Community Intravenous Therapy Program and a treatment plan for foot infections in persons with diabetes: A clinical perspective
|
|
|
- Daisy Haynes
- 5 years ago
- Views:
Transcription
1 HOME AND OUTPATIENT USE OF PARENTERAL ANTIBIOTICS Community Intravenous Therapy Program and a treatment plan for foot infections in persons with diabetes: A clinical perspective John M Embil MD 1,2, Shurjeel H Choudhri MD 1, Glenna Germaine RN 3, Theresa Imlah RN 3, Frank Duerksen MD 2,4, Marie Darcel RN 2, Hank Fong MD 2,5, Joshua Koulack MD 2,5, Alfred Gin Pharm D 6, Sheryl Stern MD 7, J Neil Simonsen MD 1,2, Godfrey KM Harding MD 1, Lindsay E Nicolle MD 1,2 Diabetes is a multi system disease that can lead to complications such as peripheral neuropathy and peripheral vascular disease. These two complications can synergistically lead to the formation of ulcerations in the feet and lower extremities of people with diabetes. Should an ulceration develop, it may be a self-limited process healing spontaneously, or it may lead to more serious complications, such as infection of the skin, soft tissue, bone, sepsis, and possibly amputation of toes, foot or lower extremity. In 1991, 57% of all amputations involving lower extremities in Manitoba were in people with diabetes. Lower extremity amputations were 10 times higher among people with diabetes than those without diabetes. In 1991, the prevalence of diabetes in adult Manitobans was as follows: First Nations individuals 12% males and 20% females; non-first Nations individuals 7% males and 6.4% females. The Manitoba Health Services Commission record for 1993 to 1994 show 16% of lower extremity amputations in Manitoba were among First Nations individuals, and 84% were among non-first Nations individuals (J Blanchard, personal communication). Despite great advances made in the treatment of diabetes, significant morbidity and mortality still occurs with this disease. Factors which influence the predisposition for infection include neuropathy which may lead to ulcerations; autonomic insufficiency leading to dry, cracked skin that serves as a portal for infection; vasculopathy leading to ischemia and decreased wound healing capacity; and immunopathy as a consequence of altered neutrophil function. These factors, combined with a lack of or inadequate knowledge of diabetes, can lead to serious complications. Thus, it is critical to identify people with diabetes at risk of foot complications and prevent the complications. Unfortunately, some individuals present with a foot complication as their first presentation of diabetes. In all individuals, it is important to treat quickly 1 Departments of Medicine and Medical Microbiology, Section of Infectious Diseases, University of Manitoba; 2 Health Sciences Centre Diabetic Foot and Complicated Wound Clinic; 3 Community Intravenous Therapy Program; 4 Department of Surgery, Section of Orthopedics, University of Manitoba; 5 Department of Surgery, Section of Vascular Surgery, University of Manitoba; 6 Department of Pharmaceutical Services, Health Sciences Centre; 7 Department of Diagnostic Imaging, Section of Nuclear Medicine, University of Manitoba, Winnipeg, Manitoba Correspondence and reprints: Dr John M Embil, Infection Control Unit, MS Sherbrook Street, Health Centre, Winnipeg, Manitoba R3A 1R9. Telephone , fax , jembil@hsc.mb.ca Can J Infect Dis Vol 11 Suppl A January/February A
2 Embil et al and effectively the underlying infection, be it skin, soft tissue and/or bone. The goal is to minimize the risk of amputation. THE COMMUNITY INTRAVENOUS THERAPY PROGRAMME The current approaches that exist for providing therapy to people with diabetes with lower extremity infections are: oral antimicrobials administered as an outpatient; parenteral antimicrobials delivered as an inpatient; parenteral antimicrobials delivered as an inpatient therapy but then switched to oral therapy at the time of discharge; or parenteral antimicrobials administered through the Community Intravenous Therapy Program (CITP). Parenteral medications administered in the outpatient setting have been shown to be safe, effective and convenient for individuals who are clinically stable with regard to their underlying disease process. In addition, cost savings are also realized (1-3). The CITP was established in the early 1980s as an adjunctive measure to patient care to prevent admission to hospital and to facilitate discharge from hospital. Criteri to establish the eligibility of an individual to receive parenteral antimicrobials administered through the CITP are as follows. The patient is clinically stable and can be discharged from hospital and requires ongoing parenteral antimicrobial therapy. Oral medications are not suitable for treatment of the current infection either because the microorganism that has been recovered from the wound is resistant to currently available oral antimicrobials or the patient is unable to tolerate oral medication. The patient must be compliant with non weight bearing, leg elevation and all other aspects of therapy that will be performed as an outpatient. More aggressive adjunctive therapy such as additional surgical debridement of skin, soft tissue or bone has either already been performed or is not necessary. The patient must be closely followed by his or her physician to ensure that the therapy for the underlying process is achieving the desired results. The patient must be compliant with the policies and procedures of the CITP. The home and social circumstances must be conducive to receiving therapy through CITP. Each request for the CITP is reviewed on a case by case basis by the CITP team consisting of: CITP nursing staff, pharmacists, pharmacy technicians, and infectious disease consultants. The CITP reserves the right to seek the input of an infectious disease consultant before enrolling a patient on the program. INFECTIONS IN THE LOWER EXTREMITIES OF PEOPLE WITH DIABETES Infections in the lower extremities of people with diabetes can be divided into those which are mild, moderate and severe and may involve skin, soft tissue, and/or bone. Numerous reports outline the management of infections in the lower extremities of people with diabetes (4-9, unpublished data). Uncomplicated lower extremity infections in people with diabetes are usually caused by aerobic Gram-positive cocci and respond well to oral outpatient therapy (4). A variety of antibiotics exist that are well tolerated orally, and can achieve suitable serum and bone levels for the treatment of deep seated infections (10). The management of osteomyelitis in the foot of PWD is more complicated, and numerous approaches have been recommended, ranging from prolonged parenteral therapy to initial parenteral therapy followed by oral antimicrobial therapy (OAT) or exclusively OAT (5-9, unpublished data). It is important to differentiate between wound infection and colonization. Infections are usually associated with purulent discharge, edema, erythema and occasionally pain, and bacteria may be recovered from the wound base. With colonization, bacteria will be recovered from swabs of the wound base but the other signs of infection are absent. Superficial skin and soft tissue infections may arise as a consequence of direct trauma and contiguous spread of organisms. If the infection is not controlled and the ulceration progresses, the underlying bone may become involved. Initially, aerobic Gram-positive bacteria such as Staphylococcus aureus and Streptococcus species are the most frequently isolated organisms. As the ulceration persists, more necrotic tissue is present, and Gram-negative and anaerobic bacteria soon predominate in the wound. Specimens for culture are best obtained from infected tissue that does not communicate with the skin surface. The ideal specimen for culture assessment of infection is a curettage specimen from the base of the ulcer or bone biopsy specimens if osteomyelitis is suspected. If such specimens are not available, cultures of purulent exudate from within the ulcer base or sinuses may be an alternative. Before appropriate therapy can be provided, it is important to establish the status of the lower extremity of a person with diabetes as it relates to infection. Issues that must be considered are: The patient must be emotionally and psychologically prepared to try therapy administered through CITP. Telephone access must be available. The safety of the CITP team must be ensured when visiting the patient s dwelling. extent of infection mild, moderate, severe; presence of underlying ulcerations; presence of neuropathy; adequacy of circulation; 50A Can J Infect Dis Vol 11 Suppl A January/February 2000
3 CITP TABLE 1A Antibiotic therapy for infected ulcerations in the lower extremity of people with diabetes Skin and soft tissue Type of infection Medication Dosage ($) cost ($) Daily cost Total daily Mild infections are deemed to be neither limb nor life-threatening processes. They are usually associated with cellulitis surrounding an ulceration. A small amount of purulent material may be present at the base of the ulcer. The most likely organisms are aerobic Gram-positive cocci. Patients with these infections can frequently be treated as outpatients with oral therapy. Moderate infections can range from plantar abscesses to more significant cellulitis with tissue necrosis and deep seated infection. Antimicrobial regimens should be effective against staphylococci, streptococci, anaerobes, and common Enterobacteriaceae species. Patients who are not toxic can be treated with local incision and drainage and oral antimicrobial therapy. Patients who are critically ill or toxic: are best treated with parenteral therapy until stable, then switch to oral therapy. Severe infections: Patients with severe diabetic foot infections have limb- or life-threatening infections requiring immediate hospitalization and parenteral antimicrobial therapy. Early surgical debridement and drainage of abscesses is critical. Cloxacillin Cephalexin TMP/SMX Clindamycin Amoxicillin-clavulinic acid TMP/SMX and TMP/SMX and Ciprofloxacin and Ciprofloxacin and Amoxicillin-clavulinic acid Managed as per severe infections, see below Clindamycin and gentamicin Cefotetan Cefazolin and Piperacillin and tazobactam Clindamycin and ceftriaxone Imipenem/cilistatin Meropenem 500 mg po qid 500 mg po qid 500/125 mg po tid 500 mg po tid 500 mg po bid 750 mg po bid 500/125 mg po tid IV 600 mg Q8h IV 80 mg Q8h IV 2 g Q12h IV 2 g Q8h IV 500 mg Q8h IV g Q6h IV 600 mg Q8h IV 1 g Q24h IV 500/500 mg Q6h IV 1 g Q8h As per daily cost As per daily cost *If in doubt about the most appropriate antibiotic for the management of the diabetic foot infection, discussion with an infectious disease consultant may be prudent. Before antimicrobials are used in the person with diabetes, an evaluation of renal function must be undertaken to best guide appropriate dosing. This is particularly important with the aminoglycosides. Dosages shown are for normal renal function. If using aminoglycosides it is imperative that the renal function and drug levels be monitored closely.; Approximate daily cost for oral therapy excludes the dispensing fee. These are 1998 costs based upon the Manitoba Drug Benefits and Interchangeability Formulary and the Manufacturer s recommended dosing regimen and listed price. In some instances, a higher dose of ciprofloxacin may be necessary. Other quinolone antimicrobial agents may be considered as alternatives, but a review of product monographs is necessary to establish optimal doses. ds Double strength; IV intravenous; po By mouth; TMP/SMX Trimethoprim/sulfamethoxazole presence of underlying osteomyelitis; and adjunctive measures. The suggestions that follow for investigations, dressings and therapeutic interventions have been kept as simple as possible. The suggestions are to be used in conjunction with appropriate management of the underlying diabetes and other metabolic abnormalities. Extent of infection: Tables 1A and 1B summarize the classification of infections in the lower extremities of people with diabetes and provides treatment suggestions. It is important to recall that it is advisable to use wound or bone cultures to help guide antimicrobial choices. Figure 1 provides a simplified algorithm to help determine the most appropriate treatment regimens for patients presenting with diabetic foot infections. Neuropathy: A history of foot numbness, lack of sensation, prior amputation of the contralateral lower extremity or toes on either extremity, and prior foot ulcerations should raise the suspicion that an individual lacks protective sensation. Callouses may result from unrelieved pressure and may also lead to ulcerations due to undermining of the underlying skin. The loss of pain perception due to neuropathy leads to increased susceptibility to mechanical and thermal trauma. Injury, ulcerations and subsequent infection may go unnoticed in the insensate foot. At every office visit, people with diabetes should be asked whether they are inspecting their feet regularly, and whether they have a current ulceration of their feet. Adequacy of circulation: For resolution of infection and promotion of wound healing, adequate circulation is necessary. If pulses are not palpable in the lower extremity, it is important to obtain an estimate of the adequacy of circulation. The ankle brachial index is a noninvasive method where comparison of Can J Infect Dis Vol 11 Suppl A January/February A
4 Embil et al TABLE 1B Antibiotic therapy for infected ulcerations in the lower extremity of people with diabetes Type of infection Medication Dosage ($) cost ($) Daily cost Total daily Osteomyelitis is a frequent complication of diabetic foot ulcerations. Antimicrobial choices must be guided by culture data. Monotherapy may be used based upon clinical assessment and culture results. Oral therapy: Osteomyelitis may be managed with long term oral antimicrobial therapy with agents that are well absorbed from the gastrointestinal tract and have good distribution to bone and tissue. Parenteral therapy: In some cases, parenteral therapy may be necessary. Although multiple parenteral regimens exist, only those which may be easily administered through the Community Intravenous Therapy Program are noted here. Aminoglycosidebased regimens are avoided for prolonged treatment courses because of potential complications. The duration of parenteral therapy is guided by clinical response and every attempt should be made to use oral regimens when possible. TMP/SMX and TMP/SMX and Amoxicillin-clavulinic acid Ciprofloxacin and Ciprofloxacin and Ciprofloxacin and Cefazolin and Cefotetan Piperacillin and tazobactam Clindamycin and ceftriaxone Ceftriaxone and 500 mg po tid 500/125 mg p tid 500 mg po bid 500 mg po tid 500 mg po bid 750 mg po bid IV 2 g Q8h IV 500 mg Q8h or 500 mg po tid IV 2 g Q12h IV g Q6h IV 600 mg Q8h IV 1 g Q24h IV 1 g Q24h IV 500 mg Q8h or 500 mg po tid *If in doubt about the most appropriate antibiotic for the management of the diabetic foot infection, discussion with an infectious disease consultant may be prudent. Before antimicrobials are used in the person with diabetes, an evaluation of renal function must be undertaken to best guide appropriate dosing. This is particularly important with the aminoglycosides. Dosages shown are for normal renal function. If using aminoglycosides it is imperative that the renal function and drug levels be monitored closely. Approximate daily cost for oral therapy excludes the dispensing fee. These are 1998 costs based upon the Manitoba Drug Benefits and Interchangeability Formulary and the Manufacturer s recommended dosing regimen and listed price. In some instances, a higher dose of ciprofloxacin may be necessary. Other quinolone antimicrobial agents may be considered as alternatives, but a review of product monographs is necessary to establish optimal doses. ds Double strength; IV intravenous; po By mouth; TMP/SMX Trimethoprim/sulfamethoxazole Figure 1) Algorithm for the selection of antimicrobial therapy. *See Table 1 for antimicrobial choices either the dorsalis pedis or posterior tibial blood pressure is made to the brachial artery blood pressure. Ankle brachial indexes below 0.5 indicate significant reduction in large blood vessel flow, corresponding with severe peripheral vascular disease (11). Ratios of less than 0.3 are associated with rest pain and limb-threatening ischemia (12). In some clinical presentations, ischemia is suspected even where an adequate ankle brachial index has been documented. This may be due to noncompressible vessels as a consequence of calcification (13). It may be prudent to proceed to angiography in these situations. Status of bone: The diagnosis of osteomyelitis in the person with diabetes with a foot infection is difficult because it may be difficult to use standard clinical criteria. Individuals with soft tissue infections or skin ulcerations that have been present for several weeks are at high risk of contiguous bone involvement, particularly if these lesions are located over a bony prominence (5). Clinical findings that can be used to determine the pres- TABLE 2 Imaging techniques for identifying osteomyelitis in the feet of people with diabetes Test modality Mean sensitivity (range) (%) Mean specificity (range) (%) Positive predictive value (%) Plain radiography 60 (28-93) 60 (50-92) Technicium bone scan 86 (68-100) 45 (0-79) Indium white blood cell scan 89 (45-100) 78 (29-100) Magnetic resonance imaging 99 (29-100) 83 (71-100) Modified from references (6,16,18-20) 52A Can J Infect Dis Vol 11 Suppl A January/February 2000
5 CITP TABLE 3 Diabetic foot ulcer management suggestions Grade Wagner classification Management suggestion Grade 0 Skin intact, no open lesions. Callous may be present under weight bearing areas. Callouses may act as abnormal pressure points leading to ulceration of the underlying skin. Nonblanching erythema may be present as a consequence of unrelieved pressure Callouses should be pared Footwear should be fitted for proper weight displacement Grade 1 Grade 2 Grade 3 Grade 4 Superficial skin ulceration, often seen under high pressure areas (metatarsal heads, toes) Deeper ulceration, usually associated with infection/cellulitis. The ulceration does not extend to bone Ulcerations extend to deeper tissue layers such as bone. If bone can be probed at the base of an ulceration, it is likely that osteomyelitis is present. Localized gangrene (toes, forefoot, heel) Callouses should be pared to expose the ulcer base. Deep swabs or currettage specimen from ulcer base should be taken for bacterial culture to determine the etiology of underlying infection. Clean with saline for 5 to 10 mins with dressing changes daily. A hydroactive gel (Duoderm [Hydroactive Gel, Convatec, Montreal, Quebec], Intrasite [Intrasite Gel, Smith and Nephew, Lachine, Quebec]or Tegagel [3M, London, Ontario]) covered by a clean gauze is the simplest approach, saline wet to dry dressings are an alternative. Should necrotic tissue be present or the wound be dirty, a gauze moistened with one-quarter strength Eusol can be applied twice daily. If Eusol is used, petroleum jelly must be used to protect the skin surrounding the ulceration. Prolonged use of Eusol must be avoided because it may be toxic to granulation tissue. Once the wound is clean and provided that granulation tissue is present, hydroactive gel should be substituted for the Eusol. Infected ulcers (cellulitis) will require systemic antibiotics. Antibiotic choice can be guided by appropriately collected swabs for culture. Radiographs should be obtained to exclude unsuspected bone infection (if this is detected, the ulcer should be considered a grade 3 lesion). Pressure relief is essential for the healing of these lesions; this can be accomplished by appropriate footwear, crutches, wheelchairs and casting. If casting is considered, it must be applied by an experienced individual and monitored on a regular basis. These ulcers are deeper and often penetrate to subcutaneous tissue with local infection but have no bony involvement. These ulcerations are managed in a fashion similar to grade 1 lesions. Some advocate aggressive surgical debridement of all infected bone; however, in many cases, osteomyelitis may be treated conservatively. Appropriate systemic antimicrobials must be administered for a prolonged period. Antimicrobials may be administered orally in most patients. Only in very rare instances is the home intravenous therapy program is necessary for the management of osteomyelitis in individuals with diabetes. Noninvasive assessment of the adequacy of peripheral circulation (ankle brachial index) should be performed. Radiographs should be obtained of the affected foot to rule out foreign bodies and gas, and to establish the magnitude of bony involvement. A surgical opinion may be necessary if vascular insufficiency is present or if resection of infected bone and gangrenous material is necessary. Management should be as for a grade 3 ulceration. An urgent noninvasive assessment of a peripheral circulation and vascular surgical opinion are indicated; an angiogram may be needed. Angioplasty or by-pass surgery may be required if a suitable stenotic lesion is demonstrated on angiography. Some individuals may have vascular disease that is not amenable to any revascularization procedure. Local surgery to remove gangrenous tissue may be attempted; however, single ischemic toes should be kept dry and may be left to mummify and auto-amputate. Grade 5 Gangrene of entire foot Patients with more extensive gangrene require urgent assessment as outlined for grade 4 lesions. These individuals will require control of diabetes and infection, and will require foot-preserving surgery or amputation, guided by the level and adequacy of circulation. ence of osteomyelitis are that the larger and deeper an ulceration is, the more likely an underlying osteomyelitis will be present (14). In another study, all ulcers in which bone was exposed either visibly or by probing had underlying osteomyelitis (15). Imaging techniques for the diagnosis of osteomyelitis vary with a wide range of sensitivity, specificity and positive predictive value. The plain radiograph, for instance, will only demonstrate bony abnormalities related to osteomyelitis 10 to 20 days after the bone infection has occurred and 40% to 70% of the bone has been resorbed (5). Although the plain radiograph findings are not pathognomonic for infection, a diagnosis of probable osteomyelitis can be made when classic radiological findings are noted (5). If plain radiographs are being used for the diagnosis of osteomyelitis, it is important to obtain a base- Can J Infect Dis Vol 11 Suppl A January/February A
6 Embil et al Figure 2) Community Intravenous Therapy Program (CITP) form for foot infections in people with diabetes. HgB Hemoglobin; HgB A1C Glycosylated hemoglobin; WBC White blood cell count; ptl Platelets, ESR Erythrocyte sedimentation rate line radiograph and then follow it with another plain radiograph in 10 to 21 days to determine whether the typical bony abnormalities are present. Table 2 demonstrates the available imaging techniques for identifying osteomyelitis in the foot of people with diabetes. Initial screening investigations for osteomyelitis include the erythrocyte sedimentation rate and a plain radiograph of the affected area. A three-phase technetium bone scan (Tc-99m MDP) is sensitive for diagnosing osteomyelitis but suffers from poor specificity in diabetic foot infections due to frequent false positives from overlying soft tissue hyperemia (16). The simplest approach is to obtain a baseline x- ray and then repeat it in two to three weeks. In that intervening period, osteomyelitis should be visible radiographically. If clinical suspicion persists, a bone scan combined with a gallium scan or white blood cell study, if equivocal, may be warranted (16). The addition of gallium or white blood cell scanning to the three-phase bone scan yields improved specificity while maintaining sensitivity. Adjunctive therapy: In addition to the antimicrobial therapy outlined in Tables 1A and 1B, ongoing care of the wound or foot ulcer is necessary. Table 3 demonstrates some suggestions for the management of these wounds. It is not clear what role, if any, topical antimicrobials play in the management of foot lesions of people with diabetes. There are insufficient, well controlled data to support the routine use of topical enzymatic debriding agents, such as collagenase, at this time. Duration of therapy: Based upon the preceding considerations, antimicrobial therapy can be initiated as outlined in Table 1. The vast majority of mild infections can be treated with a two-week course of appropriate culture-guided OAT (4). If a culture is not available, empirical therapy will be needed. If an infection is acute and the ulcer has been present for less that two to three weeks, the most likely pathogens are S aureus and Streptococcus species (groups A and B). Therapy with a betalactam, such as cloxacillin or cephalexin, would be appropriate (Table 1). If the lesion has been present for a more prolonged period, the presence of a mixed flora of microorganisms is likely and empirical therapy with trimethoprim/sulphamethoxazole or cephalexin would be appropriate (Table 1). Treatment choices are shown in Table 1. Moderate infections range from those in which the patients are not toxic and can be treated with local incision, drainage and OAT, to those in patients who are critically ill or toxic and who require incision, drainage, debridement and parenteral therapy. In those individuals with severe infections, parenteral therapy is necessary. Once the acute infection has been stabilized and an assessment of whether an underlying bone infection is present, it is prudent to step down the patient s care to oral 54A Can J Infect Dis Vol 11 Suppl A January/February 2000
7 CITP Figure 3) Nursing care plan for lower extremity infections in people with diabetes. therapy if possible. If an underlying osteomyelitis is present, in the vast majority of cases, the infection can be treated with a prolonged course of antimicrobial therapy appropriately guided by culture data as outlined in Tables 1A and 1B. The ideal duration of therapy for the treatment of osteomyelitis in the lower extremities of people with diabetes has not been precisely established. Surgical debridement, where necessary, must be adequate to remove devitalized tissue. It has been traditionally recommended that four to six weeks of parenteral therapy are sufficient. These recommendations have been based upon experimental animal models (19). However, combined regimens of parenteral therapy followed by prolonged oral therapy have had good results as have prolonged courses of OAT (20). Prolonged appropriate OAT may be an alternative to parenteral therapy for osteomyelitis (6-10, unpublished data). The decision that remains is whether to use parenteral antimicrobial therapy administered at home or whether the patient should receive an oral antimicrobial that is well absorbed from the gastrointestinal tract and which achieves high serum levels (10,21). Selecting the most appropriate antimicrobial is important because prolonged duration of therapy will be required (22). It is believed that for most antimicrobials, the concentrations achieved in bone are similar to those achieved in serum (19,21,22). The decision to use OAT for the treatment of osteomyelitis must take into account that regular follow-up of the patient with regards to their lower extremity is critical. It is important to follow the erythrocyte sedimentation rate as a marker of decreasing inflamma- Can J Infect Dis Vol 11 Suppl A January/February A
8 Embil et al tion and serial plain radiographs to ensure that bone healing and remodelling is occurring. These measures can help guide the total duration of therapy and detect relapses. If the patient does not improve or deteriorates after the initiation of OAT, re-evaluation of the treatment is critical to ensure that the appropriate therapy has been selected according to the culture data or perhaps aggressive debridement of the bone is necessary as is ensuring adequacy of circulation. USING THE CITP Before a person with diabetes with a lower extremity infection is enrolled in the CITP, the checklist in Figure 2 is completed to ensure that all the necessary background information is available. Once a patient is enrolled into the CITP, the program staff work in conjunction with the Home Care and Victorian Order of Nurses Visiting Services to ensure that the patient is managing with the prescribed therapy and that the intravenous catheter is working correctly. The routine visits are also an ideal opportunity for ongoing evaluation of the lower extremity infection and wound. Figure 3 demonstrates the nursing care plan. CONCLUSIONS Although persons with diabetes, and acute skin and soft tissue infections can be managed in hospital, they may also be managed through the CITP provided that the patient satisfies all of the criteria for participation. For osteomyelitis, which is a chronic and indolent process, our experience has shown that osteomyelitis of the foot has been successfully treated with OAT in the vast majority of cases (80.2%) which were reviewed in a large retrospective study. In this study, 116 foci of osteomyelitis were considered in 325 persons with diabetes who presented to a multidisciplinary foot clinic for assessment and management. There were 10 foci of osteomyelitis which failed to heal with OAT. The reason for failure was that the microorganisms were resistant to the available oral antimicrobials in six patients, patient noncompliance with OAT occurred with two patients, one patient developed an allergy to the oral antimicrobials and one patient had a profoundly ischemic limb that subsequently went to amputation (unpublished data). It is, therefore, important that all parameters of the patient's lower extremity and patient compliance be considered before enrolling an individual in an ambulatory intravenous therapy program. Prolonged OAT may be an alternative to parenteral therapy for the management of osteomyelitis in the foot of the person with diabetes. ACKNOWLEDGEMENTS: The authors thank Mrs Sandra Brown and Mrs Carolyn Cooper for preparing this document. REFERENCES 1. Grayson ML, Silvers J, Turnidge J. Home intravenous antibiotic therapy: A safe and effective alternative to inpatient therapy. Med J Aust 1995;162: Milkovich G. Cost and benefits. Hosp Pract 1993;3(Suppl 1): Eisenberg JN, Kitz DS. Savings from outpatient antibiotic therapy for osteomyelitis: Economic analysis of a therapeutic strategy. JAMA 1986;225: Lipsky BA, Pecoraro RE, Larson SA, et al. Outpatient management of uncomplicated lower-extremity infections in diabetic patients. Arch Intern Med 1990;150: Lipsky BA. Osteomyelitis of the foot in diabetic patients. Clin Infect Dis 1997;25: Pittet D, Wyssa B, Herter-Clavel C, et al. Outcome of diabetic foot infection treated conservatively. A retrospective cohort study with long-term follow-up. Arch Intern Med 1999;159: Wilson KH, Kauffman CA. Oral antibiotic therapy for osteomyelitis of the foot in diabetic patients. South Med J 1985;78: Venkatesan P, Lawn S, MacFarlane RM, et al. Conservative management of osteomyelitis in the feet of diabetic patients. Diabetic Med 1997;14: Peterson LR, Lissack LM, Canter K, et al. Therapy of lower extremity infections with ciprofloxacin in patients with diabetes mellitus, peripheral vascular disease or both. Am J Med 1989;86: MacGregor RR, Graziani AL. Oral administration of antibiotics: A rational alternative to the parenteral route. Clin Infect Dis 1997;24: Orchard TJ, Strandness DE Jr on behalf of the participants. Assessment of peripheral vascular disease in diabetes. Report and recommendation of an International Work Shop sponsored by the American Heart Association and the American Diabetes Association, September 18 to New Orleans, Louisiana. Circulation 1993;88: Barner MG, Kaiser GC, William VL. Blood flow in the diabetic leg. Circulation 1971;43: Takolander R, Rauwerda JA. The use of non-invasive vascular assessment in diabetic patients with foot lesions. Diabetic Med 1996;13: Newman LG, Waller J, Palestro CJ, et al. Unsuspected osteomyelitis in diabetic foot ulcers: Diagnosing and monitoring by leukocyte scanning with indium In 111 oxyquinonlone. JAMA 1991;226: Grayson ML, Gibbons GW, Balogh K, et al. Probing to bone in infected pedal ulcers. JAMA 1995;273: Keenan AM, Tindel NL, Alavi A. Diagnosing pedal osteomyelitis in diabetic patients using current scintigraphic techniques. Arch Intern Med 1989;149: Schauwecker DS. Osteomyelitis: diagnosis with In-111-labled leukocytes. Radiology 1989;171: Shults DW, Hunter GC, McIntyre KE, et al. Value of radiographs and bone scans in determining the need for therapy in diabetic patients with foot ulcers. Am J Surg 1989;158: Norden CW. Lessons learned from animal models of osteomyelitis. Rev Infect Dis 1988;10: Bamberger DM, Duas GP, Gerding DM. Osteomyelitis in the feet of diabetic patients. Am J Med 1987;83: Fitzgerald RH. Antibiotic distribution in normal and osteomyelitic bone. Orthop Clin North Am 1984;15: Gentry LO, Rodrigues GG. Oral ciprofloxacin compared with parenteral antibiotics in the treatment of osteomyelitis. Antimicrob Agents Chemother 1990;34: Perioperative nursing. In: Nettina SM, ed. The Lippincott Manual of Nursing Practice, 6th edn. Philadelphia: JB Lippincott Company, A Can J Infect Dis Vol 11 Suppl A January/February 2000
9 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections
 Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Foot infections in persons with diabetes are
 DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29
 PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29 be present. Hospitalization is required to treat the infection as well as systemic sequelae. Patients with poor vascular
PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29 be present. Hospitalization is required to treat the infection as well as systemic sequelae. Patients with poor vascular
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Introduction. Epidemiology Pathophysiology Classification Treatment
 Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH)
 Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Foot infections are now among the most
 Article Progress in a pedestrian problem: A review of the revised Infectious Diseases Society of America diabetic foot infection guidelines Benjamin A Lipsky This article was first published in The Diabetic
Article Progress in a pedestrian problem: A review of the revised Infectious Diseases Society of America diabetic foot infection guidelines Benjamin A Lipsky This article was first published in The Diabetic
Definitions and criteria
 Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
Objectives. Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection
 Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Front line management of the Diabetic Foot
 Front line management of the Diabetic Foot n o ti e b a i D + s te k o Sm = g in p Am a t u Sam Fratesi MD Smoking + diabetes = amputation Almost 2 million Canadians have diabetes In amputated diabetics
Front line management of the Diabetic Foot n o ti e b a i D + s te k o Sm = g in p Am a t u Sam Fratesi MD Smoking + diabetes = amputation Almost 2 million Canadians have diabetes In amputated diabetics
2008 American Medical Association and National Committee for Quality Assurance. All Rights Reserved. CPT Copyright 2007 American Medical Association
 Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
Transmetatarsal amputation in an at-risk diabetic population: a retrospective study
 The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
Antimicrobial Guidelines for the Empirical Management of Diabetic Foot Infections
 Antimicrobial Guidelines for the Empirical Management of Diabetic Foot Infections Version 7.2 PAGL Inclusion Approved at January 2017 PGC APPROVED BY: TRUST REFERENCE: B3/2017 AWP REF: UHL Policies and
Antimicrobial Guidelines for the Empirical Management of Diabetic Foot Infections Version 7.2 PAGL Inclusion Approved at January 2017 PGC APPROVED BY: TRUST REFERENCE: B3/2017 AWP REF: UHL Policies and
My Diabetic Patient Has No Pulses; What Should I Do?
 Emily Malgor, MD Assistant Professor of Surgery University of Oklahoma, Oklahoma City My Diabetic Patient Has No Pulses; What Should I Do? There are no disclosures. Background Diabetes affects 387 million
Emily Malgor, MD Assistant Professor of Surgery University of Oklahoma, Oklahoma City My Diabetic Patient Has No Pulses; What Should I Do? There are no disclosures. Background Diabetes affects 387 million
Wounds and Infections: Wound Management From the ID Physician Standpoint. Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department
 Wounds and Infections: Wound Management From the ID Physician Standpoint Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department Objectives Distinguish between colonization, critical
Wounds and Infections: Wound Management From the ID Physician Standpoint Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department Objectives Distinguish between colonization, critical
L APPROCCIO AL TRATTAMENTO DEL PIEDE DIABETICO INFETTO
 L APPROCCIO AL TRATTAMENTO DEL PIEDE DIABETICO INFETTO Dott.ssa Fabrizia Toscanella Resp. Centro Prevenzione e Cura del Piede Diabetico Villa Tiberia Hospital, Roma LA CLINICA NEL DIABETE: INCONTRO TRA
L APPROCCIO AL TRATTAMENTO DEL PIEDE DIABETICO INFETTO Dott.ssa Fabrizia Toscanella Resp. Centro Prevenzione e Cura del Piede Diabetico Villa Tiberia Hospital, Roma LA CLINICA NEL DIABETE: INCONTRO TRA
Aetiology Macroangiopathy occurs mainly distally ie Popliteal artery There is arterial wall calcification Microangiopathy is less common
 DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
Limb Salvage in Diabetic Ischemic Foot. Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017
 Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Determining Wound Diagnosis and Documentation Tips Job Aid
 Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Management Of The Diabetic foot
 Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Insights on Diabetic Foot Management in UK
 Insights on Diabetic Foot Management in UK Presented by Helen CHU KEC POD I / TKOH POD i/c 2015/16 Overseas Corporate Scholarship Program for podiatrists in Diabetic Foot Management London / Leicester,
Insights on Diabetic Foot Management in UK Presented by Helen CHU KEC POD I / TKOH POD i/c 2015/16 Overseas Corporate Scholarship Program for podiatrists in Diabetic Foot Management London / Leicester,
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
Infections Amenable to OPAT. (Nabin Shrestha + Ajay Mathur)
 3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR
 ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
Wound Classification. Overview
 Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Root Cause Analysis for nontraumatic
 Root Cause Analysis for nontraumatic amputations 2016 (Full Data) Date Richard Leigh and Stella Vig, Co-Chairs London SCN Footcare Network October 2015 Outline of London RCA 2016 London Hospitals invited
Root Cause Analysis for nontraumatic amputations 2016 (Full Data) Date Richard Leigh and Stella Vig, Co-Chairs London SCN Footcare Network October 2015 Outline of London RCA 2016 London Hospitals invited
1 of :19
 1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
Charcot Arthropathy of the Foot & Ankle. MTAPA Annual Meeting June 2018 Emily Harnden, MD
 Charcot Arthropathy of the Foot & Ankle MTAPA Annual Meeting June 2018 Emily Harnden, MD Background Disclosures None Learning Objectives Define the disease Recognize presenting signs/symptoms for proper
Charcot Arthropathy of the Foot & Ankle MTAPA Annual Meeting June 2018 Emily Harnden, MD Background Disclosures None Learning Objectives Define the disease Recognize presenting signs/symptoms for proper
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
Practical guidelines on the management and prevention of the diabetic foot 2011
 DIABETES/METABOLISM RESEARCH AND REVIEWS Diabetes Metab Res Rev 2012; 28(Suppl 1): 225 231. Published online in Wiley Online Library (wileyonlinelibrary.com).2253 IWGDF GUIDELINES Practical guidelines
DIABETES/METABOLISM RESEARCH AND REVIEWS Diabetes Metab Res Rev 2012; 28(Suppl 1): 225 231. Published online in Wiley Online Library (wileyonlinelibrary.com).2253 IWGDF GUIDELINES Practical guidelines
Case Presentation. The Failure to Diagnose Sepsis. chills. pain out of proportion to mechanism. low-grade fever. tachycardia that does not make sense
 Case Presentation The Failure to Diagnose Sepsis Sepsis is a regular visitor in the news as cases of flesh-eating bacteria and the dramatic speed with which victims deteriorate hit the headlines. The failure
Case Presentation The Failure to Diagnose Sepsis Sepsis is a regular visitor in the news as cases of flesh-eating bacteria and the dramatic speed with which victims deteriorate hit the headlines. The failure
Root Cause Analysis The Tools. Angie Abbott Head of Podiatry and Orthotics Torbay and Southern Devon
 Root Cause Analysis The Tools Angie Abbott Head of Podiatry and Orthotics Torbay and Southern Devon Why do RCA s? To understand if the amputation was avoidable or unavoidable Learn and improve Identify
Root Cause Analysis The Tools Angie Abbott Head of Podiatry and Orthotics Torbay and Southern Devon Why do RCA s? To understand if the amputation was avoidable or unavoidable Learn and improve Identify
Diabetes Foot Screening and Risk Stratification Tool
 Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
I have no financial interests to disclose in regards to this lecture.
 Evaluation and Treatment of Diabetic Foot Ulcerations John M. Giurini, D.P.M. Associate Professor in Surgery Harvard Medical School Disclosure Statement I have no financial interests to disclose in regards
Evaluation and Treatment of Diabetic Foot Ulcerations John M. Giurini, D.P.M. Associate Professor in Surgery Harvard Medical School Disclosure Statement I have no financial interests to disclose in regards
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Case Report Sacral Emphysematous Osteomyelitis Caused by Escherichia coli after Arthroscopy of the Knee
 Case Reports in Orthopedics Volume 2016, Article ID 1961287, 4 pages http://dx.doi.org/10.1155/2016/1961287 Case Report Sacral Emphysematous Osteomyelitis Caused by Escherichia coli after Arthroscopy of
Case Reports in Orthopedics Volume 2016, Article ID 1961287, 4 pages http://dx.doi.org/10.1155/2016/1961287 Case Report Sacral Emphysematous Osteomyelitis Caused by Escherichia coli after Arthroscopy of
Wound culture. (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center
 Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Pressure Injury Complications: Diagnostic Dilemmas
 Pressure Injury Complications: Diagnostic Dilemmas Aimée D. Garcia, MD, CWS, FACCWS Associate Professor, Department of Medicine, Geriatrics Section Baylor College of Medicine Medical Director, Wound Clinic
Pressure Injury Complications: Diagnostic Dilemmas Aimée D. Garcia, MD, CWS, FACCWS Associate Professor, Department of Medicine, Geriatrics Section Baylor College of Medicine Medical Director, Wound Clinic
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
MICHIGAN MEDICINE GUIDELINES FOR TREATMENT OF URINARY TRACT INFECTIONS IN ADULTS
 When to Order a Urine Culture: Asymptomatic bacteriuria is often treated unnecessarily, and accounts for a substantial burden of unnecessary antimicrobial use. National guidelines recommend against testing
When to Order a Urine Culture: Asymptomatic bacteriuria is often treated unnecessarily, and accounts for a substantial burden of unnecessary antimicrobial use. National guidelines recommend against testing
Abscess. A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body.
 Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
Microbiology and Treatment of Diabetic Foot Infections
 Microbiology and Treatment of Diabetic Foot Infections 18 Adolf W. Karchmer Abstract Foot infections in diabetic patients are a major source of morbidity and an important proximate cause of amputations.
Microbiology and Treatment of Diabetic Foot Infections 18 Adolf W. Karchmer Abstract Foot infections in diabetic patients are a major source of morbidity and an important proximate cause of amputations.
JMSCR Vol 06 Issue 03 Page March 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i3.55 Thesis Paper A Prospective Comparative
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i3.55 Thesis Paper A Prospective Comparative
Case Report Acute Haematogenous Metacarpal Osteomyelitis in Children: A Case Report and Review of Literature
 Case Reports in Infectious Diseases Volume 2011, Article ID 674820, 4 pages doi:10.1155/2011/674820 Case Report Acute Haematogenous Metacarpal Osteomyelitis in Children: A Case Report and Review of Literature
Case Reports in Infectious Diseases Volume 2011, Article ID 674820, 4 pages doi:10.1155/2011/674820 Case Report Acute Haematogenous Metacarpal Osteomyelitis in Children: A Case Report and Review of Literature
ABSTRACT. KEY WORDS antibiotics; prophylaxis; hysterectomy
 Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
CLI Therapy- LINCed Multi disciplinary discussions on CLI
 CLI Therapy- LINCed Multi disciplinary discussions on CLI Critical limb ischemia and managing the infected wound Michiel Schreve North West Clinics Alkmaar, The Netherlands Disclosure Speaker name: Michiel
CLI Therapy- LINCed Multi disciplinary discussions on CLI Critical limb ischemia and managing the infected wound Michiel Schreve North West Clinics Alkmaar, The Netherlands Disclosure Speaker name: Michiel
EMPIRICAL TREATMENT OF SELECT INFECTIONS ADULT GUIDELINES. Refer to VIHA Algorithm for the empiric treatment of Urinary Tract Infection
 URINARY TRACT Refer to VIHA Algorithm for the empiric treatment of Urinary Tract Infection and Asymptomatic Bacteriuria on the VIHA Intranet: https://intranet.viha.ca/departments/pharmacy/clinical_pharmacy/pages/infec
URINARY TRACT Refer to VIHA Algorithm for the empiric treatment of Urinary Tract Infection and Asymptomatic Bacteriuria on the VIHA Intranet: https://intranet.viha.ca/departments/pharmacy/clinical_pharmacy/pages/infec
Diabetic foot problems
 Diabetic foot problems: inpatient management of diabetic foot problems NICE clinical guideline Draft, November 20 This guideline was developed following the NICE short clinical guideline Issue process.
Diabetic foot problems: inpatient management of diabetic foot problems NICE clinical guideline Draft, November 20 This guideline was developed following the NICE short clinical guideline Issue process.
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme
 Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Arterial Studies And The Diabetic Foot Patient
 Arterial Studies And The Patient George L. Berdejo, BA, RVT, FSVU gberdejo@wphospital.org Disclosures I have nothing to disclose! Diabetes mellitus continues to grow in global prevalence and to consume
Arterial Studies And The Patient George L. Berdejo, BA, RVT, FSVU gberdejo@wphospital.org Disclosures I have nothing to disclose! Diabetes mellitus continues to grow in global prevalence and to consume
Osteomieliti STEOMIE
 OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
Osteomyelitis Samir S. Shah, MD, MSCE
 Osteomyelitis Samir S. Shah, MD, MSCE Professor, Department of Pediatrics University of Cincinnati College of Medicine Director, Division of Hospital Medicine Attending Physician in Infectious Diseases
Osteomyelitis Samir S. Shah, MD, MSCE Professor, Department of Pediatrics University of Cincinnati College of Medicine Director, Division of Hospital Medicine Attending Physician in Infectious Diseases
Rapid Recovery Hyperbarics 9439 Archibald Ave. Suite 104 Rancho Cucamonga CA,
 Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Diabetic Foot Complications
 Diabetic Foot Complications Podiatry Specialty Clinic YKHC Bethel, Alaska August 1-3, 2017 Charles C. Edwards, DPM Alaska Native Tribal Health Consortium Peripheral Neuropathy Diabetic Peripheral Neuropathy
Diabetic Foot Complications Podiatry Specialty Clinic YKHC Bethel, Alaska August 1-3, 2017 Charles C. Edwards, DPM Alaska Native Tribal Health Consortium Peripheral Neuropathy Diabetic Peripheral Neuropathy
Model of Care for the Diabetic Foot
 Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES
 ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
INVESTIGATING: WOUND INFECTION
 INVESTIGATING: WOUND INFECTION Diagnosing infection in surgical and other wounds involves nurses being able to observe the clinical signs in a wound rather than simply obtaining positive microbiology results
INVESTIGATING: WOUND INFECTION Diagnosing infection in surgical and other wounds involves nurses being able to observe the clinical signs in a wound rather than simply obtaining positive microbiology results
The Results Of Maggot Debridement Therapy In The Ischemic Leg: A Study On 89 Patients With 89 Wounds On The Lower Leg Treated With Maggots
 ISPUB.COM The Internet Journal of Surgery Volume 9 Number 1 The Results Of Maggot Debridement Therapy In The Ischemic Leg: A Study On 89 Patients With 89 Wounds On The Lower Leg Treated With Maggots P
ISPUB.COM The Internet Journal of Surgery Volume 9 Number 1 The Results Of Maggot Debridement Therapy In The Ischemic Leg: A Study On 89 Patients With 89 Wounds On The Lower Leg Treated With Maggots P
-> Education -> Excellence
 Quality Conference 5/2557 Extravasations: Event -> Education -> Excellence รศ.นพ. รว ศ เร องตระก ล สาขาว ชาก มารศ ลยศาสตร ภาควชาศลยศาสตร Extravasations: Event 1. Thrombophlebitis - superficial vein 2.
Quality Conference 5/2557 Extravasations: Event -> Education -> Excellence รศ.นพ. รว ศ เร องตระก ล สาขาว ชาก มารศ ลยศาสตร ภาควชาศลยศาสตร Extravasations: Event 1. Thrombophlebitis - superficial vein 2.
Wound Assessment Report
 Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Osteomyelitis Revisited
 Osteomyelitis Revisited Alan Jay Block, DPM, MS, FASPS, FACFAS Co-Chairman My Leg My Choice Assistant Professor Dept Of Orthopeadics The Ohio State University Medical Board Kent State University Editor-in
Osteomyelitis Revisited Alan Jay Block, DPM, MS, FASPS, FACFAS Co-Chairman My Leg My Choice Assistant Professor Dept Of Orthopeadics The Ohio State University Medical Board Kent State University Editor-in
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems
 Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
Bacterial Burden (Bioburden) The metabolic load imposed by bacteria in tissue.
 Glossary Ankle Brachial Index (ABI) Is a numerical figure which indicates a quantifiable pressure index. The pressure index is determined by means of Doppler Ultra Sound. The ABI is obtained by dividing
Glossary Ankle Brachial Index (ABI) Is a numerical figure which indicates a quantifiable pressure index. The pressure index is determined by means of Doppler Ultra Sound. The ABI is obtained by dividing
ESSENTIALS OF WOUND CARE PRINCIPLES AND TECHNIQUES. Abilio A. Coello MD FACS Miami Vascular Specialists Miami Cardiac & Vascular Institute
 ESSENTIALS OF WOUND CARE PRINCIPLES AND TECHNIQUES Abilio A. Coello MD FACS Miami Vascular Specialists Miami Cardiac & Vascular Institute Abilio Coello, MD No Relevant Financial Relationship Reported MANTRAS
ESSENTIALS OF WOUND CARE PRINCIPLES AND TECHNIQUES Abilio A. Coello MD FACS Miami Vascular Specialists Miami Cardiac & Vascular Institute Abilio Coello, MD No Relevant Financial Relationship Reported MANTRAS
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
December 3, 2015 Severe Sepsis and Septic Shock Antibiotic Guide
 Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma)
 A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma) The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of two specialist
A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma) The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of two specialist
General surgery department of SGMU Lecturer ass. Khilgiyaev R.H. Anaerobic infection. Gas gangrene
 Anaerobic infection Gas gangrene Anaerobic bacteria Anaerobic bacteria are the most numerous inhabitants of the normal gastrointestinal tract, including the mouth Bacteroides fragilis and Clostridium The
Anaerobic infection Gas gangrene Anaerobic bacteria Anaerobic bacteria are the most numerous inhabitants of the normal gastrointestinal tract, including the mouth Bacteroides fragilis and Clostridium The
Disclosures. Critical Limb Ischemia. Vascular Testing in the CLI Patient. Vascular Testing in Critical Limb Ischemia UCSF Vascular Symposium
 Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
Nuclear medicine and Prosthetic Joint Infections
 Nuclear medicine and Prosthetic Joint Infections Christophe Van de Wiele, M.D., Ph.D. Department of Nuclear Medicine, University Hospital Ghent, Belgium Orthopedic prostheses: world market 1996 Prosthetic
Nuclear medicine and Prosthetic Joint Infections Christophe Van de Wiele, M.D., Ph.D. Department of Nuclear Medicine, University Hospital Ghent, Belgium Orthopedic prostheses: world market 1996 Prosthetic
Use of Vacuum-assisted Wound Closure to Manage Limb Wounds in Patients Suffering from Acute Necrotizing Fasciitis
 Original Article Use of Vacuum-assisted Wound Closure to Manage Limb Wounds in Patients Suffering from Acute Necrotizing Fasciitis Wen-Shyan Huang, Shang-Chin Hsieh, Chun-Sheng Hsieh, Jen-Yu Schoung and
Original Article Use of Vacuum-assisted Wound Closure to Manage Limb Wounds in Patients Suffering from Acute Necrotizing Fasciitis Wen-Shyan Huang, Shang-Chin Hsieh, Chun-Sheng Hsieh, Jen-Yu Schoung and
CASE 1: TYPE-II DIABETIC FOOT ULCER
 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
Cellulitis: a practical guide
 Cellulitis: a practical guide Dr John Day Consultant in Infectious Diseases & General Medicine Southend University Hospital NHS Foundation Trust 77 yr old retired civil servant A&E presentation c/o rigors
Cellulitis: a practical guide Dr John Day Consultant in Infectious Diseases & General Medicine Southend University Hospital NHS Foundation Trust 77 yr old retired civil servant A&E presentation c/o rigors
Current Vascular and Endovascular Management in Diabetic Vasculopathy
 Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Surgical Off-loading. Reiber et al Goals of Diabetic Foot Surgery 4/28/2012. The most common causal pathway to a diabetic foot ulceration
 Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
ORIGINAL INVESTIGATION. A Retrospective Cohort Study With Long-term Follow-up
 ORIGINAL INVESTIGATION Outcome of Diabetic Foot Infections Treated Conservatively A Retrospective Cohort Study With Long-term Follow-up Didier Pittet, MD, MS; Blaise Wyssa, MD; Catherine Herter-Clavel,
ORIGINAL INVESTIGATION Outcome of Diabetic Foot Infections Treated Conservatively A Retrospective Cohort Study With Long-term Follow-up Didier Pittet, MD, MS; Blaise Wyssa, MD; Catherine Herter-Clavel,
Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA
 Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA Charcot 1. What is it? (definition) & Who gets it? (epidemiology
Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA Charcot 1. What is it? (definition) & Who gets it? (epidemiology
AGONY FEET. The. of the. Prevention and management of diabetic foot ulcers
 The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
Wound Care Evaluation by Kris Dalseg MS PT CWS CLT
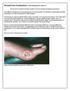 Wound Care Evaluation by Kris Dalseg MS PT CWS CLT This document is intended to describe a standard wound care evaluation for healthcare practitioners. In healthcare, all aspects of our treatment have
Wound Care Evaluation by Kris Dalseg MS PT CWS CLT This document is intended to describe a standard wound care evaluation for healthcare practitioners. In healthcare, all aspects of our treatment have
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Open Fractures. Ria Dindial. Photo courtesy pic2fly.com
 Open Fractures Ria Dindial Photo courtesy pic2fly.com CLINICAL PEARL TYPE WOUND DESCRIPTION OTHER CRITERIA I < 1cm (puncture wounds) - II 1-10 cm - IIIA >10 cm, coverage available Segmental fractures,
Open Fractures Ria Dindial Photo courtesy pic2fly.com CLINICAL PEARL TYPE WOUND DESCRIPTION OTHER CRITERIA I < 1cm (puncture wounds) - II 1-10 cm - IIIA >10 cm, coverage available Segmental fractures,
a Total Hip Prosthesis by Clostridum perfringens. A Case Report
 Haematogenous Infection of a Total Hip Prosthesis by Clostridum perfringens. A Case Report CHAPTER 5 CHAPTER 5 5.1. Introduction In orthopaedic surgery, an infection of a prosthesis is a very serious,
Haematogenous Infection of a Total Hip Prosthesis by Clostridum perfringens. A Case Report CHAPTER 5 CHAPTER 5 5.1. Introduction In orthopaedic surgery, an infection of a prosthesis is a very serious,
Case Report Perforation of an Occult Carcinoma of the Prostate as a Rare Differential Diagnosis of Subcutaneous Emphysema of the Leg
 Case Reports in Orthopedics Volume 2016, Article ID 5430637, 5 pages http://dx.doi.org/10.1155/2016/5430637 Case Report Perforation of an Occult Carcinoma of the Prostate as a Rare Differential Diagnosis
Case Reports in Orthopedics Volume 2016, Article ID 5430637, 5 pages http://dx.doi.org/10.1155/2016/5430637 Case Report Perforation of an Occult Carcinoma of the Prostate as a Rare Differential Diagnosis
Osteomyelitis Revisited
 Osteomyelitis Revisited Alan Jay Block, DPM, MS, FASPS, FACFAS Assistant Professor Dept Of Orthopeadics The Ohio State University Medical Board Kent State University Editor-in -Chief The Journal of the
Osteomyelitis Revisited Alan Jay Block, DPM, MS, FASPS, FACFAS Assistant Professor Dept Of Orthopeadics The Ohio State University Medical Board Kent State University Editor-in -Chief The Journal of the
North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance)
 North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance) Introduction OPAT services provide intravenous (IV) antibiotics to patients
North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance) Introduction OPAT services provide intravenous (IV) antibiotics to patients
Case Study 2 - Mr J. Medical history
 Case Study 2 - Mr J A 54 year-old male was referred to the podiatrist at Coast Provincial General Hospital Diabetic Clinic, for management of active foot disease. The patient s presenting complaint was
Case Study 2 - Mr J A 54 year-old male was referred to the podiatrist at Coast Provincial General Hospital Diabetic Clinic, for management of active foot disease. The patient s presenting complaint was
