Assessment of Nasal Function After Tip Surgery With a Cephalic Hinged Flap of the Lateral Crura: A Randomized Clinical Trial
|
|
|
- Sarah Garrett
- 5 years ago
- Views:
Transcription
1 529647AESXXX / X Aesthetic Surgery JournalAmali et al research-article2014 INTERNATIONAL CONTRIBUTION Rhinoplasty Assessment of Nasal Function After Tip Surgery With a Cephalic Hinged Flap of the Lateral Crura: A Randomized Clinical Trial Amin Amali, MD; Amir A. Sazgar, MD; and Mehrdad Jafari, MD Functional and aesthetic nasal surgeries are inextricably linked. This fact has become increasingly evident within the past decade, during which the principle of tissue conservation has permeated the surgical philosophy of reductive rhinoplasty. 1,2 Tissue conservation has been primarily adopted within the domain of dorsal reduction surgery, yet the same principles hold true in tip modification, or tipplasty. 3 For instance, emphasis was once placed on tip reduction techniques that achieved short-term and cosmetic goals often at the expense of harm to the support mechanisms of the tip. As knowledge of the structural and dynamic roles of cartilaginous tip support has grown, a Aesthetic Surgery Journal 2014, Vol. 34(5) The American Society for Aesthetic Plastic Surgery, Inc. Reprints and permission: journalspermissions.nav DOI: / X Abstract Background: Postrhinoplasty nasal obstruction has been ascribed to either postreductive narrowing of the midvault or dynamic collapse resulting from lateral wall insufficiency. Recently, clinicians have reported on various surgical techniques that maximally preserve alar cartilage integrity, unlike the earlier popular methods of tip reduction surgery. Objectives: The authors compared the effects of 2 rhinoplasty techniques: a cephalic trim (CT) of the lateral crura (LC) and a horizontal resection with cephalic hinged flap (HRCH) of the LC of the lower lateral cartilage (LLC). Methods: Fifty-two patients who presented with a bulbous nasal tip deformity were randomly assigned to 1 of 2 groups and underwent either CT of the LC or HRCH. Effects of the procedures were evaluated by both acoustic rhinometry (AR; first and second minimal cross-sectional areas [MCA1 and MCA2, respectively]) and by subjective scoring on a global nasal obstruction visual analog scale (VAS). Assessments were made before and after rhinoplasty. Results: MCA1 and MCA2 were increased after both CT and HRCH. This increase was significant on the right side for both CT (P <.001) and HRCH (P =.001), but the increase on the left side was significant only for HRCH. Conclusions: The improvement noted in breathing quality by VAS and AR suggests that a hinged flap may be effective in reconstructing the internal nasal valve. Level of Evidence: 3 Keywords rhinoplasty, alar cartilage, nasal valve area, cephalic trim, horizontal resection, cephalic hinged flap, lateral crura, tip-plasty, tip modification, acoustic rhinometry Accepted for publication October 21, better understanding has developed of the consequences that surgical modifications may have on dynamic nasal airflow. 1,2 From the Department of Otorhinolaryngology, Head and Neck Surgery at Vali-Asr Hospital, Tehran University of Medical Sciences, Tehran, Iran. Corresponding Author: Dr Amir A. Sazgar, Department of Otorhinolaryngology, Head and Neck Surgery, Vali-Asr Hospital, Imam Khomeini Medical Complex, Tehran University of Medical Sciences, Dr. Gharib Avenue, Keshavarz Boulevard, Tehran , Iran. asazgar@sina.tums.ac.ir
2 688 Aesthetic Surgery Journal 34(5) Despite normal conformation of the septum and turbinate, many patients exhibit some nasal obstruction after rhinoplasty. This generally has been ascribed to either postreductive narrowing of the midvault or dynamic collapse due to insufficiency of the lateral wall. 4,5 The internal valve region refers to the area between the caudal end of the upper lateral cartilage (ULC) and the cartilaginous septum and includes the circumferential neighboring structures in the nasal airway. Narrowing at this location can lead to compromised airflow. Lateral wall insufficiency is caused by weakness of the lateral nasal wall, which collapses during negative pressure generation from inhalation. 5-7 The intervalve region refers to the area between the external and internal valves, immediately superior to the lateral crura (LC) of the lower lateral cartilage (LLC) and corresponding to the supra-alar crease. This area is naturally devoid of cartilaginous support and therefore is subject to collapse after tip maneuvers. 1,8,9 Recently, many clinicians have reported on a variety of surgical techniques that maximize the preservation of tip structure Unlike earlier popular methods such as cephalic excision of the LLC, separation of the LLC and ULC, creation of an interrupted strip, and formation of loose or free cartilage edges, these newer techniques have been applied in an effort to reinforce LLC durability and to simultaneously provide aesthetic correction. In the present study, we introduce new modifications for tip-plasty. Instead of reduction surgery, we focus on conservative measures aimed at stabilizing and reorienting the cartilaginous structures and support. 15,17,18 With this technique, the cephalic portion is turned inward as a hinged flap in various ways (rather than cephalic excision of the LC of the LLC), as determined by the specific type of tip deformity, and subsequently is stabilized with nonabsorbable mattress sutures. The cosmetic and anatomic results of these techniques have been presented in earlier studies 15,17-19 ; however, potential effects on the nasal valve area (NVA) warrant additional investigation. In this study, we demonstrate the effects of the hinged flap in the horizontal resection with cephalic hinged flap (HRCH) technique on the NVA, based on subjective (patient self-assessment of global nasal obstruction with a visual analog scale [VAS]) and objective acoustic rhinometry(ar) measures. MEthods This randomized, double-blind, controlled clinical trial was conducted at Vali-Asr Hospital, Tehran University of Medical Sciences, Iran, between March 2011 and February The study design was approved by the Institutional Review Board and Ethics Committee of Tehran University of Medical Sciences. Fifty-two patients, each of whom provided informed consent for the procedures, were selected for study participation based on inclusion and exclusion criteria by each of the authors in the clinics. All patients were white, and no other ethnicity was represented in this study. Patients with a bulbous tip deformity, defined as an angle of diversion >30 and/or a tip-defining point distance >4 mm, were included in the study and were randomly assigned to receive either cephalic trim (CT; n = 26) or HRCH (n = 26). In all cases, correction of the deformity was performed during open rhinoplasty. Excluded from the study were patients who had undergone revision rhinoplasty, patients with additional deformities (such as saddle nose, rhinosinusitis, and nasal polyposis), and patients with any local or systemic disease that affected the nose and/or paranasal sinuses. Also excluded were patients with more-than-mild septal deviation or deviations that involved the NVA. Surgical Techniques Surgical techniques for both patient groups included routine open rhinoplasty maneuvers such as ULC spreader grafts, medial and lateral osteotomies, and dorsal hump reduction. As previously described for the HRCH technique, 15 the LC and ULC were not separated in the scroll area. The LC and middle crura were demarcated horizontally by 2 lines, and at least 7 to 8 mm of cartilage was preserved caudally. Two horizontal excisions were planned, the width and shape of which were determined by the anatomy and degree of the deformity. A 3- or 4-mm horizontal excision was usually sufficient. The cartilage was incised with a No. 15 scalpel blade, and the cartilage between the 2 cuts was excised and the remnants of the LC of the LLC were preserved. Unlike other techniques featuring turn-in flaps, the skin and mucosal lining inside the ala were not undermined beyond the area in which the cartilage was excised. Next, the cephalic portion was turned in as a hinged flap and stabilized with 5-0 nonabsorbable mattress sutures (Ethicon Endo-Surgery GmbH, Norderstedt, Germany). Three mattress sutures were sufficient to fix the rotated cephalic portion. For the CT technique, the LC and ULC were separated in the scroll area. The cartilage was incised with a No. 15 scalpel blade, preserving at least 7 to 8 mm of cartilage caudally, and the cartilage of the cephalic part was excised. Evaluation AR was performed preoperatively and at least 1 year postrhinoplasty with an A1 acoustic rhinometer (GM Instruments, Kilwinning, Scotland) by 1 physician (A.A.). The patient was seated in an upright position in a quiet room. The temperature in the room ranged from 20 C to 25 C. A round plastic nosepiece with a 13-mm inner
3 Amali et al 689 diameter and a 7-mm opening was placed. Each side of the nose was measured separately, with care taken to fit the nosepiece tightly to the nostril without distorting the anatomy. Four measurements, obtained at half-second intervals, were taken on each side. The measurements were considered valid if the 4 curves showed no deviation from each other, from the nostril to the end of the C-notch, with a divergence of 20% maximally from the middle curve to the curves posterior end, and no crossover. The data calculated by the A1 acoustic rhinometer software (GM Instruments) were then documented. The physician (A.A.) who performed the pre- and postoperative AR was blinded to which tip-plasty technique was performed on each patient. The first and second minimal cross-sectional areas (MCA1 and MCA2) were measured for all patients. Both preoperatively and 1 year postoperatively, patients self-scored their global nasal obstruction on a VAS from 0 to 10 (0 = no obstruction, 10 = total obstruction). Data Analysis To determine the study s sample size, we consulted a professional biostatistics expert. The sample size was calculated with the power of 80% to include at least 26 subjects in each group. Data were presented as means (± standard deviation [SD]). For each study group, measurements were compared before and after surgery with a paired sample t test. To compare the 2 different surgical techniques, postoperative measurements were subtracted from preoperative measurements, and the differences determined for each group were compared with an independent t test. An adjusted comparison was performed via analysis of covariance (ANCOVA) with SPSS version 18 (SPSS, Inc, an IBM Company, Chicago, Illinois). Significance was defined as P <.05. REsuLts All 52 patients completed the study (26 in each group). There were no statistically significant differences between the study groups with respect to age (t = 1.618, P =.112) or sex (χ 2 = 0.746, P =.338). The mean (SD) age in the CT and HRCH groups was 22.8 (5.4) years and 25.5 (6.2) years, respectively. The CT group included 18 (69.2%) women, and the HRCH group included 15 (57.7%) women. The mean follow-up period was 15.7 months for the entire study population, (range, 12-20) months for the CT group, and (range, 12-20) months for the HRCH group. No patient experienced complications postoperatively. (Clinical photographs are shown in Figures 1 and 2.) First and second minimal cross-sectional areas (MCA1 and MCA2, respectively) increased after CT and HRCH. This increase was significant on the right side in both the CT (P <.001) and HRCH (P =.001) groups (Figure 3, Table 1). However, on the left side, the change was significant only in the HRCH group (P <.001; Figure 4, Table 1). As shown in Table 2, MCA1 of the left side increased by 6.27% and 37.08% in the CT and HRCH groups, respectively (P =.013). On the right side, MCA1 increased by 13.39% and 44.56% in the CT and HRCH groups, respectively (P =.028). MCA2 of the left side increased by 31.08% and % in the CT and HRCH groups, respectively (P <.005). On the right side, MCA2 increased by 77.76% and % in the CT and HRCH groups respectively; the difference was not statistically significant (P =.138). Based on preoperative and postoperative patient self-assessments with the VAS, both groups experienced decreased nasal obstruction following the surgery (Table 1). This decrease was not statistically significant between the 2 surgical methods for the left side (P =.336) or the right side (P =.831) (Table 2). discussion The results of this study indicated improvement in both subjective assessment of breathing quality and objective measurement of cross-sectional areas (especially on the left side) following tip-plasty in which a cephalic hinged flap of the LC was placed (Table 1). As suggested by our initial hypothesis, this technique may provide satisfactory clinical and aesthetic outcomes. The improvements noted in breathing quality and AR measurements suggest that hinged flaps may be effective in reconstructing the internal nasal valve (Figure 5). In the past 2 decades, clinical application of acoustic rhinometry (AR) has expanded. Clinically relevant studies are now available for septoplasty, turbinateplasty, sinus surgery, and facial cosmetic surgery AR provides an outline of the cross-sectional areas within the nose and the volume of the nasal cavity. The advantages associated with AR include time efficiency and the need for only minimal patient cooperation. Researchers have correlated a crosssectional area measured by computed tomography with a cross section measured by AR. 24 In addition, views obtained by magnetic resonance imaging (MRI) have been correlated with cross-sectional areas as measured by AR in the decongested nose. The hinged flap, first introduced in 2010, is believed to reduce nasal tip volume while maintaining support and strength in the nasal tip. 15,17 The preserved cephalic portion of the LC, when rotated and secured with sutures, provides additional tip support to the tripod. (The conjoined medial crura forms 1 leg of the tripod, and each of the lower lateral crus forms the other 2 legs.) In a crosssectional cadaveric study, Sazgar et al 19 showed that hinged flaps prevent posterior and caudal displacement of the LC s caudal portion. Applying a practical classification
4 690 Aesthetic Surgery Journal 34(5) Figure 1. (A, C) This 24-year-old man presented for rhinoplasty involving horizontal resection with cephalic hinged flap of the lateral crura. (B, D) The same patient, 14 months postoperatively. system for tip-plasty, Sazgar and Most 18 studied and discussed the aesthetic results of this particular technique. Separation of the ULC and LLC, and consequent destruction of the scroll area in combination with wide mucosal undermining, is a common technique of previously studied rhinoplasty approaches However, we did not apply these maneuvers in the hinged flap technique. Compared with other LLC flaps, such as turn-in, turn-out, and sliding flaps, the orientation and position of the hinged flap have differed in our hands. 19 There is evidence that the hinged flap effectively improves the airway. Data from our cross-sectional cadaveric study 19
5 Amali et al 691 Figure 2. (A, C) Preoperatively, this 29-year-old woman presented with a bulbous droopy tip for rhinoplasty involving horizontal resection with cephalic hinged flap of the lateral crura. (B, D) The same patient, 1 year postoperatively. indicated that the hinged flap prevents posterior and caudal displacement of the LC s caudal portion. The space beneath the alpha angle formed by the connection of the hinged flap and the caudal part of the LC of the LLC was added to the valve area on the hinged flap side (Figure 5). Our present study demonstrates that this new surgical intervention for management of the LC does not adversely affect nasal airway function. According to both subjective and objective measurements, nasal airway patency was improved postoperatively in both the CT and HRCH groups. The fact that the increase was not statistically significant on the CT group s left side may relate to the small sample size. The percentage of increase was larger in the HRCH group for both MCA1 and MCA2. However, the difference was not statistically significant on the right side for MCA2, which also may be attributable to the small sample size. Another reason for the
6 692 Aesthetic Surgery Journal 34(5) Figure 3. (A) Preoperative and (B) postoperative acoustic rhinometry graphs for the right nasal cavity of a 24-year-old man who underwent open rhinoplasty with cephalic trim of the lateral crura. First and second minimal cross-sectional areas (MCA1 and MCA2) are indicated. Different solid colors show 4 times of acoustic rhinometry examination, and the dotted line is the baseline exam of the device. Figure 4. (A) Preoperative and (B) postoperative acoustic rhinometry graphs for the left nasal cavity of a 29-year-old man who underwent open rhinoplasty with the horizontal resection with cephalic hinged flap technique. The minimal crosssectional area was noted at the second valley, the deepest valley on the graph, which corresponds with the internal nasal valve. Different solid colors show 4 times of acoustic rhinometry examination, and the dotted line is the baseline exam of the device.
7 Amali et al 693 Table 1. Preoperative and Postoperative Comparisons of MCA1, MCA2, and VAS Scores for the CT and HRCH Techniques CT (n = 26) HRCH (n = 26) Before After P Before After P MCA1 Left (0.197) (0.223) (0.186) (0.255) <.001 Right (0.129) (0.156) < (0.241) (0.331) <.001 MCA2 Left (0.455) (0.373) (0.511) (0.494) <.001 Right (0.513) (0.584) (0.745) (0.724) <.001 VAS score for nasal obstruction Left 4.19 (3.35) 1.42 (1.77) < (3.61) 1.00 (1.17) <.001 Right 3.12 (2.78) 0.92 (1.41) < (3.13) 0.88 (1.53) <.001 Data are means (SD); P is calculated as the difference between pre- and postoperative (1 year) measurements by paired sample t test. VAS scores ranged from 0 to 10. CT, cephalic trim; HRCH, horizontal resection with cephalic hinged flap; MCA1, first minimal cross-sectional area; MCA2, second minimal cross-sectional area; VAS, visual analog scale. Table 2. Comparison of Surgical Results After the CT and HRCH Techniques MCA1 difference between the right and left sides might relate to septal deviations. It is noteworthy that bilateral ULC spreader grafts or flaps are routine procedures for all of our rhinoplasty patients. de Pochat et al 25 demonstrated that open-structure rhinoplasty with placed spreader grafts is effective in reconstructing the internal nasal valve, with significant improvement of a mean MCA on AR. Because all patients in the present study underwent this procedure, the statistical significance of the difference between the HRCH and CT groups may relate to the difference in the technique applied to the LLCs. CT (n = 26) HRCH (n = 26) Unadjusted P Adjusted P Difference, Mean (SD) Change, % Difference, Mean (SD) Change, % Left (0.212) (0.226) Right (0.118) (0.260) MCA2 Left (0.341) (0.530) Right (0.523) (0.603) VAS score for nasal obstruction a Left 2.77 (2.87) 2.81 (2.74) Right 2.19 (2.19) 2.38 (2.89) The unadjusted P represents the comparison of postoperative results of CT and HRCH techniques by the independent t test; the adjusted P represents the comparison of postoperative results of CT and HRCH techniques by analysis of covariance. CT, cephalic trim; HRCH, horizontal resection with cephalic hinged flap; MCA1, first minimal cross-sectional area; MCA2, second minimal cross-sectional area; VAS, visual analog scale. a Percentage of change was not calculated for VAS assessment because some patients selected 0 preoperatively (on a scale of 0 to 10). An obvious limitation of this clinical study is the small study population. Because our study was performed in an academic teaching hospital, finding patients who fit our specific inclusion criteria was a challenge. We believe that future studies with larger sample sizes may help to confirm the results of this study. As with all studies involving AR, concerns about intraobserver variability exist. We attempted to address this potential limitation by having a single otolaryngologist (A.A.), who was blinded to the patients study group assignments, perform all AR tests.
8 694 Aesthetic Surgery Journal 34(5) Figure 5. Schematic postoperative cross section of the nose, as viewed through the nasal valve area. Note the small crosssectional area and partial obstruction by cephalic trim on the right side. On the left side, a cephalic hinged flap of the lateral crura (LC) has been created. Note each side s position of the caudal part of the LC. Also shown are the nasal septum (S), upper lateral cartilage (ULC), caudal part of the LC, the hinged flap, the angle between the hinged flap and ULC, and the angle between the hinged flap and caudal part of the LC. (Illustration by Christine Gralapp, MA, CMI, chrisgralapp.com) conclusions Most postrhinoplasty tip abnormalities occur secondary to loss of tip support and to excessive LLC resection. Because the hinged flap procedure can be performed in individuals who have weak cartilage and wide LC, such complications may be avoided. The hinged flap is an option in nasal tip reduction surgery that may improve long-term aesthetic and functional outcomes through NVA preservation. Future studies with longer follow-up periods and larger sample sizes are warranted to further elucidate the effectiveness of this technique as a replacement for LLC CT. Acknowledgment The authors thank Dr Sam P. Most, Professor of Otolaryngology Head and Neck Surgery at Stanford University Medical Center, Stanford, California, for sharing his opinions and clinical experiences. disclosures The authors declared no potential conflicts of interest with respect to the research, authorship, and publication of this article. Funding The authors received no financial support for the research, authorship, and publication of this article. REFEREncEs 1. Kim DW, Rodriguez-Bruno K. Functional rhinoplasty. Facial Plast Surg Clin North Am. 2009;17: Tardy ME Jr, Thomas RJ. Rhinoplasty, surgical philosophy. In: Cummings CW, ed. Otolaryngology Head and Neck Surgery. Pennsylvania, PA: Mosby; 2010: Yoo S, Most SP. Nasal airway preservation using the autospreader technique: analysis of outcomes using a diseasespecific quality-of-life instrument. Arch Facial Plast Surg. 2011;13: Most SP. Analysis of outcomes after functional rhinoplasty using a disease-specific quality of life instrument. Arch Facial Plast Surg. 2006;8: Constantlan MB. Valvular incompetence is most likely cause of postrhinoplasty airway problems. Aesthetic Surg J. 1998;18: Fischer H, Gubisch W. Nasal valves: importance and surgical procedures. Facial Plast Surg. 2006;22: Spielmann PM, White PS, Hussain SS. Surgical techniques for the treatment of nasal valve collapse: a systematic review. Laryngoscope. 2009;119: Christophel JJ, Park SS. Complications in rhinoplasty. Facial Plast Surg Clin North Am. 2009;17: Ballert JA, Park SS. Functional rhinoplasty: treatment of the dysfunctional nasal sidewall. Facial Plast Surg. 2006;22: Massiha H. Elliptical horizontal excision and repair of alar cartilage in open-approach rhinoplasty to correct cartilaginous tip deformities. Plast Reconstr Surg. 1998;101:
9 Amali et al Regalado-Briz A. Aesthetic rhinoplasty with maximum preservation of alar cartilages: experience with 52 consecutive cases. Plast Reconstr Surg. 1999;103: Janis J, Trussler A, Ghavami A, Marin V, Rohrich RJ, Gunter JP. Lower lateral crural turnover flap in open rhinoplasty. Plast Reconstr Surg. 2009;123: Murakami CS, Barrera JE, Most SP. Preserving structural integrity of the alar cartilage in aesthetic rhinoplasty using a cephalic turn-in flap. Arch Facial Plast Surg. 2009;11: Ozmen S, Eryilmaz T, Sencan A, et al. Sliding alar cartilage (SAC): a new technique for nasal tip surgery. Ann Surg. 2009;63: Sazgar AA. Horizontal reduction using a cephalic hinged flap of the lateral crura: a method to treat the bulbous nasal tip. Aesthetic Plast Surg. 2010;34: Gruber RP, Zang A, Mohebali K. Preventing alar retraction by preservation of the lateral crus. Plast Reconstr Surg. 2010;126: Sazgar AA. Lateral crural setback with cephalic turn-in flap: a method to treat the drooping nose. Arch Facial Plast Surg. 2010;12: Sazgar AA, Most SP. Stabilization of nasal tip support in nasal tip reduction surgery. Otolaryngol Head Neck Surg. 2011;145: Sazgar AA, Woodard C, Most SP. Preservation of the nasal valve area with a lateral crural hinged flap: a cadaveric study. Aesthetic Plast Surg. 2012;36: Skouras A, Noussios G, Chouridis P, Argyriou N, Kontzoglou G. Acoustic rhinometry to evaluate plastic surgery results of the nasal septum. B-ENT. 2009;5: Kemker B, Liu X, Gungor A, Moinuddin R, Corey JP. Effect of nasal surgery on the nasal cavity as determined by acoustic rhinometry. Otolaryngol Head Neck Surg. 1999;121: Grymer LF. Reduction rhinoplasty and nasal patency: change in the cross-sectional area of the nose evaluated by acoustic rhinometry. Laryngoscope. 1995;105: Hormozi AK, Toosi AB. Rhinometry: an important clinical index for evaluation of the nose before and after rhinoplasty. Aesthetic Plast Surg. 2008;32: Terheyden H, Maune S, Mertens J, Hilberg O. Acoustic rhinometry: validation by three-dimensionally reconstructed computer tomographic scans. J Appl Physiol. 2000;89: de Pochat VD, Alonso N, Mendes RR, Cunha MS, Menezes JV. Nasal patency after open rhinoplasty with spreader grafts. J Plast Reconstr Aesthetic Surg. 2012;65:
Comparison of the Effects of Spreader Graft and Overlapping Lateral Crural Technique on Rhinoplasty by Rhinomanometry
 Original Article 99 Comparison of the Effects of Spreader Graft and Overlapping Lateral Crural Technique on Rhinoplasty by Rhinomanometry Mahmoud Omranifard, Hosein Abdali, Mehdi Rasti Ardakani, Amiryousef
Original Article 99 Comparison of the Effects of Spreader Graft and Overlapping Lateral Crural Technique on Rhinoplasty by Rhinomanometry Mahmoud Omranifard, Hosein Abdali, Mehdi Rasti Ardakani, Amiryousef
Surgical Treatment of Nasal Obstruction
 Surgical Treatment of Nasal Obstruction P. Daniel Knott, MD FACS Director, Division of Facial Plastic and Reconstructive Surgery Department of Otolaryngology/Head and Neck Surgery UCSF Medical Center Nothing
Surgical Treatment of Nasal Obstruction P. Daniel Knott, MD FACS Director, Division of Facial Plastic and Reconstructive Surgery Department of Otolaryngology/Head and Neck Surgery UCSF Medical Center Nothing
Nasal Soft-Tissue Triangle Deformities
 339 Hossam M.T. Foda, MD 1 1 Division of Facial Plastic Surgery, Otolaryngology Department, Alexandria Medical School, Alexandria, Egypt Facial Plast Surg 2016;32:339 344. Address for correspondence Hossam
339 Hossam M.T. Foda, MD 1 1 Division of Facial Plastic Surgery, Otolaryngology Department, Alexandria Medical School, Alexandria, Egypt Facial Plast Surg 2016;32:339 344. Address for correspondence Hossam
The overprojected ( Pinocchio ) tip and the ptotic
 Featured Operative Technique Management of the Overprojected Nose and Ptotic Nasal Tip William E. Silver, MD, FCS; and Giancarlo F. Zuliani, MD The overprojected ( Pinocchio ) tip and the ptotic tip are
Featured Operative Technique Management of the Overprojected Nose and Ptotic Nasal Tip William E. Silver, MD, FCS; and Giancarlo F. Zuliani, MD The overprojected ( Pinocchio ) tip and the ptotic tip are
Fibular Bone Graft for Nasal Septal Reconstruction: A Case Report
 220 Nasal septal reconstruction Case Report Fibular Bone Graft for Nasal Septal Reconstruction: A Case Report Yakup Cil1* Diyarbakır Military Hospital, Department of Plastic Surgery 21000 Diyarbakır, Turkey
220 Nasal septal reconstruction Case Report Fibular Bone Graft for Nasal Septal Reconstruction: A Case Report Yakup Cil1* Diyarbakır Military Hospital, Department of Plastic Surgery 21000 Diyarbakır, Turkey
Nasal Valve Obstruction
 Nasal Valve Obstruction J RANDALL JORDAN, MD, FACS Facial Plastic Surgery Department of Otolaryngology and Communicative Disorders University of Mississippi Medical School Disclosures Financial- none Off-label-none
Nasal Valve Obstruction J RANDALL JORDAN, MD, FACS Facial Plastic Surgery Department of Otolaryngology and Communicative Disorders University of Mississippi Medical School Disclosures Financial- none Off-label-none
ORIGINAL ARTICLE. Surgery for the Dysfunctional Nasal Valve
 Surgery for the Dysfunctional Nasal Valve Cadaveric Analysis and Clinical Outcomes Rodney J. Schlosser, MD; Stephen S. Park, MD ORIGINAL ARTICLE Objectives: To quantify changes in the cross-sectional area
Surgery for the Dysfunctional Nasal Valve Cadaveric Analysis and Clinical Outcomes Rodney J. Schlosser, MD; Stephen S. Park, MD ORIGINAL ARTICLE Objectives: To quantify changes in the cross-sectional area
The Effectiveness of Modified Vertical Dome Division Technique in Reducing Nasal Tip Projection in Rhinoplasty
 IJMS Vol 36, No 3, September 2011 Original Article The Effectiveness of Modified Vertical Dome Division Technique in Reducing Nasal Tip Projection in Rhinoplasty Behrooz Gandomi 1, Mohammad Hossein Arzaghi
IJMS Vol 36, No 3, September 2011 Original Article The Effectiveness of Modified Vertical Dome Division Technique in Reducing Nasal Tip Projection in Rhinoplasty Behrooz Gandomi 1, Mohammad Hossein Arzaghi
There are numerous suture techniques described for nasal. Septocolumellar Suture in Closed Rhinoplasty ORIGINAL ARTICLE
 ORIGINAL ARTICLE Erdem Tezel, MD, and Ayhan Numanoğlu, MD Abstract: Several surgeons advise a variety of tip sutures and describe their own techniques in open approach. Septocolumellar suture is one of
ORIGINAL ARTICLE Erdem Tezel, MD, and Ayhan Numanoğlu, MD Abstract: Several surgeons advise a variety of tip sutures and describe their own techniques in open approach. Septocolumellar suture is one of
Use of tent-pole graft for setting columella-lip angle in rhinoplasty
 Agrawal et al. Plast Aesthet Res 2018;5:13 DOI: 10.20517/2347-9264.2018.17 Plastic and Aesthetic Research Letter to Editor Open Access Use of tent-pole graft for setting columella-lip angle in rhinoplasty
Agrawal et al. Plast Aesthet Res 2018;5:13 DOI: 10.20517/2347-9264.2018.17 Plastic and Aesthetic Research Letter to Editor Open Access Use of tent-pole graft for setting columella-lip angle in rhinoplasty
Scientific Forum. Nostrilplasty: Raising, Lowering, Widening, and Symmetry Correction of the Alar Rim
 Nostrilplasty: Raising, Lowering, Widening, and Symmetry Correction of the lar Rim Richard Ellenbogen, MD; and Greg azell, MD ackground: lthough the alar rim has frequently been neglected in correction
Nostrilplasty: Raising, Lowering, Widening, and Symmetry Correction of the lar Rim Richard Ellenbogen, MD; and Greg azell, MD ackground: lthough the alar rim has frequently been neglected in correction
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
Rhinoplasty - Tip Augmentation by Extended Columellar Strip
 World Articles of Ear, Nose and Throat ---------------------Page 1 Rhinoplasty - Tip Augmentation by Extended Columellar Strip Authors: Vikas Sinha*, Viral A. Chhaya**, Dilavar A. Barot***, Keyur Mehta****,
World Articles of Ear, Nose and Throat ---------------------Page 1 Rhinoplasty - Tip Augmentation by Extended Columellar Strip Authors: Vikas Sinha*, Viral A. Chhaya**, Dilavar A. Barot***, Keyur Mehta****,
Preserving normal nasal function and controlling COSMETIC
 COSMETIC Dorsal Aesthetic Lines in Rhinoplasty: A Quantitative Outcome-Based Assessment of the Component Dorsal Reduction Technique Ali Mojallal, M.D., Ph.D. Da Ouyang, M.D. Michel Saint-Cyr, M.D. Nam
COSMETIC Dorsal Aesthetic Lines in Rhinoplasty: A Quantitative Outcome-Based Assessment of the Component Dorsal Reduction Technique Ali Mojallal, M.D., Ph.D. Da Ouyang, M.D. Michel Saint-Cyr, M.D. Nam
Analyzing and controlling nasal tip projection COSMETIC. A Multivariate Analysis of Nasal Tip Deprojection
 COSMETIC A Multivariate Analysis of Nasal Tip Deprojection Jacob G. Unger, M.D. Michael R. Lee, M.D. Robert K. Kwon, M.D. Rod J. Rohrich, M.D. Dallas, Texas Background: Projection of the nasal tip is a
COSMETIC A Multivariate Analysis of Nasal Tip Deprojection Jacob G. Unger, M.D. Michael R. Lee, M.D. Robert K. Kwon, M.D. Rod J. Rohrich, M.D. Dallas, Texas Background: Projection of the nasal tip is a
Radiofrequency Thermotherapy vs Bone-Anchored Suspension for Treatment of Lateral Nasal Wall Insufficiency A Randomized Clinical Trial
 Research Original Investigation Radiofrequency Thermotherapy vs Bone-Anchored Suspension for Treatment of Lateral Nasal Wall Insufficiency A Randomized Clinical Trial Joshua D. Weissman, MD; Sam P. Most,
Research Original Investigation Radiofrequency Thermotherapy vs Bone-Anchored Suspension for Treatment of Lateral Nasal Wall Insufficiency A Randomized Clinical Trial Joshua D. Weissman, MD; Sam P. Most,
Rhinoplasty and the Nasal Valve January 2008
 TITLE: Rhinoplasty and the Nasal Valve SOURCE: Grand Rounds Presentation, The University of Texas Medical Branch, Dept. of Otolaryngology DATE: January 16, 2008 RESIDENT PHYSICIAN: Jeffrey Buyten, MD FACULTY
TITLE: Rhinoplasty and the Nasal Valve SOURCE: Grand Rounds Presentation, The University of Texas Medical Branch, Dept. of Otolaryngology DATE: January 16, 2008 RESIDENT PHYSICIAN: Jeffrey Buyten, MD FACULTY
Correction of the Retracted Alar Base
 218 William D. Losquadro, M.D. 1 Anthony Bared, M.D. 2 Dean M. Toriumi, M.D. 2 1 Mount Kisco Medical Group, Katonah, New York 2 Division of Facial Plastic and Reconstructive Surgery, Department of Otolaryngology
218 William D. Losquadro, M.D. 1 Anthony Bared, M.D. 2 Dean M. Toriumi, M.D. 2 1 Mount Kisco Medical Group, Katonah, New York 2 Division of Facial Plastic and Reconstructive Surgery, Department of Otolaryngology
Fundamental to the evolution of rhinoplasty COSMETIC. Classifying Deformities of the Columella Base in Rhinoplasty.
 COSMETIC Classifying Deformities of the Columella Base in Rhinoplasty Michael R. Lee, M.D. Georges Tabbal, M.D. T. Jonathan Kurkjian, M.D. Jason Roostaeian, M.D. Rod J. Rohrich, M.D. Dallas, Texas Background:
COSMETIC Classifying Deformities of the Columella Base in Rhinoplasty Michael R. Lee, M.D. Georges Tabbal, M.D. T. Jonathan Kurkjian, M.D. Jason Roostaeian, M.D. Rod J. Rohrich, M.D. Dallas, Texas Background:
Surface Aesthetics in Tip Rhinoplasty: A Step-by-Step Guide
 537643AESXXX10.1177/1090820X14537643Aesthetic Surgery JournalÇakır et al research-article2014 INTERNATIONAL CONTRIBUTION Featured Operative Technique Surface Aesthetics in Tip Rhinoplasty: A Step-by-Step
537643AESXXX10.1177/1090820X14537643Aesthetic Surgery JournalÇakır et al research-article2014 INTERNATIONAL CONTRIBUTION Featured Operative Technique Surface Aesthetics in Tip Rhinoplasty: A Step-by-Step
Surgical Management of Nasal Airway Obstruction
 Surgical Management of Nasal Airway Obstruction John F. Teichgraeber, MD a, Ronald P. Gruber, MD b, Neil Tanna, MD, MBA c, * KEYWORDS Nasal obstruction Nasal breathing Septal deviation Nasal valve narrowing
Surgical Management of Nasal Airway Obstruction John F. Teichgraeber, MD a, Ronald P. Gruber, MD b, Neil Tanna, MD, MBA c, * KEYWORDS Nasal obstruction Nasal breathing Septal deviation Nasal valve narrowing
Spreader Graft in Closed Rhinoplasty: The Rail Spreader
 Original Article 515 Spreader Graft in Closed Rhinoplasty: The Rail Spreader Alberto Scattolin, MD 1 Niana Orlando, MD 1 Luca D Ascanio, MD 2 1 Department of Otolaryngology, Villa Donatello Clinic, Piazzale
Original Article 515 Spreader Graft in Closed Rhinoplasty: The Rail Spreader Alberto Scattolin, MD 1 Niana Orlando, MD 1 Luca D Ascanio, MD 2 1 Department of Otolaryngology, Villa Donatello Clinic, Piazzale
Component Rhinoplasty
 18 Original Article Component Rhinoplasty Muhammad Humayun Mohmand*, Muhammad Ahmad Cosmetic Plastic Surgeon, La Chirurgie, Islamabad Cosmetic Surgery Centre, Islamabad, Pakistan ABSTRACT BACKGROUND According
18 Original Article Component Rhinoplasty Muhammad Humayun Mohmand*, Muhammad Ahmad Cosmetic Plastic Surgeon, La Chirurgie, Islamabad Cosmetic Surgery Centre, Islamabad, Pakistan ABSTRACT BACKGROUND According
ORIGINAL ARTICLE. Quantitative Study of Nasal Tip Support and the Effect of Reconstructive Rhinoplasty. accomplish both an excellent
 ORIGINAL ARTICLE Quantitative Study of and the Effect of Reconstructive Rhinoplasty Holger G. Gassner, MD; William J. Remington, MD; David A. Sherris, MD Objectives: To develop a method to quantify nasal
ORIGINAL ARTICLE Quantitative Study of and the Effect of Reconstructive Rhinoplasty Holger G. Gassner, MD; William J. Remington, MD; David A. Sherris, MD Objectives: To develop a method to quantify nasal
Effect of Depressor Septi Resection in Rhinoplasty on Upper Lip Length
 Research Original Investigation Effect of Depressor Septi Resection in Rhinoplasty on Upper Lip Length Yan Ho, MD; Robert Deeb, MD; Richard Westreich, MD; William Lawson, MD, DDS IMPORTANCE Resection of
Research Original Investigation Effect of Depressor Septi Resection in Rhinoplasty on Upper Lip Length Yan Ho, MD; Robert Deeb, MD; Richard Westreich, MD; William Lawson, MD, DDS IMPORTANCE Resection of
A new classification system of nasal contractures
 Original Article J Cosmet Med 2017;1(2):106-111 https://doi.org/10.25056/jcm.2017.1.2.106 pissn 2508-8831, eissn 2586-0585 A new classification system of nasal contractures Geunuck Chang 1, Donghak Jung
Original Article J Cosmet Med 2017;1(2):106-111 https://doi.org/10.25056/jcm.2017.1.2.106 pissn 2508-8831, eissn 2586-0585 A new classification system of nasal contractures Geunuck Chang 1, Donghak Jung
Endoscopic septoplasty
 Endoscopic septoplasty Claudiu Manea, MD, PhD University of Medicine and Pharmacy Carol Davila, Bucharest, Romania Septal deviation is a common clinical finding in patients reporting nasal obstruction.
Endoscopic septoplasty Claudiu Manea, MD, PhD University of Medicine and Pharmacy Carol Davila, Bucharest, Romania Septal deviation is a common clinical finding in patients reporting nasal obstruction.
Dubai Standards of Care (Septoplasty)
 Dubai Standards of Care 2017 (Septoplasty) Preface Ear, nose and throat disorders are the most common problem dealt with in daily practice. In Dubai, the management of ear, nose and throat disorders were
Dubai Standards of Care 2017 (Septoplasty) Preface Ear, nose and throat disorders are the most common problem dealt with in daily practice. In Dubai, the management of ear, nose and throat disorders were
Absorbable Nasal Implant for Treatment of Nasal Valve Collapse
 NOTE: This policy is not effective until March 1, 2019. Medical Policy Manual Surgery, Policy No. 209 Absorbable Nasal Implant for Treatment of Nasal Valve Collapse Next Review: November 2019 Last Review:
NOTE: This policy is not effective until March 1, 2019. Medical Policy Manual Surgery, Policy No. 209 Absorbable Nasal Implant for Treatment of Nasal Valve Collapse Next Review: November 2019 Last Review:
Achieving a consistent functional and aesthetic
 Special Topic Simplifying the Management of Caudal Septal Deviation in Rhinoplasty Fadi C. Constantine, M.D. Jamil Ahmad, M.D. Palmyra Geissler, M.D. Rod J. Rohrich, M.D. Dallas, Texas; and Mississauga,
Special Topic Simplifying the Management of Caudal Septal Deviation in Rhinoplasty Fadi C. Constantine, M.D. Jamil Ahmad, M.D. Palmyra Geissler, M.D. Rod J. Rohrich, M.D. Dallas, Texas; and Mississauga,
The upper buccal sulcus approach, an alternative for post-trauma rhinoplasty
 British Journal of Plastic Surgery (2003), 56, 218 223 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00117-6 The
British Journal of Plastic Surgery (2003), 56, 218 223 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00117-6 The
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY THE NASAL SEPTUM IN RHINOPLASTY: BASIC SEPTOPLASTY TECHNIQUES FWA Otten Introduction Septal corrections form an important step in rhinoplastic
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY THE NASAL SEPTUM IN RHINOPLASTY: BASIC SEPTOPLASTY TECHNIQUES FWA Otten Introduction Septal corrections form an important step in rhinoplastic
Secondary rhinoplasty
 Free full text on www.ijps.org Secondary rhinoplasty Gaith Shubailat American Board of Plastic Surgery Address for correspondence: Gaith Shubailat, P. O. Box 5180, Amman, Jordan 11183. E-mail: gaith@shubailat.com
Free full text on www.ijps.org Secondary rhinoplasty Gaith Shubailat American Board of Plastic Surgery Address for correspondence: Gaith Shubailat, P. O. Box 5180, Amman, Jordan 11183. E-mail: gaith@shubailat.com
Essentials of Septorhinoplasty
 Essentials of Septorhinoplasty von Hans Behrbohm, Eugene Tardy 1. Auflage Essentials of Septorhinoplasty Behrbohm / Tardy schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG Thematische
Essentials of Septorhinoplasty von Hans Behrbohm, Eugene Tardy 1. Auflage Essentials of Septorhinoplasty Behrbohm / Tardy schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG Thematische
Update on the Evidence for Functional Rhinoplasty Techniques
 Update on the Evidence for Functional Rhinoplasty Techniques David Chan, MD 1 and Taha Z. Shipchandler, MD, FACS 1 1. Division of Facial Plastic & Reconstructive Surgery, Department of Otolaryngology,,
Update on the Evidence for Functional Rhinoplasty Techniques David Chan, MD 1 and Taha Z. Shipchandler, MD, FACS 1 1. Division of Facial Plastic & Reconstructive Surgery, Department of Otolaryngology,,
Evaluation With Acoustic Rhinometry of Patients Undergoing Sinonasal Surgery
 ORIGINAL ARTICLE Evaluation With Acoustic Rhinometry of Patients Undergoing Sinonasal Surgery R L A Raja Ahmad, MS (ORL)*, B S Gendeh, MS (ORL)** Department of Otolaryngology-Head & Neck Surgery, Kulliyyah
ORIGINAL ARTICLE Evaluation With Acoustic Rhinometry of Patients Undergoing Sinonasal Surgery R L A Raja Ahmad, MS (ORL)*, B S Gendeh, MS (ORL)** Department of Otolaryngology-Head & Neck Surgery, Kulliyyah
We conducted a contemporary review covering advances and trends in primary
 JOURNAL CLUB CONTEMPORARY REVIEW Contemporary Review of Rhinoplasty Patrick C. Angelos, MD; Mark J. Been, MD; Dean M. Toriumi, MD We conducted a contemporary review covering advances and trends in primary
JOURNAL CLUB CONTEMPORARY REVIEW Contemporary Review of Rhinoplasty Patrick C. Angelos, MD; Mark J. Been, MD; Dean M. Toriumi, MD We conducted a contemporary review covering advances and trends in primary
There is no uniform grading system for nasal dorsal deformities currently in general use
 ORIGINAL ARTICLE A Grading System for Nasal Dorsal Deformities Matthew A. Kienstra, MD; Holger G. Gassner, MD; David A. Sherris, MD; Eugene B. Kern, MD There is no uniform grading system for nasal dorsal
ORIGINAL ARTICLE A Grading System for Nasal Dorsal Deformities Matthew A. Kienstra, MD; Holger G. Gassner, MD; David A. Sherris, MD; Eugene B. Kern, MD There is no uniform grading system for nasal dorsal
Alar Batten Cartilage Graft: Treatment of Internal and External Nasal Valve Collapse
 Aesth Plast Surg (2009) 33:625 634 DOI 10.1007/s00266-009-9349-5 ORIGINAL ARTICLE Alar Batten Cartilage Graft: Treatment of Internal and External Nasal Valve Collapse Valerio Cervelli Æ Diana Spallone
Aesth Plast Surg (2009) 33:625 634 DOI 10.1007/s00266-009-9349-5 ORIGINAL ARTICLE Alar Batten Cartilage Graft: Treatment of Internal and External Nasal Valve Collapse Valerio Cervelli Æ Diana Spallone
Modified Endonasal Tongue-in-Groove Technique
 Rapid Communication 569 Sameep Kadakia, MD 1 Alexander Ovchinsky, MD 1 1 Department of Otolaryngology - Head and Neck Surgery, New York Eye and Ear Infirmary of Mount Sinai, New York, New York Facial Plast
Rapid Communication 569 Sameep Kadakia, MD 1 Alexander Ovchinsky, MD 1 1 Department of Otolaryngology - Head and Neck Surgery, New York Eye and Ear Infirmary of Mount Sinai, New York, New York Facial Plast
Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair
 Original Article Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair Yoon Seok Lee 1, Dong Hyeok Shin 1, Hyun Gon Choi 1, Jee Nam Kim 1, Myung Chul
Original Article Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair Yoon Seok Lee 1, Dong Hyeok Shin 1, Hyun Gon Choi 1, Jee Nam Kim 1, Myung Chul
Comparison of Aesthetic and Functional Outcomes of Spreader Graft and Autospreader Flap in Rhinoplasty
 Original Article 133 Comparison of Aesthetic and Functional Outcomes of Spreader Graft and Autospreader Flap in Rhinoplasty Seyed Esmail Hassanpour 1, Ataollah Heidari* 1, Seyed Mehdi Moosavizadeh 1, Mohammad
Original Article 133 Comparison of Aesthetic and Functional Outcomes of Spreader Graft and Autospreader Flap in Rhinoplasty Seyed Esmail Hassanpour 1, Ataollah Heidari* 1, Seyed Mehdi Moosavizadeh 1, Mohammad
The Use of Spreader Grafts and Columellar Strut as Septal Extention Graft in Dorsal Nasal Deviation
 Med. J. Cairo Univ., Vol. 83, No. 1, September: 585-589, 2015 www.medicaljournalofcairouniversity.net The Use of Spreader Grafts and Columellar Strut as Septal Extention Graft in Dorsal Nasal Deviation
Med. J. Cairo Univ., Vol. 83, No. 1, September: 585-589, 2015 www.medicaljournalofcairouniversity.net The Use of Spreader Grafts and Columellar Strut as Septal Extention Graft in Dorsal Nasal Deviation
The Onlay Folded Flap (OFF): A New Technique for Nasal Tip Surgery
 DOI 10.1007/s00266-010-9562-2 ORIGINAL ARTICLE The Onlay Folded Flap (OFF): A New Technique for Nasal Tip Surgery Hani Abou Mayaleh Received: 11 April 2010 / Accepted: 15 July 2010 Ó Springer Science+Business
DOI 10.1007/s00266-010-9562-2 ORIGINAL ARTICLE The Onlay Folded Flap (OFF): A New Technique for Nasal Tip Surgery Hani Abou Mayaleh Received: 11 April 2010 / Accepted: 15 July 2010 Ó Springer Science+Business
MedStar Health considers Septoplasty-Rhinoplasty medically necessary for the following indications:
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.038.MH Septoplasty-Rhinoplasty This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.038.MH Septoplasty-Rhinoplasty This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
Intermediate Osteotomy and other Unique Techniques used in Reduction Rhinoplasty
 Niveditha J Sagar, Chidananda R Devasamudra Original article 10.5005/jp-journals-10013-1254 Intermediate Osteotomy and other Unique Techniques used in Reduction Rhinoplasty 1 Niveditha J Sagar, 2 Chidananda
Niveditha J Sagar, Chidananda R Devasamudra Original article 10.5005/jp-journals-10013-1254 Intermediate Osteotomy and other Unique Techniques used in Reduction Rhinoplasty 1 Niveditha J Sagar, 2 Chidananda
Nose Reshaping (Rhinoplasty)
 Nose Reshaping (Rhinoplasty) Are you interested in improving the appearance of your nose? If so, you re not alone. Nose reshaping, or rhinoplasty, is one of the most common plastic surgery procedures performed
Nose Reshaping (Rhinoplasty) Are you interested in improving the appearance of your nose? If so, you re not alone. Nose reshaping, or rhinoplasty, is one of the most common plastic surgery procedures performed
Compared with other ethnicities, Asians have
 Original Article Correction of Asian Short Nose with Lower Lateral Cartilage Repositioning and Ear Cartilage Grafting Jin Suk Byun, MD, PhD* Kenneth K. Kim, MD, FACS, Background: Asians with short nose
Original Article Correction of Asian Short Nose with Lower Lateral Cartilage Repositioning and Ear Cartilage Grafting Jin Suk Byun, MD, PhD* Kenneth K. Kim, MD, FACS, Background: Asians with short nose
The Precision of Template Rhinoplasty
 The Precision of Template Rhinoplasty Paul O Keeffe Sydney www.oknoses.com.au Disclosure of Relevant Financial Interests Nothing to disclose Objective To determine a new stable nose profile Calculate soft
The Precision of Template Rhinoplasty Paul O Keeffe Sydney www.oknoses.com.au Disclosure of Relevant Financial Interests Nothing to disclose Objective To determine a new stable nose profile Calculate soft
The Beneficial Effects of Postrhinoplasty TapingFact or Fiction? Kyle A. Belek, MD, Ronald P. Gruber, MD
 The Beneficial Effects of Postrhinoplasty TapingFact or Fiction? Kyle A. Belek, MD, Ronald P. Gruber, MD Rhinoplasty The Beneficial Effects of Postrhinoplasty Taping: Fact or Fiction? Kyle A. Belek, MD;
The Beneficial Effects of Postrhinoplasty TapingFact or Fiction? Kyle A. Belek, MD, Ronald P. Gruber, MD Rhinoplasty The Beneficial Effects of Postrhinoplasty Taping: Fact or Fiction? Kyle A. Belek, MD;
Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K.
 05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
Combining Rhinoplasty with Septal Perforation Repair
 Combining Rhinoplasty with Septal Perforation Repair Hossam M.T. Foda, M.D. 1 and Emad A. Magdy, M.D. 1 ABSTRACT A combined septal perforation repair and rhinoplasty was performed in 80 patients presenting
Combining Rhinoplasty with Septal Perforation Repair Hossam M.T. Foda, M.D. 1 and Emad A. Magdy, M.D. 1 ABSTRACT A combined septal perforation repair and rhinoplasty was performed in 80 patients presenting
implementation of modern rhinoplasty techniques to yield an aesthetic result well balanced with other facial components.
 : J Dentistry and Otolaryngology Volume 14 Issue 3 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online ISSN: 2249-4618 & Print
: J Dentistry and Otolaryngology Volume 14 Issue 3 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online ISSN: 2249-4618 & Print
Shamouelian et al.: Rethinking Nasal Tip Support: A Finite Element Analysis
 The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Rethinking Nasal Tip Support: A Finite Element Analysis David Shamouelian, MD; Ryan P. Leary, MD; Cyrus T.
The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Rethinking Nasal Tip Support: A Finite Element Analysis David Shamouelian, MD; Ryan P. Leary, MD; Cyrus T.
Closed rhinoplasty. Yadranko Ducic, MD, MSc, FRCS(C), FACS, Robert DeFatta, MD, PhD. From the Center for Aesthetic Surgery, Colleyville, Texas.
 Operative Techniques in Otolaryngology (2007) 18, 233-242 Closed rhinoplasty Yadranko Ducic, MD, MSc, FRCS(C), FACS, Robert DeFatta, MD, PhD From the Center for Aesthetic Surgery, Colleyville, Texas. KEYWORDS
Operative Techniques in Otolaryngology (2007) 18, 233-242 Closed rhinoplasty Yadranko Ducic, MD, MSc, FRCS(C), FACS, Robert DeFatta, MD, PhD From the Center for Aesthetic Surgery, Colleyville, Texas. KEYWORDS
UNCORRECTED PROOF. The conchal cartilage graft in nasal reconstruction * ARTICLE IN PRESS. Armando Boccieri*, Alessandro Marano 1
 Journal of Plastic, Reconstructive & Aesthetic Surgery (2006) -, -e- 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47
Journal of Plastic, Reconstructive & Aesthetic Surgery (2006) -, -e- 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47
Extracorporeal Septoplasty: Assessing Functional Outcomes Using the Validated Nasal Obstruction Symptom Evaluation Score over a 3-Year Period
 RECONSTRUCTIVE Extracorporeal Septoplasty: Assessing Functional Outcomes Using the Validated Nasal Obstruction Symptom Evaluation Score over a 3-Year Period Steven Ross Mobley, M.D. Jennifer Long, M.D.
RECONSTRUCTIVE Extracorporeal Septoplasty: Assessing Functional Outcomes Using the Validated Nasal Obstruction Symptom Evaluation Score over a 3-Year Period Steven Ross Mobley, M.D. Jennifer Long, M.D.
Specially Processed Heterogenous Bone and Cartilage Transplants in Nasal Surgery
 Specially Processed Heterogenous Bone and Cartilage Transplants in Nasal Surgery By GRAEME M. CLARK (Melbourne) IN nasal surgery, cartilage or bone transplants are required for support or correction of
Specially Processed Heterogenous Bone and Cartilage Transplants in Nasal Surgery By GRAEME M. CLARK (Melbourne) IN nasal surgery, cartilage or bone transplants are required for support or correction of
Mastering Rhinoplasty: A Comprehensive Atlas of Surgical Techniques with Integrated Video Clips. Rollin K. Daniel
 Mastering Rhinoplasty: A Comprehensive Atlas of Surgical Techniques with Integrated Video Clips Rollin K. Daniel Rollin K. Daniel Mastering Rhinoplasty A Comprehensive Atlas of Surgical Techniques with
Mastering Rhinoplasty: A Comprehensive Atlas of Surgical Techniques with Integrated Video Clips Rollin K. Daniel Rollin K. Daniel Mastering Rhinoplasty A Comprehensive Atlas of Surgical Techniques with
Triple Plane Dissection in Open Primary Rhinoplasty in Middle Eastern Noses
 Triple Plane Dissection in Open Primary Rhinoplasty in Middle Eastern Noses Ahmed Elshahat, MD Plastic Surgery Department, Faculty of Medicine, Ain Shams University; and Eldemerdash Hospital, Cairo, Egypt
Triple Plane Dissection in Open Primary Rhinoplasty in Middle Eastern Noses Ahmed Elshahat, MD Plastic Surgery Department, Faculty of Medicine, Ain Shams University; and Eldemerdash Hospital, Cairo, Egypt
Augmentation Rhinoplasty with Rib Cartilage Graft
 Elaine Marie A. Lagura, MD Eduardo C. Yap, MD Anna Victoria G. Garcia, MD Augmentation Rhinoplasty with Rib Cartilage Graft Department of Otolaryngology Head and Neck Surgery Ospital ng Makati ABSTRACT
Elaine Marie A. Lagura, MD Eduardo C. Yap, MD Anna Victoria G. Garcia, MD Augmentation Rhinoplasty with Rib Cartilage Graft Department of Otolaryngology Head and Neck Surgery Ospital ng Makati ABSTRACT
Regina Rodman, MD Faculty Mentor: Tamara Watts, MD PhD The University of Texas Medical Branch (UTMB Health) Department of Otolaryngology Grand Rounds
 Regina Rodman, MD Faculty Mentor: Tamara Watts, MD PhD The University of Texas Medical Branch (UTMB Health) Department of Otolaryngology Grand Rounds Presentation March 29, 2012 Anatomic landmarks Photography
Regina Rodman, MD Faculty Mentor: Tamara Watts, MD PhD The University of Texas Medical Branch (UTMB Health) Department of Otolaryngology Grand Rounds Presentation March 29, 2012 Anatomic landmarks Photography
RHINOPLASTY (NOSE RE-SHAPING)
 PROCEDURE FACT SHEET PLASTIC SURGERY RHINOPLASTY (NOSE RE-SHAPING) This is a guide for people who are considering having a nose re-shaping (Rhinoplasty) operation. We advise that you talk to a plastic
PROCEDURE FACT SHEET PLASTIC SURGERY RHINOPLASTY (NOSE RE-SHAPING) This is a guide for people who are considering having a nose re-shaping (Rhinoplasty) operation. We advise that you talk to a plastic
ORIGINAL ARTICLE. Reconstruction of the Nasal Columella. David A. Sherris, MD; Jon Fuerstenberg, MD; Daniel Danahey, MD, PhD; Peter A.
 ORIGINAL ARTICLE Reconstruction of the Nasal Columella David A. Sherris, MD; Jon Fuerstenberg, MD; Daniel Danahey, MD, PhD; Peter A. Hilger, MD Objective: To report techniques successful for nasal columella
ORIGINAL ARTICLE Reconstruction of the Nasal Columella David A. Sherris, MD; Jon Fuerstenberg, MD; Daniel Danahey, MD, PhD; Peter A. Hilger, MD Objective: To report techniques successful for nasal columella
Reconstruction of Dorsal and/or Caudal Nasal Septum Deformities With Septal Battens or by Septal Replacement: An Overview and Comparison of Techniques
 The Laryngoscope Lippincott Williams & Wilkins, Inc. 2006 The American Laryngological, Rhinological and Otological Society, Inc. Reconstruction of Dorsal and/or Caudal Nasal Septum Deformities With Septal
The Laryngoscope Lippincott Williams & Wilkins, Inc. 2006 The American Laryngological, Rhinological and Otological Society, Inc. Reconstruction of Dorsal and/or Caudal Nasal Septum Deformities With Septal
New Instruments for Submembranous Dissection in Rhinoplasty
 Letter to the Editor New Instruments for Submembranous Dissection in Rhinoplasty Aesthetic Surgery Journal 2017, Vol 37(7) NP73 NP78 2017 The American Society for Aesthetic Plastic Surgery, Inc. Reprints
Letter to the Editor New Instruments for Submembranous Dissection in Rhinoplasty Aesthetic Surgery Journal 2017, Vol 37(7) NP73 NP78 2017 The American Society for Aesthetic Plastic Surgery, Inc. Reprints
Thomas T. Jeneby, M.D Wurzbach Suite 801 San Antonio, TX /
 Nose reshaping, or rhinoplasty, is one of the most common plastic surgery procedures performed today. Often, the structure or size of the nose is not proportionate with the other features on the face.
Nose reshaping, or rhinoplasty, is one of the most common plastic surgery procedures performed today. Often, the structure or size of the nose is not proportionate with the other features on the face.
Patient profile, indications, complications and Evaluation of Septoplasty outcome in a Base Hospital in Sri Lanka
 Patient profile, indications, complications and Evaluation of Septoplasty outcome in a Base Hospital in Sri Lanka Rubasinghe M.S., De Silva M.D.K., Wanasinghe W.M.S.C.L., De Livera R.J.K., Wimalaratna
Patient profile, indications, complications and Evaluation of Septoplasty outcome in a Base Hospital in Sri Lanka Rubasinghe M.S., De Silva M.D.K., Wanasinghe W.M.S.C.L., De Livera R.J.K., Wimalaratna
Rod J. Rohrich, M.D., Larry H. Hollier, Jr., M.D., Jeffrey E. Janis, M.D., and John Kim, M.D.
 Techniques in Cosmetic Surgery Rhinoplasty with Advancing Age Rod J. Rohrich, M.D., Larry H. Hollier, Jr., M.D., Jeffrey E. Janis, M.D., and John Kim, M.D. Houston and Dallas, Texas Rhinoplasty in the
Techniques in Cosmetic Surgery Rhinoplasty with Advancing Age Rod J. Rohrich, M.D., Larry H. Hollier, Jr., M.D., Jeffrey E. Janis, M.D., and John Kim, M.D. Houston and Dallas, Texas Rhinoplasty in the
The Crooked Nose and its Functional Surgical Correction
 The Crooked Nose and its Functional Surgical Correction Armando González Romero Introduction The nose is a highly specialized organ of the respiratory system and is essential for homeostasis. The pathological
The Crooked Nose and its Functional Surgical Correction Armando González Romero Introduction The nose is a highly specialized organ of the respiratory system and is essential for homeostasis. The pathological
Comparative Scar Analysis Between V and Inverted-V Incision in Open Rhinoplasty of Patients Referred to Rasht Amir-Almomenin Hospital
 Journal of Research in Medical and Dental Sciences 2018, Volume 6, Issue 3, Page No: 45-49 Copyright CC BY-NC-ND 4.0 Available Online at: www.jrmds.in eissn No. 2347-2367: pissn No. 2347-2545 Comparative
Journal of Research in Medical and Dental Sciences 2018, Volume 6, Issue 3, Page No: 45-49 Copyright CC BY-NC-ND 4.0 Available Online at: www.jrmds.in eissn No. 2347-2367: pissn No. 2347-2545 Comparative
Allen L. Van Beek, M.D., Agnieszka S. Hatfield, M.D., and Ellie Schnepf, B.S.N.
 CME Cleft Rhinoplasty Allen L. Van Beek, M.D., Agnieszka S. Hatfield, M.D., and Ellie Schnepf, B.S.N. Edina and Minneapolis, Minn. Learning Objectives: After studying this article, the participant should
CME Cleft Rhinoplasty Allen L. Van Beek, M.D., Agnieszka S. Hatfield, M.D., and Ellie Schnepf, B.S.N. Edina and Minneapolis, Minn. Learning Objectives: After studying this article, the participant should
Bony hump reduction is an integral part of classic
 Rhinoplasty Nasal Hump Reduction With Powered Micro Saw Osteotomy INTERNATIONAL CONTRIBUTION Yakup Avşar, MD Background: Hump reduction with manual osteotomy is an invasive procedure in aesthetic rhinoplasty.
Rhinoplasty Nasal Hump Reduction With Powered Micro Saw Osteotomy INTERNATIONAL CONTRIBUTION Yakup Avşar, MD Background: Hump reduction with manual osteotomy is an invasive procedure in aesthetic rhinoplasty.
Shuttle Lifting of the Nose: A Minimally Invasive Approach for Nose Reshaping
 INTERNATIONAL CONTRIBUTION Rhinoplasty Shuttle Lifting of the Nose: A Minimally Invasive Approach for Nose Reshaping Kemal Tunc Tiryaki, MD Aesthetic Surgery Journal 30(2) 176 185 2010 The American Society
INTERNATIONAL CONTRIBUTION Rhinoplasty Shuttle Lifting of the Nose: A Minimally Invasive Approach for Nose Reshaping Kemal Tunc Tiryaki, MD Aesthetic Surgery Journal 30(2) 176 185 2010 The American Society
Medical Policy. MP Absorbable Nasal Implant for Treatment of Nasal Valve Collapse
 Medical Policy MP 7.01.163 BCBSA Ref. Policy: 7.01.163 Last Review: 10/18/2018 Effective Date: 01/25/2019 Section: Surgery Related Policies 9.01.502 Experimental / Investigational Services DISCLAIMER Our
Medical Policy MP 7.01.163 BCBSA Ref. Policy: 7.01.163 Last Review: 10/18/2018 Effective Date: 01/25/2019 Section: Surgery Related Policies 9.01.502 Experimental / Investigational Services DISCLAIMER Our
Changing the Convexity and Concavity of Nasal Cartilages and Cartilage Grafts with Horizontal Mattress Sutures: Part I. Experimental Results
 Cosmetic Changing the Convexity and Concavity of Nasal Cartilages and Cartilage Grafts with Horizontal Mattress Sutures: Part I. Experimental Results Ronald P. Gruber, M.D., Farzad Nahai, M.D., Michael
Cosmetic Changing the Convexity and Concavity of Nasal Cartilages and Cartilage Grafts with Horizontal Mattress Sutures: Part I. Experimental Results Ronald P. Gruber, M.D., Farzad Nahai, M.D., Michael
Acoustic rhinometry and rhinomanometry as objective tools for the assessment of nasal patency in nasal septal surgery
 Romanian Journal of Rhinology, Vol. 7, No. 25, January-March 2017 Original study Acoustic rhinometry and rhinomanometry as objective tools for the assessment of nasal patency in nasal septal surgery Frodita
Romanian Journal of Rhinology, Vol. 7, No. 25, January-March 2017 Original study Acoustic rhinometry and rhinomanometry as objective tools for the assessment of nasal patency in nasal septal surgery Frodita
Plastic Surgeon, Middlesbrough General Hospital, Stockton Children's Hospital, Newcastle Regional Hospital Board
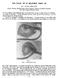 THE NASAL TIP IN BILATERAL HARE LIP By J. POTTER, F.R.C.S.Ed. Plastic Surgeon, Middlesbrough General Hospital, Stockton Children's Hospital, Newcastle Regional Hospital Board IN the problem of the bilateral
THE NASAL TIP IN BILATERAL HARE LIP By J. POTTER, F.R.C.S.Ed. Plastic Surgeon, Middlesbrough General Hospital, Stockton Children's Hospital, Newcastle Regional Hospital Board IN the problem of the bilateral
Nasal obstruction is one of the most common complaints of patients
 Augmenting the nasal airway: Beyond septoplasty Patrick Simon, M.D., and Douglas Sidle, M.D., F.A.C.S. ABSTRACT Background: Nasal airway obstruction is a common complaint of patients presenting to otolaryngology
Augmenting the nasal airway: Beyond septoplasty Patrick Simon, M.D., and Douglas Sidle, M.D., F.A.C.S. ABSTRACT Background: Nasal airway obstruction is a common complaint of patients presenting to otolaryngology
ORIGINAL ARTICLE. patients with impaired nasalbreathingandaestheticdiscomfortduetostenosisofthenasalvestibule.
 ORIGINAL ARTICLE Postoperative Management of Nasal Vestibular Stenosis The Custom-made Vestibular Device Dirk-Jan Menger, MD; Peter J. F. M. Lohuis, MD, PhD; Steven Kerssemakers, MD; Gilbert J. Nolst Trenité,
ORIGINAL ARTICLE Postoperative Management of Nasal Vestibular Stenosis The Custom-made Vestibular Device Dirk-Jan Menger, MD; Peter J. F. M. Lohuis, MD, PhD; Steven Kerssemakers, MD; Gilbert J. Nolst Trenité,
19, 2006 RESIDENT PHYSICIAN:
 TITLE: Rhinoplasty SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 19, 2006 RESIDENT PHYSICIAN: Alan L. Cowan, M.D. FACULTY ADVISOR: David C. Teller, M.D. SERIES EDITORS: Francis
TITLE: Rhinoplasty SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 19, 2006 RESIDENT PHYSICIAN: Alan L. Cowan, M.D. FACULTY ADVISOR: David C. Teller, M.D. SERIES EDITORS: Francis
RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP. By MICHAL KRAUSS. Plastic Surgery Hospital, Polanica-Zdroj, Poland
 RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP By MICHAL KRAUSS Plastic Surgery Hospital, Polanica-Zdroj, Poland RECONSTRUCTION of the nose is one of the composite procedures in
RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP By MICHAL KRAUSS Plastic Surgery Hospital, Polanica-Zdroj, Poland RECONSTRUCTION of the nose is one of the composite procedures in
Guide to Writing Oral Protocols
 Guide to Writing Oral Protocols CONTENTS PAGE Structure and Purpose of the Oral Examination 2 When Planning a Protocol 2 Selecting Photos, Illustrations, and Other Art 2 Standard Views for Major Facial
Guide to Writing Oral Protocols CONTENTS PAGE Structure and Purpose of the Oral Examination 2 When Planning a Protocol 2 Selecting Photos, Illustrations, and Other Art 2 Standard Views for Major Facial
Revision of the Cleft Lip Nose
 Revision of the Cleft Lip Nose Tom D. Wang, MD, FACS* Professor and Chief of Facial Plastic & Reconstructive Surgery Department of Otolaryngology / Head & Neck Surgery Oregon Health & Science University
Revision of the Cleft Lip Nose Tom D. Wang, MD, FACS* Professor and Chief of Facial Plastic & Reconstructive Surgery Department of Otolaryngology / Head & Neck Surgery Oregon Health & Science University
Perichondrium Graft: Harvesting and Indications in Nasal Surgery. Armando Boccieri, MD, and Tito M. Marianetti, MD
 ORIGINAL ARTICLE Perichondrium Graft: Harvesting and Indications in Nasal Surgery Armando Boccieri, MD, and Tito M. Marianetti, MD Abstract: Irregularities in the nasal contour of patients who underwent
ORIGINAL ARTICLE Perichondrium Graft: Harvesting and Indications in Nasal Surgery Armando Boccieri, MD, and Tito M. Marianetti, MD Abstract: Irregularities in the nasal contour of patients who underwent
Alireza Bakhshaeekia and Sina Ghiasi-hafezi. 1. Introduction. 2. Patients and Methods
 Plastic Surgery International Volume 0, Article ID 4578, 4 pages doi:0.55/0/4578 Clinical Study Comparing the Alteration of Nasal Tip Sensibility and Sensory Recovery Time following Open Rhinoplasty with
Plastic Surgery International Volume 0, Article ID 4578, 4 pages doi:0.55/0/4578 Clinical Study Comparing the Alteration of Nasal Tip Sensibility and Sensory Recovery Time following Open Rhinoplasty with
Computational Fluid Dynamic Analysis of Nasal Airway Model
 Computational Fluid Dynamic Analysis of Nasal Airway Model Shubham Singhmar, Deepak Duhan, Rishabh Thakur Student, Department of mechanical engineering, Chandigarh University, India Student, Department
Computational Fluid Dynamic Analysis of Nasal Airway Model Shubham Singhmar, Deepak Duhan, Rishabh Thakur Student, Department of mechanical engineering, Chandigarh University, India Student, Department
Jae Hee Kim, Dong Ju Jung, Hyo Seong Kim, Chang Hyun Kim, Tae Yeon Kim
 Analysis of the Development of the Nasal Septum and Measurement of the Harvestable Septal Cartilage in Koreans Using Three-Dimensional Facial Bone Computed Tomography Scanning Jae Hee Kim, Dong Ju Jung,
Analysis of the Development of the Nasal Septum and Measurement of the Harvestable Septal Cartilage in Koreans Using Three-Dimensional Facial Bone Computed Tomography Scanning Jae Hee Kim, Dong Ju Jung,
Immediate Functional and Cosmetic Open Rhinoplasty Following Acute Nasal Fractures: Our Experience With Asian Noses
 INTERNATIONAL CONTRIBUTION Rhinoplasty Immediate Functional and Cosmetic Open Rhinoplasty Following Acute Nasal Fractures: Our Experience With Asian Noses Aesthetic Surgery Journal 33(4) 505 515 2013 The
INTERNATIONAL CONTRIBUTION Rhinoplasty Immediate Functional and Cosmetic Open Rhinoplasty Following Acute Nasal Fractures: Our Experience With Asian Noses Aesthetic Surgery Journal 33(4) 505 515 2013 The
Occipital flattening in the infant skull
 Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Correction of Secondary Deformities of the Cleft Lip Nose
 CME Correction of Secondary Deformities of the Cleft Lip Nose Samuel Stal, M.D., and Larry Hollier, M.D. Learning Objectives: After studying this article, the practitioner should be able to: 1. Describe
CME Correction of Secondary Deformities of the Cleft Lip Nose Samuel Stal, M.D., and Larry Hollier, M.D. Learning Objectives: After studying this article, the practitioner should be able to: 1. Describe
This article presents a new surgical technique for reconstruction of the nasal dorsum
 New Technique for Reconstruction of the Nasal orsum Underlay utografting Farahmand Sabeti, M; bbas Nadimi Tehrani, M ORIGINL RTILE This article presents a new surgical technique for reconstruction of the
New Technique for Reconstruction of the Nasal orsum Underlay utografting Farahmand Sabeti, M; bbas Nadimi Tehrani, M ORIGINL RTILE This article presents a new surgical technique for reconstruction of the
Dome Division: A Viable Technique Today?
 664 Rapid Communication Dome Division: A Viable Technique Today? Armando Boccieri, MD 1 Sebastiano Sciuto, MD 1 Valerio Cervelli, MD 2 Michele Pascali, MD, PhD 2 1 Department of Facial Plastic Surgery,
664 Rapid Communication Dome Division: A Viable Technique Today? Armando Boccieri, MD 1 Sebastiano Sciuto, MD 1 Valerio Cervelli, MD 2 Michele Pascali, MD, PhD 2 1 Department of Facial Plastic Surgery,
Ideas and Innovations
 Ideas and Innovations First Female-to-Male Facial Confirmation Surgery with Description of a New Procedure for Masculinization of the Thyroid Cartilage (Adam s Apple) Jordan C. Deschamps-Braly, M.D. Caitlin
Ideas and Innovations First Female-to-Male Facial Confirmation Surgery with Description of a New Procedure for Masculinization of the Thyroid Cartilage (Adam s Apple) Jordan C. Deschamps-Braly, M.D. Caitlin
Advances of Plastic & Reconstructive Surgery
 Chapter 1 Advances of Plastic & Reconstructive Surgery Cleft lip nasal deformity: Analysis and treatment Martínez-Capoccioni Gabriel*; Martín-Martín Carlos Servizo Galego de Saúde, Service of ENT Head
Chapter 1 Advances of Plastic & Reconstructive Surgery Cleft lip nasal deformity: Analysis and treatment Martínez-Capoccioni Gabriel*; Martín-Martín Carlos Servizo Galego de Saúde, Service of ENT Head
Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A.
 UvA-DARE (Digital Academic Repository) Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A. Link to publication Citation for published
UvA-DARE (Digital Academic Repository) Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A. Link to publication Citation for published
Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear
 The British Association of Plastic Surgeons (2004) 57, 238 244 Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear Yong Oock Kim*, Beyoung Yun Park, Won Jae Lee Institute
The British Association of Plastic Surgeons (2004) 57, 238 244 Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear Yong Oock Kim*, Beyoung Yun Park, Won Jae Lee Institute
부비동내시경수술후비음도변화. Effects of Endoscopic Sinus Surgery on Nasality 동헌종 김선일 권중근 윤영선 강수미 추광철
 KISEP Rhinology Korean J Otolaryngol 1999;42:871-5 부비동내시경수술후비음도변화 동헌종 김선일 권중근 윤영선 강수미 추광철 Effects of Endoscopic Sinus Surgery on Nasality Hun-Jong Dhong, MD, Sun-Il Kim, MD, Joong-Keun Kwon, MD, Young-Sun
KISEP Rhinology Korean J Otolaryngol 1999;42:871-5 부비동내시경수술후비음도변화 동헌종 김선일 권중근 윤영선 강수미 추광철 Effects of Endoscopic Sinus Surgery on Nasality Hun-Jong Dhong, MD, Sun-Il Kim, MD, Joong-Keun Kwon, MD, Young-Sun
CHAPTER 17 FACIAL AESTHETIC SURGERY. Christopher C. Surek, DO and Mohammed S. Alghoul, MD. I. BROW LIFT (Figures 1 and 2)
 CHAPTER 17 FACIAL AESTHETIC SURGERY Christopher C. Surek, DO and Mohammed S. Alghoul, MD I. BROW LIFT (Figures 1 and 2) A. Open Coronal Brow Lift Technique 1. Coronal incision is made in the hair-bearing
CHAPTER 17 FACIAL AESTHETIC SURGERY Christopher C. Surek, DO and Mohammed S. Alghoul, MD I. BROW LIFT (Figures 1 and 2) A. Open Coronal Brow Lift Technique 1. Coronal incision is made in the hair-bearing
