Contemporary Burden and Correlates of Symptomatic Paroxysmal Supraventricular Tachycardia
|
|
|
- Jerome Banks
- 5 years ago
- Views:
Transcription
1 Contemporary Burden and Correlates of Symptomatic Paroxysmal Supraventricular Tachycardia Alan S. Go, MD; Mark A. Hlatky, MD; Taylor I. Liu, MD, PhD; Dongjie Fan, MSPH; Elisha A. Garcia, BS; Sue Hee Sung, MPH; Matthew D. Solomon, MD, PhD Background- Contemporary data about symptomatic paroxysmal supraventricular tachycardia (PSVT) epidemiology are limited. We characterized prevalence and correlates of symptomatic PSVT within a large healthcare delivery system and estimated national PSVT burden. Methods and Results- We identified adults with an encounter for potential PSVT between 2010 and 2015 in Kaiser Permanente Northern California, excluding those with prior known atrial fibrillation or atrial flutter. We adjudicated medical records, ECGs, and other monitoring data to estimate positive predictive values for targeted International Classification of Diseases (ICD), 9th and 10th Revisions codes in inpatient, emergency department, and outpatient settings. Combinations of diagnosis codes and settings were used to calculate PSVT prevalence, and PSVT correlates were identified using multivariable regression. We estimated national rates by applying prevalence estimates in Kaiser Permanente to 2010 US Census data. The highest positive predictive values included codes for PSVT in the emergency department (82%), unspecified cardiac dysrhythmia in the emergency department (27%), anomalous atrioventricular excitation as a primary inpatient diagnosis (33%), and unspecified paroxysmal tachycardia as a primary inpatient diagnosis (23%). Prevalence of symptomatic PSVT was 140 per (95% confidence interval, ) and was higher for individuals who were older, women, white or black, or who had valvular heart disease, heart failure, diabetes mellitus, lung disease, or prior bleeding. We estimate the national prevalence of symptomatic PSVT to be 168 per (95% confidence interval, ). Conclusions- Selected diagnostic codes in inpatient and emergency department settings may be useful to identify symptomatic PSVT episodes. We project that at least 0.168% of US adults experience symptomatic PSVT, and certain characteristics can identify people at higher risk. ( J Am Heart Assoc. 2018;7:e DOI: /JAHA ) Key Words: elderly epidemiology incidence sex differences supraventricular tachycardia Paroxysmal supraventricular tachycardia (PSVT) other than atrial fibrillation or atrial flutter includes a heterogeneous set of conditions involving abnormal automaticity (eg, focal ectopic atrial tachycardia, multifocal atrial tachycardia, and junctional tachycardia) and abnormal reentry (eg, From the Division of Research, Kaiser Permanente Northern California, Oakland, CA (A.S.G., M.A.H., D.F., E.A.G., S.H.S., M.D.S.); Departments of Epidemiology, Biostatistics and Medicine, University of California, San Francisco, CA (A.S.G.); Departments of Health Research and Policy (A.S.G., M.A.H.) and Medicine (Cardiovascular Medicine) (M.A.H.), Stanford University, Stanford, CA; Department of Cardiac Electrophysiology, Kaiser Permanente Santa Clara Medical Center, Santa Clara, CA (T.I.L.); Department of Cardiology, Kaiser Permanente Oakland Medical Center, Oakland, CA (M.D.S.). Correspondence to: Alan S. Go, MD, Division of Research, Kaiser Permanente Northern California, 2000 Broadway, Oakland, CA alan.s.go@kp.org Received April 28, 2018; accepted May 28, ª 2018 The Authors. Published on behalf of the American Heart Association, Inc., by Wiley. This is an open access article under the terms of the Creative Commons Attribution License, which permits use, distribution and reproduction in any medium, provided the original work is properly cited. atrioventricular nodal reentrant tachycardia and atrioventricular reentrant tachycardia with accessory pathways). PSVTs are managed using a variety of approaches depending on the underlying mechanism and the clinical stability and frequency of episodes. 1 PSVTs can have a negative effect on patient quality of life by causing symptoms during episodes (eg, palpitations, chest pain, dizziness, syncope, and shortness of breath), by imposing restrictions on patient activities, and by leading to medication-related side effects. Despite symptomatic PSVTs being considered the most frequent indication for catheter ablation procedures, reliable, contemporary data on the population burden of PVSTs are quite limited. The most frequently quoted estimate of PSVT prevalence in the United States is based on a study from the Marshfield Clinic, in central Wisconsin, using data from January 1979 through June After standardizing to the age and sex distribution in the US adult population, the investigators projected prevalent cases and incident cases per year of PSVT in the United States. 2 This study was limited by its relatively small sample size, inclusion of a DOI: /JAHA Journal of the American Heart Association 1
2 selected midwestern community that is not representative of the broad racial/ethnic diversity in the United States, and data that no longer reflect contemporary practice. During the past 25 years, there have been increases in heart failure, hypertension, diabetes mellitus, and obesity, all of which may have affected the prevalence of PSVT. In addition, this study relied on International Classification of Diseases (ICD) diagnostic codes found in electronic health records and billing claims data that are readily available from health systems but also showed low accuracy for the evaluated codes in validation studies. In contrast, population estimates based on highly selected patients referred for catheter ablation or other electrophysiology procedures benefit from more accurate patient identification but are likely biased by omitting the large majority of medically managed PSVT patients. Patient factors associated with the development of symptomatic PSVT are also poorly understood. Data from Marshfield Clinic suggested that female sex, older age, and the presence of clinical cardiovascular disease were each associated with higher risk of presenting with PSVT. 2 In addition, it is possible that atrioventricular nodal reentrant tachycardia and atrioventricular reentrant tachycardia may be more common in younger individuals. 2 The relative frequency of PSVT mediated by an accessory pathway may also be lower with increasing age. 2 To address the limitations of existing data on contemporary PSVT, we examined its epidemiology and risk factors among a large, community-based population with broad demographic diversity and used these data to estimate the national burden of symptomatic PSVT. Methods Clinical Perspective What Is New? This study provides contemporary, community-based information on the accuracy of diagnostic codes to identify episodes of symptomatic paroxysmal supraventricular tachycardia and on the national burden of symptomatic paroxysmal supraventricular tachycardia. What Are the Clinical Implications? Several patient subgroups (older age, female, black race, Hispanic ethnicity, valvular heart disease, heart failure, diabetes mellitus, lung disease, bleeding history) experience a higher burden of symptomatic episodes of paroxysmal supraventricular tachycardia. The data, analytic methods, and study materials will not be made available to other researchers for purposes of reproducing the results or replicating the procedure. Source Population The source population for the PREEMPT (Population-Based Risk and Epidemiology of Paroxysmal Supraventricular Tachycardias) study included members of Kaiser Permanente Northern California (KPNC), an integrated healthcare delivery system that provides comprehensive medical care to >4.2 million people. The KPNC membership is highly representative of the local and statewide population with respect to age, sex, race/ethnicity, and socioeconomic status. 3 5 The study was approved by the KPNC institutional review board, and a waiver of informed consent was obtained given the nature of the study. Identification of PSVT Episodes We searched electronic health records from January 1, 2010, and December 31, 2015, for diagnostic codes suggestive of symptomatic PSVT encounters in the inpatient, emergency department and outpatient clinic settings. We identified encounters with ICD-9 codes (anomalous atrioventricular excitation), (PSVT), (paroxysmal tachycardia, unspecified), (supraventricular premature beats), (other specified cardiac dysrhythmias), (cardiac dysrhythmia, unspecified), (tachycardia, unspecified), and (palpitations). 2 After October 1, 2015, when KPNC adopted ICD-10 codes, we examined encounters for I45.6 (preexcitation syndrome), I47.1 (supraventricular tachycardia), I47.9 (paroxysmal tachycardia, unspecified), I49.1 (atrial premature depolarization), I49.8 (other specified cardiac arrhythmias), I49.9 (cardiac arrhythmia, unspecified), R00.0 (tachycardia, unspecified), and R00.2 (palpitations). Validation of PSVT Diagnostic Codes We assessed the validity of diagnostic codes for potential PSVT episodes by reviewing a stratified random sample of up to 150 electronic medical records for each diagnostic code; these were further stratified by healthcare setting (inpatient, emergency department, and outpatient). Physician adjudicators reviewed relevant medical records, including 12-lead ECG, reports from long-term rhythm monitoring recorders (eg, 24-hour Holter, event loop recorder, patch-based electrocardiographic monitoring solutions), electrophysiology procedure reports, and physician progress notes. A symptomatic PSVT episode required evidence of >30-second duration during the specific clinical encounter documented in any setting and/or captured with ECG monitoring or electrophysiology procedure; if available, the specific type of PSVT was documented using standardized criteria. A documented prior history of PSVT was not considered a valid outcome. DOI: /JAHA Journal of the American Heart Association 2
3 Patient Characteristics We collected information on patient age, sex and self-reported race/ethnicity from health plan databases. The presence of chronic kidney disease was based on an estimated glomerular filtration rate <60 ml/min per 1.73 m 2 using the Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) estimating equation. 6 Diabetes mellitus status was determined based on ICD diagnostic codes, laboratory results, or receipt of diabetes mellitus specific medications within a regional diabetes mellitus registry. 7 Hypertension was determined based on >2 outpatient diagnoses or 1 diagnosis and receipt of antihypertensive therapy. 8 Coronary heart disease was defined as a history of hospitalization for acute myocardial infarction or the receipt of coronary artery bypass surgery or percutaneous coronary intervention. 8,9 Heart failure was defined as hospitalization with a primary discharge diagnosis of heart failure or 3 outpatient encounters coded for heart failure using relevant ICD codes, with at least 1 visit being to a cardiologist. 10 Statistical Analysis All analyses were performed using SAS, version 9.3 (SAS Institute). In our validation study, we calculated the positive predictive value (PPV) and associated 95% confidence interval (CI) for each diagnostic code and clinical setting combination and reported results if they met the following criteria: total number of reviewed encounters >10 for the diagnostic code/ setting combination and having a PPV >15% for the diagnostic code/setting combination. Using our final PSVT episode identification algorithm, we next calculated the period prevalence of symptomatic PSVT episodes (per ) with associated CIs among adults aged 18 years in the KPNC population. To calculate incidence of symptomatic PSVT episodes, we repeated analyses after excluding any people in the source population who met diagnostic criteria for PSVT up to 4 years before study entry. For both prevalence and incidence during the study period, we conducted subgroup analyses by age, sex, race/ethnicity, and the presence or absence of chronic kidney disease, diabetes mellitus, hypertension, coronary heart disease, and heart failure. Finally, to estimate the national burden of PSVT episodes, we calculated age- and sex-adjusted prevalence of symptomatic PSVT episodes in the United States by applying the KPNC age- and sex-stratified prevalence estimates to US Census data from Results Accuracy of Diagnostic Codes for PSVT in Different Care Settings We adjudicated a sample of 1238 potential symptomatic PSVT episodes across inpatient, emergency department, and outpatient visit settings that met our eligibility criteria but subsequently excluded 418 encounters with combinations of code and care settings that could not provide reliable estimates. Among the remaining 820 encounters, 223 (27%; 95% CI, 24% 29%) were confirmed to be episodes of symptomatic PSVT, with wide variation in the PPV across different combinations of codes and settings (Table 1). The highest PPVs were for the ICD-9/10 codes for PSVT recorded in the inpatient or emergency department setting, followed by anomalous atrioventricular excitation in the inpatient or emergency department setting and unspecified cardiac dysrhythmia in the emergency department setting (Table 1). Most of the 223 confirmed symptomatic PSVT episodes were classified as unspecified PSVT (65.5%), with the remainder being specific PSVT subtypes based on available diagnostic information: preexcitation syndrome/wolff Parkinson White syndrome (14%), atrioventricular nodal reentry tachycardia (8.1%), ectopic atrial tachycardia (4.9%), multifocal atrial tachycardia (2.2%), atrioventricular reentry tachycardia (1.3%), atrioventricular junctional tachycardia (1.3%), and other specified cardiac dysrhythmias (1.8%). Period Prevalence of PSVT We estimated the period prevalence of symptomatic PSVT in the KPNC population to be 140 per members (95% CI, ) based on the subset of diagnostic code/setting combinations that met our minimum criteria in terms of PPV and frequency of occurrence (Figure). The prevalence significantly differed across patient subgroups. Prevalence of symptomatic PSVT was substantially higher with older age, with a >20-fold higher prevalence for participants aged 65 years compared with those aged 18 to 24 years (Table 2). Symptomatic PSVT prevalence was also higher in women than in men and in individuals who were black or white compared with Asian/Pacific Islanders (Table 2). A higher prevalence of symptomatic PSVT was also observed among patients with chronic kidney disease, diabetes mellitus, hypertension, coronary heart disease, and heart failure (Table 2). Incidence of PSVT We estimated the incidence of symptomatic PSVT episodes after excluding patients with evidence of having had diagnosed PSVT before entering the cohort. The incidence of presumed new symptomatic PSVT episodes between 2010 and 2015 was 73 per (95% CI, 53 92), with variations among patient subgroups similar to those observed for prevalence during the study period (Table 2). DOI: /JAHA Journal of the American Heart Association 3
4 Table 1. PPV of Diagnostic Codes for Symptomatic PSVT Episodes ( ) ICD Code Description Setting Charts Reviewed Confirmed PSVT Episode PPV, % 95 (CI) Anomalous atrioventricular excitation Inpatient primary Inpatient secondary Emergency Outpatient I45.6 Preexcitation syndrome Inpatient primary 0 N/A N/A N/A Emergency Outpatient PSVT Inpatient primary Inpatient secondary Emergency Outpatient I47.1 Supraventricular tachycardia Inpatient primary Inpatient secondary Emergency Outpatient Paroxysmal tachycardia, unspecified Inpatient primary Inpatient secondary Emergency Outpatient I47.9 Paroxysmal tachycardia, unspecified Inpatient primary Emergency Outpatient Supraventricular premature beats Inpatient primary Inpatient secondary Emergency Outpatient I49.1 Atrial premature depolarization Inpatient primary 0 N/A N/A N/A Emergency Outpatient Other specified cardiac dysrhythmias Inpatient primary Inpatient secondary Emergency Outpatient I49.8 Other specified cardiac arrhythmias Inpatient primary 0 N/A N/A N/A Emergency 0 N/A N/A N/A Outpatient Continued DOI: /JAHA Journal of the American Heart Association 4
5 Table 1. Continued ICD Code Description Setting National Burden of PSVT Based on the age- and sex-adjusted prevalence estimates found in KPNC, we estimate the US prevalence of symptomatic PSVT in 2010 to be 168 per (95% CI, ). This translated to an estimated (95% CI, ) affected adult Americans. Discussion In a large, diverse, community-based population receiving care within an integrated healthcare delivery system, we found several combinations of diagnosis codes and care settings to have acceptable predictive value for identifying valid symptomatic, sustained PSVT episodes. We estimated a prevalence of 140 per and an incidence of 73 per in our study population, with notably higher burden in older people, women, those of white or black race, and those with Charts Reviewed Confirmed PSVT Episode PPV, % 95 (CI) Cardiac dysrhythmia, unspecified Inpatient primary Inpatient secondary Emergency Outpatient I49.9 Cardiac arrhythmia, unspecified Inpatient primary Inpatient secondary Emergency Outpatient Tachycardia, unspecified Inpatient primary Inpatient secondary Emergency Outpatient R00.0 Tachycardia, unspecified Inpatient primary Inpatient secondary Emergency Outpatient Palpitations Inpatient primary Inpatient secondary Emergency Outpatient R00.2 Palpitations Inpatient primary Emergency Outpatient Total CI indicates confidence interval; ICD, International Classification of Diseases; N/A, not available; PPV, positive predictive value; PSVT, paroxysmal supraventricular tachycardia. cardiovascular disease (coronary disease or heart failure) or major cardiovascular risk factors (chronic kidney disease, diabetes mellitus, or hypertension). Furthermore, we projected that at least Americans experience symptomatic, sustained PSVT. We found high PPV for the specific PSVT codes (427.0 in ICD-9 and I47.1 in ICD-10) in the emergency department because most of these encounters included ECG confirmation of sustained regular narrow-complex tachycardia that then reverted spontaneously or after specific treatment (eg, intravenous adenosine). The PPV of ICD-9 code for anomalous atrioventricular conduction was also high in the emergency department setting, where it appears to identify episodes of acute, sustained, symptomatic PSVT. Among inpatients, a primary diagnosis of PSVT also appears to have higher PPV because patients were admitted for specific treatment. A secondary diagnosis of PSVT had substantially DOI: /JAHA Journal of the American Heart Association 5
6 Figure. Prevalence and incidence of symptomatic paroxysmal supraventricular tachycardia (other than atrial fibrillation or atrial flutter) within Kaiser Permanente Northern California ( ). lower PPV than a primary diagnosis in the inpatient setting. Finally, all codes for PSVT in the outpatient setting had low PPV, probably reflecting a problem list diagnosis of uncertain reliability rather than a specific encounter for a symptomatic arrhythmia. Codes for palpitations, atrial premature contractions, unspecific tachycardias, and other specified cardiac arrhythmias all had low PPV for identifying symptomatic PSVT in all care settings. Consequently, it is important to consider the setting of care as well as the diagnostic code for reliable identification of symptomatic PSVT episodes. Very limited data exist about the epidemiology of PSVT in the general US population. In the Marshfield Epidemiologic Study Area, potential cases of PSVT between 1979 and 1993 in Wisconsin were identified using selected ICD-9 codes (426.7, 427.0, 427.2, 427.6, 427.9, 785.0, 785.1) found in databases from the Marshfield Clinic. 2 Among 2223 potential prevalent cases of PSVT, 600 patients had medical records and ECGs available, and 31 cases (PPV 5.2%) were confirmed and considered clinically significant based on having associated symptoms or requiring specific acute or long-term therapy. Based on the weighted sampling design, the Marshfield investigators estimated the prevalence of PSVT to be 225 per people, with higher prevalence in those aged 65 years (616 per ) versus <65 years (165 per ) and in women (256 per ) compared with men (194 per ). Among 1163 people who had potential incident PSVT between July 1991 and June 1993, 33 were confirmed cases (PPV 2.8%) for an estimated incidence of 35 per people. Finally, the authors extrapolated their findings to the 1990 US population and projected that PSVT affected Americans, with an Table 2. Prevalence and Incidence of Symptomatic PSVT Episodes by Patient Subgroup ( ) Period Prevalence Per (95% CI) Incidence Per (95% CI) Overall ( ) 72.7 ( ) Age, y ( ) 14.8 ( ) ( ) 34.1 ( ) ( ) 96.7 ( ) ( ) ( ) Sex Men ( ) 61.9 ( ) Women ( ) 83.1 ( ) Race White ( ) ( ) Black ( ) ( ) Asian/Pacific Islander 92.7 ( ) ( ) Chronic kidney disease Yes ( ) ( ) No ( ) 66.5 ( ) Diabetes mellitus Yes ( ) ( ) No ( ) 66.4 ( ) Hypertension Yes ( ) ( ) No 94.9 ( ) 53.9 ( ) Coronary heart disease Yes ( ) ( ) No ( ) 71.3 ( ) Heart failure Yes ( ) ( ) No ( ) 70.5 ( ) CI indicates confidence interval. estimated new cases per year. 2 Although this study provided important insights into population-based epidemiology of PSVT, it also highlighted the low PPV of the studied ICD-9 codes for clinically significant PSVT and was limited by the small sample size, restricted racial/ethnic diversity, lack of detail about the specific type of PSVT, and earlier study period that may not reflect contemporary epidemiology. Murman et al reported on the frequency of emergency department visits for supraventricular tachycardia in the United States based on data between 1993 and 2003 from the National Hospital Ambulatory Medical Care Survey. 11 The DOI: /JAHA Journal of the American Heart Association 6
7 occurrence of supraventricular tachycardia related visits was based on ICD-9 codes or found in probabilityweighted samples of emergency department visits. The authors estimated that visits in US emergency departments may be related to supraventricular tachycardia (estimated 18 visits per US people; 95% CI, ). The annual visit rate was higher for individuals aged 65 years (39 per ) than for those aged <65 years (15 per ) and higher for women (26 per ) than for men (11 per ). 11 The study was limited by evaluating only encounters in the emergency department, use of administrative codes without medical records review to confirm the presence and duration of arrhythmia, the relatively small number of cases identified in their sample, and the use of data from an earlier time period that may not be fully generalizable to the current era. Our study was strengthened by rigorous review of relevant medical records using standardized criteria to estimate the true PPV of available ICD-9 and ICD-10 diagnostic codes suggestive of potential symptomatic PSVT observed in different care settings. Our source population was large, ethnically diverse, and highly representative of the surrounding and statewide adult populations. We were also able to estimate PSVT burden across important patient demographic and clinical subgroups. Our study also had several limitations. We focused on identification of any PSVT unrelated to atrial fibrillation or atrial flutter, but this includes a heterogeneous set of conditions, and we had limited available data and precision to examine more specific PSVT types. Given that we applied a minimum threshold for acceptable PPV and frequency for selecting the diagnostic code/care setting combinations, we may have missed cases of true symptomatic PSVT. This includes patients who had symptomatic PSVT but had spontaneous resolution before the arrhythmia was able to be confirmed. Patients with symptomatic PSVT but who did not seek out medical care also would not have been captured. We used diagnostic codes to exclude patients with atrial flutter, but given the potential for misclassification, we may have excluded patients who actually had a non atrial flutter PSVT. Collectively, this would lead to our estimates being conservative. In contrast, the limited precision in the PPV for some of our included code/setting combinations may contribute to an overestimate in the actual burden of PSVT. Furthermore, in calculating incident PSVT, we searched up to 4 years before the index date, which may have overestimated the true incidence of PSVT. Our findings also may not be fully generalizable to other health systems, geographic areas, or uninsured people. Finally, it is important to emphasize that we identified episodes of care for sustained, symptomatic PSVT and not for individuals who may have had PSVT in the past but for whom it was not an active problem. In summary, we provide new, contemporary information about the variable accuracy of diagnostic codes in different clinical care settings and updated estimates of the burden of symptomatic PSVT episodes within the United States. In addition, selected demographic and clinical characteristics can identify people who experience a higher burden of symptomatic PSVT. Sources of Funding This work was supported by a research grant from Milestone Pharmaceuticals. Disclosures Drs Go, Hlatky and Solomon have received research funding from Milestone Pharmaceuticals for this study. The remaining authors have no disclosures to report. References 1. Page RL, Joglar JA, Caldwell MA, Calkins H, Conti JB, Deal BJ, Estes NA III, Field ME, Goldberger ZD, Hammill SC, Indik JH, Lindsay BD, Olshansky B, Russo AM, Shen WK, Tracy CM, Al-Khatib SM ACC/AHA/HRS guideline for the management of adult patients with supraventricular tachycardia: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. Circulation. 2016;133:e506 e Orejarena LA, Vidaillet H Jr, DeStefano F, Nordstrom DL, Vierkant RA, Smith PN, Hayes JJ. Paroxysmal supraventricular tachycardia in the general population. J Am Coll Cardiol. 1998;31: Krieger N. Overcoming the absence of socioeconomic data in medical records: validation and application of a census-based methodology. Am J Public Health. 1992;82: Gordon NP. Characteristics of Adult Health Plan Members in the Northern California Region Membership, as Estimated From the 2011 Member Health Survey. Oakland, CA: Division of Research, Kaiser Permanente Medical Care Program; Koebnick C, Langer-Gould AM, Gould MK, Chao CR, Iyer RL, Smith N, Chen W, Jacobsen SJ. Sociodemographic characteristics of members of a large, integrated health care system: comparison with US Census Bureau data. Perm J. 2012;16: Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF, Feldman HI, Kusek JW, Eggers P, Van Lente F, Greene T, Coresh J; Collaboration C-ECKDE. A new equation to estimate glomerular filtration rate. Ann Intern Med. 2009;150: Karter AJ, Warton EM, Lipska KJ, Ralston JD, Moffet HH, Jackson GG, Huang ES, Miller DR. Development and validation of a tool to identify patients with type 2 diabetes at high risk of hypoglycemia-related emergency department or hospital use. JAMA Intern Med. 2017;177: Go AS, Chertow GM, Fan D, McCulloch CE, Hsu CY. Chronic kidney disease and the risks of death, cardiovascular events, and hospitalization. N Engl J Med. 2004;351: Yeh RW, Sidney S, Chandra M, Sorel M, Selby JV, Go AS. Population trends in the incidence and outcomes of acute myocardial infarction. N Engl J Med. 2010;362: Gurwitz JH, Magid DJ, Smith DH, Goldberg RJ, McManus DD, Allen LA, Saczynski JS, Thorp ML, Hsu G, Sung SH, Go AS. Contemporary prevalence and correlates of incident heart failure with preserved ejection fraction. Am J Med. 2013;126: Murman DH, McDonald AJ, Pelletier AJ, Camargo CA Jr. U.S. emergency department visits for supraventricular tachycardia, Acad Emerg Med. 2007;14: DOI: /JAHA Journal of the American Heart Association 7
ATRIAL FIBRILLATION AND ETHNICITY. Elsayed Z Soliman MD, MSc, MS Director, Epidemiological Cardiology Research Center (EPICARE)
 ATRIAL FIBRILLATION AND ETHNICITY Elsayed Z Soliman MD, MSc, MS Director, Epidemiological Cardiology Research Center (EPICARE) Atrial fibrillation (AF) and ethnicity The known The unknown The paradox Why
ATRIAL FIBRILLATION AND ETHNICITY Elsayed Z Soliman MD, MSc, MS Director, Epidemiological Cardiology Research Center (EPICARE) Atrial fibrillation (AF) and ethnicity The known The unknown The paradox Why
Hypertension Update 2014:
 GSHTP Webinar Hypertension Update 2014: The Kaiser Permanente Northern California Experience Presented by: Marc Jaffe, MD Associate Clinical Professor of Medicine, UCSF Kaiser Permanente Northern California
GSHTP Webinar Hypertension Update 2014: The Kaiser Permanente Northern California Experience Presented by: Marc Jaffe, MD Associate Clinical Professor of Medicine, UCSF Kaiser Permanente Northern California
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
CLINICAL MEDICAL POLICY
 Policy Name: Policy Number: Responsible Department(s): CLINICAL MEDICAL POLICY Single-use Ambulatory Electrocardiographic Monitors (e.g., Zio Patch) MP-076-MD-DE Medical Management Provider Notice Date:
Policy Name: Policy Number: Responsible Department(s): CLINICAL MEDICAL POLICY Single-use Ambulatory Electrocardiographic Monitors (e.g., Zio Patch) MP-076-MD-DE Medical Management Provider Notice Date:
Chapter 1: CKD in the General Population
 Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With Over half of patients from the Medicare 5% sample (restricted to age 65 and older) have a diagnosis of chronic kidney disease (), cardiovascular disease,
Chapter 2: Identification and Care of Patients With Over half of patients from the Medicare 5% sample (restricted to age 65 and older) have a diagnosis of chronic kidney disease (), cardiovascular disease,
Use of Real-World Data for Population Surveillance and Monitoring. Kasia Lipska, MD Yale School of Medicine November 17 th, 2018.
 Use of Real-World Data for Population Surveillance and Monitoring Kasia Lipska, MD Yale School of Medicine November 17 th, 2018 Grants: NIH Disclosures Consultant: Health Services Advisory Group (HSAG)
Use of Real-World Data for Population Surveillance and Monitoring Kasia Lipska, MD Yale School of Medicine November 17 th, 2018 Grants: NIH Disclosures Consultant: Health Services Advisory Group (HSAG)
Wan-Ting, Lin 2017/11/21. JAMA Intern Med. doi: /jamainternmed Published online August 21, 2017.
 Development and Validation of a Tool to Identify Patients With Type 2 Diabetes at High Risk of Hypoglycemia-Related Emergency Department or Hospital Use Andrew J. Karter, PhD; E. Margaret Warton, MPH;
Development and Validation of a Tool to Identify Patients With Type 2 Diabetes at High Risk of Hypoglycemia-Related Emergency Department or Hospital Use Andrew J. Karter, PhD; E. Margaret Warton, MPH;
Asymptomatic WPW Syndrome; Observation or Ablation? 전남대학교병원순환기내과 박형욱
 Asymptomatic WPW Syndrome; Observation or Ablation? 전남대학교병원순환기내과 박형욱 Let It Be? Vs. Just Do It? Natural history of asymptomatic WPW Incidence of sudden cardiac death in natural history studies involving
Asymptomatic WPW Syndrome; Observation or Ablation? 전남대학교병원순환기내과 박형욱 Let It Be? Vs. Just Do It? Natural history of asymptomatic WPW Incidence of sudden cardiac death in natural history studies involving
CMS Limitations Guide - Cardiovascular Services
 CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
ACC/AHA Guidelines for Ambulatory Electrocardiography: Executive Summary and Recommendations
 (Circulation. 1999;100:886-893.) 1999 American Heart Association, Inc. ACC/AHA Practice Guidelines ACC/AHA Guidelines for Ambulatory Electrocardiography: Executive Summary and Recommendations A Report
(Circulation. 1999;100:886-893.) 1999 American Heart Association, Inc. ACC/AHA Practice Guidelines ACC/AHA Guidelines for Ambulatory Electrocardiography: Executive Summary and Recommendations A Report
Ambulatory Cardiac Monitors and Outpatient Telemetry Corporate Medical Policy
 Ambulatory Cardiac Monitors and Outpatient Telemetry Corporate Medical Policy File Name: Ambulatory Event Monitors and Mobile Cardiac Outpatient Telemetry File Code: UM.SPSVC.13 Origination: 10/2015 Last
Ambulatory Cardiac Monitors and Outpatient Telemetry Corporate Medical Policy File Name: Ambulatory Event Monitors and Mobile Cardiac Outpatient Telemetry File Code: UM.SPSVC.13 Origination: 10/2015 Last
USRDS UNITED STATES RENAL DATA SYSTEM
 USRDS UNITED STATES RENAL DATA SYSTEM Chapter 2: Identification and Care of Patients With CKD Over half of patients from the Medicare 5 percent sample have either a diagnosis of chronic kidney disease
USRDS UNITED STATES RENAL DATA SYSTEM Chapter 2: Identification and Care of Patients With CKD Over half of patients from the Medicare 5 percent sample have either a diagnosis of chronic kidney disease
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Community-based incidence of acute renal failure
 original article http://www.kidney-international.org & 2007 International Society of Nephrology Community-based incidence of acute renal failure C-y Hsu 1, CE McCulloch 2, D Fan 3, JD Ordoñez 4, GM Chertow
original article http://www.kidney-international.org & 2007 International Society of Nephrology Community-based incidence of acute renal failure C-y Hsu 1, CE McCulloch 2, D Fan 3, JD Ordoñez 4, GM Chertow
Incidence and timing of potentially high-risk arrhythmias detected through long term continuous ambulatory electrocardiographic monitoring
 Solomon et al. BMC Cardiovascular Disorders (2016) 16:35 DOI 10.1186/s12872-016-0210-x RESEARCH ARTICLE Incidence and timing of potentially high-risk arrhythmias detected through long term continuous ambulatory
Solomon et al. BMC Cardiovascular Disorders (2016) 16:35 DOI 10.1186/s12872-016-0210-x RESEARCH ARTICLE Incidence and timing of potentially high-risk arrhythmias detected through long term continuous ambulatory
The objective of this study was to determine the longterm
 The Natural History of Lone Atrial Flutter Brief Communication Sean C. Halligan, MD; Bernard J. Gersh, MBChB, DPhil; Robert D. Brown Jr., MD; A. Gabriela Rosales, MS; Thomas M. Munger, MD; Win-Kuang Shen,
The Natural History of Lone Atrial Flutter Brief Communication Sean C. Halligan, MD; Bernard J. Gersh, MBChB, DPhil; Robert D. Brown Jr., MD; A. Gabriela Rosales, MS; Thomas M. Munger, MD; Win-Kuang Shen,
Wellness Coaching for People with Prediabetes
 Wellness Coaching for People with Prediabetes PUBLIC HEALTH RESEARCH, PRACTICE, AND POLICY Volume 12, E207 NOVEMBER 2015 ORIGINAL RESEARCH Wellness Coaching for People With Prediabetes: A Randomized Encouragement
Wellness Coaching for People with Prediabetes PUBLIC HEALTH RESEARCH, PRACTICE, AND POLICY Volume 12, E207 NOVEMBER 2015 ORIGINAL RESEARCH Wellness Coaching for People With Prediabetes: A Randomized Encouragement
Automatic External Defibrillators
 Last Review Date: April 21, 2017 Number: MG.MM.DM.10dC3v4 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: April 21, 2017 Number: MG.MM.DM.10dC3v4 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Title: Automatic External Defibrillators Division: Medical Management Department: Utilization Management
 Retired Date: Page 1 of 7 1. POLICY DESCRIPTION: Automatic External Defibrillators 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management, Pharmacy,
Retired Date: Page 1 of 7 1. POLICY DESCRIPTION: Automatic External Defibrillators 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management, Pharmacy,
Does quality of life predict morbidity or mortality in patients with atrial fibrillation (AF)?
 Does quality of life predict morbidity or mortality in patients with atrial fibrillation (AF)? Erika Friedmann a, Eleanor Schron, b Sue A. Thomas a a University of Maryland School of Nursing; b NEI, National
Does quality of life predict morbidity or mortality in patients with atrial fibrillation (AF)? Erika Friedmann a, Eleanor Schron, b Sue A. Thomas a a University of Maryland School of Nursing; b NEI, National
Arrhythmia Care in the DGH What Still Needs to be Done? Dr. Sundeep Puri Consultant Cardiologist
 Arrhythmia Care in the DGH What Still Needs to be Done? Dr. Sundeep Puri Consultant Cardiologist LOTS!!! This presentation confines itself to the situation in the North West. The views expressed are my
Arrhythmia Care in the DGH What Still Needs to be Done? Dr. Sundeep Puri Consultant Cardiologist LOTS!!! This presentation confines itself to the situation in the North West. The views expressed are my
Cardiac Dysrhythmias and Sports
 Sudden unexpected death during athletic participation is the overriding consideration in advising individuals with dysrhythmias about participation in sports. The incidence of sudden death is 1 to 2 per
Sudden unexpected death during athletic participation is the overriding consideration in advising individuals with dysrhythmias about participation in sports. The incidence of sudden death is 1 to 2 per
Atrial Fibrillation and Common Supraventricular Tachycardias. Sunil Kapur MD
 Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
WPW syndrome and AVRT
 WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
Creating Devices for Personalized Health Monitoring: Cardiovascular Monitoring Case Studies
 University of Massachusetts Medical School escholarship@umms UMass Center for Clinical and Translational Science Research Retreat 2014 UMass Center for Clinical and Translational Science Research Retreat
University of Massachusetts Medical School escholarship@umms UMass Center for Clinical and Translational Science Research Retreat 2014 UMass Center for Clinical and Translational Science Research Retreat
CLINICAL RESEARCH STUDY
 CLINICAL RESEARCH STUDY Contemporary Prevalence and Correlates of Incident Heart Failure with Preserved Ejection Fraction Jerry H. Gurwitz, MD, a,b,c David J. Magid, MD, MPH, d,e,f David H. Smith, RPh,
CLINICAL RESEARCH STUDY Contemporary Prevalence and Correlates of Incident Heart Failure with Preserved Ejection Fraction Jerry H. Gurwitz, MD, a,b,c David J. Magid, MD, MPH, d,e,f David H. Smith, RPh,
Electrophysiology and Cathether Ablation: Historical Evolution. Saverio Iacopino, MD, FACC, FESC
 Electrophysiology and Cathether Ablation: Historical Evolution Saverio Iacopino, MD, FACC, FESC Historical Evolution ü 1967 ü 1968 ü 1969 ü 1973 ü 1979 Durrer D et al. first described initiation and termination
Electrophysiology and Cathether Ablation: Historical Evolution Saverio Iacopino, MD, FACC, FESC Historical Evolution ü 1967 ü 1968 ü 1969 ü 1973 ü 1979 Durrer D et al. first described initiation and termination
Mission Statement for our Arrhythmia Care
 Mission Statement for our Arrhythmia Care We are dedicated to provide a compassionate and an outstanding care for patients with cardiac arrhythmias. We will be utilizing the cutting edge and the most advanced
Mission Statement for our Arrhythmia Care We are dedicated to provide a compassionate and an outstanding care for patients with cardiac arrhythmias. We will be utilizing the cutting edge and the most advanced
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
SUPPLEMENTARY DATA. Table of Contents
 Table of Contents Supplemental Figure S1. Kaiser Permanente Diabetes Registry Patient Flow Diagram Supplemental Table S1. Diagnostic and procedure codes and frequency of events during follow-up for outcomes
Table of Contents Supplemental Figure S1. Kaiser Permanente Diabetes Registry Patient Flow Diagram Supplemental Table S1. Diagnostic and procedure codes and frequency of events during follow-up for outcomes
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients with CKD
 Chapter 2: Identification and Care of Patients with CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients with CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Cardiovascular Disease
 Cardiovascular Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars on the 3 rd Wednesday of each month to address topics related to risk adjustment
Cardiovascular Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars on the 3 rd Wednesday of each month to address topics related to risk adjustment
EPIDEMIOLOGY OF ARRHYTHMIAS AND OUTCOMES IN CKD & DIALYSIS KDIGO. Wolfgang C. Winkelmayer, MD, ScD Baylor College of Medicine Houston, Texas
 EPIDEMIOLOGY OF ARRHYTHMIAS AND OUTCOMES IN CKD & DIALYSIS Wolfgang C. Winkelmayer, MD, ScD Baylor College of Medicine Houston, Texas Disclosure of Interests AstraZeneca (scientific advisory board) Bayer
EPIDEMIOLOGY OF ARRHYTHMIAS AND OUTCOMES IN CKD & DIALYSIS Wolfgang C. Winkelmayer, MD, ScD Baylor College of Medicine Houston, Texas Disclosure of Interests AstraZeneca (scientific advisory board) Bayer
OP Chest Pain General Data Element List. All Records All Records. All Records All Records All Records. All Records. All Records.
 Material inside brackets ([and]) is new to this Specifications Manual version. Hospital Outpatient Quality Measures Chest Pain (CP) Set Measure ID # OP-4 * OP-5 * Measure Short Name Aspirin at Arrival
Material inside brackets ([and]) is new to this Specifications Manual version. Hospital Outpatient Quality Measures Chest Pain (CP) Set Measure ID # OP-4 * OP-5 * Measure Short Name Aspirin at Arrival
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Chapter 2: Identification and Care of Patients With Chronic Kidney Disease
 Chapter 2: Identification and Care of Patients With Chronic Kidney Disease Introduction The examination of care in patients with chronic kidney disease (CKD) is a significant challenge, as most large datasets
Chapter 2: Identification and Care of Patients With Chronic Kidney Disease Introduction The examination of care in patients with chronic kidney disease (CKD) is a significant challenge, as most large datasets
Diabetes and Prior Coronary Heart Disease are Not Necessarily Risk Equivalent for Future Coronary Heart Disease Events
 Diabetes and Prior Coronary Heart Disease are Not Necessarily Risk Equivalent for Future Coronary Heart Disease Events Jamal S. Rana, MD, PhD 1,2,3,5, Jennifer Y. Liu, MPH 3, Howard H. Moffet, MPH 3, Marc
Diabetes and Prior Coronary Heart Disease are Not Necessarily Risk Equivalent for Future Coronary Heart Disease Events Jamal S. Rana, MD, PhD 1,2,3,5, Jennifer Y. Liu, MPH 3, Howard H. Moffet, MPH 3, Marc
Mortality following acute myocardial infarction (AMI) in
 In-Hospital Mortality Among Patients With Type 2 Diabetes Mellitus and Acute Myocardial Infarction: Results From the National Inpatient Sample, 2000 2010 Bina Ahmed, MD; Herbert T. Davis, PhD; Warren K.
In-Hospital Mortality Among Patients With Type 2 Diabetes Mellitus and Acute Myocardial Infarction: Results From the National Inpatient Sample, 2000 2010 Bina Ahmed, MD; Herbert T. Davis, PhD; Warren K.
Quality Payment Program: Cardiology Specialty Measure Set
 Measure Title * Reportable via PINNACLE α Reportable via Diabetes Collaborative CQMC v1.0 Measure High Priority Measure Cross Cutting Measure Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor
Measure Title * Reportable via PINNACLE α Reportable via Diabetes Collaborative CQMC v1.0 Measure High Priority Measure Cross Cutting Measure Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor
CATHETER ABLATION FOR TACHYCARDIAS
 190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
the ECG, 6 mg of intravenous adenosine was administered as a fast bolus through a large bore intravenous cannula in
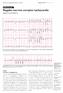 (arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
(arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
Catheter Ablation: Atrial fibrillation (AF) is the most common. Another Option for AF FAQ. Who performs ablation for treatment of AF?
 : Another Option for AF Atrial fibrillation (AF) is a highly common cardiac arrhythmia and a major risk factor for stroke. In this article, Dr. Khan and Dr. Skanes detail how catheter ablation significantly
: Another Option for AF Atrial fibrillation (AF) is a highly common cardiac arrhythmia and a major risk factor for stroke. In this article, Dr. Khan and Dr. Skanes detail how catheter ablation significantly
Paramedic Rounds. Tachyarrhythmia's. Sean Sutton Dallas Wood
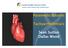 Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010
 Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010 AF Stat is sponsored by sanofi-aventis, U.S. LLC, which provided funding for this report. Avalere
Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010 AF Stat is sponsored by sanofi-aventis, U.S. LLC, which provided funding for this report. Avalere
Digitalis has been used for >200 years to treat patients with
 Original Article Effectiveness and Safety of Digoxin Among Contemporary Adults With Incident Systolic Heart Failure James V. Freeman, MD, MPH; Jingrong Yang, MA; Sue Hee Sung, MPH; Mark A. Hlatky, MD;
Original Article Effectiveness and Safety of Digoxin Among Contemporary Adults With Incident Systolic Heart Failure James V. Freeman, MD, MPH; Jingrong Yang, MA; Sue Hee Sung, MPH; Mark A. Hlatky, MD;
CATHETER ABLATION CODING & REIMBURSEMENT GUIDE. Updated September 2018
 CATHETER ABLATION CODING & REIMBURSEMENT GUIDE Updated September 2018 TABLE OF CONTENTS Diagnosis Codes...3 ICD-10-CM Diagnosis Codes Coverage for Catheter Ablation Procedures....4 Medicare Other Payers
CATHETER ABLATION CODING & REIMBURSEMENT GUIDE Updated September 2018 TABLE OF CONTENTS Diagnosis Codes...3 ICD-10-CM Diagnosis Codes Coverage for Catheter Ablation Procedures....4 Medicare Other Payers
ECTOPIC BEATS: HOW MANY COUNT?
 ECTOPIC BEATS: HOW MANY COUNT? Rupert FG Simpson, 1 Jessica Langtree, 2 *Andrew RJ Mitchell 2 1. King s College Hospital, London, UK 2. Jersey General Hospital, Jersey, UK *Correspondence to mail@jerseycardiologist.com
ECTOPIC BEATS: HOW MANY COUNT? Rupert FG Simpson, 1 Jessica Langtree, 2 *Andrew RJ Mitchell 2 1. King s College Hospital, London, UK 2. Jersey General Hospital, Jersey, UK *Correspondence to mail@jerseycardiologist.com
ECG Workshop. Jared W Magnani, MD, MSc University of Pittsburgh UPMC Heart and Vascular Institute Pittsburgh, PA March 24, 2017
 ECG Workshop Jared W Magnani, MD, MSc University of Pittsburgh UPMC Heart and Vascular Institute Pittsburgh, PA March 24, 2017 Overview and Objectives Review a differential for supraventricular tachycardia
ECG Workshop Jared W Magnani, MD, MSc University of Pittsburgh UPMC Heart and Vascular Institute Pittsburgh, PA March 24, 2017 Overview and Objectives Review a differential for supraventricular tachycardia
Chapter 3: Morbidity and Mortality
 Chapter 3: Morbidity and Mortality Introduction In this chapter we evaluate the morbidity and mortality of chronic kidney disease (CKD) patients continuously enrolled in Medicare. Each year s analysis
Chapter 3: Morbidity and Mortality Introduction In this chapter we evaluate the morbidity and mortality of chronic kidney disease (CKD) patients continuously enrolled in Medicare. Each year s analysis
Chapter 4: Cardiovascular Disease in Patients with CKD
 Chapter 4: Cardiovascular Disease in Patients with CKD The prevalence of cardiovascular disease (CVD) was 65.8% among patients aged 66 and older who had chronic kidney disease (CKD), compared to 31.9%
Chapter 4: Cardiovascular Disease in Patients with CKD The prevalence of cardiovascular disease (CVD) was 65.8% among patients aged 66 and older who had chronic kidney disease (CKD), compared to 31.9%
PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS. HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate
 PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate Measure Title Description Measure Type Data Source Level of Analysis Numerator HRS-3:
PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate Measure Title Description Measure Type Data Source Level of Analysis Numerator HRS-3:
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint
 CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation
 The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
Supplementary Online Content
 1 Supplementary Online Content Friedman DJ, Piccini JP, Wang T, et al. Association between left atrial appendage occlusion and readmission for thromboembolism among patients with atrial fibrillation undergoing
1 Supplementary Online Content Friedman DJ, Piccini JP, Wang T, et al. Association between left atrial appendage occlusion and readmission for thromboembolism among patients with atrial fibrillation undergoing
Process Measure: Screening for Adult Obstructive Sleep Apnea
 Process Measure: Screening for Adult Obstructive Sleep Apnea Measure Description Description Type of Measure All patients aged 18 years and older at high risk for obstructive sleep apnea (OSA) with documentation
Process Measure: Screening for Adult Obstructive Sleep Apnea Measure Description Description Type of Measure All patients aged 18 years and older at high risk for obstructive sleep apnea (OSA) with documentation
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
had non-continuous enrolment in Medicare Part A or Part B during the year following initial admission;
 Effectiveness and cost-effectiveness of implantable cardioverter defibrillators in the treatment of ventricular arrhythmias among Medicare beneficiaries Weiss J P, Saynina O, McDonald K M, McClellan M
Effectiveness and cost-effectiveness of implantable cardioverter defibrillators in the treatment of ventricular arrhythmias among Medicare beneficiaries Weiss J P, Saynina O, McDonald K M, McClellan M
ECG S: A CASE-BASED APPROACH December 6,
 ECG S: A CASE-BASED APPROACH December 6, 2018 1 Faculty Disclosure Faculty: Lorne Gula MD, FRCPC Professor, Western University Cardiologist, Hearth Rhythm Specialist Director, Electrophysiology Laboratory,
ECG S: A CASE-BASED APPROACH December 6, 2018 1 Faculty Disclosure Faculty: Lorne Gula MD, FRCPC Professor, Western University Cardiologist, Hearth Rhythm Specialist Director, Electrophysiology Laboratory,
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
Chronic kidney disease (CKD) has received
 Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
Results from RE-LY and RELY-ABLE
 Results from RE-LY and RELY-ABLE Assessment of the safety and efficacy of dabigatran etexilate (Pradaxa ) in longterm stroke prevention EXECUTIVE SUMMARY Dabigatran etexilate (Pradaxa ) has shown a consistent
Results from RE-LY and RELY-ABLE Assessment of the safety and efficacy of dabigatran etexilate (Pradaxa ) in longterm stroke prevention EXECUTIVE SUMMARY Dabigatran etexilate (Pradaxa ) has shown a consistent
Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts Future Cardiovascular Events
 Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
MEDICAL POLICY SUBJECT: AMBULATORY EVENT MONITORS
 MEDICAL POLICY SUBJECT: AMBULATORY EVENT MONITORS PAGE: 1 OF: 8 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: AMBULATORY EVENT MONITORS PAGE: 1 OF: 8 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Procedural Complications, Rehospitalizations, and Repeat Procedures After Catheter Ablation for Atrial Fibrillation
 Journal of the American College of Cardiology Vol. 59, No. 2, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2011.08.068
Journal of the American College of Cardiology Vol. 59, No. 2, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2011.08.068
Prior Authorization Flexeril/Amrix (cyclobenzaprine) 2017
 Drugs Requiring Prior Authorization Label Name GCN AMRIX ER 15 MG CAPSULE 97959 AMRIX ER 30 MG CAPSULE 97960 CYCLOBENZAPRINE 10 MG TABLET 18020 CYCLOBENZAPRINE 5 MG TABLET 12805 CYCLOBENZAPRINE 7.5 MG
Drugs Requiring Prior Authorization Label Name GCN AMRIX ER 15 MG CAPSULE 97959 AMRIX ER 30 MG CAPSULE 97960 CYCLOBENZAPRINE 10 MG TABLET 18020 CYCLOBENZAPRINE 5 MG TABLET 12805 CYCLOBENZAPRINE 7.5 MG
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
TAB 7: SUB TAB: AMI/CHEST PAIN Specifications & Paper Tools
 TAB 7: SUB TAB: AMI/CHEST PAIN Specifications & Paper Tools Material inside brackets ([and]) is new to this Specifications Manual version. Hospital Outpatient Quality Measures Acute Myocardial Infarction
TAB 7: SUB TAB: AMI/CHEST PAIN Specifications & Paper Tools Material inside brackets ([and]) is new to this Specifications Manual version. Hospital Outpatient Quality Measures Acute Myocardial Infarction
Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care AF symptoms Tachycardia
 Supplementary Table S1 International Classification of Disease 10 (ICD-10) codes Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care I48 AF
Supplementary Table S1 International Classification of Disease 10 (ICD-10) codes Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care I48 AF
Supplementary Online Content
 Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Tachycardias II. Štěpán Havránek
 Tachycardias II Štěpán Havránek Summary 1) Supraventricular (supraventricular rhythms) Atrial fibrillation and flutter Atrial ectopic tachycardia / extrabeats AV nodal reentrant a AV reentrant tachycardia
Tachycardias II Štěpán Havránek Summary 1) Supraventricular (supraventricular rhythms) Atrial fibrillation and flutter Atrial ectopic tachycardia / extrabeats AV nodal reentrant a AV reentrant tachycardia
A DIGITAL, END-TO-END, NATIONWIDE, PRAGMATIC TRIAL OF SCREENING FOR UNDIAGNOSED ATRIAL FIBRILLATION: PRIMARY RESULTS OF THE mstops TRIAL
 A DIGITAL, END-TO-END, NATIONWIDE, PRAGMATIC TRIAL OF SCREENING FOR UNDIAGNOSED ATRIAL FIBRILLATION: PRIMARY RESULTS OF THE mstops TRIAL Steven R. Steinhubl, MD @stevesteinhubl Scripps Translational Science
A DIGITAL, END-TO-END, NATIONWIDE, PRAGMATIC TRIAL OF SCREENING FOR UNDIAGNOSED ATRIAL FIBRILLATION: PRIMARY RESULTS OF THE mstops TRIAL Steven R. Steinhubl, MD @stevesteinhubl Scripps Translational Science
AF Today: W. For the majority of patients with atrial. are the Options? Chris Case
 AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
ACTIVITY DISCLAIMER DISCLOSURE. Craig Barstow, MD, FAAFP. Learning Objectives. Associated Session(s) Arrhythmias and Dysrhythmias: PBL
 ACTIVITY DISCLAIMER Arrhythmias and Dysrhythmias: PBL Craig Barstow, MD, FAAFP The material presented here is being made available by the American Academy of Family Physicians for educational purposes
ACTIVITY DISCLAIMER Arrhythmias and Dysrhythmias: PBL Craig Barstow, MD, FAAFP The material presented here is being made available by the American Academy of Family Physicians for educational purposes
Zio System Publications. Peer-reviewed publications demonstrating the clinical validity and utility of the Zio system
 Zio System Publications Peer-reviewed publications demonstrating the clinical validity and utility of the Zio system Contents Electrocardiographic Responses to Deer Hunting in Men and Women. Wilderness
Zio System Publications Peer-reviewed publications demonstrating the clinical validity and utility of the Zio system Contents Electrocardiographic Responses to Deer Hunting in Men and Women. Wilderness
Chapter 4: Cardiovascular Disease in Patients With CKD
 Chapter 4: Cardiovascular Disease in Patients With CKD Introduction Cardiovascular disease is an important comorbidity for patients with chronic kidney disease (CKD). CKD patients are at high-risk for
Chapter 4: Cardiovascular Disease in Patients With CKD Introduction Cardiovascular disease is an important comorbidity for patients with chronic kidney disease (CKD). CKD patients are at high-risk for
Cardiac Event Monitors
 Last Review Date: July 14, 2017 Number: MG.MM.DM.18aCv2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: July 14, 2017 Number: MG.MM.DM.18aCv2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Trends in Basal Cell Carcinoma Incidence and Identification of High-Risk Subgroups,
 Research Original Investigation Trends in Basal Cell Carcinoma Incidence and Identification of High-Risk Subgroups, 1998-2012 Maryam M. Asgari, MD, MPH; Howard H. Moffet, MPH; G. Thomas Ray, MBA; Charles
Research Original Investigation Trends in Basal Cell Carcinoma Incidence and Identification of High-Risk Subgroups, 1998-2012 Maryam M. Asgari, MD, MPH; Howard H. Moffet, MPH; G. Thomas Ray, MBA; Charles
Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B. Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D.
 Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D. SUMMARY This report documents a case which showed type
Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D. SUMMARY This report documents a case which showed type
Use of Medications for Secondary Prevention After Coronary Bypass Surgery Compared With Percutaneous Coronary Intervention
 Journal of the American College of Cardiology Vol. 61, No. 3, 2013 2013 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2012.10.018
Journal of the American College of Cardiology Vol. 61, No. 3, 2013 2013 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2012.10.018
MEDICAL POLICY Cardiac Event Monitors/ Cardiac Event Detection
 POLICY: PG0039 ORIGINAL EFFECTIVE: 10/01/11 LAST REVIEW: 12/12/17 MEDICAL POLICY Cardiac Event Monitors/ Cardiac Event Detection GUIDELINES This policy does not certify benefits or authorization of benefits,
POLICY: PG0039 ORIGINAL EFFECTIVE: 10/01/11 LAST REVIEW: 12/12/17 MEDICAL POLICY Cardiac Event Monitors/ Cardiac Event Detection GUIDELINES This policy does not certify benefits or authorization of benefits,
Chapter 3: Morbidity and Mortality in Patients with CKD
 Chapter 3: Morbidity and Mortality in Patients with CKD In this 2017 Annual Data Report (ADR) we introduce analysis of a new dataset. To provide a more comprehensive examination of morbidity patterns,
Chapter 3: Morbidity and Mortality in Patients with CKD In this 2017 Annual Data Report (ADR) we introduce analysis of a new dataset. To provide a more comprehensive examination of morbidity patterns,
Table S1: Diagnosis and Procedure Codes Used to Ascertain Incident Hip Fracture
 Technical Appendix Table S1: Diagnosis and Procedure Codes Used to Ascertain Incident Hip Fracture and Associated Surgical Treatment ICD 9 Code Descriptions Hip Fracture 820.XX Fracture neck of femur 821.XX
Technical Appendix Table S1: Diagnosis and Procedure Codes Used to Ascertain Incident Hip Fracture and Associated Surgical Treatment ICD 9 Code Descriptions Hip Fracture 820.XX Fracture neck of femur 821.XX
Asymptomatic patient with WPW
 Asymptomatic patient with WPW Dimosthenis Avramidis, MD. Arrythmiologist Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital Athens Greece Preexcitation
Asymptomatic patient with WPW Dimosthenis Avramidis, MD. Arrythmiologist Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital Athens Greece Preexcitation
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Quality Payment Program: Cardiology Specialty Measure Set
 Quality Payment Program: Cardiology Specialty Set Title Number CMS Reporting Method(s) Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor or Angiotensin Receptor Blocker (ARB) Therapy for
Quality Payment Program: Cardiology Specialty Set Title Number CMS Reporting Method(s) Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor or Angiotensin Receptor Blocker (ARB) Therapy for
Chapter 4: Cardiovascular Disease in Patients With CKD
 Chapter 4: Cardiovascular Disease in Patients With CKD The prevalence of cardiovascular disease is 68.8% among patients aged 66 and older who have CKD, compared to 34.1% among those who do not have CKD
Chapter 4: Cardiovascular Disease in Patients With CKD The prevalence of cardiovascular disease is 68.8% among patients aged 66 and older who have CKD, compared to 34.1% among those who do not have CKD
Chronic Kidney Disease is Associated with Cognitive Decline: the Northern Manhattan Study (NOMAS) Seattle VA Chief of Medicine Rounds June 9, 2009
 Chronic Kidney Disease is Associated with Cognitive Decline: the Northern Manhattan Study (NOMAS) Seattle VA Chief of Medicine Rounds June 9, 2009 Minesh Khatri Internal Medicine R2 Background Patients
Chronic Kidney Disease is Associated with Cognitive Decline: the Northern Manhattan Study (NOMAS) Seattle VA Chief of Medicine Rounds June 9, 2009 Minesh Khatri Internal Medicine R2 Background Patients
Real-World Insights from GARFIELD-AF Registry Presented at ESC Congress 2017
 Real-World Insights from GARFIELD-AF Registry Presented at ESC Congress 2017 One of the aims of GARFIELD-AF is to assist physicians in their understanding of the risk of stroke in patients with atrial
Real-World Insights from GARFIELD-AF Registry Presented at ESC Congress 2017 One of the aims of GARFIELD-AF is to assist physicians in their understanding of the risk of stroke in patients with atrial
GE Healthcare. The GE EK-Pro Arrhythmia Detection Algorithm for Patient Monitoring
 GE Healthcare The GE EK-Pro Arrhythmia Detection Algorithm for Patient Monitoring Table of Contents Arrhythmia monitoring today 3 The importance of simultaneous, multi-lead arrhythmia monitoring 3 GE EK-Pro
GE Healthcare The GE EK-Pro Arrhythmia Detection Algorithm for Patient Monitoring Table of Contents Arrhythmia monitoring today 3 The importance of simultaneous, multi-lead arrhythmia monitoring 3 GE EK-Pro
Prevalence (%) Table S4 Prevalence of AF in women and men, age- specific Study name/country Study population Study period Age group
 Table S4 Prevalence of AF in and men, age- specific Study name/country Yunnan Province, China Random sample of government Guo (2015) 1 medical insurance plan Age 20 years Spain Gomez- Doblas (2014) 2 The
Table S4 Prevalence of AF in and men, age- specific Study name/country Yunnan Province, China Random sample of government Guo (2015) 1 medical insurance plan Age 20 years Spain Gomez- Doblas (2014) 2 The
Transcoronary Chemical Ablation of Atrioventricular Conduction
 757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
Chapter 5: Acute Kidney Injury
 Chapter 5: Acute Kidney Injury In 2015, 4.3% of Medicare fee-for-service beneficiaries experienced a hospitalization complicated by Acute Kidney Injury (AKI); this appears to have plateaued since 2011
Chapter 5: Acute Kidney Injury In 2015, 4.3% of Medicare fee-for-service beneficiaries experienced a hospitalization complicated by Acute Kidney Injury (AKI); this appears to have plateaued since 2011
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh
 Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Atrial Fibrillation. Ivan Anderson, MD RIHVH Cardiology
 Atrial Fibrillation Ivan Anderson, MD RIHVH Cardiology Outline Definition and Pathophysiology Rate versus rhythm control Rate control thresholds (how much is enough) Anti-coagulation CHADS2VASc score HASBLED
Atrial Fibrillation Ivan Anderson, MD RIHVH Cardiology Outline Definition and Pathophysiology Rate versus rhythm control Rate control thresholds (how much is enough) Anti-coagulation CHADS2VASc score HASBLED
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Risk Factors for Ischemic Stroke: Electrocardiographic Findings
 Original Articles 232 Risk Factors for Ischemic Stroke: Electrocardiographic Findings Elley H.H. Chiu 1,2, Teng-Yeow Tan 1,3, Ku-Chou Chang 1,3, and Chia-Wei Liou 1,3 Abstract- Background: Standard 12-lead
Original Articles 232 Risk Factors for Ischemic Stroke: Electrocardiographic Findings Elley H.H. Chiu 1,2, Teng-Yeow Tan 1,3, Ku-Chou Chang 1,3, and Chia-Wei Liou 1,3 Abstract- Background: Standard 12-lead
