Results of single and bilateral lung transplantation in 131 consecutive recipients
|
|
|
- Diane Davidson
- 5 years ago
- Views:
Transcription
1 Results of single and bilateral lung transplantation in 131 consecutive recipients We reviewed results of the first 131 recipients who received a single or bilateral sequential lung transplant at Barnes Hospital between July 1, 1988, and July 31, Follow-up data were complete as of January 1, 1993, for a minimum of 5 months' follow-up for all surviving recipients. There were 11 hospital deaths for an overall 92 % hospital survival. Thirteen late deaths occurred and 107 (81 %) recipients remain alive with a median follow-up period of 19 months. One hundred nineteen recipients survived at least 3 months after transplantation, and for this group factors that might influence long-term results were evaluated. The prevalence of pathologically proved bronchiolitis obliterans was 18.5 %. Functional deterioration, which may not correlate with pathologic findings, was evaluated with a recently developed bronchiolitis obliterans syndrome staging system. Factors not influencing longterm outcome included the number of early rejection episodes, matching donor and recipient cytomegalovirus antibody status, or underlying diagnosis. Patients undergoing single lung transplantation for primary pulmonary hypertension or Eisenmenger's syndrome had results similar to those of other diagnostic groups. Furthermore, the hemodynamic improvement previously reported for this group of patients after single lung transplantation has been maintained at long-term follow-up. The shortage of donor organs and the need for improved methods for diagnosis and management of chronic rejection remain the most challenging problems in lung transplantation. (J THORAC CARDIOV ASC SURG 1994; 107:460-71) Joel D. Cooper, MD, G. Alexander Patterson, MD, Elbert P. Trulock, MD (by invitation), and the Washington University Lung Transplant Group, St. Louis, Mo. In the nearly 10 years since successful isolated lung transplantation was first achieved, lung transplantation has become established at numerous centers throughout the world with early success rates approaching that of other organ transplants. More than 2000 single or bilaterallung transplantation have been reported to date to the St. Louis International Lung Transplant Registry. Of this number, 66% have been performed in the past 24 months; thus reports of long-term results with current indications and current techniques are limited. Our own previous reports have focused primarily on indications, technique, From the Departments of Surgery and Medicine and the Divisions of Cardiothoracic Surgery and Pulmonary Medicine and Critical Care, Washington University School of Medicine, St. Louis, Mo. Read at the Seventy-third Annual Meeting of The American Association for Thoracic Surgery, Chicago, Ill., April 25-28, Address for reprints: Joel D. Cooper, MD, Professor of Surgery, Division of Cardiothoracic Surgery, Suite 3108, Queeny Tower, One Barnes Hospital Plaza, St. Louis, MO Copyright@) 1994 by Mosby-Year Book, Inc /94 $ /6/52062 postoperative care, and perioperative mortality. This report summarizes our experience to date and examines factors that may influence the long-term outcome. Patients and methods All lung transplantations performed at Barnes Hospital between the initiation of the program in July 1988 and July 31, 1992, were reviewed. During this time 142 lung transplantations were performed in 138 patients. Included are eight en bloc double lung procedures performed in the initial year with a mortality of 75%. This led us to abandon this procedure and to develop the bilateral sequential technique. The remaining 130 patients who received either a single or bilateral lung transplant, and one double lung recipient who subsequently received a bilateral retransplant 17 months later, form the basis of this report. Follow-up data were complete as of January 1, 1993, giving a minimum follow-up period of 5 months for all surviving recipients. Recipient selection. In general, we have reserved transplantation for patients whose disability and rate of disease progression suggest that life expectancy is limited to a range of 12 to 24 months. Such individuals are usually oxygen dependent and demonstrate deterioration of pulmonary function and increasing oxygen requirements. Recipients with chronic obstructive pulmonary disease or Cl'l-antitrypsin-related emphysema gen- 460
2 The Journal of Thoracic and Volume 107, Number 2 Cooper et al Time 20 Waiting in 15 Days Successive Groups of 10 Patients Fig. 1. Average waiting time for successive groups of 10 recipients each between July 1, 1988, and August erally have a first-second vital capacity of less than 20% predicted. Individuals with restrictive lung disease have a forced expiratory volume in 1 second (FEY 1 ) of 1.2 L oriess and have arterial oxygen desaturation with mild exercise in the presence of oxygen administration. For patients with cystic fibrosis no simple algorithm exists to predict life expectancy, although a recent publication has demonstrated a significant correlation between the FEY 1 and life expectancy. 1 We have found thatthe need for oxygen administration, a decline in nutritional status, and the need for increasing hospitalization for recurrent pulmonary infection all suggest limited life expectancy in this disease. A recent study of the natural history of patients with primary pulmonary hypertension indicates a mean life expectancy of 2.8 years from the time of diagnosis. 2 Increased right atrial pressure, diminished cardiac output, and increasing ventricular failure all adversely affect prognosis. During the initial 18 months of the program, ventilator dependency was considered a contraindication to transplantation. This restriction was subsequently eliminated and four of the recipients underwent transplantation while ventilator dependent, the period of time on the ventilator ranging from 5 days to 3 months. All four underwent successful bilateral sequential lung transplantation. Donor selection. The lack of suitable donor lungs is currently the major obstacle to more widespread application of lung transplantation. Suitable lungs are more difficult to obtain than other organs because of the susceptibility of the lungs to infection and edema under the circumstances surrounding brain death. We require that the donor chest x-ray film be clear of pulmonary infiltrates and that the arterial oxygen tension exceed 300 mm Hg with an inspired oxygen fraction of 1.0 and 5 cm H 2 0 of positive end-expiratory pressure. Furthermore, examination with a bronchoscope should reveal no grossly purulent secretions or suggestion of aspiration. We estimate that no more than 10% to 20% of organ donors have lungs suitable for transplantation. We have attempted to liberalize criteria for donor lungs as much as possible and will, on occasion, use a lung with a small contusion, lungs with a mild infiltrate thought to be due to edema, and lungs from donors with a suboptimal oxygen tension when this is thought to be caused by pulmonary edema. We have recently reviewed our experience with suboptimal donors and have found equivalent early results with respect to hospital mortality compared with optimal donors. However, for recipients with a diagnosis of pulmonary hypertension or Eisenmenger's syndrome, we have used only optimal donors, preferably with an ischemic time of less than 6 hours. The heparinized donor is given an injection of 500 f.lg of prostaglandin E\, directly into the pulmonary artery over 15 seconds. Pulmonary preservation is then achieved by a cold flush through a large-bore catheter in the donor pulmonary artery. The flushing solution consists of 3 L of Euro-Collins solution to which has been added 56 ml of 50% glucose and 8 meg of magnesium sulfate per Ii tel Waiting period. The average waiting time for a transplant has steadily risen since the onset of our lung transplant program. Fig. 1 illustrates the average waiting time for each successive group of 10 recipients. This figure is based on the first 140 lung transplantations of all types performed at our institution. As is seen in this figure, the average waiting time has risen from 65 days to 272 days over this 4V2-year period. Technique of lung transplantation. Our techniques for unilateral and bilateral sequential lung replacement have previously been described. 3 4 The single lung transplant operation is performed through a posterolateral thoracotomy, whereas the sequential bilateral procedure is performed through a bilateral transverse thoracosternotomy. Both procedures use essentially the same technique for extraction and implantation. The airway anastomoses in this series include three different techniques. All three use a running suture of absorbable monofilament suture to the membranous portion of the anastomosis. For the cartilaginous portion of the anastomoses, three different techniques were used, including end-to-end anastomoses with simple interrupted sutures, figure-of-eight sutures with slight overlap of the cartilaginous portions, or the use of an intussuscepting horizontal mattress technique with either the donor or the recipient end intussuscepted into the opposite airway for a distance of one cartilaginous ring. The majority of airway anastomoses in the series were wrapped within an omental pedicle. However, approximately 25% of the procedures, done in the later part of the series, used anastomotic wrapping with either local peribronchial and mediastinal tissues or a pedicle fashioned from the pericardial fat pad. Immunosuppression. Our immunosuppressive regimen has been based on the routine use of cyclosporine, azathioprine, and prednisone. For the first 3 years of our program, routine postoperative prednisone administration was avoided for the initial 5 postoperative days. In the most recent year, half of the patients were started on prednisone on the first postoperative day
3 4 6 2 Cooper et al. The Journal of Thoracic and February 1994 Table I. Indications for transplantation (n = 131) Single lung Bilateral lung Diagnoses No. (n = 73) (n = 58) COPD ai-antitrypsin emphysema Cystic fibrosis PPH/Eisenmenger's IPF Other COPD, Chronic obstructive pulmonary disease; PPH, primary pulmonary hypertension; IPF, idiopathic pulmonary fibrosis. whereas the other half received no routine prednisone until the fifth day. The details of the immunosuppressive regimen are as follows: Preoperative Azathioprine-2 mg/kg intravenously I to 2 hours before induction of anesthesia. Postoperative Antilymphocyte globulin (Minnesota equine)-15 mg/kg per 24 hours intravenously for 5 days. Azathioprine-2 mg/kg intravenously or orally. Cyclosporine-constant intravenous infusion of 3 to 4 mg/hr. Convert to oral dosage as soon as tolerated and adjust intravenous and oral dose according to serum cyclosporine levels (target levels of 400 ng/ ttl by radioimmunoassay on whole blood). Steroids-No "routine" steroids for the first 5 days. Prednisone 0.5 mg/kg per day beginning on postoperative day 5 to 7. Approximately 20 patients in the last year of this series received methylprednisolone 1 mg/kg per day for the first 4 postoperative days and then received prednisone 0.5 mg/kg per day as was used in the patients noted earlier. Because the Minnesota equine product is no longer available, we currently use a commercial antithymocyte preparation (Atgam, Upjohn Company, Kalamazoo, Mich.). After discharge from hospital, the immunosuppression protocol is unchanged for the first 3 months. Between the third and sixth months, the prednisone dose is tapered from 0.5 mg/kg to date down to a dose of 12.5 to 15 mg/day. By the end of the first year, this is further tapered to an average dose of 12.5 to 15 mg on alternate days. Azathioprine dose is maintained at 2 mg/kg per day unless leukopenia develops, in which case the dose is appropriately adjusted. The cyclosporine level is maintained in the upper therapeutic range for the first year. Thereafter, the cyclosporine dose is tapered to produce a blood level in the mid therapeutic range unless dose reduction is necessitated by elevated serum creatinine values. For proved or presumed episodes of chronic rejection, a boost in the steroid dose has been the primary mode of therapy. This usually is in the form of three bolus doses of methylprednisolone on successive days, with or without a concomitant boost and taper of the daily prednisone dose. Bronchoscopic surveillance. Patients undergo initial evaluation with a fiberoptic bronchoscope before leaving the operating room and again on the first postoperative day. A bronchoscopic study is also performed just before extubation. In the third postoperative week, usually just before discharge from the hospital, patients are examined with a bronchoscope under local anesthesia and protocol trans bronchial biopsies are performed. After discharge, a bronchoscopic study with transbronchial biopsy and bronchoalveolar lavage is performed whenever indicated by clinical parameters such as dyspnea, hypoxemia, decline in FEY \, radiographic infiltrate, or unexplained fever. Routine protocol transbronchial biopsy specimens and bronchoalveolar lavage are obtained at 3, 6,12, 18, and 24 months and annually thereafter. Biopsy specimens were graded according to the working formulation for the standardization of nomenclature in the diagnosis of heart and lung rejection reported by the Lung Rejection Study Group. 5 According to this formulation, bronchiolitis obliterans is characterized by the presence of fibrosis and scarring of airways (category C under the working formulation). Assessment of chronic allograft dysfunction and of bronchiolitis obliterans. It has become apparent that a uniform, objective method for evaluating functional outcome and comparing results between different centers is required. To address this issue a consensus conference was held in St. Louis in February 1993 to develop a working formulation for clinical staging of chronic dysfunction in lung allografts. The results of that conference were reported to the annual meeting of the International Society for Heart and Lung Transplantation in April According to this working formulation, lung allograft function is characterized by the ratio of the current FEY I to the highest baseline FEY 1 established after transplantation. On the basis of this ratio, four stages of lung allograft dysfunction, known as bronchiolitis obliterans syndrome (BOS), are described: stage 0, greater than 80%; stage 1,66% to 80%; stage 2, 51 % to 65%; and stage 3, 50% or less. For each stage there is a subcategory of either a or b depending on whether or not a histologic diagnosis of obliterative bronchiolitis has ever been obtained. Subcategory a indicates no such evidence while b indicates the contrary. BOS is widely presumed to be related to chronic rejection, but this is as yet unproved. For evaluation of long-term results in this series, each recipient's most recent BOS stage was determined. Results Technical details. Between July 1, 1988, and July 31, 1992, 134 single or bilateral transplant operations were performed in 131 patients. Seventy-three recipients received a single lung and 58 received a bilateral lung transplant. Of the three second transplant operations, two were done within days of the initial procedure, one for primary graft failure and one for airway necrosis. The third repeat transplant operation was a bilateral sequential transplantation performed for bronchiolitis obliterans 17 months after an en-bloc double lung transplantation. The ischemic time for the single lung transplantations was an average of 4 hours 30 minutes (range 2 hours 48 minutes to 7 hours 35 minutes). For the bilateral transplantations, the mean ischemic time for the first lung was 4 hours 50 minutes (range 2 hours to 6 hours) while the ischemic time for the second lung was an average of 7 hours 15 minutes (range 3 hours 15 minutes to 10 hours 33 minutes).
4 The Journal of Thoracic and Volume 107, Number 2 Cooper et at Table II. Causes of postoperative deaths (n = 11) Sepsis Cardiac Aspergillus infection ARDS of uncertain cause Airway complication ARDS, Adult respiratory distress syndrome. The indications and types of transplantations are shown in Table I. All transplant procedures were performed with cardiopulmonary bypass available on a standby basis. Twenty-two of the single lung transplantations were performed in the presence of systemic pulmonary artery pressure, 19 for primary pulmonary hypertension or Eisenmenger's syndrome, and three in patients with systemic pulmonary pressure caused by other underlying lung diseases. For these 22 transplantations, cardiopulmonary bypass was routinely used. In the remaining 51 single lung transplantations, cardiopulmonary bypass was used in only one patient. In this patient, bypass was required to control an injury to the pulmonary artery incurred during initial dissection. For the 58 bilateral procedures, cardiopulmonary bypass was used in 17 patients (30%). In most of these instances, bypass was used during implantation of the second lung because diversion of the entire cardiac output to the newly implanted lung occasionally results in significant pulmonary hypertension and concomitant edema and hypoxemia. Under these circumstances, partial cardiopulmonary bypass was established via right atrial and ascending aortic cannulation. Morbidity and mortality. Eleven (8%) of the 131 recipients died in the hospital after transplantation, for a overall 92% hospital survival. The causes of the hospital deaths are shown in Table II. For the 120 patients who were discharged from the hospital, the average stay in the intensive care unit was 5.6 days with a median of 3 days. Seventy-two percent of recipients left the intensive care unit by the fourth day. The average stay in the hospital was 26 days (median 22 days). There have been 13 late deaths as of January 1,1993. Ten of these occurred within 12 months of transplantation, and the remaining two occurred between 13 and 40 months after the operation. The causes of late deaths are shown in Table III. The most common cause was chronic rejection or infection related to augmented immunosuppression for treatment of chronic rejection. One hundred seven (81.6%) recipients remain alive. The average follow-up time for this group of patients is as follows: 1 to Table III. Cause of late deaths (n = 14) Chronic rejection and/or associated infections Renal failure, recurrent pulmonary sepsis Chronic pulmonary sepsis Perforated ulcer Chronic CMV infection Cancer of the pancreas Bronchovascular fistula Refractory seizures Marasmus 12 months, 33 patients; 13 to 24 months, 31 patients; 25 to 36 months, 30 patients; and 37 to 48 months, 12 patients. The median period of follow-up is 19 months. Survival by transplantation type and diagnosis. Fig. 2 demonstrates the actuarial survival curve for all 131 patients as well as for those having either single lung or bilateral lung transplantations. For the entire group, the I-year actuarial survival was 82% and the 2-year actuarial survival was 81 %. Patients receiving single lung transplants had a higher survival than those receiving bilateral transplants, primarily because of a reduced hospital mortality (5% for single lung transplant versus 12% for bilaterallung transplant). Fig. 3 demonstrates the overall survival curves for major diagnoses. The hospital mortality varied from 4% for (Xl-antitrypsin emphysema to 14% for idiopathic pulmonary fibrosis. Airway complications. Healing problems with the airway anastomosis were identified in 25 of the 131 patients in this series for an overall prevalence of 19%. In 12 patients, endoscopic evidence of necrosis or partial anastomotic separation was identified, necessitating no treatment and resulting in no apparent complication. In the remaining 13 patients (10%), a significant airway complication resulted. These are identified in Table IV. A detailed analysis of airway complications in this series of patients will be published separately. No correlation has been recognized between surgical technique, length of ischemic time, or immunosuppressive regimen and the subsequent development of an airway complication. Prevalence of bronchiolitis obliterans and chronic allograft dysfunction in long-term survivors. One hundred nineteen recipients have survived more than 3 months, and in this group the prevalence of histologically proved bronchiolitis obliterans and the prevalence of chronic allograft dysfunction were evaluated with the BOS scoring system. One hundred sixteen of the 119 patients underwent bronchoscopy with transbronchial biopsy, the average being 5.2 transbronchoscopic procedures per patient (range 2 to 11). An average of 10 biopsy specimens were obtained with each procedure. 6
5 ,...~~~.~.~.~.~.~ Cooper et al. The Journal of Thoracic and February ~"""""""""""""""""""""""""" - ~ ~S: n 49 (87%) S: n 26 (87%) - -.~ '--.,..:.:..; S T: n=80 (82%) T: n=45 (81 %) u ~: ~~.3.1..(:.6.~~... ~: ~:=.1.~.<?3.%) r 0.6 v v Single (n=73) Bilateral (n=58) --- Combined (n=131) o ~ o Days Alive (1 year) (2 years) Fig. 2. Actuarial survival curve for first consecutive 131 recipients of single or bilateral lung transplant COPD:n=24 (94% COPD: n=14 94%) PH: n=13..!!!..4~ PH: n=l!j!i~...,,~.... S u CF: n=ll (78% CF: n=5 (78%) r ~.. ~..., A-1 :n=19 (73%) A-1: n=13 (73%) v --- COPD (n=36) IPF: n=8 (73%) IPF: n=4 (73%) --- A-1 EMP (n=32) v 0.4 a --- CF (n=20) I PPHIElsen (n=19) IPF (n=13) Days Alive (1 year) 730 (2 years) Fig. 3. Actuarial survival curve for major diagnostic groups receiving single or bilateral lung transplant between July 1, 1988 and July 31, COPD, Chronic obstructive pulmonary disease; A-I EMP, ai-antitrypsin emphysema; CF, cystic fibrosis; PPH, primary pulmonary hypertension; IPF, idiopathic pulmonary fibrosis; PH, pulmonary hypertension; Eisen, Eisenmenger's syndrome. Of the 119 three-month survivors, 22 had a pathologic diagnosis of obliterative bronchiolitis on one or more occasions, for an overall prevalence of 18.5%. The BOS score was based on the patient's most recent puhnonary function study (as of January 1, 1993) or the last pulmonary function study before death in patients who have died. Of the 120 hospital survivors, 27% showed clinical evidence of chronic allograft dysfunction, namely, stages I, II, or III. The BOS distribution was as follows: stage 0, 87 patients (73%); stage I, 2 patients (1.7%); stage II, 26 patients (21.8%); and stage III, 4 patients (3.4%). Altogether, 38 recipients had deterioration in function of one or more stages at some time after transplantation. Of these, 11 patients (29%) showed subsequent improvement of one or more stages as follows: Improvement by one stage, five patients; improvement by two stages, four patients; and improvement by three stages, two patients. Of the 11 patients showing functional decline followed by improvement, five had a pathologically confirmed diagnosis of bronchiolitis obliterans. Fig. 4 demonstrates the sequential FEV I measurements in one such patient who received a single lung transplant for chronic obstructive pulmonary disease 4
6 The Journal of Thoracic and Volume 107, Number 2 Cooper et al FEV 1 (liters) I I ~ I ".. '\ 4 B.C '\ V " c t B:C I' '" J IV I a a Time - Months Fig. 4. The FEY" in liters, from sequential pulmonary function studies in a 61-year-old man undergoing single lung transplantation for chronic obstructive pulmonary disease. A progressive decline in the FEY, began at 24 months and at 30 months after transplantation. The FEY, was 53% with a previously established posttransplant baseline value. Arrows indicate timing of transbronchial biopsies that demonstrated obliterative bronchiolitis (B.o.). With augmented immunosuppression there has been a complete reversal of the functional loss. years ago. Lung function began to deteriorate 21 months after transplantation and the FEV, reached a low point of 53% of baseline 30 months after transplantation. Transbronchial biopsies confirmed the presence of bronchiolitis obliterans at 26 months and at 30 months. From 26 months onward, the patient received a total of eight courses of augmented steroids and two course of cytolytic therapy. His pulmonary function has gradually recovered to its baseline value. Relation of long-term function to early rejection. Data for the 119 patients who survived 3 months or more was analyzed for the number of 3-day courses of methylprednisolone administered during the first 30 hospital days, for presumed acute rejection. The diagnosis of acute rejection continues to rest primarily on clinical grounds, including one or more of the following: elevation of temperature by 0.5 C; fall in oxygen tension at rest or on exercise compared with previous values at an equivalent inspired oxygen fraction; radiographic development of hilar "flare" or hazy basal infiltrate. A significant improvement after the initial bolus dose of methylprednisolone, coupled with the absence of any evidence of other contributing factors, such as infection or fluid retention, is considered confirmation of acute rejection and is the indication for additional bolus doses of methylprednisolone on the next 2 consecutive days. The use of trans bronchial biopsy in the initial 3 weeks continues to have limited application for the diagnosis of rejection. Only three recipients (2.5%) failed to receive a course of methylprednisolone, confirming the very high predilection for acute rejection after lung transplantation. The average number of methylprednisolone courses was 2.1 per patient. Table V demonstrates the relation between Table IV. Airway complications in 131 patients receiving single or bilateral transplantation Complication Death Stricture or malacia necessitating stent Stricture necessitating dilation Air leak necessitating chest tube No Patients % the number of acute rejection episodes and the current functional status based on the staging of BOS. As can be seen from Table V, no apparent correlation exists to date between the number of early rejection episodes and the ultimate functional outcome. It is intriguing to note that the six patients who received four courses of methylprednisolone in the first 30 days are currently in BOS stage 0 and in fact have never deteriorated below stage O. The numbers in this group, however, are too small to be meaningful Relation of functional status to type of transplantation and to underlying diagnosis. The prevalence of pathologically proved bronchiolitis obliterans and the current BOS stage were compared between recipients of single and bilateral transplants who survived 3 months or more (n = 119). The results are shown in Table VI and demonstrate no significant difference by either assessment between the single lung and the bilateral lung recipients. A similar comparison was made according to recipient diagnosis. The results are demonstrated in Table VII. No statistically significant difference exists between any of the groups.
7 4 6 6 Cooper et al. The Journal of Thoracic and February 1994 Table V. Relation between courses of methylprednisolone in the first 30 days and current BOS stage Courses of Patients Current methylprednisolone No. % BOS stage I Table VI. Influence of type of transplantation on chronic graft dysfunction and biopsy-proved BO Type of transplantation Single lung (n = 68) Bilateral lung (n = 51) BO, Bronchiolitis obliterans. MeanBOS stage Prevalence of BO (%) \ It has been suggested that bronchiolitis obliterans is more prevalent after transplantation for pulmonary hypertension.* To test this hypothesis, we compared the BOS stage and the prevalence of bronchiolitis obliterans between all hospital survivors having a single lung transplant for pulmonary hypertension and those having a single lung transplant for any other diagnosis. The mean BOS stage for the two groups was 0.83 versus 0.54, and the prevalence of biopsy-proved bronchiolitis obliterans was 22.2% versus 18.0%. No statistically significant difference was detected between the two groups of patients for either assessment. Influence of cytomegalovirus matching on outcome. The effect of donor-recipient matching regarding cytomegalovirus (CMV) antibody status was evaluated in terms of prevalence of subsequent CMV infection, average number of such infections per patient, prevalence of pathologically proved bronchiolitis obliterans, and the functional outcome in terms ofbos stage. The results are shown in Table VIII. The number of CMV infections was based on a decision to treat the recipient with a course of ganciclovir, usually for the presence of CMV in the buffy coat or in bronchoalveolar lavage fluid in association with clinical symptoms, or for biopsy-proved CMV pneumonitis. As can be seen from Table VIII, only 2 of 26 CMV -negative recipients who received CMV-negative organs subse- *Shumway SJ, Hertz MI, Jessurun J, N akhleh R, Petty M, Bolman RM. Obliterative bronchiolitis after lung or heart-lung transplantation for primary pulmonary hypertension. Unpublished data. Table VII. Influence of type of transplantation on chronic graft dysfunction and biopsy-proved BO for the major diagnostic groups M eanbos Prevalence of Recipient diagnosis stage BO (%) COPD (n= 39) aq -Antitrypsin emphysema (n = 22) 0.54 \8.2 Cystic fibrosis (n = 18) PPH/ Eisenmenger's (n = 18) IPF (n = 12) COPD, Chronic obstructive pulmonary disease; PPH, primary pulmonary hypertension; IPF, idiopathic pulmonary fibrosis. quently had CMV infection. These infections occurred at 9 and 26 months after transplantation, respectively. On the other hand, 23 of the 26 CMV-negative recipients who received an organ from a CMV -positive donor had a subsequent CMV infection. The average number of CMV infections per patient in this group was 1.9. The donor-recipient CMV matching had no influence on the prevalence of biopsy-proved bronchiolitis obliterans or on functional BOS stage at most recent follow-up. Late immunosuppression. Fig. 5 demonstrates the number of courses of heightened steroid administration given to the 119 operative survivors after the first postoperative month for treatment of suspected or proved rejection. As can be seen, 18 patients ( 15%) received no subsequent courses of augmented steroid therapy, whereas eight patients received between seven and eleven courses. The median was two courses per patient. When heightened steroid administration failed to stabilize or reverse chronic allograft dysfunction, a course of cytolytic therapy in the form of Minnesota equine antilymphoblast globulin, antithymocyte globulin, or OKT3 was administered. The number of such courses administered to the 119 hospital survivors after the first month is depicted in Table IX. As can be seen, 99 (83%) of the recipients received no cytolytic therapy after the first month. Long-term follow-up of patients with pulmonary hypertension. Assessment of long-term functional outcome after single lung transplantation for pulmonary hypertension has included periodic cardiac catheterization with measurement of pulmonary artery pressure, cardiac output, and pulmonary vascular resistance. We? have previously reported the satisfactory hemodynamic results produced by single lung transplantation for pulmonary hypertension. In this series, 17 such recipients had at least one posttransplantation catheterization. For these patients, the mean pulmonary artery pressure was 66 mm Hg before the operation and 22 mm Hg at most recent follow-up (mean follow-up time is 15 months). The
8 The Journal of Thoracic and Volume 107, Number 2 Cooper et al # of 1 Patients 10 o # of Courses Fig. 5. Frequency distribution of the number of courses of steroid therapy administered after the first month for presumed or proved rejection. Eighteen patients received no courses of augmented steroids, whereas eight patients received seven or more such courses. Table VIII. Influence of recipient-donor CMV status No. of Patients with CMV infection Recipient/donor patients No. % NIN NIP PIN PIP Average No. of Prevalence of BO infections per patient No. % BaS stage I N, Negative; P, positive; BO, bronchiolitis obliterans. Table IX. Cytolytic therapy administered after the first month to 119 hospital survivors No. of courses o No. of patients o Table X. Mean hemodynamics in pulmonary hypertension group Preop. evaluation 12 wk 1 yr 2 yr Parameter (n= 16) (n = 16) (n =8) (n = 8) Mean PAP (mm Hg) Cardiac output PVR (Wood units) PAP, Pulmonary artery pressure; PVR, pulmonary vascular resistance. hemodynamic results at 12 weeks, 1 year, and 2 years for the 18 hospital survivors is shown in Table X. The pulmonary artery pressures have not risen over time and exercise capacity in this group of patients has been equivalent to that achieved by other groups of lung transplant recipients, as shown in Table XI. On the other hand, the physiologic consequences of chronic allograft dysfunction may be significantly greater in this group of patients than in other transplant recipients. After single lung transplantation for pulmonary hypertension, greater than 90% of the blood flow is diverted to the transplanted lung because of the high vascular resistance in the native lung. However, the native lung remains more compliant than the transplanted lung, probably caused in part at least by the relative absence of pulmonary blood flow. Thus, under normal circumstances, the native lung receives more than 50% of the minute ventilation in such patients. When chronic rejection develops in the transplanted lung, its compliance further diminishes. This results in a further increase in the percent of minute ventilation going to the native lung and this in turn may produce hypercarbia and reduced oxygenation. Discussion Over the past 10 years, techniques for lung transplantation have been refined, indications have been broadened, and postoperative care has become less complicated. Of the more than 40 lung transplantations worldwide, attempted between 1963 and 1983, only one recipient was discharged from the hospital and no long-term survivals resulted. In contrast, hospital survival rates of 80% to 90% are now routinely reported from many centers, and a
9 4 6 8 Cooper et al. The Journal of Thoracic and February 1994 Table XI. Mean six-minute walk distance (m) Diagnosis At initial evaluation 12 wk 1 yr 2 yr COPD I ai-antitrypsin emphysema Single lung transplant Bilateral lung transplant Cystic fibrosis Idiopathic pulmonary hypertension Pulmonary hypertension number of lung transplant recipients continue to enjoy good health 7 and 8 years after the operation. There are a variety of reasons why our own results and those of others have improved in recent years. For the most part, we have maintained rigorous recipient selection criteria. With the exception of those patients with pulmonary hypertension, individuals who are considered acceptable are those who, despite their end-stage lung disease, are able to participate in a progressive pulmonary rehabilitation program that builds strength and endurance before transplantation. 8 Thus individuals who are bedridden and unable to temporarily relocate to St. Louis in an outpatient setting are not considered. Many recipients are significantly below ideal body weight, and every effort is made to correct this during the preoperative rehabilitation phase of our program. Whereas the patients requiring steroid administration were formerly not considered, we have, in the past several years, considered candidates whose daily prednisone requirement is 10 mg/day. Our requirement that all patients must relocate to St. Louis for at least several months before anticipated transplantation may represent a selection bias at the outset. However, after relocation in St. Louis, many recipients have significant deterioration and require hospitalization. It is from this group that we have performed transplantation in a small number of patients receiving mechanical ventilatory support. Technical advances have also reduced postoperative mortality. Early experience with en-bloc double lung transplantation was favorable, with five of the original seven recipients receiving this procedure currently alive and well 6 years or more after their transplantation. However, the broadening of indications to older patients and to patients with cystic fibrosis hospitalized at the time of transplantation for acute deterioration resulted in an operative mortality of 75%. This was dramatically reduced by application of the bilateral sequential single lung transplantation, with 7 of the 58 bilateral procedures reported in this series resulting in a hospital fatality. Application of single lung transplantation in patients previously thought eligible for only bilateral lung replace- ment has also reduced operative mortality and increased 1- and 2-year survival in our program. The issue of single versus bilateral lung transplantation for patients with chronic obstructive lung disease remains controversial. A single lung transplant has the advantage of reduced early mortality, more efficient use of donor organs, and a reduced waiting period. However, as would be expected, long-term exercise tolerance is greater after bilateral lung transplantation (see Table XI). We continue to use bilateral transplantation for obstructive lung disease when the recipient's chest is especially large, for example, in a tall male recipient. The frequency of donor ischemic airway complications has also been reduced. In the early years of our transplant experience, we favored routine use of an omental wrap around the bronchial anastomosis and strict avoidance of perioperative routine steroid administration. We no longer believe that either factor is critical. Weare currently reviewing our experience with regard to the issues of early steroid administration, technique of bronchial anastomosis, and use of an omental pedicle. The results will be submitted for publication in the near future. However, none of these factors currently appears to influence the prevalence of airway complications. The reduction in complications is likely due to improved donor lung preservation, resulting in decreased postoperative allograft dysfunction, improved management of infectious complications, and early recognition and prompt treatment of acute rejection. As a result of all these factors, time on a ventilator, number of days spent in the intensive care unit, and overall hospital stay have all been significantly shortened. Improved prophylaxis against infection has reduced the prevalence of bacterial, viral, and Pneumocystis infection. Patients with cystic fibrosis are at considerable risk for postoperative sepsis and their preoperative and postoperative antibiotic management requires particular attention. At the present time, we do not attempt trans~ plantation in patients with cystic fibrosis at a time when their organisms are resistant to all antibiotics. When this occurs, antibiotic therapy is generally modified or withdrawn in the hopes of altering the sensitivity of the predominant organisms. Sepsis was the most common cause of early and late mortality, although in the later group death from sepsis was usually associated with heightened immunosuppression for chronic rejection. Donor availability remains a critical problem. The average waiting time for patients recently listed in our program is significantly longer than that experienced by patients in our early experience. This represents a particular problem for patients with primary pulmonary hyper-
10 The Journal of Thoracic and Volume 107, Number 2 Cooper et al tension. Life expectancy in this group of patients is quite limited, and sudden death while on the transplant waiting list is not uncommon. We reviewed the waiting time for such patients from the time of our first single lung transplantation for pulmonary hypertension, in November 1989, up to January 1, During this time, 23 patients received a single lung transplant for pulmonary hypertension or Eisenmenger's syndrome with a mean waiting time of 5.2 months. During the same period of time, 12 such individuals on the waiting list died after a mean of only 1.9 months following acceptance for transplantation. As of January 1993, there were 13 such recipients awaiting transplantation and their mean waiting time averaged 7.7 months. When these figures are compared with our current average waiting time of 7 to 9 months, it can be appreciated that the anticipated death rate on the waiting list for patients with pulmonary hypertension will continue to rise significantly. Our experience with pulmonary hypertension recipients argues for a review of the current policy for lung distribution in the United States. The current allocation system is based, first, on proximity to the donor location (less than 500 miles) and, second, on time waiting for those within the 500-mile radius. Clearly, additional factors need to be considered, with particular reference to the nature and severity of the recipient's disease and the influence that this has on life expectancy. The development of chronic allograft dysfunction remains a serious problem for clinical lung transplantation. Such dysfunction is often associated with bronchiolitis obliterans, and it is widely presumed that this condition is likely due to chronic rejection. However, the clinical manifestations associated with such dysfunction mayor may not parallel the pathologic findings on either trans bronchial biopsy or open lung biopsy. In some cases, pathologic findings of bronchiolitis obliterans are associated with no clinical or functional deterioration in graft performance. In other cases, severe and progressive deterioration of graft function, strongly suggestive of chronic rejection and not attributable to any other cause, may be associated with the absence of significant pathologic findings. It was for this reason that the recent consensus conference, sponsored by the International Society of Heart and Lung Transplantation, concluded that a standard, uniform method for assessing long-term results of lung transplantation should be based primarily on functional outcome, at least for the time being. The resultant categorization of BOS provides lung transplant programs around the world the opportunity to compare results and treatment strategies for this condition. In reviewing our own experience, with respect to subsequent development of the BOS, several interesting observations can be made. In a number of patients, the BOS, even in the presence of biopsy-proved bronchiolitis obliterans, showed reversibility over time. In most patients, the reversibility was achieved by augmentation of immunosuppression. This review also provided us an opportunity to cast doubt on several notions with respect to the influence of a variety of factors on subsequent development on BOS. We anticipated that the number of early postoperative rejection episodes would show a positive correlation with the subsequent development of BOS. However, in this series, no such evidence was found. In fact, the six patients who had the highest number of early rejection episodes have shown no sign of late allograft dysfunction. Also of interest is our experience with the effect of CMV matching. It has been reported that patients having postoperative CMV infection are more likely to have subsequent bronchiolitis obliterans. In our earlier experience, we made no effort to match donor and recipient CMV status, although recently we have tried whenever possible to place CMV-negative organs into CMV-negative recipients. This policy is based on the reduced prevalence of CMV infection among CMV-negative recipients who receive CMV-negative donor organs in comparison with the almost universal prevalence of CMV infections when such recipients receive organs from a CMV-positive donor. However, despite the difference in postoperative CMV infections in these two groups of patients, there was no difference in the BOS scores between the matched and the mismatched CMV recipients. Our experience to date shows no correlation between the number of early rejection episodes, CMV matching, or type of transplantation (single versus bilateral) on the subsequent degree of allograft dysfunction, or prevalence of bronchiolitis obliterans. In view of a median follow-up of only 19 months, these conclusions must be considered tentative until confirmed by a longer period of follow-up. It is reassuring that with a minimum follow-up of 5 months and a median follow-up of 19 months, 75% of our recipients have experienced no (73%) or minimal (1.7%) evidence of BOS. On the other hand, 25% of patients have had severe impairment of function at one time or another as a result of BOS. Some of these patients did in fact have a reversible course, whereas others had significant morbidity and mortality often as a result of opportunistic infections occurring during augmented immunosuppression. The problem of progressive BOS remains that most significant obstacle to achievement of long-term success in clinical lung transplantation. Although the early survival figures after lung transplantation appear optimistic, there is no doubt that the long-term survival curve will steadily decline over time as has been the case with all
11 4 7 0 Cooper et al. The Journal of Thoracic and February 1994 other organ transplants. At this point, we estimate that the current 5-year survival will be between 50% and 60%. As is true for all other organ transplants, there is urgent need for improved immunosuppressive agents. The induction of specific tolerance, long the dream of transplant surgeons, may be on the horizon. Somewhat further off may be the era of routine xenografting, the ultimate solution to the inadequate supply of donor organs. In the meantime, the decision as to how to distribute the limited and precious supply of donor organs and how to best diagnose and treat chronic rejection will remain among the most vexing dilemmas associated with organ transplantation. We are indebted to Mary Pohl, RN, Kate Sanders, RN, Laura Ochoa, RN, Chris Boudrexl, RN, and Dru Straatman, RN, for their assistance in assembling the data used for this report, and to Kathy Stroud for her assistance in preparing the manuscript. This report represents the combined effort of members of the Washington University Lung Transplant team, among whom are thefollowing: Surgery-Joel Cooper, MD, G. Alexander Patterson, MD, Michael Pasque, MD, Charles Huddleston, MD, and Sudhir Sundaresan, MD; Pulmonary Medicine-Elbert Trulock, MD, Neil Ettinger, MD; Anesthesiology-Anastasios Triantafillou, MD, Robert Cerza, MD, George Despotis, MD, Robert Forstot, MD, Charles Hogue, MD, Demetrios Lappas, MD, and Charles Pond, M.D.; Coordinators-Chris Boudrexl, RN, Laura Ochoa, RN, Greg Richardson, RN, Kate Sanders, RN, Dru Straatman, RN; Pulmonary Rehabilitation-Dottie Biggar, RN, Kelly Walsh, PT, Carles Collins, PT, Betty Mercer. RRT, Larry Sylvester, RRT, Yvonne Sledge, RRT, and Diane Lorenz, RRT; Nutrition-Kathy Nuetzel, RD; Chaplain-Cheryl Palmar; Psychology-Deborah Schlitt, PhD. The authors, members of the transplant team, and transplant patients are grateful to the dedicated nursing staff of the thoracic surgical service, the cardiothoracic intensive care unit, the cardiothoracic operating suite, and to the cardiothoracic fellows for their tireless dedication, which has been so essential to the success of the lung transplant program. REFERENCES 1. Kerem E, Reisman J, Corey M, Canny GJ, Levison H. Prediction of mortality in patients with cystic fibrosis. N Engl J Med 1992;326: D'Alonzo GE, Barst RJ, Ayres SM, et al. Survival in patients with primary pulmonary hypertension. Ann Intern Med 1991;115: Pasque MK, Cooper JD, Kaiser LR, Haydock DA, Triantafillou A, Trulock EP. Improved technique for bilateral lung transplantation: rationale and initial clinical experience. Ann Thorac Surg 1990;49: Cooper JD. The evolution of technique and indications for lung transplantation. Ann Surg 1990;212: Yousem SA, Berry GJ, Brunt EM, et al. A working formulation for the standardization of nomenclature in the diagnosis of heart and lung rejection: lung rejection study group. J Heart Transplant 1990;9: Cooper JD, Billingham M, Egan T, et al. A working formulation for the standardization of nomenclature and for clinical staging of chronic dysfunction in lung allografts. J Heart Lung Transplant 1993;12: Pasque MK, Trulock EP, Kaiser LR, Cooper JD. Singlelung transplantation for pulmonary hypertension: threemonth hemodynamic follow-up. Circulation 1991;84: Biggar DG, Malen JF, Trulock EP, Cooper J. Pulmonary rehabilitation before and after lung transplantation. In: Principles and practice of pulmonary rehabilitation. Philadelphia: WB Saunders, 1993; Discussion Dr. Thomas M. Egan (Chapel Hill, N.c.). I have a couple of questions about your data. First of all, have you had any patients with biopsy-proved bronchiolitis obliterans who by the classification scheme for clinical disease do not have BOS? Presumably the one patient whose pulmonary function has returned to baseline values would be one of those. How many other patients have biopsy-proved bronchiolitis obliterans who in fact do not have symptoms? Have you found that the prevalence of BOS is related to the diagnosis category or age of the recipients? Finally, you cited a mean follow-up of 16 months for patients with primary pulmonary hypertension. Could you speculate on the impact of the development of bronchiolitis obliterans in patients with that degree of ventilation-perfusion mismatch at the outset? Dr. Cooper. Yes, we have some patients with proved bronchiolitis obliterans who have not shown any clinical deterioration. It was the discrepancy between the pathologic condition and the clinical picture that led to this functional classification. The condition of the man who had the functional decline and the confirming biopsy subsequently improved. Others who have had positive biopsies, category C under the staging formulation, have not had a significant decline in function. We have seen the discrepancy both ways. I cannot supply specific numbers. We have analyzed the prevalence of both BOS and pathologically proved bronchiolitis obliterans. There is no relation to the original disease. We particularly evaluated pulmonary hypertension and compared all patients receiving single lung transplants for pulmonary hypertension with all other single lung recipients in our program, and the prevalence of pathologically proved bronchiolitis obliterans or of BOS functional decline was the same for both groups. That is true of all subcategories. Finally, I would put in a word of caution regarding pulmonary hypertension. We believe that single lung transplantation for pulmonary hypertension can be done with a good success rate. However, you need the best donors and the shortest ischemic times, and the patients present a number of postoperative problems. The technique has worked out very well in our hands and has helped us to perform transplantation in more patients in a short time. You have pointed out one of the long-term problems, and this problem will surface any time single and bilateral transplants are compared, but particularly when single lung transplantation for pulmonary hypertension is evaluated. Bronchiolitis obliterans causes a far worse physiologic consequence in the patient with primary pulmonary hypertension than in any other group
Prevalence and Outcome of Bronchiolitis Obliterans Syndrome After Lung Transplantation
 Prevalence and Outcome of Bronchiolitis Obliterans Syndrome After Lung Transplantation Sudhir Sundaresan, MD, Elbert P. Trulock, MD, Thallachallour Mohanakumar, PhD, Joel D. Cooper, MD, G. Alexander Patterson,
Prevalence and Outcome of Bronchiolitis Obliterans Syndrome After Lung Transplantation Sudhir Sundaresan, MD, Elbert P. Trulock, MD, Thallachallour Mohanakumar, PhD, Joel D. Cooper, MD, G. Alexander Patterson,
The 1-year survival rate approaches 80% for patients
 Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Evolution of Surgical Therapies for End-Stage Cardiopulmonary Failure. Heart Failure at the Shoe XI October 5, 2012
 Evolution of Surgical Therapies for End-Stage Cardiopulmonary Failure Heart Failure at the Shoe XI October 5, 2012 Robert S.D. Higgins, MD, MSHA Executive Director, Comprehensive Transplant Center Evolution
Evolution of Surgical Therapies for End-Stage Cardiopulmonary Failure Heart Failure at the Shoe XI October 5, 2012 Robert S.D. Higgins, MD, MSHA Executive Director, Comprehensive Transplant Center Evolution
Single-lung transplantation in the setting of aborted bilateral lung transplantation
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2011 Single-lung transplantation in the setting of aborted bilateral lung transplantation Varun Puri Tracey Guthrie
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2011 Single-lung transplantation in the setting of aborted bilateral lung transplantation Varun Puri Tracey Guthrie
Thirteen-Year Experience in Lung Transplantation for Emphysema
 Thirteen-Year Experience in Lung Transplantation for Emphysema Stephen D. Cassivi, MD, Bryan F. Meyers, MD, Richard J. Battafarano, MD, Tracey J. Guthrie, RN, Elbert P. Trulock, MD, John P. Lynch, MD,
Thirteen-Year Experience in Lung Transplantation for Emphysema Stephen D. Cassivi, MD, Bryan F. Meyers, MD, Richard J. Battafarano, MD, Tracey J. Guthrie, RN, Elbert P. Trulock, MD, John P. Lynch, MD,
BILATERAL VERSUS SINGLE LUNG TRANSPLANTATION FOR CHRONIC OBSTRUCTIVE PULMONARY DISEASE
 BILATERAL VERSUS SINGLE LUNG TRANSPLANTATION FOR CHRONIC OBSTRUCTIVE PULMONARY DISEASE Joseph E. Bavaria, MD Robert Kotloff, MD Harold Palevsky, MD Bruce Rosengard, MD John R. Roberts, MD Peter M. Wahl,
BILATERAL VERSUS SINGLE LUNG TRANSPLANTATION FOR CHRONIC OBSTRUCTIVE PULMONARY DISEASE Joseph E. Bavaria, MD Robert Kotloff, MD Harold Palevsky, MD Bruce Rosengard, MD John R. Roberts, MD Peter M. Wahl,
Does the Presence of Preoperative Mild or Moderate Coronary Artery Disease Affect the Outcomes of Lung Transplantation?
 Does the Presence of Preoperative Mild or Moderate Coronary Artery Disease Affect the Outcomes of Lung Transplantation? Cliff K. Choong, FRACS, Bryan F. Meyers, MD, Tracey J. Guthrie, BSN, Elbert P. Trulock,
Does the Presence of Preoperative Mild or Moderate Coronary Artery Disease Affect the Outcomes of Lung Transplantation? Cliff K. Choong, FRACS, Bryan F. Meyers, MD, Tracey J. Guthrie, BSN, Elbert P. Trulock,
RISK FACTORS FOR THE DEVELOPMENT OF BRONCHIOLITIS OBLITERANS SYNDROME AFTER LUNG TRANSPLANTATION
 Illllll RISK FACTORS FOR THE DEVELOPMENT OF BRONCHIOLITIS OBLITERANS SYNDROME AFTER LUNG TRANSPLANTATION Timothy J. Kroshus, MD Vibhu R. Kshettry, MD Kay Savik, MS Ranjit John, MD Marshall I. Hertz, MD
Illllll RISK FACTORS FOR THE DEVELOPMENT OF BRONCHIOLITIS OBLITERANS SYNDROME AFTER LUNG TRANSPLANTATION Timothy J. Kroshus, MD Vibhu R. Kshettry, MD Kay Savik, MS Ranjit John, MD Marshall I. Hertz, MD
Clinical- Pathologic Conference
 Clinical- Pathologic Conference Clinical-pathologic conference in general thoracic surgery: Bilateral lung transplantation for sarcoidosis with aspergilloma G. Alexander Patterson, MD From the Washington
Clinical- Pathologic Conference Clinical-pathologic conference in general thoracic surgery: Bilateral lung transplantation for sarcoidosis with aspergilloma G. Alexander Patterson, MD From the Washington
Reperfusion Injury Significantly Impacts Clinical Outcome After Pulmonary Transplantation
 Reperfusion Injury Significantly Impacts Clinical Outcome After Pulmonary Transplantation Robert C. King, MD, Oliver A. R. Binns, MD, Filiberto Rodriguez, MD, R. Chai Kanithanon, BA, Thomas M. Daniel,
Reperfusion Injury Significantly Impacts Clinical Outcome After Pulmonary Transplantation Robert C. King, MD, Oliver A. R. Binns, MD, Filiberto Rodriguez, MD, R. Chai Kanithanon, BA, Thomas M. Daniel,
INTERNET-BASED HOME MONITORING OF PULMONARY FUNCTION AFTER LUNG TRANSPLANTATION. 2000, 25 patients underwent heart lung (HLT) or bilateral-lung (BLT)
 Online Supplement for: INTERNET-BASED HOME MONITORING OF PULMONARY FUNCTION AFTER LUNG TRANSPLANTATION METHODS Patients Between the start of the study in June 1998 and the end of the study in September
Online Supplement for: INTERNET-BASED HOME MONITORING OF PULMONARY FUNCTION AFTER LUNG TRANSPLANTATION METHODS Patients Between the start of the study in June 1998 and the end of the study in September
R replacement that uses a sequential implantation. Bilateral Sequential Lung Transplantation: The Procedure of Choice for Double-Lung Replacement
 Bilateral Sequential Lung Transplantation: The Procedure of Choice for Double-Lung Replacement Larry R. Kaiser, MD, Michael K. Pasque, MD, Elbert P. Trulock, MD, Donald E. Low, MD, Carolyn M. Dresler,
Bilateral Sequential Lung Transplantation: The Procedure of Choice for Double-Lung Replacement Larry R. Kaiser, MD, Michael K. Pasque, MD, Elbert P. Trulock, MD, Donald E. Low, MD, Carolyn M. Dresler,
Pressure to expand the donor pool has affected all
 Effect of Donor Age and Ischemic Time on Intermediate Survival and Morbidity After Lung Transplantation* Dan M. Meyer, MD; Leah E. Bennett, PhD; Richard J. Novick, MD; and Jeffrey D. Hosenpud, MD Background:
Effect of Donor Age and Ischemic Time on Intermediate Survival and Morbidity After Lung Transplantation* Dan M. Meyer, MD; Leah E. Bennett, PhD; Richard J. Novick, MD; and Jeffrey D. Hosenpud, MD Background:
Analysis of time-dependent risks for infection, rejection, and death after pulmonary transplantation
 Cardiac and Pulmonary Replacement Analysis of time-dependent risks for infection, rejection, and death after pulmonary transplantation Infection and rejection remain the greatest threats to the survival
Cardiac and Pulmonary Replacement Analysis of time-dependent risks for infection, rejection, and death after pulmonary transplantation Infection and rejection remain the greatest threats to the survival
Citation for published version (APA): Ouwens, J. P. (2002). The Groningen lung transplant program: 10 years of experience Groningen: s.n.
 University of Groningen The Groningen lung transplant program Ouwens, Jan Paul IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen The Groningen lung transplant program Ouwens, Jan Paul IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
E most common indication for bilateral lung transplantation.
 Double-Lung Transplantation in Mechanically Ventilated Patients With Cystic Fibrosis Gilbert Massard, MD, Hani Shennib, MD, Dominique Metras, MD, Jean Camboulives, MD, Laurent Viard, MD, David S. Mulder,
Double-Lung Transplantation in Mechanically Ventilated Patients With Cystic Fibrosis Gilbert Massard, MD, Hani Shennib, MD, Dominique Metras, MD, Jean Camboulives, MD, Laurent Viard, MD, David S. Mulder,
06/04/2013 ISHLT. 2 International Conference on Respiratory Physiotherapy ARIR Genova, March 21 23, 2013
 LUNG TRANSPLANTS The Journal of Heart and Lung Transplantation, 2012 2 International Conference on Respiratory Physiotherapy ARIR Genova, March 21 23, 2013 LUNG TRANSPLANTATION:STATE OF THE ART L. Santambrogio
LUNG TRANSPLANTS The Journal of Heart and Lung Transplantation, 2012 2 International Conference on Respiratory Physiotherapy ARIR Genova, March 21 23, 2013 LUNG TRANSPLANTATION:STATE OF THE ART L. Santambrogio
Citation for published version (APA): Ouwens, J. P. (2002). The Groningen lung transplant program: 10 years of experience Groningen: s.n.
 University of Groningen The Groningen lung transplant program Ouwens, Jan Paul IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen The Groningen lung transplant program Ouwens, Jan Paul IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ
 Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ Art of Good Cooking Good Ingredient Good donor + OK recipient Good technique Good team Good timing Good
Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ Art of Good Cooking Good Ingredient Good donor + OK recipient Good technique Good team Good timing Good
LONG-TERM RESULTS OF CARDIAC TRANSPLANTATION IN PATIENTS OLDER THAN SIXTY YEARS
 LONG-TERM RESULTS OF CARDIAC TRANSPLANTATION IN PATIENTS OLDER THAN SIXTY YEARS Advanced age has traditionally been a contraindication to cardiac transplantation. We have, however, offered cardiac transplantation
LONG-TERM RESULTS OF CARDIAC TRANSPLANTATION IN PATIENTS OLDER THAN SIXTY YEARS Advanced age has traditionally been a contraindication to cardiac transplantation. We have, however, offered cardiac transplantation
L dure for patients with end-stage pulmonary disease.
 HOW TO DO IT Donor Lung Procurement: Assessment and Operative Technique Sudhir Sundaresan, MD, Gregory D. Trachiotis, MD, Motoi Aoe, MD, G. Alexander Patterson, MD, and Joel D. Cooper, MD Division of Cardiothoracic
HOW TO DO IT Donor Lung Procurement: Assessment and Operative Technique Sudhir Sundaresan, MD, Gregory D. Trachiotis, MD, Motoi Aoe, MD, G. Alexander Patterson, MD, and Joel D. Cooper, MD Division of Cardiothoracic
Lung transplantation has become a feasible option. Bronchiolitis Obliterans Syndrome and Additional Costs of Lung Transplantation*
 Bronchiolitis Obliterans Syndrome and Additional Costs of Lung Transplantation* Jan W. K. van den Berg, MD, PhD; Petra J. van Enckevort, PhD; Elisabeth M. TenVergert, PhD; Dirkje S. Postma, MD, PhD; Wim
Bronchiolitis Obliterans Syndrome and Additional Costs of Lung Transplantation* Jan W. K. van den Berg, MD, PhD; Petra J. van Enckevort, PhD; Elisabeth M. TenVergert, PhD; Dirkje S. Postma, MD, PhD; Wim
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Lung Allograft Dysfunction
 Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Objectives: The objective of this study was to examine the long-term patient outcomes of lung transplantation in a single center.
 Twenty-year experience of lung transplantation at a single center: Influence of recipient diagnosis on long-term survival Marc de Perrot, MD Cecilia Chaparro, MD Karen McRae, MD Thomas K. Waddell, MD Denis
Twenty-year experience of lung transplantation at a single center: Influence of recipient diagnosis on long-term survival Marc de Perrot, MD Cecilia Chaparro, MD Karen McRae, MD Thomas K. Waddell, MD Denis
Lung Transplantation in the United States,
 American Journal of Transplantation 2009; 9 (Part 2): 942 958 Wiley Periodicals Inc. No claim to original US government works Journal compilation C 2009 The American Society of Transplantation and the
American Journal of Transplantation 2009; 9 (Part 2): 942 958 Wiley Periodicals Inc. No claim to original US government works Journal compilation C 2009 The American Society of Transplantation and the
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Ontario s Referral and Listing Criteria for Adult Heart Transplantation
 Ontario s Referral and Listing Criteria for Adult Heart Transplantation Version 3.0 Trillium Gift of Life Network Adult Heart Transplantation Referral & Listing Criteria PATIENT REFERRAL CRITERIA: The
Ontario s Referral and Listing Criteria for Adult Heart Transplantation Version 3.0 Trillium Gift of Life Network Adult Heart Transplantation Referral & Listing Criteria PATIENT REFERRAL CRITERIA: The
End-stage pulmonary vascular disease occurs in a. Lung Transplantation for Pulmonary Vascular Disease
 ORIGINAL ARTICLES: GENERAL THORACIC Lung Transplantation for Pulmonary Vascular Disease Eric N. Mendeloff, MD, Bryan F. Meyers, MD, Thoralf M. Sundt, MD, Tracey J. Guthrie, BSN, Stuart C. Sweet, MD, Maite
ORIGINAL ARTICLES: GENERAL THORACIC Lung Transplantation for Pulmonary Vascular Disease Eric N. Mendeloff, MD, Bryan F. Meyers, MD, Thoralf M. Sundt, MD, Tracey J. Guthrie, BSN, Stuart C. Sweet, MD, Maite
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Progression pattern of restrictive allograft syndrome after lung transplantation
 http://www.jhltonline.org FEATURED ARTICLES Progression pattern of restrictive allograft syndrome after lung transplantation Masaaki Sato, MD, PhD, a,b David M. Hwang, MD, PhD, a Thomas K. Waddell, MD,
http://www.jhltonline.org FEATURED ARTICLES Progression pattern of restrictive allograft syndrome after lung transplantation Masaaki Sato, MD, PhD, a,b David M. Hwang, MD, PhD, a Thomas K. Waddell, MD,
Chapter 4 Section 24.1
 Surgery Chapter 4 Section 24.1 Issue Date: October 27, 1995 Authority: 32 CFR 199.4(e)(5) 1.0 CPT 1 PROCEDURE CODES 32850-32854, 33930-33935 2.0 DIAGNOSTIC RELATED GROUPS (DRGs) 495 for lung transplant.
Surgery Chapter 4 Section 24.1 Issue Date: October 27, 1995 Authority: 32 CFR 199.4(e)(5) 1.0 CPT 1 PROCEDURE CODES 32850-32854, 33930-33935 2.0 DIAGNOSTIC RELATED GROUPS (DRGs) 495 for lung transplant.
TREATMENT OF REFRACTORY ACUTE ALLOGRAFT REJECTION WITH AEROSOLIZED CYCLOSPORINE IN LUNG TRANSPLANT RECIPIENTS
 TREATMENT OF REFRACTORY ACUTE ALLOGRAFT REJECTION WITH AEROSOLIZED CYCLOSPORINE IN LUNG TRANSPLANT RECIPIENTS Robert J. Keenan, MD Aldo Iacono, MD James H. Dauber, MD Adriana Zeevi, PhD Samuel A. Yousem,
TREATMENT OF REFRACTORY ACUTE ALLOGRAFT REJECTION WITH AEROSOLIZED CYCLOSPORINE IN LUNG TRANSPLANT RECIPIENTS Robert J. Keenan, MD Aldo Iacono, MD James H. Dauber, MD Adriana Zeevi, PhD Samuel A. Yousem,
CHAPTER 3 SECTION 1.6B HEART-LUNG AND LUNG TRANSPLANTATION TRICARE POLICY MANUAL M, MARCH 15, 2002 SURGERY AND RELATED SERVICES
 TRICARE POLICY MANUAL 6010.47-M, MARCH 15, 2002 SURGERY AND RELATED SERVICES CHAPTER 3 SECTION 1.6B ISSUE DATE: October 27, 1995 AUTHORITY: 32 CFR 199.4(e)(5) I. CODES A. CPT 1 Procedure Codes 33930, 33935,
TRICARE POLICY MANUAL 6010.47-M, MARCH 15, 2002 SURGERY AND RELATED SERVICES CHAPTER 3 SECTION 1.6B ISSUE DATE: October 27, 1995 AUTHORITY: 32 CFR 199.4(e)(5) I. CODES A. CPT 1 Procedure Codes 33930, 33935,
Single-lung retransplantation for late graft failure.
 Eur Resplr J, 1993, 6, 1202-1206 Printed in UK all rights reserved Copyright ERS Journals Ltd 1993 European Respiratory Journal ISSN 0903 1936 Single-lung retransplantation for late graft failure M. Foumier*,
Eur Resplr J, 1993, 6, 1202-1206 Printed in UK all rights reserved Copyright ERS Journals Ltd 1993 European Respiratory Journal ISSN 0903 1936 Single-lung retransplantation for late graft failure M. Foumier*,
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: heart_lung_transplantation 5/1985 6/2018 6/2019 6/2018 Description of Procedure or Service Combined heart/lung
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: heart_lung_transplantation 5/1985 6/2018 6/2019 6/2018 Description of Procedure or Service Combined heart/lung
H tients with end-stage pulmonary hypertension was
 Pediatric Lung Transplantation for Pulmonary Hypertension and Congenital Heart Disease Thomas L. Spray, MD, George B. Mallory, MD, Charles E. Canter, MD, Charles B. Huddleston, MD, and Larry R. Kaiser,
Pediatric Lung Transplantation for Pulmonary Hypertension and Congenital Heart Disease Thomas L. Spray, MD, George B. Mallory, MD, Charles E. Canter, MD, Charles B. Huddleston, MD, and Larry R. Kaiser,
Original Policy Date
 MP 7.03.07 Heart/Lung Transplant Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
MP 7.03.07 Heart/Lung Transplant Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
Lung transplantation for individuals with endstage
 CARDIOPULMONARY BYPASS IS ASSOCIATED WITH EARLY ALLOGRAFT DYSFUNCTION BUT NOT DEATH AFTER DOUBLE-LUNG TRAPLANTATION James S. Gammie, MD Jung Cheul Lee, MD Si M. Pham, MD Robert J. Keenan, MD Robert J.
CARDIOPULMONARY BYPASS IS ASSOCIATED WITH EARLY ALLOGRAFT DYSFUNCTION BUT NOT DEATH AFTER DOUBLE-LUNG TRAPLANTATION James S. Gammie, MD Jung Cheul Lee, MD Si M. Pham, MD Robert J. Keenan, MD Robert J.
Living lobar lung transplantation was developed as an alternative
 Living Lobar Lung Transplantation Michael K. McLean, MD, Mark L. Barr, MD, and Vaughn A. Starnes, MD Living lobar lung transplantation was developed as an alternative to cadaver lung transplantation because
Living Lobar Lung Transplantation Michael K. McLean, MD, Mark L. Barr, MD, and Vaughn A. Starnes, MD Living lobar lung transplantation was developed as an alternative to cadaver lung transplantation because
CARDIOVASCULAR SURGERY
 Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
Certified Clinical Transplant Nurse (CCTN) * Detailed Content Outline
 I. PRETRANSPLANTATION CARE 9 11 3 23 A. Evaluate End-Stage Organ Failure 1 1 1 3 1. History and physical assessment 2. Vital signs and / or hemodynamic parameters 3. Lab values 4. Diagnostic tests B. Monitor
I. PRETRANSPLANTATION CARE 9 11 3 23 A. Evaluate End-Stage Organ Failure 1 1 1 3 1. History and physical assessment 2. Vital signs and / or hemodynamic parameters 3. Lab values 4. Diagnostic tests B. Monitor
Idiopathic pulmonary fibrosis (IPF) is a major type. A New Treatment Strategy for Advanced Idiopathic Interstitial Pneumonia*
 A New Treatment Strategy for Advanced Idiopathic Interstitial Pneumonia* Living-Donor Lobar Lung Transplantation Hiroshi Date, MD; Yasushi Tanimoto, MD; Keiji Goto, MD; Ichiro Yamadori, MD; Motoi Aoe,
A New Treatment Strategy for Advanced Idiopathic Interstitial Pneumonia* Living-Donor Lobar Lung Transplantation Hiroshi Date, MD; Yasushi Tanimoto, MD; Keiji Goto, MD; Ichiro Yamadori, MD; Motoi Aoe,
LIVING-DONOR LOBAR LUNG TRANSPLANTATION EXPERIENCE: INTERMEDIATE RESULTS
 LIVING-DONOR LOBAR LUNG TRANSPLANTATION EXPERIENCE: INTERMEDIATE RESULTS Vaughn A. Starnes Mark L. Barr Robbin G. Cohen Jeffrey A. Hagen Winfield J. Wells Monica V. Horn Felicia A. Schenkel Objective:
LIVING-DONOR LOBAR LUNG TRANSPLANTATION EXPERIENCE: INTERMEDIATE RESULTS Vaughn A. Starnes Mark L. Barr Robbin G. Cohen Jeffrey A. Hagen Winfield J. Wells Monica V. Horn Felicia A. Schenkel Objective:
T evolved from en bloc heart-lung transplantation to en
 Double-Lung Transplantation in Children: A Report of 20 Cases Dominique Mktras, MD, Hani Shennib, MD, Bernard Kreitmann, MD, Jean Camboulives, MD, Laurent Viard, MD, Michel Carcassonne, MD, Roger Giudicelli,
Double-Lung Transplantation in Children: A Report of 20 Cases Dominique Mktras, MD, Hani Shennib, MD, Bernard Kreitmann, MD, Jean Camboulives, MD, Laurent Viard, MD, Michel Carcassonne, MD, Roger Giudicelli,
Living-donor lobar lung transplantation (LDLLT) was developed by. Living-donor lobar lung transplantation for various lung diseases.
 Cardiothoracic Transplantation Date et al Living-donor lobar lung transplantation for various lung diseases Hiroshi Date, MD, a Motoi Aoe, MD, a Itaru Nagahiro, MD, a Yoshifumi Sano, MD, a Akio Andou,
Cardiothoracic Transplantation Date et al Living-donor lobar lung transplantation for various lung diseases Hiroshi Date, MD, a Motoi Aoe, MD, a Itaru Nagahiro, MD, a Yoshifumi Sano, MD, a Akio Andou,
Glossary. Anesthesiologist A doctor who puts you or parts of your body to sleep during surgery.
 1-Glossary Glossary Acute rejection A type of rejection that occurs when immune cells from your body attack the transplanted organ(s). Acute rejection may occur at any time after a transplant. But it usually
1-Glossary Glossary Acute rejection A type of rejection that occurs when immune cells from your body attack the transplanted organ(s). Acute rejection may occur at any time after a transplant. But it usually
Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600
 Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Preoperative Workup for Pulmonary Resection. Kristen Bridges, M.D. Richmond University Medical Center January 21, 2016
 Preoperative Workup for Pulmonary Resection Kristen Bridges, M.D. Richmond University Medical Center January 21, 2016 Patient Presentation 50 yo male with 70 pack year smoking history Large R hilar lung
Preoperative Workup for Pulmonary Resection Kristen Bridges, M.D. Richmond University Medical Center January 21, 2016 Patient Presentation 50 yo male with 70 pack year smoking history Large R hilar lung
Heart/Lung Transplant
 Medical Policy Manual Transplant, Policy No. 03 Heart/Lung Transplant Next Review: March 2019 Last Review: April 2018 Effective: June 1, 2018 IMPORTANT REMINDER Medical Policies are developed to provide
Medical Policy Manual Transplant, Policy No. 03 Heart/Lung Transplant Next Review: March 2019 Last Review: April 2018 Effective: June 1, 2018 IMPORTANT REMINDER Medical Policies are developed to provide
Lung Transplantation A look Inside A Surgeon s Perspective
 Lung Transplantation A look Inside A Surgeon s Perspective Hassan Nemeh, MD Henry Ford Hospital Michigan Society of Respiratory Care Spring Conference 2016 Historical background Alexis Carrel 1905 Reported
Lung Transplantation A look Inside A Surgeon s Perspective Hassan Nemeh, MD Henry Ford Hospital Michigan Society of Respiratory Care Spring Conference 2016 Historical background Alexis Carrel 1905 Reported
Reduction in Airway Complications After Lung Transplantation With Novel Anastomotic Technique
 Reduction in Airway Complications After Lung Transplantation With Novel Anastomotic Technique Elizabeth FitzSullivan, MD, Cynthia J. Gries, MD, Patrick Phelan, MD, Farhood Farjah, MD, Erin Gilbert, MD,
Reduction in Airway Complications After Lung Transplantation With Novel Anastomotic Technique Elizabeth FitzSullivan, MD, Cynthia J. Gries, MD, Patrick Phelan, MD, Farhood Farjah, MD, Erin Gilbert, MD,
Clinical Policy: Heart-Lung Transplant Reference Number: CP.MP.132
 Clinical Policy: Reference Number: CP.MP.132 Effective Date: 01/18 Last Review Date: 05/18 Coding Implications Revision Log Description Heart-lung transplantation is treatment of choice for patients with
Clinical Policy: Reference Number: CP.MP.132 Effective Date: 01/18 Last Review Date: 05/18 Coding Implications Revision Log Description Heart-lung transplantation is treatment of choice for patients with
SINCE the introduction of Imuran and
 Cadaveric Renal Transplantation With Cyclosporin-A and Steroids T. R. Hakala, T. E. Starzl, J. T. Rosenthal, B. Shaw, and S. watsuki SNCE the introduction of muran and prednisone in 1961, and despite the
Cadaveric Renal Transplantation With Cyclosporin-A and Steroids T. R. Hakala, T. E. Starzl, J. T. Rosenthal, B. Shaw, and S. watsuki SNCE the introduction of muran and prednisone in 1961, and despite the
We have no disclosures
 Pulmonary Artery Pressure Changes Differentially Effect Survival in Lung Transplant Patients with COPD and Pulmonary Hypertension: An Analysis of the UNOS Registry Kathryn L. O Keefe MD, Ahmet Kilic MD,
Pulmonary Artery Pressure Changes Differentially Effect Survival in Lung Transplant Patients with COPD and Pulmonary Hypertension: An Analysis of the UNOS Registry Kathryn L. O Keefe MD, Ahmet Kilic MD,
Induction Immunosuppression With Rabbit Antithymocyte Globulin in Pediatric Liver Transplantation
 LIVER TRANSPLANTATION 12:1210-1214, 2006 ORIGINAL ARTICLE Induction Immunosuppression With Rabbit Antithymocyte Globulin in Pediatric Liver Transplantation Ashesh Shah, 1 Avinash Agarwal, 1 Richard Mangus,
LIVER TRANSPLANTATION 12:1210-1214, 2006 ORIGINAL ARTICLE Induction Immunosuppression With Rabbit Antithymocyte Globulin in Pediatric Liver Transplantation Ashesh Shah, 1 Avinash Agarwal, 1 Richard Mangus,
Policy Specific Section: May 16, 1984 April 9, 2014
 Medical Policy Heart Transplant Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Transplant Original Policy Date: Effective Date: May 16, 1984 April 9, 2014 Definitions
Medical Policy Heart Transplant Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Transplant Original Policy Date: Effective Date: May 16, 1984 April 9, 2014 Definitions
Donor-specific cytotoxic T lymphocytes (CTL) are
 CYTOTOXIC T LYMPHOCYTES DIRECTED AGAINST DONOR HLA CLASS I ANTIGENS ON AIRWAY EPITHELIAL CELLS ARE PRESENT IN BRONCHOALVEOLAR LAVAGE FLUID FROM LUNG TRANSPLANT RECIPIENTS DURING ACUTE REJECTION Jun Nakajima,
CYTOTOXIC T LYMPHOCYTES DIRECTED AGAINST DONOR HLA CLASS I ANTIGENS ON AIRWAY EPITHELIAL CELLS ARE PRESENT IN BRONCHOALVEOLAR LAVAGE FLUID FROM LUNG TRANSPLANT RECIPIENTS DURING ACUTE REJECTION Jun Nakajima,
Bilateral Versus Single Lung Transplant for Idiopathic Pulmonary Fibrosis
 ArtIcle Bilateral Versus Single Lung Transplant for Idiopathic Pulmonary Fibrosis Sven Lehmann, 1* Madlen Uhlemann, 2* Sergey Leontyev, 1 Joerg Seeburger, 1 Jens Garbade, 1 Denis R. Merk, 1 Hartmuth B.
ArtIcle Bilateral Versus Single Lung Transplant for Idiopathic Pulmonary Fibrosis Sven Lehmann, 1* Madlen Uhlemann, 2* Sergey Leontyev, 1 Joerg Seeburger, 1 Jens Garbade, 1 Denis R. Merk, 1 Hartmuth B.
Use of the Total Artificial Heart in the Failing Fontan Circulation J William Gaynor, M.D.
 Use of the Total Artificial Heart in the Failing Fontan Circulation J William Gaynor, M.D. Daniel M. Tabas Endowed Chair in Pediatric Cardiothoracic Surgery at The Children s Hospital of Philadelphia The
Use of the Total Artificial Heart in the Failing Fontan Circulation J William Gaynor, M.D. Daniel M. Tabas Endowed Chair in Pediatric Cardiothoracic Surgery at The Children s Hospital of Philadelphia The
5/15/2018. Background. Disclosure Statement
 5/15/218 Efficacy of Bronchoscopically-Administered in the Setting of Primary Graft Dysfunction after Lung Transplantation Primary Investigator: Sana Ahmed, PharmD Research Associates: Matthew Soto-Arenall,
5/15/218 Efficacy of Bronchoscopically-Administered in the Setting of Primary Graft Dysfunction after Lung Transplantation Primary Investigator: Sana Ahmed, PharmD Research Associates: Matthew Soto-Arenall,
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
Patient Name: MRN: DOB: Treatment Location:
 Page 1 of 5 I. TO (Required) This Section is required to be completed by all patients who undergo kidney transplant surgery. I hereby consent to and authorize Dr. and his/her assistant(s), including supervised
Page 1 of 5 I. TO (Required) This Section is required to be completed by all patients who undergo kidney transplant surgery. I hereby consent to and authorize Dr. and his/her assistant(s), including supervised
Heart/Lung Transplant. Populations Interventions Comparators Outcomes Individuals: With end-stage cardiac and pulmonary disease.
 Protocol Heart/Lung Transplant (70308) Medical Benefit Effective Date: 04/01/14 Next Review Date: 01/19 Preauthorization Yes Review Dates: 01/10, 01/11, 01/12, 01/13, 01/14, 01/15, 01/16, 01/17, 01/18
Protocol Heart/Lung Transplant (70308) Medical Benefit Effective Date: 04/01/14 Next Review Date: 01/19 Preauthorization Yes Review Dates: 01/10, 01/11, 01/12, 01/13, 01/14, 01/15, 01/16, 01/17, 01/18
Lung Transplantation. Introduction. Current Status
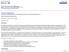 Page 1 of 24 To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/436545 Lung Transplantation This activity is made possible
Page 1 of 24 To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/436545 Lung Transplantation This activity is made possible
The Pulmonary Pathology of Iatrogenic Immunosuppression. Kevin O. Leslie, M.D. Mayo Clinic Scottsdale
 The Pulmonary Pathology of Iatrogenic Immunosuppression Kevin O. Leslie, M.D. Mayo Clinic Scottsdale The indications for iatrogenic immunosuppression Autoimmune/inflammatory disease Chemotherapy for malignant
The Pulmonary Pathology of Iatrogenic Immunosuppression Kevin O. Leslie, M.D. Mayo Clinic Scottsdale The indications for iatrogenic immunosuppression Autoimmune/inflammatory disease Chemotherapy for malignant
Lung and Lobar Lung Transplant. Populations Interventions Comparators Outcomes Individuals: With end-stage pulmonary disease
 Protocol Lung and Lobar Lung Transplant (70307) Medical Benefit Effective Date: 07/01/14 Next Review Date: 03/19 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 03/13, 03/14, 03/15, 03/16,
Protocol Lung and Lobar Lung Transplant (70307) Medical Benefit Effective Date: 07/01/14 Next Review Date: 03/19 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 03/13, 03/14, 03/15, 03/16,
The diagnosis and treatment of cardiac rejection is
 ORIGINAL ARTICLES: CARDIOVASCULAR Routine Surveillance Endomyocardial Biopsy: Late Rejection After Heart Transplantation David A. Heimansohn, MD, Robert J. Robison, MD, John M. Paris III, MD, Robert G.
ORIGINAL ARTICLES: CARDIOVASCULAR Routine Surveillance Endomyocardial Biopsy: Late Rejection After Heart Transplantation David A. Heimansohn, MD, Robert J. Robison, MD, John M. Paris III, MD, Robert G.
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Liver Transplantation
 1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
Alpha-1 Antitrypsin Deficiency Alpha-1 Lung Disease
 Alpha-1 Antitrypsin Deficiency Alpha-1 Lung Disease Chronic obstructive pulmonary disease (COPD) affects millions of people each year. Chronic means long term, obstructive means it is hard to get air in
Alpha-1 Antitrypsin Deficiency Alpha-1 Lung Disease Chronic obstructive pulmonary disease (COPD) affects millions of people each year. Chronic means long term, obstructive means it is hard to get air in
Positioning Biologics in Ulcerative Colitis
 Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency
 Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency Ken-ichi ASANO, M.D., Masahiko WASHIO, M.D., and Shoji EGUCHI, M.D. SUMMARY (1) Surgical results of
Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency Ken-ichi ASANO, M.D., Masahiko WASHIO, M.D., and Shoji EGUCHI, M.D. SUMMARY (1) Surgical results of
Methods ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE
 ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE Li-Hui Soh, Chih-Feng Chian, Wen-Lin Su, Horng-Chin Yan, Wann-Cherng Perng, and Chin-Pyng Wu Background
ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE Li-Hui Soh, Chih-Feng Chian, Wen-Lin Su, Horng-Chin Yan, Wann-Cherng Perng, and Chin-Pyng Wu Background
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Lung Transplantation for Primary and Secondary Pulmonary Hypertension
 Lung Transplantation for Primary and Secondary Pulmonary Hypertension John V. Conte, MD, Marvin J. Borja, BS, Chandrahas B. Patel, BS, Steven C. Yang, MD, Rajiv M. Jhaveri, MD, and Jonathan B. Orens, MD
Lung Transplantation for Primary and Secondary Pulmonary Hypertension John V. Conte, MD, Marvin J. Borja, BS, Chandrahas B. Patel, BS, Steven C. Yang, MD, Rajiv M. Jhaveri, MD, and Jonathan B. Orens, MD
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Preoperative Pulmonary Evaluation. Michelle Zetoony, DO, FCCP, FACOI Board Certified Pulmonary, Critical Care, Sleep and Internal Medicine
 Preoperative Pulmonary Evaluation Michelle Zetoony, DO, FCCP, FACOI Board Certified Pulmonary, Critical Care, Sleep and Internal Medicine No disclosures related to this lecture. Objectives Identify pulmonary
Preoperative Pulmonary Evaluation Michelle Zetoony, DO, FCCP, FACOI Board Certified Pulmonary, Critical Care, Sleep and Internal Medicine No disclosures related to this lecture. Objectives Identify pulmonary
Extreme pulmonary hypertension caused by mitral valve disease
 British Heart Journal, I975, 37, 74-78. Extreme pulmonary hypertension caused by mitral valve disease Natural history and results of surgery C. Ward and B. W. Hancock From the Cardio-Thoracic Unit, Northern
British Heart Journal, I975, 37, 74-78. Extreme pulmonary hypertension caused by mitral valve disease Natural history and results of surgery C. Ward and B. W. Hancock From the Cardio-Thoracic Unit, Northern
NHS. Living-donor lung transplantation for end-stage lung disease. National Institute for Health and Clinical Excellence. Issue date: May 2006
 NHS National Institute for Health and Clinical Excellence Issue date: May 2006 Living-donor lung transplantation for end-stage Understanding NICE guidance information for people considering the procedure,
NHS National Institute for Health and Clinical Excellence Issue date: May 2006 Living-donor lung transplantation for end-stage Understanding NICE guidance information for people considering the procedure,
Heart/Lung Transplant. Description
 Subject: Heart/Lung Transplant Page: 1 of 10 Last Review Status/Date: March 2016 Heart/Lung Transplant Description The heart/lung transplantation involves a coordinated triple operative procedure consisting
Subject: Heart/Lung Transplant Page: 1 of 10 Last Review Status/Date: March 2016 Heart/Lung Transplant Description The heart/lung transplantation involves a coordinated triple operative procedure consisting
Chapter 6: Transplantation
 Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Subclinical Problems in the ICU:
 Subclinical Problems in the ICU: Corticosteroid Insufficiency C. S. Cutillar, M.D., FPCP, FPSEM Associate Professor Cebu Institute of Medicine H-P-A Axis during Critical Illness CRH ACTH H-P-A Axis during
Subclinical Problems in the ICU: Corticosteroid Insufficiency C. S. Cutillar, M.D., FPCP, FPSEM Associate Professor Cebu Institute of Medicine H-P-A Axis during Critical Illness CRH ACTH H-P-A Axis during
Transplant in Pediatric Heart Failure
 Transplant in Pediatric Heart Failure Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart and Lung Transplantation
Transplant in Pediatric Heart Failure Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart and Lung Transplantation
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Bronchiolitis obliterans syndrome (BOS) results in a
 Ischemia-Reperfusion Injury After Lung Transplantation Increases Risk of Late Bronchiolitis Obliterans Syndrome Steven M. Fiser, MD, Curtis G. Tribble, MD, Stewart M. Long, MD, Aditya K. Kaza, MD, John
Ischemia-Reperfusion Injury After Lung Transplantation Increases Risk of Late Bronchiolitis Obliterans Syndrome Steven M. Fiser, MD, Curtis G. Tribble, MD, Stewart M. Long, MD, Aditya K. Kaza, MD, John
ISPUB.COM. Rare Cases: Tracheal/bronchial Obstruction. O Wenker, L Moehn, C Portera, G Walsh HISTORY ADMISSION
 ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
Pediatric Kidney Transplantation
 Pediatric Kidney Transplantation Vikas Dharnidharka, MD, MPH Associate Professor Division of Pediatric Nephrology Conflict of Interest Disclosure Vikas Dharnidharka, MD, MPH Employer: University of Florida
Pediatric Kidney Transplantation Vikas Dharnidharka, MD, MPH Associate Professor Division of Pediatric Nephrology Conflict of Interest Disclosure Vikas Dharnidharka, MD, MPH Employer: University of Florida
Living lobar lung transplantation was introduced in 1993 in response. A decade of living lobar lung transplantation: Recipient outcomes GTS
 A decade of living lobar lung transplantation: Recipient outcomes Vaughn A. Starnes, MD Michael E. Bowdish, MD Marlyn S. Woo, MD Richard G. Barbers, MD Felicia A. Schenkel, RN Monica V. Horn, RN Renzo
A decade of living lobar lung transplantation: Recipient outcomes Vaughn A. Starnes, MD Michael E. Bowdish, MD Marlyn S. Woo, MD Richard G. Barbers, MD Felicia A. Schenkel, RN Monica V. Horn, RN Renzo
Fariba Rezaeetalab Associate Professor,Pulmonologist
 Fariba Rezaeetalab Associate Professor,Pulmonologist rezaitalabf@mums.ac.ir Patient related risk factors Procedure related risk factors Preoperative risk assessment Risk reduction strategies Age Obesity
Fariba Rezaeetalab Associate Professor,Pulmonologist rezaitalabf@mums.ac.ir Patient related risk factors Procedure related risk factors Preoperative risk assessment Risk reduction strategies Age Obesity
PCI in Patients with Transplant Coronary Artery Disease. Michael S. Lee, MD, FACC, FSCAI Assistant Professor UCLA School of Medicine
 PCI in Patients with Transplant Coronary Artery Disease Michael S. Lee, MD, FACC, FSCAI Assistant Professor UCLA School of Medicine Faculty Disclosure Honararia for Boston Scientific, BMS, Daiichi Sankyo,
PCI in Patients with Transplant Coronary Artery Disease Michael S. Lee, MD, FACC, FSCAI Assistant Professor UCLA School of Medicine Faculty Disclosure Honararia for Boston Scientific, BMS, Daiichi Sankyo,
Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation
 Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation Gabriel Loor, MD Baylor St. Lukes Medical Center Surgical Director Lung Transplantation Co-chief Section of Adult Cardiac
Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation Gabriel Loor, MD Baylor St. Lukes Medical Center Surgical Director Lung Transplantation Co-chief Section of Adult Cardiac
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS
 REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
Disclosures. Transplanting Interstitial Lung Disease. Lung Transplantation. Indications. I have nothing to disclose. Adult Lung Transplants
 Transplanting Interstitial Lung Disease Steven Hays, MD Associate Professor Medical Director, Lung Transplantation UCSF Medical Center Disclosures I have nothing to disclose Adult Lung Transplants Number
Transplanting Interstitial Lung Disease Steven Hays, MD Associate Professor Medical Director, Lung Transplantation UCSF Medical Center Disclosures I have nothing to disclose Adult Lung Transplants Number
Postlung Transplant Survival is Equivalent Regardless of Cytomegalovirus Match Status
 Postlung Transplant Survival is Equivalent Regardless of Cytomegalovirus Match Status Mark J. Russo, MD, MS, David I. Sternberg, MD, Kimberly N. Hong, MHSA, Robert A. Sorabella, BA, Alan J. Moskowitz,
Postlung Transplant Survival is Equivalent Regardless of Cytomegalovirus Match Status Mark J. Russo, MD, MS, David I. Sternberg, MD, Kimberly N. Hong, MHSA, Robert A. Sorabella, BA, Alan J. Moskowitz,
Endobronchial valve insertion to reduce lung volume in emphysema
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
Prapaporn Pornsuriyasak, M.D. Pulmonary and Critical Care Medicine Ramathibodi Hospital
 Prapaporn Pornsuriyasak, M.D. Pulmonary and Critical Care Medicine Ramathibodi Hospital Only 20-30% of patients with lung cancer are potential candidates for lung resection Poor lung function alone ruled
Prapaporn Pornsuriyasak, M.D. Pulmonary and Critical Care Medicine Ramathibodi Hospital Only 20-30% of patients with lung cancer are potential candidates for lung resection Poor lung function alone ruled
Management of a Patient after the Bidirectional Glenn
 Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
