New Daily Persistent Headache in Children and Adolescents
|
|
|
- Jeffery Simpson
- 6 years ago
- Views:
Transcription
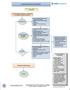
1 Curr Neurol Neurosci Rep (2010) 10: DOI /s New Daily Persistent Headache in Children and Adolescents Eric P. Baron & A. David Rothner Published online: 24 February 2010 # Springer Science+Business Media, LLC 2010 Abstract New daily persistent headache (NDPH) is a form of chronic daily headache (CDH) that may have features of both migraine and tension-type headache. In contrast with other types of CDH, NDPH is characterized by patients recalling the specific date their unremitting daily headache began. In comparison, chronic tension-type headache and chronic migraine are preceded by a gradually increasing frequency of headache. After several months, all three of these CDH forms often have a similar phenotype, making early history a key to diagnosing NDPH. Evaluations to exclude secondary causes are necessary but usually negative. NDPH is difficult to treat and requires a multimodal approach. Questions regarding NDPH remain unanswered. Additional prospective studies are necessary xsto further understand, characterize, diagnose, and treat NDPH. Keywords New daily persistent headache. Chronic daily headache. Children. Adolescents. Chronic migraine. Chronic tension-type headache E. P. Baron (*) Department of Neurology, Center for Headache and Pain/T33, Cleveland Clinic Neurological Institute, 9500 Euclid Avenue, Cleveland, OH 44195, USA barone2@ccf.org A. D. Rothner Center for Pediatric Neurology/S60, Cleveland Clinic Neurological Institute, 9500 Euclid Avenue, Cleveland, OH 44195, USA rothned@ccf.org Introduction New daily persistent headache (NDPH), first described in 1986 [1], is one of four types of chronic daily headache (CDH); the others are transformed (chronic) migraine (CM), chronic tension-type headache (CTTH), and hemicrania continua (HC) [2]. CDH is defined as a headache lasting more than 4 h/day on more than 15 days/month for more than 3 months. According to the International Classification of Headache Disorders II [3], NDPH is a headache that is present daily within 3 days of onset and is unremitting for more than 3 months. It must have two of the following four pain characteristics: bilateral location, pressing/tightening (nonpulsating) quality, mild or moderate intensity, and not aggravated by routine physical activity such as walking. It must have both of the following: no more than one of photophobia, phonophobia, or mild nausea, and neither moderate or severe nausea nor vomiting. It cannot be attributed to any other disorder. Most patients with NDPH have a headache that begins abruptly and resembles tension-type headache with variably superimposed migrainous features. The patient often remembers the exact date the headache began, which is the single most useful clue in making the diagnosis. In fact, proposals have been made to classify NDPH based on the abrupt onset of an unremitting CDH alone, regardless of pain phenotypes, because there are many overlapping features between migraine and tension-type headache [4 ]. The gradually increasing frequency of CTTH and CM is contrasted with the abrupt onset of NDPH, as illustrated in Fig. 1. In a study of mostly adult NDPH patients, 82% remembered the exact date their headache began [5], whereas a study of children and adolescents with NDPH reported 48.1% could recall the month their headaches
2 128 Curr Neurol Neurosci Rep (2010) 10: Fig. 1 Onset of chronic tensiontype headache (CTTH) and chronic migraine (CM) compared with that of new daily persistent headache (NDPH). CTTH and CM both have a gradual increase in frequency (A), whereas NDPH has an abrupt onset (B) began [4 ]. Additionally, about 30% of patients with NDPH have a family history of headache, usually migraine. In our experience, there often is a history of occasional mild headaches or occasional migraine before the onset of NDPH. Comorbid symptoms in pediatric NDPH patients include sleep disturbance in at least two thirds (especially delay in falling asleep), dizziness, generalized weakness, visual disturbances such as blurred vision, abdominal pain, occasional vomiting, sore neck muscles, difficulty concentrating, fatigue, and other nonspecific symptoms [6, 7]. Mood disorders such as anxiety and depression sometimes are associated with NDPH, although these often follow months of persistent symptoms rather than being a preexisting or early symptom [6]. Frequent school absences and overuse of over-the-counter medications commonly are seen. In one study, nine of 34 pediatric patients (26%) with NDPH had excessive school absences (>15 absences/year due to headache) and nine of 34 (26%) overused analgesics three or more times weekly for longer than 6 months [7]. In addition, we find that many patients are straight-a students and are overcommitted to multiple activities outside school. They experience higher stress levels related to maintaining their good grades and extracurricular activities. Some patients coexist with their daily headache and do not overuse medications, miss school, have a drop in grades, or have a decrease in extracurricular activities. Others frequently overuse medications, miss school, drop their grades, decrease their extracurricular activities, and are more severely affected. The explanation behind these clinical differences is unknown and requires further research. Epidemiology In general population studies, CDH is estimated to affect 4% to 5% of adults [8, 9] and 1% of adolescents [10]. Prevalence rates have been reported as 2.4% in girls and 0.8% in boys [11]. Prevalence rates of NDPH in the general population have been reported at 0.03% [12] to 0.1% [9]. In tertiary headache centers, CDH is seen in 30% of patients [13]. Of these patients, NDPH is diagnosed more frequently in children and adolescents than in adults [6]. NDPH has been estimated to occur in 1.7% to 10.8% of adults with CDH [14, 15], and in 13% to 35% of children with CDH [16 18]. It is more common in females, with the female/male ratio in adults at 2.5:1 [5] and in children and adolescents at 1.8:1 [4 ]. It has an earlier age of onset in women (ages 16 35) than in men (ages 26 45) [5]. One study of 680 pediatric headache clinic patients reported 189 (28%) with tension-type headache, 34 of whom met NDPH criteria [7]. This represented 5% of the entire headache population studied and 18% of the CDH patients, consistent with other prevalence studies. Of these NDPH patients, 24 were female and ten male, consistent with prior studies. Pathophysiology The pathophysiology of NDPH is unknown, although some general associations have been made with infection, extracranial surgery, stressful life events, hypothyroidism, hypertension, analgesic overuse, and frequent caffeine use [5, 19 21]. In one study of 34 pediatric headache patients with NDPH, five (15%) had a preceding infection, five (15%) had a preceding mild to moderate head injury, and four had significant psychosocial issues [7]. Another study reported that in 23% of patients, NDPH was preceded by mild head trauma [18]. Overall, infections seem to be most frequently associated with NDPH. One study reported 27 of 32 NDPH patients (84%) with evidence of active Epstein- Barr virus infection [22]. An episode of influenza or a cold preceded NDPH onset in 30% of patients in one study [23] and 43% in another [18]. Other infectious associations have been made with herpes simplex virus,
3 Curr Neurol Neurosci Rep (2010) 10: cytomegalovirus, Salmonella, adenovirus, Toxoplasma, and herpes zoster [1, 20, 24]. Given the variety of infectious associations, it has been postulated that the nonspecific inflammatory response initiated by the infection, rather than the infectious agent itself, may be the trigger [6]. In children, the most frequent triggers for NDPH have been reported to include febrile illness, minor head trauma, and extracranial surgery [18]. No inciting factor was identified in 12% of NDPH patients in one study [18], although a Japanese study of NDPH reported that precipitating events could not be identified in 65% of patients [25]. The latter is more consistent with our clinical practice. Evaluation History and examination are the most critical aspects in evaluating NDPH, particularly when the patient reports a specific date the headache began. The recollection of a specific date of onset is characteristic and the most useful clue to diagnosis. The other three types of CDH (CTTH, CM, and HC) should be ruled out, and history alone should differentiate these. Although HC is included in this CDH group, some authorities feel it should be excluded. HC presents much differently and usually can be separated easily from the other three types of CDH given its characteristic unilateral location, autonomic features, and absolute response to indomethacin. For these reasons, we exclude it from our discussion of CDH. The remaining three CDH types (NDPH, CTTH, and CM) all have variably overlapping symptoms, making the history of abrupt onset the most useful diagnostic clue. After several months of symptoms, all three of these types often have the same phenotype, suggesting there are several ways to get to CDH, but once there, the phenotype is the same. Patients with NDPH should have no symptoms of increased intracranial pressure or other neurologic symptoms. Their symptoms should not be progressive. They should have a normal general and neurologic examination and no papilledema. Any secondary headache may come on suddenly, so it is imperative to rule out secondary causes of new-onset daily headache. Secondary causes of NDPH include cerebral venous sinus thrombosis, low or high cerebrospinal fluid (CSF) pressure, carotid or vertebral dissection, vasculitis or other vascular disorders, toxins, sphenoid sinusitis, temporomandibular joint disease, congenital abnormalities (eg, symptomatic Chiari malformation), metabolic disorders, endocrine disorders (eg, Hashimoto s thyroiditis), hormonal changes, neoplasm, infection (particularly viral), and posttraumatic headache [26]. Routine blood work should be checked and should include thyroid studies, sedimentation rates, complete blood count, and complete metabolic profile. Additional testing should be tailored toward information discovered during history taking and examination, such as symptoms of autoimmune processes and specific infections (eg, Lyme disease). Diagnostic studies, although frequently pursued, have a low diagnostic yield in the setting of a negative history and neurologic examination. Although electroencephalography may be considered if there is concern about seizures or a focal lesion, it is not routinely indicated. According to the American Academy of Neurology practice parameters, neuroimaging should not be done routinely in children with recurrent headaches and normal neurologic examinations [27]. The variables predicting space-occupying lesions include headache of less than 1 month s duration, absence of family history of migraine, abnormal neurologic examination, gait abnormalities, and seizures [27]. Despite these recommendations, neuroimaging is performed frequently, usually because of parental anxiety and medicolegal concerns. In general, an abrupt onset of daily headache warrants neuroimaging, and an MRI of the brain is preferable to CT. Adding magnetic resonance angiography (MRA) and magnetic resonance venography (MRV) is a reasonable consideration based on the clinical presentation. Overall, neuroimaging likely will be normal, unless there is a history suggesting a secondary cause, or focal neurologic symptoms or signs are present. In one study, neuroimaging with CT or MRI was performed in 30 children with CDH and a normal neurologic examination, and five children (16.6%) had abnormal findings [28]. These findings included arachnoid cysts, Chiari I malformations, sinus disease, occult vascular malformations, and dilated Virchow-Robin spaces, all of which were considered incidental and unrelated to the headache [28]. In another study, 49 patients with NDPH underwent MRI or CT [5]. Of these, 66% had normal results, whereas the remainder had nonspecific and unrelated findings [5]. In another study, 241 of 681 pediatric headache clinic patients underwent MRI (218) or CT (23) of the brain [29]. Of these, 46 (19%) had benign abnormalities that did not change management, including sinus disease, Chiari I malformations, nonspecific white matter abnormalities, venous angiomas, arachnoid cysts, enlarged Virchow-Robin spaces, pineal cysts, mega cisterna magna, fenestration of the proximal basilar artery, and periventricular leukomalacia. In addition, 23 patients (9.5%) had findings requiring a change in management, including sinus disease, tumors, old infarcts, Chiari I malformations, moyamoya disease, intracranial vascular stenosis, internal jugular vein occlusion, arteriovenous malformation, demyelinating disease, and intracerebral hemorrhage. Ultimately, this study concluded that approximately 20% of pediatric headache patients with neuroimaging have benign imaging findings that do not result in a change in headache management. Furthermore, imaging
4 130 Curr Neurol Neurosci Rep (2010) 10: findings requiring a change in management are rare in the absence of abnormal neurologic symptoms and signs, occurring in only 1.2% of patients. Lumbar puncture is not indicated unless the history suggests a possible infectious, inflammatory, or pressurerelated etiology. Caution is advised in obese and very anxious patients because falsely elevated opening pressures may be seen, resulting in a misdiagnosis of idiopathic intracranial hypertension (pseudotumor cerebri). Sedation and fluoroscopy should be considered in this setting to avoid falsely elevated pressures, or as we refer to it, pseudo-pseudotumor. Case Presentation A 15-year-old girl presented with her parents for evaluation of daily headaches over a 1-year period. Both the patient and her parents were very anxious. She reported that her headaches began on November 19 of the previous year. Neither she nor her parents could recall any changes in her routine or other obvious reasons to explain her new headache. They did recall that she left school early the day before the headache began because of mild flulike symptoms, which resolved quickly. The patient was otherwise healthy but had rare normal, mild headaches during periods in which she was stressed with schoolwork. She was a straight-a student and involved in multiple afterschool activities. Her mother had episodic migraine. The patient described her headache as a dull, pressing sensation throughout her head. The pain fluctuated between mild and moderate but never became severe. Despite this fluctuation, she admitted that she had not had a headachefree day since the headaches began, and there was some level of discomfort 24 hours a day, 7 days a week. The patient had occasional photophobia when her headache became stronger but no phonophobia, nausea, or vomiting. She felt that her concentration was impaired. The patient s vital signs and general examination were normal, except for some mild tenderness over the cervical paraspinal musculature. Detailed neurologic and funduscopic examinations were normal. She recently had had an extensive workup, which was unremarkable. Routine blood work included thyroid studies, inflammatory markers, complete blood count, and metabolic profile. Neuroimaging included MRI, MRA, and MRV of the brain, which demonstrated a small arachnoid cyst. One physician stated that the headaches may be the result of this cyst and would have to be followed up with serial MRI. The patient and her parents were very anxious about this cyst as the cause of her headaches. The patient had trials of topiramate and gabapentin and had been using over-the-counter medications most days of the week for the previous 6 months. Her school absences had increased to more than 15 days in the prior 3 months. She was drinking soda more frequently because she was tired from staying up so late trying to catch up with missed schoolwork, and she had stopped exercising. This patient s CDH was consistent with NDPH. Her treatment required a multimodal approach, which began by reassuring the patient and her parents that there was no evidence of a tumor or any life-threatening neurologic disease and that the arachnoid cyst was incidental, common, and unrelated. They were given information about NDPH and instructions for routine daily activity, sleep, and dietary changes, including avoidance of caffeine, chocolate, nitrates, and monosodium glutamate. Because of the tenderness in the patient s neck musculature, she was prescribed physical therapy. An exercise routine was started, and pharmacotherapy was initiated with a trial of amitriptyline. Counseling was begun, and behavioral techniques focused on treating stress were discussed. The patient s parents were instructed not to allow her to miss school because of headache. She was told to limit the use of over-the-counter medications to 2 days/week or 10 days/month. Alternative therapies including supplements, acupuncture, and yoga were discussed. Follow-up was arranged in 6 weeks. Treatment Clinically, NDPH is difficult to treat, and patients with this disorder must be followed up closely. Nonpharmacologic treatments are integral to optimize the possibility of a good outcome. These treatment include confident reassurance, patient and parent education, institution of a regular schedule for eating and sleeping, a good diet with plenty of fluids, counseling for the patient and his/her family, avoidance of school absences, identification of stressors, discontinuation of over-the-counter medications, and initiation of other behavioral strategies, such as biofeedback. If the patient is overweight (ie, has a body mass index > 25), a weight loss program should be initiated. Parental enmeshment and psychopathology may contribute to CDH; therefore, parental counseling may be required. Pharmacologic therapies for NDPH are the same as those used for other CDH types and for migraine prevention. The most commonly used medications include the tricyclic antidepressants (amitriptyline) and antiepileptics (topiramate, valproic acid, gabapentin). For amitriptyline, we use a starting dose of 5 mg and 1 mg/kg per day as an initial target dose. For teens and preteens, we typically begin with 5 mg at bedtime and increase the dosage by 5 mg every 2 weeks to a goal of 20 mg at bedtime. The patient is then seen in follow-up, and the dosage is adjusted. In thin patients, we often use cyproheptadine because it also
5 Curr Neurol Neurosci Rep (2010) 10: increases appetite and improves sleep. We begin with 2 mg at bedtime and increase the dosage by 2 mg every 2 weeks to a goal of 6 mg at bedtime. We frequently use melatonin, 3 mg taken 2 hours before bedtime, in patients who have difficulty falling asleep and titrate the dosage to 9 mg as needed. Additional treatments with reported benefit, but insufficient data, include propranolol, selective serotonin reuptake inhibitors, muscle relaxants, and indomethacin. Botulinum toxin is reported to be safe and effective compared with both placebo and topiramate for CM in adults [30, 31], and successful treatment of intractable migraine and CDH in adolescents also is reported [32]. These findings suggest a potential role for botulinum toxin in treating NDPH, and success has been reported for this indication in adults [33 ]. Alternative therapies reported to be useful include riboflavin, butterbur, coenzyme Q10, magnesium, massage, acupuncture, exercise, physical therapy, weight loss, and yoga. At our center, patients who are refractory to the aforementioned treatments are offered a 3-week intensive multimodal inpatient rehabilitation program. An interesting but unconfirmed study reported elevated CSF tumor necrosis factor-α (TNF-α) levels in NDPH and treatment-refractory CM [34]. Doxycycline, a TNF-α inhibitor, was given to four patients with refractory NDPH and elevated CSF TNF-α levels who had failed at least five preventatives, infusion therapy, and inpatient treatments [35]. Treatment consisted of doxycycline, 100 mg by mouth twice daily, in an open-label fashion. All patients had a positive response to treatment: two became pain-free, one had 80% improvement, and one had a greater than 50% reduction in frequency of severe pain episodes. Onset of action was about 2 months, although one patient responded within 2 weeks. Prognosis Data regarding prognosis in NDPH are sparse, and more data are required. It has been suggested that there are two forms of NDPH. One typically resolves without therapy within several months, and the other is a more refractory form resistant to aggressive treatment [3, 23]. Unfortunately, the refractory form seems to be the most frequently encountered in our practice. In his original paper, Vanast [1] appeared to describe the milder, benign form, in which 73% to 86% of patients have headache resolution in 3 24 months, regardless of treatment [23]. From our experience, risk factors for chronification of NDPH include female sex, straight-a report cards, excess extracurricular activities, poor sleep, a disordered home life, medication overuse, obesity, caffeine, poor diet, stressful life events, head injury, and insufficient exercise and fluids. In general, 30% of children and adolescents seem to improve in 3 months to 4 months, even without intensive treatment, and the rest continue to have CDH indefinitely. Still, 78% may be significantly improved within 2 years [36]. Conclusions NDPH is a form of CDH that may combine features of both migraine and tension-type headache. In contrast to other CDH types, NDPH often has the characteristic clinical feature of the patient being able to recall the specific date his or her unremitting headache began. Given this characteristic history, along with overlapping migrainous and tension-type features, consideration should be given to some revisions of NDPH criteria. Many NDPH patients have more than one migrainous feature, although the criteria allow for only one. This makes diagnosis by strict criteria more difficult and leads to diagnostic uncertainty for both physicians and patients. In addition, after several months, NDPH, CTTH, and CM have similar phenotypes and are hard to differentiate. NDPH has an abrupt onset and is unremitting from the start, whereas CTTH and CM typically have a steadily increasing frequency before occurring daily. For this reason, diagnosis of NDPH can be made earlier than the criteria s minimum of 3 months duration of headache. A minimum of 1 month would be more reasonable for NDPH, because its onset is so characteristic. More patients would then fulfill the diagnostic criteria earlier, allowing them to receive adequate treatment sooner. The current 3-month criterion leaves patients with suspected NDPH in a quandary with an uncertain diagnosis and anxiety while they wait to meet the criterion, when they could be starting the multimodal approach required to optimally treat NDPH and to prevent further comorbidities. Patients with NDPH often undergo extensive evaluations, most of which are negative and unremarkable. The disorder often is difficult to treat and requires a multimodal approach. There are still many unanswered questions regarding NDPH; further study is necessary to better understand, characterize, diagnose, and treat it. Prospective, multi-institutional studies are warranted to better define the clinical features and etiologic factors (physical, psychological, environmental, or others) of this disorder and to determine the value of various diagnostic tests. Studies also are needed to compare nonpharmacologic, alternative, and pharmacologic treatment strategies and to better identify prognostic factors while eliminating institutional or regional bias. Disclosure Dr. Rothner received a grant from GlaxoSmithKline for research on Treximet in adolescents. No other potential conflicts of interest relevant to this article were reported.
6 132 Curr Neurol Neurosci Rep (2010) 10: References Papers of particular interest, published recently, have been highlighted as: Of importance 1. Vanast WJ: New daily persistent headaches: definition of a benign syndrome. Headache 1986, 26: Siberstein SD, Lipton RB, Solomon S, et al.: Classification of daily and near-daily headaches: proposed revisions to the IHS criteria. Headache 1994, 34: Headache Classification Subcommittee of the International Headache Society: The International Classification of Headache Disorders: 2nd edition. Cephalalgia 2004, 24(Suppl 1): Kung E, Tepper SJ, Rapoport AM, et al.: New daily persistent headache in the paediatric population. Cephalalgia 2009, 29: This article presents the most recent NDPH epidemiology data in a pediatric headache clinic population. It also proposes that NDPH be classified by abrupt onset of daily headache, given that its phenotype is similar to that of other forms of CDH. 5. Li D, Rozen TD: The clinical characteristics of new daily persistent headache. Cephalalgia 2002, 22: Mack KJ: New daily persistent headache in children and adults. Curr Pain Headache Rep 2009, 13: Abdelsalam HHM, Guo Y, Rothner AD: New daily persistent headache in children and adolescents [abstract]. Ann Neurol 2004, 56:S83 S Scher AI, Stewart WF, Liberman J, et al.: Prevalence of frequent headache in a population sample. Headache 1998, 38: Castillo J, Munoz P, Guitera V, et al.: Kaplan Award Epidemiology of chronic daily headache in the general population. Headache 1999, 39: Winner P, Lewis DW, Rothner AD: Headache in Children and Adolescents, edn 2. New York: BC Decker Inc.; Wang SJ, Fuh JL, Lu SR, et al.: Chronic daily headache in adolescents: prevalence, impact, and medication overuse. Neurology 2006, 66: Grande RB, Aaseth K, Lundqvist C, et al.: Prevalence of new daily persistent headache in the general population. The Akershus study of chronic headache. Cephalalgia 2009, 29: Winner P, Gladstein J. Chronic daily headache in pediatric practice. Curr Opin Neurol 2002, 15: Bigal ME, Lipton RB, Tepper SJ, et al.: Primary chronic daily headache and its subtypes in adolescents and adults. Neurology 2004, 63: Bigal ME, Sheftell FD, Rapoport AM, et al.: Chronic daily headache in a tertiary care population: correlation between the International Headache Society diagnostic criteria and proposed revisions of criteria for chronic daily headache. Cephalalgia 2002, 22: Gladstein J, Holden EW: Chronic daily headache in children and adolescents: a 2-year prospective study. Headache 1996, 36: Koenig MA, Gladstein J, McCarter RJ, et al.: Chronic daily headache in children and adolescents presenting to tertiary headache clinics. Headache 2002, 42: Mack KJ: What incites new daily persistent headache in children? Pediatr Neurol 2004, 31: Bigal ME, Sheftell FD, Rapoport AM, et al.: Chronic daily headache: identification of factors associated with induction and transformation. Headache 2002, 42: Santoni JR, Santoni-Williams CJ: Headache and painful lymphadenopathy in extracranial or systemic infection: etiology of new daily persistent headaches. Intern Med 1993, 32: Stewart WF, Scher AI, Lipton RB: Stressful life events and risk of chronic daily headache: results from the frequent headache epidemiology study. Cephalalgia 2001, 21: Diaz-Mitoma F, Vanast WJ, Tyrrell DL: Increased frequency of Epstein-Barr virus excretion in patients with new daily persistent headaches. Lancet 1987, 1: Rozen TD: New daily persistent headache. Curr Pain Headache Rep 2003, 7: Meineri P, Torre E, Rota E, et al.: New daily persistent headache: clinical and serological characteristics in a retrospective study. Neurol Sci 2004, 25(Suppl 3):S281 S Takase Y, Nakano M, Tatsumi C: Primary new daily persistent headache (NDPH): clinical characteristics of forty-three cases in Japan. Rinsho Shinkeigaku 2003, 43: Pascual J: Other primary headaches. Neurol Clin 2009, 27: Lewis DW, Ashwal S, Dahl G, et al.: Practice parameter: evaluation of children and adolescents with recurrent headaches: report of the Quality Standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child Neurology Society. Neurology 2002, 59: Lewis DW, Dorbad D: The utility of neuroimaging in the evaluation of children with migraine or chronic daily headache who have normal neurological examinations. Headache 2000, 40: Schwedt TJ, Guo Y, Rothner AD: Benign imaging abnormalities in children and adolescents with headache. Headache 2006, 46: Mathew NT, Jaffri SF: A double-blind comparison of onabotulinumtoxina (BOTOX) and topiramate (TOPAMAX) for the prophylactic treatment of chronic migraine: a pilot study. Headache 2009, 49: This study reported similar efficacy between topiramate and botulinum toxin for CM prophylaxis. 31. Freitag FG, Diamond S, Diamond M, et al.: Botulinum Toxin Type A in the treatment of chronic migraine without medication overuse. Headache 2008, 48: Chan VW, McCabe EJ, MacGregor DL: Botox treatment for migraine and chronic daily headache in adolescents. J Neurosci Nurs 2009, 41: Spears RC: Efficacy of botulinum toxin type A in new daily persistent headache. J Headache Pain 2008, 9: This article provides a description of successful treatment of NDPH with botulinum toxin. 34. Rozen T, Swidan SZ: Elevation of CSF tumor necrosis factor alpha levels in new daily persistent headache and treatment refractory chronic migraine. Headache 2007, 47: Rozen TD: Doxycycline for treatment resistant new daily persistent headache [abstract]. Headache 2008, 48: Wintrich S, Rothner AD: Prognosis of new daily persistent headache in children and adolescents [abstract]. Submitted for presentation at the 62nd Annual Meeting of the American Academy of Neurology. Toronto, Canada; April 10 17, 2010.
Prevalence of new daily persistent headache in the general population. The Akershus study of chronic headachecha_
 doi:10.1111/j.1468-2982.2009.01842.x Prevalence of new daily persistent headache in the general population. The Akershus study of chronic headachecha_1842 1149..1155 RB Grande 1,2, K Aaseth 1,3, C Lundqvist
doi:10.1111/j.1468-2982.2009.01842.x Prevalence of new daily persistent headache in the general population. The Akershus study of chronic headachecha_1842 1149..1155 RB Grande 1,2, K Aaseth 1,3, C Lundqvist
Headaches in the Pediatric Emergency Dept
 Headaches in Children February 23, 2011 Jinny Tavee, MD Associate Professor Neuromuscular Center Cleveland Clinic Foundation Cleveland, OH 1 Headaches in the Pediatric Emergency Dept Burton Gutierrez Kan
Headaches in Children February 23, 2011 Jinny Tavee, MD Associate Professor Neuromuscular Center Cleveland Clinic Foundation Cleveland, OH 1 Headaches in the Pediatric Emergency Dept Burton Gutierrez Kan
New daily persistent headache: Should migrainous features be incorporated?
 Original Article New daily persistent headache: Should migrainous features be incorporated? Cephalalgia 31(15) 1561 1569! International Headache Society 2011 Reprints and permissions: sagepub.co.uk/journalspermissions.nav
Original Article New daily persistent headache: Should migrainous features be incorporated? Cephalalgia 31(15) 1561 1569! International Headache Society 2011 Reprints and permissions: sagepub.co.uk/journalspermissions.nav
Index. Prim Care Clin Office Pract 31 (2004) Note: Page numbers of article titles are in boldface type.
 Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Clinical Characteristics of Chronic Daily Headache Patients Visit to University Hospital
 Clinical Characteristics of Chronic Daily Headache Patients Visit to University Hospital Jin-Kuk Do, M.D., Hee-Jong Oh, M.D., Dong-Kuck Lee, M.D. Department of Neurology, Taegu Hyosung Catholic University
Clinical Characteristics of Chronic Daily Headache Patients Visit to University Hospital Jin-Kuk Do, M.D., Hee-Jong Oh, M.D., Dong-Kuck Lee, M.D. Department of Neurology, Taegu Hyosung Catholic University
PREVALENCE BY HEADACHE TYPE
 CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation.
 I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
A case of a patient with chronic headache. Focus on Migraine. None related to the presentation Grants to conduct clinical trials from: Speaker bureau:
 Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Chronic Daily Headaches
 Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา
 ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
10/17/2017 CHRONIC MIGRAINES BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES PATIENT CASE EPIDEMIOLOGY EPIDEMIOLOGY
 BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES JENNIFER SHIN, PHARMD PGY2 AMBULATORY CARE PHARMACY RESIDENT COMMUNITYCARE HEALTH CENTERS PHARMACOTHERAPY ROUNDS OCTOBER 20, 2017
BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES JENNIFER SHIN, PHARMD PGY2 AMBULATORY CARE PHARMACY RESIDENT COMMUNITYCARE HEALTH CENTERS PHARMACOTHERAPY ROUNDS OCTOBER 20, 2017
Neurological Dilemmas in Primary Care
 Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
Psychiatric Comorbidity in Transformed Migraine: Presentation, Treatment, Impact and Outcome
 Jefferson Journal of Psychiatry Volume 23 Issue 1 Article 3 December 2010 Psychiatric Comorbidity in Transformed Migraine: Presentation, Treatment, Impact and Outcome Muhammad A. Abbas M.D Thomas Jefferson
Jefferson Journal of Psychiatry Volume 23 Issue 1 Article 3 December 2010 Psychiatric Comorbidity in Transformed Migraine: Presentation, Treatment, Impact and Outcome Muhammad A. Abbas M.D Thomas Jefferson
Neuroimaging in Migraine Critically Appraised Topic (CAT)
 Neuroimaging in Migraine Critically Appraised Topic (CAT) PICOT Question: Does a head CT scan compared to no head CT scan change the management of a child with migraine? Clinical bottom line based on literature
Neuroimaging in Migraine Critically Appraised Topic (CAT) PICOT Question: Does a head CT scan compared to no head CT scan change the management of a child with migraine? Clinical bottom line based on literature
CHRONIC HEADACHES IN CHILDHOOD
 CHRONIC HEADACHES IN CHILDHOOD EDWIN LIU, MD PEDIATRIC NEUROLOGISTS OF PALM BEACH PEDIATRIC SLEEP CENTERS OF FLORIDA ASSISTANT CLINICAL PROFESSOR FSU ASSISTANT CLINICAL PROFESSOR NOVA SOUTHEASTERN PEDIATRIC
CHRONIC HEADACHES IN CHILDHOOD EDWIN LIU, MD PEDIATRIC NEUROLOGISTS OF PALM BEACH PEDIATRIC SLEEP CENTERS OF FLORIDA ASSISTANT CLINICAL PROFESSOR FSU ASSISTANT CLINICAL PROFESSOR NOVA SOUTHEASTERN PEDIATRIC
6/2/2017. Objectives. Statement of Problem: Migraine Headaches Are Common. Chronic Headache In Pediatrics, Botox and Beyond
 Chronic Headache In Pediatrics, Botox and Beyond Ken Mack MD PhD Mayo Clinic 2015 MFMER slide-1 Objectives Understand pediatric chronic headache presentations Review evidence for the treatment of chronic
Chronic Headache In Pediatrics, Botox and Beyond Ken Mack MD PhD Mayo Clinic 2015 MFMER slide-1 Objectives Understand pediatric chronic headache presentations Review evidence for the treatment of chronic
By Nathan Hall Associate Editor
 By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache
 MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache Measure Description Percentage of patients age 18 years old and older diagnosed with migraine headache whose migraine frequency is 4 migraine
MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache Measure Description Percentage of patients age 18 years old and older diagnosed with migraine headache whose migraine frequency is 4 migraine
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, II. Management of Refractory Headaches
 Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headaches in Children and Adolescents. Paul Shillito
 Headaches in Children and Adolescents Paul Shillito Topics For Discussion What s different about childhood migraine Chronic daily headache (CDH) Tumours and other things to worry about Management of childhood
Headaches in Children and Adolescents Paul Shillito Topics For Discussion What s different about childhood migraine Chronic daily headache (CDH) Tumours and other things to worry about Management of childhood
MIGRAINE A MYSTERY HEADACHE
 MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
Chronic Migraine in Primary Care. December 11 th, 2017 Werner J. Becker University of Calgary
 Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Outpatient Headache Care Guideline
 1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
Case Presentation. Case Presentation. Case Presentation. Truths about Headaches (2017) Most headaches were muscle-tension headaches
 Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
HEADACHES THE RED FLAGS
 HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert
 Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Update on Diagnosis and Management of Migraines
 Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
Inpatient Treatment of Status Migraine With Dihydroergotamine in Children and Adolescents
 Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
Intracranial hypertension and headache. Daniel Tibussek, MD
 Intracranial hypertension and headache. Daniel Tibussek, MD none Disclosures Overview Case Clinical presentation of pediatric PTC Nomenclature, Definition What is intracranial hypertension? Diagnostic
Intracranial hypertension and headache. Daniel Tibussek, MD none Disclosures Overview Case Clinical presentation of pediatric PTC Nomenclature, Definition What is intracranial hypertension? Diagnostic
Migraine in Children. Germano Falcao, MD Pediatric Neurology 03/07/2014
 Migraine in Children Germano Falcao, MD Pediatric Neurology 03/07/2014 Headaches in Children One of the most common concerns reported by children 3% for children age 3-7 years 4-11% for children age 7-11
Migraine in Children Germano Falcao, MD Pediatric Neurology 03/07/2014 Headaches in Children One of the most common concerns reported by children 3% for children age 3-7 years 4-11% for children age 7-11
Hemicrania continua-like headache associated with carotid dissection may respond to indomethacin
 Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology January 2007 Hemicrania continua-like headache associated with carotid dissection may
Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology January 2007 Hemicrania continua-like headache associated with carotid dissection may
Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE
 Headache in children and adolescents Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE Dept. of Psychiatry of Childhood and Adolescence Medical University of Vienna, Vienna, Austria Impact
Headache in children and adolescents Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE Dept. of Psychiatry of Childhood and Adolescence Medical University of Vienna, Vienna, Austria Impact
Headaches in Pregnancy Before, During, and After
 Headaches in Pregnancy Before, During, and After Robert Kaniecki, MD Director, UPMC Headache Center Assistant Professor of Neurology University of Pittsburgh Headaches and Pregnancy Pre-pregnancy counseling
Headaches in Pregnancy Before, During, and After Robert Kaniecki, MD Director, UPMC Headache Center Assistant Professor of Neurology University of Pittsburgh Headaches and Pregnancy Pre-pregnancy counseling
Preventive treatment of migraine. Rebecca Burch, MD Brigham and Women s Faulkner Hospital Harvard Medical School Boston, MA
 Preventive treatment of migraine Rebecca Burch, MD Brigham and Women s Faulkner Hospital Harvard Medical School Boston, MA No disclosures Disclosures Many preventive treatments for migraine are not FDA-approved
Preventive treatment of migraine Rebecca Burch, MD Brigham and Women s Faulkner Hospital Harvard Medical School Boston, MA No disclosures Disclosures Many preventive treatments for migraine are not FDA-approved
Faculty Disclosure. Karen L. Bremer, MD. Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest.
 Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
Headache Mary D. Hughes, MD Neuroscience Associates
 Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
How do we treat migraine? New SIGN Guidelines
 How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
11/10/2017. THE BRIDGE Course Objectives. THE BRIDGE Course Objectives
 THE BRIDGE Course Objectives Describe clinical characteristics associated with migraine diagnosis in adult and pediatric populations. Identify barriers and risk factors impacting the clinical course of
THE BRIDGE Course Objectives Describe clinical characteristics associated with migraine diagnosis in adult and pediatric populations. Identify barriers and risk factors impacting the clinical course of
Lynne Kerr, MD May 2014
 Lynne Kerr, MD May 2014 Headache is one of top 5 health problems in children 2 nd most common diagnosis in the peds neurology outpatient clinic 14 year old girl severe headache Headaches 1-2 times/month
Lynne Kerr, MD May 2014 Headache is one of top 5 health problems in children 2 nd most common diagnosis in the peds neurology outpatient clinic 14 year old girl severe headache Headaches 1-2 times/month
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy
 HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
What is the Effectiveness of OnabotulinumtoxinA (Botox ) in Reducing the Number of Chronic Migraines (CM) in Patients Years Old?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 What is the Effectiveness of OnabotulinumtoxinA
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 What is the Effectiveness of OnabotulinumtoxinA
Headache. Section 1. Migraine headache. Clinical presentation
 Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Migraine Types and Triggering Factors in Children
 original ARTICLE Migraine Types and Triggering Factors in Children How to Cite this Article: Nejad Biglari H, Karimzadeh P, Mohammadi Kord-kheyli M, Hashemi SM. Migraine Types and Triggering Factors in
original ARTICLE Migraine Types and Triggering Factors in Children How to Cite this Article: Nejad Biglari H, Karimzadeh P, Mohammadi Kord-kheyli M, Hashemi SM. Migraine Types and Triggering Factors in
Differentiating Migraine from Other Headache Types to Target Treatment Peter J. Goadsby, MD, PhD
 Differentiating Migraine from Other Headache Types to Target Treatment Peter J. Goadsby, MD, PhD University of California, San Francisco San Francisco, CA King's College London London, England Learning
Differentiating Migraine from Other Headache Types to Target Treatment Peter J. Goadsby, MD, PhD University of California, San Francisco San Francisco, CA King's College London London, England Learning
Long-Term Care Updates
 Long-Term Care Updates September 2017 By Lindsay Slowiczek, PharmD Migraines are often considered to be a condition affecting younger or middle-aged patients, during which patients experience episodic,
Long-Term Care Updates September 2017 By Lindsay Slowiczek, PharmD Migraines are often considered to be a condition affecting younger or middle-aged patients, during which patients experience episodic,
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
Khalil Zahra, M.D Neuro-interventional radiology
 Khalil Zahra, M.D Neuro-interventional radiology 1 Disclosure None 2 Outline Etiology and pathogensis Imaging techniques and Features Literature review Treatment modalities Endovascular techniques Long
Khalil Zahra, M.D Neuro-interventional radiology 1 Disclosure None 2 Outline Etiology and pathogensis Imaging techniques and Features Literature review Treatment modalities Endovascular techniques Long
How could I be having migraine when I don't have a headache?
 Migraine Your doctor thinks you may have migraine. Classic migraine attacks start with visual symptoms (often zig-zag colored lights or flashes of light expanding to one side over 10-30 minutes) followed
Migraine Your doctor thinks you may have migraine. Classic migraine attacks start with visual symptoms (often zig-zag colored lights or flashes of light expanding to one side over 10-30 minutes) followed
Migraine Headache Prophylaxis in Adolescents
 I Migraine Headache Prophylaxis in Adolescents It s estimated that up to 28 percent of adolescents between the ages of 15 and 19 (mostly females) are affected by migraine (Lewis, Yonker, Winner, & Sowell,
I Migraine Headache Prophylaxis in Adolescents It s estimated that up to 28 percent of adolescents between the ages of 15 and 19 (mostly females) are affected by migraine (Lewis, Yonker, Winner, & Sowell,
Post-infectious headache: a reactive headache?
 J Headache Pain (2011) 12:467 473 DOI 10.1007/s10194-011-0346-0 ORIGINAL Post-infectious headache: a reactive headache? Sanjay Prakash Niyati Patel Purva Golwala Rushad Patell Received: 21 March 2011 /
J Headache Pain (2011) 12:467 473 DOI 10.1007/s10194-011-0346-0 ORIGINAL Post-infectious headache: a reactive headache? Sanjay Prakash Niyati Patel Purva Golwala Rushad Patell Received: 21 March 2011 /
July 2012 Target Population. Adult patients 18 years or older in primary care settings.
 Guideline for Primary Care Management of Headache in Adults July 2012 Target Population Adult patients 18 years or older in primary care settings. Exclusions: This guideline does not provide recommendations
Guideline for Primary Care Management of Headache in Adults July 2012 Target Population Adult patients 18 years or older in primary care settings. Exclusions: This guideline does not provide recommendations
Strategies in Migraine Care
 Strategies in Migraine Care Julie L. Roth, MD Rhode Island Hospital Assistant Professor, Neurology The Warren Alpert Medical School of Brown University March 28, 2015 Financial Disclosures None. Objectives
Strategies in Migraine Care Julie L. Roth, MD Rhode Island Hospital Assistant Professor, Neurology The Warren Alpert Medical School of Brown University March 28, 2015 Financial Disclosures None. Objectives
Proposed Project Scope. OPTIMAL USE OnabotulinumtoxinA for the Prevention of Chronic Migraine Clinical Evidence, Policies and Practice
 Proposed Project Scope OPTIMAL USE OnabotulinumtoxinA for the Prevention of Chronic Migraine Clinical Evidence, Policies and Practice May 2018 1. BACKGROUND AND RATIONALE Migraine is a common, debilitating
Proposed Project Scope OPTIMAL USE OnabotulinumtoxinA for the Prevention of Chronic Migraine Clinical Evidence, Policies and Practice May 2018 1. BACKGROUND AND RATIONALE Migraine is a common, debilitating
Dubai Standards of Care (Migraine)
 Dubai Standards of Care 2018 (Migraine) Preface Migraine is one of the most common problem dealt with in daily practice. In Dubai, the management of migraine is done through various different strategies.
Dubai Standards of Care 2018 (Migraine) Preface Migraine is one of the most common problem dealt with in daily practice. In Dubai, the management of migraine is done through various different strategies.
Is Topiramate Effective in Preventing Pediatric Migraines?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 Is Topiramate Effective in Preventing
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 Is Topiramate Effective in Preventing
Tension-type Headaches
 Stress-related Diseases Tension-type Headaches JMAJ 45(5): 202 206, 2002 Koji TSUBOI Professor, Department of Psychosomatic Medicine, School of Medicine, Toho University Abstract: Tension-type headaches
Stress-related Diseases Tension-type Headaches JMAJ 45(5): 202 206, 2002 Koji TSUBOI Professor, Department of Psychosomatic Medicine, School of Medicine, Toho University Abstract: Tension-type headaches
UNDERSTANDING CHRONIC MIGRAINE. Learn about diagnosis, management, and treatment options for this headache condition
 UNDERSTANDING CHRONIC MIGRAINE Learn about diagnosis, management, and treatment options for this headache condition 1 What We re Going to Cover Today The symptoms and phases of migraine Differences between
UNDERSTANDING CHRONIC MIGRAINE Learn about diagnosis, management, and treatment options for this headache condition 1 What We re Going to Cover Today The symptoms and phases of migraine Differences between
Treatment Of Medication. Overuse Headache
 7 November 2012 BASH GPwSI Meeting Lecture title... Treatment Of Medication Dr... Overuse Headache Dr Marcus Lewis Dr... The National Migraine Centre International Headache Society Diagnostic criteria
7 November 2012 BASH GPwSI Meeting Lecture title... Treatment Of Medication Dr... Overuse Headache Dr Marcus Lewis Dr... The National Migraine Centre International Headache Society Diagnostic criteria
Headache. Karen Thaxter
 Headache Karen Thaxter An eight year old girl is taken to her paediatrician because she has been complaining of almost daily pain at the back of her head for the past 4 months. She states that each headache
Headache Karen Thaxter An eight year old girl is taken to her paediatrician because she has been complaining of almost daily pain at the back of her head for the past 4 months. She states that each headache
Recognition and treatment of medication overuse headache
 Recognition and treatment of medication overuse headache Marcus Lewis MA, MRCGP, DRCOG, DFSRH 20 Mean weekly headache index 15 10 5 Medication overuse headache is a common condition responsible for a high
Recognition and treatment of medication overuse headache Marcus Lewis MA, MRCGP, DRCOG, DFSRH 20 Mean weekly headache index 15 10 5 Medication overuse headache is a common condition responsible for a high
Atypical presentations of cluster headache
 Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 200222Original ArticleAtypical presentations in cluster headachetd Rozen Atypical presentations of cluster headache TD Rozen Department
Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 200222Original ArticleAtypical presentations in cluster headachetd Rozen Atypical presentations of cluster headache TD Rozen Department
UTILIZATION MANAGEMENT POLICY AND PROCEDURE MANUAL
 University of Florida, Pediatric Integrated Care System UTILIZATION MANAGEMENT POLICY AND PROCEDURE MANUAL Policy: Program(s): Approval Criteria for Neuroimaging of Headaches Title XIX and Title XXI Effective
University of Florida, Pediatric Integrated Care System UTILIZATION MANAGEMENT POLICY AND PROCEDURE MANUAL Policy: Program(s): Approval Criteria for Neuroimaging of Headaches Title XIX and Title XXI Effective
Aleksandra Radojičić. Headache Center, Neurology Clinic, Clinical Center of Serbia
 European Headache School Belgrade 2012 MEDICATION OVERUSE HEADACHE Aleksandra Radojičić Headache Center, Neurology Clinic, Clinical Center of Serbia Historical data First cases were described in XVII century
European Headache School Belgrade 2012 MEDICATION OVERUSE HEADACHE Aleksandra Radojičić Headache Center, Neurology Clinic, Clinical Center of Serbia Historical data First cases were described in XVII century
Prednisone vs. placebo in withdrawal therapy following medication overuse headache
 doi:10.1111/j.1468-2982.2007.01488.x Prednisone vs. placebo in withdrawal therapy following medication overuse headache L Pageler 1,2, Z Katsarava 2, HC Diener 2 & V Limmroth 1,2 1 Department of Neurology,
doi:10.1111/j.1468-2982.2007.01488.x Prednisone vs. placebo in withdrawal therapy following medication overuse headache L Pageler 1,2, Z Katsarava 2, HC Diener 2 & V Limmroth 1,2 1 Department of Neurology,
Medication overuse headache: a critical review of end points in recent follow-up studies
 J Headache Pain (2010) 11:373 377 DOI 10.1007/s10194-010-0221-4 REVIEW ARTICLE Medication overuse headache: a critical review of end points in recent follow-up studies Knut Hagen Rigmor Jensen Magne Geir
J Headache Pain (2010) 11:373 377 DOI 10.1007/s10194-010-0221-4 REVIEW ARTICLE Medication overuse headache: a critical review of end points in recent follow-up studies Knut Hagen Rigmor Jensen Magne Geir
Clinical case. Clinical case 3/15/2018 OVERVIEW. Refractory headaches and update on novel treatment. Refractory headache.
 OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
10/13/17. Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD
 Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD } Depomed Consultant 2014 to present } Avanir Consultant 2014 to present } Amgen
Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD } Depomed Consultant 2014 to present } Avanir Consultant 2014 to present } Amgen
Discussion Questions WHAT ARE SOME POSSIBLE CAUSES OF HER PAIN? WHAT ELSE WOULD YOU LIKE TO KNOW
 CLINICAL CASES Case: Ms. FM Case: Ms. FM Ms. FM is a 37-year-old school teacher Under your care for 10 years Unremarkable past history Was in minor car accident 4 months ago Has had progressive generalized
CLINICAL CASES Case: Ms. FM Case: Ms. FM Ms. FM is a 37-year-old school teacher Under your care for 10 years Unremarkable past history Was in minor car accident 4 months ago Has had progressive generalized
Headaches in Children: Clinical Pearls and Recent Advances. Paras M Bhattarai MD, MBA McLane Children s Hospital December 7, 2018
 Headaches in Children: Clinical Pearls and Recent Advances Paras M Bhattarai MD, MBA McLane Children s Hospital December 7, 2018 Conflict of Interest : None Question: How many patients with headaches have
Headaches in Children: Clinical Pearls and Recent Advances Paras M Bhattarai MD, MBA McLane Children s Hospital December 7, 2018 Conflict of Interest : None Question: How many patients with headaches have
UCNS Course A Review of ICHD-3b
 UCNS Course A Review of ICHD-3b Andrew D. Hershey, M.D., Ph.D., FAHS Endowed Chair and Director of Neurology Director, Cincinnati Children s Headache Center Professor of Neurology and Pediatrics University
UCNS Course A Review of ICHD-3b Andrew D. Hershey, M.D., Ph.D., FAHS Endowed Chair and Director of Neurology Director, Cincinnati Children s Headache Center Professor of Neurology and Pediatrics University
HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in
 HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in Anesthesia and Neurology Harvard Medical School Limited time
HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in Anesthesia and Neurology Harvard Medical School Limited time
Current Migraine Treatment Therapy. Daniel Kassicieh, DO, FAAN
 Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
Evaluating an Apparent Unprovoked First Seizure in Adults
 Evaluating an Apparent Unprovoked First Seizure in Adults Case Presentation A 52 year old woman is brought to the emergency room after a witnessed seizure. She was shopping at the local mall when she was
Evaluating an Apparent Unprovoked First Seizure in Adults Case Presentation A 52 year old woman is brought to the emergency room after a witnessed seizure. She was shopping at the local mall when she was
An Overview of MOH. ALAN M. Rapoport, M.D. Clinical Professor of Neurology The David Geffen School of Medicine at UCLA Los Angeles, California
 An Overview of MOH IHS ASIAN HA MASTERS SCHOOL MARCH 24, 2013 ALAN M. Rapoport, M.D. Clinical Professor of Neurology The David Geffen School of Medicine at UCLA Los Angeles, California President-Elect
An Overview of MOH IHS ASIAN HA MASTERS SCHOOL MARCH 24, 2013 ALAN M. Rapoport, M.D. Clinical Professor of Neurology The David Geffen School of Medicine at UCLA Los Angeles, California President-Elect
Levetiracetam in the Preventive Treatment of Transformed Migraine: A Prospective, Open-Label, Pilot Study
 VOLUME 66, NUMBER 3, MAY/JUNE 2005 Levetiracetam in the Preventive Treatment of Transformed Migraine: A Prospective, Open-Label, Pilot Study Alan M. Rapoport, MD1,2; Fred D. Sheftell, MD2,3; Stewart J.
VOLUME 66, NUMBER 3, MAY/JUNE 2005 Levetiracetam in the Preventive Treatment of Transformed Migraine: A Prospective, Open-Label, Pilot Study Alan M. Rapoport, MD1,2; Fred D. Sheftell, MD2,3; Stewart J.
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Quality ID #419: Overuse Of Neuroimaging For Patients With Primary Headache And A Normal Neurological Examination National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL
Quality ID #419: Overuse Of Neuroimaging For Patients With Primary Headache And A Normal Neurological Examination National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
Headache in an Italian pediatric emergency department
 J Headache Pain (2008) 9:83 87 DOI 10.1007/s10194-008-0014-1 ORIGINAL Headache in an Italian pediatric emergency department Paola Scagni Æ Rosaura Pagliero Received: 2 October 2007 / Revised: 3 January
J Headache Pain (2008) 9:83 87 DOI 10.1007/s10194-008-0014-1 ORIGINAL Headache in an Italian pediatric emergency department Paola Scagni Æ Rosaura Pagliero Received: 2 October 2007 / Revised: 3 January
Lynda J. Krasenbaum, MSN, ANP BC. Associate Director New York Headache Center
 Diagnosing Headache in Adults and Adolescents Lynda J. Krasenbaum, MSN, ANP BC Associate Director New York Headache Center New York, New York Learning Objectives Understand the diagnostic challenges of
Diagnosing Headache in Adults and Adolescents Lynda J. Krasenbaum, MSN, ANP BC Associate Director New York Headache Center New York, New York Learning Objectives Understand the diagnostic challenges of
Diagnosing headache. The clinician should approach the diagnosis of. Secondary headache. Primary headache. Blue and red flag headaches
 Headache THEME Diagnosing headache BACKGROUND A systematic approach to the diagnosis of primary and secondary headache disorders requires the measurement of the frequency and the duration of headache.
Headache THEME Diagnosing headache BACKGROUND A systematic approach to the diagnosis of primary and secondary headache disorders requires the measurement of the frequency and the duration of headache.
Status Epilepticus in Children
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PAEDIATRIC ACUTE CARE GUIDELINE. Headache. This document should be read in conjunction with this DISCLAIMER
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline. Scottish intercollegiate Guidelines Network SIGN
 A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
TIA: Updates and Management 2008
 TIA: Updates and Management 2008 S. Andrew Josephson, MD Department of Neurology, Neurovascular Division University of California San Francisco Commonly Held TIA Misconceptions TIA is easy to diagnose
TIA: Updates and Management 2008 S. Andrew Josephson, MD Department of Neurology, Neurovascular Division University of California San Francisco Commonly Held TIA Misconceptions TIA is easy to diagnose
MIGRAINE UPDATE. Objectives & Disclosures. Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment.
 MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
GENERAL APPROACH AND CLASSIFICATION OF HEADACHES
 GENERAL APPROACH AND CLASSIFICATION OF HEADACHES CLASSIFICATION Headache is one of the most common medical complaints. Most of the population will have experienced headache, and over 5% will seek medical
GENERAL APPROACH AND CLASSIFICATION OF HEADACHES CLASSIFICATION Headache is one of the most common medical complaints. Most of the population will have experienced headache, and over 5% will seek medical
Cluster headache associated with acute maxillary sinusitis.
 Cluster headache associated with acute maxillary sinusitis. Edvardsson, Bengt Published in: SpringerPlus DOI: 10.1186/2193-1801-2-509 2013 Link to publication Citation for published version (APA): Edvardsson,
Cluster headache associated with acute maxillary sinusitis. Edvardsson, Bengt Published in: SpringerPlus DOI: 10.1186/2193-1801-2-509 2013 Link to publication Citation for published version (APA): Edvardsson,
Specific Objectives A. Topics to be lectured and discussed at the plenary sessions
 Specific Objectives A. Topics to be lectured and discussed at the plenary sessions 0. Introduction: Good morning ICHD-III! Let s start at the very beginning. When you read you begin with A-B-C, so when
Specific Objectives A. Topics to be lectured and discussed at the plenary sessions 0. Introduction: Good morning ICHD-III! Let s start at the very beginning. When you read you begin with A-B-C, so when
RISK FACTORS AND PROGNOSIS OF CHRONIC MIGRAINE
 RISK FACTORS AND PROGNOSIS OF CHRONIC MIGRAINE Gretchen E. Tietjen, MD University of Toledo Toledo, Ohio Learning objectives At the conclusion of this presentation, participants should be able to: 1. Understand
RISK FACTORS AND PROGNOSIS OF CHRONIC MIGRAINE Gretchen E. Tietjen, MD University of Toledo Toledo, Ohio Learning objectives At the conclusion of this presentation, participants should be able to: 1. Understand
Neurological disorders. Headache (chronic tension-type) Search date December 2013 Mona Ghadiri-Sani and Nicholas Silver ...
 Headache (chronic tensiontype) Search date December 213 Mona GhadiriSani and Nicholas Silver.................................................. ABSTRACT INTRODUCTION: Chronic tensiontype headache (CTTH)
Headache (chronic tensiontype) Search date December 213 Mona GhadiriSani and Nicholas Silver.................................................. ABSTRACT INTRODUCTION: Chronic tensiontype headache (CTTH)
Common Headaches. Types and Natural Treatments
 Common Headaches Types and Natural Treatments by Heidi Fritz, MA, ND Bolton Naturopathic Clinic 64 King St W, Bolton, Ontario, L7E1C7 www.boltonnaturopathic.ca Three Common Types of Headaches Headaches
Common Headaches Types and Natural Treatments by Heidi Fritz, MA, ND Bolton Naturopathic Clinic 64 King St W, Bolton, Ontario, L7E1C7 www.boltonnaturopathic.ca Three Common Types of Headaches Headaches
Recent Advances in Neurology Difficult Cases
 Patient X: History Part 1 Recent Advances in Neurology Difficult Cases Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Brain Center Previously healthy 14-year old
Patient X: History Part 1 Recent Advances in Neurology Difficult Cases Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Brain Center Previously healthy 14-year old
Secondary Headaches: A Strategic Approach. Emerg Med 40(4):18, 2008
 Secondary Headaches: A Strategic Approach Emerg Med 40(4):18, 2008 Headaches are common complaints in the emergency department, but the causes of secondary headaches are often misdiagnosed. The authors
Secondary Headaches: A Strategic Approach Emerg Med 40(4):18, 2008 Headaches are common complaints in the emergency department, but the causes of secondary headaches are often misdiagnosed. The authors
What is IIH? Idiopathic Intracranial Hypertension (IIH)
 What is IIH? Idiopathic Intracranial Hypertension (IIH) What is Idiopathic Intracranial Hypertension? Idiopathic intracranial hypertension (IIH), also known as benign intracranial hypertension or pseudotumour
What is IIH? Idiopathic Intracranial Hypertension (IIH) What is Idiopathic Intracranial Hypertension? Idiopathic intracranial hypertension (IIH), also known as benign intracranial hypertension or pseudotumour
NEURO QUIZ 45 EHLERS DANLOS SYNDROME
 NEURO QUIZ 45 EHLERS DANLOS SYNDROME Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D START 1. Regarding
NEURO QUIZ 45 EHLERS DANLOS SYNDROME Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D START 1. Regarding
Headaches in Children
 How common are headaches? What is the impact? Very common! 20% of kids from preschool through teenage report frequent or severe headaches in any given year 2 Headaches are more common in children who have
How common are headaches? What is the impact? Very common! 20% of kids from preschool through teenage report frequent or severe headaches in any given year 2 Headaches are more common in children who have
MIGRAINES RESEARCH PRESENTATION ONE
 MIGRAINES RESEARCH PRESENTATION ONE GROUP 4 Miguel Cardoso, Shara Chowdhury, Sabrina Musto, Harpreet Pabla, Ojan Yarkhani. LIFESCI 4M03 Research Seminar Instructor Dr. Daniel Yang 1 EPIDEMIOLOGY The incidence,
MIGRAINES RESEARCH PRESENTATION ONE GROUP 4 Miguel Cardoso, Shara Chowdhury, Sabrina Musto, Harpreet Pabla, Ojan Yarkhani. LIFESCI 4M03 Research Seminar Instructor Dr. Daniel Yang 1 EPIDEMIOLOGY The incidence,
