Neonatal Jaundice HOPE. Doa'a Al Zou'bi & Nadeen Al-share'
|
|
|
- Anthony Barrett
- 6 years ago
- Views:
Transcription
1 Neonatal Jaundice HOPE Doa'a Al Zou'bi & Nadeen Al-share'
2 Neonatal Jaundice Hyperbilirubinemia is a newborn hemolytic disease. Hyperbilirubinemia is a very common disease affect 60% of all term babies and 80% of all preterm. Bilirubin Metabolism RBCs Hemoglobin Heme & globin ( protein ). Bilirubin is a product of heme catabolism 80% coming from hemoglobin breakdown and 20% from cytochromes metabolism. Two steps for birubin production : First step Heme [ 1 gram ] biliverdin + carbon monoxide ( CO ) By Heme oxygenase enzyme. ( carbon monoxide measurement can idicate the rate of bilirubin production) Second step Biliverdin bilirubin ( Indirect ) [ 35 gram ] by biliverdin reductase. (( One gram of hemoglobin produces 35 mg of bilirubin )) This Bilirubin has 3 distinct features : 1. Lipid soluble / Water insoluble << this limits its excretion. 2. Unconjugated / reacts as Indirect agent in Bergh test. 3. Toxic to CNS ( free bilirubin can cross the blood brain barrier ) and may cause Kernicterus. Bilirubin either to bind albumin and so become inactive, if not bind albumin ; free bilirubin become available to enter CNS. it may not bind or displaced by drug as sulfisoxazole.
3 In hepatocyte ; bilirubin bind to Ligandin (cytoplasm liver protein ) in a process called Conjugation by UDP- glucuronsyltransferese enzyme giving Bilirubin Diglucuronid (direct). Bilirubin Diglucuronid has 3 district features : 1. Water Soluble. 2. Conjugated / reacts as Direct agent in Bergh test. 3. Excreted in bile and urine. Most of Bilirubin Diglucuronid excreted in bile then to small intestine and by the effect of gut microflora converted to Sterobilinogen that excreted in stool and give it dark color, and to Urobilinogen which excreted in urine. This excretion limit the bilirubin reabsorption. Intestinal mucosa have glcorunodase enzyme, this enzyme deconjugate some direct bilirubin, this result in indirect bilirubin which can reabsorbed by intestinal cells and go to circulation again, this called enterohepatic cirulation. Direct bilirubin can`t be absorbed by intestinal cells ** Any problem in any of these steps will lead to elevation of bilirubin level ( Hperbilirubinemia ) / Jaundice Clinical Manifestation : Jaundice may be present at birth or may appear at any time during the neonatal period Cephalocaudal progression. Dermal pressure can help to reveal the anatomic progression of jaundice Clinical examination cannot be depended on to estimate serum levels especially in babies with dark skin. Jaundice from deposition of indirect bilirubin in the skin tends to appear bright yellow or orange. Jaundice (yellowish discoloration of skin and sclera ) appear on physical exam when TSB is 5 mg/dl in newborns Conjugated ( Direct ) Vs. un conjugated ( indirect ) : Unconjugated Hyperbilirubinemia
4 Hemolysis present Blood group incompatibility Hemolysis absent Physiologic jaundice (common cause ) Infections(sepsis ) RBC enzyme defect Hemoglobinopathy RBC membrane disorders breast milk jaundice Polycythemia Internal hemorrhage Hypothyroidism gilbert and crigler najjar syndrome stenosis pyloric Conjugated Hperbilirubinemia Common Uncommon TORCH Infection Cystic Fibrosis Neonatal hepatitis Biliary Atresia Sepsis Inborn Error of Metabolism Hperalimentation cholestasis (parenteral nutrition ) Alpha one Antitrypsin deficiency result of : 1. Increased RBCs mass, so increase bilirubin production. 2. Shortened RBC life span to instead of 120 days.
5 3. Hepatic immaturity of lingandin & glucuronosyl transferase. 4. Increase enterohepatic circulation of bilirubin due to absence of anerobic flora in the neonatal intestine. 5. More in Greek and Asian infants. - Maximum intensity by 4th-5th day in term & 7th day in preterm Clinical picture : 1. Visible jaundice appearing after 24 hours of age ( NOT in the first day ) - Serum level less than 15 ( peak ) ** past lec. 2. (NELSON ) Peak Indirect bilirubin level of no more than 12 mg/dl on day 3 of life. ( direct hyperbilitubinemia always pathological ) * in preterm the peak is 15mg/dl in the 5 th day. * in breast milk fed is 15-17mg/dl, higher in breast milkfed infants than in formula-fed infants because of decreased fluid intake. 3. Disappearance without treatment by 7 th or 10 th day of life 4. Total bilirubin rises by < 5 mg/dl (86 mmol/l) per day Clinical Picture : 1. Occur in the 1 st 24 hours 2. Persist for more than 14 days. 3. Bilirubin level is rising at greater rate than 0.5 mg/dl. 4. Peak is more than 13 mg/dl in term infant. 5. There are signs of underlying illness ( ex : anemia, hepatosplenomegaly ). 6. Dark urine and caly ( acholic ) stool. Result of :
6 Pathological Unconjugated Hypebilirubinemia Overproduction of bilirubin Decrease rate of conjugation Hemolytic causes High reticylocyte count Non-hemolytic Nr. reticylocyte count * Crigle-Nijjar * Gilbert * Hypothyroidism?? 1- Immune- Mediated + direct antibodies ( DAT, coomb ) test 1- Extravascular : Cephalohematoma, intracranial hemorrhage,extensive brusing 2- Non-Immune - direct antibodies ( DAT, coomb ) test 3- pt. with bacterial & viral sepsis. 2- Polycythemia 3- Exaggarated enterohepatic circulation : Bowel obstruction, fuctional ilius 4- Breast milk associated
7 1- Decrease Rate of conjugation : Crigle-Najjar Syndrome Rare & serious inherited form of nonhemolytic jaundice. UDPGT deficiency: Crigler-Najjar syndrome type I (complete deficiency, autosomal recessive) and type II (partial deficiency, autosomal dominant). Autosomal dominant form respond to phenobarb ( which increase enzyme activity ), autosomal recessive form does not respond to phenobarb. Both are rare but can cause sever unconjugated Hperbilirubinemia, bilirubin encephalopathy & death if untreated. Liver transplantation is curative. Gilbert Disease Is due to mutation of the promotor region of UDPGT, lead to dec. hepatic UDPGT activity, result in mild unconjugated hyperbilirubinemia. 2- Over production of bilirubin : Hemolytic Causes : 1- Antibody-me v diated hemolysis (Coombs test positive) a. Rh Isoimmunization The fetus is Rhesus positive and the mother Rhesus negative. The mother have been sensitized in a previous pregnancy by the passage of fetal red blood cells into her circulation, either at delivery or during a threatened miscarriage. Most Rh-negative women have no anti-rh antibodies at the time of their first pregnancy,,,so usually it is a disease of a second & subsequent pregnancies. It increases in severity with each immunized pregnancy because of increased maternal IgG antibody production. Most Rh disease can be prevented by treating the mother during pregnancy or promptly (within 72 hours) after childbirth,,, by
8 giving the mother an intramuscular injection of anti-rh antibodies (Rho(D) Immune Globulin), by this the fetal Rhesus D positive erythrocytes are destroyed before her immune system can discover them. Neonates are often anemic at birth, and hemolysis rapidly causes hyperbilirubinemia and more severe anemia. The most severe form of Rh isoimmunization, erythroblastosis fetalis, is characterized by life-threatening anemia, generalized edema, and fetal or neonatal heart failure. Without antenatal intervention, fetal or neonatal death may result. The cornerstone of antenatal management is transfusion of the fetus with Rh-negative cells, either directly into the umbilical vein or into the fetal abdominal cavity. Phototherapy is usually started in these infants upon delivery, with exchange transfusion given if needed. Intravenous immune globulin (IVIG; g/kg) given to the infant as soon as the diagnosis is made decreases the need for exchange transfusion. Ongoing hemolysis occurs until all maternal antibody is gone; therefore, these infants require monitoring for 2 3 months for anemia severe enough to require transfusion. Most Rh disease can be prevented by giving high-titer Rho (D) immune globulin to the Rh negative woman after invasive procedures during pregnancy or after miscarriage, abortion, or delivery of an Rh-positive infant. b. ABO blood group incompatibility ** This finding can accompany any pregnancy in a type O mother. Hemolysis is usually mild, but the severity is unpredictable because of variability in the amount of naturally occurring maternal anti-a or anti-b IgG antibodies. Because many mothers who have blood group O have IgG antibodies to A and B before pregnancy, the firstborn infant of A or B blood type may be affected. In contrast to Rh disease, ABO hemolytic disease does not become more severe with subsequent pregnancies. Hemolysis with ABO incompatibility is less severe than hemolysis in Rh-sensitized pregnancy, either because the anti-a or anti-b antibody may bind to nonerythrocytic cells that contain A or B antigen or because fetal
9 erythrocytes have fewer A or B antigenic determinants than they have Rh sites. With the declining incidence of Rh hemolytic disease, ABO incompatibility has become the most common cause of neonatal hyperbilirubinemia requiring therapy-currently accounting for approximately 20% of clinically significant jaundice in the newborn. " Causes : Environmental exposure Anti-A and anti-b antibodies are usually IgM and do not pass through the placenta, but some mothers "naturally" have IgG anti-a or IgG anti-b antibodies, which can pass through the placenta. Exposure to A-antigens and B-antigens, which are both widespread in nature, usually leads to the production of IgM anti-a and IgM anti-b antibodies but occasionally IgG antibodies are produced. Fetal-maternal transfusion Some mothers may be sensitized by fetal-maternal transfusion of ABO incompatible red blood and produce immune IgG antibodies against the antigen they do not have and their baby does. For example, when a mother of genotype OO (blood group O) carries a fetus of genotype AO (blood group A) she may produce IgG anti-a antibodies. The father will either have blood group A, with genotype AA or AO, or more rarely, have blood group AB, with genotype AB. Blood transfusion It would be very rare for ABO sensitization to be caused by therapeutic blood transfusion as a great deal of effort and checking is done to ensure that blood is ABO compatible between the recipient and the donor. " WIKI 2- Non-immune hemolysis ( comb test negative ) Abnormal red cell shapes: spherocytosis, elliptocytosis, pyknocytosis, stomatocytosis.
10 Red cell enzyme abnormalities: glucose-6-phosphate dehydrogenase deficiency, pyruvate kinase deficiency, hexokinase, deficiency, other metabolic defects. Breast milk jaundice Breast fed jaundice Breast Milk Jaundice Jaundice related to milk nature. The etiology of breast-milk jaundice attributed to the presence of glucuronidase in breast milk,which increase enterohepatic circulation Unconjugated hyperbilirubinemia without evidence of hemolysis in the 1 st and 2 nd weeks of life. Bilirubin levels rarely increase to more than 20 mg/dl. Interruption of breastfeeding for 1 to 2 days results in a rapid decline of bilirubin levels, which do not increase significantly after breastfeeding resumes but, Generally mild and does not require intervention it should be monitored to ensure it remains uncongujated and does not increase. Breast feeding can continue with expectation of resolution by 12 weeks. If the diagnosis of breast milk jaundice is made there is no need to stop breast feeding routinely, if the TSB level is low.but if the TSB reach levels which needs treatment ( phototherapy ) the physician should consider stopping breast milk feeding. Although uncommon, kernicterus can occur in patients with breastmilk jaundice. Breast Fed Jaundice Jaundice related to feeding technique
11 Occurs in 1 st few days. Baby is not having enough feeding, so increase dehydration, decrease bowel motion and increase enterohepatic circulation. Treated by increase feeding frequency or using bottle feeding. Remember : Jaundice of the 1 st day of life is always pathological. Lab investigations for unconjugated hyperbilirubinemia : 1. TSB (total Serum Bilirubin) if more than 5mg/dl of 1 st To convert from Micromol to dl : micromole = dl/17. day of life, we depend on it to determine if we need therapy and which type of therapy needed. Values in mg/dl or micromol/l ; then do : 2. Blood typing 3. CBC ( complete blood cell count ) 4. Blood film 5. Coombs test & Reticulocyte count ( for hemolytic anemia). Diagnosis : Total serum Bilirubin ( TSB). Transcutaneous measurement of bilirubin. ETCO, end tidal carbon monoxide. Visible jaundice with a TSB greater than 5 mg/dl before 24 hours of age is most commonly a result of significant hemolysis. Or internat hemorrhage. Evaluation of Hyperalbuminemia Because most newborns are discharged at hours of age, before physiologic jaundice peaks and before maternal milk supply is established, a predischarge TSB or a transcutaneous bilirubin measurement (TcB) may help predict which infants are at risk for severe hyperbilirubinemia. In all infants, an assessment of risk for severe hyperbilirubinemia should be performed before discharge. Risk Factors for Development of Severe Hyperbilirubinemia in Infants of 35 or More Week's Gestation : Jaundice observed in the first 24 h
12 Blood group incompatibility with other known hemolytic disease (G6PD deficiency) Gestational age wk Previous sibling received phototherapy Cephalohematoma Exclusive breastfeeding, if nursing is not going well and weight loss is excessive. Management of UnConjugated Hyperbilirubinemia Phototherapy An effective and safe method for reducing indirect bilirubin levels, particularly when initiated before serum bilirubin increases to levels associated with kernicterus. In term infants, phototherapy is begin when indirect bilirubin levels are between mg/dl. Phototherapy is initiated in premature infants when bilirubin is at lower levels, to prevent bilirubin from reaching high concentration necessitating exchange transfusion. Blue lights and white light are effective in reducing bilirubin levels, light must be in range of nm wavelength baby, but being away from baby by 20cm By that Bilirubin transformed into isomers that are water soluble and easily excreted. Complication of phototherapy : 1. Water loss, diarrhea, dehydration. 2. Macular rash. 3. Retinal damage. 4. Lethargy. 5. Skin bronzing noted in direct jaundice. 6. Separation between the infant and his mother. Exchange Transfusion
13 Usually is reserved for infants with dangerously high indirect bilirubin levels who are at risk for kernicterus. As a rule of thumb, a level of 20mg/dl for indiect reacting bilirubin is the exchange number for infant with hemolysis who weigh more than 2000g. Asymptomatic infant with physiological or breast milk jaundice may not require exchange transfusion unless the indirect bilirubin level exceed 25 mg/dl. The exchangeable level of indirect bilirubin for other infants may be estimated by calculating 10% of the birth weight in grams: the level in an infant weighing 1500 g would be 15 mg/dl. Infants weighing less than 1000 g usually do not require an exchange transfusion until the bilirubin level exceeds 10 mg/dl. The exchange is performed through an umbilical venous catheter placed in the inferior vena cava, the level of serum bilirubin immediately declines after the exchange to levels that are half of those before the exchange. Complication of exchange transfusion : 1. Related to blood (transfusion reaction, metabolic instability, infections) 2. Related to catheter (vessel perforation, hemorrhage) 3. Related to procedure (Hypotension). IV albumin In case of sever hypoalbumenemia IV Ig ( Intravenous immunoglobulin ) Decrease the need of exchange transfusion in ABO & Rh hemolysis unresponsive to double phototherapy,, because it reduce hemolysis. ( Dose g/kg/dose repeat in 12 hrs) Note : double phototherapy means usage of two sources of light 1. Over-head light source.
14 2. Fiber-Optic blanket directly on skin. Metaloporphyrin Inhibit heme oxygenase enzyme. Data on efficacy, toxicity, and long-term benefit are currently being evaluated Never physiological, always pathological. Not neurotoxic because conjugated bilirubin can't pass the BBB. Signifies serious underlying disorders involve : cholestasis or hepatocellular injury. Investigations for conjugated hyperbilirubinemia : 1. Unconjugated bilirubin ( more than 20% of total serum bilirubin ). 2. Liver enzyme. 3. Metabolic screening test as ; congenital hypothyroidism and galactosemia. 4. Hepatic ultrasound. 5. Sweat chloride test. Treatment of unconjugated hyperbilirubinemia : Not phototherapy nor Exchange transfusion, instead treat the underlying cause Kernicterus Kernicterus, or bilirubin encephalopathy, is a neurologic syndrome resulting from the deposition of unconjugated (indirect) bilirubin in the basal ganglia and brainstem nuclei.
15 Lipid soluble, unconjugated, indirect bilirubin fraction is toxic to the developing CNS, occur when indirect bilirubin concentration are high and exceed the binding capacity of albumin. Kernicterus result when indirect bilirubin is deposited in brain cells and disturbs neuronal metabolism and function, especially in the basal ganglia. Indirect bilirubin may cross the BBB because of its lipid solubility. Usually it dose NOT develop in term infant when bilirubin level are less than mg/dl, but the incidence increases as serum bilirubin level exceed 25mg/dl. Kernicterus may be noted at bilirubin level less than 20mg/dl in the presence of sepsis, meningitis, hemolysis, asphyxia, hypoxia, hypothermia, bilirubin displacing drug, prematurity, other risk factors for kernicterus in term infant and hemolysis jaundice noted within 24 hours of birth. Kernicterus has developed in extremely immature infant weighing less than 1000g when bilirubin levels are less than 10mg/dl ; because more permeable BBB associated with prematurity. Clinical Feature Early signs of kernicterus ( noted after day 4 of life ), include : 1. Lethargy, drowsiness, irritability. 2. Poor moro reflex, Poor feeding. 3. High pitched cry and emesis may also be present. Early signs of kernicterus occasionally may be reversed by immediately instituting an exchange transfusion Later signs include : 1. Bulging fontanel. 2. Opisthotonic posturing. 3. Pulmonary Hemorrhage 4. Fever. 5. Hypertonicity. 6. Seziure. Root Causes for Kernicterus by AAP A Hospital discharge before 48 hours of life
16 No early follow up (especially for infants born at 35 to 37 weeks gestational age) Failure to check the bilirubin in Jaundiced infant in the first 24hr Failure to recognize the presence of risk factors for hyperbilirubinemia CASE : a pt. 20 day old has jaundice,, Take History : Postnatal history 1) Onset ( if in first 24 hr of life or appear after the 7 th day it suggests pathological process ), and progression 2) Loss of stool color ( obstructive jaundice ) 3) Breastfeeding, oral intake, activity (dehydration and low caloric intake increase bilirubin level, decrease activity suggest sepsis ) 4) Greater than average weight loss (>8%) 5) Maternal blood group, Gestational age 6) Infections or fever, General activity 7) Medications? (newborn or mother) e.g sulfa drugs can displace bilirubin from its binding site on albumin. 8) Symptoms or signs of metabolic disease (eg, galactosemia) (direct) 9) Symptoms or signs of hypothyroidism Family History 10) Previous sibling with neonatal jaundice. 11) Other family members with jaundice Anemia or splenectomy or known heredity for hemolytic disorders 12) Liver disease History of pregnancy & delivery 13) Maternal illness suggestive of viral or other infection 14) Maternal drug intake 15) Delayed cord clamping 16) Birth trauma with bruising 17) Results of newborn screening tests (if done ) Important physical examination you should do :
17 In most infants, yellow color is the only finding on physical examination. General : Does the child look well or unwell? Vitals: If febrile, the newborn will require a full septic work-up. In hemolytic states, there can be an increase in heart rate and respiration rate as well as poor perfusion Growth Parameters : excessive weight loss or insufficient weight gain may point to dehydration Head and neck : look for pallor and jaundice,look for cephalohematoma or bruising Cardiovascular : Severe haemolytic processes can result in heart failure. Abdomen: Check for hepatomegaly and splenomegaly. Neurologic: Level of consciousness,posture, Ant.fontanel, gross motor movements, tone, primitive reflexes, quality of the cry, cranial nerves and observe for any abnormal movements what's your DDx? Timing of Jaundice and Differential Diagnosis : - Early Jaundice ( in the 1 st two days ) : usually due to acute hemolytic condition as ABO or RH incompatibility. - Jaundice between 3 rd and 10 th day : may be due to physiological jaundice, infant of diabetic mother, cephalohematoma, infection or asphyxia. - Late onset or prolonged jaundice beyond 14 days : may be due to biliary atresia, galactosemia, hepatitis, or infection Finally, the END :D Resources : Nelson, past lec., Dr.Mahdi Al Shboul's slides, current Done by your colleagues from HOPE batch / 2010 : Doa'a Samarah Al Zou'bi & Nadeen Alshare' ) ق ل ه ل ي س ت و ي ال ذ ين ي ع ل م ون و ال ذ ين ال ي ع ل م ون (
Clinical evaluation Jaundice skin and mucous membranes
 JAUNDICE Framework The definition of Neonatal Jaundice Billirubin Metabolism Special characteristic in neonates Dangerous of the Hyperbillirubinemia The diseases in relation with Neonatal Jaundice Objectives:
JAUNDICE Framework The definition of Neonatal Jaundice Billirubin Metabolism Special characteristic in neonates Dangerous of the Hyperbillirubinemia The diseases in relation with Neonatal Jaundice Objectives:
Neonatal Jaundice Hyperbilirubinemia
 Neonatal Jaundice Hyperbilirubinemia Dr. Abdulrahman Al Nemri, MD Chairman Pediatric Department Associate Professor of Pediatric Consultant Neonatologist 100 $ questions on Neonatal Jaundice (NJ) 1. What
Neonatal Jaundice Hyperbilirubinemia Dr. Abdulrahman Al Nemri, MD Chairman Pediatric Department Associate Professor of Pediatric Consultant Neonatologist 100 $ questions on Neonatal Jaundice (NJ) 1. What
Approach to the management of Hyperbilirubinemia in Term Newborn Infant
 Approach to the management of Hyperbilirubinemia in Term Newborn Infant Mohammad Bagher Hosseini MD Neonatologist Assosiated professor of Tabriz University of Medical science May 2011 Case1 You are called
Approach to the management of Hyperbilirubinemia in Term Newborn Infant Mohammad Bagher Hosseini MD Neonatologist Assosiated professor of Tabriz University of Medical science May 2011 Case1 You are called
Safe and Healthy Beginnings. M. Jeffrey Maisels MD William Beaumont Hospital Royal Oak, MI
 Safe and Healthy Beginnings M. Jeffrey Maisels MD William Beaumont Hospital Royal Oak, MI jmaisels@beaumont.edu Risk Factors There are 2 kinds Those that increase the risk of subsequently developing a
Safe and Healthy Beginnings M. Jeffrey Maisels MD William Beaumont Hospital Royal Oak, MI jmaisels@beaumont.edu Risk Factors There are 2 kinds Those that increase the risk of subsequently developing a
11/8/12. KERNICTERUS: The reason we have to care about bilirubin. MANAGING JAUNDICE IN THE BREASTFEEDING INFANT AKA: Lack of Breastfeeding Jaundice
 MANAGING JAUNDICE IN THE BREASTFEEDING INFANT AKA: Lack of Breastfeeding Jaundice November 16, 2012 Orange County Lawrence M. Gartner, M.D. University of Chicago and Valley Center, California KERNICTERUS:
MANAGING JAUNDICE IN THE BREASTFEEDING INFANT AKA: Lack of Breastfeeding Jaundice November 16, 2012 Orange County Lawrence M. Gartner, M.D. University of Chicago and Valley Center, California KERNICTERUS:
Breastfeeding, Jaundice and Hyperbilirubinemia in the Newborn. Jeremy Jones, DO Oklahoma State University Center for Health Sciences
 Breastfeeding, Jaundice and Hyperbilirubinemia in the Newborn Jeremy Jones, DO Oklahoma State University Center for Health Sciences Table of Contents Learning Objectives Practice Gap The Newborn Baby and
Breastfeeding, Jaundice and Hyperbilirubinemia in the Newborn Jeremy Jones, DO Oklahoma State University Center for Health Sciences Table of Contents Learning Objectives Practice Gap The Newborn Baby and
An Approach to Jaundice Block 10. Dr AJ Terblanche Department of Paediatrics and Child Health
 An Approach to Jaundice Block 10 Dr AJ Terblanche Department of Paediatrics and Child Health JAUNDICE (ICTERUS) Yellow discoloration skin, sclerae, mucous membranes Observed 60% term, 80% preterm infants
An Approach to Jaundice Block 10 Dr AJ Terblanche Department of Paediatrics and Child Health JAUNDICE (ICTERUS) Yellow discoloration skin, sclerae, mucous membranes Observed 60% term, 80% preterm infants
Definition of bilirubin Bilirubin metabolism
 Definition of bilirubin Bilirubin metabolism obilirubin formation otransport of bilirubin in plasma ohepatic bilirubin transport oexcretion through intestine Other substances conjugated by glucuronyl transferase.
Definition of bilirubin Bilirubin metabolism obilirubin formation otransport of bilirubin in plasma ohepatic bilirubin transport oexcretion through intestine Other substances conjugated by glucuronyl transferase.
HEMOLYSIS AND JAUNDICE:
 1 University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL SEMINAR HEMOLYSIS AND JAUNDICE: An overview
1 University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL SEMINAR HEMOLYSIS AND JAUNDICE: An overview
PAEDIATRIC ACUTE CARE GUIDELINE. Jaundice Neonatal
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Jaundice Neonatal Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Jaundice Neonatal Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read
Crash Cart therapy for Severe Jaundice. Dr Sandeep Kadam Neonatologist Pune
 Crash Cart therapy for Severe Jaundice Dr Sandeep Kadam Neonatologist Pune Objectives Assessment & stabilization Role of Investigations Management principles Steps for a crash-cart approach Assess Risk
Crash Cart therapy for Severe Jaundice Dr Sandeep Kadam Neonatologist Pune Objectives Assessment & stabilization Role of Investigations Management principles Steps for a crash-cart approach Assess Risk
What to Do when the Lights Don t Work- Neonatal Hyperbilirubinemia
 What to Do when the Lights Don t Work- Neonatal Hyperbilirubinemia Dr G Elske Hildes-Ripstein Dept of Child Health and Pediatrics University of Manitoba, College of Medicine Annual Scientific Assembly;
What to Do when the Lights Don t Work- Neonatal Hyperbilirubinemia Dr G Elske Hildes-Ripstein Dept of Child Health and Pediatrics University of Manitoba, College of Medicine Annual Scientific Assembly;
Immunohematology (Introduction)
 Modified from Serotonin version Immunohematology (Introduction) References: -Blood Groups and Red Cell Antigens (Laura Dean) -Cellular and molecular immunology, 8 th edition Introduction to replace blood
Modified from Serotonin version Immunohematology (Introduction) References: -Blood Groups and Red Cell Antigens (Laura Dean) -Cellular and molecular immunology, 8 th edition Introduction to replace blood
Immunohematology (Introduction) References: -Blood Groups and Red Cell Antigens (Laura Dean) -Cellular and molecular immunology, 8 th edition
 Immunohematology (Introduction) References: -Blood Groups and Red Cell Antigens (Laura Dean) -Cellular and molecular immunology, 8 th edition Introduction to replace blood lost by hemorrhage or to correct
Immunohematology (Introduction) References: -Blood Groups and Red Cell Antigens (Laura Dean) -Cellular and molecular immunology, 8 th edition Introduction to replace blood lost by hemorrhage or to correct
Jaundice in newborn babies under 28 days
 Jaundice in newborn babies under days NICE guideline: short version Draft for consultation, January 0 This guideline covers the care of newborn babies (from birth to days) with jaundice. Who is it for?
Jaundice in newborn babies under days NICE guideline: short version Draft for consultation, January 0 This guideline covers the care of newborn babies (from birth to days) with jaundice. Who is it for?
Table 1. Agents to be avoided in G6PD Deficiency Patients MANAGEMENT OF NNJ
 NEONATAL JAUNDICE What is jaundice? Jaundice is apparent clinically when the level of bilirubin in the serum rises above 85µmol/l (5mg/dl). Physiological jaundice is a reflection of the bilirubin load
NEONATAL JAUNDICE What is jaundice? Jaundice is apparent clinically when the level of bilirubin in the serum rises above 85µmol/l (5mg/dl). Physiological jaundice is a reflection of the bilirubin load
The Lecture s topics
 The Lecture s topics Blood groups -ABO system *Transfusion reaction -Rhesus factor *Hemolytic disease of newborn Blood transfusion and Tissue transplant The ABO System Discovered in 1901 by Dr. Karl Landsteiner
The Lecture s topics Blood groups -ABO system *Transfusion reaction -Rhesus factor *Hemolytic disease of newborn Blood transfusion and Tissue transplant The ABO System Discovered in 1901 by Dr. Karl Landsteiner
HEMOLYSIS & JAUNDICE: An Overview
 HEMOLYSIS & JAUNDICE: An Overview University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL MBBS III
HEMOLYSIS & JAUNDICE: An Overview University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL MBBS III
Immunohaematology: a branch of immunology that deals with the immunologic properties of blood.
 1 Immunohaematology: a branch of immunology that deals with the immunologic properties of blood. The red blood cells have on their surface hundreds of antigens and according to the antigen on their surface
1 Immunohaematology: a branch of immunology that deals with the immunologic properties of blood. The red blood cells have on their surface hundreds of antigens and according to the antigen on their surface
Revised Authors: Malathi Balasundaram MD, Vinod K. Bhutani, MD, FAAP
 Severe Hyperbilirubinemia Prevention (SHP Toolkit) Revised Authors: Malathi Balasundaram MD, Vinod K. Bhutani, MD, FAAP Original Authors: Richard Bell, MD, Lisa Bollman, RN, CPHQ, Courtney Nisbet, RN,
Severe Hyperbilirubinemia Prevention (SHP Toolkit) Revised Authors: Malathi Balasundaram MD, Vinod K. Bhutani, MD, FAAP Original Authors: Richard Bell, MD, Lisa Bollman, RN, CPHQ, Courtney Nisbet, RN,
Risk Factors ff Jaundice in Neonates at DHQ Teaching Hospital Dera Ghazi Khan
 ORIGINAL ARTICLE Risk Factors ff Jaundice in Neonates at DHQ Teaching Hospital Dera Ghazi Khan SHAKEEL AHMED 1, MUKHTAR AHMAD 2, TAYYABA RAFIQUE 3 ABSTRACT Background: Jaundice is the yellow discoloration
ORIGINAL ARTICLE Risk Factors ff Jaundice in Neonates at DHQ Teaching Hospital Dera Ghazi Khan SHAKEEL AHMED 1, MUKHTAR AHMAD 2, TAYYABA RAFIQUE 3 ABSTRACT Background: Jaundice is the yellow discoloration
Cord blood bilirubin used as an early predictor of hyperbilirubinemia
 International Journal of Contemporary Pediatrics Ramamoorthy K et al. Int J Contemp Pediatr. 218 Jul;5(4):128-1285 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article
International Journal of Contemporary Pediatrics Ramamoorthy K et al. Int J Contemp Pediatr. 218 Jul;5(4):128-1285 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article
Recent Advances in Understanding Neonatal Hemolytic Disease
 Does this Sound FUN or BOARING? Recent Advances in Understanding Neonatal Hemolytic Disease Robert D. Christensen MD Neonatology/Hematology/Oncology Disclosure Statement No financial relationship with
Does this Sound FUN or BOARING? Recent Advances in Understanding Neonatal Hemolytic Disease Robert D. Christensen MD Neonatology/Hematology/Oncology Disclosure Statement No financial relationship with
BCM 317 LECTURE OJEMEKELE O.
 BCM 317 LECTURE BY OJEMEKELE O. JAUNDICE Jaundice is yellowish discoloration of the skin, sclera and mucous membrane, resulting from an increased bilirubin concentration in the body fluid. It is usually
BCM 317 LECTURE BY OJEMEKELE O. JAUNDICE Jaundice is yellowish discoloration of the skin, sclera and mucous membrane, resulting from an increased bilirubin concentration in the body fluid. It is usually
Prolonged Neonatal Jaundice
 Prolonged Neonatal Jaundice Ahmed Laving KPA Annual Scientific Conference 2018 Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Case Presentation
Prolonged Neonatal Jaundice Ahmed Laving KPA Annual Scientific Conference 2018 Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Case Presentation
LIVER FUNCTION TESTS
 LIVER FUNCTION TESTS A- Metabolic Functions of the Liver: 1. The liver plays a major role in carbohydrate, lipid and protein homeostasis, with the processes of glycolysis, the Krebs cycle, gluconeogenesis,
LIVER FUNCTION TESTS A- Metabolic Functions of the Liver: 1. The liver plays a major role in carbohydrate, lipid and protein homeostasis, with the processes of glycolysis, the Krebs cycle, gluconeogenesis,
Low temperature < 96.8 F (36.0 C) rectally that doesn't respond to warming
 Jaundice - Newborn Office Hours Telephone Triage Protocols Pediatric 2018 DEFINITION The skin has turned a yellow color At higher bilirubin levels, the whites of the eyes also turn yellow Included: Home
Jaundice - Newborn Office Hours Telephone Triage Protocols Pediatric 2018 DEFINITION The skin has turned a yellow color At higher bilirubin levels, the whites of the eyes also turn yellow Included: Home
CHAPTER 10 BLOOD GROUPS: ABO AND Rh
 CHAPTER 10 BLOOD GROUPS: ABO AND Rh The success of human blood transfusions requires compatibility for the two major blood group antigen systems, namely ABO and Rh. The ABO system is defined by two red
CHAPTER 10 BLOOD GROUPS: ABO AND Rh The success of human blood transfusions requires compatibility for the two major blood group antigen systems, namely ABO and Rh. The ABO system is defined by two red
RHESUS BLOOD GROUP SYSTEM (Author: Alvine Janse van Rensburg; ND Biomedical Technology-Microbiology, Haematology, Chemistry)
 RHESUS BLOOD GROUP SYSTEM (Author: Alvine Janse van Rensburg; ND Biomedical Technology-Microbiology, Haematology, Chemistry) Introduction The term Rh refers to a complex blood group system that comprised
RHESUS BLOOD GROUP SYSTEM (Author: Alvine Janse van Rensburg; ND Biomedical Technology-Microbiology, Haematology, Chemistry) Introduction The term Rh refers to a complex blood group system that comprised
Determination of effect of low dose vs moderate dose clofibrate on decreasing serum bilirubin in healthy term neonates
 Original Article Iran J Ped June 2007, Vol 17 (No 2), Pp:108-112 Determination of effect of low dose vs moderate dose clofibrate on decreasing serum bilirubin in healthy term neonates Mohammad Ashkan Moslehi
Original Article Iran J Ped June 2007, Vol 17 (No 2), Pp:108-112 Determination of effect of low dose vs moderate dose clofibrate on decreasing serum bilirubin in healthy term neonates Mohammad Ashkan Moslehi
Dr. Shiva Nazari Assistant Professor of Pediatric Oncologist & Hematologist Shahid Beheshti Medical Science University Mofid Children s Hospital
 Dr. Shiva Nazari Assistant Professor of Pediatric Oncologist & Hematologist Shahid Beheshti Medical Science University Mofid Children s Hospital Reduction in the normal red cell survival (120 days) RBC
Dr. Shiva Nazari Assistant Professor of Pediatric Oncologist & Hematologist Shahid Beheshti Medical Science University Mofid Children s Hospital Reduction in the normal red cell survival (120 days) RBC
GUIDELINE FOR THE MANAGEMENT OF PROLONGED JAUNDICE IN BABIES. All babies admitted to hospital with prolonged jaundice
 GUIDELINE FOR THE MANAGEMENT OF PROLONGED JAUNDICE IN BABIES Reference No: Prolonged Jaundice Version No: 1 Applicable to All babies admitted to hospital with prolonged jaundice Classification of document:
GUIDELINE FOR THE MANAGEMENT OF PROLONGED JAUNDICE IN BABIES Reference No: Prolonged Jaundice Version No: 1 Applicable to All babies admitted to hospital with prolonged jaundice Classification of document:
Around million aged erythrocytes/hour are broken down.
 Anemia Degradation ofheme Around 100 200 million aged erythrocytes/hour are broken down. The degradation process starts in reticuloendothelial cells in the spleen, liver, and bone marrow. [1] The tetrapyrrole
Anemia Degradation ofheme Around 100 200 million aged erythrocytes/hour are broken down. The degradation process starts in reticuloendothelial cells in the spleen, liver, and bone marrow. [1] The tetrapyrrole
WHAT IT MEANS or WHY YOU DO IT
 WHAT IT MEANS or WHY YOU DO IT Dr. Patrick Sauer Billings Clinic Pediatrics Objective Increase understanding of prenatal tests Increase understanding of routine newborn procedures Increase knowledge to
WHAT IT MEANS or WHY YOU DO IT Dr. Patrick Sauer Billings Clinic Pediatrics Objective Increase understanding of prenatal tests Increase understanding of routine newborn procedures Increase knowledge to
Severe neonatal hyperbilirubinemia leading to exchange transfusion
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Severe neonatal hyperbilirubinemia leading to exchange transfusion Downloaded from mjiri.iums.ac.ir
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Severe neonatal hyperbilirubinemia leading to exchange transfusion Downloaded from mjiri.iums.ac.ir
A STUDY OF REBOUND HYPERBILIRUBINEMIA IN POST PHOTOTHERAPY NEONATES
 wjpmr, 2017,3(8), 226-235 SJIF Impact Factor:.103 Arakhita et al. WORLD JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH www.wjpmr.com Research Article ISSN 255-3301 WJPMR A STUDY OF REBOUND HYPERBILIRUBINEMIA
wjpmr, 2017,3(8), 226-235 SJIF Impact Factor:.103 Arakhita et al. WORLD JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH www.wjpmr.com Research Article ISSN 255-3301 WJPMR A STUDY OF REBOUND HYPERBILIRUBINEMIA
Anatomy and Physiology
 Anatomy and Physiology For The First Class 2 nd Semester Erythrocytes = Red Blood Cells (RBC) Erythrocytes = Red Blood Cells Red blood cells are biconcave discs, they have no nucleus and cytoplasmic organelles.
Anatomy and Physiology For The First Class 2 nd Semester Erythrocytes = Red Blood Cells (RBC) Erythrocytes = Red Blood Cells Red blood cells are biconcave discs, they have no nucleus and cytoplasmic organelles.
Background OVER 30 ISSUES IDENTIFIED! Key opportunities. What we ve done. October 31, 2012
 Background Hyperbilirubinemia: Developed by CMNRP s Jaundice Working Group Strategic planning meeting of CMNRP and its committees Multiple tables identified jaundice as a problem/priority Opportunity to
Background Hyperbilirubinemia: Developed by CMNRP s Jaundice Working Group Strategic planning meeting of CMNRP and its committees Multiple tables identified jaundice as a problem/priority Opportunity to
Comparison of Two Phototherapy Methods (Prophylactic vs Therapeutic) for Management of Hyperbilirubinemia in Very Low Birth Weight Newborns
 Original Article Iran J Pediatr Dec 2011; Vol 21 (No 4), Pp: 425-430 Comparison of Two Phototherapy Methods (Prophylactic vs Therapeutic) for Management of Hyperbilirubinemia in Very Low Birth Weight Newborns
Original Article Iran J Pediatr Dec 2011; Vol 21 (No 4), Pp: 425-430 Comparison of Two Phototherapy Methods (Prophylactic vs Therapeutic) for Management of Hyperbilirubinemia in Very Low Birth Weight Newborns
JAUNDICE. Zdeněk Fryšák 3rd Clinic of Internal Medicine Nephrology-Rheumatology-Endocrinology Faculty Hospital Olomouc
 JAUNDICE Zdeněk Fryšák 3rd Clinic of Internal Medicine Nephrology-Rheumatology-Endocrinology Faculty Hospital Olomouc Definition of Jaundice Icterus A yellowish staining of the skin, sclerae and deeper
JAUNDICE Zdeněk Fryšák 3rd Clinic of Internal Medicine Nephrology-Rheumatology-Endocrinology Faculty Hospital Olomouc Definition of Jaundice Icterus A yellowish staining of the skin, sclerae and deeper
Original Article Effect of Intravenous Fluid Supplementation on Serum Bilirubin Level in Jaundiced Healthy Neonates during Conventional Phototherapy
 Original Article Effect of Intravenous Fluid Supplementation on Serum Bilirubin Level in Jaundiced Healthy Neonates during Conventional Phototherapy Abstract R. Iranpour MD*, R. Nohekhan MD**, I. Haghshenas
Original Article Effect of Intravenous Fluid Supplementation on Serum Bilirubin Level in Jaundiced Healthy Neonates during Conventional Phototherapy Abstract R. Iranpour MD*, R. Nohekhan MD**, I. Haghshenas
BIOL 2458 CHAPTER 19 Part 1 SI 1. List the types of extracellular fluids. 2. Intracellular fluid makes up of the body fluids. Where is it found?
 BIOL 2458 CHAPTER 19 Part 1 SI 1 1. Extracellular fluid makes up of the body fluids. List the types of extracellular fluids. 2. Intracellular fluid makes up of the body fluids. Where is it found? 3. In
BIOL 2458 CHAPTER 19 Part 1 SI 1 1. Extracellular fluid makes up of the body fluids. List the types of extracellular fluids. 2. Intracellular fluid makes up of the body fluids. Where is it found? 3. In
Erythrocyte sedimentation rate. Hemolysis. Blood groups. Erythrocyte sedimentation rate (ESR)
 Erythrocyte sedimentation rate. Hemolysis. Blood groups. Erythrocyte sedimentation rate (ESR) Definition: The erythrocyte sedimentation rate (ESR), also called a sedimentation rate, sed rate, or Biernacki
Erythrocyte sedimentation rate. Hemolysis. Blood groups. Erythrocyte sedimentation rate (ESR) Definition: The erythrocyte sedimentation rate (ESR), also called a sedimentation rate, sed rate, or Biernacki
Glucose-6-Phosphate Dehydrogenase
 Glucose-6-Phosphate Dehydrogenase Is the major enzyme in the pentose phosphate pathway (also called the phosphogluconate pathway or the hexose monophosphate shunt) which is a metabolic pathway parallel
Glucose-6-Phosphate Dehydrogenase Is the major enzyme in the pentose phosphate pathway (also called the phosphogluconate pathway or the hexose monophosphate shunt) which is a metabolic pathway parallel
Immunohematology. Done by : Zaid Al-Ghnaneem
 Immunohematology Done by : Zaid Al-Ghnaneem Hello everyone, in this sheet we will talk mainly about immunohematology which is the reactions between our immune system with Antigens found mainly within blood
Immunohematology Done by : Zaid Al-Ghnaneem Hello everyone, in this sheet we will talk mainly about immunohematology which is the reactions between our immune system with Antigens found mainly within blood
Doaa Kotkot. Somaya Alkiswani. Nayef
 6 Doaa Kotkot Somaya Alkiswani Nayef Heme Synthesis In the previous lecture we talked about heme synthesis and we said that the rate limiting step is the condensation of Glycine + Succinyl CoA to produce
6 Doaa Kotkot Somaya Alkiswani Nayef Heme Synthesis In the previous lecture we talked about heme synthesis and we said that the rate limiting step is the condensation of Glycine + Succinyl CoA to produce
Management. (By the World Health Organization according to the magnitude of the enzyme deficiency and the severity of hemolysis)
 Glucose-6-Phosphate Dehydrogenase (G6PD) Deficiency Management Definition: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is an inherited disorder caused by a genetic defect in the red blood cell
Glucose-6-Phosphate Dehydrogenase (G6PD) Deficiency Management Definition: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is an inherited disorder caused by a genetic defect in the red blood cell
Acute Bilirubin Encephalopathy in Healthy Term Neonates Requiring Exchange Transfusion
 Iranian Journal of Neonatology 8 Acute Bilirubin Encephalopathy in Healthy Term Neonates Requiring Exchange Transfusion Seyedeh Fatemeh Khatami* 1, Pouya Parvaresh 2 *1-Department of Pediatrics, Division
Iranian Journal of Neonatology 8 Acute Bilirubin Encephalopathy in Healthy Term Neonates Requiring Exchange Transfusion Seyedeh Fatemeh Khatami* 1, Pouya Parvaresh 2 *1-Department of Pediatrics, Division
-Liver function tests -
 -Liver function tests - Biochimestry teamwork Osamah Al-Jarallah Abdulaziz Al-Shamlan Abdullah Al-Mazyad Turki Al-Otaibi Khalid Al-Khamis Saud Al-awad KhaledAlmohaimede Meshal Al-Otaibi Al-Anood Asiri
-Liver function tests - Biochimestry teamwork Osamah Al-Jarallah Abdulaziz Al-Shamlan Abdullah Al-Mazyad Turki Al-Otaibi Khalid Al-Khamis Saud Al-awad KhaledAlmohaimede Meshal Al-Otaibi Al-Anood Asiri
The Child with a Hematologic Alteration
 47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
Pathophysiology I Liver and Biliary Disease
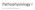 Pathophysiology I Liver and Biliary Disease The Liver The liver is located in the right upper portion of the abdominal cavity just beneath the right side of the rib cage. The liver has many functions that
Pathophysiology I Liver and Biliary Disease The Liver The liver is located in the right upper portion of the abdominal cavity just beneath the right side of the rib cage. The liver has many functions that
CrackCast Episode 28 Jaundice
 CrackCast Episode 28 Jaundice Episode overview: 1) Describe heme metabolism 2) List common pre-hepatic/hepatic/post-hepatic causes of jaundice Wisecracks: 1) What are clinical signs of liver disease? 2)
CrackCast Episode 28 Jaundice Episode overview: 1) Describe heme metabolism 2) List common pre-hepatic/hepatic/post-hepatic causes of jaundice Wisecracks: 1) What are clinical signs of liver disease? 2)
Standard of Newborn Care in the Age of Birth Plans. Stephanie Deal, MD Tiffany McKee-Garrett, MD
 Standard of Newborn Care in the Age of Birth Plans Stephanie Deal, MD Tiffany McKee-Garrett, MD Disclosure We have no relevant financial relationships with the manufacturers(s) of any commercial products(s)
Standard of Newborn Care in the Age of Birth Plans Stephanie Deal, MD Tiffany McKee-Garrett, MD Disclosure We have no relevant financial relationships with the manufacturers(s) of any commercial products(s)
ABO/Rh Blood Group System. A. Amirzargar
 ABO/Rh Blood Group System A. Amirzargar Carl Landsteiner: 1. Discovered the ABO Blood Group System in 1901 2. He and five co-workers began mixing each others red blood cells and serum together and inadvertently
ABO/Rh Blood Group System A. Amirzargar Carl Landsteiner: 1. Discovered the ABO Blood Group System in 1901 2. He and five co-workers began mixing each others red blood cells and serum together and inadvertently
Direct Antiglobulin Test (DAT)
 Exercise 8 Direct Antiglobulin Test (DAT) Objectives 1. State the purpose for performing the DAT. 2. State what a positive DAT indicates. 3. List the reagents which are used for performing the DAT. 4.
Exercise 8 Direct Antiglobulin Test (DAT) Objectives 1. State the purpose for performing the DAT. 2. State what a positive DAT indicates. 3. List the reagents which are used for performing the DAT. 4.
O 2 O 2 O 2. Haemoglobin
 O 2 O 2 O 2 Haemoglobin O 2 O 2 O 2 98% travels in oxyhaemoglobin (in red blood cells) 2% is dissolved in plasma (compared to carbon dioxide, oxygen is relatively insoluble in plasma) O 2 is not very soluble
O 2 O 2 O 2 Haemoglobin O 2 O 2 O 2 98% travels in oxyhaemoglobin (in red blood cells) 2% is dissolved in plasma (compared to carbon dioxide, oxygen is relatively insoluble in plasma) O 2 is not very soluble
Bilirubin Metabolism. Prof. Dr. Hedef Dhafir El-Yassin. 1 Prof. Dr. El-Yassin
 Bilirubin Metabolism Prof. Dr. Hedef Dhafir El-Yassin 1 Prof. Dr. El-Yassin Objectives: 1. To outline the basic metabolic pathway of bilirubin breakdown and conjugation 2. To state the basic metabolic
Bilirubin Metabolism Prof. Dr. Hedef Dhafir El-Yassin 1 Prof. Dr. El-Yassin Objectives: 1. To outline the basic metabolic pathway of bilirubin breakdown and conjugation 2. To state the basic metabolic
Transfusion Reactions. Directed by M-azad March 2012
 Transfusion Reactions Directed by M-azad March 2012 Transfusion Reactions are Adverse reactions associated with the transfusion of blood and its components Transfusion reactions Non-threatening to fatal
Transfusion Reactions Directed by M-azad March 2012 Transfusion Reactions are Adverse reactions associated with the transfusion of blood and its components Transfusion reactions Non-threatening to fatal
PRACTICE GUIDELINES WOMEN S HEALTH PROGRAM
 C Title: NEWBORN: HYPOGLYCEMIA IN NEONATES BORN AT 35+0 WEEKS GESTATION AND GREATER: DIAGNOSIS AND MANAGEMENT IN THE FIRST 72 HOURS Authorization Section Head, Neonatology, Program Director, Women s Health
C Title: NEWBORN: HYPOGLYCEMIA IN NEONATES BORN AT 35+0 WEEKS GESTATION AND GREATER: DIAGNOSIS AND MANAGEMENT IN THE FIRST 72 HOURS Authorization Section Head, Neonatology, Program Director, Women s Health
Neonatal Seizure. Dr.Nawar Yahya. Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan. Supervised by:
 Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Interpreting Liver Function Tests
 PSH Clinical Guidelines Statement 2017 Interpreting Liver Function Tests Dr. Asad A Chaudhry Consultant Hepatologist, Chaudhry Hospital, Gujranwala, Pakistan. Liver function tests (LFTs) generally refer
PSH Clinical Guidelines Statement 2017 Interpreting Liver Function Tests Dr. Asad A Chaudhry Consultant Hepatologist, Chaudhry Hospital, Gujranwala, Pakistan. Liver function tests (LFTs) generally refer
Average adult = 8-10 pints of blood. Functions:
 Average adult = 8-10 pints of blood Functions: Transports nutrients, oxygen, cellular waste products, and hormones Aids in distribution of heat Regulates acid-base balance Helps protect against infection
Average adult = 8-10 pints of blood Functions: Transports nutrients, oxygen, cellular waste products, and hormones Aids in distribution of heat Regulates acid-base balance Helps protect against infection
C. treatment with Desferal (deferoxamine mesylate USP, iron-chelating agent)
 HEMOLYTIC ANEMIAS Single choice tests 1. Select the clinical manifestation that is not characteristic for the hemolytic crisis: A. decrease of the red blood cell count B. reticulocytosis C. jaundice D.
HEMOLYTIC ANEMIAS Single choice tests 1. Select the clinical manifestation that is not characteristic for the hemolytic crisis: A. decrease of the red blood cell count B. reticulocytosis C. jaundice D.
Jaundice including Vitamin K Deficiency Bleeding in the Newborn Policy
 This is an official Northern Trust policy and should not be edited in any way Jaundice including Vitamin K Deficiency Bleeding in the Newborn Policy Reference Number: NHSCT/10/320 Target audience: Paediatrics,
This is an official Northern Trust policy and should not be edited in any way Jaundice including Vitamin K Deficiency Bleeding in the Newborn Policy Reference Number: NHSCT/10/320 Target audience: Paediatrics,
HEPETIC SYSTEMS BIOCHEMICAL HEPATOCYTIC SYSTEM HEPATOBILIARY SYSTEM RETICULOENDOTHELIAL SYSTEM
 EVALUATION OF LIVER FUNCTION R. Mohammadi Biochemist (Ph.D.) Faculty member of Medical Faculty HEPETIC SYSTEMS BIOCHEMICAL HEPATOCYTIC SYSTEM HEPATOBILIARY SYSTEM RETICULOENDOTHELIAL SYSTEM METABOLIC FUNCTION
EVALUATION OF LIVER FUNCTION R. Mohammadi Biochemist (Ph.D.) Faculty member of Medical Faculty HEPETIC SYSTEMS BIOCHEMICAL HEPATOCYTIC SYSTEM HEPATOBILIARY SYSTEM RETICULOENDOTHELIAL SYSTEM METABOLIC FUNCTION
Liver Function Tests
 Liver Function Tests The liver is of vital importance in intermediary metabolism and in the detoxification and elimination of toxic substances. Damage to the organ may not obviously affects its activity
Liver Function Tests The liver is of vital importance in intermediary metabolism and in the detoxification and elimination of toxic substances. Damage to the organ may not obviously affects its activity
ABO Hemolytic Disease of the Newborn
 ABO Hemolytic Disease of the Newborn A Retrospective Analysis of 5 Cases D. ROBERT DUOUR,.D. AND W. PATRICK ONOGHAN, PH.D. Dufour, D. Robert and onaghan, W. Patrick: ABO hemolytic disease of the newborn.
ABO Hemolytic Disease of the Newborn A Retrospective Analysis of 5 Cases D. ROBERT DUOUR,.D. AND W. PATRICK ONOGHAN, PH.D. Dufour, D. Robert and onaghan, W. Patrick: ABO hemolytic disease of the newborn.
Human Blood Groups. ABO Blood Grouping 5/1/12. Dr Badri Paudel Landsteiner s Rule
 Human Blood Groups ABO Blood Grouping Dr Badri Paudel www.badripaudel.com RBC membranes have glycoprotein an:gens on their external surfaces These an:gens are: Unique to the individual Recognized as foreign
Human Blood Groups ABO Blood Grouping Dr Badri Paudel www.badripaudel.com RBC membranes have glycoprotein an:gens on their external surfaces These an:gens are: Unique to the individual Recognized as foreign
Cardiovascular System: Blood Physiology Study Guide, Chapter 13 Cardiovascular System: Blood Part I. Clinical Applications
 Name: Cardiovascular System: Blood Physiology Study Guide, Chapter 13 Cardiovascular System: Blood Part I. Clinical Applications Lab Day/Time: 1 1. Mrs. Carlyle is pregnant for the first time. Her blood
Name: Cardiovascular System: Blood Physiology Study Guide, Chapter 13 Cardiovascular System: Blood Part I. Clinical Applications Lab Day/Time: 1 1. Mrs. Carlyle is pregnant for the first time. Her blood
CORD BLOOD TESTING AND HDFN A CASE STUDY. Eric Rosa, MLS (ASCP) CM University of Kansas Hospital April 20, 2016
 CORD BLOOD TESTING AND HDFN A CASE STUDY Eric Rosa, MLS (ASCP) CM University of Kansas Hospital April 20, 2016 BACKGROUND KU Hospital policy: run ABO/Rh (front) type + Direct Antiglobulin test on cord
CORD BLOOD TESTING AND HDFN A CASE STUDY Eric Rosa, MLS (ASCP) CM University of Kansas Hospital April 20, 2016 BACKGROUND KU Hospital policy: run ABO/Rh (front) type + Direct Antiglobulin test on cord
Cardiovascular System Module 2: Blood Typing *
 OpenStax-CNX module: m49688 1 Cardiovascular System Module 2: Blood Typing * Donna Browne Based on Blood Typing by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
OpenStax-CNX module: m49688 1 Cardiovascular System Module 2: Blood Typing * Donna Browne Based on Blood Typing by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
BILIARY ATRESIA. What is biliary atresia?
 The Childhood Liver Disease Research Network strives to provide information and support to individuals and families affected by liver disease through its many research programs. BILIARY ATRESIA What is
The Childhood Liver Disease Research Network strives to provide information and support to individuals and families affected by liver disease through its many research programs. BILIARY ATRESIA What is
Hematology Revision. By Dr.AboRashad . Mob
 1 1- Hb A2 is consisting of: a) 3 ά chains and 2 γ chains b) 2 ά chains and 2 β chains c) 2 ά chains and 2 δ chains** d) 2 ά chains and 3 δ chains e) 3 ά chains and 2 δ chains 2- The main (most) Hb found
1 1- Hb A2 is consisting of: a) 3 ά chains and 2 γ chains b) 2 ά chains and 2 β chains c) 2 ά chains and 2 δ chains** d) 2 ά chains and 3 δ chains e) 3 ά chains and 2 δ chains 2- The main (most) Hb found
Enzymatic Conversion of Heme to Bilirubin in Normal and Starved Fetuses and Newborn Rats
 Pediat. Res. (5/197-201 (1972) Bilirubin heme oxygenase developmental liver biochemistry spleen Enzymatic Conversion of Heme to Bilirubin in Normal and Starved Fetuses and Newborn Rats M. MICHAEL THALER
Pediat. Res. (5/197-201 (1972) Bilirubin heme oxygenase developmental liver biochemistry spleen Enzymatic Conversion of Heme to Bilirubin in Normal and Starved Fetuses and Newborn Rats M. MICHAEL THALER
Department of Pediatrics, Coimbatore Medical College Hospital, Coimbatore, Tamilnadu, India Correspondence to: Senthilkumar P,
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 8 Ver. VIII (Aug. 2017), PP 40-45 www.iosrjournals.org A Randomized Trial of Intravenous Fluid
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 8 Ver. VIII (Aug. 2017), PP 40-45 www.iosrjournals.org A Randomized Trial of Intravenous Fluid
The American Academy of Pediatrics (AAP) requested
 AMERICAN ACADEMY OF PEDIATRICS TECHNICAL REPORT Stanley Ip, MD; Mei Chung, MPH; John Kulig, MD, MPH; Rebecca O Brien, MD; Robert Sege, MD, PhD; Stephan Glicken, MD; M. Jeffrey Maisels, MB, BCh; and Joseph
AMERICAN ACADEMY OF PEDIATRICS TECHNICAL REPORT Stanley Ip, MD; Mei Chung, MPH; John Kulig, MD, MPH; Rebecca O Brien, MD; Robert Sege, MD, PhD; Stephan Glicken, MD; M. Jeffrey Maisels, MB, BCh; and Joseph
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia. Abdallah Abbadi
 Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Biochemical Investigations in Liver Disease. Dr Roshitha de Silva Department of Pathology Faculty of Medicine University of Kelaniya
 Biochemical Investigations in Liver Disease Dr Roshitha de Silva Department of Pathology Faculty of Medicine University of Kelaniya Biochemical markers Albumin ALP ALT, AST Gamma-glutamyl transpeptidase
Biochemical Investigations in Liver Disease Dr Roshitha de Silva Department of Pathology Faculty of Medicine University of Kelaniya Biochemical markers Albumin ALP ALT, AST Gamma-glutamyl transpeptidase
TOXIC AND NUTRITIONAL DISORDER MODULE
 TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
Fluid supplementation in term neonates with severe hyperbilirubinemia: a randomized controlled trial study
 International Journal of Contemporary Pediatrics Bandyopadhyay A et al. Int J Contemp Pediatr. 2017 May;4(3):853-857 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article
International Journal of Contemporary Pediatrics Bandyopadhyay A et al. Int J Contemp Pediatr. 2017 May;4(3):853-857 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article
IMMU 7630 Fall 2012 IMMUNOHEMATOLOGY
 IMMUNOHEMATOLOGY GENERAL PRINCIPLES. Blood transfusion has been practical since the 1920s, when its relatively simple rules were worked out. It is possible because what you re really doing most of the
IMMUNOHEMATOLOGY GENERAL PRINCIPLES. Blood transfusion has been practical since the 1920s, when its relatively simple rules were worked out. It is possible because what you re really doing most of the
Blood Typing * OpenStax. 1 Antigens, Antibodies, and Transfusion Reactions
 OpenStax-CNX module: m46708 1 Blood Typing * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By the end of this section, you will be able
OpenStax-CNX module: m46708 1 Blood Typing * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By the end of this section, you will be able
Bile pigments, porphyrins. 1 Bile pigments
 ÚSTAV LÉKAŘSKÉ BIOCHEMIE A LABORATORNÍ DIAGNOSTIKY 1. LF UK Bile pigments Porphyrins General Medicine Lenka Fialová & Martin Vejražka translated and edited by Jan Pláteník 2016/2017 1 Bile pigments Bile
ÚSTAV LÉKAŘSKÉ BIOCHEMIE A LABORATORNÍ DIAGNOSTIKY 1. LF UK Bile pigments Porphyrins General Medicine Lenka Fialová & Martin Vejražka translated and edited by Jan Pláteník 2016/2017 1 Bile pigments Bile
Biochemistry Liver Function Tests (LFTs)
 HbA NH 2 H 2 O 2 KClO3 Cl 2 O 7 PO 4 CH2O NAOH KMnO 4 M E D I C I N E KING SAUD UNIVERSITY Co 2 COOH MgCl 2 H 2 O Important Extra Information Doctors slides Doctors notes SO 2 HCN CCl 4 CuCl 2 SiCl 4 Biochemistry
HbA NH 2 H 2 O 2 KClO3 Cl 2 O 7 PO 4 CH2O NAOH KMnO 4 M E D I C I N E KING SAUD UNIVERSITY Co 2 COOH MgCl 2 H 2 O Important Extra Information Doctors slides Doctors notes SO 2 HCN CCl 4 CuCl 2 SiCl 4 Biochemistry
Prof. Dr. Hedef Dhafir El-Yassin. Prof. Dr. El-Yassin
 Prof. Dr. Hedef Dhafir El-Yassin 1 1. To define jaundice 2. To describe the types of jaundice 3. To tabulate and evaluate Laboratory results in all types of jaundice 2 } This is a condition where there
Prof. Dr. Hedef Dhafir El-Yassin 1 1. To define jaundice 2. To describe the types of jaundice 3. To tabulate and evaluate Laboratory results in all types of jaundice 2 } This is a condition where there
Anemia (3).ms Hemolytic Anemia. Abdallah Abbadi Feras Fararjeh
 Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Immunity. Acquired immunity differs from innate immunity in specificity & memory from 1 st exposure
 Immunity (1) Non specific (innate) immunity (2) Specific (acquired) immunity Characters: (1) Non specific: does not need special recognition of the foreign cell. (2) Innate: does not need previous exposure.
Immunity (1) Non specific (innate) immunity (2) Specific (acquired) immunity Characters: (1) Non specific: does not need special recognition of the foreign cell. (2) Innate: does not need previous exposure.
Liver function and clinical chemistry of liver
 INTRODUCTION Liver function and clinical chemistry of liver The liver plays a major role in carbohydrate, lipid and protein metabolism with the processes of glycolysis, the Krebs cycle,,homeostasis synthesis
INTRODUCTION Liver function and clinical chemistry of liver The liver plays a major role in carbohydrate, lipid and protein metabolism with the processes of glycolysis, the Krebs cycle,,homeostasis synthesis
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
HEMOLYTIC ANEMIA Anemia of increased destruction Normochromic, normochromic anemia Shortened RBC survival Reticulocytosis - Response to increased RBC
 HEMOLYTIC ANEMIAS Edited by: GR. Bahoush, MD. HEMOLYTIC ANEMIA Anemia of increased destruction Normochromic, normochromic anemia Shortened RBC survival Reticulocytosis - Response to increased RBC destruction
HEMOLYTIC ANEMIAS Edited by: GR. Bahoush, MD. HEMOLYTIC ANEMIA Anemia of increased destruction Normochromic, normochromic anemia Shortened RBC survival Reticulocytosis - Response to increased RBC destruction
OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General
![OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General](/thumbs/85/91909911.jpg) OB Well Baby Nursery Admission (Term) [3040000234] For specialty focused order sets for your patient, refer to: 3040000424 Neonatal Circumcision Order Set 3040000522 Neonatal Herpes Viral Order Set 3040000524
OB Well Baby Nursery Admission (Term) [3040000234] For specialty focused order sets for your patient, refer to: 3040000424 Neonatal Circumcision Order Set 3040000522 Neonatal Herpes Viral Order Set 3040000524
Management of Indirect Neonatal Hyperbilirubinemia
 Quality Department Guidelines for Clinical Care Inpatient Hyperbilirubinemia Guideline Team Team Leaders Nicole S Sroufe, MD, MPH Pediatric Emergency Medicine Jennifer L Vredeveld, MD Internal Medicine,
Quality Department Guidelines for Clinical Care Inpatient Hyperbilirubinemia Guideline Team Team Leaders Nicole S Sroufe, MD, MPH Pediatric Emergency Medicine Jennifer L Vredeveld, MD Internal Medicine,
Summary of Changes: References/content updated to reflect most current standards of practice.
 Alaska Native Medical Center: Mother Baby Unit Guideline: Neonatal Hypoglycemia Subject: Neonatal Hypoglycemia REVISION DATE: Jan 2015,12/2011, 02/2009, 11, 2007, 07/2007,04/2001, 04/1999 REPLACES: NSY:
Alaska Native Medical Center: Mother Baby Unit Guideline: Neonatal Hypoglycemia Subject: Neonatal Hypoglycemia REVISION DATE: Jan 2015,12/2011, 02/2009, 11, 2007, 07/2007,04/2001, 04/1999 REPLACES: NSY:
Jaundice. Agnieszka Dobrowolska- Zachwieja, MD, PhD
 Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Approach to the Patient with Liver Disease
 Approach to the Patient with Liver Disease Diagnosis of liver disease Careful history taking Physical examination Laboratory tests Radiologic examination and imaging studies Liver biopsy Liver diseases
Approach to the Patient with Liver Disease Diagnosis of liver disease Careful history taking Physical examination Laboratory tests Radiologic examination and imaging studies Liver biopsy Liver diseases
TRANSFUSION REACTIONS
 14 TRANSFUSION REACTIONS 14.1 INTRODUCTION Transfusion of blood and blood products are reported to cause reactions during or after procedure specially in patients who receive multiple transfusions. These
14 TRANSFUSION REACTIONS 14.1 INTRODUCTION Transfusion of blood and blood products are reported to cause reactions during or after procedure specially in patients who receive multiple transfusions. These
Ashley Robson Canyon Creek Dr. Mckinney, TX 75070
 1 Ashley Robson 2212 Canyon Creek Dr. Mckinney, TX 75070 September 2 nd 2014 Debra Brandon PhD, RN, CCNS, FAAN Duke University School of Nursing Durham, NC Dear Mrs. Brandon- I would like the opportunity
1 Ashley Robson 2212 Canyon Creek Dr. Mckinney, TX 75070 September 2 nd 2014 Debra Brandon PhD, RN, CCNS, FAAN Duke University School of Nursing Durham, NC Dear Mrs. Brandon- I would like the opportunity
6. Production or formation of plasma protein and clotting factors and heparin.
 Liver function test Clinical pathology dr. Ali H. Liver function test The liver has many vital physiologic functions involving synthesis, excretion, and storage. When a disease process damages cells within
Liver function test Clinical pathology dr. Ali H. Liver function test The liver has many vital physiologic functions involving synthesis, excretion, and storage. When a disease process damages cells within
LIVER FUNCTION TESTS
 LIVER FUNCTION TESTS TtáxÜ `A TuwxÄté Å? c{w Assistant professor of Medical Biochemistry Zagazig University, Egypt University of Bisha, KSA aaserabdelazim@yahoo.com 3/20/2018 of Clinical Medical Biochemistry
LIVER FUNCTION TESTS TtáxÜ `A TuwxÄté Å? c{w Assistant professor of Medical Biochemistry Zagazig University, Egypt University of Bisha, KSA aaserabdelazim@yahoo.com 3/20/2018 of Clinical Medical Biochemistry
