Characteristics of post-traumatic headaches in children following mild traumatic brain injury and their response to treatment: a prospective cohort
|
|
|
- Barnard Chapman
- 5 years ago
- Views:
Transcription
1 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Characteristics of post-traumatic headaches in children following mild traumatic brain injury and their response to treatment: a prospective cohort ANDREA KUCZYNSKI 1 SUSAN CRAWFORD 2 LISA BODELL 2 DEBORAH DEWEY 1,2 KAREN M BARLOW 1,2 1 University of Calgary, Calgary, AB; 2 Alberta Children s Hospital Research Institute, Calgary, AB, Canada. Correspondence to Dr Karen Maria Barlow, Alberta Children s Hospital, C Shaganappi Trail NW, Calgary, Alberta, CA T3B 6A8, Canada. karen.barlow@albertahealthservices.ca This article is commented on by Mack on pages of this issue. PUBLICATION DATA Accepted for publication 24th January Published online 5th April ABBREVIATIONS mtbi Mild traumatic brain injury PCS Post-concussion syndrome PCSI Post Concussive Symptom Inventory PTH Post-traumatic headache AIM Post-traumatic headaches (PTHs) following mild traumatic brain injury (mtbi) are common; however, few studies have examined the characteristics of PTHs or their response to treatment. The aims of this study were (1) to describe the clinical characteristics of PTH in a prospective cohort of children presenting to a paediatric emergency department with mtbi, and (2) to evaluate the response of PTH to treatment. METHOD The emergency department cohort was obtained from a prospective longitudinal cohort study of symptoms following mtbi (n=670; 385 males, 285 females) and a comparison group of children with extracranial injury (n=120; 61 males, 59 females). A retrospective chart review of a separate cohort of children from a brain injury clinic (the treatment cohort) treated for PTH was performed (n=44; 29 females, 15 males; mean age 14y 1mo, SD 3y 1mo). The median time since injury was 6.9 months (range 1 29mo). The mean follow-up interval after treatment started was 5.5 weeks (SD 4.3wks). RESULTS Among the emergency department cohort (n=39; 20 males, 19 females; mean age 11y 1mo, SD 4y 3mo) 11% of children were symptomatic with PTHs at a mean of 15.8 days (SD 11.6d) post injury. Three months post injury, 7.8% of children complained of headaches; of those, 56% had pre-existing headaches and 18% had experienced migraine before the injury. Although headache type varied, 55% met the criteria for migraine. A family or past medical history of migraine was present in 82% of cases. Among the treatment cohort, medications included amitriptyline, flunarizine, topiramate, and melatonin, with an overall response rate of 64%. CONCLUSION This is the first prospective cohort study to describe the clinical characteristics of PTHs following mtbi in children. Migraine was the most common headache type seen; other headaches included tension-type, cervicogenic, and occipital neuralgias, and 64% responded to treatment. Referral to a headache specialist should be considered, especially when the features are not typical of one of the primary headache disorders. Mild traumatic brain injury (mtbi) accounts for 70 to 90% of all traumatic brain injuries, and many children who experience an mtbi continue to have symptoms for over 3 months. 1,2 As many as one in five children will experience an mtbi by the age of 10 years, and this incidence may be increasing. 3 Until recently, mtbi was thought to have no long-term consequences; however, in the past few years we have seen a dramatic increase in the medical literature and wider media on the potential medical and psychosocial problems associated with mtbi. Our previous research demonstrated that 11% of children who present to an emergency department with mtbi experience post-concussion symptoms for 3 months or longer, and 2% of children have symptoms that persist for over a year. 2 Common postconcussion symptoms include somatic complaints (e.g. headaches, dizziness, nausea, fatigue, sleep disturbances, photo/phonophobia), cognitive deficits (e.g. poor concentration, memory problems, slowed thinking), and emotional symptoms (e.g. depression, irritability). Although routine neurological investigations are often normal, the child and his or her family are often significantly debilitated. 4 Post-traumatic headaches (PTHs) are one of the most common symptoms following mtbi, and perhaps the most disabling. The International Headache Society criteria (2nd edition; IHCD-II) define PTHs as headaches, with no typical characteristics known, which occur within 7 days of a traumatic brain injury and are either acute, where the headache resolves within 3 months of the trauma, or chronic where the headache persists for more than 3 months. 5 PTH accounts for 4% of headache disorders seen in tertiary 636 DOI: /dmcn The Authors. Developmental Medicine & Child Neurology 2013 Mac Keith Press
2 headache clinics, 6 but there are few reports on the prevalence and clinical characteristics in children The medical literature on PTH in children includes only 818 children with mtbi surprisingly few considering that one in five children experiences an mtbi by the age of 10 years. 7,11,15 18 The prevalence of PTH in children with mtbi in these studies varied between 9% and 72% depending on the clinical cohort, research methods, and follow-up period. Our study aimed to add significantly to the current body of literature regarding PTH in children by investigating the prevalence and clinical characteristics of the disorder in a prospective cohort of children with mtbi who presented at a paediatric emergency department. There are no controlled trials or reports of how children with PTH respond to the varying pharmacological treatment strategies. Furthermore, there are no placebo-controlled pharmacological intervention studies for the treatment of PTH in adults. 19 To our knowledge, only three studies have examined the response to such preventative therapies. Erickson 14 reported that treatment with topiramate was associated with a significant decline in PTH burden (49% response rate) compared with treatment with low-dose tricyclic antidepressant (28% response rate). Packard 20 analysed the response to divalproex sodium in 100 patients and found a mild to moderate response in 60%; and Saran 21 evaluated amitriptyline in 12 patients with depression and PTH in comparison with 12 patients with primary depression, and found no reduction in headache burden. The aims of this study were twofold: first, to describe the prevalence and clinical characteristics of PTH in a prospective cohort of children with mtbi; second, to evaluate the response of paediatric PTH to treatment in a cohort of children seen in a brain injury clinic. METHOD Cohort of emergency department attendees The cohort of emergency department attendees was obtained from a prospective cohort study of symptom survival following mtbi without extracranial injury in children between July 2005 and June Any child (aged 0 18y) who presented to the emergency department having experienced an mtbi without extracranial injury was included in the study. mtbi was defined as a Glasgow Coma Scale score of 13 to 15, loss of consciousness or altered mental state lasting less than 20 minutes, absence of focal neurological deficits, and post-traumatic amnesia lasting for less than 24 hours. 12 We identified 1264 children, and 670 (53%) consented to participate in the study. A comparison group of children with extracranial injuries was identified in the emergency department (n=120; 61 males, 59 females). We have reported the details of the methods and the comparison group in a previous study. 2 All participants were interviewed by telephone 7 to 10 days after injury and follow-up continued monthly until symptoms resolved (n=670; 385 males, 285 females). The percentage of children lost to follow-up was 13% in the mtbi group and 10% in the comparison group of children with extracranial injuries. What this paper adds 7.8% of children reported headaches 3 months after mtbi. A family or past medical history of migraine was present in 82%. Migraine was most frequent (54%), but other headache types were also common. 64% of children responded to conventional treatments for headache disorders. Referral to headache specialist is appropriate where symptoms persist. Headache was evaluated using the Post Concussive Symptom Inventory (PCSI), where symptoms are rated as 0, never a problem ; 1, rarely a problem ; 2, sometimes a problem ; 3, often a problem ; and 4, always a problem. Pre-injury symptoms, including headache, were also evaluated at 7 to 10 days post injury using the PCSI (pre-injury) questionnaire. If symptoms persisted at 2 months post injury, an appointment with a neurologist was offered (n=52). Thirty-nine of 52 children (75%) with chronic PTH were seen and a standard questionnaire and examination, including headache characterization, was performed (Table I). Treatment cohort To examine the treatment response, a separate cohort of children with mtbi attending a paediatric brain injury clinic was identified. A standardized questionnaire eliciting acute injury details, post-concussive symptoms, headache characteristics, and family history was completed for all children with mtbi referred to this clinic. Ninety-two children with Table I: Demographic and injury details of children with persistent headaches following mtbi from a prospective emergency department cohort and children receiving prophylactic treatment for post-traumatic headache seen in a paediatric brain injury clinic Patient characteristics Prospective emergency department cohort with persistent PTH (n=39) Clinic treatment cohort (n=44) Age (y) Mean 11.1 Mean 14.1 <0.01 (SD 4.3) (SD 3.1) Female/Males 19/20 29/ Time since injury (mo) Median 2 Median 6.9 <0.01 (range ) (range 1 29) Loss of consciousness Neuroimaging 5 24 Abnormal neuroimaging 1 9 Mechanism of injury Sport-related Fall 11 5 Motor vehicle accident 3 9 Abusive 0 5 Struck by object 3 0 Pre-existing headache disorder Migraine 12 6 Non-specific headache 6 10 Family history of migraine Pre-existing headache and/or family history of migraine p Post-traumatic Headaches in Children Andrea Kuczynski et al. 637
3 persistent post-concussion syndrome (PCS) were seen between 2007 and June Children who received prophylactic treatment for headaches which met the ICHD-II criteria for PTH were identified (n=44). The clinical characteristics and response to treatment of PTH were recorded. PTHs were subclassified using the ICHD-II modified for children by a neurologist with expertise in headache disorders. 22 The clinical characteristics are presented in Table II. Monthly follow-up was carried out (mean 5.5wks; SD 4.3wks; median 4wks; interquartile range [IQR] 3wks) until symptoms resolved. Migrainous headaches lacking one diagnostic criterion were classified as Table II: Clinical characteristics of post-traumatic headache persisting for longer than 3 months in children following mild traumatic brain injury in a prospective emergency department cohort and a treatment cohort Emergency department prospective cohort (n=39) n Treatment cohort (n=44) n Location Frontal Temporal 7 6 Holocephalic 5 9 Retro-orbital 3 4 Occipital 2 7 Associated neck pain 2 7 Type of pain Pulsatile 11 8 Pressure 3 5 Squeezing 2 2 Sharp/stabbing 5 9 Unable to describe 17 Associated features Nausea Vomiting 4 11 Photophobia Phonophobia Visual aura 3 14 Vertigo 2 7 Exacerbated by exercise 2 17 Other features Orthostatic hypotensive 6 3 symptoms Depression 2 7 Other mood changes Cognitive problems Length of headache Minutes h h 13 1 >4h 7 18 Frequency of headaches Daily Three or more/week 5 8 Headache classification Migraine (with or without aura) Tension-type 2 4 Occipital neuralgia 1 1 Vestibular disorder 2 1 Cervicogenic 1 2 Headache associated with 2 6 mood disorder Primary exertion headache 2 Mixed headaches 4 Medication overuse 2 2 Unclassifiable 8 17 probable migraine, 22 and those lacking two diagnostic criteria were denoted as unclassified. A reduction in headache frequency of 50% or greater, together with a functional improvement, was considered significant. An unknown response was documented when patients discontinued medication early or where there was a loss to follow-up. This study was approved by the University of Calgary Conjoint Health Research Ethics Board. Guidelines for treatment Patients were advised to avoid analgesic (such as acetaminophen and ibuprofen) overuse by limiting their use to a maximum of two or three times per week or eight times per month, and to avoid any opiate medications. Light exercise was encouraged if PCS persisted for 3 months or longer post injury. Prophylactic medications were selected based on comorbidities by a neurologist with expertise in acquired brain injury and headache disorders. Melatonin or amitriptyline was typically prescribed if sleep disruption was a significant comorbidity. Melatonin was started at 3mg and increased to a maximum of 10mg. Amitriptyline was started at 5mg and titrated to a maximum of 1mg/kg depending on response. 23 Topiramate is often used when obesity is a comorbidity and was avoided as a first-line prophylactic medication if the mtbi was associated with significant cognitive dysfunction. It was commenced at 12.5mg/day and slowly titrated to 1.5 2mg/kg/day to a maximum of 200mg/day. 24 Valproic acid is not used as a first-line medication in our paediatric clinic. A reduction in headache frequency of 50% or greater was defined as a successful response to treatment. Prophylactic medications were continued for 3 months following headache resolution and then gradually discontinued. Typically, efficacy is assessed after 2 to 3 months, and to allow medication to be changed if necessary. Statistical analysis The Statistical Package for the Social Sciences (version 19.0; SPSS Inc., Chicago, IL, USA) was used for the statistical analysis. The Kolmogorov Smirnov test was used to determine which variables were normally distributed and which were not. In the case of normally distributed data, t-tests and analysis of covariance were used to examine group differences, whereas v 2 tests and the Wilcoxon- Mann Whitney U test were used to conduct group comparisons on non-normally distributed data. Logistic regression was used to examine whether symptom resolution (i.e. treatment response status) was predicted by time in follow-up. RESULTS Cohort of emergency department attendees Initial follow-up Twenty per cent of the mtbi cohort and 16% of the extracranial injury cohort had pre-existing headaches. Seventy-five children (11%; 95% confidence interval [CI] %) in the mtbi population-based cohort were 638 Developmental Medicine & Child Neurology 2013, 55:
4 symptomatic with acute PTH at a mean of 15.8 days (SD 11.6d; median 14d; IQR 9d) post injury. The headaches were rated as 2.5 (SD 0.98; median 2; IQR 2) on the PCSI (when compared with pre-injury status). 3-month follow-up Fifty-two children with mtbi (7.8%; 95% CI %) were symptomatic with chronic PTH at 3 months post injury and with headaches rated as 2 (SD 0.85; median 2; IQR 2) on the PCSI. Headache was more commonly reported in those children who continued to have PCS over time. PTHs were present in 75% of children with symptoms at 6 months post injury, and 100% of children with symptoms at 1 year post injury. Thirty-nine out of 52 children with persistent PCS (20 males, 19 females; mean age 11y 1mo, SD 4y 3mo) were evaluated in the clinic. Thirteen families declined to participate. The demographic and injury details are shown in Table I. The characteristics of the headaches are shown in Table II. Daily headache was reported in 44% of children, and 18% had headaches lasting longer than 4 hours. Fiftyone per cent had pre-existing headaches, and 31% had migraine/probable migraine pre-injury. Forty-four per cent of children satisfied criteria for migraine (one with aura) and 3% for probable migraine; in 8% headache was unclassified. Ten children had a new-onset migraine-like disorder attributed to the mtbi, four of whom had a family history of migraine. Treatment cohort Forty-four children with PTH seen in a brain injury clinic (29 females, 15 males; mean age 14y 1mo, SD 3y 1mo) and who received prophylactic medication for their headaches were studied to determine their response to treatment. The demographic, clinical, and headache details are presented in Tables I and II. These children were older and had symptoms for a longer period (p<0.01) than the children in the emergency department cohort, but otherwise their clinical characteristics were similar. Sixty-one per cent (95% CI 47 74%) experienced daily headaches post injury. Headaches satisfied criteria for migraine in 39% of children, and 9% were classified as chronic tension-type headaches (Table II). Twenty-three per cent of children had pre-existing headaches, and 14% had migraine or probable migraine pre-injury. Overall, 64% of the treatment cohort had a successful response to medication. Twenty-two children (50%) reported a marked reduction in the frequency of their headaches post treatment. Forty-five per cent reported complete resolution of their headaches with treatment, and in six children (14%) the headache frequency decreased to one to three headaches a week. Three children (7%) continued to have severe persisting headaches but did not wish to pursue further medical treatment strategies. The length of time in follow-up was not a significant predictor of symptom resolution (i.e. treatment response status; model v 2 (1) =0.341; p=0.559). Melatonin was found to improve headaches significantly in 9 out of 12 children (75%). A total of 13 out of 18 patients (68%) reported a good effect with amitriptyline (Fig. 1). Seventeen children (39%) received more than one treatment. Indomethacin successfully treated stabbing headache in two children, and in another child occipital neuralgia responded to injections of lidocaine and triamcinolone. Other treatments included self-referred complementary and alternative therapies (16%), physiotherapy (9%), and biofeedback therapy (11%). DISCUSSION To our knowledge, this is the first study to describe the characteristics of PTHs in a large consecutive cohort of children with mtbi, and to document the response of PTH to treatment in a paediatric brain injury clinic cohort. We demonstrated that PTH is common: 11% of all children complain of increased headaches 2 weeks following mtbi and 7.8% at 3 months post injury. This prevalence suggests that PTH is a frequent problem that continues for a long period following injury. Of those Number of patients Unknown No response Partial response Full respone Amitryptiline Nortryptiline Flunarizine Topiramate Melatonin Medication Figure 1: Bar chart demonstrating the response to the most common medications used in the treatment cohort. Post-traumatic Headaches in Children Andrea Kuczynski et al. 639
5 children who reported PCS symptoms in the 3-month period following mtbi, 50% complained of a significant increase in headaches compared with their pre-injury status. PTHs continue to be a significant cause of morbidity in children in whom PCS persists: the proportion of children complaining of headache increased over time, and 100% of symptomatic children at 12 months post injury complained of headaches. This may explain why previous cohorts have reported such variable rates of PTH, for example ranging from 22.5% in studies examining outcome at 2 months to 72% when outcome was evaluated at 1 year following adult mild head injury. 6 In the present study, we found a 7.8% prevalence of increased headache frequency and/or severity at 3 months following mtbi, which is similar to the findings of a previous prospective study by Kirk et al. 17 Blume et al. 7 reported that mtbi is a risk factor for headaches at 3 months post injury (relative risk 1.7; 95% CI ); however, they found that 43% of children with mtbi reported any headache at 3 months post injury, compared with 26.2% of children with an arm injury an increase of 16%. Unfortunately, Blume et al. 7 do not report the prevalence of pre-injury headaches in their sample, which is potentially significant as this is a risk factor for PCS and PTH following mtbi 25 ; nor do they comment on the characteristics of the headaches. Our previous study found that age and severity of the injury, but not sex, were significant risk factors for symptom persistence. 2 In keeping with this, patients in this separate treatment cohort were older and more likely to have experienced a loss of consciousness at the time of injury (p<0.01), and neuroimaging was performed in 54%. This study is the first to present the clinical characteristics of PTH and to further subclassify the headaches using the ICHD-II for children. A wide range of headache characteristics were seen. Headache satisfying criteria for migraine (with or without aura) was the most common type of headache seen (54%), and tension-type headaches were reported in 5% of these children (Table II). Only one previous report characterized PTH in children: of 11 children, five had migraine, five had tension-type headaches, and one child had mixed headaches. 17 Adult cohorts vary markedly in the type of headaches seen depending on whether the patients are selected from headache clinics or have traumatic brain injury: the prevalence of migraine-like headaches ranges from 2 to 41% and of tension-type headaches from 7 to 96%. 6,9,19 In our study, 47% of children with PTH had a history of migraines, although these may not have been recognized previously. Of particular relevance in paediatric practice, in which migraine becomes more problematic in adolescence, is that 82% of the children with persistent headaches in the emergency department cohort and 57% of those in the treatment cohort reported having either pre-existing headache disorders or a family history of migraine. Medication overuse headache (5%) and chronic tensiontype headaches (5%) were seen less commonly than in previous studies. 6 These differences could be a result of the triage and initial evaluation process in our brain injury clinic. For example, patients who are referred to the clinic are contacted within 1 week of referral and families are educated about mtbi and advised of the potential for medication overuse headache, especially after the acute post-injury period has passed. It is also possible that children may differ from adults in the types of headaches they develop following mtbi, or are less likely than adults to develop chronic tension-type headaches. Twenty-one per cent of headaches in the emergency department cohort and 39% of headaches in the treatment cohort were unclassifiable using the ICHD-II, and the only consistent feature in this group was the mtbi. Less common types of headaches were also found in both cohorts, for example cervicogenic headache, occipital neuralgia, exertion headache, and idiopathic stabbing headache. The morbidity associated with PTH was significant. Among the emergency department and clinic cohorts, 44% and 61% of children respectively, were experiencing daily headaches. The children with these types of headache responded well to recognized treatments. This demonstrates that referral to a neurologist or headache specialist is appropriate where symptoms persist. This treatment case series provides additional evidence on the treatment of PTH. Packard 20 retrospectively analysed the response to sodium valproate in a clinic cohort of adult patients with PTH. Improvement was based on patient estimate and a moderate response was reported as a 50% or greater improvement in the headaches. Packard found that 60% had a mild/moderate response, although 14% of patients stopped the medication because of side effects. Sodium valproate is not routinely used to treat headache in our clinic because of the incidence of side effects. 26,27 Erickson 14 reported the efficacy of various treatments used for PTH in US military service members. There was an overall treatment response of 35%, and topiramate was found to be more effective than amitriptyline/ nortriptyline, propranolol, or valproate. As blast-related mtbi accounted for 77% of patients in the Erickson study, it is hard to extrapolate these results to childhood, especially as the mechanism of injury is very different to the fall and sport-related mtbi seen in children and young people. There are no previous studies reporting the response of PTH to treatment in children. We used a variety of treatments depending on the headache characteristics and comorbidities, such as sleep dysfunction (for which amitriptyline or melatonin was more commonly chosen), cognitive dysfunction (in which case topiramate would be avoided), and stabbing headache or Valsalva-induced headaches (treated with indomethacin). However, the numbers receiving individual treatments were small. In contrast to Erickson s study, amitriptyline was effective with 13 out of 19 children (68%) having a positive response and 47% of children reporting no headaches post treatment. Melatonin was also effective in 75% of children. Overall, we found 640 Developmental Medicine & Child Neurology 2013, 55:
6 that 64% of children documented a response to treatment (Fig. 1). We acknowledge the following limitations of this study. The numbers of children receiving individual treatments were small, and it is, therefore, not possible to draw conclusions about relative efficacy of the different agents. Another weakness of this study is the lack of a headache diary and disability score to assess the degree of functional impairment associated with the headaches and treatment response. Further, as this complex population has significant comorbidities (especially mood and cognitive dysfunction), a comprehensive paediatric quality of life measure would also have been useful. Finally, this is an observational, uncontrolled study. Although the children were reviewed at 6.9 months (SD 8.1mo) post injury and the response rates are likely to be higher than what would be expected for the natural history of PCS alone, future studies should ideally be placebo controlled. 2 CONCLUSION In summary, 7.8% of children still report PTH 3 months after mtbi. A family or past medical history of migraine headache was present in 82%. Although migraine headache is the most common type of headache, other cephalgias are not infrequent. Referral to a headache specialist should be considered, especially when the features are not typical of one of the primary headache disorders. Treatment should be tailored to headache type as well as comorbidity. Further research is required to evaluate treatment options in PTH, although our research suggests that children respond to many of the therapies commonly used to treat headache disorders. ACKNOWLEDGMENTS This research was supported by the Alberta Children s Hospital Foundation (RT34396). REFERENCES 1. Langlois JA, Rutland-Brown W, Thomas KE. The incidence of traumatic brain injury among children in the United States: differences by race. J Head Trauma Rehabil 2005; 3: Barlow KM, Crawford S, Stevenson A, Sandhu SS, Belanger F, Dewey D. Epidemiology of postconcussion syndrome in pediatric mild traumatic brain injury. Pediatrics 2010; 126: e Lincoln AE, Caswell SV, Almquist JL, Dunn RE, Norris JB, Hinton RY. Trends in concussion incidence in high school sports: a prospective 11-year study. Am J Sports Med 2011; 39: McCrory P, Meeuwisse W, Johnston K, et al. Consensus statement on concussion in sport the Third International Conference on Concussion in Sport held in Zurich, November Phys Sportsmed 2009; 37: Olesen J. The international classification of headache disorders, 2nd edition (ICHD-II). Rev Neurol (Paris) 2005; 161: Lew HL, Lin PH, Fuh JL, Wang SJ, Clark DJ, Walker WC. Characteristics and treatment of headache after traumatic brain injury: a focused review. Am J Phys Med Rehabil 2006; 85: Blume HK, Vavilala MS, Jaffe KM, et al. Headache after pediatric traumatic brain injury: a cohort study. Pediatrics 2012; 129: e Radanov B, Ludin HP. [Sequelae of craniocerebral injuries in a neurologic patient sample an attempt at interpreting post-traumatic headache]. Fortschr Neurol Psychiatr 1986; 54: [In German]. 9. Baandrup L, Jensen R. Chronic post-traumatic headache a clinical analysis in relation to the International Headache Classification, 2nd edition. Cephalalgia 2005; 25: Nampiaparampil DE. Prevalence of chronic pain after traumatic brain injury: a systematic review. JAMA 2008; 300: Necajauskaite O, Endziniene M, Jurieniene K. Prevalence, clinical features and accompanying signs of post-traumatic headache in children. Medicina (Kaunas) 2005; 41: Gladstone J. From psychoneurosis to ICHD-2: an overview of the state of the art in post-traumatic headache. Headache 2009; 49: Evans RW, Evans RW. Persistent post-traumatic headache, postconcussion syndrome, and whiplash injuries: the evidence for a non-traumatic basis with an historical review. Headache 2010; 50: Erickson JC. Treatment outcomes of chronic post-traumatic headaches after mild head trauma in US soldiers: an observational study. Headache 2011; 51: Collins MW, Field M, Lovell MR, et al. Relationship between postconcussion headache and neuropsychological test performance in high school athletes. Am J Sports Med 2003; 31: Hawley CA. Reported problems and their resolution following mild, moderate, and severe traumatic brain injury amongst children and adolescents in the UK. Brain Inj 2003; 17: Kirk C, Nagiub G, Abu-Arafeh I. Chronic post-traumatic headache after head injury in children and adolescents. Dev Med Child Neurol 2008; 50: Necajauskaite O, Endziniene M, Jureniene K. The prevalence, course and clinical features of post-concussion syndrome in children. Medicina (Kaunas) 2005; 41: Watanabe TK, Bell KR, Walker WC, Schomer K. Systematic review of interventions for post-traumatic headache. PM R 2012; 4: Packard RC. Treatment of chronic daily posttraumatic headache with divalproex sodium. Headache 2000; 40: Saran A. Antidepressants not effective in headache associated with minor closed head injury. Int J Psychiatry Med 1988; 18: Hershey AD, Winner P, Kabbouche MA, et al. Use of the ICHD-II criteria in the diagnosis of pediatric migraine. Headache 2005; 45: Hershey AD, Powers SW, Bentti AL, Degrauw TJ. Effectiveness of amitriptyline in the prophylactic management of childhood headaches. Headache 2000; 40: Hershey AD, Powers SW, Vockell AL, LeCates S, Kabbouche M. Effectiveness of topiramate in the prevention of childhood headaches. Headache 2002; 42: Lau B, Lovell MR, Collins MW, Pardini J. Neurocognitive and symptom predictors of recovery in high school athletes. Clin J Sport Med 2009; 19: Price KE, Pearce RE, Garg UC, et al. Effects of valproic acid on organic acid metabolism in children: a metabolic profiling study. Clin Pharmacol Ther 2011; 89: Blaw ME, Belknap WM. Valproate hepatotoxicity. Pediatr Neurol 1985; 1: 320. Post-traumatic Headaches in Children Andrea Kuczynski et al. 641
Mild Traumatic Brain Injury (mtbi): An Occupational Dilemma
 Mild Traumatic Brain Injury (mtbi): An Occupational Dilemma William H. Cann, MD MPH Occupational Medicine Trainee Occupational Medicine Trainee University of Washington Disclosures None This presentation
Mild Traumatic Brain Injury (mtbi): An Occupational Dilemma William H. Cann, MD MPH Occupational Medicine Trainee Occupational Medicine Trainee University of Washington Disclosures None This presentation
Mild traumatic brain injury (mtbi) has been increasingly. Follow-up issues in children with mild traumatic brain injuries
 clinical article J Neurosurg Pediatr 18:224 230, 2016 Follow-up issues in children with mild traumatic brain injuries Katarzyna Kania, MPH, 1 Kashif Ajaz Shaikh, MD, 1,2 Ian Kainoa White, MD, 1,2 and Laurie
clinical article J Neurosurg Pediatr 18:224 230, 2016 Follow-up issues in children with mild traumatic brain injuries Katarzyna Kania, MPH, 1 Kashif Ajaz Shaikh, MD, 1,2 Ian Kainoa White, MD, 1,2 and Laurie
Sport Related Concussion Update 2017
 Sport Related Concussion Update 2017 HAYLEY QUELLER, MD ST. CHARLES ORTHOPEDICS, SPORTS MEDICINE DIRECTOR THINKSMART! CONCUSSION MANAGEMENT, CO-DIRECTOR Consensus Statement: 5 th Annual Meeting, Berlin
Sport Related Concussion Update 2017 HAYLEY QUELLER, MD ST. CHARLES ORTHOPEDICS, SPORTS MEDICINE DIRECTOR THINKSMART! CONCUSSION MANAGEMENT, CO-DIRECTOR Consensus Statement: 5 th Annual Meeting, Berlin
Neurological Findings & Symptoms Associated with Acute Combat related Concussion: Disclosures. Impact of Migraine and Other Co morbidities
 Neurological Findings & Symptoms Associated with Acute Combat related Concussion: Impact of Migraine and Other Co morbidities COL Beverly R. Scott Madigan Healthcare System Disclosures The views expressed
Neurological Findings & Symptoms Associated with Acute Combat related Concussion: Impact of Migraine and Other Co morbidities COL Beverly R. Scott Madigan Healthcare System Disclosures The views expressed
The Value of Rest. Makdissi- Zurich A brief period of rest is important in the acute period following concussion.
 Treatment 2 The Value of Rest Makdissi- Zurich 2012 A brief period of rest is important in the acute period following concussion. There is no evidence however that prolonged rest is beneficial for athletes
Treatment 2 The Value of Rest Makdissi- Zurich 2012 A brief period of rest is important in the acute period following concussion. There is no evidence however that prolonged rest is beneficial for athletes
6/2/2017. Objectives. Statement of Problem: Migraine Headaches Are Common. Chronic Headache In Pediatrics, Botox and Beyond
 Chronic Headache In Pediatrics, Botox and Beyond Ken Mack MD PhD Mayo Clinic 2015 MFMER slide-1 Objectives Understand pediatric chronic headache presentations Review evidence for the treatment of chronic
Chronic Headache In Pediatrics, Botox and Beyond Ken Mack MD PhD Mayo Clinic 2015 MFMER slide-1 Objectives Understand pediatric chronic headache presentations Review evidence for the treatment of chronic
PEDIATRIC SPORTS RELATED CONCUSSIONS
 Anna Mazur, PhD PEDIATRIC SPORTS RELATED CONCUSSIONS Disclosure No financial interests or funding 1 Presentation Outline Prevalence Predicting recovery: Post Traumatic Amnesia and Loss of Consciousness
Anna Mazur, PhD PEDIATRIC SPORTS RELATED CONCUSSIONS Disclosure No financial interests or funding 1 Presentation Outline Prevalence Predicting recovery: Post Traumatic Amnesia and Loss of Consciousness
Mild Head Trauma and Chronic Headaches in Returning US Soldiers. Brett J. Theeler, MD; Jay C. Erickson, MD, PhD
 Headache 2009 the Authors Journal compilation 2009 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2009.01345.x Published by Wiley Periodicals, Inc. Research Submission Mild Head Trauma
Headache 2009 the Authors Journal compilation 2009 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2009.01345.x Published by Wiley Periodicals, Inc. Research Submission Mild Head Trauma
Disclosures. Objectives 11/10/2017. Research funding: Consultant and advisory: NIDILRR Wadsworth Foundation. Allergan Amgen Lilly Teva
 AHS Scottsdale Headache Symposium 2017 Long Term Management of Posttraumatic Headache Sylvia Lucas MD, PhD, FAHS Clinical Professor of Neurology & Neurological Surgery Adjunct, Rehabilitation Medicine
AHS Scottsdale Headache Symposium 2017 Long Term Management of Posttraumatic Headache Sylvia Lucas MD, PhD, FAHS Clinical Professor of Neurology & Neurological Surgery Adjunct, Rehabilitation Medicine
IT S ALL IN YOUR HEAD!
 IT S ALL IN YOUR HEAD! CARING FOR CONCUSSIONS IN YOUR COMMUNITY Stephen K Stacey, DO CPT, MC, USA OUTLINE Definition Epidemiology Diagnosis Evaluation Recovery Sequelae Prevention Resources for providers
IT S ALL IN YOUR HEAD! CARING FOR CONCUSSIONS IN YOUR COMMUNITY Stephen K Stacey, DO CPT, MC, USA OUTLINE Definition Epidemiology Diagnosis Evaluation Recovery Sequelae Prevention Resources for providers
and present Date: Amended January 2015
 and present Concussionn Guidelines in the GAA 2013 2016 Adopted by LGFA Date: Amended January 2015 Table of Contents Summary Principles... 2 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
and present Concussionn Guidelines in the GAA 2013 2016 Adopted by LGFA Date: Amended January 2015 Table of Contents Summary Principles... 2 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
Chronic Migraine in Primary Care. December 11 th, 2017 Werner J. Becker University of Calgary
 Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Review of: NATA Position Statement Management of Sport Concussion.
 Review of: NATA Position Statement Management of Sport Concussion www.csm-institute.com Topics: Education and Prevention Documentation and Legal Aspects Evaluation and RTP Other Considerations Strength
Review of: NATA Position Statement Management of Sport Concussion www.csm-institute.com Topics: Education and Prevention Documentation and Legal Aspects Evaluation and RTP Other Considerations Strength
Centers for Disease Control and Prevention Guideline on the Diagnosis and Management of Mild Traumatic Brain Injury Among Children September 2018
 Centers for Disease Control and Prevention Guideline on the Diagnosis and Management of Mild Traumatic Brain Injury Among Children September 2018 Nothing to Disclose CDC Guidelines- Objective Question-
Centers for Disease Control and Prevention Guideline on the Diagnosis and Management of Mild Traumatic Brain Injury Among Children September 2018 Nothing to Disclose CDC Guidelines- Objective Question-
Recurrent Headaches in Children -- An Analysis of 47 Cases
 ---------------------------------------------- Recurrent Headaches in Children -- An Analysis of Cases I H M I Hussain, MRCP Neurology Unit Paediatric Institute, Kuala Lumpur Hospital, )aian Pahang, 50586
---------------------------------------------- Recurrent Headaches in Children -- An Analysis of Cases I H M I Hussain, MRCP Neurology Unit Paediatric Institute, Kuala Lumpur Hospital, )aian Pahang, 50586
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert
 Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Director of Athletics
 3341-8-1 Concussion Management Policy. Applicability Intercollegiate Athletics Responsible Unit Policy Administrator Intercollegiate Athletics/Director of Athletics Director of Athletics (A) Policy Purpose
3341-8-1 Concussion Management Policy. Applicability Intercollegiate Athletics Responsible Unit Policy Administrator Intercollegiate Athletics/Director of Athletics Director of Athletics (A) Policy Purpose
Learning objectives 6/20/2018
 Cognitive impairment of patients with chronic migraine, in a neuropsychological assessment, does not depend on the use of topiramate or comorbidities Ferreira KS, MD, PhD Professor, Neurology Clinic, Medicine
Cognitive impairment of patients with chronic migraine, in a neuropsychological assessment, does not depend on the use of topiramate or comorbidities Ferreira KS, MD, PhD Professor, Neurology Clinic, Medicine
Physiotherapy management of concussion
 Physiotherapy management of concussion Ms. Mairead Daly, Senior Physiotherapist, Bon Secours Health System Saturday November 17 th Silver Springs Hotel Cork Concussion Physiotherapy Assessment and Management
Physiotherapy management of concussion Ms. Mairead Daly, Senior Physiotherapist, Bon Secours Health System Saturday November 17 th Silver Springs Hotel Cork Concussion Physiotherapy Assessment and Management
Inpatient Treatment of Status Migraine With Dihydroergotamine in Children and Adolescents
 Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
How do we treat migraine? New SIGN Guidelines
 How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
Concussion. James R. Borchers, MD, MPH
 Concussion James R. Borchers, MD, MPH Associate Clinical Professor Director, Division of Sports Medicine, Department of Family Medicine Head Team Physician, Athletic Department Jameson Crane Sports Medicine
Concussion James R. Borchers, MD, MPH Associate Clinical Professor Director, Division of Sports Medicine, Department of Family Medicine Head Team Physician, Athletic Department Jameson Crane Sports Medicine
The Paradox of Predicting Persistent Concussion Symptoms in Children and Adolescents
 The Paradox of Predicting Persistent Concussion Symptoms in Children and Adolescents Roger Zemek, MD, FRCPC Director, Pediatric Emergency Research Children s Hospital of Eastern Ontario Assistant Professor,
The Paradox of Predicting Persistent Concussion Symptoms in Children and Adolescents Roger Zemek, MD, FRCPC Director, Pediatric Emergency Research Children s Hospital of Eastern Ontario Assistant Professor,
Concussions. Recognition, Management, and Care
 Concussions Recognition, Management, and Care Sports Concussion: Complex, pathophysiological process affecting the brain, induced by traumatic bio-mechanical forces. 1 1.6-3.8 million concussions occur
Concussions Recognition, Management, and Care Sports Concussion: Complex, pathophysiological process affecting the brain, induced by traumatic bio-mechanical forces. 1 1.6-3.8 million concussions occur
A prospective study of prevalence and characterization of headache following mild traumatic brain injury
 Original Article A prospective study of prevalence and characterization of headache following mild traumatic brain injury Cephalalgia 2014, Vol 34(2) 93 102! International Headache Society 2013 Reprints
Original Article A prospective study of prevalence and characterization of headache following mild traumatic brain injury Cephalalgia 2014, Vol 34(2) 93 102! International Headache Society 2013 Reprints
Research Article Detecting Migraine in Patients with Mild Traumatic Brain Injury Using Three Different Headache Measures
 Behavioural Neurology Volume 2015, Article ID 693925, 7 pages http://dx.doi.org/10.1155/2015/693925 Research Article Detecting Migraine in Patients with Mild Traumatic Brain Injury Using Three Different
Behavioural Neurology Volume 2015, Article ID 693925, 7 pages http://dx.doi.org/10.1155/2015/693925 Research Article Detecting Migraine in Patients with Mild Traumatic Brain Injury Using Three Different
Outpatient Headache Care Guideline
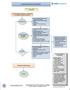 1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
Complexity and Challenges of Return to Play After a Mild Traumatic Brain Injury
 Complexity and Challenges of Return to Play After a Mild Traumatic Brain Injury Kristina Wilson, MD, MPH, CAQSM, FAAP Medical Director, Pediatric and Adolescent Sports Medicine and Sports Physical Thearpy
Complexity and Challenges of Return to Play After a Mild Traumatic Brain Injury Kristina Wilson, MD, MPH, CAQSM, FAAP Medical Director, Pediatric and Adolescent Sports Medicine and Sports Physical Thearpy
Pre and Post Concussion Management
 Pre and Post Concussion Management Timothy A. Tolbert, Ph.D., ATC Clinical Coordinator Marshall University Athletic Training Program 1 Concussion A complex pathophysiological process affecting the brain,
Pre and Post Concussion Management Timothy A. Tolbert, Ph.D., ATC Clinical Coordinator Marshall University Athletic Training Program 1 Concussion A complex pathophysiological process affecting the brain,
Copyright 2009 ACNN 1
 1 The focus of this information is children who have previously been evaluated and have an established diagnosis of concussion. The information contained herein is not intended for acute concussion management.
1 The focus of this information is children who have previously been evaluated and have an established diagnosis of concussion. The information contained herein is not intended for acute concussion management.
Concussion Management and Update. Objectives
 Concussion Management and Update Ricardo Guirola MD M Ed Pediatric Rheumatology Primary Care Sports Medicine Objectives Review definition, signs and symptoms Discuss the initial evaluation of a patient
Concussion Management and Update Ricardo Guirola MD M Ed Pediatric Rheumatology Primary Care Sports Medicine Objectives Review definition, signs and symptoms Discuss the initial evaluation of a patient
USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG)
 USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG) Note: The intent of this CPG is to serve as general guidance for medics and medical officers. It
USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG) Note: The intent of this CPG is to serve as general guidance for medics and medical officers. It
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation.
 I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
An overview of concussion. Concussion is a form of brain trauma that is mild in nature, rarely life-threatening and usually
 - Name of Disorder: Concussion - Essay Title : An overview of concussion - Title: Mr First Name: Stefan Surname: Dimou Qualifications: BBiomed - Institution: 1- Westmead Clinical School, Sydney Medical
- Name of Disorder: Concussion - Essay Title : An overview of concussion - Title: Mr First Name: Stefan Surname: Dimou Qualifications: BBiomed - Institution: 1- Westmead Clinical School, Sydney Medical
Heads Up: Concussion Management. Laurel Short, MSN, FNP-c
 Heads Up: Concussion Management Laurel Short, MSN, FNP-c Diclosure I have no current affiliation or financial interest with any grantor or commercial interests that may have direct interest in the subject
Heads Up: Concussion Management Laurel Short, MSN, FNP-c Diclosure I have no current affiliation or financial interest with any grantor or commercial interests that may have direct interest in the subject
Community Partnerships for Youth Concussion Care: Power of the Medical Neighborhood
 Community Partnerships for Youth Concussion Care: Power of the Medical Neighborhood Gerard A. Gioia, Ph.D. Pediatric Neuropsychologist Chief, Division of Pediatric Neuropsychology Director, Safe Concussion
Community Partnerships for Youth Concussion Care: Power of the Medical Neighborhood Gerard A. Gioia, Ph.D. Pediatric Neuropsychologist Chief, Division of Pediatric Neuropsychology Director, Safe Concussion
A case of a patient with chronic headache. Focus on Migraine. None related to the presentation Grants to conduct clinical trials from: Speaker bureau:
 Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Concussion Guidelines in the GAA
 And present Concussion Guidelines in the GAA 2013 2016 Page 1 of 13 Position Statement Concussion Guidelines 2013 2016 Summary Principles... 3 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
And present Concussion Guidelines in the GAA 2013 2016 Page 1 of 13 Position Statement Concussion Guidelines 2013 2016 Summary Principles... 3 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
2014 Concussion Connection
 Concussion Connection is an online resource that strives to provide education and awareness about concussions while being a support for athletes as they recover from one or more concussions. Concussion
Concussion Connection is an online resource that strives to provide education and awareness about concussions while being a support for athletes as they recover from one or more concussions. Concussion
Clinical Profiles and Recovery Trajectories Concussion Management
 Disclosures and Recovery Trajectories Concussion Management I have no disclosures Aimee Custer, PsyD, LP Clinical Sports Neuropsychologist The following slides are property of Aimee Custer, PsyD. Do not
Disclosures and Recovery Trajectories Concussion Management I have no disclosures Aimee Custer, PsyD, LP Clinical Sports Neuropsychologist The following slides are property of Aimee Custer, PsyD. Do not
CONCUSSION MANAGEMENT PROTOCOL 2015
 301-333 Terminal Avenue, Vancouver, BC Canada V6A 4C1 t: 604.568.1135 f: 604.568.1639 e: info@canadasnowboard.ca www.canadasnowboard.ca CONCUSSION MANAGEMENT PROTOCOL 2015 A CONCUSSION is a disturbance
301-333 Terminal Avenue, Vancouver, BC Canada V6A 4C1 t: 604.568.1135 f: 604.568.1639 e: info@canadasnowboard.ca www.canadasnowboard.ca CONCUSSION MANAGEMENT PROTOCOL 2015 A CONCUSSION is a disturbance
POST CONCUSSION SYMPTOM SCALE
 CONCUSSION INITIAL VISIT FORM Demographics Patient Name: Date of Consultation: DOB: Sex: Age: Who referred you to our clinic? Primary Care Physician: Pharmacy Name/Address: Your E-mail Address: Preferred
CONCUSSION INITIAL VISIT FORM Demographics Patient Name: Date of Consultation: DOB: Sex: Age: Who referred you to our clinic? Primary Care Physician: Pharmacy Name/Address: Your E-mail Address: Preferred
No relevant financial relationships to be discussed, directly or indirectly, referred to or illustrated with or without recognition within the
 No relevant financial relationships to be discussed, directly or indirectly, referred to or illustrated with or without recognition within the presentation. 24 year old Olympic ice hockey player gets hit
No relevant financial relationships to be discussed, directly or indirectly, referred to or illustrated with or without recognition within the presentation. 24 year old Olympic ice hockey player gets hit
Carleton College Concussion Safety Protocol
 Carleton College Introduction Carleton College is committed to ensuring the health and safety of its student-athletes. To this end, and in accordance with NCAA legislation [Division III Constitution 3.2.4.16],
Carleton College Introduction Carleton College is committed to ensuring the health and safety of its student-athletes. To this end, and in accordance with NCAA legislation [Division III Constitution 3.2.4.16],
Guideline for Concussion/Mild Traumatic Brain Injury and Persistent Symptoms. Patient Version
 Guideline for Concussion/Mild Traumatic Brain Injury and Persistent Symptoms 3 rd Edition - for adults, +18 years of age Patient Version This guideline has been created to help with management of concussion/mild
Guideline for Concussion/Mild Traumatic Brain Injury and Persistent Symptoms 3 rd Edition - for adults, +18 years of age Patient Version This guideline has been created to help with management of concussion/mild
Why It s Not Just a Concussion
 Why It s Not Just a Concussion Connecticut Concussion Task Force www.connecticutconcussiontaskforce.org Facts About Concussion Concussions are injuries to the brain The Centers for Disease Control (CDC)
Why It s Not Just a Concussion Connecticut Concussion Task Force www.connecticutconcussiontaskforce.org Facts About Concussion Concussions are injuries to the brain The Centers for Disease Control (CDC)
Mild TBI (Concussion) Not Just Less Severe But Different
 Mild TBI (Concussion) Not Just Less Severe But Different Disclosures Funded research: 1. NIH: RO1 Physiology of concussion 2016-2021, Co-PI, $2,000,000 2. American Medical Society of Sports Medicine: RCT
Mild TBI (Concussion) Not Just Less Severe But Different Disclosures Funded research: 1. NIH: RO1 Physiology of concussion 2016-2021, Co-PI, $2,000,000 2. American Medical Society of Sports Medicine: RCT
Concussion Management. Michael Reardon, M.D. April 24,2016
 Concussion Management Michael Reardon, M.D. April 24,2016 Objectives Understand what a concussion is Know how to recognize it Understand the differential diagnosis Know how to manage and treat symptoms
Concussion Management Michael Reardon, M.D. April 24,2016 Objectives Understand what a concussion is Know how to recognize it Understand the differential diagnosis Know how to manage and treat symptoms
Sports Concussions: Return to Learn
 Sports Concussions: Return to Learn Jonathan Santana, DO Adolescent & Sports Medicine Objectives Be able to perform a brief cognitive assessment in the athlete with a head injury Be able to prescribe return
Sports Concussions: Return to Learn Jonathan Santana, DO Adolescent & Sports Medicine Objectives Be able to perform a brief cognitive assessment in the athlete with a head injury Be able to prescribe return
Introduction To Mild TBI. Not Just Less Severe But Different
 Introduction To Mild TBI Not Just Less Severe But Different Purpose Provide a discussion of issues related to diagnostic criteria for mild brain injury and concussion To present incidence data on MTBI
Introduction To Mild TBI Not Just Less Severe But Different Purpose Provide a discussion of issues related to diagnostic criteria for mild brain injury and concussion To present incidence data on MTBI
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา
 ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
Emotional Symptoms in Athletes With PCS. David Westerdahl, MD FAAFP Cleveland Clinic Florida 6/24/2012
 Emotional Symptoms in Athletes With PCS David Westerdahl, MD FAAFP Cleveland Clinic Florida 6/24/2012 Objectives Discuss Post-Concussion symptoms and functional problems Identify pre-injury factors that
Emotional Symptoms in Athletes With PCS David Westerdahl, MD FAAFP Cleveland Clinic Florida 6/24/2012 Objectives Discuss Post-Concussion symptoms and functional problems Identify pre-injury factors that
Is Topiramate Effective in Preventing Pediatric Migraines?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 Is Topiramate Effective in Preventing
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 Is Topiramate Effective in Preventing
Sports Related Concussion. Joshua T. Williams, PT, DPT, OCS, SCS, CSCS
 Sports Related Concussion Joshua T. Williams, PT, DPT, OCS, SCS, CSCS Concussion & Traumatic Brain Injury Glasgow Coma Scale Minimal Mild Mod Severe? Sports concussion Severe GCS 8 Moderate GCS 9-12 Mild
Sports Related Concussion Joshua T. Williams, PT, DPT, OCS, SCS, CSCS Concussion & Traumatic Brain Injury Glasgow Coma Scale Minimal Mild Mod Severe? Sports concussion Severe GCS 8 Moderate GCS 9-12 Mild
Zonisamide for migraine prophylaxis in refractory patients
 Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology March 2006 Zonisamide for migraine prophylaxis in refractory patients Avi Ashkenazi
Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology March 2006 Zonisamide for migraine prophylaxis in refractory patients Avi Ashkenazi
Mild Traumatic Brain Injury in Sports, Daily Life, and Military Service
 Mild Traumatic Brain Injury in Sports, Daily Life, and Military Service Grant L. Iverson, Ph.D. Professor, Department of Physical Medicine and Rehabilitation, Harvard Medical School; Director, MassGeneral
Mild Traumatic Brain Injury in Sports, Daily Life, and Military Service Grant L. Iverson, Ph.D. Professor, Department of Physical Medicine and Rehabilitation, Harvard Medical School; Director, MassGeneral
Prednisone vs. placebo in withdrawal therapy following medication overuse headache
 doi:10.1111/j.1468-2982.2007.01488.x Prednisone vs. placebo in withdrawal therapy following medication overuse headache L Pageler 1,2, Z Katsarava 2, HC Diener 2 & V Limmroth 1,2 1 Department of Neurology,
doi:10.1111/j.1468-2982.2007.01488.x Prednisone vs. placebo in withdrawal therapy following medication overuse headache L Pageler 1,2, Z Katsarava 2, HC Diener 2 & V Limmroth 1,2 1 Department of Neurology,
Current Migraine Treatment Therapy. Daniel Kassicieh, DO, FAAN
 Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
Physical and Psychological Factors in Persistent Concussion Symptoms
 Physical and Psychological Factors in Persistent Concussion Symptoms 11/5/17 Elizabeth Pieroth, PsyD, ABPP Board Certified Neuropsychologist Associate Director NorthShore Sports Concussion Program Disclosures
Physical and Psychological Factors in Persistent Concussion Symptoms 11/5/17 Elizabeth Pieroth, PsyD, ABPP Board Certified Neuropsychologist Associate Director NorthShore Sports Concussion Program Disclosures
Seth Smith MD, PharmD. Thank You!
 Seth Smith MD, PharmD Thank You! Concussion Headlines!!! Concussion Headlines!!! Concussion rules put kids health before winning games The Miami Herald 8/21/12 FHSAA's implementation of legislation goes
Seth Smith MD, PharmD Thank You! Concussion Headlines!!! Concussion Headlines!!! Concussion rules put kids health before winning games The Miami Herald 8/21/12 FHSAA's implementation of legislation goes
Beyond the Basics, Bringing Concussion Out of the Dark
 Beyond the Basics, Bringing Concussion Out of the Dark Objectives Recognize different types of concussion based on symptomatology Identify risk factors for prolonged recovery after a concussion Predict
Beyond the Basics, Bringing Concussion Out of the Dark Objectives Recognize different types of concussion based on symptomatology Identify risk factors for prolonged recovery after a concussion Predict
Concussion Update and Case Presentations
 Concussion Update and Case Presentations Cayce Onks, DO, MS, ATC Associate Professor Primary Care Sports Medicine Penn State Concussion Program Departments of Family Medicine and Orthopaedics I have no
Concussion Update and Case Presentations Cayce Onks, DO, MS, ATC Associate Professor Primary Care Sports Medicine Penn State Concussion Program Departments of Family Medicine and Orthopaedics I have no
TRAUMATIC BRAIN INJURY
 Psychiatry and Addictions Case Conference UW Medicine Psychiatry and Behavioral Sciences TRAUMATIC BRAIN INJURY GARY STOBBE, MD UNIVERSITY OF WASHINGTON GENERAL DISCLOSURES The University of Washington
Psychiatry and Addictions Case Conference UW Medicine Psychiatry and Behavioral Sciences TRAUMATIC BRAIN INJURY GARY STOBBE, MD UNIVERSITY OF WASHINGTON GENERAL DISCLOSURES The University of Washington
Concussion: Pressure to Play in Sports: Can We Trust What the Athlete Tells Us? How I Manage Concussion: A Neuropsychologist s Perspective
 How I Manage Concussion: A Neuropsychologist s Perspective Jamie Pardini, Ph.D. UPMC Concussion Program University of Pittsburgh Medical Center Department of Orthopaedic Surgery UPMC Sports Concussion
How I Manage Concussion: A Neuropsychologist s Perspective Jamie Pardini, Ph.D. UPMC Concussion Program University of Pittsburgh Medical Center Department of Orthopaedic Surgery UPMC Sports Concussion
Disclosures. Objectives 2/15/2014. Wright, Concussion Assessment, Management and Return to Sports
 Concussion Assessment, Management and Return to Sports Wendy L. Wright, MS, APRN, FNP, FAANP Adult/Family Nurse Practitioner Owner Wright & Associates Family Healthcare Amherst Owner Wright & Associates
Concussion Assessment, Management and Return to Sports Wendy L. Wright, MS, APRN, FNP, FAANP Adult/Family Nurse Practitioner Owner Wright & Associates Family Healthcare Amherst Owner Wright & Associates
The headache profile of idiopathic intracranial hypertension
 The headache profile of idiopathic intracranial hypertension Michael Wall CEPHALALGIA Wall M. The headache profile of idiopathic intracranial hypertension. Cephalalgia 1990;10:331-5. Oslo. ISSN 0333-1024
The headache profile of idiopathic intracranial hypertension Michael Wall CEPHALALGIA Wall M. The headache profile of idiopathic intracranial hypertension. Cephalalgia 1990;10:331-5. Oslo. ISSN 0333-1024
Life After Concussion:
 Life After Concussion: Self Management Strategies Kira Heaton, Occupational Therapist Jamie Dunnett, Physical Therapist Presenters: Jamie Dunnett Kira Heaton Doctor of Physical Therapy CBI Health Group
Life After Concussion: Self Management Strategies Kira Heaton, Occupational Therapist Jamie Dunnett, Physical Therapist Presenters: Jamie Dunnett Kira Heaton Doctor of Physical Therapy CBI Health Group
1. Injury Description
 ACUTE CONCUSSION EVALUATION (ACE) Physician/Clinician Office Version Gerard Gioia, PhD 1 & Micky Collins, PhD 2 1 Children's National Medical Center 2 University of Pittsburgh Medical Center Patient Name
ACUTE CONCUSSION EVALUATION (ACE) Physician/Clinician Office Version Gerard Gioia, PhD 1 & Micky Collins, PhD 2 1 Children's National Medical Center 2 University of Pittsburgh Medical Center Patient Name
NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY
 NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY February 2015 New Zealand Rugby League Medical panel The aim of the policy is to provide information on concussion to all those involved in rugby
NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY February 2015 New Zealand Rugby League Medical panel The aim of the policy is to provide information on concussion to all those involved in rugby
Index. Prim Care Clin Office Pract 31 (2004) Note: Page numbers of article titles are in boldface type.
 Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
BELMONT ABBEY COLLEGE ATHLETIC TRAINING CONCUSSION MANAGEMENT PLAN. Revised September 7, 2016
 BELMONT ABBEY COLLEGE ATHLETIC TRAINING CONCUSSION MANAGEMENT PLAN Revised September 7, 2016 I. Introduction The Belmont Abbey College Athletic Training Department remains committed to ensuring the health
BELMONT ABBEY COLLEGE ATHLETIC TRAINING CONCUSSION MANAGEMENT PLAN Revised September 7, 2016 I. Introduction The Belmont Abbey College Athletic Training Department remains committed to ensuring the health
Migraine in Children. Germano Falcao, MD Pediatric Neurology 03/07/2014
 Migraine in Children Germano Falcao, MD Pediatric Neurology 03/07/2014 Headaches in Children One of the most common concerns reported by children 3% for children age 3-7 years 4-11% for children age 7-11
Migraine in Children Germano Falcao, MD Pediatric Neurology 03/07/2014 Headaches in Children One of the most common concerns reported by children 3% for children age 3-7 years 4-11% for children age 7-11
Headache. Karen Thaxter
 Headache Karen Thaxter An eight year old girl is taken to her paediatrician because she has been complaining of almost daily pain at the back of her head for the past 4 months. She states that each headache
Headache Karen Thaxter An eight year old girl is taken to her paediatrician because she has been complaining of almost daily pain at the back of her head for the past 4 months. She states that each headache
Controversy One: Headache and Disability. Robert Shapiro, MD, PhD University of Vermont
 Controversy One: Headache and Disability Robert Shapiro, MD, PhD University of Vermont Southern Headache Society Orlando, FL, Sept 21, 2013 Disclosures Consulting within the past 12 months: Transcept Pharmaceuticals
Controversy One: Headache and Disability Robert Shapiro, MD, PhD University of Vermont Southern Headache Society Orlando, FL, Sept 21, 2013 Disclosures Consulting within the past 12 months: Transcept Pharmaceuticals
Migraine Types and Triggering Factors in Children
 original ARTICLE Migraine Types and Triggering Factors in Children How to Cite this Article: Nejad Biglari H, Karimzadeh P, Mohammadi Kord-kheyli M, Hashemi SM. Migraine Types and Triggering Factors in
original ARTICLE Migraine Types and Triggering Factors in Children How to Cite this Article: Nejad Biglari H, Karimzadeh P, Mohammadi Kord-kheyli M, Hashemi SM. Migraine Types and Triggering Factors in
CONCUSSION AWARENESS, MANAGEMENT, AND ASSESSMENT FROM AN ATHLETIC TRAINER
 CONCUSSION AWARENESS, MANAGEMENT, AND ASSESSMENT FROM AN ATHLETIC TRAINER Dr. Ryan Krzyzanowicz, DAT, ATC Clinical Associate Professor Program Director - Athletic Training Education University at Buffalo
CONCUSSION AWARENESS, MANAGEMENT, AND ASSESSMENT FROM AN ATHLETIC TRAINER Dr. Ryan Krzyzanowicz, DAT, ATC Clinical Associate Professor Program Director - Athletic Training Education University at Buffalo
ADHD and Concussion. Mary Alexis Iaccarino, MD
 ADHD and Concussion Mary Alexis Iaccarino, MD Department of Physical Medicine and Rehabilitation Harvard Medical School Spaulding Rehabilitation Hospital MassGeneral Hospital for Children Sport Concussion
ADHD and Concussion Mary Alexis Iaccarino, MD Department of Physical Medicine and Rehabilitation Harvard Medical School Spaulding Rehabilitation Hospital MassGeneral Hospital for Children Sport Concussion
Neuropsychology of TBI & PTSD
 Neuropsychology of TBI & PTSD George S. Serna, Ph.D. Louis Stokes VA Medical Center TBI: The Signature Injury of the Iraq/Afghanistan War Veteran? 19% - 30% of OEF/OIF veterans reported some level of TBI
Neuropsychology of TBI & PTSD George S. Serna, Ph.D. Louis Stokes VA Medical Center TBI: The Signature Injury of the Iraq/Afghanistan War Veteran? 19% - 30% of OEF/OIF veterans reported some level of TBI
MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache
 MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache Measure Description Percentage of patients age 18 years old and older diagnosed with migraine headache whose migraine frequency is 4 migraine
MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache Measure Description Percentage of patients age 18 years old and older diagnosed with migraine headache whose migraine frequency is 4 migraine
Approved for public release; distribution unlimited
 Award Number: W81XWH-10-1-1021 TITLE: Post-traumatic Headache and Psychological Health: Mindfulness Training for Mild Traumatic Brain Injury PRINCIPAL INVESTIGATOR: Sutapa Ford, PhD CONTRACTING ORGANIZATION:
Award Number: W81XWH-10-1-1021 TITLE: Post-traumatic Headache and Psychological Health: Mindfulness Training for Mild Traumatic Brain Injury PRINCIPAL INVESTIGATOR: Sutapa Ford, PhD CONTRACTING ORGANIZATION:
Concussion: The Basics. Bill Meehan, MD Micheli Center for Sports Injury Prevention Sports Concussion Clinic, Boston Children s Hospital
 Concussion: The Basics Bill Meehan, MD Micheli Center for Sports Injury Prevention Sports Concussion Clinic, Boston Children s Hospital Definition Working definition Characteristics Trauma Impulse
Concussion: The Basics Bill Meehan, MD Micheli Center for Sports Injury Prevention Sports Concussion Clinic, Boston Children s Hospital Definition Working definition Characteristics Trauma Impulse
Neuropsychological Sequale of Mild Traumatic Brain Injury. Professor Magdalena Mateo. Megan Healy
 Neuropsychological Sequale of Mild Traumatic Brain Injury Professor Magdalena Mateo Megan Healy Abstract: Studies have proven that mild traumatic brain injuries (MTBI), commonly known as concussions, can
Neuropsychological Sequale of Mild Traumatic Brain Injury Professor Magdalena Mateo Megan Healy Abstract: Studies have proven that mild traumatic brain injuries (MTBI), commonly known as concussions, can
Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE
 Headache in children and adolescents Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE Dept. of Psychiatry of Childhood and Adolescence Medical University of Vienna, Vienna, Austria Impact
Headache in children and adolescents Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE Dept. of Psychiatry of Childhood and Adolescence Medical University of Vienna, Vienna, Austria Impact
Study No.:MPX Title: Rationale: Phase: IIB Study Period: Study Design: Centres: Indication: Treatment: Objectives:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, II. Management of Refractory Headaches
 Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
5/15/13. Disclosure. Objectives. Pharmacological Management of Concussion. Anthony P. Kontos, PhD
 Pharmacological Management of Concussion Anthony P. Kontos, PhD Assistant Research Director UPMC Sports Medicine Concussion Program Associate Professor Department of Orthopaedic Surgery University of Pittsburgh
Pharmacological Management of Concussion Anthony P. Kontos, PhD Assistant Research Director UPMC Sports Medicine Concussion Program Associate Professor Department of Orthopaedic Surgery University of Pittsburgh
Treatable Concussion Complications
 Treatable Concussion Complications Sue Kirelik, MD Center for Concussion November 13, 2015 www.rockymountainhospitalforchildren.com Objectives Review the presentation of common concussion complications
Treatable Concussion Complications Sue Kirelik, MD Center for Concussion November 13, 2015 www.rockymountainhospitalforchildren.com Objectives Review the presentation of common concussion complications
Unsuspected Post-Concussive Symptoms (PCS) in Children Requiring Cervical Spine Clearance
 Unsuspected Post-Concussive Symptoms (PCS) in Children Requiring Cervical Spine Clearance Becky Cook, DNP, CNP, RN Kaaren Shebesta MSN, CNP, RN Mary Ellen Watts, BSN, RN Erin Butt, MSN, CNP, RN Suzanne
Unsuspected Post-Concussive Symptoms (PCS) in Children Requiring Cervical Spine Clearance Becky Cook, DNP, CNP, RN Kaaren Shebesta MSN, CNP, RN Mary Ellen Watts, BSN, RN Erin Butt, MSN, CNP, RN Suzanne
Cinnarizine versus Topiramate in Prophylaxis of Migraines among Children and Adolescents: A Randomized, Double-Blind Clinical Trial
 original ARTICLE Cinnarizine versus Topiramate in Prophylaxis of Migraines among Children and Adolescents: A Randomized, Double-Blind Clinical Trial How to Cite This Article: Ashrafi MR, Najafi Z, Shafiei
original ARTICLE Cinnarizine versus Topiramate in Prophylaxis of Migraines among Children and Adolescents: A Randomized, Double-Blind Clinical Trial How to Cite This Article: Ashrafi MR, Najafi Z, Shafiei
Characteristics of posttraumatic headache following mild traumatic brain injury in military personnel in Iran
 Environ Health Prev Med (2014) 19:422 428 DOI 10.1007/s12199-014-0409-3 REGULAR ARTICLE Characteristics of posttraumatic headache following mild traumatic brain injury in military personnel in Iran Saeid
Environ Health Prev Med (2014) 19:422 428 DOI 10.1007/s12199-014-0409-3 REGULAR ARTICLE Characteristics of posttraumatic headache following mild traumatic brain injury in military personnel in Iran Saeid
Disclosure Statement. Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk.
 Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Disclosures. Objectives 6/2/2017
 Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Concussion guidance. Introduction CONCUSSION FACTS
 Introduction This World Rugby Concussion Guidance document has been developed to provide guidance and information to persons involved in the non-elite level of the game of Rugby regarding concussion and
Introduction This World Rugby Concussion Guidance document has been developed to provide guidance and information to persons involved in the non-elite level of the game of Rugby regarding concussion and
The Components of an Objective IME
 The Components of an Objective IME Presented By: Lee H. Doppelt, PhD Brought to you by: Today s Topics Appropriate and ethical communication with IME providers IME providers standards of conduct requirement
The Components of an Objective IME Presented By: Lee H. Doppelt, PhD Brought to you by: Today s Topics Appropriate and ethical communication with IME providers IME providers standards of conduct requirement
Neurological disorders. Headache (chronic tension-type) Search date December 2013 Mona Ghadiri-Sani and Nicholas Silver ...
 Headache (chronic tensiontype) Search date December 213 Mona GhadiriSani and Nicholas Silver.................................................. ABSTRACT INTRODUCTION: Chronic tensiontype headache (CTTH)
Headache (chronic tensiontype) Search date December 213 Mona GhadiriSani and Nicholas Silver.................................................. ABSTRACT INTRODUCTION: Chronic tensiontype headache (CTTH)
Duration and Course of Post-Concussive Symptoms
 ARTICLE Duration and Course of Post-Concussive Symptoms AUTHORS: Matthew A. Eisenberg, MD, William P. Meehan III, MD, and Rebekah Mannix, MD, MPH Division of Emergency Medicine, Boston Children s Hospital,
ARTICLE Duration and Course of Post-Concussive Symptoms AUTHORS: Matthew A. Eisenberg, MD, William P. Meehan III, MD, and Rebekah Mannix, MD, MPH Division of Emergency Medicine, Boston Children s Hospital,
UCNS Course A Review of ICHD-3b
 UCNS Course A Review of ICHD-3b Andrew D. Hershey, M.D., Ph.D., FAHS Endowed Chair and Director of Neurology Director, Cincinnati Children s Headache Center Professor of Neurology and Pediatrics University
UCNS Course A Review of ICHD-3b Andrew D. Hershey, M.D., Ph.D., FAHS Endowed Chair and Director of Neurology Director, Cincinnati Children s Headache Center Professor of Neurology and Pediatrics University
Sam Schimelpfenig, MD, FAAP Team Physician, University of Sioux Falls Avera Medical Group
 Sam Schimelpfenig, MD, FAAP Team Physician, University of Sioux Falls Avera Medical Group Understand the basic management principles of sports-related concussions Review some of the current literature
Sam Schimelpfenig, MD, FAAP Team Physician, University of Sioux Falls Avera Medical Group Understand the basic management principles of sports-related concussions Review some of the current literature
Concussions and Mild Traumatic Brain Injury
 Concussions and Mild Traumatic Brain Injury Nancy Mann, MD, Paradigm Medical Director Fellow, American Academy of Physical Medicine and Rehabilitation Nancy Mann, MD Specializes in traumatic brain injury
Concussions and Mild Traumatic Brain Injury Nancy Mann, MD, Paradigm Medical Director Fellow, American Academy of Physical Medicine and Rehabilitation Nancy Mann, MD Specializes in traumatic brain injury
Disclosure Statement. Objectives. Micky Collins May Rehabilitation and Treatment of Sports Concussion: What are we Learning?
 Rehabilitation and Treatment of Sports Concussion: What are we Learning? Micky Collins, Ph.D. University of Pittsburgh Medical Center Associate Professor Department of Orthopaedic Surgery Department of
Rehabilitation and Treatment of Sports Concussion: What are we Learning? Micky Collins, Ph.D. University of Pittsburgh Medical Center Associate Professor Department of Orthopaedic Surgery Department of
