Diabetología. Insulinoma. Diagnostic criteria and treatment Insulinoma. Criterios diagnósticos y tratamiento. Seminars on diabetes.
|
|
|
- Virgil Hoover
- 5 years ago
- Views:
Transcription
1 avances en Diabetología Av Diabetol. 2009;25:293-9 Seminars on diabetes Insulinoma. Diagnostic criteria and treatment Insulinoma. Criterios diagnósticos y tratamiento M. Diéguez Felechosa, M. Riestra Fernández, E. Menéndez Torre Endocrinology and Nutrition Service. Central University Hospital of Asturias. Oviedo Abstract Insulinomas are rare islet cell tumors of the pancreas. Ninety percent are sporadic, usually single and small. The autonomous insulin secretion results in hypoglycaemia, mostly fasting hypoglycaemia, with neuroglucopenic symptoms. Biochemical diagnosis is established by demonstrating an endogenous hyperinsulinism pattern during a spontaneous or fasting-induced episode of hypoglycaemia. High resolution computer tomography and endoscopic ultrasonography are the preferred imaging techniques for diagnosis before surgery, localizing almost 100% of tumors. Other procedures are used only in selected cases. Surgery removal of insulinoma is the treatment of choice resulting in high overall cure rates. In cases of refractory hypoglycaemia medical management using drugs as diazoxide may be used. Currently, novel therapeutic approaches are being developed. Keywords: hypoglycaemia, hiperinsulinism, insulinoma, pancreatic neuroendocrine tumors. Resumen Los insulinomas son tumores poco frecuentes derivados de las células beta de los islotes pancreáticos. En el 90% de los casos son esporádicos, únicos y de pequeño tamaño. La secreción autónoma de insulina da lugar a hipoglucemias, preferentemente de ayuno, con síntomas neuroglucopénicos. El diagnóstico bioquímico se basa en la demostración de un patrón de hiperinsulinismo endógeno durante un episodio de hipoglucemia espontánea o inducida por el ayuno. La tomografía computarizada de alta resolución y la ecografía endoscópica constituyen los métodos de elección para el diagnóstico prequirúrgico, ya que localizan prácticamente el 100% de los tumores; otras técnicas se reservan para casos seleccionados. La cirugía es el tratamiento de elección, con la que se obtienen altas tasas de curación. Para el control de la hipoglucemia refractaria se utilizan determinados fármacos, como el diazóxido. Actualmente, se encuentran en fase de desarrollo nuevas estrategias terapéuticas. Palabras clave: hipoglucemia, hiperinsulinismo, insulinoma, tumores neuroendocrinos del páncreas. Introduction The insulinoma is the most frequent functioning pancreatic endocrinous tumor. It is characterized by the autonomous production of insulin by the beta cells of the pancreatic islets. Its incidence is of 4 cases per million of population and year, with a peak between the third and Date received: May 13 th 2009 Date accepted: May 28 th 2009 Correspondence: E. Menéndez Torre. Servicio de Endocrinología y Nutrición. Hospital Universitario Central de Asturias. Julián Clavería, s/n Oviedo. edelmiro.menendez@sespa.princast.es List of acronyms quoted in the text: CT: computed tomography; EH: endogenous hyperinsulinism; 18 F-DOPA PET: positron emission tomography with fluor-18-l-dihydroxiphenilalanine; HH: hyperinsulinemic hypoglycemia; ILS: intraoperatory laparoscopic ultrasonography; MEN: multiple endocrinous neoplasia; MR: magnetic resonance. sixth decades of life, though it might be diagnosed at any age. Most of the series describe a slight predominance in women. The 90% of the insulinomas are unique tumors, with a size lower than 2 cm and of benign nature. They are located in the same way in the head, the body and the pancreatic tail. They are sporadic, but in 6% of the cases they are part of the multiple endocrinous neoplasia type 1 (MEN 1), especially in young patients, with multiple tumors or that associate other endocrinous pathologies. 1 The malignant insulinoma is less frequent (5-12% of the cases) and there are not anatomopathological criteria for its diagnosis. The diagnosis of the malignity is based on the demonstration of the existence of metastasis, in most of the cases of ganglionary or hepatic nature, which are present at the moment of the diagnosis
2 Av Diabetol. 2009;25:293-9 Clinical report The hypoglycemia diagnosis is based on the documentation of the triad of Whippel: low level of plasmatic glucose with symptoms and / or signs of hypoglycemia that are solved after the normalization of the glycemia. The insulinoma is, after the factitious hypoglycemia, the most frequent cause of hypoglycemia in the apparent healthy patient. 3 It produces a fasting hypoglycemia of a characteristic way, usually at dawn, during fasting period and after physical exercise. 4 It is important to remember that the patients with insulinoma might show also a postprandial hypoglycemia. The 75% of the patients show hypoglycemia only during fasting periods, 21% associates postprandial hypoglycemias and 6% only postprandial hypoglycemias. 3 The clinical expression of insulinoma is often unspecific and variable, even in a same patient, entailing, a mean delay in the diagnosis of 2 years together with the difficulty of documenting hypoglycemias. 5 The adrenergic manifestations of hypoglycemia (perspiration, trembling, palpitations, hunger, diaphoresis...) might be absent. The picture is characterized by neuroglycopenic manifestations (changes in the mood state, behavior alterations, weakness, and visual symptoms, reduction of the conscious level and seizure disorders) and it is usual that the patient does not remember the event. 6 It is frequent that the patients with insulinoma are wrongly diagnosed of neurological or psychiatric processes. The hypoglycemia shall be part of the differential diagnosis of the refractory epilepsy. 7 Biochemical diagnosis The diagnosis of insulinoma is based on the demonstration of endogenous hyperinsulinism (EH) during a spontaneous hypoglycemia or induced by the fasting. The criteria for the diagnosis of EH have been modified during the last years. Classically, the criteria defined by Marks and Teale in 1996 and then by Service in 1999, are based on the existence of inappropriately high levels of insulin and C-peptide coinciding with hypoglycemia. 8,9 Afterwards, other measurement parameters have been added, as the pro-insulin levels, considering the higher proportion of this substance secreted in patients with insulinoma, the beta-hydroxibutyrate, as marker of ketosis response during fasting period, and the response of the glycemia after the stimulation with glucagon. This last one allows determining the hepatic reserves of glucagon after the fasting period depleted in healthy individuals. The determination of the oral hypoglycemiant is added to this (sulphonylureas in urine) and the anti-insulin antibodies. These parameters have demonstrated a great diagnostic validity in order to determine the differential diagnosis of EH. 3,10,11 Since it is difficult to document a hypoglycemic event spontaneously or after night fasting, the hypoglycemia has to be induced by means of a controlled fasting in most of the patients. The fasting test of 72 hours is still the reference pattern for the insulinoma diagnosis. It is an expensive procedure that requires several days of hospitalization, but it is usually well tolerated by the patients. Though most of the patients experiment hypoglycemia before 72 hours (33% in 12 hours, 65% in 24 hours, 84% in 36 hours and 93% in 48 hours), a reduced number (7%) present insulinoma and negative fasting test after 48 hours. 3 Moreover, a complete suppression of the beta cell in healthy individuals is achieved only after 72 hours of fasting. Therefore, with the aim of achieving the maximum diagnosis precision, the performance of the test of 72 hours is recommended. The negativity of the fasting test in a patient with insulinoma is exceptional. The protocol of the fasting test performance is detailed in table 1. The fasting test is positive when a hypoglycemia is recorded with a EH biochemical pattern (insulin 3 μu/ ml, C-peptide 0.2 nmol/l, pro-insulin 5 pmol/l, beta-hydroxibutyrate 2.7 mmol/l, glucose response after i.v. infusion of glucagon >25 mg/dl). 10 The pro-insulin and the C-peptide are the most precise markers, with a sensitivity and a specificity close to 100%. The insulin levels and the ratio glucose/pro-insulin, pro-insulin/insulin and glucose/insulin have a lower diagnostic value, therefore its systematic use is not recommended at present. 11 The development of hypoglycemia is not a sufficient criterion to give as positive the fasting test, due to the superposition with healthy individuals, especially in young women and children. 10 Differential diagnosis The differential diagnosis of the insulinoma is performed with the other causes of hyperinsulinemic hypoglycemia (HH) in apparently healthy individuals. The facticious hypoglycemia produced an undistinguishable biochemical pattern by the abrupt determination of sulphonylure- 294
3 Seminars on diabetes Insulinoma. Diagnostic criteria and treatment. M. Diéguez Felechosa, et al. Table 1. Fasting test of 72 hours 10 Record the 72 hours of fasting as from the last performed intake Suspend all the non-necessary medication The patient can drink water and teas Motivate the patient to keep himself active during the day Serial blood extractions each 6 hours, determining plasmatic glucose first until it decreases below 60 mg/dl and then analyze the insulin, the pro-insulin, the C-peptide and the betahydroxibutyrate sample and perform extractions each 1-2 hours End the fasting after 72 hours or when the glycemia is lower than 45 mg/dl and the patient shows symptoms and/or signs of hypoglycemia. A low value of isolated glycemia without symptoms and/or signs of hypoglycemia are not an indication to interrupt the test. Should it be justified to interrupt it considering the presence of clinical hypoglycemia signs with glycemia values between 45 and 55 mg/dl At the end of the fasting, take a sample for the determination of glucose, insulin, pro-insulin C-peptide and beta-hydroxibutyrate and administer 1 mg i.v. of glucagon, recording the glycemia response after 10, 20 and 30 minutes To determine the concentrations of anti-insulin anti-bodies and sulphonylureas in urine during the test as, but the drug can be measured in urine. The C-peptide will be suppressed in the cases of exogenous administration of insulin (table 2). The nesidioblastosis or islet cell hyperplasia is not so frequent due to HH in adults. It might be congenital (related to mutations in the insulin receptor) or induced by the abrupt determination of sulphonylureas or the surgery of gastric derivation. Unlike the insulinoma, the hypoglycemia is of postprandial presentation, and the fasting test is negative. The usual imaging techniques are negative; therefore one has to resort to more sensitive methods in order to determine the diagnosis. The non insulinoma pancreatic hypoglycemia (diffuse hypertrophy of the islets cells) and hypoglycemia of autoimmune origin are exceptional. 12 Localization At present we count with a multitude of techniques to determine the localization of the insulinoma. By means of the use of intraoperatory ultrasounds and the pancreatic palpation by an experienced surgeon, 100% of the insulinomas are detected. 13 The intraoperatory echography has a sensitivity higher than 95% and it also provides anatomic information when localizing the duct system and the intra-pancreatic vessels, allowing to plan the type of surgery and reduce the number of complications. The 75% of the tumors are identified by means of pancreatic palpation (it shows limitations in the small tumors), of soft consistency and deep situation in the pancreas. 14 Since the high precision of the intraoperatory methods, the discussion is focused on the role of the pre-surgery diagnosis. Most of the authors support the pre-surgery localization as it allows planning the type of intervention, choosing a laparoscopic approach, shortening the surgi- Tabla 2. Biochemical pattern of insulinoma and differential diagnosis of the hyperinsulinemic hypoglycemia 10 Glucose (mg/dl) Insulin (μu/ml) Pro-insulin (pmo/l) C-peptide (nmo/l) Beta-hydroxibutyrate (mmol/l) Glycemia increase after glucagon (mg/dl) Anti-insulin Sulphonylureas anti-bodies in urine Insulinoma < ,2 2,7 25 Negative Negative Nesidioblastosis < ,2 2,7 25 Negative Negative Facticious hypoglycemia by insulin Facticious hypoglycemia by sulphonylureas Non-insulinoma hypoglycemia syndrome Autoimmune hypoglycemia <55 3 <5 <0,2 2,7 25 Negative Negative < ,2 2,7 25 Negative Positive < ,2 2,7 25 Negative Negative <55 3 Variable Variable 2,7 25 Positive Negative 295
4 Av Diabetol. 2009;25:293-9 cal time and reducing the morbimortality Moreover, the pre-surgical extension study by means of computed tomography (CT) or magnetic resonance (MR) allows performing the screening of the metastasis and its performance is indicated in all the cases with insulinoma. The pre-surgical diagnosis of 100% of the patients can be achieved with the current methods (75% though noninvasive methods). 3 The diagnostic precision of the conventional imaging techniques (abdominal echography, CT) is limited, with a sensitivity of 50-60%. 15 These techniques detect preferably tumors >2 cm of easy intraoperatory diagnosis. The new multi-cut helicoidal CT allow to diagnose 94% of the cases, 14 and are included within the option diagnosis methods (figure 1). The modern equipments of MR with the use of gadolinium, contrary to the other techniques, offer a better performance in the small and multiple tumors (<1 cm). 14 Among the invasive techniques, the endoscopic echography is the choice technique, recommended by most of the authors. 3 It diagnoses % of the tumors located in the head or the pancreas body, though it is less sensitive for the lesions in the tail (60%). It allows the collection of biopsies and provides excellent anatomic information. The intraductal echography improves the diagnosis precision, but due to its complexity it is reserved for selected cases. The gammagraphy with octreotide has a limited value in the insulinoma study as less than 50% of the cases express receptors of the somatostatine The positron emission tomography (PET) with fluor-18-l-dihydroxyphenylalanine ( 18 F-DOPA) is a technique which is used in the diagnosis of neuro-endocrinous tumors. This technique localizes a great sensitivity of pancreatic tissue that produces the insulin in patients with insulinoma or hyperplasia of beta cells, due to the capacity of the endocrine pancreas to capture and descarboxilate L-DOPA. It has demonstrated a higher validity as regards to the CT or MR in small series and has a promising future in the functional study of the pancreatic tissue, but the study of greater series is necessary to validate its diagnostic precision. 17 The arteriography is an invasive technique and not free from complications, with a variable sensitivity, in the region of 60%, dependent on the tumor size and the level of vascularization, and its use is being abandoned as one disposes of other diagnosis methods. 14 Figure 1. Angio-CT of the insulinoma. Angio-CT of high resolution (hepatopancreatic window) in which an insulinoma of 14 mm is identified in the pancreas head, increased uptake in arterial phase The selective intra-arterial stimulation with calcium, by means of the measurement of insulinemia in the suprahepatic veins and the record of insulin secretion in specific territories is getting an increasing protagonism in the regional diagnosis of the insulinoma. Its sensitivity is of 90%, clearly higher than the echography, the CT and the MR. 18 The access is through the femoral route and the venous catheter is placed (Swan Ganz catheter) in the suprahepatic vein for the collection of insulinemia samples. Through the arterial catheter the stimulation takes place selectively with calcium gluconate in the arteries that irrigate the pancreatic head (gastroduodenal and superior mesenteric) the body and the tail (splenic artery) and samples are collected in venous blood of basal insulinemia, after 30, 60 and 120 minutes. The tumoral cells of an insulinoma have an exaggerated response to the calcium stimulation. When stimulating through the gastroduodenal or superior mesenteric artery, the insulinemia rises more than 2-folds over the basal level, the tumor will be localized in the pancreas head or neck. If when stimulating the splenic artery the described effect is produced, the tumor will be localized in the body and the tail of the pancreas. To summarize, the performance of a pre-surgical study with multi-cut helicoidal CT and endoscopic echography allows the localization of the insulinoma with a sensitivity of 100% and a specificity of 95%. 14 The PET with 18 F-DOPA and the rest of the invasive procedures (arteriography and selective intra-artery stimulation with calcium), due to its high cost and its scarce accessibility, are reserved for patients with biochemical EH confirmation when the rest of the studies are negative, 296
5 Seminars on diabetes Insulinoma. Diagnostic criteria and treatment. M. Diéguez Felechosa, et al. and in patients with MEN 1 or with multiple tumors suspicion. Treatment The surgical extirpation of the insulinoma is the choice treatment and the only healing one, achieving remission rates of 75-98%. 19 The surgery might be either open or laparoscopic. The enucleation and the pancreatic resection by laparoscopy have been performed with success at many sites and they offer all the advantages of a minimally invasive surgery, with a lower hospital stay and a faster recovery. Though the complications are relatively frequent as the pancreatic fistula (from 18 to 33%, according to the series), they do not entail neither increase of morbidity nor hospitalization days. 20 The intra-operatory laparoscopic ultrasonography (US Lap) might facilitate the localization of the lesion and minimize the need of conversion to open surgery. The laparoscopy shall not be done in case of tumors localized in the pancreatic head, given the high risk of hemorrhage that it entails (up to 20-40% of the cases), so this route should be reserved for the patients with solitary lesions in the body and tail of the pancreas who have not undergone another pancreatic intervention previously and an experienced team should do it. The enucleation is indicated in small tumors located at least at 2-3 mm of the principal pancreatic conduct. The recent guidelines suggest that it is sufficient with the enucleation if the lesion is superficial and is clearly defined in the intra-operatory process. The widened resection is recommended when the tumor invades the pancreatic conduct or the big vessels, or when malignity is suspected by invasion of the peripheral tissues, dilatation of the pancreatic conduct or affectation of the lymphatic ganglions. The different options of resection include the distal pancreatectomy (with or without splenectomy), the technique of Whipple or the almost total pancreatectomy, according to the localization of the insulinoma. The intra-operatory determination of the insulinemia levels might be useful to ensure the complete resection of the tumor. 21 In patients with MEN 1 syndrome, the insulinomas are usually multiple up to 59% of the cases versus only 5% in the rest of the patients. Therefore, and considering the high index of post-surgical relapses, it is recommended to perform a subtotal distal pancreatectomy together with the enucleation of the tumors that are located in the pancreas head. 22 A new localization diagnosis should be done in patients with persistent hypoglycemia after surgery and an intervention is recommended by means of the laparotomy. With the application of new techniques of pre-operation localization, especially the combinations of helicoidal CT and endoscopic ultrasonography (with sensitivity close to 100%), a few hidden insulinoma are left out. If the tumor cannot be identified, the blind pancreatic resection is not recommended and the patient shall be re-evaluated in order to verify the diagnosis. 23 The 91% of the intervened patients keep remission criteria 6 months after the surgery. From these ones, 11% experience a recurrent hypoglycemia during the follow-up. Relapses can occur up to 18 years after the intervention. The accumulated incidence of recurrences is of 6% after 10 years and 8% after 20 years. In patients with MEN 1, the recurrence index is higher, reaching 21% after 10 years. 24 The survival of the patients who underwent surgery is similar to the general population. However, it worsens significantly in advanced age patients and in the patients who show a malignant insulinoma, though it seems to have a long natural history in patients with metastatic disease and more than 20 years of follow-up. 18 Treatment of the hepatic metastasis The liver is the most common place where the insulinoma metastasis are located, for which there are several direct therapeutic modalities. The hepatic resection is indicated in the absence of diffuse lesions in both lobules, previous hepatic failure and extensive extra-hepatic metastasis (pulmonary, peritoneal...), obtaining higher survival indexes, though the healing is only achieved in 15% of the patients. The therapeutic embolization of the hepatic artery causes necrosis of the tumoral tissue without damaging the healthy hepatic tissue. The selective embolization, with or without infusion of chemotherapeutic substances, is used as palliative techniques in patients with symptomatic hepatic metastasis who are not candidates to surgery. The radiofrequency and the cryoablation might be performed subcutaneously or by laparoscopic route, entailing a lower morbidity than the resection of the metastasis or the arterial embolization; there 297
6 Av Diabetol. 2009;25:293-9 Demonstration of hyperinsulinemic hypoglycemia Spontaneous hypoglycemia Open Yes Surgery Hypoglycemia confirmation (triad of Whipper) Localization diagnosis Laparoscopic Fasting test High resolution CT Localization Endoscopic echography Figure 2. Diagnosis algorhythm of insulinoma treatment (own elaboration). MR: magnetic resonance; 18 F-DOPA PET: positron emission tomography with fluor-18-l-dihydroxyphylalanine are no data available about the efficacy at long term. The hepatic transplant has been done in a few patients and the follow-up duration is insufficient to show data about the healing possibility. As regards to the chemotherapy, the traditional choice regime has been the streptotozotocine and the doxorubicin, though its modest efficiency (achieves between 10 and 40% of tumoral remission) and its toxicity has promoted the development of new therapeutic agents, as the angiogenesis inhibitors. Medical treatment The medical treatment of the insulinoma has to be taken into account in patients with hidden insulinoma, in those who are not candidates to surgery or reject them, and in those who have a non-resectable metastatic disease. The Yes No Localization Night fasting No MR 18 F-DOPA PET Arteriography Arterial stimulation with calcium Practical considerations The insulinomas are generally unique and small sized sporadic tumors in the 90% of the cases. The fasting test of 72 hours is still the reference pattern in the diagnosis. The values of pro-insulin and C-peptide are those to be taken into account due to their high sensitivity and specifi city. The combination of helicoidal CT and endoscopic ultrasonography allows determining a pre-surgical diagnosis in most of the cases. The choice treatment is the surgical resection of the tumor. therapeutic options to prevent the symptomatic hypoglycemia are as follows: The diazoxide ( mg/day) increases the plasmatic concentration of glucose reducing the insulin secretion, and up to 50% of the patients achieve an improvement in the control of their hypoglycemias. The edema, the gastrointestinal disorders and the hypertricosis are described as side effects. The octreotide inhibits the secretion of the growth hormone, but it also inhibits the secretion of TSH, insulin and glucagon in high doses. Its efficacy is limited in the insulinoma. However, it is a reasonable alternative in patients with persistent refractory hypoglycemia as regards to the treatment with diazoxide. The lanreotide is another analogue of the somatostatin that seems to have a similar effect to the octreotide and offers the advantage of having a long-acting release form. The everolimus is an immunosupressor drug with antiangiogenic effect, with promising results in the glycemic control and the tumoral reduction in patients with malignant insulinoma, even in clinical trials. 25 Figure 2 shows the diagnosis algorhythm that has to be followed before the suspicion of insulinoma. Conclusions The biochemical diagnosis and localization of the insulinoma is complex. It requires specific analytical and technical determinations, invasive some times. Almost the total diagnosis of the tumors is achieved with the current methods; therefore the hidden insulinomas are exceptional. The surgery offers high healing rates and the rest of the therapeutic options remain relegated to a second background. 298
7 Seminars on diabetes Insulinoma. Diagnostic criteria and treatment. M. Diéguez Felechosa, et al. Declaration of potential conflict of interests M. Diéguez, M. Riestra and E. Menéndez state that there are no conflicts of interest as regards to this article. References 1. Sitges-Serra A, Fernández-Cruz L. Tumores endocrinos del páncreas. Manual de la Asociación Española de Cirujanos. Madrid: Ed. Panamericana; p Hirsberg B, Cochran C, Skarulis M, Libutti S, Alexander R, Wood B, et al. Malignant insulinoma. Cancer. 2005;104: Kimberly A, Placzkowski K, Vella A, Thompson G, Grant C, Service F. Secular Trends in the presentation and management of functioning insulinoma at the Mayo Clinic, J Clin Endocrinol Metab. 2009;94: Suzuki K, Miyamoto M, Miyamoto T, Hirata K. Insulinoma with earlymorning abnormal behavior. Intern Med. 2007;46: Tucker ON, Crotty PL, Conlon KC. The management of insulinoma. Br J Surg. 2006;93: Dizon AM, Kowalyk S, Hoogwerf BJ. Neuroglycopenic and other symptoms in patients with insulinomas. Am J Med. 1999;106: O Sullivan SS, Redmond J. Insulinoma presenting as refractory late-onset epilepsy. Epilepsia. 2005;46: Marks V, Teale JD. Investigation of hypoglycaemia. Clin Endocrinol. 1996;44: Service E. Diagnostic approach to adults with hypoglycaemic disorders. Endocrinol Metab Clin North Am. 1999;28: Cryer P, Axelrod L, Grossman A, Heller S, Montori V, Seaquist E. Evaluation and management of adult hypoglycemic disorders: an Endocrine Society Clinical Practice Guideline. J Clin Endocrinol Metab, 2009;94: Vezzosi D, Bennet A, Fauvel F, Caron P. Insulin, C-peptide and proinsulin for the biochemical diagnosis fo hypoglycaemia related to endogenous hyperinsulinism. J Clin Endocrinol Metab. 2007;157: Cryer PE. Homeostasis de la glucosa e hipoglucemia. En: Kronenberg H, Melmed S, Polonsky K, Larsen PR, eds. Williams Textbook of Endocrinology, 11 th ed. Barcelona: Elservier; p Boukhman M, Karam J, Shaver J, Siperstein A, DeLorimier A, Clark O. Localization of insulinomas. Arch Surg. 1999;134: Bassam A, Joe B. Occult sporadic insulinoma. Localization and surgical strategy. World J Gastroenterol. 2008;14: Service FJ, McMahon MM, O Brien PC, Ballard DJ. Functioning insulinomaincidence, recurrence and long-term survival of patients: a 60-year study. Mayo Clin Proc. 1991;66: Priego P, Sanjuanbenito A, Martínez Molina E, Lobo E, García Teruel D, Morales V. Manejo diagnóstico y terapéutico del insulinoma pancreático. Rev Esp Enferm Dig. 2007;99: Kauhanen S, Seppänen M, Minn H, Gullichsen R, Salonen A, Alanen K. Fluorine-18-L-dihydroxyphenylalanine (18F-DOPA) positron emission tomography as a tool to localize an insulinoma or ß-cell hyperplasia in adult patients. J Clin Endocrinol Metab. 2009;92: Guettier JM, Kam A, Chang R, Skarulis MC, Cochran C, Alexander HR. Localization of insulinomas to regions of the pancreas by intraarterial calcium stimulation: the NIH Experience. J Clin Endocrinol Metab. 2009;94: Service F, Natt N. The prolonged fast. J Clin Endocrinol Metab. 2000;85: Gama R, Teale JD, Marks V. Clinical and laboratory investigation of adult spontaneous hypoglycaemia. J Clin Pathol. 2003;56: Hirshberg B, Livi A, Bartlett DL, Libutti SK, Alexander HR, Doppman JL. The diagnostic test for insulinoma. J Clin Endocrinol Metab. 2000;85: Murat A, Pervin I, Komsuoglu, Sener S. Insulinoma in differential diagnosis of seizure disorder. J Neuropsychiatry Clin Neurosci. 2006;18: Service FJ, O Brien PC. Increasing serum betahydroxybutyrate concentrations during the 72-hour fast: evidence against hyperinsulinemic hypoglycemia. J Clin Endocrinol Metab. 2005;90: Service FJ, Dale ASD, Elveback LR, Jiang NS. Insulinoma: clinical and diagnostic features of 60 consecutives cases. Mayo Clin Proc. 1976;51: Kulke MH, Bergsland EK, Yao JC. Glycemic control in patients with insulinoma treated with everolimus. N Engl J Med. 2009;360:
HYPOGLYCEMIA and neuroglycopenic symptoms
 0021-972X/00/$03.00/0 Vol. 85, No. 9 The Journal of Clinical Endocrinology & Metabolism Printed in U.S.A. Copyright 2000 by The Endocrine Society Forty-Eight-Hour Fast: The Diagnostic Test for Insulinoma
0021-972X/00/$03.00/0 Vol. 85, No. 9 The Journal of Clinical Endocrinology & Metabolism Printed in U.S.A. Copyright 2000 by The Endocrine Society Forty-Eight-Hour Fast: The Diagnostic Test for Insulinoma
Pancreatic Insulinoma Presenting. with Episodes of Hypoinsulinemic. Hypoglycemia in Elderly ---- A Case Report
 2008 19 432-436 Pancreatic Insulinoma Presenting with Episodes of Hypoinsulinemic Hypoglycemia in Elderly ---- A Case Report Chieh-Hsiang Lu 1, Shih-Che Hua 1, and Chung-Jung Wu 2,3 1 Division of Endocrinology
2008 19 432-436 Pancreatic Insulinoma Presenting with Episodes of Hypoinsulinemic Hypoglycemia in Elderly ---- A Case Report Chieh-Hsiang Lu 1, Shih-Che Hua 1, and Chung-Jung Wu 2,3 1 Division of Endocrinology
An Unusual Case of Concurrent Insulinoma and Nesidioblastosis
 CASE REPORT An Unusual Case of Concurrent Insulinoma and Nesidioblastosis Elizabeth Bright 1, Giuseppe Garcea 1, Seok L Ong 1, Webster Madira 2, David P Berry 1, Ashley R Dennison 1 Departments of 1 Hepatobiliary
CASE REPORT An Unusual Case of Concurrent Insulinoma and Nesidioblastosis Elizabeth Bright 1, Giuseppe Garcea 1, Seok L Ong 1, Webster Madira 2, David P Berry 1, Ashley R Dennison 1 Departments of 1 Hepatobiliary
Management of Pancreatic Islet Cell Tumors
 Management of Pancreatic Islet Cell Tumors Ravi Dhanisetty, MD November 5, 2009 Morbidity and Mortality Conference Case Presentation 42 yr female with chronic abdominal pain. PMHx: Uterine fibroids Medications:
Management of Pancreatic Islet Cell Tumors Ravi Dhanisetty, MD November 5, 2009 Morbidity and Mortality Conference Case Presentation 42 yr female with chronic abdominal pain. PMHx: Uterine fibroids Medications:
Endocrine topic reviews. Artit Sangkakam, MD 19, september 2013
 Endocrine topic reviews Artit Sangkakam, MD 19, september 2013 Hypoglycemia in Non-DM Definition In diabetic mellitus : Plasma glucose 70 mg/dl In Non-diabetic mellitus : Plasma glucose 55 mg/dl Normal
Endocrine topic reviews Artit Sangkakam, MD 19, september 2013 Hypoglycemia in Non-DM Definition In diabetic mellitus : Plasma glucose 70 mg/dl In Non-diabetic mellitus : Plasma glucose 55 mg/dl Normal
Insulin, C-peptide and proinsulin for the biochemical diagnosis of hypoglycaemia related to endogenous hyperinsulinism
 European Journal of Endocrinology (2007) 157 75 83 ISSN 0804-4643 CLINICAL STUDY Insulin, C-peptide and proinsulin for the biochemical diagnosis of hypoglycaemia related to endogenous hyperinsulinism D
European Journal of Endocrinology (2007) 157 75 83 ISSN 0804-4643 CLINICAL STUDY Insulin, C-peptide and proinsulin for the biochemical diagnosis of hypoglycaemia related to endogenous hyperinsulinism D
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
An Unexpected Cause of Hypoglycemia
 An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
Unusual Pancreatic Neoplasms RTC 2/11/2011
 Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Research Article Arterial Calcium Stimulation with Hepatic Venous Sampling in the Localization Diagnosis of Endogenous Hyperinsulinism
 International Endocrinology Volume 2016, Article ID 4581094, 6 pages http://dx.doi.org/10.1155/2016/4581094 Research Article Arterial Calcium Stimulation with Hepatic Venous Sampling in the Localization
International Endocrinology Volume 2016, Article ID 4581094, 6 pages http://dx.doi.org/10.1155/2016/4581094 Research Article Arterial Calcium Stimulation with Hepatic Venous Sampling in the Localization
Insulinoma Presenting with Reactive Hypoglycemia: Evaluating the Effect of Tumor Resection via Continuous Glucose Monitoring
 doi: 10.2169/internalmedicine.8766-16 http://internmed.jp CASE REPORT Insulinoma Presenting with Reactive Hypoglycemia: Evaluating the Effect of Tumor Resection via Continuous Glucose Monitoring Tomohiko
doi: 10.2169/internalmedicine.8766-16 http://internmed.jp CASE REPORT Insulinoma Presenting with Reactive Hypoglycemia: Evaluating the Effect of Tumor Resection via Continuous Glucose Monitoring Tomohiko
Hypoglycaemic disorders
 Hypoglycaemic disorders 1. Hypoglycaemia in patients with diabetes mellitus 2. Hypoglycaemia in non-diabetic patients 3. Clinical, laboratory and imaging diagnosis 4. Case report 5. GLP-1 receptor scintigraphy
Hypoglycaemic disorders 1. Hypoglycaemia in patients with diabetes mellitus 2. Hypoglycaemia in non-diabetic patients 3. Clinical, laboratory and imaging diagnosis 4. Case report 5. GLP-1 receptor scintigraphy
A Case of Insulinoma Presenting with Reactive Hypoglycemia: Evaluating the Effect of Tumor Resection via Continuous Glucose Monitoring
 doi: 10.2169/internalmedicine.8766-16 Intern Med Advance Publication http://internmed.jp CASE REPORT A Case of Insulinoma Presenting with Reactive Hypoglycemia: Evaluating the Effect of Tumor Resection
doi: 10.2169/internalmedicine.8766-16 Intern Med Advance Publication http://internmed.jp CASE REPORT A Case of Insulinoma Presenting with Reactive Hypoglycemia: Evaluating the Effect of Tumor Resection
Clinical Implications of Various Criteria for the Biochemical Diagnosis of Insulinoma
 Original Article Endocrinol Metab ;9:98-5 http://dx.doi.org/./enm..9..98 pissn -59X eissn -5978 Clinical Implications of Various Criteria for the Biochemical Diagnosis of Chang Ho Ahn, Lee-Kyung Kim, Jie
Original Article Endocrinol Metab ;9:98-5 http://dx.doi.org/./enm..9..98 pissn -59X eissn -5978 Clinical Implications of Various Criteria for the Biochemical Diagnosis of Chang Ho Ahn, Lee-Kyung Kim, Jie
David Bruyette, DVM, DACVIM Medical Director
 VCAWLAspecialty.com David Bruyette, DVM, DACVIM Medical Director The pancreas is made up of endocrine and exocrine tissue. The endocrine pancreas is composed of islets of Langerhans, which make up approximately
VCAWLAspecialty.com David Bruyette, DVM, DACVIM Medical Director The pancreas is made up of endocrine and exocrine tissue. The endocrine pancreas is composed of islets of Langerhans, which make up approximately
A Rare Case Report - Big Insulinoma of Pancreas
 A Rare Case Report - Big Insulinoma of Pancreas Dr Vikalap Gupta 1, Prof Dr Brijesh Sharma 2 Abstract: Insulinomas account for 60% of islet cell tumours (ICT) and are typically hypervascular, solitary
A Rare Case Report - Big Insulinoma of Pancreas Dr Vikalap Gupta 1, Prof Dr Brijesh Sharma 2 Abstract: Insulinomas account for 60% of islet cell tumours (ICT) and are typically hypervascular, solitary
Color Codes Pathology and Genetics Medicine and Clinical Pathology Surgery Imaging
 Saturday, November 5, 2005 8:30-10:30 a. m. Poorly Differentiated Endocrine Carcinomas Chairman: E. Van Cutsem, Leuven, Belgium 9:00-9:30 a. m. Working Group Sessions Pathology and Genetics Group leaders:
Saturday, November 5, 2005 8:30-10:30 a. m. Poorly Differentiated Endocrine Carcinomas Chairman: E. Van Cutsem, Leuven, Belgium 9:00-9:30 a. m. Working Group Sessions Pathology and Genetics Group leaders:
Insulinoma - 72 hour Fast Protocol - RNS Endocrinology
 Page 1 of 9 - RNS Endocrinology Test name 72 hour fast Alternate test names. Related Tests Mixed meal test Indication(s) Differential diagnosis of causes of hypoglycaemia. Hypoglycaemia is rare in persons
Page 1 of 9 - RNS Endocrinology Test name 72 hour fast Alternate test names. Related Tests Mixed meal test Indication(s) Differential diagnosis of causes of hypoglycaemia. Hypoglycaemia is rare in persons
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear
 Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Case Report Metastatic Insulinoma Managed with Radiolabeled Somatostatin Analog
 Case Reports in Endocrinology Volume 2013, Article ID 252159, 4 pages http://dx.doi.org/10.1155/2013/252159 Case Report Metastatic Insulinoma Managed with Radiolabeled Somatostatin Analog Ricardo Costa,
Case Reports in Endocrinology Volume 2013, Article ID 252159, 4 pages http://dx.doi.org/10.1155/2013/252159 Case Report Metastatic Insulinoma Managed with Radiolabeled Somatostatin Analog Ricardo Costa,
HEPATIC METASTASES. We can state 3 types of metastases depending on their treatment options:
 HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
Introduction SHORT COMMUNICATION
 Diabetologia (2005) 48: 2236 2240 DOI 10.1007/s00125-005-1933-x SHORT COMMUNICATION M. E. Patti. G. McMahon. E. C. Mun. A. Bitton. J. J. Holst. J. Goldsmith. D. W. Hanto. M. Callery. R. Arky. V. Nose.
Diabetologia (2005) 48: 2236 2240 DOI 10.1007/s00125-005-1933-x SHORT COMMUNICATION M. E. Patti. G. McMahon. E. C. Mun. A. Bitton. J. J. Holst. J. Goldsmith. D. W. Hanto. M. Callery. R. Arky. V. Nose.
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
APPROACH TO ORGANIC HYPERINSULINISM IN PATIENTS WITH DIABETES MELLITUS
 Vuk Vrhovac University Clinic, Dugi dol 4a, Zagreb, Croatia Review Received: March 15, 2007 Accepted: April 2, 2007 APPROACH TO ORGANIC HYPERINSULINISM IN PATIENTS Marija Požgaj-Šepec, Lea Duvnjak, Nikica
Vuk Vrhovac University Clinic, Dugi dol 4a, Zagreb, Croatia Review Received: March 15, 2007 Accepted: April 2, 2007 APPROACH TO ORGANIC HYPERINSULINISM IN PATIENTS Marija Požgaj-Šepec, Lea Duvnjak, Nikica
Diagnosis and localisation of insulinoma: the value of modern magnetic resonance imaging in conjunction with calcium stimulation catheterisation
 European Journal of Endocrinology (2010) 162 971 978 ISSN 0804-4643 CLINICAL STUDY Diagnosis and localisation of insulinoma: the value of modern magnetic resonance imaging in conjunction with calcium stimulation
European Journal of Endocrinology (2010) 162 971 978 ISSN 0804-4643 CLINICAL STUDY Diagnosis and localisation of insulinoma: the value of modern magnetic resonance imaging in conjunction with calcium stimulation
Original Article. Insulinoma: how reliable is the biochemical evidence? Introduction. Case report. Abstract. NK Chammas 1, JD Teale 2 and JD Quin 1
 Insulinoma: how reliable is the biochemical evidence? NK Chammas 1, JD Teale 2 and JD Quin 1 Original Article Abstract Addresses 1 The Royal Sussex County Hospital Eastern Road, Brighton, UK 2 SAS Peptide
Insulinoma: how reliable is the biochemical evidence? NK Chammas 1, JD Teale 2 and JD Quin 1 Original Article Abstract Addresses 1 The Royal Sussex County Hospital Eastern Road, Brighton, UK 2 SAS Peptide
Hypoglycemia in congenital hyperinsulinism
 How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
Venous sampling technique in Endocrinology: a renewed technique
 Venous sampling technique in Endocrinology: a renewed technique Poster No.: C-0682 Congress: ECR 2014 Type: Educational Exhibit Authors: M. E. Rodriguez Cabillas 1, J. Garcia Villanego 2, I. Olea Comas
Venous sampling technique in Endocrinology: a renewed technique Poster No.: C-0682 Congress: ECR 2014 Type: Educational Exhibit Authors: M. E. Rodriguez Cabillas 1, J. Garcia Villanego 2, I. Olea Comas
- Prof. Dr. A.A.R. Starke Dr. Christiane Saddig Heinrich-Heine-Universität Düsseldorf Medizinische Klinik
 www.insulinoma.net - www.gep-net.com Prof. Dr. A.A.R. Starke Dr. Christiane Saddig Heinrich-Heine-Universität Düsseldorf Medizinische Klinik Insulinoma "endogenous hyperinsulinism", autonomous inadaequate
www.insulinoma.net - www.gep-net.com Prof. Dr. A.A.R. Starke Dr. Christiane Saddig Heinrich-Heine-Universität Düsseldorf Medizinische Klinik Insulinoma "endogenous hyperinsulinism", autonomous inadaequate
Surgery in Congenital Hyperinsulinismless. Winfried Barthlen
 Surgery in Congenital Hyperinsulinismless may be more Winfried Barthlen congenital hyperinsulinism - very rare (1:40.000) - uncontrolled insulin secretion - life threatening hypoglycemia symptoms - unconsciousness,
Surgery in Congenital Hyperinsulinismless may be more Winfried Barthlen congenital hyperinsulinism - very rare (1:40.000) - uncontrolled insulin secretion - life threatening hypoglycemia symptoms - unconsciousness,
Drs Maaz Sohail, FAU Resident and Bryan Vinik, Endocrinology
 Drs Maaz Sohail, FAU Resident and Bryan Vinik, Endocrinology HPI: 75M referred for hypoglycemia with symptoms that started 18 months ago. Patient states that after drinking wine at night he would up confused
Drs Maaz Sohail, FAU Resident and Bryan Vinik, Endocrinology HPI: 75M referred for hypoglycemia with symptoms that started 18 months ago. Patient states that after drinking wine at night he would up confused
Diagnosis and treatment of pancreatic insulinoma
 1130-0108/2007/99/4/218-222 REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS Copyright 2007 ARÁN EDICIONES, S. L. REV ESP ENFERM DIG (Madrid) Vol. 99. N. 4, pp. 218-222, 2007 Diagnosis and treatment of pancreatic
1130-0108/2007/99/4/218-222 REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS Copyright 2007 ARÁN EDICIONES, S. L. REV ESP ENFERM DIG (Madrid) Vol. 99. N. 4, pp. 218-222, 2007 Diagnosis and treatment of pancreatic
Managing Congenital Hyperinsulinism in the Neonatal Period Vall d Hebron Hospital s Approach and Experience
 Managing Congenital Hyperinsulinism in the Alejandro Vargas Pieck Miquel Gussinyer Canadell María Clemente León Diego Yeste Fernández Universidad Autónoma de Barcelona Antonio Carrascosa Lezcano The first
Managing Congenital Hyperinsulinism in the Alejandro Vargas Pieck Miquel Gussinyer Canadell María Clemente León Diego Yeste Fernández Universidad Autónoma de Barcelona Antonio Carrascosa Lezcano The first
Pancreatic Lesions. Valerie Jefford Pediatric Surgery Rounds June 6, 2003
 Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
NEUROENDOCRINE CARCINOID TUMORS PANCREATIC NEUROENDOCRINE TUMORS
 University of Miami Jackson Memorial Hospital Role of the Surgeon in the Approach to Neuroendocrine tumors Dido Franceschi, MD Professor of Surgery University of Miami Karzinoide Siegfried Oberndorfer,
University of Miami Jackson Memorial Hospital Role of the Surgeon in the Approach to Neuroendocrine tumors Dido Franceschi, MD Professor of Surgery University of Miami Karzinoide Siegfried Oberndorfer,
Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Patient Demographics 5/12/2016
 Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Pediatric Endocrine Nursing Society May 14, 2016 Enyo Dzata, MSN, CRNP Congenital Hyperinsulinism Center Division
Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Pediatric Endocrine Nursing Society May 14, 2016 Enyo Dzata, MSN, CRNP Congenital Hyperinsulinism Center Division
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14
 Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
SHORT COMMUNICATION. J. C. Reubi & A. Perren & R. Rehmann & B. Waser & E. Christ & M. Callery & A. B. Goldfine & M. E. Patti
 Diabetologia (2010) 53:2641 2645 DOI 10.1007/s00125-010-1901-y SHORT COMMUNICATION Glucagon-like peptide-1 (GLP-1) receptors are not overexpressed in pancreatic islets from patients with severe hyperinsulinaemic
Diabetologia (2010) 53:2641 2645 DOI 10.1007/s00125-010-1901-y SHORT COMMUNICATION Glucagon-like peptide-1 (GLP-1) receptors are not overexpressed in pancreatic islets from patients with severe hyperinsulinaemic
Overview. o Limitations o Normal regulation of blood glucose o Definition o Symptoms o Clinical forms o Pathophysiology o Treatment.
 Pål R. Njølstad MD PhD KG Jebsen Center for Diabetes Research University of Bergen, Norway Depertment of Pediatrics Haukeland University Hospital Broad Institute of Harvard & MIT Cambridge, MA, USA Hypoglycemia
Pål R. Njølstad MD PhD KG Jebsen Center for Diabetes Research University of Bergen, Norway Depertment of Pediatrics Haukeland University Hospital Broad Institute of Harvard & MIT Cambridge, MA, USA Hypoglycemia
Neuroendocrine Tumors
 Neuroendocrine Tumors Neuroendocrine tumors arise from cells that release a hormone in response to a signal from the nervous system. Neuro refers to the nervous system. Endocrine refers to the hormones.
Neuroendocrine Tumors Neuroendocrine tumors arise from cells that release a hormone in response to a signal from the nervous system. Neuro refers to the nervous system. Endocrine refers to the hormones.
Insulin levels measured with an insulin-specific assay in patients with fasting hypoglycaemia related to endogenous hyperinsulinism
 European Journal of Endocrinology (2003) 149 413 419 ISSN 0804-4643 CLINICAL STUDY Insulin levels measured with an insulin-specific assay in patients with fasting hypoglycaemia related to endogenous hyperinsulinism
European Journal of Endocrinology (2003) 149 413 419 ISSN 0804-4643 CLINICAL STUDY Insulin levels measured with an insulin-specific assay in patients with fasting hypoglycaemia related to endogenous hyperinsulinism
Medicine. Intraoperative portal vein insulin assay combined with occlusion of the pancreas for complex pancreatogenous hypoglycemia Two cases report
 Clinical Case Report Medicine Intraoperative portal vein insulin assay combined with occlusion of the pancreas for complex pancreatogenous hypoglycemia Two cases report Zhiying Yang (MD), Haidong Tan (MD),
Clinical Case Report Medicine Intraoperative portal vein insulin assay combined with occlusion of the pancreas for complex pancreatogenous hypoglycemia Two cases report Zhiying Yang (MD), Haidong Tan (MD),
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear
 Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Use of Lanreotide (long acting Somatostatin analogue) in Congenital Hyperinsulinism (CHI)
 Use of Lanreotide (long acting Somatostatin analogue) in Congenital Hyperinsulinism (CHI) Dr Pratik Shah Clinical Research fellow in Hyperinsulinism Clinical Molecular Genetics Unit Institute of Child
Use of Lanreotide (long acting Somatostatin analogue) in Congenital Hyperinsulinism (CHI) Dr Pratik Shah Clinical Research fellow in Hyperinsulinism Clinical Molecular Genetics Unit Institute of Child
PET Scan in Practice for CHI
 PET Scan in Practice for CHI - Basics, strength and weakness - Oliver Blankenstein Institute for Experimental Paediatric Endocrinology Charité-Universitätsmedizin Berlin U N I V E R S I T Ä T S M E D I
PET Scan in Practice for CHI - Basics, strength and weakness - Oliver Blankenstein Institute for Experimental Paediatric Endocrinology Charité-Universitätsmedizin Berlin U N I V E R S I T Ä T S M E D I
Evaluation of Suspected Pancreatic Cancer
 Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Supplementary Appendix
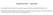 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Baidal DA, Ricordi C, Berman DM, et al. Bioengineering of an
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Baidal DA, Ricordi C, Berman DM, et al. Bioengineering of an
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
[ ] 169 NICTH Nadler WH Wolfer JA NICTH. (nonislet cell tumor. (hypoglycemia) (nonislet cell tumor hypoglycemia, NICTH)
![[ ] 169 NICTH Nadler WH Wolfer JA NICTH. (nonislet cell tumor. (hypoglycemia) (nonislet cell tumor hypoglycemia, NICTH) [ ] 169 NICTH Nadler WH Wolfer JA NICTH. (nonislet cell tumor. (hypoglycemia) (nonislet cell tumor hypoglycemia, NICTH)](/thumbs/92/107875530.jpg) [] 169 1 2 2 2 (nonislet cell tumor hypoglycemia, NICTH) (paraneoplastic syndrome) NICTH (macromolecules insulin-like growth factor-ii, big IGF-II)Big IGF-II (tumor burden) NICTH NICTH 2016; 26: 169-78
[] 169 1 2 2 2 (nonislet cell tumor hypoglycemia, NICTH) (paraneoplastic syndrome) NICTH (macromolecules insulin-like growth factor-ii, big IGF-II)Big IGF-II (tumor burden) NICTH NICTH 2016; 26: 169-78
Case Report Hypoglycemic Syndrome in a Patient with Proinsulin-Only Secreting Pancreatic Adenoma (Proinsulinoma)
 Hindawi Publishing Corporation Case Reports in Medicine Volume 2011, Article ID 930904, 5 pages doi:10.1155/2011/930904 Case Report Hypoglycemic Syndrome in a Patient with Proinsulin-Only Secreting Pancreatic
Hindawi Publishing Corporation Case Reports in Medicine Volume 2011, Article ID 930904, 5 pages doi:10.1155/2011/930904 Case Report Hypoglycemic Syndrome in a Patient with Proinsulin-Only Secreting Pancreatic
Diagnosis abnormal morphology and /or abnormal biochemistry
 Diagnosis abnormal morphology and /or abnormal biochemistry MEN 1 GEP Tumours Pancreatico-Nodal (-Duodenal) Affects 35-80% of MEN1 patients Functioning or non functioning Hyperplasia microadenoma macrotumours
Diagnosis abnormal morphology and /or abnormal biochemistry MEN 1 GEP Tumours Pancreatico-Nodal (-Duodenal) Affects 35-80% of MEN1 patients Functioning or non functioning Hyperplasia microadenoma macrotumours
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Hypoglycaemia in nondiabetic patients
 clinical Ching Luen Ng Hypoglycaemia in nondiabetic patients An evidence based approach Background Hypoglycaemia can have serious consequences for patients. Hypoglycaemia in nondiabetic patients is not
clinical Ching Luen Ng Hypoglycaemia in nondiabetic patients An evidence based approach Background Hypoglycaemia can have serious consequences for patients. Hypoglycaemia in nondiabetic patients is not
Congenital hyperinsulinism
 SWISS SOCIETY OF NEONATOLOGY Winner of the Case of the Year Award 2012 Congenital hyperinsulinism FEBRUARY 2012 2 Morgillo D, Berger TM, Caduff JH, Barthlen W, Mohnike K, Mohnike W, Neonatal and Pediatric
SWISS SOCIETY OF NEONATOLOGY Winner of the Case of the Year Award 2012 Congenital hyperinsulinism FEBRUARY 2012 2 Morgillo D, Berger TM, Caduff JH, Barthlen W, Mohnike K, Mohnike W, Neonatal and Pediatric
A case of non-islet cell tumor hypoglycemia associated with pancreatic neuroendocrine tumor
 Case Report Page 1 of 5 A case of non-islet cell tumor hypoglycemia associated with pancreatic neuroendocrine tumor Agron Ylli 1, Gerond Husi 1, Renta Sanxhaku 1, Ditila Doracaj 2, Gentian Vyshka 2, Ruden
Case Report Page 1 of 5 A case of non-islet cell tumor hypoglycemia associated with pancreatic neuroendocrine tumor Agron Ylli 1, Gerond Husi 1, Renta Sanxhaku 1, Ditila Doracaj 2, Gentian Vyshka 2, Ruden
Surgical Therapy of GEP-NET: An Overview
 Surgical Therapy of GEP-NET: An Overview Pierce K.H Chow MBBS, MMed, FRCSE, FAMS, PhD Professor, Duke-NUS Graduate School of Medicine Senior Consultant Surgeon, Singapore General Hospital Visiting Senior
Surgical Therapy of GEP-NET: An Overview Pierce K.H Chow MBBS, MMed, FRCSE, FAMS, PhD Professor, Duke-NUS Graduate School of Medicine Senior Consultant Surgeon, Singapore General Hospital Visiting Senior
Neuro-endocrine and pancreatic non-adenocarcinomas. Marc Engelbrecht, AMC, Amsterdam
 Neuro-endocrine and pancreatic non-adenocarcinomas Marc Engelbrecht, AMC, Amsterdam Pancreatic Tumors q Epithelial Exocrine q Mesenchymal Ductal Adenocarcinoma (85-95%) Metastasis Lymfoma Acinar Cell Carcinoma
Neuro-endocrine and pancreatic non-adenocarcinomas Marc Engelbrecht, AMC, Amsterdam Pancreatic Tumors q Epithelial Exocrine q Mesenchymal Ductal Adenocarcinoma (85-95%) Metastasis Lymfoma Acinar Cell Carcinoma
MD Spiral CT appearances of pancreatic tail insulinoma
 Article ID: WMC004688 ISSN 2046-1690 MD Spiral CT appearances of pancreatic tail insulinoma Peer review status: No Corresponding Author: Dr. Atanas D Hilendarov, MD, Medical University, Volga 49, ap.14,
Article ID: WMC004688 ISSN 2046-1690 MD Spiral CT appearances of pancreatic tail insulinoma Peer review status: No Corresponding Author: Dr. Atanas D Hilendarov, MD, Medical University, Volga 49, ap.14,
Endoscopic ultrasound-guided ethanol ablation therapy for pancreatic insulinoma: an unusual strategy
 Endoscopic ultrasound-guided ethanol ablation therapy for pancreatic insulinoma: an unusual strategy Adriana de Sousa Lages 1, Isabel Paiva 1, Patrícia Oliveira 1, Francisco Portela 2 and Francisco Carrilho
Endoscopic ultrasound-guided ethanol ablation therapy for pancreatic insulinoma: an unusual strategy Adriana de Sousa Lages 1, Isabel Paiva 1, Patrícia Oliveira 1, Francisco Portela 2 and Francisco Carrilho
Glucose-Responsive Insulinoma in a Patient with Postprandial Hypoglycemia in the Morning
 CASE REPORT Glucose-Responsive Insulinoma in a Patient with Postprandial Hypoglycemia in the Morning Keiji Iida 1, Takeshi Ohara 1, Yasuhisa Hino 1, Masahide Nobuhara 2, Jun Ishida 2 and Kazuo Chihara
CASE REPORT Glucose-Responsive Insulinoma in a Patient with Postprandial Hypoglycemia in the Morning Keiji Iida 1, Takeshi Ohara 1, Yasuhisa Hino 1, Masahide Nobuhara 2, Jun Ishida 2 and Kazuo Chihara
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Gastrinoma: Medical Management. Haley Gallup
 Gastrinoma: Medical Management Haley Gallup Also known as When to put your knife down Gastrinoma Definition and History Diagnosis Historic Management Sporadic vs MEN-1 Defining surgical candidates Nonsurgical
Gastrinoma: Medical Management Haley Gallup Also known as When to put your knife down Gastrinoma Definition and History Diagnosis Historic Management Sporadic vs MEN-1 Defining surgical candidates Nonsurgical
Update on Surgical Management of NETs
 Update on Surgical Management of Neuroendocrine Tumors James R. Howe, M.D. Director, Surgical Oncology and Endocrine Surgery University of Iowa College of Medicine Distribution of NETs 2000-2004 27% ---
Update on Surgical Management of Neuroendocrine Tumors James R. Howe, M.D. Director, Surgical Oncology and Endocrine Surgery University of Iowa College of Medicine Distribution of NETs 2000-2004 27% ---
AN ARGUMENT FOR SURGERY FOR GASTRINOMA. Lauren Wilson R1 General Surgery
 AN ARGUMENT FOR SURGERY FOR GASTRINOMA Lauren Wilson R1 General Surgery WHAT IS A GASTRINOMA? Gastrin secreting cells derived from multipotential stem cells of endodermal origin or enteroendocrine cells
AN ARGUMENT FOR SURGERY FOR GASTRINOMA Lauren Wilson R1 General Surgery WHAT IS A GASTRINOMA? Gastrin secreting cells derived from multipotential stem cells of endodermal origin or enteroendocrine cells
Difficulties in localization and treatment of insulinomas in
 Postgrad Med J (1992) 68, 196-200 The Fellowship of Postgraduate Medicine, 1992 Missed Diagnosis Difficulties in localization and treatment of insulinomas in type 1 multiple endocrine adenomatosis (MEA)
Postgrad Med J (1992) 68, 196-200 The Fellowship of Postgraduate Medicine, 1992 Missed Diagnosis Difficulties in localization and treatment of insulinomas in type 1 multiple endocrine adenomatosis (MEA)
Evaluation and Management of Adult Hypoglycemic Disorders: An Endocrine Society Clinical Practice Guideline
 SPECIAL FEATURE Clinical Practice Guideline Evaluation and Management of Adult Hypoglycemic Disorders: An Endocrine Society Clinical Practice Guideline Philip E. Cryer, Lloyd Axelrod, Ashley B. Grossman,
SPECIAL FEATURE Clinical Practice Guideline Evaluation and Management of Adult Hypoglycemic Disorders: An Endocrine Society Clinical Practice Guideline Philip E. Cryer, Lloyd Axelrod, Ashley B. Grossman,
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
Hyperinsulinemic Hypoglycemia with Nesidioblastosis after Gastric-Bypass Surgery
 The new england journal of medicine brief report Hyperinsulinemic Hypoglycemia with Nesidioblastosis after Gastric-Bypass Surgery Geoffrey J. Service, M.D., Geoffrey B. Thompson, M.D., F. John Service,
The new england journal of medicine brief report Hyperinsulinemic Hypoglycemia with Nesidioblastosis after Gastric-Bypass Surgery Geoffrey J. Service, M.D., Geoffrey B. Thompson, M.D., F. John Service,
WHAT IS YOUR DIAGNOSIS?
 WHAT IS YOUR DIAGNOSIS? An 8 year old, female neutered cross breed dog was presented to the R(D)SVS Internal Medicine Service following a 2 month history of ataxia and collapsing episodes which occurred
WHAT IS YOUR DIAGNOSIS? An 8 year old, female neutered cross breed dog was presented to the R(D)SVS Internal Medicine Service following a 2 month history of ataxia and collapsing episodes which occurred
GEP NEN. Personalised approach. Curative and Palliative Surgery. ESMO Preceptorship Programme Neuroendocrine Neoplasms Lugano April 2018
 GEP NEN Personalised approach Curative and Palliative Surgery ESMO Preceptorship Programme Neuroendocrine Neoplasms Lugano 13 14 April 2018 Professor Andrea Frilling Department of Surgery and Cancer Imperial
GEP NEN Personalised approach Curative and Palliative Surgery ESMO Preceptorship Programme Neuroendocrine Neoplasms Lugano 13 14 April 2018 Professor Andrea Frilling Department of Surgery and Cancer Imperial
Chronic Pancreatitis: Surgical Options. W. Charles Conway MD, FACS Upper GI/HPB Surgical Oncology Ochsner Medical Center New Orleans, LA
 Chronic Pancreatitis: Surgical Options W. Charles Conway MD, FACS Upper GI/HPB Surgical Oncology Ochsner Medical Center New Orleans, LA Chronic Pancreatitis Recurrent, debilitating abdominal pain with
Chronic Pancreatitis: Surgical Options W. Charles Conway MD, FACS Upper GI/HPB Surgical Oncology Ochsner Medical Center New Orleans, LA Chronic Pancreatitis Recurrent, debilitating abdominal pain with
Chief of Endocrinology East Orange General Hospital
 Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Intraoperative staging of GIT cancer using Intraoperative Ultrasound
 Intraoperative staging of GIT cancer using Intraoperative Ultrasound Thesis For Fulfillment of MSc Degree In Surgical Oncology By Abdelhalim Salah Abdelhalim Moursi M.B.B.Ch (Cairo University ) Supervisors
Intraoperative staging of GIT cancer using Intraoperative Ultrasound Thesis For Fulfillment of MSc Degree In Surgical Oncology By Abdelhalim Salah Abdelhalim Moursi M.B.B.Ch (Cairo University ) Supervisors
Hepatobiliary and Pancreatic Malignancies
 Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated.
 A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
Two clinical cases of insulinoma misdiagnosed as psychiatric conditions
 ACTA BIOMED 2005; 76; 118-122 Mattioli 1885 C A S E R E P O R T Two clinical cases of insulinoma misdiagnosed as psychiatric conditions Giovita Antonella Piccillo, Angelo Musco, Silvia Manfrini 1, Enrico
ACTA BIOMED 2005; 76; 118-122 Mattioli 1885 C A S E R E P O R T Two clinical cases of insulinoma misdiagnosed as psychiatric conditions Giovita Antonella Piccillo, Angelo Musco, Silvia Manfrini 1, Enrico
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012
 Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
5/17/2013. Pancreatic Cancer. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Case presentation. Differential diagnosis
 Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Pancreaticoduodenectomy
 Pancreaticoduodenectomy A Valuable Surgery Paul Montero PGY-III September 11, 2006 Overview Brief History Perils of Early Pancreaticoduodenectomy (PD) Improvements Quality of Life after PD Widened Indications
Pancreaticoduodenectomy A Valuable Surgery Paul Montero PGY-III September 11, 2006 Overview Brief History Perils of Early Pancreaticoduodenectomy (PD) Improvements Quality of Life after PD Widened Indications
Clinical Features and Causes of Endogenous Hyperinsulinemic Hypoglycemia in Korea
 Original Article Epidemiology Diabetes Metab J 2015;39:126-131 http://dx.doi.org/10.4093/dmj.2015.39.2.126 pissn 2233-6079 eissn 2233-6087 DIABETES & METABOLISM JOURNAL Clinical Features and Causes of
Original Article Epidemiology Diabetes Metab J 2015;39:126-131 http://dx.doi.org/10.4093/dmj.2015.39.2.126 pissn 2233-6079 eissn 2233-6087 DIABETES & METABOLISM JOURNAL Clinical Features and Causes of
Remission in Non-Operated Patients with Diffuse Disease and Long-Term Conservative Treatment.
 5th Congenital Hyperinsulinism International Family Conference Milan, September 17-18 Remission in Non-Operated Patients with Diffuse Disease and Long-Term Conservative Treatment. PD Dr. Thomas Meissner
5th Congenital Hyperinsulinism International Family Conference Milan, September 17-18 Remission in Non-Operated Patients with Diffuse Disease and Long-Term Conservative Treatment. PD Dr. Thomas Meissner
Usefulness of the octreotide test in Japanese patients for predicting the presence/absence of somatostatin receptor 2 expression in insulinomas
 2016, 63 (2), 135-142 Original Usefulness of the octreotide test in Japanese patients for predicting the presence/absence of somatostatin receptor 2 expression in insulinomas Akinobu Nakamura 1), Tomoko
2016, 63 (2), 135-142 Original Usefulness of the octreotide test in Japanese patients for predicting the presence/absence of somatostatin receptor 2 expression in insulinomas Akinobu Nakamura 1), Tomoko
GLP-1 agonists. Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK
 GLP-1 agonists Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What do GLP-1 agonists do? Physiology of postprandial glucose regulation Meal ❶ ❷ Insulin Rising plasma
GLP-1 agonists Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What do GLP-1 agonists do? Physiology of postprandial glucose regulation Meal ❶ ❷ Insulin Rising plasma
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
Long standing insulinoma: two case reports and review of the literature
 DOI 10.1186/s13104-015-1424-1 CASE REPORT Open Access Long standing insulinoma: two case reports and review of the literature Mohamed Tarchouli 1*, Abdelmounaim Ait Ali 1, Moulay Brahim Ratbi 1, Mohamed
DOI 10.1186/s13104-015-1424-1 CASE REPORT Open Access Long standing insulinoma: two case reports and review of the literature Mohamed Tarchouli 1*, Abdelmounaim Ait Ali 1, Moulay Brahim Ratbi 1, Mohamed
Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234)
 Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland. In patients
Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland. In patients
Case Report Metastatic Insulinoma in a Patient with Type 2 Diabetes Mellitus: Case Report and Review of the Literature
 International Endocrinology Volume 2011, Article ID 124078, 5 pages doi:10.1155/2011/124078 Case Report Metastatic Insulinoma in a Patient with Type 2 Diabetes Mellitus: Case Report and Review of the Literature
International Endocrinology Volume 2011, Article ID 124078, 5 pages doi:10.1155/2011/124078 Case Report Metastatic Insulinoma in a Patient with Type 2 Diabetes Mellitus: Case Report and Review of the Literature
Case report. Stelios Fountoulakis, 1 Dimosthenis Malliopoulos, 1 Labrini Papanastasiou, 1 Theodora Pappa, 2 George Karydas, 3 George Piaditis 1
 HORMONES Case report Reversal of impaired counterregulatory cortisol response following diazoxide treatment in a patient with non insulinoma pancreatogenous hypoglycemia syndrome: Case report and overview
HORMONES Case report Reversal of impaired counterregulatory cortisol response following diazoxide treatment in a patient with non insulinoma pancreatogenous hypoglycemia syndrome: Case report and overview
PANCREATIC CANCER GUIDELINES
 PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
PET IMAGING (POSITRON EMISSION TOMOGRAPY) FACT SHEET
 Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Outline. Parathyroid Localization Studies. Mira Milas MD, FACS Associate Professor of Surgery Director, The Thyroid Center
 Parathyroid Localization Studies Mira Milas MD, FACS Associate Professor of Surgery Director, The Thyroid Center Outline Clinical Context of Primary Hyperparathyroidism Ultrasound, Sestamibi, and Other
Parathyroid Localization Studies Mira Milas MD, FACS Associate Professor of Surgery Director, The Thyroid Center Outline Clinical Context of Primary Hyperparathyroidism Ultrasound, Sestamibi, and Other
Pancreatic Cancer. What is pancreatic cancer?
 Scan for mobile link. Pancreatic Cancer Pancreatic cancer is a tumor of the pancreas, an organ that is located behind the stomach in the abdomen. Pancreatic cancer does not always cause symptoms until
Scan for mobile link. Pancreatic Cancer Pancreatic cancer is a tumor of the pancreas, an organ that is located behind the stomach in the abdomen. Pancreatic cancer does not always cause symptoms until
New and Emerging Therapies for Type 2 DM
 Dale Clayton MHSc, MD, FRCPC Dalhousie University/Capital Health April 28, 2011 New and Emerging Therapies for Type 2 DM The science of today, is the technology of tomorrow. Edward Teller American Physicist
Dale Clayton MHSc, MD, FRCPC Dalhousie University/Capital Health April 28, 2011 New and Emerging Therapies for Type 2 DM The science of today, is the technology of tomorrow. Edward Teller American Physicist
PNET 3/7/2015. GI and Pancreatic NETs. The Postgraduate Course in Breast and Endocrine Surgery. Decision Tree. GI and Pancreatic NETs.
 GI and Pancreatic NETs The Postgraduate Course in Breast and Endocrine Surgery Disclosures Ipsen NET Advisory Board Marines Memorial Club and Hotel San Francisco, CA Eric K Nakakura San Francisco, CA March
GI and Pancreatic NETs The Postgraduate Course in Breast and Endocrine Surgery Disclosures Ipsen NET Advisory Board Marines Memorial Club and Hotel San Francisco, CA Eric K Nakakura San Francisco, CA March
Long-term treatment with Lanreotide in CHI
 Long-term treatment with Lanreotide in CHI Oliver Blankenstein Institute for Experimental Paediatric Endocrinology Charité-Universitätsmedizin Berlin U N I V E R S I T Ä T S M E D I Z I N B E R L I N 5
Long-term treatment with Lanreotide in CHI Oliver Blankenstein Institute for Experimental Paediatric Endocrinology Charité-Universitätsmedizin Berlin U N I V E R S I T Ä T S M E D I Z I N B E R L I N 5
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: ENDOCRINE 5-May-2013 DEVELOPED BY: Jonathan Serpell
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: ENDOCRINE 5-May-2013 DEVELOPED BY: Jonathan Serpell
21/07/2017. CS Verbeke. Non-neoplastic disease of the pancreas PATHOLOGY OF NON-NEOPLASTIC PANCREATIC DISEASES
 Non-neoplastic disease of the pancreas No indication for surgical resection of non-neoplastic disease (except end-stage chronic pancreatitis) Unexpected benign disease in 5-13% of pancreatic resections
Non-neoplastic disease of the pancreas No indication for surgical resection of non-neoplastic disease (except end-stage chronic pancreatitis) Unexpected benign disease in 5-13% of pancreatic resections
For The Management Of. Hypoglycemia
 Guidelines For The Management Of Hypoglycemia By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Dr.Layla Al-Shahrabani F.R.C.P (UK) Director of Clinical Affairs Kurdistan Higher Council For
Guidelines For The Management Of Hypoglycemia By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Dr.Layla Al-Shahrabani F.R.C.P (UK) Director of Clinical Affairs Kurdistan Higher Council For
Usefulness of hemoglobin A1c and glycated albumin measurements for insulinoma screening: an observational case-control study
 Torimoto et al. BMC Cancer (2019) 19:174 https://doi.org/10.1186/s12885-019-5389-7 RESEARCH ARTICLE Open Access Usefulness of hemoglobin A1c and glycated albumin measurements for insulinoma screening:
Torimoto et al. BMC Cancer (2019) 19:174 https://doi.org/10.1186/s12885-019-5389-7 RESEARCH ARTICLE Open Access Usefulness of hemoglobin A1c and glycated albumin measurements for insulinoma screening:
