Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, conta
|
|
|
- Florence Eugenia Sparks
- 5 years ago
- Views:
Transcription
1 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at ORIGINAL RESEARCH NEURORADIOLOGY Safety of Unprotected Carotid Artery Stent Placement in Symptomatic and Asymptomatic Patients: A Retrospective Analysis of 30-day Combined Adverse Outcomes 1 Franco Perona, MD Giorgio Castellazzi, MD Luca Valvassori, MD Edoardo Boccardi, MD Laura de Girolamo, PhD Gian Paolo Cornalba, MD Krishna Kandarpa, MD, PhD 1 From the Departments of Radiology (F.P., G.C.) and Research (L.d.G.), I.R.C.C.S. Galeazzi Orthopaedic Institute, Via Riccardo Galeazzi 4, Milan, Italy; Department of Neuroradiology, Ospedale Niguarda, Milan, Italy (L.V., E.B.); Department of Diagnostic and Interventional Radiology, University of Milan, School of Medicine, San Paolo Hospital, Milan, Italy (G.P.C.); and Department of Radiology, University of Massachusetts Medical School, Worcester, Mass (K.K.). From the 2006 RSNA Annual Meeting. Received January 9, 2008; revision requested February 29; revision received June 3; accepted June 17; final version accepted July 3. Address correspondence to F.P. ( franco.perona@yahoo.it ). Purpose: Materials and Methods: Results: Conclusion: To retrospectively evaluate the outcome of carotid artery stent placement (CAS) without the use of embolic protection devices (EPDs) in a large cohort of patients. Institutional review board approval and informed consent from all patients were obtained. Preprocedure color Doppler ultrasonography (US), magnetic resonance (MR) imaging, or computed tomography (CT) were used to evaluate stenosis severity (70% or greater). Clinical findings and combined 30-day complication rates in 400 patients (289 men, 111 women; mean age, 73 years 8 [standard deviation]) who underwent unprotected CAS for asymptomatic (n 156; 39%) or symptomatic (n 244, 61%) stenoses were analyzed. Follow-up at 30 days included neurologic evaluation and color Doppler US. Self-expanding stents were successfully deployed in 397 of 400 (99.25%) patients. Among the 397 patients, nine (2.27%) major complications (all in patients with prior symptoms) had occurred at 30 days, including three (0.76%) major (all in patients who had stopped antiplatelet prophylaxis) and six (1.5%) minor strokes three intraprocedural and three delayed. Minor complications included 16 (4%) transient ischemic attacks, four in asymptomatic and 12 in symptomatic patients. The 30-day combined adverse outcomes (transient ischemic attack, ipsilateral stroke, death) were significantly correlated with prior presence of symptoms (symptomatic, 8.6%; asymptomatic, 2.6%; P.03). Stent placement without EPD was performed with a high technical success rate. For asymptomatic patients, the combined 30-day adverse-outcomes rate was within the limits recommended by the American Heart Association for carotid endarterectomy and compared favorably with results reported for CAS with EPD. When a transient ischemic attack is excluded, the 30-day combined death and stroke rate among patients with prior symptoms also compared favorably with published results. RSNA, 2008 RSNA, Radiology: Volume 250: Number 1 January 2009
2 During the past several years, carotid artery stent placement (CAS) has emerged as an effective alternative to carotid endarterectomy (1 3). However, the major concern about this procedure is the potential distal embolization of particles from the treated site during or after the procedure (4,5). To prevent distal embolization, cerebral embolic protection devices (EPDs) have been developed, but published data to date do not clearly demonstrate the usefulness or safety with respect to clinical complications (6). CAS with EPD is associated with a reduction of intraprocedural cerebral embolization (3 5). However, the use of EPDs increases the procedural complexity and risk of embolization during device manipulation (6 8). Other disadvantages include filter obstruction with embolic material, with subsequent stasis of blood flow, vascular wall damage, and other nonneurologic complications that may require device removal (9 12). Since EPDs are expensive and prolong procedure time, it is important to determine the clinical value of this practice (6). The purpose of our study was to retrospectively evaluate the outcome of CAS without the use of EPDs in a large cohort of patients. Materials and Methods Advance in Knowledge We found no differences in efficacy or safety of carotid artery stent placement (CAS) without embolic protection devices in asymptomatic patients between our study and the published literature about CAS. Patient Selection and Evaluation Between June 1, 1997, and June 1, 2005, a total of 400 patients who met the inclusion and/or exclusion criteria (289 men, 111 women; mean age, 73 years 8 [standard deviation]; range, years; for men mean age 73 5 years, range 65 81; for women mean age 72 2, range 68 77) underwent CAS at two centers (Department of Radiology, I.R.C.C.S. Galeazzi Orthopaedic Institute: 158 patients; Department of Neuroradiology, Niguarda Hospital: 242 patients). We did not screen all consecutive patients ourselves. The patients were referred to us by physicians who were instructed about our inclusion and/or exclusion criteria. All these 400 patients were re-confirmed for inclusion by the authors who performed the stent placement. The study was conducted with institutional review board approval, and a written informed consent was obtained from all patients. All patients were evaluated clinically prior to the procedure by either an interventional radiologist or an interventional neuroradiologist and also a neurologist and an anesthesiologist. The following lesion selection criteria were used. Stenoses greater than 70% (in diameter) in symptomatic and in asymptomatic patients were considered for treatment. Exceptions (31 of 400 cases, 7.8%) were made for stenoses of 60% 70% severity when there was a contralateral carotid occlusion, both for asymptomatic and symptomatic patients. The following patient selection criteria were used. Inclusion criteria were (a) age older than 18 years, (b) unilateral or bilateral atherosclerotic or restenotic lesions in native carotid arteries and (c) symptoms plus stenosis of more than 70% in luminal diameter or (d) no symptoms plus stenosis more than 80% of the luminal diameter. Exclusion criteria were (a) evolving stroke or a recent stroke within the previous 7 days, (b) transient ischemic cerebral event within the last 24 hours, (c) allergy to any study medications or material, (d) renal insufficiency (creatinine level higher than 2 mg/dl [176.8 mol/l]), (e) suspicion of fresh thrombus at the internal carotid artery stenosis, or (f) occlusion of target vessel. Implication for Patient Care CAS without embolic protection devices decreases procedure time and eliminates potential filterrelated complications and cost. Moreover, our exclusion criteria required us to wait a minimum of 7 days after symptoms before performing carotid stent placement. However, as is the local practice, we wait approximately 3 weeks for patients with extensive stroke (documented on magnetic resonance [MR] or computed tomographic [CT] images) to allow healing of the blood-brain barrier and to avoid potential hemorrhagic complications due to early reperfusion. These patients are hospitalized, maintained on aspirin, and otherwise treated medically. At baseline, 156 of 400 (39%) patients presented with asymptomatic and 244 of 400 (61%) presented with symptomatic stenoses. Among patients with symptoms, 102 (41.80%) had amaurosis fugax, 94 (38.52%) had previous transient ischemic attack (TIA), and 48 (19.67%) had a stroke. All of the asymptomatic patients had severe internal carotid artery stenoses (70% 80%), and 68 of them also had the following concomitant conditions: hostile necks (radical neck surgery and radiation therapy, n 11), postcarotid endarterectomy restenosis (n 14), or a planned major operation (coronary bypass, n 29; aortic valve replacement, n 5; abdominal aorto-femoral bypass, n 9). As noted in Table 1 (items evaluated by F.P., L.V., and E.B., each of whom had more than 20 years of expe- Published online before print /radiol Radiology 2009; 250: Abbreviations: CAS carotid artery stent placement EPD embolic protection device TIA transient ischemic attack Author contributions: Guarantors of integrity of entire study, F.P., G.P.C., K.K.; study concepts/study design or data acquisition or data analysis/interpretation, all authors; manuscript drafting or manuscript revision for important intellectual content, all authors; approval of final version of submitted manuscript, all authors; literature research, F.P., G.C., G.P.C.; clinical studies, F.P., L.V., E.B., K.K.; experimental studies, F.P., G.C., L.V., E.B., L.d.G., G.P.C.; statistical analysis, L.V., E.B., L.d.G., K.K.; and manuscript editing, F.P., G.C., L.d.G., G.P.C., K.K. Authors stated no financial relationship to disclose. Radiology: Volume 250: Number 1 January
3 rience in vascular imaging and interventions), 15 of 46 contralateral occlusions and 10 of 54 contralateral stenoses (of any severity) were noted in asymptomatic patients. Demographic data, including co-morbidities and atherosclerotic risk factors, are summarized in Table 1. Clinical outcomes and the combined (TIA, ipsilateral stroke, death) 30-day adverse outcome rates for all treated patients were analyzed. Carotid Artery Imaging As is the practice in our community, all carotid lesions were initially evaluated with color Doppler ultrasonography (US) with high-frequency probes. Stenosis severity was quantified on the basis of peak systolic velocities measured at the stenosis or immediately distally (velocity 210 m/sec, corresponding to 70% diameter stenosis). Preprocedure MR imaging of the brain and MR angiography of the aortic arch vessels and carotid arteries were performed in 384 patients. Sixteen patients who were not eligible for MR imaging (13 had cardiac pacemakers, two had thalassemia major, and one had an incompatible crystalline lens implant) were examined with CT angiography. Any high or calcified lesions, difficult for color Doppler US evaluation, were diagnosed with MR angiography or CT angiography. During the procedure, all lesions were evaluated with intraarterial digital subtraction angiography prior to stent placement and were confirmed to meet eligible stenosis severity in all cases. Germany) for at least 3 days before the procedure. All procedures were performed without sedation, except for eight patients who needed light sedation (intravenous benzodiazapam) to relieve their anxiety. During the procedure, a bolus of U of heparin was administered. Heparin doses were adjusted to achieve an intraprocedural activated clotting time of 300 seconds. At the end of the procedure, the introducer was removed after activated clotting time was restored to 200 seconds or less. After the procedure, ticlopidine hydrochloride prophylaxis was prescribed for 2 months and was only discontinued (10 days) prior to any elective surgery. Aspirin was prescribed for life. After heparinization, a diagnostic catheter was placed in the common carotid artery over a guidewire, with the tip below the lesion. Digital subtraction angiograms of the carotid bifurcation (bi-plane), the intracranial segment of the internal carotid artery and cerebral circulation, were then obtained. After angiographic evaluation, the catheter was exchanged for a soft-tip 6-F guiding catheter (Envoy; Cordis/Johnson & Johnson, Miami, Fla) placed in the common carotid artery. EPDs were not used. Subsequently, the lesion was gently crossed by using a small array of inch guidewires (BMW 0.014, Abbott-Guidant, Abbott Park, Ill; V-18, Boston Scientific, Natick, Mass), Table 1 the choice was determined according to the arterial anatomy. Predilatation 3 4-mm PTA balloon catheters (Gazelle or Ultrasoft; Boston Scientific) were used in 24 of 400 (6%) patients. All patients were treated with a stent (Carotid Wallstent; Boston Scientific) that was 7 9 mm in diameter by 4 6 cm in length and was placed across the bifurcation. After deployment, stent dilation was performed in the majority of cases (394 of 400, 98.5%) by using low-profile monorail 5 7-mm percutaneous transluminal angioplasty balloon catheters (Gazelle or Ultrasoft; Boston Scientific). Intraarterial digital subtraction angiography was performed on procedure completion, as was done at baseline. Patient Monitoring Patients were monitored during the interventional procedure with regular recording of vital signs; the cardiac rhythm was monitored continuously and neurologic assessment was performed before and after intervention (end of the procedure and after 3, 6, and 12 hours). Intravenous atropine, up to 2 mg, was administered as necessary for bradycardia. Follow-up Patients were followed up for 30-day postprocedure adverse outcomes (Table 2, data evaluated by F.P., L.V., E.B.) with a neurologic examination performed by two independent neu- Stent Placement Protocol Study patients had been preselected by their referring physicians who determined them to be unsuitable for surgical revascularization for a variety of reasons, including risk and patient preference. All patients were again clinically evaluated for suitability, and CAS was performed by a senior interventional radiologist (F.P.) and two senior interventional neuroradiologists (L.V., E.B.) by using a standardized protocol. Patients were pretreated with 75 mg/d of ticlopidine hydrochloride (Tiklid; Sanofi Synthelabo, Milan, Italy) and 160 mg/d of aspirin (Bayer Health Care AG, Berlin, Patient Characteristics Characteristic Symptomatic Asymptomatic P Value Total no. of patients 244 (61) 156 (39) No. of men (total no. 289) 184 (75.4) 105 (67.3).10 No. of women (total no. 111) 60 (24.6) 51 (32.7).10 Hypertension 138 (56.6) 112 (71.8).003 Hyperlipidemia 120 (49.2) 100 (64.1).005 Tobacco use 70 (28.7) 50 (32.1).55 Diabetes 96 (39.3) 32 (20.5).0001 Peripheral vascular disease 214 (87.7) 104 (66.7).0001 Coronary artery disease 88 (36.1) 84 (53.8).001 Chronic obstructive pulmonary disease 54 (22.1) 38 (24.4).61 Contralateral occlusion 31 (12.7) 15 (9.6).43 Contralateral stenosis 44 (18) 10 (6.4).002 Note. Data in parentheses are percentages. 180 Radiology: Volume 250: Number 1 January 2009
4 rologists, as well as with color Doppler US of the treated lesion. TIA and minor and major strokes were defined as follows (9): TIA was a focal retinal or hemispheric event from which the patient made a complete recovery within 24 hours; a minor stroke was any new neurologic deficit (either ocular or cerebral) that persisted for more than 24 hours and that resolved completely within 30 days or increased by three or fewer points according to the National Institutes of Health Stroke Scale, or NIHSS; and a major stroke was as any new neurologic deficit that persisted after 30 days or increased by four or more points according to the NIHSS. Statistical Methods Correlation of 30-day adverse outcomes (TIA, stroke, death) with patient characteristics was assessed with an 2 test. A P value of less than.05 was considered to indicate a statistically significant difference. Results There were no statistically significant differences in sex or age distribution, or most clinical morbidities, between symptomatic and asymptomatic patients (Table 1). However, hypertension, hyperlipidemia, and coronary artery disease were more prevalent in the asymptomatic group (potentially placing them at a greater risk for an adverse cardiovascular event), whereas diabetes and peripheral vascular disease were more prevalent in the symptomatic group. There was also a greater Table 2 30-day Combined (TIA, Ipsilateral Stroke, Death) Adverse Outcomes Event Asymptomatic Patients (n 155) Symptomatic Patients (n 242) Total (n 397) TIA 4 (2.6) 12 (5) 16 (4) Stroke 0 (0) 9 (3.7) 9 (2.3) Death 0 (0) 0 (0) 0 (0) Total* 4 (2.6) 21 (8.7) 25 (6.3) Note. Data in parentheses are percentages. * Difference between asymptomatic and symptomatic patients was significant, P.021. incidence of contralateral stenoses (of any severity) in the symptomatic group (P.002). However, the presence of a contralateral stenoses or occlusion did not influence outcome in a relevant way. Mild chronic renal insufficiency (creatinine levels of mg/dl [ mol/l]) was found in 42 of 400 patients (10.5%) who were included. The carotid stents were successfully deployed in 397 of 400 (99.25%) patients. The stent could not be deployed successfully in three (0.75%) patients: two because of extremely tortuous carotid arteries and one because of a severe calcified stenosis. All three patients subsequently underwent successful carotid endarterectomy. In three other patients, there were severe stenoses of the mid-portion of the common carotid artery associated with internal carotid artery stenosis, two overlapping stents had to be implanted to fully cover these lesions. After the procedure, all patients showed satisfactory improvement of the internal carotid artery lumen diameter. Minimal residual stenoses of 15% 25% were observed in 34 of 397 (8.6%) patients; in the rest of the patients (363 of 397, 91.4%), no residual stenosis was founded on the final control angiogram. In the total cohort of treated patients (n 397), CAS without the use of EPD resulted in a 30-day major adverse outcome rate of 2.3% (nine of 397; all strokes; Table 2). No deaths were observed. Three patients (0.76%) had delayed, non procedure-related major strokes: one at day 2, one at day 8, and one at day 10 after the procedure. In all three cases, the patients had interrupted prescribed antiplatelet prophylaxis on their own volition. We also observed six (1.5%) minor strokes: three (0.76%) intraprocedural and three delayed one after 24 hours and two after 36 hours. Two of the three intraprocedural strokes resulted in mild contralateral arm hemiparesis. The third patient had contralateral arm weakness and quadrant-anopsia that completely resolved within 3 weeks. The latter three delayed (non procedure-related) minor strokes were attributed to short-term stent occlusions: one successfully resolved at 24 hours after surgical removal of the stent and subsequent carotid endarterectomy; the other two one after 48 hours and one after 7 days resolved spontaneously on continued dual antiplatelet (aspirin and ticlopidine) therapy. Minor complications included 16 (4%) TIAs, which were detected clinically 2 4 days after CAS. All resolved on continued antiplatelet prophylaxis and conservative management. The combined 30-day adverse outcome rate defined as the occurrence of any TIA, stroke, or death was significantly greater (P.03) among symptomatic (8.6%) than asymptomatic (2.6%) patients. Only four of the 12 TIAs, and none of the nine strokes, occurred in asymptomatic patients. The incidence of 30-day adverse outcomes was independent of patient sex and age and presence or absence of contralateral lesions (Table 3). Discussion The North American Symptomatic Carotid Endarterectomy Trial (13) and Asymptomatic Carotid Atherosclerosis Study, or ACAS (14), set the bar for acceptable periprocedural complication rates for carotid endarterectomy. ACAS identified a limited benefit relative to periprocedural risk of carotid endarterectomy in asymptomatic patients, discouraging revascularization unless the risk is below 3%. The American Heart Association guidelines for carotid endarterectomy reflect these studies and recommend an upper limit of perioperative risk of 6% for symptomatic patients and of 3% for asymptomatic patients. Competing treatment modalities, Radiology: Volume 250: Number 1 January
5 such as CAS, have had to adhere to these limits to gain widespread acceptance. CAS trials that have used EPDs have demonstrated equivalence with carotid endarterectomy (2,3) by achieving equal or superior periprocedural risk. While the Stenting and Angioplasty with Protection in Patients at High Risk for Endarterectomy (SAPPHIRE) trial (3) established equivalence in high-risk patients, the Stent-supported Percutaneous Angioplasty of the Carotid Artery vs Endarterectomy (SPACE) trial (15), which used protection in 27% of the cases, set out to achieve the same in low-risk patients but failed to do so because it was statistically underpowered. Of importance, a subgroup analysis of SPACE data failed to show any added benefit with embolic protection. Also, data from the lead-in phase of the ongoing Carotid Revascularization vs Stent Trial (16) and the Acculink for Revascularization of Carotid high-risk Patients registry data (6) failed to demonstrate a statistically significant difference between protected and unprotected CAS. It is argued by some that the relative risk reduction provided by an EPD may be as low as 25%, perhaps because the devices themselves serve as sources for cerebral embolization during manipulation or removal (6). In general, 30-day adverse outcomes (stroke, death) rate for CAS is 2.4% 11% without protection and 1.2% 7% with protection (17). Thus, there continues to be controversy regarding the benefit of these expensive devices. Our analysis of 400 sequential patients treated with CAS without the use of EPD showed a technical success rate of 99.25%. This rate compares favorably with rates of 99.5% (10) and 99.2% (9) reported by others. Not surprisingly, we found a higher 30-day combined adverse outcome rate in our patients who had prior symptoms compared with those who did not. The observed rate of 2.6% among asymptomatic patients was low and within the limits recommended by the American Heart Association for carotid endarterectomy (18) and was comparable or superior to the results of studies that used EPD during CAS (9,10,18,19). Stroke, as well as other transient ischemic events, occurred in few cases, supporting the safety and effectiveness of our standard procedural protocol, which includes meticulous attention to guidewire and catheter manipulation, stent deployment, intraprocedural anticoagulation, and postprocedure dual antiplatelet therapy. Our exclusion criteria required us to wait a minimum of 7 days after symptoms before performing carotid stent placement and 3 weeks for patients with extensive stroke. Our conservative approach to these patients by avoidance of earlier intervention may have contributed to minimizing complications. However, since we did not have a CAS-with-EPD control group, we cannot rule out the possibility that such protection could potentially have further reduced our complication rates. The TIA (4.9%) and stroke (3.7%) rates noted in our symptomatic patients were inferior to those reported in similar patients treated with EPD (10) 0.4% and 1.2%, respectively. Clearly, EPD use must be seriously considered for symptomatic patients. As reported in the SAPPHIRE trial (3), the combined 30-day death and stroke rate among high-risk asymptomatic patients was 5.4% with protected CAS and 10.2% for carotid endarterectomy. The combined (TIA, stroke, death) adverse event rate of 2.6% for asymptomatic patients undergoing CAS without EPD in our study compares very favorably with this report. The SPACE trial (20) has reported a 30-day ipsilateral ischemic stroke or death rate of 6.84% by using protected CAS in low-risk symptomatic patients. We report a combined rate of stroke and death of 3.7% (nine of 242) in symptomatic patients undergoing CAS without EPD. In light of the above data, it appears that routine use of EPDs should be questioned at least in patients who are asymptomatic prior to CAS. The use of EPDs is not without risk. The complexity of the procedure is increased, and several unprotected steps are still present during device introduction and retrieval. Furthermore, although a reduction in macroemboli has Table 3 30-day Adverse Outcomes according to Sex, Age, and State of Contralateral Carotid Artery Characteristic No. of Patients* Total No. P Value Sex Male 19 (6.6) Female 6 (5.4) 111 Age (y) (5.2) (9.0) 111 Contralateral occlusion Yes 3 (6.5) No 22 (6.2) 354 Contralateral stenosis Yes 6 (11.1) No 19 (5.5) 346 * Data in parentheses are percentages. been observed, there is a reported increase in the number of microemboli (7). Moreover, pre-dilation may be required to accommodate the EPDs, which range 3 4-F in size (11,21). Cremonesi et al report a 33% pre-dilation rate with EPD use (10), far greater than the 6% rate in our experience. Also, in one older study, EPD placement was unsuccessful in up to 20% of patients (22). Later studies have had much higher EPD deployment success rates (3). Others have reported that occlusion by the EPD may not be well tolerated (12). Rare complications of EPD include arterial dissection, entrapment or dislodgment of the system, and vessel spasm (6,10). The use of EPD has become a common practice during CAS for the presumed added safety in all patients. Several ongoing trials on CAS have incorporated protection devices in their procedure protocols. Superior efficacy or safety of any particular kind of protection system has not been established (23). However, EPDs do not necessarily reduce the overall rate of complications in all patients. Kastrup et al (19) showed that the proportion and total number of silent ischemic lesions on diffusion-weighted MR images were not 182 Radiology: Volume 250: Number 1 January 2009
6 significantly different with or without EPD use in older patients and those with asymptomatic lesions. The low intraprocedural complication rate observed in our study may be associated with several factors. Low-profile devices were used, pre-dilation of the lesions was avoided whenever possible, and stents were expanded to lower their nominal diameter. These technical practices may in part have contributed to our acceptably low complication rates. Concerning postprocedural complications, adherence to the dual antiplatelet treatment regimen appeared to be crucial, as major strokes occurred only in patients who interrupted antiplatelet prophylaxis on their own. There is an ongoing debate regarding the optimal form of protection to be used during CAS for instance filter devices or flow reversal (6,17). All such devices add time to an already complex procedure; it should be noted that prolonging procedure time could increase the risk of a serious complication (24). There is certainly potential for improvement in both endovascular devices and carotid stent placement techniques. CAS can potentially be improved with newer low-profile flexible introduction systems and greater stent flexibility to allow easier navigation through tortuous vessels for proper positioning and deployment. Various protection devices and techniques are being developed and existing ones are being improved, aiming at minimizing the severe consequences when embolic debris overwhelms the distal bed. These future devices may be much safer to use. Our retrospective analysis supports the hypothesis that the routine use of currently available EPDs during CAS, certainly in asymptomatic patients, should be questioned. Current controversy over this issue merits further evaluation through prospective randomized trials a prospect that seems unlikely given the current unquestioning enthusiasm for technologies (25) such EPDs. Our study had limitations. This was a medium-sized two-center retrospective analysis that had all the known limitations of such studies. Furthermore, there was no control group in which EPD was used, which limited the robustness of our conclusions. We also did not objectively document any silent embolic event by using MR or CT. Nevertheless, our study serves to generate a hypothesis that can only be satisfactorily proved with a prospectively designed, large, multicenter, randomized, controlled trial. In conclusion, our study suggests that CAS without protection devices can be performed in selected asymptomatic patients with complication rates well within published and currently accepted limits of efficacy and safety. References 1. Diethrich EB, Ndiaye M, Reid DB. Stenting in the carotid artery: initial experience in 110 patients. J Endovasc Surg 1996;3: CARESS Steering Committee. Carotid revascularization using endarterectomy or stenting systems (CARESS): phase I clinical trial. J Endovasc Ther 2003;10: Yadav JS, Wholey MH, Kuntz RE, et al. Protected carotid-artery stenting versus endarterectomy in high-risk patients. N Engl J Med 2004;351: Al-Mubarak N, Roubin GS, Vitek JJ, et al. Effect of the distal-balloon protection system on microembolization during carotid stenting. Circulation 2001;104: Kastrup A, Groschel K, Krapf H, et al. Early outcome of carotid angioplasty and stenting with and without cerebral protection devices: a systematic review of the literature. Stroke 2003;34: Cloft HJ. Distal protection: maybe less than you think. AJNR Am J Neuroradiol 2008;29: Vos JA, van den Berg JC, Ernst SM, et al. Carotid angioplasty and stent placement: comparison of transcranial Doppler US data and clinical outcome with and without filtering cerebral protection devices in 509 patients. Radiology 2005;234: Hammer FD, Lacroix V, Duprez T, et al. Cerebral microembolization after protected carotid artery stenting in surgical high-risk patients: results of a 2-year prospective study. J Vasc Surg 2005;42: Castriota F, Cremonesi A, Manetti R, et al. Impact of cerebral protection devices on early outcome of carotid stenting. J Endovasc Ther 2002;9: Cremonesi A, Manetti R, Setacci F, et al. Clinical advantages and complications of embolic protection devices in 442 consecutive patients. Stroke 2003;34: Eckert B, Zeumer H. Editorial comment: carotid artery stenting with or without protection devices? strong opinions, poor evidence! Stroke 2003;34: Reimers B, Schluter M, Castriota F, et al. Routine use of cerebral protection during carotid artery stenting: results of a multicenter registry of 753 patients. Am J Med 2004;116: Beneficial effect of carotid endarterectomy in symptomatic patients with high-grade carotid stenosis. North American Symptomatic Carotid Endarterectomy Trial Collaborators. N Engl J Med 1991;325: Endarterectomy for asymptomatic carotid artery stenosis. Executive Committee for the Asymptomatic Carotid Atherosclerosis Study. JAMA 1995; 273: Ringleb PA, Allenberg J, Bruckmann H, et al. 30 day results from the SPACE trial of stentprotected angioplasty versus carotid endarterectomy in symptomatic patients: a randomised non-inferiority trial. Lancet 2006;368: Hobson RW, Howard VJ, Roubin GS, et al. Credentialing of surgeons as interventionalist for carotid artery stenting: experience from the lead-in phase of CREST. J Vasc Surg 2004;40: Goodney PP, Schermehorn ML, Powell RJ. Current status of carotid artery stenting. J Vasc Surg 2006;43: Biller J, Feinberg WM, Castaldo JE, et al. Guidelines for carotid endarterectomy: a statement for healthcare professionals from a special writing group of the Stroke Council, American Heart Association. Stroke 1998;29: Kastrup A, Gröschel K, Schulz JB, et al. Clinical predictors of transient ischemic attack, stroke, or death within 30 days of carotid angioplasty and stenting. Stroke 2005;36: Ringleb PA, Kunze A, Allenberg JR, et al. The Stent-Supported Percutaneous Angioplasty of the Carotid Artery vs Endarterectomy Trial. Cerebrovasc Dis 2004;18: Sztriha LK, Vörös E, Sas K, et al. Favorable early outcome of carotid artery stenting without protection devices. Stroke 2004;35: Jaeger H, Mathias K, Drescher R, et al. Clinical results of cerebral protection with a filter device during stent implantation of the carotid artery. Cardiovasc Intervent Radiol 2001;24: Iyer V, De Donato G, Deloose K, et al. The type of embolic protection does not influence the outcome in carotid artery stenting. J Vasc Surg 2007;46: Tan WA, Bates MC, Wholey MH. Cerebral protection systems for distal emboli during carotid artery interventions. J Interv Cardiol 2001;14: Leff B, Finucane TE. Gizmo idolatry. JAMA 2008;299: Radiology: Volume 250: Number 1 January
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
Two major randomised trials concerning the surgical treatment of carotid artery stenosis
 944 * See end of article for authors affiliations c CAROTID Correspondence to: Dr Carlo Di Mario, Royal Brompton Hospital, Sydney Street, London SW3 6NP, UK; c.dimario@rbh.nthames.nhs.uk General cardiology
944 * See end of article for authors affiliations c CAROTID Correspondence to: Dr Carlo Di Mario, Royal Brompton Hospital, Sydney Street, London SW3 6NP, UK; c.dimario@rbh.nthames.nhs.uk General cardiology
Carotid Artery Stenting
 Carotid Artery Stenting Natural history of the carotid stenosis Asymptomatic 80% carotid stenosis - 6% risk of stroke / year Symptomatic carotid stenosis have 10% risk of CVA at one year and 40% at 5 years
Carotid Artery Stenting Natural history of the carotid stenosis Asymptomatic 80% carotid stenosis - 6% risk of stroke / year Symptomatic carotid stenosis have 10% risk of CVA at one year and 40% at 5 years
AN ASSESSMENT OF INTER-RATER RELIABILITY IN THE TREATMENT OF CAROTID ARTERY STENOSIS
 Pak Heart J ORIGINAL ARTICLE AN ASSESSMENT OF INTER-RATER RELIABILITY IN THE TREATMENT OF CAROTID ARTERY STENOSIS 1 2 3 4 5 Abhishek Nemani, Arshad Ali, Arshad Rehan, Ali Aboufaris, Jabar Ali 1-4 Guthrie
Pak Heart J ORIGINAL ARTICLE AN ASSESSMENT OF INTER-RATER RELIABILITY IN THE TREATMENT OF CAROTID ARTERY STENOSIS 1 2 3 4 5 Abhishek Nemani, Arshad Ali, Arshad Rehan, Ali Aboufaris, Jabar Ali 1-4 Guthrie
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Safety of Latest-Generation Self-expanding Stents in Patients With NASCET-Ineligible Severe Symptomatic Extracranial Internal Carotid Artery Stenosis Italo Linfante, MD; Joshua A.
ORIGINAL CONTRIBUTION Safety of Latest-Generation Self-expanding Stents in Patients With NASCET-Ineligible Severe Symptomatic Extracranial Internal Carotid Artery Stenosis Italo Linfante, MD; Joshua A.
Limitations of Other Embolic Protection Devices - Filters. Carotid Stenting with Flow Reversal. Limitations of Distal Occlusion
 Carotid Stenting with Flow Reversal Marc Schermerhorn, MD Division of Vascular and Endovascular Surgery Beth Israel Deaconess Center Boston, MA Limitations of Other Embolic Protection Devices - Filters
Carotid Stenting with Flow Reversal Marc Schermerhorn, MD Division of Vascular and Endovascular Surgery Beth Israel Deaconess Center Boston, MA Limitations of Other Embolic Protection Devices - Filters
Endovascular treatment for pseudoocclusion of the internal carotid artery
 Endovascular treatment for pseudoocclusion of the internal carotid artery Daqiao Guo, Xiao Tang, Weiguo Fu Institute of Vascular Surgery, Fudan University, Department of Vascular Surgery, Zhongshan Hospital
Endovascular treatment for pseudoocclusion of the internal carotid artery Daqiao Guo, Xiao Tang, Weiguo Fu Institute of Vascular Surgery, Fudan University, Department of Vascular Surgery, Zhongshan Hospital
Assessment of the procedural etiology of stroke resulting from carotid artery stenting
 Assessment of the procedural etiology of stroke resulting from carotid artery stenting 1. Study Purpose and Rationale: A. Background Stroke is the 3 rd leading cause of death in the United States and carries
Assessment of the procedural etiology of stroke resulting from carotid artery stenting 1. Study Purpose and Rationale: A. Background Stroke is the 3 rd leading cause of death in the United States and carries
CASE REPORT. Department of Neurosurgery, Kariya Toyota General Hospital, Kariya, Japan ABSTRACT
 Nagoya J. Med. Sci. 79. 559 ~ 564, 2017 doi:10.18999/nagjms.79.4.559 CASE REPORT Crevice sign as an indicator of plaque laceration associated with postoperative severe thromboembolism after carotid artery
Nagoya J. Med. Sci. 79. 559 ~ 564, 2017 doi:10.18999/nagjms.79.4.559 CASE REPORT Crevice sign as an indicator of plaque laceration associated with postoperative severe thromboembolism after carotid artery
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Carotid Artery Stenting
 Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Update on Carotid Stenting. John R. Laird Cardiovascular Research Institute Washington Hospital Center
 Update on Carotid Stenting John R. Laird Cardiovascular Research Institute Washington Hospital Center Carotid Stenting What a Crazy Idea! Pathogenesis of stroke Does it make sense to think that expansion
Update on Carotid Stenting John R. Laird Cardiovascular Research Institute Washington Hospital Center Carotid Stenting What a Crazy Idea! Pathogenesis of stroke Does it make sense to think that expansion
CAROTID STENTING A 2009 UPDATE. Hoang Duong, MD Director of Interventional Neuroradiology Memorial Regional Hospital
 CAROTID STENTING A 2009 UPDATE Hoang Duong, MD Director of Interventional Neuroradiology Memorial Regional Hospital TREATMENT FOR CAROTID STENOSIS Best medical management Antiplatelet therapy Antihypertensive
CAROTID STENTING A 2009 UPDATE Hoang Duong, MD Director of Interventional Neuroradiology Memorial Regional Hospital TREATMENT FOR CAROTID STENOSIS Best medical management Antiplatelet therapy Antihypertensive
Carotid artery stenting in the elderly: the time has come
 88 Journal of Geriatric Cardiology June 2007 Vol 4 No 2 Symposium: Review Article Carotid artery stenting in the elderly: the time has come Dipsu Patel, Neil E Strickman St. Luke s Episcopal Hospital/Texas
88 Journal of Geriatric Cardiology June 2007 Vol 4 No 2 Symposium: Review Article Carotid artery stenting in the elderly: the time has come Dipsu Patel, Neil E Strickman St. Luke s Episcopal Hospital/Texas
Treatment Considerations for Carotid Artery Stenosis. Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery
 Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
CAROTID ARTERY ANGIOPLASTY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis
 HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
Special Topic Section
 Special Topic Section Cerebrovasc Dis 2004;18:69 74 DOI: 10.1159/000078753 Received: March 8, 2004 Accepted: March 8, 2004 Published online: June 1, 2004 International Carotid Stenting Study: Protocol
Special Topic Section Cerebrovasc Dis 2004;18:69 74 DOI: 10.1159/000078753 Received: March 8, 2004 Accepted: March 8, 2004 Published online: June 1, 2004 International Carotid Stenting Study: Protocol
Although CAS is increasingly used to treat extracranial carotid
 ORIGINAL RESEARCH H.J. Kim H.J. Lee J.H. Yang I.S. Yeo J.S. Yi I.W. Lee S.B. Lee S.Y. Ryu J.K. Kim P.S. Yang The Influence of Carotid Artery Catheterization Technique on the Incidence of Thromboembolism
ORIGINAL RESEARCH H.J. Kim H.J. Lee J.H. Yang I.S. Yeo J.S. Yi I.W. Lee S.B. Lee S.Y. Ryu J.K. Kim P.S. Yang The Influence of Carotid Artery Catheterization Technique on the Incidence of Thromboembolism
Clinical Predictors of Transient Ischemic Attack, Stroke, or Death Within 30 Days of Carotid Angioplasty and Stenting
 Clinical Predictors of Transient Ischemic Attack, Stroke, or Death Within 30 Days of Carotid Angioplasty and Stenting Andreas Kastrup, MD; Klaus Gröschel, MD; Jörg B. Schulz, MD; Thomas Nägele, MD; Ulrike
Clinical Predictors of Transient Ischemic Attack, Stroke, or Death Within 30 Days of Carotid Angioplasty and Stenting Andreas Kastrup, MD; Klaus Gröschel, MD; Jörg B. Schulz, MD; Thomas Nägele, MD; Ulrike
Carotid Artery Stent: Is it ready for prime time?
 2010 CATH LAB SYMPOSIUM Carotid Artery Stent: Is it ready for prime time? Luis F. Tami, MD, FACC, FSCAI Interventional Cardiology and Vascular Medicine Memorial Regional Hospital August 2010 CAE and CAS
2010 CATH LAB SYMPOSIUM Carotid Artery Stent: Is it ready for prime time? Luis F. Tami, MD, FACC, FSCAI Interventional Cardiology and Vascular Medicine Memorial Regional Hospital August 2010 CAE and CAS
SAMMPRIS. Stenting and Aggressive Medical Management for Preventing Recurrent Stroke and Intracranial Stenosis. Khalil Zahra, M.D
 SAMMPRIS Stenting and Aggressive Medical Management for Preventing Recurrent Stroke and Intracranial Stenosis Khalil Zahra, M.D Major points Patients with recent TIA or stroke and intra-cranial artery
SAMMPRIS Stenting and Aggressive Medical Management for Preventing Recurrent Stroke and Intracranial Stenosis Khalil Zahra, M.D Major points Patients with recent TIA or stroke and intra-cranial artery
Small in-stent Low Density on CT Angiography after Carotid Artery Stenting
 www.centauro.it Interventional Neuroradiology 14 (Suppl. 2): 41-46, 2008 Small in-stent Low Density on CT Angiography after Carotid Artery Stenting MIKA OKAHARA 1, HIRO KIYOSUE 2, JUNJI KASHIWAGI 1, SHINYA
www.centauro.it Interventional Neuroradiology 14 (Suppl. 2): 41-46, 2008 Small in-stent Low Density on CT Angiography after Carotid Artery Stenting MIKA OKAHARA 1, HIRO KIYOSUE 2, JUNJI KASHIWAGI 1, SHINYA
Disclosures. CREST Trial: Summary. Lecture Outline 4/16/2015. Cervical Atherosclerotic Disease
 Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary
 SOCIETY FOR VASCULAR SURGERY DOCUMENT Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary John J. Ricotta, MD, a Ali AbuRahma, MD, FACS, b
SOCIETY FOR VASCULAR SURGERY DOCUMENT Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary John J. Ricotta, MD, a Ali AbuRahma, MD, FACS, b
Carotid Artery Stenting
 Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Artery Stenting Today: A Few Updating Remarks
 Carotid Artery Stenting Today: A Few Updating Remarks Camilo R. Gomez, MD, MBA Director, Alabama Neurological Institute Birmingham, Alabama Disclaimer & Warning Company Pharmaceutical BMS-Sanofi-Aventis
Carotid Artery Stenting Today: A Few Updating Remarks Camilo R. Gomez, MD, MBA Director, Alabama Neurological Institute Birmingham, Alabama Disclaimer & Warning Company Pharmaceutical BMS-Sanofi-Aventis
New Trials in Progress: ACT 1. Jon Matsumura, MD Cannes, France June 28, 2008
 New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
Slide 1. Slide 2 Conflict of Interest Disclosure. Slide 3 Stroke Facts. The Treatment of Intracranial Stenosis. Disclosure
 Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO
 Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
AN EXPERIENCE WITH ANGIOPLASTY AND STENTING OF CAROTID ARTERY STENOSIS WITH EMBOLIC PROTECTION DEVICES
 Arch Iranian Med 2006; 9 (2): 138 143 Original Article AN EXPERIENCE WITH ANGIOPLASTY AND STENTING OF CAROTID ARTERY STENOSIS WITH EMBOLIC PROTECTION DEVICES Ali-Mohammad Haji-Zeinali MD *, Davood Kazemi-Saleh
Arch Iranian Med 2006; 9 (2): 138 143 Original Article AN EXPERIENCE WITH ANGIOPLASTY AND STENTING OF CAROTID ARTERY STENOSIS WITH EMBOLIC PROTECTION DEVICES Ali-Mohammad Haji-Zeinali MD *, Davood Kazemi-Saleh
Carlo Setacci Chief Department of Surgery Vascular and Endovascular Unit University of Siena
 Which carotid procedures are required to grade the stroke risk? Carlo Setacci Chief Department of Surgery Vascular and Endovascular Unit University of Siena Faculty disclosure Carlo Setacci I have no financial
Which carotid procedures are required to grade the stroke risk? Carlo Setacci Chief Department of Surgery Vascular and Endovascular Unit University of Siena Faculty disclosure Carlo Setacci I have no financial
Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease
 AJNR Am J Neuroradiol 26:385 389, February 2005 Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease Tomoyuki Tsumoto
AJNR Am J Neuroradiol 26:385 389, February 2005 Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease Tomoyuki Tsumoto
More than strokes occur
 Surgery vs Stent: Treatment for Carotid Artery Disease Imad A. Alhaddad, MD ABSTRACT PURPOSE: This article summarizes and compares the roles of surgery and stent in the management of carotid artery disease.
Surgery vs Stent: Treatment for Carotid Artery Disease Imad A. Alhaddad, MD ABSTRACT PURPOSE: This article summarizes and compares the roles of surgery and stent in the management of carotid artery disease.
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk
 Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk Amy B. Reed, MD, a Peter Gaccione, MA, b Michael Belkin, MD, b Magruder C. Donaldson, MD, b John A. Mannick, MD,
Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk Amy B. Reed, MD, a Peter Gaccione, MA, b Michael Belkin, MD, b Magruder C. Donaldson, MD, b John A. Mannick, MD,
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Carotid Artery Revascularization: Current Strategies. Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014
 Carotid Artery Revascularization: Current Strategies Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014 Disclosures None 1 Stroke in 2014 Stroke kills almost
Carotid Artery Revascularization: Current Strategies Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014 Disclosures None 1 Stroke in 2014 Stroke kills almost
Extracranial Carotid Artery Stenting With or Without Distal Protection Device
 Extracranial Carotid Artery Stenting With or Without Distal Protection Device Eak-Kyun Shin MD. Professor of Medicine Division of Cardiology, Heart Center, Gil Medical Center Gacheon Medical School Incheon,
Extracranial Carotid Artery Stenting With or Without Distal Protection Device Eak-Kyun Shin MD. Professor of Medicine Division of Cardiology, Heart Center, Gil Medical Center Gacheon Medical School Incheon,
Carotid Artery Stenting (CAS) Pathophysiology. Technical Considerations. Plaque characteristics: relevant concepts. CAS and CEA
 Carotid Artery Stenting (CAS) Carotid Artery Stenting for Stroke Risk Reduction Matthew A. Corriere MD, MS, RPVI Assistant Professor of Surgery Department of Vascular and Endovascular Surgery Rationale:
Carotid Artery Stenting (CAS) Carotid Artery Stenting for Stroke Risk Reduction Matthew A. Corriere MD, MS, RPVI Assistant Professor of Surgery Department of Vascular and Endovascular Surgery Rationale:
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
CAROTID ANGIOPLASTY AND STENTING UNDER PROTECTION IS BECOMING THE GOLD STANDARD TREATMENT IN HIGH AND LOW RISK PATIENTS
 CAROTID ANGIOPLASTY AND STENTING UNDER PROTECTION IS BECOMING THE GOLD STANDARD TREATMENT IN HIGH AND LOW RISK PATIENTS M. HENRY* MD, I. HENRY MD A. POLYDOROU MD, A.D. POLYDOROU MD M. HUGEL RN NANCY FRANCE
CAROTID ANGIOPLASTY AND STENTING UNDER PROTECTION IS BECOMING THE GOLD STANDARD TREATMENT IN HIGH AND LOW RISK PATIENTS M. HENRY* MD, I. HENRY MD A. POLYDOROU MD, A.D. POLYDOROU MD M. HUGEL RN NANCY FRANCE
Peter A. Soukas, M.D., FACC, FSVM, FSCAI, RPVI
 Peter A. Soukas, M.D., FACC, FSVM, FSCAI, RPVI Director, Peripheral Vascular Interventional Laboratory Director, Vascular & Endovascular Medicine Fellowship Program Assistant Professor of Medicine The
Peter A. Soukas, M.D., FACC, FSVM, FSCAI, RPVI Director, Peripheral Vascular Interventional Laboratory Director, Vascular & Endovascular Medicine Fellowship Program Assistant Professor of Medicine The
Multicenter Evaluation of Carotid Artery Stenting With a Filter Protection System
 Journal of the American College of Cardiology Vol. 39, No. 5, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)01692-3
Journal of the American College of Cardiology Vol. 39, No. 5, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)01692-3
Original Article. Abstract. Introduction. Patients and Methods:
 Original Article Endovascular stenting for carotid artery stenosis: Results of local experience at Aga Khan University Hospital, Karachi Muhammad Azeem Uddin, Tanveer ul Haq, Ishtiaque Ahmed Chishty, Zafar
Original Article Endovascular stenting for carotid artery stenosis: Results of local experience at Aga Khan University Hospital, Karachi Muhammad Azeem Uddin, Tanveer ul Haq, Ishtiaque Ahmed Chishty, Zafar
03/30/2016 DISCLOSURES TO OPERATE OR NOT THAT IS THE QUESTION CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE
 CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
BULgarian Carotid Artery Stenting versus Surgery Study (BULCASSS): Randomized single center trial
 BULgarian Carotid Artery Stenting versus Surgery Study (): Randomized single center trial Ivo Petrov, M. Konteva, H. Dimitrov, K. Kichukov Tokuda Hospital Sofia Cardiology Department Background Carotid
BULgarian Carotid Artery Stenting versus Surgery Study (): Randomized single center trial Ivo Petrov, M. Konteva, H. Dimitrov, K. Kichukov Tokuda Hospital Sofia Cardiology Department Background Carotid
Cerebral hyperperfusion syndrome after carotid angioplasty
 case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
Carotid Endarterectomy vs. Carotid artery Stenting (Surgeon Perspective)
 Carotid Endarterectomy vs. Carotid artery Stenting (Surgeon Perspective) T-Woei Tan, MD, FACS, RPVI Assistant Professor of Surgery Vascular and Endovascular Surgery Louisiana State University Health -
Carotid Endarterectomy vs. Carotid artery Stenting (Surgeon Perspective) T-Woei Tan, MD, FACS, RPVI Assistant Professor of Surgery Vascular and Endovascular Surgery Louisiana State University Health -
Carotid Artery Stenting Versus
 Carotid Artery Stenting Versus Carotid Endarterectomy Seong-Wook Park, MD, PhD, FACC,, Seoul, Korea Stroke & Carotid artery stenosis Stroke & Carotid artery stenosis Cerebrovascular disease is one of the
Carotid Artery Stenting Versus Carotid Endarterectomy Seong-Wook Park, MD, PhD, FACC,, Seoul, Korea Stroke & Carotid artery stenosis Stroke & Carotid artery stenosis Cerebrovascular disease is one of the
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Algorithmic selection of emboli protection device during the procedure of carotid artery stunting
 Algorithmic selection of emboli protection device during the procedure of carotid artery stunting Yasuhiro Kawabata, Tetsuya Tsukahara, Shunichi Fukuda, Tomokazu Aoki, Satoru Kawarazaki Department of Neurosurgery,
Algorithmic selection of emboli protection device during the procedure of carotid artery stunting Yasuhiro Kawabata, Tetsuya Tsukahara, Shunichi Fukuda, Tomokazu Aoki, Satoru Kawarazaki Department of Neurosurgery,
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH
 ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
Management of Carotid Disease CHRISTOPHER LAU PGY-3 BROOKLYN VA
 Management of Carotid Disease CHRISTOPHER LAU PGY-3 BROOKLYN VA SUNY DOWNSTATE MEDICAL CENTER Case 61 year old male referred to Vascular Surgery for left internal carotid stenosis Presented with transient
Management of Carotid Disease CHRISTOPHER LAU PGY-3 BROOKLYN VA SUNY DOWNSTATE MEDICAL CENTER Case 61 year old male referred to Vascular Surgery for left internal carotid stenosis Presented with transient
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Outcome
 Measure #344: Rate of Carotid Artery Stenting (CAS) for Asymptomatic Patients, Without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Effective Clinical
Measure #344: Rate of Carotid Artery Stenting (CAS) for Asymptomatic Patients, Without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Effective Clinical
Carotid Artery Stent Placement with Distal Balloon Protection: Technical Considerations
 AJNR Am J Neuroradiol 26:854 861, April 2005 Carotid Artery Stent Placement with Distal Balloon Protection: Technical Considerations Jiri J. Vitek, Nadim Al-Mubarak, Sriram S. Iyer, and Gary S. Roubin
AJNR Am J Neuroradiol 26:854 861, April 2005 Carotid Artery Stent Placement with Distal Balloon Protection: Technical Considerations Jiri J. Vitek, Nadim Al-Mubarak, Sriram S. Iyer, and Gary S. Roubin
Evaluation of a new micromesh carotid stent with Optical Coherence Tomography.
 Evaluation of a new micromesh carotid stent with Optical Coherence Tomography. Technical case report. J. Lemoine,S. Myla,Z. Chati,R.Aslam, M.Amor Clinic Louis Pasteur,Essey les Nancy.France Disclosure
Evaluation of a new micromesh carotid stent with Optical Coherence Tomography. Technical case report. J. Lemoine,S. Myla,Z. Chati,R.Aslam, M.Amor Clinic Louis Pasteur,Essey les Nancy.France Disclosure
Elective stenting of carotid artery stenosis in patients with severe coronary artery disease
 European Heart Journal (1998) 19, 1365 1370 Article No. hj981048 Elective stenting of carotid artery stenosis in patients with severe coronary artery disease J. Waigand, C. M. Gross, F. Uhlich, J. Krämer,
European Heart Journal (1998) 19, 1365 1370 Article No. hj981048 Elective stenting of carotid artery stenosis in patients with severe coronary artery disease J. Waigand, C. M. Gross, F. Uhlich, J. Krämer,
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million life insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
ORIGINAL PAPER. Overlap stenting for in-stent restenosis after carotid artery stenting
 Nagoya J. Med. Sci. 78. 143 ~ 149, 2016 ORIGINAL PAPER Overlap stenting for in-stent restenosis carotid artery stenting Masahiro Nishihori 1,2, Tomotaka Ohshima 1, Taiki Yamamoto 1, Shunsaku Goto 1, Toshihisa
Nagoya J. Med. Sci. 78. 143 ~ 149, 2016 ORIGINAL PAPER Overlap stenting for in-stent restenosis carotid artery stenting Masahiro Nishihori 1,2, Tomotaka Ohshima 1, Taiki Yamamoto 1, Shunsaku Goto 1, Toshihisa
Contemporary Management of Carotid Disease What We Know So Far
 Contemporary Management of Carotid Disease What We Know So Far Ammar Safar, MD, FSCAI, FACC, FACP, RPVI Interventional Cardiology & Endovascular Medicine Disclosers NONE Epidemiology 80 % of stroke are
Contemporary Management of Carotid Disease What We Know So Far Ammar Safar, MD, FSCAI, FACC, FACP, RPVI Interventional Cardiology & Endovascular Medicine Disclosers NONE Epidemiology 80 % of stroke are
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACAS (Asymptomatic Carotid Atherosclerosis Study), 65 66 ACST (Asymptomatic Carotid Surgery Trial), 6 7, 65, 75 Age factors, in carotid
Index Note: Page numbers of article titles are in boldface type. A ACAS (Asymptomatic Carotid Atherosclerosis Study), 65 66 ACST (Asymptomatic Carotid Surgery Trial), 6 7, 65, 75 Age factors, in carotid
The CARENET all-comer trial using the CGuard micronet covered carotid embolic prevention stent
 The CARENET all-comer trial using the CGuard micronet covered carotid embolic prevention stent 6 month data Piotr Musialek, MD DPhil FESC Jagiellonian University Dept. of Cardiac & Vascular Diseases John
The CARENET all-comer trial using the CGuard micronet covered carotid embolic prevention stent 6 month data Piotr Musialek, MD DPhil FESC Jagiellonian University Dept. of Cardiac & Vascular Diseases John
Disclosures. State of the Art Management of Carotid Stenosis. NIH funding for clinical trials Consultant for Scientia Vascular and Medtronic
 State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
Carotid Revascularization
 Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Management of combined coronary & carotid disease
 Management of combined coronary & carotid disease Combined Carotid and coronary artery diseases Frequent combination Fear of imminent death psychologically traumatic for the patients and their families
Management of combined coronary & carotid disease Combined Carotid and coronary artery diseases Frequent combination Fear of imminent death psychologically traumatic for the patients and their families
Roadsaver the paradigm shift in carotid artery treatment. G. Torsello Münster
 Roadsaver the paradigm shift in carotid artery treatment G. Torsello Münster Disclosure Speaker name:...g. Torsello... I have the following potential conflicts of interest to report: Consulting Employment
Roadsaver the paradigm shift in carotid artery treatment G. Torsello Münster Disclosure Speaker name:...g. Torsello... I have the following potential conflicts of interest to report: Consulting Employment
Carotid Stenosis (carotid artery disease)
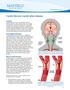 1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
MINERVA MEDICA COPYRIGHT. Alarge body of evidence is now available on evaluation. Embolism to the brain during carotid stenting
 J VASC ENDOVASC SURG 2006;13:131-5 Aim. Stenting of carotid arteries is at risk for embolic complication with cerebral ischemia. The aim of this study was to assess the prevalence, quality and clinical
J VASC ENDOVASC SURG 2006;13:131-5 Aim. Stenting of carotid arteries is at risk for embolic complication with cerebral ischemia. The aim of this study was to assess the prevalence, quality and clinical
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million Life Insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
Carotid Stenting and Surgery in 2016 in Russia
 Carotid Stenting and Surgery in 2016 in Russia Novosibirsk research institute of circulation pathology named by Meshalkin, Novosibirsk, Russia Starodubtsev V., Karpenko A., Ignatenko P. Annually in Russia
Carotid Stenting and Surgery in 2016 in Russia Novosibirsk research institute of circulation pathology named by Meshalkin, Novosibirsk, Russia Starodubtsev V., Karpenko A., Ignatenko P. Annually in Russia
TCAR: TransCarotid Artery Revascularization Angela A. Kokkosis, MD, RPVI, FACS
 TCAR: TransCarotid Artery Revascularization Angela A. Kokkosis, MD, RPVI, FACS Assistant Professor of Surgery Director of Carotid Interventions Division of Vascular & Endovascular Surgery Stony Brook University
TCAR: TransCarotid Artery Revascularization Angela A. Kokkosis, MD, RPVI, FACS Assistant Professor of Surgery Director of Carotid Interventions Division of Vascular & Endovascular Surgery Stony Brook University
Patients with symptomatic atherosclerotic stenosis of the
 ORIGINAL RESEARCH B. Du E.H.C. Wong W.-J. Jiang Long-Term Outcome of Tandem Stenting for Stenoses of the Intracranial Vertebrobasilar Artery and Vertebral Ostium BACKGROUND AND PURPOSE: Patients with symptomatic
ORIGINAL RESEARCH B. Du E.H.C. Wong W.-J. Jiang Long-Term Outcome of Tandem Stenting for Stenoses of the Intracranial Vertebrobasilar Artery and Vertebral Ostium BACKGROUND AND PURPOSE: Patients with symptomatic
RCSIsmjoriginal article
 Percutaneous transluminal carotid artery angioplasty and stenting Abstract heading Background: Carotid angioplasty with stenting is becoming a more popular treatment option for severe carotid occlusive
Percutaneous transluminal carotid artery angioplasty and stenting Abstract heading Background: Carotid angioplasty with stenting is becoming a more popular treatment option for severe carotid occlusive
NCDR CARE Registry Carotid Artery Revascularization and Endarterectomy Registry Carotid Artery Stenting Form v1.09
 NCDR CARE Registry Carotid Artery Revascularization and Endarterectomy Registry Carotid Artery Stenting Fm v1.09 A. PARTICIPANT ADMINISTRATION Participant ID 1000 : Participant Name 1010 : Medicare Provider
NCDR CARE Registry Carotid Artery Revascularization and Endarterectomy Registry Carotid Artery Stenting Fm v1.09 A. PARTICIPANT ADMINISTRATION Participant ID 1000 : Participant Name 1010 : Medicare Provider
SCAI Fall Fellows Course Subclavian/Innominate Case Presentation
 SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
Review of clinical carotid stent procedural & long-term outcomes in. symptomatic asymptomatic. patients
 Review of clinical carotid stent procedural & long-term outcomes in symptomatic asymptomatic patients 1 Conflict of Interest Statement Within the past 12 months, I or my spouse have had a financial interest/arrangement
Review of clinical carotid stent procedural & long-term outcomes in symptomatic asymptomatic patients 1 Conflict of Interest Statement Within the past 12 months, I or my spouse have had a financial interest/arrangement
Carotid. The. Issue. Now approved by the FDA, carotid stenting moves into the spotlight in endovascular care.
 The Carotid Issue 33 Carotid Revascularization in 2004 By Thomas G. Brott, MD; Jamie Roberts, LPN, CRC; Robert W. Hobson II, MD; and Susan Hughes, BSN Now approved by the FDA, carotid stenting moves into
The Carotid Issue 33 Carotid Revascularization in 2004 By Thomas G. Brott, MD; Jamie Roberts, LPN, CRC; Robert W. Hobson II, MD; and Susan Hughes, BSN Now approved by the FDA, carotid stenting moves into
a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers
 The study a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers Conflict of interest have the following potential conflicts of interest to report: Consulting
The study a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers Conflict of interest have the following potential conflicts of interest to report: Consulting
ENDOVASCULAR THERAPIES FOR ACUTE STROKE
 ENDOVASCULAR THERAPIES FOR ACUTE STROKE Cerebral Arteriogram Cerebral Anatomy Cerebral Anatomy Brain Imaging Acute Ischemic Stroke (AIS) Therapy Main goal is to restore blood flow and improve perfusion
ENDOVASCULAR THERAPIES FOR ACUTE STROKE Cerebral Arteriogram Cerebral Anatomy Cerebral Anatomy Brain Imaging Acute Ischemic Stroke (AIS) Therapy Main goal is to restore blood flow and improve perfusion
Balloon-expandable closed-cell stents were introduced
 Designing the Ideal Stent Stent cell geometry and its clinical significance in carotid stenting. BY MARK H. WHOLEY, MD, AND ENDER A. FINOL, PHD Balloon-expandable closed-cell stents were introduced for
Designing the Ideal Stent Stent cell geometry and its clinical significance in carotid stenting. BY MARK H. WHOLEY, MD, AND ENDER A. FINOL, PHD Balloon-expandable closed-cell stents were introduced for
Carotid Imaging. Dr Andrew Farrall. Consultant Neuroradiologist
 20121123 SSCA http://www.neuroimage.co.uk/network Andrew Farrall Carotid Imaging Dr Andrew Farrall Consultant Neuroradiologist SFC Brain Imaging Research Centre (www.sbirc.ed.ac.uk), SINAPSE Collaboration
20121123 SSCA http://www.neuroimage.co.uk/network Andrew Farrall Carotid Imaging Dr Andrew Farrall Consultant Neuroradiologist SFC Brain Imaging Research Centre (www.sbirc.ed.ac.uk), SINAPSE Collaboration
Filters versus Occlusion Balloons during CAS Is there a clear preference?
 Washington TCT 2005 Filters versus Occlusion Balloons during CAS Is there a clear preference? K. Mathias Department of Radiology Teaching Hospital of Dortmund - Germany Presenter Disclosure Information
Washington TCT 2005 Filters versus Occlusion Balloons during CAS Is there a clear preference? K. Mathias Department of Radiology Teaching Hospital of Dortmund - Germany Presenter Disclosure Information
UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE?
 UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE? Richard W. Petrella M.D. FACP,FACC,FASCI DEPARTMENT CHAIRMAN CVM&S UPMC HAMOT MEDICAL CENTER 1 LEARNING OBJECTIVES REVIEW THE RISK FACTORS FOR
UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE? Richard W. Petrella M.D. FACP,FACC,FASCI DEPARTMENT CHAIRMAN CVM&S UPMC HAMOT MEDICAL CENTER 1 LEARNING OBJECTIVES REVIEW THE RISK FACTORS FOR
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Case Closed Closed cell stent technology
 Sponsored by Boston Scientific Corporation Case Closed Closed cell stent technology for carotid artery disease. Innovations in device technologies have helped to raise the bar for clinical efficacy in
Sponsored by Boston Scientific Corporation Case Closed Closed cell stent technology for carotid artery disease. Innovations in device technologies have helped to raise the bar for clinical efficacy in
William A. Gray MD System Chief of Cardiovascular Services, Main Line Health President, Lankenau Heart Institute Wynnewood, PA USA
 William A. Gray MD System Chief of Cardiovascular Services, President, Wynnewood, PA USA What are the possible causes of stroke in CAS? Operator error Technique (balloon sizing, wire misadventure, EPD
William A. Gray MD System Chief of Cardiovascular Services, President, Wynnewood, PA USA What are the possible causes of stroke in CAS? Operator error Technique (balloon sizing, wire misadventure, EPD
Carotid angioplasty with internal carotid artery flow reversal is well tolerated in the awake patient
 Carotid angioplasty with internal carotid artery flow reversal is well tolerated in the awake patient Enrique Criado, MD, a Manuel Doblas, MD, b Juan Fontcuberta, MD, b Antonio Orgaz, MD, b Angel Flores,
Carotid angioplasty with internal carotid artery flow reversal is well tolerated in the awake patient Enrique Criado, MD, a Manuel Doblas, MD, b Juan Fontcuberta, MD, b Antonio Orgaz, MD, b Angel Flores,
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
Why I m afraid of occlusive devices
 Why I m afraid of occlusive devices Cannes 28.06.2008 Carlo Cernetti Cardiology Department Mirano (Venice) MEET 2008 CANNES I HAVE NOT FINACIAL INTEREST/ARRANGEMENT OR AFFILIATION CONFLICT Obstructive
Why I m afraid of occlusive devices Cannes 28.06.2008 Carlo Cernetti Cardiology Department Mirano (Venice) MEET 2008 CANNES I HAVE NOT FINACIAL INTEREST/ARRANGEMENT OR AFFILIATION CONFLICT Obstructive
APPENDIX A NORTH AMERICAN SYMPTOMATIC CAROTID ENDARTERECTOMY TRIAL
 APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
Original paper. Introduction. Aim. Material and methods
 Original paper Comparison of anti-embolic protection with proximal balloon occlusion and filter devices during carotid artery stenting: clinical and procedural outcomes Ersan Tatli 1, Ali Buturak 2, Yasemin
Original paper Comparison of anti-embolic protection with proximal balloon occlusion and filter devices during carotid artery stenting: clinical and procedural outcomes Ersan Tatli 1, Ali Buturak 2, Yasemin
ESC Heart & Brain Workshop
 ESC Heart & Brain Workshop The role of vascular surgeon in stroke prevention Barbara Rantner, MD, PhD, Department of Vascular Surgery, Medical University Innsbruck, Innsbruck, Austria Supported by Bayer,
ESC Heart & Brain Workshop The role of vascular surgeon in stroke prevention Barbara Rantner, MD, PhD, Department of Vascular Surgery, Medical University Innsbruck, Innsbruck, Austria Supported by Bayer,
New concepts for filter protection during CAS: double filtration. Alberto Cremonesi MD, FESC
 New concepts for filter protection during CAS: double filtration Alberto Cremonesi MD, FESC First Experience with the PALADIN Carotid Post-Dilation Balloon with Integrated Embolic Protection Alberto Cremonesi
New concepts for filter protection during CAS: double filtration Alberto Cremonesi MD, FESC First Experience with the PALADIN Carotid Post-Dilation Balloon with Integrated Embolic Protection Alberto Cremonesi
Techniques for Carotid Interventon
 Techniques for Carotid Interventon Jay S. Yadav MD Cleveland, Ohio Disclosures Inventor of Angioguard; fixed and recurring payments from JNJ Advisor: JNJ, Guidant Understand the Patient What is the Cause
Techniques for Carotid Interventon Jay S. Yadav MD Cleveland, Ohio Disclosures Inventor of Angioguard; fixed and recurring payments from JNJ Advisor: JNJ, Guidant Understand the Patient What is the Cause
Carotid Endarterectomy versus Carotid Angioplasty Cui Bono *
 Eur J Vasc Endovasc Surg (2010) 39, S44eS48 Carotid Endarterectomy versus Carotid Angioplasty Cui Bono * W.S. Moore* Division of Vascular Surgery, David Geffen School of Medicine at UCLA, 200 UCLA Medical
Eur J Vasc Endovasc Surg (2010) 39, S44eS48 Carotid Endarterectomy versus Carotid Angioplasty Cui Bono * W.S. Moore* Division of Vascular Surgery, David Geffen School of Medicine at UCLA, 200 UCLA Medical
CHALLENGING ILIAC ACCESSES AND THROMBOSIS PREVENTION
 CHALLENGING ILIAC ACCESSES AND THROMBOSIS PREVENTION ARMANDO MANSILHA MD, PhD, FEBVS UNIVERSITY HOSPITAL - PORTO Disclosure of Interest Speaker name: ARMANDO MANSILHA I have the following potential conflicts
CHALLENGING ILIAC ACCESSES AND THROMBOSIS PREVENTION ARMANDO MANSILHA MD, PhD, FEBVS UNIVERSITY HOSPITAL - PORTO Disclosure of Interest Speaker name: ARMANDO MANSILHA I have the following potential conflicts
