Glycaemic control in type 1 diabetes mellitus among children and adolescents in a resource limited setting in Dar es Salaam - Tanzania
|
|
|
- Beverley Garrett
- 5 years ago
- Views:
Transcription
1 Noorani et al. BMC Endocrine Disorders (2016) 16:29 DOI /s y RESEARCH ARTICLE Glycaemic control in type 1 diabetes mellitus among children and adolescents in a resource limited setting in Dar es Salaam - Tanzania Mariam Noorani 1*, Kaushik Ramaiya 2 and Karim Manji 3 Open Access Abstract Background: Type 1 Diabetes Mellitus is a rapidly growing problem in Tanzania. Children and adolescents with type 1 diabetes have previously been found to have poor glycaemic control and high prevalence of complications. Strict glycaemic control reduces the incidence and progression of chronic complications. The aim of this study was to identify the factors associated with glycaemic control among children and adolescents. Methods: A cross sectional study was done at the diabetes clinic for children and adolescents. Data on socioeconomic, demographic and diabetes specific variables including adherence, diabetes knowledge, caregivers knowledge and their involvement in the care of the child was obtained. Glycaemic control was assessed by measuring glycosylated hemoglobin. (HbA1C). Linear regression analysis was done to determine factors associated with glycaemic control Results: Seventy-five participants were recruited into the study (51 % males). The mean HbA1c was 11.1 ± 2.1 %. Children aged <10 years were found to have a significantly better glycaemic control (9.8 %) as compared to year olds (11.5 %) and >14 year olds (11.4 %) (P value = 0.022). Sixty-eight percent of patients had good adherence to insulin while adherence to blood glucose monitoring regimen was 48 % and to diet control was 28 %. Younger age, having the mother as the primary caregiver, better caregiver knowledge of diabetes, better adherence to blood glucose monitoring regimen and diabetes duration of less than 1 year were associated with better glycaemic control. In multivariate analysis, age, adherence to blood glucose monitoring regimen and the mother as the primary caregiver were found to independently predict glycaemic control (R 2 = 0.332, p value = 0.00). Conclusions: Children and adolescents with type 1 diabetes in Dar es Salaam have poor glycaemic control. In order to improve metabolic control, adherence to blood glucose monitoring should be encouraged and caregivers encouraged to participate in care of their children especially the adolescents. Keywords: Type 1 diabetes mellitus, Children, Adolescents, Tanzania, Glycaemic control, Adherence * Correspondence: mariamnoorani@yahoo.com 1 Aga Khan Hospital, PO Box 2289Barrack Obama Drive, Dar-es-Salaam, Tanzania Full list of author information is available at the end of the article 2016 The Author(s). Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Noorani et al. BMC Endocrine Disorders (2016) 16:29 Page 2 of 8 Background Type 1 diabetes mellitus (T1DM) is a rapidly growing problem in Tanzania and Africa as a whole. The incidence in some African countries was found to range between 4.4/100,000 in Algeria to 20/100,000 in Morocco. [1] In sub Saharan Africa, few studies have been done but estimates from Sudan showed an increased incidence from 9.5/100,000 in 1991 to 10.3/100,000 in In Tanzania, the incidence was estimated to be 1.5/ 100,000 per year in 1991 [2]. In Dar es Salaam, a high prevalence of chronic complications has been described. The prevalence of retinopathy was 22 % and that of micro-albuminuria, which is a marker of nephropathy, was 29 % [3]. As demonstrated in the Diabetes Control and Complication Trial, (DCCT) strict glycaemic control has been shown to reduce the long term complications of type 1 diabetes [4]. Recommendations from the DCCT were to maintain the glycosylated hemoglobin (HbA1c) below 7 %. However, due to the risk of hypoglycemia unawareness in children, the American Diabetes Association (ADA) recommends an HbA1c of between 7.5 and 8.5 % for children less than 6 years. For those between 6 and 12 years, a level of <8 % is recommended while for those >12 years, a level of <7.5 % is considered optimal. Glycaemic control in type 1 diabetics in Dar es Salaam was previously found to be very poor with mean HbA1c of %. This was in a survey carried out on children and adolescents aged 5 to 18 years at the Muhimbili National Hospital clinic for diabetes [3]. Other studies from the East African region have also demonstrated poor control. In a Kenyan study, the median HbA1c was found to be 11.1 % in children and adolescents with T1DM [5]. Various risk factors and challenges have been described that are associated with glycaemic control. Some of these include socio-demographic variables such as age of the child, socioeconomic status, and family structure [6 8]. Other diabetes related factors such as duration of diabetes, adherence and caregiver involvement in the child s care have also been significantly associated with glycaemic control [9, 10] Most of these studies were done in Europe and North America and very little data exists about risk factors in low resource settings in sub Saharan Africa. The aim of this study was to identify the factors associated with glycaemic control in children and adolescents with diabetes in Dar es Salaam. This will help to implement targeted interventions to improve control in this population and prevent chronic complications. Methods This cross-sectional study was carried out over a 6 month period from October 2010 to March 2011 at the diabetic clinic for children and adolescents at Muhimbili National Hospital in Dar es Salaam. This clinic runs once every week on Mondays since its inception in Patients are managed by a team of 2 nurses, 2 pediatricians trained in endocrinology and 3 support staff. All children and adolescents attending the clinic are provided with insulin at no cost through the International Diabetes Federation (IDF), Life for a child program. In addition, they are provided with glucose monitors, strips and diaries for selfmonitoring and recording of blood glucose at home. They are encouraged to monitor their glucose at least 3 times a week at specified times and to record the readings in their diaries. HbA1c is measured for all patients every 3 6 months and the screening for retinopathy, nephropathy and neuropathy done yearly. Patients and guardians are also given diabetes education and advice on appropriate nutrition. All children and adolescents up to and including 18 years of age were eligible for inclusion in the study if consent was provided by the parent/guardian or assent by the adolescent. Those who were newly diagnosed or who had been on treatment for less than 3 months were excluded. All children actively attending the diabetes clinic were recruited in the study, therefore sample size was not calculated. Data was collected using a structured questionnaire. For children older than 10 years, one section of the questionnaire assessing diabetes knowledge was administered separately to the child and parent/guardian. The questionnaire was translated into the local language, Kiswahili and had the following 3 components: 1. Socio demographic and background information 2. Diabetes knowledge of children/adolescents and caregivers: This was assessed by use of the Michigan Diabetes Research and Training Center s brief diabetes knowledge test. [11] This was a multiple choice questionnaire which was modified, translated and back translated into Kiswahili. A total of 14 questions out of the 23 item questionnaire were used. Nine questions were omitted because they were not applicable to our patient population. The results of the test were scored based on percentage of correct responses. 3. Diabetes related practices: a. Insulin adherence: This was determined by the number of insulin doses missed in the last 1 week and was graded as follows: Good: no missed doses
3 Noorani et al. BMC Endocrine Disorders (2016) 16:29 Page 3 of 8 Average: between 1 and 3 missed doses Poor: >3 missed doses b. Dietary adherence: This was assessed by use of a 24 h dietary recall. All meals and snacks eaten in the last 24 h prior to the clinic visit were documented and adherence was graded based on a score derived from the dietary guidelines given at the clinic: Component: Score Meal frequency: 3 meals and 3 snacks OR 3 meals and 2 snacks 4 3 meals and 1 snack 3 3 meals only 2 < 3 meals 1 Meal content: (lunch and dinner)- score each meal separately then divide by 2 All components (carbohydrates, proteins, vegetables) 4 Carbohydrates and vegetables 3 Carbohydrates and protein 2 Only carbohydrates 1 Forbidden foods: Each time a forbidden food is consumed 1 Interpretation: Maximum score: 8 <4 poor 4 6 average >6 good c. Blood glucose monitoring (BGM) adherence: This was graded as follows Good: 3 times a week Average: 1 2 times a week Poor: none d. Caregiver involvement in diabetes related tasks: This was assessed by using a scale graded as minimal, moderate or optimal involvement. This was modified from the scale used in the study by Anderson et al. [7] Involvement in insulin injections was determined by the number of doses in the last 24 h injected or supervised by the caregiver. Involvement Minimal Moderate Optimal Number of injections supervised in the last 24 h None 1 - for those on a 2 injection regimen 1 or 2 - for those on a multiple dose regimen All injections Involvement in BGM was determined by the degree of participation of the caregiver in the task Involvement Minimal Moderate Optimal Participation of caregiver No participation Reminds the child to check blood glucose Enters glucose level in the diary Asks child about the blood glucose level Sets up the meter Does the finger prick Supervises the task e. Insulin storage: this was classified as refrigeration, storage in a pot of cold water or storage at room temperature. Glycaemic control was determined by measurement of glycosylated hemoglobin levels (HbA1c). This was determined on all children and adolescents from January to March 2011 using a DCA analyzer. Socio demographic characteristics and diabetes specific variables were summarized using frequency distribution tables. Mean and median was calculated for continuous data. Association between variables was tested by use of chi square and fishers exact tests. Means were compared using students T- test and ANOVA (analysis of variance). Multivariate linear regression analysis was performed to determine factors independently associated with glycaemic control. A p value of less than or equal to 0.05 was considered statistically significant. Epi Info software version and SPSS version 16 were used for data processing. Ethical issues Ethical clearance was granted by the Muhimbili University of Health and Allied Sciences (MUHAS) Institutional review Board ( and the Muhimbili National Hospital. Children who were able to provide assent were requested along with consent from caretakers. After the data was collected and results obtained for HBA1c, participants were further counseled and educated on the same. Hurdles to good glycaemic control were individualized and measures to improve instituted after the data was collected. Results During the study period (October 2010 to March 2011), 90 children and adolescents aged up to 18 years inclusive were registered at the clinic. Of these, 5 did not attend clinic during the study duration, 5 had diabetes
4 Noorani et al. BMC Endocrine Disorders (2016) 16:29 Page 4 of 8 for less than 3 months and 2 did not consent. Seventyeight were included in the study. Three of these did not come for the HbA1c testing and were excluded from final analysis. The mean age was 13.4 ± 3.9 years (median: 14.1, range: years) with an almost equal sex distribution (50.7 % males). Thirty eight (50.7 %) children were >14 years of age. Most of the children (68 %) were on a multiple daily insulin injection regimen. The socio demographic and diabetes specific characteristics of study participants are summarized in Table 1. The mean HbA1c was 11.1 ± 2.1 %. There was no difference in the mean HbA1c between males and females. Table 1 Socio demographic and diabetes specific characteristics of the participants Characteristics Frequency Median N =75 % (range) Age (years) 14.1 (3.5, 18.9) < > Sex Male Female Family structure 2 parent family Single parent Not living with parents Orphan Primary caregiver Mother Father Sibling Other Caregiver education No formal education Primary Secondary Tertiary Duration of DM (years) 3.17 (0.33,11.2) < > Insulin dose (units/kg body wt/day) 1.0 (0.24,2.0) Insulin regimen 2 daily injections Multiple daily injections However, children in the younger age group (<10 years) had a significantly lower mean HbA1c as compared to the older children. Children with mothers as the primary caregivers had a significantly lower mean HbA1c as compared to those whose caregivers were a father, a sibling or another family member. The family structure of the patient and the education level of the caregiver were not significantly associated with glycaemic control. (Table 2) Shorter duration of disease was associated with significantly lower HbA1c levels. Children who had T1DM for less than 1 year had a mean HbA1c that was 2 % lower than those with disease for a longer duration (p value = 0.011). The insulin regimen used did not influence the HbA1c. Children who were on the multiple daily insulin injection regimens had an equal mean HbA1c as compared to those who were on 2 daily injections. The mean diabetes knowledge score of parents/caregivers was 70 ± 15 % while assessment of diabetes knowledge of the adolescent revealed a similar mean score of 70.3 ± 15.9 %. Simple linear regression analysis found diabetes knowledge of caregivers to be significantly associated with HbA1c. (r2 = 0.07, p value = 0.036). Knowledge of children was not associated with HbA1c (p value = 0.868) Adherence to the insulin regimen was found to be good in majority of study participants (68 %). Reasons cited for poor adherence included forgetfulness and Table 2 Factors associated with Glycaemic control Characteristics Mean HbA1c (% ± 2SD) P value a Age group < 10 years 9.8 ± b years 11.5 ± 2.1 > 14 years 11.4 ± 2.0 Sex Male 11.0 ± Female 11.1 ± 2.0 Family structure 2 parent family 10.9 ± Other 11.3 ± 2.2 Primary caregiver Mother 10.7 ± b Other 11.8 ± 2.0 Caregiver education None/Primary 11.3 ± Secondary/tertiary 10.7 ± 2.1 a Calculated using students t test and ANOVA b Statistically significant
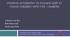
5 Noorani et al. BMC Endocrine Disorders (2016) 16:29 Page 5 of 8 inconvenience in injecting insulin at school and other public places. Forty-eight percent of children reported good adherence to the BGM regimen prescribed at the clinic while 24 and 28 % reported average and poor adherence respectively. The most common reason for poor adherence was unavailability of BGM strips. Dietary adherence was average in most of the patients (57.3 %). Difficulty in reducing carbohydrate quantity was a common problem encountered by most adolescents. Adherence is summarized in Fig 1. The mean HbA1c did not differ with adherence to diet and insulin. Adherence to BGM regimen was associated with lower mean HbA1c in those with average adherence as compared to those with poor adherence. (10.1 ± 2.1 vs 11.7 ± 2.1, p value 0.061) Caregiver involvement in diabetes related tasks of the child varied with the type of task. In the task of insulin injection, 44 % of caregivers exhibited optimal involvement as compared to only 29.3 % in the task of BGM. Caregiver involvement in diabetes related tasks was not significantly associated with HbA1c. Insulin was reported to be stored in the fridge by 65.3 % of participants; either their own or a neighbors. Thirty-two percent stored it in a pot of water while the remaining 2.7 % kept the vials at room temperature. The difference in the mean HbA1c between those who stored insulin in the fridge and in a pot of water was not statistically significant (11.1 vs %, p value = 0.85). To determine predictors of glycaemic control, a multivariate regression analysis was performed using variables that had a significant association with HbA1c (p < 0.05) and those that approached statistical significance (P < 0.1) in bi-variate analysis The variables tested in the multivariate analysis were: age of the child, primary caregiver, diabetes knowledge of caregiver, duration of disease and adherence to BGM regimen. Results of the multivariate analysis are shown in Table 3. Discussion The mean glycaemic control in this study was 11.1 ± 2.1 %. The factors that were significantly associated with glycaemic control were age, adherence to blood glucose monitoring regimen and primary caregiver. There is a marginal increase in the mean HbA1C from the mean of ± 2.09 which was reported at the same center by Majaliwa et al. in 2006 [3]. This increase is alarming because the previous study was done in the setting of very poor insulin supplies and unavailability of BGM at home. Despite major progress in the availability of insulin and blood glucose monitors, glycaemic control showed no improvement. This points to the existence of other underlying factors which have yet to be identified that are contributing to poor glycaemic control. Results of the DCCT demonstrated that every 1 % decrease in HbA1c results in a 40 % reduced risk of developing retinopathy. The importance of lowering the level of HbA1c in our population of type 1 diabetics cannot be overemphasized [4]. Very few studies have been done in Africa documenting glycaemic control. A Kenyan study by Ngwiri also showed poor glycaemic control with a median HbA1C of 12.1 % [5]. A study by Pillay et al. from South Africa documented a mean HbA1C of 9.7 % in children with T1DM aged 6 10 years [12]. This is similar to the mean HbA1c in children <10 years in the current study (9.83 %). Younger age has consistently been found to be associated with better glycaemic control in several studies [6, 7]. This may be attributed to more parental supervision in this age group. Adolescents with T1DM have been reported to have poor glycaemic control [10]. The poor glycaemic control Fig. 1 Adherence to diet, insulin and blood glucose monitoring
6 Noorani et al. BMC Endocrine Disorders (2016) 16:29 Page 6 of 8 Table 3 Multivariate analysis of the significant factors associated with glycaemic control Variable Beta P value (standardized coefficients) Age of patient a Duration of DM Primary caregiver (mother/other) a Adherence to BGM regimen (poor/good) Adherence to BGM regimen (poor/average) a Diabetes knowledge of caregiver a Statistically significant DM diabetes mellitus, BGM blood glucose monitoring The independent variables in the model predicted 33.2 % of the variance in HbA1c (R 2 = 0.332, p value = 0.000) with increasing age as demonstrated in the current study may be due to the onset of puberty and the hormonal changes that happen at this age. Elevated levels of growth hormone and reduced level of insulin like growth factor may contribute to weight gain in adolescent girls. This in turn, results in altered eating habits and missed insulin doses. In addition, psychological and social stressors in this age group may also contribute to poor glycaemic control. This is thought to be mediated by stress hormones such as cortisol and catecholamines which increase blood glucose. Reduced parental supervision and more independent control of the disease may also contribute to worsening control. The role of the family in the management of T1DM in children and adolescents has been described. In a study by Thompson et al., children from single parent families had a significantly higher HbA1c as compared to those from 2 parent families [13]. This was also demonstrated in a study by Araujo et al. in Argentina [8]. In the current study however, children from 2 parent families did not have significantly better glycaemic control. This could be explained by the role that parents play in caring for a sick child in the African societies, where it is the primary responsibility of the mother to care for sick children. Indeed this was demonstrated by the significantly lower mean HbA1c (10.8 %) in children whose primary caregiver was the mother as compared to % in those who had a primary caregiver other than the mother. The mean duration of diabetes in our population was 3.74 years. Children with duration of <1 year had significantly better mean HbA1c compared to those with duration >1 year. This is a common finding in newly diagnosed diabetics due to the honeymoon effect ; this is a period of relatively good glycaemic control that occurs due to residual beta cell function in the 1st year following diagnosis and initiation of treatment. In multivariate analysis, however, duration of DM did not significantly predict HbA1c. This is contrary to many studies which have reported diabetes duration as a significant predictor of HbA1c [6, 7, 14] The lack of association between duration and HbA1C in our study could be explained by the overall poor glycaemic control which may mask any impact of duration on the disease. In our study, majority of the children (68 %) were on a multiple insulin injection regimen. This is currently one of the recommended modes of treatment of T1DM, the other being the continuous subcutaneous insulin infusion (CSII) using a pump [15]. However, the mean HbA1c in this group did not differ from those on the conventional 2 daily insulin injection regimen. This finding is surprising given the important role of prandial insulin in lowering blood glucose. It could be explained by the suboptimal adherence to the insulin regimen and missing of the lunchtime insulin dose. Around 30 % of children reported missing one or more doses of insulin per week due to inconvenience in injecting in public places. Diabetes education is a key component in the management of T1DM. Education of both the caregiver and the child is important to ensure adherence to the multiple diabetes related tasks. In the current study population the mean parental knowledge score was 70 ± 15 %. This indicates a significant deficit in knowledge. Higher parent diabetes knowledge scores were associated with a significantly lower HbA1c. These results were similar to those in a study by Butler et al. [16] where higher parental diabetes specific knowledge was significantly correlated with a lower HbA1c. In another study by Stallwood et al. [17], parental diabetes knowledge was tested using the Michigan Diabetes Research and Training Centre s brief knowledge test using all the 23 items in the questionnaire unlike the current study where we used 14 out of 23. The mean parental score in that study was 74 % and higher scores were correlated to lower HbA1c s. The mean diabetes knowledge score of the youth was similar to that of the parents but did not show association with age or with HbA1c. This finding emphasizes the key role of optimizing parental knowledge to achieve better control in the child. There was varying adherence to the different treatment modalities. Best adherence was observed to the insulin regimen (68 %) followed by BGM (48 %) and lastly diet (28 %). This reflects the underlying importance patients given to insulin administration and the relative complacency to the other modes of treatment. The lack of a regular supply of BGM consumables could also contribute to poor adherence Overall, better adherence in the diet and insulin regimen domains did not translate to better glycaemic
7 Noorani et al. BMC Endocrine Disorders (2016) 16:29 Page 7 of 8 control. However, adherence to BGM was significantly associated with HbA1c in multivariate analysis. The adherence and glycaemic control link has been examined in several studies including a meta - analysis carried out by Hood et al. [9] This meta - analysis demonstrated an effect size of 0.28 (CI 0.32, 0.24). This implies that better adherence leads to lower HbA1c. This meta-analysis did not demonstrate any association between socio-demographic or disease specific variables on the overall effect size. A study by Mehta et al. examining dietary adherence showed that a higher dietary score was associated with lower HbA1c [18]. The absence of significant association between HbA1c and adherence to insulin and diet in our study may be explained by the method used to assess adherence which was primarily self-reporting. This method is prone to recall bias and misreporting and this may have resulted in falsely elevated adherence levels. Other studies have used caloric counting to assess dietary adherence; this however is not applicable in our population. BGM adherence can be determined by data from blood glucose meter downloads. In the current study population however, this was not practical because most patients did not carry meters to the clinic during visits. The recommended method of insulin storage is refrigeration at a temperature of 2-8 C for unopened vials of insulin. Open vials may be kept at room temperature but must be used within 1 month. Due to the low availability of refrigerators, 32 % of our patients with diabetes store their insulin in a pot of water which is kept cool by use of charcoal to absorb heat. The method of insulin storage did not significantly affect glycaemic control. This may be explained on the basis of the limited insulin stocks available to the patients, which usually do not last more than 1 month. Multivariate analysis of variables associated with glycaemic control found 3 main predictors of HbA1c: age, primary caregiver and adherence to BGM regimen The limitations in this study were the cross sectional design which is not the best design to demonstrate relationships between variables and the small study population. Effort was made to recruit all eligible participants who met inclusion criteria. Despite the small number, we believe the results of this study provide the much needed data to improve glycaemic control in resource limited settings like ours. Conclusions In conclusion, we found that metabolic control is very poor in our population of type 1 diabetics with overall poor adherence. Factors associated with poor control include older age, a caregiver other than the mother and poor adherence to BGM. In order to improve metabolic control, more frequent BGM should be encouraged and regular supply of glucose monitoring strips ensured. Emphasis needs to be put on adherence counseling and active participation of caregivers in diabetes related tasks of their children. Close follow up of the adolescents is necessary as this group is the most vulnerable to poor control. Abbreviations T1DM, Type 1 Diabetes Mellitus; DCCT, Diabetes Control and Complications trial; ADA, American Diabetes Association; HbA1c, Glycosylated Hemoglobin; BGM, Blood Glucose Monitoring; MUHAS, Muhimbili University of Health and Allied Sciences. Acknowledgements The authors acknowledge the inputs and assistance by Prof. Karim Hirji (Epidemiologist), Dr. Edna Majaliwa (Pediatric endocrinologist), Sister Licoco of the Diabetes Clinic, The Tanzania Diabetes Association for facilitating the HbA1c measurements, Prof. Le Blanc, Dr D Opondo and the children and their care-takers. Funding This study was funded independently by the primary researcher. Lab investigation was done with assistance by the Tanzania Diabetes Association. Availability of data and materials Data will not be publicly shared but is available on request. Authors contributions MN was the primary researcher and data collector. KR and KM assisted with the study design, data analysis and manuscript write up. All authors read and approved the final manuscript. Competing interests The authors declare that they have no competing interests. Consent for publication Not applicable. Ethics approval and consent to participate Ethical clearance was granted by the Muhimbili University of Health and Allied Sciences (MUHAS) Institutional review Board ( and the Muhimbili National Hospital. Written informed consent was obtained by parents/guardians and assent from adolescents. Author details 1 Aga Khan Hospital, PO Box 2289Barrack Obama Drive, Dar-es-Salaam, Tanzania. 2 Hindu Mandal Hospital, PO Box 581Chusi Street, Dar-es-Salaam, Tanzania. 3 Muhimbili University of Health and Allied Sciences, PO Box 65001UN Road, Dar-es-Salaam, Tanzania. Received: 29 January 2016 Accepted: 24 May 2016 References 1. Majaliwa ES, Elusiyan BE, Adesiyun OO, Laigong P, Adeniran AK, Kandi CM, et al. Type 1 diabetes mellitus in the African population: epidemiology and management challenges. Acta Biomed. 2008;79(3): Swai AB, Lutale JL, McLarty DG. Prospective study of incidence of juvenile diabetes mellitus over 10 years in Dar es Salaam, Tanzania. BMJ. 1993; 306(6892): Majaliwa ES, Munubhi E, Ramaiya K, Mpembeni R, Sanyiwa A, Mohn A, et al. Survey on acute and chronic complications in children and adolescents with type 1 diabetes at Muhimbili National Hospital in Dar es Salaam, Tanzania. Diabetes Care. 2007;30(9): The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med. 1993;329(14):
8 Noorani et al. BMC Endocrine Disorders (2016) 16:29 Page 8 of 8 5. Ngwiri T, Were F, Predieri B, Ngugi P, Iughetti L. Glycemic Control in Kenyan Children and Adolescents with Type 1 Diabetes Mellitus. Int J Endocrinol. 2015;2015: Published online 2015 Oct 1. doi: /2015/ Rosilio M, Cotton JB, Wieliczko MC, Gendrault B, Carel JC, Couvaras O, et al. Factors associated with glycemic control. A cross-sectional nationwide study in 2,579 French children with type 1 diabetes. The French Pediatric Diabetes Group. Diabetes Care. 1998;21(7): McKinney PA, Feltbower RG, Stephenson CR, Reynolds C. Children and young people with diabetes in Yorkshire: a population-based clinical audit of patient data 2005/2006. Diabet Med. 2008;25(11): Araujo MB, Mazza CS. Assessment of risk factors of poor metabolic control in type 1 diabetic children assisted in a public hospital in Argentina. Pediatr Diabetes. 2008;9(5): Hood KK, Peterson CM, Rohan JM, Drotar D. Association between adherence and glycemic control in pediatric type 1 diabetes: a metaanalysis. Pediatrics. 2009;124(6):e Anderson B, Ho J, Brackett J, Finkelstein D, Laffel L. Parental involvement in diabetes management tasks: relationships to blood glucose monitoring adherence and metabolic control in young adolescents with insulindependent diabetes mellitus. J Pediatr. 1997;130(2): Fitzgerald JT, Funnell MM, Hess GE, Barr PA, Anderson RM, Hiss RG, et al. The reliability and validity of a brief diabetes knowledge test. Diabetes Care. 1998;21(5): Pillay KME, Naidoo KL. Dietary intake and metabolic control of children aged six to ten with type 1 diabetes mellitus in KwaZulu-Natal. S Afr J Clin Nutr. 2009;22(2): Thompson SJ, Auslander WF, White NH. Comparison of single-mother and two-parent families on metabolic control of children with diabetes. Diabetes Care. 2001;24(2): Craig ME, Handelsman P, Donaghue KC, Chan A, Blades B, Laina R, et al. Predictors of glycaemic control and hypoglycaemia in children and adolescents with type 1 diabetes from NSW and the ACT. Med J Aust. 2002;177(5): Silverstein J, Klingensmith G, Copeland KC, et al. American Diabetes Association. Care of children and adolescents with type 1 diabetes: a statement of the American Diabetes Association. Diabetes Care. 2005;28: Butler DA, Zuehlke JB, Tovar A, Volkening LK, Anderson BJ, Laffel LM. The impact of modifiable family factors on glycemic control among youth with type 1 diabetes. Pediatr Diabetes. 2008;9(4 Pt 2): Stallwood L. Relationship between caregiver knowledge and socioeconomic factors on glycemic outcomes of young children with diabetes. J Spec Pediatr Nurs. 2006;11(3): Mehta SN, Volkening LK, Anderson BJ, Nansel T, Weissberg-Benchell J, Wysocki T, et al. Dietary behaviors predict glycemic control in youth with type 1 diabetes. Diabetes Care. 2008;31(7): Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
Factors associated with poor glycemic control among children with type 1 diabetes at Zawia province
 Factors associated with poor glycemic control among children with type 1 diabetes at Zawia province Dr Aboulgasem EM Elgerbi, Faculty of Medicine Pediatric Department Zawia University ABSTRACT : Type 1
Factors associated with poor glycemic control among children with type 1 diabetes at Zawia province Dr Aboulgasem EM Elgerbi, Faculty of Medicine Pediatric Department Zawia University ABSTRACT : Type 1
Research Article Measures of Adherence and Challenges in Using Glucometer Data in Youth with Type 1 Diabetes: Rethinking the Value of Self-Report
 Hindawi Diabetes Research Volume 2017, Article ID 1075428, 4 pages https://doi.org/10.1155/2017/1075428 Research Article Measures of Adherence and Challenges in Using Glucometer Data in Youth with Type
Hindawi Diabetes Research Volume 2017, Article ID 1075428, 4 pages https://doi.org/10.1155/2017/1075428 Research Article Measures of Adherence and Challenges in Using Glucometer Data in Youth with Type
Counting the Carbs, Fat and Protein in Type 1 Diabetes Translating the Research into Clinical Practice
 Welcome to Allied Health Telehealth Virtual Education Counting the Carbs, Fats and Protein in Type 1 Diabetes Translating the Research into Clinical Practice Dr Carmel Smart, PhD Senior Specialist Paediatric
Welcome to Allied Health Telehealth Virtual Education Counting the Carbs, Fats and Protein in Type 1 Diabetes Translating the Research into Clinical Practice Dr Carmel Smart, PhD Senior Specialist Paediatric
Approach to the Young child & Parent with Child with DM Best Structure for Continued Care
 Approach to the Young child & Parent with Child with DM Best Structure for Continued Care M.S. Limbe MD Paediatric Endcocrinologist Aga Khan University Hospital, Nairobi Approach to the Young Child & Parent
Approach to the Young child & Parent with Child with DM Best Structure for Continued Care M.S. Limbe MD Paediatric Endcocrinologist Aga Khan University Hospital, Nairobi Approach to the Young Child & Parent
Current Glucometers. Junior s s Glucose Log. All have advantages and disadvantages Answer 2
 Diabetes Dilemmas: Using Technology To Solve Clinical Conundrums Stephen E. Gitelman, MD UCSF A teenager with type 1 diabetes for 5 years comes into your office for a follow- up visit. You want to review
Diabetes Dilemmas: Using Technology To Solve Clinical Conundrums Stephen E. Gitelman, MD UCSF A teenager with type 1 diabetes for 5 years comes into your office for a follow- up visit. You want to review
DIAGNOSIS OF DIABETES NOW WHAT?
 DIAGNOSIS OF DIABETES NOW WHAT? DISCUSS GOALS FOR DIABETES CARE IDENTIFY COMMON COMPLIANCE- ADHERENCE ISSUES DESCRIBE TECHNOLOGY TO ASSIST AND / OR IMPROVE DIABETES CARE WHAT DO WE WANT OUR PATIENTS TO
DIAGNOSIS OF DIABETES NOW WHAT? DISCUSS GOALS FOR DIABETES CARE IDENTIFY COMMON COMPLIANCE- ADHERENCE ISSUES DESCRIBE TECHNOLOGY TO ASSIST AND / OR IMPROVE DIABETES CARE WHAT DO WE WANT OUR PATIENTS TO
Research Article Glycemic Control in Kenyan Children and Adolescents with Type 1 Diabetes Mellitus
 International Endocrinology Volume 2015, Article ID 761759, 7 pages http://dx.doi.org/10.1155/2015/761759 Research Article Glycemic Control in Kenyan Children and Adolescents with Type 1 Diabetes Mellitus
International Endocrinology Volume 2015, Article ID 761759, 7 pages http://dx.doi.org/10.1155/2015/761759 Research Article Glycemic Control in Kenyan Children and Adolescents with Type 1 Diabetes Mellitus
An Evaluation of the Barriers to Patient use of Glucometer Control Solutions: A Survey of Patients, Pharmacists, and Providers
 AADE14 ANNUAL MEETING & EXHIBITION AUGUST 6-9, 2014 ORLANDO, FL An Evaluation of the Barriers to Patient use of Glucometer s: A Survey of Patients, Pharmacists, and Providers Katherine S. O Neal, Pharm.D.,
AADE14 ANNUAL MEETING & EXHIBITION AUGUST 6-9, 2014 ORLANDO, FL An Evaluation of the Barriers to Patient use of Glucometer s: A Survey of Patients, Pharmacists, and Providers Katherine S. O Neal, Pharm.D.,
I. Promoting Student Independence
 The Nursing Support Services (NSS) Coordinator provides support according to the Provincial Standards: Supporting Students with Type 1 Diabetes in the School Setting. The NSS Coordinator delegates specific
The Nursing Support Services (NSS) Coordinator provides support according to the Provincial Standards: Supporting Students with Type 1 Diabetes in the School Setting. The NSS Coordinator delegates specific
RELATIONSHIPS BETWEEN QUALITY OF LIFE, FAMILY FACTORS, ADHERENCE, AND GLYCEMIC CONTROL IN PEDIATRIC PATIENTS WITH TYPE 1 DIABETES MELLITUS
 RELATIONSHIPS BETWEEN QUALITY OF LIFE, FAMILY FACTORS, ADHERENCE, AND GLYCEMIC CONTROL IN PEDIATRIC PATIENTS WITH TYPE 1 DIABETES MELLITUS By JAY B. ST. AMANT A DISSERTATION PRESENTED TO THE GRADUATE SCHOOL
RELATIONSHIPS BETWEEN QUALITY OF LIFE, FAMILY FACTORS, ADHERENCE, AND GLYCEMIC CONTROL IN PEDIATRIC PATIENTS WITH TYPE 1 DIABETES MELLITUS By JAY B. ST. AMANT A DISSERTATION PRESENTED TO THE GRADUATE SCHOOL
Diabetes II Insulin pumps; Continuous glucose monitoring system (CGMS) Ernest Asamoah, MD FACE FACP FRCP (Lond)
 Diabetes II Insulin pumps; Continuous glucose monitoring system (CGMS) Ernest Asamoah, MD FACE FACP FRCP (Lond) 9501366-011 20110401 Objectives Understand the need for insulin pumps and CGMS in managing
Diabetes II Insulin pumps; Continuous glucose monitoring system (CGMS) Ernest Asamoah, MD FACE FACP FRCP (Lond) 9501366-011 20110401 Objectives Understand the need for insulin pumps and CGMS in managing
Guidelines for managing the health care needs of children and young persons with diabetes in education
 Guidelines for managing the health care needs of children and young persons with diabetes in education Contents Page: Page Number 1.0 Introduction 1 2.0 The Care Management Plan 2 2.1 Blood Glucose monitoring
Guidelines for managing the health care needs of children and young persons with diabetes in education Contents Page: Page Number 1.0 Introduction 1 2.0 The Care Management Plan 2 2.1 Blood Glucose monitoring
Effective Health Care Program
 Comparative Effectiveness Review Number 57 Effective Health Care Program Methods for Insulin Delivery and Glucose Monitoring: Comparative Effectiveness Executive Summary Background Diabetes mellitus is
Comparative Effectiveness Review Number 57 Effective Health Care Program Methods for Insulin Delivery and Glucose Monitoring: Comparative Effectiveness Executive Summary Background Diabetes mellitus is
CLINICAL UTILITY OF CONTINUOUS SUBCUTANEOUS INSULIN INFUSION IN PATIENTS WITH TYPE 1 DIABETES: A MACEDONIAN REPORT
 University Department of Endocrinology, Diabetes and Metabolic Disorders, Medical Faculty, Sv. Kiril I Metodij University, Skopje, Macedonia Scientific Paper Received: February 19, 2007 Accepted: March
University Department of Endocrinology, Diabetes and Metabolic Disorders, Medical Faculty, Sv. Kiril I Metodij University, Skopje, Macedonia Scientific Paper Received: February 19, 2007 Accepted: March
for school staff Developed for Chicago Public Schools by: LaRabida Children s Hospital and Children s Memorial Hospital November 18, 2011
 1 Diabetes Education for school staff Developed for Chicago Public Schools by: LaRabida Children s Hospital and Children s Memorial Hospital November 18, 2011 Chicago Public Schools Office of Special Education
1 Diabetes Education for school staff Developed for Chicago Public Schools by: LaRabida Children s Hospital and Children s Memorial Hospital November 18, 2011 Chicago Public Schools Office of Special Education
Quarterly Visits with Glycated Hemoglobin Monitoring: The Sweet Spot for Glycemic Control in Youth with Type 1 Diabetes
 Page 1 of 16 Diabetes Care 1 Quarterly Visits with Glycated Hemoglobin Monitoring: The Sweet Spot for Glycemic Control in Youth with Type 1 Diabetes Running title: Visit Frequency and Glycemic Control
Page 1 of 16 Diabetes Care 1 Quarterly Visits with Glycated Hemoglobin Monitoring: The Sweet Spot for Glycemic Control in Youth with Type 1 Diabetes Running title: Visit Frequency and Glycemic Control
Original Article. Pediatric Diabetes
 Pediatric Diabetes 2009: 10: 455 460 doi: 10.1111/j.1399-5448.2009.00506.x All rights reserved # 2009 The Authors Journal compilation # 2009 Blackwell Munksgaard Pediatric Diabetes Original Article Feeding
Pediatric Diabetes 2009: 10: 455 460 doi: 10.1111/j.1399-5448.2009.00506.x All rights reserved # 2009 The Authors Journal compilation # 2009 Blackwell Munksgaard Pediatric Diabetes Original Article Feeding
Y. P. Wu 1,2, M. E. Hilliard 1,2, J. Rausch 2, L. M. Dolan 3,4 and K. K. Hood 5. Abstract. Introduction. Diabet. Med. 30, (2013)
 Research: Educational and Psychological Issues Family involvement with the diabetes regimen in young people: the role of adolescent depressive symptoms Y. P. Wu 1,2, M. E. Hilliard 1,2, J. Rausch 2, L.
Research: Educational and Psychological Issues Family involvement with the diabetes regimen in young people: the role of adolescent depressive symptoms Y. P. Wu 1,2, M. E. Hilliard 1,2, J. Rausch 2, L.
Takashi Yagisawa 1,2*, Makiko Mieno 1,3, Norio Yoshimura 1,4, Kenji Yuzawa 1,5 and Shiro Takahara 1,6
 Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
A hemodialysis cohort study of protocolbased anticoagulation management
 DOI 10.1186/s13104-017-2381-7 BMC Research Notes RESEARCH ARTICLE A hemodialysis cohort study of protocolbased anticoagulation management S. Lamontagne 1,2*, Tinzar Basein 3, Binyue Chang 3 and Lakshmi
DOI 10.1186/s13104-017-2381-7 BMC Research Notes RESEARCH ARTICLE A hemodialysis cohort study of protocolbased anticoagulation management S. Lamontagne 1,2*, Tinzar Basein 3, Binyue Chang 3 and Lakshmi
Insulin Delivery and Glucose Monitoring Methods for Diabetes Mellitus: Comparative Effectiveness
 Insulin Delivery and Glucose Monitoring Methods for Diabetes Mellitus: Comparative Effectiveness Prepared for: Agency for Healthcare Research and Quality (AHRQ) www.ahrq.gov Outline of Material Introduction
Insulin Delivery and Glucose Monitoring Methods for Diabetes Mellitus: Comparative Effectiveness Prepared for: Agency for Healthcare Research and Quality (AHRQ) www.ahrq.gov Outline of Material Introduction
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Afrezza Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Afrezza (human insulin) Prime Therapeutics will review Prior Authorization requests Prior Authorization
Afrezza Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Afrezza (human insulin) Prime Therapeutics will review Prior Authorization requests Prior Authorization
Diabetes Technology Continuous Subcutaneous Insulin Infusion Therapy And Continuous Glucose Monitoring In Adults: An Endocrine Society Clinical
 Diabetes Technology Continuous Subcutaneous Insulin Infusion Therapy And Continuous Glucose Monitoring In Adults: An Endocrine Society Clinical Practice Guideline Task Force Members Anne Peters, MD (Chair)
Diabetes Technology Continuous Subcutaneous Insulin Infusion Therapy And Continuous Glucose Monitoring In Adults: An Endocrine Society Clinical Practice Guideline Task Force Members Anne Peters, MD (Chair)
2016 Diabetes Management Plan
 Early childhood education and care setting 2016 Diabetes Management Plan Insulin pump therapy [to be used in conjunction with Action Plan] Name of child: Date of birth: Name of centre: Age : This plan
Early childhood education and care setting 2016 Diabetes Management Plan Insulin pump therapy [to be used in conjunction with Action Plan] Name of child: Date of birth: Name of centre: Age : This plan
Continuous Glucose Monitoring System
 Continuous Glucose Monitoring System Policy Number: Original Effective Date: MM.02.003 03/13/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 4/1/2018 Section: DME Place(s)
Continuous Glucose Monitoring System Policy Number: Original Effective Date: MM.02.003 03/13/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 4/1/2018 Section: DME Place(s)
Insulin Pumps - External
 Insulin Pumps - External Policy Number: Original Effective Date: MM.01.004 04/01/2011 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/20174/1/2018 Section: DME Place(s) of
Insulin Pumps - External Policy Number: Original Effective Date: MM.01.004 04/01/2011 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/20174/1/2018 Section: DME Place(s) of
Chapter 3 - Does Low Well-being Modify the Effects of
 Chapter 3 - Does Low Well-being Modify the Effects of PRISMA (Dutch DESMOND), a Structured Selfmanagement-education Program for People with Type 2 Diabetes? Published as: van Vugt M, de Wit M, Bader S,
Chapter 3 - Does Low Well-being Modify the Effects of PRISMA (Dutch DESMOND), a Structured Selfmanagement-education Program for People with Type 2 Diabetes? Published as: van Vugt M, de Wit M, Bader S,
Diabetes Update and DKA Queensland Paediatric Society of QLD Dr. Jason Yates Paediatric Endocrinologist
 Diabetes Update and DKA Queensland Paediatric Society of QLD 2018 Dr. Jason Yates Paediatric Endocrinologist Type 1 Diabetes - Paediatrics Most common Paediatric endocrine presentation >90% of all Paediatric
Diabetes Update and DKA Queensland Paediatric Society of QLD 2018 Dr. Jason Yates Paediatric Endocrinologist Type 1 Diabetes - Paediatrics Most common Paediatric endocrine presentation >90% of all Paediatric
ATHLETES & PRESCRIBING PHYSICIANS PLEASE READ
 ATHLETES & PRESCRIBING PHYSICIANS PLEASE READ USADA can grant a Therapeutic Use Exemption (TUE) in compliance with the World Anti- Doping Agency International Standard for TUEs. The TUE application process
ATHLETES & PRESCRIBING PHYSICIANS PLEASE READ USADA can grant a Therapeutic Use Exemption (TUE) in compliance with the World Anti- Doping Agency International Standard for TUEs. The TUE application process
Sponsor / Company: Sanofi Drug substance(s): Insulin Glargine (HOE901) Insulin Glulisine (HMR1964)
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Lars Jacobsson 1,2,3* and Jan Lexell 1,3,4
 Jacobsson and Lexell Health and Quality of Life Outcomes (2016) 14:10 DOI 10.1186/s12955-016-0405-y SHORT REPORT Open Access Life satisfaction after traumatic brain injury: comparison of ratings with the
Jacobsson and Lexell Health and Quality of Life Outcomes (2016) 14:10 DOI 10.1186/s12955-016-0405-y SHORT REPORT Open Access Life satisfaction after traumatic brain injury: comparison of ratings with the
Accuracy of verbal self-reported blood glucose in teenagers with type I diabetes at diabetes ski camp
 Chae et al. Journal of Diabetes & Metabolic Disorders 2014, 13:14 RESEARCH ARTICLE Open Access Accuracy of verbal self-reported blood glucose in teenagers with type I diabetes at diabetes ski camp Matthew
Chae et al. Journal of Diabetes & Metabolic Disorders 2014, 13:14 RESEARCH ARTICLE Open Access Accuracy of verbal self-reported blood glucose in teenagers with type I diabetes at diabetes ski camp Matthew
Faculty of Health Sciences, The University Of Adelaide, Adelaide, South Australia.
 The effectiveness of continuous subcutaneous insulin pumps with continuous glucose monitoring in outpatient adolescents with type 1 diabetes: A systematic review Erin Matsuda RN MSN PNP-BC 1 erin.matsuda@samuelmerritt.edu
The effectiveness of continuous subcutaneous insulin pumps with continuous glucose monitoring in outpatient adolescents with type 1 diabetes: A systematic review Erin Matsuda RN MSN PNP-BC 1 erin.matsuda@samuelmerritt.edu
Continuous Glucose Monitoring System
 Continuous Glucose Monitoring System Policy Number: Original Effective Date: MM.02.003 03/13/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2017 Section: DME Place(s)
Continuous Glucose Monitoring System Policy Number: Original Effective Date: MM.02.003 03/13/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2017 Section: DME Place(s)
Approximately one third of the 15.7 million Americans who are estimated to have diabetes
 Diabetes is a very serious illness and too many people are neglecting their condition. Approximately one third of the 15.7 million Americans who are estimated to have diabetes are unaware of their condition.
Diabetes is a very serious illness and too many people are neglecting their condition. Approximately one third of the 15.7 million Americans who are estimated to have diabetes are unaware of their condition.
Continuous Glucose Monitoring System
 Continuous Glucose Monitoring System Policy Number: Original Effective Date: MM.02.003 03/13/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2016 Section: DME Place(s)
Continuous Glucose Monitoring System Policy Number: Original Effective Date: MM.02.003 03/13/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2016 Section: DME Place(s)
DIABETES MANAGEMENT PLAN 2017
 EARLY CHILDHOOD EDUCATION AND CARE SETTING Insulin pump therapy Use in conjunction with Action Plan DIABETES MANAGEMENT PLAN 2017 Name of child: Name of centre: of birth: Age: This plan should be reviewed
EARLY CHILDHOOD EDUCATION AND CARE SETTING Insulin pump therapy Use in conjunction with Action Plan DIABETES MANAGEMENT PLAN 2017 Name of child: Name of centre: of birth: Age: This plan should be reviewed
Initiation of insulin adjustment for carbohydrate at onset of diabetes in children using a home-based education programme with a bolus calculator
 Initiation of insulin adjustment for carbohydrate at onset of diabetes in children using a home-based education programme with a bolus calculator H Thom 1 BSc (Hons), Paediatric Diabetes Dietitian S Greene
Initiation of insulin adjustment for carbohydrate at onset of diabetes in children using a home-based education programme with a bolus calculator H Thom 1 BSc (Hons), Paediatric Diabetes Dietitian S Greene
Diabetes Medical Management Plan
 SCHOOL DISTRICT OF LEE COUNTY HEALTH SERVICES Print Form Date of Plan Diabetes Medical Management Plan This plan should be completed by the student's personal health care team and parents/guardian. It
SCHOOL DISTRICT OF LEE COUNTY HEALTH SERVICES Print Form Date of Plan Diabetes Medical Management Plan This plan should be completed by the student's personal health care team and parents/guardian. It
Carbohydrate Counting In Type 1 Diabetes: What Do We Know?
 Carbohydrate Counting In Type 1 Diabetes: What Do We Know? Gail Spiegel, MS RD CDE Barbara Davis Center for Childhood Diabetes Keystone, CO July 2012 Outline Why Count Carbs? Carb counting intervention
Carbohydrate Counting In Type 1 Diabetes: What Do We Know? Gail Spiegel, MS RD CDE Barbara Davis Center for Childhood Diabetes Keystone, CO July 2012 Outline Why Count Carbs? Carb counting intervention
DIABETES MANAGEMENT PLAN 2017
 SCHOOL SETTING Multiple daily injections Use in conjunction with Action Plan DIABETES MANAGEMENT PLAN 2017 Name of student: Name of school: of birth: Grade/Year: This plan should be reviewed and updated
SCHOOL SETTING Multiple daily injections Use in conjunction with Action Plan DIABETES MANAGEMENT PLAN 2017 Name of student: Name of school: of birth: Grade/Year: This plan should be reviewed and updated
University College Hospital. Blood glucose and HbA 1 c targets
 University College Hospital Blood glucose and HbA 1 c targets Children & Young People s Diabetes Service The diabetes team at UCLH aims to help every child and young person with Type 1 Diabetes to safely
University College Hospital Blood glucose and HbA 1 c targets Children & Young People s Diabetes Service The diabetes team at UCLH aims to help every child and young person with Type 1 Diabetes to safely
Treatment guideline for adult patients with type 1 diabetes?
 Treatment guideline for adult patients with type 1 diabetes? Jae Hyeon Kim Division of Endocrinology and Metabolism, Samsung Medical Center, Sungkyunkwan University School of Medicine ICDM 2014 Treatment
Treatment guideline for adult patients with type 1 diabetes? Jae Hyeon Kim Division of Endocrinology and Metabolism, Samsung Medical Center, Sungkyunkwan University School of Medicine ICDM 2014 Treatment
Continuous Glucose Monitoring Devices Pharmacy Policy
 Line of Business: All Line of Business Effective date: August 16, 2017 Revision date: August 16, 2017 Continuous Glucose Monitoring Devices Pharmacy Policy This policy has been developed through review
Line of Business: All Line of Business Effective date: August 16, 2017 Revision date: August 16, 2017 Continuous Glucose Monitoring Devices Pharmacy Policy This policy has been developed through review
State of California Health and Human Services Agency Department of Health Care Services
 State of California Health and Human Services Agency Department of Health Care Services JENNIFER KENT Director EDMOND G. BROWN JR Governor DATE: N.L.: 03-0317 Index: Benefits TO: ALL COUNTY CALIFORNIA
State of California Health and Human Services Agency Department of Health Care Services JENNIFER KENT Director EDMOND G. BROWN JR Governor DATE: N.L.: 03-0317 Index: Benefits TO: ALL COUNTY CALIFORNIA
TUE Physician Guidelines Medical Information to Support the Decisions of TUE Committees Diabetes Mellitus DIABETES MELLITUS
 DIABETES MELLITUS 1. Introduction Diabetes is a global epidemic with 415 million people affected worldwide equivalent to the total population of the USA, Canada and Mexico. In recognition of this, the
DIABETES MELLITUS 1. Introduction Diabetes is a global epidemic with 415 million people affected worldwide equivalent to the total population of the USA, Canada and Mexico. In recognition of this, the
DIABETES MANAGEMENT PLAN 2017
 SCHOOL SETTING Insulin pump therapy Use in conjunction with Action Plan DIABETES MANAGEMENT PLAN 2017 Name of student: Name of school: Date of birth: Grade/Year: Insulin pump model: This plan should be
SCHOOL SETTING Insulin pump therapy Use in conjunction with Action Plan DIABETES MANAGEMENT PLAN 2017 Name of student: Name of school: Date of birth: Grade/Year: Insulin pump model: This plan should be
Role of Academia In Achieving Targets in Diabetes Care
 Role of Academia In Achieving Targets in Diabetes Care Disclosures Member of NovoNordisk, Lilly, Metavention, Sanofi, and Janssen Diabetes Advisory Boards Role of Academia in Discovering New Treatments
Role of Academia In Achieving Targets in Diabetes Care Disclosures Member of NovoNordisk, Lilly, Metavention, Sanofi, and Janssen Diabetes Advisory Boards Role of Academia in Discovering New Treatments
[Frida Svendsen and Jennifer Southern] University of Oxford
![[Frida Svendsen and Jennifer Southern] University of Oxford [Frida Svendsen and Jennifer Southern] University of Oxford](/thumbs/95/124874384.jpg) In adolescents with poorly controlled type 1 diabetes mellitus, could a bionic, bihormonal pancreas provide better blood glucose control than continuous subcutaneous insulin infusion therapy? [Frida Svendsen
In adolescents with poorly controlled type 1 diabetes mellitus, could a bionic, bihormonal pancreas provide better blood glucose control than continuous subcutaneous insulin infusion therapy? [Frida Svendsen
2016 Diabetes Management Plan for school Insulin pump therapy [to be used in conjunction with Action Plan]
![2016 Diabetes Management Plan for school Insulin pump therapy [to be used in conjunction with Action Plan] 2016 Diabetes Management Plan for school Insulin pump therapy [to be used in conjunction with Action Plan]](/thumbs/95/124187673.jpg) 2016 Diabetes Management Plan for school Insulin pump therapy [to be used in conjunction with Action Plan] Name of student: Date of birth: Name of school: Grade/Year : Insulin pump model: This plan should
2016 Diabetes Management Plan for school Insulin pump therapy [to be used in conjunction with Action Plan] Name of student: Date of birth: Name of school: Grade/Year : Insulin pump model: This plan should
UTILIZING ACTIGRAPHY TO EXAMINE SLEEP IN YOUNG CHILDREN WITH TYPE 1 DIABETES
 UTILIZING ACTIGRAPHY TO EXAMINE SLEEP IN YOUNG CHILDREN WITH TYPE 1 DIABETES Jadienne Lord, B.A. Beth Malow, M.D. Sarah Jaser, Ph.D. Vanderbilt University Medical Center Ian M. Burr Division of Pediatric
UTILIZING ACTIGRAPHY TO EXAMINE SLEEP IN YOUNG CHILDREN WITH TYPE 1 DIABETES Jadienne Lord, B.A. Beth Malow, M.D. Sarah Jaser, Ph.D. Vanderbilt University Medical Center Ian M. Burr Division of Pediatric
Objectives. Objectives. Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015
 Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
INSULIN THERAY دکتر رحیم وکیلی استاد غدد ومتابولیسم کودکان دانشگاه علوم پزشکی مشهد
 INSULIN THERAY DIABETES1 IN TYPE دکتر رحیم وکیلی استاد غدد ومتابولیسم کودکان دانشگاه علوم پزشکی مشهد Goals of management Manage symptoms Prevent acute and late complications Improve quality of life Avoid
INSULIN THERAY DIABETES1 IN TYPE دکتر رحیم وکیلی استاد غدد ومتابولیسم کودکان دانشگاه علوم پزشکی مشهد Goals of management Manage symptoms Prevent acute and late complications Improve quality of life Avoid
DIABETES MANAGEMENT PLAN 2017
 SCHOOL SETTING Multiple daily injections Use in conjunction with Action Plan DIABETES MANAGEMENT PLAN 2017 Name of student: Name of school: of birth: Grade/Year: This plan should be reviewed and updated
SCHOOL SETTING Multiple daily injections Use in conjunction with Action Plan DIABETES MANAGEMENT PLAN 2017 Name of student: Name of school: of birth: Grade/Year: This plan should be reviewed and updated
Monitoring in Type 2 Diabetes. Learning Outcomes. Type 2 Diabetes. Senga Hunter Community Diabetes Specialist Nurse
 Monitoring in Type 2 Diabetes Senga Hunter Community Diabetes Specialist Nurse Learning Outcomes Understand why blood monitoring is necessary Understand the blood tests for monitoring diabetes Understand
Monitoring in Type 2 Diabetes Senga Hunter Community Diabetes Specialist Nurse Learning Outcomes Understand why blood monitoring is necessary Understand the blood tests for monitoring diabetes Understand
Ensuring Safe Physical Activity in Children and Adolescents With Type 1 Diabetes
 Ensuring Safe Physical Activity in Children and Adolescents With Type 1 Diabetes FACULTY ADVISOR Lori Laffel, MD, MPH Professor, Pediatrics Harvard Medical School Chief, Pediatric, Adolescent and Young
Ensuring Safe Physical Activity in Children and Adolescents With Type 1 Diabetes FACULTY ADVISOR Lori Laffel, MD, MPH Professor, Pediatrics Harvard Medical School Chief, Pediatric, Adolescent and Young
DISCLAIMER: ECHO Nevada emphasizes patient privacy and asks participants to not share ANY Protected Health Information during ECHO clinics.
 DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
ADAG Study Group Data Links A1C Levels with Empirically Measured Blood Glucose Values - New Treatment Guidelines Will Now be Needed
 529638DSTXXX10.1177/1932296814529638Journal of Diabetes Science and TechnologyKlonoff research-article2014 Editorial ADAG Study Group Data Links A1C Levels with Empirically Measured Blood Glucose Values
529638DSTXXX10.1177/1932296814529638Journal of Diabetes Science and TechnologyKlonoff research-article2014 Editorial ADAG Study Group Data Links A1C Levels with Empirically Measured Blood Glucose Values
By: Kokeb T. January, 2016.
 Pre-ART nutritional status and its association with mortality in adult patients enrolled on ART at Fiche Hospital in North Shoa, Oromia Region, Ethiopia: retrospective cohort study. By: Kokeb T. January,
Pre-ART nutritional status and its association with mortality in adult patients enrolled on ART at Fiche Hospital in North Shoa, Oromia Region, Ethiopia: retrospective cohort study. By: Kokeb T. January,
SCIENTIFIC STUDY REPORT
 PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
Chapter 37: Exercise Prescription in Patients with Diabetes
 Chapter 37: Exercise Prescription in Patients with Diabetes American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
Chapter 37: Exercise Prescription in Patients with Diabetes American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
Quality of life among youth with poorly controlled Type 1 diabetes: role of family conflict and sharing of treatment responsibility
 Quality of life among youth with poorly controlled Type 1 diabetes: role of family conflict and sharing of treatment responsibility Melissa Cousino* 1, Rebecca Hazen 2,3, Sarah MacLeish 2,4, Rose Gubitosi-Klug
Quality of life among youth with poorly controlled Type 1 diabetes: role of family conflict and sharing of treatment responsibility Melissa Cousino* 1, Rebecca Hazen 2,3, Sarah MacLeish 2,4, Rose Gubitosi-Klug
Comparative Effectiveness and Safety of Insulin Delivery and Glucose Monitoring Methods for Diabetes Mellitus
 Draft Comparative Effectiveness Review Number XX Comparative Effectiveness and Safety of Insulin Delivery and Glucose Monitoring Methods for Diabetes Mellitus Prepared for: Agency for Healthcare Research
Draft Comparative Effectiveness Review Number XX Comparative Effectiveness and Safety of Insulin Delivery and Glucose Monitoring Methods for Diabetes Mellitus Prepared for: Agency for Healthcare Research
Diabetes in Underserved Youth. Antoinette Moran, MD University of Minnesota
 Diabetes in Underserved Youth Antoinette Moran, MD University of Minnesota In the last 3 years Dr. Moran has Disclosures Served on an DSMB for Novo Nordisk Served on advisory boards for Debiopharm, Vertex,
Diabetes in Underserved Youth Antoinette Moran, MD University of Minnesota In the last 3 years Dr. Moran has Disclosures Served on an DSMB for Novo Nordisk Served on advisory boards for Debiopharm, Vertex,
This certificate-level program is non-sponsored.
 Program Name: Diabetes Education : A Comprehensive Review Module 5 Intensive Insulin Therapy Planning Committee: Michael Boivin, B. Pharm. Johanne Fortier, BSc.Sc, BPh.LPh, CDE Carlene Oleksyn, B.S.P.
Program Name: Diabetes Education : A Comprehensive Review Module 5 Intensive Insulin Therapy Planning Committee: Michael Boivin, B. Pharm. Johanne Fortier, BSc.Sc, BPh.LPh, CDE Carlene Oleksyn, B.S.P.
DIABETES MANAGEMENT PLAN 2017
 SCHOOL SETTING Twice daily injections Use in conjunction with management plan DIABETES MANAGEMENT PLAN 2017 Name of student: Name of school: of birth: Grade/Year: This plan should be reviewed and updated
SCHOOL SETTING Twice daily injections Use in conjunction with management plan DIABETES MANAGEMENT PLAN 2017 Name of student: Name of school: of birth: Grade/Year: This plan should be reviewed and updated
student is independent staff to supervise student is independent staff to supervise student is independent staff to supervise student is independent
 Diabetes Medical Management Plan This plan as well as school medication forms, self authorization and dietary forms should be completed by the student s personal health care team and parents/guardian.
Diabetes Medical Management Plan This plan as well as school medication forms, self authorization and dietary forms should be completed by the student s personal health care team and parents/guardian.
Clinical Study Influence of the Type of Basal Insulin and Other Variables on Clinical Outcomes in Children with Newly Diagnosed Type 1 Diabetes
 ISRN Pediatrics, Article ID 758343, 6 pages http://dx.doi.org/10.1155/2014/758343 Clinical Study Influence of the Type of Basal Insulin and Other Variables on Clinical Outcomes in Children with Newly Diagnosed
ISRN Pediatrics, Article ID 758343, 6 pages http://dx.doi.org/10.1155/2014/758343 Clinical Study Influence of the Type of Basal Insulin and Other Variables on Clinical Outcomes in Children with Newly Diagnosed
15 th Annual DAFNE collaborative meeting Tuesday 28 th June 2016
 15 th Annual DAFNE collaborative meeting Tuesday 28 th June 2016 Sponsored by: Abbott Diabetes Care and Lilly Diabetes Type 1 and exercise Royal Berkshire Hospital Centre for Diabetes and Endocrinology
15 th Annual DAFNE collaborative meeting Tuesday 28 th June 2016 Sponsored by: Abbott Diabetes Care and Lilly Diabetes Type 1 and exercise Royal Berkshire Hospital Centre for Diabetes and Endocrinology
ORIGINAL INVESTIGATION. Use of a Blood Glucose Monitoring Manual to Enhance Monitoring Adherence in Adults With Diabetes
 ORIGINAL INVESTIGATION Use of a Blood Glucose Monitoring Manual to Enhance Monitoring Adherence in Adults With Diabetes A Randomized Controlled Trial Elaine C. Moreland, MD; Lisa K. Volkening, BA; Margaret
ORIGINAL INVESTIGATION Use of a Blood Glucose Monitoring Manual to Enhance Monitoring Adherence in Adults With Diabetes A Randomized Controlled Trial Elaine C. Moreland, MD; Lisa K. Volkening, BA; Margaret
Correct Site Rotation
 Injection Techniques Questionnaire (ITQ) WorldWide Results 2014-2015 Correct Site Rotation BACKGROUND Correct Rotation = at least 1 cm between successive injections Lipohypertrophy and Observed Correct
Injection Techniques Questionnaire (ITQ) WorldWide Results 2014-2015 Correct Site Rotation BACKGROUND Correct Rotation = at least 1 cm between successive injections Lipohypertrophy and Observed Correct
LAURA BIMBO WILLIAMS UNIVERSITY OF FLORIDA
 EXECUTIVE FUNCTIONING, PARENTING STRESS, AND FAMILY FACTORS AS PREDICTORS OF DIABETES MANAGEMENT IN PEDIATRIC PATIENTS WITH TYPE 1 DIABETES USING INTENSIVE INSULIN REGIMENS By LAURA BIMBO WILLIAMS A DISSERTATION
EXECUTIVE FUNCTIONING, PARENTING STRESS, AND FAMILY FACTORS AS PREDICTORS OF DIABETES MANAGEMENT IN PEDIATRIC PATIENTS WITH TYPE 1 DIABETES USING INTENSIVE INSULIN REGIMENS By LAURA BIMBO WILLIAMS A DISSERTATION
Development of a New Fear of Hypoglycemia Scale: Preliminary Results
 Development of a New Fear of Hypoglycemia Scale: Preliminary Results Jodi L. Kamps, 1 PHD, Michael C. Roberts, 2 PHD, ABPP, and R. Enrique Varela, 3 PHD 1 Children s Hospital of New Orleans, 2 University
Development of a New Fear of Hypoglycemia Scale: Preliminary Results Jodi L. Kamps, 1 PHD, Michael C. Roberts, 2 PHD, ABPP, and R. Enrique Varela, 3 PHD 1 Children s Hospital of New Orleans, 2 University
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE GUIDANCE EXECUTIVE (GE)
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE GUIDANCE EXECUTIVE (GE) Review of TA151 Continuous subcutaneous insulin infusion for the treatment of diabetes mellitus This guidance was issued in
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE GUIDANCE EXECUTIVE (GE) Review of TA151 Continuous subcutaneous insulin infusion for the treatment of diabetes mellitus This guidance was issued in
TUEC Guidelines Medical Information to Support the Decisions of TUE Committees Diabetes Mellitus DIABETES MELLITUS
 DIABETES MELLITUS 1. Introduction Diabetes is a global epidemic with 415 million people affected worldwide equivalent to the total population of the USA, Canada and Mexico. In recognition of this, the
DIABETES MELLITUS 1. Introduction Diabetes is a global epidemic with 415 million people affected worldwide equivalent to the total population of the USA, Canada and Mexico. In recognition of this, the
In general: Hypoglycemia is common in insulin treated diabetes, but may also occur in people on oral medications, especially sulfonylureas/glinides.
 1 2 3 In general: Hypoglycemia is common in insulin treated diabetes, but may also occur in people on oral medications, especially sulfonylureas/glinides. 4 Answer: b and c Many alcohol containing drinks
1 2 3 In general: Hypoglycemia is common in insulin treated diabetes, but may also occur in people on oral medications, especially sulfonylureas/glinides. 4 Answer: b and c Many alcohol containing drinks
1995 The Diabetes Control and Complications Trial: Implications for Children and Adolescents
 ADS Position Statements 1995 The Diabetes Control and Complications Trial: Implications for Children and Adolescents Jennifer Couper, Timothy Jones, Kim Donaghue, Caroline Clarke, Michael Thomsett, Martin
ADS Position Statements 1995 The Diabetes Control and Complications Trial: Implications for Children and Adolescents Jennifer Couper, Timothy Jones, Kim Donaghue, Caroline Clarke, Michael Thomsett, Martin
Type 2 Diabetes Mellitus in Adolescents PHIL ZEITLER MD, PHD SECTION OF ENDOCRINOLOGY DEPARTMENT OF PEDIATRICS UNIVERSITY OF COLORADO DENVER
 Type 2 Diabetes Mellitus in Adolescents PHIL ZEITLER MD, PHD SECTION OF ENDOCRINOLOGY DEPARTMENT OF PEDIATRICS UNIVERSITY OF COLORADO DENVER Yes! Is Type 2 diabetes the same in kids as in adults? And No!
Type 2 Diabetes Mellitus in Adolescents PHIL ZEITLER MD, PHD SECTION OF ENDOCRINOLOGY DEPARTMENT OF PEDIATRICS UNIVERSITY OF COLORADO DENVER Yes! Is Type 2 diabetes the same in kids as in adults? And No!
Screening for diabetes
 Screening for diabetes Peggy Odegard, Pharm.D, BCPS, CDE What are your risks? 1 Diabetes Mellitus A problem with glucose regulation type 1= pancreas cannot produce insulin so total insulin deficiency,
Screening for diabetes Peggy Odegard, Pharm.D, BCPS, CDE What are your risks? 1 Diabetes Mellitus A problem with glucose regulation type 1= pancreas cannot produce insulin so total insulin deficiency,
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus
 Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
Survey on Acute and Chronic Complications in Children and Adolescents with Type 1 Diabetes at Muhimbili National Hospital in Dar es Salaam, Tanzania
 Diabetes Care In Press, published online June 11, 2007 Survey on Acute and Chronic Complications in Children and Adolescents with Type 1 Diabetes at Muhimbili National Hospital in Dar es Salaam, Tanzania
Diabetes Care In Press, published online June 11, 2007 Survey on Acute and Chronic Complications in Children and Adolescents with Type 1 Diabetes at Muhimbili National Hospital in Dar es Salaam, Tanzania
APPENDIX American Diabetes Association. Published online at
 APPENDIX 1 INPATIENT MANAGEMENT OF TYPE 2 DIABETES No algorithm applies to all patients with diabetes. These guidelines apply to patients with type 2 diabetes who are not on glucocorticoids, have no
APPENDIX 1 INPATIENT MANAGEMENT OF TYPE 2 DIABETES No algorithm applies to all patients with diabetes. These guidelines apply to patients with type 2 diabetes who are not on glucocorticoids, have no
1. What s the point of a network the case for research? 2. How to use CSII effectively
 1. What s the point of a network the case for research? 2. How to use CSII effectively John Pickup King s College London Faculty of Medicine Guy s Hospital, London What should an insulin pump network do?
1. What s the point of a network the case for research? 2. How to use CSII effectively John Pickup King s College London Faculty of Medicine Guy s Hospital, London What should an insulin pump network do?
Advances in Diabetes Care Technologies
 1979 Advances in Diabetes Care Technologies 2015 Introduction Insulin pump use: ~ 20% - 30% of patients with T1DM < 1% of insulin-treated patients with T2DM 2007 FDA estimates ~375,000 insulin pumps for
1979 Advances in Diabetes Care Technologies 2015 Introduction Insulin pump use: ~ 20% - 30% of patients with T1DM < 1% of insulin-treated patients with T2DM 2007 FDA estimates ~375,000 insulin pumps for
Paolo Di Bartolo U.O di Diabetologia Dip. Malattie Digestive & Metaboliche AULS Prov. di Ravenna. Ipoglicemie e Monitoraggio Glicemico
 Paolo Di Bartolo U.O di Diabetologia Dip. Malattie Digestive & Metaboliche AULS Prov. di Ravenna Ipoglicemie e Monitoraggio Glicemico Management of Hypoglycaemia.if hypoglycemia is a problem, the principles
Paolo Di Bartolo U.O di Diabetologia Dip. Malattie Digestive & Metaboliche AULS Prov. di Ravenna Ipoglicemie e Monitoraggio Glicemico Management of Hypoglycaemia.if hypoglycemia is a problem, the principles
Standards of Care for Students with Type 1 Diabetes in School
 Standards of Care for Students with Type 1 Diabetes in School Purpose: To acknowledge and clarify the essential partnerships among parents or caregivers, students and school personnel in the care of students
Standards of Care for Students with Type 1 Diabetes in School Purpose: To acknowledge and clarify the essential partnerships among parents or caregivers, students and school personnel in the care of students
THE SHEFFIELD AREA PRESCRIBING GROUP. Position Statement for Prescribing of Freestyle Libre In Type 1 Diabetes. Date: March 2018.
 THE SHEFFIELD AREA PRESCRIBING GROUP Position Statement for Prescribing of Freestyle Libre In Type 1 Diabetes Date: March 2018 Overview Freestyle Libre is a flash glucose sensor device that measures *interstitial
THE SHEFFIELD AREA PRESCRIBING GROUP Position Statement for Prescribing of Freestyle Libre In Type 1 Diabetes Date: March 2018 Overview Freestyle Libre is a flash glucose sensor device that measures *interstitial
METABOLIC CONTROL OF TYPE 1 DIABETES IN CHILDREN TREATED WITH INSULIN PUMP THERAPY
 & METABOLIC CONTROL OF TYPE 1 DIABETES IN CHILDREN TREATED WITH INSULIN PUMP THERAPY Sniježana Hasanbegović*, Edo Hasanbegović Paediatric Clinic, University of Sarajevo Clinics Centre, Patriotske lige
& METABOLIC CONTROL OF TYPE 1 DIABETES IN CHILDREN TREATED WITH INSULIN PUMP THERAPY Sniježana Hasanbegović*, Edo Hasanbegović Paediatric Clinic, University of Sarajevo Clinics Centre, Patriotske lige
Commissioning Policy Individual Funding Request
 Commissioning Policy Individual Funding Request Continuous Glucose Monitors Prior Approval Policy Date Adopted: 13 October 2017 Version: 1718.2 Document Control Title of document Continuous Glucose Monitors
Commissioning Policy Individual Funding Request Continuous Glucose Monitors Prior Approval Policy Date Adopted: 13 October 2017 Version: 1718.2 Document Control Title of document Continuous Glucose Monitors
This Diabetes Policy should be read in conjunction with the Dealing with Medical Conditions Policy of Auburn South Preschool.
 DIABETES POLICY Mandatory Quality Area 2 The content of this policy was developed for ELAA by advocacy and diabetes educators at Diabetes Australia Vic and the Royal Children s Hospital Melbourne s manager
DIABETES POLICY Mandatory Quality Area 2 The content of this policy was developed for ELAA by advocacy and diabetes educators at Diabetes Australia Vic and the Royal Children s Hospital Melbourne s manager
The Diamond Study: Continuous Glucose Monitoring In Patients on Mulitple Daily Insulin Injections
 8/5/217 The Diamond Study: Continuous Glucose Monitoring In Patients on Mulitple Daily Insulin Injections Richard M. Bergenstal, MD Executive Director International Diabetes Center at Park Nicollet Minneapolis,
8/5/217 The Diamond Study: Continuous Glucose Monitoring In Patients on Mulitple Daily Insulin Injections Richard M. Bergenstal, MD Executive Director International Diabetes Center at Park Nicollet Minneapolis,
Childhood Obesity and Type II Diabetes: A Rising Epidemic
 Childhood Obesity and Type II Diabetes: A Rising Epidemic Charli Oquin, MS, APRN, PNP, NCSN, CNA Presentation Texas Association of Perianesthesia Nurses (TAPAN) September, 2010 National Initiatives Addressing
Childhood Obesity and Type II Diabetes: A Rising Epidemic Charli Oquin, MS, APRN, PNP, NCSN, CNA Presentation Texas Association of Perianesthesia Nurses (TAPAN) September, 2010 National Initiatives Addressing
Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based screw insertion into locking plates
 Ioannou et al. Journal of Orthopaedic Surgery and Research (2016) 11:118 DOI 10.1186/s13018-016-0458-y RESEARCH ARTICLE Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based
Ioannou et al. Journal of Orthopaedic Surgery and Research (2016) 11:118 DOI 10.1186/s13018-016-0458-y RESEARCH ARTICLE Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based
Evaluation of the Impact of a Diabetes Education Curriculum for School Personnel on Disease Knowledge and Confidence in Caring for Students
 Cedarville University DigitalCommons@Cedarville Pharmacy Practice Faculty Publications Department of Pharmacy Practice - Evaluation of the Impact of a Diabetes Education Curriculum for School Personnel
Cedarville University DigitalCommons@Cedarville Pharmacy Practice Faculty Publications Department of Pharmacy Practice - Evaluation of the Impact of a Diabetes Education Curriculum for School Personnel
TO BE COMPLETED BY LICENSED HEALTH CARE PROFESSIONAL
 PART I OFFICE OF CATHOLIC SCHOOLS DIOCESE OF ARLINGTON DIABETES MEDICAL MANAGEMENT PLAN Page 1 of 5 TO BE COMPLETED BY PARENT OR GUARDIAN Student School Date of Birth Date of Diagnosis Grade/ Teacher Physical
PART I OFFICE OF CATHOLIC SCHOOLS DIOCESE OF ARLINGTON DIABETES MEDICAL MANAGEMENT PLAN Page 1 of 5 TO BE COMPLETED BY PARENT OR GUARDIAN Student School Date of Birth Date of Diagnosis Grade/ Teacher Physical
Disease Detectives Investigate Outbreaks of Salmonella enteritidis
 2018 DISEASE DETECTIVES SAMPLE FOODBORNE ILLNESS Disease Detectives Investigate Outbreaks of Salmonella enteritidis As population growth continues demand for food production will also increase. Avenues
2018 DISEASE DETECTIVES SAMPLE FOODBORNE ILLNESS Disease Detectives Investigate Outbreaks of Salmonella enteritidis As population growth continues demand for food production will also increase. Avenues
Diabetic Neuropathy: Discordance between Symptoms and Electrophysiological Testing in Saudi Diabetics
 Bahrain Medical Bulletin, Vol.24, No.1, March 2002 Diabetic Neuropathy: Discordance between Symptoms and Electrophysiological Testing in Saudi Diabetics Daad H Akbar, FRCP(UK), Arab Board, Saudi Board
Bahrain Medical Bulletin, Vol.24, No.1, March 2002 Diabetic Neuropathy: Discordance between Symptoms and Electrophysiological Testing in Saudi Diabetics Daad H Akbar, FRCP(UK), Arab Board, Saudi Board
SCHOOL HEALTH PLAN: DIABETES
 BRANDON FLORENCE MCLAURIN NORTHWEST PELAHATCHIE RANKIN COUNTY SCHOOL DISTRICT GREAT TO BEST PISGAH PUCKETT RICHLAND RANKIN COUNTY SCHOOL DISTRICT SCHOOL HEALTH PLAN: DIABETES of Plan: Effective s: This
BRANDON FLORENCE MCLAURIN NORTHWEST PELAHATCHIE RANKIN COUNTY SCHOOL DISTRICT GREAT TO BEST PISGAH PUCKETT RICHLAND RANKIN COUNTY SCHOOL DISTRICT SCHOOL HEALTH PLAN: DIABETES of Plan: Effective s: This
DIABETES POLICY. Mandatory Quality Area 2
 DIABETES POLICY Mandatory Quality Area 2 PURPOSE To ensure that enrolled children with type 1 diabetes and their families are supported, while children are being educated and cared for by the service.
DIABETES POLICY Mandatory Quality Area 2 PURPOSE To ensure that enrolled children with type 1 diabetes and their families are supported, while children are being educated and cared for by the service.
