Use of protease inhibitors has remarkably improved
|
|
|
- Holly Charles
- 5 years ago
- Views:
Transcription
1 Mechanisms for the Deterioration in Glucose Tolerance Associated With HIV Protease Inhibitor Regimens Hans J. Woerle, 1 Peter R. Mariuz, 1 Christian Meyer, 1 Richard C. Reichman, 1 Emilia M. Popa, 1 Jean M. Dostou, 1 Stephen L. Welle, 1,2 and John E. Gerich 1 The mechanisms responsible for the deterioration in glucose tolerance associated with protease inhibitor containing regimens in HIV infection are unclear. Insulin resistance has been implicated as a major factor, but the affected tissues have not been identified. Furthermore, -cell function has not been evaluated in detail. The present study was therefore undertaken to assess the effects of protease inhibitor containing regimens on hepatic, muscle, and adipose tissue insulin sensitivity as well as pancreatic -cell function. We evaluated -cell function in addition to glucose production, glucose disposal, and free fatty acid (FFA) turnover using the hyperglycemic clamp technique in combination with isotopic measurements in 13 HIV-infected patients before and after 12 weeks of treatment and in 14 normal healthy volunteers. -Cell function and insulin sensitivity were also assessed by homeostasis model assessment (HOMA). Treatment increased fasting plasma glucose concentrations in all subjects (P < 0.001). Insulin sensitivity as assessed by HOMA and clamp experiments decreased by 50% (P < 0.003). Postabsorptive glucose production was appropriately suppressed for the prevailing hyperinsulinemia, whereas glucose clearance was reduced (P < 0.001). -Cell function decreased by 50% (P 0.002), as assessed by HOMA, and firstphase insulin release decreased by 25%, as assessed by clamp data (P 0.002). Plasma FFA turnover and clearance both increased significantly (P < 0.001). No differences at or in responses after treatment were observed between drug naïve patients who were started on a nucleoside reverse transcriptase inhibitor (NRTI) plus a protease inhibitor and patients who had been on long-term NRTI treatment and had a protease inhibitor added. The present study indicates that protease inhibitor containing regimens impair glucose tolerance in HIV-infected patients by two mechanisms: 1) inducement of peripheral insulin resistance in skeletal muscle and adipose tissue and 2) impairment of the ability of the -cell to compensate. Diabetes 52: , 2003 From the 1 Department of Medicine, University of Rochester School of Medicine, Rochester, New York; and the 2 Department of Pharmacology and Physiology, University of Rochester School of Medicine, Rochester, New York Address correspondence and reprint requests to John E. Gerich, University of Rochester School of Medicine, 601 Elmwood Ave., Box MED/CRC, Rochester, NY johngerich@compuserve.com. Received for publication 10 May 2002 and accepted in revised form 2 January R.C.R. has received financial support from GlaxoSmithKline, Agouron Pharmaceuticals, MedImmue, Triangle Pharmaceuticals, and Gilead Sciences. CT, computer tomography; FFA, free fatty acid; HLS, HIV-lipodystrophy syndrome; HOMA, homeostasis model assessment; HPLC, high-performance liquid chromatography; IGT, impaired glucose tolerance; IS HOMA, insulin sensitivity measured by HOMA; NRTI, nucleoside reverse transcriptase inhibitor; SA, specific activity; SECR homa, -cell function measured by HOMA. Use of protease inhibitors has remarkably improved long-term survival after HIV infection (1,2). However, up to 60% of HIV-infected patients treated with these agents develop either impaired glucose tolerance (IGT) or type 2 diabetes (3 6), and it now appears to be well established that regimens including protease inhibitors are associated with insulin resistance (2,5,7,8). Noor et al. (9,10) have shown that acute and 4-week protease inhibitor exposure of normal volunteers reduces glucose disposal during euglycemichyperinsulinemic clamp experiments. Moreover, in vitro studies have demonstrated that protease inhibitors reduce insulin-stimulated glucose uptake in adipocytes and skeletal muscle (11,12). Knowledge of the mechanisms responsible for deterioration in glucose tolerance during protease inhibitor containing regimens is still incomplete. It is unclear whether protease inhibitors adversely affect pancreatic -cell function (4,8) and what effect they have on glucose production and free fatty acid (FFA) turnover. Protease inhibitors are aspartate endopeptidase inhibitors (13 15). Because an aspartate endopeptidase is involved in converting proinsulin to insulin, the observation that plasma proinsulin levels are increased in protease inhibitor treated patients (5) suggests that these drugs may directly impair pancreatic -cell function. Increased plasma FFA levels have been found in protease inhibitor treated patients (16), and it is not known whether this is due to increased release or decreased utilization. This study was undertaken to prospectively assess the effect of protease inhibitor based treatment regimens on pancreatic -cell function and to determine the sites of insulin resistance. We studied 13 HIV-infected subjects with normal glucose tolerance before and after 12 weeks of protease inhibitor based treatment and 14 healthy normal volunteers using hyperglycemic clamp experiments in combination with isotopic determination of glucose and FFA turnover. Eight of the patients had been on a chronic regimen containing nucleoside reverse transcriptase inhibitors (NRTIs) to which a protease inhibitor was added, and five patients were drug naïve and were started on a combination of an NRTI and a protease inhibitor. RESEARCH DESIGN AND METHODS Informed written consent was obtained from 13 HIV-infected otherwise healthy subjects and 14 HIV-negative normal volunteers after the protocol had been approved by the University of Rochester Institutional Review Board. Subjects were recruited in the Infectious Disease Clinic based on plans for 918 DIABETES, VOL. 52, APRIL 2003
2 H.J. WOERLE AND ASSOCIATES TABLE 1 Antiviral therapy before and after starting protease inhibitors Subject Pre-PI treatment Post-PI treatment Age Sex Race 1 Nevirapine, stavudine, lamivudine Stavudine, lamivudine, nelfinavir 53 M AA 2 Efavirenz, abacavir, stavudine Lamivudine, zidovudine, nelfinavir 35 F C 3 Nevirapine, stavudine, lamivudine Lamivudine, stavudine, nelfinavir 46 F H 4 Nevirapine, stavudine, lamivudine Stavudine, lamivudine, indinavir, ritonavir 47 F AA 5 Efavirenz, abacavir, stavudine Abacavir, stavudine, saquinavir 38 F AA 6 Stavudine, lamivudine, nevirapine Stavudine, lamivudine, saquinavir, ritonavir 31 M AA 7 Stavudine, lamivudine, efavirenz Stavudine, lamivudine, nelfinavir 40 F C 8 Nevirapine, stavudine, lamivudine Stavudine, lamivudine, nelfinavir 50 M C 9 None Stavudine, lamivudine, nelfinavir 47 M AA 10 None Stavudine, lamivudine, nelfinavir 46 M H 11 None Stavudine, lamivudine, nelfinavir 32 F AA 12 None Zidovudine, lamivudine, nelfinavir 39 M AA 13 None Lopinavir, efavirenz, lamivudine, ritonavir 38 F C Normal volunteers (N 14) F/8M 3AA/10C/1H Data are means SD unless otherwise indicated. AA, African-American; C, Caucasian; H, Hispanic; PI, protease inhibitor. initiation of protease inhibitor treatment. All subjects had normal routine laboratory screening results including normal liver function tests and urinalysis. None of the subjects had a family history of diabetes. Normal glucose tolerance had been ascertained by fasting plasma glucose levels 6 mmol/l and plasma glucose levels 7.8 mmol/l 2 h after a 75-g oral glucose load (17). The drug that patients received was based on the clinical judgment of their physician. Table 1 gives the drug regimens of individual patients before and after protease inhibitor treatment. Eight subjects (NRTI pretreated) had been on a combination therapy of nucleoside analogues and a non-nrti for at least 12 months; the NRTIs were continued throughout the study, the non-nrti was discontinued, and a protease inhibitor was added. Five subjects (NRTI naïve), who were drug naïve, were started on two NRTIs plus a protease inhibitor. Thus, during the treatment phase all patients were on a combination of a protease inhibitor and NRTIs. None of the subjects experienced any subcutaneous fat wasting before or throughout the study. All were studied on three occasions: once before initiation of protease inhibitor treatment and at 6 and 12 weeks thereafter. Only results of those before and at 12 weeks are reported. Subjects consumed a weight maintenance diet containing g carbohydrate at least 3 days before the first hyperglycemic clamp experiment and throughout the whole 12-week study period. On each study occasion subjects were admitted to the clinical research center at 5:00 P.M. the day before the experiment. Between 6:00 P.M. and 7:00 P.M. a standard dinner (10 kcal/kg: 50% carbohydrate, 35% fat, and 15% protein) was given. At 5:00 A.M. the following morning, primed-continuous infusions of [6,6-2 H 2 ]glucose (24 mol/kg, 0.24 mol kg 1 min 1 ) and [9,10-3 H]palmitate (0.8 Ci/min) were started via a forearm vein. At 6:00 A.M. a retrograde venous catheter was inserted into a dorsal hand vein and maintained in a thermoregulated box at 65 C to obtain arterialized blood samplings (18). After allowing at least 2 h to achieve isotopic steady state, samples for substrate enrichments, specific activities, plasma glucose, FFAs, glycerol, insulin, glucagon, C-peptide, and proinsulin concentrations were collected at 30, 15, and 0 min. Just before beginning the clamp, subjects took their medications. Subsequently, a primed (150 mg/kg body wt) 20% glucose infusion was given and plasma glucose levels were clamped at 10 mmol/l (180 mg/dl) for 3 h (19). Plasma insulin, proinsulin, and C-peptide concentrations were measured at 2.5, 5.0, 7.5, 10, 15, 30, 60, 90, 120, 140, 160, and 180 min. Samples for plasma glucose, FFA, glucagon, glycerol concentrations, enrichments, and specific activities (SAs) were collected during the last hour of the clamp at 20-min intervals (120, 140, 160, and 180 min). Plasma glucose was measured at 5-min intervals throughout for adjustments of glucose infusion rates using a glucose analyzer (YSI Glucose Analyzer; Yellow Springs Instruments). Plasma insulin (Linco Research), proinsulin (Linco Research), C-peptide (Diagnostic Product), and glucagon (Linco Research) were measured by standard radioimmunoassays. Plasma FFA levels were measured by an enzymatic calorimetric method (NEFAC; Wako Pure Chemical). Plasma glycerol concentrations were determined by standard microfluorometric assays (20). HbA 1c was determined by high-performance liquid chromatography (HPLC). Plasma [6,6-2 H 2 ]glucose enrichments were measured by gas chromatography mass spectroscopy (21), and plasma palmitate concentrations and SAs were determined by a previously described HPLC technique (22) with coefficients of variation of 3.8 and 2.3%, respectively. Total body fat and fat-free mass was determined by bioimpedance measurements (23). Calculations. First-phase insulin release was calculated as the sum of the increments of C-peptide above at 2.5, 5.0, 7.5, and 10 min. Secondphase insulin release was calculated as the average C-peptide concentration during the last hour of the clamp (24). Insulin sensitivity index (25) was calculated by dividing the average glucose infusion rate during the last hour of the clamp ( mol kg 1 min 1 ) by the product of the average plasma insulin (pmol/l) and glucose (mmol/l) concentration during the same time interval (25). -Cell function and insulin sensitivity were also assessed by using HOMA as previously described (26). Insulin sensitivity (IS HOMA ) was calculated as IS HOMA 1/(135 insulin glucose), i.e., the inverse of insulin resistance. -Cell function (SECR homa ) was calculated as SECR homa C-peptide 3.33/(GLUC 3.5), where C-peptide (pmol/l) represents the average fasting plasma C-peptide concentration and GLUC (mmol/l) the average fasting plasma glucose concentration (27). C-peptide was used in place of the originally proposed plasma insulin because of changes in insulin metabolism induced by protease inhibitor treatment as described below. To evaluate the appropriateness of changes in -cell function in relation to changes in insulin sensitivity, the disposition index (28) was calculated as the product of -cell function and insulin sensitivity determined during the clamp experiments. During the basal state before the clamp, rates of appearance and disappearance (turnover) of FFA were calculated using the steady-state equation for the infusion of radioactive isotopes Ra(Rd) F/SA (29), where Ra represents the rate of appearance, Rd the rate of disappearance, F the infusion rate of tracer (dpm min 1 kg 1 ), and SA the specific activity (dpm mol 1 ). For glucose turnover, isotope enrichments (%) were substituted for SAs and corrected for the proportion of infused [6,6-2 H 2 ]glucose by subtracting its infusion rate from Ra(Rd). Glucose enrichments and palmitate SAs were not significantly different from one another, indicating that isotopic steady state had been achieved. Because there is evidence that NRTIs may be associated with insulin resistance (30), subjects were divided into two groups. Group 1 (NRTI pretreated, n 8) had been on an NRTI and had a protease inhibitor added; group 2 (NRTI naïve, n 5) had been drug naïve and were started on an NRTI and a protease inhibitor. The data of these groups were compared in an attempt to factor out the effects of protease inhibitors. Furthermore, data of NRTI pretreated volunteers was compared with those of 14 healthy subjects to determine whether NRTI pretreatment had effects on insulin sensitivity and -cell function. Unless specified otherwise, data are given as the mean SE and were initially evaluated by ANOVA for repeated measurements followed by Wilcoxon s matched pairs test comparing data with results after 12 weeks of treatment. Mann-Whitney tests were used to compare changes between the groups during the treatment period as well as data. Correlations between variables were performed using Spearman s regression analysis. DIABETES, VOL. 52, APRIL
3 PROTEASE INHIBITOR INDUCED GLUCOSE INTOLERANCE TABLE 2 Body composition, viral load, and CD 4 counts Baseline 12 weeks BMI (kg/m 2 ) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.34 Lean body mass (kg) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.62 Body fat (kg) NRTI pretreated NRTI naïve Both Normal volunteers groups CD 4 counts NRTI pretreated NRTI naïve Both groups 0.73 Viral load NRTI pretreated NRTI naïve Both groups 0.82 TABLE 3 HbA 1c, fasting plasma glucose, insulin, glucagon, C-peptide, and proinsulin Before 12 weeks HbA 1c (%) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.91 Glucose (mmol/l) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.59 Plasma insulin (pmol/l) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.08 Plasma glucagon (pg/ml) NRTI pretreated NRTI naïve Both Normal volunteers 70 6 groups 0.98 Plasma C-peptide (nmol/l) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.34 Plasma proinsulin (pmol/l) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.87 RESULTS Body composition, waist-to-hip ratio, viral loads, and CD 4 counts Baseline characteristics of the groups did not differ except that the NRTI-naïve subjects had lower initial body fat. During 12 weeks of treatment, BMI, total body fat, and lean body mass did not change in either group; viral load decreased by 80% in both groups (P 0.001) (Table 2). HbA 1c, fasting plasma glucose, insulin, glucagon, C- peptide, proinsulin, glycerol, FFAs, and plasma lipids Baseline values, which were comparable with those of the normal volunteers, and responses during treatment in NRTI-pretreated and NRTI-naïve groups were not significantly different (Tables 3 and 4). After 12 weeks of treatment, fasting plasma glucose increased in all subjects (P 0.001). Fasting plasma insulin also increased (P 0.001). In contrast, fasting plasma C-peptide and proinsulin did not change (both P 0.61). Consequently, both the plasma C-peptide to insulin ratio and the plasma proinsulin to insulin ratio decreased (both P 0.007). The plasma C-peptide to proinsulin ratio and plasma glucagon remained unchanged (P 0.59 and 0.69, respectively). Fasting plasma glycerol increased (P 0.02), whereas plasma FFAs, triglycerides, and total and HDL cholesterol remained unchanged (all P 0.13). However, plasma LDL cholesterol increased slightly but significantly (P 0.03). -Cell function and insulin sensitivity HOMA. Baseline values and responses to treatment were not significantly different in NRTI-pretreated and NRTInaïve subjects. At, both groups had comparable insulin sensitivity and -cell function with those of normal volunteers. After 12 weeks of treatment, both insulin sensitivity and pancreatic -cell function decreased significantly (P and 0.003, respectively) (Tables 5 and 6 and Fig. 1). Hyperglycemic clamp experiments Insulin sensitivity. Plasma glucose, insulin, C-peptide, and proinsulin concentrations and glucose infusion rates are given in Fig. 1. Plasma glucose levels were not significantly different in clamps performed at and 12 weeks in all groups. The insulin sensitivity index calculated by dividing the glucose infusion rates by the product of plasma glucose and insulin concentrations were comparable with those of the normal volunteers, and responses to treatment were not significantly different in NRTI-pretreated and NRTI-naïve subjects. The insulin sensitivity index decreased significantly after treatment (P 0.001). -Cell function. At, both first- and second-phase insulin release was normal in both patient groups. After treatment, first-phase insulin release decreased signifi- 920 DIABETES, VOL. 52, APRIL 2003
4 H.J. WOERLE AND ASSOCIATES TABLE 4 Plasma glycerol, FFAs, triglycerides, total cholesterol, and LDL and HDL cholesterol Before 12 weeks Plasma glycerol ( mol/l) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.08 Plasma FFA ( mol/l) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.26 Total cholesterol (mg/dl) NRTI pretreated NRTI naïve Both groups 0.98 HDL (mg/dl) NRTI pretreated NRTI naïve Both groups 0.81 LDL (mg/dl) NRTI pretreated NRTI naïve Both groups 0.92 Triglycerides (mg/dl) NRTI pretreated NRTI naïve Both groups 0.35 cantly in both groups to a comparable extent (P 0.002). Second-phase insulin release did not change in either group. However, the disposition index, calculated from second-phase insulin release, decreased significantly and to comparable extents in both groups (P 0.001), indicating lack of appropriate -cell compensation. Systemic glucose and FFA turnovers and clearances. Baseline values and responses to treatment did not differ among the patient groups. Fasting plasma glucose turnover, which was normal at, decreased significantly after treatment (P 0.002). The product of basal plasma insulin and glucose turnover, an index of the appropriateness of endogenous glucose production for the prevailing insulinemia, remained unchanged in both groups, suggesting appropriate suppression of endogenous glucose production. Glucose clearance, which was normal at, decreased significantly (P 0.001), indicating peripheral insulin resistance. Although plasma FFA concentrations did not change as indicated above, both fasting plasma FFA turnover and clearance increased significantly after treatment (both P 0.001) (Table 7). DISCUSSION This study was undertaken to assess the effect of protease inhibitor based treatment on pancreatic -cell function and to determine mechanisms and sites of insulin resistance induced by these agents. We studied 13 asymptomatic HIV-infected individuals before and after addition of a protease inhibitor, mainly nelfinavir (n 8). Eight of the subjects had already been on NRTI-containing antiviral regimens and the remaining five had been drug naïve, but for clinical reasons were started on both a protease inhibitor and NRTI. Some studies have suggested that NRTIs may cause insulin resistance, whereas others have not (30 32). To factor out the effect of protease inhibitor and NRTI treatment, we analyzed these groups separately. At, -cell function and insulin sensitivity did not differ between groups or when compared with a group of matched normal volunteers. This suggests either that the previous long-term NRTI treatment had not affected either -cell function or insulin sensitivity or that, if it had, its effect was too small to be detected given the number of subjects studied. Responses during treatment with either addition of a protease inhibitor alone or with the addition of both a protease inhibitor and NRTIs were comparable. This suggests that the effects we observed when adding a protease inhibitor to long-term NRTI treatment or when starting both types of agents were primarily those of the protease inhibitors as previously suggested (7). After 12 weeks of treatment, we found a deterioration in glucose tolerance in all subjects, as indicated by increased fasting plasma glucose levels. Insulin sensitivity decreased TABLE 5 HOMA assessment of -cell function and insulin sensitivity Baseline 12 weeks -Cell function (pmol/l mmol/l) NRTI pretreated 2, , NRTI naïve 1, Both 2, , Normal volunteers 1, groups 0.10 Insulin sensitivity (pmol/l 1 mmol/l 1 ) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.98 DIABETES, VOL. 52, APRIL
5 PROTEASE INHIBITOR INDUCED GLUCOSE INTOLERANCE TABLE 6 Hyperglycemic clamp assessment of -cell function and insulin Baseline 12 weeks First-phase insulin release (nmol/l) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.85 Second-phase insulin release (nmol/l) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.25 Glucose infusion rates ( mol kg 1 min 1 ) NRTI pretreated NRTI naïve Both Normal volunteers 50 6 p groups 0.83 Plasma insulin (pmol/l) NRTI pretreated , NRTI naïve Both Normal volunteers groups 0.83 Insulin sensitivity index (ml kg 1 min 1 ) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.32 Disposition index (ml pmol/l kg 1 min 1 nmol/l 1 ) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.26 by 40 50% as determined by HOMA and the hyperglycemic clamp technique. Overall pancreatic -cell function, as assessed by HOMA, and first-phase insulin release, assessed during hyperglycemic clamp experiments, decreased significantly. Second-phase insulin release during the hyperglycemic clamp experiments was not reduced in an absolute sense but with use of the disposition index, an assessment of the appropriateness of -cell function for a given degree of insulin resistance, it was found to be reduced significantly. Thus, it appears that first-phase insulin release was more severely affected than secondphase insulin release. Our results thus confirm that protease inhibitor treatment of HIV-infected individuals is associated with insulin resistance (2,7,33); furthermore, our results demonstrate that this insulin resistance is not accompanied by an appropriate compensatory increase in insulin secretion. Indeed, there was a strong correlation between deterioration of the disposition index and the increase in fasting plasma glucose concentrations (r 0.645). Various protease inhibitors (indinavir, nelfinavir, lopinovir, saquinavir, and ritonavir) have been reported to cause insulin resistance either in vivo or in vitro (1,5,12,34,35). It has been suggested that inducement of insulin resistance by protease inhibitors may be a class effect (33), although these agents may differ in the extent to which they affect insulin sensitivity (7). However, our study was not designed or powered to detect differences in magnitude among these agents, but rather to assess the mechanisms responsible for the associated deterioration in glucose tolerance. Since most of our subjects received nelfinavir, the conclusion of a class effect must be drawn with caution. Regarding the mechanisms/sites of insulin resistance induced by protease inhibitor treatment, we found a reduction in glucose disposal, whereas glucose production appeared to be appropriately reduced for the prevailing plasma insulin concentration. Under euglycemic-hyperinsulinemic clamp conditions, most glucose disposal occurs in skeletal muscle (25). Indinavir has been shown to inhibit muscle glucose transport (36). Our results thus provide additional evidence that these agents reduce skeletal muscle insulin sensitivity. Furthermore, our findings suggest that there was also insulin resistance in adipose tissue. Although plasma FFA concentrations did not change, plasma glycerol concentra- 922 DIABETES, VOL. 52, APRIL 2003
6 H.J. WOERLE AND ASSOCIATES FIG. 1. Plasma glucose, insulin, C-peptide, and proinsulin concentrations and glucose infusion rates in HIV subjects pre- and posttreatment and in normal volunteers. tions and plasma FFA turnover increased. Because this occurred in the face of increased plasma insulin levels, these observations provide evidence for impaired suppression of lipolysis by insulin. The latter is consistent with recent reports that nelfinavir, saquinavir, and ritonavir increase lipolysis (11,35,37). We found no alteration of plasma lipids except for an increase in LDL cholesterol. Previous studies have found no effect of indinavir and ritonavir on LDL cholesterol in normal volunteers, whereas in HIV-infected individuals protease inhibitors appear to consistently increase LDL cholesterol and have variable effects on triglycerides (9,38,39). Recently, the HIV-lipodystrophy syndrome (HLS), a condition characterized by changes in body fat redistribution, peripheral and facial fat loss, dyslipidemia, and insulin resistance has been associated with protease inhibitor and NRTI therapy (40). It has been suggested that the changes in lipid metabolism associated with the HLS may be at least partially responsible for a deterioration in glucose tolerance (41). We did not find any significant changes in body fat content and lean body mass or any clinical signs of fat redistribution in our patients either before or after treatment. However, we did not assess changes in body fat distribution with magnetic resonance imaging or computer tomography (CT). Thus, we cannot exclude that subtle changes in body composition might have occurred. However, changes in glucose tolerance have been reported to take place with protease inhibitors without detectable changes in body composition determined by CT (9). However, we did find an increase in FFA turnover and clearance after treatment. Recently, Sekhar et al. (42) provided strong evidence that the HLS is associated with increased FFA turnover and suggested that this reflected ongoing fat redistribution. Thus, the increased FFA turnover that we found in the absence of obvious lipodystrophy may be an early indicator for changes in lipid metabolism, which might eventually lead to the development of lipodystrophy. On the other hand, the increased FFA turnover may simply reflect insulin resistance accompanying the treatment unrelated to the HLS. Nevertheless, the insulin resistance in type 2 diabetes is characterized by normal FFA turnover and reduced FFA clearance (43,44). The molecular mechanism for the deterioration in pancreatic -cell function found in the present study and in a preliminary report in nelfinavir-treated rats (45) remains to be elucidated. It had been initially speculated that protease inhibitors may impair -cell function by inhibiting one of the endopeptidases involved in the cleavage of proinsulin to insulin (4), because increased plasma insulin to proinsulin ratios were found in protease inhibitor treated patients (5). In the present studies we found the opposite. Moreover, subsequent studies (46) in which islet cells were incubated with protease inhibitors did not show any adverse effect on the conversion of proinsulin to insulin. Thus, endopeptidase inhibition does not seem to be involved. There is evidence, however, that insulin itself may be important for maintaining normal -cell function based on the finding of reduced insulin release in mice with knockout of the insulin receptor and insulin receptor substrate-2 (47). Conceivably, therefore, the same mechanism by which protease inhibitor containing regimens cause insulin resistance in the peripheral tissues might be operative in the pancreatic -cell. It is noteworthy that in the present study the ratio of plasma proinsulin to plasma insulin and the ratio of plasma C-peptide to plasma insulin both decreased significantly with treatment, whereas the ratio of plasma proinsulin to plasma C-peptide was unaltered. Because insulin and C-peptide are secreted from the -cell in equimolar amounts, changes in the ratio of plasma C-peptide to plasma insulin would reflect a change in the clearance of insulin or C-peptide. The above findings are therefore DIABETES, VOL. 52, APRIL
7 PROTEASE INHIBITOR INDUCED GLUCOSE INTOLERANCE TABLE 7 Baseline systemic glucose and FFA turnover and clearance Before 12 weeks Glucose turnover ( mol kg 1 min 1 ) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.08 Glucose turnover plasma insulin ( mol kg 1 min 1 pmol/l 1 ) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.34 Glucose clearance (ml kg 1 min 1 ) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.93 FFA turnover NRTI pretreated NRTI naïve Both Normal volunteers groups 0.15 FFA clearance (ml kg 1 min 1 ) NRTI pretreated NRTI naïve Both Normal volunteers groups 0.06 consistent with the conclusion that insulin clearance had been reduced. If C-peptide clearance been altered, one would expect to find a change in the plasma proinsulin to plasma C-peptide ratio. The practical significance of this finding is that changes in plasma insulin concentrations cannot be used as an index of -cell function during treatment with protease inhibitor containing regimens. In conclusion, the present study indicates that protease inhibitor containing regimens impair glucose tolerance in HIV-infected patients by two mechanisms: 1) inducement of peripheral insulin resistance in skeletal muscle and adipose tissue and 2) reduction in pancreatic -cell function. There are several clinical implications of this study. First, use of these regimens may cause deterioration of glycemic control in patients with preexisting diabetes. Second, because these regimens appear to induce insulin resistance predominantly in skeletal muscle and adipose tissue, antidiabetic agents that exert their major action on peripheral tissues rather than on the liver (e.g., thiazolidinediones) would appear advantageous (48). Third, because first-phase insulin release appears to be more severely impaired than second-phase insulin release, secretagogues such as the meglitinides, which primarily improve firstphase insulin release (49), may be preferable to sulfonylureas, which apparently only affect second-phase insulin release (49). ACKNOWLEDGMENTS This work was supported in part by Division of Research Resources GCRC Grant 5MO1 RR 00044, the National Institute of Diabetes and Digestive and Kidney Diseases Grant DK (to J.E.G.), and NIAID grant AI (to R.C.R.). We thank Mary Little for her excellent editorial assistance and the nursing and laboratory staff of the General Clinical Research Center for their superb help. REFERENCES 1. Flexner C: HIV-protease inhibitors. N Engl J Med 338: , Hruz P, Murata H, Mueckler M: Adverse metabolic consequences of HIV protease inhibitor therapy: the search for a central mechanism. Am J Physiol Endocrinol Metab 280:E549 E553, Lee E, Walmsley S, Fantus I: New-onset diabetes mellitus associated with protease inhibitor therapy in an HIV-positive patient: case report and review. CMAJ 161: , Visnegarwala F, Krause K, Musher D: Severe diabetes associated with protease inhibitor therapy. Ann Intern Med 127:947, Behrens G, Dejam A, Schmidt H, Balks H, Brabant G, Korner T, Stoll M, Schmidt R: Impaired glucose tolerance, beta cell function and lipid metabolism in HIV patients under treatment with protease inhibitors. AIDS 13:F63 F70, Tsiodras S, Mantzoros C, Hammer S, Samore M: Effects of protease inhibitors on hyperglycemia, hyperlipidemia, and lipodystrophy: a 5-year cohort study. Arch Intern Med 160: , Jain R, Furfine E, Pedneault L, White A, Lenhard J: Metabolic complica- 924 DIABETES, VOL. 52, APRIL 2003
8 H.J. WOERLE AND ASSOCIATES tions associated with antiretroviral therapy. Antiviral Res 51: , Dube M, Edmondson-Melancon H, Qian D, Aqeel R, Johnson D, Buchanan T: Prospective evaluation of the effect of initiating indinavir-based therapy on insulin sensitivity and B-cell function in HIV-infected patients. J Acquir Immune Defic Syndr 27: , Noor M, Lo J, Mulligan K, Schwartz J, Halvorsen R, Schambelan M, Grunfeld C: Metabolic effects of indinavir in healthy HIV-seronegative men. AIDS 15:F11 F18, Noor M, Seneviratne T, Aweeka F, Lo J, Schwarz J, Mulligan K, Schambelan M, Grunfeld C: Indinavir acutely inhibits insulin-stimulated glucose disposal in humans: a randomized, placebo-controlled study. AIDS 16:F1 F8, Rudich A, Vanounou S, Riesenberg K, Porat M, Tirosh A, Harman-Boehm I, Greenberg AS, Schlaeffer F, Bashan N: The HIV protease inhibitor nelfinavir induces insulin resistance and increases basal lipolysis in 3T3 L1 adipocytes. Diabetes 50: , Nolte L, Yarasheski K, Kawanaka K, Fisher J, Le N, Holloszy J: The HIV protease inhibitor indinavir decreases insulin- and contraction-stimulated glucose transport in skeletal muscle. Diabetes 50: , Seelmeier S, Schmidt H, Turk V, von der Helm K: Human immunodeficiency virus has an aspartic-type protease that can be inhibited by pepstatin A. Proc Natl Acad Sci U S A 85: , Kohl N, Diehl R, Rands E, Davis L, Hanobik M, Wolanski B, Dixon R: Expression of active human immunodeficiency virus type 1 protease by noninfectious chimeric virus particles. J Virol 65: , DiIanni C, Davis L, Holloway M, Herber W, Darke P, Kohl N, Dixon R: Characterization of an active single polypeptide form of the human immunodeficiency virus type 1 protease. J Biol Chem 265: , Nolan D, Mallal S: Getting to the HAART of insulin resistance. AIDS 15: , World Health Organization: WHO Expert Committee on Diabetes Mellitus. Second Report. Geneva, World Health Org., 1980 (Tech. Rep. Ser., no. 646) 18. Liu D, Moberg E, Kollind M, Lins P, Adamson U, MacDonald I: Arterial, arterialized venous, venous and capillary blood glucose measurements in normal man during hyperinsulinaemic euglycaemia and hypoglycaemia. Diabetologia 35: , Mitrakou A, Vuorinen-Markkola H, Raptis G, Toft I, Mokan M, Strumph P, Pimenta W, Veneman T, Jenssen T, Bolli G, Korytkowski M, Yki-Jarvinen H, Gerich J: Simultaneous assessment of insulin secretion and insulin sensitivity using a hyperglycemic clamp. J Clin Endo Metab 75: , Nurjhan N, Kennedy F, Consoli A, Martin C, Miles J, Gerich J: Quantification of the glycolytic origin of plasma glycerol: implications for the use of the rate of appearance of plasma glycerol as an index of lipolysis in vivo. Metabolism 37: , Wolfe R: Radioactive and Stable Isotope Tracers in Biomedicine: Principles and Practice of Kinetic Analysis. New York, Wiley-Liss, Miles J, Ellman M, McLean K, Jensen M: Validation of a new method for determination of free fatty acid turnover. Am J Physiol 252:E431 E438, Thomas B, Cornish B, Ward L: Bioelectrical impedance analysis for measurement of body fluid volumes: a review. J Clin Eng 17: , Pimenta W, Kortytkowski M, Mitrakou A, Jenssen T, Yki-Jarvinen H, Evron W, Dailey G, Gerich J: Pancreatic beta-cell dysfunction as the primary genetic lesion in NIDDM. JAMA 273: , DeFronzo R: Glucose intolerance and aging: evidence for tissue insensitivity to insulin. Diabetes 28: , Matthews D, Hosker J, Rudenski A, Naylor B, Treacher D, Turner R: Homeostasis model assessment: insulin resistance and -cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28: , Stumvoll M, Mitrakou A, Pimenta W, Jenssen T, Yki-Järvinen H, Van Haeften T, Renn W, Gerich J: Use of the oral glucose tolerance test to assess insulin release and insulin sensitivity. Diabetes Care 23: , Kahn S, Prigeon R, McCulloch D, Boyko E, Bergman R, Schwartz M, Neifing J, Ward W, Beard J, Palmer J, Porte D: Quantification of the relationship between insulin sensitivity and beta-cell function in human subjects: evidence for a hyperbolic function. Diabetes 42: , Wolfe R: Isotopic measurement of glucose and lactate kinetics. Ann Med 22: , Hadigan C, Corcoran C, Stanley T, Piecuch S, Klibanski A, Grinspoon S: Fasting hyperinsulinemia in human immunodeficiency virus-infected men: relationship to body composition, gonadal function, and protease inhibitor use. J Clin Endocrinol Metab 85:35 41, Saint-Marc T, Partisani M, Poizot-Martin I, Bruno F, Rouviere O, Lang J-M, Gastaut J-A, Touraine J-L: A syndrome of peripheral fat wasting (lipodystrophy) in patients receiving long-term nucleoside analogue therapy. AIDS 13: , Mallal S, John M, Moore C, James I, McKinnon E: Contribution of nucleoside analogue reverse transcriptase inhibitors to subcutaneous fat wasting in patients with HIV infection. AIDS 14: , Max B, Sherer R: Management of the adverse effects of antiretroviral therapy and medication adherence. Clin Infect Dis 30 (Suppl. 2):S96 S116, Murata H, Hruz P, Mueckler M: The mechanism of insulin resistance caused by HIV protease inhibitor therapy. J Biol Chem 275: , Ranganathan S, Kern P: The HIV protease inhibitor saquinavir impairs lipid metabolism and glucose transport in cultured adipocytes. J Endocrinol 172: , Martínez E, Conget I, Lozano L, Casamitjana R, Gatell J: Reversion of metabolic abnormalities after switching from HIV-1 protease inhibitors to nevirapine. AIDS 13: , Lenhard J, Furfine E, Jain R, Ittoop O, Orband-Miller L, Blanchard S, Paulik M, Weiel J: HIV protease inhibitors block adipogenesis and increase lipolysis in vitro. Antiviral Res 47: , Purnell J, Zambon A, Knopp R, Pizzuti D, Achari R, Leonard J, Locke C, Brunzell J: Effect of ritonavir on lipids and post-heparin lipase activities in normal subjects. AIDS 14:51 57, Periard D, Telenti A, Sudre P, Cheseaux J, Halfon P, Reymond M, Marcovina S, Glauser M, Nicod P, Darioli R, Mooser V: Atherogenic dyslipidemia in HIV-infected individuals treated with protease inhibitors: the Swiss HIV Cohort Study. Circulation 100: , Tözsér J: HIV inhibitors: problems and reality. Ann N Y Acad Sci 946: , Stricker R, Goldberg B: Fat accumulation and HIV-1 protease inhibitors. Lancet 352:1392, Sekhar R, Jahoor F, White A, Pownall H, Visnegarwala F, Rodriguez- Barradas M, Sharma M, Reeds P, Balasubramanyam A: Metabolic basis of HIV-lipodystrophy syndrome. Am J Physiol Endocrinol Metab 283:E332 E337, Meyer C, Stumvoll M, Nadkarni V, Dostou J, Mitrakou A, Gerich J: Abnormal renal and hepatic glucose metabolism in type 2 diabetes mellitus. J Clin Invest 102: , Taskinen M, Bogardus C, Kennedy A, Howard B: Multiple disturbances of free fatty acid metabolism in noninsulin dependent diabetes. J Clin Invest 76: , Shankar S, Wu Y, Zhu J, Baron A, Dube M, Shankar R: Nelfinavir impairs insulin secretion and paradoxically enhances insulin sensitivity (Abstract). Diabetes 50 (Suppl. 2):A321, Danoff A, Ling W: Protease inhibitors do not interfere with prohormone processing. Ann Intern Med 132:330, Kadowaki T: Insights into insulin resistance and type 2 diabetes from knockout mouse models. J Clin Invest 106: , Walli R, Michl G, Muhlbayer D, Brinkmann L, Goebel F: Effects of troglitazone on insulin sensitivity in HIV-infected patients with protease inhibitor-associated diabetes mellitus. Res Exp Med (Berl) 199: , Lebovitz H: Insulin secretogogues: old and new. Diab Rev 7: , 1999 DIABETES, VOL. 52, APRIL
Mechanisms and Strategies for Insulin Resistance in Acquired Immune Deficiency Syndrome
 SUPPLEMENT ARTICLE Mechanisms and Strategies for Insulin Resistance in Acquired Immune Deficiency Syndrome Steven Grinspoon Harvard Medical School, Massachusetts General Hospital, Program in Nutritional
SUPPLEMENT ARTICLE Mechanisms and Strategies for Insulin Resistance in Acquired Immune Deficiency Syndrome Steven Grinspoon Harvard Medical School, Massachusetts General Hospital, Program in Nutritional
Is Reduced First-Phase Insulin Release the Earliest Detectable Abnormality in Individuals Destined to Develop Type 2 Diabetes?
 Is Reduced First-Phase Insulin Release the Earliest Detectable Abnormality in Individuals Destined to Develop Type 2 Diabetes? John E. Gerich Insulin is released from the pancreas in a biphasic manner
Is Reduced First-Phase Insulin Release the Earliest Detectable Abnormality in Individuals Destined to Develop Type 2 Diabetes? John E. Gerich Insulin is released from the pancreas in a biphasic manner
28 Regulation of Fasting and Post-
 28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
Glimepiride Improves Both First and Second Phases of Insulin Secretion in Type 2 Diabetes. Diabetes Care 25: , 2002
 Emerging Treatments and Technologies O R I G I N A L A R T I C L E Glimepiride Improves Both First and Second Phases of Insulin Secretion in Type 2 Diabetes MARY KORYTKOWSKI, MD 1 ABRAHAM THOMAS, MD 2
Emerging Treatments and Technologies O R I G I N A L A R T I C L E Glimepiride Improves Both First and Second Phases of Insulin Secretion in Type 2 Diabetes MARY KORYTKOWSKI, MD 1 ABRAHAM THOMAS, MD 2
Effect of Aging on Glucose Homeostasis. Accelerated deterioration of -cell function in individuals with impaired glucose tolerance
 Pathophysiology/Complications B R I E F R E P O R T Effect of Aging on Glucose Homeostasis Accelerated deterioration of -cell function in individuals with impaired glucose tolerance ERVIN SZOKE, MD 1 MUHAMMAD
Pathophysiology/Complications B R I E F R E P O R T Effect of Aging on Glucose Homeostasis Accelerated deterioration of -cell function in individuals with impaired glucose tolerance ERVIN SZOKE, MD 1 MUHAMMAD
Antiviral Therapy 11:
 Antiviral Therapy 11:529 535 Incidence of and risk factors for insulin resistance in treatment-naive HIV-infected patients 48 weeks after starting highly active antiretroviral therapy Rosario Palacios
Antiviral Therapy 11:529 535 Incidence of and risk factors for insulin resistance in treatment-naive HIV-infected patients 48 weeks after starting highly active antiretroviral therapy Rosario Palacios
Metabolic Abnormalities Associated with the Use of Protease Inhibitors and Non-nucleoside Reverse Transcriptase Inhibitors
 American Journal of Infectious Diseases 2 (3): 159-166, 2006 ISSN 1553-6203 2006 Science Publications Metabolic Abnormalities Associated with the Use of Protease Inhibitors and Non-nucleoside Reverse Transcriptase
American Journal of Infectious Diseases 2 (3): 159-166, 2006 ISSN 1553-6203 2006 Science Publications Metabolic Abnormalities Associated with the Use of Protease Inhibitors and Non-nucleoside Reverse Transcriptase
The oral meal or oral glucose tolerance test. Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol
 Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol Minimal Model Assessment of -Cell Responsivity and Insulin Sensitivity in Nondiabetic Individuals Chiara Dalla Man,
Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol Minimal Model Assessment of -Cell Responsivity and Insulin Sensitivity in Nondiabetic Individuals Chiara Dalla Man,
Associations among Body Mass Index, Insulin Resistance, and Pancreatic ß-Cell Function in Korean Patients with New- Onset Type 2 Diabetes
 ORIGINAL ARTICLE korean j intern med 2012;27:66-71 pissn 1226-3303 eissn 2005-6648 Associations among Body Mass Index, Insulin Resistance, and Pancreatic ß-Cell Function in Korean Patients with New- Onset
ORIGINAL ARTICLE korean j intern med 2012;27:66-71 pissn 1226-3303 eissn 2005-6648 Associations among Body Mass Index, Insulin Resistance, and Pancreatic ß-Cell Function in Korean Patients with New- Onset
Validation of a novel index to assess insulin resistance of adipose tissue lipolytic activity in. obese subjects
 Validation of a novel index to assess insulin resistance of adipose tissue lipolytic activity in obese subjects Elisa Fabbrini, MD, PhD; Faidon Magkos, PhD; Caterina Conte, MD; Bettina Mittendorfer, PhD;
Validation of a novel index to assess insulin resistance of adipose tissue lipolytic activity in obese subjects Elisa Fabbrini, MD, PhD; Faidon Magkos, PhD; Caterina Conte, MD; Bettina Mittendorfer, PhD;
TOXICITY, TOLERABILITY, AND ADHERENCE TO THERAPY
 SAFETY AND TOLERABILITY OF CURRENTLY AVAILABLE ANTIRETROVIRAL AGENTS * Esteban Martinez, MD, PhD ABSTRACT Safety and tolerability are important factors to consider when instituting or modifying therapy
SAFETY AND TOLERABILITY OF CURRENTLY AVAILABLE ANTIRETROVIRAL AGENTS * Esteban Martinez, MD, PhD ABSTRACT Safety and tolerability are important factors to consider when instituting or modifying therapy
The Lipid-Lowering Efficacy of Switching Within Non-Nucleoside Reverse Transcriptase Inhibitors in HIV-Infected Patients
 American Journal of Infectious Diseases 4 (2): 147-151, 2008 ISSN 1553-6203 2008 Science Publications The Lipid-Lowering Efficacy of Switching Within Non-Nucleoside Reverse Transcriptase Inhibitors in
American Journal of Infectious Diseases 4 (2): 147-151, 2008 ISSN 1553-6203 2008 Science Publications The Lipid-Lowering Efficacy of Switching Within Non-Nucleoside Reverse Transcriptase Inhibitors in
Metabolic Abnormalities and Cardiovascular Disease Risk Factors in Adults with Human Immunodeficiency Virus Infection and Lipodystrophy
 HIV/AIDS MAJOR ARTICLE Metabolic Abnormalities and Cardiovascular Disease Risk Factors in Adults with Human Immunodeficiency Virus Infection and Lipodystrophy Colleen Hadigan, 1,4 James B. Meigs, 3 Colleen
HIV/AIDS MAJOR ARTICLE Metabolic Abnormalities and Cardiovascular Disease Risk Factors in Adults with Human Immunodeficiency Virus Infection and Lipodystrophy Colleen Hadigan, 1,4 James B. Meigs, 3 Colleen
Adeterioration in -cell function is an independent
 Relationships Among Age, Proinsulin Conversion, and -Cell Function in Nondiabetic Humans Andreas Fritsche, Alexander Madaus, Norbert Stefan, Otto Tschritter, Elke Maerker, Anna Teigeler, Hans Häring, and
Relationships Among Age, Proinsulin Conversion, and -Cell Function in Nondiabetic Humans Andreas Fritsche, Alexander Madaus, Norbert Stefan, Otto Tschritter, Elke Maerker, Anna Teigeler, Hans Häring, and
ALIPODYSTROPHY SYNDROME
 PRELIMINARY COMMUNICATION in the Treatment of HIV Lipodystrophy Syndrome A Randomized Controlled Trial Colleen Hadigan, MD Colleen Corcoran, NP Nesli Basgoz, MD Benjamin Davis, MD Paul Sax, MD Steven Grinspoon,
PRELIMINARY COMMUNICATION in the Treatment of HIV Lipodystrophy Syndrome A Randomized Controlled Trial Colleen Hadigan, MD Colleen Corcoran, NP Nesli Basgoz, MD Benjamin Davis, MD Paul Sax, MD Steven Grinspoon,
Higher Risk of Hyperglycemia in HIV-Infected Patients Treated with Didanosine Plus Tenofovir
 6131_06_p333-337 4/5/06 10:28 AM Page 333 AIDS RESEARCH AND HUMAN RETROVIRUSES Volume 22, Number 4, 2006, pp. 333 337 Mary Ann Liebert, Inc. Higher Risk of Hyperglycemia in HIV-Infected Patients Treated
6131_06_p333-337 4/5/06 10:28 AM Page 333 AIDS RESEARCH AND HUMAN RETROVIRUSES Volume 22, Number 4, 2006, pp. 333 337 Mary Ann Liebert, Inc. Higher Risk of Hyperglycemia in HIV-Infected Patients Treated
Glucagon secretion in relation to insulin sensitivity in healthy subjects
 Diabetologia (2006) 49: 117 122 DOI 10.1007/s00125-005-0056-8 ARTICLE B. Ahrén Glucagon secretion in relation to insulin sensitivity in healthy subjects Received: 4 July 2005 / Accepted: 12 September 2005
Diabetologia (2006) 49: 117 122 DOI 10.1007/s00125-005-0056-8 ARTICLE B. Ahrén Glucagon secretion in relation to insulin sensitivity in healthy subjects Received: 4 July 2005 / Accepted: 12 September 2005
Decreased Non-Insulin Dependent Glucose Clearance Contributes to the Rise in FPG in the Non-Diabetic Range.
 Diabetes Care Publish Ahead of Print, published online November 13, 2007 Decreased Non-Insulin Dependent Glucose Clearance Contributes to the Rise in FPG in the Non-Diabetic Range. Rucha Jani, M.D., Marjorie
Diabetes Care Publish Ahead of Print, published online November 13, 2007 Decreased Non-Insulin Dependent Glucose Clearance Contributes to the Rise in FPG in the Non-Diabetic Range. Rucha Jani, M.D., Marjorie
Decreased Non Insulin-Dependent Glucose Clearance Contributes to the Rise in Fasting Plasma Glucose in the Nondiabetic Range
 Pathophysiology/Complications O R I G I N A L A R T I C L E Decreased Non Insulin-Dependent Glucose Clearance Contributes to the Rise in Fasting Plasma Glucose in the Nondiabetic Range RUCHA JANI, MD MARJORIE
Pathophysiology/Complications O R I G I N A L A R T I C L E Decreased Non Insulin-Dependent Glucose Clearance Contributes to the Rise in Fasting Plasma Glucose in the Nondiabetic Range RUCHA JANI, MD MARJORIE
Alterations in lipid kinetics in men with HIV-dyslipidemia
 Am J Physiol Endocrinol Metab 285: E490 E497, 2003. First published May 13, 2003; 10.1152/ajpendo.00118.2003. Alterations in lipid kinetics in men with HIV-dyslipidemia D. N. Reeds, B. Mittendorfer, B.
Am J Physiol Endocrinol Metab 285: E490 E497, 2003. First published May 13, 2003; 10.1152/ajpendo.00118.2003. Alterations in lipid kinetics in men with HIV-dyslipidemia D. N. Reeds, B. Mittendorfer, B.
Tesamorelin Clinical Data Overview Jean-Claude Mamputu, PhD Senior Medical Advisor, Theratechnologies
 Tesamorelin Clinical Data Overview Jean-Claude Mamputu, PhD Senior Medical Advisor, Theratechnologies Copyright 2016. All Rights Reserved. Property of Theratechnologies Inc. Mechanism of Action of Tesamorelin
Tesamorelin Clinical Data Overview Jean-Claude Mamputu, PhD Senior Medical Advisor, Theratechnologies Copyright 2016. All Rights Reserved. Property of Theratechnologies Inc. Mechanism of Action of Tesamorelin
Original article The effect of tenofovir disoproxil fumarate on whole-body insulin sensitivity, lipids and adipokines in healthy volunteers
 Antiviral Therapy 21 15:227 233 (doi: 1.3851/IMP1518) Original article The effect of tenofovir disoproxil fumarate on whole-body insulin sensitivity, lipids and adipokines in healthy volunteers Paul A
Antiviral Therapy 21 15:227 233 (doi: 1.3851/IMP1518) Original article The effect of tenofovir disoproxil fumarate on whole-body insulin sensitivity, lipids and adipokines in healthy volunteers Paul A
Adjusting Glucose-Stimulated Insulin Secretion for Adipose Insulin Resistance: An Index of b-cell Function in Obese Adults
 Diabetes Care 1 Adjusting Glucose-Stimulated Insulin Secretion for Adipose Insulin Resistance: An Index of b-cell Function in Obese Adults DOI: 10.2337/dc13-3011 Steven K. Malin, 1,2 Sangeeta R. Kashyap,
Diabetes Care 1 Adjusting Glucose-Stimulated Insulin Secretion for Adipose Insulin Resistance: An Index of b-cell Function in Obese Adults DOI: 10.2337/dc13-3011 Steven K. Malin, 1,2 Sangeeta R. Kashyap,
Antisense Mediated Lowering of Plasma Apolipoprotein C-III by Volanesorsen Improves Dyslipidemia and Insulin Sensitivity in Type 2 Diabetes
 Antisense Mediated Lowering of Plasma Apolipoprotein C-III by Volanesorsen Improves Dyslipidemia and Insulin Sensitivity in Type 2 Diabetes Digenio A, et al. Table of Contents Detailed Methods for Clinical
Antisense Mediated Lowering of Plasma Apolipoprotein C-III by Volanesorsen Improves Dyslipidemia and Insulin Sensitivity in Type 2 Diabetes Digenio A, et al. Table of Contents Detailed Methods for Clinical
Diabetes: Definition Pathophysiology Treatment Goals. By Scott Magee, MD, FACE
 Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
Molecular Mechanisms for Altered Glucose Homeostasis in HIV Infection
 American Journal of Infectious Diseases 2 (3): 187-192, 2006 ISSN 1553-6203 2006 Science Publications Molecular Mechanisms for Altered Glucose Homeostasis in HIV Infection Paul W Hruz Department of Pediatrics,
American Journal of Infectious Diseases 2 (3): 187-192, 2006 ISSN 1553-6203 2006 Science Publications Molecular Mechanisms for Altered Glucose Homeostasis in HIV Infection Paul W Hruz Department of Pediatrics,
HIV Infection as a Chronic Disease. Howard Libman, MD Beth Israel Deaconess Medical Center Harvard Medical School
 HIV Infection as a Chronic Disease Howard Libman, MD Beth Israel Deaconess Medical Center Harvard Medical School Role of Primary Care Approximately 50,000 patients are diagnosed with HIV infection annually
HIV Infection as a Chronic Disease Howard Libman, MD Beth Israel Deaconess Medical Center Harvard Medical School Role of Primary Care Approximately 50,000 patients are diagnosed with HIV infection annually
S K Mastan etal Der Pharmacia Lettre; 2009, 1 (1):
 Relative potency of protease inhibitors on glucose-insulin homeostasis, hemoglobin and glycosylated hemoglobin in normal rats SK Mastan 1, 2*, K Eswar Kumar 1 1 Pharmacology Division, University College
Relative potency of protease inhibitors on glucose-insulin homeostasis, hemoglobin and glycosylated hemoglobin in normal rats SK Mastan 1, 2*, K Eswar Kumar 1 1 Pharmacology Division, University College
Colleen Hadigan, 1 Shafali Jeste, 1 Ellen J. Anderson, 2 Rita Tsay, 3 Helen Cyr, 3 and Steven Grinspoon 1. Kenneth H. Mayer, Section Editor
 HIV/AIDS Kenneth H. Mayer, Section Editor MAJOR ARTICLE Modifiable Dietary Habits and Their Relation to Metabolic Abnormalities in Men and Women with Human Immunodeficiency Virus Infection and Fat Redistribution
HIV/AIDS Kenneth H. Mayer, Section Editor MAJOR ARTICLE Modifiable Dietary Habits and Their Relation to Metabolic Abnormalities in Men and Women with Human Immunodeficiency Virus Infection and Fat Redistribution
ARIC Manuscript Proposal # 985. PC Reviewed: 12/15/03 Status: A Priority: 2 SC Reviewed: 12/16/03 Status: A Priority: 2
 ARIC Manuscript Proposal # 985 PC Reviewed: 12/15/03 Status: A Priority: 2 SC Reviewed: 12/16/03 Status: A Priority: 2 1.a. Full Title: Association between family history of type 2 Diabetes Mellitus, the
ARIC Manuscript Proposal # 985 PC Reviewed: 12/15/03 Status: A Priority: 2 SC Reviewed: 12/16/03 Status: A Priority: 2 1.a. Full Title: Association between family history of type 2 Diabetes Mellitus, the
Supplemental Table 1. Clinical and epidemiological characteristics of the
 Tendeiro et al. Supplemental Digital Content 1_ Page 2 of 1 Supplemental Table 1. Clinical and epidemiological characteristics of the therapy naïve and treated infected individuals. a Number [male/female]
Tendeiro et al. Supplemental Digital Content 1_ Page 2 of 1 Supplemental Table 1. Clinical and epidemiological characteristics of the therapy naïve and treated infected individuals. a Number [male/female]
Metabolic Syndrome Update The Metabolic Syndrome: Overview. Global Cardiometabolic Risk
 Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
The dramatic immunologic and clinical benefits associated
 Postprandial Lipoprotein Changes in Patients Taking Antiretroviral Therapy for HIV Infection James H. Stein, Michelle A. Merwood, Jennifer B. Bellehumeur, Patrick E. McBride, Donald A. Wiebe, James M.
Postprandial Lipoprotein Changes in Patients Taking Antiretroviral Therapy for HIV Infection James H. Stein, Michelle A. Merwood, Jennifer B. Bellehumeur, Patrick E. McBride, Donald A. Wiebe, James M.
Perspectives Management of Dyslipidemia and Other Cardiovascular Risk Factors in HIV-Infected Patients: Case-based Review
 International AIDS Society USA Topics in HIV Medicine Perspectives Management of Dyslipidemia and Other Cardiovascular Risk Factors in HIV-Infected Patients: Case-based Review Many HIV-infected patients
International AIDS Society USA Topics in HIV Medicine Perspectives Management of Dyslipidemia and Other Cardiovascular Risk Factors in HIV-Infected Patients: Case-based Review Many HIV-infected patients
A Genetic Test to Screen for Abacavir Hypersensitivity Reactions
 The Future of Pharmacogenetics in HIV Clinical Care A Genetic Test to Screen for Abacavir Hypersensitivity Reactions Evan Collins & Misty Bath CANAC/ACIIS 15 th Annual Conference Vancouver, BC April 2007
The Future of Pharmacogenetics in HIV Clinical Care A Genetic Test to Screen for Abacavir Hypersensitivity Reactions Evan Collins & Misty Bath CANAC/ACIIS 15 th Annual Conference Vancouver, BC April 2007
Determining pancreatic -cell compensation for changing insulin sensitivity using an oral glucose tolerance test
 Am J Physiol Endocrinol Metab 307: E822 E829, 2014. First published September 2, 2014; doi:10.1152/ajpendo.00269.2014. Determining pancreatic -cell compensation for changing insulin sensitivity using an
Am J Physiol Endocrinol Metab 307: E822 E829, 2014. First published September 2, 2014; doi:10.1152/ajpendo.00269.2014. Determining pancreatic -cell compensation for changing insulin sensitivity using an
JAIDS Journal of Acquired Immune Deficiency Syndromes 31: Lippincott Williams & Wilkins, Inc., Philadelphia. Rapid Communications
 JAIDS Journal of Acquired Immune Deficiency Syndromes 31:257 275 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Rapid Communications Management of Metabolic Complications Associated With Antiretroviral
JAIDS Journal of Acquired Immune Deficiency Syndromes 31:257 275 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Rapid Communications Management of Metabolic Complications Associated With Antiretroviral
Cardiovascular Disease Risk Factors Among HIV Patients
 ISSN: 23776196 The American Journal of SCIENCE AND MEDICAL RESEARCH, 1(1), 92100 Research Article Cardiovascular Disease Risk Factors Among HIV Patients Open Access P. Sanjeev Reddy Government Junior College,
ISSN: 23776196 The American Journal of SCIENCE AND MEDICAL RESEARCH, 1(1), 92100 Research Article Cardiovascular Disease Risk Factors Among HIV Patients Open Access P. Sanjeev Reddy Government Junior College,
Body-composition measurements as predictors of glucose and insulin abnormalities in HIV-positive men 1 3
 Body-composition measurements as predictors of glucose and insulin abnormalities in HIV-positive men 1 3 Gary Meininger, Colleen Hadigan, Petra Rietschel, and Steven Grinspoon ABSTRACT Background: Fat
Body-composition measurements as predictors of glucose and insulin abnormalities in HIV-positive men 1 3 Gary Meininger, Colleen Hadigan, Petra Rietschel, and Steven Grinspoon ABSTRACT Background: Fat
Diabetes Care 24:89 94, 2000
 Pathophysiology/Complications O R I G I N A L A R T I C L E Insulin Resistance and Insulin Secretory Dysfunction Are Independent Predictors of Worsening of Glucose Tolerance During Each Stage of Type 2
Pathophysiology/Complications O R I G I N A L A R T I C L E Insulin Resistance and Insulin Secretory Dysfunction Are Independent Predictors of Worsening of Glucose Tolerance During Each Stage of Type 2
Skeletal muscle metabolism was studied by measuring arterio-venous concentration differences
 Supplemental Data Dual stable-isotope experiment Skeletal muscle metabolism was studied by measuring arterio-venous concentration differences across the forearm, adjusted for forearm blood flow (FBF) (1).
Supplemental Data Dual stable-isotope experiment Skeletal muscle metabolism was studied by measuring arterio-venous concentration differences across the forearm, adjusted for forearm blood flow (FBF) (1).
IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA
 UNIGASTRO Il fegato come centrale metabolica e i fattori di danno oltre ai virus epatitici IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA Dr Elisabetta Bugianesi Divisione di Gastro-Epatologia
UNIGASTRO Il fegato come centrale metabolica e i fattori di danno oltre ai virus epatitici IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA Dr Elisabetta Bugianesi Divisione di Gastro-Epatologia
Alternative insulin delivery systems: how demanding should the patient be?
 Diabetologia (1997) 4: S97 S11 Springer-Verlag 1997 Alternative insulin delivery systems: how demanding should the patient be? K.S. Polonsky, M. M. Byrne, J. Sturis Department of Medicine, The University
Diabetologia (1997) 4: S97 S11 Springer-Verlag 1997 Alternative insulin delivery systems: how demanding should the patient be? K.S. Polonsky, M. M. Byrne, J. Sturis Department of Medicine, The University
Diabetes mellitus. Treatment
 Diabetes mellitus Treatment Recommended glycemic targets for the clinical management of diabetes(ada) Fasting glycemia: 80-110 mg/dl Postprandial : 100-145 mg/dl HbA1c: < 6,5 % Total cholesterol: < 200
Diabetes mellitus Treatment Recommended glycemic targets for the clinical management of diabetes(ada) Fasting glycemia: 80-110 mg/dl Postprandial : 100-145 mg/dl HbA1c: < 6,5 % Total cholesterol: < 200
Liver Toxicity in Epidemiological Cohorts
 SUPPLEMENT ARTICLE Liver Toxicity in Epidemiological Cohorts Stephen Becker Pacific Horizon Medical Group, San Francisco, California Hepatotoxicity has been demonstrated to be associated with antiretroviral
SUPPLEMENT ARTICLE Liver Toxicity in Epidemiological Cohorts Stephen Becker Pacific Horizon Medical Group, San Francisco, California Hepatotoxicity has been demonstrated to be associated with antiretroviral
Importance of Obtaining Independent Measures of Insulin Secretion and Insulin Sensitivity During the Same Test
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Importance of Obtaining Independent Measures of Insulin Secretion and Insulin Sensitivity During the Same Test Results with
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Importance of Obtaining Independent Measures of Insulin Secretion and Insulin Sensitivity During the Same Test Results with
Adverse metabolic consequences of HIV protease inhibitor therapy: the search for a central mechanism
 Am J Physiol Endocrinol Metab 280: E549 E553, 2001. invited review Adverse metabolic consequences of HIV protease inhibitor therapy: the search for a central mechanism PAUL W. HRUZ, 1,2 HARUHIKO MURATA,
Am J Physiol Endocrinol Metab 280: E549 E553, 2001. invited review Adverse metabolic consequences of HIV protease inhibitor therapy: the search for a central mechanism PAUL W. HRUZ, 1,2 HARUHIKO MURATA,
Insulin resistance might play an important
 Pathophysiology/Complications O R I G I N A L A R T I C L E Quantitative Insulin Sensitivity Check Index and the Reciprocal Index of Homeostasis Model Assessment in Normal Range Weight and Moderately Obese
Pathophysiology/Complications O R I G I N A L A R T I C L E Quantitative Insulin Sensitivity Check Index and the Reciprocal Index of Homeostasis Model Assessment in Normal Range Weight and Moderately Obese
Ischemic Cardiovascular Disease in Persons with Human Immunodeficiency Virus Infection
 HIV/AIDS MAJOR ARTICLE Ischemic Cardiovascular Disease in Persons with Human Immunodeficiency Virus Infection Max H. David, 1,3 Richard Hornung, 2 and Carl J. Fichtenbaum 1 1 Department of Medicine, Division
HIV/AIDS MAJOR ARTICLE Ischemic Cardiovascular Disease in Persons with Human Immunodeficiency Virus Infection Max H. David, 1,3 Richard Hornung, 2 and Carl J. Fichtenbaum 1 1 Department of Medicine, Division
Fig. S1. REGN1500 reduces plasma levels of cholesterol, TG and NEFA in WT and Ldlr -/- mice. (A) WT
 Figure Legends for Supplementary Figures. Fig. S1. REGN15 reduces plasma levels of cholesterol, TG and NEF in WT and Ldlr -/- mice. () WT and Ldlr -/- mice were injected with control IgG or REGN15 (1 mg/kg)
Figure Legends for Supplementary Figures. Fig. S1. REGN15 reduces plasma levels of cholesterol, TG and NEF in WT and Ldlr -/- mice. () WT and Ldlr -/- mice were injected with control IgG or REGN15 (1 mg/kg)
Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption),
 Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption), in which blood glucose predominantly originates from
Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption), in which blood glucose predominantly originates from
ΛΟΙΜΩΞΗ HIV. Ιγνάτιος Οικονομίδης,MD,FESC Β Πανεπιστημιακή Καρδιολογική
 ΛΟΙΜΩΞΗ HIV Ιγνάτιος Οικονομίδης,MD,FESC Β Πανεπιστημιακή Καρδιολογική Κλινική, Νοσοκομείο «Αττικόν» Infection Acute Myocardial Infarction p er 100,000 HIV/AIDS discharg es 800 700 600 500 400 300 200
ΛΟΙΜΩΞΗ HIV Ιγνάτιος Οικονομίδης,MD,FESC Β Πανεπιστημιακή Καρδιολογική Κλινική, Νοσοκομείο «Αττικόν» Infection Acute Myocardial Infarction p er 100,000 HIV/AIDS discharg es 800 700 600 500 400 300 200
The effects of protease inhibitors on basal and. lipid metabolism, insulin binding and signaling.
 The effects of protease inhibitors on basal and insulin-stimulated lipid metabolism, insulin binding, and signaling Catarina Cammalleri*, and Ralph J. Germinario 1, *,,, ** Lady Davis Institute,* SMBD-Jewish
The effects of protease inhibitors on basal and insulin-stimulated lipid metabolism, insulin binding, and signaling Catarina Cammalleri*, and Ralph J. Germinario 1, *,,, ** Lady Davis Institute,* SMBD-Jewish
To put lipid-related complications seen in
 MANAGING REGIMEN DIFFICULTIES: MEETING THE CHALLENGES OF SAFETY AND TOLERABILITY * Simon A. Mallal, MBBS, FRACP, FRCPA ABSTRACT HIV-infected patients who are naive to antiretroviral therapy usually demonstrate
MANAGING REGIMEN DIFFICULTIES: MEETING THE CHALLENGES OF SAFETY AND TOLERABILITY * Simon A. Mallal, MBBS, FRACP, FRCPA ABSTRACT HIV-infected patients who are naive to antiretroviral therapy usually demonstrate
Inflammation & Type 2 Diabetes Prof. Marc Y. Donath
 Inflammation & Type 2 Diabetes 1, MD Chief Endocrinology, Diabetes & Metabolism University Hospital Basel Petersgraben 4 CH-431 Basel, Switzerland MDonath@uhbs.ch Innate immunity as a sensor of metabolic
Inflammation & Type 2 Diabetes 1, MD Chief Endocrinology, Diabetes & Metabolism University Hospital Basel Petersgraben 4 CH-431 Basel, Switzerland MDonath@uhbs.ch Innate immunity as a sensor of metabolic
Review Article The Effects of Thiazolidinediones on Metabolic Complications and Lipodystrophy in HIV-Infected Patients
 Hindawi Publishing Corporation PPAR Research Volume 2009, Article ID 373524, 15 pages doi:10.1155/2009/373524 Review Article The Effects of Thiazolidinediones on Metabolic Complications and Lipodystrophy
Hindawi Publishing Corporation PPAR Research Volume 2009, Article ID 373524, 15 pages doi:10.1155/2009/373524 Review Article The Effects of Thiazolidinediones on Metabolic Complications and Lipodystrophy
Diabetes Care 35: , 2012
 Pathophysiology/Complications O R I G I N A L A R T I C L E Multiorgan Insulin Sensitivity in Lean and Obese Subjects CATERINA CONTE, MD 1,2 ELISA FABBRINI, MD, PHD 1,3 MARLEEN KARS, MD, PHD 1,4 1 BETTINA
Pathophysiology/Complications O R I G I N A L A R T I C L E Multiorgan Insulin Sensitivity in Lean and Obese Subjects CATERINA CONTE, MD 1,2 ELISA FABBRINI, MD, PHD 1,3 MARLEEN KARS, MD, PHD 1,4 1 BETTINA
Importance of quantifying insulin secretion in relation to insulin sensitivity to accurately assess beta cell function in clinical studies
 European Journal of Endocrinology (2004) 150 97 104 ISSN 0804-4643 REVIEW Importance of quantifying insulin secretion in relation to insulin sensitivity to accurately assess beta cell function in clinical
European Journal of Endocrinology (2004) 150 97 104 ISSN 0804-4643 REVIEW Importance of quantifying insulin secretion in relation to insulin sensitivity to accurately assess beta cell function in clinical
FreeStyle Mini Blood Glucose Results Are Accurate and Suitable for Use in Glycemic Clamp Protocols
 Journal of Diabetes Science and Technology Volume 2, Issue 5, September 2008 Diabetes Technology Society CLINICAL APPLICATIONS FreeStyle Mini Blood Glucose Results Are Accurate and Suitable for Use in
Journal of Diabetes Science and Technology Volume 2, Issue 5, September 2008 Diabetes Technology Society CLINICAL APPLICATIONS FreeStyle Mini Blood Glucose Results Are Accurate and Suitable for Use in
Effects of growth hormone secretagogue receptor agonist and antagonist in nonobese type 2 diabetic MKR mice
 Effects of growth hormone secretagogue receptor agonist and antagonist in nonobese type 2 diabetic MKR mice Rasha Mosa (MBCHC, M.D, PhD candidate) School of Biomedical Sciences University of Queensland
Effects of growth hormone secretagogue receptor agonist and antagonist in nonobese type 2 diabetic MKR mice Rasha Mosa (MBCHC, M.D, PhD candidate) School of Biomedical Sciences University of Queensland
Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus
 Emerging Science Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus George Wolf Insulin resistance is defined as the reduced responsiveness to normal circulating
Emerging Science Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus George Wolf Insulin resistance is defined as the reduced responsiveness to normal circulating
Glucose-dependent arginine stimulation test for characterization of islet function: studies on reproducibility and priming effect of arginine
 Diabetologia (1998) 41: 772±777 Ó Springer-Verlag 1998 Glucose-dependent arginine stimulation test for characterization of islet function: studies on reproducibility and priming effect of arginine H. Larsson,
Diabetologia (1998) 41: 772±777 Ó Springer-Verlag 1998 Glucose-dependent arginine stimulation test for characterization of islet function: studies on reproducibility and priming effect of arginine H. Larsson,
The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans
 The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Seoul National University College of Medicine Plasma glucose
The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Seoul National University College of Medicine Plasma glucose
SYNOPSIS OF RESEARCH REPORT (PROTOCOL BC20779)
 TITLE OF THE STUDY / REPORT No. / DATE OF REPORT INVESTIGATORS / CENTERS AND COUNTRIES Clinical Study Report Protocol BC20779: Multicenter, double-blind, randomized, placebo-controlled, dose ranging phase
TITLE OF THE STUDY / REPORT No. / DATE OF REPORT INVESTIGATORS / CENTERS AND COUNTRIES Clinical Study Report Protocol BC20779: Multicenter, double-blind, randomized, placebo-controlled, dose ranging phase
IGFs are regulators of processes like growth and. Genetic Factors and Insulin Secretion Gene Variants in the IGF Genes
 Genetic Factors and Insulin Secretion Gene Variants in the IGF Genes Leen M. t Hart, 1 Andreas Fritsche, 2 Ingrid Rietveld, 3 Jacqueline M. Dekker, 4 Giel Nijpels, 4 Fausto Machicao, 2 Michael Stumvoll,
Genetic Factors and Insulin Secretion Gene Variants in the IGF Genes Leen M. t Hart, 1 Andreas Fritsche, 2 Ingrid Rietveld, 3 Jacqueline M. Dekker, 4 Giel Nijpels, 4 Fausto Machicao, 2 Michael Stumvoll,
NAFLD AND TYPE 2 DIABETES
 NAFLD AND TYPE 2 DIABETES Sonia Caprio, MD STOPNASH Symposium on the Origin and Pathways of Nonalcoholic Steatohepatitis Washington 7, 215 Global Projection of Diabetes Hossain P et al. N Engl J Med 27;356:213
NAFLD AND TYPE 2 DIABETES Sonia Caprio, MD STOPNASH Symposium on the Origin and Pathways of Nonalcoholic Steatohepatitis Washington 7, 215 Global Projection of Diabetes Hossain P et al. N Engl J Med 27;356:213
THE metabolic abnormalities of non-insulin-dependent
 55 THE NEW ENGLAND JOURNAL OF MEDICINE Aug. 31, 1995 METABOLIC EFFECTS OF METFORMIN IN NON-INSULIN-DEPENDENT DIABETES MELLITUS MICHAEL STUMVOLL, M.D., NURJAHAN NURJHAN, PH.D., GABRIELE PERRIELLO, M.D.,
55 THE NEW ENGLAND JOURNAL OF MEDICINE Aug. 31, 1995 METABOLIC EFFECTS OF METFORMIN IN NON-INSULIN-DEPENDENT DIABETES MELLITUS MICHAEL STUMVOLL, M.D., NURJAHAN NURJHAN, PH.D., GABRIELE PERRIELLO, M.D.,
Metabolic defects underlying dyslipidemia in abdominal obesity
 Metabolic defects underlying dyslipidemia in abdominal obesity Professor Marja-Riitta Taskinen Department of Medicine, Division of Cardiology Helsinki University Hospital, Finland Disclosures: Honorariums/
Metabolic defects underlying dyslipidemia in abdominal obesity Professor Marja-Riitta Taskinen Department of Medicine, Division of Cardiology Helsinki University Hospital, Finland Disclosures: Honorariums/
Insulin resistance by homeostasis model assessment in HIV-infected patients on highly active antiretroviral therapy: cross-sectional study
 Guillen et al. Diabetology & Metabolic Syndrome (2015) 7:49 DOI 10.1186/s13098-015-0046-z DIABETOLOGY & METABOLIC SYNDROME RESEARCH Open Access Insulin resistance by homeostasis model assessment in HIV-infected
Guillen et al. Diabetology & Metabolic Syndrome (2015) 7:49 DOI 10.1186/s13098-015-0046-z DIABETOLOGY & METABOLIC SYNDROME RESEARCH Open Access Insulin resistance by homeostasis model assessment in HIV-infected
Diabetes 2013: Achieving Goals Through Comprehensive Treatment. Session 2: Individualizing Therapy
 Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Adiponectin, TG/HDL-cholesterol index and hs-crp. Predictors of insulin resistance.
 ORIGINAL ARTICLE Adiponectin, TG/HDL-cholesterol index and hs-crp. Predictors of insulin resistance. Bonneau GA y Pedrozo WR 1 Ministry of Public Health, Province of Misiones, 2 School of Exact, Chemical
ORIGINAL ARTICLE Adiponectin, TG/HDL-cholesterol index and hs-crp. Predictors of insulin resistance. Bonneau GA y Pedrozo WR 1 Ministry of Public Health, Province of Misiones, 2 School of Exact, Chemical
Research Article Metabolic Disorders in HIV-Infected Adolescents Receiving Protease Inhibitors
 Hindawi BioMed Research International Volume 2017, Article ID 7481597, 14 pages https://doi.org/10.1155/2017/7481597 Research Article Metabolic Disorders in HIV-Infected Adolescents Receiving Protease
Hindawi BioMed Research International Volume 2017, Article ID 7481597, 14 pages https://doi.org/10.1155/2017/7481597 Research Article Metabolic Disorders in HIV-Infected Adolescents Receiving Protease
NOTICE TO PHYSICIANS. Division of AIDS (DAIDS), National Institute of Allergy and Infectious Diseases, National Institutes of Health
 NOTICE TO PHYSICIANS DATE: March 10, 2003 TO: FROM: SUBJECT: HIV/AIDS Health Care Providers Division of AIDS (DAIDS), National Institute of Allergy and Infectious Diseases, National Institutes of Health
NOTICE TO PHYSICIANS DATE: March 10, 2003 TO: FROM: SUBJECT: HIV/AIDS Health Care Providers Division of AIDS (DAIDS), National Institute of Allergy and Infectious Diseases, National Institutes of Health
Supplementary information
 Supplementary information Dose-response Curve Slope Sets Class-Specific Limits on Inhibitory Potential of Anti-HIV Drugs Lin Shen 1,2, Susan Peterson 1, Ahmad R. Sedaghat 1, Moira A. McMahon 1,2, Marc
Supplementary information Dose-response Curve Slope Sets Class-Specific Limits on Inhibitory Potential of Anti-HIV Drugs Lin Shen 1,2, Susan Peterson 1, Ahmad R. Sedaghat 1, Moira A. McMahon 1,2, Marc
GS-8374, a Novel HIV Protease Inhibitor, Does Not Alter Glucose Homeostasis in Cultured Adipocytes or in a Healthy-Rodent Model System
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 2011, p. 1377 1382 Vol. 55, No. 4 0066-4804/11/$12.00 doi:10.1128/aac.01184-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. GS-8374,
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 2011, p. 1377 1382 Vol. 55, No. 4 0066-4804/11/$12.00 doi:10.1128/aac.01184-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. GS-8374,
Diabetes Care 32: , 2009
 Pathophysiology/Complications O R I G I N A L A R T I C L E Primary Defects in -Cell Function Further Exacerbated by Worsening of Insulin Resistance Mark the Development of Impaired Glucose Tolerance in
Pathophysiology/Complications O R I G I N A L A R T I C L E Primary Defects in -Cell Function Further Exacerbated by Worsening of Insulin Resistance Mark the Development of Impaired Glucose Tolerance in
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
A Pilot Study of Exercise Training to Reduce Trunk Fat in Adults With HIV Associated Fat Redistribution
 A Pilot Study of Exercise Training to Reduce Trunk Fat in Adults With HIV Associated Fat Redistribution Ronenn Roubenoff, Lauren Weiss, Ann McDermott, Tanya Heflin, Gregory J. Cloutier, Michael Wood and
A Pilot Study of Exercise Training to Reduce Trunk Fat in Adults With HIV Associated Fat Redistribution Ronenn Roubenoff, Lauren Weiss, Ann McDermott, Tanya Heflin, Gregory J. Cloutier, Michael Wood and
Multiple Factors Should Be Considered When Setting a Glycemic Goal
 Multiple Facts Should Be Considered When Setting a Glycemic Goal Patient attitude and expected treatment effts Risks potentially associated with hypoglycemia, other adverse events Disease duration Me stringent
Multiple Facts Should Be Considered When Setting a Glycemic Goal Patient attitude and expected treatment effts Risks potentially associated with hypoglycemia, other adverse events Disease duration Me stringent
Insulin secretion, insulin sensitivity, and hepatic insulin extraction in first-degree relatives of type 2 diabetic patients
 Brazilian Journal of Medical and Biological Research (2003) 36: 301-308 First-degree relatives of type 2 diabetic patients ISSN 0100-879X 301 Insulin secretion, insulin sensitivity, and hepatic insulin
Brazilian Journal of Medical and Biological Research (2003) 36: 301-308 First-degree relatives of type 2 diabetic patients ISSN 0100-879X 301 Insulin secretion, insulin sensitivity, and hepatic insulin
18. PANCREATIC FUNCTION AND METABOLISM. Pancreatic secretions ISLETS OF LANGERHANS. Insulin
 18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
la prise en charge du diabète de
 N21 XIII Congrès National de Diabétologie, 29 mai 2011, Alger Intérêt et place des Anti DPP4 dans la prise en charge du diabète de type 2 Nicolas PAQUOT, MD, PhD CHU Sart-Tilman, Université de Liège Belgique
N21 XIII Congrès National de Diabétologie, 29 mai 2011, Alger Intérêt et place des Anti DPP4 dans la prise en charge du diabète de type 2 Nicolas PAQUOT, MD, PhD CHU Sart-Tilman, Université de Liège Belgique
Introduction ORIGINAL RESEARCH. Bilal A. Omar 1, Giovanni Pacini 2 & Bo Ahren 1. Abstract
 ORIGINAL RESEARCH Physiological Reports ISSN 2051-817X Impact of glucose dosing regimens on modeling of glucose tolerance and b-cell function by intravenous glucose tolerance test in diet-induced obese
ORIGINAL RESEARCH Physiological Reports ISSN 2051-817X Impact of glucose dosing regimens on modeling of glucose tolerance and b-cell function by intravenous glucose tolerance test in diet-induced obese
METABOLISM CATABOLIC Carbohydrates Lipids Proteins
 Index: - Overview: Catabolism and Anabolism. Few concepts:, NADPH. - Overview: Metabolism glucose, fatty acids and amino acids. - Table summary: Principal anabolic and catabolic pathways, and their main
Index: - Overview: Catabolism and Anabolism. Few concepts:, NADPH. - Overview: Metabolism glucose, fatty acids and amino acids. - Table summary: Principal anabolic and catabolic pathways, and their main
Treatment of respiratory virus infection Influenza A & B Respiratory Syncytial Virus (RSV)
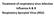 Treatment of respiratory virus infection Influenza A & B Respiratory Syncytial Virus (RSV) Amantadine and Rimantadine Use is limited to Influenza A infection. Very effective in preventing infection if
Treatment of respiratory virus infection Influenza A & B Respiratory Syncytial Virus (RSV) Amantadine and Rimantadine Use is limited to Influenza A infection. Very effective in preventing infection if
Metabolic Syndrome. DOPE amines COGS 163
 Metabolic Syndrome DOPE amines COGS 163 Overview - M etabolic Syndrome - General definition and criteria - Importance of diagnosis - Glucose Homeostasis - Type 2 Diabetes Mellitus - Insulin Resistance
Metabolic Syndrome DOPE amines COGS 163 Overview - M etabolic Syndrome - General definition and criteria - Importance of diagnosis - Glucose Homeostasis - Type 2 Diabetes Mellitus - Insulin Resistance
Muscle and Liver Insulin Resistance Indexes Derived From the Oral Glucose Tolerance Test
 Pathophysiology/Complications O R I G I N A L A R T I C L E Muscle and Liver Insulin Resistance Indexes Derived From the Oral Glucose Tolerance Test MUHAMMAD A. ABDUL-GHANI, MD, PHD MASAFUMI MATSUDA, MD
Pathophysiology/Complications O R I G I N A L A R T I C L E Muscle and Liver Insulin Resistance Indexes Derived From the Oral Glucose Tolerance Test MUHAMMAD A. ABDUL-GHANI, MD, PHD MASAFUMI MATSUDA, MD
Pathogenesis of Diabetes Mellitus
 Pathogenesis of Diabetes Mellitus Young-Bum Kim, Ph.D. Associate Professor of Medicine Harvard Medical School Definition of Diabetes Mellitus a group of metabolic diseases characterized by hyperglycemia
Pathogenesis of Diabetes Mellitus Young-Bum Kim, Ph.D. Associate Professor of Medicine Harvard Medical School Definition of Diabetes Mellitus a group of metabolic diseases characterized by hyperglycemia
0.14 ( 0.053%) UNAIDS 10% (94) ( ) (73-94/6 ) 8,920
 0.14 UNAIDS 0.053% 2 250 60 10% 94 73 20 73-94/6 8,920 12 43 Public Health Service Task Force Recommendations 5-10% for Use of Antiretroviral Drugs in 10-20% Pregnant HIV-1-Infected Women for Maternal
0.14 UNAIDS 0.053% 2 250 60 10% 94 73 20 73-94/6 8,920 12 43 Public Health Service Task Force Recommendations 5-10% for Use of Antiretroviral Drugs in 10-20% Pregnant HIV-1-Infected Women for Maternal
Hormonal and Metabolic Disorders of Human Immunodeficiency Virus Infection and Substance Abuse
 American Journal of Infectious Diseases 2 (3): 125-129, 2006 ISSN 1553-6203 2006 Science Publications Hormonal and Metabolic Disorders of Human Immunodeficiency Virus Infection and Substance Abuse Jag
American Journal of Infectious Diseases 2 (3): 125-129, 2006 ISSN 1553-6203 2006 Science Publications Hormonal and Metabolic Disorders of Human Immunodeficiency Virus Infection and Substance Abuse Jag
IN THE EARLY 1980s, it was demonstrated that insulin
 0013-7227/03/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 88(3):1264 1270 Printed in U.S.A. Copyright 2003 by The Endocrine Society doi: 10.1210/jc.2002-021547 Increased Insulin Sensitivity
0013-7227/03/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 88(3):1264 1270 Printed in U.S.A. Copyright 2003 by The Endocrine Society doi: 10.1210/jc.2002-021547 Increased Insulin Sensitivity
Didactic Series. Lipohypertrophy in HIV
 Didactic Series Lipohypertrophy in HIV Daniel Lee, MD Clinical Professor of Medicine UCSD Medical Center Owen Clinic August 14th, 2014 ACCREDITATION STATEMENT: University of California, San Diego School
Didactic Series Lipohypertrophy in HIV Daniel Lee, MD Clinical Professor of Medicine UCSD Medical Center Owen Clinic August 14th, 2014 ACCREDITATION STATEMENT: University of California, San Diego School
Comorbidities: a moving area. Paul De Munter ARC Leuven BREACH
 Comorbidities: a moving area Paul De Munter ARC Leuven BREACH 27-11-2015 Contents Introduction Comorbidities Cardiovascular disease and lipids Diabetes mellitus Hepatitis C Frailty Conclusion Introduction
Comorbidities: a moving area Paul De Munter ARC Leuven BREACH 27-11-2015 Contents Introduction Comorbidities Cardiovascular disease and lipids Diabetes mellitus Hepatitis C Frailty Conclusion Introduction
Lipids Carbohydrate Protein. Fatty Acids Glycerol. Mono/di-saccarides. Aminoacids. Fat Liver Muscle. Triglycerides Glycogen Protein
 Lipids Carbohydrate Protein Fatty Acids Glycerol Mono/di-saccarides Fat Liver Muscle Aminoacids Triglycerides Glycogen Protein Microvascular Macrovascular Diabetes-specific Diabetes-enhanced HbA1c 5.7(6.0)
Lipids Carbohydrate Protein Fatty Acids Glycerol Mono/di-saccarides Fat Liver Muscle Aminoacids Triglycerides Glycogen Protein Microvascular Macrovascular Diabetes-specific Diabetes-enhanced HbA1c 5.7(6.0)
Terapia antirretroviral inicial y de rescate: Utilidad actual y futura de nuevos medicamentos
 Terapia antirretroviral inicial y de rescate: Utilidad actual y futura de nuevos medicamentos (Antiretroviral Therapy Present and Future Prospects of Antiretroviral Drugs in Initial and Salvage Therapy)
Terapia antirretroviral inicial y de rescate: Utilidad actual y futura de nuevos medicamentos (Antiretroviral Therapy Present and Future Prospects of Antiretroviral Drugs in Initial and Salvage Therapy)
Effect of Cobalt Chloride on Blood Glucose, Plasma Insulin and Lipids in Rabbits.
 Effect of Cobalt Chloride on Blood Glucose, Plasma Insulin and Lipids in Rabbits. Masayoshi Ohmichi, Hiroyuki Morita, Yoko Onuma and Shigeo Koike Department of Hygiene, School of Medicine, Showa University,
Effect of Cobalt Chloride on Blood Glucose, Plasma Insulin and Lipids in Rabbits. Masayoshi Ohmichi, Hiroyuki Morita, Yoko Onuma and Shigeo Koike Department of Hygiene, School of Medicine, Showa University,
Cardiovascular Risk and Body-Fat Abnormalities in HIV-Infected Adults
 The new england journal of medicine review article From the Program in Nutritional Metabolism and the Neuroendocrine Unit, Massachusetts General Hospital and Harvard Medical School, Boston (S.G.); and
The new england journal of medicine review article From the Program in Nutritional Metabolism and the Neuroendocrine Unit, Massachusetts General Hospital and Harvard Medical School, Boston (S.G.); and
Antiretroviral treatment outcomes after the introduction of tenofovir in the public-sector in South Africa
 Antiretroviral treatment outcomes after the introduction of tenofovir in the public-sector in South Africa Alana T Brennan, Kate Shearer, Mhairi Maskew, Prudence Ive, Ian Sanne, Matthew P Fox Health Economics
Antiretroviral treatment outcomes after the introduction of tenofovir in the public-sector in South Africa Alana T Brennan, Kate Shearer, Mhairi Maskew, Prudence Ive, Ian Sanne, Matthew P Fox Health Economics
Continuing Education for Pharmacy Technicians
 Continuing Education for Pharmacy Technicians HIV/AIDS TREATMENT Michael Denaburg, Pharm.D. Birmingham, AL Objectives: 1. Identify drugs and drug classes currently used in the management of HIV infected
Continuing Education for Pharmacy Technicians HIV/AIDS TREATMENT Michael Denaburg, Pharm.D. Birmingham, AL Objectives: 1. Identify drugs and drug classes currently used in the management of HIV infected
Induction of Long-term Glycemic Control in Newly Diagnosed Type 2 Diabetic Patients Is Associated With Improvement of -Cell Function
 Clinical Care/Education/Nutrition O R I G I N A L A R T I C L E Induction of Long-term Glycemic Control in Newly Diagnosed Type 2 Diabetic Patients Is Associated With Improvement of -Cell Function YANBING
Clinical Care/Education/Nutrition O R I G I N A L A R T I C L E Induction of Long-term Glycemic Control in Newly Diagnosed Type 2 Diabetic Patients Is Associated With Improvement of -Cell Function YANBING
