SUCCESS IN THE DEVELOPMENT
|
|
|
- Eustace Caldwell
- 5 years ago
- Views:
Transcription
1 REVIEW ARTICLE Mesh in the Hiatus A Controversial Issue Eduardo M. Targarona, MD, PhD; Gali Bendahan, MD; Carmen Balague, MD, PhD; Jordi Garriga, MD; Manuel Trias, MD, PhD Objective: To analyze the experience acquired to date on the use of prosthetic mesh to prevent recurrence after laparoscopic repair of paraesophageal hernia. Data Sources: Current English-language literature review. Study Selection: Case reports, series, and opinion articles on the use of mesh for paraesophageal hernia repair. Data Extraction and Synthesis: Study type and results were analyzed. Most articles were short case series. Few comparative or randomized trials assessing the procedure have been published to date. The information available showed that the use of a mesh for hiatal repair was safe and prevented recurrence. However, data on the longterm results were lacking, and infrequent but severe complications may arise. Conclusions: The mesh should be used selectively, and the decision to proceed should be based on clinical experience. In light of the evidence available, however, it appears to be safe, and the fears expressed in the past have not been confirmed. Arch Surg. 2004;139: Author Affiliations: Service of Surgery, Hospital de Sant Pau, Autonomous University of Barcelona, Barcelona, Spain. SUCCESS IN THE DEVELOPMENT of laparoscopic fundoplication has made this procedure a valid alternative to medical therapy for the treatment of gastroesophageal reflux. Thanks to the experience acquired, the laparoscopic approach is now used to treat more complex situations, such as paraesophageal hernia (PEH) or type III (mixed) hiatal hernia. 1-8 The results of several series have shown that laparoscopic repair is also feasible and safe, despite the increased technical difficulty, and its immediate and short-term results are excellent 9-43 (Table 1). However, the incidence of recurrences may be high: as much as 42% in one series (Table 2). See Invited Critique on page 1296 One of the most demanding laparoscopic technical steps is crural closure, especially when the gap is wide and the closure inevitably entails a tension repair. Some authors recommend the use of prosthetic mesh to reinforce the hiatal closure (Table 3 and Table 4), but others argue against it. This review analyzes the experience accumulated so far on the use of mesh to reinforce the hiatus to prevent recurrence after laparoscopic repair of PEH. THE PROBLEM Laparoscopic repair of PEH and mixed hiatal hernias is a feasible, safe, but complex procedure. The experience during the past 15 years suggests that viscera reduction, sac excision, retrogastric crural closure, and fundoplication are the key technical factors. 1-8 Fixation of the gastric plicature, abdominal wall gastropexy, and gastrostomy are more controversial technical steps for maintaining the stomach in place in the abdomen. Although controlled comparative trials with the open approach are lacking (Table 4), the immediate clinical outcome of laparoscopic PEH repair is highly satisfactory. However, the recurrence rate is higher than expected after midterm follow-up as high as 42% when compared with the open approach (Table 5) and some authors have suggested that the laparoscopic approach is unsuitable. 17 The main reason for the failure of the hiatal repair is tension. Recurrence has been related to the mean diameter of the hiatus ( 10 cm in some cases). Another factor is the anatomy of the pillars. The hiatal crus is a fleshy structure without tendinous reinforcement. Standard sutures may cut the muscle, and when the hiatus is particularly wide and the pillars are approached, the lateral 1286
2 Table 1. Results of Laparoscopic Repair of PEH (Series With More Than 20 Cases) Source N Conversion Morbidity Mortality Mean Stay, d Mean Follow-up, mo Recurrence Good or Fair Outcome Comment Huntington, (2) 4 (7) NA Occ SE + ACR + FP Perdikis et al, (3) 9 (14) (13) 60 (92) 0 PCR + FP Edye et al, (5) 10 (17) 1 (2) NA 38 8 (14) NA 1 (2) SE + PCR + FP Gantert et al, (9) 5 (9) 1 (2) 3 11 NA 50 (91) 0 SE + PCR + FP Watson et al, (23) 11 (13) NA (1) 80 (93) 0 SE + PCR + FP Wu et al, (3) 6 (16) 2 (5) (24) 30 (79) 5 (13) Several repairs Horgan et al, (5) 1 (2) 1 (2) (12) NA Occ SE + PCR + FP Swanstrom et al, (12) (8) NA NA SE + PCR + FP Hashemi et al, (8) 3 (12) NA 20 (77) 0 SE + PCR + FP Peet et al, (14) 1 (5) 0 NA 24 5 (22) NA 3 (14) SE + PCR + FP + fixation Dahlberg et al, (5) 5 (14) 2 (5) (14) 32 (87) Occ SE + PCR + FP Wiechmann et al, (10) 1 (2) NA NA 19 4 (7) NA 0 SE + PCR + FP Velanovich and 31 5 (16) 3 (10) 1 (3) NA 24 NA NA NA Several repairs Karmy-Jones, Khaitan et al, (19) 6 (19) (40) NA NA SE + PCR + FP Pierre et al, (1.5) 57 (28.1) 1 (0.5) (2.0) 170 (83.7) 22 (10.8) SE + PCR + collis Mattar et al, (2.2) 14 (10.3) 3 (2.2) (30.1) NA 0 Several repairs Diaz et al, (2.6) 20 (17.2) 2 (1.7) (31.9) 9 (7.8) Occ SE + PCR + FP + fixation Targarona et al, NA 4 30 NA NA NA None Leeder et al, (8) 7 (13) 1 (2) (9) 41 (77) 14 (26) Several repairs Ponsky et al, (11) (4) NA PCR + Toupet + fixation Jobe et al, (7) 11 (20) (32) 45 (80) 6 (11) Hill repair Keidar and Szold, (3) 5 (15) 1 (3) (15) 28 (84) 28 (30) SE + PCR + FP Range (0-23) (0-28) (0-5.4) 2-4 (0-40) (77-94) (0-30) Abbreviations: ACR, anterior crural repair; FP, fundoplication; NA, not available; Occ, occasionally; PCR, posterior crural repair; PEH, paraesophageal hernia; SE, sac excision. Mesh Used Table 2. Recurrence After Surgical Treatment of PEH in Series With Systematic Radiologic Control Source of Patients With Esophagogram Recurrence, PEH Recurrence, No. Sliding, No. Symptoms, Mesh Type Open Surgery Luostarinen et al, /22 (86) 8 (42) (37) ±Pledget Laparoscopy Wu et al, /38 (92) 8 (23) (34) NA Hashemi et al, /27 (78) 9 (43) NA NA 8 (38) Pledget Wiechmann et al, /60 (73) 3 (7) (100) NA Khaitan et al, /25 (60) 6 (40) (50) Pledget Jobe et al, /52 (65) 11 (32) (65) Pledget 4cm Mattar et al, /125 (26) 11 (34) NA NA 14 (44) Pledget Keidar and Szold, NA 21 (15) (40) NA Diaz et al, /96 (69) 21 (32) (62) NA Tagarona et al, /37 (81) 6 (20) (50) NA Abbreviations: NA, not available; PEH, paraesophageal hernia. portions of the diaphragm near the crura become tense, with a potential risk of disruption. Currently, all hernia repairs are tension free (for example, the Lichtenstein repair or ventral hernia repair). However, performing a tension-free repair in the hiatus is technically very demanding, because of the oblique situation of the pillars and the difficulty of fixing the mesh. Furthermore, the hiatus is a complex anatomic structure in which the esophagus moves during respiratory excursion of the diaphragm, 96 whereas in inguinal or ventral hernia repair the mesh passively supports the intra-abdominal viscera. This means that any prosthetic mesh will be in contact with the esophagus, and so there is a theoretical risk of esophageal erosion and complication. This fact along with evidence of mechanical complications after placement of mesh for repair of abdominal wall defects and complications with mechanical devices located in the cardia (such as the Angelchik device and with the bands used in treatment of morbid obesity 100 ) seems to argue against the placement of foreign bodies in the hiatus. However, some surgeons report that the use of mesh in the hiatus is safe and the outcome acceptable (Tables 3 and 4). 1287
3 Table 3. Results of the Use of Mesh for PEH Repair Source N Morbidity Mortality Mean Stay, d Mean Follow-up, mo GI Tract Symptoms Recurrence Comment Open Surgery Carlson et al, (45) 1 (2) (10) 0 Onlay (polypropylene) Laparoscopy Kuster and Gilroy, (17) (17) Reduction + mesh + fixation (no sac excision) Edelman, (40) 1 (20) 4 NA NA 0 Mesh tension-free + FP + gastrostomy Pitcher et al, NA 0 ACR, FP, PTFE Oddsdottir et al, (20) 0 NA 9 1 (10) 0 Pledget, SE + PCR + FP Behrns and Schlinkert, NA 6 NA 0 Replacement mesh Huntington, (12) 0 NA Right crus patch (polypropylene) Paul et al, Anterior, tension-free, PTFE Frantzides and Carlson, Onlay PTFE Willekes et al, (27) 0 3 NA NA 0 Onlay PTFE, no CR ± FP Wu et al, (16) 2 (5) (5) 9 (24) Several repairs ± mesh Hawasli and Zonca, (4) (30) 0 SE + free tension onlay mesh + fixation (polypropylene) Basso et al, (4) (9) 0 Tension-free (polypropylene) Lambert and Huddart, (14) 0 0 NA 1 (14) 0 Onlay (polypropylene) Meyer et al, (10) SE + CR + FP + mesh (polypropylene 50%, PTFE 50%) Casaccia et al, (12) SE + tension-free + FP (composite A-shaped mesh) Kamolz et al, NA NA 0 None Ponsky et al, NA Tension-free + gastropexy Champion and Rock, (40) 1 (2) SE + CR + FP + buttress mesh Oelschlager et al, (11) NA 8 NA 1 (11) SE + PCR + FP (biomaterial mesh) Leeder et al, NA NA (14) 2 (14) Several techniques (U-shaped mesh) Keidar and Szold, NA NA 1 (10) SE + PCR + FP (PTFE + polypropylene) Granderath et al, (4) 0 NA SE + PCR + FP + onlay (polypropylene) Abbreviations: ACR, anterior crural repair; CR, crural repair; FP, fundoplication; NA, not available; PCR, posterior crural repair; PEH, paraesophageal hernia; PTFE, polytef; SE, sac excision. RECURRENCES Analysis of recurrences shows different patterns for time of presentation and shape (Table 2). Immediate recurrent hernias are usually secondary to total disruption of the hiatal closure with a relapsing PEH. Long-term recurrences may adopt several patterns: complete recurrent PEH, fundoplication migration, or a small sliding hernia, without a clear recurrence of the paraesophageal sac. In the latter subgroup, the incidence of symptoms is variable, and most are identified only by esophagogram. Recurrences of symptoms are treated surgically. However, there is tacit agreement that nonsymptomatic recurrences, especially in cases of small sliding hernias, do not require repair. Recurrent hernias of any type should be considered as technical failures, although the longterm outcome of asymptomatic recurrent hernias is unknown. METHODS A systematic PubMed search looking for all of the studies published in English in relation to treatment of paraesophageal and mixed hiatal hernias was performed. Particular attention was paid to the use of meshes for reinforcement of the hiatal repair. SURGICAL TECHNIQUE The most controversial issue in the use of prostheses in the hiatus is the surgical technique. Several models have been proposed. Tension-Free Techniques One tension-free technique is anterior placement of a triangular piece of mesh, proposed by Paul et al 52 (Figure 1). A triangular or semilunar polytef patch is placed to occlude the anterior segment of the hiatus and fixed with staples or stitches. The stomach is fixed to the abdomen and a fundoplication is added. For posterior placement of a triangular piece of mesh (Figure 2), the aim is the same as in the technique for anterior placement. Kuster and Gilroy 46 proposed a posterior segmental occlusion, occluding the base of the pillar overture, and placing the esophagus anteriorly, fixing the mesh with staples or stitches. Fixation to the abdominal wall or a gastrostomy is also performed. A third technique involves onlay of a piece of mesh, with a hole facilitating the passage of the esophagus. The mesh covers the whole of the hiatal defect, and no attempt is made to close the hiatus (Figure 3). There are several shapes of mesh designed to allow the passage of the esophagus and to facilitate fixation (eg, U shape, 22,53 A shape 59 )(Figure 4). Basso et al 101 also proposed covering the mesh with autologous flaps of peritoneal tissue obtained from the hernia sac. Casaccia et al
4 Table 4. Results of Comparative Studies of PEH Repair Source and Type Operative Mean Mean Good or of Repair N Time, min Conversion Morbidity Mortality Stay, d Follow-up, mo Recurrence Fair Outcome Reoperation Comment Laparoscopy vs Laparoscopy + Mesh Basso et al, * Laparoscopy (1) 5 (8) NA (14) NA 6 (9) None Laparoscopy + mesh (4) NA 0 Tension-free (polypropylene) Hui et al, * Laparoscopy (8) 3 (25) NA (100) NA SE + PCR + FP (PTFE + polypropylene) Laparoscopy + mesh NA 2 (17) NA (100) NA SE + PCR + FP Kamolz et al, * Laparoscopy (9) 95 (95) 6 (6) PCR + FP Laparoscopy + mesh NA 95 (95) 1 (1) PCR + FP + mesh polypropylene Frantzides et al, Laparoscopy 36 NA 0 1 (3) NA NA 40 8 (22) NA 4 (11) SE + PCR + FP Laparoscopy + mesh 36 NA 0 1 (3) NA NA 40 0 NA 1 (3) SE + PCR + FP + PTFE Open Surgery vs Laparoscopy Kuster and Gilroy, Open NA NA NA NA 2 (7) ACR 16, PCR 11, FP 7 Laparoscopic (17) 1 (17) (17) NA 0 Reduction + mesh + fixation Schauer et al, Open NA 15 (60) NA NA 21 (84) NA None Laparoscopic (4) 20 (29) NA 5 13 NA 66 (94) NA PCR + FP ± mesh Hashemi et al, Open NA NA 1 (4) (16) 22 (88) NA SE + PCR + FP Laparoscopic (8) 3 (12) (42) 20 (77) NA SE + PCR + FP (pledget) Abbreviations: ACR, anterior crural repair; FP, fundoplication; NA, not available; PCR, posterior crural repair; PEH, paraesophageal hernia; PTFE, polytef; SE, sac excision. *Nonrandomized; included all types of hiatal hernias. Prospective randomized trial. recently proposed a composite polytef-polypropylene A- shaped mesh. This mesh was designed according to the strength lines of the hiatus and produced good results after 8 months of follow-up. A piece of mesh may be placed just covering the defect below the esophagus, overlapping both pillars laterally. This was described by Basso et al 56 (Figure 5). In another technique, after a standard closure of the hiatus, a relaxing incision lateral to the right crura is placed, and a patch is fixed with stitches or staples covering the diaphragmatic defect (Figure 6). Described by Huntington in 1997, 51 it has been also proposed by Horgan et al. 15 Non Tension-Free Techniques Figure 1. Tension-free repair: anterior placement of a triangular piece of mesh. 39 Simple crural closure with either simple stitches (Figure 7) or a continuous suture (Figure 8) is the most common method for hiatal closure. In 1992, Cuschieri et al 102 described the first specific method for hiatal closure, using a continuous suture. Other non tension-free techniques are reinforcement of the crural closure, to avoid the cutting effect of the stitches; simple stitches with Teflon or Dacron pledgets 18,29 (Figure 9); a polypropylene strip along the crura to hold the stitches (Figure 10); and a piece of polypropylene mesh covering both edges of the pillars. The stitches close the hiatus including the mesh and tissue, as proposed by Kamolz et al 60 (Figure 11). A buttress mesh technique has also been described. A long strip of mesh is placed below the esophagus, covering the pillar closure (Figure 12). The advantage is that it avoids the encircling of the esophagus, reducing the risk of dysphagia or erosion. Champion and Rock 61 reported good results in a series of 52 cases, with a recurrence rate of 2%, although esophagography was performed in only 52% of cases. Placement of onlay mesh around the esophagus with a hole in the middle, once the defect has been closed, has been used (Figure 13). There are also preshaped meshes designed to adapt anatomically to the characteristics of the anatomic area 31,62 (Figure 4). 1289
5 Table 5. Results of the Open Approach for PEH Repair Source N Mean Mean Morbidity Mortality Stay, d Follow-up, mo Recurrence Good or Fair Outcome Collis Reoperation Comment Skinner and Belsey, (8-13)* 1 (1.2) NA 60 2 (7-21)* 7 (88) (Mark IV) NA NA Thor, Mark IV (60%) Hill and Tobias, NA NA NA NA NA NA Lap, SE + ACR Wichterman et al, (17) 1 (4) NA 62 0 NA NA 2 (7) Lap, SE + CR + FP + fixation Pearson et al, (11) 1 (2) NA 72 2 (4) 36 (68) (70) 2 (4) Thor, gastroplasty + Belsey Ellis et al, (24) 1 (2) (10) (88) NA 4 (8) Lap, ACR + fixation Treacy and Jamieson, NA 1 (2) NA NA 8 (81) 6 (45) NA 0 Lap, SE + PCR + FP Menguy, NA NA NA NA NA NA Lap, SE + ACR + fixation Ackermann et al, NA 1 (2) NA (50) 34 (85) NA NA Lap, CR + fixation ± FP Haas et al, (17) 5 (17) 11 9 NA 24 (83) 0 0 SE + PCR + FP Harriss et al, (12) 2 (8) NA 48 NA 22 (88) 0 0 Thor, ES + CP + FP Allen et al, (27) 0 11 (9) 42 NA 111 (93) 78 (66) 1 (1) Thor, Collis-Nissen Williamson et al, NA NA NA (10) 99 (83) NA NA Lap, fixation ± Nissen Myers et al, (38) NA NA 67 1 (3) 31 (84) NA NA SE + ACR + fixation ± FP Altorki et al, NA 1 (2) NA 45 4 (9) 42 (89) NA 0 Thor, Belsey Mark IV, Nissen Luostarinen et al, (23) 0 NA 37 9 (41) 21 (95) NA NA Lap, PCR ± FP (some pledget) Carlson et al, (45) 1 (2) NA NA NA Lap, PCR + mesh + gastrostomy Maziak et al, (19) 2 (2) NA 93 2 (2) 75 (80) 70 (74) 5 (5) Thor + Belsey Mark IV Geha et al, (6) 2 (2) NA NA 0 96 (96) NA NA 80% Abd, reduction + fixation Rogers et al, (8) (2) 51 (85) NA NA Thor, CP ± FP Low and Simchuk, (16) NA NA NA NA Hill procedure Range (6-45) (0-19) 5-12 (1.6-50) (68-95) Abbreviations: Abd, abdominal; ACR, anterior crural repair; FP, fundoplication; Lap, laparotomy; NA, not available; PCR, posterior crural repair; PEH, paraesophageal hernia; SE, sac excision; Thor, thoracotomy. *Range indicates simple closure vs Belsey Mark IV operation. Indicates of those with fundoplication. Indicates of those without fundoplication. Figure 2. Tension-free repair: posterior placement of a triangular piece of mesh. 46 Other Maneuvers Additional maneuvers for fixing the stomach in the abdominal cavity include a range of techniques, such as fixation of the fundoplication to the diaphragm, fixation of the gastric body to the Figure 3. Tension-free repair: onlay piece of mesh, with a hole facilitating the passage of the esophagus. abdominal wall, and gastrostomy. 103,104 Fundoplication itself may have some fixation effect. Some authors have proposed that the Toupet technique may avoid recurrence because the posterior placement of the fundus covers the crural closure and fixes it to 1290
6 Figure 4. Shapes of mesh designed to allow passage of the esophagus and to facilitate fixation (U shape, 22,53 A shape 59 ). Figure 6. Tension-free repair. After a standard closure of the hiatus, a relaxing incision lateral to the right crura is performed, and a patch is fixed with stitches or staples covering the diaphragmatic defect. 15,51 Figure 5. Tension-free repair: piece of mesh just covering the defect below the esophagus, overlapping both pillars laterally. 56 the diaphragm. 1,3 However, there are no definitive data from randomized trials to support any of these measures. REPAIR MATERIAL The prostheses available for hiatal reinforcement are made of a range of materials. Most authors agree that the material used should be nonresorbable, because resorbable material (polyglycolic acid) loses its mechanical properties as it is resorbed. Nonresorbable material may be made of polypropylene, polytef, or composite (polytef plus polypropylene; C. R. Bard, Inc, Murray Hill, NJ). Recently, a nonresorbable material of biological origin has been used (Surgisis; Cook Biotech Incorporated, West Lafayette, Ind). 62 The crucial aspect of the material used to reinforce the hiatus is stiffness. The advantages of polytef are its softness and its lower capacity to induce adhesions. The different surfaces prevent tight adhesions to the visceral face of the mesh, and the texture of the free margin in near contact with the esophagus is potentially less dangerous. However, the handling and sewing of the mesh may be more difficult than when polypropylene is used. The main drawback of polypropylene is the stiffness of the margins and the possibility that the esophagus will be eroded. Experience with mixed mesh or with material of biological origin is scarce. RESULTS Most of the clinical results of the use of mesh in the hiatus come from short series of patients, although the midterm Figure 7. Non tension-free repair: simple crural closure with simple stitches. follow-up is often adequate (up to 5 years). No long-term experience (up to 10 years) is available. Mesh has been used mostly in adults, although there is some experience in the pediatric setting as well. Overall results are plotted in Table 2; tolerance is good and the recurrence rate and morbidity are both low. Three comparative studies have been published (Table 3), but only 1 was a prospective randomized trial. In addition, 2 of the comparative trials included patients with all types of hiatal hernias, and only 1 focused on PEH hernia repair. Basso et al 56 compared simple and tensionfree closures using an onlay piece of polypropylene, dividing their personal series chronologically into 2 parts. Kamolz et al 60 compared simple closure with a reinforcement procedure that put the stitches over a piece of polypropylene covering the hiatal closure. Neither study was randomized; they were merely comparisons of initial experiences withoutmeshwithmorerecentexperienceswithmesh. They 1291
7 Figure 8. Non tension-free repair: simple crural closure with continuous suture. 102 Figure 10. Non tension-free repair with reinforcement of the crural closure, using a polypropylene strip along the crura to hold the stitches. Figure 9. Non tension-free repair with reinforcement of the crural closure to avoid the cutting effect of the stitches, using simple stitches with Teflon or Dacron pledgets. 18,29 also counted hiatal repair of all types, including type I hernias or pure gastroesophageal reflux disease without hernia. Mesh placement was followed by reductions in the incidence of recurrences, without specific morbidity. Frantzides et al 65 showed the results of a prospective randomized trial comparing simple closure with polytef onlay reinforcement for PEH hernia repair, in cases with hiatus wider than 8 cm. Recurrences were significantly reduced after mesh placement (20% vs 0%; P.001), without long-term sequel, after a 40-month follow-up period. The main drawback with the use of mesh in the hiatus is the risk of local complications (fibrosis and adhesions, erosion, or perforation). Nonetheless, the incidence of mesh-related complications in the hiatus is currently less than 2%, although no reports on longterm outcome ( 10 years) are available. Figure 11. Non tension-free repair with reinforcement of the crural closure, using a polypropylene piece of mesh covering both edges of the pillars. 60 Mesh placed in the hiatus may induce complications because of the type of mesh or the device used for fixation. Some complications may be related to local fibrosis (dysphagia) or to the erosion of the digestive lumen. Others may be induced by the device applied to fix the mesh, especially whenstaplesortackersareused,andinjurytothevitalstructures surrounding the hiatus may occur. Teflon pledgets may also erode the fundus or induce fibrous retraction and dysphagia. Table 6 shows the incidence of complications of this type in reports published to date Mesh has also beenusedinpediatriccases,withoutlong-termproblems. 52,109 COMMENT Surgical treatment of PEH and type III mixed hernias has been a challenging chapter in digestive surgery for the past 1292
8 30 years (Table 4). The treatment used to be offered to a subset of elderly patients, some of them particularly frail and, in some cases, associated with urgent situations such as gastric volvulus or gastric incarceration. However, the results from centers with wide experience showed low morbidity and good long-term outcome after standard open transthoracic or transabdominal approaches, although in most series the results were merely assessed on the basis of the presence or absence of symptoms without any anatomic (radiologic) evaluation. 110 The experience available shows the efficacy of the laparoscopic approach for treatment of PEH. 111,112 Despite the increased intraoperative technical difficulty, and although there are no comparative randomized trials with the open approach to conclusively determine their relative merits, the immediate outcome clearly endorses this minimally invasive approach in a population that is typically at higher risk than conventional patients with GERD or small type I hiatal hernia. The large number of series published in recent years (20 series related to the open approach in 33 years, compared with 46 series in 12 years for the laparoscopic approach) bears witness to the success of, and the interest in, the application of laparoscopic techniques in PEH repair. Most accepted technical rules for the surgical treatment of PEH include stomach reduction, sac excision, and closureofthehiataldefect onoccasionmorethan8cmwide with or without the addition of some type of fixation. The controversy arises after the definitive observation of a variable recurrence rate (up to 42%) when a routine radiologic follow-up is done. Some authors have suggested that alternative approaches (open or thoracic) may be better for this disease. Arguments put forward to account for this unacceptably high recurrence rate include the learning curve due to the technical difficulty of the procedure, poor technical crural closure, or a short esophagus. The learning curve for a difficult laparoscopic procedure undoubtedly plays a role, and it has been observed in several large series that the recurrence rate falls as surgeons gain experience. The significance of a short esophagus continues to be a controversial issue. It has been considered as a potential cause of failure, but most patients with PEH do not have advanced gastroesophageal reflux disease with esophageal scarring. The need to perform a Collis gastroplasty to lengthen the esophagus variedfrom0%to70%intheseriesanalyzed,andasyetthere isnoclearagreementonwhetherthistechnicalstepisneeded during PEH repair. Clearly, as with other abdominal wall defects, the aim is to achieve adequate closure. In contrast to the accepted standard concept for inguinal or ventral hernia, which is tension free, the most widely supported approach is to close the hiatus under tension, with the obvious risk of disruption. The rationale for this judgment is that, unlike the abdomen or groin, in which the aim of repair is to achieve passive containment, the cardial region including the hiatus and the gastroesophageal junction is a highly dynamic anatomic area and so anatomic repair is justified. However, since PEH repair causes wideranging anatomic distortion and the risk of disruption is high, reinforcement with mesh is a logical forward step. Hiatal closure is occasionally difficult. Surgeons who are in general against the placement of mesh in the hiatus are sometimes obliged to use the procedure to correct Figure 12. Non tension-free repair with reinforcement of the crural closure using buttress mesh. A long strip of mesh is placed below the esophagus, covering the pillar closure. 61 Figure 13. Non tension-free repair with reinforcement of the crural closure. Onlay mesh is placed around the esophagus once the defect has been closed. 31,62 the defect, because of either the size of the defect or the technical impossibility of proceeding otherwise. There are no clear reasons for the differences in outcome after open or laparoscopic approach to PEH. Possibly the final results of laparoscopic repair are not as good because the laparoscopic approach is more technically demanding. However, systematic evaluation with radiologic esophagogram, including asymptomatic patients, has shown a higher number of recurrences. Haas et al 75 found an anatomic recurrence rate of 42% after systematic radiologic evaluation. This suggests that the problem may also have been evident in the open-procedure era, but has only become relevant today since the increase in laparoscopic procedures and the possibility of more detailed study. One of the main arguments against mesh placement has been the emergence of complications due mainly to vis- 1293
9 Table 6. Complications in Relation to Prosthesis Placement for Surgical Repair of Hiatal Hernia Source No. With Complication/Total Complication Open Surgery Carlson et al, /44 (2.3) Esophageal erosion 29 mo after mesh placement Laparoscopy Edelman, /5 (20.0) Dysphagia and fibrosis after tension-free repair with mesh + FP + gastrostomy; reoperation for esophageal stenosis Trus et al, /76 (1.3) Dysphagia, mesh extraction Schauer et al, /70 (1.4) Late esophageal perforation (ischemia), mesh (PTFE) extraction Kemppainen and Kiviluoto, NA Cardiac tamponade secondary to mesh fixation with tacker Peet et al, /22 (4.5) Dysphagia and adherences secondary to crural closure, reinforcement with Dacron strips Baladas et al, /734 (0.1) Gastroesophageal fistula secondary to FP reinforced by Teflon pledgets Arendt et al, NA Dysphagia; transmural migration of Teflon pledgets into esophagus 9 y after FP Abbreviations: FP, fundoplication; NA, data not available; PTFE, polytef. ceral erosion, a risk that is intrinsically related to the existence of a foreign body. On the basis of this rationale, many surgeons consider routine placement contraindicated. However, there are clear differences between the placement of mesh and insertion of an Angelchik device or bands used for gastric banding in obese patients. The latter devices are placed directly over the cardia, maintaining a sustained and continued tension and favoring potential erosion; in contrast, mesh in the hiatus for reinforcement of the diaphragmatic closure is placed outside the esophagus and direct contact is avoided. Although several serious complications have been reported, the morbidity rate associated with mesh placement is low (Table 6). No objective information is available to guide the choice of material. Most authors prefer soft materials with less intense fibrotic response such as polytef rather than polypropylene, but no comparative trials of the materials have been performed. Complications have been reported with the use of both types of mesh. No long-term follow-up data on this issue are available; experience with other types of material such as combined mesh types or biomaterials is limited, and the follow-up periods are short. Another controversial point is whether the use of mesh for hiatal repair in PEH should be routine or selective. The local conditions of the hiatus after sac excision may cause differences in the results, and sometimes, although the hernia sac is large, the pillars are of good quality and can be approached without difficulty. There are no studies investigating predictive factors for recurrence after laparoscopic repair of PEH, which may involve the anatomic features of the hiatus (such as the size of the gap, tension, or diaphragmatic weakness), the type of repair (single stitches, pledget, etc), additional fixation maneuvers (Toupet, fixation, gastrostomy, etc), and patient characteristics (heavy work, constipation, chronic cough, etc). Some authors recommend a tailored approach, placing a mesh in cases at major risk of recurrence, and its use seems more advisable in the case of reoperations. However, the decision clearly depends on the experience of the surgeon. The final answers to our questions should come from analysis of the long-term follow-up over 5 years of series of patients in whom mesh has been placed, and randomized trials of suitable design to provide answers regarding the controversial technical aspects (type of mesh, location, selective vs routine, additional maneuvers [fixation], Collis esophageal lengthening, etc). At present, the information available shows that the use of a mesh for hiatal repair after laparoscopic repair of PEH is safe and prevents hernia recurrence. However, information on the long-term results is lacking; severe complications may arise, albeit infrequently. A selective use based on clinical experience is recommended, as the technique appears to be safe, and the fears expressed at earlier stages of its development have not been confirmed. Accepted for Publication: January 19, Correspondence: Eduardo M. Targarona, MD, PhD, Service of Surgery, Hospital de Sant Pau, Padre Claret 167, Barcelona, Spain (etargarona@hsp.santpau.es). Acknowledgment: Isabel Salgado drew the illustrations for the figures in this article. REFERENCES 1. Cuesta MA, Peet DL, Klinkerberg-Knol EC. Laparoscopic treatment of large hiatal hernias. Semin Laparosc Surg. 1999;6: Floch N. Paraesophageal hernias: current concepts. J Clin Gastroenterol. 1999; 29: Hashemi M, Sillin LF, Peters JH. Current concepts in the management of paraesophageal hiatal hernia. J Clin Gastroenterol. 1999;29: Buenaventura PO, Schauer PR, Keena RJ, Luketich JD. Laparoscopic repair of giant paraesophageal hernia. Semin Thorac Cardiovasc Surg. 2000;12: Freeman ME, Hinder RA. Laparoscopic paraesophageal hernia repair. Semin Laparosc Surg. 2001;8: Landrenau RJ. Surgical management of paraesophageal herniation. In: Nyhus LM, Baker RJ, Fischer JE, eds. Mastery of Surgery. 3rd ed. Boston, Mass: Little Brown & Co Inc; 1997: Litle VR, Buenaventura PO, Luketich JD. Laparoscopic repair of giant paraesophageal hernia. Adv Surg. 2001;35: Oelschlager BK, Pellegrini CA. Paraesophageal hernias: open, laparoscopic, or thoracic repair. Chest Surg Clin N Am. 2001;11: Huntington TR. Short-term outcomes of laparoscopic paraesophageal hernia repair: a case series of 58 consecutive patients. Surg Endosc. 1997;11: Perdikis G, Hinder RA, Filipi CJ, et al. Laparoscopic paraesophageal hernia repair. Arch Surg. 1997;132: Edye MB, Canin-Endres J, Gattorno F, Salky BA. Durability of laparoscopic repair of paraesophageal hernia. Ann Surg. 1998;228: Gantert WA, Patti MG, Arcerito M, et al. Laparoscopic repair of paraesophageal hiatal hernias. J Am Coll Surg. 1998;186: Watson DI, Davies N, Devitt PG, Jamieson GG. Importance of dissection of the hernial sac in laparoscopic surgery for large hiatal hernias. Arch Surg. 1999; 134: Wu JS, Dunnegan DL, Soper NJ. Clinical and radiologic assessment of laparoscopic paraesophageal hernia repair. Surg Endosc. 1999;13:
10 15. Horgan S, Eubanks TR, Jacobsen G, Omelanczuk P, Pellegrini CA. Repair of paraesophageal hernias. Am J Surg. 1999;177: Swanstrom LL, Jobe BA, Kinzie LR, Horvath KD. Oesophageal motility and outcome following laparoscopic paraesophageal hernia repair and fundoplication. Am J Surg. 1999;177: Hashemi M, Peters JH, DeMeester TR, et al. Laparoscopic repair of large type III hiatal hernia: objective follow up reveals high recurrence rate. J Am Coll Surg. 2000;190: Peet DL, Klinkerberg-Knol EC, Alonso A, Sietses C, Eijsbouts QAJ, Cuesta MA. Laparoscopic treatment of large paraesophageal hernias. Surg Endosc. 2000; 14: Dahlberg PS, Deschamps C, Miller DL, Allen MS, Nichols FC, Pairolero PC. Laparoscopic repair of large paraesophageal hiatal hernia. Ann Thorac Surg. 2001;72: Wiechmann RJ, Ferguson MK, Naunheim KS, et al. Laparoscopic management of giant paraesophageal herniation. Ann Thorac Surg. 2001;71: Velanovich V, Karmy-Jones R. Surgical management of paraesophageal hernias: outcome and quality of life analysis, with invited commentary. Dig Surg. 2001;18: Khaitan L, Houston H, Sharp K, Holzman M, Richards W. Laparoscopic paraesophageal hernia repair has an acceptable recurrence rate. Am Surg. 2002; 68: Pierre AF, Luketich JD, Fernando HC, et al. Results of laparoscopic repair of giant paraesophageal hernias: 200 consecutive patients. Ann Thorac Surg. 2002; 74: Mattar SG, Bowers SP, Galloway KD, Hunter CD, Smith CD. Long-term outcome of laparoscopic repair of paraesophageal hernia. Surg Endosc. 2002; 16: Diaz S, Brunt M, Klingensmith ME, Frisella PM, Soper NJ. Laparoscopic paraesophageal hernia repair, a challenging operation: medium-term outcome of 116 patients. J Gastrointest Surg. 2003;7: Targarona EM, Novell J, Vela S, et al. Mid-term analysis of safety and quality of life after the laparoscopic repair of paraesophageal hiatal hernia. Surg Endosc. 2004;18: Leeder PC, Smith G, Dehn TCB. Laparoscopic management of large paraesophageal hiatal hernia. Surg Endosc. 2003;17: Ponsky J, Rosen M, Fanning A, Malm J. Anterior gastropexy may reduce the recurrence after laparoscopic paraesophageal hernia repair. Surg Endosc. 2003; 17: Jobe BA, Aye RW, Deveney CW, Domreis JS, Hill LD. Laparoscopic management of giant type III hiatal hernia and short oesophagus: objective follow up at three years. J Gastrointest Surg. 2002;6: Keidar A, Szold A. Laparoscopic repair of paraesophageal hernia with selective use of mesh. Surg Laparosc Endosc Percutan Tech. 2003;13: Athanasakis H, Tzortzinis A, Tsiaoussis J, Vassilakis JS, Xynos E. Laparoscopic repair of paraesophageal hernia. Endoscopy. 2001;33: Cloyd DW. Laparoscopic repair of incarcerated paraesophageal hernias. Surg Endosc. 1994;8: Coster DD. Laparoscopic paraesophageal hernia repair using Surgi-pro mesh [letter]. Surg Laparosc Endosc. 1996;6: Johnson PE, Presuad M, Mitchell T. Laparoscopic anterior gastropexy for treatment of paraesophageal hernias. Surg Laparosc Endosc. 1994;4: Katkhouda N, Mavor E, Achanta K, et al. Laparoscopic repair of chronic intrathoracic gastric volvulus. Surgery. 2000;128: Kercher KW, Matthews BD, Ponsky JL, et al. Minimally invasive management of paraesophageal herniation in the high-risk surgical patient. Am J Surg. 2001; 182: Koger KE, Stone JM. Laparoscopic reduction of acute gastric volvulus. Am Surg. 1993;59: Krahenbuhl L, Schafer M, Farhadi J, Renzulli P, Seiler C, Buchler MW. Laparoscopic treatment of large paraesophageal hernia with totally intrathoracic stomach. J Am Coll Surg. 1998;187: Luketich JD, Raja S, Fernando HC, et al. Laparoscopic repair of giant paraesophageal hernia: 100 consecutive cases. Ann Surg. 2000;232: Medina L, Peetz M, Ratzer E, Fenoglio M. Laparoscopic paraesophageal hernia repair. JSLS. 1998;2: Mosnier H, Leport J, Aubert A, Guibert L, Caronia F. Videolaparoscopic treatment of paraesophageal hiatal hernia [in French]. Chirurgie. 1998;123: Rosati R, Bona S, Fumagalli U, Chella B, Peracchia A. Laparoscopic treatment of paraesophageal and large mixed hiatal hernias. Surg Endosc. 1996;10: Tabet J, Lacy AM, Grande L, et al. Paraesophageal hernias in elderly patients: an indication for laparoscopic surgery. Rev Esp Enferm Dig. 1996;88: Luostarinen M, Rantalainen M, Helve O, Reinikainen P, Isolauri J. Late results of paraesophageal hiatus hernia repair with funduplication. Br J Surg. 1998; 85: Carlson MA, Condon RE, Ludwig KA, Schulte WJ. Management of intrathoracic stomach with polypropylene mesh prosthesis reinforced transabdominal hiatus hernia repair. J Am Coll Surg. 1998;187: Kuster GG, Gilroy S. Laparoscopic technique for repair of paraesophageal hiatal hernias. J Laparoendosc Surg. 1993;3: Edelman DS. Laparoscopic paraesophageal hernia repair with mesh. Surg Laparosc Endosc. 1995;5: Pitcher DE, Curet MJ, Vogt DM, Mason J, Zucker KA. Successful repair of praesophageal hernia. Arch Surg. 1995;130: Oddsdottir M, Franco AL, Laycock WA, Waring JP, Hunter JG. Laparoscopic repair of paraesophageal hernia: new access, old technique. Surg Endosc. 1995; 9: Behrns KE, Schlinkert RT. Laparoscopic management of paraesophageal hernia: early results. J Laparoendosc Surg. 1996;6: Huntington TR. Laparoscopic mesh repair of the oesophageal hiatus. J Am Coll Surg. 1997;184: Paul MG, De Rosa RP, Petrucci PE, Palmer ML, Danovitch SH. Laparoscopic tension-free repair of large paraesophageal hernias. Surg Endosc. 1997; 11: Frantzides CT, Carlson MA. Prosthetic reinforcement of posterior cruroplasty during laparoscopic hiatal herniorraphy. Surg Endosc. 1997;11: Willekes CL, Edoga JK, Freeza EE. Laparoscopic repair of paraesophageal hernia. Ann Surg. 1997;225: Hawasli A, Zonca S. Laparoscopic repair of paraesophageal hiatal hernia. Am Surg. 1998;64: Basso N, DeLeo A, Genco A, et al. 360 Degrees laparoscopic fundoplication with tension free hiatoplasty in the treatment of symptomatic gastroesophageal reflux disease. Surg Endosc. 2000;14: Lambert AW, Huddart SN. Mesh hiatal reinforcement in Nissen fundoplication. Pediatr Surg Int. 2001;17: Meyer C, Bufffler A, Rohr S, Lima MC. Le traitement laparoscopique des hernies hiatales de gran taille avec mise en place d une prothese: a propos de dix cas. Ann Chir. 2002;127: Casaccia M, Torelli P, Panaro F, Cavaliere D, Ventura A, Valente U. Laparoscopic physiologic hiatoplasty for hiatal hernia: new composite A -shaped mesh. Surg Endosc. 2002;16: Kamolz T, Granderath FA, Basmmer T, Pasiut M, Pointner R. Dysphagiaandquality of life after laparoscopic Nissen funduplication in patients with and without prosthetic reinforcement of the hiatal crura. Surg Endosc. 2002;16: Champion JK, Rock D. Laparoscopic mesh cruroplasty for large paraesophageal hernias. Surg Endosc. 2003;17: Oelschlager BK, Barreca M, Chang L, Pellegrini CA. The use of small intestine submucosa in the repair of paraesophageal hernias: initial observation of a new technique. Am J Surg. 2003;186: Granderath FA, Kamolz T, Schweiger UM, Pointner R. Laparoscopic refundoplication with prosthetic hiatal closure for recurrent hiatal hernia after primary failed antireflux surgery. Arch Surg. 2003;138: Hui TT, David T, Spyrou M, Phillips EH. Mesh crural repair of large paraesophageal hiatal hernias. Am Surg. 2001;67: Frantzides CT, Madan AK, Carlson MA, Stavropoulos GP. A prospective, randomised trial of laparoscopic polytetrafluoroethylene (PTFE) patch repair vs simple cruroplasty for large hiatal hernia. Arch Surg. 2002;137: Schauer PR, Ikramuddin S, McLaughlin RH, et al. Comparison of laparoscopic versus open repair of paraesophageal hernia. Am J Surg. 1998;176: Skinner DB, Belsey RH. Surgical management of esophageal reflux and hiatus: long-term results with 1030 patients. J Thorac Cardiovasc Surg. 1967;53: Hill LD, Tobias JA. Paraesophageal hernia. Arch Surg. 1968;96: Wichterman K, Geha AS, Cahow CE, Baue AE. Giant paraesophageal hiatus hernia with intrathoracic stomach and colon: the case for early repair. Surgery. 1979;86: Pearson FG, Cooper JD, Ilves R, Todd TRJ, Jamieson WRE. Massive hiatal hernia with incarceration: a report of 53 cases. Ann Thorac Surg. 1983;35: Ellis FH Jr, Crozier RE, Shea JA. Paraesophageal hiatus hernia. Arch Surg. 1986; 121: Treacy PJ, Jamieson GG. An approach to the management of paraoesophageal hiatus hernias. Aust NZJSurg. 1987;57: Menguy R. Surgical management of large paraesophageal hernia with complete intrathoracic stomach. World J Surg. 1988;12: Ackermann C, Bally H, Harder F. Paraesophageal hiatal hernia risks and surgical indications. Helv Chir Acta. 1989;56: Haas O, Rat P, Christophe M, Friedman S, Favre JP. Surgical results of intrathoracic gastric volvulus complicating hiatal hernia. Br J Surg. 1990;77: Harriss DR, Graham TR, Galea M, Salama FD. Paraoesophageal hiatal hernias: when to operate. J R Coll Surg Edinb. 1992;37: Allen MS, Trastek VF, Deschamps C, Pairolero PC. Intrathoracic stomach: presentation and results of operation. J Thorac Cardiovasc Surg. 1993;105: Williamson WA, Ellis FH, Streitz JM, Shahian DM. Paraesophageal hiatal hernia: is an antireflux procedure necessary? Ann Thorac Surg. 1993;56: Myers GA, Harms BA, Starling JR. Management of paraesophageal hernia with a selective approach to antireflux surgery. Am J Surg. 1995;170: Altorki NK, Yankelevitz D, Skinner DB. Massive hiatal hernias: the anatomic basis of repair. J Thorac Cardiovasc Surg. 1998;115: Maziak DE, Todd TR, Pearson FG. Massive hiatus hernia: evaluation and surgical management. J Thorac Cardiovasc Surg. 1998;115: Geha AS, Massad MG, Snow NJ, Baue AE. A 32-year experience in 100 patients with giant paraesophageal hernia: the case for abdominal approach and selective antireflux repair. Surgery. 2000;128: Rogers ML, Duffy JP, Beggs FD, Salama FD, Knowles KR, Morgan WE. Surgical treatment of para-oesophageal hiatal hernia. Ann R Coll Surg Engl. 2001; 83: Low DE, Simchuk EJ. Effect of paraesophageal hernia repair on pulmonary function. Ann Thorac Surg. 2002;74: Carlson MA, Richards CG, Frantzides CT. Laparoscopic prosthetic reinforcement of hiatal herniorraphy. Dig Surg. 1999;16: Willwerth BM. Gastric complications associated with paraesophageal herniation. Am Surg. 1974;40: Wo JM, Branum GD, Hunter JG, Trus TN, Mauren SJ, Waring P. Clinical fea- 1295
11 tures of type III (mixed) paraesophageal hernias. Am J Gastroenterol. 1996; 91: Ellis FH. Controversies regarding the management of hiatus hernia. Am J Surg. 1980;139: Boerema I. Hiatus hernia: repair by right-sided, subhepatic, anterior gastropexy. Surgery. 1969;65: Carter R, Brewer LD, Hinshaw A. Acute gastric volvulus. Am J Surg. 1980;140: Hallissey MT, Ratliff DA, Temple JG. Paraoesophageal hiatus hernia: surgery for all ages. Ann R Coll Surg Engl. 1992;74: Hill LD. Incarcerated paraesophageal hernia: a surgical emergency. Am J Surg. 1973;126: Teague WJ, Ackroyd R, Watson DI, Devitt PG. Changing patterns in the management of gastric volvulus over 14 years. Br J Surg. 2000;87: Stylopoulos N, Gazelle GS, Rattner DW. Paraesophageal hernias: operation or observation? Ann Surg. 2002;236: Pros I, Targarona EM, Angás J, et al. Tratamiento quirúrgico del vólvulo gástrico. Cir Esp. 1992;51: Caskey CI, Zerhouni EA, Fishman EK, Rahmouni AD. Aging of the diaphragm: a CT study. Radiology. 1989;171: Purkiss SF, Argano VA, Kuo J, Lewis CT. Oesophageal erosion of an Angelchik prosthesis: surgical management using fundoplication. Eur J Cardiothorac Surg. 1992;6: Crookes PF, DeMeester TR. The Angelchik prosthesis: what have we learned in fifteen years? Ann Thorac Surg. 1994;57: Benjamin SB, Kerr R, Cohen D, Motaparthy V, Castell DO. Complications of the Angelchik antireflux prosthesis. Ann Intern Med. 1984;100: Abu-Abeid S, Keidar A, Gavert N, Blanc A, Szold A. The clinical spectrum of band erosion following laparoscopic adjustable silicone gastric banding for morbid obesity. Surg Endosc. 2003;17: Basso N, Rosato P, De Leo A, Genco A, Rea S, Neri T. Tension-free hiatoplasty, gastrophrenic anchorage, and 360 fundoplication in the laparoscopic treatment of paraesophageal hernia. Surg Laparosc Endosc Percutan Tech. 1999; 9: Cuschieri A, Shimi S, Nathanson LK. Laparoscopic reduction, crural repair and fundoplication of large hiatal hernia. Am J Surg. 1992;163: Agwunobi AO, Bancewicz J, Attwood SEA. Simple laparoscopic gastropexy as the initial treatment of paraesophageal hiatal hernia. Br J Surg. 1998;85: Casabella F, Sinanan M, Horgan S, Pellegrini CA. Systematic use of gastric fundoplication in laparoscopic repair of paraesophageal hernias. Am J Surg. 1996; 171: Trus TL, Bax T, Richardson WS, et al. Complications of laparoscopic paraesophageal hernia repair. J Gastrointest Surg. 1997;1: Kemppainen E, Kiviluoto T. Fatal cardiac tamponade after emergency tension free repair of a large paraesophageal hernia. Surg Endosc. 2000;14: Baladas HG, Smith GS, Richardson MA, Dempsey MB, Falk GL. Esophagogastric fistula secondary to teflon pledget: a rare complication following laparoscopic fundoplication. Dis Esophagus. 2000;13: Arendt T, Stuber E, Monig H, Folsch UR, Katsoulis S. Dysphagia due to transmural migration of surgical material into the esophagus nine years after Nissen fundoplication. Gastrointest Endosc. 2000;51: Simpson B, Ricketts RR, Parker PM. Prosthetic patch stabilization of crural repair in antireflux surgery in children. Am Surg. 1998;64: Ludemann R, Watson DI, Jamieson GG. Influence of follow-up methodology and completeness on apparent clinical outcome of funduplication. Am J Surg. 2003;186: Terry M, Smith CD, Branum GD, Galloway K, Waring JP, Hunter JG. Outcomes of laparoscopic fundoplication for gastroesophageal reflux disease and paraesophageal hernia. Surg Endosc. 2001;15: Trus TL, Laycock WS, Waring JP, Branum GD, Hunter JG. Improvement in quality of life measures after laparoscopic antireflux surgery. Ann Surg. 1999; 229: Invited Critique T his review article by Targarona et al is a meta-analysis of reports using mesh in complex paraesophageal and mixed hiatal hernias, with recurrence being the end point. Therein lies my first concern with this article. This complex disorder is more than recurrences and mesh erosion. A review article should cover all important parameters, which, in this case, include postoperative dysphagia (10%), gas bloating (8%), patient satisfaction, nausea, early satiety, and the recurrence of symptoms absent recurrent hernia, since half of these patients have resumed taking antireflux medications within 3 to 5 years after surgery. I am also troubled by 2 other observations: first, the authors do not present any data from their own experience, and second, none of the 4 coauthors is credited with a single publication in the 112 citations in the bibliography. I personally feel that credibility is an issue with review articles, because the reader infers some measure of expertise by the authors. The authors list 13 variations using mesh, which confirms the complexity of this anatomy and the need for creativity among even the most experienced laparoscopic surgeons. One should be wary of dogma in this setting. Their argument against using mesh is scientifically unfounded and, short of using autologous tissues, closure in many of these patients is impossible otherwise. They are correct in their observation that there are too few studies extending over a long enough period to make definitive statements about recurrence rates, which may lead to the real take-home message from this article: surgeons need to include all of the variables listed above in their follow-up to make the data meaningful for patients, clinicians, and health care planners, who may ultimately rule on reimbursement for this diagnosis because of the large number of patients affected. Eddie L. Hoover, MD Correspondence: Dr Hoover, Department of Surgery, Buffalo VA Medical Center, 3495 Bailey Ave, Buffalo, NY (Eddie.Hoover@med.va.gov). 1296
Traditional surgical treatment of large diaphragmatic. Laparoscopic Repair of Large Paraesophageal Hiatal Hernia
 Laparoscopic Repair of Large Paraesophageal Hiatal Hernia Peter S. Dahlberg, MD, Claude Deschamps, MD, Daniel L. Miller, MD, Mark S. Allen, MD, Francis C. Nichols, MD, and Peter C. Pairolero, MD Division
Laparoscopic Repair of Large Paraesophageal Hiatal Hernia Peter S. Dahlberg, MD, Claude Deschamps, MD, Daniel L. Miller, MD, Mark S. Allen, MD, Francis C. Nichols, MD, and Peter C. Pairolero, MD Division
Hannes J. Larusson Æ Urs Zingg Æ Dieter Hahnloser Æ Karen Delport Æ Burkhardt Seifert Æ Daniel Oertli
 World J Surg (2009) 33:980 985 DOI 10.1007/s00268-009-9958-9 Predictive Factors for Morbidity and Mortality in Patients Undergoing Laparoscopic Paraesophageal Hernia Repair: Age, ASA Score and Operation
World J Surg (2009) 33:980 985 DOI 10.1007/s00268-009-9958-9 Predictive Factors for Morbidity and Mortality in Patients Undergoing Laparoscopic Paraesophageal Hernia Repair: Age, ASA Score and Operation
ORIGINAL ARTICLE. Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation
 ORIGINAL ARTICLE Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation Preliminary Results of a Prospective Randomized Functional and Clinical
ORIGINAL ARTICLE Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation Preliminary Results of a Prospective Randomized Functional and Clinical
Metaanalysis of Recurrence After Laparoscopic Repair of Paraesophageal Hernia
 SCIENTIFIC PAPER Metaanalysis of Recurrence After Laparoscopic Repair of Paraesophageal Hernia Munir Ahmad Rathore, FRCS, Syed Imran Hussain Andrabi, FRCS, Muhammad Iqbal Bhatti, MRCS, Syed Muzahir Hussain
SCIENTIFIC PAPER Metaanalysis of Recurrence After Laparoscopic Repair of Paraesophageal Hernia Munir Ahmad Rathore, FRCS, Syed Imran Hussain Andrabi, FRCS, Muhammad Iqbal Bhatti, MRCS, Syed Muzahir Hussain
Crural Buttressing: Why, When, and with What
 Crural Buttressing: Why, When, and with What Michael Maddaus, MD Professor of Surgery Garamella Lynch Jensen Chair in Thoracic Surgery Division of General Thoracic and Foregut Surgery University of Minnesota
Crural Buttressing: Why, When, and with What Michael Maddaus, MD Professor of Surgery Garamella Lynch Jensen Chair in Thoracic Surgery Division of General Thoracic and Foregut Surgery University of Minnesota
Paraesophageal hernias typically occur in older patients, Open Repair of Paraesophageal Hernia: Reassessment of Subjective and Objective Outcomes
 Open Repair of Paraesophageal Hernia: Reassessment of Subjective and Objective Outcomes Donald E. Low, MD, FACS, and Trisha Unger, MD Section of General Thoracic Surgery, Virginia Mason Medical Center,
Open Repair of Paraesophageal Hernia: Reassessment of Subjective and Objective Outcomes Donald E. Low, MD, FACS, and Trisha Unger, MD Section of General Thoracic Surgery, Virginia Mason Medical Center,
Mid-term results of robot-assisted laparoscopic repair of large hiatal hernia; a symptomatic and radiological prospective cohort study
 Chapter 8 Mid-term results of robot-assisted laparoscopic repair of large hiatal hernia; a symptomatic and radiological prospective cohort study WA Draaisma HG Gooszen IAMJ Broeders Department of Surgery,
Chapter 8 Mid-term results of robot-assisted laparoscopic repair of large hiatal hernia; a symptomatic and radiological prospective cohort study WA Draaisma HG Gooszen IAMJ Broeders Department of Surgery,
Hiatal hernias may be classified. hiatal hernia DESCRIPTION AND IDENTIFICATION. This article is the first in a twopart series about these somewhat
 paraesophagealh hiatal hernia Leslie K Browder, MD, and Alex G Little, MD DESCRIPTION AND IDENTIFICATION Hiatal hernias may be classified as four types. The most common, Type I, may present as gastroesophageal
paraesophagealh hiatal hernia Leslie K Browder, MD, and Alex G Little, MD DESCRIPTION AND IDENTIFICATION Hiatal hernias may be classified as four types. The most common, Type I, may present as gastroesophageal
ORIGINAL ARTICLE. Laparoscopic Refundoplication With Prosthetic Hiatal Closure for Recurrent Hiatal Hernia After Primary Failed Antireflux Surgery
 ORIGINL RTICLE Laparoscopic Refundoplication With Prosthetic Hiatal Closure for Recurrent Hiatal Hernia fter Primary Failed ntireflux Surgery Frank. Granderath, MD; Thomas Kamolz, PhD; Ursula M. Schweiger,
ORIGINL RTICLE Laparoscopic Refundoplication With Prosthetic Hiatal Closure for Recurrent Hiatal Hernia fter Primary Failed ntireflux Surgery Frank. Granderath, MD; Thomas Kamolz, PhD; Ursula M. Schweiger,
Laparoscopic Paraesophageal Hernia Repair with Acellular Dermal Matrix Cruroplasty
 SCIENTIFIC PAPER Laparoscopic Paraesophageal Hernia Repair with Acellular Dermal Matrix Cruroplasty Dennis F. Diaz, MD, J. Scott Roth, MD ABSTRACT Background: Laparoscopic paraesophageal hernia repair
SCIENTIFIC PAPER Laparoscopic Paraesophageal Hernia Repair with Acellular Dermal Matrix Cruroplasty Dennis F. Diaz, MD, J. Scott Roth, MD ABSTRACT Background: Laparoscopic paraesophageal hernia repair
Paraesophageal Hernia
 Paraesophageal Hernia Inderpal (Netu) S. Sarkaria, M.D. Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Speaker/Education: Intuitive
Paraesophageal Hernia Inderpal (Netu) S. Sarkaria, M.D. Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Speaker/Education: Intuitive
Secrets for successful laparoscopic antireflux surgery: mesh hiatoplasty
 Review Article Page 1 of 6 Secrets for successful laparoscopic antireflux surgery: mesh hiatoplasty H. Alejandro Rodriguez, Brant K. Oelschlager Department of Surgery, University of Washington, Seattle,
Review Article Page 1 of 6 Secrets for successful laparoscopic antireflux surgery: mesh hiatoplasty H. Alejandro Rodriguez, Brant K. Oelschlager Department of Surgery, University of Washington, Seattle,
Chapter 10. Summary, discussion and conclusions
 Chapter 10 Summary, discussion and conclusions The studies presented in this thesis have addressed the current status of conventional and minimally invasive techniques for esophageal surgery, especially
Chapter 10 Summary, discussion and conclusions The studies presented in this thesis have addressed the current status of conventional and minimally invasive techniques for esophageal surgery, especially
Full incorporation of Strattice Reconstructive Tissue Matrix in a reinforced hiatal hernia repair: a case report
 Freedman Journal of Medical Case Reports 2012, 6:234 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Full incorporation of Strattice Reconstructive Tissue Matrix in a reinforced hiatal hernia repair:
Freedman Journal of Medical Case Reports 2012, 6:234 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Full incorporation of Strattice Reconstructive Tissue Matrix in a reinforced hiatal hernia repair:
Anatomical failure following laparoscopic antireflux surgery (LARS); does it really matter?
 The Royal College of Surgeons of England GASTROINTESTINAL SURGERY doi 10.1308/003588410X12518836440126 Anatomical failure following laparoscopic antireflux surgery (LARS); does it really matter? N DUNNE
The Royal College of Surgeons of England GASTROINTESTINAL SURGERY doi 10.1308/003588410X12518836440126 Anatomical failure following laparoscopic antireflux surgery (LARS); does it really matter? N DUNNE
A 25-year experience with open primary transthoracic repair of paraesophageal hiatal hernia
 A 25-year experience with open primary transthoracic repair of paraesophageal hiatal hernia Himanshu J. Patel, MD Bethany B. Tan, MD John Yee, MD Mark B. Orringer, MD Mark D. Iannettoni, MD Objective:
A 25-year experience with open primary transthoracic repair of paraesophageal hiatal hernia Himanshu J. Patel, MD Bethany B. Tan, MD John Yee, MD Mark B. Orringer, MD Mark D. Iannettoni, MD Objective:
2 Paraesophageal Hiatus Hernia
 2 Paraesophageal Hiatus Hernia Luigi Bonavina Pearls and Pitfalls Paraesophageal (type II) hiatus hernia represents a distinct anatomic and clinic entity requiring a unique therapeutic strategy, and is
2 Paraesophageal Hiatus Hernia Luigi Bonavina Pearls and Pitfalls Paraesophageal (type II) hiatus hernia represents a distinct anatomic and clinic entity requiring a unique therapeutic strategy, and is
Open versus Laparoscopic Hiatal Hernia Repair
 SCIENTIFIC PAPER Open versus Laparoscopic Hiatal Hernia Repair Terrence M. Fullum, MD, Tolulope A. Oyetunji, MD, MPH, Gezzer Ortega, MD, MPH, Daniel D. Tran, MD, Ian M. Woods, BS, Olusola Obayomi-Davies,
SCIENTIFIC PAPER Open versus Laparoscopic Hiatal Hernia Repair Terrence M. Fullum, MD, Tolulope A. Oyetunji, MD, MPH, Gezzer Ortega, MD, MPH, Daniel D. Tran, MD, Ian M. Woods, BS, Olusola Obayomi-Davies,
Preliminary Study of Hiatal Hernia Repair Using Polyglycolic Acid: Trimethylene Carbonate Mesh
 SCIENTIFIC PAPER Preliminary Study of Hiatal Hernia Repair Using Polyglycolic Acid: Trimethylene Carbonate Mesh James M. Massullo, MD, Tejinder P. Singh, MD, Ward J. Dunnican, MD, Brian R. Binetti, MD
SCIENTIFIC PAPER Preliminary Study of Hiatal Hernia Repair Using Polyglycolic Acid: Trimethylene Carbonate Mesh James M. Massullo, MD, Tejinder P. Singh, MD, Ward J. Dunnican, MD, Brian R. Binetti, MD
Paraesophageal hiatal hernias (type II, III, IV) are. Effect of Paraesophageal Hernia Repair on Pulmonary Function
 Effect of Paraesophageal Hernia Repair on Pulmonary Function Donald E. Low, MD, and Eric J. Simchuk, MD Section of General Thoracic Surgery, Virginia Mason Medical Center, Seattle, Washington Background.
Effect of Paraesophageal Hernia Repair on Pulmonary Function Donald E. Low, MD, and Eric J. Simchuk, MD Section of General Thoracic Surgery, Virginia Mason Medical Center, Seattle, Washington Background.
ORIGINAL SCIENTIFIC ARTICLES
 ORIGINAL SCIENTIFIC ARTICLES Biologic Prosthesis to Prevent Recurrence after Laparoscopic Paraesophageal Hernia Repair: Long-term Follow-up from a Multicenter, Prospective, Randomized Trial Brant K Oelschlager,
ORIGINAL SCIENTIFIC ARTICLES Biologic Prosthesis to Prevent Recurrence after Laparoscopic Paraesophageal Hernia Repair: Long-term Follow-up from a Multicenter, Prospective, Randomized Trial Brant K Oelschlager,
Short-term results after laparoscopic repair of giant hiatal hernias with pledgeted sutures: a retrospective analysis
 https://doi.org/10.1007/s10029-019-01890-3 ORIGINAL ARTICLE Short-term results after laparoscopic repair of giant hiatal hernias with pledgeted sutures: a retrospective analysis M. Weitzendorfer 1 R. Pfandner
https://doi.org/10.1007/s10029-019-01890-3 ORIGINAL ARTICLE Short-term results after laparoscopic repair of giant hiatal hernias with pledgeted sutures: a retrospective analysis M. Weitzendorfer 1 R. Pfandner
Histologic results 1 year after bioprosthetic repair of paraesophageal hernia in a canine model
 Surg Endosc (2006) 20: 1693 1697 DOI: 10.1007/s00464-006-0680-5 Ó Springer Science+Business Media, Inc. 2006 Histologic results 1 year after bioprosthetic repair of paraesophageal hernia in a canine model
Surg Endosc (2006) 20: 1693 1697 DOI: 10.1007/s00464-006-0680-5 Ó Springer Science+Business Media, Inc. 2006 Histologic results 1 year after bioprosthetic repair of paraesophageal hernia in a canine model
Laparoscopic Management of Giant Paraesophageal Herniation
 Laparoscopic Management of Giant Paraesophageal Herniation Robert J. Wiechmann, MD, Mark K. Ferguson, MD, Keith S. Naunheim, MD, Paul McKesey, Steven J. Hazelrigg, MD, Tibetha S. Santucci, RN, Robin S.
Laparoscopic Management of Giant Paraesophageal Herniation Robert J. Wiechmann, MD, Mark K. Ferguson, MD, Keith S. Naunheim, MD, Paul McKesey, Steven J. Hazelrigg, MD, Tibetha S. Santucci, RN, Robin S.
Outcomes After Minimally Invasive Reoperation for Gastroesophageal Reflux Disease
 Outcomes After Minimally Invasive Reoperation for Gastroesophageal Reflux Disease James D. Luketich, MD, Hiran C. Fernando, FRCS, FRCSEd, Neil A. Christie, FRCS(C), Percival O. Buenaventura, MD, Sayeed
Outcomes After Minimally Invasive Reoperation for Gastroesophageal Reflux Disease James D. Luketich, MD, Hiran C. Fernando, FRCS, FRCSEd, Neil A. Christie, FRCS(C), Percival O. Buenaventura, MD, Sayeed
Today, laparoscopic Nissen fundoplication can be performed with a 0.35%
 General Thoracic Surgery Whitson et al Wedge gastroplasty and reinforced crural repair: Important components of laparoscopic giant or recurrent hiatal hernia repair Bryan A. Whitson, MD, Chuong D. Hoang,
General Thoracic Surgery Whitson et al Wedge gastroplasty and reinforced crural repair: Important components of laparoscopic giant or recurrent hiatal hernia repair Bryan A. Whitson, MD, Chuong D. Hoang,
The impact of fibrin glue in the prevention of failure after Nissen fundoplication
 Scandinavian Journal of Surgery 100: 181 18, 011 The impact of fibrin glue in the prevention of failure after Nissen fundoplication T. Rantanen 1,, P. Neuvonen 1, M. Iivonen 1, 3, T. Tomminen 1, N. Oksala
Scandinavian Journal of Surgery 100: 181 18, 011 The impact of fibrin glue in the prevention of failure after Nissen fundoplication T. Rantanen 1,, P. Neuvonen 1, M. Iivonen 1, 3, T. Tomminen 1, N. Oksala
ORIGINAL ARTICLE. Myriam J. Curet, MD, FACS; Robert K. Josloff, MD; Othmar Schoeb, MD; Karl A. Zucker, MD
 ORIGINAL ARTICLE Laparoscopic Reoperation for Failed Antireflux Procedures Myriam J. Curet, MD, FACS; Robert K. Josloff, MD; Othmar Schoeb, MD; Karl A. Zucker, MD Background: Laparoscopic fundoplication
ORIGINAL ARTICLE Laparoscopic Reoperation for Failed Antireflux Procedures Myriam J. Curet, MD, FACS; Robert K. Josloff, MD; Othmar Schoeb, MD; Karl A. Zucker, MD Background: Laparoscopic fundoplication
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Clinical Study Hiatus Hernia Repair with Bilateral Oesophageal Fixation
 Surgery Research and Practice Volume 2015, Article ID 693138, 5 pages http://dx.doi.org/10.1155/2015/693138 Clinical Study Hiatus Hernia Repair with Bilateral Oesophageal Fixation Rajith Mendis, 1 Caran
Surgery Research and Practice Volume 2015, Article ID 693138, 5 pages http://dx.doi.org/10.1155/2015/693138 Clinical Study Hiatus Hernia Repair with Bilateral Oesophageal Fixation Rajith Mendis, 1 Caran
Causes of Long-Term Dysphagia After Laparoscopic Nissen Fundoplication
 SCIENTIFIC PAPER Causes of Long-Term Dysphagia After Laparoscopic Nissen Fundoplication Kazuyoshi Sato, MD, PhD, Ziad T. Awad, MD, Charles J. Filipi, MD, Mohamed A. Selima, MD, Judd E. Cummings, Steve
SCIENTIFIC PAPER Causes of Long-Term Dysphagia After Laparoscopic Nissen Fundoplication Kazuyoshi Sato, MD, PhD, Ziad T. Awad, MD, Charles J. Filipi, MD, Mohamed A. Selima, MD, Judd E. Cummings, Steve
PAPER. Is the Use of a Bougie Necessary for Laparoscopic Nissen Fundoplication?
 PAPER Is the Use of a Bougie Necessary for Laparoscopic Nissen Fundoplication? Yuri W. Novitsky, MD; Kent W. Kercher, MD; Mark P. Callery, MD; Donald R. Czerniach, MD; John J. Kelly, MD; Demetrius E. M.
PAPER Is the Use of a Bougie Necessary for Laparoscopic Nissen Fundoplication? Yuri W. Novitsky, MD; Kent W. Kercher, MD; Mark P. Callery, MD; Donald R. Czerniach, MD; John J. Kelly, MD; Demetrius E. M.
ORIGINAL PAPER. Mesh hiatal reinforcement in laparoscopic Nissen fundoplication for neurologically impaired children is safe and feasible
 Nagoya J. Med. Sci. 79. 427 ~ 433, 2017 doi:10.18999/nagjms.79.4.427 ORIGINAL PAPER Mesh hiatal reinforcement in laparoscopic Nissen fundoplication for neurologically impaired children is safe and feasible
Nagoya J. Med. Sci. 79. 427 ~ 433, 2017 doi:10.18999/nagjms.79.4.427 ORIGINAL PAPER Mesh hiatal reinforcement in laparoscopic Nissen fundoplication for neurologically impaired children is safe and feasible
4/24/2015. History of Reflux Surgery. Recent Innovations in the Surgical Treatment of Reflux
 Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Early View Article: Online published version of an accepted article before publication in the final form.
 Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title:
Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title:
Endoscopic vs Surgical Therapies for GERD: Is it Time to Put down the Scalpel?
 Endoscopic vs Surgical Therapies for GERD: Is it Time to Put down the Scalpel? Brian R. Smith, MD, FACS, FASMBS Associate Professor of Surgery & General Surgery Residency Program Director UC Irvine Medical
Endoscopic vs Surgical Therapies for GERD: Is it Time to Put down the Scalpel? Brian R. Smith, MD, FACS, FASMBS Associate Professor of Surgery & General Surgery Residency Program Director UC Irvine Medical
Paraoesophageal Hernia
 Paraoesophageal Hernia Grand Round Adam Cichowitz Surgical Registrar Paraoesophageal Hernia Type of hiatal hernia Transdiaphragmatic migration of abdominal content gastric fundus gastric body pylorus colon
Paraoesophageal Hernia Grand Round Adam Cichowitz Surgical Registrar Paraoesophageal Hernia Type of hiatal hernia Transdiaphragmatic migration of abdominal content gastric fundus gastric body pylorus colon
Reoperative Antireflux Surgery for Failed Fundoplication: An Analysis of Outcomes in 275 Patients
 Reoperative Antireflux Surgery for Failed Fundoplication: An Analysis of Outcomes in 275 Patients Omar Awais, DO, James D. Luketich, MD, Matthew J. Schuchert, MD, Christopher R. Morse, MD, Jonathan Wilson,
Reoperative Antireflux Surgery for Failed Fundoplication: An Analysis of Outcomes in 275 Patients Omar Awais, DO, James D. Luketich, MD, Matthew J. Schuchert, MD, Christopher R. Morse, MD, Jonathan Wilson,
Laparoscopic management of totally intra-thoracic stomach with chronic volvulus
 Online Submissions: http://www.wjgnet.com/esps/ wjg@wjgnet.com doi:10.3748/wjg.v19.i35.5848 World J Gastroenterol 2013 September 21; 19(35): 5848-5854 ISSN 1007-9327 (print) ISSN 2219-2840 (online) 2013
Online Submissions: http://www.wjgnet.com/esps/ wjg@wjgnet.com doi:10.3748/wjg.v19.i35.5848 World J Gastroenterol 2013 September 21; 19(35): 5848-5854 ISSN 1007-9327 (print) ISSN 2219-2840 (online) 2013
Prevalence, outcomes, and a risk benefit analysis of diaphragmatic hernia admissions: An examination of the National Inpatient Sample database
 Prevalence, outcomes, and a risk benefit analysis of diaphragmatic hernia admissions: An examination of the National Inpatient Sample database Subroto Paul, MD, a Farooq M. Mirza, MD, a Abu Nasar, MS,
Prevalence, outcomes, and a risk benefit analysis of diaphragmatic hernia admissions: An examination of the National Inpatient Sample database Subroto Paul, MD, a Farooq M. Mirza, MD, a Abu Nasar, MS,
Surgical treatment for gastroesophageal reflux GENERAL THORACIC SURGERY
 GENERAL THORACIC SURGERY EARLY EXPERIENCE AND LEARNING CURVE ASSOCIATED WITH LAPAROSCOPIC NISSEN FUNDOPLICATION Claude Deschamps, MD Mark S. Allen, MD Victor F. Trastek, MD Julie O. Johnson, RN Peter C.
GENERAL THORACIC SURGERY EARLY EXPERIENCE AND LEARNING CURVE ASSOCIATED WITH LAPAROSCOPIC NISSEN FUNDOPLICATION Claude Deschamps, MD Mark S. Allen, MD Victor F. Trastek, MD Julie O. Johnson, RN Peter C.
Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms
 MINI-REVIEW Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms M Anvari. Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms. Can J Gastroenterol
MINI-REVIEW Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms M Anvari. Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms. Can J Gastroenterol
! "! # $% : 2000!!,!!&/ +& # )012.A C 'B " ;BDB
 *! "! # $% :.) '(,(!.( 112 ', " # '- : # +( 2000!!,!!/ + # )012!! 5!-.0( +( 1 ' 4 32005 +!% 9!! 38! 9, 5 : $. 67.+ ;2 8 3'( 3$0$!!>$- (%66) $= 1% '7 4 78-18 +( - ' :< #( @; 36, 3? / +.(%34) 42!, B : 7
*! "! # $% :.) '(,(!.( 112 ', " # '- : # +( 2000!!,!!/ + # )012!! 5!-.0( +( 1 ' 4 32005 +!% 9!! 38! 9, 5 : $. 67.+ ;2 8 3'( 3$0$!!>$- (%66) $= 1% '7 4 78-18 +( - ' :< #( @; 36, 3? / +.(%34) 42!, B : 7
LAPAROSCOPIC HELLER MYOTOMY WITH FUNDOPLICATION FOR ACHALASIA
 LAPAROSCOPIC HELLER MYOTOMY WITH FUNDOPLICATION FOR ACHALASIA I-Rue Lai, 1 Wei-Jei Lee, 1,2 and Ming-Te Huang 2 Background and Purpose: Laparoscopic Heller cardiomyotomy for the treatment of achalasia
LAPAROSCOPIC HELLER MYOTOMY WITH FUNDOPLICATION FOR ACHALASIA I-Rue Lai, 1 Wei-Jei Lee, 1,2 and Ming-Te Huang 2 Background and Purpose: Laparoscopic Heller cardiomyotomy for the treatment of achalasia
TITLE. Suture cruroplasty versus prosthetic hiatal herniorrhaphy for large hiatal hernia: A meta-analysis and
 TITLE Suture cruroplasty versus prosthetic hiatal herniorrhaphy for large hiatal hernia: A meta-analysis and systematic review of randomized controlled trials AUTHORS (EMAILS) Muhammed Ashraf Memon, MBBS,
TITLE Suture cruroplasty versus prosthetic hiatal herniorrhaphy for large hiatal hernia: A meta-analysis and systematic review of randomized controlled trials AUTHORS (EMAILS) Muhammed Ashraf Memon, MBBS,
Combined Treatment of Symptomatic Massive Paraesophageal Hernia in the Morbidly Obese
 SCIENTIFIC PAPER Combined Treatment of Symptomatic Massive Paraesophageal Hernia in the Morbidly Obese George Kasotakis, MD, Sumeet K. Mittal, MD, Ranjan Sudan, MD ABSTRACT Introduction: Repair of large
SCIENTIFIC PAPER Combined Treatment of Symptomatic Massive Paraesophageal Hernia in the Morbidly Obese George Kasotakis, MD, Sumeet K. Mittal, MD, Ranjan Sudan, MD ABSTRACT Introduction: Repair of large
Gastroesophageal reflux disease (GERD) is the most common
 Laparoscopic Nissen Fundoplication Swee H. Teh, MD, FRCSI, FACS, John G. Hunter, MD, FACS Gastroesophageal reflux disease (GERD) is the most common disorder of the esophagus and gastroesophageal junction,
Laparoscopic Nissen Fundoplication Swee H. Teh, MD, FRCSI, FACS, John G. Hunter, MD, FACS Gastroesophageal reflux disease (GERD) is the most common disorder of the esophagus and gastroesophageal junction,
Combined Collis-Nissen Reconstruction. of the esophagogastric junction at. Mark B. Orringer, M.D., and Herbert Sloan, M.D.
 Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Upside-down stomach results of mini-invasive surgical therapy
 Original paper Videosurgery Upside-down stomach results of mini-invasive surgical therapy Radek Vrba 1, Rene Aujesky 1, Katherine Vomackova 1, Lenka Zbrozkova 2, Cestmir Neoral 1 1 1 st Department of Surgery,
Original paper Videosurgery Upside-down stomach results of mini-invasive surgical therapy Radek Vrba 1, Rene Aujesky 1, Katherine Vomackova 1, Lenka Zbrozkova 2, Cestmir Neoral 1 1 1 st Department of Surgery,
The laparoscopic hiatoplasty with antireflux surgery is a safe and effective procedure to repair giant hiatal hernia
 Marano et al. BMC Surgery 2014, 14:1 RESEARCH ARTICLE Open Access The laparoscopic hiatoplasty with antireflux surgery is a safe and effective procedure to repair giant hiatal hernia Luigi Marano *, Michele
Marano et al. BMC Surgery 2014, 14:1 RESEARCH ARTICLE Open Access The laparoscopic hiatoplasty with antireflux surgery is a safe and effective procedure to repair giant hiatal hernia Luigi Marano *, Michele
Early View Article: Online published version of an accepted article before publication in the final form.
 Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Case Reports and Images (IJCRI) Type of Article: Case Report
Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Case Reports and Images (IJCRI) Type of Article: Case Report
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control
 ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
Laparoscopic Sleeve Gastrectomy: Symptoms of Gastroesophageal Reflux can be Reduced by Changes in Surgical Technique
 OBES SURG (2012) 22:1874 1879 DOI 10.1007/s11695-012-0746-5 CLINICAL RESEARCH Laparoscopic Sleeve Gastrectomy: Symptoms of Gastroesophageal Reflux can be Reduced by Changes in Surgical Technique Jorge
OBES SURG (2012) 22:1874 1879 DOI 10.1007/s11695-012-0746-5 CLINICAL RESEARCH Laparoscopic Sleeve Gastrectomy: Symptoms of Gastroesophageal Reflux can be Reduced by Changes in Surgical Technique Jorge
Symptomatic outcome following laparoscopic anterior 180 partial fundoplication: Our initial experience
 International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD
 Esophagus Anatomy/Physiology Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD Manometry Question 50 years old female with chest pain and dysphagia. Manometry
Esophagus Anatomy/Physiology Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD Manometry Question 50 years old female with chest pain and dysphagia. Manometry
Gastroesophageal Reflux Disease, Paraesophageal Hernias &
 530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
Laparoscopic repair of secondary parahiatal hernia with incarceration of the stomach: a case report
 Takemura et al. Journal of Medical Case Reports 2013, 7:50 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Laparoscopic repair of secondary parahiatal hernia with incarceration of the stomach:
Takemura et al. Journal of Medical Case Reports 2013, 7:50 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Laparoscopic repair of secondary parahiatal hernia with incarceration of the stomach:
Large Hiatal Hernia with Floppy Fundus: Clinical and Radiographic Findings
 Radiography of Hiatal Hernia Gastrointestinal Imaging Clinical Observations Steven Y. Huang 1 Marc S. Levine 1 Stephen E. Rubesin 1 David A. Katzka 2 Igor Laufer 1 Huang SY, Levine MS, Rubesin SE, Katzka
Radiography of Hiatal Hernia Gastrointestinal Imaging Clinical Observations Steven Y. Huang 1 Marc S. Levine 1 Stephen E. Rubesin 1 David A. Katzka 2 Igor Laufer 1 Huang SY, Levine MS, Rubesin SE, Katzka
PeriOperative Concerns for Anti Reflux Procedure Patients
 PeriOperative Concerns for Anti Reflux Procedure Patients Kevin Gillian, M.D., F.A.C.S. VHC Heartburn Center Director GERD word association Heartburn Chest pain Spicy food Tums Purple pills How big a problem
PeriOperative Concerns for Anti Reflux Procedure Patients Kevin Gillian, M.D., F.A.C.S. VHC Heartburn Center Director GERD word association Heartburn Chest pain Spicy food Tums Purple pills How big a problem
Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery
 SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
2015 General Surgery Survival Guide
 2015 General Surgery Survival Guide Chapter 10: Hernia Repair Know What to Look for When Coding Hernia Repair Reporting hernia repair can be tricky. But if you know what to look for then half the work
2015 General Surgery Survival Guide Chapter 10: Hernia Repair Know What to Look for When Coding Hernia Repair Reporting hernia repair can be tricky. But if you know what to look for then half the work
7/2/2015. Incidence. *Mudge M et al, Br. J. Surg, 1985, 72:70-71
 Ventral Hernia Repair: Revisonal Surgery Natan Zundel MD FACS Professor of Surgery Vice-Chairman Department of Surgery FIU Herbert Wertheim College of Medicine. Miami Florida DISCLOSURE Ethicon Endosurgery
Ventral Hernia Repair: Revisonal Surgery Natan Zundel MD FACS Professor of Surgery Vice-Chairman Department of Surgery FIU Herbert Wertheim College of Medicine. Miami Florida DISCLOSURE Ethicon Endosurgery
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
Management of acute upside-down stomach
 Schiergens et al. BMC Surgery 2013, 13:55 CASE REPORT Open Access Management of acute upside-down stomach Tobias S Schiergens 1*, Michael N Thomas 1, Thomas P Hüttl 2 and Wolfgang E Thasler 1 Abstract
Schiergens et al. BMC Surgery 2013, 13:55 CASE REPORT Open Access Management of acute upside-down stomach Tobias S Schiergens 1*, Michael N Thomas 1, Thomas P Hüttl 2 and Wolfgang E Thasler 1 Abstract
ORIGINAL ARTICLE. Laparoscopic Antireflux Surgery in the Treatment of Gastroesophageal Reflux in Patients With Barrett Esophagus
 ORIGINAL ARTICLE Laparoscopic Antireflux Surgery in the Treatment of Gastroesophageal Reflux in Patients With Barrett Esophagus Patrick Yau, MD, FRCSC; David I. Watson, MBBS, MD, FRACS; Peter G. Devitt,
ORIGINAL ARTICLE Laparoscopic Antireflux Surgery in the Treatment of Gastroesophageal Reflux in Patients With Barrett Esophagus Patrick Yau, MD, FRCSC; David I. Watson, MBBS, MD, FRACS; Peter G. Devitt,
Congenital hiatus hernia: A case series. Department of Pediatric Surgery, Afyon Kocatepe University Faculty of Medicine, Afyonkarahisar, Turkey
 Orıgınal Article PEDIATRIC SURGERY North Clin Istanb 2018 doi: 10.14744/nci.2017.58672 UNCORRECTED PROOF Congenital hiatus hernia: A case series Didem Baskin Embleton, 1 Ahmet Ali Tuncer, 1 Mehmet Surhan
Orıgınal Article PEDIATRIC SURGERY North Clin Istanb 2018 doi: 10.14744/nci.2017.58672 UNCORRECTED PROOF Congenital hiatus hernia: A case series Didem Baskin Embleton, 1 Ahmet Ali Tuncer, 1 Mehmet Surhan
ORIGINAL ARTICLE. Surgical Reintervention After Antireflux Surgery for Gastroesophageal Reflux Disease
 ORIGINAL ARTICLE Surgical Reintervention After Antireflux Surgery for Gastroesophageal Reflux Disease A Prospective Cohort Study in 130 Patients Edgar J. B. Furnée, MD; Werner A. Draaisma, MD, PhD; Ivo
ORIGINAL ARTICLE Surgical Reintervention After Antireflux Surgery for Gastroesophageal Reflux Disease A Prospective Cohort Study in 130 Patients Edgar J. B. Furnée, MD; Werner A. Draaisma, MD, PhD; Ivo
Hernia. emoryhealthcare.org
 Hernia Have you noticed a bulge or pain in your abdominal wall or groin? If so you may have a hernia. You may be in the process of confirming this diagnosis with your Primary Care Physician or already
Hernia Have you noticed a bulge or pain in your abdominal wall or groin? If so you may have a hernia. You may be in the process of confirming this diagnosis with your Primary Care Physician or already
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
Clinical Study Congenital Paraesophageal Hernia with Intrathoracic Gastric Volvolus in Two Sisters
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 856568, 5 pages doi:10.5402/2011/856568 Clinical Study Congenital Paraesophageal Hernia with Intrathoracic Gastric Volvolus
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 856568, 5 pages doi:10.5402/2011/856568 Clinical Study Congenital Paraesophageal Hernia with Intrathoracic Gastric Volvolus
Medical Policy Manual. Topic: Gastric Reflux Surgery Date of Origin: November Section: Surgery Last Reviewed Date: March 2014
 Medical Policy Manual Topic: Gastric Reflux Surgery Date of Origin: November 2012 Section: Surgery Last Reviewed Date: March 2014 Policy No: 186 Effective Date: May 1, 2014 IMPORTANT REMINDER Medical Policies
Medical Policy Manual Topic: Gastric Reflux Surgery Date of Origin: November 2012 Section: Surgery Last Reviewed Date: March 2014 Policy No: 186 Effective Date: May 1, 2014 IMPORTANT REMINDER Medical Policies
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: A rare case of Type
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: A rare case of Type
Gastroplasty with Partial or Total Plication for Gastroesophageal Reflux: Manometric and ph-metric Postoperative Studies
 Gastroplasty with Partial or Total Plication for Gastroesophageal Reflux: Manometric and ph-metric Postoperative Studies Francisco Paris, M.D., Manuel Tomas-Ridocci, M.D., Adolfo Benages, M.D., Angel G.
Gastroplasty with Partial or Total Plication for Gastroesophageal Reflux: Manometric and ph-metric Postoperative Studies Francisco Paris, M.D., Manuel Tomas-Ridocci, M.D., Adolfo Benages, M.D., Angel G.
Collis gastroplasty: why, when and how?
 Mini-Review Page 1 of 7 Collis gastroplasty: why, when and how? Pietro Riva 1,2, Lee L. Swanström 2,3 1 Department of General Surgery, Humanitas Research Hospital, Rozzano (Milano), Italy; 2 Institute
Mini-Review Page 1 of 7 Collis gastroplasty: why, when and how? Pietro Riva 1,2, Lee L. Swanström 2,3 1 Department of General Surgery, Humanitas Research Hospital, Rozzano (Milano), Italy; 2 Institute
Unilateral Versus Bilateral Wrap Crural Fixation in Laparoscopic Nissen Fundoplication for Children
 SCIENTIFIC PAPER Unilateral Versus Bilateral Wrap Crural Fixation in Laparoscopic Nissen Fundoplication for Children Mohamed E. Hassan, MD, PhD, FEBPS ABSTRACT Introduction: Gastroesophageal reflux (GERD)
SCIENTIFIC PAPER Unilateral Versus Bilateral Wrap Crural Fixation in Laparoscopic Nissen Fundoplication for Children Mohamed E. Hassan, MD, PhD, FEBPS ABSTRACT Introduction: Gastroesophageal reflux (GERD)
Achalasia is a primary esophageal motility disorder of unknown
 Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Approximately 40% of US adults have reflux symptoms at least. Reoperative laparoscopic fundoplication for the treatment of failed fundoplication GTS
 Papasavas et al General Thoracic Surgery Reoperative laparoscopic fundoplication for the treatment of failed fundoplication Pavlos K. Papasavas, MD a Woodrow W. Yeaney, MD b Rodney J. Landreneau, MD b
Papasavas et al General Thoracic Surgery Reoperative laparoscopic fundoplication for the treatment of failed fundoplication Pavlos K. Papasavas, MD a Woodrow W. Yeaney, MD b Rodney J. Landreneau, MD b
2018 REIMBURSEMENT GUIDE
 TABLE OF CONTENTS: Component Separation Technique and Hiatal Hernia Repair...08 Hernia Repair...03 Laparoscopic Repair Hernia...06 Stoma Procedures...11 Level II Codes...13 -PCS Codes...14 Modifiers...13
TABLE OF CONTENTS: Component Separation Technique and Hiatal Hernia Repair...08 Hernia Repair...03 Laparoscopic Repair Hernia...06 Stoma Procedures...11 Level II Codes...13 -PCS Codes...14 Modifiers...13
Subjective outcome after laparoscopic hiatal hernia repair for intrathoracic stomach
 Langenbecks Arch Surg (2017) 402:521 530 DOI 10.1007/s00423-016-1504-2 ORIGINAL ARTICLE Subjective outcome after laparoscopic hiatal hernia repair for intrathoracic stomach P. S. S. Castelijns 1 & J. E.
Langenbecks Arch Surg (2017) 402:521 530 DOI 10.1007/s00423-016-1504-2 ORIGINAL ARTICLE Subjective outcome after laparoscopic hiatal hernia repair for intrathoracic stomach P. S. S. Castelijns 1 & J. E.
Intrathoracic fundoplication for reflux stricture
 Thorax 1983;38:36-40 Intrathoracic fundoplication for reflux stricture associated with short oesophagus K MOGHISSI From the Humberside Cardiothoracic Surgical Centre, Castle Hill Hospital, Cottingham,
Thorax 1983;38:36-40 Intrathoracic fundoplication for reflux stricture associated with short oesophagus K MOGHISSI From the Humberside Cardiothoracic Surgical Centre, Castle Hill Hospital, Cottingham,
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
ORIGINAL ARTICLE. National-Based Analysis of Laparoscopic and Open Fundoplications
 ORIGINAL ARTICLE Complications in Antireflux Surgery National-Based Analysis of Laparoscopic and Open Fundoplications Tuomo K. Rantanen, MD, PhD; Niku K. J. Oksala, MD, PhD; Anni K. Oksala, MD, PhD; Jarmo
ORIGINAL ARTICLE Complications in Antireflux Surgery National-Based Analysis of Laparoscopic and Open Fundoplications Tuomo K. Rantanen, MD, PhD; Niku K. J. Oksala, MD, PhD; Anni K. Oksala, MD, PhD; Jarmo
Failure of antireflux operations or hiatal hernia repairs. Outcomes After Esophagectomy in Patients With Prior Antireflux or Hiatal Hernia Surgery
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
34 yo M presented in ER of KCH at 7/06/10 Painful lump lt groin + vomiting Pain started 2 hrs before presentation. PMH known left inguinal hernia PSH
 Case Presentation 34 yo M presented in ER of KCH at 7/06/10 Painful lump lt groin + vomiting Pain started 2 hrs before presentation. PMH known left inguinal hernia PSH negative NKDA Case Presentation VS:
Case Presentation 34 yo M presented in ER of KCH at 7/06/10 Painful lump lt groin + vomiting Pain started 2 hrs before presentation. PMH known left inguinal hernia PSH negative NKDA Case Presentation VS:
The New England Journal of Medicine
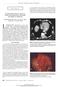 Brief Report GASTROPERICARDIAL FISTULA AFTER LAPAROSCOPIC SURGERY FOR REFLUX DISEASE In the emergency room, the patient was initially given sublingual nitroglycerin, but his blood pressure fell to 92/60
Brief Report GASTROPERICARDIAL FISTULA AFTER LAPAROSCOPIC SURGERY FOR REFLUX DISEASE In the emergency room, the patient was initially given sublingual nitroglycerin, but his blood pressure fell to 92/60
Falk Symposium, , , Portorož. Physiology of Swallowing and Anti-Gastroesophageal. Reflux-Mechanisms. Mechanisms: C.
 Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Technique Guide. Bard MK Hernia Repair. Featuring Modified Onflex Mesh SOFT TISSUE REPAIR. Anterior Approach to a Preperitoneal Inguinal Hernia Repair
 Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
5 Principles of Successful Surgical Anti-Reflux Procedures
 5 Principles of Successful Surgical Anti-Reflux Procedures Federico Cuenca-Abente, Brant K. Oelschlager, and Carlos A. Pellegrini Gastroesophageal reflux disease (GERD) is the most common gastrointestinal
5 Principles of Successful Surgical Anti-Reflux Procedures Federico Cuenca-Abente, Brant K. Oelschlager, and Carlos A. Pellegrini Gastroesophageal reflux disease (GERD) is the most common gastrointestinal
Objectives. Hesselbach s Triangle 11/30/2009. Myopectineal Orifice of Fruchaud. Hernias: Who, What, When, Where, Why?
 Objectives Hernias: Who, What, When, Where, Why? J. Scott Roth, MD Chief, Gastrointestinal Surgery Director, Minimally Invasive Surgery University of Kentucky June 16, 2009 Identify patients at risk for
Objectives Hernias: Who, What, When, Where, Why? J. Scott Roth, MD Chief, Gastrointestinal Surgery Director, Minimally Invasive Surgery University of Kentucky June 16, 2009 Identify patients at risk for
The Belsey Mark IV: an operation with an enduring role in the management of complicated hiatal hernia
 Markakis et al. BMC Surgery 0, :4 RESEARCH ARTCLE Open Access The Belsey Mark V: an operation with an enduring role in the management of complicated hiatal hernia Charalampos Markakis *, Periklis Tomos,
Markakis et al. BMC Surgery 0, :4 RESEARCH ARTCLE Open Access The Belsey Mark V: an operation with an enduring role in the management of complicated hiatal hernia Charalampos Markakis *, Periklis Tomos,
L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO
 L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO GASTROESOFAGEO Greta Saino University of Milan Department of Biomedical Sciences for Health Division of General Surgery IRCCS Policlinico San Donato TOP TEN
L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO GASTROESOFAGEO Greta Saino University of Milan Department of Biomedical Sciences for Health Division of General Surgery IRCCS Policlinico San Donato TOP TEN
Diaphragmatic Hernia Presenting With Intrathoracic Perforation
 ISPUB.COM The Internet Journal of Surgery Volume 2 Number 1 Diaphragmatic Hernia Presenting With Intrathoracic Perforation A ERDOGAN Citation A ERDOGAN.. The Internet Journal of Surgery. 2000 Volume 2
ISPUB.COM The Internet Journal of Surgery Volume 2 Number 1 Diaphragmatic Hernia Presenting With Intrathoracic Perforation A ERDOGAN Citation A ERDOGAN.. The Internet Journal of Surgery. 2000 Volume 2
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT
 STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
The Influence of Operation Technique on Long-Term Results of Achalasia Treatment
 56 :56-60 The Influence of Operation Technique on Long-Term Results of Achalasia Treatment Mindaugas Kiudelis, Kristina Mechonosina, Antanas Mickevičius, Almantas Maleckas, Žilvinas Endzinas Department
56 :56-60 The Influence of Operation Technique on Long-Term Results of Achalasia Treatment Mindaugas Kiudelis, Kristina Mechonosina, Antanas Mickevičius, Almantas Maleckas, Žilvinas Endzinas Department
Pain after laparoscopic antireflux surgery
 REVIEW Ann R Coll Surg Engl 2014; 96: 95 100 doi 10.1308/003588414X13824511649256 Pain after laparoscopic antireflux surgery DM Bunting, L Szczebiot, PM Peyser Royal Cornwall Hospitals NHS Trust, UK ABSTRACT
REVIEW Ann R Coll Surg Engl 2014; 96: 95 100 doi 10.1308/003588414X13824511649256 Pain after laparoscopic antireflux surgery DM Bunting, L Szczebiot, PM Peyser Royal Cornwall Hospitals NHS Trust, UK ABSTRACT
Physiologic Mechanism and Preoperative Prediction of New-Onset Dysphagia After Laparoscopic Nissen Fundoplication
 Physiologic Mechanism and Preoperative Prediction of New-Onset Dysphagia After Laparoscopic Nissen Fundoplication Dennis Blom, M.D., Jeffrey H. Peters, M.D., Tom R. DeMeester, M.D., Peter F. Crookes, M.D.,
Physiologic Mechanism and Preoperative Prediction of New-Onset Dysphagia After Laparoscopic Nissen Fundoplication Dennis Blom, M.D., Jeffrey H. Peters, M.D., Tom R. DeMeester, M.D., Peter F. Crookes, M.D.,
MINIMALLY INVASIVE ESOPHAGECTOMY FOR CANCER: where do we stand?
 MINIMALLY INVASIVE ESOPHAGECTOMY FOR CANCER: where do we stand? Ph Nafteux, MD Copenhagen, Nov 3rd 2011 Department of Thoracic Surgery, University Hospitals Leuven, Belgium W. Coosemans, H. Decaluwé, Ph.
MINIMALLY INVASIVE ESOPHAGECTOMY FOR CANCER: where do we stand? Ph Nafteux, MD Copenhagen, Nov 3rd 2011 Department of Thoracic Surgery, University Hospitals Leuven, Belgium W. Coosemans, H. Decaluwé, Ph.
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER AUGMENTATION FOR THE TREATMENT OF GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
Laparoscopic Crural Repair With Simultaneous Sleeve Gastrectomy: A Way in Gastroesophageal Reflux Disease Treatment Associated With Morbid Obesity
 J Minim Invasive Surg Sci.2012;1(2): 67-73. Journal of Minimally Invasive Surgical Sciences www.minsurgery.com Laparoscopic Crural Repair With Simultaneous Sleeve Gastrectomy: A Way in Gastroesophageal
J Minim Invasive Surg Sci.2012;1(2): 67-73. Journal of Minimally Invasive Surgical Sciences www.minsurgery.com Laparoscopic Crural Repair With Simultaneous Sleeve Gastrectomy: A Way in Gastroesophageal
