PATIENT-IMPACT SCORECARD
|
|
|
- Blaise Owen
- 5 years ago
- Views:
Transcription
1 UNDERSTANDING THE GSC PATIENT-IMPACT SCORECARD What is the GSC Patient-Impact Scorecard? The GSC Patient-Impact Scorecard shows pharmacy performance scores for GSC patients during the period indicated. It helps pharmacies identify what they re already doing well and potential areas for improvement. Performance information for your pharmacy is available on your Patient-Impact Scorecard approximately six weeks after the end of the measurement period. For example, a scorecard available in May includes prescription drug claims activity through March 31. Scorecards are updated and available from GSC monthly. Performance scores are calculated based upon claims adjudicated through the GSC Advantage system. De-identified GSC claims data is transferred to Pharmacy Quality Solutions (PQS) to use in their EQuIPP dashboard for analysis, then pharmacy performance results are transferred to GSC for Scorecard distribution. Score information is also posted on each pharmacy s EQuIPP dashboard. The Scorecard provides a high-level overview of pharmacy performance more detailed information relative to the pharmacy s performance, including benchmarks and non-adherence or disease management gaps, is available on the EQuIPP dashboard. We strongly encourage all pharmacies to sign up with EQuIPP to obtain in-depth insight into their performance and opportunities for improvement. Once your pharmacy signs up with EQuIPP, GSC will stop sending you a Scorecard. Note that after the initial implementation period, performance information will only be accessible through the EQuIPP dashboard. GSC will stop sending Scorecards after December What information is found on the GSC Patient-Impact Scorecard? On your scorecard you will find the following information: Pharmacy information such as name, address, and provider number Measurement period For each measure: A description of the measure Your pharmacy score GSC s goal The provincial average The number of GSC patients attributed to your pharmacy that are included in the score The gap between your score and the goal, if applicable Your pharmacy s overall score The provincial overall score average Understanding the GSC Patient-Impact Scorecard 1
2 Understanding Measurement Period The measurement period for the GSC Patient-Impact Scorecard is based on a rolling six-month period. For example, a Scorecard with a measurement period of June 2015 November 2015 includes performance scores based on claims data from June 1, 2015, through November 30, As a new Scorecard is generated monthly, the performance scores will be refreshed based on a new rolling six-month measurement period. Quality Measure and Overall Score Calculations There are three primary types of measures and an overall score: 1. Adherence Measures (Proportion of Days Covered or PDC) Hypertension (RASA) PDC Cholesterol PDC Diabetes PDC 2. Disease Management Measures Statin Use in Persons with Diabetes (SUPD) Asthma Suboptimal Control Asthma Absence of Controller Therapy GSC Cardiovascular Health Coaching 3. Patient Safety Measures High-risk Medication Use in the Elderly (HRM) An overall score that reflects performance across all of the quality measures is calculated based upon a composite of the individual performance measures. OVERALL SCORE: 3.5 Provincial Average: 3.0 YOUR PHARMACY VERSUS GOAL VERSUS OTHERS AVERAGE (PROVINCIAL) ADHERENCE Hypertension (RASA) PDC % 93.4% 90.8% Cholesterol PDC % 92.3% 89.5% Diabetes PDC % 92.0% 88.7% DISEASE MANAGEMENT Statin Use in Diabetes Asthma Suboptimal Control Asthma Absence of Controller Therapy GSC Cardiovascular Health Coaching % 77.8% 75.4% % 16.7% 60.2% 31.1% 10 0% 20.0% 24.8% % 10.0% 4.3% 6.3% SAFETY High-risk Medications 12 0% 7.7% 9.9% Understanding the GSC Patient-Impact Scorecard 2
3 Understanding Adherence (PDC) Measures Adherence or PDC measures assess the percentage of patients with prescription claims for the same drug or for another drug in the same therapeutic class, within a measurement period. The PDC threshold is the level above which the medication has a reasonable likelihood of achieving the most clinical benefit (at or greater than 80%). The PDC methodology is a standard method used to measure medication adherence and is specified within the adherence measures endorsed by the Pharmacy Quality Alliance (the organization that developed the measures). Minimum requirements for a patient to be eligible for the adherence measures include: Patient must have at least two fills in the measurement period regardless of the day supply of the prescription fills The first fill of the applicable medication (class) must be at least 91 days prior to the end of the measurement period The therapeutic categories covered by the PDC measures included in the Patient-Impact Scorecard are: Cholesterol PDC: Statins Diabetes PDC: Non-insulin diabetes medications (including biguanides, sulfonylureas, DPP-4 inhibitors, TZDs, GLP-1 receptor agonists (or incretin mimetics), meglitinides, and SGLT2 inhibitors). Patients who receive an insulin product are excluded from the Diabetes PDC measure Hypertension (RASA) PDC: Renin angiotensin system antagonists (including ACE inhibitors, ARBs, and direct renin inhibitors) PDC is calculated by dividing the number of days in period covered into the number of days in period x 100%. The numerator (number of days in period covered ) is equal to the number of days covered by the prescription fills (based on day supply) during the period. This is NOT a sum of day supply, but a summation of time arrays to reflect days supplied for each fill, thus removing any overlap of prescription fills. The denominator (number of days in period) is the number of days from when the prescription is first filled during the measurement period to the end of the measurement period. PDC calculation is performed for each individual patient. An adherent patient has an individual PDC score that is greater than or equal to 80 per cent. In other words, they have at least 80 per cent of their eligible days covered by medication for the target therapeutic category. The pharmacy s performance score reflects the percentage of adherent patients at that pharmacy, i.e., those who have an individual PDC score greater than or equal to 80 per cent. Adherence or PDC performance scores are better when they are higher. This means that patients at that pharmacy are more adherent to their medication. Hypertension (RASA) PDC % 93.4% Understanding the GSC Patient-Impact Scorecard 3
4 This pharmacy s performance score for the Hypertension (RASA) PDC measure is displayed as 95.4 per cent. This means that 95.4 per cent of the pharmacy s 65 patients are considered adherent (65 x 95.4% = 62 patients). Or, that 62 out of 65 patients have a Proportion of Days Covered (PDC) score greater than or equal to 80 per cent. In this scenario, the pharmacy would have three (65 eligible patients minus 62 patients that are adherent) patients that are non-adherent. Knowing this information enables the pharmacist to attend to these three patients and their reasons for non-adherence. Patient Attribution for Adherence (PDC) Measures Adherence measures use an encounter-based attribution method. In other words, the pharmacy that filled the most prescription claims within the measurement period for the target therapeutic category will be assigned responsibility for the patient. If a patient fills the same number of prescriptions during the measurement period at multiple pharmacies, the patient will be attributed to the pharmacy that completed the most recent fill. All paid prescription drug claims adjudicated through the drug plan, regardless of the dispensing pharmacy, will be counted towards the patient s PDC calculation. Understanding the Statin Use in Persons with Diabetes Measure The SUPD measure identifies the percentage of patients age who were dispensed a medication for treatment of diabetes that were also dispensed a statin medication. This therapy recommendation is based on the updated guidelines by the 2013 Canadian Diabetes Association Clinical Practice Guidelines and 2016 Canadian Cardiovascular Society Guidelines for the Management of Dyslipidemia for the Prevention of Cardiovascular Disease in the Adult. The SUPD measure was developed and is endorsed by the Pharmacy Quality Alliance. The SUPD performance score is better when it is higher. This means that diabetic patients at the pharmacy receive recommended primary prevention therapy with statins more often. Statin Use in Diabetes % 77.8% This pharmacy s performance score for the SUPD measure is displayed as 79.2 per cent. This means that 79.2 per cent of the pharmacy s 24 patients filled a statin along with their medications for diabetes treatment. In this scenario, the pharmacy would have five patients (24 patients, 20.8 per cent not on a statin) to evaluate for a new statin therapy. Understanding the GSC Patient-Impact Scorecard 4
5 Patient Attribution for the SUPD Measure For the SUPD measure, the pharmacy that first fills the statin medication for the patient is assigned responsibility for the patient. If a diabetic patient does not have a statin medication in their profile, the pharmacy that filled the most diabetic medications (including insulin) for the patient within the measurement period is assigned responsibility. It only takes one fill for a statin medication within the measurement period for the patient to be considered compliant with the SUPD measure. Understanding the Asthma Therapy Measures The patient population included in the two asthma measures include patients 6-50 years of age with asthma defined as patients with consecutive fills of asthma medications during the measurement year. Excluded from the measure are those patients with at least one fill in the measurement year for one of the following: COPD medication Cystic fibrosis agent Nasal steroid medication Two asthma measures are reported: Suboptimal Control: This measure refers to the percentage of patients with persistent asthma who were dispensed more than three canisters* of a short-acting beta2 agonist inhaler during the same 90-day period. Absence of Controller Therapy: This measure refers to the percentage of patients meeting the numerator for the Suboptimal Control rate (i.e., those with more than three canisters of short-acting beta2 agonist inhalers during a 90-day period), who did not receive controller therapy (e.g., inhaled corticosteroids, long-acting beta-agonists, leukotriene inhibitors, or xanthines) during the same 90-day period. Example 1: Asthma Suboptimal Control % 16.7% 60.2% This pharmacy s performance score for the Suboptimal Control measure is 76.9 per cent. This number means that 76.9 per cent of the pharmacy s 13 patients with persistent asthma have been dispensed more than three canisters of short-acting beta2 agonist inhalers during the same 90-day period. In this scenario the pharmacy would have 10 patients (13 patients, 76.9 per cent dispensed more than three canisters of short-acting beta2 agonist inhalers dispensed) to evaluate for asthma control. Example 2: Asthma Absence of Controller Therapy 10 0% 20.0% *Note: This is a count of canisters dispensed, not prescriptions filled. If a patient received two canisters at one fill, it counts as two canisters. Understanding the GSC Patient-Impact Scorecard 5
6 This pharmacy s performance score for the Absence of Controller Therapy measure is zero per cent. This number means that all of the pharmacy s 10 patients that were dispensed more than three canisters of short-acting beta2 agonist inhalers during the same 90-day period received controller therapy. The intended goal for these two measures is to have a lower performance score. Patient Attribution for the Asthma Measures For the Asthma measures, the pharmacy that fills the majority of the asthma medications for an individual patient is assigned responsibility for that patient. The pharmacy has responsibility for a patient across both measures. Understanding the GSC Cardiovascular Health Coaching Measure The patient population included in the GSC Cardiovascular Health Coaching (CHC) measure refers to the percentage of eligible patients who received at least one coaching session during the measurement period. Refer to GSC s Cardiovascular Health Coaching program information on providerconnect for patient eligibility and other program details. GSC Cardiovascular Health Coaching % 10.0% 4.3% This pharmacy s performance score for the CHC measure is 5.7 per cent. This number means that two patients eligible for CHC (35 patients, 5.7 per cent) received at least one coaching session. The pharmacy has an opportunity to engage 33 patients (35 eligible patients minus two who have already received at least one coaching session) in the Cardiovascular Health Coaching program. Please note that Pharmacist Health Coaching is a reimbursed pharmacy service. More details around this program are available at providerconnect.ca. Patient Attribution for the GSC Cardiovascular Health Coaching Measure The pharmacy assigned the CHC opportunity will be the pharmacy that has filled the majority of total prescription claims for the patient. In the event of a tie for total prescription claims across more than one pharmacy, the pharmacy with the most recent date of service for the claim will be assigned the CHC opportunity. For a pharmacy that completed a CHC service, the patient will be attributed to the pharmacy associated with the claim for the first CHC service within the measurement period, based on date of service. Understanding the GSC Patient-Impact Scorecard 6
7 Understanding the High-risk Medication Use in the Elderly Measure The High-risk Medication Use in the Elderly (HRM) measure looks at the percentage of patients 65 years of age and older who received two or more prescription fills for the same high-risk medication (HRM) during the measurement period. The list of medications in this measure was derived from a subset of the Beers List, which is maintained by the American Geriatrics Society. The medications on this list are intended to represent medications that have more significant risk of causing adverse outcomes when used in elderly patients. Some medications on the HRM drug list are only considered an HRM when used for a specific duration or at a specific dose per day. The HRM measure is endorsed and maintained by the Pharmacy Quality Alliance. The HRM measure is better when the performance score is lower. This means that fewer patients at the pharmacy are filling potentially inappropriate medications based on their age. High-risk Medications 12 0% 7.7% This pharmacy s performance score for the HRM measure is displayed as zero per cent. This means that none of the pharmacy s 12 patients have filled two or more prescriptions for a medication on the HRM list. Being proactive is key for this measure. Ideally, the pharmacist intervenes before the second prescription is dispensed. Once the patient fills the second prescription for an HRM, no change can be made to improve the patient s performance for this measure during the current measurement period. Patient Attribution for the HRM Measure Patient safety measures, such as the HRM Measure, use an event-based attribution. The pharmacy that fills the second fill of an HRM (or the fill for the requisite dose or duration, depending on the medication) is assigned responsibility for the patient for the HRM measure. If a patient has prescriptions, but no HRM fills, the pharmacy filling the most prescription claims for all medications within the measurement period will be assigned responsibility for the patient. The intended goal for this measure is to have a lower performance score. Understanding Benchmark Scores In addition to your pharmacy performance scores, the Patient-Impact Scorecard shows two other benchmark scores, a GSC-established goal and a provincial average score. These benchmark scores help add context to your pharmacy s performance, which helps you understand how you perform relative to other pharmacies. Understanding the GSC Patient-Impact Scorecard 7
8 Understanding the Overall Score The overall score reflects pharmacy performance across all of the quality measures. For a pharmacy to have an overall score calculated, they will have to have performance information available for at least three or more individual quality measures with at least 10 or more patients eligible for each measure. The overall score is calculated based upon a composite of the individual performance measures with variable weighting applied: Single-weighted measures: Hypertension (RASA) PDC Cholesterol PDC Diabetes PDC Double-weighted measures: Statin Use in Persons with Diabetes (SUPD) Asthma Suboptimal Control Asthma Absence of Controller Therapy GSC Cardiovascular Health Coaching High-risk medication Use in the Elderly (HRM) Double-weighted measures have been selected based on GSC s and the pharmacy profession s common goal to support the evolution of pharmacy practice towards the delivery of high-quality patient care. To calculate the overall score, a star rating, based on percentiles, is assigned to all qualifying measures. Weighting is then applied to calculate an overall star rating (from one to five stars). OVERALL SCORE: 4.5 Provincial Average: 3.0 YOUR PHARMACY VERSUS GOAL VERSUS OTHERS AVERAGE (PROVINCIAL) ADHERENCE Hypertension (RASA) PDC % 93.4% 90.8% Cholesterol PDC % 92.3% 89.5% Diabetes PDC % 92.0% 4.5% 88.7% DISEASE MANAGEMENT Statin Use in Diabetes Asthma Suboptimal Control Asthma Absence of Controller Therapy GSC Cardiovascular Health Coaching % 77.8% 75.4% 0 N/A 16.7% N/A N/A 0 N/A 20.0% N/A N/A 4 0.0% 10.0% 10.0% 0.0% SAFETY High-risk Medications % 7.7% 0.4% 9.9% Understanding the GSC Patient-Impact Scorecard 8
9 Calculation of overall score: QUALIFYING MEASURE MEASURE-LEVEL STAR RATING WEIGHTING Hypertension (RASA) PDC 5 star Single Cholesterol PDC 5 star Single Statin Use in Diabetes 5 star Double High Risk Medication 3 star Double = 4.333, rounded to 4.5 stars 6 Understanding the GSC Patient-Impact Scorecard 9
Disease Management. Measures At A Glance
 s At A Glance Updated: 11/2/2017 Page 1 of 7 Cross Cutting Mandatory s (4) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual
s At A Glance Updated: 11/2/2017 Page 1 of 7 Cross Cutting Mandatory s (4) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual
Disease Management. Measures At A Glance
 s At A Glance Updated: 11/01/2018 URAC 2018 Page 1 of 7 Cross-Cutting Mandatory s (3) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on
s At A Glance Updated: 11/01/2018 URAC 2018 Page 1 of 7 Cross-Cutting Mandatory s (3) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on
Understanding Your Patient Care Opportunity Report (PCOR)
 Understanding Your Patient Care Opportunity Report (PCOR) Use your January/February 208 PCOR to help improve performance on Medicare Part D Clinical Star Ratings measures. Your January/February 208 Patient
Understanding Your Patient Care Opportunity Report (PCOR) Use your January/February 208 PCOR to help improve performance on Medicare Part D Clinical Star Ratings measures. Your January/February 208 Patient
Pharmacy Benefit Management
 Benefit Management Measures At A Glance Updated: 10/8/2015 Page 1 of 7 Benefit Management Mandatory Measures (6) Note: Mandatory measures are those measures that are a requirement of accreditation and
Benefit Management Measures At A Glance Updated: 10/8/2015 Page 1 of 7 Benefit Management Mandatory Measures (6) Note: Mandatory measures are those measures that are a requirement of accreditation and
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis.
 Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DESCRIPTION NUMERATOR DENOMINATOR DM2012-12 Portion of Days Covered
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DESCRIPTION NUMERATOR DENOMINATOR DM2012-12 Portion of Days Covered
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis.
 COMMUNITY PHARMACY V1.1 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. # NAME DESCRIPTION NUMERATOR DENOMINATOR
COMMUNITY PHARMACY V1.1 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. # NAME DESCRIPTION NUMERATOR DENOMINATOR
9/25/15. Pharmacy Quality Measures: Financial Support. Learning Objectives. Speaker Disclosure. Access to Preferred Networks and Clinical Performance
 Pharmacy Quality Measures: Action Steps for Improvement Financial Support Financial support was provided for this activity through an unrestricted grant from Health Mart Systems, Inc. Christine Jacobson
Pharmacy Quality Measures: Action Steps for Improvement Financial Support Financial support was provided for this activity through an unrestricted grant from Health Mart Systems, Inc. Christine Jacobson
MEASURE STEWARD Pharmacy Quality Alliance (PQA) D ATA SOURCE Enrollment; U R A C DOMAIN Engagement & Experience of Care
 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DM2012-12 DTM2015-01 Portion of Days Covered (PDC) Adherence
MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DM2012-12 DTM2015-01 Portion of Days Covered (PDC) Adherence
Mail Service Pharmacy
 Mail Service s At A Glance Disclaimer: reserves the right to update its measures and measure sets to maintain measure relevancy and to remedy any unintended consequences that may arise during implementation.
Mail Service s At A Glance Disclaimer: reserves the right to update its measures and measure sets to maintain measure relevancy and to remedy any unintended consequences that may arise during implementation.
STARS SYSTEM 5 CATEGORIES
 TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
Drug Therapy Management
 Measures At A Glance Updated: 11/01/2018 2018 Page 1 of 9 Mandatory Measures (10) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to on an annual
Measures At A Glance Updated: 11/01/2018 2018 Page 1 of 9 Mandatory Measures (10) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to on an annual
2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT
 2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT December 2017 Table of Contents Executive Summary... 1 Pharmacy Benefit Management Organization Characteristics...
2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT December 2017 Table of Contents Executive Summary... 1 Pharmacy Benefit Management Organization Characteristics...
Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015
 Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015 Amerivantage is an HMO plan with a contract with the New Mexico Medicare program.
Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015 Amerivantage is an HMO plan with a contract with the New Mexico Medicare program.
Star Measures At-A-Glance Guide
 Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At WellCare, we value
Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At WellCare, we value
PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter
 Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Medicare Star Ratings and the Shift to Quality- Based Payment Models. David Nau, RPh, PhD, FAPhA PQS President
 Medicare Star Ratings and the Shift to Quality- Based Payment Models David Nau, RPh, PhD, FAPhA PQS President The shift to Value-Driven Healthcare The U.S. health care system is rapidly moving to value-based
Medicare Star Ratings and the Shift to Quality- Based Payment Models David Nau, RPh, PhD, FAPhA PQS President The shift to Value-Driven Healthcare The U.S. health care system is rapidly moving to value-based
Commercial Business Measurement Period Handbook For Patient-Centered Primary Care
 Commercial Business Measurement Period Handbook For Patient-Centered Primary Care Measurement Period beginning: 07/01/16 CB Version 070116 V1 Introduction: Welcome to your Commercial Business Measurement
Commercial Business Measurement Period Handbook For Patient-Centered Primary Care Measurement Period beginning: 07/01/16 CB Version 070116 V1 Introduction: Welcome to your Commercial Business Measurement
HEADED FOR HEDIS AND REACHING FOR THE STARS: THE PHARMACIST S ROLE IN POPULATION HEALTH MANAGEMENT
 HEADED FOR HEDIS AND REACHING FOR THE STARS: THE PHARMACIST S ROLE IN POPULATION HEALTH MANAGEMENT Desola Davis, PharmD, BCPS, BCACP Dalia Zall, PharmD 1 Copyright 2017 Kaiser Foundation Health Plan, Inc.
HEADED FOR HEDIS AND REACHING FOR THE STARS: THE PHARMACIST S ROLE IN POPULATION HEALTH MANAGEMENT Desola Davis, PharmD, BCPS, BCACP Dalia Zall, PharmD 1 Copyright 2017 Kaiser Foundation Health Plan, Inc.
Commercial Business Measurement Period Handbook-Medical Cost Target Model For Enhanced Personal Health Care Measurement Period beginning: 01/1/17
 Commercial Business Measurement Period Handbook-Medical Cost Target Model For Enhanced Personal Health Care Measurement Period beginning: 01/1/17 CBMCT Version 010117 V3 Introduction: Welcome to your Commercial
Commercial Business Measurement Period Handbook-Medical Cost Target Model For Enhanced Personal Health Care Measurement Period beginning: 01/1/17 CBMCT Version 010117 V3 Introduction: Welcome to your Commercial
Star Measures At-A-Glance Guide
 Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At Easy Choice, we
Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At Easy Choice, we
2018 P4P Overview 0518.PR.P.PP.1 6/18
 2018 P4P Overview Agenda MHS Pay For Performance (P4P) Ambetter P4P Program Secure Web Reporting Question and Answer What You Will Learn 1. Measure Overviews & Specifications 2. Documentation Requirements
2018 P4P Overview Agenda MHS Pay For Performance (P4P) Ambetter P4P Program Secure Web Reporting Question and Answer What You Will Learn 1. Measure Overviews & Specifications 2. Documentation Requirements
This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings.
 2019 HEDIS AT-A-GLANCE GUIDE STAR MEASURES This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. At WellCare, we value everything
2019 HEDIS AT-A-GLANCE GUIDE STAR MEASURES This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. At WellCare, we value everything
6/18/2015. Disclosure. Objectives. Star Ratings. Understand the current climate of healthcare reform
 Star Ratings John A. Galdo, Pharm.D., BCPS, CGP (Jake) Assistant Professor of Pharmacy Practice Community Practice Residency Director jgaldo@samford.edu Disclosure I do not have (nor does any immediate
Star Ratings John A. Galdo, Pharm.D., BCPS, CGP (Jake) Assistant Professor of Pharmacy Practice Community Practice Residency Director jgaldo@samford.edu Disclosure I do not have (nor does any immediate
Commercial Business Medical Cost Target
 Commercial Business Medical Cost Target Measurement Period Handbook For Enhanced Personal Health Care Measurement Period beginning: April 1, 2018 CBMCT 040118 V3 Introduction Welcome to your Commercial
Commercial Business Medical Cost Target Measurement Period Handbook For Enhanced Personal Health Care Measurement Period beginning: April 1, 2018 CBMCT 040118 V3 Introduction Welcome to your Commercial
Commercial Business Medical Cost Target
 Commercial Business Medical Cost Target Measurement Period Handbook For Enhanced Personal Health Care Measurement Period beginning: April 1, 2018 CBMCT 040118 V1 Introduction Welcome to your Commercial
Commercial Business Medical Cost Target Measurement Period Handbook For Enhanced Personal Health Care Measurement Period beginning: April 1, 2018 CBMCT 040118 V1 Introduction Welcome to your Commercial
Condition/Procedure Measure Compliance Criteria Reference Attribution Method
 Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Alabama Medicaid Pharmacy Override
 Alabama Medicaid Pharmacy Override Therapeutic Duplication, Early Refill, Maximum Unit, Prescription Limit Switchover, Dispense as Written, Accumulation Edit, Maintenance Supply Opt Out, and Maximum Cost
Alabama Medicaid Pharmacy Override Therapeutic Duplication, Early Refill, Maximum Unit, Prescription Limit Switchover, Dispense as Written, Accumulation Edit, Maintenance Supply Opt Out, and Maximum Cost
PHARMACY QUALITY MEASURES: Improving Performance Playbook
 PHARMACY QUALITY MEASURES: Improving Performance Playbook Table of Contents How to Use This Resource 4 Why Performance Measures Matter to Your Pharmacy 5 The Medicare Star Ratings System 5 For More Information
PHARMACY QUALITY MEASURES: Improving Performance Playbook Table of Contents How to Use This Resource 4 Why Performance Measures Matter to Your Pharmacy 5 The Medicare Star Ratings System 5 For More Information
Quality ID #444 (NQF 1799): Medication Management for People with Asthma National Quality Strategy Domain: Efficiency and Cost Reduction
 Quality ID #444 (NQF 1799): Medication Management for People with Asthma National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Quality ID #444 (NQF 1799): Medication Management for People with Asthma National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Asthma Population Management: Identifying Persistent Asthma, Defining High Risk Asthma, and Measuring Quality of Asthma Care
 Asthma Population Management: Identifying Persistent Asthma, Defining High Risk Asthma, and Measuring Quality of Asthma Care Michael Schatz, MD, MS Allergy Department Kaiser Permanente, San Diego, CA Constructs
Asthma Population Management: Identifying Persistent Asthma, Defining High Risk Asthma, and Measuring Quality of Asthma Care Michael Schatz, MD, MS Allergy Department Kaiser Permanente, San Diego, CA Constructs
New Measure Recommended for Endorsement by PQA
 New Measure Recommended for Endorsement by PQA Measure: Statin Use in Persons with Diabetes Description: The percentage of patients ages 40 75 years who were dispensed a medication for diabetes that receive
New Measure Recommended for Endorsement by PQA Measure: Statin Use in Persons with Diabetes Description: The percentage of patients ages 40 75 years who were dispensed a medication for diabetes that receive
USING MTM TO IMPROVE STAR RATINGS : CASE STUDIES
 USING MTM TO IMPROVE STAR RATINGS : CASE STUDIES Sept 13, 2015 Amanda Applegate, PharmD, BCACP Disclosures Nothing to disclose Learning Objectives Describe how MTM can improve star ratings Discuss strategies
USING MTM TO IMPROVE STAR RATINGS : CASE STUDIES Sept 13, 2015 Amanda Applegate, PharmD, BCACP Disclosures Nothing to disclose Learning Objectives Describe how MTM can improve star ratings Discuss strategies
116th Annual Convention
 116th Annual Convention Date: Tuesday, October 21, 2014 Time: 8:30 am 10:00 am Location: Austin Convention Center, Room 17AB, Level 4 Title: Activity Type: Speaker: Medicare Part D Star Ratings What They
116th Annual Convention Date: Tuesday, October 21, 2014 Time: 8:30 am 10:00 am Location: Austin Convention Center, Room 17AB, Level 4 Title: Activity Type: Speaker: Medicare Part D Star Ratings What They
A COMPREHENSIVE APPROACH TO MANAGING DIABETES
 A COMPREHENSIVE APPROACH TO MANAGING DIABETES Programs and services to help individuals avoid costly complications and improve outcomes 2 0 1 8 ENTER Supporting each member with targeted guidance and services.
A COMPREHENSIVE APPROACH TO MANAGING DIABETES Programs and services to help individuals avoid costly complications and improve outcomes 2 0 1 8 ENTER Supporting each member with targeted guidance and services.
The clinical quality measures as selected by the Clinical Management subcommittee for 2016 for the adult population are:
 For 2016 the Clinical Integration Program is moving its clinical quality measures from the Verisk Healthcare Quality and Risk Measures to the National Committee for Quality Assurance HEDIS based measures.
For 2016 the Clinical Integration Program is moving its clinical quality measures from the Verisk Healthcare Quality and Risk Measures to the National Committee for Quality Assurance HEDIS based measures.
INCRETIN THERAPY ROUNDTABLE: Putting recommendations into practice. Program guide
 INCRETIN THERAPY ROUNDTABLE: Putting recommendations into practice Program guide 1 TABLE OF CONTENTS Objectives. 2 Case study and interactive questions... 3 Top 5 clinical tips..... 11 OBJECTIVES After
INCRETIN THERAPY ROUNDTABLE: Putting recommendations into practice Program guide 1 TABLE OF CONTENTS Objectives. 2 Case study and interactive questions... 3 Top 5 clinical tips..... 11 OBJECTIVES After
Section II: Detailed Measure Specifications
 Section II: Detailed Measure Specifications Provide sufficient detail to describe how a measure would be calculated from the recommended data sources, uploading a separate document (+ Upload attachment)
Section II: Detailed Measure Specifications Provide sufficient detail to describe how a measure would be calculated from the recommended data sources, uploading a separate document (+ Upload attachment)
Canadian Diabetes Association 2013
 Spring 2014 Canadian Diabetes Association 2013 clinical practice guidelines - Do claims data align to the guidelines? Canadian Diabetes Association 2013 clinical practice guidelines - Do claims data align
Spring 2014 Canadian Diabetes Association 2013 clinical practice guidelines - Do claims data align to the guidelines? Canadian Diabetes Association 2013 clinical practice guidelines - Do claims data align
Optum Research Database Proportion of asthma patients with prescription fills for rescue and controller medications by year,
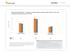 ASTHMA CHART 1 Optum Research Database Proportion of asthma patients with prescription fills for rescue and controller medications by year, 215-216 7 6 5 4 3 2 1 1 Controller medication 1 Rescue medication
ASTHMA CHART 1 Optum Research Database Proportion of asthma patients with prescription fills for rescue and controller medications by year, 215-216 7 6 5 4 3 2 1 1 Controller medication 1 Rescue medication
PCMH 2018 Enrollment and Update August 25, 2017
 PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
Your Partnership in Health Report: Chronic Conditions ABC Company and Kaiser Permanente
 Your Partnership in Health Report: s ABC Company and Kaiser Permanente Measurement Period: JUL-01-2012 through JUN-30-2013 Report Date: DEC-31-2013 Commercial All Members Partnership in Health (PIH) reports:
Your Partnership in Health Report: s ABC Company and Kaiser Permanente Measurement Period: JUL-01-2012 through JUN-30-2013 Report Date: DEC-31-2013 Commercial All Members Partnership in Health (PIH) reports:
Proposed Changes to Existing Measure for HEDIS : Adherence to Antipsychotic Medications for Individuals With Schizophrenia (SAA)
 Proposed Changes to Existing Measure for HEDIS 1 2020: Adherence to Antipsychotic Medications for Individuals With Schizophrenia (SAA) NCQA seeks comments on proposed modifications to the HEDIS Health
Proposed Changes to Existing Measure for HEDIS 1 2020: Adherence to Antipsychotic Medications for Individuals With Schizophrenia (SAA) NCQA seeks comments on proposed modifications to the HEDIS Health
5 x 7 spiral bound - prints front and back sheets - 1/1 - black MEASURE DESCRIPTION
 Requirements for Meeting Clinical Goals - Last Updated 11-1-2016 TABLE OF CONTENTS MEASURE ABBREVIATION AAB ABA ADD AMM AMR ART BCS CBP CCS CDC CDC CDC CDC CHL CWP CIS COL FUH IMA IET LBP MPM MEASURE DESCRIPTION
Requirements for Meeting Clinical Goals - Last Updated 11-1-2016 TABLE OF CONTENTS MEASURE ABBREVIATION AAB ABA ADD AMM AMR ART BCS CBP CCS CDC CDC CDC CDC CHL CWP CIS COL FUH IMA IET LBP MPM MEASURE DESCRIPTION
Population Health: Update on HEDIS measures
 Population Health: Update on HEDIS measures Office of Evidence-Based Practice Quality Management Division U.S. Army Medical Command April 2010 January 2010 Updates - MHSPHP MHSPHP Methods document is posted
Population Health: Update on HEDIS measures Office of Evidence-Based Practice Quality Management Division U.S. Army Medical Command April 2010 January 2010 Updates - MHSPHP MHSPHP Methods document is posted
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications
 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications Fidelis SecureCare strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications Fidelis SecureCare strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
Frequently Asked Questions for Ontario Pharmacists: Blood Glucose Test Strip Reimbursement Policy
 Ontario Public Drug Programs, Ministry of Health and Long-Term Care Frequently Asked Questions for Ontario Pharmacists: Blood Glucose Test Strip Reimbursement Policy 1. Why is the ministry introducing
Ontario Public Drug Programs, Ministry of Health and Long-Term Care Frequently Asked Questions for Ontario Pharmacists: Blood Glucose Test Strip Reimbursement Policy 1. Why is the ministry introducing
Definitions of chronic conditions used to define the number of serious comorbidities in the study.
 Supplementary Table 1 Definitions of chronic conditions used to define the number of serious comorbidities in the study. Comorbidity ICD-9 Code Description CAD/MI 410.x Acute myocardial infarction 411.x
Supplementary Table 1 Definitions of chronic conditions used to define the number of serious comorbidities in the study. Comorbidity ICD-9 Code Description CAD/MI 410.x Acute myocardial infarction 411.x
Outcomes Summary. February 3-6, 2016 Keystone, Colorado
 Outcomes Summary February 3-6, 2016 Keystone, Colorado Executive Summary Activity Details Background: The National Jewish Health Annual The Pulmonary and Allergy Update highlights insights and recent advances
Outcomes Summary February 3-6, 2016 Keystone, Colorado Executive Summary Activity Details Background: The National Jewish Health Annual The Pulmonary and Allergy Update highlights insights and recent advances
Provider STAR Ratings Quick Reference Guide 2016 Dates of Service. Updated January 20, 2016
 Provider STAR Ratings Quick Reference Guide 2016 Dates of Service Updated January 20, 2016 Adult BMI (Body Mass Index) Assessment (ABA) EXCLUSIONS: Members who have a diagnosis of pregnancy during the
Provider STAR Ratings Quick Reference Guide 2016 Dates of Service Updated January 20, 2016 Adult BMI (Body Mass Index) Assessment (ABA) EXCLUSIONS: Members who have a diagnosis of pregnancy during the
Pharmacy Technician Course
 Pharmacy Technician Course VERSION HISTORY SECTION 1: History and Scope of the Pharmacy Technician Scope of the Pharmacy Technician Section 1 Quiz Check Your Knowledge Section 1 Quiz Answers SECTION 2:
Pharmacy Technician Course VERSION HISTORY SECTION 1: History and Scope of the Pharmacy Technician Scope of the Pharmacy Technician Section 1 Quiz Check Your Knowledge Section 1 Quiz Answers SECTION 2:
2014 Physician Quality Reporting System Data Collection Form: Asthma (for patients aged 5-64)
 2014 Physician Quality Reporting System Data Collection Form: Asthma (for patients aged 5-64) Physician Name: Patient Name: Last First MI Date of Birth: / / mm dd yyyy Gender: M F Patient Insured - Traditional
2014 Physician Quality Reporting System Data Collection Form: Asthma (for patients aged 5-64) Physician Name: Patient Name: Last First MI Date of Birth: / / mm dd yyyy Gender: M F Patient Insured - Traditional
Legislative & Regulatory Update Brad Young, RxPlus Government Affairs
 Legislative & Regulatory Update 2018 Brad Young, RxPlus Government Affairs Disclosures Brad Young reports no actual or potential conflicts of interest associated with this presentation. 2 Learning Objectives
Legislative & Regulatory Update 2018 Brad Young, RxPlus Government Affairs Disclosures Brad Young reports no actual or potential conflicts of interest associated with this presentation. 2 Learning Objectives
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #52 (NQF 0102): Chronic Obstructive Pulmonary Disease (COPD): Long-Acting Inhaled Bronchodilator Therapy National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL
Quality ID #52 (NQF 0102): Chronic Obstructive Pulmonary Disease (COPD): Long-Acting Inhaled Bronchodilator Therapy National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL
Texas Vendor Drug Program. Formulary Drug Index File Layout. Layout effective: Jul. 2, 2018 Document update: Oct. 1, 2018
 Texas Vendor Drug Program Formulary Drug Index File Layout Layout effective: Jul. 2, 2018 Document update: Oct. 1, 2018 The Vendor Drug Program provides a weekly update of resource data available for download
Texas Vendor Drug Program Formulary Drug Index File Layout Layout effective: Jul. 2, 2018 Document update: Oct. 1, 2018 The Vendor Drug Program provides a weekly update of resource data available for download
Bridges to Excellence Chronic Obstructive Pulmonary Disease Care Recognition Program Guide
 Bridges to Excellence Chronic Obstructive Pulmonary Disease Care Recognition Program Guide Altarum Bridges to Excellence 3520 Green Court, Suite 300 Ann Arbor, MI 48105 bte@altarum.org www.bridgestoexcellence.org
Bridges to Excellence Chronic Obstructive Pulmonary Disease Care Recognition Program Guide Altarum Bridges to Excellence 3520 Green Court, Suite 300 Ann Arbor, MI 48105 bte@altarum.org www.bridgestoexcellence.org
2017 PCP INCENTIVE AWARD PROGRAM MEASURES & TIPS
 Childhood Immunization Status (CIS) Combo 10 Immunizations for Adolescents (IMA) Combo 1 Lead Screening in Children (LSC) Immunizations completed prior to a child turning 2 years of age in 2017 as follows:
Childhood Immunization Status (CIS) Combo 10 Immunizations for Adolescents (IMA) Combo 1 Lead Screening in Children (LSC) Immunizations completed prior to a child turning 2 years of age in 2017 as follows:
SUMMARY TABLE OF MEASURE CHANGES
 Summary Table of Measure 1 SUMMARY TABLE OF MEASURE CHANGES Guidelines for Physician Measurement Adult BMI Assessment Weight Assessment and Counseling for Nutrition and Physical Activity for Children/Adolescents
Summary Table of Measure 1 SUMMARY TABLE OF MEASURE CHANGES Guidelines for Physician Measurement Adult BMI Assessment Weight Assessment and Counseling for Nutrition and Physical Activity for Children/Adolescents
Step 2: Identify patients who were dispensed at least two consecutive fills for any asthma medication (Table ACT-A: Asthma
 NATIONAL QUALITY FORUM Measure Submission and Evaluation Worksheet 5.0 This form contains the information submitted by measure developers/stewards, organized according to NQF s measure evaluation criteria
NATIONAL QUALITY FORUM Measure Submission and Evaluation Worksheet 5.0 This form contains the information submitted by measure developers/stewards, organized according to NQF s measure evaluation criteria
16 th Annual IHA Stakeholders Meeting Session 2C
 16 th Annual IHA Stakeholders Meeting Session 2C September 19, 2017 Hilton Los Angeles Airport Thank you to our Content Partner: Medication Adherence AppleCare Pharmacy Programs Confidential and proprietary.
16 th Annual IHA Stakeholders Meeting Session 2C September 19, 2017 Hilton Los Angeles Airport Thank you to our Content Partner: Medication Adherence AppleCare Pharmacy Programs Confidential and proprietary.
The BlueCompare SM Physician Designation Program
 The BlueCompare SM Physician Designation Program Continuing escalation of health care costs has driven premiums and medical expenses to higher and higher levels each year, motivating employers and consumers
The BlueCompare SM Physician Designation Program Continuing escalation of health care costs has driven premiums and medical expenses to higher and higher levels each year, motivating employers and consumers
Medicare Shared Savings Program Quality Measure Benchmarks for the 2014 and 2015 Reporting Years
 Medicare Shared Savings Program Quality Measure Benchmarks for the 2014 and 2015 Reporting Years Introduction This document describes methods for calculating the quality performance benchmarks for Accountable
Medicare Shared Savings Program Quality Measure Benchmarks for the 2014 and 2015 Reporting Years Introduction This document describes methods for calculating the quality performance benchmarks for Accountable
Comprehensive Research Plan: Inhaled corticosteroids + long-acting beta agonists (ICS+LABA) for the treatment of asthma
 Comprehensive Research Plan: Inhaled corticosteroids + long-acting beta agonists (ICS+LABA) for the treatment of asthma Pharmacoepidemiology Unit July 10, 2014 30 Bond Street, Toronto ON, M5B 1W8 www.odprn.ca
Comprehensive Research Plan: Inhaled corticosteroids + long-acting beta agonists (ICS+LABA) for the treatment of asthma Pharmacoepidemiology Unit July 10, 2014 30 Bond Street, Toronto ON, M5B 1W8 www.odprn.ca
Quality Corp Measures Description and Methodologies
 Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Quality Corp Measures Description and Methodologies
 Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
ASSOCIATION OF ASTHMA CONTROL WITH HEALTH CARE UTILIZATION A PROSPECTIVE EVALUATION
 Online Supplement for: ASSOCIATION OF ASTHMA CONTROL WITH HEALTH CARE UTILIZATION A PROSPECTIVE EVALUATION METHODS Population The Northwest Region of Kaiser Permanente (KPNW) is a large, federally qualified,
Online Supplement for: ASSOCIATION OF ASTHMA CONTROL WITH HEALTH CARE UTILIZATION A PROSPECTIVE EVALUATION METHODS Population The Northwest Region of Kaiser Permanente (KPNW) is a large, federally qualified,
Kentucky Department for Medicaid Services Pharmacy and Therapeutics Advisory Committee Recommendations
 Kentucky Department for Medicaid Services Pharmacy and March 15, 2018 The following chart provides a summary of the recommendations that were made by the Pharmacy and Therapeutics (P&T) Advisory Committee
Kentucky Department for Medicaid Services Pharmacy and March 15, 2018 The following chart provides a summary of the recommendations that were made by the Pharmacy and Therapeutics (P&T) Advisory Committee
Capital Health Plan CMS Star Ratings Strategies for Improvement
 Capital Health Plan CMS Star Ratings Strategies for Improvement ESTRELLITA REDMON, MD, MBA MEDICAL DIRECTOR The Ultimate Goal Outline Current 5 Star Plans CHP History Importance of Ratings Part C and Part
Capital Health Plan CMS Star Ratings Strategies for Improvement ESTRELLITA REDMON, MD, MBA MEDICAL DIRECTOR The Ultimate Goal Outline Current 5 Star Plans CHP History Importance of Ratings Part C and Part
New Product to Market: Trelegy Ellipta Magellan Health, Inc. All rights reserved.
 Drug Review and The following tables list the Agenda items as well as the that are scheduled to be presented and reviewed at the March 15, 2018 meeting of the Pharmacy and Therapeutics Advisory Committee.
Drug Review and The following tables list the Agenda items as well as the that are scheduled to be presented and reviewed at the March 15, 2018 meeting of the Pharmacy and Therapeutics Advisory Committee.
MEDICAL ASSISTANCE BULLETIN
 ISSUE DATE January 6, 2016 SUBJECT EFFECTIVE DATE January 20, 2016 MEDICAL ASSISTANCE BULLETIN NUMBER *See below BY Prior Authorization of COPD Agents Pharmacy Service Leesa M. Allen, Deputy Secretary
ISSUE DATE January 6, 2016 SUBJECT EFFECTIVE DATE January 20, 2016 MEDICAL ASSISTANCE BULLETIN NUMBER *See below BY Prior Authorization of COPD Agents Pharmacy Service Leesa M. Allen, Deputy Secretary
Medicare STRIDE SM Physician Quality Program 2019 Program Overview
 Medicare STRIDE SM Quality Program 2019 Program Overview Health Services- Managed by Network Medical Management 2019 Program 1 Medicare Advantage Quality Program Program Overview The Plan will support
Medicare STRIDE SM Quality Program 2019 Program Overview Health Services- Managed by Network Medical Management 2019 Program 1 Medicare Advantage Quality Program Program Overview The Plan will support
Bridges to Excellence Asthma Care Recognition Program Guide for Patients 5 years of age and older
 Bridges to Excellence Asthma Care Recognition Program Guide for Patients 5 years of age and older Altarum Bridges to Excellence 3520 Green Court, Suite 300 Ann Arbor, MI 48105 bte@altarum.org www.bridgestoexcellence.org
Bridges to Excellence Asthma Care Recognition Program Guide for Patients 5 years of age and older Altarum Bridges to Excellence 3520 Green Court, Suite 300 Ann Arbor, MI 48105 bte@altarum.org www.bridgestoexcellence.org
Community Pharmacy Asthma Audit 2016/17. Contents
 Community Pharmacy Contents Community Pharmacy... 1 Executive Summary... 2 Introduction... 4 Background... 4 Method... 5 Results... 5 Section One: Community Pharmacy Guidelines Awareness and Training...
Community Pharmacy Contents Community Pharmacy... 1 Executive Summary... 2 Introduction... 4 Background... 4 Method... 5 Results... 5 Section One: Community Pharmacy Guidelines Awareness and Training...
Clinical Quality Measures Summary of Upcoming Enhancements
 Upcoming coding enhancements will impact the logic behind the clinical quality indicators applicable to your practice specialty. Please refer to this grid for a summary of the coding enhancements and some
Upcoming coding enhancements will impact the logic behind the clinical quality indicators applicable to your practice specialty. Please refer to this grid for a summary of the coding enhancements and some
SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES
 Summary Table of Measures, Product Lines and Changes 1 SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES General Guidelines for Data Collection and Reporting Guidelines for Calculations and Sampling
Summary Table of Measures, Product Lines and Changes 1 SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES General Guidelines for Data Collection and Reporting Guidelines for Calculations and Sampling
Adherence to asthma controller medication regimens
 Respiratory Medicine (2005) 99, 1263 1267 Adherence to asthma controller medication regimens D.A. Stempel a,, S.W. Stoloff b, J.R. Carranza Rosenzweig c, R.H. Stanford c, K.L. Ryskina d, A.P. Legorreta
Respiratory Medicine (2005) 99, 1263 1267 Adherence to asthma controller medication regimens D.A. Stempel a,, S.W. Stoloff b, J.R. Carranza Rosenzweig c, R.H. Stanford c, K.L. Ryskina d, A.P. Legorreta
Rich Segal, R.Ph., Ph.D. Professor and Associate Dean University of Florida
 Exploring Barriers to Medication Adherence and Strategies for Improving Adherence for Asthma Rich Segal, R.Ph., Ph.D. Professor and Associate Dean University of Florida Presentation Objectives Understand
Exploring Barriers to Medication Adherence and Strategies for Improving Adherence for Asthma Rich Segal, R.Ph., Ph.D. Professor and Associate Dean University of Florida Presentation Objectives Understand
Changes for Physician Measurement 2018
 Changes for Physician Measurement 2018 Measure Name Guidelines for Physician Measurement Effectiveness of Care Changes Revised the Systematic Sampling Methodology to require organizations to report using
Changes for Physician Measurement 2018 Measure Name Guidelines for Physician Measurement Effectiveness of Care Changes Revised the Systematic Sampling Methodology to require organizations to report using
Clinical Integration Quality Measures
 Clinical Integration Quality Measures Valley Integrated Care Network (VIPN) is physician-driven, with physicians determining which quality measures will be used to improve overall quality of care. Purpose:
Clinical Integration Quality Measures Valley Integrated Care Network (VIPN) is physician-driven, with physicians determining which quality measures will be used to improve overall quality of care. Purpose:
Kentucky Department for Medicaid Services. Drug Review Options
 Kentucky Department for Medicaid Services Drug Review Options The following chart lists the agenda items scheduled and the options submitted for review at the March 18, 2010 meeting of the Pharmacy and
Kentucky Department for Medicaid Services Drug Review Options The following chart lists the agenda items scheduled and the options submitted for review at the March 18, 2010 meeting of the Pharmacy and
Impact and Value of Pharmacist Interventions in Different Settings
 Impact and Value of Pharmacist Interventions in Different Settings Cheryl Pegus MD MPH Chief Medical Officer Walgreen Co. March 15, 2011 Chronic Care Management Today: The Challenge Less Effective Lower
Impact and Value of Pharmacist Interventions in Different Settings Cheryl Pegus MD MPH Chief Medical Officer Walgreen Co. March 15, 2011 Chronic Care Management Today: The Challenge Less Effective Lower
Reduction of High Risk Medications Using A Quality Initiative Perspective
 Reduction of High Risk Medications Using A Quality Initiative Perspective Richard Mueller PharmD, MBA, MS, Director of Pharmacy Dianne Hempel BSN, RN Quality Improvement Coordinator Objectives Learn what
Reduction of High Risk Medications Using A Quality Initiative Perspective Richard Mueller PharmD, MBA, MS, Director of Pharmacy Dianne Hempel BSN, RN Quality Improvement Coordinator Objectives Learn what
Quality Indicator Physician Medicare HEDIS, HOS, CAHPS and Part D Safety Measures Guide for 2017
 Quality Indicator Physician Medicare HEDIS, HOS, CAHPS and Part D Safety s Guide for 2017 Note: HEDIS codes can change from year to year. The codes in this document are from the HEDIS 2017 specifications.
Quality Indicator Physician Medicare HEDIS, HOS, CAHPS and Part D Safety s Guide for 2017 Note: HEDIS codes can change from year to year. The codes in this document are from the HEDIS 2017 specifications.
2016 General Practice/Family Practice Preferred Specialty Measure Set
 1 0059 5 0081 41 N/A 50 N/A 65 0069, EHR 66 0002, EHR Effective Clinical Care Effective Clinical Care Effective Clinical Care Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients
1 0059 5 0081 41 N/A 50 N/A 65 0069, EHR 66 0002, EHR Effective Clinical Care Effective Clinical Care Effective Clinical Care Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients
2018 Blue Cross NC. Provider Quality Pocket Guide
 2018 Blue Cross NC Provider Quality Pocket Guide 5 x 7 spiral bound - prints front and back sheets - 1/1 - black Requirements for Meeting Clinical Goals - Last Updated October 2017 TABLE OF CONTENTS MEASURE
2018 Blue Cross NC Provider Quality Pocket Guide 5 x 7 spiral bound - prints front and back sheets - 1/1 - black Requirements for Meeting Clinical Goals - Last Updated October 2017 TABLE OF CONTENTS MEASURE
Diabetes update - Diagnosis and Treatment
 Diabetes update - Diagnosis and Treatment Eugene J Barrett, MD,PhD Madge Jones Professor of Medicine Director, University of Virginia Diabetes Center Disclosures - None Case 1 - Screening for Diabetes
Diabetes update - Diagnosis and Treatment Eugene J Barrett, MD,PhD Madge Jones Professor of Medicine Director, University of Virginia Diabetes Center Disclosures - None Case 1 - Screening for Diabetes
Plan Change Alert. New Market Priced Drug (MPD) Program Effective 11/1/2016. Alaska United Food and Commercial Workers Trust
 Plan Change Alert New Market Priced Drug (MPD) Program Effective 11/1/2016 Plan Sponsor Alaska United Food and Commercial Workers Trust Geographic Area Alaska Number of Participants Serviced 2,000 Announcement
Plan Change Alert New Market Priced Drug (MPD) Program Effective 11/1/2016 Plan Sponsor Alaska United Food and Commercial Workers Trust Geographic Area Alaska Number of Participants Serviced 2,000 Announcement
LOUISIANA MEDICAID PROGRAM ISSUED: 02/01/12 REPLACED: 02/01/94 CHAPTER 5: PROFESSIONAL SERVICES SECTION 5.1: COVERED SERVICES PAGE(S) 6
 Diabetes Education Management Training Diabetes self management training (DSMT) is a collaborative process through which recipients with diabetes gain knowledge and skills needed to modify behavior and
Diabetes Education Management Training Diabetes self management training (DSMT) is a collaborative process through which recipients with diabetes gain knowledge and skills needed to modify behavior and
This standard is not designed to be prescriptive of how, when or in what format training is delivered although, some guidelines are included.
 Using Medicines (or medicines refresher) This is a training standard developed for the National Training Service (NTS) Alliance. This standard has been written in consultation with subject matter experts.
Using Medicines (or medicines refresher) This is a training standard developed for the National Training Service (NTS) Alliance. This standard has been written in consultation with subject matter experts.
Cost-Motivated Treatment Changes in Commercial Claims:
 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non- Medical Switching August 2017 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non-Medical
Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non- Medical Switching August 2017 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non-Medical
Section 1: 1: Trends. Section 2: 2: Comparisons to to Overall Portland Area Area Results for for
 Section 1: 1: Trends 2 Patients in the Diabetes Register 3 Diabetes Type 3 Gender of Patients with Diabetes 4 Age of Patients with Diabetes 4 Duration of Diabetes 5 Weight Control 6 Hemoglobin A1c 7 Blood
Section 1: 1: Trends 2 Patients in the Diabetes Register 3 Diabetes Type 3 Gender of Patients with Diabetes 4 Age of Patients with Diabetes 4 Duration of Diabetes 5 Weight Control 6 Hemoglobin A1c 7 Blood
Commercial HMO/POS Effectiveness of Care Measure
 Commercial HMO/POS Effectiveness of Care Measure HEDIS 2017 NCQA Quality Compass National Average Adult BMI Assessment 91.85% 76.17% Weight Assessment and Counseling for Nutrition and Physical Activity
Commercial HMO/POS Effectiveness of Care Measure HEDIS 2017 NCQA Quality Compass National Average Adult BMI Assessment 91.85% 76.17% Weight Assessment and Counseling for Nutrition and Physical Activity
Supplementary Online Content
 Supplementary Online Content Choudhry NK, Krumme AA, Ercole PM, et al. Effect of reminder devices on medication adherence: the REMIND randomized clinical trial. JAMA Int Med. Published online February
Supplementary Online Content Choudhry NK, Krumme AA, Ercole PM, et al. Effect of reminder devices on medication adherence: the REMIND randomized clinical trial. JAMA Int Med. Published online February
CASE A2 Managing Between-meal Hypoglycemia
 Managing Between-meal Hypoglycemia 1 I would like to discuss this case of a patient who, overall, was doing well on her therapy until she made an important lifestyle change to lose weight. This is a common
Managing Between-meal Hypoglycemia 1 I would like to discuss this case of a patient who, overall, was doing well on her therapy until she made an important lifestyle change to lose weight. This is a common
Texas Vendor Drug Program. Formulary Delimited File Layout. April 26, 2017
 Texas Vendor Drug Program Formulary Delimited File Layout April 26, 2017 The Vendor Drug Program provides a weekly update of resource data available for download from txvendordrug.com/resources/downloads.
Texas Vendor Drug Program Formulary Delimited File Layout April 26, 2017 The Vendor Drug Program provides a weekly update of resource data available for download from txvendordrug.com/resources/downloads.
ANALYSIS OF KENTUCKY MEDICAID MANAGED CARE VERSUS FEE-FOR- SERVICE SYSTEMS: MEDICATION ADHERENCE IN PATIENTS WITH PREVALENT CHRONIC DISEASES
 University of Kentucky UKnowledge Theses and Dissertations--Pharmacy College of Pharmacy 2016 ANALYSIS OF KENTUCKY MEDICAID MANAGED CARE VERSUS FEE-FOR- SERVICE SYSTEMS: MEDICATION ADHERENCE IN PATIENTS
University of Kentucky UKnowledge Theses and Dissertations--Pharmacy College of Pharmacy 2016 ANALYSIS OF KENTUCKY MEDICAID MANAGED CARE VERSUS FEE-FOR- SERVICE SYSTEMS: MEDICATION ADHERENCE IN PATIENTS
STEP THERAPY PROGRAM
 STEP THERAPY PROGRAM Step Therapy Program Certain prescription drugs call for a more detailed assessment to help ensure that they represent reasonable treatment. For these drugs, Great-West s Special Authorization
STEP THERAPY PROGRAM Step Therapy Program Certain prescription drugs call for a more detailed assessment to help ensure that they represent reasonable treatment. For these drugs, Great-West s Special Authorization
PROVIDER GUIDE Required information on targeted HEDIS and Part D measures
 PROVIDER GUIDE Required information on targeted HEDIS and Part D measures Visit www.atriohp.com/star-ratings-program for full measure descriptions. Contact QI@atriohp.com with any questions. Adult Body
PROVIDER GUIDE Required information on targeted HEDIS and Part D measures Visit www.atriohp.com/star-ratings-program for full measure descriptions. Contact QI@atriohp.com with any questions. Adult Body
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual
 Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Subject: Canadian Diabetes Association Feedback on New Drugs for Type 2 Diabetes: Second-Line Therapy: A Therapeutic Review Update
 February 3, 2017 Canadian Agency for Drugs and Technologies in Health (CADTH) 865 Carling Avenue, Suite 600 Ottawa, Ontario K1S 5S8 Subject: Canadian Diabetes Association Feedback on New Drugs for Type
February 3, 2017 Canadian Agency for Drugs and Technologies in Health (CADTH) 865 Carling Avenue, Suite 600 Ottawa, Ontario K1S 5S8 Subject: Canadian Diabetes Association Feedback on New Drugs for Type
