left ventricular assist device
|
|
|
- Elfreda Garrison
- 6 years ago
- Views:
Transcription
1 Caring for patients with a left ventricular assist device Thorough knowledge of left ventricular assist devices makes caring for these patients a rewarding challenge. By Heather Martonik, MSN, RN NEARLY 6 MILLION Americans suffer from heart failure (HF). The American Heart Association predicts that the number of individuals diagnosed with HF will increase 46% by HF can t be cured, but it can be managed with medications until it reaches an advanced stage. At that point, a heart transplant or an implanted left ventricular assist device (LVAD) is the only long-term option for survival. A continuous-flow pump, the LVAD directs blood from the left ventricle to the ascending aorta. (See Understanding the LVAD.) The Food and Drug Administration (FDA) first approved the LVAD for patients waiting for heart transplants; when used for this purpose, the device is considered a bridge to transplant. While a heart transplant is optimal, demand for donor hearts far exceeds supply. For that reason, LVADs have become increasingly popular as a destination therapy. The HeartMate II by Thoratec is the only FDA-approved LVAD for destination therapy. Since 2006, more than 20,000 patients have received LVADs as destination therapy, and this number is expected to increase. For this reason, nurses need to become more knowledgeable about and confident in caring for patients with these devices. This article discusses nursing care of patients with LVADs for destination therapy, including device and medication management, potential complications, patient education, and psychosocial support for patients, home caregivers, and nurses. Illustration: Wikipedia, Blausen Medical Communications, Inc. LEARNING OBJECTIVES 1. Describe the assessment of patients with a left ventricular assist device (LVAD). 2. Discuss nursing management of patients with an LVAD. 3. State possible complications from an LVAD. The author and planners of this CNE activity have disclosed no relevant financial relationships with any commercial companies pertaining to this activity. See the last page of the article to learn how to earn CNE credit. Expiration: 5/1/20 CNE 1.49 contact hours Who benefits from an LVAD? Although no stringent patient-selection guidelines exist, a provider usually refers a patient for an LVAD when advanced HF no longer responds to inotropic drugs or surgical interventions, such as valve repair. Patient evaluation for an LVAD includes nutritional status, end-organ function, right ventricular function, and signs or symptoms of infection. Patients also should be screened for depression and other psychological problems. The selection process includes determining if a home caregiver is willing and able to care for the patient around the clock for at least 3 to 6 months after surgery. Home caregivers must learn how to care for the device and assist patients. Caregiver responsibilities include helping patients manage their LVAD, monitoring for infection, changing driveline dressings, managing medications, assisting with activities of daily living, and providing transportation to and from medical appointments. Depending on the patient s needs and whether complications occur, caregiving may be needed for the rest of the patient s life. Approval for an LVAD typically occurs over several meetings between the patient and family and a team consisting of a cardiologist, a cardiothoracic surgeon, an LVAD (or VAD) coordinator, a social worker, and a palliative care provider. Many VAD coordinators are RNs who have special training in these devices. Based on the team s recommendation, the cardiothoracic surgeon will ultimately decide if the patient is a candidate for an LVAD. Proper assessment Caring for the hospitalized patient 20 American Nurse Today Volume 12, Number 5 AmericanNurseToday.com
2 with an LVAD begins with a thorough assessment of both the patient and LVAD. Monitor blood pressure and mean arterial pressure (MAP); the goal is 60 mm Hg to 90 mm Hg. Elevated MAP decreases flow and perfusion. If MAP is too high, the patient may require antihypertensive drugs, such as metoprolol, hydralazine, and isosorbide dinitrate. These drugs may need to be adjusted until the goal MAP is reached. Always check with the provider before holding any medications due to a low MAP. Check the LVAD each time you assess the patient s vital signs. You will hear the continuous humming sound of the pump when auscultating the heart. Make sure the batterycharging station is plugged into the wall and at least two spare batteries are in the charge station; a green light indicates a full charge. Additional safety checks include assessing the driveline to ensure it s securely in place and confirming there s a backup system controller in the room. The LVAD may be connected to the power module, which is plugged into the wall; or, to allow more mobility, the patient may wear the batteries in a holster. When the device is plugged into the module, several numbers on the system monitor indicate pump flow, pump speed, pulse index, and power. (See The 4 Ps of the LVAD.) If the patient is wearing a battery holster, the numbers must be read from the controller. Understanding the LVAD A left ventricular assist device (LVAD) is a continuous-flow pump that connects the left ventricle to the ascending aorta via an internal cannula. The illustration below shows the elements of the pump. To power the LVAD, a percutaneous lead (driveline) exits the abdominal wall and connects to a system controller and a power module that remains plugged into a wall outlet. Patients also can connect their LVAD to two lithium-ion batteries. They may wear the batteries on a belt or a vest for increased mobility. Batteries last approximately 12 to 14 hours. The system controller has approximately 15 minutes of battery life, but never rely on it for battery power. Patients have a set of two backup batteries, a charging station, and a shower bag to keep the controller dry while showering. Caution them not to swim or soak in a bath or hot tub. Percutaneous lead exiting the body Image from Abbott. All rights reserved. Used with permission. Aorta HeartMate II LVAD Heart Power lead Technical care of the LVAD The LVAD requires regular care and system checks, including powersource changes, daily self-tests, and driveline dressing changes. Performing these tasks in the hospital provides teaching opportunities for patients and caregivers. (See Essential education for patients and caregivers.) Switching power sources Patients and caregivers can learn how to change between batteries and the power module by watching you do it, so try to do it the same way every time. For example, always change out the white power cables first and then the black. To change from one power source to the other, push the connectors of the white cables together and turn counterclockwise to disconnect. To reconnect, align the half moons on the connectors, push them together, and turn clockwise until they re flush. Repeat the same steps with the black cables. Think power, patient, power to remind yourself to disconnect and reconnect one power source at a time. Never disconnect both sets of cables at the same time; this essentially leaves the patient without a power source. The system controller provides power for a limited time, but never rely on it. Tell the patient the device will sound an alarm when changing between power sources. AmericanNurseToday.com May 2017 American Nurse Today 21
3 Performing a daily self-test Teach the patient to perform a daily self-test to ensure the LVAD is working properly. When the patient presses and holds the battery button on the system controller, the screen displays Self Test. If the panel is working properly, the audio alarm will sound and control panel alarms will light up. These alarms include power and battery alarms, a red heart (hazard) alarm, and a wrench (advisory) alarm. Changing the driveline dressing Assess the driveline site during each patient assessment, or more frequently if you re concerned about dislodgment. Except under special circumstances, the driveline dressings must be changed daily or every other day, depending on the pro - vider s order and how long the patient has had the LVAD. (See How to change a driveline dressing.) Ultimately, you re responsible for ensuring the dressing change is completed; however, if you or the VAD coordinator have trained and observed the patient and caregiver changing the dressing, you can let them do it. Medication management Patients with LVADs are typically prescribed several medications, including anticoagulants, antiplatelet agents, antihypertensives, antiarrhythmics, fluids, and electrolytes. Anticoagulants and antiplatelets Anticoagulants and antiplatelets (for example, heparin, warfarin, and aspirin) help prevent pump thrombosis. However, these drugs increase hemorrhage risk. Antihypertensives Adequate blood pressure (typically, a MAP between 60 mm Hg and 90 mm Hg) helps maintain sufficient pump flow. Commonly prescribed antihypertensive drugs include: vasodilators, such as hydralazine and isosorbide dinitrate The 4 Ps of the LVAD Monitor these key parameters on your patient s left ventricular assist device (LVAD). Pump flow is an estimate of cardiac output based on pump speed and power. It typically ranges from 4 to 6 L/minute. Pump flow is influenced by mean arterial pressure (MAP); a higher MAP increases pump flow, and a lower MAP decreases it. Pump speed indicates the speed at which the LVAD rotors are spinning. The usual range is 8,600 to 9,800 rpm. Pulse index (PI) is a measurement of flow through the pump and is determined by pump speed and the patient s native heart function. PI typically ranges from 3 to 7. Lower values reflect less native heart function and greater reliance on the pump, while higher values reflect more native heart function and less support by the pump. Power is the amount of wattage (W) the device needs to maintain speed and flow. The normal range is 4 to 7 W. beta blockers, such as metoprolol and carvedilol angiotensin-converting enzyme (ACE) inhibitors, such as lisinopril. Always monitor heart rate and blood pressure when giving these medications. Fluid and electrolyte replacement Most patients with HF are restricted to 2 L of fluid per day. For patients with LVADs, who depend on adequate volume and pressure to maintain flow, you may need to push fluids to achieve the best filling pressures. For patients with long-term HF, provide education to ensure they don t become dehydrated after receiving the device. The decision to push fluids depends on the patient s hemodynamic status. Signs of compromised fluid status include decreased pump flow and pulse index, as well as increased hemoglobin and hematocrit. Common indications of fluid overload, which can lead to right ventricular failure, include weight gain, edema, and shortness of breath, all of which indicate increased preload. Keeping electrolytes, such as potassium, magnesium, sodium, and calcium, within normal ranges helps prevent arrhythmias. Check your patient s basic metabolic panel, comprehensive blood count, prothrombin time, and international normalized ratio (INR) daily. Managing complications Common LVAD complications include infection, pump thrombus, hemorrhage, arrhythmias, and suction events. Infection Several factors put patients with LVADs at high risk for infection for example, malnutrition. Potential sources of infection include ventilators, central venous catheters, peripheral I.V. lines, and indwelling urinary catheters. Keep in mind that all hospital patients are at risk for methicillin-resistant Staphylococcus aureus infection and Clostridium difficile infection, as well as pressure injuries, which can become infected. After surgery, driveline infections are common. To help prevent these infections, provide thorough patient and caregiver education on performing driveline dressing changes. Pump thrombus Signs and symptoms of pump throm - bus include increased heart rate, shortness of breath, increased pulse pressure, and a steady increase in pump power over several days. If the pump is completely occluded by a clot, the pump flow rate decreases. Notify the provider immediately if the patient experiences any of these problems. Treatment of pump thrombus involves anticoagulant or antiplatelet therapy, direct infusion of a local thrombolytic into the LVAD, or 22 American Nurse Today Volume 12, Number 5 AmericanNurseToday.com
4 Essential education for patients and caregivers Educating the patient, family, and home caregivers about proper care of the left ventricular assist device (LVAD) helps everyone feel more comfortable with the device and can reduce complications. Encourage patients and caregivers to handle the LVAD equipment soon after surgery so they become comfortable with it. Teach the patient and caregiver how to change the driveline dressing and have them perform a dressing change for you. Use the teach-back method when educating about signs and symptoms of infection and ways to reduce risks. Advise patients and caregivers to change the power source (see the photo below) the same way every time. For example, teach them to disconnect and connect the white cables first and then the black cables. Provide education about the purpose of medications, what to do if the patient misses a dose, and adverse reactions to report to the provider. Teach patients and caregivers to take the patient s vital signs and explain the normal ranges for heart rate and blood pressure. Ensure patients and caregivers know how to respond to LVAD alarms. Explain what to do if an emergency occurs. Emphasize the importance of notifying the local power company about the LVAD to ensure the home is a priority for power restoration if an outage occurs. pump replacement. To avoid these problems, monitor lab values to help ensure the patient s INR is in the therapeutic range, typically 2 to 3. Hemorrhage Lifelong anticoagulant use puts patients at risk for hemorrhage, especially stroke or GI bleeding. Signs and symptoms of GI bleeding are frank red to black tarry stools, a significant drop in hematocrit, decreased oxygen saturation, pallor, and dizziness. Anticoagulant therapy may need to be adjusted, and the patient may require blood products. Suction event A suction event occurs when pressure inside the ventricles drops too Power source for LVAD Photo from Abbott. All rights reserved. Used with permission. low, causing the internal cannula to adhere to the left ventricular septum. This typically results from hypovolemia. Other causes include high pump speed and poor internal cannula positioning. A suction event isn t life-threatening in itself but can lead to ventricular arrhythmias, such as ventricular tachycardia. Notify the provider immediately if you suspect a suction event. Treatment may include pushing fluids to restore ventricular pressure, treating the cause of hypovolemia (such as over-diuresis or GI loss), or surgery to restore proper cannula positioning. Arrhythmias Arrhythmias, such as ventricular tachycardia and atrial fibrillation, are common in LVAD patients. Many of these patients had a pacemaker placed before surgery to treat atrial fibrillation. After LVAD placement, arrhythmias are medically managed with antiarrhythmic agents, such as amiodarone and digoxin. For a newonset arrhythmia, assess the patient to see if he or she is stable or symptomatic, check electrolyte levels, and notify the provider. Contact the provider and VAD coordinator immediately if the patient experiences symptomatic or sustained ventricular tachycardia (longer than 30 seconds) or ventricular fibrillation. If the patient becomes unresponsive, call a code blue. Avoid chest compressions except as a last resort because they can dislodge the LVAD and cause irreparable damage. Give medications per advanced cardiac life support protocol. You can leave the pump running during defibrillation. Psychosocial support Patients with LVADs experience many physical and emotional changes. Although there are many physiological benefits (increased energy, reduced shortness of breath), patients may become depressed or even suicidal. Many patients feel socially isolated and express frustration over loss of control and dependency on family and caregivers. Others may be afraid of their device. Assess patients for depression on admission and throughout their hospital stay. Ask how they re managing daily life using open-ended questions, such as: How has your life changed since receiving an LVAD? What are your greatest concerns after leaving the hospital? How will you cope with these concerns? What are some benefits and challenges you ve experienced since receiving your LVAD? AmericanNurseToday.com May 2017 American Nurse Today 23
5 Teach coping skills, such as journaling, meditation, art therapy, prayer, and the importance of reaching out to others. Patients with LVADs can offer significant support to one another, so provide information about support groups. Caring for the home caregiver Caregiving can be burdensome. Many caregivers express fear of the LVAD, regret taking on the role, or experience depression and anxiety. They need support, even if the patient has had an LVAD for a long time. Provide caregivers with resources for support groups where they can receive encouragement and respite care. Self-care for the nurse Many nurses who are new to caring for patients with LVADs express anxiety over caring for this patient population. Make sure you re up-to-date with your employer s standard education on LVADs. Refamiliarize yourself with the equipment and ask to shadow a nurse who s caring for a patient with an LVAD. Ask for help from someone who s more experienced. VAD coordinators are excellent sources of support, so find out who s on call and how to reach him or her. In many cases, nurses who care for patients with LVADs get to know them and their families well and may experience grief if a patient becomes seriously ill or dies. If you feel you re experiencing grief or burnout, reach out to a trusted coworker, manager, or counselor. Spend days off doing something enjoyable, such as spending quality time with family, friends, or a pet. Treat yourself to a massage or a relaxing bath, go outside, take a yoga class, or meditate. Most important, never forget why you became a nurse. Rewarding challenge As the population of patients with How to change a driveline dressing Use Remove the old dressing and assess the exit site for signs of infection. Ensure the exit site is clean and dry, with no redness or drainage. Using a back-and-forth motion, clean the area surrounding the exit site with chlorhexidine, moving from the area immediately around the driveline exit site outward. Don t use a circular motion, as this increases infection risk. Clean the driveline with a new chlorhexidine swab, sweeping away from the exit site to prevent bacteria from traveling up the driveline. Fold a 2" x 2" gauze pad and tuck it underneath the driveline; cover it with another 2" x 2" gauze pad. low-adherent tape to cover the gauze pads, tearing one side just enough to tuck under the driveline. Ensure a proper securement device is intact and placed several inches lateral from the driveline exit site. It should provide just enough slack to the driveline so it s not taut. advanced HF increases, nurses in all healthcare settings need to become familiar with the care of patients with LVADs, including device assessment and management, potential complications, and patient and caregiver education and support. Caring for the patient with an LVAD can be challenging, but it s also immensely rewarding. Heather Martonik is a registered nurse in the coronary care unit at the Pulse Heart Institute at Multi- Care Health System in Tacoma, Washington. Selected references Benjamin EJ, Blaha MJ, Chiuve SE, et al. Heart disease and stroke statistics 2017 update: A report from the American Heart Association. Circulation. 2017;135(10):e Brouwers C, Denollet J, Caliskan K, et al. Psychological distress in patients with a left ventricular assist device and their partners: An exploratory study. Eur J Cardiovasc Nurs. 2015;14(1): Bruce CR, Delgado E, Kostick K, et al. Ventricular assist devices: A review of psychosocial risk factors and their impact on outcomes. J Card Fail. 2014;20(12): Doty D. Ventricular assist device and destination therapy candidates from preoperative selection through end of hospitalization. Crit Care Nurs Clin North Am. 2015;27(4): Hohner E, Crow J, Moranville MP. Medication management for left ventricular assist device thrombosis. Am J Health Syst Pharm. 2015;72(13): Jennings DL, Jones MC, Lanfear DE. Assessment of the heart failure pharmacotherapy of patients with continuous flow left-ventricular assist devices. Int J Artif Organs. 2012;35(3): Magid M, Jones J, Allen LA, et al. The perceptions of important elements of caregiving for a left ventricular assist device patient: A qualitative meta-synthesis. J Cardiovasc Nurs. 2016;31(3): Marcuccilli L, Casida JJ, Bakas T, Pagani FD. Family caregivers inside perspectives: Caring for an adult with a left ventricular assist device as a destination therapy. Prog Transplant. 2014;24(4): Miller LW, Guglin M. Patient selection for ventricular assist devices: A moving target. J Am Coll Cardiol. 2013;61(12): Modica M, Ferratini M, Torri A, et al. Quality of life and emotional distress early after left ventricular assist device implant: A mixedmethod study. Artif Organs. 2015;39(3): Ottenberg AL, Cook KE, Topazian RJ, et al. Choices for patients without a choice : Interviews with patients who received a left ventricular assist device as destination therapy. Circ Cardiovasc Qual Outcomes. 2014;7(3): Park SJ, Milano CA, Tatooles AJ, et al. Outcomes in advanced heart failure patients with left ventricular assist devices for destination therapy. Circ Heart Fail. 2012;5(2): Rommel JJ, O'Neill TJ, Lishmanov A, et al. The role of heart failure pharmacotherapy after left ventricular assist device support. Heart Fail Clin. 2014;10(4): Thoratec Corporation. HeartMate II LVAS clinical operation & patient management ENGLISH.pdf Thoratec Corporation. Proven alternative for advanced heart failure. medical-professionals 24 American Nurse Today Volume 12, Number 5 AmericanNurseToday.com
6 POST-TEST Caring for patients with a left ventricular assist device Earn contact hour credit online at CNE: 1.49 contact hours CNE Provider accreditation The American Nurses Association s Center for Continuing Education and Professional Development is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. ANCC Provider Number Contact hours: 1.49 ANA s Center for Continuing Education and Professional Development is approved by the California Board of Registered Nursing, Provider Number CEP6178 for 1.79 contact hours. Post-test passing score is 80%. Expiration: 5/1/20 ANA Center for Continuing Education and Professional Development s accredited provider status refers only to CNE activities and does not imply that there is real or implied endorsement of any product, service, or company referred to in this activity nor of any company subsidizing costs related to the activity. The author and planners of this CNE activity have disclosed no relevant financial relationships with any commercial companies pertaining to this CNE. See the banner at the top of this page to learn how to earn CNE credit. Please mark the correct answer online. 1. George Davidson,* a 60-year-old man with severe heart failure, is on the heart transplant list. As a bridge, he receives a left ventricular assist device (LVAD). You are Mr. Davidson s nurse today. You know you need to monitor his mean arterial pressure, which should be kept at a. 20 mm Hg to 40 mm Hg. b. 30 mm Hg to 60 mm Hg. c. 60 mm Hg to 90 mm Hg. d. 90 mm Hg to 100 mm Hg. 2. Which of the following would alert you to a possible safety issue with Mr. Davidson s LVAD? a. An additional system controller in the room b. Continuous humming sound on auscultation c. Two batteries in the charging station d. Yellow light on the battery charging station 3. When explaining the LVAD to Mr. Davidson, you tell him that it a. connects the right ventricle to the ascending aorta. b. connects the left ventricle to the ascending aorta. c. uses an external cannula for connecting the ventricle to the aorta. d. provides intermittant pump flow via three lithium-ion batteries. 4. Which statement about the pump flow reading on Mr. Davidson s LVAD display is correct? a. A higher MAP will reduce pump flow. b. It usually ranges from 2 to 4 L/minute. c. It s an estimate of cardiac output based on pump speed and power. d. It reflects the amount of wattage needed to maintain flow. 5. Mr. Davidson s pulse index is 4, which tells you a. it is lower than the usual range of 6 to 8. b. it is unaffected by the pump speed. c. he has more native heart function, so he has less reliance on the LVAD. d. he has less native heart function, so he has greater reliance on the LVAD. 6. Mr. Davidson s wife Amelia will be his caregiver at home. When teaching her how to change between batteries and the power module, you tell her to a. alternate the order in which the power cables are changed. b. change the white power cables first and then the black. c. turn the cable connectors clockwise to disconnect them. d. turn the cable connectors counterclockwise to reconnect. 7. When teaching Ms. Davidson how to change a driveline dressing, you instruct her to a. use chlorhexidine to clean the exit site area from outward towards the exit site. b. use a circular motion to clean the exit site area with chlorhexidine. c. clean the driveline using the same chlorhexidine swab, sweeping towards the exit site. d. clean the driveline with a new chlorhexidine swab, sweeping away from the exit site. 8. Which of the following statements about the driveline dressing change is correct? a. Use low-adherent tape to cover the gauze pad on the driveline, tearing one side just enough to tuck under the driveline. b. Use high-adhesive tape to cover the gauze pad on the driveline, tearing two sides just enough to tuck under the driveline. c. A securement device should be placed one inch from the driveline exit site. d. The securement device should be placed so that it keeps the driveline taut. 9. Which do you need to consider about Mr. Davidson s fluids? a. Symptoms of fluid overload are dangerous for patients with an LVAD because they can decrease preload. b. Common indicators of fluid overload include weight loss, pulmonary edema, and shortness of breath. c. He may need more fluids than typical patients with heart failure to achieve the best filling pressures. d. Signs of compromised fluid status include increased pump flow and pulse index. 10. Mr. Davidson says he is short of breath, and his heart rate and pulse pressure have increased. You note that there has been a steady increase in pump power during the week. Based on these findings, you suspect a. suction event. b. pump thrombosis. c. hemorrhage. d. driveline infection. 11. You alert Mr. Davidson s physician to the potential problem, which is resolved. Later that day, you act as a preceptor to a nurse who has not yet cared for a patient with an LVAD. As you re discussing Mr. Davidson s needs, you note that his international normalized ratio should be kept in the therapeutic range, typically a. 1 to 1.25 b. 1.5 to 2. c. 2 to 3. d. 4 to Mr. Davidson experiences a cardiac arrest. You know to a. leave the pump on during defibrillation. b. turn the pump off during defibrillation. c. begin chest compressions immediately and avoid interrupting them. d. avoid the use of advanced cardiac life support medications. 13. Which of the following could cause a suction event for Mr. Davidson? a. Hypovolemia b. Pump speed of 8,800 rpm c. Poor external cannula position d. Pump speed of 8,600 rpm 14. Which statement about the psychological needs for Mr. and Ms. Davidson is NOT correct? a. Patients with an LVAD, as well as their families, require minimal psychological support. b. Although LVADs provide many benefits, patients may become depressed or even suicidal. c. Patients should be assessed for depression on admission and throughout their hospital stay. d. Families of patients with an LVAD may benefit from support groups and respite care. *Names used are fictitious. AmericanNurseToday.com May 2017 American Nurse Today 25
EMS: Care of the VAD Patient. Brittany Butzler BSN RN VAD Coordinator Froedtert and the Medical College of WI
 EMS: Care of the VAD Patient Brittany Butzler BSN RN VAD Coordinator Froedtert and the Medical College of WI Disclosure No relevant financial relationships by planners or presenters Left Ventricular Assist
EMS: Care of the VAD Patient Brittany Butzler BSN RN VAD Coordinator Froedtert and the Medical College of WI Disclosure No relevant financial relationships by planners or presenters Left Ventricular Assist
EMS and Nursing Considerations in VAD Patient Care
 EMS and Nursing Considerations in VAD Patient Care B R I T T A N Y B U T Z L E R B S N R N V A D C O O R D I N A T O R F R O E D T E R T A N D T H E M E D I C A L C O L L E G E O F W I 1 0 / 2 5 / 1 8
EMS and Nursing Considerations in VAD Patient Care B R I T T A N Y B U T Z L E R B S N R N V A D C O O R D I N A T O R F R O E D T E R T A N D T H E M E D I C A L C O L L E G E O F W I 1 0 / 2 5 / 1 8
FEATURE. 58 EMERGENCY MEDICINE I FEBRUARY
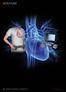 FEATURE 58 EMERGENCY MEDICINE I FEBRUARY 2016 www.emed-journal.com Troubleshooting the Left Ventricular Assist Device Alicia S. Devine, JD, MD In an update and complement to a previously published article,
FEATURE 58 EMERGENCY MEDICINE I FEBRUARY 2016 www.emed-journal.com Troubleshooting the Left Ventricular Assist Device Alicia S. Devine, JD, MD In an update and complement to a previously published article,
Is a LVAD the Right Treatment for Me? Decision Aid
 Is a LVAD the Right Treatment for Me? Decision Aid patienteducation.osumc.edu 2 Making an Informed Decision Review this book We give you this information to help you understand what the LVAD treatment
Is a LVAD the Right Treatment for Me? Decision Aid patienteducation.osumc.edu 2 Making an Informed Decision Review this book We give you this information to help you understand what the LVAD treatment
1/21/2016. HeartMate II Indications for Use. Ventricular Assist Device Overview. Jon G. Echterling MSN, CCRN, FNP-BC. Learning Objectives
 Ventricular Assist Device Overview Jon G. Echterling MSN, CCRN, FNP-BC February 5, 2016 Learning Objectives Identify the components and operation of the HeartMate II LVAD Describe the path blood follows
Ventricular Assist Device Overview Jon G. Echterling MSN, CCRN, FNP-BC February 5, 2016 Learning Objectives Identify the components and operation of the HeartMate II LVAD Describe the path blood follows
STATE OF OKLAHOMA 2014 EMERGENCY MEDICAL SERVICES PROTOCOLS
 5M VENTRICULAR ASSIST DEVICE (VAD) MANAGEMENT ADULT EMERGENCY MEDICAL DISPATCHER EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC A Ventricular Assist Device, or VAD, is a mechanical
5M VENTRICULAR ASSIST DEVICE (VAD) MANAGEMENT ADULT EMERGENCY MEDICAL DISPATCHER EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC A Ventricular Assist Device, or VAD, is a mechanical
Facts. STRONG Risk Factors for HF* LVAD, BiVAD, RVAD, HVAD 10/21/ million adults in the US have heart failure.
 10/21/18 1 Facts 5.8 million adults in the US have heart failure. About ½ of those who have HF have a 5 year life expectancy. STRONG Risk Factors for HF* Coronary Heart Disease/MI/Afib COPD Renal Failure
10/21/18 1 Facts 5.8 million adults in the US have heart failure. About ½ of those who have HF have a 5 year life expectancy. STRONG Risk Factors for HF* Coronary Heart Disease/MI/Afib COPD Renal Failure
Left Ventricular Assist Devices LVAD. North Country EMS Program Agency 3/21/12
 Left Ventricular Assist Devices LVAD North Country EMS Program Agency 3/21/12 Objectives Describe indications for and functions of ventricular assist devices (LVAD) Differentiate assessment findings of
Left Ventricular Assist Devices LVAD North Country EMS Program Agency 3/21/12 Objectives Describe indications for and functions of ventricular assist devices (LVAD) Differentiate assessment findings of
Modern Left Ventricular Assist Devices (LVAD) : An Intro, Complications, and Emergencies
 Modern Left Ventricular Assist Devices (LVAD) : An Intro, Complications, and Emergencies ERIC T. ROME D.O. HEART FAILURE, MECHANICAL ASSISTANCE AND TRANSPLANTATION CVI Left Ventricular Assist Device An
Modern Left Ventricular Assist Devices (LVAD) : An Intro, Complications, and Emergencies ERIC T. ROME D.O. HEART FAILURE, MECHANICAL ASSISTANCE AND TRANSPLANTATION CVI Left Ventricular Assist Device An
About Your Ventricular Assist Device (VAD) Surgery
 About Your Ventricular Assist Device (VAD) Surgery Why do I need surgery for a Heart Pump or Ventricular Assist Device (VAD)? VAD s may help you live longer. These electric powered heart pumps are put
About Your Ventricular Assist Device (VAD) Surgery Why do I need surgery for a Heart Pump or Ventricular Assist Device (VAD)? VAD s may help you live longer. These electric powered heart pumps are put
CHANGING THE WAY HEART FAILURE IS TREATED. VAD Therapy
 CHANGING THE WAY HEART FAILURE IS TREATED VAD Therapy VAD THERAPY IS BECOMING AN ESSENTIAL PART OF HEART FAILURE PROGRAMS AROUND THE WORLD. Patients with advanced heart failure experience an impaired quality
CHANGING THE WAY HEART FAILURE IS TREATED VAD Therapy VAD THERAPY IS BECOMING AN ESSENTIAL PART OF HEART FAILURE PROGRAMS AROUND THE WORLD. Patients with advanced heart failure experience an impaired quality
Exploring Options. A decision aid for Left Ventricular Assist Device (LVAD) as Destination Therapy A device for patients with advanced heart failure
 A decision aid for Left Ventricular Assist Device (LVAD) as Destination Therapy A device for patients with advanced heart failure Exploring Options You are being considered for an LVAD. This booklet is
A decision aid for Left Ventricular Assist Device (LVAD) as Destination Therapy A device for patients with advanced heart failure Exploring Options You are being considered for an LVAD. This booklet is
Exploring Options. A decision aid for Left Ventricular Assist Device (LVAD) A device for patients with advanced heart failure
 A decision aid for Left Ventricular Assist Device (LVAD) A device for patients with advanced heart failure Exploring Options You are being considered for an LVAD. This booklet is designed to help you understand
A decision aid for Left Ventricular Assist Device (LVAD) A device for patients with advanced heart failure Exploring Options You are being considered for an LVAD. This booklet is designed to help you understand
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Continuing Education Packet January-Feb 2018 Ventricular Assist Devices
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Continuing Education Packet January-Feb 2018 Ventricular Assist Devices Simply a ventricular assist device (VAD) is an implantable mechanical
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Continuing Education Packet January-Feb 2018 Ventricular Assist Devices Simply a ventricular assist device (VAD) is an implantable mechanical
LIVING A MORE ACTIVE LIFE. with the HeartMate 3 LVAD for the treatment of advanced heart failure RON. Recipient
 LIVING A MORE ACTIVE LIFE with the HeartMate 3 LVAD for the treatment of advanced heart failure RON HeartMate 3 LVAD Recipient What is HEART FAILURE? Heart failure sometimes called a weak heart occurs
LIVING A MORE ACTIVE LIFE with the HeartMate 3 LVAD for the treatment of advanced heart failure RON HeartMate 3 LVAD Recipient What is HEART FAILURE? Heart failure sometimes called a weak heart occurs
Exploring Options. A decision aid for Left Ventricular Assist Device (LVAD) A device for patients with advanced heart failure
 A decision aid for Left Ventricular Assist Device (LVAD) A device for patients with advanced heart failure Exploring Options You are being considered for an LVAD. This booklet is designed to help you understand
A decision aid for Left Ventricular Assist Device (LVAD) A device for patients with advanced heart failure Exploring Options You are being considered for an LVAD. This booklet is designed to help you understand
UNIVERSITY OF UTAH HEALTH CARE HOSPITALS AND CLINICS
 UNIVERSITY OF UTAH HEALTH CARE HOSPITALS AND CLINICS CARDIAC MECHANICAL SUPPORT PROGRAM GUIDELINES CARDIAC MECHANICAL SUPPORT: LVAD BASICS FREQUENT SCENARIOS AND TROUBLESHOOTING Review Date: July 2011
UNIVERSITY OF UTAH HEALTH CARE HOSPITALS AND CLINICS CARDIAC MECHANICAL SUPPORT PROGRAM GUIDELINES CARDIAC MECHANICAL SUPPORT: LVAD BASICS FREQUENT SCENARIOS AND TROUBLESHOOTING Review Date: July 2011
Jarvik 2000 VAS LAVENDER LAVENDER LAVENDER LAVENDER LAVENDER. 1. Can I do external CPR? Yes, only as a last resort.
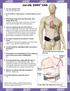 1. Can I do external CPR? Yes, only as a last resort. 2. If not, is there a hand pump or external device to use? No. 3. If the device slows down (low flow state), what alarms will go off? No alarm for
1. Can I do external CPR? Yes, only as a last resort. 2. If not, is there a hand pump or external device to use? No. 3. If the device slows down (low flow state), what alarms will go off? No alarm for
Giving your heart strength. Ventricular Assist Device.
 Giving your heart strength. Ventricular Assist Device. 1 National leader in Ventricular Assist Devices Although you may be nervous when considering heart surgery, you can rest assured knowing that UR Medicine
Giving your heart strength. Ventricular Assist Device. 1 National leader in Ventricular Assist Devices Although you may be nervous when considering heart surgery, you can rest assured knowing that UR Medicine
Is it time to consider a HEARTMATE LEFT VENTRICULAR ASSIST DEVICE (LVAD)?
 Is it time to consider a HEARTMATE LEFT VENTRICULAR ASSIST DEVICE (LVAD)? A treatment for advanced heart failure. LAURA HeartMate II LVAD Recipient What is HEART FAILURE? Heart failure sometimes called
Is it time to consider a HEARTMATE LEFT VENTRICULAR ASSIST DEVICE (LVAD)? A treatment for advanced heart failure. LAURA HeartMate II LVAD Recipient What is HEART FAILURE? Heart failure sometimes called
LVAD, RVAD, BiVAD, Total Artificial Heart
 UW MEDICINE PATIENT EDUCATION Mechanical Circulatory Support (MCS) Surgery: LVAD, RVAD, BiVAD, Total Artificial Heart Your follow-up care This handout explains follow-up care after your mechanical circulatory
UW MEDICINE PATIENT EDUCATION Mechanical Circulatory Support (MCS) Surgery: LVAD, RVAD, BiVAD, Total Artificial Heart Your follow-up care This handout explains follow-up care after your mechanical circulatory
LVAD in a Community Hospital Are You Prepared?
 LVAD in a Community Hospital Are You Prepared? Class: C75M119 LVAD ~ Left Ventricular Assist Device A mechanical circulatory support (MCS) pump Supports the damaged heart Reestablished normal hemodynamics
LVAD in a Community Hospital Are You Prepared? Class: C75M119 LVAD ~ Left Ventricular Assist Device A mechanical circulatory support (MCS) pump Supports the damaged heart Reestablished normal hemodynamics
Going Home with the Heartware (HVAD) LVAD
 Going Home with the Heartware (HVAD) LVAD While living at home with your ventricular assist device (VAD), it is vital that you follow these instructions. You must know and understand the warnings and cautions
Going Home with the Heartware (HVAD) LVAD While living at home with your ventricular assist device (VAD), it is vital that you follow these instructions. You must know and understand the warnings and cautions
Perioperative Management of the Mechanical Circulatory Support Patient. American Association of Thoracic Surgeons Allied Health Symposium May 4, 2013
 Perioperative Management of the Mechanical Circulatory Support Patient American Association of Thoracic Surgeons Allied Health Symposium May 4, 2013 Disclosures None 2012 MFMER slide-2 Objectives Review
Perioperative Management of the Mechanical Circulatory Support Patient American Association of Thoracic Surgeons Allied Health Symposium May 4, 2013 Disclosures None 2012 MFMER slide-2 Objectives Review
Going Home with the HeartMate 3 LVAD
 Going Home with the HeartMate 3 LVAD While living at home with your ventricular assist device (VAD), it is vital that you follow these instructions. You must know and understand the warnings and cautions
Going Home with the HeartMate 3 LVAD While living at home with your ventricular assist device (VAD), it is vital that you follow these instructions. You must know and understand the warnings and cautions
07/17/2014. Thursday, July 17, 14
 HENRY FORD HOSPITAL Ventricular Assist Device Emergency Response Cheryl Smith, R.N., B.S.N. VAD Coordinator Henry Ford Health System 1 WHAT IS A VAD? What is a VAD? How does it work? 1 Pulsatile, Volume
HENRY FORD HOSPITAL Ventricular Assist Device Emergency Response Cheryl Smith, R.N., B.S.N. VAD Coordinator Henry Ford Health System 1 WHAT IS A VAD? What is a VAD? How does it work? 1 Pulsatile, Volume
DEMYSTIFYING VADs. Nicolle Choquette RN MN Athabasca University
 DEMYSTIFYING VADs Nicolle Choquette RN MN Athabasca University Objectives odefine o Heart Failure o VAD o o o o Post Operative Complications Acute Long Term Nursing Interventions What is Heart Failure?
DEMYSTIFYING VADs Nicolle Choquette RN MN Athabasca University Objectives odefine o Heart Failure o VAD o o o o Post Operative Complications Acute Long Term Nursing Interventions What is Heart Failure?
ECMO Extracorporeal Membrane Oxygenation
 ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
Atrial fibrillation. Understanding NICE guidance
 Understanding NICE guidance Information for people who use NHS services Atrial fibrillation NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Understanding NICE guidance Information for people who use NHS services Atrial fibrillation NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Knowing your treatment options can give you hope for a longer, better life
 Heart failure is a deadly disease Knowing your treatment options can give you hope for a longer, better life With heart failure, it was not a matter of if I would get worse; it was a matter of when, and
Heart failure is a deadly disease Knowing your treatment options can give you hope for a longer, better life With heart failure, it was not a matter of if I would get worse; it was a matter of when, and
Admission of patient CVICU and hemodynamic monitoring
 Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Ventricular Assist Devices and Emergency Services
 Ventricular Assist Devices and Emergency Services Margaret Murray, DNP, FAHA Clinical Nurse Specialist- Cardiac Surgery, Cardiac Transplant and Ventricular Assist Devices ma.murray@hosp.wisc.edu Janean
Ventricular Assist Devices and Emergency Services Margaret Murray, DNP, FAHA Clinical Nurse Specialist- Cardiac Surgery, Cardiac Transplant and Ventricular Assist Devices ma.murray@hosp.wisc.edu Janean
How does the heart work? The heart is muscle whose main function is a pump; to push blood the rest of your body.
 1 You have a condition called atrial fibrillation. I would like you to learn more about this condition. You should read about it below, and can also watch an Internet program about it. After reading about
1 You have a condition called atrial fibrillation. I would like you to learn more about this condition. You should read about it below, and can also watch an Internet program about it. After reading about
เอกราช อร ยะช ยพาณ ชย
 30 July 2016 เอกราช อร ยะช ยพาณ ชย Heart Failure and Transplant Cardiology aekarach.a@chula.ac.th Disclosure Speaker, CME service: Merck, Otsuka, Servier Consultant, non-cme service: Novartis, Menarini
30 July 2016 เอกราช อร ยะช ยพาณ ชย Heart Failure and Transplant Cardiology aekarach.a@chula.ac.th Disclosure Speaker, CME service: Merck, Otsuka, Servier Consultant, non-cme service: Novartis, Menarini
Heart Failure. Symptoms and Treatments. FloridaHospital.com
 Heart Failure Symptoms and Treatments FloridaHospital.com Understanding Heart Failure According to the American Heart Association, one in five people over age 40 will develop heart failure. Right now,
Heart Failure Symptoms and Treatments FloridaHospital.com Understanding Heart Failure According to the American Heart Association, one in five people over age 40 will develop heart failure. Right now,
Cardiovascular Emergencies. Chapter 12
 Cardiovascular Emergencies Chapter 12 Cardiovascular Emergencies Cardiovascular disease (CVD) claimed 931,108 lives in the US during 2001. 2,551 per day Almost two people per minute! CVD accounts for 38.5%
Cardiovascular Emergencies Chapter 12 Cardiovascular Emergencies Cardiovascular disease (CVD) claimed 931,108 lives in the US during 2001. 2,551 per day Almost two people per minute! CVD accounts for 38.5%
Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know!
 Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know! Matthew A. Wanat, PharmD, BCPS, BCCCP, FCCM Clinical Assistant Professor University of Houston College of Pharmacy Clinical Pharmacy
Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know! Matthew A. Wanat, PharmD, BCPS, BCCCP, FCCM Clinical Assistant Professor University of Houston College of Pharmacy Clinical Pharmacy
Treatment Options Not Not access
 Treatment Options Treatment options for Chronic Kidney Disease (CKD) CKD is a permanent condition. Treatment will: Help the patient feel better Not cure the disease Not make the kidneys start working again
Treatment Options Treatment options for Chronic Kidney Disease (CKD) CKD is a permanent condition. Treatment will: Help the patient feel better Not cure the disease Not make the kidneys start working again
LVAD in a Community Hospital Are You Prepared?
 LVAD in a Community Hospital Are You Prepared? Class: C75M119 Objectives Describe the principles of destination LVAD in advanced heart failure Discuss emergency management of LVAD patient Outline a plan
LVAD in a Community Hospital Are You Prepared? Class: C75M119 Objectives Describe the principles of destination LVAD in advanced heart failure Discuss emergency management of LVAD patient Outline a plan
Ventricular Assisting Devices in the Cathlab. Unrestricted
 Ventricular Assisting Devices in the Cathlab Unrestricted What is a VAD? A single system device that is surgically attached to the left ventricle of the heart and to the aorta for left ventricular support
Ventricular Assisting Devices in the Cathlab Unrestricted What is a VAD? A single system device that is surgically attached to the left ventricle of the heart and to the aorta for left ventricular support
Ventricular Assist Device (VAD)
 Ventricular Assist Device (VAD) Pre-operative Education Handbook FHTransplant.com 1 Table of Contents 3 Contact Information 4 Advanced Heart Failure, Cardiac Transplant and Circulatory Assist Device Program
Ventricular Assist Device (VAD) Pre-operative Education Handbook FHTransplant.com 1 Table of Contents 3 Contact Information 4 Advanced Heart Failure, Cardiac Transplant and Circulatory Assist Device Program
AUTOLOGS TM ATLAS ON DEMAND DATA WITH EVERY PATIENT VISIT
 AUTOLOGS TM ATLAS ON DEMAND DATA WITH EVERY PATIENT VISIT Introduction The Autologs Atlas will guide your introduction to our new Autologs service and the information recorded by the HeartWare HVAD TM
AUTOLOGS TM ATLAS ON DEMAND DATA WITH EVERY PATIENT VISIT Introduction The Autologs Atlas will guide your introduction to our new Autologs service and the information recorded by the HeartWare HVAD TM
QUICK REFERENCE HEARTWARE HVAD PUMP FLOW INDEX
 QUICK REFERENCE HEARTWARE HVAD PUMP FLOW INDEX LOW PULSATILITY, LOW FLOW HVAD waveforms do NOT conform to a single, classic appearance, and are not intended for diagnostic purposes. Waveforms represent
QUICK REFERENCE HEARTWARE HVAD PUMP FLOW INDEX LOW PULSATILITY, LOW FLOW HVAD waveforms do NOT conform to a single, classic appearance, and are not intended for diagnostic purposes. Waveforms represent
Ventricular Assist Device Technology in the Rehabilitation World
 Ventricular Assist Device Technology in the Rehabilitation World MARCIA STAHOVICH, RN, CCRN MAUREEN LE DANSEUR, MSN, RN, CNS-BC, CRRN SHARP MEMORIAL HOSPITAL SAN DIEGO, CA Disclosures: Marcia Speakers
Ventricular Assist Device Technology in the Rehabilitation World MARCIA STAHOVICH, RN, CCRN MAUREEN LE DANSEUR, MSN, RN, CNS-BC, CRRN SHARP MEMORIAL HOSPITAL SAN DIEGO, CA Disclosures: Marcia Speakers
EMT. Chapter 14 Review
 EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
VAD Program Alert: Practice Change regarding CPR
 VAD Program Alert: Practice Change regarding CPR March 2018 Background The left ventricular assist device (LVAD) is a mechanical internal heart pump used to treat heart failure. The pump provides continuous
VAD Program Alert: Practice Change regarding CPR March 2018 Background The left ventricular assist device (LVAD) is a mechanical internal heart pump used to treat heart failure. The pump provides continuous
12.1 Apply Your Knowledge How long does an ambulatory monitor typically remain on a patient?
 1 2 3 4 5 6 7 Learning Outcomes (Cont d) 12.4 Educate the patient about ambulatory monitoring. 12.5 Prepare a patient for application of an ambulatory monitor. 12.6 Describe the procedure for applying
1 2 3 4 5 6 7 Learning Outcomes (Cont d) 12.4 Educate the patient about ambulatory monitoring. 12.5 Prepare a patient for application of an ambulatory monitor. 12.6 Describe the procedure for applying
Mechanical Circulatory Support in the Management of Heart Failure
 Mechanical Circulatory Support in the Management of Heart Failure Feras Bader, MD, MS, FACC Associate Professor of Medicine Director, Heart Failure and Transplant Cleveland Clinic Abu Dhabi Chairman, Heart
Mechanical Circulatory Support in the Management of Heart Failure Feras Bader, MD, MS, FACC Associate Professor of Medicine Director, Heart Failure and Transplant Cleveland Clinic Abu Dhabi Chairman, Heart
Guide to Cardiology Care at Scripps
 Guide to Cardiology Care at Scripps Cardiology is the word in health care associated with heart, but the body s vascular system is also an important part of heart care. Your body has more than 60,000 miles
Guide to Cardiology Care at Scripps Cardiology is the word in health care associated with heart, but the body s vascular system is also an important part of heart care. Your body has more than 60,000 miles
LVAD Complications, Recovery
 LVAD Complications, Recovery Abbas Ardehali, M.D., F.A.C.S. Professor of Surgery and Medicine, Division of Cardiac Surgery William E. Connor Chair in Cardiothoracic Transplantation Director, UCLA Heart,
LVAD Complications, Recovery Abbas Ardehali, M.D., F.A.C.S. Professor of Surgery and Medicine, Division of Cardiac Surgery William E. Connor Chair in Cardiothoracic Transplantation Director, UCLA Heart,
X-Plain Pacemaker Reference Summary
 X-Plain Pacemaker Reference Summary Introduction A pacemaker is a device that regulates the heart beat. More than half a million Americans use a pacemaker. If your doctor recommends that you have a pacemaker,
X-Plain Pacemaker Reference Summary Introduction A pacemaker is a device that regulates the heart beat. More than half a million Americans use a pacemaker. If your doctor recommends that you have a pacemaker,
To standardize wound care and prevent infection in compromised patients who have a Berlin Heart Ventricular Assist Device (VAD).
 PURPOSE To standardize wound care and prevent infection in compromised patients who have a Berlin Heart Ventricular Assist Device (VAD). POLICY STATEMENTS Dressing change should be done no sooner than
PURPOSE To standardize wound care and prevent infection in compromised patients who have a Berlin Heart Ventricular Assist Device (VAD). POLICY STATEMENTS Dressing change should be done no sooner than
Performance and Quality Measures 1. NQF Measure Number. Coronary Artery Disease Measure Set
 Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
The Counter HF Clinical Study for Heart Failure
 The Counter HF Clinical Study for Heart Failure CAUTION: C-Pulse is an investigational device. It is limited by Federal (or United States) Law to investigational use only. 13-111-B Agenda Heart Failure
The Counter HF Clinical Study for Heart Failure CAUTION: C-Pulse is an investigational device. It is limited by Federal (or United States) Law to investigational use only. 13-111-B Agenda Heart Failure
Cardiac Resynchronisation Therapy Defibrillator (CRT-D)
 Patient information Cardiac Resynchronisation Therapy Defibrillator (CRT-D) i Important information for all patients requiring resynchronisation therapy. Golden Jubilee National Hospital Agamemnon Street
Patient information Cardiac Resynchronisation Therapy Defibrillator (CRT-D) i Important information for all patients requiring resynchronisation therapy. Golden Jubilee National Hospital Agamemnon Street
Heart failure is the final common
 CARDIOLOGY PATIENT PAGE Ventricular Assist Devices Important Information for Patients and Families Michael M. Givertz, MD Heart failure is the final common pathway for many chronic heart diseases. With
CARDIOLOGY PATIENT PAGE Ventricular Assist Devices Important Information for Patients and Families Michael M. Givertz, MD Heart failure is the final common pathway for many chronic heart diseases. With
RESTRICTIVE CARDIOMYOPATHY
 RESTRICTIVE CARDIOMYOPATHY Restrictive cardiomyopathy (RCM) is a rare form of heart muscle disease that is characterized by restrictive filling of the ventricles. In this disease the contractile function
RESTRICTIVE CARDIOMYOPATHY Restrictive cardiomyopathy (RCM) is a rare form of heart muscle disease that is characterized by restrictive filling of the ventricles. In this disease the contractile function
From Recovery to Transplant: One Patient's Journey
 From Recovery to Transplant: One Patient's Journey Tonya Elliott, RN, MSN Assist Device and Thoracic Transplant Coordinator Inova Transplant Center at Inova Fairfax Hospital Falls Church, VA Introduction
From Recovery to Transplant: One Patient's Journey Tonya Elliott, RN, MSN Assist Device and Thoracic Transplant Coordinator Inova Transplant Center at Inova Fairfax Hospital Falls Church, VA Introduction
STROKE INTRODUCTION OBJECTIVES. When the student has finished this module, he/she will be able to:
 STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. There are two types of stroke, but both types of stroke cause the same type of
STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. There are two types of stroke, but both types of stroke cause the same type of
HEART FAILURE PHARMACOLOGY. University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
Destination Therapy SO MUCH DATA IN SUCH A SMALL DEVICE. HeartWare HVAD System The ONLY intrapericardial VAD approved for DT.
 DT Destination Therapy SO MUCH DATA IN SUCH A SMALL DEVICE. HeartWare HVAD System The ONLY intrapericardial VAD approved for DT. ONLY WE HAVE THIS BREADTH OF CLINICAL EVIDENCE TO SUPPORT DESTINATION THERAPY.
DT Destination Therapy SO MUCH DATA IN SUCH A SMALL DEVICE. HeartWare HVAD System The ONLY intrapericardial VAD approved for DT. ONLY WE HAVE THIS BREADTH OF CLINICAL EVIDENCE TO SUPPORT DESTINATION THERAPY.
Artificial Heart Program
 Artificial Heart Program Provider Review: General VAD Overview Indications for VAD Bridge to transplant (BTT) historically most common (~80%) allow rehab from severe CHF while awaiting donor Bridge to
Artificial Heart Program Provider Review: General VAD Overview Indications for VAD Bridge to transplant (BTT) historically most common (~80%) allow rehab from severe CHF while awaiting donor Bridge to
NO Pulse! No Problem!
 NO Pulse! No Problem! Trauma Patients with an Artificial Heart Joan Somes RN-BC, PhD, CEN, CPEN, FAEN, NRP with a side dish of: Stop The Bleed! Disclosures 40 yrs. Emergency Dept. RN HealthEast Part time
NO Pulse! No Problem! Trauma Patients with an Artificial Heart Joan Somes RN-BC, PhD, CEN, CPEN, FAEN, NRP with a side dish of: Stop The Bleed! Disclosures 40 yrs. Emergency Dept. RN HealthEast Part time
A SIMPLE SOLUTION FOR CARDIAC MONITORING
 A SIMPLE SOLUTION FOR CARDIAC MONITORING SEEQ Mobile Cardiac Telemetry System Actual size. NOW THERE S AN EXTERNAL HEART MONITOR THAT S AS SIMPLE TO WEAR AS A BANDAGE It s called the SEEQ Mobile Cardiac
A SIMPLE SOLUTION FOR CARDIAC MONITORING SEEQ Mobile Cardiac Telemetry System Actual size. NOW THERE S AN EXTERNAL HEART MONITOR THAT S AS SIMPLE TO WEAR AS A BANDAGE It s called the SEEQ Mobile Cardiac
Understanding the Pediatric Ventricular Assist Device
 Understanding the Pediatric Ventricular Assist Device W. James Parks, MSc., MD Pediatric Cardiologist Assistant Professor of Pediatrics and Radiology Children s Healthcare of Atlanta Sibley Heart Center
Understanding the Pediatric Ventricular Assist Device W. James Parks, MSc., MD Pediatric Cardiologist Assistant Professor of Pediatrics and Radiology Children s Healthcare of Atlanta Sibley Heart Center
ICD Implantation Patient Information
 Melbourne Heart Rhythm ICD Implantation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers (the right atrium
Melbourne Heart Rhythm ICD Implantation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers (the right atrium
Cardiac Drugs: Chapter 9 Worksheet Cardiac Agents. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate.
 Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Our Commitment to Quality and Patient Safety Core Measures
 Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Information for patients, parents and guardians. Your child s doctor has recommended that your child has a procedure called an ablation.
 Having an ablation Information for patients, parents and guardians Your child s doctor has recommended that your child has a procedure called an ablation. An ablation is a treatment for an abnormal heartbeat.
Having an ablation Information for patients, parents and guardians Your child s doctor has recommended that your child has a procedure called an ablation. An ablation is a treatment for an abnormal heartbeat.
Please check appropriate box: Right Left Bilateral Not Applicable
 Patient Label Here UNIVERSITY MEDICAL CENTER DISCLOSURE AND CONSENT - MEDICAL AND SURGICAL PROCEDURES TO THE PATIENT: You have the right as a patient to be informed about your condition and the recommended
Patient Label Here UNIVERSITY MEDICAL CENTER DISCLOSURE AND CONSENT - MEDICAL AND SURGICAL PROCEDURES TO THE PATIENT: You have the right as a patient to be informed about your condition and the recommended
The Adolescent and Adult Congenital Heart Disease Program
 The Adolescent and Adult Congenital Heart Disease Program The Heart Center at Nationwide Children s Hospital & The Ohio State University D- Transposition of the Great Vessels D- transposition of the great
The Adolescent and Adult Congenital Heart Disease Program The Heart Center at Nationwide Children s Hospital & The Ohio State University D- Transposition of the Great Vessels D- transposition of the great
Relax and Learn At the Farm 2012
 Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Drainage Frequency: PATIENT GUIDE. Dressing Frequency: Every Drainage Weekly Drainage. Physician Contact Information. Dr. Phone:
 Drainage Frequency: PATIENT GUIDE Dressing Frequency: Every Drainage Weekly Drainage Physician Contact Information Dr. Phone: CHEST DRAINAGE Pleural Space Insertion Site Cuff Exit Site Catheter Valve Connector
Drainage Frequency: PATIENT GUIDE Dressing Frequency: Every Drainage Weekly Drainage Physician Contact Information Dr. Phone: CHEST DRAINAGE Pleural Space Insertion Site Cuff Exit Site Catheter Valve Connector
Hemodynamic Monitoring and Circulatory Assist Devices
 Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
LEFT VENTRICULAR ASSIST DEVICES WHERE DOES PALLIATIVE MEDICINE FIT?
 Glennan Center for Geriatrics and Gerontology LEFT VENTRICULAR ASSIST DEVICES WHERE DOES PALLIATIVE MEDICINE FIT? April 7, 21016 Marissa Galicia Castillo, MD Medical Director, Sentara Norfolk General Hospital
Glennan Center for Geriatrics and Gerontology LEFT VENTRICULAR ASSIST DEVICES WHERE DOES PALLIATIVE MEDICINE FIT? April 7, 21016 Marissa Galicia Castillo, MD Medical Director, Sentara Norfolk General Hospital
About atrial fibrillation (AFib) Atrial Fibrillation (AFib) What is AFib? What s the danger? Who gets AFib?
 Understanding AFib Atrial Fibrillation (AFib) About AFib 3 How Your Heart Works 4 Types of AFib 5 Symptoms 5 Risk Factors 5 How is AFib Diagnosed? 6 Treatment 6 What to Ask Your Doctor 7 A normal heartbeat
Understanding AFib Atrial Fibrillation (AFib) About AFib 3 How Your Heart Works 4 Types of AFib 5 Symptoms 5 Risk Factors 5 How is AFib Diagnosed? 6 Treatment 6 What to Ask Your Doctor 7 A normal heartbeat
Module 10 Troubleshooting Guide
 Module 10 Troubleshooting Guide Your safety and wellbeing are our priority. Issues can occur during your treatment and it is important that you recognize the symptoms. This guide will teach you how to
Module 10 Troubleshooting Guide Your safety and wellbeing are our priority. Issues can occur during your treatment and it is important that you recognize the symptoms. This guide will teach you how to
Cardiac Resynchronisation Therapy Patient Information
 Melbourne Heart Rhythm Cardiac Resynchronisation Therapy Patient Information Normal Heart Function The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two
Melbourne Heart Rhythm Cardiac Resynchronisation Therapy Patient Information Normal Heart Function The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two
Living well with Heart Failure. Annabel Sturges Heart Failure Specialist Nurse Frimley Park Hospital
 Living well with Heart Failure Annabel Sturges Heart Failure Specialist Nurse Frimley Park Hospital How the Normal Heart works.. The Heart is a string muscular pump Its job is to pump the right amount
Living well with Heart Failure Annabel Sturges Heart Failure Specialist Nurse Frimley Park Hospital How the Normal Heart works.. The Heart is a string muscular pump Its job is to pump the right amount
Lesson 4-3: Cardiac Emergencies. CARDIAC EMERGENCIES Angina, AMI, CHF and AED
 Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
UW MEDICINE PATIENT EDUCATION. Hemodialysis. A treatment option for kidney disease. Treatment Options for Kidney Disease
 UW MEDICINE PATIENT EDUCATION Hemodialysis A treatment option for kidney disease Class Goals 1. Understand the purpose and care of blood access. 2. Understand the purpose and basic principles of hemodialysis.
UW MEDICINE PATIENT EDUCATION Hemodialysis A treatment option for kidney disease Class Goals 1. Understand the purpose and care of blood access. 2. Understand the purpose and basic principles of hemodialysis.
Diagnosis of Device Thrombosis
 Diagnosis of Device Thrombosis Andrew Civitello MD, FACC Medical Director, Heart Transplant Program Director, Fellowship Co-Director, Baylor St. Luke's Medical Center / Texas Heart Institute Trends in
Diagnosis of Device Thrombosis Andrew Civitello MD, FACC Medical Director, Heart Transplant Program Director, Fellowship Co-Director, Baylor St. Luke's Medical Center / Texas Heart Institute Trends in
HIP REPLACEMENT SURGERY
 HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
Nursing Process Focus: Patients Receiving Heparin
 Obtain complete heath history including allergies, drug history and possible drug Assess baseline coagulation studies and CBC. Assess for history of bleeding disorders, GI bleeding, cerebral bleed, recent
Obtain complete heath history including allergies, drug history and possible drug Assess baseline coagulation studies and CBC. Assess for history of bleeding disorders, GI bleeding, cerebral bleed, recent
Suprapubic and Mitrofanoff Catheter Care
 Urinary catheters are tubes that drain urine from your child s bladder. There are many different types of urinary catheters. Your nurse will teach you how to care for these catheters. Here is information
Urinary catheters are tubes that drain urine from your child s bladder. There are many different types of urinary catheters. Your nurse will teach you how to care for these catheters. Here is information
MONITORING PATIENTS WITH A TEMPORARY EXTERNAL EPICARDIAL PACEMAKER PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES
 PURPOSE Guidelines for caring for and monitoring patients with a temporary external epicardial pacemaker. Epicardial pacemaker monitoring is performed on a continuous basis by a nurse to evaluate the effectiveness
PURPOSE Guidelines for caring for and monitoring patients with a temporary external epicardial pacemaker. Epicardial pacemaker monitoring is performed on a continuous basis by a nurse to evaluate the effectiveness
Treatment choices for someone with Stage 5 kidney disease are:
 Information for patients about advanced kidney disease Dialysis and non-dialysis treatments DOCUMENT PREPARED FOR This information is to help you understand some key issues about dialysis; it is designed
Information for patients about advanced kidney disease Dialysis and non-dialysis treatments DOCUMENT PREPARED FOR This information is to help you understand some key issues about dialysis; it is designed
How to prevent blood clots whilst in hospital and after your return home
 How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
What You Need to Know about a Kidney Transplant
 Page 1 of 5 What You Need to Know about a Kidney Transplant This information will help you understand the risks, benefits and possible complications involved in a kidney transplant. Please read it carefully.
Page 1 of 5 What You Need to Know about a Kidney Transplant This information will help you understand the risks, benefits and possible complications involved in a kidney transplant. Please read it carefully.
LVADs, Supraglottic Airways and CPAP
 LVADs, Supraglottic Airways and CPAP David M. Landsberg, MD, FF/EMT-P, FACP, FCCP Chief of Medicine Crouse Hospital Associate Professor of Medicine and Emergency Medicine Upstate 38MD-1, 83MD-1, 98MD-4
LVADs, Supraglottic Airways and CPAP David M. Landsberg, MD, FF/EMT-P, FACP, FCCP Chief of Medicine Crouse Hospital Associate Professor of Medicine and Emergency Medicine Upstate 38MD-1, 83MD-1, 98MD-4
1. Wounds may be left exposed with some ointment applied to the stitch line:
 GENERAL AFTERCARE AT HOME Elevation If you have had surgery to your face or the chest area it is important that you try to elevate this area in the first couple of days as there is the tendency to swelling.
GENERAL AFTERCARE AT HOME Elevation If you have had surgery to your face or the chest area it is important that you try to elevate this area in the first couple of days as there is the tendency to swelling.
Less Invasive Ventricular Enhancement For Heart Attack Patients. Revivent TC TransCatheter Ventricular Enhancement System
 For Heart Attack Patients Revivent TC TransCatheter Ventricular Enhancement System This patient booklet is for those who have suffered a heart attack resulting in damage to the left side of the heart causing
For Heart Attack Patients Revivent TC TransCatheter Ventricular Enhancement System This patient booklet is for those who have suffered a heart attack resulting in damage to the left side of the heart causing
Atrial Fibrillation. Damage to your heart caused by a heart attack or rheumatic heart disease
 Atrial Fibrillation GENERAL INFORMATION: What is atrial fibrillation? Atrial fibrillation is a condition that causes the atria (top chambers of the heart) to shake or quiver. Normally, there is 1 contraction
Atrial Fibrillation GENERAL INFORMATION: What is atrial fibrillation? Atrial fibrillation is a condition that causes the atria (top chambers of the heart) to shake or quiver. Normally, there is 1 contraction
Atrial Fibrillation Information for patients
 be informed about... Atrial Fibrillation Information for patients Atrial fibrillation (AF) is an abnormal heart rhythm. This pamphlet answers some questions you may have about AF, and gives an overview
be informed about... Atrial Fibrillation Information for patients Atrial fibrillation (AF) is an abnormal heart rhythm. This pamphlet answers some questions you may have about AF, and gives an overview
Module 7 Your Blood Work
 Module 7 Your Blood Work Every month you will need to collect a sample of your blood just before you start dialysis, and depending on your doctor s recommendation, at the end of your dialysis treatment.
Module 7 Your Blood Work Every month you will need to collect a sample of your blood just before you start dialysis, and depending on your doctor s recommendation, at the end of your dialysis treatment.
Disclosures. No disclosures to report
 Disclosures No disclosures to report Update on MOMENTUM 3 Trial: The Final Word? Francis D. Pagani MD PhD Otto Gago MD Professor of Cardiac Surgery University of Michigan Ann Arbor, Michigan, USA LVAD
Disclosures No disclosures to report Update on MOMENTUM 3 Trial: The Final Word? Francis D. Pagani MD PhD Otto Gago MD Professor of Cardiac Surgery University of Michigan Ann Arbor, Michigan, USA LVAD
Chapter 10. Learning Objectives. Learning Objectives 9/11/2012. Congestive Heart Failure
 Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Acute Arrhythmias in the Hospitalized Patient
 Acute Arrhythmias in the Hospitalized Patient Gregory M Marcus, MD, MAS Associate Professor of Medicine Division of Cardiology University of California, San Francisc Disclosures Medtronic: Research Support
Acute Arrhythmias in the Hospitalized Patient Gregory M Marcus, MD, MAS Associate Professor of Medicine Division of Cardiology University of California, San Francisc Disclosures Medtronic: Research Support
FAILURE. Matt Beecroft, MD
 FAILURE Matt Beecroft, MD 64 yo male with no real PMH Sitting on couch when sudden onset SOB Says he s been sweaty FIRST PATIENT OF THE WEEKEND HR 131, RR 28, 132/96, 93% RE-EXAM BP 229/130, HR 180s
FAILURE Matt Beecroft, MD 64 yo male with no real PMH Sitting on couch when sudden onset SOB Says he s been sweaty FIRST PATIENT OF THE WEEKEND HR 131, RR 28, 132/96, 93% RE-EXAM BP 229/130, HR 180s
