Clinical- Pathologic Conference
|
|
|
- Sheena Neal
- 5 years ago
- Views:
Transcription
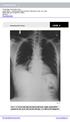
1 Clinical- Pathologic Conference Clinical-pathologic conference in general thoracic surgery: Bilateral lung transplantation for sarcoidosis with aspergilloma G. Alexander Patterson, MD From the Washington University School of Medicine, Barnes-Jewish Hospital, St Louis, Mo. This case is available for further study on the World Wide Web at: Participants From the Washington University School of Medicine, Barnes-Jewish Hospital, St Louis, Missouri Thoracic Surgery Dr G. Alexander Patterson Dr Anna Maria Ciccone Radiology Dr Harvey Glazer Pulmonary Medicine Dr Elbert Trulock Surgical Pathology Dr Jon Ritter Case Presentation Dr Ciccone: The patient is a 47-year-old man who was hospitalized 16 years ago for asthma. He had a less than complete response to initial therapy, and his treating physician s inclination at that time was that he had tuberculosis. That same year, a diagnosis of sarcoidosis was established after a lung biopsy. He had a history of systemic hypertension, osteoporosis, and gout. His condition remained stable until 3 years ago, at which time his symptoms of dyspnea worsened. He required increasing supplemental oxygen. Two years ago he was seen, evaluated, and eventually listed for bilateral lung transplantation. By spirometry, the forced expiratory volume in 1 second was only 0.55 L, 16% of predicted, and the forced vital capacity was 1.81 L, or 44% of predicted. Six months ago he was hospitalized for an exacerbation of his respiratory symptoms. He was treated and enrolled in our pulmonary rehabilitation program. On physical examination, the patient had poor chest excursion and coarse breath sounds bilaterally. The remainder of his physical examination was unremarkable. Perhaps we could review the relevant radiographic findings. Dr Glazer: Chest radiograph and computed tomographic images demonstrate findings consistent with the clinical diagnosis of end-stage sarcoidosis. The chest radiograph (Figure 1) shows extensive bullous formation and scarring, predominantly in the mid and upper lungs, with compensatory hyperinflation in the lower lungs. Superior retraction of the hila is seen. An opacity is seen within the dependent portion of a large cystic space in the left upper hemithorax, likely representing a fungus ball. Similar findings are seen on the computed tomographic scan (Figure 2). Large cystic spaces are noted with central bronchial distortion and angulation. A dependent opacity, likely a fungus ball, is seen within a large cystic space in the left lung. Dr Patterson: Dr Glazer, we typically think of sarcoidosis as being an inflammatory fibrotic lung disease. This certainly is not the picture of classic pulmonary fibrosis with decreased lung volumes. Would you describe the radiographic findings as being typical of a diagnosis of sarcoidosis? Dr Glazer: End-stage sarcoidosis is characterized by a variety of findings, including bronchial distortion, linear opacities, peripheral honeycombing, and in From the Washington University School of Medicine, Barnes-Jewish Hospital, St Louis, Mo. Received for publication Oct 12, 2001; accepted for publication Oct 31, Address for reprints: G. Alexander Patterson, MD, Washington University School of Medicine, Department of Cardiothoracic Surgery, One Barnes Hospital Plaza, Suite 3108 Queeny Tower, St Louis, MO ( pattersona@msnotes.wustl.edu). J Thorac Cardiovasc Surg 2002;124:171-5 Copyright 2002 by The American Association for Thoracic Surgery /2002 $ /1/ doi: /mtc The Journal of Thoracic and Cardiovascular Surgery Volume 124, Number 1 171
2 Clinical-Pathologic Conference Patterson et al Figure 1. Chest radiograph demonstrates extensive bullous formation and associated hyperinflation. Upper lobe scarring with hilar retraction is seen. An opacity (arrow), likely a fungus ball, is seen within a large cystic space in the left upper hemithorax. Figure 2. Computed tomographic image confirms dependent opacity (arrows), likely a fungus ball, in a large cystic space in the left hemithorax. Bronchial distortion (arrowheads) is also noted. some patients, large cystic/bullous spaces. As in this patient, the findings usually predominate in the upper lung zones with compensatory hyperinflation in the lower lungs. In some cases, conglomerate masses of fibrosis may be seen. The combination of upper lobe fibrosis, central bronchial distortion, and cystic spaces is a known manifestation of severe end-stage pulmonary sarcoidosis. Associated fungus ball formation is a widely described complication. Dr Ciccone: How does the diagnosis of sarcoidosis influence evaluation for lung transplantation, and does the presence of aspergilloma affect eligibility for subsequent transplantation? Dr Trulock: This patient underwent the standard evaluation protocol that has been used in our institution for a number of years. He had no contraindication to transplantation, such as coexisting malignant disease or other major medical problems. Transplantation was appropriate because his disease had progressed to severe pulmonary impairment despite medical treatment. Sarcoidosis is one of the diseases that is known to recur in the allograft. In most cases the recurrence has been an incidental discovery on transbronchial biopsy specimens that were obtained to monitor for rejection, and recurrence has not been associated with an adverse outcome. Hence, sarcoidosis itself is not a contraindication to transplantation. The aspergilloma in the left upper lobe presented a significant dilemma. The aspergilloma was asymptomatic at the time of evaluation, and it did not cause any clinical problems during the waiting period. At the time of his evaluation, itraconazole treatment was begun as a cautionary measure to limit the likelihood of complications while awaiting transplantation and to provide antifungal coverage for the transplant operation. Airway contamination by Aspergillus is not unusual among potential transplant recipients with bronchiectasis, such as those with cystic fibrosis. Our approach is the same in these patients. Itraconazole therapy is begun during the waiting period and continued for 3 months after transplantation and until posttransplantation bronchoscopic cultures are negative for Aspergillus. Dr Patterson: I think we could be criticized for doing a transplant operation in a patient with an active aspergilloma. We actually spent considerable time considering this patient s management in advance of this transplant. We thought that one option was to drain the aspergilloma cavity by cavernostomy. However, we concluded that the morbidity of this procedure and the unknown date of transplant might cause some complications. We therefore elected to make an effort to deal with the aspergilloma cavity at the time of transplant. The operation was specifically tailored to deal with the aspergilloma cavity in the safest possible way at the time of lung extraction. Dr Ciccone: A suitable donor was identified in Duluth, Minnesota. Donor PaO 2 at an FIO 2 of 100% was 448 mm Hg. Examination with a flexible bronchoscope demonstrated purulent secretions in the left lower lobe. In addition, the donor chest x-ray film demonstrated some volume loss in the hemithorax and a double density behind the left side of the heart, suggestive of left lower lobe atelectasis. Nonetheless, at the time of direct inspection, the lungs including the left lower lobe appeared to be of suitable quality for transplantation. The lungs were preserved by means of standard preservation techniques. The lungs were harvested en bloc 172 The Journal of Thoracic and Cardiovascular Surgery July 2002
3 Patterson et al Clinical-Pathologic Conference Figure 3. The initial postoperative chest radiograph (A) demonstrates moderate left perihilar and left basilar opacity, likely representing edema and atelectasis. Pneumonia could have a similar radiographic appearance. Improvement was noted by the third postoperative day (B). and separated into separate lung grafts on arrival at Barnes- Jewish Hospital. Recipient quantitative ventilation/perfusion imaging demonstrated 75% and 25% perfusion to the right and left lungs, respectively. The operation was commenced via a left posterolateral thoracotomy. After donor lung arrival, the left lung was extracted. The resection over the area of the fungus ball was conducted in an extrapleural plane. During ex vivo examination, the donor left lower lobe was somewhat atelectatic. There was a significant amount of purulent secretion in the donor left lower lobe. Nonetheless, we proceeded with implantation. The anterior cartilaginous airway was closed with interrupted figure-of-8 sutures of 4-0 polydioxanone (PDS; Ethicon, Inc, Somerville, NJ). Peribronchial soft tissue was approximated anteriorly to cover the bronchial anastomosis. The pulmonary artery and left atrial anastomoses were performed in standard fashion. After the lung had been deaired, clamps were removed, the Figure 4. Sections of the hilar lymph nodes showing marked elastosis and sclerosis. lung was reflected anteriorly, and the membranous airway was closed with a continuous suture. The donor left lower lobe did not inflate as easily as the upper lobe. However, gas exchange was satisfactory. After chest closure, the patient was turned supine and, via a right anterolateral thoracotomy, the recipient right lung was extracted and the donor right lung implanted via a standard technique. Immediate postoperative gas exchange was excellent, with a PaO 2 on 100% FIO 2 of 508 mm Hg. The patient was extubated on the third postoperative day. On the seventh postoperative day he was reintubated after an episode of atrial fibrillation and hypoxia. He was extubated on the ninth postoperative day and discharged from the hospital on the fourteenth postoperative day. Perhaps we could ask Dr Glazer to comment on the early postoperative chest x-ray films. Dr Glazer: The initial postoperative chest radiograph demonstrates moderate left perihilar and left basilar opacity likely representing edema and atelectasis, although pneumonia could have a similar radiographic appearance (Figure 3, A). Improvement is seen by the third postoperative day (Figure 3, B). Dr Ciccone: Dr Patterson, could you give us some insight as to the operative approach in this particular patient and the impact of the marginal lung on that selection? Dr Patterson: Our usual practice is to conduct bilateral sequential single lung transplants through an anterolateral approach. Historically, these procedures were performed through bilateral anterolateral thoracotomies with a transverse sternotomy (clamshell incision). However, for 5 years we have been routinely avoiding sternal division. Currently we conduct the vast majority of these bilateral procedures through separate anterolateral thoracotomies, irrespective of the recipient diagnosis. However, in this patient we believed there was a specific indication for a posterolateral approach on the left. In view of the extensive pleural fibrosis associated with the aspergilloma and the absolute requirement to conduct the left lung The Journal of Thoracic and Cardiovascular Surgery Volume 124, Number 1 173
4 Clinical-Pathologic Conference Patterson et al Figure 5. Photomicrograph of larger airways with intramural sclerosis. Figure 7. Terminal bronchiole surrounded by sclerosis with adjacent parenchymal emphysema. Figure 6. Sclerosis surrounding a small airway. Figure 8. Section of a bulla wall. explant without opening the aspergilloma, I thought that a posterolateral thoracotomy was the only suitable option. The bilateral transplant procedure can be easily initiated through this posterolateral approach. Indeed, we have used this approach in a number of other circumstances, typically in the situation of significant mediastinal shift associated with such lateral displacement of the heart that an anterior approach would provide unsafe exposure to the hilum. I really do not think there is any problem conducting the posterolateral thoracotomy first, implanting the first lung, then turning the patient supine for conduct of the second lung transplant. The only disadvantage is the inevitable delay of separate wound closure, dressing, and patient repositioning. The marginal donor did present some difficulties. I had underestimated the degree of left lower lobe pneumonitis. Nonetheless, the immediate intraoperative and early postoperative allograph function was very satisfactory. Over a 2- to 3-week follow-up period, the left lower lobe pneumonitis cleared quite nicely, ultimately providing the patient with a satisfactory result. Dr Ciccone: Perhaps at this point we could have the pathologist present the findings on this patient. Dr Ritter: This patient had a history of a right upper lobe transbronchial biopsy in 1985, which showed noncaseating granulomata. Furthermore, a bone marrow biopsy in 1993 showed multiple noncaseating epithelioid granulomas throughout the bone marrow compartment. No microorganisms were identified in either specimen. Sections of the hilar lymph nodes show marked elastosis and sclerosis (Figure 4). There is scant remaining lymphoid tissue. The contour of the sclerosis suggests burnt-out granulomas; however, there is no active granulomatous inflammation in the lymph nodes. Sections of the large airways show marked peribronchiolar sclerosis with deposition of elastotic material (Figure 5). This sclerosis extends into the smaller airways (Figures 6 and 7). The sclerosis has a similar quality to that seen in the lymph nodes. We speculate that this may also represent burnt-out granulomatous disease. However, multiple sections do not reveal any active granulomatous inflammation. The surrounding 174 The Journal of Thoracic and Cardiovascular Surgery July 2002
5 Patterson et al Clinical-Pathologic Conference Figure 9. Sections of the wall of the aspergillus cavity showing mixed inflammatory infiltrate. Figure 11. High-magnification view of branching hyphae. Figure 10. Low-magnification view of bulla contents showing inflammatory debris and hyphae. lung parenchyma (Figure 7) shows emphysema. Multiple bullae are present (Figure 8). One of the bullae became the site of a noninvasive aspergilloma. Sections of the wall of this cavity show a mixed inflammatory infiltrate consisting primarily of plasma cells and scattered neutrophils (Figure 9). At low power, the hyphal nature of the contents of this bulla can be appreciated (Figure 10). At high power, it can be seen that these hyphae are branching at 45 angles, a characteristic of Aspergillus (Figure 11). Sections through one of the larger pulmonary arteries (Figure 12) show intimal thickening, suggesting pulmonary hypertension. In summary, the findings include peculiar sclerosis in lymph nodes and along airways. There were pulmonary artery hypertensive changes. Distal bullous disease was also seen. These features are compatible with a diagnosis of advanced sarcoidosis. Dr Patterson: In view of these pathologic findings, perhaps Dr Trulock might wish to comment regarding the Figure 12. Sections through one of the larger pulmonary arteries showing intimal thickening. security of the original diagnosis. In the absence of granulomatous inflammation, is there any reason to doubt the diagnosis of sarcoidosis? Dr Trulock: The diagnosis of sarcoidosis is quite secure. A prior lung biopsy demonstrated noncaseating granuloma. Furthermore, the clinical course and radiographic features are consistent with the diagnosis of sarcoidosis. Dr Ciccone: At present the patient is doing well 4 months after lung transplant. At the most recent follow-up examination, spirometry showed a forced vital capacity of 3.13 L or 76% predicted and a forced expiratory volume in 1 second of 2.60 L or 78% predicted. Resting room air pulse oximetry was 98%. During a 6-minute walk test, he covered a distance of 1200 feet and maintained an arterial oxygen saturation of 96% without supplemental oxygen. He continues to have ongoing subjective improvement in his level of exertional tolerance. He walks three times weekly for 1 hour on a flat surface covering approximately 2 miles. He is free of pulmonary symptoms. The Journal of Thoracic and Cardiovascular Surgery Volume 124, Number 1 175
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Interesting Cases. Pulmonary
 Interesting Cases Pulmonary 54M with prior history of COPD, hep B/C, and possible history of TB presented with acute on chronic dyspnea, and productive cough Hazy opacity overlying the left hemithorax
Interesting Cases Pulmonary 54M with prior history of COPD, hep B/C, and possible history of TB presented with acute on chronic dyspnea, and productive cough Hazy opacity overlying the left hemithorax
10/17/2016. Nuts and Bolts of Thoracic Radiology. Objectives. Techniques
 Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
4/16/2017. Learning Objectives. Interpretation of the Chest Radiograph. Components. Production of the Radiograph. Density & Appearance
 Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Lung Allograft Dysfunction
 Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
The 1-year survival rate approaches 80% for patients
 Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Living lobar lung transplantation was developed as an alternative
 Living Lobar Lung Transplantation Michael K. McLean, MD, Mark L. Barr, MD, and Vaughn A. Starnes, MD Living lobar lung transplantation was developed as an alternative to cadaver lung transplantation because
Living Lobar Lung Transplantation Michael K. McLean, MD, Mark L. Barr, MD, and Vaughn A. Starnes, MD Living lobar lung transplantation was developed as an alternative to cadaver lung transplantation because
Evolution of Surgical Therapies for End-Stage Cardiopulmonary Failure. Heart Failure at the Shoe XI October 5, 2012
 Evolution of Surgical Therapies for End-Stage Cardiopulmonary Failure Heart Failure at the Shoe XI October 5, 2012 Robert S.D. Higgins, MD, MSHA Executive Director, Comprehensive Transplant Center Evolution
Evolution of Surgical Therapies for End-Stage Cardiopulmonary Failure Heart Failure at the Shoe XI October 5, 2012 Robert S.D. Higgins, MD, MSHA Executive Director, Comprehensive Transplant Center Evolution
August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker. Michael B. Gotway, MD
 August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ USA Clinical History: A 55 year old woman presented
August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ USA Clinical History: A 55 year old woman presented
FOREIGN BODY ASPIRATION in children. Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital
 FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Acute and Chronic Lung Disease
 KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
Signs in Chest Radiology
 Signs in Chest Radiology Jonathan H. Chung, MD Disclosures No pertinent disclosures Jonathan H. Chung, MD Assistant Professor Institute t of fadvanced d Biomedical Imaging National Jewish Health Denver,
Signs in Chest Radiology Jonathan H. Chung, MD Disclosures No pertinent disclosures Jonathan H. Chung, MD Assistant Professor Institute t of fadvanced d Biomedical Imaging National Jewish Health Denver,
Bronchial syndrome. Atelectasis Draining bronchus Bronchiectasis
 Bronchial syndrome Atelectasis Draining bronchus Bronchiectasis Etienne Leroy Terquem Pierre L Her SPI / ISP Soutien Pneumologique International / International Support for Pulmonology Atelectasis Consequence
Bronchial syndrome Atelectasis Draining bronchus Bronchiectasis Etienne Leroy Terquem Pierre L Her SPI / ISP Soutien Pneumologique International / International Support for Pulmonology Atelectasis Consequence
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1).
 PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
Chest Radiology Interpretation: Findings of Tuberculosis
 Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
SURGERY FOR GIANT BULLOUS EMPHYSEMA
 SURGERY FOR GIANT BULLOUS EMPHYSEMA Dr. Carmine Simone Head, Division of Critical Care & Thoracic Surgeon Department of Surgery December 15, 2006 OVERVIEW Introduction Classification Patient selection
SURGERY FOR GIANT BULLOUS EMPHYSEMA Dr. Carmine Simone Head, Division of Critical Care & Thoracic Surgeon Department of Surgery December 15, 2006 OVERVIEW Introduction Classification Patient selection
An Image Repository for Chest CT
 An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
HYPERSENSITIVITY PNEUMONITIS
 HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
Chest radiograph of an. asymptomatic man. Case report. Case history
 Eleftheria Chaini 1, Niki Giannakou 2, Dimitra Haini 3, Anna Maria Athanassiadou 4, Angelos Tsipis 4, Nikolaos D. Hainis 5 elhaini@otenet.gr 1 Pulmonary Dept, Corfu General Hospital, Kontokali, Greece.
Eleftheria Chaini 1, Niki Giannakou 2, Dimitra Haini 3, Anna Maria Athanassiadou 4, Angelos Tsipis 4, Nikolaos D. Hainis 5 elhaini@otenet.gr 1 Pulmonary Dept, Corfu General Hospital, Kontokali, Greece.
R replacement that uses a sequential implantation. Bilateral Sequential Lung Transplantation: The Procedure of Choice for Double-Lung Replacement
 Bilateral Sequential Lung Transplantation: The Procedure of Choice for Double-Lung Replacement Larry R. Kaiser, MD, Michael K. Pasque, MD, Elbert P. Trulock, MD, Donald E. Low, MD, Carolyn M. Dresler,
Bilateral Sequential Lung Transplantation: The Procedure of Choice for Double-Lung Replacement Larry R. Kaiser, MD, Michael K. Pasque, MD, Elbert P. Trulock, MD, Donald E. Low, MD, Carolyn M. Dresler,
Idiopathic Pulmonary of Care
 Chapter 6.1 Living Medical etextbook A Digital Tool at the Point of Care From Projects In Knowledge Pulmonology Idiopathic Pulmonary Fibrosis @Point of Care IPF Case Study: Typical Presentation, Role of
Chapter 6.1 Living Medical etextbook A Digital Tool at the Point of Care From Projects In Knowledge Pulmonology Idiopathic Pulmonary Fibrosis @Point of Care IPF Case Study: Typical Presentation, Role of
8/14/2017. Objective: correlate radiographic findings of common lung diseases to actual lung pathologic features
 What is that lung disease? Pulmonary Patterns & Correlated Pathology Dr. Russell Tucker, DACVR Objective: correlate radiographic findings of common lung diseases to actual lung pathologic features Improved
What is that lung disease? Pulmonary Patterns & Correlated Pathology Dr. Russell Tucker, DACVR Objective: correlate radiographic findings of common lung diseases to actual lung pathologic features Improved
Single-lung transplantation in the setting of aborted bilateral lung transplantation
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2011 Single-lung transplantation in the setting of aborted bilateral lung transplantation Varun Puri Tracey Guthrie
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2011 Single-lung transplantation in the setting of aborted bilateral lung transplantation Varun Puri Tracey Guthrie
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
L dure for patients with end-stage pulmonary disease.
 HOW TO DO IT Donor Lung Procurement: Assessment and Operative Technique Sudhir Sundaresan, MD, Gregory D. Trachiotis, MD, Motoi Aoe, MD, G. Alexander Patterson, MD, and Joel D. Cooper, MD Division of Cardiothoracic
HOW TO DO IT Donor Lung Procurement: Assessment and Operative Technique Sudhir Sundaresan, MD, Gregory D. Trachiotis, MD, Motoi Aoe, MD, G. Alexander Patterson, MD, and Joel D. Cooper, MD Division of Cardiothoracic
Original Report. Fibrosis of the Upper Lobes: A Newly Identified Late-Onset Complication After Lung Transplantation?
 Downloaded from www.ajronline.org by 148.251.232.83 on 05/04/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Eli Konen 1,2 Gordon L. Weisbrod 1 Smita Pakhale
Downloaded from www.ajronline.org by 148.251.232.83 on 05/04/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Eli Konen 1,2 Gordon L. Weisbrod 1 Smita Pakhale
CASE REPORTS. Idiopathic Unilateral Hyperlucent Lung
 CASE REPORTS Idiopathic Unilateral Hyperlucent Lung The Swyer-James Syndrome J. Judson McNamara, M.D., Harold C. Urschel, M.D., J. H. Arndt, M.D., Herman Ulevitch, M.D., and W. B. Kingsley, M.D. I diopathic
CASE REPORTS Idiopathic Unilateral Hyperlucent Lung The Swyer-James Syndrome J. Judson McNamara, M.D., Harold C. Urschel, M.D., J. H. Arndt, M.D., Herman Ulevitch, M.D., and W. B. Kingsley, M.D. I diopathic
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/23566
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/23566
CASE REPORTS. Inflammatory Polyp of the Bronchus. V. K. Saini, M.S., and P. L. Wahi, M.D.
 CASE REPORTS V. K. Saini, M.S., and P. L. Wahi, M.D. I n 1932 Jackson and Jackson [l] first reported a number of clinical cases under the title Benign Tumors of the Trachea and Bronchi with Especial Reference
CASE REPORTS V. K. Saini, M.S., and P. L. Wahi, M.D. I n 1932 Jackson and Jackson [l] first reported a number of clinical cases under the title Benign Tumors of the Trachea and Bronchi with Especial Reference
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
The radiological differential diagnosis of the UIP pattern
 5th International Conference on Idiopathic Pulmonary Fibrosis, Modena, 2015, June 12th The radiological differential diagnosis of the UIP pattern Simon Walsh King s College Hospital Foundation Trust London,
5th International Conference on Idiopathic Pulmonary Fibrosis, Modena, 2015, June 12th The radiological differential diagnosis of the UIP pattern Simon Walsh King s College Hospital Foundation Trust London,
Pneumothorax: A Rare Presentation of. Pulmonary Mycetoma. Prem Parkash Gupta* Sanjay Fotedar* Dipti Agarwal** Kuldeep Saini* Sarita Magu***
 Pneumothorax: A Rare Presentation of Pulmonary Mycetoma Prem Parkash Gupta* Sanjay Fotedar* Dipti Agarwal** Kuldeep Saini* Sarita Magu*** Departments of *Respiratory Medicine, **Physiology, and ***Radiodiagnosis,
Pneumothorax: A Rare Presentation of Pulmonary Mycetoma Prem Parkash Gupta* Sanjay Fotedar* Dipti Agarwal** Kuldeep Saini* Sarita Magu*** Departments of *Respiratory Medicine, **Physiology, and ***Radiodiagnosis,
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations
 Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
Median Sternotomy for Pneumonectomy in Patients With Pulmonary Complications of Tuberculosis
 Median Sternotomy for Pneumonectomy in Patients With Pulmonary Complications of Tuberculosis Cliff P. Connery, MD, James Knoetgen III, MD, Constantine E. Anagnostopoulos, MD, and Madeline V. Svitak, BS,
Median Sternotomy for Pneumonectomy in Patients With Pulmonary Complications of Tuberculosis Cliff P. Connery, MD, James Knoetgen III, MD, Constantine E. Anagnostopoulos, MD, and Madeline V. Svitak, BS,
Interpreting thoracic x-ray of the supine immobile patient: Syllabus
 Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!!
 The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer
 Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Open Lung Biopsy for Diffuse Infiltrative Lung Disease
 Open Lung Biopsy for Diffuse Infiltrative Lung Disease Vijay Chechani, MD, Rodney J. Landreneau, MD, and Shabbir S. Shaikh, MD Division of Pulmonary Medicine, Department of Medicine, and Division of Cardiothoracic
Open Lung Biopsy for Diffuse Infiltrative Lung Disease Vijay Chechani, MD, Rodney J. Landreneau, MD, and Shabbir S. Shaikh, MD Division of Pulmonary Medicine, Department of Medicine, and Division of Cardiothoracic
Lung Cancer: Determining Resectability
 Lung Cancer: Determining Resectability Leslie E. Quint lequint@umich.edu No disclosures Lung Cancer: Determining Resectability AIM: Review imaging features that suggest resectability / unresectability
Lung Cancer: Determining Resectability Leslie E. Quint lequint@umich.edu No disclosures Lung Cancer: Determining Resectability AIM: Review imaging features that suggest resectability / unresectability
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA
 Thor-ax (1954), 9, 304. PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA W. J. HANBURY, R. J. R. CURETON, AND G. SIMON From St. Bartholomew's Hospital, London BY (RECEIVED FOR PUBLICATION JUNE
Thor-ax (1954), 9, 304. PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA W. J. HANBURY, R. J. R. CURETON, AND G. SIMON From St. Bartholomew's Hospital, London BY (RECEIVED FOR PUBLICATION JUNE
Tuberculosis - clinical forms. Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases
 Tuberculosis - clinical forms Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases 1 TB DISEASE Primary Post-primary (Secondary) Common primary forms Primary complex Tuberculosis of the intrathoracic
Tuberculosis - clinical forms Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases 1 TB DISEASE Primary Post-primary (Secondary) Common primary forms Primary complex Tuberculosis of the intrathoracic
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
06/04/2013 ISHLT. 2 International Conference on Respiratory Physiotherapy ARIR Genova, March 21 23, 2013
 LUNG TRANSPLANTS The Journal of Heart and Lung Transplantation, 2012 2 International Conference on Respiratory Physiotherapy ARIR Genova, March 21 23, 2013 LUNG TRANSPLANTATION:STATE OF THE ART L. Santambrogio
LUNG TRANSPLANTS The Journal of Heart and Lung Transplantation, 2012 2 International Conference on Respiratory Physiotherapy ARIR Genova, March 21 23, 2013 LUNG TRANSPLANTATION:STATE OF THE ART L. Santambrogio
Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600
 Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
October 2012 Imaging Case of the Month. Michael B. Gotway, MD Associate Editor Imaging. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
S and secondary spontaneous pneumothorax. Primary
 Secondary Spontaneous Pneumothorax Fumihiro Tanaka, MD, Masatoshi Itoh, MD, Hiroshi Esaki, MD, Jun Isobe, MD, Youichiro Ueno, MD, and Ritsuko Inoue, MD Department of Thoracic and Cardiovascular Surgery,
Secondary Spontaneous Pneumothorax Fumihiro Tanaka, MD, Masatoshi Itoh, MD, Hiroshi Esaki, MD, Jun Isobe, MD, Youichiro Ueno, MD, and Ritsuko Inoue, MD Department of Thoracic and Cardiovascular Surgery,
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Lung Cancer Screening in the Midwest of the US: When Histoplasmosis Complicates the Picture
 Cronicon OPEN ACCESS EC PULMONOLOGY AND RESPIRATORY MEDICINE Case Report Lung Cancer Screening in the Midwest of the US: When Histoplasmosis Complicates the Picture Swan Lee 1 and Rolando Sanchez Sanchez
Cronicon OPEN ACCESS EC PULMONOLOGY AND RESPIRATORY MEDICINE Case Report Lung Cancer Screening in the Midwest of the US: When Histoplasmosis Complicates the Picture Swan Lee 1 and Rolando Sanchez Sanchez
Tests Your Pulmonologist Might Order. Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital
 Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
CONSULTATION DURING SURGERY / NOT A FINAL DIAGNOSIS. FROZEN SECTION DIAGNOSIS: - A. High grade sarcoma. Wait for paraffin sections results.
 Pathology Report Date: 3/5/02 A, B. Biopsy right distal femur- high grade spindle cell sarcoma Immunohistochemistry studies are pending to further classify the nature of the tumor. CONSULTATION DURING
Pathology Report Date: 3/5/02 A, B. Biopsy right distal femur- high grade spindle cell sarcoma Immunohistochemistry studies are pending to further classify the nature of the tumor. CONSULTATION DURING
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lung_volume_reduction_surgery 4/1996 3/2018 3/2019 3/2018 Description of Procedure or Service Emphysema is
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lung_volume_reduction_surgery 4/1996 3/2018 3/2019 3/2018 Description of Procedure or Service Emphysema is
Primary chondrosarcoma of lung
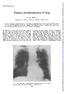 Thorax,(1970), 25, 366. Primary chondrosarcoma of lung G. M. REES Department of Surgery, Brompton Hospital, Lontdonl, S.W.3 A case of primary chondrosarcoma of the lung is described in a 64-year-old man.
Thorax,(1970), 25, 366. Primary chondrosarcoma of lung G. M. REES Department of Surgery, Brompton Hospital, Lontdonl, S.W.3 A case of primary chondrosarcoma of the lung is described in a 64-year-old man.
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis)
 Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Radiological conference. Left upper lobe collapse. Citation Hong Kong Practitioner, 1998, v. 20 n. 9, p
 Title Radiological conference. Left upper lobe collapse Author(s) Wong, LLS; Peh, WCG Citation Hong Kong Practitioner, 1998, v. 20 n. 9, p. 513-517 Issued Date 1998 URL http://hdl.handle.net/10722/44672
Title Radiological conference. Left upper lobe collapse Author(s) Wong, LLS; Peh, WCG Citation Hong Kong Practitioner, 1998, v. 20 n. 9, p. 513-517 Issued Date 1998 URL http://hdl.handle.net/10722/44672
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Does the Presence of Preoperative Mild or Moderate Coronary Artery Disease Affect the Outcomes of Lung Transplantation?
 Does the Presence of Preoperative Mild or Moderate Coronary Artery Disease Affect the Outcomes of Lung Transplantation? Cliff K. Choong, FRACS, Bryan F. Meyers, MD, Tracey J. Guthrie, BSN, Elbert P. Trulock,
Does the Presence of Preoperative Mild or Moderate Coronary Artery Disease Affect the Outcomes of Lung Transplantation? Cliff K. Choong, FRACS, Bryan F. Meyers, MD, Tracey J. Guthrie, BSN, Elbert P. Trulock,
Radiology of the respiratory disease
 Radiology of the respiratory disease [ Color index: Important Notes Extra ] [ Editing file Feedback Share your notes Shared notes ] Resources: - 435 Slides - 434 Team - 435 Notes Done by: - Mai Alageel
Radiology of the respiratory disease [ Color index: Important Notes Extra ] [ Editing file Feedback Share your notes Shared notes ] Resources: - 435 Slides - 434 Team - 435 Notes Done by: - Mai Alageel
Thoracoplasty for the Management of Postpneumonectomy Empyema
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 9 Number 2 Thoracoplasty for the Management of Postpneumonectomy Empyema S Mullangi, G Diaz-Fuentes, S Khaneja Citation S Mullangi,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 9 Number 2 Thoracoplasty for the Management of Postpneumonectomy Empyema S Mullangi, G Diaz-Fuentes, S Khaneja Citation S Mullangi,
A Case of Pediatric Plasma Cell Granuloma
 August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
CLINICAL FEATURES IN PULMONARY TUBERCULOSIS
 CLINICAL FEATURES IN PULMONARY TUBERCULOSIS Dr. Amitesh Aggarwal Department of Medicine Tuberculosis Captain of all the Men of Death Great White Plague devastating effect on society 100 years ago one in
CLINICAL FEATURES IN PULMONARY TUBERCULOSIS Dr. Amitesh Aggarwal Department of Medicine Tuberculosis Captain of all the Men of Death Great White Plague devastating effect on society 100 years ago one in
New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma
 July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
GOALS AND OBJECTIVES FOR THORACIC PATHOLOGY ROTATION
 GOALS AND OBJECTIVES FOR THORACIC PATHOLOGY ROTATION LEVEL: PGY2, PGY3, PGY5 A number of these rotations are introductory in nature, as they are major subspecialties, and are followed by two more blocks
GOALS AND OBJECTIVES FOR THORACIC PATHOLOGY ROTATION LEVEL: PGY2, PGY3, PGY5 A number of these rotations are introductory in nature, as they are major subspecialties, and are followed by two more blocks
Case 1: Question. 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule
 HRCT WORK SHOP Case 1 Case 1: Question 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule Case 1: Question 1.2 What is the diagnosis? 1. Hypersensitivity
HRCT WORK SHOP Case 1 Case 1: Question 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule Case 1: Question 1.2 What is the diagnosis? 1. Hypersensitivity
Lung Cancer Clinical Guidelines: Surgery
 Lung Cancer Clinical Guidelines: Surgery 1 Scope of guidelines All Trusts within Manchester Cancer are expected to follow this guideline. This guideline is relevant to: Adults (18 years and older) with
Lung Cancer Clinical Guidelines: Surgery 1 Scope of guidelines All Trusts within Manchester Cancer are expected to follow this guideline. This guideline is relevant to: Adults (18 years and older) with
Pulmonary Pearls. Medical Pearls. Case 1: Case 1 (cont.): Case 1: What is the Most Likely Diagnosis? Case 1 (cont.):
 Pulmonary Pearls Christopher H. Fanta, MD Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Medical Pearls Definition: Medical fact that is
Pulmonary Pearls Christopher H. Fanta, MD Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Medical Pearls Definition: Medical fact that is
Ontario s Referral and Listing Criteria for Adult Lung Transplantation
 Ontario s Referral and Listing Criteria for Adult Lung Transplantation Version 3.0 Trillium Gift of Life Network Adult Lung Transplantation Referral & Listing Criteria PATIENT REFERRAL CRITERIA: The patient
Ontario s Referral and Listing Criteria for Adult Lung Transplantation Version 3.0 Trillium Gift of Life Network Adult Lung Transplantation Referral & Listing Criteria PATIENT REFERRAL CRITERIA: The patient
CALGARY ZONE PULMONARY REFERRAL QUICK REFERENCE
 CALGARY ZONE PULMONARY REFERRAL QUICK REFERENCE EMERGENCY (Patient needs to be seen immediately) Hemoptysis (Active & 2 TBSP per day) Hypoxemia (if resting O2 SAT 85%) Pulmonary embolism (Acute - known
CALGARY ZONE PULMONARY REFERRAL QUICK REFERENCE EMERGENCY (Patient needs to be seen immediately) Hemoptysis (Active & 2 TBSP per day) Hypoxemia (if resting O2 SAT 85%) Pulmonary embolism (Acute - known
Canadian Trauma Trials Collaborative. Occult Pneumothorax in Critical Care (OPTICC): Standardized Data Collection Sheet
 Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Lung Surgery: Thoracoscopy
 Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss?
 ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
Subject Index. Bacterial infection, see Suppurative lung disease, Tuberculosis
 Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Case of the Day Chest
 Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Congenital Lung Malformations: Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Introduction to Radiology for TB Nurses
 Introduction to Radiology for TB Nurses Juzar Ali, MD; FRCP(C); FCCP May 4, 2018 Essential Skills for the TB Nurse Case Manager Little Rock, AR May 3 4, 2017 Juzar Ali, MD; FRCP(C); FCCP has the following
Introduction to Radiology for TB Nurses Juzar Ali, MD; FRCP(C); FCCP May 4, 2018 Essential Skills for the TB Nurse Case Manager Little Rock, AR May 3 4, 2017 Juzar Ali, MD; FRCP(C); FCCP has the following
Thoracic sarcoidosis: Pictoral review of typical and atypical findings
 Thoracic sarcoidosis: Pictoral review of typical and atypical findings Poster No.: C-0804 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: A. Ferreira, J. Calha; Lisbon/PT Keywords: Sarcoidosis,
Thoracic sarcoidosis: Pictoral review of typical and atypical findings Poster No.: C-0804 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: A. Ferreira, J. Calha; Lisbon/PT Keywords: Sarcoidosis,
Living-donor lobar lung transplantation (LDLLT) was developed by. Living-donor lobar lung transplantation for various lung diseases.
 Cardiothoracic Transplantation Date et al Living-donor lobar lung transplantation for various lung diseases Hiroshi Date, MD, a Motoi Aoe, MD, a Itaru Nagahiro, MD, a Yoshifumi Sano, MD, a Akio Andou,
Cardiothoracic Transplantation Date et al Living-donor lobar lung transplantation for various lung diseases Hiroshi Date, MD, a Motoi Aoe, MD, a Itaru Nagahiro, MD, a Yoshifumi Sano, MD, a Akio Andou,
Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis?
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
Breast Sarcoidosis Appearing as a Primary Manifestation of Sarcoidosis: A Case Report 1
 Breast Sarcoidosis Appearing as a Primary Manifestation of Sarcoidosis: A Case Report 1 Hye-Jeong Lee, M.D., Eun-Kyung Kim, M.D., Min Jung Kim, M.D., Ki Keun Oh, M.D., Se Hoon Kim, M.D. 2 Breast sarcoidosis
Breast Sarcoidosis Appearing as a Primary Manifestation of Sarcoidosis: A Case Report 1 Hye-Jeong Lee, M.D., Eun-Kyung Kim, M.D., Min Jung Kim, M.D., Ki Keun Oh, M.D., Se Hoon Kim, M.D. 2 Breast sarcoidosis
NONE OVERVIEW FINANCIAL DISCLOSURES UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF (UIP) FOR PATHOLOGISTS. IPF = Idiopathic UIP Radiologic UIP Path UIP
 UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
LOBECTOMY COMBINED WITH VOLUME REDUCTION FOR PATIENTS WITH LUNG CANCER AND ADVANCED EMPHYSEMA
 LOBECTOMY COMBINED WITH VOLUME REDUCTION FOR PATIENTS WITH LUNG CANCER AND ADVANCED EMPHYSEMA Steven R. DeMeester, MD* G. Alexander Patterson, MD R. Sudhir Sundaresan, MD Joel D. Cooper, MD Objective:
LOBECTOMY COMBINED WITH VOLUME REDUCTION FOR PATIENTS WITH LUNG CANCER AND ADVANCED EMPHYSEMA Steven R. DeMeester, MD* G. Alexander Patterson, MD R. Sudhir Sundaresan, MD Joel D. Cooper, MD Objective:
Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis?
 1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
FUNDAMENTALS OF CXR INTERPRETATION THE BASICS
 FUNDAMENTALS OF CXR INTERPRETATION THE BASICS PART I QUALITY ASSESSMENT 1 PATIENT-DEPENDENT FACTORS 3 REVIEW OF IMPORTANT ANATOMY 7 LUNGS AND PLEURA 11 DIAPHRAGMS 13 BONES AND SOFT TISSUES 14 A BRIEF LOOK
FUNDAMENTALS OF CXR INTERPRETATION THE BASICS PART I QUALITY ASSESSMENT 1 PATIENT-DEPENDENT FACTORS 3 REVIEW OF IMPORTANT ANATOMY 7 LUNGS AND PLEURA 11 DIAPHRAGMS 13 BONES AND SOFT TISSUES 14 A BRIEF LOOK
