as they were not at risk for the study outcomes (death and kidney graft loss) until after their pancreas transplantation. Other factors contributing to the risk of kidney graft loss following pancreas transplantation included older kidney donor age (HR 1.01, 95% CI 1.003, 1.03, p = 0.011), the use of kidneys from expanded criteria donor (ECD) and/or donor after cardiac death (DCD) (HR 2.38, 95% CI 1.63, 3.48, p < 0.001), and the use of alemtuzumab as an induction agent at the time of kidney transplantation (HR 3.11, 95% CI 1.24, 7.76, p = 0.015). On the other hand, older recipient age and higher renal function at the time of pancreas transplantation were associated with reduced risk of subsequent kidney graft loss (Table 2). The duration of diabetes exposure up to the time of kidney transplantation did not appear to negatively impact kidney graft survival post-pancreas transplantation. Furthermore, the time interval between kidney and pancreas transplantation did not appear to be associated with increased risk of death when the era effect was incorporated into the model (Table 3). Other factors that negatively affected patient survival included older recipient age at the time of pancreas transplantation (HR 1.03, 95% CI 1.01, 1.06, p = 0.002), previous dialysis history (HR 1.74, 95% CI 1.30, 2.33, p < 0.001), history of peripheral vascular disease (HR 1.58, 95% CI 1.17, 2.79, p = 0.003), history of coronary artery disease (HR 1.51, 95% CI 1.16, 1.97, p = 0.002), and African American kidney donor (HR 1.95, 405
4 Luan et al. Table 1. Demographic and baseline characteristics of study patient population Group 1 Group 2 Group 3 N = 726 N = 592 N = 535 p Age, yr (SD) 40.9 (7.9) 41.1 (7.8) 42.9 (6.9) <0.001 Gender: male (%) 416 (57.3) 354 (59.8) 308 (57.6) Race: African American (%) 45 (6.2) 52 (8.8) 38 (7.1) BMI, kg/m 2 (SD) 24.9 (4.1) 25.5 (4.2) 25.1 (4.2) Duration of diabetes at kidney transplant, yr (SD) 26.2 (7.9) 25.0 (7.9) 24.8 (6.5) Dialysis history, yes (%) 493 (67.9) 434 (73.3) 448 (83.7) <0.001 Angina/coronary artery disease, yes (%) 129 (17.8) 103 (17.4) 81 (15.1) History of blood transfusion, yes (%) 301 (41.5) 267 (45.1) 282 (52.7) <0.001 Peripheral vascular disease, yes (%) 60 (8.2) 66 (11.2) 65 (12.2) Cerebrovascular disease, yes (%) 19 (2.6) 20 (3.4) 14 (2.6) History of hypertension, yes (%) 574 (79.1) 465 (78.6) 379 (70.8) Kidney donor type (%) Living 561 (77.3) 428 (72.3) 324 (60.6) <0.001 SCD 142 (19.6) 136 (23.0) 139 (26.0) ECD or DCD 23 (3.2) 28 (4.7) 72 (13.5) Kidney donor age, yr (SD) 40.1 (12.5) 38.5 (12.6) 34.9 (13.5) <0.001 Pancreas donor age, yr (SD) 26.8 (10.9) 26.0 (10.4) 26.1 (11.1) Kidney donor race: African American (%) 38 (5.2) 35 (5.9) 25 (4.7) Kidney donor gender: male (%) 274 (46.3) 326 (44.9) 270 (50.5) Era of kidney transplant: 1995 or earlier (%) 18 (2.5) 45 (7.6) 305 (57.0) <0.001 egfr 6 months post-kidney transplant, ml/min (SD) 58.8 (19.0) 60.0 (17.9) 59.4 (17.5) egfr at pancreas transplantation, ml/min (SD) 61.4 (17.6) 61.6 (17.6) 57.2 (18.2) <0.001 HLA mismatches at kidney transplantation (SD) 2.78 (1.81) 2.66 (1.85) 2.42 (1.80) HLA mismatches at pancreas transplantation (SD) 3.8 (1.4) 4.0 (1.3) 3.9 (1.5) Peak PRA at pancreas transplantation (SD) 7.5 (18.0) 9.7 (21.2) 11.9 (23.0) Bladder drainage of pancreas, yes (%) 278 (38.3) 180 (30.4) 359 (48.4) <0.001 CNIs at kidney transplantation (%) None 38 (5.2) 30 (5.1) 14 (2.6) <0.001 Cyclosporine 262 (36.1) 279 (47.2) 437 (81.7) Tacrolimus 426 (58.7) 283 (47.8) 84 (15.7) Anti-metabolites at kidney transplantation (%) None 57 (7.9) 43 (7.3) 54 (10.1) <0.001 Mycophenolates 535 (73.7) 434 (73.3) 172 (32.2) Sirolimus/everolimus 70 (9.6) 42 (7.1) 22 (4.1) Imuran and others 64 (8.8) 73 (12.3) 287 (53.6) Steroids at kidney transplantation, yes (%) 678 (93.4) 577 (97.5) 528 (98.7) <0.001 Induction at kidney transplantation (%) None 323 (44.5) 294 (49.7) 384 (71.8) <0.001 ATG/Thymoglobulin 228 (31.4) 129 (21.8) 95 (17.8) Anti-IL2 receptor antibodies 151 (20.8) 161 (27.2) 56 (10.5) Alemtuzumab 24 (3.3) 8 (1.4) 0 (0) CNIs at pancreas transplantation (%) None 64 (8.8) 60 (10.1) 40 (7.5) Cyclosporine 75 (10.3) 89 (15.0) 70 (13.1) Tacrolimus 587 (80.9) 443 (74.8) 425 (79.4) Anti-metabolites at pancreas transplantation (%) None 83 (11.4) 58 (9.8) 49 (9.2) Mycophenolates 566 (78.0) 473 (79.9) 413 (77.2) Sirolimus/everolimus 65 (9.0) 49 (8.3) 59 (11.0) Imuran/others 12 (1.7) 12 (2.0) 14 (2.6) Steroids at pancreas transplantation, yes (%) 674 (92.8) 562 (94.9) 506 (94.6) Induction at pancreas transplantation (%) None 193 (26.6) 152 (25.7) 134 (25.1) <0.001 ATG/thymoglobulin 382 (52.6) 298 (50.4) 277 (51.7) Anti-IL2 receptor antibodies 83 (11.4) 104 (17.6) 100 (18.7) Alemtuzumab 68 (9.4) 38 (6.4) 24 (4.5) BMI, body mass index; HLA, human leukocyte antigens; PRA, panel reactive antibodies; SCD, standard criteria donor; ECD, expanded criteria donor; DCD, donor after cardiac death; egfr, estimated glomerular filtration rate; ATG, anti-thymocyte globulin. 406
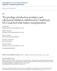
5 Time interval and PAK transplantation A Composite event-free survival B Kidney graft survival C Patients survival 100% 80% 60% 40% 20% 0% 100% 80% 60% 40% 20% 0% 100% 80% 60% 40% 20% 0% LogRank, p = 0.01 < 1 year 1 to < 3 years = > 3 years Years after pancreas transplantation LogRank, p < < 1 year 1 to < 3 years = > 3 years Years after pancreas transplantation LogRank, p < < 1 year 1 to < 3 years = > 3 years Years after pancreas transplantation Fig. 1. Kaplan Meier survival analyses among three groups of pancreas after kidney transplant patients: (A) composite eventfree survival, (B) death-censored kidney graft survival and (C) patient survival. 95% CI 1.29, 2.94, p = 0.001). Higher body mass index and renal function at the time of pancreas transplantation were associated with lower risk of death (HR 0.95, 95% CI 0.93, 0.98, p = and HR 0.99, 95% CI 0.98, 0.994, p < 0.001, respectively). Although the changing in renal function over the time, expressed as the slop, was not significantly different among the three groups (0.24 ± 4.42, 0.18 ± 1.70, and )0.03 ± 0.39 for patients from Groups 1, 2, and 3, respectively, p = 0.25), egfr at the time of pancreas transplantation was significantly lower for PAK patients from Group 3 and was independently associated with post-pancreas transplant outcomes. We further investigated the impact of actual egfr divided according to three tertiles (Table 4). Patients in the highest tertile had egfr equal to or >65 ml/min, those in the midtertile between 50 and <65 ml/min, and those in the lowest tertile <50 ml/min. Using patients in the highest tertile as a reference group, patients with egfr in the mid- and lower tertiles had 27% and 93% higher risk of death-censored kidney graft loss (p = 0.19 and p < 0.001, respectively). Similarly, patients with egfr in the mid- and lower tertiles had 51% and 95% higher risk of death (p = and p < 0.001, respectively). Discussion This study demonstrates that the time interval between kidney and pancreas transplantation independently impacts the clinical outcome of PAK transplantation, in particular, death-censored kidney graft survival. There appears to be a threshold effect, namely, a time interval equal to or greater than three yr between the two transplant events was associated with a significant increase in the risk of death-censored kidney graft loss that was independent of kidney function at the time of pancreas transplantation. Speculation on possible mechanisms for this negative effect of longer time interval could involve the progressive development of kidney graft injuries with the time, immunologic or not such as subclinical acute rejection, calcineurin inhibitor (CNI) nephrotoxicity, and continued exposure to the diabetic environment, etc. (10 14). On the other hand, the time interval did not appear to negatively impact patient survival following pancreas transplant when the effect of era in which kidney transplantation was performed was taken into consideration. In addition, renal function at the time of pancreas transplantation played an important role in determining the clinical outcome of post-pancreas transplantation. These findings should help the transplant community to provide appropriate counseling for qualified type 1 diabetic kidney transplant patients in pursue of pancreas transplantation. PAK transplantation is one of the pancreas transplant modalities endorsed by the American Diabetes Association for qualified patients with diabetic end-stage renal disease (ESRD) who had a successful kidney transplant (2). As the life-saving property of a kidney transplant has been firmly established (15), the major advantage of PAK transplantation is to allow patients with type 1 407
6 Luan et al. Table 2. Clinical correlates of kidney graft loss following pancreas transplantation Variables Hazard ratio 95% CI p Model 1 a Years between transplantations 0.07 <1 yr Ref. Ref. Ref. 1 to <3 yr , yr , Duration of diabetes , at kidney transplant (yr) Age at pancreas , 0.98 <0.001 transplantation (yr) egfr at pancreas , transplantation (ml/min) Kidney donor age (yr) , Kidney donor type <0.001 Living Ref. Ref. Ref. SCD , ECD or DCD , 3.48 <0.001 Induction at kidney 0.07 transplant None Ref. Ref. Ref. ATG/thymoglobulin , Anti-IL 2 receptor , antibodies Alemtuzumab , Model 2 b Months between transplantations All , <0.001 <1 yr , to <3 yr , yr , SCD, standard criteria donor; ECD, expanded criteria donor; DCD, donor after cardiac death; egfr, estimated glomerular filtration rate; ATG, anti-thymocyte globulin. a Time interval as categorical variable. b Time intervals as continuous variable. Table 3. Clinical correlates of death following pancreas transplantation Variables Hazard ratio 95% CI p Model 1 a Years between transplantations 0.24 <1 yr Ref. Ref. Ref. 1 to <3 yr , yr , Age at pancreas , transplantation (yr) Recipient BMI at , pancreas transplantation (kg/m 2 ) egfr at pancreas , <0.001 transplantation (ml/min) History of peripheral , vascular disease, yes History of coronary , artery disease, yes African American , kidney donor, yes Dialysis history, yes , Induction at pancreas <0.001 transplantation None Ref. Ref. Ref. ATG/thymoglobulin , Anti-IL 2 receptor , antibodies Alemtuzumab , Model 2 b Months between transplantations , BMI, body mass index; egfr, estimated glomerular filtration rate; ATG, antithymocyte globulin. a Time interval as a categorical variable. b Time intervals as continuous variable. diabetic ESRD to receive a living donor kidney transplant as soon as this is available, while still having the possibility of receiving a pancreas transplant later on. This approach also has the potential to increase both the deceased donor kidney and pancreas pools (16). Notwithstanding this benefit, one of the main concerns of this approach is the potentially negative effect that pancreas transplantation can have on the function and the lifespan of previous kidney transplant (1, 6, 15). A few studies have addressed the question of whether the time interval elapsed between the two transplant procedures impacts the outcome of PAK transplantation (7, 8). Chronic kidney allograft injuries, in the form of interstitial fibrosis and tubular atrophy, can be detected as early as within the first year of kidney transplantation, either as a result of undetected subclinical acute rejection or CNI nephrotoxicity, and increase progressively with time (10, 13, 14, 17). Furthermore, continued diabetes exposure following kidney transplantation has also been shown to cause renal transplant injuries (11, 12). In one study, PAK transplant recipients who received a pancreas transplant with a time interval between the two transplant procedures greater than four months had no difference in outcomes when compared with those with a time interval less than four months (7). On the other hand, one recent study involving 126 PAK transplant recipients reported that a time interval greater than one yr between kidney and Table 4. Renal function at pancreas transplant and clinical outcome Renal function a (mean ± SD, ml/min) Adjusted HR 95% CI p Kidney graft failure egfr 65 (79.5 ± 15.4) Ref. Ref. Ref. egfr 50 to <65 (56.9 ± 4.4) , egfr <50 (42.9 ± 5.0) , 2.77 <0.001 Death egfr 65 (79.5 ± 15.4) Ref. Ref. Ref. egfr 50 to <65 (56.9 ± 4.4) , egfr <50 (42.9 ± 5.0) , 2.62 <0.001 a Abbreviated Modification of Diet in Renal Disease formula. egfr, estimated glomerular filtration rate. 408
7 Time interval and PAK transplantation pancreas transplantation affected subsequent uncensored kidney graft loss but the impact on death-censored graft survival and patient survival was not separately addressed and the direction of such effect was not clear from their analyses (8). Thus, our study provides additional information that may be helpful in the assessment of the benefit and risk when PAK transplantation is considered. The importance of renal function prior to PAK transplantation on the subsequent kidney graft survival has been recognized by several investigators (1, 8, 18). Our study is in full agreement with these previous observations, and in addition, we demonstrated that the levels of kidney function at the time of PAK transplantation, independent of time interval between kidney and pancreas transplantation, impact the risk of death, which is consistent with similar observation among kidney transplant patients (19). Although we did not identify a threshold of renal function levels below which PAK transplantation should not be recommended, an appropriate counseling for patients seeking a PAK transplant with emphasis on the degree of renal function should be provided. Our study has several major limitations. First, as this is a retrospective national registry data analysis, the bias in patient selection for pancreas transplantation and post-transplant care by individual transplant centers could not be accounted for. For the same reason, the conclusion relies heavily on the accuracy of data collection from individual transplant centers reported to OPTN/ SRTR. Second, separation of patients into three groups was somewhat arbitrary and without a particular rationale; thus, as a consequence, the patients from the three groups were dissimilar on many aspects. In particular, patients from Group 3 were more likely to have their kidney transplant from an early era (prior to 1995) and had more frequent use of cyclosporine as the initial CNI and less use of mycophenolates as an anti-proliferative agent. Although we adjusted for these and other variables in our multivariate analyses, this adjustment may have not eliminated the impact stemmed from the difference in care and in immunosuppressive regimens over the years. Third, the lack of detailed and important clinical information regarding clinical events such as the occurrence of biopsy proven rejection, CNI nephrotoxicity and infection, the degree of glycemia control and the presence of proteinuria prior to pancreas transplantation, etc., prevents us from pinpointing the specific mechanisms of our findings. Finally, our observations do not address the question whether having a pancreas transplant is better than not having it when the waiting time for a pancreas transplant is long and renal function is suboptimal. Thus, the time interval need not be used as a sole criteria to determine whether a qualified type 1 diabetic kidney transplant patient should receive a pancreas transplant or not. Rather, it should be considered in conjunction with many other factors such as the stability of kidney transplant and the degree of renal function as our study shows that better renal function was associated with good clinical outcome following pancreas transplantation. In conclusion, longer time interval beyond three yr following kidney transplantation and reduced renal function were independently associated with an increased risk of kidney graft loss in PAK transplant recipients. Thus, reducing the waiting time for qualified type 1 diabetic kidney transplant patients and optimizing their renal function prior to pancreas transplantation should be emphasized. Acknowledgements The data reported in this article have been supplied by the Arbor Research Collaborative for Health (Arbor Research) as the contractor for the Scientific Registry of Transplant Recipients (SRTR). The interpretation and reporting of these data are the responsibility of the author(s) and in no way should be seen as an official policy of or interpretation by the SRTR or the US Government. Portion of material was presented as an oral presentation in American Transplant Congress 2010, San Diego, California, May 1 5, References 1. Larson TS, Bohorquez H, Rea DJ et al. Pancreasafter-kidney transplantation: an increasingly attractive alternative to simultaneous pancreas-kidney transplantation. Transplantation 2004: 77: Robertson P, Davis C, Larsen J, Stratta R, Sutherland DE. Pancreas transplantation in type 1 diabetes. Diabetes Care 2004: 27(Suppl 1): S Kleinclauss F, Fauda M, Sutherland DE et al. Pancreas after living donor kidney transplants in diabetic patients: impact on long-term kidney graft function. Clin Transplant 2009: 23: McCullough KP, Keith DS, Meyer KH, Stock PG, Brayman KL, Leichtman AB. Kidney and pancreas transplantation in the United States, : access for patients with diabetes and end-stage renal disease. Am J Transplant 2009: 9(4 Pt 2): Fridell JA, Joseph Tector A, Mangus RS, Kazimi MM, Hollinger EF, Vianna RM. A new vascular approach to the modified multivisceral graft procurement. Clin Transplant 2009: 23: Venstrom JM, McBride MA, Rother KI, Hirshberg B, Orchard TJ, Harlan DM. Survival after pancreas transplantation in patients with diabetes and preserved kidney function. JAMA 2003: 290: Humar A, Sutherland DE, Ramcharan T, Gruessner RW, Gruessner AC, Kandaswamy R. Optimal timing 409
8 Luan et al. for a pancreas transplant after a successful kidney transplant. Transplantation 2000: 70: Pavlakis M, Khwaja K, Mandelbrot D et al. Renal allograft failure predictors after PAK transplantation: results from the New England Collaborative Association of Pancreas Programs. Transplantation 2010: 89: Dickinson DM, Ellison MD, Webb RL. Data sources and structure. Am J Transplant 2003: 3(Suppl 4): Nankivell BJ, Borrows RJ, Fung CL, OÕconnell PJ, Allen RD, Chapman JR. The natural history of chronic allograft nephropathy. N Engl J Med 2003: 349: Yamamoto I, Yamamoto H, Mitome J et al. Secondary focal segmental glomerulosclerosis following kidney transplantation in a patient with type I diabetes mellitus. Clin Transplant 2006: 20(Suppl 15): Salifu MO, Nicastri AD, Markell MS, Ghali H, Sommer BG, Friedman EA. Allograft diabetic nephropathy may progress to end-stage renal disease. Pediatr Transplant 2004: 8: Nankivell BJ, Borrows RJ, Fung CL, OÕconnell PJ, Allen RD, Chapman JR. Natural history, risk factors, and impact of subclinical rejection in kidney transplantation. Transplantation 2004: 78: Baboolal K, Jones GA, Janezic A, Griffiths DR, Jurewicz WA. Molecular and structural consequences of early renal allograft injury. Kidney Int 2002: 61: Wolfe RA, Ashby VB, Milford EL et al. Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N Engl J Med 1999: 341: Weiss AS, Smits G, Wiseman AC. Simultaneous pancreas-kidney versus deceased donor kidney transplant: can a fair comparison be made? Transplantation 2009: 87: Kaneku HK, Terasaki PI. Thirty year trend in kidney transplants: UCLA and UNOS Renal Transplant Registry. Clin Transpl 2006: Hariharan S, Pirsch JD, Lu CY et al. Pancreas after kidney transplantation. J Am Soc Nephrol 2002: 13: Meier-Kriesche HU, Baliga R, Kaplan B. Decreased renal function is a strong risk factor for cardiovascular death after renal transplantation. Transplantation 2003: 75:
Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
 Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Influence of Recipient Race on the Outcome of Simultaneous Pancreas and Kidney Transplantation
 American Journal of Transplantation 2010; 10: 2074 2081 Wiley Periodicals Inc. C 2010 The Authors Journal compilation C 2010 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2010; 10: 2074 2081 Wiley Periodicals Inc. C 2010 The Authors Journal compilation C 2010 The American Society of Transplantation and the American Society of Transplant
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
Article. Simultaneous Pancreas Kidney Transplant versus Other Kidney Transplant Options in Patients with Type 2 Diabetes
 Article Simultaneous Pancreas Kidney Transplant versus Other Kidney Transplant Options in Patients with Type 2 Diabetes Alexander C. Wiseman* and Jane Gralla Summary Background and objectives Current organ
Article Simultaneous Pancreas Kidney Transplant versus Other Kidney Transplant Options in Patients with Type 2 Diabetes Alexander C. Wiseman* and Jane Gralla Summary Background and objectives Current organ
J Am Soc Nephrol 14: , 2003
 J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
Should Pediatric Patients Wait for HLA-DR-Matched Renal Transplants?
 American Journal of Transplantation 2008; 8: 2056 2061 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2008; 8: 2056 2061 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
Pancreas After Islet Transplantation: A First Report of the International Pancreas Transplant Registry
 American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
 Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
Chapter 6: Transplantation
 Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Kidney and Pancreas Transplantation in the United States,
 American Journal of Transplantation 2006; 6 (Part 2): 1153 1169 Blackwell Munksgaard No claim to original US government works Journal compilation C 2006 The American Society of Transplantation and the
American Journal of Transplantation 2006; 6 (Part 2): 1153 1169 Blackwell Munksgaard No claim to original US government works Journal compilation C 2006 The American Society of Transplantation and the
Access and Outcomes Among Minority Transplant Patients, , with a Focus on Determinants of Kidney Graft Survival
 American Journal of Transplantation 2010; 10 (Part 2): 1090 1107 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
American Journal of Transplantation 2010; 10 (Part 2): 1090 1107 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
Literature Review Transplantation
 Literature Review 2010- Transplantation Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney and Pancreas Transplant Programs University of
Literature Review 2010- Transplantation Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney and Pancreas Transplant Programs University of
Long-Term Renal Allograft Survival in the United States: A Critical Reappraisal
 American Journal of Transplantation 2011; 11: 450 462 Wiley Periodicals Inc. C 2010 The Authors Journal compilation C 2010 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2011; 11: 450 462 Wiley Periodicals Inc. C 2010 The Authors Journal compilation C 2010 The American Society of Transplantation and the American Society of Transplant
Prevalence and Outcomes of Multiple-Listing for Cadaveric Kidney and Liver Transplantation
 American Journal of Transplantation 24; 4: 94 1 Blackwell Munksgaard Copyright C Blackwell Munksgaard 23 doi: 1.146/j.16-6135.23.282.x Prevalence and Outcomes of Multiple-Listing for Cadaveric Kidney and
American Journal of Transplantation 24; 4: 94 1 Blackwell Munksgaard Copyright C Blackwell Munksgaard 23 doi: 1.146/j.16-6135.23.282.x Prevalence and Outcomes of Multiple-Listing for Cadaveric Kidney and
The New Kidney Allocation System: What You Need to Know. Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health
 The New Kidney Allocation System: What You Need to Know Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health ~6% of patients die each year on the deceased donor waiting
The New Kidney Allocation System: What You Need to Know Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health ~6% of patients die each year on the deceased donor waiting
Simultaneous Pancreas Kidney Transplantation:
 Simultaneous Pancreas Kidney Transplantation: What is the added advantage, and for whom? Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney
Simultaneous Pancreas Kidney Transplantation: What is the added advantage, and for whom? Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney
Literature Review: Transplantation July 2010-June 2011
 Literature Review: Transplantation July 2010-June 2011 James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Kidney Transplant Top 10 List: July Kidney
Literature Review: Transplantation July 2010-June 2011 James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Kidney Transplant Top 10 List: July Kidney
Are two better than one?
 Are two better than one? Disclosures Ryutaro Hirose, MD Professor in Clinical Surgery University of California, San Francisco I have no relevant disclosures related to this presentation The PROBLEM There
Are two better than one? Disclosures Ryutaro Hirose, MD Professor in Clinical Surgery University of California, San Francisco I have no relevant disclosures related to this presentation The PROBLEM There
Kidney Transplant Outcomes In Elderly Patients. Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania
 Kidney Transplant Outcomes In Elderly Patients Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Case Discussion 70 year old Asian male, neuropsychiatrist, works full
Kidney Transplant Outcomes In Elderly Patients Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Case Discussion 70 year old Asian male, neuropsychiatrist, works full
Obesity has become an epidemic in the United States
 Original Clinical ScienceçGeneral Selected Mildly Obese Donors Can Be Used Safely in Simultaneous Pancreas and Kidney Transplantation Tarek Alhamad, MD, MS, 1,2 Andrew F. Malone, MD, 1 Krista L. Lentine,
Original Clinical ScienceçGeneral Selected Mildly Obese Donors Can Be Used Safely in Simultaneous Pancreas and Kidney Transplantation Tarek Alhamad, MD, MS, 1,2 Andrew F. Malone, MD, 1 Krista L. Lentine,
Trends in Organ Donation and Transplantation in the United States,
 American Journal of Transplantation 2010; 10 (Part 2): 961 972 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
American Journal of Transplantation 2010; 10 (Part 2): 961 972 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
For more information about how to cite these materials visit
 Author(s): Silas P. Norman, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Silas P. Norman, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Long-term prognosis of BK virus-associated nephropathy in kidney transplant recipients
 Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
OUT OF DATE. Choice of calcineurin inhibitors in adult renal transplantation: Effects on transplant outcomes
 nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
Reduced graft function (with or without dialysis) vs immediate graft function a comparison of long-term renal allograft survival
 Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Current status of kidney and pancreas transplantation in the United States,
 American Journal of Transplantation 25; 5 (Part 2): 94 915 Blackwell Munksgaard Blackwell Munksgaard 25 Current status of kidney and pancreas transplantation in the United States, 1994 23 Gabriel M. Danovitch
American Journal of Transplantation 25; 5 (Part 2): 94 915 Blackwell Munksgaard Blackwell Munksgaard 25 Current status of kidney and pancreas transplantation in the United States, 1994 23 Gabriel M. Danovitch
Progress in Pediatric Kidney Transplantation
 Send Orders for Reprints to reprints@benthamscience.net The Open Urology & Nephrology Journal, 214, 7, (Suppl 2: M2) 115-122 115 Progress in Pediatric Kidney Transplantation Jodi M. Smith *,1 and Vikas
Send Orders for Reprints to reprints@benthamscience.net The Open Urology & Nephrology Journal, 214, 7, (Suppl 2: M2) 115-122 115 Progress in Pediatric Kidney Transplantation Jodi M. Smith *,1 and Vikas
Improved patient survival with simultaneous pancreas and kidney transplantation in recipients with diabetic end-stage renal disease
 Diabetologia (2013) 56:1364 1371 DOI 10.1007/s00125-013-2888-y ARTICLE Improved patient survival with simultaneous pancreas and kidney transplantation in recipients with diabetic end-stage renal disease
Diabetologia (2013) 56:1364 1371 DOI 10.1007/s00125-013-2888-y ARTICLE Improved patient survival with simultaneous pancreas and kidney transplantation in recipients with diabetic end-stage renal disease
Impact of graft implantation order on graft survival in simultaneous pancreas kidney transplantation
 Transplant International ORIGINAL ARTICLE Impact of graft implantation order on graft survival in simultaneous pancreas kidney transplantation Nadja Niclauss, Beno^ıt Bedat, Philippe Morel, Axel Andres,
Transplant International ORIGINAL ARTICLE Impact of graft implantation order on graft survival in simultaneous pancreas kidney transplantation Nadja Niclauss, Beno^ıt Bedat, Philippe Morel, Axel Andres,
Kidney and Pancreas Transplantation in the United States, : Access for Patients with Diabetes and End-Stage Renal Disease
 American Journal of Transplantation 29; 9 (Part 2): 894 96 Wiley Periodicals Inc. No claim to original US government works Journal compilation C 29 The American Society of Transplantation and the American
American Journal of Transplantation 29; 9 (Part 2): 894 96 Wiley Periodicals Inc. No claim to original US government works Journal compilation C 29 The American Society of Transplantation and the American
BK virus infection in renal transplant recipients: single centre experience. Dr Wong Lok Yan Ivy
 BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
Geographic Differences in Event Rates by Model for End-Stage Liver Disease Score
 American Journal of Transplantation 2006; 6: 2470 2475 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2006; 6: 2470 2475 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
Acute rejection and late renal transplant failure: Risk factors and prognosis
 Nephrol Dial Transplant (2004) 19 [Suppl 3]: iii38 iii42 DOI: 10.1093/ndt/gfh1013 Acute rejection and late renal transplant failure: Risk factors and prognosis Luis M. Pallardo Mateu 1, Asuncio n Sancho
Nephrol Dial Transplant (2004) 19 [Suppl 3]: iii38 iii42 DOI: 10.1093/ndt/gfh1013 Acute rejection and late renal transplant failure: Risk factors and prognosis Luis M. Pallardo Mateu 1, Asuncio n Sancho
The Role of Kidney-Pancreas Transplantation in Diabetic Kidney Disease
 Curr Diab Rep (2010) 10:385 391 DOI 10.1007/s11892-010-0136-0 The Role of Kidney-Pancreas Transplantation in Diabetic Kidney Disease Alexander C. Wiseman Published online: 27 July 2010 # The Author(s)
Curr Diab Rep (2010) 10:385 391 DOI 10.1007/s11892-010-0136-0 The Role of Kidney-Pancreas Transplantation in Diabetic Kidney Disease Alexander C. Wiseman Published online: 27 July 2010 # The Author(s)
Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function
 ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
Allogeneic Pancreas Transplant. Description
 Subject: Allogeneic Pancreas Transplant Page: 1 of 12 Last Review Status/Date: June 2015 Allogeneic Pancreas Transplant Description Transplantation of a normal pancreas is a treatment method for patients
Subject: Allogeneic Pancreas Transplant Page: 1 of 12 Last Review Status/Date: June 2015 Allogeneic Pancreas Transplant Description Transplantation of a normal pancreas is a treatment method for patients
Incidence of Rejection in Renal Transplant Surgery in the LVHN Population Leading to Graft Failure: 6 Year Review
 Incidence of Rejection in Renal Transplant Surgery in the LVHN Population Leading to Graft Failure: 6 Year Review Jessica Ludolph 1 Lynsey Biondi, MD 1,2 and Michael Moritz, MD 1,2 1 Department of Surgery,
Incidence of Rejection in Renal Transplant Surgery in the LVHN Population Leading to Graft Failure: 6 Year Review Jessica Ludolph 1 Lynsey Biondi, MD 1,2 and Michael Moritz, MD 1,2 1 Department of Surgery,
Wait List Management. John J. Friedewald, Darshika Chhabra, and Baris Ata. The US Transplant System. National Wait List
 Wait List Management John J. Friedewald, Darshika Chhabra, and Baris Ata 4 Abbreviations CDC Centers for Disease Control and Prevention CPRAs Calculated panel reactive antibodies DCD Donation after cardiac
Wait List Management John J. Friedewald, Darshika Chhabra, and Baris Ata 4 Abbreviations CDC Centers for Disease Control and Prevention CPRAs Calculated panel reactive antibodies DCD Donation after cardiac
The Art and Science of Increasing Authorization to Donation
 The Art and Science of Increasing Authorization to Donation OPO Metrics: The Good, The Bad, and The Maybe Charlotte Arrington, MPH Arbor Research Collaborative for Health Alan Leichtman, MD University
The Art and Science of Increasing Authorization to Donation OPO Metrics: The Good, The Bad, and The Maybe Charlotte Arrington, MPH Arbor Research Collaborative for Health Alan Leichtman, MD University
KIDNEY TRANSPLANTATION IS THE
 ORIGINAL CONTRIBUTION Deceased-Donor Characteristics and the Survival Benefit of Kidney Transplantation Robert M. Merion, MD Valarie B. Ashby, MA Robert A. Wolfe, PhD Dale A. Distant, MD Tempie E. Hulbert-Shearon,
ORIGINAL CONTRIBUTION Deceased-Donor Characteristics and the Survival Benefit of Kidney Transplantation Robert M. Merion, MD Valarie B. Ashby, MA Robert A. Wolfe, PhD Dale A. Distant, MD Tempie E. Hulbert-Shearon,
Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation
 Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation July 26, 2006 Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation A paper prepared
Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation July 26, 2006 Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation A paper prepared
Association of Kidney Transplantation with Survival in Patients with Long Dialysis Exposure
 Article Association of Kidney Transplantation with Survival in Patients with Long Dialysis Exposure Caren Rose,* Jagbir Gill,* and John S. Gill* Abstract Background and objectives Evidence that kidney
Article Association of Kidney Transplantation with Survival in Patients with Long Dialysis Exposure Caren Rose,* Jagbir Gill,* and John S. Gill* Abstract Background and objectives Evidence that kidney
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29755 holds various files of this Leiden University dissertation. Author: Moes, Dirk Jan Alie Roelof Title: Optimizing immunosuppression with mtor inhibitors
Cover Page The handle http://hdl.handle.net/1887/29755 holds various files of this Leiden University dissertation. Author: Moes, Dirk Jan Alie Roelof Title: Optimizing immunosuppression with mtor inhibitors
Transplant Update New Kidney Allocation System Transplant Referral Strategies. Antonia Harford, MD University of New Mexico
 Transplant Update New Kidney Allocation System Transplant Referral Strategies Antonia Harford, MD University of New Mexico Financial Disclosures Doctor Harford has received financial support for dialysis
Transplant Update New Kidney Allocation System Transplant Referral Strategies Antonia Harford, MD University of New Mexico Financial Disclosures Doctor Harford has received financial support for dialysis
Kidney Transplant in the Elderly. Robert Santella, M.D., F.A.C.P.
 Kidney Transplant in the Elderly! Robert Santella, M.D., F.A.C.P. Incident Rate of ESRD by Age Age 75+ 65-74 From US Renal Data System, 2012 Should there be an age limit? Various guidelines: Canadian,
Kidney Transplant in the Elderly! Robert Santella, M.D., F.A.C.P. Incident Rate of ESRD by Age Age 75+ 65-74 From US Renal Data System, 2012 Should there be an age limit? Various guidelines: Canadian,
The New Kidney Allocation Policy: Implications for Your Patients and Your Practice
 The New Kidney Allocation Policy: Implications for Your Patients and Your Practice Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Explain
The New Kidney Allocation Policy: Implications for Your Patients and Your Practice Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Explain
MORTALITY IN PATIENTS ON DIALYSIS AND TRANSPLANT RECIPIENTS
 MORTALITY IN PATIENTS ON DIALYSIS AND TRANSPLANT RECIPIENTS COMPARISON OF MORTALITY IN ALL PATIENTS ON DIALYSIS, PATIENTS ON DIALYSIS AWAITING TRANSPLANTATION, AND RECIPIENTS OF A FIRST CADAVERIC TRANSPLANT
MORTALITY IN PATIENTS ON DIALYSIS AND TRANSPLANT RECIPIENTS COMPARISON OF MORTALITY IN ALL PATIENTS ON DIALYSIS, PATIENTS ON DIALYSIS AWAITING TRANSPLANTATION, AND RECIPIENTS OF A FIRST CADAVERIC TRANSPLANT
Transplant International. Impact of graft implantation order on graft survival in simultaneous pancreas-kidney transplantation.
 Draft Manuscript for Review Impact of graft implantation order on graft survival in simultaneous pancreas-kidney transplantation. Journal: Manuscript ID TRI-OA--0.R Manuscript Type: Original Article Date
Draft Manuscript for Review Impact of graft implantation order on graft survival in simultaneous pancreas-kidney transplantation. Journal: Manuscript ID TRI-OA--0.R Manuscript Type: Original Article Date
Echocardiography analysis in renal transplant recipients
 Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Metabolic Control Improves Long-Term Renal Allograft and Patient Survival in Type 1 Diabetes
 Metabolic Control Improves Long-Term Renal Allograft and Patient Survival in Type 1 Diabetes Christian Morath,* Martin Zeier,* Bernd Döhler, Jan Schmidt, Peter P. Nawroth, and Gerhard Opelz Departments
Metabolic Control Improves Long-Term Renal Allograft and Patient Survival in Type 1 Diabetes Christian Morath,* Martin Zeier,* Bernd Döhler, Jan Schmidt, Peter P. Nawroth, and Gerhard Opelz Departments
OPTN/SRTR 2016 Annual Data Report: Preface
 OPTN/SRTR 2016 Annual Data Report: Preface This Annual Data Report of the US Organ Procurement and Transplantation Network (OPTN) and the Scientific Registry of Transplant Recipients (SRTR) is the twenty-sixth
OPTN/SRTR 2016 Annual Data Report: Preface This Annual Data Report of the US Organ Procurement and Transplantation Network (OPTN) and the Scientific Registry of Transplant Recipients (SRTR) is the twenty-sixth
Clinical Study Over Ten-Year Kidney Graft Survival Determinants
 International Nephrology Volume 2012, Article ID 302974, 5 pages doi:10.1155/2012/302974 Clinical Study Over Ten-Year Kidney Graft Survival Determinants Anabela Malho Guedes, 1, 2 Jorge Malheiro, 1 Isabel
International Nephrology Volume 2012, Article ID 302974, 5 pages doi:10.1155/2012/302974 Clinical Study Over Ten-Year Kidney Graft Survival Determinants Anabela Malho Guedes, 1, 2 Jorge Malheiro, 1 Isabel
Simultaneous kidney and pancreas (SPK) transplantation
 Original Clinical ScienceçGeneral A Reassessment of the Survival Advantage of Simultaneous Kidney-Pancreas Versus Kidney-Alone Transplantation Randall S. Sung, 1 Min Zhang, 2 Douglas E. Schaubel, 2 Xu
Original Clinical ScienceçGeneral A Reassessment of the Survival Advantage of Simultaneous Kidney-Pancreas Versus Kidney-Alone Transplantation Randall S. Sung, 1 Min Zhang, 2 Douglas E. Schaubel, 2 Xu
kidney OPTN/SRTR 2012 Annual Data Report:
 kidney wait list 18 deceased donation 22 live donation 24 transplant 26 donor-recipient matching 28 outcomes 3 pediatric transplant 33 Medicare data 4 transplant center maps 43 A. J. Matas1,2, J. M. Smith1,3,
kidney wait list 18 deceased donation 22 live donation 24 transplant 26 donor-recipient matching 28 outcomes 3 pediatric transplant 33 Medicare data 4 transplant center maps 43 A. J. Matas1,2, J. M. Smith1,3,
Short-term and Long-term Survival of Kidney Allograft Cure Model Analysis
 TRANSPLANTATION Short-term and Long-term Survival of Kidney Allograft Cure Model Analysis Moghaddameh Mirzaee, 1 Jalal Azmandian, 2 Hojjat Zeraati, 1 Mahmood Mahmoodi, 1 Kazem Mohammad, 1 Abbas Etminan,
TRANSPLANTATION Short-term and Long-term Survival of Kidney Allograft Cure Model Analysis Moghaddameh Mirzaee, 1 Jalal Azmandian, 2 Hojjat Zeraati, 1 Mahmood Mahmoodi, 1 Kazem Mohammad, 1 Abbas Etminan,
Organ donation and transplantation trends in the United States, 2001
 American Journal of Transplantation 2003; 3 (Suppl. 4): 7 12 Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1601-2577 Organ donation and transplantation trends in the United States, 2001 Friedrich
American Journal of Transplantation 2003; 3 (Suppl. 4): 7 12 Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1601-2577 Organ donation and transplantation trends in the United States, 2001 Friedrich
Allocation of deceased donor kidneys. Phil Clayton NSW Renal Group 14 June 2012
 Allocation of deceased donor kidneys Phil Clayton NSW Renal Group 14 June 2012 Outline Why study kidney allocation? Equity vs utility Current Australian model Previous work in Australia US allocation research
Allocation of deceased donor kidneys Phil Clayton NSW Renal Group 14 June 2012 Outline Why study kidney allocation? Equity vs utility Current Australian model Previous work in Australia US allocation research
Clinical correlates, outcomes and healthcare costs associated with early mechanical ventilation after kidney transplantation
 The American Journal of Surgery (2013) 206, 686-692 Association of Women Surgeons: Clinical Science Clinical correlates, outcomes and healthcare costs associated with early mechanical ventilation after
The American Journal of Surgery (2013) 206, 686-692 Association of Women Surgeons: Clinical Science Clinical correlates, outcomes and healthcare costs associated with early mechanical ventilation after
Transplant Options for Patients: Choices and Consequences. Olwyn Johnston Medical Director Kidney Transplantation Vancouver General Hospital
 Transplant Options for Patients: Choices and Consequences Olwyn Johnston Medical Director Kidney Transplantation Vancouver General Hospital BC Kidney Days October 6 th 2017 Non contributory Conflict of
Transplant Options for Patients: Choices and Consequences Olwyn Johnston Medical Director Kidney Transplantation Vancouver General Hospital BC Kidney Days October 6 th 2017 Non contributory Conflict of
HLA-Matched Kidney Transplantation in the Era of Modern Immunosuppressive Therapy
 HLA-Matched Kidney Transplantation in the Era of Modern Immunosuppressive Therapy Arun Amatya, MD; Sandy Florman, MD; Anil Paramesh, MD; Anup Amatya, PhD Jennifer McGee, MD; Mary Killackey, MD; Quing Ren,
HLA-Matched Kidney Transplantation in the Era of Modern Immunosuppressive Therapy Arun Amatya, MD; Sandy Florman, MD; Anil Paramesh, MD; Anup Amatya, PhD Jennifer McGee, MD; Mary Killackey, MD; Quing Ren,
Controversies in Renal Transplantation. The Controversial Questions. Patrick M. Klem, PharmD, BCPS University of Colorado Hospital
 Controversies in Renal Transplantation Patrick M. Klem, PharmD, BCPS University of Colorado Hospital The Controversial Questions Are newer immunosuppressants improving patient outcomes? Are corticosteroids
Controversies in Renal Transplantation Patrick M. Klem, PharmD, BCPS University of Colorado Hospital The Controversial Questions Are newer immunosuppressants improving patient outcomes? Are corticosteroids
Topic: Pancreas Transplant Date of Origin: January Section: Transplant Last Reviewed Date: August 2013
 Medical Policy Manual Topic: Pancreas Transplant Date of Origin: January 1996 Section: Transplant Last Reviewed Date: August 2013 Policy No: 6 Effective Date: November 1, 2013 IMPORTANT REMINDER Medical
Medical Policy Manual Topic: Pancreas Transplant Date of Origin: January 1996 Section: Transplant Last Reviewed Date: August 2013 Policy No: 6 Effective Date: November 1, 2013 IMPORTANT REMINDER Medical
Donor Quality Assessment
 Donor Quality Assessment Francesc Moreso, MD, PhD Renal Transplant Unit Hospital Universitari Vall d Hebron Barcelona. Spain 4/9/2017 Donor Quality Assessment 1 What is the problem? Across all age ranges,
Donor Quality Assessment Francesc Moreso, MD, PhD Renal Transplant Unit Hospital Universitari Vall d Hebron Barcelona. Spain 4/9/2017 Donor Quality Assessment 1 What is the problem? Across all age ranges,
Acute Pancreas Allograft Rejection Is Associated With Increased Risk of Graft Failure in Pancreas Transplantation
 American Journal of Transplantation 2013; 13: 1019 1025 Wiley Periodicals Inc. C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12167
American Journal of Transplantation 2013; 13: 1019 1025 Wiley Periodicals Inc. C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12167
HHS Public Access Author manuscript Kidney Int. Author manuscript; available in PMC 2015 September 01.
 Kidney transplant results in children: progress made, but blacks lag behind Vikas R. Dharnidharka, MD, MPH 1 and Michael E. Seifert, MD 1,2 1 Division of Pediatric Nephrology, Washington University School
Kidney transplant results in children: progress made, but blacks lag behind Vikas R. Dharnidharka, MD, MPH 1 and Michael E. Seifert, MD 1,2 1 Division of Pediatric Nephrology, Washington University School
Update on Kidney Allocation
 Update on Kidney Allocation 23rd Annual Conference Association for Multicultural Affairs in Transplantation Silas P. Norman, M.D., M.P.H. Associate Professor Division of Nephrology September 23, 2015 Disclosures
Update on Kidney Allocation 23rd Annual Conference Association for Multicultural Affairs in Transplantation Silas P. Norman, M.D., M.P.H. Associate Professor Division of Nephrology September 23, 2015 Disclosures
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 2, by the Massachusetts Medical Society VOLUME 342 M ARCH 2, 2 NUMBER 9 IMPROVED GRAFT SURVIVAL AFTER RENAL TRANSPLANTATION IN THE UNITED STATES, 1988 TO
The New England Journal of Medicine Copyright, 2, by the Massachusetts Medical Society VOLUME 342 M ARCH 2, 2 NUMBER 9 IMPROVED GRAFT SURVIVAL AFTER RENAL TRANSPLANTATION IN THE UNITED STATES, 1988 TO
User Guide. A. Program Summary B. Waiting List Information C. Transplant Information
 User Guide This report contains a wide range of useful information about the kidney transplant program at (FLMR). The report has three main sections: A. Program Summary B. Waiting List Information The
User Guide This report contains a wide range of useful information about the kidney transplant program at (FLMR). The report has three main sections: A. Program Summary B. Waiting List Information The
Receiving a Kidney Transplant in the Ninth Decade of Life
 Trends Edmund in Transplant. Huang and 2011;5:121-7 Suphamai Bunnapradist: Receiving a Kidney Transplant in the Ninth Decade of Life Receiving a Kidney Transplant in the Ninth Decade of Life Edmund Huang
Trends Edmund in Transplant. Huang and 2011;5:121-7 Suphamai Bunnapradist: Receiving a Kidney Transplant in the Ninth Decade of Life Receiving a Kidney Transplant in the Ninth Decade of Life Edmund Huang
Outcomes of Adult Dual Kidney Transplants by KDRI in the United States
 American Journal of Transplantation 2013; 13: 2433 2440 Wiley Periodicals Inc. Brief Communication C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons
American Journal of Transplantation 2013; 13: 2433 2440 Wiley Periodicals Inc. Brief Communication C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons
James E. Cooper, M.D. Assistant Professor, University of Colorado at Denver Division of Renal Disease and Hypertension, Kidney and PancreasTransplant
 James E. Cooper, M.D. Assistant Professor, University of Colorado at Denver Division of Renal Disease and Hypertension, Kidney and PancreasTransplant Program Has no real or apparent conflicts of interest
James E. Cooper, M.D. Assistant Professor, University of Colorado at Denver Division of Renal Disease and Hypertension, Kidney and PancreasTransplant Program Has no real or apparent conflicts of interest
COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS
 COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS A COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS KEVIN C. MANGE, M.D.,
COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS A COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS KEVIN C. MANGE, M.D.,
Determinants of Discard of Expanded Criteria Donor Kidneys: Impact of Biopsy and Machine Perfusion
 American Journal of Transplantation 2008; 8: 783 792 Blackwell Munksgaard C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant Surgeons
American Journal of Transplantation 2008; 8: 783 792 Blackwell Munksgaard C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant Surgeons
TRANSPLANTATION IN DIABETIC PATIENTS. A.Tarik Kizilisik, MD, MSc, FACS, FICS Director & Primary Transplant Surgeon Lutheran Transplant Center
 TRANSPLANTATION IN DIABETIC PATIENTS A.Tarik Kizilisik, MD, MSc, FACS, FICS Director & Primary Transplant Surgeon Lutheran Transplant Center Diabetes is the pandemic of the new millennium 24 million diabetics
TRANSPLANTATION IN DIABETIC PATIENTS A.Tarik Kizilisik, MD, MSc, FACS, FICS Director & Primary Transplant Surgeon Lutheran Transplant Center Diabetes is the pandemic of the new millennium 24 million diabetics
Kidney vs. Liver: Where are We Really with Allocation in Kidney Transplantation?
 Kidney vs. Liver: Where are We Really with Allocation in Kidney Transplantation? Mark D. Stegall,, MD Chair, UNOS/OPTN Kidney Allocation Review Subcommittee Different Allocation Factors Liver Wait list
Kidney vs. Liver: Where are We Really with Allocation in Kidney Transplantation? Mark D. Stegall,, MD Chair, UNOS/OPTN Kidney Allocation Review Subcommittee Different Allocation Factors Liver Wait list
The privilege of induction avoidance and calcineurin inhibitors withdrawal in 2 haplotype HLA matched white kidney transplantation
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 The privilege of induction avoidance and calcineurin inhibitors withdrawal in 2 haplotype HLA matched white
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 The privilege of induction avoidance and calcineurin inhibitors withdrawal in 2 haplotype HLA matched white
Hasan Fattah 3/19/2013
 Hasan Fattah 3/19/2013 AASK trial Rational: HTN is a leading cause of (ESRD) in the US, with no known treatment to prevent progressive declines leading to ESRD. Objective: To compare the effects of 2 levels
Hasan Fattah 3/19/2013 AASK trial Rational: HTN is a leading cause of (ESRD) in the US, with no known treatment to prevent progressive declines leading to ESRD. Objective: To compare the effects of 2 levels
journal of medicine The new england
 The new england journal of medicine established in 1812 february 5, 2004 vol. 350 no. 6 Effect of Changing the Priority for HLA Matching on the Rates and Outcomes of Kidney Transplantation in Minority
The new england journal of medicine established in 1812 february 5, 2004 vol. 350 no. 6 Effect of Changing the Priority for HLA Matching on the Rates and Outcomes of Kidney Transplantation in Minority
Association of Center Volume with Outcome After Liver and Kidney Transplantation
 American Journal of Transplantation 2004; 4: 920 927 Blackwell Munksgaard Copyright C Blackwell Munksgaard 2004 doi: 10.1111/j.1600-6143.2004.00462.x Association of Center Volume with Outcome After Liver
American Journal of Transplantation 2004; 4: 920 927 Blackwell Munksgaard Copyright C Blackwell Munksgaard 2004 doi: 10.1111/j.1600-6143.2004.00462.x Association of Center Volume with Outcome After Liver
Management of Rejection
 Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation
 Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation Titte R Srinivas, MD, FAST Medical Director, Kidney and Pancreas Transplant Programs Objectives: Describe trends
Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation Titte R Srinivas, MD, FAST Medical Director, Kidney and Pancreas Transplant Programs Objectives: Describe trends
A Lifetime of Allograft Function with Kidneys from Older Donors
 A Lifetime of Allograft Function with Kidneys from Older Donors Caren Rose,* Elke Schaeffner, Ulrich Frei, Jagbir Gill,* and John S. Gill* *Division of Nephrology, University of British Columbia, Vancouver,
A Lifetime of Allograft Function with Kidneys from Older Donors Caren Rose,* Elke Schaeffner, Ulrich Frei, Jagbir Gill,* and John S. Gill* *Division of Nephrology, University of British Columbia, Vancouver,
Outcomes of living donor kidney transplantation in diabetic patients: age and sex matched comparison with non-diabetic patients
 ORIGINAL ARTICLE Korean J Intern Med 2018;33:356-366 Outcomes of living donor kidney transplantation in diabetic patients: age and sex matched comparison with non-diabetic patients Chung Hee Baek 1, Hyosang
ORIGINAL ARTICLE Korean J Intern Med 2018;33:356-366 Outcomes of living donor kidney transplantation in diabetic patients: age and sex matched comparison with non-diabetic patients Chung Hee Baek 1, Hyosang
Should red cells be matched for transfusions to patients listed for renal transplantation?
 Should red cells be matched for transfusions to patients listed for renal transplantation? Dr M.Willicombe Imperial College Renal and Transplant Centre, Hammersmith Hospital Should red cells be matched
Should red cells be matched for transfusions to patients listed for renal transplantation? Dr M.Willicombe Imperial College Renal and Transplant Centre, Hammersmith Hospital Should red cells be matched
The Kidney Allocation System Changed in a Substantive Way on December 5, Your Patients Have Been, and Will Be, Affected by These Changes
 The Kidney Allocation System Changed in a Substantive Way on December 5, 2014 Your Patients Have Been, and Will Be, Affected by These Changes 1 The New Kidney Allocation System Terms of Importance Pediatric
The Kidney Allocation System Changed in a Substantive Way on December 5, 2014 Your Patients Have Been, and Will Be, Affected by These Changes 1 The New Kidney Allocation System Terms of Importance Pediatric
Allogeneic Pancreas Transplant
 Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14, 05/15, 05/16,
Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14, 05/15, 05/16,
The CARI Guidelines Caring for Australians with Renal Impairment. Assessment of donors with sub-optimal kidney function/structure GUIDELINES
 Assessment of donors with sub-optimal kidney function/structure Date written: June 2004 Final submission: April 2005 GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR
Assessment of donors with sub-optimal kidney function/structure Date written: June 2004 Final submission: April 2005 GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR
Does Kidney Donor Risk Index implementation lead to the transplantation of more and higher-quality donor kidneys?
 Nephrol Dial Transplant (2017) 32: 1934 1938 doi: 10.1093/ndt/gfx257 Advance Access publication 21 August 2017 Does Kidney Donor Risk Index implementation lead to the transplantation of more and higher-quality
Nephrol Dial Transplant (2017) 32: 1934 1938 doi: 10.1093/ndt/gfx257 Advance Access publication 21 August 2017 Does Kidney Donor Risk Index implementation lead to the transplantation of more and higher-quality
Home Hemodialysis or Transplantation of the Treatment of Choice for Elderly?
 Home Hemodialysis or Transplantation of the Treatment of Choice for Elderly? Miklos Z Molnar, MD, PhD, FEBTM, FERA, FASN Associate Professor of Medicine Division of Nephrology, Department of Medicine University
Home Hemodialysis or Transplantation of the Treatment of Choice for Elderly? Miklos Z Molnar, MD, PhD, FEBTM, FERA, FASN Associate Professor of Medicine Division of Nephrology, Department of Medicine University
Concepts for Kidney Allocation
 ORGAN PROCUREMENT AND TRANSPLANTATION NETWORK Concepts for Kidney Allocation The Organ Procurement and Transplantation Network (OPTN) is seeking feedback regarding the use of two concepts in the allocation
ORGAN PROCUREMENT AND TRANSPLANTATION NETWORK Concepts for Kidney Allocation The Organ Procurement and Transplantation Network (OPTN) is seeking feedback regarding the use of two concepts in the allocation
Allogeneic Pancreas Transplant
 Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14 The following
Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14 The following
Intruduction PSI MODE OF ACTION AND PHARMACOKINETICS
 Multidisciplinary Insights on Clinical Guidance for the Use of Proliferation Signal Inhibitors in Heart Transplantation Andreas Zuckermann, MD et al. Department of Cardio-Thoracic Surgery, Medical University
Multidisciplinary Insights on Clinical Guidance for the Use of Proliferation Signal Inhibitors in Heart Transplantation Andreas Zuckermann, MD et al. Department of Cardio-Thoracic Surgery, Medical University
Kidney Transplant Outcomes for Prolonged Cold Ischemic Times in the Context of Kidney Paired Donation
 Kidney Transplant Outcomes for Prolonged Cold Ischemic Times in the Context of Kidney Paired Donation by Yayuk Joffres Thesis Submitted in Partial Fulfillment of the Requirements for the Degree of Master
Kidney Transplant Outcomes for Prolonged Cold Ischemic Times in the Context of Kidney Paired Donation by Yayuk Joffres Thesis Submitted in Partial Fulfillment of the Requirements for the Degree of Master
Kidney Allograft Fibrosis and Atrophy Early After Living Donor Transplantation
 American Journal of Transplantation 2005; 5: 1130 1136 Blackwell Munksgaard Copyright C Blackwell Munksgaard 2005 doi: 10.1111/j.1600-6143.2005.00811.x Kidney Allograft Fibrosis and Atrophy Early After
American Journal of Transplantation 2005; 5: 1130 1136 Blackwell Munksgaard Copyright C Blackwell Munksgaard 2005 doi: 10.1111/j.1600-6143.2005.00811.x Kidney Allograft Fibrosis and Atrophy Early After
What is the Best Induction Immunosuppression Regimen in Kidney Transplantation? Richard Borrows: Queen Elizabeth Hospital Birmingham
 What is the Best Induction Immunosuppression Regimen in Kidney Transplantation? Richard Borrows: Queen Elizabeth Hospital Birmingham SYMPHONY Study Ekberg et al. NEJM 2008 Excluded: DCD kidneys; CIT>30hours;
What is the Best Induction Immunosuppression Regimen in Kidney Transplantation? Richard Borrows: Queen Elizabeth Hospital Birmingham SYMPHONY Study Ekberg et al. NEJM 2008 Excluded: DCD kidneys; CIT>30hours;
chapter seven transplantation page
 chapter seven There been times that I thought I couldn t last for long But now I think I m able to carry on It s been a long, a long time coming But I know a change gonna come, oh yes it will Sam Cooke,
chapter seven There been times that I thought I couldn t last for long But now I think I m able to carry on It s been a long, a long time coming But I know a change gonna come, oh yes it will Sam Cooke,
Kidney Allocation- Will it ever be fair? Peter G Stock MD, PhD UCSF Department of Surgery. Would you accept this offer?
 Kidney Allocation- Will it ever be fair? Peter G Stock MD, PhD UCSF Department of Surgery Question 1: A 19 y/o deceased donor kidney (O mismatch) from NYC is allocated to a 72 y/o highly sensitized caucasian
Kidney Allocation- Will it ever be fair? Peter G Stock MD, PhD UCSF Department of Surgery Question 1: A 19 y/o deceased donor kidney (O mismatch) from NYC is allocated to a 72 y/o highly sensitized caucasian
Alfonso H. Santos Jr., Michael J. Casey, and Karl L. Womer
 Hindawi Journal of Transplantation Volume 217, Article ID 8132672, 1 pages https://doi.org/1.1155/217/8132672 Research Article Analysis of Risk Factors for Kidney Retransplant Outcomes Associated with
Hindawi Journal of Transplantation Volume 217, Article ID 8132672, 1 pages https://doi.org/1.1155/217/8132672 Research Article Analysis of Risk Factors for Kidney Retransplant Outcomes Associated with
Mortality After Kidney Transplantation: A Comparison Between the United States and Canada
 American Journal of Transplantation 2006; 6: 109 114 Blackwell Munksgaard C 2005 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/j.1600-6143.2005.01141.x
American Journal of Transplantation 2006; 6: 109 114 Blackwell Munksgaard C 2005 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/j.1600-6143.2005.01141.x
