Migraine is a common recurrent neurological disorder with
|
|
|
- Kristopher Randall
- 5 years ago
- Views:
Transcription
1 Review Article Department Part 1: Diagnosis, General Management, and Role of Dopamine Antagonists and NSAIDs Vongvaivanich K, MD Kiratikorn Vongvaivanich, MD 1 Keywords: treatment for migraine headache, migraine headache in emergency 1 Comprehensive Headache Clinic, Bangkok Hospital, Bangkok Hospital Group, Bangkok, Thailand. Migraine is a common recurrent neurological disorder with a high impact and is debilitating. Approximately 14.7% of the global population has migraine (an estimated 6% in men and up to 18% in women). 1 A recent report ranked migraine headache as the third most common disease in the world (behind dental caries and tension type headache). 2 On the basis of migraine attack disability alone, migraine was ranked seventh highest among years of life lost to disability). 1,2 Recent data from US public health cause of emergency department (ED) visits in the United States, estimated to account for over 4 million visits annually (1.2% of outpatient visits). The burden of headache was highest in females aged 18-44, where the 3-month prevalence of migraine or severe headache was 26.1% and head pain was the third leading cause of ED visits. 3 Most migraineurs who visit ED for treatment generally have severe and/or prolonged symptoms concomitant with nausea/ vomiting, and usual acute medications are not effective. Over half of the patients use simple analgesics to treat their headache attack but often to no effect. 4 Migraine-specific medications (triptans or ergotamine) have been used only in a few patients. 5 The goal of ED therapy is to deliver medicines with rapid, complete relief of pain and associated migraine symptoms, restore functional ability, with minimum adverse effects and without recurrence of headache after ED discharge. 6 Intravenous medications dopamine antagonists, NSAIDs, opioids, magnesium, valproate, and corticosteroids. This paper consists of 2 parts; part 1 reviews the role of dopamine antagonists, NSAIDs, and opioids that are available in Thailand for migraine treatment in ED. Diagnosis of migraine in the emergency setting *Address Correspondence to author: Kiratikorn Vongvaivanich, MD Comprehensive Headache Clinic, Bangkok Hospital 2 Soi Soonvijai 7, New Petchburi Rd., Bangkok 10310, Thailand. kiratikorn.vo@bangkokhospital.com Received: January 6, 2014 Revision received: January 6, 2014 Accepted after revision: January 10, 2014 Bangkok Med J 2014;7: E-journal: the diagnosis and rule out life-threatening causes of secondary headaches such as subarachnoid hemorrhage, arterial dissection, tion, and elevated or low intracranial pressure. The clinical characteristics of secondary cause of headache can be memorized from the mnemonic SNOOP4 : Systemic symptoms (fever, weight loss) or Systemic disease (malignancy) Neurologic symptoms or signs Onset sudden (acute or thunderclap headache) Onset after age 50 years Previous headache history (new or different) Progressive Precipitation by Valsalva (cough, bend) Postural 86 The Bangkok Medical Journal Vol. 7; February 2014
2 Department Part 1: Diagnosis, General Management, and Role of Dopamine Antagonists and NSAIDs If one or more of the SNOOP4 features are present, the diagnostic tests including neuroimaging (computed tomography or magnetic resonance imaging), lumbar puncture, and blood tests may be considered. 7 Migraine is diagnosed by clinical criteria provided 3 rd 8 Migraine headache is characterized by unilateral location, pulsating quality, moderate to severe intensity, aggravated by routine physical activity, and accompanied by photophobia (sensitivity to light) and phonophobia (sensitivity to sound) or nausea and/or vomiting. The accurate diagnosis of headache can be troublesome at the ED due to the severity of the migraine attack, the associated symptoms especially nausea and/or vomiting that might require emergency treatment, and also because administered migraine screener (ID-Migraine), consisting of questions on disability, nausea, and photophobia, is a valid and reliable screening instrument for migraine headaches in the primary care setting. The test outcome is positive when the answer is yes for at least two out of the three questions. (Table 2) The study role of ID-Migraine in emergency departments showed that the ID-Migraine exhibited a high sensitivity 10 A negative ID Migraine score, less than 2 positive responses, 23%. 11 Management for acute migraine in the emergency room The patient should be assessed for volume depletion occurs in approximately 70% of migraineurs. In those who experienced nausea or vomiting, % indicated that it interfered with their ability to take their oral migraine medication. 12,13 useful for rehydration and in avoiding postural hypotension associated with dopamine antagonist treatment and provides some degree of renal protection if non-steroidal 14,15 A quiet, darkened and comfortable area in ED can provide Dopamine plays an important role in migraine pathogenesis probably by acting on central pain control pathways and on cranial blood vessels. 16 Recent genetic studies show evidence of genetic polymorphism of the dopaminergic and dopamine transporter genes. 17,18 The dopamine the migraine attack and the levels correlate with the severity of pain. Dopamine antagonists are very useful in rescue treatment of migraine and appear to be equivalent to the ergotamine) in migraine pain relief. 20 There are 2 major subclasses of neuroleptics, the phenothiazines group (e.g., prochlorperazine, chlorpromazine, promethazine, and methotrimeprazine) and the butyrophenones group (droperidol and haloperidol). Metoclopramide is in its own third class. The phenothiazines, chlorpromazine and prochlorperazine, were commonly used in ED. Thirteen trials showed that phenothiazines were markedly more success, but not different for headache relief. The clinical 21 Neuroleptics act on the postsynaptic dopamine D2 receptor in the hypothalamus, limbic system, periaqueductal grey, and basal ganglia. Neuroleptics also have anticholinergic, antiadrenergic, anti-serotonergic and antihistaminergic effects. The most common side effects of neuroleptics are sedation and drowsiness due to blockage of muscarinic cholinergic and histamine receptors. Extrapyramidal side effects dystonia and akathisia are commonly seen in parenteral form and more often with prochlorperazine. Dystonia and akathisia can be prevented by premedication with anticholinergic agents (e.g., benztropine, diphen- antagonist effects, postural hypotension can occur but is infrequently reported in phenothiazine. Neuroleptic malignant syndrome, which is characterized by fever, rigidity, confusion, and autonomic function instability, is a rare side effect. Droperidol and haloperidol can cause QT interval prolongation that increases risk of fatal ventricular arrhythmias and cardiac arrest Several randomized controlled trials and head-to-head migraine. 20 Pool clinical analysis showed the success rate of acute migraine treatment is 81% for chlorpromazine 23 In a randomized controlled trial in an emergency room setting, chlorpromazine at dose 0.1 pain score compared with placebo in 128 migraineurs. Pain free at 1 hour for migraine with aura (66.7% in chlorpromazine group vs. 6.7% in placebo; p < 0.01) and migraine without aura (63.2% vs. 10%; p < 0.01). 24 In comparison trials, pain reduction (VAS) was greater for chlorpromazine 0.1mg/kg IV (up to 3 doses) than meperidine 0.4 mg/kg IV plus diphenhydramine 25mg (VAS vs ; p < 0.05). 25 Chlorpromazine 12.5 mg IV (could be repeated up to 37.5mg) was compared The Bangkok Medical Journal Vol. 7; February
3 Vongvaivanich K Table 1: The International Classication of Headache Disorders, 3 rd edition (beta version) for migraine without aura and migraine with aura. Migraine without aura Diagnostic criteria: A. At least ve attacks 1 fullling criteria B-D B. Headache attacks lasting 4-72 hours (untreated or unsuccessfully treated) 2,3 C. Headache has at least two of the following four characteristics: 1. unilateral location 2. pulsating quality 3. moderate or severe pain intensity 4. aggravation by or causing avoidance of routine physical activity (e.g. walking or climbing stairs) D. During headache at least one of the following: 1. nausea and/or vomiting 2. photophobia and phonophobia Migraine with aura Diagnostic criteria: A. At least two attacks fullling criteria B and C B. One or more of the following fully reversible aura symptoms: 1. visual 2. Sensory 3. speech and/or language 4. motor 5. brainstem 6. retinal C. At least two of the following four characteristics: 1. at least one aura symptom spreads gradually over 5 minutes, and/or two or more symptoms occur in succession 2. each individual aura symptom lasts 5-60 minutes1 3. at least one aura symptom is unilateral2 4. the aura is accompanied, or followed within 60 minutes, by headache D. Not better accounted for by another ICHD-3 diagnosis, and transient ischemic attack has been excluded. E. Not accounted for by another ICHD-3 diagnosis Note: 1. One or a few migraine attacks may be difcult to distinguish from symptomatic migraine-like attacks. Furthermore, the nature of a single or a few attacks may be difcult to understand. Therefore, at least ve attacks are required. Individuals who otherwise meet criteria for 1.1 Migraine without aura but have had fewer than ve attacks, should be coded Probable migraine without aura. 2. When the patient falls asleep during a migraine attack and wakes up without it, duration of the attack is reckoned until the time of waking. 3. In children and adolescents (aged under 18 years), attacks may last 2-72 hours (the evidence for untreated durations of less than 2 hours in children has not been substantiated). Note: 1. When, for example, three symptoms occur during an aura, the acceptable maximal duration is 3x60 minutes. Motor symptoms may last up to 72 hours. 2. Aphasia is always regarded as a unilateral symptom; dysarthria may or may not be. Table 2: The ID-Migraine. - During the last 3 months, did you have the following with your headaches: You felt nauseated or sick to your stomach ( ) Yes ( ) No Light bothered you (a lot more than when you don t have headaches) ( ) Yes ( ) No Your headaches limited your ability to work, study or do what you needed to do for at least one day. ( ) Yes ( ) No 88 The Bangkok Medical Journal Vol. 7; February 2014
4 Department Part 1: Diagnosis, General Management, and Role of Dopamine Antagonists and NSAIDs with lidocaine 50mg IV (could be repeated up to 150 be repeated once). Pain reduction (11 PPS) was greater - p < 0.05). 26 Chlorpromazine 12.5 mg IV (could be repeated up to 37.5mg) was compared with sumatriptan SQ 6mg. At 2 hours, there was no difference in pain reduction (VAS) (chlorpromazine mm vs. sumatriptan mm) Metoclopramide is widely available, inexpensive, and commonly used for the treatment of nausea, vomiting, and gastroparesis. In addition to dopamine antagonists, metoclopramide also has serotonin antagonist effect. congestive heart failure and liver disease), lower seizure threshold, mild sedation and extrapyramidal side effects. Meta-analysis from 13 randomized controlled trials for parenteral metoclopramide in acute migraine showed metoclopramide is an effective treatment for migraine headache in adults and should be considered as a primary agent in the treatment of acute migraine in emergency departments. 28 Metoclopramide 10mg IV showed superior to placebo in three studies for all outcomes related to pain and nausea. Pooled data from three studies showed that 28 Metoclopramide was more effective than placebo in reducing nausea in four studies. Three studies compared metoclopramide with other neuroleptics (chlorpromazine and prochlorperazine). 30,33,34 These studies suggested that metoclopramide was less effective in relieving pain and nausea than phenothiazine. Pooled results from all three studies showed that patients who received metoclopramide were more likely to require 28 In comparison to non-emetics, metoclopramide 10mg IV was similar in pain reduction to metoclopramide plus ibuprofen 600 mg PO (VAS -75 vs. -50) but VAS reduction was larger than ibuprofen alone or placebo. Patients in the metoclo- rescue drugs. 31 Metoclopramide 10mg IV was compared with magnesium 2g IV and with placebo. Pain reduction was similar in three groups but in metoclopramide and magnesium groups the requirement of rescue medications was less than in placebo (38% and 44% vs. 65% in placebo; p = 0.04). 34 Metoclopramide 20mg IV plus diphenhydramine 25mg IV (dose up to 4 times) was found to be superior to sumatriptan 6mg SQ as a percentage of not for 1 hour (p = 0.22) and 24 hours (p = 0.23). 36 trial of 356 patients, intravenous metoclopramide 10mg p = vs. 20% vs. 21%). The most common adverse event was similar rates across doses mainly by blocking D2 dopamine receptor with some in 500 ml normal saline (NSS) IV was compared with placebo NSS 500 ml IV. Pain reduction (VAS) was greater with haloperidol (from 7.7 to 2.3; p < ) compared to placebo (from 7.2 to 6.3; p < 0.01). Eighty percent who received haloperidol felt marked relief from pain, whereas only 15% responded to placebo (p < ). The common side effects were motor agitation (akathisia) in 53% and drowsiness in 53%. Sixteen percent of the patients considered the side effects intolerable and were unwilling to be treated with haloperidol in the future. 38 Due to black box warnings for prolonged QTc, together with high incidence of sedation and akathisia, haloperidol should be reserved for use only when other rescue medications failed to relieve headache. Electrocardiogram (ECG) should be done before and after treatment. Pretreatment with IV fluid and an anticholinergic (benztropine, trihexyphenidyl, diphenhydramine or benzodiazepine) are recommended. 20 NSAIDs inhibit both cyclooxygenase-1 (COX1) and cascade and thereby prostaglandin synthesis, and platelet aggregation associated with the release of vasoactive agents that are involved in initiation and prolongation of migraine. - Ketorolac is a NSAID with strong analgesic activity. Ketorolac attenuates moderate to severe pain especially in patients with migraine headache and is usually as effective as an opioid. The analgesic effect of ketorolac tends to be slower in onset than that of morphine or meperidine but persists longer. 40 Most adverse events involve the gastrointestinal tract (GI), ranging from mild upset to ulceration and hemorrhage. Overall, parenteral ketorolac is associated with only a slightly increased risk of GI or operative site bleeding compared to opioids (OR 1.30 and 1.02, respectively). The risk of bleeding is strongly linked to increased age, high dosage and treatment for more than 5 days. 41 All NSAIDs have the potential to cause nephropathies, but these occur more frequently in patients with hypovolemia or patients with hemodynamic compromise. 42 The Bangkok Medical Journal Vol. 7; February 2014
5 Vongvaivanich K The total daily dosage of parenteral ketorolac should renal impairment or body weight < 50kg. Ketorolac is contraindicated in patients with congestive heart failure, hepatic impairment, hypertension or conditions that may lead to a reduction in blood volume and in those who are hypersensitive to NSAIDs. Ketorolac should not be co-administered with other NSAIDs, probenecid, pentoxifylline or lithium and should be administered cautiously to patients on anticoagulation therapy (including low dose heparin). 40 it is used in up to 16% of ED visits for migraine. 43 The of migraine. A recent systematic review which included 8 RCTs (321 patients) examined the effectiveness of ketorolac in acute migraine and suggested ketorolac is associated with pain reduction in adult migraine attack patients. 44 to meperidine ( mg IM) in pain score reduction at 60 minutes (weight mean difference (WMD) 0.44; p = 0.35). Due to risk of abuse and addiction associated with meperidine, ketorolac is a migraine who were treated with narcotic agents showed an increased likelihood to return to the ED within 7 days. 45 A single study demonstrated that ketorolac IV 30mg 46 Ketorolac has not been compared with other more effective routes patients have often used triptans as an abortive agent before ED arrival. Two studies compared IV ketorolac with IV phenothiazines (prochlorperazine and chlorpromazine). The pool analysis found no statistical difference in geneity was high, trends may suggest phenothiazines are more effective. 47,48 - Parecoxib is a cyclooxygenase-2 (COX-2) specific inhibitor widely used for acute pain in ED. In animal protein extravasation (PPE) in rat dura mater and reduced expression of c-fos within the ipsilateral trigeminal nucleus correlated with migraine pathophysiology. Only one nous parecoxib, oral fast-dissolving tablet of rizatriptan, and subcutaneous injection of sumatriptan in patients with acute migraine. Using the visual analog scale for pain intensity at baseline before and then after the drug intake at intervals of 20, 30, 60, and 120 minutes, rizatriptan 10mg 6mg, and parecoxib was more effective than sumatriptan at 20 and 30 minutes after drug administration. 50 Opioids have long been used to treat various types of pain include headache. Parenteral opioids are very frequently used in the ED setting, for example for more than 50% of all migraine visits to EDs in US and in Canada. 51,52 Opioids can modulate nociceptive input to the spinal trigeminal nucleus (nucleus caudalis) but they have no effect on neurovascular inflammation in migraine pathophysiology. 53 A large US population-based study demonstrated that opioid use is common for the acute treatment of migraine. Approximately 30% of the popu- currently using opioids. Around 16% of current opioid users were dependent. Opioid use for migraine is associated with more severe headache-related disability, symptomology, comorbidities (depression, anxiety, and cardiovascular disease), and greater health-care resource utilization for headache. 54 The major concern about the use of opioids in acute migraine attack regards the possible association with an increased risk of medication overuse of short-acting opioids may be associated with worsening based and population-based longitudinal studies support an association between CM and opioids use. 55 In the American Migraine Prevalence and Prevention (AMPP) study, the risk of CM is higher for opioids use (with an OR = 1.48). Critical level of exposure is around 8 days per month, and the effect is more evident in men (OR = 2.76) than in women (OR = 1.28). 56 occur with even brief durations of narcotic treatment. Of patients who were exposed to opioids, their pain thresholds declined, and their pain sensitivity, pain location, and pain intensity increased to any stimulus. The phenomenon doses of opioids, but the basic pathophysiology is different from tolerance. 57 cholecystokinin up-regulation in the rostral ventromedial medulla (RVM), peripheral expression of calcitonin-gene related peptide (CGRP) in primary afferent neurons is up-regulated, there is an increase in dynorphin, pro- receptors, and activation of glia cell via the toll-like neuroexcitatory substances. 58 Opioids are pro-nociceptive, prevent reversal of migraine central sensitization, and interfere with triptan effectiveness. Adverse effects of opioids include sedation, respiratory depression, bradycardia and hypotension, seizure, in addition to long term dependence. - Meperidine is the opioid most frequently used and most studied for headache treatment in ED. 60 In a meta- The Bangkok Medical Journal Vol. 7; February 2014
6 Department Part 1: Diagnosis, General Management, and Role of Dopamine Antagonists and NSAIDs less pyramidal side effects than antiemetics, and similar ketorolac. 61 A review of 75 studies of rescue therapy for acute migraine found opioids (meperidine, tramadol, and nalbuphine) were superior to placebo in relieving migraine pain, although meperidine combined with promethazine was not. Meperidine 75mg was superior to ketorolac 30 mg IM but was similar to ketorolac 60mg IM even when combined with an antihistamine. Meperidine 75mg IM or 62 - Tramadol hydrogen chloride is an atypical opioid that has relatively weak mu opioid receptor binding properties and also inhibits serotonin and norepinephrine re-uptake. Tramadol is better tolerated than other opioids because of its low impact on the respiratory, cardiac, and gastrointestinal systems at therapeutic doses. 63 Tramadol 100mg IV was compared with placebo (NSS) IV. Pain reduction (VAS) at 1 hour was greater in the tramadol group (70.6% vs. 35.3%, p=0.04) but the percent pain free at 1 hour was not p=0.40). Side effects were not observed at 1 hour. 64 In the prospective, randomized, double-blind study, tramadol 100 mg IM was compared with diclofenac sodium 75mg IM; headache relief was the same in both groups (80%). 65 Conclusion Migraine is a common disabling disorder. Migraine attacks with moderate to severe pain and other debilitating associated symptoms such as nausea, vomiting, photophobia, and phonophobia that lead to emergency room visits. Detailed history taking, physical examination, and appropriate diagnostic tools should rule out secondary headache. The mnemonic SNOOP4 is a useful for recognizing secondary causes of headache. ID-migraine, the short 3 item questionnaire, is recommended as a can be useful in patients with nausea and vomiting, and to prevent postural hypotension in patients who will be administered a dopamine antagonist. Dopamine antagonists (chlorpromazine and metoclopramide) are very effective in rescue migraine treatment. Effective doses of chlorpromazine in migraine ranged from 0.1mg/kg to 37.5mg administered intravenously or in pain relief was up to 80%. Metoclopramide 10mg IV had an average pain relief of 70%. The most common adverse effects of dopamine antagonists were drowsiness, postural hypotension, and akathisia. Dopamine antag- migraine attack in ED. Ketorolac, the parenteral NSAID, should be considered a second line rescue treatment in ED. The recommended ketorolac dose is 30mg IV or 60mg IM. Average percentages of pain relief of ketorolac are 60% for ketorolac 30mg IV and 37% for ketorolac 60mg IM. Ketorolac and meperidine had similar pain scores at 60 minutes and ketorolac was not different from phenothiazines in pain relief at 60 minutes. Adverse effects were risk of GI bleeding and nephropathies that increased with age, high dosages, and prolonged use for more than 5 days. of meperidine 75mg IM is similar to ketorolac 60mg IM meperidine is 58%. Tramadol 100mg IM had similar included sedation, dizziness, GI discomfort, nausea and vomiting, and akathisia (less than neuroleptics). Opioids are not recommended for rescue migraine treatment due to a high rate of headache recurrence, increased risk of medication overuse, chronic migraine transformation, opioid-induced hyperalgesia, central sensitization, nausea and dizziness, and raised concerns for overuse and abuse. References Burden of Disease Study Steiner TJ, Stovner LJ, Birbeck GL. Migraine: the seventh disabler. impact, and treatment of migraine and severe headaches in the United States: a review of statistics from national surveillance studies. 2013;53: Diamond M, Cady R. Initiating and optimizing acute therapy 2005;118:18S-27S. underutilization of headache medications in a university hospital emergency department. 2007;47: gency department-based migraine research: an analysis of commonly used clinical trial outcome measures. The Bangkok Medical Journal Vol. 7; February 2014
7 Vongvaivanich K 7. Dodick DW. Clinical clues and clinical rules: primary versus secondary headache. Adv. 2003;3: rd edition (beta version). tered screener for migraine in primary care: the ID Migraine validation study. 2003;61: Mostardini C, d Agostino VC, Dugoni DE, et al. A possible role of ID-Migraine in the emergency department: study of an emergency department out-patient population. accuracy of the ID Migraine: a systematic review and meta-analysis. 2011;51: Silberstein SD. Migraine symptoms: Results of a survey of self-reported migraineurs. 13. Silberstein S. Gastrointestinal manifestations of migraine: meeting the treatment challenges. 2013;53: Logan P, Lewis D. Chlorpromazine in migraine. 15. Shrestha M, Singh R, Moreden J, et al. Ketorolac vs. chlorpromazine in the treatment of acute migraine without aura. A prospective, randomized, double-blind trial. toms in migraine. 2013;34:S gene variants in migraine susceptibility. 2013;15: Todt U, Netzer C, Toliat M, et al. New genetic evidence for involvement of the dopamine system in migraine with aura. Hum Genet tyrosine and 3,4-dihydroxyphenyl-acetic acid levels in migraine patients. 20. Kelley NE, Tepper DE. Rescue therapy for acute migraine, part 2: neuroleptics, antihistamines, and others. 21. Bigal ME. Phenothiazines in migraine treatment. Curr 2010;14: Marmura J. Use of dopamine antagonists in treatment of migraine. 2012;14: of phenothiazines for the treatment of acute migraine: a meta-analysis. 24. Bigal ME, Bordini CA, Speciali JG. Intravenous chlorpromazine in the emergency department treatment of migraine: A randomized controlled trial. 2002;23: Lane PL, McLellan BA, Baggoley CJ. Comparative drinate in migraine headache. 26. Bell R, Montoya D, Shuaib A, et al. A comparative trial of three agents in the treatment of acute migraine headache. 27. Kelly AM, Ardagh M, Curry C, et al. Intravenous chlorpromazine vs. intramuscular sumatriptan for acute migraine. 28. Colman I, Brown MD, Innes GD, et al. Parenteral metoclopramide for acute migraine: meta-analysis of randomised controlled trials. double-blind study of metoclopramide hydrochloride for the control of migraine in the emergency department. placebo-controlled evaluation of prochlorperazine versus metoclopramide for emergency department treatment of migraine headache. double blind study of metoclopramide in the treatment of migraine attacks. of metoclopramide in the treatment of migraine headache. 33. Jones J, Pack S, Chun E. Intramuscular prochlorperazine versus metoclopramide as single-agent therapy for the treatment of acute migraine headache. 34. Cameron JD, Lane PL, Speechley M. Intravenous chlorpromazine vs. intravenous metoclopramide in acute migraine headache. placebo-controlled study of intravenous magnesium sulfate vs. metoclopramide in the management of acute migraine attacks in the Emergency Department. clopramide vs. sumatriptan for the emergency department treatment of migraines. 2005;64: trial. 2011;57: peridol in the acute treatment of migraine: a randomized, double-blind, placebo-controlled study. 2006; 46: in the context of migraine. 2001;53: Gillis JC, Brogden RN. Ketorolac. A reappraisal of its pharmacodynamic and pharmacokinetic properties and therapeutic use in pain management. 41. Strom BL, Berlin la, Kinman JL, et al. Parenteral ketorolac and risk of gastrointestinal and operative site bleeding: a post marketing surveillance study DuBose lr TO, Molony DA, Verani R, et al. Nephrotoxicity 344: Vinson DR. Treatment patterns of isolated benign headache in US emergency departments. 44. Taggart E, Doran S, Kokotillo A, et al. Ketorolac in the treatment of acute migraine: a systematic review. 2013;53: Colman I, Rothney A, Wright S, et al. Use of narcotic analgesics in the emergency department treatment of migraine headache. 46. Meredith JT, Wait S, Brewer KL. A prospective doubleblind study of nasal sumatriptan versus IV ketorolac in migraine. 2003;21: The Bangkok Medical Journal Vol. 7; February 2014
8 Department Part 1: Diagnosis, General Management, and Role of Dopamine Antagonists and NSAIDs 47. Seim MB, March JA, Dunn KA. Intravenous ketorolac vs. intravenous prochlorperazine for the treatment of migraine headaches. 48. Shrestha M, Singh R, Moreden J, et al. Ketorolac vs. chlorpromazine in the treatment of acute migraine without aura. A prospective, randomized, double-blind trial. parecoxib on plasma protein extravasation and c-fos expression in the rat. 2006;46: and rizatriptan in the treatment of acute migraine attacks. 51. Vinson DR. Treatment patterns of isolated benign headache in US emergency departments. 52. Colman I, Rothney A, Wright SC, et al. Use of narcotic analgesics in the emergency department treatment of migraine headache. 2014;54: dependence among persons with migraine: results of the AMPP study. 2012;52: Bigal ME, Lipton RB. Excessive opioid use and the development of chronic migraine. 56. Bigal ME, Serrano D, Buse D, et al. Acute migraine medications and evolution from episodic to chronic migraine: a longitudinal population-based study. 2008; 48: in humans: Molecular mechanisms and clinical considerations. 58. Tepper SJ. Opioids should not be used in migraine. 2012;52:30-4. of primary headache disorders after emergency depart- and functional outcomes. 2008;52: migraine: a meta-analysis of randomized controlled trials. 2008;52: Tepper DE, Kelley NE. Rescue therapy for acute migraine, part 3: Opioids, NSAIDs, steroids, and postdischarge medications. 2012;52: ment of headache. intravenous tramadol for acute migraine pain in adults: A single-blind, prospective, randomized, placebo-controlled clinical trial. 65. Engindeniz Z, Demircan C, Karli N, et al. Intramuscular tramadol vs. diclofenac sodium for the treatment of acute migraine attacks in emergency department: A prospective, randomized, double-blind study. 2005;6: The Bangkok Medical Journal Vol. 7; February 2014
Adult & Pediatric Patients. Stanford Health Care, Division Pain Medicine
 Acute Treatment Strategies in Adult & Pediatric Patients Theresa Mallick Searle, MS, RN BC, ANP BC Disclosures Speakers Bureau: Allergan, Depomed Acute Treatment Strategies in Adult & Pediatric Patients
Acute Treatment Strategies in Adult & Pediatric Patients Theresa Mallick Searle, MS, RN BC, ANP BC Disclosures Speakers Bureau: Allergan, Depomed Acute Treatment Strategies in Adult & Pediatric Patients
ADVANCES IN MIGRAINE MANAGEMENT
 ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
Faculty Disclosures. Learning Objectives. Acute Treatment Strategies
 WWW.AMERICANHEADACHESOCIETY.ORG Acute Treatment Strategies Content developed by: Lawrence C. Newman, MD, FAHS Donna Gutterman, PharmD Faculty Disclosures LAWRENCE C. NEWMAN, MD, FAHS Dr. Newman has received
WWW.AMERICANHEADACHESOCIETY.ORG Acute Treatment Strategies Content developed by: Lawrence C. Newman, MD, FAHS Donna Gutterman, PharmD Faculty Disclosures LAWRENCE C. NEWMAN, MD, FAHS Dr. Newman has received
Treatment of Headache in the ED
 Treatment of Headache in the ED Benjamin W. Friedman, MD, MS, FAAEM Associate professor of Emergency Medicine Albert Einstein College of Medicine Montefiore Medical Center Disclosure Topics of Discussion
Treatment of Headache in the ED Benjamin W. Friedman, MD, MS, FAAEM Associate professor of Emergency Medicine Albert Einstein College of Medicine Montefiore Medical Center Disclosure Topics of Discussion
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation.
 I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
MIGRAINE UPDATE. Objectives & Disclosures. Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment.
 MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in
 HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in Anesthesia and Neurology Harvard Medical School Limited time
HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in Anesthesia and Neurology Harvard Medical School Limited time
Specific Care Question : Question Originator: Plain Language Summary from The Office of Evidence Based Practice: Conditional Recommendation
 Ketorolac for Refractory Migraine in the ED Specific Care Question : In the pediatric patient diagnosed with refractory migraine is ketorolac an effective treatment? Question Originator: Migraine Therapy
Ketorolac for Refractory Migraine in the ED Specific Care Question : In the pediatric patient diagnosed with refractory migraine is ketorolac an effective treatment? Question Originator: Migraine Therapy
Inpatient Treatment of Status Migraine With Dihydroergotamine in Children and Adolescents
 Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline. Scottish intercollegiate Guidelines Network SIGN
 A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
ISSN doi: /head VC 2015 American Headache Society Published by Wiley Periodicals, Inc.
 ISSN 0017-8748 Headache doi: 10.1111/head.12746 VC 2015 American Headache Society Published by Wiley Periodicals, Inc. Review Article Acute Treatment Therapies for Pediatric Migraine: A Qualitative Systematic
ISSN 0017-8748 Headache doi: 10.1111/head.12746 VC 2015 American Headache Society Published by Wiley Periodicals, Inc. Review Article Acute Treatment Therapies for Pediatric Migraine: A Qualitative Systematic
A case of a patient with chronic headache. Focus on Migraine. None related to the presentation Grants to conduct clinical trials from: Speaker bureau:
 Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Prevention of Antineoplastic Medication induced Nausea and Vomiting in Pediatric Cancer Patients
 Prevention of Antineoplastic Medication induced Nausea and Vomiting in Pediatric Cancer Patients Done by :Meznah Zaid Al-Mutairi Pharm.D Candidate PNU University College of Pharmacy Introduction Nausea
Prevention of Antineoplastic Medication induced Nausea and Vomiting in Pediatric Cancer Patients Done by :Meznah Zaid Al-Mutairi Pharm.D Candidate PNU University College of Pharmacy Introduction Nausea
Dose: Metoclopramide -0.1 mg/kg (max 10 mg) IV, over 15 minutes
 Metoclopramide for Refractory Migraine in the ED Specific Care Question : In the pediatric patient diagnosed with refractory migraine, is metoclopramide an effective treatment? Question Originator: Migraine
Metoclopramide for Refractory Migraine in the ED Specific Care Question : In the pediatric patient diagnosed with refractory migraine, is metoclopramide an effective treatment? Question Originator: Migraine
Faculty Disclosure. Karen L. Bremer, MD. Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest.
 Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
What A Headache! Theresa Biesiada March 8, 2012
 What A Headache! Theresa Biesiada March 8, 2012 Objectives Describe the EM relevance of headaches and migraines Discuss the rationale for steroid therapy Review the evidence Conclusions My inspiration
What A Headache! Theresa Biesiada March 8, 2012 Objectives Describe the EM relevance of headaches and migraines Discuss the rationale for steroid therapy Review the evidence Conclusions My inspiration
Disclosures. Objectives 6/2/2017
 Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache
 MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
Inpatient Treatment of Refractory Headache
 Inpatient Treatment of Refractory Headache MaryAnn Mays, MD Headache Center Center for Neurological Restoration Neurological Institute Cleveland Clinic Disclosures Speakers Bureau for Allergan, Teva, and
Inpatient Treatment of Refractory Headache MaryAnn Mays, MD Headache Center Center for Neurological Restoration Neurological Institute Cleveland Clinic Disclosures Speakers Bureau for Allergan, Teva, and
Active ingredients: Metoclopramide Hydrochloride mg Equivalent to metoclopramide hydrochloride anhydrous mg
 Name Primperan 10 mg / 2 ml Metoclopramide hydrochloride anhydrous Solution for I.M. or I.V. injection (Ampoules) Composition Each 2 ml ampoule contains: Active ingredients: Metoclopramide Hydrochloride.
Name Primperan 10 mg / 2 ml Metoclopramide hydrochloride anhydrous Solution for I.M. or I.V. injection (Ampoules) Composition Each 2 ml ampoule contains: Active ingredients: Metoclopramide Hydrochloride.
Paediatric headaches. Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services. Brevity, levity, repetition
 Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
Update on Diagnosis and Management of Migraines
 Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, II. Management of Refractory Headaches
 Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Measure Components Numerator Statement
 MEASURE #5: OVERUSE OF OPIOID CONTAINING MEDICATIONS FOR PRIMARY HEADACHE DISORDERS Headache For Quality Improvement Only. Not to be used for Public Reporting or Accountability Measure Description Percentage
MEASURE #5: OVERUSE OF OPIOID CONTAINING MEDICATIONS FOR PRIMARY HEADACHE DISORDERS Headache For Quality Improvement Only. Not to be used for Public Reporting or Accountability Measure Description Percentage
Migraine Management. Roger Cady, MD Headache Care Center Springfield, MO
 Migraine Management Roger Cady, MD Headache Care Center Springfield, MO Disclosures Objectives The evolution of migraine From benign episodic (benign) headache to potentially a devastating chronic disease
Migraine Management Roger Cady, MD Headache Care Center Springfield, MO Disclosures Objectives The evolution of migraine From benign episodic (benign) headache to potentially a devastating chronic disease
HEADACHE. Dr Nick Pendleton. September Headache
 HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
PAEDIATRIC ACUTE CARE GUIDELINE. Headache. This document should be read in conjunction with this DISCLAIMER
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
25/09/2018 HEADACHE. Dr Nick Pendleton
 HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital
 Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital Honorarium from Current Pain and Headache Reports; Section Editor Unusual
Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital Honorarium from Current Pain and Headache Reports; Section Editor Unusual
ACUTE TREATMENT FOR MIGRAINE. Cristina Tassorelli
 The European Headache School 2012 ACUTE TREATMENT FOR MIGRAINE Cristina Tassorelli Headache Science Centre, IRCCS Neurological Institute C. Mondino Foundation - Pavia University Centre for Adaptive Disorders
The European Headache School 2012 ACUTE TREATMENT FOR MIGRAINE Cristina Tassorelli Headache Science Centre, IRCCS Neurological Institute C. Mondino Foundation - Pavia University Centre for Adaptive Disorders
Index. Prim Care Clin Office Pract 31 (2004) Note: Page numbers of article titles are in boldface type.
 Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Clinical Learning Days November 10, 2017
 Migraine Clinical Learning Days November 10, 2017 Alyssa Lettich. MD Neurosciences Institute/Neurosciences Clinical Program Medical Director Headache Disclosures: none Learning Objectives: At the conclusion
Migraine Clinical Learning Days November 10, 2017 Alyssa Lettich. MD Neurosciences Institute/Neurosciences Clinical Program Medical Director Headache Disclosures: none Learning Objectives: At the conclusion
Outpatient Headache Care Guideline
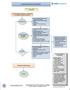 1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
Disclosures. Triptans for Kids 5/16/13
 5/16/13 Disclosures Triptans for Kids Amy A. Gelfand, MD GelfandA@neuropeds.ucsf.edu Departments of Neurology and Pediatrics UCSF Child Neurology and Headache Center I receive grant funding from: NIH/NINDS
5/16/13 Disclosures Triptans for Kids Amy A. Gelfand, MD GelfandA@neuropeds.ucsf.edu Departments of Neurology and Pediatrics UCSF Child Neurology and Headache Center I receive grant funding from: NIH/NINDS
MIGRAINE A MYSTERY HEADACHE
 MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
disease or in clients who consume alcohol on a regular basis. bilirubin
 NON-OPIOID Acetaminophen(Tylenol) Therapeutic class: Analgesic, antipyretic Aspirin (ASA, Acetylsalicylic Acid) Analgesic, NSAID, antipyretic Non-Opioid Analgesics COMMON USES WHAT I NEED TO KNOW AS A
NON-OPIOID Acetaminophen(Tylenol) Therapeutic class: Analgesic, antipyretic Aspirin (ASA, Acetylsalicylic Acid) Analgesic, NSAID, antipyretic Non-Opioid Analgesics COMMON USES WHAT I NEED TO KNOW AS A
SUMAVEL DOSEPRO (sumatriptan succinate) solution for injection
 SUMAVEL DOSEPRO (sumatriptan succinate) solution for injection Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit
SUMAVEL DOSEPRO (sumatriptan succinate) solution for injection Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit
ONZETRA XSAIL (sumatriptan) nasal powder
 ONZETRA XSAIL (sumatriptan) nasal powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
ONZETRA XSAIL (sumatriptan) nasal powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
Abstract The aim of this prospective,
 J Headache Pain (2005) 6:143 148 DOI 10.1007/s10194-005-0169-y ORIGINAL Zulfi Engindeniz Celaleddin Demircan Necdet Karli Erol Armagan Mehtap Bulut Tayfun Aydin Mehmet Zarifoglu Intramuscular tramadol
J Headache Pain (2005) 6:143 148 DOI 10.1007/s10194-005-0169-y ORIGINAL Zulfi Engindeniz Celaleddin Demircan Necdet Karli Erol Armagan Mehtap Bulut Tayfun Aydin Mehmet Zarifoglu Intramuscular tramadol
Current Migraine Treatment Therapy. Daniel Kassicieh, DO, FAAN
 Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
Migraine much more than just a headache
 Migraine much more than just a headache Session hosted by Teva UK Limited PUU4 11:15 12:15 UK/NHSS/18/0021b Date of Preparation: August 2018 The views expressed in this presentation are those of the speaker
Migraine much more than just a headache Session hosted by Teva UK Limited PUU4 11:15 12:15 UK/NHSS/18/0021b Date of Preparation: August 2018 The views expressed in this presentation are those of the speaker
Sumatriptan Tablets, Nasal Spray (Imitrex), Nasal Powder (Onzetra Xsail), sumatriptan and naproxen sodium (Treximet tablets)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 0 Subject: Sumatriptan Page: 1 of 6 Last Review Date: November 30, 2018 Sumatriptan Description Sumatriptan
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 0 Subject: Sumatriptan Page: 1 of 6 Last Review Date: November 30, 2018 Sumatriptan Description Sumatriptan
Nausea and Vomiting in Palliative Care
 Nausea and Vomiting in Palliative Care Definitions Nausea - an unpleasant feeling of the need to vomit Vomiting - the expulsion of gastric contents through the mouth, caused by forceful and sustained contraction
Nausea and Vomiting in Palliative Care Definitions Nausea - an unpleasant feeling of the need to vomit Vomiting - the expulsion of gastric contents through the mouth, caused by forceful and sustained contraction
Headache. Section 1. Migraine headache. Clinical presentation
 Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
How do we treat migraine? New SIGN Guidelines
 How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
MEASURE #1: MEDICATION PRESCRIBED FOR ACUTE MIGRAINE ATTACK Headache
 MEASURE #1: MEDICATION PRESCRIBED FOR ACUTE MIGRAINE ATTACK Headache Measure Description Percentage of patients age 12 years and older with a diagnosis of migraine who were prescribed a guideline recommended
MEASURE #1: MEDICATION PRESCRIBED FOR ACUTE MIGRAINE ATTACK Headache Measure Description Percentage of patients age 12 years and older with a diagnosis of migraine who were prescribed a guideline recommended
Controlling Migraine Pain
 Migraine Stats Controlling Migraine Pain Alan Zacharias, M.D. Associated Neurologists, Boulder Community Health 303-622-3365 Women 15% Men 5% Usually starts in 2 nd and 3 rd Decade Major Impact on days
Migraine Stats Controlling Migraine Pain Alan Zacharias, M.D. Associated Neurologists, Boulder Community Health 303-622-3365 Women 15% Men 5% Usually starts in 2 nd and 3 rd Decade Major Impact on days
10/13/17. Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD
 Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD } Depomed Consultant 2014 to present } Avanir Consultant 2014 to present } Amgen
Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD } Depomed Consultant 2014 to present } Avanir Consultant 2014 to present } Amgen
Migraine Management. Jane Melling Headache nurse Mater Misericordiae Hospital
 Migraine Management Jane Melling Headache nurse Mater Misericordiae Hospital Migraine facts Among the most common disorders of the nervous system 3 rd most prevalent medical disorder on the planet (lancet
Migraine Management Jane Melling Headache nurse Mater Misericordiae Hospital Migraine facts Among the most common disorders of the nervous system 3 rd most prevalent medical disorder on the planet (lancet
Overuse of barbiturate and opioid containing medications for primary headache disorders Description
 Measure Title Overuse of barbiturate and opioid containing medications for primary headache disorders Description Percentage of s age 12 years and older with a diagnosis of primary headache who were prescribed
Measure Title Overuse of barbiturate and opioid containing medications for primary headache disorders Description Percentage of s age 12 years and older with a diagnosis of primary headache who were prescribed
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centers: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
PAIN. Physiology of pain relating to pain management
 PAIN Physiology of pain relating to pain management What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) The generation of pain
PAIN Physiology of pain relating to pain management What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) The generation of pain
10/31/2017 PRIMARY CARE AND HEADACHE DISCLOSURES WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Primary Care 67%
 PRIMARY CARE AND HEADACHE Sonja Potrebic MD PhD Regional Headache Specialist Kaiser LAMC 1 WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Column1 Primary Care 67% Primary Care Headache Specialty Other
PRIMARY CARE AND HEADACHE Sonja Potrebic MD PhD Regional Headache Specialist Kaiser LAMC 1 WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Column1 Primary Care 67% Primary Care Headache Specialty Other
The best defense is a good offense. Optimizing the Acute Treatment of Migraine. Disclosures 11/10/2017
 Optimizing the Acute Treatment of Migraine Brian M. Plato, DO, FAHS Norton Neuroscience Institute Louisville, KY Disclosures Speakers Bureau (personal): Allergan, Depomed, Avanir Research Funding (paid
Optimizing the Acute Treatment of Migraine Brian M. Plato, DO, FAHS Norton Neuroscience Institute Louisville, KY Disclosures Speakers Bureau (personal): Allergan, Depomed, Avanir Research Funding (paid
Dosing & Administration
 Dosing & Administration REAL LIFE. REAL RESULTS. INDICATION INVEGA SUSTENNA (paliperidone palmitate) is indicated for the treatment of: Schizophrenia. Schizoaffective disorder as monotherapy and as an
Dosing & Administration REAL LIFE. REAL RESULTS. INDICATION INVEGA SUSTENNA (paliperidone palmitate) is indicated for the treatment of: Schizophrenia. Schizoaffective disorder as monotherapy and as an
Migraine: pharmacotherapy in the emergency department
 J Accid Emerg Med 2000;17:241 245 241 Department of Emergency Medicine, Western Hospital, Footscray 3011, Australia Correspondence to: Professor Kelly, Director of Emergency Medicine (Anne-Maree.Kelly@
J Accid Emerg Med 2000;17:241 245 241 Department of Emergency Medicine, Western Hospital, Footscray 3011, Australia Correspondence to: Professor Kelly, Director of Emergency Medicine (Anne-Maree.Kelly@
A Prospective, Randomized Trial of Intravenous Prochlorperazine Versus Subcutaneous Sumatriptan in Acute Migraine Therapy in the Emergency Department
 PAIN MANAGEMENT/ORIGINAL RESEARCH A Prospective, Randomized Trial of Intravenous Prochlorperazine Versus Subcutaneous Sumatriptan in Acute Migraine Therapy in the Emergency Department Mark A. Kostic, MD,
PAIN MANAGEMENT/ORIGINAL RESEARCH A Prospective, Randomized Trial of Intravenous Prochlorperazine Versus Subcutaneous Sumatriptan in Acute Migraine Therapy in the Emergency Department Mark A. Kostic, MD,
MIGRAINE A CAUSE OF INTENSE THROBBING; A MINI REVIEW
 IJBPAS, January, 2016, 5(1): 87-92 ISSN: 2277 4998 MIGRAINE A CAUSE OF INTENSE THROBBING; A MINI REVIEW MUHAMMAD ZAMAN 1*, RABIA HASSAN 1, MUHAMMAD SHAFEEQ UR RAHMAN 2, MUHAMMAD HAFIZ ARSHAD 3, SYED ATIF
IJBPAS, January, 2016, 5(1): 87-92 ISSN: 2277 4998 MIGRAINE A CAUSE OF INTENSE THROBBING; A MINI REVIEW MUHAMMAD ZAMAN 1*, RABIA HASSAN 1, MUHAMMAD SHAFEEQ UR RAHMAN 2, MUHAMMAD HAFIZ ARSHAD 3, SYED ATIF
What is the Effectiveness of OnabotulinumtoxinA (Botox ) in Reducing the Number of Chronic Migraines (CM) in Patients Years Old?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 What is the Effectiveness of OnabotulinumtoxinA
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 What is the Effectiveness of OnabotulinumtoxinA
MIGRAINE ASSOCIATION OF IRELAND
 MIGRAINE ASSOCIATION OF IRELAND HEADACHE IN MEN: THE FACTS This leaflet was composed by Paolo Rossi M.D., Ph.D. of the European Headache Alliance to mark European Migraine Day of Action 2014. Why a leaflet
MIGRAINE ASSOCIATION OF IRELAND HEADACHE IN MEN: THE FACTS This leaflet was composed by Paolo Rossi M.D., Ph.D. of the European Headache Alliance to mark European Migraine Day of Action 2014. Why a leaflet
MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache
 MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache Measure Description Percentage of patients age 18 years old and older diagnosed with migraine headache whose migraine frequency is 4 migraine
MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache Measure Description Percentage of patients age 18 years old and older diagnosed with migraine headache whose migraine frequency is 4 migraine
UPDATE IN MIGRAINE MANAGEMENT
 UPDATE IN MIGRAINE MANAGEMENT Eric P. Baron, DO Cleveland Clinic Neurological Institute Center for Neurological Restoration Headache and Chronic Pain Medicine barone2@ccf.org @Neuralgroover Disclosures
UPDATE IN MIGRAINE MANAGEMENT Eric P. Baron, DO Cleveland Clinic Neurological Institute Center for Neurological Restoration Headache and Chronic Pain Medicine barone2@ccf.org @Neuralgroover Disclosures
DISCLAIMER: ECHO Nevada emphasizes patient privacy and asks participants to not share ANY Protected Health Information during ECHO clinics.
 DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
BJF Acute Pain Team Formulary Group
 Title Analgesia Guidelines for Acute Pain Management (Adults) in BGH Document Type Issue no Clinical guideline Clinical Governance Support Team Use Issue date April 2013 Review date April 2015 Distribution
Title Analgesia Guidelines for Acute Pain Management (Adults) in BGH Document Type Issue no Clinical guideline Clinical Governance Support Team Use Issue date April 2013 Review date April 2015 Distribution
Sumatriptan Tablets, Nasal Spray (Imitrex), Nasal Powder (Onzetra Xsail), sumatriptan and naproxen sodium (Treximet tablets)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 05.70.10 Subject: Sumatriptan Page: 1 of 6 Last Review Date: March 16, 2018 Sumatriptan Description Sumatriptan
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 05.70.10 Subject: Sumatriptan Page: 1 of 6 Last Review Date: March 16, 2018 Sumatriptan Description Sumatriptan
Management of headache
 Management of headache TJ Steiner Imperial College London Based on European principles of management of common headache disorders TJ Steiner, K Paemeleire, R Jensen, D Valade, L Savi, MJA Lainez, H-C Diener,
Management of headache TJ Steiner Imperial College London Based on European principles of management of common headache disorders TJ Steiner, K Paemeleire, R Jensen, D Valade, L Savi, MJA Lainez, H-C Diener,
Migraine: Developing Drugs for Acute Treatment Guidance for Industry
 Migraine: Developing Drugs for Acute Treatment Guidance for Industry U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and Research (CDER) February 2018
Migraine: Developing Drugs for Acute Treatment Guidance for Industry U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and Research (CDER) February 2018
PAIN PODCAST SHOW NOTES:
 PAIN PODCAST SHOW NOTES: Dallas Holladay, DO Ultrasound Fellow Cook County Hospital Rush University Medical Center Jonathan D. Alterie, DO PGY-2, Emergency Medicine Midwestern University An overview of
PAIN PODCAST SHOW NOTES: Dallas Holladay, DO Ultrasound Fellow Cook County Hospital Rush University Medical Center Jonathan D. Alterie, DO PGY-2, Emergency Medicine Midwestern University An overview of
Chronic Daily Headaches
 Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Antidepressants: Prof. Riyadh Al_Azzawi F.R.C.Psych
 Antidepressants: Prof. Riyadh Al_Azzawi F.R.C.Psych A. Heterocyclic antidepressants: (tricyclic and tetracyclic ), e.g.amitryptaline,imipramine. B. Monoamine oxidase inhibitors(m.a.o.i), e.g.phenelzine.
Antidepressants: Prof. Riyadh Al_Azzawi F.R.C.Psych A. Heterocyclic antidepressants: (tricyclic and tetracyclic ), e.g.amitryptaline,imipramine. B. Monoamine oxidase inhibitors(m.a.o.i), e.g.phenelzine.
Chapter 161 Antipsychotics
 Chapter 161 Antipsychotics Episode Overview Extrapyramidal syndromes are a common complication of antipsychotic medications. First line treatment is benztropine or diphenhydramine. Lorazepam is used in
Chapter 161 Antipsychotics Episode Overview Extrapyramidal syndromes are a common complication of antipsychotic medications. First line treatment is benztropine or diphenhydramine. Lorazepam is used in
Daniel Kassicieh, DO, FAAN
 Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraine is a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality but high morbidity 38 million Americans
Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraine is a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality but high morbidity 38 million Americans
Chronic Migraine in Primary Care. December 11 th, 2017 Werner J. Becker University of Calgary
 Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
TRAPADOL INJECTION FOR I.V./I.M. USE ONLY
 TRAPADOL INJECTION FOR I.V./I.M. USE ONLY Composition : Each 2ml. contains : Tramadol Hydrochloride I.P. Water for injection I.P. 100mg. q.s. CLINICAL PHARMACOLOGY : Pharmacodynamics Tramadol is a centrally
TRAPADOL INJECTION FOR I.V./I.M. USE ONLY Composition : Each 2ml. contains : Tramadol Hydrochloride I.P. Water for injection I.P. 100mg. q.s. CLINICAL PHARMACOLOGY : Pharmacodynamics Tramadol is a centrally
Zomig. Zomig / Zomig-ZMT (zolmitriptan) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.22 Subject: Zomig Page: 1 of 5 Last Review Date: November 30, 2018 Zomig Description Zomig / Zomig-ZMT
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.22 Subject: Zomig Page: 1 of 5 Last Review Date: November 30, 2018 Zomig Description Zomig / Zomig-ZMT
Prevention and Treatment of Migraines CAITLIN BARNES, PHARM.D. CANDIDATE AMBULATORY CARE JOE CAMMILLERI, PHARM.D. NATOHYA MALLORY, PHARM.D.
 Prevention and Treatment of Migraines CAITLIN BARNES, PHARM.D. CANDIDATE AMBULATORY CARE JOE CAMMILLERI, PHARM.D. NATOHYA MALLORY, PHARM.D. Objectives Present patient case Review epidemiology/pathophysiology
Prevention and Treatment of Migraines CAITLIN BARNES, PHARM.D. CANDIDATE AMBULATORY CARE JOE CAMMILLERI, PHARM.D. NATOHYA MALLORY, PHARM.D. Objectives Present patient case Review epidemiology/pathophysiology
GI Pharmacology -4 Irritable Bowel Syndrome and Antiemetics. Dr. Alia Shatanawi
 GI Pharmacology -4 Irritable Bowel Syndrome and Antiemetics Dr. Alia Shatanawi 11-04-2018 Drugs used in Irritable Bowel Syndrome Idiopathic, chronic, relapsing disorder characterized by abdominal discomfort
GI Pharmacology -4 Irritable Bowel Syndrome and Antiemetics Dr. Alia Shatanawi 11-04-2018 Drugs used in Irritable Bowel Syndrome Idiopathic, chronic, relapsing disorder characterized by abdominal discomfort
Elements for a Public Summary Overview of disease epidemiology
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Acute pain usually responds to medication and should settle in less than three months. Inadequate pain relief may lead to other
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Acute pain usually responds to medication and should settle in less than three months. Inadequate pain relief may lead to other
New Zealand Data Sheet
 Arrow - Sumatriptan Sumatriptan Injection 6mg/0.5mL Presentation New Zealand Data Sheet ARROW SUMATRIPTAN Injection 6mg/0.5mL is a clear, colourless to pale yellow solution in a prefilled syringe. Uses
Arrow - Sumatriptan Sumatriptan Injection 6mg/0.5mL Presentation New Zealand Data Sheet ARROW SUMATRIPTAN Injection 6mg/0.5mL is a clear, colourless to pale yellow solution in a prefilled syringe. Uses
Case Presentation. Case Presentation. Case Presentation. Truths about Headaches (2017) Most headaches were muscle-tension headaches
 Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Clinical case. Clinical case 3/15/2018 OVERVIEW. Refractory headaches and update on novel treatment. Refractory headache.
 OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
Migraine Management. Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital
 Migraine Management Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital Referral Criteria for Migraine Migraine Management Migraine Diagnosis Spot on Health Migraine pathway
Migraine Management Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital Referral Criteria for Migraine Migraine Management Migraine Diagnosis Spot on Health Migraine pathway
Comparison of Intravenous Metoclopramide and Acetaminophen in Primary Headaches: a Randomized Controlled Trial
 1 Emergency (2015); 3 (*): ***-*** ORIGINAL RESEARCH Comparison of Intravenous Metoclopramide and Acetaminophen in Primary Headaches: a Randomized Controlled Trial Gholamreza Faridaalaee 1, Seyed Hesam
1 Emergency (2015); 3 (*): ***-*** ORIGINAL RESEARCH Comparison of Intravenous Metoclopramide and Acetaminophen in Primary Headaches: a Randomized Controlled Trial Gholamreza Faridaalaee 1, Seyed Hesam
Overview INTRODUCTION 3/15/2018. Headache Emergencies. Other way to differentiate between them? Is there an easy way to differentiate between them?
 Overview Headache Emergencies Primary versus Secondary headache disorder Red flags 4 cases of unusual headache emergencies Disclaimer: we will not talk about brain bleed as patients usually go the ED.
Overview Headache Emergencies Primary versus Secondary headache disorder Red flags 4 cases of unusual headache emergencies Disclaimer: we will not talk about brain bleed as patients usually go the ED.
NOTOPAIN CAPLETS. Diclofenac Sodium + Paracetamol. Composition. Each tablet contains: Diclofenac Sodium BP 50mg Paracetamol BP 500mg.
 NOTOPAIN CAPLETS Diclofenac Sodium + Paracetamol Composition Each tablet contains: Diclofenac Sodium BP 50mg Paracetamol BP 500mg Pharmacology Phamacodynamics Diclofenac relieves pain and inflammation
NOTOPAIN CAPLETS Diclofenac Sodium + Paracetamol Composition Each tablet contains: Diclofenac Sodium BP 50mg Paracetamol BP 500mg Pharmacology Phamacodynamics Diclofenac relieves pain and inflammation
HEADACHES THE RED FLAGS
 HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker
 PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
Managing Headache in Acute Medicine. Ben Lovell Consultant Physician in Acute Medicine University College London Hospital
 Managing Headache in Acute Medicine Ben Lovell Consultant Physician in Acute Medicine University College London Hospital Some ED headache stats Arrive by ambulance 31% Median age 39 Worst ever headache
Managing Headache in Acute Medicine Ben Lovell Consultant Physician in Acute Medicine University College London Hospital Some ED headache stats Arrive by ambulance 31% Median age 39 Worst ever headache
ACUTE MIGRAINE: OLD AND NEW DRUGS JOHN ROBROCK MD FORT WILLIAM FAMILY HEALTH TEAM
 ACUTE MIGRAINE: OLD AND NEW DRUGS JOHN ROBROCK MD FORT WILLIAM FAMILY HEALTH TEAM Conflict of Interest Declaration: Nothing to Disclose Presenter: John Robrock, MD Title of Presentation: Acute Migraine:
ACUTE MIGRAINE: OLD AND NEW DRUGS JOHN ROBROCK MD FORT WILLIAM FAMILY HEALTH TEAM Conflict of Interest Declaration: Nothing to Disclose Presenter: John Robrock, MD Title of Presentation: Acute Migraine:
Parenteral Dihydroergotamine for Acute Migraine Headache: A Systematic Review of the Literature
 NEUROLOGY/ORIGINAL RESEARCH Parenteral Dihydroergotamine for Acute Migraine Headache: A Systematic Review of the Literature Ian Colman, MSc Michael D. Brown, MD, MSc Grant D. Innes, MD Eric Grafstein,
NEUROLOGY/ORIGINAL RESEARCH Parenteral Dihydroergotamine for Acute Migraine Headache: A Systematic Review of the Literature Ian Colman, MSc Michael D. Brown, MD, MSc Grant D. Innes, MD Eric Grafstein,
Acute Migraine Treatment: What you and your family should know to help you make the best choices with your doctor
 Acute Migraine Treatment: What you and your family should know to help you make the best choices with your doctor TAKE CONTROL OF YOUR MIGRAINES! ABOUT THIS PATIENT GUIDE: Migraine attacks are often debilitating
Acute Migraine Treatment: What you and your family should know to help you make the best choices with your doctor TAKE CONTROL OF YOUR MIGRAINES! ABOUT THIS PATIENT GUIDE: Migraine attacks are often debilitating
Migraine is is one of the most common chronic neurological
 Review Article Rescue Treatment for Migraine Headache in Emergency Department Part 2: Role of Antiepileptic, Magnesium, Corticosteroids, and Discharge Care Abstract Migraine is a common chronic neurological
Review Article Rescue Treatment for Migraine Headache in Emergency Department Part 2: Role of Antiepileptic, Magnesium, Corticosteroids, and Discharge Care Abstract Migraine is a common chronic neurological
PREVALENCE BY HEADACHE TYPE
 CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy
 HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
Pain therapeutics. Acetaminophen/NSAIDs Acute pain Osteoarthritis Migraine Acute Gout Neuropathic pain
 Pain therapeutics Acetaminophen/NSAIDs Acute pain Osteoarthritis Migraine Acute Gout Neuropathic pain James McCormack, Pharm.D. Professor Faculty of Pharmaceutical Sciences, UBC Common types of pain killers
Pain therapeutics Acetaminophen/NSAIDs Acute pain Osteoarthritis Migraine Acute Gout Neuropathic pain James McCormack, Pharm.D. Professor Faculty of Pharmaceutical Sciences, UBC Common types of pain killers
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Balanced Analgesia With NSAIDS and Coxibs. Raymond S. Sinatra MD, Ph.D
 Balanced Analgesia With NSAIDS and Coxibs Raymond S. Sinatra MD, Ph.D Prostaglandins and Pain The primary noxious mediator released from damaged tissue is prostaglandin (PG) PG is responsible for nociceptor
Balanced Analgesia With NSAIDS and Coxibs Raymond S. Sinatra MD, Ph.D Prostaglandins and Pain The primary noxious mediator released from damaged tissue is prostaglandin (PG) PG is responsible for nociceptor
Symptom Management. Thomas McKain, MD, ABFM, ABHPM Medical Director
 Symptom Management Nausea & Vomiting Thomas McKain, MD, ABFM, ABHPM Medical Director Mr. Jones has nausea and vomiting. May I initiate Compazine from the Comfort Pak? Objectives 1. Delineate the Differential
Symptom Management Nausea & Vomiting Thomas McKain, MD, ABFM, ABHPM Medical Director Mr. Jones has nausea and vomiting. May I initiate Compazine from the Comfort Pak? Objectives 1. Delineate the Differential
Primary Care Adult Headache Management Pathway (formerly North West Headache Management Guideline for Adults) Version 1.0
 Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
