Secrets for successful laparoscopic antireflux surgery: mesh hiatoplasty
|
|
|
- Jeremy Baker
- 5 years ago
- Views:
Transcription
1 Review Article Page 1 of 6 Secrets for successful laparoscopic antireflux surgery: mesh hiatoplasty H. Alejandro Rodriguez, Brant K. Oelschlager Department of Surgery, University of Washington, Seattle, WA, USA Contributions: (I) Conception and design: All authors; (II) Administrative support: None; (III) Provision of study materials or patients: None; (IV) Collection and assembly of data: None; (V) Data analysis and interpretation: None; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Brant K. Oelschlager, MD, FACS. Byers Endowed Professor of Esophageal Research; Chief, Division of General Surgery; Director, Center for Esophageal and Gastric Surgery; University of Washington, 1959 NE Pacific St, Box , Seattle, WA 98195, USA. brant@uw.edu. Abstract: Repair of hiatal hernias is associated with an elevated recurrence rate, a fact that has long driven modifications to surgical technique. During the past 20 years, reinforcement of the repair with mesh has formed the basis of many of these modifications. However, despite early success, the use of synthetic and biologic mesh at the hiatus has been found to carry increased complication and high long-term recurrence rates, respectively. In this article, we review available evidence as well as our current practice for meshreinforced hiatal hernia repair. Keywords: Hiatal hernia; paraesophageal hernia; mesh hiatoplasty Received: 18 January 2017; Accepted: 19 January 2017; Published: 06 April doi: /ales View this article at: Introduction The role of the esophageal hiatus in preventing gastroesophageal reflux was first established in the mid-twentieth century by British surgeon Phillip Allison (1). Based on his observations, Allison devised an operation that would re-establish normal anatomy through suture of the diaphragmatic crura posterior to the esophagus and fixation of the cardia to the diaphragm on the abdominal side (2). During the same decade, Rudolph Nissen noted that plication of the fundus around the distal esophagus eliminated symptoms of gastro-esophageal reflux (3). These two concepts, closure of the hiatus and creation of a flapvalve mechanism, have since formed the basis of anti-reflux procedures. Significant progress has been made in anti-reflux surgery since the time of Allison and Nissen. With the introduction of minimally invasive techniques to foregut surgery, patients no longer have to endure large abdominal or thoracic incisions. Recent population-based analysis has shown a decrease in the morbidity-mortality of hiatal hernia repair over the last 20 years, with the lowest risk in those treated by laparoscopy (4). Despite these advances, recurrence of hiatal hernias (with its associated risk of recurrent GERD) remains common (5). This fact has driven many to seek improvements in technique, notably by addition of prosthetic material (mesh) to the repair. The challenge of recurrence The esophageal hiatus is subject to constant diaphragmatic movement, positive pressure from the abdomen, and negative pressure from the mediastinum. These conditions set the stage for recurrence of hiatal or paraesophageal hernias after surgical repair. Indeed, the Allison procedure fell into disuse after he reported on a nearly 50% recurrence rate for hiatal hernia at the 1973 meeting of the American Surgical Association. Allison carefully documented recurrence as demonstrated by barium swallow studies, and was the first to point out that the rate of recurrence increases over time (6). Difficulties in hiatal hernia repair were not unique to the Allison technique, as evidenced by Ronald Belsey s work. Belsey s Mark IV repair, described
2 Page 2 of 6 Annals of Laparoscopic and Endoscopic Surgery, 2017 in 1967, was the culmination of a technique that evolved (Marks I III) over years of trial and error and methodical observation. Recurrence rate for the Mark IV repair was noted to be 7%, with 50% of patients having undergone barium swallow at least a year after their operation (7). Only Hill s 1977 description of his median arcuate ligament repair stood out in reporting a 0% recurrence rate (8). However, there were few studies in the open era to track large scale outcomes, and even fewer that tracked anatomic ones. As such, subsequent reports of the Hill repair found recurrence nearing 20% in those who underwent radiologic follow-up (9). The laparoscopic approach to hiatal hernia repair was first described in the early 1990 s (10). This approach offered patients the known advantages of minimally invasive surgery while allowing surgeons to follow the tenets of successful hiatal hernia repair, namely esophageal mobilization, excision of the hernia sac and closure of the diaphragmatic crura (11). With this renewed enthusiasm for hiatal hernia repair, came more studies evaluating outcomes and anatomic failure. Despite coming under fire initially for increased recurrence rate when compared to open surgery, the laparoscopic technique has continued to be favored by most high volume centers (12-14), as the outcomes now appear similar to open approaches. Use of mesh at the esophageal hiatus Non-absorbable mesh The success of prosthetic material for repair of abdominal wall hernias suggested that the same tension-free concept could be applied to the esophageal hiatus. Kuster and Gilroy first reported placement of mesh at the hiatus in In their technique, a polyester mesh was placed anterior to the esophagus as a bridge repair (15). Many others soon followed suit, with case series documenting the use of mesh (most commonly polypropylene and PTFE) placed in a variety of configurations, including O-shaped (encircling the esophagus), U-shaped, anteriorly placed triangle and posteriorly placed rectangle (16-19). These techniques were found to be associated with decreased recurrence (20,21). However, it was soon found that the use of non-absorbable mesh was linked to unique complications, of which the most troubling were esophageal stricture and erosion of mesh into the esophagus (22,23). Some groups have reported low incidence of dysphagia and continue to advocate for the use of non-absorbable mesh at the hiatus (24-26). This remains a controversial topic as mesh erosion into the esophageal lumen has been associated with catastrophic consequences (i.e., need for esophago-gastrectomy) (19,22,27). Absorbable mesh In an effort to take advantage of the benefits of prosthetic material while avoiding complications associated with nonabsorbable mesh, our group was an early adopter of the use of absorbable (biologic) mesh at the hiatus. After our initial results showed a promising safety profile and low recurrence rate (28), we designed a multicenter randomized controlled trial comparing sutured repair to closure reinforced with biologic mesh (small intestinal submucosa, Surgisis, Cook Surgical). At 6-month follow-up, we found that compared to suture repair, use of biologic mesh was associated with a nearly three-fold reduction in recurrence (9% vs. 24%) (29). These encouraging results were later tempered by our 5-year follow-up, in which we found similar recurrence rates between both groups (54% vs. 59%) (30). The outcomes of this study led us to take a selective approach to the placement of biologic mesh at the hiatus. A recent report aimed to compare results over two types of biologic mesh (both composed of acellular human dermis) in 54 patients. Overall recurrence rate was 14% at 6-month follow-up and no significant differences were found between the two groups (31). A European observational study compared results between patients who underwent suture-only repair and repair buttressed with a biosynthetic mesh. Overall recurrence was higher in the suture-only group (9.7% vs. 18.6%) at a median follow up of 24 months. However, when recurrence-free probability was estimated, the benefit of mesh largely diminished over time (32). Thus results from these studies have largely confirmed our findings, i.e., placing biologic mesh is superior in terms of short-term recurrence, an advantage which decreases over time. There are very few head-to-head studies comparing synthetic and biologic mesh at the hiatus. The one randomized controlled trial to do so found similar 6-month recurrence rates in three groups studied: suture only repair, biologic mesh repair and non-absorbable mesh repair. This study is ongoing and its long-term results should shed further light into the complication and recurrence profiles of each type of repair (33).
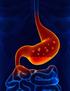
3 Annals of Laparoscopic and Endoscopic Surgery, 2017 Page 3 of 6 Figure 1 Port placement for laparoscopic hiatal hernia repair. Figure 2 U-shaped mesh placed at the hiatus. Note superior anchoring sutures. Surgeon s left hand Liver retractor Camera port Surgeon s right hand Assistant esophageal hiatus. We start the procedure by reducing as much hernia contents as possible. If the stomach is not easily reducible, no further attempts are made at this point. An incision of the sac over the left crus is made, which will enhance visualization when completing ligation of the short gastric vessels. These are taken down using the Ligasure device (Covidien, Boulder, CO, USA). Once the fundus is completely free of attachments, the areolar plane between the hernia sac and the left crus is entered. At this point, adequate identification and dissection of planes is crucial as it allows better identification of mediastinal structures, including the pleura. From the left crus, dissection of the hernia sac is carried over to the right in a counterclockwise fashion. This usually allows for full reduction of hernia contents and sac. The anterior vagus is identified and protected before reduction of the hernia sac. With the stomach in an intra-abdominal position, a Penrose drain is placed around the GE junction. This will allow traction of the esophagus during mediastinal mobilization. The esophagus can be readily mobilized from its mediastinal attachments with a combination of blunt and energy dissection. At least 3 cm of intra-abdominal esophagus should be obtained. Closure of the hiatus is usually achieved through posterior 2-0 silk sutures. Anterior stitches may also be placed if the esophagus is deemed to be angulated by only posterior sutures. We do this over a 52-Fr lighted bougie. We routinely perform a 360-degree Nissen fundoplication unless otherwise contraindicated. In patients with ineffective motility as demonstrated by high-resolution manometry, it is our preference to perform a partial (Toupet) fundoplication. Surgical technique The patient is placed in a supine, split-leg position. Both arms are tucked and safety straps are placed around the patients thighs. The surgeon stands at the foot of the table, with an assistant standing on the patient s left side. Pneumoperitoneum is obtained with a Veres needle placed through a left subcostal incision. We place our first trocar in the same location using an 11-mm optical port. We place three additional ports as seen in Figure 1. Additionally, a Nathanson liver retractor (Mediflex, Islandia, NY, USA) is placed in a subxiphoid location. A steep reverse Trendelenburg position allows visualization of the The difficult hiatal closure As previously mentioned, our approach to placing mesh is highly selective and the decision is mostly based on intraoperative findings. If the operating surgeon considers that the repair is being made under tension, a biologic mesh is placed to buttress the repair. We either cut the mesh in a U shape (Figure 2), which completely covers the hiatal closure, or in a C shape (Figure 3) to cover the posterior closure, anterior hiatus and right crus. The mesh is secured through superior sutures placed on both sides of the hiatus with additional fixation achieved by applying fibrin glue to the entire mesh (Figure 4).
4 Page 4 of 6 Annals of Laparoscopic and Endoscopic Surgery, 2017 Figure 3 C-shaped mesh placed at the hiatus. Figure 5 Relaxing incision created 2 cm lateral to the edge of the right crus. and complications are rarely life threatening (34,35). The opposite is true in hiatal hernia repair. The reported rate of complications from tacks at the hiatus is low, however they are associated with grim complications such as pericardial injury and consequent cardiac tamponade. Various reported cases have only been diagnosed on autopsy (36-38). We therefore advocate for extreme care when suturing mesh at the diaphragm (taking very superficial bites just to encourage scarring to the diaphragm) and avoiding fixation by tacks at all costs. Figure 4 Fibrin glue is applied for additional mesh fixation. In rare occasions, excessive tension at the hiatus will make it impossible or near impossible to adequately bring the crura together. In those instances, we perform a diaphragmatic relaxing incision on the right side. In this technique, a full thickness incision is made 2 cm lateral to the edge of the right crus (Figure 5). A biologic mesh is then placed in the C shape, which covers both the incision and the crural closure. The mesh is secured to the diaphragm with 4 5 stitches and fibrin glue. Conclusions and future directions While preventing recurrences is a major point of emphasis for hiatal hernia repair, the success of prosthetic material for abdominal wall surgery has not been duplicated for operations at the hiatus. The incompletely realized quest for reduction of complications and recurrence will likely drive many improvements in the years to come. Current evidence supports the use of absorbable mesh to reduce short-term recurrence, though strategies for reducing longterm recurrences are lacking. Tips, tricks and pitfalls Use of tacks to for mesh fixation Non-absorbable or absorbable tacks are widely used for mesh fixation in ventral and inguinal hernia repair. While there is concern for chronic pain and higher recurrence rate, tacks have been found to be at least as safe as suture fixation, Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare.
5 Annals of Laparoscopic and Endoscopic Surgery, 2017 Page 5 of 6 References 1. Stylopoulos N, Rattner DW. The history of hiatal hernia surgery: from Bowditch to laparoscopy. Ann Surg 2005;241: Allison PR. Reflux esophagitis, sliding hiatal hernia, and the anatomy of repair. Surg Gynecol Obstet 1951;92: Nissen R. Eine einfache operation zur beeinflussung der refluxoesophagitis. Schweiz Med Wochenschr 1956;86: Kaplan JA, Schecter S, Lin MY, et al. Morbidity and Mortality Associated With Elective or Emergency Paraesophageal Hernia Repair. JAMA Surg 2015;150: Tam V, Winger DG, Nason KS. A systematic review and meta-analysis of mesh vs suture cruroplasty in laparoscopic large hiatal hernia repair. Am J Surg 2016;211: Allison PR. Hiatus hernia: a 20-year retrospective survey. Ann Surg 1973;178: Skinner DB, Belsey RH. Surgical management of esophageal reflux and hiatus hernia. Long-term results with 1,030 patients. J Thorac Cardiovasc Surg 1967;53: Hill LD. Progress in the surgical management of hiatal hernia. World J Surg 1977;1: Aye RW, Rehse D, Blitz M, et al. The Hill antireflux repair at 5 institutions over 25 years. Am J Surg 2011;201: Cuschieri A, Shimi S, Nathanson LK. Laparoscopic reduction, crural repair, and fundoplication of large hiatal hernia. Am J Surg 1992;163: Oddsdottir M, Franco AL, Laycock WS, et al. Laparoscopic repair of paraesophageal hernia. New access, old technique. Surg Endosc 1995;9: Mattar SG, Bowers SP, Galloway KD, et al. Long-term outcome of laparoscopic repair of paraesophageal hernia. Surg Endosc 2002;16: Levy G, Aye RW, Farivar AS, et al. A Combined Nissen Plus Hill Hybrid Repair for Paraesophageal Hernia Improves Clinical Outcomes and Reduces Long-Term Recurrences Compared with Laparoscopic Nissen Alone. J Gastrointest Surg 2017;21: Oelschlager BK, Petersen RP, Brunt LM, et al. Laparoscopic Paraesophageal Hernia Repair: Defining Long-Term Clinical and Anatomic Outcomes. J Gastrointest Surg 2012;16: Kuster GG, Gilroy S. Laparoscopic technique for repair of paraesophageal hiatal hernias. J Laparoendosc Surg 1993;3: Frantzides CT, Carlson MA. Prosthetic reinforcement of posterior cruroplasty during laparoscopic hiatal herniorrhaphy. Surg Endosc 1997;11: Edelman DS. Laparoscopic paraesophageal hernia repair with mesh. Surg Laparosc Endosc 1995;5: Pitcher DE, Curet MJ, Martin DT, et al. Successful laparoscopic repair of paraesophageal hernia. Arch Surg 1995;130: Targarona EM, Bendahan G, Balague C, et al. Mesh in the hiatus: a controversial issue. Arch Surg 2004;139: Frantzides CT, Madan AK, Carlson MA, et al. A prospective, randomized trial of laparoscopic polytetrafluoroethylene (PTFE) patch repair vs simple cruroplasty for large hiatal hernia. Arch Surg 2002;137: Granderath FA, Schweiger UM, Kamolz T, et al. Laparoscopic antireflux surgery with routine meshhiatoplasty in the treatment of gastroesophageal reflux disease. J Gastrointest Surg 2002;6: Tatum RP, Shalhub S, Oelschlager BK, et al. Complications of PTFE Mesh at the Diaphragmatic Hiatus. J Gastrointest Surg 2008;12: Stadlhuber RJ, Sherif AE, Mittal SK, et al. Mesh complications after prosthetic reinforcement of hiatal closure: a 28-case series. Surg Endosc 2009;23: Granderath FA, Carlson MA, Champion JK, et al. Prosthetic closure of the esophageal hiatus in large hiatal hernia repair and laparoscopic antireflux surgery. Surg Endosc 2006;20: Antoniou SA, Antoniou GA, Koch OO, et al. Lower recurrence rates after mesh-reinforced versus simple hiatal hernia repair: a meta-analysis of randomized trials. Surg Laparosc Endosc Percutan Tech 2012;22: Müller-Stich BP, Linke GR, Senft J, et al. Laparoscopic Mesh-augmented Hiatoplasty With Cardiophrenicopexy Versus Laparoscopic Nissen Fundoplication for the Treatment of Gastroesophageal Reflux Disease. Ann Surg 2015;262:721-5; discussion Priego P, Perez de Oteyza J, Galindo J, et al. Longterm results and complications related to Crurasoft mesh repair for paraesophageal hiatal hernias. Hernia 2017;21: Oelschlager BK, Barreca M, Chang L, et al. The use of small intestine submucosa in the repair of paraesophageal hernias: initial observations of a new technique. Am J Surg 2003;186: Oelschlager BK, Pellegrini CA, Hunter J, et al. Biologic
6 Page 6 of 6 Annals of Laparoscopic and Endoscopic Surgery, 2017 prosthesis reduces recurrence after laparoscopic paraesophageal hernia repair: a multicenter, prospective, randomized trial. Ann Surg 2006;244: Oelschlager BK, Pellegrini CA, Hunter JG, et al. Biologic prosthesis to prevent recurrence after laparoscopic paraesophageal hernia repair: long-term follow-up from a multicenter, prospective, randomized trial. J Am Coll Surg 2011;213: Ward KC, Costello KP, Baalman S, et al. Effect of acellular human dermis buttress on laparoscopic hiatal hernia repair. Surg Endosc 2015;29: Asti E, Lovece A, Bonavina L, et al. Laparoscopic management of large hiatus hernia: five-year cohort study and comparison of mesh-augmented versus standard crura repair. Surg Endosc 2016;30: Watson DI, Thompson SK, Devitt PG, et al. Laparoscopic Repair of Very Large Hiatus Hernia With Sutures Versus Absorbable Mesh Versus Nonabsorbable Mesh. Ann Surg 2015;261: Kitamura RK, Choi J, Lynn E, et al. Suture versus tack fixation of mesh in laparoscopic umbilical hernia repair. JSLS 2013;17: Muysoms F, Vander Mijnsbrugge G, Pletinckx P, et al. Randomized clinical trial of mesh fixation with double crown versus sutures and tackers in laparoscopic ventral hernia repair. Hernia 2013;17: Frantzides CT, Welle SN. Cardiac tamponade as a lifethreatening complication in hernia repair. Surgery 2012;152: Thijssens K, Hoff C, Meyerink J. Tackers on the diaphragm. Lancet 2002;360: McClellan JM, Nelson D, Martin M. Hemopericardium after laparoscopic perihiatal procedures: high index of suspicion facilitates early diagnosis and successful nonoperative management. Surg Obes Relat Dis 2016;12:e doi: /ales Cite this article as: Rodriguez HA, Oelschlager BK. Secrets for successful laparoscopic antireflux surgery: mesh hiatoplasty..
Crural Buttressing: Why, When, and with What
 Crural Buttressing: Why, When, and with What Michael Maddaus, MD Professor of Surgery Garamella Lynch Jensen Chair in Thoracic Surgery Division of General Thoracic and Foregut Surgery University of Minnesota
Crural Buttressing: Why, When, and with What Michael Maddaus, MD Professor of Surgery Garamella Lynch Jensen Chair in Thoracic Surgery Division of General Thoracic and Foregut Surgery University of Minnesota
Laparoscopic Paraesophageal Hernia Repair with Acellular Dermal Matrix Cruroplasty
 SCIENTIFIC PAPER Laparoscopic Paraesophageal Hernia Repair with Acellular Dermal Matrix Cruroplasty Dennis F. Diaz, MD, J. Scott Roth, MD ABSTRACT Background: Laparoscopic paraesophageal hernia repair
SCIENTIFIC PAPER Laparoscopic Paraesophageal Hernia Repair with Acellular Dermal Matrix Cruroplasty Dennis F. Diaz, MD, J. Scott Roth, MD ABSTRACT Background: Laparoscopic paraesophageal hernia repair
Full incorporation of Strattice Reconstructive Tissue Matrix in a reinforced hiatal hernia repair: a case report
 Freedman Journal of Medical Case Reports 2012, 6:234 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Full incorporation of Strattice Reconstructive Tissue Matrix in a reinforced hiatal hernia repair:
Freedman Journal of Medical Case Reports 2012, 6:234 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Full incorporation of Strattice Reconstructive Tissue Matrix in a reinforced hiatal hernia repair:
ORIGINAL SCIENTIFIC ARTICLES
 ORIGINAL SCIENTIFIC ARTICLES Biologic Prosthesis to Prevent Recurrence after Laparoscopic Paraesophageal Hernia Repair: Long-term Follow-up from a Multicenter, Prospective, Randomized Trial Brant K Oelschlager,
ORIGINAL SCIENTIFIC ARTICLES Biologic Prosthesis to Prevent Recurrence after Laparoscopic Paraesophageal Hernia Repair: Long-term Follow-up from a Multicenter, Prospective, Randomized Trial Brant K Oelschlager,
ORIGINAL ARTICLE. Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation
 ORIGINAL ARTICLE Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation Preliminary Results of a Prospective Randomized Functional and Clinical
ORIGINAL ARTICLE Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation Preliminary Results of a Prospective Randomized Functional and Clinical
Paraesophageal Hernia
 Paraesophageal Hernia Inderpal (Netu) S. Sarkaria, M.D. Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Speaker/Education: Intuitive
Paraesophageal Hernia Inderpal (Netu) S. Sarkaria, M.D. Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Speaker/Education: Intuitive
ORIGINAL ARTICLE. Laparoscopic Refundoplication With Prosthetic Hiatal Closure for Recurrent Hiatal Hernia After Primary Failed Antireflux Surgery
 ORIGINL RTICLE Laparoscopic Refundoplication With Prosthetic Hiatal Closure for Recurrent Hiatal Hernia fter Primary Failed ntireflux Surgery Frank. Granderath, MD; Thomas Kamolz, PhD; Ursula M. Schweiger,
ORIGINL RTICLE Laparoscopic Refundoplication With Prosthetic Hiatal Closure for Recurrent Hiatal Hernia fter Primary Failed ntireflux Surgery Frank. Granderath, MD; Thomas Kamolz, PhD; Ursula M. Schweiger,
ORIGINAL PAPER. Mesh hiatal reinforcement in laparoscopic Nissen fundoplication for neurologically impaired children is safe and feasible
 Nagoya J. Med. Sci. 79. 427 ~ 433, 2017 doi:10.18999/nagjms.79.4.427 ORIGINAL PAPER Mesh hiatal reinforcement in laparoscopic Nissen fundoplication for neurologically impaired children is safe and feasible
Nagoya J. Med. Sci. 79. 427 ~ 433, 2017 doi:10.18999/nagjms.79.4.427 ORIGINAL PAPER Mesh hiatal reinforcement in laparoscopic Nissen fundoplication for neurologically impaired children is safe and feasible
2 Paraesophageal Hiatus Hernia
 2 Paraesophageal Hiatus Hernia Luigi Bonavina Pearls and Pitfalls Paraesophageal (type II) hiatus hernia represents a distinct anatomic and clinic entity requiring a unique therapeutic strategy, and is
2 Paraesophageal Hiatus Hernia Luigi Bonavina Pearls and Pitfalls Paraesophageal (type II) hiatus hernia represents a distinct anatomic and clinic entity requiring a unique therapeutic strategy, and is
Short-term results after laparoscopic repair of giant hiatal hernias with pledgeted sutures: a retrospective analysis
 https://doi.org/10.1007/s10029-019-01890-3 ORIGINAL ARTICLE Short-term results after laparoscopic repair of giant hiatal hernias with pledgeted sutures: a retrospective analysis M. Weitzendorfer 1 R. Pfandner
https://doi.org/10.1007/s10029-019-01890-3 ORIGINAL ARTICLE Short-term results after laparoscopic repair of giant hiatal hernias with pledgeted sutures: a retrospective analysis M. Weitzendorfer 1 R. Pfandner
Clinical Study Hiatus Hernia Repair with Bilateral Oesophageal Fixation
 Surgery Research and Practice Volume 2015, Article ID 693138, 5 pages http://dx.doi.org/10.1155/2015/693138 Clinical Study Hiatus Hernia Repair with Bilateral Oesophageal Fixation Rajith Mendis, 1 Caran
Surgery Research and Practice Volume 2015, Article ID 693138, 5 pages http://dx.doi.org/10.1155/2015/693138 Clinical Study Hiatus Hernia Repair with Bilateral Oesophageal Fixation Rajith Mendis, 1 Caran
Nissen Fundoplication
 Nissen Fundoplication By Donna Weldon Nissen fundoplication is a surgical procedure used to treat gastroesophageal reflux disease, or GERD, and hiatus hernias. For GERD, is it usually performed when medical
Nissen Fundoplication By Donna Weldon Nissen fundoplication is a surgical procedure used to treat gastroesophageal reflux disease, or GERD, and hiatus hernias. For GERD, is it usually performed when medical
Laparoscopic Sleeve Gastrectomy: Symptoms of Gastroesophageal Reflux can be Reduced by Changes in Surgical Technique
 OBES SURG (2012) 22:1874 1879 DOI 10.1007/s11695-012-0746-5 CLINICAL RESEARCH Laparoscopic Sleeve Gastrectomy: Symptoms of Gastroesophageal Reflux can be Reduced by Changes in Surgical Technique Jorge
OBES SURG (2012) 22:1874 1879 DOI 10.1007/s11695-012-0746-5 CLINICAL RESEARCH Laparoscopic Sleeve Gastrectomy: Symptoms of Gastroesophageal Reflux can be Reduced by Changes in Surgical Technique Jorge
Preliminary Study of Hiatal Hernia Repair Using Polyglycolic Acid: Trimethylene Carbonate Mesh
 SCIENTIFIC PAPER Preliminary Study of Hiatal Hernia Repair Using Polyglycolic Acid: Trimethylene Carbonate Mesh James M. Massullo, MD, Tejinder P. Singh, MD, Ward J. Dunnican, MD, Brian R. Binetti, MD
SCIENTIFIC PAPER Preliminary Study of Hiatal Hernia Repair Using Polyglycolic Acid: Trimethylene Carbonate Mesh James M. Massullo, MD, Tejinder P. Singh, MD, Ward J. Dunnican, MD, Brian R. Binetti, MD
Repair of giant paraesophageal hernias, once considered a
 Robotic-Assisted Giant Paraesophageal Hernia Repair and Nissen Fundoplication Justin Karush, DO *, and Inderpal S. Sarkaria, MD, FACS Repair of giant paraesophageal hernias, once considered a relatively
Robotic-Assisted Giant Paraesophageal Hernia Repair and Nissen Fundoplication Justin Karush, DO *, and Inderpal S. Sarkaria, MD, FACS Repair of giant paraesophageal hernias, once considered a relatively
Achalasia is a primary esophageal motility disorder of unknown
 Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Traditionally, surgical antireflux therapy has been
 Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
TITLE. Suture cruroplasty versus prosthetic hiatal herniorrhaphy for large hiatal hernia: A meta-analysis and
 TITLE Suture cruroplasty versus prosthetic hiatal herniorrhaphy for large hiatal hernia: A meta-analysis and systematic review of randomized controlled trials AUTHORS (EMAILS) Muhammed Ashraf Memon, MBBS,
TITLE Suture cruroplasty versus prosthetic hiatal herniorrhaphy for large hiatal hernia: A meta-analysis and systematic review of randomized controlled trials AUTHORS (EMAILS) Muhammed Ashraf Memon, MBBS,
Combined Collis-Nissen Reconstruction. of the esophagogastric junction at. Mark B. Orringer, M.D., and Herbert Sloan, M.D.
 Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
4/24/2015. History of Reflux Surgery. Recent Innovations in the Surgical Treatment of Reflux
 Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Traditional surgical treatment of large diaphragmatic. Laparoscopic Repair of Large Paraesophageal Hiatal Hernia
 Laparoscopic Repair of Large Paraesophageal Hiatal Hernia Peter S. Dahlberg, MD, Claude Deschamps, MD, Daniel L. Miller, MD, Mark S. Allen, MD, Francis C. Nichols, MD, and Peter C. Pairolero, MD Division
Laparoscopic Repair of Large Paraesophageal Hiatal Hernia Peter S. Dahlberg, MD, Claude Deschamps, MD, Daniel L. Miller, MD, Mark S. Allen, MD, Francis C. Nichols, MD, and Peter C. Pairolero, MD Division
Histologic results 1 year after bioprosthetic repair of paraesophageal hernia in a canine model
 Surg Endosc (2006) 20: 1693 1697 DOI: 10.1007/s00464-006-0680-5 Ó Springer Science+Business Media, Inc. 2006 Histologic results 1 year after bioprosthetic repair of paraesophageal hernia in a canine model
Surg Endosc (2006) 20: 1693 1697 DOI: 10.1007/s00464-006-0680-5 Ó Springer Science+Business Media, Inc. 2006 Histologic results 1 year after bioprosthetic repair of paraesophageal hernia in a canine model
Gastroesophageal reflux disease (GERD) is the most common
 Laparoscopic Nissen Fundoplication Swee H. Teh, MD, FRCSI, FACS, John G. Hunter, MD, FACS Gastroesophageal reflux disease (GERD) is the most common disorder of the esophagus and gastroesophageal junction,
Laparoscopic Nissen Fundoplication Swee H. Teh, MD, FRCSI, FACS, John G. Hunter, MD, FACS Gastroesophageal reflux disease (GERD) is the most common disorder of the esophagus and gastroesophageal junction,
PeriOperative Concerns for Anti Reflux Procedure Patients
 PeriOperative Concerns for Anti Reflux Procedure Patients Kevin Gillian, M.D., F.A.C.S. VHC Heartburn Center Director GERD word association Heartburn Chest pain Spicy food Tums Purple pills How big a problem
PeriOperative Concerns for Anti Reflux Procedure Patients Kevin Gillian, M.D., F.A.C.S. VHC Heartburn Center Director GERD word association Heartburn Chest pain Spicy food Tums Purple pills How big a problem
ORIGINAL ARTICLE. Myriam J. Curet, MD, FACS; Robert K. Josloff, MD; Othmar Schoeb, MD; Karl A. Zucker, MD
 ORIGINAL ARTICLE Laparoscopic Reoperation for Failed Antireflux Procedures Myriam J. Curet, MD, FACS; Robert K. Josloff, MD; Othmar Schoeb, MD; Karl A. Zucker, MD Background: Laparoscopic fundoplication
ORIGINAL ARTICLE Laparoscopic Reoperation for Failed Antireflux Procedures Myriam J. Curet, MD, FACS; Robert K. Josloff, MD; Othmar Schoeb, MD; Karl A. Zucker, MD Background: Laparoscopic fundoplication
5 Principles of Successful Surgical Anti-Reflux Procedures
 5 Principles of Successful Surgical Anti-Reflux Procedures Federico Cuenca-Abente, Brant K. Oelschlager, and Carlos A. Pellegrini Gastroesophageal reflux disease (GERD) is the most common gastrointestinal
5 Principles of Successful Surgical Anti-Reflux Procedures Federico Cuenca-Abente, Brant K. Oelschlager, and Carlos A. Pellegrini Gastroesophageal reflux disease (GERD) is the most common gastrointestinal
Cardiac tamponade as a life-threatening complication after laparoscopic mesh hiatal hernia repair
 www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Cardiac tamponade as a life-threatening complication after laparoscopic mesh hiatal hernia repair Dimitar Penchev, Georgi Kotashev, Georgi
www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Cardiac tamponade as a life-threatening complication after laparoscopic mesh hiatal hernia repair Dimitar Penchev, Georgi Kotashev, Georgi
Mid-term results of robot-assisted laparoscopic repair of large hiatal hernia; a symptomatic and radiological prospective cohort study
 Chapter 8 Mid-term results of robot-assisted laparoscopic repair of large hiatal hernia; a symptomatic and radiological prospective cohort study WA Draaisma HG Gooszen IAMJ Broeders Department of Surgery,
Chapter 8 Mid-term results of robot-assisted laparoscopic repair of large hiatal hernia; a symptomatic and radiological prospective cohort study WA Draaisma HG Gooszen IAMJ Broeders Department of Surgery,
7/2/2015. Incidence. *Mudge M et al, Br. J. Surg, 1985, 72:70-71
 Ventral Hernia Repair: Revisonal Surgery Natan Zundel MD FACS Professor of Surgery Vice-Chairman Department of Surgery FIU Herbert Wertheim College of Medicine. Miami Florida DISCLOSURE Ethicon Endosurgery
Ventral Hernia Repair: Revisonal Surgery Natan Zundel MD FACS Professor of Surgery Vice-Chairman Department of Surgery FIU Herbert Wertheim College of Medicine. Miami Florida DISCLOSURE Ethicon Endosurgery
Collis gastroplasty: why, when and how?
 Mini-Review Page 1 of 7 Collis gastroplasty: why, when and how? Pietro Riva 1,2, Lee L. Swanström 2,3 1 Department of General Surgery, Humanitas Research Hospital, Rozzano (Milano), Italy; 2 Institute
Mini-Review Page 1 of 7 Collis gastroplasty: why, when and how? Pietro Riva 1,2, Lee L. Swanström 2,3 1 Department of General Surgery, Humanitas Research Hospital, Rozzano (Milano), Italy; 2 Institute
Endoscopic vs Surgical Therapies for GERD: Is it Time to Put down the Scalpel?
 Endoscopic vs Surgical Therapies for GERD: Is it Time to Put down the Scalpel? Brian R. Smith, MD, FACS, FASMBS Associate Professor of Surgery & General Surgery Residency Program Director UC Irvine Medical
Endoscopic vs Surgical Therapies for GERD: Is it Time to Put down the Scalpel? Brian R. Smith, MD, FACS, FASMBS Associate Professor of Surgery & General Surgery Residency Program Director UC Irvine Medical
The impact of fibrin glue in the prevention of failure after Nissen fundoplication
 Scandinavian Journal of Surgery 100: 181 18, 011 The impact of fibrin glue in the prevention of failure after Nissen fundoplication T. Rantanen 1,, P. Neuvonen 1, M. Iivonen 1, 3, T. Tomminen 1, N. Oksala
Scandinavian Journal of Surgery 100: 181 18, 011 The impact of fibrin glue in the prevention of failure after Nissen fundoplication T. Rantanen 1,, P. Neuvonen 1, M. Iivonen 1, 3, T. Tomminen 1, N. Oksala
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Hannes J. Larusson Æ Urs Zingg Æ Dieter Hahnloser Æ Karen Delport Æ Burkhardt Seifert Æ Daniel Oertli
 World J Surg (2009) 33:980 985 DOI 10.1007/s00268-009-9958-9 Predictive Factors for Morbidity and Mortality in Patients Undergoing Laparoscopic Paraesophageal Hernia Repair: Age, ASA Score and Operation
World J Surg (2009) 33:980 985 DOI 10.1007/s00268-009-9958-9 Predictive Factors for Morbidity and Mortality in Patients Undergoing Laparoscopic Paraesophageal Hernia Repair: Age, ASA Score and Operation
Anatomical failure following laparoscopic antireflux surgery (LARS); does it really matter?
 The Royal College of Surgeons of England GASTROINTESTINAL SURGERY doi 10.1308/003588410X12518836440126 Anatomical failure following laparoscopic antireflux surgery (LARS); does it really matter? N DUNNE
The Royal College of Surgeons of England GASTROINTESTINAL SURGERY doi 10.1308/003588410X12518836440126 Anatomical failure following laparoscopic antireflux surgery (LARS); does it really matter? N DUNNE
Combined Treatment of Symptomatic Massive Paraesophageal Hernia in the Morbidly Obese
 SCIENTIFIC PAPER Combined Treatment of Symptomatic Massive Paraesophageal Hernia in the Morbidly Obese George Kasotakis, MD, Sumeet K. Mittal, MD, Ranjan Sudan, MD ABSTRACT Introduction: Repair of large
SCIENTIFIC PAPER Combined Treatment of Symptomatic Massive Paraesophageal Hernia in the Morbidly Obese George Kasotakis, MD, Sumeet K. Mittal, MD, Ranjan Sudan, MD ABSTRACT Introduction: Repair of large
Gastroesophageal Reflux Disease, Paraesophageal Hernias &
 530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
Causes of Long-Term Dysphagia After Laparoscopic Nissen Fundoplication
 SCIENTIFIC PAPER Causes of Long-Term Dysphagia After Laparoscopic Nissen Fundoplication Kazuyoshi Sato, MD, PhD, Ziad T. Awad, MD, Charles J. Filipi, MD, Mohamed A. Selima, MD, Judd E. Cummings, Steve
SCIENTIFIC PAPER Causes of Long-Term Dysphagia After Laparoscopic Nissen Fundoplication Kazuyoshi Sato, MD, PhD, Ziad T. Awad, MD, Charles J. Filipi, MD, Mohamed A. Selima, MD, Judd E. Cummings, Steve
PAPER. Is the Use of a Bougie Necessary for Laparoscopic Nissen Fundoplication?
 PAPER Is the Use of a Bougie Necessary for Laparoscopic Nissen Fundoplication? Yuri W. Novitsky, MD; Kent W. Kercher, MD; Mark P. Callery, MD; Donald R. Czerniach, MD; John J. Kelly, MD; Demetrius E. M.
PAPER Is the Use of a Bougie Necessary for Laparoscopic Nissen Fundoplication? Yuri W. Novitsky, MD; Kent W. Kercher, MD; Mark P. Callery, MD; Donald R. Czerniach, MD; John J. Kelly, MD; Demetrius E. M.
Intrathoracic fundoplication for reflux stricture
 Thorax 1983;38:36-40 Intrathoracic fundoplication for reflux stricture associated with short oesophagus K MOGHISSI From the Humberside Cardiothoracic Surgical Centre, Castle Hill Hospital, Cottingham,
Thorax 1983;38:36-40 Intrathoracic fundoplication for reflux stricture associated with short oesophagus K MOGHISSI From the Humberside Cardiothoracic Surgical Centre, Castle Hill Hospital, Cottingham,
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Hiatal hernias may be classified. hiatal hernia DESCRIPTION AND IDENTIFICATION. This article is the first in a twopart series about these somewhat
 paraesophagealh hiatal hernia Leslie K Browder, MD, and Alex G Little, MD DESCRIPTION AND IDENTIFICATION Hiatal hernias may be classified as four types. The most common, Type I, may present as gastroesophageal
paraesophagealh hiatal hernia Leslie K Browder, MD, and Alex G Little, MD DESCRIPTION AND IDENTIFICATION Hiatal hernias may be classified as four types. The most common, Type I, may present as gastroesophageal
L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO
 L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO GASTROESOFAGEO Greta Saino University of Milan Department of Biomedical Sciences for Health Division of General Surgery IRCCS Policlinico San Donato TOP TEN
L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO GASTROESOFAGEO Greta Saino University of Milan Department of Biomedical Sciences for Health Division of General Surgery IRCCS Policlinico San Donato TOP TEN
Use of laparoscopy in general surgical operations at academic centers
 Surgery for Obesity and Related Diseases 9 (2013) 15 20 Original article Use of laparoscopy in general surgical operations at academic centers Ninh T. Nguyen, M.D. a, *, Brian Nguyen, B.S. a, Anderson
Surgery for Obesity and Related Diseases 9 (2013) 15 20 Original article Use of laparoscopy in general surgical operations at academic centers Ninh T. Nguyen, M.D. a, *, Brian Nguyen, B.S. a, Anderson
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Early View Article: Online published version of an accepted article before publication in the final form.
 Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title:
Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title:
Outcomes After Minimally Invasive Reoperation for Gastroesophageal Reflux Disease
 Outcomes After Minimally Invasive Reoperation for Gastroesophageal Reflux Disease James D. Luketich, MD, Hiran C. Fernando, FRCS, FRCSEd, Neil A. Christie, FRCS(C), Percival O. Buenaventura, MD, Sayeed
Outcomes After Minimally Invasive Reoperation for Gastroesophageal Reflux Disease James D. Luketich, MD, Hiran C. Fernando, FRCS, FRCSEd, Neil A. Christie, FRCS(C), Percival O. Buenaventura, MD, Sayeed
The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control
 ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER AUGMENTATION FOR THE TREATMENT OF GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
Objectives. Hesselbach s Triangle 11/30/2009. Myopectineal Orifice of Fruchaud. Hernias: Who, What, When, Where, Why?
 Objectives Hernias: Who, What, When, Where, Why? J. Scott Roth, MD Chief, Gastrointestinal Surgery Director, Minimally Invasive Surgery University of Kentucky June 16, 2009 Identify patients at risk for
Objectives Hernias: Who, What, When, Where, Why? J. Scott Roth, MD Chief, Gastrointestinal Surgery Director, Minimally Invasive Surgery University of Kentucky June 16, 2009 Identify patients at risk for
Paraesophageal hiatal hernias (type II, III, IV) are. Effect of Paraesophageal Hernia Repair on Pulmonary Function
 Effect of Paraesophageal Hernia Repair on Pulmonary Function Donald E. Low, MD, and Eric J. Simchuk, MD Section of General Thoracic Surgery, Virginia Mason Medical Center, Seattle, Washington Background.
Effect of Paraesophageal Hernia Repair on Pulmonary Function Donald E. Low, MD, and Eric J. Simchuk, MD Section of General Thoracic Surgery, Virginia Mason Medical Center, Seattle, Washington Background.
Unilateral Versus Bilateral Wrap Crural Fixation in Laparoscopic Nissen Fundoplication for Children
 SCIENTIFIC PAPER Unilateral Versus Bilateral Wrap Crural Fixation in Laparoscopic Nissen Fundoplication for Children Mohamed E. Hassan, MD, PhD, FEBPS ABSTRACT Introduction: Gastroesophageal reflux (GERD)
SCIENTIFIC PAPER Unilateral Versus Bilateral Wrap Crural Fixation in Laparoscopic Nissen Fundoplication for Children Mohamed E. Hassan, MD, PhD, FEBPS ABSTRACT Introduction: Gastroesophageal reflux (GERD)
NIH Public Access Author Manuscript Arch Surg. Author manuscript; available in PMC 2013 April 01.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Surg. 2012 April ; 147(4): 352 357. doi:10.1001/archsurg.2012.17. Do large hiatal hernias affect esophageal peristalsis? Sabine
NIH Public Access Author Manuscript Published in final edited form as: Arch Surg. 2012 April ; 147(4): 352 357. doi:10.1001/archsurg.2012.17. Do large hiatal hernias affect esophageal peristalsis? Sabine
Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD
 Esophagus Anatomy/Physiology Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD Manometry Question 50 years old female with chest pain and dysphagia. Manometry
Esophagus Anatomy/Physiology Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD Manometry Question 50 years old female with chest pain and dysphagia. Manometry
Technique Guide. Bard MK Hernia Repair. Featuring Modified Onflex Mesh SOFT TISSUE REPAIR. Anterior Approach to a Preperitoneal Inguinal Hernia Repair
 Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Metaanalysis of Recurrence After Laparoscopic Repair of Paraesophageal Hernia
 SCIENTIFIC PAPER Metaanalysis of Recurrence After Laparoscopic Repair of Paraesophageal Hernia Munir Ahmad Rathore, FRCS, Syed Imran Hussain Andrabi, FRCS, Muhammad Iqbal Bhatti, MRCS, Syed Muzahir Hussain
SCIENTIFIC PAPER Metaanalysis of Recurrence After Laparoscopic Repair of Paraesophageal Hernia Munir Ahmad Rathore, FRCS, Syed Imran Hussain Andrabi, FRCS, Muhammad Iqbal Bhatti, MRCS, Syed Muzahir Hussain
The Influence of Operation Technique on Long-Term Results of Achalasia Treatment
 56 :56-60 The Influence of Operation Technique on Long-Term Results of Achalasia Treatment Mindaugas Kiudelis, Kristina Mechonosina, Antanas Mickevičius, Almantas Maleckas, Žilvinas Endzinas Department
56 :56-60 The Influence of Operation Technique on Long-Term Results of Achalasia Treatment Mindaugas Kiudelis, Kristina Mechonosina, Antanas Mickevičius, Almantas Maleckas, Žilvinas Endzinas Department
Symptomatic outcome following laparoscopic anterior 180 partial fundoplication: Our initial experience
 International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic insertion of a magnetic titanium ring for gastrooesophageal reflux
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic insertion of a magnetic titanium ring for gastrooesophageal reflux
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
The current status of magnetic sphincter augmentation in the management of gastroesophageal reflux disease
 Review Article Page 1 of 9 The current status of magnetic sphincter augmentation in the management of gastroesophageal reflux disease Mazen R. Al-Mansour, Kyle A. Perry, Jeffrey W. Hazey Division of General
Review Article Page 1 of 9 The current status of magnetic sphincter augmentation in the management of gastroesophageal reflux disease Mazen R. Al-Mansour, Kyle A. Perry, Jeffrey W. Hazey Division of General
Hernia. emoryhealthcare.org
 Hernia Have you noticed a bulge or pain in your abdominal wall or groin? If so you may have a hernia. You may be in the process of confirming this diagnosis with your Primary Care Physician or already
Hernia Have you noticed a bulge or pain in your abdominal wall or groin? If so you may have a hernia. You may be in the process of confirming this diagnosis with your Primary Care Physician or already
Innovations in Surgical Therapy for GERD: A tale of two therapies
 Innovations in Surgical Therapy for GERD: A tale of two therapies Brian E. Louie MD, FACS, FRCSC, MHA, MPH Director, Thoracic Research and Education Co-Director, Minimally Invasive Thoracic Surgery Program
Innovations in Surgical Therapy for GERD: A tale of two therapies Brian E. Louie MD, FACS, FRCSC, MHA, MPH Director, Thoracic Research and Education Co-Director, Minimally Invasive Thoracic Surgery Program
! "! # $% : 2000!!,!!&/ +& # )012.A C 'B " ;BDB
 *! "! # $% :.) '(,(!.( 112 ', " # '- : # +( 2000!!,!!/ + # )012!! 5!-.0( +( 1 ' 4 32005 +!% 9!! 38! 9, 5 : $. 67.+ ;2 8 3'( 3$0$!!>$- (%66) $= 1% '7 4 78-18 +( - ' :< #( @; 36, 3? / +.(%34) 42!, B : 7
*! "! # $% :.) '(,(!.( 112 ', " # '- : # +( 2000!!,!!/ + # )012!! 5!-.0( +( 1 ' 4 32005 +!% 9!! 38! 9, 5 : $. 67.+ ;2 8 3'( 3$0$!!>$- (%66) $= 1% '7 4 78-18 +( - ' :< #( @; 36, 3? / +.(%34) 42!, B : 7
Laparoscopic management of totally intra-thoracic stomach with chronic volvulus
 Online Submissions: http://www.wjgnet.com/esps/ wjg@wjgnet.com doi:10.3748/wjg.v19.i35.5848 World J Gastroenterol 2013 September 21; 19(35): 5848-5854 ISSN 1007-9327 (print) ISSN 2219-2840 (online) 2013
Online Submissions: http://www.wjgnet.com/esps/ wjg@wjgnet.com doi:10.3748/wjg.v19.i35.5848 World J Gastroenterol 2013 September 21; 19(35): 5848-5854 ISSN 1007-9327 (print) ISSN 2219-2840 (online) 2013
Reflux Control Following Gastroplasty
 ORIGINAL ARTICLES Reflux Control Following Gastroplasty Robert D. Henderson, M.B.,.F.R.C.S.(C) ABSTRACT A Belsey gastroplasty was performed on 135 patients, 132 of whom were available for follow-up. Despite
ORIGINAL ARTICLES Reflux Control Following Gastroplasty Robert D. Henderson, M.B.,.F.R.C.S.(C) ABSTRACT A Belsey gastroplasty was performed on 135 patients, 132 of whom were available for follow-up. Despite
Congenital hiatus hernia: A case series. Department of Pediatric Surgery, Afyon Kocatepe University Faculty of Medicine, Afyonkarahisar, Turkey
 Orıgınal Article PEDIATRIC SURGERY North Clin Istanb 2018 doi: 10.14744/nci.2017.58672 UNCORRECTED PROOF Congenital hiatus hernia: A case series Didem Baskin Embleton, 1 Ahmet Ali Tuncer, 1 Mehmet Surhan
Orıgınal Article PEDIATRIC SURGERY North Clin Istanb 2018 doi: 10.14744/nci.2017.58672 UNCORRECTED PROOF Congenital hiatus hernia: A case series Didem Baskin Embleton, 1 Ahmet Ali Tuncer, 1 Mehmet Surhan
2018 REIMBURSEMENT GUIDE
 TABLE OF CONTENTS: Component Separation Technique and Hiatal Hernia Repair...08 Hernia Repair...03 Laparoscopic Repair Hernia...06 Stoma Procedures...11 Level II Codes...13 -PCS Codes...14 Modifiers...13
TABLE OF CONTENTS: Component Separation Technique and Hiatal Hernia Repair...08 Hernia Repair...03 Laparoscopic Repair Hernia...06 Stoma Procedures...11 Level II Codes...13 -PCS Codes...14 Modifiers...13
Today, laparoscopic Nissen fundoplication can be performed with a 0.35%
 General Thoracic Surgery Whitson et al Wedge gastroplasty and reinforced crural repair: Important components of laparoscopic giant or recurrent hiatal hernia repair Bryan A. Whitson, MD, Chuong D. Hoang,
General Thoracic Surgery Whitson et al Wedge gastroplasty and reinforced crural repair: Important components of laparoscopic giant or recurrent hiatal hernia repair Bryan A. Whitson, MD, Chuong D. Hoang,
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: A rare case of Type
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: A rare case of Type
ORIGINAL ARTICLE. in which elements of the abdominal cavity herniate. Anatomic disruption of the esophagogastric junction (EGJ), phrenoesophageal
 ORIGINAL ARTICLE Effects of on Esophageal Peristalsis Sabine Roman, MD, PhD; Peter J. Kahrilas, MD; Leila Kia, MD; Daniel Luger, BA; Nathaniel Soper, MD; John E. Pandolfino, MD Hypothesis: Anatomic changes
ORIGINAL ARTICLE Effects of on Esophageal Peristalsis Sabine Roman, MD, PhD; Peter J. Kahrilas, MD; Leila Kia, MD; Daniel Luger, BA; Nathaniel Soper, MD; John E. Pandolfino, MD Hypothesis: Anatomic changes
Falk Symposium, , , Portorož. Physiology of Swallowing and Anti-Gastroesophageal. Reflux-Mechanisms. Mechanisms: C.
 Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD)
 Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD) Policy Number: 7.01.137 Last Review: 02/2018 Origination: 02/2014 Next Review: 02/2019 Policy Blue Cross and Blue
Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD) Policy Number: 7.01.137 Last Review: 02/2018 Origination: 02/2014 Next Review: 02/2019 Policy Blue Cross and Blue
Complications of Intrathoraac Nissen Fundoplication
 Complications of Intrathoraac Nissen Fundoplication Kamal A. Mansour, M.D., Harry G. Burton, M.D., Joseph I. Miller, Jr., M.D., and Charles R. Hatcher, Jr., M.D. ABSTRACT This report details our experience
Complications of Intrathoraac Nissen Fundoplication Kamal A. Mansour, M.D., Harry G. Burton, M.D., Joseph I. Miller, Jr., M.D., and Charles R. Hatcher, Jr., M.D. ABSTRACT This report details our experience
Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms
 MINI-REVIEW Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms M Anvari. Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms. Can J Gastroenterol
MINI-REVIEW Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms M Anvari. Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms. Can J Gastroenterol
The Emergency Hernia or The call you don t want at 2:00 a.m.*
 or The call you don t want at 2:00 a.m.* *Or even at 8:00 a.m. Michael G. Sarr, MD Professor of Surgery Mayo Clinic South Canada WEST CANADA EAST CANADA Clinical talk Hernias Inguinal Umbilical Incisional
or The call you don t want at 2:00 a.m.* *Or even at 8:00 a.m. Michael G. Sarr, MD Professor of Surgery Mayo Clinic South Canada WEST CANADA EAST CANADA Clinical talk Hernias Inguinal Umbilical Incisional
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Robotics in General Surgery. Objectives
 Robotics in General Surgery Jennifer S. Schwartz, MD Assistant Professor of Surgery Department of Surgery Division of General & Gastrointestinal Surgery The Ohio State University Wexner Medical Center
Robotics in General Surgery Jennifer S. Schwartz, MD Assistant Professor of Surgery Department of Surgery Division of General & Gastrointestinal Surgery The Ohio State University Wexner Medical Center
Gastroesophageal Reflux Disease
 gastrointestinal tract and abdomen Gastroesophageal Reflux Disease and Hiatal Hernia James A. Rydlewicz, MD, Matthew R. Pittman, MD, and Kyle A. Perry, MD Gastroesophageal reflux disease (GERD) was not
gastrointestinal tract and abdomen Gastroesophageal Reflux Disease and Hiatal Hernia James A. Rydlewicz, MD, Matthew R. Pittman, MD, and Kyle A. Perry, MD Gastroesophageal reflux disease (GERD) was not
A video demonstration of the Li s anastomosis the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma
 Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Facing Surgery for GERD (Gastroesophageal
 Facing Surgery for GERD (Gastroesophageal Reflux Disease)? Learn about minimally invasive da Vinci Surgery The Conditions: GERD, Hiatal Hernia Gastroesophageal reflux disease or GERD is a common digestive
Facing Surgery for GERD (Gastroesophageal Reflux Disease)? Learn about minimally invasive da Vinci Surgery The Conditions: GERD, Hiatal Hernia Gastroesophageal reflux disease or GERD is a common digestive
2015 General Surgery Survival Guide
 2015 General Surgery Survival Guide Chapter 10: Hernia Repair Know What to Look for When Coding Hernia Repair Reporting hernia repair can be tricky. But if you know what to look for then half the work
2015 General Surgery Survival Guide Chapter 10: Hernia Repair Know What to Look for When Coding Hernia Repair Reporting hernia repair can be tricky. But if you know what to look for then half the work
LAPAROSOPIC VERSUS OPEN FOUDOPLICATION
 LAPAROSOPIC VERSUS OPEN FOUDOPLICATION Dr. ADIL K. SALLOM, MRCS, D.MAS Member Royal College ofssurgeons of Ireland Fellow ship of Arab board of medical specialization Member of world association of laparoscopic
LAPAROSOPIC VERSUS OPEN FOUDOPLICATION Dr. ADIL K. SALLOM, MRCS, D.MAS Member Royal College ofssurgeons of Ireland Fellow ship of Arab board of medical specialization Member of world association of laparoscopic
Laparoscopic Management of Giant Paraesophageal Herniation
 Laparoscopic Management of Giant Paraesophageal Herniation Robert J. Wiechmann, MD, Mark K. Ferguson, MD, Keith S. Naunheim, MD, Paul McKesey, Steven J. Hazelrigg, MD, Tibetha S. Santucci, RN, Robin S.
Laparoscopic Management of Giant Paraesophageal Herniation Robert J. Wiechmann, MD, Mark K. Ferguson, MD, Keith S. Naunheim, MD, Paul McKesey, Steven J. Hazelrigg, MD, Tibetha S. Santucci, RN, Robin S.
SUCCESS IN THE DEVELOPMENT
 REVIEW ARTICLE Mesh in the Hiatus A Controversial Issue Eduardo M. Targarona, MD, PhD; Gali Bendahan, MD; Carmen Balague, MD, PhD; Jordi Garriga, MD; Manuel Trias, MD, PhD Objective: To analyze the experience
REVIEW ARTICLE Mesh in the Hiatus A Controversial Issue Eduardo M. Targarona, MD, PhD; Gali Bendahan, MD; Carmen Balague, MD, PhD; Jordi Garriga, MD; Manuel Trias, MD, PhD Objective: To analyze the experience
Robotic-assisted McKeown esophagectomy
 Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Perhaps the most controversial of new laparoscopic operations is the repair of the inguinal hernia. The
 JOURNAL OF LAPAROENDOSCOPIC SURGERY Volume 2, Number 6, 1992 Mary Ann Liebert, Inc., Publishers Extraperitoneal Endoscopie Inguinal Hernia Repair GEORGE S. FERZLI, M.D., F.A.C.S., AZIZ MASSAD, M.D., and
JOURNAL OF LAPAROENDOSCOPIC SURGERY Volume 2, Number 6, 1992 Mary Ann Liebert, Inc., Publishers Extraperitoneal Endoscopie Inguinal Hernia Repair GEORGE S. FERZLI, M.D., F.A.C.S., AZIZ MASSAD, M.D., and
Surgical treatment for gastroesophageal reflux GENERAL THORACIC SURGERY
 GENERAL THORACIC SURGERY EARLY EXPERIENCE AND LEARNING CURVE ASSOCIATED WITH LAPAROSCOPIC NISSEN FUNDOPLICATION Claude Deschamps, MD Mark S. Allen, MD Victor F. Trastek, MD Julie O. Johnson, RN Peter C.
GENERAL THORACIC SURGERY EARLY EXPERIENCE AND LEARNING CURVE ASSOCIATED WITH LAPAROSCOPIC NISSEN FUNDOPLICATION Claude Deschamps, MD Mark S. Allen, MD Victor F. Trastek, MD Julie O. Johnson, RN Peter C.
Paraoesophageal Hernia
 Paraoesophageal Hernia Grand Round Adam Cichowitz Surgical Registrar Paraoesophageal Hernia Type of hiatal hernia Transdiaphragmatic migration of abdominal content gastric fundus gastric body pylorus colon
Paraoesophageal Hernia Grand Round Adam Cichowitz Surgical Registrar Paraoesophageal Hernia Type of hiatal hernia Transdiaphragmatic migration of abdominal content gastric fundus gastric body pylorus colon
Medicine. Emanuele Asti, MD, Gianluca Bonitta, MSc, Andrea Lovece, MD, Veronica Lazzari, MD, Luigi Bonavina, MD, PhD, FACS. Observational Study
 Observational Study Medicine Longitudinal comparison of quality of life in patients undergoing laparoscopic Toupet fundoplication versus magnetic sphincter augmentation Observational cohort study with
Observational Study Medicine Longitudinal comparison of quality of life in patients undergoing laparoscopic Toupet fundoplication versus magnetic sphincter augmentation Observational cohort study with
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Guiding Principles. Trans-oral Incisionless Fundoplication (TIF) for GERD: When, Why & How 4/6/18
 Gastroesophageal Reflux Disease Shaping the Future of GERD Management Treating patients with the TIF procedure using the EsophyX device (EndoGastric Solutions) Gonzalo Pandolfi, MD Trans-oral Incisionless
Gastroesophageal Reflux Disease Shaping the Future of GERD Management Treating patients with the TIF procedure using the EsophyX device (EndoGastric Solutions) Gonzalo Pandolfi, MD Trans-oral Incisionless
LAPAROSCOPIC HELLER MYOTOMY WITH FUNDOPLICATION FOR ACHALASIA
 LAPAROSCOPIC HELLER MYOTOMY WITH FUNDOPLICATION FOR ACHALASIA I-Rue Lai, 1 Wei-Jei Lee, 1,2 and Ming-Te Huang 2 Background and Purpose: Laparoscopic Heller cardiomyotomy for the treatment of achalasia
LAPAROSCOPIC HELLER MYOTOMY WITH FUNDOPLICATION FOR ACHALASIA I-Rue Lai, 1 Wei-Jei Lee, 1,2 and Ming-Te Huang 2 Background and Purpose: Laparoscopic Heller cardiomyotomy for the treatment of achalasia
Robotic-assisted Roux-en-Y gastric bypass in a patient with situs inversus. Anji Wall, Zuliang Feng & Willie Melvin. Journal of Robotic Surgery
 Robotic-assisted Roux-en-Y gastric bypass in a patient with situs inversus Anji Wall, Zuliang Feng & Willie Melvin Journal of Robotic Surgery ISSN 1863-2483 Volume 8 Number 2 J Robotic Surg (2014) 8:169-171
Robotic-assisted Roux-en-Y gastric bypass in a patient with situs inversus Anji Wall, Zuliang Feng & Willie Melvin Journal of Robotic Surgery ISSN 1863-2483 Volume 8 Number 2 J Robotic Surg (2014) 8:169-171
Putting Chronic Heartburn On Ice
 Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
Minimal vs extensive esophageal mobilization during laparoscopic fundoplication: a prospective randomized trial
 Journal of Pediatric Surgery (2011) 46, 163 168 www.elsevier.com/locate/jpedsurg Minimal vs extensive during laparoscopic fundoplication: a prospective randomized trial Shawn D. St. Peter a,, Douglas C.
Journal of Pediatric Surgery (2011) 46, 163 168 www.elsevier.com/locate/jpedsurg Minimal vs extensive during laparoscopic fundoplication: a prospective randomized trial Shawn D. St. Peter a,, Douglas C.
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
