Review Article Combination Therapy for Diabetic Macular Edema
|
|
|
- Angela Holmes
- 5 years ago
- Views:
Transcription
1 Ophthalmology Volume 2012, Article ID , 6 pages doi: /2012/ Review Article Combination Therapy for Diabetic Macular Edema Dinah Zur and Anat Loewenstein Department of Ophthalmology, Tel Aviv Medical Center, Sackler Faculty of Medicine, Tel Aviv University, Tel Aviv, Israel Correspondence should be addressed to Anat Loewenstein, anatl@tasmc.health.gov.il Received 1 August 2011; Accepted 25 December 2011 Academic Editor: Chi-Chao Chan Copyright 2012 D. Zur and A. Loewenstein. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Diabetic macular edema is a main reason for visual loss in diabetic patients. Until recent years, macular laser photocoagulation was the only available therapy. The awareness that inflammation is an important factor in the pathogenetic process of DME gave reason for intravitreal treatment with corticosteroids. The introduction of anti-vegf drugs brought a revolutionary change in the treatment of DME. This paper will review the important clinical trials with an emphasis on combination therapies. 1. Introduction Diabetic maculopathy is the main reason for visual loss in patients with diabetic retinopathy, besides proliferative diabetic retinopathy [1 3]. If left untreated, 25 30% of patients affected by diabetic macular edema (DME) experience a 15- letter decrease in visual acuity (VA) score within 3 years [4]. Strict control of glucose levels and blood pressure significantly reduces and delays the onset and severity of diabetic retinopathy [5, 6]. Available therapies include macular laser photocoagulation, corticosteroids, and anti-vegf drugs. However, single treatments are often not effective enough to control DME during the entire course of the disease which can be very long. The multifactorial complex pathogenetic mechanisms require a comprehensive approach. This paper will review the major trials and recent evidence evaluating both monotherapy and combination treatment for DME. 2. Available Monotherapies 2.1. Macular Laser Photocoagulation. Macular laser photocoagulation is a standard of care since shown in 1985 by the early treatment of diabetic retinopathy study (ETDRS) to reduce the risk of moderate visual loss in patients with clinically significant macular edema (CSME) by nearly 50% at3years.however,visualacuity(va)improvementat3 years, i.e., 15-letter gain, was found in less than 3% of cases [7]. This apparently slight improvement may be caused by the fact that 85% of patients had good entry vision ( 20/40). Still, 40% of those with entry VA 20/40 improved 1 or more lines. Yet, it should be considered that a notable number of patients stayed unresponsive to photocoagulation. As explicated below, the DRCR.net found focal/grid laser to be of greater benefit than monotherapy with triamcinolone [8]. With emergence of anti-vegf treatment options the role of macular laser took a back seat in the treatment strategy Intravitreal Corticosteroids. The pathogenesis of DME is multifactorial. Breakdown of the blood-retina barrier increases retinal capillary permeability leading to retinal edema [9 11]. Inflammation is an eminent factor in this process, in particular via leukostasis within retinal capillaries [12]. The anti-inflammatory activity of corticosteroids is related to several paths of action: corticosteroids interfere with regulatory components of gene expression and inhibit the expression of proinflammatory genes as TNFα and other cytokines [13]. At the same time they induce gene functioning of anti-inflammatory factors, inhibit the phospholipase A 2 pathway, and reduce leucocyte chemotaxis. Vitreous fluid levels of ICAM-1, IL-6, IL-8, and MCP-1 were found to be elevated in DME patients [14, 15]. On the other hand VEGF plays a major role in breakdown of the blood-retina barrier [16, 17]. Corticosteroids inhibit the expression of VEGF and VEGF gene [18, 19].
2 2 Ophthalmology A multicenter randomized clinical trial by the Diabetic Retinopathy Clinical Research Network (DRCR.net) included 840 eyes and evaluated 1 mg and 4 mg doses of preservative-free triamcinolone compared with focal/grid photocoagulation for DME [20]. At four months, the 4 mg triamcinolone group had better visual acuity but by one year there were no significant differences. After 16 months and until the primary outcome visit at 2 years, mean visual acuity was better in the laser group than in the two triamcinolone groups. OCT results correlated with visual acuity. Recently, the DRCR.net published follow-up results of the third year. Findings were consistent with the 2-year results. More eyes in all groups improved than worsened. However, patients in the laser group had a benefit of +5 letters from baseline compared to the triamcinolone groups which stayed without change [8]. Expectedly, elevation of intraocular pressure and the need for cataract surgery were higher in the 4 mg triamcinolone group. These complications were likewise described in other studies [21, 22] Intravitreal Anti-VEGF Treatment. A multitude of proinflammatory cytokines are involved in the development and progression of DME [23]. VEGF has been linked to leakage of retinal vessels and hence to the formation of retinal edema [24]. This was the rationale for testing anti-vegf drugs for the treatment of DME Ranibizumab. The Safety and Efficacy of Ranibizumab in Diabetic Macular Edema (RESOLVE Study) multicenter, randomized, and double masked evaluated the efficacy and safety of intravitreal ranibizumab (0.3 or 0.5 mg) compared with sham treatment (no ocular injection) in 151 eyes with DME over 12 months [25]. After three monthly injections treatment could be stopped or reinitiated with an opportunity for rescue macular laser photocoagulation. The dose could be doubled after one month. Results showed a significant and continuous improvement in BCVA and central retinal thickness for ranibizumab versus sham. The phase III RIDE and RISE studies evaluated the efficacy and safety of ranibizumab for DME. RISE (n = 377) and RIDE (n = 382) are both double-blinded, sham-controlled randomized studies with a followup of 36 months. Patients received monthly injections of 0.3 mg ranibizumab, 0.5 mg ranibizumab, or sham. PRP was allowed when indicated, and rescue macular laser was permitted from month 3 onwards. 24-month results were recently presented [26]. In the RISE study, as twice as many patients in the ranibizumab groups gained 15 letters compared to the sham group (44.8%, 39.2%, and 18.1% in the ranibizumab 0.3 mg, 0.5 mg, and sham group, resp.). Results were similar in patients with better or less controlled glycemia. The RIDE study showed similar findings, but there was a clearer benefit for patients treated with 0.5 mg ranibizumab. Moreover, in the ranibizumab groups there were significantly more patients that achieved VA 20/40 compared to sham (60% and 63.2% versus 37.8% in RISE and 54.4% and 62.2% versus 34.6% in RIDE). Ranibizumab injections also reduced the percentage of patients progressing to proliferative diabetic retinopathy Bevacizumab. The Pan-American Collaborative Retina Study Group (PACORES) reviewed 139 eyes with DME at 11 centers which received at least one bevacizumab injection of 1.25 or 2.5 mg with a minimum followup of 24 months [27]. Results showed that at 24 months 44.6% eyes remained stable, 51.8% improved 2 or more ETDRS lines, and 3.6% decreased 2 or more lines. Anatomic changes on OCT paralleled overall functional improvement. The Bevacizumab or Laser Therapy in the Management of Diabetic Macular Edema study (BOLT study) is to date the most meaningful study concerning Bevacizumab for DME [28]. As a prospective and masked clinical trial with followup of 12 months it randomized 80 patients with CSME and at least one prior macular laser photocoagulation to Bevacizumab injections given every 6 weeks or laser treatment performed every 4 months. There was a clear benefit for the Bevacizumab group regarding BCVA improvement and CMT decrease versus the laser group. 3. Combination Therapy 3.1. Intravitreal Triamcinolone plus Macular Laser Photocoagulation. A randomized controlled trial evaluated the clinical outcome of macular laser photocoagulation after intravitreal triamcinolone acetonide (IVTA) for diffuse DME [29]. 86 eyes were included and randomized to two groups: the laser group patients underwent IVTA and macular grid photocoagulation 3 weeks afterward; the control group patients were treated with IVTA only. The interval of 3 weeks was chosen because of maximal therapeutic effects of IVTA at that time point. Mean CMT was 538 μ at baseline, 250 μ after 3 weeks, 295 and 301 μ at 3 and 6 months after IVTA in the laser group versus 510, 227, 302, and 437 μ in the control group. Visual acuities were significantly better in the laser group after 3 and 6 months. Though followup was short, it seems that combination therapy maintains reduced CMT three months after IVTA injection. As expected, almost 40% of patients in both groups suffered IOP rise above 21 mmhg; one patient was referred to trabeculectomy Intravitreal Ranibizumab plus Macular Laser Photocoagulation (READ2). The multicenter, prospective, randomized Ranibizumab for Edema of the macula in Diabetes-2 (READ2) study (phase II) compared the efficacy of intravitreal ranibizumab with focal/grid laser and a combination of both in 126 patients with DME [30]. Patients in the ranibizumab group received 0.5 mg ranibizumab at baseline and at months 1, 3, and 5. The laser group was treated with focal/grid laser photocoagulation at baseline and at month 3 if needed. The combination treatment consisted of focal/grid laser and ranibizumab injections at baseline and at month 3. After the primary endpoint at 6 months, all patients could receive ranibizumab injections according to retreatment criteria: patients in the ranibizumab group
3 Ophthalmology 3 could have ranibizumab injections, patients in the laser group could have laser or ranibizumab, and patients in the combination group could have laser plus ranibizumab or ranibizumab alone. At month 6, the ranibizumab group gained significantly more BCVA than the laser and the combination group: 22% improved 3 lines compared to 0% and 8%, respectively. At two years, the visual outcome was not significantly different in the three groups; the percentages of patients who gained 3 lines rose to 24, 18, and 26. The mean improvement of BCVA was 7.4, 0.5, and 3.8 letters, respectively, at 6 months and 7.7, 5.1, and 6.8 letters at two years. 45%, 44%, and 35% reached a Snellen equivalent of 20/40 or better. Though there was a substantial decrease of mean foveal thickness in the ranibizumab group at 6-month, it increased during the further followup. In contrast, there was a constant decline in the two other groups during 24 months. This implicates that additional macular laser photocoagulation is auxiliary to decrease persistent or recurrent DME and to reduce the number of required injections. Furthermore the results show that patients with recurrent or persistent DME after 6 months ranibizumab treatment maintain their visual acuity gain by means of treatment continuation every two months during a period of 18 months. Patients treated previously by macular laser photocoagulation experienced a significant improvement of visual acuity after 18 months of ranibizumab treatment Ranibizumab plus Prompt or Deferred Macular Laser Photocoagulation versus Triamcinolone plus Macular Laser Photocoagulation (DRCR.Net). The DRCR.net conducted a multicenter, randomized clinical trial which included 854 eyes of 691 patients [31]. Eyes were randomized into four treatment groups: prompt laser with sham injection, 0.5 mg of ranibizumab with prompt laser, 0.5 mg of ranibizumab with laser deferred for at least 24 weeks, and 4 mg of triamcinolone with prompt laser. At one year, the two groups treated with ranibizumab had a significant change in mean VA from baseline. The triamcinolone and laser alone groups did not show a significant change in VA. Likewise, significantly more patients gained 10 letters in the two ranibizumab groups than in the laser alone group (50% and 47% versus 28%), and less patients lost 10 letters (4% and 3% versus 13%). Notably, a subgroup analysis of pseudophakic eyes in the triamcinolone group showed similar results as for those in the ranibizumab groups. OCT results paralleled visual acuity Ranibizumab plus Macular Laser Photocoagulation (RESTORE). Similarly, the RESTORE study was a randomized, double-masked, multicenter phase III study over 12 months that compared ranibizumab + sham laser and ranibizumab + laser with laser + sham injection for DME in 345 patients [32]. Ranibizumab or sham injections were given monthly for three months and then PRN; laser or sham laser was given at baseline and then PRN after an interval of at least three months. In the ranibizumab and ranibizumab + laser groups a rapid improvement of VA was observed 50 os Figure 1: Fundus photograph of the left eye from a patient with severe NPDR and CSME. 07: os Figure 2: Late phase of fluorescence angiography shows macular leakage with a petalloid pattern. Note multiple microaneurysms and diffuse hyperfluorescence superotemporal to optic disc. after one month which continued up to three months and was sustained until month 12 (6.8 ± 8.3 and6.4 ± 11.8 letter gain, resp.), (Figure 3). The laser group maintained stable VA and gained 0.9 letters at month 12. Likewise, the percentage of patients reaching VA 20/40 was greater in the two ranibizumab groups (53% in the ranibizumab group and 44.9% in the ranibizumab + laser group versus 23.6% in the laser group). Accordingly, CMT decreased significantly in the two laser groups. This study evaluated also healthrelated quality of life by means of a questionnaire and found a greater improvement in the two ranibizumab groups. The number of PRN injections was about four in all three groups; the need for PRN laser was also similar in all groups. Summing up, ranibizumab monotherapy and combination with laser treatment are superior to laser treatment alone for DME. No differences in efficacy were found between the two ranibizumab groups PRP plus Macular Laser Photocoagulation plus Ranibizumab or Triamcinolone. The DRCR.net recently published short-term results (14 weeks) of a phase 3, randomized, multicenter, clinical trial which addressed DME in conjunction with panretinal photocoagulation (PRP) [33]. The study included 340 eyes with CSME and severe NPDR or PDR (Figure 1). Patients were randomized to receive sham injections or 0.5 mg ranibizumab at baseline and at 4 weeks
4 4 Ophthalmology (a) (b) Figure 3: High-resolution OCT of the right eye of a patient with CSME. (a) shows loss of foveal contour and cystoid edema. (b) One month after intravitreal avastin injection foveal contour is restored, retinal thickening decreased significantly, and there are no cystoids spaces detected anymore. or 4 mg IVTA at baseline and sham injection at 4 weeks. Macular laser was performed within 3 to 10 days, and PRP was initiated immediately or within 14 days of the baseline injection. Mean change in visual acuity letter score from baseline was significantly better in the ranibizumab and IVTA groups. These two groups also had a greater proportion of eyes which improved 10 letters and a lower proportion of eyes which worsened 10 letters at 14 weeks. CMT changes behaved similarly. After 14 weeks of followup patients were evaluated after 56 weeks for safety information. At this point, differences were not maintained. decrease of CMT at 6 weeks-without a significant difference between the groups. Based upon the finding that visual outcome at 24 months was better for patients treated with bevacizumab (alone or in combination with IVTA) than with laser, the authors recommend considering bevacizumab as a first-line treatment. The addition of IVTA did not have an adjunctive effect. However, it should be noted that the study did not assess combination of macular laser with bevacizumab or IVTA as done by the DRCR.net. Another limiting factor is the relative short followup Intravitreal Bevacizumab plus Triamcinolone. A clinical trial by Soheilian et al. randomized 150 eyes with naı ve CSME into three groups: Bevacizumab + sham laser, bevacizumab + IVTA + sham laser, and macular laser photocoagulation + sham injection [34]. Retreatment was performed at 12 weeks as needed. Change in BCVA at 24 weeks as the primary outcome measure showed a significant improvement in the bevacizumab groups at all follow-up visits up to 36 weeks. There was no significant difference between the bevacizumab and the combination group. The laser group did not have a significant VA change. A statistically significant greater percentage of patients gained 2 lines in the bevacizumab groups whereas a greater percentage of patients lost 2 lines in the laser group. All groups experienced a significant 3.7. Bevacizumab plus Macular Laser Photocoagulation. A smaller clinical trial including 62 eyes with diffuse DME evaluated the efficacy of combined bevacizumab plus macular laser photocoagulation versus each alone as primary treatment [35]. At month 1, patients in the bevacizumab group and in the combined group experienced significant reduction in CMT in contrast to patients treated by laser only. Accordingly, the two groups treated with bevacizumab had significant improvement of VA whereas the laser group did not have significant change. After three and six months, decrease of CMT was significant only in the combined group. A trend towards advantage for combined treatment was also noticed with VA improvement and decrease of macular leakage on FA (Figure 2). At six months, VA even regressed to
5 Ophthalmology 5 baseline values in the laser and bevacizumab groups whereas the improvement in the combined group was not statistically significant. It should be noted that there was no masking by sham treatment in this study. 4. Discussion Since the results of the ETDRS, macular laser photocoagulation has been considered the mainstay of treatment for DME although visual outcomes have not been satisfactory [4]. The introduction of intravitreal corticosteroids and anti- VEGF treatments changed the perspective on macular edema in general and on DME in particular. Though the studies mentioned above had different designs, some findings are consistent. Ranibizumab monotherapy and ranibizumab in combination with laser are more effective than macular laser photocoagulation monotherapy. For bevacizumab, superiority has been shown for combination with macular laser photocoagulation to each of them alone. The additive synergistic effect of laser to anti-vegf treatment can be explained by several mechanisms. Decreased foveal thickness facilitates laser treatment and reduces the need for high laser energy. Furthermore, more marked and prolonged reduction in macular thickness is achieved. Bevacizumab and ranibizumab downregulate VEGF and reduce capillary permeability. However, VEGF is only one factor in a complex pathogenetic process, and macular hypoxia as an underlying problem is not addressed. This may explain the rapid recurrence of macular edema a few weeks after injection when VEGF levels again increase in the vitreous. Grid laser photocoagulation decreases oxygen consumption by destroying photoreceptors. Hence, combining anti-vegf with laser photocoagulation is a complementary treatment with high efficacy in treating DME and decreasing recurrence. Combination therapy of IVTA plus macular laser is more effective than either monotherapy and may be comparable to anti-vegf plus laser in pseudophakic patients. The success of this combination therapy may be due to several mechanisms: IVTA decreases foveal thickness and allows more precise and effective macular laser photocoagulation with lower energy levels needed. Furthermore, steroids might promote the formation of mature laser scars. A deterioration of macular edema is a well-known complication of laser treatment. Intravitreal therapeutic levels of steroids seem to be protective and even modulate the RPE modeling after laser. PRP frequently causes exacerbation of DME. Prompt laser with IVTA or ranibizumab treatment results in better visual acuity and reduced CMT in the short term. Though intravitreal corticosteroids and anti-vegf drugs have different ways of action there was no adjunctive effect found with combination therapy. Since macular laser photocoagulation was first established by the ETDRS, treatment strategy for DME has essentially changed. Different treatment approaches reflect the complex pathogenesis of the disease. However, refractory cases still exist even with combination therapies. Due to heterogeneity among patients there will be no ideal treatment regimen for everybody. Further investigation of additional treatment options is needed in order to optimize therapy. References [1] Y. M. Paulus and R. F. Gariano, Diabetic retinopathy: a growing concern in an aging population, Geriatrics, vol. 64, no. 2, pp , [2] A. D. Deshpande, M. Harris-Hayes, and M. Schootman, Epidemiology of diabetes and diabetes-related complications, Physical Therapy, vol. 88, no. 11, pp , [3] R. Klein, M. D. Knudtson, K. E. Lee, R. Gangnon, and B. E. K. Klein, The wisconsin epidemiologic study of diabetic retinopathy XXIII: the twenty-five-year incidence of macular edema in persons with type 1 diabetes, Ophthalmology, vol. 116, no. 3, pp , [4] Early treatment diabetic retinopathy study research group: photocoagulation for diabetic macular edema: early treatment diabetic retinopathy study report number 1, Archives of Ophthalmology, vol. 103, no. 12, pp , [5] Diabetes Control and Complications Trial Research Group, The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulindependent diabetes mellitus, The New England Medicine, vol. 329, pp , [6] UK Prospective Diabetes Study Group, Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38, British Medical Journal, vol. 317, pp , [7] Early treatment diabeticretinopathy study research group: photocoagulation for diabetic macular edema: early treatment diabetic retinopathy study report number 1, Archives of Ophthalmology, vol. 103, no. 12, pp , [8] Diabetic Retinopathy Clinical Research Network (DRCR.net), R. W. Beck, A. R. Edwards et al., Three-year follow-up of a randomized trial comparing focal/grid photocoagulation and intravitreal triamcinolone for diabeticmacular edema, Archives of Ophthalmology, vol. 127, no. 3, pp , [9] L. P. Aiello, S. E. Bursell, A. Clermont et al., Vascular endothelial growth factor-induced retinal permeability is mediated by protein kinase C in vivo and suppressed by an orally effective β-isoform-selective inhibitor, Diabetes, vol. 46, no. 9, pp , [10] D.A.Antonetti,A.J.Barber,L.A.Hollinger,E.B.Wolpert,and T. W. Gardner, Vascular endothelial growth factor induces rapid phosphorylation of tight junction proteins occludin and zonula occluden 1. A potential mechanism for vascular permeability in diabetic retinopathy and tumors, Biological Chemistry, vol. 274, no. 33, pp , [11] D.R.Senger,S.J.Galli,A.M.Dvorak,C.A.Perruzzi,V.Susan Harvey, and H. F. Dvorak, Tumor cells secrete a vascular permeability factor that promotes accumulation of ascites fluid, Science, vol. 219, no. 4587, pp , [12] T. S. Kern, Contributions of inflammatory processes to the development of the early stages of diabetic retinopathy, Experimental diabetes research, vol. 2007, p , [13] L. G. Tsaprouni, K. Ito, N. Punchard, and I. M. Adcock, Triamcinolone acetonide and dexamethasome suppress TNF-αinduced histone H4 acetylation on lysine residues 8 and 12 in mononuclear cells, Annals of the New York Academy of Sciences, vol. 973, pp , 2002.
6 6 Ophthalmology [14] T. Yoshimura, K.-H. Sonoda, M. Sugahara et al., Comprehensive analysis of inflammatory immune mediators in vitreoretinal diseases, Plos ONE, vol. 4, no. 12, [15] H. Funatsu, H. Noma, T. Mimura, S. Eguchi, and S. Hori, Association of vitreous inflammatory factors with diabetic macular edema, Ophthalmology, vol. 116, no. 1, pp , [16] D. A. Antonetti, A. J. Barber, S. Khin, E. Lieth, J. M. Tarbell, and T. W. Gardner, Vascular permeability in experimental diabetes is associated with reduced endothelial occludin content. Vascular endothelial growth factor decreases occludin in retinal endothelial cells, Diabetes, vol. 47, no. 12, pp , [17] A. M. Joussen, V. Poulaki, M. L. Le et al., A central role for inflammation in the pathogenesis of diabetic retinopathy, The FASEB Journal, vol. 18, no. 12, pp , [18] M. Nauck, G. Karakiulakis, A. Perruchoud, E. Papakonstantinou, and M. Roth, Corticosteroids inhibit the expression of the vascular endothelial growth factor gene in human vascular smooth muscle cells, European Pharmacology, vol. 341, no. 2-3, pp , [19] M. Nauck, M. Roth, M. Tamm et al., Induction of vascular endothelial growth factor by platelet-activating factor and platelet-derived growth factor is downregulated by corticosteroids, American Respiratory Cell and Molecular Biology, vol. 16, no. 4, pp , [20] Diabetic Retinopathy Clinical Research Network, A randomized trial comparing intravitreal triamcinolone acetonide and focal/grid photocoagulation for diabetic macular edema, Ophthalmology, vol. 115, no. 9, pp , [21] J. B. Jonas, I. Kreissig, and R. Degenring, Intraocular pressure after intravitreal injection of triamcinolone acetonide, British Ophthalmology, vol. 87, no. 1, pp , [22] J. B. Jonas, R. Degenring, U. Vossmerbauemer, and B. Kamppeter, Frequency of cataract surgery after intravitreal injection of high-dosage triamcinolone acetonide, European Ophthalmology, vol. 15, no. 4, pp , [23] L. P. Aiello, S. E. Bursell, A. Clermont et al., Vascular endothelial growth factor-induced retinal permeability is mediated by protein kinase C in vivo and suppressed by an orally effective β-isoform-selective inhibitor, Diabetes, vol. 46, no. 9, pp , [24] Q. D. Nguyen, S. Tatlipinar, S. M. Shah et al., Vascular endothelial growth factor is a critical stimulus for diabetic macular edema, American Ophthalmology, vol. 142, no. 6, pp. 961 e4, [25] P. Massin, F. Bandello, J. G. Garweg et al., Safety and efficacy of ranibizumab in diabetic macular edema (RESOLVE study): a 12-month, randomized, controlled, double-masked, multicenter phase II study, Diabetes Care, vol. 33, no. 11, pp , [26] D. S. Boyer, J. Sy, A. C. Rundle et al., Ranibizumab for Vision Loss due to Diabetic Macular Edema Results of two Phase III Randomized trials, American Diabetes Association 71st Scientific Sessions, San Diego, Calif, USA, [27] J. F. Arevalo, J. G. Sanchez, L. Wu et al., Primary intravitreal bevacizumab for diffuse diabetic macular edema: the Pan- American collaborative retina study group at 24 months: the Pan-American collaborative retina study group at 24 months, Ophthalmology, vol. 116, no. 8, pp , [28] M. Michaelides, A. Kaines, R. D. Hamilton et al., A prospective randomized trial of intravitreal bevacizumab or laser therapy in the management of diabetic macular edema (BOLT Study). 12-month data: report 2, Ophthalmology, vol. 117, no. 6, pp , [29] W.K.Se,H.-S.Sa,Y.C.Hee,andI.K.Jong, Maculargrid photocoagulation after intravitreal triamcinolone acetonide for diffuse diabetic macular edema, Archives of Ophthalmology, vol. 124, no. 5, pp , [30] Q. D. Nguyen, S. M. Shah, A. A. Khwaja et al., Two-year outcomes of the ranibizumab for edema of the macula in diabetes (READ-2) study, Ophthalmology, vol. 117, no. 11, pp , [31] M. J. Elman, N. M. Bressler, H. Qin et al., Expanded 2-year follow-up of ranibizumab plus prompt or deferred laser or triamcinolone plus prompt laser for diabetic macular edema, Ophthalmology, vol. 118, no. 4, pp , [32] P. Mitchell, F. Bandello, U. Schmidt-Erfurth et al., The RESTORE study: ranibizumab monotherapy or combined with laser versus laser monotherapy for diabetic macular edema, Ophthalmology, vol. 118, no. 4, pp , [33] J. Googe, A. J. Brucker, N. M. Bressler et al., Randomized trial evaluating short-term effects of intravitreal ranibizumab or triamcinolone acetonide on macular edema after focal/grid laser for diabetic macular edema in eyes also receiving panretinal photocoagulation, Retina, vol. 31, no. 6, pp , [34] M. Soheilian, A. Ramezani, A. Obudi et al., Randomized trial of intravitreal bevacizumab alone or combined with triamcinolone versus macular photocoagulation in diabetic macular edema, Ophthalmology, vol. 116, no. 6, pp , [35] K. A. Solaiman, M. M. Diab, and M. Abo-Elenin, Intravitreal bevacizumab and/or macular photocoagulation as a primary treatment for diffusediabetic macular edema, Retina, vol. 30, no. 10, pp , 2010.
7 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA
 Basrah Journal Of Surgery EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA Salah Zuhair Abed Al-Asadi MB,ChB, FICMS, Lecturer, Department of Surgery, College
Basrah Journal Of Surgery EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA Salah Zuhair Abed Al-Asadi MB,ChB, FICMS, Lecturer, Department of Surgery, College
Diabetic Retinopathy: Recent Advances in Treatment and Treatment Approaches
 Diabetic Retinopathy: Recent Advances in Treatment and Treatment Approaches Dr. David Wong Associate Professor Retina Specialist, Department of Ophthalmology & Vision Sciences, University of Toronto, Canada
Diabetic Retinopathy: Recent Advances in Treatment and Treatment Approaches Dr. David Wong Associate Professor Retina Specialist, Department of Ophthalmology & Vision Sciences, University of Toronto, Canada
Clinical Trials in Diabetic Retinopathy. Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D.
 1 Clinical Trials in Diabetic Retinopathy 2018 Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D. Bascom Palmer Eye Institute 900 N.W. 17th Street Miami, FL 33136 Phone: (305) 326-6118 Fax: (305) 326-6417
1 Clinical Trials in Diabetic Retinopathy 2018 Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D. Bascom Palmer Eye Institute 900 N.W. 17th Street Miami, FL 33136 Phone: (305) 326-6118 Fax: (305) 326-6417
Review Article Combination of Anti-VEGF and Laser Photocoagulation for Diabetic Macular Edema: A Review
 Hindawi Ophthalmology Volume 2017, Article ID 2407037, 7 pages https://doi.org/10.1155/2017/2407037 Review Article Combination of Anti-VEGF and Laser Photocoagulation for Diabetic Macular Edema: A Review
Hindawi Ophthalmology Volume 2017, Article ID 2407037, 7 pages https://doi.org/10.1155/2017/2407037 Review Article Combination of Anti-VEGF and Laser Photocoagulation for Diabetic Macular Edema: A Review
Anti Vascular Endothelial Growth Factor Pharmacotherapy for Diabetic Macular Edema
 Ophthalmic Technology Assessment Anti Vascular Endothelial Growth Factor Pharmacotherapy for Diabetic Macular Edema A Report by the American Academy of Ophthalmology Allen C. Ho, MD, Ingrid U. Scott, MD,
Ophthalmic Technology Assessment Anti Vascular Endothelial Growth Factor Pharmacotherapy for Diabetic Macular Edema A Report by the American Academy of Ophthalmology Allen C. Ho, MD, Ingrid U. Scott, MD,
New Developments in the treatment of Diabetic Retinopathy
 New Developments in the treatment of Diabetic Retinopathy B. Jeroen Klevering University Medical Centre Nijmegen - The Netherlands Topics Management of diabetic retinopathy Interventions a. primary (prevention)
New Developments in the treatment of Diabetic Retinopathy B. Jeroen Klevering University Medical Centre Nijmegen - The Netherlands Topics Management of diabetic retinopathy Interventions a. primary (prevention)
Diabetic Macular Edema Treatment in the 21st Century
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
The Diabetic Retinopathy Clinical Research Network. Management of DME in Eyes with PDR
 The Diabetic Retinopathy Clinical Research Network Management of DME in Eyes with PDR 1 What Has Been Learned? Diabetic Retinopathy Treatment Protocol F: Results suggest that clinically meaningful differences
The Diabetic Retinopathy Clinical Research Network Management of DME in Eyes with PDR 1 What Has Been Learned? Diabetic Retinopathy Treatment Protocol F: Results suggest that clinically meaningful differences
Clinical Study Switch to Aflibercept in Diabetic Macular Edema Patients Unresponsive to Previous Anti-VEGF Therapy
 Hindawi Ophthalmology Volume 2017, Article ID 5632634, 4 pages https://doi.org/10.1155/2017/5632634 Clinical Study Switch to Aflibercept in Diabetic Macular Edema Patients Unresponsive to Previous Anti-VEGF
Hindawi Ophthalmology Volume 2017, Article ID 5632634, 4 pages https://doi.org/10.1155/2017/5632634 Clinical Study Switch to Aflibercept in Diabetic Macular Edema Patients Unresponsive to Previous Anti-VEGF
ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS
 ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Diabetic maculopathy 11/ An update on. Miss Vasuki Sivagnanavel
 Miss Vasuki Sivagnanavel Consultant Ophthalmologist An update on Diabetic maculopathy Despite advances in the management of diabetes, diabetic retinopathy is already the commonest cause of blindness among
Miss Vasuki Sivagnanavel Consultant Ophthalmologist An update on Diabetic maculopathy Despite advances in the management of diabetes, diabetic retinopathy is already the commonest cause of blindness among
ANTI-VEGF THERAPY FOR DIABETIC MACULAR EDEMA
 January/February 2015 Supplement to ANTI-VEGF THERAPY FOR DIABETIC MACULAR EDEMA A roundtable discussion with Franck Fajnkuchen, MD, and Paolo Lanzetta, MD Case report by Paolo Lanzetta, MD The answers
January/February 2015 Supplement to ANTI-VEGF THERAPY FOR DIABETIC MACULAR EDEMA A roundtable discussion with Franck Fajnkuchen, MD, and Paolo Lanzetta, MD Case report by Paolo Lanzetta, MD The answers
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
ILUVIEN IN DIABETIC MACULAR ODEMA
 1 ILUVIEN IN DIABETIC MACULAR ODEMA Marie Tsaloumas Consultant Ophthalmic Surgeon Queen Elizabeth Hospital, Birmingham bars conference 2104 1 2 Declaration of interest I have sat on Advisory boards for
1 ILUVIEN IN DIABETIC MACULAR ODEMA Marie Tsaloumas Consultant Ophthalmic Surgeon Queen Elizabeth Hospital, Birmingham bars conference 2104 1 2 Declaration of interest I have sat on Advisory boards for
Diabetic retinopathy (DR) progressively
 FOCUS ON DIABETIC MACULAR EDEMA * Frederick L. Ferris III, MD ABSTRACT The current state of treatment for diabetic macular edema (DME) is focused on slowing the rate of vision loss through assessment of
FOCUS ON DIABETIC MACULAR EDEMA * Frederick L. Ferris III, MD ABSTRACT The current state of treatment for diabetic macular edema (DME) is focused on slowing the rate of vision loss through assessment of
Diabetic Retinopathy: Managing the Extremes. J. Michael Jumper, MD West Coast Retina
 Diabetic Retinopathy: Managing the Extremes J. Michael Jumper, MD West Coast Retina Case 1: EC 65 y.o. HM No vision complaints Meds: Glyburide Metformin Pioglitazone Va: 20/20 OU 20/20 Case 2: HS 68 y.o.
Diabetic Retinopathy: Managing the Extremes J. Michael Jumper, MD West Coast Retina Case 1: EC 65 y.o. HM No vision complaints Meds: Glyburide Metformin Pioglitazone Va: 20/20 OU 20/20 Case 2: HS 68 y.o.
COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY
 Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington
 Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington I Jay M. Haynie, OD, FAAO have received honoraria from the following companies: Reichert Technologies Notal Vision Carl Zeiss Meditec
Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington I Jay M. Haynie, OD, FAAO have received honoraria from the following companies: Reichert Technologies Notal Vision Carl Zeiss Meditec
Combination Treatment of Diabetic Macular Edema with Anti-Vascular Endothelial Growth Factor and Steroids: Analysis of DRCR.
 REVIEW ARTICLE Combination Treatment of Diabetic Macular Edema with Anti-Vascular Endothelial Growth Factor and Steroids: Analysis of DRCR.net Protocol U Cindy Ung 1, Kareem Moussa 1, Yoshihiro Yonekawa
REVIEW ARTICLE Combination Treatment of Diabetic Macular Edema with Anti-Vascular Endothelial Growth Factor and Steroids: Analysis of DRCR.net Protocol U Cindy Ung 1, Kareem Moussa 1, Yoshihiro Yonekawa
Supplement to March Ranibizumab for Visual Impairment in DME: An Overview of The Evidence SPONSORED BY NOVARTIS PHARMA AG
 Supplement to March 2018 Ranibizumab for Visual Impairment in DME: An Overview of The Evidence SPONSORED BY NOVARTIS PHARMA AG Ranibizumab for Visual Impairment in DME: An Overview of The Evidence BY PROF.
Supplement to March 2018 Ranibizumab for Visual Impairment in DME: An Overview of The Evidence SPONSORED BY NOVARTIS PHARMA AG Ranibizumab for Visual Impairment in DME: An Overview of The Evidence BY PROF.
Diabetic Retinopatathy
 Diabetic Retinopatathy Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl Zeiss Meditec Arctic DX Macula Risk Advanced
Diabetic Retinopatathy Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl Zeiss Meditec Arctic DX Macula Risk Advanced
Paradigm Shift in the treatment of Diabetic Retinopathy. Haytham I. S. Salti, MD Associate Professor
 Paradigm Shift in the treatment of Diabetic Retinopathy Haytham I. S. Salti, MD Associate Professor Disclosure No financial interests related to the subject matter of this talk This presentation includes
Paradigm Shift in the treatment of Diabetic Retinopathy Haytham I. S. Salti, MD Associate Professor Disclosure No financial interests related to the subject matter of this talk This presentation includes
THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION
 THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION MOESTIDJAB DEPARTMENT OF OPHTHALMOLOGY SCHOOL OF MEDICINE AIRLANGGA UNIVERSITY DR SOETOMO HOSPITAL SURABAYA INTRODUCTION
THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION MOESTIDJAB DEPARTMENT OF OPHTHALMOLOGY SCHOOL OF MEDICINE AIRLANGGA UNIVERSITY DR SOETOMO HOSPITAL SURABAYA INTRODUCTION
Persistent Macular Thickening After Ranibizumab Treatment for Diabetic Macular Edema With Vision Impairment
 9:30 AM Persistent Macular Thickening After Ranibizumab Treatment for Diabetic Macular Edema With Vision Impairment Lee Jampol, MD OBJECTIVE To assess subsequent visual and anatomic outcomes of eyes with
9:30 AM Persistent Macular Thickening After Ranibizumab Treatment for Diabetic Macular Edema With Vision Impairment Lee Jampol, MD OBJECTIVE To assess subsequent visual and anatomic outcomes of eyes with
Review Article Anti-VEGF for the Management of Diabetic Macular Edema
 Immunology Research, Article ID 632307, 8 pages http://dx.doi.org/10.1155/2014/632307 Review Article Anti-VEGF for the Management of Diabetic Macular Edema Francisco Rosa Stefanini, 1,2 Emmerson Badaró,
Immunology Research, Article ID 632307, 8 pages http://dx.doi.org/10.1155/2014/632307 Review Article Anti-VEGF for the Management of Diabetic Macular Edema Francisco Rosa Stefanini, 1,2 Emmerson Badaró,
Clinical Outcomes After Intravitreal Bevacizumab Injection for Diabetic Macular Edema
 Original Article Clinical Outcomes After Intravitreal Bevacizumab Injection for Diabetic Macular Edema Karen Joyce G. Castro, MD, Marie Joan V. Loy, MD International Eye Institute St. Luke s Medical Center
Original Article Clinical Outcomes After Intravitreal Bevacizumab Injection for Diabetic Macular Edema Karen Joyce G. Castro, MD, Marie Joan V. Loy, MD International Eye Institute St. Luke s Medical Center
1/25/2018. Case Management Strategies in Diabetic Retinopathy. Case Study #1: Severe DME. DDOS: 3/31/2016 Va 20/400. Disclosures
 Case Management Strategies in Diabetic Retinopathy Disclosures No financial conflict of interest Will discuss off label use of intraocular Bevacizumab (Avastin) for Diabetic Retinopathy Sundeep Dev, MD
Case Management Strategies in Diabetic Retinopathy Disclosures No financial conflict of interest Will discuss off label use of intraocular Bevacizumab (Avastin) for Diabetic Retinopathy Sundeep Dev, MD
Treatment for Central-Involved Diabetic Macular Edema in Eyes with Very Good Visual Acuity
 Diabetic Retinopathy Clinical Research Network Treatment for Central-Involved Diabetic Macular Edema in Eyes with Very Good Visual Acuity Version 3.0 April 18, 2014 Treatment of CIDME in Eyes with Good
Diabetic Retinopathy Clinical Research Network Treatment for Central-Involved Diabetic Macular Edema in Eyes with Very Good Visual Acuity Version 3.0 April 18, 2014 Treatment of CIDME in Eyes with Good
12-month results of the standardised combination therapy for diabetic macular oedema: intravitreal bevacizumab and navigated retinal photocoagulation
 Clinical science 1 Department of Ophthalmology, Jacobs Retina Center at Shiley Eye Center, University of California San Diego, La Jolla, CA, USA 2 Ophthalmological Unit, Department of Clinical Sciences
Clinical science 1 Department of Ophthalmology, Jacobs Retina Center at Shiley Eye Center, University of California San Diego, La Jolla, CA, USA 2 Ophthalmological Unit, Department of Clinical Sciences
A retrospective nonrandomized study was conducted at 3
 Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Scott M. Pfahler D.O. Dayton Vitreo-Retinal Associates AOCOO-HNS Palm Springs, CA 2012
 Scott M. Pfahler D.O. Dayton Vitreo-Retinal Associates AOCOO-HNS Palm Springs, CA 2012 Proliferative Diabetic Retinopathy Laser Treatments Medical Treatment Surgical Treatment Diabetic Macular Edema Laser
Scott M. Pfahler D.O. Dayton Vitreo-Retinal Associates AOCOO-HNS Palm Springs, CA 2012 Proliferative Diabetic Retinopathy Laser Treatments Medical Treatment Surgical Treatment Diabetic Macular Edema Laser
Case Report Inherent Challenges in Managing Long Standing Refractory Diabetic Macular Edema
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Report Inherent Challenges in Managing Long Standing Refractory Diabetic Macular Edema V Swetha E Jeganathan 1,2 * and Karen Madill 3 1 Department of Ophthalmology,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Report Inherent Challenges in Managing Long Standing Refractory Diabetic Macular Edema V Swetha E Jeganathan 1,2 * and Karen Madill 3 1 Department of Ophthalmology,
Kyungmin Lee, Heeyoung Chung, Youngsuk Park, Joonhong Sohn. HanGil Eye Hospital, Incheon, Korea
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):298-305 http://dx.doi.org/10.3341/kjo.2014.28.4.298 Original Article Efficacy of Intravitreal Anti-vascular Endothelial Growth Factor or
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):298-305 http://dx.doi.org/10.3341/kjo.2014.28.4.298 Original Article Efficacy of Intravitreal Anti-vascular Endothelial Growth Factor or
Intravitreal Ranibizumab or Triamcinolone Acetonide in Combination with Laser Photocoagulation for Diabetic Macular Edema
 Diabetic Retinopathy Clinical Research Network Intravitreal Ranibizumab or Triamcinolone Acetonide in Combination with Laser Photocoagulation for Diabetic Macular Edema Version 6.0 May 21, 2010 Note: See
Diabetic Retinopathy Clinical Research Network Intravitreal Ranibizumab or Triamcinolone Acetonide in Combination with Laser Photocoagulation for Diabetic Macular Edema Version 6.0 May 21, 2010 Note: See
Vitrectomy Combined with Intravitreal Triamcinolone Acetonide Injection and Macular Laser Photocoagulation for Nontractional Diabetic Macular Edema
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(3):186-193 http://dx.doi.org/10.3341/kjo.2013.27.3.186 Original Article Vitrectomy Combined with Intravitreal Triamcinolone Acetonide Injection
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(3):186-193 http://dx.doi.org/10.3341/kjo.2013.27.3.186 Original Article Vitrectomy Combined with Intravitreal Triamcinolone Acetonide Injection
Diabetic Retinopathy Clinical Research Network
 Diabetic Retinopathy Clinical Research Network Short-term Evaluation of Combination Corticosteroid+Anti- VEGF Treatment for Persistent Central-Involved Diabetic Macular Edema Following Anti-VEGF Therapy
Diabetic Retinopathy Clinical Research Network Short-term Evaluation of Combination Corticosteroid+Anti- VEGF Treatment for Persistent Central-Involved Diabetic Macular Edema Following Anti-VEGF Therapy
Recalcitrant Diabetic Macular Oedema: Therapeutic Options
 December 2007 A. Giridhar et al. - Recalcitrant DME 451 CONSULTATION S E C T I O N Recalcitrant Diabetic Macular Oedema: Therapeutic Options Dr. Cyrus M Shroff 1, Dr. N S Muralidhar 2, Dr. R Narayanan
December 2007 A. Giridhar et al. - Recalcitrant DME 451 CONSULTATION S E C T I O N Recalcitrant Diabetic Macular Oedema: Therapeutic Options Dr. Cyrus M Shroff 1, Dr. N S Muralidhar 2, Dr. R Narayanan
Diabetic eye disease. Diabetic retinopathy. Sam S. Dahr, M.D. Retina Center of Oklahoma.
 Diabetic eye disease Sam S. Dahr, M.D. Retina Center of Oklahoma www.rcoklahoma.com Downloaded from: The Retina (on 28 May 2007 12:48 AM) 2007 Elsevier Diabetic retinopathy Downloaded from: The Retina
Diabetic eye disease Sam S. Dahr, M.D. Retina Center of Oklahoma www.rcoklahoma.com Downloaded from: The Retina (on 28 May 2007 12:48 AM) 2007 Elsevier Diabetic retinopathy Downloaded from: The Retina
Yule Xu, Ao Rong, Yanlong Bi, and Wei Xu. 1. Introduction
 Ophthalmology Volume 2016, Article ID 2143082, 7 pages http://dx.doi.org/10.1155/2016/2143082 Research Article Intravitreal Conbercept Injection with and without Grid Laser Photocoagulation in the Treatment
Ophthalmology Volume 2016, Article ID 2143082, 7 pages http://dx.doi.org/10.1155/2016/2143082 Research Article Intravitreal Conbercept Injection with and without Grid Laser Photocoagulation in the Treatment
Philadelphia College of Osteopathic Medicine. Heather Bladek Philadelphia College of Osteopathic Medicine,
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 In Adult Patients With Diabetic Macular
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 In Adult Patients With Diabetic Macular
Macular edema (ME) is the most common
 MANAGEMENT OF RETINAL VEIN OCCLUSIONS * Peter A. Campochiaro, MD ABSTRACT Macular edema (ME) is the most common cause of reduced vision in patients with retinal vein occlusions (RVOs). The primary cause
MANAGEMENT OF RETINAL VEIN OCCLUSIONS * Peter A. Campochiaro, MD ABSTRACT Macular edema (ME) is the most common cause of reduced vision in patients with retinal vein occlusions (RVOs). The primary cause
An updated review of long-term outcomes from randomized controlled trials in approved pharmaceuticals for diabetic macular edema
 Review Article An updated review of long-term outcomes from randomized controlled trials in approved pharmaceuticals for diabetic macular edema Jia-Kang Wang 1,2,3,4, Tzu-Lun Huang 1,5, Pei-Yuan Su 1,4,6,
Review Article An updated review of long-term outcomes from randomized controlled trials in approved pharmaceuticals for diabetic macular edema Jia-Kang Wang 1,2,3,4, Tzu-Lun Huang 1,5, Pei-Yuan Su 1,4,6,
CENTENE PHARMACY AND THERAPEUTICS NEW DRUG REVIEW 2Q17 April May
 BRAND NAME Lucentis GENERIC NAME ranibizumab MANUFACTURER Genentech, Inc. DATE OF APPROVAL June 30, 2006 PRODUCT LAUNCH DATE July 13, 2006 REVIEW TYPE Review type 1 (RT1): New Drug Review Full review of
BRAND NAME Lucentis GENERIC NAME ranibizumab MANUFACTURER Genentech, Inc. DATE OF APPROVAL June 30, 2006 PRODUCT LAUNCH DATE July 13, 2006 REVIEW TYPE Review type 1 (RT1): New Drug Review Full review of
VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT
 The Professional Medical Journal DOI: 10.17957/TPMJ/16.2856 ORIGINAL PROF-2856 VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT 1. MBBS.FCPS Assistant Professor Ophthalmology Independent
The Professional Medical Journal DOI: 10.17957/TPMJ/16.2856 ORIGINAL PROF-2856 VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT 1. MBBS.FCPS Assistant Professor Ophthalmology Independent
Protocol. This trial protocol has been provided by the authors to give readers additional information about their work.
 Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: The Diabetic Retinopathy Clinical Research Network. Aflibercept, bevacizumab,
Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: The Diabetic Retinopathy Clinical Research Network. Aflibercept, bevacizumab,
Targeting Inflammation in Diabetic Macular Edema: From Basic Science to Clinical Trials to Clinical Practice
 Targeting Inflammation in Diabetic Macular Edema: From Basic Science to Clinical Trials to Clinical Practice Baruch D Kuppermann, MD, PhD Professor of Ophthalmology and Biomedical Engineering Director,
Targeting Inflammation in Diabetic Macular Edema: From Basic Science to Clinical Trials to Clinical Practice Baruch D Kuppermann, MD, PhD Professor of Ophthalmology and Biomedical Engineering Director,
Opthea Initiates OPT-302 Diabetic Macular Edema Clinical Trial
 ASX and Media Release 3 January 2018 Opthea Initiates OPT-302 Diabetic Macular Edema Clinical Trial Melbourne, Australia; January 3 2018 Opthea Limited (ASX:OPT), a late stage biopharmaceutical company
ASX and Media Release 3 January 2018 Opthea Initiates OPT-302 Diabetic Macular Edema Clinical Trial Melbourne, Australia; January 3 2018 Opthea Limited (ASX:OPT), a late stage biopharmaceutical company
Treatment of Diabetic Macular Edema without Intravitreal injections
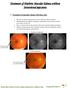 Treatment of Diabetic Macular Edema without Intravitreal injections 1. Treatment of macular edema with laser only This 60 year old female presented on 02-01-2007 for retinal evaluation. She had proliferative
Treatment of Diabetic Macular Edema without Intravitreal injections 1. Treatment of macular edema with laser only This 60 year old female presented on 02-01-2007 for retinal evaluation. She had proliferative
Posterior Segment Diabetic Macular Oedema
 Posterior Segment Diabetic Macular Oedema Evidence for Anti-vascular Endothelial Growth Factor Treatment of Diabetic Macular Oedema Francesco Bandello, 1 Umberto De Benedetto, 1 Karl Anders Knutsson, 1
Posterior Segment Diabetic Macular Oedema Evidence for Anti-vascular Endothelial Growth Factor Treatment of Diabetic Macular Oedema Francesco Bandello, 1 Umberto De Benedetto, 1 Karl Anders Knutsson, 1
Case Report Increase in Central Retinal Edema after Subthreshold Diode Micropulse Laser Treatment of Chronic Central Serous Chorioretinopathy
 Case Reports in Ophthalmological Medicine Volume 2015, Article ID 813414, 4 pages http://dx.doi.org/10.1155/2015/813414 Case Report Increase in Central Retinal Edema after Subthreshold Diode Micropulse
Case Reports in Ophthalmological Medicine Volume 2015, Article ID 813414, 4 pages http://dx.doi.org/10.1155/2015/813414 Case Report Increase in Central Retinal Edema after Subthreshold Diode Micropulse
SUMMARY. Heather Casparis, MD,* and Neil M. Bressler, MD MARINA AND ANCHOR
 The following are summaries of selected presentations and posters from the American Society of Retina Specialists and European VitreoRetinal Society Annual Meeting held September 9 13, 2006, in Cannes,
The following are summaries of selected presentations and posters from the American Society of Retina Specialists and European VitreoRetinal Society Annual Meeting held September 9 13, 2006, in Cannes,
Facts About Diabetic Eye Disease
 Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Past ocular history. DME Case 1. Patient presents blurred VA. Hemoglobin A1c 11.5% -- patient states sugars have not been in good control
 Past ocular history Patient presents blurred VA DME Case 1 Hemoglobin A1c 11.5% -- patient states sugars have not been in good control PDR with macular edema OU Rishi Singh MD Cleveland Clinic OD OS 1
Past ocular history Patient presents blurred VA DME Case 1 Hemoglobin A1c 11.5% -- patient states sugars have not been in good control PDR with macular edema OU Rishi Singh MD Cleveland Clinic OD OS 1
The Era of anti- - - VEGF Kirk L. Halvorson, OD
 The Era of anti- - - VEGF Kirk L. Halvorson, OD Introduction: Anti- - - Vascular Endothelial Growth Factor (Anti- - - VEGF) medication is a relatively a new line of medications used in treating a variety
The Era of anti- - - VEGF Kirk L. Halvorson, OD Introduction: Anti- - - Vascular Endothelial Growth Factor (Anti- - - VEGF) medication is a relatively a new line of medications used in treating a variety
EU Regulatory workshop Ophthalmology clinical development and scientific advice. Industry view on DME and macular edema secondary to RVO
 EU Regulatory workshop Ophthalmology clinical development and scientific advice. Industry view on DME and macular edema secondary to RVO Yehia Hashad, M.D. Vice President and Global Therapeutic Area Head
EU Regulatory workshop Ophthalmology clinical development and scientific advice. Industry view on DME and macular edema secondary to RVO Yehia Hashad, M.D. Vice President and Global Therapeutic Area Head
Retina Diabetic Macular Edema
 Retina Diabetic Macular Edema ILUVIEN A New Approach to the Treatment of Diabetic Macula Edema Pravin U Dugel, MD 1 and Richard Parrish, MD 2 1. Retinal Consultants of Arizona, Phoenix, Arizona, US; Clinical
Retina Diabetic Macular Edema ILUVIEN A New Approach to the Treatment of Diabetic Macula Edema Pravin U Dugel, MD 1 and Richard Parrish, MD 2 1. Retinal Consultants of Arizona, Phoenix, Arizona, US; Clinical
Diabetic Retinopathy Clinical Research Network
 Diabetic Retinopathy Clinical Research Network Intravitreal Ranibizumab or Triamcinolone Acetonide as Adjunctive Treatment to Panretinal Photocoagulation for Proliferative Diabetic Retinopathy Version
Diabetic Retinopathy Clinical Research Network Intravitreal Ranibizumab or Triamcinolone Acetonide as Adjunctive Treatment to Panretinal Photocoagulation for Proliferative Diabetic Retinopathy Version
New developments in the treatment of diabetic macular edema: latest clinical evidence
 Review: Clinical Trial Outcomes New developments in the treatment of diabetic macular edema: latest clinical evidence Clin. Invest. (2012) 2(1), 89 105 Diabetic retinopathy is a major cause of blindness
Review: Clinical Trial Outcomes New developments in the treatment of diabetic macular edema: latest clinical evidence Clin. Invest. (2012) 2(1), 89 105 Diabetic retinopathy is a major cause of blindness
Diabetic Retinopathy A Presentation for the Public
 Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
Clinical Case Presentation. Branch Retinal Vein Occlusion. Sarita M. Registered Nurse Whangarei Base Hospital
 Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
New Insights on Treating Diabetic Retinopathy & Diabetic Macular Edema from the 2018 AAO Meeting
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Overview of the Pathogenesis of Diabetic Retinopathy
 Activity presentations are considered intellectual property. These slides may not be published or posted online without permission from Vindico Medical Education (cme@vindicocme.com). Please be respectful
Activity presentations are considered intellectual property. These slides may not be published or posted online without permission from Vindico Medical Education (cme@vindicocme.com). Please be respectful
Updates and Controversies
 Updates and Controversies Philippine Journal of OPHTHALMOLOGY Vascular endothelial growth factor (VEGF) and inflammation. VEGF-A circulates normally in the body and is essential in endothelial cell growth.
Updates and Controversies Philippine Journal of OPHTHALMOLOGY Vascular endothelial growth factor (VEGF) and inflammation. VEGF-A circulates normally in the body and is essential in endothelial cell growth.
CSME BCVA. OCT Bevacizumab CMT CMT BCVA. BCVA LogMAR. p CMT NPDR PDR PDR. Bevacizumab PDR FDA. Ranibizumab. Bevacizumab.
 email: rezaj76@yahoo.com Bevacizumab FDA mg Ranibizumab - Bevacizumab NPDR PDR PDR PDR CSME FAZFA BCVA CMT OCT Bevacizumab BCVA CMT BCVA LogMAR p CMT p CSME CRVO CSME BRVO CRVOBRVO (fovea avascular zone)
email: rezaj76@yahoo.com Bevacizumab FDA mg Ranibizumab - Bevacizumab NPDR PDR PDR PDR CSME FAZFA BCVA CMT OCT Bevacizumab BCVA CMT BCVA LogMAR p CMT p CSME CRVO CSME BRVO CRVOBRVO (fovea avascular zone)
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient
 Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
ORIGINAL RESEARCH ARTICLE
 EJO ISSN 1120-6721 Eur J Ophthalmol 2017; 27 (3): 357-362 DOI: 10.5301/ejo.5000929 ORIGINAL RESEARCH ARTICLE Diabetic macular edema outcomes in eyes treated with fluocinolone acetonide 0.2 µg/d intravitreal
EJO ISSN 1120-6721 Eur J Ophthalmol 2017; 27 (3): 357-362 DOI: 10.5301/ejo.5000929 ORIGINAL RESEARCH ARTICLE Diabetic macular edema outcomes in eyes treated with fluocinolone acetonide 0.2 µg/d intravitreal
Efficacy of intravitreal bevacizumab (Avastin TM ) for shortterm treatment of diabetic macular edema
 111 ORIGINAL Efficacy of intravitreal bevacizumab (Avastin TM ) for shortterm treatment of diabetic macular edema Toshihiko Nagasawa, Takeshi Naito, Shingo Matsushita, Hiroyuki Sato, Takashi Katome, and
111 ORIGINAL Efficacy of intravitreal bevacizumab (Avastin TM ) for shortterm treatment of diabetic macular edema Toshihiko Nagasawa, Takeshi Naito, Shingo Matsushita, Hiroyuki Sato, Takashi Katome, and
Diabetic Retinopathy Clinical Research Network
 Diabetic Retinopathy Clinical Research Network Prompt Panretinal Photocoagulation Versus Intravitreal Ranibizumab with Deferred Panretinal Photocoagulation for Proliferative Diabetic Retinopathy Version
Diabetic Retinopathy Clinical Research Network Prompt Panretinal Photocoagulation Versus Intravitreal Ranibizumab with Deferred Panretinal Photocoagulation for Proliferative Diabetic Retinopathy Version
FLUOCINOLONE ACETONIDE: STEROID LONG ACTING
 FLUOCINOLONE ACETONIDE: STEROID LONG ACTING Giuseppe Querques, MD PhD Department of Ophthalmology, IRCCS Ospedale San Raffaele, University Vita Salute San Raffaele, Milan, Italy Financial Disclosure ADVISORY
FLUOCINOLONE ACETONIDE: STEROID LONG ACTING Giuseppe Querques, MD PhD Department of Ophthalmology, IRCCS Ospedale San Raffaele, University Vita Salute San Raffaele, Milan, Italy Financial Disclosure ADVISORY
Does Ranibizumab Improve Best Corrected Visual Acuity in Adults with Diabetic Macular Edema Compared to Those without Ranibizumab?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 Does Ranibizumab Improve Best Corrected
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 Does Ranibizumab Improve Best Corrected
Diabetic retinopathy (DR) is the leading PROCEEDINGS EVIDENCE-BASED DATA IN THE TREATMENT OF DIABETIC RETINOPATHY*
 EVIDENCE-BASED DATA IN THE TREATMENT OF DIABETIC RETINOPATHY* Lloyd Paul Aiello, MD, PhD, and Jennifer K. Sun, MD, MPH ABSTRACT There is a wide array of research into the pathophysiology and treatment
EVIDENCE-BASED DATA IN THE TREATMENT OF DIABETIC RETINOPATHY* Lloyd Paul Aiello, MD, PhD, and Jennifer K. Sun, MD, MPH ABSTRACT There is a wide array of research into the pathophysiology and treatment
INTRODUCTION. Trans Am Ophthalmol Soc 2010;108:62-76
 INTERPRETING THICKNESS CHANGES IN THE DIABETIC MACULA: THE PROBLEM OF SHORT- TERM VARIATION IN OPTICAL COHERENCE TOMOGRAPHY MEASURED MACULAR THICKENING (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) BY
INTERPRETING THICKNESS CHANGES IN THE DIABETIC MACULA: THE PROBLEM OF SHORT- TERM VARIATION IN OPTICAL COHERENCE TOMOGRAPHY MEASURED MACULAR THICKENING (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) BY
Molecular Biology of Diabetic Retinopathy
 Opportunities for Therapeutic Intervention: Molecular Biology of Diabetic Retinopathy Jointly sponsored by The Dulaney Foundation and DIABETIC MICROVASCULAR COMPLICATIONS TODAY. Release Date: January 2006.
Opportunities for Therapeutic Intervention: Molecular Biology of Diabetic Retinopathy Jointly sponsored by The Dulaney Foundation and DIABETIC MICROVASCULAR COMPLICATIONS TODAY. Release Date: January 2006.
HHS Public Access Author manuscript J Vitreoretin Dis. Author manuscript; available in PMC 2017 November 03.
 Prediction of Anti-VEGF Response in Diabetic Macular Edema After 1 Injection Ankoor R. Shah, M.D. 1,2, Yoshihiro Yonekawa, M.D. 3,7, Bozho Todorich, M.D. Ph.D. 3,7, Lily Van Laere, M.D. 3, Rehan Hussain,
Prediction of Anti-VEGF Response in Diabetic Macular Edema After 1 Injection Ankoor R. Shah, M.D. 1,2, Yoshihiro Yonekawa, M.D. 3,7, Bozho Todorich, M.D. Ph.D. 3,7, Lily Van Laere, M.D. 3, Rehan Hussain,
Diabetic Retinopathy Clinical Research Network
 Diabetic Retinopathy Clinical Research Network A Randomized Trial Comparing Intravitreal Triamcinolone Acetonide and Laser Photocoagulation for Diabetic Macular Edema Version 6.0 July 20, 2007 Triamcinolone
Diabetic Retinopathy Clinical Research Network A Randomized Trial Comparing Intravitreal Triamcinolone Acetonide and Laser Photocoagulation for Diabetic Macular Edema Version 6.0 July 20, 2007 Triamcinolone
Randomized Trial Evaluating Short- Term Effects of Intravitreal Ranibizumab or Triamcinolone Acetonide on Macular
 Randomized Trial Evaluating Short- Term Effects of Intravitreal Ranibizumab or Triamcinolone Acetonide on Macular Edema After Focal/grid Laser for Diabetic Macular Edema in Eyes Also Receiving Panretinal
Randomized Trial Evaluating Short- Term Effects of Intravitreal Ranibizumab or Triamcinolone Acetonide on Macular Edema After Focal/grid Laser for Diabetic Macular Edema in Eyes Also Receiving Panretinal
Diabetic retinopathy (DR) represents a
 THE MOLECULAR BIOLOGY OF DIABETIC RETINOPATHY: OPPORTUNITIES FOR THERAPEUTIC INTERVENTION Lloyd P. Aiello, MD, PhD ABSTRACT Hyperglycemia is the principal underlying cause of diabetic microvascular complications,
THE MOLECULAR BIOLOGY OF DIABETIC RETINOPATHY: OPPORTUNITIES FOR THERAPEUTIC INTERVENTION Lloyd P. Aiello, MD, PhD ABSTRACT Hyperglycemia is the principal underlying cause of diabetic microvascular complications,
Anti VEGF Agents in Retinal Disorders Current Scenario
 Retina Anti VEGF Agents in Retinal Disorders Current Scenario Charu Gupta MS Charu Gupta MS, Cyrus M. Shroff MD Shroff Eye Centre, New Delhi T is a group of proteins involved in the regulation of angiogenesis,
Retina Anti VEGF Agents in Retinal Disorders Current Scenario Charu Gupta MS Charu Gupta MS, Cyrus M. Shroff MD Shroff Eye Centre, New Delhi T is a group of proteins involved in the regulation of angiogenesis,
Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England. Retinal Vein Occlusion (RVO) with Macular oedema (MO)
 Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England (Royal Victoria Infirmary, Sunderland Eye Infirmary, James Cook University Hospital, Darlington Memorial Hospital, University Hospital
Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England (Royal Victoria Infirmary, Sunderland Eye Infirmary, James Cook University Hospital, Darlington Memorial Hospital, University Hospital
Cataract and Diabetic macular edema: What should I do?
 Cataract and Diabetic macular edema: What should I do? Irini Chatziralli Ophthalmic Surgeon, University Scholar 2 nd Department of Ophthalmology, University of Athens (Director: Prof P. Theodossiadis)
Cataract and Diabetic macular edema: What should I do? Irini Chatziralli Ophthalmic Surgeon, University Scholar 2 nd Department of Ophthalmology, University of Athens (Director: Prof P. Theodossiadis)
Diabetic Retinopathy Update 2017
 Diabetic Retinopathy Update 2017 Basis for DR management standards for past 40 years Diabetic Retinopathy Study (DRS) 1971-1989 and Early Treatment of Diabetic Retinopathy Study (ETDRS) 1979-1990 Sundeep
Diabetic Retinopathy Update 2017 Basis for DR management standards for past 40 years Diabetic Retinopathy Study (DRS) 1971-1989 and Early Treatment of Diabetic Retinopathy Study (ETDRS) 1979-1990 Sundeep
Charles C. Wykoff MD PhD Rahul N. Khurana MD
 HDWallpapers Suprachoroidal Triamcinolone Acetonide with & without Intravitreal Aflibercept for DME: Results of the 6 Month Prospective Phase 1/2 Hulk trial Blanton Eye Institute Charles C. Wykoff MD PhD
HDWallpapers Suprachoroidal Triamcinolone Acetonide with & without Intravitreal Aflibercept for DME: Results of the 6 Month Prospective Phase 1/2 Hulk trial Blanton Eye Institute Charles C. Wykoff MD PhD
Intravitreal versus Posterior Subtenon Injection of Triamcinolone Acetonide for Diabetic Macular Edema
 Intravitreal versus Posterior Subtenon Injection of Triamcinolone Acetonide for Diabetic Macular Edema Young Jae Choi, MD, In Kyung Oh, MD, Jae Ryung Oh, MD, PhD, Kuhl Huh, MD, PhD Department of Ophthalmology,
Intravitreal versus Posterior Subtenon Injection of Triamcinolone Acetonide for Diabetic Macular Edema Young Jae Choi, MD, In Kyung Oh, MD, Jae Ryung Oh, MD, PhD, Kuhl Huh, MD, PhD Department of Ophthalmology,
Original Article. Authors
 Original Article APMC-303 Efficacy of Intra-Vitreal Bevacizumab Combined with Phaco- Emulsification in the Prophylaxis of Macular Edema in Patients with Non-Proliferative Diabetic Retinopathy Muhammad
Original Article APMC-303 Efficacy of Intra-Vitreal Bevacizumab Combined with Phaco- Emulsification in the Prophylaxis of Macular Edema in Patients with Non-Proliferative Diabetic Retinopathy Muhammad
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Health Technology Appraisal. Aflibercept for treating diabetic macular oedema.
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Health Technology Appraisal Aflibercept for treating diabetic macular oedema Final scope Final remit/appraisal objective To appraise the clinical and cost
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Health Technology Appraisal Aflibercept for treating diabetic macular oedema Final scope Final remit/appraisal objective To appraise the clinical and cost
 Research Article http://www.alliedacademies.org/clinical-ophthalmology-and-vision-science/ A 2-year retrospective study of the treatment of retinal vein occlusion with dexamethasone 0.7 mg intravitreal
Research Article http://www.alliedacademies.org/clinical-ophthalmology-and-vision-science/ A 2-year retrospective study of the treatment of retinal vein occlusion with dexamethasone 0.7 mg intravitreal
Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema
 Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
OCT Assessment of the Vitreoretinal Relationship in CSME
 December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
Case Report Macular Oedema Related to Idiopathic Macular Telangiectasia Type 1 Treated with Dexamethasone Intravitreal Implant (Ozurdex)
 Case Reports in Ophthalmological Medicine, Article ID 231913, 5 pages http://dx.doi.org/10.1155/2014/231913 Case Report Macular Oedema Related to Idiopathic Macular Telangiectasia Type 1 Treated with Dexamethasone
Case Reports in Ophthalmological Medicine, Article ID 231913, 5 pages http://dx.doi.org/10.1155/2014/231913 Case Report Macular Oedema Related to Idiopathic Macular Telangiectasia Type 1 Treated with Dexamethasone
Long-Term Follow-Up of Patient with Diabetic Macular Edema Receiving Fluocinolone Acetonide Intravitreal Implant
 Ophthalmol Ther (2015) 4:51 58 DOI 10.1007/s40123-015-0028-0 CASE REPORT Long-Term Follow-Up of Patient with Diabetic Macular Edema Receiving Fluocinolone Acetonide Intravitreal Implant Thomas Bertelmann
Ophthalmol Ther (2015) 4:51 58 DOI 10.1007/s40123-015-0028-0 CASE REPORT Long-Term Follow-Up of Patient with Diabetic Macular Edema Receiving Fluocinolone Acetonide Intravitreal Implant Thomas Bertelmann
A Phase 2 Evaluation of Anti-VEGF Therapy for Diabetic Macular Edema: Bevacizumab (Avastin)
 Diabetic Retinopathy Clinical Research Network A Phase 2 Evaluation of Anti-VEGF Therapy for Diabetic Macular Edema: Bevacizumab (Avastin) Version1.2 April 27, 2006 Avastin Protocol 4-27-06 V1.2.doc Contact
Diabetic Retinopathy Clinical Research Network A Phase 2 Evaluation of Anti-VEGF Therapy for Diabetic Macular Edema: Bevacizumab (Avastin) Version1.2 April 27, 2006 Avastin Protocol 4-27-06 V1.2.doc Contact
Dexamethasone implant in diabetic macular edema in real-life situations
 (2016) 30, 426 430 2016 Macmillan Publishers Limited All rights reserved 0950-222X/16 www.nature.com/eye CLINICAL STUDY 1 Smt. Kanuri Santhamma Retina Vitreous Centre, L.V. Prasad Institute, Hyderabad,
(2016) 30, 426 430 2016 Macmillan Publishers Limited All rights reserved 0950-222X/16 www.nature.com/eye CLINICAL STUDY 1 Smt. Kanuri Santhamma Retina Vitreous Centre, L.V. Prasad Institute, Hyderabad,
Intravitreal Corticosteroids in the Management of Diabetic Macular Edema
 Curr Ophthalmol Rep (2013) 1:144 149 DOI 10.1007/s40135-013-0015-3 DIABETIC RETINOPATHY: MEDICAL AND SURGICAL THERAPIES (PK KAISER, SECTION EDITOR) Intravitreal Corticosteroids in the Management of Diabetic
Curr Ophthalmol Rep (2013) 1:144 149 DOI 10.1007/s40135-013-0015-3 DIABETIC RETINOPATHY: MEDICAL AND SURGICAL THERAPIES (PK KAISER, SECTION EDITOR) Intravitreal Corticosteroids in the Management of Diabetic
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
Front Line Diabetic Retinopathy What Not to Miss and Why
 Front Line Diabetic Retinopathy What Not to Miss and Why David M Brown MD FACS Clinical Professor of Ophthalmology Blanton Eye Institute, Houston Methodist Hospital Baylor College of Medicine Retina Consultants
Front Line Diabetic Retinopathy What Not to Miss and Why David M Brown MD FACS Clinical Professor of Ophthalmology Blanton Eye Institute, Houston Methodist Hospital Baylor College of Medicine Retina Consultants
Diabetic Retinopathy. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
