Changes in parathyroid hormone and body mass index and the association with mortality in dialysis patients
|
|
|
- Lizbeth Mitchell
- 5 years ago
- Views:
Transcription
1 Nephrol Dial Transplant (2011) 26: doi: /ndt/gfq541 Advance Access publication 14 September 2010 Changes in parathyroid hormone and body mass index and the association with mortality in dialysis patients Christiane Drechsler 1,2, Diana C. Grootendorst 1, Elisabeth W. Boeschoten 3, Raymond T. Krediet 4, Christoph Wanner 2, Friedo W. Dekker 1 and for the NECOSAD study group 1 Department of Clinical Epidemiology, LUMC, Leiden, The Netherlands, 2 Division of Nephrology, University of Würzburg, Germany, 3 Hans Mak Institute, Naarden, The Netherlands and 4 Department of Nephrology, AMC, Amsterdam, The Netherlands Correspondence and offprint requests to: Christiane Drechsler; c.drechsler@gmx.net Abstract Background. Obesity is associated with secondary hyperparathyroidism in the general population. It is unknown whether body mass index (BMI) affects parathyroid hormone (PTH) level and its association with mortality in dialysis patients. Methods. From a prospective cohort study of incident dialysis patients in the Netherlands (NECOSAD), we selected all patients with recorded BMI and PTH at 3 months (baseline) after the start of dialysis [n = 1628, age 59 ± 15 years, BMI 24.7 ± 4.1 kg/m 2, median PTH 13.0 (interquartile range ) pmol/l]. We assessed associations between BMI and PTH at baseline and between their changes over 3 months by correlation and linear regression analyses. The effect of the changes in PTH on all-cause mortality during a subsequent mean follow-up of 3.2 ± 2 years was assessed by Cox regression analyses. Results. Median PTH levels at baseline were lowest in underweight patients (10.2 pmol/l), followed by normal weight (12.1 pmol/l), overweight (14.0 pmol/l) and obese patients (17.5 pmol/l). The associations were similar in diabetic and non-diabetic patients. A 5% decrease in BMI (n = 101) over 3 months was accompanied by a 26% decrease in PTH (PTH ratio 0.74; P = 0.039), whereas a 5% increase in BMI (n = 143) was associated with an 11% increase in PTH (PTH ratio 1.11; P = 0.026). Compared to patients with stable PTH levels, patients with decreasing PTH in the presence of weight loss showed a 2-fold higher mortality (hazard ratio 2.02, 95% confidence interval ; P < 0.001), in contrast to those with decreasing PTH in the absence of weight loss. Additional analyses showed that the weight loss was responsible for increased deaths. Conclusions. PTH is associated with BMI and its longitudinal changes in dialysis patients, both in patients with and without diabetes mellitus. An increased mortality seen for patients with concurrent decreases in PTH and BMI was explained by the weight loss, representing an important confounder for outcome analyses according to levels of PTH. Low and decreasing PTH levels may be symptoms of wasting, which should be taken into account in the care of dialysis patients. Keywords: body mass index; epidemiology; dialysis; mortality; parathyroid hormone Introduction Disturbances of mineral metabolism are common in patients undergoing maintenance dialysis. Secondary hyperparathyroidism develops early in the progression of chronic kidney disease (CKD) and worsens with advanced stages of the disease [1 5]. A variety of complications may develop, including bone demineralization, soft tissue and vascular calcification, anaemia, cognitive dysfunction and muscle and skin complaints [6]. Furthermore, high levels of parathyroid hormone (PTH) have been found associated with an increased mortality in patients with CKD [7 10]. On the other hand, mineral disorders may also occur with low levels of PTH. In this context, adynamic bone disease has been reported as an important and serious complication [11,12]. It has been shown that low levels of PTH are also associated with an increased mortality in dialysis patients [13 15]. The pathophysiology thereby is not clear, pointing out the need to identify risk factors that lead to alterations in PTH metabolism and associated mortality risk. Nutritional status may impact on PTH metabolism, since obesity has been found related to increased levels of PTH in the general population [16 18] and in pre-dialysis patients [19]. It is unknown whether obesity is a risk factor for high PTH levels in dialysis patients. In contrast, dialysis patients suffer to a considerable extent from wasting, which is a complex process of muscle loss, poor food intake, inflammation and the development of comorbidities [20]. Underweight, frequently observed in patients with the wasting syndrome, has been shown to be associated with a high mortality in dialysis patients [21]. Considering The Author Published by Oxford University Press on behalf of ERA-EDTA. All rights reserved. For Permissions, please journals.permissions@oxfordjournals.org
2 Changes in PTH, BMI, and mortality in dialysis patients 1341 the interrelations between body mass index (BMI) and mineral metabolism in the general population, it is speculated that underweight and weight loss may result in low levels of PTH. This, in turn, may have a different impact on mortality as compared to low levels of PTH that are unrelated to wasting and either physiologic or intentionally achieved by medication. The aim of this study was 3-fold. First, to investigate the association of BMI with levels of PTH in end-stage renal disease (ESRD) patients starting dialysis; second, to assess the relation of longitudinal changes in BMI with changes in PTH; and third, to assess the potential impact of changing PTH on mortality in dialysis patients, analysing data of a prospective multicentre cohort study of incident dialysis patients in the Netherlands. Materials and methods Study design NECOSAD is an observational prospective follow-up study in which incident dialysis patients have been enrolled in 38 participating dialysis centres since 1997 in the Netherlands. Study visits took place at the start of dialysis, at 3 months, 6 months and subsequently at 6-month intervals until the date of loss to follow-up (death, kidney transplantation or transfer to a non-participating dialysis centre) or the end of the follow-up at 1 January Baseline demographic and clinical data were obtained between 4 weeks prior to and 2 weeks after the start of long-term dialysis treatment. Blood and 24-h urine samples were obtained at all visits. For the present analysis, baseline is defined as 3 months after the start of dialysis treatment, when the patients fluid and metabolic conditions had stabilized. Patients Patients with ESRD who were at least 18 years old and started long-term dialysis therapy for the first time were invited to participate in NECOSAD. In the present analysis, all patients with recorded height, weight and measurements of PTH at 3 months after initiation of dialysis were included. The medical ethical committees of the participating centres approved the study, and all patients gave their written informed consent before inclusion. Data collection Demographic and clinical data included age, sex, ethnicity, smoking habits, primary kidney disease and comorbidity. Primary kidney diseases and causes of death were classified according to the coding system of the European Renal Association European Dialysis and Transplant Association (ERA EDTA). Diagnoses of comorbid conditions were reported by the patients nephrologists and used to calculate the comorbidity score according to Khan. Plasma calcium, phosphorus, intact PTH and albumin were measured at 3 and at 6 months after the initiation of dialysis by standard laboratory techniques in the different centres. Height and weight were measured after dialysis sessions, and BMI was calculated as weight (kilograms) divided by height (metres) squared. Blood pressure was measured in sitting position. Statistical analyses Mean values with standard deviations (SD) were calculated for continuous variables and median values with interquartile range (IQR) as appropriate. Categorical variables were expressed as proportions. BMI at baseline was categorized into four groups, with obesity being defined as a BMI 30 kg/m 2 and overweight as a BMI between 25 and 30 kg/m 2. Because of the lack of appropriate standards for dialysis patients [20], normal weight was defined as a BMI between 20 and 25 kg/m 2 (reference group) and underweight as <20 kg/m 2. First, we assessed the association of BMI with PTH at baseline using correlation and linear regression analyses. Levels of PTH were logarithmically transformed and used as the dependent variable. The analyses were adjusted for age, sex, primary kidney disease, dialysis modality, diabetes mellitus, cardiovascular disease and levels of calcium and phosphate. Since BMI is generally higher and PTH lower in diabetic patients as compared to non-diabetic patients, we investigated potential effect modification by the disease and repeated the analyses in strata of diabetes mellitus. Second, we performed longitudinal analyses of the relation between BMI and PTH. We calculated the relative change in BMI from 3 months (baseline) until the next available follow-up visit at 6months(BMI 6m /BMI baseline ). This time period was examined in line with the suggestions by an expert panel to assess clinically meaningful changes in weight [20]. Accordingly, we divided the patients into three categories: patients with a decreasing BMI 5%, patients with a stable BMI ± 5% and patients with an increasing BMI 5%. Similarly, we assessed the relative change in PTH from baseline (PTH 6m /PTH baseline ). Linear regression analyses were then used to assess the association of the change in BMI with the change in PTH and adjusted for the confounders mentioned above. Finally, we investigated the potential impact of this association on mortality in dialysis patients. Death rates according to the change in PTH from baseline (tertiles) were determined by Cox regression analyses, under consideration of changes in weight. In particular, we evaluated patients with decreasing PTH according to the presence or absence of weight loss. Hazard ratios (HR) and 95% confidence intervals (CI) were calculated for analyses, which were performed both univariately and adjusted for confounders. Additional adjustments were performed for the year of starting dialysis treatment, in order to take into account potential differences in therapy, which may arise with the long-term recruitment of patients into the study. Statistical analyses were performed with SPSS version Results Patients A total of 1916 patients with ESRD who started long-term dialysis were included and still participated in NECOSAD at 3 months after the initiation of dialysis therapy (baseline). Of the 1724 patients presenting with recorded height and weight, 1628 patients had measurements of PTH available at baseline and were included in the present analysis. Mean age of the patients was 59 ± 15 years, mean BMI was 24.7 ± 4.1 kg/m 2 andmedianpthwas13.0(iqr ) pmol/l. With higher BMI at baseline, more patients had diabetes and cardiovascular disease, and fewer patients had renal vascular diseases as primary kidney disease (Table 1). The percentage of male patients was smaller in underweight and in obese patients compared to patients with normal weight. Association of BMI with PTH Median PTH levels at baseline were lowest in underweight patients (10.2 pmol/l), followed by normal weight (12.1 pmol/l), overweight (14.0 pmol/l) and obese patients (17.5 pmol/l). The levels of PTH and BMI were correlated, both when used as continuous variables (both log transformed, Pearson correlation coefficient r =0.1,P< 0.001) and with BMI as a categorical variable (Spearman correlation coefficient r = 0.1, P < 0.001). The PTH levels as derived from adjusted linear regression analyses were significantly higher by 51% in obese patients and by 18% in overweight patients as compared to patients with normal weight. In line with this, PTH levels were 18% lower in underweight as compared to normal weight patients. Additional adjustments for the year of starting dialysis did not
3 1342 C. Drechsler et al. Table 1. Baseline patient characteristics, presented per BMI category; study population, n = 1628 BMI (kg/m 2 ) Characteristic Whole group < (n = 1628) (n = 153) (n = 819) (n = 499) (n = 157) Age (years) 59.5 (15.1) 54.4 (18.1) 59.5 (15.8) 61.0 (13.0) 59.9 (12.9) Gender (% men) Dialysis modality (% HD) BMI (kg/m 2 ) (1.0) 22.7 (1.4) 27.1 (1.4) 33.4 (3.3) Primary kidney disease Diabetes mellitus (%) Glomerulonephritis (%) Renal vascular disease (%) Comorbidity Diabetes mellitus a (%) Cardiovascular disease (%) Comorbidity Khan score Low (%) Intermediate (%) High (%) Systolic blood pressure (mm Hg) 149 (24) 146 (25) 149 (24) 150 (23) 151 (24) Diastolic blood pressure (mm Hg) 83 (13) 83 (15) 83 (14) 83 (13) 83 (13) Albumin (g/dl) 3.6 (0.5) 3.5 (0.6) 3.6 (0.5) 3.7 (0.5) 3.6 (0.5) Calcium (mmol/l) 2.4 (0.3) 2.4 (0.3) 2.4 (0.3) 2.4 (0.2) 2.4 (0.3) Phosphate (mmol/l) 1.8 (0.6) 1.8 (0.6) 1.8 (0.6) 1.8 (0.5) 1.8 (0.5) Values are presented as means (SD) or %. To convert serum cholesterol in mg/dl to mmol/l, multiply by ; albumin in g/dl to g/l, multiply by 10. Abbreviations: BMI = body mass index; HD = haemodialysis; BP = blood pressure. a Numbers include patients who have diabetes mellitus as their primary kidney disease. change the results. The associations were similar in the analyses stratified for diabetes mellitus, whereby overweight and obese patients with the disease generally had lower levels of PTH than patients without the disease. The levels of PTH and differences over the categories of BMI are shown in Table 2. Longitudinal changes of BMI and PTH Of all 1628 patients with available BMI and PTH at baseline, a total of 1437 had both measurements also available at the subsequent follow-up visit, taking place at 6 months Table 2. Baseline PTH and adjusted differences in PTH over categories of BMI, n = 1628 BMI (kg/m 2 ) after the initiation of dialysis. These were included in the longitudinal analyses. Median PTH at follow-up was 11.7 (IQR ) pmol/l, i.e. 90% of the median PTH level at baseline (13.0 pmol/l). The changes in PTH levels from baseline (ratio PTH 6m / baseline ) were significantly correlated with the changes in BMI from baseline, both when used as continuous variables (both log transformed; Pearson correlation coefficient r = 0.14, P < 0.001) and with BMI as a categorical variable (Spearman correlation coefficient r = 0.13, P < 0.001). In quantitative terms, patients with a stable BMI (ratio BMI 6m/baseline , group 1, n = 1197) showed stable PTH levels (median ratio PTH 6m / baseline < (n = 153) (n = 819) (n = 499) (n = 157) Whole study population Baseline PTH (IQR; pmol/l) 10.2 ( ) 12.1 ( ) 14.0 ( ) 17.5 ( ) Adjusted b difference in PTH 18% 0 a +18% +51% P-value <0.001 With diabetes mellitus Baseline PTH (IQR; pmol/l) 10.7 ( ) 12.5 ( ) 11.0 ( ) 15.6 ( ) Adjusted c difference in PTH % 15% 0 a +21% +35% P-value Without diabetes mellitus Baseline PTH (IQR; pmol/l) 10.0 ( ) 12.1 ( ) 16.0 ( ) 18.6 ( ) Adjusted c difference in PTH % 19% 0 a +17% +66% P-value <0.001 a Patients with a body mass index 20 and <25 were used as the reference group. b Adjustments were made for age, sex, primary kidney disease, dialysis modality, diabetes mellitus, cardiovascular disease calcium and phosphate levels. c Adjustments were made for age, sex, primary kidney disease, dialysis modality, cardiovascular disease calcium and phosphate levels.
4 Changes in PTH, BMI, and mortality in dialysis patients , IQR ). Compared to these patients, the adjusted PTH ratio for patients with a 5% decrease in BMI (group 2, n = 101) was significantly lower by 19% [PTH ratio group2-vs (95% CI 0.67; 0.99), P = 0.039], representing a meaningful decrease. Accordingly, the adjusted PTH ratio for patients with a 5% increase in BMI (group 3, n = 143) was markedly higher by 22% [PTH ratio group3-vs (95% CI 1.02; 1.44), P = 0.026], representing a significant increase. These ratios translate into absolute numbers by considering the change in PTH of the reference group (PTH 6m / baseline 0.91): a 5% decrease in BMI (n = 101) was accompanied by an adjusted 26% decrease in PTH (PTH 6m / baseline group2 = 0.81 * 0.91 = 0.74), whereas a 5% increase in BMI (n = 143) was associated with an 11% increase in PTH (PTH 6m / baseline group3 = 1.22 * 0.91 = 1.11) (Figure 1). In stratified analyses, patients with diabetes mellitus showed a decrease in median PTH levels from 12.7 (IQR ) pmol/l at baseline to 9.5 (IQR ) pmol/l at follow-up. In contrast, the median PTH levels in patients without diabetes mellitus did not meaningfully alter, being 13.0 (IQR ) pmol/l at baseline and 12.0 (IQR ) pmol/l at follow-up. The longitudinal associations between changes in BMI and PTH applied to both groups (diabetic and non-diabetic patients) and were more pronounced in diabetic patients (Figure 1). Regarding patients with diabetes mellitus, a 5% decrease in BMI was accompanied by an adjusted 48% decrease in PTH, whereas a 5% increase in BMI was associated with a 13% increase in PTH. The changes in PTH for non-diabetic patients were a 19% decrease (in the presence of weight loss) and a 10% increase (in the presence of weight gain), respectively. Fig. 1. Relative change in PTH levels (PTH 6m/baseline ) in groups of BMI change (decreasing/stable/increasing BMI). Mortality risks of changing BMI and PTH Patients were divided into tertiles according to the relative change in PTH from baseline (PTH 6m / baseline ). The tertiles corresponded to a PTH ratio of 0.64 (Tertile 1, n = 479), PTH ratio of > (Tertile 2, n = 479) and a PTH ratio >1.20 (Tertile 3, n = 479). The majority of the patients with significant weight loss (58 out of the 101 patients with a decrease in BMI 5%) were among the lowest tertile of PTH change. These patients were subgrouped separately. Compared to patients with stable PTH (Tertile 2), those with decreasing PTH in the presence of weight loss (n = 58) had a 2-fold increased mortality (HR 2.02, 95% CI ), while patients with decreasing PTH in the absence of weight loss (n = = 421) were not at increased risk of death (HR 0.94, 95% CI ) (Table 3 and Figure 2). The results persisted after multivariable adjustments and additional inclusion of the year of the start of dialysis into the analysis. Furthermore, we performed additional analyses to investigate the separate effects of weight loss and PTH decrease, allowing for further insight into why patients with both a decrease in PTH and BMI had an increased mortality. Four categories were formed and evaluated according to changes in BMI and/or PTH, whereby patients with stable or increasing PTH (Tertiles 2 and 3 of PTH change) were not differentiated due to the similar mortality risks in the previous analyses. The groups were (i) patients with neither decrease in BMI or PTH (PTH ratio Tertiles 2 and 3, no weight loss, n = 915, reference), (ii) only a decrease in BMI (PTH ratio Tertiles 2 and 3, presence of weight loss, n = 43), (iii) only a decrease in PTH (PTH ratio Tertile 1, no weight loss, n = 421) and (iv) both a decrease in BMI and PTH (PTH ratio Tertile 1, presence of weight loss, n = 58). Compared to the reference group 1, patients with both a decrease in BMI and PTH (group 4) had similar mortality risks to the patients with only a decrease in BMI (group 2). The hazard ratios were 2.17 ( ) and 2.05 ( ), respectively, partly attenuating after multivariable adjustments [1.55 ( ) and 1.91 ( )]. In contrast, patients with only a decrease in PTH (group 3) were not at increased risk of death [HR adjusted 0.95 ( )]. Discussion In this prospective cohort study of incident dialysis patients, BMI was associated with PTH at baseline. Underweight patients had the lowest levels of PTH, followed by normal weight, overweight and obese patients. Furthermore, longitudinal changes in BMI over 3 months of follow-up were paralleled by longitudinal changes in PTH. Weight loss during follow-up was accompanied by decreases in PTH, while weight gain resulted in increases of PTH. Considering decreases in PTH, the relation with BMI strongly affected the outcome: compared to patients with stable PTH levels, patients with decreasing PTH associated with weight loss had a >2-fold higher risk of death, while those with decreasing PTH in the absence of weight loss did not. Additional analyses showed that the weight loss was responsible for increased deaths. Obesity has been shown to be a risk factor for secondary hyperparathyroidism in the general population [16]. Similarly, a higher BMI was found to be associated with higher PTH levels in men with CKD not yet on dialysis [19]. In line with this, our study extends the previous findings, showing that the association of high BMI with PTH also holds true for the dialysis population and in particular applies to both diabetic and non-diabetic patients. This is important, as diabetic patients usually present with higher
5 1344 C. Drechsler et al. Table 3. Mortality (hazard ratio and 95% CI) according to the change in PTH from baseline, n = 1437 Tertiles of PTH change (ratio PTH 6m/baseline ) Model Tertile PTH ratio 0.64 n = 479 Tertile 2 Tertile 3 PTH ratio > PTH ratio >1.20 n = 479 n = 479 Crude 1.04 ( ) P = a 0.92 ( ) P = 0.44 Adjusted b 1.02 ( ) P = a 1.09 ( ) P = 0.42 With weight loss n = 58 Without weight loss n = 421 Crude 2.02 ( ) P < ( ) P = a 0.92 ( ) P = 0.44 Adjusted b 1.54 ( ) P = ( ) P = a 1.08 ( ) P = 0.47 a Patients with a PTH ratio > were used as the reference group. b Adjustments were made for age, sex, primary kidney disease, dialysis modality, diabetes mellitus, cardiovascular disease, calcium and phosphate levels. weight but lower PTH levels than non-diabetic patients [22]. Our findings therefore show that weight similarly relates to PTH in both patient groups and does not play a Fig. 2. (A) Kaplan Meier curves for all-cause mortality in tertiles of the relative change in PTH from baseline (PTH 6m/baseline ). Tertile 1 = decreasing PTH (PTH ratio 0.64, n =479);Tertile2=stablePTH (PTH ratio > , n = 479); Tertile 3 = increasing PTH (PTH ratio >1.20, n = 479). (B) Kaplan Meier curves for all-cause mortality in tertiles of the relative change in PTH from baseline (PTH 6m/baseline ), differentiating the Tertile 1 with decreasing PTH levels according to the presence or absence of weight loss. Tertile 1 = decreasing PTH and presence of weight loss (n = 58); Tertile 1 = decreasing PTH and absence of weight loss (n = 421); Tertile 2 = stable PTH (n = 479); Tertile 3 = increasing PTH (n = 479). major role in explaining the differences in PTH levels between diabetic and non-diabetic patients. The mechanisms underlying the association between BMI and PTH are not yet known in detail. One possible link may be 25 (OH) vitamin D levels, which were shown to be lower in persons with higher BMI in the general population [16,18,23 25]. Patients with a high BMI possibly experience less sun exposure due to lower mobility and clothing habits, leading to a lower bioavailability of vitamin D [25,26]. In addition, obesity potentially results in a higher storage of vitamin D in adipose tissue, further contributing to lower circulating levels of vitamin D. In this context, one study measuring body composition by dual-energy X-ray absorptiometry showed that total body fat is even better than BMI when related to hyperparathyroidism, suggesting that fat cells play a main role for vitamin D availability [18]. Finally, a higher body weight may impose a greater strain on the skeleton, potentially resulting in decreased skeletal responses to the actions of PTH [16]. This, in turn, may lead to compensatory higher PTH levels. Furthermore, we showed that underweight was related to low PTH levels and that weight loss was paralleled by a decrease in PTH. These data extend results from prior studies in the general population, where weight loss achieved by intestinal bypass surgery in obese people was shown to lower their PTH levels [27]. Importantly, this present observation in renal patients may provide a link to explain why low levels of PTH were related to an increased mortality in some previous studies of dialysis patients [13 15]. In contrast to intentional weight loss in the studies of the general population [27], partly achieved by dietary or surgical interventions, weight loss in patients with CKD most likely occurs unintentionally in the context of wasting. Wasting is common in patients with CKD or ESRD and represents a severe and complex process of muscle loss, poor food intake, inflammation and the development of comorbidities. The decrease in PTH, accompanying the weight loss, may be interpreted as a symptom of an underlying illness (wasting), which is associated with a high mortality [28]. In the additional analyses, we found that compared to the patients with neither decrease in BMI nor PTH, those with both a decrease in PTH and BMI had a 2-fold increased risk of death, which was similar to those with only a decrease in BMI. The results therefore
6 Changes in PTH, BMI, and mortality in dialysis patients 1345 suggest that the weight loss was mainly responsible for the increased mortality in patients with concurrent decreases in PTH and BMI. Thus, decreasing levels of PTH that are potentially found to be linked to an increased mortality may in the presence of weight loss represent a surrogate of the wasting process, which is responsible for the increased deaths. The link between wasting and PTH has also been proposed by one recent study finding different mortality risks according to levels of PTH before and after adjustments of markers of the wasting syndrome [29]. Our analyses extend the current knowledge by particularly considering longitudinal changes. We believe that the findings are important for any future studies investigating relations of PTH with mortality, as the BMI and its changes should be taken into account. This can particularly be supported by the fact that weight loss largely explained the increased death of patients with the combined decrease in PTH and BMI. Thus, decreasing levels of PTH linked to a high rate of death may in the presence of weight loss represent a surrogate of the wasting process [30]. This proposed link between wasting and low and decreasing PTH levels can be supported by further evidence. Wasting was found to be associated with adynamic bone disease [11,12,31,32]. Furthermore, inflammation, which often accompanies the wasting syndrome, has, in vitro, been shown to suppress PTH [33,34]. Finally, leptin, as a key anorexigenic hormone potentially involved in wasting, was shown to have antiosteogenic properties and to decrease bone mass [35]. While decreases in PTH may be warranted in the context of intentional interventions, e.g. by medication, decreasing PTH can also occur in different circumstances. Our study shows that for the evaluation and treatment of bone metabolism in dialysis patients, it is therefore especially important to consider nutritional status among the reasons for decreases in PTH. These may completely differently relate to outcome, depending on the circumstances, such as the concurrent presence or absence of weight loss. Potential limitations of our study need to be acknowledged. We did not have information on vitamin D levels, which may potentially provide further insight into the mechanisms underlying the associations seen. The measurements of PTH were not centrally performed but by various first-generation immunometric PTH assays depending on the different participating centres. With central measurements, the associations could even have been stronger. Despite the measurements in several laboratories, however, we still were able to detect the presented effects. Finally, due to the observational design, causality cannot be inferred. The strengths of this study include the favourable design of incident dialysis patients reducing selection, the high number of participants and the longitudinal measures of BMI and PTH. Conclusion In conclusion, PTH is associated with BMI and its longitudinal changes in dialysis patients, both in patients with and without diabetes mellitus. Weight loss during followup was accompanied by decreases in PTH, while weight gain resulted in increases in PTH. An increased mortality seen for patients with concurrent decreases in PTH and BMI was explained by the weight loss, representing an important confounder for outcome analyses according to levels of PTH. Low and decreasing PTH levels may be symptoms of wasting, which should be taken into account in the care of dialysis patients. Acknowledgements. C.D. is grateful to the ERA EDTA for the support with a research fellowship. We thank the investigators and study nurses of the participating dialysis centres and the data managers of the NECOSAD study for collection and management of the data. NECOSAD study investigators include Apperloo AJ, Bijlsma JA, Boekhout M, Boer WH, Büller HR, de Charro FTH, de Fijter CWH, Doorenbos CJ, Fagel WJ, Feith GW, Frenken LAM, Gerlag PGG, Gorgels JPMC, Grave W, Huisman RM, Jager KJ, Jie K, Koning-Mulder WAH, Koolen MI, Kremer Hovinga TK, Lavrijssen ATJ, Luik AJ, Parlevliet KJ, Raasveld MHM, Schonck MJM, Schuurmans MMJ, Siegert CEH, Stegeman CA, Stevens P, Thijssen JGP, Valentijn RM, van Buren M, van den Dorpel MA, van der Boog PJM, van der Meulen J, van der Sande FM, van Es A, van Geelen JACA, Vastenburg GH, Verburgh CA, Vincent HH and Vos PF. Conflict of interest statement. None declared. References 1. De Boer I, Gorodetskaya I, Young B et al. The severity of secondary hyperparathyroidism in chronic renal insufficiency is GFR-dependent, race-dependent, and associated with cardiovascular disease. J Am Soc Nephrol 2002; 13: Fajtova VT, Sayegh MH, Hickey N et al. Intact parathyroid hormone levels in renal insufficiency. Calcif Tissue Int 1995; 57: Levin A, Bakris GL, Molitch M et al. Prevalence of abnormal serum vitamin D, PTH, calcium, and phosphorus in patients with chronic kidney disease: results of the study to evaluate early kidney disease. Kidney Int 2007; 71: Martinez I, Saracho R, Montenegro J et al. The importance of dietary calcium and phosphorous in the secondary hyperparathyroidism of patients with early renal failure. Am J Kidney Dis 1997; 29: Pitts TO, Piraino BH, Mitro R et al. Hyperparathyroidism and 1,25- dihydroxyvitamin D deficiency in mild, moderate, and severe renal failure. J Clin Endocrinol Metab 1988; 67: Noordzij M, Boeschoten EW, Bos WJ et al. Disturbed mineral metabolism is associated with muscle and skin complaints in a prospective cohort of dialysis patients. Nephrol Dial Transplant 2007; 22: Block GA, Klassen PS, Lazarus JM et al. Mineral metabolism, mortality, and morbidity in maintenance hemodialysis. J Am Soc Nephrol 2004; 15: Melamed ML, Eustace JA, Plantinga L et al. Changes in serum calcium, phosphate, and PTH and the risk of death in incident dialysis patients: a longitudinal study. Kidney Int 2006; 70: Tentori F, Blayney MJ, Albert JM et al. Mortality risk for dialysis patients with different levels of serum calcium, phosphorus, and PTH: the Dialysis Outcomes and Practice Patterns Study (DOPPS). Am J Kidney Dis 2008; 52: Young EW, Albert JM, Satayathum S et al. Predictors and consequences of altered mineral metabolism: the Dialysis Outcomes and Practice Patterns Study. Kidney Int 2005; 67: Coen G, Ballanti P, Bonucci E et al. Bone markers in the diagnosis of low turnover osteodystrophy in haemodialysis patients. Nephrol Dial Transplant 1998; 13: Sherrard DJ, Hercz G, Pei Y et al. The spectrum of bone disease in end-stage renal failure an evolving disorder. Kidney Int 1993; 43:
7 1346 A. Kirkpantur et al. 13. Avram MM, Sreedhara R, Avram DK et al. Enrollment parathyroid hormone level is a new marker of survival in hemodialysis and peritoneal dialysis therapy for uremia. Am J Kidney Dis 1996; 28: Avram MM, Mittman N, Myint MM et al. Importance of low serum intact parathyroid hormone as a predictor of mortality in hemodialysis and peritoneal dialysis patients: 14 years of prospective observation. Am J Kidney Dis 2001; 38: Guh JY, Chen HC, Chuang HY et al. Risk factors and risk for mortality of mild hypoparathyroidism in hemodialysis patients. Am J Kidney Dis 2002; 39: Bell NH, Epstein S, Greene A et al. Evidence for alteration of the vitamin D-endocrine system in obese subjects. J Clin Invest 1985; 76: Bolland MJ, Grey AB, Gamble GD et al. Association between primary hyperparathyroidism and increased body weight: a metaanalysis. J Clin Endocrinol Metab 2005; 90: Snijder MB, van Dam RM, Visser M et al. Adiposity in relation to vitamin D status and parathyroid hormone levels: a population-based study in older men and women. J Clin Endocrinol Metab 2005; 90: Kovesdy CP, Ahmadzadeh S, Anderson JE et al. Obesity is associated with secondary hyperparathyroidism in men with moderate and severe chronic kidney disease. Clin J Am Soc Nephrol 2007; 2: Fouque D, Kalantar-Zadeh K, Kopple J et al. A proposed nomenclature and diagnostic criteria for protein-energy wasting in acute and chronic kidney disease. Kidney Int 2008; 73: de Mutsert R, Snijder MB, van der Sman-de Beer F et al. Association between body mass index and mortality is similar in the hemodialysis population and the general population at high age and equal duration of follow-up. J Am Soc Nephrol 2007; 18: Avram MM. Lower parathyroid hormone and creatinine in diabetic uremia. Contrib Nephrol 1980; 20: Kamycheva E, Sundsfjord J, Jorde R. Serum parathyroid hormone level is associated with body mass index. The 5th Tromso study. Eur J Endocrinol 2004; 151: Nephrol Dial Transplant (2011) 26: doi: /ndt/gfq539 Advance Access publication 2 September Parikh SJ, Edelman M, Uwaifo GI et al. The relationship between obesity and serum 1,25-dihydroxy vitamin D concentrations in healthy adults. J Clin Endocrinol Metab 2004; 89: Wortsman J, Matsuoka LY, Chen TC et al. Decreased bioavailability of vitamin D in obesity. Am J Clin Nutr 2000; 72: Liel Y, Ulmer E, Shary J et al. Low circulating vitamin D in obesity. Calcif Tissue Int 1988; 43: Olmos JM, Vazquez LA, Amado JA et al. Mineral metabolism in obese patients following vertical banded gastroplasty. Obes Surg 2008; 18: de Mutsert R, Grootendorst DC, Boeschoten EWet al. Subjective global assessment of nutritional status is strongly associated with mortality in chronic dialysis patients. Am J Clin Nutr 2009; 89: Dukkipati R, Kovesdy CP, Colman S et al. Association of relatively low serum parathyroid hormone with malnutrition-inflammation complex and survival in maintenance hemodialysis patients. J Ren Nutr 2010; 20: Drechsler C, Krane V, Grootendorst DC et al. The association between parathyroid hormone and mortality in dialysis patients is modified by wasting. Nephrol Dial Transplant 2009; 24: Andress DL. Adynamic bone in patients with chronic kidney disease. Kidney Int 2008; 73: Sanchez-Gonzalez MC, Lopez-Barea F, Bajo MA et al. Serum albumin levels, an additional factor implicated in hyperparathyroidism outcome in peritoneal dialysis: a prospective study with paired bone biopsies. Adv Perit Dial 2006; 22: Carlstedt E, Ridefelt P, Lind L et al. Interleukin-6 induced suppression of bovine parathyroid hormone secretion. Biosci Rep 1999; 19: Nielsen PK, Rasmussen AK, Butters R et al. Inhibition of PTH secretion by interleukin-1 beta in bovine parathyroid glands in vitro is associated with an up-regulation of the calcium-sensing receptor mrna. Biochem Biophys Res Commun 1997; 238: Elefteriou F, Takeda S, Ebihara K et al. Serum leptin level is a regulator of bone mass. Proc Natl Acad Sci USA 2004; 101: Received for publication: ; Accepted in revised form: Serum fibroblast growth factor-23 (FGF-23) levels are independently associated with left ventricular mass and myocardial performance index in maintenance haemodialysis patients Alper Kirkpantur 1, Mustafa Balci 2, Oguz Alp Gurbuz 3, Baris Afsar 4, Basol Canbakan 1, Ramazan Akdemir 2 and Mehmet Deniz Ayli 1 1 Nephrology, Ministry of Health, Diskapi Training and Research Hospital, Ankara, Turkey, 2 Cardiology, Ministry of Health, Diskapi Training and Research Hospital, Ankara, Turkey, 3 Infectious Diseases, Ministry of Health, Diskapi Training and Research Hospital, Ankara, Turkey and 4 Nephrology, Ministry of Health, Zonguldak Training and Research Hospital, Zonguldak, Turkey Correspondence and offprint requests to: Alper Kirkpantur; alperkirkpantur@yahoo.com Abstract Background. Fibroblast growth factor-23 (FGF-23) is a phosphorus-regulating substance. Circulating FGF-23 levels increase markedly in dialysis patients and are independently associated with increased risk of mortality. Given the fact that cardiovascular disease is the leading The Author Published by Oxford University Press on behalf of ERA-EDTA. All rights reserved. For Permissions, please journals.permissions@oxfordjournals.org
Muscle mass depletion and weight loss are associated with increased mortality in hemodialysis patients, independent of body mass index
 4 Muscle mass depletion and weight loss are associated with increased mortality in hemodialysis patients, independent of body mass index R. de Mutsert D.C. Grootendorst E.W. Boeschoten R.T. Krediet S.
4 Muscle mass depletion and weight loss are associated with increased mortality in hemodialysis patients, independent of body mass index R. de Mutsert D.C. Grootendorst E.W. Boeschoten R.T. Krediet S.
A positive effect of AII inhibitors on peritoneal membrane function in long-term PD patients
 Nephrol Dial Transplant (2009) 24: 272 277 doi: 10.1093/ndt/gfn421 Advance Access publication 30 July 2008 Original Article A positive effect of AII inhibitors on peritoneal membrane function in long-term
Nephrol Dial Transplant (2009) 24: 272 277 doi: 10.1093/ndt/gfn421 Advance Access publication 30 July 2008 Original Article A positive effect of AII inhibitors on peritoneal membrane function in long-term
Similar Survival on Automated Peritoneal Dialysis and Continuous Ambulatory Peritoneal Dialysis in a Large Prospective Cohort
 Similar Survival on Automated Peritoneal Dialysis and Continuous Ambulatory Peritoneal Dialysis in a Large Prospective Cohort Wieneke Marleen Michels,* Marion Verduijn, Elisabeth Wilhelmina Boeschoten,
Similar Survival on Automated Peritoneal Dialysis and Continuous Ambulatory Peritoneal Dialysis in a Large Prospective Cohort Wieneke Marleen Michels,* Marion Verduijn, Elisabeth Wilhelmina Boeschoten,
Effects of Diabetes Mellitus, Age, and Duration of Dialysis on Parathormone in Chronic Hemodialysis Patients. Hamid Nasri 1, Soleiman Kheiri 2
 Saudi J Kidney Dis Transplant 2008;19(4):608-613 2008 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Original Article Effects of Diabetes Mellitus, Age, and
Saudi J Kidney Dis Transplant 2008;19(4):608-613 2008 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Original Article Effects of Diabetes Mellitus, Age, and
Time trends in initiation and dose of dialysis in end-stage renal disease patients in The Netherlands
 Nephrol Dial Transplant (2003) 18: 552 558 Original Article Time trends in initiation and dose of dialysis in end-stage renal disease patients in The Netherlands Fabian Termorshuizen 1, Johanna C. Korevaar
Nephrol Dial Transplant (2003) 18: 552 558 Original Article Time trends in initiation and dose of dialysis in end-stage renal disease patients in The Netherlands Fabian Termorshuizen 1, Johanna C. Korevaar
Renal Association Clinical Practice Guideline in Mineral and Bone Disorders in CKD
 Nephron Clin Pract 2011;118(suppl 1):c145 c152 DOI: 10.1159/000328066 Received: May 24, 2010 Accepted: December 6, 2010 Published online: May 6, 2011 Renal Association Clinical Practice Guideline in Mineral
Nephron Clin Pract 2011;118(suppl 1):c145 c152 DOI: 10.1159/000328066 Received: May 24, 2010 Accepted: December 6, 2010 Published online: May 6, 2011 Renal Association Clinical Practice Guideline in Mineral
Glycaemic control and serum intact parathyroid hormone levels in diabetic patients on haemodialysis therapy
 Nephrol Dial Transplant (2008) 23: 315 320 doi: 10.1093/ndt/gfm639 Advance Access publication 23 October 2007 Original Article Glycaemic control and serum intact parathyroid hormone levels in diabetic
Nephrol Dial Transplant (2008) 23: 315 320 doi: 10.1093/ndt/gfm639 Advance Access publication 23 October 2007 Original Article Glycaemic control and serum intact parathyroid hormone levels in diabetic
The CARI Guidelines Caring for Australasians with Renal Impairment. Biochemical Targets. Calcium GUIDELINES
 Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Biochemical Targets CARMEL HAWLEY (Woolloongabba, Queensland) GRAHAME ELDER (Westmead, New South Wales) Calcium GUIDELINES
Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Biochemical Targets CARMEL HAWLEY (Woolloongabba, Queensland) GRAHAME ELDER (Westmead, New South Wales) Calcium GUIDELINES
Improvement in Pittsburgh Symptom Score Index After Initiation of Peritoneal Dialysis
 Advances in Peritoneal Dialysis, Vol. 24, 2008 Matthew J. Novak, 1 Heena Sheth, 2 Filitsa H. Bender, 1 Linda Fried, 1,3 Beth Piraino 1 Improvement in Pittsburgh Symptom Score Index After Initiation of
Advances in Peritoneal Dialysis, Vol. 24, 2008 Matthew J. Novak, 1 Heena Sheth, 2 Filitsa H. Bender, 1 Linda Fried, 1,3 Beth Piraino 1 Improvement in Pittsburgh Symptom Score Index After Initiation of
Introduction/objective: Adinamic bone disease (ABD) is a common finding in peritoneal. dialysis (PD) and is associated with a
 Original Article Low-calcium peritoneal dialysis solution is effective in bringing PTH levels to the range recommended by current guidelines in patients with PTH levels < 150 pg/dl Authors Thyago Proença
Original Article Low-calcium peritoneal dialysis solution is effective in bringing PTH levels to the range recommended by current guidelines in patients with PTH levels < 150 pg/dl Authors Thyago Proença
( ) , (Donabedian, 1980) We would not choose any treatment with poor outcomes
 ..., 2013 Amgen. 1 ? ( ), (Donabedian, 1980) We would not choose any treatment with poor outcomes 1. :, 2. ( ): 3. :.,,, 4. :, [Biomarkers Definitions Working Group, 2001]., (William M. Bennet, Nefrol
..., 2013 Amgen. 1 ? ( ), (Donabedian, 1980) We would not choose any treatment with poor outcomes 1. :, 2. ( ): 3. :.,,, 4. :, [Biomarkers Definitions Working Group, 2001]., (William M. Bennet, Nefrol
Peritoneal Dialysis Adequacy: Not Just Small- Solute Clearance
 Advances in Peritoneal Dialysis, Vol. 24, 2008 Rajesh Yalavarthy, Isaac Teitelbaum Peritoneal Dialysis Adequacy: Not Just Small- Solute Clearance Two indices of small-solute clearance, Kt/V urea and creatinine
Advances in Peritoneal Dialysis, Vol. 24, 2008 Rajesh Yalavarthy, Isaac Teitelbaum Peritoneal Dialysis Adequacy: Not Just Small- Solute Clearance Two indices of small-solute clearance, Kt/V urea and creatinine
The CARI Guidelines Caring for Australasians with Renal Impairment. Serum phosphate GUIDELINES
 Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Serum phosphate GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions
Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Serum phosphate GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions
Excess mortality due to interaction between proteinenergy wasting, inflammation and cardiovascular disease in chronic dialysis patients
 7 Excess mortality due to interaction between proteinenergy wasting, inflammation and cardiovascular disease in chronic dialysis patients R. de Mutsert D.C. Grootendorst J. Axelsson E.W. Boeschoten R.T.
7 Excess mortality due to interaction between proteinenergy wasting, inflammation and cardiovascular disease in chronic dialysis patients R. de Mutsert D.C. Grootendorst J. Axelsson E.W. Boeschoten R.T.
HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE ON MAINTENANCE DIALYSIS THERAPY
 UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
Social support predicts survival in dialysis patients
 Nephrol Dial Transplant (2007) 22: 845 850 doi:10.1093/ndt/gfl700 Advance Access publication 12 December 2006 Original Article Social support predicts survival in dialysis patients Melissa S. Y. Thong
Nephrol Dial Transplant (2007) 22: 845 850 doi:10.1093/ndt/gfl700 Advance Access publication 12 December 2006 Original Article Social support predicts survival in dialysis patients Melissa S. Y. Thong
CLINICAL PRACTICE GUIDELINE CKD-MINERAL AND BONE DISORDERS (CKD-MBD) Final Version (01/03/2015)
 CLINICAL PRACTICE GUIDELINE CKD-MINERAL AND BONE DISORDERS (CKD-MBD) Final Version (01/03/2015) Dr Simon Steddon, Consultant Nephrologist, Guy s and St Thomas NHS Foundation Trust, London Dr Edward Sharples,
CLINICAL PRACTICE GUIDELINE CKD-MINERAL AND BONE DISORDERS (CKD-MBD) Final Version (01/03/2015) Dr Simon Steddon, Consultant Nephrologist, Guy s and St Thomas NHS Foundation Trust, London Dr Edward Sharples,
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Aspetti nutrizionali nel paziente in emodialisi cronica
 Aspetti nutrizionali nel paziente in emodialisi cronica Enrico Fiaccadori enrico.fiaccadori@unipr.it Università degli Studi di Parma Agenda Diagnosis of protein-energy wasting (PEW) in ESRD on HD Epidemiology
Aspetti nutrizionali nel paziente in emodialisi cronica Enrico Fiaccadori enrico.fiaccadori@unipr.it Università degli Studi di Parma Agenda Diagnosis of protein-energy wasting (PEW) in ESRD on HD Epidemiology
Calcium x phosphate product
 Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Calcium x phosphate product GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL
Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Calcium x phosphate product GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL
TO EAT OR NOT TO EAT DURING HEMODIALYSIS TREATMENT?
 TO EAT OR NOT TO EAT DURING HEMODIALYSIS TREATMENT? Rana G. Rizk, PhD, MPH, LD Maastricht University, The Netherlands November, 2017 Learning objectives Review the evidence behind benefits and concerns
TO EAT OR NOT TO EAT DURING HEMODIALYSIS TREATMENT? Rana G. Rizk, PhD, MPH, LD Maastricht University, The Netherlands November, 2017 Learning objectives Review the evidence behind benefits and concerns
Malnutrition and inflammation in peritoneal dialysis patients
 Kidney International, Vol. 64, Supplement 87 (2003), pp. S87 S91 Malnutrition and inflammation in peritoneal dialysis patients PAUL A. FEIN, NEAL MITTMAN, RAJDEEP GADH, JYOTIPRAKAS CHATTOPADHYAY, DANIEL
Kidney International, Vol. 64, Supplement 87 (2003), pp. S87 S91 Malnutrition and inflammation in peritoneal dialysis patients PAUL A. FEIN, NEAL MITTMAN, RAJDEEP GADH, JYOTIPRAKAS CHATTOPADHYAY, DANIEL
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
Therapeutic golas in the treatment of CKD-MBD
 Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
PART ONE. Peritoneal Kinetics and Anatomy
 PART ONE Peritoneal Kinetics and Anatomy Advances in Peritoneal Dialysis, Vol. 22, 2006 Paul A. Fein, Irfan Fazil, Muhammad A. Rafiq, Teresa Schloth, Betty Matza, Jyotiprakas Chattopadhyay, Morrell M.
PART ONE Peritoneal Kinetics and Anatomy Advances in Peritoneal Dialysis, Vol. 22, 2006 Paul A. Fein, Irfan Fazil, Muhammad A. Rafiq, Teresa Schloth, Betty Matza, Jyotiprakas Chattopadhyay, Morrell M.
White Rose Research Online URL for this paper: Version: Accepted Version
 This is a repository copy of Effect on mortality of elective parathyroid surgery in one hundred and three patients with chronic kidney disease : our experience. White Rose Research Online URL for this
This is a repository copy of Effect on mortality of elective parathyroid surgery in one hundred and three patients with chronic kidney disease : our experience. White Rose Research Online URL for this
How is the dialysis patient different?
 How is the dialysis patient different? Mihály Tapolyai, MD, FASN, FACP Fresenius Medical Care SOTE, Budapest; Hungary Minneapolis VAMC, Minneapolis, MN; USA How is the dialysis patient different? Dialysis
How is the dialysis patient different? Mihály Tapolyai, MD, FASN, FACP Fresenius Medical Care SOTE, Budapest; Hungary Minneapolis VAMC, Minneapolis, MN; USA How is the dialysis patient different? Dialysis
Magnetic resonance imaging, image analysis:visual scoring of white matter
 Supplemental method ULSAM Magnetic resonance imaging, image analysis:visual scoring of white matter hyperintensities (WMHI) was performed by a neuroradiologist using a PACS system blinded of baseline data.
Supplemental method ULSAM Magnetic resonance imaging, image analysis:visual scoring of white matter hyperintensities (WMHI) was performed by a neuroradiologist using a PACS system blinded of baseline data.
1. Reggie J. Divina, M.D. (1) 2. Fe S. Felicilda, M.D., DPBCN (1,2) 3. Rufino E. Chan, M.D. (1) 4. Luisito O. Llido, M.D.
 82 TITLE: Nutritional status of hemodialysis patients in the Philippines: a cross sectional survey in four out- patient dialysis centers Submitted: January 10, 2010 Posted: August 30, 2010 AUTHOR(S) 1.
82 TITLE: Nutritional status of hemodialysis patients in the Philippines: a cross sectional survey in four out- patient dialysis centers Submitted: January 10, 2010 Posted: August 30, 2010 AUTHOR(S) 1.
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
Improved survival of type 2 diabetic patients on renal replacement therapy in Finland
 Nephrol Dial Transplant (2010) 25: 892 896 doi: 10.1093/ndt/gfp555 Advance Access publication 21 October 2009 Improved survival of type 2 diabetic patients on renal replacement therapy in Finland Marjo
Nephrol Dial Transplant (2010) 25: 892 896 doi: 10.1093/ndt/gfp555 Advance Access publication 21 October 2009 Improved survival of type 2 diabetic patients on renal replacement therapy in Finland Marjo
S150 KEEP Analytical Methods. American Journal of Kidney Diseases, Vol 55, No 3, Suppl 2, 2010:pp S150-S153
 S150 KEEP 2009 Analytical Methods American Journal of Kidney Diseases, Vol 55, No 3, Suppl 2, 2010:pp S150-S153 S151 The Kidney Early Evaluation program (KEEP) is a free, communitybased health screening
S150 KEEP 2009 Analytical Methods American Journal of Kidney Diseases, Vol 55, No 3, Suppl 2, 2010:pp S150-S153 S151 The Kidney Early Evaluation program (KEEP) is a free, communitybased health screening
Analytical Methods: the Kidney Early Evaluation Program (KEEP) The Kidney Early Evaluation program (KEEP) is a free, community based health
 Analytical Methods: the Kidney Early Evaluation Program (KEEP) 2000 2006 Database Design and Study Participants The Kidney Early Evaluation program (KEEP) is a free, community based health screening program
Analytical Methods: the Kidney Early Evaluation Program (KEEP) 2000 2006 Database Design and Study Participants The Kidney Early Evaluation program (KEEP) is a free, community based health screening program
Setting the standard
 SCLEROSTIN in NEPHROLOGY MOST REFERENCED OPTIMIZED FOR CLINICAL SAMPLES Setting the standard for clinical research. SCLEROSTIN A BONE-RELATED PROTEIN URINE PROTOCOL AVAILABLE Sclerostin ELISA - Assay Characteristics
SCLEROSTIN in NEPHROLOGY MOST REFERENCED OPTIMIZED FOR CLINICAL SAMPLES Setting the standard for clinical research. SCLEROSTIN A BONE-RELATED PROTEIN URINE PROTOCOL AVAILABLE Sclerostin ELISA - Assay Characteristics
Predictive Factors for Withdrawal from Peritoneal Dialysis: A Retrospective Cohort Study at Two Centers in Japan
 Advances in Peritoneal Dialysis, Vol. 33, 2017 Yasuhiro Taki, 1 Tsutomu Sakurada, 2 Kenichiro Koitabashi, 2 Naohiko Imai, 1 Yugo Shibagaki 2 Predictive Factors for Withdrawal from Peritoneal Dialysis:
Advances in Peritoneal Dialysis, Vol. 33, 2017 Yasuhiro Taki, 1 Tsutomu Sakurada, 2 Kenichiro Koitabashi, 2 Naohiko Imai, 1 Yugo Shibagaki 2 Predictive Factors for Withdrawal from Peritoneal Dialysis:
Secondary Hyperparathyroidism: Where are we now?
 Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Mehruba Alam Ananna, Wasim Md. Mohosin Ul Haque, Muhammad Abdur Rahim, Tufayel Ahmed Chowdhury, Tabassum Samad, Md. Mostarshid Billah, Sarwar Iqbal
 Original Article Correlation of serum intact parathyroid hormone and alkaline phosphatase in diabetic chronic kidney disease stage 3 to 5 patients with mineral bone disorders Mehruba Alam Ananna, Wasim
Original Article Correlation of serum intact parathyroid hormone and alkaline phosphatase in diabetic chronic kidney disease stage 3 to 5 patients with mineral bone disorders Mehruba Alam Ananna, Wasim
Nutrition and Renal Disease Update
 Nutrition and Renal Disease Update Denis FOUQUE Department of Nephrology Centre de Recherche en Nutrition Humaine University Claude Bernard Lyon - France What have we learned? 1. Chronic kidney disease:
Nutrition and Renal Disease Update Denis FOUQUE Department of Nephrology Centre de Recherche en Nutrition Humaine University Claude Bernard Lyon - France What have we learned? 1. Chronic kidney disease:
Prevalence of malnutrition in dialysis
 ESPEN Congress Cannes 2003 Organised by the Israel Society for Clinical Nutrition Education and Clinical Practice Programme Session: Nutrition and the Kidney Malnutrition and Haemodialysis Doctor Noël
ESPEN Congress Cannes 2003 Organised by the Israel Society for Clinical Nutrition Education and Clinical Practice Programme Session: Nutrition and the Kidney Malnutrition and Haemodialysis Doctor Noël
Effects of Body Size and Body Composition on Survival in Hemodialysis Patients
 J Am Soc Nephrol 14: 2366 2372, 2003 Effects of Body Size and Body Composition on Survival in Hemodialysis Patients SRINIVASAN BEDDHU,* LISA M. PAPPAS, NIRUPAMA RAMKUMAR, and MATTHEW SAMORE *Renal Section,
J Am Soc Nephrol 14: 2366 2372, 2003 Effects of Body Size and Body Composition on Survival in Hemodialysis Patients SRINIVASAN BEDDHU,* LISA M. PAPPAS, NIRUPAMA RAMKUMAR, and MATTHEW SAMORE *Renal Section,
The Parsabiv Beginner s Book
 The Parsabiv Beginner s Book A quick guide to help you learn about your treatment with Parsabiv and what to expect Indication Parsabiv (etelcalcetide) is indicated for the treatment of secondary hyperparathyroidism
The Parsabiv Beginner s Book A quick guide to help you learn about your treatment with Parsabiv and what to expect Indication Parsabiv (etelcalcetide) is indicated for the treatment of secondary hyperparathyroidism
Assessment of Osteoporosis Risk Factors in Low Socioeconomic Status Hemodialysis Patients in Jeddah
 World Journal of Medical Sciences 1 (4): 438-443, 015 ISSN 1817-3055 IDOSI Publications, 015 DOI: 10.589/idosi.wjms.015.1.4.1154 Assessment of Osteoporosis Risk Factors in Low Socioeconomic Status Hemodialysis
World Journal of Medical Sciences 1 (4): 438-443, 015 ISSN 1817-3055 IDOSI Publications, 015 DOI: 10.589/idosi.wjms.015.1.4.1154 Assessment of Osteoporosis Risk Factors in Low Socioeconomic Status Hemodialysis
Individual Study Table Referring to Part of Dossier: Volume: Page:
 Synopsis Abbott Laboratories Name of Study Drug: Paricalcitol Capsules (ABT-358) (Zemplar ) Name of Active Ingredient: Paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For
Synopsis Abbott Laboratories Name of Study Drug: Paricalcitol Capsules (ABT-358) (Zemplar ) Name of Active Ingredient: Paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For
Vitamin D supplementation of professionally active adults
 Vitamin D supplementation of professionally active adults VITAMIN D MINIMUM, MAXIMUM, OPTIMUM FRIDAY, SEPTEMBER 22 ND 2017 Samantha Kimball, PhD, MLT Research Director Pure North S Energy Foundation The
Vitamin D supplementation of professionally active adults VITAMIN D MINIMUM, MAXIMUM, OPTIMUM FRIDAY, SEPTEMBER 22 ND 2017 Samantha Kimball, PhD, MLT Research Director Pure North S Energy Foundation The
METABOLISM AND NUTRITION WITH PD OBESITY. Rajnish Mehrotra Harborview Medical Center University of Washington, Seattle
 METABOLISM AND NUTRITION WITH PD OBESITY Rajnish Mehrotra Harborview Medical Center University of Washington, Seattle 1 Body Size in Patients New to Dialysis United States Body Mass Index, kg/m2 33 31
METABOLISM AND NUTRITION WITH PD OBESITY Rajnish Mehrotra Harborview Medical Center University of Washington, Seattle 1 Body Size in Patients New to Dialysis United States Body Mass Index, kg/m2 33 31
Low cholesterol in dialysis patients causal factor for mortality or an effect of confounding?
 Nephrol Dial Transplant (2011) 26: 3325 3331 doi: 10.1093/ndt/gfr008 Advance Access publication 28 February 2011 Low cholesterol in dialysis patients causal factor for mortality or an effect of confounding?
Nephrol Dial Transplant (2011) 26: 3325 3331 doi: 10.1093/ndt/gfr008 Advance Access publication 28 February 2011 Low cholesterol in dialysis patients causal factor for mortality or an effect of confounding?
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients. Int.J.Curr.Res.Aca.Rev.2016; 4(11):
 Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
ISN Mission: Advancing the diagnosis, treatment and prevention of kidney diseases in the developing and developed world
 ISN Mission: Advancing the diagnosis, treatment and prevention of kidney diseases in the developing and developed world Nutrition in Kidney Disease: How to Apply Guidelines to Clinical Practice? T. Alp
ISN Mission: Advancing the diagnosis, treatment and prevention of kidney diseases in the developing and developed world Nutrition in Kidney Disease: How to Apply Guidelines to Clinical Practice? T. Alp
Haemodiafiltration - the case against. Prof Peter G Kerr Professor/Director of Nephrology Monash Health
 Haemodiafiltration - the case against Prof Peter G Kerr Professor/Director of Nephrology Monash Health Know your opposition.. Haemodiafiltration NB: pre or post-dilution What is HDF how is it different
Haemodiafiltration - the case against Prof Peter G Kerr Professor/Director of Nephrology Monash Health Know your opposition.. Haemodiafiltration NB: pre or post-dilution What is HDF how is it different
Advances in Peritoneal Dialysis, Vol. 22, 2006
 Advances in Peritoneal Dialysis, Vol. 22, 2006 M. Carmen Sánchez González, 1 Fernando López Barea, 2 M. Auxiliadora Bajo, 1 Rafael Selgas, 1 for the Collaborators of the Multicenter Study Group* Serum
Advances in Peritoneal Dialysis, Vol. 22, 2006 M. Carmen Sánchez González, 1 Fernando López Barea, 2 M. Auxiliadora Bajo, 1 Rafael Selgas, 1 for the Collaborators of the Multicenter Study Group* Serum
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Concern about the decreasing use of peritoneal dialysis
 Page 1 of 8 Peritoneal Dialysis International Peritoneal Dialysis International, Vol. 30, pp. doi: 10.3747/pdi.2008.00277 0896-8608/10 $3.00 +.00 Copyright 2010 International Society for Peritoneal Dialysis
Page 1 of 8 Peritoneal Dialysis International Peritoneal Dialysis International, Vol. 30, pp. doi: 10.3747/pdi.2008.00277 0896-8608/10 $3.00 +.00 Copyright 2010 International Society for Peritoneal Dialysis
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Predictors of Patient Survival in Continuous Ambulatory Peritoneal Dialysis 10-Year Experience in 2 Major Centers in Tehran
 Dialysis Predictors of Patient Survival in Continuous Ambulatory Peritoneal Dialysis 10-Year Experience in 2 Major Centers in Tehran Monir Sadat Hakemi, 1 Mehdi Golbabaei, 2 Amirahmad Nassiri, 3 Mandana
Dialysis Predictors of Patient Survival in Continuous Ambulatory Peritoneal Dialysis 10-Year Experience in 2 Major Centers in Tehran Monir Sadat Hakemi, 1 Mehdi Golbabaei, 2 Amirahmad Nassiri, 3 Mandana
UC Irvine ICTS Publications
 UC Irvine ICTS Publications Title Comparative Mortality-Predictability Using Alkaline Phosphatase and Parathyroid Hormone in Patients on Peritoneal Dialysis and Hemodialysis Permalink https://escholarship.org/uc/item/2732k730
UC Irvine ICTS Publications Title Comparative Mortality-Predictability Using Alkaline Phosphatase and Parathyroid Hormone in Patients on Peritoneal Dialysis and Hemodialysis Permalink https://escholarship.org/uc/item/2732k730
02/27/2018. Objectives. To Replace or Not to Replace: Nutritional Vitamin D in Dialysis.
 To Replace or Not to Replace: Nutritional Vitamin D in Dialysis. Michael Shoemaker-Moyle, M.D. Assistant Professor of Clinical Medicine Objectives Review Vitamin D Physiology Review Current Replacement
To Replace or Not to Replace: Nutritional Vitamin D in Dialysis. Michael Shoemaker-Moyle, M.D. Assistant Professor of Clinical Medicine Objectives Review Vitamin D Physiology Review Current Replacement
PREVALENCE AND PATTERNS OF HYPERPARATHYROIDISM AND MINERAL BONE DISEASE IN PATIENTS WITH CHRONIC KIDNEY DISEASE AT KENYATTA NATIONAL HOSPITAL
 PREVALENCE AND PATTERNS OF HYPERPARATHYROIDISM AND MINERAL BONE DISEASE IN PATIENTS WITH CHRONIC KIDNEY DISEASE AT KENYATTA NATIONAL HOSPITAL DR. ANNE MUGERA The Problem Chronic Kidney disease is a worldwide
PREVALENCE AND PATTERNS OF HYPERPARATHYROIDISM AND MINERAL BONE DISEASE IN PATIENTS WITH CHRONIC KIDNEY DISEASE AT KENYATTA NATIONAL HOSPITAL DR. ANNE MUGERA The Problem Chronic Kidney disease is a worldwide
New biological targets for CKD- MBD: From the KDOQI to the
 New biological targets for CKD- MBD: From the KDOQI to the KDIGO Guillaume JEAN, MD. Centre de Rein Artificiel, 42 avenue du 8 mai 1945, Tassin la Demi-Lune, France. E-mail : guillaume-jean-crat@wanadoo.fr
New biological targets for CKD- MBD: From the KDOQI to the KDIGO Guillaume JEAN, MD. Centre de Rein Artificiel, 42 avenue du 8 mai 1945, Tassin la Demi-Lune, France. E-mail : guillaume-jean-crat@wanadoo.fr
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Economic evaluation of end stage renal disease treatment Ardine de Wit G, Ramsteijn P G, de Charro F T
 Economic evaluation of end stage renal disease treatment Ardine de Wit G, Ramsteijn P G, de Charro F T Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion
Economic evaluation of end stage renal disease treatment Ardine de Wit G, Ramsteijn P G, de Charro F T Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion
The Effect of Residual Renal Function at the Initiation of Dialysis on Patient Survival
 ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.1.55 The Effect of Residual Renal Function at the Initiation of Dialysis on Patient Survival Seoung Gu Kim 1 and Nam Ho Kim 2 Department of Internal Medicine,
ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.1.55 The Effect of Residual Renal Function at the Initiation of Dialysis on Patient Survival Seoung Gu Kim 1 and Nam Ho Kim 2 Department of Internal Medicine,
Ying-Ping Sun, Wen-Jun Yang, Su-Hua Li, Yuan-yuan Han, and Jian Liu
 Hindawi BioMed Research International Volume 2017, Article ID 2516934, 5 pages https://doi.org/10.1155/2017/2516934 Research Article Clinical Epidemiology of Mineral Bone Disorder Markers in Prevalent
Hindawi BioMed Research International Volume 2017, Article ID 2516934, 5 pages https://doi.org/10.1155/2017/2516934 Research Article Clinical Epidemiology of Mineral Bone Disorder Markers in Prevalent
Variable Included. Excluded. Included. Excluded
 Table S1. Baseline characteristics of patients included in the analysis and those excluded patients because of missing baseline serumj bicarbonate levels, stratified by dialysis modality. Variable HD patients
Table S1. Baseline characteristics of patients included in the analysis and those excluded patients because of missing baseline serumj bicarbonate levels, stratified by dialysis modality. Variable HD patients
(n=6279). Continuous variables are reported as mean with 95% confidence interval and T1 T2 T3. Number of subjects
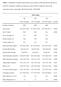 Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Trial to Reduce. Aranesp* Therapy. Cardiovascular Events with
 Trial to Reduce Cardiovascular Events with Aranesp* Therapy John J.V. McMurray, Hajime Uno, Petr Jarolim, Akshay S. Desai, Dick de Zeeuw, Kai-Uwe Eckardt, Peter Ivanovich, Andrew S. Levey, Eldrin F. Lewis,
Trial to Reduce Cardiovascular Events with Aranesp* Therapy John J.V. McMurray, Hajime Uno, Petr Jarolim, Akshay S. Desai, Dick de Zeeuw, Kai-Uwe Eckardt, Peter Ivanovich, Andrew S. Levey, Eldrin F. Lewis,
Mineral and bone disorder (MBD) affects the majority
 Consistent Control of Mineral and Bone Disorder in Incident Hemodialysis Patients Mark D. Danese,* Vasily Belozeroff, Karen Smirnakis, and Kenneth J. Rothman *Outcomes Insights, Inc., Newbury Park, California;
Consistent Control of Mineral and Bone Disorder in Incident Hemodialysis Patients Mark D. Danese,* Vasily Belozeroff, Karen Smirnakis, and Kenneth J. Rothman *Outcomes Insights, Inc., Newbury Park, California;
J Am Soc Nephrol 15: , 2004
 J Am Soc Nephrol 15: 1061 1070, 2004 Relative Contribution of Residual Renal Function and Different Measures of Adequacy to Survival in Hemodialysis Patients: An analysis of the Netherlands Cooperative
J Am Soc Nephrol 15: 1061 1070, 2004 Relative Contribution of Residual Renal Function and Different Measures of Adequacy to Survival in Hemodialysis Patients: An analysis of the Netherlands Cooperative
Aetiology versus Prediction - correct for Confounding? Friedo Dekker ERA-EDTA Registry / LUMC
 Aetiology versus Prediction - correct for Confounding? Friedo Dekker ERA-EDTA Registry / LUMC Aetiology Study effect of a risk factor on an outcome Consider potential confounding: other risk factor for
Aetiology versus Prediction - correct for Confounding? Friedo Dekker ERA-EDTA Registry / LUMC Aetiology Study effect of a risk factor on an outcome Consider potential confounding: other risk factor for
Home Hemodialysis or Transplantation of the Treatment of Choice for Elderly?
 Home Hemodialysis or Transplantation of the Treatment of Choice for Elderly? Miklos Z Molnar, MD, PhD, FEBTM, FERA, FASN Associate Professor of Medicine Division of Nephrology, Department of Medicine University
Home Hemodialysis or Transplantation of the Treatment of Choice for Elderly? Miklos Z Molnar, MD, PhD, FEBTM, FERA, FASN Associate Professor of Medicine Division of Nephrology, Department of Medicine University
Pre-ESRD Changes in Body Weight and Survival in Nursing Home Residents Starting Dialysis
 CJASN epress. Published on September 5, 2013 as doi: 10.2215/CJN.01410213 Article Pre-ESRD Changes in Body Weight and Survival in Nursing Home Residents Starting Dialysis Shobha Stack,* Glenn M. Chertow,*
CJASN epress. Published on September 5, 2013 as doi: 10.2215/CJN.01410213 Article Pre-ESRD Changes in Body Weight and Survival in Nursing Home Residents Starting Dialysis Shobha Stack,* Glenn M. Chertow,*
PART FOUR. Metabolism and Nutrition
 PART FOUR Metabolism and Nutrition Advances in Peritoneal Dialysis, Vol. 23, 2007 Alicja E. Grzegorzewska, Monika Mĺot Michalska Serum Level of Intact Parathyroid Hormone and Other Markers of Bone Metabolism
PART FOUR Metabolism and Nutrition Advances in Peritoneal Dialysis, Vol. 23, 2007 Alicja E. Grzegorzewska, Monika Mĺot Michalska Serum Level of Intact Parathyroid Hormone and Other Markers of Bone Metabolism
Type of arteriovenous vascular access and association with patency and mortality
 Ocak et al. BMC Nephrology 2013, 14:79 RESEARCH ARTICLE Type of arteriovenous vascular access and association with patency and mortality Gürbey Ocak 1, Joris I Rotmans 2, Carla Y Vossen 1,3, Frits R Rosendaal
Ocak et al. BMC Nephrology 2013, 14:79 RESEARCH ARTICLE Type of arteriovenous vascular access and association with patency and mortality Gürbey Ocak 1, Joris I Rotmans 2, Carla Y Vossen 1,3, Frits R Rosendaal
Original Article. Sean F. Leavey 2, Keith McCullough 1, Erwin Hecking 3, David Goodkin 4, Friedrich K. Port 2 and Eric W. Young 1,2.
 Nephrol Dial Transplant (2001) 16: 2386 2394 Original Article Body mass index and mortality in healthier as compared with sicker haemodialysis patients: results from the Dialysis Outcomes and Practice
Nephrol Dial Transplant (2001) 16: 2386 2394 Original Article Body mass index and mortality in healthier as compared with sicker haemodialysis patients: results from the Dialysis Outcomes and Practice
Narender Goel et al. Middletown Medical PC, Montefiore Medical Center & Albert Einstein College of Medicine, New York
 Narender Goel et al. Middletown Medical PC, Montefiore Medical Center & Albert Einstein College of Medicine, New York 4th International Conference on Nephrology & Therapeutics September 14, 2015 Baltimore,
Narender Goel et al. Middletown Medical PC, Montefiore Medical Center & Albert Einstein College of Medicine, New York 4th International Conference on Nephrology & Therapeutics September 14, 2015 Baltimore,
The CARI Guidelines Caring for Australians with Renal Impairment. Cardiovascular Risk Factors
 Cardiovascular Risk Factors ROB WALKER (Dunedin, New Zealand) Lipid-lowering therapy in patients with chronic kidney disease Date written: January 2005 Final submission: August 2005 Author: Rob Walker
Cardiovascular Risk Factors ROB WALKER (Dunedin, New Zealand) Lipid-lowering therapy in patients with chronic kidney disease Date written: January 2005 Final submission: August 2005 Author: Rob Walker
Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis
 Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis Seoung Woo Lee Div. Of Nephrology and Hypertension, Dept. of Internal Medicine, Inha Unv. College of Medicine, Inchon, Korea
Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis Seoung Woo Lee Div. Of Nephrology and Hypertension, Dept. of Internal Medicine, Inha Unv. College of Medicine, Inchon, Korea
CLINICAL RESEARCH STUDY
 CLINICAL RESEARCH STUDY Phosphorus and Risk of Renal Failure in Subjects with Normal Renal Function John J. Sim, MD, a Simran K. Bhandari, MD, a Ning Smith, PhD, b Joanie Chung, MS, b In Lu A. Liu, MS,
CLINICAL RESEARCH STUDY Phosphorus and Risk of Renal Failure in Subjects with Normal Renal Function John J. Sim, MD, a Simran K. Bhandari, MD, a Ning Smith, PhD, b Joanie Chung, MS, b In Lu A. Liu, MS,
End stage renal disease and Protein Energy wasting
 End stage renal disease and Protein Energy wasting Dr Goh Heong Keong MBBS,MRCP(UK) www.passpaces.com/kidney.htm Introduction Chronic kidney disease- increasing health burden in many countries. The estimated
End stage renal disease and Protein Energy wasting Dr Goh Heong Keong MBBS,MRCP(UK) www.passpaces.com/kidney.htm Introduction Chronic kidney disease- increasing health burden in many countries. The estimated
Risks and benefits of weight loss: challenges to obesity research
 European Heart Journal Supplements (2005) 7 (Supplement L), L27 L31 doi:10.1093/eurheartj/sui083 Risks and benefits of weight loss: challenges to obesity research Donna Ryan* Pennington Biomedical Research
European Heart Journal Supplements (2005) 7 (Supplement L), L27 L31 doi:10.1093/eurheartj/sui083 Risks and benefits of weight loss: challenges to obesity research Donna Ryan* Pennington Biomedical Research
... . : ... PTH.
 IRMA Email msarookhani@qumsacir * CRD GFR D [1,25OH 2 D 3 ] SHPT GFR» «KDOQI SHPT Ca * P P P Selectra Overt HPT = = Ca * P P > GM II DSL i IRMA ± ± ± Ca * P % % % % % % % % % % % % % % % % pgml = = > ±
IRMA Email msarookhani@qumsacir * CRD GFR D [1,25OH 2 D 3 ] SHPT GFR» «KDOQI SHPT Ca * P P P Selectra Overt HPT = = Ca * P P > GM II DSL i IRMA ± ± ± Ca * P % % % % % % % % % % % % % % % % pgml = = > ±
17 th Annual Meeting of JSHDF, Sept 3-4, 2011
 17 th Annual Meeting of JSHDF, Sept 3-4, 2011 Sug Kyun Shin 1, JY Moon 2, SW Han 3, DH Yang 4, SH Lee 2, HC Park 5, JK Kim 6 and YI Jo 7 1 Nephrology, NHIC Ilsan Hospital, 2 Kyunghee University Hospital
17 th Annual Meeting of JSHDF, Sept 3-4, 2011 Sug Kyun Shin 1, JY Moon 2, SW Han 3, DH Yang 4, SH Lee 2, HC Park 5, JK Kim 6 and YI Jo 7 1 Nephrology, NHIC Ilsan Hospital, 2 Kyunghee University Hospital
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Prof. Samir Morcos Rafla Alexandria Univ. Cardiology Dept.
 Obesity as a risk factor for Atrial Fibrillation Prof. Samir Morcos Rafla Alexandria Univ. Cardiology Dept. CardioAlex 2010 smrafla@hotmail.com 1 Obesity has reached epidemic proportions in the United
Obesity as a risk factor for Atrial Fibrillation Prof. Samir Morcos Rafla Alexandria Univ. Cardiology Dept. CardioAlex 2010 smrafla@hotmail.com 1 Obesity has reached epidemic proportions in the United
Cardiovascular Mortality: General Population vs ESRD Dialysis Patients
 Cardiovascular Mortality: General Population vs ESRD Dialysis Patients Annual CVD Mortality (%) 100 10 1 0.1 0.01 0.001 25-34 35-44 45-54 55-64 66-74 75-84 >85 Age (years) GP Male GP Female GP Black GP
Cardiovascular Mortality: General Population vs ESRD Dialysis Patients Annual CVD Mortality (%) 100 10 1 0.1 0.01 0.001 25-34 35-44 45-54 55-64 66-74 75-84 >85 Age (years) GP Male GP Female GP Black GP
A n aly tical m e t h o d s
 a A n aly tical m e t h o d s If I didn t go to the screening at Farmers Market I would not have known about my kidney problems. I am grateful to the whole staff. They were very professional. Thank you.
a A n aly tical m e t h o d s If I didn t go to the screening at Farmers Market I would not have known about my kidney problems. I am grateful to the whole staff. They were very professional. Thank you.
Krediet slide di 18
 1 di 18 Assessment of fluid status in PD patients Raymond T. Krediet, Amsterdam, Netherlands Chairs:Walther H. Boer, Utrecht, The Netherlands F. Fevzi Ersoy, Antalya, Turkey Prof. Raymond T. Krediet DDivision
1 di 18 Assessment of fluid status in PD patients Raymond T. Krediet, Amsterdam, Netherlands Chairs:Walther H. Boer, Utrecht, The Netherlands F. Fevzi Ersoy, Antalya, Turkey Prof. Raymond T. Krediet DDivision
What Are the Targets in CKD-MBD?
 Knowledge Exchange 2016 Paris, France, September 30, 2016 Date of preparation: Nov 2016 Item job code: INTSP/C-ANPROM/FOS/16/0025 Cristina Ortiz Jorge B Cannata-Andía Bone and Mineral Research Unit Hospital
Knowledge Exchange 2016 Paris, France, September 30, 2016 Date of preparation: Nov 2016 Item job code: INTSP/C-ANPROM/FOS/16/0025 Cristina Ortiz Jorge B Cannata-Andía Bone and Mineral Research Unit Hospital
Evidence Table. Study Type: Randomized controlled trial. Study Aim: To compare frequent nocturnal hemodialysis and conventional in-center dialysis.
 Evidence Table Clinical Area: Reference: Frequent home dialysis Culleton BF, Walsh M, Klarenbach SW et al. Effect of frequent nocturnal hemodialysis vs conventional hemodialysis on left ventricular mass
Evidence Table Clinical Area: Reference: Frequent home dialysis Culleton BF, Walsh M, Klarenbach SW et al. Effect of frequent nocturnal hemodialysis vs conventional hemodialysis on left ventricular mass
Pediatric Nutrition and Kidney Disease
 Pediatric Nutrition and Kidney Disease Loai Eid, MD, MSHS, FAAP Consultant Pediatric Nephrologist Pediatric Nephrology & Hypertension Division Chief Dubai Hospital - DHA 26 th October, 2017 Objectives
Pediatric Nutrition and Kidney Disease Loai Eid, MD, MSHS, FAAP Consultant Pediatric Nephrologist Pediatric Nephrology & Hypertension Division Chief Dubai Hospital - DHA 26 th October, 2017 Objectives
Advances in Peritoneal Dialysis, Vol. 29, 2013
 Advances in Peritoneal Dialysis, Vol. 29, 2013 Takeyuki Hiramatsu, 1 Takahiro Hayasaki, 1 Akinori Hobo, 1 Shinji Furuta, 1 Koki Kabu, 2 Yukio Tonozuka, 2 Yoshiyasu Iida 1 Icodextrin Eliminates Phosphate
Advances in Peritoneal Dialysis, Vol. 29, 2013 Takeyuki Hiramatsu, 1 Takahiro Hayasaki, 1 Akinori Hobo, 1 Shinji Furuta, 1 Koki Kabu, 2 Yukio Tonozuka, 2 Yoshiyasu Iida 1 Icodextrin Eliminates Phosphate
Chronic Kidney Disease
 Chronic Kidney Disease Chronic Kidney Disease (CKD) Guideline (2010) Chronic Kidney Disease CKD: Executive Summary of Recommendations (2010) Executive Summary of Recommendations Below are the major recommendations
Chronic Kidney Disease Chronic Kidney Disease (CKD) Guideline (2010) Chronic Kidney Disease CKD: Executive Summary of Recommendations (2010) Executive Summary of Recommendations Below are the major recommendations
Cinacalcet treatment in advanced CKD - is it justified?
 Cinacalcet treatment in advanced CKD - is it justified? Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia TSN Congress October 21, 2017, Antalya Session Objectives From ROD to
Cinacalcet treatment in advanced CKD - is it justified? Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia TSN Congress October 21, 2017, Antalya Session Objectives From ROD to
Lucia Cea Soriano 1, Saga Johansson 2, Bergur Stefansson 2 and Luis A García Rodríguez 1*
 Cea Soriano et al. Cardiovascular Diabetology (2015) 14:38 DOI 10.1186/s12933-015-0204-5 CARDIO VASCULAR DIABETOLOGY ORIGINAL INVESTIGATION Open Access Cardiovascular events and all-cause mortality in
Cea Soriano et al. Cardiovascular Diabetology (2015) 14:38 DOI 10.1186/s12933-015-0204-5 CARDIO VASCULAR DIABETOLOGY ORIGINAL INVESTIGATION Open Access Cardiovascular events and all-cause mortality in
New Medicines Profile. December 2013 Issue No. 13/04. Colestilan
 New Medicines Profile December 2013 Issue. 13/04 Concise evaluated information to support the managed entry of new medicines in the NHS Summary (BindRen ) is an oral, non-absorbed, non-calcium, nonmetallic
New Medicines Profile December 2013 Issue. 13/04 Concise evaluated information to support the managed entry of new medicines in the NHS Summary (BindRen ) is an oral, non-absorbed, non-calcium, nonmetallic
Nutritional Considerations with Obesity and Bariatric Surgery. Presented by Dr. Ron Grabowski
 Nutritional Considerations with Obesity and Bariatric Surgery Presented by Dr. Ron Grabowski January 25, 2010 Nutritional Considerations with Obesity and Bariatric Surgery Presented by Dr. Ron Grabowski
Nutritional Considerations with Obesity and Bariatric Surgery Presented by Dr. Ron Grabowski January 25, 2010 Nutritional Considerations with Obesity and Bariatric Surgery Presented by Dr. Ron Grabowski
Should cinacalcet be used in patients who are not on dialysis?
 Should cinacalcet be used in patients who are not on dialysis? Jorge B Cannata-Andía and José Luis Fernández-Martín Affiliations: Bone and Mineral Research Unit. Hospital Universitario Central de Asturias.
Should cinacalcet be used in patients who are not on dialysis? Jorge B Cannata-Andía and José Luis Fernández-Martín Affiliations: Bone and Mineral Research Unit. Hospital Universitario Central de Asturias.
Macro- and Micronutrient Homeostasis in the Setting of Chronic Kidney Disease. T. Alp Ikizler, MD Vanderbilt University Medical Center
 Macro- and Micronutrient Homeostasis in the Setting of Chronic Kidney Disease T. Alp Ikizler, MD Vanderbilt University Medical Center Nutrition and Chronic Kidney Disease What is the disease itself and
Macro- and Micronutrient Homeostasis in the Setting of Chronic Kidney Disease T. Alp Ikizler, MD Vanderbilt University Medical Center Nutrition and Chronic Kidney Disease What is the disease itself and
INFLUENCE OF LOW PROTEIN DIET IN IMPROVING ANEMIA TREATED WITH ERYTHROPOETIN
 INFLUENCE OF LOW PROTEIN DIET IN IMPROVING ANEMIA TREATED WITH ERYTHROPOETIN, Idrizi A, Barbullushi M, Gjyzari A, Duraku A Department of Nephrology, University Hospital Center, Tirana, Albania Introduction
INFLUENCE OF LOW PROTEIN DIET IN IMPROVING ANEMIA TREATED WITH ERYTHROPOETIN, Idrizi A, Barbullushi M, Gjyzari A, Duraku A Department of Nephrology, University Hospital Center, Tirana, Albania Introduction
