Lorazepam vs Diazepam for Pediatric Status Epilepticus A Randomized Clinical Trial
|
|
|
- Marian Byrd
- 5 years ago
- Views:
Transcription
1 Research Original Investigation vs for Pediatric Status Epilepticus A Randomized Clinical Trial James M. Chamberlain, MD; Pamela Okada, MD; Maija Holsti, MD; Prashant Mahajan, MD, MBA; Kathleen M. Brown, MD; Cheryl Vance, MD; Victor Gonzalez, MD; Richard Lichenstein, MD; Rachel Stanley, MD, MPH; David C. Brousseau, MD, MPH; Joseph Grubenhoff, MD; Roger Zemek, MD; David W. Johnson, MD; Traci E. Clemons, PhD; Jill Baren, MD, MPH; for the Pediatric Emergency Care Applied Research Network (PECARN) IMPORTANCE Benzodiazepines are considered first-line therapy for pediatric status epilepticus. Some studies suggest that lorazepam may be more effective or safer than diazepam, but lorazepam is not Food and Drug Administration approved for this indication. Supplemental content at jama.com OBJECTIVE To test the hypothesis that lorazepam has better efficacy and safety than diazepam for treating pediatric status epilepticus. DESIGN, SETTING, AND PARTICIPANTS This double-blind, randomized clinical trial was conducted from March 1, 2008, to March 14, Patients aged 3 months to younger than 18 years with convulsive status epilepticus presenting to 1 of 11 US academic pediatric emergency departments were eligible. There were 273 patients; 140 randomized to diazepam and 133 to lorazepam. INTERVENTIONS Patients received either 0.2 mg/kg of diazepam or 0.1 mg/kg of lorazepam intravenously, with half this dose repeated at 5 minutes if necessary. If status epilepticus continued at 12 minutes, fosphenytoin was administered. MAIN OUTCOMES AND MEASURES The primary efficacy outcome was cessation of status epilepticus by 10 minutes without recurrence within 30 minutes. The primary safety outcome was the performance of assisted ventilation. Secondary outcomes included rates of seizure recurrence and sedation and times to cessation of status epilepticus and return to baseline mental status. Outcomes were measured 4 hours after study medication administration. RESULTS Cessation of status epilepticus for 10 minutes without recurrence within 30 minutes occurred in 101 of 140 (72.1%) in the diazepam group and 97 of 133 (72.9%) in the lorazepam group, with an absolute efficacy difference of 0.8% (95% CI, 11.4% to 9.8%). Twenty-six patients in each group required assisted ventilation (16.0% given diazepam and 17.6% given lorazepam; absolute risk difference, 1.6%; 95% CI, 9.9% to 6.8%). There were no statistically significant differences in secondary outcomes except that lorazepam patients were more likely to be sedated (66.9% vs 50%, respectively; absolute risk difference, 16.9%; 95% CI, 6.1% to 27.7%). CONCLUSIONS AND RELEVANCE Among pediatric patients with convulsive status epilepticus, treatment with lorazepam did not result in improved efficacy or safety compared with diazepam. These findings do not support the preferential use of lorazepam for this condition. TRIAL REGISTRATION clinicaltrials.gov Identifier: NCT JAMA. 2014;311(16): doi: /jama Author Affiliations: Author affiliations are listed at the end of this article. Group Information: The Pediatric Emergency Care Applied Research Network (PECARN) members are listed at the end of the article. Corresponding Author: James M. Chamberlain, MD, Division of Emergency Medicine, Children s National Medical Center, 111 Michigan Ave NW, Washington, DC (jchamber@childrensnational.org) jama.com
2 vs for Pediatric SE Original Investigation Research Status epilepticus occurs approximately times in children annually in the United States, 1 and4to8children per 1000 have an episode of status epilepticus before age 15 years. 2 Rapid control of status epilepticus is desirable to avoid permanent neuronal injury and acute lifethreatening complications such as respiratory failure. Benzodiazepines are widely used as first-line pharmacologic agents, achieving lasting seizure control in up to 80% of patients. 3,4 Respiratory depression and failure are the most common life-threatening complications of benzodiazepine treatment in status epilepticus; data on its safety in children are limited. 5 and lorazepam are both effective in treating pediatric status epilepticus. 6 The Food and Drug Administration (FDA) has approved diazepam for the treatment of status epilepticus in children. However, despite many experts advocating its use, 5-9 lorazepam is not yet FDA approved for this indication. Potential advantages proposed in some studies of lorazepam include improved effectiveness in terminating convulsions, 10 longer duration of action compared with diazepam, 11 and lower incidence of respiratory depression. 4,12 Specific pediatric data comparing diazepam with lorazepam suggest that lorazepam might be superior, but they are limited to reports from single institutions or retrospective studies with small sample sizes, thus limiting generalizability. 12,13 A registry study of childhood convulsive status epilepticus in North London found lorazepam more effective than diazepam in stopping status epilepticus, but these data are difficult to interpret because lorazepam was administered intravenously while diazepam was administered rectally. 14 Other pediatric studies have found that the 2 medications are similar in efficacy 15,16 but there may be differences in safety. 12,16 Thus, there is no conclusive evidence to support lorazepam as a superior treatment and there is little consensus as to which is the preferred agent. 17 The Best Pharmaceuticals for Children Act was enacted to enhance pediatric clinical studies, leading to new pediatric labeling in accordance with FDA regulations. as a therapy for pediatric status epilepticus was chosen as a priority off-patent medication for which pediatric studies are needed. The purpose of this study was to test the hypothesis that lorazepam is superior in efficacy (primary efficacy hypothesis) and safety (primary safety hypothesis) to diazepam for the treatment of pediatric status epilepticus. Methods We conducted a double-blind, randomized clinical trial to compare the efficacy and safety of intravenous lorazepam with diazepam in children presenting to the emergency department (ED) with generalized convulsive status epilepticus. (PECARN); subsequently, we included 3 additional sites to enhance enrollment. Study Participants Children aged 3 months to younger than 18 years were eligible for inclusion if they exhibited generalized tonic-clonic status epilepticus. Status epilepticus was defined as either (1) 3 or more convulsions within the preceding hour and currently experiencing a convulsion; (2) 2 or more convulsions in succession with no recovery of consciousness and currently experiencing a convulsion; or (3) a current single convulsion of at least 5 minutes duration. Seizures may have started focally and then generalized; however, to be included, the patients had to have loss of consciousness and generalized tonicclonic seizures. These definitions are consistent with current standards for therapy. 7,18,19 Patients were excluded if they met any of the following criteria prior to medication administration: known pregnancy; hypotension; significant cardiac dysrhythmia; need for emergent surgical intervention and general anesthesia; known contraindication to benzodiazepine use; or benzodiazepine use within the preceding 7 days, including use of anticonvulsant medications by ambulance personnel. Patients were terminated from the study (early terminators) if the investigators discovered 1 of the exclusionary criteria after receiving study medication or if the family refused participation in the study. Efficacy and safety data were retained from early terminators in accordance with FDA regulations. Informed Consent Recognizing the need to include status epilepticus in patients with previously undiagnosed seizure disorders, patients were enrolled using the Exception from Informed Consent for Emergency Research, 21 CFR This federal regulation allows emergency research without prior consent under limited conditions and requires additional safeguards to protect the well-being of patients. 20 Thus, patients were randomized and treated prior to consent. After stabilization of the patient s clinical condition in conjunction with family support through the period of crisis, we approached families to discuss the study and obtain written consent for continued participation and collection of blood specimens for pharmacokinetic analyses. Patients from neurology practices with a known history of epilepsy were approached to obtain prospective informed consent prior to an actual episode of status epilepticus whenever possible. The FDA, the study sponsor (Eunice Kennedy Shriver National Institute of Child Health and Human Development), an external expert ethics advisory panel, and the institutional research review boards of the participating centers approved the Exception from Informed Consent for Emergency Research plan for the study. Setting We enrolled patients at 11 large academic pediatric hospitals in the United States. Initial recruitment of sites was from the Pediatric Emergency Care Applied Research Network Randomization and Study Medication Administration An age-stratified, permuted block randomization (1:1) scheme with block sizes of 4 in 3 age groups 3 months to younger than 3 years, 3 years to younger than 13 years, and jama.com JAMA April 23/30, 2014 Volume 311, Number
3 Research Original Investigation vs for Pediatric SE 13 years to younger than 18 years was incorporated. These age groups were chosen at the request of an expert panel of the FDA, which commissioned this trial. A medication nurse or pharmacist selected a vial of study medication from the medication-dispensing system sequentially based on the patient s age group. The medication nurse or pharmacist, independent of the treating team at the patient s bedside, used a dosing card to prepare the study medication based on estimated patient weight to deliver a final dose of 0.2 mg/kg of diazepam (maximum dose, 8 mg) or 0.1 mg/kg of lorazepam (maximum dose, 4 mg). To maintain blinding of the bedside clinicians, diluent was added to lorazepam so that the final medication volume was the same for both medications. Opaque syringe cylinders were used to prevent visualizing the medication. The medication was handed to the treating team, who administered it by slow intravenous (IV) push for 1 minute. The end of the IV push was defined as time 0. If a second dose was required for ongoing convulsions at 5 minutes, the dispensing and administration processes were repeated using half the initial dose. 21 If the patient had ongoing status epilepticus at 12 minutes, IV fosphenytoin or phenytoin, 15 to 20 mg/kg, was administered; phenobarbital, 15 to 20 mg/kg, was used if the patient was allergic to phenytoin. At 20 minutes, open-label treatment with anticonvulsants of choice based on clinician preference was allowed. Determination of Study Outcomes Efficacy The primary efficacy outcome was defined as cessation of status epilepticus within 10 minutes of the initial dose of study medication and a sustained absence of convulsions for 30 minutes. The end of status epilepticus was defined as the time when generalized convulsive activity stopped, provided that it was followed by return of consciousness within the 4-hour follow-up period. Recurrence of generalized convulsions without return of consciousness was considered ongoing status. Secondary efficacy end points included response latency (time to cessation of convulsions), need for a second dose of study medication, need for additional anticonvulsant medications for ongoing status, and sustained absence of convulsions for 60 minutes and 4 hours after receiving the study medication. Safety The primary safety outcome was severe respiratory depression within 4 hours of initial medication, which was defined as the need for assisted ventilation (bag-valve-mask ventilation or endotracheal intubation). Secondary safety end points included aspiration pneumonia, any degree of respiratory depression, time to return to baseline mental status, and sedation or agitation, as measured by the Riker Sedation- Agitation Scale. 22 The Riker scale ranges from 1 (deeply sedated, no response to stimuli) to 7 (dangerously agitated), with 4 representing normal baseline mental status (neither sedated nor agitated). The Riker scale was modified for use in preverbal children (etable in Supplement) and demonstrated internal and external validity prior to this study (data available on request). Patients were followed up for adverse events for up to 24 hours or until hospital discharge, whichever came first. A follow-up phone call was performed at 30 days to determine whether adverse events occurred after hospital discharge. All study outcomes were determined by the treating attending physician and were reviewed by the site principal investigator and the study principal investigator. Statistical Analyses The primary efficacy outcome included all patients who were randomized and met the definition of generalized convulsive status epilepticus. This group was defined because some patients received study medication but were not in generalized status. For patients who were enrolled more than once, only the first visit was included. For the primary safety outcome, an intention-to-treat analysis, including all randomized patients, was used. Additionally, per-protocol analyses of efficacy outcomes to account for 64 patients with significant protocol deviations were performed. Predefined protocol deviations included study medication dose administration outside a margin of ±30% of the desired dose, a second dose of study medication more than 9 minutes after the first dose, administration of a secondary anticonvulsant before 10 minutes, benzodiazepines within 2 hours prior to enrollment, and IV extravasation. Protocol violations also included 15 patients who were systematically randomized incorrectly because of a pharmacy error at a single site. Time to cessation of convulsions, time to new seizure activity, and time to recovery to baseline mental status are reported as median and interquartile range. Cox proportional hazards regression models for time-to-event analyses were developed for these secondary outcomes. The assumptions for proportional hazards models were met for all time-to-event outcomes. Patients who received second-line or third-line medications, paralytic agents, or coma induction were censored at the time of these medications. Independent factors in the Cox proportional hazards regression model included treatment assignment and treatment hospital; treatment hospital had no effect. Kaplan-Meier survival curves were constructed for each treatment group. All analyses were performed for the overall treatment groups and for each age stratum. Sample-size estimates were based on the primary efficacy outcome and an expected efficacy of diazepam of 60% based on previous literature. 15,16 With a 2-sided alpha of.05, the study had 80% power to detect an absolute difference in efficacy of at least 17% with 120 patients in each group. 23 Based on a planned interim analysis after enrollment of 50%, the independent data monitoring committee recommended increasing the sample size to 131 in each group. 24 All analyses were performed using SAS version 9.2 (SAS Institute Inc). Results A total of 310 patients were randomized, of whom 273 patients met the definition of generalized convulsive status epi JAMA April 23/30, 2014 Volume 311, Number 16 jama.com
4 vs for Pediatric SE Original Investigation Research Figure. CONSORT Diagram of Participants in the Pediatric Seizure Study Patients assessed for eligibility Excluded 4357 Not actively seizing 6729 Did not meet other inclusion criteria 4 Parent refused participation 230 Potentially eligible but missed by emergency department or study staff 310 Randomized 162 Randomized to receive diazepam 148 Randomized to receive lorazepam 162 Included in the safety analysis 148 Included in the safety analysis 140 Included in the primary efficacy analysis 22 Excluded 18 Did not have status epilepticus 4 Duplicate participant 133 Included in the primary efficacy analysis 15 Excluded (1 patient is in both categories) 13 Did not have status epilepticus 3 Duplicate participant 102 Included in per-protocol analysis 38 Excluded (patients may have >1 protocol deviation) 3 Received benzodiazepine prior to randomization 10 Received study medication outside of 30% dosing margin 13 Received late administration of second dose of study medication 1 Received phenytoin immediately after first study medication dose 1 Received open label benzodiazepine after first medication dose 3 Had infiltration of study medication intravenous line 10 Site randomization errors 107 Included in per-protocol analysis 26 Excluded (patients may have >1 protocol deviation) 13 Received study medication outside of 30% margin 6 Received late administration of second dose of study medication 1 Received early administration of second dose of study medication 1 Received phenytoin immediately after first study medication dose 2 Received open label benzodiazepine after first medication dose 6 Site randomization errors lepticus (140 taking diazepam and 133 taking lorazepam). The Figure depicts the CONSORT diagram for all patients. Table 1 displays the patient characteristics of the randomized patients and Table 2 shows the seizure etiologies in the 2 treatment groups. There were no significant baseline differences in patient characteristics or the distribution of seizure etiologies between the treatment groups. There were no significant differences in the primary efficacy and safety outcomes. Cessation of status epilepticus within 10 minutes without recurrence within 30 minutes occurred in 101 patients (72.1%) in the diazepam group compared with 97 patients (72.9%) in the lorazepam group (Table 3; absolute efficacy difference, 0.8%; 95% CI, 11.4% to 9.8%). Twenty-six patients in each group required assisted ventilation (16.0% in the diazepam vs 17.6% in the lorazepam groups; absolute risk difference, 1.6%; 95% CI, 9.9% to 6.8%). These findings were consistent in per-protocol analyses after excluding 64 additional patients with significant protocol deviations, also shown in Table 3. The most common protocol violations were study medication dose outside the 30% margin (n = 27), late administration of the second dose of study medication (n = 21), incorrect randomization (n = 15), receipt of a benzodiazepine within 2 hours prior to enrollment (n = 4), IV extravasation (n = 3), and early administration of secondary medications (n = 3). Secondary study outcomes are shown in Table 3. The rates of recurrent generalized convulsions within 60 minutes, excluding patients who failed the primary outcome, were 10.9% for diazepam and 10.3% for lorazepam and the rates of recurrence within 4 hours were 38.6% and 39.2%, respectively. Data on the precise time of cessation of status epilepticus were available in 266 of 273 patients (97.4%). The median time to termination of status epilepticus was 2.5 minutes (interquartile range, minutes) in the diazepam group and 2.0 minutes (interquartile range, minutes) in the lorazepam group (P =.80). The only statistically significant difference between treatment groups in any of the secondary outcomes was in the incidence of sedation, which occurred in 81 of 162 diazepam patients (50%) and 99 of 148 lorazepam patients (66.9%) (absolute risk difference, 16.9%; 95% CI, 6.1%-27.7%). Survival analyses showed no statistically significant differences between groups in response latency (hazard ratio, 0.99; 95% CI, ; P =.92; efigure 1 in Supplement) or time to recurrence of seizures (hazard ratio, 1.04; 95% CI, ; P =.81; efigure 2 in Supplement). There was a significant difference favoring the diazepam arm in time to return to baseline mental status (hazard ratio, 1.96; 95% CI, ; P =.0004; efigure 3 in Supplement). There were no significant differences in efficacy between treatments when com- jama.com JAMA April 23/30, 2014 Volume 311, Number
5 Research Original Investigation vs for Pediatric SE Table 1. Characteristics of Randomized Patients a Age3moto<3y Age3to<13y Age 13y Overall Characteristic (n = 77) (n = 71) (n = 68) (n = 63) (n = 17) (n = 14) (n = 162) (n = 148) Age, mean (SD), y 1.4 (0.7) 1.4 (0.7) 6.1 (2.5) 6.3 (2.6) 15.9 (3.7) 15.5 (1.6) 4.9 (4.9) 4.8 (4.6) Median (range) 1.3 ( ) 1.3 ( ) 5.2 ( ) 5.8 ( ) 14.6 ( ) 15.9 ( ) 3.2 ( ) 3.1 ( ) Male, No. (%) 41 (53.2) 33 (46.5) 35 (51.5) 30 (47.6) 11 (64.7) 5 (35.7) 87 (53.7) 68 (45.9) Ethnicity, No. (%) Hispanic/Latino 30 (39.0) 20 (28.2) 19 (27.9) 21 (33.3) 2 (11.8) 3 (21.4) 51 (31.5) 44 (29.7) Not reported 2 (2.6) 1 (1.4) 3 (4.4) 2 (3.2) 2 (11.8) 1 (7.1) 7 (4.3) 4 (2.7) Race/ethnicity, No. (%) American Indian/ Alaska Native (1.6) 1 (5.9) 0 1 (0.6) 1 (0.7) Asian 3 (3.9) 1 (1.4) 1 (1.5) 2 (3.2) (2.5) 3 (2.0) Black/African American Native Hawaiian/ Pacific Islander 26 (33.8) 27 (38.0) 23 (33.8) 23 (36.5) 5 (29.4) 7 (50.0) 54 (33.3) 57 (38.5) 1 (1.3) 0 1 (1.5) (7.1) 2 (1.2) 1 (0.7) White 38 (49.4) 31 (43.7) 34 (50.0) 33 (52.4) 9 (52.9) 4 (28.6) 81 (50.0) 68 (45.9) More than 1 race 5 (6.5) 8 (11.3) 3 (4.4) 2 (3.2) (4.9) 10 (6.8) Other 4 (5.2) 2 (2.8) 4 (5.9) 1 (1.6) 2 (11.8) 1 (7.1) 10 (6.2) 4 (2.7) Not reported 0 2 (2.8) 2 (2.9) 1 (1.6) 0 1 (7.1) 2 (1.2) 4 (2.7) a None of the differences were statistically significant. paring subgroups of primary etiology. The point estimate for overall efficacy for febrile seizures was lower than for other etiologies but was not statistically significant (65.2% vs 76.1%; absolute efficacy difference, 10.9%; 95% CI, 22.6% to 0.74%). Discussion The results of this randomized clinical trial do not support the hypothesis that lorazepam is superior to diazepam for the treatment of pediatric status epilepticus of at least 5 minutes duration. Both medications were effective in stopping status epilepticus in more than 70% of cases and had rates of severe respiratory depression of less than 20%. There were no statistically significant differences in either primary or secondary efficacy and safety outcomes, with the exception of higher rates and duration of sedation for lorazepam. Our results are similar to several previous studies of benzodiazepines for status epilepticus in children. In a single-site quasirandomized study 16 of IV lorazepam compared with diazepam in 61 children, efficacy was 70% and 65%, respectively, similar to our results. Qureshi et al 15 performed a pediatric medical record audit after a protocol change from IV diazepam to IV lorazepam and found a success rate of 65% in both groups. While a randomized trial (RAMPART [Rapid Anticonvulsant Medication Prior to Arrival Trial]) 25 of adults and children found, overall, that intramuscular midazolam initiated in the prehospital setting stopped more seizures at arrival to the ED than intravenous lorazepam (73% vs 63%), subgroup analysis of the 149 children enrolled showed similar results (70% vs 68%, respectively) for the 2 medications. The overall rate of intubation (14% in each group) was also similar to the overall rates of severe respiratory depression in our study (17%). Previous studies of adults with status epilepticus have found consistent, but statistically nonsignificant, trends toward superiority of lorazepam over diazepam with respect to efficacy. Treiman et al 26 enrolled 518 adults with both overt and subtle status; in the subgroup of patients with overt status epilepticus, success rates were 65% for the lorazepam group and 56% for the diazepam plus phenytoin group. Alldredge at al 23 enrolled 205 adults with status epilepticus in the prehospital setting and found success rates for lorazepam and diazepam of 59% and 43%, respectively. In this study, both medications were superior to placebo for both efficacy and safety. Similarly, a smaller study of 78 adults found success rates for lorazepam and diazepam of 89% and 76%, respectively. 10 These trials found similar safety rates for both medications. 10,23,26 Our study s results contrast with several retrospective studies in children, which suggested that lorazepam was more effective in stopping convulsions or had lower rates of respiratory depression. 12,13 This study was designed to improve on the limitations of previous studies. First, it was a randomized clinical trial rather than a retrospective review or quasi-experimental trial. Second, a second dose was administered, when needed, at half the initial dose based on pharmacokinetic models derived in a previous study. 21 Finally, medications were administered as a slow IV 1656 JAMA April 23/30, 2014 Volume 311, Number 16 jama.com
6 vs for Pediatric SE Original Investigation Research Table 2. Seizure Etiology by Treatment Group a No. (%) Age3moto<3y Age3to<13y Age 13y Overall Variable (n = 72) (n = 62) (n = 55) (n = 60) (n = 13) (n = 11) (n = 140) (n = 133) Febrile 36 (50.0) 32 (51.6) 13 (23.6) 8 (13.3) (35.0) 40 (30.1) Low levels of anti-epileptic drugs 2 (2.8) 4 (6.5) 8 (14.5) 9 (15.0) 2 (15.4) 0 12 (8.6) 13 (9.8) Acute symptomatic 13 (18.1) 7 (11.3) 8 (14.5) 8 (13.3) 2 (15.4) 0 23 (16.4) 15 (11.3) Head injury 3 (4.2) 1 (1.6) 0 2 (3.3) (2.1) 3 (2.3) CNS infection 1 (1.4) 1 (1.6) 3 (5.5) 1 (1.7) (2.9) 2 (1.5) Acute hypoxic/ ischemic insult 2 (2.8) (1.4) 0 Hypoglycemia Electrolyte abnormality 0 2 (3.2) (1.5) Brain tumor 1 (1.4) 0 1 (1.8) 0 1 (7.7) 0 3 (2.1) 0 Acute vascular event Alcohol or other drug toxicity 0 1 (1.6) (0.8) 1 (1.4) (0.7) 0 Other 5 (6.9) 2 (3.2) 4 (7.3) 5 (8.3) 1 (7.7) 0 10 (7.1) 7 (5.3) Remote symptomatic 5 (6.9) 6 (9.7) 7 (12.7) 6 (10.0) 1 (7.7) 2 (18.2) 13 (9.3) 14 (10.5) Past hypoxic/ ischemic insult 2 (2.8) 0 1 (1.8) 1 (1.7) 0 1 (9.1) 3 (2.1) 2 (1.5) Past head injury 0 1 (1.6) 1 (1.8) (0.7) 1 (0.8) Past brain surgery 0 1 (1.6) 0 1 (1.7) (1.5) Other 3 (4.2) 4 (6.5) 5 (9.1) 4 (6.7) 1 (7.7) 1 (9.1) 9 (6.4) 9 (6.8) Idiopathic 14 (19.4) 13 (21.0) 15 (27.3) 24 (40.0) 8 (61.5) 7 (63.6) 37 (26.4) 44 (33.1) Other 2 (2.8) 0 4 (7.3) 4 (6.7) 0 2 (18.2) 6 (4.3) 6 (4.5) Abbreviation: CNS, central nervous system a None of the differences were statistically significant. push for 1 minute. In contrast, retrospective studies cannot ensure that dosing was given in such a standardized manner. Our study results are also different than the populationbased study by Chin et al. 14 They showed that lorazepam was far more effective than diazepam; however, lorazepam was administered intravenously and diazepam rectally, making a direct comparison difficult. Compared with previous studies of status epilepticus in children, this study was larger and is further strengthened by the multicenter design across 11 geographically diverse pediatric academic hospitals. Furthermore, the use of Exception from Informed Consent for Emergency Research helped prevent selection bias by allowing the inclusion of patients without previous seizures. Prior prehospital care was controlled for by excluding all patients who had received a benzodiazepine in the previous 7 days, including ambulance administration, allowing for an uncontaminated examination of efficacy and safety. The methods used incorporated a standardized assessment of sedation, using the validated Riker scale, and are a strength of this study as compared with previous studies. The study results have important implications for both prehospital and ED care. can be stored without refrigeration and thus has been used as the treatment of choice in many prehospital systems. The results of this study do not support the superiority of lorazepam over diazepam as a firstline agent for pediatric status epilepticus. Taken together with the results of the RAMPART trial, 25 it would appear that either diazepam, lorazepam, or midazolam could be chosen as a reasonable first-line therapy. The study has several potential limitations. First, electroencephalogram monitoring was not used to determine the termination of status epilepticus. Instead, clinical criteria were used, which is consistent with previous studies. 10,12,13,23 Electroencephalogram monitoring is not readily available in most EDs and is not clinically useful except in rare circumstances or unusual forms of status epilepticus. Second, this study was designed as a superiority trial rather than a noninferiority trial. Therefore, failure to demonstrate a difference between treatment groups should not be construed to mean that lorazepam is statistically equivalent to diazepam. Although the point estimates for both efficacy and safety outcomes are similar in the 2 groups, the confidence intervals suggest that one medication could be superior in efficacy by as much as approximately 10% to 11% and in safety by approximately 7% to jama.com JAMA April 23/30, 2014 Volume 311, Number
7 Research Original Investigation vs for Pediatric SE Table 3. Primary and Secondary Efficacy and Safety Outcomes a No./Total No. (%) Age3moto<3y Age3to<13y Age 13y Overall Outcome Primary Outcomes Efficacy 48/72 38/62 44/55 49/60 9/13 10/11 101/140 97/133 (66.7) (61.3) (80.0) (81.7) (69.2) (90.9) (72.1) (72.9) Efficacy (per-protocol population) Need for assisted ventilation (all randomized patients) Secondary Outcomes Patients requiring only a single dose of study medication Patients requiring a second dose of study medication Patients requiring study medication plus additional anticonvulsant medication(s) Patients responding to fosphenytoin or phenytoin within 10 min Recurrence within 1h Recurrence within 4h Any respiratory depression (all severities) Sedation (Riker score <3) Aspiration pneumonia 35/48 (72.9) 11/77 (14.3) 41/72 (56.9) 27/72 (37.5) 15/72 (20.8) 6/15 (40.0) 6/48 (12.5) 23/48 (47.9) 38/77 (49.4) 35/77 (45.5) 32/48 (66.7) 16/71 (22.5) 34/62 (54.8) 25/62 (40.3) 15/62 (24.2) 2/15 (13.3) 3/38 (7.9) 25/38 (65.8) 32/71 (45.1) 0/77 1/71 (1.4) 36/43 (83.7) 12/68 (17.6) 37/55 (67.3) 14/55 (25.5) 4/55 (7.3) 44/50 (88.0) 10/63 (15.9) 38/60 (63.3) 17/60 (28.3) 6/60 (10.0) 0/4 1/6 (16.7) 5/44 (11.4) 11/44 (25.0) 33/68 (48.5) 44/71 (62.0) b 38/68 (55.9) 1/68 (1.5) 6/49 (12.2) 12/49 (24.5) 21/63 (33.3) 7/11 (63.6) 3/17 (17.6) 9/13 (69.2) 1/13 (7.7) 2/13 (15.4) 9/9 (100.0) 78/102 (76.5) 0/14 26/162 (16.0) 8/11 (72.7) 2/11 (18.2) 87/140 (62.1) 42/140 (30.0) 0/11 21/140 (15.0) 0/2 NA 6/21 (28.6) 0/9 1/10 (10.0) 5/9 (55.6) 3/17 (17.6) 47/63 8/17 (74.6) b (47.1) 1/63 (1.6) 1/17 (5.9) 1/10 (10.0) 1/14 (7.1) 8/14 (57.1) 11/101 (10.9) 39/101 (38.6) 74/162 (45.7) 81/162 (50.0) 0/14 2/162 (1.2) Secondary Time Outcomes, Median (IQR), min No. of noncensored patients Time to status epilepticus cessation Time to recovery from sedation 3.0 ( ) ( ) 4.0 ( ) 60.0 ( ) 2.0 ( ) ( ) 2.0 ( ) ( ) 3.0 ( ) 10.5 ( ) 1.0 ( ) 5.0 ( ) 2.5 ( ) ( ) 85/107 (79.4) 26/148 (17.6) 80/133 (60.2) 44/133 (33.1) 21/133 (15.8) 3/21 (14.3) 10/97 (10.3) 38/97 (39.2) 54/148 (36.5) 99/148 (66.9) b 2/148 (1.4) 2.0 ( ) ( ) Abbreviations: IQR, interquartile range; NA, not applicable. a Efficacy analysis includes all patients who received study medication and were experiencing generalized convulsive SE. Patients who were enrolled more than once were only included for the first visit. The per-protocol analysis excludes patients with significant protocol deviations (see Methods section). b P < %. Third, prehospital treatment by paramedics is an effective therapy 25 and is becoming more common. While excluding patients receiving benzodiazepines in the previous 7 days permitted a cleaner analysis of efficacy, we did not study the efficacy or safety of lorazepam or diazepam for patients requiring additional benzodiazepine treatment in the ED after receiving prehospital treatment. Fourth, the duration of status epilepticus prior to treatment in the cohort was not characterized because duration of status epilepticus prior to hospital arrival is often not available or reliable by historical report. Finally, protocol deviations were common in this study and reflect the often unpredictable practice of emergency medicine, including incomplete or inaccurate initial information available in emergency situations, incorrect weight estimation, and IV infiltration during infusion. However, it is reassuring that the results of the per-protocol analysis are consistent with overall results. The results suggest future research opportunities. For example, more efforts are required to ensure patient safety 1658 JAMA April 23/30, 2014 Volume 311, Number 16 jama.com
8 vs for Pediatric SE Original Investigation Research and the prevention of adverse events, especially in the emergency care setting. 27,28 Failure of efficacy was observed in approximately 1 in 4 children and severe respiratory depression rate in approximately 1 in 6. Future trials should consider newer medications and novel interventions targeting those at highest risk for medication failure or respiratory depression. Conclusions Among pediatric patients with convulsive status epilepticus, treatment with lorazepam did not result in improved efficacy or safety compared with diazepam. These findings do not support the preferential use of lorazepam for this condition. ARTICLE INFORMATION Author Affiliations: Division of Emergency Medicine, Children s National Medical Center, Washington, DC (Chamberlain, Brown); The Pediatric Emergency Care Applied Research Network (PECARN) (Chamberlain, Holsti, Mahajan, Brown, Vance, Gonzalez, Stanley, Brousseau, Grubenhoff, Baren); University of Texas, Southwestern, Dallas (Okada); Department of Pediatrics, University of Utah, Salt Lake City (Holsti); Department of Pediatrics, Children s Hospital of Michigan, Detroit (Mahajan); University of California, Davis, Sacramento (Vance); Baylor College of Medicine, Houston, Texas (Gonzalez); Department of Pediatrics, University of Maryland, Baltimore (Lichenstein); University of Michigan, Ann Arbor (Stanley); Department of Pediatrics, Medical College of Wisconsin, Milwaukee (Brousseau); Children s Hospital of Colorado, Denver (Grubenhoff); Department of Pediatrics, Children s Hospital of Eastern Ontario, Ottawa, Ontario, Canada (Zemek); Alberta Children s Hospital, Calgary, Alberta, Canada (Johnson); The EMMES Corp, Rockville, Maryland (Clemons); Department of Pediatrics, The Children s Hospital of Philadelphia, Philadelphia, Pennsylvania (Baren). Author Contributions: Drs Chamberlain and Clemons had full access to all of the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Chamberlain, Holsti, Mahajan, Brown, Baren. Acquisition, analysis, or interpretation of data: All authors. Drafting of the manuscript: Chamberlain, Brown, Grubenhoff, Zemek. Critical revision of the manuscript for important intellectual content: Chamberlain, Okada, Holsti, Mahajan, Brown, Vance, Gonzalez, Lichenstein, Stanley, Brousseau, Zemek, Johnson, Clemons, Baren. Statistical analysis: Clemons. Obtained funding: Chamberlain, Brown. Administrative, technical, or material support: Okada, Holsti, Vance, Gonzalez, Stanley, Brousseau, Grubenhoff, Baren. Study supervision: Chamberlain, Okada, Holsti, Mahajan, Brown, Baren. Conflict of Interest Disclosures: All authors have completed and submitted the ICMJE Form for Disclosure of Potential Conflicts of Interest. Dr Okada reported having received grants from the Eunice Kennedy Shriver National Institute of Child Health and Human Development/Children s National Health Center during the conduct of the study. Drs Mahajan, Lichenstein, and Grubenhoff reported having received grants from the National Institutes of Health during the conduct of the study. Dr Brousseau reported consulting for Mast Therapeutics. No other disclosures were reported. Funding/Support: This study was funded by grant HHSN C from the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD). The Pediatric Emergency Care Applied Research Network (PECARN) is supported by cooperative agreements U03MC00001, U03MC00003, U03MC00006, U03MC00007, and U03MC00008 from the Emergency Medical Services for Children (EMSC) program of the Maternal and Child Health Bureau (MCHB), Health Resources and Services Administration, Department of Health and Human Services. The Best Pharmaceuticals for Children Act Data Coordinating Center for this study was the EMMES Corp and was funded by the NICHD under a separate contract. Role of the Sponsors: The Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) had a role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication. The NICHD commissioned an expert panel of ethicists, regulatory experts, and attorneys to advise the investigators on the proper conduct of the Exception from Informed Consent; convened the Data Safety Monitoring Board; contracted with the Data Coordinating Center to provide data management and data analysis and to aid with interpretation of study results; reviewed the final manuscript prior to submission; and approved the final manuscript prior to submission. Group Information: The Pediatric Emergency Care Applied Research Network (PECARN) includes the following investigators: Best Pharmaceuticals for Children Act (BPCA) Data Coordinating Center (DCC): The EMMES Corp: D. King, C. Kim, K. Martz, and J. Zhao. BPCA Data Monitoring Committee (DMC): P. Walson (chair), K. Weise, A. Das, D. Venzon, B. Wiedermann, G. Koren, C. Vocke, A. Thompson, N. Harris, M. Riddle, L. Brown, P. Swerdlow, and A. Zajicek. Participating centers and site investigators: Children s Hospital, Boston: L. Nigrovic; Children s Hospital of Buffalo: K. Lillis; Children s Hospital of Michigan: P. Mahajan; Children s Hospital of New York Presbyterian: M. Sonnett; Children s Hospital of Philadelphia: K. Shaw; Children s Memorial Hospital: E. Powell; Children s National Medical Center: K. Brown; Cincinnati Children s Hospital Medical Center: R. Ruddy; DeVos Children s Hospital: J. Hoyle; Hurley Medical Center: D. Borgialli; Jacobi Medical Center: Y. Atherly-John; Medical College of Wisconsin/Children s Hospital of Wisconsin: M. Gorelick; University of California Davis Medical Center: E. Andrada; University of Michigan: R. Stanley; University of Rochester: G. Conners; University of Utah/Primary Children s Medical Center: C. Pruitt; Washington University/St. Louis Children s Hospital: D. Jaffe; University of Maryland: R. Lichenstein. PECARN Steering Committee: P. Dayan (chair); E. Alpern, L. Bajaj, K. Brown, D. Borgialli, J. Chamberlain, J. M. Dean, M. Gorelick, D. Jaffe, N. Kuppermann, M. Kwok, R. Lichenstein, K. Lillis, P. Mahajan, D. Monroe, L. Nigrovic, E. Powell, A. Rogers, R. Ruddy, R. Stanley, M. Tunik. MCHB/EMSC liaisons: D. Kavanaugh and H. Park. PECARN Data Coordinating Center (DCC): J. M. Dean, H. Gramse, R. Holubkov, A. Donaldson, C. Olson, S. Zuspan, and R. Enriquez. Feasibility and Budget Subcommittee (FABS): K. Brown, S. Goldfarb (co-chairs); E. Crain, E. Kim, S. Krug, D. Monroe, D. Nelson, M. Berlyant, and S. Zuspan. Grants and Publications Subcommittee (GAPS): M. Gorelick (chair); L. Alpern, J. Anders, D. Borgialli, L. Cimpello, A. Donaldson, G. Foltin, F. Moler, and K. Shreve. Protocol Review and Development Subcommittee (PRADS): L. Nigrovic (chair); J. Chamberlain, P. Dayan, JM. Dean, R. Holubkov, D. Jaffe, E. Powell, K. Shaw, R. Stanley, and M. Tunik. Quality Assurance Subcommittee (QAS): K. Lillis (chair); E. Alessandrini, S. Blumberg, R. Enriquez, R. Lichenstein, P. Mahajan, R. McDuffie, R. Ruddy, B. Thomas, and J. Wade. Safety and Regulatory Affairs Subcommittee (SRAS): W. Schalick, J. Hoyle, (co-chairs); S. Atabaki, K. Call, H. Gramse, M. Kwok, A. Rogers, D. Schnadower, and N. Kuppermann. REFERENCES 1. US Department of Health and Human Services national statistics. /HCUPnet.jsp. Accessed July 5, Shinnar S, Berg AT, Moshe SL, et al. The risk of seizure recurrence after a first unprovoked afebrile seizure in childhood: an extended follow-up. Pediatrics. 1996;98(2, pt 1): De Negri M, Baglietto MG. Treatment of status epilepticus in children. Paediatr Drugs. 2001;3(6): Treiman DM. The role of benzodiazepines in the management of status epilepticus. Neurology. 1990;40(5)(suppl 2): Mitchell WG. Status epilepticus and acute repetitive seizures in children, adolescents, and young adults: etiology, outcome, and treatment. Epilepsia. 1996;37(suppl 1):S74-S Appleton R, Choonara I, Martland T, Phillips B, Scott R, Whitehouse W. The treatment of convulsive status epilepticus in children: The Status Epilepticus Working Party, Members of the Status Epilepticus Working Party. Arch Dis Child. 2000;83(5): Manno EM. New management strategies in the treatment of status epilepticus. Mayo Clin Proc. 2003;78(4): Bleck TP. Management approaches to prolonged seizures and status epilepticus. Epilepsia. 1999;40(suppl 1):S59-S63, discussion S64-S Sabo-Graham T, Seay AR. Management of status epilepticus in children. Pediatr Rev. 1998;19(9): , quiz 310. jama.com JAMA April 23/30, 2014 Volume 311, Number
9 Research Original Investigation vs for Pediatric SE 10. Leppik IE, Derivan AT, Homan RW, Walker J, Ramsay RE, Patrick B. Double-blind study of lorazepam and diazepam in status epilepticus. JAMA. 1983;249(11): Cock HR, Schapira AHV. A comparison of lorazepam and diazepam as initial therapy in convulsive status epilepticus. QJM. 2002;95(4): Chiulli DA, Terndrup TE, Kanter RK. The influence of diazepam or lorazepam on the frequency of endotracheal intubation in childhood status epilepticus.jemerg Med. 1991;9(1-2): Giang DW, McBride MC. versus diazepam for the treatment of status epilepticus. Pediatr Neurol. 1988;4(6): Chin RF, Neville BG, Peckham C, Wade A, Bedford H, Scott RC. Treatment of community-onset, childhood convulsive status epilepticus: a prospective, population-based study [published correction appears in Lancet Neurol. 2008;7(9):771]. Lancet Neurol. 2008;7(8): Qureshi A, Wassmer E, Davies P, Berry K, Whitehouse WP. Comparative audit of intravenous lorazepam and diazepam in the emergency treatment of convulsive status epilepticus in children.seizure. 2002;11(3): Appleton R, Sweeney A, Choonara I, Robson J, Molyneux E. versus diazepam in the acute treatment of epileptic seizures and status epilepticus. Dev Med Child Neurol. 1995;37(8): Martland T, Baxter P, Rittey C. Is there an agreed treatment for children in status epilepticus? Dev Med Child Neurol. 1998;40(4): Lowenstein DH. Status epilepticus: an overview of the clinical problem. Epilepsia. 1999;40(suppl 1):S3-S8, discussion S21-S Appleton R, Choonara I, Martland T, Phillips B, Scott R, Whitehouse W. The treatment of convulsive status epilepticus in children: The Status Epilepticus Working Party. Arch Dis Child. 2000;83(5): Food and Drug Administration. Guidance for institutional review boards, clinical investigators, and sponsors: Exception from Informed Consent Requirements for Emergency Research. March /RegulatoryInformation/Guidances /UCM pdf. Accessed April 13, Chamberlain JM, Capparelli EV, Brown KM, et al; Pediatric Emergency Care Applied Research Network (PECARN). Pharmacokinetics of intravenous lorazepam in pediatric patients with and without status epilepticus. J Pediatr. 2012;160(4): , e Riker RR, Picard JT, Fraser GL. Prospective evaluation of the Sedation-Agitation Scale for adult critically ill patients. Crit Care Med. 1999;27(7): Alldredge BK, Gelb AM, Isaacs SM, et al. A comparison of lorazepam, diazepam, and placebo for the treatment of out-of-hospital status epilepticus. N Engl J Med. 2001;345(9): Chen YHJ, DeMets DL, Lan KKG. Increasing the sample size when the unblinded interim result is promising. Stat Med.2004;23(7): Silbergleit R, Durkalski V, Lowenstein D, et al; NETT Investigators. Intramuscular versus intravenous therapy for prehospital status epilepticus.nengl J Med. 2012;366(7): Treiman DM, Meyers PD, Walton NY, et al; Veterans Affairs Status Epilepticus Cooperative Study Group. A comparison of four treatments for generalized convulsive status epilepticus. N Engl J Med. 1998;339(12): Woods D, Thomas E, Holl J, Altman S, Brennan T. Adverse events and preventable adverse events in children.pediatrics. 2005;115(1): Krug SE, Frush K; Committee on Pediatric Emergency Medicine, American Academy of Pediatrics. Patient safety in the pediatric emergency care setting. Pediatrics. 2007;120(6): JAMA April 23/30, 2014 Volume 311, Number 16 jama.com
1. What is the comparative efficacy of IV lorazepam and IV diazepam for the treatment of febrile seizures in children (less than 12 years of age)?
 Title: The Use of Lorazepam for Febrile Seizures in Children Date: 25 January 2008 Context and policy issues: Febrile seizures are the most common form of childhood seizures, affecting approximately 2
Title: The Use of Lorazepam for Febrile Seizures in Children Date: 25 January 2008 Context and policy issues: Febrile seizures are the most common form of childhood seizures, affecting approximately 2
Stop the Status: Improving Outcomes in Pediatric Epilepsy Syndromes. Michelle Welborn, PharmD ICE Alliance
 Stop the Status: Improving Outcomes in Pediatric Epilepsy Syndromes Michelle Welborn, PharmD ICE Alliance Overview Seizures and Epilepsy Syndromes Seizure Emergencies Febrile Seizures Critical Population
Stop the Status: Improving Outcomes in Pediatric Epilepsy Syndromes Michelle Welborn, PharmD ICE Alliance Overview Seizures and Epilepsy Syndromes Seizure Emergencies Febrile Seizures Critical Population
Accounting for Repeat Enrollments During an Emergency Clinical Trial: The Rapid Anticonvulsant Medications Prior to Arrival Trial (RAMPART)
 RESEARCH METHODS &STATISTICS Accounting for Repeat Enrollments During an Emergency Clinical Trial: The Rapid Anticonvulsant Medications Prior to Arrival Trial (RAMPART) William J. Meurer, MD, MS, Robert
RESEARCH METHODS &STATISTICS Accounting for Repeat Enrollments During an Emergency Clinical Trial: The Rapid Anticonvulsant Medications Prior to Arrival Trial (RAMPART) William J. Meurer, MD, MS, Robert
Challenges in the Design and Analysis of Non-Inferiority Trials: A Case Study. Key Points from FDA Guidance
 Challenges in the Design and Analysis of Non-Inferiority Trials: A Case Study Valerie Durkalski NETT Statistical and Data Management Center (NINDS U01 NS059041) Division of Biostatistics & Epidemiology
Challenges in the Design and Analysis of Non-Inferiority Trials: A Case Study Valerie Durkalski NETT Statistical and Data Management Center (NINDS U01 NS059041) Division of Biostatistics & Epidemiology
NMDOH digital library; keywords searched: pre-hospital, benzodiazepine, emergency medical technician, treatment of seizures, status epilepticus.
 Background Literature Review and Recommendations Administration of Benzodiazepines by EMT -I in the pre-hospital setting EMS Bureau Protocol Review Steering Committee Status epilepticus is a recognized
Background Literature Review and Recommendations Administration of Benzodiazepines by EMT -I in the pre-hospital setting EMS Bureau Protocol Review Steering Committee Status epilepticus is a recognized
A Shot in the Arm for Prehospital Status Epilepticus: The RAMPART Study
 Current Literature In Clinical Science A Shot in the Arm for Prehospital Status Epilepticus: The RAMPART Study Intramuscular Versus Intravenous Therapy for Prehospital Status Epilepticus. Silbergleit R,
Current Literature In Clinical Science A Shot in the Arm for Prehospital Status Epilepticus: The RAMPART Study Intramuscular Versus Intravenous Therapy for Prehospital Status Epilepticus. Silbergleit R,
Lieven Lagae Department of Paediatric Neurology Leuven University Leuven, Belgium. Management of acute seizure settings from infancy to adolescence
 Lieven Lagae Department of Paediatric Neurology Leuven University Leuven, Belgium Management of acute seizure settings from infancy to adolescence Consequences of prolonged seizures Acute morbidity and
Lieven Lagae Department of Paediatric Neurology Leuven University Leuven, Belgium Management of acute seizure settings from infancy to adolescence Consequences of prolonged seizures Acute morbidity and
Department of Clinical Pharmacy, University of Colorado, Skaggs School of Pharmacy and Pharmaceutical Sciences, Aurora, CO 6
 American Epilepsy Society Guideline Evidence-Based Guideline: Treatment of Convulsive Status Epilepticus in Children and Adults: Report of the Guideline Committee of the American Epilepsy Society Tracy
American Epilepsy Society Guideline Evidence-Based Guideline: Treatment of Convulsive Status Epilepticus in Children and Adults: Report of the Guideline Committee of the American Epilepsy Society Tracy
Simple Protocol & Bayesian Design: Established Status Epilepticus Treatment Trial (ESETT)
 Simple Protocol & Bayesian Design: Established Status Epilepticus Treatment Trial (ESETT) Jaideep Kapur on behalf of ESETT invertigator University of Virginia Status epilepticus is a condition resulting
Simple Protocol & Bayesian Design: Established Status Epilepticus Treatment Trial (ESETT) Jaideep Kapur on behalf of ESETT invertigator University of Virginia Status epilepticus is a condition resulting
abstract ARTICLE BACKGROUND AND OBJECTIVES: Convulsive seizures account for 15% of pediatric air transports.
 Seizure Treatment in Children Transported to Tertiary Care: Recommendation Adherence and Outcomes Heather M. Siefkes, MD, MSCI, a, b Maija Holsti, MD, MPH, c Denise Morita, MD, d Lawrence J. Cook, PhD,
Seizure Treatment in Children Transported to Tertiary Care: Recommendation Adherence and Outcomes Heather M. Siefkes, MD, MSCI, a, b Maija Holsti, MD, MPH, c Denise Morita, MD, d Lawrence J. Cook, PhD,
First Line Therapy in Acute Seizure Management. William Dalsey, MD, FACEP
 First Line Therapy in Acute Seizure Management Case Presentation A 32-year old male intravenous drug user was brought to the ED having had a witnessed generalized tonic-clonic seizure 10 minutes prior
First Line Therapy in Acute Seizure Management Case Presentation A 32-year old male intravenous drug user was brought to the ED having had a witnessed generalized tonic-clonic seizure 10 minutes prior
Inappropriate emergency management of status epilepticus in children contributes to need for intensive care
 1584 PAPER Inappropriate emergency management of status epilepticus in children contributes to need for intensive care R F M Chin, L Verhulst, B G R Neville, M J Peters, R C Scott... See end of article
1584 PAPER Inappropriate emergency management of status epilepticus in children contributes to need for intensive care R F M Chin, L Verhulst, B G R Neville, M J Peters, R C Scott... See end of article
What Are the Best Non-IV Parenteral Options for a Seizing Patient? William C. Dalsey, MD, MBA, FACEP
 What Are the Best Non-IV Parenteral Options for a Seizing Patient? A 32-year old male intravenous drug user was brought to the ED having had a witnessed generalized tonic-clonic seizure 10 minutes prior
What Are the Best Non-IV Parenteral Options for a Seizing Patient? A 32-year old male intravenous drug user was brought to the ED having had a witnessed generalized tonic-clonic seizure 10 minutes prior
Early termination of prolonged epileptic
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e Early termination of prolonged epileptic seizures in response to intravenous administration of benzodiazepines by paramedics in the prehospital setting
T h e n e w e ngl a nd j o u r na l o f m e dic i n e Early termination of prolonged epileptic seizures in response to intravenous administration of benzodiazepines by paramedics in the prehospital setting
Rescue medications. What are rescue medications? Ideal rescue medication. Why use rescue medications?
 Rescue medications Out-of-hospital treatment of prolonged seizures or acute repetitive seizures What are rescue medications? Medicines used to terminate a prolonged seizure or acute repetitive seizures
Rescue medications Out-of-hospital treatment of prolonged seizures or acute repetitive seizures What are rescue medications? Medicines used to terminate a prolonged seizure or acute repetitive seizures
A comparison of lorazepam and diazepam as initial therapy in convulsive status epilepticus
 Q J Med 2002; 95:225 231 A comparison of lorazepam and diazepam as initial therapy in convulsive status epilepticus H.R. COCK 1 and A.H.V. SCHAPIRA 1,2 From the 1 Department of Clinical and Experimental
Q J Med 2002; 95:225 231 A comparison of lorazepam and diazepam as initial therapy in convulsive status epilepticus H.R. COCK 1 and A.H.V. SCHAPIRA 1,2 From the 1 Department of Clinical and Experimental
A bs tr ac t. n engl j med 366;7 nejm.org february 16,
 The new england journal of medicine established in 1812 february 16, 2012 vol. 366 no. 7 Intramuscular versus Intravenous Therapy for Prehospital Status Epilepticus Robert Silbergleit, M.D., Valerie Durkalski,
The new england journal of medicine established in 1812 february 16, 2012 vol. 366 no. 7 Intramuscular versus Intravenous Therapy for Prehospital Status Epilepticus Robert Silbergleit, M.D., Valerie Durkalski,
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kuppermann N, Ghetti S, Schunk JE, et al. Clinical trial of
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kuppermann N, Ghetti S, Schunk JE, et al. Clinical trial of
Status Epilepticus: Implications Outside the Neuro-ICU
 Status Epilepticus: Implications Outside the Neuro-ICU Jeffrey M Singh MD Critical Care and Neurocritical Care Toronto Western Hospital October 31 st, 2014 Disclosures I (unfortunately) have no disclosures
Status Epilepticus: Implications Outside the Neuro-ICU Jeffrey M Singh MD Critical Care and Neurocritical Care Toronto Western Hospital October 31 st, 2014 Disclosures I (unfortunately) have no disclosures
Emergency Medicine Updates. Dr. Timothy Cobb March 1, 2018
 Emergency Medicine Updates Dr. Timothy Cobb March 1, 2018 Topics Chest pain Renal colic Atrial fibrillation Pediatric head trauma Asymptomatic hypertension Chest Pain Non traumatic chest pain 2nd most
Emergency Medicine Updates Dr. Timothy Cobb March 1, 2018 Topics Chest pain Renal colic Atrial fibrillation Pediatric head trauma Asymptomatic hypertension Chest Pain Non traumatic chest pain 2nd most
Outline. What is a seizure? What is epilepsy? Updates in Seizure Management Terminology, Triage & Treatment
 Outline Updates in Seizure Management Terminology, Triage & Treatment Joseph Sullivan, MD! Terminology! Videos of different types of seizures! Diagnostic evaluation! Treatment options! Acute! Maintenance
Outline Updates in Seizure Management Terminology, Triage & Treatment Joseph Sullivan, MD! Terminology! Videos of different types of seizures! Diagnostic evaluation! Treatment options! Acute! Maintenance
The New England Journal of Medicine
 The New England Journal of Medicine Copyright 21 by the Massachusetts Medical Society VOLUME 345 A UGUST 3, 21 NUMBER 9 A COMPARISON OF LORAZEPAM, DIAZEPAM, AND FOR THE TREATMENT OF OUT-OF-HOSPITAL STATUS
The New England Journal of Medicine Copyright 21 by the Massachusetts Medical Society VOLUME 345 A UGUST 3, 21 NUMBER 9 A COMPARISON OF LORAZEPAM, DIAZEPAM, AND FOR THE TREATMENT OF OUT-OF-HOSPITAL STATUS
Performance of the Pediatric Glasgow Coma Scale Score in the Evaluation of Children With Blunt Head Trauma
 ORIGINAL CONTRIBUTION Performance of the Pediatric Glasgow Coma Scale Score in the Evaluation of Children With Blunt Head Trauma Dominic A. Borgialli, DO, MPH, Prashant Mahajan, MD, MPH, MBA, John D. Hoyle,
ORIGINAL CONTRIBUTION Performance of the Pediatric Glasgow Coma Scale Score in the Evaluation of Children With Blunt Head Trauma Dominic A. Borgialli, DO, MPH, Prashant Mahajan, MD, MPH, MBA, John D. Hoyle,
A Comparison of Buccal Midazolam and Intravenous Diazepam for the Acute Treatment of Seizures in Children
 Original Article Iran J Pediatr Sep 2012; Vol 22 (No 3), Pp: 303-308 A Comparison of Buccal Midazolam and Intravenous Diazepam for the Acute Treatment of Seizures in Children Seyed-Hassan Tonekaboni 1,2,
Original Article Iran J Pediatr Sep 2012; Vol 22 (No 3), Pp: 303-308 A Comparison of Buccal Midazolam and Intravenous Diazepam for the Acute Treatment of Seizures in Children Seyed-Hassan Tonekaboni 1,2,
Can t Stop the Seizing!
 Can t Stop the Seizing! Joseph Miller, MD, MS MCEP Critical Care March, 2019 Objectives Describe the importance of time to treatment Delineate treatment based on best evidence Describe novel diagnostic
Can t Stop the Seizing! Joseph Miller, MD, MS MCEP Critical Care March, 2019 Objectives Describe the importance of time to treatment Delineate treatment based on best evidence Describe novel diagnostic
Established Status Epilepticus Treatment Trial (ESETT)
 Established Status Epilepticus Treatment Trial (ESETT) A multicenter, randomized, blinded, comparative effectiveness study of fosphenytoin, valproic acid, or levetiracetam in the emergency department treatment
Established Status Epilepticus Treatment Trial (ESETT) A multicenter, randomized, blinded, comparative effectiveness study of fosphenytoin, valproic acid, or levetiracetam in the emergency department treatment
B GÜRBÜZ, F GÜRBÜZ, A CAYIR, A DE. Key words. Introduction
 HK J Paediatr (new series) 2016;21:79-85 Evaluation of Aetiological Causes, Clinical Features, Treatment and Prognosis in Patients Diagnosed with and Treated for Status Epilepticus: An Epidemiological
HK J Paediatr (new series) 2016;21:79-85 Evaluation of Aetiological Causes, Clinical Features, Treatment and Prognosis in Patients Diagnosed with and Treated for Status Epilepticus: An Epidemiological
The fitting child. Dr Chris Bird MRCPCH DTMH, Locum consultant, Paediatric Emergency Medicine
 The fitting child Dr Chris Bird MRCPCH DTMH, Locum consultant, Paediatric Emergency Medicine What I am not Detail from The Neurologist, Jose Perez The sacred disease Epilepsy comes from the ancient Greek
The fitting child Dr Chris Bird MRCPCH DTMH, Locum consultant, Paediatric Emergency Medicine What I am not Detail from The Neurologist, Jose Perez The sacred disease Epilepsy comes from the ancient Greek
Epilepsy CASE 1 Localization Differential Diagnosis
 2 Epilepsy CASE 1 A 32-year-old man was observed to suddenly become unresponsive followed by four episodes of generalized tonic-clonic convulsions of the upper and lower extremities while at work. Each
2 Epilepsy CASE 1 A 32-year-old man was observed to suddenly become unresponsive followed by four episodes of generalized tonic-clonic convulsions of the upper and lower extremities while at work. Each
PFIZER INC. Study Initiation Date: 15 June 1995; Completion Date: 22 April 1996
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. PROPRIETARY DRUG NAME /GENERIC DRUG NAME: Cerebyx /fosphenytoin
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. PROPRIETARY DRUG NAME /GENERIC DRUG NAME: Cerebyx /fosphenytoin
WHOLE LOTTA SHAKIN GOIN ON
 WHOLE LOTTA SHAKIN GOIN ON ADAM M. YATES, MD FACEP ASSOCIATE CHIEF OF EMERGENCY SERVICES UPMC MERCY SEIZURE DEFINITIONS Partial(focal) only involves part of the brain General Involves entire brain Simple
WHOLE LOTTA SHAKIN GOIN ON ADAM M. YATES, MD FACEP ASSOCIATE CHIEF OF EMERGENCY SERVICES UPMC MERCY SEIZURE DEFINITIONS Partial(focal) only involves part of the brain General Involves entire brain Simple
Peer Reviewed Title: Journal Issue: Author: Publication Date: Permalink: Author Bio: Keywords:
 Peer Reviewed Title: Prehospital Care for the Adult and Pediatric Seizure Patient: Current Evidence Based Recommendations Journal Issue: Western Journal of Emergency Medicine: Integrating Emergency Care
Peer Reviewed Title: Prehospital Care for the Adult and Pediatric Seizure Patient: Current Evidence Based Recommendations Journal Issue: Western Journal of Emergency Medicine: Integrating Emergency Care
ESETT ELIGIBILITY OVERVIEW. James Chamberlain, MD
 ESETT ELIGIBILITY OVERVIEW James Chamberlain, MD Eligibility Age Convulsive Status Benzos Not excluded Eligibility Age 2 years to < 18 years (Pediatric) 18 years to 65 years (Adult) > 65 years (Geriatric)
ESETT ELIGIBILITY OVERVIEW James Chamberlain, MD Eligibility Age Convulsive Status Benzos Not excluded Eligibility Age 2 years to < 18 years (Pediatric) 18 years to 65 years (Adult) > 65 years (Geriatric)
Refractory Status Epilepticus in Children: What are the Options?
 Refractory Status Epilepticus in Children: What are the Options? Weng Man Lam, PharmD, BCPS, BCPPS PICU Clinical Pharmacy Specialist Memorial Hermann Texas Medical Center November 11, 2017 Objectives 1.
Refractory Status Epilepticus in Children: What are the Options? Weng Man Lam, PharmD, BCPS, BCPPS PICU Clinical Pharmacy Specialist Memorial Hermann Texas Medical Center November 11, 2017 Objectives 1.
Seizure remission in adults with long-standing intractable epilepsy: An extended follow-up
 Epilepsy Research (2010) xxx, xxx xxx journal homepage: www.elsevier.com/locate/epilepsyres Seizure remission in adults with long-standing intractable epilepsy: An extended follow-up Hyunmi Choi a,, Gary
Epilepsy Research (2010) xxx, xxx xxx journal homepage: www.elsevier.com/locate/epilepsyres Seizure remission in adults with long-standing intractable epilepsy: An extended follow-up Hyunmi Choi a,, Gary
Information for Year 1 ITU Training (basic):
 Disclaimer: The Great Ormond Street Paediatric Intensive Care Training Programme was developed in 2004 by the clinicians of that Institution, primarily for use within Great Ormond Street Hospital and the
Disclaimer: The Great Ormond Street Paediatric Intensive Care Training Programme was developed in 2004 by the clinicians of that Institution, primarily for use within Great Ormond Street Hospital and the
Prevalence of Brain Injuries and Recurrence of Seizures in Children With Posttraumatic Seizures
 ORIGINAL CONTRIBUTION Prevalence of Brain Injuries and Recurrence of Seizures in Children With Posttraumatic Seizures Mohamed K. Badawy, MD, Peter S. Dayan, MD, MSc, Michael G. Tunik, MD, Frances M. Nadel,
ORIGINAL CONTRIBUTION Prevalence of Brain Injuries and Recurrence of Seizures in Children With Posttraumatic Seizures Mohamed K. Badawy, MD, Peter S. Dayan, MD, MSc, Michael G. Tunik, MD, Frances M. Nadel,
Pediatric 9-1-1: Show Me the Evidence!
 Pediatric 9-1-1: Show Me the Evidence! Toni Gross, MD, MPH Phoenix Children s Hospital Division of Emergency Medicine National Association of EMS Physicians, Pediatric Committee Chair Overview EMS history
Pediatric 9-1-1: Show Me the Evidence! Toni Gross, MD, MPH Phoenix Children s Hospital Division of Emergency Medicine National Association of EMS Physicians, Pediatric Committee Chair Overview EMS history
Downloaded from jssu.ssu.ac.ir at 0:37 IRST on Sunday February 17th 2019
 -2384 2 *. : 4 :. 2 / 4 3 6/. ( /) : 6 /4. 6. 00 92 6. 0 :. :. 0 :. International league Against Epilepsy (ILAE) First Unprovoked Seizure (FUS) 24 () (2) 20.. 2 3-4. (). : -* - 0 626024: 0 626024 : E-mial:
-2384 2 *. : 4 :. 2 / 4 3 6/. ( /) : 6 /4. 6. 00 92 6. 0 :. :. 0 :. International league Against Epilepsy (ILAE) First Unprovoked Seizure (FUS) 24 () (2) 20.. 2 3-4. (). : -* - 0 626024: 0 626024 : E-mial:
ESETT OUTCOMES. Investigator Kick-off Meeting Robert Silbergleit, MD
 ESETT OUTCOMES Investigator Kick-off Meeting Robert Silbergleit, MD Primary objective The primary objective is to determine the most effective and/or the least effective treatment of benzodiazepinerefractory
ESETT OUTCOMES Investigator Kick-off Meeting Robert Silbergleit, MD Primary objective The primary objective is to determine the most effective and/or the least effective treatment of benzodiazepinerefractory
CrackCast Episode 18 Seizures
 CrackCast Episode 18 Seizures Episode overview: 1) Define status epilepticus 2) List the doses of common medications used for status epilepticus 3) List 10 differential diagnoses for seizures 4) List 10
CrackCast Episode 18 Seizures Episode overview: 1) Define status epilepticus 2) List the doses of common medications used for status epilepticus 3) List 10 differential diagnoses for seizures 4) List 10
Refractory Seizures. Dr James Edwards EMCORE May 30th 2014
 Refractory Seizures Dr James Edwards EMCORE May 30th 2014 Refractory Seizures Seizures are a common presentation to the ED and some patients will have multiple seizures or have a reduced level of consciousness
Refractory Seizures Dr James Edwards EMCORE May 30th 2014 Refractory Seizures Seizures are a common presentation to the ED and some patients will have multiple seizures or have a reduced level of consciousness
Status Epilepticus. Ednea Simon, MD Swedish Pediatric Neuroscience Center
 Status Epilepticus Ednea Simon, MD Swedish Pediatric Neuroscience Center 1 Status Epilepticus Status epilepticus (SE) is a condition resulting either from failure of the mechanisms responsible for seizure
Status Epilepticus Ednea Simon, MD Swedish Pediatric Neuroscience Center 1 Status Epilepticus Status epilepticus (SE) is a condition resulting either from failure of the mechanisms responsible for seizure
WATCHMAN PROTECT AF Study Rev. 6
 WATCHMAN PROTECT AF Study Rev. 6 Protocol Synopsis Title WATCHMAN Left Atrial Appendage System for Embolic PROTECTion in Patients with Atrial Fibrillation (PROTECT AF) Sponsor Atritech/Boston Scientific
WATCHMAN PROTECT AF Study Rev. 6 Protocol Synopsis Title WATCHMAN Left Atrial Appendage System for Embolic PROTECTion in Patients with Atrial Fibrillation (PROTECT AF) Sponsor Atritech/Boston Scientific
Status Epilepticus in Children
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
ORIGINAL CONTRIBUTION. Abstract
 ORIGINAL CONTRIBUTION Comparison of Clinician Suspicion Versus a Clinical Prediction Rule in Identifying Children at Risk for Intra-abdominal Injuries After Blunt Torso Trauma Prashant Mahajan, MD, MPH,
ORIGINAL CONTRIBUTION Comparison of Clinician Suspicion Versus a Clinical Prediction Rule in Identifying Children at Risk for Intra-abdominal Injuries After Blunt Torso Trauma Prashant Mahajan, MD, MPH,
11/1/2018 STATUS EPILEPTICUS DISCLOSURE SPEAKER FOR SUNOVION AND UCB PHARMACEUTICALS. November is National Epilepsy Awareness Month
 STATUS EPILEPTICUS ALBERTO PINZON, MD, MSBE, PhD November is National Epilepsy Awareness Month DISCLOSURE SPEAKER FOR SUNOVION AND UCB PHARMACEUTICALS 1 SEIZURE A transient occurrence of signs and/or symptoms
STATUS EPILEPTICUS ALBERTO PINZON, MD, MSBE, PhD November is National Epilepsy Awareness Month DISCLOSURE SPEAKER FOR SUNOVION AND UCB PHARMACEUTICALS 1 SEIZURE A transient occurrence of signs and/or symptoms
Continuing Medical Education Activity in Academic Emergency Medicine
 CONTINUING MEDICAL EDUCATION Continuing Medical Education Activity in Academic Emergency Medicine CME Editor: Hal Thomas, MD Authors: Kenneth Yen, MD, MS, Nathan Kuppermann, MD, MPH, Kathleen Lillis, MD,
CONTINUING MEDICAL EDUCATION Continuing Medical Education Activity in Academic Emergency Medicine CME Editor: Hal Thomas, MD Authors: Kenneth Yen, MD, MS, Nathan Kuppermann, MD, MPH, Kathleen Lillis, MD,
Disclosures. What is Status Epilepticus? Purpose of Today s Discussion. Nothing to Disclose. How do I recognize Status Epilepticus?
 Disclosures Nothing to Disclose Neurologic Emergencies SID W. ATKINSON MD Chief, Division of Child Neurology, and Developmental Pediatrics Purpose of Today s Discussion Understand 2 Neurologic Emergencies
Disclosures Nothing to Disclose Neurologic Emergencies SID W. ATKINSON MD Chief, Division of Child Neurology, and Developmental Pediatrics Purpose of Today s Discussion Understand 2 Neurologic Emergencies
Status Epilepticus in Children. Azhar Daoud Professor of Child Neurology Jordan Univ of science and Tech
 Status Epilepticus in Children Azhar Daoud Professor of Child Neurology Jordan Univ of science and Tech Status epilepticus (SE) presents in a multitude of forms, dependent on etiology and patient age
Status Epilepticus in Children Azhar Daoud Professor of Child Neurology Jordan Univ of science and Tech Status epilepticus (SE) presents in a multitude of forms, dependent on etiology and patient age
JPPT Brief Review Article
 Brief Review Article Treatment of Acute Seizures: Is Intranasal Midazolam a Viable Option? Lesley K. Humphries, PharmD 1 and Lea S. Eiland, PharmD 2,3 1 Department of Pharmacy, Rockingham Memorial Hospital,
Brief Review Article Treatment of Acute Seizures: Is Intranasal Midazolam a Viable Option? Lesley K. Humphries, PharmD 1 and Lea S. Eiland, PharmD 2,3 1 Department of Pharmacy, Rockingham Memorial Hospital,
Treatment adherence and outcomes in the management of convulsive status epilepticus in the emergency room
 Original article Epileptic Disord 2007; 9 (1): 43-50 Treatment adherence and outcomes in the management of convulsive status epilepticus in the emergency room Taim Muayqil, Brian H. Rowe, S. Nizam Ahmed
Original article Epileptic Disord 2007; 9 (1): 43-50 Treatment adherence and outcomes in the management of convulsive status epilepticus in the emergency room Taim Muayqil, Brian H. Rowe, S. Nizam Ahmed
Comparison of Prediction Rules and Clinician Suspicion for Identifying Children With Clinically Important Brain Injuries After Blunt Head Trauma
 ORIGINAL CONTRIBUTION Comparison of Prediction Rules and Clinician Suspicion for Identifying Children With Clinically Important Brain Injuries After Blunt Head Trauma Shireen M. Atabaki, MD, MPH, John
ORIGINAL CONTRIBUTION Comparison of Prediction Rules and Clinician Suspicion for Identifying Children With Clinically Important Brain Injuries After Blunt Head Trauma Shireen M. Atabaki, MD, MPH, John
Title 1 Descriptive title identifying the study design, population, interventions, and, if applicable, trial acronym
 SPIRIT 2013 Checklist: Recommended items to address in a clinical trial protocol and related documents* Section/item Item No Description Addressed on page number Administrative information Title 1 Descriptive
SPIRIT 2013 Checklist: Recommended items to address in a clinical trial protocol and related documents* Section/item Item No Description Addressed on page number Administrative information Title 1 Descriptive
Pain Rating Scale GG. PAIN MANAGEMENT (NEW 10) 1. Initiate General Patient Care.
 GG. PAIN MANAGEMENT (NEW 10) 1. Initiate General Patient Care. 2. Presentation Pain may be present in many different conditions. Management of pain in the field can help to reduce suffering, make transport
GG. PAIN MANAGEMENT (NEW 10) 1. Initiate General Patient Care. 2. Presentation Pain may be present in many different conditions. Management of pain in the field can help to reduce suffering, make transport
Efficacy and Safety of Diclofenac Potassium 25 mg Tablet Taken Three Times Daily in Subjects With Acute Joint Pain
 Page 1 of 8 A service of the U.S. National Institutes of Health Try our beta test site Trial record 1 of 1 for: 853-P-401 Previous Study Return to List Next Study Efficacy and Safety of Taken Three Times
Page 1 of 8 A service of the U.S. National Institutes of Health Try our beta test site Trial record 1 of 1 for: 853-P-401 Previous Study Return to List Next Study Efficacy and Safety of Taken Three Times
BIBLIOGRAPHIC REFERENCE TABLE FOR SODIUM VALPROATE IN CHILDHOOD EPILEPSY
 BIBLIOGRAPHIC REFERENCE TABLE FOR SODIUM VALPROATE IN CHILDHOOD EPILEPSY Bibliographic Marson AG et al. for (Review). The Cochrane 2000 De Silva M et al. Romised or for childhood. Lancet, 1996; 347: 709-713
BIBLIOGRAPHIC REFERENCE TABLE FOR SODIUM VALPROATE IN CHILDHOOD EPILEPSY Bibliographic Marson AG et al. for (Review). The Cochrane 2000 De Silva M et al. Romised or for childhood. Lancet, 1996; 347: 709-713
Epilepsy and EEG in Clinical Practice
 Mayo School of Professional Development Epilepsy and EEG in Clinical Practice November 10-12, 2016 Hard Rock Hotel at Universal Orlando Orlando, FL Course Directors Jeffrey Britton, MD and William Tatum,
Mayo School of Professional Development Epilepsy and EEG in Clinical Practice November 10-12, 2016 Hard Rock Hotel at Universal Orlando Orlando, FL Course Directors Jeffrey Britton, MD and William Tatum,
RESEARCH ARTICLE MIDAZOLAM EFFICACY AND SIDE EFFECTS IN GENERALIZED AND PARTIAL REFRACTORY STATUS EPILEPTICUS IN CHILDREN
 RESEARCH ARTICLE MIDAZOLAM EFFICACY AND SIDE EFFECTS IN GENERALIZED AND PARTIAL REFRACTORY STATUS EPILEPTICUS IN CHILDREN M.R. Salehi Omran MD 1, M.R. Edraki MD 2 1. Associate Professor, Pediatric neurologist,
RESEARCH ARTICLE MIDAZOLAM EFFICACY AND SIDE EFFECTS IN GENERALIZED AND PARTIAL REFRACTORY STATUS EPILEPTICUS IN CHILDREN M.R. Salehi Omran MD 1, M.R. Edraki MD 2 1. Associate Professor, Pediatric neurologist,
Multicenter cohort study of in-hospital pediatric cardiac arrest*
 Feature Articles Multicenter cohort study of in-hospital pediatric cardiac arrest* Kathleen L. Meert, MD, FCCM; Amy Donaldson, MS; Vinay Nadkarni, MD, FCCM; Kelly S. Tieves, DO; Charles L. Schleien, MD,
Feature Articles Multicenter cohort study of in-hospital pediatric cardiac arrest* Kathleen L. Meert, MD, FCCM; Amy Donaldson, MS; Vinay Nadkarni, MD, FCCM; Kelly S. Tieves, DO; Charles L. Schleien, MD,
Midazolam for seizures: Buccal administration
 Midazolam for seizures: Buccal administration Rationale Buccal Midazolam is a convenient and efficient method used to treat prolonged seizures and status epilepticus in children. It can be used in hospital
Midazolam for seizures: Buccal administration Rationale Buccal Midazolam is a convenient and efficient method used to treat prolonged seizures and status epilepticus in children. It can be used in hospital
Chapter 15. Seizures. Learning Objectives. Learning Objectives 9/11/2012
 Chapter 15 Seizures Learning Objectives Demonstrate proper procedure for rectal administration of diazepam, and discuss why rectal administration is sometimes necessary for patient having a seizure Discuss
Chapter 15 Seizures Learning Objectives Demonstrate proper procedure for rectal administration of diazepam, and discuss why rectal administration is sometimes necessary for patient having a seizure Discuss
5/23/14. Febrile seizures: Who need further workup? Afebrile seizures: Who needs imaging? Status epilepticus: Most effective treatments
 Febrile seizures: Who need further workup? Afebrile seizures: Who needs imaging? Status epilepticus: Most effective treatments Andi Marmor, MD, MSEd Associate Professor, Pediatrics University of California,
Febrile seizures: Who need further workup? Afebrile seizures: Who needs imaging? Status epilepticus: Most effective treatments Andi Marmor, MD, MSEd Associate Professor, Pediatrics University of California,
CHAIR SUMMIT 7TH ANNUAL #CHAIR2014. Master Class for Neuroscience Professional Development. September 11 13, Westin Tampa Harbour Island
 #CHAIR2014 7TH ANNUAL CHAIR SUMMIT Master Class for Neuroscience Professional Development September 11 13, 2014 Westin Tampa Harbour Island Sponsored by #CHAIR2014 Clinical Case Challenge: Seizure Emergency
#CHAIR2014 7TH ANNUAL CHAIR SUMMIT Master Class for Neuroscience Professional Development September 11 13, 2014 Westin Tampa Harbour Island Sponsored by #CHAIR2014 Clinical Case Challenge: Seizure Emergency
Talk outline. Some definitions. Emergency epilepsy now what? Recognising seizure types. Dr Richard Perry. Management of status epilepticus
 Emergency epilepsy now what? Dr Richard Perry Imperial College NHS Trust Imperial College Talk outline Recognising seizure types Management of status epilepticus Some definitions Epileptic seizure A clinical
Emergency epilepsy now what? Dr Richard Perry Imperial College NHS Trust Imperial College Talk outline Recognising seizure types Management of status epilepticus Some definitions Epileptic seizure A clinical
2018 American Academy of Neurology
 Practice Guideline Update Efficacy and Tolerability of the New Antiepileptic Drugs I: Treatment of New-Onset Epilepsy Report by: Guideline Development, Dissemination, and Implementation Subcommittee of
Practice Guideline Update Efficacy and Tolerability of the New Antiepileptic Drugs I: Treatment of New-Onset Epilepsy Report by: Guideline Development, Dissemination, and Implementation Subcommittee of
SAGE-547 for super-refractory status epilepticus
 NIHR Innovation Observatory Evidence Briefing: April 2017 SAGE-547 for super-refractory status epilepticus NIHRIO (HSRIC) ID: 10866 NICE ID: 8456 Status epilepticus is a single epileptic seizure lasting
NIHR Innovation Observatory Evidence Briefing: April 2017 SAGE-547 for super-refractory status epilepticus NIHRIO (HSRIC) ID: 10866 NICE ID: 8456 Status epilepticus is a single epileptic seizure lasting
Management of Suspected Opioid Overdose With Naloxone by EMS Personnel
 Management of Suspected Opioid Overdose With Naloxone by EMS Personnel DATE: January 10, 2018 PRESENTED BY: Roger Chou, M. D., Director, Pacific Northwest Evidence - based Practice Center Purpose of Report
Management of Suspected Opioid Overdose With Naloxone by EMS Personnel DATE: January 10, 2018 PRESENTED BY: Roger Chou, M. D., Director, Pacific Northwest Evidence - based Practice Center Purpose of Report
Clopidogrel and Aspirin in Acute Ischemic Stroke and TIA: Final Results of the POINT Trial
 Clopidogrel and Aspirin in Acute Ischemic Stroke and TIA: Final Results of the POINT Trial S. Claiborne Johnston, 1 J. Donald Easton, 2 Mary Farrant, 2 William Barsan, 3 Robin A. Conwit, 4 Jordan J. Elm,
Clopidogrel and Aspirin in Acute Ischemic Stroke and TIA: Final Results of the POINT Trial S. Claiborne Johnston, 1 J. Donald Easton, 2 Mary Farrant, 2 William Barsan, 3 Robin A. Conwit, 4 Jordan J. Elm,
S (17) Reference: YAJEM 57199
 Accepted Manuscript Should patients with complex febrile seizure be admitted for further management? Heather Olson, Tiffany Rudloe, Tobias Loddenkemper, Marvin B. Harper, Amir A. Kimia PII: S0735-6757(17)31061-6
Accepted Manuscript Should patients with complex febrile seizure be admitted for further management? Heather Olson, Tiffany Rudloe, Tobias Loddenkemper, Marvin B. Harper, Amir A. Kimia PII: S0735-6757(17)31061-6
June 30 (Fri), Teaching Session 1. New definition & epilepsy classification. Chairs Won-Joo Kim Ran Lee
 June 30 (Fri), 2017 Teaching Session 1 New definition & epilepsy classification Chairs Won-Joo Kim Ran Lee Teaching Session 1 TS1-1 Introduction of new definition of epilepsy Sung Chul Lim Department of
June 30 (Fri), 2017 Teaching Session 1 New definition & epilepsy classification Chairs Won-Joo Kim Ran Lee Teaching Session 1 TS1-1 Introduction of new definition of epilepsy Sung Chul Lim Department of
Intervention [5] Comparison [6]
![Intervention [5] Comparison [6] Intervention [5] Comparison [6]](/thumbs/86/94005273.jpg) Cowan LD. The epidemiology of the epilepsies in children. Mental Retardation and Developmental Disabilities Res Reviews, 2002; 8: 171-181 Review article Paediatric patients Discusses incidence and prevalence
Cowan LD. The epidemiology of the epilepsies in children. Mental Retardation and Developmental Disabilities Res Reviews, 2002; 8: 171-181 Review article Paediatric patients Discusses incidence and prevalence
Hope for New Treatments for Acute Repetitive Seizures
 Current Literature In Clinical Science Hope for New Treatments for Acute Repetitive Seizures A Double-Blind, Randomized, Placebo-Controlled Trial of a Diazepam Auto-Injector Administered by Caregivers
Current Literature In Clinical Science Hope for New Treatments for Acute Repetitive Seizures A Double-Blind, Randomized, Placebo-Controlled Trial of a Diazepam Auto-Injector Administered by Caregivers
Status Epilepticus: A refresher. Objectives
 Status Epilepticus: A refresher Ruben D. Villanueva, Pharm.D., BCPS OU Medical Center Trauma ICU Pharmacist Objectives Define seizures, convulsive and non convulsive status epilepticus, and refractory
Status Epilepticus: A refresher Ruben D. Villanueva, Pharm.D., BCPS OU Medical Center Trauma ICU Pharmacist Objectives Define seizures, convulsive and non convulsive status epilepticus, and refractory
Turning Up the Heat on the Impact of Febrile Status Epilepticus
 Current Literature In Clinical Science Turning Up the Heat on the Impact of Febrile Status Epilepticus MRI Abnormalities Following Febrile Status Epilepticus in Children: The FEBSTAT Study. Shinnar S,
Current Literature In Clinical Science Turning Up the Heat on the Impact of Febrile Status Epilepticus MRI Abnormalities Following Febrile Status Epilepticus in Children: The FEBSTAT Study. Shinnar S,
The New England Journal of Medicine A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES
 A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES JOHN F. ANNEGERS, PH.D., W. ALLEN HAUSER, M.D., SHARON P. COAN, M.S., AND WALTER A. ROCCA, M.D., M.P.H. ABSTRACT Background The risk
A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES JOHN F. ANNEGERS, PH.D., W. ALLEN HAUSER, M.D., SHARON P. COAN, M.S., AND WALTER A. ROCCA, M.D., M.P.H. ABSTRACT Background The risk
Alotaibi, Khalid Nijr (2017) Convulsive status epilepticus in children. PhD thesis, University of Nottingham.
 Alotaibi, Khalid Nijr (2017) Convulsive status epilepticus in children. PhD thesis, University of Nottingham. Access from the University of Nottingham repository: http://eprints.nottingham.ac.uk/38829/1/khalid%20final%20thesis%20nov%202016.pdf
Alotaibi, Khalid Nijr (2017) Convulsive status epilepticus in children. PhD thesis, University of Nottingham. Access from the University of Nottingham repository: http://eprints.nottingham.ac.uk/38829/1/khalid%20final%20thesis%20nov%202016.pdf
Lesson learnt from big trials. Sung Phil Chung, MD Gangnam Severance Hospital, Yonsei Univ.
 Lesson learnt from big trials Sung Phil Chung, MD Gangnam Severance Hospital, Yonsei Univ. Trend of cardiac arrest research 1400 1200 1000 800 600 400 200 0 2008 2009 2010 2011 2012 2013 2014 2015 2016
Lesson learnt from big trials Sung Phil Chung, MD Gangnam Severance Hospital, Yonsei Univ. Trend of cardiac arrest research 1400 1200 1000 800 600 400 200 0 2008 2009 2010 2011 2012 2013 2014 2015 2016
Paediatrica Indonesiana. Predictive factors for recurrent febrile seizures in children
 Paediatrica Indonesiana VOLUME 52 November NUMBER 6 Original Article Predictive factors for recurrent febrile seizures in children Pengekuten T. Marudur, Elisabeth S. Herini, Cahya Dewi Satria Abstract
Paediatrica Indonesiana VOLUME 52 November NUMBER 6 Original Article Predictive factors for recurrent febrile seizures in children Pengekuten T. Marudur, Elisabeth S. Herini, Cahya Dewi Satria Abstract
FEBRILE SEIZURES. IAP UG Teaching slides
 FEBRILE SEIZURES 1 DEFINITION Febrile seizures are seizures that occur between the age of 6 and 60 months with a temperature of 38 C or higher, that are not the result of central nervous system infection
FEBRILE SEIZURES 1 DEFINITION Febrile seizures are seizures that occur between the age of 6 and 60 months with a temperature of 38 C or higher, that are not the result of central nervous system infection
NASDAQ: ZGNX. Company Presentation. October 2017
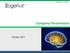 NASDAQ: ZGNX Company Presentation October 2017 2 Forward Looking Statement Zogenix cautions you that statements included in this presentation that are not a description of historical facts are forward-looking
NASDAQ: ZGNX Company Presentation October 2017 2 Forward Looking Statement Zogenix cautions you that statements included in this presentation that are not a description of historical facts are forward-looking
The Management of Refractory Status Epilepticus: An Update
 Epilepsia, 47(Suppl. 1):35 40, 2006 Blackwell Publishing, Inc. C International League Against Epilepsy The Management of Refractory Status Epilepticus: An Update Daniel H. Lowenstein Department of Neurology,
Epilepsia, 47(Suppl. 1):35 40, 2006 Blackwell Publishing, Inc. C International League Against Epilepsy The Management of Refractory Status Epilepticus: An Update Daniel H. Lowenstein Department of Neurology,
Impact of an Interactive Online Nursing Educational Module on Insulin Errors in Hospitalized Pediatric Patients
 Diabetes Care Publish Ahead of Print, published online May 26, 2010 Impact of an Interactive Online Nursing Educational Module on Insulin Errors in Hospitalized Pediatric Patients Short Title: Impact of
Diabetes Care Publish Ahead of Print, published online May 26, 2010 Impact of an Interactive Online Nursing Educational Module on Insulin Errors in Hospitalized Pediatric Patients Short Title: Impact of
Supplementary Online Content
 Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Can Status Epilepticus Sometimes Just Be a Long Seizure?
 Current Literature In Clinical Science Can Status Epilepticus Sometimes Just Be a Long Seizure? Unprovoked Status Epilepticus: The Prognosis for Otherwise Normal Children With Focal Epilepsy. Camfield
Current Literature In Clinical Science Can Status Epilepticus Sometimes Just Be a Long Seizure? Unprovoked Status Epilepticus: The Prognosis for Otherwise Normal Children With Focal Epilepsy. Camfield
Status epilepticus (SE) is a condition that commonly
 Status Epilepticus in the Pediatric Emergency Department Joshua Goldstein, MD Status epilepticus (SE) is a common childhood condition often seen by emergency physicians. It occurs at a frequency of between
Status Epilepticus in the Pediatric Emergency Department Joshua Goldstein, MD Status epilepticus (SE) is a common childhood condition often seen by emergency physicians. It occurs at a frequency of between
The risk of epilepsy following
 ~~ Article abstract41 cohort of 666 children who had convulsions with fever were followed to determine the risks of subsequent epilepsy High risks were found in children with preexisting cerebral palsy
~~ Article abstract41 cohort of 666 children who had convulsions with fever were followed to determine the risks of subsequent epilepsy High risks were found in children with preexisting cerebral palsy
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Clinical Study Underestimated Rate of Status Epilepticus according to the Traditional Definition of Status Epilepticus
 e Scientific World Journal Volume 2015, Article ID 801834, 5 pages http://dx.doi.org/10.1155/2015/801834 Clinical Study Underestimated Rate of Status Epilepticus according to the Traditional Definition
e Scientific World Journal Volume 2015, Article ID 801834, 5 pages http://dx.doi.org/10.1155/2015/801834 Clinical Study Underestimated Rate of Status Epilepticus according to the Traditional Definition
PROTOCOL. Francesco Brigo, Luigi Giuseppe Bongiovanni
 COMMON REFERENCE-BASED INDIRECT COMPARISON META-ANALYSIS OF INTRAVENOUS VALPROATE VERSUS INTRAVENOUS PHENOBARBITONE IN GENERALIZED CONVULSIVE STATUS EPILEPTICUS PROTOCOL Francesco Brigo, Luigi Giuseppe
COMMON REFERENCE-BASED INDIRECT COMPARISON META-ANALYSIS OF INTRAVENOUS VALPROATE VERSUS INTRAVENOUS PHENOBARBITONE IN GENERALIZED CONVULSIVE STATUS EPILEPTICUS PROTOCOL Francesco Brigo, Luigi Giuseppe
CONVULSIONS - AFEBRILE
 Incidence All Children require Management Recurrence Risk Indications for starting therapy Starting Anticonvulsant medication Criteria for Referral to Paediatric Neurology Useful links References Appendix
Incidence All Children require Management Recurrence Risk Indications for starting therapy Starting Anticonvulsant medication Criteria for Referral to Paediatric Neurology Useful links References Appendix
Identification of children at very low risk of clinically-important brain injuries after head trauma: a prospective cohort study
 Identification of children at very low risk of clinically-important brain injuries after head trauma: a prospective cohort study Nathan Kuppermann, James F Holmes, Peter S Dayan, John D Hoyle, Jr, Shireen
Identification of children at very low risk of clinically-important brain injuries after head trauma: a prospective cohort study Nathan Kuppermann, James F Holmes, Peter S Dayan, John D Hoyle, Jr, Shireen
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
A Fully Magnetically Levitated Left Ventricular Assist Device. Final Report of the MOMENTUM 3 Trial
 A Fully Magnetically Levitated Left Ventricular Assist Device Final Report of the MOMENTUM 3 Trial Mandeep R. Mehra, MD, Nir Uriel, MD, Joseph C. Cleveland, Jr., MD, Daniel J. Goldstein, MD, National Principal
A Fully Magnetically Levitated Left Ventricular Assist Device Final Report of the MOMENTUM 3 Trial Mandeep R. Mehra, MD, Nir Uriel, MD, Joseph C. Cleveland, Jr., MD, Daniel J. Goldstein, MD, National Principal
Emergency Management of Paediatric Status Epilepticus. Dr. Maggie Yau Department of Paediatrics Prince of Wales Hospital
 Emergency Management of Paediatric Status Epilepticus Dr. Maggie Yau Department of Paediatrics Prince of Wales Hospital Definition (ILAE 2015) After t1 failure of the mechanisms responsible for seizure
Emergency Management of Paediatric Status Epilepticus Dr. Maggie Yau Department of Paediatrics Prince of Wales Hospital Definition (ILAE 2015) After t1 failure of the mechanisms responsible for seizure
Shands Jacksonville Department of Pharmacy
 Shands Jacksonville Department of Pharmacy Medication Use Evaluation: IV Levetiracetam Evaluation Time Period: 05/27/2013 06/24/2013 Important Aspect of Care: Care of Patients, Medication Use, Prescribing
Shands Jacksonville Department of Pharmacy Medication Use Evaluation: IV Levetiracetam Evaluation Time Period: 05/27/2013 06/24/2013 Important Aspect of Care: Care of Patients, Medication Use, Prescribing
Emergency treatment of acute seizures and status epilepticus
 78 Arch Dis Child 1998;79:78 83 CURRET TOPIC Department of Paediatrics, University of Cambridge School of inical Medicine, Cambridge CB2 2QQ, UK R C Tasker Emergency treatment of acute seizures and status
78 Arch Dis Child 1998;79:78 83 CURRET TOPIC Department of Paediatrics, University of Cambridge School of inical Medicine, Cambridge CB2 2QQ, UK R C Tasker Emergency treatment of acute seizures and status
Accuracy of the Urinalysis for Urinary Tract Infections in Febrile Infants 60 Days and Younger
 Accuracy of the Urinalysis for Urinary Tract Infections in Febrile Infants 60 Days and Younger Leah Tzimenatos, MD, a Prashant Mahajan, MD, MPH, MBA, b Peter S. Dayan, MD, MSc, c Melissa Vitale, MD, d
Accuracy of the Urinalysis for Urinary Tract Infections in Febrile Infants 60 Days and Younger Leah Tzimenatos, MD, a Prashant Mahajan, MD, MPH, MBA, b Peter S. Dayan, MD, MSc, c Melissa Vitale, MD, d
Management of Complex Febrile Seizures
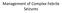 Management of Complex Febrile Seizures An 13 month old girl presents to the ED after having a shaking episode at home. Mom describes shaking of both arms and legs, lasting 20 minutes. The child has no
Management of Complex Febrile Seizures An 13 month old girl presents to the ED after having a shaking episode at home. Mom describes shaking of both arms and legs, lasting 20 minutes. The child has no
