Prognostic significance of blood pressure measured in the office, at home and during ambulatory monitoring in older patients in general practice
|
|
|
- Alexis Dorsey
- 6 years ago
- Views:
Transcription
1 (2005) 19, & 2005 Nature Publishing Group All rights reserved /05 $ ORIGINAL ARTICLE Prognostic significance of blood pressure measured in the office, at home and during ambulatory monitoring in older patients in general practice RH Fagard, C Van Den Broeke and P De Cort Department of Molecular and Cardiovascular Research, Hypertension and Cardiovascular Rehabilitation Unit, Faculty of Medicine, University of Leuven, UZ Gasthuisberg, Leuven, Belgium The purpose of the study was to assess the prognostic significance of out-of-the-office blood pressure (BP) measurement in older patients in general practice, and to compare the results for BP measured in the office, at home and during 24-h ambulatory monitoring. All registerd patients who were 60 years or older were eligible for the study, except when bedridden, demented or admitted in a home for sick elderly people, or when they had suffered a myocardial infarction or stroke. After baseline measurements in , incidence of major cardiovascular events (cardiovascular death, myocardial infarction and stroke) was ascertained in and related to the BPs by use of multivariate Cox regression analysis. Age of the 391 patients averaged 7179 years; 40% were men. During median follow-up of 10.9 years, 86 patients (22%) suffered a cardiovascular event. The adjusted relative hazard rate, associated with a 1 s.d. increment in systolic BP was 1.13 for office BP (NS), and, respectively, 1.32, 1.33 and 1.42, for home, daytime and night time BP (Pp0.01 for all). Results were similar for diastolic BP. The prognostic significance of all out-of-the-office BPs was independent of office BP. The prognostic value of home BP was equal to (systolic) or even better (diastolic) than that of daytime BP. Night time BP predicted cardiovascular events independent of all other BPs. Prognosis of whitecoat hypertension was similar to that of true normotension, but better than in sustained hypertension. In conclusion, the prognostic value of home BP is better than that of office BP in older patients in primary care, and is at least equal to that of daytime ambulatory BP. The prognosis of patients with white-coat hypertension is similar to that of true normotensives. (2005) 19, doi: /sj.jhh ; published online 16 June 2005 Keywords: ambulatory blood pressure; cardiovascular events; home blood pressure; office blood pressure; prognosis; white-coat hypertension Introduction Most of the management of hypertension occurs in the primary care setting, in which decisions on antihypertensive treatment are mainly based on blood pressure (BP) measurements in the office. In the last decade, a number of studies have reported on the prognostic significance of out-of-the-office BP and showed that out-of-the-office BP has greater Correspondence: Professor RH Fagard, Department of Molecular and Cardiovascular Research, Hypertension and Cardiovascular Rehabilitation Unit, Faculty of Medicine, University of Leuven, UZ Gasthuisberg Hypertensie, Herestraat 49, KU Leuven, B-3000 Leuven, Belgium. robert.fagard@uz.kuleuven.ac.be The study was presented at the 14th European Meeting on Hypertension, Paris, France, June 13 17, Received 16 February 2005; revised and accepted 17 May 2005; published online 16 June 2005 prognostic value than office or clinic BP These studies have been perfomed in the population, 3,5 in the elderly, 10 in hypertensive individuals in general, 1,2,4,7,11,13,15 in patients with isolated systolic hypertension, 8,9 in hypertensives under treatment 12,14 and in patients with refractory hypertension. 6 Out-of-the-office BP was assessed by ambulatory BP monitoring in all but two of these studies, in which home BP measurement was used. 5,14 In addition, only one study addressed this issue in general practice. 14 The study population was restricted to treated elderly hypertensives and out-of-the-office BP was assessed by home BP measurements. There are currently no data on ambulatory BP monitoring and outcome in primary care. Furthermore, the prognostic value of BP measured in the office, at home and during ambulatory monitoring has not been directly compared in the same study population. In the late
2 s, we designed a study in which BP was measured in the office, in the patient s usual living situation at home and by ambulatory BP monitoring in older patients in one general practice. Our primary aim was to compare the prognostic significance of the three types of BP measurement in this setting. In addition, the data allowed us to compare the outcome of white-coat hypertensives with true normotensives recruited from the same population, whereas most studies except one 14 recruited hypertensives and normotensive controls from different populations. 2,10,13,15 The importance of the issue is highlighted by the high prevalence of hypertension in older patients in the primary care setting, which amounted to 74% based on office BP measurement in 3761 patients in 253 general practices in Belgium. 17 Materials and methods The study protocol was approved by the institutional Ethics Committee and all participants gave informed consent. The study was performed in one primary care practice in Flanders, Belgium, in which 2044 patients were registered, of whom 462 were at least 60 years old. Patients were excluded from the current study when they were bedridden, demented, admitted in a home for sick elderly people or had suffered a myocardial infarction or a stroke. Baseline examinations were performed between November 1990 and May Patients were visited at home or contacted by telephone to explain the study protocol, which involved a visit to the office, a home visit and 24-h ambulatory BP monitoring. The office and home visits were performed within 2 weeks and in random order. The office visit consisted of a medical history, including medication and smoking habits, a standardized clinical examination and measurements of height, weight, heart rate and BP. After 5 min of rest, BP was measured three times in the sitting position by the auscultatory technique using a mercury sphygmomanometer and an appropriately sized cuff. BP was measured on the right arm, except when BP was lower by X10 mmhg on the right arm than on the left arm. Finally, a blood sample was taken for measurement of serum cholesterol. The same BP measurements were performed at the patient s home; the patient was informed on the date a few days before the visit. Office and home BPs were always measured by the same investigator, most often by the primary care physician, otherwise by one assistant physician. We used the average of the three sitting BPs for all analyses involving office and home BP. Finally, 24-h ambulatory BP monitoring was performed by use of the Spacelabs or device, with appropriate cuff size. BP was measured every 15 min from 0800 to 2200 h and every 30 min from 2200 to 0600 h. For the analysis, daytime BP was defined as the weighted average of all measurements between 1000 and 2000 h; night time was taken from 0000 to 0600 h. 18 We also divided the patients into four subgroups on the basis of office BP and daytime ambulatory BP. Office BP was considered normal when systolic BP was o140 mmhg and diastolic BP o90 mmhg; the cut off values for daytime ambulatory BP were 135 and 85 mmhg, respectively. 19 True normotension was defined as a normal office and ambulatory BP, and sustained hypertension corresponded to an elevated office and ambulatory BP. White-coat hypertension and masked hypertension were defined as isolated office and isolated ambulatory hypertension, respectively. Follow-up The vital and health status of the patients was ascertained between January 2002 and December The aggregate of stroke, myocardial infarction and cardiovascular death was the primary end point of the current study. All events were corroborated by the investigators according to established criteria 20 and without knowledge of the baseline data. Statistical analysis Database management and statistical analyses were performed using SAS software, version 6.12 (SAS Institute Inc.). Data are reported as mean7standard deviation (s.d.) or as percentages. BP measurements in different conditions were compared by use of paired t-tests and relationships between BPs by univariate regression analysis. Differences among groups were analysed by analysis of variance and Scheffe s multiple means test. The w 2 -test was used for categorical data. We used Cox regression analysis to assess the prognostic significance of baseline characteristics and of the various BPs. For BP, the relative hazard rates (RHR) represent the risk associated with a 1 s.d. increment in BP. In multivariate Cox regression analysis, we adjusted for age, gender, body mass index (BMI), use of BP-lowering drugs, smoking, serum total cholesterol and diabetes at baseline. To assess whether the effect was independent from other BP measurements, we performed additional consecutive adjustments for the other BPs. We also assessed the prognostic significance of white-coat hypertension, masked hypertension and sustained hypertension in comparison with true normotension. A two-tailed value of Pp0.05 was considered significant. Results Patients Of the 462 patients, 42 patients (9.1%) were not eligible because they were bedridden (n ¼ 3), demented (n ¼ 2), admitted in a home for sick elderly people (n ¼ 7), or had suffered a myocardial infarction (n ¼ 16), a stroke (n ¼ 12) or both (n ¼ 2) at entry.
3 Since the main aim of the study was to compare the prognostic value of different BP measurements, only patients in whom at least two types of BP measurement were available were retained for the analyses. On this basis we excluded 20 of the 420 patients (4.8%) because only one type of BP was available, mainly due to lack of collaboration or to failed BP measurements. Finally, nine of the 400 remaining patients (2.2%) were lost to follow-up. Patient characteristics at baseline Table 1 summarizes the general characteristics of the 391 remaining patients. The oldest patient was 99 years old. Women were on average 3.0 years older than men (Po0.001). All systolic BPs were significantly different from one another (Po0.001), except office and home BP (P ¼ 0.54). The paired differences for diastolic BP were significant (Po0.01), except for the comparison of office and daytime BP (P ¼ 0.20). The regression equations and coefficients of determination of the relationships between office, home, daytime and night time BP are given in Table 2. All systolic BPs increased significantly with age ( þ 0.12prp þ 0.25; Pp0.05). Office, home and daytime diastolic BP decreased with age ( 0.13prp 0.24; Pp0.01), but this was not the case for night time BP (P ¼ 0.65). The night day ratio of systolic (r ¼þ0.31; Po0.001) and of diastolic BP (r ¼þ0.21; Po0.001) was higher in older than in younger subjects. 803 Table 1 Baseline characteristics of all patients and of untreated and treated patients, and univariate relative hazard rates for cardiovascular events for all patients All Untreated Treated RHR (95% CI) Number (%) 391 (100) 265 (68) 126 (32) Age (year) * 3.03 ( )*** Gender, men (n (%)) 157 (40) 126 (48) 31 (25)*** 1.21 ( ) NS Body mass index (kg/m 2 ) *** 0.92 ( ) NS Current smokers (n (%)) 74 (19) 62 (23) 12 (9.5)*** 1.19 ( ) NS Serum cholesterol concentration (mmol/l) NS 0.79 ( )* Diabetes mellitus (n (%)) 33 (8.4) 19 (7.2) 14 (11) NS 2.70 ( )*** Blood pressure (mmhg) a Systolic Office *** 1.44 ( )*** Home *** 1.63 ( )*** Daytime *** 1.46 ( )*** Night time *** 1.89 ( )*** Night/day ratio NS 1.63 ( )*** Diastolic Office ** 0.78 ( )* Home NS 1.17 ( ) NS Daytime NS 0.93 ( ) NS Night time NS 1.28 ( )* Night/day ratio NS 1.49 ( )*** Values are means7s.d. or number (percentages). Relative hazard rates (RHR) (95% CI) reflect the risk associated with a 1 s.d. increment for a continuous variable and with presence vs absence for a dichotomous variable. n: number of patients. *Pp0.05; **Pp0.01; ***Pp0.001; NS P40.05, for respectively, the comparison of treated and untreated patients, and the relative hazard rates. a Number of BP measurements: office: 376; home: 373; daytime: 374; night time: 364. Table 2 Relationships between different methods of BP measurement BP measurement n Systolic BP Diastolic BP Intercept Slope R 2 * Intercept Slope R 2 * Home vs office Daytime vs office Night time vs office Daytime vs home Night time vs home Daytime vs night time Abbreviations: BP: blood pressure; n: number or BP measurements in each comparison; R 2 : coefficient of determination. *Po0.001 for all coefficients of determination.
4 804 As shown in Table 1, patients under antihypertensive treatment were older, comprised more women than men, and had higher BMI and systolic BP than the untreated patients. Office hypertension, defined as sitting systolic BPX140 mmhg or diastolic BPX90 mmhg or taking antihypertensive drugs, was present in 62% of the patients, of whom 54% were on antihypertensive therapy. Finally, Table 3 summarizes baseline characteristics in the four subgroups according to office BP and daytime ambulatory BP, irrespective of antihypertensive treatment. Follow-up Median follow-up after the baseline examinations was 10.9 (range: ) years and total follow-up amounted to 3378 patient-years. Overall, 165 patients died, 69 from a cardiovascular cause and 92 from a noncardiovascular cause; the cause of death could not be identified in four cases. Noncardiovascular causes of death included cancer (n ¼ 33), internal diseases (n ¼ 52) and peri-operative death (n ¼ 7). The primary end point comprised 86 first cardiovascular events. Among the 31 first nonfatal events, there were 13 strokes and 18 myocardial infarctions. The first event was cardiovascular death in 55 patients (stroke: 11; myocardial infarction: five; sudden death: 18; congestive heart failure: 17; peripheral vascular disease: two; cardiac surgery: one; and pulmonary embolism: one). Table 1 gives the crude RHRs for the primary endpoint for patient characteristics and BP. Age, diabetes mellitus and all systolic BPs were highly significant predictors in univariate analysis. Table 4 gives the adjusted RHRs for the various systolic and diastolic BPs. All BPs independently predicted cardiovascular events, except office BP. Among the covariates, only age, gender and diabetes at baseline were significant in the multivariate Cox models. The risk of a cardiovascular event increased by B15% per 1 year increment in age (Po0.001), was B3 times higher in men than in women (Pp0.01), and B2 times greater in diabetics than in nondiabetics (0.01oPo0.10). Table 5 summarizes the RHRs after additional consecutive adjustment for other BP measurements. Home BP, and daytime and night time ambulatory BP predicted cardiovascular events, independent Table 4 Adjusted relative hazard rates for cardiovascular events with different methods of BP measurement BP measurement a Relative hazard rate (95% CI) P-value Systolic Office 1.13 ( ) 0.34 Home 1.32 ( ) 0.01 Daytime 1.33 ( ) o0.01 Night time 1.42 ( ) o0.001 Diastolic Office 1.04 ( ) 0.73 Home 1.40 ( ) Daytime 1.26 ( ) 0.05 Night time 1.40 ( ) o0.01 Relative hazard rates are for each 1 s.d. increment in BP, with adjustment for age, gender, BMI, use of BP-lowering drugs, smoking, serum total cholesterol and diabetes at baseline. a Number of BP measurements: office: 376, home: 373, daytime: 374, night time: 364. Table 3 Baseline characteristics in four subgroups, classified according to office and daytime ambulatory BP, irrespective of antihypertensive treatment NT WCHT MHT SHT P-value* Number (% of all patients) 136 (38) 87 (24) 31 (8.6) 105 (29) Age (year) Gender, men (n (%)) 65 (48) 24 (28) a 17 (55) 37 (35) Body mass index (kg/m 2 ) Current smokers (n (%)) 35 (26) 7 (8.0) a 9 (29) 13 (12) o0.001 Serum cholesterol concentration (mmol/l) a,b Diabetes mellitus (n (%)) 6 (4.4) 9 (10) 0 (0) 13 (12) 0.03 Use of BP-lowering drugs (n (%)) 19 (14) 37 (43) a 9 (29) 51 (49) a o0.001 Blood pressure (mmhg) Office Systolic a b a,b,c (o0.001) Diastolic a a,c (o0.001) Daytime Systolic a a,b a,b,c (o0.001) Diastolic a,b a,b (o0.001) Results are for 359 patients in whom both office BP and daytime ambulatory BP were available. Values are means7s.d. or numbers (percentages). n: number of patients; NT: normotension; WCHT: white-coat hypertension; MHT: masked hypertension; SHT: sustained hypertension. Statistical analysis: *overall P-value; a,b,c refer to significant differences between groups (Pp0.05); a compared with NT; b compared with WCHT; c compared with MHT.
5 Table 5 Relative hazard rates for cardiovascular events with different methods of BP measurement, after additional consecutive adjustment for other BP measurements 805 BP measurement a Relative risks (95% CI) Adjusted for Office Home Daytime Night time Systolic BP Office 0.91 NS ( ) 0.92 NS ( ) 0.96 NS ( ) Home 1.42* ( ) 1.26 NS ( ) 1.24 NS ( ) Daytime 1.40** ( ) 1.19 NS ( ) 1.21 NS ( ) Night time 1.43** ( ) 1.30* ( ) 1.32* ( ) Diastolic BP Office 0.81 NS ( ) 0.81 NS ( ) 0.81 NS ( ) Home 1.55*** ( ) 1.37** ( ) 1.37** ( ) Daytime 1.44** ( ) 1.09 NS ( ) 1.12 NS ( ) Night time 1.49** ( ) 1.30* ( ) 1.32* ( ) Relative hazard rates are for each one standard deviation increment in BP with adjustment for age, gender, BMI, use of BP-lowering drugs, smoking, serum cholesterol and diabetes at baseline, and with additional consecutive adjustment for other BPs. *Pp0.05; **Pp0.01; ***Pp0.001; NS P a Number of subjects in analyses with simultaneous inclusion of office and home BP: 358; office and daytime BP: 359; office and night time BP: 352; home and daytime BP: 356; home and night time BP: 347; daytime and night time BP: 364. of office BP. Diastolic but not systolic home BP added prognostic precision to daytime and night time ambulatory BP. Finally, the predictive value of night time BP was independent of all other BP measurements. Whereas the night day ratio of systolic and diastolic BP predicted cardiovascular events before adjustment (Table 1), the RHR was only significant for systolic BP after adjustment (RHR for þ 1 s.d.: 1.24; 95% CI, ; Po0.05). However, the RHR was no longer significant (P ¼ 0.16) after additional adjustment for mean 24-h BP. Figure 1 shows the RHRs for the different types of hypertension vs subjects with normal BP. In the analysis on all patients, with adjustment for covariates including antihypertensive treatment, the risk for cardiovascular events was similar in white-coat hypertension and true normotension (P ¼ 0.85). The risk of sustained hypertension was 2.54 times greater than that of normotension (P ¼ 0.005) and 2.16 times greater than in white-coat hypertensives (95% CI, ; P ¼ 0.01). Results were similar in untreated subjects. The risk ratio of B1.5 of masked hypertension vs normotension did not reach statistical significance. Discussion The major findings of the present study are (1) that the superiority of out-of-the-office BP over office BP for the prediction of cardiovascular events also applies to older patients in general practice; (2) that the prognostic value of BP measured in the patient s home is at least equal to that of daytime ambulatory BP; (3) that night time BP is a better predictor of cardiovascular events than daytime Figure 1 Relative hazard rates (RHR) for cardiovascular events, and 95% confidence intervals (95% CI) of white-coat hypertension (WCHT), masked hypertension (MHT) and sustained hypertension (SHT) vs normotension (NT), in all patients (K) and in untreated patients (J), with adjustment for age, gender, BMI, smoking, serum total cholesterol, diabetes at baseline in all analyses, and antihypertensive treatment in the analyses on all patients. Results are for 359 patients in whom both office BP and daytime ambulatory BP were available. Ne: number of events; Np: number of patients. BP; (4) that the outcome of white-coat hypertensives is similar to that of normotensives; and (5) that the prognosis of sustained hypertension is worse than that of normotension and white-coat hypertension. The observation that the BP measured by the family physician in the office was not independently
6 806 predictive for future cardiovascular events, whereas the BP measured by the same investigator in the patient s usual living situation by the same methodology was predictive, suggests that the person who measured the BP and the number of measurements were of less importance than the circumstances of the measurement to explain the difference in prognostic power between home and office BP. Average diastolic BP was significantly lower at home than in the office. However, systolic BP was similar in the two conditions, suggesting that the visit to the office influenced BP to variable extents in individual patients with consequent loss of predictive power. The fact that office BP did not predict the incidence of cardiovascular events after control for a number of covariates is compatible with most reports on out-of-the-office BP 3,5,7,11,14 with few exceptions. 12 The significant prognostic value of home BP in elderly patients registered in primary care extends the findings of Ohkubo et al 5 and of Bobrie et al. 14 These authors observed in a Japanese rural population 5 and in treated elderly hypertensives in general practice in France, 14 that selfmeasured home BP, by use of an automated device, significantly predicted cardiovascular mortality and/or morbidity, independent of a number of confounders and screening 5 or office 14 BP, which were not significant predictors by themselves. The present study confirms in the primary care setting that ambulatory BP is a better predictor of cardiovascular events than office BP. 1 4,6 13 However, the prognostic value of BP measured by the physician during one home visit was at least similar to that of daytime ambulatory BP. We also considered the prognostic significance of various types of hypertension. The classification was based on office BP and daytime ambulatory BP, for which normal values have been established. 19 The results confirm that patients with hypertension in the office and out-of-the office have a greater incidence of cardiovascular events than true normotensives and/or white-coat hypertensives. 2,4,6,9 11,14 It is, however, less well known if the prognosis of white-coat hypertensives differs from that of true normotensives, in which the selection of the study populations in previous studies has to be taken into account. Studies that recruited white-coat hypertensives and normotensives from different populations found that the incidence of cardiovascular events or stroke was similar in these two groups, 2,10,15 or that the risk was higher in white-coat hypertension. 13 In our study and in that of Bobrie et al, 14 normotensives and hypertensives were drawn from the same study population and both studies concluded that prognosis was similar in the two groups. Only a small number of our patients had a normal office BP and an elevated ambulatory BP, and the contention that patients with so-called masked hypertension have a worse prognosis than normotensive subjects 14,21 cannot be confirmed nor refuted in the current study. Studies that reported on daytime and night time BP separately found that both BPs carried significant prognostic information. 3,7,8,12 Staessen et al 8 directly compared the prognostic value of the two BPs and found that night time BP was a better predictor than daytime BP in older patients with isolated systolic hypertension. We confirmed this finding in an elderly population in primary care. Results on the nocturnal fall of BP or on the night day ratio are not consistent. Some studies observed a significantly better prognosis in patients with a greater decline in night time BP 2,8,22 but this was not confirmed by others. 12,23,24 We found that a lower night day ratio of systolic BP was indeed associated with a lower incidence of cardiovascular events, but this was no longer significant after additional adjustment for the average 24-h BP. Several limitations have to be considered. In the current study, home BP was the BP measured by the investigator in the patient s home, whereas other studies on the prognostic significance of home BP reported on self-measured BP by use of an automated device. 5,14 Office BP was the average of three BPs during one visit, whereas guidelines recommend BP measurements at several visits, at least for the initial patient evaulation. 25 In addition, Bovet et al 26 showed that triplicate readings on two visits could be a minimal strategy for assessing adequately the prevalence of hypertension at the population level. However, it is not certain if the results of population studies apply to the primary care situation of our study, in which registered patients were familiar with the physician, the technique and the circumstances of the BP measurement. Moreover, also home BP consisted of three BP measurements during one single visit, and did predict the incidence of cardiovascular events. A number of patients were on antihypertensive treatment at baseline but it is unlikely that this influenced the results. Use of BP-lowering drugs was included as a covariate in the analyses, but never reached statistical significance in the multivariate models, and separate analyses in untreated patients yielded What is known on this topic and what this study adds What is known on this topic Out-of-the-office BP had greater prognostic value than office BP in different populations, but there are few data in the primary care setting. Whereas most studies used ambulatory BP monitoring only two studies used BP measurements in the patient s home. Prognosis of white-coat hypertension is worse than that of sustained hypertension, but it is not well known if prognosis differs from that of true normotensives. What this study adds Both ambulatory BP and home BP have greater prognostic value than office BP in older patients registered in general practice. The prognostic value of BP measured in the patients home is at least equal to that of ambulatory BP. The outcome of white-coat hypertensives is similar to that of true normotensives.
7 similar results. In fact, the prognostic significance of the out-of-the-office BP has not only been shown in untreated subjects but also in hypertensive patients under treatment. 6,12,14 Finally, as in the other studies except in one controlled trial, 8,9 the management of hypertension and other clinical conditions was not standardized during follow-up. A number of patients were institutionalized, treated in other general practices or moved out of the area, and some were unavailable for follow-up. Acknowledgements We gratefully acknowledge the secretarial assistance of N Ausseloos. References 1 Perloff D, Sokolow M, Cowan RM, Juster RP. Prognostic value of ambulatory BP measurements: further analysis. J Hypertens 1989; 7(Suppl 3): S3 S10. 2 Verdecchia P et al. Ambulatory BP: an independent predictor of prognosis in essential hypertension. Hypertension 1994; 24: Ohkubo T et al. Prediction of mortality by ambulatory BP monitoring versus screening BP measurements: a pilot study in Ohasama. J Hypertens 1997; 15: Khattar RS, Senior R, Lahiri A. Cardiovascular outcome in white-coat versus sustained mild hypertension: a 10-year follow-up study. Circulation 1998; 98: Ohkubo T et al. Home BP measurement has a stronger predictive power for mortality than does screening BP measurement: a population-based observation in Ohasama, Japan. J Hypertens 1998; 16: Redon J et al. Prognostic value of ambulatory blood pressure monitoring in refractory hypertension: a prospective study. Hypertension 1998; 31: Khattar RS et al. Prediction of coronary and cerebrovascular morbidity and mortality by direct continuous ambulatory BP monitoring in essential hypertension. Circulation 1999; 100: Staessen JA et al. Predicting cardiovascular risk using conventional and ambulatory blood pressure in older patients with systolic hypertension. JAMA 1999; 282: Fagard RH et al. Response to antihypertensive therapy in older patients with sustained and nonsustained systolic hypertension. Circulation 2000; 102: Kario K et al. Silent and clinically overt stroke in older Japanese subjects with white-coat and sustained hypertension. J Am Coll Cardiol 2001; 38: Celis H et al. Cardiovascular risk in white-coat and sustained hypertensive patients. Blood Pressure 2002; 11: Clement DL et al. Prognostic value of ambulatory blood pressure recordings in patients with treated hypertension. N Engl J Med 2003; 348: Gustavsen PH, Hoegholm A, Bang LE, Kristensen KS. White-coat hypertension is a cardiovascular risk factor: a 10-year follow-up study. J Hum Hypertens 2003; 17: Bobrie G et al. Cardiovascular prognosis of masked hypertension detected by blood pressure self-measurement in elderly treated hypertensive patients. JAMA 2004; 17: Pierdomenico SD et al. Cardiovascular and renal events in uncomplicated mild hypertensive patients with sustained and white-coat hypertension. Am J Hypertens 2004; 17: Fagard RH, Celis H. Prognostic significance of various characteristics of out-of-the-office blood pressure. J Hypertens 2004; 22: Fagard RH, Van den Enden M, Leeman M, Warling X. Survey on treatment of hypertension and implementation of World Health Organization/International Society of Hypertension risk stratification in primary care in Belgium. J Hypertens 2002; 20: Fagard R, Brguljan J, Thijs L, Staessen J. Prediction of the actual awake and asleep blood pressures by various methods of 24-h pressure analysis. J Hypertens 1996; 14: O Brien E et al. European Society of Hypertension recommendations for conventional, ambulatory and home blood pressure measurement. J Hypertens 2003; 21: Staessen JA et al. Randomized double-blind comparison of placebo and active treatment for older patients with isolated systolic hypertension. Lancet 1997; 350: Bjorklund K et al. Isolated ambulatory hypertension predicts cardiovascular morbidity in elderly men. Circulation 2003; 107: Ohkubo T et al. Prognostic significance of the nocturnal decline in blood pressure in individuals with and without high 24-h blood pressure: the Ohasama study. J Hypertens 2002; 20: Khattar RS et al. Effect of aging on the prognostic significance of ambulatory systolic, diastolic, and pulse pressure in essential hypertension. Circulation 2001; 104: Bjorklund K et al. Prognostic significance of 24-h ambulatory blood pressure characteristics for cardiovascular morbidity in a population of elderly men. J Hypertens 2004; 22: Guidelines Committee European Society of Hyypertension European Society of Cardiology guidelines for the management of arterial hypertension. J Hypertens 2003; 21: Bovet P et al. Assessisng the prevalence of hypertension in populations: are we doing it right? J Hypertens 2003; 21:
a Hypertension and Cardiovascular Rehabilitation Unit, Faculty of Medicine, Received 2 June 2008 Revised 1 July 2008 Accepted 9 July 2008
 Original article 325 Prognostic significance of ambulatory blood pressure in hypertensive patients with history of cardiovascular disease Robert H. Fagard a, Lutgarde Thijs a, Jan A. Staessen a, Denis
Original article 325 Prognostic significance of ambulatory blood pressure in hypertensive patients with history of cardiovascular disease Robert H. Fagard a, Lutgarde Thijs a, Jan A. Staessen a, Denis
ANTIHYPERTENSIVE DRUG THERAPY IN CONSIDERATION OF CIRCADIAN BLOOD PRESSURE VARIATION*
 Progress in Clinical Medicine 1 ANTIHYPERTENSIVE DRUG THERAPY IN CONSIDERATION OF CIRCADIAN BLOOD PRESSURE VARIATION* Keishi ABE** Asian Med. J. 44(2): 83 90, 2001 Abstract: J-MUBA was a large-scale clinical
Progress in Clinical Medicine 1 ANTIHYPERTENSIVE DRUG THERAPY IN CONSIDERATION OF CIRCADIAN BLOOD PRESSURE VARIATION* Keishi ABE** Asian Med. J. 44(2): 83 90, 2001 Abstract: J-MUBA was a large-scale clinical
Journal of the American College of Cardiology Vol. 46, No. 3, by the American College of Cardiology Foundation ISSN /05/$30.
 Journal of the American College of Cardiology Vol. 46, No. 3, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.03.070
Journal of the American College of Cardiology Vol. 46, No. 3, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.03.070
Journal of Hypertension 2004, 22: a Hypertension and Cardiovascular Rehabilitation Unit, Catholic University of
 Original article 81 Relationship between ambulatory blood pressure and followup clinic blood pressure in elderly patients with systolic hypertension Robert H. Fagard a, Jan A. Staessen a, Lutgarde Thijs
Original article 81 Relationship between ambulatory blood pressure and followup clinic blood pressure in elderly patients with systolic hypertension Robert H. Fagard a, Jan A. Staessen a, Lutgarde Thijs
Slide notes: References:
 1 2 3 Cut-off values for the definition of hypertension are systolic blood pressure (SBP) 135 and/or diastolic blood pressure (DBP) 85 mmhg for home blood pressure monitoring (HBPM) and daytime ambulatory
1 2 3 Cut-off values for the definition of hypertension are systolic blood pressure (SBP) 135 and/or diastolic blood pressure (DBP) 85 mmhg for home blood pressure monitoring (HBPM) and daytime ambulatory
ORIGINAL ARTICLE AMBULATORY BLOOD PRESSURE IN OBESITY. Introduction. Patients and Methods
 Vol. 2, Issue 1, pages 31-36 ORIGINAL ARTICLE AMBULATORY BLOOD PRESSURE IN OBESITY By Alejandro de la Sierra, MD Luis M. Ruilope, MD Hypertension Units, Hospital Clinico, Barcelona & Hospital 12 de Octubre,
Vol. 2, Issue 1, pages 31-36 ORIGINAL ARTICLE AMBULATORY BLOOD PRESSURE IN OBESITY By Alejandro de la Sierra, MD Luis M. Ruilope, MD Hypertension Units, Hospital Clinico, Barcelona & Hospital 12 de Octubre,
Ambulatory Blood Pressure and Prognosis
 Ambulatory Blood Pressure and Prognosis Daytime and Nighttime Blood Pressure as Predictors of Death and Cause-Specific Cardiovascular Events in Hypertension Robert H. Fagard, Hilde Celis, Lutgarde Thijs,
Ambulatory Blood Pressure and Prognosis Daytime and Nighttime Blood Pressure as Predictors of Death and Cause-Specific Cardiovascular Events in Hypertension Robert H. Fagard, Hilde Celis, Lutgarde Thijs,
High-dose monotherapy vs low-dose combination therapy of calcium channel blockers and angiotensin receptor blockers in mild to moderate hypertension
 (2005) 19, 491 496 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE High-dose monotherapy vs low-dose combination therapy of calcium channel blockers
(2005) 19, 491 496 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE High-dose monotherapy vs low-dose combination therapy of calcium channel blockers
Ambulatory blood pressure (ABP) may be normal in
 Response to Antihypertensive Therapy in Older Patients With Sustained and Nonsustained Systolic Hypertension Robert H. Fagard, MD; Jan A. Staessen, MD; Lutgarde Thijs, BSc; Jerzy Gasowski, MD; Christopher
Response to Antihypertensive Therapy in Older Patients With Sustained and Nonsustained Systolic Hypertension Robert H. Fagard, MD; Jan A. Staessen, MD; Lutgarde Thijs, BSc; Jerzy Gasowski, MD; Christopher
24-uur ambulante bloeddrukmeting versus thuisbloedrukmeting
 2017 Dementia 24-uur ambulante bloeddrukmeting versus thuisbloedrukmeting Wat gebruiken in de klinische praktijk? Jan A. Staessen, MD, PhD KU Leuven jan.staessen@kuleuven.be BPM Key messages to be made
2017 Dementia 24-uur ambulante bloeddrukmeting versus thuisbloedrukmeting Wat gebruiken in de klinische praktijk? Jan A. Staessen, MD, PhD KU Leuven jan.staessen@kuleuven.be BPM Key messages to be made
Overview of the outcome trials in older patients with isolated systolic hypertension
 Journal of Human Hypertension (1999) 13, 859 863 1999 Stockton Press. All rights reserved 0950-9240/99 $15.00 http://www.stockton-press.co.uk/jhh Overview of the outcome trials in older patients with isolated
Journal of Human Hypertension (1999) 13, 859 863 1999 Stockton Press. All rights reserved 0950-9240/99 $15.00 http://www.stockton-press.co.uk/jhh Overview of the outcome trials in older patients with isolated
University of Padova, Padua, Italy, and HARVEST Study Group, Italy
 University of Padova, Padua, Italy, and HARVEST Study Group, Italy ISOLATED SYSTOLIC HYPERTENSION IN THE YOUNG DOES NOT IMPLY AN INCREASED RISK OF FUTURE HYPERTENSION NEEDING TREATMENT Mos L, Saladini
University of Padova, Padua, Italy, and HARVEST Study Group, Italy ISOLATED SYSTOLIC HYPERTENSION IN THE YOUNG DOES NOT IMPLY AN INCREASED RISK OF FUTURE HYPERTENSION NEEDING TREATMENT Mos L, Saladini
Assessing Blood Pressure for Clinical Research: Pearls & Pitfalls
 Assessing Blood Pressure for Clinical Research: Pearls & Pitfalls Anthony J. Viera, MD, MPH, FAHA Department of Family Medicine Hypertension Research Program UNC School of Medicine Objectives Review limitations
Assessing Blood Pressure for Clinical Research: Pearls & Pitfalls Anthony J. Viera, MD, MPH, FAHA Department of Family Medicine Hypertension Research Program UNC School of Medicine Objectives Review limitations
Low fractional diastolic pressure in the ascending aorta increased the risk of coronary heart disease
 (2002) 16, 837 841 & 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Low fractional diastolic pressure in the ascending aorta increased the risk
(2002) 16, 837 841 & 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Low fractional diastolic pressure in the ascending aorta increased the risk
AGING, BLOOD PRESSURE & CARDIOVASCULAR DISEASE EVENT RISK. Michael Smolensky, Ph.D. The University of Texas Austin & Houston
 AGING, BLOOD PRESSURE & CARDIOVASCULAR DISEASE EVENT RISK Michael Smolensky, Ph.D. The University of Texas Austin & Houston Disclosures Partner: Circadian Ambulatory Diagnostics Consultant: Spot On Sciences
AGING, BLOOD PRESSURE & CARDIOVASCULAR DISEASE EVENT RISK Michael Smolensky, Ph.D. The University of Texas Austin & Houston Disclosures Partner: Circadian Ambulatory Diagnostics Consultant: Spot On Sciences
Use of ambulatory and home blood pressure (BP) measurements
 Long-Term Risk of Mortality Associated With Selective and Combined Elevation in Office, Home, and Ambulatory Blood Pressure Giuseppe Mancia, Rita Facchetti, Michele Bombelli, Guido Grassi, Roberto Sega
Long-Term Risk of Mortality Associated With Selective and Combined Elevation in Office, Home, and Ambulatory Blood Pressure Giuseppe Mancia, Rita Facchetti, Michele Bombelli, Guido Grassi, Roberto Sega
OBJECTIVES BACKGROUND METHODS RESULTS CONCLUSIONS
 Journal of the American College of Cardiology Vol. 38, No. 1, 2001 2001 by the American College of Cardiology ISSN 0735-1097/01/$20.00 Published by Elsevier Science Inc. PII S0735-1097(01)01325-0 Silent
Journal of the American College of Cardiology Vol. 38, No. 1, 2001 2001 by the American College of Cardiology ISSN 0735-1097/01/$20.00 Published by Elsevier Science Inc. PII S0735-1097(01)01325-0 Silent
Importance of Ambulatory Blood Pressure Monitoring in Adolescents
 Importance of Ambulatory Blood Pressure Monitoring in Adolescents Josep Redon, MD, PhD, FAHA Internal Medicine Hospital Clinico Universitario de Valencia University of Valencia CIBERObn Instituto de Salud
Importance of Ambulatory Blood Pressure Monitoring in Adolescents Josep Redon, MD, PhD, FAHA Internal Medicine Hospital Clinico Universitario de Valencia University of Valencia CIBERObn Instituto de Salud
Protocol. Automated Ambulatory Blood Pressure Monitoring for the Diagnosis of Hypertension in Patients with Elevated Office Blood Pressure
 Automated Ambulatory Blood Monitoring for the Diagnosis of Hypertension in Patients with Elevated Office Blood (10102) Medical Benefit Effective Date: 07/01/14 Next Review Date: 03/15 Preauthorization
Automated Ambulatory Blood Monitoring for the Diagnosis of Hypertension in Patients with Elevated Office Blood (10102) Medical Benefit Effective Date: 07/01/14 Next Review Date: 03/15 Preauthorization
Association of Isolated Systolic, Isolated Diastolic, and Systolic-Diastolic Masked Hypertension With Carotid Artery Intima-Media Thickness
 ORIGINAL PAPER Association of Isolated Systolic, Isolated Diastolic, and Systolic-Diastolic Masked Hypertension With Carotid Artery Intima-Media Thickness Efstathios Manios, MD; 1 Fotios Michas, MD; 1
ORIGINAL PAPER Association of Isolated Systolic, Isolated Diastolic, and Systolic-Diastolic Masked Hypertension With Carotid Artery Intima-Media Thickness Efstathios Manios, MD; 1 Fotios Michas, MD; 1
Dementia Retinal arteriolar narrowing and HT. What comes first?
 Dementia 2016 Retinal arteriolar narrowing and HT What comes first? Jan A. Staessen, MD, PhD University of Leuven / Maastricht University jan.staessen@med.kuleuven.be / ja.staessen@maastrichtuniversity.nl
Dementia 2016 Retinal arteriolar narrowing and HT What comes first? Jan A. Staessen, MD, PhD University of Leuven / Maastricht University jan.staessen@med.kuleuven.be / ja.staessen@maastrichtuniversity.nl
Prognostic significance of blood pressure measured on rising
 (2001) 15, 413 417 2001 Nature Publishing Group All rights reserved 0950-9240/01 $15.00 www.nature.com/jhh ORIGINAL ARTICLE Prognostic significance of blood pressure measured on rising P Gosse, C Cipriano,
(2001) 15, 413 417 2001 Nature Publishing Group All rights reserved 0950-9240/01 $15.00 www.nature.com/jhh ORIGINAL ARTICLE Prognostic significance of blood pressure measured on rising P Gosse, C Cipriano,
Effects of exercise, diet and their combination on blood pressure
 (2005) 19, S20 S24 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Effects of exercise, diet and their combination on blood pressure Department
(2005) 19, S20 S24 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Effects of exercise, diet and their combination on blood pressure Department
DIFFERENTE RELAZIONE TRA VALORI PRESSORI E MASSA VENTRICOLARE SX NEI DUE SESSI IN PAZIENTI IPERTESI.
 DIFFERENTE RELAZIONE TRA VALORI PRESSORI E MASSA VENTRICOLARE SX NEI DUE SESSI IN PAZIENTI IPERTESI. Franco Cipollini, Carlo Porta, Enrica Arcangeli, Carla Breschi, & Giuseppe Seghieri Azienda USL 3, Ambulatorio
DIFFERENTE RELAZIONE TRA VALORI PRESSORI E MASSA VENTRICOLARE SX NEI DUE SESSI IN PAZIENTI IPERTESI. Franco Cipollini, Carlo Porta, Enrica Arcangeli, Carla Breschi, & Giuseppe Seghieri Azienda USL 3, Ambulatorio
Ambulatory arterial stiffness index as a predictor of cardiovascular events.
 Ambulatory arterial stiffness index as a predictor of cardiovascular events. A meta-analysis of longitudinal studies. Konstantinos Aznaouridis, Charalambos Vlachopoulos, Christodoulos Stefanadis. 1 st
Ambulatory arterial stiffness index as a predictor of cardiovascular events. A meta-analysis of longitudinal studies. Konstantinos Aznaouridis, Charalambos Vlachopoulos, Christodoulos Stefanadis. 1 st
Hospital and 1-year outcome after acute myocardial infarction in patients with diabetes mellitus and hypertension
 (2003) 17, 665 670 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Hospital and 1-year outcome after acute myocardial infarction in patients with
(2003) 17, 665 670 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Hospital and 1-year outcome after acute myocardial infarction in patients with
ORIGINAL INVESTIGATION. Prognosis of Isolated Systolic and Isolated Diastolic Hypertension as Assessed by Self-Measurement of Blood Pressure at Home
 Prognosis of Isolated Systolic and Isolated Diastolic Hypertension as Assessed by Self-Measurement of Blood Pressure at Home The Ohasama Study ORIGINAL INVESTIGATION Atsushi Hozawa, MD; Takayoshi Ohkubo,
Prognosis of Isolated Systolic and Isolated Diastolic Hypertension as Assessed by Self-Measurement of Blood Pressure at Home The Ohasama Study ORIGINAL INVESTIGATION Atsushi Hozawa, MD; Takayoshi Ohkubo,
Normal Ambulatory Blood Pressure: A Clinical-Practice- Based Analysis of Recent American Heart Association Recommendations
 The American Journal of Medicine (2006) 119, 69.e13-69.e18 CLINICAL RESEARCH STUDY Normal Ambulatory Blood Pressure: A Clinical-Practice- Based Analysis of Recent American Heart Association Recommendations
The American Journal of Medicine (2006) 119, 69.e13-69.e18 CLINICAL RESEARCH STUDY Normal Ambulatory Blood Pressure: A Clinical-Practice- Based Analysis of Recent American Heart Association Recommendations
Prevalence, awareness, treatment and control of hypertension in employees of factories of Northern Greece: the Naoussa study
 (2004) 18, 623 629 & 2004 Nature Publishing Group All rights reserved 0950-9240/04 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Prevalence, awareness, treatment and control of hypertension in employees of
(2004) 18, 623 629 & 2004 Nature Publishing Group All rights reserved 0950-9240/04 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Prevalence, awareness, treatment and control of hypertension in employees of
Is Traditional Clinic Blood Pressure Dead?
 Royal College of Physicans May 16 th 2017 Is Traditional Clinic Blood Pressure Dead? Professor Bryan Williams MD FRCP FAHA FESC Chair of Medicine UCL Director National Institute for Health Research Biomedical
Royal College of Physicans May 16 th 2017 Is Traditional Clinic Blood Pressure Dead? Professor Bryan Williams MD FRCP FAHA FESC Chair of Medicine UCL Director National Institute for Health Research Biomedical
White coat and masked hypertension
 White coat and masked hypertension Conflict of interest Support from Spacelabs, Microlife. Honoraria from Novartis, Elpen, Boeringer-Ingelheim, CANA, Lilly, MSD, Sanofi, Menarini, Ciezi, Astra-Zeneca.
White coat and masked hypertension Conflict of interest Support from Spacelabs, Microlife. Honoraria from Novartis, Elpen, Boeringer-Ingelheim, CANA, Lilly, MSD, Sanofi, Menarini, Ciezi, Astra-Zeneca.
& Wilkins. a Division of Cardiology, Schulich Heart Centre, b Institute for Clinical and
 Original article 333 Optimum frequency of office blood pressure measurement using an automated sphygmomanometer Martin G. Myers a, Miguel Valdivieso a and Alexander Kiss b,c Objective To determine the
Original article 333 Optimum frequency of office blood pressure measurement using an automated sphygmomanometer Martin G. Myers a, Miguel Valdivieso a and Alexander Kiss b,c Objective To determine the
Blood Pressure Targets in Diabetes
 Stockholm, 29 th August 2010 ESC Meeting Blood Pressure Targets in Diabetes Peter M Nilsson, MD, PhD Department of Clinical Sciences University Hospital, Malmö Sweden Studies on BP in DM2 ADVANCE RCT (Lancet
Stockholm, 29 th August 2010 ESC Meeting Blood Pressure Targets in Diabetes Peter M Nilsson, MD, PhD Department of Clinical Sciences University Hospital, Malmö Sweden Studies on BP in DM2 ADVANCE RCT (Lancet
ESM1 for Glucose, blood pressure and cholesterol levels and their relationships to clinical outcomes in type 2 diabetes: a retrospective cohort study
 ESM1 for Glucose, blood pressure and cholesterol levels and their relationships to clinical outcomes in type 2 diabetes: a retrospective cohort study Statistical modelling details We used Cox proportional-hazards
ESM1 for Glucose, blood pressure and cholesterol levels and their relationships to clinical outcomes in type 2 diabetes: a retrospective cohort study Statistical modelling details We used Cox proportional-hazards
How well do office and exercise blood pressures predict sustained hypertension? A Dundee Step Test Study
 (2000) 14, 429 433 2000 Macmillan Publishers Ltd All rights reserved 0950-9240/00 $15.00 www.nature.com/jhh ORIGINAL ARTICLE How well do office and exercise blood pressures predict sustained hypertension?
(2000) 14, 429 433 2000 Macmillan Publishers Ltd All rights reserved 0950-9240/00 $15.00 www.nature.com/jhh ORIGINAL ARTICLE How well do office and exercise blood pressures predict sustained hypertension?
Blood Pressure Targets: Where are We Now?
 Blood Pressure Targets: Where are We Now? Diana Cao, PharmD, BCPS-AQ Cardiology Assistant Professor Department of Clinical & Administrative Sciences California Northstate University College of Pharmacy
Blood Pressure Targets: Where are We Now? Diana Cao, PharmD, BCPS-AQ Cardiology Assistant Professor Department of Clinical & Administrative Sciences California Northstate University College of Pharmacy
BRIEF COMMUNICATIONS. KEY WORDS: Ambulatory blood pressure monitoring, placebo effect, antihypertensive drug trials.
 AJH 1995; 8:311-315 BRIEF COMMUNICATIONS Lack of Placebo Effect on Ambulatory Blood Pressure Giuseppe Mancia, Stefano Omboni, Gianfranco Parati, Antonella Ravogli, Alessandra Villani, and Alberto Zanchetti
AJH 1995; 8:311-315 BRIEF COMMUNICATIONS Lack of Placebo Effect on Ambulatory Blood Pressure Giuseppe Mancia, Stefano Omboni, Gianfranco Parati, Antonella Ravogli, Alessandra Villani, and Alberto Zanchetti
Ambulatory Blood Pressure Monitoring Clinical Practice Recommendations
 Acta Medica Marisiensis 2016;62(3):350-355 DOI: 10.1515/amma-2016-0038 UPDATE Ambulatory Blood Pressure Monitoring Clinical Practice Recommendations Mako Katalin *, Ureche Corina, Jeremias Zsuzsanna University
Acta Medica Marisiensis 2016;62(3):350-355 DOI: 10.1515/amma-2016-0038 UPDATE Ambulatory Blood Pressure Monitoring Clinical Practice Recommendations Mako Katalin *, Ureche Corina, Jeremias Zsuzsanna University
Managing HTN in the Elderly: How Low to Go
 Managing HTN in the Elderly: How Low to Go Laxmi S. Mehta, MD, FACC The Ohio State University Medical Center Assistant Professor of Clinical Internal Medicine Clinical Director of the Women s Cardiovascular
Managing HTN in the Elderly: How Low to Go Laxmi S. Mehta, MD, FACC The Ohio State University Medical Center Assistant Professor of Clinical Internal Medicine Clinical Director of the Women s Cardiovascular
Validation of the SEJOY BP-1307 upper arm blood pressure monitor for home. blood pressure monitoring according to the European Society of Hypertension
 Validation of the SEJOY BP-1307 upper arm blood pressure monitor for home blood pressure monitoring according to the European Society of Hypertension International Protocol revision 2010 Short title: Validation
Validation of the SEJOY BP-1307 upper arm blood pressure monitor for home blood pressure monitoring according to the European Society of Hypertension International Protocol revision 2010 Short title: Validation
Does Antihypertensive Drug Class Affect Day-to-Day Variability of Self-Measured Home Blood Pressure? The HOMED-BP Study
 Does Antihypertensive Drug Class Affect Day-to-Day Variability of Self-Measured Home Blood Pressure? The HOMED-BP Study Kei Asayama, MD, PhD; Takayoshi Ohkubo, MD, PhD; Tomohiro Hanazawa, MS; Daisuke Watabe,
Does Antihypertensive Drug Class Affect Day-to-Day Variability of Self-Measured Home Blood Pressure? The HOMED-BP Study Kei Asayama, MD, PhD; Takayoshi Ohkubo, MD, PhD; Tomohiro Hanazawa, MS; Daisuke Watabe,
Ambulatory blood pressure as a predictor of cardiovascular risk
 Review paper Ambulatory blood pressure as a predictor of cardiovascular risk Ankur Sethi, Rohit R. Arora Department of Cardiology, Rosalind Franklin University, Chicago Medical School, North Chicago, IL,
Review paper Ambulatory blood pressure as a predictor of cardiovascular risk Ankur Sethi, Rohit R. Arora Department of Cardiology, Rosalind Franklin University, Chicago Medical School, North Chicago, IL,
Risk Stratification of ACS Patients. Frans Van de Werf, MD, PhD University of Leuven, Belgium
 Risk Stratification of ACS Patients Frans Van de Werf, MD, PhD University of Leuven, Belgium Which type of ACS patients are we talking about to day? 4/14/2011 STEMI and NSTEMI in the NRMI registry from
Risk Stratification of ACS Patients Frans Van de Werf, MD, PhD University of Leuven, Belgium Which type of ACS patients are we talking about to day? 4/14/2011 STEMI and NSTEMI in the NRMI registry from
The accurate measurement of blood pressure
 Position Paper ASH Position Paper: Home and Ambulatory Blood Pressure Monitoring When and How to Use Self (Home) and Ambulatory Blood Pressure Monitoring Thomas G. Pickering, MD, D Phil; 1 William B. White,
Position Paper ASH Position Paper: Home and Ambulatory Blood Pressure Monitoring When and How to Use Self (Home) and Ambulatory Blood Pressure Monitoring Thomas G. Pickering, MD, D Phil; 1 William B. White,
Antihypertensive Trial Design ALLHAT
 1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
Comparison of arbitrary definitions of circadian time periods with those determined by wrist actigraphy in analysis of ABPM data
 Journal of Human Hypertension (1999) 13, 449 453 1999 Stockton Press. All rights reserved 0950-9240/99 $12.00 http://www.stockton-press.co.uk/jhh ORIGINAL ARTICLE Comparison of arbitrary definitions of
Journal of Human Hypertension (1999) 13, 449 453 1999 Stockton Press. All rights reserved 0950-9240/99 $12.00 http://www.stockton-press.co.uk/jhh ORIGINAL ARTICLE Comparison of arbitrary definitions of
80 Appendix A. Fig. A.1 Repository of ABPM information containing measurements of the BP
 Appendix A In the first part of the research for developing the initial classifier the data base of 30 patients monitoring during 5 days with 4 readings at day was created for use in the model. The measures
Appendix A In the first part of the research for developing the initial classifier the data base of 30 patients monitoring during 5 days with 4 readings at day was created for use in the model. The measures
Talking about blood pressure
 Talking about blood pressure Mrs Khan 56 BP 158/99 BMI 32 Total cholesterol 5.4 (HDL 0.8) HbA1c 43 She has been promising to do more exercise and eat more healthily for the last 2 years but her weight
Talking about blood pressure Mrs Khan 56 BP 158/99 BMI 32 Total cholesterol 5.4 (HDL 0.8) HbA1c 43 She has been promising to do more exercise and eat more healthily for the last 2 years but her weight
Many observational studies evaluating the changing pattern
 Effect of Aging on the Prognostic Significance of Ambulatory Systolic, Diastolic, and Pulse Pressure in Essential Hypertension Rajdeep S. Khattar, BM, MRCP; John D. Swales, MA, MD, FRCP; Caroline Dore,
Effect of Aging on the Prognostic Significance of Ambulatory Systolic, Diastolic, and Pulse Pressure in Essential Hypertension Rajdeep S. Khattar, BM, MRCP; John D. Swales, MA, MD, FRCP; Caroline Dore,
Clinical Updates in the Treatment of Hypertension JNC 7 vs. JNC 8. Lauren Thomas, PharmD PGY1 Pharmacy Practice Resident South Pointe Hospital
 Clinical Updates in the Treatment of Hypertension JNC 7 vs. JNC 8 Lauren Thomas, PharmD PGY1 Pharmacy Practice Resident South Pointe Hospital Objectives Review the Eighth Joint National Committee (JNC
Clinical Updates in the Treatment of Hypertension JNC 7 vs. JNC 8 Lauren Thomas, PharmD PGY1 Pharmacy Practice Resident South Pointe Hospital Objectives Review the Eighth Joint National Committee (JNC
Ambulatory BP Monitoring: Getting the Diagnosis of Hypertension Right. Anthony J. Viera, MD, MPH, FAHA Professor and Chair
 Ambulatory BP Monitoring: Getting the Diagnosis of Hypertension Right Anthony J. Viera, MD, MPH, FAHA Professor and Chair Objectives Review limitations of office BP in making a correct diagnosis of hypertension
Ambulatory BP Monitoring: Getting the Diagnosis of Hypertension Right Anthony J. Viera, MD, MPH, FAHA Professor and Chair Objectives Review limitations of office BP in making a correct diagnosis of hypertension
Time of day for exercise on blood pressure reduction in dipping and nondipping hypertension
 (2005) 19, 597 605 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE on blood pressure reduction in dipping and nondipping hypertension S Park,
(2005) 19, 597 605 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE on blood pressure reduction in dipping and nondipping hypertension S Park,
Hypertension and Cardiovascular Disease
 Hypertension and Cardiovascular Disease Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic,
Hypertension and Cardiovascular Disease Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic,
Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial
 Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial Sripal Bangalore, MD, MHA, Chuan-Chuan Wun, PhD, David A DeMicco, PharmD,
Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial Sripal Bangalore, MD, MHA, Chuan-Chuan Wun, PhD, David A DeMicco, PharmD,
Prevention of Atrial Fibrillation and Heart Failure in the Hypertensive Patient
 Prevention of Atrial Fibrillation and Heart Failure in the Hypertensive Patient The Issue of Primary Prevention of A.Fib. (and Heart Failure) and not the Prevention of Recurrent A.Fib. after Electroconversion
Prevention of Atrial Fibrillation and Heart Failure in the Hypertensive Patient The Issue of Primary Prevention of A.Fib. (and Heart Failure) and not the Prevention of Recurrent A.Fib. after Electroconversion
Value of cardiac rehabilitation Prof. Dr. L Vanhees
 Session: At the interface of hypertension and coronary heart disease haemodynamics, heart and hypertension Value of cardiac rehabilitation Prof. Dr. L Vanhees ESC Stockholm August 2010 Introduction There
Session: At the interface of hypertension and coronary heart disease haemodynamics, heart and hypertension Value of cardiac rehabilitation Prof. Dr. L Vanhees ESC Stockholm August 2010 Introduction There
Appendix F: Clinical evidence tables
 378 Appendix F: F.1 Blood pressure variability STUDY 1 P. M. Rothwell, S. C. Howard, E. Dolan, E. O'Brien, J. E. Dobson, B. Dahlof, N. R. Poulter, and P. S. Sever. Effects of beta blockers and calciumchannel
378 Appendix F: F.1 Blood pressure variability STUDY 1 P. M. Rothwell, S. C. Howard, E. Dolan, E. O'Brien, J. E. Dobson, B. Dahlof, N. R. Poulter, and P. S. Sever. Effects of beta blockers and calciumchannel
Recently, there is growing evidence that arterial
 AJH 2004; 17:439 445 Sleep Pulse Pressure and Awake Mean Pressure as Independent Predictors for Stroke in Older Hypertensive Patients Kazuomi Kario, Joji Ishikawa, Kazuo Eguchi, Masato Morinari, Satoshi
AJH 2004; 17:439 445 Sleep Pulse Pressure and Awake Mean Pressure as Independent Predictors for Stroke in Older Hypertensive Patients Kazuomi Kario, Joji Ishikawa, Kazuo Eguchi, Masato Morinari, Satoshi
Todd S. Perlstein, MD FIFTH ANNUAL SYMPOSIUM
 Todd S. Perlstein, MD FIFTH ANNUAL SYMPOSIUM Faculty Disclosure I have no financial interest to disclose No off-label use of medications will be discussed FIFTH ANNUAL SYMPOSIUM Recognize changes between
Todd S. Perlstein, MD FIFTH ANNUAL SYMPOSIUM Faculty Disclosure I have no financial interest to disclose No off-label use of medications will be discussed FIFTH ANNUAL SYMPOSIUM Recognize changes between
OHTAC Recommendation: Twenty-Four-Hour Ambulatory Blood Pressure Monitoring in Hypertension. Ontario Health Technology Advisory Committee
 OHTAC Recommendation: Twenty-Four-Hour Ambulatory Blood Pressure Monitoring in Hypertension Ontario Health Technology Advisory Committee May 2012 Background Hypertension in Canada Hypertension occurs when
OHTAC Recommendation: Twenty-Four-Hour Ambulatory Blood Pressure Monitoring in Hypertension Ontario Health Technology Advisory Committee May 2012 Background Hypertension in Canada Hypertension occurs when
Automated Ambulatory Blood Pressure Monitoring for the Diagnosis of Hypertension in Patients with Elevated Office Blood Pressure
 Automated Ambulatory Blood Pressure Monitoring for the Diagnosis of Hypertension in Patients with Elevated Office Blood Pressure Policy Number: 1.01.02 Last Review: 9/2014 Origination: 1/1989 Next Review:
Automated Ambulatory Blood Pressure Monitoring for the Diagnosis of Hypertension in Patients with Elevated Office Blood Pressure Policy Number: 1.01.02 Last Review: 9/2014 Origination: 1/1989 Next Review:
Carlos A. Segre, Rubens K. Ueno, Karim R. J. Warde, Tarso A. D. Accorsi, Márcio H. Miname, Chang K. Chi, Angela M. G. Pierin, Décio Mion Júnior
 Original Article White-coat Hypertension and Normotension in the League of Hypertension of the Hospital das Clínicas, FMUSP. Prevalence, Clinical and Demographic Characteristics Carlos A. Segre, Rubens
Original Article White-coat Hypertension and Normotension in the League of Hypertension of the Hospital das Clínicas, FMUSP. Prevalence, Clinical and Demographic Characteristics Carlos A. Segre, Rubens
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association
 Ambulatory Blood Pressure Monitoring Page 1 of 14 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Ambulatory Blood Pressure Monitoring Professional Institutional
Ambulatory Blood Pressure Monitoring Page 1 of 14 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Ambulatory Blood Pressure Monitoring Professional Institutional
Int. J. Pharm. Sci. Rev. Res., 36(1), January February 2016; Article No. 06, Pages: JNC 8 versus JNC 7 Understanding the Evidences
 Research Article JNC 8 versus JNC 7 Understanding the Evidences Anns Clara Joseph, Karthik MS, Sivasakthi R, Venkatanarayanan R, Sam Johnson Udaya Chander J* RVS College of Pharmaceutical Sciences, Coimbatore,
Research Article JNC 8 versus JNC 7 Understanding the Evidences Anns Clara Joseph, Karthik MS, Sivasakthi R, Venkatanarayanan R, Sam Johnson Udaya Chander J* RVS College of Pharmaceutical Sciences, Coimbatore,
The aims of the present study were to assess whether treated hypertensive subjects presented an excess of
 Article number = 0397 Original article Why cardiovascular mortality is higher in treated hypertensives versus subjects of the same age, in the general population Athanase Benetos, Frédérique Thomas, Kathryn
Article number = 0397 Original article Why cardiovascular mortality is higher in treated hypertensives versus subjects of the same age, in the general population Athanase Benetos, Frédérique Thomas, Kathryn
1. Department of Gynecology and Obstetrics, St. Joseph's Hospital Berlin Tempelhof, Germany
 Page 1 of 9 Validation of the TONOPORT VI ambulatory blood pressure monitor, according to the European Society of Hypertension International Protocol revision 2010 Michael Abou-Dakn 1, Cornelius Döhmen
Page 1 of 9 Validation of the TONOPORT VI ambulatory blood pressure monitor, according to the European Society of Hypertension International Protocol revision 2010 Michael Abou-Dakn 1, Cornelius Döhmen
Prevalence, awareness, treatment and control of hypertension in North America, North Africa and Asia
 (2004) 18, 545 551 & 2004 Nature Publishing Group All rights reserved 0950-9240/04 $30.00 www.nature.com/jhh REVIEW ARTICLE Prevalence, awareness, treatment and control of hypertension in North America,
(2004) 18, 545 551 & 2004 Nature Publishing Group All rights reserved 0950-9240/04 $30.00 www.nature.com/jhh REVIEW ARTICLE Prevalence, awareness, treatment and control of hypertension in North America,
Ambulatory Blood Pressure and Cardiovascular Events in Chronic Kidney Disease. Rajiv Agarwal, MD
 Ambulatory Blood Pressure and Cardiovascular Events in Chronic Kidney Disease Rajiv Agarwal, MD Summary: Hypertension is an important risk factor for adverse cardiovascular and renal outcomes, particularly
Ambulatory Blood Pressure and Cardiovascular Events in Chronic Kidney Disease Rajiv Agarwal, MD Summary: Hypertension is an important risk factor for adverse cardiovascular and renal outcomes, particularly
Contents. Version 1.0: 01/02/2010 Protocol# ISRCTN Page 1 of 7
 Contents 1. INTRODUCTION... 2 2. STUDY SYNOPSIS... 2 3. STUDY OBJECTIVES... 2 3.1. Primary Objective... 2 3.2. Secondary Objectives... 2 3.3. Assessment of Objectives... 3 3.4. Change the Primary Objective
Contents 1. INTRODUCTION... 2 2. STUDY SYNOPSIS... 2 3. STUDY OBJECTIVES... 2 3.1. Primary Objective... 2 3.2. Secondary Objectives... 2 3.3. Assessment of Objectives... 3 3.4. Change the Primary Objective
Prediction of Cardiovascular Disease in suburban population of 3 municipalities in Nepal
 Prediction of Cardiovascular Disease in suburban population of 3 municipalities in Nepal Koju R, Gurung R, Pant P, Humagain S, Yogol CM, Koju A, Manandhar K, Karmacharya B, Bedi TRS Address for Correspondence:
Prediction of Cardiovascular Disease in suburban population of 3 municipalities in Nepal Koju R, Gurung R, Pant P, Humagain S, Yogol CM, Koju A, Manandhar K, Karmacharya B, Bedi TRS Address for Correspondence:
Conventional and Ambulatory Blood Pressure as Predictors of Retinal Arteriolar Narrowing
 Online Supplement and Ambulatory as Predictors of Retinal Arteriolar Narrowing Fang-Fei Wei 1, Zhen-Yu Zhang 1, Lutgarde Thijs 1, Wen-Yi Yang 1, Lotte Jacobs 1, Nicholas Cauwenberghs 1, Yu-Mei Gu 1, Tatiana
Online Supplement and Ambulatory as Predictors of Retinal Arteriolar Narrowing Fang-Fei Wei 1, Zhen-Yu Zhang 1, Lutgarde Thijs 1, Wen-Yi Yang 1, Lotte Jacobs 1, Nicholas Cauwenberghs 1, Yu-Mei Gu 1, Tatiana
가정혈압의활용 CARDIOVASCULAR CENTER. Wook Bum Pyun M.D., Ph.D. HOME BLOOD PRESSURE MONITORING. Ewha Womans University, school of Medicine
 가정혈압의활용 HOME BLOOD PRESSURE MONITORING CARDIOVASCULAR CENTER Wook Bum Pyun M.D., Ph.D. pwb423@ewha.ac.kr Ewha Womans University, school of Medicine Non-Invasive Blood Pressure Measurement 5-20% Resistant
가정혈압의활용 HOME BLOOD PRESSURE MONITORING CARDIOVASCULAR CENTER Wook Bum Pyun M.D., Ph.D. pwb423@ewha.ac.kr Ewha Womans University, school of Medicine Non-Invasive Blood Pressure Measurement 5-20% Resistant
J-curve Revisited. An Analysis of Blood Pressure and Cardiovascular Events in the Treating to New Targets (TNT) Trial
 J-curve Revisited An Analysis of Blood Pressure and Cardiovascular Events in the Treating to New Targets (TNT) Trial Sripal Bangalore, MD, MHA, Franz H Messerli, MD, Chuan-Chuan Wun, PhD, Andrea L. Zuckerman,
J-curve Revisited An Analysis of Blood Pressure and Cardiovascular Events in the Treating to New Targets (TNT) Trial Sripal Bangalore, MD, MHA, Franz H Messerli, MD, Chuan-Chuan Wun, PhD, Andrea L. Zuckerman,
Prevention of Heart Failure: What s New with Hypertension
 Prevention of Heart Failure: What s New with Hypertension Ali AlMasood Prince Sultan Cardiac Center Riyadh 3ed Saudi Heart Failure conference, Jeddah, 13 December 2014 Background 20-30% of Saudi adults
Prevention of Heart Failure: What s New with Hypertension Ali AlMasood Prince Sultan Cardiac Center Riyadh 3ed Saudi Heart Failure conference, Jeddah, 13 December 2014 Background 20-30% of Saudi adults
and bias, which are known to be present in self-home and in professional office BP measurements taken using the auscultatory technique [7].
![and bias, which are known to be present in self-home and in professional office BP measurements taken using the auscultatory technique [7]. and bias, which are known to be present in self-home and in professional office BP measurements taken using the auscultatory technique [7].](/thumbs/86/94636218.jpg) Devices and technology 37 Validation of the A&D UM-11 professional hybrid device for office blood pressure measurement according to the International Protocol George S. Stergiou, Periklis P. Giovas, Charilaos
Devices and technology 37 Validation of the A&D UM-11 professional hybrid device for office blood pressure measurement according to the International Protocol George S. Stergiou, Periklis P. Giovas, Charilaos
Risk Assessment of developing type 2 diabetes mellitus in patient on antihypertensive medication
 41 Research Article Risk Assessment of developing type 2 diabetes mellitus in patient on antihypertensive medication Amarjeet Singh*, Sudeep bhardwaj, Ashutosh aggarwal Department of Pharmacology, Seth
41 Research Article Risk Assessment of developing type 2 diabetes mellitus in patient on antihypertensive medication Amarjeet Singh*, Sudeep bhardwaj, Ashutosh aggarwal Department of Pharmacology, Seth
The incidence of transient myocardial ischemia,
 AJH 1999;12:50S 55S Heart Rate and the Rate-Pressure Product as Determinants of Cardiovascular Risk in Patients With Hypertension William B. White Inability to supply oxygen to the myocardium when demand
AJH 1999;12:50S 55S Heart Rate and the Rate-Pressure Product as Determinants of Cardiovascular Risk in Patients With Hypertension William B. White Inability to supply oxygen to the myocardium when demand
Nomogram of the Relation of Brachial-Ankle Pulse Wave Velocity with Blood Pressure
 801 Original Article Nomogram of the Relation of Brachial-Ankle Pulse Wave Velocity with Blood Pressure Akira YAMASHINA, Hirofumi TOMIYAMA, Tomio ARAI, Yutaka KOJI, Minoru YAMBE, Hiroaki MOTOBE, Zydem
801 Original Article Nomogram of the Relation of Brachial-Ankle Pulse Wave Velocity with Blood Pressure Akira YAMASHINA, Hirofumi TOMIYAMA, Tomio ARAI, Yutaka KOJI, Minoru YAMBE, Hiroaki MOTOBE, Zydem
The problem of uncontrolled hypertension
 (2002) 16, S3 S8 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh The problem of uncontrolled hypertension Department of Public Health and Clinical Medicine, Norrlands
(2002) 16, S3 S8 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh The problem of uncontrolled hypertension Department of Public Health and Clinical Medicine, Norrlands
Diabetologia 9 Springer-Verlag 1991
 Diabetologia (1991) 34:590-594 0012186X91001685 Diabetologia 9 Springer-Verlag 1991 Risk factors for macrovascular disease in mellitus: the London follow-up to the WHO Multinational Study of Vascular Disease
Diabetologia (1991) 34:590-594 0012186X91001685 Diabetologia 9 Springer-Verlag 1991 Risk factors for macrovascular disease in mellitus: the London follow-up to the WHO Multinational Study of Vascular Disease
Prognostic Value of Cardiopulmonary Exercise Testing in Patients with Atrial Fibrillation
 Prognostic Value of Cardiopulmonary Exercise Testing in Patients with Atrial Fibrillation Hidekazu Tsuneoka 1)2), Akira Koike 2), Osamu Nagayama 2), Koji Sakurada 2), Hitoshi Sawada 2), Kazutaka Aonuma
Prognostic Value of Cardiopulmonary Exercise Testing in Patients with Atrial Fibrillation Hidekazu Tsuneoka 1)2), Akira Koike 2), Osamu Nagayama 2), Koji Sakurada 2), Hitoshi Sawada 2), Kazutaka Aonuma
CONGESTIVE HEART FAILURE
 ORIGINAL CONTRIBUTION Diurnal Blood Pressure Pattern and Risk of Congestive Heart Failure Erik Ingelsson, MD, PhD Kristina Björklund-Bodegård, MD, PhD Lars Lind, MD, PhD Johan Ärnlöv, MD, PhD Johan Sundström,
ORIGINAL CONTRIBUTION Diurnal Blood Pressure Pattern and Risk of Congestive Heart Failure Erik Ingelsson, MD, PhD Kristina Björklund-Bodegård, MD, PhD Lars Lind, MD, PhD Johan Ärnlöv, MD, PhD Johan Sundström,
Arterial Age and Shift Work
 340 Arterial Age and Shift Work Ioana Mozos 1*, Liliana Filimon 2 1 Department of Functional Sciences, Victor Babes University of Medicine and Pharmacy, Timisoara, Romania 2 Department of Occupational
340 Arterial Age and Shift Work Ioana Mozos 1*, Liliana Filimon 2 1 Department of Functional Sciences, Victor Babes University of Medicine and Pharmacy, Timisoara, Romania 2 Department of Occupational
Echocardiographic definition of left ventricular hypertrophy in the hypertensive: which method of indexation of left ventricular mass?
 Journal of Human Hypertension (1999) 13, 505 509 1999 Stockton Press. All rights reserved 0950-9240/99 $12.00 http://www.stockton-press.co.uk/jhh ORIGINAL ARTICLE Echocardiographic definition of left ventricular
Journal of Human Hypertension (1999) 13, 505 509 1999 Stockton Press. All rights reserved 0950-9240/99 $12.00 http://www.stockton-press.co.uk/jhh ORIGINAL ARTICLE Echocardiographic definition of left ventricular
THE NEW ARMENIAN MEDICAL JOURNAL DISTRIBUTION, AWARENESS, TREATMENT, AND CONTROL OF ARTERIAL HYPERTENSION IN YEREVAN (ARMENIA)
 THE NEW ARMENIAN MEDICAL JOURNAL Vol.5 (2011), Nо 2, p.29-34 DISTRIBUTION, AWARENESS, TREATMENT, AND CONTROL OF ARTERIAL HYPERTENSION IN YEREVAN (ARMENIA) Zelveian P.H. 1, 2, Podosyan G.A. 2 1 Institute
THE NEW ARMENIAN MEDICAL JOURNAL Vol.5 (2011), Nо 2, p.29-34 DISTRIBUTION, AWARENESS, TREATMENT, AND CONTROL OF ARTERIAL HYPERTENSION IN YEREVAN (ARMENIA) Zelveian P.H. 1, 2, Podosyan G.A. 2 1 Institute
(n=6279). Continuous variables are reported as mean with 95% confidence interval and T1 T2 T3. Number of subjects
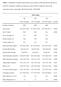 Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Since 1980, obesity has more than doubled worldwide, and in 2008 over 1.5 billion adults aged 20 years were overweight.
 Impact of metabolic comorbidity on the association between body mass index and health-related quality of life: a Scotland-wide cross-sectional study of 5,608 participants Dr. Zia Ul Haq Doctoral Research
Impact of metabolic comorbidity on the association between body mass index and health-related quality of life: a Scotland-wide cross-sectional study of 5,608 participants Dr. Zia Ul Haq Doctoral Research
T. Suithichaiyakul Cardiomed Chula
 T. Suithichaiyakul Cardiomed Chula The cardiovascular (CV) continuum: role of risk factors Endothelial Dysfunction Atherosclerosis and left ventricular hypertrophy Myocardial infarction & stroke Endothelial
T. Suithichaiyakul Cardiomed Chula The cardiovascular (CV) continuum: role of risk factors Endothelial Dysfunction Atherosclerosis and left ventricular hypertrophy Myocardial infarction & stroke Endothelial
ARIC Manuscript Proposal # PC Reviewed: 2/10/09 Status: A Priority: 2 SC Reviewed: Status: Priority:
 ARIC Manuscript Proposal # 1475 PC Reviewed: 2/10/09 Status: A Priority: 2 SC Reviewed: Status: Priority: 1.a. Full Title: Hypertension, left ventricular hypertrophy, and risk of incident hospitalized
ARIC Manuscript Proposal # 1475 PC Reviewed: 2/10/09 Status: A Priority: 2 SC Reviewed: Status: Priority: 1.a. Full Title: Hypertension, left ventricular hypertrophy, and risk of incident hospitalized
The role of physical activity in the prevention and management of hypertension and obesity
 The 1 st World Congress on Controversies in Obesity, Diabetes and Hypertension (CODHy) Berlin, October 26-29 2005 The role of physical activity in the prevention and management of hypertension and obesity
The 1 st World Congress on Controversies in Obesity, Diabetes and Hypertension (CODHy) Berlin, October 26-29 2005 The role of physical activity in the prevention and management of hypertension and obesity
Within-Home Blood Pressure Variability on a Single Occasion Has Clinical Significance
 Published online: May 12, 2016 2235 8676/16/0041 0038$39.50/0 Mini-Review Within-Home Blood Pressure Variability on a Single Occasion Has Seiichi Shibasaki a, b Satoshi Hoshide b Kazuomi Kario b a Department
Published online: May 12, 2016 2235 8676/16/0041 0038$39.50/0 Mini-Review Within-Home Blood Pressure Variability on a Single Occasion Has Seiichi Shibasaki a, b Satoshi Hoshide b Kazuomi Kario b a Department
Central pressures and prediction of cardiovascular events in erectile dysfunction patients
 Central pressures and prediction of cardiovascular events in erectile dysfunction patients N. Ioakeimidis, K. Rokkas, A. Angelis, Z. Kratiras, M. Abdelrasoul, C. Georgakopoulos, D. Terentes-Printzios,
Central pressures and prediction of cardiovascular events in erectile dysfunction patients N. Ioakeimidis, K. Rokkas, A. Angelis, Z. Kratiras, M. Abdelrasoul, C. Georgakopoulos, D. Terentes-Printzios,
A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes
 A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Hypotheses: Among individuals with type 2 diabetes, the risks of major microvascular
A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Hypotheses: Among individuals with type 2 diabetes, the risks of major microvascular
MEDICAL POLICY SUBJECT: AUTOMATED AMBULATORY BLOOD PRESSURE MONITORING
 MEDICAL POLICY SUBJECT: AUTOMATED AMBULATORY 02/19/09 PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: AUTOMATED AMBULATORY 02/19/09 PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Online Supplementary Material
 Section 1. Adapted Newcastle-Ottawa Scale The adaptation consisted of allowing case-control studies to earn a star when the case definition is based on record linkage, to liken the evaluation of case-control
Section 1. Adapted Newcastle-Ottawa Scale The adaptation consisted of allowing case-control studies to earn a star when the case definition is based on record linkage, to liken the evaluation of case-control
Does masked hypertension exist in healthy volunteers and apparently well-controlled hypertensive patients?
 O R I G I N A L A R T I C L E Does masked hypertension exist in healthy volunteers and apparently well-controlled hypertensive patients? I. Aksoy, J. Deinum, J.W.M. Lenders, Th. Thien *# Department of
O R I G I N A L A R T I C L E Does masked hypertension exist in healthy volunteers and apparently well-controlled hypertensive patients? I. Aksoy, J. Deinum, J.W.M. Lenders, Th. Thien *# Department of
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
Biases in clinical research. Seungho Ryu, MD, PhD Kanguk Samsung Hospital, Sungkyunkwan University
 Biases in clinical research Seungho Ryu, MD, PhD Kanguk Samsung Hospital, Sungkyunkwan University Learning objectives Describe the threats to causal inferences in clinical studies Understand the role of
Biases in clinical research Seungho Ryu, MD, PhD Kanguk Samsung Hospital, Sungkyunkwan University Learning objectives Describe the threats to causal inferences in clinical studies Understand the role of
White-Coat and Masked Hypertension
 White-Coat and Masked Hypertension Long-Term Risk of Sustained Hypertension in White-Coat or Masked Hypertension Giuseppe Mancia, Michele Bombelli, Rita Facchetti, Fabiana Madotto, Fosca Quarti-Trevano,
White-Coat and Masked Hypertension Long-Term Risk of Sustained Hypertension in White-Coat or Masked Hypertension Giuseppe Mancia, Michele Bombelli, Rita Facchetti, Fabiana Madotto, Fosca Quarti-Trevano,
DEPARTMENT OF GENERAL MEDICINE WELCOMES
 DEPARTMENT OF GENERAL MEDICINE WELCOMES 1 Dr.Mohamed Omar Shariff, 2 nd Year Post Graduate, Department of General Medicine. DR.B.R.Ambedkar Medical College & Hospital. 2 INTRODUCTION Leading cause of global
DEPARTMENT OF GENERAL MEDICINE WELCOMES 1 Dr.Mohamed Omar Shariff, 2 nd Year Post Graduate, Department of General Medicine. DR.B.R.Ambedkar Medical College & Hospital. 2 INTRODUCTION Leading cause of global
