Prevention of Aspiration
|
|
|
- Maude Foster
- 5 years ago
- Views:
Transcription
1 1 Prevention of Aspiration Scope and Impact of Problem Critically ill patients have an increased risk for aspirating oropharyngeal secretions and regurgitated gastric contents. For those who are tube-fed, aspiration of gastric contents is of greater concern. While witnessed large-volume aspirations occur occasionally, small-volume clinically silent aspirations are far more common. For example, a laboratory study identified frequent microaspirations in approximately half of a large population of critically ill, mechanically ventilated patients who were receiving tube feedings. 1 In the same study, risk for pneumonia was about 4 times greater in patients identified as frequent aspirators. Because no bedside tests are currently available to detect microaspirations, efforts to prevent or minimize aspiration take on added importance. Expected Practice Maintain head-of-bed elevation at an angle of 30 to 45 degrees, unless contraindicated. [Level B] Use sedatives as sparingly as feasible. [Level C] For tube-fed patients, assess placement of the feeding tube at 4-hour intervals. [Level C] For patients receiving gastric tube feedings, assess for gastrointestinal intolerance to the feedings at 4- hour intervals. [Level C] For tube-fed patients, avoid bolus feedings in those at high risk for aspiration. [Level E] Consult with physician about obtaining a swallowing assessment before oral feedings are started for recently extubated patients who have experienced prolonged intubation. [Level C] Maintain endotracheal cuff pressures at an appropriate level, and ensure that secretions are cleared from above the cuff before it is deflated. [Level B] Supporting Evidence Head-of-Bed Elevation There is evidence that a sustained supine position (zero-degree head-of-bed elevation) increases gastroesophageal reflux and the probability for aspiration; for example, using a radioactive-labeled formula, endobronchial counts were higher when patients were lying flat in bed (zero degree) compared to when they were in a semirecumbent (45-degree) position. 2 Thus, elevating the head of the bed to an angle of 30 to 45 degrees, unless contraindicated, is recommended for patients at high risk for aspiration pneumonia (eg, a patient receiving mechanical ventilation and/or one who has a feeding tube in place). 3,4 Although effectiveness of the reverse Trendelenberg position in minimizing aspiration has not been studied, it is likely to produce similar results to an elevated backrest position. 4 1 of 6 Issued November 2011
2 2 Sedation Sedation causes reduced cough and gag reflexes and can interfere with the patient s ability to handle oropharyngeal secretions and refluxed gastric contents; in addition, sedation may slow gastric emptying. 5,6 To reduce the risk for aspiration, it is prudent to use the smallest effective level of sedation. Assess Feeding-Tube Placement at Regular Intervals Expert panels recommend that correct feeding-tube placement be verified at regular intervals to minimize the risk for aspiration. 3,4,7 If feedings are administered at the wrong site (such as the esophagus, or even the stomach of a patient who requires small-bowel feedings), the risk for aspiration is increased. 8 It is not uncommon for feeding tubes to become malpositioned during routine use. For example, in a study of 201 critically ill patients, it was found that the distal tips of 24 of 116 feeding tubes originally positioned in the small bowel were displaced upward into the gastrointestinal tract (23 into the stomach and 1 into the esophagus). 9 Assess for Gastrointestinal Intolerance to Tube Feedings Tube-fed patients who experience frequent regurgitation and aspiration of gastric contents are at increased risk for poor respiratory outcomes. 1 Guidelines developed jointly by the Society of Critical Care Medicine and the American Society for Parenteral and Enteral Nutrition recommend that patients be monitored for tolerance to enteral feedings by noting abdominal distention, complaints of abdominal pain, observing for passage of flatus and stool, and monitoring gastric residual volumes. 10 Because gastric distention predisposes to regurgitation, it is recommended that gastric residual volumes (GRVs) be measured every 4 hours in critically ill patients. 4 Practice varies widely in regard to GRVs; however, 200 ml and 250 ml are frequently cited values for initial concern. 11,12 In a study of 206 critically ill patients, 2 or more GRVs of at least 200 ml and 1 or more GRVs of at least 250 ml were found significantly more often in patients who experienced frequent aspiration. 11 Prokinetics are sometimes advocated to improve gastric emptying when GRVs exceed a stipulated value. Several sources recommend that feedings be stopped when GRVs exceed 500 ml. 4,7 In a study of gastrointestinal (GI) symptoms in critically ill patients, investigators found that those with 2 or more simultaneous GI symptoms (such as high gastric aspirate volume, absent or abnormal bowel sounds, vomiting/regurgitation, diarrhea, bowel distension, and gastrointestinal bleeding) were less likely to have successful enteral feedings than those with fewer than 2 GI symptoms (84% vs 12.2%, respectively, p <.001). 13 Although bedside assessments for GI function such as GRVs and abdominal girth are difficult to evaluate, they are frequently used in combination to provide an estimate of GI tolerance to enteral feedings. Small bowel feeding with the tube s ports situated at or below the Ligament of Treitz is strongly recommended for patients with persistent intolerance to gastric feedings and documented aspiration. 7 Avoid Bolus Tube Feedings in Patients at High Risk for Aspiration An expert panel has concluded that no recommendation can be made regarding the best type of formula delivery method (continuous or intermittent). 3 Also, no guidelines exist for bolus feedings. On the basis of logic, 2 of 6 Issued November 2011
3 3 however, administering an entire 4-hour volume of formula over a period of a few minutes is more likely to predispose to regurgitation of gastric contents than is the steady administration of the same volume over a period of 4 hours. Continuous feedings are used in most critical care units. Supportive of this action is a small study of neurologically impaired adult patients; aspiration was observed more frequently in those with intermittent feedings (3 of 17) than in those who received continuous feedings (1 of 17). 17 It is possible that the bolus method of feeding may decrease the lower esophageal pressure and thus predispose patients to reflux and aspiration. 18 Other researchers reported that adult burn patients who received continuous tube feedings had less stool frequency and less time required to reach nutritional goals than did intermittently fed patients. 19 Swallowing Assessment Before Oral Feedings for Recently Extubated Patients Tracheal intubation interferes with overall swallowing physiology. 20 Thus, it is reasonable to expect some degree of swallowing impairment when patients are initially extubated. A systematic literature review found that recently extubated patients were at increased risk for swallowing difficulties; more than 20% of the patients in many of the reviewed studies experienced dysphagia. 21 Management of Endotracheal Tubes A persistent low cuff pressure (< 20 cm H 2 O) predisposes patients to pneumonia, presumably by predisposing to aspiration of oropharyngeal secretions and/or refluxed gastric contents. 22 To minimize aspiration of secretions pooled above the endotracheal tube s cuff, hypopharyngeal suctioning should be performed before deflating the cuff. 3 Actions for Nursing Practice Maintain head-of-bed elevation at an angle of 30 to 45 degrees, unless contraindicated If backrest elevation is not tolerated, consider use of the reverse Trendelenberg position to elevate the head of the bed, unless contraindicated. If necessary to lower the head of bed for a procedure or a medical contraindication, return the patient to a head-of-bed elevated position as soon as feasible. Use sedatives as sparingly as feasible Use an appropriate sedation scale to guide the administration of sedatives. Consider clinical situations that affect the need for sedatives. For tube-fed patients, assess feeding-tube placement at 4-hour intervals to ensure the tube has remained in the desired location. Observe for a change in length of the external portion of the feeding tube, as determined by movement of the marked portion of the tube. Review routine chest and abdominal x-ray reports to look for notations about tube location. 3 of 6 Issued November 2011
4 4 Observe changes in volume of aspirate from the feeding tube; a large increase in volume may signal the upward dislocation of a small-bowel feeding tube into the stomach. If ph strips are available, measure the ph of feeding-tube aspirates if feedings are interrupted for more than a few hours. Also, observe the appearance of feeding-tube aspirates if feedings are interrupted for more than a few hours. Obtain an x-ray to confirm tube position if there is doubt about the tube s position. For patients receiving gastric tube feedings, assess for intolerance to feedings every 4 hours by monitoring GRVs, abdominal discomfort, nausea/vomiting, and abdominal girth/tension Although it is easier to withdraw gastric contents from large-bore feeding tubes than from small-bore tubes, it is important to measure residual volumes from all types of gastric tubes, including gastrostomy tubes. o A 60 ml syringe is most suitable for measuring residual volumes. o It is helpful to inject 30 ml of air before attempting to aspirate fluid from flexible, small-diameter tubes. o Withdraw as much fluid as possible to make an accurate assessment. o It may be helpful to reposition the patient to facilitate withdrawal of fluid from the tube (for example, turning the patient from side to side may allow the feeding tube s ports to enter a pool of gastric fluid). If patients are able to communicate, ask if they are experiencing abdominal discomfort or nausea. If vomiting is present, feedings should be stopped, and the physician notified. Palpate the abdomen for firmness; a millimeter tape may be used to measure abdominal girth. Evaluate the significance of a single abnormal finding, such as a high GRV, in relation to other indicators of GI intolerance to tube feedings, such as abdominal distention, abdominal discomfort, and nausea and vomiting. Although clinicians disagree about the necessity for small bowel feedings to minimize aspiration risk in all critically ill patients, small bowel feedings have been recommended when patients are intolerant of gastric feedings or when they have documented aspiration. 7 For tube-fed patients, avoid bolus feedings for those at high risk for aspiration As indicated above, it is better to introduce feedings evenly over a period of hours to minimize risk for regurgitation and aspiration of gastric contents. Consult with a dietitian and a physician about the best feeding method for individual patients. Consult with the patient s physician about obtaining a swallowing assessment before beginning oral feedings for a recently extubated patient who has undergone prolonged intubation As indicated above, studies have shown that patients may experience dysphagia following extubation, especially if intubation has been prolonged. As such, it is prudent to observe for swallowing problems before introducing oral feedings. If a swallowing assessment is needed, it will likely be performed by a speech pathologist. 4 of 6 Issued November 2011
5 5 Maintain endotracheal cuff pressures at an appropriate level The American Thoracic Society recommends that endotracheal tube cuff pressure be maintained at > 20 cm H 2 O to prevent leakage of secretions around the cuff into the lower respiratory tract. 23 Moreover, it has been recommended that cuff pressure be maintained at < 30 cm H 2 O to prevent tracheal injury. 24 To minimize aspiration of pooled secretions from above the cuff, hypopharyngeal suctioning is recommended before the cuff is deflated. 3 AACN Levels of Evidence Level A Meta-analysis of quantitative studies or metasynthesis of qualitative studies with results that consistently support a specific action, intervention, or treatment Level B Well-designed, controlled studies with results that consistently support a specific action, intervention, or treatment Level C Qualitative studies, descriptive or correlational studies, integrative reviews, systematic reviews, or randomized controlled trials with inconsistent results Level D Peer-reviewed professional and organizational standards with the support of clinical study recommendations Level E Multiple case reports, theory-based evidence from expert opinions, or peer-reviewed professional organizational standards without clinical studies to support recommendations Level M Manufacturer s recommendations only Need More Information or Help? Contact a clinical practice specialist for additional information ( then select Practice Resource Network and Ask the Clinical Practice Team. References 1. Metheny NA, Clouse RE, Chang YH, Stewart BJ, Oliver DA, Kollef MH. Tracheobronchial aspiration of gastric contents in critically ill tube-fed patients: frequency, outcomes, and risk factors. Crit Care Med. 2006;34(4): Torres A, Serra-Bailles J, Ros E, Piera C, et al. Pulmonary aspiration of gastric contents in patients receiving mechanical ventilation: the effect of body position. Ann Intern Med. 1992; 116(7): Tablan OC, Anderson LJ, Besser R, Bridges C, Hajjeh R. Guidelines for preventing health-care associated pneumonia, 2003: recommendations of CDC and the Healthcare Infection Control Practices Advisory Committee. MMWR Recomm Rep. 2004;53(RR-3): Bankhead R, Boullata J, Brantley S, et al. Enteral nutrition practice recommendations. JPEN J Parenter Enteral Nutr. 2009;33(2): Nishino T. Physiological and pathophysiological implications of upper airway reflexes in humans. Jpn J Physiol. 2000;50(1): Kao CH, ChangLai SP, Chieng PU, Yen TC. Gastric emptying in head-injured patients. Am J Gastroenterol. 1998;93(7): McClave SA, DeMeo MT, DeLegge MH, et al. North American summit on aspiration in the critically ill patient: consensus statement. JPEN J Parenter Enteral Nutr. 2002;26(6 Suppl):S80-S Metheny NA, Clouse RE, Clark JM, Reed L, Wehrle MA, Wiersema L. ph testing of feeding-tube aspirates to determine placement. Nutr Clin Pract. 1994;9(5): of 6 Issued November 2011
6 6 9. Metheny NA, Schnelker R, McGinnis J, et al. Indicators of tubesite during feedings. J Neurosci Nurs. 2005;37(6): McClave SA, Martindale RG, Vanek VW, et al. Guidelines for the provision and assessment of nutrition support therapy in the adult critically ill patient: Society of Critical Care Medicine (SCCM) and American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.). JPEN J Parenter Enteral Nutr. 2009;33(3): Metheny NA, Schallom L, Oliver DA, Clouse RE. Gastric residual volume and aspiration in critically ill patients receiving gastric feedings. Am J Crit Care. 2008;17(5): Pinilla JC, Samphire J, Arnold C, Liu L, Thiessen B. Comparison of gastrointestinal tolerance to two feeding protocols in critically ill patients: a prospective, randomized controlled trial. JPEN J Parenter Enteral Nutr. 2001;25(2): Reintam A, Parm P, Kitus R, Kern H, Starkopf J. Gastrointestinal symptoms in intensive care patients. Acta Anaesthesiol Scand. 2009;53(3): O Meara D, Mireles-Cabodevila E, Frame F, et al. Evaluation of delivery of enteral nutrition in critically ill patients receiving mechanical ventilation. Am J Crit Care. 2008;17(1): Chan LN. A gutsy move : Tackling enteral feeding intolerance in critically ill patients. Nutr Clin Pract. 2010;25(1): Btaiche IF, Chan LN, Pleva M, Kraft MD. Critical illness, gastrointestinal complications, and medication therapy during enteral feeding in critically ill adult patients. Nutr Clin Pract. 2010;25(1): Kocan MJ, Hickisch SM. A comparison of continuous and intermittent enteral nutrition in NICU patients. J Neurosci Nurs. 1986;18(6): Coben RM, Weintraub A, DiMarino AJ Jr, Cohen S. Gastroesophageal reflux during gastrostomy feeding. Gastroenterology. 1994;106: Hiebert JM, Brown A, Anderson RG, Halfacre S, Rodeheaver GT, Edlich RF. Comparison of continuous vs intermittent tube feedings in adult burn patients. JPEN J Parenter Enteral Nutr. 1981;5(1): Tolep K, Getch CL, Criner GJ. Swallowing dysfunction in patients receiving prolonged mechanical ventilation. Chest. 1996;109(1): Skoretz SA, Flowers HL, Martino R. The incidence of dysphagia following endotracheal intubation: a systematic review. Chest. 2010;137(3): Rello J, Sonora R, Jubert P, Artigas A, Rue M, Valles J. Pneumonia in intubated patients: role of respiratory airway care. Am J Respir Crit Care Med. 1996;154(1): American Thoracic Society, Infectious Diseases Society of America. Guidelines for the management of adults with hospital-acquired, ventilator-associated, and healthcare-associated pneumonia. Am J Respir Crit Care Med. 2005;171(4): Lorente L, Blot S, Rello J. New issues and controversies in the prevention of ventilator-associated pneumonia. Am J Respir Crit Care Med. 2010;182(7): of 6 Issued November 2011
AACN Practice Alert. Prevention of Aspiration in Adults
 AACN Practice Alert Prevention of Aspiration in Adults Scope and Impact of the Problem Critically ill patients are at increased risk of aspirating oropharyngeal secretions and regurgitated gastric contents.
AACN Practice Alert Prevention of Aspiration in Adults Scope and Impact of the Problem Critically ill patients are at increased risk of aspirating oropharyngeal secretions and regurgitated gastric contents.
Issues in Enteral Feeding: Aspiration
 Issues in Enteral Feeding: Aspiration A webinar for HealthTrust Members February 11, 2019 Co-sponsored by HealthTrust and V NOS Continuing Education Provider Presented by: Kathleen Stoessel, RN, BSN, MS
Issues in Enteral Feeding: Aspiration A webinar for HealthTrust Members February 11, 2019 Co-sponsored by HealthTrust and V NOS Continuing Education Provider Presented by: Kathleen Stoessel, RN, BSN, MS
5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes May 2015
 5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes May 2015 2015 Recommendation: Based on 3 level 2 studies, a gastric residual volume of either 250 or 500
5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes May 2015 2015 Recommendation: Based on 3 level 2 studies, a gastric residual volume of either 250 or 500
STRATEGIES TO IMPROVE ENTERAL FEEDING TOLERANCE. IS IT WORTH IT? ENGELA FRANCIS RD(SA)
 STRATEGIES TO IMPROVE ENTERAL FEEDING TOLERANCE. IS IT WORTH IT? ENGELA FRANCIS RD(SA) DEFINITION OF ENTERAL FEEDING INTOLERANCE Gastrointestinal feeding intolerance are usually defined as: High gastric
STRATEGIES TO IMPROVE ENTERAL FEEDING TOLERANCE. IS IT WORTH IT? ENGELA FRANCIS RD(SA) DEFINITION OF ENTERAL FEEDING INTOLERANCE Gastrointestinal feeding intolerance are usually defined as: High gastric
5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes March 2013
 5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes March 203 NEW SECTION in 203 Recommendation: There are insufficient data to make a recommendation for not
5.5 Strategies to Optimize the Delivery of EN: Use of and Threshold for Gastric Residual Volumes March 203 NEW SECTION in 203 Recommendation: There are insufficient data to make a recommendation for not
IS YOUR CUFF DOING THE JOB?
 MICROCUFF * Endotracheal Tubes IS YOUR CUFF DOING THE JOB? Polyurethane cuff and subglottic secretion drainage help prevent early- and late-onset VAP 1 LEADING AUTHORITIES: SUBGLOTTIC SUCTIONING IS A BEST
MICROCUFF * Endotracheal Tubes IS YOUR CUFF DOING THE JOB? Polyurethane cuff and subglottic secretion drainage help prevent early- and late-onset VAP 1 LEADING AUTHORITIES: SUBGLOTTIC SUCTIONING IS A BEST
ASPEN Safe Practices for Enteral Nutrition Therapy
 ASPEN Safe Practices for Enteral Nutrition Therapy Ainsley Malone, MS, RDN, CNSC, FAND, FASPEN Nutrition Support Dietitian Mt. Carmel West Hospital ASPEN Clinical Practice Specialist Disclosure I have
ASPEN Safe Practices for Enteral Nutrition Therapy Ainsley Malone, MS, RDN, CNSC, FAND, FASPEN Nutrition Support Dietitian Mt. Carmel West Hospital ASPEN Clinical Practice Specialist Disclosure I have
Division of Acute Care Surgery Clinical Practice Policies, Guidelines, and Algorithms: Enteral Nutrition Algorithm Clinical Practice Guideline
 Division of Acute Care Surgery Clinical Practice Policies, Guidelines, and Algorithms: Enteral Nutrition Algorithm Clinical Practice Guideline Original Date: 08/2011 Purpose: To promote the early use of
Division of Acute Care Surgery Clinical Practice Policies, Guidelines, and Algorithms: Enteral Nutrition Algorithm Clinical Practice Guideline Original Date: 08/2011 Purpose: To promote the early use of
Chapter 29 Gastrointestinal Intubation
 Chapter 29 Gastrointestinal Intubation Intubation Intubation: placement of a tube into a body structure Types of intubation Orogastric: mouth to stomach Nasogastric: nose to stomach Nasointestinal: nose
Chapter 29 Gastrointestinal Intubation Intubation Intubation: placement of a tube into a body structure Types of intubation Orogastric: mouth to stomach Nasogastric: nose to stomach Nasointestinal: nose
5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric May 2015
 5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric May 2015 2015 Recommendation: Based on 16 level 2 studies, small bowel feeding compared to gastric feeding
5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric May 2015 2015 Recommendation: Based on 16 level 2 studies, small bowel feeding compared to gastric feeding
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: ADMINISTRATION OF A FEEDING (CONTINUOUS OR INTERMITTENT) OR MEDICATION VIA A GASTROSTOMY TUBE-ADULT Nursing DATE: REVIEWED: PAGES: 07/82
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: ADMINISTRATION OF A FEEDING (CONTINUOUS OR INTERMITTENT) OR MEDICATION VIA A GASTROSTOMY TUBE-ADULT Nursing DATE: REVIEWED: PAGES: 07/82
5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric February 2014
 5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric February 2014 2013 Recommendation: Based on 15 level 2 studies, small bowel feeding compared to gastric feeding
5.3 Strategies to Optimize Delivery and Minimize Risks of EN: Small Bowel Feeding vs. Gastric February 2014 2013 Recommendation: Based on 15 level 2 studies, small bowel feeding compared to gastric feeding
GASTRIC RESIDUAL VOLUME AND ASPIRATION PATIENTS RECEIVING GASTRIC FEEDINGS IN CRITICALLY ILL. Pulmonary Critical Care. 1.0 Hour
 Pulmonary Critical Care GASTRIC RESIDUAL VOLUME AND ASPIRATION IN CRITICALLY ILL PATIENTS RECEIVING GASTRIC FEEDINGS By Norma A. Metheny, RN, PhD, Lynn Schallom, RN, MSN, CCNS, CCRN, Dana A. Oliver, MPH,
Pulmonary Critical Care GASTRIC RESIDUAL VOLUME AND ASPIRATION IN CRITICALLY ILL PATIENTS RECEIVING GASTRIC FEEDINGS By Norma A. Metheny, RN, PhD, Lynn Schallom, RN, MSN, CCNS, CCRN, Dana A. Oliver, MPH,
Interesting Case Series. Pulmonary Injury Secondary to Feeding Tube Misplacement
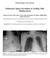 Interesting Case Series Pulmonary Injury Secondary to Feeding Tube Misplacement Thomas R. Resch, MD, Leigh A. Price, MD, and Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS Johns Hopkins Burn Center, The
Interesting Case Series Pulmonary Injury Secondary to Feeding Tube Misplacement Thomas R. Resch, MD, Leigh A. Price, MD, and Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS Johns Hopkins Burn Center, The
1.40 Prevention of Nosocomial Pneumonia
 1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
Feeding Protocols Enteral or Parenteral. AM Poleÿ 2012
 Practical aspects on Feeding Protocols Enteral or Parenteral AM Poleÿ 2012 Enteral Feeding Facts A reduction in mortality Prophylaxis for stress ulcers Full-strength Time to start enteral nutrition If
Practical aspects on Feeding Protocols Enteral or Parenteral AM Poleÿ 2012 Enteral Feeding Facts A reduction in mortality Prophylaxis for stress ulcers Full-strength Time to start enteral nutrition If
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Why You Switched to the Tiger 2 Self-Advancing Nasal Jejunal Feeding Tube
 Why You Switched to the Tiger 2 Self-Advancing Nasal Jejunal Feeding Tube Ease of Use Self-advancing technology minimises hands-on time for clinicians. Requires no additional devices or costly capital
Why You Switched to the Tiger 2 Self-Advancing Nasal Jejunal Feeding Tube Ease of Use Self-advancing technology minimises hands-on time for clinicians. Requires no additional devices or costly capital
COMMUNICATION. Communication and Swallowing post Tracheostomy. Role of SLT. Impact of Tracheostomy. Normal Speech. Facilitating Communication
 Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
PERFORMANCE UNDER PRESSURE.
 PERFORMANCE UNDER PRESSURE. IntelliCuff Cuff Pressure Controller and SubG Endotracheal Tube Smart technology to help reduce risk of VAP and tracheal injuries Replace Complexity with Efficiency. Managing
PERFORMANCE UNDER PRESSURE. IntelliCuff Cuff Pressure Controller and SubG Endotracheal Tube Smart technology to help reduce risk of VAP and tracheal injuries Replace Complexity with Efficiency. Managing
5.4 Strategies to optimize delivery and minimize risks of Enteral Nutrition: Body position January 31 st, 2009
 5.4 Strategies to optimize delivery and minimize risks of Enteral Nutrition: Body position January 31 st, 2009 Recommendation: Based on 1 level 1 and 1 level 2 study, we recommend that critically ill patients
5.4 Strategies to optimize delivery and minimize risks of Enteral Nutrition: Body position January 31 st, 2009 Recommendation: Based on 1 level 1 and 1 level 2 study, we recommend that critically ill patients
VAP Prevention bundles
 VAP Prevention bundles Dr. Shafiq A.Alimad MD Head of medical department at USTH YICID workshop, 15-12-2014 Care Bundles What are they & why use them? What are Care Bundles? Types of Care Bundles available
VAP Prevention bundles Dr. Shafiq A.Alimad MD Head of medical department at USTH YICID workshop, 15-12-2014 Care Bundles What are they & why use them? What are Care Bundles? Types of Care Bundles available
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation David A. Muir Course Outline Physiology of Swallow
 Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Diarrhea may be: Acute (short-term, usually lasting several days), which is usually related to bacterial or viral infections.
 Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Nutrient intake is considered part of the global resuscitation
 Prospective Randomized Control Trial of Intermittent Versus Continuous Gastric Feeds for Critically Ill Trauma Patients Jana B. A. MacLeod, MD, Jennifer Lefton, RD, CNSD, Doug Houghton, MSN, Christina
Prospective Randomized Control Trial of Intermittent Versus Continuous Gastric Feeds for Critically Ill Trauma Patients Jana B. A. MacLeod, MD, Jennifer Lefton, RD, CNSD, Doug Houghton, MSN, Christina
Home Total Parenteral Nutrition for Adults
 Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
Nutrition in critical illness:
 Nutrition in critical illness: from theory to daily practice Aim of the presentation Summarize the guidelines for the provision and assessment of nutrition support therapy in the adult critically ill patient.
Nutrition in critical illness: from theory to daily practice Aim of the presentation Summarize the guidelines for the provision and assessment of nutrition support therapy in the adult critically ill patient.
American College of Surgeons Critical Care Review Course 2012: Infection Control
 American College of Surgeons Critical Care Review Course 2012: Infection Control Overview: I. Central line associated blood stream infection (CLABSI) II. Ventilator associated pneumonia (VAP) I. Central
American College of Surgeons Critical Care Review Course 2012: Infection Control Overview: I. Central line associated blood stream infection (CLABSI) II. Ventilator associated pneumonia (VAP) I. Central
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Wali R Johnson et. al. / International Journal of New Technologies in Science and Engineering Vol. 2, Issue 4, October 2015, ISSN
 Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis.
 Page 1 of 6 Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis. Case Report Mohd Basri bin Mat Nor. Department of Anaesthesiology
Page 1 of 6 Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis. Case Report Mohd Basri bin Mat Nor. Department of Anaesthesiology
ENTERAL FEEDING GUIDELINES INTRODUCTION
 INTRODUCTION Enteral feeding is defined as the administration of nutrients directly into the gastrointestinal (GI) tract. If the patient is unable to meet his/her nutritional requirements with oral diet/nutritional
INTRODUCTION Enteral feeding is defined as the administration of nutrients directly into the gastrointestinal (GI) tract. If the patient is unable to meet his/her nutritional requirements with oral diet/nutritional
Intermittent and Bolus Methods of Feeding in Critical Care
 Intermittent and Bolus Methods of Feeding in Critical Care Satomi Ichimaru a * and Teruyoshi Amagai b a Department of Nutrition Management, Kobe City Medical Center General Hospital, Kobe, Hyogo, Japan
Intermittent and Bolus Methods of Feeding in Critical Care Satomi Ichimaru a * and Teruyoshi Amagai b a Department of Nutrition Management, Kobe City Medical Center General Hospital, Kobe, Hyogo, Japan
Current concepts in Critical Care Nutrition
 Current concepts in Critical Care Nutrition Dr.N.Ramakrishnan AB (Int Med), AB (Crit Care), MMM, FACP, FCCP, FCCM Director, Critical Care Services Apollo Hospitals, Chennai Objectives Why? Enteral or Parenteral
Current concepts in Critical Care Nutrition Dr.N.Ramakrishnan AB (Int Med), AB (Crit Care), MMM, FACP, FCCP, FCCM Director, Critical Care Services Apollo Hospitals, Chennai Objectives Why? Enteral or Parenteral
Vanderbilt University Medical Center Trauma ICU Nutrition Management Guidelines
 Vanderbilt University Medical Center Trauma ICU Nutrition Management Guidelines Trauma Critical Care Nutrition Guidelines Clinical judgment may supersede guidelines as patient circumstances warrant ASSESSMENT
Vanderbilt University Medical Center Trauma ICU Nutrition Management Guidelines Trauma Critical Care Nutrition Guidelines Clinical judgment may supersede guidelines as patient circumstances warrant ASSESSMENT
3.2 Nutritional Prescription of Enteral Nutrition: Achieving Target Dose of Enteral Nutrition March 2013
 . Nutritional Prescription of Enteral Nutrition: Achieving Target Dose of Enteral Nutrition March 01 There were no new randomized controlled trials since the 009 update and hence there are no changes to
. Nutritional Prescription of Enteral Nutrition: Achieving Target Dose of Enteral Nutrition March 01 There were no new randomized controlled trials since the 009 update and hence there are no changes to
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
Enteral Nutrition: Whom, Why, When, What and Where to Feed?
 Meier RF, Reddy BR, Soeters PB (eds): The Importance of Nutrition as an Integral Part of Disease Management. Nestlé Nutr Inst Workshop Ser, vol 82, pp 53 59, (DOI: 10.1159/000382002) Nestec Ltd., Vevey/S.
Meier RF, Reddy BR, Soeters PB (eds): The Importance of Nutrition as an Integral Part of Disease Management. Nestlé Nutr Inst Workshop Ser, vol 82, pp 53 59, (DOI: 10.1159/000382002) Nestec Ltd., Vevey/S.
5.1 Strategies to Optimize Delivery and Minimize Risks of EN: Feeding Protocols March 2013
 5.1 Strategies to Optimize Delivery and Minimize Risks of EN: Feeding Protocols March 2013 There were no new randomized controlled trials since the 2009 update and hence there are no changes to the following
5.1 Strategies to Optimize Delivery and Minimize Risks of EN: Feeding Protocols March 2013 There were no new randomized controlled trials since the 2009 update and hence there are no changes to the following
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
Key findings, outcomes or recommendations
 Reference (include title, author, journal title, year of publication, volume and issue, pages) Evidence level (I-VII) Key findings, outcomes or recommendations ASPEN Safe Practices for Enteral Nutrition
Reference (include title, author, journal title, year of publication, volume and issue, pages) Evidence level (I-VII) Key findings, outcomes or recommendations ASPEN Safe Practices for Enteral Nutrition
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Targeted literature review:
 Targeted literature review: What are the key infection prevention and control recommendations to inform a minimising ventilator associated pneumonia (VAP) quality improvement tool? Part of HAI Delivery
Targeted literature review: What are the key infection prevention and control recommendations to inform a minimising ventilator associated pneumonia (VAP) quality improvement tool? Part of HAI Delivery
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient
 CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Overview. Chapter 37. Advanced Airway Techniques. Sellick Maneuver 9/11/2012
 Chapter 37 Advanced Airway Techniques Slide 1 Sellick Maneuver Purpose Anatomic Location Technique Special Considerations Overview Advanced Airway Management of Adults Esophageal Tracheal Combitubes Tracheal
Chapter 37 Advanced Airway Techniques Slide 1 Sellick Maneuver Purpose Anatomic Location Technique Special Considerations Overview Advanced Airway Management of Adults Esophageal Tracheal Combitubes Tracheal
L.Mageswary Dietitian Hospital Selayang
 L.Mageswary Dietitian Hospital Selayang 14 15 AUG ASMIC 2015 Learning Objectives 1. To understand the importance of nutrition support in ICU 2. To know the right time to feed 3. To understand the indications
L.Mageswary Dietitian Hospital Selayang 14 15 AUG ASMIC 2015 Learning Objectives 1. To understand the importance of nutrition support in ICU 2. To know the right time to feed 3. To understand the indications
Back to Basics: What Imaging Test should I order? Jeanne G. Hill, M.D. Pediatric Radiology Medical University of South Carolina
 Back to Basics: What Imaging Test should I order? Jeanne G. Hill, M.D. Pediatric Radiology Medical University of South Carolina Disclosure Neither I nor any member of my immediate family has a relevant
Back to Basics: What Imaging Test should I order? Jeanne G. Hill, M.D. Pediatric Radiology Medical University of South Carolina Disclosure Neither I nor any member of my immediate family has a relevant
Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Pediatric Critically Ill Patient: ASPEN-SCCM 2017
 Number of Patients Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Pediatric Critically Ill Patient: ASPEN-SCCM 2017 Jorge A. Coss-Bu, MD Associate Professor of Pediatrics
Number of Patients Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Pediatric Critically Ill Patient: ASPEN-SCCM 2017 Jorge A. Coss-Bu, MD Associate Professor of Pediatrics
5.2 Strategies to Optimize Delivery and Minimize Risks of EN: Motility Agents May 2015
 5.2 Strategies to Optimize Delivery and Minimize Risks of EN: Motility Agents May 2015 There were no new randomized controlled trials since the 2009 and 2013 updates and hence there are no changes to the
5.2 Strategies to Optimize Delivery and Minimize Risks of EN: Motility Agents May 2015 There were no new randomized controlled trials since the 2009 and 2013 updates and hence there are no changes to the
3.2 Nutritional Prescription of Enteral Nutrition: Enhanced Dose of Enteral Nutrition May 2015
 . Nutritional Prescription of Enteral Nutrition: Enhanced Dose of Enteral Nutrition May 015 015 Recommendation: Based on 1 level 1 study, level studies and cluster randomized controlled trials, when starting
. Nutritional Prescription of Enteral Nutrition: Enhanced Dose of Enteral Nutrition May 015 015 Recommendation: Based on 1 level 1 study, level studies and cluster randomized controlled trials, when starting
VOLUME-BASED VS. RATE-BASED FEEDING
 VOLUME-BASED VS. RATE-BASED FEEDING Amanda Holyk Critical Care Pharmacist Mount Nittany Medical Center Society of Critical Care Medicine Annual Symposium November 10, 2017 0 Disclosure I have no actual
VOLUME-BASED VS. RATE-BASED FEEDING Amanda Holyk Critical Care Pharmacist Mount Nittany Medical Center Society of Critical Care Medicine Annual Symposium November 10, 2017 0 Disclosure I have no actual
PREPARING FOR REFLUX TESTING. Bravo Reflux Testing System. A simple way to evaluate your gastroesophageal reflux symptoms
 PREPARING FOR REFLUX TESTING Bravo Reflux Testing System A simple way to evaluate your gastroesophageal reflux symptoms HOW IT WORKS The test involves a miniature ph capsule, which is approximately the
PREPARING FOR REFLUX TESTING Bravo Reflux Testing System A simple way to evaluate your gastroesophageal reflux symptoms HOW IT WORKS The test involves a miniature ph capsule, which is approximately the
Gastric versus Jejunal Feeding: Evidence or Emotion?
 Carol Rees Parrish, R.D., M.S., Series Editor Gastric versus Jejunal Feeding: Evidence or Emotion? Joe Krenitsky Delivery of enteral feeding into the small bowel has been suggested as a strategy to reduce
Carol Rees Parrish, R.D., M.S., Series Editor Gastric versus Jejunal Feeding: Evidence or Emotion? Joe Krenitsky Delivery of enteral feeding into the small bowel has been suggested as a strategy to reduce
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY
 SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
Gastrointestinal Feedings Post Op: What s the deal on beginning oral feedings?
 Gastrointestinal Feedings Post Op: What s the deal on beginning oral feedings? Kate Willcutts, DCN, RD, CNSC University of Virginia Health System Charlottesville, VA kfw3w@virginia.edu Objectives 1. Discuss
Gastrointestinal Feedings Post Op: What s the deal on beginning oral feedings? Kate Willcutts, DCN, RD, CNSC University of Virginia Health System Charlottesville, VA kfw3w@virginia.edu Objectives 1. Discuss
Metabolic Control in Critical Care: Nutrition Therapy
 LOGO Metabolic Control in Critical Care: Nutrition Therapy ผศ.นพ.พรพจน เปรมโยธ น สาขาโภชนาการคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร ศ ร ราชพยาบาล 2016 SCCM/ASPEN Guidelines Nutrition Therapy in the ICU
LOGO Metabolic Control in Critical Care: Nutrition Therapy ผศ.นพ.พรพจน เปรมโยธ น สาขาโภชนาการคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร ศ ร ราชพยาบาล 2016 SCCM/ASPEN Guidelines Nutrition Therapy in the ICU
WHEN To Initiate Parenteral Nutrition A Frequent Question With New Answers
 WHEN To Initiate Parenteral Nutrition A Frequent Question With New Answers Ainsley Malone, MS, RD, LD, CNSC, FAND, FASPEN Dubai International Nutrition Conference 2018 Disclosures No commercial relationship
WHEN To Initiate Parenteral Nutrition A Frequent Question With New Answers Ainsley Malone, MS, RD, LD, CNSC, FAND, FASPEN Dubai International Nutrition Conference 2018 Disclosures No commercial relationship
Gastric Residuals in Preterm Infants
 Neonatal Nursing Education Brief: Gastric Residuals in the Preterm Infant https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Neonatal Nursing Education Brief: Gastric Residuals in the Preterm Infant https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
PRODUCTS FOR THE DIFFICULT AIRWAY. Courtesy of Cook Critical Care
 PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
The Roles and Responsibilities of Nurse Before and After Laparoscopic Urologic Surgery
 + The Roles and Responsibilities of Nurse Before and After Laparoscopic Urologic Surgery Elif GEZGINCI Gulhane Military Medical Academy School of Nursing Ankara 1 + 2 PREOPERATİVE + Preoperative (Patient
+ The Roles and Responsibilities of Nurse Before and After Laparoscopic Urologic Surgery Elif GEZGINCI Gulhane Military Medical Academy School of Nursing Ankara 1 + 2 PREOPERATİVE + Preoperative (Patient
NO DISCLOSURES 5/9/2015
 Annette Stralovich-Romani, RD, CNSC Adult Critical Care Nutritionist UCSF Medical Center NO DISCLOSURES Incidence & consequences of malnutrition Underfeeding in the ICU Causes/ consequences Nutrition intervention
Annette Stralovich-Romani, RD, CNSC Adult Critical Care Nutritionist UCSF Medical Center NO DISCLOSURES Incidence & consequences of malnutrition Underfeeding in the ICU Causes/ consequences Nutrition intervention
Speech and Language Therapy in Critical Care
 Speech and Language Therapy in Critical Care Sarah Eli, MSc, MRCSLT, MHPC Specialist Speech and Language Therapist in Critical Care Sarah.Eli@royalberkshire.nhs.uk Why do We Need SLT in Critical Care Key
Speech and Language Therapy in Critical Care Sarah Eli, MSc, MRCSLT, MHPC Specialist Speech and Language Therapist in Critical Care Sarah.Eli@royalberkshire.nhs.uk Why do We Need SLT in Critical Care Key
Ventilator-Associated Pneumonia Prevention Bundle 2010 Revised Edition (JSICM-VAP Bundle)
 1 Ventilator-Associated Pneumonia Prevention Bundle 2010 Revised Edition (JSICM-VAP Bundle) Committee on ICU Evaluation Japanese Society of Intensive Care Medicine 2 I. Ensuring hand hygiene Hand washing
1 Ventilator-Associated Pneumonia Prevention Bundle 2010 Revised Edition (JSICM-VAP Bundle) Committee on ICU Evaluation Japanese Society of Intensive Care Medicine 2 I. Ensuring hand hygiene Hand washing
Chapter 14: Training in Radiology. DDSEP Chapter 1: Question 12
 DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
Information about Feeding Tubes
 Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA
 RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
INTRODUCTION TO UPPER ENDOSCOPY
 INTRODUCTION TO UPPER ENDOSCOPY Satish Nagula, MD Associate Professor of Medicine Icahn School of Medicine at Mount Sinai NYSGE First Year Fellows Course July 14, 2018 Early endoscopes 1805: Bozzini Lichtleiter
INTRODUCTION TO UPPER ENDOSCOPY Satish Nagula, MD Associate Professor of Medicine Icahn School of Medicine at Mount Sinai NYSGE First Year Fellows Course July 14, 2018 Early endoscopes 1805: Bozzini Lichtleiter
Western General Hospital Tubefeeding Group Radiologically Inserted Gastrostomy Protocol, October 2008
 Lothian University Hospitals Division Western General Hospital Protocol for the Care of Radiologically Inserted Gastrostomy Tube 14 FG Medicina G Tube CARE OF PATIENT FOLLOWING TUBE INSERTION OBSERVATIONS
Lothian University Hospitals Division Western General Hospital Protocol for the Care of Radiologically Inserted Gastrostomy Tube 14 FG Medicina G Tube CARE OF PATIENT FOLLOWING TUBE INSERTION OBSERVATIONS
[No conflicts of interest]
![[No conflicts of interest] [No conflicts of interest]](/thumbs/86/94144068.jpg) [No conflicts of interest] Patients and staff at: Available evidence pre-calories Three meta-analyses: Gramlich L et al. Does enteral nutrition compared to parenteral nutrition result in better outcomes
[No conflicts of interest] Patients and staff at: Available evidence pre-calories Three meta-analyses: Gramlich L et al. Does enteral nutrition compared to parenteral nutrition result in better outcomes
A Case of Severe Neonatal Dysphagia: Experience and Reason
 A Case of Severe Neonatal Dysphagia: Experience and Reason The Contemporary Management of Aerodigestive Disease in Children 2 nd Aerodigestive Meeting Vanderbilt University, Nashville, TN Friday, November
A Case of Severe Neonatal Dysphagia: Experience and Reason The Contemporary Management of Aerodigestive Disease in Children 2 nd Aerodigestive Meeting Vanderbilt University, Nashville, TN Friday, November
Understanding GERD. & Stretta Therapy. GERD (gĕrd): Gastroesophageal Reflux Disease
 Understanding GERD & Stretta Therapy GERD (gĕrd): Gastroesophageal Reflux Disease What is GERD? When the muscle between your stomach and esophagus is weak, stomach contents like acid or bile can reflux
Understanding GERD & Stretta Therapy GERD (gĕrd): Gastroesophageal Reflux Disease What is GERD? When the muscle between your stomach and esophagus is weak, stomach contents like acid or bile can reflux
Reluctance or refusal to feed or eat. Understanding Feeding Aversion in a City Full of Foodies. Presentation Outline. Learning Objectives
 Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Tracheoesophageal Fistula and Esophageal Atresia
 Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
HOMES AND SENIORS SERVICES. APPROVAL DATE: February 2011 REVISION DATE: January 2015; July 2018
 POLICY: Page 1 of 6 A resident requiring enteral (tube) feeding as a sole source or adjunctive nutrition support have access to a comprehensive enteral feeding program and receive appropriate support from
POLICY: Page 1 of 6 A resident requiring enteral (tube) feeding as a sole source or adjunctive nutrition support have access to a comprehensive enteral feeding program and receive appropriate support from
The effectiveness of ultrasonography in verifying the placement of a nasogastric tube in patients with low consciousness at an emergency center
 Kim et al. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine 2012, 20:38 ORIGINAL RESEARCH Open Access The effectiveness of ultrasonography in verifying the placement of a nasogastric
Kim et al. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine 2012, 20:38 ORIGINAL RESEARCH Open Access The effectiveness of ultrasonography in verifying the placement of a nasogastric
The Laryngeal Mask and Other Supraglottic Airways: Application to Clinical Airway Management
 The Laryngeal Mask and Other Supraglottic Airways: Application to Clinical Airway Management D. John Doyle MD PhD FRCPC Department of General Anesthesiology Cleveland Clinic Foundation 9500 Euclid Avenue
The Laryngeal Mask and Other Supraglottic Airways: Application to Clinical Airway Management D. John Doyle MD PhD FRCPC Department of General Anesthesiology Cleveland Clinic Foundation 9500 Euclid Avenue
The value of bowel sound assessment in predicting feeding intolerance in critically ill patients
 Crit Care & Shock (2011) 14:65-69 The value of bowel sound assessment in predicting feeding intolerance in critically ill patients Abdullah AlShimemeri, Maram Sakkijha, Samir Haddad, Yaseen Arabi Abstract
Crit Care & Shock (2011) 14:65-69 The value of bowel sound assessment in predicting feeding intolerance in critically ill patients Abdullah AlShimemeri, Maram Sakkijha, Samir Haddad, Yaseen Arabi Abstract
PARENTERAL NUTRITION THERAPY
 UnitedHealthcare Benefits of Texas, Inc. 1. UnitedHealthcare of Oklahoma, Inc. 2. UnitedHealthcare of Oregon, Inc. UnitedHealthcare of Washington, Inc. UnitedHealthcare West BENEFIT INTERPRETATION POLICY
UnitedHealthcare Benefits of Texas, Inc. 1. UnitedHealthcare of Oklahoma, Inc. 2. UnitedHealthcare of Oregon, Inc. UnitedHealthcare of Washington, Inc. UnitedHealthcare West BENEFIT INTERPRETATION POLICY
A NEW direction for subglottic secretion management
 A NEW direction for subglottic secretion management The SIMEX Subglottic Aspiration System, cuff M and cuff S are the most advanced solution for the aspiration of subglottic secretion, featuring all new
A NEW direction for subglottic secretion management The SIMEX Subglottic Aspiration System, cuff M and cuff S are the most advanced solution for the aspiration of subglottic secretion, featuring all new
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
KIMBERLY-CLARK* MICROCUFF* Endotracheal Tube.. Revolutionary cuff material designed to reduce micro-aspiration
 KIMBERLY-CLARK* MICROCUFF* Endotracheal Tube.. Revolutionary cuff material designed to reduce micro-aspiration Ventilator-Associated Pneumonia VAP is a major clinical concern...... associated with high
KIMBERLY-CLARK* MICROCUFF* Endotracheal Tube.. Revolutionary cuff material designed to reduce micro-aspiration Ventilator-Associated Pneumonia VAP is a major clinical concern...... associated with high
Gastric residual volume management in critically ill mechanically ventilated patients: A literature review
 598451PSH0010.1177/2010105815598451Proceedings of Singapore HealthcareGuo research-article2015 Review Article PROCEEDINGS OF SINGAPORE HEALTHCARE Gastric residual volume management in critically ill mechanically
598451PSH0010.1177/2010105815598451Proceedings of Singapore HealthcareGuo research-article2015 Review Article PROCEEDINGS OF SINGAPORE HEALTHCARE Gastric residual volume management in critically ill mechanically
UMC HEALTH SYSTEM Lubbock, Texas :
 Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
SUBGLOTTIC SECRETION REMOVAL:
 ARROW REGIONAL TELEFLEX ANAESTHESIA ISIS Nullan utpat, Better vulputpatie access. ero Best dion practice. ulputat SUBGLOTTIC SECRETION REMOVAL: A VAP REDUCTION STRATEGY Ventilator-Associated Pneumonia
ARROW REGIONAL TELEFLEX ANAESTHESIA ISIS Nullan utpat, Better vulputpatie access. ero Best dion practice. ulputat SUBGLOTTIC SECRETION REMOVAL: A VAP REDUCTION STRATEGY Ventilator-Associated Pneumonia
CARDIAC EMERGENCIES Other Cardiac Dysrhythmias C9
 CARDIAC EMERGENCIES Other Cardiac Dysrhythmias C9 ATRIAL FLUTTER Variable rate depending on block. Atrial rate between 250-350, saw-tooth pattern. (see Appendix B for energy settings for bi-phasic low
CARDIAC EMERGENCIES Other Cardiac Dysrhythmias C9 ATRIAL FLUTTER Variable rate depending on block. Atrial rate between 250-350, saw-tooth pattern. (see Appendix B for energy settings for bi-phasic low
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
GET THE. Suction port. Subglottic secretions. VAP incidence and mortality. Pathogenesis and risk factors. Subglottic secretions drainage (SSD)
 GET THE FACTS The facts about ventilator-associated pneumonia () and subglottic secretions drainage (SSD) incidence and mortality is the second most common nosocomial infection in the United States. It
GET THE FACTS The facts about ventilator-associated pneumonia () and subglottic secretions drainage (SSD) incidence and mortality is the second most common nosocomial infection in the United States. It
Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST
 Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST Objectives Gain a general understanding of normal swallowing Gain
Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST Objectives Gain a general understanding of normal swallowing Gain
Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased
 1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Nutrition support in adults: oral supplements, enteral and parenteral feeding.
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Pediatric ER Half-day Rounds October 12, 2011 Dr. Karen Bailey
 Pediatric ER Half-day Rounds October 12, 2011 Dr. Karen Bailey Objectives to identify various enteral and vascular access lines what do they look like? indications & contraindications proper placement
Pediatric ER Half-day Rounds October 12, 2011 Dr. Karen Bailey Objectives to identify various enteral and vascular access lines what do they look like? indications & contraindications proper placement
Having a PEG tube inserted Information for patients and carers
 Sunderland Day Case Centre Endoscopy Having a PEG tube inserted Information for patients and carers www.medway.nhs.uk Checklist Things to remember before your procedure Read the booklet carefully. Fill
Sunderland Day Case Centre Endoscopy Having a PEG tube inserted Information for patients and carers www.medway.nhs.uk Checklist Things to remember before your procedure Read the booklet carefully. Fill
LMA Supreme Second Seal. Maintain the airway. Manage gastric contents. Meet NAP4 recommendations.
 LMA Supreme Second Seal Maintain the airway. Manage gastric contents. Meet NAP4 recommendations. A proven double seal The importance of the Second Seal (oesophageal seal) is significant: it can minimise
LMA Supreme Second Seal Maintain the airway. Manage gastric contents. Meet NAP4 recommendations. A proven double seal The importance of the Second Seal (oesophageal seal) is significant: it can minimise
