GLAUCOMA FOLLOWING CATARACT SURGERY IN CHILDREN: SURGICALLY MODIFIABLE RISK FACTORS
|
|
|
- Bertram Poole
- 6 years ago
- Views:
Transcription
1 GLAUCOMA FOLLOWING CATARACT SURGERY IN CHILDREN: SURGICALLY MODIFIABLE RISK FACTORS BY Mary Gilbert Lawrence MD MPH,* Natalia Y. Kramarevsky MD, Stephen P. Christiansen MD, Martha M. Wright MD, Terri L. Young MD, AND C. Gail Summers MD ABSTRACT Purpose: To determine the incidence of glaucoma following cataract surgery in children and to identify surgically modifiable risk factors that may influence the development of glaucoma in these eyes. Methods: All lensectomies performed in patients 18 years old or younger over a 7-year period (1995 through 2001) were identified by conducting a database search. A retrospective chart review was performed for every patient identified. Data extraction included patient s age at surgery, intraocular lens implantation at cataract extraction, date of glaucoma onset, and length of followup. Statistical methods included risk ratio calculations and Kaplan-Meier analyses for the time to glaucoma for eyes undergoing lensectomy. Results: We identified 116 eyes of 79 children in whom lensectomy was performed. The median age at cataract surgery was 178 days (~6 months). Mean follow-up time was 2.7 years. The overall incidence of glaucoma was 11%. Kaplan-Meier analysis demonstrated that eyes operated on at less than 30 days of age were statistically more likely to develop glaucoma than eyes operated on at age 30 days or older (P <.001). For those operated on at less than 30 days of age, the risk ratio was 11.8 for subsequent glaucoma development compared with those operated on at 30 days of age or older. Forty-nine eyes (42%) had primary intraocular lens implantation, and none of these developed glaucoma (P =.001). Conclusions: Timing of surgery at less than 30 days of age and lack of implantation of an intraocular lens at lensectomy were both associated with an increased risk of subsequent glaucoma. Knowledge of modifiable risk factors is essential to allow ophthalmic surgeons to make cogent decisions regarding the care of children with cataracts. Trans Am Ophthalmol Soc 2005;103:46-55 INTRODUCTION Early detection and surgical treatment of pediatric cataracts have greatly improved the visual prognosis in children with this congenital and/or developmental condition over the past several decades. 1 Despite these advances, the development of subsequent glaucoma remains one of the most frequent serious complications following lensectomy in children, with reported incidence rates varying between 0 and 32% of eyes Aphakic glaucoma in infants and children may present early in the postoperative course after lensectomy, or it may present years later. This condition can be difficult to manage, and parents should be counseled about the risk of developing this complication and its consequences. Reported risk factors for the development of pediatric aphakic glaucoma include ocular morphologic findings such as microphthalmia, persistent hyperplastic primary vitreous, small corneal diameter, and type of cataract. 9,17 Other risk factors, relating to the surgical procedure itself, have also been reported and include the timing of surgery (patient s age at surgery) 7,8,11,14 and lack of implantation of an intraocular lens Whereas the occurrence of glaucoma following cataract extraction has long been recognized, 22 the study of factors that are modifiable by the ophthalmic surgeon deserves further evaluation. Knowledge of best practices has the potential to result in improved visual outcomes for these children. We undertook this study to determine the overall incidence of glaucoma following cataract surgery in a cohort of children, and to identify and quantify surgeon-modifiable risk factors that might influence the development of glaucoma in these eyes. METHODS SUBJECTS Approval of the Fairview University Medical Center Institutional Review Board was obtained before initiation of the study. All cataract extractions performed in patients 18 years old or younger over a 7-year period from January 1995 through December 2001 by surgeons in the Department of Ophthalmology at the University of Minnesota were identified by database search for all procedures From the Departments of Ophthalmology (Dr Lawrence, Dr Kramarevsky, Dr Christiansen, Dr Wright, Dr Young, Dr Summers) and Pediatrics (Dr Christiansen, Dr Young, Dr Summers), University of Minnesota, Minneapolis, Minnesota. This project was supported in part by an unrestricted grant to the University of Minnesota, Department of Ophthalmology, from Research to Prevent Blindness, Inc, New York, New York. *Presenter. Bold type indicates AOS member. Trans Am Ophthalmol Soc / Vol 103/
2 Lawrence, Kramarevsky, Christiansen et al with CPT codes 66840, 66850, 66983, 66984, and A chart review was performed for every case identified. Eyes with traumatic cataract, preexisting glaucoma, and other serious ocular malformations, including anterior segment dysgenesis, Lowe syndrome, and persistent fetal vasculature, were excluded. Data extraction included patient age at surgery, intraocular lens implantation at cataract extraction, date of glaucoma onset, and length of follow-up. We designated cases as having glaucoma on the basis of the attending ophthalmologist s recorded decision to start long-term glaucoma medications, perform glaucoma surgery, or refer to a glaucoma specialist. SURGICAL TECHNIQUE Lensectomies were performed through a standard limbal or pars plana incision. Posterior capsulotomies and anterior vitrectomies were performed with automated vitrectomy instrumentation. Forty-nine eyes (42%) had intraocular lens implantation at the time of lensectomy. Topical corticosteroids were routinely used postoperatively. For those without intraocular lens implantation, contact lens fitting was usually performed 1 week postoperatively. STATISTICAL ANALYSIS The Kaplan-Meier method was used to evaluate the time to glaucoma for all eyes in the study. The analysis was also stratified by the patient s age at surgery (<30 days, 30 days) and intraocular lens implantation. These subgroups were compared using the log-rank test, and a P value less than.05 was considered statistically significant. Risk ratios were calculated for the following variables: age at surgery, gender, and intraocular lens implantation at the time of lensectomy. Only patients followed for more than 12 months were included for calculation of risk ratios. RESULTS The data from 116 lensectomies in 79 patients were included in this study. All surgeries were performed for congenital or developmental cataracts. Thirty-six patients (46%) were male, and the median age at cataract surgery was 178 days (~6 months). Mean follow-up time was 2.7 years. Forty-nine eyes (42%) underwent primary intraocular lens implantation. Thirteen eyes developed glaucoma, for an overall incidence of glaucoma of 11%. Table 1 shows the clinical features of each of the 13 eyes that developed subsequent glaucoma. Ten of the 13 eyes with glaucoma EYE OD or OS TABLE 1. CLINICAL FEATURES OF EYES THAT DEVELOPED SUBSEQUENT GLAUCOMA UNILATERAL OR BILATERAL CATARACT TIMING OF LENSECTOMY (PATIENT S AGE IN DAYS) IOL GLAUCOMA ONSET (DAYS AFTER LENSECTOMY) GLAUCOMA SURGICAL TREATMENT (NO.) MOST RECENT VISUAL ACUITY 1* OS B 9 N 26 Y (2) 20/710 (OU) 2 OD U 17 N 82 Y (3) NA 3 OS U 16 N 254 N Enucleated 4 OD B 18 N 1,871 Y (1) 20/20 5 OD U 19 N 90 Y (2) NA 6 OD U 20 N 148 Y (1) 20/200 7 OD U 21 N 50 N NA (phthisis) 8 OD U 23 N 1,942 N 20/25 9 OD B 26 N 56 N 20/360 (OU) 10* OD B 27 N 8 Y (3) 20/710 (OU) 11 OS U 48 N 62 Y (3) 20/ OS U 213 N 183 Y (1) 20/ OD U 503 N 1,308 N 20/125 B = bilateral IOL = intraocular lens implantation at the time of lensectomy N = no NA = not available OD = right eye OS = left eye U = unilateral Y = yes *Eyes 1 and 10 belong to same patient. underwent lensectomy at less than 30 days of age. None had intraocular lens implantation at initial lensectomy. Eight of 13 eyes required at least one glaucoma surgery, and of those, three required three glaucoma surgeries. (Glaucoma surgeries included Trans Am Ophthalmol Soc / Vol 103/
3 Glaucoma Following Cataract Surgery In Children: Surgically Modifiable Risk Factors trabeculotomies, goniotomies, trabeculectomies, and shunt procedures.) The final recorded visual acuity in eyes that developed subsequent glaucoma ranged from 20/20 to no light perception (due to enucleation). Two eyes had final visual acuities better than 20/60, two eyes had visual acuities between 20/60 and 20/180, five eyes had visual acuities between 20/200 and 20/3000, three eyes did not have vision recorded in the chart, and one eye was eventually enucleated. In our series, the earliest diagnosis of glaucoma was 8 days after lensectomy (Table 1, eye 10); the latest diagnosis was made 1,942 days after surgery in the middle of the fifth year (Table 1, eye 8). The mean time between cataract surgery and the detection of glaucoma was 468 days (~1 year, 3 months). The Kaplan-Meier curve of time to glaucoma for the overall pediatric lensectomy cohort is shown in Figure 1. By 5 years after lensectomy, approximately 70% of the cohort remained glaucoma-free. FIGURE 1 Kaplan-Meier analysis of glaucoma incidence of overall pediatric lensectomy cohort (n = 116 eyes). FIGURE 2 Number of eyes undergoing lensectomy, by month, for the first 24 months of life. All 13 eyes that subsequently developed glaucoma were operated on within this time period. Of the 24 eyes operated on within the first month of life, 10 (42%) subsequently developed glaucoma. TIMING OF LENSECTOMY The timing of lensectomy in our series ranged from 4 days to 17.5 years of age. The median age at surgery was 21 days for those that developed glaucoma and 208 days (~7 months) for those that did not develop glaucoma. All eyes that subsequently developed glaucoma were operated on within the first 24 months of life. The number of eyes undergoing lensectomy, by month, for the first 2 years of life is shown in Figure 2. Of the eyes operated on during the first month of life, 42% (10 of 24) developed glaucoma. Risk factor analysis is shown in Table 2. The total number of eyes with at least 1 year of follow-up was 86. Eyes that underwent RISK FACTOR TABLE 2. RISK FACTOR ANALYSIS FOR GLAUCOMA DEVELOPMENT (N = 86) CASES OF GLAUCOMA (N = 13) CASES WITHOUT GLAUCOMA (N = 73) RISK RATIO P* IOL implantation 0 (0%) 34 (46.6%) Undefined.001 Age at surgery (<30 days) 10 (76.9%) 9 (12.3%) 11.8 <.001 Gender 7 (53.8%) 34 (46.6%) IOL = intraocular lens. P value was determined from the chi-square or Fisher s exact test. Trans Am Ophthalmol Soc / Vol 103/
4 Lawrence, Kramarevsky, Christiansen et al lensectomy when the infant was less than 30 days of age were 11.8 times more likely to develop glaucoma than eyes that underwent surgery when infants were more than 1 month of age (P <.001). The Kaplan-Meier analysis of glaucoma incidence stratified by timing of surgery, shown in Figure 3, also showed a statistically significant difference in events (P <.001). By 5 years after surgery, approximately one fourth of eyes operated on within the first month of life were glaucoma-free. FIGURE 3 Kaplan-Meier analysis of glaucoma incidence stratified by age at surgery (P value of the log-rank test: <.001). PRIMARY INTRAOCULAR LENS IMPLANTATION Intraocular lens implantation at the time of lensectomy was performed in 49 eyes (42%). The median age at surgery for the pseudophakic group was 4.53 years, with a range of 37 days to 17.5 years. No cases of lensectomy with primary intraocular lens implantation developed glaucoma. Sixty-seven eyes (58%) had no intraocular lens implanted at the time of lensectomy. The median age at surgery for the aphakic group was 88 days (~3 months), with a range of 4 days to 6.1 years. Risk factor analysis for primary intraocular lens implantation is shown in Table 2. In no cases of lensectomy with primary intraocular lens implantation did glaucoma develop. Because of this, the risk ratio was undefined; however, intraocular lens implantation appeared to have a protective effect (P =.001). Kaplan-Meier analysis showed a statistically significant difference in glaucoma incidence by 5 years postoperatively (P =.002), as shown in Figure 4. RELATIVE SIGNIFICANCE OF THE TREATMENT FACTORS To determine which of the two factors, either timing of surgery or implantation of an intraocular lens, had more impact on the occurrence of glaucoma, we separated the eyes into subgroups defined by these two variables. (A factorial analysis could not be performed because no cases of glaucoma occurred in pseudophakic eyes.) Table 3 shows the subgroup analysis of the incidence of glaucoma in aphakic eyes that underwent surgery at 30 days of age or older (9.1%) and in those that had surgery at less than 30 days of age (39.1%). The rate of glaucoma in the subgroups was compared using the chi-square test and was statistically significantly different between the subgroups (P =.016). Both treatment variables appeared to have a substantial effect, but timing of surgery seemed to have a larger impact on glaucoma rates. Trans Am Ophthalmol Soc / Vol 103/
5 Glaucoma Following Cataract Surgery In Children: Surgically Modifiable Risk Factors FIGURE 4 Kaplan-Meier analysis of glaucoma incidence stratified by intraocular lens implantation at the time of lensectomy (P value of the log-rank test:.002). TABLE 3. SUBGROUP ANALYSIS FOR GLAUCOMA DEVELOPMENT: IOL IMPLANTATION VERSUS TIMING OF SURGERY IN EYES THAT DEVELOPED GLAUCOMA SUBGROUP TREATMENT VARIABLES GLAUCOMA INCIDENCE 1 IOL and age 30 days 0/49 (0%) 2* No IOL and age 30 days 4/44 (9.1%) 3* No IOL and age <30 days 9/23 (39.1%) IOL = intraocular lens. The pairwise comparison between subgroups 2 and 3 was statistically significant (P value of the chi-square:.016). DISCUSSION The current study is a retrospective analysis of childhood cataract surgery performed at our institution over a 6-year period. It is limited by variable follow-up of patients and incomplete data available in the medical records. Multiple surgeons performing somewhat different lensectomy techniques may also compromise the data. Microphthalmia, microcornea, extent of pupillary dilation at the time of surgery, 10 type of cataract, 9 amount of residual lens tissue, and gonioscopic findings, 23 although previously reported to be risk factors for glaucoma, were inconsistently documented in our medical records and thus were not included in our data collection. Despite these limitations, our series represents one of the only studies to focus on surgeon-modifiable variables. We analyzed our data to determine whether two treatment variables determined by the ophthalmologist s treatment plan timing of surgery and intraocular lens implantation showed statistical significance for the development of glaucoma. Both of these modifiable factors showed significant impact on glaucoma incidence. Trans Am Ophthalmol Soc / Vol 103/
6 Lawrence, Kramarevsky, Christiansen et al The relative risk ratio for development of glaucoma in children undergoing surgery before the age of 1 month was This supports previously published reports showing a significantly higher rate of glaucoma in patients undergoing surgery at younger ages. The series reported by Keech and coworkers in showed an overall glaucoma incidence of 11% and age less than 8 weeks to be a significant risk factor. Magnusson and colleagues 8 reported a Swedish cohort with a 12% glaucoma incidence and age at lensectomy of less than 10 days to be a significant risk factor. Early surgery was also shown to be a significant risk factor in a series reported by Vishwanath and associates 11 from the Great Ormond Street Hospital in London, leading them to pose the question, Should we delay congenital cataract surgery until four weeks old? In contrast, Watts and coworkers, 14 using classification and regression trees analysis, found a higher incidence of glaucoma among infants operated on between 13.5 days and 43 days of life than among those operated on under 14 days of age. They concluded that the first 2 weeks of life were the most favorable time to perform lensectomy. In our series, seven eyes were operated on during the first 2 weeks of life, one of which developed glaucoma, so our data do not confirm a safe window with respect to glaucoma development within the first 2 weeks of life. Of the eyes that developed subsequent glaucoma, however, 9 of 13 (69%) were operated on between 16 and 27 days of life Other studies reporting no association with age at surgery included fewer patients who underwent early surgery or did not analyze data regarding timing of surgery. 5,9,24 Timing of surgery can have a major impact on long-term visual prognosis in eyes with congenital cataracts. Surgery performed after 6 to 8 weeks of age may result in deprivation of visual stimuli and less favorable visual outcomes It is now generally accepted practice that lensectomy in the pediatric population be performed as early as possible to maximize visual functioning and minimize the effects of amblyopia and nystagmus. With the mounting evidence that timing the lensectomy within the first few weeks of life may lead to a higher incidence of glaucoma, perhaps pediatric ophthalmologists should consider delaying surgery until 30 days of life. A randomized, prospective study may be optimal to reduce the inherent biases of retrospective analyses and, may help to determine if it is the timing of the surgery per se that leads to the increased rate of glaucoma, or if the increased rate of glaucoma is due to intrinsic factors associated with eyes that are brought to surgery earlier. Our study also demonstrated that primary intraocular lens implantation during lensectomy may be associated with a significantly decreased risk of subsequent glaucoma development. Asrani and colleagues 28 recently reported a retrospective analysis of two large databases from multiple centers in the United States that suggested a reduced incidence of glaucoma in the primary pseudophakic eyes (0.3%), compared with those that were left aphakic (11.3%). In contrast, Lambert and coworkers 20 compared outcomes in children with and without primary intraocular lens implantation in lensectomies performed within the first 6 months of life. They found that the intraocular lens group had higher rates of complications requiring reoperation, including two of 12 that required glaucoma surgery. Our study lends more evidence to confirm Asrani and coworkers suggestions that primary intraocular lens implantation may be protective for the development of glaucoma. Possible biases that may confound the findings of our study include detection bias and selection bias. Infants are more likely to be operated on earlier when their cataract is detected and referred earlier, such as when there is a family history of congenital cataract. Are we preferentially selecting infants with worse disease or those that may have a known familial genetic predisposition for the group that has a higher incidence of glaucoma? Do infants who are diagnosed earlier have more involvement of a single disease process that involves the trabecular outflow channels and hence the higher rate of glaucoma? Although it is tempting to propose a single disease entity that would account for both congenital cataract and glaucoma, other investigators have felt that the glaucoma appears to develop only if, and after, lensectomy is performed. 29,30 Our study excluded eyes in which a diagnosis of glaucoma had been made prior to the lensectomy and thus does not shed new light on this question. The pathogenesis of pediatric aphakic glaucoma is not well understood. In very young, small eyes, with a smaller pupil, perhaps the surgery is more difficult and may lead to more retained lens material and hence greater postoperative inflammation. The role of postoperative use of corticosteroids should also be considered. 11 The finding that aphakic glaucoma is detected, in some cases, years after lensectomy and discontinuation of corticosteroids, with the intervening period documented by normal intraocular pressures and no uveitis, would make this cause unlikely for most cases. Perhaps the cause is some aspect of the actual surgery, in combination with an early period of sensitivity that lasts about 30 days. It is possible that a structural change in the trabecular meshwork, or its supporting beams, may occur during the surgery or afterwards, when the lens is removed. The lack of structural rigidity in very young eyes may lead to either collapse or stretching of the trabecular meshwork during surgery, causing permanent physiologic damage or disrupted maturation of the meshwork. The role of the stretch of the zonular fibers, and hence the ciliary processes, when an intraocular lens is inserted, and the lack thereof in aphakic eyes, should also be considered. The role of vitreous chemical components has also been suggested. 19 In conclusion, we found that lensectomy performed during the first 30 days of life was associated with a higher risk of subsequent glaucoma than surgery performed later. In our series, the implantation of an intraocular lens at the time of lensectomy was associated with a lower rate of subsequent glaucoma. The independent contribution of each of these treatment variables could not be determined in this study, but both factors appear to exert an effect. Although it may be tempting to delay cataract surgery until after 30 days of age and to consider primarily implanting an intraocular lens in very young infants, prospective randomized studies will be needed to corroborate or refute these findings and, may help to elucidate mechanisms of the pathogenesis of this challenging disease. Knowledge of modifiable risk factors is essential to allow pediatric ophthalmic surgeons to make cogent decisions regarding the care of children with cataracts. Trans Am Ophthalmol Soc / Vol 103/
7 Glaucoma Following Cataract Surgery In Children: Surgically Modifiable Risk Factors ACKNOWLEDGMENTS We thank Bruce Lindgren, Director of the Biostatistics Consulting Lab, Division of Biostatistics at the University of Minnesota School of Public Health, for his invaluable biostatistics advice. REFERENCES 1. Biglan A. Outcome of treatment for bilateral congenital cataracts. Trans Am Ophthalmol Soc 1992;90: Crouch ER, Crouch ER Jr, Pressman SH. Prospective analysis of pediatric pseudophakia: myopic shift and postoperative outcomes. J AAPOS 2002;6: Pressman SH, Crouch ER. Pediatric aphakic glaucoma. Ann Ophthalmol 1983;5: Francois J. Glaucoma and uveitis after congenital cataract surgery. Ann Ophthalmol 1971;3: Chrousos GA, Parks MM, O Neill JF. Incidence of chronic glaucoma, retinal detachment and secondary membrane surgery in pediatric aphakic patients. Ophthalmology 1984;91: O Keefe MO, Mulvihill A, Yeoh PL. Visual outcome and complications of bilateral intraocular lens implantation in children. J Cataract Refract Surg 2000;26: Keech RV, Tongue AC, Scott WE. Complications after surgery for congenital and infantile cataracts. Am J Ophthalmol 1989;108: Magnusson G, Abrahamsson M, Sjostrand J. Glaucoma following congenital cataract surgery: an 18-year longitudinal followup. Acta Ophthalmol Scand 2000;78: Parks MM, Johnson DA, Reed GW. Long-term visual results and complications in children with aphakia: a function of cataract type. Ophthalmology 1993;100: Mills MD, Robb RM. Glaucoma following childhood cataract surgery. J Pediatr Ophthalmol Strabismus 1994;31: Vishwanath M, Cheong-Leen R, Russell-Eggitt I, et al. Is early surgery for congenital cataract a risk factor for glaucoma? Br J Ophthalmol 2004;88: Robb RM, Peterson RA. Outcome of treatment for bilateral congenital cataracts. Ophthalmic Surg 1992;23: Chen TC, Bhatia LS, Walton DS. Complications of pediatric lensectomy in 193 eyes. Ophthalmic Surg Lasers Imaging 2005;36: Watts P, Abdolell M, Levin AV. Complications in infants undergoing surgery for congenital cataract in the first 12 weeks of life: Is early surgery better? J AAPOS 2003;7: Simon JW, Mehta N, Simmons ST, et al. Glaucoma after pediatric lensectomy/vitrectomy. Ophthalmology 1991;98: Miyahara S, Amino K, Tanihara H. Glaucoma secondary to pars plana lensectomy for congenital cataract. Graefes Arch Clin Exp Ophthalmol 2002;240: Egbert JE, Wright MM, Dahlhauser KF, et al. A prospective study of ocular hypertension and glaucoma after pediatric cataract surgery. Ophthalmology 1995;102: Johnson CP, Keech RV. Prevalence of glaucoma after surgery for PHPV and infantile cataracts. J Pediatr Ophthalmol Strabismus 1996;33: Asrani SG, Wilensky JT. Glaucoma after congenital cataract surgery. Ophthalmology 1995;102: Lambert SR, Buckley EG, Plager DA, et al. Unilateral intraocular lens implantation during the first six months of life. J AAPOS 1999;3: Plager DA, Yang S, Neely D, et al. Complications in the first year following cataract surgery with and without IOL in infants and children. J AAPOS 2002;6: Chandler PA. Surgery of the lens in infancy and childhood. Arch Ophthalmol 1951;45: Walton DS. Pediatric aphakic glaucoma: a study of 65 patients. Trans Am Ophthalmol Soc 1995;93: Phelps CD, Arafat NI. Open-angle glaucoma following surgery for congenital cataracts. Arch Ophthalmol 1977;95: Elston JS, Timms C. Clinical evidence for the onset of the sensitive period in infancy. Br J Ophthalmol 1992;76: Birch EE, Stager DR. Prevalence of good visual acuity following surgery for congenital unilateral cataract. Arch Ophthalmol 1988;106: Ellemberg D, Lewis TL, Mauer D, et al. Spatial and temporal vision in patients treated for bilateral congenital cataracts. Vis Res 1999;39: Asrani S, Freedman S, Hasselblad V, et al. Does primary intraocular lens implantation prevent aphakic glaucoma in children? J AAPOS 2000;4: Phelps CD, Arafat NI. Open-angle glaucoma following surgery for congenital cataracts. Arch Ophthalmol 1977;95: Mori M, Keech RV, Scott WE. Glaucoma and ocular hypertension in pediatric patients with cataracts. J AAPOS 1997;1: PEER DISCUSSION DR M. EDWARD WILSON. The prognosis for a child born today with a congenital cataract is much improved because of improvements in surgical treatment, earlier detection of the cataracts, and more successful treatment of associated amblyopia. Trans Am Ophthalmol Soc / Vol 103/
8 Lawrence, Kramarevsky, Christiansen et al However, the incidence of glaucoma after congenital cataract surgery has remained high, especially for the children with dense cataracts present at birth who need surgical intervention early in life. Dr Lawrence and co-workers have analyzed 116 eyes from 79 patients operated for childhood cataracts in the first 18 years of life. While the overall incidence of glaucoma was 11%, the incidence among those children operated for truly congenital cataracts in the first month of life was 38%. As pointed out by Dr Lawrence, 50 75% of these children may have developed glaucoma by 5 years after surgery. The most important question this paper asks is whether the glaucoma incidence can be reduced by altering something we, as surgeons, do when we remove the congenital cataract. In the author s series, surgery in the first 30 days of life was highly correlated with glaucoma development. In my practice, I usually delay surgery until the 5 th week of life based on work published by Birch and co-workers 1 that documented no benefit to operating earlier than 6 weeks in unilateral congenital cataracts. Since this change in my practice pattern, I have not seen a decrease in the incidence of aphakic glaucoma. It has been suggested that intraocular lens implantation (IOL) may help decrease the incidence of glaucoma since none of the implanted eyes developed glaucoma. However, there is no evidence that the IOL group is comparable, in this series, to the non-iol group. Eyes at the highest risk for glaucoma were not selected to receive an IOL. If visually significant cataracts present at birth are likely to both be operated early and left aphakic, these treatment choices will be highly correlated with glaucoma even if, in reality, it is the mere existence of the severe cataract at birth that carries the risk. Dr Rupal Trivedi and I recently presented an analysis of 561 eyes I had operated for childhood cataract using very similar exclusion criteria applied in Dr Lawrence s study (unpublished data presented at the 2005 annual meeting of the AAPOS). We found 10 eyes with glaucoma among the IOL group. All had been operated before 4.5 months of life. The incidence of glaucoma when surgery was performed in the first 4.5 months of life was the same whether an IOL was implanted or not. Glaucoma developed in 24.3% (10 of 41) in the IOL group and 19.6% (9 of 46) in the aphakic group. Also, for eyes having surgery in the first 4.5 months of life, microcornea and microphthalmia were common but neither corneal diameter nor axial lengths were predictive of glaucoma. Finding surgically modifiable risk factors is important. However, I suspect that neither a delay of the cataract surgery nor the implantation of an IOL will lower the incidence of glaucoma in babies at the highest risk for this potentially blinding complication. REFERENCE 1. Birch EE, Stager DR. The critical period for surgical treatment of dense congenital unilateral cataract. Invest Ophthalmol Vis Sci. 1996;37: DR DAN B JONES. Perhaps it is in the written manuscript, but I have not heard your definition of glaucoma and how it was determined. How was the pressure measured and was any attention given to pachymetry in this group? In summarizing the 3 groups, you had a total of 116 eyes and then discussed these by age group. You ve got 37 patients who had bilateral cataracts and it may not be fair to combine them in looking at group analysis. What happened in the children that had bilateral cataracts in terms of incidence of glaucoma? DR DOUGLAS R. ANDERSON. Might there be a correlation between implantation or non-implantation of an intraocular lens and early surgery? Or are they independent factors? Then the question is whether or not we can do something to prevent glaucoma. The two things that might be suggested are, do not operate before 30 days and be sure to place an intraocular lens. The problem with concluding either from a retrospective study is that there must be some reason why the surgeon is reluctant to place a lens in an eye when he does surgery on a very young infant, and if these features do correlate, it is difficult to conclude that which recommendation (operate later, place a lens) is relevant; perhaps it is satisfactory to operate early if you place a lens, for example. Another relationship that is difficult to discern from the available data is whether the decision not to place an intraocular lens might be related to the nature of the eye or the nature of the cataract; and the features of the eye or cataract that lead to that decision may correlate with a tendency to have glaucoma. The glaucoma was perhaps not the result of deciding not to place an intraocular lens. The same might be said for early surgery, whether there was some reason the surgeon felt compelled to operate earlier than 30 days in some cases, and others were delayed to 6 weeks. The apparent urgency may reflect a different type of congenital defect, one associated with glaucoma. In either case, it is interesting to contemplate that changing surgical habits (operate later, use a lens) might help avoid glaucoma, but one would have to be prepared for possible disappointment, to find that such changes did not reduce the incidence of glaucoma. DR ELIAS I.TRABOULSI. My own data supports that implantation of an intraocular lens in infants less than 2 years of age may be protective of glaucoma. We presented a poster at the American Association for Pediatric Ophthalmologists and Strabismus annual meeting this year with about 20 eyes in each of two groups: with and without IOL; 6 eyes of those who did not have an IOL developed glaucoma versus none in the group with an intraocular lens. However, this was a retrospective study and suffers from the same deficiencies as the other studies. A current infantile aphakia treatment study is looking at the implantation of intraocular lenses in unilateral cataracts under the age of 6 months in a prospective manner and hopefully will provide some of those answers. Additional data from Europe in large numbers of patients also supports the fact that the implantation of an intraocular lens may be protective of glaucoma. I agree with Dr Wilson that there is no rush in doing the surgery and I tend to delay surgery until into the second month. Trans Am Ophthalmol Soc / Vol 103/
9 Glaucoma Following Cataract Surgery In Children: Surgically Modifiable Risk Factors DR ALLAN J. FLACH. Did any of these children with the cataracts have a syndrome of any sort, such as rubella or galactosemia? Could some of these have been traumatic? If any of these factors were present, could that have affected the tendency towards glaucoma? Is there any explanation for the cataracts in your study? DR MALCOLM R. ING. Was there a matching of the age, the range of age of implantation, and the mean age between the two groups? Was the length of follow up similar between the two groups? How often should you measure the intraocular pressure in a pediatric patient with or without an implant? What method would you use to measure the pressure? Are you satisfied with a Tonopen? Will you do a full general anesthetic? Do you also have a category of ocular hypertension? I have noted that sometimes in a bilateral case, one eye will show an elevation of the tension months or years ahead of the other one and this alerts me that that eye may be going into glaucoma. DR GERHARD W. CIBIS. How often should you measure intraocular pressures from a medical/legal perspective? When do you have to consider anesthesia, etc? Another question relates to the pars plicata approach. You indicated that you could not report whether the surgical approach was anterior or pars plana. Dr Gholam Peyman pointed out that the pars plana doesn t develop until 6 years of age, so you re actually going through the pars plicata in these young patients. I have a personal bias in my practice that the pars plicata is a better approach than an anterior approach in terms of less glaucoma, but I have no statistics at this time. DR ROBERT N. WEINREB. I would like to suggest for consideration another modifiable risk factor: topical steroids. I assume that you used glaucoma as a surrogate for intraocular pressure. Cursory observation of the data in the young group, the less-than-30-daysold children, suggests a large number who develop glaucoma rather rapidly, compared to the group that had the delayed surgery. Might topical steroids have caused the increase in intraocular pressure? Might these young individuals be particularly sensitive to intraocular pressure? It might be possible that the young individual is not only more sensitive with an immediate increase in intraocular pressure but perhaps the trabecular meshwork cells can be damaged by topical steroids, and this is manifested as a late pressure rise. DR FREDERICK L. FERRIS. You present Kaplan-Meier curves, but the late 3-5 year rates are probably terribly unstable, because one event was causing about a 10-15% change. Your rates to one, maybe two years, are probably fairly stable. Regarding the intraocular lens issue, did you say that there was about a 9% risk in the older children without IOLs compared with 0% for those with IOLs? It wasn t clear whether that was statistically significant; if it is not, I m not sure you have grounds to say that IOL itself is protective. There was also the issue of selection bias as to who is chosen for IOL versus who is not. This may have a lot more to do with the apparent protection than the IOL itself. Did you look at factors associated with having an IOL or not? DR ROBERT C. DREWS. Was the incidence of glaucoma with cataract before surgery really 0%? DR ALBERT W. BIGLAN. The literature that encourages us to perform cataract surgery within the first weeks of life really needs to be reevaluated. Perhaps we should wait as Dr Wilson has pointed out and as Stager s paper (Birch EE, Stager, DR. Invest Ophthalmol Vis Sci 1996; 37: ) and others to delaying the surgery until after 30 days following term delivery. Measurement of central corneal thickness with pachymetry has become the standard for adult care. Pachymetry measurements of the central corneal thickness in children should be included in the evaluations. The pachymetry that I have performed on my pediatric aphakic patients indicates that these corneas are extremely thick, around 600 microns. Although Dr Evelyn Paysse has published some data to the contrary, I have found that the normal eye, or the non-cataractous eye in the monocular cases, also shows a tendency toward increased thickness. I would encourage you to add these measurements to your study if possible. You have not described the type of glaucoma early in life. Is the mechanism angle-closure, or is it open angle? I will be anxious to see the gonioscopy results in the written manuscript. DR JOHN F. O NEILL. In my experiences, there was a very significant relationship between unilateral cataracts, microphthalmia, and the incidence of glaucoma, and I had not heard about these conditions in your presentation. DR ROBERT L. STAMPER. Some care has to be exercised in interpreting pachymetry readings in these children, because the surgical intervention of cataract surgery itself may influence the pachymetry reading. I suspect that the relationships that we found for pachymetry and intraocular pressure as measured by some instrumentation in adults who have not had surgery, or perhaps, less invasive surgery, may not be valid in these children who have had some pretty profound surgical manipulation. DR MARY G. LAWRENCE. For the purposes of this study, we were only looking at post-operative glaucoma development. We did not include any eyes that had glaucoma prior to lensectomy. Eyes were designated as having glaucoma based on information written in the chart. This included eyes that were started on long-term glaucoma medicines, referred to a glaucoma specialist, or had glaucoma surgery performed. If there was an immediate, short-lived, post-operative rise in intraocular pressure (IOP), or if there was increased IOP in the setting of concomitant steroid medication, the designation of glaucoma was not given. We excluded all eyes with a syndrome such as Persistent Hyperplastic Primary Vitreous and Lowe Syndrome. However, we could not be sure about microcornea or microphthalmia. In this retrospective study, not all patients had axial lengths evaluated and not all patients had corneal diameters recorded. But, any eye with a documented recognized syndrome that may have been associated with another type of glaucoma was excluded. Eyes with traumatic cataract were also excluded. The disease process that causes bilateral cataracts may be completely different than the mechanism that causes a unilateral cataract. Our study did not address these differences. This may need further evaluation. Trans Am Ophthalmol Soc / Vol 103/
10 Lawrence, Kramarevsky, Christiansen et al In answer to Dr Ferris question, IOL implantation, as a separate risk factor, was statistically significant. The largest bias in our study was selection bias. Is the timing of surgery, per se, causing increased glaucoma or is it due to intrinsic factors associated with eyes that are brought to surgery earlier? A retrospective study cannot really answer that question. The median age of the pseudophakic group was 4. 5 years at the time of surgery, and the median age of the aphakic group was 88 days (about 3 months). There s a big difference in those two groups. An NEI study with Dr Scott Lambert as the Principal Investigator is looking at approximately 100 patients with unilateral cataracts over a 4-year time frame. I understand that they are not looking specifically at timing of surgery, but are looking at IOL implantation. Dr Cibis asked how often intraocular pressures should be taken in these patients. I am not a pediatric ophthalmologist but rather a glaucoma specialist, so I would prefer intraocular pressure (IOP) be assessed more frequently than less frequently. In light of the North American and European studies published over that past years, showing that overall glaucoma incidence after pediatric lensectomy ranges from about 10 to 20 percent, I might suggest that an IOP measurement be attempted at most visits after lensectomy for the patient s lifetime. Clinical standards for frequency of care, however, are best developed by a consensus of ophthalmologists who routinely perform pediatric lensectomies. Please note that I did not perform any of the lensectomies, and I did not follow these children post-operatively. Some were referred to me only when they developed more severe glaucoma. Regarding the best device for the measurement of IOP, I think that, of the commonly available instruments, a Goldman tonometer gives the most accurate IOP measurement. A Tonopen, however, is easier to use in some children, and also gives quite accurate data. Dr Gail Summers, a member of our department and co-author of this paper, is highly accurate (to within a few millimeters mercury) in performing digital palpation pressure on these small children. Because she is so accurate, palpation of the eye is probably all that is needed in her patients. I d suggest taking IOP measurement using whatever is most accurate and expedient in your own practice settings. Certainly, something is better than nothing. To address the expert witness concerns, our study was aimed at starting to develop an evidence-based approach, so that we, as surgeons, can make better decisions to maximize the long-term outcome for children with cataracts. As of now, we have conscientiously evaluated a relatively large data set, and, with your help, are beginning to ask more questions. Our study adds to the literature but is not definitive at this stage. Retrospective studies often raise questions that future prospective randomized clinical trials can answer more authoritatively. It is our hope that this paper will spawn more studies that will corroborate or refute our findings regarding surgeon modifiable variables. Trans Am Ophthalmol Soc / Vol 103/
A phakic glaucoma is an established complication following
 905 EXTENDED REPORT Is early surgery for congenital cataract a risk factor for glaucoma? M Vishwanath, R Cheong-Leen, D Taylor, I Russell-Eggitt, J Rahi... See end of article for authors affiliations...
905 EXTENDED REPORT Is early surgery for congenital cataract a risk factor for glaucoma? M Vishwanath, R Cheong-Leen, D Taylor, I Russell-Eggitt, J Rahi... See end of article for authors affiliations...
Glaucoma after Congenital Cataract Surgery
 Glaucoma after Congenital Cataract Surgery Mahmoodreza Panahi Bazaz, MD 1 Farideh Sharifipour, MD 2 Mitra Zamani, MD 2 Ali Sadeghi, MD 3 Hossein Roostai, MD 3 Seyed Mahmood Latifi, MSc 4 Abstract Purpose:
Glaucoma after Congenital Cataract Surgery Mahmoodreza Panahi Bazaz, MD 1 Farideh Sharifipour, MD 2 Mitra Zamani, MD 2 Ali Sadeghi, MD 3 Hossein Roostai, MD 3 Seyed Mahmood Latifi, MSc 4 Abstract Purpose:
RISK FACTORS FOR THE DEVELOPMENT OF APHAKIC GLAUCOMA AFTER CONGENITAL CATARACT SURGERY
 RISK FACTORS FOR THE DEVELOPMENT OF APHAKIC GLAUCOMA AFTER CONGENITAL CATARACT SURGERY BY Teresa C. Chen MD,* Lini S. Bhatia MD, Elkan F. Halpern PhD, AND David S. Walton, MD ABSTRACT Purpose: It is well
RISK FACTORS FOR THE DEVELOPMENT OF APHAKIC GLAUCOMA AFTER CONGENITAL CATARACT SURGERY BY Teresa C. Chen MD,* Lini S. Bhatia MD, Elkan F. Halpern PhD, AND David S. Walton, MD ABSTRACT Purpose: It is well
Complication and Visual Outcome after Peadiatric Cataract Surgery with or Without Intra Ocular Lens Implantation
 Original Article Complication and Visual Outcome after Peadiatric with or Without Intra Ocular Lens Implantation Mazhar-ul-Hasan, Umair A. Qidwai, Aziz-ur-Rehman, Nasir Bhatti, Rashid H. Alvi Pak J Ophthalmol
Original Article Complication and Visual Outcome after Peadiatric with or Without Intra Ocular Lens Implantation Mazhar-ul-Hasan, Umair A. Qidwai, Aziz-ur-Rehman, Nasir Bhatti, Rashid H. Alvi Pak J Ophthalmol
Paediatric cataract pathogenesis and management
 Paediatric cataract pathogenesis and management Dr. Kavitha Kalaivani. N Paediatric ophthalmology Sankara Nethralaya February 28-2017 Incidence... 1 to 13 per 10 000 live births 1 200,000 children blind
Paediatric cataract pathogenesis and management Dr. Kavitha Kalaivani. N Paediatric ophthalmology Sankara Nethralaya February 28-2017 Incidence... 1 to 13 per 10 000 live births 1 200,000 children blind
GLAUCOMA CONTINUES TO
 CLINICAL SCIENCES Aphakic Glaucoma After Congenital Cataract Surgery Teresa C. Chen, MD; David S. Walton, MD; Lini S. Bhatia, MD Objective: To describe the largest series of patients who developed aphakic
CLINICAL SCIENCES Aphakic Glaucoma After Congenital Cataract Surgery Teresa C. Chen, MD; David S. Walton, MD; Lini S. Bhatia, MD Objective: To describe the largest series of patients who developed aphakic
The incidence of glaucoma following paediatric cataract surgery: a 20-year retrospective study
 (2010) 24, 1366 1375 & 2010 Macmillan Publishers Limited All rights reserved 0950-222X/10 $32.00 www.nature.com/eye CLINICAL STUDY The incidence of glaucoma following paediatric cataract surgery: a 20-year
(2010) 24, 1366 1375 & 2010 Macmillan Publishers Limited All rights reserved 0950-222X/10 $32.00 www.nature.com/eye CLINICAL STUDY The incidence of glaucoma following paediatric cataract surgery: a 20-year
Incidence of Early Onset Glaucoma after Infant Cataract Extraction With and Without
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 Title: Incidence of Early Onset Glaucoma after Infant Cataract Extraction With and Without Intraocular Lens Implantation Authors: Inez B.Y. Wong, FRCSEd(Ophth),
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 Title: Incidence of Early Onset Glaucoma after Infant Cataract Extraction With and Without Intraocular Lens Implantation Authors: Inez B.Y. Wong, FRCSEd(Ophth),
Title: Fitting Gas Permeable Contact Lenses on Aphakic Infants with Congenital Cataracts: Case Report
 Title: Fitting Gas Permeable Contact Lenses on Aphakic Infants with Congenital Cataracts: Case Report I. Case History Patient demographics: 9-month-old Caucasian female Purpose of visit/chief Complaint:
Title: Fitting Gas Permeable Contact Lenses on Aphakic Infants with Congenital Cataracts: Case Report I. Case History Patient demographics: 9-month-old Caucasian female Purpose of visit/chief Complaint:
Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age
 Original Article Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age Suma Ganesh 1, Reena Gupta 2, Sumita Sethi 3, Chandra Gurung 4, Raman Mehta 5 1,5 Dr. Shroff s Charitable
Original Article Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age Suma Ganesh 1, Reena Gupta 2, Sumita Sethi 3, Chandra Gurung 4, Raman Mehta 5 1,5 Dr. Shroff s Charitable
Lessons learned about cataract surgery in infants from the Infant Aphakia Treatment Study
 1 April 4, 2017 Lessons learned about cataract surgery in infants from the Infant Aphakia Treatment Study Summary: The workshop will present the latest findings from the Infant Aphakia Treatment Study
1 April 4, 2017 Lessons learned about cataract surgery in infants from the Infant Aphakia Treatment Study Summary: The workshop will present the latest findings from the Infant Aphakia Treatment Study
Predicting Factor of Visual Outcome in Unilateral Idiopathic Cataract Surgery in Patients Aged 3 to 10 Years
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(4):273-280 https://doi.org/10.3341/kjo.2017.0113 Original Article Predicting Factor of Visual Outcome in Unilateral Idiopathic Cataract Surgery
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(4):273-280 https://doi.org/10.3341/kjo.2017.0113 Original Article Predicting Factor of Visual Outcome in Unilateral Idiopathic Cataract Surgery
Incidence and Risk Factors of Early-onset Glaucoma following Pediatric Cataract Surgery in Egyptian Children: One-year Study
 Ghada I Gawdat et al ORIGINAL ARTICLE 10.5005/jp-journals-10028-1229 following Pediatric Cataract Surgery in Egyptian Children: One-year Study 1 Ghada I Gawdat, 2 Maha M Youssef, 3 Nermeen M Bahgat, 4
Ghada I Gawdat et al ORIGINAL ARTICLE 10.5005/jp-journals-10028-1229 following Pediatric Cataract Surgery in Egyptian Children: One-year Study 1 Ghada I Gawdat, 2 Maha M Youssef, 3 Nermeen M Bahgat, 4
Shedding Light on Pediatric Cataracts. Kimberly G. Yen, MD Associate Professor of Ophthalmology Texas Children s Hospital
 Shedding Light on Pediatric Cataracts Kimberly G. Yen, MD Associate Professor of Ophthalmology Texas Children s Hospital A newborn infant presents with bilateral white cataracts. What is the best age to
Shedding Light on Pediatric Cataracts Kimberly G. Yen, MD Associate Professor of Ophthalmology Texas Children s Hospital A newborn infant presents with bilateral white cataracts. What is the best age to
Pediatric cataract. Nikos Kozeis MD, PhD, FICO, FEBO, MRCOphth. Surgical challenges and postoperative complications
 Pediatric cataract Surgical challenges and postoperative complications Nikos Kozeis MD, PhD, FICO, FEBO, MRCOphth Consultant Paediatric Ophthalmologist Thessaloniki, Greece Pediatric Cataract 2.4 / 10000
Pediatric cataract Surgical challenges and postoperative complications Nikos Kozeis MD, PhD, FICO, FEBO, MRCOphth Consultant Paediatric Ophthalmologist Thessaloniki, Greece Pediatric Cataract 2.4 / 10000
Retinal detachment following surgery for congenital cataract: presentation and outcomes
 (2005) 19, 317 321 & 2005 Nature Publishing Group All rights reserved 0950-222X/05 $30.00 www.nature.com/eye Retinal detachment following surgery for congenital cataract: presentation and outcomes D Yorston,
(2005) 19, 317 321 & 2005 Nature Publishing Group All rights reserved 0950-222X/05 $30.00 www.nature.com/eye Retinal detachment following surgery for congenital cataract: presentation and outcomes D Yorston,
Learn Connect Succeed. JCAHPO Regional Meetings 2015
 Learn Connect Succeed JCAHPO Regional Meetings 2015 Pediatric Cataracts: Complicated Cases and Controversies M. Edward Wilson, M.D. N. Edgar Miles Professor of Ophthalmology and Pediatrics Storm Eye Institute
Learn Connect Succeed JCAHPO Regional Meetings 2015 Pediatric Cataracts: Complicated Cases and Controversies M. Edward Wilson, M.D. N. Edgar Miles Professor of Ophthalmology and Pediatrics Storm Eye Institute
The Evolving Story of Aphakic and Pseudophakic Glaucoma after Cataract Surgery in Children: What s New?
 358 Kerala Journal of Ophthalmology Vol. XXI, No. 4 MAJOR REVIEW The Evolving Story of Aphakic and Pseudophakic Glaucoma after Cataract Surgery in Children: What s New? Dr. Ghada Abdel Hafez MD, Dr. Rupal
358 Kerala Journal of Ophthalmology Vol. XXI, No. 4 MAJOR REVIEW The Evolving Story of Aphakic and Pseudophakic Glaucoma after Cataract Surgery in Children: What s New? Dr. Ghada Abdel Hafez MD, Dr. Rupal
Visual Function Following Congenital Cataract Surgery
 Visual Function Following Congenital Cataract Surgery Misao Yamamoto, Murat Dogru, Makoto Nakamura, Hiroko Shirabe, Yasutomo Tsukahara, Yoshibumi Sekiya Department of Ophthalmology, Kobe University School
Visual Function Following Congenital Cataract Surgery Misao Yamamoto, Murat Dogru, Makoto Nakamura, Hiroko Shirabe, Yasutomo Tsukahara, Yoshibumi Sekiya Department of Ophthalmology, Kobe University School
Posterior Chamber Intraocular Lens Implantation in Pediatric Cataract with Microcornea and/or Microphthalmos
 Posterior Chamber Intraocular Lens Implantation in Pediatric Cataract with Microcornea and/or Microphthalmos Young Suk Yu, MD 1,2, Seong-Joon Kim, MD 1,2, Ho Kyoung Choung, MD 3 Department of Ophthalmology,
Posterior Chamber Intraocular Lens Implantation in Pediatric Cataract with Microcornea and/or Microphthalmos Young Suk Yu, MD 1,2, Seong-Joon Kim, MD 1,2, Ho Kyoung Choung, MD 3 Department of Ophthalmology,
IOL Power Calculation for Children
 1 IOL Power Calculation for Children Rupal H. Trivedi, MD MSCR M. Edward Wilson, MD The authors have no financial interest in the subject matter of this presentation. Intraocular lens (IOL) implantation
1 IOL Power Calculation for Children Rupal H. Trivedi, MD MSCR M. Edward Wilson, MD The authors have no financial interest in the subject matter of this presentation. Intraocular lens (IOL) implantation
Among adults, it is well-known that the risk of retinal
 Lens Risk of Retinal Detachment After Pediatric Cataract Surgery Birgitte Haargaard, 1,2 Elisabeth W. Andersen, 1 Anna Oudin, 1 Gry Poulsen, 1 Jan Wohlfahrt, 1 Morten la Cour, 2 and Mads Melbye 1 1 Department
Lens Risk of Retinal Detachment After Pediatric Cataract Surgery Birgitte Haargaard, 1,2 Elisabeth W. Andersen, 1 Anna Oudin, 1 Gry Poulsen, 1 Jan Wohlfahrt, 1 Morten la Cour, 2 and Mads Melbye 1 1 Department
Postcataract surgery outcome in a series of infants and children with Down syndrome
 The Children s University Hospital, Temple Street, Dublin 1, Ireland Correspondence to: Professor M O Keefe, Eye Department, The Children s University Hospital, Temple Street, Dublin 1, Ireland; mokeefe@materprivate.ie
The Children s University Hospital, Temple Street, Dublin 1, Ireland Correspondence to: Professor M O Keefe, Eye Department, The Children s University Hospital, Temple Street, Dublin 1, Ireland; mokeefe@materprivate.ie
Paediatric cataract: IOL vs aphakia. Νikolas G. Ziakas Aristotle University of Thessaloniki
 Paediatric cataract: IOL vs aphakia Νikolas G. Ziakas Aristotle University of Thessaloniki 2017 Cataract surgery in children The aim of pediatric cataract surgery is to provide and maintain a clear visual
Paediatric cataract: IOL vs aphakia Νikolas G. Ziakas Aristotle University of Thessaloniki 2017 Cataract surgery in children The aim of pediatric cataract surgery is to provide and maintain a clear visual
Treating Amblyopia in Aphakic and Pseudophakic Children
 Treating Amblyopia in Aphakic and Pseudophakic Children Scott R. Lambert, M.D. ABSTRACT Introduction Amblyopia is the leading cause of reduced vision in children following cataract surgery. It may develop
Treating Amblyopia in Aphakic and Pseudophakic Children Scott R. Lambert, M.D. ABSTRACT Introduction Amblyopia is the leading cause of reduced vision in children following cataract surgery. It may develop
One-Year Strabismus Outcomes in the Infant Aphakia Treatment Study
 One-Year Strabismus Outcomes in the Infant Aphakia Treatment Study Erick D. Bothun, University of Minnesota Julia Cleveland, Emory University Michael Lynn, Emory University Stephen P. Christiansen, Boston
One-Year Strabismus Outcomes in the Infant Aphakia Treatment Study Erick D. Bothun, University of Minnesota Julia Cleveland, Emory University Michael Lynn, Emory University Stephen P. Christiansen, Boston
Journal of Ophthalmology & Clinical Research
 Research Article Primary and Secondary Intraocular Lens Implantation in Congenital Cataract Surgery: A Retrospective Comparative Study of the Visual Outcomes Alhawsawi Abrar 1*, Alhibshi Nizar 2, Maniyar
Research Article Primary and Secondary Intraocular Lens Implantation in Congenital Cataract Surgery: A Retrospective Comparative Study of the Visual Outcomes Alhawsawi Abrar 1*, Alhibshi Nizar 2, Maniyar
The Management of Infant Aphakia
 The Management of Infant Aphakia Christina Twardowski O.D., FAAO Please silence all mobile devices and remove items from chairs so others can sit. Unauthorized recording of this session is prohibited.
The Management of Infant Aphakia Christina Twardowski O.D., FAAO Please silence all mobile devices and remove items from chairs so others can sit. Unauthorized recording of this session is prohibited.
Pediatric Eye Disease Investigator Group. Pediatric Cataract Surgery Outcomes Registry. Version 1.0 December 2, 2011
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Pediatric Eye Disease Investigator Group Pediatric Cataract Surgery Outcomes Registry Version 1.0 December 2, 2011 Print Date: 03/06/12
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Pediatric Eye Disease Investigator Group Pediatric Cataract Surgery Outcomes Registry Version 1.0 December 2, 2011 Print Date: 03/06/12
Visual Impairment Secondary to Congenital Cataracts: A Case Report
 Visual Impairment Secondary to Congenital Cataracts: A Case Report Karen Kehbein, OD Big Rapids, Michigan Abstract Background: Congenital cataracts can lead to severe effects on the development of the
Visual Impairment Secondary to Congenital Cataracts: A Case Report Karen Kehbein, OD Big Rapids, Michigan Abstract Background: Congenital cataracts can lead to severe effects on the development of the
Structural changes of the anterior chamber following cataract surgery during infancy
 Structural changes of the anterior chamber following cataract surgery during infancy Matthew Nguyen, Emory University Marla Shainberg, Emory University Allen Beck, Emory University Scott Lambert, Emory
Structural changes of the anterior chamber following cataract surgery during infancy Matthew Nguyen, Emory University Marla Shainberg, Emory University Allen Beck, Emory University Scott Lambert, Emory
Objectives. Tubes, Ties and Videotape: Financial Disclosure. Five Year TVT Results IOP Similar
 Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
The outcome of congenital cataract surgery in Kuwait
 Saudi Journal of Ophthalmology (2011) 25, 295 299 King Saud University Saudi Journal of Ophthalmology www.saudiophthaljournal.com www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE The outcome of congenital
Saudi Journal of Ophthalmology (2011) 25, 295 299 King Saud University Saudi Journal of Ophthalmology www.saudiophthaljournal.com www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE The outcome of congenital
Institution: Glick Eye Institute, Department of Ophthalmology, Indiana University School of Medicine
 Comparison of Circumferential and Traditional Trabeculotomy in Pediatric Glaucoma Maria E. Lim MD, Daniel E. Neely MD, Jingyun Wang, PhD, Kathryn M. Haider MD, Heather A. Smith MD, David A. Plager MD Glick
Comparison of Circumferential and Traditional Trabeculotomy in Pediatric Glaucoma Maria E. Lim MD, Daniel E. Neely MD, Jingyun Wang, PhD, Kathryn M. Haider MD, Heather A. Smith MD, David A. Plager MD Glick
Evaluation of Changing Axial Length in Eyes after Paediatric Cataract Surgery.
 DOI: 10.21276/aimdr.2018.4.5.OT1 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Evaluation of Changing Axial Length in Eyes after Paediatric Cataract Surgery. Mamta Singh 1, B P Sinha 2, Deepak
DOI: 10.21276/aimdr.2018.4.5.OT1 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Evaluation of Changing Axial Length in Eyes after Paediatric Cataract Surgery. Mamta Singh 1, B P Sinha 2, Deepak
2/26/2017. Sameh Galal. M.D, FRCS Glasgow. Lecturer of Ophthalmology Research Institute of Ophthalmology
 Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Lens Embryology. Lens. Pediatric Cataracts. Cataract 2/15/2017. Lens capsule size is fairly constant. Stable vs. progressive
 Lens Embryology Catherine O. Jordan M.D. Surface ectoderm overlying optic vesicle Day 28 begins to form End of week 5 lens vesicle is formed Embryonic nucleus formed at week 7 Weeks 12-14 anterior Y and
Lens Embryology Catherine O. Jordan M.D. Surface ectoderm overlying optic vesicle Day 28 begins to form End of week 5 lens vesicle is formed Embryonic nucleus formed at week 7 Weeks 12-14 anterior Y and
Sensorimotor outcomes by age 5 years after monocular cataract surgery in the Infant Aphakia Treatment Study (IATS)
 Sensorimotor outcomes by age 5 years after monocular cataract surgery in the Infant Aphakia Treatment Study (IATS) Erick D. Bothun, University of Minnesota Michael Lynn, Emory University Stephen P. Christiansen,
Sensorimotor outcomes by age 5 years after monocular cataract surgery in the Infant Aphakia Treatment Study (IATS) Erick D. Bothun, University of Minnesota Michael Lynn, Emory University Stephen P. Christiansen,
Cataract is one of the major causes of childhood. Primary Intraocular Lens Implantation for Unilateral Idiopathic Cataract in Children
 Original Article 52 Primary Intraocular Lens Implantation for Unilateral Idiopathic Cataract in Children Meng-Ling Yang 1,2, MD; Ken-Kuo Lin 2, MD; Chiun-Ho Hou 2, MD; Yu-Sung Liang 3, MD; Jiahn-Shing
Original Article 52 Primary Intraocular Lens Implantation for Unilateral Idiopathic Cataract in Children Meng-Ling Yang 1,2, MD; Ken-Kuo Lin 2, MD; Chiun-Ho Hou 2, MD; Yu-Sung Liang 3, MD; Jiahn-Shing
Vanderbilt Eye Institute Clinical Trials
 April, 2010 Vanderbilt Eye Institute Clinical Trials Ophthalmology Actively Recruiting Studies For information on our clinical trials and other studies, please contact: Sandy Owings, COA, CCRP Clinic Director
April, 2010 Vanderbilt Eye Institute Clinical Trials Ophthalmology Actively Recruiting Studies For information on our clinical trials and other studies, please contact: Sandy Owings, COA, CCRP Clinic Director
Characteristics of Children With Primary Congenital Glaucoma Receiving Trabeculotomy and Goniotomy
 Characteristics of Children With Primary Congenital Glaucoma Receiving Trabeculotomy and Goniotomy Lekha Mukkamala, MD; Robert Fechtner, MD; Bart Holland, MPH, PhD; Albert S. Khouri, MD ABSTRACT Purpose:
Characteristics of Children With Primary Congenital Glaucoma Receiving Trabeculotomy and Goniotomy Lekha Mukkamala, MD; Robert Fechtner, MD; Bart Holland, MPH, PhD; Albert S. Khouri, MD ABSTRACT Purpose:
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs
 The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation
 Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation Masaru Inatani*, Hidenobu Tanihara, Takahito Muto*, Megumi Honjo*,
Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation Masaru Inatani*, Hidenobu Tanihara, Takahito Muto*, Megumi Honjo*,
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Childhood Glaucoma. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Childhood Glaucoma. These podcasts are designed to give medical students an overview of key topics in pediatrics.
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Management of Congenital Cataract Surgery. Dr. Vaishali Vasavada, MS. Dr. Abhay R. Vasavada, MS, FRCS (England) Raghudeep Eye Hospital, India
 Management of Congenital Cataract Surgery Dr. Vaishali Vasavada, MS Dr. Abhay R. Vasavada, MS, FRCS (England) Raghudeep Eye Hospital, India Congenital cataract surgery is a complex issue best left to surgeons
Management of Congenital Cataract Surgery Dr. Vaishali Vasavada, MS Dr. Abhay R. Vasavada, MS, FRCS (England) Raghudeep Eye Hospital, India Congenital cataract surgery is a complex issue best left to surgeons
Early Treatment of Congenital Unilateral Cataract Minimizes Unequal Competition
 Early Treatment of Congenital Unilateral Cataract Minimizes Unequal Competition 12 Eileen E. Birch, 12 David Stager? Joel Leffler? and David Weakley 23 PURPOSE. Dense congenital unilateral cataracts may
Early Treatment of Congenital Unilateral Cataract Minimizes Unequal Competition 12 Eileen E. Birch, 12 David Stager? Joel Leffler? and David Weakley 23 PURPOSE. Dense congenital unilateral cataracts may
CLINICAL SCIENCES. Glaucoma-Related Adverse Events in the Infant Aphakia Treatment Study
 ONLINE FIRST CLINICAL SCIENCES Glaucoma-Related Adverse Events in the Infant Aphakia Treatment Study 1-Year Results Allen D. Beck, MD; Sharon F. Freedman, MD; Michael J. Lynn, MS; Erick Bothun, MD; Daniel
ONLINE FIRST CLINICAL SCIENCES Glaucoma-Related Adverse Events in the Infant Aphakia Treatment Study 1-Year Results Allen D. Beck, MD; Sharon F. Freedman, MD; Michael J. Lynn, MS; Erick Bothun, MD; Daniel
Saemah Nuzhat Zafar, Sorath Noorani Siddiqui, Ayesha Khan 1
 Original Article Effects of Artisan aphakic intraocular lens on central corneal thickness and intra ocular pressure in pediatric eyes with crystalline subluxated lenses Saemah Nuzhat Zafar, Sorath Noorani
Original Article Effects of Artisan aphakic intraocular lens on central corneal thickness and intra ocular pressure in pediatric eyes with crystalline subluxated lenses Saemah Nuzhat Zafar, Sorath Noorani
Case Study. Monocular Malignant Melanoma
 Case Study Monocular Malignant Melanoma Case History A 52 year old Caucasian female presented with a number of naevi on the skin and a right ciliary body malignant melanoma twelve years ago and had an
Case Study Monocular Malignant Melanoma Case History A 52 year old Caucasian female presented with a number of naevi on the skin and a right ciliary body malignant melanoma twelve years ago and had an
Refractive Changes after Removal of Anterior IOLs in Temporary Piggyback IOL Implantation for Congenital Cataracts
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(2):93-97 http://dx.doi.org/10.3341/kjo.2013.27.2.93 Original Article Refractive Changes after Removal of Anterior IOLs in Temporary Piggyback
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(2):93-97 http://dx.doi.org/10.3341/kjo.2013.27.2.93 Original Article Refractive Changes after Removal of Anterior IOLs in Temporary Piggyback
Open globe injuries in children: factors predictive of a poor final visual acuity
 (2009) 23, 621 625 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Open globe injuries in children: factors predictive of a poor final visual acuity A Gupta,
(2009) 23, 621 625 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Open globe injuries in children: factors predictive of a poor final visual acuity A Gupta,
Pediatric Cataract Surgery: Consensus And Controversies
 Major Review Satish Thomas, MD (AIIMS) DNB Pediatric Cataract Surgery: Consensus And Controversies Abstract Pediatric cataract surgery has improved significantly in terms of outcome over the last 2 decades
Major Review Satish Thomas, MD (AIIMS) DNB Pediatric Cataract Surgery: Consensus And Controversies Abstract Pediatric cataract surgery has improved significantly in terms of outcome over the last 2 decades
Anterior segment imaging
 Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
Role of ultrasound in congenital cataract: Our experience
 Role of ultrasound in congenital cataract: Our experience Ayat Aziz Al-Alwan (1) Hazim Kamil Haddad (1) Rana Ahmad Alkrimeen (1) Mohammad Jalal Alsa aideh (2) Mu taz Ghalib Halasah (1) (1) Jordanian Royal
Role of ultrasound in congenital cataract: Our experience Ayat Aziz Al-Alwan (1) Hazim Kamil Haddad (1) Rana Ahmad Alkrimeen (1) Mohammad Jalal Alsa aideh (2) Mu taz Ghalib Halasah (1) (1) Jordanian Royal
Trabeculectomy combined with cataract extraction: a follow-up study
 British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
Practical Care of the Cataract Patient with Retinal Disease
 Practical Care of the Cataract Patient with Retinal Disease Brooks R. Alldredge, OD, FAAO Kelly L. Cyr, OD, FAAO The Retina Center Eye Associates of New Mexico 4411 The 25 Way NE, Suite 325 Albuquerque,
Practical Care of the Cataract Patient with Retinal Disease Brooks R. Alldredge, OD, FAAO Kelly L. Cyr, OD, FAAO The Retina Center Eye Associates of New Mexico 4411 The 25 Way NE, Suite 325 Albuquerque,
Management of monocular congenital cataracts
 Management of monocular congenital cataracts SCOTT R. LAMBERT Scott R. Lambert, MD Emory Eye Center Emory University School of Medicine 1365-B Clifton Road, NE Suite 4610 Atlanta GA 30322, USA Tel: +1
Management of monocular congenital cataracts SCOTT R. LAMBERT Scott R. Lambert, MD Emory Eye Center Emory University School of Medicine 1365-B Clifton Road, NE Suite 4610 Atlanta GA 30322, USA Tel: +1
OVERVIEW OF OCULAR MANAGEMENT IN MARFAN SYNDROME
 OVERVIEW OF OCULAR MANAGEMENT IN MARFAN SYNDROME Prepared by: Deborah Alcorn, MD, Dianna Milewicz, MD, and Irene H Maumenee, MD OCULAR FEATURES OF MARFAN SYNDROME Marfan syndrome is a dominantly inherited
OVERVIEW OF OCULAR MANAGEMENT IN MARFAN SYNDROME Prepared by: Deborah Alcorn, MD, Dianna Milewicz, MD, and Irene H Maumenee, MD OCULAR FEATURES OF MARFAN SYNDROME Marfan syndrome is a dominantly inherited
ASCRS 2016 Instructional Course Mastering Femtosecond Laser Assisted Phacoemulsification. An Evidence-Based Review
 ASCRS 2016 Instructional Course 07-410 Mastering Femtosecond Laser Assisted Phacoemulsification An Evidence-Based Review TIMOTHY V ROBERTS MBBS (NSW), MMed (Syd), FRANZCO, FRACS, GAICD Vision Eye Institute,
ASCRS 2016 Instructional Course 07-410 Mastering Femtosecond Laser Assisted Phacoemulsification An Evidence-Based Review TIMOTHY V ROBERTS MBBS (NSW), MMed (Syd), FRANZCO, FRACS, GAICD Vision Eye Institute,
Persistent Hyperplastic Primary Vitreous Found at the Time of Cataract Surgery in an Adult
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Report Persistent Hyperplastic Primary Vitreous Found at the Time of Cataract Surgery in an Adult Ming Chen 1, John Drouilhet 2 and Justin Karlin 3 * 1 University
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Report Persistent Hyperplastic Primary Vitreous Found at the Time of Cataract Surgery in an Adult Ming Chen 1, John Drouilhet 2 and Justin Karlin 3 * 1 University
SUMMARY: 1) Why is pediatric vision screening important?
 SUMMARY: In January 2016 a new joint policy statement from the American Academy of Pediatrics (AAP), American Academy of Ophthalmology (AAO), American Association for Pediatric Ophthalmology and Strabismus
SUMMARY: In January 2016 a new joint policy statement from the American Academy of Pediatrics (AAP), American Academy of Ophthalmology (AAO), American Association for Pediatric Ophthalmology and Strabismus
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Cataract Extraction and Primary Hydrophobic Acrylic Intraocular Lens Implantation in Infants
 Cataract Extraction and Primary Hydrophobic Acrylic Intraocular Lens Implantation in Infants Samuray Tuncer, MD, Ahmet Gucukoglu, MD and Nilufer Gozum, MD Purpose: We sought to report the incidence of
Cataract Extraction and Primary Hydrophobic Acrylic Intraocular Lens Implantation in Infants Samuray Tuncer, MD, Ahmet Gucukoglu, MD and Nilufer Gozum, MD Purpose: We sought to report the incidence of
WGA. The Global Glaucoma Network
 The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz)
 PATIENT INFORMATION BOOKLET PAGE 1 OF 32 VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL
PATIENT INFORMATION BOOKLET PAGE 1 OF 32 VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL
Primary Angle Closure Glaucoma
 www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Goals. Glaucoma PARA PEARL TO DO. Vision Loss with Glaucoma
 Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Bilateral Microphthalmos Associated with Papillomacular Fold, Severe Hyperopia and Steep Cornea
 Bilateral Microphthalmos Associated with Papillomacular Fold, Severe Hyperopia and Steep Cornea Mojtaba Abrishami, MD 1 Alireza Maleki, MD 2 Ali Hamidian-Shoormasti, MD 3 Mostafa Abrishami, MD 4 Abstract
Bilateral Microphthalmos Associated with Papillomacular Fold, Severe Hyperopia and Steep Cornea Mojtaba Abrishami, MD 1 Alireza Maleki, MD 2 Ali Hamidian-Shoormasti, MD 3 Mostafa Abrishami, MD 4 Abstract
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Intraocular lens implantation in unilateral congenital cataract with minimal levels of persistent fetal vasculature in the first 18 months of life
 Matsuo SpringerPlus 2014, 3:361 a SpringerOpen Journal RESEARCH Open Access Intraocular lens implantation in unilateral congenital cataract with minimal levels of persistent fetal vasculature in the first
Matsuo SpringerPlus 2014, 3:361 a SpringerOpen Journal RESEARCH Open Access Intraocular lens implantation in unilateral congenital cataract with minimal levels of persistent fetal vasculature in the first
THE OUTCOME OF STRABISMUS SURGERY IN CHILDHOOD EXOTROPIA
 THE OUTCOME OF STRABISMUS SURGERY IN CHILDHOOD EXOTROPIA J. M. KEENAN and H. E. WILLSHAW Birmingham SUMMARY The results of squint surgery in 42 children with primary, non-paralytic, childhood are analysed.
THE OUTCOME OF STRABISMUS SURGERY IN CHILDHOOD EXOTROPIA J. M. KEENAN and H. E. WILLSHAW Birmingham SUMMARY The results of squint surgery in 42 children with primary, non-paralytic, childhood are analysed.
Glaucoma. Cornea. Iris
 Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
GENERAL INFORMATION GLAUCOMA GLAUCOMA
 GENERAL INFORMATION GLAUCOMA GLAUCOMA WHAT IS GLAUCOMA? Glaucoma is commonly known as the sneak thief of sight because it can cause irreversible vision loss without any obvious symptoms. The term glaucoma
GENERAL INFORMATION GLAUCOMA GLAUCOMA WHAT IS GLAUCOMA? Glaucoma is commonly known as the sneak thief of sight because it can cause irreversible vision loss without any obvious symptoms. The term glaucoma
Pediatric traumatic cataract Presentation and Management. Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017
 Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T.
 STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
Eye diseases in infancy and early childhood
 Eye diseases in infancy and early childhood Contents: a. Visual development and assessment of vision in infancy and childhood. b. The infant with whitish pupil. c. The infant with watery eye. d. Prematurity
Eye diseases in infancy and early childhood Contents: a. Visual development and assessment of vision in infancy and childhood. b. The infant with whitish pupil. c. The infant with watery eye. d. Prematurity
Contact Lenses for Infants: Indication, Evaluation, and Technique
 Contact Lenses for Infants: Indication, Evaluation, and Technique Elaine Chen, OD, FAAO, FSLS Southern California College of Optometry Marshall B. Ketchum University Maureen Plaumann, OD, FAAO The Ohio
Contact Lenses for Infants: Indication, Evaluation, and Technique Elaine Chen, OD, FAAO, FSLS Southern California College of Optometry Marshall B. Ketchum University Maureen Plaumann, OD, FAAO The Ohio
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Pachymetry Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Pachymetry Professional Institutional Original Effective Date: March 11, 2004 Original Effective
Pachymetry Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Pachymetry Professional Institutional Original Effective Date: March 11, 2004 Original Effective
Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures
 Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
IMPLANTATION OF AN INTRAOCUlar
 CLINICAL SCIENCES Keratometry in Pediatric Eyes With Cataract Rupal H. Trivedi, MD, MSCR; M. Edward Wilson, MD Objectives: To report the keratometry data of pediatric cataractous eyes (randomly selected
CLINICAL SCIENCES Keratometry in Pediatric Eyes With Cataract Rupal H. Trivedi, MD, MSCR; M. Edward Wilson, MD Objectives: To report the keratometry data of pediatric cataractous eyes (randomly selected
Temporary Piggyback Intraocular Lens Implantation Versus Single Intraocular Lens Implantation in Congenital Cataracts: Long-Term Clinical Outcomes
 Lens Temporary Piggyback Intraocular Lens Implantation Versus Single Intraocular Lens Implantation in Congenital Cataracts: Long-Term Clinical Outcomes Sungsoon Hwang, 1 Dong Hui Lim, 1,2 Soomin Lee, 1
Lens Temporary Piggyback Intraocular Lens Implantation Versus Single Intraocular Lens Implantation in Congenital Cataracts: Long-Term Clinical Outcomes Sungsoon Hwang, 1 Dong Hui Lim, 1,2 Soomin Lee, 1
Endo Optiks. Clinical Publication Summaries
 Endo Optiks Clinical Publication Summaries Effective. Safe. Simple. Four scientific studies demonstrating the proven clinical benefits of combined ECP and cataract surgery. ECP is an Effective, Safe, and
Endo Optiks Clinical Publication Summaries Effective. Safe. Simple. Four scientific studies demonstrating the proven clinical benefits of combined ECP and cataract surgery. ECP is an Effective, Safe, and
SILICONE OIL INJECTION INDUCED GLAUCOMA: INCIDENCE AND MANAGEMENT
 SILICONE OIL INJECTION INDUCED GLAUCOMA: INCIDENCE AND MANAGEMENT Ahmad Elsayed Hudieb Department of Ophthalmology Faculty of Medicine, Al- Azhar University ABSTRACT Purpose: Intravitreal silicone oil
SILICONE OIL INJECTION INDUCED GLAUCOMA: INCIDENCE AND MANAGEMENT Ahmad Elsayed Hudieb Department of Ophthalmology Faculty of Medicine, Al- Azhar University ABSTRACT Purpose: Intravitreal silicone oil
Glaucoma What You Should Know
 Glaucoma What You Should Know U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute The National Eye Institute (NEI) conducts and supports research that leads
Glaucoma What You Should Know U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute The National Eye Institute (NEI) conducts and supports research that leads
The visual outcome after implantation of the Multifocal Intra Ocular Lens. Dr.Bhargav Dave National Institute of Ophthalmology Pune
 The visual outcome after implantation of the Multifocal Intra Ocular Lens Dr.Bhargav Dave National Institute of Ophthalmology Pune 1 The era of cataract surgery has come leaps and bounds since the inception
The visual outcome after implantation of the Multifocal Intra Ocular Lens Dr.Bhargav Dave National Institute of Ophthalmology Pune 1 The era of cataract surgery has come leaps and bounds since the inception
Prakash S 1*, Giridhar 2, Harshila Jain 3. Original Research Article. Abstract
 Original Research Article Efficacy of plasma knife assisted posterior capsulotomy versus manual primary posterior capsulorhexis in preventing visual axis opacification in pediatric cataract surgery: A
Original Research Article Efficacy of plasma knife assisted posterior capsulotomy versus manual primary posterior capsulorhexis in preventing visual axis opacification in pediatric cataract surgery: A
Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature of
 1.2.4 OPHTHALMOLOGICAL ABNORMALITIES Ocular abnormalities are well documented in patients with NPS 6 62 81 95. 1.2.4.1 Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature
1.2.4 OPHTHALMOLOGICAL ABNORMALITIES Ocular abnormalities are well documented in patients with NPS 6 62 81 95. 1.2.4.1 Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature
Anisometropia at Age 5 Years After Unilateral Intraocular Lens Implantation During Infancy in the Infant Aphakia Treatment Study
 Anisometropia at Age 5 Years After Unilateral Intraocular Lens Implantation During Infancy in the Infant Aphakia Treatment Study David Weakley, University of Texas Southwestern Medical Center George A
Anisometropia at Age 5 Years After Unilateral Intraocular Lens Implantation During Infancy in the Infant Aphakia Treatment Study David Weakley, University of Texas Southwestern Medical Center George A
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
Landmark Tube Trials
 SECTION EDITOR: BARBARA SMIT, MD, PhD Landmark Tube Trials A review of key findings from recent multicenter randomized clinical trials involving tube shunts. BY AMBIKA HOGUET, MD, AND STEVEN J. GEDDE,
SECTION EDITOR: BARBARA SMIT, MD, PhD Landmark Tube Trials A review of key findings from recent multicenter randomized clinical trials involving tube shunts. BY AMBIKA HOGUET, MD, AND STEVEN J. GEDDE,
WORLD GLAUCOMA WEEK What is Glaucoma? Can I develop glaucoma if I have increased eye pressure?
 WORLD GLAUCOMA WEEK What is Glaucoma? Glaucoma is a group of diseases that damage the optic nerve and can result in gradual vision loss and blindness. However, with early detection and treatment, you can
WORLD GLAUCOMA WEEK What is Glaucoma? Glaucoma is a group of diseases that damage the optic nerve and can result in gradual vision loss and blindness. However, with early detection and treatment, you can
CHARTING THE NEW COURSE FOR MIGS
 CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
THE CHRONIC GLAUCOMAS
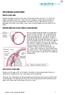 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
A Retrospective Analysis of Refractive Changes in Pediatric Pseudophakia
 43 Abstract A Retrospective Analysis of Refractive Changes in Pediatric Pseudophakia Manmitha Reddy Muppidi, Sairani Karanam, Akhil Bevara Sankara Eye Hospital, Pedakakani, Guntur, Andhra Pradesh, India
43 Abstract A Retrospective Analysis of Refractive Changes in Pediatric Pseudophakia Manmitha Reddy Muppidi, Sairani Karanam, Akhil Bevara Sankara Eye Hospital, Pedakakani, Guntur, Andhra Pradesh, India
Clinical study of traumatic cataract and its management
 Clinical study of traumatic cataract and its management Original article Manjula Mangane, M.R. Pujari, Chethan N. Murthy Department of Ophthalmology, Basaweshwar Teaching and General Hospital, Gulbarga,
Clinical study of traumatic cataract and its management Original article Manjula Mangane, M.R. Pujari, Chethan N. Murthy Department of Ophthalmology, Basaweshwar Teaching and General Hospital, Gulbarga,
Chronicity. Narrow Minded. Course Outline. Acute angle closure. Subacute angle closure. Classification of Angle Closure 5/19/2014
 Chronicity Narrow Minded The management of narrow angles in the optometric practice Acute Subacute Chronic Aaron McNulty, OD, FAAO Course Outline Classification of Angle Closure Evaluation of narrow angles
Chronicity Narrow Minded The management of narrow angles in the optometric practice Acute Subacute Chronic Aaron McNulty, OD, FAAO Course Outline Classification of Angle Closure Evaluation of narrow angles
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
