intermediate hyperglycaemia
|
|
|
- Jewel Washington
- 5 years ago
- Views:
Transcription
1 Initiating interventions in people with intermediate hyperglycaemia ( pre-diabetes ) Intermediate hyperglycaemia is a state of raised glycaemic levels in a person without diabetes. It is an independent risk-factor for type 2 diabetes and cardiovascular disease. The primary aim of management of intermediate hyperglycaemia is to prevent progression to diabetes. Intervention involves structured lifestyle changes, and for people with a high risk of progression to diabetes who do not achieve normoglycaemia, treatment with metformin. 36
2 What constitutes intermediate hyperglycaemia? Diabetes is diagnosed with an HbA 1c level of 50 mmol/ mol or greater (and, if measured, a fasting blood glucose 7.0mmol/L). 1, 2 This is the glycaemic level at which the incidence of moderate diabetic retinopathy begins to rise exponentially. 2 In an asymptomatic person, a result greater than 50 mmol/mol should be repeated to confirm the diagnosis. Intermediate hyperglycaemia is a biochemical state in which a person has glucose levels above the normal range, but does not yet meet the criteria for a diagnosis of diabetes. In New What s in a name? Intermediate hyperglycaemia versus pre-diabetes The term pre-diabetes is controversial: in 1980 the World Health Organisation (WHO) recommended against its use as not all people with borderline glycaemic levels progress to diabetes. In 2006 the WHO again discouraged the use of the term pre-diabetes and instead suggested intermediate hyperglycaemia to signify impaired fasting glucose (IFG) and impaired glucose tolerance (IGT). 3 The 2012 NICE guidelines (United Kingdom) refer to increased risk of type 2 diabetes rather than pre-diabetes. 4 Zealand intermediate hyperglycaemia is defined as an HbA 1c level of mmol/mol (and, if measured, a fasting blood glucose of mmol/l). 1, 2 Unlike diabetes, repeat testing is not required to confirm intermediate hyperglycaemia. A single HbA 1c result between mmol/mol in a person who is not acutely ill or who does not have a condition * that may affect HbA 1c levels is sufficient. HbA 1c should then be monitored every six to 12 months, unless there are intervening symptoms. 2 HbA 1c is most frequently requested in the context of a cardiovascular disease (CVD) risk assessment. If a person is identified as having intermediate hyperglycaemia, and they are in the targeted age range, they should have a full CVD risk assessment, including investigation of lipid levels, if this was not done at the same time as the HbA 1c test. In New Zealand, normoglycaemia is defined as an HbA 1c level below 40 mmol/mol (and, if measured, a fasting blood glucose 6.0mmol/L). 1, 2 For further information on the use of HbA 1c to diagnose diabetes, see: The new role of HbA 1c in diagnosing type 2 diabetes, BPJ 42 (Feb, 2012) and Understanding the new HbA 1c units for the diagnosis of Type 2 diabetes, Braatvedt G et al, NZMJ 2012;125(1362). * For example high red blood cell turnover, iron or B12 supplementation or recent blood transfusion can falsely lower HbA 1c levels and severe anaemia, B12 or folate deficiency, chronic alcoholism, chronic renal failure or certain haemoglobinopathies can falsely raise HbA 1c levels. Intermediate hyperglycaemia is an independent risk-factor for diabetes Approximately 5 10% of people with intermediate hyperglycaemia progress to diabetes every year, but 5 10% will revert back to normogylcaemia. 5, 6 However, in the longterm, up to 70% of people with intermediate hyperglycaemia will eventually develop type 2 diabetes. 7 This represents a relative risk for type 2 diabetes six times greater for people with intermediate hyperglycaemia than those with normogylcaemia. 5 Intermediate hyperglycaemia should be viewed as a continuous scale rather than a discrete variable, i.e. those at the higher end of the mmol/mol range have a much greater risk of developing diabetes than those at the lower end. The risk of having a high glycaemic level remains, even for people who have undergone proven prevention such as bariatric surgery. 8 In addition, other factors play an important part in assessing an individual s risk of progressing to diabetes, including: Age Weight and BMI Physical activity Diet Ethnicity Māori, Pacific and South-Asian people have an increased risk of diabetes BPJ Issue 48 37
3 Smoking status three-fold increase in risk of progression to diabetes Family history of diabetes Increased blood pressure Increased lipid levels Certain conditions, such as polycystic ovary syndrome (see sidebar) There are a number of tools for assessing who is at risk of developing diabetes, and helping to determine the pre-test probability of a diagnosis in people who have not had a recent HbA 1c test. The most practical tools incorporate information readily available to primary care and have a high specificity for future diabetes progression. 9 These prediction tools have not been validated in high risk ethnicities in New Zealand, therefore a single tool cannot be recommended above any other for this population. However, viewing the patient s risk in light of the above risk factors is likely to be beneficial in assessing the likelihood of progression to diabetes. Many vascular complications begin before HbA 1c reaches diabetic levels While diabetes is defined by the threshold where the prevalence of moderate diabetic retinopathy begins to increase exponentially, many of the underlying pathophysiological processes associated with diabetes begin during the intermediate hyperglycaemic stage. This includes nephropathy, chronic kidney disease, neuropathy, retinopathy, cardiovascular disease and overall mortality. 10 Similarly, increased vascular risk remains even in people with diabetes who have achieved target glycaemic levels below the diagnostic threshold for diabetes. 11 Early management is particularly important among highrisk groups as complications develop earlier, often before a diagnosis of diabetes is made, although this could be a result of either lower testing rates (meaning longer unmanaged time with hyperglycaemia) or a greater actual risk. For example, in a New Zealand study of 4269 Māori, of the participants identified as having clinical diabetes, 29.6% already had established microalbuminuria, and 7.7% albuminuria, at diagnosis. 12 Management of intermediate hyperglycaemia reduces progression to diabetes The identification and management of people with intermediate hyperglycaemia should be viewed as an opportunity to halt progression to diabetes and to reduce the risk of diabetes related complications. Intervention with lifestyle changes, and initiation of metformin where appropriate, can reduce the number of people progressing to clinical diabetes by 30 60%. 6, 13 Treatment is considered to be both safe and cost-effective The Diabetes Prevention Program, a large United States study of early prevention, found that 5% of people in the lifestyle intervention group and 7.8% of people in the metformin group (no lifestyle changes) developed clinical diabetes each year, compared to 11% of those in the placebo group (Figure 1). 6 Lifestyle intervention was more advantageous than metformin in people aged over 60 years and those with a lower body-mass index. 6 People who achieved even one normoglycaemic result during the study period had a significantly lower long-term risk of progressing to diabetes. 16 In the Diabetes Prevention Program, women with a history of gestational diabetes and current intermediate hyperglycaemia showed significant benefit from both lifestyle intervention and metformin. Each intervention reduced the relative risk of progression to diabetes by approximately 50% compared with the placebo group. In contrast, this reduction was 49% for lifestyle and 14% for metformin in women without a history of gestational diabetes. 17 Overall, it is estimated that the number of people with intermediate hyperglycaemia who need to be treated for three years in order to prevent one case of diabetes is 6.9 for lifestyle intervention and 13.9 for metformin. 6 Treatment goal: agree on a target HbA 1c level There is no defined treatment target in people with intermediate hyperglycaemia, therefore a target should be individually agreed upon between the patient and the doctor. Ideally the goal of treatment should be regression to normoglycaemia, in which case an HbA 1c target of < 40 mmol/ mol should be aimed for, as this is associated with significant reductions in long-term diabetes risk. 15 However, for many people delaying and slowing the progression to diabetes is a more realistic target and is still likely to be beneficial. Repeat testing of HbA 1c is recommended every 6 12 months, unless there are intervening symptoms. 20 N.B It is critical that HbA 1c level targets are not the only goal set, weight loss and exercise goals should be part of the treatment process. 38 BPJ Issue 48
4 Cumulative Incidence of Diabetes (%) Time (Years) Placebo Metformin Lifestyle Figure 1: The cumulative incidence of diabetes based on intervention 6 Lifestyle intervention for everyone Most people with raised glycaemic levels will benefit from advice on an intensive programme of lifestyle changes. 4 The two most important modifiable risk factors for diabetes development are obesity and physical inactivity. 7 Target goals should be set for weight, weekly physical activity level and diet, e.g. fat intake, fibre intake and total kilojoules. Key advice includes encouraging people to: 4 Undertake a minimum of 150 minutes of moderate intensity physical activity per week Gradually lose weight to reach and maintain a BMI within the healthy range Increase consumption of whole grains, vegetables and other foods that are high in dietary fibre Reduce the total amount of fat in their diet Eat less saturated fat Some practices may consider addressing lifestyle interventions with patients in a group setting. Key components of a successful programme include: 4 Participants meet at least eight times over 9 18 months Participants have at least 16 hours of educational time, either in the group or on a one-to-one basis Follow-up sessions should be offered regularly, e.g. every three months, for at least two years after the programme Behavioural change techniques should be used in conjunction with diet and exercise advice, e.g. setting short and long-term goals, identifying triggers Referral to a dietitian for further advice and guidance is likely to be beneficial, although waiting times for publically funded services and the cost of private services may be an issue for some people. In the Finnish Diabetes Prevention study, achievement of lifestyle intervention goals resulted in a reduction of 58% in the risk of progression to diabetes. 18 Achieving each individual goal (e.g. exercise, reducing fat in the diet) was independently associated with reduced risk of progression to diabetes. For example, a 5% reduction in weight significantly reduced the overall risk of developing diabetes (odds ratio of 0.3 compared to no weight loss). 18 In the Diabetes Prevention Program study population, it was found that even a small weight loss, e.g. 1 kg, resulted in a significant reduction in the risk of progression to diabetes. 6 For further information on lifestyle interventions see: Addressing weight issues in young people and families in New Zealand. BPJ 45 (Aug, 2012) and Promoting healthy lifestyles for Pacific peoples BPJ 32 (Nov, 2010). Add metformin if lifestyle intervention is insufficient After approximately six months of lifestyle intervention, people who do not show glycaemic improvement, gain weight or are unable to adhere to recommendations may be offered metformin as an adjunct to lifestyle intervention. BPJ Issue 48 39
5 The role of metformin in women with polycystic ovary syndrome Polycystic ovary syndrome (PCOS) is a group of disorders that result in inappropriate gonadotropin secretion, usually from the ovaries but technically from anywhere along the hypothalamic-pituitary-ovarian (HPO) axis. It is common, affecting between 5 10% of women of reproductive age. 19 The syndrome is characterised by a varying combination of menstrual dysfunction (typically oligo-ovulation or anovulation manifested by oligoamenorrhea), hyperandrogenism and polycystic ovaries on ultrasound. Insulin resistance is common in women with PCOS, along with an increased risk of developing type 2 diabetes and cardiovascular disease. Annual HbA 1c testing is recommended, but there is very little evidence for measurement of plasma insulin in women with PCOS. The role of metformin in women with PCOS is controversial. Metformin is potentially useful for maintaining satisfactory glycaemic levels and in increasing fertility, although evidence of effect has been difficult to find until recently. The PCOSMIC trial, a New Zealand trial investigating the use of metformin and clomiphene in women with PCOS, found that metformin increased the pregnancy rate, and that clomiphene plus metformin was more effective than either metformin or clomiphene alone. 21 A long-term United States study found that metformin improved the metabolic profile of women with PCOS over a 36-month treatment course, particularly improving circulating HDLcholesterol, diastolic blood pressure and BMI. 19 At present, there is no recommendation to treat all women with PCOS with metformin, nor is it an approved indication for metformin. However, women with PCOS and an HbA 1c level > 40 mmol/mol are likely to benefit from use of metformin, in addition to lifestyle interventions. In addition, most women with polycystic ovary syndrome and raised glycaemic levels are likely to benefit from a trial with metformin (see The role of metformin in women with polycystic ovary syndrome ). 19 Women with a history of gestational diabetes and current intermediate hyperglycaemia are also likely to particularly benefit from metformin. 17 Because the benefits of metformin are not maintained after cessation, it is important that diet and lifestyle management is continued during metformin treatment in order to address and improve the underlying obesogenic behaviours that contribute to intermediate hyperglycaemia and diabetes. Long-term primary prevention can then be maintained even after medicine cessation. How to prescribe metformin for intermediate hyperglycaemia Intermediate hyperglycaemia is not an approved use for metformin, but it can be prescribed fully subsidised for this indication and there is strong clinical evidence to justify its use. Metformin can be commenced at a low dose, e.g. 500 mg once daily, and increased gradually, e.g. over several weeks, as tolerated to a maximum of 2 g daily if required. 4 Lactic acidosis has been reported in people taking metformin who have reduced renal function. Although the risk may be overstated, at present it is recommended that the dose of metformin should be reduced if renal function deteriorates, and people who decline to an egfr < 30 ml/min/1.73m 2 or are at risk of rapid decline in renal function should cease treatment. 1 A Cochrane review of 96,295 patients found no incidences of lactic acidosis in people taking metformin, even in those who had a contraindication to metformin, such as renal insufficiency. 22 Consider a maximum daily dose of 1 g metformin in patients with egfr ml/min/1.73m 2. However, in patients who are obese, egfr may be an underestimate of their true creatinine clearance, and this group is likely to benefit most from metformin. Therefore metformin doses may not have to be reduced in obese patients with egfr in the ml/ min/1.73m2 range. If required, consider using the Cockcroft- Gault equation to calculate a more accurate value for creatinine clearance in these patients. As metformin is primarily cleared by the kidneys, all patients taking metformin should have their renal function monitored annually and more frequently if clinically indicated. 40 BPJ Issue 48
6 For further information on egfr and kidney disease, see Making a difference in chronic kidney disease. BPJ 22 (Jul, 2012) and Acute-on-chronic kidney disease: prevention, diagnosis, management and referral in primary care, BPJ 46 (Sept, 2012). Compliance and adverse effects of metformin need to be monitored Metformin is generally well tolerated. The most common reported adverse effect is gastrointestinal disturbance. Other adverse effects include anorexia, nausea, taste disturbance and decreased vitamin-b12 absorption. Regularly follow-up to ensure that metformin is being taken as prescribed and that adverse effects are not affecting adherence. Metformin may need to be continued long-term Metformin should be given initially for six to 12 months. 4 For many people metformin will need to be continued long-term. If no effect is seen with metformin, consider stopping the medicine, but continue with lifestyle interventions. 4 If, despite metformin treatment, the patient progresses to diabetes, other medicines, e.g. sulphonylureas or insulin, may need to be added if glycaemic control cannot be achieved with metformin alone. ACKNOWLEDGEMENT: Thank you to Dr Brandon Orr-Walker, Endocrinologist, Middlemore Hospital, Auckland and Dr Kirsten Coppell, Senior Research Fellow, Edgar National Centre for Diabetes Research, Dunedin School of Medicine, University of Otago for expert guidance in developing this article. References 1. New Zealand Gudelines Group. New Zealand primary care handbook rd ed. Wellington: New Zealand Guidelines Group; New Zealand Society for the Study of Diabetes (NZSSD). NZSSD position statement on the diagnosis of, and screening for, Type 2 diabetes. NZSSD; Available from: (Accessed Nov, 2012). 3. World Health Organisation (WHO). Definition and diagnosis of diabetes mellitus and intermediate hyperglycaemia: report of a WHO/ IDF consultation. WHO, Geneva; Available from: (Accessed Nov, 2012). 4. Chatterton H, Younger T, Fischer A, et al. Risk identification and interventions to prevent type 2 diabetes in adults at high risk: summary of NICE guidance. BMJ 2012;345:e Twigg S, Kamp M, Davis T, et al. Prediabetes: a position statement from the Australian Diabetes Society and Australian Diabetes Educators Association. Med J Aust 2007;186(9): Diabetes Prevention Program Research Group. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 2002;346: Tabák AG, Herder C, Rathmann W, et al. Prediabetes: a high-risk state for diabetes development. The Lancet 2012;379(9833): Carlsson L, Peltonen M, Ahlin S, et al. Bariatric surgery and prevention of type 2 diabetes in Swedish obese subjects. N Eng J Med 2012;367: Abbasi A, Peelen L, Corpeleijn E, et al. Prediction models for risk of developing type 2 diabetes: systematic literature search and independent external validation study. BMJ 2012;345:e Bertram MY, Vos T. Quantifying the duration of pre-diabetes. Aust NZ J Publ Heal 2010;34(3): Sarwar N, Gao P, Seshasai S, et al. Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies. Lancet 2010;375(9733): Simmons D, Rush E, Crook N. Prevalence of undiagnosed diabetes, impaired glucose tolerance, and impaired fasting glucose among Maori in Te Wai o Rona: Diabetes Prevention Strategy. N Z Med J 2009;122(1288): Gillies C, Abrams K, Lambert P, et al. Pharmacological and lifestyle interventions to prevent or delay type 2 diabetes in people with impaired glucose tolerance: systematic review and meta analysis. BMJ 2007;334: Fradkin J, Robberts B, Rodgers G. What s preventing us from preventing type 2 diabetes? N Engl J Med 2012;367: Bertram M, Lim S, Barendregt J, Vos T. Assessing the cost-effectiveness of drug and lifestyle intervention following opportunistic screening for pre-diabetes in primary care. Diabetologia 2010;53(5): Perreault L, Pan Q, Mather KJ, et al. Effect of regression from prediabetes to normal glucose regulation on long-term reduction in diabetes risk: results from the Diabetes Prevention Program Outcomes Study. The Lancet 2012;379(9833): Ratner R, Christophi C, Metzger B, et al. Prevention of diabetes in women with a history of gestational diabetes: effects of metformin and lifestyle interventions. J Clin Endocrinol Metab 2008;93(12): Tuomilehto J, Lindström J, Eriksson JG, et al. Prevention of Type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N Eng J Med 2001;344(18): Lucidi R. Polycystic Ovarian Syndrome. Medscape Reference; Available from: (Accessed Nov, 2012). 20. Braatvedt G, Cundy T, Crooke M, et al. Understanding the new HbA1c units for the diagnosis of Type 2 diabetes. N Z Med J 2012;125(1362):In press. 21. Johnson N, Stewart A, Falkiner J, et al. PCOSMIC: a multi-centre randomized trial in women with Polycystic Ovary Syndrome evaluating metformin for infertility with clomiphene. Hum Reprod 2010;25(7): Salpeter S, Greyber E, Pasternak G, Salpeter E. Risk of fatal and nonfatal lactic acidosis with metformin use in type 2 diabetes mellitus. Cochrane Database Syst Rev ;(4):CD BPJ Issue 48 41
Diabetes Mellitus. Eiman Ali Basheir. Mob: /1/2019
 Diabetes Mellitus Eiman Ali Basheir Mob: 091520385 27/1/2019 Learning Outcomes Discuss the WHO criteria for Diabetes Mellitus diagnosis Describe the steps taken to confirm diagnosis Interpret GTT. Discuss
Diabetes Mellitus Eiman Ali Basheir Mob: 091520385 27/1/2019 Learning Outcomes Discuss the WHO criteria for Diabetes Mellitus diagnosis Describe the steps taken to confirm diagnosis Interpret GTT. Discuss
Pre-diabetes. Dr Neel Basudev. GPSI Lambeth DICT, Diabetes Lead Lambeth CCG
 Pre-diabetes Dr Neel Basudev GPSI Lambeth DICT, Diabetes Lead Lambeth CCG The Prevention of Diabetes Where has this come from? Pre-diabetes mellitus (PDM) Term introduced by Tommy G. Thompson (Health &
Pre-diabetes Dr Neel Basudev GPSI Lambeth DICT, Diabetes Lead Lambeth CCG The Prevention of Diabetes Where has this come from? Pre-diabetes mellitus (PDM) Term introduced by Tommy G. Thompson (Health &
Polycystic Ovary Syndrome
 What is the polycystic ovary syndrome? Polycystic Ovary Syndrome The polycystic ovary syndrome (PCOS) is a clinical diagnosis characterized by the presence of two or more of the following features: irregular
What is the polycystic ovary syndrome? Polycystic Ovary Syndrome The polycystic ovary syndrome (PCOS) is a clinical diagnosis characterized by the presence of two or more of the following features: irregular
Metformin should be considered in all patients with type 2 diabetes unless contra-indicated
 November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
What s new in cardiovascular disease risk assessment and management for primary care clinicians
 Cardiovascular system What s new in cardiovascular disease risk assessment and management for primary care clinicians The recently released 2018 Cardiovascular Disease Risk Assessment and Management for
Cardiovascular system What s new in cardiovascular disease risk assessment and management for primary care clinicians The recently released 2018 Cardiovascular Disease Risk Assessment and Management for
Impaired Glucose Tolerance
 Page 1 of 6 Impaired Glucose Tolerance If you have impaired glucose tolerance, your blood glucose is raised beyond the normal range but it is not so high that you have diabetes. However, if you have impaired
Page 1 of 6 Impaired Glucose Tolerance If you have impaired glucose tolerance, your blood glucose is raised beyond the normal range but it is not so high that you have diabetes. However, if you have impaired
SHORT COMMUNICATION. G. Joshy & P. Dunn & M. Fisher & R. Lawrenson
 Diabetologia (2009) 52:1474 1478 DOI 10.1007/s00125-009-1380-1 SHORT COMMUNICATION Ethnic differences in the natural progression of nephropathy among diabetes patients in New Zealand: hospital admission
Diabetologia (2009) 52:1474 1478 DOI 10.1007/s00125-009-1380-1 SHORT COMMUNICATION Ethnic differences in the natural progression of nephropathy among diabetes patients in New Zealand: hospital admission
Diabetes Mellitus Aeromedical Considerations. Aviation Medicine Seminar Bucharest, Romania. 11 th to 15 th November 2013
 Diabetes Mellitus Aeromedical Considerations Aviation Medicine Seminar Bucharest, Romania. 11 th to 15 th November 2013 Metabolic, Nutritional or Endocrine disorders Applicants with metabolic, nutritional
Diabetes Mellitus Aeromedical Considerations Aviation Medicine Seminar Bucharest, Romania. 11 th to 15 th November 2013 Metabolic, Nutritional or Endocrine disorders Applicants with metabolic, nutritional
Why is Earlier and More Aggressive Treatment of T2 Diabetes Better?
 Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
Chapter 7: Diabetes. Diabetes mellitus is a major and increasing health problem in New Zealand.
 Key points Chapter 7: mellitus is a major and increasing health problem in New Zealand. Around 1 in 27 adults (3.7%) in the 1996/97 Health Survey reported that they had been diagnosed with diabetes. Mäori
Key points Chapter 7: mellitus is a major and increasing health problem in New Zealand. Around 1 in 27 adults (3.7%) in the 1996/97 Health Survey reported that they had been diagnosed with diabetes. Mäori
PREDIABETES TESTING SERVICES
 PREDIABETES TESTING SERVICES ASSESSING DIABETES RISK IN ASYMPTOMATIC ADULTS Depending upon population characteristics, up to 70% of individuals with prediabetes will ultimately progress to diabetes at
PREDIABETES TESTING SERVICES ASSESSING DIABETES RISK IN ASYMPTOMATIC ADULTS Depending upon population characteristics, up to 70% of individuals with prediabetes will ultimately progress to diabetes at
3. Metformin therapy for PCOS
 1. Introduction The key clinical features of polycystic ovary syndrome (PCOS) are hyperandrogenism (hirsutism, acne, alopecia) and menstrual irregularity with associated anovulatory infertility. 1 The
1. Introduction The key clinical features of polycystic ovary syndrome (PCOS) are hyperandrogenism (hirsutism, acne, alopecia) and menstrual irregularity with associated anovulatory infertility. 1 The
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus
 Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead
 Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead Today s Presentation HbA1c & diagnosing Diabetes What is Impaired Glucose & IGR? Implications
Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead Today s Presentation HbA1c & diagnosing Diabetes What is Impaired Glucose & IGR? Implications
Diagnostic criteria for diabetes Routine cases and Non-diabetic hyperglycaemia adapted with permission from Royal Devon and Exeter
 Diagnostic criteria for diabetes Routine cases and Non-diabetic hyperglycaemia adapted with permission from Royal Devon and Exeter Diabetes may be diagnosed on any of the following criteria (WHO 2006,
Diagnostic criteria for diabetes Routine cases and Non-diabetic hyperglycaemia adapted with permission from Royal Devon and Exeter Diabetes may be diagnosed on any of the following criteria (WHO 2006,
Pre-diabetes: Information for primary care practitioners
 Pre-diabetes: Information for primary care practitioners Michelle Barker 2005 Important Messages This booklet is based on three key messages for patients. 1. Pre-diabetes is a serious condition with a
Pre-diabetes: Information for primary care practitioners Michelle Barker 2005 Important Messages This booklet is based on three key messages for patients. 1. Pre-diabetes is a serious condition with a
EXENATIDE (BYETTA ) PROTOCOL, 5mcg and 10mcg SC injection pre-filled pens
 EXENATIDE (BYETTA ) PROTOCOL, 5mcg and 10mcg SC injection pre-filled pens This document should be read in conjunction with the current Summary of Product Characteristics http://www.medicines.org.uk 1.
EXENATIDE (BYETTA ) PROTOCOL, 5mcg and 10mcg SC injection pre-filled pens This document should be read in conjunction with the current Summary of Product Characteristics http://www.medicines.org.uk 1.
Goals of today s talk. How to Stop Prediabetes from Becoming Diabetes. Goals of today s talk. Type 2 diabetes mellitus
 Goals of today s talk How to Stop Prediabetes from Becoming Diabetes Zara Frankel, MD Boulder Creek Family Medicine 303-720-6956 Diabetes is a devastating disease Prediabetes and diabetes are on different
Goals of today s talk How to Stop Prediabetes from Becoming Diabetes Zara Frankel, MD Boulder Creek Family Medicine 303-720-6956 Diabetes is a devastating disease Prediabetes and diabetes are on different
EFFECTIVE SHARE CARE AGREEMENT. FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY
 Specialist details Patient identifier Name Tel: EFFECTIVE SHARE CARE AGREEMENT FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY The aim of Effective Shared Care Guidelines
Specialist details Patient identifier Name Tel: EFFECTIVE SHARE CARE AGREEMENT FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY The aim of Effective Shared Care Guidelines
SIGN 149 Risk estimation and the prevention of cardiovascular disease. Quick Reference Guide July Evidence
 SIGN 149 Risk estimation and the prevention of cardiovascular disease Quick Reference Guide July 2017 Evidence ESTIMATING CARDIOVASCULAR RISK R Individuals with the following risk factors should be considered
SIGN 149 Risk estimation and the prevention of cardiovascular disease Quick Reference Guide July 2017 Evidence ESTIMATING CARDIOVASCULAR RISK R Individuals with the following risk factors should be considered
CVD, diabetes renal disease
 Testing for CVD, diabetes renal disease and in elderly people As people age and their co-morbidities and medicine use increases, decisions about medical management change. There is limited evidence of
Testing for CVD, diabetes renal disease and in elderly people As people age and their co-morbidities and medicine use increases, decisions about medical management change. There is limited evidence of
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc)
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Guideline for the Investigation and Management of Polycystic Ovary Syndrome Author: Contact Name and Job Title
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Guideline for the Investigation and Management of Polycystic Ovary Syndrome Author: Contact Name and Job Title
TREATMENTS FOR TYPE 2 DIABETES. Susan Henry Diabetes Specialist Nurse
 TREATMENTS FOR TYPE 2 DIABETES Susan Henry Diabetes Specialist Nurse How can we improve outcomes in Type 2 diabetes? Earlier diagnosis Better patient education Stress central role of lifestyle management
TREATMENTS FOR TYPE 2 DIABETES Susan Henry Diabetes Specialist Nurse How can we improve outcomes in Type 2 diabetes? Earlier diagnosis Better patient education Stress central role of lifestyle management
Diabetes Mellitus: A Cardiovascular Disease
 Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
Donna Tomky, MSN, C-ANP, CDE, FAADE Albuquerque, New Mexico
 Donna Tomky, MSN, C-ANP, CDE, FAADE Albuquerque, New Mexico Presented in Collaboration with New Mexico Health Care Takes On Diabetes Discuss the burden and challenges prediabetes presents in New Mexico.
Donna Tomky, MSN, C-ANP, CDE, FAADE Albuquerque, New Mexico Presented in Collaboration with New Mexico Health Care Takes On Diabetes Discuss the burden and challenges prediabetes presents in New Mexico.
Implementing Type 2 Diabetes Prevention Programmes
 Implementing Type 2 Diabetes Prevention Programmes Jaakko Tuomilehto Department of Public Health University of Helsinki Helsinki, Finland FIN-D2D Survey 2004 Prevalence of previously diagnosed and screen-detected
Implementing Type 2 Diabetes Prevention Programmes Jaakko Tuomilehto Department of Public Health University of Helsinki Helsinki, Finland FIN-D2D Survey 2004 Prevalence of previously diagnosed and screen-detected
CHAPTER 1. What is diabetes?
 14 What is diabetes? People with type 1 diabetes, can live healthy and fulfilling lives with the provision of an uninterrupted supply of insulin and blood glucose testing equipment, when combined with
14 What is diabetes? People with type 1 diabetes, can live healthy and fulfilling lives with the provision of an uninterrupted supply of insulin and blood glucose testing equipment, when combined with
Community Based Diabetes Prevention
 Community Based Diabetes Prevention Melanie Davies Professor of Diabetes Medicine Outline NIHR Programme Grant proposal and update to progress The Vascular Check programme HbA1c debate Algorithm to detect
Community Based Diabetes Prevention Melanie Davies Professor of Diabetes Medicine Outline NIHR Programme Grant proposal and update to progress The Vascular Check programme HbA1c debate Algorithm to detect
Frailty and Type 2 Diabetes Guidelines for clinicians
 H.G. WELLS PROJECT Frailty and Type 2 Diabetes Guidelines for clinicians Victoria Ruszala victoria.ruszala@nhs.net H.G. Wells Project team Dugal T, Partington E. Kernow CCG Diabetes and Frailty Guideline
H.G. WELLS PROJECT Frailty and Type 2 Diabetes Guidelines for clinicians Victoria Ruszala victoria.ruszala@nhs.net H.G. Wells Project team Dugal T, Partington E. Kernow CCG Diabetes and Frailty Guideline
Type 2 diabetes how to prevent it? East of England Diabetes Mellitus Transformation and Sustainability Network 28 th March 2018
 Type 2 diabetes how to prevent it? East of England Diabetes Mellitus Transformation and Sustainability Network 28 th March 2018 Dr Charles Bodmer Consultant Clinical Lead Dr Sonica Goel GP Clinical Lead
Type 2 diabetes how to prevent it? East of England Diabetes Mellitus Transformation and Sustainability Network 28 th March 2018 Dr Charles Bodmer Consultant Clinical Lead Dr Sonica Goel GP Clinical Lead
Polycystic ovarian syndrome Can lifestyle modifications help?? Dr Saloni Assistant Professor, Deptt of OBG BPSGMC for Women, Khanpur Kalan
 Polycystic ovarian syndrome Can lifestyle modifications help?? Dr Saloni Assistant Professor, Deptt of OBG BPSGMC for Women, Khanpur Kalan Life-long condition Hirsutism Menstrual irregularities? Pronounced
Polycystic ovarian syndrome Can lifestyle modifications help?? Dr Saloni Assistant Professor, Deptt of OBG BPSGMC for Women, Khanpur Kalan Life-long condition Hirsutism Menstrual irregularities? Pronounced
National Institute for Health and Care Excellence. Type 2 diabetes. Stakeholder Comments Draft Guideline
 National Institute for Health and Care Excellence Type 2 diabetes Stakeholder Comments Draft Guideline NOTE: NICE is unable to accept comments from non-registered organisations or individuals. If you wish
National Institute for Health and Care Excellence Type 2 diabetes Stakeholder Comments Draft Guideline NOTE: NICE is unable to accept comments from non-registered organisations or individuals. If you wish
NHS Greater Glasgow & Clyde Managed Clinical Network for Diabetes
 Guidelines for the Diagnosis of Diabetes Mellitus NHS Greater Glasgow & Clyde Managed Clinical Network for Diabetes Lead Authors: Dr Brian Kennon, Dr David Carty June 2015 Review due: December 2016 Diagnosis
Guidelines for the Diagnosis of Diabetes Mellitus NHS Greater Glasgow & Clyde Managed Clinical Network for Diabetes Lead Authors: Dr Brian Kennon, Dr David Carty June 2015 Review due: December 2016 Diagnosis
Diabetes Diagnosis 2011 Does your patient have diabetes?
 Diabetes Diagnosis 2011 Does your patient have diabetes? Dr Rick Cutfield Physician and Endocrinologist Waitemata District Health Board Mercy Specialist Centre Case 1: A 24 year old stockcar driver presents
Diabetes Diagnosis 2011 Does your patient have diabetes? Dr Rick Cutfield Physician and Endocrinologist Waitemata District Health Board Mercy Specialist Centre Case 1: A 24 year old stockcar driver presents
New PCOS guidelines: What s relevant to general practice
 New PCOS guidelines: What s relevant to general practice Dr Michael Costello Fertility Specialist IVF Australia UNSW Royal Hospital for Women Sydney How do we know if something is new? Louvre Museum, Paris
New PCOS guidelines: What s relevant to general practice Dr Michael Costello Fertility Specialist IVF Australia UNSW Royal Hospital for Women Sydney How do we know if something is new? Louvre Museum, Paris
Type 2 Diabetes. Stopping Smoking. Consider referral to smoking cessation. Consider referring for weight management advice.
 Type 2 Diabetes Stopping Smoking Consider referral to smoking cessation BMI > 25 kg m² Set a weight loss target of a 5-10% reduction Consider referring for weight management advice Control BP to
Type 2 Diabetes Stopping Smoking Consider referral to smoking cessation BMI > 25 kg m² Set a weight loss target of a 5-10% reduction Consider referring for weight management advice Control BP to
bpac better e m dicine
 bpac nz better medicin e bpac nz Development Team: Rachael Clarke Sonia Ross Dr Trevor Walker David Woods bpac nz Clinical Advisory Group (laboratory programme): Tracey Barron Dr Dave Colquhoun Michele
bpac nz better medicin e bpac nz Development Team: Rachael Clarke Sonia Ross Dr Trevor Walker David Woods bpac nz Clinical Advisory Group (laboratory programme): Tracey Barron Dr Dave Colquhoun Michele
Why Do We Care About Prediabetes?
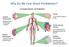 Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Polycystic Ovary Syndrome (PCOS)
 Polycystic Ovary Syndrome (PCOS) What are Polycystic Ovaries? Polycystic ovaries are slightly larger than normal ovaries and have twice the number of follicles (small cysts). Polycystic ovaries are very
Polycystic Ovary Syndrome (PCOS) What are Polycystic Ovaries? Polycystic ovaries are slightly larger than normal ovaries and have twice the number of follicles (small cysts). Polycystic ovaries are very
Other targets will be set as data become available and the NBCSP is established.
 Target revision No revision of the target is required at this stage. Trends will need to be monitored with the change in ethnicity coding as there may be a need to set separate targets for Mäori. Other
Target revision No revision of the target is required at this stage. Trends will need to be monitored with the change in ethnicity coding as there may be a need to set separate targets for Mäori. Other
Manipal & Apollo Spectra Hospital. Special Interest:Laparoscopy & Bariatric Surgery
 Name: Dr M G Bhat Designation: Consultant Surgeon Affiliation: Manipal & Apollo Spectra Hospital Special Interest:Laparoscopy & Bariatric Surgery When should we suggest Bariatric Surgery in PCOD? 17 June
Name: Dr M G Bhat Designation: Consultant Surgeon Affiliation: Manipal & Apollo Spectra Hospital Special Interest:Laparoscopy & Bariatric Surgery When should we suggest Bariatric Surgery in PCOD? 17 June
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Diabetes dietary review Potential output: Recommendations
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Diabetes dietary review Potential output: Recommendations
Metformin Hydrochloride
 Metformin Hydrochloride 500 mg, 850 mg, 500 mg LA and 750 mg LA Tablet Description Informet is a preparation of metformin hydrochloride that belongs to a biguanide class of oral antidiabetic drugs. Metformin
Metformin Hydrochloride 500 mg, 850 mg, 500 mg LA and 750 mg LA Tablet Description Informet is a preparation of metformin hydrochloride that belongs to a biguanide class of oral antidiabetic drugs. Metformin
Polycystic ovary syndrome in young women - new ideas
 Polycystic ovary syndrome in young women - new ideas Disclosures Minor shareholder IVF clinic Grant support MSD, Merck and Ferring Grant support NHMRC Perspective is everything in PCOS Peacock s 2013 Polycystic
Polycystic ovary syndrome in young women - new ideas Disclosures Minor shareholder IVF clinic Grant support MSD, Merck and Ferring Grant support NHMRC Perspective is everything in PCOS Peacock s 2013 Polycystic
Barns Medical Practice Service Specification: Diabetes
 Barns Medical Practice Service Specification: Diabetes DEVELOPED June 2017 REVIEW DATE June 2019 Introduction Diabetes mellitus is a life-long progressive condition that can be controlled but not cured.
Barns Medical Practice Service Specification: Diabetes DEVELOPED June 2017 REVIEW DATE June 2019 Introduction Diabetes mellitus is a life-long progressive condition that can be controlled but not cured.
Amenorrhoea: polycystic ovary syndrome
 There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES
 Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES Objectives u At conclusion of the lecture the participant will be able to: 1. Differentiate between the classifications of diabetes
Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES Objectives u At conclusion of the lecture the participant will be able to: 1. Differentiate between the classifications of diabetes
The new face of diabetes care in New Zealand
 UPFRONT The new face of diabetes care in New Zealand ON 1 JULY, 2012 the Get Checked programme, under which diabetes follow-up care in New Zealand is funded, will cease to exist. In its place will be the
UPFRONT The new face of diabetes care in New Zealand ON 1 JULY, 2012 the Get Checked programme, under which diabetes follow-up care in New Zealand is funded, will cease to exist. In its place will be the
Insulin Initiation, titration & Insulin switch in the Primary Care-KISS
 Insulin Initiation, titration & Insulin switch in the Primary Care-KISS Rotorua GP CME 9 June 2012 Dr Kingsley Nirmalaraj FRACP Endocrinologist, BOPDHB & Suite 9, Promed House, Tenth Ave, Tauranga Linda
Insulin Initiation, titration & Insulin switch in the Primary Care-KISS Rotorua GP CME 9 June 2012 Dr Kingsley Nirmalaraj FRACP Endocrinologist, BOPDHB & Suite 9, Promed House, Tenth Ave, Tauranga Linda
Weight management IN ADULTS ASSESS MANAGE MONITOR MAINTAIN. Proceed to stage 2: Assess. Reassess. Obese. Overweight
 Weight management IN ADULTS MONITOR MANAGE MAINTAIN Monitor weight and calculate body mass index (BMI) opportunistically (ideally annually) or as needed. Overweight 5 kg/m If weight is increasing, or BMI
Weight management IN ADULTS MONITOR MANAGE MAINTAIN Monitor weight and calculate body mass index (BMI) opportunistically (ideally annually) or as needed. Overweight 5 kg/m If weight is increasing, or BMI
5.2 Key priorities for implementation
 5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
GESTATIONAL DIABETES for GP Obstetric Shared Care Accreditation Seminar. Simon Kane March 2016
 GESTATIONAL DIABETES for GP Obstetric Shared Care Accreditation Seminar Simon Kane March 2016 Objectives History and definitions Definition and Australian data Pathophysiology and prevalence Rationale
GESTATIONAL DIABETES for GP Obstetric Shared Care Accreditation Seminar Simon Kane March 2016 Objectives History and definitions Definition and Australian data Pathophysiology and prevalence Rationale
Diabetes and Hypertension
 Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
The Pursuit of Prevention of Renal failure in an imperfect world-is it possible in the 21 st century?
 The Pursuit of Prevention of Renal failure in an imperfect world-is it possible in the 21 st century? By: Baskar, WDHB, Renal Service Auckland New Zealand Presented at : 4 th International Conference on
The Pursuit of Prevention of Renal failure in an imperfect world-is it possible in the 21 st century? By: Baskar, WDHB, Renal Service Auckland New Zealand Presented at : 4 th International Conference on
What is polycystic ovary syndrome? What are polycystic ovaries? What are the symptoms of PCOS?
 What is polycystic ovary syndrome? Polycystic ovary syndrome (PCOS) is a condition which can affect a woman s menstrual cycle, fertility, hormones and aspects of her appearance. It can also affect your
What is polycystic ovary syndrome? Polycystic ovary syndrome (PCOS) is a condition which can affect a woman s menstrual cycle, fertility, hormones and aspects of her appearance. It can also affect your
Diabetes Educator. Australian. Diabetes in Pregnancy. Policy Discussion. GDM Model of Care the Role of the Credentialled Diabetes Educator
 Australian Diabetes Educator Volume 17, Number 3, August 2014 Diabetes in Pregnancy GDM Model of Care the Role of the Credentialled Diabetes Educator GDM a New Era in Diagnosis and the Impact for Diabetes
Australian Diabetes Educator Volume 17, Number 3, August 2014 Diabetes in Pregnancy GDM Model of Care the Role of the Credentialled Diabetes Educator GDM a New Era in Diagnosis and the Impact for Diabetes
Mr Rab Burtun. Dr David Kim. 8:30-10:30 WS #2: Diabetes Basic 11:00-13:00 WS #9: Diabetes Basic (Repeated)
 Dr David Kim Endocrinologist and General Physician Waitemata DHB and Apollo Specialist Clinic Albany Auckland Mr Rab Burtun Diabetes Nurse Specialist Waitemata DHB Waitakere Hospital Auckland 8:30-10:30
Dr David Kim Endocrinologist and General Physician Waitemata DHB and Apollo Specialist Clinic Albany Auckland Mr Rab Burtun Diabetes Nurse Specialist Waitemata DHB Waitakere Hospital Auckland 8:30-10:30
Information for you. What is polycystic ovary syndrome? Polycystic ovary syndrome: what it means for your long-term health
 aashara Polycystic ovary syndrome: what it means for your long-term health Information for you Published in February 2005, minor amendments in June 2005 Revised 2009 What is polycystic ovary syndrome?
aashara Polycystic ovary syndrome: what it means for your long-term health Information for you Published in February 2005, minor amendments in June 2005 Revised 2009 What is polycystic ovary syndrome?
Diabesity. Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs
 Diabesity Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs Abdominal obesity Low HDL, high LDL, and high triglycerides HTN High blood glucose (F>100l,
Diabesity Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs Abdominal obesity Low HDL, high LDL, and high triglycerides HTN High blood glucose (F>100l,
Polycystic ovary syndrome (PCOS)
 Information for patients Polycystic ovary syndrome (PCOS) What is polycystic ovary syndrome? Polycystic ovary syndrome (PCOS) is a condition which can affect a woman s menstrual cycle, fertility, hormones
Information for patients Polycystic ovary syndrome (PCOS) What is polycystic ovary syndrome? Polycystic ovary syndrome (PCOS) is a condition which can affect a woman s menstrual cycle, fertility, hormones
Diabetes and Kidney Disease. Kris Bentley Renal Nurse practitioner 2018
 Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS
 IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
Standards of Medical Care in Diabetes 2016
 Standards of Medical Care in Diabetes 2016 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking
Standards of Medical Care in Diabetes 2016 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking
Diabetes and Kidney Disease: Time to Act. Your Guide to Diabetes and Kidney Disease
 Diabetes and Kidney Disease: Time to Act Your Guide to Diabetes and Kidney Disease Diabetes is fast becoming a world epidemic Diabetes is reaching epidemic proportions worldwide. Every year more people
Diabetes and Kidney Disease: Time to Act Your Guide to Diabetes and Kidney Disease Diabetes is fast becoming a world epidemic Diabetes is reaching epidemic proportions worldwide. Every year more people
American Academy of Insurance Medicine
 American Academy of Insurance Medicine October 2012 Dr. Alison Moy Liberty Mutual Dr. John Kirkpatrick Thrivent Financial for Lutherans 1 59 year old male, diagnosed with T2DM six months ago Nonsmoker
American Academy of Insurance Medicine October 2012 Dr. Alison Moy Liberty Mutual Dr. John Kirkpatrick Thrivent Financial for Lutherans 1 59 year old male, diagnosed with T2DM six months ago Nonsmoker
Metabolic Syndrome. Shon Meek MD, PhD Mayo Clinic Florida Endocrinology
 Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Cardiovascular Disease Risk Assessment and Management for Primary Care
 Cardiovascular Disease Risk Assessment and Management for Primary Care 2018 Released 2018 health.govt.nz Acknowledgements With thanks to the consumers and sector stakeholders who contributed during workshops/discussions
Cardiovascular Disease Risk Assessment and Management for Primary Care 2018 Released 2018 health.govt.nz Acknowledgements With thanks to the consumers and sector stakeholders who contributed during workshops/discussions
Scottish Diabetes Survey 2012
 Scottish Diabetes Survey 2012 Scottish Diabetes Survey Monitoring Group 1 Scottish Diabetes Survey Monitoring Group Contents Foreword... 3 Executive Summary... 5 Prevalence... 6 Undiagnosed diabetes...
Scottish Diabetes Survey 2012 Scottish Diabetes Survey Monitoring Group 1 Scottish Diabetes Survey Monitoring Group Contents Foreword... 3 Executive Summary... 5 Prevalence... 6 Undiagnosed diabetes...
Implementation of HbA1c as a Diagnostic Test in New Zealand
 Implementation of HbA1c as a Diagnostic Test in New Zealand Chris Florkowski MD MRCP(UK) FRACP FRCPA FFSc Consultant in Chemical Pathology, Canterbury Health Laboratories Diabetes Physician, Christchurch
Implementation of HbA1c as a Diagnostic Test in New Zealand Chris Florkowski MD MRCP(UK) FRACP FRCPA FFSc Consultant in Chemical Pathology, Canterbury Health Laboratories Diabetes Physician, Christchurch
Diabetic Nephropathy. Objectives:
 There are, in truth, no specialties in medicine, since to know fully many of the most important diseases a man must be familiar with their manifestations in many organs. William Osler 1894. Objectives:
There are, in truth, no specialties in medicine, since to know fully many of the most important diseases a man must be familiar with their manifestations in many organs. William Osler 1894. Objectives:
Hot Topics in Diabetic Kidney Disease a primary care perspective
 Hot Topics in Diabetic Kidney Disease a primary care perspective DR SARAH DAVIES GP PARTNER WITH SPECIAL INTEREST IN DIABETES, CARDIFF DUK CLINICAL CHAMPION NB MEDICAL HOT TOPICS PRESENTER AND DIABETES
Hot Topics in Diabetic Kidney Disease a primary care perspective DR SARAH DAVIES GP PARTNER WITH SPECIAL INTEREST IN DIABETES, CARDIFF DUK CLINICAL CHAMPION NB MEDICAL HOT TOPICS PRESENTER AND DIABETES
Diabetes Prevention in Wisconsin. American Diabetes Association 2017 Professional Diabetes Education Conference March 17, 2017 Middleton, WI
 Diabetes Prevention in Wisconsin American Diabetes Association 2017 Professional Diabetes Education Conference March 17, 2017 Middleton, WI Presenter Disclosure Information In compliance with the accrediting
Diabetes Prevention in Wisconsin American Diabetes Association 2017 Professional Diabetes Education Conference March 17, 2017 Middleton, WI Presenter Disclosure Information In compliance with the accrediting
Diabetes Prevention in Wisconsin
 Diabetes Prevention in Wisconsin American Diabetes Association 2017 Professional Diabetes Education Conference March 17, 2017 Middleton, WI Presenter Disclosure Information In compliance with the accrediting
Diabetes Prevention in Wisconsin American Diabetes Association 2017 Professional Diabetes Education Conference March 17, 2017 Middleton, WI Presenter Disclosure Information In compliance with the accrediting
DIABETES A BITESIZE GUIDE EVERYTHING YOU NEED TO KNOW ABOUT DIABETES
 DIABETES A BITESIZE GUIDE EVERYTHING YOU NEED TO KNOW ABOUT DIABETES TABLE OF CONTENTS 3 INTRODUCTION 4 SO, WHAT IS DIABETES? 6 DIFFERENT TYPES 7 TYPE 1 DIABETES 8 TYPE 2 DIABETES 9 GESTATIONAL 10 SYMPTOMS
DIABETES A BITESIZE GUIDE EVERYTHING YOU NEED TO KNOW ABOUT DIABETES TABLE OF CONTENTS 3 INTRODUCTION 4 SO, WHAT IS DIABETES? 6 DIFFERENT TYPES 7 TYPE 1 DIABETES 8 TYPE 2 DIABETES 9 GESTATIONAL 10 SYMPTOMS
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus
 Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
Monthly WellPATH Spotlight November 2016: Diabetes
 Monthly WellPATH Spotlight November 2016: Diabetes DIABETES RISK FACTORS & SELF CARE TIPS Diabetes is a condition in which the body does not produce enough insulin or does not use the insulin produced
Monthly WellPATH Spotlight November 2016: Diabetes DIABETES RISK FACTORS & SELF CARE TIPS Diabetes is a condition in which the body does not produce enough insulin or does not use the insulin produced
Clinical Practice Guidelines for Diabetes Management
 Clinical Practice Guidelines for Diabetes Management Diabetes is a disease in which blood glucose levels are above normal. Over the years, high blood glucose damages nerves and blood vessels, which can
Clinical Practice Guidelines for Diabetes Management Diabetes is a disease in which blood glucose levels are above normal. Over the years, high blood glucose damages nerves and blood vessels, which can
New Treatments for Type 2 diabetes. Nandini Seevaratnam April 2016 Rushcliffe Patient Forum
 New Treatments for Type 2 diabetes Nandini Seevaratnam April 2016 Rushcliffe Patient Forum Overview Growing population of Type 2 diabetes Basic science on what goes wrong Current treatments Why there is
New Treatments for Type 2 diabetes Nandini Seevaratnam April 2016 Rushcliffe Patient Forum Overview Growing population of Type 2 diabetes Basic science on what goes wrong Current treatments Why there is
Diabetes is a condition with a huge health impact in Asia. More than half of all
 Interventions to Change Health Behaviors and Prevention Rob M. van Dam, PhD Diabetes is a condition with a huge health impact in Asia. More than half of all people with diabetes live today in Asian countries,
Interventions to Change Health Behaviors and Prevention Rob M. van Dam, PhD Diabetes is a condition with a huge health impact in Asia. More than half of all people with diabetes live today in Asian countries,
Presenter Disclosure Information
 Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
13 th Annual Women s Health Day PCOS. Saturday 02/09/2017 Dr Mathias Epee-Bekima O&G Consultant KEMH
 13 th Annual Women s Health Day PCOS Saturday 02/09/2017 Dr Mathias Epee-Bekima O&G Consultant KEMH Learning objectives Perform the appropriate investigations in women where there is a clinical suspicion
13 th Annual Women s Health Day PCOS Saturday 02/09/2017 Dr Mathias Epee-Bekima O&G Consultant KEMH Learning objectives Perform the appropriate investigations in women where there is a clinical suspicion
Adult Diabetes Clinician Guide NOVEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
Polycystic Ovary Syndrome (PCOS):
 Polycystic Ovary Syndrome (PCOS): Current diagnosis and treatment Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the end of this presentation,
Polycystic Ovary Syndrome (PCOS): Current diagnosis and treatment Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the end of this presentation,
Case study: Lean adult with no complications, newly diagnosed with type 2 diabetes
 Case study: Lean adult with no complications, newly diagnosed with type 2 diabetes Authored by Clifford Bailey and James LaSalle on behalf of the Global Partnership for Effective Diabetes Management. The
Case study: Lean adult with no complications, newly diagnosed with type 2 diabetes Authored by Clifford Bailey and James LaSalle on behalf of the Global Partnership for Effective Diabetes Management. The
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme
 Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Primary prevention of CVD Potential output:
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Primary prevention of CVD Potential output:
Why Screen at 23? What can YOU do?
 Why Screen at 23? Every 1 in 2 Asian American adults has diabetes or prediabetes. More than half of Asian Americans did not know they have type 2 diabetes or prediabetes. Asian Americans can develop diabetes
Why Screen at 23? Every 1 in 2 Asian American adults has diabetes or prediabetes. More than half of Asian Americans did not know they have type 2 diabetes or prediabetes. Asian Americans can develop diabetes
1. Which one of the following patients does not need to be screened for hyperlipidemia:
 Questions: 1. Which one of the following patients does not need to be screened for hyperlipidemia: a) Diabetes mellitus b) Hypertension c) Family history of premature coronary disease (first degree relatives:
Questions: 1. Which one of the following patients does not need to be screened for hyperlipidemia: a) Diabetes mellitus b) Hypertension c) Family history of premature coronary disease (first degree relatives:
Macronutrients and Dietary Patterns for Glucose Control
 제 20 회대한당뇨병학회춘계학술대회 Macronutrients and Dietary Patterns for Glucose Control 2017.5.13 서울대학교병원임정현 Conflict of interest disclosure None Committee of Scientific Affairs Contents Review of Nutrition Recommendation
제 20 회대한당뇨병학회춘계학술대회 Macronutrients and Dietary Patterns for Glucose Control 2017.5.13 서울대학교병원임정현 Conflict of interest disclosure None Committee of Scientific Affairs Contents Review of Nutrition Recommendation
Diabetes in Renal Patients. Contents. Understanding Diabetic Nephropathy
 Diabetes in Renal Patients Contents Understanding Diabetic Nephropathy What effect does CKD have on a patient s diabetic control? Diabetic Drugs in CKD and Dialysis Patients Hyper and Hypoglycaemia in
Diabetes in Renal Patients Contents Understanding Diabetic Nephropathy What effect does CKD have on a patient s diabetic control? Diabetic Drugs in CKD and Dialysis Patients Hyper and Hypoglycaemia in
Absolute cardiovascular disease risk management
 Quick reference guide for health professionals Absolute cardiovascular disease risk management This quick reference guide is for use by health professionals for primary prevention of cardiovascular disease
Quick reference guide for health professionals Absolute cardiovascular disease risk management This quick reference guide is for use by health professionals for primary prevention of cardiovascular disease
ERBP Guideline on management of diabetics with advanced CKD
 ERBP Guideline on management of diabetics with advanced CKD ERBP Mission improve the outcome of patients with kidney disease in a sustainable way, through enhancing the accessibility of knowledge on patient
ERBP Guideline on management of diabetics with advanced CKD ERBP Mission improve the outcome of patients with kidney disease in a sustainable way, through enhancing the accessibility of knowledge on patient
6.1. Feeding specifications for people with diabetes mellitus type 1
 6 Feeding 61 Feeding specifications for people with diabetes mellitus type 1 It is important that the food intake of people with DM1 is balanced, varied and that it meets the caloric needs, and takes into
6 Feeding 61 Feeding specifications for people with diabetes mellitus type 1 It is important that the food intake of people with DM1 is balanced, varied and that it meets the caloric needs, and takes into
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE. Type 2 diabetes: the management of type 2 diabetes (update)
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Type 2 diabetes: the management of type 2 diabetes (update) 1.1 Short title Type 2 diabetes (update) 2 Background a) The National
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Type 2 diabetes: the management of type 2 diabetes (update) 1.1 Short title Type 2 diabetes (update) 2 Background a) The National
INJECTABLE THERAPIES IN DIABETES. Barbara Ann McKee Diabetes Specialist Nurse
 INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
APPENDIX 2F Management of Cholesterol
 Patients with established CVD: Coronary heart disease Cerebrovascular disease Peripheral vascular disease APPEDIX 2F Management of Cholesterol Patients at high risk of cardiovascular events: Chronic kidney
Patients with established CVD: Coronary heart disease Cerebrovascular disease Peripheral vascular disease APPEDIX 2F Management of Cholesterol Patients at high risk of cardiovascular events: Chronic kidney
Disclosures. Nutrition & Menopause. What changes? Mindless Eating 10/6/2017. I have no disclosures
 I have no disclosures Disclosures Nutrition & Menopause Making changes when you can t eat like a 25 year old, and get away with it.. What changes? Social situation Family and family meals Activity levels
I have no disclosures Disclosures Nutrition & Menopause Making changes when you can t eat like a 25 year old, and get away with it.. What changes? Social situation Family and family meals Activity levels
Dept of Diabetes Main Desk
 Dept of Diabetes Main Desk 01202 448060 Glucose management in Type 2 Diabetes in Adults The natural history of type 2 diabetes is for HbA1c to deteriorate with time. A stepwise approach to treatment is
Dept of Diabetes Main Desk 01202 448060 Glucose management in Type 2 Diabetes in Adults The natural history of type 2 diabetes is for HbA1c to deteriorate with time. A stepwise approach to treatment is
Objectives. Objectives. Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015
 Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
