Transradial Approach for Mechanical Thrombectomy of Posterior Circulation Stroke
|
|
|
- Stuart Ryan
- 5 years ago
- Views:
Transcription
1 Journal of Neuroendovascular Therapy 2018; 12: Online January 18, 2018 DOI: /jnet.tn Transradial Approach for Mechanical Thrombectomy of Posterior Circulation Stroke Taichiro Mizokami, 1 Takeshi Uwatoko, 2 Takashi Furukawa, 1 Eiji Higashi, 2 Yusuke Sakaki, 2 Natsuki Suetsugi, 3 Yuichiro Takamatsu, 1 Kenichi Matsumoto, 1 Hiroshi Takashima, 3 Hiroshi Sugimori, 2 and Shuji Sakata 1 Objective: We report the mechanical thrombectomy (MT) of posterior circulation large vessel occlusion (pc-lvo) in which the transradial approach (TRA) was selected as an initial approach route to reduce the duration of treatment. Case Presentation: We performed MT using the TRA for four patients with pc-lvo between November 2015 and March The TRA was used as an initial approach route in patients in whom preoperative MRI showed that the right vertebral artery (VA) was predominant. In all patients, the procedure could be accomplished without changing the approach route. Thrombolysis in Cerebral Infarction (TICI) 2b or better recanalization was achieved in all patients (100%), and TICI 3 recanalization in three patients (75%). Mean time from radial artery puncture to initial intracranial angiography and to the effective recanalization was 7.3 ± 1.5 and 28.8 ± 6.2 minutes, respectively. There was no complication at the site of puncture. Conclusion: Recanalization was promptly and effectively achieved by the MT of pc-lvo using the TRA. The results suggest that TRA can be utilized as an initial access route in patients in whom an approach to the right VA is possible. Keywords transradial approach, posterior circulation stroke, endovascular treatment, acute ischemic stroke, mechanical thrombectomy Introduction The development of thrombectomy devices, such as stent retrievers and large aspiration catheters, and evidence on efficacy have rapidly promoted the widespread application of endovascular treatment in clinical practice. 1,2) With respect to thrombectomy or the recanalization rate, favorable results have been consistently obtained, but we have often encountered patients in whom it was difficult to guide 1 Department of Neurosurgery, Saga-Ken Medical Center Koseikan, Saga, Saga, Japan 2 Department of Cerebrovascular Disease, Saga-Ken Medical Center Koseikan, Saga, Saga, Japan 3 Department of Neurology, Saga-Ken Medical Center Koseikan, Saga, Saga, Japan Received: August 12, 2017; Accepted: December 17, 2017 Corresponding author: Taichiro Mizokami. Saga-ken Medical Center Koseikan, 400 Nakabaru, Kase, Saga , Japan mizmiztaich@gmail.com This work is licensed under a Creative Commons Attribution-NonCommercial- NoDerivatives International License The Japanese Society for Neuroendovascular Therapy a guiding catheter into an occluded blood vessel, with an increase in the number of patients to be treated by this therapy. 3 6) Several studies reported that recanalization should be promptly performed to treat posterior circulation large vessel occlusion (pc-lvo), as indicated for the anterior circulation. 7,8) However, when selecting the transfemoral approach (TFA) for patients in whom an approach to the right vertebral artery (VA) is necessary, a specific interval is sometimes required until reaching due to the tortuosity of the aortic arch. We speculated that the transradial approach (TRA) might be useful in patients in whom an approach to the right VA is necessary, and treated them using the TRA. We examined the efficacy and safety of the TRA for the mechanical thrombectomy (MT) of pc-lvo. Case Presentation Of 80 patients who underwent acute-phase MT in our hospital between November 2013 and March 2017, pc-lvo was observed in nine patients (12.5%). In these patients, the posterior circulation Alberta Stroke Program Early CT score (pc-aspects) 9) and degree of left/right VA development were evaluated on preoperative MRI. 314
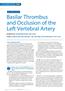
2 TRA for MT of Posterior Circulation Stroke When MRA showed that the right VA was predominant, the radial artery was used as the site of puncture after confirming a positive reaction on the Allen test. When the left VA was predominant, endovascular treatment was started using the femoral artery. When the degree of VA development was similar between the left and right sides, the operator selected a blood vessel to be punctured. The interval between arterial puncture and initial intracranial angiography through a guiding catheter was defined as the access time. Success or failure in recanalization was evaluated using the Thrombolysis in Cerebral Infarction (TICI) classification. 10) The interval from arterial puncture until TICI 2b or better recanalization was defined as the time to recanalization. For four patients, MT was performed through the right VA using the TRA. These patients showed positive reactions on the Allen test. The mean age was 82.0 ± 10.7 years. The preoperative Glasgow Coma Scale (GCS) score was 6.5 ± 4.4, and the preoperative National Institute of Health Stroke Scale (NIHSS) score was 21.0 ± The pc- ASPECTS was 6.5 ± 3.3. Intravenous thrombolysis with recombinant tissue plasminogen activator (rt-pa) was performed in three patients (75%). In three patients with out-of-hospital onset, the mean interval from onset until arrival was 86.7 ± 50.3 minutes, and that from arrival until arterial puncture was ± 73.6 minutes. In one patient with in-hospital onset, the interval from onset until arterial puncture was 125 minutes. The occluded blood vessels were P1 segment of the posterior cerebral artery (PCA) in two patients, basilar trunk in one patient, and basilar tip in one patient. In all patients, it was possible to start thrombectomy without changing the approach route. The mean access time was 7.3 ± 1.5 minutes. TICI 3 recanalization was achieved in three patients (75%), and TICI 2b recanalization in one patient (25%). The mean time to recanalization was 28.8 ± 6.2 minutes. Under local anesthesia, radial artery puncture was performed using a 21G puncture needle. After a 4 Fr. sheath was inserted, it was exchanged for a guiding catheter using a guidewire. As a guiding catheter, a guiding sheath was used in all patients. An ASAHI FUBUKI Dilator 6 Fr. (Asahi Intecc, Aichi, Japan) was adopted for the first patient, and an ASAHI FUBUKI Dilator 4 Fr. was used in the subsequent three patients. Concerning devices for thrombectomy, a stent retriever was selected for patients with proximal occlusion of the basilar trunk or those in whom the thrombus volume was expected to be large, and an aspiration catheter for those with distal occlusion involving the basilar tip. A Trevo XP ProVue Retriever 4 20 mm (Stryker, Kalamazoo, MI, USA) was combined with a Penumbra 3MAX (Penumbra, Alameda, CA, U.S.A.) in one patient. A Penumbra 4MAX was used in one patient, and a Penumbra 3MAX in two patients. The mean frequency of the procedure was 1.8 ± 1.0 times. For all patients, hemostasis was performed using a TR band (Terumo Corporation, Tokyo, Japan). Concerning the outcome, the mean GCS score at 24 hours after treatment was 12.5 ± 4.4, and the mean NIHSS score was 16.5 ± A favorable outcome was achieved in one patient (20.0%), with a modified Rankin Scale (mrs) score of 2 after 3 months. There was no complication at the site of puncture in any patient treated using the TRA. The details are shown in Table 1. During the same period, the MT of pc-lvo via the TFA was performed for five patients in our hospital. For all patients, an access to the left VA was selected. The mean access time was 11.0 ± 5.2 minutes. TICI 2a recanalization was achieved in one patient (20%), and TICI 2b recanalization in four patients (80%). In the latter, the mean time to recanalization was 35.5 ± 14.9 minutes. Regarding devices for thrombectomy, a 5MAX ACE was used in one patient, a 3MAX in one patient, the combination of a 4MAX and Trevo XP ProVue Retriever 4 x 20 mm in two patients, and the combination of a 4MAX and Solitaire FR 4 20 mm (Medtronic, Minneapolis, MN, USA) in one patient. The mean frequency of the procedure was 2.8 ± 1.5 times. As a complication at the site of puncture, a retroperitoneal hematoma was noted in one patient (20.0%). As shown in Table 2, the treatment results were compared between the TRA and TFA. Representative case Our case is an 86-year-old male. Consciousness disorder occurred while having a meal. He was brought to our hospital by ambulance 80 minutes after onset. The consciousness level on arrival was E1V1M3 by the GCS score, and the NIHSS score was 31. On MRI diffusion-weighted images (DWIs), high-signal-intensity areas were partially detected in the left occipital lobe and pons. Small highsignal-intensity areas were also detected in the midbrain and bilateral thalamus, and the pc-aspects was 2 (Fig. 1A and 1B). On intracranial MRA, the basilar artery was not visualized (Fig. 1C). On cervical MRA, the right VA was visualized, but the left VA was not (Fig. 1D). The platelet count was 30000/µL, which did not meet indication criteria of the intravenous thrombolysis with rt-pa, and thus it was not performed. Although the condition was 315
3 Mizokami T, et al. Table 1 Summary of the patients selected for the transradial approach Post-GCS mrs Number of procedure Device Guiding sheath TICI Time to recanalization Access time Door to puncture Onset IV rt-pa Location to door pc- ASPECTS Pre- NIHSS Pre- GCS No Age 3 E1V1M4 5 Trevo 4 20, 3MAX 1 86 E1V1M No BA trunk b FUBUKI Dilator4 Fr. 4MAX 1 E4V4M E1V1M Yes PCA (P1) FUBUKI Dilator6 Fr. 3MAX 1 E4V5M E3V4M Yes BA tip FUBUKI Dilator4 Fr. 3MAX 2 E4V5M E1V1M3 5 6 Yes PCA (P1) FUBUKI Dilator4 Fr. Mean Patient 3 was in hospital onset ischemic stroke. BA: basilar artery; Fr.: French; GCS: Glasgow Coma Scale; IV: intravenous infusion; mrs: modified Rankin Scale; NIHSS: National Institute of Health Stroke Scale; PCA: posterior cerebral artery; pc-aspects: the posterior circulation Alberta Stroke Program Early CT score; rt-pa: recombinant tissue plasminogen activator; TICI: thrombolysis in cerebral infarction severe, the patient was diagnosed as complete basilar artery occlusion, and MT was considered to be necessary. Based on preoperative MRA information, an approach from the radial artery to the right VA was selected. The interval from hospital arrival until arterial puncture was 95 minutes. Under local anesthesia, the radial artery was punctured using a 21G needle, and a 4 Fr. sheath (Terumo Corporation) was inserted. Subsequently, it was exchanged for an ASAHI FUBUKI Dilator 4 Fr. using Radiofocus wire (Terumo Corporation). The dilator was removed, and a guiding catheter was inserted into the right VA through the right subclavian artery using a 4 Fr. OK-2 M (Cathex, Tokyo, Japan) as an inner catheter (Fig. 1E and 1F). Intracranial angiography was performed 8 minutes after arterial puncture. At the basilar trunk, a thrombus was detected, and anterograde blood flow was blocked (Fig. 1G). As the thrombus volume was expected to be large, a stent retriever was selected. A Marksman (Medtronic) was guided into the right PCA, and thrombectomy was performed using a Trevo XP ProVue Retriever 4 20 mm. Anterograde blood flow from the basilar artery to the right PCA was resumed at 24 minutes after arterial puncture. Still the thrombus involving the basilar tip to P1 segment of the left PCA remained; therefore, thrombectomy was performed using a Penumbra 3MAX. A delay in left PCA blood flow was noted, and treatment was completed with TICI 2b recanalization (Fig. 1H). Hemostasis with a TR band was conducted. After surgery, no improvement in consciousness disorder was observed. The mrs score after 3 months was 5. Discussion For endovascular treatment in acute ischemic stroke, a reduction in the interval from the onset of cerebral infarction until recanalization significantly contributes to an improvement in the outcome; it is important to shorten the duration of treatment. 1,2) The interval from the start of treatment until an access by a guiding catheter to an occluded blood vessel is an important factor for shortening the duration of treatment. However, other factors, such as aortic tortuosity, prolong the access time in some patients. Ribo et al. 6) reported that the recanalization rate was low in patients with an access time of 30 minutes, and that many patients showed an unfavorable outcome. According to several studies, the route was changed, or the use of devices was devised in such patients. 3 6,11) Of patients with pc-lvo, the prognosis becomes unfavorable in approximately 90% when recanalization is 316
4 TRA for MT of Posterior Circulation Stroke Table 2 Procedural outcomes of TRA and TFA total TRA TFA n:9 n:4 n:5 Age 75.7 ± ± ± 9.8 Access time 9.3 ± ± ± 5.2 Time to recanalization 40.4 ± ± ± 14.9 TICI 2b or 3(%) 8 (88.9) 4 (100) 4 (80.0) TICI 3(%) 3 (33.3) 3 (75.0) 0 (0) Number of the procedure 2.2 ± ± ± 1.5 Access site complication (%) 1 (11.1) 0 (0) 1 (20.0) TFA: transfemoral approach; TICI: thrombolysis in cerebral infarction; TRA: transradial approach Fig. 1 (A and B) The diffusion-weighted MRI showed ischemic stroke at the left occipital lobe, mid brain, and bilateral thalamus. (C) The intracranial MRA showed basilar artery occlusion. (D) The cervical MRA showed the right vertebral artery that is the dominant side (arrow). (E and F) The guiding catheter was navigated into the right vertebral artery via the transradial approach. (G and H) The DSA showed the basilar trunk was occluded by the thrombus (arrowhead) and TICI 2b reperfusion was achieved after thrombectomy. TICI: thrombolysis in cerebral infarction not achieved. On the other hand, recent studies indicated that the endovascular treatment related effective recanalization rate was approximately 70% 80%, and that a favorable outcome was achieved in 30% 40%. 7,8,12,13) Concerning the MT of pc-lvo, some studies reported that prompt, effective recanalization of occluded blood vessels contributed to the prognosis, as demonstrated for anterior circulation; a fast access route with a high success rate should be selected. 7,8) In the field of cerebral endovascular treatment for cerebral aneurysms or VA stenosis, the success rates of transradial or -brachial approaches are high, suggesting their efficacy ) These approaches have the following merits: direct cannulation from the subclavian artery to the VA is possible regardless of the aortic tortuosity, and a guiding catheter stays stable after insertion. According to previous studies of endovascular treatment for acute ischemic stroke, TRA and transbrachial 317
5 Mizokami T, et al. approach was chosen only for patients who switched from unsuccessful TFA. 4 6) Haussen et al. 4) reported 15 patients who underwent endovascular treatment for acute ischemic stroke via the TRA. In 12 of these, the TFA was unsuccessful, requiring a switch to the TRA. They suggested the TRA as an alternative and useful method for patients in whom the TFA is difficult. Furthermore, 10 patients had posterior circulation stroke, and the TRA was more appropriate. To our knowledge, this is the first report predominantly selecting the TRA rather than the TFA in MT of pc-lvo which allows an approach to the right VA. When performing MT, the selection of an initial approach route is an influential for the duration of treatment; it should be carefully selected. 2) Cerebral endovascular treatment has been performed via the TFA in many cases. For patients with pc-lvo, an access to the left VA via the TFA may be an initial access route if an approach to the left VA is possible. On the other hand, there are differences in the difficulty of an access to the right VA via the TFA, depending on the position of the bifurcation between the aorta and brachiocephalic trunk; this may prolong the duration of treatment or contribute to the instability of a guiding catheter. We selected the TRA as an initial access route for patients requiring an access to the right VA, considering more prompt recanalization and the stability of a guiding catheter. In all patients for whom the TRA was selected, treatment was possible. Furthermore, the access time, time to recanalization, and effective recanalization rate were similar to those in patients in whom an access to the left VA via the TFA was used during the same period in our institution. An access to the right VA via the TRA is a prompt, safe, and effective method in patients in whom an access to the right VA is possible, while the TRA to the left VA is not appropriate for endovascular treatment for the following reasons: puncture is complex, and the TFA is easy. When adopting the TRA, 4 Fr. and 6 Fr. guiding sheaths were used. A Stent Retriever and Penumbra 3MAX are available for 4 Fr. guiding sheaths. In addition to the former, a Penumbra 5MAX ACE and Penumbra 4MAX are available for 6 Fr. guiding sheaths. We performed treatment with a Penumbra 4MAX using a 6 Fr. guiding sheath for one patient in the initial phase. However, we currently consider that treatment with a Stent Retriever or Penumbra 3MAX is possible. When conducting the endovascular treatment of pc-lvo via the TRA, treatment is started using a 4 Fr. guiding sheath. With respect to the selection of devices for thrombectomy, a stent retriever was selected for patients with proximal occlusion of the basilar trunk or VA or those in whom the thrombus volume was expected to be large, and an aspiration catheter for those with distal occlusion of the basilar tip or PCA. Balloon guiding catheters, 18) which are useful for treating the anterior circulation occlusion, are not used for the treatment of the posterior circulation occlusion due to the presence of contralateral VA blood flow and a small VA diameter. Concerning the site of puncture, the radial artery, where the incidence of puncture-site complications is lower than at the brachial artery, is adopted, 19) as IV rt-pa therapy is combined in many cases. Recently, MRI has been skipped to reduce the time of examination in the treatment of the anterior circulation occlusion. 20) However, posterior circulation stroke causes various neurologic symptoms; therefore, endovascular treatment is performed after a definitive diagnosis is made based on MRI findings. In this study, an improvement in the GCS score was achieved immediately after MT in three of the four patients. However, three of the four patients showed unfavorable outcomes; deaths were related to a low pc-aspects, advanced age, and postoperative aspiration pneumonia. pc-lvo uniformly leads to an unfavorable outcome if recanalization is not achieved. Therefore, treatment must be indicated for a larger number of patients, and serious stroke-related complications may occur, raising issues. In the MT of pc-lvo, the limitations of the initial TRA include the prolongation of the puncture time, flexion of the brachial artery, and a vasospasm-related delay in approaching. Furthermore, the course of the subclavian artery or bifurcation angle between the subclavian and VAs may make the approach difficult in some patients. Although there are strategies to overcome these problems, the TRA should be promptly switched to other approaches, such as the TFA, for time-sensitive MT. Therefore, disinfection at the femoral artery region or draping beforehand is effective. However, the number of patients in this study was small, and a larger number of patients should be examined in the future. Conclusion In four patients in whom the MT of pc-lvo was started via the TRA, recanalization was promptly and effectively achieved without changing the approach route, suggesting the usefulness of this approach method. 318
6 TRA for MT of Posterior Circulation Stroke Disclosure Statement There is no conflict of interest for the first author and coauthors. References 1) Badhiwala JH, Nassiri F, Alhazzani W, et al: Endovascular thrombectomy for acute ischemic stroke: a meta-analysis. JAMA 2015; 314: ) Saver JL, Goyal M, van der Lugt A, et al: Time to treatment with endovascular thrombectomy and outcomes from ischemic stroke: a meta-analysis. JAMA 2016; 316: ) Tokunaga S, Tsurusaki Y, Sambongi Y, et al: Ballooninflation anchoring technique for insertion of a guiding catheter in acute mechanical thrombectomy. JNET 2017; 11: ) Haussen DC, Nogueira RG, DeSousa KG, et al: Transradial access in acute ischemic stroke intervention. J Neurointerv Surg 2016; 8: ) Okawa M, Tateshima S, Liebeskind D, et al: Successful recanalization for acute ischemic stroke via the transbrachial approach. J Neurointerv Surg 2016; 8: ) Ribo M, Flores A, Rubiera M, et al: Difficult catheter access to the occluded vessel during endovascular treatment of acute ischemic stroke is associated with worse clinical outcome. J Neurointerv Surg 2013; 5: i70 i73. 7) Mokin M, Sonig A, Sivakanthan S, et al: Clinical and procedural predictors of outcomes from the endovascular treatment of posterior circulation strokes. Stroke 2016; 47: ) Vergouwen MD, Algra A, Pfefferkorn T, et al: Time is brain(stem) in basilar artery occlusion. Stroke 2012; 43: ) Tei H, Uchiyama S, Usui T, et al: Posterior circulation ASPECTS on diffusion-weighted MRI can be a powerful marker for predicting functional outcome. J Neurol 2010; 257: ) Higashida RT, Furlan AJ, Roberts H, et al: Trial design and reporting standards for intra-arterial cerebral thrombolysis for acute ischemic stroke. Stroke 2003; 34: e109 e ) Yoshimura S, Enomoto Y, Kitajima H, et al: Carotidcompression technique for the insertion of guiding catheters. AJNR Am J Neuroradiol 2006; 27: ) Singer OC, Berkefeld J, Nolte CH, et al: Mechanical recanalization in basilar artery occlusion: the ENDOSTROKE study. Ann Neurol 2015; 77: ) Eom YI, Hwang YH, Hong JM, et al: Forced arterial suction thrombectomy with the penumbra reperfusion catheter in acute basilar artery occlusion: a retrospective comparison study in 2 Korean university hospitals. AJNR Am J Neuroradiol 2014; 35: ) Horton TG, Kalapos P, Cockroft KM: Brachial artery approach for endovascular treatment of posterior circulation intracranial vascular disease: technique and application in 5 cases. J Stroke Cerebrovasc Dis 2012; 21: ) Iwata T, Mori T, Miyazaki Y, et al: Anatomical features of the vertebral artery for transbrachial direct cannulation of a guiding catheter to perform coil embolization of cerebral aneurysms in the posterior cerebral circulation. Interv Neuroradiol 2015; 21: ) Gao F, Lo WJ, Sun X, et al: Selective use of transradial access for endovascular treatment of severe intracranial vertebrobasilar artery stenosis. Clin Neurol Neurosurg 2015; 134: ) Mizokami T, Uwatoko T, Inoue K, et al: Transbrachial coil embolization for posterior circulation aneurysm in elderly patients using a 4 Fr. guiding sheath. JNET 2016; 10: ) Nguyen TN, Malisch T, Castonguay AC, et al: Balloon guide catheter improves revascularization and clinical outcomes with the solitaire device: analysis of the North American solitaire acute stroke registry. Stroke 2014; 45: ) Kiemeneij F, Laarman GJ, Odekerken D, et al: A randomized comparison of percutaneous transluminal coronary angioplasty by the radial, brachial and femoral approaches: the access study. J Am Coll Cardiol 1997; 29: ) Menon BK, Almekhlafi MA, Pereira VM, et al: Optimal workflow and process-based performance measures for endovascular therapy in acute ischemic stroke: analysis of the Solitaire FR thrombectomy for acute revascularization study. Stroke 2014; 45:
Thrombectomy in Octogenarians in the Era of Stent Retriever: Is an Age Limit Necessary?
 Journal of Neuroendovascular Therapy 2017; 11: 563 569 Online July 10, 2017 DOI: 10.5797/jnet.oa.2017-0031 Thrombectomy in Octogenarians in the Era of Stent Retriever: Is an Age Limit Necessary? Yosuke
Journal of Neuroendovascular Therapy 2017; 11: 563 569 Online July 10, 2017 DOI: 10.5797/jnet.oa.2017-0031 Thrombectomy in Octogenarians in the Era of Stent Retriever: Is an Age Limit Necessary? Yosuke
Successful Endovascular Revascularization of Acute Basilar Artery Occlusion Approached via an Aberrant Right Subclavian Artery
 Journal of Neuroendovascular Therapy 2017; 11: 416 420 Online April 27, 2017 DOI: 10.5797/jnet.cr.2016-0109 Successful Endovascular Revascularization of Acute Basilar Artery Occlusion Approached via an
Journal of Neuroendovascular Therapy 2017; 11: 416 420 Online April 27, 2017 DOI: 10.5797/jnet.cr.2016-0109 Successful Endovascular Revascularization of Acute Basilar Artery Occlusion Approached via an
Endovascular Treatment for Acute Ischemic Stroke: Considerations from Recent Randomized Trials
 Published online: March 13, 2015 1664 9737/15/0034 0115$39.50/0 Review Endovascular Treatment for Acute Ischemic Stroke: Considerations from Recent Randomized Trials Manabu Shirakawa a Shinichi Yoshimura
Published online: March 13, 2015 1664 9737/15/0034 0115$39.50/0 Review Endovascular Treatment for Acute Ischemic Stroke: Considerations from Recent Randomized Trials Manabu Shirakawa a Shinichi Yoshimura
Perils of Mechanical Thrombectomy in Acute Asymptomatic Large Vessel Occlusion
 Perils of Mechanical Thrombectomy in Acute Asymptomatic Large Vessel Occlusion Aman B. Patel, MD Robert & Jean Ojemann Associate Professor Director, Cerebrovascular Surgery Director, Neuroendovascular
Perils of Mechanical Thrombectomy in Acute Asymptomatic Large Vessel Occlusion Aman B. Patel, MD Robert & Jean Ojemann Associate Professor Director, Cerebrovascular Surgery Director, Neuroendovascular
Stroke Clinical Trials Update Transitioning to an Anatomic Diagnosis in Ischemic Stroke
 Stroke Clinical Trials Update Transitioning to an Anatomic Diagnosis in Ischemic Stroke Alexander A. Khalessi MD MS Director of Endovascular Neurosurgery Surgical Director of NeuroCritical Care University
Stroke Clinical Trials Update Transitioning to an Anatomic Diagnosis in Ischemic Stroke Alexander A. Khalessi MD MS Director of Endovascular Neurosurgery Surgical Director of NeuroCritical Care University
Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous Internal Carotid Artery Dissections
 Journal of Neuroendovascular Therapy 2017; 11: 437 442 Online June 13, 2017 DOI: 10.5797/jnet.tn.2016-0059 Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous
Journal of Neuroendovascular Therapy 2017; 11: 437 442 Online June 13, 2017 DOI: 10.5797/jnet.tn.2016-0059 Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
 Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
Three Cases with Wide-necked Cerebral Aneurysms in Whom the T-stent Technique Was Useful
 DOI: 10.5797/jnet.tn.2017-0127 Three Cases with Wide-necked Cerebral Aneurysms in Whom the T-stent Technique Was Useful Yusuke Morinaga, Hayatsura Hanada, Ayumu Eto, Takafumi Mitsutake, Fumihiro Hiraoka,
DOI: 10.5797/jnet.tn.2017-0127 Three Cases with Wide-necked Cerebral Aneurysms in Whom the T-stent Technique Was Useful Yusuke Morinaga, Hayatsura Hanada, Ayumu Eto, Takafumi Mitsutake, Fumihiro Hiraoka,
Endovascular Therapy for Acute Ischemic Stroke: Reducing Door-to-puncture Time
 DOI: 10.5797/jnet.oa.2016-0140 Endovascular Therapy for Acute Ischemic Stroke: Reducing Door-to-puncture Time Yoichi Morofuji, 1,2 Nobutaka Horie, 1,2 Yohei Tateishi, 2,3 Minoru Morikawa, 4 Eisaku Sadakata,
DOI: 10.5797/jnet.oa.2016-0140 Endovascular Therapy for Acute Ischemic Stroke: Reducing Door-to-puncture Time Yoichi Morofuji, 1,2 Nobutaka Horie, 1,2 Yohei Tateishi, 2,3 Minoru Morikawa, 4 Eisaku Sadakata,
Mechanical Thrombectomy of Large Vessel Occlusions Using Stent Retriever Devices
 Mechanical Thrombectomy of Large Vessel Occlusions Using Stent Retriever Devices Joey English MD, PhD Medical Director, Neurointerventional Services California Pacific Medical Center Hospitals, San Francisco,
Mechanical Thrombectomy of Large Vessel Occlusions Using Stent Retriever Devices Joey English MD, PhD Medical Director, Neurointerventional Services California Pacific Medical Center Hospitals, San Francisco,
Acute basilar artery occlusion (BAO) is associated with a very
 ORIGINAL RESEARCH INTERVENTIONAL Acute Basilar Artery Occlusion: Outcome of Mechanical Thrombectomy with Solitaire Stent within 8 Hours of Stroke Onset J.M. Baek, W. Yoon, S.K. Kim, M.Y. Jung, M.S. Park,
ORIGINAL RESEARCH INTERVENTIONAL Acute Basilar Artery Occlusion: Outcome of Mechanical Thrombectomy with Solitaire Stent within 8 Hours of Stroke Onset J.M. Baek, W. Yoon, S.K. Kim, M.Y. Jung, M.S. Park,
Endovascular Treatment for Acute Ischemic Stroke
 ular Treatment for Acute Ischemic Stroke Vishal B. Jani MD Assistant Professor Interventional Neurology, Division of Department of Neurology. Creighton University/ CHI health Omaha NE Disclosure None 1
ular Treatment for Acute Ischemic Stroke Vishal B. Jani MD Assistant Professor Interventional Neurology, Division of Department of Neurology. Creighton University/ CHI health Omaha NE Disclosure None 1
Basilar artery stenosis with bilateral cerebellar strokes on coumadin
 Qaisar A. Shah, MD Patient Profile 68 years old female with a history of; Basilar artery stenosis with bilateral cerebellar strokes on coumadin Diabetes mellitus Hyperlipidemia Hypertension She developed
Qaisar A. Shah, MD Patient Profile 68 years old female with a history of; Basilar artery stenosis with bilateral cerebellar strokes on coumadin Diabetes mellitus Hyperlipidemia Hypertension She developed
Update on Early Acute Ischemic Stroke Interventions
 Update on Early Acute Ischemic Stroke Interventions Diana Goodman MD Lead Neurohospitalist Maine Medical Center Assistant Professor of Neurology, Tufts University School of Medicine I have no disclosures
Update on Early Acute Ischemic Stroke Interventions Diana Goodman MD Lead Neurohospitalist Maine Medical Center Assistant Professor of Neurology, Tufts University School of Medicine I have no disclosures
PARADIGM SHIFT FOR THROMBOLYSIS IN PATIENTS WITH ACUTE ISCHAEMIC STROKE, FROM EXTENSION OF THE TIME WINDOW TO RAPID RECANALISATION AFTER SYMPTOM ONSET
 PARADIGM SHIFT FOR THROMBOLYSIS IN PATIENTS WITH ACUTE ISCHAEMIC STROKE, FROM EXTENSION OF THE TIME WINDOW TO RAPID RECANALISATION AFTER SYMPTOM ONSET Hye Seon Jeong, *Jei Kim Department of Neurology and
PARADIGM SHIFT FOR THROMBOLYSIS IN PATIENTS WITH ACUTE ISCHAEMIC STROKE, FROM EXTENSION OF THE TIME WINDOW TO RAPID RECANALISATION AFTER SYMPTOM ONSET Hye Seon Jeong, *Jei Kim Department of Neurology and
Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge Procedure Using the Coil Mass as a Support
 Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
Single Pass MCA Revascularization with Trevo
 Single Pass MCA Revascularization with Trevo By Concentric Medical ProVueTM Retriever Case Reported By Sascha Prothmann, MD Klinikum rechts der Isar, Munich, Germany Images contained herein courtesy of
Single Pass MCA Revascularization with Trevo By Concentric Medical ProVueTM Retriever Case Reported By Sascha Prothmann, MD Klinikum rechts der Isar, Munich, Germany Images contained herein courtesy of
Neuro-vascular Intervention in Stroke. Will Adams Consultant Neuroradiologist Plymouth Hospitals NHS Trust
 Neuro-vascular Intervention in Stroke Will Adams Consultant Neuroradiologist Plymouth Hospitals NHS Trust Stroke before the mid 1990s Swelling Stroke extension Haemorrhagic transformation Intravenous thrombolysis
Neuro-vascular Intervention in Stroke Will Adams Consultant Neuroradiologist Plymouth Hospitals NHS Trust Stroke before the mid 1990s Swelling Stroke extension Haemorrhagic transformation Intravenous thrombolysis
ACUTE ISCHEMIC STROKE. Current Treatment Approaches for Acute Ischemic Stroke
 ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
Predictors of Poor Outcome after Successful Mechanical Thrombectomy in Patients with Acute Anterior Circulation Stroke
 THIEME Original Article 139 Predictors of Poor Outcome after Successful Mechanical Thrombectomy in Patients with Acute Anterior Circulation Stroke Yosuke Tajima 1 Michihiro Hayasaka 1 Koichi Ebihara 1
THIEME Original Article 139 Predictors of Poor Outcome after Successful Mechanical Thrombectomy in Patients with Acute Anterior Circulation Stroke Yosuke Tajima 1 Michihiro Hayasaka 1 Koichi Ebihara 1
Endovascular Stroke Therapy
 Endovascular Stroke Therapy Update with Emphasis on Practical Clinical and Imaging Considerations Sachin Kishore Pandey, MD, FRCPC Disclosures I have no relevant financial disclosures or conflict of interest
Endovascular Stroke Therapy Update with Emphasis on Practical Clinical and Imaging Considerations Sachin Kishore Pandey, MD, FRCPC Disclosures I have no relevant financial disclosures or conflict of interest
A Patient with Cerebral Embolism Related to Trousseau s Syndrome
 Journal of Neuroendovascular Therapy 2017; 11: 575 580 Online July 11, 2017 DOI: 10.5797/jnet.cr.2017-0008 A Patient with Cerebral Embolism Related to Trousseau s Syndrome Yosuke Nishimuta, 1 Tetsuya Nagayama,
Journal of Neuroendovascular Therapy 2017; 11: 575 580 Online July 11, 2017 DOI: 10.5797/jnet.cr.2017-0008 A Patient with Cerebral Embolism Related to Trousseau s Syndrome Yosuke Nishimuta, 1 Tetsuya Nagayama,
UPDATES IN INTRACRANIAL INTERVENTION Jordan Taylor DO Metro Health Neurology 2015
 UPDATES IN INTRACRANIAL INTERVENTION Jordan Taylor DO Metro Health Neurology 2015 NEW STUDIES FOR 2015 MR CLEAN ESCAPE EXTEND-IA REVASCAT SWIFT PRIME RECOGNIZED LIMITATIONS IV Alteplase proven benefit
UPDATES IN INTRACRANIAL INTERVENTION Jordan Taylor DO Metro Health Neurology 2015 NEW STUDIES FOR 2015 MR CLEAN ESCAPE EXTEND-IA REVASCAT SWIFT PRIME RECOGNIZED LIMITATIONS IV Alteplase proven benefit
SEE IT. BELIEVE IT. THE CONFIDENCE OF CLARITY. Solitaire Platinum. Revascularization Device
 SEE IT. BELIEVE IT. THE CONFIDENCE OF CLARITY. Revascularization THE CONFIDENCE OF CLARITY. The key features that make the device effective have been retained including our unique Parametric overlapping
SEE IT. BELIEVE IT. THE CONFIDENCE OF CLARITY. Revascularization THE CONFIDENCE OF CLARITY. The key features that make the device effective have been retained including our unique Parametric overlapping
ORIGINAL RESEARCH. Gabriel A. Vidal, MD, 1,2 James M. Milburn, MD 3
 ORIGINAL RESEARCH Ochsner Journal 16:486 491, 2016 Ó Academic Division of Ochsner Clinic Foundation The Penumbra 5MAX ACE Catheter Is Safe, Efficient, and Cost Saving as a Primary Mechanical Thrombectomy
ORIGINAL RESEARCH Ochsner Journal 16:486 491, 2016 Ó Academic Division of Ochsner Clinic Foundation The Penumbra 5MAX ACE Catheter Is Safe, Efficient, and Cost Saving as a Primary Mechanical Thrombectomy
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Thrombectomy using Trevo ProVue Stent Retriever Devices after Recombinant Tissue Plasminogen Activator Thrombolysis for Acute Basilar Artery Occlusion during Vertebral Artery Dissection Joe
CASE REPORT Thrombectomy using Trevo ProVue Stent Retriever Devices after Recombinant Tissue Plasminogen Activator Thrombolysis for Acute Basilar Artery Occlusion during Vertebral Artery Dissection Joe
Mechanical Thrombectomy: Where Are We Now? T. Adam Oliver, MD Tallahassee Neurological Clinic Tallahassee, Florida TMH Neurosymposium June 11, 2016
 Mechanical Thrombectomy: Where Are We Now? T. Adam Oliver, MD Tallahassee Neurological Clinic Tallahassee, Florida TMH Neurosymposium June 11, 2016 none DISCLOSURES Where did we come from? Spiotta, et
Mechanical Thrombectomy: Where Are We Now? T. Adam Oliver, MD Tallahassee Neurological Clinic Tallahassee, Florida TMH Neurosymposium June 11, 2016 none DISCLOSURES Where did we come from? Spiotta, et
Mechanical thrombectomy beyond the 6 hours. Mahmoud Rayes, MD Medical Director, Stroke program Greenville Memorial Hospital
 Mechanical thrombectomy beyond the 6 hours Mahmoud Rayes, MD Medical Director, Stroke program Greenville Memorial Hospital Disclosures None Worldwide statistics 1 IN 6 people will have a stroke at some
Mechanical thrombectomy beyond the 6 hours Mahmoud Rayes, MD Medical Director, Stroke program Greenville Memorial Hospital Disclosures None Worldwide statistics 1 IN 6 people will have a stroke at some
Successful Clot Retrieval Therapy of Cerebral Embolism in a Pediatric Patient with Ventricular Assist Device: A Case Report
 Journal of Neuroendovascular Therapy 2017; 11: 29 34 Online November 9, 2016 DOI: 10.5797/jnet.cr.2016-0063 Successful Clot Retrieval Therapy of Cerebral Embolism in a Pediatric Patient with Ventricular
Journal of Neuroendovascular Therapy 2017; 11: 29 34 Online November 9, 2016 DOI: 10.5797/jnet.cr.2016-0063 Successful Clot Retrieval Therapy of Cerebral Embolism in a Pediatric Patient with Ventricular
Acute brain vessel thrombectomie: when? Why? How?
 Acute brain vessel thrombectomie: when? Why? How? Didier Payen, MD, Ph D Université Paris 7 Département Anesthesiologie-Réanimation Univ Paris 7; Unité INSERM 1160 Hôpital Lariboisière AP-HParis current
Acute brain vessel thrombectomie: when? Why? How? Didier Payen, MD, Ph D Université Paris 7 Département Anesthesiologie-Réanimation Univ Paris 7; Unité INSERM 1160 Hôpital Lariboisière AP-HParis current
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACAS (Asymptomatic Carotid Atherosclerosis Study), 65 66 ACST (Asymptomatic Carotid Surgery Trial), 6 7, 65, 75 Age factors, in carotid
Index Note: Page numbers of article titles are in boldface type. A ACAS (Asymptomatic Carotid Atherosclerosis Study), 65 66 ACST (Asymptomatic Carotid Surgery Trial), 6 7, 65, 75 Age factors, in carotid
Advances in Neuro-Endovascular Care for Acute Stroke
 Advances in Neuro-Endovascular Care for Acute Stroke Ciarán J. Powers, MD, PhD, FAANS Associate Professor Program Director Department of Neurological Surgery Surgical Director Comprehensive Stroke Center
Advances in Neuro-Endovascular Care for Acute Stroke Ciarán J. Powers, MD, PhD, FAANS Associate Professor Program Director Department of Neurological Surgery Surgical Director Comprehensive Stroke Center
Distal Mechanical Thrombectomy in Acute Ischemic Stroke Method and Benefit. Hans Henkes, Wiebke Kurre Stuttgart, Germany
 Distal Mechanical Thrombectomy in Acute Ischemic Stroke Method and Benefit Hans Henkes, Wiebke Kurre Stuttgart, Germany 1 Thrombectomy... with stent-retrievers is an evidence based therapy for intracranial
Distal Mechanical Thrombectomy in Acute Ischemic Stroke Method and Benefit Hans Henkes, Wiebke Kurre Stuttgart, Germany 1 Thrombectomy... with stent-retrievers is an evidence based therapy for intracranial
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Basilar Thrombus and Occlusion of the Left Vertebral Artery
 WHAT WOULD YOU DO? Basilar Thrombus and Occlusion of the Left Vertebral Artery MODERATOR: GUILHERME DABUS, MD, FAHA PANEL: DONALD FREI, MD; ANSAAR T. RAI, MD, MBA; AND SUDHAKAR R. SATTI, MD CASE PRESENTATION
WHAT WOULD YOU DO? Basilar Thrombus and Occlusion of the Left Vertebral Artery MODERATOR: GUILHERME DABUS, MD, FAHA PANEL: DONALD FREI, MD; ANSAAR T. RAI, MD, MBA; AND SUDHAKAR R. SATTI, MD CASE PRESENTATION
ORIGINAL PAPER. 8-F balloon guide catheter for embolization of anterior circulation aneurysms: an institutional experience in 152 patients
 Nagoya J. Med. Sci. 79. 435 ~ 441, 2017 doi:10.18999/nagjms.79.4.435 ORIGINAL PAPER 8-F balloon guide catheter for embolization of anterior circulation aneurysms: an institutional experience in 152 patients
Nagoya J. Med. Sci. 79. 435 ~ 441, 2017 doi:10.18999/nagjms.79.4.435 ORIGINAL PAPER 8-F balloon guide catheter for embolization of anterior circulation aneurysms: an institutional experience in 152 patients
Patient selection for i.v. thrombolysis and thrombectomy
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 8 Acute treatment and early secondary prevention of stroke Level 2 Patient selection for
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 8 Acute treatment and early secondary prevention of stroke Level 2 Patient selection for
Broadening the Stroke Window in Light of the DAWN Trial
 Broadening the Stroke Window in Light of the DAWN Trial South Jersey Neurovascular and Stroke Symposium April 26, 2018 Rohan Chitale, MD Assistant Professor of Neurological Surgery Vanderbilt University
Broadening the Stroke Window in Light of the DAWN Trial South Jersey Neurovascular and Stroke Symposium April 26, 2018 Rohan Chitale, MD Assistant Professor of Neurological Surgery Vanderbilt University
Historical. Medical Policy
 Medical Policy Subject: Mechanical Embolectomy for Treatment of Acute Stroke Policy #: SURG.00098 Current Effective Date: 01/01/2016 Status: Revised Last Review Date: 08/06/2015 Description/Scope This
Medical Policy Subject: Mechanical Embolectomy for Treatment of Acute Stroke Policy #: SURG.00098 Current Effective Date: 01/01/2016 Status: Revised Last Review Date: 08/06/2015 Description/Scope This
A Novel Technique of Microcatheter Shaping with Cerebral Aneurysmal Coil Embolization: In Vivo Printing Method
 Journal of Neuroendovascular Therapy 2017; 11: 48 52 Online November 28, 2016 DOI: 10.5797/jnet.tn.2016-0051 A Novel Technique of Microcatheter Shaping with Cerebral Aneurysmal Coil Embolization: In Vivo
Journal of Neuroendovascular Therapy 2017; 11: 48 52 Online November 28, 2016 DOI: 10.5797/jnet.tn.2016-0051 A Novel Technique of Microcatheter Shaping with Cerebral Aneurysmal Coil Embolization: In Vivo
The prognosis for acute basilar artery occlusion (BAO) is
 Published July 17, 2014 as 10.3174/ajnr.A4045 ORIGINAL RESEARCH INTERVENTIONAL Forced Arterial Suction Thrombectomy with the Penumbra Reperfusion Catheter in Acute Basilar Artery Occlusion: A Retrospective
Published July 17, 2014 as 10.3174/ajnr.A4045 ORIGINAL RESEARCH INTERVENTIONAL Forced Arterial Suction Thrombectomy with the Penumbra Reperfusion Catheter in Acute Basilar Artery Occlusion: A Retrospective
Stroke Cart Improves Efficiency in Acute Ischemic Stroke Intervention
 Stroke Cart Improves Efficiency in Acute Ischemic Stroke Intervention MR Amans, F Settecase, R Darflinger, M Alexander, A Nicholson, DL Cooke, SW Hetts, CF Dowd, RT Higashida, VV Halbach Interventional
Stroke Cart Improves Efficiency in Acute Ischemic Stroke Intervention MR Amans, F Settecase, R Darflinger, M Alexander, A Nicholson, DL Cooke, SW Hetts, CF Dowd, RT Higashida, VV Halbach Interventional
Primary manual aspiration thrombectomy (MAT) for acute ischemic stroke: safety, feasibility and outcomes in 112 consecutive patients
 1 Department of Neurosurgery, University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania, USA 2 Department of Neurology, Stroke Institute, University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania,
1 Department of Neurosurgery, University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania, USA 2 Department of Neurology, Stroke Institute, University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania,
Interventional Treatment of Stroke
 Interventional Treatment of Stroke Andrew F. Ducruet, MD Barrow Neurological Institute 2018 BNI Stroke Rehab Symposium October 13, 2018 Disclosures Consultant: Medtronic, Penumbra, Cerenovus Lecture Overview
Interventional Treatment of Stroke Andrew F. Ducruet, MD Barrow Neurological Institute 2018 BNI Stroke Rehab Symposium October 13, 2018 Disclosures Consultant: Medtronic, Penumbra, Cerenovus Lecture Overview
Pseudoaneurysm Formation after Repetitive Suction Thrombectomy Using a Penumbra Suction Catheter
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2016.18.3.296 Case Report Pseudoaneurysm Formation after Repetitive Suction Thrombectomy
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2016.18.3.296 Case Report Pseudoaneurysm Formation after Repetitive Suction Thrombectomy
Mechanical thrombectomy in Plymouth. Will Adams. Will Adams
 Mechanical thrombectomy in Plymouth Will Adams Will Adams History Intra-arterial intervention 1995 (NINDS) iv tpa improved clinical outcome in patients treated within 3 hours of ictus but limited recanalisation
Mechanical thrombectomy in Plymouth Will Adams Will Adams History Intra-arterial intervention 1995 (NINDS) iv tpa improved clinical outcome in patients treated within 3 hours of ictus but limited recanalisation
Acute Stroke Treatment: Current Trends 2010
 Acute Stroke Treatment: Current Trends 2010 Helmi L. Lutsep, MD Oregon Stroke Center Oregon Health & Science University Overview Ischemic Stroke Neuroprotectant trials to watch for IV tpa longer treatment
Acute Stroke Treatment: Current Trends 2010 Helmi L. Lutsep, MD Oregon Stroke Center Oregon Health & Science University Overview Ischemic Stroke Neuroprotectant trials to watch for IV tpa longer treatment
ENDOVASCULAR THERAPIES FOR ACUTE STROKE
 ENDOVASCULAR THERAPIES FOR ACUTE STROKE Cerebral Arteriogram Cerebral Anatomy Cerebral Anatomy Brain Imaging Acute Ischemic Stroke (AIS) Therapy Main goal is to restore blood flow and improve perfusion
ENDOVASCULAR THERAPIES FOR ACUTE STROKE Cerebral Arteriogram Cerebral Anatomy Cerebral Anatomy Brain Imaging Acute Ischemic Stroke (AIS) Therapy Main goal is to restore blood flow and improve perfusion
Overview. Introduction. New Interventions for Acute Stroke. New Approaches to hemorrhagic Strokes
 Overview New Interventions for Acute Stroke Paula Eboli, MD Department of Neurosurgery Rockwood Clinic, Deaconess Hospital Introduction New Approaches to hemorrhagic Strokes New Approaches to Ischemic
Overview New Interventions for Acute Stroke Paula Eboli, MD Department of Neurosurgery Rockwood Clinic, Deaconess Hospital Introduction New Approaches to hemorrhagic Strokes New Approaches to Ischemic
Acute basilar artery occlusion (BAO) carries a high morbidity
 ORIGINAL RESEARCH INTERVENTIONAL Combined Use of Mechanical Thrombectomy with Angioplasty and Stenting for Acute Basilar Occlusions with Underlying Severe Intracranial Vertebrobasilar Stenosis: Preliminary
ORIGINAL RESEARCH INTERVENTIONAL Combined Use of Mechanical Thrombectomy with Angioplasty and Stenting for Acute Basilar Occlusions with Underlying Severe Intracranial Vertebrobasilar Stenosis: Preliminary
Endovascular Treatment of Ischemic Stroke
 Endovascular Treatment of Ischemic Stroke William Thorell, MD Associate Professor Neurosurgery UNMC Co-Director Stroke and Neurovascular Center Nebraska Medicine Overview Definitions of terms Review basic
Endovascular Treatment of Ischemic Stroke William Thorell, MD Associate Professor Neurosurgery UNMC Co-Director Stroke and Neurovascular Center Nebraska Medicine Overview Definitions of terms Review basic
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Stent Retriever-Mediated Manual Aspiration Thrombectomy for Acute Ischemic Stroke
 Published online: October 7, 2016 Original Paper Stent Retriever-Mediated Manual Aspiration Thrombectomy for Acute Ashutosh P. Jadhav a, b Amin Aghaebrahim a Anat Horev d Dan-Victor Giurgiutiu c Andrew
Published online: October 7, 2016 Original Paper Stent Retriever-Mediated Manual Aspiration Thrombectomy for Acute Ashutosh P. Jadhav a, b Amin Aghaebrahim a Anat Horev d Dan-Victor Giurgiutiu c Andrew
UNIVERSITY HOSPITAL UDINE/ITALY A SINGLE CENTRE EXPERIENCE IN STROKE TREATMET WITH EMBOTRAP II. TECHNOLOGY BASE ON CLOT RESEARCH
 UNIVERSITY HOSPITAL UDINE/ITALY A SINGLE CENTRE EXPERIENCE IN STROKE TREATMET WITH EMBOTRAP II. TECHNOLOGY BASE ON CLOT RESEARCH Massimo Sponza, Vladimir Gavrilović RIPERFUSION THERAPY Intraovenous thrombolysis
UNIVERSITY HOSPITAL UDINE/ITALY A SINGLE CENTRE EXPERIENCE IN STROKE TREATMET WITH EMBOTRAP II. TECHNOLOGY BASE ON CLOT RESEARCH Massimo Sponza, Vladimir Gavrilović RIPERFUSION THERAPY Intraovenous thrombolysis
A Patient with Stenosis of the Cervical Internal Carotid Artery in Whom Hyperperfusion Syndrome Occurred after Staged Angioplasty
 DOI: 10.5797/jnet.cr.2017-0043 A Patient with Stenosis of the Cervical Internal Carotid Artery in Whom Hyperperfusion Syndrome Occurred after Staged Angioplasty Jun Niimi, Kenta Tasaka, Fumio Nemoto, Takuya
DOI: 10.5797/jnet.cr.2017-0043 A Patient with Stenosis of the Cervical Internal Carotid Artery in Whom Hyperperfusion Syndrome Occurred after Staged Angioplasty Jun Niimi, Kenta Tasaka, Fumio Nemoto, Takuya
Stroke Treatment Beyond Traditional Time Windows. Rishi Gupta, MD, MBA
 Stroke Treatment Beyond Traditional Time Windows Rishi Gupta, MD, MBA Director, Stroke and Neurocritical Care Endovascular Neurosurgery Wellstar Health System THE PAST THE PRESENT 2015 American Heart Association/American
Stroke Treatment Beyond Traditional Time Windows Rishi Gupta, MD, MBA Director, Stroke and Neurocritical Care Endovascular Neurosurgery Wellstar Health System THE PAST THE PRESENT 2015 American Heart Association/American
Mechanical Endovascular Reperfusion Therapy
 Get With the Guidelines Stroke Mechanical Endovascular Reperfusion Therapy February 1, 2017 Speaker Lee H. Schwamm, MD Executive Vice Chairman and Director of Stroke/TeleStroke Services, Department of
Get With the Guidelines Stroke Mechanical Endovascular Reperfusion Therapy February 1, 2017 Speaker Lee H. Schwamm, MD Executive Vice Chairman and Director of Stroke/TeleStroke Services, Department of
Acute Ischemic Stroke Imaging. Ronald L. Wolf, MD, PhD Associate Professor of Radiology
 Acute Ischemic Stroke Imaging Ronald L. Wolf, MD, PhD Associate Professor of Radiology Title of First Slide of Substance An Illustrative Case 2 Disclosures No financial disclosures Off-label uses of some
Acute Ischemic Stroke Imaging Ronald L. Wolf, MD, PhD Associate Professor of Radiology Title of First Slide of Substance An Illustrative Case 2 Disclosures No financial disclosures Off-label uses of some
Endovascular Procedures (Angioplasty and/or Stenting) for Intracranial Arterial Disease (Atherosclerosis and Aneurysms)
 Endovascular Procedures (Angioplasty and/or Stenting) for Intracranial Arterial Disease (Atherosclerosis and Aneurysms) Policy Number: 2.01.54 Last Review: 11/2018 Origination: 4/2006 Next Review: 11/2019
Endovascular Procedures (Angioplasty and/or Stenting) for Intracranial Arterial Disease (Atherosclerosis and Aneurysms) Policy Number: 2.01.54 Last Review: 11/2018 Origination: 4/2006 Next Review: 11/2019
Disclosure. Advances in Interventional Neurology. Disclosure. Natural History of Disease 3/15/2018. Vishal B. Jani MD
 Advances in Interventional Neurology Disclosure Vishal B. Jani MD Medical Director Vascular Neurology Consultant Interventional Neurology CHI Health Assistant Professor, Creighton University School of
Advances in Interventional Neurology Disclosure Vishal B. Jani MD Medical Director Vascular Neurology Consultant Interventional Neurology CHI Health Assistant Professor, Creighton University School of
Strokecenter Key lessons of MR CLEAN study
 Strokecenter Key lessons of MR CLEAN study Diederik Dippel Disclosures Funded by the Dutch Heart Foundation Nominal, unrestricted grants from AngioCare BV Medtronic/Covidien/EV3 MEDAC Gmbh/LAMEPRO Penumbra
Strokecenter Key lessons of MR CLEAN study Diederik Dippel Disclosures Funded by the Dutch Heart Foundation Nominal, unrestricted grants from AngioCare BV Medtronic/Covidien/EV3 MEDAC Gmbh/LAMEPRO Penumbra
Trans-radial Carotid Artery Stenting in a Patient with Abdominal Aortic Occlusion
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2016.18.2.129 Case Report Trans-radial Carotid Artery Stenting in a Patient with
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2016.18.2.129 Case Report Trans-radial Carotid Artery Stenting in a Patient with
Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital
 Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital Disclosures Penumbra, Inc. research grant (significant) for
Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital Disclosures Penumbra, Inc. research grant (significant) for
Intro: Slide 1. Slide 2. Slide 3. Basic understanding of interventional radiology. Gain knowledge of key terms and phrases
 Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Mechanical thrombectomy with stent retriever in acute ischemic stroke: first results.
 Mechanical thrombectomy with stent retriever in acute ischemic stroke: first results. Poster No.: C-0829 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. H. J. Voormolen, T. Van der Zijden, I. Baar,
Mechanical thrombectomy with stent retriever in acute ischemic stroke: first results. Poster No.: C-0829 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. H. J. Voormolen, T. Van der Zijden, I. Baar,
CAROTID ARTERY STENTING TECHNICALS ASPECTS. Symposium Abbott Vascular CANNES MEET 2008 Drs V PIRET, P BERGERON
 CAROTID ARTERY STENTING TECHNICALS ASPECTS Symposium Abbott Vascular CANNES MEET 2008 Drs V PIRET, P BERGERON POINTS TO DISCUSS TO CAS INDICATIONS CONTRA INDICATIONS ANATOMICAL CONSIDERATION TECHNICS CAS
CAROTID ARTERY STENTING TECHNICALS ASPECTS Symposium Abbott Vascular CANNES MEET 2008 Drs V PIRET, P BERGERON POINTS TO DISCUSS TO CAS INDICATIONS CONTRA INDICATIONS ANATOMICAL CONSIDERATION TECHNICS CAS
Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis
 HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
Single-stage Coil Embolization for Kissing Aneurysms of the Internal Carotid Artery Using Enterprise Stent: Three Cases Reports
 Journal of Neuroendovascular Therapy 2018; 12: 6 13 Online September 21, 2017 DOI: 10.5797/jnet.oa.2017-0017 Single-stage Coil Embolization for Kissing Aneurysms of the Internal Carotid Artery Using Enterprise
Journal of Neuroendovascular Therapy 2018; 12: 6 13 Online September 21, 2017 DOI: 10.5797/jnet.oa.2017-0017 Single-stage Coil Embolization for Kissing Aneurysms of the Internal Carotid Artery Using Enterprise
Acute Management of Stroke due to Intracranial Steno-occlusion. Joon-Tae Kim, MD, PhD Department of Neurology Chonnam National University Hospital
 Acute Management of Stroke due to Intracranial Steno-occlusion Joon-Tae Kim, MD, PhD Department of Neurology Chonnam National University Hospital None Disclosure Contents Current status of acute management
Acute Management of Stroke due to Intracranial Steno-occlusion Joon-Tae Kim, MD, PhD Department of Neurology Chonnam National University Hospital None Disclosure Contents Current status of acute management
12/4/2017. Disclosures. Study organization. Stryker Medtronic Penumbra Viz Route 92. Data safety monitoring board Tudor G.
 12/4/2017 Update on Stroke Trials:Extending the Window DWI or CTP Assessment with Clinical Mismatch in the Triage of Wake-Up and Late Presenting Strokes Undergoing Neurointervention with Trevo NP001713
12/4/2017 Update on Stroke Trials:Extending the Window DWI or CTP Assessment with Clinical Mismatch in the Triage of Wake-Up and Late Presenting Strokes Undergoing Neurointervention with Trevo NP001713
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Managing the Measures: A Serious Look at Key Abstraction Concepts for the Comprehensive Stroke (CSTK) Measure Set Session 2
 Managing the Measures: A Serious Look at Key Abstraction Concepts for the Comprehensive Stroke (CSTK) Measure Set Session 2 January 28, 2015 1 to 3 PM Central Time Continuing Education Credit This course
Managing the Measures: A Serious Look at Key Abstraction Concepts for the Comprehensive Stroke (CSTK) Measure Set Session 2 January 28, 2015 1 to 3 PM Central Time Continuing Education Credit This course
Solitaire FR Revascularization Device
 Solitaire FR Revascularization Device FEATURING PARAMETRIC DESIGN Restore. Retrieve. Revive. 5 Revolutionizing Mechanical Thrombectomy with Parametric Design Solitaire FR Device The Solitaire FR revascularization
Solitaire FR Revascularization Device FEATURING PARAMETRIC DESIGN Restore. Retrieve. Revive. 5 Revolutionizing Mechanical Thrombectomy with Parametric Design Solitaire FR Device The Solitaire FR revascularization
Endovascular stroke research after MRCLEAN. W. van Zwam
 1 Endovascular stroke research after MRCLEAN W. van Zwam 2 Layout 1. What do we know by now 2. Next research questions Anesthesia Aspiration 3. Ongoing and future research Dutch initiatives 3 4 N=70 Intervention
1 Endovascular stroke research after MRCLEAN W. van Zwam 2 Layout 1. What do we know by now 2. Next research questions Anesthesia Aspiration 3. Ongoing and future research Dutch initiatives 3 4 N=70 Intervention
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Endovascular Treatment for Acute Ischemic Stroke: Curtis A. Given II, MD Co-Director, Neurointerventional Services Baptist Physician Lexington
 Endovascular Treatment for Acute Ischemic Stroke: Curtis A. Given II, MD Co-Director, Neurointerventional Services Baptist Physician Lexington Disclosures: SWIFT PRIME site (Medtronic) Physician Proctor
Endovascular Treatment for Acute Ischemic Stroke: Curtis A. Given II, MD Co-Director, Neurointerventional Services Baptist Physician Lexington Disclosures: SWIFT PRIME site (Medtronic) Physician Proctor
The Effect of Diagnostic Catheter Angiography on Outcomes of Acute Ischemic Stroke Patients Being Considered for Endovascular Treatment
 The Effect of Diagnostic Catheter Angiography on Outcomes of Acute Ischemic Stroke Patients Being Considered for Endovascular Treatment Adnan I. Qureshi, MD 1, Muhammad A. Saleem, MD 1, Emrah Aytaç, MD
The Effect of Diagnostic Catheter Angiography on Outcomes of Acute Ischemic Stroke Patients Being Considered for Endovascular Treatment Adnan I. Qureshi, MD 1, Muhammad A. Saleem, MD 1, Emrah Aytaç, MD
Endovascular Treatment Updates in Stroke Care
 Endovascular Treatment Updates in Stroke Care Autumn Graham, MD April 6-10, 2017 Phoenix, AZ Endovascular Treatment Updates in Stroke Care Autumn Graham, MD Associate Professor of Clinical Emergency Medicine
Endovascular Treatment Updates in Stroke Care Autumn Graham, MD April 6-10, 2017 Phoenix, AZ Endovascular Treatment Updates in Stroke Care Autumn Graham, MD Associate Professor of Clinical Emergency Medicine
Coil Embolization of Cerebral Tiny Aneurysms
 Journal of Neuroendovascular Therapy 2016; 10: 243 248 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0035 Coil Embolization of Cerebral Tiny Aneurysms Terumasa Kuroiwa, 1 Fuminori Shimizu, 2 Taro Yamashita,
Journal of Neuroendovascular Therapy 2016; 10: 243 248 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0035 Coil Embolization of Cerebral Tiny Aneurysms Terumasa Kuroiwa, 1 Fuminori Shimizu, 2 Taro Yamashita,
Clinical Characteristics of Patients with Embolic Stroke of Undetermined Source Treated by Endovascular Recanalization Therapy
 DOI: 10.5797/jnet.oa.2017-0101 Clinical Characteristics of Patients with Embolic Stroke of Undetermined Source Treated by Endovascular Recanalization Therapy Ryota Kurogi, 1 Tomoyuki Tsumoto, 1 Yuichi
DOI: 10.5797/jnet.oa.2017-0101 Clinical Characteristics of Patients with Embolic Stroke of Undetermined Source Treated by Endovascular Recanalization Therapy Ryota Kurogi, 1 Tomoyuki Tsumoto, 1 Yuichi
In acute ischemic stroke, recanalization of an occluded cerebral
 ORIGINAL RESEARCH INTERVENTIONAL Double Solitaire Mechanical Thrombectomy in Acute Stroke: Effective Rescue Strategy for Refractory Artery Occlusions? J. Klisch, V. Sychra, C. Strasilla, C.A. Taschner,
ORIGINAL RESEARCH INTERVENTIONAL Double Solitaire Mechanical Thrombectomy in Acute Stroke: Effective Rescue Strategy for Refractory Artery Occlusions? J. Klisch, V. Sychra, C. Strasilla, C.A. Taschner,
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
Toshiaki Bando, Yoji Kuramoto, Narihide Shinoda, Shinya Hori, Kazuyuki Mikami, Daisuke Shimo, Takahiro Kuroyama, and Yasushi Ueno
 DOI: 10.5797/jnet.tn.2016-0141 Two Cases of Cerebral Venous Sinus Thrombosis Successfully Recanalized by the Concomitant Use of an Aspiration through the Guiding Catheter and Stent Thrombectomy Device
DOI: 10.5797/jnet.tn.2016-0141 Two Cases of Cerebral Venous Sinus Thrombosis Successfully Recanalized by the Concomitant Use of an Aspiration through the Guiding Catheter and Stent Thrombectomy Device
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Stroke Update Elaine J. Skalabrin MD Medical Director and Neurohospitalist Sacred Heart Medical Center Stroke Center
 Stroke Update 2015 Elaine J. Skalabrin MD Medical Director and Neurohospitalist Sacred Heart Medical Center Stroke Center Objectives 1. Review successes in systems of care approach to acute ischemic stroke
Stroke Update 2015 Elaine J. Skalabrin MD Medical Director and Neurohospitalist Sacred Heart Medical Center Stroke Center Objectives 1. Review successes in systems of care approach to acute ischemic stroke
TRANSRADIAL CARDIAC CATHETERIZATION. Amanda Ryan, DO, Interventional Cardiologist Heart Care Centers of Florida April 13, 2013
 TRANSRADIAL CARDIAC CATHETERIZATION Amanda Ryan, DO, Interventional Cardiologist Heart Care Centers of Florida April 13, 2013 TOPICS Historical perspective and current trends Rationale Bleeding for the
TRANSRADIAL CARDIAC CATHETERIZATION Amanda Ryan, DO, Interventional Cardiologist Heart Care Centers of Florida April 13, 2013 TOPICS Historical perspective and current trends Rationale Bleeding for the
Mechanical Thrombectomy Using a Solitaire Stent in Acute Ischemic Stroke; Initial Experience in 40 Patients
 Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2012.14.3.164 Original Article Mechanical Thrombectomy Using a Solitaire Stent in
Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2012.14.3.164 Original Article Mechanical Thrombectomy Using a Solitaire Stent in
The DAWN of a New Era for Wake-up Stroke
 The DAWN of a New Era for Wake-up Stroke Alan H. Yee, D.O. Stroke and Critical Care Neurology Department of Neurology University of California Davis Medical Center Objectives Review Epidemiology and Natural
The DAWN of a New Era for Wake-up Stroke Alan H. Yee, D.O. Stroke and Critical Care Neurology Department of Neurology University of California Davis Medical Center Objectives Review Epidemiology and Natural
Balloon Angioplasty for Intracranial Atherosclerotic Disease: a Multicenter Study
 Balloon Angioplasty for Intracranial Atherosclerotic Disease: a Multicenter Study Lakshmi Sudha Prasanna Karanam 1, Mukesh Sharma 2, Anand Alurkar 3, Sridhar Reddy Baddam 1, Vijaya Pamidimukkala 1, and
Balloon Angioplasty for Intracranial Atherosclerotic Disease: a Multicenter Study Lakshmi Sudha Prasanna Karanam 1, Mukesh Sharma 2, Anand Alurkar 3, Sridhar Reddy Baddam 1, Vijaya Pamidimukkala 1, and
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
2017 Cardiology Survival Guide
 2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
MAXIMIZE RADIAL SOLUTIONS TO PERIPHERAL CHALLENGES
 MAXIMIZE RADIAL SOLUTIONS TO PERIPHERAL CHALLENGES PUSHING BOUNDARIES Terumo Interventional Systems is committed to your success with innovative procedural solutions and ongoing support for your most challenging
MAXIMIZE RADIAL SOLUTIONS TO PERIPHERAL CHALLENGES PUSHING BOUNDARIES Terumo Interventional Systems is committed to your success with innovative procedural solutions and ongoing support for your most challenging
Endovascular Procedures for Intracranial Arterial Disease (Atherosclerosis and Aneurysms)
 Last Review Status/Date: December 2016 Page: 1 of 49 Arterial Disease (Atherosclerosis and Description Intracranial arterial disease includes thromboembolic events, vascular stenoses, and aneurysms. Endovascular
Last Review Status/Date: December 2016 Page: 1 of 49 Arterial Disease (Atherosclerosis and Description Intracranial arterial disease includes thromboembolic events, vascular stenoses, and aneurysms. Endovascular
Interventional Stroke Treatment
 Interventional Stroke Treatment Vishal B. Jani MD Medical Director Vascular Neurology Consultant Interventional Neurology CHI Health Assistant Professor, Creighton University School of Medicine Omaha,
Interventional Stroke Treatment Vishal B. Jani MD Medical Director Vascular Neurology Consultant Interventional Neurology CHI Health Assistant Professor, Creighton University School of Medicine Omaha,
Prevention and Management of Vascular Complications Related to Transcatheter Aortic Valve Implantation
 Prevention and Management of Vascular Complications Related to Transcatheter Aortic Valve Implantation Marco Roffi Division of Cardiology University Hospital Geneva, Switzerland Disclosure Speaker name:...marco
Prevention and Management of Vascular Complications Related to Transcatheter Aortic Valve Implantation Marco Roffi Division of Cardiology University Hospital Geneva, Switzerland Disclosure Speaker name:...marco
Michael Horowitz, MD Pittsburgh, PA
 Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Extra- and intracranial tandem occlusions in the anterior circulation - clinical outcome of endovascular treatment in acute major stroke.
 Extra- and intracranial tandem occlusions in the anterior circulation - clinical outcome of endovascular treatment in acute major stroke. Poster No.: C-1669 Congress: ECR 2014 Type: Scientific Exhibit
Extra- and intracranial tandem occlusions in the anterior circulation - clinical outcome of endovascular treatment in acute major stroke. Poster No.: C-1669 Congress: ECR 2014 Type: Scientific Exhibit
Supplementary Online Content
 Supplementary Online Content Badhiwala JH, Nassiri F, Alhazzani W, et al. Endovascular Thrombectomy for Acute Ischemic Stroke: A Meta-analysis. JAMA. doi:10.1001/jama.2015.13767. etable 1. The modified
Supplementary Online Content Badhiwala JH, Nassiri F, Alhazzani W, et al. Endovascular Thrombectomy for Acute Ischemic Stroke: A Meta-analysis. JAMA. doi:10.1001/jama.2015.13767. etable 1. The modified
New Stroke Interventions. Scott L. Zuckerman M.D. Vanderbilt Neurosurgery
 New Stroke Interventions Scott L. Zuckerman M.D. Vanderbilt Neurosurgery Agenda Clot Retrieval Devices Merci Penumbra Stent Retrievers Solitaire Trevo New Technology Funnel ReCover MERCI Retriever (2004)
New Stroke Interventions Scott L. Zuckerman M.D. Vanderbilt Neurosurgery Agenda Clot Retrieval Devices Merci Penumbra Stent Retrievers Solitaire Trevo New Technology Funnel ReCover MERCI Retriever (2004)
