Giorgio Sandrini Armando Perrotta Cristina Tassorelli Paola Torelli Filippo Brighina Grazia Sances Giuseppe Nappi
|
|
|
- Jacob Dennis
- 5 years ago
- Views:
Transcription
1 J Headache Pain (2011) 12: DOI /s z ORIGINAL Botulinum toxin type-a in the prophylactic treatment of medication-overuse headache: a multicenter, double-blind, randomized, placebo-controlled, parallel group study Giorgio Sandrini Armando Perrotta Cristina Tassorelli Paola Torelli Filippo Brighina Grazia Sances Giuseppe Nappi Received: 1 February 2011 / Accepted: 26 March 2011 / Published online: 16 April 2011 The Author(s) This article is published with open access at Springerlink.com Abstract Medication-overuse headache (MOH) represents a severely disabling condition, with a low response to prophylactic treatments. Recently, consistent evidences have emerged in favor of botulinum toxin type-a (onabotulinum toxin A) as prophylactic treatment in chronic migraine. In a 12-week double-blind, parallel group, placebo-controlled study, we tested the efficacy and safety of onabotulinum toxin A as prophylactic treatment for MOH. A total of 68 patients were randomized (1:1) to onabotulinum toxin A (n = 33) or placebo (n = 35) treatment and received 16 intramuscular injections. The primary efficacy end point was mean change from baseline in the frequency of headache days for the 28-day period ending with week 12. Electronic supplementary material The online version of this article (doi: /s z) contains supplementary material, which is available to authorized users. A. Perrotta (&) G. Sances G. Nappi Headache Science Center, IRCCS C. Mondino Institute of Neurology Foundation, Via Mondino 2, Pavia, Italy armando.perrotta@uniroma1.it A. Perrotta Headache Clinic, IRCCS Mediterranean Neurological Institute Neuromed, Pozzilli, Isernia, Italy G. Sandrini C. Tassorelli Headache Science Center, IRCCS C. Mondino Institute of Neurology Foundation, University of Pavia, Via Mondino 2, Pavia, Italy P. Torelli Headache Centre, Department of Neuroscience, University of Parma, Parma, Italy F. Brighina Department of Clinical Neurosciences, University of Palermo, Palermo, Italy No significant differences between onabotulinum toxin A and placebo treatment were detected in the primary (headache days) end point (12.0 vs. 15.9; p = 0.81). A significant reduction was recorded in the secondary end point, mean acute pain drug consumption at 12 weeks in onabotulinum toxin A-treated patients when compared with those with placebo (12.1 vs. 18.0; p = 0.03). When we considered the subgroup of patients with pericranial muscle tenderness, we recorded a significant improvement in those treated with onabotulinum toxin A compared to placebo treated in both primary (headache days) and secondary end points (acute pain drug consumption, days with drug consumption), as well as in pain intensity and disability measures (HIT-6 and MIDAS) at 12 weeks. Onabotulinum toxin A was safe and well tolerated, with few treatment-related adverse events. Few subjects discontinued due to adverse events. Our data identified the presence of pericranial muscle tenderness as predictor of response to onabotulinum toxin A in patients with complicated form of migraine such as MOH, the presence of pericranial muscle tenderness and support it as prophylactic treatment in these patients. Keywords Botulinum toxin type-a Medication-overuse headache Prophylactic treatment Migraine Pericranial muscle tenderness Introduction The 2nd edition of the International Headache Society s International Classification of Headache Disorders (ICHD- II, IHS 2004) [1] introduced the term medication-overuse headache (MOH: code 8.2, ICHD-II) to indicate a chronic daily headache condition in which an excessive intake of symptomatic drugs has played a role in the chronification,
2 428 J Headache Pain (2011) 12: and in which a clear relationship between increased drug intake and worsening of the headache is detectable [2]. The prevalence of MOH ranges from 1 to 5% in the general population [3, 4], rising to 10% in headache clinic patients [5] and to 80% among patients with chronic migraine in a tertiary headache center population [6]. MOH represents a severely disabling condition affecting social life and work ability, with a low response to prophylactic treatments in the absence of a concomitant drug withdrawal treatment (see [7] for review), but also with a very high incidence of relapse (between 30 and 50% of patients) within the first year after withdrawal treatment [8]. Intramuscular injections of botulinum toxin type-a (onabotulinum toxin A) has been employed to treat headache pain including episodic migraine [9, 10] and chronic tension-type headache [11 13] without univocal results as prophylactic treatment and chronic daily headaches not responding to previous prophylactic treatments with encouraging results [14]. On the contrary, growing consistent evidences are emerging in favor of onabotulinum toxin A as prophylactic treatment in chronic migraine (1.5.1, ICHD-II) [15 17] and, in particular, in subgroups of patients with cutaneous allodynia, pericranial muscular tenderness [18] or specific types of headache pain such as the so defined imploding and ocular pain [19, 20]. To explain the prophylactic effect of onabotulinum toxin A, it has been hypothesized that this neurotoxin could prevent or reduce the abnormal peripheral sensory signals from the pericranial muscles to the central nervous system and/or inhibit the sensitization of nociceptive neurons in the dorsal horn [21]. As in chronic daily headache, including MOH patients with migraine as primary headache, both pericranial muscle tenderness [22] and sensitization of the pain pathways at the trigeminal [23] and spinal levels [24] has been demonstrated, one would predict that in these patients onabotulinum toxin A would further improve the benefit of the withdrawal treatment and so facilitate the reversion to an episodic form of headache. Our study was aimed to evaluate in a multicenter, doubleblind placebo-controlled study the efficacy and safety of onabotulinum toxin A as prophylactic treatment for patients with MOH with migraine as primary headache, as well as to address if specific features such as cephalic allodynia, pericranial muscle tenderness, type of headache pain or of drug overuse may influence the response to onabotulinum toxin A. Materials and methods Study design The enrollment phase was conducted from January 2006 to July 2008 at: The Headache Science Center, IRCCS C. Fig. 1 Study design Mondino Institute of Neurology Foundation, Pavia, Italy; Headache Center, University of Parma, Parma, Italy; Headache Center, University of Palermo, Palermo, Italy. The study had a 4-week baseline screening phase (referred to as baseline) and a 12-week double-blind, parallel group, placebo-controlled phase with one injection cycle at day 0 of the double-blind phase, followed by a 12-week, open-label phase (details will be described separately) (Fig. 1). All the potential participants were selected from among patients on the waiting list for a consultation in outpatient headache clinics of the participating center. All the patients enrolled in the study filled in a daily headache diary (mailed) to record their headache symptoms and acute treatments every day for at least 2 months before the start of the baseline period (4 weeks) and for the entire period of the study. The study was conducted in accordance with the Declaration of Helsinki Ethical Principles and Good Clinical Practices and was approved at each site by an independent local ethics committee. Written informed consent was obtained from each participant prior to any study-related procedures. Study population Eligible patients were men or women aged years with a history of headache, fulfilling the diagnostic criteria for migraine without aura (coded as 1.1) [1] as primary headache plus medication-overuse headache (coded as 8.2) [1, 2] with C15 headache days every 4 weeks in the past 3 months and with each headache day consisting of C4 h of continuous headache prevalent with migraine features. Exclusion criteria were definite or suspected diagnosis of pathologies affecting neuromuscular function including, myasthenia gravis, Eaton Lambert syndrome and amyotrophic lateral sclerosis, and presence of cervical pathologies or other factors liable to give rise to pericranial muscle disorders. Further exclusion criteria included: other primary or secondary headaches, including a history of complicated
3 J Headache Pain (2011) 12: migraine (i.e., migrainous infarction, hemiplegic migraine, basilar migraine or ophthalmoplegic migraine); any serious systemic or neurological diseases or psychiatric disorders, including depression (Beck s Depression Inventory score [17 at day 1 of baseline); temporo-mandibular disorder, fibromyalgia, complex regional pain syndrome or neuropathic pain [25 27]; use of prophylactic medications for headaches, use of opiates, antidepressants, benzodiazepines, hormones, muscle relaxants and agents that may interfere with neuromuscular function within 4 weeks of day 1 of the baseline; previous exposure to any botulinum toxin serotype for other pathological conditions or for other purposes. Women of childbearing potential were required to have negative urine pregnancy test. Females who were pregnant, nursing or planning a pregnancy during the study, or who were unable or unwilling to use a reliable form of contraception during the study were excluded. Randomization, stratification and study treatment At the end of the baseline period, patients meeting the inclusion/exclusion criteria were admitted as inpatients (ordinary hospitalization or day hospital) and treated with standard withdrawal therapy for detoxification for 8 ± 2 days [28]. Patients were stratified based on the type and frequency of acute drug overused during baseline, in order to balance their distribution within the two study groups. The project statistician created a randomized treatment allocation schedule using a computer random number generator. Both the patient and principal investigator, as well as the co-investigators who administered the treatment and assessed the safety and outcomes and the sponsor of the study, were blinded as to the identity of the randomized study medication. Blinding was maintained by having a designated pharmacist (the only person to have access to the randomization list), who provided the principal investigator or study co-ordinator with a vial containing the study medication labeled with the patient s sequential identification number from the randomized allocation schedule. All patients remained double blinded until the last patient had completed the study. The blind code could be broken by the principal investigator only for safety concern. During the second day of hospitalization, all patients were randomized (1:1) in a double-blind fashion to onabotulinum toxin A (BOTOX, Allergan Inc., Irvine, CA, USA) or placebo treatment and received 16 (8 on the right and 8 on the left) intramuscular injections in the following muscles: frontalis (2 injection points), corrugators (1 injection point), temporalis (1 injection point), cervical paraspinal (2 injection points) and trapezius (2 injection points) for a total of 100 U for patients. Intramuscular injections were administered using a sterile 30-gauge, 0.5 inch needle and 0.2 ml (saline dilution) of onabotulinum toxin A (5 U) or placebo at each site, except for the trapezius where we administered 0.4 ml of onabotulinum toxin A (10 U). Patients were discharged and reassessed after 4, 8 and 12 weeks as outpatients. At the end of the study, all the onabotulinum toxin A responder patients were offered entry into a 12-week open-label follow-up phase to receive a second injection cycle (Fig. 1). All patients, including those who were not willing to participate in the long-term study, were re-assessed in a follow-up visit at 12 months. During the withdrawal treatment, to mitigate possible rebound effects, the patients received twice a day, intravenous infusion of a saline solution plus a vitamin complex (B12, folic acid, PP, C), glutatione 600 mg, alizapride 0.25 mg and clordemetildiazepam (0.25 mg for the first 3 days, then gradually reduced until withdrawal in 4 days). Breakthrough migraine attacks were treated with ketoprofene, 100 mg i.m., as a rescue medication. Safety was assessed by reports of adverse events, physical and neurological examination and laboratory tests. After treatment at day 0, adverse events were recorded and documented with information regarding the date of onset, severity, duration, resolution date, relationship with study treatment, treatment required and outcome. Outcome measures The primary efficacy end point was mean change from baseline in frequency of headache days for the 28-day period ending with week 12. A headache day was defined as a calendar day (00:00 to 23:59) when the patient reported not \4 h of headache. Secondary efficacy end points were mean change from baseline in acute headache pain medication intakes and in days with acute headache medication consumption at 4, 8 and 12 weeks after onabotulinum toxin A administration. The intensity of the headache pain was evaluated by a 0 10 numerical rating scale (NRS) score. The analysis included two assessments of disability measured by Headache Impact Test (HIT)-6 score and Migraine Disability Assessment Scale (MIDAS) administered at 4 and 12 week after onabotulinum toxin A administration. Patients were subdivided into subgroups based on the presence/absence of cephalic cutaneous allodynia measured by a prospective clinical questionnaire [29], pericranial muscle tenderness, assessed by palpation and type of migraine pain (exploding, imploding, ocular) [19] at baseline. Other efficacy analysis included the incidence of subjects with no less than 50% decrease from baseline in the frequency of headache days for the 28-day period ending with week 12 (primary end point) and during the whole observed period from 4 to 12 weeks.
4 430 J Headache Pain (2011) 12: Statistical analysis Data analysis was performed using non-parametric statistics. Ordinal measurements, including age, headache days, acute headache medication intake, days with drug consumption, pain intensity and disability scales (MIDAS and HIT-6), were compared between groups using Mann Whitney test. Ordinal measurements before and after treatment were compared using ANOVA for repeated measures. For post hoc analysis of group mean differences, we used Student s t test with Bonferroni correction. Nominal data were analyzed using v 2 test. The level of significance was set at All statistics were calculated using the SPSS (16.0) program for Windows (SPSS, Chicago, IL, USA). Results Demographic and baseline characteristics Of the 145 patients screened, 68 were randomized to onabotulinumtoxina (n = 33) or placebo (n = 35). Twelve (17.7%) subjects discontinued prior to week 12, six (8.8%) randomized to onabotulinum toxin A and six (8.8%) to placebo, and 56 (82.3%) completed the study, 27 (48.2%) randomized to onabotulinum toxin A and 29 (51.7%) to placebo. As a consequence, the number of participants was small and represented a limitation of the present work. In subjects who dropped-out, discontinuation was due to being lost to follow-up (1 onabotulinum toxin A; 2 placebo); adverse events (2 onabotulinum toxin A; 0 placebo) or personal reasons (3 onabotulinum toxin A; 4 placebo). Demographic and clinical characteristics of the study population at baseline are reported in Table 1. Headache pain intensity and assessment of disability (MIDAS and HIT-6) at baseline were reported as Online Resource 1. The prevalence of cutaneous allodynia, pericranial muscle tenderness, type of migraine pain and drug overuse is summarized in Table 2. There were no betweengroup significant differences at baseline for demographic and clinical characteristics (Table 1), as well as for headache pain intensity and disability measurements (MIDAS and HIT-6) (Online Resource 1). Outcome measures Overall subjects When the whole group of randomized subjects (onabotulinum toxin A and placebo) was considered, despite a clear tendency of onabotulinum toxin A-treated subjects to show better results than placebo-treated subjects, no significant differences were detected in primary (headache days) and Table 1 Demographic and clinical characteristics of the study population at baseline and at 4, 8 and 12 weeks BoNTA (n = 27) Placebo (n = 29) p values Mean age 48.5 ± 9.2 (28 65) 49.0 ± 10.1 (28 64) (years) Female Duration (years) Mean headache days/28 days Baseline 24.2 ± 5.0 (14 30) 25.5 ± 5.6 (15 30) ± 8.2 (0 30) 19.0 ± 9.6 (0 30) ± 9.1 (1 30) 18.0 ± 9.5 (0 30) ± 9.0 (4 30) 15.9 ± 9.5 (0 30) Mean acute pain drug consumption/28 days Baseline 31.0 ± 12.7 (12 60) 34.7 ± 18.5 (12 90) ± 12.8 (0 56) 19.6 ± 15.3 (0 60) ± 14.3 (2 60) 19.0 ± 15.5 (0 60) ± 14.6 (0 58) 18.0 ± 14.4 (0 90) Mean days with acute pain drug consumption/28 days Baseline 22.7 ± 6.4 (12 30) 23.6 ± 6.6 (12 30) ± 9.0 (0 30) 15.3 ± 10.1 (0 30) ± 9.5 (1 30) 15.1 ± 10.2 (0 30) ± 10.1 (2 30) 14.3 ± 9.1 (0 30) Table 2 Headache characteristics of the study population at baseline BoNTA (n = 27) Placebo (n = 29) Headache characteristics Cutaneous allodynia 21 (77.8%) 25 (86.2%) Pericranial muscle tenderness 14 (51.9%) 15 (51.7%) Exploding pain 12 (44.4%) 10 (34.5%) Imploding pain 13 (48.1%) 14 (48.3%) Ocular pain 2 (7.4%) 5 (17.2%) Drug overused Combination 5 (18.5%) 6 (20.7%) Ergot 1 (3.7%) 1 (3.4%) FANS 10 (37.0%) 13 (44.8%) Triptans 11 (40.7%) 9 (31.0%) secondary (acute pain drug consumption, days with acute pain drug consumption) end points, pain intensity and headache impact on functioning (HIT-6 and MIDAS), except for a significant reduction in mean acute pain drug consumption at 12 weeks in the onabotulinum toxin A-treated compared to placebo-treated patients (Table 1). Subjects with pericranial muscle tenderness and cephalic allodynia Significant differences in onabotulinum toxin A-treated versus placebo-treated patients were observed for primary
5 J Headache Pain (2011) 12: and secondary end points at 12 weeks in those with pericranial muscle tenderness. In patients with pericranial muscle tenderness, onabotulinum toxin A-treatment was found to show, when compared with placebo treatment, a significant reduction in frequency of headache days (primary end point) (Fig. 2), as well as in both headache pain medication intake (Fig. 3) and days with acute headache medication consumption (Fig. 4) for the 28-day period at 12 weeks. Furthermore, a statistical significant reduction in scores for pain intensity as well as for disability measures, MIDAS and HIT-6, were detected at both 4 and 12 weeks in onabotulinum toxin A-treated when compared with placebo-treated patients (Online Resource 2 Figs. 1 3). No differences were detected at any time point between the onabotulinum toxin A- and placebo-treated subjects in primary and secondary end points, as well as in pain intensity and headache impact on functioning scores in subgroups of patients with cephalic allodynia (all p [ 0.05). Fig. 4 Secondary end point: mean change (±SE) from baseline in days with acute headache medication consumption in MOH patients with pericranial muscle tenderness Subjects with exploding versus imploding/ocular headache In the subgroups of randomized subjects based on the type of headache pain (exploding and imploding/ocular), no significant differences were found between onabotulinum toxin A- and placebo-treated patients, except for a significantly better mean MIDAS score at 4 (p = 0.012) and 12 (p = 0.008) weeks in the exploding pain subgroup that had onabotulinum toxin A treatment when compared with placebo treatment. Responders versus non-responders Fig. 2 Primary end point: mean change (±SE) from baseline in frequency of headache days for the 28-day period in MOH patients with pericranial muscle tenderness A significantly greater percentage of onabotulinum toxin A-treated than placebo-treated patients had at least a 50% decrease from baseline in the frequency of headache days when both headache days at 12 weeks (Z =-2.915; p = 0.004) and that across all time points (Z = 2.121; p = 0.034) were considered (Fig. 5). Fig. 3 Secondary end point: mean change (±SE) from baseline in acute headache pain medication intake for the 28-day period in MOH patients with pericranial muscle tenderness Fig. 5 Percentage of patients with at least a 50% decrease from baseline in the frequency of headache days across all time points and at 12 weeks in BoNTA and placebo treated
6 432 J Headache Pain (2011) 12: Safety A total of 16 (28.5%) subjects in the randomized population experienced adverse events. Treatment-related adverse events were reported in 25.9% of the onabotulinum toxin A-treated (7 patients) and in 17.2% of the placebo-treated (5 patients) patients. Two patients randomized to onabotulinum toxin A (7.4%) discontinued due to adverse events (neck pain). No clinically significant serious adverse events were reported in any of the 56 subjects. Most common adverse events ([5%) were pain at the site of injection and muscular weakness, all of which resolved without sequelae. Discussion The study evaluated the efficacy and safety of onabotulinum toxin A as prophylactic treatment in MOH patients with migraine as primary headache, reporting on clinical features that could play as predictors of response to onabotulinum toxin A. Results showed that when the whole group of randomized subjects was considered, a significant reduction in mean acute pain drug consumption at 12 weeks, as well as a clear but not significant trend toward better clinical results across all time points in primary and other secondary end points in favor of onabotulinum toxin A-treated when compared with placebo-treated patients was observed. It is worth noting that a significantly greater percentage of onabotulinum toxin A-treated with respect to placebo-treated patients showed 50% or more improvement in the primary end point (mean headache days), both when the 12-week time point and the entire post-treatment period, from 4 to 12 weeks, were considered. The most relevant result of the study emerged when the subgroup of patients with muscular tenderness was considered. In this case, a significant improvement in both primary (mean headache days) and secondary end points (mean drugs consumption and mean days with consumption) at 12 weeks, as well as in pain intensity and headache impact on functioning (HIT-6 and MIDAS) across all time points (4 and 12 weeks) was found. The analysis of the results should take into account some questions. The sample size was not sufficient to reach an adequate statistical power and we could only speculate on the results. In this sense, the lack of significance in the primary end point in the whole population could be a consequence of a small sample size. However, a clear trend toward a better performance of the onabotulinum toxin A-treated patients across all time points and for all considered parameters, including pain perception and disability measures, was detected. There were no significant differences favoring placebo for any efficacy variable at any time point in the study. Furthermore, the proportion of responders was clearly in favor of onabotulinum toxin A-treated. In addition, as the patients underwent withdrawal treatment due to a medication-overuse, the role of this treatment in the clinical improvement should be taken into account. Withdrawal treatment represents a pivotal strategy to treat patients with MOH [28] and this is also confirmed from the clear clinical improvement observed in MOH patients treated with placebo. However, as the intake of acute pain medication and the withdrawal treatment were similar between the groups (placebo and onabotulinum toxin A), but the proportion of responders was clearly in favor of the onabotulinum toxin A treated, we hypothesized that the injection of onabotulinum toxin A could be responsible for this further significant clinical improvement detectable in MOH patients treated with onabotulinum toxin A. Another relevant result is the statistically significant improvement in patients-reported quality of life measures, such as HIT-6 and MIDAS scores, observed in onabotulinum toxin A-treated patients with pericranial muscle tenderness and muscular allodynia when compared with the placebo treated. Treatment-related adverse events were reported in 25.9% of the onabotulinum toxin A-treated (7 patients), and 7.4% of the onabotulinum toxin A-treated patients (2 patients) discontinued due to treatment-related adverse events. No clinically significant serious adverse events were reported in any of the 56 subjects. These data confirm the favorable safety profile of onabotulinum toxin A injected into the head and neck muscles. Our data confirm and support previous clinical trial findings obtained in patients with chronic migraine in which only two-thirds overused acute pain medication during the baseline period [15 17]. As the presence of medication overuse represents a risk factor for the development of chronification [3, 6] as well as a factor that reduces the efficacy of the prophylactic treatment [8], the success rate of preventing migraine attacks using onabotulinum toxin A in our MOH samples could be considered a further confirmation of the efficacy of this treatment in chronic migraine prophylaxis and, in particular, in patients with peculiar clinical characteristics such as pericranial muscle tenderness. From a pathophysiological point of view, as in a previous study, we demonstrate that the withdrawal treatment reduces both the clinical severity as well as the sensitization in pain processing that take place in patients with MOH [24]. We hypothesize that, in view of these results, onabotulinum toxin A could influence, through the inhibition of peripheral sensitization [21], the central mechanisms responsible for the facilitation in pain processing, which contribute to the development and maintenance of chronification in these patients.
7 J Headache Pain (2011) 12: In conclusion, our data permit the identification as predictor of clinical response to onabotulinum toxin A in patients with complicated form of migraine such as MOH, the presence of pericranial muscle tenderness and so to support it as prophylactic treatment in patients with these features. Acknowledgments Irvine, CA, USA. Conflict of interest The study was sponsored by Allergan, Inc., None. Open Access This article is distributed under the terms of the Creative Commons Attribution License which permits any use, distribution and reproduction in any medium, provided the original author(s) and source are credited. References 1. Headache Classification Subcommittee of the International Headache Society (2004) The international classification of headache disorders: 2nd edition. Cephalalgia 24(Suppl 1): Headache Classification Committee of the International Headache Society (2006) New appendix criteria open for a broader concept of chronic migraine. Cephalalgia 26: Zwart JA, Dyb G, Hagen K, Svebak S, Holmen J (2003) Analgesic use: a predictor of chronic pain and medication overuse headache: the head-hunt study. Neurology 61(2): Colas R, Munoz P, Temprano R, Gomez C, Pascual J (2004) Chronic daily headache with analgesic overuse: epidemiology and impact on quality of life. Neurology 62(8): Dowson AJ (2003) Analysis of the patients attending a specialist UK headache clinic over a 3-year period. Headache 43: Sances G, Ghiotto N, Loi M, Guaschino E, Marchioni E, Catarci T, Nappi G (2005) A CARE: pathway in medication-overuse headache: the experience of the Headache Centre in Pavia. J Headache Pain 6(4): Nappi G, Perrotta A, Rossi P, Sandrini G (2008) Chronic daily headache. Expert Rev Neurother 8(3): Review 8. Katsarava Z, Muessig M, Dzagnidze A, Fritsche G, Diener HC, Limmroth V (2005) Medication overuse headache: rates and predictors for relapse in a 4-year prospective study. Cephalalgia 25: Aurora SK, Gawel M, Brandes JL, Pokta S, VanDenburgh AM (2007) Botulinum toxin type A prophylactic treatment of episodic migraine: a randomized, double-blind, placebo-controlled exploratory study. Headache 47: Relja M, Poole AC, Schoenen J, Pascual J, Lei X, Thompson C (2007) A multicentre, double-blind, randomized, placebo-controlled, parallel group study of multiple treatments of botulinum toxin type A (BoNTA) for the prophylaxis of episodic migraine headaches. Cephalalgia 27: Schulte-Mattler WJ, Krack P, BoNTTH Study Group (2004) Treatment of chronic tension-type headache with botulinum toxin A: a randomized, double-blind, placebo-controlled multicenter study. Pain 109(1 2): Padberg M, de Bruijn SF, de Haan RJ, Tavy DL (2004) Treatment of chronic tension-type headache with botulinum toxin: a double-blind, placebo-controlled clinical trial. Cephalalgia 24(8): Silberstein SD, Gobel H, Jensen R et al (2006) Botulinum toxin type A in the prophylactic treatment of chronic tension-type headache: a multicentre, double-blind, randomized, placebocontrolled, parallel-group study. Cephalalgia 26: Aurora SK, Dodick DW, Turkel CC, DeGryse RE, Silberstein SD, Lipton RB, Diener HC, Brin MF (2010) PREEMPT 1 Chronic Migraine Study Group. Onabotulinum toxin A for treatment of chronic migraine: results from the double-blind, randomized, placebo-controlled phase of the PREEMPT 1 trial. Cephalalgia 30(7): Farinelli I, Coloprisco G, De Filippis S, Martelletti P (2006) Long-term benefits of botulinum toxin type A (BOTOX) in chronic daily headache: a five-year long experience. J Headache Pain 7(6): Diener HC, Dodick DW, Aurora SK, Turkel CC, DeGryse RE, Lipton RB, Silberstein SD, Brin MF (2010) PREEMPT 2 Chronic Migraine Study Group. Onabotulinum toxin A for treatment of chronic migraine: results from the double-blind, randomized, placebo-controlled phase of the PREEMPT 2 trial. Cephalalgia 30(7): Dodick DW, Turkel CC, DeGryse RE, Aurora SK, Silberstein SD, Lipton RB, Diener HC, Brin MF (2010) PREEMPT Chronic Migraine Study Group. Onabotulinum toxin A for treatment of chronic migraine: pooled results from the double-blind, randomized, placebo-controlled phases of the PREEMPT clinical program. Headache 50(6): Mathew NT, Kailasam J, Meadors L (2008) Predictors of response to botulinum toxin type A (BoNTA) in chronic daily headache. Headache 48(2): Jakubowski M, McAllister PJ, Bajwa ZH, Ward TN, Smith P, Burstein R (2006) Exploding vs. imploding headache in migraine prophylaxis with botulinum toxin A. Pain 125(3): Burstein R, Dodick D, Silberstein S (2009) Migraine prophylaxis with botulinum toxin A is associated with perception of headache. Toxicon 54(5): Aoki KR (2005) Review of a proposed mechanism for the antinociceptive action of botulinum toxin type A. Neurotoxicology 26: Mongini F, Ciccone G, Deregibus A, Ferrero L, Mongini T (2004) Muscle tenderness in different headache types and its relation to anxiety and depression. Pain 112(1 2): Ayzenberg I, Obermann M, Nyhuis P, Gastpar M, Limmroth V, Diener HC, Kaube H, Katsarava Z (2006) Central sensitization of the trigeminal and somatic nociceptive systems in medication overuse headache mainly involves cerebral supraspinal structures. Cephalalgia 26(9): Perrotta A, Serrao M, Sandrini G, Burstein R, Sances G, Rossi P, Bartolo M, Pierelli F, Nappi G (2010) Sensitisation of spinal cord pain processing in medication overuse headache involves supraspinal pain control. Cephalalgia 30(3): Wolfe F, Smythe HA, Yunus MB, Bennett RM, Bombardier C, Goldenberg DL et al (1990) The American College of Rheumatology 1990 criteria for the classification of fibromyalgia: report of the Multicenter Criteria Committee. Arthritis Rheum 33: Bruehl S, Harden RN, Galer BS, Saltz S, Bertram M, Backonja M et al (1999) External validation of IASP diagnostic criteria for complex regional pain syndrome and proposed research diagnostic criteria. International Association for the Study of Pain. Pain 81: Cruccu G, Anand P, Attal N, Garcia-Larrea L, Haanpää M, Jørum E et al (2004) EFNS guidelines on neuropathic pain assessment. Eur J Neurol 11: Ghiotto N, Sances G, Galli F, Tassorelli C, Guaschino E, Sandrini G, Nappi G (2009) Medication overuse headache and applicability of the ICHD-II diagnostic criteria: 1-year follow-up study (CARE I protocol). Cephalalgia 29(2): Mathew NT, Kailasam J, Seifert T (2004) Clinical recognition of allodynia in migraine. Neurology 63(5):
Does analgesic overuse matter? Response to OnabotulinumtoxinA in patients with chronic migraine with or without medication overuse
 DOI 10.1186/s40064-015-1386-8 RESEARCH Open Access Does analgesic overuse matter? Response to OnabotulinumtoxinA in patients with chronic migraine with or without medication overuse Fayyaz Ahmed *, Hassan
DOI 10.1186/s40064-015-1386-8 RESEARCH Open Access Does analgesic overuse matter? Response to OnabotulinumtoxinA in patients with chronic migraine with or without medication overuse Fayyaz Ahmed *, Hassan
A two years open-label prospective study of OnabotulinumtoxinA 195 U in medication overuse headache: a real-world experience
 Negro et al. The Journal of Headache and Pain (2016) 17:1 DOI 10.1186/s10194-016-0591-3 RESEARCH ARTICLE A two years open-label prospective study of OnabotulinumtoxinA 195 U in medication overuse headache:
Negro et al. The Journal of Headache and Pain (2016) 17:1 DOI 10.1186/s10194-016-0591-3 RESEARCH ARTICLE A two years open-label prospective study of OnabotulinumtoxinA 195 U in medication overuse headache:
Medication overuse headache: a critical review of end points in recent follow-up studies
 J Headache Pain (2010) 11:373 377 DOI 10.1007/s10194-010-0221-4 REVIEW ARTICLE Medication overuse headache: a critical review of end points in recent follow-up studies Knut Hagen Rigmor Jensen Magne Geir
J Headache Pain (2010) 11:373 377 DOI 10.1007/s10194-010-0221-4 REVIEW ARTICLE Medication overuse headache: a critical review of end points in recent follow-up studies Knut Hagen Rigmor Jensen Magne Geir
Prednisone vs. placebo in withdrawal therapy following medication overuse headache
 doi:10.1111/j.1468-2982.2007.01488.x Prednisone vs. placebo in withdrawal therapy following medication overuse headache L Pageler 1,2, Z Katsarava 2, HC Diener 2 & V Limmroth 1,2 1 Department of Neurology,
doi:10.1111/j.1468-2982.2007.01488.x Prednisone vs. placebo in withdrawal therapy following medication overuse headache L Pageler 1,2, Z Katsarava 2, HC Diener 2 & V Limmroth 1,2 1 Department of Neurology,
Aleksandra Radojičić. Headache Center, Neurology Clinic, Clinical Center of Serbia
 European Headache School Belgrade 2012 MEDICATION OVERUSE HEADACHE Aleksandra Radojičić Headache Center, Neurology Clinic, Clinical Center of Serbia Historical data First cases were described in XVII century
European Headache School Belgrade 2012 MEDICATION OVERUSE HEADACHE Aleksandra Radojičić Headache Center, Neurology Clinic, Clinical Center of Serbia Historical data First cases were described in XVII century
David W. Dodick M.D. Professor Director of Headache Medicine Department of Neurology Mayo Clinic Phoenix Arizona USA
 Headache Masters School 2013 in Asia Sunday March 24, 2013 Procedural Medicine Workshop Onabotulinumtoxin A: Evidence, Injection Technique, and Mechanism of Action David W. Dodick M.D. Professor Director
Headache Masters School 2013 in Asia Sunday March 24, 2013 Procedural Medicine Workshop Onabotulinumtoxin A: Evidence, Injection Technique, and Mechanism of Action David W. Dodick M.D. Professor Director
OnabotulinumtoxinA treatment for chronic migraine: experience in 52 patients treated with the PREEMPT paradigm
 Pedraza et al. SpringerPlus (2015) 4:176 DOI 10.1186/s40064-015-0957-z a SpringerOpen Journal RESEARCH Open Access OnabotulinumtoxinA treatment for chronic migraine: experience in 52 patients treated with
Pedraza et al. SpringerPlus (2015) 4:176 DOI 10.1186/s40064-015-0957-z a SpringerOpen Journal RESEARCH Open Access OnabotulinumtoxinA treatment for chronic migraine: experience in 52 patients treated with
OnabotulinumtoxinA 155 U in medication overuse headache: a two years prospective study
 OnabotulinumtoxinA 155 U in medication overuse headache: a two years prospective study The Harvard community has made this article openly available. Please share how this access benefits you. Your story
OnabotulinumtoxinA 155 U in medication overuse headache: a two years prospective study The Harvard community has made this article openly available. Please share how this access benefits you. Your story
Expert Opinion. OnabotulinumtoxinA for Chronic Migrainehead_2071 CLINICAL HISTORY. Andrew Blumenfeld, MD; Randolph W. Evans, MD
 142..148 Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.02081.x Published by Wiley Periodicals, Inc. Expert Opinion OnabotulinumtoxinA for Chronic Migrainehead_2071
142..148 Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.02081.x Published by Wiley Periodicals, Inc. Expert Opinion OnabotulinumtoxinA for Chronic Migrainehead_2071
Mark W. Green, MD, FAAN
 Mark W. Green, MD, FAAN Professor of Neurology, Anesthesiology, and Rehabilitation Medicine Director of Headache and Pain Medicine Icahn School of Medicine at Mt Sinai New York Pain-sensitive structures
Mark W. Green, MD, FAAN Professor of Neurology, Anesthesiology, and Rehabilitation Medicine Director of Headache and Pain Medicine Icahn School of Medicine at Mt Sinai New York Pain-sensitive structures
What is the Effectiveness of OnabotulinumtoxinA (Botox ) in Reducing the Number of Chronic Migraines (CM) in Patients Years Old?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 What is the Effectiveness of OnabotulinumtoxinA
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 What is the Effectiveness of OnabotulinumtoxinA
The majority of primary headaches fall into
 NEUROTOXINS Neurotoxins: Expanding Uses of Neuromodulators in Medicine Headache Edward Nahabet, BA Jeffrey E. Janis, MD, FACS Bahman Guyuron, MD, FACS Cleveland and Columbus, Ohio Summary: Over the course
NEUROTOXINS Neurotoxins: Expanding Uses of Neuromodulators in Medicine Headache Edward Nahabet, BA Jeffrey E. Janis, MD, FACS Bahman Guyuron, MD, FACS Cleveland and Columbus, Ohio Summary: Over the course
Signe B Munksgaard, Lars Bendtsen and Rigmor H Jensen. Introduction. Original Article
 Original Article Detoxification of medication-overuse headache by a multidisciplinary treatment programme is highly effective: A comparison of two consecutive treatment methods in an open-label design
Original Article Detoxification of medication-overuse headache by a multidisciplinary treatment programme is highly effective: A comparison of two consecutive treatment methods in an open-label design
Defining the Differences Between Episodic Migraine and Chronic Migraine
 Curr Pain Headache Rep (2012) 16:86 92 DOI 10.1007/s11916-011-0233-z CHRONIC DAILY HEADACHE (SJ WANG, SECTION EDITOR) Defining the Differences Between Episodic Migraine and Chronic Migraine Zaza Katsarava
Curr Pain Headache Rep (2012) 16:86 92 DOI 10.1007/s11916-011-0233-z CHRONIC DAILY HEADACHE (SJ WANG, SECTION EDITOR) Defining the Differences Between Episodic Migraine and Chronic Migraine Zaza Katsarava
Botulinum Neurotoxin for Chronic Migraine and Trigeminal Neuralgia
 Botulinum Neurotoxin for Chronic Migraine and Trigeminal Neuralgia David W. Dodick, MD Professor Department of Neurology, Mayo Clinic Phoenix Arizona, USA Onabotulinumtoxin A is the only botulinum toxin
Botulinum Neurotoxin for Chronic Migraine and Trigeminal Neuralgia David W. Dodick, MD Professor Department of Neurology, Mayo Clinic Phoenix Arizona, USA Onabotulinumtoxin A is the only botulinum toxin
National Institute for Health and Clinical Excellence. Single Technology Appraisal (STA)
 National Institute for Health and Clinical Excellence Comment 1: the draft remit Single Technology Appraisal (STA) Botulinum toxin type A for the prophylaxis of headaches in adults with chronic migraine
National Institute for Health and Clinical Excellence Comment 1: the draft remit Single Technology Appraisal (STA) Botulinum toxin type A for the prophylaxis of headaches in adults with chronic migraine
Is OnabotulinumtoxinA Good for Other Head and Face Pain? Disclosures BoNT/A for non- CM Botulinum neurotoxin (BoNT) in clinical use for headache >20
 1 2 3 4 5 6 Is OnabotulinumtoxinA Good for Other Head and Face Pain? Disclosures BoNT/A for non- CM Botulinum neurotoxin (BoNT) in clinical use for headache >20 years Efficacy of BoNT type A (onabotulinumtoxina,
1 2 3 4 5 6 Is OnabotulinumtoxinA Good for Other Head and Face Pain? Disclosures BoNT/A for non- CM Botulinum neurotoxin (BoNT) in clinical use for headache >20 years Efficacy of BoNT type A (onabotulinumtoxina,
Research Submission. Accepted for publication December 14, 2004.
 Research Submission Botulinum Toxin Type A for the Prophylaxis of Chronic Daily Headache: Subgroup Analysis of Patients Not Receiving Other Prophylactic Medications: A Randomized Double-Blind, Placebo-Controlled
Research Submission Botulinum Toxin Type A for the Prophylaxis of Chronic Daily Headache: Subgroup Analysis of Patients Not Receiving Other Prophylactic Medications: A Randomized Double-Blind, Placebo-Controlled
2 nd Resubmission. 13 January 2017
 2 nd Resubmission botulinum toxin A, 50 Allergan units, 100 Allergan units, 200 Allergan units, powder for solution for injection (Botox ) SMC No. (692/11) Allergan Limited 13 January 2017 The Scottish
2 nd Resubmission botulinum toxin A, 50 Allergan units, 100 Allergan units, 200 Allergan units, powder for solution for injection (Botox ) SMC No. (692/11) Allergan Limited 13 January 2017 The Scottish
Long-term benefits of botulinum toxin type A (BOTOX) in chronic daily headache: a five-year long experience
 J Headache Pain (26) 7:47 412 DOI 1.17/s1194-6-344-9 RAPID COMMUNICATION Ivano Farinelli Gabriella Coloprisco Sergio De Filippis Paolo Martelletti Long-term benefits of botulinum toxin type A (BOTOX) in
J Headache Pain (26) 7:47 412 DOI 1.17/s1194-6-344-9 RAPID COMMUNICATION Ivano Farinelli Gabriella Coloprisco Sergio De Filippis Paolo Martelletti Long-term benefits of botulinum toxin type A (BOTOX) in
Aalborg Universitet. Botulinum neurotoxin A for chronic migraine headaches Cairns, Brian Edwin; Gazerani, Parisa. Published in: Pain Management
 Aalborg Universitet Botulinum neurotoxin A for chronic migraine headaches Cairns, Brian Edwin; Gazerani, Parisa Published in: Pain Management DOI (link to publication from Publisher): 10.2217/PMT.14.30
Aalborg Universitet Botulinum neurotoxin A for chronic migraine headaches Cairns, Brian Edwin; Gazerani, Parisa Published in: Pain Management DOI (link to publication from Publisher): 10.2217/PMT.14.30
Medication overuse headache is a severe chronic pain condition that is preventable and treatable. An International Experience
 Medication overuse headache is a severe chronic pain condition that is preventable and treatable An International Experience C. Tassorelli Chair of Neurolgy, Department of Brain and Behavioral Sciences,
Medication overuse headache is a severe chronic pain condition that is preventable and treatable An International Experience C. Tassorelli Chair of Neurolgy, Department of Brain and Behavioral Sciences,
Botulinum toxin type A is currently being
 EMERGING PREVENTIVE OPTIONS FOR CHRONIC DAILY HEADACHE * David W. Dodick, MD, FRCP(C), FACP ABSTRACT Approximately 3% to 5% of the population is affected by headaches on a daily or almost daily basis.
EMERGING PREVENTIVE OPTIONS FOR CHRONIC DAILY HEADACHE * David W. Dodick, MD, FRCP(C), FACP ABSTRACT Approximately 3% to 5% of the population is affected by headaches on a daily or almost daily basis.
A one-year prospective costing study of botulinum toxin type A treatment of chronic tension headache
 J Headache Pain (2004) 5:192 196 DOI 10.1007/s10194-004-0100-3 ORIGINAL Fabio Palazzo Francesco S. Mennini Laura Fioravanti Laura Piasini Gabriella Coloprisco Paolo Martelletti A one-year prospective costing
J Headache Pain (2004) 5:192 196 DOI 10.1007/s10194-004-0100-3 ORIGINAL Fabio Palazzo Francesco S. Mennini Laura Fioravanti Laura Piasini Gabriella Coloprisco Paolo Martelletti A one-year prospective costing
10/17/2017 CHRONIC MIGRAINES BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES PATIENT CASE EPIDEMIOLOGY EPIDEMIOLOGY
 BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES JENNIFER SHIN, PHARMD PGY2 AMBULATORY CARE PHARMACY RESIDENT COMMUNITYCARE HEALTH CENTERS PHARMACOTHERAPY ROUNDS OCTOBER 20, 2017
BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES JENNIFER SHIN, PHARMD PGY2 AMBULATORY CARE PHARMACY RESIDENT COMMUNITYCARE HEALTH CENTERS PHARMACOTHERAPY ROUNDS OCTOBER 20, 2017
Treatment Of Medication. Overuse Headache
 7 November 2012 BASH GPwSI Meeting Lecture title... Treatment Of Medication Dr... Overuse Headache Dr Marcus Lewis Dr... The National Migraine Centre International Headache Society Diagnostic criteria
7 November 2012 BASH GPwSI Meeting Lecture title... Treatment Of Medication Dr... Overuse Headache Dr Marcus Lewis Dr... The National Migraine Centre International Headache Society Diagnostic criteria
Chronic Migraine in Primary Care. December 11 th, 2017 Werner J. Becker University of Calgary
 Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
An Overview of MOH. ALAN M. Rapoport, M.D. Clinical Professor of Neurology The David Geffen School of Medicine at UCLA Los Angeles, California
 An Overview of MOH IHS ASIAN HA MASTERS SCHOOL MARCH 24, 2013 ALAN M. Rapoport, M.D. Clinical Professor of Neurology The David Geffen School of Medicine at UCLA Los Angeles, California President-Elect
An Overview of MOH IHS ASIAN HA MASTERS SCHOOL MARCH 24, 2013 ALAN M. Rapoport, M.D. Clinical Professor of Neurology The David Geffen School of Medicine at UCLA Los Angeles, California President-Elect
medications. This was an openlabel study consisting of patients with migraines who historically failed to respond to oral triptan
 J Headache Pain (2007) 8:13 18 DOI 10.1007/s10194-007-0354-7 ORIGINAL Seymour Diamond Fred G. Freitag Alexander Feoktistov George Nissan Sumatriptan 6 mg subcutaneous as an effective migraine treatment
J Headache Pain (2007) 8:13 18 DOI 10.1007/s10194-007-0354-7 ORIGINAL Seymour Diamond Fred G. Freitag Alexander Feoktistov George Nissan Sumatriptan 6 mg subcutaneous as an effective migraine treatment
Field testing of the ICHD-3β and expert opinion criteria for chronic migraine
 Jiang et al. The Journal of Headache and Pain (2016) 17:85 DOI 10.1186/s10194-016-0678-x The Journal of Headache and Pain RESEARCH ARTICLE Open Access Field testing of the ICHD-3β and expert opinion criteria
Jiang et al. The Journal of Headache and Pain (2016) 17:85 DOI 10.1186/s10194-016-0678-x The Journal of Headache and Pain RESEARCH ARTICLE Open Access Field testing of the ICHD-3β and expert opinion criteria
Preventive Effect of Greater Occipital Nerve Block on Severity and Frequency of Migraine Headache
 Global Journal of Health Science; Vol. 6, No. 6; 2014 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Preventive Effect of Greater Occipital Nerve Block on Severity
Global Journal of Health Science; Vol. 6, No. 6; 2014 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Preventive Effect of Greater Occipital Nerve Block on Severity
A Multi-Center Double-Blind Pilot Comparison of OnabotulinumtoxinA and Topiramate for the Prophylactic Treatment of Chronic Migrainehead_
 Headache 2010 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2010.01796.x Published by Wiley Periodicals, Inc. Research Submission A Multi-Center Double-Blind Pilot Comparison of OnabotulinumtoxinA
Headache 2010 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2010.01796.x Published by Wiley Periodicals, Inc. Research Submission A Multi-Center Double-Blind Pilot Comparison of OnabotulinumtoxinA
Effectiveness of Pharmacological Treatments in Imploding vs. Exploding Headaches
 Effectiveness of Pharmacological Treatments in Imploding vs. Exploding Headaches Item Type Thesis Authors Hunt, Megan Publisher The University of Arizona. Rights Copyright is held by the author. Digital
Effectiveness of Pharmacological Treatments in Imploding vs. Exploding Headaches Item Type Thesis Authors Hunt, Megan Publisher The University of Arizona. Rights Copyright is held by the author. Digital
Chronic daily headache (CDH), defined
 FINDING A FIT: STRATEGIES FOR CHRONIC MIGRAINE PROPHYLAXIS David W. Dodick, MD, FRCP(C), FACP ABSTRACT Chronic daily headache (CDH) affects approximately 4% to 5% of the population and is responsible for
FINDING A FIT: STRATEGIES FOR CHRONIC MIGRAINE PROPHYLAXIS David W. Dodick, MD, FRCP(C), FACP ABSTRACT Chronic daily headache (CDH) affects approximately 4% to 5% of the population and is responsible for
NIH Public Access Author Manuscript Curr Pain Headache Rep. Author manuscript; available in PMC 2014 May 22.
 NIH Public Access Author Manuscript Published in final edited form as: Curr Pain Headache Rep. 2009 December ; 13(6): 463 469. Tension-type Headache With Medication Overuse: Pathophysiology and Clinical
NIH Public Access Author Manuscript Published in final edited form as: Curr Pain Headache Rep. 2009 December ; 13(6): 463 469. Tension-type Headache With Medication Overuse: Pathophysiology and Clinical
Chronic migraine plus medication overuse headache: two entities or not?
 J Headache Pain (2011) 12:593 601 DOI 10.1007/s10194-011-0388-3 REVIEW ARTICLE Chronic migraine plus medication overuse headache: two entities or not? Andrea Negro Paolo Martelletti Received: 7 June 2011
J Headache Pain (2011) 12:593 601 DOI 10.1007/s10194-011-0388-3 REVIEW ARTICLE Chronic migraine plus medication overuse headache: two entities or not? Andrea Negro Paolo Martelletti Received: 7 June 2011
Recognition and treatment of medication overuse headache
 Recognition and treatment of medication overuse headache Marcus Lewis MA, MRCGP, DRCOG, DFSRH 20 Mean weekly headache index 15 10 5 Medication overuse headache is a common condition responsible for a high
Recognition and treatment of medication overuse headache Marcus Lewis MA, MRCGP, DRCOG, DFSRH 20 Mean weekly headache index 15 10 5 Medication overuse headache is a common condition responsible for a high
INDIVIDUAL STUDY TABLE REFERRING TO PART OF THE DOSSIER Volume: Page:
 SYNOPSIS Protocol No.: TOPMAT-MIG-303 EudraCT No.: 2005-000321-29 Title of Study: A double-blind, randomised, placebo-controlled, multicentre study to investigate the efficacy and tolerability of in prolonged
SYNOPSIS Protocol No.: TOPMAT-MIG-303 EudraCT No.: 2005-000321-29 Title of Study: A double-blind, randomised, placebo-controlled, multicentre study to investigate the efficacy and tolerability of in prolonged
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, II. Management of Refractory Headaches
 Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 CGRP Page 1 of 13 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: CGRP (calcitonin gene-related peptide) Prime Therapeutics will review Prior Authorization requests
CGRP Page 1 of 13 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: CGRP (calcitonin gene-related peptide) Prime Therapeutics will review Prior Authorization requests
OnabotulinumtoxinA in the treatment of patients with chronic migraine: clinical evidence and experience
 731521TAN0010.1177/1756285617731521Therapeutic Advances in Neurological DisordersC-C Chiang and AJ Starling research-article2017 Therapeutic Advances in Neurological Disorders Review OnabotulinumtoxinA
731521TAN0010.1177/1756285617731521Therapeutic Advances in Neurological DisordersC-C Chiang and AJ Starling research-article2017 Therapeutic Advances in Neurological Disorders Review OnabotulinumtoxinA
Atenolol in the prophylaxis of chronic migraine: a 3-month open-label study
 Edvardsson SpringerPlus 2013, 2:479 a SpringerOpen Journal RESEARCH Open Access Atenolol in the prophylaxis of chronic migraine: a 3-month open-label study Bengt Edvardsson Abstract Background: Chronic
Edvardsson SpringerPlus 2013, 2:479 a SpringerOpen Journal RESEARCH Open Access Atenolol in the prophylaxis of chronic migraine: a 3-month open-label study Bengt Edvardsson Abstract Background: Chronic
Psychiatric Comorbidity in Transformed Migraine: Presentation, Treatment, Impact and Outcome
 Jefferson Journal of Psychiatry Volume 23 Issue 1 Article 3 December 2010 Psychiatric Comorbidity in Transformed Migraine: Presentation, Treatment, Impact and Outcome Muhammad A. Abbas M.D Thomas Jefferson
Jefferson Journal of Psychiatry Volume 23 Issue 1 Article 3 December 2010 Psychiatric Comorbidity in Transformed Migraine: Presentation, Treatment, Impact and Outcome Muhammad A. Abbas M.D Thomas Jefferson
Specific Objectives A. Topics to be lectured and discussed at the plenary sessions
 Specific Objectives A. Topics to be lectured and discussed at the plenary sessions 0. Introduction: Good morning ICHD-III! Let s start at the very beginning. When you read you begin with A-B-C, so when
Specific Objectives A. Topics to be lectured and discussed at the plenary sessions 0. Introduction: Good morning ICHD-III! Let s start at the very beginning. When you read you begin with A-B-C, so when
Physiotherapy for tension-type headache: a controlled study
 Blackwell Science, LtdOxford, UKCHACephalalgia1468-2982Blackwell Science, 232412936Original ArticlePhysiotherapy for tension-type headachep Torelli et al. Physiotherapy for tension-type headache: a controlled
Blackwell Science, LtdOxford, UKCHACephalalgia1468-2982Blackwell Science, 232412936Original ArticlePhysiotherapy for tension-type headachep Torelli et al. Physiotherapy for tension-type headache: a controlled
6/20/2018 PROCEDURAL TREATMENTS FOR HEADACHE. Case study: Emily. Diary
 Headache severity (Scale 0 10) Topiramate started on July 20, D/C July 29 Amitriptyline initiated, D/C on Sep 23 PROCEDURAL TREATMENTS FOR HEADACHE Andrew M. Blumenfeld Director of the Headache Center
Headache severity (Scale 0 10) Topiramate started on July 20, D/C July 29 Amitriptyline initiated, D/C on Sep 23 PROCEDURAL TREATMENTS FOR HEADACHE Andrew M. Blumenfeld Director of the Headache Center
Early treatment of a migraine attack while pain is still mild increases the efficacy of sumatriptan
 Blackwell Science, LtdOxford, UKCHACephalalgia1468-2982Blackwell Science, 20042411925933Original ArticleEarly treatment of migraine with sumatriptanj Scholpp et al. Early treatment of a migraine attack
Blackwell Science, LtdOxford, UKCHACephalalgia1468-2982Blackwell Science, 20042411925933Original ArticleEarly treatment of migraine with sumatriptanj Scholpp et al. Early treatment of a migraine attack
Botox for Chronic Migraine: Tips and Tricks
 Botox for Chronic Migraine: Tips and Tricks Ten Questions for Andrew M. Blumenfeld, MD Andrew M. Blumenfeld is director of The Headache Center of Southern California. Most of his research has focused on
Botox for Chronic Migraine: Tips and Tricks Ten Questions for Andrew M. Blumenfeld, MD Andrew M. Blumenfeld is director of The Headache Center of Southern California. Most of his research has focused on
Chronic Migraine: Epidemiology and Disease Burden
 Curr Pain Headache Rep (2011) 15:70 78 DOI 10.1007/s11916-010-0157-z Chronic Migraine: Epidemiology and Disease Burden Aubrey N. Manack & Dawn C. Buse & Richard B. Lipton Published online: 10 November
Curr Pain Headache Rep (2011) 15:70 78 DOI 10.1007/s11916-010-0157-z Chronic Migraine: Epidemiology and Disease Burden Aubrey N. Manack & Dawn C. Buse & Richard B. Lipton Published online: 10 November
A new questionnaire for assessment of adverse events associated with triptans: methods of assessment influence the results. Preliminary results
 J Headache Pain (2004) 5:S112 S116 DOI 10.1007/s10194-004-0123-4 Michele Feleppa Fred D. Sheftell Luciana Ciannella Amedeo D Alessio Giancarlo Apice Nino N. Capobianco Donato M.T. Saracino Walter Di Iorio
J Headache Pain (2004) 5:S112 S116 DOI 10.1007/s10194-004-0123-4 Michele Feleppa Fred D. Sheftell Luciana Ciannella Amedeo D Alessio Giancarlo Apice Nino N. Capobianco Donato M.T. Saracino Walter Di Iorio
Preventive Effect of Greater Occipital Nerve Block on Severity and Frequency of Migraine Headache
 Proceeding S.Z.P.G.M.I. Vol: 31(2): pp. 75-79, 2017. Preventive effect of Greater Occipital Nerve Block on Severity and Frequency of Migraine Headache Dr. Syed Mehmood Ali, Dr. Mudassar Aslam, Dr. Dawood
Proceeding S.Z.P.G.M.I. Vol: 31(2): pp. 75-79, 2017. Preventive effect of Greater Occipital Nerve Block on Severity and Frequency of Migraine Headache Dr. Syed Mehmood Ali, Dr. Mudassar Aslam, Dr. Dawood
Inpatient Treatment of Status Migraine With Dihydroergotamine in Children and Adolescents
 Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 CGRP Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: CGRP (calcitonin gene-related peptide) Prime Therapeutics will review Prior Authorization requests
CGRP Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: CGRP (calcitonin gene-related peptide) Prime Therapeutics will review Prior Authorization requests
Medical Policy. Description/Scope. Position Statement. Rationale
 Subject: Document#: Current Effective Date: 06/28/2017 Status: Reviewed Last Review Date: 05/04/2017 Description/Scope This document addresses occipital nerve stimulation (ONS), which involves delivering
Subject: Document#: Current Effective Date: 06/28/2017 Status: Reviewed Last Review Date: 05/04/2017 Description/Scope This document addresses occipital nerve stimulation (ONS), which involves delivering
10/13/17. Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD
 Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD } Depomed Consultant 2014 to present } Avanir Consultant 2014 to present } Amgen
Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD } Depomed Consultant 2014 to present } Avanir Consultant 2014 to present } Amgen
Treatment of withdrawal headache in patients with medication overuse headache: a pilot study
 Cevoli et al. The Journal of Headache and Pain (2017) 18:56 DOI 10.1186/s10194-017-0763-9 The Journal of Headache and Pain RESEARCH ARTICLE Open Access Treatment of withdrawal headache in patients with
Cevoli et al. The Journal of Headache and Pain (2017) 18:56 DOI 10.1186/s10194-017-0763-9 The Journal of Headache and Pain RESEARCH ARTICLE Open Access Treatment of withdrawal headache in patients with
Topiramate plus nortriptyline in the preventive treatment of migraine: a controlled study for nonresponders
 J Headache Pain (2012) 13:53 59 DOI 10.1007/s10194-011-0395-4 ORIGINAL Topiramate plus nortriptyline in the preventive treatment of migraine: a controlled study for nonresponders Abouch Valenty Krymchantowski
J Headache Pain (2012) 13:53 59 DOI 10.1007/s10194-011-0395-4 ORIGINAL Topiramate plus nortriptyline in the preventive treatment of migraine: a controlled study for nonresponders Abouch Valenty Krymchantowski
Botulinum toxin type A for the prevention of headaches in adults with chronic migraine
 Botulinum toxin type A for the prevention of headaches in adults with chronic migraine Issued: June 2012 guidance.nice.org.uk/ta260 NICE has accredited the process used by the Centre for Health Technology
Botulinum toxin type A for the prevention of headaches in adults with chronic migraine Issued: June 2012 guidance.nice.org.uk/ta260 NICE has accredited the process used by the Centre for Health Technology
Medication-overuse headache: epidemiology, diagnosis and treatment
 522683TAW0010.1177/2042098614522683Kristoffersen and LundqvistES Kristoffersen and C Lundqvist research-article2014 Therapeutic Advances in Drug Safety Review Medication-overuse headache: epidemiology,
522683TAW0010.1177/2042098614522683Kristoffersen and LundqvistES Kristoffersen and C Lundqvist research-article2014 Therapeutic Advances in Drug Safety Review Medication-overuse headache: epidemiology,
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache
 MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
RISK FACTORS AND PROGNOSIS OF CHRONIC MIGRAINE
 RISK FACTORS AND PROGNOSIS OF CHRONIC MIGRAINE Gretchen E. Tietjen, MD University of Toledo Toledo, Ohio Learning objectives At the conclusion of this presentation, participants should be able to: 1. Understand
RISK FACTORS AND PROGNOSIS OF CHRONIC MIGRAINE Gretchen E. Tietjen, MD University of Toledo Toledo, Ohio Learning objectives At the conclusion of this presentation, participants should be able to: 1. Understand
Is Yoga an Effective Treatment for Reducing the Frequency of Episodic Migraine?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is Yoga an Effective Treatment for Reducing
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is Yoga an Effective Treatment for Reducing
Migraine and hormonal contraceptives
 Migraine and hormonal contraceptives Department of Community Medicine, Systems Epidemiology University of Tromsø, November 2017 Nora Stensland Bugge Medical research student Presentation outline What is
Migraine and hormonal contraceptives Department of Community Medicine, Systems Epidemiology University of Tromsø, November 2017 Nora Stensland Bugge Medical research student Presentation outline What is
Migraine: Developing Drugs for Acute Treatment Guidance for Industry
 Migraine: Developing Drugs for Acute Treatment Guidance for Industry U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and Research (CDER) February 2018
Migraine: Developing Drugs for Acute Treatment Guidance for Industry U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and Research (CDER) February 2018
Proposed Project Scope. OPTIMAL USE OnabotulinumtoxinA for the Prevention of Chronic Migraine Clinical Evidence, Policies and Practice
 Proposed Project Scope OPTIMAL USE OnabotulinumtoxinA for the Prevention of Chronic Migraine Clinical Evidence, Policies and Practice May 2018 1. BACKGROUND AND RATIONALE Migraine is a common, debilitating
Proposed Project Scope OPTIMAL USE OnabotulinumtoxinA for the Prevention of Chronic Migraine Clinical Evidence, Policies and Practice May 2018 1. BACKGROUND AND RATIONALE Migraine is a common, debilitating
MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache
 MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache Measure Description Percentage of patients age 18 years old and older diagnosed with migraine headache whose migraine frequency is 4 migraine
MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache Measure Description Percentage of patients age 18 years old and older diagnosed with migraine headache whose migraine frequency is 4 migraine
BOTULINUM TOXIN THERAPY FOR CERVICOGENIC HEADACHE AND NECK PAIN
 BOTULINUM TOXIN THERAPY FOR CERVICOGENIC HEADACHE AND NECK PAIN Dr. Laxman Bahroo Director; Botulinum Toxin Clinic Director; Neurology Residency Program Associate Professor of Neurology Objectives Discuss
BOTULINUM TOXIN THERAPY FOR CERVICOGENIC HEADACHE AND NECK PAIN Dr. Laxman Bahroo Director; Botulinum Toxin Clinic Director; Neurology Residency Program Associate Professor of Neurology Objectives Discuss
Rizatriptan vs. ibuprofen in migraine: a randomised placebo-controlled trial
 J Headache Pain (2007) 8:175 179 DOI 10.1007/s10194-007-0386-7 ORIGINAL Usha Kant Misra Jayantee Kalita Rama Kant Yadav Rizatriptan vs. ibuprofen in migraine: a randomised placebo-controlled trial Received:
J Headache Pain (2007) 8:175 179 DOI 10.1007/s10194-007-0386-7 ORIGINAL Usha Kant Misra Jayantee Kalita Rama Kant Yadav Rizatriptan vs. ibuprofen in migraine: a randomised placebo-controlled trial Received:
Charly Gaul Christina van Doorn Nadine Webering Martha Dlugaj Zaza Katsarava Hans-Christoph Diener Günther Fritsche. Introduction
 J Headache Pain (2011) 12:475 483 DOI 10.1007/s10194-011-0348-y ORIGINAL Clinical outcome of a headache-specific multidisciplinary treatment program and adherence to treatment recommendations in a tertiary
J Headache Pain (2011) 12:475 483 DOI 10.1007/s10194-011-0348-y ORIGINAL Clinical outcome of a headache-specific multidisciplinary treatment program and adherence to treatment recommendations in a tertiary
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา
 ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
The effects of greater occipital nerve block and trigger point injection on brush allodynia and pain in migraine
 Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology April 2005 The effects of greater occipital nerve block and trigger point injection
Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology April 2005 The effects of greater occipital nerve block and trigger point injection
Per cent of patients with chronic migraine who responded per onabotulinumtoxina treatment cycle: PREEMPT
 Migraine 1 Department of Neurology, Thomas Jefferson University, Philadelphia, Pennsylvania, USA 2 Department of Neurology, Mayo Clinic Arizona, Phoenix, Arizona, USA 3 Department of Neurology and Neurological
Migraine 1 Department of Neurology, Thomas Jefferson University, Philadelphia, Pennsylvania, USA 2 Department of Neurology, Mayo Clinic Arizona, Phoenix, Arizona, USA 3 Department of Neurology and Neurological
Application of ICHD 2nd edition criteria for primary headaches with the aid of a computerised, structured medical record for the specialist
 J Headache Pain (2005) 6:205 210 DOI 10.1007/s10194-005-0186-x ICHD-II: EVALUATION AND PROPOSALS Paola Sarchielli Mauro Pedini Andrea Alberti Cristiana Rossi Antonio Baldi Ilenia Corbelli Paolo Calabresi
J Headache Pain (2005) 6:205 210 DOI 10.1007/s10194-005-0186-x ICHD-II: EVALUATION AND PROPOSALS Paola Sarchielli Mauro Pedini Andrea Alberti Cristiana Rossi Antonio Baldi Ilenia Corbelli Paolo Calabresi
MEASURE #9: MIGRAINE OR CERVICOGENIC HEADACHE RELATED DISABILITY FUNCTIONAL STATUS Headache Quality Improvement Only
 MEASURE #9: MIGRAINE OR CERVICOGENIC HEADACHE RELATED DISABILITY FUNCTIONAL STATUS Headache Quality Improvement Only Measure Description Percentage of patients age 6 years old and older who have a diagnosis
MEASURE #9: MIGRAINE OR CERVICOGENIC HEADACHE RELATED DISABILITY FUNCTIONAL STATUS Headache Quality Improvement Only Measure Description Percentage of patients age 6 years old and older who have a diagnosis
Psychiatric disorders in chronic daily headache: detection by means of the SCID interview
 J Headache Pain (2000) 1:S33 S37 Springer-Verlag 2000 Francomichele Puca Mario Guazzelli Vittorio Sciruicchio Giuseppe Libro Paola Sarchielli Susanna Russo Andrea Alberti Giorgio Zanchin Cinzia Schianchi
J Headache Pain (2000) 1:S33 S37 Springer-Verlag 2000 Francomichele Puca Mario Guazzelli Vittorio Sciruicchio Giuseppe Libro Paola Sarchielli Susanna Russo Andrea Alberti Giorgio Zanchin Cinzia Schianchi
Classification of headaches
 Classification of headaches Jasna Zidverc Trajković Headache center Headache in adults: 1-year prevalence 13.4 Kryst 35.9 Miranda 28.7 Jaillard 87.3 O Brien 63.1 Wiehe 37.3 Lavados 59.7 Schwartz 76.0 Boardman
Classification of headaches Jasna Zidverc Trajković Headache center Headache in adults: 1-year prevalence 13.4 Kryst 35.9 Miranda 28.7 Jaillard 87.3 O Brien 63.1 Wiehe 37.3 Lavados 59.7 Schwartz 76.0 Boardman
Caspian Journal of Neurological Sciences "Caspian J Neurol Sci" Journal Homepage:
 Caspian Journal of Neurological Sciences "Caspian J Neurol Sci" Journal Homepage: http://cjns.gums.ac.ir Research aper: or for Treatment of Medication Overuse Headache: A Randomized, Double- Blind Clinical
Caspian Journal of Neurological Sciences "Caspian J Neurol Sci" Journal Homepage: http://cjns.gums.ac.ir Research aper: or for Treatment of Medication Overuse Headache: A Randomized, Double- Blind Clinical
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Value of postmarketing surveillance studies in achieving a complete picture of antimigraine agents: using almotriptan as an example
 J Headache Pain (2006) 7:27 33 DOI 10.1007/s10194-006-0266-6 ORIGINAL Julio Pascual Hans-Christoph Diener Hélène Massiou Value of postmarketing surveillance studies in achieving a complete picture of antimigraine
J Headache Pain (2006) 7:27 33 DOI 10.1007/s10194-006-0266-6 ORIGINAL Julio Pascual Hans-Christoph Diener Hélène Massiou Value of postmarketing surveillance studies in achieving a complete picture of antimigraine
Guidelines of the International Headache Society for controlled trials of preventive treatment of chronic migraine in adults
 Original Article Guidelines of the International Headache Society for controlled trials of preventive treatment of chronic migraine in adults Cephalalgia 0(0) 1 18! International Headache Society 2018
Original Article Guidelines of the International Headache Society for controlled trials of preventive treatment of chronic migraine in adults Cephalalgia 0(0) 1 18! International Headache Society 2018
ACUTE TREATMENT FOR MIGRAINE. Cristina Tassorelli
 The European Headache School 2012 ACUTE TREATMENT FOR MIGRAINE Cristina Tassorelli Headache Science Centre, IRCCS Neurological Institute C. Mondino Foundation - Pavia University Centre for Adaptive Disorders
The European Headache School 2012 ACUTE TREATMENT FOR MIGRAINE Cristina Tassorelli Headache Science Centre, IRCCS Neurological Institute C. Mondino Foundation - Pavia University Centre for Adaptive Disorders
Despite the widespread use of triptans ... REPORTS... Almotriptan: A Review of Pharmacology, Clinical Efficacy, and Tolerability
 ... REPORTS... Almotriptan: A Review of Pharmacology, Clinical Efficacy, and Tolerability Randal L. Von Seggern, PharmD, BCPS Abstract Objective: This article summarizes preclinical and clinical data for
... REPORTS... Almotriptan: A Review of Pharmacology, Clinical Efficacy, and Tolerability Randal L. Von Seggern, PharmD, BCPS Abstract Objective: This article summarizes preclinical and clinical data for
Botox (Botulinum toxin type A) in the prophylaxis of headaches in chronic migraine
 Botox (Botulinum toxin type A) in the prophylaxis of headaches in chronic migraine Manufacturer responses to clarification questions from the Evidence Review Group November 2011 Clarification on manufacturer
Botox (Botulinum toxin type A) in the prophylaxis of headaches in chronic migraine Manufacturer responses to clarification questions from the Evidence Review Group November 2011 Clarification on manufacturer
Decision-making deficit in chronic migraine patients with medication overuse
 DOI 10.1007/s10072-012-1071-4 ORAL COMMUNICATIONS Decision-making deficit in chronic migraine patients with medication overuse B. Biagianti L. Grazzi O. Gambini S. Usai R. Muffatti S. Scarone G. Bussone
DOI 10.1007/s10072-012-1071-4 ORAL COMMUNICATIONS Decision-making deficit in chronic migraine patients with medication overuse B. Biagianti L. Grazzi O. Gambini S. Usai R. Muffatti S. Scarone G. Bussone
Chronic migraine classification: current knowledge and future perspectives
 J Headache Pain (2011) 12:585 592 DOI 10.1007/s10194-011-0393-6 REVIEW ARTICLE Chronic migraine classification: current knowledge and future perspectives Gian Camillo Manzoni Vincenzo Bonavita Gennaro
J Headache Pain (2011) 12:585 592 DOI 10.1007/s10194-011-0393-6 REVIEW ARTICLE Chronic migraine classification: current knowledge and future perspectives Gian Camillo Manzoni Vincenzo Bonavita Gennaro
Botulinum toxins: abobotulinumtoxina (Dysport ), incobotulinumtoxina (Xeomin ), onabotulinumtoxina (Botox ), & rimabotulinumtoxinb (Myobloc )
 Botulinum toxins: abobotulinumtoxina (Dysport ), incobotulinumtoxina (Xeomin ), onabotulinumtoxina (Botox ), & rimabotulinumtoxinb (Myobloc ) These services may or may not be covered by your HealthPartners
Botulinum toxins: abobotulinumtoxina (Dysport ), incobotulinumtoxina (Xeomin ), onabotulinumtoxina (Botox ), & rimabotulinumtoxinb (Myobloc ) These services may or may not be covered by your HealthPartners
Get ahead of the ACHE: Monoclonal Antibodies in Migraine Prevention
 Get ahead of the ACHE: Monoclonal Antibodies in Migraine Prevention Amanda Janisch, PharmD PGY2 Ambulatory Care Pharmacy Resident MCHS SWMN, Mankato, MN 2018 MFMER slide-1 Disclosures No financial interest
Get ahead of the ACHE: Monoclonal Antibodies in Migraine Prevention Amanda Janisch, PharmD PGY2 Ambulatory Care Pharmacy Resident MCHS SWMN, Mankato, MN 2018 MFMER slide-1 Disclosures No financial interest
11/10/2017 HEADACHE INJECTIONS WORKSHOP. Comprehensive Migraine Education Program Procedural Curriculum Developers. Disclosures
 HEADACHE INJECTIONS WORKSHOP Saturday, November 18 and Sunday, November 19 Scottsdale Headache Symposium Comprehensive Migraine Education Program Procedural Curriculum Developers PROGRAM CHAIRS David W.
HEADACHE INJECTIONS WORKSHOP Saturday, November 18 and Sunday, November 19 Scottsdale Headache Symposium Comprehensive Migraine Education Program Procedural Curriculum Developers PROGRAM CHAIRS David W.
Harold G. Wolff Lecture Award Winner
 Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01217.x Published by Wiley Periodicals, Inc. Harold G. Wolff Lecture Award Winner
Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01217.x Published by Wiley Periodicals, Inc. Harold G. Wolff Lecture Award Winner
Guidance for Industry Migraine: Developing Drugs for Acute Treatment
 Guidance for Industry Migraine: Developing Drugs for Acute Treatment DRAFT GUIDANCE This guidance document is being distributed for comment purposes only. Comments and suggestions regarding this draft
Guidance for Industry Migraine: Developing Drugs for Acute Treatment DRAFT GUIDANCE This guidance document is being distributed for comment purposes only. Comments and suggestions regarding this draft
Prevalence of new daily persistent headache in the general population. The Akershus study of chronic headachecha_
 doi:10.1111/j.1468-2982.2009.01842.x Prevalence of new daily persistent headache in the general population. The Akershus study of chronic headachecha_1842 1149..1155 RB Grande 1,2, K Aaseth 1,3, C Lundqvist
doi:10.1111/j.1468-2982.2009.01842.x Prevalence of new daily persistent headache in the general population. The Akershus study of chronic headachecha_1842 1149..1155 RB Grande 1,2, K Aaseth 1,3, C Lundqvist
Measure Components Numerator Statement
 MEASURE #5: OVERUSE OF OPIOID CONTAINING MEDICATIONS FOR PRIMARY HEADACHE DISORDERS Headache For Quality Improvement Only. Not to be used for Public Reporting or Accountability Measure Description Percentage
MEASURE #5: OVERUSE OF OPIOID CONTAINING MEDICATIONS FOR PRIMARY HEADACHE DISORDERS Headache For Quality Improvement Only. Not to be used for Public Reporting or Accountability Measure Description Percentage
Efficacy of Levetiracetam: A Review of Three Pivotal Clinical Trials
 Epilepsia, 42(Suppl. 4):31 35, 2001 Blackwell Science, Inc. International League Against Epilepsy Efficacy of : A Review of Three Pivotal Clinical Trials Michael Privitera University of Cincinnati Medical
Epilepsia, 42(Suppl. 4):31 35, 2001 Blackwell Science, Inc. International League Against Epilepsy Efficacy of : A Review of Three Pivotal Clinical Trials Michael Privitera University of Cincinnati Medical
Comparison of dynamic (brush) and static (pressure) mechanical allodynia in migraine
 Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology July 2006 Comparison of dynamic (brush) and static (pressure) mechanical allodynia in
Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology July 2006 Comparison of dynamic (brush) and static (pressure) mechanical allodynia in
Development of Kappa Opioid Receptor Antagonists for Prophylactic Treatment of Migraine
 Development of Kappa Opioid Receptor Antagonists for Prophylactic Treatment of Migraine Item Type text; Electronic Thesis Authors Frank, Larry Robert Jr. Publisher The University of Arizona. Rights Copyright
Development of Kappa Opioid Receptor Antagonists for Prophylactic Treatment of Migraine Item Type text; Electronic Thesis Authors Frank, Larry Robert Jr. Publisher The University of Arizona. Rights Copyright
PDFlib PLOP: PDF Linearization, Optimization, Protection. Page inserted by evaluation version
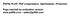 PDFlib PLOP: PDF Linearization, Optimization, Protection Page inserted by evaluation version www.pdflib.com sales@pdflib.com Headache 2008 the Authors Journal compilation 2008 American Headache Society
PDFlib PLOP: PDF Linearization, Optimization, Protection Page inserted by evaluation version www.pdflib.com sales@pdflib.com Headache 2008 the Authors Journal compilation 2008 American Headache Society
Controversy One: Headache and Disability. Robert Shapiro, MD, PhD University of Vermont
 Controversy One: Headache and Disability Robert Shapiro, MD, PhD University of Vermont Southern Headache Society Orlando, FL, Sept 21, 2013 Disclosures Consulting within the past 12 months: Transcept Pharmaceuticals
Controversy One: Headache and Disability Robert Shapiro, MD, PhD University of Vermont Southern Headache Society Orlando, FL, Sept 21, 2013 Disclosures Consulting within the past 12 months: Transcept Pharmaceuticals
The frequency with which migraine attacks
 STRATEGIES TO PREVENT MIGRAINE * Sheena K. Aurora, MD ABSTRACT Patients who suffer from daily or near-daily headaches may experience significant disability and interference in all aspects of their professional
STRATEGIES TO PREVENT MIGRAINE * Sheena K. Aurora, MD ABSTRACT Patients who suffer from daily or near-daily headaches may experience significant disability and interference in all aspects of their professional
UNDERSTANDING CHRONIC MIGRAINE. Learn about diagnosis, management, and treatment options for this headache condition
 UNDERSTANDING CHRONIC MIGRAINE Learn about diagnosis, management, and treatment options for this headache condition 1 What We re Going to Cover Today The symptoms and phases of migraine Differences between
UNDERSTANDING CHRONIC MIGRAINE Learn about diagnosis, management, and treatment options for this headache condition 1 What We re Going to Cover Today The symptoms and phases of migraine Differences between
