PPG DGBI QOL PGSAS-45. Keywords ORIGINAL ARTICLE. Gastric Cancer (2016) 19: DOI /s
|
|
|
- Junior Foster
- 5 years ago
- Views:
Transcription
1 Gastric Cancer (2016) 19: DOI /s ORIGINAL ARTICLE Assessment of postoperative quality of life following pyloruspreserving gastrectomy and Billroth-I distal gastrectomy in gastric cancer patients: results of the nationwide postgastrectomy syndrome assessment study Junya Fujita Masazumi Takahashi Takashi Urushihara Kazuaki Tanabe Yasuhiro Kodera Takeyoshi Yumiba Hideo Matsumoto Akinori Takagane Chikara Kunisaki Koji Nakada Received: 26 August 2014 / Accepted: 30 December 2014 / Published online: 31 January 2015 The International Gastric Cancer Association and The Japanese Gastric Cancer Association 2015 Abstract Background Pylorus-preserving gastrectomy (PPG) is increasingly being used to treat early gastric cancer in the middle third of the stomach, with the hope of ameliorating postoperative dysfunction and improving quality of life (QOL). We evaluated symptoms of postgastrectomy syndrome (PGS) and QOL by means of a newly developed integrated questionnaire, the Postgastrectomy Syndrome Assessment Scale-45 (PGSAS-45), and compared PPG with Billroth-I distal gastrectomy (DGBI). Methods The PGSAS-45 consists of 45 items, including items from the SF-8 and GSRS instruments, as well as 22 newly selected items. It was designed to assess the severity of PGS and the living status and QOL of gastrectomized patients. The nationwide PGSAS surveillance study enrolled 2,368 gastric cancer patients who underwent J. Fujita (&) Department of Surgery, NTT West Osaka Hospital, Karasugatsuji Tennoji-ku, Osaka , Japan j.fujita@mhc.west.ntt.co.jp M. Takahashi Division of Gastroenterological Surgery, Yokohama Municipal Citizen s Hospital, Yokohama, Japan T. Urushihara Department of Gastroenterological, Breast and Transplant Surgery, Hiroshima Prefectural Hospital, Hiroshima, Japan K. Tanabe Department of Gastroenterological and Transplant Surgery, Institute of Biomedical and Health Sciences, Hiroshima University, Hiroshima, Japan Y. Kodera Department of Gastroenterological Surgery, Nagoya University Graduate School of Medicine, Nagoya, Japan various types of gastrectomy. In this study we analyzed 313 PPG patients and 909 DGBI patients. Results Body weight loss was -6.9 % in the PPG group and -7.9 % in the DGBI group (P = 0.052). The PPG group scored better on the diarrhea subscale (PPG; 1.8 vs. DGBI; 2.1, P \ ), dumping subscale (1.8 vs. 2.0, P = 0.003), and frequency of additional meals (1.8 vs. 1.9, P = 0.034). Multiple regression analysis revealed that age and the preservation of the celiac branch of the vagus nerve were independent factors predicting diarrhea and dumping. Conclusions It has been suggested that PPG is superior to DGBI for ameliorating PGS. Preservation of the celiac branch of the vagus nerve is recommended to reduce postoperative disorders regardless of the reconstruction method used. Keywords PPG DGBI QOL PGSAS-45 T. Yumiba Department of Surgery, Kenporen Osaka Central Hospital, Osaka, Japan H. Matsumoto Department of Digestive Surgery, Kawasaki Medical School, Kurashiki, Japan A. Takagane Department of Surgery, Hakodate Goryoukaku Hospital, Hakodate, Japan C. Kunisaki Department of Surgery, Gastroenterological Center, Yokohama City University Medical Center, Yokohama, Japan K. Nakada Department of Surgery, The Jikei University School of Medicine, Tokyo, Japan
2 QOL comparison of PPG and DGBI 303 Introduction The radical surgical treatment of gastric cancer requires resection of a large portion of the stomach as well as regional lymphadenectomy. It is well known that gastric resection and reconstruction of the gastrointestinal tract result in a variety of functional and physiological disorders. These unpleasant alimentary and/or systemic symptoms are collectively referred to as postgastrectomy syndrome (PGS) [1, 2]. A recent report from the Japanese nationwide gastric cancer registry showed that patients with early gastric cancer (EGC) accounted for approximately 60 % of all gastric cancer patients who underwent gastrectomy, and the 5-year survival rate of EGC patients exceeded 90 % [3]. It is important to determine which gastrectomy operations can most minimize PGS, as EGC patients can survive for a long period of time following surgery. The Billroth-I (BI) method is one of the most commonly performed reconstruction procedures following distal gastrectomy (DG) in gastric cancer patients. In Japan, the number of surgeons who prefer Roux-en-Y (RY) anastomosis has been increasing recently; however, the majority of medical institutions still select BI for reconstruction after DG (DGBI). The questionnaire survey regarding the reconstruction methods after gastrectomy conducted in Japan showed that BI was selected as the first choice for DG in 77 % of Japanese institutions, RY in 21 %, and BII in 0.7 % [4]. The operative simplicity and physiological passage of the diet through the duodenum are regarded as merits of DGBI, although postoperative reflux symptoms, esophagitis, and remnant gastritis were found to be significantly more frequent in BI patients compared with those receiving RY, indicating that the bile reflux, which is attributed to the direct anastomosis between the gastric stump and duodenum, is one of the disadvantages of DGBI [5, 6]. Pylorus-preserving gastrectomy (PPG) was initially devised for resection of gastric ulcers by Maki and colleagues in 1967 [7], but it has recently been applied to EGC patients with the intention of attenuating PGS by maintaining pyloric function [8, 9]. With accumulation of data demonstrating acceptable long-term survival following PPG in EGC patients [10 12], the Japanese gastric cancer treatment guidelines (version 3) recognized PPG as an alternative to conventional DGBI for ct1n0 tumors located in the middle third of the stomach [13]. It is important to determine whether PPG is superior to DGBI in terms of comprehensively ameliorating PGS and improving QOL after gastrectomy. The postgastrectomy syndrome assessment scale-45 (PGSAS-45) was newly developed by the Japanese Postgastrectomy Syndrome Working Party (JPGSWP) as an integrated questionnaire designed to assess postgastrectomy-specific clinical symptoms and QOL [14]. The JPGSWP also conducted multiinstitutional nationwide surveillance to investigate long-term symptoms, living status and QOL following various types of gastrectomy. In the present study we used the PGSAS-45 to compare PPG and DGBI and evaluate the advantages of PPG as a function-preserving gastrectomy technique. Patients and methods Patients Patient eligibility criteria were: (1) diagnosis of pathologically confirmed stage IA or IB gastric cancer; (2) first-time gastrectomy status; (3) age C20 and B75 years; (4) no history of chemotherapy; (5) no recurrence or distant metastasis; (6) gastrectomy conducted 1 or more years prior to enrollment date; (7) performance status (PS) B1 on the Eastern Cooperative Oncology Group (ECOG) scale; (8) full capacity to understand and respond to the questionnaire; (9) no history of other diseases or surgeries that might influence responses to the questionnaire; (10) no presence of organ failure or mental illness; (11) written informed consent. Patients with dual malignancies or with concomitant resection of other organs (with co-resection equivalent to cholecystectomy being the exception) were excluded. QOL assessment The PGSAS-45 is an integrated questionnaire to assess the living status and the QOL in postgastrectomy patients, as described previously [14]. It consists of eight items from the Short-Form Health Survey (SF-8), 15 items from the Gastrointestinal Symptom Rating Scale (GSRS), and 22 items originally proposed by the JPGSWP members (Table 1). The items of the PGSAS-45 were classified into three domains, i.e., the symptom, living status, and QOL domains. The QOL domain consists of SF-8 and three of the dissatisfaction items; the living status domain consists of meal-associated items and ability to work. The symptom domain is composed of 23 symptom-related items clustered into seven symptom subscales (SS), i.e., the esophageal reflux SS, abdominal pain SS, meal-related distress SS, indigestion SS, diarrhea SS, constipation SS, and dumping SS. In items 1 8, 34, 35, and 38 40, higher scores indicate better outcomes; in items 9 28, 30, 31, 33, and 41 45, higher scores indicate worse outcomes. Study methods This is a retrospective cross-sectional study conducted by continuous sampling from a central registration system for
3 304 J. Fujita et al. Table 1 Structure of postgastrectomy syndrome assessment scale-45 (PGSAS-45) (domains/subdomains/items/subscales) Domains Subdomains Items Subscales QOL SF-8 (QOL) 1 Physical functioning* Physical component summary* (items 1 8) 2 Role physical* Mental component summary* (items 1 8) 3 Bodily pain* 4 General health* 5 Vitality* 6 Social functioning* 7 Role emotional* 8 Mental health* Symptoms GSRS (symptoms) 9 Abdominal pains Esophageal reflux subscale (items 10, 11, 13, 24) 10 Heartburn Abdominal pain subscale (items 9, 12, 28) 11 Acid regurgitation Meal-related distress subscale (items 25 27) 12 Sucking sensations in the epigastrium Indigestion subscale (items 14 17) 13 Nausea and vomiting Diarrhea subscale (items 19, 20, 22) 14 Borborygmus Constipation subscale (items 18, 21, 23) 15 Abdominal distension Dumping subscale (items 30, 31, 33) 16 Eructation 17 Increased flatus Total symptom score (above seven subscales) 18 Decreased passage of stool 19 Increased passage of stool 20 Loose stool 21 Hard stool 22 Urgent need for defecation 23 Feeling of incomplete evacuation Symptoms 24 Bile regurgitation 25 Sense of food sticking 26 Postprandial fullness 27 Early satiation 28 Lower abdominal pain 29 Number and type of early dumping symptoms 30 Early dumping general symptoms 31 Early dumping abdominal symptoms 32 Number and type of late dumping symptoms 33 Late dumping symptoms Living status Meals (amount) 1 34 Ingested amount of food per meal* 35 Ingested amount of food per day* 36 Frequency of main meals 37 Frequency of additional meals Meals (quality) 38 Appetite* Quality of ingestion subscale* (items 38 40) 39 Hunger feeling* 40 Satiety feeling* Meals (amount) 2 41 Necessity for additional meals Social activity 42 Ability to work QOL Dissatisfaction (QOL) 43 Dissatisfaction with symptoms Dissatisfaction for daily life subscale (items 43 45) 44 Dissatisfaction at the meals 45 Dissatisfaction at working PGSAS-45 postgastrectomy syndrome assessment scale-45, SF-8 short form-8, QOL quality of life, GSRS gastrointestinal symptom rating scale. In items or subscales with *, higher scores indicate better conditions. In items or subscales without *, higher scores indicate worse conditions. Each subscale is calculated as the mean of its composite items or subscales, except the physical and mental component summaries of SF-8. Items 29 and 32 do not have scores; these items were analyzed separately
4 QOL comparison of PPG and DGBI 305 participant enrollment. The questionnaire was distributed to all eligible patients as they presented to the participating clinics, and patients were instructed to send the forms directly by mail to the data center. All QOL data from the questionnaires were matched with individual patient data collected via case report forms. The postoperative body weight was measured at the time of enrollment in the study. Between July 2009 and December 2010, a total of 2,922 patients from 52 institutions were enrolled in the PGSAS surveillance study (Fig. 1). A total of 2,520 (86 %) answers were retrieved, but of these 152 cases were excluded because of: age C76 years (n = 90), postoperative period \1 year (n = 29), concomitant resection of other organs (n = 8), and other factors (n = 25). As a result, 2,368 (81 %) patients were determined to be eligible for the inclusion criteria. Among the eligible 2,368 responders, 393 patients underwent total gastrectomy, 909 DGBI, 475 DGRY, 313 PPG, 193 proximal gastrectomy, and 85 local gastric resection. In the present study, 909 patients who underwent DGBI and 313 patients who underwent PPG were subjected to the analysis. This study was registered with the University Hospital Medical Information Network s Clinical Trials Registry (UMIN-CTR; registration no ). The study protocol was approved by the institutional review board at each of the participating institutions. Written informed consent was obtained from all enrolled patients. TGRY 393 Ques onnaire handed 2922 Retrieved 2520 (86%) Analyzed 2368 (81%) DGRY 475 DGBI 909 Conven onal gastrectomy Not retrieved 402 (14%) Excluded 152 (5%) age 76< : 90 postopera ve period 1 yr> : 29 resec on of other organs : 8 others : 25 PPG 313 PG 193 Func on-preserving gastrectomy Fig. 1 Outline of the study. TG Total gastrectomy with Roux-en-Y reconstruction, DGRY distal gastrectomy with Roux-en-Y reconstruction, DGBI distal gastrectomy with Billroth I reconstruction, PPG pylorus-preserving gastrectomy, PG proximal gastrectomy, LR local resection LR 85 Statistics Statistical analyses were performed by the biostatisticians mainly using StatView for Windows, version 5.0 (SAS Institute, Inc.). Statistical methods included the t test and chi-squared test. In the case of P \ 0.1 by univariate analysis, Cohen s d was calculated. Main outcome measures that exhibited significant variations in univariate analysis were further analyzed using multiple regression analysis; P \ 0.05 was considered statistically significant. In the case of P \ 0.1 in multiple regression analysis, a standardization coefficient of regression (b), decision coefficient (R 2 ), and P value are shown in Table 4. Cohen s d, b, and R 2 measure effect sizes. Interpretation of effect sizes were C0.2 small, C0.5 medium, and C0.8 large in Cohen s d; C0.1 small, C0.3 medium, and C0.5 large in b; C0.02 small, C0.13 medium, and C0.26 large in R 2. Results Patients characteristics The patient characteristics are shown in Table 2. In the patient backgrounds there were no significant differences between the two groups except for gender where the proportion of males was higher in the DGBI group. In terms of the approach of surgery, the ratio of laparoscopic operations was similar in the two groups. The more extensive lymphadenectomy was conducted in DGBI patients compared with PPG patients, namely, almost all of the patients in the PPG group underwent BD1 dissection, while 36 % of the patients in the DGBI group underwent D2 dissection (P \ ). The celiac branch of the vagus nerve was preserved in 14.6 % in DGBI and 68.0 % in PPG (P \ ). The size of the remnant stomach was significantly larger in the PPG than in the DGBI patients. The mean of the postoperative period at the time of enrollment in this study was 40.7 months and 38.4 months for DGBI and PPG, respectively. Main outcome measures Seven symptom SSs, the total symptom score, items representing the amount of food, quality of ingestion SS, items and SS representing dissatisfaction with life, the physical component summary (PCS) and mental component summary (MCS) from the PGSAS-45, and change in body weight at the enrollment were selected as the main outcome measures in this study based on the results of the validation analysis of PGSAS-45 as reported previously (Table 3) [14]. The results of the univariate analysis of the
5 306 J. Fujita et al. Table 2 Patient characteristics DGBI PPG P value Number of patients Postoperative period 40.7? 30.7 a 38.4? 27.7 C0.1 (months) Age 61.6? 9.1 a 61.5? 8.7 a C0.1 Gender Male Female Preoperative BMI b 22.7? 3.0 a 22.7? 3.0 a C0.1 Postoperative BMI b 20.9? 2.8 a 21.1? 2.6 a C0.1 Approach Open C0.1 Laparoscopic Extent of lymph node dissection c D1[ 4 39 \ D1 8 6 D1a D1b D Celiac branch of the vagal nerve Preserved \ Divided Combined resection None Gallbladder Spleen 0 0 Miscellaneous 4 0 Size of remnant stomach \ Over half Around one-third Less than one-quarter a Mean ± SD b Body mass index c According to the Japanese gastric cancer treatment guidelines main outcome measures comparing DGBI with PPG are shown in Table 3. Regarding the symptom domain, PPG patients had significantly lower scores (indicating better conditions) in the diarrhea and dumping SSs, although there were no differences in the other symptom SSs or in the total symptom score between the two groups. The loss of body weight was marginally greater for DGBI than PPG, -7.9 % and -6.9 %, respectively (P = 0.052). Although the ingested amount of food per meal was not different in the two groups, the necessity for an additional meal was statistically higher in the DGBI group compared with the PPG group (P = 0.034). There were no differences in the quality of ingestion, dissatisfactions categorized in the QOL domain, or the PCS and MCS of SF-8 between the two groups. Next we conducted a multiple regression analysis for the diarrhea SS, dumping SS, and necessity for an additional meal by adding the type of gastrectomy, postoperative period, age, gender, surgical approach, and celiac branch preservation as explanatory variables (Table 4). Younger age and division of the celiac branch were detected as common and significant independent factors predicting diarrhea and dumping, but the type of gastrectomy was not. Female gender and younger age were detected as a significant independent factor for deteriorating dumping. As for living status, male gender, a longer postoperative period, a laparoscopic approach, PPG and younger age acted independently to reduce the necessity for an additional meal. Outcome measures of singular symptom items The results of each singular score among GSRS and PGSAS-45 specific symptom items are shown in Table 5. All of the component items of the diarrhea SS, namely increased passage of stools, loose stools, urgent need for defecation, and all of the component items of the dumping SS, namely early dumping general symptoms, early dumping abdominal symptoms, and late dumping symptoms, were significantly better in the PPG group compared with the DGBI group. The only worse score in PPG than DGBI was eructation (P = ). Discussion In recent years, PPG has been widely used in EGC patients as a function-preserving surgery that aims to reduce PGS and improve postoperative QOL. It is anticipated that preservation of the pyloric sphincter may attenuate rapid gastric emptying and suppress dumping symptomatology, which is one of the most unpleasant sequelae after gastrectomy and substantially affects QOL [15, 16]. Thus far, several studies have used various methods to assess the superiority of PPG over DGBI for reducing dumping [17 23]. We developed the PGSAS-45 as a comprehensive evaluation tool specific to PGS. It contains three items that evaluate the intensity of dumping symptoms: early dumping general, early dumping abdominal, and late dumping. In the current study we analyzed these outcomes in detail with a large number of patients and found that the scores for each of these three items were significantly lower in the PPG than in the DGBI group. Our results confirmed those of other investigators showing the superiority of PPG over DGBI in terms of dumping symptoms. In addition, we found that the PPG group scored
6 QOL comparison of PPG and DGBI 307 Table 3 Univariate analysis of main outcome measures following distal gastrectomy (DGBI) and pylorus-preserving gastrecrtomy (PPG) procedures Domains Subdomains Main outcome measures DGBI PPG Univariate analysis Mean SD Mean SD P-value Cohen s d Symptoms PGSAS subscales Esophageal reflux subscale (items 10, 11, C0.1 13, 24) (GSRS and PGSAS items) Abdominal pain subscale (items 9, 12, 28) C0.1 Meal-related distress subscale (items 25 27) C0.1 Indigestion subscale (items 14 17) C0.1 Diarrhea subscale (items 19, 20, 22) \ Constipation subscale (items 18, 21, 23) C0.1 Dumping subscale (items 30, 31, 33) Total Total symptom score C0.1 Living Body weight Change in body weight -7.9 % 8.1 % -6.9 % 7.0 % (0.13) Status Meals(amount) Ingested amount of food per meal C0.1 Necessity for additional meals (0.14) Meals(quality) Quality of ingestion subscale* (items 38 40) C0.1 Social activity Ability to work C0.1 QOL Dissatisfaction Dissatisfaction with symptoms C0.1 Dissatisfaction at the meal C0.1 Dissatisfaction at working C0.1 SF-8 Dissatisfaction for daily life subscale (items 43 45) Physical component summary (PCS)* (items 1 8) Mental component summary (MCS)* (items 1 8) C C C0.1 The interpretation of effect size Cohen s d (None-very small) (\0.20) Small C0.20 Medium C0.50 Large C0.80 Integrated subscales are underlined in the table. Outcome measures with *, higher score indicating better condition. Outcome measures without *, higher score indicating worse condition. Each subscale is calculated as the mean of composed items or subscales, except PCS or MCS of SF-8 significantly lower on the diarrhea subscale of the PGSAS- 45 than the DGBI group. These results indicated that by preventing the rapid evacuation of the contents of the remnant stomach into the small intestine, PPG might reduce the incidence of increased passage of stool, loose stool, and urgent need for defecation. A secondary advantage of PPG with regard to postoperative function is that it is thought to suppress duodenogastric reflux. It has been widely reported that the incidence of bile regurgitation and remnant gastritis is significantly lower in PPG than DGBI patients as assessed by endoscopic examination [15, 18, 24]. Nevertheless, in the present study there were no significant differences between the two groups in the scores of items associated with gastritis and bile reflux. Namely, the suppression of bile reflux by PPG did not decrease symptomatic complaints. Since the visceral sensation to chemical stimulants such as bile and acid is mediated primarily by vagal input, our findings may be explained at least in part by the loss of this input to the remnant stomach due to perigastric lymph node dissection. Even though there were no differences in symptoms between the PPG and DGBI groups, we still should pay attention to latent injuries to the remnant gastric mucosa. Long-term observations are needed to evaluate the histological influence of these procedures on the remnant stomach and any secondary carcinogenesis. Another expected advantage of PPG is prandial and nutritional improvement. Reduced food intake and loss of
7 308 J. Fujita et al. Table 4 Multivariate analysis of main outcome measures Celiac branch of the vagal nerve (preserved) Age (years) Gender (male) Approach (laparoscopic) Postoperative period (months) Main outcome measures Type of gastrectomy (DGBI) b P value b P value b P value b P value b P value b P value R 2 P value Diarrhea SS C0.1 C \ C0.1 C \ Dumping SS C0.1 C \ C0.1 (-0.078) \ Necessity for additional meals (0.093) (-0.115) (0.063) \ C \ Interpretation of effect size b R 2 (None-very small) \(0.100) \(0.020) Small C0.100 C0.020 Medium C0.300 C0.130 Large C0.500 C0.260 Multiple regression analysis was performed if the P value of the item/subscale in the univariate analysis was P \ Integrated subscales are underlined in the table. If b is positive, the score of the outcome measure of the patients belonging to the category in (parentheses) is higher in cases when the factor is a nominal scale, and the score of the outcome measure of patients with larger values is higher in cases when the factor is a numeral scale body weight greatly influence living status and QOL in patients who undergo gastrectomy. In general, PPG enables conservation of a relatively large gastric remnant compared to conventional DG. Because the present study was retrospective in design and we did not control the extent of gastric excision, the sizes of the remnant stomach differed significantly between the two groups. In the PPG group, at least half of the original stomach was preserved in 24 % of patients, in contrast to only 3 % of patients in the DGBI group. This may be the primary reason why PPG patients required fewer additional meals and why body weight loss was smaller in the PPG than the DGBI group (- 6.9 ± 7.0 % vs ± 8.1 %, P = 0.052). Namikawa et al. [25] used the PGSAS-45 to conduct a more detailed analysis of PPG patients and reported that larger proximal gastric remnants resulted in less body weight loss and dissatisfaction at meals and in daily life. Despite these positive findings, a typical adverse outcome after PPG is delayed gastric emptying. This occurs significantly more frequently in the early postoperative period in PPG patients than in those undergoing DGBI and is generally recognized as a PPG-specific complication [26]. Food residue was frequently observed in the remnant stomach in PPG patients even several years after surgery [24], although this disorder gradually improves over time. We evaluated symptoms of delayed gastric emptying using the postprandial fullness and early satiation items of the PGSAS-45 and found no significant differences between the PPG and DGBI group for either item. As the average postoperative period of the PPG patients was 38.4 months, we consider that delayed gastric emptying caused by PPG resolved over this period of time. Multiple regression analysis revealed that younger age and female gender were independent factors influencing PGSAS-45 symptom scores of diarrhea and dumping, and longer postoperative periods attenuated the need for additional meals. Taken together, these findings suggest that relatively young female EGC patients might be good candidates for function-preserving surgery that can minimize these postoperative disorders. Recently, gastrectomy with preservation of the celiac branch of the vagus nerve has become widely used in EGC patients. The celiac branch innervates the upper gastrointestinal organs, such as the stomach, duodenum, jejunum, and pancreas, and some of these organs physiological functions are regulated by the afferent-efferent network of the vagus nerve connecting the hypothalamus and visceral organs. In an experimental study using a canine model, Ando et al. [27] demonstrated that section of the celiac branch decreased the postprandial motility of the duodenum and jejunum. Other investigators also showed that denervation of the celiac branch influenced the regulation of hormonal secretion. Kinami et al. [28] reported that
8 QOL comparison of PPG and DGBI 309 Table 5 Univariate analysis of other outcome measures (symptoms) Subdomains Items Univariate analysis DGBI PPG Mean SD Mean SD P value Cohen s d GSRS items Abdominal pain C0.1 Heartburn C0.1 Acid regurgitation C0.1 Sucking sensations in the epigastrium C0.1 Nausea and vomiting C0.1 Borborygmus C0.1 Abdominal distension C0.1 Eructation Increased flatus C0.1 Decreased passage of stools C0.1 Increased passage of stools Loose stools Hard stools C0.1 Urgent need for defecation \ Feeling of incomplete evacuation C0.1 PGSAS specific items Bile regurgitation C0.1 Sense of food sticking C0.1 Postprandial fullness C0.1 Early satiation C0.1 Lower abdominal pains Early dumping general symptoms Early dumping abdominal symptoms Late dumping symptoms section of the celiac branch during gastrectomy impaired the secretion of insulin in response to glucagon administration, and Takiguchi et al. [29] recently demonstrated that denervation of the celiac branch disturbed postprandial changes in ghrelin secretion. As described above, preservation of the celiac branch might be beneficial for maintaining physiologic functions, but the practical efficacy of this surgical procedure in gastrectomy has not been fully elucidated [30, 31]. In the present study, 71 % of PPG patients and 15 % of DGBI patients underwent preservation of the celiac branch. Multivariable regression analysis revealed that preservation of the celiac branch significantly affected the dumping SS and diarrhea SS scores, although the method of reconstruction (PPG vs. DGBI) was not an independent factor predicting these symptoms. These findings strongly suggest that the celiac branch of the vagus nerve should be preserved whenever possible regardless of which reconstruction method is preferred. In contrast to the differences in symptom scores between PPG and DGBI, we did not detect any differences between the two approaches in terms of general QOL scores on the PGSAS-45. One reason may be that the effect size of the difference for each symptom item was relatively small, represented as Cohen s d values of , which might result in a lack of total improvement in the general QOL scores. Similar findings were observed in other series of the PGSAS study, i.e., DGBI vs. DG Roux-en-Y [5] and total gastrectomy vs. proximal gastrectomy [32]. Our work has several limitations that may be attributed to the retrospective design of the study. The PPG surgical procedures conducted in this study were considerably lacking in uniformity; specifically, the following factors varied widely among institutions and surgeons: the extent of lymphadenectomy, size of the remnant stomach, length of the pyloric cuff, surgical approach (open or laparoscopic), method of anastomosis (hand sewn or stapling), and preservation of the vagus nerve and infrapyloric vessels. All of these factors are known to substantially influence postoperative dysfunction following PPG [33]. Another weakness of this study was the sizable variation in the postoperative period of the enrolled patients. Determining the optimal time point to evaluate the postoperative change of QOL properly is a matter of concern. In addition, there might also be a slight placebo effect, as the PPG
9 310 J. Fujita et al. patients probably were told that this operation was used with the intention to reduce postoperative symptoms. Future prospective controlled studies are desired that provide the most suitable uniform surgery in each study group and have appropriate timing for the assessment. In conclusion, we demonstrated that PPG patients in this study had superior results compared to DGBI patients in terms of suppressing postoperative dumping symptoms, diarrhea, and the need for additional food. Preservation of the celiac branch of the vagus nerve is recommended either in DGBI or PPG for EGC. Acknowledgments This study was supported by a grant from Jikei University and the Japanese Society for Gastro-Surgical Pathophysiology. The authors thank all physicians who participated in this study and the patients whose cooperation made it possible. Conflict of interest The authors declare no conflicts of interest with regard to this manuscript. References 1. Bolton JS, Conway WC 2nd. Postgastrectomy syndromes. The Surgical Clinics of North America. 2011;91(5): Carvajal SH, Mulvihill SJ. Postgastrectomy syndromes: dumping and diarrhea. Gastroenterol Clin North Am. 1994;23(2): Nashimoto A, Akazawa K, Isobe Y, Miyashiro I, Katai H, Kodera Y, et al. Gastric cancer treated in 2002 in Japan: 2009 annual report of the JGCA nationwide registry. Gastric Cancer. 2013;16(1): Kumagai K, Shimizu K, Yokoyama N, Aida S, Arima S, Aikou T. Questionnaire survey regarding the current status and controversial issues concerning reconstruction after gastrectomy in Japan. Surg Today. 2012;42(5): Terashima M, Tanabe K, Yoshida M, Kawahira H, Inada T, Okabe H, et al. Postgastrectomy syndrome assessment scale (PGSAS)-45 and changes in body weight are useful tools for evaluation of reconstruction methods following distal Gastrectomy. Ann Surg Oncol. 2014;21(Suppl 3): Hirao M, Takiguchi S, Imamura H, Yamamoto K, Kurokawa Y, Fujita J, et al. Comparison of Billroth I and Roux-en-Y reconstruction after distal gastrectomy for gastric cancer: one-year postoperative effects assessed by a multi-institutional RCT. Ann Surg Oncol. 2013;20(5): Maki T, Shiratori T, Hatafuku T, Sugawara K. Pylorus-preserving gastrectomy as an improved operation for gastric ulcer. Surgery. 1967;61(6): Kodama M, Koyama K. Indications for pylorus preserving gastrectomy for early gastric cancer located in the middle third of the stomach. World J Surg. 1991;15(5): (Discussion 33 34). 9. Isozaki H, Okajima K, Momura E, Ichinona T, Fujii K, Izumi N, et al. Postoperative evaluation of pylorus-preserving gastrectomy for early gastric cancer. Br J Sur. 1996;83(2): Morita S, Katai H, Saka M, Fukagawa T, Sano T, Sasako M. Outcome of pylorus-preserving gastrectomy for early gastric cancer. Br J Surg. 2008;95(9): Hiki N, Sano T, Fukunaga T, Ohyama S, Tokunaga M, Yamaguchi T. Survival benefit of pylorus-preserving gastrectomy in early gastric cancer. J Am Coll Surg. 2009;209(3): Matsuki A, Nashimoto A, Yabusaki H, Nakagawa S. Long-term clinical outcome and survival after pylorus-preserving gastrectomy. Hepatogastroenterology. 2012;59(118): Japanese Gastric Cancer Association. Japanese gastric cancer treatment guidelines 2010 (ver. 3). Gastric Cancer Off J Int Gastric Cancer Assoc Japan Gastric Cancer Assoc. 2011;14(2): Nakada K, Ikeda M, Takahashi M, Kinami S, Yoshida M, U- enosono Y, et al. Characteristics and clinical relevance of postgastrectomy syndrome assessment scale (PGSAS)-45: newly developed integrated questionnaires for assessment of living status and quality of life in postgastrectomy patients. Gastric Cancer. 2014;. doi: /s Imada T, Rino Y, Takahashi M, Suzuki M, Tanaka J, Shiozawa M, et al. Postoperative functional evaluation of pylorus-preserving gastrectomy for early gastric cancer compared with conventional distal gastrectomy. Surgery. 1998;(2): Nishikawa K, Kawahara H, Yumiba T, Nishida T, Inoue Y, Ito T, et al. Functional characteristics of the pylorus in patients undergoing pylorus preserving gastrectomy for early gastric cancer. Surgery. 2002;131(6): Nakane Y, Akehira K, Inoue K, Iiyama H, Sato M, Masuya Y, et al. Postoperative evaluation of pylorus-preserving gastrectomy for early gastric cancer. Hepatogastroenterology. 2000;47(32): Yamaguchi T, Ichikawa D, Kurioka H, Ikoma H, Koike H, Otsuji E, et al. Postoperative clinical evaluation following pylorus-preserving gastrectomy. Hepatogastroenterology. 2004;51(57): Shibata C, Shiiba KI, Funayama Y, Ishii S, Fukushima K, Mizoi T, et al. Outcomes after pylorus-preserving gastrectomy for early gastric cancer: a prospective multicenter trial. World J Surg. 2004;28(9): Nunobe S, Sasako M, Saka M, Fukagawa T, Katai H, Sano T. Symptom evaluation of long-term postoperative outcomes after pylorus-preserving gastrectomy for early gastric cancer. Gastric Cancer. 2007;10(3): de Park J, Lee HJ, Jung HC, Kim WH, Lee KU, Yang HK. Clinical outcome of pylorus-preserving gastrectomy in gastric cancer in comparison with conventional distal gastrectomy with Billroth I anastomosis. World J Surg. 2008;32(6): Mine S, Sano T, Tsutsumi K, Murakami Y, Ehara K, Saka M, et al. Large-scale investigation into dumping syndrome after gastrectomy for gastric cancer. J Am Coll Surg. 2010;211(5): Urushihara T, Sumimoto K, Shimokado K, Kuroda Y. Gastric motility after laparoscopically assisted distal gastrectomy, with or without preservation of the pylorus, for early gastric cancer, as assessed by digital dynamic x-ray imaging. Surg Endosc. 2004;18(6): Nagano H, Ohyama S, Sakamoto Y, Ohta K, Yamaguchi T, Muto T, et al. The endoscopic evaluation of gastritis, gastric remnant residue, and the incidence of secondary cancer after pyloruspreserving and transverse gastrectomies. Gastric Cancer. 2004;7(1): Namikawa T, Hiki N, Kinami S, Okabe H, Urushihara T, Kawahira H, et al. Factors that minimize postgastrectomy symptoms following pylorus-preserving gastrectomy: assessment using a newly developed scale (PGSAS-45). Gastric Cancer. 2014;. doi: /s y. 26. Suh YS, Han DS, Kong SH, Kwon S, Shin CI, Kim WH, et al. Laparoscopy-assisted pylorus-preserving gastrectomy is better than laparoscopy-assisted distal gastrectomy for middle-third early gastric cancer. Ann Surg. 2014;259(3): Ando H, Mochiki E, Ohno T, Kogure N, Tanaka N, Tabe Y, et al. Effect of distal subtotal gastrectomy with preservation of the celiac branch of the vagus nerve to gastrointestinal function: an experimental study in conscious dogs. Ann Surg. 2008;247(6):
10 QOL comparison of PPG and DGBI Kinami S, Miwa K, Sato T, Miyazaki I. Section of the vagal celiac branch in man reduces glucagon-stimulated insulin release. J Auton Nerv Syst. 1997;64(1): Takiguchi S, Hiura Y, Takahashi T, Kurokawa Y, Yamasaki M, Nakajima K, et al. Preservation of the celiac branch of the vagus nerve during laparoscopy-assisted distal gastrectomy: impact on postprandial changes in ghrelin secretion. World J Surg. 2013;37(9): Tokunaga M, Hiki N, Fukunaga T, Ohyama S, Nunobe S, Yamada K, et al. Is preservation of the celiac branch of the vagal nerve effective in preventing stasis following pylorus-preserving gastrectomy? Hepatogastroenterology. 2011;58( ): Yamada H, Kojima K, Inokuchi M, Kawano T, Sugihara K. Efficacy of celiac branch preservation in Roux-en-y reconstruction after laparoscopy-assisted distal gastrectomy. Surgery. 2011;149(1): Takiguchi N, Takahashi M, Ikeda M, Inagawa S, Ueda S, Nobuoka T, et al. Long-term quality-of-life comparison of total gastrectomy and proximal gastrectomy by Postgastrectomy Syndrome Assessment Scale (PGSAS-45): a nationwide multiinstitutional study. Gastric Cancer. 2014;. doi: /s Hiki N, Nunobe S, Kubota T, Jiang X. Function-preserving gastrectomy for early gastric cancer. Ann Surg Oncol. 2013;20(8):
Factors that minimize postgastrectomy symptoms following pylorus-preserving gastrectomy: assessment using a newly developed scale (PGSAS-45)
 Gastric Cancer (2015) 18:397 406 DOI 10.1007/s10120-014-0366-y ORIGINAL ARTICLE Factors that minimize postgastrectomy symptoms following pylorus-preserving gastrectomy: assessment using a newly developed
Gastric Cancer (2015) 18:397 406 DOI 10.1007/s10120-014-0366-y ORIGINAL ARTICLE Factors that minimize postgastrectomy symptoms following pylorus-preserving gastrectomy: assessment using a newly developed
ORIGINAL ARTICLE. Gastric Cancer (2015) 18: DOI /s
 Gastric Cancer (2015) 18:675 681 DOI 10.1007/s10120-014-0407-6 ORIGINAL ARTICLE Evaluation of postgastrectomy symptoms after distal gastrectomy with Billroth-I reconstruction using the Postgastrectomy
Gastric Cancer (2015) 18:675 681 DOI 10.1007/s10120-014-0407-6 ORIGINAL ARTICLE Evaluation of postgastrectomy symptoms after distal gastrectomy with Billroth-I reconstruction using the Postgastrectomy
Preservation of the celiac branch of the vagal nerve for pylorus preserving gastrectomy: is it meaningful?
 Gastric Cancer (2018) 21:516 523 https://doi.org/10.1007/s10120-017-0776-8 ORIGINAL ARTICLE Preservation of the celiac branch of the vagal nerve for pylorus preserving gastrectomy: is it meaningful? Haruna
Gastric Cancer (2018) 21:516 523 https://doi.org/10.1007/s10120-017-0776-8 ORIGINAL ARTICLE Preservation of the celiac branch of the vagal nerve for pylorus preserving gastrectomy: is it meaningful? Haruna
ORIGINAL ARTICLE. Observational Study
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v22.i40.8978 World J Gastroenterol 2016 October 28; 22(40): 8978-8990 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v22.i40.8978 World J Gastroenterol 2016 October 28; 22(40): 8978-8990 ISSN 1007-9327
Kendai Kaneshima 1, Akiyoshi Seshimo 1, Kunitomo Miyake 1, Shingo Kameoka 1, Satoru Shimizu 2
 Int Surg 2015;100:1429 1434 DOI: 10.9738/INTSURG-D-14-00263.1 Examination of the Relationship Between Postoperative Quality of Life and Gastric Emptying Function After Pylorus-Preserving Gastrectomy and
Int Surg 2015;100:1429 1434 DOI: 10.9738/INTSURG-D-14-00263.1 Examination of the Relationship Between Postoperative Quality of Life and Gastric Emptying Function After Pylorus-Preserving Gastrectomy and
ORIGINAL ARTICLE. Feasibility of Pylorus-Preserving Gastrectomy With a Wider Scope of Lymphadenectomy
 ORIGINAL ARTICLE Feasibility of Pylorus-Preserving Gastrectomy With a Wider Scope of Lymphadenectomy Donglin Zhang, MD; Shouji Shimoyama, MD; Michio Kaminishi, MD Objective: To demonstrate the feasibility
ORIGINAL ARTICLE Feasibility of Pylorus-Preserving Gastrectomy With a Wider Scope of Lymphadenectomy Donglin Zhang, MD; Shouji Shimoyama, MD; Michio Kaminishi, MD Objective: To demonstrate the feasibility
Introduction. Original Article
 pissn : 2093-582X, eissn : 2093-5641 J Gastric Cancer 2016;16(2):93-97 http://dx.doi.org/10.5230/jgc.2016.16.2.93 Original Article Non-Randomized Confirmatory Trial of Laparoscopy-Assisted Total Gastrectomy
pissn : 2093-582X, eissn : 2093-5641 J Gastric Cancer 2016;16(2):93-97 http://dx.doi.org/10.5230/jgc.2016.16.2.93 Original Article Non-Randomized Confirmatory Trial of Laparoscopy-Assisted Total Gastrectomy
Function-preserving surgery for gastric cancer: current status and future perspectives
 Review Article Function-preserving surgery for gastric cancer: current status and future perspectives Souya Nunobe, Naoki Hiki Department of Gastroenterological surgery, Cancer Institute Ariake Hospital,
Review Article Function-preserving surgery for gastric cancer: current status and future perspectives Souya Nunobe, Naoki Hiki Department of Gastroenterological surgery, Cancer Institute Ariake Hospital,
The detection rate of early gastric cancer has been increasing owing to advances in
 Focused Issue of This Month Sung Hoon Noh, MD, ph.d Department of Surgery, Yonsei University College of Medicine E - mail : sunghoonn@yuhs.ac J Korean Med Assoc 2010; 53(4): 306-310 Abstract The detection
Focused Issue of This Month Sung Hoon Noh, MD, ph.d Department of Surgery, Yonsei University College of Medicine E - mail : sunghoonn@yuhs.ac J Korean Med Assoc 2010; 53(4): 306-310 Abstract The detection
Function-Preserving Surgery in Gastric Cancer
 REVIEW ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(4):141-147 Journal of Minimally Invasive Surgery Function-Preserving Surgery in Gastric Cancer Jan Andrew D. Bueno, M.D. 1,2,
REVIEW ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(4):141-147 Journal of Minimally Invasive Surgery Function-Preserving Surgery in Gastric Cancer Jan Andrew D. Bueno, M.D. 1,2,
Risk Factors for Gallstone Formation after Surgery for Gastric Cancer
 pissn : 93-82X, eissn : 93-641 J Gastric Cancer 16;16(2):98-14 http://dx.doi.org/1.23/jgc.16.16.2.98 Original Article Risk Factors for Gallstone Formation after Surgery for Gastric Cancer Dong Jin Park
pissn : 93-82X, eissn : 93-641 J Gastric Cancer 16;16(2):98-14 http://dx.doi.org/1.23/jgc.16.16.2.98 Original Article Risk Factors for Gallstone Formation after Surgery for Gastric Cancer Dong Jin Park
Factors for Postoperative Gallstone Occurrence in Patients with Gastric Cancer: a Meta-analysis
 RESEARCH ARTICLE Factors for Postoperative Gallstone Occurrence in Patients with Gastric Cancer: a Meta-analysis Xiang-Jun Chen, Nian Li, Ying-De Huang, Shuang Ren, Fang Liu, Lian Chen, Yong Wang, Min
RESEARCH ARTICLE Factors for Postoperative Gallstone Occurrence in Patients with Gastric Cancer: a Meta-analysis Xiang-Jun Chen, Nian Li, Ying-De Huang, Shuang Ren, Fang Liu, Lian Chen, Yong Wang, Min
Prognosis of Patients With Gastric Cancer Who Underwent Proximal Gastrectomy
 Int Surg 2012;97:275 279 Prognosis of Patients With Gastric Cancer Who Underwent Proximal Gastrectomy Masahide Ikeguchi, Abdul Kader, Seigo Takaya, Youji Fukumoto, Tomohiro Osaki, Hiroaki Saito, Shigeru
Int Surg 2012;97:275 279 Prognosis of Patients With Gastric Cancer Who Underwent Proximal Gastrectomy Masahide Ikeguchi, Abdul Kader, Seigo Takaya, Youji Fukumoto, Tomohiro Osaki, Hiroaki Saito, Shigeru
Akiko Serizawa *, Kiyoaki Taniguchi, Takuji Yamada, Kunihiko Amano, Sho Kotake, Shunichi Ito and Masakazu Yamamoto
 Serizawa et al. Surgical Case Reports (2018) 4:88 https://doi.org/10.1186/s40792-018-0494-4 CASE REPORT Successful conversion surgery for unresectable gastric cancer with giant paraaortic lymph node metastasis
Serizawa et al. Surgical Case Reports (2018) 4:88 https://doi.org/10.1186/s40792-018-0494-4 CASE REPORT Successful conversion surgery for unresectable gastric cancer with giant paraaortic lymph node metastasis
Research Article Meta-Analysis and Systemic Review of Different Reconstruction Methods for Gastric Carcinoma Following Distal Gastrectomy
 Cronicon OPEN ACCESS CANCER Research Article Meta-Analysis and Systemic Review of Different Reconstruction Methods for Gastric Carcinoma Following Distal Shuailong Yang, Fangfang Chen, Shuyi Wang, Haibin
Cronicon OPEN ACCESS CANCER Research Article Meta-Analysis and Systemic Review of Different Reconstruction Methods for Gastric Carcinoma Following Distal Shuailong Yang, Fangfang Chen, Shuyi Wang, Haibin
Intraabdominal Roux-en-Y reconstruction with a novel stapling technique after laparoscopic distal gastrectomy
 Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Seiichiro Kanaya Yuichiro Kawamura Hironori Kawada Hironori Iwasaki Takashi Gomi Seiji Satoh Ichiro Uyama
 Gastric Cancer (2011) 14:365 371 DOI 10.1007/s10120-011-0054-0 ORIGINAL ARTICLE The delta-shaped anastomosis in laparoscopic distal gastrectomy: analysis of the initial 100 consecutive procedures of intracorporeal
Gastric Cancer (2011) 14:365 371 DOI 10.1007/s10120-011-0054-0 ORIGINAL ARTICLE The delta-shaped anastomosis in laparoscopic distal gastrectomy: analysis of the initial 100 consecutive procedures of intracorporeal
Omentum-preserving gastrectomy for advanced gastric cancer: a propensity-matched retrospective cohort study
 Gastric Cancer (213) 16:383 388 DOI 1.17/s112-12-198-6 ORIGINAL ARTICLE Omentum-preserving gastrectomy for advanced gastric cancer: a propensity-matched retrospective cohort study Shinichi Hasegawa Chikara
Gastric Cancer (213) 16:383 388 DOI 1.17/s112-12-198-6 ORIGINAL ARTICLE Omentum-preserving gastrectomy for advanced gastric cancer: a propensity-matched retrospective cohort study Shinichi Hasegawa Chikara
Clinical features of gastric emptying after distal gastrectomy
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 https://doi.org/10.4174/astr.2017.93.6.310 Annals of Surgical Treatment and Research Clinical features of gastric emptying after distal gastrectomy Dae
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 https://doi.org/10.4174/astr.2017.93.6.310 Annals of Surgical Treatment and Research Clinical features of gastric emptying after distal gastrectomy Dae
Vagus Nerve Preservation Selectively Restores Visceral Fat Volume in Patients with Early Gastric Cancer who Underwent Gastrectomy
 Journal of Surgical Research 173, 60 67 (2012) doi:10.1016/j.jss.2010.08.040 Vagus Nerve Preservation Selectively Restores Visceral Fat Volume in Patients with Early Gastric Cancer who Underwent Gastrectomy
Journal of Surgical Research 173, 60 67 (2012) doi:10.1016/j.jss.2010.08.040 Vagus Nerve Preservation Selectively Restores Visceral Fat Volume in Patients with Early Gastric Cancer who Underwent Gastrectomy
Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer
 Med. Bull. Fukuoka Univ. 39 3/4 251 256 2012 Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer Tatsuya HASHIMOTO,
Med. Bull. Fukuoka Univ. 39 3/4 251 256 2012 Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer Tatsuya HASHIMOTO,
Kikuchi et al. BMC Surgery (2017) 17:72 DOI /s
 Kikuchi et al. BMC Surgery (2017) 17:72 DOI 10.1186/s12893-017-0268-0 RESEARCH ARTICLE Open Access Management of early gastric cancer that meet the indication for radical lymph node dissection following
Kikuchi et al. BMC Surgery (2017) 17:72 DOI 10.1186/s12893-017-0268-0 RESEARCH ARTICLE Open Access Management of early gastric cancer that meet the indication for radical lymph node dissection following
Background. compared with LTG and LPG, so it may be a better treatment option for cstage I proximal gastric carcinoma.
 Gastric Cancer (2018) 21:500 507 https://doi.org/10.1007/s10120-017-0755-0 ORIGINAL ARTICLE Short term outcomes and nutritional status after laparoscopic subtotal gastrectomy with a very small remnant
Gastric Cancer (2018) 21:500 507 https://doi.org/10.1007/s10120-017-0755-0 ORIGINAL ARTICLE Short term outcomes and nutritional status after laparoscopic subtotal gastrectomy with a very small remnant
Risk Factors for Para-aortic Lymph Node Metastasis of Gastric Cancer from a Randomized Controlled Trial of JCOG9501
 Risk Factors for Para-aortic Lymph Node Metastasis of Gastric Cancer from a Randomized Controlled Trial of JCOG9501 Eiji Nomura 1, Mitsuru Sasako 2, Seiichiro Yamamoto 3, Takeshi Sano 2, Toshimasa Tsujinaka
Risk Factors for Para-aortic Lymph Node Metastasis of Gastric Cancer from a Randomized Controlled Trial of JCOG9501 Eiji Nomura 1, Mitsuru Sasako 2, Seiichiro Yamamoto 3, Takeshi Sano 2, Toshimasa Tsujinaka
Long-term outcomes of Roux-en-Y and Billroth-I reconstruction after laparoscopic distal gastrectomy
 Gastric Cancer (2013) 16:67 73 DOI 10.1007/s10120-012-0154-5 ORIGINAL ARTICLE Long-term outcomes of Roux-en-Y and Billroth-I reconstruction after laparoscopic distal gastrectomy Mikito Inokuchi Kazuyuki
Gastric Cancer (2013) 16:67 73 DOI 10.1007/s10120-012-0154-5 ORIGINAL ARTICLE Long-term outcomes of Roux-en-Y and Billroth-I reconstruction after laparoscopic distal gastrectomy Mikito Inokuchi Kazuyuki
Theoretical therapeutic impact of lymph node dissection on adenocarcinoma and squamous cell carcinoma
 Gastric Cancer (2016) 19:143 149 DOI 10.1007/s10120-014-0439-y ORIGINAL ARTICLE Theoretical therapeutic impact of lymph node dissection on adenocarcinoma and squamous cell carcinoma of the esophagogastric
Gastric Cancer (2016) 19:143 149 DOI 10.1007/s10120-014-0439-y ORIGINAL ARTICLE Theoretical therapeutic impact of lymph node dissection on adenocarcinoma and squamous cell carcinoma of the esophagogastric
gastric cancer; lymph node dissection;
 Yonago Acta Medica 18;61:175 181 Original Article Therapeutic Value of Lymph Node Dissection Along the Superior Mesenteric Vein and the Posterior Surface of the Pancreatic Head in Gastric Cancer Located
Yonago Acta Medica 18;61:175 181 Original Article Therapeutic Value of Lymph Node Dissection Along the Superior Mesenteric Vein and the Posterior Surface of the Pancreatic Head in Gastric Cancer Located
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Satisfactory surgical outcome of T2 gastric cancer after modified D2 lymphadenectomy
 Original Article Satisfactory surgical outcome of T2 gastric cancer after modified D2 lymphadenectomy Shupeng Zhang 1, Liangliang Wu 2, Xiaona Wang 2, Xuewei Ding 2, Han Liang 2 1 Department of General
Original Article Satisfactory surgical outcome of T2 gastric cancer after modified D2 lymphadenectomy Shupeng Zhang 1, Liangliang Wu 2, Xiaona Wang 2, Xuewei Ding 2, Han Liang 2 1 Department of General
OPERATIVE TREATMENT OF ULCER DISEASE
 Página 1 de 8 Copyright 2001 Lippincott Williams & Wilkins Greenfield, Lazar J., Mulholland, Michael W., Oldham, Keith T., Zelenock, Gerald B., Lillemoe, Keith D. Surgery: Scientific Principles & Practice,
Página 1 de 8 Copyright 2001 Lippincott Williams & Wilkins Greenfield, Lazar J., Mulholland, Michael W., Oldham, Keith T., Zelenock, Gerald B., Lillemoe, Keith D. Surgery: Scientific Principles & Practice,
SUPPLEMENTARY INFORMATION Associated with
 Table1: Rome III and Rome IV diagnostic criteria for IBS, functional constipation and functional dyspepsia. Rome III diagnostic criteria 1,2 Rome IV diagnostic criteria 3,4 Diagnostic criteria for IBS
Table1: Rome III and Rome IV diagnostic criteria for IBS, functional constipation and functional dyspepsia. Rome III diagnostic criteria 1,2 Rome IV diagnostic criteria 3,4 Diagnostic criteria for IBS
Risk factors for lymph node metastasis in histologically poorly differentiated type early gastric cancer
 498 Original article Risk factors for lymph node metastasis in histologically poorly differentiated type early gastric cancer Authors C. Kunisaki 1, M. Takahashi 2, Y. Nagahori 3, T. Fukushima 3, H. Makino
498 Original article Risk factors for lymph node metastasis in histologically poorly differentiated type early gastric cancer Authors C. Kunisaki 1, M. Takahashi 2, Y. Nagahori 3, T. Fukushima 3, H. Makino
Correspondence should be addressed to Kazuhito Yajima;
 Case Reports in Surgery Volume 2016, Article ID 9357659, 5 pages http://dx.doi.org/10.1155/2016/9357659 Case Report A Case of Laparoscopic Resection for Carcinoma of the Gastric Remnant following Proximal
Case Reports in Surgery Volume 2016, Article ID 9357659, 5 pages http://dx.doi.org/10.1155/2016/9357659 Case Report A Case of Laparoscopic Resection for Carcinoma of the Gastric Remnant following Proximal
Changes of Quality of Life after Gastric Cancer Surgery
 J Gastric Cancer 2012;12(3):194-200 http://dx.doi.org/10.5230/jgc.2012.12.3.194 Original Article Changes of Quality of Life after Gastric Cancer Surgery Horyon Kong, Oh Kyung Kwon 1, and Wansik Yu 1 Department
J Gastric Cancer 2012;12(3):194-200 http://dx.doi.org/10.5230/jgc.2012.12.3.194 Original Article Changes of Quality of Life after Gastric Cancer Surgery Horyon Kong, Oh Kyung Kwon 1, and Wansik Yu 1 Department
--Manuscript Draft-- Laparoscopic gastrectomy, Postoperative pancreatic fistula, Pancreatic injury. Tokyo Medical and Dental University Tokyo, JAPAN
 International Surgery Intraoperative pancreatic injury gives rise to severe postoperative pancreatic fistula: results of a review of unedited videos of the laparoscopic surgical procedures --Manuscript
International Surgery Intraoperative pancreatic injury gives rise to severe postoperative pancreatic fistula: results of a review of unedited videos of the laparoscopic surgical procedures --Manuscript
Michael A. Choti, MD, FACS Department of Surgery Johns Hopkins Medicine, Baltimore, MD
 Michael A. Choti, MD, FACS Department of Surgery Johns Hopkins Medicine, Baltimore, MD Surgical Therapy of Gastric Cancer CLINICAL QUESTIONS 1. How much of the stomach should be removed? 2. How many lymph
Michael A. Choti, MD, FACS Department of Surgery Johns Hopkins Medicine, Baltimore, MD Surgical Therapy of Gastric Cancer CLINICAL QUESTIONS 1. How much of the stomach should be removed? 2. How many lymph
pissn: , eissn: Yonsei Med J 55(1): , 2014
 Original Article http://dx.doi.org/10.3349/ymj.2014.55.1.162 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 55(1):162-169, 2014 Totally Laparoscopic Roux-en-Y Gastrojejunostomy after Laparoscopic Distal
Original Article http://dx.doi.org/10.3349/ymj.2014.55.1.162 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 55(1):162-169, 2014 Totally Laparoscopic Roux-en-Y Gastrojejunostomy after Laparoscopic Distal
Postoperative morbidity in elderly patients after gastric cancer surgery
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Postoperative morbidity in elderly patients after gastric cancer surgery Tomoyuki Wakahara, Nozomi Ueno, Tetsuo Maeda, Kiyonori Kanemitsu, Takuro
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Postoperative morbidity in elderly patients after gastric cancer surgery Tomoyuki Wakahara, Nozomi Ueno, Tetsuo Maeda, Kiyonori Kanemitsu, Takuro
Postgastrectomy Syndromes
 Postgastrectomy Syndromes Postgastrectomy syndromes are iatrogenic conditions that may arise from partial gastrectomies, independent of whether the gastric surgery was initially performed for peptic ulcer
Postgastrectomy Syndromes Postgastrectomy syndromes are iatrogenic conditions that may arise from partial gastrectomies, independent of whether the gastric surgery was initially performed for peptic ulcer
Survival benefit of bursectomy in patients with resectable gastric cancer: interim analysis results of a randomized controlled trial
 Gastric Cancer (2012) 15:42 48 DOI 10.1007/s10120-011-0058-9 ORIGINAL ARTICLE Survival benefit of bursectomy in patients with resectable gastric cancer: interim analysis results of a randomized controlled
Gastric Cancer (2012) 15:42 48 DOI 10.1007/s10120-011-0058-9 ORIGINAL ARTICLE Survival benefit of bursectomy in patients with resectable gastric cancer: interim analysis results of a randomized controlled
Tornado Roux-en-Y anastomosis in laparoscopy-assisted distal gastrectomy
 Gastric Cancer (2008) 11: 181 185 DOI 10.1007/s10120-008-0474-7 Technical note 2008 by International and Japanese Gastric Cancer Associations Tornado Roux-en-Y anastomosis in laparoscopy-assisted distal
Gastric Cancer (2008) 11: 181 185 DOI 10.1007/s10120-008-0474-7 Technical note 2008 by International and Japanese Gastric Cancer Associations Tornado Roux-en-Y anastomosis in laparoscopy-assisted distal
Long-Hai Cui, Sang-Yong Son, Ho-Jung Shin, Cheulsu Byun, Hoon Hur, Sang-Uk Han, and Yong Kwan Cho
 Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 1803851, 6 pages https://doi.org/10.1155/2017/1803851 Clinical Study Billroth II with Braun Enteroenterostomy Is a Good Alternative
Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 1803851, 6 pages https://doi.org/10.1155/2017/1803851 Clinical Study Billroth II with Braun Enteroenterostomy Is a Good Alternative
Diagnostic accuracy of T stage of gastric cancer from the view point of application of laparoscopic proximal gastrectomy
 MOLECULAR AND CLINICAL ONCOLOGY 8: 773-778, 2018 Diagnostic accuracy of T stage of gastric cancer from the view point of application of laparoscopic proximal gastrectomy KEITA KOUZU, HIRONORI TSUJIMOTO,
MOLECULAR AND CLINICAL ONCOLOGY 8: 773-778, 2018 Diagnostic accuracy of T stage of gastric cancer from the view point of application of laparoscopic proximal gastrectomy KEITA KOUZU, HIRONORI TSUJIMOTO,
Effectiveness of Gastric Neurostimulation in Patients With Gastroparesis
 SCIENTIFIC PAPER Effectiveness of Gastric Neurostimulation in Patients With Gastroparesis Jeremy Ross, MS, Mario Masrur, MD, Raquel Gonzalez-Heredia, MD, E. Fernando Elli, MD ABSTRACT Background: Patients
SCIENTIFIC PAPER Effectiveness of Gastric Neurostimulation in Patients With Gastroparesis Jeremy Ross, MS, Mario Masrur, MD, Raquel Gonzalez-Heredia, MD, E. Fernando Elli, MD ABSTRACT Background: Patients
Laparoscopic gastrectomy for remnant gastric cancer: a comprehensive review and case series
 Gastric Cancer (2016) 19:287 292 DOI 10.1007/s10120-014-0451-2 ORIGINAL ARTICLE Laparoscopic gastrectomy for remnant gastric cancer: a comprehensive review and case series Shigeru Tsunoda Hiroshi Okabe
Gastric Cancer (2016) 19:287 292 DOI 10.1007/s10120-014-0451-2 ORIGINAL ARTICLE Laparoscopic gastrectomy for remnant gastric cancer: a comprehensive review and case series Shigeru Tsunoda Hiroshi Okabe
JKSS INTRODUCTION. Ki Han Kim, Min Chan Kim, Ghap Joong Jung ORIGINAL ARTICLE
 J Korean Surg Soc 2012;83:274-280 http://dx.doi.org/10.4174/jkss.2012.83.5.274 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Risk factors associated with
J Korean Surg Soc 2012;83:274-280 http://dx.doi.org/10.4174/jkss.2012.83.5.274 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Risk factors associated with
Safety of Laparoscopy Assisted Gastrectomy for Gastric Cancer, Including Advanced Cancers
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 215;18(3):79-85 Journal of Minimally Invasive Surgery Safety of Laparoscopy Assisted Gastrectomy for Gastric Cancer, Including Advanced
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 215;18(3):79-85 Journal of Minimally Invasive Surgery Safety of Laparoscopy Assisted Gastrectomy for Gastric Cancer, Including Advanced
Original article. Introduction
 Gastric Cancer (2010) 13: 238 244 DOI 10.1007/s10120-010-0565-0 Original article 2010 by International and Japanese Gastric Cancer Associations Safety and feasibility of laparoscopy-assisted distal gastrectomy
Gastric Cancer (2010) 13: 238 244 DOI 10.1007/s10120-010-0565-0 Original article 2010 by International and Japanese Gastric Cancer Associations Safety and feasibility of laparoscopy-assisted distal gastrectomy
ORIGINAL ARTICLE. International Journal of Surgery
 International Journal of Surgery (2013) 11(S1), S104 S109 Contents lists available at ScienceDirect International Journal of Surgery journal homepage: www.journal-surgery.net ORIGINAL ARTICLE Quality of
International Journal of Surgery (2013) 11(S1), S104 S109 Contents lists available at ScienceDirect International Journal of Surgery journal homepage: www.journal-surgery.net ORIGINAL ARTICLE Quality of
Complications Leading Reoperation after Gastrectomy in Patients with Gastric Cancer: Frequency, Type, and Potential Causes
 J Gastric Cancer 2013;13(4):242-246 http://dx.doi.org/10.5230/jgc.2013.13.4.242 Original Article Complications Leading Reoperation after Gastrectomy in Patients with Gastric Cancer: Frequency, Type, and
J Gastric Cancer 2013;13(4):242-246 http://dx.doi.org/10.5230/jgc.2013.13.4.242 Original Article Complications Leading Reoperation after Gastrectomy in Patients with Gastric Cancer: Frequency, Type, and
Surgical Outcomes From Laparoscopic Distal Gastrectomy and Roux-en-Y Reconstruction: Evolution in a Totally Intracorporeal Technique
 ORIGINAL ARTICLE Surgical Outcomes From Laparoscopic Distal Gastrectomy and Roux-en-Y Reconstruction: Evolution in a Totally Intracorporeal Technique George Bouras, MRCS, Sang-Woong Lee, MD, PhD, Eiji
ORIGINAL ARTICLE Surgical Outcomes From Laparoscopic Distal Gastrectomy and Roux-en-Y Reconstruction: Evolution in a Totally Intracorporeal Technique George Bouras, MRCS, Sang-Woong Lee, MD, PhD, Eiji
Surgical Treatment of Gastric Cancer
 SMGr up Surgical Treatment of Gastric Cancer Igor Correia de Farias 1 *, Maria Luiza Leite de Medeiros 2, Wilson Luiz da Costa Júnior 1, Heber Salvador de Castro Ribeiro 1, Alessandro Landskron Diniz 1,
SMGr up Surgical Treatment of Gastric Cancer Igor Correia de Farias 1 *, Maria Luiza Leite de Medeiros 2, Wilson Luiz da Costa Júnior 1, Heber Salvador de Castro Ribeiro 1, Alessandro Landskron Diniz 1,
Clinicopathological Characteristics and Outcome Indicators of Stage II Gastric Cancer According to the Japanese Classification of Gastric Cancer
 Clinicopathological Characteristics and Outcome Indicators of Stage II Gastric Cancer According to the Japanese Classification of Gastric Cancer HITOSHI OJIMA 1, KEN-ICHIRO ARAKI 1, TOSHIHIDE KATO 1, KAORI
Clinicopathological Characteristics and Outcome Indicators of Stage II Gastric Cancer According to the Japanese Classification of Gastric Cancer HITOSHI OJIMA 1, KEN-ICHIRO ARAKI 1, TOSHIHIDE KATO 1, KAORI
Technique. Matthew Bettendorf, MD Essentia Health Duluth Clinic. Laparoscopic approach One 12mm port, Four 5mm ports
 Matthew Bettendorf, MD Essentia Health Duluth Clinic Technique Laparoscopic approach One 12mm port, Four 5mm ports Single staple line with no anastamosis 85% gastrectomy Goal to remove
Matthew Bettendorf, MD Essentia Health Duluth Clinic Technique Laparoscopic approach One 12mm port, Four 5mm ports Single staple line with no anastamosis 85% gastrectomy Goal to remove
Determining the Optimal Surgical Approach to Esophageal Cancer
 Determining the Optimal Surgical Approach to Esophageal Cancer Amit Bhargava, MD Attending Thoracic Surgeon Department of Cardiovascular and Thoracic Surgery Open Esophagectomy versus Minimally Invasive
Determining the Optimal Surgical Approach to Esophageal Cancer Amit Bhargava, MD Attending Thoracic Surgeon Department of Cardiovascular and Thoracic Surgery Open Esophagectomy versus Minimally Invasive
M. Nakamura 1, M. Nakamori 1,T.Ojima 1, M. Iwahashi 1, T. Horiuchi 6, Y. Kobayashi 2, N. Yamade 3, K. Shimada 4,M.Oka 5 and H.
 Randomized clinical trial Randomized clinical trial comparing long-term quality of life for Billroth I versus Roux-en-Y reconstruction after distal gastrectomy for gastric cancer M. Nakamura 1, M. Nakamori
Randomized clinical trial Randomized clinical trial comparing long-term quality of life for Billroth I versus Roux-en-Y reconstruction after distal gastrectomy for gastric cancer M. Nakamura 1, M. Nakamori
Recent Evolution of Surgical Treatment for Gastric Cancer in Korea
 J Gastric Cancer 2011;11(1):1-6 DOI:10.5230/jgc.2011.11.1.1 Review Article Recent Evolution of Surgical Treatment for Gastric Cancer in Korea Ji Yeong An, Jae-Ho Cheong, Woo Jin Hyung, and Sung Hoon Noh
J Gastric Cancer 2011;11(1):1-6 DOI:10.5230/jgc.2011.11.1.1 Review Article Recent Evolution of Surgical Treatment for Gastric Cancer in Korea Ji Yeong An, Jae-Ho Cheong, Woo Jin Hyung, and Sung Hoon Noh
Positive impact of adding No.14v lymph node to D2 dissection on survival for distal gastric cancer patients after surgery with curative intent
 Original Article Positive impact of adding No.14v lymph node to D2 dissection on survival for distal gastric cancer patients after surgery with curative intent Yuexiang Liang 1,2 *, Liangliang Wu 1 *,
Original Article Positive impact of adding No.14v lymph node to D2 dissection on survival for distal gastric cancer patients after surgery with curative intent Yuexiang Liang 1,2 *, Liangliang Wu 1 *,
Case Report Late Onset Remnant Gastric Cancer with Afferent Loop Syndrome 47 Years after Billroth II Surgery
 Case Reports in Surgery Volume 2015, Article ID 730897, 4 pages http://dx.doi.org/10.1155/2015/730897 Case Report Late Onset Remnant Gastric Cancer with Afferent Loop Syndrome 47 Years after Billroth II
Case Reports in Surgery Volume 2015, Article ID 730897, 4 pages http://dx.doi.org/10.1155/2015/730897 Case Report Late Onset Remnant Gastric Cancer with Afferent Loop Syndrome 47 Years after Billroth II
2 Yu Ohkura. Hisahiro Hosogi. 2 Masaki Ueno
 Gastric Cancer (2017) 20:528 535 DOI 10.1007/s10120-016-0624-2 ORIGINAL ARTICLE Proximal gastrectomy with exclusion of no. 3b lesser curvature lymph node dissection could be indicated for patients with
Gastric Cancer (2017) 20:528 535 DOI 10.1007/s10120-016-0624-2 ORIGINAL ARTICLE Proximal gastrectomy with exclusion of no. 3b lesser curvature lymph node dissection could be indicated for patients with
A Proposed Strategy for Treatment of Superficial Carcinoma. in the Thoracic Esophagus Based on an Analysis. of Lymph Node Metastasis
 Kitakanto Med J 2002 ; 52 : 189-193 189 A Proposed Strategy for Treatment of Superficial Carcinoma in the Thoracic Esophagus Based on an Analysis of Lymph Node Metastasis Susumu Kawate,' Susumu Ohwada,'
Kitakanto Med J 2002 ; 52 : 189-193 189 A Proposed Strategy for Treatment of Superficial Carcinoma in the Thoracic Esophagus Based on an Analysis of Lymph Node Metastasis Susumu Kawate,' Susumu Ohwada,'
Early and long term outcomes of endoscopic submucosal dissection for early gastric cancer in a large patient series
 594 Early and long term outcomes of endoscopic submucosal dissection for early gastric cancer in a large patient series KEN OHNITA 1, HAJIME ISOMOTO 1, SABURO SHIKUWA 2, HIROYUKI YAJIMA 1, HITOMI MINAMI
594 Early and long term outcomes of endoscopic submucosal dissection for early gastric cancer in a large patient series KEN OHNITA 1, HAJIME ISOMOTO 1, SABURO SHIKUWA 2, HIROYUKI YAJIMA 1, HITOMI MINAMI
Present and Future Status of Gastric Cancer Surgery
 Review Article Jpn J Clin Oncol 2011;41(3)307 313 doi:10.1093/jjco/hyq240 Advance Access Publication 17 January 2011 Present and Future Status of Gastric Cancer Surgery Makoto Saka *, Shinji Morita, Takeo
Review Article Jpn J Clin Oncol 2011;41(3)307 313 doi:10.1093/jjco/hyq240 Advance Access Publication 17 January 2011 Present and Future Status of Gastric Cancer Surgery Makoto Saka *, Shinji Morita, Takeo
Is There any Role of Visceral Fat Area for Predicting Difficulty of Laparoscopic Gastrectomy for Gastric Cancer?
 pissn : 2093-582X, eissn : 2093-5641 J Gastric Cancer 2015;15(3):151-158 http://dx.doi.org/10.5230/jgc.2015.15.3.151 Original Article Is There any Role of Visceral Fat Area for Predicting Difficulty of
pissn : 2093-582X, eissn : 2093-5641 J Gastric Cancer 2015;15(3):151-158 http://dx.doi.org/10.5230/jgc.2015.15.3.151 Original Article Is There any Role of Visceral Fat Area for Predicting Difficulty of
Impact of comorbidities on postoperative complications in patients undergoing laparoscopyassisted gastrectomy for gastric cancer
 Inokuchi et al. BMC Surgery 2014, 14:97 RESEARCH ARTICLE Open Access Impact of comorbidities on postoperative complications in patients undergoing laparoscopyassisted gastrectomy for gastric cancer Mikito
Inokuchi et al. BMC Surgery 2014, 14:97 RESEARCH ARTICLE Open Access Impact of comorbidities on postoperative complications in patients undergoing laparoscopyassisted gastrectomy for gastric cancer Mikito
Minimally invasive function-preserving surgery based on sentinel node concept in early gastric cancer
 Review Article Minimally invasive function-preserving surgery based on sentinel node concept in early gastric cancer Hiroya Takeuchi, Yuko Kitagawa Department of Surgery, Keio University School of Medicine,
Review Article Minimally invasive function-preserving surgery based on sentinel node concept in early gastric cancer Hiroya Takeuchi, Yuko Kitagawa Department of Surgery, Keio University School of Medicine,
Comparison of Short-Term Postoperative Outcomes in Totally Laparoscopic Distal Gastrectomy Versus Laparoscopy-Assisted Distal Gastrectomy
 J Gastric Cancer 2014;14(2):105-110 http://dx.doi.org/10.5230/jgc.2014.14.2.105 Original Article Comparison of Short-Term Postoperative Outcomes in Totally Laparoscopic Distal Gastrectomy Versus Laparoscopy-Assisted
J Gastric Cancer 2014;14(2):105-110 http://dx.doi.org/10.5230/jgc.2014.14.2.105 Original Article Comparison of Short-Term Postoperative Outcomes in Totally Laparoscopic Distal Gastrectomy Versus Laparoscopy-Assisted
MATERIALS AND METHODS Patients
 Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
Risk factors for non-curative resection of early gastric neoplasms with endoscopic submucosal dissection: Analysis of 1,123 lesions
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 9: 1209-1214, 2015 Risk factors for non-curative resection of early gastric neoplasms with endoscopic submucosal dissection: Analysis of 1,123 lesions TATSUYA TOYOKAWA
EXPERIMENTAL AND THERAPEUTIC MEDICINE 9: 1209-1214, 2015 Risk factors for non-curative resection of early gastric neoplasms with endoscopic submucosal dissection: Analysis of 1,123 lesions TATSUYA TOYOKAWA
Won Ho Han1, Amir Ben Yehuda2, Deok-Hee Kim1, Seung Geun Yang1, Bang Wool Eom1, Hong Man Yoon1, Young-Woo Kim1, Keun Won Ryu1 View this article at:
 Original Article A comparative study of totally laparoscopic distal gastrectomy versus laparoscopic-assisted distal gastrectomy in gastric cancer patients: Short-term operative outcomes at a high-volume
Original Article A comparative study of totally laparoscopic distal gastrectomy versus laparoscopic-assisted distal gastrectomy in gastric cancer patients: Short-term operative outcomes at a high-volume
Which is better long-term survival of gastric cancer patients with Billroth I or Billroth II reconstruction after distal gastrectomy?
 Ann. Cancer Res. Ther. Vol. 21, No. 1, pp. 2-25, 213 Which is better long-term survival of gastric cancer patients with Billroth I or Billroth II reconstruction after distal gastrectomy? Impact on 2-year
Ann. Cancer Res. Ther. Vol. 21, No. 1, pp. 2-25, 213 Which is better long-term survival of gastric cancer patients with Billroth I or Billroth II reconstruction after distal gastrectomy? Impact on 2-year
Long-Term Outcomes of Proximal Gastrectomy versus Total Gastrectomy for Upper-Third Gastric Cancer
 J Gastric Cancer 2014;14(4):246-251 http://dx.doi.org/10.5230/jgc.2014.14.4.246 Original Article Long-Term Outcomes of Proximal Gastrectomy versus Total Gastrectomy for Upper-Third Gastric Cancer Myoung
J Gastric Cancer 2014;14(4):246-251 http://dx.doi.org/10.5230/jgc.2014.14.4.246 Original Article Long-Term Outcomes of Proximal Gastrectomy versus Total Gastrectomy for Upper-Third Gastric Cancer Myoung
STOMACH and DUODENUM DISEASE
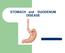 STOMACH and DUODENUM DISEASE STOMACH ANATOMY In the living and upright posture, the stomach is a j-shaped. It has two surfaces, two curvatures and two openings. Esophagus Fundus cardia Pylorus B o d y
STOMACH and DUODENUM DISEASE STOMACH ANATOMY In the living and upright posture, the stomach is a j-shaped. It has two surfaces, two curvatures and two openings. Esophagus Fundus cardia Pylorus B o d y
Laparoscopy-assisted distal gastrectomy for early gastric cancer poses few limitations for selected elderly patients: a single-center experience
 Anegawa et al. Surgical Case Reports (2016) 2:56 DOI 10.11/s407-016-0183-0 CASE REPORT Laparoscopy-assisted distal gastrectomy for early gastric cancer poses few limitations for selected elderly patients:
Anegawa et al. Surgical Case Reports (2016) 2:56 DOI 10.11/s407-016-0183-0 CASE REPORT Laparoscopy-assisted distal gastrectomy for early gastric cancer poses few limitations for selected elderly patients:
Gastric cancer treatment: similarity and difference between China and Korea
 Review Article Gastric cancer treatment: similarity and difference between China and Korea Kun Yang 1,2, Jian-Kun Hu 1,2 1 Department of Gastrointestinal Surgery, West China Hospital, Sichuan University,
Review Article Gastric cancer treatment: similarity and difference between China and Korea Kun Yang 1,2, Jian-Kun Hu 1,2 1 Department of Gastrointestinal Surgery, West China Hospital, Sichuan University,
Incidence of metachronous gastric cancer in the remnant stomach after synchronous multiple cancer surgery
 Gastric Cancer (2014) 17:61 66 DOI 10.1007/s10120-013-0261-y ORIGINAL ARTICLE Incidence of metachronous gastric cancer in the remnant stomach after synchronous multiple cancer surgery Isao Nozaki Shinji
Gastric Cancer (2014) 17:61 66 DOI 10.1007/s10120-013-0261-y ORIGINAL ARTICLE Incidence of metachronous gastric cancer in the remnant stomach after synchronous multiple cancer surgery Isao Nozaki Shinji
Department of Surgery, Aizu Central Hospital, Fukushima
 Case Reports Resection of Asynchronous Quadruple Advanced Colonic Carcinomas Followed by Reconstruction with Ileal Interposition between the Transverse Colon and Rectum Sho Mineta 1, Kimiyoshi Shimanuki
Case Reports Resection of Asynchronous Quadruple Advanced Colonic Carcinomas Followed by Reconstruction with Ileal Interposition between the Transverse Colon and Rectum Sho Mineta 1, Kimiyoshi Shimanuki
Perigastric lymph node metastases in gastric cancer: comparison of different staging systems
 Gastric Cancer (1999) 2: 201 205 Original article 1999 by International and Japanese Gastric Cancer Associations Perigastric lymph node metastases in gastric cancer: comparison of different staging systems
Gastric Cancer (1999) 2: 201 205 Original article 1999 by International and Japanese Gastric Cancer Associations Perigastric lymph node metastases in gastric cancer: comparison of different staging systems
Postgastrectomy and Postvagotomy Syndromes
 H. D. Becker W.F. Caspary Postgastrectomy and Postvagotomy Syndromes With 84 Figures (Mainly in Two Colors) Springer-Verlag Berlin Heidelberg New York 1980 Professor Dr. med. H. D. Becker KlInik und PolIklImk
H. D. Becker W.F. Caspary Postgastrectomy and Postvagotomy Syndromes With 84 Figures (Mainly in Two Colors) Springer-Verlag Berlin Heidelberg New York 1980 Professor Dr. med. H. D. Becker KlInik und PolIklImk
Prognostic factors in stage IB gastric cancer
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i21.6580 World J Gastroenterol 2014 June 7; 20(21): 6580-6585 ISSN 1007-9327 (print)
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i21.6580 World J Gastroenterol 2014 June 7; 20(21): 6580-6585 ISSN 1007-9327 (print)
Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer
 Review Article Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer Hideki Sunagawa, Takahiro Kinoshita Gastric Surgery Division,
Review Article Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer Hideki Sunagawa, Takahiro Kinoshita Gastric Surgery Division,
A Multicenter Study on Oncologic Outcome of Laparoscopic Gastrectomy for Early Cancer in Japan
 ORIGINAL ARTICLES A Multicenter Study on Oncologic Outcome of Seigo Kitano, MD, PhD,* Norio Shiraishi, MD, PhD,* Ichiro Uyama, MD, PhD, Kenichi Sugihara, MD, PhD, Nobuhiko Tanigawa, MD, PhD, and the Japanese
ORIGINAL ARTICLES A Multicenter Study on Oncologic Outcome of Seigo Kitano, MD, PhD,* Norio Shiraishi, MD, PhD,* Ichiro Uyama, MD, PhD, Kenichi Sugihara, MD, PhD, Nobuhiko Tanigawa, MD, PhD, and the Japanese
Comparative study of clinical efficacy of laparoscopy-assisted radical gastrectomy versus open radical gastrectomy for advanced gastric cancer
 Comparative study of clinical efficacy of laparoscopy-assisted radical gastrectomy versus open radical gastrectomy for advanced gastric cancer L.M. Wu, X.J. Jiang, Q.F. Lin and C.X. Jian Department of
Comparative study of clinical efficacy of laparoscopy-assisted radical gastrectomy versus open radical gastrectomy for advanced gastric cancer L.M. Wu, X.J. Jiang, Q.F. Lin and C.X. Jian Department of
Commonly Performed Bariatric Procedures in Singapore. Lin Jinlin Associate Consultant General, Upper GI and Bariatric Surgery Changi General Hospital
 Commonly Performed Bariatric Procedures in Singapore Lin Jinlin Associate Consultant General, Upper GI and Bariatric Surgery Changi General Hospital Scope 1. Introduction 2. Principles of bariatric surgery
Commonly Performed Bariatric Procedures in Singapore Lin Jinlin Associate Consultant General, Upper GI and Bariatric Surgery Changi General Hospital Scope 1. Introduction 2. Principles of bariatric surgery
Splenic hilar dissection in the treatment of proximal advanced gastric cancer: what is an adequate strategy?
 Editorial Splenic hilar dissection in the treatment of proximal advanced gastric cancer: what is an adequate strategy? Takahiro Kinoshita Gastric Surgery Division, National Cancer Center Hospital East,
Editorial Splenic hilar dissection in the treatment of proximal advanced gastric cancer: what is an adequate strategy? Takahiro Kinoshita Gastric Surgery Division, National Cancer Center Hospital East,
Multicenter study of the long-term outcomes of endoscopic submucosal dissection for early gastric cancer in patients 80 years of age or older
 Gastric Cancer (2012) 15:70 75 DOI 10.1007/s10120-011-0067-8 ORIGINAL ARTICLE Multicenter study of the long-term outcomes of endoscopic submucosal dissection for early gastric cancer in patients 80 years
Gastric Cancer (2012) 15:70 75 DOI 10.1007/s10120-011-0067-8 ORIGINAL ARTICLE Multicenter study of the long-term outcomes of endoscopic submucosal dissection for early gastric cancer in patients 80 years
Characteristics of intramural metastasis in gastric cancer. Tatsuya Hashimoto Kuniyoshi Arai Yuichi Yamashita Yoshiaki Iwasaki Tsunekazu
 ORIGINAL ARTICLE Characteristics of intramural metastasis in gastric cancer Tatsuya Hashimoto Kuniyoshi Arai Yuichi Yamashita Yoshiaki Iwasaki Tsunekazu Hishima Author for correspondence: T. Hashimoto
ORIGINAL ARTICLE Characteristics of intramural metastasis in gastric cancer Tatsuya Hashimoto Kuniyoshi Arai Yuichi Yamashita Yoshiaki Iwasaki Tsunekazu Hishima Author for correspondence: T. Hashimoto
Risk factors for complications during surgical treatment of remnant gastric cancer
 Gastric Cancer (2015) 18:390 396 DOI 10.1007/s10120-014-0369-8 ORIGINAL ARTICLE Risk factors for complications during surgical treatment of remnant gastric cancer In Gyu Kwon In Cho Yoon Young Choi Woo
Gastric Cancer (2015) 18:390 396 DOI 10.1007/s10120-014-0369-8 ORIGINAL ARTICLE Risk factors for complications during surgical treatment of remnant gastric cancer In Gyu Kwon In Cho Yoon Young Choi Woo
سرطان المعدة. Gastric Cancer حمود حامد
 سرطان المعدة Gastric Cancer ا أ لستاذ الدك تور حمود حامد عميد كلية الطب البشري بجامعة دمشق Epidemiology second leading cause of cancer death and fourth most common cancer worldwide Overall declining Histologic
سرطان المعدة Gastric Cancer ا أ لستاذ الدك تور حمود حامد عميد كلية الطب البشري بجامعة دمشق Epidemiology second leading cause of cancer death and fourth most common cancer worldwide Overall declining Histologic
Clinical Significance of the Pattern of Lymph Node Metastasis Depending on the Location of Gastric Cancer
 J Gastric Cancer 2011;11(2):86-93 DOI:10.5230/jgc.2011.11.2.86 Original Article Clinical Significance of the Pattern of Lymph Node Metastasis Depending on the Location of Gastric Cancer Ki Bin Han, You
J Gastric Cancer 2011;11(2):86-93 DOI:10.5230/jgc.2011.11.2.86 Original Article Clinical Significance of the Pattern of Lymph Node Metastasis Depending on the Location of Gastric Cancer Ki Bin Han, You
Post-discharge Self-management of Food Intake in Distal Gastrectomy Patients
 Post-discharge Self-management of Food Intake in Distal Gastrectomy Patients Masumi Yamaguchi 1), Yayoi Kamakura 2), Junko Fukada 2), Masahiko Yoneda 2), Yoshitaka Yamamura 3), Hisae Kanada 3) Key Words
Post-discharge Self-management of Food Intake in Distal Gastrectomy Patients Masumi Yamaguchi 1), Yayoi Kamakura 2), Junko Fukada 2), Masahiko Yoneda 2), Yoshitaka Yamamura 3), Hisae Kanada 3) Key Words
Evaluation of the delta-shaped anastomosis in laparoscopic distal gastrectomy: midterm results of a comparison with Roux-en-Y anastomosis
 Surg Endosc (2014) 28:2137 2144 DOI 10.1007/s00464-014-3445-6 and Other Interventional Techniques Evaluation of the delta-shaped anastomosis in laparoscopic distal gastrectomy: midterm results of a comparison
Surg Endosc (2014) 28:2137 2144 DOI 10.1007/s00464-014-3445-6 and Other Interventional Techniques Evaluation of the delta-shaped anastomosis in laparoscopic distal gastrectomy: midterm results of a comparison
Indian Journal of Medical Research and Pharmaceutical Sciences July 2017;4(7) ISSN: ISSN: DOI: /zenodo Impact Factor: 3.
 GALLBLADDER DISEASES ASSOCIATED WITH LAPAROSCOPIC SLEEVE GASTRECTOMY IN JORDAN, PILOT STUDY Dr. Osama T. Abu Salem*, Dr. Ibrahim Al Gwairy, Dr. Ramadan Al Hasanat & Dr. Talal Jalabneh** *Consultant Gneral
GALLBLADDER DISEASES ASSOCIATED WITH LAPAROSCOPIC SLEEVE GASTRECTOMY IN JORDAN, PILOT STUDY Dr. Osama T. Abu Salem*, Dr. Ibrahim Al Gwairy, Dr. Ramadan Al Hasanat & Dr. Talal Jalabneh** *Consultant Gneral
Outcome after emergency surgery in patients with a free perforation caused by gastric cancer
 experimental and therapeutic medicine 1: 199-203, 2010 199 Outcome after emergency surgery in patients with a free perforation caused by gastric cancer Hironori Tsujimoto 1, Shuichi Hiraki 1, Naoko Sakamoto
experimental and therapeutic medicine 1: 199-203, 2010 199 Outcome after emergency surgery in patients with a free perforation caused by gastric cancer Hironori Tsujimoto 1, Shuichi Hiraki 1, Naoko Sakamoto
Impact of conversion during laparoscopic gastrectomy on outcomes of patients with gastric cancer
 JBUON 2017; 22(4): 926-931 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Impact of conversion during laparoscopic gastrectomy on outcomes of
JBUON 2017; 22(4): 926-931 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Impact of conversion during laparoscopic gastrectomy on outcomes of
Approaches to Surgical Treatment of Gastric Cancer. Byrne Lee, MD FACS Chief, Mixed Tumor Surgery Service
 Approaches to Surgical Treatment of Gastric Cancer Byrne Lee, MD FACS Chief, Mixed Tumor Surgery Service Disclosures I do not have anything to disclose Outline Background Diagnosis Histology Staging Surgery
Approaches to Surgical Treatment of Gastric Cancer Byrne Lee, MD FACS Chief, Mixed Tumor Surgery Service Disclosures I do not have anything to disclose Outline Background Diagnosis Histology Staging Surgery
Significance of the lymph nodes in the 7th station in rational dissection for metastasis of distal gastric cancer with different T categories
 Original Article Significance of the lymph nodes in the 7th station in rational dissection for metastasis of distal gastric cancer with different T categories Wu Song, Yulong He, Shaochuan Wang, Weiling
Original Article Significance of the lymph nodes in the 7th station in rational dissection for metastasis of distal gastric cancer with different T categories Wu Song, Yulong He, Shaochuan Wang, Weiling
A case of local recurrence and distant metastasis following curative endoscopic submucosal dissection of early gastric cancer
 Gastric Cancer (2015) 18:188 192 DOI 10.1007/s10120-014-0341-7 CASE REPORT A case of local recurrence and distant metastasis following curative endoscopic submucosal dissection of early gastric cancer
Gastric Cancer (2015) 18:188 192 DOI 10.1007/s10120-014-0341-7 CASE REPORT A case of local recurrence and distant metastasis following curative endoscopic submucosal dissection of early gastric cancer
Completely laparoscopic extraperigastric lymph node dissection for gastric malignancies located in the middle or lower third of the stomach
 Gastric Cancer (1999) 2: 186 190 Technical note 1999 by International and Japanese Gastric Cancer Associations Completely laparoscopic extraperigastric lymph node dissection for gastric malignancies located
Gastric Cancer (1999) 2: 186 190 Technical note 1999 by International and Japanese Gastric Cancer Associations Completely laparoscopic extraperigastric lymph node dissection for gastric malignancies located
Risk factors for recurrence of gastric cancer after curative laparoscopic gastrectomy
 79 ORIGINAL Risk factors for recurrence of gastric cancer after curative laparoscopic gastrectomy Hideya Kashihara, Mitsuo Shimada, Kozo Yoshikawa, Jun Higashijima, Takuya Tokunaga, Masaaki Nishi, and
79 ORIGINAL Risk factors for recurrence of gastric cancer after curative laparoscopic gastrectomy Hideya Kashihara, Mitsuo Shimada, Kozo Yoshikawa, Jun Higashijima, Takuya Tokunaga, Masaaki Nishi, and
